Review Article Lower Urinary Tract Dysfunction in Pelvic Gynecologic Cancer: The Role of Urodynamics
|
|
|
- Brandon Owens
- 6 years ago
- Views:
Transcription
1 Hindawi Publishing Corporation Advances in Urology Volume 2014, Article ID , 6 pages Review Article Lower Urinary Tract Dysfunction in Pelvic Gynecologic Cancer: The Role of Urodynamics Fouad Aoun, 1,2 Alexandre Peltier, 1,2 and Roland van Velthoven 1,2 1 Jules Bordet Institute, 1 Rue Héger Bordet, 1000 Brussels, Belgium 2 Université Libre de Bruxelles, 50 Franklin Roosevelt Avenue, 1050 Brussels, Belgium Correspondence should be addressed to Fouad Aoun; fouad.aoun@bordet.be Received 18 June 2014; Revised 1 November 2014; Accepted 3 November 2014; Published 23 November 2014 Academic Editor: Matthew Rutman Copyright 2014 Fouad Aoun et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. The exact incidence of lower urinary tract dysfunction is not known and its pathogenesis is not completely understood. Advances in urodynamic assessment and widespread availability of a standardized technique have facilitated its exploration prior to and subsequent to the surgical management of patients with gynecologic pelvic cancer. We performed a PubMed and Medline literature search using the following keywords: bladder dysfunction, urinary dysfunction, and urodynamics and all these terms in combination with radical hysterectomy in order to analyze the role of urodynamics in patients with pelvic gynecologic cancer in the preoperative as well as in the early and late postoperative settings. 1. Introduction Gynecologic cancer confers a large burden among women worldwide. In 2015, it is estimated that 101,080 women in the United States will be diagnosed with a gynecologic cancer [1]. The incidence of gynecologic cancer will continue to increase over the next 40 years but the mortality rates will decrease perhaps due to an increase in cure rates [1, 2]. In fact, the prognosis of localized gynecologic cancer is excellent with 5-year survival rates >90% [2, 3]. Radical pelvic surgery represents the cornerstone in the management of these tumors. However, radical pelvic surgery is associated with a significant amount of complications and a negative impact on quality of life [4]. Owing to the anatomical location of female reproductive organs in the pelvis, radical treatment of gynecologic cancer has understandably been associated with urological complications [5]. Injuries of the lower urinary tract and the ureters can occur during surgery and lymph node dissection. Extensiveradicalgynecologicsurgerycanalsodamagepelvic nerves and vascular supply of the lower urinary tract as well as pelvic floor muscles and attachments resulting in lower urinary tract dysfunction (LUTD). This abnormality represents the most common complication after radical pelvic surgery for gynecologic cancers. However, there is significant variation in the incidence of LUTD among different studies and limited information on the pathophysiology of LUTD after this kind of surgery. New advent in urodynamic technology, especially the advent of the multichannel recording, has led to the improvement in understanding the changes in the bladder and urethral functions that occurred after radical gynecologic surgery [6]. In this review, we give a critical analysis on the evidence for LUTD after pelvic surgery for gynecologic cancer. Emphasis will be placed on the contribution of urodynamic investigation in understanding the mechanisms that lead to such disorders and in improving short- and long-term outcomes. We performed a PubMed and Medline literature search using the following keywords: bladder and radical hysterectomy and urinary dysfunction and radical hysterectomy. Significant results and citations were reviewed manually by the authors. 2. Incidence of LUTD after Radical Gynecologic Surgery The incidence of clinically significant LUTD varies among different studies from 8 to 80% [7]. This wide range in the literature is due to variable evaluation and definition
2 2 Advances in Urology of LUTD, different operation techniques, variable follow-up time, and unstandardized urodynamic investigations. In fact, very few studies used previously validated questionnaire to assess LUTD after gynecologic cancer surgery. Some studies based their evaluation on institutional internal instruments or a simple evaluation by the surgeon in the immediate postoperative period or in the outclinic consultation [8, 9]. Some authors used observational surveys with previously validated instruments sent to patients at home and evaluating retrospectively their symptoms and their quality of life [10]. Others utilized telephone interviews with the same instruments to evaluate the incidence of LUTD [11]. Moreover, the definition of LUTD varies enormously among the studies. It includes the inability to empty the bladder, dysuria, increased frequency of urination, increased micturition urgency, nocturia, bladder sensory loss, abdominal straining on micturition, urge incontinence, and stress incontinence. Another important point relates to the use of urodynamics as an assessment tool for urinary functional outcome. Complete urodynamic data are lacking in all studies published before the standardization of urodynamic disturbances according to the International Continence Society (ICS) classification [12]. Preoperative and postoperative complete urodynamic explorations are necessary to evaluate the incidence of LUTD relatedtosurgerybecauseupto80%ofpatientsalreadyhad some degree of bladder dysfunction before surgery [13]. The incidence of LUTD is higher in all studies using urodynamics but the clinical significance of these findings is still lacking. Some studies used postvoid residual urine volume or the need of clean intermittent catheterization or straining to void as assessment tools to detect clinically significant LUTD [14, 15]. The follow-up timing seems to be the major factor influencing the wide range of incidence of LUTD reported in literature. One year is mandatory to assess the incidence of long-term LUTD after pelvic cancer surgery. Studies with follow-up >1 year revealed a low rate of LUTD with respect to those with shorter follow-up [16]. Another limitation in the published literature is the retrospective design of the studies with a variable follow-up and a small sample size. In a review by Plotti et al., only two studies out of 19 were found to be of good quality being prospective with a sample size >50 patients and a follow-up >1 year[7]. Finally, in several studies, the importance of LUTD correlates with the anatomical extent of resection and nerve preservation. A recent meta-analysis demonstrated lower incidence of LUTD following nerve sparing radical hysterectomy compared to conventional radical hysterectomy [17]. However, there are no standardized techniques for the nerve sparing approach. Urinary functional outcome varies according to the technique used and the different approaches to clear the ligament and thelymphnodesfromthenerves.laparoscopicandrobotic approaches appear to facilitate the preservation of pelvic nerves by allowing a fine and precise dissection in a magnified operative field and are associated with better functional outcomes [18 20]. Unilateral nerve sparing approach is also associated with lower incidence of LUTD demonstrating that unilateral nerve injury could be partially compensated by the nervous supply from the other side [21, 22]. In addition, there are different neural injuries with different prognosis. The injury could be a temporary blockade of signal transmission without axon lesion (neurapraxia) with functional disorders resolving hours to weeks following surgery. It could be a transection of the axon with intact nerve sheets (axonotmesis) allowing regeneration at the site of the injury and distal to the injury with a nerve growth velocity varying from 0.25 mm/day to 4 mm/day. A complete transection of the nerves including their sheets is also possible with no potential to regenerate [23]. The mechanism is even more complex because injury of vascular supply to these nerves is as much important as injuries to the nerves themselves [24]. The combination of stretch and ischemia makes the nerve more vulnerable to injury. It appears that to obtain optimal functional results avoiding nerve handling in nerve sparing approach should be mandatory. Finally, nerve injury is not the only mechanism responsible for LUTD after radical hysterectomy as demonstrated by the higher incidence of LUTD following class 4 nerve-sparing radical hysterectomy. Direct surgical injury to the bladder wall, lymph stasis, interruption of the blood supply, and fibrosis of the urethra also play a role [25, 26]. Stress urinary incontinence (SUI) and voiding and/or storage dysfunction increased significantly following radical pelvic surgery. LUTD is a common finding in the early postoperative period. Its incidence has been reported between 70 and 85% of cases in the literature [27 31]. With adequate urological care, bladder dysfunction resolves spontaneously within 6 to 12 months in 70% of cases [32, 33]. Early LUTD is characterized by decreased bladder capacity, detrusor underactivity, and diminished bladder sensation which causes voiding dysfunction and may require urethral catheterization [34, 35]. Late dysfunction usually reveals voiding difficulty with abdominal straining, decreased bladder compliance, detrusor overactivity, and urinary incontinence [27, 28]. For example, the overall incidence of urodynamic LUTD afterradicalhysterectomyis72%.intheearlypostoperative period, detrusor dysfunction with low compliance is found in 24.4% (range: 18% 73%) of cases, mixed urinary incontinence in 24.5% (range: 11% 50%), and SUI in 40% (range: 11% 81%) [7]. Studies with a follow-up >12 months after primary radical surgery reported that the abovementioned ratesarereducedto35%,17%,and38%,respectively,and 16% of women experience LUTD severe enough to seek medical care [32]. Two postoperative factors modify the natural history of the functional urinary outcome. The first is clean intermittent catheterization and the second is adjuvant radiotherapy which increases the incidence of LUTD and constitutes a confusion factor for studies with a long-term follow-up [36, 37]. 3. Importance of Urodynamics in Radical Gynecologic Surgery Inthelastyears,advancesinurodynamicassessmenttechniques, especially the advent of the multichannel recording, and widespread availability of a standardized technique have facilitated exploration of LUTD prior to and subsequent to
