A quick guide for health professionals
|
|
|
- Elvin Elliott
- 5 years ago
- Views:
Transcription
1 A quick guide for health professionals
2 Background Most cancer survivors will not have any long-term lower GI consequences of their cancer or its treatment. However, some will develop problems including chronic diarrhoea, faecal incontinence, urgency, pain, bleeding and excessive flatulence, particularly following pelvic radiotherapy and surgery [1]. For these people quality of life can be severely affected. Chronic GI symptoms often affect those who have been treated with pelvic radiotherapy for urological cancers (30% have chronic GI symptoms affecting quality of life) [1], gynaecological cancers (40%) and colorectal cancers (up to 66%) [1]. These symptoms may arise as new symptoms several years after cancer treatment has ended. The content of this Quick Guide is based on The Practical Management of the Gastrointestinal Symptoms of Pelvic Radiation Disease [2], by Andreyev et al, (often referred to as the bowel algorithm found to be effective in the ORBIT study [3], a randomised controlled trial) which can be downloaded at: For further information, please refer to the British Society of Gastroenterology Practice guidance on the management of acute and chronic gastrointestinal problems arising as a result of treatment for cancer. [4]
3 Contents This guide is designed to be used systematically, by working through Step 1, Step 2 (if you are in a position to do so) and Step 3 in consecutive order. Step 1 Identify patients experiencing chronic GI problems Is the patient currently undergoing cancer treatment? Key questions to identify chronic GI problems Basic assessment Rectal bleeding Medical history Bowel and/or food diary Provide basic advice and treatment Information Lifestyle Dietary advice Stool bulking agents or anti-diarrhoeals Access to public toilets Bowel training Pelvic floor exercises P4 P4 P5 P5 P6 P6 P6 P6 P7 If symptoms do not improve, go to Step 2, if you are in a position to do so, or go straight to Step 3 Step 2 Further investigation and treatment of GI problems Investigation and management of: Rectal bleeding Faecal incontinence Urgency Diarrhoea Constipation Abdominal pain Painful bowel movements P8 P9 P9 P10 P11 P11 P12 If sympoms do not improve, go to Step 3 Step 3 Referral to a gastroenterologist or other specialist Who to refer to Information to include in referral Useful organisations P13 P13 P14
4 Step 1 Identify patients experiencing chronic GI problems If recurrent disease is suspected refer urgently to the oncology team If the patient is currently undergoing cancer treatment refer to cancer treatment unit or acute oncology team. Acute GI side-effects due to infection, perforation, haemorrhage or bowel obstruction are oncological emergencies and require immediate attention. Trigger questions: The following questions should be asked regularly to any patient who has had pelvic radiotherapy. If a person answers yes to any of the following proceed immediately to Basic assessment below. 1 Are you woken up at night to have a bowel movement? 2 Do you need to rush to the toilet to have a bowel movement? 3 Do you ever have bowel leakage, soiling or a loss of control over your bowels? 4 Do you have any bowel symptoms preventing you from living a full life? Basic assessment Rectal bleeding? Yes? go immediately to or straight to Step 3 Step 2 (if you are in a position to follow the algorithm) Rectal bleeding following radiotherapy is common, although it is usually mild and often does not need significant treatment, it should always be investigated to determine the cause and contributing factors. This should include at least a flexible sigmoidoscopy. Medical History A drug history can help to identify and rule out any possible drug-induced GI sideeffects caused by opioids, ondansetron, anti-muscarinic drugs, loperamide, iron supplements, PPIs, laxatives, beta-blockers, metformin and selenium. Recommend keeping a bowel and/or food diary This can help to identify whether certain foods trigger GI symptoms. A food and symptoms diary template is available from Macmillan ( 4
5 Step 1 Provide basic advice and treatment Information to support self-management Further information for people experiencing GI problems following cancer treatment is available to order or download for free from be.macmillan Managing the late effects of pelvic radiotherapy in men (Order Code: MAC13825) Managing the late effects of pelvic radiotherapy in women (Order Code: MAC13826) Managing the late effects of bowel cancer treatment (Order Code: MAC12162) Promoting health and wellbeing Physical activity: Information and advice during and following cancer treatment is provided in the Macmillan Cancer Support booklet Move More (order code MAC13314). Alcohol consumption: Patients should be encouraged to limit alcohol intake and include one or two alcohol-free days each week. Stress: can worsen GI symptoms, consider relaxation classes, counselling, psychological support or complementary therapies. Information about local cancer information and support centres can be found on the Macmillan website. Dietary advice: After treatment, cancer survivors should follow the recommendations for cancer prevention as set out in the World Cancer Research Fund UK Recommendations (2013). If dietary changes are made, they should be done in a systematic way and should initially always be for a trial period. If symptoms do not improve dramatically, the dietary change may not provide any benefit and may actually restrict the person s nutritional intake. If you are making long term dietary changes referral to a dietitian may be beneficial. Specific dietary advice can be found below: Excessive fibre is a common cause of GI problems, especially following pelvic radiotherapy. A reduction in fibre may be beneficial. Inadequate fibre intake can also exacerbate GI symptoms. Patients should be advised that if they plan to increase the amount of fibre in their diet, they should also increase their fluid intake. High fat, caffeine and alcohol intake, artificial sweeteners and carbonated drinks can contribute to bloating, excessive flatulence and diarrhoea. Patients may develop carbohydrate intolerances including lactose or fructose intolerances. If a suspected food intolerance has been confirmed, referral to a dietitian is advised. Skipping meals may make bowel habits unpredictable. So patients may be advised to eat at regular times. If patients are losing weight as a result of their GI problems, referral to a dietitian should be considered. 5
6 Step 1 Stool bulking agents or anti-diarrhoeal medications Stool bulking agents - Fibre supplements are useful in relieving constipation or tenesmus. For excessive flatulence, a non-fermentable fibre supplement such as Normacol (sterculia) is recommended, as this is less likely to cause flatulence that may occur with other forms of fibre supplements or dietary fibre. Anti-diarrhoeal medications - Loperamide can be used in cases of chronic diarrhoea after all reasonable measures have been taken to address the underlying causes. For adults, an appropriate initial dose is 1-2mg once or twice a day, subsequently adjusted according to response and given in up to 4 divided doses a day for maintenance; up to a maximum of 16mg daily. Using smaller doses of Loperamide liquid (0.5-1mg) half an hour before meals can be helpful as it reduces the gastrocolic reflex triggered by eating. An additional dose before bed time or half an hour before leaving home may also be useful. Access to toilet facilities Patients suffering from urgency or bowel incontinence often feel anxious about going out and should be advised on toilet accessibility including: local authority websites and toilet apps, toilet cards to help them gain access to a toilet not normally accessible, purchasing a Radar NKS key from Disability Rights UK offering access to locked public toilets across the UK. 6
