Pleural effusion occurs in up to 89% of patients
|
|
|
- Preston Webb
- 5 years ago
- Views:
Transcription
1 Symptomatic Persistent Post-Coronary Artery Bypass Graft Pleural Effusions Requiring Operative Treatment* Clinical and Histologic Features Y. C. Gary Lee, MBChB; Marcelo A. C. Vaz, MD; Kim A. Ely, MD; Edward C. McDonald, MD; Philip J. Thompson, MBBS, FCCP; Jonathan C. Nesbitt, MD, FCCP; and Richard W. Light, MD, FCCP Background: More than 85 of patients develop pleural effusions after coronary artery bypass grafting (CABG). Although the majority resolve spontaneously, post-cabg effusions can persist. The cause of these persistent effusions is unknown, and the histology of the pleural changes has seldom been reported. Objectives: To describe the patient characteristics and pathologic condition of the pleural tissues in patients with persistent post-cabg effusions. Subjects: Eight patients with persistent post-cabg effusions who underwent thoracoscopy or thoracotomy over a 2-year period by one thoracic surgeon. These eight patients were selected as having undergone CABG > 2 months before their thoracic surgery and had no other identifiable causes of effusion. Results: The median time from CABG to pleural surgery was 132 days (range, 74 to 2,258 days). The median left ventricular ejection fraction was 57 (range, 15 to 70). All patients were dyspneic and had large (> 25 of the hemithorax) effusions on chest radiograph. All effusions persisted after two or more thoracenteses. Pleural effusion was left sided in three patients and bilateral in five patients. Pleural fluid was characterized by lymphocytosis (82 to 99). Four of the eight patients had a visceral peel and trapped lung requiring decortication. Seven of the eight biopsy specimens showed pleural thickening characterized by dense fibrous tissues with associated mononuclear cell infiltration, while the eighth biopsy specimen showed only clotted blood. The degree of inflammation and fibrosis correlated with the interval between CABG and pleural surgery. Early post-cabg patients displayed more inflammation, with abundant lymphocytes in nodular configuration deep in the fibrous tissues away from the surface. Abundant keratinpositive, spindle-shaped cells were present in the fibrous tissues. Late cases showed predominantly mature fibrosis. Conclusions: Persistent post-cabg effusion can occur. Pleural fluids and pleural tissue in early-stage lesions were characterized by lymphocytosis. With time, the inflammatory changes were replaced by fibrosis that resulted in dyspnea and, at times, trapped lungs requiring surgical intervention. (CHEST 2001; 119: ) Key words: coronary artery bypass grafting; pathology; pleural effusion Abbreviation: CABG coronary artery bypass grafting Pleural effusion occurs in up to 89 of patients during the first week after coronary artery bypass grafting (CABG). 1 Most of these effusions are small, self-limiting, and do not require interventions. 2 However, chronic, persistent post-cabg effusions have been reported. 3 7 The etiology of these persistent effusions remains unknown. We report the clinical and pleural histologic features of eight patients who had persistent post- CABG pleural effusions and underwent thoracos- *From the Departments of Pulmonary Medicine (Dr. Lee) and Pathology (Dr. McDonald) and Cardiovascular Surgical Associates (Dr. Nesbitt), Saint Thomas Hospital, Nashville, TN; the Pulmonary Division (Dr. Vaz), Heart Institute (INCOR), University of Sao Paulo Medical School, Sao Paulo, Brazil; the Departments of Pathology (Dr. Ely) and Medicine (Dr. Light), Vanderbilt University, Nashville, TN; and the Department of Medicine (Dr. Thompson), University of Western Australia, Perth, Australia. Supported by the Saint Thomas Foundation, Nashville, TN, and United States-New Zealand Fulbright Graduate Award (Dr. Lee). Manuscript received February 29, 2000; revision accepted September 25, Correspondence to: Y. C. Gary Lee, MBChB, Department of Pulmonary Medicine, Saint Thomas Hospital, 4220 Harding Rd, Nashville, TN 37202; ycgarylee@hotmail.com CHEST / 119 / 3/ MARCH,
2 copy or thoracotomy from 10 weeks to 6 years after their CABG. Materials and Methods All patients who underwent thoracoscopy or thoracotomy for pleural effusion performed by one thoracic surgeon (J.C.N.) in our institute between October 1, 1997, and October 1, 1999, and who had previous histories of CABG were identified. Their medical records, chest radiographs, laboratory results, and surgical records were reviewed. Post-CABG effusion was defined as a pleural effusion that developed within the first 2 months after CABG where no other causes were identified. s were contacted by telephone at the end of October 1999 (2 to 12 months after their thoracoscopy or thoracotomy), regarding whether they had further needs of thoracentesis. This study was approved by the Institutional Review Board of Saint Thomas Hospital. Clinical Data Eight patients who underwent video-assisted thoracoscopy or thoracotomy for investigation or management of persistent post- CABG pleural effusions were identified. Their pleural tissues from open biopsy were independently examined. The pleural fluid result of one of the patients (patient 7) has been included in a previous publication. 7 None of the eight patients had radiologic evidence of pleural effusion before their CABG. Two patients had mild chronic renal impairment (serum creatinine, 1.6 mg/dl and 1.7 mg/dl, respectively) not severe enough to explain their effusions. None of these patients had a history of connective tissue diseases, hepatic cirrhosis, recent pneumonia, significant asbestos exposure, or use of drugs associated with pleural effusions. Pathology Pleural tissues obtained during thoracoscopy or thoracotomy were reviewed. The slides were stained with hematoxylin-eosin and cytokeratin stains (for immunoreactivity against AE1/AE3 and a low-molecular-weight cytokeratin, CAM-5.2). Immunohistochemical analysis with L26 (pan B-cell specific marker) and UCHL1 (pan T-cell-specific marker) was also performed. Results Six male and two female patients was included. Median age was 69 years (range, 47 to 88 years) at the time of thoracoscopy or thoracotomy, with the median interval from CABG to thoracoscopy/thoracotomy being 132 days (range, 74 to 2,258 days). All the patients complained of dyspnea, one had a cough, and two reported weight loss. None of the patients had pleuritic chest pain or fever. Two patients were receiving warfarin (patients 2 and 3), while the remaining six patients were receiving aspirin. 2 also had an aortic valve replacement at the time of CABG. The demographics of these patients, the intervals between CABG and first evidence of pleural effusion as well as between CABG and first thoracentesis, the preoperative left ventricular ejection fractions (measured on echocardiography or during cardiac catheterization), and types of bypass grafts are presented in Table 1. All patients had large ( 25 of the hemithorax) effusions on chest radiograph. The pleural effusion was left sided in three patients and bilateral in five patients. All effusions persisted after two or more thoracenteses. Two patients (patients 2 and 7) also underwent tube thoracostomy before their thoracic surgery. The radiographic abnormalities and number of thoracenteses received are reported in Table 2. The thoracentesis results were available in four patients (Table 3). Lymphocytosis (82 to 99) was a common feature in all these four effusions. 8 underwent her CABG in June Bilateral effusions (right side more than left) were diagnosed 4 weeks after CABG, and she received the first thoracentesis at the same time. She underwent a further thoracentesis for symptomatic dyspnea in early 1993, and thereafter two additional right-sided thoracenteses over the following 5 years at times of increasing dyspnea. In August 1998, she was referred for surgical evaluation. No other etiology for the effusions was identified during the 6 years of her disease course. 7 had a CABG operation in October 1996, after which he developed bilateral Table 1 Demographics, Left Ventricular Ejection Fraction, and Type of Surgical Grafts* Sex/Age at Pleural Surgery, yr Time When Effusion First Noticed (Days After CABG), Time to First Thoracentesis (Days After CABG), Time Between CABG and Pleural Surgery (Days), Left Ventricular Ejection Fraction, Re-do CABG IMA Graft, SV Graft, RA Graft, 1 M/ No M/ Yes M/ No M/ No F/ No M/ Yes M/ No F/ , No * M male; F female; IMA internal mammary artery; SV saphenous vein; RA radial artery. 796 Clinical Investigations
