We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
|
|
|
- Madison Gibson
- 5 years ago
- Views:
Transcription
1 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3, , M Open access books available International authors and editors Downloads Our authors are among the 154 Countries delivered to TOP 1% most cited scientists 12.2% Contributors from top 500 universities Selection of our books indexed in the Book Citation Index in Web of Science Core Collection (BKCI) Interested in publishing with us? Contact book.department@intechopen.com Numbers displayed above are based on latest data collected. For more information visit
2 Robotic Sacrocolpopexy and Sacrocervicopexy for the Correction of Pelvic Organ Prolapse James C Brien 1, Michael D Fabrizio 1 and James C Lukban 2 1 Department of Urology, Eastern Virginia Medical School, Norfolk, Virginia, 2 Division of Urogynecology, Eastern Virgina Medical School, Norfolk, Virginia, USA 7 1. Introduction The lifetime risk for undergoing a single operation for prolapse (or incontinence) is 11%, with the National Center for Health Statistics reporting 400,000 procedures for these conditions performed annually.[1] Swift et al. described the epidemiologic distribution of pelvic organ prolapse (POP) in a sample of 1004 women presenting for an annual gynecologic exam, evaluated with a validated staging system (Pelvic Organ Prolapse Quantification System or POP-Q).[2,3] Despite a relatively young mean age of 42.7 years, clinically significant (Stage II or greater) vaginal wall descensus was identified in 37% of subjects. In a larger study as part of the Women s Health Initiative, those between the ages of 50 and 79 were screened for POP through a non-validated system.[4] Of 16,616 subjects with no previous hysterectomy, 41.1% had some form of prolapse, while 38% of 10,727 hysterectomized women exhibited POP. The true incidence of POP is likely higher, as many women may not report their condition due to embarrassment, or they may feel that such changes are a normal part of aging. 2. Anatomy of the pelvic floor The pelvic floor is comprised of layers of connective tissue and muscle that provide support to the pelvic viscera. The urethra, vagina and rectum are attached to the pelvic sidewalls by the endopelvic fascia, which in turn is supported by the pelvic floor musculature (PFM).[5] The PFM consists of the levator ani (pubococcygeus and iliococcygeus) and coccygeus muscles, providing tonic support to the endoplvic fascia and viscera through a preponderance of type I (slow twitch) fibers.[6] Thus, a robust PFM is essential in maintaining the position of the viscera within the pelvis. 3. Etiology of pelvic organ prolapse Pelvic organ prolpase represents an attenuation or disruption of the connective tissue comprising the pubocervical endopelvic fascia anteriorly or rectovaginal endopelvic fascia posteriorly, manifesting as anterior or posterior vaginal wall prolapse, respectively. Additionally, a weak or torn cardinal - uterosacral ligament complex may lead to vaginal Source: Robot Surgery, Book edited by: Seung Hyuk Baik, ISBN , pp. 172, January 2010, INTECH, Croatia, downloaded from SCIYO.COM
3 110 Robot Surgery apex (cuff post hysterectomy or cervix) descent. Predominant risk factors for POP include age and parity, with partial denervation of the PFM proven to be the result of parturition, senescence, or some combination.[7,8] As the PFM becomes weak, support to the endopelvic fascia and viscera is lost, placing the connective tissue at risk for attenuation and/or discrete breaks with resultant POP. When encountered in a younger subject, POP may reasonably be the sequela of acute obstetric trauma, or the result of a genetic alteration in the proportion of fascial collagen subtypes.[9] 4. Considerations prior to surgical correction of pelvic organ prolapse The goal of POP repair is to restore pelvic anatomy, and facilitate normal visceral and sexual function. To this end, the surgeon must consider, first and foremost, the integrity of the vaginal apex. The Surgery for Pelvic Organ Prolapse Committee of the 3rd International Consultation on Incontinence noted, the apex is the keystone of pelvic organ support. [10] Additionally, they concluded that anterior and posterior repairs are doomed to fail unless the apex is adequately supported. While multiple approaches exist to address vaginal apical prolapse, choosing the optimal repair is critical to a successful outcome. In the following text, we will discuss several methods for the repair of apical descensus, examine the surgical evolution from vaginal and abdominal surgery to laparoscopic and robotic approaches, and describe our technique of robot assisted laparoscopic sacrocolpopexy and sacrocervicopexy. 5. Transvaginal surgery for apical prolapse Uterosacral ligament suspension is an intraperitoneal technique in which the remnants of the ureterosacral ligaments are brought together with permanent suture, and subsequently attached to the vaginal apices bilaterally employing delayed absorbable stitch. Recurrent apical prolapse following this procedure has been reported between 1% and 18%, with the anterior segment found to be the most common site of persistent prolapse.[11,12] Overall, reported patient satisfaction is high, with a re-operation rate of 5.5% in one series.[13] Although bowel injury and bleeding complications are relatively infrequent, ureteral injury or kinking has been reported to be as high as 11%, emphasizing the importance of interrogating the ureters endoscopically after suspension.[12,13] Sacrospinous ligament fixation involves an extraperitoneal rectovaginal dissection with support of the vaginal apex through attachment to the sacrospinous ligament either unilaterally or bilaterally. Exposing the ischial spine and ligament may, at times, be a challenge, with the attendant risk of neurovascular trauma. The surgeon must avoid the hypogastic plexus, the inferior gluteal and internal pudendal vessels, and the pudendal and sciatic nerves. Outcomes are variable, with recurrence ranging from 3-30%. [14-16] Additional potential complications include gluteal pain and rectal injury. Iliococcygeus fascial suspension is also an extraperitoneal technique performed through a posterior vaginal incision. Dissection is carried out laterally and cephalad until the iliococcygeus musculature is identified, at which point an absorbable suture is placed through the fascia and ipsilateral vaginal apex bilaterally. While Shull and colleagues reported recurrence as low as 5% with low complication rates compared to other transvaginal approaches, the potential for hemorrhagic morbidity exists, with one author reporting an average estimated blood loss (EBL) of 358 ml.[17,18]
4 Robotic Sacrocolpopexy and Sacrocervicopexy for the Correction of Pelvic Organ Prolapse Transvaginal mesh repairs The introduction of a variety of mesh products has been implemented for the repair of stress urinary incontinence as well as POP. Although a thorough review of this modality is beyond the scope of this chapter, a brief account of contemporary outcomes will be discussed. Several synthetic graft materials have been used historically including expanded PTFE and polyester, with polypropylene being the dominant synthetic used in contemporary kits due its macroporous nature, allowing for tissue in-growth and minimal inflammatory response.[19,20] Commercial kits, designed to allow for minimally invasive mesh insertion, include Elevate (American Medical Systems, Minnetonka, MN, USA) and Gynecare Prolift System (Ethicon Women s Health and Urology, Somerville, NJ, USA), along with several other products and approaches for mesh support of the vaginal apex. In a review of clinical trials and observational studies addressing apical prolapse repair, Diwadkar and colleagues included 3,425 patients from 24 studies employing vaginal mesh kits, reporting a low rate of reoperation for recurrent POP (1.3 % at 17 months), with an overall complication rate (14.5 %) similar to traditional vaginal (15.3 %) and abdominal (17.1%) approaches.[21] However, the majority of complications associated with mesh kits required surgical intervention under general anesthesia (8.5 %), due in part to mesh erosion (vaginal exposure of synthetic material). In a retrospective review comparing outcomes following Prolift mesh repair, uterosacral ligament suspension and abdominal sacrocolpopexy, no difference in operative success (% with Stage 0 or I at follow-up) was observed between the three groups; however, mean change in apical support was significantly better after abdominal sacrocolpopexy compared to transvaginal mesh repair and uterosacral ligament suspension.[22] 7. Abdominal surgery for apical prolapse High uterosacral ligament suspension, similar to its vaginal counterpart, involves suspension of the vaginal apex to plicated ureterosacral ligaments. After entrance into the abdomen, the cul-de-sac is obliterated to address any co-existing enterocele. Subsequently, the apex of the vagina is exposed and reapproximated to the plicated uterosacral ligaments. Abdominal sacral colpopexy (ASC) involves securing the apex of the vagina to the sacral promonatory with intervening mesh. After a laparotomy incision is made and hysterectomy performed (if uterus present), the vagina is elevated with an end-to-end anastomosis (EEA) sizer followed by dissection of the vesicovaginal and rectovaginal spaces. The anterior and posterior leafs of a Y-shaped polypropylene mesh are sutured to the anterior and posterior vaginal walls, respectively. After opening the peritoneum over the sacral promontory, multiple nonabsorbable sutures are placed through the anterior longitudinal ligament, and secured to the single tail of the Y. Lastly, the peritoneum over the sacrum and vaginal apex is closed. Several studies document durable success following ASC, with recurrent prolapse ranging from 1-7% at long term follow up.[23,24] A recent Cochrane Review of the Surgical Management of Pelvic Organ Prolapse concluded that ASC was superior to sacrospinous fixation, exhibiting a lower rate of recurrent prolapse and less postoperative dyspareunia. [25] Abdominal sacrocolpopexy, however, was associated with longer operative time, longer recovery time and higher costs. Complications are infrequent, and include injury to bowel and bladder, with the potential for significant hemorrhage from presacral vessels. While