3 Advances in Urology 3 the surgical management of patients with gynecologic pelvic cancer In the Preoperative Phase. LUTD and abnormal urodynamic findings are common in patients with gynecologic pelvic cancer prior to surgical treatment. Lin et al. showed that only 17% of patients with cervical cancer had normal urodynamic findings before radical hysterectomy [13]. The authors reported voiding LUTS in 10%, storage LUTS in 45%, and both voiding and storage LUTS in 28%. In addition, 37% had genuine stress urinary incontinence, 8% urge urinary incontinence, and 6% mixed urinary incontinence [13]. However, controversies in the literature surround the causal relationship between LUTD and pelvic gynecologic cancer. The increased rate of urodynamic abnormalities prior to surgery was not associated with the stage of the disease according to one study [6]. The authors concluded that LUTD in patients with pelvic gynecologic malignancies is not due to neurologic damage [6]. It is noteworthy to mention that gynecologic malignancies occur in a group of women at risk of LUTD. Parity, age, and menopausal status might be possible factors contributing to the increased rate of LUTD. A match pair analysis between urodynamic findings in women scheduled to radical pelvic gynecologic surgery compared towomeningeneralpopulationwithoutpelvicmalignancy wouldbeofgreatvalueinunderstandinglutdduetothe presence of the pelvic malignancy. Urodynamic assessment before surgery is not systematically recommended for all women to be treated by radical hysterectomy. Furthermore, the evidence supporting its use in the preoperative settings in symptomatic women is lacking. However, preoperative urodynamic assessment for patients included in clinical trials is mandatory in order to understand the effect of surgery on the lower urinary tract. Comparison of preoperative and postoperative urodynamic parameters had contributed to the understanding of a part of the pathophysiology of LUTD after radical hysterectomy. In fact, more nerves are damaged during radical hysterectomy than during simple hysterectomy and the increased rate of LUTD and urodynamic abnormalities after radical hysterectomy compared to simple hysterectomy had led to the development of nerve sparing techniques [38, 39]. In a recent comparative urodynamic study, Maneschi et al. found only mild functional impairments in the postoperative period after nerve-sparing radical hysterectomy in 15 patients [40]. These results support the neurologic origin of LUTD after gynecologic radical pelvic surgery. 3.2.IntheEarlyPostoperativePhase. During the early postoperative phase, bladder function is reported to be affected in 70 85% of patients with a significant reduction of bladder compliance and a significant reduction of maximal urethral closure pressure [5, 16, 41]. The pathogenesis of this condition is not completely elucidated and appears to be multifactorial. In the past, several urodynamic studies were carried out to explain bladder dysfunctions after radical gynecologic pelvic surgery. They had defined well the changes in urodynamic parameters and their incidence. In 1949, Halter and Richter reported a cystometric demonstration of a hypertonic bladder with reduced capacity in the early postoperative period [42]. Their findings have been confirmed by a number of authors. For some authors, hypertonic bladder dysfunction was the result of an increase in myogenic tonicity of the detrusor muscle secondary to the trauma of operation and prolonged catheter drainage [43]. For others, the dysfunction was attributed to partial peripheral neurologic denervation with parasympathetic dominance, and they ascribed little significance to the role of the sympathetic innervations [44, 45]. In more recent studies combining cystometry and electromyography, the presence of normal sphincter function and the absence of a decrease in bladder pressure when treated with a parasympatholytic drug had suggested that bladder dysfunction was not a result of parasympathetic dominance [43]. The role of sympathetic system in the pathophysiology of the early postoperative dysfunction was corroborated by the studies of Forney and Low et al. [46, 47]. The authors showed that the compromise of sympathetic β-adrenergic function during storage phase causes consequent low bladder compliance. Furthermore, the loss of sympathetic αadrenergic stimulation may have an excitatory effect on parasympathetic transmission to the detrusor muscle during urine storage and a permanent relaxation of the bladder neck and the proximal urethra, explaining the high incidence of the detrusor dyssynergia and the urinary stress incontinence after radical pelvic surgery. They concluded that sympathetic loss plays a major role in postoperative bladder changes. Standardization of urodynamic studies in the late 1990 contributedtotheemergenceofanewtheory [48]. Bladder dysfunction may be due to the unmasking of intrinsic detrusor activity, characterized by loss of β-adrenergic innervations with subsequent α-adrenergic hyperinnervation, or due to the impact of residual sympathetic innervations [49, 50]. In fact, the significant decrease of the maximal urethral closure pressure encountered in the early postoperative period could be attributed to the damage of the pelvic plexus and pudendal nerves with loss of periurethral tone. The loss of sympathetic adrenergic stimulation may have an excitatory effect on parasympathetic transmission to the detrusor muscle during urine storage and may lead to permanent relaxation of the bladder neck and the proximal urethra. These alterations could contribute to the characterization of urinary stress incontinence and detrusor overactivity and incontinence after radical pelvic surgery. Furthermore, in a recent study, Axelsen and Petersen confirmed the crucial role of the urethral sphincter mechanism [51]. They had reported no differences in urodynamic findings between continent and incontinent women after radical hysterectomy except for an overall difference in the intraurethral pressure [51]. Hamada et al. found urodynamic correlation between the severity of the incontinence and reduction of bladder compliance [49]. With the advent of β-agonists, it would be interesting to test its effectiveness in patients after radical hysterectomy. Inhibition of relaxation of the detrusor muscle by a βagonist in the filling phase should result in reduced bladder compliance and urinary incontinence. Another emerging concept, based on decentralization rather than complete denervation, is gaining place due to
4 4 Advances in Urology studies on animal models. It was hypothesized that damage to the afferent nerves leads to reduced and abnormal afferent input into the central nervous system, and this could interfere with the normal function of the pontine micturition center [9, 52]. Close cooperation between the gynecologists and the urologists is an essential prerequisite of good practice for the adequate management of LUTD in the early postoperative phase. The best treatment option for bladder emptying and significant postvoid residue is clean intermittent catheterization [8]. Abdominal straining to facilitate emptying the bladder is not recommended, as it leads to increased bladder pressure, increased risk of vesicoureteral reflux, and pressure propagation to the kidneys, potentially resulting in renal damage in the long term. Voiding without abdominal pressure enhances recovery of bladder function after radical hysterectomy [36]. Adequate postoperative bladder care can help to restore bladder function within 12 months of surgery. The daily frequency of clean intermittent catheterization is dependent on the residual urine volume and occurrence of spontaneous micturition. A permanent indwelling or suprapubic catheter should be avoided as long as possible as these can lead to complications such as urinary leakage, untreatable infections, bladder stones, fibrotic bladder, and bladder carcinoma In the Late Postoperative Phase. Spontaneous recovery of bladder function is generally to be expected within 6 12 months after surgery [32, 33]. The mechanisms of spontaneous recovery are complicated. It could be attributed to plasticity reorganization which occurs at multiple levels in the central and peripheral nervous system in response to peripheral injuries [9]. In a feline model, ablation of the pelvic plexus with early widespread degeneration of intrinsic axons andmusclecellswasfollowedafter10weeksbyaperiodof restitution of cholinergic axon terminals, increase in adrenergic and copeptidergic axons, and muscle cell regeneration [52]. However, persistent late changes are reported in 30 to 50% of studies [36, 37]. In routine practice, the persistence of symptoms beyond 12 months is indicative of worse functional prognosis. Urodynamic studies had played a major role in understanding the natural history of postoperative LUTD. In all studies with long-term urodynamic assessment, bladder compliance is improved and maximal urethral closure pressure is stabilized from the third postoperative month. Another important point related to the use of urodynamics as an assessment tool for surgical functional outcome is low incidence of normal detrusor function in long-term studies. Benedetti-Panici et al. reported normal detrusor function in 24% of their patients 1 year after surgery. They have found acontractile detrusor in 2% of patients, overactive detrusor in 21%, urodynamic stress incontinence in 29%, and mixed incontinence in 24% [16]. The high rate of urodynamic abnormalities in their series is due in part to their rigorous observation protocol and systematic urodynamic evaluation of all patients. In clinical practice, these abnormalities arerarelyassociatedwithsevereclinicalmanifestationsas demonstrated by the study of Pieterse et al. [53]. It seems also that cancer patients deal with urinary symptoms better than noncancer patients given the relatively high level of distress that is usually present regarding their underlying malignant disease compared to the other symptoms [16]. In contrast, improvement of clinical symptoms alone is not always synonym of improved bladder function. It could be the result of compensatory factors such as abdominal straining, substitute sensation, and voiding technique. Such patients are always susceptible to lower urinary tract decompensation and upper urinary tract deterioration especially if not diagnosed at time [54]. The role of urodynamic investigation is to detect these potentially dangerous situations by demonstrating subclinical modifications in bladder function and/or urethral closure pressure. 4. Conclusion LUTD is the most common complication after pelvic gynecologic surgery and it alters significantly the quality of life of thesurvivingpatients.thepathophysiologyiscomplexand incompletely elucidated. Urodynamic investigations played a major role in understanding the neurologic mechanisms underlying the dysfunction. These findings had led to the modification of the procedure in order to minimize urologic functional outcomes. Urodynamics played also a major role in characterizing postoperative disorder allowing a better urologic care modifying long-term LUTD and renal deterioration. Electrophysiologic studies and video-urodynamic recordings by characterizing, in a clinical trial, neurophysiologic and anatomic parameters would certainly help elucidate the mechanisms of LUTD following pelvic gynecologic cancer surgery. Conflict of Interests The authors, Fouad Aoun, Roland van Velthoven, and Alexandre Peltier, declare that they have no conflict of interests. References [1] A. H. Wallace, L. J. Havrilesky, F. A. Valea, J. C. Barnett, A. Berchuck, and E. R. Myers, Projecting the need for gynecologic oncologists for the next 40 years, Obstetrics and Gynecology, vol. 116, no. 6, pp , [2] Institut de Veille Sanitaire (InVS) and Institut National du Cancer (INCa), Réseau Francim, Institut National de la Santé et de la Recherche Médicale (Inserm), Hospices Civils de Lyon (HCL), Projections de l incidence et de la Mortalité par Cancer en France, [3] M.Arbyn,X.Castellsagué, S. de sanjosé et al., Worldwide burden of cervical cancer in 2008, Annals of Oncology,vol.22,no. 12, Article ID mdr015, pp , [4] J. Wu, X. Liu, K. Hua, C. Hu, X. Chen, and X. Lu, Effect of nerve-sparing radical hysterectomy on bladder function recovery and quality of life in patients with cervical carcinoma, International Journal of Gynecological Cancer,vol.20,no.5,pp , 2010.
