Homocysteinuria is a rare inborn error of metabolism that
|
|
|
- Elisabeth Nelson
- 5 years ago
- Views:
Transcription
1 Increased Serum Homocysteine and Sudden Death Resulting from Coronary Atherosclerosis With Fibrous Plaques Allen P. Burke, V. Fonseca, Frank Kolodgie, Arthur Zieske, Louis Fink, Renu Virmani Introduction Modest elevations of total homocysteine have been associated with increased risk for coronary atherosclerosis but correlation between elevated homocysteine and plaque morphology has not been described in humans. Methods We determined serum homocysteine at postmortem from 87 men with coronary thrombus (62 of whom were diagnosed as acute), from 35 men with severe coronary disease without thrombus, and from 46 controls. In coronary deaths, atherosclerotic plaques at the sites of maximal luminal narrowing of the four epicardial coronary arteries were classified as fibrous plaques, fibrous cap atheromas, thin-cap atheromas, and healed ruptures, and macrophage infiltration was assessed semiquantitatively. Results Median serum homocysteine postmortem as a result of acute thrombus was 10.4 mol/l (P 0.4 versus controls), 12.1 mol/l in men with organized thrombi (P 0.1 versus controls), 15.6 mol/l in men without thrombus (P versus controls), and 9.8 mol/l in controls. The median homocysteine was 12.1 mol/l in 65 men with healed infarcts (P 0.03 versus controls). The number of fibrous plaques was associated with log-normalized homocysteine (P 0.004), independent of age, albumin, smoking, hypertension, and serum cholesterol. Homocysteine levels in the upper tertile ( 15 mol/l) were associated with sudden death without acute or organized thrombus (odds ratio 3.8, P 0.03) independent of age and other risk factors; the coexistence of diabetes increased the association (odds ratio 25.1, P 0.009, versus lowest tertile 8.5 mol/l). Conclusions Increased serum homocysteine is associated with sudden death in the absence of acute coronary thrombosis, especially with concomitant diabetes, and with the presence of lipid-poor, fibrous plaques. (Arterioscler Thromb Vasc Biol. 2002;22: ) Key Words: homocysteine diabetes coronary artery disease sudden death thrombosis Homocysteinuria is a rare inborn error of metabolism that is a result of cystathionine -synthase deficiency and results in a high ( 100 mol per liter) plasma homocysteine and premature mortality resulting from thromboembolic events. 1 The mechanism of thrombosis is unclear but may be related to an effect of homocysteine on coagulation, decreased resistance of the endothelium to thrombosis, and inhibition of nitric oxide mediated vasodilation. In contrast, modest elevations of total homocysteine between 10 to 100 mol per liter are due to variations in vitamin B intake and genetic factors, particularly 5,10-methylenetetrahydrofolate reductase polymorphism. 2 There has been a link between modest elevations of total homocysteine with acute myocardial infarction, 3 stroke, 4 aortic atherosclerosis, 5 and mortality in patients with known coronary artery disease. 6 Because thrombosis is a component of the progression of atherosclerosis, small increases in total homocysteine may accelerate atherosclerosis by a thrombotic mechanism. 7 However, mechanisms independent of thrombosis may play a role in homocysteine-mediated atherogenesis, 8 and unstable coronary syndromes are not always associated with elevations of total homocysteine. 9 There has as yet been no study measuring total homocysteine in sudden coronary death victims or studies correlating total homocysteine with coronary plaque morphology. In patients who die suddenly of coronary artery disease, the coronary findings are heterogeneous. Potential mechanisms for sudden death caused by severe coronary disease include plaque rupture or erosion with luminal thrombosis and nonthrombotic mechanisms in patients without arterial thrombi, which may include myocardial factors such as hypertrophy and healed infarcts and coronary spasm overlying stable plaque. 10 The purpose of this study was to compare homocysteine levels in men who died suddenly with coronary thrombosis or with severe coronary artery disease without thrombosis to a control set of men who died of noncoronary causes. In addition, the types of coronary plaque are be correlated with homocysteine levels using a recent classification adapted from morphological studies of sudden-death victims. 11 The results of these data will demonstrate whether Received July 1, 2002; revision accepted July 29, From the Department of Cardiovascular Pathology, Armed Forces Institute of Pathology, Washington, DC (R.V., A.P.B., F.K.); the Veteran s Affairs Medical Center (L.F., V.F.), Little Rock, Ark; and Louisiana State University (A.Z.), New Orleans, La. Correspondence to Renu Virmani, MD, Chairperson, Department of Cardiovascular Pathology, Armed Forces Institute of Pathology, Washington, DC. virmani@afip.osd.mil 2002 American Heart Association, Inc. Arterioscler Thromb Vasc Biol. is available at DOI: /01.ATV
2 Burke et al Homocysteine and Sudden Coronary Death 1937 elevations of homocysteine that have been seen in patients with severe coronary disease correlate with coronary thrombosis or stable plaque and whether homocysteine is elevated in patients who die suddenly with severe coronary disease compared with controls. Materials and Methods Cardiac Dissection Hearts from 122 men who died suddenly of severe coronary artery disease were studied. Risk factor data without homocysteine analysis, definitions of sudden coronary death, and cardiac dissection techniques have been reported previously for these cases. 7,10 In addition, sera and risk factor data were obtained from 46 male control noncoronary deaths. The epicardial arteries of the study patients were evaluated at 3- to 4-mm intervals and each segment with a gross estimation of 50 cross-sectional luminal narrowing or evidence of thrombus were studied histologically. Morphological Analysis We assessed the relationship of homocysteine levels to the nature of the culprit lesion, whether a fibrous plaque, acute thrombus (rupture or acute plaque erosion), organized thrombus, or no significant coronary lesion in the case of control patients. Stable culprit plaque was defined as one or more segments with 75 crosssectional area luminal narrowing (severe coronary disease) in the absence of acute coronary thrombus. Coronary deaths with stable culprit plaque were subclassified as cases of healed infarcts (area of fibrosis 1 cm in greatest diameter) with or without organizing or organized thrombi; stable plaque with or without organizing or old coronary thrombi but absence of healed infarction; and 75 cross-sectional area luminal narrowing and absence of healed infarction and organizing or organized thrombi. Acute ruptures and erosions were defined as previously reported. 12 We also assessed the relationship of homocysteine to quantitation of types of plaques in hearts with severe coronary disease. Plaques were classified as predominantly fibrous plaque when the plaque consisted of fibrous tissue, smooth muscle cells, few macrophages with or without calcification, fibrous cap atheroma with a lipid-rich necrotic core, thin-cap atheroma, recanalized thrombus, and healed plaque rupture, as previously described. 11 In the coronary cases, 11 4 sections (excluding acute thrombi) were examined. Fibrous plaque denoted an absence of a lipid-rich core and 0 to 1 semiquantitative analysis of macrophage infiltrates (see below). Fibroatheroma, in contrast, demonstrated a core filled with cholesterol clefts and macrophage cellular debris. Thin-cap atheroma denoted an area of thinning over the lipid core and was focally 65 m in thickness, as previously defined. 10 A semiquantitative assessment of macrophage infiltration, assessed by avidin biotin immunohistochemical staining for CD68 (Dako, Carpinteria, Calif, 1:200), was assessed as follows: 0, rare or few macrophages; 1, isolated macrophages limited to surface plaque; 2, isolated macrophages present throughout the plaque and surrounding lipid core; 3, focal clusters of macrophages within the fibrous cap and within lipid core; and 4, sheets of macrophages within the fibrous cap and diffuse CD68 staining within lipid core. Healed ruptures were determined by staining with Sirius Red and assessing breaks in the fibrous cap using polarized light. 7 The numbers of each of these plaques were counted in each specimen, and these values compared among groups of men with and without serum homocysteine elevation. Determination of Homocysteine Total serum homocysteine cysteine, mixed disulfides, and proteinbound homocysteine was measured by high-performance liquid chromatography, coupled with fluorescence detectometer, on autopsy sera. 13 In all cases, blood was centrifuged and separated into serum at the time of autopsy and frozen at 70 C and batched for measurement of homocysteine. Determination of Other Risk Factors In addition to homocysteine, the interaction of other traditional risk factors was assessed. Diabetes mellitus was determined based on history and percent glycohemoglobin determination on postmortem red blood cells. Greater than 8 glycohemoglobin indicated glucose intolerance and 10 indicated overt diabetes. 14 Cigarette smoking was determined based on history and postmortem evaluation of thiocyanate. Total and HDL cholesterol and serum albumin were measured as previously described. 15,16 Hypertensive renovascular changes were identified based on previous criteria. 