Comparison of long-term results of above-the-knee femoro-popliteal bypass with autogenous vein and polytetrafluoroethylene grafts
|
|
|
- Baldwin Blair
- 5 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE pissn eissn Annals of Surgical Treatment and Research Comparison of long-term results of above-the-knee femoro-popliteal bypass with autogenous vein and polytetrafluoroethylene grafts Seon-Hee Heo, Yang-Jin Park, Shin-Young Woo, Dong-Ik Kim, Young-Wook Kim Division of Vascular Surgery, Department of Surgery, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Korea Purpose: To analyze the long-term results of above-the-knee femoro-popliteal bypass (ATKFPB) with vein grafts compared with polytetrafluoroethylene (PTFE) grafts. Methods: A database of patients with chronic atherosclerotic occlusive disease who underwent ATKFPB was retrospectively reviewed. Characteristics of patient and arterial lesion, and follow-up results were compared between vein grafts and PTFE grafts. Graft patency was determined by periodic examinations of duplex ultrasonography or CT angiograms. Graft patency and limb salvage rates were calculated using the Kaplan-Meier method. Results: In total, 253 ATKFPBs (107 vein grafts; 146 PTFE grafts; critical limb ischemia, 32%) were performed on 228 patients (mean age, 68.5 years; male, 87.7%). No significant differences were observed between the two groups with respect to demographic characteristics, characteristics of arterial lesions, or distal runoff score. During the mean followup period of 41 months (range, months), 14.5% patients died, and 94% of all limbs were available for follow-up. The primary patency rates were not significantly different between the two groups at 10 years after treatment (75% vs. 42%, P = 0.330). However, the primary-assisted patency rates (88% vs. 42%, P = 0.003) and secondary patency rates (91% vs. 49%, P = 0.013) were significantly higher in the vein grafts compared with the PTFE grafts. Graft occlusion developed more often in the PTFE grafts (5.6% vs. 20.5%, P = 0.001). When graft occlusion occurred, acute limb ischemia was significantly more frequent in the PTFE grafts than in the vein grafts (0% vs. 53%, P = 0.027). Conclusion: After ATKFPB, autologous vein grafts showed significantly better long-term results compared with PTFE grafts. [Ann Surg Treat Res 2015;88(1):28-34] Key Words: Comparative study, Vascular graft occlusion, Peripheral arterial occlusive disease INTRODUCTION Even though endovascular therapy can be successfully performed with various kinds of balloons, stents, or stent grafts, lower extremity arterial bypass (LEAB) surgery remains the most viable treatment option for patients with atherosclerotic arterial occlusive disease, particularly those with diffuse and long segment lesions of the superficial femoral artery (SFA) [1]. The superiority of vein grafts to prosthetic grafts has been well proven in below-the-knee arterial bypass [2-4]. However, previous studies have shown mixed results in above-the-knee femoro-popliteal bypass (ATKFPB) [5-12]. One prospective randomized trial [9] that compared graft patency at two years after ATKFPB reported no statistically significant difference in primary or secondary patency rate between vein grafts and polytetrafluoroethylene (PTFE) grafts. Other randomized Received June 9, 2014, Revised July 26, 2014, Accepted August 1, 2014 Corresponding Author: Young-Wook Kim Division of Vascular Surgery, Department of Surgery, Samsung Medical Center, Sungkyunkwan University School of Medicine, 81 Irwon-ro, Gangnam-gu, Seoul , Korea Tel: , Fax: ywkim@skku.edu Copyright c 2015, the Korean Surgical Society cc Annals of Surgical Treatment and Research is an Open Access Journal. All articles are distributed under the terms of the Creative Commons Attribution Non- Commercial License ( which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. 28
2 Seon-Hee Heo, et al: Above-the-knee femoro-popliteal bypass: vein vs. PTFE grafts controlled trials [6,7,11,13,14] that compared long-term patency rates reported significantly higher patency rates of vein grafts compared with PTFE grafts. Most studies comparing the efficacy of these two types of grafts have been based on graft patency [5-13]. However, graft recommendations should not be based solely on the superiority of graft patency. Approximately 10 years ago, Jackson et al. [15] reported different clinical features in cases of LEAB graft occlusion that had received vein grafts versus those that had received prosthetic grafts; moreover, PTFE graft is associated with a higher risk of ischemic complications from graft occlusion than are vein grafts. However, few reports have investigated the clinical consequences of graft occlusion. In this retrospective review, we compare the long-term patency rates of ATKFPB with vein grafts versus PFTE grafts. We also compare the clinical outcomes of graft occlusions in these two groups. METHODS Study design, patients, and data collection We retrospectively reviewed a database of patients with chronic atherosclerotic occlusive lesions who underwent ATKFPB at a single institute during the past 10 years (September 2003 through February 2014). Patients with nonatherosclerotic occlusive disease who underwent LEAB were excluded from this study. The decision to insert a bypass conduit during ATKFPB was left to the surgeon. In total, 107 autogenous vein grafts and 146 PTFE grafts were performed. All vein grafts used the reversed great saphenous vein as the conduit. The prosthetic grafts were either external supported or smooth PTFE grafts (Gore-tex, W. L. Gore & Associates Inc., Newark, DE, USA) that were 7 or 8 mm in diameter. Between-group differences in preoperative demographic data, clinical features, distal runoff artery status, adjunctive procedures, and procedural details were compared. The distal runoff score was calculated according to the reporting standards on preoperative angiograms as outlined by the Joint Council of the Society for Vascular Surgery and the North American Chapter of the International Society for Cardiovascular surgery [16]. Postoperatively, all patients with vein grafts except one were prescribed single antiplatelet therapy unless contraindicated. Moreover, 126 patients (vein grafts, 11.2% vs. PTFE grafts, 57.7%; P < 0.001) were prescribed warfarin due to concomitant cardiac arrhythmia or to prevent graft thrombosis. For graft surveillance, periodic examinations of duplex ultrasonography scans were performed by experienced vascular technicians at one month postsurgery and then every 3 6 months throughout the first 12 months postsurgery; after this period, examinations were performed every 6 12 months. The graft surveillance procedures were identical for the two groups. Primary, primary-assisted, secondary patency rates of the grafts, and cumulative limb salvage rates were compared and the clinical courses of target limbs were also compared between the vein graft and PTFE graft groups in patients with graft occlusion. Data analysis and statistical methods Either Student t-test or the Mann-Whitney test was used to compare descriptive variables between the two groups. The chi-square or Fisher exact test was used to compare categorical data. Primary, primary-assisted, secondary patency, and limb salvage rates were calculated using the Kaplan-Meier method, and the log-rank test was used to examine differences between the two groups. Statistical analysis was performed with IBM Table 1. Comparison of preoperative demographic and clinical characteristics Characteristic Vein graft PTFE graft (n = 107 limbs) (n = 146 limbs) P-value Age (yr) 68.6 ± ± Male sex 90 (84.1) 132 (90.4) Body mass index (kg/m 2 ) 22.8 ± ± Indication for bypass Claudication 72 (67.3) 100 (68.5) CLI 35 (32.7) 46 (31.5) Rest pain 9 (8.4) 14 (9.6) Nonhealing ulcer 11 (10.3) 15 (10.3) Gangrene 15 (14.0) 17 (11.6) Distal runoff score a) 3.9 ± ± TASC class b) Class B 0 (0) 1 (0.7) Class C 17 (16.7) 37 (25.9) Class D 85 (83.3) 105 (73.4) Comorbidity/risk factor Hypertension 78 (72.9) 114 (78.1) Diabetes mellitus 43 (40.2) 61 (41.8) Hyperlipidemia 37 (34.6) 57 (39.0) Smoking 66 (61.7) 94 (64.4) Ischemic heart disease 32 (29.9) 44 (30.1) Chronic renal failure 9 (8.4) 8 (5.5) Laboratory finding Total cholesterol (mg/dl) ± ± LDL cholesterol (mg/dl) ± ± CRP (mg/dl) 1.4 ± ± Values are presented as mean ± standard deviation or number of limbs (%). PTFE, polytetrafluoroethylene; CLI, critical limb ischemia; TASC, transatlantic society consensus; LDL, low-density lipoprotein. a) Calculated according to the Joint Council of the Society for Vascular Surgery and the North American Chapter of the International Society for Cardiovascular Surgery reporting standards, b) TASC class followed TASC II classification, Annals of Surgical Treatment and Research 29
