For personal use only CONTROVERSIES IN PELVIC SURGERY
|
|
|
- Colin Atkins
- 6 years ago
- Views:
Transcription
1 For mass reproduction, content licensing and permissions contact Dowden Health Media. OBG MANAGEMENT NEW VIDEO ONLINE Copyright Dowden Health Media For personal use only This posthysterectomy prolapse clearly requires surgical correction, but the route of operation and the specific repair depend on the surgeon s expertise and the patient s symptoms, health, and desire for coitus IN THIS ARTICLE What is the best operation for advanced prolapse? Page 77 Are unaugmented repairs doomed to fail? Page 78 Are kits the new standard? Page 80 The Golden Rule of surgery Page 84 CONTROVERSIES IN PELVIC SURGERY Pelvic organ prolapse: Which operation for which patient? The stream of new technologies seems never-ending. That s part of the problem. The more numerous the choices of surgical techniques for pelvic organ prolapse, the less agreement there is on which operation is best. Further complicating the picture is the industry s push to consider augmentation with synthetic or biologic materials on an almost routine basis. Few scientific comparisons of the various approaches have been performed, however. To help shed some light on surgical decision-making, we convened an expert panel to review published data and explore our experience with selected procedures. What to consider before choosing a procedure A woman s desires regarding sexual activity are a critical piece of information, just as are her general health and history of pelvic surgery. It also helps to know which symptoms of her prolapse and related pelvic floor disorders she finds most bothersome. KARRAM: When a woman with symptomatic pelvic organ prolapse desires surgical correction, what factors do you explore before deciding which procedure to use? IMAGE: TODD BUCK 72 OBG MANAGEMENT May 2006
2 BRUBAKER: I make an effort to determine the woman s readiness to undergo surgery and her expectations for it, as well as any concomitant pelvic floor or medical/surgical conditions. Other important factors that I consider include her pelvic surgical history specifically, whether she has undergone earlier continence and/or prolapse repairs and the presence of any materials in the proposed surgical site, especially foreign bodies that may limit dissection planes or have eroded into pelvic viscera. I also consider her desire (or lack of it) for sexual activity, and her preferred route of surgical access. Patient s lifestyle should sway surgical decision PARAISO: I take into account her age and stage of prolapse; vaginal length; innervation of the pelvic floor; hormonal status; desire for uterine preservation and coitus; symptoms of sexual, urinary, or bowel dysfunction; and any comorbidities that influence her eligibility for anesthesia or chronically increase intra-abdominal pressure. Connective tissue disorders are also important, as are any coexisting medical conditions that impede healing. Lifestyle has an impact, too, especially if she regularly performs heavy manual labor. After assessing the patient s history and performing an examination, I target the prolapse and functional symptoms and correlating anatomic defects that exacerbate her quality of life. I tailor her surgical therapy in order to correct her symptoms and minimize compensatory defects and de novo dysfunction. Ask her to prioritize her complaints SHULL: I have the patient list her complaints in order of their severity and impact on her lifestyle. Next, I complete a detailed pelvic exam, including use of a mirror to demonstrate the findings to her. If appropriate, I test bladder or bowel function. At that point, we discuss what I think are appropriate options, although in some situations I may not be able to treat all her complaints with equal success. KARRAM: I think prioritizing the patient s complaints is a good idea. My foremost aim is to determine what the woman is most bothered by. If it is prolapse symptoms such as pressure and tissue protrusion, with no functional derangements, I try to ensure that my surgical repair provides durable support but does not create de novo derangements such as stress incontinence. So, for example, I try to determine whether she has preexisting stress incontinence that is masked by the prolapse. Correlation between prolapse and dysfunction can be weak Obviously, if the patient has many functional derangements associated with the prolapse symptoms, the preoperative consultation becomes much more complicated. Although the complexity may not change my surgical approach, I think it is important for the patient to understand that the correlation between anatomic OUR EXPERT PANELISTS Moderator Mickey Karram, MD, Director of Urogynecology, Good Samaritan Hospital, Cincinnati, and Professor of Obstetrics and Gynecology, University of Cincinnati. Linda Brubaker, MD, MS, Assistant Dean of Clinical and Translational Research, and Professor and Director, Division of Female Pelvic Medicine and Reconstructive Pelvic Surgery, Departments of Obstetrics & Gynecology and Urology, Loyola University Health System, Chicago. Marie Fidela Paraiso, MD, Co-Director of Female Pelvic Medicine and Reconstructive Surgery, Department of Obstetrics and Gynecology and the Urological Institute, The Cleveland Clinic, Cleveland, Ohio. Bob L. Shull, MD, Vice Chairman, Department of Obstetrics and Gynecology, and Chief, Section of Female Pelvic Medicine and Pelvic Reconstructive Surgery, Scott & White Health Care System, Temple, Tex. My foremost aim is to determine what the woman is most bothered by Mickey Karram, MD May 2006 OBG MANAGEMENT 73
3 Pelvic organ prolapse: Which operation for which patient? I probably perform 98% of reconstructive cases transvaginally Bob L. Shull, MD descent and the functional derangement may not be very good. As previously mentioned, I make a point to ask about sexual function. If the woman is elderly and has no intention of being sexually active again, I may consider a very tight or obliterative repair because these are much less invasive than conventional repairs. Is one surgical route superior? There is no consensus among experts as to the preferred route of surgery for advanced pelvic organ prolapse. KARRAM: Numerous vaginal, abdominal, and laparoscopic procedures have been described. Which route do you prefer? BRUBAKER: I don t prefer any laparoscopic procedures, but I am flexible about vaginal or abdominal approaches. Among vaginal procedures, I prefer uterosacral suspension at the time of hysterectomy, or the Michigan modification of sacrospinous ligament suspension when the patient has already undergone hysterectomy. As for abdominal procedures, I prefer sacrocolpopexy with Mersilene mesh. In my hands, these reconstructive procedures give predictable results that allow me to appropriately counsel patients preoperatively. KARRAM: Why do you dislike the laparoscopic approach? BRUBAKER: It is not a matter of dislike, but a matter of getting the most reliable result for my patient. When scientific evidence from well-done clinical trials demonstrates the equivalency of laparoscopic procedures, I fully anticipate incorporating them into my practice. Similarly, the novel use of the robot may be useful in reconstructive pelvic surgery. Laparoscopic repair can produce good results in the right hands PARAISO: I prefer the laparoscopic and vaginal routes. In fact, I have converted most abdominal procedures to laparoscopic access. I have nearly 10 years of experience with laparoscopic sacrocolpopexy, with excellent success. My colleagues and I did a cohort study that showed equal cure rates for this procedure, compared with open sacrocolpopexy. 1 I also have had great success with the vaginal route when performing uterosacral vaginal vault suspensions. Patients are referred to me or seek me out specifically for minimally invasive procedures, so the majority of operations I perform are laparoscopic procedures with or without vaginal procedures, or vaginal procedures alone. Vaginal approach is possible in high percentage of cases SHULL: I probably perform 98% of reconstructive cases transvaginally. If the woman has urinary incontinence as well as prolapse, I usually perform a midurethral sling procedure along with the repair. KARRAM: I do roughly 90% of prolapse repairs transvaginally. For the last 6 to 8 years, my colleagues and I have utilized a high uterosacral vaginal vault suspension to support the vaginal cuff. We do so in conjunction with a modified internal McCall-type procedure to obliterate the cul-de-sac. We also do site-specific anterior and posterior colporrhaphy as needed, and a synthetic midurethral sling if the patient has stress incontinence. In very young patients (under 35 years of age) or those who have substantial recurrent prolapse or a prolapsed foreshortened vagina, we consider abdominal sacrocolpopexy with synthetic mesh as our primary operation. In such cases, we commonly perform retropubic repair for incontinence and paravaginal defects, as well as posterior repair and perineorrhaphy. I have very little experience with laparoscopic prolapse repairs. Abdominal sacrocolpopexy is anatomically superior KARRAM: Dr. Brubaker, you just chaired a consensus panel on pelvic organ prolapse 74 OBG MANAGEMENT May 2006
