International Journal of Health Sciences and Research ISSN:
|
|
|
- Bruno Bennett
- 5 years ago
- Views:
Transcription
1 International Journal of Health Sciences and Research ISSN: Original Research Article Effect of Pelvic Floor Muscle Training Based on Severity of Incontinence on Dr. Zarna Ronak Shah 1, Dr. Priyanshu V. Rathod 2 1 Junior Lecturer, SBB College of Physiotherapy, V.S.General Hospital, Ahmedabad. 2 Principal, School of Physiotherapy, R.K.University, Rajkot. Corresponding Author: Dr. Zarna Ronak Shah ABSTRACT Background: Urinary Incontinence is widely prevalent in females but poorly diagnosed. Several studies all around the world have already proven the effect of physiotherapy management in females with stress urinary incontinence. In India, since last 10 years the awareness and education regarding physiotherapy in SUI has increased. Still limited evidences in India, and acceptance of this problem by majority of females lead to low level of evidence based practice. The cultural, economic and religious scenario of Indian women is very different than that of western or other developed countries. So there is immense need to work on these areas, define a protocol of exercise for them and to see the efficacy of this protocol on incontinence episodes in women with SUI. Aim: To evaluate the effect of Pelvic Floor Muscle Training (PFMT) based on severity of incontinence on incontinence episodes in women with Stress Urinary Incontinence. Materials and Methods: Total 65 subjects were recruited according to inclusion criteria for an experimental study which was set up at SBB College of Physiotherapy, V.S.General Hospital Campus and Shruti nursing home, Naranpura, Ahmedabad. Each subject received 6 weeks of home based PFMT based on severity of incontinence which was decided by Incontinence Severity Index. Pre and post data were taken and further analysis was done using SPSS The outcome measure used was voiding diary (Number of incontinence episodes per week and frequency of micturition per day). Results and Discussion: Level of significance was set at 5%. Wilcoxon test was used to compare the pre and post data for all the subjects. The hypothesis is proven with Z = and Z = for frequency and number of leakages respectively. p < shows highly significant difference between two groups. Conclusions: Six weeks home based PFMT based on severity of incontinence is effective in reducing no. of leakages per week and frequency of micturition per day in female with SUI. Key words: Pelvic Floor Muscle Training, No. of leakages, Frequency of micturition, voiding diary, Stress Urinary Incontinence. INTRODUCTION Stress Urinary Incontinence (SUI) is the non-volitional leakage of urine on effort or exertion, sneezing, coughing, or laughing. [1] These activities increase the intra-abdominal pressure. This overcomes the sphincter closure mechanism when a bladder contraction is not present. Weak pelvic floor muscles (PFM) are frequently the cause behind the leakage of urine in such condition. According to most of the studies, the prevalence of urinary incontinence in [2] women varies between 10 to 40%. Approximately 50 million people worldwide suffer from UI wherein a woman to man ratio is 2:1. [3] In a survey done in Asia, prevalence of UI in India was 12%. [4] A International Journal of Health Sciences & Research ( 120
2 study done in Tamil Nadu in 2009 has estimated that amongst 197 women surveyed about 41(20.8%) were found to have UI. [5] Out of these 41 women more than 50% had SUI. Pelvic Floor Muscle Training (PFMT) should be the first line treatment for stress incontinence, as it has no serious adverse effects. However, the training needs proper instruction and close follow-up to be effective. [6] Several studies all around the world have already proven the effect of physiotherapy management in females with SUI. In India, since last 10 years the awareness and education regarding physiotherapy in SUI has increased. Still limited evidences in India, and acceptance of this problem by majority of females lead to low level of evidence based practice. The cultural, economic and religious scenario of Indian women is very different than that of western or other developed countries. So there is immense need to work on these areas, define a protocol of exercise for them and to see the efficacy of this protocol on females with SUI. So, the objective of the study was to see the effect of PFMT based on severity of incontinence on incontinence episodes in women with SUI. It has been hypothesised that the PFMT given in this study is effective in reducing the no of leakages per week and frequency of micturition per day in female with SUI. METHODOLOGY It was an experimental clinical trial where source of data was department of Obstetrics and Gynaecology, Sheth Chinai maternity home, V.S.General Hospital and menopause health club of Ahmedabad. Apart from this, several awareness programs were conducted by the principal investigator to get maximum subjects from different parts of Ahmedabad. Many private gynaecologists also referred patients with SUI. The data was primary which was collected by the principal investigator. This study was conducted from January 2013 to Dec 2015.The intervention period was of 6 weeks. Subjects were asked to perform the exercises at home for one to three times in a day depending on severity of incontinence which was decided by Incontinence Severity Index. [7,8] The females with confirm case of stress urinary incontinence (confirmation of diagnosis was made by cough stress test either by gynaecologist or principal investigator) and having slight, moderate and severe incontinence as per Incontinence Severity Impact scale [7,8] were included. Female with prolapsed perineal organs, neurogenic bladder, pregnancy, Acute Urinary Tract Infection and Incontinence Severity Index score 0 (No incontinence) or 12 (very severe incontinence) were excluded. MINI tab software was used to decide the sample size. Difference of means of pre and post no. of leakages (17-6 = 11) taken from pilot study and keeping 80% power of study sample size was calculated and found to be 33. Sample size recorded in the study is 73 by purposive sampling. Procedure Ethical clearance from the local ethics committee of S.B.B. College of physiotherapy was taken in Dec, 2012 (PTC/IEC/59/ ) under a broad titled study Efficacy of Physiotherapy Management in women with SUI. The study has passed through Institutional Review Board of RK University, Rajkot and has been approved. The study is part of a broad study Efficacy of Physiotherapy Management in women with SUI which has been registered under CTRI. The registration no. of the trial is CTRI/2016/12/ International Journal of Health Sciences & Research ( 121
3 Total 140 females reported having urinary leakage problem. Subjective screening was done by screening form made by principal investigator. Out of them 50 subjects screened out due to urinary problems other than incontinence Remaining 90 females were recruited for objective screening by ISI and clinical confirmation by cough test Out of them 15 were excluded (7 cough test negative, 5 ISI score= 0, 3 ISI score = 12) Remaining 75 females with confirmed diagnosis of SUI were included (45 subjects by primary investigators and 30 by gynaecologist). Informed consent for participation in study was taken and PT management was given for 6 weeks. Out of them 2 subjects withdrew due to lack of interest Total 65 subjects finished the study protocol and data was analysed (8 subjects of pilot study are excluded) Fig 1: Flow chart of procedure The ISI is an ordinal scale having two questions regarding the frequency of leakage and quantity of leakage. The scale was translated in Gujarati by principal investigator. According to the answers by patients, the score is calculated by multiplying two scores of two questions. The score ranges from 0 to 12, 0 meaning no incontinence and 12 meaning very severe incontinence. 1 2 score means slight, 3 4 means moderate and 6 8 means severe incontinence. Sandvik et al in 1993 have validated the scale to measure severity of incontinence in women with urinary incontinence. [7,8] Subjects with score 0 and score 12 on ISI were excluded. The screened subjects were then made to perform cough test. Cough test was done with full bladder. Subjects were asked to cough in crook lying position and urine leakage was observed. Leakage of urine while coughing indicates positive cough test. The cough test has shown good sensitivity and specificity in the diagnosis of SUI. [9-11] The clinically confirmed cases of SUI (positive cough test) were then explained and asked to sign the consent form and then included in the study and were given 6 weeks home based physiotherapy management which included pelvic floor muscle training and life style modification. The treatment was given at different places according to the convenience of subjects. These places include S.B.B. college of Physiotherapy and other private set ups of gynaecologists. Before starting the main study a pilot study was done on 8 subjects. These subjects were asked to keep records of frequency of micturition and no. of leakages on a self-made voiding diary. It was observed that self-made diaries were very different for all subjects and so to maintain uniformity and objectivity, voiding diaries were provided to all subjects after the pilot study. These 8 pilot study subjects were not included in the study. Subjects were given 7 days voiding diary prepared in Gujarati language and were asked to record their no. of leakages and frequency of micturition at first and last week of treatment. The physiotherapy management based on severity of incontinence was given in the International Journal of Health Sciences & Research ( 122