3 Annals of Surgical Treatment and Research 2015;88(1):28-34 SPSS Statistics ver (IBM Co., Armonk, NY, USA). P-values of <0.05 were considered to be significant. RESULTS Among the 253 ATKFPBs performed for 228 patients (mean age, 68.5 years; range, years; male, 87.7%), reversed great saphenous vein grafts were performed on 107 limbs (42.3%) and PTFE grafts were used on 146 limbs (57.7%). The patient characteristics of the two groups are compared in Table 1. No significant differences regarding demographic features, surgical indications, distal runoff scores, coexisting morbidities, or risk factors were observed between the two groups. With respect to the transatlantic society consensus (TASC) classes in the two groups, all patients except one showed class C or D lesions according to the TASC II classification scheme. The details of the ATKFPB procedures in the two groups of patients, including the frequencies of previous interventions, inflow procedures, proximal anastomosis sites, adjuvant procedures, and postoperative Table 2. Comparison of procedural details of above-theknee femoro-popliteal bypass Variable Vein graft PTFE graft (n = 107 limbs) (n = 146 limbs) P-value Redo bypass 5 (4.7) 3 (2.1) Previous endovascular 6 (5.6) 6 (4.1) intervention SFA stenting 3 (50.0) 2 (33.3) SFA balloon angioplasty 3 (50.0) 4 (66.7) Inflow procedure 46 (43.0) 51 (34.9) Aorto-femoral bypass 2 (4.3) 3 (2.1) Femoro-femoral bypass 16 (34.8) 19 (13.0) Axillo-bifemoral bypass 0 (0) 1 (0.7) Ilio-femoral bypass 4 (8.7) 3 (2.1) Iliac stenting or PTA 30 (65.2) 29 (19.8) Proximal anastomosis site Femoral artery 107 (100) 137 (93.8) Inflow graft 0 (0) 9 (6.2) Adjuvant procedure 12 (11.2) 35 (24.0) Femoral artery 11 (10.3) 32 (21.9) Endarterectomy 11 (100) 31 (96.9) Thrombectomy 0 (0) 1 (3.1) Popliteal artery 1 (0.9) 4 (2.7) Endarterectomy 1 (100) 3 (75.0) Thrombectomy 0 (0) 1 (25.0) Postop antithrombotic medication Aspirin 106 (99.1) 135 (92.5) Aspirin & clopidogrel 0 (0) 3 (2.1) Warfarin 12 (11.2) 114 (57.7) <0.001 Values are presented as number of limbs (%). PTFE, polytetrafluoroethylene; SFA, superficial femoral artery; PTA, percutaneous transluminal angioplasty. antithrombotic medications, are summarized in Table 2. In the PTFE grafts group, proximal anastomosis of the ATKFPB was more frequently performed at the inflow graft; moreover, adjuvant femoral endarterectomies were also more frequently performed in this group. During the postoperative follow-up period (mean, 41 ± 32 months; range, months), 33 patients (14.5%) died, and 15 Patency rate Primary patency_vein Primary patency_ptfe Primary-assisted patency_vein Secondary patency_vein Secondary patency_ptfe Follow-up (mo) Fig. 1. Comparison of patency rates between vein grafts and polytetrafluoroethylene (PTFE) grafts following above-theknee femoro-popliteal bypass grafting. Table 3. Comparison of the long-term results Variable Vein graft PTFE graft (n = 107 limbs) (n = 146 limbs) P-value No. of patients Death during follow-up 13 (12.1) 20 (13.7) Lost to follow-up 7 (6.5) 8 (5.5) Duration of follow-up (mo) 42.3 ± ± Graft or anastomosis stenosis 15 (14.0) 3 (2.1) <0.001 Open surgical treatment 3 (20.0) 0 (0) Endovascular treatment 7 (46.7) 1 (33.3) Graft occlusion 6 (5.6) 30 a) (20.5) Time to detection (mo) 28.6 ± ± <6 After bypass 1 (16.7) 6 (20.0) After bypass 5 (83.3) 24 (80.0) Clinical feature of graft occlusion Asymptomatic 1 (16.7) 2 (6.7) Recurrent claudication 5 (83.3) 12 (40.0) Acute limb ischemia 0 (0) 16 (53.3) Treatment Graft thrombectomy 0 (0) 13 (43.3) Graft revision 0 (0) 2 (6.7) Redo bypass 2 (33.3) 4 (13.3) Results in limb loss 0 (0) 7 (4.8) Values are presented as number of limbs (%) or mean ± standard deviation. a) One patient who presented with acute leg ischemia due to polytetrafluoroethylene (PTFE) graft occlusion and infection included. 30
4 Seon-Hee Heo, et al: Above-the-knee femoro-popliteal bypass: vein vs. PTFE grafts Cumulative limb salvage rate Fig. 2. Comparison of cumulative limb salvage rates between the vein graft and the polytetrafluoroethylene (PTFE) graft groups following above-the-knee femoro-popliteal bypass grafting. grafts (5.9%) were lost to follow-up. The graft patency rates of the vein graft and PTFE graft groups are compared in Fig. 1. No significant difference in primary patency (75% vs. 59% at 5 years; 75% vs. 42% at 10 years, P = 0.330) was observed between the two groups. However, primary-assisted (88% vs. 59% at 5 years; 88% vs. 42% at 10 years, P = 0.003) and secondary graft patency rates (91% vs. 76% at 5 years; 91% vs. 49% at 10 years, P = 0.013) were significantly higher in the vein graft group at 10 years after ATKFPB. During the follow-up period, graft (or anastomotic site) stenosis (n = 18, 7.1%) was more frequently detected in the vein graft group (vein grafts, 14.0% vs. PTFE grafts, 2.1%; P < 0.001), whereas graft occlusions (n = 36, 14.2%) were more frequently detected in the PTFE graft group (vein grafts, 5.6% vs. PTFE grafts, 20.5%; P = 0.001). The clinical features of graft occlusions also differed between the two groups. All vein graft occlusions (n = 6, 5.6%) presented as recurrent leg claudication, with the exception of one asymptomatic limb. In contrast, PTFE graft occlusion more often presented as acute limb ischemia (vein graft, 0% vs. PTFE grafts, 53.3%; P = 0.027) (Table 3). Despite various treatments of the graft occlusions, limb loss occurred significantly more frequently in the PTFE graft group than in the vein graft group (vein grafts, 0% vs. PTFE grafts, 4.8%; P = 0.019) (Table 3, Fig. 2). DISCUSSION Follow-up (mo) Vein PTFE P = (log-rank test) LEAB is still used as the last option for arterial reconstruction in patients with symptomatic, diffuse atherosclerotic occlusive disease; LEAB is typically performed as a primary or secondary procedure following failed endovascular or open surgical procedures [1,17,18]. Although an autologous saphenous vein is generally the conduit of choice in distal leg bypass surgery, the superiority of vein grafts to prosthetic grafts in ATKFPB has been disputed. Several previous prospective randomized controlled trials have reported different follow-up results after comparing vein grafts and prosthetic grafts in ATKFPB. However, this issue has become less important as endovascular therapy has become a more relevant treatment for SFA lesions. In a prospective randomized trial comparing vein grafts with PTFE grafts in ATKFPB, Burger et al. [9] reported no significant differences in the primary and secondary patency rates at two years after bypass surgery (83% vs. 67%, P = 0.065; 83% vs. 77%, P = 0.298). Veith et al. [14] also reported in a randomized controlled study that the 4-year graft patencies of patients who underwent ATKFPB with autogenous saphenous vein grafts versus those with PTFE grafts were not significantly different (68% vs. 38%, P = 0.25). In another randomized trial comparing vein graft, human umbilical vein graft, and PTFE graft outcomes after ATKFPB, similar 2-year patency rates were reported (saphenous vein, 81%; human umbilical vein, 70%; PTFE, 69%); however, that study found a significantly higher 5-year patency rate of saphenous vein grafts compared with PTFE grafts (73% vs. 39%, P < 0.01) [11]. The data presented by Tilanus et al. [19] also support the superior long-term patency of vein grafts compared to prosthetic grafts in ATKFPB (70% vs. 37%, P < 0.001). In the present study, we did not observe a statistically significant difference in the long-term primary patency rates of vein grafts compared with PTFE grafts (75% vs. 42%, P = 0.330) at 10 years after graft implantation. However, we did find that the primary-assisted patency and secondary patency rates of the vein grafts were significantly higher at 10 years compared with those of the PTFE grafts (primary-assisted patency, 88% vs. 42%, P = 0.003; secondary patency, 91% vs. 49%, P = 0.013) (Fig. 1). The discrepant results of the primary patency rates compared with those of the primary-assisted and secondary patency rates may be attributed to the higher rate of detection and revision of the failing grafts in the vein graft group compared with the PTFE graft group (14.0% vs. 2.1%, P < 0.001). Given that SFA lesions that require ATKFPB are as not as diffuse or atherosclerotic as SFA lesions that require distal leg bypass grafting, it was not surprising that we observed a significant difference in the limb salvage rates between the two groups (Fig. 2). The clinical results of patients with graft occlusions also revealed that patients in the PTFE graft group exhibited poorer clinical outcomes, including a higher frequency of acute limb ischemia (0% vs. 53.3%, P = 0.027). The poorer late clinical outcomes of the PTFE grafts may be attributed to differences in biological impact on the surrounding native arteries from the autogenous vein graft. This hypothesis is supported by the higher frequency of sudden occlusion associated with PTFE graft (vein graft, 5.6% vs. PTFE Annals of Surgical Treatment and Research 31
5 Annals of Surgical Treatment and Research 2015;88(1):28-34 A B C C Fig. 3. Diagnosis and treatment of a failing vein graft: (A) femoro-popliteal vein graft showing stenosis close to the site of proximal anastomosis on a contrast angiogram; (B) stenotic vein graft showing a high peak systolic velocity (451 cm/sec) on a duplex ultrasonography scan; (C) vein graft stenosis; and (D) vein patch angioplasty for the treatment of the failing graft [22]. graft, 20.5%; P = 0.001) and the more frequent graft narrowing in vein grafts (vein graft, 14.0% vs. PTFE graft, 2.1%; P < 0.001) (Fig. 3). These findings may be due to sudden thrombosis, which occurs more frequently in prosthetic grafts than in vein grafts, in which intimal hyperplasia is the major cause of late graft occlusion [20]. As reported in previous studies [15,21], rapid revascularization is required to manage the impact of sudden graft thrombosis on the local collateral circulation and the persistence of foreign graft material in tissues. Such events may lead to higher limb loss rates in cases of prosthetic graft occlusion compared with those of vein graft occlusion. According to our assessment of LEAB results, limb salvage rather than graft patency shows a more striking difference between the two groups, particularly in the context of the preservation of a painless and functioning limb that does not require reintervention. From this point of view, our retrospective analysis leads us to recommend vein grafts rather 32 than PTFE grafts as bypass conduits for ATKFPB. Furthermore, the importance of postoperative surveillance of vein grafts and early treatment of failing vein grafts is highlighted by our analysis, which revealed a higher assisted primary graft patency rate in the vein graft group, in accordance with previous studies [15,22]. Moreover, the argument that PTFE grafts should be used in ATKFPB in order to preserve the great saphenous vein for future coronary artery bypass grafting (CABG) has become less convincing due to the availability of improved conduits for CABG and the increasing incidence of percutaneous coronary artery intervention [23,24]. This study was somewhat limited by its retrospective design; moreover, patients who underwent ATKFPB were not allocated randomly into the vein graft group or the PTFE group. In summary, this study shows that long-term patency rates and clinical outcomes after ATKFPB were significantly better