3 Table 2 Radiographic Appearances and of Thoracenteses Prior to Pleural Surgery Side of Effusion Cardiomegaly Loculations Effusion Size, * Left Thoracentesis, Right Thoracentesis, 1 Left only No No Left more than right No No Right more than left Yes No Left only No Yes Left only No No Right more than left No Yes Right more than left No No Right more than left No No *The size of the effusion indicates the largest size of the effusion on radiographs during the period between CABG and pleural surgery. (right side more than left) pleural effusions before his hospital discharge. The effusions were rapidly reaccumulating and required frequent thoracentesis for symptomatic relief. Diuretics and a short course of oral corticosteroids offered no apparent benefit. In February 1997, he received bilateral tube thoracostomy drainage. He underwent unsuccessful chemical pleurodeses with talc slurry to the right pleural space and, later, doxycycline to the left pleural space. In March 1997, he underwent a right thoracoscopy and parietal pleurectomy. Despite that, he continued to suffer from recurrent bilateral effusions (right side more than left). In April 1999, he underwent a right thoracotomy, pleurectomy, and mechanical pleurodesis (under J.C.N.). Extensive investigations did not reveal the etiology of the effusions. The macroscopic and microscopic examinations of the pleura also failed to demonstrate any specific cause for his effusion. 6 had poor left ventricular function with an ejection fraction of 15, but his effusion was bloody and he had thickened pleura and trapped lung, features not usually associated with effusions because of congestive cardiac failure. It is possible, however, that congestive cardiac failure could be a contributing factor to his pleural effusion. A summary of the surgical procedures and intraoperative findings of the eight patients are summarized in Table 4. Four of the patients (50) had trapped lungs requiring decortication. All patients had intraoperative findings suggestive of a chronic inflammatory process, with no macroscopic features of an acute process or of malignancies. None of the patients had further recurrence of their effusions after their thoracoscopy or thoracotomy (follow-up period, 2 to 18 months; median, 12 months). Pleural Histology The pleural biopsy samples showed a spectrum of changes that roughly correlated with the interval between CABG and thoracotomy/thoracoscopy. Cases in which this period was short (eg, 6 months) displayed a predominance of inflammation with dense cellular infiltrates, especially lymphocytes, and relatively little pleural fibrosis (Fig 1). As the interval increased, the biopsy samples showed progressively less inflammation, decreased density of the cellular infiltrate, and increased amounts of fibrosis. The pleura was markedly thickened with the increased amount of dense fibrous tissues (Fig 2). The fibrous component was typically paucicellular, but did contain collections of entrapped cells that were cytokeratin immunoreactive, compatible with mesothelial cells. In the samples obtained relatively soon after Table 3 Characteristics of the Pleural Fluid of the Four s Whose Thoracentesis Results Were Available* Side of Thoracentesis Effusion WBC Count, Cells/ L Lym, PMN, Mono, Eos, Baso, RBC Count, Cells/ L LDH, IU/L Protein, mg/l 5 Left Nonbloody 1, Right Bloody , Right Nonbloody 2, , Right Nonbloody , *Lym lymphocytes; PMN polymorphonuclear leukocytes; Mono monocytes; Eos eosinophils; Baso basophils; LDH lactate dehydrogenase. CHEST / 119 / 3/ MARCH,
4 Table 4 Types of Pleural Surgery Performed and the Operative Findings Surgery Side Procedure Pleurodesis Loculation Visceral Peel Trapped Lung 1 Thoracotomy Left Decortication and Nil Nil Yes Yes pleurectomy 2 Thoracoscopy Bilateral Pleural debridment and Nil Yes Nil Nil evacuation of hemothorax 3 Thoracoscopy Right Pleurodesis Mechanical abrasion plus talc Nil Nil Nil 4 Thoracotomy Left Decortication Nil Nil Yes Yes 5 Thoracoscopy Left Pleurodesis Mechanical abrasion plus talc Nil Nil Nil 6 Thoracoscopy Right Diagnostic only Nil Yes Yes Yes 7 Thoracotomy Right Decortication and Mechanical abrasion plus talc Nil Nil Nil pleurectomy 8 Thoracotomy Right Decortication and pleurectomy Nil Yes Yes Yes CABG, the inflammatory cell infiltrate was concentrated deep in the fibrous tissue and away from the mesothelial layer. It consisted predominantly of lymphocytes that focally tended toward a nodular configuration (Fig 3). Immunohistochemical analysis with L26 (pan B-cell-specific marker) and UCHL1 (pan T-cell-specific marker) demonstrated a mixed population of lymphocytes with a predominance of B cells. Small numbers of reactive plasma cells were also present. One sample of the pleura represented material from a patient with a hemothorax (patient 2) and consisted entirely of blood clots. No granulomata or malignant changes were observed in any of the pleural biopsy specimens. Discussion We presented the clinical and pathologic features of eight patients who had persistent post-cabg Figure 1. Pleural biopsy specimen in a patient who underwent CABG 6 months before the thoracoscopy. Notice that the pleura was relatively thin with little fibrosis. The pleural tissue displayed a predominance of inflammation with dense cellular infiltrates (hematoxylin-eosin, original 40). pleural effusions that failed to resolve with repeated thoracenteses and eventually required surgical intervention. The pleural biopsy samples of these patients demonstrated a spectrum of histologic changes that roughly correlated with the interval between CABG and pleural surgery, and likely represent the temporal evolution of this condition. Inflammation and lymphocytosis were the characteristics in the early phase. With time, these changes were replaced by mature fibrosis, which in some cases resulted in trapped lungs and required decortication. Pleural effusion is very common after CABG surgery and can be detected in approximately 90 of patients within the first week of operation. 1 While most of these effusions are small and self-limiting, large and persistent pleural effusions have been reported. 7 The etiology of post-cabg effusions and the reasons why some effusions persist while most resolve remain unknown. None of these patients had other identifiable risk factors for pleural effusion, and the temporal relationship of the onset of effusion and CABG suggested a causal relationship. The lack of pleuritic symptoms or fever and the duration of the effusion virtually excluded post-cardiac injury syndrome. None of the eight patients we described had clinical evidence of pericardial disease or congestive cardiac failure. No other causes were found during the disease course or from thoracoscopy/thoracotomy to explain the effusions. Open pleural biopsy specimens failed to demonstrate any specific cause (eg, malignancy) for these effusions, and there was no recurrence of the effusion after the surgical intervention. Large post-cabg effusions can be categorized into early- and late-phase effusions. 7 The early ones are usually related with surgical trauma and peak in size within the first month after surgery. These effusions are bloody with associated eosinophilia. The late-phase post-cabg effusions are different in that they usually reach maximum size after the first 798 Clinical Investigations
5 Figure 2. Pleural biopsy specimen in a patient who underwent CABG 2 years before the thoracoscopy. The pleura was markedly thickened, with a significantly larger amount of dense fibrous tissue. There were relatively little inflammatory changes (hematoxylin-eosin, original 40). postoperative month. The pleural fluids often appear nonbloody and are characterized by significant lymphocytosis. 6,7 The latter feature has led to the speculation of an immunologic basis of these late-phase post-cabg pleural effusions. Little is known about the histologic changes of the pleura in patients with persistent post-cabg effusions. Areno et al 8 described the histology of one patient 2 years after CABG. The parietal pleura was thickened and showed evidence of chronic pleuritis with nests of lymphocytes. 8 Kollef 3 described another patient 3 months after CABG who had a closed pleural biopsy specimen showing chronic inflammation and a mesothelial cyst. Our samples confirmed that lymphocytosis was the key feature on the early biopsy tissues as well as in the pleural fluids. We further defined that the lymphocytes were predominantly B cells and that these lymphocytic infiltrates subsided with time. The trigger for the intense inflammation and lymphocytic infiltration is unknown. The exact etiologic role of these lymphocytes also warrants further evaluation. All of the patients in our series had symptomatic, large pleural effusions that failed to resolve after at least two thoracenteses. Those with long intervals after CABG were more likely to have evidence of visceral peel and trapped lung that required decortication. This was confirmed by the pleural biopsy samples, which demonstrated that patients with a longer interval after CABG had more pleural fibrosis and thickening. The source of the fibrosis remains unclear. While infiltrating fibroblasts can produce the fibrosis, mesothelial cells have also been shown to produce collagen, 9 11 which may in part contribute to the fibrotic process. Four of the patients we described had visceral peel and trapped lungs. Full reexpansion was achieved in three of these four patients after decortication. Of all the cases of persistent post-cabg effusions reported, most resolved with thoracentesis. 