7 Step 1 Practical advice Bowel training Patients can be advised to go to the toilet at regular times each day (such as after meals). Adopting the correct position on the lavatory may help to trigger bowel movements [2]. 1 Sitting on the toilet, lean forward with your forearms resting on your thighs and use a low footrest to raise your feet off the floor. 2 Relax and lower the shoulders. Breathe slowly, regularly and gently do not hold your breath as this will encourage straining. Try and stay as relaxed as possible. 3 Try and brace your abdominal muscles. This is best done by putting your hands on your waist. Expand your waist and feel your hands being pushed out sideways. Concentrate on relaxing your anus to allow the stool to pass. Only push down from above once your anus is relaxed. 4 Relax very slightly for 1 second maintaining pressure but without the push. 5 Then brace outwards and push down once again. 6 Repeat steps 1-5 The brace position 1 Knees higher than hips 2 Lean forward and put elbows on your knees 3 Relax shoulders 4 Bulge out your abdomen 1 Foot rest Pelvic floor exercises Cancer treatments such as pelvic radiotherapy or hormone treatment may weaken pelvic floor muscles. Exercises that strengthen muscles around the rectum, anus and anterior pelvic floor can help with reducing faecal urgency, leakage and incontinence. Detailed instructions are available in Managing the Late Effects of Pelvic Radiotherapy in Men/Women (MAC13825/13826). 1 Sit, stand or lie with your knees slightly apart. Tighten and pull up your bottom muscles as tightly as you can. Hold for at least five seconds and then relax for at least ten seconds. Repeat at least five times. This will work on the strength of your muscles. 2 Next, pull the muscles up to about half of their maximum squeeze. See how long you can hold this for. Then relax for at least ten seconds. Repeat at least five times. This will work on the endurance or staying power of your muscles and will improve their coordination. 3 Pull up the muscles as quickly and tightly as you can and then relax and then pull up again, and see how many times you can do this before you get tired. Try at least five quick pull-ups. 4 Repeat exercises 1, 2, and 3 at least ten times every day. 5 As the muscles get stronger, you will find that you can hold for longer than five seconds, and that you can do more pull-ups each time without the muscle getting tired. 7
8 Step 2 Further Investigation and management If the advice and basic interventions in Step 1 do not improve symptoms, the following investigations and treatments may be necessary. If it is not possible to undertake/ request the suggested tests and interventions please go straight to Step 3. A) Rectal bleeding Blood tests required Abnormal result Action Haemoglobin RBC indices Platelets If heavy bleeding has occured, check clotting and haematinics If Hb <80g/l Anaemic but Hb >80g/l Check ferritin, transferrin saturation, RBC folate and vitamin B12 levels and consider referring patient for blood transfusion where clinically appropriate. If iron deficient, consider iron supplements. If unexplained, refer patient for upper GI endoscopy and colonoscopy. Check ferritin, transferrin saturation, RBC folate and vitamin B12 levels. Replace if necessary and monitor response. If unexplained, refer patients for upper GI endoscopy and colonoscopy/ CT pneumocolon. Other abnormal results Follow routine treatment for abnormal blood results. (For more information, refer to full algorithm [2] ) Consider the following investigations or referrals: Flexible sigmoidoscopy Colonoscopy Optimise bowel function and stool consistency If it is dark bleeding consider the following investigations or referrals: Colonoscopy Upper GI endoscopy (for more information, refer to the full bowel algorithm [2] which can be downloaded at 8
9 Step 2 B) Faecal incontinence/leakage and urgency (without diarrhoea) Tests required Routine blood tests Full blood count Electrolytes Urea and Liver function tests Glucose Calcium Additional blood tests Erythrocyte sedimentation C-reactive protein (CRP) RBC folate Iron studies Vitamin B12 Thyroid function tests Coeliac serology (TTG, IgA) Magnesium Abnormal result Abnormal haemoglobin levels/ anaemia Abnormal liver function tests Elevated ESR/CRP RBC folate deficiency Action See table A Refer patient for liver ultrasound and liver screening, including Hepatitis B and C serology, ferritin, alpha feta protein, alpha 1 antitrypsin, liver auto-antibodies, total cholesterol and triglycerides, immunoglobulins. If unexplained refer to gastroenterology. Consider the following: Infection, including small intestinal bacterial overgrowth (SIBO) Inflammation, including IBD; refer to gastroenterology for diagnosis. Recurrent malignancy; refer to oncology Non-GI causes (e.g. rheumatoid arthritis, vasculitis, connective tissue disorders). Consider referring patient to a dietitian for specialist dietetic advice/supplementation. Other tests Rectal examination Anoscopy Flexible simoidoscopy Abnormal coeliac serology Pelvic floor dysfunction with radiation protopathy and faecal incontinence OR anal sphincter defect Presence of other contributing factors If IgA deficient, request IgG coeliac screen. If TTG elevated, refer to gastroenterology to confirm with duodenal biopsy. Refer patient to a dietitian for specialist dietetic advice. Recommend pelvic floor and toileting exercises Prescribe a stool bulking agent ± anti-diarrhoeal medication Prescribe anti-diarrhoeal medication ± stimulant laxative suppositories/enemas. Consider the use of a topical sympathomimetic agent (e.g. phenylephrine). Advise patient on perianal skin care. Refer patient for biofeedback services (if available). If cause is unrelated to radiotherapy (e.g. childbirth, previous sphincter surgery), refer to specialist team for management of faecal incontinence. Presence of other mucus discharge Refer patient to a dietitian for a detailed dietary review. Recommend pelvic floor and toileting exercises. If due to haemorrhoids, consider local treatment If newly diagnosed neoplasm, refer urgently to oncology, requesting appointment within 2 weeks. If due to rectal mucosal prolapse, ulceration or if cause unknown, refer to gastroenterology. Consider the following investigations or referrals if you are in a position to do so (for more information, refer to the full algorithm [2] ): Endo anal ultrasound AND Anorectal physiology 9
10 Step 2 C) Diarrhoea (type 6-7 stool Bristol Stool Chart) Tests required Routine and additional blood tests Abnormal result Action See table B Stool sample for microscopy, culture and Clostridium Difficile toxin Stools contain pathogen Treat as recommended by microbiologists and local protocols. Stool sample for faecal elastase Exocrine pancreatic insufficiency (EPI) Initiate pancreatic enzyme replacement therapy. Consider long-term multivitamin and trace element supplementation. Refer patient to a dietitian (Step 3) if dietary advice necessary. Refer to gastroenterology (Step 3) if symptoms do not improve. Consider the following investigations or referrals if you are in a position to do so (for more information, refer to the full algorithm [2] ): Upper GI endoscopy with duodenal aspirate and biopsies AND/OR Glucose hydrogen/methane breath test Carbohydrate challenge SeHCAT scan Flexible sigmoidoscopy with biopsies from non-irradiated bowel (avoid biopsies from areas irradiated in sigmoid and rectum) If all tests are negative but symptoms persist, consider the following: Symptomatic treatment with anti-diarrhoeal medication Trial of low-dose tricyclic antidepressants Biofeedback 10
11 Step 2 D) Constipation (type 1-2 stool Bristol Stool Chart) Tests required Rectal examination Abnormal result Anal fissure Action 1 Initially, treat with a topical healing agent such as GTN or diltiazem gel for 8 weeks. 2 Prescribe a stool bulking/softening agent ± short term topical local anaesthesic. 3 If recurrent, consider referral for botulinum toxin treatment. 4 If fissure has not healed after two months, refer to gastroenterology. Routine and additional blood tests See table B Abdominal x-ray Faecal loading/faecal impaction 1 Full bowel clearance e.g. Picolax, Klean-Prep. 2 Prescribe maintenance bulk laxative. 3 Recommend pelvic floor and toileting exercises Consider the following investigations or referrals if you are in a position to do so (for more information, refer to the full algorithm [2] ): Colonoscopy CT pneumocolon if new onset Flexible sigmoidoscopy for long standing problems E) Abdominal pain Tests required Routine blood tests and calcium, ESR and CRP Abnormal result Action See table B Abdominal x-ray Faecal loading/ faecal impaction 1 Full bowel clearance e.g. Picolax, Klean-Prep. 2 Prescribe maintenance bulk laxative. 3 Recommend toileting exercises Consider the following investigations or referrals if you are in a position to do so (for more information, refer to the full algorithm [2] ): Upper GI endoscopy with duodenal aspirate and biopsies ± Glucose hydrogen/methane breath test Flexible sigmoidoscopy Ultrasound of biliary tree and small bowel (if no recent CT scan of abdomen and pelvis) 11
