Clinical Study Comparison of Clinical Outcomes Using Elevate Anterior versus Perigee System Devices for the Treatment of Pelvic Organ Prolapse
|
|
|
- Ashlee Page
- 5 years ago
- Views:
Transcription
1 Hindawi Publishing Corporation BioMed Research International Volume 2015, Article ID , 7 pages Clinical Study Comparison of Clinical Outcomes Using Elevate Anterior versus Perigee System Devices for the Treatment of Pelvic Organ Prolapse Cheng-Yu Long, 1,2 Chiu-Lin Wang, 2 Ming-Ping Wu, 3 Chin-Hu Wu, 1 Kun-Ling Lin, 1 Cheng-Min Liu, 1 Eing-Mei Tsai, 1 and Ching-Ju Shen 1 1 Department of Obstetrics and Gynecology, Kaohsiung Medical University Hospital, Kaohsiung Medical University, 100 Ziyou 1st Road, Kaohsiung City 80756, Taiwan 2 Department of Obstetrics and Gynecology, Kaohsiung Municipal Hsiao-Kang Hospital, Kaohsiung Medical University, 100 Ziyou 1st Road, Kaohsiung City 80756, Taiwan 3 Department of Obstetrics and Gynecology, Chi Mei Foundation Hospital, Tainan, Taiwan Correspondence should be addressed to Ching-Ju Shen; chenmed.tw@yahoo.com.tw Received 8 October 2014; Revised 11 January 2015; Accepted 12 January 2015 Academic Editor: Stefan Rimbach Copyright 2015 Cheng-Yu Long et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Objective. This study aims to compare clinical outcomes using the Perigee versus Elevate anterior devices for the treatment of pelvic organ prolapse (POP). Study Design. One hundred and forty-one women with POP stages II to IV were scheduled for either Perigee (n =91) or Elevate anterior device (n =50). Preoperative and postoperative assessments included pelvic examination, urodynamic study, and a personal interview about quality of life and urinary symptoms. Results. Despite postoperative point C of Elevate group being significantly deeper than the Perigee group (median: 7.5 versus 6; P < 0.01), the 1-year success rates for two groups were comparable (P > 0.05). Apart from urgency incontinence, women with advanced POP experienced significant resolution of irritating and obstructive symptoms after both procedures (P < 0.05), generating the improvement in postoperative scores of Urogenital Distress Inventory (UDI-6) and Incontinence Impact Questionnaire (IIQ-7) (P < 0.01). On urodynamics, only theresidual urinedecreased significantly following thesetwo procedures (P < 0.05). Women undergoing Perigee mesh experienced significantly higher visual analogue scale (VAS) scores and vaginal extrusion rates compared with the Elevate anterior procedure (P < 0.05). Conclusions. With comparable success rates, the Elevate procedure has advantages over the Perigee surgery with lower extrusion rate and postoperative day 1 VAS scores. 1. Introduction It has been estimated that a lifetime risk of undergoing primary surgery for pelvic organ prolapse (POP) or urine incontinence for a woman is about 11% [1]. Despite the fact that anterior colporrhaphies have been the empirical treatment of POP for a long time, it carries a higher failure rate [1]. Thus, surgery with mesh or graft materials has gained more and more popularity over the last decade due to the excellent short-term cure rate, especially in the anterior compartment [2, 3]. The Perigee (AMS, Inc., Minnetonka, MN, USA) system is one kind of the synthetic mesh kits recently launched and adopted in pelvic reconstruction for the treatment of anterior vaginal wall prolapse. The Elevate anterior (AMS, Inc., Minnetonka, MN, USA) device is the next generation of the Perigee system, claiming the use of a type I polypropylene Intepro Lite mesh and single vaginal incision in this newer procedure. The Perigee mesh is anchored using trocar passes through the obturator foramen and the latter mesh with hooksisreachedwithdirectpenetrationtotheobturator fascia and sacrospinous ligament [4, 5]. Therefore, the Elevate anterior mesh provides both anterior and apical support, which is important due to the notable reports of compensatory recurrence rates after POP surgery [6].
2 2 BioMed Research International However, the United States Food and Drug Administration (FDA) announced a public health notification regarding serious complications associated with transvaginal placement of surgical mesh in repair of POP and stress urinary incontinence (SUI) in 2011 July [7]. Indeed,the FDA warning hascausedfurthercautionwhenselectingthetypeofmesh kits.wehadpublishedapilotstudycomparingclinicaloutcomes using Perigee and/or Apogee versus Prolift anterior and/or posterior devices for the treatment of POP [8]. This time, we wonder whether the newer Elevate device offers a safer and less painful procedure and whether this would be more durable. In reviewing the literature, limited data are available on the comparisons of efficacy and safety between these two graft-reinforced POP surgeries. Accordingly, we evaluated our experience with the focus on safety, clinical outcomes, and urodynamic findings following these two procedures. 2. Materials and Methods From June 2004 to December 2012, two hundred consecutive symptomatic women with stage II or greater anterior/apical compartment prolapse defined by the POP quantification (POP-Q) staging system [9] were referred for cystocele repair using Perigee or Elevate anterior system devices (120 Perigee; 80 Elevate devices) to our hospital. Concomitant anti-incontinence sling surgeries, including tension-free vaginal tape (TVT;GynecareTVT,Ethicon,Inc.,Piscataway,NJ,USA), TVT-O (Gynecare TVT-Obturator System, Ethicon, Inc., Somerville, NJ, USA), Monarc (AMS, Inc., Minnetonka, MN, USA), and Ajust (C.R. Bard, Inc., Murray Hill, NJ, USA), were performed in patients with current or occult urodynamic stress incontinence (USI). Fifty-nine women were excluded from our study due to various reasons, including incomplete medical records (n =24;fifteen women in the Perigee group, nine in the Elevate group) and inadequacy or loss of followup (n =35;twenty-fivewomeninthePerigeegroup,tenin the Elevate group). Finally, the remaining 141 women were divided into the Perigee group (n =91)and the Elevate group (n =50). Preoperative and postoperative assessments included pelvic examination using the POP-Q staging system, urodynamic study, and a personal interview to evaluate the short forms of Urogenital Distress Inventory (UDI-6), Incontinence Impact Questionnaire (IIQ-7) [10], and urinary symptoms with the standardized questionnaire taking into account the 2002 ICS definitions [11]. Women were asked to fill out the VAS (visual analogue scale) scores during the postoperative day 1 rounds. Urodynamic studies were performed according to the recommendations by the International Continence Society [12] with a 6-channel urodynamic monitor (MMS; UD2000, Enschede, Netherlands). USI was defined as involuntary urinary loss with cough in the absence of detrusor contractions during cystometry. The diagnosis of occult USI was made by the occurrence of urinary leakage during the reduction of prolapse. Any uninhibited detrusor contraction during filling cystometry was deemed positive for idiopathic detrusor overactivity (DO) Operative Technique: Perigee Device. Firstly, an anterior vaginal vertical incision was opened from the bladder neck toward the anterior fornix of the vagina. After hydrodissection, the paravesical space was created on both sides in order to put the index finger behind the obturator foramen. During the Perigee procedure, superior trocars were inserted through the upper medial angle of the obturator foramen at the level of the clitoris, and the inferior trocars were inserted 2 cm inferior and 1 cm lateral to the upper incisions. All trocars were passed through the arcus tendineus fascia pelvisandemergeinthevaginalwound.themesharmsof Perigee devices were attached to the corresponding passers andbroughtoutoftheskinwounds[4] Operative Technique: Elevate Device. After hydrodissection and separation of the paravesical fascia and vaginal mucosa, the Elevate anterior mesh with bilateral upper and lower arms was pushed to the obturator fascia and sacrospinous ligaments, respectively. Graft anchorage was performed via self-fixating tips, which avoided blind trocar passage through the obturator and perirectal fossa seen in Perigee mesh kit techniques. Then, cystoscopy was performed to exclude any bladder injury and to confirm intact ureters. The synthetic mesh was put under the bladder base and anchored with 2-0 PDS (polydioxanone) sutures proximally and distally. The vaginal wound was closed with 3-0 polyglactin sutures. The skin wounds were closed using Dermabond and vaginal packing was placed for hours. Operative time was calculated from the first incision of anterior vaginal wall to the end of wound closure. All patients were administered antibiotics (intravenous Cefazolin 1 g; Cefamezin,Fujisawa,Tokyo,Japan)beforeoperation.The surgeries were carried out with the women under spinal, epidural, or general anesthesia. All procedures were finished mainly by the first author (Cheng-Yu Long), with individual experience of over 400 transvaginal mesh repairs. Postoperative follow-up was scheduled at 1, 3, 6, and 12 months and then yearly thereafter. All POP-Q measurements were made by the first author. Surgical failure was defined as the most distal portion of prolapse over stage II or more, regardless of primary or de novo site. The International Urogynecological Association (IUGA)/International Continence Society (ICS) scale is used for the classification of the meshrelated complications [13].EthicalapprovalbytheInstitutional Review Board of our hospitals had been obtained for data analysis. Statistical calculations were performed using Student s t-test, Mann-Whitney U test, McNemar s or Wilcoxon signed rank test for continuous variables, and the chi-square or Fisher s exact test for categorical variables. A P < 0.05 was considered statistically significant. We assessed the power of tests for differentiating the surgical outcome between groups, and power analysis showed that around women in each group would have a power of 80%. Although some comparisons, such as DO rates, could not reach sufficient power due to the limited numbers of the Elevate group, we utilized multiple parameters of POP-Q system to evaluate the postoperative change. We found with >40 women in each group that there was a power of over 85% for discrimination.
