Comparison of abdominal and perineal procedures for complete rectal prolapse: an analysis of 104 patients
|
|
|
- Donna Heath
- 6 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE pissn eissn Annals of Surgical Treatment and Research Comparison of abdominal and perineal procedures for complete rectal prolapse: an analysis of 104 patients Jong Lyul Lee, Sung Soo Yang 1, In Ja Park, Chang Sik Yu, Jin Cheon Kim Department of Surgery, Asan Medical Center, University of Ulsan College of Medicine, Seoul, 1 Department of Surgery, Ulsan University Hospital, University of Ulsan College of Medicine, Ulsan, Korea Purpose: Selecting the best surgical approach for treating complete rectal prolapse involves comparing the operative and functional outcomes of the procedures. The aims of this study were to evaluate and compare the operative and functional outcomes of abdominal and perineal surgical procedures for patients with complete rectal prolapse. Methods: A retrospective study of patients with complete rectal prolapse who had operations at a tertiary referral hospital and a university hospital between March 1990 and May 2011 was conducted. Patients were classified according to the type of operation: abdominal procedure (AP) (n = 64) or perineal procedure (PP) (n = 40). The operative outcomes and functional results were assessed. Results: The AP group had the younger and more men than the PP group. The AP group had longer operation times than the PP group (165 minutes vs. 70 minutes; P = 0.001) and longer hospital stays (10 days vs. 7 days; P = 0.001), but a lower overall recurrence rate (6.3% vs. 15.0%; P = 0.14). The overall rate of the major complication was similar in the both groups (10.9% vs. 6.8%; P = 0.47). The patients in the AP group complained more frequently of constipation than of incontinence, conversely, in the PP group of incontinence than of constipation. Conclusion: The two approaches for treating complete rectal prolapse did not differ with regard to postoperative morbidity, but the overall recurrence tended to occur frequently among patients in the PP group. Functional results after each surgical approach need to be considered for the selection of procedure. [Ann Surg Treat Res 2014;86(5): ] Key Words: Rectal prolapse, Abdomen, Perineum, Procedure INTRODUCTION Rectal prolapse is a socially debilitating condition, characterized by rectal protrusion through the anus [1]. Complete rectal prolapse is full-thickness rectal wall prolapse. It is usually associated with a long history of constipation, and with varying degrees of faecal incontinence [2,3]. For this reason, when surgeons select which operational procedure to use, they should consider not only functional results following surgery but also other facts about the patient such as age, sex, comorbidity and the extent of prolapse. In addition, the recurrence, morbidity and mortality rates associated with each procedure need to be considered. Although more than 100 different procedures for the treatment of complete rectal prolapse were described in the 20th century [4-6], the procedures fall into two broad categories, according to whether the route of access is abdominal or perineal [6]. Complete rectal prolapse has been studied in various subjects, and some studies have compared abdominal and perineal procedures [1,6]. Abdominal procedures (APs) generally offer lower rates of recurrence but are associated with Received November 27, 2013, Revised January 6, 2014, Accepted February 4, 2014 Corresponding Author: Jin Cheon Kim Department of Surgery, Asan Medical Center, Institute of Innovative Cancer Research, University of Ulsan College of Medicine, 88 Olympic-ro 43-gil, Songpa-gu, Seoul , Korea Tel: , Fax: jckim@amc.seoul.kr A poster was presented on this work at the 45th Korean Society of Coloproctology Annual Meeting, Seoul, Korea, 6 to 8 April, Copyright c 2014, the Korean Surgical Society cc Annals of Surgical Treatment and Research is an Open Access Journal. All articles are distributed under the terms of the Creative Commons Attribution Non- Commercial License ( which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. Annals of Surgical Treatment and Research 249
2 Annals of Surgical Treatment and Research 2014;86(5): higher morbidity rates than perineal procedures [1,3,7]. These results might help to select suitable operative procedures for patients with complete rectal prolapse. In this study we aimed to evaluate and compare the patient factors, operative and functional outcomes of both procedures used to treat patients with complete rectal prolapse. METHODS The medical records of all patients who had primary operation for complete rectal prolapse at a tertiary referral hospital and a university hospital between March 1990 and May 2011 were reviewed retrospectively. The study was approved by the Institutional Review Boards. Of 127 patients, 19 (9 abdominal and 10 perineal) were excluded because follow-up was less than six months and they could not be contacted by telephone and 4 who underwent Thiersch s operation were also excluded. Follow-up data were obtained from medical records and from standardized telephone interviews in May and June For patients who had died or whose personal information was lost at the time of the telephone interview, we used the data recorded at the previous follow-up. The 104 eligible patients were divided into two groups: those who had an AP (n = 64) and those who had a perineal procedure (PP) (n = 40). The operations were performed by four colorectal surgeons (A, B, C, and D). The indication of surgical treatment was the patient s distress related to complete rectal prolapse in the entire patient. The APs included open and laparoscopic rectopexy (modified Ripstein s method) with or without resection. The modified Ripstein s method was performed as follows; posterior fixation of the knitted monofilament polypropylene mesh (Marlex mesh, C.R. Bard, Inc., Murray Hill, NJ, USA) to the sacrum with attachment of the ends of the mesh to the rectum laterally [8], in open as well as laparoscopic surgery. The PPs included Delorme s and Altemeier s procedures. The operative outcomes analyzed were operation time, length of hospital stay, complications, and recurrence rate. Recorded functional outcomes were constipation, incontinence and manometric results. Constipation was evaluated using the scoring system of Agachan et al. [9], and faecal incontinence was evaluated using the Wexner score [10]. The constipation and incontinence outcomes were categorized as: none, improved, same, or worse. A same or worse outcome was defined as persistent constipation or incontinence compared with the preoperative condition. Of 70 patients at a tertiary referral hospital, 36 patients agreed with the manometric assessment and manometric values were measured at two time points, preoperative and postoperative period. Postoperative measurement was usually checked between 3 and 6 months after operation. The complications were divided into four categories, based on their timing and severity: immediate major or minor complications (within two months of operation), and delayed major or minor complications (two months or more after operation). Major complications were defined as those requiring surgical intervention or hospitalization. Minor complications were defined as those not requiring surgical intervention or hospital admission. Recurrence of rectal prolapse at the follow-up examination or telephone interview was defined as either a recurring full-thickness prolapse, or the recurrence of prolapsed symptoms. Table 1. Baseline characteristics of patients with complete rectal prolapse who underwent an abdominal or perineal procedure Characteristic Abdominal procedure (n = 64) Perineal procedure (n = 40) P-value Age (yr) 52 ± ± 12 <0.001* Sex Female/male 28/36 (43.8/56.3) 27/13 (67.5/32.5) <0.001* Reducible, yes 61 (95.3) 38 (95.0) 0.94 Presence of comorbidity a) 32 (50.0) 24 (60.0) 0.32 Prolapsed length (cm) 6.25 ± ± Duration of prolapse (yr) 11 ± ± Main reason for operation 0.29 History of constipation 17 (26.6) 16 (40.0) History of incontinence 13 (20.3) 12 (27.5) Prolapse 17 (26.6) 3 (7.5) Others b) 17 (26.6) 10 (25.0) Anesthesia type, general 64 (100) 15 (37.5) <0.001* Values are presented as mean ± standard deviation or no. of patients (%). a) Cardiovascular diseases, chronic obstructive lung diseases, diabetes mellitus, and chronic hepatitis. b) Anal bleeding, incarcerated rectum, anal pain, and recurrence of prolapse and/or symptoms. *Statistically significant. 250
3 Jong Lyul Lee, et al: Abdominal and perineal procedures for complete rectal prolapse The patient groups were compared using the chi-square test for proportions or Fisher exact test, as appropriate. The preand postoperative manometric values were compared using an unpaired Student t-test. Univariate analysis using binary logistic regression was used to assess the risk of delayed major complication. The 5-year recurrence-free period (RFP) was calculated using the Kaplan-Meier method and compared using the log rank test. Statistical significance was defined as P <0.05, and all analyses were performed using the IBM SPSS ver (IBM Co., Armonk, NY, USA). RESULTS Patient characteristics The median follow-up period was 26 months (interquartile range [IQR], 7 87 months) in the AP group and 22 months (IQR, 8 65 months) in the PP group. The PP group had older (67 years vs. 52 years; P < 0.001) and contained more women than the AP group (67.5% vs. 43.8%, P < 0.001). The AP group tended to have longer prolapsed pre-operative bowel lengths without significance (6.25 cm vs cm, P = 0.07) (Table 1). The two groups had similar preoperative parameters: reducibility, presence of comorbidity, duration of prolapse, and main reason for the operation (Table 1). Of the 64 patients treated with AP, 62 underwent rectopexy (16 rectopexies with resection); of these, 26 used a laparoscopic approach (20 cases of rectopexy and six rectopexies with resection). Two patients underwent open anterior resection. Of the 40 patients treated with PP, 36 underwent Delorme s procedure and four had Altemeier s procedure (Table 2). There were no postoperative deaths in either group. Operative outcomes and recurrence The AP group had longer operation times and hospital stays than the PP group, but similar relief of symptoms. The recurrence outcomes showed a lower overall recurrence rate (6.3% vs. 15.0%, P = 0.14) and a higher 5-year RFP (89.3% vs. 79.4%, P = 0.13) in the AP group compared with the PP group (Table 3). The characteristics of recurrence differed between the two groups. In the AP group, recurrence depended on the early experience of the surgeons, because it occurred in one of the four patients (25%) who underwent open posterior rectopexy in 1997 to 1998, and this was when two colorectal surgeons began performing these operations. By contrast, there was no recurrence in any of the patients whose open posterior Table 2. Surgical methods for patients with complete rectal prolapse and surgical details by four surgeons Operation type Surgeon A Surgeon B Surgeon C Surgeon D Total Posterior rectopexy 16 (15.4) 2 (1.9) 2 (1.9) 6 (5.8) 26 (25.0) Resection c rectopexy - 5 (4.8) 4 (3.9) 1 (0.9) 10 (9.6) Resection, only (1.9) - 2 (1.9) Lap-rectopexy (19.2) 20 (19.2) Lap-resection c rectopexy - 3 (2.9) 2 (1.9) 1 (0.9) 6 (5.8) Delorme s procedure 8 (7.7) 12 (11.5) 9 (8.7) 7 (6.7) 36 (34.6) Altemeier s procedure (1.9) 2 (1.9) 4 (3.9) Values are presented as no. of patients (%). Lap-rectopexy, laparoscopic posterior rectopexy; Lap-resection c rectopexy, laparoscopic resection with posterior rectopexy. Table 3. Clinical and functional outcomes of patients with complete rectal prolapse who underwent an abdominal or perineal procedure Variable Abdominal procedure (n = 64) Perineal procedure (n = 40) P-value Operation time (min) 165 ± ± 38 <0.001* Hospital stay (day) 10 ± 4 7 ± 2 <0.001* Functional outcomes 21 (32.8) 17 (41.4) Persistent a) constipation 13 (20.3) 6 (15.0) Persistent a) incontinence 8 (12.5) 11 (27.5) Overall recurrence 4 (6.3) 6 (15.0) year RFP (%) 89.3 ± ± Values are presented as mean ± standard deviation or no. of patients (%). RFP, recurrence-free period. a) Constipation and incontinence was the same or worse after the operation. *Statistically significant. Annals of Surgical Treatment and Research 251