12 Step 2 F) Painful bowel movements Tests required Medication assessment Visual assessment Abnormal result Patient on nicorandil Haemorrhoids Action Consider alternative medication 1 Prescribe a stool bulking/softening agent ± short term topical local anaesthesic. 2 Consider referral to gastroenterology for surgical review of grade 3 or 4 haemorrhoids. Anoscopy and flexible sigmoidoscopy Anal fissure Anorectal fistula Anorectal abscess or ulcer Mucosal prolapse/ solitary rectal ulcer 1 Initially, treat with a topical healing agent such as GTN or diltiazem gel for 8 weeks. 2 Prescribe a stool bulking/ softening agent ± short term topical local anaesthesic. 3 If recurrent, consider referral for botulinum toxin treatment. 4 If fissure has not healed after two months, refer to gastroenterology. 1 Refer patient for Pelvic MRI 2 Refer to gastroenterology. Refer urgently to gastroenterology Refer to gastroenterology Neoplastic ulcer Refer urgently to oncology, requesting appointment within 2 weeks. Radiation-related ulceration Do NOT biopsy. 1 Sucralfate enemas. 2 Consider stool bulking/softening agents 3 Antibiotics. 4 Refer to gastroenterology Consider the following investigations or referrals if you are in a position to do so (for more information, refer to the full algorithm [2] ): MRI If all tests are negative but symptoms persist, consider the following: 1 Investigation under anaesthesia 2 Pelvic floor and toileting exercises 3 Stool bulking agent ± laxative 4 Referral for acupuncture 5 Referral to specialist pain team for further assessment 6 Low-dose anti-depressant 7 Agent for neuropathic pain 8 Referral for a urological/gynaecological opinion 12
13 Step 3 Referral to a gastroenterologist or other specialist If the symptoms do not improve following Step 1 and Step 2 patients will require referral to gastroenterology or other specialist departments. For guidance on where to refer see below: Suspected diagnosis Referral Suspected diagnosis of cancer or recurrent disease Refer to appropriate oncology team within two weeks High dietary fibre intake Carbohydrate intolerance Coeliac disease Other nutritional problems Refer to dietitian Rectal bleeding GI symptoms persisting following interventions Bile acid malabsorption Pancreatic insufficiency Inflammatory Bowel Disease Refer to a gastroenterologist Information to include in the referral Reports and results for tests that have been carried out in Step 2 such as endoscopy and histology reports if biopsies were carried out. Details of GI symptoms leading to the referral. Previous tumour type/location. Oncology treatment, including treatment type, duration and date at which treatment ended. Be aware A patient may believe that nothing can be done and may therefore need reassurance that there are specialist treatments that can help to manage their symptoms. Consider further referrals to continence services, physiotherapy and psychology to manage the impact of these symptoms. 13
14 Useful organisations Bladder and Bowel Foundation Bowel Cancer UK British Association for Counselling and Psychotherapy Crohn s and Colitis UK Disability Rights UK Macmillan Cancer Support Maggie s Cancer Caring Centres Pelvic Radiation Disease Association Prostate Cancer UK Relate Jo s Cervical Cancer Trust References [1] Macmillan Cancer Support. Throwing Light on the Consequences of Cancer and its Treatment [2] Andreyev et al. The practical management of the gastrointestinal symptoms of pelvic radiation disease. Frontline Gastroenterology 2015;6(1): [3] Andreyev HJ et al. Algorithm-based management of patients with gastrointestinal symptoms in patients after pelvic radiation treatment (ORBIT): a randomised controlled trial, The Lancet 2013;, 382: [4] Andreyev HJ, Davidson S, Gillespie C, et al. Practice guidance on the management of acute and chronic gastrointestinal problems arising as a result of treatment for cancer Gut 2012; 61:
15 Acknowledgements and special thanks for reviewing this document: Dr Jervoise Andreyev, Consultant Gastroenterologist, The Royal Marsden NHS Foundation Trust Dr Clare Donnellan, Consultant Gastroenterologist, Leeds Teaching Hospitals NHS Trust Karen Morgan, Macmillan Consultant Radiographer, Taunton and Somerset NHS Foundation Trust Ann Muls, Macmillan Nurse Consultant (GI Consequences of Cancer Treatment), The Royal Marsden NHS Foundation Trust Dr Claire Taylor, Macmillan Nurse Consultant in Colorectal Cancer, London North West Healthcare NHS Trust And the Macmillan GP Advisors Dr Charles Campion-Smith, Dr Terry Bowley, Dr Anthony Cunliffe and Dr David Linden This guide was produced in June To be reviewed in June
16 As a healthcare professional, you know cancer doesn t just affect your patients physically. It can affect everything their relationships, finances, work. But maybe you feel like there aren t enough hours in the day to spend as long as you d like with them, or to answer all their questions. That s where we come in. We re here to provide extra support to your patients with cancer, and their loved ones. Whether it s offering benefits advice, help returning to work, or support with getting active again we re here to help you give your patients the energy and inspiration they need to feel more in control of their lives. Right from the moment they re diagnosed, through treatment and beyond. To find out more about how we can help, visit macmillan.org.uk. And please let your patients know they can contact us on if they need support. Printed using sustainable material. Please recycle. Macmillan Cancer Support, registered charity in England and Wales (261017), Scotland (SC039907) and the Isle of Man (604). MAC15384_0615
Guide to managing Gastrointestinal Pelvic Radiation Disease (PRD) using Algorithm V7 (January 2011)
 Guide to managing Gastrointestinal Pelvic Radiation Disease (PRD) using Algorithm V7 (January 2011) This algorithm is particularly designed to help clinical nurse specialists working in conjunction with
Guide to managing Gastrointestinal Pelvic Radiation Disease (PRD) using Algorithm V7 (January 2011) This algorithm is particularly designed to help clinical nurse specialists working in conjunction with
Late effects of treatment for colorectal cancer. Claire Taylor Macmillan Nurse Consultant St Mark s Hospital
 Late effects of treatment for colorectal cancer Claire Taylor Macmillan Nurse Consultant St Mark s Hospital The number of people living with cancer is set to double from 2m to 4m by 2030 Source: Maddams
Late effects of treatment for colorectal cancer Claire Taylor Macmillan Nurse Consultant St Mark s Hospital The number of people living with cancer is set to double from 2m to 4m by 2030 Source: Maddams
Anal sphincter exercises. Information for patients Sheffield Teaching Hospitals
 Anal sphincter exercises Information for patients Sheffield Teaching Hospitals Anal sphincter exercises to help lessen leakage from the bowel Sphincter exercises, when practiced correctly, can build up
Anal sphincter exercises Information for patients Sheffield Teaching Hospitals Anal sphincter exercises to help lessen leakage from the bowel Sphincter exercises, when practiced correctly, can build up
Obstructive Defaecation
 Oxford Pelvic Floor Service Obstructive Defaecation Information for patients page 2 What is obstructive defaecation? Obstructive defaecation is the inability to pass stools (open your bowels). This is
Oxford Pelvic Floor Service Obstructive Defaecation Information for patients page 2 What is obstructive defaecation? Obstructive defaecation is the inability to pass stools (open your bowels). This is
Irritable bowel syndrome in adults
 Irritable bowel syndrome in adults NICE provided the content for this booklet which is independent of any company or product advertised Welcome In February 2008, NICE published a clinical guideline on
Irritable bowel syndrome in adults NICE provided the content for this booklet which is independent of any company or product advertised Welcome In February 2008, NICE published a clinical guideline on
Biofeedback Program. GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1
 Biofeedback Program GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1 Biofeedback Checklist Bristol Stool Form Scale Digestive process 4F s Fibre, Fluid, Fitness,
Biofeedback Program GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1 Biofeedback Checklist Bristol Stool Form Scale Digestive process 4F s Fibre, Fluid, Fitness,
Faecal Incontinence Information Leaflet THE DIGESTIVE SYSTEM
 THE DIGESTIVE SYSTEM This factsheet is about faecal incontinence Faecal (or anal) incontinence is the loss of stool, liquid or gas from the bowel at an undesirable time. Males and females of any age may