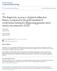
3 BioMed Research International 3 Table 1: Clinical background of patients with pelvic organ prolapse in both groups. Data are given as mean ± standard deviation, median [range], or n (%). Perigee (n =91) Elevate (n =50) P values Mean age (years) 61.0 ± ± Mean parity 3.4 ± ± Mean BMI (kg/m 2 ) 23.7 ± ± Menopause 72 (79.1) 44 (88.0) 0.19 Current hormone therapy 5 (5.5) 4 (8.0) 0.72 Diabetes mellitus 10 (11.0) 9 (18.0) 0.14 Hypertension 20 (22.0) 18 (36.0) 0.07 History of hysterectomy 9 (9.9) 10 (20.0) 0.09 History of POP repair 3 (3.3) 5 (10.0) 0.13 POP Stage 2 20 (22.0) 10 (20.0) 0.78 Stage 3 66 (72.5) 38 (76.0) 0.65 Stage 4 5 (5.5) 2 (4.0) 1.0 Concomitant procedures Posterior repair 3 (3.3) 2 (4.0) 1.0 Vaginal hysterectomy 17 (18.7) 16 (32.0) 0.07 Midurethral sling 58 (63.7) 27 (54.0) 0.26 BMI, body mass index; POP, pelvic organ prolapse; Student s t-test; Chisquare test; Fisher s exact test. 3. Results Participant characteristics of both groups are compared in Table 1. There was no difference between the two groups with regard to age, parity, current hormone use, diabetes, hypertension, prior history of hysterectomy or POP repair, POP stages, and concomitant procedures (P > 0.05). As for the POP-Q analysis, there was a significant improvement at points Aa, Ba, C, Ap, and Bp (P < 0.01) inbothgroups except for total vaginal length (P > 0.05; Table 2). Moreover, postoperative point C of the Elevate group was significantly deeper than that in the Perigee group (P < 0.01) (Figure 1). Other POP-Q points between the two groups did not differ significantly (P > 0.05). The 1-year success rate was comparableinbothgroups(p > 0.05; Table 2). The prevalence of urinary symptoms in both groups, including urinary frequency, SUI, incomplete bladder emptying, urinary hesitancy, and nocturia, was found to be significantly lower following surgery (P < 0.01). As expected, postoperative UDI-6 and IIQ-7 scores of both groups improved in a significant manner (P < 0.01).However,therateofurgency urinary incontinence did not show statistical significance in both groups (P > 0.05)(Table 3). The percentage of DO decreased significantly postoperatively only in the Perigee group (P = 0.002; Table 4), but this wasnotthecaseintheelevategroup(p > 0.05; Table 4). As for urodynamic parameters, including maximum flow rate, residual urine, maximum cystometric capacity, functional 0 H Aa = Ba Ap = Bp Perigee procedure Elevate anterior procedure C H: hymeneal ring C: cervix or vaginal cuff Figure 1: Postoperative point C of the Elevate group was significantly deeper than that in the Perigee group. urethral length, maximum urethral closure pressure, and urethral closure area, they did not show significant changes in either group (P > 0.05). Only the residual urine decreased significantly following these two procedures (P < 0.05; Table 4). The Perigee procedure had a shorter operative time than did the Elevate procedure, but this did not reach significant difference (P = 0.07). With regard to intraoperative complications including bladder injury, rectal injury, and transfusion, none was suspected and confirmed by cystoscopic and rectal examinations. All postoperative complications in both groups included urinary tract infection (11.7% versus 16.7%), voiding dysfunction (difficulty initiating the void) (3.3% versus 2.1%), pelvic hematoma in none (0%), and dyspareunia (16.5% versus 12%). Chi-square and Fisher s exact tests showed no significant differences between both devices in intraoperative and postoperative comparisons (P > 0.05). However, women undergoing Perigee mesh experienced significantly higher VAS scores (3.9 ± 0.8 versus 2.6 ± 1.5; P < 0.01) (Table 5)comparedwiththeElevate anterior procedure. The rate of vaginal extrusion was borderline significantly higher in the Perigee group (10/91; 11% versus 1/50; 2%; P = 0.05) (Table 5). All patients were initially treated conservatively with estrogen vaginal cream. However, eight of them (seven in the Perigee group, one in Elevate group) subsequently needed excisions of the exposed mesh. One woman with Perigee mesh had persistent extrusion requiring repeat excision after 3 months. According to the mesh-related complications by ICS/IUGA scale, we found that one woman ofelevategroupwas3bt3s1,andtheremaining10women of Perigee group were as follows: two with 2BT2S1, two with 2BT3S1, five with 2AT3S1, and one with 7AT2S3.
4 4 BioMed Research International Table 2: Pelvic organ prolapse quantification (POP-Q) values in both groups before and 1 year after surgery. Data are given as median (range) or n [%]. POP-Q parameters (cm) Perigee (n =91) Elevate(n =50) Pre-op Post-op P values Pre-op Post-op P values P values # Aa 2 (0 3) 2( 1 3) # < ( 2 3) 2( 3 1.5) # < # Ba 2.5 ( 1 4) 2( 1 5) # < ( 1 4) 2( 3 1.5) # < # C 1( 3 5) 6( 5 8) # < ( 5 2) 7.5 ( 9 6) # <0.001 <0.01 # Ap 1( 2 3) 2( 3 0) # < ( 3 0) 2( 3 2) # # Bp 1( 2 4) 2( 5 0) # < ( 2 1) 2( 3 2) # < # Tvl 8 (5 9) 8 (6 9) # (7 10) 8.5 (8 10.5) # # Success rate 85 [93.4] 47 [94] 1.0 Pre-op, preoperative; Post-op, postoperative; Tvl, total vaginal length. Wilcoxon signed rank test; # Mann-Whitney U test; Fisher s exact test. Table 3: Urinary symptoms of patients with pelvic organ prolapse in both groups before and 6 months after surgery. Data are given as n (%). Symptoms Perigee (n =91) Elevate(n =50) Pre-op Post-op P value Pre-op Post-op P value Urinary frequency 51 (56.0) 16 (17.6) < (48) 5 (10) <0.01 SUI 59 (64.8) 16 (17.6) < (64) 7 (50) <0.01 UUI 35 (38.5) 27 (29.7) (28) 11 (22) 0.38 Incomplete emptying 65 (71.4) 11 (12.1) < (74) 9 (18) <0.01 Urinary hesitancy 53 (58.2) 9 (9.9) < (62) 7 (14) <0.01 Nocturia 53 (58.2) 43 (47.3) (78) 28 (56) <0.01 UDI ± ± 1.8 < ± ± 3.4 <0.01 IIQ ± ± 1.9 < ± ± 3.1 <0.01 SUI, stress urinary incontinence; UUI, urgency urinary incontinence; UDI-6, Urogenital Distress Inventory; IIQ-7, Incontinence Impact Questionnaire. McNemar s test; Paired t-test. Table4:Urodynamicchangesinbothgroupsbeforeand6monthsaftersurgery.Dataaregivenasn (%) or mean ± standard deviation. Parameters Perigee (n =91) Elevate(n =50) Pre-op Post-op P value Pre-op Post-op P value DO 31 (34.1) 12 (13.2) (34.0) 11 (22.0) 0.29 Qmax (ml/s) 18.6 ± ± ± ± RU (ml) 63.1 ± ± ± ± FS (ml) ± ± ± ± MCC (ml) ± ± ± ± Pdet (cmh 2 O) 26.5 ± ± ± ± FUL (mm) 24.6 ± ± ± ± MUCP (cmh 2 O) 56.3 ± ± ± ± UCA (mmcmh 2 O) ± ± ± ± DO, detrusor overactivity; Qmax, maximum flow rate; RU, residual urine; FS, first sensation to void; MCC, maximum cystometric capacity; Pdet, detrusor pressure at peak flow; FUL, functional urethral length; MUCP, maximum urethral closure pressure; UCA, urethral closure area. McNemar s test; Paired t-test. Statistical significance. 4. Discussion The surgical efficacy of anatomical correction was comparable in both groups at 1-year follow-up. Although earlier launch of the Perigee device had the longer follow-up time in our series, we only reviewed its postoperative 1-year POP- Q data to match the Elevate group. The 1-year success rate of 94% for our Elevate anterior group is slightly higher than another study by Rapp et al. [5], but lower than the data of Lo et al. [14]. Both reported the 90.5% cure rates at 2-year followup and 96.9% at 1-year follow-up, respectively. This may be due to the different study periods and subjects. We found that younger (mean age of 61.7 years) and slimmer (mean BMI of 24) women were enrolled in our study.
