Assia A. Stepanian, MD*, John R. Miklos, MD, Robert D. Moore, DO, and T. Fleming Mattox, MD
|
|
|
- Terence Bates
- 5 years ago
- Views:
Transcription
1 Risk of Mesh Extrusion and Other Mesh-Related Complications After Laparoscopic Sacral Colpopexy with or without Concurrent Laparoscopic-Assisted Vaginal Hysterectomy: Experience of 402 Patients Assia A. Stepanian, MD*, John R. Miklos, MD, Robert D. Moore, DO, and T. Fleming Mattox, MD From the Center for Women s Care and Reproductive Surgery, Atlanta, GA (Dr. Stepanian); Atlanta Urogynecology Associates, Atlanta, GA (Drs. Miklos and Moore); and the Carolina Continence Center, Greenville, South Carolina (Dr. Mattox). ABSTRACT Keywords: Study Objective: To estimate the incidence of mesh-related complications including mesh erosion/extrusion rates in patients undergoing laparoscopic sacral colpopexy, with or without concurrent hysterectomy, using macroporous soft polypropylene mesh. Design: Historical cohort study (Canadian Task Force classification II-2). Setting: Private urogynecology clinic. Patients: A total of 446 consecutive patients with uterovaginal or vaginal vault prolapse underwent laparoscopic sacral colpopexy with use of macroporous soft polypropylene mesh from January 2003 through January In all, 402 consecutive patients met enrollment criteria. Two groups of patients were identified: (1) those receiving concurrent hysterectomy (n 130); and (2) those with a history of hysterectomy (n 272). Interventions: Patients were treated with laparoscopic sacral colpopexy with use of macroporous soft polypropylene mesh in conjunction with other laparoscopic and/or vaginal procedures. Measurements and Main Results: Data were collected in the form of chart reviews and patient questionnaires. Comparisons were made between groups 1 and 2. Patient demographics, history, mesh erosion/extrusion rates, and mesh-related complications were analyzed. Length of follow-up was 1 to 54 months with a median follow-up time of 12 months. No statistically significant differences existed between 2 groups in rates of mesh erosion/extrusion or other mesh-related complications. Overall vaginal mesh erosion/extrusion rate was 1.2% (95% CI 0.5% 2.7%) with an associated mesh revision rate of 1.2% (95% CI 0.5% 2.7%). Patients with concurrent hysterectomy had an erosion/extrusion rate of 2.3% (3/130) as compared with 0.7% (2/272) in patients with a history of hysterectomy, p.18. No cases of mesh erosion through organs and tissues other than vaginal mucosa were observed. Cuff abscess occurred in 1 patient with concurrent hysterectomy, with an overall infection rate of 0.3% (95% CI 0.01% 1.2%). One more patient developed an inflammatory reaction to the mesh. Excision of exposed mesh was performed in all 5 patients with mesh extrusion. Vaginal approach to excision was uniformly used. Laparoscopic removal of the entire mesh took place in 4 patients with persistent pelvic pain, in 1 patient with cuff abscess, and in one patient with a questionable mesh reaction. An estimated 975 to patients were required in each group to achieve power to detect a statistically significant difference in rate of mesh-related complications in this study. Conclusion: Risk of mesh extrusion or other mesh-related complications after laparoscopic sacral colpopexy using soft macroporous Y-shaped polypropylene mesh is about 1% in our study. No significant increase in risk of mesh-related complications was observed in patients receiving concurrent hysterectomy when compared with patients who had a previous hysterectomy. The sample size of almost 2000 patients was needed to detect a statistically significant difference in rate of mesh-extrusion in this study. Journal of Minimally Invasive Gynecology (2008) 15, AAGL. All rights reserved. Laparoscopy; Sacral colpopexy; Mesh erosion; Mesh extrusion; Infection; Hysterectomy; Mesh; Uterovaginal prolapse; Pelvic organ prolapse; Pelvic floor relaxation; Vaginal vault prolapse The authors have no commercial, proprietary, or financial interest in the products or companies described in this article. Corresponding author: Assia A. Stepanian, MD, Center for Women s Care and Reproductive Surgery, 1140 Hammond Drive, Suite F-6230, Atlanta, GA cwcassia@mindspring.com Submitted August 14, Accepted for publication November 21, Available at and /$ -see front matter 2008 AAGL. All rights reserved. doi: /j.jmig
2 Stepanian et al. Mesh-Related Complications 189 One of the first descriptions of sacral colpopexy, using an intervening graft between the vagina and the sacrum, was described in 1962 [1]. Sacral colpopexy is considered one of the most effective operations for treatment of vaginal vault prolapse [2]. In an attempt to minimize morbidity and maintain high cure rates, the laparoscopic approach to this procedure was first described in 1994 to 1995 [3 5]. Published anatomic apical cure rates for sacral colpopexy performed via laparotomy range between 78% to 100% [6], and via laparoscopy the anatomic cure rate is quoted as 90% to 100% [3,7,8]. Despite its high cure rate, sacral colpopexy can have concerning postoperative complications. One of the most common postoperative complications is mesh extrusion through the vaginal epithelium. Mesh erosion/extrusion usually occurs in the first couple of years, whereas infection is noted soon after surgery. Delayed complications, however, have been described [9,10]. A comprehensive review on abdominal sacral colpopexy reported an overall mesh erosion rate of 3.4% [6]. It was suggested that the procedure should not be performed at the time of hysterectomy in an attempt to reduce bacterial contamination of the prosthetic material [11]. Reports have compared the incidence of mesh erosion in abdominal sacral colpopexy with and without concomitant hysterectomy [12 16]. The results of these studies are not consistent. Three studies suggest an association between hysterectomy [12 14] and mesh erosion and the other 2 do not show such an association [15,16]. A comparison has not been made for the incidence of mesh erosion/extrusion in laparoscopic sacral colpopexy with and without concurrent hysterectomy. In fact, one of the retrospective cohort studies excluded patients who underwent a laparoscopic sacral colpopexy, suggesting that the laparoscopic approach would taint the data [15]. The objective of this study was to estimate incidence of mesh-related complications in women undergoing laparoscopic sacral colpopexy with and without simultaneous laparoscopic-assisted vaginal hysterectomy. Materials and Methods Study Design After receiving institutional review board approval, a historical cohort analysis of office and hospital records was performed for all patients who underwent laparoscopic sacral colpopexy from January 2003 through January 2007 at our institution. In all, 446 consecutive patients with uterovaginal or vaginal vault prolapse were treated with laparoscopic sacral colpopexy in conjunction with other laparoscopic and/or vaginal procedures. Data were collected in the form of chart reviews and patient questionnaires. A total of 10 patients with mesh of types other than Y-shaped polypropylene mesh, 11 patients with no follow-up information, and 2 patients with inconsistent data were excluded, as were 21 patients with laparoscopic sacral colpopexy without hysterectomy. A total of 402 remaining patients were enrolled. Two groups of patients were formed: (1) those receiving concurrent hysterectomy (n 130); and (2) those with a history of hysterectomy (n 272). Patient demographics, history, mesh erosion/extrusion rates, and mesh-related complications were analyzed. Median length of follow-up was 12 months (range: 1 54 months). Statistical Analysis A sample size calculation was performed using 2-sided 2 test with power selected at.80 (.20) and.05. Mesh erosion/extrusion rate was selected as the primary outcome. For power analysis we selected a study [12] that used the same type of mesh in both previous and concurrent hysterectomy groups and stated that one (0.8%) of 121 patients in a previous hysterectomy group and 3 (13.6%) of 22 patients in a concurrent total abdominal hysterectomy (TAH) group developed mesh erosion through the vaginal mucosa, revealing a statistically significant difference between 2 groups. Applying the 2 statistic to compare mesh erosion/extrusion rate between previous and concurrent hysterectomy groups in patients undergoing sacral colpopexy, 70 patients were needed in each group to achieve a confidence level of 95% (2-sided.05) and a power of 80% (.2). The 2 study groups were compared using Fisher exact test for proportions and Student s t test for means. Any p values less than.05 were considered indicative of statistical significance. Fisher exact 95% CIs were calculated for proportions. To estimate the number of patients in our study needed to achieve the power to detect a statistically significant difference for each complication studied we used a 2-sided Fisher exact test,.05, and equal numbers per group (nquery Advisor software Version 4.0; Boston, MA). Kaplan-Meier survival analysis was used to assess time to mesh-related complication; the 2 study groups were compared using the log rank test. All analyses were conducted using statistical software (SAS, Version 9; SAS Institute, Cary, NC). Surgical Technique All patients received 1 dose of antibiotic preoperatively. The procedure was performed using 4 trocars in the following locations: 10-mm trocar in the inferior border of the umbilicus; 10-mm trocar at approximately the level of the umbilicus in the left midclavicular line; 5-mm trocar suprapubically in the midline; and another 5-mm trocar at the level of the umbilicus at the right midclavicular line. Each patient was placed in dorsal lithotomy position and carbon dioxide was insufflated to an intraabdominal pressure of 10 mm Hg. The small bowel was mobilized out of the cul-desac and placed into the right upper quadrant. After the completion of the laparoscopic aspect of laparoscopic-assisted vaginal hysterectomy (if required), closure of the vaginal cuff was performed via a vaginal approach. Inter-
