The surgical technique and initial outcomes of Anatolian neobladder: a novel technique of ileal neobladder after radical cystectomy
|
|
|
- Wilfred Johns
- 5 years ago
- Views:
Transcription
1 Talat et al. BMC Urology (2018) 18:94 TECHNICAL ADVANCE Open Access The surgical technique and initial outcomes of Anatolian neobladder: a novel technique of ileal neobladder after radical cystectomy Z. Talat, B. Onal, B. Cetinel, C. Demirdag, S. Citgez * and C. Dogan Abstract Background: We describe a detailed novel step-by-step approach for creation of an ileal neobladder and compare the outcomes with standart neobladder. Methods: Between August 2009 and January 2016, 36 consecutive patients with bladder cancer underwent radical cystectomy and orthotopic urinary diversion with an ileal neobladder. A novel technique of ileal neobladder construction, called the Anatolian neobladder, was designed by a single surgeon (ZT). Demographics and clinical data were collected. Perioperative, oncologic, and functional outcomes were reported. Complications were graded as early or late. These outcomes were compared with patients who underwent standard neobladder during this period in our center. Results: The operation was technically successful in all cases. Early postoperative complications occurred in 33.3% of the patients. Daytime continence was achieved successfully in 83.3% of the patients. No patient had severe metabolic acidosis. Six patients (16.6%) died during follow-up, five due to metastatic bladder cancer and one due to a cardiac problem. There was no any statistically significant difference between novel technique and standard neobladder for oncological and functional outcomes. Conclusions: The Anatolian ileal neobladder is as feasible and safe as standard neobladder technique for urinary diversioninpatientswithbladdercancer undergoing radical cystectomy. Keywords: Bladder cancer, Orthotopic neobladder, Radical cystectomy, Ileal neobladder Background Orthotopic neobladders are constructed for urinary diversion after radical cystectomy. An orthotopic neobladder should achieve several normal bladder characteristics, including a continence mechanism, adequate capacity at a low pressure, and an antireflux mechanism for preventing upper urinary tract dilatation [1]. Camey first described an orthotopic neobladder in which a small tubular bowel segment was used as a bladder substitute by anastomosing it directly to the urethra without detubularization [2]. Since this version was described, many different types of orthotopic neobladders have been described, consisting of different gastrointestinal segments [3 5]. Intestinal detubularization plays an important role in the formation of low pressure and * Correspondence: drsinharib@yahoo.com Department of Urology, Istanbul University-Cerrahpasa, Cerrahpasa Medical Faculty, Fatih, Istanbul, Turkey adequate bladder volume. Based on this, various techniques have been acceptable using different types of bowel segments (ileum, ileo-colon, colon, sigmoid) and ureterointestinal anastomosis. Studer et al. reported use of a detubularized ileal pouch as a bladder substitute in patients with an intact urethra after cystectomy [6]. There is no agreement on the significant advantage of a single technique over another, despite the description of each technique by the investigators. We present our experience with a new surgical technique for ileal neobladder creation using 45 cm of ileum. The neobladder is constructed in a simple triangular configuration without a chimney. A spherical apex segment forms the neourethra at the bottom, which provides a sufficient part for anastomosis. The surgical technique, perioperative complications, and medium-term results, including cancer control and continence, are described. The Author(s) Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
2 Talat et al. BMC Urology (2018) 18:94 Page 2 of 9 The outcomes of were compared with patients who underwent standard neobladder in our center. Methods Patients A total of 52 patients (36 with novel technique, 16 with standard neobladder) with a preoperative diagnosis of invasive bladder cancer who were treated at our center between August 2009 and January 2016 were studied (Table 1). All patients underwent radical cystectomy and urinary diversion with creation of an orthotopic neobladder made of terminal ileum. Their charts were reviewed for preoperative (age, sex, disease status, creatinine level), perioperative (operative time, complications, morbidity), and postoperative (imaging methods, laboratory results, continence, complications, morbidity) data. Patients followed for less than 1 year were not included. Measurements The patients had high-grade recurrent stage T1, T2, or T3 bladder cancer. Preoperative imaging studies, including chest x-ray, and abdominal and pelvic computerized tomography (CT), indicated node-negative disease with no evidence of distant metastases in all patients. We used seftriaxone + metronidazol for antibiotic prophylaxis in patients. Single J stents were removed at postoperative 8th 10th days. Foley catheter was removed at postoperative 21st day after cystogram was performed. Patients were evaluated initially 4 weeks postoperatively and then at three-month intervals. CT and laboratory investigations were performed at each visit. We used routine cystogram postoperative 2. month to see the bladder capacity and check if there is any reflux. Complications were graded as early (grouped based on the modified Clavien system) or late (defined as those occurring more than 1 month postoperatively) [7]. Patients with complications underwent additional imaging studies, including excretory urography, voiding cystourethrography or renal scan, as needed. Continence was evaluated by patient self-report during the Table 1 The preoperative findings Novel technique (Anatolian neobladder) (n = 36) Standard technique (Studer neobladder) (n = 16) p Age, years, mean ± SD 54.7 ± ± Sex > Male 34 (94.4%) 15 (93.7%) -Female 2 (5.6%) 1 (6.3%) ASA 2 (1 3) 2 (1 3) 0.77 Chemotherapy -Neo-adjuvant 9 (25%) 4 (25%) > Adjuvant 2 (5.5%) 1 (6.2%) > 0.99 follow-up visits and International Consultation on Incontinence Questionnaire Short Form (ICIQ-SF). If the patient uses more than 1 pad per day, he/she is considered to be an incontinent. Urodynamic evaluation was performed in patients with daytime incontinence. The outcomes were compared with standard neobladder [6]. Statistical analysis Statistical analysis was done with SPSS for Windows 10.0 (SPSS,Inc.,Chicago,IL,USA).Continuousandnon-continuous numeric variables were described as median (Range). The Mann-Whitney U test was used to compare continuous and non-continuous numeric variables. Kaplan Meier analysis was used to calculate overall survival (OS). P < 0.05 was considered statistically significant. Surgical technique A 45 cm ileal segment was separated, starting at an appropriate point 15 to 20 cm from the ileocecal junction to avoid gastrointestinal problems postoperatively (Fig. 1). The intestinal continuity was rebuilt by an end-to-end anastomosis with surgical staplers (Fig. 2). The whole separated ileal segment was cut at the antimesenteric border for detubularization. Proximal and distal sides of the ileal loop were anastomosed side-to-side and a bagel-shaped detubularized ileal segment was formed (Figs. 3 and 4). Three identical points, starting from the medial border of the anastomosis segment, were identified and united at the center. Then, the medial edges of the ileal loop were Fig. 1 A 45 cm ileal segment was selected, starting at an appropriate point 15 to 20 cm from the ileocecal junction
3 Talat et al. BMC Urology (2018) 18:94 Page 3 of 9 Fig. 2 The intestinal continuity is rebuilt by an end-to-end anastomosis with surgical staplers joined by a running through-and-through suture of 3 0 polyglactin continuously, resulting in a goosefoot image in the centrum (Fig. 5). After this stage, a triangular configuration was formed. Also, three points from the lateral side of the detubularized ileal loop were identified and united at the center, and the lateral edges of the ileal loop were sutured continuously with 3 0 polyglactin, leaving the lower part of the reservoir open for the urethroileal anastomosis. Both ureters were spatulated and anastomosed end-to-side to the neobladder over appropriate single J stents with an antireflux mechanism (Fig. 6). The ureteral Fig. 3 The whole separated ileal segment is cut at the antimesenteric border for detubularization Fig. 4 A bagel-shaped detubularized ileal segment is formed stents were fixed to the ileal mucosa and taken out of the pouch by stabbing the anterior wall of the reservoir (Fig. 7). The urethroileal anastomosis was performed over a transurethral 22-French catheter with six to eight 3 0 polyglactin sutures. The pelvis was drained with a 28-French tube drain. Results Median follow-up was 44 months (range, months). The operation was technically successful in all cases. There were no intraoperative or perioperative deaths. Mean operative time was 5.5 h (range, h) and 5.6 h (4 7 h) for novel technique and standard technique, respectively (p < 0.001). There were no severe intraoperative complications. Mean amount of blood loss was 550 ml ( ml) and 580 ml ( ml), for novel technique and standard technique, respectively (p = 0.22). The perioperative and postoperative outcomes were given in Table 2. Kaplan Meier analysis of overall survival (OS) for two techniques was showed in Fig. 8. Early postoperative complications were occurred in 33.3% and 31.2% of the patients, for novel technique and standard technique, respectively (p = 0.55). According to the Clavien classification of surgical complications, a Grade 2 urinary infection occurred in 5 patients (13.8%) and 2 patients (12.5%) for novel technique and standard technique, respectively, all of whom improved with antibiotic treatment. Grade 2 paralytic ileus occurred in 3 patients (8.3%) and 1 patient (6.2) for novel technique and standard technique, respectively; however, open surgery was not required in any patient. Late complications were noted in 6 patients (16.6%) and 3 patients for novel