THE DIGESTIVE SYSTEM This factsheet is about faecal incontinence Faecal (or anal) incontinence is the loss of stool, liquid or gas from the bowel at an undesirable time. Males and females of any age may
Guidance on managing gastro-intestinal consequences of colorectal cancer and its treatments
 Guidance on managing gastro-intestinal consequences of colorectal cancer and its treatments 1. Background The number of people living with and beyond cancer continues to increase on a yearly basis in the
Guidance on managing gastro-intestinal consequences of colorectal cancer and its treatments 1. Background The number of people living with and beyond cancer continues to increase on a yearly basis in the
Pelvic floor exercises for women. Information for patients Continence Service
 Pelvic floor exercises for women Information for patients Continence Service page 2 of 8 Why do I need to do pelvic floor exercises? Many women experience pelvic floor problems at some time during their
Pelvic floor exercises for women Information for patients Continence Service page 2 of 8 Why do I need to do pelvic floor exercises? Many women experience pelvic floor problems at some time during their
Recent developments in radiotherapy and management of bowel toxicity
 The Roy al Marsden Recent developments in radiotherapy and management of bowel toxicity Dr Alexandra Taylor Radiotherapy for cervical cancer Historical perspective 1901 First use of radium for cervical
The Roy al Marsden Recent developments in radiotherapy and management of bowel toxicity Dr Alexandra Taylor Radiotherapy for cervical cancer Historical perspective 1901 First use of radium for cervical
Constipation Information Leaflet THE DIGESTIVE SYSTEM. gutscharity.org.uk
 THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Constipation Constipation is a symptom that can mean different things to different people but the usual
THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Constipation Constipation is a symptom that can mean different things to different people but the usual
Bowel cancer risk in the under 50s. Greg Rubin Professor of General Practice and Primary Care
 Bowel cancer risk in the under 50s Greg Rubin Professor of General Practice and Primary Care Prevalence of GI problems in the consulting population Thompson et al, Gut 2000 Number of patients % of patients
Bowel cancer risk in the under 50s Greg Rubin Professor of General Practice and Primary Care Prevalence of GI problems in the consulting population Thompson et al, Gut 2000 Number of patients % of patients
What you can expect at your doctors
 What you can expect at your doctors Investigations and Procedures Tests are not always necessary Current guidelines encourage gastroenterologists to make a positive diagnosis of Irritable Bowel Syndrome
What you can expect at your doctors Investigations and Procedures Tests are not always necessary Current guidelines encourage gastroenterologists to make a positive diagnosis of Irritable Bowel Syndrome
Clinical problems related to GI involvement in SSc
 Clinical problems related to GI involvement in SSc Incontinence Abdominal pain/distension Gastro-oesophageal Diarrhoea Weight loss/al Issues Constipation Management of incontinence Establish diagnosis
Clinical problems related to GI involvement in SSc Incontinence Abdominal pain/distension Gastro-oesophageal Diarrhoea Weight loss/al Issues Constipation Management of incontinence Establish diagnosis
Pelvic Floor Exercises
 Directorate of Women, Children and Surgical Services Burton and District Urogynaecology Centre A Nationally Accredited Urogynaecology Unit Pelvic Floor Exercises You have been given this leaflet because
Directorate of Women, Children and Surgical Services Burton and District Urogynaecology Centre A Nationally Accredited Urogynaecology Unit Pelvic Floor Exercises You have been given this leaflet because
Anorectal physiology test
 Anorectal physiology test We hope this factsheet will help to answer some of your questions about having an anorectal physiology test. If you have any further questions or concerns, please don t hesitate
Anorectal physiology test We hope this factsheet will help to answer some of your questions about having an anorectal physiology test. If you have any further questions or concerns, please don t hesitate
A guide to Anoplasty (anal surgery)
 Saint Mary s Hospital Newborn Intensive Care Unit Information for Parents A guide to Anoplasty (anal surgery) Introduction This information leaflet is designed to help parents and families to care for
Saint Mary s Hospital Newborn Intensive Care Unit Information for Parents A guide to Anoplasty (anal surgery) Introduction This information leaflet is designed to help parents and families to care for
Uterus (Womb) Rectum. Another problem could be the sensation of something coming down at the birth canal or back passage (prolapse).
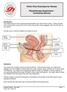 Pelvic Floor Exercises for Women Physiotherapy Department Continence Service Introduction This leaflet tells you how to exercise and strengthen your pelvic floor muscles. These muscles form a broad sling
Pelvic Floor Exercises for Women Physiotherapy Department Continence Service Introduction This leaflet tells you how to exercise and strengthen your pelvic floor muscles. These muscles form a broad sling
Sphincter exercises for people with bowel control problems. Information for patients. Physiotherapy Department
 Sphincter exercises for people with bowel control problems Information for patients Physiotherapy Department 01625 661481 @EastCheshireNHS Leaflet Ref: 11229 Published: June 18 Review: 31/0/5/2021 Page
Sphincter exercises for people with bowel control problems Information for patients Physiotherapy Department 01625 661481 @EastCheshireNHS Leaflet Ref: 11229 Published: June 18 Review: 31/0/5/2021 Page
Guideline scope Diverticular disease: diagnosis and management
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Diverticular disease: diagnosis and management The Department of Health in England has asked NICE to develop a clinical guideline on diverticular
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Diverticular disease: diagnosis and management The Department of Health in England has asked NICE to develop a clinical guideline on diverticular
The Pelvic Floor Muscles - a Guide for Women
 The Pelvic Floor Muscles - a Guide for Women This booklet is supported by WWWWW Wellbeing of Women Registered Charity No. 239281 www.wellbeingofwomen.org.uk Introduction Up to a third of all women experience
The Pelvic Floor Muscles - a Guide for Women This booklet is supported by WWWWW Wellbeing of Women Registered Charity No. 239281 www.wellbeingofwomen.org.uk Introduction Up to a third of all women experience
Promoting Continence with Physiotherapy
 A Common problem for Men and women Promoting Continence with Physiotherapy This leaflet contains information about physiotherapy advice and treatment for anyone with bladder and bowel problems. This may
A Common problem for Men and women Promoting Continence with Physiotherapy This leaflet contains information about physiotherapy advice and treatment for anyone with bladder and bowel problems. This may
South Yorkshire, Bassetlaw and North Derbyshire Cancer Alliance
 South Yorkshire, Bassetlaw and North Derbyshire Cancer Alliance Patient Details: Patient Name Address DOB Home Tel. No. Mobile Tel. No. Preferred Tel. No. Main Spoken Language Transport needed? Registered
South Yorkshire, Bassetlaw and North Derbyshire Cancer Alliance Patient Details: Patient Name Address DOB Home Tel. No. Mobile Tel. No. Preferred Tel. No. Main Spoken Language Transport needed? Registered
Side effects of brachytherapy
 Side effects of brachytherapy Dr Arian Barnardo BM BMedSci MD FRCP AGAF Consultant Gastroenterologists & BCSP Endoscopist Anal pain & Rectal bleeding Rectal bleeding not everything is oncological Side
Side effects of brachytherapy Dr Arian Barnardo BM BMedSci MD FRCP AGAF Consultant Gastroenterologists & BCSP Endoscopist Anal pain & Rectal bleeding Rectal bleeding not everything is oncological Side
Pelvic Floor Exercises
 Pelvic Floor Exercises Physiotherapy Department Patient information leaflet Up to a third of women experience a problem with their pelvic floor muscles at some point during their life. The muscles can
Pelvic Floor Exercises Physiotherapy Department Patient information leaflet Up to a third of women experience a problem with their pelvic floor muscles at some point during their life. The muscles can
Prevention of Bowel Cancer: which patients do I send for colonoscopy?