5 112 Robot Surgery mesh erosion has historically been higher with ASC employing small pore multifilament material, rates of apical exposure of graft have been 5% or less with the use of polypropylene.[26] Given the durability of ASC, such an approach is considered by many to represent the gold standard in the treatment of apical prolapse. In considering the attendant risks of open abdominal procedures and the availability of burgeoning technology, practitioners have made the logical progression to a less invasive approach using minimally invasive instrumentation in the performance of sacrocolpopexy. 8. Laparoscopic sacrocolpopexy (LSC) The concept and surgical technique of LSC is similar to that of its open counterpart. With the introduction of laparoscopy to vaginal reconstruction, many studies have been published evaluating the efficacy and safety of LSC as compared to ASC. Overall, LSC appears to be durable, with a low rate of recurrence (0-4%),[28-30] exhibiting favorable quality of life outcomes[28] and high patient satisfaction (96%).[30] Complications are overall infrequent, and include erosions (0-9%), dysparunia (1%), spondylitis (<1%), partial small bowel obstruction (0-4%) and a low conversion to open rate of 2.2%.[28-31] Reported operative times have ranged from 97 min to 219 minutes depending on surgeon experience.[29-30] In two retrospective comparative trials, LSC was associated with lower EBL, shorter hospital stay and increased time in the operating room (OR) as compared to ASC.[27,29] From this data, we may conclude LSC to be non-inferior to it s open counterpart with a low incidence of adverse events. 9. Robot assisted laparoscopic sacral colpopexy and cervicopexy (RALSC) The da Vinci surgical system (Intuitive Surgical, Sunnyvale, CA, USA) has augmented traditional laparoscopy adding three-dimensional vision, wristed instrumentation with seven degrees of freedom (versus 3 degrees with laparoscopy) and improved surgical ergonomics. Specific to sacrocolpopexy, the addition of the 4 th arm adds facilitation of sigmoid colon reflection. Robot assist laparoscopic sacrocolpopexy (RALSC) has been found to have similar outcomes to its pure laparoscopic predecessor. Efficacy appears durable with one non-comparative study of 30 patients reporting 6% recurrence at 24 months,[32] and surgical failure in two additional studies ranging from 0-4.7% at shorter follow up.[33,34] Such data are comparable to the 7% rate of recurrence reported in a large series of open sacralcolpopexy by Snyder and Krantz.[24] Daneshgardi and colleagues evaluated preoperative and postoperative POP-Q values in patients undergoing RALSC, reporting not only an overall improvement in global POP-Q scores, but statistically significant improvement of anterior, posterior and apical POP-Q scores separately. Mesh erosion rates are comparable to an open incidence of 7% reported by Kohli and colleagues.[37] Length of hospital stay in 4 series ranges from days[32,33,35,38] with operative times ranging minutes.[32,34-36,38] One series reported a 25% decrease in procedure time after the initial 10 cases, suggesting a steep, but short learning curve.[36] Complications of RALSC are comparable to LSC. Ureteral injury, enterotomy and cystotomy are infrequent (0-1.2%) as is post op small bowel obstruction (4.7%).[32,34,36] While no randomized-controlled trials comparing RALSC to LSC have been published to our
6 Robotic Sacrocolpopexy and Sacrocervicopexy for the Correction of Pelvic Organ Prolapse 113 knowledge, a retrospective comparison of RALSC with ASC by Geller et al.found the former to be associated with slightly better postoperative POP-Q C (apex) improvement, less EBL and shorter hospital stay. While RALSC was observed to have longer operative times, there was no significant difference with respect to intraoperative or postoperative complications between the two groups.[38] 10. Description of RALSC The patient is given appropriate antibiotic prophylaxis in the preoperative area and sequential pneumatic compression devices are applied for deep venous thrombosis prophylaxis. After intubation, the patient is placed in low - lithotomy position and straps are placed across the shoulders and chest in a criss - cross pattern to secure the patient on the table. The arms are padded and tucked. See Figure 1 for operating room configuration. After prepping and draping of the abdomen, perineum and vagina, a foley catheter is placed. A Veress needle may be inserted through the umbilicus (or just cephalad) to facilitate insufflation of the abdomen, or the initial trocar may be introduced under direct vision employing a clear blunt tipped device with lens inside prior to introduction of gas. In patients suspected of having significant midline abdominal adhesions, one may enter the abdomen with a 5 mm laparoscope loaded into a 5 mm clear blunt-tipped trocar at Palmer s point (3 cm below the left costal margin in the mid-clavicular line) to visualize subsequent midline trocar placement.[39] The initial 12 mm camera port is inserted no less than 15 cm and no greater than 22 cm from the pubic symphysis in the midline. Prior to placement of lateral trocars, the patient is placed in a steep Trendelenburg tilt. With full insufflation (not to exceed 15 mm Hg), measurements are made on the anterior abdomen to ensure appropriate placement of subsequent trocars, and avoid collision of the robotic arms (Fig. 2). Two lateral 8 mm ports are then placed 10 cm inferolateral to the camera port in the direction of the ipsilateral anterior superior iliac spine (ports 1 and 2). A 3rd 8 mm port is placed 8 10 cm superolateral to port 2 (port 3) and a 12 mm assistant port is placed 8 cm lateral to port 1. The robot is docked and ports secured (Fig. 3). The sigmoid is reflected with the fourth arm employing a non-fenestrated grasper in the open position, facilitatating visualization of the sacrum. If the sigmoid shows significant redundancy, additional retraction may be provided by the introduction of a 0 polypropylene suture on a straight needle passed percutaneously through the left lower abdomen to tether the sigmoid. Several passes are made through the appendices epiploicae and the needle re-passed to exit the abdomen at a point 1 cm lateral to its site of entry. The sigmoid is placed on gentle traction to complete exposure. The peritoneum over the promontory is then incised, with dissection carried out distally to the pelvis in between the right ureter and rectosigmoid. The pre-sacral fat is cleared and the anterior longitudinal ligament exposed (Fig. 4). This area should be well inspected for presacral vessels, the inadvertent injury to which may lead to troublesome bleeding. Should this occur we prefer the use of bipolar cautery or Ligasure (Covidien, Norwalk, CT, USA) to control hemorrhage. Using an EEA placed transvaginally, the apex is identified and peritoneum over the cuff incised, allowing for dissection of the vesicovaginal and rectovaginal spaces (Fig. 5). A
7 114 Robot Surgery polypropylene Y- shaped mesh is then passed through the assistant port. The mesh is tailored to ensure coverage of the anterior vaginal wall to a point just above the trigone, and the posterior wall to the level of the perineal body. The anterior limb is secured to the anterior vagina with 6 interrupted sutures of expanded PTFE or braided polyester suture (Fig. 6). Similarly, the posterior limb of the mesh is sutured to the posterior vagina, employing 8 sutures of the same (Fig. 7). Care is taken not to pass the stitch through full thickness vagina. Next, the single arm of the Y- mesh is brought to the sacral promontory. Excess mesh is trimmed to the appropriate length (Fig. 8). Once the appropriate tension is set the, the mesh may be held with fixed tension with the fourth arm and sutured to the promontory with 2 to 4 interrupted sutures of expanded PTFE or braided polyester (Fig. 9). Finally, the peritoneum is closed over the mesh to avoid bowel adhesions, potential erosion or small bowel obstruction (Fig. 10). This is accomplished with a running absorbable suture with a Lapra-Ty (Ethicon Endo-Surgery, Albuquerque, NM, USA) fixed to the end (we prefer 2-0 piloglecaprone 25 stitch due to its relatively short persistence and ability to slide). The abdomen is inspected for bleeding or any unrecognized visceral injury. The vagina is inspected to confirm the apex is well supported. The camera and robotic ports are subsequently decoupled from robotic arms and all ports removed under direct endoscopic visualization. We close both 12 mm ports with an interrupted suture of 0 polyglactin suture using the Carter-Thomason CloseSure System (Inlet Medical, Eden Prarie, MN, USA). Patients are evaluated for ureteral patency postoperatively with cystoscopy following the intravenous administration of indigo carmine. An anti-incontinence procedure may also be performed at this time if stress urinary incontinence has been diagnosed preoperatively on urodynamic testing with prolapse reduction. 11. Innovations in robotic surgical techniques for apex suspension Traditional docking of the robot patient cart often restricts access to the patient s perineum, a potential problem in those patients requiring concomitant vaginal and intracorporeal approaches. In this situation, side docking should be considered. Proper docking requires the patient cart to be aligned with the ipsilateral anterior superior iliac spine and midline camera port. Additionally, this technique may require lateral displacement of the 3 rd robotic port, with the 4 th port placed in the horizontal plane slightly above the camera site, bisecting the camera and 3 rd ports (Fig. 11). We have recently adopted this technique for cases requiring simultaneous perineal and intraabdominal access, including robotic assisted laparoscopic creation of an ileal neovagina, finding overall good range of motion and relative ease of set up. 12. Conclusion While level 1 evidence favors outcomes of abdominal sacrocolpopexy over sacrospinous ligament repairs, this comes with the attendant morbidity of a traditional open abdominal procedure. Robot assisted laparoscopic sacrocolpopexy offers the ability to support the apex in a fashion similar to the open approach with equal efficacy. This technique offers the advantages of a minimally invasive option using a modality the traditional open surgeon can adopt with a demonstrated steep but short learning curve.
