A Case of Massive Pulmonary Embolism in Systemic Lupus Erythematosus without Antiphospholipid Antibody
|
|
|
- Julianna Hubbard
- 5 years ago
- Views:
Transcription
1 Journal of Rheumatic Diseases Vol. 22, No. 2, April, Case Report A Case of Massive Pulmonary Embolism in Systemic Lupus Erythematosus without Antiphospholipid Antibody Jae-Hyun Jung, Min-Gu Lee, Ju-Sung Sim, Tae-Hyun Kim, Hong-Kwon Oh, Jong Dae Ji, Young Ho Lee Division of Rheumatology, Department of Internal Medicine, Korea University College of Medicine, Seoul, Korea Patients with systemic lupus erythematosus (SLE) are at an increased risk of developing thromboses with antiphospholipid antibodies (apl). The presence of apl is related to an increased risk of thrombotic events. However, thromboembolic events can occur in SLE patients without apl, and pulmonary emboli are rarely reported manifestations of SLE without apl. Here, we report on a case of massive pulmonary embolism in a 58-year-old woman with apl-negative SLE. She presented with chest pain and dyspnea, and chest computed tomography (CT) and lung perfusion ventilation scans showed pulmonary thromboembolism. She was administered thrombolytic agents, heparin, and warfarin. Two months later, no remarkable residual thromboembolism was observed on chest CT. (J Rheum Dis 2015;22: ) Key Words. Pulmonary embolism, Systemic lupus erythematosus, Antiphospholipid antibodies INTRODUCTION Systemic lupus erythematosus (SLE) is a prototypic autoimmune disease in which immune regulation is disrupted, leading to intense inflammation and multiple organ damage. Although extraordinary improvement in its prognosis and survival rate has been accomplished, throughout the SLE disease course, patients deal with possibility of disease activity, infections, irreversible organ damage, and severe clinical manifestations, i.e., thromboses, which impair their quality of life and survival rate. These thromboembolic events occur especially in patients with antiphospholipid antibodies (apl). apl syndrome (APS) is characterized by venous and arterial thromboses, obstetric morbidity, and the presence of apl, including lupus anticoagulant, anticardiolipin antibodies (acl), and/or antibodies primarily directed against β2-glycoprotein I (β2gpi) [1]. Among SLE patients, the prevalence of apl is substantially higher, ranging from 12% to 30% for acl [2]. However, thromboembolic events can occur in SLE patients without apl, and pulmonary emboli are rarely reported manifestations of apl-negative SLE [3]. Though pulmonary thromboembolism is rarely reported apl-negative SLE patients, it can appear acutely and be fatal. Pulmonary thromboembolism, however, can disappear if it is quickly diagnosed and treated, so clinicians should consider thromboembolism event when they exam all SLE patients. In this article, we describe a case of massive pulmonary embolism that developed in an apl-negative SLE patient. CASE REPORT A 58-year-old female with a 3-year history of macular erythema and wrist and shoulder pain was admitted to the hospital emergency room with chief complains of fever and myalgia. The patient had been diagnosed with SLE approximately 2 months previously. Fluorescent antinuclear antibody results were positive (1:1,280, diffuse type). Anti-ds-DNA antibody titers were elevated (8.68 IU/mL). Other autoimmune markers, including anti-sm, Received:February 3, 2014, Revised (1st) April 8, 2014, (2nd) April 28, 2014, Accepted:May 14, 2014 Corresponding to:young Ho Lee, Division of Rheumatology, Department of Internal Medicine, Korea University Anam Hospital, Korea University College of Medicine, 73 Inchon-ro, Seongbuk-gu, Seoul , Korea. lyhcgh@korea.ac.kr pissn: X, eissn: Copyright c 2015 by The Korean College of Rheumatology. All rights reserved. This is a Free Access article, which permits unrestricted non-commerical use, distribution, and reproduction in any medium, provided the original work is properly cited. 106
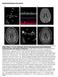
2 A Pulmonary Embolism in Antiphospholipid Antibody-negative SLE anti-rnp, anti-ssb, and anti-ssa antibodies, were all negative. She had been diagnosed with SLE on the basis of skin lesions, oral ulcer, arthritis, and presence of antinuclear antibodies. She was being treated with 10 mg prednisolone once daily and 200 mg hydroxychloroquine per day. She was a non-smoker and her body mass index was 23.5 (control, 18.5 to 24.9). She did not have hypertension, diabetes mellitus, dyslipidemia or the evidences of cancer, which were risk factors of pulmonary embolism, but one year later she has got diabetes mellitus. Upon presentation, the patient complained of acute onset of fever, was diagnosed with acute pyelonephritis, was given ciprofloxacin, and the pyelonephritis symptoms improved. Her ongoing prednisolone dose was increased to 30 mg daily owing to skin lesions and arthritis. On the 5th day of admission, she complained of dizziness. Brain magnetic resonance imaging diffusion was performed, which showed acute or recent infarction on the right lower pons and medulla; she was therefore administered 100 mg aspirin once daily. On the 23rd day of admission, however, she had developed sudden chest pain and dyspnea. Physical examination revealed unilateral rales in the right lung base. Laboratory tests showed that the D-dimer level was increased to 3.10 μg/ml (normal, <0.5 μg/ml). However, test results for apl were negative: lupus anticoagulant was negative, the acl immunoglobulin (Ig) M level was 0.5 U/mL (normal, <7 U/mL), the acl Ab IgG level was 1.0 U/mL (normal, <10 U/mL), the anti-phos- Figure 1. Spiral chest computed tomography showing pulmonary thromboembolism in the right pulmonary artery (A) and chest computed tomography showing the absence of remarkable residual thromboembolism (B). Figure 2. Perfusion ventilation scintigraphy showing segmental perfusion defects in the right lung and normal tracer distribution in the left lung
3 Jae-Hyun Jung et al. pholipid Ab IgM level was <0.5 U/mL (normal, <10 U/mL), and the anti-phospholipid Ab IgG level was 0.7 U/mL (normal, <10 U/mL). The anti-β2gpi Ab was not checked in this patient. Other laboratory test results were unremarkable, except for a 34% decrease in protein S (control, 58.7% to 119.2%) and increased anti-ds-dna of 9.5 IU/mL: the FDP level was 3.97 μg/dl (normal, <5 μg/ dl), the fibrinogen level was mg/dl (control, 230 to 480 mg/dl), the protein C level was 81% (control, 7% to 130%), the antithrombin III level was 84% (control, 70% to 120%), the C3 level was 86.6 mg/dl (control, 88 to 201 mg/dl), and the C4 level was 28.3 mg/dl (control, 16 to 47 mg/dl). Chest radiography showed right pleural effusion and spiral contrast-enhanced chest computed tomography (CT) revealed large filling defects in the right main pulmonary artery that continued through the right pulmonary arterial branch of the upper and lower lobe (Figure 1A). Prominent large defects were noted at the bifurcation area. The dense parenchymal opacity in the right lower lobe was compatible with infarction. A lung perfusion ventilation scan was performed, which showed significant perfusion defects in the right lung and normal tracer distribution in the left lung (Figure 2). On transthoracic echocardiography, mild mitral regurgitation was detected. Left and right ventricle function was normal. Color Doppler sonography of the lower extremities was also performed, which revealed deep thrombosis in the right peroneal vein and the absence of deep thrombosis in the veins of both lower extremities. Pulmonary thromboembolism was diagnosed, and the patient was administered intravenous recombinant tissue-type plasminogen activator (100 mg alteplase) and was started on subcutaneous low-molecular-weight heparin ( mg enoxaparin) and 5 mg oral warfarin. The next day, she did not complain of dyspnea and chest pain. She was discharged home with warfarin anticoagulation (international normalized ratio [INR], 2.5 to 3.5) to be re-evaluated as an outpatient. Two months later, no remarkable residual thromboembolism was observed on chest CT (Figure 1B). DISCUSSION SLE is a chronic inflammatory autoimmune disorder that affects multiple organ systems. Pulmonary involvement usually develops late in the disease course and can affect any part of the pulmonary system, including the airways, lung parenchyma, pulmonary vasculature, pleura, and diaphragm [4]. Patients with SLE are at increased risk of venous thromboembolism, with a prevalence of 9% [5], and patients with apl have an even higher increased risk of 35% to 42% [6]. apl may be present in up to two-thirds of patients with lupus [7]. APS is characterized by arterial and venous thrombosis, which leads to an increased risk of thromboembolic events and recurrent fetal loss in