6,12,13 Only one case of trapped lung from persistent post-cabg effusion had previously been described. 12 In that patient, decortication performed 4 months after CABG was also successful in restoring reexpansion. Cohen and Finch 5 described two patients with loculated post-cabg effusions who were treated successfully with intrapleural urokinase. It was not certain whether they had trapped lungs. In cases in which fluid reaccumulation continues for 6 months, consideration should be given to more aggressive intervention that may help prevent the eventual development of trapped lungs. Pleurecotomy or surgical pleurodesis with talc with or without mechanical abrasion appeared effective in controlling the effusion in the patients we described. None had further recurrence of pleural effusion afterwards. There are some limitations to this present study. It is a retrospective review, and not all the patients pleural fluid analyses were available. Post-CABG pleural effusion is a diagnosis of exclusion. Although there are no other identifiable causes for the effusion in any of our patients, other etiologies cannot be fully excluded. While none of the patients had recurrence of symptoms or required further thoracentesis after thoracoscopy or thoracotomy, no radiographs were obtained. Hence, we cannot fully exclude the possibility of asymptomatic recurrence of the effusions. Also, our method of identifying patients may well have underestimated the true incidence of persistent post-cabg effusions requiring surgical intervention. Figure 3. Histologic section of the pleura showing the lymphoid aggregates deep in the fibrous tissues away from the mesothelial layer (hematoxylin-eosin, original 40). CHEST / 119 / 3/ MARCH,
6 In conclusion, we demonstrated that persistent post-cabg pleural effusion can occur and, in some cases, require surgical intervention. The number of cases of persistent post-cabg effusion may rise as more CABG procedures are performed each year. Increased awareness and recognition of this syndrome is important. If the effusion persists 6 months, surgical intervention should be considered, as it is effective in decorticating any trapped lung and in preventing reaccumulation of the effusions. ACKNOWLEDGMENT: The authors thank Dr. Kirk Lane for his advice and assistance in the preparation of this article. References 1 Vargas FS, Cukier A, Hueb W, et al. Relationship between pleural effusion and pericardial involvement after myocardial revascularization. Chest 1994; 105: Hurlbut D, Myers ML, Lefcoe M, et al. Pleuropulmonary morbidity: internal thoracic artery versus saphenous vein graft. Ann Thorac Surg 1990; 50: Kollef MH. Symptomatic pleural effusion after coronary artery revascularization: unsuspected pleural injury from internal mammary artery resection. South Med J 1993; 86: Kollef MH. Chronic pleural effusion after coronary artery revascularization with the internal mammary artery. Chest 1990; 97: Cohen ML, Finch IJ. Transcatheter intrapleural urokinase for loculated pleural effusion. Chest 1994; 105: Kim YK, Mohsenifar Z, Koerner SK. Lymphocytic pleural effusion in postpericardiotomy syndrome. Am Heart J 1988; 115: Light RW, Rogers JT, Cheng DS, et al. Large pleural effusions occurring after coronary artery bypass grafting. Ann Intern Med 1999; 130: Areno JP, McCartney JP, Eggerstedt J, et al. Persistent pleural effusions after coronary bypass surgery. Chest 1998; 114: Owens MW, Grimes SR. Pleural mesothelial cell response to inflammation: tumor necrosis factor-induced mitogenesis and collagen synthesis. Am J Physiol 1993; 265:L382 L Owens MW, Milligan SA, Grisham MB. Inhibition of pleural mesothelial cell collagen synthesis by nitric oxide. Free Radic Biol Med 1996; 21: Bauman MH, Heinrich K, Sahn SA, et al. Pleural macrophages differentially alter mesothelial cell growth and collagen production. Inflammation 1993; 17: Kollef MH, Peller T, Knodel A, et al. Delayed pleuropulmonary complications following coronary artery revascularization with the internal mammary artery. Chest 1988; 94: Kollef MH. Trapped lung syndrome after cardiac surgery: a potentially preventable complication of pleural injury. Heart Lung 1990; 19: Clinical Investigations
Alfonso Fiorelli 1, Francesco Caronia 2, Aldo Prencipe 3, Mario Santini 1, Brendon Stiles 4. Evidenced-Based Clinical Problem Solving Article
 Evidenced-Based Clinical Problem Solving Article The role of video-assisted thoracoscopic surgery for management of symptomatic pleural effusion after coronary artery bypass surgery: a best evidence topic
Evidenced-Based Clinical Problem Solving Article The role of video-assisted thoracoscopic surgery for management of symptomatic pleural effusion after coronary artery bypass surgery: a best evidence topic
Bacterial pneumonia with associated pleural empyema pleural effusion
 EMPYEMA Synonyms : - Parapneumonic effusion - Empyema thoracis - Bacterial pneumonia - Pleural empyema, pleural effusion - Lung abscess - Complicated parapneumonic effusions (CPE) 1 Bacterial pneumonia
EMPYEMA Synonyms : - Parapneumonic effusion - Empyema thoracis - Bacterial pneumonia - Pleural empyema, pleural effusion - Lung abscess - Complicated parapneumonic effusions (CPE) 1 Bacterial pneumonia
Management of Pleural Effusion
 Management of Pleural Effusion Development of Pleural Effusion pulmonary capillary pressure (CHF) capillary permeability (Pneumonia) intrapleural pressure (atelectasis) plasma oncotic pressure (hypoalbuminemia)
Management of Pleural Effusion Development of Pleural Effusion pulmonary capillary pressure (CHF) capillary permeability (Pneumonia) intrapleural pressure (atelectasis) plasma oncotic pressure (hypoalbuminemia)
APPROACH TO PLEURAL EFFUSIONS. Raed Alalawi, MD, FCCP
 APPROACH TO PLEURAL EFFUSIONS Raed Alalawi, MD, FCCP CASE 65-year-old woman with H/O breast cancer presented with a 1 week H/O progressively worsening exersional dyspnea. Physical exam: Diminished breath
APPROACH TO PLEURAL EFFUSIONS Raed Alalawi, MD, FCCP CASE 65-year-old woman with H/O breast cancer presented with a 1 week H/O progressively worsening exersional dyspnea. Physical exam: Diminished breath
Dr. A.Torossian, M.D., Ph. D. Department of Respiratory Diseases
 Pleural effusions Dr. A.Torossian, M.D., Ph. D. Department of Respiratory Diseases A pleural effusion is an abnormal collection of fluid in the pleural space resulting from excess fluid production or decreased
Pleural effusions Dr. A.Torossian, M.D., Ph. D. Department of Respiratory Diseases A pleural effusion is an abnormal collection of fluid in the pleural space resulting from excess fluid production or decreased
Diagnostic Approach to Pleural Effusion
 Diagnostic Approach to Pleural Effusion Objectives Define the leading causes of pleural effusion Classify the type of effusion Identify procedures and tests associated with diagnosis 2 Agenda Basic anatomy
Diagnostic Approach to Pleural Effusion Objectives Define the leading causes of pleural effusion Classify the type of effusion Identify procedures and tests associated with diagnosis 2 Agenda Basic anatomy
Malignant Effusions. Anantham Devanand Respiratory and Critical Care Medicine Singapore General Hospital
 Malignant Effusions Anantham Devanand Respiratory and Critical Care Medicine Singapore General Hospital Malignant Effusions Definition: Presence of malignant cells in the pleural space 75% are caused by
Malignant Effusions Anantham Devanand Respiratory and Critical Care Medicine Singapore General Hospital Malignant Effusions Definition: Presence of malignant cells in the pleural space 75% are caused by
EFFECTIVENESS OF TALC SLURRY IN PRODUCING PLEURODESIS: A STUDY IN RABBITS
 Trakia Journal of Sciences, Vol. 5, No. 3-4, pp 7-11, 2007 Copyright 2007 Trakia University Available online at: http://www.uni-sz.bg ISSN 1312-1723 Original Contribution EFFECTIVENESS OF TALC SLURRY IN
Trakia Journal of Sciences, Vol. 5, No. 3-4, pp 7-11, 2007 Copyright 2007 Trakia University Available online at: http://www.uni-sz.bg ISSN 1312-1723 Original Contribution EFFECTIVENESS OF TALC SLURRY IN
Manejo Práctico del Derrame Pleural
 Manejo Práctico del Derrame Pleural San José, Costa Rica Junio 29, 2017 Rodrigo Cartín Ceba, MD, MSc Consultant, Pulmonary and Critical Care Medicine Associate Professor of Medicine Mayo Clinic 2010 MFMER
Manejo Práctico del Derrame Pleural San José, Costa Rica Junio 29, 2017 Rodrigo Cartín Ceba, MD, MSc Consultant, Pulmonary and Critical Care Medicine Associate Professor of Medicine Mayo Clinic 2010 MFMER