6 Seon-Hee Heo, et al: Above-the-knee femoro-popliteal bypass: vein vs. PTFE grafts with vein grafts compared with PTFE grafts. In addition, this study highlights the importance of postoperative vein graft surveillance and treatment of failing grafts for successfully preventing graft failure. Accordingly, we propose that ATKFPB with a vein graft and postoperative graft surveillance should remain the preferred treatment for patients with diffuse, long occlusive lesions of the SFA. CONFLICTS OF INTEREST No potential conflict of interest relevant to this article was reported. REFERENCES 1. Norgren L, Hiatt WR, Dormandy JA, Nehler MR, Harris KA, Fowkes FG, et al. Inter-Society Consensus for the Management of Peripheral Arterial Disease (TASC II). Eur J Vasc Endovasc Surg 2007;33 Suppl 1:S Bergan JJ, Veith FJ, Bernhard VM, Yao JS, Flinn WR, Gupta SK, et al. Randomization of autogenous vein and polytetrafluorethylene grafts in femoral-distal reconstruction. Surgery 1982;92: Londrey GL, Ramsey DE, Hodgson KJ, Bark meier LD, Sumner DS. Infrapopliteal bypass for severe ischemia: comparison of autogenous vein, composite, and prosthetic grafts. J Vasc Surg 1991;13: Sayers RD, Raptis S, Berce M, Miller JH. Long-term results of femorotibial bypass with vein or polytetrafluoroethylene. Br J Surg 1998;85: Abbott WM, Green RM, Matsumoto T, Wheeler JR, Miller N, Veith FJ, et al. Pro sthetic above-knee femoropopliteal bypass grafting: results of a multicenter ran domized prospective trial. Above-Knee Femoropopliteal Study Group. J Vasc Surg 1997;25: AbuRahma AF, Robinson PA, Holt SM. Prospective controlled study of polytetrafluoroethylene versus saphenous vein in claudicant patients with bilateral above knee femoropopliteal bypasses. Surgery 1999;126: Ballotta E, Renon L, Toffano M, Da Giau G. Prospective randomized study on bilateral above-knee femoropopliteal revascularization: polytetrafluoroethylene gra ft versus reversed saphenous vein. J Vasc Surg 2003;38: Berglund J, Bjorck M, Elfstrom J; SWE- DVASC Femoro-popliteal Study Gro up. Long-term results of above knee femoropopliteal bypass depend on indi cation for surgery and graft-material. Eur J Vasc Endovasc Surg 2005;29: Burger DH, Kappetein AP, Van Bockel JH, Breslau PJ. A prospective randomized trial comparing vein with polytetra fluoroethylene in above-knee femoropopliteal bypass grafting. J Vasc Surg 2000;32: Green RM, Abbott WM, Matsumoto T, Wheeler JR, Miller N, Veith FJ, et al. Prosthetic above-knee femoropopliteal by pass grafting: five-year results of a random ized trial. J Vasc Surg 2000;31: Johnson WC, Lee KK. A comparative evalu ation of polytetrafluoroethylene, um bilical vein, and saphenous vein bypass grafts for femoral-popliteal aboveknee revascularization: a prospective ran domized Department of Veterans Affairs cooperative study. J Vasc Surg 2000; 32: Klinkert P, Schepers A, Burger DH, van Bockel JH, Breslau PJ. Vein versus polytetrafluoroethylene in above-knee femoropopliteal bypass grafting: five-year results of a randomized controlled trial. J Vasc Surg 2003;37: Klinkert P, Post PN, Breslau PJ, van Bockel JH. Saphenous vein versus PTFE for above-knee femoropopliteal bypass. A review of the literature. Eur J Vasc Endovasc Surg 2004;27: Veith FJ, Gupta SK, Ascer E, White-Flores S, Samson RH, Scher LA, et al. Six-year prospective multicenter randomized compa rison of autologous saphenous vein and expanded polytetrafluoroethylene grafts in infrainguinal arterial reconstructions. J Vasc Surg 1986;3: Jackson MR, Belott TP, Dickason T, Kaiser WJ, Modrall JG, Valentine RJ, et al. The consequences of a failed femoropopliteal bypass grafting: comparison of saphenous vein and PTFE grafts. J Vasc Surg 2000;32: ; Rutherford RB, Baker JD, Ernst C, Johnston KW, Porter JM, Ahn S, et al. Recommended standards for reports dealing with lower extremity ischemia: revised version. J Vasc Surg 1997;26: Smolock CJ, Anaya-Ayala JE, Kaufman Y, Bavare CS, Patel MS, El-Sayed HF, et al. Cu rrent efficacy of open and endovascular inter ventions for advanced superficial femo ral artery occlusive disease. J Vasc Surg 2013;58: e Adam DJ, Beard JD, Cleveland T, Bell J, Bradbury AW, Forbes JF, et al. Bypass versus angioplasty in severe ischaemia of the leg (BASIL): multicentre, randomised controlled trial. Lancet 2005;366: Tilanus HW, Obertop H, Van Urk H. Saphenous vein or PTFE for femoropopliteal bypass. A prospective randomized trial. Ann Surg 1985;202: John TG, Stonebridge PA, Kelman J, Murie JA, Jenkins AM, Ruckley CV. Above-knee femoropopliteal bypass grafts and the consequences of graft failure. Ann R Coll Surg Engl 1993;75: Pereira CE, Albers M, Romiti M, Brochado- Neto FC, Pereira CA. Meta-analysis of femo ropopliteal bypass grafts for lower extremity arterial insufficiency. J Vasc Annals of Surgical Treatment and Research 33
7 Annals of Surgical Treatment and Research 2015;88(1):28-34 Surg 2006;44: Park KM, Park YJ, Yang SS, Kim DI, Kim YW. Treatment of failing vein grafts in patients who underwent lower extremity arterial bypass. J Korean Surg Soc 2012;83: Poletti LF, Matsuura JH, Dattilo JB, Posner MP, Lee HM, Scouvart M, et al. Should vein be saved for future operations? A 15- year review of infrainguinal bypasses and the subsequent need for autogenous vein. Ann Vasc Surg 1998;12: Sterpetti AV, Schultz RD, Feldhaus RJ, Peetz DJ Jr. Seven-year experience with polytetrafluoroethylene as above-knee femoropopliteal bypass graft. Is is worth while to preserve the autologous saphenous vein? J Vasc Surg 1985;2:
John E. Campbell, MD Assistant Professor of Surgery and Medicine Department of Vascular Surgery West Virginia University, Charleston Division
 John E. Campbell, MD Assistant Professor of Surgery and Medicine Department of Vascular Surgery West Virginia University, Charleston Division John Campbell, MD For the 12 months preceding this CME activity,
John E. Campbell, MD Assistant Professor of Surgery and Medicine Department of Vascular Surgery West Virginia University, Charleston Division John Campbell, MD For the 12 months preceding this CME activity,
Long-term Results of Above Knee Femoro-popliteal Bypass Depend on Indication for Surgery and Graft-material
 Eur J Vasc Endovasc Surg 29, 412 418 (2005) doi:10.1016/j.ejvs.2004.12.023, available online at http://www.sciencedirect.com on Long-term Results of Above Knee Femoro-popliteal Bypass Depend on Indication
Eur J Vasc Endovasc Surg 29, 412 418 (2005) doi:10.1016/j.ejvs.2004.12.023, available online at http://www.sciencedirect.com on Long-term Results of Above Knee Femoro-popliteal Bypass Depend on Indication
Ten year outcomes after bypass surgery in aortoiliac occlusive disease
 J Korean Surg Soc 2012;82:365-369 http://dx.doi.org/10.4174/jkss.2012.82.6.365 ORIGINAL ARTICLE JKSS Journal of the Korean Surgical Society pissn 2233-7903 ㆍ eissn 2093-0488 Ten year outcomes after bypass
J Korean Surg Soc 2012;82:365-369 http://dx.doi.org/10.4174/jkss.2012.82.6.365 ORIGINAL ARTICLE JKSS Journal of the Korean Surgical Society pissn 2233-7903 ㆍ eissn 2093-0488 Ten year outcomes after bypass
Vasile Goldiş Western University of Arad Faculty of Medicine, Pharmacy and Dental Medicine, Arad, Romania
 ENDOVASCULAR TREATMENT FOR VASCULAR GRAFT RESTENOSIS Bogdan Totolici 1, Francisca Blanca Călinescu 1*, Ionel Droc 2, Carmen Neamţu 1 1 Vasile Goldiş Western University of Arad Faculty of Medicine, Pharmacy
ENDOVASCULAR TREATMENT FOR VASCULAR GRAFT RESTENOSIS Bogdan Totolici 1, Francisca Blanca Călinescu 1*, Ionel Droc 2, Carmen Neamţu 1 1 Vasile Goldiş Western University of Arad Faculty of Medicine, Pharmacy
Do the newest grafts achieve comparable results to saphenous vein bypass? THE HEPARIN-BONDED eptfe GRAFT. C. Pratesi
 Do the newest grafts achieve comparable results to saphenous vein bypass? THE HEPARIN-BONDED eptfe GRAFT C. Pratesi Department of Vascular Surgery University of Florence-Italy www.chirvasc-unifi.it FEMORO-POPLITEAL
Do the newest grafts achieve comparable results to saphenous vein bypass? THE HEPARIN-BONDED eptfe GRAFT C. Pratesi Department of Vascular Surgery University of Florence-Italy www.chirvasc-unifi.it FEMORO-POPLITEAL
Comparing vein with collagen impregnated woven polyester prosthesis in above-knee femoropopliteal bypass grafting
 International Journal of Surgery (2007) 5, 109e113 www.theijs.com Comparing vein with collagen impregnated woven polyester prosthesis in above-knee femoropopliteal bypass grafting A. Mohammadi Tofigh a,
International Journal of Surgery (2007) 5, 109e113 www.theijs.com Comparing vein with collagen impregnated woven polyester prosthesis in above-knee femoropopliteal bypass grafting A. Mohammadi Tofigh a,
Endovascular Should Be Considered First Line Therapy
 Revascularization of Patients with Critical Limb Ischemia Endovascular Should Be Considered First Line Therapy Michael Conte David Dawson David L. Dawson, MD Revised Presentation Title A Selective Approach
Revascularization of Patients with Critical Limb Ischemia Endovascular Should Be Considered First Line Therapy Michael Conte David Dawson David L. Dawson, MD Revised Presentation Title A Selective Approach
Maximally Invasive Vascular Surgery for the Treatment of Critical Limb Ischemia
 Maximally Invasive Vascular Surgery for the Treatment of Critical Limb Ischemia Traci A. Kimball, MD Department of Surgery Grand Rounds Septemember 13, 2010 Overview Defining Critical Limb Ischemia Epidemiology
Maximally Invasive Vascular Surgery for the Treatment of Critical Limb Ischemia Traci A. Kimball, MD Department of Surgery Grand Rounds Septemember 13, 2010 Overview Defining Critical Limb Ischemia Epidemiology
Comparison Of Primary Long Stenting Versus Primary Short Stenting For Long Femoropopliteal Artery Disease (PARADE)
 Comparison Of Primary Long Stenting Versus Primary Short Stenting For Long Femoropopliteal Artery Disease (PARADE) Young-Guk Ko, M.D. Severance Cardiovascular Hospital, Yonsei University Health System,
Comparison Of Primary Long Stenting Versus Primary Short Stenting For Long Femoropopliteal Artery Disease (PARADE) Young-Guk Ko, M.D. Severance Cardiovascular Hospital, Yonsei University Health System,
Popliteal Bypass Versus Percutaneous Transluminal
 501591SJS102410.1177/1457496913501591The treatment of occlusive superficial femoral artery diseaseh. Linnakoski, et al. 2013 ORIGINAL ARTICLE Scandinavian Journal of Surgery 102: 227 233, 2013 Comparison
501591SJS102410.1177/1457496913501591The treatment of occlusive superficial femoral artery diseaseh. Linnakoski, et al. 2013 ORIGINAL ARTICLE Scandinavian Journal of Surgery 102: 227 233, 2013 Comparison
Remote Endarterectomy Update
 Remote Endarterectomy Update An endovascular alternative to bypass? BY JOHN D. MARTIN, MD Treating the superficial femoral artery (SFA) is still one of the most highly debated topics among vascular specialists.
