Association of overactive bladder and stress urinary incontinence in rats with pudendal
|
|
|
- Dale Cunningham
- 6 years ago
- Views:
Transcription
1 Page 1 of 33 Articles in PresS. Am J Physiol Regul Integr Comp Physiol (March 12, 2008). doi: /ajpregu Association of overactive bladder and stress urinary incontinence in rats with pudendal nerve ligation injury Akira Furuta, 1, 3 Masafumi Kita, 1 Yasuyuki Suzuki, 3 Shin Egawa, 3 Michael B. Chancellor, 1 William C. de Groat, 2 Naoki Yoshimura 1, 2 1 Department of Urology and 2 Pharmacology, University of Pittsburgh School of Medicine, Pittsburgh, Pennsylvania; and 3 Department of Urology, The Jikei University School of Medicine, Tokyo, Japan Running head: OAB and SUI after pudendal nerve injury Correspondence to: Naoki Yoshimura, MD, PhD Department of Urology, University of Pittsburgh School of Medicine Suite 700, Kaufmann Medical Building, 3471 Fifth Avenue, Pittsburgh, PA Phone: Fax: nyos@pitt.edu Copyright 2008 by the American Physiological Society.
2 Page 2 of 33 2 ABSTRACT Approximately one-third of patients with stress urinary incontinence (SUI) also suffer from urgency incontinence that is one of the major symptoms of overactive bladder (OAB) syndrome. Pudendal nerve injury has been recognized as a possible cause for both SUI and OAB. Therefore, we investigated the effects of pudendal nerve ligation (PNL) on bladder function and urinary continence in female Sprague-Dawley rats. Conscious cystometry with or without capsaicin pretreatment (125 mg/kg s.c.), leak point pressures (LPPs), contractile responses of bladder muscle strips to carbachol or phenylephrine, and levels of nerve growth factor (NGF) protein and mrna in the bladder were compared in sham and PNL rats 4 weeks after the injury. Urinary frequency detected by a reduction in intercontraction intervals and voided volume was observed in PNL rats compared with sham rats, but it was not seen in PNL rats with capsaicin pretreatment that desensitizes C-fiber afferent pathways. LPPs in PNL rats were significantly decreased compared with sham rats. The contractile responses of detrusor muscle strips to phenylephrine, but not to carbachol, were significantly increased in PNL rats. The levels of NGF protein and mrna in the bladder of PNL rats were significantly increased compared with sham rats. These results suggest that pudendal nerve neuropathy induced by PNL may be one of the potential risk factors for OAB as well as SUI. Somato-visceral cross sensitization between somatic (pudendal) and visceral (bladder) sensory pathways that increases NGF expression and 1 -adrenoceptormediated contractility in the bladder may be involved in this pathophysiological mechanism.
3 Page 3 of 33 3 Keywords: overactive bladder, urinary incontinence, pudendal nerve injury, nerve growth factor, cross-talk sensitization
4 Page 4 of 33 4 INTRODUCTION Overactive bladder (OAB) syndrome is defined as a symptom complex of urgency usually associated with daytime frequency and nocturia, with or without urgency incontinence (1). The prevalence of OAB is approximately 17% of the general adult population (30, 48). In addition, 25% of women from 20 years of age live with urinary incontinence, in which a half of all urinary incontinence is stress urinary incontinence (SUI), 11% urgency and 36% mixed incontinence (14), indicating that approximately one-third of patients with SUI also suffer from urgency incontinence, one of the major symptoms of OAB. Main risk factors for SUI defined as involuntary loss of urine secondary to an increase in abdominal pressure during events such as sneezing, coughing or laughing include parity, age and obesity (7). Childbirth injury to muscles, connective tissues and nerves seems to be the most important risk factor for lifetime incontinence because damage of pudendal nerves innervating to the external urethral sphincter is often found in SUI patients (4, 43, 44, 49) and about 30% of mothers become urinary incontinent after their first vaginal delivery (28). In addition, it has been reported that patients with pudendal nerve entrapment that induces compression or stretching of the pudendal nerve at the ischial spine or in Alcock s canal exhibit urgency, urinary incontinence (stress, urgency and mixed types), and chronic pelvic pain such as vulvodynia, perineal pain and proctalgia (3, 36). These findings raise the possibility that pudendal nerve injury that damages the urethral continence mechanisms to induce SUI is also involved in OAB pathogenesis.
5 Page 5 of 33 5 Since the pudendal nerve carries motor and sensory fibers, injury to this nerve can affect both efferent and afferent pathways. Reflex interaction between pelvic organs, necessary for the normal regulation of sexual, bladder and bowel function, is likely mediated by the convergence of afferent pathways in the spinal cord or innervation of multiple organs by the same primary afferent neurons (10, 16). Because a neural substrate for pelvic organ reflex interaction or cross-talk exists under normal conditions, alterations in this cross-talk by injury or disease may play a role in the development of pelvic organ dysfunction (35, 37). Thus, there is the possibility that pudendal nerve injury can induce increased activity of bladder C-fiber afferent pathways, which is reportedly involved in the development of OAB (8, 53). Nerve growth factor (NGF) may be an important factor inducing afferent sensitization and OAB symptoms. Increased NGF levels have been found in the bladder of patients with idiopathic OAB (23), and intravesical application of NGF or injection of a viral vector encoding for NGF into the bladder wall induces OAB in rats (11, 20). Moreover, NGF may play an important role in somato-visceral cross sensitization because intravesical application of NGF induces hyperalgesia of the hind limb (an example of viscerosomatic convergence or cross-talk) (15), and injection of NGF-encoding vectors into the bladder wall enhances the responses to colorectal distension (an example of viscerovisceral convergence or cross-talk) (5). Therefore, the present study first examined whether PNL was able to induce OAB and SUI conditions using cystometry and leak point pressure (LPP) measurements, respectively. We also examined the effects of capsaicin pretreatment that induces C-fiber desensitization on bladder activity and the levels of NGF protein and mrna in the
6 Page 6 of 33 6 bladder to clarify whether sensitization of C-fiber afferent pathways and increased bladder NGF levels were involved in PNL-induced bladder overactivity. In addition, the responses of detrusor muscle strips to muscarinic or 1 -adrenoceptor (AR) stimulation were also studied to investigate changes in detrusor contractility after PNL. MATERIALS AND METHODS Pudendal nerve ligation injury. Eighty adult female Sprague-Dawley rats weighing g were divided into pudendal nerve ligation injury (PNL, n = 40) and sham operated control groups (sham, n = 40). In PNL rats, under isoflurane (Hospira, Lake Forest, IL, USA) anesthesia, pudendal nerves were exposed bilaterally near the internal iliac vessels through a lower midline abdominal incision (26) and ligated with 4-0 silk threads to compress approximately a half of the nerve s diameter. Sham rats underwent the same procedures without ligation. After the surgery, the animals were treated with ampicillin (100 mg/kg sc, Fort Dodge Animal Health Inc., Fort Dodge, IA, USA) and buprenorphine (0.5 mg/kg sc, Pharmaceuticals, Richmond, VA, USA) for 3 days. All experiments were conducted in accordance with institutional guidelines and approved by the University of Pittsburgh Institutional Animal Care and Use Committee. Conscious cystometry with or without capsaicin pretreatment. Conscious cystometry was performed in 8 sham and 8 PNL rats 4 weeks after the operation. Under isoflurane anesthesia, the bladder was exposed through a lower midline abdominal incision and a polyethylene (PE) -50 catheter (Clay Adams, Parsippany, NJ, USA) was implanted into the bladder through the bladder dome. The intravesical catheter was passed through the abdominal wound when the wound was closed with sutures, and local
7 Page 7 of 33 7 anesthetics (EMLA cream, AstraZeneca, Wilmington, DE, USA) were applied to the abdominal wound. The animals were then placed in a restraining cage and allowed to recover from anesthesia, so that cystometry was performed while they were awake. The intravesical catheter was connected via three-way stopcocks to a pressure transducer (Transbridge 4M, World Precision Instruments, Sarasota, FL, USA) and a syringe pump (Harvard Apparatus, Holliston, MA, USA). Saline was infused at 0.04 ml per minute for about 2 hours until rhythmic bladder contractions became stable. Cystometric parameters were then measured during saline infusion for 1 to 2 hours to evaluate bladder function. In another group of animals, conscious cystometry was performed in 8 sham and 8 PNL rats after the pretreatment with capsaicin (125 mg/kg sc, Sigma, St. Louis, MO, USA) 4 days prior to cystometry under isoflurane anesthesia to examine whether PNL-induced changes in bladder activity was mediated by activation of capsaicin sensitive C-fiber afferent pathways (27). An eye wipe test was performed on each unanesthetized animal just before the experiment to evaluate the effectiveness of capsaicin pretreatment as previously described (9). Saline voided from the urethral orifice was collected and measured to determine voided volume (VV). After constant voided volumes were collected the infusion was stopped and post-void residual volume (RV) was measured by dropping the catheter and withdrawing intravesical fluid through the catheter by gravity. Voiding efficiency (VE) was calculated with the formula, VV / (VV + RV) 100. Intercontraction interval (ICI), baseline pressure (BP), voiding threshold pressure (TP) and maximal voiding pressure (MVP) were also recorded using a data-acquisition software (sampling at 40 Hz, Chart,
8 Page 8 of 33 8 ADInstruments, Castle Hill NSW, Australia) on a computer system equipped with an analog-to-digital converter (PowerLab, ADInstruments). Leak point pressure (LPP) measurement. LPPs were measured using the vertical tilt table/intravesical pressure clamp method (21) in another group of animals (8 sham and 8 PNL rats) 4 weeks after the surgery. Under isoflurane anesthesia, the animals underwent spinal cord transection at the T8-9 level after laminectomy to eliminate spontaneous reflex voiding mediated by spino-bulbo-spinal pathways passing through a micturition center in the pons. This manipulation does not interfere with urethral reflexes induced by bladder distension, which are predominantly organized in the lumbosacral spinal cord (12, 18). The bladder was exposed through a lower midline abdominal incision and a PE-90 catheter was implanted into the bladder through the bladder dome. Feces were removed from the distal colon through a small incision in the colon wall. After the surgery, isoflurane anesthesia was turned off and replaced with urethane anesthesia (1.2 g/kg sc, Sigma). The animals were then mounted on a tilt table and placed in the vertical position. Intravesical pressure was clamped by connecting the bladder catheter to a saline reservoir (60ml syringe, BD Franklin Lakes, NJ, USA) and a pressure transducer (Transbridge 4M, World Precision Instruments) via three-way stopcocks, and recorded using a Chart software on a PowerLab system (sampling at 10 Hz, ADInstruments). The reservoir was mounted on a metered vertical pole for controlled height adjustment. Intravesical pressure was increased in 2.5 cm steps from zero upward until visual identification of leakage of fluid from the urethral orifice. The pressure at leak point was regarded as LPP. The average of three consecutive LPPs was taken as a data point for each animal. In addition to the measurement of LPPs, all the
9 Page 9 of 33 9 bladders were dissected and weighed to examine whether PNL induced bladder hypertrophy. Bladder muscle strip study. The bladders of 8 sham and 8 PNL rats 4 weeks after the operation were harvested. Transverse muscle strips (2 8 mm) of the posterior wall of the bladder were prepared in a cold Krebs-Henseleit (K-H) solution composed of 118 mm NaCl, 4.7 mm KCl, 2.5 mm CaCl 2, 1.2 mm MgSO 4, 25 mm NaHCO 3, 1.2 mm KH 2 PO 4 and 10 mm glucose. Muscle strips were then suspended in a 30 ml organ bath filled with K-H solution at 37 C and gassed with a 95% O 2 and 5% CO 2 mixture. Contractile responses were monitored with a pressure transducer (Transbridge 4M, World Precision Instruments) and recorded using a Chart software on a PowerLab system (sampling at 40 Hz, ADInstruments). Each strip was adjusted to a resting tension of 1 g and then allowed to equilibrate for at least 60 minutes. After the responses to 80 mm KCl were assessed, cumulative concentration-dependent contractions induced by carbachol (10-8 to 10-4 M, Sigma), a muscarinic receptor agonist, and phenylephrine (10-7 to 10-3 M, Sigma), an 1 -AR agonist, were recorded in a stepwise manner after the response to the previous concentration had reached a plateau. Contractile responses were expressed as a percent of the response to 80 mm KCl, and contractile forces were calculated as grams of active force per cross-sectional area using the following formula, weight / (length 1.05), where 1.05 is the assumed density of muscles (32). EC 50 values that are the concentration required to produce 50% of the maximal contractile response were obtained from contractile response curves with an iterative non-linear least square curve-fitting program using a Prism program (GraphPad Software, San Diego, CA, USA).
