The use of intraoperative cystoscopy in major vaginal and urogynecologic surgeries
|
|
|
- Kelley Dennis
- 5 years ago
- Views:
Transcription
1 The use of intraoperative cystoscopy in major vaginal and urogynecologic surgeries Christina H. Kwon, MD, Roger P. Goldberg, MD, MPH, Sumana Koduri, MD, and Peter K. Sand, MD Evanston, Ill OBJECTIVE: Our purpose was to examine the frequency of significant intraoperative cystoscopic findings during major vaginal reconstructive and urogynecologic surgeries. STUDY DESIGN: The records of 526 consecutive women who underwent routine cystoscopy with intravenous injection of indigo carmine at the time of their urogynecologic and major vaginal reconstructive procedures between January 1, 1997, and April 20, 2001, were reviewed. We determined the incidence of significant cystoscopic findings and their effect on intraoperative management. Two-tailed t tests and logistic regression analyses were used to compare characteristics between the groups with and without significant cystoscopic findings. RESULTS: During the 526 operations, 26 significant findings (4.9%) were unsuspected before cystoscopy and 15 (2.9%) of these findings were operative injuries that required intervention. Seventy-nine subjects (15.0%) had no anti-incontinence operation performed. Of these patients, there was one partial ureteral obstruction from an anterior colporrhaphy (1.3%). Seven of 184 Burch procedures (3.8%) resulted in injuries to the lower urinary tract, of which 3 (1.6%) required intervention that were unrecognized before cystoscopy. Seven of the 15 cases resulting in changes in intraoperative management were caused by anterior colporrhaphy sutures (2.0% of all anterior colporrhaphies). There were no unrecognized injuries that caused morbidity after surgery. There were no significant differences between patients with abnormal and normal cystoscopic findings in regard to mean age, weight, parity, estimated blood loss, previous surgery, or previous incontinence surgeries. No complications or morbidity occurred as a direct result of intraoperative cystoscopy. CONCLUSION: Intraoperative cystoscopy with intravenous indigo carmine is a safe and effective way to detect injury of the lower urinary tract. Cystoscopy detected unsuspected operative injuries in 2.9%. In cases that did not involve anti-incontinence procedures, the rate of injury was 1.3%. With a significant rate of detection, cystoscopy allows for immediate recognition and easier repair of lower urinary tract injury, lowering the patient s risk for morbidity. Anterior colporrhaphy was the most common cause of unrecognized ureteral compromise. ( 2002;187: ) Key words: Cystoscopy, urinary tract injuries, vaginal surgery, incontinence operation Injury to the lower urinary tract has been reported to occur during almost every type of gynecologic procedure. 1 Early recognition of injury and repair during the primary surgery most often results in less morbidity for the patient, more successful outcome, and increased ease of repair. 2 This is true especially during anti-incontinence and complex pelvic reconstructive surgeries, where the potential for injury is higher, and routine intraoperative cystoscopy appears to be warranted. 3-5 Some studies have shown a risk of up to 11% for unrecognized ureteral injuries 6 and up to 6% for vesical injuries 5 discovered on From the Evanston Continence Center, Evanston Northwestern Healthcare, Northwestern University Medical School. Presented at the Twenty-eighth Annual Meeting of the Society of Gynecologic Surgeons, Dallas, Tex, March 4-6, Reprint requests: Christina Kwon, Evanston Continence Center, 1000 Central St, Suite 730, Evanston, IL , Mosby, Inc. All rights reserved /2002 $ /6/ doi: /mob routine intraoperative cystoscopy. Whether routine cystoscopy should be performed during all major gynecologic procedures is still a matter of debate. This study represents the largest series of patients evaluated to date. Our service routinely performs cystoscopy after all anti-incontinence and pelvic reconstructive operations. We hoped to determine what our injury rate is after our procedures, specifically those that would have been undetected without the use of cystoscopy and possibly identify any procedures that might be associated with a particularly high risk for injury. We also attempted to identify characteristics that could predict preoperatively those patients at higher risk for injury. Material and methods The charts of 526 patients who underwent anti-incontinence or pelvic reconstructive surgery during the period of January 1, 1997, and April 20, 2001, were reviewed. All of these women had routine cystoscopy with intravenous indigo carmine performed after their anti-incontinence 1466
2 Volume 187, Number 6 Kwon et al 1467 Table I. Vaginal reconstructive procedures performed Table II. Anti-incontinence/urogynecologic procedures Vaginal reconstructive procedures No. Incontinence/urogynecologic procedures No. Hysterectomy 196 Vaginal hysterectomy 163 Total abdominal hysterectomy 31 Laparoscopically assisted vaginal hysterectomy 2 Paravaginal repair 121 Abdominal paravaginal repair 82 Vaginal paravaginal repair 39 Culdoplasty 267 Vaginal culdoplasty 237 Abdominal culdoplasty 30 Posterior colporrhaphy 417 Anterior colporrhaphy 346 Vaginal apex suspension 195 Sacrospinous vaginal vault suspension 152 Iliococcygeous suspension 34 Abdominal sacral colpopexy 9 Colpocleisis 1 Retropubic urethropexy 183 Abdominal Burch 147 Vaginal Burch 34 Laparoscopic Burch 2 Transvaginal suburethral sling 137 Fascial suburethral sling 30 Fascial patch bone anchor sling 15 Vaginal wall bone anchor sling 12 Vesica bone anchor sling 10 Pereyra bone anchor sling 7 TVT 31 Urethral diverticulectomy 7 Kelly Kennedy plication 5 Sling revision 3 Needle urethropexy 2 Durasphere injection 2 Excision of protogen mesh and repair 2 Ingleman Sundberg 2 Abdominal vesicovaginal fistula repair 1 or pelvic reconstruction operation. Transurethral cystoscopy was performed with a 21F 70-degree cystoscope. The bladder was systematically inspected for the presence of injury or foreign material. Ureteral patency was assessed after performance of the anti-incontinence procedure, culdoplasty, or anterior vaginal wall reconstructive procedure by the strong efflux of indigo-carmine stained urine from both ureteral orifices. Preoperative variables such as age, parity, menopausal status, estimated blood loss, previous pelvic surgeries, and previous incontinence surgeries were recorded from each subject s medical record when available. Information regarding history of previous surgery was unavailable for seven women, but none of these seven had significant findings on cystoscopy and were therefore included in the analysis. Two-tailed t tests and logistic regression analysis were used to compare characteristics between groups with and without significant cystoscopic findings. Results Four hundred forty-seven women (85.0%) underwent vaginal reconstructive and anti-incontinence procedures. Seventy-nine women (15.0%) had no anti-incontinence procedures performed during their reconstructive operations. These vaginal reconstructive procedures are detailed in Table I. Table II lists the anti-incontinence and urogynecologic procedures performed. All procedures were performed under the direct supervision of the senior author (P. K. S.). Two hundred seventy-seven women had a history of previous pelvic surgery (Table III). Seventy-nine of these operations were prior anti-incontinence procedures. Of 526 women, 32 (6.0%) had significant findings on cystoscopy. Of these 32, 3 had received a diagnosis before surgery (Hunner s ulcer, Protogen mesh erosion, intravesical bladder tacks from previous laparoscopic retropubic urethropexy). Three intraoperative cystotomies occurred during abdominal retropubic urethropexies in women with prior pelvic surgery that were detected before cystoscopy. A total of 26 significant findings (4.9%) were unsuspected before cystoscopy. Of these 26, 15 (2.9%) were a result of operative injury that required intervention. These findings included 6 ureters (1.7%) that were kinked and obstructed during 346 anterior colporrhaphies. Intravesical sutures from abdominal Burch procedures were noted in 2 women (1.1%). The bladder was puckered in 2 cases, which was relieved by removal and replacement of an anterior colporrhaphy suture in one case and a paravaginal repair suture in another. Bladder punctures were noted during a vesica procedure and a tension-free transvaginal tape (TVT) procedure that only required removal of the suture/graft delivery system. Two unrecognized cystotomies occurred that required repair, one caused by an abdominal Burch procedure and the other by a vaginal wall bone anchored sling procedure. One suture line was revised during an abdominal vesicovaginal fistula repair because of insufficient closure. These findings are listed in Table IV. Eleven cases (2.1%) had occult cystoscopic findings that were not caused by the operative procedure or did not require intraoperative intervention (Table V). Two cases required biopsy, one for a suspicious bladder polyp and one case with fibrinous adhesions seen within the bladder. Pathology results for both cases returned with benign findings. In three cases, slow or no ureteral efflux was noted unilaterally but required only temporary ureteral catheterization or intraoperative intravenous pyelogram with no suture revision needed. Three cases had puckering of the bladder wall, but no suture seen. Two cases had findings consistent with inadvertent passage of a needle or instrument but no repair was needed. One case had delayed left ureteral efflux in comparison