3 190 Journal of Minimally Invasive Gynecology, Vol 15, No 2, March/April 2008 Fig. 1. Steps of laparoscopic sacral colpopexy: anterior (A) and posterior (B) dissection of peritoneum overlying vaginal vault; exposure of anterior ligament of sacrum (C); fixation of anterior and posterior leafs of mesh to anterior (D) and posterior (E) aspects of vaginal cuff, respectively; fixation of mesh to anterior ligament of sacrum (F). rupted figure-of-eight stitches of 0-polyglaction suture were used to close the cuff. A vaginal probe was used to elevate the vaginal apex, and the peritoneum overlying the vault was dissected anteriorly exposing the pubocervical fascia (Fig. 1A). Posterior dissection was performed to delineate the apex of the rectovaginal fascia (Fig. 1B). If a large enterocele was encountered, it was resected to prevent suturing of the mesh to the excessive vaginal epithelium. The peritoneum over the sacral promontory was incised longitu-
4 Stepanian et al. Mesh-Related Complications 191 Table 1 Demographics Variable Concomitant hysterectomy n 130 H/o hysterectomy n 272 Age, y, mean SD (95% CI) ( ) ( ) Weight, lb, mean SD (95% CI) ( ) ( ) Largest birth weight, g, mean SD (95% CI) ( ) ( ) Patients with largest birth weight 4000 g 30.4% 28.4%.70 (34/112) (63/222) Gravidity median (range) 3 (0 10) 3 (0 8).94 Parity median (range) 2 (0 9) 2 (0 6).79 Race, No. (%) Caucasian 17 (93.6) 239 (96.8).001 African American 7 (5.6) 4 (1.6) Other 1 (0.8) 4 (1.6) Estrogen users, No. (%) 35 (26.9) 120 (44.1).001 Menopausal status, No. (%) Premenopausal 27 (25.5) 22 (9.0).001 Perimenopausal 7 (6.6) 6 (2.5) Postmenopausal 72 (67.9) 216 (88.5) H/o History of. Fisher s exact, p dinally (Fig. 1C), and the peritoneal incision was extended into the cul-de-sac. The anterior ligament of the sacral promontory was exposed through blunt dissection. A15-3- to 4-cm polypropylene mesh fashioned in a Y shape was used to secure the pubocervical fascia anteriorly and the rectovaginal fascia posteriorly. The anterior leaf of the mesh was routinely secured to the proximal 4 to 5 cm of the vaginal cuff using 6 interrupted stitches of nonabsorbable suture, 2-0 polyester (Fig. 1D). The posterior leaf of the mesh was routinely secured using 6 to 8 interrupted stitches of the same suture (Fig. 1E). The long arm of the Y-shaped mesh graft was then secured to the anterior ligament of the sacrum using either 2 or 3 interrupted nonabsorbable sutures or titanium tacks (Fig. 1F). Polypropylene mesh was extraperitonealized using absorbable suture of 2-0 poliglecaprone along the previously made peritoneal incision. Additional surgical repairs such as enterocele repair, retropubic urethropexy, slings, paravaginal repairs, and posterior repairs were performed in most cases. Cystoscopy was performed in all cases to confirm ureteral patency and bladder integrity. All patients received a 1-week course of antibiotics postoperatively. Estrogen vaginal cream was used postoperatively in all patients with preoperatively noted vaginal mucosal atrophy. Results Records were reviewed for 402 patients meeting study criteria. In all, 130 patients with concurrent hysterectomy and 272 patients with a previous hysterectomy were followed up postoperatively for 1 to 54 months. The demographic data, including age, ethnicity, gravidity and parity, weight, largest birth weight inclusive of deliveries via cesarean section, and estrogen-containing preparation use, are shown in Table 1. Data comparing patients surgical history in each group are provided in Table 2. Estimation of the incidence of mesh-related complications including mesh erosion/extrusion was the primary focus of this study. Demographics No statistically significant differences existed between the groups in patients weight, largest birth weight, gravidity, parity, and steroid drug use. Patients in previous hysterectomy group were older ( [95% CI ] vs [95% CI ] years, p.002), used more estrogen supplementation (44.1% [120 of 272] vs 26.9% [35 of 130], p.001), and were more often postmenopausal (216 of 272 vs 72 of 130, p.001). Although ethnicity was not statistically different in the 2 groups, the prevalence of a Caucasian population in this study was evident, with 93.6% Caucasian patients in the concomitant hysterectomy group and 96.8% Caucasian patients in the history of hysterectomy group. Histories Table 2 shows significant differences in number of pelvic and abdominal procedures, with higher rate observed in previous hysterectomy group. In comparison with 13 (10%) patients in concurrent hysterectomy group, 237 (87%) patients in previous hysterectomy group had undergone pelvic floor reconstructive procedures before sacral colopexy.
5 192 Journal of Minimally Invasive Gynecology, Vol 15, No 2, March/April 2008 Table 2 Surgical history Procedure Concomitant hysterectomy n 130 (%) Previous hysterectomy n 272 (%) A&P repair 1 (0.8) 31 (11.4).001 SCP 0 (0) 3 (1.1).55 PVR 2 (1.5) 16 (5.9).07 AR 0 (0.9) 19 (7.0).001 PR 5 (3.8) 33 (12.1).006 Enterocele repair 1 (0.8) 17 (6.3).010 Urethral support 2 (1.5) 55 (20.2).001 Sling-2 Sling-33 Burch-12 Raz-6 MMK-6 Bladder support 2 (1.5) 39 (14.3).001 Surgery for VVP 0 (0) 27 (9.9).001 or UVP Abdominoplasty 3 (2.3) 25 (9.2).011 Cesarean section 6 (4.6) 11 (4.0).60 Hernia repair 5 (3.8) 22 (8.1).14 Adhesiolysis 3 (2.3) 20 (7.4).019 Appendectomy 21 (16.2) 54 (19.9).41 Other abdominal 5 (3.8) 11 (4.0) 1.00 surgeries Total No. of pelvic floor procedures 13 (10) 237 (87.1).001 Fisher s exact, p A&P anterior and posterior; AR anterior repair; MMK-6 Marshall-Marchetti-Kranz operation; PR posterior repair; PVR paravaginal repair; SCP sacral colpopexy; UVP uterovaginal prolapse; VVP vaginal vault prolapse. Types of Mesh Used Only cases in which macroporous polypropylene Y mesh was used were included in the study: 171 patients had laparoscopic sacral colpopexy performed with IntePro (American Medical Systems, Minnetonka, MN) and 231 with Gynemesh (Gynecare Inc., Menlo Park, CA). No statistically significant differences were established between the study groups on the basis of types of meshes used, p.67. Complications As shown in Table 3, no statistically significant differences existed between 2 groups in rates of mesh erosion/ extrusion through vaginal epithelium, mesh-associated infection, mesh reaction, pain at the apex requiring treatment, and mesh revision or removal. Risk of mesh erosion/extrusion in the prior hysterectomy group was 0.7% (2/272) as compared with 2.3% (3/130) in patients with concurrent hysterectomy, p.18. The overall mesh erosion/extrusion rate was 1.2% (95% CI 0.5% 2.7%). Each patient with mesh erosion/extrusion was initially treated with a 6-week course of estrogen and antibiotic vaginal creams. None of these patients was cured with this therapy, uniformly requiring surgical treatment, and subsequently leading to an overall excision of exposed mesh rate of 1.2% (95% CI 0.5% 2.7%). The rate of excision did not differ between the 2 compared groups, and equaled 0.7% and 2.3% in previous hysterectomy and concomitant hys- Table 3 Complications Complication Overall complication rate (n 402) No. rate (95% CI) Concomitant hysterectomy (n 130) No. (rate) Previous hysterectomy (n 272) No. (rate) Fisher s exact, p Mesh extrusion ( ) (2.3) (0.7) Excision of exposed mesh ( ) (2.3) (0.7) Pain at apex ( ) (0.8) (1.5) Reoperation for pain at apex ( ) (0.8) (1.1) Infection ( ) (0.8) Questionable mesh reaction ( ) (0.4) Reoperation for mesh-related complications, total ( ) (3.9) (2.2) Bleeding/hematoma ( ) (0.8) (0.7) Ileus/SBO ( ) (2.3) (2.2) Injury to bladder ( ) (2.2) Injury to bowel ( ) (1.1) Injury to ureter ( ) (0.4) SBO small bowel obstruction.