5 BioMed Research International 5 Table 5: Intraoperative, postoperative, and mesh-related complications of patients with pelvic organ prolapse in both groups. Data are given as n (%). Perigee (n =91) Elevate (n =50) P values Intraoperative complications Operative time (minutes) 35.3 ± ± # Bladder injury 0 0 Rectal injury 0 0 Blood transfusion 0 0 Postoperative complications Post-op day 1 VAS scores 3.9 ± ± 1.5 <0.01 # Urinary tract infection 9 (11.7) 8 (16.7) 0.29 Voiding dysfunction 2 (3.3) 4 (2.1) 0.19 Perineal hematoma 0 0 Dyspareunia 15 (16.5) 6 (12) 0.25 Mesh complications Vaginal extrusion 10 (11) 1 (2) 0.05 Bladder extrusion 0 0 Post-op, postoperative; VAS, visual analogue scale. # Student s t-test; Chi-square test; Fisher s exact test. With insignificant difference of total vaginal length, we found that postoperative point C of the Elevate group was significantly deeper than that in the Perigee group, in accordance with another study [14]. A possibility was that anchorage of lower arms of the Elevate anterior mesh to sacrospinous ligament provided better postoperative support of the apical compartment. However, it is hard to draw a conclusion due to the shorter follow-up time and limited case numbers. With the advance of mesh materials for the treatment of anterior vaginal prolapse, synthetic mesh has the advantages of durability and strength over traditional anterior colporrhaphy [3].However,anumberofreportedmeshcomplications between 2008 and 2010 provoked a series of actions by the FDA that resulted in reclassifying mesh kits to class III devices and requiring these manufacturers of these commercial kits to conduct research studies about their device if they desired to continue selling their devices in the market [7]. The Elevate anterior system device was launched in November 2010, and it is the next generation of the Perigee system. We questioned whether the newer Elevate device provides a safer, more durable, and less painful procedure; therefore, we included these two former and latter marketed kits of the same manufacturer for comparison in this study. Lo et al. found that Elevate mesh caused a significantly higher rate of de novo SUI postoperatively than did the Perigee device [14], but we did not meet this condition. A possibility was that over half (60.3%; 85/141) of our women underwent concomitant anti-incontinence surgery. Interestingly, a recent study showed that the rate of overactive bladder (OAB) symptoms may be higher significantly when TVT and POP repair were performed together [15]. We did not find these results. A possibility was that most of our women underwent the minisling or transobturator tape rather than TVT procedure. The horizontal shape of the minisling or TOT tape may be less obstructive [16, 17] andunlikelyto cause irritating symptoms. However, whether the TOT is more suitable in women with preoperative OAB symptoms remains unclear. It is well known that severe POP could cause bladder outlet obstruction by urethral kinking or external compression [18], which can promote uninhibited detrusor contractions. Our findings of postoperative improvement in irritating and obstructive symptoms after mesh repair might be partly related to the release of urethral obstruction. This also contributedtotheimprovementofdoandurogenitaldistress questionnaires in a significant manner. Despite the changes in DO of Elevate patients not being significant, larger sample size may shed more light upon this condition. In theory, lower uroflow rate and higher postvoid residual urine on urodynamics could be improved after the POP surgery. However, we did not find any significant change in all urodynamic parameters postoperatively except for the decrease of residual urine, in accordance with our previous study [19]. Urodynamic study might not have been sensitive enough to identify minimal changes in all dysfunctional voiding. Another possibility was that not every woman experienced stage IV advanced POP in this study. The use of blind trocars of commercial kits has arisen some concerns [7]. A review study revealed a total of 1.9% of visceral injury during anterior and/or posterior 2ndgeneration mesh repair [20]. Thus, the newer Elevate mesh is designed for no blind or external trocar passage potentially minimizingtheriskoftissuetraumaduetoitssingleincision procedure. We were fortunate to avoid these complications completely in both groups. Besides, the Perigee procedure had shorter but not significant operative time than the Elevate procedure, indicating that the authors may be more comfortable with the former mesh as a result of longer experience. Mesh extrusion refers to the mesh pushing itself out of the tissue and producing a protrusion, whereas mesh erosion refers to the destruction of the vaginal layer covering the mesh, which usually migrates into the vaginal lumen [21]. In theory, the less the amount of mesh placed, the lower the rate of extrusion occurring. As expected, the vaginal extrusion rate for the Perigee group (11%; 10/91) was higher than the Elevate group (2%; 1/50), this possibly being related to the use of a type I Intepro Lite mesh with lower molecular weight in this newer procedure. Lo et al. also obtained similar results (4.9% for Perigee and 0% for Elevate group) [14]. In addition, wefoundanotheradvantageoftheelevatedeviceisthat all needles pass through a single vaginal incision, noticeably minimizing its postoperative pain scores. We found the conservative management of vaginal extrusion was disappointing in this study. Although all women received initial treatment with estrogen vaginal cream, over half (55.6%; 6/11) subsequently needed excision of the exposed mesh. A previous study concluded that mesh extrusion after prolapse surgery is more likely to occur with
6 6 BioMed Research International concomitant hysterectomy [22]. Similar results were obtained in our study; four mesh extrusions occurred in Perigee patients undergoing concomitant hysterectomy (4/17; 23.5%) and another 6 in Perigee women without hysterectomy (6/74; 8.1%). A flaw of this study was that heterogeneous study population included women having more than one compartment repair and those with and without anti-incontinence sling surgery. However, it would be difficult to select a patient population undergoing anterior mesh alone. In conclusion, the results of our study suggested that Perigee and Elevate anterior devices for POP repair had comparable success rates and intraoperative complications. However, the Elevate procedure has advantages over the Perigee surgery with lower extrusion rate and postoperative day 1 VAS scores. Although the Elevate anterior mesh created a deeper anatomical position of cervix or vaginal cuff, it did not appear to have asignificantimpactonfunctionaloutcome.womenwith advanced prolapse could experience significant improvement of obstructive and irritating symptoms after transvaginal mesh repair. More prospective randomized studies and longer follow-up time of functional and anatomical results are urgently needed to guide the appropriate use of mesh by gynecologists and urologists in the future. Conflict of Interests The authors declare that there is no conflict of interests regarding the publication of this paper. Acknowledgments The authors appreciate that this study was supported by the grants from Kaohsiung Municipal Hsiao Kang Hospital (kmhk ) and the statistical work by the Department of Research Education and Training. References [1] A. L. Olsen, V. J. Smith, J. O. Bergstrom, J. C. Colling, and A. L. Clark, Epidemiology of surgically managed pelvic organ prolapse and urinary incontinence, Obstetrics and Gynecology,vol. 89,no.4,pp ,1997. [2] M. Abdel-Fattah and I. Ramsay, Retrospective multicentre study of the new minimally invasive mesh repair devices for pelvic organ prolapse, BJOG,vol.115,no.1,pp.22 30,2008. [3] D. Altman, T. Väyrynen, M. E. Engh, S. Axelsen, and C. Falconer, Anterior colporrhaphy versus transvaginal mesh for pelvic-organ prolapse, The New England Journal of Medicine, vol.364,no.19,pp ,2011. [4] C.-Y. Long, C.-S. Hsu, M.-Y. Jang, C.-M. Liu, P.-H. Chiang, and E.-M. Tsai, Comparison of clinical outcome and urodynamic findings using perigee and/or Apogee versus prolift anterior and/or posterior system devices for the treatment of pelvic organ prolapse, International Urogynecology Journal and Pelvic Floor Dysfunction,vol.22,no.2,pp ,2011. [5]D.E.Rapp,A.B.King,B.Rowe,andJ.P.Wolters, Comprehensive evaluation of anterior elevate system for the treatment of anterior and apical pelvic floor descent: 2-year followup, Journal of Urology,vol.191,no.2,pp ,2014. [6] M.I.Withagen,A.L.Milani,J.W.deLeeuw,andM.E.Vierhout, Development of de novo prolapse in untreated vaginal compartments after prolapse repair with and without mesh: a secondary analysis of a randomised controlled trial, BJOG,vol. 119, no. 3, pp , [7] United States Food and Drug Administration, FDA Safety Communication: Update on Serious Complications Associated with Transvaginal Placement of Surgical Mesh for Pelvic Organ Prolapse, United States Food and Drug Administration, 2011, ucm htm. [8] C.-Y. Long, C.-S. Hsu, M.-Y. Jang, C.-M. Liu, P.-H. Chiang, and E.-M. Tsai, Comparison of clinical outcome and urodynamic findings using perigee and/or Apogee versus prolift anterior and/or posterior system devices for the treatment of pelvic organ prolapse, International Urogynecology Journal, vol. 22, no. 2, pp , [9] R. C. Bump, A. Mattiasson, K. Bo et al., The standardization of terminology of female pelvic organ prolapse and pelvic floor dysfunction, American Journal of Obstetrics & Gynecology, vol. 175, no. 1, pp , [10] J.S.Uebersax,J.F.Wyman,S.A.Shumakeretal., Shortforms to assess life quality and symptom distress for urinary incontinence in women: the incontinence impact questionnaire and the urogenital distress inventory, Neurourology and Urodynamics,vol.14,no.2,pp ,1995. [11] P. Abrams, L. Cardozo, M. Fall et al., The standardisation of terminology of lower urinary tract function: report from the standardisation sub-committee of the international continence society, Neurourology and Urodynamics,vol.21,no.2,pp , [12] P.Abrams,J.G.Blaivas,S.L.Stanton,andJ.T.Andersen, The standardisation of terminology of lower urinary tract function. The International Continence Society Committee on Standardisation of Terminology, Scandinavian Journal of Urology and Nephrology. Supplement, vol. 114, pp. 5 19, [13] B. T. Haylen, R. M. Freeman, S. E. Swift et al., An international urogynecological association (IUGA)/International Continence Society (ICS) joint terminology and classification of the complications related directly to the insertion of prostheses (meshes, implants, tapes) and grafts in female pelvic flo, Neurourology and Urodynamics,vol.30,no.1,pp.2 12,2011. [14] T.-S. Lo, N. Bt Karim, E. F. M. Cortes, P.-Y. Wu, Y.-H. Lin, and Y. L. Tan, Comparison between Elevate Anterior/Apical system and Perigee system in pelvic organ prolapse surgery: clinical and sonographic outcomes, International Urogynecology Journal, vol.26,no.3,pp ,2015. [15] I. Diez-Itza, I. Aizpitarte, A. Becerro, and C. Sarasqueta, Incidence of overactive bladder after vaginal hysterectomy and associated repairs for pelvic organ prolapse, Gynecologic and Obstetric Investigation,vol.68,no.1,pp.65 70,2009. [16] C.Y.Long,C.S.Hsu,T.S.Lo,C.M.Liu,Y.H.Chen,andE.M. Tsai, Ultrasonographic assessment of tape location following tension-free vaginal tape and transobturator tape procedure, Acta Obstetricia et Gynecologica Scandinavica,vol.87,no.1,pp , [17] C.-Y. Long, C.-S. Hsu, M.-P. Wu, C.-M. Liu, T.-N. Wang, and E.-M. Tsai, Comparison of tension-free vaginal tape and transobturator tape procedure for the treatment of stress urinary incontinence, Current Opinion in Obstetrics and Gynecology, vol.21,no.4,pp ,2009.