5 Advances in Urology 5 [5] M. A. Zullo, N. Manci, R. Angioli, L. Muzii, and P. B. Panici, Vesical dysfunctions after radical hysterectomy for cervical cancer: a critical review, Critical Reviews in Oncology/ Hematology,vol.48,no.3,pp ,2003. [6] H.H.Lin,B.C.Sheu,M.C.Lo,andS.C.Huang, Abnormal urodynamic findings after radical hysterectomy or pelvic irradiation for cervical cancer, International Journal of Gynecology and Obstetrics, vol. 63, no. 2, pp , [7] F. Plotti, R. Angioli, M. A. Zullo et al., Update on urodynamic bladder dysfunctions after radical hysterectomy for cervical cancer, Critical Reviews in Oncology/Hematology, vol. 80, no. 2, pp , [8] F.-C. Chuang and H.-C. Kuo, Management of lower urinary tract dysfunction after radical hysterectomy with or without radiotherapy for uterine cervical cancer, Journal of the Formosan Medical Association,vol.108,no.8,pp ,2009. [9] G.-D. Chen, L.-Y. Lin, P.-H. Wang, and H.-S. Lee, Urinary tract dysfunction after radical hysterectomy for cervical cancer, Gynecologic Oncology, vol. 85, no. 2, pp , [10]R.A.Brooks,J.D.Wright,M.A.Powelletal., Long-term assessment of bladder and bowel dysfunction after radical hysterectomy, Gynecologic Oncology, vol. 114, no. 1, pp , [11] S. Kives and G. Lefebvre, Supracervical hysterectomy, The Society of Obstetricians and Gynaecologists of Canada Clinical Practice Guideline no. 238, [12]P.Abrams,L.Cardozo,M.Falletal., Thestandardisationof terminology in lower urinary tract function: report from the standardisation sub-committee of the International Continence Society, Urology,vol.61,no.1,pp.37 49,2003. [13] H.-H. Lin, H.-J. Yu, B.-C. Sheu, and S.-C. Huang, Importance of urodynamic study before radical hysterectomy for cervical cancer, Gynecologic Oncology,vol.81,no.2,pp ,2001. [14] D. Querleu, F. Narducci, V. Poulard et al., Modified radical vaginal hysterectomy with or without laparoscopic nervesparing dissection: a comparative study, Gynecologic Oncology, vol.85,no.1,pp ,2002. [15] J.B.Trimbos,C.P.Maas,M.C.Deruiter,A.A.W.Peters,and G. G. Kenter, A nerve-sparing radical hysterectomy: guidelines and feasibility in Western patients, International Journal of Gynecological Cancer, vol. 11, no. 3, pp , [16] P. Benedetti-Panici, M. A. Zullo, F. Plotti, N. Manci, L. Muzii, and R. Angioli, Long-term bladder function in patients with locally advanced cervical carcinoma treated with neoadjuvant chemotherapy and type 3 4 radical hysterectomy, Cancer,vol. 100, no. 10, pp , [17] Y. Long, D.-S. Yao, X.-W. Pan, and T.-Y. Ou, Clinical efficacy and safety of nerve-sparing radical hysterectomy for cervical cancer: a systematic review and meta-analysis, PLoS ONE,vol. 9,no.4,ArticleIDe94116,2014. [18] N.Y.Park,G.O.Chong,D.G.Hong,Y.L.Cho,I.S.Park,and Y. S. Lee, Oncologic results and surgical morbidity of laparoscopic nerve-sparing radical hysterectomy in the treatment of figo stage ib cervical cancer: long-term follow-up, International JournalofGynecologicalCancer, vol. 21, no. 2, pp , [19] S. P. Puntambekar, A. Patil, S. N. Joshi, N. V. Rayate, S. S. Puntambekar, and G. A. Agarwal, Preservation of autonomic nerves in laparoscopic total radical hysterectomy, Journal of Laparoendoscopic & Advanced Surgical Techniques, vol.20,no. 10, pp , [20] J. F. Magrina, W. Pawlina, R. M. Kho, and P. M. Magtibay, Robotic nerve-sparing radical hysterectomy: feasibility and technique, Gynecologic Oncology, vol. 121, no. 3, pp , [21] T. Kato, G. Murakami, and Y. Yabuki, A new perspective on nerve-sparing radical hysterectomy: nerve topography and over-preservation of the cardinal ligament, Japanese Journal of Clinical Oncology,vol.33,no.11,pp ,2003. [22]T.Zhu,A.J.Yu,H.F.Shouetal., Feasibilityofunilateralor bilateral nerve-sparing radical hysterectomy in patients with cervical cancer and evaluation of the post-surgery recovery of the bladder and rectal function, Chinese Journal of Oncology, vol. 33, no. 1, pp , [23] M. Eicke, R. Hohenfellner, and J. Leissner, Nerve injuries in urologic surgery, in Advanced Urologic Surgery, vol. 75, pp , Blackwell, [24] D. W. Zochodne, Nerve and ganglion blood flow in diabetes: an appraisal, International Review of Neurobiology,vol.50,pp , [25] G. Ralph, K. Tamussino, and W. Lichtenegger, Urodynamics following radical abdominal hysterectomy for cervical cancer, Archives of Gynecology and Obstetrics, vol.243,no.4,pp , [26] N. Kadar, N. Saliba, and J. H. Nelson, The frequency, causes and prevention of severe urinary dysfunction after radical hysterectomy, British Journal of Obstetrics and Gynaecology, vol. 90, no. 9, pp , [27] J. P. Forney, The effect of radical hysterectomy on bladder physiology, American Journal of Obstetrics and Gynecology,vol. 138, no. 4, pp , [28]R.J.Scotti,A.Bergman,N.N.Bhatia,andD.R.Ostergard, Urodynamic changes in urethrovesical function after radical hysterectomy, Obstetrics and Gynecology,vol.68,no.1,pp , [29] J. A. Low, G. M. Mauger, and J. A. Carmichael, The effect of Wertheim hysterectomy upon bladder and urethral function, American Journal of Obstetrics and Gynecology, vol.139,no.7, pp , [30] G. Ralph, R. Winter, L. Michelitsch, and K. Tamussino, Radicality of parametrial resection and dysfunction of the lower urinary tract after radical hysterectomy, European Journal of Gynaecological Oncology,vol.12,no.1,pp.27 30,1991. [31] K. Charoenkwan and S. Pranpanas, Prevalence and characteristics of late postoperative voiding dysfunction in earlystage cervical cancer patients treated with radical hysterectomy, Asian Pacific Journal of Cancer Prevention,vol.8,no.3,pp , [32] R. Naik, J. Nwabinelli, C. Mayne et al., Prevalence and management of (non-fistulous) urinary incontinence in women following radical hysterectomy for early stage cervical cancer, European Journal of Gynaecological Oncology,vol.22,no.1,pp , [33] K. S. Jackson and R. Naik, Pelvic floor dysfunction and radical hysterectomy, International Journal of Gynecological Cancer, vol.16,no.1,pp ,2006. [34] L.-Y. Lin, J.-H. Wu, C.-W. Yang, B.-C. Sheu, and H.-H. Lin, Impact of radical hysterectomy for cervical cancer on urodynamic findings, International Urogynecology Journal and Pelvic Floor Dysfunction,vol.15,no.6,pp ,2004. [35] T.-Y. Chuang, K.-J. Yu, I.-W. Penn, Y.-C. Chang, P.-H. Lin, and Y.-A. Tsai, Neurourological changes before and after radical hysterectomy in patients with cervical cancer, Acta Obstetricia et Gynecologica Scandinavica,vol.82,no.10,pp ,2003.
6 6 Advances in Urology [36] Y.Oda,Y.Todo,S.Hanleyetal., Riskfactorsforpersistentlow bladder compliance after radical hysterectomy, International Journal of Gynecological Cancer, vol. 21, no. 1, pp , [37] M.H.Hazewinkel,M.A.G.Sprangers,J.vanderVeldenetal., Long-term cervical cancer survivors suffer from pelvic floor symptoms: a cross-sectional matched cohort study, Gynecologic Oncology,vol.117,no.2,pp ,2010. [38] S. Butler-Manuel, L. Buttery, R. AHern, J. Polak, and D. Barton, Pelvic nerve plexus trauma at radical hysterectomy and simple hysterectomy: the nerve content of the uterine supporting ligaments, Cancer, vol. 89, pp , [39] S. A. Butler-Manuel, L. D. K. Buttery, R. P. A Hern, J. M. Polak, and D. P. J. Barton, Pelvic nerve plexus trauma at radical andsimplehysterectomy:aquantitativestudyofnervetypes in the uterine supporting ligaments, Journal of the Society for Gynecologic Investigation,vol.9,no.1,pp.47 56,2002. [40] F. Maneschi, P. Ianiri, M. Sarno, F. Gagliardi, and P. B. Panici, Nerve-sparing class III-IV radical hysterectomy: urodynamic study and surgical technique, International Journal of Gynecological Cancer,vol.22,no.4,pp ,2012. [41] F. Raspagliesi, A. Ditto, F. Hanozet et al., Nerve-sparing radical hysterectomy in cervical cancer: evolution of concepts, Gynecologic Oncology,vol.107,no.1,pp.S119 S121,2007. [42] A. C. Fraser, The late effects of Wertheim s hysterectomy on the urinary tract, The Journal of Obstetrics and Gynaecology of the British Commonwealth,vol.73,no.6,pp ,1966. [43] J. C. Seski and A. C. Diokno, Bladder dysfunction after radical abdominal hysterectomy, American Journal of Obstetrics & Gynecology,vol.128,no.6,pp ,1977. [44] B. E. Glahn, The neurogenic factor in vesical dysfunction following radical hysterectomy for carcinoma of the cervix., Scandinavian Journal of Urology and Nephrology, vol.4,no.2, pp , [45] D. L. Barclay and J. J. Roman-Lopez, Bladder dysfunction after Schauta hysterectomy. One year follow up, The American Journal of Obstetrics and Gynecology,vol.123,no.5,pp , [46] J. P. Forney, The effect of radical hysterectomy on bladder physiology, American Journal of Obstetrics & Gynecology, vol. 138, no. 4, pp , [47] J. A. Low, G. M. Mauger, and J. A. Carmichael, The effect of Wertheim hysterectomy upon bladder and urethral function, The American Journal of Obstetrics and Gynecology,vol.139,no. 7,pp ,1981. [48] D. Griffiths, K. Höfner, R. van Mastrigt, H. J. Rollema, A. Spångberg, and D. Gleason, Standardization of terminology of lower urinary tract function: pressure-flow studies of voiding, urethral resistance, and urethral obstruction, Neurourology and Urodynamics,vol.16,no.1,pp.1 18,1997. [49] K. Hamada, T. Kihana, M. Kataoka et al., Urinary disturbance after therapy for cervical cancer: urodynamic evaluation and β2-agonist medication, International Urogynecology Journal and Pelvic Floor Dysfunction,vol.10,no.6,pp ,1999. [50] K. Maman, S. Aballea, J. Nazir et al., Comparative efficacy and safety of medical treatments for the management of overactive bladder: a systematic literature review and mixed treatment comparison, European Urology,vol.65,no.4,pp ,2013. [51] S. M. Axelsen and L. K. Petersen, Urogynaecological dysfunction after radical hysterectomy, European Journal of Surgical Oncology,vol.32,no.4,pp ,2006. [52] A. Haferkamp, J. Dörsam, N. M. Resnick, S. V. Yalla, and A. Elbadawi, Structural basis of neurogenic bladder dysfunction III. Intrinsic detrusor innervation, The Journal of Urology,vol. 169, no. 2, pp , [53] Q. D. Pieterse, C. P. Maas, M. M. Ter Kuile et al., An observational longitudinal study to evaluate miction, defecation, and sexual function after radical hysterectomy with pelvic lymphadenectomy for early-stage cervical cancer, International Journal of Gynecological Cancer, vol.16,no.3,pp , [54] M. H. Hazewinkel, L. Gietelink, J. van der Velden, M. P. M. Burger, J. Stoker, and J.-P. W. R. Roovers, Renal ultrasound to detect hydronephrosis: a need for routine imaging after radical hysterectomy? Gynecologic Oncology,vol.124,no.1,pp.83 86, 2012.
Management of Lower Urinary Tract Dysfunction After Radical Hysterectomy With or Without Radiotherapy for Uterine Cervical Cancer
 ORIGINAL ARTICLE Management of Lower Urinary Tract Dysfunction After Radical Hysterectomy With or Without Radiotherapy for Uterine Cervical Cancer Fei-Chi Chuang, 1 Hann-Chorng Kuo 2 * Background/Purpose:
ORIGINAL ARTICLE Management of Lower Urinary Tract Dysfunction After Radical Hysterectomy With or Without Radiotherapy for Uterine Cervical Cancer Fei-Chi Chuang, 1 Hann-Chorng Kuo 2 * Background/Purpose:
The Neurogenic Bladder
 The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
The Management of Female Urinary Incontinence. Part 1: Aetiology and Investigations
 The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
NEUROGENIC BLADDER. Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph
 NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
Neurogenic bladder. Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder.
 Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
A prospective study of nerve-sparing radical hysterectomy for uterine cervical carcinoma in Taiwan
 Available online at www.sciencedirect.com Taiwanese Journal of Obstetrics & Gynecology 51 (2012) 55e59 Original Article A prospective study of nerve-sparing radical hysterectomy for uterine cervical carcinoma
Available online at www.sciencedirect.com Taiwanese Journal of Obstetrics & Gynecology 51 (2012) 55e59 Original Article A prospective study of nerve-sparing radical hysterectomy for uterine cervical carcinoma
Neuropathic Bladder. Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014
 Neuropathic Bladder Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014 Plan Physiology- bladder and sphincter behaviour in neurological disease Clinical consequences of Symptoms
Neuropathic Bladder Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014 Plan Physiology- bladder and sphincter behaviour in neurological disease Clinical consequences of Symptoms
This Special Report supplement
 ...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
Guidelines on Neurogenic Lower Urinary Tract Dysfunction
 Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION
 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E. Chartier-Kastler, G. Kramer, A. Mattiasson, J-J. Wyndaele Introduction NLUTD (neurogenic lower urinary
GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E. Chartier-Kastler, G. Kramer, A. Mattiasson, J-J. Wyndaele Introduction NLUTD (neurogenic lower urinary
Vesical dysfunctions after radical hysterectomy for cervical cancer: a critical review
 Critical Reviews in Oncology/Hematology 48 (2003) 287 293 Vesical dysfunctions after radical hysterectomy for cervical cancer: a critical review Marzio Angelo Zullo, Natalina Manci, Roberto Angioli, Ludovico
Critical Reviews in Oncology/Hematology 48 (2003) 287 293 Vesical dysfunctions after radical hysterectomy for cervical cancer: a critical review Marzio Angelo Zullo, Natalina Manci, Roberto Angioli, Ludovico
Urodynamics in Neurological Lower Urinary Tract Dysfunction. Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne
 Urodynamics in Neurological Lower Urinary Tract Dysfunction Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne Learning Objectives Review functional neurology relevant to lower
Urodynamics in Neurological Lower Urinary Tract Dysfunction Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne Learning Objectives Review functional neurology relevant to lower
THE RISK OF URINARY RETENTION AFTER NERVE-SPARING SURGERY FOR DEEP INFILTRATING ENDOMETRIOSIS: A SYSTEMATIC REVIEW AND META-ANALYSIS
 THE RISK OF URINARY RETENTION AFTER NERVE-SPARING SURGERY FOR DEEP INFILTRATING ENDOMETRIOSIS: A SYSTEMATIC REVIEW AND META-ANALYSIS JOSÉ ANACLETO RESENDE JR (Urology) LUCIANA CAVALINI (Epidemiology) CLAUDIO
THE RISK OF URINARY RETENTION AFTER NERVE-SPARING SURGERY FOR DEEP INFILTRATING ENDOMETRIOSIS: A SYSTEMATIC REVIEW AND META-ANALYSIS JOSÉ ANACLETO RESENDE JR (Urology) LUCIANA CAVALINI (Epidemiology) CLAUDIO
Recommandations de prise en charge des vessies neurogènes EAU 2006
 Annexe 4-1 Recommandations de prise en charge des vessies neurogènes EAU 2006 (Version courte) 685 686 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E.
Annexe 4-1 Recommandations de prise en charge des vessies neurogènes EAU 2006 (Version courte) 685 686 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E.
Normal micturition involves complex
 NEW TARGET FOR INTERVENTION: THE NEUROUROLOGY CONNECTION * Donald R. Ostergard, MD, FACOG ABSTRACT Urine storage and release are under the control of the parasympathetic, sympathetic, and somatic nervous
NEW TARGET FOR INTERVENTION: THE NEUROUROLOGY CONNECTION * Donald R. Ostergard, MD, FACOG ABSTRACT Urine storage and release are under the control of the parasympathetic, sympathetic, and somatic nervous
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist
 Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Summary. Neuro-urodynamics. The bladder cycle. and voiding. 14/12/2015. Neural control of the LUT Initial assessment Urodynamics
 Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
Review Article Pelvic Floor Dysfunction, Body Excreta Incontinence and Continence
 Cronicon OPEN ACCESS GYNAECOLOGY Review Article Pelvic Floor Dysfunction, Body Excreta Incontinence and Continence Abdel Karim M El Hemaly 1 * and Laila ASE Mousa 1 1 Professor of Obstetrics and gynaecology,
Cronicon OPEN ACCESS GYNAECOLOGY Review Article Pelvic Floor Dysfunction, Body Excreta Incontinence and Continence Abdel Karim M El Hemaly 1 * and Laila ASE Mousa 1 1 Professor of Obstetrics and gynaecology,
Clinical Study Cough Test during Tension-Free Vaginal Tape Procedure in Preventing Postoperative Urinary Retention
 Advances in Urology Volume 2013, Article ID 797854, 4 pages http://dx.doi.org/10.1155/2013/797854 Clinical Study Cough Test during Tension-Free Vaginal Tape Procedure in Preventing Postoperative Urinary
Advances in Urology Volume 2013, Article ID 797854, 4 pages http://dx.doi.org/10.1155/2013/797854 Clinical Study Cough Test during Tension-Free Vaginal Tape Procedure in Preventing Postoperative Urinary
John Laughlin 4 th year Cardiff University Medical Student
 John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
What should we consider before surgery? BPH with bladder dysfunction. Inje University Sanggye Paik Hospital Sung Luck Hee
 What should we consider before surgery? BPH with bladder dysfunction Inje University Sanggye Paik Hospital Sung Luck Hee Diagnostic tests in three categories Recommendation: there is evidence to support
What should we consider before surgery? BPH with bladder dysfunction Inje University Sanggye Paik Hospital Sung Luck Hee Diagnostic tests in three categories Recommendation: there is evidence to support
Post operative voiding dysfunction and the Value of Urodynamics. Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist
 Post operative voiding dysfunction and the Value of Urodynamics Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist Learning objectives: v Pathophysiology of post op voiding dysfunction.
Post operative voiding dysfunction and the Value of Urodynamics Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist Learning objectives: v Pathophysiology of post op voiding dysfunction.
Dysfunctional voiding
 Dysfunctional voiding The importance of assessment, diagnosis and treatment of dysfunctional voiding and its role in recurrent UTI Dr Dean Wallace Consultant Paediatric Nephrologist RMCH Objectives Development
Dysfunctional voiding The importance of assessment, diagnosis and treatment of dysfunctional voiding and its role in recurrent UTI Dr Dean Wallace Consultant Paediatric Nephrologist RMCH Objectives Development
URINARY INCONTINENCE. Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara
 URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
Spinal Cord Injury. R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH
 Spinal Cord Injury R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH SCI 800 1000 new cases per year in UK Car accidents 35%
Spinal Cord Injury R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH SCI 800 1000 new cases per year in UK Car accidents 35%
Ben Herbert Alex Wojtowicz
 Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Overactive Bladder: Diagnosis and Approaches to Treatment
 Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline
 Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline TARGET POPULATION Eligibility Decidable (Y or N) Inclusion
Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline TARGET POPULATION Eligibility Decidable (Y or N) Inclusion
Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests. Amelyn R.
 Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests Amelyn R. Rafael, MD 1 Functions of the Urinary Bladder 1. storage of urine 150 cc 1 st urge
Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests Amelyn R. Rafael, MD 1 Functions of the Urinary Bladder 1. storage of urine 150 cc 1 st urge
TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION Author : SIMONA T RADAELLI Categories : Vets Date : July
Vet Times The website for the veterinary profession https://www.vettimes.co.uk TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION Author : SIMONA T RADAELLI Categories : Vets Date : July
Definitions of IC: U.S. perspective. Edward Stanford MD MS FACOG FACS Western Colorado
 Definitions of IC: U.S. perspective Edward Stanford MD MS FACOG FACS Western Colorado PURPOSE OF A DEFINITION? Identifies with specificity those patients who are most likely to have the disease. Identifies
Definitions of IC: U.S. perspective Edward Stanford MD MS FACOG FACS Western Colorado PURPOSE OF A DEFINITION? Identifies with specificity those patients who are most likely to have the disease. Identifies
Management of Female Stress Incontinence
 Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Dr. Aso Urinary Symptoms
 Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS
 Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
GUIDELINES ON NEURO-UROLOGY
 GUIDELINES ON NEURO-UROLOGY (Text update pril 2014) J. Pannek (co-chair), B. Blok (co-chair), D. Castro-Diaz, G. del Popolo, J. Groen, G. Karsenty, T.M. Kessler, G. Kramer, M. Stöhrer Eur Urol 2009 Jul;56(1):81-8
GUIDELINES ON NEURO-UROLOGY (Text update pril 2014) J. Pannek (co-chair), B. Blok (co-chair), D. Castro-Diaz, G. del Popolo, J. Groen, G. Karsenty, T.M. Kessler, G. Kramer, M. Stöhrer Eur Urol 2009 Jul;56(1):81-8
Bladder dysfunction in ALD and AMN
 Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
NEUROMODULATION FOR UROGYNAECOLOGISTS
 NEUROMODULATION FOR UROGYNAECOLOGISTS Introduction The pelvic floor is highly complex structure made up of skeletal and striated muscle, support and suspensory ligaments, fascial coverings and an intricate
NEUROMODULATION FOR UROGYNAECOLOGISTS Introduction The pelvic floor is highly complex structure made up of skeletal and striated muscle, support and suspensory ligaments, fascial coverings and an intricate
Urogynecology in EDS. Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018
 Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Urinary incontinence (UI) affects as many
 EXPLORING NEW HORIZONS IN STRESS INCONTINENCE: THE NEUROUROLOGY CONNECTION W. Glenn Hurt, MD* ABSTRACT As many as one-third of women are affected by urinary incontinence, the most common of which being
EXPLORING NEW HORIZONS IN STRESS INCONTINENCE: THE NEUROUROLOGY CONNECTION W. Glenn Hurt, MD* ABSTRACT As many as one-third of women are affected by urinary incontinence, the most common of which being
Neuroanatomy, Neurophysiology and Clinical Presentation of Visceral Urological Pain
 Neuroanatomy, Neurophysiology and Clinical Presentation of Visceral Urological Pain Prof Dr K. Everaert Functional urology Department of Urology Ghent University Hospital Gent, Belgium Chronic pelvic pain
Neuroanatomy, Neurophysiology and Clinical Presentation of Visceral Urological Pain Prof Dr K. Everaert Functional urology Department of Urology Ghent University Hospital Gent, Belgium Chronic pelvic pain
THE ACONTRACTILE BLADDER - FACT OR FICTION?