addition to the presence of apl or lupus anticoagulant. Pulmonary APS manifestations include embolism and infarction, increased pulmonary artery pressure secondary to thromboembolism, and pulmonary microvascular thrombosis. Pulmonary embolism occurs in 30% of patients and originates from the calf veins, inferior vena cava, tricuspid valve vegetation, or right intracardiac thromboses in many cases. Traditionally, elevated levels of apls are associated with the increased thrombotic risk that is characteristic of APL. However, as always in real clinical practice, there are often discrepancies between antibody levels and clinical disease presentation [8]. In addition, it is not unusual to find patients with clinical features suggestive of APS who are persistently negative for the criteria acl, anti-β2gpi, and lupus anticoagulant tests [9]. Seronegative APS (SNAPS) was first introduced in 2003 by Hughes and Khamashta [8]. Rodriguez-Garcia et al. [10] reported no significant differences in the frequency of thrombotic events or obstetric morbidity in patients with SNAPS versus those with seropositive APS. Platelets are the most important components in maintaining homeostasis and play an important role in the development of arterial thrombosis and atherosclerosis. Thrombosis can occur because of either a reactive process or manifestation of a clonal hematopoietic disorder. Thrombocytosis usually develops secondary to a disease process such as inflammation or trauma and is accordingly termed reactive thrombocytosis, in which the platelet count increases temporarily during the active phase of the disease. Thrombosis occurs in the blood flow by the interaction and coexistence of vascular, cellular, and humoral factors. Such factors that play important roles in the pathophysiology of thrombosis include endothelial damage, vascular stasis, and alterations in relevant blood components, which are known as Virchow s triad. In rheumatic disorders, both thrombocytosis and thrombosis can be observed and may lead to severe complications [11]. SLE is generally associated with thrombocytopenia rather 108 J Rheum Dis Vol. 22, No. 2, April, 2015
4 A Pulmonary Embolism in Antiphospholipid Antibody-negative SLE than thrombocytosis, but thrombosis can also be observed in SLE. The most common cause of thrombosis in SLE is apl; however, thromboses in SLE patients may result from diverse mechanisms, including inflammatory, primarily thrombotic, or atherosclerotic processes. The relevance of each mechanism may vary throughout the disease course, thus atherosclerosis seems to predominate late in the evolution of the disease. Hereditary factors such as protein C, protein S or antithrombin III deficiency, factor V-leiden, prothrombin, or methylene tetrahydrofolate reductase may be involved in the etiology of thrombosis. Protein C, fibrinogen, D-dimer, and homocysteine levels are increased in SLE patients, which can cause thrombosis. In addition, inflammatory cytokines are major mediators involved in the activation of the coagulation cascade. Inflammatory mediators can elevate the platelet count, platelet reactivity, and fibrinogen concentration; downregulate natural anticoagulant mechanisms; initiate the coagulation cascade; facilitate propagation of the coagulant response; and impair fibrinolysis. Patients with autoimmune diseases, particularly SLE, are at an increased risk of developing thromboses. SLE diagnosis is the single most common variable associated with venous and arterial thromboses. Patients with SLE-related venous thromboses show vasculitis and disease activity, whereas dyslipidemia, central nervous system involvement, and disease activity are associated with arterial thromboses [12]. The patient of this case has no genetic risk factors of pulmonary embolism, which are genetic thrombophilia, antithrombin III deficiency, protein C deficiency, plasminogen deficiency and etc. She also did not have acquired risk factors except stroke developed in hospital. Acquired risk factors of pulmonary embolism include advanced age, obesity, immobilization, major surgery, trauma, congestive cardiac failure, myocardial infarction, smoking, stroke, malignity, chemotherapy, central venous catheter, pregnancy, puerperality, the use of oral contraceptives and hormone replacement, previous pulmonary emboli/deep vein thrombosis, antiphospholipid syndrome, chronic obstructive pulmonary disease and medical conditions requiring hospitalization. In the International Stroke Trial, the incidence of pulmonary embolism after a stroke was 0.8% at 2 weeks [13]. Her pulmonary embolism could be developed by stroke event, but cerebral infarction occurred during admission period and she had not any risk factors of infarction. So we can think that stroke and pulmonary embolism were affected with SLE itself. Management of pulmonary thromboembolism in SLE patients is the same in patients with APS as in the general population. Patients require anticoagulation treatment with heparin followed by warfarin. It is recommended that an INR ranging between 2.5 and 3.5 be maintained [14]. SLE patients are at an increased risk of developing thromboses with or without apl. Clinicians should be aware that even if SLE patients do not have apl, thrombosis can develop and be fatal. SUMMARY Thromboembolic events can occur in SLE patients without apl, and pulmonary emboli are rarely reported manifestations of SLE without apl. Thus, we report a case of massive pulmonary embolism in a 58-year-old woman with apl-negative SLE. CONFLICT OF INTEREST No potential conflict of interest relevant to this article was reported. REFERENCES 1. Rezaei N, Yeganeh MZ, Ahmadi F. Antiphospholipid antibody syndrome presenting with pulmonary embolism. Tanaffos 2008;7: Levine JS, Branch DW, Rauch J. The antiphospholipid syndrome. N Engl J Med 2002;346: Matta BN, Uthman I, Taher AT, Khamashta MA. The current standing of diagnosis of antiphospholipid syndrome associated with systemic lupus erythematosus. Expert Rev Clin Immunol 2013;9: Gari AG, Telmesani A, Alwithenani R. Pulmonary manifestations of systemic lupus erythematosus. In: Almoallim H, ed. Systemic lupus erythematosus. Rijeka, Croatia, InTech, 2012, p Gladman DD, Urowitz MB. Venous syndromes and pulmonary embolism in systemic lupus erythematosus. Ann Rheum Dis 1980;39: Love PE, Santoro SA. Antiphospholipid antibodies: anticardiolipin and the lupus anticoagulant in systemic lupus erythematosus (SLE) and in non-sle disorders. Prevalence and clinical significance. Ann Intern Med 1990;112: Ruiz-Irastorza G, Egurbide MV, Ugalde J, Aguirre C. High impact of antiphospholipid syndrome on irreversible organ damage and survival of patients with systemic lupus erythematosus. Arch Intern Med 2004;164: Hughes GR, Khamashta MA. Seronegative antiphospholipid syndrome. Ann Rheum Dis 2003;62: Mahler M, Norman GL, Meroni PL, Khamashta M. Autoantibodies to domain 1 of beta 2 glycoprotein 1: a promising candidate biomarker for risk management in antiphospholipid syndrome. Autoimmun Rev 2012;12: Rodriguez-Garcia JL, Bertolaccini ML, Cuadrado MJ, Sanna 109
5 Jae-Hyun Jung et al. G, Ateka-Barrutia O, Khamashta MA. Clinical manifestations of antiphospholipid syndrome (APS) with and without antiphospholipid antibodies (the so-called 'seronegative APS'). Ann Rheum Dis 2012;71: Cipil H, Kargili A, Senaran H, Uz E, Kasapoglu B, Alici Ö, et al. Thrombosis and thrombocytosis in a thousand rheumatologic cases. New J Med 2011;28: Romero-Díaz J, García-Sosa I, Sánchez-Guerrero J. Thrombosis in systemic lupus erythematosus and other autoimmune diseases of recent onset. J Rheumatol 2009;36: Çobanoğlu U. Risk factor for pulmonary embolism. In: Çobanoğlu U, ed. Pulmonary embolism. Rijeka, Croatia, InTech, 2012, p Espinosa G, Cervera R, Font J, Asherson RA. The lung in the antiphospholipid syndrome. Ann Rheum Dis 2002;61: J Rheum Dis Vol. 22, No. 2, April, 2015
Mabel Labrada, MD Miami VA Medical Center
 Mabel Labrada, MD Miami VA Medical Center *1-Treatment for acute DVT with underlying malignancy is for 3 months. *2-Treatment of provoked acute proximal DVT can be stopped after 3months of treatment and
Mabel Labrada, MD Miami VA Medical Center *1-Treatment for acute DVT with underlying malignancy is for 3 months. *2-Treatment of provoked acute proximal DVT can be stopped after 3months of treatment and
Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria
 Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria Farjah H AlGahtani Associate professor,md,mph Leukemia,Lymphoma in adolescent,thromboembolic
Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria Farjah H AlGahtani Associate professor,md,mph Leukemia,Lymphoma in adolescent,thromboembolic
Are there still any valid indications for thrombophilia screening in DVT?