4 Talat et al. BMC Urology (2018) 18:94 Page 4 of 9 Fig. 5 Three identical points, starting from the medial border of the anastomosis segment, are identified and united at the center, and the medial edges of the ileal loop are joined technique and standard technique, respectively; urinary infection in three (8.3%) for novel technique and 1 patient for standard technique, and incisional hernia in one (2.7%) for novel technique. The latter patient required additional surgical treatment. Stenosis of the ureterointestinal anastomosis in one patient (2.7%) for novel technique and 1 patient (6.2%) for standard technique were repaired with open surgery. There were no metabolic complications. An intravenous pyelogram (IVP) was performed when necessary (Fig. 9). Ureteral stenosis in one patient (2.7%) for novel technique and 1 (6.2%) for standard neobladder were treated endoscopically. The perioperative admission rate was found 27.7% and 25% for novel technique and standard technique, respectively. Six patients (16.6%) in novel technique and 3 patients (18.7%) in standard technique died during follow-up. Five of them in novel technique died because of recurrent bladder cancer and one of unrelated cancer. Also, 2 of them in novel technique died because of recurrent bladder cancer and one of unrelated cancer. Continence improved by stages with time and most patients became continent within a mean of 3.5 months (range, 1 12 months) postoperatively for both two techniques. Self-catheterization was performed before bedtime to improve nighttime continence until patients regained Fig. 6 Both ureters are spatulated and anastomosed end-to-side to the neobladder over appropriate single J stents with an antireflux mechanism
5 Talat et al. BMC Urology (2018) 18:94 Page 5 of 9 Fig. 7 The triangular-shaped Anatolian pouch is formed. The ureteral stents are fixed to the ileal mucosa and taken out of the pouch by stabbing the anterior wall of the reservoir. The urethroileal anastomosis is performed over a transurethral 22-French catheter with six to eight 3 0 polyglactin sutures continence. Complete daytime continence was achieved in 32 of the 36 patients (88.8%) and 14 of the 16 patients (87.5%) for novel technique and standard technique, respectively (p = 0.89). Nighttime continence was achieved in 20 (55.5%) and 9 (56.2%) patients, for novel technique and standard technique, respectively (p = 0.96). Urodynamic evaluation was performed in four patients of novel technique (Fig. 10) and revealed urodynamic stress incontinence in two and low pressure low flow in two. Discussion Various types of orthotopic neobladders are used as a method of urinary diversion after radical cystectomy. Although new neobladder techniques have been described, it is still controversial as to how best to shape it. A normal neobladder should be safe and easy to create. Ideally, it should have low pressure. It should also be of the appropriate capacity. There should be no reflux in the upper urinary tract and the development of stricture Table 2 The perioperative and postoperative outcomes Novel technique (Anatolian Neobladder) (n = 36) Standard technique (Studer neobladder) (n = 16) p Bleeding (ml) 550 ( ) 580 ( ) 0.22 Operation time (h) 5.5 (4 6.5) 5.6 (4 7) < Hospitalization time (day) 7.3 (6 20) 7.3 (5 14) 0.80 Early postoperative complications 12 (33.3%) 5 (31.2%) Urinary infection (Grade 2 a ) 5 (13.8%) 2 (12.5%) -Paralytic ileus (Grade 2 a ) 3 (8.3%) 1 (6.2%) -Skin infection (Grade 2 a ) 4 (11.1%) 2 (12.5%) Late postoperative complications 6 (16.6%) 3 (18.7%) Urinary infection 3 (8.3%) 1 (6.2%) -Incisional hernia 1 (2.7%) -Urethro-neobladder stenosis 1 (2.7%) 1 (6.2%) -Uretero-neobladder stenosis 1 (2.7%) 1 (6.2%) Survival time (months) (95%CI) 71.6 ( ) 69.1 ( ) 0.72 Perioperative admission rate 27.7% 25.0% 0.84 Postmictuonal residual urine (ml) 2. month Postoperative ICIQ-SF score 2.7 (0 21) 2.6 (0 21) 0.72 Continence improved -Daytime continence 32/36 (88.8%) 14/16 (87.5%) Nighttime continence 20/36 (55.5%) 9/16 (56.2%) 0.96 a According to the Clavien classification of surgical complications
6 Talat et al. BMC Urology (2018) 18:94 Page 6 of 9 Fig. 8 Kaplan Meier analysis of overall survival (OS) in the ureters should be prevented. In addition, day- and nighttime continence should be ensured [8]. The Studer neobladder and other ileo-colonic neobladder techniques which are known for long term outcomes are the most frequently performed methods [5, 6, 9 11]. The Studer technique has these characteristics and has significant advantages [6]. Generally, surgeons adopt one or two techniques that are suitable for them. As surgeons perform a significant number of these reconstructive techniques per year, it is reasonable for them to adopt a technique that is appropriate, easy to perform and long-term results are known. Our clinic is a high volume center for radical cystectomy (> 25) and a mean of 30 patients underwent this operation within a year. These reasons prompted us to design a new neobladder construction. In our novel technique, the operative time is acceptable. The main advantage of this technique is that a simple shape, like an original bladder configuration, is constructed. The ileal segment used for the ureteroileal anastomosis is formed spontaneously and the ureters are anastomosed to the bottom of the neobladder without creating a chimney (Fig. 7). Residual urine volume was not significant in patients due to the bladder configuration. In the Anatolian neobladder, we fixed both upper Fig. 9 IVP shows no dilatation of the upper urinary tract system
7 Talat et al. BMC Urology (2018) 18:94 Page 7 of 9 Fig. 10 Urodynamic evaluation was performed in a patient with daytime incontinence during follow-up. The cystometric image also is seen in the Figure corners of the ileal pouch to the psoas muscles. In our opinion, this was another factor that led to good emptying of the neobladder. The ureters were anastomosed to the neobladder according to the technique of Abol-Eneim and Ghoneim [12]. We anastomosed the spatulated end of the ureters to the intestinal mucosa using a direct mucosa-to-mucosa and inverted ureteral nipple technique. Use of an isoperistaltic limb of ileum as an antireflux mechanism offers the advantage of an easily constructed ureterointestinal anastomosis with a low incidence of reflux and confusion of the upper tracts. To date, of 72 renal units, there is no confusion of any renal unit. This rate of upper tract preservation is acceptable. Before removing the Foley catheters postoperatively, we routinely perform cystography to demonstrate no reflux in the renal units. There were no severe intraoperative complications in our study. Mean blood loss was 550 ml (range, ) and 580 ml ( ml), for novel technique and standard technique, respectively and there were no statistically significant differences between two techniques (P = 0.22). Protection of the upper urinary tract is a critical point during orthotopic neobladder reconstructions. In our study, urinary infection occurred in eight patients (22.2%), all of whom improved with medical treatment. Rogers and Scardino used a modification of the Studer technique and reported acute pyelonephritis in two of 20 patients (10%) [13]. In another study, Yoneda et al. used a modified Studer technique and reported acute pyelonephritis in 27% of the patients [14]. Our series had a similar rate of pyelonephritis and there was no statistically difference for postoperative urinary infection rates between novel technique and standard neobladder in this study. Paralytic ileus occurred in three patients (8.3%) for novel technique and in 1 (6.2%) for standard neobladder, but open surgery was not required in any patient. Incisional hernia in one patient required additional surgery. No other late complications occurred. Stenosis of the uretero-neobladder anastomosis in one patient (2.7%) for novel technique and 1 patient for standard technique (6.2%), were treated by additional open surgery. Ureterointestinal anastomosis should prevent stenosis and obstruction [15]. Stenosis of the urethra in one patient (2.7%) for novel technique and 1 patient (6.2%) for standard technique, were treated endoscopically. Authors should remember that the rate of complications after radical cystectomy and orthotopic urinary diversion is not to be underestimated. In the review published by Faba et al., they stated that the complications were significant after cystectomy and orthotopic urinary diversion and they were not as low as in previous publications [16]. It was emphasized that complications were encountered in the 20th year after the operation and therefore follow-up should be done. In our study, there were no metabolic complications. Use of the terminal ileum was not advocated because of the potential risk of vitamin B12 and bile acid malabsorption, and resultant diarrhea [17]. Exclusion of the ileocecal valve from the normal alimentary tract and interference with feces transit time also may account for diarrhea in these patients. There are several reports of metabolic acidosis occurring in patients during follow-up [5, 6]. Hautmann et al. reported that 48% of patients with an ileal neobladder required alkalizing treatment for acidotic imbalance [5]. Gakis et al. described the advantages of using a terminal ileal segment for orthotopic urinary diversion [17]. Metabolic consequences due to bowel wall secretion and urinary reabsorption from the intestinal reservoir can be compensated best in the terminal ileum or jejunum. As a result, the terminal ileal segment is the most ideally suited bowel segment for orthotopic urinary diversion. There were no metabolic complications in our patients during the early follow-up period. We routinely evaluated laboratory values and replaced vitamin B and sodium bicarbonate if necessary during long-term follow-up.