8 Robotic Sacrocolpopexy and Sacrocervicopexy for the Correction of Pelvic Organ Prolapse References [1] Olsen AL, Smith VJ, Bergsrom JO et al. Epidemiology of surgically managed pelvic organ prolpase and urinary incontinence. Obstet Gynecol 1997; 89:501 [2] Swift S, Woodman R, O Boyle A et al. Pelvic Organ Support Study (POSST): the distribution, clinical definition, and epidemiologic condition of pelvic organ support defects. Am J Obstet Gynecol 2005; 192:795 [3] Bump RC, Mattiasson A, Bo K et al. The standardization of terminology of female pelvic organ prolapse and pelvic floor dysfunction. Am J Obstet Gynecol 1996; 175:10 [4] Hendrix SL, Clark A, Nygaard I et al. Pelvic organ prolapse in the Women s Heath Initiative: gravity and gravidity. Am J Obstet Gynecol 2002; 186:1160 [5] Delancey JOL. Surgical anatomy of the female pelvis, In: Rock JA, Thompson JD, eds. TeLinde s Operative Gynecology, ed 8. Philadelphia: Lippincott-Raven; 1997:63-93 [6] Gosling JA, Dixon JS, Critchley HOD et al. A comparative study of the human external sphincter and periurethral levator ani muscles. Br J Urol 1981;53:35-41 [7] Allen RE, Hosker GL, Smith ARB et al. Pelvic floor damage and childbirth: a neurophysiological study. Br J Obstet Gynaecol 1990;97: [8] Smith ARB, Hosker GL, Warrell DW. The role of partial denervation of the pelvic floor in the etiology of genitourinary prolapse and stress incontinence of urine. A neurophysiological study. Br J Obstet Gynaecol 1989;96:24-28 [9] Chen HY, Chung YW, Lin WY et al. Collagen type 3 alpha 1 polymorphism and risk of pelvic organ prolapse. Int J Gynecol Obstet 2008;103:55-58 [10] Brubaker L, Bump R, Fynes M et al. Surgery for Pelvic Organ Prolapse, In: Abrams P, Cardozo L, Khoury S et al. editors. Incontinence, Management. Third International Consultation on Incontinence. Vol. 2, Monaco: International Continence Society pp , chapter 21 [11] Shull BL, Bachofen C, Coats KW, et al. A transvaginal approach to repair of apical and other associated sites of pelvic organ prolapse with uterosacral ligaments. Am J Obstet Gynecol 2000;183:1365 [12] Barber MD, Visco AG, Weidner AC et al. Bilateral uterosacral ligament vaginal vault suspension with site-specific endopelvic fascia defect repair for treatment of pelvic organ prolapse. Am J Obstet Gynecol 2000;183: 1402 [13] Karram M, Goldwasser S, Kleeman S et al. High uterosacral vaginal vault suspension with fascial reconstruction for vaginal repair of enterocele and vaginal vault prolapse. Am J Obstet Gynecol 2001;185:1339 [14] Richter K, Albright W. Long-term results following fixation of the vagina on the sacrospinous ligament by the vaginal route. Am J Obstet Gynecol 1981; 151: 811 [15] Nichols DH. Sacrospinous fixation for massive eversion of the vagina. Am J Obstet Gynecol 1982; 142:901 [16] Sze E, Miklos J, Patroll L, et al. Sacrospinous ligament fixation with transvaginal needle suspension for advanced pelvic organ prolapse and stress incontinence. Obstet Gynecol 1997; 98: 94 [17] Shull BL, Capen CV, Riggs MW, et al. Bilateral attachment of the vaginal cuff to iliococcygeus fascia: an effective method of cuff suspension. Am J Obstet Gynecol.1993; 168:1669 [18] Meeks GR, Washburne JF, McGehee RP, et al.. Repair of vaginal vault prolapse by suspension of the vagina to the iliococcygeus (prespinous) fascia. Am J Obstet Gynecol 1994; 171:
9 116 Robot Surgery [19] Amid PK. Classification of biomaterials and their complications in abdominal wall hernia surgery. Hernia 1997;1: 15 [20] Cosson M, Debodinance P, Boukerrou M, et al. Mechanical properties of synthetic implants used in the repair of prolapse and urinary incontinence in women: which is the ideal material? Int Urogynecol J Pelvic Floor Dysfunct. 2003; 14:169 [21] Diwadkar GB, Barber MD, Feiner B, et al. Complication and reoperation rates after apical vaginal prolapse surgical repair: a systematic review. Obstet Gynecol 2009; 113: 367 [22] Sanses TVD, Shahryarinejad A, Molden S, et al. Anatomic outcomes of vaginal mesh procedure (Prolift) compared with uterosacral ligament suspension and abdominal sacrocolpopexy for pelvic organ prolapse: a Fellow s Pelvic Research Network study. Am J Obstet Gynecol 2009 [23] Timmons MC, Addison WA, Addison SB, et al. Abdominal sacral colpopexy in 163 women with post hysterectomy vaginal vault prolapse and enterocele. Evolution of operative techniques. J Reprod Med 1992; 37: 323 [24] Snyder TE, Krantz KE. Abdominal-retroperitoneal sacral colpopexy for the correction of vaginal prolpase. Obstet Gynecol 1991; 77:944 [25] Maher C, Baessler K, Glazener CMA et al. Surgical management of pelvic organ prolapse in women (Review). The Cochrane Collaboration. The Cochrane Library 2007, Issue 2 [26] Cundiff GW, Varner E, Visco AG, Zyczynski HM, Nager CW, Norton PA, Schaffer J, Brown MB, Brubaker L; Pelvic Floor Disorders Network. Am J Obstet Gynecol 2008; 199:e1-5. [27] Paraiso MFR, Walters MD, Rackley RR et al. Laparoscopic and abdominal sacral colpopexy: A comparative cohort study. Am J Obstet Gynecol 2005; 192:1752 [28] Sarlos D, Brandner S, Kots L et al. Laparoscopic sacrocolpopexy for uterine and posthysterectomy prolapse: anatomical results, quality of life and perioperative outcome - a prospective study with 101 cases. Int Urogynecol J Pelvic Floor Dysfunct 2008; 19:1415 [29] Hsiao KC, Latchamsetty K, Govier FE et al. Comparison of laparoscopic and abdominal sacrocolpopexy for the treatment of vaginal vault prolapse. J Endourol 2007;21:926 [30] Rozet F, Mandron E, Arroyo C et al. Laparoscopic sacral colpopexy approach for gentiourinary prolapse: experience with 363 cases. Eur Urol 2005;47:230 [31] Ross JW, Preston M. Laparoscopic sacrocolpopexy for severe vaginal vault prolapse: five-year outcome. J Minim Invasive Gynecol 2005;12:221 [32] Elliott DS, Krambeck AE, Chow GK. Long-term results of robotic assisted laparoscopic sacrocolpopexy for the treatment of high grade vaginal vault prolpase. J Urol 2006;176:655 [33] Di Marco DS, Chow GK, Gettman MT et al. Robotic-assisted laparoscopic sacrocolpopexy for treatment of vaginal vault prolapse. Urology 2004;63:373 [34] Kramer BA, Whelan CM, Powell TM et al. Robotic-assisted laparoscopic sacrocolpopexy as management for pelvic organ prolpase. J Endourol 2009;23:655 [35] Daneshgari F, Kefer JC, Moore C et al. Robotic abdominal sacrocolpopexy/ sacrouteropexy repair of advanced female pelvic organ prolapse (POP): utilizing POP-quantification-based staging and outcomes. BJU Int. 2007; 100: 875
10 Robotic Sacrocolpopexy and Sacrocervicopexy for the Correction of Pelvic Organ Prolapse 117 [36] Akl MN, Long JB, Giles DL et al. Robotic assisted sacrocolpopexy: technique and learning curve. Surg Endosc 2009 (27) [37] Kohli N, Walsh PM, Roat TW et al. Mesh erosion after abdominal sacrocolpopexy. Obstet Gynecol 1998;92:999 [38] Geller EJ, Siddiqui NY, Wu JM et al. Soft-term outcomes of robotic sacrocolpopexy compared with abdominal sacrocolpopexy. Obstet Gynecol 2008;112:1198 [39] Chang FH, Lee CL, Soong YK. Use of Palmer s Point for Insertion of the Operative Laparoscope in Patients with Severe Pelvic Adhesions: Experience of Seventeen Cases. J Am Assoc Gynecol Laparosc 1994;1:S7 Figures Fig. 1. Operating room configuration