 THE ACONTRACTILE BLADDER - FACT OR FICTION? Jacob Golomb Department of Urology Chaim Sheba Medical Center Tel Hashomer NEUROGENIC UNDERACTIVE DETRUSOR Central (complete/incomplete): Spinal cord injury-
THE ACONTRACTILE BLADDER - FACT OR FICTION? Jacob Golomb Department of Urology Chaim Sheba Medical Center Tel Hashomer NEUROGENIC UNDERACTIVE DETRUSOR Central (complete/incomplete): Spinal cord injury-
Survey on micturition disorders, surgical procedures and therapeutic approaches in patients treated for gynecologic cancers in clinical settings
 Cancer Reports and Reviews Research Article ISSN: 2513-9290 Survey on micturition disorders, surgical procedures and therapeutic approaches in patients treated for gynecologic cancers in clinical settings
Cancer Reports and Reviews Research Article ISSN: 2513-9290 Survey on micturition disorders, surgical procedures and therapeutic approaches in patients treated for gynecologic cancers in clinical settings
MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH
 MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH INTRODUCTION (1) Part of male sexual reproductive organ Size
MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH INTRODUCTION (1) Part of male sexual reproductive organ Size
Physiologic Anatomy and Nervous Connections of the Bladder
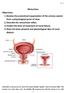 Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
PRE-OPERATIVE URODYNAMIC
 PRE-OPERATIVE URODYNAMIC STUDIES: IS THERE VALUE IN PREDICTING POST-OPERATIVE STRESS URINARY INCONTINENCE IN WOMEN UNDERGOING PROLAPSE SURGERY? Dr K Janse van Rensburg Dr JA van Rensburg INTRODUCTION POP
PRE-OPERATIVE URODYNAMIC STUDIES: IS THERE VALUE IN PREDICTING POST-OPERATIVE STRESS URINARY INCONTINENCE IN WOMEN UNDERGOING PROLAPSE SURGERY? Dr K Janse van Rensburg Dr JA van Rensburg INTRODUCTION POP
INCONTINENCE. Continence and Pelvic Floor Rehabilitation TYPES OF INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE 11/08/2015
 INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
Sexual function after partial cystectomy and urothelial stripping in a 32-year-old woman with radiation cystitis
 CHAPTER 8 Sexual function after partial cystectomy and urothelial stripping in a 32-year-old woman with radiation cystitis Based on: Elzevier HW, Gaarenstroom KN, Lycklama à Nijeholt AAB. Sexual function
CHAPTER 8 Sexual function after partial cystectomy and urothelial stripping in a 32-year-old woman with radiation cystitis Based on: Elzevier HW, Gaarenstroom KN, Lycklama à Nijeholt AAB. Sexual function
Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M.
 UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
Glossary of terms Urinary Incontinence
 Patient Information English Glossary of terms Urinary Incontinence Anaesthesia (general, spinal, or local) Before a procedure you will get medication to make sure that you don t feel pain. Under general
Patient Information English Glossary of terms Urinary Incontinence Anaesthesia (general, spinal, or local) Before a procedure you will get medication to make sure that you don t feel pain. Under general
Urogynecology ICD-9 to ICD-10 Crosswalks
 1100 Wayne Ave, Suite 825 Silver Spring, MD 20910 301.273.0570 Fax 301.273.0778 info@augs.org www.augs.org Urogynecology ICD-9 to ICD-10 Crosswalks ICD 9 ICD 9 Description ICD 10 Code ICD 10 Description
1100 Wayne Ave, Suite 825 Silver Spring, MD 20910 301.273.0570 Fax 301.273.0778 info@augs.org www.augs.org Urogynecology ICD-9 to ICD-10 Crosswalks ICD 9 ICD 9 Description ICD 10 Code ICD 10 Description
What We Have Learned from Over 1400 Radical Hysterectomy Operations in Chiang Mai University Hospital
 Thai Journal of Obstetrics and Gynaecology April 2008, Vol. 16, pp. 79-8561-167 SPECIAL ARTICLE What We Have Learned from Over 1400 Radical Hysterectomy Operations in Chiang Mai University Hospital Jatupol
Thai Journal of Obstetrics and Gynaecology April 2008, Vol. 16, pp. 79-8561-167 SPECIAL ARTICLE What We Have Learned from Over 1400 Radical Hysterectomy Operations in Chiang Mai University Hospital Jatupol
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics. Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital
 Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
Urodynamic study before and after radical porstatectomy 가톨릭의대성바오로병원김현우
 Urodynamic study before and after radical porstatectomy 가톨릭의대성바오로병원김현우 Introduction Radical prostatectomy - treatment of choice for patients with localized prostate cancer. Urinary incontinence and/or
Urodynamic study before and after radical porstatectomy 가톨릭의대성바오로병원김현우 Introduction Radical prostatectomy - treatment of choice for patients with localized prostate cancer. Urinary incontinence and/or
Tools for Evaluation. Urodynamics Case Studies. Case 1. Evaluation. Case 1. Bladder Diary SUI 19/01/2018
 Urodynamics Case Studies Christopher K. Payne, MD Vista Urology & Pelvic Pain Partners Emeritus Professor of Urology, Stanford University Tools for Evaluation Ears, Eyes, and Brain Bladder diary Stress
Urodynamics Case Studies Christopher K. Payne, MD Vista Urology & Pelvic Pain Partners Emeritus Professor of Urology, Stanford University Tools for Evaluation Ears, Eyes, and Brain Bladder diary Stress
Male LUTS. Dr. Brian Ho. Division of Urology Department of Surgery Queen Mary Hospital
 Male LUTS Dr. Brian Ho Division of Urology Department of Surgery Queen Mary Hospital Mr. Siu M/78 Known to have HT & DM since 2008 on follow up with General ut-patient Clinic (GPC) Noticed to have worsening
Male LUTS Dr. Brian Ho Division of Urology Department of Surgery Queen Mary Hospital Mr. Siu M/78 Known to have HT & DM since 2008 on follow up with General ut-patient Clinic (GPC) Noticed to have worsening
CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1
 1 CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1 35 years old man, who previously has been completely healthy, was shot twice in the neck
1 CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1 35 years old man, who previously has been completely healthy, was shot twice in the neck
Objectives. Prevalence of Urinary Incontinence URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS
 URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
Overactive bladder can result from one or more of the following causes:
 Overactive bladder can affect people of any age; however, it is more common in older people. Effective treatments are available and seeing your doctor for symptoms of overactive bladder often results in
Overactive bladder can affect people of any age; however, it is more common in older people. Effective treatments are available and seeing your doctor for symptoms of overactive bladder often results in
Case Based Urology Learning Program
 Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 23 CBULP 2011 077 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 23 CBULP 2011 077 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Practical urodynamics What PA s need to know. Gary E. Lemack, MD Professor of Urology and Neurology
 Practical urodynamics What PA s need to know Gary E. Lemack, MD Professor of Urology and Neurology Urodynamics essential elements Urethral catheter Fill rate Catheter size Intravesical pressure measurements
Practical urodynamics What PA s need to know Gary E. Lemack, MD Professor of Urology and Neurology Urodynamics essential elements Urethral catheter Fill rate Catheter size Intravesical pressure measurements
Video-urodynamics. P J R Shah Institute of Urology and UCH
 Video-urodynamics P J R Shah Institute of Urology and UCH Bladder Function Storage Capacity and Pressure Emptying Pressure/flow/emptying URODYNAMIC INVESTIGATIONS Free urine flow rate Urethral pressure
Video-urodynamics P J R Shah Institute of Urology and UCH Bladder Function Storage Capacity and Pressure Emptying Pressure/flow/emptying URODYNAMIC INVESTIGATIONS Free urine flow rate Urethral pressure
Urodynamic and electrophysiological investigations in neuro-urology
 Urodynamic and electrophysiological investigations in neuro-urology Pr. Gerard Amarenco Neuro-Urology and Pelvic-Floor Investigations Department Tenon Hospital, Assistance Publique Hôpitaux de Paris, Er6,
Urodynamic and electrophysiological investigations in neuro-urology Pr. Gerard Amarenco Neuro-Urology and Pelvic-Floor Investigations Department Tenon Hospital, Assistance Publique Hôpitaux de Paris, Er6,
GUIDELINES ON NEURO-UROLOGY
 GUIDELINES ON NEURO-UROLOGY (Limited text update March 2015) B. Blok (Co-chair), J. Pannek (Co-chair), D. Castro Diaz, G. del Popolo, J. Groen, T. Gross (Guidelines ssociate), R. Hamid, G. Karsenty, T.M.