 Carotid artery stenosis and risk of stroke Are there still any valid indications for thrombophilia screening in DVT? Armando Mansilha MD, PhD, FEBVS Faculty of Medicine of University of Porto Munich, 2016
Carotid artery stenosis and risk of stroke Are there still any valid indications for thrombophilia screening in DVT? Armando Mansilha MD, PhD, FEBVS Faculty of Medicine of University of Porto Munich, 2016
Approach to Thrombosis
 Approach to Thrombosis Theera Ruchutrakool, M.D. Division of Hematology Department of Medicine Siriraj Hospital Faculty of Medicine Mahidol University Approach to Thrombosis Thrombosis: thrombus formation
Approach to Thrombosis Theera Ruchutrakool, M.D. Division of Hematology Department of Medicine Siriraj Hospital Faculty of Medicine Mahidol University Approach to Thrombosis Thrombosis: thrombus formation
Thrombophilia. Diagnosis and Management. Kevin P. Hubbard, DO, FACOI
 Thrombophilia Diagnosis and Management Kevin P. Hubbard, DO, FACOI Clinical Professor of Medicine Kansas City University of Medicine and Biosciences-College of Osteopathic Medicine Kansas City, Missouri
Thrombophilia Diagnosis and Management Kevin P. Hubbard, DO, FACOI Clinical Professor of Medicine Kansas City University of Medicine and Biosciences-College of Osteopathic Medicine Kansas City, Missouri
Thrombophilia. Dr. A Sarrafnejad PhD Dep. Immunology School of public health TUMS
 Autoimmune Thrombophilia Dr. A Sarrafnejad PhD Dep. Immunology School of public health TUMS Saraf@sina.tums.ac.ir Acquired Thrombophilia HIT PNH Cyckle cell Anemia Myeloproliferative lf Diseases Thrombocytosis
Autoimmune Thrombophilia Dr. A Sarrafnejad PhD Dep. Immunology School of public health TUMS Saraf@sina.tums.ac.ir Acquired Thrombophilia HIT PNH Cyckle cell Anemia Myeloproliferative lf Diseases Thrombocytosis
Handbook for Venous Thromboembolism
 Handbook for Venous Thromboembolism Gregory Piazza Benjamin Hohlfelder Samuel Z. Goldhaber Handbook for Venous Thromboembolism Gregory Piazza Cardiovascular Division Harvard Medical School Brigham and
Handbook for Venous Thromboembolism Gregory Piazza Benjamin Hohlfelder Samuel Z. Goldhaber Handbook for Venous Thromboembolism Gregory Piazza Cardiovascular Division Harvard Medical School Brigham and
A Case of Antiphospholipid Syndrome Refractory to Secondary Anticoagulating Prophylaxis after Deep Vein Thrombosis- Pulmonary Embolism
 CASE REPORT http://dx.doi.org/10.4046/trd.2014.77.6.274 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2014;77:274-278 A Case of Antiphospholipid Syndrome Refractory to Secondary Anticoagulating
CASE REPORT http://dx.doi.org/10.4046/trd.2014.77.6.274 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2014;77:274-278 A Case of Antiphospholipid Syndrome Refractory to Secondary Anticoagulating
Lupus as a risk factor for cardiovascular disease
 Lupus as a risk factor for cardiovascular disease SØREN JACOBSEN Department Rheumatology, Rigshospitalet Søren Jacobsen Main sponsors: Gigtforeningen Novo Nordisk Fonden Rigshospitalet Disclaimer: Novo
Lupus as a risk factor for cardiovascular disease SØREN JACOBSEN Department Rheumatology, Rigshospitalet Søren Jacobsen Main sponsors: Gigtforeningen Novo Nordisk Fonden Rigshospitalet Disclaimer: Novo
Thrombophilia: To test or not to test
 Kenneth Bauer, MD Harvard Medical School, Boston, MA Professor of Medicine VA Boston Healthcare System Chief, Hematology Section Beth Israel Deaconess Medical Center, Boston, MA Director, Thrombosis Clinical
Kenneth Bauer, MD Harvard Medical School, Boston, MA Professor of Medicine VA Boston Healthcare System Chief, Hematology Section Beth Israel Deaconess Medical Center, Boston, MA Director, Thrombosis Clinical
VENOUS THROMBOEMBOLISM AND CORONARY ARTERY DISEASE: IS THERE A LINK?
 VENOUS THROMBOEMBOLISM AND CORONARY ARTERY DISEASE: IS THERE A LINK? Ayman El-Menyar (1), MD, Hassan Al-Thani (2),MD (1)Clinical Research Consultant, (2) Head of Vascular Surgery, Hamad General Hospital
VENOUS THROMBOEMBOLISM AND CORONARY ARTERY DISEASE: IS THERE A LINK? Ayman El-Menyar (1), MD, Hassan Al-Thani (2),MD (1)Clinical Research Consultant, (2) Head of Vascular Surgery, Hamad General Hospital
Antiphospholipid Syndrome Handbook
 Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, Oier Ateka-Barrutia, and Munther A. Khamashta Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, MD, PhD Lupus Research Unit The Rayne
Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, Oier Ateka-Barrutia, and Munther A. Khamashta Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, MD, PhD Lupus Research Unit The Rayne
February 2016, Volume: 8, Issue: 2, Pages: , DOI:
 Electronic Physician (ISSN: 2008-5842) http://www.ephysician.ir February 2016, Volume: 8, Issue: 2, Pages: 1874-1879, DOI: http://dx.doi.org/10.19082/1874 Pulmonary embolism in an adolescent girl with
Electronic Physician (ISSN: 2008-5842) http://www.ephysician.ir February 2016, Volume: 8, Issue: 2, Pages: 1874-1879, DOI: http://dx.doi.org/10.19082/1874 Pulmonary embolism in an adolescent girl with
Dr. Rami M. Adil Al-Hayali Assistant Professor in Medicine
 Dr. Rami M. Adil Al-Hayali Assistant Professor in Medicine Venous thromboembolism: pulmonary embolism (PE) deep vein thrombosis (DVT) 1% of all patients admitted to hospital 5% of in-hospital mortality
Dr. Rami M. Adil Al-Hayali Assistant Professor in Medicine Venous thromboembolism: pulmonary embolism (PE) deep vein thrombosis (DVT) 1% of all patients admitted to hospital 5% of in-hospital mortality
CARDIAC PROBLEMS IN PREGNANCY
 CARDIAC PROBLEMS IN PREGNANCY LAS VEGAS, NEVADA, USA 27 February 1 March 2016 SUCCESSFUL TREATMENT WITH RECOMBINANT TISSUE PLASMINOGEN ACTIVATOR OF MASSIVE PULMONARY EMBOLISM IN THE 16 TH WEEK OF PREGNANCY
CARDIAC PROBLEMS IN PREGNANCY LAS VEGAS, NEVADA, USA 27 February 1 March 2016 SUCCESSFUL TREATMENT WITH RECOMBINANT TISSUE PLASMINOGEN ACTIVATOR OF MASSIVE PULMONARY EMBOLISM IN THE 16 TH WEEK OF PREGNANCY
Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations
 08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
October 2017 Pulmonary Embolism
 October 2017 Pulmonary Embolism Prof. Ahmed BaHammam, FRCP, FCCP Professor of Medicine College of Medicine King Saud University 1 Objectives Epidemiology Pathophysiology Diagnosis Massive PE Treatment
October 2017 Pulmonary Embolism Prof. Ahmed BaHammam, FRCP, FCCP Professor of Medicine College of Medicine King Saud University 1 Objectives Epidemiology Pathophysiology Diagnosis Massive PE Treatment
The Antiphospholipid Syndrome
 The Antiphospholipid Syndrome 1 / 6 2 / 6 3 / 6 The Antiphospholipid Syndrome Antiphospholipid antibody syndrome (commonly called antiphospholipid syndrome or APS) is an autoimmune disease present mostly
The Antiphospholipid Syndrome 1 / 6 2 / 6 3 / 6 The Antiphospholipid Syndrome Antiphospholipid antibody syndrome (commonly called antiphospholipid syndrome or APS) is an autoimmune disease present mostly
How long to continue anticoagulation after DVT?