6 Stepanian et al. Mesh-Related Complications 193 Table 4 Number of patients needed to achieve power in current study Complication Overall complication rate (n 402) No. rate (95% CI) Power of current study (%) Mesh extrusion ( ) Excision of exposed mesh ( ) Pain at apex ( ) Reoperation for pain at apex ( ) Infection ( ) Questionable mesh reaction ( ) Reoperation, total (1.4, 4.7) Sample size (No. of patients) needed/group terectomy groups, respectively (p.18). No cases of mesh erosion through organs and tissues other than vaginal mucosa were observed in this study. Our study did not suggest an association between concomitant procedures and the location of the exposed mesh. In 5 patients with identified mesh extrusion, exposed mesh was noted in 2 patients at the apex itself, in 2 patients within 2.5 cm from the apex, and in 1 patient at 0.5 to 1 cm posterior to the apex. Three of these patients had concurrent paravaginal repair and posterior repair, 1 patient had enterocele repair, and 4 had urethral support procedures. Two patients had had pelvic floor reconstructive procedures performed before sacral colpopexy, and 2 different patients had abdominoplasty. No statistically significant differences were established between 2 groups in pain at the vaginal apex. Four of 272 patients in a previous hysterectomy group and 1 of 130 patients in a concurrent hysterectomy group (1.5% and 0.8%, respectively) (p 1.0) developed pain at the apex with the overall rate of 1.2% (95% CI 0.5% 2.7%). Mesh was entirely removed in 4 of 5 patients with pain at the apex, establishing an overall rate of 1% (95% CI 0.3% 2.4%), with a 1.1% rate of removal in prior hysterectomy group and a 0.8% rate in concomitant hysterectomy group, p.60. Cuff abscess occurred in 1 patient with concomitant hysterectomy, and in no patients in the other group, establishing the overall infection rate of 0.3% (95% CI 0.01% 1.2%), p.32. A questionable mesh reaction was observed in one patient in a previous hysterectomy group, and in no other groups, leading to overall mesh reaction rate of 0.3% (95% CI 0.01% 1.2%), with no statistically significant differences between the 2 studied groups, p Both of the above patients had their mesh removed. Total reoperation rate for mesh-associated complications, including excision of exposed mesh and removal of mesh, was 2.2% in prior hysterectomy group and 3.9% in patients with concurrent hysterectomy (6 of 272 and 5 of 130 patients, respectively). This established a p value of.27 and revealed absence of statistically significant difference. Nonmesh-Related Complications As seen in Table 3, preoperative complications observed in the current study include hematoma formation 0.75% (95% CI 0.15% 2.17%); ileus/small bowel obstruction 2.24% (95% CI 1.03% 4.21%); and injuries to bladder 1.49% (95% CI 0.55% 3.22%), ureters 0.25% (95% CI 0.01% 1.38%), and small bowel 0.75% (95% CI 0.15% 2.17%). In all 3 cases of reoperation for small bowel obstruction, mesh was not located in proximity to the obstructed area. In fact, in 1 case, the area of obstruction was in a side of the abdomen contralateral to mesh location. Estimation of Sample Size Needed to Achieve Power As shown in Table 4, because the power of this study for mesh extrusion is 48%, the number of patients needed to achieve a statistically significant difference in mesh extrusion alone equaled 975 for each group of patients. This required enrollment of at least 1950 patients. Length of Follow-up The length of follow-up was variable, with the range of 1 to 54 months and median of 12 months. No statistically significant difference existed between the 2 groups with regard to time to mesh-related complications (Fig. 2). At 24 months, the previous hysterectomy group and concomitant hysterectomy group had estimated proportions of and without mesh-related complications, respectively. Discussion Multiple procedures for uterovaginal and vaginal vault prolapse have been successfully performed laparoscopically. Recently conducted comparative cohort analysis indicated the comparable aspects of laparoscopic and open
7 194 Journal of Minimally Invasive Gynecology, Vol 15, No 2, March/April 2008 Fig. 2. Kaplan-Meier survival analysis and log rank test. No statistically significant difference between 2 groups existed with regard to time to mesh-related complications. At 24 months, history of (H/O) and concomitant hysterectomy groups had estimated proportions of and without mesh-related complications, respectively. abdominal approaches to sacral colpopexy with respect to clinical outcomes and safety whereas the laparoscopic approach offers the benefits of minimally invasive surgery [17]. In addition to providing minimally invasive access to the peritoneal cavity [18], the laparoscopic approach to sacral colpopexy contributes to superior visualization of the operative field because of magnification of the image, concentration of the light at the site of surgical action, and visualization of the tissue and instruments at selected distances [5,19]. An essential role in success and safety of sacral colpopexy is attributed to the selection of an appropriate graft material. Since the beginning of this study, all of our patients have been treated with macroporous, monofilament, soft polypropylene meshes, classified as type I [20]. Larger pores of these mesh materials, greater than 75 nm, allow macrophage and leukocyte migration and, thus, reduce infection [21,22]. Presence of large pores also improves flexibility of the mesh [23,24] and promotes tissue ingrowths and collagen deposition [25]. Polypropylene material has the lowest stiffness compared with other prosthesis and leads to the development of well-organized, fibrous, mature connective tissue [26]. Mesh erosion/extrusion is a complication that is seen in between 0.8% and 19% of cases of abdominal sacral colpopexy during the follow-up time of 0 to 74 months [16,22] and between 0.9% and 8% of cases of laparoscopic sacral colpopexy at 13.5 months to 5 years of follow-up [8,17,27]. Patients with mesh erosion/extrusion most often have newonset blood-tinged vaginal discharge and nonspecific pelvic pain usually occurring between 4 and 20 months [22]. Other described sequelae of mesh extrusion include sinus tract formation [28], abscess [29], and sacral osteomyelitis [29]. The suggested causal factors for mesh extrusion or exposure are synthetic meshes of types other than type I [21], atrophic vaginal mucosa, placement of the sutures at often devascularized and thin vaginal apex [9,30], and placement of mesh under tension [31]. The last factor results in exposure of the posterior aspect of the vaginal apex to abdominal pressure and leads to subsequent mesh exposure in this region. In an attempt to prevent vaginal mesh erosion/ extrusion, we: (1) avoided placing sutures at the vaginal cuff itself; (2) improved vaginal mucosal status by administering vaginal estrogen cream; (3) used perioperative antibiotics; (4) chose macroporous soft polypropylene mesh; (5) reduced significant enterocele and avoided it when placing mesh fixation sutures; and (6) placed this mesh in a tensionfree pattern to maintain natural orientation of the vagina [18,31]. Aspecialplaceintheliteratureisdevotedtostudiesaddressing the effect of concomitant hysterectomy on risk of mesh erosion/extrusion. Our investigation of the current literature did not identify studies on laparoscopic sacral colpopexy in which mesh-associated complications were compared between previous and concomitant hysterectomy groups. One study noted a statistically significant (p.04), 7-fold increased risk of mesh erosion in patients who underwent abdominal sacral colpopexy with concomitant total abdominal hysterectomy in comparison with women who had previous hysterectomy and concomitant supracervical hysterectomy. Range of follow-up in this study was 0.3 to 63.3 months [14]. Another study stratified patients according to the type of concurrent hysterectomy to evaluate the effect of supracervical hysterectomy on the risk of mesh erosion. That study also revealed a higher risk of mesh erosion in the concomitant total abdominal hysterectomy group (10.5%) as compared with a 3.6% mesh erosion rate in patients with concurrent supracervical hysterectomy, but the study lacked the power to achieve statistical significance [32]. A low, 0.8% overall rate of vaginal mesh erosion was documented in a study at 0 to 74 months of follow-up [16]. They explained such a high success of prevention of mesh extrusion by repairing the vaginal cuff in 2 layers. No incidence of mesh erosion was noted in a concurrent abdominal hysterectomy group. Mesh erosion was reported, however, in 1 patient with previous hysterectomy. Based on retrospective analysis of 363 cases of laparoscopic sacral colpopexy with average follow-up duration of 14.6 months, a similarly low overall rate of mesh extrusion (0.9%) was reported. Results were explained by tacking the posterior mesh to the levator ani musculature, avoiding posterior vaginal erosion, by careful dissection of levator ani and vagina, and, finally, by reperitonealization [8]. One study revealed that in women on estrogen therapy hysterectomy was associated with higher risk of mesh erosion [15]. The authors explained this association, however, by the possible presence of vaginal mucosal atrophy as an indication for estrogen use. Review of the records of our patients who developed mesh extrusion indicated that es-