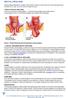
4 Annals of Surgical Treatment and Research 2014;86(5): rectopexy was carried out by a colorectal surgeon who had enough experience for posterior rectopexy before included period. In addition, recurrence occurred in one of the five patients (20%) who underwent laparoscopic posterior rectopexy in 2002 to 2004, when laparoscopic surgery for colorectal disease was started to be performed at our institution. The overall recurrence rate for the laparoscopic approach in our institution between 2005 and 2011 was 6.7% (1/15), which is consistent with the overall recurrence rates of APs performed previously in our institution. In the PP group, recurrence depended on the type of operative procedure. Recurrence occurred in one of the four patients (25.0%) who underwent Altemeier s procedure, whereas only five of the 36 patients (13.9%) who underwent Delorme s procedure had recurrence. Compared open posterior rectopexy, which was used the most in AP, with Delorme s operation in PP, the results were similar to those between the AP and PP group. The group that underwent Delorme s operation was older (68 years vs. 51 years, P < 0.001) and contained more women than the open rectopexy group (63.9% vs. 41.3%, P = 0.04). The two groups had similar preoperative parameters like a comparison of the AP and PP group. The open posterior rectopexy group had longer operation times (164 minutes vs. 66 minutes, P < 0.001) and hospital stays (11 days vs. 7 days, P < 0.001) than the Delorme s group, but had similar rates of minor and major complication (minor: 10% vs. 7%, P = 0.78; major: 2% vs. 4%, P = 0.59). Recurrence developed less frequently in the open posterior rectopexy group than in the Delorme s operation group (3.8% vs. 13.9%, P = 0.187). A summary of the analysis of complications is presented in Table 4. There were no cardiac, respiratory or renal complications in either group. The frequencies of the four categories of complication were similar in the both groups. Univariate analysis showed no significant association between the operative approach and the frequencies of the four categories of complication. However, in the AP group, delayed major complications occurred more frequently among patients combined with resection than rectopexy-only cases (35.3% vs. 8.5%, P = 0.009). Functional outcomes Persistent constipation or incontinence after surgery was observed in 21 patients in the AP group and in 17 patients in the PP group. In the AP group there were more complaints of constipation than of incontinence; by contrast, the patients in the PP group complained more frequently of incontinence than of constipation. The difference of persistent constipation between two groups was not statistically significant (P = 0.49), but persistent incontinence between two groups were marginally different (P = 0.054) (Table 3). With regard to the manometric results, both groups exhibited higher mean postoperative maximal resting pressure (MRP) than before the operation (Fig. 1) (preoperative vs. Table 4. Postoperative complications in patients with complete rectal prolapse who underwent an abdominal or perineal procedure Variable Abdominal procedure (n = 64) Perineal procedure (n = 40) P-value Immediate a) minor c) complications 12 (18.8) 5 (12.5) 0.40 Wound infection 4 2 (D) Urinary retention 4 (1 OR, 1 OPR, 2 LPR) 1 (D) Anal pain during defecation 3 1 Temporary hematochezia 1 1 Immediate a) major d) complications 4 (5.8) 1 (2.5) 0.38 Ileus 3 (2 OR, 1 OPR) Anastomosis site leakage 1 (LRPR) Anal stricture 1 (D) Delayed b) minor c) complications 6 (9.4) 2 (5.0) 0.42 Urinary retention 2 0 Sexual dysfunction 4 2 Anal pain 1 2 Delayed b) major d) complications 9 (14.1) 3 (7.5) 0.30 Ileus 2 (ORPR) Anastomosis stricture 3 (2 ORPR, 1 LRPR) 2 (D) Incisional hernia 3 (2 ORPR, 1 OPR) Recto-vaginal fistula 1 (ORPR) Rectal perforation 1 (D) OR, open resection; OPR, open posterior rectopexy; LPR, laparoscopic posterior rectopexy; LRPR, laparoscopic resection with posterior rectopexy; ORPR, open resection with posterior rectopexy; D, Delorme s procedure. a) Within 2 months of the operation. b) More than 2 months after the operation. c) Did not require surgical intervention or hospital admission. d) Required surgical intervention or hospitalization. 252
5 Jong Lyul Lee, et al: Abdominal and perineal procedures for complete rectal prolapse Fig. 1. Pre- and postoperative manometric results in the abdominal (A) and perineal procedure (B) groups. The postoperative values were generally obtained between three and six months after the operation. For both groups, the mean maximal resting pressure (MRP) after the operation was higher than the preoperative MRP. The other manometric values did not changed significantly in either group. MSP, maximal squeezing pressure; MSV, minimal sensory volume; UV, urgent need to defecate volume; MTV, maximal tolerance volume; SL, sphincter length; HPZ, high-pressure zone. postoperative; AP group: 24.6 mmhg vs mmhg, respectively; PP group: 16.7 mmhg vs mmhg, respectively). However, the postoperative MRP values were still below the normal MRP range. The pre- and postoperative measurement of other manometric values remained unchanged in both groups. These included maximal squeezing pressure, minimal sensory volume, maximal tolerance volume, urgent need to defecate volume, high-pressure zone length and sphincter length (Fig. 1). DISCUSSION Several operational procedures for complete rectal prolapse have been performed in our institution over the past two decades. Delorme s procedure was the most commonly performed in our institution throughout the entire study period. By contrast, the type of AP has changed during the last decade because laparoscopy has been increasingly used since 2002: two laparoscopic procedures (22.2% of all APs) were introduced in 2002 and half of the patients who underwent AP in 2010 had laparoscopic procedures. Although several different procedures were performed, the current study compared the AP and PP groups. Before the comparison of the AP group and the PP group, the current study showed that the relationship between gender and the incidence of rectal prolapse in Korea was very different to that in the West. According to a western review [11], rectal prolapse is more common in women, and more than 80% of patients are female. A Korean study, however, reported similar incidences in men and women [12]. Among the patients who were treated surgically for complete rectal prolapse in the current study, there were similar numbers of females and males (female/male ratio, 52.8%/47.2%), but the proportion of women among the elderly patients aged 70 or older was about 80% (female/male ratio, 80.6%/19.4%). This means the incidence in young male patients is relatively high in Korea. Another Korean study demonstrated that the age of onset for male was lower, the duration of symptoms was longer, and surgery in male was performed younger than in female (mean age, 51 years vs. 64 years) but the severities of incontinence and constipation were lower in male [13]. What makes this difference in incidence among the Korean and the Western is not clear though we suspected the life style which apt to strain in one of the reason. Further study is needed to investigate the incidence of complete rectal prolapse in Korea because the current study was not population-based. In the current study, the AP group was younger and had a longer prolapsed length of rectum than the PP group. The choice of approach was generally influenced by a clinical preference for a PP because of age and/or pre-existing conditions [7]. Our data suggest that in our institution the age of the patient and Annals of Surgical Treatment and Research 253
6 Annals of Surgical Treatment and Research 2014;86(5): the prolapsed length were major considerations in selecting the operation type, as in other studies [6,11,14]. However, there was no significant association between the four complication categories and patient factors (age, sex, reducibility, comorbidity, prolapsed length, duration of disease, main reason for operation, and operation types). Patients in the PP group had shorter hospital stays, shorter operation times, and higher recurrence rates than patients who had an AP, as shown in previous studies [3,4,15-19]. The PP group was followed up for a shorter time (a median of 4 months less than the AP group), so the recurrence rate at set intervals would be higher for the PP patients. When we analyzed the relationship between the recurrence and the operative approach, the current study showed that recurrences were correlated with the surgeon s early experience in the AP group and the operative method in the PP group. Our observations suggest that surgeons increased familiarity with APs (both open operations and laparoscopy) might be associated with lower recurrence. Some studies [20,21] suggested that the learning curve for AP might be responsible for recurrences. In the PP group, the recurrence rates are consistent with the rates that have been reported previously: 0% 20% for Altemeier s procedure [22], and 4% 38% for Delorme s procedure [11]. In the current study, AP combined with resection was a risk factor of the delayed major complications; six of the seven patients (85.7%) experienced delayed major complications (rectopexy only vs. resection; odd ratio, 0.19). Resection procedures are reported to significantly reduce constipation in patients who complain of this symptom before surgery [4], but surgeons should be aware of the tendency for delayed major complications. Persistent constipation was more common than persistent incontinence in the AP group, although this was not statistically significant. In contrast, persistent incontinence tended to be more frequent than persistent constipation in the PP group. This may indicate that the presence of constipation or incontinence before surgery influenced the choice of operative approach. Especially, surgeon would note higher rate of persistent incontinence in the PP group than in the AP group. In the current study, manometric measurements revealed that the pre- and postoperative measurement of all manometric values except MRP value remained unchanged in both groups and the postoperative MRP values were still below the normal MRP range. Therefore, this study could not suggest whether manometric studies for complete rectal prolapse could predict functional outcomes. A recent study [23] suggested