 How long to continue anticoagulation after DVT? Dr. Nihar Ranjan Pradhan M.S., DNB (Vascular Surgery), FVES(UK) Consultant Vascular Surgeon Apollo Hospital, Jubilee Hills, Hyderabad (Formerly Faculty in
How long to continue anticoagulation after DVT? Dr. Nihar Ranjan Pradhan M.S., DNB (Vascular Surgery), FVES(UK) Consultant Vascular Surgeon Apollo Hospital, Jubilee Hills, Hyderabad (Formerly Faculty in
Sindrome da anticorpi antifosfolipidi: clinica e terapia. Vittorio Pengo Clinical Cardiology, Padova, Italy
 Sindrome da anticorpi antifosfolipidi: clinica e terapia Vittorio Pengo Clinical Cardiology, Padova, Italy Revised Classification Criteria for the Antiphospholipid Syndrome J Thromb Haemost 2006;4:295-306
Sindrome da anticorpi antifosfolipidi: clinica e terapia Vittorio Pengo Clinical Cardiology, Padova, Italy Revised Classification Criteria for the Antiphospholipid Syndrome J Thromb Haemost 2006;4:295-306
Case Report Lower Limb Ischemia: Aortoiliac Thrombosis Related to Antiphospholipid Syndrome (APS) Case Report and Review of the Literature
 Case Reports in Surgery Volume 2013, Article ID 536971, 4 pages http://dx.doi.org/10.1155/2013/536971 Case Report Lower Limb Ischemia: Aortoiliac Thrombosis Related to Antiphospholipid Syndrome (APS) Case
Case Reports in Surgery Volume 2013, Article ID 536971, 4 pages http://dx.doi.org/10.1155/2013/536971 Case Report Lower Limb Ischemia: Aortoiliac Thrombosis Related to Antiphospholipid Syndrome (APS) Case
Mortality in the Catastrophic Antiphospholipid Syndrome
 ARTHRITIS & RHEUMATISM Vol. 54, No. 8, August 2006, pp 2568 2576 DOI 10.1002/art.22018 2006, American College of Rheumatology Mortality in the Catastrophic Antiphospholipid Syndrome Causes of Death and
ARTHRITIS & RHEUMATISM Vol. 54, No. 8, August 2006, pp 2568 2576 DOI 10.1002/art.22018 2006, American College of Rheumatology Mortality in the Catastrophic Antiphospholipid Syndrome Causes of Death and
DVT and Pulmonary Embolus. Dr Piers Blombery BSc(Biomed), MBBS (Hons), FRACP, FRCPA Consultant Haematologist Peter MacCallum Cancer Centre
 DVT and Pulmonary Embolus Dr Piers Blombery BSc(Biomed), MBBS (Hons), FRACP, FRCPA Consultant Haematologist Peter MacCallum Cancer Centre Overview Structure of deep and superficial venous system of upper
DVT and Pulmonary Embolus Dr Piers Blombery BSc(Biomed), MBBS (Hons), FRACP, FRCPA Consultant Haematologist Peter MacCallum Cancer Centre Overview Structure of deep and superficial venous system of upper
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/21764 holds various files of this Leiden University dissertation. Author: Mos, Inge Christina Maria Title: A more granular view on pulmonary embolism Issue
Cover Page The handle http://hdl.handle.net/1887/21764 holds various files of this Leiden University dissertation. Author: Mos, Inge Christina Maria Title: A more granular view on pulmonary embolism Issue
PULMONARY EMBOLISM (PE): DIAGNOSIS AND TREATMENT
 PULMONARY EMBOLISM (PE): DIAGNOSIS AND TREATMENT OBJECTIVE: To provide a diagnostic algorithm and treatment options for patients with acute pulmonary embolism (PE). BACKGROUND: Venous thromboembolism (VTE)
PULMONARY EMBOLISM (PE): DIAGNOSIS AND TREATMENT OBJECTIVE: To provide a diagnostic algorithm and treatment options for patients with acute pulmonary embolism (PE). BACKGROUND: Venous thromboembolism (VTE)
Disclosures. Sneddon Syndrome: Untangling the Web. Case Presentation. MRI head w/ and w/o contrast. Further Workup. Further Workup 10/26/2017
 Sneddon Syndrome: Untangling the Web Sadhana Murali, MD, PGY-4 University of Wisconsin-Madison WNS Conference October 27-28, 2017 Disclosures I have no relevant financial relationships with any commercial
Sneddon Syndrome: Untangling the Web Sadhana Murali, MD, PGY-4 University of Wisconsin-Madison WNS Conference October 27-28, 2017 Disclosures I have no relevant financial relationships with any commercial
Venous thrombosis is common and often occurs spontaneously, but it also frequently accompanies medical and surgical conditions, both in the community
 Venous Thrombosis Venous Thrombosis It occurs mainly in the deep veins of the leg (deep vein thrombosis, DVT), from which parts of the clot frequently embolize to the lungs (pulmonary embolism, PE). Fewer
Venous Thrombosis Venous Thrombosis It occurs mainly in the deep veins of the leg (deep vein thrombosis, DVT), from which parts of the clot frequently embolize to the lungs (pulmonary embolism, PE). Fewer
DISCLOSURE. Presented by: Merav Sendowski, MD Oregon Health and Science University
 Thrombophilia! DISCLOSURE Presented by: Merav Sendowski, MD Oregon Health and Science University Created by: Thomas Deloughery, MD Oregon Health and Science University Current Relevant Financial Relationship(s)
Thrombophilia! DISCLOSURE Presented by: Merav Sendowski, MD Oregon Health and Science University Created by: Thomas Deloughery, MD Oregon Health and Science University Current Relevant Financial Relationship(s)
Lung diseases of Vascular Origin. By: Shefaa Qa qqa
 Lung diseases of Vascular Origin By: Shefaa Qa qqa Pulmonary Hypertension Pulmonary hypertension is defined as a mean pulmonary artery pressure greater than or equal to 25 mm Hg at rest. Based on underlying
Lung diseases of Vascular Origin By: Shefaa Qa qqa Pulmonary Hypertension Pulmonary hypertension is defined as a mean pulmonary artery pressure greater than or equal to 25 mm Hg at rest. Based on underlying
Supplemental Figures and Legends
 Supplemental Figures and Legends Online Figure 1. 18 year old female with SLE and acute homonymous hemianopsia, confusional state, and cognitive dysfunction. A. This TEE four chamber view demonstrates
Supplemental Figures and Legends Online Figure 1. 18 year old female with SLE and acute homonymous hemianopsia, confusional state, and cognitive dysfunction. A. This TEE four chamber view demonstrates
Pulmonary Thromboembolism
 Pulmonary Thromboembolism James Allen, MD Epidemiology of Pulmonary Embolism 1,500,000 new cases per year in the United States Often asymptomatic 300,000 deaths per year DVT or PE present in 10% of ICU
Pulmonary Thromboembolism James Allen, MD Epidemiology of Pulmonary Embolism 1,500,000 new cases per year in the United States Often asymptomatic 300,000 deaths per year DVT or PE present in 10% of ICU
Anti β 2. -Glycoprotein I and Antiphosphatidylserine Antibodies Are Predictors of Arterial Thrombosis in Patients With Antiphospholipid Syndrome
 Coagulation and Transfusion Medicine / PREDICTIVE VALUE OF ANTIPHOSPHOLIPID ANTIBODIES Anti β -Glycoprotein I and Antiphosphatidylserine Antibodies Are Predictors of Arterial Thrombosis in Patients With
Coagulation and Transfusion Medicine / PREDICTIVE VALUE OF ANTIPHOSPHOLIPID ANTIBODIES Anti β -Glycoprotein I and Antiphosphatidylserine Antibodies Are Predictors of Arterial Thrombosis in Patients With
Pathology of pulmonary vascular disease. Dr.Ashraf Abdelfatah Deyab. Assistant Professor of Pathology Faculty of Medicine Almajma ah University
