Guide to managing Gastrointestinal Pelvic Radiation Disease (PRD) using Algorithm V7 (January 2011)
|
|
|
- Sarah May
- 5 years ago
- Views:
Transcription
1 Guide to managing Gastrointestinal Pelvic Radiation Disease (PRD) using Algorithm V7 (January 2011) This algorithm is particularly designed to help clinical nurse specialists working in conjunction with a gastroenterologist to investigate and treat the GI symptoms of patients following pelvic radiotherapy. The basis for this guide is that: 1. Patients often have multiple symptoms 2. Many patients have more than one cause for their symptoms 3. Symptoms often have multiple causes 4. A systematic approach is needed to investigate symptoms otherwise causes are missed 5. After radiotherapy a slightly different approach may be needed to patients who have never had cancer. 6. The key to using the algorithm, is to identify patients symptoms accurately We have identified the following 23 symptoms as particularly relevant to this group of patients and present an algorithm of investigation and treatment for each one. Yes No Yes No Bleeding (rectal) Bloating Borborygmi Change in bowel habit (recent) Nausea Nocturnal need to defaecate Pain - abdomen Pain - back (new onset) Constipation Pain - perineal / anal / rectal Diarrhoea / loose stool Evacuation difficulty Faecal incontinence (soiling / leakage / pads) Flatulence (oral / rectal) Frequency of defaecation Loss of sensation of need to open bowel/ bladder Mucus Pruritus Steatorrhoea Tenesmus Urgency of defaecation Vomiting Weight loss
2 It is important that no practitioner should work with this guidance outside the scope of their competency and should ask advice about abnormal test results which they do not understand. We advise non-medically qualified personnel using this guidance to be sure from whom they can seek advice when they feel unable to deal with test findings especially those which need urgent discussions. Specific therapies are usually not listed by name but as class of potential drugs as different clinicians may have local constraints or preferences as to the medications available. Written information is often helpful to supplement the management of specific diagnoses. If local information sheets are not available, information sheets on the following disorders can be obtained from Dr. Andreyev s office at the Royal Marsden Hospital ( ). 1. Bile acid malabsorption, 2. Pancreatic insufficiency, 3. Small bowel bacterial overgrowth 4. Treatment of radiation-induced gastrointestinal bleeding 5. Toileting and pelvic floor & toileting exercises 6. Advice for those with constipation or who often need to strain Specific leaflets are also available on the following treatments. 1. Lactose free diet 2. Managing fibre in your diet 3. Taking antidiarrhoeals 4. Taking colesevelam 5. Taking normacol, 6. Using sucralfate enemas Version 7. January
3 Using the algorithm 1. identify the symptoms 2. use the algorithm to plan investigations 3. most patients have more than one symptom and so investigations need to be requested for each symptom 4. usually all investigations are ordered at the same time and the patient reviewed with all the results 5. when investigations should be ordered sequentially, the algorithm indicates this by stating 1st line, 2nd line etc 6. Treatment options are generally offered sequentially but clinical judgement should be used. Abbreviations used in the algorithm CMV CT FODMAPS HBO GI IBD MCT MRI OGD SeHCAT SIBO cytomegalovirus computer tomography fermentable oligo-, di- and mono-saccharides and polyols hyperbaric oxygen gastrointestinal inflammatory bowel disease medium chain triglycerides magnetic resonance imaging upper GI endoscopy 75 selenohomocholyltaurine small intestine bacterial overgrowth Version 7. January
4 Guideline for blood tests used within the Algorithm Routine blood screen includes: Full blood count, urea and electrolytes, glucose, calcium, liver function Additional blood screen includes: C reactive protein, coeliac serology, iron studies, red blood cell folate, thyroid function tests Action when blood tests return abnormal results Consider rechecking if clinical doubt, and seek advice for any abnormalities not considered below. Vitamin B12 deficiency 1. Recheck result once, if deficiency confirmed 2. Ask GP to start long-term intramuscular Vitamin B12 replacement after ensuring red blood folate levels are in the normal range Elevated ESR/CRP consider the following possibilities but also discuss: 1. Infection (including SIBO) 2. Inflammation (eg. IBD) 3. Recurrent malignancy 4. Non-GI cause RBC folate - deficiency Dietary advice/referral to dietician Iron studies If results suggest deficiency together with anaemia - discuss urgently If suggesting iron overload - discuss urgently Thyroid function tests If suppressed TSH: 1. Recheck result once with thyroid auto antibodies 2. Ask GP to arrange radiological imaging and arrange treatment If elevated TSH: 1. Recheck result once 2. Check morning cortisol if any possibility of Addison s disease (ie symptoms of weakness/ tiredness/ dizziness or serum sodium is at or below lower end of normal, serum potassium is at or above the upper limit of normal, or urea or creatinine are raised). 3. Start on thyroid replacement, ask GP to monitor long-term 4. Review bowel function after 6-8 weeks Version 7. January
5 Abnormal urea and electrolytes, and calcium Abnormal liver functions Will need liver screen and liver ultrasound Haemoglobin <12.5g/L If unexplained, consider OGD + Colonoscopy If iron deficient, consider iron supplements If Haemoglobin <10g/L, consider transfusion Glucose 1. If between 7.8 and 11 and no history of diabetes refer to GP 2. If > 11 and no history of diabetes discuss urgently 3. If known diabetic and >11 but < 20 inform GP 4. If >20 discuss urgently Fat soluble Vitamin and trace element levels including Vitamin A, Vitamin D, Vitamin E, INR (for Vitamin K) selenium and zinc 1. If any borderline, prescribe multivitamin + trace element supplement (eg Forceval) daily and ask GP to recheck in 12 months and monitor long-term 2. If any deficient, ask GP to prescribe replacement, monitor long-term (minimum annually) and suggest additional Forceval one daily long-term Elevated triglyceride levels Discuss Version 7. January
6 Bleeding - bright red +/- clots Check haemoglobin Check clotting and haematinics if heavy bleeding is occurring Flexible sigmoidoscopy Abnormal Radiation proctopathy with bleeding from telangiectasia Follow treatment abnormal blood results pg. 4, 5 1. No treatment if minor (give written information) 2. If significant bleeding affecting quality of life, topical therapy using sucralfate enemas +/- 4 weeks of metronidazole 3. Discuss for hyperbaric oxygen or endoscopic therapy 4. Discuss experimental agents (eg. Vitamin A, thalidomide, clot stabilizing agents) Haemorrhoidal bleeding Consider local treatment of haemorrhoids (diet, creams etc); if 3 rd degree surgical referral Primary inflammatory bowel disease 1. Send stool culture 2. Diverticular bleeding Newly diagnosed neoplasia 2nd primary / tumour recurrence / advanced polyp Viral infection (eg. CMV) If all tests are negative, but symptoms persist Consider colonoscopy Bleeding - dark bleeding Routine blood screen AND OGD + colonoscopy Abnormal Radiation induced telangiectasia in the colon or terminal ileum Follow treatment abnormal blood results pg. 4, 5 1. No treatment if minor (give written information) 2. Discuss hyperbaric oxygen or endoscopic therapy 3. Discuss experimental agents (eg. Vitamin A, thalidomide, clot stabilizing agents) Version 7. January
7 Bleeding - dark bleeding cont'd Newly diagnosed neoplasia 2nd primary / tumour recurrence / advanced polyp Primary inflammatory bowel disease Diverticular bleeding Upper GI source for bleeding 1. Send stool culture 2. Bloating / cramping. This is also the Algorithm guideline for Abdominal pain If steatorrhoea is present, or possible, also follow Algorithm Steatorrhoea 1st line: Routine blood screen AND Additional blood screen AND Abdominal X-ray Careful dietary history Careful drug history If all tests are negative, but Consider capsule endoscopy / enteroscopy symptoms persist Abnormal results Follow treatment abnormal blood results pg. 4, 5 Faecal loading (with overflow diarrhoea) Appropriate fluid and fibre intake Excessive sorbitol Excessive caffeine Bulking agent / laxatives +/- stimulant rectal enema 1. Written advice 2. Simple dietary advice 3. Referral to dietician Consider stopping opiate drugs / metformin / non steroidal anti-inflammatory drugs 2nd line: OGD and duodenal aspirate and glucose hydrogen methane breath tests SIBO (Small Intestinal Bacterial Overgrowth) Treatment for SIBO 1. Written Information Sheet AND one 7-10 day course of broad spectrum oral antibiotics 2. No improvement / rapid recurrence further 7-10 day course of second antibiotic treatment 3. If rapid recurrence discuss cyclical antibiotics / low dose continuous /intermittent antibiotics Version 7. January