that preoperative manometry could predict the fecal continence rate after proctectomy, because patients with MSP above 60 mmhg had significantly better outcomes. However, it should be noted that there was no long-term physiological follow-up of patients [23]. Further research might be needed to determine a value of physiological study as a predictor of functional outcome. A study [24], in the early 1990s, insisted that the AP would be performed when PP was failed in the results obtained from younger patients. Recently, laparoscopic ventral rectopexy (LVR) has gained wide acceptance [25] as the surgical treatment of rectal prolapse associated with low complication and recurrence rate [26]. The results of the current study might support LVR partly because the current study showed high incidence of young patients in Korea, relatively higher 5-year RFP in the AP group, and comparable complications. However, the PP would be preserved for the selected patients who should avoid general anesthesia although comparable study [27] was existed. The present study has a number of limitations that should be considered when interpreting the results. As in all retrospective observational cohort studies, there is potential for both referral and selection bias. The assessment of patients by telephone without physical examination was subjective; although it used detailed questionnaires, it was likely that recurred prolapse was underestimated by the patients. The subgroup analysis of manometric finding was restricted by the small number of patients and the limited implementation of manometry. Intervention groups in the current study were heterogeneous. For this reason, additional comparison between open posterior rectopexy and Delorme s procedure was performed. The current study, however, would provide insight into changes in procedures over time, factors influencing the choice of operative procedure, and factors affecting recurrence. In the operative management of complete rectal prolapse, there was no significant association between major or minor complications and patient factors. The AP group had similar postoperative complications compared with the PP group except AP combined with resection for a risk of delayed major complications. The overall recurrence in the PP group tended to occur frequently, compared with the AP group. Persistent constipation was more frequent in the AP group, while, persistent incontinence was more prominent in the PP group. Preoperative functional deficit and the early experience of surgeon for AP procedure, accompanied with age, comorbidities, and the length of the prolapsed rectum, would be considered for the selection of surgical procedures. CONFLICTS OF INTEREST No potential conflict of interest relevant to this article was reported. ACKNOWLEDGEMENTS This work was supported by grants from the Asan Institute for Life Sciences ( ). 254
7 Jong Lyul Lee, et al: Abdominal and perineal procedures for complete rectal prolapse REFERENCES 1. Riansuwan W, Hull TL, Bast J, Hammel JP, Church JM. Comparison of perineal operations with abdominal operations for full-thickness rectal prolapse. World J Surg 2010;34: Schultz I, Mellgren A, Dolk A, Johansson C, Holmstrom B. Long-term results and functional outcome after Ripstein rectopexy. Dis Colon Rectum 2000;43: Kim DS, Tsang CB, Wong WD, Lowry AC, Goldberg SM, Madoff RD. Complete rectal prolapse: evolution of management and results. Dis Colon Rectum 1999;42: Luukkonen P, Mikkonen U, Jarvinen H. Abdominal rectopexy with sigmoidectomy vs. rectopexy alone for rectal prolapse: a prospective, randomized study. Int J Colorectal Dis 1992;7: Finlay IG, Aitchison M. Perineal excision of the rectum for prolapse in the elderly. Br J Surg 1991;78: Brown AJ, Anderson JH, McKee RF, Finlay IG. Strategy for selection of type of operation for rectal prolapse based on clinical criteria. Dis Colon Rectum 2004;47: Fleming FJ, Kim MJ, Gunzler D, Messing S, Monson JR, Speranza JR. It s the proce dure not the patient: the operative approach is independently associated with an increased risk of complications after rectal prolapse repair. Colorectal Dis 2012;14: McMahan JD, Ripstein CB. Rectal prolapse. An update on the rectal sling procedure. Am Surg 1987;53: Agachan F, Chen T, Pfeifer J, Reissman P, Wexner SD. A constipation scoring system to simplify evaluation and management of constipated patients. Dis Colon Rectum 1996;39: Jorge JM, Wexner SD. Etiology and management of fecal incontinence. Dis Colon Rectum 1993;36: Gourgiotis S, Baratsis S. Rectal prolapse. Int J Colorectal Dis 2007;22: Yoon SG. Rectal prolapse: review according to the personal experience. J Korean Soc Coloproctol 2011;27: Yoon SG, Lee KR, Cho KA, Hwang DY, Kim KU, Kang YW, et al. Clinical and physiologic characteristics of rectal prolapse in males. J Korean Soc Colopro ctol 2000;16: Madiba TE, Baig MK, Wexner SD. Surgical management of rectal prolapse. Arch Surg 2005;140: Kuijpers HC. Treatment of complete rectal prolapse: to narrow, to wrap, to suspend, to fix, to encircle, to plicate or to resect? World J Surg 1992;16: Yakut M, Kaymakcioglu N, Simsek A, Tan A, Sen D. Surgical treatment of rectal prolapse. A retrospective analysis of 94 cases. Int Surg 1998;83: Husa A, Sainio P, von Smitten K. Abdominal rectopexy and sigmoid resec tion (Frykman-Goldberg operation) for rectal prolapse. Acta Chir Scand 1988;154: Graf W, Karlbom U, Pahlman L, Nilsson S, Ejerblad S. Functional results after abdo minal suture rectopexy for rectal pro lapse or intussusception. Eur J Surg 1996;162: Delemarre JB, Gooszen HG, Kruyt RH, Soebhag R, Geesteranus AM. The effect of posterior rectopexy on fecal continence: a prospective study. Dis Colon Rectum 1991;34: Ashari LH, Lumley JW, Stevenson AR, Stitz RW. Laparoscopically-assisted resection rectopexy for rectal prolapse: ten years experience. Dis Colon Rectum 2005;48: Ahmad M, Sileri P, Franceschilli L, Mercer- Jones M. The role of biologics in pelvic floor surgery. Colorectal Dis 2012;14 Suppl 3: Glasgow SC, Birnbaum EH, Kodner IJ, Fleshman JW, Dietz DW. Preoperative anal manometry predicts continence after perineal proctectomy for rectal prolapse. Dis Colon Rectum 2006;49: Ris F, Colin JF, Chilcott M, Remue C, Jamart J, Kartheuser A. Altemeier's procedure for rectal prolapse: analysis of longterm outcome in 60 patients. Colorec tal Dis 2012;14: Park HJ, So BJ, Jun KY. Comparative analysis of operative procedures in rectal prolapse between perineal and abdominal approach. J Korean Surg Soc 1991;40: Formijne Jonkers HA, Draaisma WA, Wexner SD, Broeders IA, Bemelman WA, Lindsey I, et al. Evaluation and surgi cal treatment of rectal prolapse: an international survey. Colorectal Dis 2013;15: D Hoore A, Cadoni R, Penninckx F. Longterm outcome of laparoscopic ventral rectopexy for total rectal prolapse. Br J Surg 2004;91: Wijffels N, Cunningham C, Dixon A, Greenslade G, Lindsey I. Laparoscopic ventral rectopexy for external rectal prolap se is safe and effective in the elderly. Does this make perineal proce dures obsolete? Colorectal Dis 2011;13: Annals of Surgical Treatment and Research 255
Prolaps: Anteriore Rektopexie nach D Hoore. Prof. Dr. med. F. Hetzer
 Prolaps: Anteriore Rektopexie nach D Hoore Prof. Dr. med. F. Hetzer franc.hetzer@spital-linth.ch Rectal prolapse pathophysiology 24 22 20 18 congenital female pathology (90%) 16 14 straining weakened pelvic
Prolaps: Anteriore Rektopexie nach D Hoore Prof. Dr. med. F. Hetzer franc.hetzer@spital-linth.ch Rectal prolapse pathophysiology 24 22 20 18 congenital female pathology (90%) 16 14 straining weakened pelvic
Summary and conclusion. Summary And Conclusion
 Summary And Conclusion Summary and conclusion Rectal prolapse remain a disorder for which no single ideal treatment was approved for all cases. Complete rectal prolapse (procidentia) is the circumferential
Summary And Conclusion Summary and conclusion Rectal prolapse remain a disorder for which no single ideal treatment was approved for all cases. Complete rectal prolapse (procidentia) is the circumferential
Rectal Prolapse: A 10-Year Experience
 24 The Ochsner Journal Volume 7, Number 1, Spring 2007 25 Rectal Prolapse: A 10-Year Experience Figure 2. Physical examination. A. Concentric folds of prolapsed rectum. B. Radial folds of hemorrhoids (mucosal
24 The Ochsner Journal Volume 7, Number 1, Spring 2007 25 Rectal Prolapse: A 10-Year Experience Figure 2. Physical examination. A. Concentric folds of prolapsed rectum. B. Radial folds of hemorrhoids (mucosal
Motility Disorders. Pelvic Floor. Colorectal Center for Functional Bowel Disorders (N = 701) January 2010 November 2011
 Motility Disorders Pelvic Floor Colorectal Center for Functional Bowel Disorders (N = 71) January 21 November 211 New Patients 35 3 25 2 15 1 5 Constipation Fecal Incontinence Rectal Prolapse Digestive-Genital
Motility Disorders Pelvic Floor Colorectal Center for Functional Bowel Disorders (N = 71) January 21 November 211 New Patients 35 3 25 2 15 1 5 Constipation Fecal Incontinence Rectal Prolapse Digestive-Genital
Rectal Prolapse: Review According to the Personal Experience
 Review Journal of the Korean Society of DOI: 10.3393/jksc.2011.27.3.107 pissn 2093-7822 eissn 2093-7830 Rectal Prolapse: Review According to the Personal Experience Department of Surgery, Seoul Song Do
Review Journal of the Korean Society of DOI: 10.3393/jksc.2011.27.3.107 pissn 2093-7822 eissn 2093-7830 Rectal Prolapse: Review According to the Personal Experience Department of Surgery, Seoul Song Do
The role of biologics in pelvic floor surgery
 Review article doi:10.1111/codi.12045 The role of biologics in pelvic floor surgery M. Ahmad*, P. Sileri, L. Franceschilli and M. Mercer-Jones* *Department of Colorectal Surgery, Queen Elizabeth Hospital,
Review article doi:10.1111/codi.12045 The role of biologics in pelvic floor surgery M. Ahmad*, P. Sileri, L. Franceschilli and M. Mercer-Jones* *Department of Colorectal Surgery, Queen Elizabeth Hospital,
LONG TERM OUTCOME OF ELECTIVE SURGERY
 LONG TERM OUTCOME OF ELECTIVE SURGERY Roberto Persiani Associate Professor Mini-invasive Oncological Surgery Unit Institute of Surgical Pathology (Dir. prof. D. D Ugo) Dis Colon Rectum, March 2000 Dis
LONG TERM OUTCOME OF ELECTIVE SURGERY Roberto Persiani Associate Professor Mini-invasive Oncological Surgery Unit Institute of Surgical Pathology (Dir. prof. D. D Ugo) Dis Colon Rectum, March 2000 Dis
Factors Influencing Morbidity after Rectopexy for Posterior Pelvic Floor Disorders
 Factors Influencing Morbidity after Rectopexy for Posterior Pelvic Floor Disorders Ayca Fatma Gultekin 1, Jean-Benoit Hardouin 2, Guilé Romain 3, Myriam Boutami 1, Paul-Antoine Lehur 1, Guillaume Meurette
Factors Influencing Morbidity after Rectopexy for Posterior Pelvic Floor Disorders Ayca Fatma Gultekin 1, Jean-Benoit Hardouin 2, Guilé Romain 3, Myriam Boutami 1, Paul-Antoine Lehur 1, Guillaume Meurette
Our Experience in Management of Complete Rectal Prolapse in Children by Delorme Procedure
 Med. J. Cairo Univ., Vol. 84, No. 1, December: 1357-1362, 2016 www.medicaljournalofcairouniversity.net Our Experience in Management of Complete Rectal Prolapse in Children by Delorme Procedure MOHAMED
Med. J. Cairo Univ., Vol. 84, No. 1, December: 1357-1362, 2016 www.medicaljournalofcairouniversity.net Our Experience in Management of Complete Rectal Prolapse in Children by Delorme Procedure MOHAMED
What the radiologist needs to know!
