CM-B 2008: Semen Analysis INTRODUCTION ANATOMY AND PHYSIOLOGY
|
|
|
- Lynn Patterson
- 5 years ago
- Views:
Transcription
1 INTRODUCTION Semen analysis is a laboratory test that is primarily used for evaluating fertility potential and for assessing success following a vasectomy procedure. The composition of semen, also known as seminal fluid, consists of spermatozoa (sperm cells) and secretions. Semen analysis is a unique laboratory test in which multiple parameters are evaluated to determine the physical and chemical properties of a seminal fluid sample. Semen analysis consists of macroscopic and microscopic examinations, which provide information on the physical, functional, and biochemical properties of seminal fluid. Within the male genital tract, various anatomical structures contribute to the formation of seminal fluid. These include the testes (testicles), epididymis, vas deferens, seminal vesicles, and prostate gland. The maturation of spermatozoa, known as spermatogenesis, is a rather intricate developmental process. In spermatogenesis, sperm cells undergo a series of changes, which result in the formation of mature motile spermatozoa. In addition, biochemical substances are secreted. These substances provide a nutrient environment for spermatozoa and as a means for transporting sperm cells. In performing semen analysis, various factors can impact the validity of the test results and can occur during the pre-analytic and analytic phases. To prevent erroneous results, it is imperative to have at a minimum: 1. Properly obtained semen sample, 2. Use of standardized test procedures, and 3. Staff proficient in the interpretation of multiple semen analysis test parameters. The main objective of this educational activity is to provide the reader with an overview of semen analysis. Information is given on recognizing factors that can adversely affect semen analysis test results and their impact on subsequent medical management of the patient. Discussion is focused on the manual methods of semen analysis that are used in most laboratories. The readers are encouraged to review the listed references for further information. This includes the most recent edition of the World Health Organization (WHO) manual (4 th edition), which is used as the main source of reference values of semen variables. 1 ANATOMY AND PHYSIOLOGY The development of mature sperm cells is a complex process involving multiple anatomic sites within the male genital tract. The illustration on the male reproductive system and spermatogenesis (Figure 1. in the Appendix) should be used as a supplement to the descriptive overview given below. Sperm maturation occurs within the scrotum, primarily within the testes and epididymides. Since the scrotum is located outside the body, it is at a lower temperature. Decreased body temperature is essential to sperm maturation. 1 - Education
2 The male hormone testosterone is produced in the testes. Within the testes are seminiferous tubules, which are coiled and convoluted. This network of tubules can be identified on microscopic examination of the testes. It is within the seminiferous tubules that sperm cell maturation occurs. In the process of sperm development, undifferentiated germ cells, or spermatogonia, undergo changes in the testes. This involves a unique form of cell division known as meiosis. Spermatogonia undergo divisions resulting in primary and secondary spermatocytes, respectively. The secondary spermatocytes undergo further meiosis and evolve into spermatids. The spermatids undergo further development into immature immotile sperm. Within the testes are sertoli cells that provide support and nourishment to the developing sperm cells. Following maturation in the testes, immature spermatozoa are carried within fluid to the epididymides. Each epididymis is also located within the scrotum. Within the epididymis, the spermatozoa undergo the final stages of maturation and become motile. Mature sperm cells remain in the epididymis until ejaculation occurs. When spermatozoa leave the epididymis, these sperm cells are carried through the vas deferens, which connects to an ejaculatory duct. Each ejaculatory duct is in proximity to the seminal vesicles and transverses into the prostate gland. The seminal vesicles and prostate glands are accessory glands in the male reproductive tract. They produce biochemical substances that provide a nutrient milieu for sperm cells. Seminal vesicles produce most of the fluid component in semen. Fructose is produced in the seminal vesicles. The prostate gland secretes protein, zinc, and enzymes, including acid phosphatase. The fluids from the prostate gland and seminal vesicles are added to the ejaculatory duct. The results of semen analysis can indicate an anatomic abnormality of the male genital tract. The absence of spermatozoa (azoospermia) or a marked decrease in the number