4 Pelvic organ prolapse: Which operation for which patient? for the International Consultation on Incontinence. This panel reviewed all the published literature on the topic. What conclusions did it reach about the various surgical procedures for pelvic organ prolapse? BRUBAKER: The big picture findings were that abdominal sacrocolpopexy is anatomically superior to the other procedures, but carries a higher rate of shortterm morbidity than transvaginal procedures. Since that panel, a review on sacrocolpopexy by Nygaard et al 2 highlighted the strengths, weaknesses, and uncertainties of this procedure. We found no indications for routine use of ancillary materials when performing primary transvaginal repairs. What is the best operation for advanced prolapse? The best procedure depends on the patient s health, type and extent of prolapse, and sexual activity. Surgical history also is key. KARRAM: Let s say a 60-year-old woman with advanced, symptomatic, primary pelvic organ prolapse presents to you for surgical treatment. The findings include posthysterectomy vaginal vault prolapse with a large cystocele, large rectocele, and an enterocele. What operation would you perform? SHULL: I would probably elect a transvaginal approach using the uterosacral ligaments to suspend the cuff and reapproximate the connective tissue of the anterior and posterior compartments. My colleagues and I described this technique. 3 PARAISO: If the patient is physically and sexually active and willing to undergo synthetic graft implantation, I would perform laparoscopic sacrocolpopexy, especially if previous transvaginal apical suspension has failed, if she has a foreshortened vagina, or if she has denervation of her pelvic floor. Check for defecatory dysfunction If it is necessary for her to manually digitate her vagina or splint her perineum to defecate, I would perform a rectocele repair and perineorrhaphy. If she is not a candidate for laparoscopic or abdominal surgery because of a history of multiple procedures for inflammatory bowel disease or severe adhesions, has not had a previous transvaginal apical suspension, and has intact pelvic floor innervation, I would perform either uterosacral vaginal vault suspension or sacrospinous ligament suspension with concomitant anterior and posterior repair. I would consider offering this patient a tension-free vaginal mesh kit procedure (with synthetic mesh) if she: has failed previous vaginal procedures, has multiple comorbidities, is not a candidate for laparoscopic or abdominal surgery, desires to remain sexually active, and is willing to use and has no contraindications to intravaginal estrogen therapy. If she does not wish to remain sexually active and is not a good operative candidate, I would offer colpectomy and colpocleisis with perineorrhaphy. Which circumstances pose special challenges? Apical suspension is a critical factor in success and durability of the surgery. KARRAM: Which segment of the pelvic floor do you find most challenging when correcting advanced pelvic organ prolapse? SHULL: My colleagues and I have reported our experience with several techniques of vaginal repair for prolapse, including sacrospinous ligament suspension, iliococcygeus fascial suspension, and uterosacral ligament suspension. When we analyzed specific sites in the vagina, the anterior compartment always had the greatest percentage of persistent or recurrent loss of support. Our best success has been with uterosacral ligament suspension. C O N T I N U E D If you get the apex up solidly, you re usually home free Linda Brubaker, MD May 2006 OBG MANAGEMENT 77
5 Pelvic organ prolapse: Which operation for which patient? Vaginal apex is key to success PARAISO: I also find the anterior segment challenging. However, if I am able to suspend the vaginal apex well, management of the anterior vaginal wall is less challenging. The anterior wall fails because treatment of high transverse cystoceles and anterior enteroceles (less commonly seen) depends on the apical suspension. Many of these defects go untreated because they are often not detected. BRUBAKER: I agree with Dr. Paraiso. If you get the apex up solidly, you re usually home free. KARRAM: Yes. If one can get good, high, durable support to the apex, the other segments of the pelvic floor are much more likely to endure. Are unaugmented repairs doomed to fail? Despite claims to the contrary, reoperation rates are low for most conventional repairs. Surgeons may be tempted to adopt graft augmentation techniques to keep up with Dr. Jones. KARRAM: As you know, there has been a recent push to consider augmenting most pelvic organ prolapse repairs with either biologic or synthetic mesh. This approach is based on a perception that conventional repairs without augmentation inevitably will fail. Do you agree with this perception? SHULL: Not based on my own experience. Mesh has been effectively and safely used for midurethral slings and abdominal sacrocolpopexies, but there are not enough data on the use of allografts, xenografts, or meshes to be able to counsel a patient properly about their safety, efficacy, or long-term effects. PARAISO: I agree that this perception is being promoted, prompting many physicians to adopt graft augmentation techniques to keep up with Dr. Jones or to offer their patients cutting-edge treatment. Despite the fact that conventional procedures are often described as having high failure rates, the reoperation rates in most series are low. Nevertheless, augmen- 78 OBG MANAGEMENT May 2006
6 Pelvic organ prolapse: Which operation for which patient? Any operation that alters the vaginal axis will seriously weaken the vagina opposite the distorted axis Mickey Karram, MD tation with biologic grafts has been widely adopted without prior investigation or data. Traditional and site-specific repairs versus graft augmentation My colleagues and I just presented a manuscript on traditional posterior colporrhaphy, site-specific rectocele repair, and sitespecific repair with graft augmentation using a porcine small intestinal submucosa bioengineered collagen matrix. The anatomic cure rate was substantially higher in the traditional and site-specific groups when compared with the graft augmentation arm, with cure rates of 86% and 78% versus 54%, respectively (P=.02). 4 Currently, my indications for a meshaugmented prolapse repair are: Nonexistent or suboptimal autologous tissue Need to augment weak or absent endopelvic tissue Connective tissue disorder Unavoidable stress on the repair (eg, chronic lifting, chronic obstructive pulmonary disease, chronic straining to defecate, obesity) Need to bridge a space such as sacral colpopexy Concern about vaginal length or caliber Denervated pelvic floor Recurrent prolapse Surgeons should not believe that graft augmentation compensates for surgical mediocrity or patient risk factors for pelvic organ prolapse. The key to success: Maintain the vaginal axis KARRAM: I don t believe all traditional repairs are bound to fail. Many factors play into recurrent prolapse. I think most people overlook the fact that the vagina is very sensitive to its axis. Any operation that alters the vaginal axis will seriously weaken the vagina opposite the distorted axis. For example, we know that sacrospinous ligament suspension retroverts the vagina and sets women up for recurrence or development of anterior vaginal wall prolapse. Another example is a Burch colposuspension that anteverts a portion of the vagina and sets patients up for posterior vaginal wall defects in the form of a rectocele and enterocele. Too much simplification I also think surgeons and device manufacturers have attempted to simplify what, in reality, is a very complicated clinical picture. So many factors are involved in the identification and appropriate utilization of support structures for a durable prolapse repair. Since Dr. Shull s popularization of a high uterosacral suspension, we have had very good long-term success with transvaginal vault repair. Also, over time I have realized that it is possible to mobilize a substantial amount of durable fascial tissue which is nothing more than the muscular lining of the vagina to appropriately support the anterior and posterior vaginal walls. That said, the results are far from perfect. I would estimate our anatomic failure rate at 15% to 20% over the long term. Does augmentation add complications? When it comes to mesh, we have to ask: Is it truly going to increase durability? If it is, is that going to be at the expense of a new set of complications such as mesh erosion or extrusion and dyspareunia? The only way to answer these questions is with a randomized trial with longterm follow-up. At this time, such data are not available. Are tension-free repair kits the wave of the future? It s not yet time to make these kits the standard, although preliminary data are promising. KARRAM: Do you think the synthetic mesh repairs now being promoted as tensionfree repairs utilizing numerous industry- CONTINUED 80 OBG MANAGEMENT May 2006