3 1468 Kwon et al December 2002 Table III. Prior surgical procedures Previous surgeries with her right side. After surgery, this patient had suprapubic and lower abdominal pain and fever develop. A pelvic ultrasound revealed an urinoma from her suprapubic catheter site and left hydronephrosis. An IVP was then performed that showed a partial ureterovesical junction obstruction with moderate left hydronephrosis. A urology consult was obtained and the patient was managed conservatively. After her suprapubic catheter was removed, she had complete resolution of her symptoms without further intervention. Of the 79 subjects with no anti-incontinence procedure performed, there was one partial ureteral obstruction from an anterior colporrhaphy (1.3%). Of 183 Burch procedures, 3 (1.6%) resulted in unrecognized injuries to the lower urinary tract before cystoscopy. Of 346 anterior colporrhaphy cases, 7 (2.0%) had ureteral compromise, making it the most common cause of intraoperative injury. There were no unrecognized injuries that caused morbidity after surgery. There were no significant differences between patients with abnormal and normal cystoscopic findings in regard to mean age, weight, parity, or estimated blood loss (Table VI). Of the 15 operative injuries, 9 (60%) of these patients had prior pelvic surgery (2 of these were previous anti-incontinence procedures). No complications or morbidity occurred as a direct result of intraoperative cystoscopy. Comment Lower urinary tract injuries are well-known complications of gynecologic surgery. The anatomic proximity of No. Hysterectomy 235 Abdominal 118 Vaginal 117 Laparoscopically assisted vaginal hysterectomy 3 Colporrhaphy (anterior or posterior) 109 Sacrospinous vaginal vault suspension 12 Needle urethropexy 23 Abdominal Burch 13 Laparoscopic Burch 2 Marshall-Marchetti-Krantz 21 Kelly Kennedy plication 13 Sling 13 Bone-anchored sling 3 Iliococcygeous vault suspension 2 Paravaginal repair 9 Abdominal sacrocolpopexy 3 Laparoscopic oophorectomy 4 Laparoscopic tubal sterilization 4 Exploratory laparotomy 2 Uterine suspension 2 Abdominal vesicovaginal fistula repair 1 Rectovaginal fistula repair (history of Crohn s disease) 1 Pelvic fracture surgery s/p motor vehicle accident 1 Aborted sling/cystotomy repair 1 Cesarean section 2 3 Vulvectomy 1 Myomectomy 1 the lower urinary tract to the reproductive organs predisposes this area to injury during gynecologic procedures. The ureter has been found to be a mean of 0.9 cm from anterior colporraphy plication sutures and a mean of 1.0 cm from the infundibulopelvic ligament when the tube and ovary are removed. 7 Cadaveric dissection of hemisected pelves have shown the mean distance from ureter to uterosacral ligament to be 0.9, 2.3, and 4.1 cm in the cervical, intermediate, and sacral portions of the uterosacral ligament, respectively. 8 Hurd et al 9 used computed pelvic tomogram studies to delineate that the ureter is located at a mean distance of 2.3 cm from the cervix, but in 12% of the women examined, this distance was 0.5 cm or less. This demonstrates the variability and sometimes extreme proximity of the ureter to the cervix. Immediate recognition and correction of lower urinary tract injury will minimize postoperative morbidity. It is the unrecognized injury of the ureter or bladder that may lead to serious morbidity, such as renal damage and urogenital fistula formation. Injuries that are detected and repaired intraoperatively reduce morbidity Although there is no substitute for meticulous operative technique and dissection, cystoscopy has been demonstrated to be an effective means to diagnose lower urinary tract injury intraoperatively. 2 Although routine cystoscopy may miss some injuries, especially those associated with necrosis or ischemia, it can provide early recognition and facilitate repair for the majority of lower urinary tract injuries. 3 Most gynecologic surgeons still do not use this technique routinely. In large retrospective reviews in which cystoscopy was not used, the rate of ureteral injury ranges from 0.2% to 0.43% In a review by Gilmour et al, 3 the incidence of bladder injury in studies performing routine cystoscopy was 4-fold higher than those studies that did not. This difference in injury rates likely reflects detection of minor injuries by cystoscopy, which may have been asymptomatic, as well as the more frequent performance of cystoscopy during surgery for incontinence or advanced pelvic organ prolapse. Currently, there is no consensus on performing routine cystoscopy during every major gynecologic and vaginal reconstructive procedure (ie, vaginal hysterectomy, anterior colporrhaphy, enterocele repair/culdoplasty, vault suspension) that is not considered to be high risk. 16 Intraoperative dissection and direct visualization can significantly reduce the risk of lower urinary tract injury during abdominal gynecologic procedures. Many of these techniques cannot be used in the vaginal approach. Palpation of the ureters transvaginally has been advocated by some for intraoperative assessment, 6 although this technique would not be able to assess bladder injury. Routine preoperative testing such as ultrasound, intravenous pyelogram, and computed tomography have not been shown to be effective in preventing urinary tract injury. 2,17,18 We found no significant differences between
4 Volume 187, Number 6 Kwon et al 1469 Table IV. Operative injuries with significant cystoscopic findings Cystoscopic findings Causative surgical procedure (No. of cases) Intraoperative intervention (No. of affected cases/total cases) Ureteral obstruction (6) Removal and replacement of suture Anterior colporrhaphy (6/346) Intravesical suture (2) Removal and replacement of suture Abdominal Burch (2/147) Puckering of bladder mucosa with Removal and replacement of suture Anterior colporrhaphy (6/346), suture seen (2) abdominal paravaginal repair (1/82) Bladder perforation (2) Removal of needle/trocar with no Vesica procedure (1/10), TVT (1/31) cystotomy repair needed Cystotomy, unrecognized (2) Repair of cystotomy Abdominal Burch (1/147), vaginal wall bone-anchored sling (1/12) Insufficient cystotomy repair (1) Revision of cystotomy closure Abdominal vesicovaginal fistula repair (1/1) Table V. Occult cystoscopic findings Cystoscopic findings (No. of cases) Intervention (No. of cases) Sluggish or no ureteral efflux (3) Ureteral stent passage and removal without suture revisions (3) Findings requiring bladder biopsy (2) Biopsy of polyp (1) Biopsy of fibrinous tissue (1) Pucker in bladder wall with no suture seen (3) None Pinpoint bleed seen at bladder neck with no suture seen (1) None 5-mm puncture noted in left dome, no repair needed (1) None Delayed left ureteral efflux (1) None, IVP done postoperatively showed partial left UVJ obstruction Table VI. Logistic regression analysis of risks for intraoperative cystoscopic findings in 526 women Group 1 Group 2 Clinical characteristic (n = 511) (n = 15) Statistical significance Age (y) 60.1 ± ± 13.1 P =.95 Parity 2.8 ± ± 1.2 P =.71 Weight (pounds) ± ± 23.7 P =.20 Estimated blood loss (ml) ± ± P =.51 Prior pelvic surgery P =.60 Data presented as mean ± SD. Group 1 = patients without cystoscopically detected operative injury; group 2 = patients with cystoscopic findings caused by operative injury. patients with and without findings on cystoscopy, although as with other studies, our relatively small numbers of injuries limits the conclusions that can be drawn. There were no preoperative identifying factors that were predictive of a higher risk of injury. In large, retrospective studies that use routine cystoscopy during anti-incontinence and pelvic reconstructive surgery, the reported lower urinary tract injury rate has ranged from 3% to 9%. 2,5 Ureteral occlusion during specific techniques, such as uterosacral vaginal vault suspension, was reported by Barber et al 6 to be as high as 11% in their series. Four percent of their patients required exploratory laparotomy and ureteroneocystomy to repair the injury. In our study, no ureteral injuries were noted in 237 vaginal culdoplasties or in 152 sacrospinous vaginal vault suspensions. These results suggest that differences in specific techniques and operator variability may account for the large disparity in rates of ureteral injury. In our study, cystoscopy revealed unsuspected findings in 4.9% of our cases. Fifteen (2.9%) of these findings were operative injuries that required intervention. In the 11 cases (2.1%) of occult cystoscopic findings, there were 3 cases (0.6%) of slow (2) or no (1) ureteral efflux unilaterally, resulting in successful retrograde ureteral catheterization assuring ureteral patency. No sutures were revised in these 3 cases. The patient with no ureteral efflux had an intraoperative IVP that showed no filling of the right kidney with cortical atrophy. A postoperative CT scan was significant for severe right renal cortical loss resulting from right ureteropelvic junction obstruction. This patient had had a prior abdominal hysterectomy. Although these 3 cases did result in increased intraoperative time, no complications or side effect resulted. Postoperatively, 1 patient developed a symptomatic urinoma from her suprapubic catheter site, with partial left urethrovesical junction obstruction found incidentally as part of her workup. Her symptoms completely resolved after the suprapubic catheter was removed. There were no injuries resulting in clinical findings that were not detected by cystoscopy.