7 BioMed Research International 7 [18] C.-Y. Long, S.-C. Hsu, T.-P. Wu, D.-J. Sun, J.-H. Su, and E.-M. Tsai, Urodynamic comparison of continent and incontinent women with severe uterovaginal prolapse, Journal of Reproductive Medicine,vol.49,no.1,pp.33 37,2004. [19] C.-Y. Long, C.-S. Hsu, C.-H. Wu, C.-M. Liu, C.-L. Wang, and E.-M. Tsai, Three-year outcome of transvaginal mesh repair for the treatment of pelvic organ prolapse, European Journal of Obstetrics Gynecology and Reproductive Biology, vol.161,no.1, pp , [20] X. Jia, C. Glazener, G. Mowatt et al., Efficacy and safety of using mesh or grafts in surgery for anterior and/or posterior vaginal wall prolapse: systematic review and meta-analysis, BJOG, vol. 115, no. 11, pp , [21] D. Zoorob and M. Karram, Management of mesh complications and vaginal constriction a urogynecology perspective, Urologic Clinics of North America, vol.39,no.3,pp , [22] M. Cervigni, F. Natale, C. Penna, M. Panei, and A. Mako, Transvaginal cystocele repair with polypropylene mesh using a tension-free technique, International Urogynecology Journal and Pelvic Floor Dysfunction,vol.19,no.4,pp ,2008.
Predictors of improved overactive bladder symptoms after transvaginal mesh repair for the treatment of pelvic organ prolapse
 DOI 10.1007/s00192-010-1312-0 ORIGINAL ARTICLE Predictors of improved overactive bladder symptoms after transvaginal mesh repair for the treatment of pelvic organ prolapse Predictors of Improved OAB after
DOI 10.1007/s00192-010-1312-0 ORIGINAL ARTICLE Predictors of improved overactive bladder symptoms after transvaginal mesh repair for the treatment of pelvic organ prolapse Predictors of Improved OAB after
Anatomical and Functional Results of Pelvic Organ Prolapse Mesh Repair: A Prospective Study of 105 Cases
 International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
Interventional procedures guidance Published: 12 October 2016 nice.org.uk/guidance/ipg566
 Single-incision short sling mesh insertion for stress urinary incontinence in women Interventional procedures guidance Published: 12 October 2016 nice.org.uk/guidance/ipg566 Your responsibility This guidance
Single-incision short sling mesh insertion for stress urinary incontinence in women Interventional procedures guidance Published: 12 October 2016 nice.org.uk/guidance/ipg566 Your responsibility This guidance
Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M.
 UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
Gökmen Sukgen, 1 Esra SaygJlJ YJlmaz, 2 and Eralp BaGer Introduction. 2. Case Presentation
 Case Reports in Obstetrics and Gynecology Volume 2016, Article ID 2906596, 4 pages http://dx.doi.org/10.1155/2016/2906596 Case Report Vaginal Hysterectomy with Anterior Four-Arm Mesh Implant Technique
Case Reports in Obstetrics and Gynecology Volume 2016, Article ID 2906596, 4 pages http://dx.doi.org/10.1155/2016/2906596 Case Report Vaginal Hysterectomy with Anterior Four-Arm Mesh Implant Technique
Evaluation of the single-incision Elevate system to treat pelvic organ prolapse: follow-up from 15 to 45 months
 Int Urogynecol J (2015) 26:1341 1346 DOI 10.1007/s00192-015-2693-x ORIGINAL ARTICLE Evaluation of the single-incision Elevate system to treat pelvic organ prolapse: follow-up from 15 to 45 months Kuan-Hui
Int Urogynecol J (2015) 26:1341 1346 DOI 10.1007/s00192-015-2693-x ORIGINAL ARTICLE Evaluation of the single-incision Elevate system to treat pelvic organ prolapse: follow-up from 15 to 45 months Kuan-Hui
High success rate and considerable adverse events of pelvic prolapse surgery with Prolift: A single center experience
 Available online at www.sciencedirect.com ScienceDirect Taiwanese Journal of Obstetrics & Gynecology 52 (2013) 389e394 Short Communication High success rate and considerable adverse events of pelvic prolapse
Available online at www.sciencedirect.com ScienceDirect Taiwanese Journal of Obstetrics & Gynecology 52 (2013) 389e394 Short Communication High success rate and considerable adverse events of pelvic prolapse
Clinical Study Cough Test during Tension-Free Vaginal Tape Procedure in Preventing Postoperative Urinary Retention
 Advances in Urology Volume 2013, Article ID 797854, 4 pages http://dx.doi.org/10.1155/2013/797854 Clinical Study Cough Test during Tension-Free Vaginal Tape Procedure in Preventing Postoperative Urinary
Advances in Urology Volume 2013, Article ID 797854, 4 pages http://dx.doi.org/10.1155/2013/797854 Clinical Study Cough Test during Tension-Free Vaginal Tape Procedure in Preventing Postoperative Urinary
This information is intended as an overview only
 This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments?
 Int Urogynecol J (2010) 21:271 278 DOI 10.1007/s00192-009-1028-1 ORIGINAL ARTICLE Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments? Mariëlla
Int Urogynecol J (2010) 21:271 278 DOI 10.1007/s00192-009-1028-1 ORIGINAL ARTICLE Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments? Mariëlla
Efficacy and Adverse Effects of Monarc Versus Tension-free Vaginal Tape Obturator: a Retrospective One-year Follow-up Study
 Efficacy and Adverse Effects of Monarc Versus Tension-free Vaginal Tape Obturator: a Retrospective One-year Follow-up Study Yvonne KY CHENG MBChB, MRCOG William WK TO MBBS, M Phil, FRCOG, FHKAM (O&G) HX
Efficacy and Adverse Effects of Monarc Versus Tension-free Vaginal Tape Obturator: a Retrospective One-year Follow-up Study Yvonne KY CHENG MBChB, MRCOG William WK TO MBBS, M Phil, FRCOG, FHKAM (O&G) HX
A PATIENT GUIDE TO Understanding Stress Urinary Incontinence
 A PATIENT GUIDE TO Understanding Stress Urinary Incontinence Q: What is SUI? A: Stress urinary incontinence is defined as the involuntary leakage of urine. The problem afflicts approximately 18 million
A PATIENT GUIDE TO Understanding Stress Urinary Incontinence Q: What is SUI? A: Stress urinary incontinence is defined as the involuntary leakage of urine. The problem afflicts approximately 18 million
One Slim Needle One Incision. One Simple Solution for Stress Urinary Incontinence. The Difference is in the Data
 CONTINENCE SOLUTIONS One Slim Needle One Incision ordering information Description US International Order Number Order Number One Simple Solution for Stress Urinary Incontinence MiniArc Single-Incision
CONTINENCE SOLUTIONS One Slim Needle One Incision ordering information Description US International Order Number Order Number One Simple Solution for Stress Urinary Incontinence MiniArc Single-Incision
PRE-OPERATIVE URODYNAMIC
 PRE-OPERATIVE URODYNAMIC STUDIES: IS THERE VALUE IN PREDICTING POST-OPERATIVE STRESS URINARY INCONTINENCE IN WOMEN UNDERGOING PROLAPSE SURGERY? Dr K Janse van Rensburg Dr JA van Rensburg INTRODUCTION POP
PRE-OPERATIVE URODYNAMIC STUDIES: IS THERE VALUE IN PREDICTING POST-OPERATIVE STRESS URINARY INCONTINENCE IN WOMEN UNDERGOING PROLAPSE SURGERY? Dr K Janse van Rensburg Dr JA van Rensburg INTRODUCTION POP
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015
 Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Content. Terminology Anatomy Aetiology Presentation Classification Management
 Prolapse Content Terminology Anatomy Aetiology Presentation Classification Management Terminology Prolapse Descent of pelvic organs into the vagina Cystocele ant. vaginal wall involving bladder Uterine
Prolapse Content Terminology Anatomy Aetiology Presentation Classification Management Terminology Prolapse Descent of pelvic organs into the vagina Cystocele ant. vaginal wall involving bladder Uterine
John Laughlin 4 th year Cardiff University Medical Student
 John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE
 493495.q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE 493495.q7:480499_P0 6/5/09 10:23 AM Page 2 What is Stress Urinary Incontinence? Urinary
493495.q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE 493495.q7:480499_P0 6/5/09 10:23 AM Page 2 What is Stress Urinary Incontinence? Urinary
Operative Approach to Stress Incontinence. Goals of presentation. Preoperative evaluation: Urodynamic Testing? Michelle Y. Morrill, M.D.