7 Pelvic organ prolapse: Which operation for which patient? Until trials are done, we won t really know how the kits with synthetic mesh compare with conventional repairs Mickey Karram, MD created kits will be the future of prolapse repair? BRUBAKER: I hope not. KARRAM: At present, I would say the answer to that question is no. However, I was very reluctant to accept synthetic midurethral slings, and they have turned out to be the standard of care. SHULL: These products are the future for surgeons who allow industry to dictate their practice styles. For those of us who are more skeptical, we will change only after there is adequate scientific information to do so. Though unproven, kits do have advantages PARAISO: I agree. Even so, in many ways, these kits make sense. Operative time is greatly reduced and incisions are small, thus offering the advantage of minimally invasive procedures. Preliminary data at 6 months show excellent anatomic outcomes. However, the graft extrusion rate is high with the kit procedures, compared with existing evidence on synthetic mesh erosion associated with abdominal and laparoscopic sacral colpopexy. In addition, current synthetic materials are not ideal. Long-term sequelae of transvaginal implantation of these meshes are not known. Nor do we have long-term data on sexual function. By and large, these procedures are blind and involve the transobturator and transgluteal (ischiorectal fossa) spaces uncharted waters for many gynecologic surgeons. Further, many gynecologic surgeons lack extensive training or experience in sacrospinous ligament suspension, iliococcygeus fascia suspension, and vaginal paravaginal defect repair, which are prerequisites for the kit procedures. Matching the kit procedure to the patient As for patient selection, women for whom previous anterior repair (with or without biologic graft), paravaginal defect repair, and apical suspension have failed, and who continue to have asymptomatic anterior vaginal wall prolapse are the best candidates for anterior kit procedures. The best candidates for posterior and apical segment kit procedures are women in whom transvaginal apical suspension has failed, and who are not suited for laparoscopic or abdominal procedures. The only impediments to widespread adoption of these procedures for years to come will be adverse events or technology so advanced it makes gene modification possible, rendering surgery obsolete. KARRAM: I think we need better and longer follow-up. Most of the surgeons currently using these procedures are proponents of the repairs, in my opinion, but until results from comparative trials become available, we won t really know how they compare to conventional repairs. Bringing up the next generation Residents need as much hands-on experience as possible, including cadaveric dissections, urodynamic labs, and urogynecologic clinics even virtual-reality models. KARRAM: How do we best train residents in the appropriate evaluation and surgical management of these very common pelvic floor disorders? BRUBAKER: Carefully and ethically. Encourage them to be good consumers of surgical literature and to resist the urge to constantly demonstrate the latest and greatest until we have solid evidence. PARAISO: Residents can learn from discussions of surgical indications prior to pelvic reconstructive procedures in which they are involved, attendance at urogynecologic clinics, urodynamic lab rotations, and study of urogynecologic learning modules and current clinical textbooks that focus on these surgeries. Given the decrease in resident work hours, which translates to fewer cases, cadaver labs are also helpful. C O N T I N U E D 82 OBG MANAGEMENT May 2006
8 Expert Peer Review These educators and researchers are among the experts who help select up-to-date, accurate, and relevant information for every issue, cover-to-cover. Harold Bivins, MD Savannah, Ga Andrew I. Brill, MD Chicago, Ill Brian C. Brost, MD Haywood Brown, MD Durham, NC James Burke II, MD Savannah, Ga David Byck, MD Savannah, Ga Frank Chervenak, MD New York, NY William A. Cliby, MD Alan H. DeCherney, MD Bethesda, Md Philip J. DiSaia, MD Orange, Calif Patrick Duff, MD Gainesville, Fla Abimbola O. Famuyide, MD Sebastian Faro, MD, PhD Houston, Tex John Gebhart, MD Martin L. Gimovsky, MD Newark, NJ Mark H. Glasser, MD San Rafael, Calif Amos Grunebaum, MD New York, NY Steven Hockstein, MD New York, NY Thomas M. Julian, MD Madison, Wis Christopher Klingele, MD Robert Kovac, MD Atlanta, Ga Franklin Loffer, MD Tucson, Ariz Anthony A. Luciano, MD New Britain, Conn Dev Maulik, MD, PhD Mineola, NY Ramon V. Meguiar, MD Savannah, Ga William H. Parker, MD Santa Monica, Calif JoAnn Rosenfeld, MD Odenton, Md Amy Rosenman, MD Santa Monica, Calif Gerard Roy, MD New Britain, Conn Hyagriv Simhan, MD Pittsburgh, Pa Anthony R. Scialli, MD Alexandria, Va Stephen B. Young, MD Worcester, Mass Carl W. Zimmerman, MD Nashville, Tenn Pelvic organ prolapse: Which operation for which patient? Virtual-reality models are being developed and will be available this decade. Golden rule of surgery: Do unto others... SHULL: I would advise residents to treat every woman as you would your wife, mother, sister, daughter, or yourself. That may mean using a consultant for some of your patients. Those of us who are teachers must use all available resources, including didactic instruction, video clips, cadaver dissection, simulators, and hands-on supervision in the operating room. Those who are learning new procedures must be willing to accept constructive comments and critically evaluate their own skills. KARRAM: I think it is important to continue training residents in the basics of pelvic floor support and anatomy. If the future involves passing needles into blind spaces, the outcomes will be disastrous if the surgeon is not comfortable with the relevant anatomy. Secondly, surgeons should maintain their skills in proven operations such as abdominal sacrocolpopexy and sacrospinous ligament suspension. As we gain experience and long-term data, other procedures can be added more easily if we have a good understanding of the conventional repairs. REFERENCES 1. Paraiso MFR, Walters MD, Rackley RR, Melek S, Hugney C. Laparoscopic and open sacral colpopexies: a cohort study. Am J Obstet Gynecol. 2005;192: Nygaard IE, McCreery R, Brubaker L, et al. Abdominal sacrocolpopexy: a comprehensive review. Obstet Gynecol. 2004;104: Shull BL, Bachofen CG, Coates KW, Kuehl TJ. A transvaginal approach to repair of apical and other associated sites of pelvic organ prolapse using uterosacral ligaments. Am J Obstet Gynecol. 2000;183: Paraiso MFR, Barber MD, Muir TW, Walters MD. Rectocele repair: a randomized trial of three surgical techniques including graft augmentation. Am J Obstet Gynecol [in press]. Dr. Karram receives grant/research support from American Medical Systems, Carbon Medical, Gynecare, and Pfizer; is a consultant to Gynecare; and is a speaker for Gynecare, Indevus, and Ortho-McNeil. Dr. Paraiso has received grant/research support from American Medical Systems and Organogenesis Inc.; and is a consultant to American Medical Systems, and Ethicon Women's Health and Urology. Dr. Brubaker and Dr. Shull report no financial relationships relevant to this article. 84 OBG MANAGEMENT May 2006
Understanding Pelvic Organ Prolapse. Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery
 Understanding Pelvic Organ Prolapse Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery Disclosures None I am the daughter of a physician assistant. Objectives List types of pelvic
Understanding Pelvic Organ Prolapse Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery Disclosures None I am the daughter of a physician assistant. Objectives List types of pelvic
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review
 Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy
 Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
International Federation of Gynecology and Obstetrics
 International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
PRACTICE BULLETIN Female Pelvic Medicine & Reconstructive Surgery Volume 23, Number 4, July/August 2017
 PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015
 Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
LAPAROSCOPIC REPAIR OF PELVIC FLOOR
 LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
9/24/2015. Pelvic Floor Disorders. Agenda. What is the Pelvic Floor? Pelvic Floor Problems
 Management of Pelvic Floor Disorders Doctor, I don t want THAT mesh! Agenda What are pelvic floor disorders (PFDs)? What are the treatment options? Expectant. Conservative. Surgical. How and when are grafts
Management of Pelvic Floor Disorders Doctor, I don t want THAT mesh! Agenda What are pelvic floor disorders (PFDs)? What are the treatment options? Expectant. Conservative. Surgical. How and when are grafts
Stop Coping. Start Living. Talk to your doctor about pelvic organ prolapse and sacrocolpopexy
 Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