 Pathology of pulmonary vascular disease Dr.Ashraf Abdelfatah Deyab Assistant Professor of Pathology Faculty of Medicine Almajma ah University Pulmonary vascular disease Type of pulmonary circulation: Types
Pathology of pulmonary vascular disease Dr.Ashraf Abdelfatah Deyab Assistant Professor of Pathology Faculty of Medicine Almajma ah University Pulmonary vascular disease Type of pulmonary circulation: Types
Anticardiolipin Antibodies in Patients With Type 2 Diabetes Mellitus
 CM&R Rapid Release. Published online ahead of print February 26, 2009 as doi:10.3121/cmr.2008.828 Original Research Anticardiolipin Antibodies in Patients With Type 2 Diabetes Mellitus José María Calvo-Romero,
CM&R Rapid Release. Published online ahead of print February 26, 2009 as doi:10.3121/cmr.2008.828 Original Research Anticardiolipin Antibodies in Patients With Type 2 Diabetes Mellitus José María Calvo-Romero,
Thursday, February 26, :00 am. Regulation of Coagulation/Disseminated Intravascular Coagulation HEMOSTASIS/THROMBOSIS III
 REGULATION OF COAGULATION Introduction HEMOSTASIS/THROMBOSIS III Regulation of Coagulation/Disseminated Coagulation necessary for maintenance of vascular integrity Enough fibrinogen to clot all vessels
REGULATION OF COAGULATION Introduction HEMOSTASIS/THROMBOSIS III Regulation of Coagulation/Disseminated Coagulation necessary for maintenance of vascular integrity Enough fibrinogen to clot all vessels
Epidemiologia e clinica del tromboembolismo venoso. Maria Ciccone Sezione di Ematologia e Fisiopatologia della Coagulazione
 Epidemiologia e clinica del tromboembolismo venoso Maria Ciccone Sezione di Ematologia e Fisiopatologia della Coagulazione Thrombophilia may present clinically as one or more of several thrombotic manifestations
Epidemiologia e clinica del tromboembolismo venoso Maria Ciccone Sezione di Ematologia e Fisiopatologia della Coagulazione Thrombophilia may present clinically as one or more of several thrombotic manifestations
Potpourri of Hematology Oncology. Jasmine Nabi, M.D. Oncology Associates Hall-Perrine Cancer Center at Mercy
 Potpourri of Hematology Oncology Jasmine Nabi, M.D. Oncology Associates Hall-Perrine Cancer Center at Mercy Lifestyle Modifications to Decrease the Risk of Colorectal Cancer Estimates for 2018 American
Potpourri of Hematology Oncology Jasmine Nabi, M.D. Oncology Associates Hall-Perrine Cancer Center at Mercy Lifestyle Modifications to Decrease the Risk of Colorectal Cancer Estimates for 2018 American
A 48-Year Old Woman with Recurrent Venous Thromboembolism and Pulmonary Artery Aneurysm
 A 48-Year Old Woman with Recurrent Venous Thromboembolism and Pulmonary Artery Aneurysm Group 10: Arjun Prasanna, Keaton Mcclure, Shruti Srikumar, Nisha Karwal Patient History: 15 months prior 48 year
A 48-Year Old Woman with Recurrent Venous Thromboembolism and Pulmonary Artery Aneurysm Group 10: Arjun Prasanna, Keaton Mcclure, Shruti Srikumar, Nisha Karwal Patient History: 15 months prior 48 year
Key words: antiphospholipid syndrome, trombosis, pathogenesis
 26. XI,. 4/2011,.,..,..,., -..,,. 2GPI. -,.,,., -,, -, -,,,,, IL-1, IL-2, IL-6, IL-8, IL-12, IL-10, TNF, INF-. :,, N. Stoilov, R. Rashkov and R. Stoilov. ANTIPHOSPHOLIPID SYNDROME HISTORICAL DATA, ETI-
26. XI,. 4/2011,.,..,..,., -..,,. 2GPI. -,.,,., -,, -, -,,,,, IL-1, IL-2, IL-6, IL-8, IL-12, IL-10, TNF, INF-. :,, N. Stoilov, R. Rashkov and R. Stoilov. ANTIPHOSPHOLIPID SYNDROME HISTORICAL DATA, ETI-
Antiphospholipid Antibody Syndrome: Management Issues for the Hematologist
 Antiphospholipid Antibody Syndrome: Management Issues for the Hematologist Wisconsin Institute of Discovery Karen Rossi/Bristol-Myers Squibb Morey A. Blinder, MD Washington University, St. Louis, MO March
Antiphospholipid Antibody Syndrome: Management Issues for the Hematologist Wisconsin Institute of Discovery Karen Rossi/Bristol-Myers Squibb Morey A. Blinder, MD Washington University, St. Louis, MO March
9/25/2013 SYSTEMIC LUPUS ERYTHEMATOSUS (SLE)
 SYSTEMIC LUPUS ERYTHEMATOSUS (SLE) 1 Other Types of Lupus Discoid Lupus Erythematosus Lupus Pernio --- Sarcoidosis Lupus Vulgaris --- Tuberculosis of the face Manifestations of SLE Fever Rashes Arthritis
SYSTEMIC LUPUS ERYTHEMATOSUS (SLE) 1 Other Types of Lupus Discoid Lupus Erythematosus Lupus Pernio --- Sarcoidosis Lupus Vulgaris --- Tuberculosis of the face Manifestations of SLE Fever Rashes Arthritis
A 50-year-old woman with syncope
 Hira Shahzad 1, Ali Bin Sarwar Zubairi 2 1 Medical College, Aga Khan University Hospital, Karachi 2 Department of Medicine, Aga Khan University Hospital, Karachi, Pakistan Ali Bin Sarwar Zubairi Associate
Hira Shahzad 1, Ali Bin Sarwar Zubairi 2 1 Medical College, Aga Khan University Hospital, Karachi 2 Department of Medicine, Aga Khan University Hospital, Karachi, Pakistan Ali Bin Sarwar Zubairi Associate
VENOUS THROMBOEMBOLISM: DURATION OF TREATMENT
 VENOUS THROMBOEMBOLISM: DURATION OF TREATMENT OBJECTIVE: To provide guidance on the recommended duration of anticoagulant therapy for venous thromboembolism (VTE). BACKGROUND: Recurrent episodes of VTE
VENOUS THROMBOEMBOLISM: DURATION OF TREATMENT OBJECTIVE: To provide guidance on the recommended duration of anticoagulant therapy for venous thromboembolism (VTE). BACKGROUND: Recurrent episodes of VTE
Updates in Diagnosis & Management of VTE
 Updates in Diagnosis & Management of VTE TRACY MINICHIELLO, MD CHIEF, ANTICOAGULATION& THROMBOSIS SERVICE-SAN FRANCISCO VAMC PROFESSOR OF MEDICINE UNIVERSITY OF CALIFORNIA, SAN FRANCISCO Financial Disclosures-NONE
Updates in Diagnosis & Management of VTE TRACY MINICHIELLO, MD CHIEF, ANTICOAGULATION& THROMBOSIS SERVICE-SAN FRANCISCO VAMC PROFESSOR OF MEDICINE UNIVERSITY OF CALIFORNIA, SAN FRANCISCO Financial Disclosures-NONE
Cardiovascular Images
 Cardiovascular Images Pulmonary Embolism Diagnosed From Right Heart Changes Seen After Exercise Stress Echocardiography Brian C. Case, MD; Micheas Zemedkun, MD; Amarin Sangkharat, MD; Allen J. Taylor,
Cardiovascular Images Pulmonary Embolism Diagnosed From Right Heart Changes Seen After Exercise Stress Echocardiography Brian C. Case, MD; Micheas Zemedkun, MD; Amarin Sangkharat, MD; Allen J. Taylor,
Lupus anticoagulant and anticardiolipin antibodies in SLE with secondary Antiphospholipid Antibody Syndrome
 Turk J Hematol 2007; 24:69-74 Turkish Society of Hematology RESEARCH ARTICLE Lupus anticoagulant and anticardiolipin antibodies in SLE with secondary Antiphospholipid Antibody Syndrome Shveta Garg, Annamma
Turk J Hematol 2007; 24:69-74 Turkish Society of Hematology RESEARCH ARTICLE Lupus anticoagulant and anticardiolipin antibodies in SLE with secondary Antiphospholipid Antibody Syndrome Shveta Garg, Annamma
Deep Vein Thrombosis
 Deep Vein Thrombosis from NHS (UK) guidelines Introduction Deep vein thrombosis (DVT) is a blood clot in one of the deep veins in the body. Blood clots that develop in a vein are also known as venous thrombosis.
Deep Vein Thrombosis from NHS (UK) guidelines Introduction Deep vein thrombosis (DVT) is a blood clot in one of the deep veins in the body. Blood clots that develop in a vein are also known as venous thrombosis.