11 118 Robot Surgery Fig. 2. Port placement for RALSC (4-arm DaVinci) Fig. 3. Patient positioning and patient cart docking of 4-arm DaVinci
12 Robotic Sacrocolpopexy and Sacrocervicopexy for the Correction of Pelvic Organ Prolapse 119 Fig. 4. Exposed anterior longitudinal ligament over sacral promontory Fig. 5. Dissecting peritoneum from vaginal cuff
13 120 Robot Surgery Fig. 6. Securing mesh to anterior vaginal wall Fig. 7. Securing mesh to posterior vaginal wall
14 Robotic Sacrocolpopexy and Sacrocervicopexy for the Correction of Pelvic Organ Prolapse 121 Fig. 8. Mesh trimmed to appropriate size Fig. 9. Securing mesh to sacral promontory
15 122 Robot Surgery Fig. 10. Closure of peritoneum over mesh Fig. 11. Alternative side-docking 4-arm DaVinci for pelvic surgery
16 Robot Surgery Edited by Seung Hyuk Baik ISBN Hard cover, 172 pages Publisher InTech Published online 01, January, 2010 Published in print edition January, 2010 Robotic surgery is still in the early stages even though robotic assisted surgery is increasing continuously. Thus, exact and careful understanding of robotic surgery is necessary because chaos and confusion exist in the early phase of anything. Especially, the confusion may be increased because the robotic equipment, which is used in surgery, is different from the robotic equipment used in the automobile factory. The robots in the automobile factory just follow a program. However, the robot in surgery has to follow the surgeon s hand motions. I am convinced that this In-Tech Robotic Surgery book will play an essential role in giving some solutions to the chaos and confusion of robotic surgery. The In-Tech Surgery book contains 11 chapters and consists of two main sections. The first section explains general concepts and technological aspects of robotic surgery. The second section explains the details of surgery using a robot for each organ system. I hope that all surgeons who are interested in robotic surgery will find the proper knowledge in this book. Moreover, I hope the book will perform as a basic role to create future prospectives. Unfortunately, this book could not cover all areas of robotic assisted surgery such as robotic assisted gastrectomy and pancreaticoduodenectomy. I expect that future editions will cover many more areas of robotic assisted surgery and it can be facilitated by dedicated readers. Finally, I appreciate all authors who sacrificed their time and effort to write this book. I must thank my wife NaYoung for her support and also acknowledge MiSun Park s efforts in helping to complete the book. How to reference In order to correctly reference this scholarly work, feel free to copy and paste the following: James C Brien, Michael D Fabrizio and James C Lukban (2010). Robotic Sacrocolpopexy and Sacrocervicopexy for the Correction of Pelvic Organ Prolapse, Robot Surgery, Seung Hyuk Baik (Ed.), ISBN: , InTech, Available from: InTech Europe University Campus STeP Ri Slavka Krautzeka 83/A Rijeka, Croatia Phone: +385 (51) InTech China Unit 405, Office Block, Hotel Equatorial Shanghai No.65, Yan An Road (West), Shanghai, , China Phone:
17 Fax: +385 (51) Fax:
18 2010 The Author(s). Licensee IntechOpen. This chapter is distributed under the terms of the Creative Commons Attribution-NonCommercial- ShareAlike-3.0 License, which permits use, distribution and reproduction for non-commercial purposes, provided the original is properly cited and derivative works building on this content are distributed under the same license.
SURGICAL. How to manage the cuff at vaginal hysterectomy. For personal use only. Copyright Dowden Health Media TECHNIQUES
 For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review
 Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
International Federation of Gynecology and Obstetrics
 International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
Paravaginal Repair: A Laparoscopic Approach
 44 Paravaginal Repair: A Laparoscopic Approach John R. Miklos and Robert Moore Atlanta Urogynecology Associates, Atlanta, Georgia, U.S.A. Neeraj Kohli Harvard University, Boston, Massachusetts, U.S.A.
44 Paravaginal Repair: A Laparoscopic Approach John R. Miklos and Robert Moore Atlanta Urogynecology Associates, Atlanta, Georgia, U.S.A. Neeraj Kohli Harvard University, Boston, Massachusetts, U.S.A.
INGUINAL HERNIA REPAIR PROCEDURE GUIDE
 ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
W23: Approaches to pelvic organ prolapse surgery Workshop Chair: Philippe Zimmern, United States 21 October :00-12:00
 W23: Approaches to pelvic organ prolapse surgery Workshop Chair: Philippe Zimmern, United States 21 October 2014 09:00-12:00 Start End Topic Speakers 09:00 09:30 Goals of repair and anatomical principles
W23: Approaches to pelvic organ prolapse surgery Workshop Chair: Philippe Zimmern, United States 21 October 2014 09:00-12:00 Start End Topic Speakers 09:00 09:30 Goals of repair and anatomical principles
Step by step High uterosacral vaginal vault suspension to repair enterocele and apical prolapse
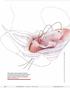 When performing high uterosacral suspension, it is possible to pass sutures through the coccygeus muscle-sacrospinous ligament complex (arrow) because a segment of the uterosacral ligament inserts into
When performing high uterosacral suspension, it is possible to pass sutures through the coccygeus muscle-sacrospinous ligament complex (arrow) because a segment of the uterosacral ligament inserts into
ROBOTIC MESH SACROCOLPOPEXY
 ROBOTIC MESH SACROCOLPOPEXY Philippe E. Zimmern, MD, FACS Professor of Urology Mesh sacrocolpopexy Background First described in 1962 by Lane Until then, treatment options were: Pessary Colpocleisis Vaginal
ROBOTIC MESH SACROCOLPOPEXY Philippe E. Zimmern, MD, FACS Professor of Urology Mesh sacrocolpopexy Background First described in 1962 by Lane Until then, treatment options were: Pessary Colpocleisis Vaginal
Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option.
 Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option. The Condition(s): Vaginal Prolapse, Uterine Prolapse Vaginal prolapse occurs when the
Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option. The Condition(s): Vaginal Prolapse, Uterine Prolapse Vaginal prolapse occurs when the
Laparoscopic Sacrocolpopexy with & without the Robot: Tips and Tricks for success and avoidance / management of complications
 Laparoscopic Sacrocolpopexy with & without the Robot: Tips and Tricks for success and avoidance / management of complications Course Faculty: Patrick Culligan, MD Peter Rosenblatt, MD What is a Sacrocolpopexy?
Laparoscopic Sacrocolpopexy with & without the Robot: Tips and Tricks for success and avoidance / management of complications Course Faculty: Patrick Culligan, MD Peter Rosenblatt, MD What is a Sacrocolpopexy?