5 1470 Kwon et al December 2002 The Burch retropubic urethropexy has been associated with a risk of urinary tract injury as high as 9%. 4 In our hands, during 184 Burch procedures (148 abdominal, 34 vaginal, 2 laparoscopic), there were three cases (1.6%) with unsuspected findings on cystoscopy, which required intervention. Our rate of injury during Burch procedures (3.8%) was lower than previously reported by some, but similar to that reported by Tulikangas et al. 19 As with their study, our rate may be lower because one senior surgeon (P. K. S.) oversaw all cases. In our series, the procedure associated with the highest rate of injury was an anterior colporrhaphy. Anterior colporrhaphy resulted in suture removal and replacement in 7 of 346 (2.0%) repairs performed. Aggressive plication of the redundant anterior endopelvic connective tissue causing ureteral kinking was the most common cause of ureteral compromise. In the 15 cases requiring an intraoperative intervention, an anterior colporrhaphy was responsible for 47% (7 of 15) of those cases. This finding is similar to that of Jabs et al 18 in which the bladder neck stitch during anterior colporrhaphy was responsible for ureteral blockage in 6 of 12 (50%) of cases that resulted in a change in management. A recent decision-analysis model was constructed to evaluate the cost-effectiveness of intraoperative cystoscopy at the time of abdominal, vaginal, and laparoscopically assisted vaginal hysterectomy. 20 By using conservative estimates of costs, ureteral injury rates at or above 1.5% during abdominal hysterectomy and 2% during vaginal hysterectomy made universal intraoperative cystoscopy cost saving. In our study, unsuspected urinary tract injury occurred as a result of the operative procedure in 2.9%, with ureteral compromise occurring in 1.1%. Although their decision-analysis examined cost-effectiveness of cystoscopy for ureteral injury only, any unrecognized lower urinary tract injury could have an impact on readmission rates as well as long-term morbidity such as intravesical stone formation or vesicovaginal fistula formation. With an unsuspected injury rate of nearly 3%, routine cystoscopy also appears to be cost-effective during the time of our pelvic surgeries. The majority of intraoperative interventions consisted of removing and replacing sutures. This is consistent with the findings of Gilmour et al, 3 who found that 69% of intraoperative management did not involve advanced urologic surgery. In our study, no patients had significant injuries to the lower urinary tract develop after surgery that were not detected at the time of surgery. We encountered three false-positive intraoperative cystoscopies during which retrograde ureteral catheterization assured ureteral patency. This low incidence (0.6%) did increase intraoperative time but did not result in any long-term morbidity for these patients. There were no complications directly caused by cystoscopy itself. The utility and benefit of performing concomitant cystoscopy at the time of urinary incontinence procedures is well accepted. 2-5,19 The consensus is not as clear during vaginal reconstructive surgery. The incidence of lower urinary tract injury detected by routine cystoscopy during gynecologic surgery varies in the literature. For example, in experienced hands, unsuspected injury rates detected by cystoscopy during Burch retropubic urethropexy varies widely from 0% to 10%. 4,19 For specific procedures such as uterosacral ligament plication or suspension, ureteral injury rates vary from 1% to as high as 11%. 6,21 In our series, we found that anterior colporrhaphy, which is not traditionally thought to place the ureter at high risk, was the most frequent offender in causing ureteral compromise or bladder injury. Clearly, rates of injury are influenced greatly by the individual techniques employed, even for similar procedures. Cystoscopy provides an easily performed test that can effectively assess the lower urinary tract, decreasing morbidity by early diagnosis. Because of the elevated risk for ureteral and bladder injury, routine intraoperative cystoscopy should be considered during all anti-incontinence and vaginal reconstructive surgeries. We thank Laxmi Atkuru for her help in data entry for this study. REFERENCES 1. Drake MJ, Noble JG. Ureteric trauma in gynecologic surgery. Int Urogynecol J Pelvic Floor Dysfunct 1998;9: Pettit PD, Petrou SP. The value of cystoscopy in major vaginal surgery. Obstet Gynecol 1994;84: Gilmour DT, Dwyer PL, Carey MP. Lower urinary tract injury during gynecologic surgery and its detection by intraoperative cystoscopy. Obstet Gynecol 1999;94: Harris RL, Cundiff GW, Theofrastous JP, Yoon H, Bump RC, Addison WA. The value of intraoperative cystoscopy in urogynecologic and reconstructive pelvic surgery. 1997;177: Stevenson KR, Cholhan HJ, Hartmann DM, Buchsbaum GM, Guzick DS. Lower urinary tract injury during the Burch procedure: is there a role for routine cystoscopy? 1999;181: Barber MD, Visco AG, Weidner AC, Amundsen CL, Bump RC. Bilateral uterosacral ligament vaginal vault suspension with sitespecific endopelvic fascia defect repair for treatment of pelvic organ prolapse. 2000;183: Stanhope CR, Wilson TO, Utz WJ, Smith LH, O Brien PC. Suture entrapment and secondary ureteral obstruction. Am J Obstet Gynecol 1991;164: Buller JL, Thompson JR, Cundiff GW, Sullivan LK, Schön Ybarra MA, Bent AE. Uterosacral ligament: description of anatomic relationships to optimize surgical safety. Obstet Gynecol 2001: 97: Hurd WW, Chee SS, Gallagher KL, Ohl DA, Hurteau JA. Location of the ureters in relation to the uterine cervix by computed tomography. 2001;184: Saidi MH, Sadler RK, Vancaillie TG, Akright BD, Farhart SA, White AM. Diagnosis and management of serious urinary complications after major operative laparoscopy. Obstet Gynecol 1996;87: Witters S, Cornelissen M, Vereecken R. Iatrogenic ureteral injury: aggressive or conservative treatment. 1986;155:582-4.
6 Volume 187, Number 6 Kwon et al Neuman M, Eidelman A, Langer R, Golan A, Bukovsky I, Caspi E. Iatrogenic injuries to the ureter during gynecologic and obstetric operations. Surg Gynecol Obstet 1991;173: Goodno JA, Powers TW, Harris VD. Ureteral injury in gynecologic surgery: a ten-year review in a community hospital. Am J Obstet Gynecol 1995;172: Daly JW, Higgins KA. Injury to the ureter during gynecologic surgical procedures. Surg Gynecol Obstet 1988;167: Onwudiegwu U, Makinde OA, Badejo OA, Okonofua FE, Ogunniyi SO. Ureteral injuries associated with gynecologic surgery. Int J Gynecol Obstet 1991;34: Wiskind AK, Thompson JD. Should cystoscopy be performed at every gynecologic operation to diagnose unsuspected ureteral injury? J Pelvic Surg 1995;3: Piscitelli JT, Simel DL, Addison WA. Who should have intravenous pyelograms before hysterectomy for benign disease? Obstet Gynecol 1987;69: Jabs CFI, Drutz HP. The role of intraoperative cystoscopy in prolapse and incontinence surgery. 2001; 185: Tulikangas PK, Weber AM, Larive AB, Walters MD. Intraoperative cystoscopy in conjunction with anti incontinence surgery. Obstet Gynecol 2000;95: Visco AG, Taber KH, Weidner AC, Barber MD, Myers ER. Costeffectiveness of universal cystoscopy to identify ureteral injury at hysterectomy. Obstet Gynecol 2001;97: Shull BL, Bachofen C, Coates KC, Kuehl TJ. A transvaginal approach to repair of apical and other associated sites of pelvic organ prolapse with uterosacral ligaments. 2000;183: Discussion DR RORY ADAM, Atlanta, Ga. Others have published on the subject of cystoscopy during pelvic surgery. Among the more recent, Harris et al 1 reported 224 patients undergoing urogynecologic surgery that had intraoperative cystoscopy. Nine unsuspected urinary tract injuries occurred, for an incidence of 4.0%. Jabs and Drutz 2 documented 12 unsuspected injuries of their 224 cases, for an incidence of 5.3%. These findings correlate well with the current paper s incidence of 4.9% of 526 patients, indeed making this the largest reported series to date. None of these studies identified any preoperative or operative characteristics that were associated with an increased risk of abnormal cystoscopic findings. Given the low rate of abnormal findings, none of the studies, including the current one, was of sufficient power to identify factors predictive of increased risk. Previous studies have looked at the Burch procedure in particular. Stevenson et al 3 reported 10 of 109 patients with urinary tract injury, for an incidence of 9.2%. They concluded that routine intraoperative cystoscopy is warranted. In a study by Klutke et al 4 no injuries were reported in 97 patients, and therefore the authors argue against routine intraoperative cystoscopy. Gill et al 5 in a recent series of 181 patients undergoing Burch colposuspensions report a 3.3% total injury rate. Of the 6 injuries, only 1 (0.5%) was not recognized before cystoscopy. This ureteral injury was said to be due to the concomitant paravaginal repair and not to the Burch procedure itself. The authors conclude that it may not be necessary to proceed with routine cystoscopy during an uncomplicated Burch urethropexy, when performed as the only procedure. 