Remote Endarterectomy Update An endovascular alternative to bypass? BY JOHN D. MARTIN, MD Treating the superficial femoral artery (SFA) is still one of the most highly debated topics among vascular specialists.
Diagnosis and Endovascular Treatment of Critical Limb Ischemia: What You Need to Know S. Jay Mathews, MD, MS, FACC
 Diagnosis and Endovascular Treatment of Critical Limb Ischemia: What You Need to Know S. Jay Mathews, MD, MS, FACC Interventional Cardiologist/Endovascular Specialist Bradenton Cardiology Center Bradenton,
Diagnosis and Endovascular Treatment of Critical Limb Ischemia: What You Need to Know S. Jay Mathews, MD, MS, FACC Interventional Cardiologist/Endovascular Specialist Bradenton Cardiology Center Bradenton,
Clinical presentation and outcome after failed infrainguinal endovascular and open revascularization in patients with chronic limb ischemia
 From the Society for Clinical Vascular Surgery Clinical presentation and outcome after failed infrainguinal endovascular and open revascularization in patients with chronic limb ischemia Hasan H. Dosluoglu,
From the Society for Clinical Vascular Surgery Clinical presentation and outcome after failed infrainguinal endovascular and open revascularization in patients with chronic limb ischemia Hasan H. Dosluoglu,
Disclosures. Objectives. Bypass vs. Endo for SFA Disease: Reaching Consensus on a Rational Approach. Christopher D. Owens, MD 4/23/2009
 Disclosures Bypass vs. Endo for SFA Disease: Reaching Consensus on a Rational Approach No disclosures No conflicts of interest Christopher D. Owens, MD Objectives Changing face of our patients presenting
Disclosures Bypass vs. Endo for SFA Disease: Reaching Consensus on a Rational Approach No disclosures No conflicts of interest Christopher D. Owens, MD Objectives Changing face of our patients presenting
Practical Point in Diabetic Foot Care 3-4 July 2017
 Diabetic Foot Ulcer : Role of Vascular Surgeon Practical Point in Diabetic Foot Care 3-4 July 2017 Supapong Arworn, MD Division of Vascular and Endovascular Surgery Department of Surgery, Chiang Mai University
Diabetic Foot Ulcer : Role of Vascular Surgeon Practical Point in Diabetic Foot Care 3-4 July 2017 Supapong Arworn, MD Division of Vascular and Endovascular Surgery Department of Surgery, Chiang Mai University
The long-term value of composite limb salvage
 The long-term value of composite limb salvage grafts for John B. Chang, MD, and Theodore A. Stein, PhD, Roslyn, N.Y. Purpose: We determined the long-term efficacy of composite grafts for limb salvage when
The long-term value of composite limb salvage grafts for John B. Chang, MD, and Theodore A. Stein, PhD, Roslyn, N.Y. Purpose: We determined the long-term efficacy of composite grafts for limb salvage when
Surgery is and Remains the Gold Standard for Limb-Threatening Ischemia
 Surgery is and Remains the Gold Standard for Limb-Threatening Ischemia Albeir Mousa, MD., FACS.,MPH., MBA Professor of Vascular and Endovascular Surgery West Virginia University Disclosure None What you
Surgery is and Remains the Gold Standard for Limb-Threatening Ischemia Albeir Mousa, MD., FACS.,MPH., MBA Professor of Vascular and Endovascular Surgery West Virginia University Disclosure None What you
A Case for Mandatory Routine Graft Surveillance of lower extremity bypass grafts. Avishai Meyer UCHSC resident, Surgery May 8, 2006
 A Case for Mandatory Routine Graft Surveillance of lower extremity bypass grafts Avishai Meyer UCHSC resident, Surgery May 8, 2006 Outline: Definition Background of terms and studies U/S surveillance What
A Case for Mandatory Routine Graft Surveillance of lower extremity bypass grafts Avishai Meyer UCHSC resident, Surgery May 8, 2006 Outline: Definition Background of terms and studies U/S surveillance What
Stratifying Management Options for Patients with Critical Limb Ischemia: When Should Open Surgery Be the Initial Option for CLI?
 Stratifying Management Options for Patients with Critical Limb Ischemia: When Should Open Surgery Be the Initial Option for CLI? Peter F. Lawrence, M.D. Gonda Vascular Center Division of Vascular Surgery
Stratifying Management Options for Patients with Critical Limb Ischemia: When Should Open Surgery Be the Initial Option for CLI? Peter F. Lawrence, M.D. Gonda Vascular Center Division of Vascular Surgery
Saphenous Vein Versus PTFE for Above-Knee Femoropopliteal Bypass. A Review of the Literature
 Eur J Vasc Endovasc Surg 27, 357 362 (2004) doi: 10.1016/j.ejvs.2003.12.027, available online at http://www.sciencedirect.com on REVIEW Saphenous Vein Versus PTFE for Above-Knee Femoropopliteal Bypass.
Eur J Vasc Endovasc Surg 27, 357 362 (2004) doi: 10.1016/j.ejvs.2003.12.027, available online at http://www.sciencedirect.com on REVIEW Saphenous Vein Versus PTFE for Above-Knee Femoropopliteal Bypass.
Femoropopliteal Above-Knee Bypass: The True Results
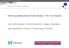 Femoropopliteal Above-Knee Bypass: The True Results Lise Pyndt Jørgensen, Camilla Rasmussen & Torben V Schroeder Rigshospitalet and University of Copenhagen, DENMARK Treatment options in the femoropopliteal
Femoropopliteal Above-Knee Bypass: The True Results Lise Pyndt Jørgensen, Camilla Rasmussen & Torben V Schroeder Rigshospitalet and University of Copenhagen, DENMARK Treatment options in the femoropopliteal
Distal By-Pass procedures can reduce limb loss
 Conventional treatment of the diabetic foot Distal By-Pass procedures can reduce limb loss Dr. Nikolaos Melas, PhD Vascular and Endovascular Surgeon Military Doctor Associate in 1st department of Surgery,
Conventional treatment of the diabetic foot Distal By-Pass procedures can reduce limb loss Dr. Nikolaos Melas, PhD Vascular and Endovascular Surgeon Military Doctor Associate in 1st department of Surgery,
Limb Salvage in Diabetic Ischemic Foot. Kritaya Kritayakirana, MD, FACS Assistant Professor Chulalongkorn University April 30, 2017
 Limb Salvage in Diabetic Ischemic Foot Kritaya Kritayakirana, MD, FACS Assistant Professor Chulalongkorn University April 30, 2017 Case Male 67 years old Underlying DM, HTN, TVD Present with gangrene
Limb Salvage in Diabetic Ischemic Foot Kritaya Kritayakirana, MD, FACS Assistant Professor Chulalongkorn University April 30, 2017 Case Male 67 years old Underlying DM, HTN, TVD Present with gangrene
Current Vascular and Endovascular Management in Diabetic Vasculopathy
 Current Vascular and Endovascular Management in Diabetic Vasculopathy Yang-Jin Park Associate professor Vascular Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine Peripheral artery
Current Vascular and Endovascular Management in Diabetic Vasculopathy Yang-Jin Park Associate professor Vascular Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine Peripheral artery
Long-term assessment of cryopreserved vein bypass grafting success
 Long-term assessment of cryopreserved vein bypass grafting success Linda Harris, MD, a Monica O Brien-Irr MS, RN, a and John J. Ricotta, MD, b Buffalo, NY Purpose: When autogenous vein is unavailable,
Long-term assessment of cryopreserved vein bypass grafting success Linda Harris, MD, a Monica O Brien-Irr MS, RN, a and John J. Ricotta, MD, b Buffalo, NY Purpose: When autogenous vein is unavailable,
Imaging Strategy For Claudication
 Who are the Debators? Imaging Strategy For Claudication Duplex Ultrasound Alone is Adequate to Select Patients for Endovascular Intervention - Pro: Dennis Bandyk MD No Disclosures PRO - Vascular Surgeon
Who are the Debators? Imaging Strategy For Claudication Duplex Ultrasound Alone is Adequate to Select Patients for Endovascular Intervention - Pro: Dennis Bandyk MD No Disclosures PRO - Vascular Surgeon
Influence of vein size (diameter) on infrapopliteal reversed vein graft patency
 Influence of vein size (diameter) on infrapopliteal reversed vein graft patency Kurt R. Wengerter, MD, Frank J. Veith, MD, Sushil K. Gupta, MD, Enrico Ascer, MD, and Steven P. Rivers, MD, New York, N.Y.