 Operative Approach to Stress Incontinence Goals of presentation Michelle Y. Morrill, M.D. Director of Urogynecology The Permanente Medical Group Kaiser, San Francisco Review preoperative care & evaluation
Operative Approach to Stress Incontinence Goals of presentation Michelle Y. Morrill, M.D. Director of Urogynecology The Permanente Medical Group Kaiser, San Francisco Review preoperative care & evaluation
Surgical repair of vaginal wall prolapse using mesh
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
Stress Incontinence. Susannah Elvy Urogynaecology CNS
 Stress Incontinence Susannah Elvy Urogynaecology CNS Definitions Prevalence Assessment Investigation Treatment Surgery Men International Continence Society define as the complaint of any involuntary leakage
Stress Incontinence Susannah Elvy Urogynaecology CNS Definitions Prevalence Assessment Investigation Treatment Surgery Men International Continence Society define as the complaint of any involuntary leakage
Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583
 Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
TVT-O versus Monarc after a 2 4-year follow-up: a prospective comparative study
 Int Urogynecol J (2009) 20:1327 1333 DOI 10.1007/s00192-009-0943-5 ORIGINAL ARTICLE TVT-O versus Monarc after a 2 4-year follow-up: a prospective comparative study R. Marijn Houwert & Charlotte Renes-Zijl
Int Urogynecol J (2009) 20:1327 1333 DOI 10.1007/s00192-009-0943-5 ORIGINAL ARTICLE TVT-O versus Monarc after a 2 4-year follow-up: a prospective comparative study R. Marijn Houwert & Charlotte Renes-Zijl
Improvements in overactive bladder syndrome after polypropylene mesh surgery for cystocele
 Australian and New Zealand Journal of Obstetrics and Gynaecology 29; 49: 226 231 DOI: 1.1111/j.1479-828X.29.965.x Blackwell Publishing Asia Original Article Improvements in overactive bladder syndrome
Australian and New Zealand Journal of Obstetrics and Gynaecology 29; 49: 226 231 DOI: 1.1111/j.1479-828X.29.965.x Blackwell Publishing Asia Original Article Improvements in overactive bladder syndrome
The Safety and Efficacy of a New Adjustable Single Incision Sling for Treatment of Female. Stress Urinary Incontinence Through 12-months of Follow-up
 Manuscript (Submit in MS Word; include Title Page and Abstract; Tables and Figures should NOT be included but attached separately) Runninghead: ALTIS SINGLE INCISION SLING The Safety and Efficacy of a
Manuscript (Submit in MS Word; include Title Page and Abstract; Tables and Figures should NOT be included but attached separately) Runninghead: ALTIS SINGLE INCISION SLING The Safety and Efficacy of a
Advanced Care for Female Overactive Bladder & Urinary Incontinence. Department of Urology Kaiser Permanente Santa Rosa
 Advanced Care for Female Overactive Bladder & Urinary Incontinence Department of Urology Kaiser Permanente Santa Rosa Goals Participants will: Review normal urinary tract anatomy and function Understand
Advanced Care for Female Overactive Bladder & Urinary Incontinence Department of Urology Kaiser Permanente Santa Rosa Goals Participants will: Review normal urinary tract anatomy and function Understand
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of infracoccygeal sacropexy using mesh to repair vaginal vault prolapse The vaginal
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of infracoccygeal sacropexy using mesh to repair vaginal vault prolapse The vaginal
Prolapse & Stress Incontinence
 Advanced Pelvic Floor Course Prolapse & Stress Incontinence OVERVIEW Day One and morning of Day Two- Pelvic Organ Prolapse The Prolapse component covers the detailed anatomy of POP including the DeLancey
Advanced Pelvic Floor Course Prolapse & Stress Incontinence OVERVIEW Day One and morning of Day Two- Pelvic Organ Prolapse The Prolapse component covers the detailed anatomy of POP including the DeLancey
PRACTICE BULLETIN Female Pelvic Medicine & Reconstructive Surgery Volume 23, Number 4, July/August 2017
 PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
What are we talking about? Symptoms. Prolapse Risk Factors. Vaginal bulge 1 Splinting. ?? Pelvic pressure Back pain 1 Urinary complaints 2
 Options for Vaginal Prolapse What are we talking about? Michelle Y. Morrill, M.D. Director of Urogynecology The Permanente Medical Group Kaiser, San Francisco Assistant Professor, Volunteer Faculty Department
Options for Vaginal Prolapse What are we talking about? Michelle Y. Morrill, M.D. Director of Urogynecology The Permanente Medical Group Kaiser, San Francisco Assistant Professor, Volunteer Faculty Department
CHAU KHAC TU M.D., Ph.D.
 CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
Treatment Outcomes of Tension-free Vaginal Tape Insertion
 Are the Treatment Outcomes of Tension-free Vaginal Tape Insertion the Same for Patients with Stress Urinary Incontinence with or without Intrinsic Sphincter Deficiency? A Retrospective Study in Hong Kong
Are the Treatment Outcomes of Tension-free Vaginal Tape Insertion the Same for Patients with Stress Urinary Incontinence with or without Intrinsic Sphincter Deficiency? A Retrospective Study in Hong Kong
Kathleen C. Kobashi, MD, FACS Head, Section of Urology and Renal Transplantation Virginia Mason Medical Center, Seattle, WA
 Kathleen C. Kobashi, MD, FACS Head, Section of Urology and Renal Transplantation Virginia Mason Medical Center, Seattle, WA Disclosures Advisory Board and/or Speaker Allergan Medtronic Astellas AUA Guidelines
Kathleen C. Kobashi, MD, FACS Head, Section of Urology and Renal Transplantation Virginia Mason Medical Center, Seattle, WA Disclosures Advisory Board and/or Speaker Allergan Medtronic Astellas AUA Guidelines
Gynecology Dr. Sallama Lecture 3 Genital Prolapse
 Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (10), Page
 The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (10), Page 5351-5355 The Efficacy of Transobturator Tape (TOT) in Treatment of Mixed Urinary Incontinence in Females Amr Mohammed Elsadek Nowier,
The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (10), Page 5351-5355 The Efficacy of Transobturator Tape (TOT) in Treatment of Mixed Urinary Incontinence in Females Amr Mohammed Elsadek Nowier,
Seventeen years follow-up of the tension-free vaginal tape procedure for female stress urinary incontinence
 Int Urogynecol J (2013) 24:1265 1269 DOI 10.1007/s00192-013-2090-2 ORIGINAL ARTICLE: EDITORS CHOICE Seventeen years follow-up of the tension-free vaginal tape procedure for female stress urinary incontinence
Int Urogynecol J (2013) 24:1265 1269 DOI 10.1007/s00192-013-2090-2 ORIGINAL ARTICLE: EDITORS CHOICE Seventeen years follow-up of the tension-free vaginal tape procedure for female stress urinary incontinence
Tian-Ni Kuo 1, Ming-Ping Wu 1,2 *
 RESEARCH LETTER THE USE OF A CONCOMITANT TENSION-FREE VAGINAL MESH TECHNIQUE AND A TENSION-FREE MIDURETHRAL SLING IN TREATING PELVIC ORGAN PROLAPSE AND OCCULT STRESS URINARY INCONTINENCE Tian-Ni Kuo 1,
RESEARCH LETTER THE USE OF A CONCOMITANT TENSION-FREE VAGINAL MESH TECHNIQUE AND A TENSION-FREE MIDURETHRAL SLING IN TREATING PELVIC ORGAN PROLAPSE AND OCCULT STRESS URINARY INCONTINENCE Tian-Ni Kuo 1,
Ben Herbert Alex Wojtowicz
 Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Tension-free Vaginal Tape for Urodynamic Stress Incontinence
 Long-term Results of Tension-free Vaginal Tape Insertion for Urodynamic Stress Incontinence in Chinese Women at Eight-year Follow-up: a Prospective Study YM CHAN MBBS, MRCOG, FHKAM (O&G), DCG, DCH, DFM,
Long-term Results of Tension-free Vaginal Tape Insertion for Urodynamic Stress Incontinence in Chinese Women at Eight-year Follow-up: a Prospective Study YM CHAN MBBS, MRCOG, FHKAM (O&G), DCG, DCH, DFM,
INJ. Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple Sutures: Surgical Technique and Results.