THROMBOSIS RISK FACTOR ASSESSMENT
 Name: Procedure: Doctor: Date: THROMBOSIS RISK FACTOR ASSESSMENT CHOOSE ALL THAT APPLY EACH RISK FACTOR REPRESENTS 1 POINT Age 41 60 years Minor Surgery Planned History of Prior Major Surgery (< 1 month)
Name: Procedure: Doctor: Date: THROMBOSIS RISK FACTOR ASSESSMENT CHOOSE ALL THAT APPLY EACH RISK FACTOR REPRESENTS 1 POINT Age 41 60 years Minor Surgery Planned History of Prior Major Surgery (< 1 month)
University Journal of Medicine and Medical Specialities
 University Journal of Medicine and Medical Specialities Volume 1 Issue 1 2015 An unusual case of SADDLE Pulmonary Thrombo Embolism Boopathirajan P Jayanthi R Stanley Medical College Abstract: Pulmonary
University Journal of Medicine and Medical Specialities Volume 1 Issue 1 2015 An unusual case of SADDLE Pulmonary Thrombo Embolism Boopathirajan P Jayanthi R Stanley Medical College Abstract: Pulmonary
Prevalence of antiphospholipid auto antibodies in patients with thrombosis
 EUROPEAN ACADEMIC RESEARCH Vol. IV, Issue 6/ September 2016 ISSN 2286-4822 www.euacademic.org Impact Factor: 3.4546 (UIF) DRJI Value: 5.9 (B+) Prevalence of antiphospholipid auto antibodies in patients
EUROPEAN ACADEMIC RESEARCH Vol. IV, Issue 6/ September 2016 ISSN 2286-4822 www.euacademic.org Impact Factor: 3.4546 (UIF) DRJI Value: 5.9 (B+) Prevalence of antiphospholipid auto antibodies in patients
Lupus Anticoagulants (LA), Antiphospholipid (APL) Antibodies & APL Syndrome: Review & Update. Antiphospholipid. Antiphospholipid
 , Antiphospholipid (APL) Antibodies & APL Syndrome: Review & Update William L. Nichols, MD Mayo Clinic College of Medicine Rochester, Minnesota USA Disclosures & Objectives (Nichols) Disclosures Relevant
, Antiphospholipid (APL) Antibodies & APL Syndrome: Review & Update William L. Nichols, MD Mayo Clinic College of Medicine Rochester, Minnesota USA Disclosures & Objectives (Nichols) Disclosures Relevant
Sinus and Cerebral Vein Thrombosis
 Sinus and Cerebral Vein Thrombosis A Summary Sinus and cerebral vein clots are uncommon. They can lead to severe headaches, confusion, and stroke-like symptoms. They may lead to bleeding into the surrounding
Sinus and Cerebral Vein Thrombosis A Summary Sinus and cerebral vein clots are uncommon. They can lead to severe headaches, confusion, and stroke-like symptoms. They may lead to bleeding into the surrounding
Pulmonary Embolism. Pulmonary Embolism. Pulmonary Embolism. PE - Clinical
 Pulmonary embolus - a practical approach to investigation and treatment Sam Janes Wellcome Senior Fellow and Respiratory Physician, University College London Background Diagnosis Treatment Common: 50 cases
Pulmonary embolus - a practical approach to investigation and treatment Sam Janes Wellcome Senior Fellow and Respiratory Physician, University College London Background Diagnosis Treatment Common: 50 cases
PE and DVT. Dr Anzo William Adiga WatsApp or Call Medical Officer/RHEMA MEDICAL GROUP
 PE and DVT Dr Anzo William Adiga WatsApp or Call +256777363201 Medical Officer/RHEMA MEDICAL GROUP OBJECTIVES DEFINE DVT AND P.E PATHOPHYSIOLOGY OF DVT CLINICAL PRESENTATION OF DVT/PE INVESTIGATE DVT MANAGEMENT
PE and DVT Dr Anzo William Adiga WatsApp or Call +256777363201 Medical Officer/RHEMA MEDICAL GROUP OBJECTIVES DEFINE DVT AND P.E PATHOPHYSIOLOGY OF DVT CLINICAL PRESENTATION OF DVT/PE INVESTIGATE DVT MANAGEMENT
Thrombosis. By Dr. Sara Mohamed Abuelgasim
 Thrombosis By Dr. Sara Mohamed Abuelgasim 1 Thrombosis Unchecked, blood coagulation would lead to dangerous occlusion of blood vessels if the protective mechanisms of coagulation factor inhibitors, blood
Thrombosis By Dr. Sara Mohamed Abuelgasim 1 Thrombosis Unchecked, blood coagulation would lead to dangerous occlusion of blood vessels if the protective mechanisms of coagulation factor inhibitors, blood
DVT Pathophysiology and Prophylaxis in Medically Hospitalized Patients. David Liff MD Oklahoma Heart Institute Vascular Center
 DVT Pathophysiology and Prophylaxis in Medically Hospitalized Patients David Liff MD Oklahoma Heart Institute Vascular Center Overview Pathophysiology of DVT Epidemiology and risk factors for DVT in the
DVT Pathophysiology and Prophylaxis in Medically Hospitalized Patients David Liff MD Oklahoma Heart Institute Vascular Center Overview Pathophysiology of DVT Epidemiology and risk factors for DVT in the
Case Report Internal Jugular Vein Thrombosis in Isolated Tuberculous Cervical Lymphadenopathy
 Volume 2016, Article ID 5184196, 4 pages http://dx.doi.org/10.1155/2016/5184196 Case Report Internal Jugular Vein Thrombosis in Isolated Tuberculous Cervical Lymphadenopathy Sanjay Khaladkar, Avadhesh
Volume 2016, Article ID 5184196, 4 pages http://dx.doi.org/10.1155/2016/5184196 Case Report Internal Jugular Vein Thrombosis in Isolated Tuberculous Cervical Lymphadenopathy Sanjay Khaladkar, Avadhesh
AMPLIADO SÍNDROME ANTIFOSFOLÍPIDO SÍNDROME DE SJÖGREN María José Cuadrado Lozano Clínica Universidad de Navarra-Madrid
 AMPLIADO SÍNDROME ANTIFOSFOLÍPIDO SÍNDROME DE SJÖGREN María José Cuadrado Lozano Clínica Universidad de Navarra-Madrid PLASMABLAST PROLIFERATION IS ASSOCIATED WITH TLR7 POLYMORPHISMS AND UPREGULATION OF
AMPLIADO SÍNDROME ANTIFOSFOLÍPIDO SÍNDROME DE SJÖGREN María José Cuadrado Lozano Clínica Universidad de Navarra-Madrid PLASMABLAST PROLIFERATION IS ASSOCIATED WITH TLR7 POLYMORPHISMS AND UPREGULATION OF
Jordan M. Garrison, MD FACS, FASMBS
 Jordan M. Garrison, MD FACS, FASMBS Peripheral Arterial Disease (PAD) Near or Complete obstruction of > 1 Peripheral Artery Peripheral Venous reflux Disease Varicose Veins Chronic Venous Stasis Ulcer Disease
Jordan M. Garrison, MD FACS, FASMBS Peripheral Arterial Disease (PAD) Near or Complete obstruction of > 1 Peripheral Artery Peripheral Venous reflux Disease Varicose Veins Chronic Venous Stasis Ulcer Disease
DVT PROPHYLAXIS IN HOSPITALIZED MEDICAL PATIENTS SAURABH MAJI SR (PULMONARY,MEDICINE)
 DVT PROPHYLAXIS IN HOSPITALIZED MEDICAL PATIENTS SAURABH MAJI SR (PULMONARY,MEDICINE) Introduction VTE (DVT/PE) is an important complication in hospitalized patients Hospitalization for acute medical illness
DVT PROPHYLAXIS IN HOSPITALIZED MEDICAL PATIENTS SAURABH MAJI SR (PULMONARY,MEDICINE) Introduction VTE (DVT/PE) is an important complication in hospitalized patients Hospitalization for acute medical illness
Risk factors for DVT. Venous thrombosis & pulmonary embolism. Anticoagulation (cont d) Diagnosis 1/5/2018. Ahmed Mahmoud, MD
 Risk factors for DVT Venous thrombosis & pulmonary embolism Ahmed Mahmoud, MD Surgery ; post op especially for long cases, pelvic operations (THR), Trauma ; long bone fractures, pelvic fractures (posterior
Risk factors for DVT Venous thrombosis & pulmonary embolism Ahmed Mahmoud, MD Surgery ; post op especially for long cases, pelvic operations (THR), Trauma ; long bone fractures, pelvic fractures (posterior
Venous thrombosis & pulmonary embolism. Ahmed Mahmoud, MD
 Venous thrombosis & pulmonary embolism Ahmed Mahmoud, MD Risk factors for DVT Surgery ; post op especially for long cases, pelvic operations (THR), Trauma ; long bone fractures, pelvic fractures (posterior
Venous thrombosis & pulmonary embolism Ahmed Mahmoud, MD Risk factors for DVT Surgery ; post op especially for long cases, pelvic operations (THR), Trauma ; long bone fractures, pelvic fractures (posterior
What are blood clots?
 What are blood clots? Dr Matthew Fay GP Principal The Willows Medical Practice- Queensbury GPwSI and Co-Founder Westcliffe Cardiology Service GP Partner Westcliffe Medical Group Created 5/31/18 Dr. Matthew
What are blood clots? Dr Matthew Fay GP Principal The Willows Medical Practice- Queensbury GPwSI and Co-Founder Westcliffe Cardiology Service GP Partner Westcliffe Medical Group Created 5/31/18 Dr. Matthew
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
Pulmonary Embolism. Thoracic radiologist Helena Lauri
 Pulmonary Embolism Thoracic radiologist Helena Lauri 8.5.2017 Statistics 1-2 out of 1000 adults annually are diagnosed with deep vein thrombosis (DVT) and/or pulmonary embolism (PE) About half of patients
Pulmonary Embolism Thoracic radiologist Helena Lauri 8.5.2017 Statistics 1-2 out of 1000 adults annually are diagnosed with deep vein thrombosis (DVT) and/or pulmonary embolism (PE) About half of patients
Index. Crit Care Clin 19 (2003)
 Crit Care Clin 19 (2003) 331 335 Index A ACVECC. See American College of Veterinary Emergency and Critical Care (ACVECC). Aging. See also Elderly; Geriatric critical care. respiratory function effects
Crit Care Clin 19 (2003) 331 335 Index A ACVECC. See American College of Veterinary Emergency and Critical Care (ACVECC). Aging. See also Elderly; Geriatric critical care. respiratory function effects
Jessica Bryan, Natalia Evans, Karlyn Henderson, & Whitney Parks
 Jessica Bryan, Natalia Evans, Karlyn Henderson, & Whitney Parks 1. What is the most common cause of death in hospitalized patients? 1. Hospital-acquired infection 2. Pulmonary embolism 3. Myocardial infarction
Jessica Bryan, Natalia Evans, Karlyn Henderson, & Whitney Parks 1. What is the most common cause of death in hospitalized patients? 1. Hospital-acquired infection 2. Pulmonary embolism 3. Myocardial infarction
Deep Vein Thrombosis and Pulmonary Embolism: Patient Information
 Deep Vein Thrombosis and Pulmonary Embolism: Patient Information A Deep Vein Thrombosis (DVT) and a Pulmonary Embolism (PE) are both disorders of unwanted blood clotting. Unwanted blood clots can occur
Deep Vein Thrombosis and Pulmonary Embolism: Patient Information A Deep Vein Thrombosis (DVT) and a Pulmonary Embolism (PE) are both disorders of unwanted blood clotting. Unwanted blood clots can occur
Daniel Egan, MD April 13, 2012
 Daniel Egan, MD April 13, 2012 Aug 2006 (at age 15): Acute unprovoked DVT in left common femoral vein Factor V Leiden heterozygous Positive lupus inhibitor Lovenox BID 2 weeks later: increased clot burden,
Daniel Egan, MD April 13, 2012 Aug 2006 (at age 15): Acute unprovoked DVT in left common femoral vein Factor V Leiden heterozygous Positive lupus inhibitor Lovenox BID 2 weeks later: increased clot burden,
Neuropsychiatric Systemic Lupus Erythematosus (NPSLE) Case presentations and topic discussion The Rheumatology Unit UMMC experience
 Neuropsychiatric Systemic Lupus Erythematosus (NPSLE) Case presentations and topic discussion The Rheumatology Unit UMMC experience References Sanna G, Bertolaccini ML. Neuropsychiatric manifestations
Neuropsychiatric Systemic Lupus Erythematosus (NPSLE) Case presentations and topic discussion The Rheumatology Unit UMMC experience References Sanna G, Bertolaccini ML. Neuropsychiatric manifestations
Genetic Tests for the Better Outcome of VTE? 서울대학교병원혈액종양내과윤성수
 Genetic Tests for the Better Outcome of VTE? 서울대학교병원혈액종양내과윤성수 Thrombophilia A hereditary or acquired disorder predisposing to thrombosis Questions Why should we test? Who should we test For what disorders?