SURGICAL. How to manage the cuff at vaginal hysterectomy. For personal use only. Copyright Dowden Health Media TECHNIQUES
 For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
What are we talking about? Symptoms. Prolapse Risk Factors. Vaginal bulge 1 Splinting. ?? Pelvic pressure Back pain 1 Urinary complaints 2
 Options for Vaginal Prolapse What are we talking about? Michelle Y. Morrill, M.D. Director of Urogynecology The Permanente Medical Group Kaiser, San Francisco Assistant Professor, Volunteer Faculty Department
Options for Vaginal Prolapse What are we talking about? Michelle Y. Morrill, M.D. Director of Urogynecology The Permanente Medical Group Kaiser, San Francisco Assistant Professor, Volunteer Faculty Department
PL Narducci Department of Obstetrics and Gynecology General Hospital San Giovanni Battista Foligno, ITALY
 NESA DAYS 2018 New European Surgical Academy Perugia, April 19-21, 2018 EXCELLENCE IN FEMALE SURGERY PROLAPSE RECONSTRUCTIVE SURGERY IN SEXUALLY ACTIVE WOMEN LAPAROSCOPIC ANTERIOR ABDOMINAL WALL COLPOPEXY
NESA DAYS 2018 New European Surgical Academy Perugia, April 19-21, 2018 EXCELLENCE IN FEMALE SURGERY PROLAPSE RECONSTRUCTIVE SURGERY IN SEXUALLY ACTIVE WOMEN LAPAROSCOPIC ANTERIOR ABDOMINAL WALL COLPOPEXY
Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583
 Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse
 ORIGINAL ARTICLE Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse Cecile A. Unger, MD, MPH, Matthew D. Barber, MD, MHS, Mark
ORIGINAL ARTICLE Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse Cecile A. Unger, MD, MPH, Matthew D. Barber, MD, MHS, Mark
Surgical repair of vaginal wall prolapse using mesh
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
Step by step High uterosacral vaginal vault suspension to repair enterocele and apical prolapse
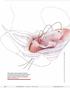 When performing high uterosacral suspension, it is possible to pass sutures through the coccygeus muscle-sacrospinous ligament complex (arrow) because a segment of the uterosacral ligament inserts into
When performing high uterosacral suspension, it is possible to pass sutures through the coccygeus muscle-sacrospinous ligament complex (arrow) because a segment of the uterosacral ligament inserts into
Gynecology Dr. Sallama Lecture 3 Genital Prolapse
 Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Current status in pelvic organ prolapse surgery: an evidence based review
 Current status in pelvic organ prolapse surgery: an evidence based review Christian Falconer, MD, PhD Department of Obstetrics and Gynecology Danderyd University Hospital Stockholm, Sweden Finnish Society
Current status in pelvic organ prolapse surgery: an evidence based review Christian Falconer, MD, PhD Department of Obstetrics and Gynecology Danderyd University Hospital Stockholm, Sweden Finnish Society
By:Dr:ISHRAQ MOHAMMED
 By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
SACROSPINOUS LIGAMENT FIXATION, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE
 Original Article, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE * ** Fauzia Rasool Memon, Mohamed Matar * Consultant Obstetrician and Gynecologist
Original Article, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE * ** Fauzia Rasool Memon, Mohamed Matar * Consultant Obstetrician and Gynecologist
Pelvic Floor. Reimbursement & Coding Guide
 Pelvic Floor Reimbursement & Coding Guide Pelvic Floor Reimbursement and Coding Guide ACell Pelvic Floor Matrix products are biologically-derived devices comprised of porcine Urinary Bladder Matrix (UBM),
Pelvic Floor Reimbursement & Coding Guide Pelvic Floor Reimbursement and Coding Guide ACell Pelvic Floor Matrix products are biologically-derived devices comprised of porcine Urinary Bladder Matrix (UBM),
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Abdominal mesh background of, 84 85 Age as factor in PFDs, 8 Anal plugs in FI management in women, 107 Anterior compartment native tissue
Index Note: Page numbers of article titles are in boldface type. A Abdominal mesh background of, 84 85 Age as factor in PFDs, 8 Anal plugs in FI management in women, 107 Anterior compartment native tissue
Introduction. Regarding the Section of the UPDATE Entitled Purpose
 Time to Rethink: an Evidence-Based Response from Pelvic Surgeons to the FDA Safety Communication: UPDATE on Serious Complications Associated with Transvaginal Placement of Surgical Mesh for Pelvic Organ
Time to Rethink: an Evidence-Based Response from Pelvic Surgeons to the FDA Safety Communication: UPDATE on Serious Complications Associated with Transvaginal Placement of Surgical Mesh for Pelvic Organ
1) What conditions is vaginal mesh used to commonly treat? Vaginal mesh is used to treat two different health issues in women:
 Vaginal Mesh Frequently Asked Questions 1) What conditions is vaginal mesh used to commonly treat? Vaginal mesh is used to treat two different health issues in women: a) stress urinary incontinence (SUI)
Vaginal Mesh Frequently Asked Questions 1) What conditions is vaginal mesh used to commonly treat? Vaginal mesh is used to treat two different health issues in women: a) stress urinary incontinence (SUI)
Innovations in mesh kit technology for vaginal wall prolapse
 Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
Prolapse & Stress Incontinence
 Advanced Pelvic Floor Course Prolapse & Stress Incontinence OVERVIEW Day One and morning of Day Two- Pelvic Organ Prolapse The Prolapse component covers the detailed anatomy of POP including the DeLancey
Advanced Pelvic Floor Course Prolapse & Stress Incontinence OVERVIEW Day One and morning of Day Two- Pelvic Organ Prolapse The Prolapse component covers the detailed anatomy of POP including the DeLancey
12/1/13. What are Pelvic Floor Disorders? What is the Pelvic Floor? Facts. Prevalence of Urinary InconOnence. What s New in Pelvic Floor Disorders?
 What are Pelvic Floor Disorders? Urinary Control Problems - InconOnence or leakage of urine Prolapse of pelvic organs - Vagina, bladder, rectum What s New in Pelvic Floor Disorders? Kimberly Kenton MD,
What are Pelvic Floor Disorders? Urinary Control Problems - InconOnence or leakage of urine Prolapse of pelvic organs - Vagina, bladder, rectum What s New in Pelvic Floor Disorders? Kimberly Kenton MD,
John Laughlin 4 th year Cardiff University Medical Student
 John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
Medium-term follow-up on use of freeze-dried, irradiated donor fascia for sacrocolpopexy and sling procedures
 Int Urogynecol J (2004) 15: 238 242 DOI 10.1007/s00192-004-1146-8 ORIGINAL ARTICLE Mary Pat FitzGerald Æ S. Renee Edwards Æ Dee Fenner Medium-term follow-up on use of freeze-dried, irradiated donor fascia
Int Urogynecol J (2004) 15: 238 242 DOI 10.1007/s00192-004-1146-8 ORIGINAL ARTICLE Mary Pat FitzGerald Æ S. Renee Edwards Æ Dee Fenner Medium-term follow-up on use of freeze-dried, irradiated donor fascia
Pelvic Organ Prolapse. Natural Solutions
 Pelvic Organ Prolapse Natural Solutions Bringing your body back to its natural state There is a very common problem affecting millions of women. Many women are too embarrassed to talk to their physicians
Pelvic Organ Prolapse Natural Solutions Bringing your body back to its natural state There is a very common problem affecting millions of women. Many women are too embarrassed to talk to their physicians
Clinical Curriculum: Urogynecology
 Updated July 201 Clinical Curriculum: Urogynecology GOAL: The primary goal of the Urogynecology rotation at the University of Alabama at Birmingham (UAB) is to train physicians to have a broad knowledge
Updated July 201 Clinical Curriculum: Urogynecology GOAL: The primary goal of the Urogynecology rotation at the University of Alabama at Birmingham (UAB) is to train physicians to have a broad knowledge
Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation
 Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation Roger P. Goldberg, MD, MPH, Sumana Koduri, MD, Robert W. Lobel, MD, Patrick J. Culligan,
Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation Roger P. Goldberg, MD, MPH, Sumana Koduri, MD, Robert W. Lobel, MD, Patrick J. Culligan,
Management of Vaginal Prolapse
 Information for Patients Saint Mary s Hospital/Trafford General Hospital Uro-gynaecology Service Management of Vaginal Prolapse Before reading this leaflet you should read What is vaginal prolapse? If
Information for Patients Saint Mary s Hospital/Trafford General Hospital Uro-gynaecology Service Management of Vaginal Prolapse Before reading this leaflet you should read What is vaginal prolapse? If
INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR SURGICAL PROCEDURES TO
 AN AMERICAN UROGYNECOLOGIC SOCIETY (AUGS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR SURGICAL PROCEDURES TO TREAT PELVIC ORGAN PROLAPSE NEED FOR A WORKING
AN AMERICAN UROGYNECOLOGIC SOCIETY (AUGS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR SURGICAL PROCEDURES TO TREAT PELVIC ORGAN PROLAPSE NEED FOR A WORKING
Bard: Continence Therapy. Stress Urinary Incontinence. Regaining Control. Restoring Your Lifestyle.
