How to Obtain Good Results with Orthotopic Bladder Substitution: The 10 Commandments
|
|
|
- Jeffery May
- 5 years ago
- Views:
Transcription
1 EUROPEAN UROLOGY SUPPLEMENTS 8 (2009) available at journal homepage: How to Obtain Good Results with Orthotopic Bladder Substitution: The 10 Commandments Richard E. Hautmann a, *, Henry Botto b, Urs E. Studer c a Department of Urology, University of Ulm, Ulm, Germany b Service d Urologie et de transplantation rénale, Hôpital Foch, Suresnes Cedex, France c Department of Urology, University of Bern, Bern, Switzerland Article info Keywords: Bladder cancer Cystectomy Neobladder Orthotopic reconstruction Urinary diversion Please visit europeanurology to read and answer questions on-line. The EU-ACME credits will then be attributed automatically. Abstract Context: The orthotopic neobladder has not only withstood the test of time but is increasingly becoming a more desirable method of urinary diversion. Complementing orthotopic neobladder features with adequate training allows patients to return to a urinary routine that is close to, if not completely, normal. Objective: The preconditions, indications, and contraindications as well as the key points of the surgical technique will be presented by researchers who pioneered this operation. Evidence acquisition: Experience with and long-term follow-up of orthotopic reconstruction is presented by surgeons at institutions that pioneered orthotopic reconstruction during the last 25 yr with a high surgical volume of radical cystectomy (RCX) and any form of urinary diversion (particularly orthotopic reconstruction). Evidence synthesis: Ten commandments were developed for achieving good results with orthotopic bladder substitution: (1) The procedure should be performed by a high-volume surgeon; (2) do not overextend the indication; (3) experience with nerve-sparing radical prostatectomy and bowel surgery is mandatory; (4) use ileum whenever possible; (5) maximum detubularisation is a must; (6) use a stented, freely refluxive ileoureterostomy; (7) the low-pressure, compliant, freely refluxive reservoir is standard; (8) be aware of myriad potential complications; (9) a full armamentarium of diversion techniques must be available; and (10) meticulous follow-up must be guaranteed. Conclusions: Continence and voiding function following orthotopic bladder substitution are determined primarily by characteristics of the reservoir and by a preserved, innervated outlet mechanism. The reservoir should be detubularised and compliant with a low end filling pressure. Ileum seems to be superior to sigmoid or stomach, which can be used when necessary but with higher incontinence rates. Reflux prevention is not a major concern and does not justify the use of an antireflux mechanism with a high complication rate. # 2009 European Association of Urology. Published by Elsevier B.V. All rights reserved. * Corresponding author. University of Ulm, Prittwitzstraße 43, Ulm, Germany. Tel ; Fax: address: richard.hautmann@uniklinik-ulm.de (R.E. Hautmann) /$ see front matter # 2009 European Association of Urology. Published by Elsevier B.V. All rights reserved. doi: /j.eursup
2 EUROPEAN UROLOGY SUPPLEMENTS 8 (2009) Introduction The orthotopic neobladder has not only withstood the test of time but is increasingly becoming a more desirable method of urinary diversion [1,2]. Complementing orthotopic neobladder features with adequate training allows patients to return to a urinary routine that is close to, if not completely, normal. Ten points, however, must be followed carefully. 2. Evidence acquisition Experience with and long-term follow-up of orthotopic reconstruction is presented by surgeons at institutions that pioneered orthotopic reconstruction during the last 25 yr with a high surgical volume of radical cystectomy (RCX) and any form of urinary diversion (particularly orthotopic reconstruction). 3. Evidence synthesis 3.1. Commandment 1: The procedure should be performed by a high-volume surgeon RCX has been assessed the highest values in terms of difficulty of surgery for any procedure in urology [3]. RCX also is the most difficult robotic procedure and is even more difficult if the diversion is performed totally intracorporeally [4]. Mortality from RCX at low-volume hospitals is 3.1% versus 0.7% at high-volume hospitals. Negative surgical margins and 10 lymph nodes removed were associated with better overall survival independent of patient age, pathologic stage, nodal status, and whether or not patients actually received neoadjuvant chemotherapy [5,6]. A local recurrence developed in 68% of margin-positive patients compared to 6% in margin-negative patients. High-volume urologists had a margin-positive rate of 4% versus 14% for low-volume urologists. The quality of the RCX, the pelvic lymph node dissection, and the urinary diversion directly affects the patient s chances of survival and is surgeon dependent. The likelihood of receiving a neobladder after RCX varies and depends on geographic, social, ethnic, and religious factors. Health care systems and referral patterns play an important role: for example, in the United States, 50% of RCX patients received a neobladder at medical centres as opposed to 15% in the Medicare population [7] Commandment 2: Do not overextend the indication During patient selection, it is essential for realistic expectations to be discussed by the patient and the surgeon. There are several contraindications for an orthotopic neobladder: Urinary stress incontinence Damaged rhabdosphincter or incompetent urethra Tumour infiltration of the distal prostatica urethra in men or the bladder neck in women Impaired renal function (serum creatinine >150 mmol/l) Severely impaired liver function Severe intestinal disease (eg, Crohn s disease) Inadequate intellectual capacity, dexterity, or mobility Incompliant patients for active postoperative reeducation and regular follow-up Impossibility of nerve-sparing surgery at least on one side. Patients aged >80 yr should not be excluded but should be very restrictively selected for an orthotopic neobladder. Achieving urinary continence for these patients might take longer than in younger patients, due to a possibly weaker rhabdosphincter muscle [8] Commandment 3: Experience with nerve-sparing radical prostatectomy and bowel surgery is mandatory For nerve-sparing surgical technique, the oncologic outcomes must be considered. First, the radical cancer resection must not be compromised by nerve-sparing surgery. Nerve sparing should only be attempted on the non tumour-bearing side. Neurovascular bundles are preserved along the prostate dorsolaterally and in the angle between prostate and bladder along the seminal vesicles. This technique improves sexual function [9] and continence, especially during the day [10]. The prostatic capsule and seminal-sparing cystectomy goes one step further than the nerve-sparing technique. It has been proposed to improve the postoperative sexual function. It succeeded for that purpose but does not really improve the continence rate [11,12]. Moreover, the oncologic results are clearly worse, with a 10 15% higher failure rate [11]. Thus, this technique seems like a step in the wrong direction [11] until we understand the oncologic failures better. Experience with bowel surgery and, more generally, with intestinal surgery is mandatory. Ileus and entero-enteral, enteropouch, or enterocutaneous fistula are among the most serious complications and could be life threatening [13]. Consequently, prevention and management are of great importance. It is also necessary to have experience in gynaecological surgery. The preservation of the anterior vaginal wall with orthotopic bladder is indicated in unifocal organ-confined tumours above the bladder base, using preoperative computed tomography scan to exclude uterine infiltration by the bladder cancer [14]. This preservation maintains vaginal length and support, has excellent functional results and acceptable complication rates, and can achieve negative margins with a low incidence of hypercontinence [15,16]. In summary, orthotopic bladder replacement after RCX could involve several surgical specialists, but all of them are part of a single team. Only one team leader is responsible for the surgery and its follow-up, and that is the urologist Commandment 4: Use ileum whenever possible A comparison of gastric, ileal, ileocolic, right colic, and sigmoid segments shows an advantage for ileum over any