Genetic Tests for the Better Outcome of VTE? 서울대학교병원혈액종양내과윤성수 Thrombophilia A hereditary or acquired disorder predisposing to thrombosis Questions Why should we test? Who should we test For what disorders?
Pathophysiology. Tutorial 3 Hemodynamic Disorders
 Pathophysiology Tutorial 3 Hemodynamic Disorders ILOs Recall different causes of thrombosis. Explain different types of embolism and their predisposing factors. Differentiate between hemorrhage types.
Pathophysiology Tutorial 3 Hemodynamic Disorders ILOs Recall different causes of thrombosis. Explain different types of embolism and their predisposing factors. Differentiate between hemorrhage types.
Interventional Treatment VTE: Radiologic Approach
 Interventional Treatment VTE: Radiologic Approach Hae Giu Lee, MD Professor, Dept of Radiology Seoul St. Mary s Hospital The Catholic University of Korea Introduction Incidence High incidence: 250,000-1,000,000/year
Interventional Treatment VTE: Radiologic Approach Hae Giu Lee, MD Professor, Dept of Radiology Seoul St. Mary s Hospital The Catholic University of Korea Introduction Incidence High incidence: 250,000-1,000,000/year
CURRENT & FUTURE THERAPEUTIC MANAGEMENT OF VENOUS THROMBOEMBOLISM. Gordon Lowe Professor of Vascular Medicine University of Glasgow
 CURRENT & FUTURE THERAPEUTIC MANAGEMENT OF VENOUS THROMBOEMBOLISM Gordon Lowe Professor of Vascular Medicine University of Glasgow VENOUS THROMBOEMBOLISM Common cause of death and disability 50% hospital-acquired
CURRENT & FUTURE THERAPEUTIC MANAGEMENT OF VENOUS THROMBOEMBOLISM Gordon Lowe Professor of Vascular Medicine University of Glasgow VENOUS THROMBOEMBOLISM Common cause of death and disability 50% hospital-acquired
Primary Care practice clinics within the Edmonton Southside Primary Care Network.
 INR Monitoring and Warfarin Dose Adjustment Last Review: November 2016 Intervention(s) and/or Procedure: Registered Nurses (RNs) adjust warfarin dosage according to individual patient International Normalized
INR Monitoring and Warfarin Dose Adjustment Last Review: November 2016 Intervention(s) and/or Procedure: Registered Nurses (RNs) adjust warfarin dosage according to individual patient International Normalized
Cardiovascular Disorders Lecture 3 Coronar Artery Diseases
 Cardiovascular Disorders Lecture 3 Coronar Artery Diseases By Prof. El Sayed Abdel Fattah Eid Lecturer of Internal Medicine Delta University Coronary Heart Diseases It is the leading cause of death in
Cardiovascular Disorders Lecture 3 Coronar Artery Diseases By Prof. El Sayed Abdel Fattah Eid Lecturer of Internal Medicine Delta University Coronary Heart Diseases It is the leading cause of death in
Diagnosis and Treatment of Deep Venous Thrombosis and Pulmonary Embolism
 Agency for Healthcare Research and Quality Evidence Report/Technology Assessment Diagnosis and Treatment of Deep Venous Thrombosis and Pulmonary Embolism Summary Number 68 Overview Venous thromboembolism
Agency for Healthcare Research and Quality Evidence Report/Technology Assessment Diagnosis and Treatment of Deep Venous Thrombosis and Pulmonary Embolism Summary Number 68 Overview Venous thromboembolism
DOWNLOAD OR READ : POSITIVE OPTIONS FOR ANTIPHOSPHOLIPID SYNDROME APS SELF HELP AND TREATMENT PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : POSITIVE OPTIONS FOR ANTIPHOSPHOLIPID SYNDROME APS SELF HELP AND TREATMENT PDF EBOOK EPUB MOBI Page 1 Page 2 positive options for antiphospholipid syndrome aps self help and treatment
DOWNLOAD OR READ : POSITIVE OPTIONS FOR ANTIPHOSPHOLIPID SYNDROME APS SELF HELP AND TREATMENT PDF EBOOK EPUB MOBI Page 1 Page 2 positive options for antiphospholipid syndrome aps self help and treatment
Thrombosis and emboli. Peter Nagy
 Thrombosis and emboli Peter Nagy A thrombus is any solid object developing from the blood in vivo within the vascular system or heart. Thrombosis is hemostasis in the wrong place. Major components, forms:
Thrombosis and emboli Peter Nagy A thrombus is any solid object developing from the blood in vivo within the vascular system or heart. Thrombosis is hemostasis in the wrong place. Major components, forms:
Hematologic Disorders. Assistant professor of anesthesia
 Preoperative Evaluation Hematologic Disorders Dr M.Razavi Assistant professor of anesthesia Anemia Evaluation needs to consider the extent and type of surgery, the anticipated blood loss, and the patient's
Preoperative Evaluation Hematologic Disorders Dr M.Razavi Assistant professor of anesthesia Anemia Evaluation needs to consider the extent and type of surgery, the anticipated blood loss, and the patient's
Deep Vein Thrombosis and Pulmonary Embolism in the Perioperative Patient
 ...PRESENTATIONS... Deep Vein Thrombosis and Pulmonary Embolism in the Perioperative Patient Based on a presentation by James E. Muntz, MD Presentation Summary Approximately 500,000 cases of deep vein
...PRESENTATIONS... Deep Vein Thrombosis and Pulmonary Embolism in the Perioperative Patient Based on a presentation by James E. Muntz, MD Presentation Summary Approximately 500,000 cases of deep vein
Case Report Catastrophic Antiphospholipid Syndrome
 Case Reports in Rheumatology Volume 2016, Article ID 4161439, 4 pages http://dx.doi.org/10.1155/2016/4161439 Case Report Catastrophic Antiphospholipid Syndrome Rawhya R. El-Shereef, 1 Zein El-Abedin, 2
Case Reports in Rheumatology Volume 2016, Article ID 4161439, 4 pages http://dx.doi.org/10.1155/2016/4161439 Case Report Catastrophic Antiphospholipid Syndrome Rawhya R. El-Shereef, 1 Zein El-Abedin, 2
Images in Cardiovascular Medicine
 Images in Cardiovascular Medicine Numerous Small Vegetations Revealing Libman-Sacks Endocarditis in Catastrophic Antiphospholipid Syndrome Hideo Yamamoto, MD; Tamaki Iwade, MD; Ryuji Nakano, MD; Masahiro
Images in Cardiovascular Medicine Numerous Small Vegetations Revealing Libman-Sacks Endocarditis in Catastrophic Antiphospholipid Syndrome Hideo Yamamoto, MD; Tamaki Iwade, MD; Ryuji Nakano, MD; Masahiro
Anticoagulants. Pathological formation of a haemostatic plug Arterial associated with atherosclerosis Venous blood stasis e.g. DVT
 Haemostasis Thrombosis Phases Endogenous anticoagulants Stopping blood loss Pathological formation of a haemostatic plug Arterial associated with atherosclerosis Venous blood stasis e.g. DVT Vascular Platelet
Haemostasis Thrombosis Phases Endogenous anticoagulants Stopping blood loss Pathological formation of a haemostatic plug Arterial associated with atherosclerosis Venous blood stasis e.g. DVT Vascular Platelet
Iron-deficiency anemia as a rare cause of cerebral venous thrombosis and pulmonary embolism. NICASTRO, Nicolas, SCHNIDER, Armin, LEEMANN, Béatrice
 Article Iron-deficiency anemia as a rare cause of cerebral venous thrombosis and pulmonary embolism NICASTRO, Nicolas, SCHNIDER, Armin, LEEMANN, Béatrice Abstract Cerebral venous thrombosis (CVT) is a
Article Iron-deficiency anemia as a rare cause of cerebral venous thrombosis and pulmonary embolism NICASTRO, Nicolas, SCHNIDER, Armin, LEEMANN, Béatrice Abstract Cerebral venous thrombosis (CVT) is a