 What the radiologist needs to know! Clare Molyneux Sam Treadway Sathi Sukumar Wal Baraza Abhiram Sharma Karen Telford University Hospital of South Manchester Manchester UK Introduction Indications Investigations
What the radiologist needs to know! Clare Molyneux Sam Treadway Sathi Sukumar Wal Baraza Abhiram Sharma Karen Telford University Hospital of South Manchester Manchester UK Introduction Indications Investigations
Clinical Study Delorme s Procedure for Complete Rectal Prolapse: A Study of Recurrence Patterns in the Long Term
 Surgery Research and Practice Volume 215, Article ID 92154, 6 pages http://dx.doi.org/1.1155/215/92154 Clinical Study Delorme s Procedure for Complete Rectal Prolapse: A Study of Recurrence Patterns in
Surgery Research and Practice Volume 215, Article ID 92154, 6 pages http://dx.doi.org/1.1155/215/92154 Clinical Study Delorme s Procedure for Complete Rectal Prolapse: A Study of Recurrence Patterns in
Anus,Rectum and Colon
 JOURNAL OF THE Anus,Rectum and Colon http://journal-arc.jp CLINICAL RESEARCH Laparoscopic ventral rectopexy with sacrocolpopexy for coexisting pelvic organ prolapse and external rectal prolapse Yoshiyuki
JOURNAL OF THE Anus,Rectum and Colon http://journal-arc.jp CLINICAL RESEARCH Laparoscopic ventral rectopexy with sacrocolpopexy for coexisting pelvic organ prolapse and external rectal prolapse Yoshiyuki
Laparoscopic Ventral. Mesh Rectopexy (LVMR)
 Laparoscopic Ventral Mesh Rectopexy (LVMR) Questions & Answers GLASGOW COLORECTAL CENTRE Ross Hall Hospital 221 Crookston Road Glasgow G52 3NQ e-mail: info@colorectalcentre.co.uk Ph: Main hospital switchboard
Laparoscopic Ventral Mesh Rectopexy (LVMR) Questions & Answers GLASGOW COLORECTAL CENTRE Ross Hall Hospital 221 Crookston Road Glasgow G52 3NQ e-mail: info@colorectalcentre.co.uk Ph: Main hospital switchboard
Repeat Single Incision Laparoscopic Surgery after Primary Single Incision Laparoscopic Surgery for Colorectal Disease
 ORIGINAL ARTICLE pissn 2234-778X eissn 2234-5248 J Minim Invasive Surg 2018;21(1):38-42 Journal of Minimally Invasive Surgery Repeat Single Incision Laparoscopic Surgery after Primary Single Incision Laparoscopic
ORIGINAL ARTICLE pissn 2234-778X eissn 2234-5248 J Minim Invasive Surg 2018;21(1):38-42 Journal of Minimally Invasive Surgery Repeat Single Incision Laparoscopic Surgery after Primary Single Incision Laparoscopic
Perineale Rektumprolapsoperation: Gute Resultate bei geringem Aufwand! F.H. Hetzer
 Perineale Rektumprolapsoperation: Gute Resultate bei geringem Aufwand! F.H. Hetzer STARR: Wunderwaffe beim Obstructed Defecation Syndrom (ODS) F.H. Hetzer Stapled TransAnal Rectal Resection STARR PPH 01
Perineale Rektumprolapsoperation: Gute Resultate bei geringem Aufwand! F.H. Hetzer STARR: Wunderwaffe beim Obstructed Defecation Syndrom (ODS) F.H. Hetzer Stapled TransAnal Rectal Resection STARR PPH 01
Pelvic Floor Disorders. Amir Darakhshan MD FRCS (Gen Surg) Consultant Colorectal and General Surgeon
 Pelvic Floor Disorders Amir Darakhshan MD FRCS (Gen Surg) Consultant Colorectal and General Surgeon What is Pelvic Floor Disorder Surgical perspective symptoms of RED, FI or prolapse on the background
Pelvic Floor Disorders Amir Darakhshan MD FRCS (Gen Surg) Consultant Colorectal and General Surgeon What is Pelvic Floor Disorder Surgical perspective symptoms of RED, FI or prolapse on the background
Robotic Ventral Rectopexy
 Robotic Ventral Rectopexy What is a robotic ventral rectopexy? The term rectopexy refers to an operation in which the rectum (the part of the bowel nearest the anus) is put back into its normal position
Robotic Ventral Rectopexy What is a robotic ventral rectopexy? The term rectopexy refers to an operation in which the rectum (the part of the bowel nearest the anus) is put back into its normal position
Delorme's operation plus sphincteroplasty for complete rectal prolapse associated with traumatic fecal incontinence
 Available online at www.jbr-pub.org Open Access at PubMed Central The Journal of Biomedical Research, 2015, 29(4):326-331 Original Article Delorme's operation plus sphincteroplasty for complete rectal
Available online at www.jbr-pub.org Open Access at PubMed Central The Journal of Biomedical Research, 2015, 29(4):326-331 Original Article Delorme's operation plus sphincteroplasty for complete rectal
Does Anastomosis Configuration Influence Long-term Outcomes in Patients With Crohn Disease?
 Original Article Ann Coloproctol 217;33(5):173-177 https://doi.org/1.3393/ac.217.33.5.173 pissn 2287-9714 eissn 2287-9722 Does Anastomosis Configuration Influence Long-term Outcomes in Patients With Crohn
Original Article Ann Coloproctol 217;33(5):173-177 https://doi.org/1.3393/ac.217.33.5.173 pissn 2287-9714 eissn 2287-9722 Does Anastomosis Configuration Influence Long-term Outcomes in Patients With Crohn
Clinical Practice Guidelines for the Treatment of Rectal Prolapse
 CLINICAL PRACTICE GUIDELINES Clinical Practice Guidelines for the Treatment of Rectal Prolapse Liliana Bordeianou, M.D., M.P.H. Ian Paquette, M.D. Eric Johnson, M.D. Stefan D. Holubar, M.D. Wolfgang Gaertner,
CLINICAL PRACTICE GUIDELINES Clinical Practice Guidelines for the Treatment of Rectal Prolapse Liliana Bordeianou, M.D., M.P.H. Ian Paquette, M.D. Eric Johnson, M.D. Stefan D. Holubar, M.D. Wolfgang Gaertner,
Acute Diverticulitis. Andrew B. Peitzman, MD Mark M. Ravitch Professor of Surgery University of Pittsburgh
 Acute Diverticulitis Andrew B. Peitzman, MD Mark M. Ravitch Professor of Surgery University of Pittsburgh Focus today: when to operate n Recurrent, uncomplicated diverticulitis; after how many episodes?
Acute Diverticulitis Andrew B. Peitzman, MD Mark M. Ravitch Professor of Surgery University of Pittsburgh Focus today: when to operate n Recurrent, uncomplicated diverticulitis; after how many episodes?
Index. Note: Page numbers of article title are in boldface type.