Influence of vein size (diameter) on infrapopliteal reversed vein graft patency Kurt R. Wengerter, MD, Frank J. Veith, MD, Sushil K. Gupta, MD, Enrico Ascer, MD, and Steven P. Rivers, MD, New York, N.Y.
Isolated femoral endarterectomy: Impact of SFA TASC classification on recurrence of symptoms and need for additional intervention
 From the Eastern Vascular Society Isolated femoral endarterectomy: Impact of SFA TASC classification on recurrence of symptoms and need for additional intervention Georges Al-Khoury, MD, Luke Marone, MD,
From the Eastern Vascular Society Isolated femoral endarterectomy: Impact of SFA TASC classification on recurrence of symptoms and need for additional intervention Georges Al-Khoury, MD, Luke Marone, MD,
Olive registry: 3-years outcome of BTK intervention in Japan. Osamu Iida, MD Kansai Rosai Hospital Amagasaki, Hyogo, Japan
 Olive registry: 3-years outcome of BTK intervention in Japan Osamu Iida, MD Kansai Rosai Hospital Amagasaki, Hyogo, Japan What is the optimal treatment for the patient with critical limb ischemia (CLI)?
Olive registry: 3-years outcome of BTK intervention in Japan Osamu Iida, MD Kansai Rosai Hospital Amagasaki, Hyogo, Japan What is the optimal treatment for the patient with critical limb ischemia (CLI)?
DCB in my practice: How the evidence influences my strategy. Yang-Jin Park
 DCB in my practice: How the evidence influences my strategy Yang-Jin Park Associate Professor Division of Vascular Surgery, Department of Surgery Samsung Medical Center Sungkyunkwan University School of
DCB in my practice: How the evidence influences my strategy Yang-Jin Park Associate Professor Division of Vascular Surgery, Department of Surgery Samsung Medical Center Sungkyunkwan University School of
Accurate Vessel Sizing Drives Clinical Results. IVUS In the Periphery
 Accurate Vessel Sizing Drives Clinical Results IVUS In the Periphery Discussion Iida O, et. al. Study Efficacy of Intravascular Ultrasound in Femoropopliteal Stenting for Peripheral Artery Disease With
Accurate Vessel Sizing Drives Clinical Results IVUS In the Periphery Discussion Iida O, et. al. Study Efficacy of Intravascular Ultrasound in Femoropopliteal Stenting for Peripheral Artery Disease With
Case Discussion. Disclosures. Critical Limb Ischemia: A Selective Approach to Revascularization Works Best 4/28/2012. None. 58 yo M, DM, CAD, HTN
 Critical Limb Ischemia: A Selective Approach to Revascularization Works Best None Disclosures Michael S. Conte MD, FACS Division of Vascular and Endovascular Surgery Co-Director, Heart and Vascular Center
Critical Limb Ischemia: A Selective Approach to Revascularization Works Best None Disclosures Michael S. Conte MD, FACS Division of Vascular and Endovascular Surgery Co-Director, Heart and Vascular Center
John E. Campbell, MD. Assistant Professor of Surgery and Medicine Department of Vascular Surgery West Virginia University, Charleston Division
 John E. Campbell, MD Assistant Professor of Surgery and Medicine Department of Vascular Surgery West Virginia University, Charleston Division John Campbell, MD For the 12 months preceding this CME activity,
John E. Campbell, MD Assistant Professor of Surgery and Medicine Department of Vascular Surgery West Virginia University, Charleston Division John Campbell, MD For the 12 months preceding this CME activity,
Endovascular treatment (EVT) has markedly advanced,
 Ann Vasc Dis Vol. 6, No. 3; 2013; pp 573 577 Online August 12, 2013 2013 Annals of Vascular Diseases doi:10.3400/avd.oa.13-00055 Original Article A Review of Surgically Treated Patients with Obstruction
Ann Vasc Dis Vol. 6, No. 3; 2013; pp 573 577 Online August 12, 2013 2013 Annals of Vascular Diseases doi:10.3400/avd.oa.13-00055 Original Article A Review of Surgically Treated Patients with Obstruction
Practical Point in Holistic Diabetic Foot Care 3 March 2016
 Diabetic Foot Ulcer : Vascular Management Practical Point in Holistic Diabetic Foot Care 3 March 2016 Supapong Arworn, MD Division of Vascular and Endovascular Surgery Department of Surgery, Chiang Mai
Diabetic Foot Ulcer : Vascular Management Practical Point in Holistic Diabetic Foot Care 3 March 2016 Supapong Arworn, MD Division of Vascular and Endovascular Surgery Department of Surgery, Chiang Mai
Clinical and morphological features of patients who underwent endovascular interventions for lower extremity arterial occlusive diseases
 Original paper Clinical and morphological features of patients who underwent endovascular interventions for lower extremity arterial occlusive diseases Sakir Arslan, Isa Oner Yuksel, Erkan Koklu, Goksel
Original paper Clinical and morphological features of patients who underwent endovascular interventions for lower extremity arterial occlusive diseases Sakir Arslan, Isa Oner Yuksel, Erkan Koklu, Goksel
Introduction. Risk factors of PVD 5/8/2017
 PATHOPHYSIOLOGY AND CLINICAL FEATURES OF PERIPHERAL VASCULAR DISEASE Dr. Muhamad Zabidi Ahmad Radiologist and Section Chief, Radiology, Oncology and Nuclear Medicine Section, Advanced Medical and Dental
PATHOPHYSIOLOGY AND CLINICAL FEATURES OF PERIPHERAL VASCULAR DISEASE Dr. Muhamad Zabidi Ahmad Radiologist and Section Chief, Radiology, Oncology and Nuclear Medicine Section, Advanced Medical and Dental
Disclosures. Talking Points. An initial strategy of open bypass is better for some CLI patients, and we can define who they are
 An initial strategy of open bypass is better for some CLI patients, and we can define who they are Fadi Saab, MD, FASE, FACC, FSCAI Metro Heart & Vascular Metro Health Hospital, Wyoming, MI Assistant Clinical
An initial strategy of open bypass is better for some CLI patients, and we can define who they are Fadi Saab, MD, FASE, FACC, FSCAI Metro Heart & Vascular Metro Health Hospital, Wyoming, MI Assistant Clinical
The ZILVERPASS study a randomized study comparing ZILVER PTX stenting with Bypass in femoropopliteal lesions
 The ZILVERPASS study a randomized study comparing ZILVER PTX stenting with Bypass in femoropopliteal lesions Dr. Sven Bräunlich Department of Angiology University-Hospital Leipzig, Germany Disclosure Speaker
The ZILVERPASS study a randomized study comparing ZILVER PTX stenting with Bypass in femoropopliteal lesions Dr. Sven Bräunlich Department of Angiology University-Hospital Leipzig, Germany Disclosure Speaker
Intercepting PAD. Playbook for Cardiovascular Care 2018 February 24, Jonathan D Woody, MD, FACS. University Surgical Vascular
 Intercepting PAD Playbook for Cardiovascular Care 2018 February 24, 2018 Jonathan D Woody, MD, FACS University Surgical Vascular Attending Vascular Surgeon - Piedmont Athens Regional Adjunct Clinical Associate
Intercepting PAD Playbook for Cardiovascular Care 2018 February 24, 2018 Jonathan D Woody, MD, FACS University Surgical Vascular Attending Vascular Surgeon - Piedmont Athens Regional Adjunct Clinical Associate
Percutaneous Angioplasty for Infrainguinal Graft-related Stenoses
 Eur J Vasc Endovasc Surg 14, 380-385 (1997) Percutaneous Angioplasty for Infrainguinal Graft-related Stenoses A. D. Houghton ~1, C. Todd 1, B. Pardy 2, P. R. Taylor ~ and J. F. Reidy ~ Departments of Surgery,
Eur J Vasc Endovasc Surg 14, 380-385 (1997) Percutaneous Angioplasty for Infrainguinal Graft-related Stenoses A. D. Houghton ~1, C. Todd 1, B. Pardy 2, P. R. Taylor ~ and J. F. Reidy ~ Departments of Surgery,
The present status of selfexpanding. for CLI: Why and when to use. Sean P Lyden MD Cleveland Clinic Cleveland, Ohio
 The present status of selfexpanding and balloonexpandable tibial BMS and DES for CLI: Why and when to use Sean P Lyden MD Cleveland Clinic Cleveland, Ohio Disclosure Speaker name: Sean Lyden, MD I have
The present status of selfexpanding and balloonexpandable tibial BMS and DES for CLI: Why and when to use Sean P Lyden MD Cleveland Clinic Cleveland, Ohio Disclosure Speaker name: Sean Lyden, MD I have
Recommendations for Follow-up After Vascular Surgery Arterial Procedures SVS Practice Guidelines
 Recommendations for Follow-up After Vascular Surgery Arterial Procedures 2018 SVS Practice Guidelines vsweb.org/svsguidelines About the guidelines Published in the July 2018 issue of Journal of Vascular
Recommendations for Follow-up After Vascular Surgery Arterial Procedures 2018 SVS Practice Guidelines vsweb.org/svsguidelines About the guidelines Published in the July 2018 issue of Journal of Vascular
Comparing patency rates between external iliac and common iliac artery stents
 Comparing patency rates between external iliac and common iliac artery stents Eugene S. Lee, MD, Carol Coleman Steenson, MD, FACR, FSCVIR, Kristina E. Trimble, Michael P. Caldwell, BS, Michael A. Kuskowski,