8 Stepanian et al. Mesh-Related Complications 195 trogenization was adequate in all patients at the time of preoperative evaluation; one patient was using estrogen preoperatively; surgical and postsurgical care was the same in each patient. Although there are no published reports on success of the conservative management of mesh erosion, transvaginal surgical excision [9,33,34] and transvaginal endoscopic techniques for removal of eroded mesh have been described [33]. Patients in our study responded well to transvaginal excision of an exposed mesh. We excised surrounding mesh granulation tissue, applied downward traction to the exposed mesh, and excised its visible fragment. The surrounding vaginal mucosa and underlying fascia were closed using interrupted stitches of delayed absorbable suture. This procedure was previously described [9,33,34]. Consistent with this study, no recurrence of mesh exposure occurred after the excision of exposed mesh; no removal of the entire mesh was necessary. In addition, previously described complications of treatment of mesh erosion were not observed, including infection, abscess, and sinus tract formation [28]. The median time to diagnosis and treatment of mesh extrusion in our study was 6 months, with a range of 3 weeks to 19 months. Studies involving various types of meshes documented a range of 6 weeks to 72 months as time to mesh exposure after sacral colpopexy [9,16,33]. A study [14] involved 121 patients with polypropylene mesh and revealed that 3 of 4 patients developed mesh extrusion/ erosion during the first 5 to 10 months of follow-up. One additional extrusion was diagnosed at 24 months after surgery. Although we have probably seen most cases that are to develop mesh extrusion in our study, potentially longer follow-up may be necessary to assess mesh-related complications with higher accuracy of detection. Conclusion The risks of mesh-related complications associated with laparoscopic sacral colpopexy were low and equal to about 1% for mesh extrusions, infection, reaction, and apical pain. We believe that low risk of mesh-related complications is the result of use of macroporous soft knitted polypropylene mesh and strict adherence to surgical techniques indicated to decrease the risk of mesh exposure and other meshrelated complications. No statistically significant differences in mesh-related complication rates between previous hysterectomy and concurrent hysterectomy groups were noted, and we could not prove that laparoscopic hysterectomy that is concurrent to laparoscopic sacral colpopexy is associated with an increased risk of mesh-associated complications. Based on our data, 975 patients were required in each group to achieve power to detect a statistically significant difference in complication rates in this study if primary outcome continues to be mesh erosion/extrusion. Although we believe in the protective effect of vaginal estrogenization in the prevention of mesh extrusion/erosion, all patients with mesh extrusion/erosion had adequate estrogenization. This suggests that adequate vaginal estrogenization status does not preclude mesh-related complications. The excision of the exposed mesh was shown to be an optimal treatment for mesh extrusions that resulted from laparoscopic sacral colpopexy. Acknowledgment We would like to thank Dawn Blackhurst, PhD, for her statistical analysis of this study. References 1. Lane FE. Repair of posthysterectomy vaginal-vault prolapse. Obstet Gynecol. 1962;20: Gadonneix P, Ercoli A, Scambia G, Villet R. The use of laparoscopic sacrocolpopexy in the management of pelvic organ prolapse. Curr Opin Obstet Gynecol. 2006;17: Nezhat CH, Nezhat F, Nezhat C. Laparoscopic sacral colpopexy for vaginal vault prolapse. Obstet Gynecol. 1994;84: Dorsey JH, Cundiff G. Laparoscopic procedures for incontinence and prolapse. Curr Opin Obstet Gynecol. 1994;6: Lyons TL. Minimally invasive treatment of urinary stress incontinence and laparoscopically directed repair of pelvic floor defects. Clin Obstet Gynecol. 1995;38: Nygaard IE, McCreery R, Brubaker L, Connolly A, Cundiff G, Weber AM, et al. Abdominal sacrocolpopexy: a comprehensive review. Obstet Gynecol. 2004;104: Antiphon P, Elard S, Benyoussef A, Fofana M, Yiou R, Gettman M, et al. Laparoscopic promontory sacral colpopexy: is the posterior, recto-vaginal, mesh mandatory? Eur Urol. 2004;45: Rozet F, Mandron E, Arroyo C, Andrews H, Cathelineau X, Mombet A, et al. Laparoscopic sacral colpopexy approach for genito-urinary prolapse; experience with 363 cases. Eur Urol. 2005;47: Kohli N, Walsh PM, Roat TW, Karram MM. Mesh erosion after abdominal sacrocolpopexy. Obstet Gynecol. 1998;92: Weidner AC, Cunfidff GW, Harris RL, Addison WA. Sacral osteomyelitis: an unusual complication of abdominal sacral colpopexy. Obstet Gynecol. 1997;90: Imparato E, Spesi G, Rovetta E, Presti M. Surgical management and prevention of vaginal vault prolapse. Surg Gynecol Obstet. 1992;175: Thompson PK, Pugmire JE, Sangi-Haghpeykar H. Abdominal sacrocolpopexy utilizing Gore-Tex in genital prolapse. J Pelvic Med Surg. 2004;10: Culligan PJ, Murphy M, Blackwell L, Hammons G, Graham C, Heit MH. Long-term success of abdominal sacral colpopexy using synthetic mesh. Am J Obstet Gynecol. 2002;187: Bensinger G, Lind L, Lesser M, Guess M, Winkler H. Abdominal sacral suspensions: analysis of complications using permanent mesh. Am J Obstet Gynecol. 2005;193: Wu JM, Wells EC, Hundley AF, Connoly AM, Williams KS, Visco AG. Mesh erosion in abdominal sacral colpopexy with and without concomitant hysterectomy. Am J Obstet Gynecol. 2006;192: Brizzolara S, Pillai-Allen A. Risk of mesh erosion with sacral colpopexy and concurrent hysterectomy. Obstet Gynecol. 2003;102: Paraiso MF, Walters MD, Rackley RR, Melek S, Hugney C. Laparoscopic and abdominal sacral colpopexies: a comparative cohort study. Am J Obstet Gynecol. 2005;192:
9 196 Journal of Minimally Invasive Gynecology, Vol 15, No 2, March/April Miklos JR, Moore RD, Kohli N. Laparoscopic surgery for pelvic support defects. Curr Opin Obstet Gynecol. 2002;14: Wattiez A, Mashiach R, Donoso M. Laparoscopic repair of vaginal vault prolapse. Curr Opin Obstet Gynecol. 2003;15: Deval B, Haab F. What s new in prolapse surgery? Curr Opin Urol. 2003;13: Birch C, Fynes MM. The role of synthetic and biological prosthesis in reconstructive pelvic floor surgery. Curr Opin Obstet Gynecol. 2002; 14: Govier FE, Kobashi KC, Kozlowski PM, Kuznetsov DD, Begley SJ, McGonigle KF, et al. High complication rate identified in sacrocolpopexy patients attributed to silicone mesh. JUrol. 2005;65: Costantini E, Lombi R, Micheli C, Parziani S, Porena M. Colposacropexy with Gore-Tex mesh in marked vaginal and uterovaginal prolapse. Eur Urol. 1998;34: Davila GW, Drutz H, Deprest J. Clinical implications of the biology of grafts: conclusions of the 2005 IUGA grafts roundtable. Int Urogynecol J. 2006;17:S51 S Davila GW, Moore RD, Giudice TP, Erickson TB. Innovations in the treatment of vaginal prolapse. OBG Manage. 2006;18:1. Available at Boulangeir L, Boukerrou M, Lambaudie E, Defossez A, Cosson M. Tissue integration and tolerance to meshes used in gynecologic surgery: an experimental study. Eur J Obstet Gynecol Reprod Biol. 2006;125: Ross JW, Preston M. Laparoscopic sacrocolopexy for severe vaginal vault prolapse: five-year outcome. J Minim Invasive Gynecol. 2005; 12: Hart SR, Weiser EB. Abdominal sacral colpopexy mesh erosion resulting in a sinus tract formation and sacral abscess. Obstet Gynecol. 2004;103: Taylor GB, Moore RD, Miklos JR. Osteomyelitis secondary to sacral colopexy mesh erosion requiring laminectomy. Obstet Gynecol. 2006; 107: Richardson AC. The anatomic defects in rectocele and enterocele. J Pelvic Surg. 1995;1: Hunt WG. Abdominal sacral colpopexies complicated by vaginal graft extrusion. Obstet Gynecol. 2004;103: Griffis K, Evers M, Terry C, Hale D. Mesh erosion and abdominal sacrocolpopexy; a comparison of total and supracervical hysterectomy. J Pelvic Med Surg. 2004;10:S15 S Timmons MC, Addison WA. Mesh erosion after abdominal sacral colpopexy. J Pelvic Surg. 1997;2: Mattox TF, Stanford EJ, Varner E. Infected abdominal sacrocolopexies: diagnosis and treatment. Int Urogynecol J Pelvic Floor Dysfunct. 2004;15:
Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse
 ORIGINAL ARTICLE Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse Cecile A. Unger, MD, MPH, Matthew D. Barber, MD, MHS, Mark
ORIGINAL ARTICLE Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse Cecile A. Unger, MD, MPH, Matthew D. Barber, MD, MHS, Mark
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review
 Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583
 Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
Paravaginal Repair: A Laparoscopic Approach
 44 Paravaginal Repair: A Laparoscopic Approach John R. Miklos and Robert Moore Atlanta Urogynecology Associates, Atlanta, Georgia, U.S.A. Neeraj Kohli Harvard University, Boston, Massachusetts, U.S.A.
44 Paravaginal Repair: A Laparoscopic Approach John R. Miklos and Robert Moore Atlanta Urogynecology Associates, Atlanta, Georgia, U.S.A. Neeraj Kohli Harvard University, Boston, Massachusetts, U.S.A.
Female Urology. The Results of Grade IV Cystocele Repair Using Mesh. Introduction ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M
 Urology Journal UNRC/IUA Vol. 1, No. 4, 263-267 Autumn 2004 Printed in IRAN Female Urology The Results of Grade IV Cystocele Repair Using Mesh ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M Department of Urology,
Urology Journal UNRC/IUA Vol. 1, No. 4, 263-267 Autumn 2004 Printed in IRAN Female Urology The Results of Grade IV Cystocele Repair Using Mesh ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M Department of Urology,
International Federation of Gynecology and Obstetrics
 International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
Prevalence and risk factors for mesh erosion after laparoscopic-assisted sacrocolpopexy
 Int Urogynecol J (2011) 22:205 212 DOI 10.1007/s00192-010-1265-3 ORIGINAL ARTICLE Prevalence and risk factors for mesh erosion after laparoscopic-assisted sacrocolpopexy Jasmine Tan-Kim & Shawn A. Menefee
Int Urogynecol J (2011) 22:205 212 DOI 10.1007/s00192-010-1265-3 ORIGINAL ARTICLE Prevalence and risk factors for mesh erosion after laparoscopic-assisted sacrocolpopexy Jasmine Tan-Kim & Shawn A. Menefee
Current status in pelvic organ prolapse surgery: an evidence based review
 Current status in pelvic organ prolapse surgery: an evidence based review Christian Falconer, MD, PhD Department of Obstetrics and Gynecology Danderyd University Hospital Stockholm, Sweden Finnish Society
Current status in pelvic organ prolapse surgery: an evidence based review Christian Falconer, MD, PhD Department of Obstetrics and Gynecology Danderyd University Hospital Stockholm, Sweden Finnish Society
ROBOTIC MESH SACROCOLPOPEXY
 ROBOTIC MESH SACROCOLPOPEXY Philippe E. Zimmern, MD, FACS Professor of Urology Mesh sacrocolpopexy Background First described in 1962 by Lane Until then, treatment options were: Pessary Colpocleisis Vaginal
ROBOTIC MESH SACROCOLPOPEXY Philippe E. Zimmern, MD, FACS Professor of Urology Mesh sacrocolpopexy Background First described in 1962 by Lane Until then, treatment options were: Pessary Colpocleisis Vaginal