of sperm cells (oligospermia) on semen analysis can signify an obstruction to the vas deferens or ejaculatory duct. These findings can prompt a more comprehensive urological evaluation for the patient. SEMINAL FLUID SPECIMEN AND SEMEN ANALYSIS In performing a semen analysis, it is crucial to maintain specimen integrity throughout all phases of testing. A suboptimal specimen can adversely affect the semen analysis results. Pre-Analytical Test Phase Patients should be instructed on specimen collection. The instructions should include an emphasis on prompt delivery of the semen sample to the laboratory, especially if collected off site and not subjecting the semen sample to extreme temperature fluctuations during transit to the laboratory. If the specimen is obtained in proximity to the laboratory, an appropriate and comfortable environment should be made available to the patient. 2 - Education
3 The following items should be included in patients instructions for collection of semen samples: The semen sample should be collected after a period of sexual abstinence of at least 48 hours, but not more than 7 days. The patient produces a semen sample by masturbation and ejaculation into a wide mouthed container. The laboratory should ensure that the containers used are not toxic to sperm prior to their usage. 1 Lubricants and condoms should not be used in specimen procurement, since these can potentially affect the validity of the test results. It is important to obtain collection of a complete semen specimen. An incomplete specimen collection may not provide accurate results. Since sperm concentration is highest in the first portion of the ejaculate, an initial loss of specimen could result in a spurious decrease in sperm count. Analytical Test Phase Semen analysis testing in the laboratory should commence within one hour of specimen procurement. The sample should be well mixed. The evaluated parameters of a semen analysis include macroscopic (visual) and microscopic examinations. The macroscopic evaluation includes: appearance, volume, liquefaction, viscosity, and ph. The microscopic examination includes sperm count, motility, and morphology. Other microscopic findings may be seen, such as sperm agglutination or the presence of other cells, (e.g. white blood cells). These findings and their potential clinical impact will be further discussed. Macroscopic Evaluation Color/Appearance The appearance of normal semen is a homogeneous gray-opalescent or creamy color. If the color is red or brownish, this may indicate the presence of blood in seminal fluid. If a semen sample appears white and turbid, this can signify inflammation and possible infection. Volume Normal volume is 2 to 5 ml. If a patient has low volume especially on repeat semen samples, this finding may indicate an anatomic abnormality of the genital tract. An increased semen volume can be seen in retrograde ejaculation. In this condition, seminal fluid, which would normally be passed through the urethra, enters into the bladder. Diagnosis is made when sperm cells are noted on urinalysis. ph Normal semen reference ph range is 7.2 to ,2 Variations in volume and low ph may be due to congenital abnormalities of the genital tract or to obstruction. A ph of 8.0 or greater can be associated with infection of the prostate, seminal vesicle, or epididymis Education
4 Liquefaction & Viscosity When ejaculated, semen has a thick consistency that reverts to a liquid. Normal seminal fluid samples should liquify within 60 minutes at room temperature, although most samples will liquify in a shorter period of time, (i.e., 15 minutes or less). In highly viscous semen, liquefaction may be incomplete. Failure of complete liquefaction can be evaluated by aspirating a portion of the semen sample into a pipette. As the sample is slowly expelled from the pipette, the semen should form small discrete droplets. Semen samples of high viscosity will not form droplets and will demonstrate an elongated thread-like consistency. Increased semen viscosity and abnormal liquefaction can affect sperm count and morphology results. Microscopic Examination Sperm Count This parameter refers to the number of sperm cells per milliliter (ml) or concentration. A sperm count or 1 density greater than 20 million sperm / ml is considered within normal limits. A counting chamber is used to assess sperm count. Different counting chambers exist, and procedures for counting spermatozoa vary among chambers. Procedural differences can include the number of fields or grids examined or the need to dilute a semen sample prior to determining the count. If the number of sperm cells varies considerably from field to field, the specimen may not be homogeneous and should be thoroughly mixed. Other factors that can contribute to count variations are specimen dilution, microscopic viewing of grids versus fields, and for some chambers, mathematical calculations. Duplicate counts of 200 spermatozoa are advised to obviate counting error. 