 Original Article Int Neurourol J 2012;16:144-148 pissn 2093-4777 eissn 2093-6931 International Neurourology Journal Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple
Original Article Int Neurourol J 2012;16:144-148 pissn 2093-4777 eissn 2093-6931 International Neurourology Journal Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Urodynamic findings in women with insensible incontinence
 bs_bs_banner International Journal of Urology (2013) 20, 429 433 doi: 10.1111/j.1442-2042.2012.03146.x Original Article: Clinical Investigation Urodynamic findings in women with insensible Benjamin M Brucker,
bs_bs_banner International Journal of Urology (2013) 20, 429 433 doi: 10.1111/j.1442-2042.2012.03146.x Original Article: Clinical Investigation Urodynamic findings in women with insensible Benjamin M Brucker,
Understanding Pelvic Organ Prolapse. Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery
 Understanding Pelvic Organ Prolapse Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery Disclosures None I am the daughter of a physician assistant. Objectives List types of pelvic
Understanding Pelvic Organ Prolapse Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery Disclosures None I am the daughter of a physician assistant. Objectives List types of pelvic
Sdefined as involuntary urine leakage
 Transobturator Tape and Female Urinary Incontinence, Follow up and Complication Swapnil Mane*, Sindhu Chandra** Abstract Stress urinary incontinence (SUI) is defined as involuntary urine leakage on exertion.
Transobturator Tape and Female Urinary Incontinence, Follow up and Complication Swapnil Mane*, Sindhu Chandra** Abstract Stress urinary incontinence (SUI) is defined as involuntary urine leakage on exertion.
Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
 Gynecol Surg (2006) 3: 88 92 DOI 10.1007/s10397-005-0168-7 ORIGINAL ARTICLE R. Oliver. C. Dasgupta. A. Coker Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
Gynecol Surg (2006) 3: 88 92 DOI 10.1007/s10397-005-0168-7 ORIGINAL ARTICLE R. Oliver. C. Dasgupta. A. Coker Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
Nine-year experience in sub-urethral prosthesis for the treatment of female stress urinary incontinence
 Nine-year experience in sub-urethral prosthesis for the treatment of female stress urinary incontinence Adrian Haşegan Department of Urology, Emergency County Hospital Sibiu, Faculty of Medicine Abstract
Nine-year experience in sub-urethral prosthesis for the treatment of female stress urinary incontinence Adrian Haşegan Department of Urology, Emergency County Hospital Sibiu, Faculty of Medicine Abstract
Urodynamics in women. Aims of Urodynamics in women. Why do Urodynamics?
 Urodynamics in women Chendrimada Madhu MD, MA, MRCOG Subspecialty Trainee in Urogynaecology Southmead Hospital 2013 Aims of Urodynamics in women n Confirmation of incontinence and its cause n Definition
Urodynamics in women Chendrimada Madhu MD, MA, MRCOG Subspecialty Trainee in Urogynaecology Southmead Hospital 2013 Aims of Urodynamics in women n Confirmation of incontinence and its cause n Definition
Efficacy and Safety of the TVT-SECUR R and Impact on Quality of Life in Women with Stress Urinary Incontinence: A 2-Year Follow-Up
 www.kjurology.org DOI:10.4111/kju.2011.52.5.335 Voiding Dysfunction Efficacy and Safety of the TVT-SECUR R and Impact on Quality of Life in Women with Stress Urinary Incontinence: A 2-Year Follow-Up Yu
www.kjurology.org DOI:10.4111/kju.2011.52.5.335 Voiding Dysfunction Efficacy and Safety of the TVT-SECUR R and Impact on Quality of Life in Women with Stress Urinary Incontinence: A 2-Year Follow-Up Yu
Bard: Continence Therapy. Stress Urinary Incontinence. Regaining Control. Restoring Your Lifestyle.
 Bard: Continence Therapy Stress Urinary Incontinence Regaining Control. Restoring Your Lifestyle. Stress Urinary Incontinence Urinary incontinence is a common problem and one that can be resolved by working
Bard: Continence Therapy Stress Urinary Incontinence Regaining Control. Restoring Your Lifestyle. Stress Urinary Incontinence Urinary incontinence is a common problem and one that can be resolved by working
Aetiology 1998 Bump & Norton Theoretical model
 Kate Lough MSc MCSP Handout IUGA Nice 2015 Physiotherapy and the Provision of Pelvic Floor Muscle Training and Lifestyle Intervention in the Conservative Management of Pelvic Organ Prolapse an evidence
Kate Lough MSc MCSP Handout IUGA Nice 2015 Physiotherapy and the Provision of Pelvic Floor Muscle Training and Lifestyle Intervention in the Conservative Management of Pelvic Organ Prolapse an evidence
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of infracoccygeal sacropexy using mesh to repair uterine prolapse Uterine prolapse
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of infracoccygeal sacropexy using mesh to repair uterine prolapse Uterine prolapse
Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M.
 UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review
 Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M.
 UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
High risk of complications with a single incision pelvic floor repair kit: results of a retrospective case series
 Int Urogynecol J (2014) 25:109 116 DOI 10.1007/s00192-013-2156-1 ORIGINAL ARTICLE High risk of complications with a single incision pelvic floor repair kit: results of a retrospective case series Stephen
Int Urogynecol J (2014) 25:109 116 DOI 10.1007/s00192-013-2156-1 ORIGINAL ARTICLE High risk of complications with a single incision pelvic floor repair kit: results of a retrospective case series Stephen
FDA & Transvaginal Mesh: What Happened? What s Next?
 FDA & Transvaginal Mesh: What Happened? What s Next? Matthew D. Barber, MD MHS Professor & Vice Chair for Clinical Research Obstetrics Gynecology & Women s Health Institute Disclosures I receive no grants,
FDA & Transvaginal Mesh: What Happened? What s Next? Matthew D. Barber, MD MHS Professor & Vice Chair for Clinical Research Obstetrics Gynecology & Women s Health Institute Disclosures I receive no grants,
Complications from permanent synthetic mesh
 Original Research Symptom Resolution After Operative Management of Complications From Transvaginal Mesh Erin C. Crosby, MD, Melinda Abernethy, MD, MPH, Mitchell B. Berger, MD, PhD, John O. DeLancey, MD,
Original Research Symptom Resolution After Operative Management of Complications From Transvaginal Mesh Erin C. Crosby, MD, Melinda Abernethy, MD, MPH, Mitchell B. Berger, MD, PhD, John O. DeLancey, MD,
I-STOP TOMS Transobturator Male Sling
 I-STOP TOMS Transobturator Male Sling The CL Medical I-STOP TOMS sling for male stress urinary incontinence was developed in France where it is widely used and is the market leader. It is constructed with
I-STOP TOMS Transobturator Male Sling The CL Medical I-STOP TOMS sling for male stress urinary incontinence was developed in France where it is widely used and is the market leader. It is constructed with
International Federation of Gynecology and Obstetrics
 International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
Efficacy and safety of Elevate system on apical and anterior compartment prolapse repair with personal technique modification
 ORIGINAL ARTICLE Vol. 43 (6): 1115-1121, November - December, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0233 Efficacy and safety of Elevate system on apical and anterior compartment prolapse repair with personal
ORIGINAL ARTICLE Vol. 43 (6): 1115-1121, November - December, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0233 Efficacy and safety of Elevate system on apical and anterior compartment prolapse repair with personal
Prolapse and Urogynae Incontinence. Lucy Tiffin and Hannah Wheldon-Holmes
 Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
Innovations in mesh kit technology for vaginal wall prolapse
 Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
Sequential Assessment of Urodynamic Findings before and aftertension-free Vaginal Tape (TVT) Operation for Female Genuine Stress Incontinence
 European Urology European Urology 45 (2004) 362 366 Sequential Assessment of Urodynamic Findings before and aftertension-free Vaginal Tape (TVT) Operation for Female Genuine Stress Incontinence Long-Yau