3 714 EUROPEAN UROLOGY SUPPLEMENTS 8 (2009) other segment with regard to function/urodynamics, transformation after exposure to urine, change in absorptive capacity, adaptation of mucosa absorptive to storage, incidence of metabolic disorders, late-volume increase, capacity at first and at maximum contraction, involuntary contractions, motor activity, distensibility, and suitability for patients with decreased kidney function [2]. Advantages were shown for ileocolic and sigmoid segments with regard to initial volume, accessibility and anastomosis, saving the ileocecal valve, and lack of vitamin B12 deficiency [2]. Comparison of gastric, ileal, ileocolic, right colic, and sigmoid segments shows that continence rates and urodynamic data were remarkably different for ileal, ileocolic, sigmoid, and gastric segments. Clear differences also appeared with regard to metabolic consequences in ileal, gastric, and colonic segments. Patient and surgeon issues were different with regard to surgeon s preference, length and ease of surgery, body image, and lowest possible complication rate Commandment 5: Maximum detubularisation is a must The difference in pressure between a tubularised and a detubularised ileal neobladder becomes obvious in the urodynamics studies (Fig. 1). The peristaltic contractions of the tubularised segment generate high peak pressures that lead to urine leakage when the bladder pressure exceeds the urethral pressure. In the detubularised reservoir, bladder pressure increases little and the bladder end filling pressure is <30 cm of water, which is less than the urethral pressure. Consider a tubular segment: Open it along the full length and fold it. By doing that, a new tubular segment is obtained with double the width, half the length, and a doubled volume. It is the same with a segment of bowel. Moreover, the body of the neobladder reservoir counteracts pressure peaks, and, thus, a large volume is obtained at low pressure. It is also possible to preserve a tubular segment for ureteral implantation, such as a short limb for a Hautmann-type neobladder or a longer tubular segment for the Studer technique. The peak pressures in connection with this tubular segment are lost in the low bladder pressure, with Fig. 1 Typical urodynamic studies of tubularised versus detubularised good segment. no clinical impact. In special cases, it is also possible to replace the ureter with a tubular segment. In conclusion, there is no reason left to use tubularised bladder Commandment 6: Use a stented, freely refluxive ileoureterostomy Conventional wisdom suggests the need for an antireflux mechanism, as reflux nephropathy can develop with highpressure neuropathic bladders. Reflux prevention in a lowpressure detubularised orthotopic reservoir, however, might not be as beneficial as anticipated. Several reasons for that exist. First, with detubularised bowel segments and the absence of any coordinated contractions, no appreciable pressure is generated. Second, an increase in intraabdominal pressure results in identical pressure rises in both the neobladder and ureters, allowing no reflux [17]. The pressure in the reservoir cannot be higher than the peristaltic force of the ureters and afferent tubular segment. Additionally, the afferent tubular segment itself has certain dynamic antireflux properties due to its coordinated peristalsis [18]. With a major pressure peak within the reservoir that exceeds the urethral closure pressure, the external sphincter generally acts as a safety valve, allowing urinary leakage and thus preventing reflux. Urine usually remains sterile within the closed system of orthotopic substitutes, and therefore nephropathy is less likely. Finally, all published antireflux techniques have a higher anastomotic stricture and eventual renal damage rate than the Nesbit technique (direct ureterointestinal anastomosis) Commandment 7: The low-pressure, compliant, freely refluxive reservoir is standard It is mandatory to avoid ileal or colonic segments that are too long because they lead to neobladder volume that is too large and, thus, to overdistension. The larger the bladder volume, the higher the rate of postvoiding residual urine and, thus, of reflux; the higher the rate of leakage, the higher the risk of metabolic disorders [19]. No more than 45 cm of ileum seems safe to avoid metabolic disorders. The rate of bacteriuria is also increased with large bladder and residual postvoiding urine. An optimal volume of 450 ml for the bladder has been advocated [20]. Whatever the detubularised technique used, training and life-long follow-up are of great importance. Training is necessary to teach and explain to the patient how to be continent, how to empty the bladder, and how to avoid overdistension. Life-long follow-up, apart from oncologic surveillance, controls these data regularly and if needed, corrects them. And remember: Confidence does not exclude surveillance. In ureteroileal anastomosis, the pressure in the lower part of the ureter is cm of water [21]. The bladder end filling pressure is 20 cm for an optimal cytometric capacity of 450 cm 3. This pressure difference is a safety margin. During the filling phase of bladder, the absence of coordinated contractions guarantees a low pressure
4 EUROPEAN UROLOGY SUPPLEMENTS 8 (2009) Fig. 2 Patient with a Z-shaped ileal bladder done in 1994 with good urethral filling, no reflux, and no postvoiding residual urine. Reprinted with permission from Elsevier [22]. reservoir. During voiding, the use of Valsalva manoeuvre increases the pressure in the bladder, the abdomen, and the renal pelvis simultaneously, keeping the safety margin. Thus, a direct ureteral neobladder anastomosis can be performed, provided that the patient is well trained and controlled (Fig. 2). Even if there is reflux during voiding, it is only transient and grade 1 without renal damage. But in the case of overdistension of the bladder, whatever the reason, reflux will occur. In summary, the low-pressure, highly compliant, freely refluxive reservoir allows a good bladder capacity without renal reflux and postresidual urine, assuming training and surveillance are well done Commandment 8: Be aware of myriad potential complications RCX is a morbid procedure, even in the most experienced hands, with contemporary single-institution series reporting postoperative complications in the range of 25 57%, inhospital mortality of 3%, and reoperative rates in the range of % [23]. The disparity in the quality of surgicalcomplication reporting in urologic oncology makes it impossible to compare the morbidity of surgical techniques and outcomes [24]. Between January 1986 and September 2008, the Department of Urology at Ulm, Germany, performed 1013 RCXs with orthotopic reconstruction. All complications within 90 d of surgery were defined, categorised into 11 categories, and classified with an established five-grade modification of the original Clavien system utilised at the Memorial Sloan-Kettering Cancer Centre (MSKCC): Grade 1 consisted of oral medication/ bedside care; grade 2 consisted of intravenous therapy, hyperalimentation, enteral feedings, or transfusions; grade 3 consisted of intubation, interventional radiology, or reoperative intervention; grade 4 consisted of organ resection or chronic disability; and grade 5 consisted of death. Results shows that only 42.4% of the patients had no early complications. Overall, 11.1% of complications were grade 1, 25.3% were grade 2, 16.7% were grade 3, 2.3% were grade 4, and 2.3% were grade 5 (Table 1) [25]. In summary, RCX and ileal neobladder formation represents major surgery with potential, relevant, early complications, even in the most experienced hands. The
5 716 EUROPEAN UROLOGY SUPPLEMENTS 8 (2009) Table 1 Grading of early complications according the modified Clavien system at the Memorial Sloan-Kettering Cancer Centre [25] Gastrointestinal 85.0 % 0.7 % 8.1 % 3.9 % 1.8 % 0.5 % Infection 75.4 % 3.8 % 15.6 % 3.6 % 0.4 % 1.3 % Wound 93.5 % 1.9 % 1.1 % 3.5 % 0.1 % 0.0 % Cardiac 97.6 % 1.2 % 0.9 % 0.1 % 0.0 % 0.2 % Genitourinary 83.8 % 3.5 % 7.1 % 5.6 % 0.0 % 0.0 % Pulmonary 95.3 % 0.3 % 1.8 % 1.7 % 0.2 % 0.8 % Bleeding 98.1 % 0.1 % 0.2 % 1.5 % 0.1 % 0.0 % Thromboembolic 97.2 % 0.7 % 1.4 % 0.2 % 0.0 % 0.5 % Neurologic 97.5 % 1.9 % 0.5 % 0.0 % 0.0 % 0.1 % Miscellaneous 90.5 % 3.0 % 1.6 % 4.9 % 0.0 % 0.0 % Surgical 96.7 % 2.1 % 0.5 % 0.6 % 0.0 % 0.1 % Total 42.4 % 11.1 % 25.3 % 16.7 % 2.3 % 2.3 % rate of severe and lethal complications, however, is acceptably low Commandment 9: A full armamentarium of diversion techniques must be available Orthotopic bladder replacement may be infeasible for anatomical and oncologic reasons. Anatomically, in the preoperative setting, it is necessary to select, together with the patient, the optimal position for a potential cutaneous urinary stoma. The position of the patient on the operating table is hyperextended to open the surgical field. For the urethral neobladder anastomosis, this position can be altered and the lower limbs are pushed up. With this change in position, the urethral stump moves upwards by a mean of 3 cm, avoiding too much tension on the urethraneobladder anastomosis. In an extreme and very uncommon situation, it could be necessary to free the right colonic junction and to move the ileum and the right colon downwards to make the urethra-neobladder anastomosis tension free or at least avoiding too much tension. When the urethral