1 Aside from technical/ procedural differences between counting chambers, intrinsic abnormalities in a given semen sample, namely increased viscosity, can affect sperm count. If no sperm cells are seen on initial examination, the semen specimen should be centrifuged and re-examined. If no spermatozoa are identified following these steps, then the absence of sperm cells should be reported. Motility This parameter determines the percentage of spermatozoa with progressive forward movement. At least five microscopic fields are examined to grade the movement of 200 spermatozoa as rapid progressive, slow progressive, non-progressive motility, or non-motility. There is subjective interpretation in grading sperm cell motility. If a large percentage of non-motile spermatozoa are present, this may signify either a sperm cell flagellum defect or the presence of dead sperm. Distinguishing between live and dead spermatozoa can 4 - Education
5 be done through a supravital stain such as eosin Y. In principle, dead spermatozoa have damaged cell membranes, which consequently take up the stain; whereas live spermatozoa have intact cell membranes and do not take up the stain. The dead sperm cells stain red and live sperm cells are unstained. Poor sperm motility can affect fertility potential. Decreased motility can impede spermatozoa from entering the cervix and moving into the fallopian tubes and ovum. Morphology A spermatozoan or sperm cell is comprised of a head, neck, acrosome, and tail. A sperm cell is generally considered normal if it has a smooth and oval head, an acrosome comprising 40-70% of the sperm head, symmetrical neck insertion into head, a midpiece with no large cytoplasmic droplets (greater than 30% of head size), and a uniform tail of regular width and length without coiling or bent configuration. In addition to these morphological criteria, there are measurement criteria pertaining to length and width of a sperm cell. 1 An ocular micrometer should be used in determining spermatozoan measurements. Sperm cells are evaluated on stained slides using bright field microscopy. At least 200 consecutive spermatozoa are examined when possible. Abnormalities of a sperm cell may involve a single region (e.g., head, tail, etc.) or involve multiple regions (e.g., head and tail, head and neck, etc.), or involve abnormal length or width. As the results of the proficiency tests indicate, participating laboratories use various classifications and stains in assessing sperm morphology. Stains include Papanicolaou, Spermac, Shorr, Wright Giemsa, and Diff-Quik. Within selected subgroups using similar classification and stain, variations in reported morphology results were noted. Adhering to standard staining protocols is important since technical deviations can affect the quality of the slide. Artifacts on the slide can interfere with accurate sperm cell interpretation. Other factors can impact sperm morphology evaluation. Sperm concentrations, particularly in the high and low ranges, can impact the quality of smear preparation. There may be a subjective interpretation of classifying sperm cells as normal or abnormal, especially if an abnormality is subtle. The Kruger (Tygerberg) classification uses strict criteria in determining whether or not spermatozoa are normal. Based on the percentage of normal spermatozoa, there are three threshold groups: 0-4% normal forms 5-14% normal forms Greater than 14% normal forms These groups are used clinically as a predictive value in determining in-vitro fertilization outcomes. 5 - Education
6 In the most recent WHO semen manual (4th edition), the reference value for normal sperm morphology has changed from that of previous editions (WHO 2 nd and 3 rd eds.). The reference value is based on strict criteria. From a clinical perspective, morphological abnormalities provide information on sperm functionality. For example, if sperm cells have significant tail defects, the migratory activity of spermatozoa through cervical mucus can be decreased. An acrosome defect may impede a sperm cell from penetrating an oocyte (egg) membrane for fertilization. Post-Analytic Test Phase In semen analysis, there can be unexpected findings that may prompt further evaluation. When sperm cells are absent (azoospermia), a fructose test can be performed to determine if a congenital abnormality or obstruction is present. As previously mentioned, fructose is produced in the seminal vesicles and secreted. A fructose level can be low if there are congential anomalies or obstruction involving the seminal vesicles, vas deferens, or ejaculatory ducts. When motile spermatozoa stick to each other, this is agglutination. Sperm cells can agglutinate in a head to head, or tail to tail, or head to tail configuration. If the sperm