5 In the current study, Kwon et al documented a total of 7 injuries of 183 (3.8%) Burch procedures. Of these, 3 injuries were undetected until cystoscopy for an incidence of 1.6%. The procedure with the highest injury rate in the current series was anterior colporrhaphy (2.0%), accounting for 46% of significant findings. This is in agreement with the findings of Jabs and Drutz 2 in which 6 of their 12 patients (50%) with abnormal cystoscopic findings required replacement of the bladder neck stitch. My questions to Dr Kwon are the following: 1. Has this information changed your intraoperative management? If so, how? 2. Was a postoperative IVP performed to rule out silent renal damage in the patients with sluggish ureteral efflux and no subsequent suture revisions? 3. At what point in the procedure do you advocate doing the cystoscopy? At the very end when the incisions are closed, or after the portion that causes the most perceived risk? The current study further supports the argument for the routine use of cystoscopy. I believe, however, that there is insufficient data, at this time, to definitively recommend the routine use of cystoscopy after all reconstructive pelvic surgeries. Having said that, many surgeons, myself included, do it regardless. Because many gynecologists believe that cystoscopy is not an option for them, we make it a point to train our residents and fellows to use intraoperative cystoscopy and to feel comfortable with its technique. This has been shown to result in subsequent granting of privileges after residency training. 6 This is the first step in ensuring the continued safety of the lower urinary tract despite the ever-increasing complexity of our surgical interventions. REFERENCES 1. Harris RL, Cundiff GW, Theofrastous JP, Yoon H, Bump RC, Addison MA. The value of intraoperative cystoscopy in urogynecologic and reconstructive pelvic surgery. 1997;177: Jabs CFI, Drutz HP. The role of intraoperative cystoscopy in prolapse and incontinence surgery. Am J Obstet Gyneco1 2001; 185: Stevenson KR, Cholhan HJ, Hartmann DM, Buchsbaum GM, Guzick DC. Lower urinary tract injury during the Burch procedure: is there a role for routine cystoscopy? 1999;181: Klutke JJ, Klutke CG, Hsieh G. Bladder injury during the Burch retropubic urethropexy: is routine cystoscopy necessary? Tech Urol 1998;4: Gill EJ, Elser DM, Bonidie MJ, Roberts KM, Hurt WG. The routine use of cystoscopy with the Burch procedure. 2001;185: Hibbert ML, Salminen ER, Dainty LA, Davis GD, Perez RP. Credentialing residents for intraoperative cystoscopy. Obstet Gynecol 2000;96: DR KWON (Closing). Although the current available literature seems to support the use of routine intraopera-
7 1472 Kwon et al December 2002 tive cystoscopy during anti-incontinence procedures, most specifically the Burch retropubic urethropexy, the routine use of cystoscopy during all reconstructive surgery is not as clear. What this study has most significantly revealed to us is that procedures such as anterior colporrhaphy, not traditionally thought to place the lower urinary tract at high risk, might actually pose the greatest risk to the patient. In terms of our own intraoperative procedures, we perform an aggressive anterior colporrhaphy, mindful that midline plication of the tissue may cause ureteral kinking. As the anterior compartment is a difficult one to treat, with a high rate of prolapse recurrence, we will continue to perform our anterior colporrhaphies and, of course, continue to perform intraoperative cystoscopy with this procedure. Postoperative IVP evaluation is obtained for patients if they develop symptoms after surgery. In the case of the patient who became symptomatic after surgery who did obtain an IVP, the partial obstruction seen was an incidental finding because her pain arose from the urinoma that developed from her suprapubic catheter placement. Her symptoms completely resolved after removal of the suprapubic catheter, and she was managed conservatively and expectantly for the hydronephrosis. We had obtained a consult from urology in this case as well, who agreed with the expectant management. No further interventions were required for this patient. We performed the cystoscopy after all anterior repair, sling sutures, and culdoplasty sutures are placed, before the closure of the anterior vaginal epithelium. Depending on the type of anti-incontinence procedure concomitantly performed, such as a TVT, cystoscopy may be repeated if performed through a separate incision from anterior colporrhaphy. This study has only further supported our practice of performing routine intraoperative cystoscopy at the time of any vaginal reconstructive surgery and antiincontinence procedure. It is a low-risk and easy to perform procedure that can prevent serious morbidity for our operative patients.
International Federation of Gynecology and Obstetrics
 International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
MIDLAND MEMORIAL HOSPITAL Delineation of Privileges FEMALE PELVIC MEDICINE AND RECONSTRUCTIVE SURGERY (UROGYNECOLOGY)
 MIDLAND MEMORIAL HOSPITAL Delineation of Privileges FEMALE PELVIC MEDICINE AND RECONSTRUCTIVE SURGERY (UROGYNECOLOGY) Physician Name: Your home for healthcare Female Pelvic Medicine and Reconstructive
MIDLAND MEMORIAL HOSPITAL Delineation of Privileges FEMALE PELVIC MEDICINE AND RECONSTRUCTIVE SURGERY (UROGYNECOLOGY) Physician Name: Your home for healthcare Female Pelvic Medicine and Reconstructive
SURGICAL. How to manage the cuff at vaginal hysterectomy. For personal use only. Copyright Dowden Health Media TECHNIQUES
 For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
For personal use only. Injury-free vaginal surgery: Case-based protective tactics
 For mass reproduction, content licensing and permissions contact Dowden Health Media. OBG MANAGEMENT Lennox Hoyte, MD Director of Female Pelvic Medicine and Reconstructive Surgery, Department of Obstetrics
For mass reproduction, content licensing and permissions contact Dowden Health Media. OBG MANAGEMENT Lennox Hoyte, MD Director of Female Pelvic Medicine and Reconstructive Surgery, Department of Obstetrics
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review
 Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation
 Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation Roger P. Goldberg, MD, MPH, Sumana Koduri, MD, Robert W. Lobel, MD, Patrick J. Culligan,
Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation Roger P. Goldberg, MD, MPH, Sumana Koduri, MD, Robert W. Lobel, MD, Patrick J. Culligan,
Paravaginal Repair: A Laparoscopic Approach
 44 Paravaginal Repair: A Laparoscopic Approach John R. Miklos and Robert Moore Atlanta Urogynecology Associates, Atlanta, Georgia, U.S.A. Neeraj Kohli Harvard University, Boston, Massachusetts, U.S.A.
44 Paravaginal Repair: A Laparoscopic Approach John R. Miklos and Robert Moore Atlanta Urogynecology Associates, Atlanta, Georgia, U.S.A. Neeraj Kohli Harvard University, Boston, Massachusetts, U.S.A.
Sara Schaenzer Grand Rounds January 24 th, 2018
 Sara Schaenzer Grand Rounds January 24 th, 2018 Bladder Anatomy Ureter Anatomy Areas of Injury Bladder: Posterior bladder wall above trigone Ureter Crosses beneath uterine vessels At pelvic brim when ligating
Sara Schaenzer Grand Rounds January 24 th, 2018 Bladder Anatomy Ureter Anatomy Areas of Injury Bladder: Posterior bladder wall above trigone Ureter Crosses beneath uterine vessels At pelvic brim when ligating
Step by step High uterosacral vaginal vault suspension to repair enterocele and apical prolapse
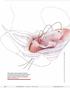 When performing high uterosacral suspension, it is possible to pass sutures through the coccygeus muscle-sacrospinous ligament complex (arrow) because a segment of the uterosacral ligament inserts into
When performing high uterosacral suspension, it is possible to pass sutures through the coccygeus muscle-sacrospinous ligament complex (arrow) because a segment of the uterosacral ligament inserts into
A trial placement of a prophylactic ureteral catheter during the excision of a huge pelvic mass with incidental cystotomy
 372 CASE REPORT TRAUMA AND RECONSTRUCTIVE UROLOGY A trial placement of a prophylactic ureteral catheter during the excision of a huge pelvic mass with incidental cystotomy Hussein Warda Department of Obstetrics
372 CASE REPORT TRAUMA AND RECONSTRUCTIVE UROLOGY A trial placement of a prophylactic ureteral catheter during the excision of a huge pelvic mass with incidental cystotomy Hussein Warda Department of Obstetrics
A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience
 Journal Of Laparoendoscopic Surgery Volume 4, Number 5, 1994 Mary Ann Liebert, Inc., Publishers A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience E.D. RIZA, M.D.(1)
Journal Of Laparoendoscopic Surgery Volume 4, Number 5, 1994 Mary Ann Liebert, Inc., Publishers A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience E.D. RIZA, M.D.(1)
We welcome comments and corrections which will be used to improve the system annually.