 Prevention of Bowel Cancer: which patients do I send for colonoscopy? Dr Chris Groves Consultant Gastroenterologist and Honorary Senior Lecturer St George s Hospital and Medical School Director, SW London
Prevention of Bowel Cancer: which patients do I send for colonoscopy? Dr Chris Groves Consultant Gastroenterologist and Honorary Senior Lecturer St George s Hospital and Medical School Director, SW London
Patient Information Leaflet. Anal Sphincter Exercises for people with leakage from the bowel
 Patient Information Leaflet Anal Sphincter Exercises for people with leakage from the bowel Anal Sphincter Exercises for people with leakage from the bowel Introduction Sphincter exercises can help you
Patient Information Leaflet Anal Sphincter Exercises for people with leakage from the bowel Anal Sphincter Exercises for people with leakage from the bowel Introduction Sphincter exercises can help you
Throwing light on the consequences of cancer and its treatment
 Throwing light on the consequences of cancer and its treatment Lesley Smith Consequences of Treatment Programme Manager at Macmillan Cancer Support & the National Cancer Survivorship Initiative The London
Throwing light on the consequences of cancer and its treatment Lesley Smith Consequences of Treatment Programme Manager at Macmillan Cancer Support & the National Cancer Survivorship Initiative The London
Going home after major gynaecological surgery. Information for patients Gynaecology
 Going home after major gynaecological surgery Information for patients Gynaecology page 2 of 16 Discharge advice following your surgery You have had a major operation. This booklet gives some useful advice
Going home after major gynaecological surgery Information for patients Gynaecology page 2 of 16 Discharge advice following your surgery You have had a major operation. This booklet gives some useful advice
Pelvic organ prolapse. Information for patients Continence Service
 Pelvic organ prolapse Information for patients Continence Service What is a pelvic organ prolapse? A pelvic organ prolapse occurs when the uterus (womb), vagina, bladder or bowel slips out of place, resulting
Pelvic organ prolapse Information for patients Continence Service What is a pelvic organ prolapse? A pelvic organ prolapse occurs when the uterus (womb), vagina, bladder or bowel slips out of place, resulting
Keep high, stay dry. Pelvic floor exercises for men
 Keep high, stay dry Pelvic floor exercises for men What is the pelvic floor? Layers of muscle stretch like a hammock from your pubic bone in the front to the bottom of your backbone (see diagram). These
Keep high, stay dry Pelvic floor exercises for men What is the pelvic floor? Layers of muscle stretch like a hammock from your pubic bone in the front to the bottom of your backbone (see diagram). These
What Is Constipation?
 CONSTIPATION What Is Constipation? Constipation is when you have infrequent or hard-to-pass bowel movements (meaning they are painful or you have to strain), have hard stools or feel like your bowel movements
CONSTIPATION What Is Constipation? Constipation is when you have infrequent or hard-to-pass bowel movements (meaning they are painful or you have to strain), have hard stools or feel like your bowel movements
PARTICULARS, SCHEDULE 2- THE SERVICES, A- SERVICE SPECIFICATIONS. A08/S/d Colorectal: Faecal Incontinence (Adult)
 A08/S/d 2013/14 NHS STANDARD CONTRACT FOR COLORECTAL: FAECAL INCONTINENCE (ADULT) PARTICULARS, SCHEDULE 2- THE SERVICES, A- SERVICE SPECIFICATIONS Service Specification No. Service Commissioner Lead Provider
A08/S/d 2013/14 NHS STANDARD CONTRACT FOR COLORECTAL: FAECAL INCONTINENCE (ADULT) PARTICULARS, SCHEDULE 2- THE SERVICES, A- SERVICE SPECIFICATIONS Service Specification No. Service Commissioner Lead Provider
Prescribing Guidance for the Treatment of Constipation in Children
 Prescribing Guidance for the Treatment of Constipation in Children Effective Date: July 2007 Reviewed: September 2009 & December 2011 Review Date: December 2013 Gateshead Medicines Management Approved
Prescribing Guidance for the Treatment of Constipation in Children Effective Date: July 2007 Reviewed: September 2009 & December 2011 Review Date: December 2013 Gateshead Medicines Management Approved
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE SCOPE. Coeliac disease: recognition, assessment and management of coeliac disease
 Appendix B: NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE 1 Guideline title SCOPE Coeliac disease: recognition, assessment and management of coeliac disease 1.1 Short title Coeliac disease 2 The remit
Appendix B: NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE 1 Guideline title SCOPE Coeliac disease: recognition, assessment and management of coeliac disease 1.1 Short title Coeliac disease 2 The remit
IMPROVING URINARY INCONTINENCE
 IMPROVING URINARY INCONTINENCE INFORMATION FOR OLDER ADULTS, FAMILIES, AND CAREGIVERS READ THIS PAMPHLET TO LEARN: What Urinary Incontinence is. How to Manage Urinary Incontinence. What Pelvic Floor Exercises
IMPROVING URINARY INCONTINENCE INFORMATION FOR OLDER ADULTS, FAMILIES, AND CAREGIVERS READ THIS PAMPHLET TO LEARN: What Urinary Incontinence is. How to Manage Urinary Incontinence. What Pelvic Floor Exercises
Pelvic floor weakness
 Information leaflet for patients Pelvic floor weakness Physiotherapy department You have been referred to this department for treatment and advice because you have one or more of the following symptoms:
Information leaflet for patients Pelvic floor weakness Physiotherapy department You have been referred to this department for treatment and advice because you have one or more of the following symptoms:
Patient Information Leaflet. Sphincter Exercises for people with Bowel Control Problems
 Patient Information Leaflet Sphincter Exercises for people with Bowel Control Problems Sphincter Exercises for people with Bowel Control Problems Introduction Sphincter exercises can help you to improve
Patient Information Leaflet Sphincter Exercises for people with Bowel Control Problems Sphincter Exercises for people with Bowel Control Problems Introduction Sphincter exercises can help you to improve
Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for women
 Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for women Introduction Many women suffer from weakness of their pelvic floor muscles. Common symptoms include: leaking urine
Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for women Introduction Many women suffer from weakness of their pelvic floor muscles. Common symptoms include: leaking urine
Lets talk about Faecal incontinence (FI) in Scleroderma
 Lets talk about Faecal incontinence (FI) in Scleroderma Dr. Shamaila Butt Gastroenterology Research Registrar GI Physiology unit University College Hospital London GI manifestations in Scleroderma Oesophagus
Lets talk about Faecal incontinence (FI) in Scleroderma Dr. Shamaila Butt Gastroenterology Research Registrar GI Physiology unit University College Hospital London GI manifestations in Scleroderma Oesophagus
Bowel Health in Adults
 Bowel Health in Adults Patient Information Contact Details: Bladder and Bowel Specialist Nurse Service First Floor New Alderley House Macclesfield District General Hospital Victoria Road Macclesfield SK10
Bowel Health in Adults Patient Information Contact Details: Bladder and Bowel Specialist Nurse Service First Floor New Alderley House Macclesfield District General Hospital Victoria Road Macclesfield SK10
Oxford Pelvic Floor Services A guide to the pelvic floor muscles. Information for men
 Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for men Introduction Many men suffer from weakness of their pelvic floor muscles. Common symptoms include: leaking urine with
Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for men Introduction Many men suffer from weakness of their pelvic floor muscles. Common symptoms include: leaking urine with
UK Inflammatory Bowel Disease Audit. A summary report on the quality of healthcare provided to people with inflammatory bowel disease
 UK Inflammatory Bowel Disease Audit A summary report on the quality of healthcare provided to people with inflammatory bowel disease Section heading UK IBD Audit summary report 2014 This summary report
UK Inflammatory Bowel Disease Audit A summary report on the quality of healthcare provided to people with inflammatory bowel disease Section heading UK IBD Audit summary report 2014 This summary report
PATIENT INFORMATION Anterior Resection After Care
 PATIENT INFORMATION Anterior Resection After Care Anatomy of your bowel Transverse colon Ascending colon Descending colon Sigmoid colon Rectum Anus Your bowel before your operation The large bowel or colon
PATIENT INFORMATION Anterior Resection After Care Anatomy of your bowel Transverse colon Ascending colon Descending colon Sigmoid colon Rectum Anus Your bowel before your operation The large bowel or colon
The York Faecal Calprotectin Care Pathway for use in primary care. James Turvill
 The York Faecal Calprotectin Care Pathway for use in primary care James Turvill NICE guidance: dg11 Faecal calprotectin (FC) testing as an option in adults with recent onset of lower gastrointestinal symptoms
The York Faecal Calprotectin Care Pathway for use in primary care James Turvill NICE guidance: dg11 Faecal calprotectin (FC) testing as an option in adults with recent onset of lower gastrointestinal symptoms
Western Health Specialist Clinics Access & Referral Guidelines
 Gastroenterology Specialist Clinics at Western Health: Western Health provides the following Specialist Clinics for patients who require assessment and management of Gastroenterology / Hepatology conditions.