Alper Toker, MD. VATS decortication. Istanbul University, Istanbul Medical School Department of Thoracic Surgery
 VATS decortication Alper Toker, MD Istanbul University, Istanbul Medical School Department of Thoracic Surgery Pleural space infection is a common pathology causing morbidity and mortality. It is a collection
VATS decortication Alper Toker, MD Istanbul University, Istanbul Medical School Department of Thoracic Surgery Pleural space infection is a common pathology causing morbidity and mortality. It is a collection
EXPERIMENTAL PLEURAL EMPYEMA PATHOLOGIC CHANGES
 Trakia Journal of Sciences, Vol. 3, No. 2, pp 61-65, 2005 Copyright 2005 Trakia University Available online at: http://www.uni-sz.bg ISSN 1312-1723 Original Contribution EXPERIMENTAL PLEURAL EMPYEMA PATHOLOGIC
Trakia Journal of Sciences, Vol. 3, No. 2, pp 61-65, 2005 Copyright 2005 Trakia University Available online at: http://www.uni-sz.bg ISSN 1312-1723 Original Contribution EXPERIMENTAL PLEURAL EMPYEMA PATHOLOGIC
Malignant Pleurisy Associated with Primary Lung Cancer Well Controlled by Pleurodesis Using Distilled Water
 CASE REPORT Malignant Pleurisy Associated with Primary Lung Cancer Well Controlled by Pleurodesis Using Distilled Water Mitsuaki Sekiya, Toshiji Ishiwata, Kaku Yoshimi, Tetsutaro Nagaoka, Yoshiteru Morio,
CASE REPORT Malignant Pleurisy Associated with Primary Lung Cancer Well Controlled by Pleurodesis Using Distilled Water Mitsuaki Sekiya, Toshiji Ishiwata, Kaku Yoshimi, Tetsutaro Nagaoka, Yoshiteru Morio,
Persistent Spontaneous Pneumothorax for Four Years: A Case Report
 303) Persistent Spontaneous Pneumothorax for Four Years: A Case Report Mizuno Y., Iwata H., Shirahashi K., Matsui M., Takemura H. Department of General and Cardiothoracic Surgery, Graduate School of Medicine,
303) Persistent Spontaneous Pneumothorax for Four Years: A Case Report Mizuno Y., Iwata H., Shirahashi K., Matsui M., Takemura H. Department of General and Cardiothoracic Surgery, Graduate School of Medicine,
A Repeat Case of Idiopathic Spontaneous Hemothorax
 Case Report A Repeat Case of Idiopathic Spontaneous Hemothorax Felix R. Gaw, MD Jack H. Bloch, MD, PhD, FACS Nolan J. Anderson, MD, FACS Spontaneous hemothorax, a collection of blood in the pleural cavity
Case Report A Repeat Case of Idiopathic Spontaneous Hemothorax Felix R. Gaw, MD Jack H. Bloch, MD, PhD, FACS Nolan J. Anderson, MD, FACS Spontaneous hemothorax, a collection of blood in the pleural cavity
Page 5. TUBERCULOSIS PLEURAL EFFUSIONS AND A CASE OF EMPYEMA NECESSITATIS (NECESSITANS) David Griffith, MD CASE HISTORY
 Page 5 TUBERCULOSIS PLEURAL EFFUSIONS AND A CASE OF EMPYEMA NECESSITATIS (NECESSITANS) David Griffith, MD CASE HISTORY A 15 year old pregnant female presented to the emergency department of a local hospital
Page 5 TUBERCULOSIS PLEURAL EFFUSIONS AND A CASE OF EMPYEMA NECESSITATIS (NECESSITANS) David Griffith, MD CASE HISTORY A 15 year old pregnant female presented to the emergency department of a local hospital
Modern Approaches to Empyema
 Modern Approaches to Empyema Amit Bhargava, MD Attending Thoracic Surgeon Assistant Professor Department of Cardiovascular and Thoracic Surgery 1 Principles of Treatment Adequate drainage Sterilization
Modern Approaches to Empyema Amit Bhargava, MD Attending Thoracic Surgeon Assistant Professor Department of Cardiovascular and Thoracic Surgery 1 Principles of Treatment Adequate drainage Sterilization
New lung lesion in a 55 year-old male treated with chemoradiation for non-small cell lung carcinoma
 July 2016 New lung lesion in a 55 year-old male treated with chemoradiation for non-small cell lung carcinoma Contributed by: Laurel Rose, MD, Resident Physician, Indiana University School of Medicine,
July 2016 New lung lesion in a 55 year-old male treated with chemoradiation for non-small cell lung carcinoma Contributed by: Laurel Rose, MD, Resident Physician, Indiana University School of Medicine,
Thoracoscopic Management of Complicated Parapneumonic Effusions in Young Children. Saeed Al Hindi, MD, CABS, FRCSI*
 Bahrain Medical Bulletin, Vol. 31, No. 4, December 2009 Thoracoscopic Management of Complicated Parapneumonic Effusions in Young Children Saeed Al Hindi, MD, CABS, FRCSI* Objective: To evaluate the role
Bahrain Medical Bulletin, Vol. 31, No. 4, December 2009 Thoracoscopic Management of Complicated Parapneumonic Effusions in Young Children Saeed Al Hindi, MD, CABS, FRCSI* Objective: To evaluate the role
EVIDENCE THAT MESOTHELIAL CELLS MAY REGULATE THE ACUTE INFLAMMATORY RESPONSE IN TALC PLEURODESIS
 ERJ Express. Published on July 26, 2006 as doi: 10.1183/09031936.06.00037906 EVIDENCE THAT MESOTHELIAL CELLS MAY REGULATE THE ACUTE INFLAMMATORY RESPONSE IN TALC PLEURODESIS Marchi E, MD; Vargas FS, MD;
ERJ Express. Published on July 26, 2006 as doi: 10.1183/09031936.06.00037906 EVIDENCE THAT MESOTHELIAL CELLS MAY REGULATE THE ACUTE INFLAMMATORY RESPONSE IN TALC PLEURODESIS Marchi E, MD; Vargas FS, MD;
Some clinical conditions such as congestive heart failure, cirrhosis, acute. Bleomycin in the treatment of 50 cases with malignant pleural effusion
 Original Article Bleomycin in the treatment of 5 cases with malignant pleural effusion Novin Nikbakhsh (MD) *1 Ali Pourhasan Amiri (MD) 2 Danial Hoseinzadeh (MD) 3 1- Department of Surgery, Babol University
Original Article Bleomycin in the treatment of 5 cases with malignant pleural effusion Novin Nikbakhsh (MD) *1 Ali Pourhasan Amiri (MD) 2 Danial Hoseinzadeh (MD) 3 1- Department of Surgery, Babol University
Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations
 08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
Well-differentiated Papillary Mesothelioma of the Pleura Diagnosed by Video-Assisted Thoracic Surgical Pleural Biopsy : A Case Report
 Showa Univ J Med Sci 25 1, 67 72, March 2013 Case Report Well-differentiated Papillary Mesothelioma of the Pleura Diagnosed by Video-Assisted Thoracic Surgical Pleural Biopsy : A Case Report Yuri TOMITA
Showa Univ J Med Sci 25 1, 67 72, March 2013 Case Report Well-differentiated Papillary Mesothelioma of the Pleura Diagnosed by Video-Assisted Thoracic Surgical Pleural Biopsy : A Case Report Yuri TOMITA
Pneumothorax and Chest Tube Problems
 Pneumothorax and Chest Tube Problems Pneumothorax Definition Air accumulation in the pleural space with secondary lung collapse Sources Visceral pleura Ruptured esophagus Chest wall defect Gas-forming
Pneumothorax and Chest Tube Problems Pneumothorax Definition Air accumulation in the pleural space with secondary lung collapse Sources Visceral pleura Ruptured esophagus Chest wall defect Gas-forming
A case of giant benign localized fibrous tumor of the pleura
 Turkish Journal of Cancer Vol.30 / No. 4/2000 A case of giant benign localized fibrous tumor of the pleura ALİ KEMAL UZUNLAR 1, MEHMET YALDIZ 1, İBRAHİM H. ÖZERCAN 2, FAHRİ YILMAZ 1, AKIN E. BALCI 3 1
Turkish Journal of Cancer Vol.30 / No. 4/2000 A case of giant benign localized fibrous tumor of the pleura ALİ KEMAL UZUNLAR 1, MEHMET YALDIZ 1, İBRAHİM H. ÖZERCAN 2, FAHRİ YILMAZ 1, AKIN E. BALCI 3 1
Pleural Fluid Analysis: Back to Basics
 Pleural Fluid Analysis: Back to Basics Tonya L. Page, MSN, RN, ACNP-BC Patrick A. Laird, DNP, RN, ACNP-BC 70 y/o female with complaints of shortness of breath and orthopnea for 1 month. Symptoms have worsened
Pleural Fluid Analysis: Back to Basics Tonya L. Page, MSN, RN, ACNP-BC Patrick A. Laird, DNP, RN, ACNP-BC 70 y/o female with complaints of shortness of breath and orthopnea for 1 month. Symptoms have worsened
The measurements of pleural fluid WBC count
 Variations in Pleural Fluid WBC Count and Differential Counts With Different Sample Containers and Different Methods* Barrett D. Conner, MD; Y. C. Gary Lee, MD; Paul Branca, MD, FCCP; Jeffrey T. Rogers,
Variations in Pleural Fluid WBC Count and Differential Counts With Different Sample Containers and Different Methods* Barrett D. Conner, MD; Y. C. Gary Lee, MD; Paul Branca, MD, FCCP; Jeffrey T. Rogers,
S and secondary spontaneous pneumothorax. Primary
 Secondary Spontaneous Pneumothorax Fumihiro Tanaka, MD, Masatoshi Itoh, MD, Hiroshi Esaki, MD, Jun Isobe, MD, Youichiro Ueno, MD, and Ritsuko Inoue, MD Department of Thoracic and Cardiovascular Surgery,
Secondary Spontaneous Pneumothorax Fumihiro Tanaka, MD, Masatoshi Itoh, MD, Hiroshi Esaki, MD, Jun Isobe, MD, Youichiro Ueno, MD, and Ritsuko Inoue, MD Department of Thoracic and Cardiovascular Surgery,
The diagnosis and management of pneumothorax
 Respiratory 131 The diagnosis and management of pneumothorax Pneumothorax is a relatively common presentation in patients under the age of 40 years (approximately, 85% of patients are younger than 40 years).
Respiratory 131 The diagnosis and management of pneumothorax Pneumothorax is a relatively common presentation in patients under the age of 40 years (approximately, 85% of patients are younger than 40 years).