Comparing patency rates between external iliac and common iliac artery stents Eugene S. Lee, MD, Carol Coleman Steenson, MD, FACR, FSCVIR, Kristina E. Trimble, Michael P. Caldwell, BS, Michael A. Kuskowski,
The ZILVERPASS study a randomized study comparing ZILVER PTX stenting with Bypass in femoropopliteal lesions Preliminary report
 The ZILVERPASS study a randomized study comparing ZILVER PTX stenting with Bypass in femoropopliteal lesions Preliminary report G. Biro, M. Bosiers on behalf of ZILVERPASS Study Group Disclosure Speaker
The ZILVERPASS study a randomized study comparing ZILVER PTX stenting with Bypass in femoropopliteal lesions Preliminary report G. Biro, M. Bosiers on behalf of ZILVERPASS Study Group Disclosure Speaker
Surgical Options for revascularisation P E T E R S U B R A M A N I A M
 Surgical Options for revascularisation P E T E R S U B R A M A N I A M The goal Treat pain Heal ulcer Preserve limb Preserve life The options Conservative Endovascular Surgical bypass Primary amputation
Surgical Options for revascularisation P E T E R S U B R A M A N I A M The goal Treat pain Heal ulcer Preserve limb Preserve life The options Conservative Endovascular Surgical bypass Primary amputation
Optimal conduit choice in the absence of singlesegment great saphenous vein for below-knee popliteal bypass
 From the Society for Vascular Surgery Optimal conduit choice in the absence of singlesegment great saphenous vein for below-knee popliteal bypass James T. McPhee, MD, Neal R. Barshes, MD, C. Keith Ozaki,
From the Society for Vascular Surgery Optimal conduit choice in the absence of singlesegment great saphenous vein for below-knee popliteal bypass James T. McPhee, MD, Neal R. Barshes, MD, C. Keith Ozaki,
Endovascular and Hybrid Treatment of TASC C & D Aortoiliac Occlusive Disease
 Endovascular and Hybrid Treatment of TASC C & D Aortoiliac Occlusive Disease Arash Bornak, MD FACS Vascular & Endovascular Surgery University of Miami Miller School of Medicine No disclosure BACKGROUND
Endovascular and Hybrid Treatment of TASC C & D Aortoiliac Occlusive Disease Arash Bornak, MD FACS Vascular & Endovascular Surgery University of Miami Miller School of Medicine No disclosure BACKGROUND
9/7/2018. Disclosures. CV and Limb Events in PAD. Challenges to Revascularization. Challenges. Answering the Challenge
 Disclosures State-of-the-Art Endovascular Lower Extremity Revascularization Promotional Speaker Jansen Pharmaceutical Promotional Speaker Amgen Pharmaceutical C. Michael Brown, MD, FACC al Cardiology Associate
Disclosures State-of-the-Art Endovascular Lower Extremity Revascularization Promotional Speaker Jansen Pharmaceutical Promotional Speaker Amgen Pharmaceutical C. Michael Brown, MD, FACC al Cardiology Associate
vs 39 p = 0.01 PTA STENT Tel:
 13 537543 24 1 FF1 19 FF 45 66 1521 81 85 65 1 vs 88 vs 56 p =.4 8mm vs 6mm 91 vs p =.4 S vs C 89 vs 39 p =.1 6mm 8mm 9 FF 8mm 13 537543 24 1 FF 1 2 3 PTA STENT TASC 3cm Tel: 76-472-1212 93-391 51 23 11
13 537543 24 1 FF1 19 FF 45 66 1521 81 85 65 1 vs 88 vs 56 p =.4 8mm vs 6mm 91 vs p =.4 S vs C 89 vs 39 p =.1 6mm 8mm 9 FF 8mm 13 537543 24 1 FF 1 2 3 PTA STENT TASC 3cm Tel: 76-472-1212 93-391 51 23 11
Iliac artery stenting in patients with poor distal runoff: Influence of concomitant infrainguinal arterial reconstruction
 Iliac artery stenting in patients with poor distal runoff: Influence of concomitant infrainguinal arterial reconstruction Carlos H. Timaran, MD, a Takao Ohki, MD, a Nicholas J. Gargiulo, III, MD, a Frank
Iliac artery stenting in patients with poor distal runoff: Influence of concomitant infrainguinal arterial reconstruction Carlos H. Timaran, MD, a Takao Ohki, MD, a Nicholas J. Gargiulo, III, MD, a Frank
PAD and CRITICAL LIMB ISCHEMIA: EVALUATION AND TREATMENT 2014
 PAD and CRITICAL LIMB ISCHEMIA: EVALUATION AND TREATMENT 2014 Van Crisco, MD, FACC, FSCAI First Coast Heart and Vascular Center, PLLC Jacksonville, FL 678-313-6695 Conflict of Interest Bayer Healthcare
PAD and CRITICAL LIMB ISCHEMIA: EVALUATION AND TREATMENT 2014 Van Crisco, MD, FACC, FSCAI First Coast Heart and Vascular Center, PLLC Jacksonville, FL 678-313-6695 Conflict of Interest Bayer Healthcare
Peripheral Arterial Disease: the growing role of endovascular management
 Peripheral Arterial Disease: the growing role of endovascular management Poster No.: C-1931 Congress: ECR 2012 Type: Educational Exhibit Authors: E. M. C. Guedes Pinto, E. Rosado, D. Penha, P. Cabral,
Peripheral Arterial Disease: the growing role of endovascular management Poster No.: C-1931 Congress: ECR 2012 Type: Educational Exhibit Authors: E. M. C. Guedes Pinto, E. Rosado, D. Penha, P. Cabral,
Brachytherapy for In-Stent Restenosis: Is the Concept Still Alive? Matthew T. Menard, M.D. Brigham and Women s Hospital Boston, Massachussetts
 Brachytherapy for In-Stent Restenosis: Is the Concept Still Alive? Matthew T. Menard, M.D. Brigham and Women s Hospital Boston, Massachussetts Disclosure Speaker name: Matthew T. Menard... x I do not have
Brachytherapy for In-Stent Restenosis: Is the Concept Still Alive? Matthew T. Menard, M.D. Brigham and Women s Hospital Boston, Massachussetts Disclosure Speaker name: Matthew T. Menard... x I do not have
THE NEW ARMENIAN MEDICAL JOURNAL
 THE NEW ARMENIAN MEDICAL JOURNAL Vol.10 (2016), Nо 1, p. 57-62 Clinical Research SHORT-TERM OUTCOMES OF ENDOVASCULAR INTERVENTION OF INFRAINGUINAL ARTERIES IN PATIENTS WITH CRITICAL LIMB ISCHEMIA Sultanyan
THE NEW ARMENIAN MEDICAL JOURNAL Vol.10 (2016), Nо 1, p. 57-62 Clinical Research SHORT-TERM OUTCOMES OF ENDOVASCULAR INTERVENTION OF INFRAINGUINAL ARTERIES IN PATIENTS WITH CRITICAL LIMB ISCHEMIA Sultanyan
Step by step Hybrid procedures in peripheral obstructive disease. Holger Staab, MD University Hospital Leipzig, Germany Clinic for Vascular Surgery
 Step by step Hybrid procedures in peripheral obstructive disease Holger Staab, MD University Hospital Leipzig, Germany Clinic for Vascular Surgery Disclosure Speaker name: H.H. Staab I have the following
Step by step Hybrid procedures in peripheral obstructive disease Holger Staab, MD University Hospital Leipzig, Germany Clinic for Vascular Surgery Disclosure Speaker name: H.H. Staab I have the following
Interventional Treatment First for CLI
 Interventional Treatment First for CLI Patrick Alexander, MD, FACC, FSCAI Interventional Cardiology Medical Director, Critical Limb Clinic Providence Heart Institute, Southfield MI 48075 Disclosures Consultant
Interventional Treatment First for CLI Patrick Alexander, MD, FACC, FSCAI Interventional Cardiology Medical Director, Critical Limb Clinic Providence Heart Institute, Southfield MI 48075 Disclosures Consultant
2-YEAR DATA SUPERA POPLITEAL REAL WORLD
 2-YEAR DATA SUPERA POPLITEAL REAL WORLD Enrique M. San Norberto. Angiology and Vascular Surgery. Valladolid University Hospital. Valladolid. Spain. Disclosure Speaker name: ENRIQUE M. SAN NORBERTO I have
2-YEAR DATA SUPERA POPLITEAL REAL WORLD Enrique M. San Norberto. Angiology and Vascular Surgery. Valladolid University Hospital. Valladolid. Spain. Disclosure Speaker name: ENRIQUE M. SAN NORBERTO I have
Dacron or PTFE for Above-knee Femoropopliteal Bypass. A Multicenter Randomised Study *
 Eur J Vasc Endovasc Surg 34, 44e49 (2007) doi:10.1016/j.ejvs.2007.01.016, available online at http://www.sciencedirect.com on Dacron or PTFE for Above-knee Femoropopliteal Bypass. A Multicenter Randomised
Eur J Vasc Endovasc Surg 34, 44e49 (2007) doi:10.1016/j.ejvs.2007.01.016, available online at http://www.sciencedirect.com on Dacron or PTFE for Above-knee Femoropopliteal Bypass. A Multicenter Randomised
Distal hybrids - an option in long SFA CTO accompanied by severely compromized crural runoff
 Distal hybrids - an option in long SFA CTO accompanied by severely compromized crural runoff P. Kuryanov, A. Lipin, A. Antropov, K. Atmadzas, A. Atmadzas, Y. Eminov, A. Borisov, R. Sobolev, A.Orlov Limb
Distal hybrids - an option in long SFA CTO accompanied by severely compromized crural runoff P. Kuryanov, A. Lipin, A. Antropov, K. Atmadzas, A. Atmadzas, Y. Eminov, A. Borisov, R. Sobolev, A.Orlov Limb
The incidence of peripheral artery disease (PAD)
 Pharmacologic Options for Treating Restenosis The role of cilostazol in the treatment of patients with infrainguinal lesions. By Osamu Iida, MD, and Yoshimitsu Soga, MD The incidence of peripheral artery
Pharmacologic Options for Treating Restenosis The role of cilostazol in the treatment of patients with infrainguinal lesions. By Osamu Iida, MD, and Yoshimitsu Soga, MD The incidence of peripheral artery
Is the preferential use of polytetrafluoroethylene grafts for femoropopliteal bypass justified?