8 Talat et al. BMC Urology (2018) 18:94 Page 8 of 9 Complete daytime continence was achieved in 32 of the 36 patients (88.8%) and 14 of the 16 patients (87.5%) for novel technique and standard technique, respectively (p = 0.89). Also, nighttime continence was achieved in 20 (55.5%) and 9 (56.2%) patients, for novel technique and standard technique, respectively (p = 0.96) and there was no statistically significant difference between two techniques. Parekh et al. reported that patients with bladder substitution achieved daytime control more rapidly than those who underwent radical prostatectomy, and stress urinary incontinence was rare [18]. Also, patient adaptation and mental capacity to understand the new bladder are important factors for achieving continence. Our success rate for achieving continence was similar to that of other studies [5, 6, 13, 15]. In addition, there was no statistically difference between our novel technique and standard technique in this study. Finally, the complication rate was acceptable, and there was no perioperative mortality for novel technique and standard technique, in this study. In addition, this bladder substitute of novel technique appears to be technically easier and safe. However, there are several limitations to our study. One limitation was that our data were collected retrospectively. Consecutively, 36 patients were included in this study and compared with 16 patients who underwent standard neobladder. However, the number of patients was limited and long-term results were not known. This might have decreased the power of the study. However, the functional results and postoperative morbidity rates in our series were acceptable. Future studies including larger series of patients should be designed prospectively to overcome existing limitations. Conclusions Our study demonstrated the feasibility of novel technique (Anatolian neobladder) in the treatment of bladder cancer after radical cystectomy. It can be an alternative to other ileal neobladder techniques. Further prospective and randomized controlled comparative studies including large series of patients are needed. Abbreviations CT: Computerized tomography; ICIQ-SF: International Consultation on Incontinence Questionnaire Short Form; OS: Overall survival Acknowledgements We would like to thank Ahmet Necati Sanli, for making the illustration of our technique. Funding No funding was obtained for this study. Also, we would like to thank Eren Esen, for performing statistical analysis of this study. Availability of data and materials The datasets analyzed during the current study available from the corresponding author on reasonable request. Authors contributions ZT, BO, BC, SC, CD1 made substantial contributions to conception and design, analysis and interpretation of data, he gave final approval of the version to be published. BO, SC, CD2 and BC made substantial contributions to conception and design, and acquisition of data. BO, BC, SC, CD1 and CD2 made substantial contributions to conception and design, was involved in drafting the manuscript and revising it critically for important intellectual content. ZT, SC, CD1, BO, BC and CD2 made substantial contributions to acquisition of data, analysis and interpretation of data, and was a major contributor in writing the manuscript. All authors above have read and approved of the final manuscript. Ethics approval and consent to participate This study was designed retrospectively and all patients signed an informed consent agreement. Approval was given by Ethical Committee of Istanbul University-Cerrahpasa, Cerrahpasa Medical Faculty of Medicine (IRB Number: 32821). Consent for publication Not applicable. Competing interests The authors declare that they have no competing interests. Publisher s Note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations. Received: 19 July 2018 Accepted: 17 October 2018 References 1. Benson MC, Seaman EK, Olsson CA. The ileal ureter neobladder is associated with a high success and a low complication rate. J Urol. 1996;155: Lilien OM, Camey M. 25-year experience with replacement of the human bladder (Camey procedure). J Urol. 2017;197(2S): Light JK, Marks JL. Total bladder replacement in the male and female using the ileocolonic segment (LeBag). Br J Urol. 1990;65(5): Melchior H, Spehr C, Knop-Wagemann I, Persson MC, Junemann KP. The continent ileal bladder for urinary tract reconstruction after cystectomy: a survey of 44 patients. J Urol. 1988;139(4): Hautmann RE, Miller K, Steiner U, Wenderworth U. The ileal neobladder: 6 years of experience with more than 200 patients. J Urol. 1993;150(1): Studer UE, Danuser H, Hochreiter W, Springer JP, Turner WH, Zingg EJ. Summary of 10 years experience with an ileal lowpressure bladder substitute combined with an afferent tubular isoperistaltic segment. World J Urol. 1996;14: Dindo D, Demartines N, Clavien PA. Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg. 2004;240: McDougal WS. Use of intestinal segments and urinary diversion. In: Walsh PC, Retik AB, Vaughan ED, Wein AJ, editors. Campbell s Urology, 8th edn. Philadelphia: Saunders, 2002, Vol 4, Chap 10, Meyer JP, Blick C, Arumainayagam N, Hurley K, Gillatt D, Persad R, Fawcett D. A three-centre experience of orthotopic neobladder reconstruction after radical cystectomy: revisiting the initial experience, and results in 104 patients. BJU Int. 2009;103: Thuroff JW, Alken P, Riedmiller H, Jacobi GH, Hohenfellner R. 100 cases of Mainz pouch: continuing experience and evolution. J Urol. 1988;140: Marshall FF, Mostwin JL, Radebaugh LC, Walsh PC, Brendler CB. Ileocolic neobladder post-cystectomy: continence and potency. J Urol. 1991;145: Abol-Eneim H, Ghoneim MA. A novel uretero-ileal reimplantation technique: the serous lined extramural tunnel. A preliminary report. J Urol. 1995;151: Rogers E, Scardino PT. A simple ileal substitute bladder after radical cystectomy. Experience with a modification of the Studer pouch. J Urol. 1995;153: Yoneda T, Igawa M, Shiina H, Shigeno K, Urakami S. Postoperative morbidity, functional results and quality of life of patients following orthotopic neobladder reconstruction. Int J Urol. 2003;10:119.
9 Talat et al. BMC Urology (2018) 18:94 Page 9 of Studer UE, Spiegel T, Casanova GA, Springer J, Gerber E, Ackermann DK, Gurtner F, Zingg EJ. Ileal bladder substitute: antireflux nipple or afferent tubular segment? Eur Urol. 1991;20(4): Faba OR, Tyson MD, Artibani W, et al. Update of the ICUD-SIU International consultation on bladder Cancer 2018: urinary diversion. World J Urol Gakis G, Stenzi A. Ileal neobladder and its variants. Eur Urol Suppl. 2010;9: Parekh DJ, Gilbert WB, Smith JA Jr. Functional lower urinary tract voiding outcomes after cystectomy and orthotopic neobladder. J Urol. 2000;163:56 9.
URINARY DIVERSIONS. Susan Hilton, MD and Nicholas Papanicolaou, MD Co-Chiefs, CT Section Hospital of the University of Pennsylvania
 URINARY DIVERSIONS Susan Hilton, MD and Nicholas Papanicolaou, MD Co-Chiefs, CT Section Hospital of the University of Pennsylvania Neither of us has any financial relationships with commercial interests
URINARY DIVERSIONS Susan Hilton, MD and Nicholas Papanicolaou, MD Co-Chiefs, CT Section Hospital of the University of Pennsylvania Neither of us has any financial relationships with commercial interests
Urethral Carcinoma Recurrence in Ileal Orthotopic Neobladder: Urethrectomy and Conversion in a Continent Pouch with Abdominal Stoma
 Case Report Urol Int 1999;62:213 216 Received: June 19, 1998 Accepted after revision: March 8, 1999 Urethral Carcinoma Recurrence in Ileal Orthotopic Neobladder: Urethrectomy and Conversion in a Continent
Case Report Urol Int 1999;62:213 216 Received: June 19, 1998 Accepted after revision: March 8, 1999 Urethral Carcinoma Recurrence in Ileal Orthotopic Neobladder: Urethrectomy and Conversion in a Continent
OUTCOME OF ORTHOTOPIC NEOBLADDER AFTER RADICAL CYSTECTOMY
 OUTCOME OF ORTHOTOPIC NEOBLADDER AFTER RADICAL CYSTECTOMY MA SALAM, MS ISLAM, MM UDDIN, MM SHAFIQUR, S HASAN, P SAHA, KR ABEDIN, GM MAULA Abstract Objective: To assess the results of patients underwent
OUTCOME OF ORTHOTOPIC NEOBLADDER AFTER RADICAL CYSTECTOMY MA SALAM, MS ISLAM, MM UDDIN, MM SHAFIQUR, S HASAN, P SAHA, KR ABEDIN, GM MAULA Abstract Objective: To assess the results of patients underwent
Comparison of Clinical and Urodynamic Outcome in Orthotopic Ileocaecal and Ileal Neobladder $
 European Urology European Urology 43 (2003) 258±262 Comparison of Clinical and Urodynamic Outcome in Orthotopic Ileocaecal and Ileal Neobladder $ YasËar BeduÈk, Kadir TuÈrkoÈlmez, SuÈmer Baltacõ, CËagÆatay
European Urology European Urology 43 (2003) 258±262 Comparison of Clinical and Urodynamic Outcome in Orthotopic Ileocaecal and Ileal Neobladder $ YasËar BeduÈk, Kadir TuÈrkoÈlmez, SuÈmer Baltacõ, CËagÆatay
Bladder replacement in men and women: when and when not? Outline. Continent Diversion History
 1 Bladder replacement in men and women: when and when not? Eila C. Skinner, MD Professor of Clinical Urology Keck USC School of Medicine Outline 1) Selection criteria for orthotopic diversion: Tumor-related
1 Bladder replacement in men and women: when and when not? Eila C. Skinner, MD Professor of Clinical Urology Keck USC School of Medicine Outline 1) Selection criteria for orthotopic diversion: Tumor-related