Vascular endothelial growth factor levels in post-cabg pleural effusions are associated with pleural inflammation and permeability
 Respiratory Medicine (2007) 101, 223 229 Vascular endothelial growth factor levels in post-cabg pleural effusions are associated with pleural inflammation and permeability Ioannis Kalomenidis a,, Georgios
Respiratory Medicine (2007) 101, 223 229 Vascular endothelial growth factor levels in post-cabg pleural effusions are associated with pleural inflammation and permeability Ioannis Kalomenidis a,, Georgios
CHRONIC PLEURAL CHANGES AFTER INTRAPLEURAL INSTILLATION OF IODPOVIDONE EXPERIMENTAL STUDY IN RABBITS
 Trakia Journal of Sciences, Vol. 9, No 1, pp 17-23, 2011 Copyright 2011 Trakia University Available online at: http://www.uni-sz.bg ISSN 1313-7050 (print) ISSN 1313-3551 (online) Original Contribution
Trakia Journal of Sciences, Vol. 9, No 1, pp 17-23, 2011 Copyright 2011 Trakia University Available online at: http://www.uni-sz.bg ISSN 1313-7050 (print) ISSN 1313-3551 (online) Original Contribution
BMC Pulmonary Medicine
 BMC Pulmonary Medicine This Provisional PDF corresponds to the article as it appeared upon acceptance. Fully formatted PDF and full text (HTML) versions will be made available soon. Pneumothorax Ex-vacuo
BMC Pulmonary Medicine This Provisional PDF corresponds to the article as it appeared upon acceptance. Fully formatted PDF and full text (HTML) versions will be made available soon. Pneumothorax Ex-vacuo
Indwelling Pleural Catheters in Malignant and Non-Malignant Disease
 Indwelling Catheters in Malignant and Non-Malignant Disease 20th Hellenic Conference November 2011 Najib Rahman Clinical Lecturer Oxford Centre for Respiratory Medicine University of Oxford, UK Najib.rahman@ndm.ox.ac.uk
Indwelling Catheters in Malignant and Non-Malignant Disease 20th Hellenic Conference November 2011 Najib Rahman Clinical Lecturer Oxford Centre for Respiratory Medicine University of Oxford, UK Najib.rahman@ndm.ox.ac.uk
PLEURAL EFFUSION. Prof. G. Zuliani
 PLEURAL EFFUSION Prof. G. Zuliani Anatomy of pleural membrane and pleural space Pleural membrane consists of parietal pleura and visceral pleura A space situated between parietal and visceral pleura is
PLEURAL EFFUSION Prof. G. Zuliani Anatomy of pleural membrane and pleural space Pleural membrane consists of parietal pleura and visceral pleura A space situated between parietal and visceral pleura is
Diagnosis of thoracic endometriosis with immunohistochemistry
 Original Article Diagnosis of thoracic endometriosis with immunohistochemistry Yo Kawaguchi 1,2, Jun Hanaoka 1, Yasuhiko Ohshio 1, Tomoyuki Igarashi 1, Keigo Okamoto 1, Ryosuke Kaku 1, Kazuki Hayashi 1,
Original Article Diagnosis of thoracic endometriosis with immunohistochemistry Yo Kawaguchi 1,2, Jun Hanaoka 1, Yasuhiko Ohshio 1, Tomoyuki Igarashi 1, Keigo Okamoto 1, Ryosuke Kaku 1, Kazuki Hayashi 1,
Pneumothorax Ex-vacuo or trapped lung in the setting of hepatic hydrothorax
 Kim et al. BMC Pulmonary Medicine 2012, 12:78 CASE REPORT Open Access Pneumothorax Ex-vacuo or trapped lung in the setting of hepatic hydrothorax Yan S Kim 1*, Irawan Susanto 1, Catherine A Lazar 1, Ali
Kim et al. BMC Pulmonary Medicine 2012, 12:78 CASE REPORT Open Access Pneumothorax Ex-vacuo or trapped lung in the setting of hepatic hydrothorax Yan S Kim 1*, Irawan Susanto 1, Catherine A Lazar 1, Ali
Lung folding simulating peripheral pulmonary
 Thorax, 1980, 35, 936-940 Lung folding simulating peripheral pulmonary neoplasm (Blesovsky's syndrome) C R PAYNE, P JAQUES, AND I From the Brompton Hospital, London H KERR ABSTRACT Six cases are reported
Thorax, 1980, 35, 936-940 Lung folding simulating peripheral pulmonary neoplasm (Blesovsky's syndrome) C R PAYNE, P JAQUES, AND I From the Brompton Hospital, London H KERR ABSTRACT Six cases are reported
MANAGEMENT OF RETAINED HAEMOTHORAX DR AG JACOBS PRINCIPAL SPECIALIST DEPARTMENT OF CARDIO THORACIC SURGERY UNIVERSITY OF PRETORIA
 MANAGEMENT OF RETAINED HAEMOTHORAX DR AG JACOBS PRINCIPAL SPECIALIST DEPARTMENT OF CARDIO THORACIC SURGERY UNIVERSITY OF PRETORIA MANAGEMENT OF RETAINED HAEMOTHORAX Retained Haemothorax Definition: Failure
MANAGEMENT OF RETAINED HAEMOTHORAX DR AG JACOBS PRINCIPAL SPECIALIST DEPARTMENT OF CARDIO THORACIC SURGERY UNIVERSITY OF PRETORIA MANAGEMENT OF RETAINED HAEMOTHORAX Retained Haemothorax Definition: Failure
Pleural fluid analysis
 Pleural fluid analysis Dr Akash Verma Senior Consultant- Department of Respiratory and Critical Care Medicine Tan Tock Seng Hospital, Singapore 308433 Adj A/Professor- Lee Kong Chian School of Medicine
Pleural fluid analysis Dr Akash Verma Senior Consultant- Department of Respiratory and Critical Care Medicine Tan Tock Seng Hospital, Singapore 308433 Adj A/Professor- Lee Kong Chian School of Medicine
Pleural Effusions. Kyle J Henry, MD Pulmonary/ CCM Fellow PGY4 (210) (602)
 Pleural Effusions Kyle J Henry, MD Pulmonary/ CCM Fellow PGY4 (210) 275 8583 (602) 202 0351 None Disclosures Objectives Understand the presentation of a pleural effusion How to diagnose and treat Differentiate
Pleural Effusions Kyle J Henry, MD Pulmonary/ CCM Fellow PGY4 (210) 275 8583 (602) 202 0351 None Disclosures Objectives Understand the presentation of a pleural effusion How to diagnose and treat Differentiate
Medical Thoracoscopy When to Choose Over a General Anaesthetic VATS
 Medical Thoracoscopy When to Choose Over a General Anaesthetic VATS SpR Training Day 07.07.14 Dr Alex West Consultant Chest/Pleural Physician Guy s and St Thomas Hospital Medical Thoracoscopy? No Just
Medical Thoracoscopy When to Choose Over a General Anaesthetic VATS SpR Training Day 07.07.14 Dr Alex West Consultant Chest/Pleural Physician Guy s and St Thomas Hospital Medical Thoracoscopy? No Just
Pleural Disease. Disclosure. Normal Pleural Anatomy. Outline. Pleural Fluid Origins: Transudates. Pleural Fluid Origins: Exudates
 Disclosure Pleural Disease Anne L Fuhlbrigge MD MS Clinical Director Division of Pulmonary and Critical Care Medicine Brigham and Women s Hospital Channing Laboratory Harvard Medical School Boston, MA
Disclosure Pleural Disease Anne L Fuhlbrigge MD MS Clinical Director Division of Pulmonary and Critical Care Medicine Brigham and Women s Hospital Channing Laboratory Harvard Medical School Boston, MA
Archived Resident Experience Report By Role
 Archived Resident Experience Report By Role Primary Procedures Program ID: 4602621046 Program Name: University of Minnesota Program At All Institutions All Attendings Resident: Sample Resident For Surgeon
Archived Resident Experience Report By Role Primary Procedures Program ID: 4602621046 Program Name: University of Minnesota Program At All Institutions All Attendings Resident: Sample Resident For Surgeon
Kathmandu University Medical Journal (2007), Vol. 5, No. 4, Issue 20,
 Kathmandu University Medical Journal (2007), Vol. 5, No. 4, Issue 20, 521-525 Empyema thoracis Original Article Singh DR 1, Joshi MR 2, Thapa P 2, Nath S 3 1 Assistant Professor, 2 Lecturer, 3 Professor,
Kathmandu University Medical Journal (2007), Vol. 5, No. 4, Issue 20, 521-525 Empyema thoracis Original Article Singh DR 1, Joshi MR 2, Thapa P 2, Nath S 3 1 Assistant Professor, 2 Lecturer, 3 Professor,
ERDHEIM-CHESTER DISEASE LUNG & HEART ISSUES
 ERDHEIM-CHESTER DISEASE LUNG & HEART ISSUES GIULIO CAVALLI, M.D. INTERNAL MEDICINE AND CLINICAL IMMUNOLOGY IRCCS SAN RAFFAELE HOSPITAL VITA-SALUTE SAN RAFFAELE UNIVERSITY MILAN, ITALY cavalli.giulio@hsr.it
ERDHEIM-CHESTER DISEASE LUNG & HEART ISSUES GIULIO CAVALLI, M.D. INTERNAL MEDICINE AND CLINICAL IMMUNOLOGY IRCCS SAN RAFFAELE HOSPITAL VITA-SALUTE SAN RAFFAELE UNIVERSITY MILAN, ITALY cavalli.giulio@hsr.it
Chapter 8. Other Important Tests and Procedures. Mosby items and derived items 2011, 2006 by Mosby, Inc., an affiliate of Elsevier Inc.