 Is the preferential use of polytetrafluoroethylene grafts for femoropopliteal bypass justified? William J. Quifiones-Baldrich, MD, Ronald W. Busuttil, MD, PhD, J. Dennis Baker, MD, Candace L. Vescera,
Is the preferential use of polytetrafluoroethylene grafts for femoropopliteal bypass justified? William J. Quifiones-Baldrich, MD, Ronald W. Busuttil, MD, PhD, J. Dennis Baker, MD, Candace L. Vescera,
Midterm results from a multicenter registry on the treatment of infrainguinal critical limb ischemia using a heparin-bonded eptfe graft
 From the Society for Vascular Surgery Midterm results from a multicenter registry on the treatment of infrainguinal critical limb ischemia using a heparin-bonded eptfe graft Raffaele Pulli, MD, a Walter
From the Society for Vascular Surgery Midterm results from a multicenter registry on the treatment of infrainguinal critical limb ischemia using a heparin-bonded eptfe graft Raffaele Pulli, MD, a Walter
Hypothesis: When compared to conventional balloon angioplasty, cryoplasty post-dilation decreases the risk of SFA nses in-stent restenosis
 Cryoplasty or Conventional Balloon Post-dilation of Nitinol Stents For Revascularization of Peripheral Arterial Segments Background: Diabetes mellitus is associated with increased risk of in-stent restenosis
Cryoplasty or Conventional Balloon Post-dilation of Nitinol Stents For Revascularization of Peripheral Arterial Segments Background: Diabetes mellitus is associated with increased risk of in-stent restenosis
Utility of new classification based on clinical and lesional factors after self-expandable nitinol stenting in the superficial femoral artery
 Utility of new classification based on clinical and lesional factors after self-expandable nitinol stenting in the superficial femoral artery Yoshimitsu Soga, MD, a Osamu Iida, MD, b Keisuke Hirano, MD,
Utility of new classification based on clinical and lesional factors after self-expandable nitinol stenting in the superficial femoral artery Yoshimitsu Soga, MD, a Osamu Iida, MD, b Keisuke Hirano, MD,
Joung Hun Byun, M.D. 1, Tae Gyu Kim, M.D. 2, Yun Gyu Song, M.D., Ph.D. 3. Introduction. CLINICAL RESEARCH
 Korean J Thorac Cardiovasc Surg 2017;50:371-377 ISSN: 2233-601X (Print) ISSN: 2093-6516 (Online) CLINICAL RESEARCH https://doi.org/10.5090/kjtcs.2017.50.5.371 Femoro-Supragenicular Popliteal Bypass with
Korean J Thorac Cardiovasc Surg 2017;50:371-377 ISSN: 2233-601X (Print) ISSN: 2093-6516 (Online) CLINICAL RESEARCH https://doi.org/10.5090/kjtcs.2017.50.5.371 Femoro-Supragenicular Popliteal Bypass with
Evidence-Based Optimal Treatment for SFA Disease
 Evidence-Based Optimal Treatment for SFA Disease Endo first Don t burn surgical bridge Don t stent if possible Javairiah Fatima, MD Assistant Professor of Surgery Division of Vascular and Endovascular
Evidence-Based Optimal Treatment for SFA Disease Endo first Don t burn surgical bridge Don t stent if possible Javairiah Fatima, MD Assistant Professor of Surgery Division of Vascular and Endovascular
The Struggle to Manage Stroke, Aneurysm and PAD
 The Struggle to Manage Stroke, Aneurysm and PAD In this article, Dr. Salvian examines the management of peripheral arterial disease, aortic aneurysmal disease and cerebrovascular disease from symptomatology
The Struggle to Manage Stroke, Aneurysm and PAD In this article, Dr. Salvian examines the management of peripheral arterial disease, aortic aneurysmal disease and cerebrovascular disease from symptomatology
Management of In-stent Restenosis after Lower Extremity Endovascular Procedures
 Management of In-stent Restenosis after Lower Extremity Endovascular Procedures Piotr Sobieszczyk, MD Associate Director, Cardiac Catheterization Laboratory Cardiovascular Division and Vascular Medicine
Management of In-stent Restenosis after Lower Extremity Endovascular Procedures Piotr Sobieszczyk, MD Associate Director, Cardiac Catheterization Laboratory Cardiovascular Division and Vascular Medicine
Predictors for adverse outcome after iliac angioplasty and stenting for limb-threatening ischemia
 Predictors for adverse outcome after iliac angioplasty and stenting for limb-threatening ischemia Carlos H. Timaran, MD, Scott L. Stevens, MD, Michael B. Freeman, MD, and Mitchell H. Goldman, MD, Knoxville,
Predictors for adverse outcome after iliac angioplasty and stenting for limb-threatening ischemia Carlos H. Timaran, MD, Scott L. Stevens, MD, Michael B. Freeman, MD, and Mitchell H. Goldman, MD, Knoxville,
Distal Percutaneous Transluminal Angioplasty Through Infrainguinal Bypass Grafts
 Eur J Vasc Endovasc Surg 23, 212 219 (2002) doi:10.1053/ejvs.2001.1584, available online at http://www.idealibrary.com on Distal Percutaneous Transluminal Angioplasty Through Infrainguinal Bypass Grafts
Eur J Vasc Endovasc Surg 23, 212 219 (2002) doi:10.1053/ejvs.2001.1584, available online at http://www.idealibrary.com on Distal Percutaneous Transluminal Angioplasty Through Infrainguinal Bypass Grafts
N. J. Lalak, MB, BS, K. C. Hanel, MB, BS, FRACS, DDU, J. Hunt, RN, and A. Morgan, RN, RVT, DMU (vasc.), Kogarah, Australia
 Duplex scan surveillance prosthetic bypass grafts of infrainguinal N. J. Lalak, MB, BS, K. C. Hanel, MB, BS, FRACS, DDU, J. Hunt, RN, and A. Morgan, RN, RVT, DMU (vasc.), Kogarah, Australia Purpose: Surveillance
Duplex scan surveillance prosthetic bypass grafts of infrainguinal N. J. Lalak, MB, BS, K. C. Hanel, MB, BS, FRACS, DDU, J. Hunt, RN, and A. Morgan, RN, RVT, DMU (vasc.), Kogarah, Australia Purpose: Surveillance
Critical Limb Ischemia: Diagnosis and Current Management
 Research Article Joseph Karam, MD Elliot J. Stephenson, MD From: Minneapolis Heart Institutet at Abbott Northwestern Hospital, Minneapolis, MN Address for correspondence: Joseph Karam, MD Minneapolis Heart
Research Article Joseph Karam, MD Elliot J. Stephenson, MD From: Minneapolis Heart Institutet at Abbott Northwestern Hospital, Minneapolis, MN Address for correspondence: Joseph Karam, MD Minneapolis Heart
Popliteal Aneurysm: When is surgical therapy indicated? PROF. GRZEGORZ OSZKINIS
 Popliteal Aneurysm: When is surgical therapy indicated? PROF. GRZEGORZ OSZKINIS Asymptomatic mass - 38-40%will develop symptoms at a rate of 14%/yr Intermittent claudic ation (chronic ischemia) - 25%-40%
Popliteal Aneurysm: When is surgical therapy indicated? PROF. GRZEGORZ OSZKINIS Asymptomatic mass - 38-40%will develop symptoms at a rate of 14%/yr Intermittent claudic ation (chronic ischemia) - 25%-40%
Peripheral Vascular Disease
 Peripheral artery disease (PAD) results from the buildup of plaque (atherosclerosis) in the arteries of the legs. For people with PAD, symptoms may be mild, requiring no treatment except modification of
Peripheral artery disease (PAD) results from the buildup of plaque (atherosclerosis) in the arteries of the legs. For people with PAD, symptoms may be mild, requiring no treatment except modification of
Lower Extremity Revascularization D oes Anesthesia Matter. Onaona Gurney PGY 4
 Lower Extremity Revascularization D oes Anesthesia Matter Onaona Gurney PGY 4 Case Presentation 89yoM PMH of HTN, DM, HLD, BPH presented to podiatry with abscess to R great toe 5 weeks prior Drained by
Lower Extremity Revascularization D oes Anesthesia Matter Onaona Gurney PGY 4 Case Presentation 89yoM PMH of HTN, DM, HLD, BPH presented to podiatry with abscess to R great toe 5 weeks prior Drained by
The Crack and Pave technique for highly resistant calcified lesions. Manuela Matschuck MD University Hospital Leipzig Department Angiology
 The Crack and Pave technique for highly resistant calcified lesions Manuela Matschuck MD University Hospital Leipzig Department Angiology Disclosure Speaker name: Dr. med. Manuela Matschuck I have the
The Crack and Pave technique for highly resistant calcified lesions Manuela Matschuck MD University Hospital Leipzig Department Angiology Disclosure Speaker name: Dr. med. Manuela Matschuck I have the
Popliteal Artery Aneurysms: Diagnosis and Repair Options
 Deepak N. Deshmukh DO April 27, 2018 Popliteal Artery Aneurysms: Diagnosis and Repair Options No Disclosures Popliteal Artery Aneurysms (PAAs) Male Predominanace Most common peripheral Aneurysm (70%) 30-50%
Deepak N. Deshmukh DO April 27, 2018 Popliteal Artery Aneurysms: Diagnosis and Repair Options No Disclosures Popliteal Artery Aneurysms (PAAs) Male Predominanace Most common peripheral Aneurysm (70%) 30-50%
Wifi classification does not predict limb amputation risk in dialysis patients following critical limb ischemia revascularization
 Wifi classification does not predict limb amputation risk in dialysis patients following critical limb ischemia revascularization A Sonetto, M Abualhin, M Gargiulo, GL Faggioli, A Stella Disclosure Speaker
Wifi classification does not predict limb amputation risk in dialysis patients following critical limb ischemia revascularization A Sonetto, M Abualhin, M Gargiulo, GL Faggioli, A Stella Disclosure Speaker
LIMB SALVAGE IN THE DIABETIC PATIENT
 LIMB SALVAGE IN THE DIABETIC PATIENT WHO? HOW? BEST? DISCLOSURES Educational grant from Cook Inc OBJECTIVES Review risk stratification and staging schemes for the threatened limb Discuss current concepts
LIMB SALVAGE IN THE DIABETIC PATIENT WHO? HOW? BEST? DISCLOSURES Educational grant from Cook Inc OBJECTIVES Review risk stratification and staging schemes for the threatened limb Discuss current concepts
4/14/2016. How Far Should We Go with the Endovascular Treatment of Advanced PAD in the Era of Health Care Reform?