By:Dr:ISHRAQ MOHAMMED
 By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
SURGICAL. How to manage the cuff at vaginal hysterectomy. For personal use only. Copyright Dowden Health Media TECHNIQUES
 For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy
 Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
With our aging population, the rate of pelvic
 Original Research Short-Term Outcomes of Robotic Sacrocolpopexy Compared With Abdominal Sacrocolpopexy Elizabeth J. Geller, MD, Nazema Y. Siddiqui, MD, Jennifer M. Wu, MD, MPH, and Anthony G. Visco, MD
Original Research Short-Term Outcomes of Robotic Sacrocolpopexy Compared With Abdominal Sacrocolpopexy Elizabeth J. Geller, MD, Nazema Y. Siddiqui, MD, Jennifer M. Wu, MD, MPH, and Anthony G. Visco, MD
Surgical repair of vaginal wall prolapse using mesh
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
Innovations in mesh kit technology for vaginal wall prolapse
 Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
PL Narducci Department of Obstetrics and Gynecology General Hospital San Giovanni Battista Foligno, ITALY
 NESA DAYS 2018 New European Surgical Academy Perugia, April 19-21, 2018 EXCELLENCE IN FEMALE SURGERY PROLAPSE RECONSTRUCTIVE SURGERY IN SEXUALLY ACTIVE WOMEN LAPAROSCOPIC ANTERIOR ABDOMINAL WALL COLPOPEXY
NESA DAYS 2018 New European Surgical Academy Perugia, April 19-21, 2018 EXCELLENCE IN FEMALE SURGERY PROLAPSE RECONSTRUCTIVE SURGERY IN SEXUALLY ACTIVE WOMEN LAPAROSCOPIC ANTERIOR ABDOMINAL WALL COLPOPEXY
Prospective study of an ultra-lightweight polypropylene Y mesh for robotic sacrocolpopexy
 Int Urogynecol J (2013) 24:1371 1375 DOI 10.1007/s00192-012-2021-7 ORIGINAL ARTICLE Prospective study of an ultra-lightweight polypropylene Y mesh for robotic sacrocolpopexy Charbel G. Salamon & Christa
Int Urogynecol J (2013) 24:1371 1375 DOI 10.1007/s00192-012-2021-7 ORIGINAL ARTICLE Prospective study of an ultra-lightweight polypropylene Y mesh for robotic sacrocolpopexy Charbel G. Salamon & Christa
Gynecology Dr. Sallama Lecture 3 Genital Prolapse
 Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
LAPAROSCOPIC REPAIR OF PELVIC FLOOR
 LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
PRACTICE BULLETIN Female Pelvic Medicine & Reconstructive Surgery Volume 23, Number 4, July/August 2017
 PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
T h e C o m p l e t e Tr e a t m e n t o f P e l v i c F l o o r P r o l a p s e by Laparoscopy Technique, Tips and Tricks
 T h e C o m p l e t e Tr e a t m e n t o f P e l v i c F l o o r P r o l a p s e by Laparoscopy Technique, Tips and Tricks R Botchorishvili, A Wattiez, G Mage, M Canis, B Rabischong, K Jardon, C Rivoire,
T h e C o m p l e t e Tr e a t m e n t o f P e l v i c F l o o r P r o l a p s e by Laparoscopy Technique, Tips and Tricks R Botchorishvili, A Wattiez, G Mage, M Canis, B Rabischong, K Jardon, C Rivoire,
Subjective and objective results 1 year after robotic sacrocolpopexy using a lightweight Y-mesh
 DOI 10.1007/s00192-013-2265-x ORIGINAL ARTICLE Subjective and objective results 1 year after robotic sacrocolpopexy using a lightweight Y-mesh Patrick J. Culligan & Emil Gurshumov & Christa Lewis & Jennifer
DOI 10.1007/s00192-013-2265-x ORIGINAL ARTICLE Subjective and objective results 1 year after robotic sacrocolpopexy using a lightweight Y-mesh Patrick J. Culligan & Emil Gurshumov & Christa Lewis & Jennifer
Understanding Pelvic Organ Prolapse. Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery
 Understanding Pelvic Organ Prolapse Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery Disclosures None I am the daughter of a physician assistant. Objectives List types of pelvic
Understanding Pelvic Organ Prolapse Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery Disclosures None I am the daughter of a physician assistant. Objectives List types of pelvic
Medium-term follow-up on use of freeze-dried, irradiated donor fascia for sacrocolpopexy and sling procedures
 Int Urogynecol J (2004) 15: 238 242 DOI 10.1007/s00192-004-1146-8 ORIGINAL ARTICLE Mary Pat FitzGerald Æ S. Renee Edwards Æ Dee Fenner Medium-term follow-up on use of freeze-dried, irradiated donor fascia
Int Urogynecol J (2004) 15: 238 242 DOI 10.1007/s00192-004-1146-8 ORIGINAL ARTICLE Mary Pat FitzGerald Æ S. Renee Edwards Æ Dee Fenner Medium-term follow-up on use of freeze-dried, irradiated donor fascia
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015
 Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Randomized trial of fascia lata and polypropylene mesh for abdominal sacrocolpopexy: 5-year follow-up
 DOI 10.1007/s00192-010-1249-3 ORIGINAL ARTICLE Randomized trial of fascia lata and polypropylene mesh for abdominal sacrocolpopexy: 5-year follow-up Susan B. Tate & Linda Blackwell & Douglas J. Lorenz
DOI 10.1007/s00192-010-1249-3 ORIGINAL ARTICLE Randomized trial of fascia lata and polypropylene mesh for abdominal sacrocolpopexy: 5-year follow-up Susan B. Tate & Linda Blackwell & Douglas J. Lorenz
Laparoscopic sacrocolpopexy for the correction of vaginal vault prolapse
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2004 Laparoscopic sacrocolpopexy for the correction of vaginal vault prolapse Chandru P. Sundaram Indiana University
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2004 Laparoscopic sacrocolpopexy for the correction of vaginal vault prolapse Chandru P. Sundaram Indiana University
Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
 Gynecol Surg (2006) 3: 88 92 DOI 10.1007/s10397-005-0168-7 ORIGINAL ARTICLE R. Oliver. C. Dasgupta. A. Coker Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
Gynecol Surg (2006) 3: 88 92 DOI 10.1007/s10397-005-0168-7 ORIGINAL ARTICLE R. Oliver. C. Dasgupta. A. Coker Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
Stop Coping. Start Living. Talk to your doctor about pelvic organ prolapse and sacrocolpopexy
 Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Laparoscopic sacrocolpopexy: an observational study of functional and anatomical outcomes
 DOI 10.1007/s00192-010-1241-y ORIGINAL ARTICLE Laparoscopic sacrocolpopexy: an observational study of functional and anatomical outcomes Natalia Price & Alex Slack & Simon R. Jackson Received: 26 April
DOI 10.1007/s00192-010-1241-y ORIGINAL ARTICLE Laparoscopic sacrocolpopexy: an observational study of functional and anatomical outcomes Natalia Price & Alex Slack & Simon R. Jackson Received: 26 April
REPAIR OF LARGE CYSTOCELE
 REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
The incidence of mesh extrusion after vaginal incontinence and pelvic floor prolapse surgery
 ORIGINAL ARTICLE The incidence of mesh extrusion after vaginal incontinence and pelvic floor prolapse surgery Seth Cohen, Elizabeth Kavaler Department of Urology, Lenox Hill Hospital, USA Correspondence:
ORIGINAL ARTICLE The incidence of mesh extrusion after vaginal incontinence and pelvic floor prolapse surgery Seth Cohen, Elizabeth Kavaler Department of Urology, Lenox Hill Hospital, USA Correspondence:
Supracervical Robotic-Assisted Laparoscopic Sacrocolpopexy for Pelvic Organ Prolapse
 SCIENTIFIC PAPER Supracervical Robotic-Assisted Laparoscopic Sacrocolpopexy for Pelvic Organ Prolapse Aaron D. Benson, MD, Brandan A. Kramer, MD, Robert O. Wayment, MD, Bradley F. Schwartz, DO ABSTRACT
SCIENTIFIC PAPER Supracervical Robotic-Assisted Laparoscopic Sacrocolpopexy for Pelvic Organ Prolapse Aaron D. Benson, MD, Brandan A. Kramer, MD, Robert O. Wayment, MD, Bradley F. Schwartz, DO ABSTRACT
Laparoscopic surgery for pelvic support defects
 ~ Laparoscopic surgery for pelvic support defects John R. Miklosa, Robert D. Mooreb and Neeraj Kohlia Reconstructive pelvic surgery for the treatment of vaginal prolapse continues to evolve as surgeons
~ Laparoscopic surgery for pelvic support defects John R. Miklosa, Robert D. Mooreb and Neeraj Kohlia Reconstructive pelvic surgery for the treatment of vaginal prolapse continues to evolve as surgeons
Tension Free Monofilament Macropore Polypropylene Mesh (Gynemesh PS) in Female Genital Prolapse Repair
 Clinical Urology Gynemesh PS in Female Genital Prolapse Repair International Braz J Urol Vol. 32 (4): 410-415, July - August, 2006 Tension Free Monofilament Macropore Polypropylene Mesh (Gynemesh PS) in
Clinical Urology Gynemesh PS in Female Genital Prolapse Repair International Braz J Urol Vol. 32 (4): 410-415, July - August, 2006 Tension Free Monofilament Macropore Polypropylene Mesh (Gynemesh PS) in
Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option.
 Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option. The Condition(s): Vaginal Prolapse, Uterine Prolapse Vaginal prolapse occurs when the
Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option. The Condition(s): Vaginal Prolapse, Uterine Prolapse Vaginal prolapse occurs when the
A Long-Term Treatment Outcome of Abdominal Sacrocolpopexy
 Original Article DOI 10.3349/ymj.2009.50.6.807 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 50(6): 807-813, 2009 A Long-Term Treatment Outcome of Abdominal Sacrocolpopexy Myung Jae Jeon, 1 Yeo Jung
Original Article DOI 10.3349/ymj.2009.50.6.807 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 50(6): 807-813, 2009 A Long-Term Treatment Outcome of Abdominal Sacrocolpopexy Myung Jae Jeon, 1 Yeo Jung
Robot Assisted Rectopexy
 1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
Complications from permanent synthetic mesh
 Original Research Symptom Resolution After Operative Management of Complications From Transvaginal Mesh Erin C. Crosby, MD, Melinda Abernethy, MD, MPH, Mitchell B. Berger, MD, PhD, John O. DeLancey, MD,
Original Research Symptom Resolution After Operative Management of Complications From Transvaginal Mesh Erin C. Crosby, MD, Melinda Abernethy, MD, MPH, Mitchell B. Berger, MD, PhD, John O. DeLancey, MD,
Vaginally-Assisted Laparoscopic Hysterosacropexy for Advanced Utero-Vaginal Prolapse: A Series of 32 Cases
 ARS Medica Tomitana - 2014; 2(77): 63-70 10.2478/arsm-2014-0012 Brătilă V. Elvira 1, Brătilă P.C. 2, Negroiu Andra-Teodora 3 Vaginally-Assisted Laparoscopic Hysterosacropexy for Advanced Utero-Vaginal
ARS Medica Tomitana - 2014; 2(77): 63-70 10.2478/arsm-2014-0012 Brătilă V. Elvira 1, Brătilă P.C. 2, Negroiu Andra-Teodora 3 Vaginally-Assisted Laparoscopic Hysterosacropexy for Advanced Utero-Vaginal
CHAU KHAC TU M.D., Ph.D.
 CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
Bowel cancer and previous mesh surgery
 Gynecol Surg (2011) 8:217 221 DOI 10.1007/s10397-010-0563-6 CASE REPORT Bowel cancer and previous mesh surgery Sapna Ahuja & Oliver Chappatte & Michael Thomas & Alistair Cook Received: 27 October 2009
Gynecol Surg (2011) 8:217 221 DOI 10.1007/s10397-010-0563-6 CASE REPORT Bowel cancer and previous mesh surgery Sapna Ahuja & Oliver Chappatte & Michael Thomas & Alistair Cook Received: 27 October 2009
Index. B Bladder, injury of, Bowel, injury of, , Brachytherapy, for cervical cancer, 357 Burns, electrosurgical,
 Perioperative Nursing Clinics 1 (2006) 375 379 Index Note: Page numbers of article titles are in boldface type. A Abdominal hysterectomy Acidosis, from insufflation, 323 Active electrode monitoring, in
Perioperative Nursing Clinics 1 (2006) 375 379 Index Note: Page numbers of article titles are in boldface type. A Abdominal hysterectomy Acidosis, from insufflation, 323 Active electrode monitoring, in
ORIGINAL ARTICLE. Alper Biler 1, I. Egemen Ertas 1, Gokhan Tosun 1, Ismet Hortu 2, Unal Turkay 3, Ozge E. Gultekin 4, Gulfem Igci 3 ABSTRACT
 ORIGINAL ARTICLE Vol. 44 (5): 996-1004, September - October, 2018 doi: 10.1590/S1677-5538.IBJU.2017.0692 Perioperative complications and short-term outcomes of abdominal, laparoscopic, and laparoscopic
ORIGINAL ARTICLE Vol. 44 (5): 996-1004, September - October, 2018 doi: 10.1590/S1677-5538.IBJU.2017.0692 Perioperative complications and short-term outcomes of abdominal, laparoscopic, and laparoscopic
Laparoscopic Sacral ColpopexyApproach for Genito-Urinary Prolapse: Experience with 363 Cases
 European Urology European Urology 47 (2005) 230 236 Laparoscopic Sacral ColpopexyApproach for Genito-Urinary Prolapse: Experience with 363 Cases Francois Rozet a, *, Eric Mandron b, Carlos Arroyo a,1,
European Urology European Urology 47 (2005) 230 236 Laparoscopic Sacral ColpopexyApproach for Genito-Urinary Prolapse: Experience with 363 Cases Francois Rozet a, *, Eric Mandron b, Carlos Arroyo a,1,
A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience
 Journal Of Laparoendoscopic Surgery Volume 4, Number 5, 1994 Mary Ann Liebert, Inc., Publishers A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience E.D. RIZA, M.D.(1)
Journal Of Laparoendoscopic Surgery Volume 4, Number 5, 1994 Mary Ann Liebert, Inc., Publishers A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience E.D. RIZA, M.D.(1)
Vaginal McCall culdoplasty versus laparoscopic uterosacral plication to prophylactically address vaginal vault prolapse
 Vaginal McCall culdoplasty versus laparoscopic uterosacral to prophylactically address vaginal vault prolapse Niblock, K., Bailie, E., McCracken, G., & Johnston, K. (2017). Vaginal McCall culdoplasty versus
Vaginal McCall culdoplasty versus laparoscopic uterosacral to prophylactically address vaginal vault prolapse Niblock, K., Bailie, E., McCracken, G., & Johnston, K. (2017). Vaginal McCall culdoplasty versus
Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation
 Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation Roger P. Goldberg, MD, MPH, Sumana Koduri, MD, Robert W. Lobel, MD, Patrick J. Culligan,
Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation Roger P. Goldberg, MD, MPH, Sumana Koduri, MD, Robert W. Lobel, MD, Patrick J. Culligan,
This information is intended as an overview only
 This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
Colorectal procedure guide
 Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Site-specific fascial defects in the diagnosis and surgical management of enterocele
 Site-specific fascial defects in the diagnosis and surgical management of enterocele John R. Miklos, MD,a Neeraj Kohli, MD,b Vincent Lucente, MD,c and William B. Safe, MDd Atlanta and Marietta, GeO1gia,
Site-specific fascial defects in the diagnosis and surgical management of enterocele John R. Miklos, MD,a Neeraj Kohli, MD,b Vincent Lucente, MD,c and William B. Safe, MDd Atlanta and Marietta, GeO1gia,
Anus,Rectum and Colon
 JOURNAL OF THE Anus,Rectum and Colon http://journal-arc.jp CLINICAL RESEARCH Laparoscopic ventral rectopexy with sacrocolpopexy for coexisting pelvic organ prolapse and external rectal prolapse Yoshiyuki
JOURNAL OF THE Anus,Rectum and Colon http://journal-arc.jp CLINICAL RESEARCH Laparoscopic ventral rectopexy with sacrocolpopexy for coexisting pelvic organ prolapse and external rectal prolapse Yoshiyuki
Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications
 Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications Karyn S. Eilber, M.D. Cedars-Sinai FPMRS Associate Professor, Cedars-Sinai Dept of Surgery Associate Director, Urology Residency
Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications Karyn S. Eilber, M.D. Cedars-Sinai FPMRS Associate Professor, Cedars-Sinai Dept of Surgery Associate Director, Urology Residency
W23: Approaches to pelvic organ prolapse surgery Workshop Chair: Philippe Zimmern, United States 21 October :00-12:00
 W23: Approaches to pelvic organ prolapse surgery Workshop Chair: Philippe Zimmern, United States 21 October 2014 09:00-12:00 Start End Topic Speakers 09:00 09:30 Goals of repair and anatomical principles
W23: Approaches to pelvic organ prolapse surgery Workshop Chair: Philippe Zimmern, United States 21 October 2014 09:00-12:00 Start End Topic Speakers 09:00 09:30 Goals of repair and anatomical principles
Female Pelvic Prolapse: Considerations on Mesh Surgery and our Experience with Prolift Mesh in 84 Women with Complicated Pelvic Prolapses
 Journal of Applied Medical Sciences, vol.5, no. 2, 2016, 19-30 ISSN: 2241-2328 (print version), 2241-2336 (online) Scienpress Ltd, 2016 Female Pelvic Prolapse: Considerations on Mesh Surgery and our Experience
Journal of Applied Medical Sciences, vol.5, no. 2, 2016, 19-30 ISSN: 2241-2328 (print version), 2241-2336 (online) Scienpress Ltd, 2016 Female Pelvic Prolapse: Considerations on Mesh Surgery and our Experience
Step by step High uterosacral vaginal vault suspension to repair enterocele and apical prolapse
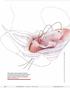 When performing high uterosacral suspension, it is possible to pass sutures through the coccygeus muscle-sacrospinous ligament complex (arrow) because a segment of the uterosacral ligament inserts into
When performing high uterosacral suspension, it is possible to pass sutures through the coccygeus muscle-sacrospinous ligament complex (arrow) because a segment of the uterosacral ligament inserts into
Anatomical and Functional Results of Pelvic Organ Prolapse Mesh Repair: A Prospective Study of 105 Cases
 International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
Sarah A. Huber, 1 LaChanda Dunlap-Wright, 2 John R. Miklos, 1 and Robert D. Moore Introduction
 Case Reports in Urology Volume 2016, Article ID 6180756, 5 pages http://dx.doi.org/10.1155/2016/6180756 Case Report Concomitant Laparoscopic Burch Urethropexy and Combined Vaginal-Laparoscopic Mesh Sling
Case Reports in Urology Volume 2016, Article ID 6180756, 5 pages http://dx.doi.org/10.1155/2016/6180756 Case Report Concomitant Laparoscopic Burch Urethropexy and Combined Vaginal-Laparoscopic Mesh Sling
Laparoscopic sacrocolpopexy: how low does the mesh go?