 Chapter 8 Other Important Tests and Procedures 1 Introduction Additional important diagnostic studies include: Sputum examination Skin tests Endoscopic examination Lung biopsy Thoracentesis Hematology,
Chapter 8 Other Important Tests and Procedures 1 Introduction Additional important diagnostic studies include: Sputum examination Skin tests Endoscopic examination Lung biopsy Thoracentesis Hematology,
DIAGNOSTIC EVALUATION OF BLOODY PLEURAL EFFUSION
 DIAGNOSTIC EVALUATION OF BLOODY PLEURAL EFFUSION Mamatha S, Manish Kumar Singh, Pravati Dutta, Rekha Manjhi, Sudarsan Pothal,Amit Kumar Jha, Nilam Nigam, Sanjay Kumar Nigam 1. Senior Resident, Department
DIAGNOSTIC EVALUATION OF BLOODY PLEURAL EFFUSION Mamatha S, Manish Kumar Singh, Pravati Dutta, Rekha Manjhi, Sudarsan Pothal,Amit Kumar Jha, Nilam Nigam, Sanjay Kumar Nigam 1. Senior Resident, Department
Posttraumatic Empyema Thoracis
 Posttraumatic Empyema Thoracis Dr AG Jacobs STEVE BIKO ACADEMIC HOSPITAL, UNIVERSITY OF PRETORIA EMPYEMA THORACIS Derived from Greek word empyein Means pus-producing Refers to accumulation of pus within
Posttraumatic Empyema Thoracis Dr AG Jacobs STEVE BIKO ACADEMIC HOSPITAL, UNIVERSITY OF PRETORIA EMPYEMA THORACIS Derived from Greek word empyein Means pus-producing Refers to accumulation of pus within
Restrictive lung diseases
 Restrictive lung diseases Restrictive lung diseases are diseases that affect the interstitium of the lung. Interstitium of the lung is the very thin walls surrounding the alveoli, it s formed of epithelium
Restrictive lung diseases Restrictive lung diseases are diseases that affect the interstitium of the lung. Interstitium of the lung is the very thin walls surrounding the alveoli, it s formed of epithelium
Pleural Empyema Joseph Junewick, MD FACR
 Pleural Empyema Joseph Junewick, MD FACR 03/19/2010 History Teenager with persistent fever and cough. Pneumonia diagnosed 1 week ago. Diagnosis Pleural Empyema Additional Clinical Surgery-Clear fluid with
Pleural Empyema Joseph Junewick, MD FACR 03/19/2010 History Teenager with persistent fever and cough. Pneumonia diagnosed 1 week ago. Diagnosis Pleural Empyema Additional Clinical Surgery-Clear fluid with
A comparison between two types of indwelling pleural catheters for management of malignant pleural effusions
 Original Article A comparison between two types of indwelling pleural catheters for management of malignant pleural effusions Sushilkumar Satish Gupta 1, Charalampos S. Floudas 2, Abhinav B. Chandra 3
Original Article A comparison between two types of indwelling pleural catheters for management of malignant pleural effusions Sushilkumar Satish Gupta 1, Charalampos S. Floudas 2, Abhinav B. Chandra 3
Interventional Pulmonary Case Based Discussions (ATS) Ali Imran Saeed, MD University of New Mexico
 Interventional Pulmonary Case Based Discussions (ATS) Ali Imran Saeed, MD University of New Mexico Objectives Interventional Pulmonary in New Mexico Interventional Pulmonary and Advanced Diagnostic Cases
Interventional Pulmonary Case Based Discussions (ATS) Ali Imran Saeed, MD University of New Mexico Objectives Interventional Pulmonary in New Mexico Interventional Pulmonary and Advanced Diagnostic Cases
Louis Saffran, MD; David E. Ost, MD, FCCP; Alan M. Fein, MD, FCCP; and Mark J. Schiff, MD
 Outpatient Pleurodesis of Malignant Pleural Effusions Using a Small-Bore Pigtail Catheter* Louis Saffran, MD; David E. Ost, MD, FCCP; Alan M. Fein, MD, FCCP; and Mark J. Schiff, MD Study objective: Patients
Outpatient Pleurodesis of Malignant Pleural Effusions Using a Small-Bore Pigtail Catheter* Louis Saffran, MD; David E. Ost, MD, FCCP; Alan M. Fein, MD, FCCP; and Mark J. Schiff, MD Study objective: Patients
Surgical treatment of empyema in children
 Surgical treatment of empyema in children Jacques Janson Pierre Goussard Cardiothoracic Surgery, Paediatric Pulmonology Tygerberg Academic Hospital University of Stellenbosch Pleural space Netter, Frank
Surgical treatment of empyema in children Jacques Janson Pierre Goussard Cardiothoracic Surgery, Paediatric Pulmonology Tygerberg Academic Hospital University of Stellenbosch Pleural space Netter, Frank
Bilateral Simultaneous Pleurodesis by Median Sternotomy for Spontaneous Pneumo thorax
 Bilateral Simultaneous Pleurodesis by Median Sternotomy for Spontaneous Pneumo thorax I. Kalnins, M.B., T. A. Torda, F.F.A.R.C.S,, and J. S. Wright, F.R.A.C.S. ABSTRACT Bilateral pleurodesis by median
Bilateral Simultaneous Pleurodesis by Median Sternotomy for Spontaneous Pneumo thorax I. Kalnins, M.B., T. A. Torda, F.F.A.R.C.S,, and J. S. Wright, F.R.A.C.S. ABSTRACT Bilateral pleurodesis by median
Assessing Cardiac Risk in Noncardiac Surgery. Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington
 Assessing Cardiac Risk in Noncardiac Surgery Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington Disclosure None. I have no conflicts of interest, financial or otherwise. CME
Assessing Cardiac Risk in Noncardiac Surgery Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington Disclosure None. I have no conflicts of interest, financial or otherwise. CME
CEU Final Exam for Code It! Sixth Edition
 CEU Final Exam for 3-2-1 Code It! Sixth Edition Note to CEU applicant In order to receive CEU credit for taking this exam, the following criteria must be met: You must be certified by AAPC prior to purchasing
CEU Final Exam for 3-2-1 Code It! Sixth Edition Note to CEU applicant In order to receive CEU credit for taking this exam, the following criteria must be met: You must be certified by AAPC prior to purchasing
BIOCHEMICAL INVESTIGATIONS IN THE DIAGNOSTICS OF CARDIOVASCULAR DISORDERS. As. MARUSHCHAK M.I.
 BIOCHEMICAL INVESTIGATIONS IN THE DIAGNOSTICS OF CARDIOVASCULAR DISORDERS As. MARUSHCHAK M.I. Heart attack symptoms Acute MI Measurement of cardiac enzyme levels Measure cardiac enzyme levels at regular
BIOCHEMICAL INVESTIGATIONS IN THE DIAGNOSTICS OF CARDIOVASCULAR DISORDERS As. MARUSHCHAK M.I. Heart attack symptoms Acute MI Measurement of cardiac enzyme levels Measure cardiac enzyme levels at regular
Rapid pleurodesis is an outpatient alternative in patients with malignant pleural effusions: a prospective randomized controlled trial
 Original Article Rapid pleurodesis is an outpatient alternative in patients with malignant pleural effusions: a prospective randomized controlled trial Serkan Özkul, Akif Turna, Ahmet Demirkaya, Burcu
Original Article Rapid pleurodesis is an outpatient alternative in patients with malignant pleural effusions: a prospective randomized controlled trial Serkan Özkul, Akif Turna, Ahmet Demirkaya, Burcu
Differential diagnosis
 Differential diagnosis Idiopathic pulmonary fibrosis (IPF) is part of a large family of idiopathic interstitial pneumonias (IIP), one of four subgroups of interstitial lung disease (ILD). Differential
Differential diagnosis Idiopathic pulmonary fibrosis (IPF) is part of a large family of idiopathic interstitial pneumonias (IIP), one of four subgroups of interstitial lung disease (ILD). Differential
PLEURAL DISEASES. (Pleural effusion & empyema) Menaldi Rasmin
 PLEURAL DISEASES (Pleural effusion & empyema) Menaldi Rasmin Department of Pulmonology & Respiratory Medicine Faculty of Medicine, University of Indonesia Introduction Pleural effusion is the most common
PLEURAL DISEASES (Pleural effusion & empyema) Menaldi Rasmin Department of Pulmonology & Respiratory Medicine Faculty of Medicine, University of Indonesia Introduction Pleural effusion is the most common
Atlas of the Vasculitic Syndromes
 CHAPTER e40 Atlas of the Vasculitic Syndromes Carol A. Langford Anthony S. Fauci Diagnosis of the vasculitic syndromes is usually based upon characteristic histologic or arteriographic findings in a patient
CHAPTER e40 Atlas of the Vasculitic Syndromes Carol A. Langford Anthony S. Fauci Diagnosis of the vasculitic syndromes is usually based upon characteristic histologic or arteriographic findings in a patient
FILED: NEW YORK COUNTY CLERK 03/05/ :02 PM INDEX NO /2015 NYSCEF DOC. NO. 439 RECEIVED NYSCEF: 03/05/2018
 Steven Markowitz, MD, DrPH Occupational & Environmental Medicine 123 7th Ayenue - PMB 140 Brooklyn, NY 11215 January 26, 2016 Amy Fair, R.N. Simmons, Hanly, Conroy Law Firm 112 Madison Avenue New York,
Steven Markowitz, MD, DrPH Occupational & Environmental Medicine 123 7th Ayenue - PMB 140 Brooklyn, NY 11215 January 26, 2016 Amy Fair, R.N. Simmons, Hanly, Conroy Law Firm 112 Madison Avenue New York,
Pneumothorax has long been listed as one of the
 Pneumothorax in Cystic Fibrosis* Patrick A. Flume, MD, FCCP Spontaneous pneumothorax is a common complication in patients with cystic fibrosis (CF). It is thought to occur more frequently in patients with