cells demonstrate a consistent pattern of agglutination on microscopic examination, this finding can indicate an immunological etiology, such as the presence of antisperm antibodies. Round cells may be seen on microscopic review. These cells may represent immature sperm cells, white blood cell leukocytes, or epithelial cells undergoing degenerative changes. If bacteria and/ or leukocytes are noted, seminal cultures should be considered for further evaluation. CLINICAL MANAGEMENT The findings of semen analysis can influence medical management of an infertile couple. In male patients with low sperm counts or abnormal sperm morphology, assisted reproductive techniques such as in-vitro fertilization or intracytoplasmic sperm injection may be used to enhance the likelihood of fertilization. SUMMARY In semen analysis, many factors during the pre-analytic and analytic test phases can impact the validity of the results. It is vital that laboratories maintain good standard consistent practices and technical competency. Since multiple factors can affect results of semen analysis, repeat testing on a different sample should be made especially prior to costly and time consuming assisted reproductive technologies and procedures. 6 - Education
7 References 1. World Health Organization (WHO). World Health Organization Laboratory Manual for Human Semen and Sperm Cervical-Mucus Interaction. 4th ed. Cambridge, UK: Cambridge University Press; Brunzel NA. Fundamentals of Urine & Body Fluid Analysis. 2 nd ed. Philadelphia, Pa: Elsevier Saunders; Fink LM, Marlar RA, Miller JL. In: McPherson RA, Pincus MR, eds. Henry s Clinical Diagnosis and Management by Laboratory Methods. 21 st ed. Philadelphia, Pa: Elsevier Churchill Livingstone; Kruger TF, Franken DR. Atlas of Human Sperm Morphology Evaluation. London: Taylor & Francis; Kjeldsberg CR, Knight JA, eds. Body Fluids. 3 rd ed. Chicago, IL. American Society of Clinical Pathologists; Menkveld R, Oettle EE, Kruger TF, Swanson RJ, Acosta AA, Oehninger S. Atlas of Human Sperm Morphology. Baltimore, Md: Williams & Wilkins; Adelman MM, Cahill EM, eds. Atlas of Sperm Morphology. Chicago, IL: ASCP Press; Education
8 Appendix Figure Education
9 Education Activity Authors Patricia A. Devine, MD, FCAP: Patricia Devine, MD, is the Medical Director of the Department of Pathology and Laboratory Medicine at Lowell General Hospital in Lowell, Massachusetts. She is a member of the Hematology and Clinical Microscopy Resource Committee for the College of American Pathologists (CAP) and has a special interest in body fluids. Roberta L. Zimmerman, MD, FCAP: Roberta L. Zimmerman, MD, is the Clinical Laboratory Director and Pathologist for Grand Itasca Clinic and Hospital in Grand Rapids, Minnesota. She also serves as Laboratory Director and consulting pathologist for three Northern Minnesota hospitals, provides coroner s autopsies for Itasca and Koochiching Counties and is a member of the Hematology and Clinical Microscopy Resource Committee for the College of American Pathologists (CAP). She has a special interest in clinical pathology, urinalysis in particular. Education Activity Contributors Eric F. Glassy, MD, FCAP: Eric F. Glassy, MD, is Medical Director at Pathology Inc., Torrance, California. He is a member of the Council on Education and is chairman of the Curriculum Committee of the College of American Pathologists (CAP). Dr. Glassy is an author/editor of several pathology books and book chapters. He is also a software programmer for pathology-related projects dealing with prostate biopsy reporting, whole slide digital imaging, and flow cytometry. Barb Flamich, MT(ASCP): Barb Flamich, MT(ASCP), is an Instructional Designer at the College of American Pathologists (CAP). 9 - Education
Abnormalities of Spermatogenesis
 Abnormalities of Spermatogenesis Male Factor 40% of the cause for infertility Sperm is constantly produced by the germinal epithelium of the testicle Sperm generation time 73 days Sperm production is thermoregulated
Abnormalities of Spermatogenesis Male Factor 40% of the cause for infertility Sperm is constantly produced by the germinal epithelium of the testicle Sperm generation time 73 days Sperm production is thermoregulated
Seminal fluid analysis
 What is semen? Semen is the fluid formed at ejaculation. Made of secretions of all the accessory glands of the male genital tract and testicular sperm component Semen quality is maintained by all the accessory
What is semen? Semen is the fluid formed at ejaculation. Made of secretions of all the accessory glands of the male genital tract and testicular sperm component Semen quality is maintained by all the accessory
Semen. Dr. Mohamed Saad Daoud
 Semen Dr. Mohamed Saad Daoud 1 Reference Books: Urinanalysis and body fluids (Susan King Strasinger- Marjorie Schaub De Lorenzo) Fifth edition Dr. Mohamed Saad Daoud 2 Diagram of the male genitalia Dr.