10 Page 10 of Emax values that are the maximal contractile response were obtained from contractile force curves. NGF protein measurement by ELISA. The bladders were removed following conscious cystometry without capsaicin pretreatment in 8 sham and 8 PNL rats 4 weeks after the operation for the measurement of NGF protein by enzyme-linked immunosorbent assay (ELISA) (40). The tissues were rapidly frozen and stored at -80 C until protein extraction. The bladders were homogenized with the buffer composed of 2.66% Trisma HCl (Sigma), 0.985% Trisma Base (Sigma), 0.5 mm phenylmethylsulfonyl fluoride (Sigma), 1 µm leupeptin (Sigma), 1 µm pepstatin A (Sigma) and 0.3 µm aprotinin (Sigma) in 400 µl. The homogenate was centrifuged at 10,000 gravity for 4 minutes, and the supernatant was diluted with 4 volumes of Dulbecco s phosphate buffer saline (Invitrogen, Carlsbad, CA, USA). The samples were acidified by 10N HCl to ph 2.0 to 3.0 for 15 minutes and then neutralized by 10N NaOH to ph 7.5 to 8.0 in order to activate the immunological recognition of all biologically active antibodies to NGF (55). After acid treatment the samples were stored at -80 C until assayed. The samples were assayed by ELISA Emax ImmunoAssay System (Promega, Madison, WI, USA) according to the manufacturer s instructions. In addition, total protein concentration in the same samples was detected with a Bradford Assay Kit (Pierce, Rockford, IL, USA). All tissue NGF values were then standardized by tissue protein levels and expressed in pg/µg total protein. NGF mrna measurement by real-time RT-PCR. The bladders were harvested from 8 sham and 8 PNL rats 4 weeks after the operation for the measurement of NGF
11 Page 11 of mrna. The tissues were rapidly frozen and stored at -80 C until RNA extraction. Total RNA was extracted from frozen tissues using TRIzol (Invitrogen) according to the manufacturer s instructions. The concentration of RNA was estimated by measuring the absorbance at 260 nm with an ELx800 system (Bio-Tec Instruments, Winooski, VT, USA). The 260/280 ratio was used to check for purity. Reverse transcription (RT) reaction mixture contained 3 µg of total RNA, 500 ng oligo(dt) 15 Primer (Promega), 0.5 mm dntp Mix (Invitrogen), 1 first strand buffer, 10 mm DTT, 20 units RNasin Ribonuclease Inhibitor (Promega) and 200 units SuperScript Reverse Transcriptase (Invitrogen) in a total volume of 20 µl. The mixture was incubated at 42 C for 50 minutes, heated to 70 C for 15 minutes to denature the RT, and then cooled to 4 C. The cdna was stored at -20 C until assayed by real-time polymerase chain reaction (PCR). The sequence of oligonucleotide primers for amplifying NGF mrna were sense; 5 - AACAGGACTCACAGGAGCAA-3, antisense; 5 -CTTCCTGCTGAGCACACACA-3 (GeneMark, Atlanta, GA, USA). Amplification of -actin mrna served as an internal standard. The primers used for -actin were 5 -CTATGAGCTGCCTGACGGTC-3, antisense; 5 -AGTTTCATGGATGCCACAGG-3, giving a 115 bp fragment. Real-time PCR was performed with QuantiTect SYBR Green PCR Kit (Qiagen, Valencia, CA, USA) using an Mx3000P QPCR system (Stratagene, La Jolla, CA, USA). The real-time PCR reaction mixture contained 1 QuantiTect SYBR Green PCR, 0.3 µm primer pairs of NGF and 1 µl cdna of the samples in a total volume of 25 µl. The mixture was heated at 95 C for 15 minutes in order to activate DNA polymerase, and then followed by 35 cycles with denaturation at 95 C for 60 seconds, annealing at 55 C for 60 seconds and extension at 72 C for 60 seconds. Each assay for the samples was performed in
12 Page 12 of duplicate wells. After PCR products had been made, melt curve protocols designed for increment temperatures of 1 C (starting at 55 C and ending at 95 C) was performed to ensure that primer-dimers and other non-specific product had been minimized or eliminated. Each copy number of the sample and housekeeping gene was calculated from its standard curve, and NGF levels of the samples were shown as relative expression with the standardization of -actin. Data analysis. All data are represented as mean values ± standard error of the mean (SEM). Statistical analyses were performed using unpaired Student s t-test in a Prism program (GraphPad Software). P<0.05 was regarded as the level of significance.
13 Page 13 of RESULTS Cystometry and LPP testing. Representative conscious cystometric recordings in sham and PNL groups were shown in Fig. 1. During cystometry, ICI and VV were significantly decreased in PNL rats compared with sham rats (ICI: PNL; ± 23.9 sec. vs Sham; ± 24.3 sec., VV: PNL; 0.30 ± 0.03 ml vs Sham; 0.41 ± 0.05 ml) whereas BP, TP, MVP, RV or VE were not different between PNL and sham rats. However, the differences of ICI and VV were not seen when PNL and sham rats were pretreated with capsaicin to desensitize C-fiber afferents (ICI: PNL; ± 11.3 sec. vs Sham; ± 56.2 sec., VV: PNL; 0.41 ± 0.02 ml vs Sham; 0.47 ± 0.06 ml). In addition, no difference was observed in any of other parameters (BP, TP, MVP, RV or VE) in sham and PNL rats with capsaicin pretreatment (Table 1). Moreover, there was no significant difference between the bladder weight of PNL (0.13 ± 0.01 g) and sham (0.12 ± 0.01 g) rats. In another group of animals, LPP was significantly decreased in PNL (31.9 ± 2.2 cmh 2 O) rats compared with sham (38.2 ± 1.5 cmh 2 O) rats 4 week after PNL (p<0.05). Contractile responses of the bladder muscle strips. An analysis of concentrationdependent responses of the bladder muscle strips from PNL and sham rats to carbachol (10-8 to 10-4 M) and phenylephrine (10-7 to 10-3 M) yielded values for functional affinity constants, EC 50, and maximal contractions, Emax, for the agonists (Table 2). EC 50 and Emax values of the detrusor responses to carbachol were similar in PNL and sham rats (Fig. 2A, B). However, EC 50 values of the detrusor responses to phenylephrine were significantly decreased in PNL (2.2 ± 1.3 µm) rats compared with sham (6.8 ± 1.4 µm) rats (Fig. 2C), and Emax values of the detrusor responses to phenylephrine were significantly increased in PNL (1.1 ± 0.1 g/mm 2 ) rats compared with sham (0.7 ± 0.1
14 Page 14 of g/mm 2 ) rats (Fig. 2D), indicating increased contractile responses of the detrusor to 1 -AR stimulation after PNL. Levels of NGF protein and mrna in the bladder. Four weeks after the operation, NGF protein levels of the bladder were significantly higher in PNL (70.9 ± 7.9 pg/µg) rats than in sham (44.8 ± 3.2 pg/µg) rats (Fig. 3A). Similarly, NGF mrna levels of the bladder were also significantly increased in PNL (2.6 ± 0.4) rats compared with sham (1.4 ± 0.2) rats (Fig. 3B). DISCUSSION The results of the present study demonstrate that: (1) pudendal nerve injury induces not only SUI indicated by reduced LPPs, but also OAB conditions indicated by reduced ICI and VV; (2) OAB induced by PNL is at least in part mediated by activation of capsaicinsensitive C-fiber afferents; (3) PNL increases the levels of NGF protein and mrna in the bladder; and (4) PNL enhances 1 -AR-mediated contractile responses of the detrusor. SUI is the most common type of urinary incontinence in women, and approximately one-third of women with urinary incontinence exhibit both SUI and urgency incontinence (i.e., mixed incontinence) (14). A recent cross sectional population-based study also has revealed that SUI is strongly associated with urgency, the primary symptom of OAB (50). The mechanisms that contribute to development of SUI and OAB symptoms in the same patients are not well understood although a pervious study has suggested that leakage of urine into the urethra (i.e., stress incontinence) may stimulate urethral afferents that induce an involuntary voiding reflex (i.e., urgency incontinence) (17). Vaginal parity has been described as one of the major risk factors inducing SUI, in addition to age and
15 Page 15 of obesity. Childbirth injury can damage muscles, connective tissues and nerves including the pudendal nerves (7, 28). Previous clinical studies in SUI patients have provided evidence of damage of pudendal nerves (4, 43, 44, 49). The results of the present study raise the possibility that the mixed stress and urgency incontinence condition is induced by pudendal nerve injury which sensitizes bladder afferent pathways and induces bladder overactivity by increasing the levels of bladder NGF. In addition, SUI conditions induced in PNL rats seem to be modest because the reduction in LPPs after PNL in the study was smaller (16% decrease) than that observed in our previous study using rats with pudendal nerve transection (22% decrease) (19). Additional evidence for a contribution of pudendal nerve injury to bladder overactivity was obtained in patients with pudendal nerve entrapment (PNE) (3, 36). The pudendal nerves which, in human, are derived from the sacral roots S2, S3 and S4 seem to be susceptible to compression or stretching because of their anatomical course (3, 39). Three main symptoms of PNE include urinary incontinence (both stress and urgency types) (74%), fecal incontinence (62%) and perineodynia (35%) that includes vulvodynia, perineal pain and proctalgia (3). Patients with PNE frequently (40%) have additional symptoms such as urinary frequency and urgency (36). Thus it seems likely that pudendal nerve injury is involved in pathogenesis of OAB symptoms such as urgency, frequency and urgency incontinence as well as SUI in patients with PNE. Although the precise mechanism inducing changes in bladder activity following pudendal nerve injury is not known, cross sensitization of sensory pathways may be involved because there is extensive convergence of afferent inputs from cutaneous, muscles and visceral tissues at the level of spinal cord and/or dorsal root ganglia (31).