4 form of pelvic floor muscle training and lifestyle modification as follows: Life style modification: o Educating women with severe (ISI = 6 8) incontinence to wear diapers. o Avoiding caffeine, and excessive fluid intake. o Weight control exercises like walking or jogging. o Asking them to go to void for every 2 hours. o Ergonomic advices of lifting heavy weight (>5 kg) so that intra abdominal pressure does not increase much and thus avoiding instances of incontinence. o Performing Pelvic Floor Muscle Training (PFMT) whenever they find time e.g. waiting at traffic signal. Pelvic floor muscle training protocol o 5 repetitions of general stretching and warm up for pelvic floor muscles and hip adductors (butterfly posture). o 10 repetition of voluntary pelvic floor muscle contraction with 5 second hold and 10 second rest, progress at 2 weeks to 10 second hold and 20 second rest. o 10 repetitions of isometrics of hip adductors and irradiation to pelvic floor muscle with 5 sec hold and 10 sec rest, progress to 10 sec hold and 20 sec rest. o 5 repetitions of transverse abdominis muscle contraction and pelvic floor muscle contraction simultaneously, 5 sec hold and 10 sec rest. o Cool down with slow stretching of adductors and perineal muscles. This treatment was properly explained and given under supervision on the very first day. The subjects were asked to carry out the treatment at home. The subjects who were slight incontinent (ISI = 1 2) were asked to perform one session a day, moderate incontinent (ISI 3 4) two sessions a day and severe incontinent (ISI 6 8) three sessions a day. Pre-treatment readings were taken at first day whereas post treatment readings were taken after 6 weeks. Though the subjects were asked to carry out regular exercises every day for 6 weeks, exercises for 5 to 6 days a week were considered. The pelvic floor muscle contractions were first taught in crook lying position. On the very first day, the physiotherapist exposed the part and checked for proper contraction. The patients were explained well how to contract the pelvic floor muscles. Once mastered, subject was asked to practice this in sitting position. Figure 2: Pelvic floor muscle contraction Figure 3: Transverse abdominis contraction and pelvic floor muscle contraction simultaneously The pelvic floor muscle contraction along with transverse abdominis contraction was performed first in lying and then in sitting. It is believed that there is cocontraction of transverses abdominis muscle during PFM contraction. [12] So, transverses International Journal of Health Sciences & Research ( 123
5 abdominis muscle contraction with PFM contraction is now incorporated into treatment protocols. [13] For this reason, transverses abdominis contraction exercise was added with PFM exercise. Figure 4: Hip adductor isometric and pelvic floor muscle contraction Figure 5: Progression in sitting The isometric exercises for hip adductor muscles were given in crook lying. Subjects were asked to press pillow between the two knees. It is believed that isometric hip adductors irradiate the contraction to pelvic floor muscles and pelvic floor muscles also contract along with it due to their biomechanical relationship. Though very less evidences are available for this, Hulme and colleagues have introduced Kegel plus hip muscle exercises including obturator muscle resisted exercise in Beyond Kegels protocol for incontinence and have proven them to be effective. [14-16] The pelvic floor muscles contraction is performed by contracting and relaxing the muscles of the pelvic floor. A correct contraction consists of a squeeze around the pelvic opening followed by an inward cranial lift. Many patients cannot perform PFM contraction easily at first time. Evidences also report difficulty in pelvic floor muscle contraction at 1 st consultation. [17,18] For such patients, vaginal palpation method was used by per vaginal finger insertion and was taught proper contractions. They were also asked to palpate their perineum while performing the exercises. The following outcome measures were taken: 1. Frequency of micturition per day 2. No. of leakages per week RESULTS Statistical analysis was done using SPSS 21.0 version. The parameters used in the study are ordinal data and so, nonparametric tests were used to analyse these data. Wilcoxon test was applied to see the pre-post difference. Table 1: Demographic details of the subjects Parameter Mean / Median SD Age (years) 1.17 BMI kg/m Number of deliveries 2 (median) ISI score 3 (median) Table 2: Difference within the group Outcome measures No. of subjects Pre treatment Post treatment Z value p value (Mean/ Median) (Mean/ Median) Frequency of micturition <0.001 No. of leakages <0.001 Table 3: Comparison between different severity groups for pre treatment-post treatment difference Outcome measure Group no. of subjects Mean/ Median SD p value Significance Frequency of micturition No No. of leakages Yes (Group 1 Slight, Group 2 Moderate and Group 3 Severe) International Journal of Health Sciences & Research ( 124
6 Table 4 : Comparison between different age groups for pre-post treatment difference. Outcome measure Group no. of subjects Mean SD p value Significance Frequency of micturition No No. of leakages No (Group 1: years, Group 2: years, Group 3: year) Table 5: Comparison between different BMI groups for pre-post treatment difference. Outcome measure Group no. of subjects Mean SD p value Significance Frequency of micturition No No. of leakages No (Group 1 Underweight, Group 2 Normal, Group 3 Overweight) Table 6: Comparison between different parity groups for pre-post treatment difference. Outcome measure Group no. of subjects Mean SD p value Significance Frequency of micturition No No. of leakages No (Group 1: 0 2 deliveries, Group 2: >2 deliveries) DISCUSSION The present study aimed to prove the effectiveness of Pelvic Floor Muscle Training based on severity of incontinence on incontinence episodes in females with SUI. Total 65 females with SUI were included in the study. These 65 females were clinically confirmed cases of SUI. Urodynamic testing was not done due to financial reasons. The subjects were given 6 weeks home based pelvic floor exercises as taught along with tips of lifestyle modifications as mentioned in methodology. The median frequency of micturition per day was 10 pre treatment and was 8 post treatment. This showed 20% improvement in frequency of micturition post treatment. The median no. of leakages per week was 3 pre-treatment, which was reduced to 1 episode per week after 6 weeks of physiotherapy. This shows 67% improvement in no. of leakages per week. This shows that leakage episodes decrease with physiotherapy management of 6 weeks. The incontinent patients had more complaints of leakage episodes than frequency. Increase in frequency does not bother them much but leakage caused several issues like wet clothes, restriction for social activities, interference in day to day life and participation restriction in society. Many women in developed countries manage to attend social gatherings wearing diapers or sanitary pads. This is not common in Indian cultural set up and so, advice to wear diaper or sanitary pad while going out was given as a part of life style modification in this study so the quality of life does not compromise. The frequency and leakage episodes were noted in voiding diary provided by the investigator to the subjects. The subjects were properly explained how to fill in the diary. Many subjects reported no leakage in a day and one or two episodes in a week and so 7 days voiding diary was chosen. The 1 week voiding diary has high test-retest reliability for micturition frequency and incontinence episodes (r = 0.91). [19] Four subjects were found to have 0 leakages per week on voiding diary but the complaint was there. It is highly possible that these subjects might not have leaked in the week when they recorded but may have leaked in some other weeks or they might have forgotten to tick in voiding diary. Other possibility of no leak may be due to the instructions to go for void every 2 hourly (timed voiding) which may have reduced their leakage episodes. International Journal of Health Sciences & Research ( 125
7 33 out of 65 subjects had zero leakages in voiding diary after 6 weeks and so we considered them as 100% cured of incontinence. 51% such subjects have been cured of incontinence episodes after 6 weeks of physiotherapy management. We can say that 51% subjects became continent. The hypothesis is proven with Z = and Z = for frequency and number of leakages respectively. p <0.001 shows highly significant difference between two groups. There was an improvement in the frequency of micturition after the physiotherapy intervention which is in accordance to the findings of Pages et al [20] and Kafri et al. Pages et al concluded that 4 weeks of group Physical Therapy in the form of pelvic floor exercises resulted in reduced daytime and nocturnal urinary frequency. Kafri [21] et al too reported the same after comparing the residual effects of a 3 month rehabilitation program and a standardized drug regime for Urge Urinary Incontinence 21 months after the intervention. In the long rehabilitation, patients maintained and also improved what achievements they had made in the intervention period while the patients on drug therapy deteriorated to initial preintervention values in urinary frequency. The improvement in the frequency of micturition can be attributed to the increase in strength of the PFM. Also, the lifestyle modifications that were taught like avoiding excessive caffeine and fluid intake may cause the improvement. However, this is contradictory to the [22] findings of Yoon HS et al who concluded bladder training to be more effective than pelvic muscle exercises in reducing urinary frequency and in increasing voided volume. However, the pelvic muscles exercise group showed greater improvement in increasing the peak and average pressures of pelvic muscle contraction. A Cochrane review done in 2010 by Dumoulin C [23] concluded that PFMT is more beneficial compared to no treatment, placebo drug, or inactive control treatments for females with SUI, MUI or UUI. Females given PFMT were more probable at reporting resolution or improvement, better QOL, lesser leakage episodes in a day and have less urine leakage on short pad tests than controls. The trials recommended that efficacy of the treatment (especially selfreported resolution/improvement) may be higher in females with SUI who have participated in a supervised PFMT program for a minimum of three months. The PFMs are helpful in maintaining continence. Activities like coughing, sneezing or laughing affect the continence system, and cause the intra-abdominal pressure to rise. This pressure is then transferred to the urethra to increase closure. But this happens only when the urethra maintains its position between the pubic symphysis (PS) and the pelvic floor. Measurements of urethral trajectory and acceleration during functional tasks such as coughing have concluded that women with SUI demonstrate a larger excursion of the urethra and/or anorectal angle (ARA) during coughing manoeuvres than their continent counterparts. So, it may be stated that the urethra is not held at its normal position posterior to the pubic symphysis to safeguard its compression against the pelvic floor during times of an increased intraabdominal pressure, which also suggests that females with SUI do not have effective endopelvic fascia (pubourethral ligaments) and/or have PFMs that are not fast enough or incapable to offer urethral support so as to press it close. A study by McLean L et al [24] in 2013 demonstrated that PFMT under supervision decreases mobility of the urethra during coughing and leads to an increase in the urethral cross-sectional area, but does not decrease the capacity of the bladder neck to extend during maximal effort valsalva manoeuvres. This shows that PFMT effectively reduces urethral excursion and enhances urethral sphincter cross-sectional area in women with SUI. International Journal of Health Sciences & Research ( 126
8 This probably contributes to a decline in the number of leakage episodes. CONCLUSION Six weeks home based PFMT based on severity of incontinence is effective in reducing no. of leakages per week and frequency of micturition per day in female with SUI. Future scopes for research: Subjects should be given adherence diaries and treatment adherence should be added as one of the parameter. REFERENCES 1. Thayer C, Cohen A. Urinary Incontinence in women guidelines, Group health Cooperative Hunskaar S, Burgio K, Diokno AC,Herzog AR, Hjalmas K, Lapitan MC. Epidemiology and natural history of urinary incontinence (UI).In: Abrams P, Cardozo L, Khoury S editor(s). Incontinence. 2 nd Edition. Health Publication Ltd, Bo Eun Kwon, Gi Yon Kim, Youn Jung Son et al Quality of life of women with urinary incontinence: A systematic literature review. International Neurourol Journal. 14(3): Ananias C. Diokno Incidence and prevalence of stress urinary incontinence. Advanced Studies in Medicine. 3(8E), S824 S Baranitharan R, Mahalakshmi V. Prevalence of type of urinary incontinence and their association with types of delivery. Indian Journal of Physiotherapy and Occupational Therapy 2009 Apr;3(4): Bo K. Pelvic floor muscle training in treatment of female stress urinary incontinence, pelvic organ prolapse and sexual dysfunction. World J Urol. 2012; 30: Sandvik H, Hunskaar S et al. Validation of a severity index in female urinary incontinence and its implementation in an epidemiological survey. J Epidemiol Community Health 1990; 47: Sandvik H, Selm A et al. A severity index for epidemiological surveys of female urinary incontinence: comparison with 48 hours pad weighing tests. Neurourol Urodyn. 2000; 19: Swift SE, Ostergard DR. Evaluation of current urodynamic test methods in the diagnosis of genuine stress incontinence. Obstetrics and Gynecology. 1995; 86: Scotti RJ, Myers DL (1993) A comparison of the cough stress test and single-channel cystometry with multichannel urodynamic evaluation in genuine stress incontinence. Obstet Gynecol 81: Wall LL, Wiskind AK, Taylor PA. Simple bladder filling with a cough stress test compared with subtracted cystometry for the diagnosis of urinary incontinence. American Journal of Obstet Gynecol. 1994; 171: Knight S, Laycock J, Naylor D: Evaluation of neuromuscular electrical stimulation in the treatment of genuine stress incontinence. Physiotherapy 1998, 84(2): Sapsford, R R, Hodges, P W, Richardson, C et al. Co activation of the abdominal and pelvic floor muscles during voluntary exercises, Neurourology and Urodynamics. 2001; 20: Donahoe-Fillmore B, Chorny W, Brahler CJ, Ingley A, Kennedy J, Osterfeld V. A comparison of two pelvic floor muscle training programs in females with stress urinary incontinence: a pilot study. The Journal of applied research. 2012; 11(2): Bo K. Hagen RH, Kvarstein B, Jorgensen j, Larsen S. pelvic floor muscle exercise for the treatment of female stress urinary incontinence: III. Effects of two different degrees of pelvic floor muscle exercises. Neurourol urodun. 1990; 9: Hulme, JA. Beyond kegels: Fabulous Four Exercises and more to prevent and treat incontinence. 3 rd Ed. Missoula Mt: Phoenix publishing co; Susanne Ahlund, Birgitta Nordgren, Eva Lotta Wilander, et al. Is home based pelvic floor muscle training International Journal of Health Sciences & Research ( 127
9 effective in treatment of urinary incontinence after birth in primiparous women? A randomized controlled trial. cite this article as doi: /aogs Benvenuti F, Caputo GM, Bandinelli S, Mayer F, Biagini C, Sommavilla A. Reeducative treatment of female genuine stress incontinence. Am J Phys Med. 1987; 66(4): Wyman JF, Choi SC, Harkins SW, Wilson MR, Fantl JA. The urinary diary in evaluation of incontinent women: A test-retest analysis. Obstetrics and Gynecology. 1988; 71: Pages IH, Jahr S, Schaufele MK, Conradi E: Comparative analysis of biofeedback and physical therapy for treatment of urinary stress incontinence in women. Am J Phys Med Rehabil. 2001; 80: Kafri R, Shames J, Raz M, Katz-Leurer M. Rehabilitation versus drug therapy for urge urinary incontinence: long-term outcomes. International Urogynecology Journal Jan. 19 (1): Yoon HS, Song HH, Ro YJ. A comparison of effectiveness of bladder training and pelvic muscle exercise on female urinary incontinence. International Journal of Nursing Studies.2003 Jan; 40(1): Dumoulin C, Hay-Smith J (2010). "Pelvic floor muscle training versus no treatment, or inactive control treatments, for urinary incontinence in women Cochrane Database Syst Rev (1): CD doi: / cd pub2. PMID McLean L, Varette K, Gentilcore- Saulnier E, Harvey MA, Baker K,Sauerbrei E. Pelvic Floor Muscle Training in Women With Stress Urinary Incontinence Causes Hypertrophy of the Urethral Sphincters and Reduces Bladder Neck Mobility During Coughing. Neurourol Urodyn November; 32(8): How to cite this article: Shah ZR, Rathod PV. Effect of pelvic floor muscle training based on severity of incontinence on incontinence episodes in women with stress urinary incontinence. Int J Health Sci Res. 2017; 7(10): *********** International Journal of Health Sciences & Research ( 128
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Screening of Immediate Post Partum Females for Urinary Incontinence Ami Vishal Mehta 1, Zarna
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Screening of Immediate Post Partum Females for Urinary Incontinence Ami Vishal Mehta 1, Zarna
URINARY INCONTINENCE AMONG OBESE WOMEN: A CROSS- SECTIONAL STUDY
 WORLD JOURNAL OF PHARMACY AND PHARMACEUTICAL SCIENCES Aisha et al. SJIF Impact Factor 6.647 Volume 6, Issue 9, 1384-1391 Research Article ISSN 2278 4357 URINARY INCONTINENCE AMONG OBESE WOMEN: A CROSS-
WORLD JOURNAL OF PHARMACY AND PHARMACEUTICAL SCIENCES Aisha et al. SJIF Impact Factor 6.647 Volume 6, Issue 9, 1384-1391 Research Article ISSN 2278 4357 URINARY INCONTINENCE AMONG OBESE WOMEN: A CROSS-
PREVENTING URINARY INCONTINENCE through PELVIC FLOOR REHABILITATION in DISABLED ELDERLY
 PREVENTING URINARY INCONTINENCE through PELVIC FLOOR REHABILITATION in DISABLED ELDERLY Paolo DI BENEDETTO Lecturer, Tor Vergata University, Rome, Italy Former Director of Rehabilitation Department Institute
PREVENTING URINARY INCONTINENCE through PELVIC FLOOR REHABILITATION in DISABLED ELDERLY Paolo DI BENEDETTO Lecturer, Tor Vergata University, Rome, Italy Former Director of Rehabilitation Department Institute
INCONTINENCE. Continence and Pelvic Floor Rehabilitation TYPES OF INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE 11/08/2015
 INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
Bill Landry BScPT, BScH, MCPA, CAFCI Family Physiotherapy Centre of London
 Bill Landry BScPT, BScH, MCPA, CAFCI blandry@fpclondon.com Family Physiotherapy Centre of London Objectives To describe the scope of post-prostatectomy incontinence To describe what s been done To provide
Bill Landry BScPT, BScH, MCPA, CAFCI blandry@fpclondon.com Family Physiotherapy Centre of London Objectives To describe the scope of post-prostatectomy incontinence To describe what s been done To provide
Pelvic Floor Exercise. Brigi0e Fung Physiotherapist
 Pelvic Floor Exercise Brigi0e Fung Physiotherapist Treatment for urinary incontinence Pelvic floor muscle exercise (Kegel, 1948) Bladder retraining Behaviour modification Treatment for urinary incontinence
Pelvic Floor Exercise Brigi0e Fung Physiotherapist Treatment for urinary incontinence Pelvic floor muscle exercise (Kegel, 1948) Bladder retraining Behaviour modification Treatment for urinary incontinence
Effects of Combined Pelvic Floor Muscle Exercises in Patient with Urinary Incontinence
 MACROJOURNALS The Journal of MacroTrends in Health and Medicine Effects of Combined Pelvic Floor Muscle Exercises in Patient with Urinary Incontinence Vjollca Ndreu*, Fatjona Kamberi*, Enkeleda Sinaj*,
MACROJOURNALS The Journal of MacroTrends in Health and Medicine Effects of Combined Pelvic Floor Muscle Exercises in Patient with Urinary Incontinence Vjollca Ndreu*, Fatjona Kamberi*, Enkeleda Sinaj*,
Effect of PFMT: Kegel, LA, USA Pelvic floor rehabilitation. Problems with systematic reviews / meta-analysis 15/10/2013
 Exercise programs for the pelvic floor evidence for an optimal program? ICS Barcelona PT-Roundtable 2013 Kari Bø Professor, PhD PT, Exercise Scientist Affiliations to disclose: Enter Organisation/relationship
Exercise programs for the pelvic floor evidence for an optimal program? ICS Barcelona PT-Roundtable 2013 Kari Bø Professor, PhD PT, Exercise Scientist Affiliations to disclose: Enter Organisation/relationship
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Effect of Tanzberger Exercises in Women with Stress Urinary Incontinence Heena A. Bhatt 1*,
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Effect of Tanzberger Exercises in Women with Stress Urinary Incontinence Heena A. Bhatt 1*,
Uterus (Womb) Rectum. Another problem could be the sensation of something coming down at the birth canal or back passage (prolapse).
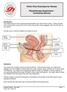 Pelvic Floor Exercises for Women Physiotherapy Department Continence Service Introduction This leaflet tells you how to exercise and strengthen your pelvic floor muscles. These muscles form a broad sling
Pelvic Floor Exercises for Women Physiotherapy Department Continence Service Introduction This leaflet tells you how to exercise and strengthen your pelvic floor muscles. These muscles form a broad sling
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives
 Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
Urinary Incontinence for the Primary Care Provider
 Urinary Incontinence for the Primary Care Provider Diana J Scott FNP-BC https://youtu.be/gmzaue1ojn4 1 Assessment of Urinary Incontinence Urge Stress Mixed Other overflow, postural, continuous, insensible,
Urinary Incontinence for the Primary Care Provider Diana J Scott FNP-BC https://youtu.be/gmzaue1ojn4 1 Assessment of Urinary Incontinence Urge Stress Mixed Other overflow, postural, continuous, insensible,
Pelvic Floor and More.. Urinary Continence. Urinary Incontinence. Normal Bladder Function
 Pelvic Floor and More.. Jo Pitts Women s and Men s Health Physiotherapist Milton Keynes University Hospital Women s and Men s Health Physiotherapy at MKUH Pregnancy-related back and pelvic girdle pain
Pelvic Floor and More.. Jo Pitts Women s and Men s Health Physiotherapist Milton Keynes University Hospital Women s and Men s Health Physiotherapy at MKUH Pregnancy-related back and pelvic girdle pain
Effect of Abdominal Versus Pelvic Floor Muscles Exercises on Vaginal and Leak Point Pressures in Mild Stress Urinary Incontinence in Obese Women
 Effect of Abdominal Versus Pelvic Floor Muscles Exercises on Vaginal and Leak Point Pressures in Mild Stress Urinary Incontinence in Obese Women 1 Dalia M. Kamel 1 Ali A. Thabet 2 Sayed A. Tantawy and
Effect of Abdominal Versus Pelvic Floor Muscles Exercises on Vaginal and Leak Point Pressures in Mild Stress Urinary Incontinence in Obese Women 1 Dalia M. Kamel 1 Ali A. Thabet 2 Sayed A. Tantawy and
Female Urinary Incontinence: What It Is and What You Can Do About It
 Female Urinary Incontinence: What It Is and What You Can Do About It Urogynecology Patient Information Sheet What is Urinary Incontinence? Stress Incontinence is a leakage of urine that occurs, for example,
Female Urinary Incontinence: What It Is and What You Can Do About It Urogynecology Patient Information Sheet What is Urinary Incontinence? Stress Incontinence is a leakage of urine that occurs, for example,
The development of a questionnaire to measure the severity of symptoms and the quality of life before and after surgery for stress incontinence
 BJOG: an International Journal of Obstetrics and Gynaecology November 2003, Vol. 110, pp. 983 988 The development of a questionnaire to measure the severity of symptoms and the quality of life before and
BJOG: an International Journal of Obstetrics and Gynaecology November 2003, Vol. 110, pp. 983 988 The development of a questionnaire to measure the severity of symptoms and the quality of life before and
Management of Female Stress Incontinence
 Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION What is the effect of retraining diaphragmatic, deep abdominal, and pelvic floor muscle (PFM) coordinated function in a graded, multi-stage, supervised
CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION What is the effect of retraining diaphragmatic, deep abdominal, and pelvic floor muscle (PFM) coordinated function in a graded, multi-stage, supervised
Dynamic rehabilitative ultrasound for pelvic floor disorders Introduction in techniques and hands-on-workshop
 Dynamic rehabilitative ultrasound for pelvic floor disorders Introduction in techniques and hands-on-workshop Bärbel Junginger, B.Sc. /physiotherapist, manualtherapist (IFOMPT) Kaven Baessler, MD, PhD
Dynamic rehabilitative ultrasound for pelvic floor disorders Introduction in techniques and hands-on-workshop Bärbel Junginger, B.Sc. /physiotherapist, manualtherapist (IFOMPT) Kaven Baessler, MD, PhD
ORIGINAL ARTICLE. Judith A. Thompson & Peter B. O Sullivan & N. Kathryn Briffa & Patricia Neumann
 Int Urogynecol J (2007) 18:779 786 DOI 10.1007/s00192-006-0225-4 ORIGINAL ARTICLE Comparison of transperineal and transabdominal ultrasound in the assessment of voluntary pelvic floor muscle contractions
Int Urogynecol J (2007) 18:779 786 DOI 10.1007/s00192-006-0225-4 ORIGINAL ARTICLE Comparison of transperineal and transabdominal ultrasound in the assessment of voluntary pelvic floor muscle contractions
Using Physiotherapy to Manage Urinary Incontinence in Women
 Using Physiotherapy to Manage Urinary Incontinence in Women Bladder control problems are common, and affect people of all ages, genders and backgrounds. These problems are referred to as urinary incontinence
Using Physiotherapy to Manage Urinary Incontinence in Women Bladder control problems are common, and affect people of all ages, genders and backgrounds. These problems are referred to as urinary incontinence
Diagnosis and Treatment of Urinary Incontinence. Urinary Incontinence
 Diagnosis and Treatment of Urinary Incontinence Leslee L. Subak, MD Professor Obstetrics, Gynecology & RS Epidemiology, Urology University of California, San Francisco Urinary Incontinence Common - 25%
Diagnosis and Treatment of Urinary Incontinence Leslee L. Subak, MD Professor Obstetrics, Gynecology & RS Epidemiology, Urology University of California, San Francisco Urinary Incontinence Common - 25%
Urinary Incontinence. Lora Keeling and Byron Neale
 Urinary Incontinence Lora Keeling and Byron Neale Not life threatening. Introduction But can have a huge impact on quality of life. Two main types of urinary incontinence (UI). Stress UI leakage on effort,
Urinary Incontinence Lora Keeling and Byron Neale Not life threatening. Introduction But can have a huge impact on quality of life. Two main types of urinary incontinence (UI). Stress UI leakage on effort,
John Laughlin 4 th year Cardiff University Medical Student
 John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
The effectiveness of pelvic floor exercises on symptoms in females with stress urinary incontinence
 Medical Communication Biosci. Biotech. Res. Comm. 11(4): 681-686 (2018) The effectiveness of pelvic floor exercises on symptoms in females with stress urinary incontinence Nitesh Malhotra 1 * and Aksh
Medical Communication Biosci. Biotech. Res. Comm. 11(4): 681-686 (2018) The effectiveness of pelvic floor exercises on symptoms in females with stress urinary incontinence Nitesh Malhotra 1 * and Aksh
Pelvic Floor Muscle Exercises and Advice for Men
 Pelvic Floor Muscle Exercises and Advice for Men (formerly ACPWH) Useful resources Websites Pelvic Obstetric & Gynaecological Physiotherapy - pogp.csp.org.uk Bladder and Bowel Foundation - www.bladderandbowelfoundation.org
Pelvic Floor Muscle Exercises and Advice for Men (formerly ACPWH) Useful resources Websites Pelvic Obstetric & Gynaecological Physiotherapy - pogp.csp.org.uk Bladder and Bowel Foundation - www.bladderandbowelfoundation.org
restore the pelvic floor
 restore the pelvic floor A non-invasive, safe, and effective treatment that improves pelvic floor muscle contraction and diminishes urine loss in pelvic floor disorders 1 has changed my life for the better.
restore the pelvic floor A non-invasive, safe, and effective treatment that improves pelvic floor muscle contraction and diminishes urine loss in pelvic floor disorders 1 has changed my life for the better.
How big is the problem? Incontinence in numbers
 How big is the problem? Incontinence in numbers Ian Milsom Gothenburg Continence Research Center (GCRC) Sahlgrenska Academy, Gothenburg University Gothenburg, Sweden If UI where a country, 2 it would be
How big is the problem? Incontinence in numbers Ian Milsom Gothenburg Continence Research Center (GCRC) Sahlgrenska Academy, Gothenburg University Gothenburg, Sweden If UI where a country, 2 it would be
The diagnostic strength of the 24-h pad test for self-reported symptoms of urinary incontinence in pregnancy and after childbirth
 Int Urogynecol J (8) 19:525 53 DOI.7/s192-7-472-z ORIGINAL ARTICLE The diagnostic strength of the 24-h pad test for self-reported symptoms of urinary incontinence in pregnancy and after childbirth Jacobus
Int Urogynecol J (8) 19:525 53 DOI.7/s192-7-472-z ORIGINAL ARTICLE The diagnostic strength of the 24-h pad test for self-reported symptoms of urinary incontinence in pregnancy and after childbirth Jacobus
IMPROVING URINARY INCONTINENCE
 IMPROVING URINARY INCONTINENCE INFORMATION FOR OLDER ADULTS, FAMILIES, AND CAREGIVERS READ THIS PAMPHLET TO LEARN: What Urinary Incontinence is. How to Manage Urinary Incontinence. What Pelvic Floor Exercises
IMPROVING URINARY INCONTINENCE INFORMATION FOR OLDER ADULTS, FAMILIES, AND CAREGIVERS READ THIS PAMPHLET TO LEARN: What Urinary Incontinence is. How to Manage Urinary Incontinence. What Pelvic Floor Exercises
Incontinence. Anatomy The human body has two kidneys. The kidneys continuously filter the blood and make urine.
 Incontinence Introduction Urinary incontinence occurs when a person cannot control the emptying of his or her urinary bladder. It can happen to anyone, but is very common in older people. Urinary incontinence
Incontinence Introduction Urinary incontinence occurs when a person cannot control the emptying of his or her urinary bladder. It can happen to anyone, but is very common in older people. Urinary incontinence
Pelvic Floor Muscle Exercises and Advice for Men
 Pelvic Floor Muscle Exercises and Advice for Men Why are my pelvic floor muscles important? Your pelvic floor muscles are important for bladder and bowel control. These muscles help to keep the bladder
Pelvic Floor Muscle Exercises and Advice for Men Why are my pelvic floor muscles important? Your pelvic floor muscles are important for bladder and bowel control. These muscles help to keep the bladder
Information on Physical Therapy For Urogynecologic Problems
 Information on Physical Therapy For Urogynecologic Problems You have scheduled an appointment for evaluation and treatment of a urogynecologic problem. Following, you will find a pelvic floor questionnaire
Information on Physical Therapy For Urogynecologic Problems You have scheduled an appointment for evaluation and treatment of a urogynecologic problem. Following, you will find a pelvic floor questionnaire
Urodynamic Tests. Department of Gynaecology. Patient Information
 Urodynamic Tests Department of Gynaecology Patient Information What are urodynamic tests? Urodynamic tests assess the dynamic function of the lower urinary tract. The tests assess 3 functions; The ability
Urodynamic Tests Department of Gynaecology Patient Information What are urodynamic tests? Urodynamic tests assess the dynamic function of the lower urinary tract. The tests assess 3 functions; The ability
Toning your pelvic floor WELCOME
 Toning your pelvic floor WELCOME Introductions Amelia Samuels, Physiotherapist, Active Rehabilitation Physiotherapy Supporting the Continence Foundation of Australia Continence Foundation of Australia
Toning your pelvic floor WELCOME Introductions Amelia Samuels, Physiotherapist, Active Rehabilitation Physiotherapy Supporting the Continence Foundation of Australia Continence Foundation of Australia
The Management of Female Urinary Incontinence. Part 1: Aetiology and Investigations
 The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
Pelvic Support Problems
 AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
Training a Wayward Bladder
 D. James Ballard, PT, DPT, GCS The University of Utah, Dept. of Physical Therapy Training a Wayward Bladder Agenda 1. Discuss urinary incontinence 2. Review pelvic floor and lower urinary tract functional
D. James Ballard, PT, DPT, GCS The University of Utah, Dept. of Physical Therapy Training a Wayward Bladder Agenda 1. Discuss urinary incontinence 2. Review pelvic floor and lower urinary tract functional
A non-invasive, safe and effective treatment that improves pelvic floor muscle contraction and diminishes urine loss in pelvic floor disorders 1
 A non-invasive, safe and effective treatment that improves pelvic floor muscle contraction and diminishes urine loss in pelvic floor disorders 1 INNOVO INNOVO has changed my life for the better. I no longer
A non-invasive, safe and effective treatment that improves pelvic floor muscle contraction and diminishes urine loss in pelvic floor disorders 1 INNOVO INNOVO has changed my life for the better. I no longer
FEMALE URINARY INCONTINENCE: WHAT IT IS AND WHAT YOU CAN DO ABOUT IT
 URO-GYNECOLOGY PATIIENT IINFORMATIION SHEET FEMALE URINARY INCONTINENCE: WHAT IT IS AND WHAT YOU CAN DO ABOUT IT What is Urinary Incontinence? Stress Incontinence is a leakage of urine that occurs, for
URO-GYNECOLOGY PATIIENT IINFORMATIION SHEET FEMALE URINARY INCONTINENCE: WHAT IT IS AND WHAT YOU CAN DO ABOUT IT What is Urinary Incontinence? Stress Incontinence is a leakage of urine that occurs, for
Urogynecology Associates of Philadelphia URODYNAMIC TESTING
 URODYNAMIC TESTING Urogynecology Associates of Philadelphia Most women with urinary incontinence will need to complete a few simple tests, performed in the office, to help your doctor assess your symptoms
URODYNAMIC TESTING Urogynecology Associates of Philadelphia Most women with urinary incontinence will need to complete a few simple tests, performed in the office, to help your doctor assess your symptoms
Stress Incontinence. Susannah Elvy Urogynaecology CNS
 Stress Incontinence Susannah Elvy Urogynaecology CNS Definitions Prevalence Assessment Investigation Treatment Surgery Men International Continence Society define as the complaint of any involuntary leakage
Stress Incontinence Susannah Elvy Urogynaecology CNS Definitions Prevalence Assessment Investigation Treatment Surgery Men International Continence Society define as the complaint of any involuntary leakage
Please complete this voiding diary and questionnaire. Bring both of them with you to your next appointment with your provider.
 Please complete this voiding diary and questionnaire. Bring both of them with you to your next appointment with your provider. To begin the diary, please choose two days when you will be at home. The two
Please complete this voiding diary and questionnaire. Bring both of them with you to your next appointment with your provider. To begin the diary, please choose two days when you will be at home. The two
Incontinence: Risks, Causes and Care
 Welcome To Incontinence: Risks, Causes and Care Presented by Kamal Masaki, MD Professor and Chair Department of Geriatric Medicine John A. Burns School of Medicine, UH Manoa September 5, 2018 10:00 11:00
Welcome To Incontinence: Risks, Causes and Care Presented by Kamal Masaki, MD Professor and Chair Department of Geriatric Medicine John A. Burns School of Medicine, UH Manoa September 5, 2018 10:00 11:00
Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN
 Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN Diane K. Newman, DNP is a Biofeedback Certified Continence Specialist. With over 35-years experience, she is an expert in the assessment and management of pelvic-floor
Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN Diane K. Newman, DNP is a Biofeedback Certified Continence Specialist. With over 35-years experience, she is an expert in the assessment and management of pelvic-floor
Role Of Pelvic Floor Muscle Therapy In Obese Perimenopausal Females With Stress Incontinence: A Randomized Control Trial
 ISPUB.COM The Internet Journal of Radiology Volume 14 Number 2 Role Of Pelvic Floor Muscle Therapy In Obese Perimenopausal Females With Stress Incontinence: A K Abdulaziz, T Hasan Citation K Abdulaziz,
ISPUB.COM The Internet Journal of Radiology Volume 14 Number 2 Role Of Pelvic Floor Muscle Therapy In Obese Perimenopausal Females With Stress Incontinence: A K Abdulaziz, T Hasan Citation K Abdulaziz,
Stress. incontinence FACTS, ADVICE, AND EXERCISES.
 Stress incontinence FACTS, ADVICE, AND EXERCISES Facts about incontinence Urinary incontinence is a common problem; one in every four women has problems with some form of leakage. Incontinence can be anything
Stress incontinence FACTS, ADVICE, AND EXERCISES Facts about incontinence Urinary incontinence is a common problem; one in every four women has problems with some form of leakage. Incontinence can be anything
CONSERVATIVE MANAGEMENT OF URINARY INCONTINENCE IN WOMEN. Riette Vosloo Physiotherapist in Women s s Health
 CONSERVATIVE MANAGEMENT OF URINARY INCONTINENCE IN WOMEN Riette Vosloo Physiotherapist in Women s s Health CONSERVATIVE TREATMENT Any therapy that does not involve Pharmacologic intervention or Surgical
CONSERVATIVE MANAGEMENT OF URINARY INCONTINENCE IN WOMEN Riette Vosloo Physiotherapist in Women s s Health CONSERVATIVE TREATMENT Any therapy that does not involve Pharmacologic intervention or Surgical
IF YOU VE GOT TO GO, WE VE GOT SOLUTIONS.
 IF YOU VE GOT TO GO, WE VE GOT SOLUTIONS. Get the facts about urinary incontinence and get real solutions. HENRY FORD PELVIC HEALTH & CONTINENCE CENTER HENRY FORD WOMEN S HEALTH SERVICES INCONVENIENCE?
IF YOU VE GOT TO GO, WE VE GOT SOLUTIONS. Get the facts about urinary incontinence and get real solutions. HENRY FORD PELVIC HEALTH & CONTINENCE CENTER HENRY FORD WOMEN S HEALTH SERVICES INCONVENIENCE?
A Stress Urinary Incontinence fact sheet for
 A Stress Urinary Incontinence fact sheet for women and teenagers What is Stress Urinary Incontinence? Get to know your gusset - the science bit Stress urinary incontinence (SUI) is defined as a sudden
A Stress Urinary Incontinence fact sheet for women and teenagers What is Stress Urinary Incontinence? Get to know your gusset - the science bit Stress urinary incontinence (SUI) is defined as a sudden
The urethral support system during pregnancy and after childbirth Wijma, Jacobus
 University of Groningen The urethral support system during pregnancy and after childbirth Wijma, Jacobus IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
University of Groningen The urethral support system during pregnancy and after childbirth Wijma, Jacobus IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
21/03/2016. The urogynaecologist approach. Urinary continence management in women: a multidisciplinary approach. Dr Anna Rosamillia
 Urinary continence management in women: a multidisciplinary approach The urogynaecologist approach Dr Anna Rosamillia What is normal bladder function? Incontinence is not normal Normal voiding is 7-8 times
Urinary continence management in women: a multidisciplinary approach The urogynaecologist approach Dr Anna Rosamillia What is normal bladder function? Incontinence is not normal Normal voiding is 7-8 times
Normal micturition involves complex
 NEW TARGET FOR INTERVENTION: THE NEUROUROLOGY CONNECTION * Donald R. Ostergard, MD, FACOG ABSTRACT Urine storage and release are under the control of the parasympathetic, sympathetic, and somatic nervous
NEW TARGET FOR INTERVENTION: THE NEUROUROLOGY CONNECTION * Donald R. Ostergard, MD, FACOG ABSTRACT Urine storage and release are under the control of the parasympathetic, sympathetic, and somatic nervous
Northwest Rehabilitation Associates, Inc.
 Pelvic Health Patient Intake Form Name: Date: Please answer the following questions as honestly and thoroughly as you can. Your responses will help us better understand your condition and provide the best
Pelvic Health Patient Intake Form Name: Date: Please answer the following questions as honestly and thoroughly as you can. Your responses will help us better understand your condition and provide the best
Urinary incontinence is a common and debilitating
 Female Urology Using the Vibrance Kegel Device With Pelvic Floor Muscle Exercise for Stress Urinary Incontinence: A Randomized Controlled Pilot Study Teng Aik Ong, Su Yen Khong, Keng Lim Ng, Jesse Ron
Female Urology Using the Vibrance Kegel Device With Pelvic Floor Muscle Exercise for Stress Urinary Incontinence: A Randomized Controlled Pilot Study Teng Aik Ong, Su Yen Khong, Keng Lim Ng, Jesse Ron
Various Types. Ralph Boling, DO, FACOG
 Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Objectives. Prevalence of Urinary Incontinence URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS
 URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
Neurourology and Urodynamics 26: (2007) ß 2007 Wiley-Liss, Inc.
 Neurourology and Urodynamics 26:486 491 (2007) Short-Term Efficacy of Group Pelvic Floor Training Under Intensive Supervision Versus Unsupervised Home Training for Female Stress Urinary Incontinence: A
Neurourology and Urodynamics 26:486 491 (2007) Short-Term Efficacy of Group Pelvic Floor Training Under Intensive Supervision Versus Unsupervised Home Training for Female Stress Urinary Incontinence: A
PELVIC HEALTH PHYSICAL THERAPY AND THE NURSE PRACTITIONER: WHAT S GOING ON DOWN THERE?
 PELVIC HEALTH PHYSICAL THERAPY AND THE NURSE PRACTITIONER: WHAT S GOING ON DOWN THERE? Kathy Curry, PT, DPT Physical Therapy Today Pelvic Health Physical Therapy () Objectives: Discuss components of pelvic
PELVIC HEALTH PHYSICAL THERAPY AND THE NURSE PRACTITIONER: WHAT S GOING ON DOWN THERE? Kathy Curry, PT, DPT Physical Therapy Today Pelvic Health Physical Therapy () Objectives: Discuss components of pelvic
Letter from the SAUGA President
 Volume3, Issue 1 February 2016 Letter from the SAUGA President Things are hotting up in Cape Town literally and figuratively!! The IUGA meeting Cape Town August 2016 now has an exciting academic programme
Volume3, Issue 1 February 2016 Letter from the SAUGA President Things are hotting up in Cape Town literally and figuratively!! The IUGA meeting Cape Town August 2016 now has an exciting academic programme
The Pelvic Floor Muscles - a Guide for Women
 The Pelvic Floor Muscles - a Guide for Women This booklet is supported by WWWWW Wellbeing of Women Registered Charity No. 239281 www.wellbeingofwomen.org.uk Introduction Up to a third of all women experience
The Pelvic Floor Muscles - a Guide for Women This booklet is supported by WWWWW Wellbeing of Women Registered Charity No. 239281 www.wellbeingofwomen.org.uk Introduction Up to a third of all women experience
Medical Policy Title: Radiofrequency ARBenefits Approval: 10/19/2011
 Medical Policy Title: Radiofrequency ARBenefits Approval: 10/19/2011 Treatment, Urinary Stress Incontinence, Transurethral Effective Date: 01/01/2012 Document: ARB0359 Revision Date: Code(s): 53860 Transurethral
Medical Policy Title: Radiofrequency ARBenefits Approval: 10/19/2011 Treatment, Urinary Stress Incontinence, Transurethral Effective Date: 01/01/2012 Document: ARB0359 Revision Date: Code(s): 53860 Transurethral
Pelvic floor weakness
 Information leaflet for patients Pelvic floor weakness Physiotherapy department You have been referred to this department for treatment and advice because you have one or more of the following symptoms:
Information leaflet for patients Pelvic floor weakness Physiotherapy department You have been referred to this department for treatment and advice because you have one or more of the following symptoms:
Look Good Feel Good. after pregnancy. Physiotherapy advice and exercises for new mums
 Look Good Feel Good after pregnancy Physiotherapy advice and exercises for new mums How to exercise after pregnancy with physiotherapy Bowel Tail Bone Uterus Bladder Pubic Bone Pelvic Floor Muscles Urethra
Look Good Feel Good after pregnancy Physiotherapy advice and exercises for new mums How to exercise after pregnancy with physiotherapy Bowel Tail Bone Uterus Bladder Pubic Bone Pelvic Floor Muscles Urethra
Pelvic Floor Muscle Exercises
 INFORMATION FOR WOMEN OF ALL AGES Pelvic Floor Muscle Exercises How to exercise and strengthen your pelvic floor muscles ASSOCIATION OF CHARTERED PHYSIOTHERAPISTS IN WOMEN S HEALTH This leaflet is supported
INFORMATION FOR WOMEN OF ALL AGES Pelvic Floor Muscle Exercises How to exercise and strengthen your pelvic floor muscles ASSOCIATION OF CHARTERED PHYSIOTHERAPISTS IN WOMEN S HEALTH This leaflet is supported
Incontinence: The silent scourge of the young and old. The International Continence Society has. In this article:
 Focus on CME at the University of Toronto Incontinence: The silent scourge of the young and old By Sender Herschorn, BSc, MDCM, FRCSC In this article: 1. What is the workup for urinary incontinence? 2.
Focus on CME at the University of Toronto Incontinence: The silent scourge of the young and old By Sender Herschorn, BSc, MDCM, FRCSC In this article: 1. What is the workup for urinary incontinence? 2.
Urogynaecology. Colm McAlinden
 Urogynaecology Colm McAlinden Definitions Urinary incontinence compliant of any involuntary leakage of urine with many different causes Two main types: Stress Urge Definitions Nocturia: More than a single
Urogynaecology Colm McAlinden Definitions Urinary incontinence compliant of any involuntary leakage of urine with many different causes Two main types: Stress Urge Definitions Nocturia: More than a single
Your pelvic floor muscles
 Continence office Ballochmyle Suite, University Hospital Ayr Telephone 019 177 Your pelvic floor muscles Advice and exercise for women Follow us on Twitter @NHSaaa Find us on Facebook at www.facebook.com/nhsaaa
Continence office Ballochmyle Suite, University Hospital Ayr Telephone 019 177 Your pelvic floor muscles Advice and exercise for women Follow us on Twitter @NHSaaa Find us on Facebook at www.facebook.com/nhsaaa
Pelvic organ prolapse. Information for patients Continence Service
 Pelvic organ prolapse Information for patients Continence Service What is a pelvic organ prolapse? A pelvic organ prolapse occurs when the uterus (womb), vagina, bladder or bowel slips out of place, resulting
Pelvic organ prolapse Information for patients Continence Service What is a pelvic organ prolapse? A pelvic organ prolapse occurs when the uterus (womb), vagina, bladder or bowel slips out of place, resulting
Pelvic Floor Rehabilitation
 Pelvic Floor Rehabilitation according to the Integral Theory Towards a more time efficient method for pelvic floor rehabilitation and with a wider symptom scope.1 Introduction The scope of traditional
Pelvic Floor Rehabilitation according to the Integral Theory Towards a more time efficient method for pelvic floor rehabilitation and with a wider symptom scope.1 Introduction The scope of traditional
The pelvic floor muscles (PFM) form
 Correlation of Digital Palpation and Transabdominal Ultrasound for Assessment of Pelvic Floor Muscle Contraction Amir Massoud Arab, PT, PhD 1 ; Roxana Bazaz Behbahani, PT, BSc 2 ; Leila Lorestani, PT,
Correlation of Digital Palpation and Transabdominal Ultrasound for Assessment of Pelvic Floor Muscle Contraction Amir Massoud Arab, PT, PhD 1 ; Roxana Bazaz Behbahani, PT, BSc 2 ; Leila Lorestani, PT,
This file was dowloaded from the institutional repository Brage NIH - brage.bibsys.no/nih
 This file was dowloaded from the institutional repository Brage NIH - brage.bibsys.no/nih Bø, K., Hilde, G., Stær-Jensen, J., Brækken, I. H. (2011). Can the Paula method facilitate co-contraction of the
This file was dowloaded from the institutional repository Brage NIH - brage.bibsys.no/nih Bø, K., Hilde, G., Stær-Jensen, J., Brækken, I. H. (2011). Can the Paula method facilitate co-contraction of the
Duloxetine in women awaiting surgery
 DOI: 1.1111/j.1471-528.6.879.x www.blackwellpublishing.com/bjog Review article H Drutz Ontario Power Generation Building, Toronto, Ontario, Canada Correspondence: Prof. Dr H Drutz, Mount Sinai Hospital,
DOI: 1.1111/j.1471-528.6.879.x www.blackwellpublishing.com/bjog Review article H Drutz Ontario Power Generation Building, Toronto, Ontario, Canada Correspondence: Prof. Dr H Drutz, Mount Sinai Hospital,
Aetiology 1998 Bump & Norton Theoretical model
 Kate Lough MSc MCSP Handout IUGA Nice 2015 Physiotherapy and the Provision of Pelvic Floor Muscle Training and Lifestyle Intervention in the Conservative Management of Pelvic Organ Prolapse an evidence
Kate Lough MSc MCSP Handout IUGA Nice 2015 Physiotherapy and the Provision of Pelvic Floor Muscle Training and Lifestyle Intervention in the Conservative Management of Pelvic Organ Prolapse an evidence
Overactive Bladder: Diagnosis and Approaches to Treatment
 Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Not a Laughing Matter
 Not a Laughing Matter How to Incorporate Pelvic Health Rehabilitation into your STAR program Nancy Corvigno MSPT PRPC Certified Star Clinician STAR Program at Griffin Hospital Survivorship Training and
Not a Laughing Matter How to Incorporate Pelvic Health Rehabilitation into your STAR program Nancy Corvigno MSPT PRPC Certified Star Clinician STAR Program at Griffin Hospital Survivorship Training and
Pelvic Floor Muscle Training Concept
 Intervention published in Trials 2015 Nov 17;16(1):524 as additional file 1 Pelvic Floor Muscle Training Concept for Women Suffering from Stress Urinary Incontinence Helena Luginbuehl 1,2, Corinne Lehmann
Intervention published in Trials 2015 Nov 17;16(1):524 as additional file 1 Pelvic Floor Muscle Training Concept for Women Suffering from Stress Urinary Incontinence Helena Luginbuehl 1,2, Corinne Lehmann
Pelvic Floor Exercises
 Directorate of Women, Children and Surgical Services Burton and District Urogynaecology Centre A Nationally Accredited Urogynaecology Unit Pelvic Floor Exercises You have been given this leaflet because
Directorate of Women, Children and Surgical Services Burton and District Urogynaecology Centre A Nationally Accredited Urogynaecology Unit Pelvic Floor Exercises You have been given this leaflet because
PRE-OPERATIVE URODYNAMIC
 PRE-OPERATIVE URODYNAMIC STUDIES: IS THERE VALUE IN PREDICTING POST-OPERATIVE STRESS URINARY INCONTINENCE IN WOMEN UNDERGOING PROLAPSE SURGERY? Dr K Janse van Rensburg Dr JA van Rensburg INTRODUCTION POP
PRE-OPERATIVE URODYNAMIC STUDIES: IS THERE VALUE IN PREDICTING POST-OPERATIVE STRESS URINARY INCONTINENCE IN WOMEN UNDERGOING PROLAPSE SURGERY? Dr K Janse van Rensburg Dr JA van Rensburg INTRODUCTION POP
Periurethral bulking injections for stress urinary incontinence
 n The Leeds Teaching Hospitals NHS Trust Periurethral bulking injections for stress urinary incontinence Information for patients Leeds Centre for Women s Health Urinary incontinence is the involuntary
n The Leeds Teaching Hospitals NHS Trust Periurethral bulking injections for stress urinary incontinence Information for patients Leeds Centre for Women s Health Urinary incontinence is the involuntary
Promoting Continence with Physiotherapy
 A Common problem for Men and women Promoting Continence with Physiotherapy This leaflet contains information about physiotherapy advice and treatment for anyone with bladder and bowel problems. This may
A Common problem for Men and women Promoting Continence with Physiotherapy This leaflet contains information about physiotherapy advice and treatment for anyone with bladder and bowel problems. This may
Disease Management. Incontinence Care. Chan Sau Kuen Continence Nurse Consultant United Christian Hospital 14/11/09
 Disease Management in Incontinence Care Chan Sau Kuen Continence Nurse Consultant United Christian Hospital 14/11/09 What is incontinence? Definition of Incontinence - Is the compliant of any involuntary
Disease Management in Incontinence Care Chan Sau Kuen Continence Nurse Consultant United Christian Hospital 14/11/09 What is incontinence? Definition of Incontinence - Is the compliant of any involuntary
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Correlation of Digital Examination Vs Perineometry in Measuring the Pelvic Floor Muscles Strength
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Correlation of Digital Examination Vs Perineometry in Measuring the Pelvic Floor Muscles Strength
Treatment Outcomes of Tension-free Vaginal Tape Insertion
 Are the Treatment Outcomes of Tension-free Vaginal Tape Insertion the Same for Patients with Stress Urinary Incontinence with or without Intrinsic Sphincter Deficiency? A Retrospective Study in Hong Kong
Are the Treatment Outcomes of Tension-free Vaginal Tape Insertion the Same for Patients with Stress Urinary Incontinence with or without Intrinsic Sphincter Deficiency? A Retrospective Study in Hong Kong
Pelvic floor exercises for women. Information for patients Continence Service
 Pelvic floor exercises for women Information for patients Continence Service page 2 of 8 Why do I need to do pelvic floor exercises? Many women experience pelvic floor problems at some time during their
Pelvic floor exercises for women Information for patients Continence Service page 2 of 8 Why do I need to do pelvic floor exercises? Many women experience pelvic floor problems at some time during their
Physical Therapy Treatment for Pelvic Floor Disorders: Interventions and Home Programs
 Physical Therapy Treatment for Pelvic Floor Disorders: Interventions and Home Programs T INA M A LLEN, PT PRPC BCB - PMD U N I V E R S I T Y O F W A S H I N G T O N M E D I C A L C E N T E R H E R M A
Physical Therapy Treatment for Pelvic Floor Disorders: Interventions and Home Programs T INA M A LLEN, PT PRPC BCB - PMD U N I V E R S I T Y O F W A S H I N G T O N M E D I C A L C E N T E R H E R M A
International Federation of Gynecology and Obstetrics
 International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
17 th European congress of Physical Rehabilitation Medicine. 38th SIMFER congress
 17 th European congress of Physical Rehabilitation Medicine 38th SIMFER congress European Rehabilitation: Quality, Evidence, Efficacy and Effectiveness Venice, May 23 27 2010 THE PHYSIATRIST AND URO-GYNECOLOGICAL
17 th European congress of Physical Rehabilitation Medicine 38th SIMFER congress European Rehabilitation: Quality, Evidence, Efficacy and Effectiveness Venice, May 23 27 2010 THE PHYSIATRIST AND URO-GYNECOLOGICAL
Urodynamic findings in women with insensible incontinence
 bs_bs_banner International Journal of Urology (2013) 20, 429 433 doi: 10.1111/j.1442-2042.2012.03146.x Original Article: Clinical Investigation Urodynamic findings in women with insensible Benjamin M Brucker,
bs_bs_banner International Journal of Urology (2013) 20, 429 433 doi: 10.1111/j.1442-2042.2012.03146.x Original Article: Clinical Investigation Urodynamic findings in women with insensible Benjamin M Brucker,
Voiding Diary. Begin recording upon rising in the morning and continue for a full 24 hours.
 Urodvnamics Your physician has scheduled you for a test called URODYNAMICS. This test is a series of different measurements of bladder function and can be used to determine the cause of a variety of bladder
Urodvnamics Your physician has scheduled you for a test called URODYNAMICS. This test is a series of different measurements of bladder function and can be used to determine the cause of a variety of bladder
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS
 Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Advanced Care for Female Overactive Bladder & Urinary Incontinence. Department of Urology Kaiser Permanente Santa Rosa
 Advanced Care for Female Overactive Bladder & Urinary Incontinence Department of Urology Kaiser Permanente Santa Rosa Goals Participants will: Review normal urinary tract anatomy and function Understand
Advanced Care for Female Overactive Bladder & Urinary Incontinence Department of Urology Kaiser Permanente Santa Rosa Goals Participants will: Review normal urinary tract anatomy and function Understand
Paediatric Urotherapy Training
 Paediatric Urotherapy Training Frances Shit NS, MSc (Hons), ET, Dept. of Surgery, PWH, CUHK HKSAR Urinary Incontinence in Children Urine leakage in a child from 5 years of age Leakage occurs on a regular
Paediatric Urotherapy Training Frances Shit NS, MSc (Hons), ET, Dept. of Surgery, PWH, CUHK HKSAR Urinary Incontinence in Children Urine leakage in a child from 5 years of age Leakage occurs on a regular
Urinary incontinence. Factsheet March Fighting for a
 Urinary incontinence Factsheet March 2013 Fighting for a Life Unlimited Urinary incontinence Introduction Women and girls with cystic fibrosis (CF) are more likely to experience urinary incontinence (UI)
Urinary incontinence Factsheet March 2013 Fighting for a Life Unlimited Urinary incontinence Introduction Women and girls with cystic fibrosis (CF) are more likely to experience urinary incontinence (UI)
Prolapse and Urogynae Incontinence. Lucy Tiffin and Hannah Wheldon-Holmes
 Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
URINARY INCONTINENCE FOR FALLS PREVENTION. by Susan Elms P.T. Elms Physiotherapy
 URINARY INCONTINENCE PHYSIOTHERAPY MANAGEMENT FOR FALLS PREVENTION by Susan Elms P.T. Elms Physiotherapy OR How to avoid the mad dash to the bathroom! INCONTINENCE INFORMATION TALK What is incontinence?
URINARY INCONTINENCE PHYSIOTHERAPY MANAGEMENT FOR FALLS PREVENTION by Susan Elms P.T. Elms Physiotherapy OR How to avoid the mad dash to the bathroom! INCONTINENCE INFORMATION TALK What is incontinence?
REVIEW OF CAUSES, EVALUATION, AND TREATMENTS URINARY INCONTINENCE 101
 REVIEW OF CAUSES, EVALUATION, AND TREATMENTS URINARY INCONTINENCE 101 March 5, 2014 Kevin E Miller, MD Department of Obstetrics and Gynecology University of Kansas School of Medicine- Wichita URINARY INCONTINENCE
REVIEW OF CAUSES, EVALUATION, AND TREATMENTS URINARY INCONTINENCE 101 March 5, 2014 Kevin E Miller, MD Department of Obstetrics and Gynecology University of Kansas School of Medicine- Wichita URINARY INCONTINENCE
Ben Herbert Alex Wojtowicz
 Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist
 Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Male Lower Urinary Tract Symptoms: Lifestyle Advice, Bladder Training and Pelvic Floor Exercises
 MALE LUTS/CUP_11_11 Male Lower Urinary Tract Symptoms: Lifestyle Advice, Bladder Training and Pelvic Floor Exercises Lower urinary tract symptoms (LUTS) include the need to pass water very frequently (frequency)
MALE LUTS/CUP_11_11 Male Lower Urinary Tract Symptoms: Lifestyle Advice, Bladder Training and Pelvic Floor Exercises Lower urinary tract symptoms (LUTS) include the need to pass water very frequently (frequency)