 ACGME Case Log Instructions: Female Pelvic Medicine and Reconstructive Surgery (FPMRS) Review Committees for Obstetrics and Gynecology, and Urology Updated July 2013 BACKGROUND The ACGME Case Log System
ACGME Case Log Instructions: Female Pelvic Medicine and Reconstructive Surgery (FPMRS) Review Committees for Obstetrics and Gynecology, and Urology Updated July 2013 BACKGROUND The ACGME Case Log System
Female Urology. The Results of Grade IV Cystocele Repair Using Mesh. Introduction ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M
 Urology Journal UNRC/IUA Vol. 1, No. 4, 263-267 Autumn 2004 Printed in IRAN Female Urology The Results of Grade IV Cystocele Repair Using Mesh ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M Department of Urology,
Urology Journal UNRC/IUA Vol. 1, No. 4, 263-267 Autumn 2004 Printed in IRAN Female Urology The Results of Grade IV Cystocele Repair Using Mesh ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M Department of Urology,
PL Narducci Department of Obstetrics and Gynecology General Hospital San Giovanni Battista Foligno, ITALY
 NESA DAYS 2018 New European Surgical Academy Perugia, April 19-21, 2018 EXCELLENCE IN FEMALE SURGERY PROLAPSE RECONSTRUCTIVE SURGERY IN SEXUALLY ACTIVE WOMEN LAPAROSCOPIC ANTERIOR ABDOMINAL WALL COLPOPEXY
NESA DAYS 2018 New European Surgical Academy Perugia, April 19-21, 2018 EXCELLENCE IN FEMALE SURGERY PROLAPSE RECONSTRUCTIVE SURGERY IN SEXUALLY ACTIVE WOMEN LAPAROSCOPIC ANTERIOR ABDOMINAL WALL COLPOPEXY
PRACTICE BULLETIN Female Pelvic Medicine & Reconstructive Surgery Volume 23, Number 4, July/August 2017
 PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
Case Based Urology Learning Program
 Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 19 CBULP 2011 044 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 19 CBULP 2011 044 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Stop Coping. Start Living. Talk to your doctor about pelvic organ prolapse and sacrocolpopexy
 Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Clinical Curriculum: Urogynecology
 Updated July 201 Clinical Curriculum: Urogynecology GOAL: The primary goal of the Urogynecology rotation at the University of Alabama at Birmingham (UAB) is to train physicians to have a broad knowledge
Updated July 201 Clinical Curriculum: Urogynecology GOAL: The primary goal of the Urogynecology rotation at the University of Alabama at Birmingham (UAB) is to train physicians to have a broad knowledge
Prevention of Surgical Injuries in Gynecology
 in Gynecology John K. Chan, M.D. Division of Gynecologic Oncology Overview Review anatomy, etiology, intraoperative, postoperative management, prevention of injuries to: 1. Urinary tract 2. Gastrointestinal
in Gynecology John K. Chan, M.D. Division of Gynecologic Oncology Overview Review anatomy, etiology, intraoperative, postoperative management, prevention of injuries to: 1. Urinary tract 2. Gastrointestinal
Gynecology Dr. Sallama Lecture 3 Genital Prolapse
 Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Clinical Study Initial Experience with Robotic Retropubic Urethropexy Compared to Open Retropubic Urethropexy
 Obstetrics and Gynecology International Volume 2013, Article ID 315680, 5 pages http://dx.doi.org/10.1155/2013/315680 Clinical Study Initial Experience with Retropubic Urethropexy Compared to Open Retropubic
Obstetrics and Gynecology International Volume 2013, Article ID 315680, 5 pages http://dx.doi.org/10.1155/2013/315680 Clinical Study Initial Experience with Retropubic Urethropexy Compared to Open Retropubic
SACROSPINOUS LIGAMENT FIXATION, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE
 Original Article, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE * ** Fauzia Rasool Memon, Mohamed Matar * Consultant Obstetrician and Gynecologist
Original Article, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE * ** Fauzia Rasool Memon, Mohamed Matar * Consultant Obstetrician and Gynecologist
Current status in pelvic organ prolapse surgery: an evidence based review
 Current status in pelvic organ prolapse surgery: an evidence based review Christian Falconer, MD, PhD Department of Obstetrics and Gynecology Danderyd University Hospital Stockholm, Sweden Finnish Society
Current status in pelvic organ prolapse surgery: an evidence based review Christian Falconer, MD, PhD Department of Obstetrics and Gynecology Danderyd University Hospital Stockholm, Sweden Finnish Society
By:Dr:ISHRAQ MOHAMMED
 By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse
 ORIGINAL ARTICLE Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse Cecile A. Unger, MD, MPH, Matthew D. Barber, MD, MHS, Mark
ORIGINAL ARTICLE Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse Cecile A. Unger, MD, MPH, Matthew D. Barber, MD, MHS, Mark
What are we talking about? Symptoms. Prolapse Risk Factors. Vaginal bulge 1 Splinting. ?? Pelvic pressure Back pain 1 Urinary complaints 2
 Options for Vaginal Prolapse What are we talking about? Michelle Y. Morrill, M.D. Director of Urogynecology The Permanente Medical Group Kaiser, San Francisco Assistant Professor, Volunteer Faculty Department
Options for Vaginal Prolapse What are we talking about? Michelle Y. Morrill, M.D. Director of Urogynecology The Permanente Medical Group Kaiser, San Francisco Assistant Professor, Volunteer Faculty Department
Recent advances have improved the
 SURGICAL TECHNIQUES BY NEERAJ KOHLI, MD, MBA, and JOHN R. MIKLOS, MD Meeting the challenge of vesicovaginal fistula repair: Conservative and surgical measures A number of simple adjustments to technique
SURGICAL TECHNIQUES BY NEERAJ KOHLI, MD, MBA, and JOHN R. MIKLOS, MD Meeting the challenge of vesicovaginal fistula repair: Conservative and surgical measures A number of simple adjustments to technique
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablation in uterine leiomyoma management, 719 723 Adnexal masses diagnosis of, 664 667 imaging in, 664 665 laboratory studies in, 665
Index Note: Page numbers of article titles are in boldface type. A Ablation in uterine leiomyoma management, 719 723 Adnexal masses diagnosis of, 664 667 imaging in, 664 665 laboratory studies in, 665
Eric R. Sokol, MD. Bio. CLINICAL OFFICES Gynecology Clinic 900 Blake Wilbur Dr. Palo Alto, CA Tel (650) Fax (650) BIO
 CLINICAL OFFICES Gynecology Clinic 900 Blake Wilbur Dr Bio Palo Alto, CA 94304 Associate Professor of Obstetrics and Gynecology (Gynecology-Urogynecology) and, by courtesy, of Urology at the Stanford University
CLINICAL OFFICES Gynecology Clinic 900 Blake Wilbur Dr Bio Palo Alto, CA 94304 Associate Professor of Obstetrics and Gynecology (Gynecology-Urogynecology) and, by courtesy, of Urology at the Stanford University
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Suture complications in a teaching institution among patients undergoing uterosacral ligament suspension with permanent braided suture
 Int Urogynecol J (2010) 21:813 818 DOI 10.1007/s00192-010-1109-1 ORIGINAL ARTICLE Suture complications in a teaching institution among patients undergoing uterosacral ligament suspension with permanent
Int Urogynecol J (2010) 21:813 818 DOI 10.1007/s00192-010-1109-1 ORIGINAL ARTICLE Suture complications in a teaching institution among patients undergoing uterosacral ligament suspension with permanent
Understanding Pelvic Organ Prolapse. Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery
 Understanding Pelvic Organ Prolapse Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery Disclosures None I am the daughter of a physician assistant. Objectives List types of pelvic
Understanding Pelvic Organ Prolapse Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery Disclosures None I am the daughter of a physician assistant. Objectives List types of pelvic
FRANZCOG Training Program Logbook Procedure List and Classification
 FRANZCOG Training Program Logbook Procedure List and Classification This logbook procedure list provides sites and trainees with the major/minor classification of procedures in the online logbook. As detailed
FRANZCOG Training Program Logbook Procedure List and Classification This logbook procedure list provides sites and trainees with the major/minor classification of procedures in the online logbook. As detailed
Avoiding and Managing Urologic Injury
 Avoiding and Managing Urologic Injury Jubilee Brown, MD Professor & Associate Director, Gynecologic Oncology Levine Cancer Institute at the Carolinas HealthCare System Charlotte, North Carolina 1 No relevant
Avoiding and Managing Urologic Injury Jubilee Brown, MD Professor & Associate Director, Gynecologic Oncology Levine Cancer Institute at the Carolinas HealthCare System Charlotte, North Carolina 1 No relevant
Chatzipapas I., Kathopoulis N., Protopapas A., Kyritsis N., Vlachos D. E., Loutradis D.
 HJOG An Obstetrics and Gynecology International Journal Research Article HJOG 2017, 16 (2), 23-28 Mobile Cystoscope Chatzipapas I., Kathopoulis N., Protopapas A., Kyritsis N., Vlachos D. E., Loutradis
HJOG An Obstetrics and Gynecology International Journal Research Article HJOG 2017, 16 (2), 23-28 Mobile Cystoscope Chatzipapas I., Kathopoulis N., Protopapas A., Kyritsis N., Vlachos D. E., Loutradis
Vaginal McCall culdoplasty versus laparoscopic uterosacral plication to prophylactically address vaginal vault prolapse
 Vaginal McCall culdoplasty versus laparoscopic uterosacral to prophylactically address vaginal vault prolapse Niblock, K., Bailie, E., McCracken, G., & Johnston, K. (2017). Vaginal McCall culdoplasty versus
Vaginal McCall culdoplasty versus laparoscopic uterosacral to prophylactically address vaginal vault prolapse Niblock, K., Bailie, E., McCracken, G., & Johnston, K. (2017). Vaginal McCall culdoplasty versus
Urethrolysis; When, Why & How. M Karram Professor of Ob/Gyn & Urology University of Cincinnati
 Urethrolysis; When, Why & How M Karram Professor of Ob/Gyn & Urology University of Cincinnati Anatomy Urethra may be fixed to the pubic bone with dense scar tissue Goal of urethrolysis is to completely
Urethrolysis; When, Why & How M Karram Professor of Ob/Gyn & Urology University of Cincinnati Anatomy Urethra may be fixed to the pubic bone with dense scar tissue Goal of urethrolysis is to completely
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015
 Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Iatrogenic Ureteral Injuries in Non Urological Surgeries: An Institutional Experience
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 11 Ver. I (Nov. 2015), PP 29-33 www.iosrjournals.org Iatrogenic Ureteral Injuries in Non Urological
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 11 Ver. I (Nov. 2015), PP 29-33 www.iosrjournals.org Iatrogenic Ureteral Injuries in Non Urological
American Journal of Obstetrics and Gynecology
 American Journal of Obstetrics and Gynecology 1 2 3 Recurrence of vaginal prolapse after total vaginal hysterectomy with concurrent vaginal uterosacral ligament suspension: comparison between normal-weight
American Journal of Obstetrics and Gynecology 1 2 3 Recurrence of vaginal prolapse after total vaginal hysterectomy with concurrent vaginal uterosacral ligament suspension: comparison between normal-weight
Daniel K Roberts MD, PhD 2014 Annual Clinical Update
 Daniel K Roberts MD, PhD 2014 Annual Clinical Update Kevin E Miller, MD Division of Female Pelvic Medicine and Reconstructive Surgery Dept. of OBGYN University of Kansas School of Medicine- Wichita at
Daniel K Roberts MD, PhD 2014 Annual Clinical Update Kevin E Miller, MD Division of Female Pelvic Medicine and Reconstructive Surgery Dept. of OBGYN University of Kansas School of Medicine- Wichita at
Long-term outcomes of modified high uterosacral ligament vault suspension (HUSLS) at vaginal hysterectomy
 Int Urogynecol J (2011) 22:577 584 DOI 10.1007/s00192-010-1325-8 ORIGINAL ARTICLE Long-term outcomes of modified high uterosacral ligament vault suspension (HUSLS) at vaginal hysterectomy Stergios K. Doumouchtsis
Int Urogynecol J (2011) 22:577 584 DOI 10.1007/s00192-010-1325-8 ORIGINAL ARTICLE Long-term outcomes of modified high uterosacral ligament vault suspension (HUSLS) at vaginal hysterectomy Stergios K. Doumouchtsis
Site-specific fascial defects in the diagnosis and surgical management of enterocele
 Site-specific fascial defects in the diagnosis and surgical management of enterocele John R. Miklos, MD,a Neeraj Kohli, MD,b Vincent Lucente, MD,c and William B. Safe, MDd Atlanta and Marietta, GeO1gia,
Site-specific fascial defects in the diagnosis and surgical management of enterocele John R. Miklos, MD,a Neeraj Kohli, MD,b Vincent Lucente, MD,c and William B. Safe, MDd Atlanta and Marietta, GeO1gia,
Surgical repair of vaginal wall prolapse using mesh
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
 Gynecol Surg (2006) 3: 88 92 DOI 10.1007/s10397-005-0168-7 ORIGINAL ARTICLE R. Oliver. C. Dasgupta. A. Coker Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
Gynecol Surg (2006) 3: 88 92 DOI 10.1007/s10397-005-0168-7 ORIGINAL ARTICLE R. Oliver. C. Dasgupta. A. Coker Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
INJ. Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple Sutures: Surgical Technique and Results.