 Bard: Continence Therapy Stress Urinary Incontinence Regaining Control. Restoring Your Lifestyle. Stress Urinary Incontinence Urinary incontinence is a common problem and one that can be resolved by working
Bard: Continence Therapy Stress Urinary Incontinence Regaining Control. Restoring Your Lifestyle. Stress Urinary Incontinence Urinary incontinence is a common problem and one that can be resolved by working
Gökmen Sukgen, 1 Esra SaygJlJ YJlmaz, 2 and Eralp BaGer Introduction. 2. Case Presentation
 Case Reports in Obstetrics and Gynecology Volume 2016, Article ID 2906596, 4 pages http://dx.doi.org/10.1155/2016/2906596 Case Report Vaginal Hysterectomy with Anterior Four-Arm Mesh Implant Technique
Case Reports in Obstetrics and Gynecology Volume 2016, Article ID 2906596, 4 pages http://dx.doi.org/10.1155/2016/2906596 Case Report Vaginal Hysterectomy with Anterior Four-Arm Mesh Implant Technique
Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M.
 UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
Dr John Short. Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch
 Dr John Short Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch 8:30-9:25 WS #142: Peeling Back the Layers - The Pelvic Floor Uncovered 9:35-10:30 WS #152:
Dr John Short Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch 8:30-9:25 WS #142: Peeling Back the Layers - The Pelvic Floor Uncovered 9:35-10:30 WS #152:
Considering Surgery for Pelvic Prolapse? Learn about minimally invasive da Vinci Surgery
 Considering Surgery for Pelvic Prolapse? Learn about minimally invasive da Vinci Surgery The Surgery: Pelvic Prolapse Surgery If you have pelvic prolapse symptoms, your doctor may suggest medicine or lifestyle
Considering Surgery for Pelvic Prolapse? Learn about minimally invasive da Vinci Surgery The Surgery: Pelvic Prolapse Surgery If you have pelvic prolapse symptoms, your doctor may suggest medicine or lifestyle
Ina S. Irabon, MD, FPOGS, FPSRM, FPSGE Obstetrics and Gynecology Reproductive Endocrinology and Infertility Laparoscopy and Hysteroscopy
 Ina S. Irabon, MD, FPOGS, FPSRM, FPSGE Obstetrics and Gynecology Reproductive Endocrinology and Infertility Laparoscopy and Hysteroscopy Comprehensive Gynecology 7 th edition, 2017 (Lobo RA, Gershenson
Ina S. Irabon, MD, FPOGS, FPSRM, FPSGE Obstetrics and Gynecology Reproductive Endocrinology and Infertility Laparoscopy and Hysteroscopy Comprehensive Gynecology 7 th edition, 2017 (Lobo RA, Gershenson
Ralph & Berryl Goldman Fellowship in Neuro urology, voiding dysfunction and bladder reconstruction
 Ralph & Berryl Goldman Fellowship in Neuro urology, voiding dysfunction and bladder reconstruction Length of fellowship: A 1 year Fellowship: This fellowship has been designed for Urology or Gynecology
Ralph & Berryl Goldman Fellowship in Neuro urology, voiding dysfunction and bladder reconstruction Length of fellowship: A 1 year Fellowship: This fellowship has been designed for Urology or Gynecology
Thesis. Reference. To mesh or not to mesh: a review of pelvic organ reconstructive surgery. DAELLENBACH, Patrick Peter
 Thesis To mesh or not to mesh: a review of pelvic organ reconstructive surgery DAELLENBACH, Patrick Peter Abstract Pelvic organ prolapse (POP) is a major health issue with a lifetime risk of undergoing
Thesis To mesh or not to mesh: a review of pelvic organ reconstructive surgery DAELLENBACH, Patrick Peter Abstract Pelvic organ prolapse (POP) is a major health issue with a lifetime risk of undergoing
Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option.
 Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option. The Condition(s): Vaginal Prolapse, Uterine Prolapse Vaginal prolapse occurs when the
Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option. The Condition(s): Vaginal Prolapse, Uterine Prolapse Vaginal prolapse occurs when the
Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications
 Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications Karyn S. Eilber, M.D. Cedars-Sinai FPMRS Associate Professor, Cedars-Sinai Dept of Surgery Associate Director, Urology Residency
Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications Karyn S. Eilber, M.D. Cedars-Sinai FPMRS Associate Professor, Cedars-Sinai Dept of Surgery Associate Director, Urology Residency
ROBOTIC MESH SACROCOLPOPEXY
 ROBOTIC MESH SACROCOLPOPEXY Philippe E. Zimmern, MD, FACS Professor of Urology Mesh sacrocolpopexy Background First described in 1962 by Lane Until then, treatment options were: Pessary Colpocleisis Vaginal
ROBOTIC MESH SACROCOLPOPEXY Philippe E. Zimmern, MD, FACS Professor of Urology Mesh sacrocolpopexy Background First described in 1962 by Lane Until then, treatment options were: Pessary Colpocleisis Vaginal
Sep \8958 Appell Dmochowski.ppt LMF 1
 Surgical Outcomes (How did we get ourselves into this mess?) Roger R. Dmochowski, MD, FACS Department of Urologic Surgery Vanderbilt University School of Medicine Nashville, Tennessee Considerations Evaluation
Surgical Outcomes (How did we get ourselves into this mess?) Roger R. Dmochowski, MD, FACS Department of Urologic Surgery Vanderbilt University School of Medicine Nashville, Tennessee Considerations Evaluation
Site-specific fascial defects in the diagnosis and surgical management of enterocele
 Site-specific fascial defects in the diagnosis and surgical management of enterocele John R. Miklos, MD,a Neeraj Kohli, MD,b Vincent Lucente, MD,c and William B. Safe, MDd Atlanta and Marietta, GeO1gia,
Site-specific fascial defects in the diagnosis and surgical management of enterocele John R. Miklos, MD,a Neeraj Kohli, MD,b Vincent Lucente, MD,c and William B. Safe, MDd Atlanta and Marietta, GeO1gia,
2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL)
 E10d 2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No.
E10d 2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No.
Laparoscopic Sacrocolpopexy vs Robotic Sacrocolpopexy
 Laparoscopic Sacrocolpopexy vs Robotic Sacrocolpopexy Magnus Murphy FRCSC Clinical Assistant Professor Department of Obstetrics and Gynecology University of Calgary Division of Urogynecology www.pelvicfloor.com
Laparoscopic Sacrocolpopexy vs Robotic Sacrocolpopexy Magnus Murphy FRCSC Clinical Assistant Professor Department of Obstetrics and Gynecology University of Calgary Division of Urogynecology www.pelvicfloor.com
Female Urology. The Results of Grade IV Cystocele Repair Using Mesh. Introduction ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M
 Urology Journal UNRC/IUA Vol. 1, No. 4, 263-267 Autumn 2004 Printed in IRAN Female Urology The Results of Grade IV Cystocele Repair Using Mesh ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M Department of Urology,
Urology Journal UNRC/IUA Vol. 1, No. 4, 263-267 Autumn 2004 Printed in IRAN Female Urology The Results of Grade IV Cystocele Repair Using Mesh ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M Department of Urology,
Optional Hands-On Laparoscopic & Robotic Suturing Techniques Workshop October 5-6, 2009 PROGRAM SCHEDULE
 22 nd ANNUAL ADVANCED TECHNIQUES IN ENDOSCOPIC AND ROBOTIC GYNECOLOGIC SURGERY Hyatt Regency Maui Resort & Spa Lahaina, Maui, Hawaii October 7-10, 2009 Optional Hands-On Laparoscopic & Robotic Suturing
22 nd ANNUAL ADVANCED TECHNIQUES IN ENDOSCOPIC AND ROBOTIC GYNECOLOGIC SURGERY Hyatt Regency Maui Resort & Spa Lahaina, Maui, Hawaii October 7-10, 2009 Optional Hands-On Laparoscopic & Robotic Suturing
FDA & Transvaginal Mesh: What Happened? What s Next?