Gastroenterology Specialist Clinics at Western Health: Western Health provides the following Specialist Clinics for patients who require assessment and management of Gastroenterology / Hepatology conditions.
Referral Criteria for Direct Access Outpatient Colonoscopy or Computed Tomography Colonography
 Referral Criteria for Direct Access Outpatient Colonoscopy or Computed Tomography Colonography 2019 Released 2019 health.govt.nz Citation: Ministry of Health. 2019. Referral Criteria for Direct Access
Referral Criteria for Direct Access Outpatient Colonoscopy or Computed Tomography Colonography 2019 Released 2019 health.govt.nz Citation: Ministry of Health. 2019. Referral Criteria for Direct Access
Constipation. What is constipation? What is the criteria for having constipation? What are the different types of constipation?
 What is constipation? is defined as having a bowel movement less than 3 times per week. It is usually associated with hard stools or difficulty passing stools. You may have pain while passing stools or
What is constipation? is defined as having a bowel movement less than 3 times per week. It is usually associated with hard stools or difficulty passing stools. You may have pain while passing stools or
Toning your pelvic floor WELCOME
 Toning your pelvic floor WELCOME Introductions Amelia Samuels, Physiotherapist, Active Rehabilitation Physiotherapy Supporting the Continence Foundation of Australia Continence Foundation of Australia
Toning your pelvic floor WELCOME Introductions Amelia Samuels, Physiotherapist, Active Rehabilitation Physiotherapy Supporting the Continence Foundation of Australia Continence Foundation of Australia
POSTNATAL EXERCISES & ADVICE. Physiotherapy Department
 POSTNATAL EXERCISES & ADVICE Physiotherapy Department This booklet provides advice and exercises to help you to get back to normal after the birth or your baby. Rest: After having your baby it is important
POSTNATAL EXERCISES & ADVICE Physiotherapy Department This booklet provides advice and exercises to help you to get back to normal after the birth or your baby. Rest: After having your baby it is important
Pelvic Floor Muscle exercises and Bladder advice
 n The Leeds Teaching Hospitals NHS Trust Pelvic Floor Muscle exercises and Bladder advice Information for patients Leeds Centre for Women s Health This leaflet aims to explain about your pelvic floor muscles,
n The Leeds Teaching Hospitals NHS Trust Pelvic Floor Muscle exercises and Bladder advice Information for patients Leeds Centre for Women s Health This leaflet aims to explain about your pelvic floor muscles,
The Late Consequences of Cancer Treatment The Impact & Management of the Late Effects of Pelvic Cancer Treatments
 The Late Consequences of Cancer Treatment The Impact & Management of the Late Effects of Pelvic Cancer Treatments Lesley Smith Consequences of Treatment Programme Manager at Macmillan Cancer Support &
The Late Consequences of Cancer Treatment The Impact & Management of the Late Effects of Pelvic Cancer Treatments Lesley Smith Consequences of Treatment Programme Manager at Macmillan Cancer Support &
Going home after major gynaecological surgery. Information for patients Gynaecology
 Going home after major gynaecological surgery Information for patients Gynaecology Discharge advice following your surgery You have had a major operation. This booklet gives some useful advice about what
Going home after major gynaecological surgery Information for patients Gynaecology Discharge advice following your surgery You have had a major operation. This booklet gives some useful advice about what
Pelvic floor muscle exercises
 Lifestyle Helpline 0800 074 8383 prostatecanceruk.org 31 Pelvic floor muscle exercises In this fact sheet: How do pelvic floor muscle exercises help with urinary problems? How do I do the exercises? More
Lifestyle Helpline 0800 074 8383 prostatecanceruk.org 31 Pelvic floor muscle exercises In this fact sheet: How do pelvic floor muscle exercises help with urinary problems? How do I do the exercises? More
Bowel Cancer Information Leaflet THE DIGESTIVE SYSTEM
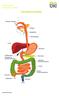 THE DIGESTIVE SYSTEM This factsheet is about bowel cancer Throughout our lives, the lining of the bowel constantly renews itself. This lining contains many millions of tiny cells, which grow, serve their
THE DIGESTIVE SYSTEM This factsheet is about bowel cancer Throughout our lives, the lining of the bowel constantly renews itself. This lining contains many millions of tiny cells, which grow, serve their
Pelvic floor exercises for women. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Pelvic floor exercises for women An information guide Pelvic Floor Exercises for Women This leaflet will provide you with information about
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Pelvic floor exercises for women An information guide Pelvic Floor Exercises for Women This leaflet will provide you with information about
EXERCISE and ADVICE. after pregnancy
 EXERCISE and ADVICE after pregnancy Contents Introduction...1 Comfort...2 Activity in the early days...3 Caesarean section operation...3 Exercises...4 Regaining your physical well-being...7 Contact information...ibc
EXERCISE and ADVICE after pregnancy Contents Introduction...1 Comfort...2 Activity in the early days...3 Caesarean section operation...3 Exercises...4 Regaining your physical well-being...7 Contact information...ibc
Physiotherapy advice following your third or fourth degree perineal tear
 Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Certain genes passed on from parent to child increase the risk of developing Crohn's disease, if the right trigger occurs.