 Index Note: Page numbers of article title are in boldface type. A Abscess(es) in Crohn s disease, 168 169 IPAA and, 110 114 as unexpected finding in colorectal surgery, 46 Adhesion(s) trocars-related laparoscopy
Index Note: Page numbers of article title are in boldface type. A Abscess(es) in Crohn s disease, 168 169 IPAA and, 110 114 as unexpected finding in colorectal surgery, 46 Adhesion(s) trocars-related laparoscopy
Laparoscopic ventral rectopexy for obstructed defecation syndrome
 Surg Endosc (2008) 22:2728 2732 DOI 10.1007/s00464-008-9771-9 Laparoscopic ventral rectopexy for obstructed defecation syndrome J. W. van den Esschert Æ A. A. W. van Geloven Æ N. Vermulst Æ A. Groenedijk
Surg Endosc (2008) 22:2728 2732 DOI 10.1007/s00464-008-9771-9 Laparoscopic ventral rectopexy for obstructed defecation syndrome J. W. van den Esschert Æ A. A. W. van Geloven Æ N. Vermulst Æ A. Groenedijk
Bowel dysfunctions following hysterectomy
 Bowel dysfunctions following hysterectomy Marco Scaglia Retrospective studies Retrospective studies 6% of patients developed new symptoms (Carlson 1994) Constipation is more common in women after hysterectomy
Bowel dysfunctions following hysterectomy Marco Scaglia Retrospective studies Retrospective studies 6% of patients developed new symptoms (Carlson 1994) Constipation is more common in women after hysterectomy
World Journal of Colorectal Surgery
 World Journal of Colorectal Surgery Volume 3, Issue 3 2013 Article 5 Closed Versus Open Lateral Internal Sphincterotomy Technique in Treatment of Anal Fissure Seyed Reza Mousavi Jr Shohada Medical Center,
World Journal of Colorectal Surgery Volume 3, Issue 3 2013 Article 5 Closed Versus Open Lateral Internal Sphincterotomy Technique in Treatment of Anal Fissure Seyed Reza Mousavi Jr Shohada Medical Center,
REVIEW ARTICLE. Surgical Management of Rectal Prolapse. the anus. 1 Complete or
 REVIEW ARTICLE Surgical Management of Rectal Prolapse Thandinkosi E. Madiba, MMed(Chir), FCS(SA); Mirza K. Baig, FRCS; Steven D. Wexner, MD, FACS, FRCS, FRCS(Edin) Background: The problem of complete rectal
REVIEW ARTICLE Surgical Management of Rectal Prolapse Thandinkosi E. Madiba, MMed(Chir), FCS(SA); Mirza K. Baig, FRCS; Steven D. Wexner, MD, FACS, FRCS, FRCS(Edin) Background: The problem of complete rectal
DIVERTICULAR DISEASE. Dr. Irina Murray Casanova PGY IV
 DIVERTICULAR DISEASE Dr. Irina Murray Casanova PGY IV Diverticular Disease Colonoscopy Abdpelvic CT Scan Surgical Indications Overall, approximately 20% of patients with diverticulitis require surgical
DIVERTICULAR DISEASE Dr. Irina Murray Casanova PGY IV Diverticular Disease Colonoscopy Abdpelvic CT Scan Surgical Indications Overall, approximately 20% of patients with diverticulitis require surgical
Longterm Complications of Hand-Assisted Versus Laparoscopic Colectomy
 Longterm Complications of Hand-Assisted Versus Laparoscopic Colectomy Toyooki Sonoda, MD, Sushil Pandey, MD, Koiana Trencheva, BSN, Sang Lee, MD, Jeffrey Milsom, MD, FACS BACKGROUND: STUDY DESIGN: Hand-assisted
Longterm Complications of Hand-Assisted Versus Laparoscopic Colectomy Toyooki Sonoda, MD, Sushil Pandey, MD, Koiana Trencheva, BSN, Sang Lee, MD, Jeffrey Milsom, MD, FACS BACKGROUND: STUDY DESIGN: Hand-assisted
UvA-DARE (Digital Academic Repository) Rectal prolapse: enlightenment of the obscure Wijffels, N.A.T. Link to publication
 UvA-DARE (Digital Academic Repository) Rectal prolapse: enlightenment of the obscure Wijffels, N.A.T. Link to publication Citation for published version (APA): Wijffels, N. A. T. (2012). Rectal prolapse:
UvA-DARE (Digital Academic Repository) Rectal prolapse: enlightenment of the obscure Wijffels, N.A.T. Link to publication Citation for published version (APA): Wijffels, N. A. T. (2012). Rectal prolapse:
Citation for published version (APA): Bartels, S. A. L. (2013). Laparoscopic colorectal surgery: beyond the short-term effects
 UvA-DARE (Digital Academic Repository) Laparoscopic colorectal surgery: beyond the short-term effects Bartels, S.A.L. Link to publication Citation for published version (APA): Bartels, S. A. L. (2013).
UvA-DARE (Digital Academic Repository) Laparoscopic colorectal surgery: beyond the short-term effects Bartels, S.A.L. Link to publication Citation for published version (APA): Bartels, S. A. L. (2013).
A Constipation Scoring System to Simplify Evaluation and Management of Constipated Patients
 A Constipation Scoring System to Simplify Evaluation and Management of Constipated Patients Feran Agachan, M.D., Teng Chen, M.D., Johann Pfeifer, M.D., Petachia Reissman, M.D., Steven D. Wexner, M.D.,
A Constipation Scoring System to Simplify Evaluation and Management of Constipated Patients Feran Agachan, M.D., Teng Chen, M.D., Johann Pfeifer, M.D., Petachia Reissman, M.D., Steven D. Wexner, M.D.,
Ein Leben nach tiefer Rektumresektion: Was erwartet unsere Patienten im Langzeitverlauf?
 Ein Leben nach tiefer Rektumresektion: Was erwartet unsere Patienten im Langzeitverlauf? Dieter Hahnloser Klinik für Viszeral- und Transplantationschirurgie UniverstätsSpital Zürich Low Rectal Resection
Ein Leben nach tiefer Rektumresektion: Was erwartet unsere Patienten im Langzeitverlauf? Dieter Hahnloser Klinik für Viszeral- und Transplantationschirurgie UniverstätsSpital Zürich Low Rectal Resection
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of laparoscopic ventral mesh rectopexy for internal rectal prolapse Internal rectal
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of laparoscopic ventral mesh rectopexy for internal rectal prolapse Internal rectal
Rectal prolapse CASE REPORT. Sekac J 1, Labas P 2, Skultety J 1, Prochotsky A 1, Skubla R 3, Okolicany R 1
 CASE REPORT Rectal prolapse Sekac J 1, Labas P 2, Skultety J 1, Prochotsky A 1, Skubla R 3, Okolicany R 1 2nd Department for Surgery, University Hospital, Bratislava, Slovakia. jaroslavsekac@yahoo.com
CASE REPORT Rectal prolapse Sekac J 1, Labas P 2, Skultety J 1, Prochotsky A 1, Skubla R 3, Okolicany R 1 2nd Department for Surgery, University Hospital, Bratislava, Slovakia. jaroslavsekac@yahoo.com
Surgery for complete(full-thickness) rectal prolapse in adults(review)
 Cochrane Database of Systematic Reviews Surgery for complete(full-thickness) rectal prolapse in adults (Review) TouS,BrownSR,NelsonRL TouS,BrownSR,NelsonRL. Surgery for complete(full-thickness) rectal
Cochrane Database of Systematic Reviews Surgery for complete(full-thickness) rectal prolapse in adults (Review) TouS,BrownSR,NelsonRL TouS,BrownSR,NelsonRL. Surgery for complete(full-thickness) rectal
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of laparoscopic ventral mesh rectopexy for internal rectal prolapse Internal rectal
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of laparoscopic ventral mesh rectopexy for internal rectal prolapse Internal rectal
Satisfaction with facial laceration repair by provider specialty in the emergency department
 Clin Exp Emerg Med 15;2(3):179-183 http://dx.doi.org/.15441/ceem.15.5 Satisfaction with facial laceration repair by provider specialty in the emergency department eissn: 2383-4625 Original Article Sang-Jae
Clin Exp Emerg Med 15;2(3):179-183 http://dx.doi.org/.15441/ceem.15.5 Satisfaction with facial laceration repair by provider specialty in the emergency department eissn: 2383-4625 Original Article Sang-Jae
Clinical Study Long-Term Outcome after Resection Rectopexy for Internal Rectal Intussusception
 International Scholarly Research Network ISRN Gastroenterology Volume 2012, Article ID 824671, 7 pages doi:10.5402/2012/824671 Clinical Study Long-Term Outcome after Resection Rectopexy for Internal Rectal
International Scholarly Research Network ISRN Gastroenterology Volume 2012, Article ID 824671, 7 pages doi:10.5402/2012/824671 Clinical Study Long-Term Outcome after Resection Rectopexy for Internal Rectal
UvA-DARE (Digital Academic Repository) Rectal prolapse: enlightenment of the obscure Wijffels, N.A.T. Link to publication
 UvA-DARE (Digital Academic Repository) Rectal prolapse: enlightenment of the obscure Wijffels, N.A.T. Link to publication Citation for published version (APA): Wijffels, N. A. T. (2012). Rectal prolapse:
UvA-DARE (Digital Academic Repository) Rectal prolapse: enlightenment of the obscure Wijffels, N.A.T. Link to publication Citation for published version (APA): Wijffels, N. A. T. (2012). Rectal prolapse:
GI Physiology - Investigating and treating patients with pelvic floor dysfunction. Lynne Smith Department of GI Physiology NGH Sheffield
 GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
High-grade hemorrhoids requiring surgical treatment are common after laparoscopic ventral mesh rectopexy
 Tech Coloproctol (2016) 20:235 242 DOI 10.1007/s10151-016-1432-8 ORIGINAL ARTICLE High-grade hemorrhoids requiring surgical treatment are common after laparoscopic ventral mesh rectopexy J. J. van Iersel
Tech Coloproctol (2016) 20:235 242 DOI 10.1007/s10151-016-1432-8 ORIGINAL ARTICLE High-grade hemorrhoids requiring surgical treatment are common after laparoscopic ventral mesh rectopexy J. J. van Iersel
Outcomes of Colostomy Reversal Procedures in Two Teaching Hospitals in Addis Ababa, Ethiopia A. Bekele, B. Kotisso, H. Biluts Correspondence to
 East and Central African Journal of Surgery http://www.bioline.org.br/js 9 Outcomes of Colostomy Reversal Procedures in Two Teaching Hospitals in Addis Ababa, Ethiopia A. Bekele, B. Kotisso, H. Biluts
East and Central African Journal of Surgery http://www.bioline.org.br/js 9 Outcomes of Colostomy Reversal Procedures in Two Teaching Hospitals in Addis Ababa, Ethiopia A. Bekele, B. Kotisso, H. Biluts
Association between Sacral Slanting and Adjacent Structures in Patients with Adolescent Idiopathic Scoliosis
 Original Article Clinics in Orthopedic Surgery 17;9:57-62 https://doi.org/10.4055/cios.17.9.1.57 Association between Sacral Slanting and Adjacent Structures in Patients with Adolescent Idiopathic Scoliosis
Original Article Clinics in Orthopedic Surgery 17;9:57-62 https://doi.org/10.4055/cios.17.9.1.57 Association between Sacral Slanting and Adjacent Structures in Patients with Adolescent Idiopathic Scoliosis
ARTIFICIAL MESH REPAIR FOR TREATMENT OF PELVIC ORGAN PROLAPSE
 Pelvic Floor Unit / Department of Gynaecology Ward 17, Singleton Hospital, Sketty, Swansea, SA2 8QA 01792 205666 Secretary Direct Line: 01792 285688. Fax: 01792 285874 ARTIFICIAL MESH REPAIR FOR TREATMENT
Pelvic Floor Unit / Department of Gynaecology Ward 17, Singleton Hospital, Sketty, Swansea, SA2 8QA 01792 205666 Secretary Direct Line: 01792 285688. Fax: 01792 285874 ARTIFICIAL MESH REPAIR FOR TREATMENT
Surgical Management of IBD in the Age of Biologics
 Surgical Management of IBD in the Age of Biologics Lisa S. Poritz, M.D Associate Professor of Surgery Division of Colon and Rectal Surgery Objectives Discuss surgical management of IBD When to operate
Surgical Management of IBD in the Age of Biologics Lisa S. Poritz, M.D Associate Professor of Surgery Division of Colon and Rectal Surgery Objectives Discuss surgical management of IBD When to operate
CHAU KHAC TU M.D., Ph.D.
 CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
TYPES OF RECTAL PROLAPSE
 RECTAL PROLPASE Rectal prolapse describes a condition where either the lining or entire wall of the rectum becomes loose and falls into, or even out of, the rectum through the anus. TYPES OF RECTAL PROLAPSE
RECTAL PROLPASE Rectal prolapse describes a condition where either the lining or entire wall of the rectum becomes loose and falls into, or even out of, the rectum through the anus. TYPES OF RECTAL PROLAPSE
JNM Journal of Neurogastroenterology and Motility
 JNM Journal of Neurogastroenterology and Motility J Neurogastroenterol Motil, Vol. 19 No. 1 January, 2013 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm.2013.19.1.78 Original Article Successful
JNM Journal of Neurogastroenterology and Motility J Neurogastroenterol Motil, Vol. 19 No. 1 January, 2013 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm.2013.19.1.78 Original Article Successful
Colostomy & Ileostomy
 Colostomy & Ileostomy Indications, problems and preference By Waleed Omar Professor of Colorectal surgery, Mansoura University. Disclosure I have no disclosures. Presentation outline Stoma: Definition
Colostomy & Ileostomy Indications, problems and preference By Waleed Omar Professor of Colorectal surgery, Mansoura University. Disclosure I have no disclosures. Presentation outline Stoma: Definition
The Younger Patients Have More Better Prognosis in Limited Disease Small Cell Lung Cancer
 ORIGINAL ARTICLE http://dx.doi.org/10.4046/trd.2016.79.4.274 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2016;79:274-281 The Younger Patients Have More Better Prognosis in Limited Disease
ORIGINAL ARTICLE http://dx.doi.org/10.4046/trd.2016.79.4.274 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2016;79:274-281 The Younger Patients Have More Better Prognosis in Limited Disease
Complete rectal prolapse, although relatively uncommon,
 ORIGINAL CONTRIBUTION Long-Term Outcome of Altemeier s Procedure for Rectal Prolapse Donato F. Altomare, M.D. 1 & GianAndrea Binda, M.D. 2 & Ezio Ganio, M.D. 3 Paola De Nardi, M.D. 4 & Paolo Giamundo,
ORIGINAL CONTRIBUTION Long-Term Outcome of Altemeier s Procedure for Rectal Prolapse Donato F. Altomare, M.D. 1 & GianAndrea Binda, M.D. 2 & Ezio Ganio, M.D. 3 Paola De Nardi, M.D. 4 & Paolo Giamundo,
Surgical Apgar Score Predicts Post- Laparatomy Complications
 ORIGINAL ARTICLE Surgical Apgar Score Predicts Post- Laparatomy Complications Dullo M 1, Ogendo SWO 2, Nyaim EO 2 1 Kitui District Hospital 2 School of Medicine, University of Nairobi Correspondence to:
ORIGINAL ARTICLE Surgical Apgar Score Predicts Post- Laparatomy Complications Dullo M 1, Ogendo SWO 2, Nyaim EO 2 1 Kitui District Hospital 2 School of Medicine, University of Nairobi Correspondence to:
Articles. Funding None.
 Bowel function after laparoscopic posterior sutured versus ventral mesh for rectal prolapse: a double-blind, randomised single-centre study Lilli Lundby, Lene H Iversen, Steen Buntzen, Pål Wara, Katrine
Bowel function after laparoscopic posterior sutured versus ventral mesh for rectal prolapse: a double-blind, randomised single-centre study Lilli Lundby, Lene H Iversen, Steen Buntzen, Pål Wara, Katrine
Innovations in Rectal Cancer Surgery
 Innovations in Rectal Cancer Surgery A. D Hoore MD PhD, EBSQ-CR, (hon)fascrs A. Wolthuis MD PhD, EBSQ-CR, FACS G. Bislenghi MD Departement of Abdominal Surgery University Hospitals Leuven, Belgium invasiveness
Innovations in Rectal Cancer Surgery A. D Hoore MD PhD, EBSQ-CR, (hon)fascrs A. Wolthuis MD PhD, EBSQ-CR, FACS G. Bislenghi MD Departement of Abdominal Surgery University Hospitals Leuven, Belgium invasiveness
Hemorrhoids. Carlos R. Alvarez-Allende PGY-III Colorectal Surgery
 Hemorrhoids Carlos R. Alvarez-Allende PGY-III Colorectal Surgery Overview Anatomy Classification Etiology Incidence Symptoms Differential Diagnosis Medical Management Surgical Management Anatomy Anal canal
Hemorrhoids Carlos R. Alvarez-Allende PGY-III Colorectal Surgery Overview Anatomy Classification Etiology Incidence Symptoms Differential Diagnosis Medical Management Surgical Management Anatomy Anal canal
WHAT IS LARS? LOW ANTERIOR RESECTIONSYNDROME. Sophie Pilkington. Colorectal Surgeon University Hospital Southampton
 WHAT IS LARS? LOW ANTERIOR RESECTIONSYNDROME Sophie Pilkington Colorectal Surgeon University Hospital Southampton INTRODUCTION UK Bowel cancer 2013 41,100 new cases INTRODUCTION UK Bowel cancer 2013 41,100
WHAT IS LARS? LOW ANTERIOR RESECTIONSYNDROME Sophie Pilkington Colorectal Surgeon University Hospital Southampton INTRODUCTION UK Bowel cancer 2013 41,100 new cases INTRODUCTION UK Bowel cancer 2013 41,100
Laparoscopic vs Robotic Rectal Cancer Surgery: Making it better!