16 Page 16 of Several examples of cross-organ sensitization have been demonstrated in the pelvic viscera including chemically-induced colitis in rats that induces urinary frequency, bladder afferent fiber hyperexcitability (35, 51), upregulation of the NGF mrna levels and mast cell infiltration in the bladder (22, 52), and increased excitability of bladder afferent neurons as well as spinal dorsal horn neurons receiving inputs from the bladder (25, 37). The NGF levels are reportedly elevated in the bladders of patients with benign prostatic hyperplasia (46), idiopathic OAB and interstitial cystitis (23). Thus, it is possible that PNL-induced irritation of pudendal nerve afferents can induce sensitization of bladder afferent pathways to increase the bladder NGF levels and elicit bladder overactivity. It has been reported that increased NGF levels in the bladder or bladder afferent pathways can induce OAB and C-fiber afferent hyperexcitability (5, 20, 42, 45, 47, 54). Because bladder overactivity in the PNL animals disappeared after capsaicin pretreatment that induces C-fiber desensitization in the present study, it seems reasonable to assume that NGF-induced C-fiber afferent hyperexcitability is also likely to be involved in PNLinduced bladder overactivity. Since there was no difference in bladder weight and postvoid residual volume between sham and PNL rats in the present study, it seems that PNL did not induce bladder outlet obstruction (BOO), which can lead to bladder hypertrophy. A previous study has also reported no changes in bladder weight in rats with pudendal nerve transection injury (34). Thus, upregualtion of bladder NGF after PNL is likely to be induced by direct sensitization of bladder afferent pathways, rather than BOO-induced bladder hypertrophy.
17 Page 17 of In the present study, 1 -AR-mediated contractility was increased in the bladder muscle strips obtained from the PNL rats, suggesting that PNL induces postjunctional changes in the bladder. 1 -ARs are expressed at low levels in normal human bladder muscles (29), the highest levels being 1D -AR (66%) followed by 1A -AR (34%) and no expression of 1B -AR (24). A 4-fold increase in -ARs has been reported in the bladder muscles of OAB patients compared with normal human bladder (38). Increased contractile responses to phenylephrine have been also demonstrated in the bladder muscle strips from patients with BOO, and these responses were inhibited by tamsulosin, an 1A and 1D -ARs antagonist (6). However, other studies on human normal and obstructed bladders do not show any differences in 1 -ARs mrna expression and function (33). Hampel et al. have reported that there are changes in 1 -AR subtype expression from 1A to 1D subtypes in the bladder muscles of rats with BOO (13). Since 1D -AR has 10 to 100-fold higher affinity for the endogenous norepinephrine and epinephrine compared with other 1 -AR subtypes (41), it is possible that upregulation of 1D in the bladder can increase contractility of bladder smooth muscles in response to sympathetic nerve activation, which occurs during urine storage. However, because there is already 1D -AR predominance in the normal human detrusor (24), increased 1D -AR expression may not be an important factor for generating OAB (2). More studies are needed to clarify the role of increased 1 -AR-mediated contractility of the detrusor in PNL-induced bladder overactivity. Perspectives and Significance. Our findings that pudendal nerve injury can induce both SUI and OAB conditions support the clinical data that approximately one-third of patients with SUI suffer from urgency incontinence (i.e., mixed incontinence) (14, 48).
18 Page 18 of The pathophysiological mechanism inducing bladder overactivity following pudendal nerve injury might be due to somato-visceral cross sensitization between pudendal and bladder afferent pathways, which induces increased levels of bladder NGF and increased responses to 1 -AR stimulation of bladder smooth muscles. Thus, pudendal nerve neuropathy could be one of the potential risk factors for not only SUI but also OAB. GRANTS This study was supported by National Institutes of Health grants (R01DK57267, R01DK68557 and P01DK44935).
19 Page 19 of REFERENCES 1. Abrams P, Cardozo L, Fall M, Griffiths D, Rosier P, Ulmsten U, van Kerrebroeck P, Victor A, and Wein A. The standardisation of terminology of lower urinary tract function: report from the Standardisation Sub-committee of the International Continence Society. Neurourol Urodyn 21: , Andersson KE. LUTS treatment: future treatment options. Neurourol Urodyn 26: , Beco J, Climov D, and Bex M. Pudendal nerve decompression in perineology: a case series. BMC Surg 4: 15, Bhatia NN and Ostergard DR. Urodynamics in women with stress urinary incontinence. Obstet Gynecol 60: , Bielefeldt K, Lamb K, and Gebhart GF. Convergence of sensory pathways in the development of somatic and visceral hypersensitivity. Am J Physiol Gastrointest Liver Physiol 291: G , Bouchelouche K, Andersen L, Alvarez S, Nordling J, and Bouchelouche P. Increased contractile response to phenylephrine in detrusor of patients with bladder outlet obstruction: effect of the alpha1a and alpha1d-adrenergic receptor antagonist tamsulosin. J Urol 173: , Bump RC and Norton PA. Epidemiology and natural history of pelvic floor dysfunction. Obstet Gynecol Clin North Am 25: , Chai TC, Gray ML, and Steers WD. The incidence of a positive ice water test in bladder outlet obstructed patients: evidence for bladder neural plasticity. J Urol 160: 34-38, 1998.
20 Page 20 of Cheng CL, Ma CP, and de Groat WC. Effect of capsaicin on micturition and associated reflexes in chronic spinal rats. Brain Res 678: , Christianson JA, Liang R, Ustinova EE, Davis BM, Fraser MO, and Pezzone MA. Convergence of bladder and colon sensory innervation occurs at the primary afferent level. Pain 128: , Chuang YC, Fraser MO, Yu Y, Chancellor MB, de Groat WC, and Yoshimura N. The role of bladder afferent pathways in bladder hyperactivity induced by the intravesical administration of nerve growth factor. J Urol 165: , de Groat WC. Anatomy of the central neural pathways controlling the lower urinary tract. Eur Urol 34 Suppl 1: 2-5, Hampel C, Dolber PC, Smith MP, Savic SL, Th roff JW, Thor KB, and Schwinn DA. Modulation of bladder alpha1-adrenergic receptor subtype expression by bladder outlet obstruction. J Urol 167: , Hannestad YS, Rortveit G, Sandvik H, and Hunskaar S. A community-based epidemiological survey of female urinary incontinence: the Norwegian EPINCONT study. Epidemiology of Incontinence in the County of Nord- Trondelag. J Clin Epidemiol 53: , Jaggar SI, Scott HC, and Rice AS. Inflammation of the rat urinary bladder is associated with a referred thermal hyperalgesia which is nerve growth factor dependent. Br J Anaesth 83: , Janig W and Koltzenburg M. On the function of spinal primary afferent fibres supplying colon and urinary bladder. J Auton Nerv Syst 30 Suppl: S89-96, 1990.
21 Page 21 of Jung SY, Fraser MO, Ozawa H, Yokoyama O, Yoshiyama M, De Groat WC, and Chancellor MB. Urethral afferent nerve activity affects the micturition reflex; implication for the relationship between stress incontinence and detrusor instability. J Urol 162: , Kakizaki H, Fraser MO, and De Groat WC. Reflex pathways controlling urethral striated and smooth muscle function in the male rat. Am J Physiol 272: R , Kwon D, Kim Y, Pruchnic R, Jankowski R, Usiene I, de Miguel F, Huard J, and Chancellor MB. Periurethral cellular injection: comparison of musclederived progenitor cells and fibroblasts with regard to efficacy and tissue contractility in an animal model of stress urinary incontinence. Urology 68: , Lamb K, Gebhart GF, and Bielefeldt K. Increased nerve growth factor expression triggers bladder overactivity. J Pain 5: , Lee JY, Cannon TW, Pruchnic R, Fraser MO, Huard J, and Chancellor MB. The effects of periurethral muscle-derived stem cell injection on leak point pressure in a rat model of stress urinary incontinence. Int Urogynecol J Pelvic Floor Dysfunct 14: 31-37; discussion 37, Liang R, Ustinova EE, Patnam R, Fraser MO, Gutkin DW, and Pezzone MA. Enhanced expression of mast cell growth factor and mast cell activation in the bladder following the resolution of trinitrobenzenesulfonic acid (TNBS) colitis in female rats. Neurourol Urodyn, 2007.
22 Page 22 of Lowe EM, Anand P, Terenghi G, Williams-Chestnut RE, Sinicropi DV, and Osborne JL. Increased nerve growth factor levels in the urinary bladder of women with idiopathic sensory urgency and interstitial cystitis. Br J Urol 79: , Malloy BJ, Price DT, Price RR, Bienstock AM, Dole MK, Funk BL, Rudner XL, Richardson CD, Donatucci CF, and Schwinn DA. Alpha1-adrenergic receptor subtypes in human detrusor. J Urol 160: , Malykhina AP, Qin C, Greenwood-van Meerveld B, Foreman RD, Lupu F, and Akbarali HI. Hyperexcitability of convergent colon and bladder dorsal root ganglion neurons after colonic inflammation: mechanism for pelvic organ crosstalk. Neurogastroenterol Motil 18: , Manzo J, Vazquez MI, Cruz MR, Hernandez ME, Carrillo P, and Pacheco P. Fertility ratio in male rats: effects after denervation of two pelvic floor muscles. Physiol Behav 68: , Masuda H, Kim JH, Kihara K, Chancellor MB, de Groat WC, and Yoshimura N. Inhibitory roles of peripheral nitrergic mechanisms in capsaicininduced detrusor overactivity in the rat. BJU Int 100: , Meyer S, Schreyer A, De Grandi P, and Hohlfeld P. The effects of birth on urinary continence mechanisms and other pelvic-floor characteristics. Obstet Gynecol 92: , Michel MC and Vrydag W. Alpha1-, alpha2- and beta-adrenoceptors in the urinary bladder, urethra and prostate. Br J Pharmacol 147 Suppl 2: S88-119, 2006.