FUNCTIONAL RESULTS OF ORTHOTOPIC ILEAL NEOBLADDER WITH SEROUS-LINED EXTRAMURAL URETERAL REIMPLANTATION: EXPERIENCE WITH 450 PATIENTS
 0022-5347/01/1655-1427/0 THE JOURNAL OF UROLOGY Vol. 165, 1427 1432, May 2001 Copyright 2001 by AMERICAN UROLOGICAL ASSOCIATION, INC. Printed in U.S.A. FUNCTIONAL RESULTS OF ORTHOTOPIC ILEAL NEOBLADDER
0022-5347/01/1655-1427/0 THE JOURNAL OF UROLOGY Vol. 165, 1427 1432, May 2001 Copyright 2001 by AMERICAN UROLOGICAL ASSOCIATION, INC. Printed in U.S.A. FUNCTIONAL RESULTS OF ORTHOTOPIC ILEAL NEOBLADDER
URINARY DIVERSIONS. Winter 2016 Dr P. O Malley
 URINARY DIVERSIONS Winter 2016 Dr P. O Malley OVERVIEW Who gets diversions? What s involved with cystectomy? What are the different types of diversions? What are the problems with various diversions? How
URINARY DIVERSIONS Winter 2016 Dr P. O Malley OVERVIEW Who gets diversions? What s involved with cystectomy? What are the different types of diversions? What are the problems with various diversions? How
Functional and Clinicopathologic Outcomes Using a Modified Vescica Ileale Padovana Technique
 Bladder Cancer 1 (2015) 73 79 DOI 10.3233/BLC-140002 IOS Press Research Report 73 Functional and Clinicopathologic Outcomes Using a Modified Vescica Ileale Padovana Technique Chandra K. Flack, M. Francesca
Bladder Cancer 1 (2015) 73 79 DOI 10.3233/BLC-140002 IOS Press Research Report 73 Functional and Clinicopathologic Outcomes Using a Modified Vescica Ileale Padovana Technique Chandra K. Flack, M. Francesca
Lower Urinary Tract Reconstruction Following Radical Cystectomy Using Ileal Neobladder with Studor Technique; 3 Years Experience
 Journal of the Egyptian Nat. Cancer Inst., Vol. 12, No. 4, December: 235-243, 2000 Lower Urinary Tract Reconstruction Following Radical Cystectomy Using Ileal Neobladder with Studor Technique; 3 Years
Journal of the Egyptian Nat. Cancer Inst., Vol. 12, No. 4, December: 235-243, 2000 Lower Urinary Tract Reconstruction Following Radical Cystectomy Using Ileal Neobladder with Studor Technique; 3 Years
Functional and Clinical Outcome of Ileal (Studer) Neo-bladder Reconstruction: Single Centre Experience from Pakistan
 ORIGINAL ARTICLE Functional and Clinical Outcome of Ileal (Studer) Neo-bladder Reconstruction: Single Centre Experience from Pakistan Syed M. Nazim, M. Hammad Ather and Farhat Abbas ABSTRACT Objective:
ORIGINAL ARTICLE Functional and Clinical Outcome of Ileal (Studer) Neo-bladder Reconstruction: Single Centre Experience from Pakistan Syed M. Nazim, M. Hammad Ather and Farhat Abbas ABSTRACT Objective:
Long-Term Results of a Prospective Randomized Study ComparingTwo Different AntirefluxTechniques in Orthotopic Bladder Substitution
 European Urology European Urology 45 (2004) 82 86 Long-Term Results of a Prospective Randomized Study ComparingTwo Different AntirefluxTechniques in Orthotopic Bladder Substitution Yasser Osman *, Hassan
European Urology European Urology 45 (2004) 82 86 Long-Term Results of a Prospective Randomized Study ComparingTwo Different AntirefluxTechniques in Orthotopic Bladder Substitution Yasser Osman *, Hassan
UTI and UrinaryTract Reconstruction
 EAU Update Series 2 (2004) 101 105 UTI and UrinaryTract Reconstruction Werner W. Hochreiter *, Sebastian Z Brun Department of Urology, University of Bern, Anna-Seiler-Haus, Inselspital, CH-3010 Bern, Switzerland
EAU Update Series 2 (2004) 101 105 UTI and UrinaryTract Reconstruction Werner W. Hochreiter *, Sebastian Z Brun Department of Urology, University of Bern, Anna-Seiler-Haus, Inselspital, CH-3010 Bern, Switzerland
Sexuality Preserving Cystectomy and Neobladder (SPCN): Functional Results of a Neobladder Anastomosed to the Prostate
 European Urology European Urology 43 (2003) 646 650 Sexuality Preserving Cystectomy and Neobladder (SPCN): Functional Results of a Neobladder Anastomosed to the Prostate W. Meinhardt *, S. Horenblas Department
European Urology European Urology 43 (2003) 646 650 Sexuality Preserving Cystectomy and Neobladder (SPCN): Functional Results of a Neobladder Anastomosed to the Prostate W. Meinhardt *, S. Horenblas Department
Orthotopic neobladder reconstruction what are the options?
 Minirev Article ORTHOTOPIC NEOBLADDER RECONSTRUCTION MEYER et al. Orthotopic neobladder reconstruction what are the options? JON-PAUL MEYER, DEREK FAWCETT*, DAVID GILLATT and RAJENDRA PERSAD Department
Minirev Article ORTHOTOPIC NEOBLADDER RECONSTRUCTION MEYER et al. Orthotopic neobladder reconstruction what are the options? JON-PAUL MEYER, DEREK FAWCETT*, DAVID GILLATT and RAJENDRA PERSAD Department
Long-Term Complications of Conduit Urinary Diversion
 Long-Term Complications of Conduit Urinary Diversion Mark S. Shimko,* Matthew K. Tollefson, Eric C. Umbreit, Sara A. Farmer, Michael L. Blute and Igor Frank From the Department of Urology (MSS, MKT, ECU,
Long-Term Complications of Conduit Urinary Diversion Mark S. Shimko,* Matthew K. Tollefson, Eric C. Umbreit, Sara A. Farmer, Michael L. Blute and Igor Frank From the Department of Urology (MSS, MKT, ECU,
Surgical Atlas Orthotopic ileal neobladder
 Surgery Illustrated ORTHOTOPIC ILEAL NEOBLADDER U.E. STUDER ET AL. Surgical Atlas Orthotopic ileal neobladder U.E. STUDER, C. VAROL and H. DANUSER University of Bern, Department of Urology, Bern, Switzerland
Surgery Illustrated ORTHOTOPIC ILEAL NEOBLADDER U.E. STUDER ET AL. Surgical Atlas Orthotopic ileal neobladder U.E. STUDER, C. VAROL and H. DANUSER University of Bern, Department of Urology, Bern, Switzerland
Department of Urology, Theodor Bilharz research Institute, Cairo, Egypt
 Surgical Technique Vol. 41 (4): 796-803, July - August, 2015 doi: 10.1590/S1677-5538.IBJU.2013.0086 Detour technique, Dipping technique, or IIeal bladder flap technique for surgical correction of uretero-ileal
Surgical Technique Vol. 41 (4): 796-803, July - August, 2015 doi: 10.1590/S1677-5538.IBJU.2013.0086 Detour technique, Dipping technique, or IIeal bladder flap technique for surgical correction of uretero-ileal
Radical cystectomy and urinary diversion: Normal anatomy and complications
 Radical cystectomy and urinary diversion: Normal anatomy and complications Poster No.: C-0648 Congress: ECR 2014 Type: Scientific Exhibit Authors: J. M. Marin, N. alegre, P. Perez Martin, A. Velarde Pedraza
Radical cystectomy and urinary diversion: Normal anatomy and complications Poster No.: C-0648 Congress: ECR 2014 Type: Scientific Exhibit Authors: J. M. Marin, N. alegre, P. Perez Martin, A. Velarde Pedraza
SEROUS LINED EXTRAMURAL ILEAL VALVE: A NEW CONTINENT URINARY OUTLET
 0022-5347/99/1613-0786$03.00/0 THE JOURNAL OF UROLOGY Vol. 161, 786 791, March 1999 Copyright 1999 by AMERICAN UROLOGICAL ASSOCIATION, INC. Printed in U.S.A. SEROUS LINED EXTRAMURAL ILEAL VALVE: A NEW
0022-5347/99/1613-0786$03.00/0 THE JOURNAL OF UROLOGY Vol. 161, 786 791, March 1999 Copyright 1999 by AMERICAN UROLOGICAL ASSOCIATION, INC. Printed in U.S.A. SEROUS LINED EXTRAMURAL ILEAL VALVE: A NEW
Comparison of Three Types of Continent Urinary Diversions in a Single Center
 Article TheScientificWorldJOURNAL (2004) 4 (S1), 135 141 ISSN 1537-744X; DOI 10.1100/tsw.2004.59 Comparison of Three Types of Continent Urinary Diversions in a Single Center Cengiz Girgin, M.D., Akif Sezer,
Article TheScientificWorldJOURNAL (2004) 4 (S1), 135 141 ISSN 1537-744X; DOI 10.1100/tsw.2004.59 Comparison of Three Types of Continent Urinary Diversions in a Single Center Cengiz Girgin, M.D., Akif Sezer,
The Studer Orthotopic Neobladder: Long-Term (More Than 10 Years) Functional Outcomes, Urodynamic Features, and Complications
 Original Article http://dx.doi.org/10.3349/ymj.2013.54.3.690 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 54(3):690-695, 2013 The Studer Orthotopic Neobladder: Long-Term (More Than 10 Years) Functional
Original Article http://dx.doi.org/10.3349/ymj.2013.54.3.690 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 54(3):690-695, 2013 The Studer Orthotopic Neobladder: Long-Term (More Than 10 Years) Functional
Department and Clinic of Urology, Medical University of Silesia, Katowice, Poland
 BioMed Research International Volume 2015, Article ID 306191, 4 pages http://dx.doi.org/10.1155/2015/306191 Clinical Study Sacrocolpopexy with Polypropylene Tape as Valuable Surgical Modification during
BioMed Research International Volume 2015, Article ID 306191, 4 pages http://dx.doi.org/10.1155/2015/306191 Clinical Study Sacrocolpopexy with Polypropylene Tape as Valuable Surgical Modification during
Recovery of sexual function after radical cystectomy with orthotopic neobladder
 Recovery of sexual function after radical cystectomy with orthotopic neobladder C. Gingu, V. Olaru, A. Dick, C. Baston, M. Crăsneanu, C. Surcel, S. Voinea, Liliana Domnişor, I. Sinescu Center of Urological
Recovery of sexual function after radical cystectomy with orthotopic neobladder C. Gingu, V. Olaru, A. Dick, C. Baston, M. Crăsneanu, C. Surcel, S. Voinea, Liliana Domnişor, I. Sinescu Center of Urological
Modified Le Bag Pouch after Radical Cystectomy: Continence, Urodynamic Results and Morbidity
 Journal of the Egyptian Nat. Cancer Inst., Vol. 22, No. 1, March: 29-39, 2010 Modified Le Bag Pouch after Radical Cystectomy: Continence, Urodynamic Results and Morbidity OMAYA A.H. NASSAR, M.D., F.R.C.S.