 FDA & Transvaginal Mesh: What Happened? What s Next? Matthew D. Barber, MD MHS Professor & Vice Chair for Clinical Research Obstetrics Gynecology & Women s Health Institute Disclosures I receive no grants,
FDA & Transvaginal Mesh: What Happened? What s Next? Matthew D. Barber, MD MHS Professor & Vice Chair for Clinical Research Obstetrics Gynecology & Women s Health Institute Disclosures I receive no grants,
Surgery for women with apical vaginal prolapse(review)
 Cochrane Database of Systematic Reviews (Review) Maher C, Feiner B, Baessler K, Christmann-Schmid C, Haya N, Brown J Maher C, Feiner B, Baessler K, Christmann-Schmid C, Haya N, Brown J.. Cochrane Database
Cochrane Database of Systematic Reviews (Review) Maher C, Feiner B, Baessler K, Christmann-Schmid C, Haya N, Brown J Maher C, Feiner B, Baessler K, Christmann-Schmid C, Haya N, Brown J.. Cochrane Database
Stephen T Jeffery. University of Cape Town, South Africa
 Stephen T Jeffery University of Cape Town, South Africa I still think there s a role for mesh in Prolapse surgery Examples of my most recent mesh cases Case 1 62 yr old Sacrocolpopexy for vault prolapse
Stephen T Jeffery University of Cape Town, South Africa I still think there s a role for mesh in Prolapse surgery Examples of my most recent mesh cases Case 1 62 yr old Sacrocolpopexy for vault prolapse
JMSCR Volume 03 Issue 03 Page March 2015
 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Quality of Life among Patients after Vaginal Hysterectomy and Pelvic Floor Repair Operation ABSTRACT Authors S Lovereen 1, F A Suchi 2,
www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Quality of Life among Patients after Vaginal Hysterectomy and Pelvic Floor Repair Operation ABSTRACT Authors S Lovereen 1, F A Suchi 2,
The UK National Prolapse Survey: 10 years on
 Int Urogynecol J (2018) 29:795 801 DOI 10.1007/s00192-017-3476-3 ORIGINAL ARTICLE The UK National Prolapse Survey: 10 years on Swati Jha 1 & Alfred Cutner 2 & Paul Moran 3 Received: 28 June 2017 /Accepted:
Int Urogynecol J (2018) 29:795 801 DOI 10.1007/s00192-017-3476-3 ORIGINAL ARTICLE The UK National Prolapse Survey: 10 years on Swati Jha 1 & Alfred Cutner 2 & Paul Moran 3 Received: 28 June 2017 /Accepted:
Urogynaecology & Prolapse. Alexander Denning and Leifa Jennings
 + Urogynaecology & Prolapse Alexander Denning and Leifa Jennings + Contents What even is prolapse / urogynaecology? Pelvic floor anatomy Prolapse Urinary incontinence Prevention The end (woot) + Urogynaecology
+ Urogynaecology & Prolapse Alexander Denning and Leifa Jennings + Contents What even is prolapse / urogynaecology? Pelvic floor anatomy Prolapse Urinary incontinence Prevention The end (woot) + Urogynaecology
Vaginal McCall culdoplasty versus laparoscopic uterosacral plication to prophylactically address vaginal vault prolapse
 Vaginal McCall culdoplasty versus laparoscopic uterosacral to prophylactically address vaginal vault prolapse Niblock, K., Bailie, E., McCracken, G., & Johnston, K. (2017). Vaginal McCall culdoplasty versus
Vaginal McCall culdoplasty versus laparoscopic uterosacral to prophylactically address vaginal vault prolapse Niblock, K., Bailie, E., McCracken, G., & Johnston, K. (2017). Vaginal McCall culdoplasty versus
A PATIENT GUIDE TO Understanding Stress Urinary Incontinence
 A PATIENT GUIDE TO Understanding Stress Urinary Incontinence Q: What is SUI? A: Stress urinary incontinence is defined as the involuntary leakage of urine. The problem afflicts approximately 18 million
A PATIENT GUIDE TO Understanding Stress Urinary Incontinence Q: What is SUI? A: Stress urinary incontinence is defined as the involuntary leakage of urine. The problem afflicts approximately 18 million
Randomized trial of fascia lata and polypropylene mesh for abdominal sacrocolpopexy: 5-year follow-up
 DOI 10.1007/s00192-010-1249-3 ORIGINAL ARTICLE Randomized trial of fascia lata and polypropylene mesh for abdominal sacrocolpopexy: 5-year follow-up Susan B. Tate & Linda Blackwell & Douglas J. Lorenz
DOI 10.1007/s00192-010-1249-3 ORIGINAL ARTICLE Randomized trial of fascia lata and polypropylene mesh for abdominal sacrocolpopexy: 5-year follow-up Susan B. Tate & Linda Blackwell & Douglas J. Lorenz
Bob L. Shull, MD Reference List
 Book Chapter Shull BL, Yandell PM. Paravaginal Defect Repair, in Telinde66Es Operative Gynecology, 2008 2008 Shull BL: Choice of Surgery for Prolapse, in Female Pelvic Reconstructive Surgery, edited by
Book Chapter Shull BL, Yandell PM. Paravaginal Defect Repair, in Telinde66Es Operative Gynecology, 2008 2008 Shull BL: Choice of Surgery for Prolapse, in Female Pelvic Reconstructive Surgery, edited by
Index. Cyclical pelvic pain, 37 Cystocele, 22, 23, 25, 48, 51, 52, 54, 56, 124, 148, 160
 A Abdominal approach, 141 Abdominal hernia s surgery, 123, 124 Abdominal sacrocolpopexy (ASC), 116, 117 Abnormal uterine bleeding, 96 Anterior compartment repair, 101, 102 Apical compartment repair, 96
A Abdominal approach, 141 Abdominal hernia s surgery, 123, 124 Abdominal sacrocolpopexy (ASC), 116, 117 Abnormal uterine bleeding, 96 Anterior compartment repair, 101, 102 Apical compartment repair, 96
Registry Protocol Research Registry (PFDR-R) Version 1.3. (August 2016)
 Registry Protocol Research Registry (PFDR-R) Version 1.3 (August 2016) Table of Contents List of Abbreviations... 4 1. Background... 5 2. Rationale... 7 3. Objectives... 8 4. Registry Design... 9 4.1 Registry
Registry Protocol Research Registry (PFDR-R) Version 1.3 (August 2016) Table of Contents List of Abbreviations... 4 1. Background... 5 2. Rationale... 7 3. Objectives... 8 4. Registry Design... 9 4.1 Registry
Two-thirds of the almost one-half million
 Minimally Invasive Surgery New data and the guidance of our professional societies are bringing us closer to clarity in understanding the superiority of minimally invasive techniques of hysterectomy Amy
Minimally Invasive Surgery New data and the guidance of our professional societies are bringing us closer to clarity in understanding the superiority of minimally invasive techniques of hysterectomy Amy
Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments?