With our aging population, the rate of pelvic
 Original Research Short-Term Outcomes of Robotic Sacrocolpopexy Compared With Abdominal Sacrocolpopexy Elizabeth J. Geller, MD, Nazema Y. Siddiqui, MD, Jennifer M. Wu, MD, MPH, and Anthony G. Visco, MD
Original Research Short-Term Outcomes of Robotic Sacrocolpopexy Compared With Abdominal Sacrocolpopexy Elizabeth J. Geller, MD, Nazema Y. Siddiqui, MD, Jennifer M. Wu, MD, MPH, and Anthony G. Visco, MD
Surgical treatments for vaginal apical prolapse
 Review Article Obstet Gynecol Sci 2016;59(4):253-260 http://dx.doi.org/10.5468/ogs.2016.59.4.253 pissn 2287-8572 eissn 2287-8580 Surgical treatments for vaginal apical prolapse Mi Kyung Kong, Sang Wook
Review Article Obstet Gynecol Sci 2016;59(4):253-260 http://dx.doi.org/10.5468/ogs.2016.59.4.253 pissn 2287-8572 eissn 2287-8580 Surgical treatments for vaginal apical prolapse Mi Kyung Kong, Sang Wook
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015
 Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy
 Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse
 ORIGINAL ARTICLE Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse Cecile A. Unger, MD, MPH, Matthew D. Barber, MD, MHS, Mark
ORIGINAL ARTICLE Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse Cecile A. Unger, MD, MPH, Matthew D. Barber, MD, MHS, Mark
LAPAROSCOPIC REPAIR OF PELVIC FLOOR
 LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
PL Narducci Department of Obstetrics and Gynecology General Hospital San Giovanni Battista Foligno, ITALY
 NESA DAYS 2018 New European Surgical Academy Perugia, April 19-21, 2018 EXCELLENCE IN FEMALE SURGERY PROLAPSE RECONSTRUCTIVE SURGERY IN SEXUALLY ACTIVE WOMEN LAPAROSCOPIC ANTERIOR ABDOMINAL WALL COLPOPEXY
NESA DAYS 2018 New European Surgical Academy Perugia, April 19-21, 2018 EXCELLENCE IN FEMALE SURGERY PROLAPSE RECONSTRUCTIVE SURGERY IN SEXUALLY ACTIVE WOMEN LAPAROSCOPIC ANTERIOR ABDOMINAL WALL COLPOPEXY
Understanding Pelvic Organ Prolapse. Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery
 Understanding Pelvic Organ Prolapse Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery Disclosures None I am the daughter of a physician assistant. Objectives List types of pelvic
Understanding Pelvic Organ Prolapse Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery Disclosures None I am the daughter of a physician assistant. Objectives List types of pelvic
Supracervical Robotic-Assisted Laparoscopic Sacrocolpopexy for Pelvic Organ Prolapse
 SCIENTIFIC PAPER Supracervical Robotic-Assisted Laparoscopic Sacrocolpopexy for Pelvic Organ Prolapse Aaron D. Benson, MD, Brandan A. Kramer, MD, Robert O. Wayment, MD, Bradley F. Schwartz, DO ABSTRACT
SCIENTIFIC PAPER Supracervical Robotic-Assisted Laparoscopic Sacrocolpopexy for Pelvic Organ Prolapse Aaron D. Benson, MD, Brandan A. Kramer, MD, Robert O. Wayment, MD, Bradley F. Schwartz, DO ABSTRACT
By:Dr:ISHRAQ MOHAMMED
 By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
Dr John Short. Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch
 Dr John Short Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch 8:30-9:25 WS #142: Peeling Back the Layers - The Pelvic Floor Uncovered 9:35-10:30 WS #152:
Dr John Short Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch 8:30-9:25 WS #142: Peeling Back the Layers - The Pelvic Floor Uncovered 9:35-10:30 WS #152:
Robot Assisted Rectopexy
 1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
Stop Coping. Start Living. Talk to your doctor about pelvic organ prolapse and sacrocolpopexy
 Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Prevalence and risk factors for mesh erosion after laparoscopic-assisted sacrocolpopexy
 Int Urogynecol J (2011) 22:205 212 DOI 10.1007/s00192-010-1265-3 ORIGINAL ARTICLE Prevalence and risk factors for mesh erosion after laparoscopic-assisted sacrocolpopexy Jasmine Tan-Kim & Shawn A. Menefee
Int Urogynecol J (2011) 22:205 212 DOI 10.1007/s00192-010-1265-3 ORIGINAL ARTICLE Prevalence and risk factors for mesh erosion after laparoscopic-assisted sacrocolpopexy Jasmine Tan-Kim & Shawn A. Menefee
REPAIR OF LARGE CYSTOCELE
 REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
 Gynecol Surg (2006) 3: 88 92 DOI 10.1007/s10397-005-0168-7 ORIGINAL ARTICLE R. Oliver. C. Dasgupta. A. Coker Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
Gynecol Surg (2006) 3: 88 92 DOI 10.1007/s10397-005-0168-7 ORIGINAL ARTICLE R. Oliver. C. Dasgupta. A. Coker Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
Original article J Bas Res Med Sci 2015; 2(2): The incidence of recurrent pelvic organ prolapse: A cross sectional study
 The incidence of recurrent pelvic organ prolapse: A cross sectional study Ashraf Direkvand-Moghadam 1, Ali Delpisheh 2, Azadeh Direkvand-Moghadam 3* 1. Psychosocial Injuries Research Center, Faculty of
The incidence of recurrent pelvic organ prolapse: A cross sectional study Ashraf Direkvand-Moghadam 1, Ali Delpisheh 2, Azadeh Direkvand-Moghadam 3* 1. Psychosocial Injuries Research Center, Faculty of
Current status in pelvic organ prolapse surgery: an evidence based review
 Current status in pelvic organ prolapse surgery: an evidence based review Christian Falconer, MD, PhD Department of Obstetrics and Gynecology Danderyd University Hospital Stockholm, Sweden Finnish Society
Current status in pelvic organ prolapse surgery: an evidence based review Christian Falconer, MD, PhD Department of Obstetrics and Gynecology Danderyd University Hospital Stockholm, Sweden Finnish Society
Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments?
 Int Urogynecol J (2010) 21:271 278 DOI 10.1007/s00192-009-1028-1 ORIGINAL ARTICLE Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments? Mariëlla
Int Urogynecol J (2010) 21:271 278 DOI 10.1007/s00192-009-1028-1 ORIGINAL ARTICLE Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments? Mariëlla
PRACTICE BULLETIN Female Pelvic Medicine & Reconstructive Surgery Volume 23, Number 4, July/August 2017
 PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
Prospective study of an ultra-lightweight polypropylene Y mesh for robotic sacrocolpopexy
 Int Urogynecol J (2013) 24:1371 1375 DOI 10.1007/s00192-012-2021-7 ORIGINAL ARTICLE Prospective study of an ultra-lightweight polypropylene Y mesh for robotic sacrocolpopexy Charbel G. Salamon & Christa
Int Urogynecol J (2013) 24:1371 1375 DOI 10.1007/s00192-012-2021-7 ORIGINAL ARTICLE Prospective study of an ultra-lightweight polypropylene Y mesh for robotic sacrocolpopexy Charbel G. Salamon & Christa
This information is intended as an overview only
 This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
Laparoscopic sacrocolpopexy for the correction of vaginal vault prolapse
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2004 Laparoscopic sacrocolpopexy for the correction of vaginal vault prolapse Chandru P. Sundaram Indiana University
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2004 Laparoscopic sacrocolpopexy for the correction of vaginal vault prolapse Chandru P. Sundaram Indiana University
Prevention of Surgical Injuries in Gynecology
 in Gynecology John K. Chan, M.D. Division of Gynecologic Oncology Overview Review anatomy, etiology, intraoperative, postoperative management, prevention of injuries to: 1. Urinary tract 2. Gastrointestinal
in Gynecology John K. Chan, M.D. Division of Gynecologic Oncology Overview Review anatomy, etiology, intraoperative, postoperative management, prevention of injuries to: 1. Urinary tract 2. Gastrointestinal
Laparoscopic sacrocolpopexy: an observational study of functional and anatomical outcomes
 DOI 10.1007/s00192-010-1241-y ORIGINAL ARTICLE Laparoscopic sacrocolpopexy: an observational study of functional and anatomical outcomes Natalia Price & Alex Slack & Simon R. Jackson Received: 26 April
DOI 10.1007/s00192-010-1241-y ORIGINAL ARTICLE Laparoscopic sacrocolpopexy: an observational study of functional and anatomical outcomes Natalia Price & Alex Slack & Simon R. Jackson Received: 26 April
Innovations in mesh kit technology for vaginal wall prolapse
 Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
NOTES FROM GUTMAN LECTURE 10/26 Use this outline to study from. As you go through Gutman s lecture, fill in the topics.
 NOTES FROM GUTMAN LECTURE 10/26 Use this outline to study from. As you go through Gutman s lecture, fill in the topics. Anatomy above the arcuate line Skin Camper s fascia Scarpa s fascia External oblique
NOTES FROM GUTMAN LECTURE 10/26 Use this outline to study from. As you go through Gutman s lecture, fill in the topics. Anatomy above the arcuate line Skin Camper s fascia Scarpa s fascia External oblique
Gynecology Dr. Sallama Lecture 3 Genital Prolapse
 Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
RECTAL INJURY IN UROLOGIC SURGERY. Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences.
 RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
Laparoscopic surgery for pelvic support defects
 ~ Laparoscopic surgery for pelvic support defects John R. Miklosa, Robert D. Mooreb and Neeraj Kohlia Reconstructive pelvic surgery for the treatment of vaginal prolapse continues to evolve as surgeons
~ Laparoscopic surgery for pelvic support defects John R. Miklosa, Robert D. Mooreb and Neeraj Kohlia Reconstructive pelvic surgery for the treatment of vaginal prolapse continues to evolve as surgeons
ISSN (o): Sacrospinous fixation: an efficient technique for prevention and treatment of vault prolapse
 Original article www.ijrhs.com ISSN (o):2321 7251 Sacrospinous fixation: an efficient technique for prevention and treatment of vault Rajshree dayanand katke 1, Usha kiran. 2 1M.D.(Obstetrics & Gynecology),
Original article www.ijrhs.com ISSN (o):2321 7251 Sacrospinous fixation: an efficient technique for prevention and treatment of vault Rajshree dayanand katke 1, Usha kiran. 2 1M.D.(Obstetrics & Gynecology),
Surgical repair of vaginal wall prolapse using mesh
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology
 Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology Ospedale San Giovanni di Dio, Gorizia, Italy ANATOMY URINARY CONTINENCE
Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology Ospedale San Giovanni di Dio, Gorizia, Italy ANATOMY URINARY CONTINENCE
Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications
 Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications Karyn S. Eilber, M.D. Cedars-Sinai FPMRS Associate Professor, Cedars-Sinai Dept of Surgery Associate Director, Urology Residency
Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications Karyn S. Eilber, M.D. Cedars-Sinai FPMRS Associate Professor, Cedars-Sinai Dept of Surgery Associate Director, Urology Residency
Vaginal McCall culdoplasty versus laparoscopic uterosacral plication to prophylactically address vaginal vault prolapse
 Vaginal McCall culdoplasty versus laparoscopic uterosacral to prophylactically address vaginal vault prolapse Niblock, K., Bailie, E., McCracken, G., & Johnston, K. (2017). Vaginal McCall culdoplasty versus
Vaginal McCall culdoplasty versus laparoscopic uterosacral to prophylactically address vaginal vault prolapse Niblock, K., Bailie, E., McCracken, G., & Johnston, K. (2017). Vaginal McCall culdoplasty versus
Site-specific fascial defects in the diagnosis and surgical management of enterocele
 Site-specific fascial defects in the diagnosis and surgical management of enterocele John R. Miklos, MD,a Neeraj Kohli, MD,b Vincent Lucente, MD,c and William B. Safe, MDd Atlanta and Marietta, GeO1gia,
Site-specific fascial defects in the diagnosis and surgical management of enterocele John R. Miklos, MD,a Neeraj Kohli, MD,b Vincent Lucente, MD,c and William B. Safe, MDd Atlanta and Marietta, GeO1gia,
Dana Alrafaiah. - Amani Nofal. - Ahmad Alsalman. 1 P a g e
 - 2 - Dana Alrafaiah - Amani Nofal - Ahmad Alsalman 1 P a g e This lecture will discuss five topics as follows: 1- Arrangement of pelvic viscera. 2- Muscles of Pelvis. 3- Blood Supply of pelvis. 4- Nerve
- 2 - Dana Alrafaiah - Amani Nofal - Ahmad Alsalman 1 P a g e This lecture will discuss five topics as follows: 1- Arrangement of pelvic viscera. 2- Muscles of Pelvis. 3- Blood Supply of pelvis. 4- Nerve
Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583
 Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
SACROSPINOUS LIGAMENT FIXATION, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE
 Original Article, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE * ** Fauzia Rasool Memon, Mohamed Matar * Consultant Obstetrician and Gynecologist
Original Article, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE * ** Fauzia Rasool Memon, Mohamed Matar * Consultant Obstetrician and Gynecologist
What are we talking about? Symptoms. Prolapse Risk Factors. Vaginal bulge 1 Splinting. ?? Pelvic pressure Back pain 1 Urinary complaints 2
 Options for Vaginal Prolapse What are we talking about? Michelle Y. Morrill, M.D. Director of Urogynecology The Permanente Medical Group Kaiser, San Francisco Assistant Professor, Volunteer Faculty Department
Options for Vaginal Prolapse What are we talking about? Michelle Y. Morrill, M.D. Director of Urogynecology The Permanente Medical Group Kaiser, San Francisco Assistant Professor, Volunteer Faculty Department
Le fort s operation for prolapse uterus: A forgotten procedure
 2017; 1(2): 52-56 ISSN (P): 2522-6614 ISSN (E): 2522-6622 Gynaecology Journal www.gynaecologyjournal.com 2017; 1(2): 52-56 Received: 12-09-2017 Accepted: 13-10-2017 Dr. Jasmine Lall 3 rd Year Resident,
2017; 1(2): 52-56 ISSN (P): 2522-6614 ISSN (E): 2522-6622 Gynaecology Journal www.gynaecologyjournal.com 2017; 1(2): 52-56 Received: 12-09-2017 Accepted: 13-10-2017 Dr. Jasmine Lall 3 rd Year Resident,
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,100 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,100 116,000 120M Open access books available International authors and editors Downloads Our
Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M.
 UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
9/24/2015. Pelvic Floor Disorders. Agenda. What is the Pelvic Floor? Pelvic Floor Problems
 Management of Pelvic Floor Disorders Doctor, I don t want THAT mesh! Agenda What are pelvic floor disorders (PFDs)? What are the treatment options? Expectant. Conservative. Surgical. How and when are grafts
Management of Pelvic Floor Disorders Doctor, I don t want THAT mesh! Agenda What are pelvic floor disorders (PFDs)? What are the treatment options? Expectant. Conservative. Surgical. How and when are grafts
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time
 EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time Menachem Alcalay,M.D, Urogynecology unit, Sheba Medical
EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time Menachem Alcalay,M.D, Urogynecology unit, Sheba Medical
Long-term outcomes of modified high uterosacral ligament vault suspension (HUSLS) at vaginal hysterectomy
 Int Urogynecol J (2011) 22:577 584 DOI 10.1007/s00192-010-1325-8 ORIGINAL ARTICLE Long-term outcomes of modified high uterosacral ligament vault suspension (HUSLS) at vaginal hysterectomy Stergios K. Doumouchtsis
Int Urogynecol J (2011) 22:577 584 DOI 10.1007/s00192-010-1325-8 ORIGINAL ARTICLE Long-term outcomes of modified high uterosacral ligament vault suspension (HUSLS) at vaginal hysterectomy Stergios K. Doumouchtsis
Factors associated with intraoperative conversion during robotic sacrocolpopexy
 ORIGINAL ARTICLE Vol. 41 (2): 319-324, March - April, 2015 doi: 10.1590/S1677-5538.IBJU.2015.02.19 Factors associated with intraoperative conversion during robotic sacrocolpopexy Brian J. Linder 1, George
ORIGINAL ARTICLE Vol. 41 (2): 319-324, March - April, 2015 doi: 10.1590/S1677-5538.IBJU.2015.02.19 Factors associated with intraoperative conversion during robotic sacrocolpopexy Brian J. Linder 1, George
Medium-term follow-up on use of freeze-dried, irradiated donor fascia for sacrocolpopexy and sling procedures
 Int Urogynecol J (2004) 15: 238 242 DOI 10.1007/s00192-004-1146-8 ORIGINAL ARTICLE Mary Pat FitzGerald Æ S. Renee Edwards Æ Dee Fenner Medium-term follow-up on use of freeze-dried, irradiated donor fascia
Int Urogynecol J (2004) 15: 238 242 DOI 10.1007/s00192-004-1146-8 ORIGINAL ARTICLE Mary Pat FitzGerald Æ S. Renee Edwards Æ Dee Fenner Medium-term follow-up on use of freeze-dried, irradiated donor fascia
A Long-Term Treatment Outcome of Abdominal Sacrocolpopexy
 Original Article DOI 10.3349/ymj.2009.50.6.807 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 50(6): 807-813, 2009 A Long-Term Treatment Outcome of Abdominal Sacrocolpopexy Myung Jae Jeon, 1 Yeo Jung
Original Article DOI 10.3349/ymj.2009.50.6.807 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 50(6): 807-813, 2009 A Long-Term Treatment Outcome of Abdominal Sacrocolpopexy Myung Jae Jeon, 1 Yeo Jung
Considering Surgery for Pelvic Prolapse? Learn about minimally invasive da Vinci Surgery
 Considering Surgery for Pelvic Prolapse? Learn about minimally invasive da Vinci Surgery The Surgery: Pelvic Prolapse Surgery If you have pelvic prolapse symptoms, your doctor may suggest medicine or lifestyle
Considering Surgery for Pelvic Prolapse? Learn about minimally invasive da Vinci Surgery The Surgery: Pelvic Prolapse Surgery If you have pelvic prolapse symptoms, your doctor may suggest medicine or lifestyle
Introduction. Regarding the Section of the UPDATE Entitled Purpose
 Time to Rethink: an Evidence-Based Response from Pelvic Surgeons to the FDA Safety Communication: UPDATE on Serious Complications Associated with Transvaginal Placement of Surgical Mesh for Pelvic Organ
Time to Rethink: an Evidence-Based Response from Pelvic Surgeons to the FDA Safety Communication: UPDATE on Serious Complications Associated with Transvaginal Placement of Surgical Mesh for Pelvic Organ
Suture complications in a teaching institution among patients undergoing uterosacral ligament suspension with permanent braided suture
 Int Urogynecol J (2010) 21:813 818 DOI 10.1007/s00192-010-1109-1 ORIGINAL ARTICLE Suture complications in a teaching institution among patients undergoing uterosacral ligament suspension with permanent
Int Urogynecol J (2010) 21:813 818 DOI 10.1007/s00192-010-1109-1 ORIGINAL ARTICLE Suture complications in a teaching institution among patients undergoing uterosacral ligament suspension with permanent
Colorectal procedure guide
 Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Clinical Curriculum: Urogynecology
 Updated July 201 Clinical Curriculum: Urogynecology GOAL: The primary goal of the Urogynecology rotation at the University of Alabama at Birmingham (UAB) is to train physicians to have a broad knowledge
Updated July 201 Clinical Curriculum: Urogynecology GOAL: The primary goal of the Urogynecology rotation at the University of Alabama at Birmingham (UAB) is to train physicians to have a broad knowledge
Ina S. Irabon, MD, FPOGS, FPSRM, FPSGE Obstetrics and Gynecology Reproductive Endocrinology and Infertility Laparoscopy and Hysteroscopy
 Ina S. Irabon, MD, FPOGS, FPSRM, FPSGE Obstetrics and Gynecology Reproductive Endocrinology and Infertility Laparoscopy and Hysteroscopy Comprehensive Gynecology 7 th edition, 2017 (Lobo RA, Gershenson
Ina S. Irabon, MD, FPOGS, FPSRM, FPSGE Obstetrics and Gynecology Reproductive Endocrinology and Infertility Laparoscopy and Hysteroscopy Comprehensive Gynecology 7 th edition, 2017 (Lobo RA, Gershenson
and recovery time have led many clinicians
 Research UROGYNECOLOGY Laparoscopic sacral colpopexy versus total vaginal mesh for vaginal vault prolapse: a randomized trial Christopher F. Maher, MD; Benjamin Feiner, MD; Eva M. DeCuyper, MD; Cathy J.