European Urology European Urology 45 (2004) 362 366 Sequential Assessment of Urodynamic Findings before and aftertension-free Vaginal Tape (TVT) Operation for Female Genuine Stress Incontinence Long-Yau
Urinary Incontinence. Lora Keeling and Byron Neale
 Urinary Incontinence Lora Keeling and Byron Neale Not life threatening. Introduction But can have a huge impact on quality of life. Two main types of urinary incontinence (UI). Stress UI leakage on effort,
Urinary Incontinence Lora Keeling and Byron Neale Not life threatening. Introduction But can have a huge impact on quality of life. Two main types of urinary incontinence (UI). Stress UI leakage on effort,
Predictors of Postoperative Voiding Dysfunction following Transobsturator Sling Procedures in Patients with Stress Urinary Incontinence
 Voiding Dysfunction INJ 2010;14:26-33 Predictors of Postoperative Voiding Dysfunction following Transobsturator Sling Procedures in Patients with Stress Urinary Incontinence Sung-Tae Cho, Hyeong-Cheol
Voiding Dysfunction INJ 2010;14:26-33 Predictors of Postoperative Voiding Dysfunction following Transobsturator Sling Procedures in Patients with Stress Urinary Incontinence Sung-Tae Cho, Hyeong-Cheol
Management of Female Stress Incontinence
 Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Tools for Evaluation. Urodynamics Case Studies. Case 1. Evaluation. Case 1. Bladder Diary SUI 19/01/2018
 Urodynamics Case Studies Christopher K. Payne, MD Vista Urology & Pelvic Pain Partners Emeritus Professor of Urology, Stanford University Tools for Evaluation Ears, Eyes, and Brain Bladder diary Stress
Urodynamics Case Studies Christopher K. Payne, MD Vista Urology & Pelvic Pain Partners Emeritus Professor of Urology, Stanford University Tools for Evaluation Ears, Eyes, and Brain Bladder diary Stress
Stop Coping. Start Living. Talk to your doctor about pelvic organ prolapse and sacrocolpopexy
 Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Comparison of midurethral sling outcomes with and without concomitant prolapse repair
 Original Article Obstet Gynecol Sci 2014;57(1):50-58 http://dx.doi.org/10.5468/ogs.2014.57.1.50 pissn 2287-8572 eissn 2287-8580 Comparison of midurethral sling outcomes with and without concomitant prolapse
Original Article Obstet Gynecol Sci 2014;57(1):50-58 http://dx.doi.org/10.5468/ogs.2014.57.1.50 pissn 2287-8572 eissn 2287-8580 Comparison of midurethral sling outcomes with and without concomitant prolapse
LONG TERM FOLLOW UP OF THE TRANSOBTURATOR TAPE PROCEDURE FOR THE TREATMENT OF STRESS URINARY INCONTINENCE IN A TERTIARY HOSPITAL IN SOUTH AFRICA
 LONG TERM FOLLOW UP OF THE TRANSOBTURATOR TAPE PROCEDURE FOR THE TREATMENT OF STRESS URINARY INCONTINENCE IN A TERTIARY HOSPITAL IN SOUTH AFRICA Dr. A. Chrysostomou MD, FCOG (SA), Mmed (WITS) Senior Specialist,
LONG TERM FOLLOW UP OF THE TRANSOBTURATOR TAPE PROCEDURE FOR THE TREATMENT OF STRESS URINARY INCONTINENCE IN A TERTIARY HOSPITAL IN SOUTH AFRICA Dr. A. Chrysostomou MD, FCOG (SA), Mmed (WITS) Senior Specialist,
CommonKnowledge. Pacific University. Gina Clark Pacific University. Lauren Murphy Pacific University. Recommended Citation.
 Pacific University CommonKnowledge PT Critically Appraised Topics School of Physical Therapy 2012 The diagnostic accuracy of patient subjective history compared to the gold standard of urodynamic testing
Pacific University CommonKnowledge PT Critically Appraised Topics School of Physical Therapy 2012 The diagnostic accuracy of patient subjective history compared to the gold standard of urodynamic testing
Retrospective study of transobturator polypropylene mesh kit for the management of pelvic organ prolapse
 Singapore Med J 212; 53(1) : 664 Retrospective study of transobturator polypropylene mesh kit for the management of pelvic organ prolapse Ganesh Raj Vaiyapuri 1, MBBS, MOG, How Chuan Han 2, MBBS, FRCOG,
Singapore Med J 212; 53(1) : 664 Retrospective study of transobturator polypropylene mesh kit for the management of pelvic organ prolapse Ganesh Raj Vaiyapuri 1, MBBS, MOG, How Chuan Han 2, MBBS, FRCOG,
Sarah A. Huber, 1 LaChanda Dunlap-Wright, 2 John R. Miklos, 1 and Robert D. Moore Introduction
 Case Reports in Urology Volume 2016, Article ID 6180756, 5 pages http://dx.doi.org/10.1155/2016/6180756 Case Report Concomitant Laparoscopic Burch Urethropexy and Combined Vaginal-Laparoscopic Mesh Sling
Case Reports in Urology Volume 2016, Article ID 6180756, 5 pages http://dx.doi.org/10.1155/2016/6180756 Case Report Concomitant Laparoscopic Burch Urethropexy and Combined Vaginal-Laparoscopic Mesh Sling
Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline
 Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline TARGET POPULATION Eligibility Decidable (Y or N) Inclusion
Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline TARGET POPULATION Eligibility Decidable (Y or N) Inclusion
Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications
 Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications Karyn S. Eilber, M.D. Cedars-Sinai FPMRS Associate Professor, Cedars-Sinai Dept of Surgery Associate Director, Urology Residency
Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications Karyn S. Eilber, M.D. Cedars-Sinai FPMRS Associate Professor, Cedars-Sinai Dept of Surgery Associate Director, Urology Residency
UroToday International Journal. Volume 4 - June 2011
 UroToday International Journal Paulo Palma, 1 Cassio Riccetto, 1 Rodrigo Castro, 2 Sebastian Altuna, 3 Viviane Herrmann, 1 Ricardo Miyaoka 1 1 Division of Female Urology, State University of Campinas (UNICAMP),
UroToday International Journal Paulo Palma, 1 Cassio Riccetto, 1 Rodrigo Castro, 2 Sebastian Altuna, 3 Viviane Herrmann, 1 Ricardo Miyaoka 1 1 Division of Female Urology, State University of Campinas (UNICAMP),
Frequency of urinary incontinence with Pelvic organ prolapse and associated factors
 ORIGINAL ARTICLE Frequency of urinary incontinence with Pelvic organ prolapse and associated factors Dr. Raheela Mohsin 1, Dr.Ayesha Saba 2, Humera Ismail 3 1 Dr. Raheela Mohsin, Aga Khan University Hospital,
ORIGINAL ARTICLE Frequency of urinary incontinence with Pelvic organ prolapse and associated factors Dr. Raheela Mohsin 1, Dr.Ayesha Saba 2, Humera Ismail 3 1 Dr. Raheela Mohsin, Aga Khan University Hospital,
Clinical Study Posterior Intravaginal Slingplasty versus Unilateral Sacrospinous Ligament Fixation in Treatment of Vaginal Vault Prolapse
 ISRN Obstetrics and Gynecology Volume 2013, Article ID 958670, 5 pages http://dx.doi.org/10.1155/2013/958670 Clinical Study Posterior Intravaginal Slingplasty versus Unilateral Sacrospinous Ligament Fixation
ISRN Obstetrics and Gynecology Volume 2013, Article ID 958670, 5 pages http://dx.doi.org/10.1155/2013/958670 Clinical Study Posterior Intravaginal Slingplasty versus Unilateral Sacrospinous Ligament Fixation
Female Pelvic Prolapse: Considerations on Mesh Surgery and our Experience with Prolift Mesh in 84 Women with Complicated Pelvic Prolapses
 Journal of Applied Medical Sciences, vol.5, no. 2, 2016, 19-30 ISSN: 2241-2328 (print version), 2241-2336 (online) Scienpress Ltd, 2016 Female Pelvic Prolapse: Considerations on Mesh Surgery and our Experience
Journal of Applied Medical Sciences, vol.5, no. 2, 2016, 19-30 ISSN: 2241-2328 (print version), 2241-2336 (online) Scienpress Ltd, 2016 Female Pelvic Prolapse: Considerations on Mesh Surgery and our Experience
Original article J Bas Res Med Sci 2015; 2(2): The incidence of recurrent pelvic organ prolapse: A cross sectional study
 The incidence of recurrent pelvic organ prolapse: A cross sectional study Ashraf Direkvand-Moghadam 1, Ali Delpisheh 2, Azadeh Direkvand-Moghadam 3* 1. Psychosocial Injuries Research Center, Faculty of
The incidence of recurrent pelvic organ prolapse: A cross sectional study Ashraf Direkvand-Moghadam 1, Ali Delpisheh 2, Azadeh Direkvand-Moghadam 3* 1. Psychosocial Injuries Research Center, Faculty of
International Federation of Gynecology and Obstetrics
 International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
Curr Opin Obstet Gynecol 21: ß 2009 Wolters Kluwer Health Lippincott Williams & Wilkins X
 Comparison of tension-free vaginal tape and transobturator tape procedure for the treatment of stress urinary incontinence Cheng-Yu Long a,b, Chun-Shuo Hsu c, Ming-Ping Wu d, Cheng-Min Liu a, Tsu-Nai Wang