Semen Dr. Mohamed Saad Daoud 1 Reference Books: Urinanalysis and body fluids (Susan King Strasinger- Marjorie Schaub De Lorenzo) Fifth edition Dr. Mohamed Saad Daoud 2 Diagram of the male genitalia Dr.
The Reproductive System
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Reproductive System 16PART A The Reproductive System Gonads primary sex organs Testes in males
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Reproductive System 16PART A The Reproductive System Gonads primary sex organs Testes in males
The Reproductive System
 Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 16 The Reproductive System Slides 16.1 16.20 Lecture Slides in PowerPoint by Jerry L. Cook The Reproductive System Gonads
Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 16 The Reproductive System Slides 16.1 16.20 Lecture Slides in PowerPoint by Jerry L. Cook The Reproductive System Gonads
Male Reproductive Physiology
 Male Reproductive Physiology Overview Anatomy Function Endocrine and spermatogenesis Testis epididymus,vas deferens,seminal vesicles and prostate Hypothalamic pituitary testicular axis Hormones of the
Male Reproductive Physiology Overview Anatomy Function Endocrine and spermatogenesis Testis epididymus,vas deferens,seminal vesicles and prostate Hypothalamic pituitary testicular axis Hormones of the
The Reproductive System
 16 PART A The Reproductive System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Reproductive
16 PART A The Reproductive System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Reproductive
Chapter 22 The Reproductive System (I)
 Chapter 22 The Reproductive System (I) An Overview of Reproductive Physiology o The Male Reproductive System o The Female Reproductive System 22.1 Reproductive System Overview Reproductive system = all
Chapter 22 The Reproductive System (I) An Overview of Reproductive Physiology o The Male Reproductive System o The Female Reproductive System 22.1 Reproductive System Overview Reproductive system = all
Male Reproductive System
 21-1 21-2 Reproductive System Male Reproductive System Genital Tract In males the testes, held outside the body in the scrotum (optimum temp of about 35 0 C), produce sperm. Sperm mature in coiled tubes
21-1 21-2 Reproductive System Male Reproductive System Genital Tract In males the testes, held outside the body in the scrotum (optimum temp of about 35 0 C), produce sperm. Sperm mature in coiled tubes
Male Reproduction Organs. 1. Testes 2. Epididymis 3. Vas deferens 4. Urethra 5. Penis 6. Prostate 7. Seminal vesicles 8. Bulbourethral glands
 Outline Terminology Human Reproduction Biol 105 Lecture Packet 21 Chapter 17 I. Male Reproduction A. Reproductive organs B. Sperm development II. Female Reproduction A. Reproductive organs B. Egg development
Outline Terminology Human Reproduction Biol 105 Lecture Packet 21 Chapter 17 I. Male Reproduction A. Reproductive organs B. Sperm development II. Female Reproduction A. Reproductive organs B. Egg development
describe the parts and function of semen and the glands that contribute to it
 You need to be able to: describe spermatogenesis (How is sperm made?) describe the anatomy of a sperm describe the parts and function of semen and the glands that contribute to it How is sperm made? Spermatogenesis
You need to be able to: describe spermatogenesis (How is sperm made?) describe the anatomy of a sperm describe the parts and function of semen and the glands that contribute to it How is sperm made? Spermatogenesis
STRUCTURE AND FUNCTION OF THE MALE REPRODUCTIVE SYSTEM
 Unit 7A STRUCTURE AND FUNCTION OF THE MALE REPRODUCTIVE SYSTEM LEARNING OBJECTIVES 1. Learn the structures of the male reproductive system. 2. Learn the functions of the male reproductive system. 3. Learn
Unit 7A STRUCTURE AND FUNCTION OF THE MALE REPRODUCTIVE SYSTEM LEARNING OBJECTIVES 1. Learn the structures of the male reproductive system. 2. Learn the functions of the male reproductive system. 3. Learn
Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization
 Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization may occur! A. Scrotum 1. Muscular pouch that holds the
Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization may occur! A. Scrotum 1. Muscular pouch that holds the
To General Embryology Dr: Azza Zaki