Research UROGYNECOLOGY Laparoscopic sacral colpopexy versus total vaginal mesh for vaginal vault prolapse: a randomized trial Christopher F. Maher, MD; Benjamin Feiner, MD; Eva M. DeCuyper, MD; Cathy J.
A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience
 Journal Of Laparoendoscopic Surgery Volume 4, Number 5, 1994 Mary Ann Liebert, Inc., Publishers A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience E.D. RIZA, M.D.(1)
Journal Of Laparoendoscopic Surgery Volume 4, Number 5, 1994 Mary Ann Liebert, Inc., Publishers A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience E.D. RIZA, M.D.(1)
Gökmen Sukgen, 1 Esra SaygJlJ YJlmaz, 2 and Eralp BaGer Introduction. 2. Case Presentation
 Case Reports in Obstetrics and Gynecology Volume 2016, Article ID 2906596, 4 pages http://dx.doi.org/10.1155/2016/2906596 Case Report Vaginal Hysterectomy with Anterior Four-Arm Mesh Implant Technique
Case Reports in Obstetrics and Gynecology Volume 2016, Article ID 2906596, 4 pages http://dx.doi.org/10.1155/2016/2906596 Case Report Vaginal Hysterectomy with Anterior Four-Arm Mesh Implant Technique
Tian-Ni Kuo 1, Ming-Ping Wu 1,2 *
 RESEARCH LETTER THE USE OF A CONCOMITANT TENSION-FREE VAGINAL MESH TECHNIQUE AND A TENSION-FREE MIDURETHRAL SLING IN TREATING PELVIC ORGAN PROLAPSE AND OCCULT STRESS URINARY INCONTINENCE Tian-Ni Kuo 1,
RESEARCH LETTER THE USE OF A CONCOMITANT TENSION-FREE VAGINAL MESH TECHNIQUE AND A TENSION-FREE MIDURETHRAL SLING IN TREATING PELVIC ORGAN PROLAPSE AND OCCULT STRESS URINARY INCONTINENCE Tian-Ni Kuo 1,
Elevate Anterior/Apical: 12-Month Data Showing Safety and Efficacy in Surgical Treatment of Pelvic Organ Prolapse
 ORIGINAL ARTICLE Elevate Anterior/Apical: 12-Month Data Showing Safety and Efficacy in Surgical Treatment of Pelvic Organ Prolapse Edward J. Stanford, MD, MS,* Robert D. Moore, DO,Þ Jan-Paul W.R. Roovers,
ORIGINAL ARTICLE Elevate Anterior/Apical: 12-Month Data Showing Safety and Efficacy in Surgical Treatment of Pelvic Organ Prolapse Edward J. Stanford, MD, MS,* Robert D. Moore, DO,Þ Jan-Paul W.R. Roovers,
Laparoscopic pectopexy: initial experience of single center with a new technique for apical prolapse surgery
 ORIGINAL ARTICLE Vol. 43 (5): 903-909, September - October, 2017 doi: 10.1590/S1677-5538.IBJU.2017.0070 Laparoscopic pectopexy: initial experience of single center with a new technique for apical surgery
ORIGINAL ARTICLE Vol. 43 (5): 903-909, September - October, 2017 doi: 10.1590/S1677-5538.IBJU.2017.0070 Laparoscopic pectopexy: initial experience of single center with a new technique for apical surgery
Robot-Assisted Gynecologic Surgery. Gynecologic Surgery
 Robot-Assisted Gynecologic Surgery Alison F. Jacoby, MD Department of Obstetrics, Gynecology and Reproductive Sciences University of California, San Francisco Robot-Assisted Gynecologic Surgery Clinical
Robot-Assisted Gynecologic Surgery Alison F. Jacoby, MD Department of Obstetrics, Gynecology and Reproductive Sciences University of California, San Francisco Robot-Assisted Gynecologic Surgery Clinical
SCIENTIFIC PAPER ABSTRACT INTRODUCTION MATERIALS AND METHODS
 SCIENTIFIC PAPER Vaginal Cuff Closure during Robotic-Assisted Total Laparoscopic Hysterectomy: Comparing Vicryl to Barbed Sutures A. Karim Nawfal, MD, David Eisenstein, MD, Evan Theoharis, MD, Marisa Dahlman,
SCIENTIFIC PAPER Vaginal Cuff Closure during Robotic-Assisted Total Laparoscopic Hysterectomy: Comparing Vicryl to Barbed Sutures A. Karim Nawfal, MD, David Eisenstein, MD, Evan Theoharis, MD, Marisa Dahlman,
Vaginally-Assisted Laparoscopic Hysterosacropexy for Advanced Utero-Vaginal Prolapse: A Series of 32 Cases
 ARS Medica Tomitana - 2014; 2(77): 63-70 10.2478/arsm-2014-0012 Brătilă V. Elvira 1, Brătilă P.C. 2, Negroiu Andra-Teodora 3 Vaginally-Assisted Laparoscopic Hysterosacropexy for Advanced Utero-Vaginal
ARS Medica Tomitana - 2014; 2(77): 63-70 10.2478/arsm-2014-0012 Brătilă V. Elvira 1, Brătilă P.C. 2, Negroiu Andra-Teodora 3 Vaginally-Assisted Laparoscopic Hysterosacropexy for Advanced Utero-Vaginal
CHAU KHAC TU M.D., Ph.D.
 CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
Female Urology. The Results of Grade IV Cystocele Repair Using Mesh. Introduction ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M
 Urology Journal UNRC/IUA Vol. 1, No. 4, 263-267 Autumn 2004 Printed in IRAN Female Urology The Results of Grade IV Cystocele Repair Using Mesh ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M Department of Urology,
Urology Journal UNRC/IUA Vol. 1, No. 4, 263-267 Autumn 2004 Printed in IRAN Female Urology The Results of Grade IV Cystocele Repair Using Mesh ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M Department of Urology,
Stephen T Jeffery. University of Cape Town, South Africa
 Stephen T Jeffery University of Cape Town, South Africa I still think there s a role for mesh in Prolapse surgery Examples of my most recent mesh cases Case 1 62 yr old Sacrocolpopexy for vault prolapse
Stephen T Jeffery University of Cape Town, South Africa I still think there s a role for mesh in Prolapse surgery Examples of my most recent mesh cases Case 1 62 yr old Sacrocolpopexy for vault prolapse
High levator myorraphy versus uterosacral ligament suspension for vaginal vault fixation: a prospective, randomized study
 Int Urogynecol J (2010) 21:515 522 DOI 10.1007/s00192-009-1064-x ORIGINAL ARTICLE High levator myorraphy versus uterosacral ligament suspension for vaginal vault fixation: a prospective, randomized study
Int Urogynecol J (2010) 21:515 522 DOI 10.1007/s00192-009-1064-x ORIGINAL ARTICLE High levator myorraphy versus uterosacral ligament suspension for vaginal vault fixation: a prospective, randomized study
RADICAL CYSTECTOMY. Solutions for minimally invasive urologic surgery
 RADICAL CYSTECTOMY Solutions for minimally invasive urologic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation Intuitive motion RADICAL CYSTECTOMY Maintains the oncologic
RADICAL CYSTECTOMY Solutions for minimally invasive urologic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation Intuitive motion RADICAL CYSTECTOMY Maintains the oncologic
Table 2. First Generated List of Expert Responses. Likert-Type Scale. Category or Criterion. Rationale or Comments (1) (2) (3) (4)
 Table 2. First Generated List of Expert Responses. Likert-Type Scale Category or Criterion Anatomical Structures and Features Skeletal Structures and Features (1) (2) (3) (4) Rationale or Comments 1. Bones
Table 2. First Generated List of Expert Responses. Likert-Type Scale Category or Criterion Anatomical Structures and Features Skeletal Structures and Features (1) (2) (3) (4) Rationale or Comments 1. Bones
Assia A. Stepanian, MD*, John R. Miklos, MD, Robert D. Moore, DO, and T. Fleming Mattox, MD
 Risk of Mesh Extrusion and Other Mesh-Related Complications After Laparoscopic Sacral Colpopexy with or without Concurrent Laparoscopic-Assisted Vaginal Hysterectomy: Experience of 402 Patients Assia A.
