Review Article Pelvic Floor Dysfunction, Body Excreta Incontinence and Continence
|
|
|
- Arlene Kelley
- 6 years ago
- Views:
Transcription
1 Cronicon OPEN ACCESS GYNAECOLOGY Review Article Pelvic Floor Dysfunction, Body Excreta Incontinence and Continence Abdel Karim M El Hemaly 1 * and Laila ASE Mousa 1 1 Professor of Obstetrics and gynaecology, Faculty of Medicine, Al Azhar University, Cairo, Egypt *Corresponding Author: Abdel Karim M El Hemaly, 1Professor of Obstetrics and gynaecology, Faculty of Medicine, Al Azhar University, Cairo, Egypt. Received: October 29, 2015; Published: November 02, 2015 Abstract Anatomy: Pelvic floor dysfunction, better called pelvic organs dysfunction, is widely present in women particularly around menopause. We believe that every organ in the body has a strong collagen chassis. Injury of the chassis will distort the organ, lead to dysfunction, abnormal position and chronic pain. The strongest layer of the pelvic floor is the second layer, which is a fibro-muscular layer. It consists of the pelvic diaphragm muscles and the strong endopelvic fascia. The endopelvic fascia consists mainly of collagen tissue and has condensation of the collagen creating the pelvic ligaments (the utero-sacral, the great transverse cervical and the pubo-vesical ligaments). The strong second layer keeps the pelvic organ s tracts in their proper site. Any weakness in the second layer leads to displacement of the pelvic organs and chronic pelvic pain. Micturition and the IUS: The internal urethral sphincter (IUS) is a collagen-muscle tissue cylinder that extends from the bladder neck down to the perineal membrane in men and women. The muscle has its nerve supply from alpha sympathetic fibers from T10- L 2. After training, in the second stage of micturition, there is high alpha sympathetic tone that keeps the IUS contracted and the urethra closed and empty all the time except on voiding. Defecation and the IAS: The internal anal sphincter (IAS) is a collagen-muscle tissue cylinder that surrounds the anal canal, with the external anal sphincter surrounding its lower part. The nerve supply to the IAS is alpha-sympathetic nerves from T 10 to L2. Training creates high alpha-sympathetic tone at the IAS that keeps it contracted and the anal canal closed and empty all the time. Pathophysiology: Injury of the pelvic collagen leads to voiding troubles, urinary incontinence (UI), fecal incontinence (FI), genital prolapse and chronic pelvic pain. Keywords: Pelvic floor dysfunction; Women; Menopause; Urinary Incontinence Introduction The pelvic floor consists of all the structures closing the pelvic outlet from the peritoneum superiorly to the skin inferiorly. It consists of three strata. The first stratum is the pelvic peritoneum. The second stratum is the pelvic diaphragm, which is a funnel-shaped fibromuscular partition. It consists of the pelvic diaphragm muscles and the endopelvic fascia. The endopelvic fascia consists mainly of collagen fibers, with its condensations, the pelvic ligaments (the utero-sacral, cardinal transverse cervical and pubo-cervical ligaments). The third stratum is the perineum, which consists of the perineal membrane, perineal muscles, fascia, and the skin. Pathophysiology: 2-29 The endopelvic fascia with its condensations, the pelvic ligaments, consists mainly of collagen. Estrogen supports the vitality and strength of the pelvic collagen, so that estrogen deficiency leads to weak atrophic pelvic ligaments with its sequel genital prolapse. The female pelvis contains three major tracts that lie on and traverse the pelvic floor. These tracts are the urinary bladder and the urethra anteriorly, the female genital tract in the middle, and the rectum and anal canal posteriorly.
2 171 We believe that every organ in the body has strong collagen chassis. Injury of the collagen chassis will lead to abnormality in the shape, site, and the functions of that organ. The contributions of the pelvic floor to the structural support and the functions of the three major tracts have been the subject of controversy. With increasing age, women can develop voiding troubles, such as urgency, overactive bladder (OAB), frequency, nocturia, and stress urinary incontinence (SUI). Other concomitant troubles that occur are genital prolapse, fecal incontinence (FI), and chronic pelvic pain (CPP). All these symptoms can be associated to a greater or lesser extent with pelvic floor defects 1. We think that these troubles are, more accurately, associated with defects in the pelvic organs 2, 5 & 8. Childbirth is the main traumatic factor to the pelvic organs and the pelvic floor. The trauma is more severe especially after difficult labor, instrumental labor, frequent and repeated labors. Infections, (uro-genital), chronic and recurrent infections, can cause degeneration of the pelvic collagen adding to its weakness. Estrogens support the pelvic collagen, so estrogen deficiency leads to its atrophy that adds to its weakness. Rarely there is congenital weakness of the collagen leading to virginal genital prolapse. Urinary Incontinence: 2, 3, 4, 5, 6, 8, 9, 10, 11, 22, 28 & 29. The internal urethral sphincter (IUS) is a collagen-muscle tissue cylinder that extends from the bladder neck down to the perineal membrane in men and women. The muscle has its nerve supply from the thoraco-lumbar alpha sympathetic chain, fibers from T10- L 2. Micturition has two stages, the first stage, before training, as the bladder is full, stretch receptors send impulses along pelvic sensory nerves, S 2, 3 & 4 to the sacral centers. The sacral para-sympathetic nerves, S 2, 3 & 4 induce contraction of the detrusor muscle and emptying of the bladder. The second stage: the mother starts to teach and train her infant/child how to hold up and not to void until she puts her/him on the pot, and with growing up, in the toilet according to social circumstances. After training, in the second stage of micturition, there will be an acquired high alpha sympathetic tone that keeps the IUS contracted and the urethra closed and empty all the time until favorable social circumstances. On desire/or need, the person voluntary will inhibit the acquired high alpha-sympathetic tone at the IUS, relaxing the sphincter allow the flow of urine. The external urethral sphincter is a voluntary muscle innervated with somatic nerves. Injury of the IUS or its nerve supply will lead to voiding troubles. The lacerations usually affect the collagen tissue layer of the IUS mostly caused by childbirth. The lacerations usually affect the whole length leading to mixed type of urinary incontinence. We can demonstrate this by pelvic floor imaging (ultrasound, MRI, CT scan). On imaging, (figures 1-7) there will be seen an open urethra with irregular torn wall. If the laceration is mainly in the upper part of the cylinder of the IUS, this will allow urine to enter the upper part of the urethra on stress, that will initiates a sudden desire to void, over active bladder (OAB) (figures 1B, 2A, 3B & 5), otherwise urine will leak, urge and urgency incontinence. If the injury affects mainly the lower part of the IUS, this will lead to genuine stress urinary incontinence (figure 4). Normally, there is contraction of the IUS due to the acquired high alpha- sympathetic tone. The urethra is closed and empty. This is in contrast to torn IUS, which affects the upper part causing OAB. There are lacerations in the walls of the IAS, and the anal canal is open Figure 1: MRI pictures of the pelvis, (A) there is lacerations of the IAS which leads to an open anal canal. There is a small funneling of the urethra. Image (B), both the IUS and the IAS are intact leading to a closed empty urethra and a closed empty anal canal. Image (C), both the IUS and the IAS are torn with an open urethra in its upper end (funneling), this leads to OAB; and an open anal canal, which leads to FI.