anastomosis is too tight, despite all of these manoeuvres, the goal of bladder replacement must be given up. Oncologically, urethral frozen section is mandatory. In men, the use of frozen section is a matter of controversy, but it seems wise to use it whenever possible [26]. When a positive margin for carcinoma in situ or major dysplasia is found, it is necessary to carry out a urethrectomy ending in a cutaneous urinary diversion. Cutaneous ureterostomy seems like the worst technique for the patient. Regarding the other techniques of cutaneous diversion, even when performed by a high-volume surgeon, some procedures are not used. Consequently, the urologist should select those techniques for which he or she is regularly trained, remembering that practice makes perfect Commandment 10: Meticulous follow-up must be guaranteed Critical components for good long-term results require not only surgical finesse but also patient compliance and meticulous postoperative care [27,28]. Immediate postoperative management should include the following steps: Subcutaneous heparin prophylaxis into the arm instead of the thigh to prevent lymphoceles Bladder substitute rinsed every 6 h, with aspiration of mucus Bowel stimulation with parasympathomimetics from day 2or3on Withdrawal of urethral stents at day 5 7 after resumed bowel activity First removal of the suprapubic tube on day 8 10 (cystogram) Withdrawal of urethral catheter on day Following catheter withdrawal, patients are carefully instructed on how to void. Initially, they are taught to empty the neobladder in a sitting position every 2 h during the day by relaxing the pelvic floor and increasing the intraabdominal pressure. The following points must be observed: Voiding without residual urine Sterile urine Alarm clock at night Venous blood gas analysis every second day Supplement of bicarbonate (2 6 g) and salt. Increase fluid intake and check body weight. Increase reservoir capacity by adhering to regular voiding intervals: at first, 2 h; thereafter, 3 h; later, 4 h. The aim is a capacity of 500 ml. Meticulous long-term follow-up is essential regarding metabolism (vitamin B12, electrolytes, base excess), continence, volume of voided urine ( ml), sterile urine, residual urine (if yes, check regular voiding intervals), and bladder neck obstruction (if yes, perform incision or resection). 4. Conclusions Continence and voiding function following orthotopic bladder substitution are determined primarily by the characteristics of the reservoir and by a preserved, innervated outlet mechanism. The reservoir should be detubularised and compliant, with a low end filling pressure. Ileum seems to be superior to sigmoid or stomach, which can be used when necessary but with higher
6 EUROPEAN UROLOGY SUPPLEMENTS 8 (2009) incontinence rates. Reflux prevention is not a major concern and does not justify the use of an antireflux mechanism with a high complication rate. Orthotopic reconstruction has passed the test of time. In these patients, life is similar to that of individuals with a native lower urinary tract. Until a better solution is devised, orthotopic reconstruction remains the best option for patients requiring RCX. Conflicts of interest The authors have nothing to disclose. Funding support None. References [1] Madersbacher S, Möhrle K, Burkhard F, Studer UE. Long-term voiding pattern of patients with ileal orthotopic bladder substitutes. J Urol 2002;167: [2] Hautmann RE. Urinary diversion: ileal conduit to neobladder. J Urol 2003;169: [3] Montie JE. Technique of radical cystectomy in the male. In: Marshall FF, Kavoussi LR, McAninch JW, Peters CA, eds. Textbook of operative urology. Philadelphia, PA: W.B. Saunders Company; p [4] Hemal AK, Abol-Enein H, Tewari A, et al. Robotic radical cystectomy and urinary diversion. Urol Clin North Am 2004;31: [5] Herr HW, Faulkner JR, Grossman HB, et al. Surgical factors influence bladder cancer outcomes: a cooperative group report. J Clin Oncol 2004;22: [6] Elting LS, Pettaway C, Bekele BN, et al. Correlation between annual volume of cystectomy, professional staffing and outcomes. Cancer 2005;104: [7] Saigal S, Gore J, Polich S, Litwin MS. Trends in reconstruction after radical cystectomy in the Medicare population. J Urol 2005;173: 487. [8] Kessler TM, Burkhard FC, Permenis P, Danuser H, Thalmann GN, Hochreiter WW. Attempted nerve-sparing surgery and age have a significant effect on urinary continence and erectile function after radical cystoprostatovesiculectomy and ileal orthotopic bladder substitution. J Urol 2004;172: [9] Hekal IA, El-Bahnasawy MS, Mosbah A, El-Assmy A, Shaaban A. Recoverability of erectile function in post-radical cystectomy patients: subjective and objective evaluations. Eur Urol 2009;55: [10] Kessler TM, Burkhard FC, Studer UE. Clinical indications and outcomes with nerve sparing cystectomy in patients with bladder cancer. Urol Clin North Am 2005;32: [11] Hautmann RE, Stein JP. Neobladder with prostatica capsule and seminal-sparing cystectomy for bladder cancer: a step in the wrong direction. Urol Clin North Am 2005;32: [12] Botto H, Sebe P, Molinié V, Herve J, Yonneau L, Lebret T. Prostatic capsule and seminal-sparing cystectomy for bladder carcinoma: initials results for selected patients. BJU Int 2004;94: [13] Studer UE, Burkhard FC, Schumacher M, et al. Twenty years experience with an ileal orthotopic low pressure bladder substitute lessons to be learned. J Urol 2006;176: [14] Ali-El-Dein B. Oncological outcome after radical cystectomy and orthotopic bladder substitution in women. Eur J Surg Oncol 2009;35: [15] Chang SS, Cole E, Cookson MS, Peterson M, Schmidt JA. Preservation of the anterior vaginal wall during female radical cystectomy with orthotopic urinary diversion: technique and results. J Urol 2002;168: [16] Abou-Elela A. Outcome of anterior vaginal wall sparing during female radical cystectomy with orthotopic urinary diversion. Eur J Surg Oncol 2008;34: [17] Studer UE, Danuser H, Thalmann GN, Springer J, Turner H. Antireflux nipples or afferent tubular segments in 70 patients with ileal low pressure bladder substitutes: long-term results of a prospective, randomized trial. J Urol 1996;156: [18] Mann FC, Bollmann JL. A method for making a satisfactory fistula at any level of the gastrointestinal tract. Ann Surg 1931;93: [19] Salomon L, Lugagne PM, Hervé JM, Lebret T, Botto H. No evidence of metabolic disorders 10 to 22 years after Camey type I ileal enterocystoplasty. J Urol 1997;157: [20] Fiona C, Burkhard C, Kessler TM, Springer J, Studer UE. Early and late urodynamic assessment of ileal orthotopic bladder substitutes combined with an afferent tubular segment. J Urol 2006;175: [21] Buzelin JM. Physiologie et explorations fonctionnelles de la voie excrétrice urinaire. Rapport au 87ème Congrès Français d Urologie; Novembre 1993; Paris, France. [22] Botto H, Hervé JM, Barré P. Entéroplastie détubulée en Z après prostato-cystectomie totale. Prog Urol 1994;4(Suppl 2): [23] Konety BR, Allareddy V, Herr H. Complications after radical cystectomy: analysis of population-based data. Urology 2006;68: [24] Donat SM. Standards for surgical complication reporting in urologic oncology: time for a change. Urology 2007;69: [25] Volkmer BG, de Petriconi RC, Hautmann RE. Lessons learned from 1000 ileal neobladders: the early complication rate. J Urol 2009;181:142. [26] Lebret T, Hervé JM, Barré P, Lugagne PM, Barbagelatta M, Botto H. Urethral recurrence in transitional cell carcinoma of the bladder. Predictive value of preoperative latero-montanal biopsies and urethral frozen sections during prostatocystectomy. Eur Urol 1998;33: [27] Thurairaja R, Burkhard FC, Studer UE. The orthotopic neobladder. BJU Int 2008;102: [28] Hautmann RE, Volkmer BG, Schumacher MC, Gschwend JE, Studer UE. Long-term results of standard procedures in urology: the ileal neobladder. World J Urol 2006;24:
Bladder replacement in men and women: when and when not? Outline. Continent Diversion History
 1 Bladder replacement in men and women: when and when not? Eila C. Skinner, MD Professor of Clinical Urology Keck USC School of Medicine Outline 1) Selection criteria for orthotopic diversion: Tumor-related
1 Bladder replacement in men and women: when and when not? Eila C. Skinner, MD Professor of Clinical Urology Keck USC School of Medicine Outline 1) Selection criteria for orthotopic diversion: Tumor-related
URINARY DIVERSIONS. Susan Hilton, MD and Nicholas Papanicolaou, MD Co-Chiefs, CT Section Hospital of the University of Pennsylvania
 URINARY DIVERSIONS Susan Hilton, MD and Nicholas Papanicolaou, MD Co-Chiefs, CT Section Hospital of the University of Pennsylvania Neither of us has any financial relationships with commercial interests
URINARY DIVERSIONS Susan Hilton, MD and Nicholas Papanicolaou, MD Co-Chiefs, CT Section Hospital of the University of Pennsylvania Neither of us has any financial relationships with commercial interests
Radical Cystectomy Often Too Late? Yes, But...