Risk of Mesh Extrusion and Other Mesh-Related Complications After Laparoscopic Sacral Colpopexy with or without Concurrent Laparoscopic-Assisted Vaginal Hysterectomy: Experience of 402 Patients Assia A.
Are effective nonsurgical treatments available for women with pelvic organ prolapse?
 Are effective nonsurgical treatments available for women with pelvic organ prolapse? For women with asymptomatic prolapse, education and reassurance are appropriate. Women may not realize that symptoms
Are effective nonsurgical treatments available for women with pelvic organ prolapse? For women with asymptomatic prolapse, education and reassurance are appropriate. Women may not realize that symptoms
The accomplished gynecologic surgeon
 For mass reproduction, content licensing and permissions contact Dowden Health Media. SURGICAL TECHNIQUES THE RETROPERITONEAL SPACE Keeping vital structures out of harm s way Knowledge of the retroperitoneal
For mass reproduction, content licensing and permissions contact Dowden Health Media. SURGICAL TECHNIQUES THE RETROPERITONEAL SPACE Keeping vital structures out of harm s way Knowledge of the retroperitoneal
Assessment of the durability of robot-assisted laparoscopic sacrocolpopexy for treatment of vaginal vault prolapse
 J Robotic Surg (2007) 1:163 168 DOI 10.1007/s11701-007-0028-8 ORIGINAL ARTICLE Assessment of the durability of robot-assisted laparoscopic sacrocolpopexy for treatment of vaginal vault prolapse Daniel
J Robotic Surg (2007) 1:163 168 DOI 10.1007/s11701-007-0028-8 ORIGINAL ARTICLE Assessment of the durability of robot-assisted laparoscopic sacrocolpopexy for treatment of vaginal vault prolapse Daniel
Posterior Deep Endometriosis. What is the best approach? Posterior Deep Endometriosis. Should we perform a routine excision of the vagina??
 Posterior Deep Endometriosis What is the best approach? Dept Gyn Obst Polyclinique Hotel Dieu CHU Clermont Ferrand France Posterior Deep Endometriosis Organs involved - Peritoneum - Uterine cervix -Rectum
Posterior Deep Endometriosis What is the best approach? Dept Gyn Obst Polyclinique Hotel Dieu CHU Clermont Ferrand France Posterior Deep Endometriosis Organs involved - Peritoneum - Uterine cervix -Rectum
Sara Schaenzer Grand Rounds January 24 th, 2018
 Sara Schaenzer Grand Rounds January 24 th, 2018 Bladder Anatomy Ureter Anatomy Areas of Injury Bladder: Posterior bladder wall above trigone Ureter Crosses beneath uterine vessels At pelvic brim when ligating
Sara Schaenzer Grand Rounds January 24 th, 2018 Bladder Anatomy Ureter Anatomy Areas of Injury Bladder: Posterior bladder wall above trigone Ureter Crosses beneath uterine vessels At pelvic brim when ligating
Total vs Subtotal Hysterectomy
 Total vs Subtotal Hysterectomy AN UNSOLVED PROBLEM? G Centini, E Zupi, A Wattiez 153 patient with 15 years of follow-up The Timeline The first successful hysterectomy (Subtotal)! First Laparoscopic Hysterectomy!
Total vs Subtotal Hysterectomy AN UNSOLVED PROBLEM? G Centini, E Zupi, A Wattiez 153 patient with 15 years of follow-up The Timeline The first successful hysterectomy (Subtotal)! First Laparoscopic Hysterectomy!
Obstetric Anal Sphincter Injury. An update on best practices. Objectives
 Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
da Vinci Hysterectomy Overview Hysterectomy Facts
 da Vinci Hysterectomy for Benign Gynecologic Conditions K. Toursarkissian,MD Beaver Medical Group Dept of OB/GYN Banning, California Overview Welcome & Introductions Hysterectomy in the US da Vinci Surgery
da Vinci Hysterectomy for Benign Gynecologic Conditions K. Toursarkissian,MD Beaver Medical Group Dept of OB/GYN Banning, California Overview Welcome & Introductions Hysterectomy in the US da Vinci Surgery
12/1/13. What are Pelvic Floor Disorders? What is the Pelvic Floor? Facts. Prevalence of Urinary InconOnence. What s New in Pelvic Floor Disorders?
 What are Pelvic Floor Disorders? Urinary Control Problems - InconOnence or leakage of urine Prolapse of pelvic organs - Vagina, bladder, rectum What s New in Pelvic Floor Disorders? Kimberly Kenton MD,
What are Pelvic Floor Disorders? Urinary Control Problems - InconOnence or leakage of urine Prolapse of pelvic organs - Vagina, bladder, rectum What s New in Pelvic Floor Disorders? Kimberly Kenton MD,
Index. Cyclical pelvic pain, 37 Cystocele, 22, 23, 25, 48, 51, 52, 54, 56, 124, 148, 160
 A Abdominal approach, 141 Abdominal hernia s surgery, 123, 124 Abdominal sacrocolpopexy (ASC), 116, 117 Abnormal uterine bleeding, 96 Anterior compartment repair, 101, 102 Apical compartment repair, 96
A Abdominal approach, 141 Abdominal hernia s surgery, 123, 124 Abdominal sacrocolpopexy (ASC), 116, 117 Abnormal uterine bleeding, 96 Anterior compartment repair, 101, 102 Apical compartment repair, 96
Technique Guide. Bard MK Hernia Repair. Featuring Modified Onflex Mesh SOFT TISSUE REPAIR. Anterior Approach to a Preperitoneal Inguinal Hernia Repair
 Bard MK Hernia Repair Featuring Modified Onflex Mesh Technique Guide Anterior Approach to a Preperitoneal Inguinal Hernia Repair SOFT TISSUE REPAIR Right Procedure. Right Product. Right Outcome. The opinions
Bard MK Hernia Repair Featuring Modified Onflex Mesh Technique Guide Anterior Approach to a Preperitoneal Inguinal Hernia Repair SOFT TISSUE REPAIR Right Procedure. Right Product. Right Outcome. The opinions
Anus,Rectum and Colon
 JOURNAL OF THE Anus,Rectum and Colon http://journal-arc.jp CLINICAL RESEARCH Laparoscopic ventral rectopexy with sacrocolpopexy for coexisting pelvic organ prolapse and external rectal prolapse Yoshiyuki
JOURNAL OF THE Anus,Rectum and Colon http://journal-arc.jp CLINICAL RESEARCH Laparoscopic ventral rectopexy with sacrocolpopexy for coexisting pelvic organ prolapse and external rectal prolapse Yoshiyuki
Childbirth, chronic coughing, heavy lifting,
 OBG MANAGEMENT BY THOMAS JULIAN, MD Pelvic-support defects: a guide to anatomy and physiology Due to high postoperative failure rates, the traditional treatment for pelvic-organ prolapse hysterectomy with
OBG MANAGEMENT BY THOMAS JULIAN, MD Pelvic-support defects: a guide to anatomy and physiology Due to high postoperative failure rates, the traditional treatment for pelvic-organ prolapse hysterectomy with
High success rate and considerable adverse events of pelvic prolapse surgery with Prolift: A single center experience
 Available online at www.sciencedirect.com ScienceDirect Taiwanese Journal of Obstetrics & Gynecology 52 (2013) 389e394 Short Communication High success rate and considerable adverse events of pelvic prolapse
Available online at www.sciencedirect.com ScienceDirect Taiwanese Journal of Obstetrics & Gynecology 52 (2013) 389e394 Short Communication High success rate and considerable adverse events of pelvic prolapse
FIG The inferior and posterior peritoneal reflection is easily
 PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
Sacral, ilioinguinal, and vasal nerve stimulation for treatment of pelvic, sacral, inguinal and testicular Pain.
 Chapter 14 Sacral, ilioinguinal, and vasal nerve stimulation for treatment of pelvic, sacral, inguinal and testicular Pain. Introduction Sacral nerve root stimulation has been recognized as a treatment
Chapter 14 Sacral, ilioinguinal, and vasal nerve stimulation for treatment of pelvic, sacral, inguinal and testicular Pain. Introduction Sacral nerve root stimulation has been recognized as a treatment
da Vinci Prostatectomy My Greek personal experience
 da Vinci Prostatectomy My Greek personal experience Vassilis Poulakis MD, PhD, FEBU Ass. Prof. of Urology Director of Urologic Clinic Doctors Hospital Athens Laparoscopy - golden standard in Urology -
da Vinci Prostatectomy My Greek personal experience Vassilis Poulakis MD, PhD, FEBU Ass. Prof. of Urology Director of Urologic Clinic Doctors Hospital Athens Laparoscopy - golden standard in Urology -