 Ultrasound Obstet Gynecol 2017; 49: 404 408 Published online 7 February 2017 in Wiley Online Library (wileyonlinelibrary.com). DOI: 10.1002/uog.15882 Laparoscopic sacrocolpopexy: how low does the mesh
Ultrasound Obstet Gynecol 2017; 49: 404 408 Published online 7 February 2017 in Wiley Online Library (wileyonlinelibrary.com). DOI: 10.1002/uog.15882 Laparoscopic sacrocolpopexy: how low does the mesh
Reconstructive Pelvic Floor Surgery: Sacrocolpopexy W43, 16 October :00-18:00
 Reconstructive Pelvic Floor Surgery: Sacrocolpopexy W43, 16 October 2012 14:00-18:00 Start End Topic Speakers 14:00 14:30 Introduction, Evidence and Applied Anatomy Salma Kayani 14:30 14:50 Applied Anatomy
Reconstructive Pelvic Floor Surgery: Sacrocolpopexy W43, 16 October 2012 14:00-18:00 Start End Topic Speakers 14:00 14:30 Introduction, Evidence and Applied Anatomy Salma Kayani 14:30 14:50 Applied Anatomy
Introduction. Regarding the Section of the UPDATE Entitled Purpose
 Time to Rethink: an Evidence-Based Response from Pelvic Surgeons to the FDA Safety Communication: UPDATE on Serious Complications Associated with Transvaginal Placement of Surgical Mesh for Pelvic Organ
Time to Rethink: an Evidence-Based Response from Pelvic Surgeons to the FDA Safety Communication: UPDATE on Serious Complications Associated with Transvaginal Placement of Surgical Mesh for Pelvic Organ
EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time
 EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time Menachem Alcalay,M.D, Urogynecology unit, Sheba Medical
EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time Menachem Alcalay,M.D, Urogynecology unit, Sheba Medical
Surgical treatments for vaginal apical prolapse
 Review Article Obstet Gynecol Sci 2016;59(4):253-260 http://dx.doi.org/10.5468/ogs.2016.59.4.253 pissn 2287-8572 eissn 2287-8580 Surgical treatments for vaginal apical prolapse Mi Kyung Kong, Sang Wook
Review Article Obstet Gynecol Sci 2016;59(4):253-260 http://dx.doi.org/10.5468/ogs.2016.59.4.253 pissn 2287-8572 eissn 2287-8580 Surgical treatments for vaginal apical prolapse Mi Kyung Kong, Sang Wook
Original article J Bas Res Med Sci 2015; 2(2): The incidence of recurrent pelvic organ prolapse: A cross sectional study
 The incidence of recurrent pelvic organ prolapse: A cross sectional study Ashraf Direkvand-Moghadam 1, Ali Delpisheh 2, Azadeh Direkvand-Moghadam 3* 1. Psychosocial Injuries Research Center, Faculty of
The incidence of recurrent pelvic organ prolapse: A cross sectional study Ashraf Direkvand-Moghadam 1, Ali Delpisheh 2, Azadeh Direkvand-Moghadam 3* 1. Psychosocial Injuries Research Center, Faculty of
Laparoscopic Sacrocolpopexy with & without the Robot: Tips and Tricks for success and avoidance / management of complications
 Laparoscopic Sacrocolpopexy with & without the Robot: Tips and Tricks for success and avoidance / management of complications Course Faculty: Patrick Culligan, MD Peter Rosenblatt, MD What is a Sacrocolpopexy?
Laparoscopic Sacrocolpopexy with & without the Robot: Tips and Tricks for success and avoidance / management of complications Course Faculty: Patrick Culligan, MD Peter Rosenblatt, MD What is a Sacrocolpopexy?
Tian-Ni Kuo 1, Ming-Ping Wu 1,2 *
 RESEARCH LETTER THE USE OF A CONCOMITANT TENSION-FREE VAGINAL MESH TECHNIQUE AND A TENSION-FREE MIDURETHRAL SLING IN TREATING PELVIC ORGAN PROLAPSE AND OCCULT STRESS URINARY INCONTINENCE Tian-Ni Kuo 1,
RESEARCH LETTER THE USE OF A CONCOMITANT TENSION-FREE VAGINAL MESH TECHNIQUE AND A TENSION-FREE MIDURETHRAL SLING IN TREATING PELVIC ORGAN PROLAPSE AND OCCULT STRESS URINARY INCONTINENCE Tian-Ni Kuo 1,
Gökmen Sukgen, 1 Esra SaygJlJ YJlmaz, 2 and Eralp BaGer Introduction. 2. Case Presentation
 Case Reports in Obstetrics and Gynecology Volume 2016, Article ID 2906596, 4 pages http://dx.doi.org/10.1155/2016/2906596 Case Report Vaginal Hysterectomy with Anterior Four-Arm Mesh Implant Technique
Case Reports in Obstetrics and Gynecology Volume 2016, Article ID 2906596, 4 pages http://dx.doi.org/10.1155/2016/2906596 Case Report Vaginal Hysterectomy with Anterior Four-Arm Mesh Implant Technique
THE USE OF PROSTHESES IN PELVIC RECONSTRUCTIVE SURGERY: JOY OR TOY?
 REVIEW ARTICLE THE USE OF PROSTHESES IN PELVIC RECONSTRUCTIVE SURGERY: JOY OR TOY? Ming-Ping Wu 1,2 * 1 Division of Urogynecology and Pelvic Floor Reconstruction, Department of Obstetrics and Gynecology,
REVIEW ARTICLE THE USE OF PROSTHESES IN PELVIC RECONSTRUCTIVE SURGERY: JOY OR TOY? Ming-Ping Wu 1,2 * 1 Division of Urogynecology and Pelvic Floor Reconstruction, Department of Obstetrics and Gynecology,
Stephen T Jeffery. University of Cape Town, South Africa
 Stephen T Jeffery University of Cape Town, South Africa I still think there s a role for mesh in Prolapse surgery Examples of my most recent mesh cases Case 1 62 yr old Sacrocolpopexy for vault prolapse
Stephen T Jeffery University of Cape Town, South Africa I still think there s a role for mesh in Prolapse surgery Examples of my most recent mesh cases Case 1 62 yr old Sacrocolpopexy for vault prolapse
SCIENTIFIC PAPER ABSTRACT INTRODUCTION MATERIALS AND METHODS
 SCIENTIFIC PAPER Vaginal Cuff Closure during Robotic-Assisted Total Laparoscopic Hysterectomy: Comparing Vicryl to Barbed Sutures A. Karim Nawfal, MD, David Eisenstein, MD, Evan Theoharis, MD, Marisa Dahlman,
SCIENTIFIC PAPER Vaginal Cuff Closure during Robotic-Assisted Total Laparoscopic Hysterectomy: Comparing Vicryl to Barbed Sutures A. Karim Nawfal, MD, David Eisenstein, MD, Evan Theoharis, MD, Marisa Dahlman,
We welcome comments and corrections which will be used to improve the system annually.
 ACGME Case Log Instructions: Female Pelvic Medicine and Reconstructive Surgery (FPMRS) Review Committees for Obstetrics and Gynecology, and Urology Updated July 2013 BACKGROUND The ACGME Case Log System
ACGME Case Log Instructions: Female Pelvic Medicine and Reconstructive Surgery (FPMRS) Review Committees for Obstetrics and Gynecology, and Urology Updated July 2013 BACKGROUND The ACGME Case Log System
One Slim Needle One Incision. One Simple Solution for Stress Urinary Incontinence. The Difference is in the Data
 CONTINENCE SOLUTIONS One Slim Needle One Incision ordering information Description US International Order Number Order Number One Simple Solution for Stress Urinary Incontinence MiniArc Single-Incision
CONTINENCE SOLUTIONS One Slim Needle One Incision ordering information Description US International Order Number Order Number One Simple Solution for Stress Urinary Incontinence MiniArc Single-Incision
Assessment of the durability of robot-assisted laparoscopic sacrocolpopexy for treatment of vaginal vault prolapse
 J Robotic Surg (2007) 1:163 168 DOI 10.1007/s11701-007-0028-8 ORIGINAL ARTICLE Assessment of the durability of robot-assisted laparoscopic sacrocolpopexy for treatment of vaginal vault prolapse Daniel
J Robotic Surg (2007) 1:163 168 DOI 10.1007/s11701-007-0028-8 ORIGINAL ARTICLE Assessment of the durability of robot-assisted laparoscopic sacrocolpopexy for treatment of vaginal vault prolapse Daniel
SACROSPINOUS LIGAMENT FIXATION, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE
 Original Article, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE * ** Fauzia Rasool Memon, Mohamed Matar * Consultant Obstetrician and Gynecologist
Original Article, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE * ** Fauzia Rasool Memon, Mohamed Matar * Consultant Obstetrician and Gynecologist
Suture complications in a teaching institution among patients undergoing uterosacral ligament suspension with permanent braided suture
 Int Urogynecol J (2010) 21:813 818 DOI 10.1007/s00192-010-1109-1 ORIGINAL ARTICLE Suture complications in a teaching institution among patients undergoing uterosacral ligament suspension with permanent
Int Urogynecol J (2010) 21:813 818 DOI 10.1007/s00192-010-1109-1 ORIGINAL ARTICLE Suture complications in a teaching institution among patients undergoing uterosacral ligament suspension with permanent
INJ. Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple Sutures: Surgical Technique and Results.
 Original Article Int Neurourol J 2012;16:144-148 pissn 2093-4777 eissn 2093-6931 International Neurourology Journal Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple
Original Article Int Neurourol J 2012;16:144-148 pissn 2093-4777 eissn 2093-6931 International Neurourology Journal Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple
What are we talking about? Symptoms. Prolapse Risk Factors. Vaginal bulge 1 Splinting. ?? Pelvic pressure Back pain 1 Urinary complaints 2
 Options for Vaginal Prolapse What are we talking about? Michelle Y. Morrill, M.D. Director of Urogynecology The Permanente Medical Group Kaiser, San Francisco Assistant Professor, Volunteer Faculty Department
Options for Vaginal Prolapse What are we talking about? Michelle Y. Morrill, M.D. Director of Urogynecology The Permanente Medical Group Kaiser, San Francisco Assistant Professor, Volunteer Faculty Department
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of sacrocolpopexy with hysterectomy using mesh to repair uterine prolapse Uterine
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of sacrocolpopexy with hysterectomy using mesh to repair uterine prolapse Uterine
A New Technique for Performing a Laparoscopic Hysterectomy Using Microlaparoscopy: Microlaparoscopic Assisted Vaginal Hysterectomy (mlavh)
 A New Technique for Performing a Laparoscopic Hysterectomy Using Microlaparoscopy: Microlaparoscopic Assisted Vaginal Hysterectomy (mlavh) ABSTRACT In an effort to further decrease patient postoperative
A New Technique for Performing a Laparoscopic Hysterectomy Using Microlaparoscopy: Microlaparoscopic Assisted Vaginal Hysterectomy (mlavh) ABSTRACT In an effort to further decrease patient postoperative
Research Article The Impact of Training Residents on the Outcome of Robotic-Assisted Sacrocolpopexy
 Minimally Invasive Surgery Volume 2012, Article ID 289342, 6 pages doi:10.1155/2012/289342 Research Article The Impact of Training Residents on the Outcome of Robotic-Assisted Sacrocolpopexy Mohamed A.