 Original Article Int Neurourol J 2012;16:144-148 pissn 2093-4777 eissn 2093-6931 International Neurourology Journal Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple
Original Article Int Neurourol J 2012;16:144-148 pissn 2093-4777 eissn 2093-6931 International Neurourology Journal Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple
A SIMPLE SURGICAL TECHNIQUE TO MINIMIZE POSTOPERATIVE URINARY RETENTION WITH A PUBOVAGINAL SLING
 Urological Neurology Brazilian Journal of Urology Official Journal of the Brazilian Society of Urology Vol. 27 (3): 275-280, May - June, 2001 A SIMPLE SURGICAL TECHNIQUE TO MINIMIZE POSTOPERATIVE URINARY
Urological Neurology Brazilian Journal of Urology Official Journal of the Brazilian Society of Urology Vol. 27 (3): 275-280, May - June, 2001 A SIMPLE SURGICAL TECHNIQUE TO MINIMIZE POSTOPERATIVE URINARY
Anatomical and Functional Results of Pelvic Organ Prolapse Mesh Repair: A Prospective Study of 105 Cases
 International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy
 Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
THE operation of reimplantation of the ureter into the bladder has undergone
 REIMPLANTATION OF THE URETER INTO THE BLADDER J. G. WARDEN, M.D., and C. C. HIGGINS, M.D. Department of Urology THE operation of reimplantation of the ureter into the bladder has undergone a stormy course
REIMPLANTATION OF THE URETER INTO THE BLADDER J. G. WARDEN, M.D., and C. C. HIGGINS, M.D. Department of Urology THE operation of reimplantation of the ureter into the bladder has undergone a stormy course
Medium-term follow-up on use of freeze-dried, irradiated donor fascia for sacrocolpopexy and sling procedures
 Int Urogynecol J (2004) 15: 238 242 DOI 10.1007/s00192-004-1146-8 ORIGINAL ARTICLE Mary Pat FitzGerald Æ S. Renee Edwards Æ Dee Fenner Medium-term follow-up on use of freeze-dried, irradiated donor fascia
Int Urogynecol J (2004) 15: 238 242 DOI 10.1007/s00192-004-1146-8 ORIGINAL ARTICLE Mary Pat FitzGerald Æ S. Renee Edwards Æ Dee Fenner Medium-term follow-up on use of freeze-dried, irradiated donor fascia
Urogynecology: Evidence-Based Clinical Practice
 Urogynecology: Evidence-Based Clinical Practice Kate H. Moore Urogynecology: Evidence-Based Clinical Practice Second Edition Kate H. Moore, MBBS, FRCOG, FRANZCOG, MD, CU Department Obstetrics & Gynaecology
Urogynecology: Evidence-Based Clinical Practice Kate H. Moore Urogynecology: Evidence-Based Clinical Practice Second Edition Kate H. Moore, MBBS, FRCOG, FRANZCOG, MD, CU Department Obstetrics & Gynaecology
This information is intended as an overview only
 This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
PUBOVAGINAL SLING IN THE TREATMENT OF STRESS URINARY INCONTINENCE FOR URETHRAL HYPERMOBILITY AND INTRINSIC SPHINCTERIC DEFICIENCY
 Urological Neurology International Braz J Urol Official Journal of the Brazilian Society of Urology PUBOVAGINAL SLING IN SUI Vol. 29 (6): 540-544, November - December, 2003 PUBOVAGINAL SLING IN THE TREATMENT
Urological Neurology International Braz J Urol Official Journal of the Brazilian Society of Urology PUBOVAGINAL SLING IN SUI Vol. 29 (6): 540-544, November - December, 2003 PUBOVAGINAL SLING IN THE TREATMENT
REPAIR OF LARGE CYSTOCELE
 REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
Are effective nonsurgical treatments available for women with pelvic organ prolapse?
 Are effective nonsurgical treatments available for women with pelvic organ prolapse? For women with asymptomatic prolapse, education and reassurance are appropriate. Women may not realize that symptoms
Are effective nonsurgical treatments available for women with pelvic organ prolapse? For women with asymptomatic prolapse, education and reassurance are appropriate. Women may not realize that symptoms
SciFed Journal of Public Health. Endoscopic Management of Obstetrical Uretero-Uterine Fistula. Case Report and Review of Literature
 SciFed Journal of Public Health Case Report Open Access Endoscopic Management of Obstetrical Uretero-Uterine Fistula. Case Report and Review of Literature * Yasin Idweini * Chairperson of Urology Department
SciFed Journal of Public Health Case Report Open Access Endoscopic Management of Obstetrical Uretero-Uterine Fistula. Case Report and Review of Literature * Yasin Idweini * Chairperson of Urology Department
Tian-Ni Kuo 1, Ming-Ping Wu 1,2 *
 RESEARCH LETTER THE USE OF A CONCOMITANT TENSION-FREE VAGINAL MESH TECHNIQUE AND A TENSION-FREE MIDURETHRAL SLING IN TREATING PELVIC ORGAN PROLAPSE AND OCCULT STRESS URINARY INCONTINENCE Tian-Ni Kuo 1,
RESEARCH LETTER THE USE OF A CONCOMITANT TENSION-FREE VAGINAL MESH TECHNIQUE AND A TENSION-FREE MIDURETHRAL SLING IN TREATING PELVIC ORGAN PROLAPSE AND OCCULT STRESS URINARY INCONTINENCE Tian-Ni Kuo 1,
Efficacy and Adverse Effects of Monarc Versus Tension-free Vaginal Tape Obturator: a Retrospective One-year Follow-up Study
 Efficacy and Adverse Effects of Monarc Versus Tension-free Vaginal Tape Obturator: a Retrospective One-year Follow-up Study Yvonne KY CHENG MBChB, MRCOG William WK TO MBBS, M Phil, FRCOG, FHKAM (O&G) HX
Efficacy and Adverse Effects of Monarc Versus Tension-free Vaginal Tape Obturator: a Retrospective One-year Follow-up Study Yvonne KY CHENG MBChB, MRCOG William WK TO MBBS, M Phil, FRCOG, FHKAM (O&G) HX
Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M.
 UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
Laparoscopic sacrocolpopexy: an observational study of functional and anatomical outcomes
 DOI 10.1007/s00192-010-1241-y ORIGINAL ARTICLE Laparoscopic sacrocolpopexy: an observational study of functional and anatomical outcomes Natalia Price & Alex Slack & Simon R. Jackson Received: 26 April
DOI 10.1007/s00192-010-1241-y ORIGINAL ARTICLE Laparoscopic sacrocolpopexy: an observational study of functional and anatomical outcomes Natalia Price & Alex Slack & Simon R. Jackson Received: 26 April
LAPAROSCOPIC REPAIR OF PELVIC FLOOR
 LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
T h e C o m p l e t e Tr e a t m e n t o f P e l v i c F l o o r P r o l a p s e by Laparoscopy Technique, Tips and Tricks
 T h e C o m p l e t e Tr e a t m e n t o f P e l v i c F l o o r P r o l a p s e by Laparoscopy Technique, Tips and Tricks R Botchorishvili, A Wattiez, G Mage, M Canis, B Rabischong, K Jardon, C Rivoire,
T h e C o m p l e t e Tr e a t m e n t o f P e l v i c F l o o r P r o l a p s e by Laparoscopy Technique, Tips and Tricks R Botchorishvili, A Wattiez, G Mage, M Canis, B Rabischong, K Jardon, C Rivoire,
* 梁景忠醫師 所有發表期刊論文 Bibliography
 * 梁景忠醫師 所有發表期刊論文 Bibliography A. First author and Corresponding author (2000- ) 1. Liang CC, Tseng CJ, Soong YK: The usefulness of cystoscopy in the staging of cervical cancer. Gynecol Oncol 76: 200-3,
* 梁景忠醫師 所有發表期刊論文 Bibliography A. First author and Corresponding author (2000- ) 1. Liang CC, Tseng CJ, Soong YK: The usefulness of cystoscopy in the staging of cervical cancer. Gynecol Oncol 76: 200-3,
Current trend in anti-incontinence surgery
 Current trend in anti-incontinence surgery 吳銘斌醫師 (Ming-Ping Wu, M.D., Ph.D.) 奇美醫院婦產部婦女泌尿暨骨盆醫學科主任台北醫學大學醫學院婦產學科副教授成功大學醫學院臨床醫學所博士 Anti-incontinence surgery Bladder buttress operation: Kelly plication Needle
Current trend in anti-incontinence surgery 吳銘斌醫師 (Ming-Ping Wu, M.D., Ph.D.) 奇美醫院婦產部婦女泌尿暨骨盆醫學科主任台北醫學大學醫學院婦產學科副教授成功大學醫學院臨床醫學所博士 Anti-incontinence surgery Bladder buttress operation: Kelly plication Needle
Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583
 Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
Gynecologic. Indiana Regional Medical Center Procedures to Labs/Tests June 1, A/P REPAIR W/SACROSP COLPOPEXY Table 1
 Indiana Regional Medical Center Procedures to Labs/Tests June 1, 2011 Gynecologic A/P REPAIR W/SACROSP COLPOPEXY Table 1 ABD SUPRACERVICAL HYSTERECTOMY Table 1 ANTERIOR POSTERIOR REPAIR Table 1 ANTERIOR
Indiana Regional Medical Center Procedures to Labs/Tests June 1, 2011 Gynecologic A/P REPAIR W/SACROSP COLPOPEXY Table 1 ABD SUPRACERVICAL HYSTERECTOMY Table 1 ANTERIOR POSTERIOR REPAIR Table 1 ANTERIOR
Complications from permanent synthetic mesh
 Original Research Symptom Resolution After Operative Management of Complications From Transvaginal Mesh Erin C. Crosby, MD, Melinda Abernethy, MD, MPH, Mitchell B. Berger, MD, PhD, John O. DeLancey, MD,
Original Research Symptom Resolution After Operative Management of Complications From Transvaginal Mesh Erin C. Crosby, MD, Melinda Abernethy, MD, MPH, Mitchell B. Berger, MD, PhD, John O. DeLancey, MD,
Interventional management of postoperative ureteric complications after pelvic surgery
 Interventional management of postoperative ureteric complications after pelvic surgery Poster No.: C-0169 Congress: ECR 2015 Type: Scientific Exhibit Authors: R. Tabashy, A. Hamed, S. El-Sebai; Cairo/EG
Interventional management of postoperative ureteric complications after pelvic surgery Poster No.: C-0169 Congress: ECR 2015 Type: Scientific Exhibit Authors: R. Tabashy, A. Hamed, S. El-Sebai; Cairo/EG
Index. B Bladder, injury of, Bowel, injury of, , Brachytherapy, for cervical cancer, 357 Burns, electrosurgical,
 Perioperative Nursing Clinics 1 (2006) 375 379 Index Note: Page numbers of article titles are in boldface type. A Abdominal hysterectomy Acidosis, from insufflation, 323 Active electrode monitoring, in
Perioperative Nursing Clinics 1 (2006) 375 379 Index Note: Page numbers of article titles are in boldface type. A Abdominal hysterectomy Acidosis, from insufflation, 323 Active electrode monitoring, in
Introduction. Regarding the Section of the UPDATE Entitled Purpose
 Time to Rethink: an Evidence-Based Response from Pelvic Surgeons to the FDA Safety Communication: UPDATE on Serious Complications Associated with Transvaginal Placement of Surgical Mesh for Pelvic Organ
Time to Rethink: an Evidence-Based Response from Pelvic Surgeons to the FDA Safety Communication: UPDATE on Serious Complications Associated with Transvaginal Placement of Surgical Mesh for Pelvic Organ
Prolapse & Stress Incontinence
 Advanced Pelvic Floor Course Prolapse & Stress Incontinence OVERVIEW Day One and morning of Day Two- Pelvic Organ Prolapse The Prolapse component covers the detailed anatomy of POP including the DeLancey
Advanced Pelvic Floor Course Prolapse & Stress Incontinence OVERVIEW Day One and morning of Day Two- Pelvic Organ Prolapse The Prolapse component covers the detailed anatomy of POP including the DeLancey
Figure 13 1 Technique of anterior repair with plication of the pubocervical fascia for cystocele repair.
 Figure 13 1 Technique of anterior repair with plication of the pubocervical fascia for cystocele repair. Figure 13 2 Technique of posterior repair with plication of the recto-vaginal fascia for rectocele
Figure 13 1 Technique of anterior repair with plication of the pubocervical fascia for cystocele repair. Figure 13 2 Technique of posterior repair with plication of the recto-vaginal fascia for rectocele
ROBOTIC MESH SACROCOLPOPEXY
 ROBOTIC MESH SACROCOLPOPEXY Philippe E. Zimmern, MD, FACS Professor of Urology Mesh sacrocolpopexy Background First described in 1962 by Lane Until then, treatment options were: Pessary Colpocleisis Vaginal
ROBOTIC MESH SACROCOLPOPEXY Philippe E. Zimmern, MD, FACS Professor of Urology Mesh sacrocolpopexy Background First described in 1962 by Lane Until then, treatment options were: Pessary Colpocleisis Vaginal
Subspecialty Procedural Volume Guidelines
 Subspecialty Review Committee for Obstetrics and Gynecology In response to requests from program directors, and in an effort to be transparent, the Review Committee for Obstetrics and Gynecology has elected
Subspecialty Review Committee for Obstetrics and Gynecology In response to requests from program directors, and in an effort to be transparent, the Review Committee for Obstetrics and Gynecology has elected
Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications
 Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications Karyn S. Eilber, M.D. Cedars-Sinai FPMRS Associate Professor, Cedars-Sinai Dept of Surgery Associate Director, Urology Residency
Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications Karyn S. Eilber, M.D. Cedars-Sinai FPMRS Associate Professor, Cedars-Sinai Dept of Surgery Associate Director, Urology Residency
Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments?
 Int Urogynecol J (2010) 21:271 278 DOI 10.1007/s00192-009-1028-1 ORIGINAL ARTICLE Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments? Mariëlla
Int Urogynecol J (2010) 21:271 278 DOI 10.1007/s00192-009-1028-1 ORIGINAL ARTICLE Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments? Mariëlla
Log Title: OBRES Gynecologic Case Log
 Log Title: OBRES Gynecologic Case Log Hospital/Institution: (Lookup) Attending Physician (Lookup) Is Patient Pregnant? ( Y or N) MEDRECNO: (text) Date (encounter) (Date) Diagnosis DX GYN Acute Pelvic Pain
Log Title: OBRES Gynecologic Case Log Hospital/Institution: (Lookup) Attending Physician (Lookup) Is Patient Pregnant? ( Y or N) MEDRECNO: (text) Date (encounter) (Date) Diagnosis DX GYN Acute Pelvic Pain
30/06/2014. Gynaecological Surgery. Mr Alfred Cutner, Consultant Gynaecologist, University College Hospital, London WHAT IS LAPAROSCOPIC SURGERY?