GUIDELINES ON NEURO-UROLOGY (Limited text update March 2015) B. Blok (Co-chair), J. Pannek (Co-chair), D. Castro Diaz, G. del Popolo, J. Groen, T. Gross (Guidelines ssociate), R. Hamid, G. Karsenty, T.M.
Physiology & Neurophysiology of lower U.T.
 Physiology & Neurophysiology of lower U.T. Classification of voiding dysfunction Evaluation of a child with voiding dysfunction Management Storage Ø Adequate volume of urine Ø At LOW pressure Ø With NO
Physiology & Neurophysiology of lower U.T. Classification of voiding dysfunction Evaluation of a child with voiding dysfunction Management Storage Ø Adequate volume of urine Ø At LOW pressure Ø With NO
lower Urinary Tract Dysfunction as Persistent Complication of Radical Hysterectomy
 lower Urinary Tract Dysfunction as Persistent Complication of Radical Hysterectomy Noritoshi Sekido," Koji Kawai, and Hideyuki Akaza Department of Urology, Institute of Clinical Medicine, University of
lower Urinary Tract Dysfunction as Persistent Complication of Radical Hysterectomy Noritoshi Sekido," Koji Kawai, and Hideyuki Akaza Department of Urology, Institute of Clinical Medicine, University of
Research Article Safety and Cost Considerations during the Introduction Period of Laparoscopic Radical Hysterectomy
 Hindawi Obstetrics and Gynecology International Volume 2017, Article ID 2103763, 6 pages https://doi.org/10.1155/2017/2103763 Research Article Safety and Cost Considerations during the Introduction Period
Hindawi Obstetrics and Gynecology International Volume 2017, Article ID 2103763, 6 pages https://doi.org/10.1155/2017/2103763 Research Article Safety and Cost Considerations during the Introduction Period
National Kidney and Urologic Diseases Information Clearinghouse
 Urodynamic Testing National Kidney and Urologic Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is the urinary tract? The urinary tract
Urodynamic Testing National Kidney and Urologic Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is the urinary tract? The urinary tract
Index. Surg Oncol Clin N Am 14 (2005) Note: Page numbers of article titles are in boldface type.
 Surg Oncol Clin N Am 14 (2005) 433 439 Index Note: Page numbers of article titles are in boldface type. A Abdominosacral resection, of recurrent rectal cancer, 202 215 Ablative techniques, image-guided,
Surg Oncol Clin N Am 14 (2005) 433 439 Index Note: Page numbers of article titles are in boldface type. A Abdominosacral resection, of recurrent rectal cancer, 202 215 Ablative techniques, image-guided,
Tension-free Vaginal Tape for Urodynamic Stress Incontinence
 Long-term Results of Tension-free Vaginal Tape Insertion for Urodynamic Stress Incontinence in Chinese Women at Eight-year Follow-up: a Prospective Study YM CHAN MBBS, MRCOG, FHKAM (O&G), DCG, DCH, DFM,
Long-term Results of Tension-free Vaginal Tape Insertion for Urodynamic Stress Incontinence in Chinese Women at Eight-year Follow-up: a Prospective Study YM CHAN MBBS, MRCOG, FHKAM (O&G), DCG, DCH, DFM,
Female Pelvic Medicine & Reconstructive Surgery
 Female Pelvic Medicine & Reconstructive Surgery APPLICATION FOR NEW FELLOWSHIP Name of Institution: McGill University Location: Royal Victoria Hospital (Glen Site), St Mary s Hospital Centre Type of Fellowship:
Female Pelvic Medicine & Reconstructive Surgery APPLICATION FOR NEW FELLOWSHIP Name of Institution: McGill University Location: Royal Victoria Hospital (Glen Site), St Mary s Hospital Centre Type of Fellowship:
Facing a Hysterectomy? If you ve been diagnosed with gynecologic cancer, learn about minimally invasive da Vinci Surgery
 Facing a Hysterectomy? If you ve been diagnosed with gynecologic cancer, learn about minimally invasive da Vinci Surgery The Surgery: Hysterectomy If you have gynecologic cancer - such as cancer of the
Facing a Hysterectomy? If you ve been diagnosed with gynecologic cancer, learn about minimally invasive da Vinci Surgery The Surgery: Hysterectomy If you have gynecologic cancer - such as cancer of the
Clean Intermittent Self-Catheterisation (CISC)
 Saint Mary s Hospital & Trafford General Hospital Uro-gynaecology Service Information for Patients Clean Intermittent Self-Catheterisation (CISC) What is catheterisation? Catheterisation involves passing
Saint Mary s Hospital & Trafford General Hospital Uro-gynaecology Service Information for Patients Clean Intermittent Self-Catheterisation (CISC) What is catheterisation? Catheterisation involves passing
Prolapse and Urogynae Incontinence. Lucy Tiffin and Hannah Wheldon-Holmes
 Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury. Original Policy Date
 MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
Disease Management. Incontinence Care. Chan Sau Kuen Continence Nurse Consultant United Christian Hospital 14/11/09
 Disease Management in Incontinence Care Chan Sau Kuen Continence Nurse Consultant United Christian Hospital 14/11/09 What is incontinence? Definition of Incontinence - Is the compliant of any involuntary
Disease Management in Incontinence Care Chan Sau Kuen Continence Nurse Consultant United Christian Hospital 14/11/09 What is incontinence? Definition of Incontinence - Is the compliant of any involuntary
SUPRAPUBIC PUNCTURE IN THE TREATMENT OF NEUROGENIC BLADDER
 SUPRAPUBIC PUNCTURE IN THE TREATMENT OF NEUROGENIC BLADDER CHARLES C. HIGGINS, M.D. W. JAMES GARDNER, M.D. WM. A. NOSIK, M.D. The treatment of "cord bladder", a disturbance of bladder function from disease
SUPRAPUBIC PUNCTURE IN THE TREATMENT OF NEUROGENIC BLADDER CHARLES C. HIGGINS, M.D. W. JAMES GARDNER, M.D. WM. A. NOSIK, M.D. The treatment of "cord bladder", a disturbance of bladder function from disease
Urodynamics in women. Aims of Urodynamics in women. Why do Urodynamics?
 Urodynamics in women Chendrimada Madhu MD, MA, MRCOG Subspecialty Trainee in Urogynaecology Southmead Hospital 2013 Aims of Urodynamics in women n Confirmation of incontinence and its cause n Definition
Urodynamics in women Chendrimada Madhu MD, MA, MRCOG Subspecialty Trainee in Urogynaecology Southmead Hospital 2013 Aims of Urodynamics in women n Confirmation of incontinence and its cause n Definition
Facing Gynecologic Surgery?