Pneumothorax in Cystic Fibrosis* Patrick A. Flume, MD, FCCP Spontaneous pneumothorax is a common complication in patients with cystic fibrosis (CF). It is thought to occur more frequently in patients with
The Portsmouth thoracoscopy experience, an evaluation of service by retrospective case note analysis
 Respiratory Medicine (2007) 101, 1021 1025 The Portsmouth thoracoscopy experience, an evaluation of service by retrospective case note analysis Sophie V. Fletcher,1, Robin J. Clark Respiratory Centre,
Respiratory Medicine (2007) 101, 1021 1025 The Portsmouth thoracoscopy experience, an evaluation of service by retrospective case note analysis Sophie V. Fletcher,1, Robin J. Clark Respiratory Centre,
Case 5 15-year-old male
 Case 5 15-year-old male Present illness: Six months ago, abnormality of ECG was incidentally detected by annual health check. His blood level of γ-gtp, HbA1c and norepinephrine were elevated; however,
Case 5 15-year-old male Present illness: Six months ago, abnormality of ECG was incidentally detected by annual health check. His blood level of γ-gtp, HbA1c and norepinephrine were elevated; however,
E valuation of the patient with a pleural effusion is
 The Diagnostic Value of Pleural Fluid ph* James T. Good, Jr., M.D.; David A. Taryle, M.D.; Robert M. Maulitz, M.D.; Robin L. Kaplan, M.D.; and Steven A. Sahn, M.D., F.C.C.P. One hundred eighty-three patients
The Diagnostic Value of Pleural Fluid ph* James T. Good, Jr., M.D.; David A. Taryle, M.D.; Robert M. Maulitz, M.D.; Robin L. Kaplan, M.D.; and Steven A. Sahn, M.D., F.C.C.P. One hundred eighty-three patients
A 70-Year-Old Woman With Dyspnea and Chest Pain
 CHEST Chest Imaging and Pathology for Clinicians A 70-Year-Old Woman With Dyspnea and Chest Pain Aarthi Ganesh, MD ; Michael Flores, MD ; Isabel Oliva, MD ; and Gordon E. Carr, MD CHEST 2014; 146 ( 1 ):
CHEST Chest Imaging and Pathology for Clinicians A 70-Year-Old Woman With Dyspnea and Chest Pain Aarthi Ganesh, MD ; Michael Flores, MD ; Isabel Oliva, MD ; and Gordon E. Carr, MD CHEST 2014; 146 ( 1 ):
Thoracic Surgery; An Overview
 Thoracic Surgery What we see Thoracic Surgery; An Overview James P. Locher, Jr, MD Methodist Cardiovascular and Thoracic Surgery Lung cancer Mets Fungus and TB Lung abcess and empyema Pleural based disease
Thoracic Surgery What we see Thoracic Surgery; An Overview James P. Locher, Jr, MD Methodist Cardiovascular and Thoracic Surgery Lung cancer Mets Fungus and TB Lung abcess and empyema Pleural based disease
The use of thrombolytics in the management of complex pleural fluid collections
 Original Article The use of thrombolytics in the management of complex pleural fluid collections Jessica Heimes 1, Hannah Copeland 2, Aditya Lulla 3, Marjulin Duldulao 4, Khaled Bahjri 5, Salman Zaheer
Original Article The use of thrombolytics in the management of complex pleural fluid collections Jessica Heimes 1, Hannah Copeland 2, Aditya Lulla 3, Marjulin Duldulao 4, Khaled Bahjri 5, Salman Zaheer
DEPARTMENT OF SURGERY CARDIOVASCULAR-THORACIC SECTION
 DEPARTMENT OF SURGERY CARDIOVASCULAR-THORACIC SECTION DIRECTIONS: This must accompany all initial applications for appointment to the Cardiovascular-Thoracic Section, Department of Surgery. Please indicate
DEPARTMENT OF SURGERY CARDIOVASCULAR-THORACIC SECTION DIRECTIONS: This must accompany all initial applications for appointment to the Cardiovascular-Thoracic Section, Department of Surgery. Please indicate
Cardiovascular Disorders Lecture 3 Coronar Artery Diseases
 Cardiovascular Disorders Lecture 3 Coronar Artery Diseases By Prof. El Sayed Abdel Fattah Eid Lecturer of Internal Medicine Delta University Coronary Heart Diseases It is the leading cause of death in
Cardiovascular Disorders Lecture 3 Coronar Artery Diseases By Prof. El Sayed Abdel Fattah Eid Lecturer of Internal Medicine Delta University Coronary Heart Diseases It is the leading cause of death in
How to Analyse Difficult Chest CT
 How to Analyse Difficult Chest CT Complex diseases are:- - Large lesion - Unusual or atypical pattern - Multiple discordant findings Diffuse diseases are:- - Numerous findings in both sides 3 basic steps
How to Analyse Difficult Chest CT Complex diseases are:- - Large lesion - Unusual or atypical pattern - Multiple discordant findings Diffuse diseases are:- - Numerous findings in both sides 3 basic steps
Understanding Pleural Mesothelioma
 Understanding Pleural Mesothelioma UHN Information for patients and families Read this booklet to learn about: What is pleural mesothelioma? What causes it? What are the symptoms? What tests are done to
Understanding Pleural Mesothelioma UHN Information for patients and families Read this booklet to learn about: What is pleural mesothelioma? What causes it? What are the symptoms? What tests are done to
UAMS MEDICAL CENTER TRAUMA SERVICES MANUAL. REVIEWED: New PAGE: 1 of 7. RECOMMENDATION(S): Dr. Michael Sutherland APPROVAL: 04/28/2016
 REVIEWED: New PAGE: 1 of 7 PURPOSE: To provide guidelines for the evaluation and management of patients with traumatic chest wall injury including rib fractures, sternal fractures, hemothorax and retained
REVIEWED: New PAGE: 1 of 7 PURPOSE: To provide guidelines for the evaluation and management of patients with traumatic chest wall injury including rib fractures, sternal fractures, hemothorax and retained
Comparison of Pleural Fluid ph Values Obtained Using Blood Gas Machine, ph Meter, and ph Indicator Strip*
 Comparison of Pleural Fluid ph Values Obtained Using Blood Gas Machine, ph Meter, and ph Indicator Strip* Dong-sheng Cheng, MD; R. Michael Rodriguez, MD; Jeffrey Rogers, RRT; Marvin Wagster; DanielL. Starnes,
Comparison of Pleural Fluid ph Values Obtained Using Blood Gas Machine, ph Meter, and ph Indicator Strip* Dong-sheng Cheng, MD; R. Michael Rodriguez, MD; Jeffrey Rogers, RRT; Marvin Wagster; DanielL. Starnes,
PLEURAL EFFUSION: DIAGNOSIS, MANAGEMENT AND DISPOSAL
 PLEURAL EFFUSION: DIAGNOSIS, MANAGEMENT AND DISPOSAL 1. This replaces the DGAFMS Medical Memorandum No.63 on Primary (Idiopathic) Pleural Effusion, which dealt with tubercular pleural effusion. 2. Normally
PLEURAL EFFUSION: DIAGNOSIS, MANAGEMENT AND DISPOSAL 1. This replaces the DGAFMS Medical Memorandum No.63 on Primary (Idiopathic) Pleural Effusion, which dealt with tubercular pleural effusion. 2. Normally
Empyema in rheumatoid arthritis
 Ann. rheum. Dis. (1975), 34, 181 Empyema in rheumatoid arthritis P. A. DIEPPE From the Brompton Hospital, Fulham Road, London Dieppe, P. A. (1975). Annals ofthe Rheumatic Diseases, 34, 181. Empyema in
Ann. rheum. Dis. (1975), 34, 181 Empyema in rheumatoid arthritis P. A. DIEPPE From the Brompton Hospital, Fulham Road, London Dieppe, P. A. (1975). Annals ofthe Rheumatic Diseases, 34, 181. Empyema in
Treatment of multiloculated empyema thoracis using minimally invasive methods
 O r i g i n a l A r t i c l e Singapore Med J 2010; 51(3) : 242 Treatment of multiloculated empyema thoracis using minimally invasive methods Metin M, Yeginsu A, Sayar A, Alzafer S, Solak O, Ozgul A, Erkorkmaz
O r i g i n a l A r t i c l e Singapore Med J 2010; 51(3) : 242 Treatment of multiloculated empyema thoracis using minimally invasive methods Metin M, Yeginsu A, Sayar A, Alzafer S, Solak O, Ozgul A, Erkorkmaz
Study of Predictors for Successful Pleurodesis in Patients with Malignant Pleural Effusion
 Med. J. Cairo Univ., Vol. 85, No. 1, March: 11-20, 2017 www.medicaljournalofcairouniversity.net Study of Predictors for Successful Pleurodesis in Patients with Malignant Pleural Effusion TALAT A. ARAFA,
Med. J. Cairo Univ., Vol. 85, No. 1, March: 11-20, 2017 www.medicaljournalofcairouniversity.net Study of Predictors for Successful Pleurodesis in Patients with Malignant Pleural Effusion TALAT A. ARAFA,
Cardiac tamponade and Pericardiocentesis Made Easy
 Cardiac tamponade and Pericardiocentesis Made Easy www.cardiconcept.com Etiology of pericardial diseases. Non Infectious cause Infectious cause European Heart Journal (2015) 36, 2921 2964 Recommendations
Cardiac tamponade and Pericardiocentesis Made Easy www.cardiconcept.com Etiology of pericardial diseases. Non Infectious cause Infectious cause European Heart Journal (2015) 36, 2921 2964 Recommendations
Phil. J. Internal Medicine, 47: 77-81, March-April, 2009 INCIDENCE OF PNEUMOTHORAX AFTER THORACENTESIS AND FACTORS ASSOCIATED WITH ITS OCCURRENCE
 Original Articles Incidence of Pneumothorax After Thoracentesis and Factors Associated with Its Occurrence 77 Phil. J. Internal Medicine, 47: 77-81, March-April, 2009 INCIDENCE OF PNEUMOTHORAX AFTER THORACENTESIS
Original Articles Incidence of Pneumothorax After Thoracentesis and Factors Associated with Its Occurrence 77 Phil. J. Internal Medicine, 47: 77-81, March-April, 2009 INCIDENCE OF PNEUMOTHORAX AFTER THORACENTESIS