Journal of the Egyptian Nat. Cancer Inst., Vol. 22, No. 1, March: 29-39, 2010 Modified Le Bag Pouch after Radical Cystectomy: Continence, Urodynamic Results and Morbidity OMAYA A.H. NASSAR, M.D., F.R.C.S.
Laparoscopic Bladder-Preserving Surgery for Enterovesical Fistula Complicated with Benign Gastrointestinal Disease
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
Original Paper. Urol Int 2002;69:
 Original Paper Urol Int 2002;69:184 189 Received: June 15, 2001 Accepted after revision: January 29, 2002 D igit al Fluorographic V ideo-u rodynam ics in t he Long-Term M orphof unct ional Evaluat ion
Original Paper Urol Int 2002;69:184 189 Received: June 15, 2001 Accepted after revision: January 29, 2002 D igit al Fluorographic V ideo-u rodynam ics in t he Long-Term M orphof unct ional Evaluat ion
FIG The inferior and posterior peritoneal reflection is easily
 PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
Bowel Function Remains Subjectively Unchanged After Ileal Resection for Construction of Continent Ileal Reservoirs
 EUROPEAN UROLOGY 60 (2011) 585 590 available at www.sciencedirect.com journal homepage: www.europeanurology.com Reconstructive Urology Bowel Function Remains Subjectively Unchanged After Ileal Resection
EUROPEAN UROLOGY 60 (2011) 585 590 available at www.sciencedirect.com journal homepage: www.europeanurology.com Reconstructive Urology Bowel Function Remains Subjectively Unchanged After Ileal Resection
Running head: Treatment modality and long term renal function in MIBC-Hamidi et al.
 Running head: Treatment modality and long term renal function in MIBC-Hamidi et al. Effect of Treatment Modality on Long Term Renal Functions in Patients With Muscle Invasive Bladder Cancer Nurullah Hamidi
Running head: Treatment modality and long term renal function in MIBC-Hamidi et al. Effect of Treatment Modality on Long Term Renal Functions in Patients With Muscle Invasive Bladder Cancer Nurullah Hamidi
SciFed Journal of Public Health. Endoscopic Management of Obstetrical Uretero-Uterine Fistula. Case Report and Review of Literature
 SciFed Journal of Public Health Case Report Open Access Endoscopic Management of Obstetrical Uretero-Uterine Fistula. Case Report and Review of Literature * Yasin Idweini * Chairperson of Urology Department
SciFed Journal of Public Health Case Report Open Access Endoscopic Management of Obstetrical Uretero-Uterine Fistula. Case Report and Review of Literature * Yasin Idweini * Chairperson of Urology Department
Urethral catheter removal 3 days after radical retropubic prostatectomy is feasible and desirable
 Urethral catheter 3 days after radical retropubic prostatectomy is feasible and desirable (2002) 5, 291 295 ß 2002 Nature Publishing Group All rights reserved 1365 7852/02 $25.00 www.nature.com/pcan JM
Urethral catheter 3 days after radical retropubic prostatectomy is feasible and desirable (2002) 5, 291 295 ß 2002 Nature Publishing Group All rights reserved 1365 7852/02 $25.00 www.nature.com/pcan JM
Florence robotic intracorporeal neobladder (FloRIN): a new reconfiguration strategy developed following the IDEAL guidelines
 Step-by-Step Florence robotic intracorporeal neobladder (FloRIN): a new reconfiguration strategy developed following the IDEAL guidelines Andrea Minervini*, Davide Vanacore*, Gianni Vittori*, Martina Milanesi*,
Step-by-Step Florence robotic intracorporeal neobladder (FloRIN): a new reconfiguration strategy developed following the IDEAL guidelines Andrea Minervini*, Davide Vanacore*, Gianni Vittori*, Martina Milanesi*,
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER
 MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
Optimal Timing of Radical Cystectomy for Patients with Invasive Transitional Cell Carcinoma of the Bladder
 Jpn J Clin Oncol 2002;32(1)14 18 Optimal Timing of Radical Cystectomy for Patients with Invasive Transitional Cell Carcinoma of the Bladder Isao Hara, Hideaki Miyake, Shoji Hara, Akinobu Gotoh, Hiroshi
Jpn J Clin Oncol 2002;32(1)14 18 Optimal Timing of Radical Cystectomy for Patients with Invasive Transitional Cell Carcinoma of the Bladder Isao Hara, Hideaki Miyake, Shoji Hara, Akinobu Gotoh, Hiroshi
Canada s first robotic-assisted totally intracorporeal orthotopic ileal neobladder
 case report Canada s first robotic-assisted totally intracorporeal orthotopic ileal neobladder Richard L. Haddad, BMED, MS (Urology), FRACS (Urology); * Patrick Richard, MD; * Franck Bladou, MD, FRCSC
case report Canada s first robotic-assisted totally intracorporeal orthotopic ileal neobladder Richard L. Haddad, BMED, MS (Urology), FRACS (Urology); * Patrick Richard, MD; * Franck Bladou, MD, FRCSC
Abstract. Original Article
 Original Article Middle East Journal of Cancer; July 2015; 6(3): 165-170 A Comparison of Early Results and Patient Satisfaction Rate between Modified Radical Cystectomy with Mainz II Urinary Diversion
Original Article Middle East Journal of Cancer; July 2015; 6(3): 165-170 A Comparison of Early Results and Patient Satisfaction Rate between Modified Radical Cystectomy with Mainz II Urinary Diversion
Ureteral Reconstruction With Bowel Segments: Experience With Eight Patients in a Single Institute
 www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.11.742 Original Article - Reconstructive Urology http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.11.742&domain=pdf&date_stamp=2014-11-16
www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.11.742 Original Article - Reconstructive Urology http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.11.742&domain=pdf&date_stamp=2014-11-16
Bricker versus Wallace anastomosis: A meta-analysis of ureteroenteric stricture rates after ileal conduit urinary diversion
 Original research Bricker versus Wallace anastomosis: A meta-analysis of ureteroenteric stricture rates after ileal conduit urinary diversion Niall F. Davis, MD; John P. Burke, MD; TED McDermott, MD; Robert
Original research Bricker versus Wallace anastomosis: A meta-analysis of ureteroenteric stricture rates after ileal conduit urinary diversion Niall F. Davis, MD; John P. Burke, MD; TED McDermott, MD; Robert
URINARY DIVERSION SURGERY: WHAT THE RADIOLOGIST NEEDS TO KNOW
 URINARY DIVERSION SURGERY: WHAT THE RADIOLOGIST NEEDS TO KNOW Poster No.: C-2327 Congress: ECR 2012 Type: Scientific Exhibit Authors: A. Salvador; Santander/ES Keywords: Urinary Tract / Bladder, CT, Complications,
URINARY DIVERSION SURGERY: WHAT THE RADIOLOGIST NEEDS TO KNOW Poster No.: C-2327 Congress: ECR 2012 Type: Scientific Exhibit Authors: A. Salvador; Santander/ES Keywords: Urinary Tract / Bladder, CT, Complications,
MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER
 10 MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER Recommendations from the EAU Working Party on Muscle Invasive and Metastatic Bladder Cancer G. Jakse (chairman), F. Algaba, S. Fossa, A. Stenzl, C. Sternberg
10 MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER Recommendations from the EAU Working Party on Muscle Invasive and Metastatic Bladder Cancer G. Jakse (chairman), F. Algaba, S. Fossa, A. Stenzl, C. Sternberg
Long-term Renal Function After Urinary Diversion by Ileal Conduit or Orthotopic Ileal Bladder Substitution
 EUROPEAN UROLOGY 61 (2012) 491 497 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Bladder Cancer Editorial by Ja Hyeon Ku and Seth P. Lerner on pp. 498 500
EUROPEAN UROLOGY 61 (2012) 491 497 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Bladder Cancer Editorial by Ja Hyeon Ku and Seth P. Lerner on pp. 498 500
PROFESSIONAL SKILLS 1 3RD YEAR SEMESTER 6 RADIOGRAPHY. THE URINARY SYSTEM Uz. Fatema shmus aldeen Tel
 PROFESSIONAL SKILLS 1 3RD YEAR SEMESTER 6 RADIOGRAPHY THE URINARY SYSTEM Uz. Fatema shmus aldeen Tel. 0925111552 Professional skills-2 THE URINARY SYSTEM The urinary system (review anatomy and physiology)
PROFESSIONAL SKILLS 1 3RD YEAR SEMESTER 6 RADIOGRAPHY THE URINARY SYSTEM Uz. Fatema shmus aldeen Tel. 0925111552 Professional skills-2 THE URINARY SYSTEM The urinary system (review anatomy and physiology)
Bladder Replacement and Urinary Diversion After Radical Cystectomy
 Arthur Grover Rider (American, 1886-1975). Spanish Boats, c.1922. Oil on canvas, 40"x 44". Courtesy of the Fleischer Museum, Scottsdale, Arizona. Bladder Replacement and Urinary Diversion After Radical
Arthur Grover Rider (American, 1886-1975). Spanish Boats, c.1922. Oil on canvas, 40"x 44". Courtesy of the Fleischer Museum, Scottsdale, Arizona. Bladder Replacement and Urinary Diversion After Radical
Chapter 8: Urinary Diversions after Cystectomy: The Association of Clinical Factors, Complications and Functional Results of Four Different Diversions
 Chapter 8: Urinary Diversions after Cystectomy: The Association of Clinical Factors, Complications and Functional Results of Four Different Diversions J.A. Nieuwenhuijzen* R.R. de Vries* A. Bex H.G. van
Chapter 8: Urinary Diversions after Cystectomy: The Association of Clinical Factors, Complications and Functional Results of Four Different Diversions J.A. Nieuwenhuijzen* R.R. de Vries* A. Bex H.G. van
Muscle-invasive bladder cancer
 Patient Information English 4 Muscle-invasive bladder cancer The underlined terms are listed in the glossary. What is muscle-invasive bladder cancer? About a quarter of patients diagnosed with bladder
Patient Information English 4 Muscle-invasive bladder cancer The underlined terms are listed in the glossary. What is muscle-invasive bladder cancer? About a quarter of patients diagnosed with bladder
ENDOSCOPIC URETERECTOMY DURING NEPHROURETERECTOMY FOR UPPER URINARY TRACT TRANSITIONAL CELL CARCINOMA
 ENDOSCOPIC URETERECTOMY DURING NEPHROURETERECTOMY FOR UPPER URINARY TRACT TRANSITIONAL CELL CARCINOMA Il. Saltirov, Ts. Petkov, G. Georgiev, K.Petkova Department of Urology and Nephrology, Military Medical
ENDOSCOPIC URETERECTOMY DURING NEPHROURETERECTOMY FOR UPPER URINARY TRACT TRANSITIONAL CELL CARCINOMA Il. Saltirov, Ts. Petkov, G. Georgiev, K.Petkova Department of Urology and Nephrology, Military Medical
Interventional management of postoperative ureteric complications after pelvic surgery
 Interventional management of postoperative ureteric complications after pelvic surgery Poster No.: C-0169 Congress: ECR 2015 Type: Scientific Exhibit Authors: R. Tabashy, A. Hamed, S. El-Sebai; Cairo/EG
Interventional management of postoperative ureteric complications after pelvic surgery Poster No.: C-0169 Congress: ECR 2015 Type: Scientific Exhibit Authors: R. Tabashy, A. Hamed, S. El-Sebai; Cairo/EG
Application of Yang-Monti Principle in Ileal Ureter Substitution: Is It a beneficial Modification?