 Facing Gynecologic Surgery? Domenico Vitobello, MD Domenico Vitobello is the medical director of the Gynecologic Unit at the Humanitas Clinical and Research Center since 2009. He has developed a comprehensive
Facing Gynecologic Surgery? Domenico Vitobello, MD Domenico Vitobello is the medical director of the Gynecologic Unit at the Humanitas Clinical and Research Center since 2009. He has developed a comprehensive
Neural control of the lower urinary tract in health and disease
 Neural control of the lower urinary tract in health and disease Jalesh N. Panicker MD, DM, FRCP Consultant Neurologist and Clinical lead in Uro-Neurology The National Hospital for Neurology and Neurosurgery
Neural control of the lower urinary tract in health and disease Jalesh N. Panicker MD, DM, FRCP Consultant Neurologist and Clinical lead in Uro-Neurology The National Hospital for Neurology and Neurosurgery
Bill Landry BScPT, BScH, MCPA, CAFCI Family Physiotherapy Centre of London
 Bill Landry BScPT, BScH, MCPA, CAFCI blandry@fpclondon.com Family Physiotherapy Centre of London Objectives To describe the scope of post-prostatectomy incontinence To describe what s been done To provide
Bill Landry BScPT, BScH, MCPA, CAFCI blandry@fpclondon.com Family Physiotherapy Centre of London Objectives To describe the scope of post-prostatectomy incontinence To describe what s been done To provide
Case Report Transurethral Incision of the Bladder Neck in a Woman with Primary Bladder Neck Obstruction after Kidney Transplantation
 Case Reports in Transplantation Volume 2015, Article ID 312084, 4 pages http://dx.doi.org/10.1155/2015/312084 Case Report Transurethral Incision of the Bladder Neck in a Woman with Primary Bladder Neck
Case Reports in Transplantation Volume 2015, Article ID 312084, 4 pages http://dx.doi.org/10.1155/2015/312084 Case Report Transurethral Incision of the Bladder Neck in a Woman with Primary Bladder Neck
Urogynaecology. Colm McAlinden
 Urogynaecology Colm McAlinden Definitions Urinary incontinence compliant of any involuntary leakage of urine with many different causes Two main types: Stress Urge Definitions Nocturia: More than a single
Urogynaecology Colm McAlinden Definitions Urinary incontinence compliant of any involuntary leakage of urine with many different causes Two main types: Stress Urge Definitions Nocturia: More than a single
Patient Expectations Following Greenlight XPS
 Patient Expectations Following Greenlight XPS 1. Hematuria it is common for men to have light pink to cherry red urine following the procedure. This small amount of blood in the urine usually resolves
Patient Expectations Following Greenlight XPS 1. Hematuria it is common for men to have light pink to cherry red urine following the procedure. This small amount of blood in the urine usually resolves
Mr. GIT KAH ANN. Pakar Klinikal Urologi Hospital Kuala Lumpur.
 Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
INTERNATIONAL SPINAL CORD INJURY DATA SETS URINARY TRACT IMAGING BASIC DATA SET - COMMENTS
 1 INTERNATIONAL SPINAL CORD INJURY DATA SETS URINARY TRACT IMAGING BASIC DATA SET - COMMENTS The working-group consists of: Fin Biering-Sørensen representing the Executive Committee of The International
1 INTERNATIONAL SPINAL CORD INJURY DATA SETS URINARY TRACT IMAGING BASIC DATA SET - COMMENTS The working-group consists of: Fin Biering-Sørensen representing the Executive Committee of The International
Serviks Kanserinde radikal cerrahide sinir koruyucu yaklaşım
 Serviks Kanserinde radikal cerrahide sinir koruyucu yaklaşım Prof. Dr. Hüsnü Çelik Başkent Üniversitesi Tıp Fakulesi Jinekolojik Onkoloji Bölümü (Adana Yerleşkesi) Maximal oncological control Minimal early
Serviks Kanserinde radikal cerrahide sinir koruyucu yaklaşım Prof. Dr. Hüsnü Çelik Başkent Üniversitesi Tıp Fakulesi Jinekolojik Onkoloji Bölümü (Adana Yerleşkesi) Maximal oncological control Minimal early
EXPERIMENTAL AND THERAPEUTIC MEDICINE 4: , 2012
 1112 Usefulness of total bladder capacity and post void residual urine volume as a predictor of detrusor overactivity with impaired contractility in stroke patients SANG HYUB LEE, JOONG GEUN LEE, GYEONG
1112 Usefulness of total bladder capacity and post void residual urine volume as a predictor of detrusor overactivity with impaired contractility in stroke patients SANG HYUB LEE, JOONG GEUN LEE, GYEONG
MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER
 10 MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER Recommendations from the EAU Working Party on Muscle Invasive and Metastatic Bladder Cancer G. Jakse (chairman), F. Algaba, S. Fossa, A. Stenzl, C. Sternberg
10 MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER Recommendations from the EAU Working Party on Muscle Invasive and Metastatic Bladder Cancer G. Jakse (chairman), F. Algaba, S. Fossa, A. Stenzl, C. Sternberg
Sequential Assessment of Urodynamic Findings before and aftertension-free Vaginal Tape (TVT) Operation for Female Genuine Stress Incontinence
 European Urology European Urology 45 (2004) 362 366 Sequential Assessment of Urodynamic Findings before and aftertension-free Vaginal Tape (TVT) Operation for Female Genuine Stress Incontinence Long-Yau
European Urology European Urology 45 (2004) 362 366 Sequential Assessment of Urodynamic Findings before and aftertension-free Vaginal Tape (TVT) Operation for Female Genuine Stress Incontinence Long-Yau
EAU GUIDELINES ON NEURO-UROLOGY
 EAU GUIDELINES ON NEURO-UROLOGY (Limited text update March 2017) B. Blok (Co-chair), J. Pannek (Co-chair) D. Castro-Diaz, G. del Popolo, J. Groen, R. Hamid, G. Karsenty, T.M. Kessler Guidelines Associates:
EAU GUIDELINES ON NEURO-UROLOGY (Limited text update March 2017) B. Blok (Co-chair), J. Pannek (Co-chair) D. Castro-Diaz, G. del Popolo, J. Groen, R. Hamid, G. Karsenty, T.M. Kessler Guidelines Associates:
Case Report Sacral Neuromodulation: Foray into Chronic Pelvic Pain in End Stage Endometriosis
 Hindawi Case Reports in Neurological Medicine Volume 2017, Article ID 2197831, 4 pages https://doi.org/10.1155/2017/2197831 Case Report Sacral Neuromodulation: Foray into Chronic Pelvic Pain in End Stage
Hindawi Case Reports in Neurological Medicine Volume 2017, Article ID 2197831, 4 pages https://doi.org/10.1155/2017/2197831 Case Report Sacral Neuromodulation: Foray into Chronic Pelvic Pain in End Stage
Prolapse & Urogynaecology. Hester Mannion and Fabi Sica
 Prolapse & Urogynaecology Hester Mannion and Fabi Sica Take home messages Prolapse and associated incontinence is very common It has a devastating effect on the QoL of the patient and their partner Strategies
Prolapse & Urogynaecology Hester Mannion and Fabi Sica Take home messages Prolapse and associated incontinence is very common It has a devastating effect on the QoL of the patient and their partner Strategies
Neurourology, especially the video urodynamic
 NEUROUROLOGIC FINDINGS WITH APPLICABILITY TO INCONTINENCE AND URETHRAL FUNCTION * Edward J. McGuire, MD ABSTRACT Neurourology is applicable to urinary incontinence and obstructive uropathy in the general
NEUROUROLOGIC FINDINGS WITH APPLICABILITY TO INCONTINENCE AND URETHRAL FUNCTION * Edward J. McGuire, MD ABSTRACT Neurourology is applicable to urinary incontinence and obstructive uropathy in the general
Prolapse and Urogynae. By Sarah Rangan & Daniel Warrell
 Prolapse and Urogynae By Sarah Rangan & Daniel Warrell Anatomy and physiology of the pelvic supports The pelvic floor supports the pelvic viscera and vaginal, urethral and rectal openings Endopelvic fascial
Prolapse and Urogynae By Sarah Rangan & Daniel Warrell Anatomy and physiology of the pelvic supports The pelvic floor supports the pelvic viscera and vaginal, urethral and rectal openings Endopelvic fascial
Management of Urinary Incontinence in Older Women. Dr. Cecilia Cheon Department of Obs. & Gyn. Queen Elizabeth Hospital
 Management of Urinary Incontinence in Older Women Dr. Cecilia Cheon Department of Obs. & Gyn. Queen Elizabeth Hospital Epidemiology Causes Investigation Treatment Conclusion Elderly Women High prevalence
Management of Urinary Incontinence in Older Women Dr. Cecilia Cheon Department of Obs. & Gyn. Queen Elizabeth Hospital Epidemiology Causes Investigation Treatment Conclusion Elderly Women High prevalence
Bladder Management. A guide for patients. Key points
 Bladder Management A guide for patients Key points Urinary issues remain one of the highest causes of readmission to hospital following Spinal Cord Injury (SCI). Following SCI most patients experience
Bladder Management A guide for patients Key points Urinary issues remain one of the highest causes of readmission to hospital following Spinal Cord Injury (SCI). Following SCI most patients experience
Neurogenic Bladder. Spina Bifida Education Day Conference SBA of Northeastern New York Albany, New York April 14, Eric Levey, M.D.
 Neurogenic Bladder Spina Bifida Education Day Conference SBA of Northeastern New York Albany, New York April 14, 2018 Eric Levey, M.D. Pediatrics & Neurodevelopmental Disabilities Chief Medical Officer,
Neurogenic Bladder Spina Bifida Education Day Conference SBA of Northeastern New York Albany, New York April 14, 2018 Eric Levey, M.D. Pediatrics & Neurodevelopmental Disabilities Chief Medical Officer,
Various Types. Ralph Boling, DO, FACOG
 Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