Comparison of tension-free vaginal tape and transobturator tape procedure for the treatment of stress urinary incontinence Cheng-Yu Long a,b, Chun-Shuo Hsu c, Ming-Ping Wu d, Cheng-Min Liu a, Tsu-Nai Wang
Overactive Bladder: Diagnosis and Approaches to Treatment
 Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Laparoscopic sacrocolpopexy: an observational study of functional and anatomical outcomes
 DOI 10.1007/s00192-010-1241-y ORIGINAL ARTICLE Laparoscopic sacrocolpopexy: an observational study of functional and anatomical outcomes Natalia Price & Alex Slack & Simon R. Jackson Received: 26 April
DOI 10.1007/s00192-010-1241-y ORIGINAL ARTICLE Laparoscopic sacrocolpopexy: an observational study of functional and anatomical outcomes Natalia Price & Alex Slack & Simon R. Jackson Received: 26 April
By:Dr:ISHRAQ MOHAMMED
 By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Urinary incontinence in women: the management of urinary incontinence in women 1.1 Short title Urinary incontinence in women
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Urinary incontinence in women: the management of urinary incontinence in women 1.1 Short title Urinary incontinence in women
Elevate Anterior/Apical: 12-Month Data Showing Safety and Efficacy in Surgical Treatment of Pelvic Organ Prolapse
 ORIGINAL ARTICLE Elevate Anterior/Apical: 12-Month Data Showing Safety and Efficacy in Surgical Treatment of Pelvic Organ Prolapse Edward J. Stanford, MD, MS,* Robert D. Moore, DO,Þ Jan-Paul W.R. Roovers,
ORIGINAL ARTICLE Elevate Anterior/Apical: 12-Month Data Showing Safety and Efficacy in Surgical Treatment of Pelvic Organ Prolapse Edward J. Stanford, MD, MS,* Robert D. Moore, DO,Þ Jan-Paul W.R. Roovers,
Trocar-guided polypropylene mesh for pelvic organ prolapse surgery perioperative morbidity and short-term outcome of the first 100 patients
 Gynecol Surg (2011) 8:165 170 DOI 10.1007/s10397-010-0628-6 ORIGINAL ARTICLE Trocar-guided polypropylene mesh for pelvic organ prolapse surgery perioperative morbidity and short-term outcome of the first
Gynecol Surg (2011) 8:165 170 DOI 10.1007/s10397-010-0628-6 ORIGINAL ARTICLE Trocar-guided polypropylene mesh for pelvic organ prolapse surgery perioperative morbidity and short-term outcome of the first
Effect of Anesthesia on Voiding Function After Tension-Free Vaginal Tape Procedure
 Effect of Anesthesia on Voiding Function After Tension-Free Vaginal Tape Procedure M. Murphy, MD, M. H. Heit, MD, MSPH, L. Fouts, MD, C. A. Graham, MD, L. Blackwell, RN, and P. J. Culligan, MD OBJECTIVE:
Effect of Anesthesia on Voiding Function After Tension-Free Vaginal Tape Procedure M. Murphy, MD, M. H. Heit, MD, MSPH, L. Fouts, MD, C. A. Graham, MD, L. Blackwell, RN, and P. J. Culligan, MD OBJECTIVE:
Current trend in anti-incontinence surgery
 Current trend in anti-incontinence surgery 吳銘斌醫師 (Ming-Ping Wu, M.D., Ph.D.) 奇美醫院婦產部婦女泌尿暨骨盆醫學科主任台北醫學大學醫學院婦產學科副教授成功大學醫學院臨床醫學所博士 Anti-incontinence surgery Bladder buttress operation: Kelly plication Needle
Current trend in anti-incontinence surgery 吳銘斌醫師 (Ming-Ping Wu, M.D., Ph.D.) 奇美醫院婦產部婦女泌尿暨骨盆醫學科主任台北醫學大學醫學院婦產學科副教授成功大學醫學院臨床醫學所博士 Anti-incontinence surgery Bladder buttress operation: Kelly plication Needle
ABSTRACT R.D. MOORE, D.O., F.A.C.O.G., F.A.C.S. DIRECTOR, ADVANCED PELVIC SURGERY DIRECTOR, UROGYNECOLOGY ATLANTA UROGYNECOLOGY ASSOCIATES ATLANTA, GA
 Single-Center Retrospective Study of the Technique, Safety, and 12-Month Efficacy of the MiniArc Single-Incision Sling: A New Minimally Invasive Procedure for Treatment of Female SUI R.D. MOORE, D.O.,
Single-Center Retrospective Study of the Technique, Safety, and 12-Month Efficacy of the MiniArc Single-Incision Sling: A New Minimally Invasive Procedure for Treatment of Female SUI R.D. MOORE, D.O.,
Risk Factors of Voiding Dysfunction and Patient Satisfaction After Tension-free Vaginal Tape Procedure
 J Korean Med Sci 2005; 20: 1006-10 ISSN 1011-8934 Copyright The Korean Academy of Medical Sciences Risk Factors of Voiding Dysfunction and Patient Satisfaction After Tension-free Vaginal Tape Procedure
J Korean Med Sci 2005; 20: 1006-10 ISSN 1011-8934 Copyright The Korean Academy of Medical Sciences Risk Factors of Voiding Dysfunction and Patient Satisfaction After Tension-free Vaginal Tape Procedure
UroToday International Journal. Volume 4 - February 2011
 UroToday International Journal Scott Serels, 1 Sandy B Nosseir, 2 Lawrence R Lind, 2 Harvey A Winkler 2 1 Bladder Control Center of Norwalk and Section of Urogynecology, Norwalk Hospital, Norwalk, CT,
UroToday International Journal Scott Serels, 1 Sandy B Nosseir, 2 Lawrence R Lind, 2 Harvey A Winkler 2 1 Bladder Control Center of Norwalk and Section of Urogynecology, Norwalk Hospital, Norwalk, CT,
Urethral pressure measurement in stress incontinence: does it help?
 Int Urol Nephrol (2009) 41:491 495 DOI 10.1007/s11255-008-9506-9 UROLOGY - ORIGINAL PAPER Urethral pressure measurement in stress incontinence: does it help? Bassem S. Wadie Æ Ahmed S. El-Hefnawy Received:
Int Urol Nephrol (2009) 41:491 495 DOI 10.1007/s11255-008-9506-9 UROLOGY - ORIGINAL PAPER Urethral pressure measurement in stress incontinence: does it help? Bassem S. Wadie Æ Ahmed S. El-Hefnawy Received:
Combined anterior trans-obturator mesh and sacrospinous ligament fixation in women with severe prolapse a case series of 30 months follow-up
 DOI 10.1007/s00192-010-1266-2 ORIGINAL ARTICLE Combined anterior trans-obturator mesh and sacrospinous ligament fixation in women with severe prolapse a case series of 30 months follow-up Tsia-Shu Lo &
DOI 10.1007/s00192-010-1266-2 ORIGINAL ARTICLE Combined anterior trans-obturator mesh and sacrospinous ligament fixation in women with severe prolapse a case series of 30 months follow-up Tsia-Shu Lo &
Pelvic Floor Ultrasound Imaging. Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague)
 Pelvic Floor Ultrasound Imaging Workshop IUGA 2015 Nice Faculty: Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague) The use of translabial ultrasound
Pelvic Floor Ultrasound Imaging Workshop IUGA 2015 Nice Faculty: Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague) The use of translabial ultrasound
AGENDA. 8:00 AM 8:30 AM Pelvic Anatomy of the Lower Urinary Tract and the Anatomy and Physiology of Continence/Incontinence Mickey M.
 Thursday, June 12, 2014 Juniper Ballroom 1: Exhibits AGENDA 6:30 AM 8:00 AM Breakfast and Exhibits EVALUATION AND MANAGEMENT OF LOWER URINARY TRACT SYMPTOMS 8:00 AM 8:30 AM Pelvic Anatomy of the Lower
Thursday, June 12, 2014 Juniper Ballroom 1: Exhibits AGENDA 6:30 AM 8:00 AM Breakfast and Exhibits EVALUATION AND MANAGEMENT OF LOWER URINARY TRACT SYMPTOMS 8:00 AM 8:30 AM Pelvic Anatomy of the Lower
1) What conditions is vaginal mesh used to commonly treat? Vaginal mesh is used to treat two different health issues in women:
 Vaginal Mesh Frequently Asked Questions 1) What conditions is vaginal mesh used to commonly treat? Vaginal mesh is used to treat two different health issues in women: a) stress urinary incontinence (SUI)
Vaginal Mesh Frequently Asked Questions 1) What conditions is vaginal mesh used to commonly treat? Vaginal mesh is used to treat two different health issues in women: a) stress urinary incontinence (SUI)
Clinical Curriculum: Urogynecology
 Updated July 201 Clinical Curriculum: Urogynecology GOAL: The primary goal of the Urogynecology rotation at the University of Alabama at Birmingham (UAB) is to train physicians to have a broad knowledge
Updated July 201 Clinical Curriculum: Urogynecology GOAL: The primary goal of the Urogynecology rotation at the University of Alabama at Birmingham (UAB) is to train physicians to have a broad knowledge
Introital ultrasound in the diagnosis of lower urinary tract symptoms following anti-incontinence surgery using a synthetic midurethral tape
 International Urogynecology Journal https://doi.org/10.1007/s00192-018-3837-6 ORIGINAL ARTICLE Introital ultrasound in the diagnosis of lower urinary tract symptoms following anti-incontinence surgery
International Urogynecology Journal https://doi.org/10.1007/s00192-018-3837-6 ORIGINAL ARTICLE Introital ultrasound in the diagnosis of lower urinary tract symptoms following anti-incontinence surgery