 ORIGINAL ARTICLE Vol. 38 (6): 779-787, November - December, 2012 Application of Yang-Monti Principle in Ileal Ureter Substitution: Is It a beneficial Modification? M. Esmat, A. Abdelaal, D. Mostafa Department
ORIGINAL ARTICLE Vol. 38 (6): 779-787, November - December, 2012 Application of Yang-Monti Principle in Ileal Ureter Substitution: Is It a beneficial Modification? M. Esmat, A. Abdelaal, D. Mostafa Department
Uroradiology For Medical Students
 Uroradiology For Medical Students Lesson 4: Cystography & Urethrography - Part 2 American Urological Association Review Cystography is useful in evaluating the bladder, the urethra and the competence of
Uroradiology For Medical Students Lesson 4: Cystography & Urethrography - Part 2 American Urological Association Review Cystography is useful in evaluating the bladder, the urethra and the competence of
Indications and effectiveness of the open surgery in vesicoureteral reflux
 Indications and effectiveness of the open surgery in vesicoureteral reflux Suzi DEMIRBAG, MD Department of Pediatric Surgery, Gulhane Military Medical Academy, Ankara, TURKEY Vesicoureteral reflux (VUR)
Indications and effectiveness of the open surgery in vesicoureteral reflux Suzi DEMIRBAG, MD Department of Pediatric Surgery, Gulhane Military Medical Academy, Ankara, TURKEY Vesicoureteral reflux (VUR)
Percutaneous Nephrolithotomy in a Patient with Mainz Pouch II Urinary Diversion: A Case Report
 198) Prague Medical Report / Vol. 117 (2016) No. 4, p. 198 203 Percutaneous Nephrolithotomy in a Patient with Mainz Pouch II Urinary Diversion: A Case Report Stavros Sfoungaristos 1, Ioannis Mykoniatis
198) Prague Medical Report / Vol. 117 (2016) No. 4, p. 198 203 Percutaneous Nephrolithotomy in a Patient with Mainz Pouch II Urinary Diversion: A Case Report Stavros Sfoungaristos 1, Ioannis Mykoniatis
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Outcome of Open Radical Cystectomy and Ileal Conduit: A Single Center Experience Mahesh Kalloli
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Outcome of Open Radical Cystectomy and Ileal Conduit: A Single Center Experience Mahesh Kalloli
Robot assisted radical cystectomy and intracorporeal urinary diversion safe and reproducible?
 18 Central European Journal of Urology O R I G I N A L P A P E R UROLOGICAL ONCOLOGY Robot assisted radical cystectomy and intracorporeal urinary diversion safe and reproducible? Allen Sim 1, Mevlana Derya
18 Central European Journal of Urology O R I G I N A L P A P E R UROLOGICAL ONCOLOGY Robot assisted radical cystectomy and intracorporeal urinary diversion safe and reproducible? Allen Sim 1, Mevlana Derya
Retroperitoneoscopic Transureteroureterostomy with Cutaneous Ureterostomy to Salvage Failed Ileal Conduit Urinary Diversion
 available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Study of the Month Retroperitoneoscopic Transureteroureterostomy with Cutaneous Ureterostomy to Salvage Failed Ileal Conduit
available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Study of the Month Retroperitoneoscopic Transureteroureterostomy with Cutaneous Ureterostomy to Salvage Failed Ileal Conduit
Postoperative Appearance and Complications of the Urinary Tract Following Surgery: A Comprehensive Review
 Postoperative Appearance and Complications of the Urinary Tract Following Surgery: A Comprehensive Review Poster No.: C-2137 Congress: ECR 2018 Type: Authors: Keywords: DOI: Educational Exhibit N. Kinger
Postoperative Appearance and Complications of the Urinary Tract Following Surgery: A Comprehensive Review Poster No.: C-2137 Congress: ECR 2018 Type: Authors: Keywords: DOI: Educational Exhibit N. Kinger
Evolution of the Neobladder: A Critical Review of Open and Intracorporeal
 Evolution of the Neobladder: A Critical Review of Open and Intracorporeal Neobladder Reconstruction Techniques Wei Shen Tan 1,2, Benjamin W Lamb 2, John D Kelly 1,2 1. Division of Surgery & Interventional
Evolution of the Neobladder: A Critical Review of Open and Intracorporeal Neobladder Reconstruction Techniques Wei Shen Tan 1,2, Benjamin W Lamb 2, John D Kelly 1,2 1. Division of Surgery & Interventional
Radical Cystectomy Often Too Late? Yes, But...
 european urology 50 (2006) 1129 1138 available at www.sciencedirect.com journal homepage: www.europeanurology.com Editorial 50th Anniversary Radical Cystectomy Often Too Late? Yes, But... Urs E. Studer
european urology 50 (2006) 1129 1138 available at www.sciencedirect.com journal homepage: www.europeanurology.com Editorial 50th Anniversary Radical Cystectomy Often Too Late? Yes, But... Urs E. Studer
Citation International journal of urology (2. Right which has been published in final f
 Title Novel constant-pressure irrigation of renal pelvic tumors after ipsila Nakamura, Kenji; Terada, Naoki; Sug Author(s) Toshinori; Matsui, Yoshiyuki; Imamu Kazutoshi; Kamba, Tomomi; Yoshimura Citation
Title Novel constant-pressure irrigation of renal pelvic tumors after ipsila Nakamura, Kenji; Terada, Naoki; Sug Author(s) Toshinori; Matsui, Yoshiyuki; Imamu Kazutoshi; Kamba, Tomomi; Yoshimura Citation
How to Obtain Good Results with Orthotopic Bladder Substitution: The 10 Commandments
 EUROPEAN UROLOGY SUPPLEMENTS 8 (2009) 712 717 available at www.sciencedirect.com journal homepage: www.europeanurology.com How to Obtain Good Results with Orthotopic Bladder Substitution: The 10 Commandments
EUROPEAN UROLOGY SUPPLEMENTS 8 (2009) 712 717 available at www.sciencedirect.com journal homepage: www.europeanurology.com How to Obtain Good Results with Orthotopic Bladder Substitution: The 10 Commandments
RECTAL INJURY IN UROLOGIC SURGERY. Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences.
 RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,700 108,500 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,700 108,500 1.7 M Open access books available International authors and editors Downloads Our
Primary Realignment of Posterior Urethral Rupture
 Urology Journal UNRC/IUA Vol. 2, No. 4, 211-215 Autumn 2005 Printed in IRAN Mehdi Salehipour, Abdolaziz Khezri, Rashid Askari,* Parham Masoudi Department of Surgery, Division of Urology, Faghihi Hospital,
Urology Journal UNRC/IUA Vol. 2, No. 4, 211-215 Autumn 2005 Printed in IRAN Mehdi Salehipour, Abdolaziz Khezri, Rashid Askari,* Parham Masoudi Department of Surgery, Division of Urology, Faghihi Hospital,
Trimodality Therapy for Muscle Invasive Bladder Cancer
 Trimodality Therapy for Muscle Invasive Bladder Cancer Brita Danielson, MD, FRCPC Radiation Oncologist, Cross Cancer Institute Assistant Professor, Department of Oncology University of Alberta Edmonton,
Trimodality Therapy for Muscle Invasive Bladder Cancer Brita Danielson, MD, FRCPC Radiation Oncologist, Cross Cancer Institute Assistant Professor, Department of Oncology University of Alberta Edmonton,
Microscopic Study of Histological Changes the Use of Ileal Mucosa as a Bladder (Radical Cystectomy - Case Report)
 Microscopic Study of Histological Changes the Use of Ileal Mucosa as a Bladder (Radical Cystectomy - Case Report) Sareh Najaf Asaadi, Hassan Morovvati, Ahmad Reza Taftachi International Journal of Advanced
Microscopic Study of Histological Changes the Use of Ileal Mucosa as a Bladder (Radical Cystectomy - Case Report) Sareh Najaf Asaadi, Hassan Morovvati, Ahmad Reza Taftachi International Journal of Advanced
Jaspreet S. Sandhu,*,, Geoffrey T. Gotto,*, Luis A. Herran, Peter T. Scardino, James A. Eastham and Farhang Rabbani
 Age, Obesity, Medical Comorbidities and Surgical Technique are Predictive of Symptomatic Anastomotic Strictures After Contemporary Radical Prostatectomy Jaspreet S. Sandhu,*,, Geoffrey T. Gotto,*, Luis
Age, Obesity, Medical Comorbidities and Surgical Technique are Predictive of Symptomatic Anastomotic Strictures After Contemporary Radical Prostatectomy Jaspreet S. Sandhu,*,, Geoffrey T. Gotto,*, Luis
Open Radical Cystectomy Tips and Tricks in Males and Females
 Open Radical Cystectomy Tips and Tricks in Males and Females Seth P. Lerner, MD, FACS Professor of Urology Beth and Dave Swalm Chair in Urologic Oncology Scott Department of Urology Baylor College of Medicine
Open Radical Cystectomy Tips and Tricks in Males and Females Seth P. Lerner, MD, FACS Professor of Urology Beth and Dave Swalm Chair in Urologic Oncology Scott Department of Urology Baylor College of Medicine
A comparison of preliminary oncologic outcome and postoperative complications between patients undergoing either open or robotic radical cystectomy
 ORIGINAL ARTICLE Vol. 42 (4): 663-670, July - August, 2016 doi: 10.1590/S1677-5538.IBJU.2015.0393 A comparison of preliminary oncologic outcome and postoperative complications between patients undergoing
ORIGINAL ARTICLE Vol. 42 (4): 663-670, July - August, 2016 doi: 10.1590/S1677-5538.IBJU.2015.0393 A comparison of preliminary oncologic outcome and postoperative complications between patients undergoing
Index. Surg Oncol Clin N Am 14 (2005) Note: Page numbers of article titles are in boldface type.
 Surg Oncol Clin N Am 14 (2005) 433 439 Index Note: Page numbers of article titles are in boldface type. A Abdominosacral resection, of recurrent rectal cancer, 202 215 Ablative techniques, image-guided,
Surg Oncol Clin N Am 14 (2005) 433 439 Index Note: Page numbers of article titles are in boldface type. A Abdominosacral resection, of recurrent rectal cancer, 202 215 Ablative techniques, image-guided,
Facing Surgery. for a Urinary Tract Condition? Learn about minimally invasive da Vinci Surgery
 Facing Surgery for a Urinary Tract Condition? Learn about minimally invasive da Vinci Surgery The Condition: Urinary Tract Obstruction Your urinary system produces, stores, and eliminates urine. It includes
Facing Surgery for a Urinary Tract Condition? Learn about minimally invasive da Vinci Surgery The Condition: Urinary Tract Obstruction Your urinary system produces, stores, and eliminates urine. It includes
1. Introduction. 2. Methods. high-risk NMIBC in men with and without a prior history of RT for PC.
 ISRN Urology Volume 2013, Article ID 405064, 5 pages http://dx.doi.org/10.1155/2013/405064 Research Article Radical Cystectomy after BCG Immunotherapy for High-Risk Nonmuscle-Invasive Bladder Cancer in
ISRN Urology Volume 2013, Article ID 405064, 5 pages http://dx.doi.org/10.1155/2013/405064 Research Article Radical Cystectomy after BCG Immunotherapy for High-Risk Nonmuscle-Invasive Bladder Cancer in
1 st Department of Urology, Gennimatas General Hospital, Aristotle University of Thessaloniki, Thessaloniki, Greece 2
 Official Journal of Korean Continence Society / Korean Society of Urological Research / The Korean Children s Continence and Enuresis Society / The Korean Association of Urogenital Tract Infection and
Official Journal of Korean Continence Society / Korean Society of Urological Research / The Korean Children s Continence and Enuresis Society / The Korean Association of Urogenital Tract Infection and
URETERORENOSCOPY: INDICATIONS AND COMPLICATIONS - A RETROSPECTIVE STUDY
 Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 9 (58) No. 2-2016 URETERORENOSCOPY: INDICATIONS AND COMPLICATIONS - A RETROSPECTIVE STUDY L. MAXIM 1,2 I.A. BĂNUŢĂ 2 I.
Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 9 (58) No. 2-2016 URETERORENOSCOPY: INDICATIONS AND COMPLICATIONS - A RETROSPECTIVE STUDY L. MAXIM 1,2 I.A. BĂNUŢĂ 2 I.
Introduction. Teck Wei Tan 1,2 Rajesh Nair 1 Sanad Saad 1 Ramesh Thurairaja 1 Muhammad Shamim Khan 1
 World Journal of Urology (2019) 37:367 372 https://doi.org/10.1007/s00345-018-2386-4 ORIGINAL ARTICLE Safe transition from extracorporeal to intracorporeal urinary diversion following robot assisted cystectomy:
World Journal of Urology (2019) 37:367 372 https://doi.org/10.1007/s00345-018-2386-4 ORIGINAL ARTICLE Safe transition from extracorporeal to intracorporeal urinary diversion following robot assisted cystectomy:
Reconstructive Surgery
 Urology Journal UNRC/IUA Vol. 2, No. 4, 206-210 Autumn 2005 Printed in IRAN Reconstructive Surgery Abdorasol Mehrsai, 1 Hooman Djaladat, 2 * Alireza Sina, 1 Sepehr Salem, 1 Gholamreza Pourmand 1 1Department
Urology Journal UNRC/IUA Vol. 2, No. 4, 206-210 Autumn 2005 Printed in IRAN Reconstructive Surgery Abdorasol Mehrsai, 1 Hooman Djaladat, 2 * Alireza Sina, 1 Sepehr Salem, 1 Gholamreza Pourmand 1 1Department
Long-Term Follow-Up on the Effects of Sigmoid-Rectal Pouch for Urinary Diversion
 UROLOGICAL ONCOLOGY Long-Term Follow-Up on the Effects of Sigmoid-Rectal Pouch for Urinary Diversion Bin Sun, Jing-Min Yan, Jian-Ye Li, He-Qing Guo, Quan Hong, Zhi-Yong Yao, Gao-Biao Zhou, Guang-Xin Pan,
UROLOGICAL ONCOLOGY Long-Term Follow-Up on the Effects of Sigmoid-Rectal Pouch for Urinary Diversion Bin Sun, Jing-Min Yan, Jian-Ye Li, He-Qing Guo, Quan Hong, Zhi-Yong Yao, Gao-Biao Zhou, Guang-Xin Pan,
Mainz Pouch II technique: 10 years experience
 Original Article 10 YEARS EXPERIENCE OF MAINZ POUCH II G. D ELIA et al. In this section, the use of the Mainz Pouch II is examined in some detail, from Mainz (where it originated), and from London. Both
Original Article 10 YEARS EXPERIENCE OF MAINZ POUCH II G. D ELIA et al. In this section, the use of the Mainz Pouch II is examined in some detail, from Mainz (where it originated), and from London. Both
THE operation of reimplantation of the ureter into the bladder has undergone
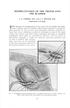 REIMPLANTATION OF THE URETER INTO THE BLADDER J. G. WARDEN, M.D., and C. C. HIGGINS, M.D. Department of Urology THE operation of reimplantation of the ureter into the bladder has undergone a stormy course
REIMPLANTATION OF THE URETER INTO THE BLADDER J. G. WARDEN, M.D., and C. C. HIGGINS, M.D. Department of Urology THE operation of reimplantation of the ureter into the bladder has undergone a stormy course
Continent urinary diversion
 Critical Reviews in Oncology/Hematology 57 (2006) 255 264 Continent urinary diversion Fiona C. Burkhard, Thomas M. Kessler, Rob Mills, Urs E. Studer Department of Urology, University of Bern, 3010 Bern,
Critical Reviews in Oncology/Hematology 57 (2006) 255 264 Continent urinary diversion Fiona C. Burkhard, Thomas M. Kessler, Rob Mills, Urs E. Studer Department of Urology, University of Bern, 3010 Bern,
Månsson, Wiking; Davidsson, Thomas; Könyves, J; Liedberg, Fredrik; Månsson, Åsa; Wullt, Björn
 Continent urinary tract reconstruction - the Lund experience. Månsson, Wiking; Davidsson, Thomas; Könyves, J; Liedberg, Fredrik; Månsson, Åsa; Wullt, Björn Published in: BJU International DOI: 10.1046/j.1464-410X.2003.04330.x
Continent urinary tract reconstruction - the Lund experience. Månsson, Wiking; Davidsson, Thomas; Könyves, J; Liedberg, Fredrik; Månsson, Åsa; Wullt, Björn Published in: BJU International DOI: 10.1046/j.1464-410X.2003.04330.x
Radical cystectomy is the mainstay of treatment for
 Potency Preserving Cystectomy With Intrafascial Prostatectomy for High Risk Superficial Bladder Cancer Paolo Puppo, Carlo Introini, Franco Bertolotto and Angelo Naselli* From the Urology Unit, Department