 Topic Page: Crohn's disease Definition: Crohn's disease from Benders' Dictionary of Nutrition and Food Technology Chronic inflammatory disease of the bowel, commonly the terminal ileum, of unknown aetiology,
Topic Page: Crohn's disease Definition: Crohn's disease from Benders' Dictionary of Nutrition and Food Technology Chronic inflammatory disease of the bowel, commonly the terminal ileum, of unknown aetiology,
Pelvic floor exercises for women. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Pelvic floor exercises for women An information guide Pelvic floor exercises for women This leaflet will provide you with information about
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Pelvic floor exercises for women An information guide Pelvic floor exercises for women This leaflet will provide you with information about
Pelvic floor exercises for anal incontinence
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Pelvic floor exercises for anal incontinence An information guide Pelvic floor exercises for anal incontinence Introduction The muscles
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Pelvic floor exercises for anal incontinence An information guide Pelvic floor exercises for anal incontinence Introduction The muscles
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Constipation: management of idiopathic constipation in children in primary and secondary care 1.1 Short title Constipation
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Constipation: management of idiopathic constipation in children in primary and secondary care 1.1 Short title Constipation
Dr David Rowbotham. The Leeds Teaching Hospitals NHS Trust NHS
 Dr David Rowbotham The Leeds Teaching Hospitals NHS Trust NHS Useful Titbits from the World of Gastroenterology David Rowbotham Clinical Director & Consultant Gastroenterologist Dept of Gastroenterology
Dr David Rowbotham The Leeds Teaching Hospitals NHS Trust NHS Useful Titbits from the World of Gastroenterology David Rowbotham Clinical Director & Consultant Gastroenterologist Dept of Gastroenterology
Delorme s Operation For Rectal Prolapse
 Delorme s Operation For Rectal Prolapse Patient Information Colorectal Surgery Author ID: NM Leaflet Number: Surg 045 Version: 3.1 Name of Leaflet: Delorme s Operation for Rectal Prolapse Date Produced:
Delorme s Operation For Rectal Prolapse Patient Information Colorectal Surgery Author ID: NM Leaflet Number: Surg 045 Version: 3.1 Name of Leaflet: Delorme s Operation for Rectal Prolapse Date Produced:
Pelvic Floor Exercises: a guide for women
 Approvals: Gynae Guidelines Group: Jul 2018 O&G SDU: Jul 2018 Clinical Guidelines Subgroup: not required BMV: Sep 2018 Equality Impact Assessment: Oct 2018 Patient Experience Group: February 2019 Division
Approvals: Gynae Guidelines Group: Jul 2018 O&G SDU: Jul 2018 Clinical Guidelines Subgroup: not required BMV: Sep 2018 Equality Impact Assessment: Oct 2018 Patient Experience Group: February 2019 Division
Clinical guideline Published: 23 February 2008 nice.org.uk/guidance/cg61
 Irritable bowel syndrome in adults: diagnosis and management Clinical guideline Published: 23 February 2008 nice.org.uk/guidance/cg61 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Irritable bowel syndrome in adults: diagnosis and management Clinical guideline Published: 23 February 2008 nice.org.uk/guidance/cg61 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Listed below are some of the words that you might come across concerning diseases and conditions of the bowels.
 Listed below are some of the words that you might come across concerning diseases and conditions of the bowels. Abscess A localised collection of pus in a cavity that is formed by the decay of diseased
Listed below are some of the words that you might come across concerning diseases and conditions of the bowels. Abscess A localised collection of pus in a cavity that is formed by the decay of diseased
Anaemia Patient information
 Anaemia Patient information What is anaemia? Anaemia is the result of either not having enough red cells to take oxygen around the body, or having faulty red cells that are unable to carry enough oxygen.
Anaemia Patient information What is anaemia? Anaemia is the result of either not having enough red cells to take oxygen around the body, or having faulty red cells that are unable to carry enough oxygen.
Returning to fitness after birth
 Returning to fitness after birth This leaflet is designed for all women, whether you have given birth vaginally or by Caesarean section. During pregnancy your body undergoes many changes to adapt to your
Returning to fitness after birth This leaflet is designed for all women, whether you have given birth vaginally or by Caesarean section. During pregnancy your body undergoes many changes to adapt to your
Robotic Ventral Rectopexy
 Robotic Ventral Rectopexy What is a robotic ventral rectopexy? The term rectopexy refers to an operation in which the rectum (the part of the bowel nearest the anus) is put back into its normal position
Robotic Ventral Rectopexy What is a robotic ventral rectopexy? The term rectopexy refers to an operation in which the rectum (the part of the bowel nearest the anus) is put back into its normal position
A Trip Through the GI Tract: Common GI Diseases and Complaints. Jennifer Curtis, MD
 A Trip Through the GI Tract: Common GI Diseases and Complaints Jennifer Curtis, MD Colon Cancer How does it develop? Most cancers arise from polyps Over time these can turn into cancer Combination of genetic
A Trip Through the GI Tract: Common GI Diseases and Complaints Jennifer Curtis, MD Colon Cancer How does it develop? Most cancers arise from polyps Over time these can turn into cancer Combination of genetic
Melbourne GI & Endoscopy
 1 Melbourne GI & Endoscopy Multi-disciplinary care for your patients Gastroenterology Hepatobiliary & upper gastrointestinal surgery Colorectal surgery Oncology Perioperative care One contact & one address
1 Melbourne GI & Endoscopy Multi-disciplinary care for your patients Gastroenterology Hepatobiliary & upper gastrointestinal surgery Colorectal surgery Oncology Perioperative care One contact & one address
Irritable Bowel Syndrome (IBS) Information Leaflet THE DIGESTIVE SYSTEM
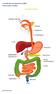 THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Irritable Bowel Syndrome (IBS) Irritable Bowel Syndrome (IBS) consists of a number of symptoms. The most
THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Irritable Bowel Syndrome (IBS) Irritable Bowel Syndrome (IBS) consists of a number of symptoms. The most
Gastrointestinal Hemorrhage, Lower
 Gastrointestinal Hemorrhage, Lower What is a lower gastrointestinal hemorrhage? A lower gastrointestinal (GI) hemorrhage, also called lower GI bleeding or rectal bleeding, is abnormal blood loss from the
Gastrointestinal Hemorrhage, Lower What is a lower gastrointestinal hemorrhage? A lower gastrointestinal (GI) hemorrhage, also called lower GI bleeding or rectal bleeding, is abnormal blood loss from the
Look Good Feel Good. after pregnancy. Physiotherapy advice and exercises for new mums
 Look Good Feel Good after pregnancy Physiotherapy advice and exercises for new mums How to exercise after pregnancy with physiotherapy Bowel Tail Bone Uterus Bladder Pubic Bone Pelvic Floor Muscles Urethra
Look Good Feel Good after pregnancy Physiotherapy advice and exercises for new mums How to exercise after pregnancy with physiotherapy Bowel Tail Bone Uterus Bladder Pubic Bone Pelvic Floor Muscles Urethra
Improving Your Bowel Function
 Improving Your Bowel Function EDUCATES, SUPPORTS AND PROMOTES SPECIALIST PHYSIOTHERAPISTS Glossary symptoms - a feeling of a physical change / bothersome change rectum/back passage - where stool / faeces
Improving Your Bowel Function EDUCATES, SUPPORTS AND PROMOTES SPECIALIST PHYSIOTHERAPISTS Glossary symptoms - a feeling of a physical change / bothersome change rectum/back passage - where stool / faeces
Sphincter exercises for people with bowel control problems
 All of our publications are available in different languages, larger print, braille (English only), audio tape or another format of your choice. Continence service Ballochmyle Suite University Hospital
All of our publications are available in different languages, larger print, braille (English only), audio tape or another format of your choice. Continence service Ballochmyle Suite University Hospital
Southern Derbyshire Shared Care Pathology Guidelines. Coeliac Disease