 FINANCIAL DISCLOSURE How Far Should We Go with the Endovascular Treatment of Advanced PAD in the Era of Health Care Reform? An Endocompetent Vascular Surgeon s View Bruce A. Perler, MD, MBA I Have No Financial
FINANCIAL DISCLOSURE How Far Should We Go with the Endovascular Treatment of Advanced PAD in the Era of Health Care Reform? An Endocompetent Vascular Surgeon s View Bruce A. Perler, MD, MBA I Have No Financial
Femoropopliteal Balloon Angioplasty vs. Bypass Surgery for CLI: A Propensity Score Analysis
 Eur J Vasc Endovasc Surg (), 78e8 Femoropopliteal Balloon vs. Bypass Surgery for CLI: A Propensity Score Analysis M. Korhonen a,b, *, F. Biancari c,m.söderström a, E. Arvela a, K. Halmesmäki a, A. Albäck
Eur J Vasc Endovasc Surg (), 78e8 Femoropopliteal Balloon vs. Bypass Surgery for CLI: A Propensity Score Analysis M. Korhonen a,b, *, F. Biancari c,m.söderström a, E. Arvela a, K. Halmesmäki a, A. Albäck
Managing Conditions Resulting from Untreated Cardiometabolic Syndrome
 Managing Conditions Resulting from Untreated Cardiometabolic Syndrome Matthew P. Namanny DO, FACOS Vascular/Endovascular Surgery Saguaro Surgical/AZ Vascular Specialist Tucson Medical Center Critical Limb
Managing Conditions Resulting from Untreated Cardiometabolic Syndrome Matthew P. Namanny DO, FACOS Vascular/Endovascular Surgery Saguaro Surgical/AZ Vascular Specialist Tucson Medical Center Critical Limb
Abstract. Key words: peripheral artery disease, lower limb, endovascular therapy, Iran
 The evaluation of the success rate, complications and midterm follow up results of patients with peripheral arterial disease of lower limb treated using endovascular therapy: A single center study Mohammad
The evaluation of the success rate, complications and midterm follow up results of patients with peripheral arterial disease of lower limb treated using endovascular therapy: A single center study Mohammad
Study population The study population comprised patients suffering from superficial femoral artery stenosis that required revascularisation.
 Maintenance of patency following remote superficial femoral artery endarterectomy Galland R B, Whiteley M S, Gibson M, Simmons M J, Torrie E P, Magee T R Record Status This is a critical abstract of an
Maintenance of patency following remote superficial femoral artery endarterectomy Galland R B, Whiteley M S, Gibson M, Simmons M J, Torrie E P, Magee T R Record Status This is a critical abstract of an
Endovascular treatment of thrombosis (acute) of aneurysm through bifurcated endoprothesis: challenge cases
 Endovascular treatment of thrombosis (acute) of aneurysm through bifurcated endoprothesis: challenge cases Fábio Luiz Costa Pereira Fabrício Machado Rossi Pablo da Silva Mendes Carlos Andre Daher Victor
Endovascular treatment of thrombosis (acute) of aneurysm through bifurcated endoprothesis: challenge cases Fábio Luiz Costa Pereira Fabrício Machado Rossi Pablo da Silva Mendes Carlos Andre Daher Victor
Critical Limb Ischemia A Collaborative Approach to Patient Care. Christopher LeSar, MD Vascular Institute of Chattanooga July 28, 2017
 Critical Limb Ischemia A Collaborative Approach to Patient Care Christopher LeSar, MD Vascular Institute of Chattanooga July 28, 2017 Surgeons idea Surgeons idea represents the final stage of peripheral
Critical Limb Ischemia A Collaborative Approach to Patient Care Christopher LeSar, MD Vascular Institute of Chattanooga July 28, 2017 Surgeons idea Surgeons idea represents the final stage of peripheral
4/23/2009. Vein Bypass Remains the Gold Standard AND We Can Improve Outcomes. Lower Extremity Revascularization Options: Key Factors to Consider
 Vein Bypass Remains the Gold Standard AND We Can Improve Outcomes Lower Extremity Revascularization Options: Key Factors to Consider General health of the patient Michael S. Conte MD Division of Vascular
Vein Bypass Remains the Gold Standard AND We Can Improve Outcomes Lower Extremity Revascularization Options: Key Factors to Consider General health of the patient Michael S. Conte MD Division of Vascular
Paclitaxel-coated versus Plain Balloon Angioplasty in the Treatment of Infrainguinal Vein Bypass Stenosis
 Paclitaxel-coated versus Plain Balloon Angioplasty in the Treatment of Infrainguinal Vein Bypass Stenosis T. Hölzenbein, A. Ugurluoglu, M. Aspalter, W. Hitzl, K. Linni Dep Vascular & Endovascular Surgery
Paclitaxel-coated versus Plain Balloon Angioplasty in the Treatment of Infrainguinal Vein Bypass Stenosis T. Hölzenbein, A. Ugurluoglu, M. Aspalter, W. Hitzl, K. Linni Dep Vascular & Endovascular Surgery
The Society for Vascular Surgery s. Objective Performance Goals for Lower Extremity Revascularization
 The Society for Vascular Surgery s Objective Performance Goals for Lower Extremity Revascularization Are Not Generalizable to Many Open Surgical Bypass Patients Encountered in Contemporary Surgical Practice
The Society for Vascular Surgery s Objective Performance Goals for Lower Extremity Revascularization Are Not Generalizable to Many Open Surgical Bypass Patients Encountered in Contemporary Surgical Practice
Popliteal-to-distal bypass for limb-threatening ischemia
 Popliteal-to-distal bypass for limb-threatening ischemia Jeffrey Marks, MD, Terry A, King, MD, Henry Baele, MD, Jeffrey Rubin, MD, and Cynthia Marmen, RN, Cleveland, Ohio In a subset of patients requiring
Popliteal-to-distal bypass for limb-threatening ischemia Jeffrey Marks, MD, Terry A, King, MD, Henry Baele, MD, Jeffrey Rubin, MD, and Cynthia Marmen, RN, Cleveland, Ohio In a subset of patients requiring
TOBA II 12-Month Results Tack Optimized Balloon Angioplasty
 TOBA II 12-Month Results Tack Optimized Balloon Angioplasty William Gray, MD System Chief, Cardiovascular Division Main Line Health, Philadelphia, PA Dissection: The Primary Mechanism of Angioplasty Lesions
TOBA II 12-Month Results Tack Optimized Balloon Angioplasty William Gray, MD System Chief, Cardiovascular Division Main Line Health, Philadelphia, PA Dissection: The Primary Mechanism of Angioplasty Lesions
Polytetrafluoroethylene (PTFE) Femorodistal Grafts with a Distal Vein Cuff for Critical Ischaemia
 Eur J Vasc Endovasc Surg 15, 449-453 (1998) Polytetrafluoroethylene (PTFE) Femorodistal Grafts with a Distal Vein Cuff for Critical Ischaemia L. D. Wijesinghe ~, D, M. Beardsmore and D, J. A. Scott Department
Eur J Vasc Endovasc Surg 15, 449-453 (1998) Polytetrafluoroethylene (PTFE) Femorodistal Grafts with a Distal Vein Cuff for Critical Ischaemia L. D. Wijesinghe ~, D, M. Beardsmore and D, J. A. Scott Department
Vascular Surgery Cases: Detours. Brian F. Stull, RDMS, RVT UNC REX Healthcare Vascular Specialists
 Vascular Surgery Cases: Detours Brian F. Stull, RDMS, RVT UNC REX Healthcare Vascular Specialists Brian.Stull@Unchealth.unc.edu Objectives Anatomy of a bypass graft Where does it connect, where does it
Vascular Surgery Cases: Detours Brian F. Stull, RDMS, RVT UNC REX Healthcare Vascular Specialists Brian.Stull@Unchealth.unc.edu Objectives Anatomy of a bypass graft Where does it connect, where does it
Pedal Bypass With Deep Venous Arterialization:
 Pedal Bypass With Deep Venous Arterialization: Long Term Result For Critical Limb Ischemia With Unreconstructable Distal Arteries Pramook Mutirangura Professor of Vascular Surgery Faculty of Medicine Siriraj
Pedal Bypass With Deep Venous Arterialization: Long Term Result For Critical Limb Ischemia With Unreconstructable Distal Arteries Pramook Mutirangura Professor of Vascular Surgery Faculty of Medicine Siriraj
Medical therapy after angioplasty / stenting
 Nurse and Technician Forum Part I Medical therapy after angioplasty / stenting Erich Minar Department Angiology Medical University Vienna Disclosure Speaker name: Erich Minar I do not have any potential
Nurse and Technician Forum Part I Medical therapy after angioplasty / stenting Erich Minar Department Angiology Medical University Vienna Disclosure Speaker name: Erich Minar I do not have any potential
Long-term outcomes after revascularization for advanced popliteal artery entrapment syndrome with segmental arterial occlusion
 Long-term outcomes after revascularization for advanced popliteal artery entrapment syndrome with segmental arterial occlusion Seong-Yup Kim, MD, Seung-Kee Min, MD, PhD, Sanghyun Ahn, MD, Sang-Il Min,
Long-term outcomes after revascularization for advanced popliteal artery entrapment syndrome with segmental arterial occlusion Seong-Yup Kim, MD, Seung-Kee Min, MD, PhD, Sanghyun Ahn, MD, Sang-Il Min,
Powerful patency. A decade of performance.
 Above-knee Data 1 Year a : 84% N=528 2 Years a : 78% N=320 3 Years a : 76% N=222 Powerful patency. A decade of performance. Below-knee Data 1 Year a : 76% N=745 2 Years a : 67% N=631 3 Years a : 60% N=477
Above-knee Data 1 Year a : 84% N=528 2 Years a : 78% N=320 3 Years a : 76% N=222 Powerful patency. A decade of performance. Below-knee Data 1 Year a : 76% N=745 2 Years a : 67% N=631 3 Years a : 60% N=477