3 172 Figure 2: MRI images, sagittal sections; Image (A) there are torn both IUS, which causes funneling of the bladder neck leading to OAB; and torn IAS that leads to FI. In image (B), there is an intact IAS with closed and empty anal canal, but there is torn IUS in its upper end causing funneling of the bladder neck that leads to urge and urgency incontinence. Figure 3: Image (A) is 3Dimension ultrasound (3DUS), that shows torn IUS with an open urethra, especially its upper end with funneling of the bladder neck. Image (B) is an MR image, which shows torn IUS, the lacerations affect the whole length. Figure 4: An image with 3DUS, that shows an open urethra with torn IUS more marked in its lower part. The patient suffers from genuine SUI.
4 173 Figure 5: An image with 3DUS, it shows an open urethra with torn IUS. The lacerations are all through the entire length of the IUS. The patient complains of mixed type of UI. Figure 6: An image with 3DUS, it shows an open anal canal with torn IAS. The lacerations are all through the entire length of the IAS, which cause FI. Figure 7: MR images (A) is sagittal section, which shows an open anal canal with torn IAS in a patient who suffers FI. Image (B) is a coronal section, which shows an open anal canal with torn IAS, with some stool leaking.
5 174 Fecal Incontinence: 2, 3, 4, 5, 7 & 14; figures 1A, B & C, 2B, 6 & 7) The internal anal sphincter (IAS) is a collagen-muscle tissue cylinder that surrounds the anal canal, with the external anal sphincter surrounding its lower part. The nerve supply to the IAS is alpha-sympathetic nerves from T10 to L2. Defecation has two stages, the first stage, before training, as the rectum is full, stretch receptors send impulses along pelvic sensory nerves, S 2, 3 & 4 to the sacral centers. The sacral para-sympathetic nerves, S 2, 3 & 4 induce contraction of the rectal and pelvic colon muscles and emptying of the rectum irrespective of time and place. The second stage: the mother starts to teach and train her infant/ child how to hold up and not to defecate until she puts her/him on the pot, and with growing up, in the toilet according to social circumstances. After training, in the second stage of defecation, there will be an acquired high alpha sympathetic tone that keeps the IAS contracted and the anal canal closed and empty all the time until favorable social circumstances. On desire/or need, the person voluntary will inhibit the acquired high alpha-sympathetic tone at the IAS, relaxing the sphincter allow the passage of flatus and/or stools. Training creates high alpha-sympathetic tone at the IAS that keeps it contracted and the anal canal closed and empty all the time. Childbirth may cause injury and lacerations of the collagen chassis of the IAS leading to its weakness and subsequent leak of flatus and/ or feces on rise of abdominal pressure, fecal incontinence (FI). Sometimes, childbirth causes complete perineal tear (third and fourth degree tear) where anal sphincters, the internal and external are torn leading to FI. Repair of the external anal sphincter and missing to repair the torn IAS explains the poor results of the repair done. Estrogen deficiency and chronic or repeated infections lead to weakness of the collagen layer of the IAS. This will aggravate the IAS weakness. Another important traumatic factor of torn weak IAS is anal intercourse. The pelvic diaphragm muscles, mainly the levator ani muscles keep an acute angle between the rectum and the anal canal during rest; this is another factor of maintaining fecal continence. On defecation the levators relaxes turning the rectum and the anal canal into one axis to facilitate the passage of flatus and/or the feces. Genital Prolapse: 4, 5, 8 & 10. The vagina is a cylinder of collagen-elastic-muscle tissues that extends from the vulva externally, in an upward and backward direction. The uterus, pierce its upper end from the front. The strong collagen sheet is an important factor of keeping the up-backward direction of the vagina. The pelvic ligaments support the upper part of the vagina and keep their site to the lateral pelvic walls. Torn weak pelvic ligaments will lead to vault and uterine prolapse. Childbirth trauma causes stretching of vaginal walls with injury of the collagen chassis leading to vaginal prolapse. The IUS is intimately lying on the anterior vaginal wall and laceration will affect its collagen chassis as well. This will lead to anterior vaginal wall prolapse and urinary incontinence, (UI). Similarly, childbirth trauma will lacerate the collagen chassis of both the posterior vaginal wall and the IAS. The result is posterior vaginal wall prolapse and fecal incontinence, (FI). Conclusion: Every body organ has a strong collagen chassis. Injury of the chassis will lead to anatomical, functional disturbances and pain until treated. The pelvic diaphragm is an essential element in keeping the pelvic organs in situ to perform their functions properly. In addition, the state of the pelvic organs and their nerve supply are essential factors in their proper anatomy and functions. Lacerations and weakness of the IUS lead to UI. Lacerations and weakness of the IAS cause FI. Lacerations of the endopelvic fascia and its condensations the pelvic ligaments induce uterine, vault prolapse and chronic pelvic pain. Lacerations and laxity of the vagina produce vaginal prolapse.
6 175 Bibliography 1. A de Boer., et al. Pelvic Organ Prolapse and Overactive Bladder, Review Article. Neurourology and Urodynamics 29.1 (2010): Abdel Karim El Hemaly., et al. Continence. International Journal of Gynecology, Obstetrics and Neonatal Care 2.2 (2015): Abdel Karim El Hemaly., et al. Continence and Incontinence: How Can You Gain Continence? Scholars press November Abdel Karim M El Hemaly., et al. Imaging of the Pelvic Floor. Current Medical Imaging Reviews 10.3 (2014): Abdel Karim M El Hemaly., et al. Pelvic Floor Dysfunction and its Reconstructive Surgery: Novel Concepts Abdel Karim M El Hemaly., et al. Micturition and Urinary Incontinence. Journal of Nephrology and Urology Research 2.1 (2014): Abdel Karim M. El Hemaly., et al. A Novel Concept on the Patho-Physiology of Defecation and Fecal Incontinence (FI) in Women- Moreover, Its Reconstructive Surgery. FECAL INCOTINENCE Causes, Management AND OUTME. INTECH Publication (2014) Abdel Karim M El Hemaly., et al. Al- Adwani in Pelvic Floor Dysfunction And Its Surgical Treatment: Novel Concepts On Pelvic Organs Dysfunction And Their Reconstructive Surgery, in Abdul Kareem A. Al- Adwani eds (2013). 9. Abdel Karim M. El Hemaly., et al. Micturition and Urinary Incontinence. Journal of Nephrology and Urology Research 2.1 (2014): Abdel Karim M El Hemaly., et al. Pelvic Floor Dysfunction, the Role of Imaging and Reconstructive Surgery. Donald School Journal of Ultrasound in Obstetrics and Gynecology 7.1 (2013): Abdel Karim M. El Hemaly., et al. Ultrasonic Assessment of the Urethra and the Vagina in Normal Continent Women and Women Suffering from Stress Urinary Incontinence and Vaginal Prolapse. Donald School Journal of Ultrasound in Obstetrics and Gynecology 5.4 (2011): Abdel Karim M. El Hemaly., et al. Ultrasound Assessment of the Internal Anal Sphincter in Women with Fecal Incontinence and Posterior Vaginal Wall Prolapse (Rectocele). Donald School Journal of Ultrasound in Obstetrics and Gynecology 5.4 (2011): Abdel Karim M. El Hemaly., et al. Imaging the Internal Urethral Sphincter and the Vagina in Normal Women and Women Suffering from Stress Urinary Incontinence and Vaginal Prolapse. Gynaecologia Et Perinatologia 18.4 (2009): Abdel Karim M. El Hemaly., et al. A Novel Concept: The Role of the internal Anal sphincter (IAS) in defecation and fecal incontinence. Gynaecologia Et Perinatologia 19.2 (2010): Abdel Karim M El Hemaly., et al. Surgical Treatment of Stress Urinary Incontinence, Fecal Incontinence and Vaginal Prolapse By A Novel Operation Urethro- Ano-Vaginoplasty. Gynaecologia Et Perinatologia 19.3 (2010): Abdel Karim M. El Hemaly., et al. Urethro-vaginoplasty. Detursor Overactivity (DO), Mixed Urinary Incontinence and Anterior Vaginal Wall Descent. 17. Abdel Karim M. El Hemaly., et al. Urethro-raphy a new technique for surgical management of Stress Urinary Incontinence. 18. Abdel Karim M. El Hemaly., et al. Urethro-raphy The New Operation for the treatment of stress urinary incontinence, SUI, detrusor instability, DI, and mixed-type of urinary incontinence; short and long term results. 19. Abdel Karim M. El Hemaly., et al. Menopause, and Voiding troubles. obgyn.net El Hemaly AKMA and Mousa LA. Micturition and Urinary Continence. International Journal of Gynecology & Obstetrics 52.3 (1996): Abdel Karim M. El Hemaly. Urinary incontinence in gynecology, a review article (2010). 22. El Hemaly AKMA. Nocturnal Enuresis: Pathogenesis and Treatment. International Urogynecology Journal - and Pelvic Floor 9.3 (1998) El Hemaly AKMA and Mousa LAE. Stress Urinary Incontinence, a New Concept. European Journal of Obstetrics & Gynecology (1996): El Hemaly AKMA and Kandil IM. Stress Urinary Incontinence SUI facts and fiction. Is SUI a puzzle?! (2010). 25. Abdel Karim El Hemaly., et al. Evidence based Facts on the Pathogenesis and Management of SUI.
7 26. Abdel Karim M. El Hemaly., et al. Urethro-plasty, a Novel Operation based on a New Concept, for the Treatment of Stress Urinary Incontinence (2010). 27. Ibrahim M Kandil., et al. Ultrasonic Assessment of the Internal Urethral Sphincter in Stress Urinary Incontinence. The Internet Journal of Gynecology and Obstetrics 2.1 (2003). 28. Abdel Karim M El Hemaly., et al. Nocturnal Enureses: A Novel Concept on its pathogenesis and Treatment. (2010). 29. Abdel Karim M El Hemaly. Nocturnal Enureses: An Update on the pathogenesis and Treatment. Psychiatric Times Volume 2 Issue 2 November 2015 All rights are reserved by Abdel Karim M El Hemaly and Laila ASE Mousa.
LAPAROSCOPIC REPAIR OF PELVIC FLOOR
 LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,100 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,100 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,100 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,100 116,000 120M Open access books available International authors and editors Downloads Our
Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology
 Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology Ospedale San Giovanni di Dio, Gorizia, Italy ANATOMY URINARY CONTINENCE
Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology Ospedale San Giovanni di Dio, Gorizia, Italy ANATOMY URINARY CONTINENCE
Ultrasonic Assessment of the Internal Urethral Sphincter in Stress Urinary Incontinence
 ISPUB.COM The Internet Journal of Gynecology and Obstetrics Volume 2 Number 1 Ultrasonic Assessment of the Internal Urethral Sphincter in Stress Urinary Incontinence I Kandil, A El Hemaly, M Radwan Citation
ISPUB.COM The Internet Journal of Gynecology and Obstetrics Volume 2 Number 1 Ultrasonic Assessment of the Internal Urethral Sphincter in Stress Urinary Incontinence I Kandil, A El Hemaly, M Radwan Citation
Gynecology Dr. Sallama Lecture 3 Genital Prolapse
 Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Urogynecology ICD-9 to ICD-10 Crosswalks
 1100 Wayne Ave, Suite 825 Silver Spring, MD 20910 301.273.0570 Fax 301.273.0778 info@augs.org www.augs.org Urogynecology ICD-9 to ICD-10 Crosswalks ICD 9 ICD 9 Description ICD 10 Code ICD 10 Description
1100 Wayne Ave, Suite 825 Silver Spring, MD 20910 301.273.0570 Fax 301.273.0778 info@augs.org www.augs.org Urogynecology ICD-9 to ICD-10 Crosswalks ICD 9 ICD 9 Description ICD 10 Code ICD 10 Description
Management of Female Stress Incontinence
 Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M.
 UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
Inferior Pelvic Border
 Pelvis + Perineum Pelvic Cavity Enclosed by bony, ligamentous and muscular wall Contains the urinary bladder, ureters, pelvic genital organs, rectum, blood vessels, lymphatics and nerves Pelvic inlet (superior
Pelvis + Perineum Pelvic Cavity Enclosed by bony, ligamentous and muscular wall Contains the urinary bladder, ureters, pelvic genital organs, rectum, blood vessels, lymphatics and nerves Pelvic inlet (superior
Content. Terminology Anatomy Aetiology Presentation Classification Management
 Prolapse Content Terminology Anatomy Aetiology Presentation Classification Management Terminology Prolapse Descent of pelvic organs into the vagina Cystocele ant. vaginal wall involving bladder Uterine
Prolapse Content Terminology Anatomy Aetiology Presentation Classification Management Terminology Prolapse Descent of pelvic organs into the vagina Cystocele ant. vaginal wall involving bladder Uterine
Urinary Bladder. Prof. Imran Qureshi
 Urinary Bladder Prof. Imran Qureshi Urinary Bladder It develops from the upper end of the urogenital sinus, which is continuous with the allantois. The allantois degenerates and forms a fibrous cord in
Urinary Bladder Prof. Imran Qureshi Urinary Bladder It develops from the upper end of the urogenital sinus, which is continuous with the allantois. The allantois degenerates and forms a fibrous cord in
Physiologic Anatomy and Nervous Connections of the Bladder
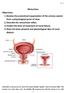 Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
Ben Herbert Alex Wojtowicz
 Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
INCONTINENCE. Continence and Pelvic Floor Rehabilitation TYPES OF INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE 11/08/2015
 INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
Dana Alrafaiah. - Amani Nofal. - Ahmad Alsalman. 1 P a g e
 - 2 - Dana Alrafaiah - Amani Nofal - Ahmad Alsalman 1 P a g e This lecture will discuss five topics as follows: 1- Arrangement of pelvic viscera. 2- Muscles of Pelvis. 3- Blood Supply of pelvis. 4- Nerve
- 2 - Dana Alrafaiah - Amani Nofal - Ahmad Alsalman 1 P a g e This lecture will discuss five topics as follows: 1- Arrangement of pelvic viscera. 2- Muscles of Pelvis. 3- Blood Supply of pelvis. 4- Nerve
Objectives. Prevalence of Urinary Incontinence URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS
 URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
Postpartum Complications
 ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
The Management of Female Urinary Incontinence. Part 1: Aetiology and Investigations
 The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
Prolapse and Urogynae. By Sarah Rangan & Daniel Warrell
 Prolapse and Urogynae By Sarah Rangan & Daniel Warrell Anatomy and physiology of the pelvic supports The pelvic floor supports the pelvic viscera and vaginal, urethral and rectal openings Endopelvic fascial
Prolapse and Urogynae By Sarah Rangan & Daniel Warrell Anatomy and physiology of the pelvic supports The pelvic floor supports the pelvic viscera and vaginal, urethral and rectal openings Endopelvic fascial
ICD-10 Common Codes for Pelvic Rehab Providers
 ICD-10 Common Codes for Pelvic Rehab Providers With ICD-10 changes taking place in 2015, we thought it would be helpful to put together a bit of a cheat sheet for our pelvic health providers. Keep in mind
ICD-10 Common Codes for Pelvic Rehab Providers With ICD-10 changes taking place in 2015, we thought it would be helpful to put together a bit of a cheat sheet for our pelvic health providers. Keep in mind
17 th European congress of Physical Rehabilitation Medicine. 38th SIMFER congress
 17 th European congress of Physical Rehabilitation Medicine 38th SIMFER congress European Rehabilitation: Quality, Evidence, Efficacy and Effectiveness Venice, May 23 27 2010 THE PHYSIATRIST AND URO-GYNECOLOGICAL
17 th European congress of Physical Rehabilitation Medicine 38th SIMFER congress European Rehabilitation: Quality, Evidence, Efficacy and Effectiveness Venice, May 23 27 2010 THE PHYSIATRIST AND URO-GYNECOLOGICAL
Prolapse and Urogynae Incontinence. Lucy Tiffin and Hannah Wheldon-Holmes
 Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
John Laughlin 4 th year Cardiff University Medical Student
 John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
Pelvic Floor Ultrasound Imaging. Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague)
 Pelvic Floor Ultrasound Imaging Workshop IUGA 2015 Nice Faculty: Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague) The use of translabial ultrasound
Pelvic Floor Ultrasound Imaging Workshop IUGA 2015 Nice Faculty: Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague) The use of translabial ultrasound
Urogynaecology & Prolapse. Alexander Denning and Leifa Jennings
 + Urogynaecology & Prolapse Alexander Denning and Leifa Jennings + Contents What even is prolapse / urogynaecology? Pelvic floor anatomy Prolapse Urinary incontinence Prevention The end (woot) + Urogynaecology
+ Urogynaecology & Prolapse Alexander Denning and Leifa Jennings + Contents What even is prolapse / urogynaecology? Pelvic floor anatomy Prolapse Urinary incontinence Prevention The end (woot) + Urogynaecology
Pelvic Floor and More.. Urinary Continence. Urinary Incontinence. Normal Bladder Function
 Pelvic Floor and More.. Jo Pitts Women s and Men s Health Physiotherapist Milton Keynes University Hospital Women s and Men s Health Physiotherapy at MKUH Pregnancy-related back and pelvic girdle pain
Pelvic Floor and More.. Jo Pitts Women s and Men s Health Physiotherapist Milton Keynes University Hospital Women s and Men s Health Physiotherapy at MKUH Pregnancy-related back and pelvic girdle pain
High-field (3T) magnetic resonance defecography with functional assessment of the evacuation phase: A pictorial essay
 High-field (3T) magnetic resonance defecography with functional assessment of the evacuation phase: A pictorial essay Poster No.: C-430 Congress: ECR 2009 Type: Educational Exhibit Topic: Abdominal and
High-field (3T) magnetic resonance defecography with functional assessment of the evacuation phase: A pictorial essay Poster No.: C-430 Congress: ECR 2009 Type: Educational Exhibit Topic: Abdominal and
By:Dr:ISHRAQ MOHAMMED
 By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
Questionnaire for Incontinent Patients
 Questionnaire for Incontinent Patients Name Date: Date of birth: weight: height: Vaginal deliveries: Caesarean Sections: profession: No Yes Sometimes Yes 50% or more Do you lose urine during sneezing or
Questionnaire for Incontinent Patients Name Date: Date of birth: weight: height: Vaginal deliveries: Caesarean Sections: profession: No Yes Sometimes Yes 50% or more Do you lose urine during sneezing or
The Egyptian Journal of Hospital Medicine (April 2018) Vol. 71 (3), Page
 The Egyptian Journal of Hospital Medicine (April 2018) Vol. 71 (3), Page 2742-2750 Role of dynamic MRI in assessment of Pelvic Floor Dysfunction in Females Nada Ahmed Hussein, Naglaa Hussein Shebrya, Nermeen
The Egyptian Journal of Hospital Medicine (April 2018) Vol. 71 (3), Page 2742-2750 Role of dynamic MRI in assessment of Pelvic Floor Dysfunction in Females Nada Ahmed Hussein, Naglaa Hussein Shebrya, Nermeen
Clinical Curriculum: Urogynecology
 Updated July 201 Clinical Curriculum: Urogynecology GOAL: The primary goal of the Urogynecology rotation at the University of Alabama at Birmingham (UAB) is to train physicians to have a broad knowledge
Updated July 201 Clinical Curriculum: Urogynecology GOAL: The primary goal of the Urogynecology rotation at the University of Alabama at Birmingham (UAB) is to train physicians to have a broad knowledge
Female Pelvic Medicine & Reconstructive Surgery
 Female Pelvic Medicine & Reconstructive Surgery APPLICATION FOR NEW FELLOWSHIP Name of Institution: McGill University Location: Royal Victoria Hospital (Glen Site), St Mary s Hospital Centre Type of Fellowship:
Female Pelvic Medicine & Reconstructive Surgery APPLICATION FOR NEW FELLOWSHIP Name of Institution: McGill University Location: Royal Victoria Hospital (Glen Site), St Mary s Hospital Centre Type of Fellowship:
ig. 2. The organs and their outlet tubes.
 Fig. 1. Birth-related laxity. The diagram shows the baby s head severely stretching ligaments and other tissues in and outside the vagina. This may cause various degrees of looseness, prolapse of the bladder
Fig. 1. Birth-related laxity. The diagram shows the baby s head severely stretching ligaments and other tissues in and outside the vagina. This may cause various degrees of looseness, prolapse of the bladder
Imaging of Pelvic Floor Weakness. Dr Susan Kouloyan-Ilic Radiologist Epworth Medical Imaging The Women s, Melbourne
 Imaging of Pelvic Floor Weakness Dr Susan Kouloyan-Ilic Radiologist Epworth Medical Imaging The Women s, Melbourne Outline Overview and Epidemiology Risk Factors, Causes and Results Review of Relevant
Imaging of Pelvic Floor Weakness Dr Susan Kouloyan-Ilic Radiologist Epworth Medical Imaging The Women s, Melbourne Outline Overview and Epidemiology Risk Factors, Causes and Results Review of Relevant
Pelvic Floor Disorders. Amir Darakhshan MD FRCS (Gen Surg) Consultant Colorectal and General Surgeon
 Pelvic Floor Disorders Amir Darakhshan MD FRCS (Gen Surg) Consultant Colorectal and General Surgeon What is Pelvic Floor Disorder Surgical perspective symptoms of RED, FI or prolapse on the background
Pelvic Floor Disorders Amir Darakhshan MD FRCS (Gen Surg) Consultant Colorectal and General Surgeon What is Pelvic Floor Disorder Surgical perspective symptoms of RED, FI or prolapse on the background
Prolapse & Urogynaecology. Hester Mannion and Fabi Sica
 Prolapse & Urogynaecology Hester Mannion and Fabi Sica Take home messages Prolapse and associated incontinence is very common It has a devastating effect on the QoL of the patient and their partner Strategies
Prolapse & Urogynaecology Hester Mannion and Fabi Sica Take home messages Prolapse and associated incontinence is very common It has a devastating effect on the QoL of the patient and their partner Strategies
Neurogenic bladder. Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder.
 Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
10/15/2012. Pelvic Pain and Dysfunction
 Pain and Holly Bommersbach PT, MPT Angela De La Cruz PT, MPT Pain which occurs in the perineal and/or anal areas Pain in the lower abdomen, low back and/or pelvic girdle Pain may often affect other areas,
Pain and Holly Bommersbach PT, MPT Angela De La Cruz PT, MPT Pain which occurs in the perineal and/or anal areas Pain in the lower abdomen, low back and/or pelvic girdle Pain may often affect other areas,
Uterine prolapse & Fistulas. Raja Nursing Instructor RN, DCHN, Post RN. BSc.N
 Uterine prolapse & Fistulas Raja Nursing Instructor RN, DCHN, Post RN. BSc.N 31/03/2016 Objectives 1. Review the anatomy & physiology of female reproductive system 2. Discuss the causes, pathophysiology,
Uterine prolapse & Fistulas Raja Nursing Instructor RN, DCHN, Post RN. BSc.N 31/03/2016 Objectives 1. Review the anatomy & physiology of female reproductive system 2. Discuss the causes, pathophysiology,
CHERRY BAKER AND TRACEY GJERTSEN BSC MCSP HCPC INTRODUCTION TO DIAMOND TRAINING REHAB AND PERFORMANCE FOR PELVIC POWER
 CHERRY BAKER AND TRACEY GJERTSEN BSC MCSP HCPC INTRODUCTION TO DIAMOND TRAINING REHAB AND PERFORMANCE FOR PELVIC POWER What is it? Where is it? Breathing Graded relaxation Incontinence Stress Incontinence
CHERRY BAKER AND TRACEY GJERTSEN BSC MCSP HCPC INTRODUCTION TO DIAMOND TRAINING REHAB AND PERFORMANCE FOR PELVIC POWER What is it? Where is it? Breathing Graded relaxation Incontinence Stress Incontinence
Pelvic Support Problems
 AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
PREVENTING URINARY INCONTINENCE through PELVIC FLOOR REHABILITATION in DISABLED ELDERLY
 PREVENTING URINARY INCONTINENCE through PELVIC FLOOR REHABILITATION in DISABLED ELDERLY Paolo DI BENEDETTO Lecturer, Tor Vergata University, Rome, Italy Former Director of Rehabilitation Department Institute
PREVENTING URINARY INCONTINENCE through PELVIC FLOOR REHABILITATION in DISABLED ELDERLY Paolo DI BENEDETTO Lecturer, Tor Vergata University, Rome, Italy Former Director of Rehabilitation Department Institute
Urogynecology Curriculum for the PGY III and IV Resident
 Urogynecology Curriculum for the PGY III and IV Resident Sinai Hospital of Baltimore Maryland Department of Obstetrics and Gynecology I. Educational Purpose: The dedicated Urogynecology rotation is intended
Urogynecology Curriculum for the PGY III and IV Resident Sinai Hospital of Baltimore Maryland Department of Obstetrics and Gynecology I. Educational Purpose: The dedicated Urogynecology rotation is intended
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives
 Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
Le fort s operation for prolapse uterus: A forgotten procedure
 2017; 1(2): 52-56 ISSN (P): 2522-6614 ISSN (E): 2522-6622 Gynaecology Journal www.gynaecologyjournal.com 2017; 1(2): 52-56 Received: 12-09-2017 Accepted: 13-10-2017 Dr. Jasmine Lall 3 rd Year Resident,
2017; 1(2): 52-56 ISSN (P): 2522-6614 ISSN (E): 2522-6622 Gynaecology Journal www.gynaecologyjournal.com 2017; 1(2): 52-56 Received: 12-09-2017 Accepted: 13-10-2017 Dr. Jasmine Lall 3 rd Year Resident,
Childbirth, chronic coughing, heavy lifting,
 OBG MANAGEMENT BY THOMAS JULIAN, MD Pelvic-support defects: a guide to anatomy and physiology Due to high postoperative failure rates, the traditional treatment for pelvic-organ prolapse hysterectomy with
OBG MANAGEMENT BY THOMAS JULIAN, MD Pelvic-support defects: a guide to anatomy and physiology Due to high postoperative failure rates, the traditional treatment for pelvic-organ prolapse hysterectomy with
Stop Coping. Start Living. Talk to your doctor about pelvic organ prolapse and sacrocolpopexy
 Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Guide to Pelvic Floor Multicompartment Scanning
 Guide to Pelvic Floor Multicompartment Scanning These guidelines have been prepared by Giulio A. Santoro, MD, PhD, Head Pelvic Floor Unit, Section of Anal Physiology and Ultrasound, Coloproctology Service,
Guide to Pelvic Floor Multicompartment Scanning These guidelines have been prepared by Giulio A. Santoro, MD, PhD, Head Pelvic Floor Unit, Section of Anal Physiology and Ultrasound, Coloproctology Service,
Glossary of terms Urinary Incontinence
 Patient Information English Glossary of terms Urinary Incontinence Anaesthesia (general, spinal, or local) Before a procedure you will get medication to make sure that you don t feel pain. Under general
Patient Information English Glossary of terms Urinary Incontinence Anaesthesia (general, spinal, or local) Before a procedure you will get medication to make sure that you don t feel pain. Under general
University of Alberta Reconstructive Urology Fellowship
 FACULTY OF MEDICINE AND DENTISTRY DEPARTMENT OF SURGERY DIVISION OF UROLOGY Keith Rourke, MD, FRCSC Reconstructive Urology Professor Chair of Academic Urology Reconstructive Urology Fellowship Director
FACULTY OF MEDICINE AND DENTISTRY DEPARTMENT OF SURGERY DIVISION OF UROLOGY Keith Rourke, MD, FRCSC Reconstructive Urology Professor Chair of Academic Urology Reconstructive Urology Fellowship Director
Accidental Bowel Leakage (Fecal Incontinence)
 Accidental Bowel Leakage (Fecal Incontinence) What is Accidental Bowel Leakage (ABL)? Accidental bowel leakage is the inability to control solid or liquid stool. This is the inability to control gas and
Accidental Bowel Leakage (Fecal Incontinence) What is Accidental Bowel Leakage (ABL)? Accidental bowel leakage is the inability to control solid or liquid stool. This is the inability to control gas and
URINARY INCONTINENCE. Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara
 URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
Female Urinary Incontinence: What It Is and What You Can Do About It
 Female Urinary Incontinence: What It Is and What You Can Do About It Urogynecology Patient Information Sheet What is Urinary Incontinence? Stress Incontinence is a leakage of urine that occurs, for example,
Female Urinary Incontinence: What It Is and What You Can Do About It Urogynecology Patient Information Sheet What is Urinary Incontinence? Stress Incontinence is a leakage of urine that occurs, for example,
Pathophysiological Rationale for Surgical Treatments of Stress Urinary Incontinence
 Pathophysiological Rationale for Surgical Treatments of Stress Urinary Incontinence Urology Grand Rounds April 6, 2005 Herman Christopher Kwan R4 A familiar case? 62 year old female initial presentation
Pathophysiological Rationale for Surgical Treatments of Stress Urinary Incontinence Urology Grand Rounds April 6, 2005 Herman Christopher Kwan R4 A familiar case? 62 year old female initial presentation
Urinary incontinence. Urology Department. Patient Information Leaflet
 Urinary incontinence Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been diagnosed with urinary incontinence. It contains information about the bladder,
Urinary incontinence Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been diagnosed with urinary incontinence. It contains information about the bladder,
Various Types. Ralph Boling, DO, FACOG
 Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Fecal Incontinence. What is fecal incontinence?
 Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
4. Know how to examine and name relevant test performed on patients
 Chapter 18 Female Urinary lncontinence Dr Zeelha Abdool Ed ucational Objectives : After completion of this chapter you should be able to: 1. Understand the pathophysiology of incontinence 2. Define and
Chapter 18 Female Urinary lncontinence Dr Zeelha Abdool Ed ucational Objectives : After completion of this chapter you should be able to: 1. Understand the pathophysiology of incontinence 2. Define and
Surgical Management for Defecation Dysfunction
 Defecatory Dysfunction Surgical Management for Defecation Dysfunction JMAJ 46(9): 378 383, 2003 Tatsuo TERAMOTO Professor, 1st Department of Surgery, School of Medicine, Toho University Abstract: Typical
Defecatory Dysfunction Surgical Management for Defecation Dysfunction JMAJ 46(9): 378 383, 2003 Tatsuo TERAMOTO Professor, 1st Department of Surgery, School of Medicine, Toho University Abstract: Typical
Ina S. Irabon, MD, FPOGS, FPSRM, FPSGE Obstetrics and Gynecology Reproductive Endocrinology and Infertility Laparoscopy and Hysteroscopy
 Ina S. Irabon, MD, FPOGS, FPSRM, FPSGE Obstetrics and Gynecology Reproductive Endocrinology and Infertility Laparoscopy and Hysteroscopy Comprehensive Gynecology 7 th edition, 2017 (Lobo RA, Gershenson
Ina S. Irabon, MD, FPOGS, FPSRM, FPSGE Obstetrics and Gynecology Reproductive Endocrinology and Infertility Laparoscopy and Hysteroscopy Comprehensive Gynecology 7 th edition, 2017 (Lobo RA, Gershenson
Pelvic floor exercises for women. Information for patients Continence Service
 Pelvic floor exercises for women Information for patients Continence Service page 2 of 8 Why do I need to do pelvic floor exercises? Many women experience pelvic floor problems at some time during their
Pelvic floor exercises for women Information for patients Continence Service page 2 of 8 Why do I need to do pelvic floor exercises? Many women experience pelvic floor problems at some time during their
Ralph & Berryl Goldman Fellowship in Neuro urology, voiding dysfunction and bladder reconstruction
 Ralph & Berryl Goldman Fellowship in Neuro urology, voiding dysfunction and bladder reconstruction Length of fellowship: A 1 year Fellowship: This fellowship has been designed for Urology or Gynecology
Ralph & Berryl Goldman Fellowship in Neuro urology, voiding dysfunction and bladder reconstruction Length of fellowship: A 1 year Fellowship: This fellowship has been designed for Urology or Gynecology
Dr. Aso Urinary Symptoms
 Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Urodynamic and electrophysiological investigations in neuro-urology
 Urodynamic and electrophysiological investigations in neuro-urology Pr. Gerard Amarenco Neuro-Urology and Pelvic-Floor Investigations Department Tenon Hospital, Assistance Publique Hôpitaux de Paris, Er6,
Urodynamic and electrophysiological investigations in neuro-urology Pr. Gerard Amarenco Neuro-Urology and Pelvic-Floor Investigations Department Tenon Hospital, Assistance Publique Hôpitaux de Paris, Er6,
This Special Report supplement
 ...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
Regulation of the Urinary Bladder Chapter 26
 Regulation of the Urinary Bladder Chapter 26 Anatomy 1. The urinary bladder is smooth muscle lined internally by transitional epithelium and externally by the parietal peritoneum. Contraction of the smooth
Regulation of the Urinary Bladder Chapter 26 Anatomy 1. The urinary bladder is smooth muscle lined internally by transitional epithelium and externally by the parietal peritoneum. Contraction of the smooth
Urinary Incontinence. Lora Keeling and Byron Neale
 Urinary Incontinence Lora Keeling and Byron Neale Not life threatening. Introduction But can have a huge impact on quality of life. Two main types of urinary incontinence (UI). Stress UI leakage on effort,
Urinary Incontinence Lora Keeling and Byron Neale Not life threatening. Introduction But can have a huge impact on quality of life. Two main types of urinary incontinence (UI). Stress UI leakage on effort,
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN
 Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN Diane K. Newman, DNP is a Biofeedback Certified Continence Specialist. With over 35-years experience, she is an expert in the assessment and management of pelvic-floor
Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN Diane K. Newman, DNP is a Biofeedback Certified Continence Specialist. With over 35-years experience, she is an expert in the assessment and management of pelvic-floor
Pelvic organ prolapse. Information for patients Continence Service
 Pelvic organ prolapse Information for patients Continence Service What is a pelvic organ prolapse? A pelvic organ prolapse occurs when the uterus (womb), vagina, bladder or bowel slips out of place, resulting
Pelvic organ prolapse Information for patients Continence Service What is a pelvic organ prolapse? A pelvic organ prolapse occurs when the uterus (womb), vagina, bladder or bowel slips out of place, resulting
Incontinence; Lets talk about it. Karanvir Virk M.D. Minimally Invasive and Pelvic Reconstructive Surgery
 Incontinence; Lets talk about it Karanvir Virk M.D. Minimally Invasive and Pelvic Reconstructive Surgery Select the most appropriate subtitle for this talk A: Bladders gone wild! B: There s no such thing
Incontinence; Lets talk about it Karanvir Virk M.D. Minimally Invasive and Pelvic Reconstructive Surgery Select the most appropriate subtitle for this talk A: Bladders gone wild! B: There s no such thing
+ Understanding Male Pelvic Health
 Understanding Male Pelvic Health Presented by: Dr. Casey M. Smith, PT, DPT, CSCS Women s Health Physical Therapy and Men s Pelvic Health Richmond, VA Objectives Review male pelvic anatomy/physiology Understand
Understanding Male Pelvic Health Presented by: Dr. Casey M. Smith, PT, DPT, CSCS Women s Health Physical Therapy and Men s Pelvic Health Richmond, VA Objectives Review male pelvic anatomy/physiology Understand
Appendix F: Continence Care and Bowel Management Program Training Presentation. Audience: For Front-line Staff Release Date: December 22, 2010
 Appendix F: Continence Care and Bowel Management Program Training Presentation Audience: For Front-line Staff Release Date: December 22, 2010 Objectives Address individual needs and preferences with respect
Appendix F: Continence Care and Bowel Management Program Training Presentation Audience: For Front-line Staff Release Date: December 22, 2010 Objectives Address individual needs and preferences with respect
The Neurogenic Bladder
 The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
Gross Anatomy of the Urinary System
 Gross Anatomy of the Urinary System Lecture Objectives Overview of the urinary system. Describe the external and internal anatomical structure of the kidney. Describe the anatomical structure of the ureter
Gross Anatomy of the Urinary System Lecture Objectives Overview of the urinary system. Describe the external and internal anatomical structure of the kidney. Describe the anatomical structure of the ureter
Table 2. First Generated List of Expert Responses. Likert-Type Scale. Category or Criterion. Rationale or Comments (1) (2) (3) (4)
 Table 2. First Generated List of Expert Responses. Likert-Type Scale Category or Criterion Anatomical Structures and Features Skeletal Structures and Features (1) (2) (3) (4) Rationale or Comments 1. Bones
Table 2. First Generated List of Expert Responses. Likert-Type Scale Category or Criterion Anatomical Structures and Features Skeletal Structures and Features (1) (2) (3) (4) Rationale or Comments 1. Bones
JMSCR Volume 03 Issue 03 Page March 2015
 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Quality of Life among Patients after Vaginal Hysterectomy and Pelvic Floor Repair Operation ABSTRACT Authors S Lovereen 1, F A Suchi 2,
www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Quality of Life among Patients after Vaginal Hysterectomy and Pelvic Floor Repair Operation ABSTRACT Authors S Lovereen 1, F A Suchi 2,
Loss of Bladder Control
 BLADDER HEALTH: Bladder Prolapse Loss of Bladder Control Bladder Prolapse Don t Let Bladder Prolapse Keep You from Enjoying Life. What is the Bladder? The bladder is a hollow, balloon-like organ made mostly
BLADDER HEALTH: Bladder Prolapse Loss of Bladder Control Bladder Prolapse Don t Let Bladder Prolapse Keep You from Enjoying Life. What is the Bladder? The bladder is a hollow, balloon-like organ made mostly
Module 3 Causes Of Urinary Incontinence
 Causes Of Urinary Incontinence V4: Last Reviewed September 2017 Learning Outcomes Appreciate the numerous requirements and skills necessary for the person to achieve and maintain urinary continence Discuss
Causes Of Urinary Incontinence V4: Last Reviewed September 2017 Learning Outcomes Appreciate the numerous requirements and skills necessary for the person to achieve and maintain urinary continence Discuss
REPRODUCTIVE SYSTEM By Dr.Ahmed Salman
 The University Of Jordan Faculty Of Medicine Anatomy Department REPRODUCTIVE SYSTEM By Dr.Ahmed Salman Assistant Professor of Anatomy &embryology Perineum It is the diamond-shaped lower end of the trunk
The University Of Jordan Faculty Of Medicine Anatomy Department REPRODUCTIVE SYSTEM By Dr.Ahmed Salman Assistant Professor of Anatomy &embryology Perineum It is the diamond-shaped lower end of the trunk
FEMALE URINARY INCONTINENCE: WHAT IT IS AND WHAT YOU CAN DO ABOUT IT
 URO-GYNECOLOGY PATIIENT IINFORMATIION SHEET FEMALE URINARY INCONTINENCE: WHAT IT IS AND WHAT YOU CAN DO ABOUT IT What is Urinary Incontinence? Stress Incontinence is a leakage of urine that occurs, for
URO-GYNECOLOGY PATIIENT IINFORMATIION SHEET FEMALE URINARY INCONTINENCE: WHAT IT IS AND WHAT YOU CAN DO ABOUT IT What is Urinary Incontinence? Stress Incontinence is a leakage of urine that occurs, for
4) Urinary Incontinence - Dr. Abeer
 4) Urinary Incontinence - Dr. Abeer INTRODUCTION Involuntary loss of urine Social and hygienic problem It affects individuals physical, psychological and social which is associated with a significant reduction
4) Urinary Incontinence - Dr. Abeer INTRODUCTION Involuntary loss of urine Social and hygienic problem It affects individuals physical, psychological and social which is associated with a significant reduction
Voiding Diary. Begin recording upon rising in the morning and continue for a full 24 hours.