 Southern Derbyshire Shared Care Pathology Guidelines Coeliac Disease Purpose of Guideline When and how to investigate patients for Coeliac Disease What the results mean When and how to refer patients Monitoring
Southern Derbyshire Shared Care Pathology Guidelines Coeliac Disease Purpose of Guideline When and how to investigate patients for Coeliac Disease What the results mean When and how to refer patients Monitoring
Dietary advice for people with Inflammatory Bowel Disease
 Dietary advice for people with Inflammatory Bowel Disease Crohn s disease and Ulcerative colitis Information for patients Name Your Dietitian Dietitian contact number: 0118 322 7116 What is Inflammatory
Dietary advice for people with Inflammatory Bowel Disease Crohn s disease and Ulcerative colitis Information for patients Name Your Dietitian Dietitian contact number: 0118 322 7116 What is Inflammatory
Chapter 34. Nursing Care of Patients with Lower Gastrointestinal Disorders
 Chapter 34 Nursing Care of Patients with Lower Gastrointestinal Disorders Lower Gastrointestinal System Small Intestines Large Intestines Rectum Anus Constipation Fecal Mass Held In Rectum Feces Become
Chapter 34 Nursing Care of Patients with Lower Gastrointestinal Disorders Lower Gastrointestinal System Small Intestines Large Intestines Rectum Anus Constipation Fecal Mass Held In Rectum Feces Become
BOWEL CANCER. Causes of bowel cancer
 A cancer is an abnormality in an organ that grows without control. The growth is often quite slow, but will continue unabated until it is detected. It can cause symptoms by its presence in the organ or
A cancer is an abnormality in an organ that grows without control. The growth is often quite slow, but will continue unabated until it is detected. It can cause symptoms by its presence in the organ or
CHRONIC DIARRHEA DR. PHILIP K. BLUSTEIN M.D. F.R.C.P.(C) DEFINITION: *LOOSE, WATERY STOOLS *MORE THAN 3 TIMES A DAY *FOR MORE THAN 4 WEEKS
 DR. PHILIP K. BLUSTEIN M.D. F.R.C.P.(C) 415 14 TH ST. NW. CALGARY AB T2N2A1 PHONE (403) 270-9555 FAX (403) 270-7479 CHRONIC DIARRHEA DEFINITION: *LOOSE, WATERY STOOLS *MORE THAN 3 TIMES A DAY *FOR MORE
DR. PHILIP K. BLUSTEIN M.D. F.R.C.P.(C) 415 14 TH ST. NW. CALGARY AB T2N2A1 PHONE (403) 270-9555 FAX (403) 270-7479 CHRONIC DIARRHEA DEFINITION: *LOOSE, WATERY STOOLS *MORE THAN 3 TIMES A DAY *FOR MORE
Daily preparation for Radiotherapy Treatment Important instructions for patients having a course of radiotherapy for cancer of the prostate
 Daily preparation for Radiotherapy Treatment Important instructions for patients having a course of radiotherapy for cancer of the prostate Sussex Cancer Care Introduction Your oncologist (specialist cancer
Daily preparation for Radiotherapy Treatment Important instructions for patients having a course of radiotherapy for cancer of the prostate Sussex Cancer Care Introduction Your oncologist (specialist cancer
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE The management of faecal incontinence in adults 1.1 Short title Faecal incontinence 2 Background (a) (b) (c) The National Institute
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE The management of faecal incontinence in adults 1.1 Short title Faecal incontinence 2 Background (a) (b) (c) The National Institute
Pelvic Floor Exercises
 Pelvic Floor Exercises Information for service users and carers RDaSH leading the way with care Pelvic Floor Muscles The pelvic floor muscles are a sling of muscles across the floor of the pelvis. The
Pelvic Floor Exercises Information for service users and carers RDaSH leading the way with care Pelvic Floor Muscles The pelvic floor muscles are a sling of muscles across the floor of the pelvis. The
Fecal Incontinence. What is fecal incontinence?
 Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
GUIDANCE ON THE INDICATIONS FOR DIAGNOSTIC UPPER GI ENDOSCOPY, FLEXIBLE SIGMOIDOSCOPY AND COLONOSCOPY
 Position Statement produced by BSG, AUGIS and ACPGBI GUIDANCE ON THE INDICATIONS FOR DIAGNOSTIC UPPER GI ENDOSCOPY, FLEXIBLE SIGMOIDOSCOPY AND COLONOSCOPY Introduction In 2011 the Independent Practice
Position Statement produced by BSG, AUGIS and ACPGBI GUIDANCE ON THE INDICATIONS FOR DIAGNOSTIC UPPER GI ENDOSCOPY, FLEXIBLE SIGMOIDOSCOPY AND COLONOSCOPY Introduction In 2011 the Independent Practice
Management Of Rectal Bleeding In The Community: How A Shared Care Approach Can Benefit Dr. Daniel Lee
 Management Of Rectal Bleeding In The Community: How A Shared Care Approach Can Benefit Dr. Daniel Lee MD, MMed (S'pore), FRCS (Edin) Associate Consultant Department of Surgery 9 January 2016 Incidence
Management Of Rectal Bleeding In The Community: How A Shared Care Approach Can Benefit Dr. Daniel Lee MD, MMed (S'pore), FRCS (Edin) Associate Consultant Department of Surgery 9 January 2016 Incidence
Irritable Bowel Syndrome
 Irritable Bowel Syndrome Dietary Management Practicalities Dearbháile O Hanlon Senior Specialist Gastroenterology Dietitian Outline Diagnosis & Red Flags Initial assessment Tips to help implement diet
Irritable Bowel Syndrome Dietary Management Practicalities Dearbháile O Hanlon Senior Specialist Gastroenterology Dietitian Outline Diagnosis & Red Flags Initial assessment Tips to help implement diet
Constipation. Information for adults. GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1
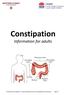 Constipation Information for adults GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1 Contents Role of the large intestine..3 Mass movements in the large intestine..4
Constipation Information for adults GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1 Contents Role of the large intestine..3 Mass movements in the large intestine..4
GPMP and TCA Coeliac disease
 MP and TCA Coeliac disease ITEM: prepares MP (721) REVIEWS MP (732) prepared TCA (723) REVIEW TCA (732) PATIENT DETAILS: DETAILS: DATE PREPARED: Does a current management plan or Team care arrangement
MP and TCA Coeliac disease ITEM: prepares MP (721) REVIEWS MP (732) prepared TCA (723) REVIEW TCA (732) PATIENT DETAILS: DETAILS: DATE PREPARED: Does a current management plan or Team care arrangement
INFORMATION FOR WOMEN FIT. following. Surgery. Advice and exercise following major gynaecological surgery
 INFORMATION FOR WOMEN FIT following Surgery Advice and exercise following major gynaecological surgery Contents Fit following Surgery Introduction...3 First day after your operation...3 Pelvic floor muscle
INFORMATION FOR WOMEN FIT following Surgery Advice and exercise following major gynaecological surgery Contents Fit following Surgery Introduction...3 First day after your operation...3 Pelvic floor muscle
Do we care enough? Solutions for GI symptoms before, during & after GI cancer
 Do we care enough? Solutions for GI symptoms before, during & after GI cancer Jervoise Andreyev Consultant Gastroenterologist in GI Consequences of Cancer Treatment 1 Jane 28, hedge fund manager felt really
Do we care enough? Solutions for GI symptoms before, during & after GI cancer Jervoise Andreyev Consultant Gastroenterologist in GI Consequences of Cancer Treatment 1 Jane 28, hedge fund manager felt really
Post Natal Exercises
 York Teaching Hospital NHS Foundation Trust Post Natal Exercises Taking care of yourself For more information, please contact: Women s Health Physiotherapy Scarborough Hospital: 01723 342259 Woodlands
York Teaching Hospital NHS Foundation Trust Post Natal Exercises Taking care of yourself For more information, please contact: Women s Health Physiotherapy Scarborough Hospital: 01723 342259 Woodlands
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
2012 update. Bowel Cancer. Information for people at increased risk of bowel cancer. Published by the New Zealand Guidelines Group
 2012 update Bowel Cancer Information for people at increased risk of bowel cancer Published by the New Zealand Guidelines Group i Contents Introduction 1 The bowel 1 Bowel cancer 3 What are the symptoms
2012 update Bowel Cancer Information for people at increased risk of bowel cancer Published by the New Zealand Guidelines Group i Contents Introduction 1 The bowel 1 Bowel cancer 3 What are the symptoms
In-patient brachytherapy for gynaecological cancer. Cancer Services Information for patients
 In-patient brachytherapy for gynaecological cancer Cancer Services Information for patients i Introduction This booklet provides information about brachytherapy (a type of internal radiotherapy). We hope
In-patient brachytherapy for gynaecological cancer Cancer Services Information for patients i Introduction This booklet provides information about brachytherapy (a type of internal radiotherapy). We hope