7,10,16 18 For determination of increased left ventricular mass, hearts were weighed to the nearest gram before fixation, after removal of intracavitary blood, pericardium, and great vessels 2 to 3 cm above the semilunar valves. Statistical Analysis Univariate comparisons of serum homocysteine were performed by Mann Whitney unpaired two group test. Because homocysteine levels are not distributed normally, log-transformed values were used for Student t test and ANOVA. In correlating culprit plaques with homocysteine tertiles, multivariate analysis was performed using logistic regression with dependent variable in the presence or absence of morphological finding (eg, presence of sudden death with stable plaque). For determination of odds ratios, serum homocysteine levels were grouped into lowest ( 8.5), middle (8.5 to 15), and upper tertiles ( 15 Mol/L). The odds ratios are presented comparing the highest versus the lowest tertile. The correlation of numbers of nonculprit plaque types with log-transformed homocysteine levels, multiple linear regression was used. Software from SAS Institute (Statview, Cary, NC), was used. Results Patient Age and Presence of Infarct The mean age of the 122 men with coronary disease was years. Of these, there were 62 acute coronary thrombi (aged 48 9 years), of which 46 were plaque ruptures (49 9 years) and 16 plaque erosions (46 9 years). An additional 25 men who died with coronary disease demonstrated organized thrombi, and 15 of the men with acute thrombi had organized thrombi as well. The mean age of the 25 men with organized thrombi was years. Thirty-five hearts in the severe coronary disease group showed no thrombi, acute or organized (mean age years, Table 1). Healed infarcts were present in 65 hearts and were distributed in all groups (mean age years) but were especially frequent in hearts with organized thrombi (Table 1). The control men were aged years and died of unnatural traumatic causes (n 36) and noncoronary cardiac causes (n 10); in no case was there 50 cross-sectional area luminal area narrowing by atherosclerotic plaque. Effect of Postmortem Interval on Homocysteine Levels By simple regression, there was no effect of postmortem interval on log-normalized homocysteine using all samples (r ) or values 15 mol/l/l (r ). Analysis of Homocysteine Levels of Coronary and Control Deaths by Culprit Plaque By univariate analysis, serum homocysteine levels were elevated in men who died with coronary disease compared with controls (median 1.05 mol/l versus 9.8 mol/ml, P 0.05, Table 1). When analyzed by culprit plaque morphology, homocysteine was especially elevated in the absence of acute or organized thrombus compared with controls (median
3 1938 Arterioscler Thromb Vasc Biol. November 2002 TABLE 1. Homocysteine Levels by Culprit Lesion Culprit lesion (n; age, y SD; healed infarcts Hcy, Median P vs Log Hcy SD Pvs Albumin, mg/dl SD htn Smokers Any thrombus (87; 49 11; 58) Acute thrombi (62; 48 9; 48) Organized thrombi (25; 50 11; 84) No thrombus (35; 53 11; 44) All coronary deaths (122) (46; 51 12) Total (168) Hcy indicates homocysteine; htn, hypertension 9.8 mol/l/l versus 15.6 mol/l/l, P 0.007, controls versus coronary deaths without thrombus). The median and mean log-transformed homocysteine levels were intermediate in the organized thrombus group, reaching borderline statistical significance (P 0.05 using log-transformed data, Table 1). Mean and median homocysteine levels were only slightly increased over controls in the acute thrombus group (P 0.1, Table 1). Although there was a significant correlation between maximal percent cross-sectional luminal narrowing and log-transformed serum homocysteine levels (P 0.03), the correlation was weak (r ). Univariate Analysis of Serum Homocysteine and Other Risk Factors There was a significant weakly positive correlation between log-transformed homocysteine and age (P 0.03, r ) and a positive but insignificant correlation with heart weight (r ), glycohemoglobin (r ), albumin (r ), presence or absence of diabetes (P 0.4), and presence of hypertension (P 0.3). There was a negative, insignificant correlation between serum homocysteine and body mass index (r ), total/hdl cholesterol ratio (r ), and cigarette smoking (P 0.7) Multivariate Analysis of Homocysteine Levels by Culprit Plaque Using multivariable analysis, including as covariates age, body mass index, serum albumin, hypertension, history of smoking, and total/hdl cholesterol ratio in all cases examined, men in the highest tertile ( 15 mol/l) of homocysteine were significantly more likely to have stable plaque without acute or organized thrombus (odds ratio 3.8, range 1.1 to 12.9, P 0.03, versus lowest tertile). When the additive effect of diabetes and homocysteine was examined, diabetic men with serum homocysteine in the upper tertile as compared with the lowest tertile ( 8.5 mol/l) were more likely to die with stable plaque (odds ratio 25.1, range 2.2 to 281, P 0.009). When the percentage of men who died without acute thrombus was plotted against the presence of diabetes and elevated homocysteine in the highest tertile, there appeared to be an additive effect of diabetes and homocysteine elevation for men who died with stable plaque without acute thrombus (Figure 1). Homocysteine Levels and the Presence of Myocardial Infarction Table 2 shows that the presence of healed infarcts was associated with elevated homocysteine. There was no difference in the control and acute infarct groups. Association Between Types of Nonculprit Plaques and Serum Homocysteine The numbers of recanalized thrombi (Figure 2A) and fibrous cap atheromas (Figure 2B) did not significantly vary by homocysteine tertile. Thin-cap atheromas were more frequent in lower tertiles of homocysteine (Figure 2C). Fibrous plaques were the most numerous in the highest tertile (Figure 2D). There were fewer healed plaque ruptures in the highest serum homocysteine tertile compared with the lowest (Figure 2E). Mean macrophage index was least in the highest tertile of homocysteine (Figure 2F). By multivariate analysis, numbers of fibrous plaques was associated with log-normalized homocysteine (P , t 2.9), independent of age, albumin, smoking, renovascular changes of hypertension, and total/hdl cholesterol. Discussion Homocysteine Levels in Sudden-Death Victims The current study demonstrates that homocysteine is elevated in sudden death as a result of severe coronary artery disease without acute or organized coronary thrombosis. In addition, this association seems to be increased if there is concomitant diabetes mellitus. Whether these data suggest that reduction of serum homocysteine may reduce the rate of sudden coronary death in men remains unknown. Whether elevated serum homocysteine may be causally associated with sudden Figure 1. The relationship of diabetes and homocysteine elevation to stable plaque. The proportion of deaths resulting from stable plaque was increased with homocysteine and diabetes, with an additive effect.
4 Burke et al Homocysteine and Sudden Coronary Death 1939 TABLE 2. Homocysteine Levels by Presence of Infarct Infarct (n; age, y SD) Hcy, Median Pvs Log Hcy SD P, vs Albumin, mg/dl SD htn Smokers Coronary disease, no infarct (49; 48 11) Coronary disease, acute infarct (8; 45 9) Coronary disease, healed infarct (65; 52 10) (46; 51 12) Total (168) death or merely a marker of a process related to sudden death is unclear. A prospective clinical study linked elevated serum homocysteine to all mortality in patients with clinically documented coronary disease, 6 suggesting that the association between homocysteine and sudden death may not be coincidental. Folsom et al, 19 however, did not show a relationship between serum homocysteine and acute coronary events independent of serum vitamin levels and vitamin use. Cross-sectional studies have demonstrated an increased risk for coronary events in patients with elevated serum homocysteine. The association between healed myocardial infarct and elevated serum homocysteine in the current study is consistent with clinical findings relating elevated serum homocysteine with a history of previous myocardial infarction. 6 The association between homocysteine and acute infarction has been questioned because of the apparent acute phase reactant effect of homocysteine, which has been suggested in a study comparing serum homocysteine at days 1 and 3 after acute infarction. 20 Other studies have suggested, however, that homocysteine is independent of C-reactive protein levels 21 and may reflect the degree of myocyte necrosis. 22 The current study demonstrates that instantaneous deaths with stable plaque in the absence of an acute or organized thrombus, which demonstrated necrosis in 2 of cases, were associated with increased homocysteine levels, unlike death as a result of acute coronary thrombi, which was associated with myocyte necrosis in 17 of patients. Therefore, it seems likely that homocysteine is a marker for stable coronary plaque, as opposed to a marker for an acute response to an inflammatory reaction secondary to acute ischemia. Figure 2. Nonculprit plaque types by homocysteine tertiles. For homocysteine, the lowest tertile was 8.5, the middle 8.5 to 15, and the upper tertile 15 Mol/L. There was no significant difference in numbers of recanalized thrombi (A) or fibrous cap atheromas with lipid cores (B). Thin-cap atheromas decreased with increasing homocysteine (C); the difference between mid- and highest tertile was significant to P 0.04(ANOVA means table, Fisher s post hoc test). Stable plaques were increased with elevated homocysteine (D); the difference between lowest tertile with the highest tertile was significant (P 0.01). There was a decrease in healed plaque ruptures with increasing homocysteine (E). Macrophage index was significantly decreased in highest tertile of homocysteine (P 0.01 versus lowest tertile) (F). Values are mean SD.
5 1940 Arterioscler Thromb Vasc Biol. November 2002 Homocysteine Is Not Associated With Acute Atherothrombosis But With Fibrous Plaque Although the current study did not measure serum levels of pyridoxal 5 -phosphate and folate, which are inversely proportional to homocysteine levels, or gather data regarding vitamin use, it provides morphological data establishing a link between homocysteine and a specific type of coronary plaque, namely fibrous plaque. In particular, there was no association in our study between fatal acute coronary thrombosis and serum homocysteine. The implications of these findings are unclear, but they may explain in part negative studies showing no association between homocysteine and acute coronary events, which are presumably triggered by atherothrombosis. 9,23 The weak association between homocysteine and organized thrombus appears contradictory, given the lack of link between homocysteine and acute thrombus. It is likely that this association is due to the fact that organized thrombi were very prevalent (84) in hearts with healed myocardial infarcts. The same mechanism associating hyperhomocysteinemia with fibrous plaque formation may be at play in scar formation in the myocardium, but this hypothesis remains speculative. Until recently, it was debated whether hyperhomocysteinemia results in increased atheroma formation, that is, is atherogenic, or whether the increased susceptibility to coronary events in patients with elevated serum homocysteine is mediated by functional abnormalities such as vasospasm. 