ORIGINAL INVESTIGATION
 ORIGINAL INVESTIGATION High Impact of Antiphospholipid Syndrome on Irreversible Organ Damage and Survival of Patients With Systemic Lupus Erythematosus Guillermo Ruiz-Irastorza, MD, PhD; Maria-Victoria
ORIGINAL INVESTIGATION High Impact of Antiphospholipid Syndrome on Irreversible Organ Damage and Survival of Patients With Systemic Lupus Erythematosus Guillermo Ruiz-Irastorza, MD, PhD; Maria-Victoria
Antiphospholipid Syndrome ( APS)
 Antiphospholipid Syndrome ( APS) Edward John Walter Bowie, MD Mayo Medical School the first to identify APS as an acquired thrombophilia Graham Robert Vivian Hughes MD FRCP Unit Rayne Institute St Thomas
Antiphospholipid Syndrome ( APS) Edward John Walter Bowie, MD Mayo Medical School the first to identify APS as an acquired thrombophilia Graham Robert Vivian Hughes MD FRCP Unit Rayne Institute St Thomas
Antiphospholipid antibodies
 CARDIOLOGY PATIENT PAGE CARDIOLOGY PATIENT PAGE Antiphospholipid Antibodies Caron P. Misita, PharmD; Stephan Moll, MD Antiphospholipid antibodies (APLAs) are proteins that may be present in the blood and
CARDIOLOGY PATIENT PAGE CARDIOLOGY PATIENT PAGE Antiphospholipid Antibodies Caron P. Misita, PharmD; Stephan Moll, MD Antiphospholipid antibodies (APLAs) are proteins that may be present in the blood and
Μακροχρόνια παρακολούθηση ασθενών με πνευμονική εμβολή
 Μακροχρόνια παρακολούθηση ασθενών με πνευμονική εμβολή Ευφροσύνη Δ. Μάναλη Λέκτορας Β Πανεπιστημιακή Πνευμονολογική Κλινική ΓΝΑ «Αττικόν» Εθνικό και Καποδιστριακό Πανεπιστήμιο Αθηνών Existing guidelines
Μακροχρόνια παρακολούθηση ασθενών με πνευμονική εμβολή Ευφροσύνη Δ. Μάναλη Λέκτορας Β Πανεπιστημιακή Πνευμονολογική Κλινική ΓΝΑ «Αττικόν» Εθνικό και Καποδιστριακό Πανεπιστήμιο Αθηνών Existing guidelines
Combined oral contraceptives and risk of venous thromboembolism: nested case control studies using the QResearch and the CPRD databases
 Combined oral contraceptives and risk of venous thromboembolism: nested case control studies using the QResearch and the CPRD databases Yana Vinogradova, Carol Coupland, Julia Hippisley-Cox Web appendix:
Combined oral contraceptives and risk of venous thromboembolism: nested case control studies using the QResearch and the CPRD databases Yana Vinogradova, Carol Coupland, Julia Hippisley-Cox Web appendix:
Epidermiology Early pulmonary embolism
 Epidermiology Early pulmonary embolism Sitang Nirattisaikul Faculty of Medicine, Prince of Songkla University 3 rd most common cause of cardiovascular death in the United States, following ischemic heart
Epidermiology Early pulmonary embolism Sitang Nirattisaikul Faculty of Medicine, Prince of Songkla University 3 rd most common cause of cardiovascular death in the United States, following ischemic heart
What s New in DVT & PE
 What s New in DVT & PE Mark Buch MD CM CCFP(EM) Attending physician Emergency Department Jewish General Hospital Family Physician and Medical Director GMF Santé Mont-Royal Objectives: Review the diagnostic
What s New in DVT & PE Mark Buch MD CM CCFP(EM) Attending physician Emergency Department Jewish General Hospital Family Physician and Medical Director GMF Santé Mont-Royal Objectives: Review the diagnostic
Acute cor pulmonale due to pulmonary tumor thrombotic microangiopathy in two patients with breast cancer
 LETTER TO THE EDITOR Korean J Intern Med 2017;32:190-194 Acute cor pulmonale due to pulmonary tumor thrombotic microangiopathy in two patients with breast cancer Sung Young Moon, Kang Hoon Lee, Jong Sik
LETTER TO THE EDITOR Korean J Intern Med 2017;32:190-194 Acute cor pulmonale due to pulmonary tumor thrombotic microangiopathy in two patients with breast cancer Sung Young Moon, Kang Hoon Lee, Jong Sik
DVT - initial management NSCCG
 Background information Information resources for patients and carers Updates to this care map Synonyms Below knee DVT and bleeding risks Patient with confirmed DVT Scan confirms superficial thrombophlebitis
Background information Information resources for patients and carers Updates to this care map Synonyms Below knee DVT and bleeding risks Patient with confirmed DVT Scan confirms superficial thrombophlebitis
Cover Page. The handle holds various files of this Leiden University dissertation
 Cover Page The handle http://hdl.handle.net/1887/40114 holds various files of this Leiden University dissertation Author: Exter, Paul L. den Title: Diagnosis, management and prognosis of symptomatic and
Cover Page The handle http://hdl.handle.net/1887/40114 holds various files of this Leiden University dissertation Author: Exter, Paul L. den Title: Diagnosis, management and prognosis of symptomatic and
ESIM 2014 Clinical Case Presentation Israel. Ben-Sasson Maayan Bnei-Zion medical center Haifa
 ESIM 2014 Clinical Case Presentation Israel Ben-Sasson Maayan Bnei-Zion medical center Haifa Presentation A 24 YO male,a ping-pong player, presented to the ER with acute onset of right upper extremity
ESIM 2014 Clinical Case Presentation Israel Ben-Sasson Maayan Bnei-Zion medical center Haifa Presentation A 24 YO male,a ping-pong player, presented to the ER with acute onset of right upper extremity
COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP)
 The European Agency for the Evaluation of Medicinal Products Evaluation of Medicines for Human Use London, 16 December 1999 COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP) NOTE FOR GUIDANCE ON CLINICAL
The European Agency for the Evaluation of Medicinal Products Evaluation of Medicines for Human Use London, 16 December 1999 COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP) NOTE FOR GUIDANCE ON CLINICAL
Proper Diagnosis of Venous Thromboembolism (VTE)
 Proper Diagnosis of Venous Thromboembolism (VTE) Whal Lee, M.D. Seoul National University Hospital Department of Radiology 2 nd EFORT Asia Symposium, 3 rd November 2010, Taipei DVT - Risk Factors Previous
Proper Diagnosis of Venous Thromboembolism (VTE) Whal Lee, M.D. Seoul National University Hospital Department of Radiology 2 nd EFORT Asia Symposium, 3 rd November 2010, Taipei DVT - Risk Factors Previous
Disclosures. DVT: Diagnosis and Treatment. Questions To Ask. Dr. Susanna Shin - DVT: Diagnosis and Treatment. Acute Venous Thromboembolism (VTE) None
 Disclosures DVT: Diagnosis and Treatment None Susanna Shin, MD, FACS Assistant Professor University of Washington Acute Venous Thromboembolism (VTE) Deep Venous Thrombosis (DVT) Pulmonary Embolism (PE)
Disclosures DVT: Diagnosis and Treatment None Susanna Shin, MD, FACS Assistant Professor University of Washington Acute Venous Thromboembolism (VTE) Deep Venous Thrombosis (DVT) Pulmonary Embolism (PE)
Cardiovascular Disease
 Cardiovascular Disease Chapter 15 Introduction Cardiovascular disease (CVD) is the leading cause of death in the U.S. One American dies from CVD every 33 seconds Nearly half of all Americans will die from
Cardiovascular Disease Chapter 15 Introduction Cardiovascular disease (CVD) is the leading cause of death in the U.S. One American dies from CVD every 33 seconds Nearly half of all Americans will die from