 european urology 50 (2006) 1129 1138 available at www.sciencedirect.com journal homepage: www.europeanurology.com Editorial 50th Anniversary Radical Cystectomy Often Too Late? Yes, But... Urs E. Studer
european urology 50 (2006) 1129 1138 available at www.sciencedirect.com journal homepage: www.europeanurology.com Editorial 50th Anniversary Radical Cystectomy Often Too Late? Yes, But... Urs E. Studer
Surgical Atlas Orthotopic ileal neobladder
 Surgery Illustrated ORTHOTOPIC ILEAL NEOBLADDER U.E. STUDER ET AL. Surgical Atlas Orthotopic ileal neobladder U.E. STUDER, C. VAROL and H. DANUSER University of Bern, Department of Urology, Bern, Switzerland
Surgery Illustrated ORTHOTOPIC ILEAL NEOBLADDER U.E. STUDER ET AL. Surgical Atlas Orthotopic ileal neobladder U.E. STUDER, C. VAROL and H. DANUSER University of Bern, Department of Urology, Bern, Switzerland
URINARY DIVERSIONS. Winter 2016 Dr P. O Malley
 URINARY DIVERSIONS Winter 2016 Dr P. O Malley OVERVIEW Who gets diversions? What s involved with cystectomy? What are the different types of diversions? What are the problems with various diversions? How
URINARY DIVERSIONS Winter 2016 Dr P. O Malley OVERVIEW Who gets diversions? What s involved with cystectomy? What are the different types of diversions? What are the problems with various diversions? How
Urethral Carcinoma Recurrence in Ileal Orthotopic Neobladder: Urethrectomy and Conversion in a Continent Pouch with Abdominal Stoma
 Case Report Urol Int 1999;62:213 216 Received: June 19, 1998 Accepted after revision: March 8, 1999 Urethral Carcinoma Recurrence in Ileal Orthotopic Neobladder: Urethrectomy and Conversion in a Continent
Case Report Urol Int 1999;62:213 216 Received: June 19, 1998 Accepted after revision: March 8, 1999 Urethral Carcinoma Recurrence in Ileal Orthotopic Neobladder: Urethrectomy and Conversion in a Continent
Cystectomies and bladder preservation: What you need to know
 Cystectomies and bladder preservation: What you need to know Robin Morash RN, BNSc, MHS Bladder Cancer Canada November 21, 2018 Presentation goals Review the options for treatment of muscle-invasive bladder
Cystectomies and bladder preservation: What you need to know Robin Morash RN, BNSc, MHS Bladder Cancer Canada November 21, 2018 Presentation goals Review the options for treatment of muscle-invasive bladder
Sexuality Preserving Cystectomy and Neobladder (SPCN): Functional Results of a Neobladder Anastomosed to the Prostate
 European Urology European Urology 43 (2003) 646 650 Sexuality Preserving Cystectomy and Neobladder (SPCN): Functional Results of a Neobladder Anastomosed to the Prostate W. Meinhardt *, S. Horenblas Department
European Urology European Urology 43 (2003) 646 650 Sexuality Preserving Cystectomy and Neobladder (SPCN): Functional Results of a Neobladder Anastomosed to the Prostate W. Meinhardt *, S. Horenblas Department
Recovery of sexual function after radical cystectomy with orthotopic neobladder
 Recovery of sexual function after radical cystectomy with orthotopic neobladder C. Gingu, V. Olaru, A. Dick, C. Baston, M. Crăsneanu, C. Surcel, S. Voinea, Liliana Domnişor, I. Sinescu Center of Urological
Recovery of sexual function after radical cystectomy with orthotopic neobladder C. Gingu, V. Olaru, A. Dick, C. Baston, M. Crăsneanu, C. Surcel, S. Voinea, Liliana Domnişor, I. Sinescu Center of Urological
Long-term Renal Function After Urinary Diversion by Ileal Conduit or Orthotopic Ileal Bladder Substitution
 EUROPEAN UROLOGY 61 (2012) 491 497 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Bladder Cancer Editorial by Ja Hyeon Ku and Seth P. Lerner on pp. 498 500
EUROPEAN UROLOGY 61 (2012) 491 497 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Bladder Cancer Editorial by Ja Hyeon Ku and Seth P. Lerner on pp. 498 500
Chapter 8: Urinary Diversions after Cystectomy: The Association of Clinical Factors, Complications and Functional Results of Four Different Diversions
 Chapter 8: Urinary Diversions after Cystectomy: The Association of Clinical Factors, Complications and Functional Results of Four Different Diversions J.A. Nieuwenhuijzen* R.R. de Vries* A. Bex H.G. van
Chapter 8: Urinary Diversions after Cystectomy: The Association of Clinical Factors, Complications and Functional Results of Four Different Diversions J.A. Nieuwenhuijzen* R.R. de Vries* A. Bex H.G. van
Koji Ichihara Hiroshi Kitamura Naoya Masumori Fumimasa Fukuta Taiji Tsukamoto
 Int J Clin Oncol (2013) 18:75 80 DOI 10.1007/s10147-011-0346-8 ORIGINAL ARTICLE Transurethral prostate biopsy before radical cystectomy remains clinically relevant for decision-making on urethrectomy in
Int J Clin Oncol (2013) 18:75 80 DOI 10.1007/s10147-011-0346-8 ORIGINAL ARTICLE Transurethral prostate biopsy before radical cystectomy remains clinically relevant for decision-making on urethrectomy in
Long-Term Results of a Prospective Randomized Study ComparingTwo Different AntirefluxTechniques in Orthotopic Bladder Substitution
 European Urology European Urology 45 (2004) 82 86 Long-Term Results of a Prospective Randomized Study ComparingTwo Different AntirefluxTechniques in Orthotopic Bladder Substitution Yasser Osman *, Hassan
European Urology European Urology 45 (2004) 82 86 Long-Term Results of a Prospective Randomized Study ComparingTwo Different AntirefluxTechniques in Orthotopic Bladder Substitution Yasser Osman *, Hassan
The Studer Orthotopic Neobladder: Long-Term (More Than 10 Years) Functional Outcomes, Urodynamic Features, and Complications
 Original Article http://dx.doi.org/10.3349/ymj.2013.54.3.690 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 54(3):690-695, 2013 The Studer Orthotopic Neobladder: Long-Term (More Than 10 Years) Functional
Original Article http://dx.doi.org/10.3349/ymj.2013.54.3.690 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 54(3):690-695, 2013 The Studer Orthotopic Neobladder: Long-Term (More Than 10 Years) Functional
Long-Term Complications of Conduit Urinary Diversion
 Long-Term Complications of Conduit Urinary Diversion Mark S. Shimko,* Matthew K. Tollefson, Eric C. Umbreit, Sara A. Farmer, Michael L. Blute and Igor Frank From the Department of Urology (MSS, MKT, ECU,
Long-Term Complications of Conduit Urinary Diversion Mark S. Shimko,* Matthew K. Tollefson, Eric C. Umbreit, Sara A. Farmer, Michael L. Blute and Igor Frank From the Department of Urology (MSS, MKT, ECU,
UTI and UrinaryTract Reconstruction
 EAU Update Series 2 (2004) 101 105 UTI and UrinaryTract Reconstruction Werner W. Hochreiter *, Sebastian Z Brun Department of Urology, University of Bern, Anna-Seiler-Haus, Inselspital, CH-3010 Bern, Switzerland
EAU Update Series 2 (2004) 101 105 UTI and UrinaryTract Reconstruction Werner W. Hochreiter *, Sebastian Z Brun Department of Urology, University of Bern, Anna-Seiler-Haus, Inselspital, CH-3010 Bern, Switzerland
Department and Clinic of Urology, Medical University of Silesia, Katowice, Poland
 BioMed Research International Volume 2015, Article ID 306191, 4 pages http://dx.doi.org/10.1155/2015/306191 Clinical Study Sacrocolpopexy with Polypropylene Tape as Valuable Surgical Modification during
BioMed Research International Volume 2015, Article ID 306191, 4 pages http://dx.doi.org/10.1155/2015/306191 Clinical Study Sacrocolpopexy with Polypropylene Tape as Valuable Surgical Modification during
MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER
 10 MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER Recommendations from the EAU Working Party on Muscle Invasive and Metastatic Bladder Cancer G. Jakse (chairman), F. Algaba, S. Fossa, A. Stenzl, C. Sternberg
10 MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER Recommendations from the EAU Working Party on Muscle Invasive and Metastatic Bladder Cancer G. Jakse (chairman), F. Algaba, S. Fossa, A. Stenzl, C. Sternberg
Bowel Function Remains Subjectively Unchanged After Ileal Resection for Construction of Continent Ileal Reservoirs
 EUROPEAN UROLOGY 60 (2011) 585 590 available at www.sciencedirect.com journal homepage: www.europeanurology.com Reconstructive Urology Bowel Function Remains Subjectively Unchanged After Ileal Resection
EUROPEAN UROLOGY 60 (2011) 585 590 available at www.sciencedirect.com journal homepage: www.europeanurology.com Reconstructive Urology Bowel Function Remains Subjectively Unchanged After Ileal Resection
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Outcome of Open Radical Cystectomy and Ileal Conduit: A Single Center Experience Mahesh Kalloli
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Outcome of Open Radical Cystectomy and Ileal Conduit: A Single Center Experience Mahesh Kalloli
Functional and Clinical Outcome of Ileal (Studer) Neo-bladder Reconstruction: Single Centre Experience from Pakistan
 ORIGINAL ARTICLE Functional and Clinical Outcome of Ileal (Studer) Neo-bladder Reconstruction: Single Centre Experience from Pakistan Syed M. Nazim, M. Hammad Ather and Farhat Abbas ABSTRACT Objective:
ORIGINAL ARTICLE Functional and Clinical Outcome of Ileal (Studer) Neo-bladder Reconstruction: Single Centre Experience from Pakistan Syed M. Nazim, M. Hammad Ather and Farhat Abbas ABSTRACT Objective:
BCAN Fall Series: Survivorship
 BCAN Fall Series: Survivorship The New Normal after Bladder Removal and Urinary Diversion Vashti Livingston RN, MS, CNS, CWOCN Ambulatory Urology MSKCC NYC livingsv@mskcc.org Disclosure None BCAN Volunteer
BCAN Fall Series: Survivorship The New Normal after Bladder Removal and Urinary Diversion Vashti Livingston RN, MS, CNS, CWOCN Ambulatory Urology MSKCC NYC livingsv@mskcc.org Disclosure None BCAN Volunteer
Radical Cystectomy A Patient s Guide
 Radical Cystectomy A Patient s Guide Introduction The urinary system, which includes the bladder, urethra, ureters, and kidneys, helps maintain stable chemical conditions in the body, stores, and eliminates