24 Animal studies have suggested the former because apoe-null mice develop larger lesions in the aorta when the diet is modified to increase serum homocysteine compared with normal levels. 25,26 Interestingly, the lesions described by Zhou et al 26 were fibrous-rich, similar to the human lesions described in the current study. The association between elevated homocysteine and fibrous plaques hearkens back to the seminal observations of McCully, 27 who described fibrocalcific plaques in patients with congenital homocysteinemia. The current study shows a marked difference in the types of plaque in men with elevations of homocysteine compared with those with hypercholesterolemia. It has been demonstrated that elevated cholesterol is associated with features of plaques that are associated with ruptures, including thincapped atheroma, acute plaque rupture, and healed plaque rupture. 7,10 The current study demonstrates that features of plaque associated with rupture are less frequent in men with elevated homocysteine levels, suggesting a different method of plaque progression. These data suggest that homocysteine may not result in plaque instability as currently understood. Therefore, efforts to reduce serum homocysteine may be complementary to lipid reduction because plaque fibrosis may occur via a distinct mechanism. One possible mechanism that may contribute to sudden death in hyperhomocystinemic patients without overt thrombosis may be endothelial dysfunction. Endothelial dysfunction is well known to occur in hyperhomocysteinemia and can be corrected by folate supplementation. 28 Interaction Between Diabetes and Hyperhomocysteinemia The observed interaction between diabetes and hyperhomocysteinemia in our study is interesting and compatible with other report in the literature. Recent studies have demonstrated that total homocysteine is an important risk factor even in patients who are already at high risk, such as those with type 2 diabetes. 29,30 In the Hoorn study, hyperhomocysteinemia increased the risk of death in all subjects, 29 but the effect was greater in patients with type 2 diabetes. Total homocysteine is frequently elevated in patients with type 2 diabetes who have coexistent cardiovascular disease. 31 In contrast, patients with diabetes without vascular disease may have low total homocysteine, but total homocysteine is still a predictor of mortality. In patients with diabetic nephropathy, the risk of mortality may be even greater 30 and recent data suggest complex derangement of homocysteine metabolism in these patients. 31 It is possible that recently described effects of glucose and insulin on homocysteine metabolism play a role in elevating homocysteine levels in diabetic patients. 32 Mechanism of Atherogenesis and Increased Homocysteine Although the current study does not address mechanisms, the observation linking increased homocysteine with fibrous plaques with or without calcification suggests, as mentioned above, a distinct mechanism of atherogenesis from that induced by hyperlipidemia, which is believed to be mediated largely by inflammatory cells, especially macrophages. Experimental studies have shown that homocysteine upregulates endothelial endoplasmic reticulum stress-response genes, 33 may induce proliferation of smooth muscle cells, 8 and results in upregulation of nuclear factor B in smooth muscle cells. 34 Although further studies relating risk factors and plaque morphology are necessary, the current study suggests, similar to previous work, that plaque morphology may reflect distinct mechanisms of atherogenesis induced by different risk factors, underscoring the heterogeneity of the atherosclerotic process. Study Limitations Because the current study uses autopsy specimens, there are inherent errors in postmortem risk-factor determinations. Although homocysteine levels increase with the duration of blood cells in contact with serum, between 1 and 25 in a 4-hour interval, we were unable to demonstrate significant increases in overall homocysteine levels with increasing postmortem intervals. Another potential confounding effect is the increase in homocysteine seen in patients with renal failure. 38 The association, however, between homocysteine and renal failure in patients with acute coronary syndromes has been shown to be minor, 39 and in the current study the associated between homocysteine and fibrous plaques appeared to be independent of renovascular hypertensive changes and serum albumin. Conclusion Elevated serum homocysteine is associated with sudden unexpected death in men and is especially associated with
6 Burke et al Homocysteine and Sudden Coronary Death 1941 diabetes. Although hyperhomocysteinuria is associated with unstable coronary syndromes, the mechanism of sudden coronary death in men with modest elevations of homocysteine does not seem to be mediated via a thrombotic mechanism. Elevated serum homocysteine is associated with an increase in fibrous plaques and a relative decrease in thin-cap atheromas, suggesting a different mechanism of atherogenesis from that of hypercholesterolemia. References 1. Mudd SH, Skovby F, Levy HL, Pettigrew KD, Wilcken B, Pyeritz RE, Andria G, Boers GH, Bromberg IL, Cerone R, Fowler B, Gröbe H, Schmidt H, Schweitzer L. The natural history of homocystinuria due to cystathionine beta-synthase deficiency. Am J Hum Genet. 1985;37: Ma J, Stampfer MJ, Hennekens CH, Frosst P, Selhub J, Horsford J, Malinow MR, Willett WC, Rozen R. Methylenetetrahydrofolate reductase polymorphism, plasma folate, homocysteine, and risk of myocardial infarction in US physicians. Circulation. 1996;94: Israelsson B, Brattstrom LE, Hultberg BL. Homocysteine and myocardial infarction. Atherosclerosis. 1988;71: Perry IJ, Refsum H, Morris RW, Ebrahim SB, Ueland PM, Shaper AG. Prospective study of serum total homocysteine concentration and risk of stroke in middle-aged British men. Lancet. 1995;346: Tribouilloy CM, Peltier M, Iannetta Peltier MC, Trojette F, Andrejak M, Lesbre JP. Plasma homocysteine and severity of thoracic aortic atherosclerosis. Chest. 2000;118: Nygård O, Nordrehaug JE, Refsum H, Ueland PM, Farstad M, Vollset SE. Plasma homocysteine levels and mortality in patients with coronary artery disease. N Engl J Med. 1997;337: Burke AP, Kolodgie FD, Farb A, Weber DK, Malcom GT, Smialek J, Virmani R. Healed plaque ruptures and sudden coronary death: evidence that subclinical rupture has a role in plaque progression. Circulation. 2001;103: Tsai JC, Perrella MA, Yoshizumi M, Hsieh CM, Haber E, Schlegel R, Lee ME. Promotion of vascular smooth muscle cell growth by homocysteine: a link to atherosclerosis. Proc Natl Acad Sci U S A. 1994;91: Verhoef P, Hennekens CH, Allen RH, Stabler SP, Willett WC, Stampfer MJ. Plasma total homocysteine and risk of angina pectoris with subsequent coronary artery bypass surgery. Am J Cardiol. 1997;79: Burke AP, Farb A, Malcom GT, Liang Y-H, Smialek J, Virmani R. Coronary risk factors and plaque morphology in patients with coronary disease dying suddenly. N Engl J Med. 1997;336: Virmani R, Kolodgie FD, Burke AP, Farb A, Schwartz SM. Lessons from sudden coronary death: a comprehensive morphological classification scheme for atherosclerotic lesions. Arterioscler Thromb Vasc Biol. 2000; 20: Farb A, Burke AP, Tang A, Liang Y-H, Mannan P, Smialek J, Virmani R. Coronary plaque erosion without rupture into a lipid core: a frequent cause of coronary thrombosis in sudden coronary death. Circulation. 1996;93: Fonseca VA, Stone A, Munshi M, Baliga BS, Aljada A, Thusu K, Fink L, Dandona P. Oxidative stress in diabetic macrovascular disease: does homocysteine play a role? South Med J. 1997;90: Burke AP, Farb A, Pestaner J, Malcom GT, Zieske A, Kutys R, Smialek J, Virmani R. Traditional risk factors and the incidence of sudden coronary death with and without coronary thrombosis in blacks. Circulation. 2002;105: McGill H, McMahan C, Malcom G, Oalmann M, Strong J. Relation of glycohemoglobin and adiposity to atherosclerosis in youth: Pathobiological Determinants of Atherosclerosis in Youth (PDAY) Research Group. Arterioscler Thromb Vasc Biol. 1995;15: Strong JP, Malcom GT, Oalmann MC. Environmental and genetic risk factors in early human atherogenesis: lessons from the PDAY study. Pathobiol Determinants Atheroscler Youth Pathol Int. 1995;45: Tracy R, Mercante D, Moncada A, Berenson G. Quantitation of hypertensive nephrosclerosis on an objective rational scale of measure in adults and children. Am J Clin Pathol. 1986;85: Virmani R, Avolio AP, Mergner WJ, Robinowitz M, Herderick EE, Cornhill JF, Guo SY, Liu TH, Ou DY, O Rourke M. Effect of aging on aortic morphology in populations with high and low prevalence of hypertension and atherosclerosis: comparison between occidental and Chinese communities. Am J Pathol. 1991;139: Folsom AR, Nieto FJ, McGovern PG, Tsai MY, Malinow MR, Eckfeldt JH, Hess DL, Davis CE. Prospective study of coronary heart disease incidence in relation to fasting total homocysteine, related genetic polymorphisms, and B vitamins: the Atherosclerosis Risk in Communities (ARIC) study. Circulation. 1998;98: Senaratne MP, Griffiths J, Nagendran J. Elevation of plasma homocysteine levels associated with acute myocardial infarction. Clin Invest Med. 2000;23: Al-Obaidi MK, Stubbs PJ, Amersey R, Noble MI. Acute and convalescent changes in plasma homocysteine concentrations in acute coronary syndromes. Heart. 2001;85: Al-Obaidi MK, Stubbs PJ, Collinson P, Conroy R, Graham I, Noble MI. Elevated homocysteine levels are associated with increased ischemic myocardial injury in acute coronary syndromes. J Am Coll Cardiol. 2000;36: Fallon UB, Ben-Shlomo Y, Elwood P, Ubbink JB, Smith GD. Homocysteine and coronary heart disease in the Caerphilly cohort: a 10 year follow up. Heart. 2001;85: Lentz SR. Does homocysteine promote atherosclerosis? Arterioscler Thromb Vasc Biol. 2001;21: Hofmann MA, Lall E, Lu Y, Gleason MR, Wolf BM, Tanji N, Ferran LJ, Kohl B, Rao V, Kiseil W, Stern DM, Schmidt AM. Hyperhomocysteinemia enhances vascular inflammation and accelerates atherosclerosis in a murine model. J Clin Invest. 2001;107: Zhou J, Moller J, Danielson CC, Bentzon J, Ravn HB, Austin RC, Falk E. Hyperhomocysteinemia promotes the development of collagen-rich and stable plaques in apoe-deficient mice. Arterioscler Thromb Vasc Biol. 2001;21: McCully KS. Vascular pathology of homocysteinemia: implications for the pathogenesis of arteriosclerosis. Am J Pathol. 