Potency Preserving Cystectomy With Intrafascial Prostatectomy for High Risk Superficial Bladder Cancer Paolo Puppo, Carlo Introini, Franco Bertolotto and Angelo Naselli* From the Urology Unit, Department
Koji Ichihara Hiroshi Kitamura Naoya Masumori Fumimasa Fukuta Taiji Tsukamoto
 Int J Clin Oncol (2013) 18:75 80 DOI 10.1007/s10147-011-0346-8 ORIGINAL ARTICLE Transurethral prostate biopsy before radical cystectomy remains clinically relevant for decision-making on urethrectomy in
Int J Clin Oncol (2013) 18:75 80 DOI 10.1007/s10147-011-0346-8 ORIGINAL ARTICLE Transurethral prostate biopsy before radical cystectomy remains clinically relevant for decision-making on urethrectomy in
Cystectomies and bladder preservation: What you need to know
 Cystectomies and bladder preservation: What you need to know Robin Morash RN, BNSc, MHS Bladder Cancer Canada November 21, 2018 Presentation goals Review the options for treatment of muscle-invasive bladder
Cystectomies and bladder preservation: What you need to know Robin Morash RN, BNSc, MHS Bladder Cancer Canada November 21, 2018 Presentation goals Review the options for treatment of muscle-invasive bladder
Pelvioureteric junction obstruction of the lower collecting system associated with incomplete ureteral duplication: A case report
 Ped Urol Case Rep 2014;1(6):11-15 DOI:10.14534/PUCR.201468061 PUCR Ped Urol Case Rep PEDIATRIC UROLOGY CASE REPORTS ISSN: 2148 2969 Journal homepage: http://www.pediatricurologycasereports.com Pelvioureteric
Ped Urol Case Rep 2014;1(6):11-15 DOI:10.14534/PUCR.201468061 PUCR Ped Urol Case Rep PEDIATRIC UROLOGY CASE REPORTS ISSN: 2148 2969 Journal homepage: http://www.pediatricurologycasereports.com Pelvioureteric
Sara Schaenzer Grand Rounds January 24 th, 2018
 Sara Schaenzer Grand Rounds January 24 th, 2018 Bladder Anatomy Ureter Anatomy Areas of Injury Bladder: Posterior bladder wall above trigone Ureter Crosses beneath uterine vessels At pelvic brim when ligating
Sara Schaenzer Grand Rounds January 24 th, 2018 Bladder Anatomy Ureter Anatomy Areas of Injury Bladder: Posterior bladder wall above trigone Ureter Crosses beneath uterine vessels At pelvic brim when ligating
CT findings in patients with Cabazitaxel induced pelvic pain and haematuria: a case series
 Malalagama et al. Cancer Imaging (2017) 17:17 DOI 10.1186/s40644-017-0119-3 CASE SERIES CT findings in patients with Cabazitaxel induced pelvic pain and haematuria: a case series Geethal N. Malalagama
Malalagama et al. Cancer Imaging (2017) 17:17 DOI 10.1186/s40644-017-0119-3 CASE SERIES CT findings in patients with Cabazitaxel induced pelvic pain and haematuria: a case series Geethal N. Malalagama
I-STOP TOMS Transobturator Male Sling
 I-STOP TOMS Transobturator Male Sling The CL Medical I-STOP TOMS sling for male stress urinary incontinence was developed in France where it is widely used and is the market leader. It is constructed with
I-STOP TOMS Transobturator Male Sling The CL Medical I-STOP TOMS sling for male stress urinary incontinence was developed in France where it is widely used and is the market leader. It is constructed with
Clinical Study of G3 Superficial Bladder Cancer without Concomitant CIS Treated with Conservative Therapy
 Jpn J Clin Oncol 2002;32(11)461 465 Clinical Study of G3 Superficial Bladder Cancer without Concomitant CIS Treated with Conservative Therapy Takashi Saika, Tomoyasu Tsushima, Yasutomo Nasu, Ryoji Arata,
Jpn J Clin Oncol 2002;32(11)461 465 Clinical Study of G3 Superficial Bladder Cancer without Concomitant CIS Treated with Conservative Therapy Takashi Saika, Tomoyasu Tsushima, Yasutomo Nasu, Ryoji Arata,
Radical Cystectomy and Orthotopic Neobladder with Prostate and Seminal Sparing inyoung Patients with Transitional Cell Carcinoma (TCC) of the Bladder
 European Urology Supplements European Urology Supplements 4 (2005) 61 66 Radical Cystectomy and Orthotopic Neobladder with Prostate and Seminal Sparing inyoung Patients with Transitional Cell Carcinoma
European Urology Supplements European Urology Supplements 4 (2005) 61 66 Radical Cystectomy and Orthotopic Neobladder with Prostate and Seminal Sparing inyoung Patients with Transitional Cell Carcinoma
Postoperative Care for Pelvic Fistulae. Peter Jeppson, MD October 3, 2017
 Postoperative Care for Pelvic Fistulae Peter Jeppson, MD October 3, 2017 No Disclosures Rational for Postoperative Care Intraoperative injury may be managed by: Identification Closure Continuous post-operative
Postoperative Care for Pelvic Fistulae Peter Jeppson, MD October 3, 2017 No Disclosures Rational for Postoperative Care Intraoperative injury may be managed by: Identification Closure Continuous post-operative
Attachment #2 Overview of Follow-up
 Attachment #2 Overview of Follow-up Provided below is a general overview of follow-up and this may vary based on specific patient or cancer characteristics. Of note, Labs and imaging can be performed closer
Attachment #2 Overview of Follow-up Provided below is a general overview of follow-up and this may vary based on specific patient or cancer characteristics. Of note, Labs and imaging can be performed closer
Presence of transient hydronephrosis immediately after surgery has a limited influence on renal function 1 year after ileal neobladder construction
 Narita et al. BMC Urology (17) 17:7 DOI 1.1186/s1894-17-63-x RESEARCH ARTICLE Presence of transient hydronephrosis immediately after surgery has a limited influence on renal function 1 year after ileal
Narita et al. BMC Urology (17) 17:7 DOI 1.1186/s1894-17-63-x RESEARCH ARTICLE Presence of transient hydronephrosis immediately after surgery has a limited influence on renal function 1 year after ileal
Clinical features and long-term outcomes of idiopathic urethrorrhagia
 The Turkish Journal of Pediatrics 2015; 57: 380-384 Original Clinical features and long-term outcomes of idiopathic urethrorrhagia Serdar Moralıoğlu, Ayşenur Cerrah-Celayir, Oktav Bosnalı Department of
The Turkish Journal of Pediatrics 2015; 57: 380-384 Original Clinical features and long-term outcomes of idiopathic urethrorrhagia Serdar Moralıoğlu, Ayşenur Cerrah-Celayir, Oktav Bosnalı Department of
Ileal Pouch Anal Anastomosis: The Preferred Method of Reconstruction after Proctocolectomy in Children
 Ileal Pouch Anal Anastomosis: The Preferred Method of Reconstruction after Proctocolectomy in Children Stephanie Jones, D.O. Surgical Fellow March 21, 2011 Ulcerative Colitis Spectrum of inflammatory bowel
Ileal Pouch Anal Anastomosis: The Preferred Method of Reconstruction after Proctocolectomy in Children Stephanie Jones, D.O. Surgical Fellow March 21, 2011 Ulcerative Colitis Spectrum of inflammatory bowel
Robotic distal ureterectomy with psoas hitch and ureteroneocystostomy: Surgical technique and outcomes
 Asian Journal of Urology (2015) 2, 123e127 HOSTED BY Available online at www.sciencedirect.com ScienceDirect journal homepage: www.elsevier.com/locate/ajur CASE REPORT Robotic distal with psoas hitch and
Asian Journal of Urology (2015) 2, 123e127 HOSTED BY Available online at www.sciencedirect.com ScienceDirect journal homepage: www.elsevier.com/locate/ajur CASE REPORT Robotic distal with psoas hitch and
Complications and Quality of Life Following Urinary Diversion After Cystectomy
 EAU Update Series EAU Update Series 3 (2005) 156 168 Complications and Quality of Life Following Urinary Diversion After Cystectomy Elmar W. Gerharz a, *, Alexander Roosen a, Wiking Månsson b a Department
EAU Update Series EAU Update Series 3 (2005) 156 168 Complications and Quality of Life Following Urinary Diversion After Cystectomy Elmar W. Gerharz a, *, Alexander Roosen a, Wiking Månsson b a Department
Radical Cystectomy A Patient s Guide
 Radical Cystectomy A Patient s Guide Introduction The urinary system, which includes the bladder, urethra, ureters, and kidneys, helps maintain stable chemical conditions in the body, stores, and eliminates
Radical Cystectomy A Patient s Guide Introduction The urinary system, which includes the bladder, urethra, ureters, and kidneys, helps maintain stable chemical conditions in the body, stores, and eliminates
Citation for published version (APA): Bartels, S. A. L. (2013). Laparoscopic colorectal surgery: beyond the short-term effects
 UvA-DARE (Digital Academic Repository) Laparoscopic colorectal surgery: beyond the short-term effects Bartels, S.A.L. Link to publication Citation for published version (APA): Bartels, S. A. L. (2013).
UvA-DARE (Digital Academic Repository) Laparoscopic colorectal surgery: beyond the short-term effects Bartels, S.A.L. Link to publication Citation for published version (APA): Bartels, S. A. L. (2013).
Point/Counterpoint: Quality of Life Considerations for Patients with Muscle Invasive Bladder Cancer Pro Trimodality Therapy
 Point/Counterpoint: Quality of Life Considerations for Patients with Muscle Invasive Bladder Cancer Pro Trimodality Therapy Kimberley S. Mak, MD, MPH Assistant Professor Boston Medical Center Boston University
Point/Counterpoint: Quality of Life Considerations for Patients with Muscle Invasive Bladder Cancer Pro Trimodality Therapy Kimberley S. Mak, MD, MPH Assistant Professor Boston Medical Center Boston University