 Introduction To General Embryology The Human Development is a continuous process that begins when an ovum from a female is fertilized by a sperm from a male. Cell division, growth and differentiation transform
Introduction To General Embryology The Human Development is a continuous process that begins when an ovum from a female is fertilized by a sperm from a male. Cell division, growth and differentiation transform
Rodriguez The Semen Analysis
 RODRIGUEZ 2016 Rodriguez 2016 The Semen Analysis DISCLOSURE "Yo divulgo que no tengo relación financiera con intereses comerciales". RODRIGUEZ 2016 Question1 Fill the Blanks with the Correct Statement
RODRIGUEZ 2016 Rodriguez 2016 The Semen Analysis DISCLOSURE "Yo divulgo que no tengo relación financiera con intereses comerciales". RODRIGUEZ 2016 Question1 Fill the Blanks with the Correct Statement
Human Reproduction. Human Reproductive System. Scrotum. Male Reproductive System
 Human Reproductive System Human Reproduction Chapter 41 Contraceptives Scrotum Testes Epididymus Vas Deferens Seminal Vesicles Prostate Gland Bulbourethral Gland Penis Scrotum Sac of smooth muscle tissue
Human Reproductive System Human Reproduction Chapter 41 Contraceptives Scrotum Testes Epididymus Vas Deferens Seminal Vesicles Prostate Gland Bulbourethral Gland Penis Scrotum Sac of smooth muscle tissue
Male Reproductive System
 Male Reproductive System The male reproductive system consists of a number of sex organs that are part of the reproductive process. The following sections describe the function of each part of the male
Male Reproductive System The male reproductive system consists of a number of sex organs that are part of the reproductive process. The following sections describe the function of each part of the male
SEMEN ANALYSIS: Sadeghi MR., (PhD).
 : What? When? How? Why? Sadeghi MR., (PhD). Clinical embryologist, Avicenna Infertility Clinic Editor in chief, Journal of Reproduction & Infertility Avicenna Research Institute : What? When? How? Why?
: What? When? How? Why? Sadeghi MR., (PhD). Clinical embryologist, Avicenna Infertility Clinic Editor in chief, Journal of Reproduction & Infertility Avicenna Research Institute : What? When? How? Why?
TECHNICAL GUIDANCE FOR THE ACCREDITATION OF ANDROLOGY LABORATORIES
 TECHNICAL GUIDANCE FOR THE ACCREDITATION OF ANDROLOGY LABORATORIES Approved By: Chief Executive Officer: Ron Josias Accreditation Executive: Mpho Phaloane Revised By: Medical Specialist Technical Committee
TECHNICAL GUIDANCE FOR THE ACCREDITATION OF ANDROLOGY LABORATORIES Approved By: Chief Executive Officer: Ron Josias Accreditation Executive: Mpho Phaloane Revised By: Medical Specialist Technical Committee
Microscope Requirements
 SEMEN EVALUATION EQUIPMENT Microscope Requirements Good quality lenses Phase-contrast preferred for % progressive motility evaluations Objectives 10X, 20X*, 40X*, 100X, minimum Heated stage preferred *Preferably
SEMEN EVALUATION EQUIPMENT Microscope Requirements Good quality lenses Phase-contrast preferred for % progressive motility evaluations Objectives 10X, 20X*, 40X*, 100X, minimum Heated stage preferred *Preferably
Female and Male Reproductive Systems
 Female and Male Reproductive Systems Reproductive System: Organs that make possible the production of offspring. Female Reproductive System Female Reproductive System: Words to be familiar with ESTROGEN
Female and Male Reproductive Systems Reproductive System: Organs that make possible the production of offspring. Female Reproductive System Female Reproductive System: Words to be familiar with ESTROGEN
Semen LEARNING OBJECTIVES KEY TERMS
 13044C11.PGS 7/11/02 4:30 PM Page 169 C H A P T E R 11 Semen LEARNING OBJECTIVES Upon completion of this chapter, the reader will be able to: 1 Describe the four components of semen with regard to source
13044C11.PGS 7/11/02 4:30 PM Page 169 C H A P T E R 11 Semen LEARNING OBJECTIVES Upon completion of this chapter, the reader will be able to: 1 Describe the four components of semen with regard to source
1. Both asexual and sexual reproduction occur in the animal kingdom
 1. Both asexual and sexual reproduction occur in the animal kingdom Asexual reproduction involves the formation of individuals whose genes all come from one parent. There is no fusion of sperm and egg.