8 Bloating / cramping cont'd Stool for faecal elastase Pancreatic insufficiency Treatment for pancreatic insufficiency 1. Written information AND 2. Pancreatic enzyme supplements +/- PPI 3. Refer to dietician: low fat predominant diet 4. Annual monitoring of fat soluble vitamins and trace elements by GP 5. Consider long-term multi vitamin + trace element supplement Dietary history +/- challenge test for carbohydrate malabsorption Ultrasound of biliary tree (+ small bowel if no recent CT scan of abdomen and pelvis) Carbohydrate intolerance Suggestive of gallstones or inflammatory bowel disease If all tests are negative, but symptoms persist Treatment for carbohydrate malabsorption Dietetic advice (eg. FODMAPS or specific carbohydrate exclusion diet) 1. Reassure 2. Antispasmodic 3. Low dose anti-depressants 4. Referral for acupuncture 5. Agent for neuropathic pain if pain severe 6. Refer to pain clinic if pain severe Borborygmi 1st line: Routine blood screen AND additional blood screen Abnormal results Follow treatment abnormal blood results pg. 4, 5 AND OGD and duodenal aspirate and biopsies and/or glucose hydrogen methane breath tests SIBO Enteric infection Treatment plan for SIBO (see 'Bloating') Treat as recommended by microbiologist Version 7. January
9 Borborygmi Cont. Carbohydrate challenge Carbohydrate malabsorption Treatment plan for carbohydrate malabsorption (see 'Bloating') 2nd line: Chromogranin A&B + Gut hormones+ Urinary 5HIAA Carcinoid syndrome If all tests are negative, but symptoms persist Reassure Change in Bowel Habit Most patients will have change in their bowel habit from preradiotherapy, but this section is to help investigate those with a sudden recent change Routine blood screen AND additional blood screen AND colonoscopy Non GI causes for symptoms Newly diagnosed neoplasia Newly diagnosed IBD If all tests are negative, but symptoms persist Reassure Version 7. January
10 Constipation This is also the Algorithm guideline for 'Evacuation difficulty' Abdominal / rectal examination AND routine blood screen AND additional blood screen Dietary/ lifestyle assessment Constipation / Evacuation disorder SIBO Dietary / lifestyle advice 1. Correct positioning +/- rectal evacuant 2. Bulk laxative +/-rectal evacuant 3. Refer for biofeedback therapy if refractory Treatment plan for SIBO (see Bloating ) Abdominal X-ray Upper GI endoscopy with duodenal aspirate and biopsies and/or glucose hydrogen (methane) breath test Non GI causes for symptoms Newly diagnosed neoplasia Newly diagnosed IBD Diarrhoea - loose / semi formed stool. Colonoscopy Routine blood screen AND additional blood screen Abnormal results Follow guidelines for abnormal blood results pg. 4, 5 See also the guideline for 'Diarrhoea watery stool' (except here colonoscopy is performed in preference to flexi sigmoidoscopy) AND serum Mg2+ Mg2+ low Coeliac screen Coeliac disease 1. If IgA deficient, request IgG Coeliac screen 2. Confirm with duodenal biopsy 3. Refer to dietician / GP for gluten free diet and annual monitoring including bone densometry Stool sample for microscopy, culture + Clostridia Difficile toxin Stool contains pathogen Treat as recommended by the microbiologist Version 7. January
11 Diarrhoea - loose / semi formed stool cont'd Upper GI endoscopy with duodenal aspirate and biopsies and/or glucose hydrogen (methane) breath test SIBO Treatment plan for SIBO (see Bloating ) This is also the guideline for 'Frequency of defaecation' and Nocturnal defaecation Lactose challenge ie. remove lactose from diet for one week and then reintroduce and/or lactose hydrogen breath test Lactose Intolerance Treatment for lactose intolerance 1. Written Information Sheet AND 2. Long term lactose free diet AND 3. Refer to dietician: diet and calcium intake Flexible sigmoidoscopy with biopsies from non-irradiated bowel (being careful to avoid biopsies from areas obviously irradiated in sigmoid and rectum) Radiation proctopathy & frequency of defaecation Radiation proctopathy and loose stool 1. Pelvic floor & toileting exercises - min. 6 weeks (Info Sheet) 2. Add stool bulking agent to pelvic floor exercise regimen 3. Anti-diarrhoeal +/- stool bulking agent +/- stimulant laxative suppository / enema 4. Low dose anti-depressant Anti-diarrhoeal +/- stool bulking agent +/- pelvic floor & toileting exercises SeHCAT scan Bile acid malabsorption Treatment for bile acid malabsorption 1. Written information and 2. Bile acid sequestrant + annual monitoring of fat soluble vitamin levels, triglycerides and trace elements 3. Add an anti-diarrhoeal agent 4. Low fat diet 5. MCT predominant diet with dietician supervision Dietary history Excess / inadequate fibre Excessive caffeine/alcohol 1. Simple advice (eg Fibre Information Sheet) 2. Dietetic review Version 7. January
12 Diarrhoea - loose / semi formed stool cont'd If all tests are negative, but symptoms persist If borderline or below normal Vitamin B12 level consider treatment for SIBO even in the absence of positive duodenal aspirate culture and negative breath test and see if Vitamin B12 corrects after treatment. Otherwise consider 1. 2nd line investigations: gut hormones / chromogranin A&B +/- urinary 5HIAA 2. Symptomatic treatment with anti-diarrhoeal agent Diarrhoea - watery stool Follow guidelines for Diarrhoea loose / semi formed stool Follow guidelines for 'Diarrhoea / loose stool' BUT as1st line: perform colonoscopy with biopsies rather than flexible sigmoidoscopy Macroscopic or microscopic colitis Organic cause Discuss results If all tests are negative, but symptoms persist Evacuation difficulty Flexible sigmoidoscopy Evacuation disorder 1. Correct positioning on lavatory +/- rectal evacuant 2. Biofeedback 3. Discuss specialist referral / specialist tests eg defaecating proctogram or balloon expulsion test Version 7. January
13 Faecal incontinence (Includes soiling, protective liners, pads) Routine blood screen AND additional blood screen Rectal examination Anoscopy Flexible sigmoidoscopy 2nd line: Endo anal ultrasound AND anorectal physiology Abnormal results Radiation proctopathy and faecal incontinence / leakage or Anal sphincter injury Loose stool Follow treatment abnormal blood results pg. 4, 5 1. Pelvic floor & toileting exercises - minimum 6 weeks (Info Sheet) 2. Stool bulking +/- anti-diarrhoeal agent 3. Anti-diarrhoeal agent +/- stimulant laxative suppositories / enemas 4. Topical sympathomimetic agent (eg. phenylephrine) 5. Referral for biofeedback 6. Discuss consideration of defunctioning surgery / sphincter repair Treatment plan for 'Diarrhoea / soft stool' Mucus discharge Treatment plan for mucus 1. Fibre Information Sheet. 2. Pelvic floor & toileting exercises minimum 6 weeks + fibre 3. Stool bulking agent and / or 4. Anti diarrhoeal agent Radiation proctopathy Mucosal prolapse Treatment plan for Faecal incontinence Discuss Unrelated to radiotherapy Discuss Version 7. January
14 Flatulence - excessive wind or can t control wind Dietary review to consider possible reduction in fibre intake Dietary - excess / deficiency of fibre - inadequate fluid intake Refer to dietician for detailed dietary review and advice Abdominal X-ray Faecal overload, constipation Stool bulking agent / laxatives if abdominal X-ray shows faecal loading (follow guidelines for 'Constipation') OGD + D2 Aspirate and/or Glucose hydrogen breath test SIBO Treat SIBO (see 'Bloating') Flexible sigmoidoscopy Organic cause - eg. IBD, neoplasia Lax sphincter muscle 1. Pelvic floor & toileting exercises - minimum 6 weeks (Info Sheet) 2. Stool bulking +/- anti-diarrhoeal agent 3. Anti-diarrhoeal agent +/- stimulant laxative suppositories / enemas 4. Referral for biofeedback Flatulence - oral (burping) Abdominal X-ray OGD +D2 asp. Glucose hydrogen/methane breath test Faecal loading See treatment plan Constipation SIBO If all tests are negative, but symptoms persist See treatment plan SIBO Bloating 1. Trial of a proton pump inhibitor 2. Discuss aerophagia with patient Version 7. January
15 Frequency of defaecation - follow guidelines for 'Diarrhoea/loose stool Loss of sensation unable to discriminate between need to defaecate and to pass urine Follow guidelines for 'Diarrhoea / loose stool' 1st line Routine blood screen AND additional blood screen AND flexible sigmoidoscopy Consider MRI pelvis Abnormal blood results Follow treatment abnormal blood results pg. 4, 5 Organic cause as above eg. IBD, neoplasia Tumour recurrence or other cause for neurological dysfunction Related to radiotherapy 1. Bulking agent + pelvic floor & toileting exercises 2. Biofeedback Mucus +/- leakage (excessive or wet wind ) Rectal examination Organic cause Trial of low fibre diet Flexible sigmoidoscopy If no improvement AND radiation proctopathy Treatment plan for mucus (see Faecal incontinence - soiling ) Version 7. January
16 Nausea Blood screen Metabolic abnormality Liver / biliary pathology Sepsis Antibiotics Urine analysis Metabolic abnormality eg glucosuria, ketonuria Infection Antibiotics Trial of proton pump inhibitor Inflammatory (acid related) Continue intermittent /lower dose proton pump inhibitor and reassess Trial of sucralfate suspension Inflammatory (acid/bile related) Continue intermittent /lower dose sucralfate suspension and reassess Endoscopy Inflammatory / ulcerative 1. Proton pump inhibitor 2. Sucralfate promotility agents 3. Promotility agents Duodenal aspirate/ glucose hydrogen methane breath test Hepatic and pancreatic ultrasound CXR/CT/MRI (including CNS) Small intestine bacterial overgrowth Biliary / hepatic/ pancreatic aetiology Local or distal infection Central nervous system pathology If all tests are negative, but symptoms persist Treatment plan for SIBO (see Bloating ) Treat appropriately Antibiotics Refer to neurology team Version 7. January
17 Nocturnal need to defecate follow guidelines for Diarrhoea Follow guidelines for 'Diarrhoea' Pain - abdomen/cramps follow guidelines for 'Bloating' Follow guidelines for 'Bloating' Pain - back (new onset) Routine blood screen AND additional blood screen Back X-ray CT/MRI/PET scan abdomen and pelvis (to restage patient) Consider a bone scan Abnormal results suggesting relapse Colonic faecal loading Consider referral back to oncologist See treatment plan for 'Constipation' Pain perineal - anal/rectal (typical proctalgia fugax) None needed for typical proctalgia fugax Rectal spasm Treatment for rectal spasm 1. Pelvic floor & toileting exercises 6 weeks 2. Inhaled beta 2 agonist 3. Low dose anti-depressants 4. Consider acupuncture Version 7. January
18 Pain perineal - anal/rectal (related to defaecation) 1st line: Anoscopy and flexible sigmoidoscopy 2nd line: MRI Fistula in ano / abscess Fissure 1. If abscess / fistula, antibiotics and surgical referral 2. If fissure, topical agent eg. diltiazem and analgesia to reduce anal spasm (8 weeks) AND consider stool bulking / softening agent +/- short term topical local anaesthetic 3. If not healed after 2 months, refer for surgical opinion Complex haemorrhoids Surgical review Ano-rectal ulceration Treat the cause, if radiation related 1. Sucralfate enemas 2. Antibiotics 3. Pentoxifylline + Vitamin E 4. Consider stool bulking / softening agent 5. Hyperbaric oxygen Pain perineal - anal/rectal (unrelated to defaecation) Also pruritis (below) 1st line: Anoscopy and flexible sigmoidoscopy Possible diagnoses as above Pain related to defaecation 2nd line: MRI No physical cause identified 1. Pelvic floor & toileting exercises minimum 6 weeks + Information Sheet 2. Low dose anti-depressants 3. Acupuncture 4. Agent for neuropathic pain 5. Consider urological/gynaecological opinion Version 7. January
19 Pruritis (perianal) If loose stool / diarrhoea is present, also see guidance for diarrhoea especially SeHCAT scan Steatorrhoea (see guidelines for 'Diarrhoea - loose stool' re prescription of anti-diarrhoeal) Visual assessment Changes of radiotherapy 1. If soiling see guidance for faecal incontinence p Topical barrier agent 3. Topical corticosteroids (trimovate) 4. No improvement - refer to dermatologist No changes of radiotherapy Refer to dermatologist Stool for faecal elastase Pancreatic insufficiency 1. Written information AND 2. Pancreatic enzyme supplements +/- PPI 3. Refer to dietician: low fat predominant diet 4. Multi vitamin and trace elements supplement 5. Annual monitoring of trace elements by GP Routine blood screens AND additional blood screen AND fat soluble vitamin levels and trace elements Addison's disease / coeliac disease / thyroid dysfunction / Vitamin B12 deficiency Follow treatment abnormal blood results pg. 4, 5 Glucose / hydrogen/ methane breath test for bacterial overgrowth and / or OGD + D2 asp and biopsies Small Intestine Bacterial Overgrowth See treatment plan SIBO Bloating' SeHCAT scan Bile acid malabsorption Treatment for Bile acid malabsorption See Diarrhoea/loose stool Tenesmus Flexible sigmoidoscopy Radiation proctopathy and tenesmus 1. Pelvic floor & toileting exercises - 6 weeks (Information Sheet) and stool bulking agent 2. Low dose anti-depressants 3. Consider acupuncture 4. Biofeedback Version 7. January
20 Urgency of defaecation - follow guidelines for diarrhoea/ loose stool Routine blood screen, AND additional blood screen Flexible sigmoidoscopy Any blood test abnormality Follow treatment abnormal blood results pg. 4, 5 Radiation proctopathy and urgency of defaecation 1. Pelvic floor & toileting exercises - 6 weeks (Information Sheet) 2. Stool bulking agent 3. Anti-diarrhoeal agent 4. Low dose anti-depressants 5. Biofeedback Vomiting Blood screen 1. Drug / medication related 2. Alcohol related 3. Metabolic 4. Endocrine Urine analysis + culture Infective Follow recommendations of microbiologist Trial of proton pump inhibitor Trial of Sucralfate suspension Endoscopy (+ duodenal aspirate) Glucose hydrogen / methane breath test / trial of antibiotics Metabolic Inflammatory (acid related) Inflammatory (acid/bile related) Inflammatory/ ulceration Small intestinal bacterial overgrowth Continue intermittent / lower dose proton pump inhibitor and reassess Continue intermittent / lower dose Sucralfate suspension and reassess Proton pump inhibitor Sucralfate Promotility agents See treatment plan for SIBO 'Bloating' Version 7. January
21 Vomiting cont'd CT/MRI Bowel obstruction Admit to hospital Consider CT MRI head Neurological disease Weight loss - unexplained Dietary review Routine blood screen AND additional blood screen OGD AND Colonoscopy CT chest abdomen and pelvis Abnormal results Organic cause No organic cause Follow treatment abnormal blood results pg. 4, 5 Refer for expert advice Refer to dietician and review regularly Any of the above symptoms requiring hospital admission Discuss Any symptoms not covered in the management plan Discuss Clinical depression Discuss Version 7. January
A quick guide for health professionals
 A quick guide for health professionals Background Most cancer survivors will not have any long-term lower GI consequences of their cancer or its treatment. However, some will develop problems including
A quick guide for health professionals Background Most cancer survivors will not have any long-term lower GI consequences of their cancer or its treatment. However, some will develop problems including
Late effects of treatment for colorectal cancer. Claire Taylor Macmillan Nurse Consultant St Mark s Hospital
 Late effects of treatment for colorectal cancer Claire Taylor Macmillan Nurse Consultant St Mark s Hospital The number of people living with cancer is set to double from 2m to 4m by 2030 Source: Maddams
Late effects of treatment for colorectal cancer Claire Taylor Macmillan Nurse Consultant St Mark s Hospital The number of people living with cancer is set to double from 2m to 4m by 2030 Source: Maddams
Clinical problems related to GI involvement in SSc
 Clinical problems related to GI involvement in SSc Incontinence Abdominal pain/distension Gastro-oesophageal Diarrhoea Weight loss/al Issues Constipation Management of incontinence Establish diagnosis
Clinical problems related to GI involvement in SSc Incontinence Abdominal pain/distension Gastro-oesophageal Diarrhoea Weight loss/al Issues Constipation Management of incontinence Establish diagnosis
Recent developments in radiotherapy and management of bowel toxicity
 The Roy al Marsden Recent developments in radiotherapy and management of bowel toxicity Dr Alexandra Taylor Radiotherapy for cervical cancer Historical perspective 1901 First use of radium for cervical
The Roy al Marsden Recent developments in radiotherapy and management of bowel toxicity Dr Alexandra Taylor Radiotherapy for cervical cancer Historical perspective 1901 First use of radium for cervical
Side effects of brachytherapy
 Side effects of brachytherapy Dr Arian Barnardo BM BMedSci MD FRCP AGAF Consultant Gastroenterologists & BCSP Endoscopist Anal pain & Rectal bleeding Rectal bleeding not everything is oncological Side
Side effects of brachytherapy Dr Arian Barnardo BM BMedSci MD FRCP AGAF Consultant Gastroenterologists & BCSP Endoscopist Anal pain & Rectal bleeding Rectal bleeding not everything is oncological Side
What you can expect at your doctors
 What you can expect at your doctors Investigations and Procedures Tests are not always necessary Current guidelines encourage gastroenterologists to make a positive diagnosis of Irritable Bowel Syndrome
What you can expect at your doctors Investigations and Procedures Tests are not always necessary Current guidelines encourage gastroenterologists to make a positive diagnosis of Irritable Bowel Syndrome
Listed below are some of the words that you might come across concerning diseases and conditions of the bowels.
 Listed below are some of the words that you might come across concerning diseases and conditions of the bowels. Abscess A localised collection of pus in a cavity that is formed by the decay of diseased
Listed below are some of the words that you might come across concerning diseases and conditions of the bowels. Abscess A localised collection of pus in a cavity that is formed by the decay of diseased
Constipation Information Leaflet THE DIGESTIVE SYSTEM. gutscharity.org.uk
 THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Constipation Constipation is a symptom that can mean different things to different people but the usual
THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Constipation Constipation is a symptom that can mean different things to different people but the usual
CHRONIC DIARRHEA DR. PHILIP K. BLUSTEIN M.D. F.R.C.P.(C) DEFINITION: *LOOSE, WATERY STOOLS *MORE THAN 3 TIMES A DAY *FOR MORE THAN 4 WEEKS
 DR. PHILIP K. BLUSTEIN M.D. F.R.C.P.(C) 415 14 TH ST. NW. CALGARY AB T2N2A1 PHONE (403) 270-9555 FAX (403) 270-7479 CHRONIC DIARRHEA DEFINITION: *LOOSE, WATERY STOOLS *MORE THAN 3 TIMES A DAY *FOR MORE
DR. PHILIP K. BLUSTEIN M.D. F.R.C.P.(C) 415 14 TH ST. NW. CALGARY AB T2N2A1 PHONE (403) 270-9555 FAX (403) 270-7479 CHRONIC DIARRHEA DEFINITION: *LOOSE, WATERY STOOLS *MORE THAN 3 TIMES A DAY *FOR MORE
Bowel cancer risk in the under 50s. Greg Rubin Professor of General Practice and Primary Care
 Bowel cancer risk in the under 50s Greg Rubin Professor of General Practice and Primary Care Prevalence of GI problems in the consulting population Thompson et al, Gut 2000 Number of patients % of patients
Bowel cancer risk in the under 50s Greg Rubin Professor of General Practice and Primary Care Prevalence of GI problems in the consulting population Thompson et al, Gut 2000 Number of patients % of patients
Guideline scope Diverticular disease: diagnosis and management
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Diverticular disease: diagnosis and management The Department of Health in England has asked NICE to develop a clinical guideline on diverticular
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Diverticular disease: diagnosis and management The Department of Health in England has asked NICE to develop a clinical guideline on diverticular
Irritable bowel syndrome in adults
 Irritable bowel syndrome in adults NICE provided the content for this booklet which is independent of any company or product advertised Welcome In February 2008, NICE published a clinical guideline on
Irritable bowel syndrome in adults NICE provided the content for this booklet which is independent of any company or product advertised Welcome In February 2008, NICE published a clinical guideline on
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Constipation: management of idiopathic constipation in children in primary and secondary care 1.1 Short title Constipation
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Constipation: management of idiopathic constipation in children in primary and secondary care 1.1 Short title Constipation
PELVIC PAIN : Gastroenterological Conditions
 PELVIC PAIN : Gastroenterological Conditions Departman Tarih Prof. A. Melih OZEL, MD Department of Gastroenterology Anadolu Medical Center Hospital Gebze Kocaeli - TURKEY Presentation plan 15 min. Introduction
PELVIC PAIN : Gastroenterological Conditions Departman Tarih Prof. A. Melih OZEL, MD Department of Gastroenterology Anadolu Medical Center Hospital Gebze Kocaeli - TURKEY Presentation plan 15 min. Introduction
Certain genes passed on from parent to child increase the risk of developing Crohn's disease, if the right trigger occurs.
 Topic Page: Crohn's disease Definition: Crohn's disease from Benders' Dictionary of Nutrition and Food Technology Chronic inflammatory disease of the bowel, commonly the terminal ileum, of unknown aetiology,
Topic Page: Crohn's disease Definition: Crohn's disease from Benders' Dictionary of Nutrition and Food Technology Chronic inflammatory disease of the bowel, commonly the terminal ileum, of unknown aetiology,
WALSALL COELIAC DISEASE FLOWCHART
 WALSALL COELIAC DISEASE FLOWCHART CLINICAL SUSPICION OF COELIAC DISEASE ( Which can present at any age ) [see Box A or Box B] DO NOT START GLUTEN FREE DIET BEFORE ANY INVESTIGATIONS Test for IgA Tissue
WALSALL COELIAC DISEASE FLOWCHART CLINICAL SUSPICION OF COELIAC DISEASE ( Which can present at any age ) [see Box A or Box B] DO NOT START GLUTEN FREE DIET BEFORE ANY INVESTIGATIONS Test for IgA Tissue
Constipation. What is constipation? What is the criteria for having constipation? What are the different types of constipation?
 What is constipation? is defined as having a bowel movement less than 3 times per week. It is usually associated with hard stools or difficulty passing stools. You may have pain while passing stools or
What is constipation? is defined as having a bowel movement less than 3 times per week. It is usually associated with hard stools or difficulty passing stools. You may have pain while passing stools or
Irritable Bowel Syndrome. Mustafa Giaffer March 2017
 Irritable Bowel Syndrome Mustafa Giaffer March 2017 Introduction First described in 1771. 50% of patients present
Irritable Bowel Syndrome Mustafa Giaffer March 2017 Introduction First described in 1771. 50% of patients present
Understanding & Alleviating Constipation. Living (Well!) with Gastroparesis Program Warm-Up Class
 Understanding & Alleviating Constipation Living (Well!) with Gastroparesis Program Warm-Up Class Please Remember The information presented is for educational purposes only and is in no way intended as
Understanding & Alleviating Constipation Living (Well!) with Gastroparesis Program Warm-Up Class Please Remember The information presented is for educational purposes only and is in no way intended as
GUIDANCE ON THE INDICATIONS FOR DIAGNOSTIC UPPER GI ENDOSCOPY, FLEXIBLE SIGMOIDOSCOPY AND COLONOSCOPY
 Position Statement produced by BSG, AUGIS and ACPGBI GUIDANCE ON THE INDICATIONS FOR DIAGNOSTIC UPPER GI ENDOSCOPY, FLEXIBLE SIGMOIDOSCOPY AND COLONOSCOPY Introduction In 2011 the Independent Practice
Position Statement produced by BSG, AUGIS and ACPGBI GUIDANCE ON THE INDICATIONS FOR DIAGNOSTIC UPPER GI ENDOSCOPY, FLEXIBLE SIGMOIDOSCOPY AND COLONOSCOPY Introduction In 2011 the Independent Practice
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE SCOPE. Coeliac disease: recognition, assessment and management of coeliac disease
 Appendix B: NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE 1 Guideline title SCOPE Coeliac disease: recognition, assessment and management of coeliac disease 1.1 Short title Coeliac disease 2 The remit
Appendix B: NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE 1 Guideline title SCOPE Coeliac disease: recognition, assessment and management of coeliac disease 1.1 Short title Coeliac disease 2 The remit
INVESTIGATIONS OF GASTROINTESTINAL DISEAS
 INVESTIGATIONS OF GASTROINTESTINAL DISEAS Lecture 1 and 2 دز اسماعيل داود فرع الطب كلية طب الموصل Radiological tests of structure (imaging) Plain X-ray: May shows soft tissue outlines like liver, spleen,
INVESTIGATIONS OF GASTROINTESTINAL DISEAS Lecture 1 and 2 دز اسماعيل داود فرع الطب كلية طب الموصل Radiological tests of structure (imaging) Plain X-ray: May shows soft tissue outlines like liver, spleen,
PELVIC PAIN : Gastroenterological Conditions
 PELVIC PAIN : Gastroenterological Conditions Departman Tarih Prof. A. Melih OZEL, MD Department of Gastroenterology Anadolu Medical Center Hospital Gebze Kocaeli - TURKEY Presentation plan 15 min. Introduction
PELVIC PAIN : Gastroenterological Conditions Departman Tarih Prof. A. Melih OZEL, MD Department of Gastroenterology Anadolu Medical Center Hospital Gebze Kocaeli - TURKEY Presentation plan 15 min. Introduction
BOWEL CANCER. Causes of bowel cancer
 A cancer is an abnormality in an organ that grows without control. The growth is often quite slow, but will continue unabated until it is detected. It can cause symptoms by its presence in the organ or
A cancer is an abnormality in an organ that grows without control. The growth is often quite slow, but will continue unabated until it is detected. It can cause symptoms by its presence in the organ or
Colon Cancer , The Patient Education Institute, Inc. oc Last reviewed: 05/17/2017 1
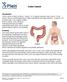 Colon Cancer Introduction Colon cancer is fairly common. About 1 in 15 people develop colon cancer. Colon cancer can be a life threatening condition that affects the large intestine. However, if it is
Colon Cancer Introduction Colon cancer is fairly common. About 1 in 15 people develop colon cancer. Colon cancer can be a life threatening condition that affects the large intestine. However, if it is
Guidance: The practical management of the gastrointestinal symptoms of pelvic radiation disease
 1 The GI and Nutrition Team, The Royal Marsden NHS Foundation Trust, London and Surrey, UK 2 King s College London, London, UK 3 Digestive Diseases Clinical Academic Unit, Barts and The London School of
1 The GI and Nutrition Team, The Royal Marsden NHS Foundation Trust, London and Surrey, UK 2 King s College London, London, UK 3 Digestive Diseases Clinical Academic Unit, Barts and The London School of
Rectal Bleeding. Exceptional healthcare, personally delivered
 Rectal Bleeding Exceptional healthcare, personally delivered Content n The surgical team has assessed you because you have had bleeding from the back passage (rectal bleeding). n But your condition needs
Rectal Bleeding Exceptional healthcare, personally delivered Content n The surgical team has assessed you because you have had bleeding from the back passage (rectal bleeding). n But your condition needs
Referral Criteria for Direct Access Outpatient Colonoscopy or Computed Tomography Colonography
 Referral Criteria for Direct Access Outpatient Colonoscopy or Computed Tomography Colonography 2019 Released 2019 health.govt.nz Citation: Ministry of Health. 2019. Referral Criteria for Direct Access
Referral Criteria for Direct Access Outpatient Colonoscopy or Computed Tomography Colonography 2019 Released 2019 health.govt.nz Citation: Ministry of Health. 2019. Referral Criteria for Direct Access
Dr David Rowbotham. The Leeds Teaching Hospitals NHS Trust NHS
 Dr David Rowbotham The Leeds Teaching Hospitals NHS Trust NHS Useful Titbits from the World of Gastroenterology David Rowbotham Clinical Director & Consultant Gastroenterologist Dept of Gastroenterology
Dr David Rowbotham The Leeds Teaching Hospitals NHS Trust NHS Useful Titbits from the World of Gastroenterology David Rowbotham Clinical Director & Consultant Gastroenterologist Dept of Gastroenterology
Prevention of Bowel Cancer: which patients do I send for colonoscopy?
 Prevention of Bowel Cancer: which patients do I send for colonoscopy? Dr Chris Groves Consultant Gastroenterologist and Honorary Senior Lecturer St George s Hospital and Medical School Director, SW London
Prevention of Bowel Cancer: which patients do I send for colonoscopy? Dr Chris Groves Consultant Gastroenterologist and Honorary Senior Lecturer St George s Hospital and Medical School Director, SW London
Chapter 34. Nursing Care of Patients with Lower Gastrointestinal Disorders
 Chapter 34 Nursing Care of Patients with Lower Gastrointestinal Disorders Lower Gastrointestinal System Small Intestines Large Intestines Rectum Anus Constipation Fecal Mass Held In Rectum Feces Become
Chapter 34 Nursing Care of Patients with Lower Gastrointestinal Disorders Lower Gastrointestinal System Small Intestines Large Intestines Rectum Anus Constipation Fecal Mass Held In Rectum Feces Become
COMMON PROBLEMS IN PAEDIATRIC GASTROENTEROLOGY AKSHAY BATRA CONSULTANT PAEDIATRIC GASTROENTEROLOGIST
 COMMON PROBLEMS IN PAEDIATRIC GASTROENTEROLOGY AKSHAY BATRA CONSULTANT PAEDIATRIC GASTROENTEROLOGIST Paediatric Gastroenterology : Referral Base Common problems Feeding difficulties in infancy Recurrent
COMMON PROBLEMS IN PAEDIATRIC GASTROENTEROLOGY AKSHAY BATRA CONSULTANT PAEDIATRIC GASTROENTEROLOGIST Paediatric Gastroenterology : Referral Base Common problems Feeding difficulties in infancy Recurrent
Gastrointestinal Hemorrhage, Lower
 Gastrointestinal Hemorrhage, Lower What is a lower gastrointestinal hemorrhage? A lower gastrointestinal (GI) hemorrhage, also called lower GI bleeding or rectal bleeding, is abnormal blood loss from the
Gastrointestinal Hemorrhage, Lower What is a lower gastrointestinal hemorrhage? A lower gastrointestinal (GI) hemorrhage, also called lower GI bleeding or rectal bleeding, is abnormal blood loss from the
Treatment of haemorrhoids. Mr Rowan Collinson FRACS Colorectal and General Surgeon Auckland
 Treatment of haemorrhoids Mr Rowan Collinson FRACS Colorectal and General Surgeon Auckland Much overlap of haemorrhoidal symptoms with other conditions Is it just the haemorrhoids? what type of haemorrhoidal
Treatment of haemorrhoids Mr Rowan Collinson FRACS Colorectal and General Surgeon Auckland Much overlap of haemorrhoidal symptoms with other conditions Is it just the haemorrhoids? what type of haemorrhoidal
The York Faecal Calprotectin Care Pathway for use in primary care. James Turvill
 The York Faecal Calprotectin Care Pathway for use in primary care James Turvill NICE guidance: dg11 Faecal calprotectin (FC) testing as an option in adults with recent onset of lower gastrointestinal symptoms
The York Faecal Calprotectin Care Pathway for use in primary care James Turvill NICE guidance: dg11 Faecal calprotectin (FC) testing as an option in adults with recent onset of lower gastrointestinal symptoms
REFERRAL GUIDELINES GASTROENTEROLOGY
 REFERRAL GUIDELINES GASTROENTEROLOGY Referral Form: The GP Referral Template is the preferred referral tool (previously known as the Victorian Statewide Referral Form) GP Referral Template This tool is
REFERRAL GUIDELINES GASTROENTEROLOGY Referral Form: The GP Referral Template is the preferred referral tool (previously known as the Victorian Statewide Referral Form) GP Referral Template This tool is
Digestion: Small and Large Intestines Pathology
 Digestion: Small and Large Intestines Pathology Dr. Ritamarie Loscalzo Medical Disclaimer: The information in this presentation is not intended to replace a one onone relationship with a qualified health
Digestion: Small and Large Intestines Pathology Dr. Ritamarie Loscalzo Medical Disclaimer: The information in this presentation is not intended to replace a one onone relationship with a qualified health
A guide to Anoplasty (anal surgery)
 Saint Mary s Hospital Newborn Intensive Care Unit Information for Parents A guide to Anoplasty (anal surgery) Introduction This information leaflet is designed to help parents and families to care for
Saint Mary s Hospital Newborn Intensive Care Unit Information for Parents A guide to Anoplasty (anal surgery) Introduction This information leaflet is designed to help parents and families to care for
Diarrhoea Mashiko Setshedi 01 Feb Practical Diagnostic Approach to Chronic
 Diarrhoea Mashiko Setshedi 01 Feb 2019 Practical Diagnostic Approach to Chronic Overview Chronic diarrhoea is common (3-5% of population) Considerable diagnostic challenge Several hundred possible differential
Diarrhoea Mashiko Setshedi 01 Feb 2019 Practical Diagnostic Approach to Chronic Overview Chronic diarrhoea is common (3-5% of population) Considerable diagnostic challenge Several hundred possible differential
Clinical Evaluation of CHRONIC DIARRHEA. By Dr. Mohamed El-Awady
 Clinical Evaluation of CHRONIC DIARRHEA By Dr. Mohamed El-Awady Definition Stool weight of more than 300 gm / 24 h more than 4 weeks (Feldman et al 2002) CLINICAL CLASSIFICATION 1) Large-Volume Versus
Clinical Evaluation of CHRONIC DIARRHEA By Dr. Mohamed El-Awady Definition Stool weight of more than 300 gm / 24 h more than 4 weeks (Feldman et al 2002) CLINICAL CLASSIFICATION 1) Large-Volume Versus
1/3/2008. Karen Burke Priscilla LeMone Elaine Mohn-Brown. Medical-Surgical Nursing Care, 2e Karen Burke, Priscilla LeMone, and Elaine Mohn-Brown
 Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 20 Caring for Clients with Bowel Disorders Diarrhea Pathophysiology Result from impaired water absorption
Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 20 Caring for Clients with Bowel Disorders Diarrhea Pathophysiology Result from impaired water absorption
RADIATION INDUCED SMALL BOWEL DISEASE. Dr Mnguni Supervisor: Dr Lohlun Radiation Oncology
 RADIATION INDUCED SMALL BOWEL DISEASE Dr Mnguni Supervisor: Dr Lohlun Radiation Oncology INTRODUCTION Radiation therapy is not regularly indicated in the treatment of small bowel disease. Reasons are complex
RADIATION INDUCED SMALL BOWEL DISEASE Dr Mnguni Supervisor: Dr Lohlun Radiation Oncology INTRODUCTION Radiation therapy is not regularly indicated in the treatment of small bowel disease. Reasons are complex
University Medical Center at Brackenridge. Gastroenterology Clinic Worksheet
 Gastroenterology Clinic Worksheet 1. GI Bleeding (occult or symptomatic) a. CBC b. Iron, Ferritin b. Medication history 2. Iron Deficiency Anemia and no evident source (if no iron deficiency consider hematological
Gastroenterology Clinic Worksheet 1. GI Bleeding (occult or symptomatic) a. CBC b. Iron, Ferritin b. Medication history 2. Iron Deficiency Anemia and no evident source (if no iron deficiency consider hematological
What is Crohn's disease?
 What is Crohn's disease? Crohn's disease is a chronic inflammatory disorder that causes inflammation of the digestive tract. It can affect any area of the GI tract, from the mouth to the anus, but it most
What is Crohn's disease? Crohn's disease is a chronic inflammatory disorder that causes inflammation of the digestive tract. It can affect any area of the GI tract, from the mouth to the anus, but it most
Gastrointestinal complications after stem cell transplantation
 Gastrointestinal complications after stem cell transplantation Jervoise Andreyev Consultant Gastroenterologist in Pelvic Radiation Disease London, UK 1 100 consecutive patient audit In hospital impact
Gastrointestinal complications after stem cell transplantation Jervoise Andreyev Consultant Gastroenterologist in Pelvic Radiation Disease London, UK 1 100 consecutive patient audit In hospital impact
Colon Investigation. Flexible Sigmoidoscopy
 Colon Investigation Flexible Sigmoidoscopy What is a flexible sigmoidoscopy? Flexible sigmoidoscopy is a frequently performed test to investigate the lower part of the bowel. This is an endoscopic test
Colon Investigation Flexible Sigmoidoscopy What is a flexible sigmoidoscopy? Flexible sigmoidoscopy is a frequently performed test to investigate the lower part of the bowel. This is an endoscopic test
What Is an Endoscopic Ultrasound (EUS)?
 ENDOSCOPIC ULTRASOUND (EUS) What Is an Endoscopic Ultrasound (EUS)? An endoscopic ultrasound (EUS) is a specialized procedure that blends: Endoscopy use of a scope to look at the inside lining of the gastrointestinal
ENDOSCOPIC ULTRASOUND (EUS) What Is an Endoscopic Ultrasound (EUS)? An endoscopic ultrasound (EUS) is a specialized procedure that blends: Endoscopy use of a scope to look at the inside lining of the gastrointestinal
Nutritional Protocol for Blood and Bone Marrow Transplantation (BMT)
 Nutritional Protocol for Blood and Bone Marrow Transplantation (BMT) Scope This protocol details pre, during and post BMT nutritional assessment and management for all forms of BMT undertaken by OxBMT,
Nutritional Protocol for Blood and Bone Marrow Transplantation (BMT) Scope This protocol details pre, during and post BMT nutritional assessment and management for all forms of BMT undertaken by OxBMT,
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Constipation: the diagnosis and management of idiopathic childhood constipation in primary and secondary care 1.1 Short title
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Constipation: the diagnosis and management of idiopathic childhood constipation in primary and secondary care 1.1 Short title
Do we care enough? Solutions for GI symptoms before, during & after GI cancer
 Do we care enough? Solutions for GI symptoms before, during & after GI cancer Jervoise Andreyev Consultant Gastroenterologist in GI Consequences of Cancer Treatment 1 Jane 28, hedge fund manager felt really
Do we care enough? Solutions for GI symptoms before, during & after GI cancer Jervoise Andreyev Consultant Gastroenterologist in GI Consequences of Cancer Treatment 1 Jane 28, hedge fund manager felt really
Western Health Specialist Clinics Access & Referral Guidelines
 Gastroenterology Specialist Clinics at Western Health: Western Health provides the following Specialist Clinics for patients who require assessment and management of Gastroenterology / Hepatology conditions.
Gastroenterology Specialist Clinics at Western Health: Western Health provides the following Specialist Clinics for patients who require assessment and management of Gastroenterology / Hepatology conditions.
Algorithms & Information Sheets
 Minor Ailment Scheme Algorithms & Information Sheets Acute Diarrhoea Diarrhoea is an increased frequency, fluidity or volume of the bowel movements with the passage of soft and watery stools as compared
Minor Ailment Scheme Algorithms & Information Sheets Acute Diarrhoea Diarrhoea is an increased frequency, fluidity or volume of the bowel movements with the passage of soft and watery stools as compared
, may spread caudally to present as a perianal abscess, laterally across the external sphincter to form an ischiorectal abscess or, rarely,
 ANORECTAL ABSCESSES , may spread caudally to present as a perianal abscess, laterally across the external sphincter to form an ischiorectal abscess or, rarely, superiorly above the anorectal junction
ANORECTAL ABSCESSES , may spread caudally to present as a perianal abscess, laterally across the external sphincter to form an ischiorectal abscess or, rarely, superiorly above the anorectal junction
Southern Derbyshire Shared Care Pathology Guidelines. Coeliac Disease
 Southern Derbyshire Shared Care Pathology Guidelines Coeliac Disease Purpose of Guideline When and how to investigate patients for Coeliac Disease What the results mean When and how to refer patients Monitoring
Southern Derbyshire Shared Care Pathology Guidelines Coeliac Disease Purpose of Guideline When and how to investigate patients for Coeliac Disease What the results mean When and how to refer patients Monitoring
Irritable Bowel Syndrome (IBS)
 Irritable Bowel Syndrome (IBS) Dr Rex J Polson 17 th January 2018 Overview Description of the condition Discussion of symptoms and investigations that may be required Discussion of management and treatment
Irritable Bowel Syndrome (IBS) Dr Rex J Polson 17 th January 2018 Overview Description of the condition Discussion of symptoms and investigations that may be required Discussion of management and treatment
Robotic Ventral Rectopexy
 Robotic Ventral Rectopexy What is a robotic ventral rectopexy? The term rectopexy refers to an operation in which the rectum (the part of the bowel nearest the anus) is put back into its normal position
Robotic Ventral Rectopexy What is a robotic ventral rectopexy? The term rectopexy refers to an operation in which the rectum (the part of the bowel nearest the anus) is put back into its normal position
MOVICOL HALF PI December MOVICOL-Half. Powder for Solution (macrogol 3350) Potassium 5.4 mmol/l. Bicarbonate 17 mmol/l
 MOVICOL -Half Powder for Solution (macrogol 3350) Product Name: Product Description: MOVICOL-Half Each sachet of MOVICOL-Half contains: Macrogol 3350 6.563 g Sodium chloride 175.4 mg Sodium bicarbonate
MOVICOL -Half Powder for Solution (macrogol 3350) Product Name: Product Description: MOVICOL-Half Each sachet of MOVICOL-Half contains: Macrogol 3350 6.563 g Sodium chloride 175.4 mg Sodium bicarbonate
This page explains some of the medical words that you may hear when you are finding out about pancreatic cancer and how it is treated.
 A-Z of medical words This page explains some of the medical words that you may hear when you are finding out about pancreatic cancer and how it is treated. Absorption: once your food has been broken down,
A-Z of medical words This page explains some of the medical words that you may hear when you are finding out about pancreatic cancer and how it is treated. Absorption: once your food has been broken down,
Prescribing Guidance for the Treatment of Constipation in Children
 Prescribing Guidance for the Treatment of Constipation in Children Effective Date: July 2007 Reviewed: September 2009 & December 2011 Review Date: December 2013 Gateshead Medicines Management Approved
Prescribing Guidance for the Treatment of Constipation in Children Effective Date: July 2007 Reviewed: September 2009 & December 2011 Review Date: December 2013 Gateshead Medicines Management Approved
Fecal Incontinence. What is fecal incontinence?
 Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
PERSISTENT DIARRHOEA. IAP UG Teaching slides
 PERSISTENT DIARRHOEA 1 DEFINITION Prolongation of acute diarrhoea / dysentery for more than 14 days Generally associated with weight loss. 2 PROTRACTED DIARRHOEA Prolongation of acute diarrhoea or dysentery
PERSISTENT DIARRHOEA 1 DEFINITION Prolongation of acute diarrhoea / dysentery for more than 14 days Generally associated with weight loss. 2 PROTRACTED DIARRHOEA Prolongation of acute diarrhoea or dysentery
Clinical guideline Published: 23 February 2008 nice.org.uk/guidance/cg61
 Irritable bowel syndrome in adults: diagnosis and management Clinical guideline Published: 23 February 2008 nice.org.uk/guidance/cg61 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Irritable bowel syndrome in adults: diagnosis and management Clinical guideline Published: 23 February 2008 nice.org.uk/guidance/cg61 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
ABDOMINAL PAIN, CHRONIC
 Introduction Incidence Aetiology Clinical Assessment Formulation Investigations Management Prognosis Conclusion References Introduction The generally accepted definition of this condition is three or more
Introduction Incidence Aetiology Clinical Assessment Formulation Investigations Management Prognosis Conclusion References Introduction The generally accepted definition of this condition is three or more
Lower GI Series. National Digestive Diseases Information Clearinghouse
 Lower GI Series National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is a lower gastrointestinal (GI) series? A lower GI
Lower GI Series National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is a lower gastrointestinal (GI) series? A lower GI
Anorectal physiology test
 Anorectal physiology test We hope this factsheet will help to answer some of your questions about having an anorectal physiology test. If you have any further questions or concerns, please don t hesitate
Anorectal physiology test We hope this factsheet will help to answer some of your questions about having an anorectal physiology test. If you have any further questions or concerns, please don t hesitate
Outcomes from treating bile acid malabsorption (BAM) using a multidisciplinary approach
 Outcomes from treating bile acid malabsorption (BAM) using a multidisciplinary approach Gupta A et al. Support Care Cancer. 2015 Oct;23(10):2881-90 Prescribing information can be found at the end of this
Outcomes from treating bile acid malabsorption (BAM) using a multidisciplinary approach Gupta A et al. Support Care Cancer. 2015 Oct;23(10):2881-90 Prescribing information can be found at the end of this
What Is Constipation?
 CONSTIPATION What Is Constipation? Constipation is when you have infrequent or hard-to-pass bowel movements (meaning they are painful or you have to strain), have hard stools or feel like your bowel movements
CONSTIPATION What Is Constipation? Constipation is when you have infrequent or hard-to-pass bowel movements (meaning they are painful or you have to strain), have hard stools or feel like your bowel movements
This is the portion of the intestine which lies between the small intestine and the outlet (Anus).
 THE COLON This is the portion of the intestine which lies between the small intestine and the outlet (Anus). 3 4 5 This part is responsible for formation of stool. The large intestine (colon- coloured
THE COLON This is the portion of the intestine which lies between the small intestine and the outlet (Anus). 3 4 5 This part is responsible for formation of stool. The large intestine (colon- coloured
Chapter 31 Bowel Elimination
 Chapter 31 Bowel Elimination Defecation Defecation: the act of expelling feces from the body Peristalsis: rhythmic contractions of intestinal smooth muscle to facilitate defecation Gastrocolic reflex:
Chapter 31 Bowel Elimination Defecation Defecation: the act of expelling feces from the body Peristalsis: rhythmic contractions of intestinal smooth muscle to facilitate defecation Gastrocolic reflex:
Bowel Cancer Information Leaflet THE DIGESTIVE SYSTEM
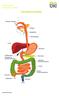 THE DIGESTIVE SYSTEM This factsheet is about bowel cancer Throughout our lives, the lining of the bowel constantly renews itself. This lining contains many millions of tiny cells, which grow, serve their
THE DIGESTIVE SYSTEM This factsheet is about bowel cancer Throughout our lives, the lining of the bowel constantly renews itself. This lining contains many millions of tiny cells, which grow, serve their
Management Of Rectal Bleeding In The Community: How A Shared Care Approach Can Benefit Dr. Daniel Lee
 Management Of Rectal Bleeding In The Community: How A Shared Care Approach Can Benefit Dr. Daniel Lee MD, MMed (S'pore), FRCS (Edin) Associate Consultant Department of Surgery 9 January 2016 Incidence
Management Of Rectal Bleeding In The Community: How A Shared Care Approach Can Benefit Dr. Daniel Lee MD, MMed (S'pore), FRCS (Edin) Associate Consultant Department of Surgery 9 January 2016 Incidence
UNDERSTANDING X-RAYS: ABDOMINAL IMAGING THE ABDOMEN
 UNDERSTANDING X-RAYS: ABDOMINAL IMAGING THE ABDOMEN Radiology Enterprises radiologyenterprises@gmail.com www.radiologyenterprises.com STOMACH AND SMALL BOWEL STOMACH AND SMALL BOWEL Swallowed air is a
UNDERSTANDING X-RAYS: ABDOMINAL IMAGING THE ABDOMEN Radiology Enterprises radiologyenterprises@gmail.com www.radiologyenterprises.com STOMACH AND SMALL BOWEL STOMACH AND SMALL BOWEL Swallowed air is a
OPIOID-INDUCED CONSTIPATION DR ANDREW DAVIES
 OPIOID-INDUCED CONSTIPATION DR ANDREW DAVIES Introduction Introduction Mean faecal weight 128 g / cap / day Mean range 51-796 g Absolute range 15-1505 g Main factors affecting mass are caloric intake,
OPIOID-INDUCED CONSTIPATION DR ANDREW DAVIES Introduction Introduction Mean faecal weight 128 g / cap / day Mean range 51-796 g Absolute range 15-1505 g Main factors affecting mass are caloric intake,
Guidelines NICE, not NICE and the Daily Mail. Dr Andy Poullis Consultant Gastroenterologist
 Guidelines NICE, not NICE and the Daily Mail 2018 Dr Andy Poullis Consultant Gastroenterologist Coeliac IBS Gall bladder polyps PEI PPI Who to test for Coeliac persistent unexplained abdominal or gastrointestinal
Guidelines NICE, not NICE and the Daily Mail 2018 Dr Andy Poullis Consultant Gastroenterologist Coeliac IBS Gall bladder polyps PEI PPI Who to test for Coeliac persistent unexplained abdominal or gastrointestinal
Medical monitoring: tests available at central hospitals
 medial monitoring: tests available at central hospitals: 1 medical monitoring: tests available at central hospitals Medical monitoring: tests available at central hospitals medial monitoring: tests available
medial monitoring: tests available at central hospitals: 1 medical monitoring: tests available at central hospitals Medical monitoring: tests available at central hospitals medial monitoring: tests available
Elderly Man With Chronic Constipation
 Elderly Man With Chronic Constipation Linda Nguyen, MD Director, Neurogastroenterology and Motility Clinical Assistant Professor Stanford University Overview Normal bowel function Defining Constipation:
Elderly Man With Chronic Constipation Linda Nguyen, MD Director, Neurogastroenterology and Motility Clinical Assistant Professor Stanford University Overview Normal bowel function Defining Constipation:
The London Gastroenterology Partnership CROHN S DISEASE
 CROHN S DISEASE What is Crohn s disease? Crohn s disease is a condition, in which inflammation develops in parts of the gut leading to symptoms such as diarrhoea, abdominal pain and tiredness. The inflammation
CROHN S DISEASE What is Crohn s disease? Crohn s disease is a condition, in which inflammation develops in parts of the gut leading to symptoms such as diarrhoea, abdominal pain and tiredness. The inflammation
Bloating, Flatulence, and
 A 45-Year-Old Man With Recurrent Abdominal Pain, Bloating, Flatulence, and Intermittent Loose Stools Anthony J. Lembo, MD Associate Professor of Medicine Harvard Medical School Director, GI Motility Laboratory
A 45-Year-Old Man With Recurrent Abdominal Pain, Bloating, Flatulence, and Intermittent Loose Stools Anthony J. Lembo, MD Associate Professor of Medicine Harvard Medical School Director, GI Motility Laboratory
Pediatric Gastroenterology Referral Guidelines
 Suggested Pre-Referral Workup This is a general suggestion of possible testing to confirm a suspected diagnosis. Although referrals will be accepted without the suggested work up being complete, to ensure
Suggested Pre-Referral Workup This is a general suggestion of possible testing to confirm a suspected diagnosis. Although referrals will be accepted without the suggested work up being complete, to ensure
8/29/2016 DIVERTICULAR DISEASE: WHAT EVERY NURSE PRACTITIONER SHOULD KNOW. LENORE LAMANNA Ed.D, ANP-C LEARNING OBJECTIVES
 DIVERTICULAR DISEASE: WHAT EVERY NURSE PRACTITIONER SHOULD KNOW LENORE LAMANNA Ed.D, ANP-C LEARNING OBJECTIVES Define Diverticular Disease Discuss Epidemiology and Pathophysiology of Diverticular disease
DIVERTICULAR DISEASE: WHAT EVERY NURSE PRACTITIONER SHOULD KNOW LENORE LAMANNA Ed.D, ANP-C LEARNING OBJECTIVES Define Diverticular Disease Discuss Epidemiology and Pathophysiology of Diverticular disease
Delorme s Operation For Rectal Prolapse
 Delorme s Operation For Rectal Prolapse Patient Information Colorectal Surgery Author ID: NM Leaflet Number: Surg 045 Version: 3.1 Name of Leaflet: Delorme s Operation for Rectal Prolapse Date Produced:
Delorme s Operation For Rectal Prolapse Patient Information Colorectal Surgery Author ID: NM Leaflet Number: Surg 045 Version: 3.1 Name of Leaflet: Delorme s Operation for Rectal Prolapse Date Produced:
Melbourne GI & Endoscopy
 1 Melbourne GI & Endoscopy Multi-disciplinary care for your patients Gastroenterology Hepatobiliary & upper gastrointestinal surgery Colorectal surgery Oncology Perioperative care One contact & one address
1 Melbourne GI & Endoscopy Multi-disciplinary care for your patients Gastroenterology Hepatobiliary & upper gastrointestinal surgery Colorectal surgery Oncology Perioperative care One contact & one address
COLORECTAL CANCER FAISALGHANISIDDIQUI MBBS; FCPS; PGDIP-BIOETHICS; MCPS-HPE
 COLORECTAL CANCER FAISALGHANISIDDIQUI MBBS; FCPS; PGDIP-BIOETHICS; MCPS-HPE PROFESSOR OF SURGERY & DIRECTOR, PROFESSIONAL DEVELOPMENT CENTRE J I N N A H S I N D H M E D I C A L U N I V E R S I T Y faisal.siddiqui@jsmu.edu.pk
COLORECTAL CANCER FAISALGHANISIDDIQUI MBBS; FCPS; PGDIP-BIOETHICS; MCPS-HPE PROFESSOR OF SURGERY & DIRECTOR, PROFESSIONAL DEVELOPMENT CENTRE J I N N A H S I N D H M E D I C A L U N I V E R S I T Y faisal.siddiqui@jsmu.edu.pk
Prescribing Guidelines on Gluten-Free products. Information for GPs
 Prescribing Guidelines on Gluten-Free products Information for GPs This guideline should be used in conjunction with NICE clinical guideline 86 Coeliac disease: recognition and assessment of coeliac disease.
Prescribing Guidelines on Gluten-Free products Information for GPs This guideline should be used in conjunction with NICE clinical guideline 86 Coeliac disease: recognition and assessment of coeliac disease.
MOVICOL Junior Powder for Solution (macrogol 3350)
 MOVICOL Junior Powder for Solution (macrogol 3350) Product Name: MOVICOL Junior Product Description: Each sachet of MOVICOL Junior contains: Macrogol 3350 Sodium chloride Sodium bicarbonate Potassium chloride
MOVICOL Junior Powder for Solution (macrogol 3350) Product Name: MOVICOL Junior Product Description: Each sachet of MOVICOL Junior contains: Macrogol 3350 Sodium chloride Sodium bicarbonate Potassium chloride
Summary of Important Points Please note that the time given to you is your arrival time and not the time of your procedure. The time taken to perform
 Summary of Important Points Please note that the time given to you is your arrival time and not the time of your procedure. The time taken to perform endoscopy procedures vary and emergency patients sometimes
Summary of Important Points Please note that the time given to you is your arrival time and not the time of your procedure. The time taken to perform endoscopy procedures vary and emergency patients sometimes
Inflammatory Bowel Disease
 Inflammatory Bowel Disease Gastroenterology Department Patient information leaflet Royal Surrey County Hospital Gastroenterology services specialises in the care and management of patients with Inflammatory
Inflammatory Bowel Disease Gastroenterology Department Patient information leaflet Royal Surrey County Hospital Gastroenterology services specialises in the care and management of patients with Inflammatory
Prepared by: Dr Katherine Brown Fir Lea House Whitecross Newquay Cornwall TR8 4LW. Date: 17/10/2016
 EXPERT MEDICAL REPORT FOR THE COURT ON BREACH OF DUTY Prepared by: Dr Katherine Brown Fir Lea House Whitecross Newquay Cornwall TR8 4LW Date: 17/10/2016 -------------------------------------------------------------------
EXPERT MEDICAL REPORT FOR THE COURT ON BREACH OF DUTY Prepared by: Dr Katherine Brown Fir Lea House Whitecross Newquay Cornwall TR8 4LW Date: 17/10/2016 -------------------------------------------------------------------
Gastroenterology. Certification Examination Blueprint. Purpose of the exam
 Gastroenterology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified gastroenterologist
Gastroenterology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified gastroenterologist
IBD 101. Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition
 IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
DOES ENTERAL NUTRITION CAUSE DIARRHOEA & LOOSE STOOLS?
 DOES ENTERAL NUTRITION CAUSE DIARRHOEA & LOOSE STOOLS? Geoffrey Axiak M.Sc. Nursing (Manchester), B.Sc. Nursing, P.G. Dip. Nutrition & Dietetics, Dip. Public Management, Cert. Clinical Nutrition (Leeds)
DOES ENTERAL NUTRITION CAUSE DIARRHOEA & LOOSE STOOLS? Geoffrey Axiak M.Sc. Nursing (Manchester), B.Sc. Nursing, P.G. Dip. Nutrition & Dietetics, Dip. Public Management, Cert. Clinical Nutrition (Leeds)
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT OF DYSPEPSIA
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT OF DYSPEPSIA o Patients of any age with ALARM signs should be referred through the 2-week referral system o Routine endoscopic investigation
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT OF DYSPEPSIA o Patients of any age with ALARM signs should be referred through the 2-week referral system o Routine endoscopic investigation
Constipation. Information for adults. GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1
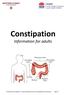 Constipation Information for adults GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1 Contents Role of the large intestine..3 Mass movements in the large intestine..4
Constipation Information for adults GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1 Contents Role of the large intestine..3 Mass movements in the large intestine..4
IBS - Definition. Chronic functional disorder of GI generally characterized by:
 IBS - Definition Chronic functional disorder of GI generally characterized by: 3500 3000 No. of Publications 2500 2000 1500 1000 Irritable Bowel syndrome Irritable Bowel Syndrome 500 0 1968-1977 1978-1987
IBS - Definition Chronic functional disorder of GI generally characterized by: 3500 3000 No. of Publications 2500 2000 1500 1000 Irritable Bowel syndrome Irritable Bowel Syndrome 500 0 1968-1977 1978-1987
Faecal Incontinence Information Leaflet THE DIGESTIVE SYSTEM
 THE DIGESTIVE SYSTEM This factsheet is about faecal incontinence Faecal (or anal) incontinence is the loss of stool, liquid or gas from the bowel at an undesirable time. Males and females of any age may
THE DIGESTIVE SYSTEM This factsheet is about faecal incontinence Faecal (or anal) incontinence is the loss of stool, liquid or gas from the bowel at an undesirable time. Males and females of any age may
Diagnosis and Management of Irritable Bowel Syndrome (IBS) For the Primary Care Provider
 Diagnosis and Management of Irritable Bowel Syndrome (IBS) For the Primary Care Provider Elizabeth Coss, MD General Gastroenterologist Audie Murphy Veterans Hospital UT Health This presentation does not
Diagnosis and Management of Irritable Bowel Syndrome (IBS) For the Primary Care Provider Elizabeth Coss, MD General Gastroenterologist Audie Murphy Veterans Hospital UT Health This presentation does not
The Digestive System or tract extends from the mouth to the anus.
 The Digestive System or tract extends from the mouth to the anus. FUNCTION The Digestive System breaks down and absorbs food materials e.g. amino acids, glucose DEFINITIONS: Ingestion: Ingestion is the
The Digestive System or tract extends from the mouth to the anus. FUNCTION The Digestive System breaks down and absorbs food materials e.g. amino acids, glucose DEFINITIONS: Ingestion: Ingestion is the
IBD 101. Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition
 IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
PATIENT HISTORY FORM
 PATIENT HISTORY FORM Date: Page 1 of 5 Last Name: First Name: Middle Initial: Referred By: Age: Primary Care Doctor: Please provide name(s) of other physician(s) that you have visited within the last year:
PATIENT HISTORY FORM Date: Page 1 of 5 Last Name: First Name: Middle Initial: Referred By: Age: Primary Care Doctor: Please provide name(s) of other physician(s) that you have visited within the last year:
Crohn's Disease. What causes Crohn s disease? What are the symptoms?
 Crohn's Disease Crohn s disease is an ongoing disorder that causes inflammation of the digestive tract, also referred to as the gastrointestinal (GI) tract. Crohn s disease can affect any area of the GI
Crohn's Disease Crohn s disease is an ongoing disorder that causes inflammation of the digestive tract, also referred to as the gastrointestinal (GI) tract. Crohn s disease can affect any area of the GI