 Laparoscopic vs Robotic Rectal Cancer Surgery: Making it better! Francis Seow- Choen Medical Director Seow-Choen Colorectal Centre Singapore In all situations: We have to use the right tool for the job
Laparoscopic vs Robotic Rectal Cancer Surgery: Making it better! Francis Seow- Choen Medical Director Seow-Choen Colorectal Centre Singapore In all situations: We have to use the right tool for the job
Treatment of Right Colonic Diverticulitis: The Role of Nonoperative Treatment
 Original Article Journal of the Korean Society of DOI: 10.3393/jksc.2010.26.6.402 pissn 2093-7822 eissn 2093-7830 Treatment of Right Colonic Diverticulitis: The Role of Nonoperative Treatment Ma Ru Kim,
Original Article Journal of the Korean Society of DOI: 10.3393/jksc.2010.26.6.402 pissn 2093-7822 eissn 2093-7830 Treatment of Right Colonic Diverticulitis: The Role of Nonoperative Treatment Ma Ru Kim,
Laparoscopic Ventral Mesh Rectopexy: Functional Outcomes after Surgery
 THIEME Original Article e205 Laparoscopic Ventral Mesh Rectopexy: Functional Outcomes after Surgery Nasir Zaheer Ahmad, FRCS 1 Samuel Stefan, MRCS 1 Vidhi Adukia, MRCS 1 Syed Abul Hassan Naqvi, FRCS 1
THIEME Original Article e205 Laparoscopic Ventral Mesh Rectopexy: Functional Outcomes after Surgery Nasir Zaheer Ahmad, FRCS 1 Samuel Stefan, MRCS 1 Vidhi Adukia, MRCS 1 Syed Abul Hassan Naqvi, FRCS 1
World Journal of Colorectal Surgery
 World Journal of Colorectal Surgery Volume 3, Issue 4 2013 Article 3 Sigmoidorectal Intussusception Presenting as Prolapse Per Anus in an Adult Venugopal Hg Hasmukh B. Vora Mahendra S. Bhavsar SMT.NHL
World Journal of Colorectal Surgery Volume 3, Issue 4 2013 Article 3 Sigmoidorectal Intussusception Presenting as Prolapse Per Anus in an Adult Venugopal Hg Hasmukh B. Vora Mahendra S. Bhavsar SMT.NHL
Viscous Fluid Retention: A New Method for Evaluating Anorectal Function
 Viscous Fluid Retention: A New Method for Evaluating Anorectal Function Michael Srensen, M.D., Tine Tetzschner, M.D., le 0. Rasmussen, M.D., John Christiansen, M.D. From the Department of Surgery D, Glostrup
Viscous Fluid Retention: A New Method for Evaluating Anorectal Function Michael Srensen, M.D., Tine Tetzschner, M.D., le 0. Rasmussen, M.D., John Christiansen, M.D. From the Department of Surgery D, Glostrup
Tertiary, regional and local pelvic floor service providers: the future. model? Andrew Williams
 Tertiary, regional and local pelvic floor service providers: the future Andrew Williams model? Pelvic Floor Unit Guy s and St Thomas NHS Foundation Trust Background 23% women suffer at least one pelvic
Tertiary, regional and local pelvic floor service providers: the future Andrew Williams model? Pelvic Floor Unit Guy s and St Thomas NHS Foundation Trust Background 23% women suffer at least one pelvic
Incidence of Colorectal Cancers- Australia. Anterior Resection 5/23/2018. What spurs us to investigate?
 Incidence of Colorectal Cancers- Australia 17,000 Colorectal cancers in 2018 20% of Colorectal cancers are in the Rectum 12.3% of all new cancers Anterior Resection Syndrome (ARS) Lisa Wilson. Colorectal
Incidence of Colorectal Cancers- Australia 17,000 Colorectal cancers in 2018 20% of Colorectal cancers are in the Rectum 12.3% of all new cancers Anterior Resection Syndrome (ARS) Lisa Wilson. Colorectal
Although disparate topics, these two different pathologic
 34 H E M O R R H O I D S A N D R E C T A L P R O L A P S E CHARLES N. HEADRICK MICHAEL J. STAMOS Although disparate topics, these two different pathologic entities are commonly misdiagnosed by both layperson
34 H E M O R R H O I D S A N D R E C T A L P R O L A P S E CHARLES N. HEADRICK MICHAEL J. STAMOS Although disparate topics, these two different pathologic entities are commonly misdiagnosed by both layperson
Stapled transanal rectal resection for obstructed defaecation syndrome
 Stapled transanal rectal resection for obstructed Issued: June 2010 www.nice.org.uk/ipg351 NHS Evidence has accredited the process used by the NICE Interventional Procedures Programme to produce interventional
Stapled transanal rectal resection for obstructed Issued: June 2010 www.nice.org.uk/ipg351 NHS Evidence has accredited the process used by the NICE Interventional Procedures Programme to produce interventional
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015
 Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Identifying predictors of success of the LIFT procedure in the treatment of fistula-in-ano: does location matter?
 Identifying predictors of success of the LIFT procedure in the treatment of fistula-in-ano: does location matter? Department of Colorectal Surgery Cleveland Clinic Florida Sami Chadi MD, Daniel Bekele
Identifying predictors of success of the LIFT procedure in the treatment of fistula-in-ano: does location matter? Department of Colorectal Surgery Cleveland Clinic Florida Sami Chadi MD, Daniel Bekele
Chapter I 7. Laparoscopic versus open elective sigmoid resection in diverticular disease: six months follow-up of the randomized control Sigma-trial
 Chapter I 7 Laparoscopic versus open elective sigmoid resection in diverticular disease: six months follow-up of the randomized control Sigma-trial Bastiaan R. Klarenbeek Roberto Bergamaschi Alexander
Chapter I 7 Laparoscopic versus open elective sigmoid resection in diverticular disease: six months follow-up of the randomized control Sigma-trial Bastiaan R. Klarenbeek Roberto Bergamaschi Alexander
PAPER. Long-term Follow-up of the Modified Delorme Procedure for Rectal Prolapse
 PAPER Long-term Follow-up of the Modified Delorme Procedure for Rectal Prolapse Brian P. Watkins, MD, MS; Jeffrey Landercasper, MD; G. Eric Belzer, MD; Paula Rechner, MD; Rebecca Knudson, BA; Marilu Bintz,
PAPER Long-term Follow-up of the Modified Delorme Procedure for Rectal Prolapse Brian P. Watkins, MD, MS; Jeffrey Landercasper, MD; G. Eric Belzer, MD; Paula Rechner, MD; Rebecca Knudson, BA; Marilu Bintz,
POSTERIOR LEVATOR REPAIR AND RECTAL SUSPENSION FOR RECURRENT RECTAL PROLAPSE: AUTHOR'S EXPERIENCE
 POSTERIOR LEVATOR REPAIR AND RECTAL SUSPENSION FOR RECURRENT RECTAL PROLAPSE: AUTHOR'S EXPERIENCE *Shyam B. Sharma 1&2 and Rahul Gupta 2 1 Department of Pediatric Surgery SMS Medical College 2 Pediatric
POSTERIOR LEVATOR REPAIR AND RECTAL SUSPENSION FOR RECURRENT RECTAL PROLAPSE: AUTHOR'S EXPERIENCE *Shyam B. Sharma 1&2 and Rahul Gupta 2 1 Department of Pediatric Surgery SMS Medical College 2 Pediatric
Bozza Programma preliminare
 Bozza Programma preliminare COLORECTAL AND PELVIC FLOOR DISORDERS FIRST INTERNATIONAL SYMPOSIUM 07-08 Ottobre 2009 - Parma MAIN PELVIC FLOOR: ANATOMY PELVIC FLOOR: NEUROPHISIOLOGY IMAGING IN PELVIC FLOOR
Bozza Programma preliminare COLORECTAL AND PELVIC FLOOR DISORDERS FIRST INTERNATIONAL SYMPOSIUM 07-08 Ottobre 2009 - Parma MAIN PELVIC FLOOR: ANATOMY PELVIC FLOOR: NEUROPHISIOLOGY IMAGING IN PELVIC FLOOR
Rectal irrigation: a useful tool in the armamentarium for functional bowel disorders
 Original article doi:10.1111/j.1463-1318.2011.02797.x Rectal irrigation: a useful tool in the armamentarium for functional bowel disorders D. S. Y. Chan*, A. Saklani, P. R. Shah, M. Lewis and P. N. Haray
Original article doi:10.1111/j.1463-1318.2011.02797.x Rectal irrigation: a useful tool in the armamentarium for functional bowel disorders D. S. Y. Chan*, A. Saklani, P. R. Shah, M. Lewis and P. N. Haray
World Journal of Colorectal Surgery
 World Journal of Colorectal Surgery Volume 6, Issue 5 2016 Article 8 Sigmoidocele: A Rare Cause Of Constipation In Males Noor Shah MD Milind Kachare MD Craig Rezac MD Rutgers Robert Wood Johnson Medical
World Journal of Colorectal Surgery Volume 6, Issue 5 2016 Article 8 Sigmoidocele: A Rare Cause Of Constipation In Males Noor Shah MD Milind Kachare MD Craig Rezac MD Rutgers Robert Wood Johnson Medical
World Journal of Colorectal Surgery
 World Journal of Colorectal Surgery Volume 6, Issue 1 Article 3 Starr Surgery In ODS: A Case Series Of 500 ODS Patients Operated At India s Largest Proctology Clinic Ashwin Dhanarajji Porwal Paresh Manilal
World Journal of Colorectal Surgery Volume 6, Issue 1 Article 3 Starr Surgery In ODS: A Case Series Of 500 ODS Patients Operated At India s Largest Proctology Clinic Ashwin Dhanarajji Porwal Paresh Manilal
Routine Internal Sphincterotomy with Hemorrhoidectomy: A Prospective Study
 Original Article DOI:./ijss// Routine Internal Hemorrhoidectomy: A Prospective Study S Harish, R Raxith Sringeri, G Ajay Associate Professor, Department of Surgery, JSS University, Mysore, Karnataka, India,
Original Article DOI:./ijss// Routine Internal Hemorrhoidectomy: A Prospective Study S Harish, R Raxith Sringeri, G Ajay Associate Professor, Department of Surgery, JSS University, Mysore, Karnataka, India,
Ischemic Stroke in Critically Ill Patients with Malignancy
 Ischemic Stroke in Critically Ill Patients with Malignancy Jeong-Am Ryu 1, Oh Young Bang 2, Daesang Lee 1, Jinkyeong Park 1, Jeong Hoon Yang 1, Gee Young Suh 1, Joongbum Cho 1, Chi Ryang Chung 1, Chi-Min
Ischemic Stroke in Critically Ill Patients with Malignancy Jeong-Am Ryu 1, Oh Young Bang 2, Daesang Lee 1, Jinkyeong Park 1, Jeong Hoon Yang 1, Gee Young Suh 1, Joongbum Cho 1, Chi Ryang Chung 1, Chi-Min
A Comparitive Study of Laying Open of Wound Vs Primary Closure In Fistula in Ano