Radical Cystectomy A Patient s Guide Introduction The urinary system, which includes the bladder, urethra, ureters, and kidneys, helps maintain stable chemical conditions in the body, stores, and eliminates
Muscle-invasive bladder cancer
 Patient Information English 4 Muscle-invasive bladder cancer The underlined terms are listed in the glossary. What is muscle-invasive bladder cancer? About a quarter of patients diagnosed with bladder
Patient Information English 4 Muscle-invasive bladder cancer The underlined terms are listed in the glossary. What is muscle-invasive bladder cancer? About a quarter of patients diagnosed with bladder
Functional and Clinicopathologic Outcomes Using a Modified Vescica Ileale Padovana Technique
 Bladder Cancer 1 (2015) 73 79 DOI 10.3233/BLC-140002 IOS Press Research Report 73 Functional and Clinicopathologic Outcomes Using a Modified Vescica Ileale Padovana Technique Chandra K. Flack, M. Francesca
Bladder Cancer 1 (2015) 73 79 DOI 10.3233/BLC-140002 IOS Press Research Report 73 Functional and Clinicopathologic Outcomes Using a Modified Vescica Ileale Padovana Technique Chandra K. Flack, M. Francesca
Retroperitoneoscopic Transureteroureterostomy with Cutaneous Ureterostomy to Salvage Failed Ileal Conduit Urinary Diversion
 available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Study of the Month Retroperitoneoscopic Transureteroureterostomy with Cutaneous Ureterostomy to Salvage Failed Ileal Conduit
available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Study of the Month Retroperitoneoscopic Transureteroureterostomy with Cutaneous Ureterostomy to Salvage Failed Ileal Conduit
FUNCTIONAL RESULTS OF ORTHOTOPIC ILEAL NEOBLADDER WITH SEROUS-LINED EXTRAMURAL URETERAL REIMPLANTATION: EXPERIENCE WITH 450 PATIENTS
 0022-5347/01/1655-1427/0 THE JOURNAL OF UROLOGY Vol. 165, 1427 1432, May 2001 Copyright 2001 by AMERICAN UROLOGICAL ASSOCIATION, INC. Printed in U.S.A. FUNCTIONAL RESULTS OF ORTHOTOPIC ILEAL NEOBLADDER
0022-5347/01/1655-1427/0 THE JOURNAL OF UROLOGY Vol. 165, 1427 1432, May 2001 Copyright 2001 by AMERICAN UROLOGICAL ASSOCIATION, INC. Printed in U.S.A. FUNCTIONAL RESULTS OF ORTHOTOPIC ILEAL NEOBLADDER
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER
 MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
Early radical cystectomy in NMIBC Marko Babjuk
 Early radical cystectomy in NMIBC Marko Babjuk Dept. of Urology, 2nd Faculty of Medicine, Hospital Motol, Praha, Czech Republic We Are The European Association of Urology We Are Urologists, residents,
Early radical cystectomy in NMIBC Marko Babjuk Dept. of Urology, 2nd Faculty of Medicine, Hospital Motol, Praha, Czech Republic We Are The European Association of Urology We Are Urologists, residents,
Do Patients Benefit from Routine Follow-up to Detect Recurrences After Radical Cystectomy and Ileal Orthotopic Bladder Substitution?
 EUROPEAN UROLOGY 58 (2010) 486 494 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Bladder Cancer Editorial by Renzo Colombo on pp. 495 497 of this issue
EUROPEAN UROLOGY 58 (2010) 486 494 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Bladder Cancer Editorial by Renzo Colombo on pp. 495 497 of this issue
Open Radical Cystectomy Tips and Tricks in Males and Females
 Open Radical Cystectomy Tips and Tricks in Males and Females Seth P. Lerner, MD, FACS Professor of Urology Beth and Dave Swalm Chair in Urologic Oncology Scott Department of Urology Baylor College of Medicine
Open Radical Cystectomy Tips and Tricks in Males and Females Seth P. Lerner, MD, FACS Professor of Urology Beth and Dave Swalm Chair in Urologic Oncology Scott Department of Urology Baylor College of Medicine
Comparison of Clinical and Urodynamic Outcome in Orthotopic Ileocaecal and Ileal Neobladder $
 European Urology European Urology 43 (2003) 258±262 Comparison of Clinical and Urodynamic Outcome in Orthotopic Ileocaecal and Ileal Neobladder $ YasËar BeduÈk, Kadir TuÈrkoÈlmez, SuÈmer Baltacõ, CËagÆatay
European Urology European Urology 43 (2003) 258±262 Comparison of Clinical and Urodynamic Outcome in Orthotopic Ileocaecal and Ileal Neobladder $ YasËar BeduÈk, Kadir TuÈrkoÈlmez, SuÈmer Baltacõ, CËagÆatay
Index. Surg Oncol Clin N Am 14 (2005) Note: Page numbers of article titles are in boldface type.
 Surg Oncol Clin N Am 14 (2005) 433 439 Index Note: Page numbers of article titles are in boldface type. A Abdominosacral resection, of recurrent rectal cancer, 202 215 Ablative techniques, image-guided,
Surg Oncol Clin N Am 14 (2005) 433 439 Index Note: Page numbers of article titles are in boldface type. A Abdominosacral resection, of recurrent rectal cancer, 202 215 Ablative techniques, image-guided,
Clinical Commissioning Policy Proposition: Robotic Assisted Surgery for Bladder Cancer
 Clinical Commissioning Policy Proposition: Robotic Assisted Surgery for Bladder Cancer Reference: NHS England B14X08 Information Reader Box (IRB) to be inserted on inside front cover for documents of 6
Clinical Commissioning Policy Proposition: Robotic Assisted Surgery for Bladder Cancer Reference: NHS England B14X08 Information Reader Box (IRB) to be inserted on inside front cover for documents of 6
The surgical technique and initial outcomes of Anatolian neobladder: a novel technique of ileal neobladder after radical cystectomy
 Talat et al. BMC Urology (2018) 18:94 https://doi.org/10.1186/s12894-018-0406-8 TECHNICAL ADVANCE Open Access The surgical technique and initial outcomes of Anatolian neobladder: a novel technique of ileal
Talat et al. BMC Urology (2018) 18:94 https://doi.org/10.1186/s12894-018-0406-8 TECHNICAL ADVANCE Open Access The surgical technique and initial outcomes of Anatolian neobladder: a novel technique of ileal
Radical cystectomy with or without urethrectomy?
 Critical Reviews in Oncology/Hematology 47 (2003) 141/145 www.elsevier.com/locate/critrevonc Radical cystectomy with or without urethrectomy? Hein Van Poppel *, Tomas Sorgeloose Division of Urology, University
Critical Reviews in Oncology/Hematology 47 (2003) 141/145 www.elsevier.com/locate/critrevonc Radical cystectomy with or without urethrectomy? Hein Van Poppel *, Tomas Sorgeloose Division of Urology, University
Orthotopic neobladder reconstruction what are the options?
 Minirev Article ORTHOTOPIC NEOBLADDER RECONSTRUCTION MEYER et al. Orthotopic neobladder reconstruction what are the options? JON-PAUL MEYER, DEREK FAWCETT*, DAVID GILLATT and RAJENDRA PERSAD Department
Minirev Article ORTHOTOPIC NEOBLADDER RECONSTRUCTION MEYER et al. Orthotopic neobladder reconstruction what are the options? JON-PAUL MEYER, DEREK FAWCETT*, DAVID GILLATT and RAJENDRA PERSAD Department
Radical cystectomy is the mainstay of treatment for
 Potency Preserving Cystectomy With Intrafascial Prostatectomy for High Risk Superficial Bladder Cancer Paolo Puppo, Carlo Introini, Franco Bertolotto and Angelo Naselli* From the Urology Unit, Department
Potency Preserving Cystectomy With Intrafascial Prostatectomy for High Risk Superficial Bladder Cancer Paolo Puppo, Carlo Introini, Franco Bertolotto and Angelo Naselli* From the Urology Unit, Department
FIG The inferior and posterior peritoneal reflection is easily
 PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
Radical cystectomy and urinary diversion: Normal anatomy and complications
 Radical cystectomy and urinary diversion: Normal anatomy and complications Poster No.: C-0648 Congress: ECR 2014 Type: Scientific Exhibit Authors: J. M. Marin, N. alegre, P. Perez Martin, A. Velarde Pedraza
Radical cystectomy and urinary diversion: Normal anatomy and complications Poster No.: C-0648 Congress: ECR 2014 Type: Scientific Exhibit Authors: J. M. Marin, N. alegre, P. Perez Martin, A. Velarde Pedraza
RADICAL PROSTATECTOMY
 Tennyson Centre Suite 19 520 South Road Kurralta Park SA 5037 P 08 8292 2399 F 08 8292 2388 admin@urologicalsolutions.com.au www.urologicalsolutions.com.au Darwin Private Hospital Suite 5 Rocklands Drive
Tennyson Centre Suite 19 520 South Road Kurralta Park SA 5037 P 08 8292 2399 F 08 8292 2388 admin@urologicalsolutions.com.au www.urologicalsolutions.com.au Darwin Private Hospital Suite 5 Rocklands Drive
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Interventional management of postoperative ureteric complications after pelvic surgery
 Interventional management of postoperative ureteric complications after pelvic surgery Poster No.: C-0169 Congress: ECR 2015 Type: Scientific Exhibit Authors: R. Tabashy, A. Hamed, S. El-Sebai; Cairo/EG
Interventional management of postoperative ureteric complications after pelvic surgery Poster No.: C-0169 Congress: ECR 2015 Type: Scientific Exhibit Authors: R. Tabashy, A. Hamed, S. El-Sebai; Cairo/EG
Department of Urology, Cochin hospital Paris Descartes University
 Technical advances in the treatment of localized prostate cancer Pr Michaël Peyromaure Department of Urology, Cochin hospital Paris Descartes University Introduction Curative treatments of localized prostate
Technical advances in the treatment of localized prostate cancer Pr Michaël Peyromaure Department of Urology, Cochin hospital Paris Descartes University Introduction Curative treatments of localized prostate
Kaiser Oakland Urology
 Kaiser Oakland Urology What is Laparoscopy? Minimally invasive surgical alternative to standard surgery How is Laparoscopy Performed? A laparoscope and video camera are used to visualize internal organs
Kaiser Oakland Urology What is Laparoscopy? Minimally invasive surgical alternative to standard surgery How is Laparoscopy Performed? A laparoscope and video camera are used to visualize internal organs
Laparoscopic Bladder-Preserving Surgery for Enterovesical Fistula Complicated with Benign Gastrointestinal Disease
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
Dr. Aso Urinary Symptoms
 Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Running head: Treatment modality and long term renal function in MIBC-Hamidi et al.