Different characteristics of tuberculous pleural effusion according to pleural fluid cellular predominance and loculation
 Original Article Different characteristics of tuberculous pleural effusion according to pleural fluid cellular predominance and loculation Jaehee Lee 1, Jae Kwang Lim 2, Seung Soo Yoo 1, Shin Yup Lee 1,
Original Article Different characteristics of tuberculous pleural effusion according to pleural fluid cellular predominance and loculation Jaehee Lee 1, Jae Kwang Lim 2, Seung Soo Yoo 1, Shin Yup Lee 1,
Pleural Disease in the Intensive Care Unit
 Chapter 115 Pleural Disease in the Intensive Care Unit Hiren J. Mehta and Michael A. Jantz Introduction Pleural disease in itself is an unusual cause for admission to the intensive care unit (ICU). Conditions
Chapter 115 Pleural Disease in the Intensive Care Unit Hiren J. Mehta and Michael A. Jantz Introduction Pleural disease in itself is an unusual cause for admission to the intensive care unit (ICU). Conditions
A Rare Case of Lymphangioleiomyomatosis in Sri Lanka
 A Rare Case of Lymphangioleiomyomatosis in Sri Lanka Author s Details: (1) Dushantha Madegedara (2) Asela Rasika Bandara (3) Sachini Seneviratne (4) Samadara Nakandala (5) Rathnayake R.M.D.H.M - (1) (2)
A Rare Case of Lymphangioleiomyomatosis in Sri Lanka Author s Details: (1) Dushantha Madegedara (2) Asela Rasika Bandara (3) Sachini Seneviratne (4) Samadara Nakandala (5) Rathnayake R.M.D.H.M - (1) (2)
TSDA ACGME Milestones
 TSDA ACGME Milestones Short MW and Edwards JA. Assessing resident milestones using a CASPE March 2012 Short MW and Edwards JA. Assessing resident milestones using a CASPE March 2012 Short
TSDA ACGME Milestones Short MW and Edwards JA. Assessing resident milestones using a CASPE March 2012 Short MW and Edwards JA. Assessing resident milestones using a CASPE March 2012 Short
Ischemic Heart Disease Interventional Treatment
 Ischemic Heart Disease Interventional Treatment Cardiac Catheterization Laboratory Procedures (N = 89) is a regional and national referral center for percutaneous coronary intervention (PCI). A total of
Ischemic Heart Disease Interventional Treatment Cardiac Catheterization Laboratory Procedures (N = 89) is a regional and national referral center for percutaneous coronary intervention (PCI). A total of
Diagnostic and Prognostic Implications of Pleural Adhesions in Malignant Effusions
 ORIGINAL ARTICLE Diagnostic and Prognostic Implications of Pleural Adhesions in Malignant Effusions Silvia Bielsa, MD,* José Martín-Juan, MD, José M. Porcel, MD,* and Francisco Rodríguez-Panadero, MD Background
ORIGINAL ARTICLE Diagnostic and Prognostic Implications of Pleural Adhesions in Malignant Effusions Silvia Bielsa, MD,* José Martín-Juan, MD, José M. Porcel, MD,* and Francisco Rodríguez-Panadero, MD Background
Ischemic Heart Disease Interventional Treatment
 Ischemic Heart Disease Interventional Treatment Cardiac Catheterization Laboratory Procedures (N = 11,61) is a regional and national referral center for percutaneous coronary intervention (PCI). A total
Ischemic Heart Disease Interventional Treatment Cardiac Catheterization Laboratory Procedures (N = 11,61) is a regional and national referral center for percutaneous coronary intervention (PCI). A total
BODY FLUID ANALYSIS. Synovial Fluid. Synovial Fluid Classification. CLS 426 Urinalysis and Body Fluid Analysis Body Fluid Lecture Session 1
 BODY FLUID ANALYSIS Synovial Fluid Serous fluids the 3 P s Peritoneal Pleural Pericardial Cerebrospinal Fluid Karen Keller, MT(ASCP), SH Synovial Fluid Lubricant and sole nutrient source of joint. Normal
BODY FLUID ANALYSIS Synovial Fluid Serous fluids the 3 P s Peritoneal Pleural Pericardial Cerebrospinal Fluid Karen Keller, MT(ASCP), SH Synovial Fluid Lubricant and sole nutrient source of joint. Normal
Giant Solitary Fibrous Tumor of the Pleura: An Analysis of Five Patients
 World J Surg (2010) 34:2553 2557 DOI 10.1007/s00268-010-0715-x Giant Solitary Fibrous Tumor of the Pleura: An Analysis of Five Patients Juntang Guo Xiangyang Chu Yu-e Sun Lianbin Zhang Naikang Zhou Published
World J Surg (2010) 34:2553 2557 DOI 10.1007/s00268-010-0715-x Giant Solitary Fibrous Tumor of the Pleura: An Analysis of Five Patients Juntang Guo Xiangyang Chu Yu-e Sun Lianbin Zhang Naikang Zhou Published
Serous fluids. Dr. Mohamed Saad Daoud
 Serous fluids 1 Reference Books: Urinanalysis and body fluids (Susan King Strasinger- Marjorie Schaub De Lorenzo) Fifth edition 2 The closed cavities of the body namely, the pleural, pericardial, and peritoneal
Serous fluids 1 Reference Books: Urinanalysis and body fluids (Susan King Strasinger- Marjorie Schaub De Lorenzo) Fifth edition 2 The closed cavities of the body namely, the pleural, pericardial, and peritoneal
Pulmonary Sarcoidosis - Radiological Evaluation
 Original Research Article Pulmonary Sarcoidosis - Radiological Evaluation Jayesh Shah 1, Darshan Shah 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident, 3 Professor and HOD Radiology Department,
Original Research Article Pulmonary Sarcoidosis - Radiological Evaluation Jayesh Shah 1, Darshan Shah 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident, 3 Professor and HOD Radiology Department,
BGS Autumn The wet lung - Pleural effusions. Nick Maskell. BGS Autumn Meeting November 2017
 The wet lung - Pleural effusions BGS Autumn Meeting November 2017 Nick Maskell Professor of Respiratory Medicine Bristol University, Bristol Conflicts of interest Prof Maskell has sat on advisory boards
The wet lung - Pleural effusions BGS Autumn Meeting November 2017 Nick Maskell Professor of Respiratory Medicine Bristol University, Bristol Conflicts of interest Prof Maskell has sat on advisory boards
The pericardial sac is composed of the outer fibrous pericardium
 Pericardiectomy for Constrictive or Recurrent Inflammatory Pericarditis Mauricio A. Villavicencio, MD, Joseph A. Dearani, MD, and Thoralf M. Sundt, III, MD Anatomy and Preoperative Considerations The pericardial
Pericardiectomy for Constrictive or Recurrent Inflammatory Pericarditis Mauricio A. Villavicencio, MD, Joseph A. Dearani, MD, and Thoralf M. Sundt, III, MD Anatomy and Preoperative Considerations The pericardial
Case 1. A 35-year-old male presented with fever, cough, and purulent sputum for one week. This was his CXR (Fig. 1.1). What is the diagnosis?
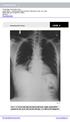 1 Interpreting Chest X-Rays CASE 1 Fig. 1.1 Case 1. A 35-year-old male presented with fever, cough, and purulent sputum for one week. This was his CXR (Fig. 1.1). What is the diagnosis? CASE 1 Interpreting
1 Interpreting Chest X-Rays CASE 1 Fig. 1.1 Case 1. A 35-year-old male presented with fever, cough, and purulent sputum for one week. This was his CXR (Fig. 1.1). What is the diagnosis? CASE 1 Interpreting
Thiazolidinedione-Associated Congestive Heart Failure and Pulmonary Edema
 Search the Journal search Advanced Search > Home Current Issue Past Issues Reprints Submissions Subscriptions Permissions About Us MAYO CLIN PROC. 2003;78:1088-1091 2003 MAYO FOUNDATION FOR MEDICAL EDUCATION
Search the Journal search Advanced Search > Home Current Issue Past Issues Reprints Submissions Subscriptions Permissions About Us MAYO CLIN PROC. 2003;78:1088-1091 2003 MAYO FOUNDATION FOR MEDICAL EDUCATION
Empyema Thoracis* Therapeutic Management and Outcome
 Empyema Thoracis* Therapeutic Management and Outcome Gregory P. LeMense, MD; Charlie Strange, MD, FCCP; and Steven A. Sahn, MD, FCCP Study objective: We evaluated treatment and outcome of patients with
Empyema Thoracis* Therapeutic Management and Outcome Gregory P. LeMense, MD; Charlie Strange, MD, FCCP; and Steven A. Sahn, MD, FCCP Study objective: We evaluated treatment and outcome of patients with
Post Pneumonic Empyema: Is There Still a Role for Surgery?
 Post Pneumonic Empyema: Is There Still a Role for Surgery? M. Blair Marshall, MD Ismael Matus, MD Chief, Thoracic Surgery Interventional Pulmonary Professor of Surgery Medicine MedStar Georgetown University
Post Pneumonic Empyema: Is There Still a Role for Surgery? M. Blair Marshall, MD Ismael Matus, MD Chief, Thoracic Surgery Interventional Pulmonary Professor of Surgery Medicine MedStar Georgetown University
Unusual Causes of Aortic Regurgitation. Case 1
 Unusual Causes of Aortic Regurgitation Judy Hung, MD Cardiology Division Massachusetts General Hospital Boston, MA No Disclosures Case 1 54 year old female with h/o cerebral aneurysm and vascular malformation
Unusual Causes of Aortic Regurgitation Judy Hung, MD Cardiology Division Massachusetts General Hospital Boston, MA No Disclosures Case 1 54 year old female with h/o cerebral aneurysm and vascular malformation