1969;56: Chambers JC, Ueland PM, Obeid OA, Wrigley J, Refsum H, Kooner JS. Improved vascular endothelial function after oral B vitamins: an effect mediated through reduced concentrations of free plasma homocysteine. Circulation. 2000;102: Hoogeveen EK, Kostense PJ, Jakobs C, Dekker JM, Nijpels G, Heine RJ, Bouter LM, Stehouwer CD. Hyperhomocysteinemia increases risk of death, especially in type 2 diabetes: 5-year follow-up of the Hoorn Study. Circulation. 2000;101: Stehouwer CD, Gall MA, Hougaard P, Jakobs C, Parving HH. Plasma homocysteine concentration predicts mortality in non-insulin-dependent diabetic patients with and without albuminuria. Kidney Int. 1999;55: Poirier LA, Brown AT, Fink LM, Wise CK, Randolph CJ, Delongchamp RR, Fonseca VA. Blood S-adenosylmethionine concentrations and lymphocyte methylenetetrahydrofolate reductase activity in diabetes mellitus and diabetic nephropathy. Metabolism. 2001;50: Dicker-Brown A, Fonseca VA, Fink LM, Kern PA. The effect of glucose and insulin on the activity of methylene tetrahydrofolate reductase and cystathionine-beta-synthase: studies in hepatocytes. Atherosclerosis. 2001;158: Kokame K, Kato H, Miyata T. Nonradioactive differential display cloning of genes induced by homocysteine in vascular endothelial cells. Methods. 1998;16: Wang G, Siow YL, O K. Homocysteine stimulates nuclear factor kappab activity and monocyte chemoattractant protein-1 expression in vascular smooth-muscle cells: a possible role for protein kinase C. Biochem J. 2000;352 Pt 3: Duarte NL, Wang XL, Wilcken DE. Effects of anticoagulant and time of plasma separation on measurement of homocysteine. Clin Chem. 2002; 48: Nauck M, Bisse E, Wieland H. Pre-analytical conditions affecting the determination of the plasma homocysteine concentration. Clin Chem Lab Med. 2001;39: Caliskan S, Kuralay F, Onvural B. Effect of anticoagulants on plasma homocysteine determination. Clin Chim Acta. 2001;309: Jacques PF, Bostom AG, Wilson PW, Rich S, Rosenberg IH, Selhub J. Determinants of plasma total homocysteine concentration in the Framingham Offspring cohort. Am J Clin Nutr. 2001;73: Jonasson T, Ohlin H, Andersson A, Arnadottir M, Hultberg B. Renal function exerts only a minor influence on high plasma homocysteine concentrations in patients with acute coronary syndromes. Clin Chem Lab Med. 2002;40:
Pathology of Vulnerable Plaque Angioplasty Summit 2005 TCT Asia Pacific, Seoul, April 28-30, 2005
 Pathology of Vulnerable Plaque Angioplasty Summit 25 TCT Asia Pacific, Seoul, April 28-3, 25 Renu Virmani, MD CVPath, A Research Service of the International Registry of Pathology Gaithersburg, MD Plaque
Pathology of Vulnerable Plaque Angioplasty Summit 25 TCT Asia Pacific, Seoul, April 28-3, 25 Renu Virmani, MD CVPath, A Research Service of the International Registry of Pathology Gaithersburg, MD Plaque
Elevated C-Reactive Protein Values and Atherosclerosis in Sudden Coronary Death. Association With Different Pathologies
 Elevated C-Reactive Protein Values and Atherosclerosis in Sudden Coronary Death Association With Different Pathologies Allen P. Burke, MD; Russell P. Tracy, PhD; Frank Kolodgie, PhD; Gray T. Malcom, PhD;
Elevated C-Reactive Protein Values and Atherosclerosis in Sudden Coronary Death Association With Different Pathologies Allen P. Burke, MD; Russell P. Tracy, PhD; Frank Kolodgie, PhD; Gray T. Malcom, PhD;
Pathology of the Vulnerable Plaque
 Journal of the American College of Cardiology Vol. 47, No. 8 Suppl C 2006 by the American College of Cardiology Foundation ISSN 0735-1097/06/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2005.10.065
Journal of the American College of Cardiology Vol. 47, No. 8 Suppl C 2006 by the American College of Cardiology Foundation ISSN 0735-1097/06/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2005.10.065
REVIEW ARTICLE. Blood Levels of Homocysteine and Increased Risks of Cardiovascular Disease
 Blood Levels of Homocysteine and Increased Risks of Cardiovascular Disease Causal or Casual? REVIEW ARTICLE William G. Christen, ScD; Umed A. Ajani, MBBS; Robert J. Glynn, ScD; Charles H. Hennekens, MD
Blood Levels of Homocysteine and Increased Risks of Cardiovascular Disease Causal or Casual? REVIEW ARTICLE William G. Christen, ScD; Umed A. Ajani, MBBS; Robert J. Glynn, ScD; Charles H. Hennekens, MD
The New England Journal of Medicine CORONARY RISK FACTORS AND PLAQUE MORPHOLOGY IN MEN WITH CORONARY DISEASE WHO DIED SUDDENLY
 CORONARY RISK FACTORS AND PLAQUE MORPHOLOGY IN MEN WITH CORONARY DISEASE WHO DIED SUDDENLY ALLEN P. BURKE, M.D., ANDREW FARB, M.D., GRAY T. MALCOM, PH.D., YOU-HUI LIANG, M.D., JOHN SMIALEK, M.D., AND RENU
CORONARY RISK FACTORS AND PLAQUE MORPHOLOGY IN MEN WITH CORONARY DISEASE WHO DIED SUDDENLY ALLEN P. BURKE, M.D., ANDREW FARB, M.D., GRAY T. MALCOM, PH.D., YOU-HUI LIANG, M.D., JOHN SMIALEK, M.D., AND RENU
Arteriosclerosis & Atherosclerosis
 Arteriosclerosis & Atherosclerosis Arteriosclerosis = hardening of arteries = arterial wall thickening + loss of elasticity 3 types: -Arteriolosclerosis -Monckeberg medial sclerosis -Atherosclerosis Arteriosclerosis,
Arteriosclerosis & Atherosclerosis Arteriosclerosis = hardening of arteries = arterial wall thickening + loss of elasticity 3 types: -Arteriolosclerosis -Monckeberg medial sclerosis -Atherosclerosis Arteriosclerosis,
Pathology of Coronary Artery Disease
 Pathology of Coronary Artery Disease Seth J. Kligerman, MD Pathology of Coronary Artery Disease Seth Kligerman, MD Assistant Professor Medical Director of MRI University of Maryland Department of Radiology
Pathology of Coronary Artery Disease Seth J. Kligerman, MD Pathology of Coronary Artery Disease Seth Kligerman, MD Assistant Professor Medical Director of MRI University of Maryland Department of Radiology
Imaging Overview for Vulnerable Plaque: Data from IVUS Trial and An Introduction to VH-IVUS Imgaging
 Imaging Overview for Vulnerable Plaque: Data from IVUS Trial and An Introduction to VH-IVUS Imgaging Gary S. Mintz,, MD Cardiovascular Research Foundation New York, NY Today, in reality, almost everything
Imaging Overview for Vulnerable Plaque: Data from IVUS Trial and An Introduction to VH-IVUS Imgaging Gary S. Mintz,, MD Cardiovascular Research Foundation New York, NY Today, in reality, almost everything
TVA_C02.qxd 8/8/06 10:27 AM Page 19 PART 2. Pathology
 TVA_C2.qxd 8/8/6 :27 AM Page 19 2 PART 2 Pathology TVA_C2.qxd 8/8/6 :27 AM Page TVA_C2.qxd 8/8/6 :27 AM Page 21 2 CHAPTER 2 The pathology of vulnerable plaque Renu Virmani, Allen P Burke, James T Willerson,
TVA_C2.qxd 8/8/6 :27 AM Page 19 2 PART 2 Pathology TVA_C2.qxd 8/8/6 :27 AM Page TVA_C2.qxd 8/8/6 :27 AM Page 21 2 CHAPTER 2 The pathology of vulnerable plaque Renu Virmani, Allen P Burke, James T Willerson,
Ischemic heart disease
 Ischemic heart disease Introduction In > 90% of cases: the cause is: reduced coronary blood flow secondary to: obstructive atherosclerotic vascular disease so most of the time it is called: coronary artery
Ischemic heart disease Introduction In > 90% of cases: the cause is: reduced coronary blood flow secondary to: obstructive atherosclerotic vascular disease so most of the time it is called: coronary artery
Vulnerable Plaque Pathophysiology, Detection, and Intervention. VP: A Local Problem or Systemic Disease. Erling Falk, Denmark
 Vulnerable Plaque Pathophysiology, Detection, and Intervention VP: A Local Problem or Systemic Disease Erling Falk, Denmark Vulnerable Plaque Pathophysiology, Detection, and Intervention VP: A Local Problem
Vulnerable Plaque Pathophysiology, Detection, and Intervention VP: A Local Problem or Systemic Disease Erling Falk, Denmark Vulnerable Plaque Pathophysiology, Detection, and Intervention VP: A Local Problem
Blood Vessels. Dr. Nabila Hamdi MD, PhD
 Blood Vessels Dr. Nabila Hamdi MD, PhD ILOs Understand the structure and function of blood vessels. Discuss the different mechanisms of blood pressure regulation. Compare and contrast the following types
Blood Vessels Dr. Nabila Hamdi MD, PhD ILOs Understand the structure and function of blood vessels. Discuss the different mechanisms of blood pressure regulation. Compare and contrast the following types
The New England Journal of Medicine ASSOCIATION BETWEEN MULTIPLE CARDIOVASCULAR RISK FACTORS AND ATHEROSCLEROSIS IN CHILDREN AND YOUNG ADULTS
 ASSOCIATION BETWEEN MULTIPLE CARDIOVASCULAR RISK FACTORS AND ATHEROSCLEROSIS IN CHILDREN AND YOUNG ADULTS GERALD S. BERENSON, M.D., SATHANUR R. SRINIVASAN, PH.D., WEIHANG BAO, PH.D., WILLIAM P. NEWMAN
ASSOCIATION BETWEEN MULTIPLE CARDIOVASCULAR RISK FACTORS AND ATHEROSCLEROSIS IN CHILDREN AND YOUNG ADULTS GERALD S. BERENSON, M.D., SATHANUR R. SRINIVASAN, PH.D., WEIHANG BAO, PH.D., WILLIAM P. NEWMAN
Left main coronary artery (LMCA): The proximal segment
 Anatomy and Pathology of Left main coronary artery G Nakazawa Tokai Univ. Kanagawa, Japan 1 Anatomy Difinition Left main coronary artery (LMCA): The proximal segment RCA AV LAD LM LCX of the left coronary
Anatomy and Pathology of Left main coronary artery G Nakazawa Tokai Univ. Kanagawa, Japan 1 Anatomy Difinition Left main coronary artery (LMCA): The proximal segment RCA AV LAD LM LCX of the left coronary
Pathophysiology of Cardiovascular System. Dr. Hemn Hassan Othman, PhD
 Pathophysiology of Cardiovascular System Dr. Hemn Hassan Othman, PhD hemn.othman@univsul.edu.iq What is the circulatory system? The circulatory system carries blood and dissolved substances to and from
Pathophysiology of Cardiovascular System Dr. Hemn Hassan Othman, PhD hemn.othman@univsul.edu.iq What is the circulatory system? The circulatory system carries blood and dissolved substances to and from
State of the Art. Advances in Cardiovascular Imaging. ESC Congres Stockholm September 1, 2010 Frank E. Rademakers, MD, PhD, FESC
 State of the Art Advances in Cardiovascular Imaging ESC Congres Stockholm September 1, 2010 Frank E. Rademakers, MD, PhD, FESC Coronary Artery Disease Content Patho Physiology Imaging requirements Economical
State of the Art Advances in Cardiovascular Imaging ESC Congres Stockholm September 1, 2010 Frank E. Rademakers, MD, PhD, FESC Coronary Artery Disease Content Patho Physiology Imaging requirements Economical
Vascular disease. Structural evaluation of vascular disease. Goo-Yeong Cho, MD, PhD Seoul National University Bundang Hospital
 Vascular disease. Structural evaluation of vascular disease Goo-Yeong Cho, MD, PhD Seoul National University Bundang Hospital resistance vessels : arteries
Vascular disease. Structural evaluation of vascular disease Goo-Yeong Cho, MD, PhD Seoul National University Bundang Hospital resistance vessels : arteries
Laboratory Bulletin...
 Laboratory Bulletin... Updates and Information from Rex Healthcare and Rex Outreach September 1997 Issue Number 24 Homocysteine and vascular risk Introduction: This past June, the New England Journal of
Laboratory Bulletin... Updates and Information from Rex Healthcare and Rex Outreach September 1997 Issue Number 24 Homocysteine and vascular risk Introduction: This past June, the New England Journal of
Elevated serum homocysteine level has a positive correlation with serum cardiac troponin I in patients with acute myocardial infarction
 Bangladesh Med Res Counc Bull 2012; 38: 9-13 Elevated serum homocysteine level has a positive correlation with serum cardiac troponin I in patients with acute myocardial infarction Abstract Alam N, Khan
Bangladesh Med Res Counc Bull 2012; 38: 9-13 Elevated serum homocysteine level has a positive correlation with serum cardiac troponin I in patients with acute myocardial infarction Abstract Alam N, Khan
EAE Teaching Course. Magnetic Resonance Imaging. Competitive or Complementary? Sofia, Bulgaria, 5-7 April F.E. Rademakers
 EAE Teaching Course Magnetic Resonance Imaging Competitive or Complementary? Sofia, Bulgaria, 5-7 April 2012 F.E. Rademakers Complementary? Of Course N Engl J Med 2012;366:54-63 Clinical relevance Treatment
EAE Teaching Course Magnetic Resonance Imaging Competitive or Complementary? Sofia, Bulgaria, 5-7 April 2012 F.E. Rademakers Complementary? Of Course N Engl J Med 2012;366:54-63 Clinical relevance Treatment
Homocysteine and ischaemic stroke in men: the Caerphilly study
 J Epidemiol Community Health 2001;55:91 96 91 Homocysteine and ischaemic stroke in men: the Caerphilly study U B Fallon, P Elwood, Y Ben-Shlomo, J B Ubbink, R Greenwood, G Davey Smith Department of Social
J Epidemiol Community Health 2001;55:91 96 91 Homocysteine and ischaemic stroke in men: the Caerphilly study U B Fallon, P Elwood, Y Ben-Shlomo, J B Ubbink, R Greenwood, G Davey Smith Department of Social
Added Value of Invasive Coronary Imaging for Plaque Rupture and Erosion
 Assessment of Coronary Plaque Rupture and Erosion Added Value of Invasive Coronary Imaging for Plaque Rupture and Erosion Yukio Ozaki, MD, PhD, FACC, FESC Cardiology Dept., Fujita Health Univ. Toyoake,
Assessment of Coronary Plaque Rupture and Erosion Added Value of Invasive Coronary Imaging for Plaque Rupture and Erosion Yukio Ozaki, MD, PhD, FACC, FESC Cardiology Dept., Fujita Health Univ. Toyoake,
2yrs 2-6yrs >6yrs BMS 0% 22% 42% DES 29% 41% Nakazawa et al. J Am Coll Cardiol 2011;57:
 Pathology of In-stent Neoatherosclerosis in BMS and DES 197 BMS, 103 SES, and 106 PES with implant duration >30 days The incidence of neoatherosclerosis was significantly greater in DES (31%) than BMS
Pathology of In-stent Neoatherosclerosis in BMS and DES 197 BMS, 103 SES, and 106 PES with implant duration >30 days The incidence of neoatherosclerosis was significantly greater in DES (31%) than BMS
Abundant evidence has accumulated supporting the association
 Folate, Vitamin B 6, and B 12 Intakes in Relation to Risk of Stroke Among Men Ka He, MD; Anwar Merchant, DMD; Eric B. Rimm, ScD; Bernard A. Rosner, PhD; Meir J. Stampfer, MD; Walter C. Willett, MD; Alberto
Folate, Vitamin B 6, and B 12 Intakes in Relation to Risk of Stroke Among Men Ka He, MD; Anwar Merchant, DMD; Eric B. Rimm, ScD; Bernard A. Rosner, PhD; Meir J. Stampfer, MD; Walter C. Willett, MD; Alberto
Chapter 43 Noninvasive Coronary Plaque Imaging
 hapter 43 Noninvasive oronary Plaque Imaging NIRUDH KOHLI The goal of coronary imaging is to define the extent of luminal narrowing as well as composition of an atherosclerotic plaque to facilitate appropriate
hapter 43 Noninvasive oronary Plaque Imaging NIRUDH KOHLI The goal of coronary imaging is to define the extent of luminal narrowing as well as composition of an atherosclerotic plaque to facilitate appropriate
The 10 th International & 15 th National Congress on Quality Improvement in Clinical Laboratories
 The 10 th International & 15 th National Congress on Quality Improvement in Clinical Laboratories Cardiac biomarkers in atherosclerosis Najma Asadi MD-APCP Ross and Colleagues in 1973: Response to Injury
The 10 th International & 15 th National Congress on Quality Improvement in Clinical Laboratories Cardiac biomarkers in atherosclerosis Najma Asadi MD-APCP Ross and Colleagues in 1973: Response to Injury
Acute coronary syndrome. Dr LM Murray Chemical Pathology Block SA
 Acute coronary syndrome Dr LM Murray Chemical Pathology Block SA13-2014 Acute myocardial infarction (MI) MI is still the leading cause of death in many countries It is characterized by severe chest pain,
Acute coronary syndrome Dr LM Murray Chemical Pathology Block SA13-2014 Acute myocardial infarction (MI) MI is still the leading cause of death in many countries It is characterized by severe chest pain,
Title for Paragraph Format Slide
 Title for Paragraph Format Slide Presentation Title: Month Date, Year Atherosclerosis A Spectrum of Disease: February 12, 2015 Richard Cameron Padgett, MD Executive Medical Director, OHVI Pt RB Age 38
Title for Paragraph Format Slide Presentation Title: Month Date, Year Atherosclerosis A Spectrum of Disease: February 12, 2015 Richard Cameron Padgett, MD Executive Medical Director, OHVI Pt RB Age 38
Myocardial Infarction
 Myocardial Infarction MI = heart attack Defined as necrosis of heart muscle resulting from ischemia. A very significant cause of death worldwide. of these deaths, 33% -50% die before they can reach the
Myocardial Infarction MI = heart attack Defined as necrosis of heart muscle resulting from ischemia. A very significant cause of death worldwide. of these deaths, 33% -50% die before they can reach the
Prevalence of Coronary Artery Disease: A Tertiary Care Hospital Based Autopsy Study
 Article History Received: 03 Feb 2016 Revised: 05 Feb 2016 Accepted: 08 Feb 2016 *Correspondence to: Dr. Alpana Jain Senior demonstrator SMS Medical College, Jaipur, Rajasthan, INDIA. dr.alpana.jain@gmail.com
Article History Received: 03 Feb 2016 Revised: 05 Feb 2016 Accepted: 08 Feb 2016 *Correspondence to: Dr. Alpana Jain Senior demonstrator SMS Medical College, Jaipur, Rajasthan, INDIA. dr.alpana.jain@gmail.com
Atherosclerotic lesions commonly classified as fatty
 Associations of Coronary Heart Disease Risk Factors With the Intermediate Lesion of Atherosclerosis in Youth Henry C. McGill, Jr, C. Alex McMahan, Arthur W. Zieske, Gregory D. Sloop, Jamie V. Walcott,
Associations of Coronary Heart Disease Risk Factors With the Intermediate Lesion of Atherosclerosis in Youth Henry C. McGill, Jr, C. Alex McMahan, Arthur W. Zieske, Gregory D. Sloop, Jamie V. Walcott,
Homocysteine is an amino acid produced as an intermediate
 CLINICAL REVIEW Homocysteine and Vascular Disease Christopher A. Friedrich, MD, PhD, and Daniel J. Rader, MD Homocysteine is an amino acid produced as an intermediate product in the metabolism of methionine,
CLINICAL REVIEW Homocysteine and Vascular Disease Christopher A. Friedrich, MD, PhD, and Daniel J. Rader, MD Homocysteine is an amino acid produced as an intermediate product in the metabolism of methionine,
Independent Risk Factors of Cardiovascular Disease Achieving Healthy Homocysteine Levels
 Independent Risk Factors of Cardiovascular Disease Achieving Healthy Homocysteine Levels AUTHORS: JON LEGERE, BRADLEY RALPH, DR. RON LEGERE 15344 N 83RD WAY, SCOTTSDALE, AZ 85260 TEL: 800.528.3144 EMAIL:
Independent Risk Factors of Cardiovascular Disease Achieving Healthy Homocysteine Levels AUTHORS: JON LEGERE, BRADLEY RALPH, DR. RON LEGERE 15344 N 83RD WAY, SCOTTSDALE, AZ 85260 TEL: 800.528.3144 EMAIL:
Plasma homocysteine concentrations in a Belgian school-age population 1 3
 Plasma homocysteine concentrations in a Belgian school-age population 1 3 Corinne De Laet, Jean-Claude Wautrecht, Daniel Brasseur, Michèle Dramaix, Jean-Marie Boeynaems, Jean Decuyper, and André Kahn ABSTRACT
Plasma homocysteine concentrations in a Belgian school-age population 1 3 Corinne De Laet, Jean-Claude Wautrecht, Daniel Brasseur, Michèle Dramaix, Jean-Marie Boeynaems, Jean Decuyper, and André Kahn ABSTRACT
Lecture 8 Cardiovascular Health Lecture 8 1. Introduction 2. Cardiovascular Health 3. Stroke 4. Contributing Factors
 Lecture 8 Cardiovascular Health 1 Lecture 8 1. Introduction 2. Cardiovascular Health 3. Stroke 4. Contributing Factors 1 Human Health: What s Killing Us? Health in America Health is the U.S Average life
Lecture 8 Cardiovascular Health 1 Lecture 8 1. Introduction 2. Cardiovascular Health 3. Stroke 4. Contributing Factors 1 Human Health: What s Killing Us? Health in America Health is the U.S Average life
10/8/2018. Lecture 9. Cardiovascular Health. Lecture Heart 2. Cardiovascular Health 3. Stroke 4. Contributing Factor
 Lecture 9 Cardiovascular Health 1 Lecture 9 1. Heart 2. Cardiovascular Health 3. Stroke 4. Contributing Factor 1 The Heart Muscular Pump The Heart Receives blood low pressure then increases the pressure
Lecture 9 Cardiovascular Health 1 Lecture 9 1. Heart 2. Cardiovascular Health 3. Stroke 4. Contributing Factor 1 The Heart Muscular Pump The Heart Receives blood low pressure then increases the pressure
The PROSPECT Trial. A Natural History Study of Atherosclerosis Using Multimodality Intracoronary Imaging to Prospectively Identify Vulnerable Plaque
 The PROSPECT Trial Providing Regional Observations to Study Predictors of Events in the Coronary Tree A Natural History Study of Atherosclerosis Using Multimodality Intracoronary Imaging to Prospectively
The PROSPECT Trial Providing Regional Observations to Study Predictors of Events in the Coronary Tree A Natural History Study of Atherosclerosis Using Multimodality Intracoronary Imaging to Prospectively
The Gender Divide Women, Men and Heart Disease February 2017
 The Gender Divide Women, Men and Heart Disease February 2017 Nandita S. Scott, MD FACC Co-Director MGH Heart Center Corrigan Women s Heart Health Program Massachusetts General Hospital Heart Disease For
The Gender Divide Women, Men and Heart Disease February 2017 Nandita S. Scott, MD FACC Co-Director MGH Heart Center Corrigan Women s Heart Health Program Massachusetts General Hospital Heart Disease For
Normal blood vessels A= artery V= vein
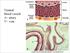 Normal blood vessels A= artery V= vein Artery (A) versus vein (V) ARTERIOSCLEROSIS Arteriosclerosis ="hardening of the arteries" arterial wall thickening and loss of elasticity. Three patterns are recognized,
Normal blood vessels A= artery V= vein Artery (A) versus vein (V) ARTERIOSCLEROSIS Arteriosclerosis ="hardening of the arteries" arterial wall thickening and loss of elasticity. Three patterns are recognized,
Part 1 Risk Factors and Atherosclerosis. LO1. Define the Different Forms of CVD
 Week 3: Cardiovascular Disease Learning Outcomes: 1. Define the difference forms of CVD 2. Describe the various risk factors of CVD 3. Describe atherosclerosis and its stages 4. Describe the role of oxidation,
Week 3: Cardiovascular Disease Learning Outcomes: 1. Define the difference forms of CVD 2. Describe the various risk factors of CVD 3. Describe atherosclerosis and its stages 4. Describe the role of oxidation,
Dyslipidemia Endothelial dysfunction Free radicals Immunologic
 ATHEROSCLEROSIS Hossein Mehrani Professor of Clinical Biochemistry Definition Atherosclerosis: Is a chronic inflammatory process characterized by plaque formation within the vessel wall of arteries and
ATHEROSCLEROSIS Hossein Mehrani Professor of Clinical Biochemistry Definition Atherosclerosis: Is a chronic inflammatory process characterized by plaque formation within the vessel wall of arteries and
Invasive Coronary Imaging Modalities for Vulnerable Plaque Detection
 Invasive Coronary Imaging Modalities for Vulnerable Plaque Detection Gary S. Mintz, MD Cardiovascular Research Foundation New York, NY Greyscale IVUS studies have shown Plaque ruptures do not occur randomly
Invasive Coronary Imaging Modalities for Vulnerable Plaque Detection Gary S. Mintz, MD Cardiovascular Research Foundation New York, NY Greyscale IVUS studies have shown Plaque ruptures do not occur randomly
1) Severe, crushing substernal chest pain 2) radiate to the neck, jaw, epigastrium, or left arm. 3- rapid and weak pulse 4- nausea (posterior MI).
 1) Severe, crushing substernal chest pain 2) radiate to the neck, jaw, epigastrium, or left arm. 3- rapid and weak pulse 4- nausea (posterior MI). 5- cardiogenic shock (massive MIs >40% of the left ventricle)
1) Severe, crushing substernal chest pain 2) radiate to the neck, jaw, epigastrium, or left arm. 3- rapid and weak pulse 4- nausea (posterior MI). 5- cardiogenic shock (massive MIs >40% of the left ventricle)
Journal of the American College of Cardiology Vol. 36, No. 4, by the American College of Cardiology ISSN /00/$20.
 Journal of the American College of Cardiology Vol. 36, No. 4, 2000 2000 by the American College of Cardiology ISSN 0735-1097/00/$20.00 Published by Elsevier Science Inc. PII S0735-1097(00)00820-2 Elevated
Journal of the American College of Cardiology Vol. 36, No. 4, 2000 2000 by the American College of Cardiology ISSN 0735-1097/00/$20.00 Published by Elsevier Science Inc. PII S0735-1097(00)00820-2 Elevated
Gary S. Mintz,, MD. IVUS Observations in Acute (vs Chronic) Coronary Artery Disease: Structure vs Function
 Gary S. Mintz,, MD IVUS Observations in Acute (vs Chronic) Coronary Artery Disease: Structure vs Function Important IVUS Observations: Remodeling Originally used (first by Glagov) ) to explain atherosclerosis
Gary S. Mintz,, MD IVUS Observations in Acute (vs Chronic) Coronary Artery Disease: Structure vs Function Important IVUS Observations: Remodeling Originally used (first by Glagov) ) to explain atherosclerosis
Assessment of plaque morphology by OCT in patients with ACS
 Assessment of plaque morphology by OCT in patients with ACS Takashi Akasaka, M.D. Department of Cardiovascular Medicine Wakayama, Japan Unstable plaque Intima Lipid core Plaque rupture and coronary events
Assessment of plaque morphology by OCT in patients with ACS Takashi Akasaka, M.D. Department of Cardiovascular Medicine Wakayama, Japan Unstable plaque Intima Lipid core Plaque rupture and coronary events
Histopathology: Vascular pathology
 Histopathology: Vascular pathology These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you need to learn about these
Histopathology: Vascular pathology These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you need to learn about these
The Effects of Hyperhomocysteinemia on the Presence, Extent, and Severity of Coronary Artery Disease
 The Effects of Hyperhomocysteinemia on the Presence, Extent, and Severity of Coronary Artery Disease Abdi BOZKURT, 1 MD, Hale TOYAKSI, 2 MD, Esmeray ACARTÜRK, 1 MD, Abdullah TULI, 2 MD, and Murat ÇAYLI,
The Effects of Hyperhomocysteinemia on the Presence, Extent, and Severity of Coronary Artery Disease Abdi BOZKURT, 1 MD, Hale TOYAKSI, 2 MD, Esmeray ACARTÜRK, 1 MD, Abdullah TULI, 2 MD, and Murat ÇAYLI,
Intermediate Methods in Epidemiology Exercise No. 4 - Passive smoking and atherosclerosis
 Intermediate Methods in Epidemiology 2008 Exercise No. 4 - Passive smoking and atherosclerosis The purpose of this exercise is to allow students to recapitulate issues discussed throughout the course which
Intermediate Methods in Epidemiology 2008 Exercise No. 4 - Passive smoking and atherosclerosis The purpose of this exercise is to allow students to recapitulate issues discussed throughout the course which
Imaging Atheroma The quest for the Vulnerable Plaque
 Imaging Atheroma The quest for the Vulnerable Plaque P.J. de Feijter 1. Department of Cardiology 2. Department of Radiology Coronary Heart Disease Remains the Leading Cause of Death in the U.S, Causing
Imaging Atheroma The quest for the Vulnerable Plaque P.J. de Feijter 1. Department of Cardiology 2. Department of Radiology Coronary Heart Disease Remains the Leading Cause of Death in the U.S, Causing
Serum Total Homocysteine and Coronary Heart Disease
 International Journal of Epidemiology O International Eptctemlotoglcal Association 1995 Vol. 24, No. 4 Printed In Great Britain Serum Total Homocysteine and Coronary Heart Disease EGIL ARNESEN,* HELGA
International Journal of Epidemiology O International Eptctemlotoglcal Association 1995 Vol. 24, No. 4 Printed In Great Britain Serum Total Homocysteine and Coronary Heart Disease EGIL ARNESEN,* HELGA
PATIENTS AND METHODS:
 BACKGROUND: Rheumatoid arthritis (RA) is a chronic systemic inflammatory disease characterized by erosive synovitis that involves peripheral joints and implicates an important influence in the quality
BACKGROUND: Rheumatoid arthritis (RA) is a chronic systemic inflammatory disease characterized by erosive synovitis that involves peripheral joints and implicates an important influence in the quality
Declaration of conflict of interest. None to declare
 Declaration of conflict of interest None to declare Risk management of coronary artery disease Arrhythmias and diabetes Hercules Mavrakis Cardiology Department Heraklion University Hospital Crete, Greece
Declaration of conflict of interest None to declare Risk management of coronary artery disease Arrhythmias and diabetes Hercules Mavrakis Cardiology Department Heraklion University Hospital Crete, Greece
Homocysteine Level and Coronary Heart Disease Incidence: A Systematic Review and Meta-analysis
 ORIGINAL ARTICLE HOMOCYSTEINE AND CORONARY HEART DISEASE RISK Homocysteine Level and Coronary Heart Disease Incidence: A Systematic Review and Meta-analysis LINDA L. HUMPHREY, MD, MPH; RONGWEI FU, PHD;
ORIGINAL ARTICLE HOMOCYSTEINE AND CORONARY HEART DISEASE RISK Homocysteine Level and Coronary Heart Disease Incidence: A Systematic Review and Meta-analysis LINDA L. HUMPHREY, MD, MPH; RONGWEI FU, PHD;
ATHEROSCLEROSIS. Secondary changes are found in other coats of the vessel wall.
 ATHEROSCLEROSIS Atherosclerosis Atherosclerosis is a disease process affecting the intima of the aorta and large and medium arteries, taking the form of focal thickening or plaques of fibrous tissue and
ATHEROSCLEROSIS Atherosclerosis Atherosclerosis is a disease process affecting the intima of the aorta and large and medium arteries, taking the form of focal thickening or plaques of fibrous tissue and
12 Lead EKG Chapter 4 Worksheet
 Match the following using the word bank. 1. A form of arteriosclerosis in which the thickening and hardening of the vessels walls are caused by an accumulation of fatty deposits in the innermost lining
Match the following using the word bank. 1. A form of arteriosclerosis in which the thickening and hardening of the vessels walls are caused by an accumulation of fatty deposits in the innermost lining
Term-End Examination December, 2009 MCC-006 : CARDIOVASCULAR EPIDEMIOLOGY
 MCC-006 POST GRADUATE DIPLOMA IN CLINICAL CARDIOLOGY (PGDCC) 00269 Term-End Examination December, 2009 MCC-006 : CARDIOVASCULAR EPIDEMIOLOGY Time : 2 hours Maximum Marks : 60 Note : There will be multiple
MCC-006 POST GRADUATE DIPLOMA IN CLINICAL CARDIOLOGY (PGDCC) 00269 Term-End Examination December, 2009 MCC-006 : CARDIOVASCULAR EPIDEMIOLOGY Time : 2 hours Maximum Marks : 60 Note : There will be multiple
Observe the effects of atherosclerosis on the coronary artery lumen
 Clumps and Bumps: A Look at Atherosclerosis Activity 4B Activity Description This activity features actual photomicrographs of coronary artery disease in young people aged 18 24 years. Students will observe
Clumps and Bumps: A Look at Atherosclerosis Activity 4B Activity Description This activity features actual photomicrographs of coronary artery disease in young people aged 18 24 years. Students will observe
Cho et al., 2009 Journal of Cardiology (2009), 54:
 Endothelial Dysfunction, Increased Carotid Artery Intima-media Thickness and Pulse Wave Velocity, and Increased Level of Inflammatory Markers are Associated with Variant Angina Cho et al., 2009 Journal
Endothelial Dysfunction, Increased Carotid Artery Intima-media Thickness and Pulse Wave Velocity, and Increased Level of Inflammatory Markers are Associated with Variant Angina Cho et al., 2009 Journal
Can IVUS Define Plaque Features that Impact Patient Care?
 Can IVUS Define Plaque Features that Impact Patient Care? A Pichard L Satler, K Kent, R Waksman, W Suddath, N Bernardo, N Weissman, M Angelo, D Harrington, J Lindsay, J Panza. Washington Hospital Center
Can IVUS Define Plaque Features that Impact Patient Care? A Pichard L Satler, K Kent, R Waksman, W Suddath, N Bernardo, N Weissman, M Angelo, D Harrington, J Lindsay, J Panza. Washington Hospital Center
Quantification of Coronary Arterial Narrowing at Necropsy in Acute Transmural Myocardial Infarction
 Quantification of Coronary Arterial Narrowing at Necropsy in Acute Transmural Myocardial Infarction Analysis and Comparison of Findings in 27 Patients and 22 Controls WILLIAM C. ROBERTS, M.D., AND ANCIL
Quantification of Coronary Arterial Narrowing at Necropsy in Acute Transmural Myocardial Infarction Analysis and Comparison of Findings in 27 Patients and 22 Controls WILLIAM C. ROBERTS, M.D., AND ANCIL
The inhibition of CETP: From simply raising HDL-c to promoting cholesterol efflux and lowering of atherogenic lipoproteins Prof Dr J Wouter Jukema
 The inhibition of CETP: From simply raising HDL-c to promoting cholesterol efflux and lowering of atherogenic lipoproteins Prof Dr J Wouter Jukema Dept Cardiology, Leiden University Medical Center, Leiden,
The inhibition of CETP: From simply raising HDL-c to promoting cholesterol efflux and lowering of atherogenic lipoproteins Prof Dr J Wouter Jukema Dept Cardiology, Leiden University Medical Center, Leiden,
High-risk vulnerable plaques. Kostis Raisakis G.Gennimatas General Hospital of Athens
 High-risk vulnerable plaques. Kostis Raisakis G.Gennimatas General Hospital of Athens Overview: 1 Definition-Pathology 2 3 Diagnostic Strategies Invasive Non Invasive Prognostic Value of Detection 4 Treatment
High-risk vulnerable plaques. Kostis Raisakis G.Gennimatas General Hospital of Athens Overview: 1 Definition-Pathology 2 3 Diagnostic Strategies Invasive Non Invasive Prognostic Value of Detection 4 Treatment
Complications of Diabetes mellitus. Dr Bill Young 16 March 2015
 Complications of Diabetes mellitus Dr Bill Young 16 March 2015 Complications of diabetes Multi-organ involvement 2 The extent of diabetes complications At diagnosis as many as 50% of patients may have
Complications of Diabetes mellitus Dr Bill Young 16 March 2015 Complications of diabetes Multi-organ involvement 2 The extent of diabetes complications At diagnosis as many as 50% of patients may have
Dr Rodney Itaki Lecturer Anatomical Pathology Discipline. University of Papua New Guinea School of Medicine & Health Sciences Division of Pathology
 Arterial Diseases Dr Rodney Itaki Lecturer Anatomical Pathology Discipline University of Papua New Guinea School of Medicine & Health Sciences Division of Pathology Disease Spectrum Arteriosclerosis Atherosclerosis
Arterial Diseases Dr Rodney Itaki Lecturer Anatomical Pathology Discipline University of Papua New Guinea School of Medicine & Health Sciences Division of Pathology Disease Spectrum Arteriosclerosis Atherosclerosis
Homocysteine is a thiol-containing amino acid derived
 Plasma Homocysteine Concentrations in the Acute and Convalescent Periods of Atherothrombotic Stroke D.J. Meiklejohn, MBChB; M.A. Vickers, MD; R. Dijkhuisen, MD; M. Greaves, PhD Background and Purpose Homocysteine
Plasma Homocysteine Concentrations in the Acute and Convalescent Periods of Atherothrombotic Stroke D.J. Meiklejohn, MBChB; M.A. Vickers, MD; R. Dijkhuisen, MD; M. Greaves, PhD Background and Purpose Homocysteine
The Framingham Coronary Heart Disease Risk Score
 Plasma Concentration of C-Reactive Protein and the Calculated Framingham Coronary Heart Disease Risk Score Michelle A. Albert, MD, MPH; Robert J. Glynn, PhD; Paul M Ridker, MD, MPH Background Although
Plasma Concentration of C-Reactive Protein and the Calculated Framingham Coronary Heart Disease Risk Score Michelle A. Albert, MD, MPH; Robert J. Glynn, PhD; Paul M Ridker, MD, MPH Background Although
( 1) Framingham Heart
 ( 1) ( 1) Framingham Heart Study [1] 1. (Am J Kidney Dis. 45: 223-232, 2005) 96 19 1 17 Framingham Heart Study ( 1) American Heart Association (1) (2) (3) (4) [2] (GFR) [3] ARIC [4] Cardiovascular Health
( 1) ( 1) Framingham Heart Study [1] 1. (Am J Kidney Dis. 45: 223-232, 2005) 96 19 1 17 Framingham Heart Study ( 1) American Heart Association (1) (2) (3) (4) [2] (GFR) [3] ARIC [4] Cardiovascular Health
Page: 1 of 11. Homocysteine Testing in the Screening, Diagnosis and Management of Cardiovascular Disease
 Last Review Status/Date: June 2015 Page: 1 of 11 Diagnosis and Management of Description Homocysteine is an amino acid found in the blood; levels are inversely correlated with folate levels. Homocysteine
Last Review Status/Date: June 2015 Page: 1 of 11 Diagnosis and Management of Description Homocysteine is an amino acid found in the blood; levels are inversely correlated with folate levels. Homocysteine
International Journal of Current Research in Medical Sciences
 International Journal of Current Research in Medical Sciences ISSN: 2454-5716 www.ijcrims.com Coden: IJCRPP(USA) Research Article http://s-o-i.org/1.15/ijcrms-2016-2-1-5 How Raised Homocysteine is Correlated
International Journal of Current Research in Medical Sciences ISSN: 2454-5716 www.ijcrims.com Coden: IJCRPP(USA) Research Article http://s-o-i.org/1.15/ijcrms-2016-2-1-5 How Raised Homocysteine is Correlated
The major strategy to prevent coronary heart disease
 Clinical Investigation and Reports Association of Coronary Heart Disease Risk Factors With Microscopic Qualities of Coronary Atherosclerosis in Youth Henry C. McGill, Jr, MD; C. Alex McMahan, PhD; Arthur
Clinical Investigation and Reports Association of Coronary Heart Disease Risk Factors With Microscopic Qualities of Coronary Atherosclerosis in Youth Henry C. McGill, Jr, MD; C. Alex McMahan, PhD; Arthur
Hyperhomocysteinemia is known to be an. Methylenetetrahydrofolate Reductase Gene Polymorphism. Relation to Blood Pressure and Cerebrovascular Disease
 AJH 1998;11:1019 1023 BRIEF COMMUNICATIONS Methylenetetrahydrofolate Reductase Gene Polymorphism Relation to Blood Pressure and Cerebrovascular Disease Yukiko Nakata, Tomohiro Katsuya, Seiju Takami, Noriyuki
AJH 1998;11:1019 1023 BRIEF COMMUNICATIONS Methylenetetrahydrofolate Reductase Gene Polymorphism Relation to Blood Pressure and Cerebrovascular Disease Yukiko Nakata, Tomohiro Katsuya, Seiju Takami, Noriyuki
Current Cholesterol Guidelines and Treatment of Residual Risk COPYRIGHT. J. Peter Oettgen, MD
 Current Cholesterol Guidelines and Treatment of Residual Risk J. Peter Oettgen, MD Associate Professor of Medicine Harvard Medical School Director, Preventive Cardiology Beth Israel Deaconess Medical Center
Current Cholesterol Guidelines and Treatment of Residual Risk J. Peter Oettgen, MD Associate Professor of Medicine Harvard Medical School Director, Preventive Cardiology Beth Israel Deaconess Medical Center
as a Mechanism of Stent Failure
 In-Stent t Neoatherosclerosis e osc e os s as a Mechanism of Stent Failure Soo-Jin Kang MD., PhD. University of Ulsan College of Medicine, Heart Institute Asan Medical Center, Seoul, Korea Disclosure I
In-Stent t Neoatherosclerosis e osc e os s as a Mechanism of Stent Failure Soo-Jin Kang MD., PhD. University of Ulsan College of Medicine, Heart Institute Asan Medical Center, Seoul, Korea Disclosure I
PATHOPHYSIOLOGY OF ACUTE CORONARY SYNDROMES
 PATHOPHYSIOLOGY OF ACUTE CORONARY SYNDROMES Brian R. Holroyd, MD, FACEP, FRCPC Professor and Director, Division of Emergency Medicine, Faculty of Medicine and Dentistry, University of Alberta, Edmonton,
PATHOPHYSIOLOGY OF ACUTE CORONARY SYNDROMES Brian R. Holroyd, MD, FACEP, FRCPC Professor and Director, Division of Emergency Medicine, Faculty of Medicine and Dentistry, University of Alberta, Edmonton,
One third to one half of the variation in vascular disease
 Plasma Homocysteine Predicts Mortality Independently of Traditional Risk Factors and C-Reactive Protein in Patients With Angiographically Defined Coronary Artery Disease Jeffrey L. Anderson, MD; Joseph
Plasma Homocysteine Predicts Mortality Independently of Traditional Risk Factors and C-Reactive Protein in Patients With Angiographically Defined Coronary Artery Disease Jeffrey L. Anderson, MD; Joseph
10/17/16. Assessing cardiovascular risk through use of inflammation testing
 Assessing cardiovascular risk through use of inflammation testing Anthony L. Lyssy, DO Medical Director and Managing Partner Diamond Physicians Dallas, TX Response to Injury Hypothesis Injury Response
Assessing cardiovascular risk through use of inflammation testing Anthony L. Lyssy, DO Medical Director and Managing Partner Diamond Physicians Dallas, TX Response to Injury Hypothesis Injury Response
THE BLOOD VESSELS. Manar hajeer, MD University of Jordan Faculty of medicine, pathology department.
 THE BLOOD VESSELS Manar hajeer, MD University of Jordan Faculty of medicine, pathology department. Vascular pathology: 1- Narrowing or complete obstruction of vessel lumina, either progressively (e.g.,
THE BLOOD VESSELS Manar hajeer, MD University of Jordan Faculty of medicine, pathology department. Vascular pathology: 1- Narrowing or complete obstruction of vessel lumina, either progressively (e.g.,
The purpose of this report is to compare the results of
 Comparison of Two Measures of Atherosclerosis in a Prospective Epidemiology Study Dwayne M. Reed, Jack P. Strong, Takuji Hayashi, W. P. ewman III, Richard E. Tracy, Miguel A. Guzman, and Grant. Stemmermann
Comparison of Two Measures of Atherosclerosis in a Prospective Epidemiology Study Dwayne M. Reed, Jack P. Strong, Takuji Hayashi, W. P. ewman III, Richard E. Tracy, Miguel A. Guzman, and Grant. Stemmermann
Key words: Risk factor. Hyperhomocysteinemia. Ischemic heart disease. Smoking.
 j c p s p September 2004 Volume 14 Number 09 September 2004 Home JCPSP Home Sep JCPSP Contents Email JCPSP HYPERHOMOCYSTEINEMIA AS A RISK FACTOR FOR ISCHEMIC HEART DISEASE Muhammad Aamir, Abdus Sattar,*
j c p s p September 2004 Volume 14 Number 09 September 2004 Home JCPSP Home Sep JCPSP Contents Email JCPSP HYPERHOMOCYSTEINEMIA AS A RISK FACTOR FOR ISCHEMIC HEART DISEASE Muhammad Aamir, Abdus Sattar,*
in a population with low plasma
 518 Cardiology, Hacettepe University Faculty of Medicine, Ankara 06100, Turkey S L Tokgözoğlu E Atalar K Aytemir N Özer K Övünç S Kes Paediatric Genetics, Hacettepe University Faculty of Medicine M Alikaşifoğlu
518 Cardiology, Hacettepe University Faculty of Medicine, Ankara 06100, Turkey S L Tokgözoğlu E Atalar K Aytemir N Özer K Övünç S Kes Paediatric Genetics, Hacettepe University Faculty of Medicine M Alikaşifoğlu
The New England Journal of Medicine
 The New England Journal of Medicine Copyright, 1997, by the Massachusetts Medical Society VOLUME 336 A PRIL 3, 1997 NUMBER 14 INFLAMMATION, ASPIRIN, AND THE RISK OF CARDIOVASCULAR DISEASE IN APPARENTLY
The New England Journal of Medicine Copyright, 1997, by the Massachusetts Medical Society VOLUME 336 A PRIL 3, 1997 NUMBER 14 INFLAMMATION, ASPIRIN, AND THE RISK OF CARDIOVASCULAR DISEASE IN APPARENTLY
CT Imaging of Atherosclerotic Plaque. William Stanford MD Professor-Emeritus Radiology University of Iowa College of Medicine Iowa City, IA
 CT Imaging of Atherosclerotic Plaque William Stanford MD Professor-Emeritus Radiology University of Iowa College of Medicine Iowa City, IA PREVALENCE OF CARDIOVASCULAR DISEASE In 2006 there were 80 million
CT Imaging of Atherosclerotic Plaque William Stanford MD Professor-Emeritus Radiology University of Iowa College of Medicine Iowa City, IA PREVALENCE OF CARDIOVASCULAR DISEASE In 2006 there were 80 million
IVUS Virtual Histology. Listening through Walls D. Geoffrey Vince, PhD The Cleveland Clinic Foundation
 IVUS Virtual Histology Listening through Walls D. Geoffrey Vince, PhD Disclosure VH is licenced to Volcano Therapeutics Grant funding from Pfizer, Inc. Grant funding from Boston-Scientific Most Myocardial
IVUS Virtual Histology Listening through Walls D. Geoffrey Vince, PhD Disclosure VH is licenced to Volcano Therapeutics Grant funding from Pfizer, Inc. Grant funding from Boston-Scientific Most Myocardial
Andrew Cohen, MD and Neil S. Skolnik, MD INTRODUCTION
 2 Hyperlipidemia Andrew Cohen, MD and Neil S. Skolnik, MD CONTENTS INTRODUCTION RISK CATEGORIES AND TARGET LDL-CHOLESTEROL TREATMENT OF LDL-CHOLESTEROL SPECIAL CONSIDERATIONS OLDER AND YOUNGER ADULTS ADDITIONAL
2 Hyperlipidemia Andrew Cohen, MD and Neil S. Skolnik, MD CONTENTS INTRODUCTION RISK CATEGORIES AND TARGET LDL-CHOLESTEROL TREATMENT OF LDL-CHOLESTEROL SPECIAL CONSIDERATIONS OLDER AND YOUNGER ADULTS ADDITIONAL
 1. Prevalence and prognostic significance of incidental cardiac troponin T elevation in ambulatory patients with stable coronary artery disease: data from the Heart and Soul study Hsieh, B.P., et al. Am
1. Prevalence and prognostic significance of incidental cardiac troponin T elevation in ambulatory patients with stable coronary artery disease: data from the Heart and Soul study Hsieh, B.P., et al. Am
Cardiovascular Disorders. Heart Disorders. Diagnostic Tests for CV Function. Bio 375. Pathophysiology
 Cardiovascular Disorders Bio 375 Pathophysiology Heart Disorders Heart disease is ranked as a major cause of death in the U.S. Common heart diseases include: Congenital heart defects Hypertensive heart
Cardiovascular Disorders Bio 375 Pathophysiology Heart Disorders Heart disease is ranked as a major cause of death in the U.S. Common heart diseases include: Congenital heart defects Hypertensive heart
For unclear reasons, only about 40% of patients with calcific aortic stenosis also have coronary
 Αθηροσκλήρωση και ασβεστοποιός στένωση της αορτικής βαλβίδας. Οµοιότητες και διαφορές Ν. Μεζίλης Κλινική «Άγιος Λουκάς» Ασβεστοποιός στένωση της αορτικής βαλβίδας: Μία ακόµα µορφή αθηρωµάτωσης; Some observations
Αθηροσκλήρωση και ασβεστοποιός στένωση της αορτικής βαλβίδας. Οµοιότητες και διαφορές Ν. Μεζίλης Κλινική «Άγιος Λουκάς» Ασβεστοποιός στένωση της αορτικής βαλβίδας: Μία ακόµα µορφή αθηρωµάτωσης; Some observations
Objectives. Acute Coronary Syndromes; The Nuts and Bolts. Overview. Quick quiz.. How dose the plaque start?
 Objectives Acute Coronary Syndromes; The Nuts and Bolts Michael P. Gulseth, Pharm. D., BCPS Pharmacotherapy II Spring 2006 Compare and contrast pathophysiology of unstable angina (UA), non-st segment elevation
Objectives Acute Coronary Syndromes; The Nuts and Bolts Michael P. Gulseth, Pharm. D., BCPS Pharmacotherapy II Spring 2006 Compare and contrast pathophysiology of unstable angina (UA), non-st segment elevation
Basic Mechanisms of Atherosclerosis and Plaque Rupture: Clinical Implications
 12 th Annual Cardiovascular Disease Prevention Symposium February 8, 2013 KEYNOTE ADDRESS Basic Mechanisms of Atherosclerosis and Plaque Rupture: Clinical Implications Ira Tabas, M.D., Ph.D. Richard J.
12 th Annual Cardiovascular Disease Prevention Symposium February 8, 2013 KEYNOTE ADDRESS Basic Mechanisms of Atherosclerosis and Plaque Rupture: Clinical Implications Ira Tabas, M.D., Ph.D. Richard J.
This review will reconsider the current paradigm for
 Lessons From Sudden Coronary Death A Comprehensive Morphological Classification Scheme for Atherosclerotic Lesions Renu Virmani, Frank D. Kolodgie, Allen P. Burke, Andrew Farb, Stephen M. Schwartz This
Lessons From Sudden Coronary Death A Comprehensive Morphological Classification Scheme for Atherosclerotic Lesions Renu Virmani, Frank D. Kolodgie, Allen P. Burke, Andrew Farb, Stephen M. Schwartz This
CAD in Chronic Kidney Disease. Kuang-Te Wang
 CAD in Chronic Kidney Disease Kuang-Te Wang InIntroduction What I am going to talk about: CKD and its clinical impact on CAD Diagnosis of CAD in CKD PCI / Revasc Outcomes in CKD CKD PCI CAD Ohtake T,
CAD in Chronic Kidney Disease Kuang-Te Wang InIntroduction What I am going to talk about: CKD and its clinical impact on CAD Diagnosis of CAD in CKD PCI / Revasc Outcomes in CKD CKD PCI CAD Ohtake T,
Cardiac Pathology & Rehabilitation
 Cardiac Pathology & Rehabilitation Which of the following best describes the physical activity performed in my leisure time? A. I perform vigorous physical activity 3X/week for 20 minutes each time B.
Cardiac Pathology & Rehabilitation Which of the following best describes the physical activity performed in my leisure time? A. I perform vigorous physical activity 3X/week for 20 minutes each time B.
Results of Ischemic Heart Disease
 Ischemic Heart Disease: Angina and Myocardial Infarction Ischemic heart disease; syndromes causing an imbalance between myocardial oxygen demand and supply (inadequate myocardial blood flow) related to
Ischemic Heart Disease: Angina and Myocardial Infarction Ischemic heart disease; syndromes causing an imbalance between myocardial oxygen demand and supply (inadequate myocardial blood flow) related to
ARIC Manuscript Proposal #1233. PC Reviewed: 4_/_10/07 Status: _A Priority: 2_ SC Reviewed: Status: Priority:
 ARIC Manuscript Proposal #1233 PC Reviewed: 4_/_10/07 Status: _A Priority: 2_ SC Reviewed: Status: Priority: 1.a. Full Title: Subclinical atherosclerosis precedes type 2 diabetes in the ARIC study cohort
ARIC Manuscript Proposal #1233 PC Reviewed: 4_/_10/07 Status: _A Priority: 2_ SC Reviewed: Status: Priority: 1.a. Full Title: Subclinical atherosclerosis precedes type 2 diabetes in the ARIC study cohort
PoS(FISBH2006)019. Imaging Vulnerable Plaque A radionuclide approach. H. William Strauss, M.D. 1
 A radionuclide approach H. William Strauss, M.D. 1 Section of Nuclear Medicine, Memorial Sloan Kettering Cancer Center, New York, NY 10021 United States E-mail: straussh@mskcc.org Frontiers in Imaging
A radionuclide approach H. William Strauss, M.D. 1 Section of Nuclear Medicine, Memorial Sloan Kettering Cancer Center, New York, NY 10021 United States E-mail: straussh@mskcc.org Frontiers in Imaging
Cardiovascular manifestations of HIV
 Cardiovascular manifestations of HIV Prabhakar Rajiah, MBBS, MD, FRCR Associate Professor of Radiology Associate Director, Cardiac CT and MRI University of Texas Southwestern Medical Center, Dallas, USA
Cardiovascular manifestations of HIV Prabhakar Rajiah, MBBS, MD, FRCR Associate Professor of Radiology Associate Director, Cardiac CT and MRI University of Texas Southwestern Medical Center, Dallas, USA
Joshua A. Beckman, MD. Brigham and Women s Hospital
 Peripheral Vascular Disease: Overview, Peripheral Arterial Obstructive Disease, Carotid Artery Disease, and Renovascular Disease as a Surrogate for Coronary Artery Disease Joshua A. Beckman, MD Brigham
Peripheral Vascular Disease: Overview, Peripheral Arterial Obstructive Disease, Carotid Artery Disease, and Renovascular Disease as a Surrogate for Coronary Artery Disease Joshua A. Beckman, MD Brigham