23 Page 23 of Milsom I, Abrams P, Cardozo L, Roberts RG, Thuroff J, and Wein AJ. How widespread are the symptoms of an overactive bladder and how are they managed? A population-based prevalence study. BJU Int 87: , Morch CD, Hu JW, Arendt-Nielsen L, and Sessle BJ. Convergence of cutaneous, musculoskeletal, dural and visceral afferents onto nociceptive neurons in the first cervical dorsal horn. Eur J Neurosci 26: , Mutoh S, Latifpour J, Saito M, and Weiss RM. Evidence for the presence of regional differences in the subtype specificity of muscarinic receptors in rabbit lower urinary tract. J Urol 157: , Nomiya M and Yamaguchi O. A quantitative analysis of mrna expression of alpha 1 and beta-adrenoceptor subtypes and their functional roles in human normal and obstructed bladders. J Urol 170: , Peng CW, Chen JJ, Chang HY, de Groat WC, and Cheng CL. External urethral sphincter activity in a rat model of pudendal nerve injury. Neurourol Urodyn 25: , Pezzone MA, Liang R, and Fraser MO. A model of neural cross-talk and irritation in the pelvis: implications for the overlap of chronic pelvic pain disorders. Gastroenterology 128: , Popeney C, Ansell V, and Renney K. Pudendal entrapment as an etiology of chronic perineal pain: diagnosis and treatment. Neurourol Urodyn, Qin C, Malykhina AP, Akbarali HI, and Foreman RD. Cross-organ sensitization of lumbosacral spinal neurons receiving urinary bladder input in rats with inflamed colon. Gastroenterology 129: , 2005.
24 Page 24 of Restorick JM and Mundy AR. The density of cholinergic and alpha and beta adrenergic receptors in the normal and hyper-reflexic human detrusor. Br J Urol 63: 32-35, Robert R, Prat-Pradal D, Labat JJ, Bensignor M, Raoul S, Rebai R, and Leborgne J. Anatomic basis of chronic perineal pain: role of the pudendal nerve. Surg Radiol Anat 20: 93-98, Sasaki K, Chancellor MB, Phelan MW, Yokoyama T, Fraser MO, Seki S, Kubo K, Kumon H, Groat WC, and Yoshimura N. Diabetic cystopathy correlates with a long-term decrease in nerve growth factor levels in the bladder and lumbosacral dorsal root Ganglia. J Urol 168: , Schwinn DA, Johnston GI, Page SO, Mosley MJ, Wilson KH, Worman NP, Campbell S, Fidock MD, Furness LM, Parry-Smith DJ, and et al. Cloning and pharmacological characterization of human alpha-1 adrenergic receptors: sequence corrections and direct comparison with other species homologues. J Pharmacol Exp Ther 272: , Seki S, Sasaki K, Fraser MO, Igawa Y, Nishizawa O, Chancellor MB, de Groat WC, and Yoshimura N. Immunoneutralization of nerve growth factor in lumbosacral spinal cord reduces bladder hyperreflexia in spinal cord injured rats. J Urol 168: , Smith AR, Hosker GL, and Warrell DW. The role of pudendal nerve damage in the aetiology of genuine stress incontinence in women. Br J Obstet Gynaecol 96: 29-32, 1989.
25 Page 25 of Snooks SJ, Swash M, Mathers SE, and Henry MM. Effect of vaginal delivery on the pelvic floor: a 5-year follow-up. Br J Surg 77: , Steers WD, Creedon DJ, and Tuttle JB. Immunity to nerve growth factor prevents afferent plasticity following urinary bladder hypertrophy. J Urol 155: , Steers WD, Kolbeck S, Creedon D, and Tuttle JB. Nerve growth factor in the urinary bladder of the adult regulates neuronal form and function. J Clin Invest 88: , Steers WD and Tuttle JB. Mechanisms of Disease: the role of nerve growth factor in the pathophysiology of bladder disorders. Nat Clin Pract Urol 3: , Stewart WF, Van Rooyen JB, Cundiff GW, Abrams P, Herzog AR, Corey R, Hunt TL, and Wein AJ. Prevalence and burden of overactive bladder in the United States. World J Urol 20: , Takahashi S, Homma Y, Fujishiro T, Hosaka Y, Kitamura T, and Kawabe K. Electromyographic study of the striated urethral sphincter in type 3 stress incontinence: evidence of myogenic-dominant damages. Urology 56: , Teleman PM, Lidfeldt J, Nerbrand C, Samsioe G, and Mattiasson A. Overactive bladder: prevalence, risk factors and relation to stress incontinence in middle-aged women. Bjog 111: , Ustinova EE, Fraser MO, and Pezzone MA. Colonic irritation in the rat sensitizes urinary bladder afferents to mechanical and chemical stimuli: an
26 Page 26 of afferent origin of pelvic organ cross-sensitization. Am J Physiol Renal Physiol 290: F , Ustinova EE, Gutkin DW, and Pezzone MA. Sensitization of pelvic nerve afferents and mast cell infiltration in the urinary bladder following chronic colonic irritation is mediated by neuropeptides. Am J Physiol Renal Physiol 292: F , Yokoyama T, Nozaki K, Fujita O, Nose H, Inoue M, and Kumon H. Role of C afferent fibers and monitoring of intravesical resiniferatoxin therapy for patients with idiopathic detrusor overactivity. J Urol 172: , Yoshimura N, Bennett NE, Hayashi Y, Ogawa T, Nishizawa O, Chancellor MB, de Groat WC, and Seki S. Bladder overactivity and hyperexcitability of bladder afferent neurons after intrathecal delivery of nerve growth factor in rats. J Neurosci 26: , Zettler C, Bridges DC, Zhou XF, and Rush RA. Detection of increased tissue concentrations of nerve growth factor with an improved extraction procedure. J Neurosci Res 46: , 1996.
27 Page 27 of FIGURE LEGENDS Fig. 1. Representative recordings of conscious cystometry in a sham rat without capsaicin pretreatment (A) and rats with pudendal nerve ligation (PNL) without (B) or with (C) capsaicin pretreatment. Intercontraction interval (ICI) and voided volume (VV) were decreased in the PNL rat without capsaicin pretreatment (B) compared with the sham rat without capsaicin pretreatment (A) (ICI: PNL; ± 26.3 vs sham; ± 36.0 sec., VV: PNL; 0.28 ± 0.03 vs sham; 0.40 ± 0.06 ml). In the PNL rat with capsaicin pretreatment (C), ICI and VV were increased to ± 69.3 sec. and 0.38 ± 0.08 ml, respectively. Fig. 2. Comparison of concentration-response curves of carbachol-induced contractions (A) and contractile forces (B) and phenylephrine-induced contractions (C) and contractile forces (D) in bladder muscle strips from sham and pudendal nerve ligation (PNL) groups. There were no significant differences between the curves of carbachol-induced contractions and contractile forces whereas there were significant differences (**p<0.01, *p<0.05) in the curves of phenylephrine-induced contractions and contractile forces between sham and PNL groups. Fig. 3. Levels of nerve growth factor (NGF) protein (A) and mrna (B) in the bladder of sham and pudendal nerve ligation (PNL) groups. Levels of NGF protein are standardized to tissue protein and expressed in pg/µg. Levels of NGF mrna are standardized to a housekeeping gene, -actin, and shown as relative expression. NGF protein levels of the bladder were significantly higher in PNL (70.9 ± 7.9 pg/µg) rats than in sham (44.8 ± 3.2
28 Page 28 of pg/µg) rats. NGF mrna levels were also significantly increased in PNL (2.6 ± 0.4) rats compared with sham (1.4 ± 0.2) rats. **p<0.01 indicates a significant difference compared with the sham group.
29 Page 29 of TABLES Table 1. Parameters of bladder activity during conscious cystometry in sham and pudendal nerve ligation (PNL) groups with or without capsaicin pretreatment. Sham PNL n BP (cmh 2 O) TP (cmh 2 O) MVP (cmh 2 O) ICI (sec.) without capsaicin ± ± ± ± ± ± ± 2.0 with capsaicin ± ± ± ± ± ± ± 2.1 without capsaicin ± ± ± ± 23.9 ## 0.30 ± 0.03 # 0.08 ± ± 3.8 with capsaicin ± ± ± ± 11.3 ** 0.41 ± 0.02 * 0.04 ± 0.01 * 88.0 ± 1.7 * VV (ml) RV (ml) VE (%) All parameters are represented as mean values ± SEM. BP: baseline pressure, TP: threshold pressure, MVP: maximal voiding pressure, ICI: intercontraction interval, VV: voided volume, RV: residual volume, VE: voiding efficiency. # p<0.05 and ## p<0.01; PNL rats without capsaicin pretreatment (PNL without capsaicin) vs sham rats without capsaicin pretreatment (Sham without capsaicin). * p<0.05 and ** p<0.01; PNL rats with capsaicin pretreatment (PNL with capsaicin) vs PNL rats without capsaicin pretreatment (PNL without capsaicin). There are no significant differences in any parameters in sham groups (with vs without capsaicin) or in capsaicin-treated groups (Sham vs PNL).
30 Page 30 of Table 2. Contractile responses of bladder muscle strips of sham and pudendal nerve ligation (PNL) groups to carbachol and phenylephrine. Carbachol Phenylephrine n EC 50 ( µm ) Emax ( g/mm2 ) Sham ± ± 0.7 PNL ± ± 0.3 Sham ± ± 0.1 PNL ± 1.3* 1.1 ± 0.1* All data are represented as mean values ± SEM. EC 50 : concentration required to produce 50% of the maximal contractile response. Emax: maximal contractile response. *p<0.05 indicates a significant difference compared with the sham group (Sham).