 Urodvnamics Your physician has scheduled you for a test called URODYNAMICS. This test is a series of different measurements of bladder function and can be used to determine the cause of a variety of bladder
Urodvnamics Your physician has scheduled you for a test called URODYNAMICS. This test is a series of different measurements of bladder function and can be used to determine the cause of a variety of bladder
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS
 Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
NEUROMODULATION FOR UROGYNAECOLOGISTS
 NEUROMODULATION FOR UROGYNAECOLOGISTS Introduction The pelvic floor is highly complex structure made up of skeletal and striated muscle, support and suspensory ligaments, fascial coverings and an intricate
NEUROMODULATION FOR UROGYNAECOLOGISTS Introduction The pelvic floor is highly complex structure made up of skeletal and striated muscle, support and suspensory ligaments, fascial coverings and an intricate
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist
 Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Over Active Pelvic Floor
 Over Active Pelvic Floor Maeve Whelan SMISCP Specialist Chartered Physiotherapist, Women s Health Background The concept of an overactive pelvic floor (OAPF) is relatively new in pelvic floor rehabilitation.
Over Active Pelvic Floor Maeve Whelan SMISCP Specialist Chartered Physiotherapist, Women s Health Background The concept of an overactive pelvic floor (OAPF) is relatively new in pelvic floor rehabilitation.
Bill Landry BScPT, BScH, MCPA, CAFCI Family Physiotherapy Centre of London
 Bill Landry BScPT, BScH, MCPA, CAFCI blandry@fpclondon.com Family Physiotherapy Centre of London Objectives To describe the scope of post-prostatectomy incontinence To describe what s been done To provide
Bill Landry BScPT, BScH, MCPA, CAFCI blandry@fpclondon.com Family Physiotherapy Centre of London Objectives To describe the scope of post-prostatectomy incontinence To describe what s been done To provide
Advanced Care for Female Overactive Bladder & Urinary Incontinence. Department of Urology Kaiser Permanente Santa Rosa
 Advanced Care for Female Overactive Bladder & Urinary Incontinence Department of Urology Kaiser Permanente Santa Rosa Goals Participants will: Review normal urinary tract anatomy and function Understand
Advanced Care for Female Overactive Bladder & Urinary Incontinence Department of Urology Kaiser Permanente Santa Rosa Goals Participants will: Review normal urinary tract anatomy and function Understand
Pelvic Floor Muscle Exercises and Advice for Men
 Pelvic Floor Muscle Exercises and Advice for Men (formerly ACPWH) Useful resources Websites Pelvic Obstetric & Gynaecological Physiotherapy - pogp.csp.org.uk Bladder and Bowel Foundation - www.bladderandbowelfoundation.org
Pelvic Floor Muscle Exercises and Advice for Men (formerly ACPWH) Useful resources Websites Pelvic Obstetric & Gynaecological Physiotherapy - pogp.csp.org.uk Bladder and Bowel Foundation - www.bladderandbowelfoundation.org
Urogynecology in EDS. Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018
 Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Northwest Rehabilitation Associates, Inc.
 Pelvic Health Patient Intake Form Name: Date: Please answer the following questions as honestly and thoroughly as you can. Your responses will help us better understand your condition and provide the best
Pelvic Health Patient Intake Form Name: Date: Please answer the following questions as honestly and thoroughly as you can. Your responses will help us better understand your condition and provide the best
Female Pelvic Relaxation
 Female Pelvic Relaxation A Primer for Women with Pelvic Organ Prolapse by Andrew L. Siegel, M.D. Board-Certified Urologist and Urological Surgeon Director, Center for Continence Care An educational service
Female Pelvic Relaxation A Primer for Women with Pelvic Organ Prolapse by Andrew L. Siegel, M.D. Board-Certified Urologist and Urological Surgeon Director, Center for Continence Care An educational service
NOTES FROM GUTMAN LECTURE 10/26 Use this outline to study from. As you go through Gutman s lecture, fill in the topics.
 NOTES FROM GUTMAN LECTURE 10/26 Use this outline to study from. As you go through Gutman s lecture, fill in the topics. Anatomy above the arcuate line Skin Camper s fascia Scarpa s fascia External oblique
NOTES FROM GUTMAN LECTURE 10/26 Use this outline to study from. As you go through Gutman s lecture, fill in the topics. Anatomy above the arcuate line Skin Camper s fascia Scarpa s fascia External oblique
Urinary Continence & Management Post Stroke
 Urinary Continence & Management Post Stroke Incontinence and Stroke occurs in greater than 50% of acute stroke patients despite the personal, economic and psychosocial impact treatment evidence specific
Urinary Continence & Management Post Stroke Incontinence and Stroke occurs in greater than 50% of acute stroke patients despite the personal, economic and psychosocial impact treatment evidence specific
Applied Anatomy and Physiology of the Pelvic Floor. Dr David Tarver Consultant Radiologist, Poole
 Applied Anatomy and Physiology of the Pelvic Floor Dr David Tarver Consultant Radiologist, Poole Pelvic Floor 1. Sacrospinous Ligament 2. Levator Ani A Puborectalis B. Pubococcygeus C. Iliococcygeus 3.
Applied Anatomy and Physiology of the Pelvic Floor Dr David Tarver Consultant Radiologist, Poole Pelvic Floor 1. Sacrospinous Ligament 2. Levator Ani A Puborectalis B. Pubococcygeus C. Iliococcygeus 3.
Loss of Bladder Control
 BLADDER HEALTH: Surgery for Urinary Incontinence Loss of Bladder Control Surgery for Urinary Incontinence Don t Let Urinary Incontinence Keep You from Enjoying Life. What is Urinary Incontinence? What
BLADDER HEALTH: Surgery for Urinary Incontinence Loss of Bladder Control Surgery for Urinary Incontinence Don t Let Urinary Incontinence Keep You from Enjoying Life. What is Urinary Incontinence? What
ORIENTING TO BISECTED SPECIMENS ON THE PELVIS PRACTICAL
 ORIENTING TO BISECTED SPECIMENS ON THE PELVIS PRACTICAL The Pelvis is just about as complicated as head and neck and considerably more mysterious. You have to be able to visualize (imagine) the underlying
ORIENTING TO BISECTED SPECIMENS ON THE PELVIS PRACTICAL The Pelvis is just about as complicated as head and neck and considerably more mysterious. You have to be able to visualize (imagine) the underlying
Perineal Electrophysiologic Tests
 Perineal disorders and emg! Perineal Electrophysiologic Tests Voiding dysfunction Stress Urinary Incontinence urgency OAB Urge Incontinence nocturia Pr. Gerard Amarenco Mixed Incontinence frequency Service
Perineal disorders and emg! Perineal Electrophysiologic Tests Voiding dysfunction Stress Urinary Incontinence urgency OAB Urge Incontinence nocturia Pr. Gerard Amarenco Mixed Incontinence frequency Service