 Gynaecological Surgery Mr Alfred Cutner, Consultant Gynaecologist, University College Hospital, London Laparoscopic surgery techniques Common complications of laparoscopic surgery Intra-operative injuries:
Gynaecological Surgery Mr Alfred Cutner, Consultant Gynaecologist, University College Hospital, London Laparoscopic surgery techniques Common complications of laparoscopic surgery Intra-operative injuries:
Gökmen Sukgen, 1 Esra SaygJlJ YJlmaz, 2 and Eralp BaGer Introduction. 2. Case Presentation
 Case Reports in Obstetrics and Gynecology Volume 2016, Article ID 2906596, 4 pages http://dx.doi.org/10.1155/2016/2906596 Case Report Vaginal Hysterectomy with Anterior Four-Arm Mesh Implant Technique
Case Reports in Obstetrics and Gynecology Volume 2016, Article ID 2906596, 4 pages http://dx.doi.org/10.1155/2016/2906596 Case Report Vaginal Hysterectomy with Anterior Four-Arm Mesh Implant Technique
Morbidity Audit and Logbook Tool SNOMED Board Reporting Terms for SET and IMG Urology ENDOSCOPIC LOWER URINARY TRACT
 ENDOSCOPIC LOWER URINARY TRACT Cystolitholapaxy Cystoscopic removal of foreign body from bladder Cystoscopic removal of ureteric stent Cystoscopy and cystodiathermy Cystoscopy and transurethral biopsy
ENDOSCOPIC LOWER URINARY TRACT Cystolitholapaxy Cystoscopic removal of foreign body from bladder Cystoscopic removal of ureteric stent Cystoscopy and cystodiathermy Cystoscopy and transurethral biopsy
Tension-free Vaginal Tape for Urodynamic Stress Incontinence
 Long-term Results of Tension-free Vaginal Tape Insertion for Urodynamic Stress Incontinence in Chinese Women at Eight-year Follow-up: a Prospective Study YM CHAN MBBS, MRCOG, FHKAM (O&G), DCG, DCH, DFM,
Long-term Results of Tension-free Vaginal Tape Insertion for Urodynamic Stress Incontinence in Chinese Women at Eight-year Follow-up: a Prospective Study YM CHAN MBBS, MRCOG, FHKAM (O&G), DCG, DCH, DFM,
JMSCR Volume 03 Issue 03 Page March 2015
 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Quality of Life among Patients after Vaginal Hysterectomy and Pelvic Floor Repair Operation ABSTRACT Authors S Lovereen 1, F A Suchi 2,
www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Quality of Life among Patients after Vaginal Hysterectomy and Pelvic Floor Repair Operation ABSTRACT Authors S Lovereen 1, F A Suchi 2,
Innovations in mesh kit technology for vaginal wall prolapse
 Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
A Midurethral Sling to Reduce Incontinence after Vaginal Prolapse Repair
 T h e n e w e ngl a nd j o u r na l o f m e dic i n e original article A Midurethral Sling to Reduce Incontinence after Vaginal Prolapse Repair John T. Wei, M.D., Ingrid Nygaard, M.D., Holly E. Richter,
T h e n e w e ngl a nd j o u r na l o f m e dic i n e original article A Midurethral Sling to Reduce Incontinence after Vaginal Prolapse Repair John T. Wei, M.D., Ingrid Nygaard, M.D., Holly E. Richter,
With our aging population, the rate of pelvic
 Original Research Short-Term Outcomes of Robotic Sacrocolpopexy Compared With Abdominal Sacrocolpopexy Elizabeth J. Geller, MD, Nazema Y. Siddiqui, MD, Jennifer M. Wu, MD, MPH, and Anthony G. Visco, MD
Original Research Short-Term Outcomes of Robotic Sacrocolpopexy Compared With Abdominal Sacrocolpopexy Elizabeth J. Geller, MD, Nazema Y. Siddiqui, MD, Jennifer M. Wu, MD, MPH, and Anthony G. Visco, MD
The incidence of mesh extrusion after vaginal incontinence and pelvic floor prolapse surgery
 ORIGINAL ARTICLE The incidence of mesh extrusion after vaginal incontinence and pelvic floor prolapse surgery Seth Cohen, Elizabeth Kavaler Department of Urology, Lenox Hill Hospital, USA Correspondence:
ORIGINAL ARTICLE The incidence of mesh extrusion after vaginal incontinence and pelvic floor prolapse surgery Seth Cohen, Elizabeth Kavaler Department of Urology, Lenox Hill Hospital, USA Correspondence:
Female Pelvic Medicine & Reconstructive Surgery
 Female Pelvic Medicine & Reconstructive Surgery APPLICATION FOR NEW FELLOWSHIP Name of Institution: McGill University Location: Royal Victoria Hospital (Glen Site), St Mary s Hospital Centre Type of Fellowship:
Female Pelvic Medicine & Reconstructive Surgery APPLICATION FOR NEW FELLOWSHIP Name of Institution: McGill University Location: Royal Victoria Hospital (Glen Site), St Mary s Hospital Centre Type of Fellowship:
Desara TV and Desara Blue TV
 Desara TV and Desara Blue TV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide Available Electronically M Manufactured
Desara TV and Desara Blue TV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide Available Electronically M Manufactured
SURGICAL PROCEDURES OPERATIONS ON THE UROGENITAL SYSTEM
 KIDNEYS AND PERINEPHRUM 1. No additional claim should be made for nephroscopy when done at the time of pyelolithotomy or nephrolithotomy. 2. In a routine surgical approach to the kidney and related procedures,
KIDNEYS AND PERINEPHRUM 1. No additional claim should be made for nephroscopy when done at the time of pyelolithotomy or nephrolithotomy. 2. In a routine surgical approach to the kidney and related procedures,
Effect of Anesthesia on Voiding Function After Tension-Free Vaginal Tape Procedure
 Effect of Anesthesia on Voiding Function After Tension-Free Vaginal Tape Procedure M. Murphy, MD, M. H. Heit, MD, MSPH, L. Fouts, MD, C. A. Graham, MD, L. Blackwell, RN, and P. J. Culligan, MD OBJECTIVE:
Effect of Anesthesia on Voiding Function After Tension-Free Vaginal Tape Procedure M. Murphy, MD, M. H. Heit, MD, MSPH, L. Fouts, MD, C. A. Graham, MD, L. Blackwell, RN, and P. J. Culligan, MD OBJECTIVE:
When the suburethral sling was first
 SURGICAL TECHNIQUES BY CHERYL IGLESIA, MD, AND MARIA PETTIT CANTER, MD Treating stress urinary incontinence with suburethral slings Recent modifications to suburethral sling procedures have brought them
SURGICAL TECHNIQUES BY CHERYL IGLESIA, MD, AND MARIA PETTIT CANTER, MD Treating stress urinary incontinence with suburethral slings Recent modifications to suburethral sling procedures have brought them
Prospective study of an ultra-lightweight polypropylene Y mesh for robotic sacrocolpopexy
 Int Urogynecol J (2013) 24:1371 1375 DOI 10.1007/s00192-012-2021-7 ORIGINAL ARTICLE Prospective study of an ultra-lightweight polypropylene Y mesh for robotic sacrocolpopexy Charbel G. Salamon & Christa
Int Urogynecol J (2013) 24:1371 1375 DOI 10.1007/s00192-012-2021-7 ORIGINAL ARTICLE Prospective study of an ultra-lightweight polypropylene Y mesh for robotic sacrocolpopexy Charbel G. Salamon & Christa
Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option.
 Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option. The Condition(s): Vaginal Prolapse, Uterine Prolapse Vaginal prolapse occurs when the
Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option. The Condition(s): Vaginal Prolapse, Uterine Prolapse Vaginal prolapse occurs when the
A New Dimension in Vesicovaginal Fistula Management: An 8-year Experience at Ramathibodi Hospital
 Original Article A New Dimension in Vesicovaginal Fistula Management: An 8-year Experience at Ramathibodi Hospital Wachira Kochakarn and Wipaporn Pummangura, 1 Division of Urology, Department of Surgery,
Original Article A New Dimension in Vesicovaginal Fistula Management: An 8-year Experience at Ramathibodi Hospital Wachira Kochakarn and Wipaporn Pummangura, 1 Division of Urology, Department of Surgery,
Urogynaecology. Colm McAlinden
 Urogynaecology Colm McAlinden Definitions Urinary incontinence compliant of any involuntary leakage of urine with many different causes Two main types: Stress Urge Definitions Nocturia: More than a single
Urogynaecology Colm McAlinden Definitions Urinary incontinence compliant of any involuntary leakage of urine with many different causes Two main types: Stress Urge Definitions Nocturia: More than a single
The number following the procedure code is the TRICARE payment group. KIDNEY
 TRICARE/CHAMPUS POLICY MANUAL 6010.47-M JUNE 25, 1999 S POLICY CHAPTER 13 SECTION 9.1 ADDENDUM 1, SECTION 8 TRICARE-APPROVED AMBULATORY SURGERY S - URINARY SYSTEM The number following the procedure code
TRICARE/CHAMPUS POLICY MANUAL 6010.47-M JUNE 25, 1999 S POLICY CHAPTER 13 SECTION 9.1 ADDENDUM 1, SECTION 8 TRICARE-APPROVED AMBULATORY SURGERY S - URINARY SYSTEM The number following the procedure code
High levator myorraphy versus uterosacral ligament suspension for vaginal vault fixation: a prospective, randomized study
 Int Urogynecol J (2010) 21:515 522 DOI 10.1007/s00192-009-1064-x ORIGINAL ARTICLE High levator myorraphy versus uterosacral ligament suspension for vaginal vault fixation: a prospective, randomized study
Int Urogynecol J (2010) 21:515 522 DOI 10.1007/s00192-009-1064-x ORIGINAL ARTICLE High levator myorraphy versus uterosacral ligament suspension for vaginal vault fixation: a prospective, randomized study
Sarah A. Huber, 1 LaChanda Dunlap-Wright, 2 John R. Miklos, 1 and Robert D. Moore Introduction
 Case Reports in Urology Volume 2016, Article ID 6180756, 5 pages http://dx.doi.org/10.1155/2016/6180756 Case Report Concomitant Laparoscopic Burch Urethropexy and Combined Vaginal-Laparoscopic Mesh Sling
Case Reports in Urology Volume 2016, Article ID 6180756, 5 pages http://dx.doi.org/10.1155/2016/6180756 Case Report Concomitant Laparoscopic Burch Urethropexy and Combined Vaginal-Laparoscopic Mesh Sling
Anterior vaginal wall prolapse occurs commonly
 Anterior vaginal wall prolapse: Innovative surgical approaches MARK D. WALTERS, MD, AND MARIE FIDELA R. PARAISO, MD Anterior vaginal wall prolapse occurs commonly and may coexist with disorders of micturition.
Anterior vaginal wall prolapse: Innovative surgical approaches MARK D. WALTERS, MD, AND MARIE FIDELA R. PARAISO, MD Anterior vaginal wall prolapse occurs commonly and may coexist with disorders of micturition.