31 Page 31 of 33 Representative recordings of conscious cystometry in a sham rat without capsaicin pretreatment (A) and rats with pudendal nerve ligation (PNL) without (B) or with (C) capsaicin pretreatment. Intercontraction interval (ICI) and voided volume (VV) were decreased in the PNL rat without capsaicin pretreatment (B) compared with the sham rat without capsaicin pretreatment (A) (ICI: PNL; vs sham; sec., VV: PNL; vs sham; ml). In the PNL rat with capsaicin pretreatment (C), ICI and VV were increased to sec. and ml, respectively. 254x190mm (96 x 96 DPI)
32 Comparison of concentration-response curves of carbachol-induced contractions (A) and contractile forces (B) and phenylephrine-induced contractions (C) and contractile forces (D) in bladder muscle strips from sham and pudendal nerve ligation (PNL) groups. There were no significant differences between the curves of carbachol-induced contractions and contractile forces whereas there were significant differences (**p<0.01, *p<0.05) in the curves of phenylephrine-induced contractions and contractile forces between sham and PNL groups. 254x190mm (96 x 96 DPI) Page 32 of 33
33 Page 33 of 33 Levels of nerve growth factor (NGF) protein (A) and mrna (B) in the bladder of sham and pudendal nerve ligation (PNL) groups. Levels of NGF protein are standardized to tissue protein and expressed in pg/:g. Levels of NGF mrna are standardized to a housekeeping gene, -actin, and shown as relative expression. NGF protein levels of the bladder were significantly higher in PNL ( pg/:g) rats than in sham ( pg/:g) rats. NGF mrna levels were also significantly increased in PNL ( ) rats compared with sham ( ) rats. **p<0.01 indicates a significant difference compared with the sham group. 254x190mm (96 x 96 DPI)
Overactive Bladder; OAB. Aδ silent C. Adenosine triphosphate; ATP SD g n Key words
 25-32 2009 SD 200-270g n 28 4 1 2 3 4 PE-50 4-5 0.25 60 C Key words acupuncture stimulation overactive bladder rat bladder irritation C C fiber Received November 17, 2008; Accepted January 9, 2009 I Overactive
25-32 2009 SD 200-270g n 28 4 1 2 3 4 PE-50 4-5 0.25 60 C Key words acupuncture stimulation overactive bladder rat bladder irritation C C fiber Received November 17, 2008; Accepted January 9, 2009 I Overactive
Naoki Wada, Seiji Matsumoto, Masafumi Kita, Kazumi Hashizume and Hidehiro Kakizaki
 bs_bs_banner International Journal of Urology (1) 1, 15 1 doi: 1.1111/iju.157 Original Article: Clinical Investigation Decreased urinary nerve growth factor reflects prostatic volume reduction and relief
bs_bs_banner International Journal of Urology (1) 1, 15 1 doi: 1.1111/iju.157 Original Article: Clinical Investigation Decreased urinary nerve growth factor reflects prostatic volume reduction and relief
Normal micturition involves complex
 NEW TARGET FOR INTERVENTION: THE NEUROUROLOGY CONNECTION * Donald R. Ostergard, MD, FACOG ABSTRACT Urine storage and release are under the control of the parasympathetic, sympathetic, and somatic nervous
NEW TARGET FOR INTERVENTION: THE NEUROUROLOGY CONNECTION * Donald R. Ostergard, MD, FACOG ABSTRACT Urine storage and release are under the control of the parasympathetic, sympathetic, and somatic nervous
This Special Report supplement
 ...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
Original Article. Annals of Rehabilitation Medicine INTRODUCTION
 Original Article Ann Rehabil Med 2014;38(3):342-346 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.3.342 Annals of Rehabilitation Medicine Phasic Changes in Bladder Compliance
Original Article Ann Rehabil Med 2014;38(3):342-346 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.3.342 Annals of Rehabilitation Medicine Phasic Changes in Bladder Compliance
Neural Control of Lower Urinary Tract Function. William C. de Groat University of Pittsburgh Medical School
 Neural Control of Lower Urinary Tract Function William C. de Groat University of Pittsburgh Medical School Disclosures Current funding: NIH Grants, DK093424, DK-091253, DK-094905, DK-090006. Other financial
Neural Control of Lower Urinary Tract Function William C. de Groat University of Pittsburgh Medical School Disclosures Current funding: NIH Grants, DK093424, DK-091253, DK-094905, DK-090006. Other financial
The influence of distal colon irritation on the changes of cystometry parameters to esophagus and colon distentions
 ORIGINAL ARTICLE Vol. 42 (3): 594-602, May - June, 2016 doi: 10.1590/S1677-5538.IBJU.2015.0238 The influence of distal colon irritation on the changes of cystometry parameters to esophagus and colon distentions
ORIGINAL ARTICLE Vol. 42 (3): 594-602, May - June, 2016 doi: 10.1590/S1677-5538.IBJU.2015.0238 The influence of distal colon irritation on the changes of cystometry parameters to esophagus and colon distentions
Definitions of IC: U.S. perspective. Edward Stanford MD MS FACOG FACS Western Colorado
 Definitions of IC: U.S. perspective Edward Stanford MD MS FACOG FACS Western Colorado PURPOSE OF A DEFINITION? Identifies with specificity those patients who are most likely to have the disease. Identifies
Definitions of IC: U.S. perspective Edward Stanford MD MS FACOG FACS Western Colorado PURPOSE OF A DEFINITION? Identifies with specificity those patients who are most likely to have the disease. Identifies
3/20/10. Prevalence of OAB Men: 16.0% Women: 16.9% Prevalence of OAB with incontinence (OAB wet) Men: 2.6% Women: 9.3% Dry. Population (millions) Wet
 1 Prevalence of OAB Men: 16.0% Women: 16.9% Stewart WF, et al. World J Urol. 2003;20:327-336. Prevalence of OAB with incontinence (OAB wet) Men: 2.6% Women: 9.3% Stewart WF, et al. World J Urol. 2003;20:327-336.
1 Prevalence of OAB Men: 16.0% Women: 16.9% Stewart WF, et al. World J Urol. 2003;20:327-336. Prevalence of OAB with incontinence (OAB wet) Men: 2.6% Women: 9.3% Stewart WF, et al. World J Urol. 2003;20:327-336.
Duloxetine in women awaiting surgery
 DOI: 1.1111/j.1471-528.6.879.x www.blackwellpublishing.com/bjog Review article H Drutz Ontario Power Generation Building, Toronto, Ontario, Canada Correspondence: Prof. Dr H Drutz, Mount Sinai Hospital,
DOI: 1.1111/j.1471-528.6.879.x www.blackwellpublishing.com/bjog Review article H Drutz Ontario Power Generation Building, Toronto, Ontario, Canada Correspondence: Prof. Dr H Drutz, Mount Sinai Hospital,
Male lower urinary tract symptoms and α 1D -adrenoceptors. and Karl-Erik Andersson 2. Winston Salem, NC, USA
 Male lower urinary tract symptoms and α 1D -adrenoceptors Osamu Ishizuka, 1 Tetsuya Imamura, 1 Yoshiki Kurizaki, 1 Osamu Nishizawa 1 and Karl-Erik Andersson 2 1 Department of Urology, Shinshu University
Male lower urinary tract symptoms and α 1D -adrenoceptors Osamu Ishizuka, 1 Tetsuya Imamura, 1 Yoshiki Kurizaki, 1 Osamu Nishizawa 1 and Karl-Erik Andersson 2 1 Department of Urology, Shinshu University
Ben Herbert Alex Wojtowicz
 Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Urethral closure mechanisms under sneeze-induced stress condition in rats: a new animal model for evaluation of stress urinary incontinence
 Am J Physiol Regul Integr Comp Physiol 285: R356 R365, 2003. First published May 15, 2003; 10.1152/ajpregu.00010.2003. Urethral closure mechanisms under sneeze-induced stress condition in rats: a new animal
Am J Physiol Regul Integr Comp Physiol 285: R356 R365, 2003. First published May 15, 2003; 10.1152/ajpregu.00010.2003. Urethral closure mechanisms under sneeze-induced stress condition in rats: a new animal
Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology
 Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology Ospedale San Giovanni di Dio, Gorizia, Italy ANATOMY URINARY CONTINENCE
Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology Ospedale San Giovanni di Dio, Gorizia, Italy ANATOMY URINARY CONTINENCE
Role of Animal Models
 Division of Urology, Department of Surgery, Duke University Medical Center Institute for Medical Research, Durham Veteran s Affairs Medical Center Role of Animal Models Matthew O. Fraser, PhD 9th Annual
Division of Urology, Department of Surgery, Duke University Medical Center Institute for Medical Research, Durham Veteran s Affairs Medical Center Role of Animal Models Matthew O. Fraser, PhD 9th Annual
What is on the Horizon in Drug Therapy for OAB?
 What is on the Horizon in Drug Therapy for OAB? K-E Andersson, MD, PhD Wake Forest Institute for Regenerative Medicine Wake Forest University School of Medicine Winston Salem, North Carolina Disclosures
What is on the Horizon in Drug Therapy for OAB? K-E Andersson, MD, PhD Wake Forest Institute for Regenerative Medicine Wake Forest University School of Medicine Winston Salem, North Carolina Disclosures
INJ. Original Article INTRODUCTION. Int Neurourol J 2011;15: pissn eissn
 Original Article Int Neurourol J 2011;15:199-205 pissn 2093-4777 eissn 2093-6931 International Neurourology Journal Effects of Spinal and Peripheral Injection of α1a or α1d Adrenoceptor Antagonists on
Original Article Int Neurourol J 2011;15:199-205 pissn 2093-4777 eissn 2093-6931 International Neurourology Journal Effects of Spinal and Peripheral Injection of α1a or α1d Adrenoceptor Antagonists on
Neurogenic bladder. Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder.
 Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Summary. Neuro-urodynamics. The bladder cycle. and voiding. 14/12/2015. Neural control of the LUT Initial assessment Urodynamics
 Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
Characterization of bladder and external urethral activity in mice with or without spinal cord injury a comparison study with rats
 Am J Physiol Regul Integr Comp Physiol 31: R752 R758, 216. First published January 27, 216; doi:1.1152/ajpregu.45.215. Characterization of bladder and external urethral activity in mice with or without
Am J Physiol Regul Integr Comp Physiol 31: R752 R758, 216. First published January 27, 216; doi:1.1152/ajpregu.45.215. Characterization of bladder and external urethral activity in mice with or without
Characterization of bladder and external urethral activity in mice with or without spinal cord injury a comparison study with rats
 Am J Physiol Regul Integr Comp Physiol 31: R752 R758, 216. First published January 27, 216; doi:1.1152/ajpregu.45.215. Characterization of bladder and external urethral activity in mice with or without
Am J Physiol Regul Integr Comp Physiol 31: R752 R758, 216. First published January 27, 216; doi:1.1152/ajpregu.45.215. Characterization of bladder and external urethral activity in mice with or without
Objectives. Prevalence of Urinary Incontinence URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS
 URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
Overactive Bladder: Diagnosis and Approaches to Treatment
 Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
The Time-Frequency Analysis of the Pudendo-to-Pudendal Nerve and Pelvic-to-Pudendal Nerve Reflexes in Anesthetized Intact Rats
 Journal of Medical and Biological Engineering, 24(1): 17-22 17 The Time-Frequency Analysis of the Pudendo-to-Pudendal Nerve and Pelvic-to-Pudendal Nerve Reflexes in Anesthetized Intact Rats Hui-Yi Chang
Journal of Medical and Biological Engineering, 24(1): 17-22 17 The Time-Frequency Analysis of the Pudendo-to-Pudendal Nerve and Pelvic-to-Pudendal Nerve Reflexes in Anesthetized Intact Rats Hui-Yi Chang
Physiologic Anatomy and Nervous Connections of the Bladder
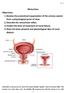 Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
The Neurogenic Bladder
 The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
Efficacy of Silodosin for Relieving Benign Prostatic Obstruction: Prospective Pressure Flow Study
 Efficacy of Silodosin for Relieving Benign Prostatic Obstruction: Prospective Pressure Flow Study Yoshihisa Matsukawa,* Momokazu Gotoh, Tomonori Komatsu, Yasuhito Funahashi, Naoto Sassa and Ryohei Hattori
Efficacy of Silodosin for Relieving Benign Prostatic Obstruction: Prospective Pressure Flow Study Yoshihisa Matsukawa,* Momokazu Gotoh, Tomonori Komatsu, Yasuhito Funahashi, Naoto Sassa and Ryohei Hattori
INCONTINENCE. Continence and Pelvic Floor Rehabilitation TYPES OF INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE 11/08/2015
 INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
Signal transduction underlying the control of urinary bladder smooth muscle tone Puspitoayu, E.
 UvA-DARE (Digital Academic Repository) Signal transduction underlying the control of urinary bladder smooth muscle tone Puspitoayu, E. Link to publication Citation for published version (APA): Puspitoayu,
UvA-DARE (Digital Academic Repository) Signal transduction underlying the control of urinary bladder smooth muscle tone Puspitoayu, E. Link to publication Citation for published version (APA): Puspitoayu,
Diagnosis and Treatment of Overactive Bladder
 Diagnosis and Treatment of Overactive Bladder Case study: Mr. Lin I I have started to rush out of meetings to go to the toilet I I need to void every one hour I I used to be quite active. This is becoming
Diagnosis and Treatment of Overactive Bladder Case study: Mr. Lin I I have started to rush out of meetings to go to the toilet I I need to void every one hour I I used to be quite active. This is becoming
Mr. GIT KAH ANN. Pakar Klinikal Urologi Hospital Kuala Lumpur.
 Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
The Evidence for Antimuscarinic Agents in Female Mixed Urinary Incontinence
 european urology supplements 5 (2006) 849 853 available at www.sciencedirect.com journal homepage: www.europeanurology.com The Evidence for Antimuscarinic Agents in Female Mixed Urinary Incontinence Stefano
european urology supplements 5 (2006) 849 853 available at www.sciencedirect.com journal homepage: www.europeanurology.com The Evidence for Antimuscarinic Agents in Female Mixed Urinary Incontinence Stefano
Safety and Pain-relief Efficacy of Urethral Catheter with Local-anesthetic Injection Port
 Shinshu Med J, 65⑹:355~359, 2017 Safety and Pain-relief Efficacy of Urethral Catheter with Local-anesthetic Injection Port Teppei Yamamoto *, Masashi Shiozaki, Yuji Shimojima, Tomomi Haba Tomohiko Oguchi,
Shinshu Med J, 65⑹:355~359, 2017 Safety and Pain-relief Efficacy of Urethral Catheter with Local-anesthetic Injection Port Teppei Yamamoto *, Masashi Shiozaki, Yuji Shimojima, Tomomi Haba Tomohiko Oguchi,
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist
 Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Urodynamic and electrophysiological investigations in neuro-urology
 Urodynamic and electrophysiological investigations in neuro-urology Pr. Gerard Amarenco Neuro-Urology and Pelvic-Floor Investigations Department Tenon Hospital, Assistance Publique Hôpitaux de Paris, Er6,
Urodynamic and electrophysiological investigations in neuro-urology Pr. Gerard Amarenco Neuro-Urology and Pelvic-Floor Investigations Department Tenon Hospital, Assistance Publique Hôpitaux de Paris, Er6,
Overactive bladder: prevalence, risk factors and relation to stress incontinence in middle-aged women.
 Overactive bladder: prevalence, risk factors and relation to stress incontinence in middle-aged women. Teleman, Pia; Lidfeldt, Jonas; Nerbrand, Christina; Samsioe, Göran; Mattiasson, Anders Published in:
Overactive bladder: prevalence, risk factors and relation to stress incontinence in middle-aged women. Teleman, Pia; Lidfeldt, Jonas; Nerbrand, Christina; Samsioe, Göran; Mattiasson, Anders Published in:
Comparison of Symptom Severity and Treatment Response in Patients with Incontinent and Continent Overactive Bladder
 European Urology European Urology 48 (2005) 110 115 Female UrologyöIncontinence Comparison of Symptom Severity and Treatment Response in Patients with Incontinent and Continent Overactive Bladder Martin
European Urology European Urology 48 (2005) 110 115 Female UrologyöIncontinence Comparison of Symptom Severity and Treatment Response in Patients with Incontinent and Continent Overactive Bladder Martin
A Novel Cystometric Model of Pelvic Floor Dysfunction After Rabbit Pelvic Floor Noxious Electrical Stimulation
 ORIGINAL ARTICLE A Novel Cystometric Model of Pelvic Floor Dysfunction After Rabbit Pelvic Floor Noxious Electrical Stimulation Amy D. Dobberfuhl, MD,* Sara Spettel, MD, Catherine Schuler, BA, Andrew H.
ORIGINAL ARTICLE A Novel Cystometric Model of Pelvic Floor Dysfunction After Rabbit Pelvic Floor Noxious Electrical Stimulation Amy D. Dobberfuhl, MD,* Sara Spettel, MD, Catherine Schuler, BA, Andrew H.
Efficacy and Adverse Effects of Solifenacin in the Treatment of Lower Urinary Tract Symptoms in Patients With Overactive Bladder
 Urol Sci 21;21(1):38 43 ORIGINAL ARTICLE Efficacy and Adverse Effects of Solifenacin in the Treatment of Lower Urinary Tract Symptoms in Patients With Overactive Bladder Yih-Chou Chen, Chia-Yen Chen, Hann-Chorng
Urol Sci 21;21(1):38 43 ORIGINAL ARTICLE Efficacy and Adverse Effects of Solifenacin in the Treatment of Lower Urinary Tract Symptoms in Patients With Overactive Bladder Yih-Chou Chen, Chia-Yen Chen, Hann-Chorng
Mechanisms of Disease: central nervous system involvement in overactive bladder syndrome
 Mechanisms of Disease: central nervous system involvement in overactive bladder syndrome Karl-Erik Andersson SUMMARY The pathophysiology of overactive bladder syndrome (OABS) and detrusor overactivity
Mechanisms of Disease: central nervous system involvement in overactive bladder syndrome Karl-Erik Andersson SUMMARY The pathophysiology of overactive bladder syndrome (OABS) and detrusor overactivity
URINARY INCONTINENCE. Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara
 URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION Author : SIMONA T RADAELLI Categories : Vets Date : July
Vet Times The website for the veterinary profession https://www.vettimes.co.uk TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION Author : SIMONA T RADAELLI Categories : Vets Date : July
Neural control of the lower urinary tract in health and disease
 Neural control of the lower urinary tract in health and disease Jalesh N. Panicker MD, DM, FRCP Consultant Neurologist and Clinical lead in Uro-Neurology The National Hospital for Neurology and Neurosurgery
Neural control of the lower urinary tract in health and disease Jalesh N. Panicker MD, DM, FRCP Consultant Neurologist and Clinical lead in Uro-Neurology The National Hospital for Neurology and Neurosurgery
A New Method for Urinary Bladder. Hyperactivity in Conscious Rats
 A New Method for Urinary Bladder Hyperactivity in Conscious Rats January 2010 Manabu MITOBE A New Method for Urinary Bladder Hyperactivity in Conscious Rats A Dissertation Submitted to the Graduate School
A New Method for Urinary Bladder Hyperactivity in Conscious Rats January 2010 Manabu MITOBE A New Method for Urinary Bladder Hyperactivity in Conscious Rats A Dissertation Submitted to the Graduate School
NEUROGENIC BLADDER. Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph
 NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
THE ACONTRACTILE BLADDER - FACT OR FICTION?
 THE ACONTRACTILE BLADDER - FACT OR FICTION? Jacob Golomb Department of Urology Chaim Sheba Medical Center Tel Hashomer NEUROGENIC UNDERACTIVE DETRUSOR Central (complete/incomplete): Spinal cord injury-
THE ACONTRACTILE BLADDER - FACT OR FICTION? Jacob Golomb Department of Urology Chaim Sheba Medical Center Tel Hashomer NEUROGENIC UNDERACTIVE DETRUSOR Central (complete/incomplete): Spinal cord injury-
Urinary nerve growth factor levels could be a biomarker for overactive bladder symptom: a meta-analysis
 Urinary nerve growth factor levels could be a biomarker for overactive bladder symptom: a meta-analysis H.C. Qu, S. Yan, X.L. Zhang, X.W. Zhu, Y.L. Liu and P. Wang Department of Urological Surgery, The
Urinary nerve growth factor levels could be a biomarker for overactive bladder symptom: a meta-analysis H.C. Qu, S. Yan, X.L. Zhang, X.W. Zhu, Y.L. Liu and P. Wang Department of Urological Surgery, The
Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial
 ORIGINAL ARTICLE Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial Tahereh Eftekhar 1, Nastaran Teimoory 1, Elahe Miri 1, Abolghasem Nikfallah 2,
ORIGINAL ARTICLE Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial Tahereh Eftekhar 1, Nastaran Teimoory 1, Elahe Miri 1, Abolghasem Nikfallah 2,
Neurophysiology of Lower Urinary Tract Function and Dysfunction Naoki Yoshimura, MD, PhD, Michael B. Chancellor, MD
 TREATMENT OF OVERACTIVE BLADDER Neurophysiology of Lower Urinary Tract Function and Dysfunction Naoki Yoshimura, MD, PhD, Michael B. Chancellor, MD Department of Urology, University of Pittsburgh, Pittsburgh,
TREATMENT OF OVERACTIVE BLADDER Neurophysiology of Lower Urinary Tract Function and Dysfunction Naoki Yoshimura, MD, PhD, Michael B. Chancellor, MD Department of Urology, University of Pittsburgh, Pittsburgh,
New Treatment Modalities for Benign Prostatic Hyperplasia. Seung-June Oh, MD Department of Urology, Seoul National University Hospital
 New Treatment Modalities for Benign Prostatic Hyperplasia Seung-June Oh, MD Department of Urology, Seoul National University Hospital Options for Treating BPH Pharmacotherapy blocker Agents for BPH + OAB
New Treatment Modalities for Benign Prostatic Hyperplasia Seung-June Oh, MD Department of Urology, Seoul National University Hospital Options for Treating BPH Pharmacotherapy blocker Agents for BPH + OAB
Impact of urethral catheterization on uroflow during pressure-flow study
 Research Report Impact of urethral catheterization on uroflow during pressure-flow study Journal of International Medical Research 2016, Vol. 44(5) 1034 1039! The Author(s) 2016 Reprints and permissions:
Research Report Impact of urethral catheterization on uroflow during pressure-flow study Journal of International Medical Research 2016, Vol. 44(5) 1034 1039! The Author(s) 2016 Reprints and permissions:
Alpha antagonists from initial concept to routine clinical practice
 european urology 50 (2006) 635 642 available at www.sciencedirect.com journal homepage: www.europeanurology.com Editorial 50th Anniversary Alpha antagonists from initial concept to routine clinical practice
european urology 50 (2006) 635 642 available at www.sciencedirect.com journal homepage: www.europeanurology.com Editorial 50th Anniversary Alpha antagonists from initial concept to routine clinical practice
The impact of overactive bladder on quality of life in south of China
 The impact of overactive bladder on quality of life in south of China Dong Chen, Yining Li * Department of Urology, Second Affiliated Hospital of Fujian Medical University, Quanzhou, 362000, China. * Corresponding
The impact of overactive bladder on quality of life in south of China Dong Chen, Yining Li * Department of Urology, Second Affiliated Hospital of Fujian Medical University, Quanzhou, 362000, China. * Corresponding
Regulation of the Urinary Bladder Chapter 26
 Regulation of the Urinary Bladder Chapter 26 Anatomy 1. The urinary bladder is smooth muscle lined internally by transitional epithelium and externally by the parietal peritoneum. Contraction of the smooth
Regulation of the Urinary Bladder Chapter 26 Anatomy 1. The urinary bladder is smooth muscle lined internally by transitional epithelium and externally by the parietal peritoneum. Contraction of the smooth
We have heard a great deal about "overactive" bladder recently. But what
 BLADDER DYSFUNCTION Differential Diagnosis and Treatment of Impaired Bladder Emptying Naoki Yoshimura, MD, PhD, Michael B. Chancellor, MD Department of Urology, University of Pittsburgh School of Medicine,
BLADDER DYSFUNCTION Differential Diagnosis and Treatment of Impaired Bladder Emptying Naoki Yoshimura, MD, PhD, Michael B. Chancellor, MD Department of Urology, University of Pittsburgh School of Medicine,
Anatomical and Functional Results of Pelvic Organ Prolapse Mesh Repair: A Prospective Study of 105 Cases
 International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
Bill Landry BScPT, BScH, MCPA, CAFCI Family Physiotherapy Centre of London
 Bill Landry BScPT, BScH, MCPA, CAFCI blandry@fpclondon.com Family Physiotherapy Centre of London Objectives To describe the scope of post-prostatectomy incontinence To describe what s been done To provide
Bill Landry BScPT, BScH, MCPA, CAFCI blandry@fpclondon.com Family Physiotherapy Centre of London Objectives To describe the scope of post-prostatectomy incontinence To describe what s been done To provide
Autonomic Nervous System Dr. Ali Ebneshahidi
 Autonomic Nervous System Dr. Ali Ebneshahidi Nervous System Divisions of the nervous system The human nervous system consists of the central nervous System (CNS) and the Peripheral Nervous System (PNS).
Autonomic Nervous System Dr. Ali Ebneshahidi Nervous System Divisions of the nervous system The human nervous system consists of the central nervous System (CNS) and the Peripheral Nervous System (PNS).
Urodynamic study before and after radical porstatectomy 가톨릭의대성바오로병원김현우
 Urodynamic study before and after radical porstatectomy 가톨릭의대성바오로병원김현우 Introduction Radical prostatectomy - treatment of choice for patients with localized prostate cancer. Urinary incontinence and/or
Urodynamic study before and after radical porstatectomy 가톨릭의대성바오로병원김현우 Introduction Radical prostatectomy - treatment of choice for patients with localized prostate cancer. Urinary incontinence and/or
CHAPTER 6. M.D. Eckhardt, G.E.P.M. van Venrooij, T.A. Boon. hoofdstuk :49 Pagina 89
 hoofdstuk 06 19-12-2001 09:49 Pagina 89 Urethral Resistance Factor (URA) Versus Schäfer s Obstruction Grade and Abrams-Griffiths (AG) Number in the Diagnosis of Obstructive Benign Prostatic Hyperplasia
hoofdstuk 06 19-12-2001 09:49 Pagina 89 Urethral Resistance Factor (URA) Versus Schäfer s Obstruction Grade and Abrams-Griffiths (AG) Number in the Diagnosis of Obstructive Benign Prostatic Hyperplasia
Urethral pressure measurement in stress incontinence: does it help?
 Int Urol Nephrol (2009) 41:491 495 DOI 10.1007/s11255-008-9506-9 UROLOGY - ORIGINAL PAPER Urethral pressure measurement in stress incontinence: does it help? Bassem S. Wadie Æ Ahmed S. El-Hefnawy Received:
Int Urol Nephrol (2009) 41:491 495 DOI 10.1007/s11255-008-9506-9 UROLOGY - ORIGINAL PAPER Urethral pressure measurement in stress incontinence: does it help? Bassem S. Wadie Æ Ahmed S. El-Hefnawy Received:
Yuan et al., Afr J Tradit Complement Altern Med. (2014) 11(4):
 IZALPININ FROM FRUITS OF ALPINIA OXYPHYLLA WITH ANTAGONISTIC ACTIVITY AGAINST THE RAT BLADDER CONTRACTILITY 120 Yuan Yuan 1,5#, Yin-Feng Tan 2,3,4#, Peng Xu 2,3,4, Hailong Li 2,3,4, Yong-Hui Li 2,3,4,
IZALPININ FROM FRUITS OF ALPINIA OXYPHYLLA WITH ANTAGONISTIC ACTIVITY AGAINST THE RAT BLADDER CONTRACTILITY 120 Yuan Yuan 1,5#, Yin-Feng Tan 2,3,4#, Peng Xu 2,3,4, Hailong Li 2,3,4, Yong-Hui Li 2,3,4,
Involuntary Detrusor Contractions: Correlation of Urodynamic Data to Clinical Categories
 Neurourology and Urodynamics 20:249±257 (2001) Involuntary Detrusor Contractions: Correlation of Urodynamic Data to Clinical Categories Lauri J. Romanzi, Asnat Groutz, Dianne M. Heritz, and Jerry G. Blaivas*
Neurourology and Urodynamics 20:249±257 (2001) Involuntary Detrusor Contractions: Correlation of Urodynamic Data to Clinical Categories Lauri J. Romanzi, Asnat Groutz, Dianne M. Heritz, and Jerry G. Blaivas*
Urinary incontinence (UI) affects as many
 EXPLORING NEW HORIZONS IN STRESS INCONTINENCE: THE NEUROUROLOGY CONNECTION W. Glenn Hurt, MD* ABSTRACT As many as one-third of women are affected by urinary incontinence, the most common of which being
EXPLORING NEW HORIZONS IN STRESS INCONTINENCE: THE NEUROUROLOGY CONNECTION W. Glenn Hurt, MD* ABSTRACT As many as one-third of women are affected by urinary incontinence, the most common of which being
Physiology & Neurophysiology of lower U.T.
 Physiology & Neurophysiology of lower U.T. Classification of voiding dysfunction Evaluation of a child with voiding dysfunction Management Storage Ø Adequate volume of urine Ø At LOW pressure Ø With NO
Physiology & Neurophysiology of lower U.T. Classification of voiding dysfunction Evaluation of a child with voiding dysfunction Management Storage Ø Adequate volume of urine Ø At LOW pressure Ø With NO
Urogynecology in EDS. Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018
 Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Flowmetry/ pelvic floor electromyographic findings in patients with detrusor overactivity
 ORIGINAL ARTICLE Vol. 41 (3): 521-526, May - June, 2015 doi: 10.1590/S1677-5538.IBJU.2014.0204 Flowmetry/ pelvic floor electromyographic findings in patients with detrusor overactivity Farshid Alizadeh
ORIGINAL ARTICLE Vol. 41 (3): 521-526, May - June, 2015 doi: 10.1590/S1677-5538.IBJU.2014.0204 Flowmetry/ pelvic floor electromyographic findings in patients with detrusor overactivity Farshid Alizadeh
Efficacy and Safety of Propiverine and Solifenacin for the Treatment of Female Patients with Overactive Bladder: A Crossover Study
 LUTS () 3, 36 4 ORIGINAL ARTICLE Efficacy and Safety of Propiverine and Solifenacin for the Treatment of Female Patients with Overactive Bladder: A Crossover Study Naoki WADA, Masaki WATANABE, Masafumi
LUTS () 3, 36 4 ORIGINAL ARTICLE Efficacy and Safety of Propiverine and Solifenacin for the Treatment of Female Patients with Overactive Bladder: A Crossover Study Naoki WADA, Masaki WATANABE, Masafumi
Chapter 23. Micturition and Renal Insufficiency
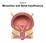 Chapter 23 Micturition and Renal Insufficiency Voiding Urine Between acts of urination, the bladder is filling. detrusor muscle relaxes urethral sphincters are tightly closed accomplished by sympathetic
Chapter 23 Micturition and Renal Insufficiency Voiding Urine Between acts of urination, the bladder is filling. detrusor muscle relaxes urethral sphincters are tightly closed accomplished by sympathetic
Diagnosis and Mangement of Nocturia in Adults
 Diagnosis and Mangement of Nocturia in Adults Christopher Chapple Professor of Urology Sheffield Teaching Hospitals University of Sheffield Sheffield Hallam University UK 23 rd October 2015 Terminology
Diagnosis and Mangement of Nocturia in Adults Christopher Chapple Professor of Urology Sheffield Teaching Hospitals University of Sheffield Sheffield Hallam University UK 23 rd October 2015 Terminology
김준철 가톨릭대학교의과대학비뇨기과학교실
 비뇨기계자율신경병증의치료 김준철 가톨릭대학교의과대학비뇨기과학교실 Introduction Urologic complications have increasingly become a concern in those affected by DM Genitourinary problems are included among these complications, related
비뇨기계자율신경병증의치료 김준철 가톨릭대학교의과대학비뇨기과학교실 Introduction Urologic complications have increasingly become a concern in those affected by DM Genitourinary problems are included among these complications, related
Bristol Urological Institute, Bristol, UK. The Warrell Unit, St Mary s Hospital, Manchester. UK.
 Disclosures Basic Principles of Urodynamics Andrew Gammie Bristol Urological Institute, Bristol, UK Albyn, Andromeda, Laborie, Mediwatch, MMS Project sponsorship T-Doc LLC Trial sponsorship with grateful
Disclosures Basic Principles of Urodynamics Andrew Gammie Bristol Urological Institute, Bristol, UK Albyn, Andromeda, Laborie, Mediwatch, MMS Project sponsorship T-Doc LLC Trial sponsorship with grateful
The new International Continence Society
 ROLE OF CYSTOMETRY IN EVALUATING PATIENTS WITH OVERACTIVE BLADDER ADAM J. FLISSER AND JERRY G. BLAIVAS ABSTRACT Overactive bladder (OAB) can be caused by a variety of conditions. We believe that cystometrography
ROLE OF CYSTOMETRY IN EVALUATING PATIENTS WITH OVERACTIVE BLADDER ADAM J. FLISSER AND JERRY G. BLAIVAS ABSTRACT Overactive bladder (OAB) can be caused by a variety of conditions. We believe that cystometrography
PHYSIOLOGICAL SOCIETY SYMPOSIUM: THE PHYSIOLOGY AND PATHOPHYSIOLOGY OF THE LOWER URINARY TRACT THE ACTIVATION OF BLADDER WALL AFFERENT NERVES
 Experimental Physiology (1999). 84, 131-136 Printed in Great Britain PHYSIOLOGICAL SOCIETY SYMPOSIUM: THE PHYSIOLOGY AND PATHOPHYSIOLOGY OF THE LOWER URINARY TRACT THE ACTIVATION OF BLADDER WALL AFFERENT
Experimental Physiology (1999). 84, 131-136 Printed in Great Britain PHYSIOLOGICAL SOCIETY SYMPOSIUM: THE PHYSIOLOGY AND PATHOPHYSIOLOGY OF THE LOWER URINARY TRACT THE ACTIVATION OF BLADDER WALL AFFERENT
Neurourology, especially the video urodynamic
 NEUROUROLOGIC FINDINGS WITH APPLICABILITY TO INCONTINENCE AND URETHRAL FUNCTION * Edward J. McGuire, MD ABSTRACT Neurourology is applicable to urinary incontinence and obstructive uropathy in the general
NEUROUROLOGIC FINDINGS WITH APPLICABILITY TO INCONTINENCE AND URETHRAL FUNCTION * Edward J. McGuire, MD ABSTRACT Neurourology is applicable to urinary incontinence and obstructive uropathy in the general
Neurological control of the bladder in health and disease
 Section 1 Chapter 1 Neurological control of pelvic organ functions Neurological control of the bladder in health and disease Derek J. Griffiths and Apostolos Apostolidis Peripheral control of micturition
Section 1 Chapter 1 Neurological control of pelvic organ functions Neurological control of the bladder in health and disease Derek J. Griffiths and Apostolos Apostolidis Peripheral control of micturition
New approaches in the pharmacological treatment of stress urinary incontinence
 International Journal of Gynecology and Obstetrics 86 Suppl. 1 (2004) S1 S5 New approaches in the pharmacological treatment of stress urinary incontinence Keywords: Stress urinary incontinence; Epidemiology;
International Journal of Gynecology and Obstetrics 86 Suppl. 1 (2004) S1 S5 New approaches in the pharmacological treatment of stress urinary incontinence Keywords: Stress urinary incontinence; Epidemiology;
Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests. Amelyn R.
 Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests Amelyn R. Rafael, MD 1 Functions of the Urinary Bladder 1. storage of urine 150 cc 1 st urge
Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests Amelyn R. Rafael, MD 1 Functions of the Urinary Bladder 1. storage of urine 150 cc 1 st urge
Prevalence of the Overactive Bladder Syndrome byapplying the International Continence Society Definition
 European Urology European Urology 48 (2005) 622 627 Female Urology ^ Incontinence Prevalence of the Overactive Bladder Syndrome byapplying the International Continence Society Definition Christian Temml
European Urology European Urology 48 (2005) 622 627 Female Urology ^ Incontinence Prevalence of the Overactive Bladder Syndrome byapplying the International Continence Society Definition Christian Temml
Various Types. Ralph Boling, DO, FACOG
 Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
The lower urinary tract is composed of the bladder and the urethra the 2
 URINARY INCONTINENCE IN WOMEN Neurophysiology of Stress Urinary Incontinence Michael B. Chancellor, MD, Naoki Yoshimura, MD, PhD Department of Urology, University of Pittsburgh School of Medicine, Pittsburgh,
URINARY INCONTINENCE IN WOMEN Neurophysiology of Stress Urinary Incontinence Michael B. Chancellor, MD, Naoki Yoshimura, MD, PhD Department of Urology, University of Pittsburgh School of Medicine, Pittsburgh,
The Praxis FES System and Bladder/Bowel Management in Patients with Spinal Cord Injury
 The Praxis FES System and Bladder/Bowel Management in Patients with Spinal Cord Injury Brian J. Benda 1, Thierry Houdayer 2, Graham Creasey 3, Randal R. Betz 1, Brian T. Smith 1 *, Therese E. Johnston
The Praxis FES System and Bladder/Bowel Management in Patients with Spinal Cord Injury Brian J. Benda 1, Thierry Houdayer 2, Graham Creasey 3, Randal R. Betz 1, Brian T. Smith 1 *, Therese E. Johnston
Training a Wayward Bladder
 D. James Ballard, PT, DPT, GCS The University of Utah, Dept. of Physical Therapy Training a Wayward Bladder Agenda 1. Discuss urinary incontinence 2. Review pelvic floor and lower urinary tract functional
D. James Ballard, PT, DPT, GCS The University of Utah, Dept. of Physical Therapy Training a Wayward Bladder Agenda 1. Discuss urinary incontinence 2. Review pelvic floor and lower urinary tract functional
Management of Female Stress Incontinence
 Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
α 1 adrenergic receptor antagonists versus placebo for female lower urinary tract symptoms: A meta analysis
 EXPERIMENTAL AND THERAPEUTIC MEDICINE 10: 251-256, 2015 α 1 adrenergic receptor antagonists versus placebo for female lower urinary tract symptoms: A meta analysis PENG ZHANG 1, WAN LI HU 1, BEI CHENG
EXPERIMENTAL AND THERAPEUTIC MEDICINE 10: 251-256, 2015 α 1 adrenergic receptor antagonists versus placebo for female lower urinary tract symptoms: A meta analysis PENG ZHANG 1, WAN LI HU 1, BEI CHENG
Antimuscarinic drugs in detrusor overactivity and the overactive bladder syndrome: motor or sensory actions?
 Review Article SENSORY ACTIONS OF ANTIMUSCARINICS FINNEY et al. Antimuscarinic drugs in detrusor overactivity and the overactive bladder syndrome: motor or sensory actions? STEVEN M. FINNEY, KARL-ERIK
Review Article SENSORY ACTIONS OF ANTIMUSCARINICS FINNEY et al. Antimuscarinic drugs in detrusor overactivity and the overactive bladder syndrome: motor or sensory actions? STEVEN M. FINNEY, KARL-ERIK
Urinary Incontinence in Women: Never an Acceptable Consequence of Aging
 Urinary Incontinence in Women: Never an Acceptable Consequence of Aging Catherine A. Matthews, MD Associate Professor Chief, Urogynecology and Pelvic Reconstructive Surgery University of North Carolina,
Urinary Incontinence in Women: Never an Acceptable Consequence of Aging Catherine A. Matthews, MD Associate Professor Chief, Urogynecology and Pelvic Reconstructive Surgery University of North Carolina,
Autonomic Nervous System
 Autonomic Nervous System Keri Muma Bio 6 Organization of the Nervous System Efferent Division Somatic Nervous System Voluntary control Effector = skeletal muscles Muscles must be excited by a motor neuron
Autonomic Nervous System Keri Muma Bio 6 Organization of the Nervous System Efferent Division Somatic Nervous System Voluntary control Effector = skeletal muscles Muscles must be excited by a motor neuron
Taking Control of your Bladder, or. Don't make me laugh when laughter isn't the best medicine: a discussion on urinary incontinence
 Taking Control of your Bladder, or Don't make me laugh when laughter isn't the best medicine: a discussion on urinary incontinence Brett Vassallo, MD, FACOG, FAC Female Pelvic Medicine and Reconstructive
Taking Control of your Bladder, or Don't make me laugh when laughter isn't the best medicine: a discussion on urinary incontinence Brett Vassallo, MD, FACOG, FAC Female Pelvic Medicine and Reconstructive
La vescica iperattiva: dalla diagnosi ai nuovi approcci terapeutici
 La Prostata nel Mirino Napoli, 1 dicembre 2016 La vescica iperattiva: dalla diagnosi ai nuovi approcci terapeutici Giorgio Annoni Cattedra e Scuola di Specializzazione in Geriatria Università degli Studi
La Prostata nel Mirino Napoli, 1 dicembre 2016 La vescica iperattiva: dalla diagnosi ai nuovi approcci terapeutici Giorgio Annoni Cattedra e Scuola di Specializzazione in Geriatria Università degli Studi
phenylephrine - phenylephrine
 * * Fischer 344 carbachol carbachol M phenylephrine - phenylephrine [ 3 H] quinuclidinyl benzilate (QNB) [ 3 H] QNB QOL quality of life 1 3) 2 Krebs-Henseleit 37 0.1 10 ml organ bath 3 7T-15-240 3 mm NaCl
* * Fischer 344 carbachol carbachol M phenylephrine - phenylephrine [ 3 H] quinuclidinyl benzilate (QNB) [ 3 H] QNB QOL quality of life 1 3) 2 Krebs-Henseleit 37 0.1 10 ml organ bath 3 7T-15-240 3 mm NaCl
Validation of a simple patient questionnaire to assist self-detection of overactive bladder
 æoriginal PAPER Validation of a simple patient questionnaire to assist self-detection of overactive bladder A study in general practice Arnfinn Seim 1, Trygve Talseth 2, Harriet Haukeland 3, Kjetil Høye
æoriginal PAPER Validation of a simple patient questionnaire to assist self-detection of overactive bladder A study in general practice Arnfinn Seim 1, Trygve Talseth 2, Harriet Haukeland 3, Kjetil Høye
Anticholinergic medication use for female overactive bladder in the ambulatory setting in the United States.
 Página 1 de 6 PubMed darifenacin vs solifenacin Display Settings:, Sorted by Recently Added Results: 5 1. Int Urogynecol J. 2013 Oct 25. [Epub ahead of print] Anticholinergic medication use for female
Página 1 de 6 PubMed darifenacin vs solifenacin Display Settings:, Sorted by Recently Added Results: 5 1. Int Urogynecol J. 2013 Oct 25. [Epub ahead of print] Anticholinergic medication use for female
Overactive bladder: current understanding and future issues
 DOI: 10.1111/j.1471-0528.2006.01081.x www.blackwellpublishing.com/bjog Review article Overactive bladder: current understanding and future issues I Milsom Department of Obstetrics and Gynecology, Sahlgrenska
DOI: 10.1111/j.1471-0528.2006.01081.x www.blackwellpublishing.com/bjog Review article Overactive bladder: current understanding and future issues I Milsom Department of Obstetrics and Gynecology, Sahlgrenska
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS
 Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
URINARY SYSTEM. Urinary System
 URINARY SYSTEM Urinary System Kidney Functions Excretion Regulation of blood volume and pressure Regulation of electrolyte and ph levels Kidney Structure Gross Anatomy Fibrous Capsule Renal Cortex Renal
URINARY SYSTEM Urinary System Kidney Functions Excretion Regulation of blood volume and pressure Regulation of electrolyte and ph levels Kidney Structure Gross Anatomy Fibrous Capsule Renal Cortex Renal
Review Article Pelvic Floor Dysfunction, Body Excreta Incontinence and Continence
 Cronicon OPEN ACCESS GYNAECOLOGY Review Article Pelvic Floor Dysfunction, Body Excreta Incontinence and Continence Abdel Karim M El Hemaly 1 * and Laila ASE Mousa 1 1 Professor of Obstetrics and gynaecology,
Cronicon OPEN ACCESS GYNAECOLOGY Review Article Pelvic Floor Dysfunction, Body Excreta Incontinence and Continence Abdel Karim M El Hemaly 1 * and Laila ASE Mousa 1 1 Professor of Obstetrics and gynaecology,
Treatment Outcomes of Tension-free Vaginal Tape Insertion
 Are the Treatment Outcomes of Tension-free Vaginal Tape Insertion the Same for Patients with Stress Urinary Incontinence with or without Intrinsic Sphincter Deficiency? A Retrospective Study in Hong Kong
Are the Treatment Outcomes of Tension-free Vaginal Tape Insertion the Same for Patients with Stress Urinary Incontinence with or without Intrinsic Sphincter Deficiency? A Retrospective Study in Hong Kong
Role of vasopressin V 1A receptor in the urethral closure reflex in rats
 Am J Physiol Renal Physiol 300: F976 F982, 2011. First published January 12, 2011; doi:10.1152/ajprenal.00658.2010. Role of vasopressin V 1A receptor in the urethral closure reflex in rats Hiroyuki Ueno,
Am J Physiol Renal Physiol 300: F976 F982, 2011. First published January 12, 2011; doi:10.1152/ajprenal.00658.2010. Role of vasopressin V 1A receptor in the urethral closure reflex in rats Hiroyuki Ueno,
Management of LUTS after TURP and MIT
 Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