 Running head: Treatment modality and long term renal function in MIBC-Hamidi et al. Effect of Treatment Modality on Long Term Renal Functions in Patients With Muscle Invasive Bladder Cancer Nurullah Hamidi
Running head: Treatment modality and long term renal function in MIBC-Hamidi et al. Effect of Treatment Modality on Long Term Renal Functions in Patients With Muscle Invasive Bladder Cancer Nurullah Hamidi
Comparison of Three Types of Continent Urinary Diversions in a Single Center
 Article TheScientificWorldJOURNAL (2004) 4 (S1), 135 141 ISSN 1537-744X; DOI 10.1100/tsw.2004.59 Comparison of Three Types of Continent Urinary Diversions in a Single Center Cengiz Girgin, M.D., Akif Sezer,
Article TheScientificWorldJOURNAL (2004) 4 (S1), 135 141 ISSN 1537-744X; DOI 10.1100/tsw.2004.59 Comparison of Three Types of Continent Urinary Diversions in a Single Center Cengiz Girgin, M.D., Akif Sezer,
Radical Cystectomy for Urothelial Carcinoma of the Bladder Without Neoadjuvant or Adjuvant Therapy: Long-Term Results in 1100 Patients
 EUROPEAN UROLOGY 61 (2012) 1039 1047 available at www.sciencedirect.com journal homepage: www.europeanurology.com Bladder Cancer Radical Cystectomy for Urothelial Carcinoma of the Bladder Without Neoadjuvant
EUROPEAN UROLOGY 61 (2012) 1039 1047 available at www.sciencedirect.com journal homepage: www.europeanurology.com Bladder Cancer Radical Cystectomy for Urothelial Carcinoma of the Bladder Without Neoadjuvant
Laparoscopic Surgery. The Da Vinci Robot. Limits of Laparoscopy. What Robotics Offers. Robotic Urologic Surgery: A New Era in Patient Care
 Laparoscopic Surgery Robotic Urologic Surgery: A New Era in Patient Care Laparoscopic technique was introduced in urologic surgery in the 1990s Benefits: Improved recovery time, decreased morbidity Matthew
Laparoscopic Surgery Robotic Urologic Surgery: A New Era in Patient Care Laparoscopic technique was introduced in urologic surgery in the 1990s Benefits: Improved recovery time, decreased morbidity Matthew
Morbidity Audit and Logbook Tool SNOMED Board Reporting Terms for SET and IMG Urology ENDOSCOPIC LOWER URINARY TRACT
 ENDOSCOPIC LOWER URINARY TRACT Cystolitholapaxy Cystoscopic removal of foreign body from bladder Cystoscopic removal of ureteric stent Cystoscopy and cystodiathermy Cystoscopy and transurethral biopsy
ENDOSCOPIC LOWER URINARY TRACT Cystolitholapaxy Cystoscopic removal of foreign body from bladder Cystoscopic removal of ureteric stent Cystoscopy and cystodiathermy Cystoscopy and transurethral biopsy
Impact of invasive bladder cancer and orthotopic urinary diversion on general health-related quality of life: An SF-36 survey
 758 Impact of invasive bladder cancer and orthotopic urinary diversion on general health-related quality of life: An SF-36 survey MINGYING YANG 1,2*, HAIFENG WANG 2*, JIANSONG WANG 2 and MINGHUI RUAN 1
758 Impact of invasive bladder cancer and orthotopic urinary diversion on general health-related quality of life: An SF-36 survey MINGYING YANG 1,2*, HAIFENG WANG 2*, JIANSONG WANG 2 and MINGHUI RUAN 1
Cystectomy and Bladder Reconstruction (Continent Urinary Diversion) Department of Urology Information for patients
 Cystectomy and Bladder Reconstruction (Continent Urinary Diversion) Department of Urology Information for patients i Introduction You and your consultant have decided that you need a cystectomy (removal
Cystectomy and Bladder Reconstruction (Continent Urinary Diversion) Department of Urology Information for patients i Introduction You and your consultant have decided that you need a cystectomy (removal
Life after Bladder Removal Selecting your best urinary diversion. Part IV: Indiana Pouch and Question & Answer Session
 Life after Bladder Removal Selecting your best urinary diversion A candid conversation with Alexander Kutikov MD Tuesday, January 24, 2017 Part IV: Indiana Pouch and Question & Answer Session Presented
Life after Bladder Removal Selecting your best urinary diversion A candid conversation with Alexander Kutikov MD Tuesday, January 24, 2017 Part IV: Indiana Pouch and Question & Answer Session Presented
Department of Urology, Theodor Bilharz research Institute, Cairo, Egypt
 Surgical Technique Vol. 41 (4): 796-803, July - August, 2015 doi: 10.1590/S1677-5538.IBJU.2013.0086 Detour technique, Dipping technique, or IIeal bladder flap technique for surgical correction of uretero-ileal
Surgical Technique Vol. 41 (4): 796-803, July - August, 2015 doi: 10.1590/S1677-5538.IBJU.2013.0086 Detour technique, Dipping technique, or IIeal bladder flap technique for surgical correction of uretero-ileal
Kelly procedure. How does the urinary system work? What is a Kelly procedure and why does my child need one?
 Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Kelly procedure This information sheet from Great Ormond Street Hospital (GOSH) explains the Kelly procedure used
Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Kelly procedure This information sheet from Great Ormond Street Hospital (GOSH) explains the Kelly procedure used
Joseph H. Williams, MD Idaho Urologic Institute St. Alphonsus Regional Medical Center September 22, 2016
 BLADDER CANCER Joseph H. Williams, MD Idaho Urologic Institute St. Alphonsus Regional Medical Center September 22, 2016 BLADDER CANCER = UROTHELIAL CANCER Antiquated term is Transitional Cell Carcinoma
BLADDER CANCER Joseph H. Williams, MD Idaho Urologic Institute St. Alphonsus Regional Medical Center September 22, 2016 BLADDER CANCER = UROTHELIAL CANCER Antiquated term is Transitional Cell Carcinoma
Guidelines on Neurogenic Lower Urinary Tract Dysfunction
 Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
Continent urinary diversion
 Critical Reviews in Oncology/Hematology 57 (2006) 255 264 Continent urinary diversion Fiona C. Burkhard, Thomas M. Kessler, Rob Mills, Urs E. Studer Department of Urology, University of Bern, 3010 Bern,
Critical Reviews in Oncology/Hematology 57 (2006) 255 264 Continent urinary diversion Fiona C. Burkhard, Thomas M. Kessler, Rob Mills, Urs E. Studer Department of Urology, University of Bern, 3010 Bern,
Original Paper. Urol Int 2002;69:
 Original Paper Urol Int 2002;69:184 189 Received: June 15, 2001 Accepted after revision: January 29, 2002 D igit al Fluorographic V ideo-u rodynam ics in t he Long-Term M orphof unct ional Evaluat ion
Original Paper Urol Int 2002;69:184 189 Received: June 15, 2001 Accepted after revision: January 29, 2002 D igit al Fluorographic V ideo-u rodynam ics in t he Long-Term M orphof unct ional Evaluat ion
Anterior urethra sparing cystoprostatectomy for bladder cancer: a 10 year, single center experience
 DOI 10.1186/s40064-015-1200-7 RESEARCH Open Access Anterior urethra sparing cystoprostatectomy for bladder cancer: a 10 year, single center experience Nozomi Hayakawa 1,2*, Nobuyuki Kikuno 1,2, Hiroki
DOI 10.1186/s40064-015-1200-7 RESEARCH Open Access Anterior urethra sparing cystoprostatectomy for bladder cancer: a 10 year, single center experience Nozomi Hayakawa 1,2*, Nobuyuki Kikuno 1,2, Hiroki
Trimodality Therapy for Muscle Invasive Bladder Cancer
 Trimodality Therapy for Muscle Invasive Bladder Cancer Brita Danielson, MD, FRCPC Radiation Oncologist, Cross Cancer Institute Assistant Professor, Department of Oncology University of Alberta Edmonton,
Trimodality Therapy for Muscle Invasive Bladder Cancer Brita Danielson, MD, FRCPC Radiation Oncologist, Cross Cancer Institute Assistant Professor, Department of Oncology University of Alberta Edmonton,
Bladder Cancer Guidelines
 Bladder Cancer Guidelines Agreed by Urology CSG: October 2011 Review Date: September 2013 Bladder Cancer 1. Referral Guidelines The following patients should be considered as potentially having bladder
Bladder Cancer Guidelines Agreed by Urology CSG: October 2011 Review Date: September 2013 Bladder Cancer 1. Referral Guidelines The following patients should be considered as potentially having bladder
Chapter 16 URINARY, SEXUAL AND REPRODUCTIVE IMPAIRMENT
 Chapter 16 URINARY, SEXUAL AND REPRODUCTIVE IMPAIRMENT Introduction This chapter provides criteria for assessing permanent impairment from entitled urinary, sexual and reproductive conditions. The chapter
Chapter 16 URINARY, SEXUAL AND REPRODUCTIVE IMPAIRMENT Introduction This chapter provides criteria for assessing permanent impairment from entitled urinary, sexual and reproductive conditions. The chapter
I-STOP TOMS Transobturator Male Sling
 I-STOP TOMS Transobturator Male Sling The CL Medical I-STOP TOMS sling for male stress urinary incontinence was developed in France where it is widely used and is the market leader. It is constructed with
I-STOP TOMS Transobturator Male Sling The CL Medical I-STOP TOMS sling for male stress urinary incontinence was developed in France where it is widely used and is the market leader. It is constructed with
PROFESSIONAL SKILLS 1 3RD YEAR SEMESTER 6 RADIOGRAPHY. THE URINARY SYSTEM Uz. Fatema shmus aldeen Tel
 PROFESSIONAL SKILLS 1 3RD YEAR SEMESTER 6 RADIOGRAPHY THE URINARY SYSTEM Uz. Fatema shmus aldeen Tel. 0925111552 Professional skills-2 THE URINARY SYSTEM The urinary system (review anatomy and physiology)
PROFESSIONAL SKILLS 1 3RD YEAR SEMESTER 6 RADIOGRAPHY THE URINARY SYSTEM Uz. Fatema shmus aldeen Tel. 0925111552 Professional skills-2 THE URINARY SYSTEM The urinary system (review anatomy and physiology)
Part II: Treatment. A Woman-to-Woman Talk with Dr. Armine Smith. Wednesday, March 8, Presented by
 Women & Bladder Cancer A Woman-to-Woman Talk with Dr. Armine Smith Wednesday, March 8, 2017 Part II: Treatment Presented by Dr. Smith is an Assistant Professor of Urology at Johns Hopkins University and
Women & Bladder Cancer A Woman-to-Woman Talk with Dr. Armine Smith Wednesday, March 8, 2017 Part II: Treatment Presented by Dr. Smith is an Assistant Professor of Urology at Johns Hopkins University and
TURP Complications & Treatments. G. Testa
 TURP Complications & Treatments G. Testa Statistics Operative mortality 0.2 per cent Most common cause of death was sepsis which occurred >1 month after surgery 77% of patients had significant pre-existing
TURP Complications & Treatments G. Testa Statistics Operative mortality 0.2 per cent Most common cause of death was sepsis which occurred >1 month after surgery 77% of patients had significant pre-existing
Index. urologic.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablative therapies, transurethral needle ablation, Adverse events, sexual side effects of BPH Aging, and incidence of BPH associated with
Index Note: Page numbers of article titles are in boldface type. A Ablative therapies, transurethral needle ablation, Adverse events, sexual side effects of BPH Aging, and incidence of BPH associated with
da Vinci Prostatectomy My Greek personal experience
 da Vinci Prostatectomy My Greek personal experience Vassilis Poulakis MD, PhD, FEBU Ass. Prof. of Urology Director of Urologic Clinic Doctors Hospital Athens Laparoscopy - golden standard in Urology -
da Vinci Prostatectomy My Greek personal experience Vassilis Poulakis MD, PhD, FEBU Ass. Prof. of Urology Director of Urologic Clinic Doctors Hospital Athens Laparoscopy - golden standard in Urology -
THE operation of reimplantation of the ureter into the bladder has undergone
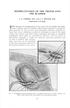 REIMPLANTATION OF THE URETER INTO THE BLADDER J. G. WARDEN, M.D., and C. C. HIGGINS, M.D. Department of Urology THE operation of reimplantation of the ureter into the bladder has undergone a stormy course
REIMPLANTATION OF THE URETER INTO THE BLADDER J. G. WARDEN, M.D., and C. C. HIGGINS, M.D. Department of Urology THE operation of reimplantation of the ureter into the bladder has undergone a stormy course
Attachment #2 Overview of Follow-up
 Attachment #2 Overview of Follow-up Provided below is a general overview of follow-up and this may vary based on specific patient or cancer characteristics. Of note, Labs and imaging can be performed closer
Attachment #2 Overview of Follow-up Provided below is a general overview of follow-up and this may vary based on specific patient or cancer characteristics. Of note, Labs and imaging can be performed closer
Attachment #2 Overview of Follow-up
 Attachment #2 Overview of Follow-up Provided below is a general overview of follow-up and this may vary based on specific patient or cancer characteristics. Of note, Labs and imaging can be performed closer
Attachment #2 Overview of Follow-up Provided below is a general overview of follow-up and this may vary based on specific patient or cancer characteristics. Of note, Labs and imaging can be performed closer
hoofdstuk :07 Pagina ix Introduction
 hoofdstuk 00 08-03-2001 15:07 Pagina ix Introduction Incontinence at pediatric age is a problem that can harm the psychological and physical development of children. Starting in 1986 we have searched for
hoofdstuk 00 08-03-2001 15:07 Pagina ix Introduction Incontinence at pediatric age is a problem that can harm the psychological and physical development of children. Starting in 1986 we have searched for
3. Urinary Catheters. Indications. Methods of Bladder Catheterization. Hashim Hashim
 3. Urinary Catheters Hashim Hashim Indications Urinary catheters are used to drain urine from the bladder. The main indications are: A. Diagnostic Measure post-void residual in the absence of ultrasound
3. Urinary Catheters Hashim Hashim Indications Urinary catheters are used to drain urine from the bladder. The main indications are: A. Diagnostic Measure post-void residual in the absence of ultrasound
CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1
 1 CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1 35 years old man, who previously has been completely healthy, was shot twice in the neck
1 CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1 35 years old man, who previously has been completely healthy, was shot twice in the neck
Percutaneous Nephrolithotomy in a Patient with Mainz Pouch II Urinary Diversion: A Case Report
 198) Prague Medical Report / Vol. 117 (2016) No. 4, p. 198 203 Percutaneous Nephrolithotomy in a Patient with Mainz Pouch II Urinary Diversion: A Case Report Stavros Sfoungaristos 1, Ioannis Mykoniatis
198) Prague Medical Report / Vol. 117 (2016) No. 4, p. 198 203 Percutaneous Nephrolithotomy in a Patient with Mainz Pouch II Urinary Diversion: A Case Report Stavros Sfoungaristos 1, Ioannis Mykoniatis
QUESTIONS TO ASK A UROLOGIST
 QUESTIONS TO ASK A UROLOGIST For the patient: You should review these questions and determine if the answers would satisfy a better understanding of what to expect and ease your concerns. If there are
QUESTIONS TO ASK A UROLOGIST For the patient: You should review these questions and determine if the answers would satisfy a better understanding of what to expect and ease your concerns. If there are
UNM SRMC UROLOGY CLINICAL PRIVILEGES.
 o o o Initial privileges (initial appointment) Renewal of privileges (reappointment) Expansion of privileges (modification) INSTRUCTIONS All new applicants must meet the following requirements as approved
o o o Initial privileges (initial appointment) Renewal of privileges (reappointment) Expansion of privileges (modification) INSTRUCTIONS All new applicants must meet the following requirements as approved
Modified Le Bag Pouch after Radical Cystectomy: Continence, Urodynamic Results and Morbidity
 Journal of the Egyptian Nat. Cancer Inst., Vol. 22, No. 1, March: 29-39, 2010 Modified Le Bag Pouch after Radical Cystectomy: Continence, Urodynamic Results and Morbidity OMAYA A.H. NASSAR, M.D., F.R.C.S.
Journal of the Egyptian Nat. Cancer Inst., Vol. 22, No. 1, March: 29-39, 2010 Modified Le Bag Pouch after Radical Cystectomy: Continence, Urodynamic Results and Morbidity OMAYA A.H. NASSAR, M.D., F.R.C.S.
The number following the procedure code is the TRICARE payment group. KIDNEY
 TRICARE/CHAMPUS POLICY MANUAL 6010.47-M JUNE 25, 1999 S POLICY CHAPTER 13 SECTION 9.1 ADDENDUM 1, SECTION 8 TRICARE-APPROVED AMBULATORY SURGERY S - URINARY SYSTEM The number following the procedure code
TRICARE/CHAMPUS POLICY MANUAL 6010.47-M JUNE 25, 1999 S POLICY CHAPTER 13 SECTION 9.1 ADDENDUM 1, SECTION 8 TRICARE-APPROVED AMBULATORY SURGERY S - URINARY SYSTEM The number following the procedure code
Bladder Sparing Treatment of Muscle Invasive Bladder Cancer
 Bladder Sparing Treatment of Muscle Invasive Bladder Cancer Pr Alexandre de la Taille CHU Mondor, Créteil INSERMU955Eq07 adelataille@hotmail.com High-Risk Invasive and Muscle-Invasive BCa Radical cystectomy
Bladder Sparing Treatment of Muscle Invasive Bladder Cancer Pr Alexandre de la Taille CHU Mondor, Créteil INSERMU955Eq07 adelataille@hotmail.com High-Risk Invasive and Muscle-Invasive BCa Radical cystectomy
OUTCOME OF ORTHOTOPIC NEOBLADDER AFTER RADICAL CYSTECTOMY
 OUTCOME OF ORTHOTOPIC NEOBLADDER AFTER RADICAL CYSTECTOMY MA SALAM, MS ISLAM, MM UDDIN, MM SHAFIQUR, S HASAN, P SAHA, KR ABEDIN, GM MAULA Abstract Objective: To assess the results of patients underwent
OUTCOME OF ORTHOTOPIC NEOBLADDER AFTER RADICAL CYSTECTOMY MA SALAM, MS ISLAM, MM UDDIN, MM SHAFIQUR, S HASAN, P SAHA, KR ABEDIN, GM MAULA Abstract Objective: To assess the results of patients underwent
Complications and Quality of Life Following Urinary Diversion After Cystectomy
 EAU Update Series EAU Update Series 3 (2005) 156 168 Complications and Quality of Life Following Urinary Diversion After Cystectomy Elmar W. Gerharz a, *, Alexander Roosen a, Wiking Månsson b a Department
EAU Update Series EAU Update Series 3 (2005) 156 168 Complications and Quality of Life Following Urinary Diversion After Cystectomy Elmar W. Gerharz a, *, Alexander Roosen a, Wiking Månsson b a Department
Muscle-invasive bladder cancer
 Patient Information English 4 Muscle-invasive bladder cancer The underlined terms are listed in the glossary. What is muscle-invasive bladder cancer? The most common type of bladder cancer is non muscle-invasive,
Patient Information English 4 Muscle-invasive bladder cancer The underlined terms are listed in the glossary. What is muscle-invasive bladder cancer? The most common type of bladder cancer is non muscle-invasive,
Complications in robotic surgery!! Review of the literature! RALP, RAPN and RARC!
 Complications in robotic surgery Review of the literature RALP, RAPN and RARC Anna Wallerstedt, MD Karolinska University Hospital Stockholm, Sweden Agenda The importance of reporting surgical complications
Complications in robotic surgery Review of the literature RALP, RAPN and RARC Anna Wallerstedt, MD Karolinska University Hospital Stockholm, Sweden Agenda The importance of reporting surgical complications
Sara Schaenzer Grand Rounds January 24 th, 2018
 Sara Schaenzer Grand Rounds January 24 th, 2018 Bladder Anatomy Ureter Anatomy Areas of Injury Bladder: Posterior bladder wall above trigone Ureter Crosses beneath uterine vessels At pelvic brim when ligating
Sara Schaenzer Grand Rounds January 24 th, 2018 Bladder Anatomy Ureter Anatomy Areas of Injury Bladder: Posterior bladder wall above trigone Ureter Crosses beneath uterine vessels At pelvic brim when ligating
Urinary incontinence. Urology Department. Patient Information Leaflet
 Urinary incontinence Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been diagnosed with urinary incontinence. It contains information about the bladder,
Urinary incontinence Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been diagnosed with urinary incontinence. It contains information about the bladder,
Optimal Timing of Radical Cystectomy for Patients with Invasive Transitional Cell Carcinoma of the Bladder
 Jpn J Clin Oncol 2002;32(1)14 18 Optimal Timing of Radical Cystectomy for Patients with Invasive Transitional Cell Carcinoma of the Bladder Isao Hara, Hideaki Miyake, Shoji Hara, Akinobu Gotoh, Hiroshi
Jpn J Clin Oncol 2002;32(1)14 18 Optimal Timing of Radical Cystectomy for Patients with Invasive Transitional Cell Carcinoma of the Bladder Isao Hara, Hideaki Miyake, Shoji Hara, Akinobu Gotoh, Hiroshi
Eiji Kikuchi, Yutaka Horiguchi, Jun Nakashima, Takashi Ohigashi, Mototsugu Oya, Ken Nakagawa, Akira Miyajima and Masaru Murai
 Assessment of Long-Term Quality of Life Using the FACT-BL Questionnaire in Patients with an Ileal Conduit, Continent Reservoir, or Orthotopic Neobladder Eiji Kikuchi, Yutaka Horiguchi, Jun Nakashima, Takashi
Assessment of Long-Term Quality of Life Using the FACT-BL Questionnaire in Patients with an Ileal Conduit, Continent Reservoir, or Orthotopic Neobladder Eiji Kikuchi, Yutaka Horiguchi, Jun Nakashima, Takashi
Point/Counterpoint: Quality of Life Considerations for Patients with Muscle Invasive Bladder Cancer Pro Trimodality Therapy
 Point/Counterpoint: Quality of Life Considerations for Patients with Muscle Invasive Bladder Cancer Pro Trimodality Therapy Kimberley S. Mak, MD, MPH Assistant Professor Boston Medical Center Boston University
Point/Counterpoint: Quality of Life Considerations for Patients with Muscle Invasive Bladder Cancer Pro Trimodality Therapy Kimberley S. Mak, MD, MPH Assistant Professor Boston Medical Center Boston University
Lymph Node Positive Bladder Cancer Treated With Radical Cystectomy and Lymphadenectomy: Effect of the Level of Node Positivity
 EUROPEAN UROLOGY 61 (2012) 1025 1030 available at www.sciencedirect.com journal homepage: www.europeanurology.com Bladder Cancer Lymph Node Positive Bladder Cancer Treated With Radical Cystectomy and Lymphadenectomy:
EUROPEAN UROLOGY 61 (2012) 1025 1030 available at www.sciencedirect.com journal homepage: www.europeanurology.com Bladder Cancer Lymph Node Positive Bladder Cancer Treated With Radical Cystectomy and Lymphadenectomy:
Motility Disorders. Pelvic Floor. Colorectal Center for Functional Bowel Disorders (N = 701) January 2010 November 2011
 Motility Disorders Pelvic Floor Colorectal Center for Functional Bowel Disorders (N = 71) January 21 November 211 New Patients 35 3 25 2 15 1 5 Constipation Fecal Incontinence Rectal Prolapse Digestive-Genital
Motility Disorders Pelvic Floor Colorectal Center for Functional Bowel Disorders (N = 71) January 21 November 211 New Patients 35 3 25 2 15 1 5 Constipation Fecal Incontinence Rectal Prolapse Digestive-Genital
Radical Perineal Prostatectomy and Simultaneous Extended Pelvic Lymph Node Dissection via the Same Incision
 european urology 52 (2007) 384 388 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Radical Perineal Prostatectomy and Simultaneous Extended Pelvic Lymph Node
european urology 52 (2007) 384 388 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Radical Perineal Prostatectomy and Simultaneous Extended Pelvic Lymph Node
Risk of in-hospital complications after radical cystectomy for urinary bladder carcinoma: population-based follow-up study of 7608 patients
 Risk of in-hospital complications after radical cystectomy for urinary bladder carcinoma: population-based follow-up study of 7608 patients Mieke van Hemelrijck, Andreas Thorstenson*, Philip Smith, Jan
Risk of in-hospital complications after radical cystectomy for urinary bladder carcinoma: population-based follow-up study of 7608 patients Mieke van Hemelrijck, Andreas Thorstenson*, Philip Smith, Jan
3.1 Investigations for Patients Presenting with Haematuria Table 1
 3.1 Investigations for Patients Presenting with Haematuria Table 1 Patients at risk of bacterial endocarditis should be given antibiotic prophylaxis as per local guidelines. Patients with heart valve replacements
3.1 Investigations for Patients Presenting with Haematuria Table 1 Patients at risk of bacterial endocarditis should be given antibiotic prophylaxis as per local guidelines. Patients with heart valve replacements
Urodynamic study before and after radical porstatectomy 가톨릭의대성바오로병원김현우
 Urodynamic study before and after radical porstatectomy 가톨릭의대성바오로병원김현우 Introduction Radical prostatectomy - treatment of choice for patients with localized prostate cancer. Urinary incontinence and/or
Urodynamic study before and after radical porstatectomy 가톨릭의대성바오로병원김현우 Introduction Radical prostatectomy - treatment of choice for patients with localized prostate cancer. Urinary incontinence and/or