 Int Urogynecol J (2010) 21:271 278 DOI 10.1007/s00192-009-1028-1 ORIGINAL ARTICLE Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments? Mariëlla
Int Urogynecol J (2010) 21:271 278 DOI 10.1007/s00192-009-1028-1 ORIGINAL ARTICLE Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments? Mariëlla
Pelvic Floor Reconstruction
 3.9 Curriculum in Urology Trauma and Reconstruction Pelvic Floor Reconstruction W. Artibani a, Stuart L. Stanton b, D. Kumar c, R. Villet d a University of Verona, Italy; b Saint George Hospital Medical
3.9 Curriculum in Urology Trauma and Reconstruction Pelvic Floor Reconstruction W. Artibani a, Stuart L. Stanton b, D. Kumar c, R. Villet d a University of Verona, Italy; b Saint George Hospital Medical
MIDLAND MEMORIAL HOSPITAL Delineation of Privileges FEMALE PELVIC MEDICINE AND RECONSTRUCTIVE SURGERY (UROGYNECOLOGY)
 MIDLAND MEMORIAL HOSPITAL Delineation of Privileges FEMALE PELVIC MEDICINE AND RECONSTRUCTIVE SURGERY (UROGYNECOLOGY) Physician Name: Your home for healthcare Female Pelvic Medicine and Reconstructive
MIDLAND MEMORIAL HOSPITAL Delineation of Privileges FEMALE PELVIC MEDICINE AND RECONSTRUCTIVE SURGERY (UROGYNECOLOGY) Physician Name: Your home for healthcare Female Pelvic Medicine and Reconstructive
Female Pelvic Prolapse: Considerations on Mesh Surgery and our Experience with Prolift Mesh in 84 Women with Complicated Pelvic Prolapses
 Journal of Applied Medical Sciences, vol.5, no. 2, 2016, 19-30 ISSN: 2241-2328 (print version), 2241-2336 (online) Scienpress Ltd, 2016 Female Pelvic Prolapse: Considerations on Mesh Surgery and our Experience
Journal of Applied Medical Sciences, vol.5, no. 2, 2016, 19-30 ISSN: 2241-2328 (print version), 2241-2336 (online) Scienpress Ltd, 2016 Female Pelvic Prolapse: Considerations on Mesh Surgery and our Experience
Female Pelvic Medicine & Reconstructive Surgery
 Female Pelvic Medicine & Reconstructive Surgery APPLICATION FOR NEW FELLOWSHIP Name of Institution: McGill University Location: Royal Victoria Hospital (Glen Site), St Mary s Hospital Centre Type of Fellowship:
Female Pelvic Medicine & Reconstructive Surgery APPLICATION FOR NEW FELLOWSHIP Name of Institution: McGill University Location: Royal Victoria Hospital (Glen Site), St Mary s Hospital Centre Type of Fellowship:
Polypropylene vaginal mesh implants for vaginal prolapse
 Polypropylene vaginal mesh implants for vaginal prolapse This statement has been developed and reviewed by the Women s Health Committee and approved by the RANZCOG Board and Council. A list of Women s
Polypropylene vaginal mesh implants for vaginal prolapse This statement has been developed and reviewed by the Women s Health Committee and approved by the RANZCOG Board and Council. A list of Women s
Are effective nonsurgical treatments available for women with pelvic organ prolapse?
 Are effective nonsurgical treatments available for women with pelvic organ prolapse? For women with asymptomatic prolapse, education and reassurance are appropriate. Women may not realize that symptoms
Are effective nonsurgical treatments available for women with pelvic organ prolapse? For women with asymptomatic prolapse, education and reassurance are appropriate. Women may not realize that symptoms
Pelvic Support Problems
 AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
Surgical treatments for vaginal apical prolapse
 Review Article Obstet Gynecol Sci 2016;59(4):253-260 http://dx.doi.org/10.5468/ogs.2016.59.4.253 pissn 2287-8572 eissn 2287-8580 Surgical treatments for vaginal apical prolapse Mi Kyung Kong, Sang Wook
Review Article Obstet Gynecol Sci 2016;59(4):253-260 http://dx.doi.org/10.5468/ogs.2016.59.4.253 pissn 2287-8572 eissn 2287-8580 Surgical treatments for vaginal apical prolapse Mi Kyung Kong, Sang Wook
Surgery for vaginal vault prolapse. Patient decision aid
 Surgery for vaginal vault prolapse Patient decision aid? i What is vaginal vault prolapse? Vaginal vault prolapse happens when the top of the vagina (the vault) slips from its normal position and sags
Surgery for vaginal vault prolapse Patient decision aid? i What is vaginal vault prolapse? Vaginal vault prolapse happens when the top of the vagina (the vault) slips from its normal position and sags
We welcome comments and corrections which will be used to improve the system annually.
 ACGME Case Log Instructions: Female Pelvic Medicine and Reconstructive Surgery (FPMRS) Review Committees for Obstetrics and Gynecology, and Urology Updated July 2013 BACKGROUND The ACGME Case Log System
ACGME Case Log Instructions: Female Pelvic Medicine and Reconstructive Surgery (FPMRS) Review Committees for Obstetrics and Gynecology, and Urology Updated July 2013 BACKGROUND The ACGME Case Log System
For personal use only. Injury-free vaginal surgery: Case-based protective tactics
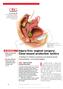 For mass reproduction, content licensing and permissions contact Dowden Health Media. OBG MANAGEMENT Lennox Hoyte, MD Director of Female Pelvic Medicine and Reconstructive Surgery, Department of Obstetrics
For mass reproduction, content licensing and permissions contact Dowden Health Media. OBG MANAGEMENT Lennox Hoyte, MD Director of Female Pelvic Medicine and Reconstructive Surgery, Department of Obstetrics
T h e C o m p l e t e Tr e a t m e n t o f P e l v i c F l o o r P r o l a p s e by Laparoscopy Technique, Tips and Tricks
 T h e C o m p l e t e Tr e a t m e n t o f P e l v i c F l o o r P r o l a p s e by Laparoscopy Technique, Tips and Tricks R Botchorishvili, A Wattiez, G Mage, M Canis, B Rabischong, K Jardon, C Rivoire,
T h e C o m p l e t e Tr e a t m e n t o f P e l v i c F l o o r P r o l a p s e by Laparoscopy Technique, Tips and Tricks R Botchorishvili, A Wattiez, G Mage, M Canis, B Rabischong, K Jardon, C Rivoire,
Tian-Ni Kuo 1, Ming-Ping Wu 1,2 *
 RESEARCH LETTER THE USE OF A CONCOMITANT TENSION-FREE VAGINAL MESH TECHNIQUE AND A TENSION-FREE MIDURETHRAL SLING IN TREATING PELVIC ORGAN PROLAPSE AND OCCULT STRESS URINARY INCONTINENCE Tian-Ni Kuo 1,
RESEARCH LETTER THE USE OF A CONCOMITANT TENSION-FREE VAGINAL MESH TECHNIQUE AND A TENSION-FREE MIDURETHRAL SLING IN TREATING PELVIC ORGAN PROLAPSE AND OCCULT STRESS URINARY INCONTINENCE Tian-Ni Kuo 1,
Complications from permanent synthetic mesh
 Original Research Symptom Resolution After Operative Management of Complications From Transvaginal Mesh Erin C. Crosby, MD, Melinda Abernethy, MD, MPH, Mitchell B. Berger, MD, PhD, John O. DeLancey, MD,
Original Research Symptom Resolution After Operative Management of Complications From Transvaginal Mesh Erin C. Crosby, MD, Melinda Abernethy, MD, MPH, Mitchell B. Berger, MD, PhD, John O. DeLancey, MD,
Surgery for stress incontinence:
 Surgery for stress incontinence: information for you aashara Published February 2005 by the RCOG Contents Key points About this information What is stress incontinence? Do I need an operation? What operation
Surgery for stress incontinence: information for you aashara Published February 2005 by the RCOG Contents Key points About this information What is stress incontinence? Do I need an operation? What operation
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablation in uterine leiomyoma management, 719 723 Adnexal masses diagnosis of, 664 667 imaging in, 664 665 laboratory studies in, 665
Index Note: Page numbers of article titles are in boldface type. A Ablation in uterine leiomyoma management, 719 723 Adnexal masses diagnosis of, 664 667 imaging in, 664 665 laboratory studies in, 665
Prospective study of an ultra-lightweight polypropylene Y mesh for robotic sacrocolpopexy
 Int Urogynecol J (2013) 24:1371 1375 DOI 10.1007/s00192-012-2021-7 ORIGINAL ARTICLE Prospective study of an ultra-lightweight polypropylene Y mesh for robotic sacrocolpopexy Charbel G. Salamon & Christa