Minimally Invasive Surgery Volume 2012, Article ID 289342, 6 pages doi:10.1155/2012/289342 Research Article The Impact of Training Residents on the Outcome of Robotic-Assisted Sacrocolpopexy Mohamed A.
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,900 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,900 116,000 120M Open access books available International authors and editors Downloads Our
Posterior Deep Endometriosis. What is the best approach? Posterior Deep Endometriosis. Should we perform a routine excision of the vagina??
 Posterior Deep Endometriosis What is the best approach? Dept Gyn Obst Polyclinique Hotel Dieu CHU Clermont Ferrand France Posterior Deep Endometriosis Organs involved - Peritoneum - Uterine cervix -Rectum
Posterior Deep Endometriosis What is the best approach? Dept Gyn Obst Polyclinique Hotel Dieu CHU Clermont Ferrand France Posterior Deep Endometriosis Organs involved - Peritoneum - Uterine cervix -Rectum
Long-term outcomes of modified high uterosacral ligament vault suspension (HUSLS) at vaginal hysterectomy
 Int Urogynecol J (2011) 22:577 584 DOI 10.1007/s00192-010-1325-8 ORIGINAL ARTICLE Long-term outcomes of modified high uterosacral ligament vault suspension (HUSLS) at vaginal hysterectomy Stergios K. Doumouchtsis
Int Urogynecol J (2011) 22:577 584 DOI 10.1007/s00192-010-1325-8 ORIGINAL ARTICLE Long-term outcomes of modified high uterosacral ligament vault suspension (HUSLS) at vaginal hysterectomy Stergios K. Doumouchtsis
Efficacy and Adverse Effects of Monarc Versus Tension-free Vaginal Tape Obturator: a Retrospective One-year Follow-up Study
 Efficacy and Adverse Effects of Monarc Versus Tension-free Vaginal Tape Obturator: a Retrospective One-year Follow-up Study Yvonne KY CHENG MBChB, MRCOG William WK TO MBBS, M Phil, FRCOG, FHKAM (O&G) HX
Efficacy and Adverse Effects of Monarc Versus Tension-free Vaginal Tape Obturator: a Retrospective One-year Follow-up Study Yvonne KY CHENG MBChB, MRCOG William WK TO MBBS, M Phil, FRCOG, FHKAM (O&G) HX
Pelvic Health Coding & Payment Quick Reference
 Payer policies will vary and should be verified prior to treatment for limitations on diagnosis, coding or site of service requirements. The coding options listed within this guide are commonly used codes
Payer policies will vary and should be verified prior to treatment for limitations on diagnosis, coding or site of service requirements. The coding options listed within this guide are commonly used codes
Desara TV and Desara Blue TV
 Desara TV and Desara Blue TV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide Available Electronically M Manufactured
Desara TV and Desara Blue TV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide Available Electronically M Manufactured
Laparoscopic sacrocolpopexy compared with open abdominal sacrocolpopexy for vault prolapse repair: a randomised controlled trial
 Int Urogynecol J (2017) 28:1469 1479 DOI 10.1007/s00192-017-3296-5 ORIGINAL ARTICLE Laparoscopic sacrocolpopexy compared with open abdominal sacrocolpopexy for vault prolapse repair: a randomised controlled
Int Urogynecol J (2017) 28:1469 1479 DOI 10.1007/s00192-017-3296-5 ORIGINAL ARTICLE Laparoscopic sacrocolpopexy compared with open abdominal sacrocolpopexy for vault prolapse repair: a randomised controlled
Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan
 Original Article Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan ABSTRACT Objective: Aim of the study was to determine
Original Article Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan ABSTRACT Objective: Aim of the study was to determine
High success rate and considerable adverse events of pelvic prolapse surgery with Prolift: A single center experience
 Available online at www.sciencedirect.com ScienceDirect Taiwanese Journal of Obstetrics & Gynecology 52 (2013) 389e394 Short Communication High success rate and considerable adverse events of pelvic prolapse
Available online at www.sciencedirect.com ScienceDirect Taiwanese Journal of Obstetrics & Gynecology 52 (2013) 389e394 Short Communication High success rate and considerable adverse events of pelvic prolapse
9/24/2015. Pelvic Floor Disorders. Agenda. What is the Pelvic Floor? Pelvic Floor Problems
 Management of Pelvic Floor Disorders Doctor, I don t want THAT mesh! Agenda What are pelvic floor disorders (PFDs)? What are the treatment options? Expectant. Conservative. Surgical. How and when are grafts
Management of Pelvic Floor Disorders Doctor, I don t want THAT mesh! Agenda What are pelvic floor disorders (PFDs)? What are the treatment options? Expectant. Conservative. Surgical. How and when are grafts
Clinical Study Initial Experience with Robotic Retropubic Urethropexy Compared to Open Retropubic Urethropexy
 Obstetrics and Gynecology International Volume 2013, Article ID 315680, 5 pages http://dx.doi.org/10.1155/2013/315680 Clinical Study Initial Experience with Retropubic Urethropexy Compared to Open Retropubic
Obstetrics and Gynecology International Volume 2013, Article ID 315680, 5 pages http://dx.doi.org/10.1155/2013/315680 Clinical Study Initial Experience with Retropubic Urethropexy Compared to Open Retropubic
Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments?
 Int Urogynecol J (2010) 21:271 278 DOI 10.1007/s00192-009-1028-1 ORIGINAL ARTICLE Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments? Mariëlla
Int Urogynecol J (2010) 21:271 278 DOI 10.1007/s00192-009-1028-1 ORIGINAL ARTICLE Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments? Mariëlla
MIDLAND MEMORIAL HOSPITAL Delineation of Privileges FEMALE PELVIC MEDICINE AND RECONSTRUCTIVE SURGERY (UROGYNECOLOGY)
 MIDLAND MEMORIAL HOSPITAL Delineation of Privileges FEMALE PELVIC MEDICINE AND RECONSTRUCTIVE SURGERY (UROGYNECOLOGY) Physician Name: Your home for healthcare Female Pelvic Medicine and Reconstructive
MIDLAND MEMORIAL HOSPITAL Delineation of Privileges FEMALE PELVIC MEDICINE AND RECONSTRUCTIVE SURGERY (UROGYNECOLOGY) Physician Name: Your home for healthcare Female Pelvic Medicine and Reconstructive
Laparoscopic vs Robotic-assisted Sacrocolpopexy
 10.5005/jp-journals-10033-1180 REVIEW ARTICLE ABSTRACT Background: Laparoscopic sacrocolpopexy has been in vogue since 1993. Robotic technique has started only since 2004. 1 In this article both the techniques
10.5005/jp-journals-10033-1180 REVIEW ARTICLE ABSTRACT Background: Laparoscopic sacrocolpopexy has been in vogue since 1993. Robotic technique has started only since 2004. 1 In this article both the techniques
For personal use only CONTROVERSIES IN PELVIC SURGERY
 For mass reproduction, content licensing and permissions contact Dowden Health Media. OBG MANAGEMENT NEW VIDEO ONLINE www.obgmanagement.com Copyright Dowden Health Media For personal use only This posthysterectomy
For mass reproduction, content licensing and permissions contact Dowden Health Media. OBG MANAGEMENT NEW VIDEO ONLINE www.obgmanagement.com Copyright Dowden Health Media For personal use only This posthysterectomy
and recovery time have led many clinicians
 Research UROGYNECOLOGY Laparoscopic sacral colpopexy versus total vaginal mesh for vaginal vault prolapse: a randomized trial Christopher F. Maher, MD; Benjamin Feiner, MD; Eva M. DeCuyper, MD; Cathy J.
Research UROGYNECOLOGY Laparoscopic sacral colpopexy versus total vaginal mesh for vaginal vault prolapse: a randomized trial Christopher F. Maher, MD; Benjamin Feiner, MD; Eva M. DeCuyper, MD; Cathy J.
Laparoscopic Compared With Robotic Sacrocolpopexy for Vaginal Prolapse A Randomized Controlled Trial
 Compared With for Vaginal Prolapse A Randomized Controlled Trial Marie Fidela R. Paraiso, MD, J. Eric Jelovsek, MD, Anna Frick, MD, MPH, Chi Chung Grace Chen, MD, and Matthew D. Barber, MD, MHS OBJECTIVE:
Compared With for Vaginal Prolapse A Randomized Controlled Trial Marie Fidela R. Paraiso, MD, J. Eric Jelovsek, MD, Anna Frick, MD, MPH, Chi Chung Grace Chen, MD, and Matthew D. Barber, MD, MHS OBJECTIVE:
For personal use only. Injury-free vaginal surgery: Case-based protective tactics
 For mass reproduction, content licensing and permissions contact Dowden Health Media. OBG MANAGEMENT Lennox Hoyte, MD Director of Female Pelvic Medicine and Reconstructive Surgery, Department of Obstetrics
For mass reproduction, content licensing and permissions contact Dowden Health Media. OBG MANAGEMENT Lennox Hoyte, MD Director of Female Pelvic Medicine and Reconstructive Surgery, Department of Obstetrics
The UK National Prolapse Survey: 10 years on
 Int Urogynecol J (2018) 29:795 801 DOI 10.1007/s00192-017-3476-3 ORIGINAL ARTICLE The UK National Prolapse Survey: 10 years on Swati Jha 1 & Alfred Cutner 2 & Paul Moran 3 Received: 28 June 2017 /Accepted:
Int Urogynecol J (2018) 29:795 801 DOI 10.1007/s00192-017-3476-3 ORIGINAL ARTICLE The UK National Prolapse Survey: 10 years on Swati Jha 1 & Alfred Cutner 2 & Paul Moran 3 Received: 28 June 2017 /Accepted:
