SEMEN ANALYSIS: Sadeghi MR., (PhD).
|
|
|
- Rosalind O’Brien’
- 6 years ago
- Views:
Transcription
1 : What? When? How? Why? Sadeghi MR., (PhD). Clinical embryologist, Avicenna Infertility Clinic Editor in chief, Journal of Reproduction & Infertility Avicenna Research Institute
2 : What? When? How? Why? Sadeghi MR., (PhD). Clinical embryologist, Editor in chief, Journal of Reproduction & Infertility
3 BACKGROUND What is semen, exactly? A mixture of seminal plasma and cells Seminal plasma contains: Prostatic fluid (~30% of the volume) Epididymal plasma (~5% of the volume) Seminal vesicle fluid (the remainder of the ejaculate) The cells are: Spermatozoa Germ line cells Leukocytes of various types Bacteria Epithelial cells Occasional red cells
4 BACKGROUND Formation of the sperm cell (1) Formed in the seminiferous e tubules, develop in close association with the Sertoli cells Start as spermatogonia (self-renewing stem cell of the male germ cell line) located on the basement membrane The transformation from the round germ cell to the sperm cell occurs during passage to the centre of the seminiferous s tubule
5 BACKGROUND Formation of the sperm cell (2) Spermatogenesis is a cascade of cell divisions: Mitosis: spermatogonia to primary spermatocytes First meiotic division: secondary spermatocytes Second meiotic division: haploid spermatids This process takes 70 ± 4 days in the human so errors will take about 3 months to show up
6 BACKGROUND Formation of the sperm cell (3) Spermiogenesis: differentiation of the round spermatid into a spermatozoon Thi i h i hi h This is the process in which sperm morphology is largely determined
7 BACKGROUND Sperm transport and seminal plasma Testicular sperm need to undergo more maturation steps before they are ready to fertilize Transported from the testes to the epididymis, where they mature, and acquire the ability to swim Then moved to the vas deferens, for storage At ejaculation, the sperm are transported out of the vas and mix with accessory gland secretions: prostatic fluid (ph slightly acidic to neutral; contains citric acid and zinc) seminal vesicle fluid (ph strongly alkaline; contains fructose)
8 BACKGROUND What the spermatozoon looks like (2) Midpiece Head Tail The human sperm cell is about 70 µm long The nucleus is in the head contains the 23 chromosomes It is the head which binds to the egg at fertilization Midpiece: the energy for motility is generated Tail: motility the beat is initiated just behind Tail: motility the beat is initiated just behind the midpiece, and then propagated along the tail
9 BACKGROUND Sperm function The ejaculated sperm pass through the cervix, then the uterus, and enter the oviduct The fertilizing sperm swims through the layers of cells around the egg (cumulus and corona), and reaches the zona pellucida The esperm then loses osesthe front membranes es of its head (the acrosome reaction ), binds to the zona, then forces its way through the zona to the egg membrane When the sperm head binds to the egg membrane, its tail stops beating, and the egg incorporates the whole sperm cell Th k th th th l d f l The egg unpacks the sperm, then the male and female pronuclei form.
10 WHY PERFORM SEMEN ANALYSIS? Diagnosis of sterility Diagnosis of infertility Prognosis for fertility Identify treatment options: surgical treatment medical treatment assisted conception treatment Therefore = a screening test to help direct management.
11 What is the standard approach to semen evaluation? International minimum standards are, by consensus, the World Health Organization s Lab Manual (Fourth edition). Focus is on standardization with expanded section on quality control. Methods amenable for use in any ( third world ) country. Basic infertility work-up.
12 What is the standard approach to semen evaluation? International minimum standards are, by consensus, the World Health Organization s Lab Manual (Fifth edition). Focus is on standardization with expanded section on quality control. Methods amenable for use in any ( third world ) country. Basic infertility work-up.
13 Sample Collection For ameaningful result, semen samples must always be collected under standardized conditions: the container has to be sterile and known NOT to be spermotoxic (i.e. provided d by the lab) themanmusthavehad3 5daysofabstinence the man must have washed his hands before collection (particularly if microbiological analysis is requested) the man must NOT have used lubricants. the sample must be kept at 37 C until analysis, which begins ideally within 30 min, but absolutely within 60 min, of ejaculation
14 Sample Handling The semen sample should be mixed gently during the liquefaction period to promote liquefaction The sample should NEVER be vortexed (the only exception is for the fixed prep for concentration assessment) The sample should NEVER be needled if it is too viscous to work with, a known volume of sperm buffer should be added and the sample mixed gently. The added volume must be included in the sperm concentration calculation
15 Macroscopic Evaluation There are several macroscopic evaluations which give useful diagnostic information about the sample: Appearance Odour Liquefaction Volume Viscosity ph
16 Macroscopic Evaluation - Appearance Swirl the sample, still in the collection jar, gently Hold the jar up to look through its bottom Note the following: Colour (normal = white to grayish-yellow) if there is blood present, it may rangefrompink to brown Opacity / translucence (normal = tends to opaque) Whether mucus streaks or cell clumps are present
17 Macroscopic Evaluation - Odour Different people have different abilities to smell semen, so this cannot be standardized However, when the lid is taken off the collection jar, it should be noted if there is a strong smell of urine or of putrefaction Samples collected after a prolonged abstinence period (i.e. several weeks) are likely to have a stronger odour
18 Macroscopic Evaluation Liquefaction & Viscosity Liquefaction is the breakdown of the gel portion of the seminal plasma the enzymes for this are in the prostatic fluid A sample with incomplete liquefaction has a gelatinous material in a liquid base this can be seen when the sample is swirled for the appearance assessment Viscosity is related to the fluid nature of the whole sample This is rated subjectively according to the length of the thread of semen produced when the sample is allowed to run back out of the volumetric pipette used to measure the ejaculate volume
19 Macroscopic Evaluation - Volume The volume of the sample should be measured to allow an accurate determination of the sperm number This is most easily assessed using a warmed disposable volumetric pipette (which is sterile and known NOT to be spermotoxic) After the sample is measured, allow it to run back into the collection jar, noting its viscosity (a normal sample will have some viscosity i.e. not watery, but it will flow easily)
20 Macroscopic Evaluation - ph ph is important because sperm die at ph < 6.9 The ph of liquefied semen is normally determined using test strips (we use EM Science ColorpHast type, ph ) We usually measure ph after volume and viscosity by touching the emptied volumetric pipette to the testt strip The normal ph range is Inflammatory disorders of the accessory glands can take the ph outside of this range
21 The wet preparation set-up Place 10µl of thoroughly mixed, liquefied semen on a microscope slide and cover with a 22x22mm No 1½ coverslip There are several important points to keep in mind: The quality of sperm motility ii is affected by temperature the lower the temperature, the poorer the motility, and then cold shock starts to occur at around 15 C. So great care must be taken to ensure that the slides and coverslips, as well as the pipette tips are kept at 37 C The assessment must start as soon as the flow stops if this is >1 minute, then a new wet prep must be made Microscope: phase contrast optics and a heated stage
22 The wet preparation assessments The characteristics assessed are: Motility (to be discussed later) Sperm aggregation (random clumping) some is normal, but large clumps (each with hundreds of sperm) is abnormal Spermagglutination (between specific sites) could suggest the presence of antisperm antibodies. Round cells: should be <1 per 40 field (~ 1 million/ml). If more abundant, a leukocyte test should be run Epithelial cells: usually present in small numbers Erythrocytes: should not be present Debris: particles smaller than sperm head, may be plentiful Bacteria and protozoa: presence indicates infection
23 Motility assessment - Background This is the first assessment made on the wet prep If >10 15% of the sperm are clumped, just assess the freeswimming sperm (and note this on the report form) A repeat assessment should be made on a second wet prep Don t estimate, count (> 4 fields and 200 sperm per prep) Use a 40 objective, and phase contrast optics Make a random selection of the fields that are assessed Assess fields that are away from the coverslip edge Count only those sperm that were in the field at one moment in time (you have to be quick!) There must be agreement to within 10% between duplicates
24 Motility assessment - types % motile=the proportion of sperm with ihtail movement Progression rating = the grade of progression shown by the majority of the sperm: this can be from 0 (all immotile) to 4 (all with rapid progression); or from a (rapid progression) to d (all immotile) Differential motility count = proportion of sperm in each of 4 motility classes (rapid progressive; slow progressive; non- progressive; immotile)
25 Motility assessment differential motility Differential motility classification is based on the distance swum over time: Rapid progressive: > 25 µm/s Slow progressive: 5 25 µm/s Non-progressive: < 5 µm/s Immotile: no flagellar movement The sperm head is about 5 µm long, so the rapid sperm have a net gain of 5 head lengths / second
26 Motility assessment monitor Alternatively, use a video monitor with a grid for the differential motility assessments so we do them off the screen. Each square is the equivalent of µm (a stage micro-meter is used to set this up) This approach is very useful for This approach is very useful for training and for QC/QA
27 Motility assessment lab sources of error Have the definitions been implemented correctly? Are staff trained to classify progression? Internal quality control? How is velocity/progression yp assessed? Effect of temperature :% motile = minimal % progressive = slight % rapid = very large Representative sample aliquots? Adequate number of sperm counted? Repeatability of duplicate counts? Calculations performed correctly? Precision of results? External quality assurance / proficiency testing? Uncertainty of results?
28 Motility assessment interpretation The WHO s Reference values for motility are: 50% or more with progressive motility; or 25% or more with rapid progressive motility Assuming that all of the collection and laboratory factors have been controlled, a poor motility result may have negative implications for fertility. However this should be confirmed by a repeat semen However, this should be confirmed by a repeat semen analysis, and the result should be interpreted with the rest of the semen analysis results
29 Sperm concentration- background Sperm count = total number of sperm in the ejaculate Sperm concentration = number of sperm per ml (not density, which is an expression of mass / unit volume) Most accurate method is volumetric dilution and haemocytometry Must use a positive displacement pipettor We make a dilution with a fixative solution (allows the assessments to be batched - usually counted within two days)
30 Sperm concentration - method Fix the haemocytometer coverslip over the chambers ensure interference fringes can be seen Vortex the fixed sample, load ~10 µl in both chambers Leave in a humid chamber for minutes Count using a 20 objective and phase contrast optics
31 Sperm concentration - haemocytometer The number of squares assessed depends on the number of sperm counted in the first large square: If < 10 counted, the whole grid is assessed If counted, 10 squares are assessed If > 40 counted 5 squares are If > 40 counted, 5 squares are assessed First large square counted
32 Sperm concentration - calculations If the counts of the two chambers are not within 5% oftheir average (i.e. the difference > 1/20 of their sum): discard, remix the sample, and set it up again If the two counts are in agreement, then the sum of the two counts is divided by the correction factor: If 2 25 squares counted, divide their sum by 10 If 2 10 squares counter, divide their sum by 4 If 2 5 squares counted, divide their sum by 2 This gives the sperm concentration in millions per ml Sperm count = concentration total volume
33 Sperm concentration lab sources of error Sample aliquot representative of ejaculate? semen homogeneous (mixed)? accurate sample aliquot (N.B. viscosity)? duplicate aliquot? Accurate dilution : volumes of sample aliquot and diluent? storage (airtight) / sperm bind to vial? Secondary sampling : mixing of diluted aliquot? duplicate aliquots? Preparation of counting chambers : good chamber design/manufacture? chamber loaded correctly &/or cover glass placed correctly? adequate minimum number of cells? repeatability of duplicate counts? Calculations C l l correct? Precision of results? Uncertainty of measurement known?
34 Sperm concentration interpretation The WHO Reference values for: Sperm concentration is > sperm/ml Sperm count is > sperm per ejaculate A persistently low sperm concentration is associated with impaired fertility If a man has a sperm concentration < sperm/ml, the WHO recommends assessment for numerical and structural abnormalities of sex chromosomes Azoospermia can indicate a failure of spermatogenesis or blockage(s) in the male tract
35 Variation in Sperm Counting
36 Sperm morphology background Morphology is even more important than motility and concentration ti Because of the small size of the human sperm head, must use an air-dried smear which has been stained The Papanicolaou method is best Prepared ed samples are assessed using a 100 oil-immersion eso objective under bright field optics The WHO recommends that 200 spermatozoa are counted per sample (and says that is better) Fields for counting must be selected at random When counting, remember about the normal distribution
37 Sperm morphology morphology types Variations of normal head shape Asymmetric insertion Non-inserted tail Distended midpiece Thin midpiece Small / large head Tapering heads Cytoplasmic Coiled Duplicate Conjoined droplet tail tail form Pyriform heads Vacuolated head Constricted Reduced acrosome Amorphous forms Dense staining Short tail Hairpin tail Terminal droplet Bent tail
38 Sperm morphology assessment Even good samples will have <20% normal forms But we know that these sperm from these samples can fertilize eggs so is the morphology any help at all? Yes it is but there are a few things to think about: The result will indicate a probability, not an absolute You have to count 200 sperm to discriminate reliably between, say, 3% and 5% ( Strict Criteria cut-off 4%) The dynamic range of 4 15% is not very large, and means that it is difficult to make a meaningful assessment
39 Diff quick staining kit
40 Sperm morphology assessment schemes vs Tygerberg scheme defines normal sperm and counts the number that meet these criteria. WHO 92 looks for, and counts, defects that might affect sperm function in each region of a sperm normal sperm are those that have no recognizable defects. Expert direct comparison study between the schemes* revealed little difference. Issues with counting error and uncertainty of measurement, especially if only 100 sperm counted. Need additional information, e.g. Acrosome Index or Teratozoospermia Index (TZI) when dynamic range of % normal forms is very limited. * Mortimer & Menkveld (2001) J. Androl. 22:
41 Sperm morphology TZI The Teratozoospermic Index is an expression of the average number of abnormalities per abnormal sperm Each sperm cell is assessed for an abnormality in the head, neck/midpiece, or tail, and for a cytoplasmic droplet If it does not have any of these abnormalities, it is normal If it does have an abnormality, it is abnormal, and we score each abnormality. So, if a cell has an abnormal head and tail, it is counted as 1 cell, and 2 abnormalities Then, (total # abnormalities) / (total # sperm) = TZI A TZI > %80 has been associated with poor sperm fertilizing p p g ability in vivo and in vitro
42 Semen biochemistry Acid phosphatase: p marker for prostatic function Citric acid: can indicate prostatic function low levels may indicate dysfunction or a prostatic duct obstruction Zinc: marker for prostatic function colorimetric assay (WHO) Fructose: marker for seminal vesicle function, and is a substrate for sperm metabolism spectrophotometric assay (WHO) α-glucosidase: secreted exclusively by the epididymis and so is a marker for epididymal function spectrophotometric assay (WHO)
43 Sperm Vitality Used in samples with low total motility y( (<50%) Distinguishes between samples with live, but immotile sperm (e.g Kartagener syndrome), and those with lots of dead sperm (could result from: sperm senescence; exposure to detergents or lubricants; or spermotoxic antibodies) Also provides a check on the accuracy of motility assessments: % live should be slightly higher than % motile U ll f d i it l t i h i Y ith Usually performed using a vital stain, such as eosin Y, with a counterstain (nigrosin) although could use a fluorescent DNA stain, such as H33258.
44 SDFA Kit Sperm DNA Fragmentation Assay Kit
45
46 Retrograde ejaculation In some men, the semen passes back into the bladder at ejaculation - this is confirmed by examination of a sample of postejaculatory urine The man must take sodium bicarbonate the day before, and the day of, his appointment to alkalinize his urine Before collection, he should pass urine and then wait until he feels there is some urine in his bladder before masturbating He then collects a urine sample for analysis Assess volume and ph of the urine Centrifuge (600gg for 10 min), resuspend pellets to a total of 20ml with sperm buffer + protein Re-spin, resuspend pellets and combine add buffer to a final volume of 1ml Perform a standard semen analysis with this suspension
47 Post-vasectomy analysis To determine the sperm concentration when few/none expected: centrifuge as much of the sample as possible (1000 g for 15 min) in a disposable conical centrifuge tube note the exact volume used Remove most of the supernatant - note volume removed Make at least 5 wet preps (10µl of resuspended pellet under a 22 22mm coverslip) Search through at least 5 wet preps If anything that looks like a sperm is seen the report is not clear Final decision is the responsibility of the embryologist
48 Always: SEMEN ANALYSIS What tests should always be done? Semen volume Sperm concentration Differential motility Morphology If there is an indication: White cells Vitality
49 RESEARCH & NEW TECHNIQUES Sperm kinematics The way sperm swim affects their fertility To get through the cervix, they have to swim in a straight path To get through the outer layer of the egg, they have to generate a lot of power this is seen as hyperactivated motility
50 RESEARCH & NEW TECHNIQUES Sperm kinematics The sperm tracks are analyzed and a number of kinematic parameters are derived, including: Velocity (VCL, VSL and VAP) Velocity ratios (expression of the path shape and regularity) Amplitude of lateral head displacement Beat/cross frequency The proportion of sperm in a sample which meet particular kinematic criteria is used to predict (failure) of: Mucus-penetrating ability Hyperactivation (a marker of sperm function)
51 RESEARCH & NEW TECHNIQUES CASA Computer-aided sperm analysis Able to assess the kinematics of hundreds of sperm in a couple of minutes Means that these tests can be part of the infertility work-up
52 STANDARDIZATION & QUALITY CONTROL Fundamental requirements of all laboratory tests : appropriate and robust methodology careful training operator experience } suitable assay control limits it regular internal comparisons regular external comparisons cost effectiveness accuracy & precision = IQC = EQA College of Reproductive Biology Inaugural Meeting, Houston, May 1997
53 CONCLUSION Semen analysis is an important laboratory test and should be thought of in the same way as any other diagnostic assay It isused in dt determining ii treatmentt tplans for infertility The results can therefore have a huge impact on the level of intervention, with the associated emotional and financial costs to the couple
54 Samples Motility No. Grade a b c d
TECHNICAL GUIDANCE FOR THE ACCREDITATION OF ANDROLOGY LABORATORIES
 TECHNICAL GUIDANCE FOR THE ACCREDITATION OF ANDROLOGY LABORATORIES Approved By: Chief Executive Officer: Ron Josias Accreditation Executive: Mpho Phaloane Revised By: Medical Specialist Technical Committee
TECHNICAL GUIDANCE FOR THE ACCREDITATION OF ANDROLOGY LABORATORIES Approved By: Chief Executive Officer: Ron Josias Accreditation Executive: Mpho Phaloane Revised By: Medical Specialist Technical Committee
Semen. Dr. Mohamed Saad Daoud
 Semen Dr. Mohamed Saad Daoud 1 Reference Books: Urinanalysis and body fluids (Susan King Strasinger- Marjorie Schaub De Lorenzo) Fifth edition Dr. Mohamed Saad Daoud 2 Diagram of the male genitalia Dr.
Semen Dr. Mohamed Saad Daoud 1 Reference Books: Urinanalysis and body fluids (Susan King Strasinger- Marjorie Schaub De Lorenzo) Fifth edition Dr. Mohamed Saad Daoud 2 Diagram of the male genitalia Dr.
Microscope Requirements
 SEMEN EVALUATION EQUIPMENT Microscope Requirements Good quality lenses Phase-contrast preferred for % progressive motility evaluations Objectives 10X, 20X*, 40X*, 100X, minimum Heated stage preferred *Preferably
SEMEN EVALUATION EQUIPMENT Microscope Requirements Good quality lenses Phase-contrast preferred for % progressive motility evaluations Objectives 10X, 20X*, 40X*, 100X, minimum Heated stage preferred *Preferably
Seminal fluid analysis
 What is semen? Semen is the fluid formed at ejaculation. Made of secretions of all the accessory glands of the male genital tract and testicular sperm component Semen quality is maintained by all the accessory
What is semen? Semen is the fluid formed at ejaculation. Made of secretions of all the accessory glands of the male genital tract and testicular sperm component Semen quality is maintained by all the accessory
Abnormalities of Spermatogenesis
 Abnormalities of Spermatogenesis Male Factor 40% of the cause for infertility Sperm is constantly produced by the germinal epithelium of the testicle Sperm generation time 73 days Sperm production is thermoregulated
Abnormalities of Spermatogenesis Male Factor 40% of the cause for infertility Sperm is constantly produced by the germinal epithelium of the testicle Sperm generation time 73 days Sperm production is thermoregulated
CM-B 2008: Semen Analysis INTRODUCTION ANATOMY AND PHYSIOLOGY
 INTRODUCTION Semen analysis is a laboratory test that is primarily used for evaluating fertility potential and for assessing success following a vasectomy procedure. The composition of semen, also known
INTRODUCTION Semen analysis is a laboratory test that is primarily used for evaluating fertility potential and for assessing success following a vasectomy procedure. The composition of semen, also known
Computer Assisted Semen Analysis. M i r a S p e r m A n a l y z e r
 Computer Assisted Semen Analysis M i r a 9 S p e r m A n a l y z e r CASA Mira9 Sperm Analyzer Mira9 (CASA) Specifications System Components 1. PC include Mira9 CASA software. 2. Mira9 special slide. 3.
Computer Assisted Semen Analysis M i r a 9 S p e r m A n a l y z e r CASA Mira9 Sperm Analyzer Mira9 (CASA) Specifications System Components 1. PC include Mira9 CASA software. 2. Mira9 special slide. 3.
Male Reproductive Physiology
 Male Reproductive Physiology Overview Anatomy Function Endocrine and spermatogenesis Testis epididymus,vas deferens,seminal vesicles and prostate Hypothalamic pituitary testicular axis Hormones of the
Male Reproductive Physiology Overview Anatomy Function Endocrine and spermatogenesis Testis epididymus,vas deferens,seminal vesicles and prostate Hypothalamic pituitary testicular axis Hormones of the
The Reproductive System
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Reproductive System 16PART A The Reproductive System Gonads primary sex organs Testes in males
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Reproductive System 16PART A The Reproductive System Gonads primary sex organs Testes in males
System overview Installation System Description System Default Settings and Loading I-Button Tests Components/Kits /Accessories Maintenance & Cleaning
 SQA-VISION TRAINING Content of Presentation System overview Installation System Description System Default Settings and Loading I-Button Tests Components/Kits /Accessories Maintenance & Cleaning SQA-Vision
SQA-VISION TRAINING Content of Presentation System overview Installation System Description System Default Settings and Loading I-Button Tests Components/Kits /Accessories Maintenance & Cleaning SQA-Vision
Sergey I. Moskovtsev and Clifford L. Librach
 Chapter 2 Methods of Sperm Vitality Assessment Sergey I. Moskovtsev and Clifford L. Librach Abstract Sperm vitality is a re fl ection of the proportion of live, membrane-intact spermatozoa determined by
Chapter 2 Methods of Sperm Vitality Assessment Sergey I. Moskovtsev and Clifford L. Librach Abstract Sperm vitality is a re fl ection of the proportion of live, membrane-intact spermatozoa determined by
The Reproductive System
 16 PART A The Reproductive System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Reproductive
16 PART A The Reproductive System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Reproductive
describe the parts and function of semen and the glands that contribute to it
 You need to be able to: describe spermatogenesis (How is sperm made?) describe the anatomy of a sperm describe the parts and function of semen and the glands that contribute to it How is sperm made? Spermatogenesis
You need to be able to: describe spermatogenesis (How is sperm made?) describe the anatomy of a sperm describe the parts and function of semen and the glands that contribute to it How is sperm made? Spermatogenesis
The Reproductive System
 Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 16 The Reproductive System Slides 16.1 16.20 Lecture Slides in PowerPoint by Jerry L. Cook The Reproductive System Gonads
Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 16 The Reproductive System Slides 16.1 16.20 Lecture Slides in PowerPoint by Jerry L. Cook The Reproductive System Gonads
Semen LEARNING OBJECTIVES KEY TERMS
 13044C11.PGS 7/11/02 4:30 PM Page 169 C H A P T E R 11 Semen LEARNING OBJECTIVES Upon completion of this chapter, the reader will be able to: 1 Describe the four components of semen with regard to source
13044C11.PGS 7/11/02 4:30 PM Page 169 C H A P T E R 11 Semen LEARNING OBJECTIVES Upon completion of this chapter, the reader will be able to: 1 Describe the four components of semen with regard to source
Male Reproduction Organs. 1. Testes 2. Epididymis 3. Vas deferens 4. Urethra 5. Penis 6. Prostate 7. Seminal vesicles 8. Bulbourethral glands
 Outline Terminology Human Reproduction Biol 105 Lecture Packet 21 Chapter 17 I. Male Reproduction A. Reproductive organs B. Sperm development II. Female Reproduction A. Reproductive organs B. Egg development
Outline Terminology Human Reproduction Biol 105 Lecture Packet 21 Chapter 17 I. Male Reproduction A. Reproductive organs B. Sperm development II. Female Reproduction A. Reproductive organs B. Egg development
Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization
 Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization may occur! A. Scrotum 1. Muscular pouch that holds the
Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization may occur! A. Scrotum 1. Muscular pouch that holds the
**Florida licensees, please note: This exercise will appear in CE Broker under the specialty of Andrology.
 EDUCATIONAL COMMENTARY SEMEN ANALYSIS AND FERTILITY Commentary provided by: Henry C. Lee, CLS, MASCP, CPHQ Laboratory Manager Arrowhead Regional Medical Center Colton, CA Educational commentary is provided
EDUCATIONAL COMMENTARY SEMEN ANALYSIS AND FERTILITY Commentary provided by: Henry C. Lee, CLS, MASCP, CPHQ Laboratory Manager Arrowhead Regional Medical Center Colton, CA Educational commentary is provided
5 15/3/2012. Malik Al-Momani
 5 15/3/2012 Malik Al-Momani بسم هللا الرحمن الرحيم Spermatogenesis Note : Please refer to slides so see photos. Quick Revision : - Testis is divided by septum into testicular lobules, inside the lobules
5 15/3/2012 Malik Al-Momani بسم هللا الرحمن الرحيم Spermatogenesis Note : Please refer to slides so see photos. Quick Revision : - Testis is divided by septum into testicular lobules, inside the lobules
To General Embryology Dr: Azza Zaki
 Introduction To General Embryology The Human Development is a continuous process that begins when an ovum from a female is fertilized by a sperm from a male. Cell division, growth and differentiation transform
Introduction To General Embryology The Human Development is a continuous process that begins when an ovum from a female is fertilized by a sperm from a male. Cell division, growth and differentiation transform
SEMEN ANALYSIS. A minimum of 2 days and a maximum of 7 days of sexual abstinence.
 2nd Symposium of the Croatian Society of Clinical Embryologists and Andrology Workshop Workstation 1 SEMEN ANALYSIS Evaluation of male fertility: Testis function and male genital tract; accessory sex glands
2nd Symposium of the Croatian Society of Clinical Embryologists and Andrology Workshop Workstation 1 SEMEN ANALYSIS Evaluation of male fertility: Testis function and male genital tract; accessory sex glands
Semen analysis report. 2nd symposium of Croatian Society of Clinical Embryologist and Andrology Workshop, Opatija, November, 2014
 Semen analysis report 2nd symposium of Croatian Society of Clinical Embryologist and Andrology Workshop, Opatija, 28-30 November, 2014 No single test or sperm parameter was found to be absolute in its
Semen analysis report 2nd symposium of Croatian Society of Clinical Embryologist and Andrology Workshop, Opatija, 28-30 November, 2014 No single test or sperm parameter was found to be absolute in its
Male reproduction. Cross section of Human Testis ผศ.ดร.พญ.ส ว ฒณ ค ปต ว ฒ ภาคว ชาสร รว ทยา คณะแพทยศาสตร ศ ร ราชพยาบาล 1. Aims
 Aims Male reproduction Male reproductive structure Spermatogenesis ส ว ฒณ ค ปต ว ฒ ห อง 216 โทร: 7578 Hypothalamo-pituitary-testicular axis Male sex hormone action Male reproductive structure Male reproductive
Aims Male reproduction Male reproductive structure Spermatogenesis ส ว ฒณ ค ปต ว ฒ ห อง 216 โทร: 7578 Hypothalamo-pituitary-testicular axis Male sex hormone action Male reproductive structure Male reproductive
Reproductive System Purpose General Structures Male Structures Functions Female Anatomy Structures Functions Clinical Applications
 The Reproductive System: Male, Ch 23 Outline of class lecture After studying the male reproductive system you should be able to: 1. Define the purpose of reproduction and identify the general organs of
The Reproductive System: Male, Ch 23 Outline of class lecture After studying the male reproductive system you should be able to: 1. Define the purpose of reproduction and identify the general organs of
Semen evaluation in domestic animals I
 Reproductive Biotechnologies Andrology I I Semen evaluation in domestic animals I Prof. Alberto Contri Different aims 1. Diagnosis 2. Handling and preservation Related to the male - Breeding soundness
Reproductive Biotechnologies Andrology I I Semen evaluation in domestic animals I Prof. Alberto Contri Different aims 1. Diagnosis 2. Handling and preservation Related to the male - Breeding soundness
Chapter 22 The Reproductive System (I)
 Chapter 22 The Reproductive System (I) An Overview of Reproductive Physiology o The Male Reproductive System o The Female Reproductive System 22.1 Reproductive System Overview Reproductive system = all
Chapter 22 The Reproductive System (I) An Overview of Reproductive Physiology o The Male Reproductive System o The Female Reproductive System 22.1 Reproductive System Overview Reproductive system = all
Animal Science 434. Sperm Head. Sperm From Different Species. Sperm Structure. Epididymis, Ejaculation and Semen. Head Acrosome Neck Middle Piece
 Sperm Structure Head Acrosome Neck Middle Piece Animal Science 434 Annulus Principal Piece Epididymis, Ejaculation and Semen End Piece Sperm From Different Species Sperm Head (Equatorial Segment) Nucleus
Sperm Structure Head Acrosome Neck Middle Piece Animal Science 434 Annulus Principal Piece Epididymis, Ejaculation and Semen End Piece Sperm From Different Species Sperm Head (Equatorial Segment) Nucleus
Welcome to chapter 2. The following chapter is called Sperm preparation for IVF and ICSI and sperm freezing. The author is Bart Desmet.
 Welcome to chapter 2. The following chapter is called Sperm preparation for IVF and ICSI and sperm freezing. The author is Bart Desmet. 1 After this chapter, the student should be able to know the different
Welcome to chapter 2. The following chapter is called Sperm preparation for IVF and ICSI and sperm freezing. The author is Bart Desmet. 1 After this chapter, the student should be able to know the different
STRUCTURE AND FUNCTION OF THE MALE REPRODUCTIVE SYSTEM
 Unit 7A STRUCTURE AND FUNCTION OF THE MALE REPRODUCTIVE SYSTEM LEARNING OBJECTIVES 1. Learn the structures of the male reproductive system. 2. Learn the functions of the male reproductive system. 3. Learn
Unit 7A STRUCTURE AND FUNCTION OF THE MALE REPRODUCTIVE SYSTEM LEARNING OBJECTIVES 1. Learn the structures of the male reproductive system. 2. Learn the functions of the male reproductive system. 3. Learn
Male Reproductive System
 21-1 21-2 Reproductive System Male Reproductive System Genital Tract In males the testes, held outside the body in the scrotum (optimum temp of about 35 0 C), produce sperm. Sperm mature in coiled tubes
21-1 21-2 Reproductive System Male Reproductive System Genital Tract In males the testes, held outside the body in the scrotum (optimum temp of about 35 0 C), produce sperm. Sperm mature in coiled tubes
Male Reproductive System
 Male Reproductive System The male reproductive system consists of a number of sex organs that are part of the reproductive process. The following sections describe the function of each part of the male
Male Reproductive System The male reproductive system consists of a number of sex organs that are part of the reproductive process. The following sections describe the function of each part of the male
Rodriguez The Semen Analysis
 RODRIGUEZ 2016 Rodriguez 2016 The Semen Analysis DISCLOSURE "Yo divulgo que no tengo relación financiera con intereses comerciales". RODRIGUEZ 2016 Question1 Fill the Blanks with the Correct Statement
RODRIGUEZ 2016 Rodriguez 2016 The Semen Analysis DISCLOSURE "Yo divulgo que no tengo relación financiera con intereses comerciales". RODRIGUEZ 2016 Question1 Fill the Blanks with the Correct Statement
Human Reproduction. Human Reproductive System. Scrotum. Male Reproductive System
 Human Reproductive System Human Reproduction Chapter 41 Contraceptives Scrotum Testes Epididymus Vas Deferens Seminal Vesicles Prostate Gland Bulbourethral Gland Penis Scrotum Sac of smooth muscle tissue
Human Reproductive System Human Reproduction Chapter 41 Contraceptives Scrotum Testes Epididymus Vas Deferens Seminal Vesicles Prostate Gland Bulbourethral Gland Penis Scrotum Sac of smooth muscle tissue
Primary sex organs (gonads): testes and ovaries. Accessory reproductive organs: ducts, glands, and external genitalia
 Male Reproductive System Primary sex organs (gonads): testes and ovaries Produce sex cells (gametes) Secrete steroid sex hormones Androgens (males) Estrogens and progesterone (females) Accessory reproductive
Male Reproductive System Primary sex organs (gonads): testes and ovaries Produce sex cells (gametes) Secrete steroid sex hormones Androgens (males) Estrogens and progesterone (females) Accessory reproductive
Study Guide Answer Key Reproductive System
 Biology 12 Human Biology Textbook: BC Biology 12 Study Guide Answer Key Reproductive System 1. Distinguish between a gamete and a gonad using specific examples from the male and female systems. Gonads
Biology 12 Human Biology Textbook: BC Biology 12 Study Guide Answer Key Reproductive System 1. Distinguish between a gamete and a gonad using specific examples from the male and female systems. Gonads
VideoTesT-Sperm 2.1 VideoTesT-Sperm 2.1 Motility Morphology Motility Standard Method Morphology Standard Method Database
 VideoTesT-Sperm 2.1 CASA is designed to equip the workplace of specialists dealing with sperm analysis. The analyzer enables experts to count the amount of spermatozoa and to estimate their motility parameters
VideoTesT-Sperm 2.1 CASA is designed to equip the workplace of specialists dealing with sperm analysis. The analyzer enables experts to count the amount of spermatozoa and to estimate their motility parameters
Importance of Papanicolaou Staining for Sperm Morphologic Analysis Comparison With an Automated Sperm Quality Analyzer
 Anatomic Pathology / Pap Staining for Sperm Morphologic Analysis Importance of Papanicolaou Staining for Sperm Morphologic Analysis Comparison With an Automated Sperm Quality Analyzer Smita Singh, MD,
Anatomic Pathology / Pap Staining for Sperm Morphologic Analysis Importance of Papanicolaou Staining for Sperm Morphologic Analysis Comparison With an Automated Sperm Quality Analyzer Smita Singh, MD,
Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature
 REPRODUCTION Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature reduction -Testes wall made of fibrous connective
REPRODUCTION Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature reduction -Testes wall made of fibrous connective
Gametogenesis. Omne vivum ex ovo All living things come from eggs.
 Omne vivum ex ovo All living things come from eggs. William Harvery, 1651 Gametogenesis This lecture is the preface, so to speak, to embryology; that is, it introduces the development of the specialized
Omne vivum ex ovo All living things come from eggs. William Harvery, 1651 Gametogenesis This lecture is the preface, so to speak, to embryology; that is, it introduces the development of the specialized
Animal Reproductive Systems. Chapter 42
 Animal Reproductive Systems Chapter 42 Impacts, Issues Male or Female? Body or Genes? Body and genes don t always match male or female characteristics also depend on hormones mutations can result in intersex
Animal Reproductive Systems Chapter 42 Impacts, Issues Male or Female? Body or Genes? Body and genes don t always match male or female characteristics also depend on hormones mutations can result in intersex
Physiologic Anatomy of the Male Sexual Organs
 Reproductive and Hormonal Functions of the Male The reproductive functions of the male can be divided into three major subdivisions: (1) spermatogenesis, which means simply the formation of sperm; (2)
Reproductive and Hormonal Functions of the Male The reproductive functions of the male can be divided into three major subdivisions: (1) spermatogenesis, which means simply the formation of sperm; (2)
Chapter 26: Reproductive Systems. Male 11/29/2015. Male reproductive system is composed of... BIO 218 Fall Gonads (testes)
 Chapter 26: Reproductive Systems BIO 218 Fall 2015 Male Male reproductive system is composed of... Gonads (testes) Duct system (epididymis, ductus deferens, ejaculatory ducts, urethra) Accessory sex glands
Chapter 26: Reproductive Systems BIO 218 Fall 2015 Male Male reproductive system is composed of... Gonads (testes) Duct system (epididymis, ductus deferens, ejaculatory ducts, urethra) Accessory sex glands
The spermatogenesis CHARACTERISTICS OF THE SPERMATOZOON 26/04/2017. Reproductive Biotechnologies Andrology I. Prof. Alberto Contri
 Reproductive Biotechnologies Andrology I The spermatogenesis Prof. Alberto Contri CHARACTERISTICS OF THE SPERMATOZOON 1) Aploid cell with high condensed DNA 2) Forward motility - flagellum 3) Enzymes for
Reproductive Biotechnologies Andrology I The spermatogenesis Prof. Alberto Contri CHARACTERISTICS OF THE SPERMATOZOON 1) Aploid cell with high condensed DNA 2) Forward motility - flagellum 3) Enzymes for
Embryology 3. Spermatogenesis:
 Embryology 3 Spermatogenesis: The 2 testis in males are each divided into lobes and lobules by connective tissue septa forming 250 lobule and in each lobule there are 1 to 4 seminefrous tubule ( so almost
Embryology 3 Spermatogenesis: The 2 testis in males are each divided into lobes and lobules by connective tissue septa forming 250 lobule and in each lobule there are 1 to 4 seminefrous tubule ( so almost
Information Sheet. Male Infertility
 Infertility National Public Awareness Campaign Information Sheet Male Infertility In approximately half of couples complaining of infertility part of the problem lies with the male. Male infertility has
Infertility National Public Awareness Campaign Information Sheet Male Infertility In approximately half of couples complaining of infertility part of the problem lies with the male. Male infertility has
1. Both asexual and sexual reproduction occur in the animal kingdom
 1. Both asexual and sexual reproduction occur in the animal kingdom Asexual reproduction involves the formation of individuals whose genes all come from one parent. There is no fusion of sperm and egg.
1. Both asexual and sexual reproduction occur in the animal kingdom Asexual reproduction involves the formation of individuals whose genes all come from one parent. There is no fusion of sperm and egg.
ANDROVISION - MORE THAN CASA
 ANDROVISION - MORE THAN CASA AndroVision CASA system with Zeiss AxioScope optics and automated ScanStage Computerized semen analysis AndroVision is a highly precise CASA* system for standardised, interactive
ANDROVISION - MORE THAN CASA AndroVision CASA system with Zeiss AxioScope optics and automated ScanStage Computerized semen analysis AndroVision is a highly precise CASA* system for standardised, interactive
Male Reproductive System
 Male Reproductive System Constitution of male reproductive system Genital gland ----testis Genital ducts epididymis / ductus deferens / urinary duct Accessory sex glands Penis prostate gland Seminal vesicle
Male Reproductive System Constitution of male reproductive system Genital gland ----testis Genital ducts epididymis / ductus deferens / urinary duct Accessory sex glands Penis prostate gland Seminal vesicle
MALE REPRODUCTIVE SYSTEM
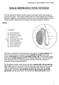 MALE REPRODUCTIVE SYSTEM The male reproductive system consists of primary sex organs (testes) and secondary or accessory sex organs. The secondary organs consist of a series of genital ducts (ductules
MALE REPRODUCTIVE SYSTEM The male reproductive system consists of primary sex organs (testes) and secondary or accessory sex organs. The secondary organs consist of a series of genital ducts (ductules
SEMEN ANALYSIS DISPOSABLES AND COMPONENTS MORE THAN JUST BASIC SEMEN ANALYSIS
 SEMEN ANALYSIS DISPOSABLES AND COMPONENTS MORE THAN JUST BASIC SEMEN ANALYSIS mot MOTILITY AND CONCENTRATION SCA Leja slides Disposable counting chambers for semen analysis, optimised for SCA. 10 micron
SEMEN ANALYSIS DISPOSABLES AND COMPONENTS MORE THAN JUST BASIC SEMEN ANALYSIS mot MOTILITY AND CONCENTRATION SCA Leja slides Disposable counting chambers for semen analysis, optimised for SCA. 10 micron
What You Need to Know
 UW MEDICINE PATIENT EDUCATION What You Need to Know Facts about male infertility This handout explains what causes male infertility, how it is diagnosed, and possible treatments. Infertility is defined
UW MEDICINE PATIENT EDUCATION What You Need to Know Facts about male infertility This handout explains what causes male infertility, how it is diagnosed, and possible treatments. Infertility is defined
6.7 IN. Continuity through Reproduction. What are the differences between male and female gametes? Discuss their formation and physical attributes.
 6.7 IN What are the differences between male and female gametes? Discuss their formation and physical attributes. Males - 4 sperm per parent cell; Females - 1 ovum per parent cell Sperm - motile (tail);
6.7 IN What are the differences between male and female gametes? Discuss their formation and physical attributes. Males - 4 sperm per parent cell; Females - 1 ovum per parent cell Sperm - motile (tail);
Reversible Conditions Organising More Information semen analysis Male Infertility at Melbourne IVF Fertility Preservation
 Male Infertility Understanding fertility in men Conceiving a baby depends on a number of factors, including healthy sperm. After a woman s age, this can be the biggest issue. Reproduction, although simple
Male Infertility Understanding fertility in men Conceiving a baby depends on a number of factors, including healthy sperm. After a woman s age, this can be the biggest issue. Reproduction, although simple
ESHRE Monographs: Manual on Basic Semen Analysis pp , Sperm morphology
 ESHRE Monographs: Manual on Basic Semen Analysis pp. 13 17, 2002 5. Sperm morphology Principles The morphology seen with the microscope is not the true morphology of a living spermatozoon, but an image
ESHRE Monographs: Manual on Basic Semen Analysis pp. 13 17, 2002 5. Sperm morphology Principles The morphology seen with the microscope is not the true morphology of a living spermatozoon, but an image
The Male Reproductive System
 The Male Reproductive System Male Reproductive System The male sex cell is a sperm cell The whole purpose is to produce and deliver sperm to the egg Structure of a Human Sperm Cell Streamlined, built to
The Male Reproductive System Male Reproductive System The male sex cell is a sperm cell The whole purpose is to produce and deliver sperm to the egg Structure of a Human Sperm Cell Streamlined, built to
Computerized semen analysis. Product features. Basic system
 AndroVision - more than CASA AndroVision CASA system with Zeiss AxioScope optics and automated ScanStage Computerized semen analysis AndroVision is a highly precise CASA* system for standardised, interactive
AndroVision - more than CASA AndroVision CASA system with Zeiss AxioScope optics and automated ScanStage Computerized semen analysis AndroVision is a highly precise CASA* system for standardised, interactive
Functions of male Reproductive System: produce gametes deliver gametes protect and support gametes
 Functions of male Reproductive System: produce gametes deliver gametes protect and support gametes Spermatogenesis occurs in the testes after puberty. From the testes they are deposited into the epididymas
Functions of male Reproductive System: produce gametes deliver gametes protect and support gametes Spermatogenesis occurs in the testes after puberty. From the testes they are deposited into the epididymas
Semen Analysis Using Hamilton-Thorne Computer Assisted Semen Analyzer (CASA)
 Semen Analysis Using Hamilton-Thorne Computer Assisted Semen Analyzer (CASA) 5 Ashok Agarwal, Sajal Gupta, and Rakesh Sharma 1 Introduction Semen analysis yields useful information about the fertility
Semen Analysis Using Hamilton-Thorne Computer Assisted Semen Analyzer (CASA) 5 Ashok Agarwal, Sajal Gupta, and Rakesh Sharma 1 Introduction Semen analysis yields useful information about the fertility
Adapted from Preg. & Part., Senger
 MALE ENDOCRINOLOGY AND SPERMATOGENESIS (Chapter 10) AVS 222 (Instructor: Dr. Amin Ahmadzadeh) I. MALE ENDOCRINOLOGY (Figure10-1 to 10-3) A. Glands and their respective hormones 1) Hypothalamic hormone:
MALE ENDOCRINOLOGY AND SPERMATOGENESIS (Chapter 10) AVS 222 (Instructor: Dr. Amin Ahmadzadeh) I. MALE ENDOCRINOLOGY (Figure10-1 to 10-3) A. Glands and their respective hormones 1) Hypothalamic hormone:
SEMEN ANALYSIS DISPOSABLES AND COMPONENTS MORE THAN JUST BASIC SEMEN ANALYSIS
 SEMEN ANALYSIS DISPOSABLES AND COMPONENTS MORE THAN JUST BASIC SEMEN ANALYSIS mot MOTILITY AND CONCENTRATION SCA Leja slides Disposable counting chambers for semen analysis, optimised for SCA. 10 micron
SEMEN ANALYSIS DISPOSABLES AND COMPONENTS MORE THAN JUST BASIC SEMEN ANALYSIS mot MOTILITY AND CONCENTRATION SCA Leja slides Disposable counting chambers for semen analysis, optimised for SCA. 10 micron
Instructions for Use. APO-AB Annexin V-Biotin Apoptosis Detection Kit 100 tests
 3URGXFW,QIRUPDWLRQ Sigma TACS Annexin V Apoptosis Detection Kits Instructions for Use APO-AB Annexin V-Biotin Apoptosis Detection Kit 100 tests For Research Use Only. Not for use in diagnostic procedures.
3URGXFW,QIRUPDWLRQ Sigma TACS Annexin V Apoptosis Detection Kits Instructions for Use APO-AB Annexin V-Biotin Apoptosis Detection Kit 100 tests For Research Use Only. Not for use in diagnostic procedures.
Chapter 14 Reproduction Review Assignment
 Date: Mark: _/45 Chapter 14 Reproduction Review Assignment Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Use the diagram above to answer the next question.
Date: Mark: _/45 Chapter 14 Reproduction Review Assignment Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Use the diagram above to answer the next question.
Human Reproductive System
 Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male=s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male=s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
Male Reproductive System. Dr Maan Al-Abbasi PhD, MSc, MBChB, MD
 Male Reproductive System Dr Maan Al-Abbasi PhD, MSc, MBChB, MD Learning Objectives 1. Describe the General Anatomy of the Male Reproductive System 2. Identify the structures that are related to the prostate.
Male Reproductive System Dr Maan Al-Abbasi PhD, MSc, MBChB, MD Learning Objectives 1. Describe the General Anatomy of the Male Reproductive System 2. Identify the structures that are related to the prostate.
Sperm Preparation for Intrauterine Insemination Using Density Gradient Separation
 Sperm Preparation for Intrauterine Insemination Using Density Gradient Separation 14 Ashok Agarwal, Sajal Gupta, and Rakesh Sharma 1 Introduction Sperm washing is performed to remove seminal plasma and
Sperm Preparation for Intrauterine Insemination Using Density Gradient Separation 14 Ashok Agarwal, Sajal Gupta, and Rakesh Sharma 1 Introduction Sperm washing is performed to remove seminal plasma and
Chapter 28: REPRODUCTIVE SYSTEM: MALE
 Chapter 28: REPRODUCTIVE SYSTEM: MALE I. FUNCTIONAL ANATOMY (Fig. 28.1) A. Testes: glands which produce male gametes, as well as glands producing testosterone 2. Seminiferous tubules (Fig.28.3; 28.5) a.
Chapter 28: REPRODUCTIVE SYSTEM: MALE I. FUNCTIONAL ANATOMY (Fig. 28.1) A. Testes: glands which produce male gametes, as well as glands producing testosterone 2. Seminiferous tubules (Fig.28.3; 28.5) a.
Grade 9 Science - Human Reproduction
 Grade 9 Science - Human Reproduction The human reproductive system is a series of organs that work together for one purpose: reproduction (creating new humans). Each part has a specific role in the reproductive
Grade 9 Science - Human Reproduction The human reproductive system is a series of organs that work together for one purpose: reproduction (creating new humans). Each part has a specific role in the reproductive
Human Reproductive System
 Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
Histology of Male Reproductive system (1)
 Histology of Male Reproductive system (1) Prof. Dr. Malak A. Al-yawer Learning Objectives At the end of this lecture, the medical student will be able to: State the organization of the testis Define seminiferous
Histology of Male Reproductive system (1) Prof. Dr. Malak A. Al-yawer Learning Objectives At the end of this lecture, the medical student will be able to: State the organization of the testis Define seminiferous
Sperm production. Sperm production. Meiosis. Mitosis. The cells of Leydig in testes secrete
 Sperm production Ductus deferens Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Sperm production Ductus deferens Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Sperm production. Sperm production. Controlling sperm production. Meiosis. Mitosis. The cells of Leydig in testes secrete
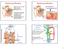 Ductus deferens Sperm production Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Ductus deferens Sperm production Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Testosterone Therapy-Male Infertility
 Testosterone Therapy-Male Infertility Testosterone Therapy-Male Infertility Many men are prescribed testosterone for a variety of reasons. Low testosterone levels (Low T) with no symptoms, general symptoms
Testosterone Therapy-Male Infertility Testosterone Therapy-Male Infertility Many men are prescribed testosterone for a variety of reasons. Low testosterone levels (Low T) with no symptoms, general symptoms
Chapter 36 Active Reading Guide Reproduction and Development
 Name: AP Biology Mr. Croft Chapter 36 Active Reading Guide Reproduction and Development Section 1 1. Distinguish between sexual reproduction and asexual reproduction. 2. Which form of reproduction: a.
Name: AP Biology Mr. Croft Chapter 36 Active Reading Guide Reproduction and Development Section 1 1. Distinguish between sexual reproduction and asexual reproduction. 2. Which form of reproduction: a.
What to do about infertility?
 What to do about infertility? Dr. M.A. Fischer Section Head, Division of Urology, Department of Surgery Assistant Clinical Professor, Department of Obstetrics and Gynecology Hamilton Health Sciences, Hamilton,
What to do about infertility? Dr. M.A. Fischer Section Head, Division of Urology, Department of Surgery Assistant Clinical Professor, Department of Obstetrics and Gynecology Hamilton Health Sciences, Hamilton,
1.0 Purpose - This procedure specifies the method for conducting analysis for semen and sperm in forensic casework.
 Procedure for Semen and Sperm Analysis 1.0 Purpose - This procedure specifies the method for conducting analysis for semen and sperm in forensic casework. 2.0 Scope - This procedure applies to those Forensic
Procedure for Semen and Sperm Analysis 1.0 Purpose - This procedure specifies the method for conducting analysis for semen and sperm in forensic casework. 2.0 Scope - This procedure applies to those Forensic
The Male Reproductive System
 The Male Reproductive System The male reproductive system Testes Genital ducts Accessory sex glands: seminal vesicles prostate bulbourethral glands External genitalia: penis Structure of the Testis Tunica
The Male Reproductive System The male reproductive system Testes Genital ducts Accessory sex glands: seminal vesicles prostate bulbourethral glands External genitalia: penis Structure of the Testis Tunica
Efferent Ducts and Epididymis
 increase) the secretion of each of the androgen regulated proteins. Regulation of spermatogenesis is therefore an extremely complex cascade of cell-cell interactions with the Leydig cells supporting germ
increase) the secretion of each of the androgen regulated proteins. Regulation of spermatogenesis is therefore an extremely complex cascade of cell-cell interactions with the Leydig cells supporting germ
SQA-V Gold Semiannual Validation/Proficiency/QC Recommendations
 MEDICAL ELECTRONIC SYSTEMS 5757 W. Century Blvd. Suite 805 Los Angeles, CA. 90045 Remember, it ALL Started with a Sperm! www.mes global.com SQA-V Gold Semiannual Validation/Proficiency/QC Recommendations
MEDICAL ELECTRONIC SYSTEMS 5757 W. Century Blvd. Suite 805 Los Angeles, CA. 90045 Remember, it ALL Started with a Sperm! www.mes global.com SQA-V Gold Semiannual Validation/Proficiency/QC Recommendations
Outline. Male Reproductive System Testes and Sperm Hormonal Regulation
 Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
Internal Fertilization
 Internal Fertilization Fertilization which takes place inside the female body is called internal fertilization(the union of the gametes within the female body after insemination) Occurs in the widest part
Internal Fertilization Fertilization which takes place inside the female body is called internal fertilization(the union of the gametes within the female body after insemination) Occurs in the widest part
Pluricyte Cardiomyocytes
 Pluricyte Cardiomyocytes Manual Version 2.1 / March 2018 Contents 1. Introduction 2 2. Equipment, Materials and Reagents 3 3. Methods 4 3.1 Coating of tissue culture plates 4 3.2 Thawing Pluricyte Cardiomyocytes
Pluricyte Cardiomyocytes Manual Version 2.1 / March 2018 Contents 1. Introduction 2 2. Equipment, Materials and Reagents 3 3. Methods 4 3.1 Coating of tissue culture plates 4 3.2 Thawing Pluricyte Cardiomyocytes
What are the main functions of the male reproductive system? 1. Produce sperm 2. Deposit sperm into the female 3. Provide a pathway for the removal
 What are the main functions of the male reproductive system? 1. Produce sperm 2. Deposit sperm into the female 3. Provide a pathway for the removal of urine Where is sperm produced? -In the 2 testes What
What are the main functions of the male reproductive system? 1. Produce sperm 2. Deposit sperm into the female 3. Provide a pathway for the removal of urine Where is sperm produced? -In the 2 testes What
Cell Divisions. The autosomes represent the whole body. * Male Sex Chromosomes: XY * Female Sex Chromosomes: XX
 Cell Divisions Each Cell (including gonads) has 46 chromosomes (23 pairs of chromosomes: 22 pairs of autosomes, 1 pair of sex chromosomes) which are located in the nucleus). The autosomes represent the
Cell Divisions Each Cell (including gonads) has 46 chromosomes (23 pairs of chromosomes: 22 pairs of autosomes, 1 pair of sex chromosomes) which are located in the nucleus). The autosomes represent the
Male Reproductive System Dr. Gary Mumaugh
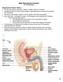 Male Reproductive System Dr. Gary Mumaugh Reproductive System Basics Primary sex organs (gonads) testes in males, ovaries in females Gonads produce sex cells called gametes (gametes means spouses) and
Male Reproductive System Dr. Gary Mumaugh Reproductive System Basics Primary sex organs (gonads) testes in males, ovaries in females Gonads produce sex cells called gametes (gametes means spouses) and
a. the tail disappears b. they become spermatids c. they undergo capacitation d. they have been stored in the uterus for several days
 (2 points each) Multiple Choice. Read each question thoroughly before answering. From the choices available, choose the answer that is the most correct. Place all answers on the accompanying answer sheet.
(2 points each) Multiple Choice. Read each question thoroughly before answering. From the choices available, choose the answer that is the most correct. Place all answers on the accompanying answer sheet.
EXPERIMENT 13: Isolation and Characterization of Erythrocyte
 EXPERIMENT 13: Isolation and Characterization of Erythrocyte Day 1: Isolation of Erythrocyte Steps 1 through 6 of the Switzer & Garrity protocol (pages 220-221) have been performed by the TA. We will be
EXPERIMENT 13: Isolation and Characterization of Erythrocyte Day 1: Isolation of Erythrocyte Steps 1 through 6 of the Switzer & Garrity protocol (pages 220-221) have been performed by the TA. We will be
RayBio Acid Phosphatase Activity Colorimetric Assay. Kit. User Manual Version 1.0 May 5, RayBiotech, Inc. Kit Protocol. (Cat#: 68CL-AcPh-S500)
 RayBio Acid Phosphatase Activity Colorimetric Assay Kit User Manual Version 1.0 May 5, 2014 RayBio Acid Phosphatase Activity Colorimetric Assay (Cat#: 68CL-AcPh-S500) RayBiotech, Inc. We Provide You With
RayBio Acid Phosphatase Activity Colorimetric Assay Kit User Manual Version 1.0 May 5, 2014 RayBio Acid Phosphatase Activity Colorimetric Assay (Cat#: 68CL-AcPh-S500) RayBiotech, Inc. We Provide You With
The new 5 th WHO manual semen parameter reference values do they help or hinder?
 The new 5 th WHO manual semen parameter reference values do they help or hinder? Roelof Menkveld, PhD Andrology Laboratory, Department of Obstetrics and Gynaecology, Tygerberg Academic Hospital and University
The new 5 th WHO manual semen parameter reference values do they help or hinder? Roelof Menkveld, PhD Andrology Laboratory, Department of Obstetrics and Gynaecology, Tygerberg Academic Hospital and University
FEMALE REPRODUCTIVE SYSTEM
 FEMALE REPRODUCTIVE SYSTEM UTERUS (made up of muscular walls, a lining called the endometrium, and a cervix. The uterus is also called womb ) houses and protects embryo/fetus/baby allows nutrient & waste
FEMALE REPRODUCTIVE SYSTEM UTERUS (made up of muscular walls, a lining called the endometrium, and a cervix. The uterus is also called womb ) houses and protects embryo/fetus/baby allows nutrient & waste
Sample Provincial exam Q s: Reproduction
 Sample Provincial exam Q s: Reproduction 11. Functions Testosterone Makes the male sex organs function normally, and also inhibits hypothalamus s release of GnRH and thus LH & FSH and thus testosterone
Sample Provincial exam Q s: Reproduction 11. Functions Testosterone Makes the male sex organs function normally, and also inhibits hypothalamus s release of GnRH and thus LH & FSH and thus testosterone
Aac Reagent Set ELISA for the detection of Acidovorax avenae subsp. citrulli Catalog number: SRA 14800
 List of contents Lot number Aac Reagent Set Item 96 wells 500 wells 1000 wells 5000 wells Capture antibody 0.150 ml 0.275 ml 0.525 ml 2.525 ml Alkaline phosphatase enzyme conjugate 0.150 ml 0.275 ml 0.525
List of contents Lot number Aac Reagent Set Item 96 wells 500 wells 1000 wells 5000 wells Capture antibody 0.150 ml 0.275 ml 0.525 ml 2.525 ml Alkaline phosphatase enzyme conjugate 0.150 ml 0.275 ml 0.525
For more information about how to cite these materials visit
 Author: A. Kent Christensen, Ph.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Share Alike 3.0 License: http://creativecommons.org/licenses/by-sa/3.0/
Author: A. Kent Christensen, Ph.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Share Alike 3.0 License: http://creativecommons.org/licenses/by-sa/3.0/
Unit 15 ~ Learning Guide
 Unit 15 ~ Learning Guide Name: INSTRUCTIONS Complete the following notes and questions as you work through the related lessons. You are required to have this package completed BEFORE you write your unit
Unit 15 ~ Learning Guide Name: INSTRUCTIONS Complete the following notes and questions as you work through the related lessons. You are required to have this package completed BEFORE you write your unit
Outline. History of sperm freezing. Testicular tissue: When and how should it be cryopreserved?
 Testicular tissue: When and how should it be cryopreserved? Greta Verheyen Centre for Reproductive Medicine UZ Brussel, Belgium ESHRE Campus Granada 25-26 March 2010 Outline History of sperm freezing Indications
Testicular tissue: When and how should it be cryopreserved? Greta Verheyen Centre for Reproductive Medicine UZ Brussel, Belgium ESHRE Campus Granada 25-26 March 2010 Outline History of sperm freezing Indications
Special Parts: Gender. Why Have Sex?
 Why Have Sex? Lots of animals clone themselves... 100% of their genes are passed on! Sex requires sharing, it s expensive (time, mate selection, special parts, prenuptial gifts...) So why do it? Special
Why Have Sex? Lots of animals clone themselves... 100% of their genes are passed on! Sex requires sharing, it s expensive (time, mate selection, special parts, prenuptial gifts...) So why do it? Special
Human Reproduction. Male & Female Systems & Menstration
 Human Reproduction Male & Female Systems & Menstration Make a Sperm & Ovum Female Mons Pubis Labia Urethra Perineum Vagina Cervix Uterus Endometrium Fallopian tubes Ovaries Ovum Male Scrotrum Testicle
Human Reproduction Male & Female Systems & Menstration Make a Sperm & Ovum Female Mons Pubis Labia Urethra Perineum Vagina Cervix Uterus Endometrium Fallopian tubes Ovaries Ovum Male Scrotrum Testicle
SISTEMA REPRODUCTOR (LA IDEA FIJA) Copyright 2004 Pearson Education, Inc., publishing as Benjamin Cummings
 SISTEMA REPRODUCTOR (LA IDEA FIJA) How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development,
SISTEMA REPRODUCTOR (LA IDEA FIJA) How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development,
Male Reproductive System
 Male Reproductive System organs that function in: gamete and hormone production not all in abdominal cavity paired testicles = controlled by LH & FSH duct systems accessory glands Testis: Gross Histology
Male Reproductive System organs that function in: gamete and hormone production not all in abdominal cavity paired testicles = controlled by LH & FSH duct systems accessory glands Testis: Gross Histology