Int Urogynecol J (2013) 24:1371 1375 DOI 10.1007/s00192-012-2021-7 ORIGINAL ARTICLE Prospective study of an ultra-lightweight polypropylene Y mesh for robotic sacrocolpopexy Charbel G. Salamon & Christa
Dear Mrs. Burch and editors of the BMJ,
 Dear Mrs. Burch and editors of the BMJ, We are pleased that our manuscript entitled: Sacrospinous hysteropexy versus vaginal hysterectomy with uterosacral ligament suspension in women with uterine prolapse
Dear Mrs. Burch and editors of the BMJ, We are pleased that our manuscript entitled: Sacrospinous hysteropexy versus vaginal hysterectomy with uterosacral ligament suspension in women with uterine prolapse
SGS Annual Course in Advanced Gynecologic Surgery New Orleans, LA
 SGS Annual Course in Advanced Gynecologic Surgery New Orleans, LA Thursday, November 29 Royal Sonesta New Orleans 7:00 7:20 am Registration and Continental Breakfast 7:20 7:30 am Welcome and Opening Remarks
SGS Annual Course in Advanced Gynecologic Surgery New Orleans, LA Thursday, November 29 Royal Sonesta New Orleans 7:00 7:20 am Registration and Continental Breakfast 7:20 7:30 am Welcome and Opening Remarks
Infracoccygeal sacropexy using mesh for uterine prolapse repair
 Infracoccygeal sacropexy using mesh for uterine Issued: January 2009 www.nice.org.uk/ipg280 NHS Evidence has accredited the process used by the NICE Interventional Procedures Programme to produce interventional
Infracoccygeal sacropexy using mesh for uterine Issued: January 2009 www.nice.org.uk/ipg280 NHS Evidence has accredited the process used by the NICE Interventional Procedures Programme to produce interventional
Robotic Ventral Rectopexy
 Robotic Ventral Rectopexy What is a robotic ventral rectopexy? The term rectopexy refers to an operation in which the rectum (the part of the bowel nearest the anus) is put back into its normal position
Robotic Ventral Rectopexy What is a robotic ventral rectopexy? The term rectopexy refers to an operation in which the rectum (the part of the bowel nearest the anus) is put back into its normal position
Pelvic Health Coding & Payment Quick Reference
 Payer policies will vary and should be verified prior to treatment for limitations on diagnosis, coding or site of service requirements. The coding options listed within this guide are commonly used codes
Payer policies will vary and should be verified prior to treatment for limitations on diagnosis, coding or site of service requirements. The coding options listed within this guide are commonly used codes
This information is intended as an overview only
 This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
Prolapse and Urogynae Incontinence. Lucy Tiffin and Hannah Wheldon-Holmes
 Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
AGENDA. 8:00 AM 8:30 AM Pelvic Anatomy of the Lower Urinary Tract and the Anatomy and Physiology of Continence/Incontinence Mickey M.
 Thursday, June 12, 2014 Juniper Ballroom 1: Exhibits AGENDA 6:30 AM 8:00 AM Breakfast and Exhibits EVALUATION AND MANAGEMENT OF LOWER URINARY TRACT SYMPTOMS 8:00 AM 8:30 AM Pelvic Anatomy of the Lower
Thursday, June 12, 2014 Juniper Ballroom 1: Exhibits AGENDA 6:30 AM 8:00 AM Breakfast and Exhibits EVALUATION AND MANAGEMENT OF LOWER URINARY TRACT SYMPTOMS 8:00 AM 8:30 AM Pelvic Anatomy of the Lower
Paravaginal Repair: A Laparoscopic Approach
 44 Paravaginal Repair: A Laparoscopic Approach John R. Miklos and Robert Moore Atlanta Urogynecology Associates, Atlanta, Georgia, U.S.A. Neeraj Kohli Harvard University, Boston, Massachusetts, U.S.A.
44 Paravaginal Repair: A Laparoscopic Approach John R. Miklos and Robert Moore Atlanta Urogynecology Associates, Atlanta, Georgia, U.S.A. Neeraj Kohli Harvard University, Boston, Massachusetts, U.S.A.
Subjective and objective results 1 year after robotic sacrocolpopexy using a lightweight Y-mesh
 DOI 10.1007/s00192-013-2265-x ORIGINAL ARTICLE Subjective and objective results 1 year after robotic sacrocolpopexy using a lightweight Y-mesh Patrick J. Culligan & Emil Gurshumov & Christa Lewis & Jennifer
DOI 10.1007/s00192-013-2265-x ORIGINAL ARTICLE Subjective and objective results 1 year after robotic sacrocolpopexy using a lightweight Y-mesh Patrick J. Culligan & Emil Gurshumov & Christa Lewis & Jennifer
Pelvic organ prolapse
 Page 1 of 11 Pelvic organ prolapse Introduction The aim of this leaflet is to give you information about a pelvic organ prolapse, its causes and available treatments but does not replace advice given by
Page 1 of 11 Pelvic organ prolapse Introduction The aim of this leaflet is to give you information about a pelvic organ prolapse, its causes and available treatments but does not replace advice given by
FDA and Mesh Complications in Vaginal Surgery
 FDA and Mesh Complications in Vaginal Surgery Response to FDA Safety Communication dated July 13, 2011 To Our Patients and Women of the Community: As many of you are aware, on July 13, 2011, the FDA released
FDA and Mesh Complications in Vaginal Surgery Response to FDA Safety Communication dated July 13, 2011 To Our Patients and Women of the Community: As many of you are aware, on July 13, 2011, the FDA released
Advanced Care for Female Overactive Bladder & Urinary Incontinence. Department of Urology Kaiser Permanente Santa Rosa
 Advanced Care for Female Overactive Bladder & Urinary Incontinence Department of Urology Kaiser Permanente Santa Rosa Goals Participants will: Review normal urinary tract anatomy and function Understand
Advanced Care for Female Overactive Bladder & Urinary Incontinence Department of Urology Kaiser Permanente Santa Rosa Goals Participants will: Review normal urinary tract anatomy and function Understand
Imaging of Pelvic Floor Weakness. Dr Susan Kouloyan-Ilic Radiologist Epworth Medical Imaging The Women s, Melbourne
 Imaging of Pelvic Floor Weakness Dr Susan Kouloyan-Ilic Radiologist Epworth Medical Imaging The Women s, Melbourne Outline Overview and Epidemiology Risk Factors, Causes and Results Review of Relevant
Imaging of Pelvic Floor Weakness Dr Susan Kouloyan-Ilic Radiologist Epworth Medical Imaging The Women s, Melbourne Outline Overview and Epidemiology Risk Factors, Causes and Results Review of Relevant
One Slim Needle One Incision. One Simple Solution for Stress Urinary Incontinence. The Difference is in the Data
 CONTINENCE SOLUTIONS One Slim Needle One Incision ordering information Description US International Order Number Order Number One Simple Solution for Stress Urinary Incontinence MiniArc Single-Incision
CONTINENCE SOLUTIONS One Slim Needle One Incision ordering information Description US International Order Number Order Number One Simple Solution for Stress Urinary Incontinence MiniArc Single-Incision
Anatomical and functional results of McCall culdoplasty in the prevention of enteroceles and vaginal vault prolapse after vaginal hysterectomy
 Int Urogynecol J (2008) 19:1007 1011 DOI 10.1007/s00192-007-0549-8 ORIGINAL ARTICLE Anatomical and functional results of McCall culdoplasty in the prevention of enteroceles and vaginal vault prolapse after
Int Urogynecol J (2008) 19:1007 1011 DOI 10.1007/s00192-007-0549-8 ORIGINAL ARTICLE Anatomical and functional results of McCall culdoplasty in the prevention of enteroceles and vaginal vault prolapse after
Pelvic organ prolapse: A primer for urologists
 review Pelvic organ prolapse: A primer for urologists Michel Bureau, MD; Kevin V. Carlson, MD Section of Urology, Department of Surgery, University of Calgary, Calgary, AB, Canada Cite as: Can Urol Assoc
review Pelvic organ prolapse: A primer for urologists Michel Bureau, MD; Kevin V. Carlson, MD Section of Urology, Department of Surgery, University of Calgary, Calgary, AB, Canada Cite as: Can Urol Assoc