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-853, p-issn: 2279-861.Volume 13, Issue 9 Ver. III (Sep. 214), PP 39-45 A Comparitive Study of Laying Open of Wound Vs Primary Closure
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-853, p-issn: 2279-861.Volume 13, Issue 9 Ver. III (Sep. 214), PP 39-45 A Comparitive Study of Laying Open of Wound Vs Primary Closure
A scoring system for the assessment of bowel and lower urinary tract symptoms in women
 BJOG: an International Journal of Obstetrics and Gynaecology April 2002, Vol. 109, pp. 424 430 A scoring system for the assessment of bowel and lower urinary tract symptoms in women L. Hiller a, H.D. Bradshaw
BJOG: an International Journal of Obstetrics and Gynaecology April 2002, Vol. 109, pp. 424 430 A scoring system for the assessment of bowel and lower urinary tract symptoms in women L. Hiller a, H.D. Bradshaw
Study of laparoscopic appendectomy: advantages, disadvantages and reasons for conversion of laparoscopic to open appendectomy
 International Surgery Journal Agrawal SN et al. Int Surg J. 2017 Mar;4(3):993-997 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20170849
International Surgery Journal Agrawal SN et al. Int Surg J. 2017 Mar;4(3):993-997 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20170849
The incidence of incisional hernias following ileostomy reversal in colorectal cancer patients treated with anterior resection
 GENERAL SURGERY Ann R Coll Surg Engl 2017; 99: 319 324 doi 10.1308/rcsann.2016.0347 The incidence of incisional hernias following ileostomy reversal in colorectal cancer patients treated with anterior
GENERAL SURGERY Ann R Coll Surg Engl 2017; 99: 319 324 doi 10.1308/rcsann.2016.0347 The incidence of incisional hernias following ileostomy reversal in colorectal cancer patients treated with anterior
SACRAL NERVE STIMULATION FOR EXPERIENCE IN CHILDREN
 SACRAL NERVE STIMULATION FOR COLORECTAL DISEASES: EXPERIENCE IN CHILDREN C. LOUIS-BORRIONE - JM. GUYS TIMONE-ENFANTS MARSEILLE SACRAL NEUROMODULATION IN CHILDREN 26 : Humphreys et al - 23 children with
SACRAL NERVE STIMULATION FOR COLORECTAL DISEASES: EXPERIENCE IN CHILDREN C. LOUIS-BORRIONE - JM. GUYS TIMONE-ENFANTS MARSEILLE SACRAL NEUROMODULATION IN CHILDREN 26 : Humphreys et al - 23 children with
Inadvertent Enterotomy in Minimally Invasive Abdominal Surgery
 SCIENTIFIC PAPER Inadvertent Enterotomy in Minimally Invasive Abdominal Surgery Steven J. Binenbaum, MD, Michael A. Goldfarb, MD ABSTRACT Background: Inadvertent enterotomy (IE) in laparoscopic abdominal
SCIENTIFIC PAPER Inadvertent Enterotomy in Minimally Invasive Abdominal Surgery Steven J. Binenbaum, MD, Michael A. Goldfarb, MD ABSTRACT Background: Inadvertent enterotomy (IE) in laparoscopic abdominal
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan
 Original Article Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan ABSTRACT Objective: Aim of the study was to determine
Original Article Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan ABSTRACT Objective: Aim of the study was to determine
Standardized Thyroid Cancer Mortality in Korea between 1985 and 2010
 Original Article Endocrinol Metab 2014;29:530-535 http://dx.doi.org/10.3803/enm.2014.29.4.530 pissn 2093-596X eissn 2093-5978 Standardized Thyroid Cancer Mortality in Korea between 1985 and 2010 Yun Mi
Original Article Endocrinol Metab 2014;29:530-535 http://dx.doi.org/10.3803/enm.2014.29.4.530 pissn 2093-596X eissn 2093-5978 Standardized Thyroid Cancer Mortality in Korea between 1985 and 2010 Yun Mi
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy
 Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
ORIGINAL RESEARCH. International Journal of Surgery
 International Journal of Surgery 11 (2013) 52e58 Contents lists available at SciVerse ScienceDirect International Journal of Surgery journal homepage: www.theijs.com Original research Comparative study
International Journal of Surgery 11 (2013) 52e58 Contents lists available at SciVerse ScienceDirect International Journal of Surgery journal homepage: www.theijs.com Original research Comparative study
Relation between the Peripherofacial Psoriasis and Scalp Psoriasis
 pissn 1013-9087ㆍeISSN 2005-3894 Ann Dermatol Vol. 28, No. 4, 2016 http://dx.doi.org/10.5021/ad.2016.28.4.422 ORIGINAL ARTICLE Relation between the Peripherofacial Psoriasis and Scalp Psoriasis Kyung Ho
pissn 1013-9087ㆍeISSN 2005-3894 Ann Dermatol Vol. 28, No. 4, 2016 http://dx.doi.org/10.5021/ad.2016.28.4.422 ORIGINAL ARTICLE Relation between the Peripherofacial Psoriasis and Scalp Psoriasis Kyung Ho
15. Prevention of UTI and lifestyle modifications
 15. Prevention of UTI and lifestyle modifications Key questions: Does improving poor voiding habits help prevent UTI recurrence? Does improving constipation help prevent UTI recurrence? Does increasing
15. Prevention of UTI and lifestyle modifications Key questions: Does improving poor voiding habits help prevent UTI recurrence? Does improving constipation help prevent UTI recurrence? Does increasing
The main issues of the rectal resection for carcinoma
 The main issues of the rectal resection for carcinoma - Level of the vessels transection and mobilisation of the splenic flexure - Lymphadenectomy - Distal margin - Parietal invasion of rectal wall - Functional
The main issues of the rectal resection for carcinoma - Level of the vessels transection and mobilisation of the splenic flexure - Lymphadenectomy - Distal margin - Parietal invasion of rectal wall - Functional
Citation Acta medica Nagasakiensia. 2003, 48
 NAOSITE: Nagasaki University's Ac Title Author(s) Surgical Strategy for Low Imperfora Anal Transplantation or Limited Pos Obatake, Masayuki; Yamashita, Hidek Norihisa; Nakagoe, Tohru Citation Acta medica
NAOSITE: Nagasaki University's Ac Title Author(s) Surgical Strategy for Low Imperfora Anal Transplantation or Limited Pos Obatake, Masayuki; Yamashita, Hidek Norihisa; Nakagoe, Tohru Citation Acta medica
Robot-assisted laparoscopic rectovaginopexy for rectal prolapse: a prospective cohort study on feasibility and safety
 J Robotic Surg (2008) 1:273 277 DOI 10.1007/s11701-007-0053-7 ORIGINL RTICLE Robot-assisted laparoscopic rectovaginopexy for rectal prolapse: a prospective cohort study on feasibility and safety Werner.
J Robotic Surg (2008) 1:273 277 DOI 10.1007/s11701-007-0053-7 ORIGINL RTICLE Robot-assisted laparoscopic rectovaginopexy for rectal prolapse: a prospective cohort study on feasibility and safety Werner.
Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583
 Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
CIC Edizioni Internazionali. original article. Transanal repair of rectocele with high frequency radio scalpel. Patients and methods.
 G Chir Vol. 39 - n. 5 - pp. 303-308 September-October 2018 Transanal repair of rectocele with high frequency radio scalpel D. SFORZA, C. BELARDI, M. PELLICCIARO, V. FILINGERI SUMMARY: Transanal repair
G Chir Vol. 39 - n. 5 - pp. 303-308 September-October 2018 Transanal repair of rectocele with high frequency radio scalpel D. SFORZA, C. BELARDI, M. PELLICCIARO, V. FILINGERI SUMMARY: Transanal repair
Outcomes of Radical Prostatectomy in Thai Men with Prostate Cancer
 Original Article Outcomes of Radical Prostatectomy in Thai Men with Prostate Cancer Sunai Leewansangtong, Suchai Soontrapa, Chaiyong Nualyong, Sittiporn Srinualnad, Tawatchai Taweemonkongsap and Teerapon
Original Article Outcomes of Radical Prostatectomy in Thai Men with Prostate Cancer Sunai Leewansangtong, Suchai Soontrapa, Chaiyong Nualyong, Sittiporn Srinualnad, Tawatchai Taweemonkongsap and Teerapon
Hester Cheung Memorial Lecture
 Hester Cheung Memorial Lecture STEVEN D WEXNER, MD, PHD (HON),FACS, FRCS, FRCS(ED) Director, Digestive Disease Center; Chairman, Department of Colorectal Surgery; Cleveland Clinic Florida Professor of
Hester Cheung Memorial Lecture STEVEN D WEXNER, MD, PHD (HON),FACS, FRCS, FRCS(ED) Director, Digestive Disease Center; Chairman, Department of Colorectal Surgery; Cleveland Clinic Florida Professor of
2/5/2016. Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach
 Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach Holly E Richter, PhD, MD, FACOG, FACS J Marion Sims Professor Obstetrics and Gynecology Professor
Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach Holly E Richter, PhD, MD, FACOG, FACS J Marion Sims Professor Obstetrics and Gynecology Professor
Factors Influencing the Prevalence of Amblyopia in Children with Anisometropia
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2010;24(4):225-229 DOI: 10.3341/kjo.2010.24.4.225 Factors Influencing the Prevalence of Amblyopia in Children with Anisometropia Original Article Chong
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2010;24(4):225-229 DOI: 10.3341/kjo.2010.24.4.225 Factors Influencing the Prevalence of Amblyopia in Children with Anisometropia Original Article Chong
STOMA SITING & PARASTOMAL HERNIA MANAGEMENT
 STOMA SITING & PARASTOMAL HERNIA MANAGEMENT Professor Hany S. Tawfik Head of the Department of Surgery & Chairman of Colorectal Surgery Unit Benha University Disclosure No financial affiliation to disclose
STOMA SITING & PARASTOMAL HERNIA MANAGEMENT Professor Hany S. Tawfik Head of the Department of Surgery & Chairman of Colorectal Surgery Unit Benha University Disclosure No financial affiliation to disclose