1. Both asexual and sexual reproduction occur in the animal kingdom Asexual reproduction involves the formation of individuals whose genes all come from one parent. There is no fusion of sperm and egg.
- production of two types of gametes -- fused at fertilization to form zygote
 Male reproductive system I. Sexual reproduction -- overview - production of two types of gametes -- fused at fertilization to form zygote - promotes genetic variety among members of a species -- each offspring
Male reproductive system I. Sexual reproduction -- overview - production of two types of gametes -- fused at fertilization to form zygote - promotes genetic variety among members of a species -- each offspring
Study Guide Answer Key Reproductive System
 Biology 12 Human Biology Textbook: BC Biology 12 Study Guide Answer Key Reproductive System 1. Distinguish between a gamete and a gonad using specific examples from the male and female systems. Gonads
Biology 12 Human Biology Textbook: BC Biology 12 Study Guide Answer Key Reproductive System 1. Distinguish between a gamete and a gonad using specific examples from the male and female systems. Gonads
6.7 IN. Continuity through Reproduction. What are the differences between male and female gametes? Discuss their formation and physical attributes.
 6.7 IN What are the differences between male and female gametes? Discuss their formation and physical attributes. Males - 4 sperm per parent cell; Females - 1 ovum per parent cell Sperm - motile (tail);
6.7 IN What are the differences between male and female gametes? Discuss their formation and physical attributes. Males - 4 sperm per parent cell; Females - 1 ovum per parent cell Sperm - motile (tail);
The spermatogenesis CHARACTERISTICS OF THE SPERMATOZOON 26/04/2017. Reproductive Biotechnologies Andrology I. Prof. Alberto Contri
 Reproductive Biotechnologies Andrology I The spermatogenesis Prof. Alberto Contri CHARACTERISTICS OF THE SPERMATOZOON 1) Aploid cell with high condensed DNA 2) Forward motility - flagellum 3) Enzymes for
Reproductive Biotechnologies Andrology I The spermatogenesis Prof. Alberto Contri CHARACTERISTICS OF THE SPERMATOZOON 1) Aploid cell with high condensed DNA 2) Forward motility - flagellum 3) Enzymes for
Animal Reproductive Systems. Chapter 42
 Animal Reproductive Systems Chapter 42 Impacts, Issues Male or Female? Body or Genes? Body and genes don t always match male or female characteristics also depend on hormones mutations can result in intersex
Animal Reproductive Systems Chapter 42 Impacts, Issues Male or Female? Body or Genes? Body and genes don t always match male or female characteristics also depend on hormones mutations can result in intersex
The beginning of puberty is marked by the progressive increase in the production of sex hormones.
 Puberty is characterized by the changes that prepare the human body for the ability to reproduce. This stage generally occurs between the ages of 10 and 14 years old. The beginning of puberty is marked
Puberty is characterized by the changes that prepare the human body for the ability to reproduce. This stage generally occurs between the ages of 10 and 14 years old. The beginning of puberty is marked
Male Reproductive System Dr. Gary Mumaugh
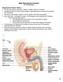 Male Reproductive System Dr. Gary Mumaugh Reproductive System Basics Primary sex organs (gonads) testes in males, ovaries in females Gonads produce sex cells called gametes (gametes means spouses) and
Male Reproductive System Dr. Gary Mumaugh Reproductive System Basics Primary sex organs (gonads) testes in males, ovaries in females Gonads produce sex cells called gametes (gametes means spouses) and
Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature
 REPRODUCTION Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature reduction -Testes wall made of fibrous connective
REPRODUCTION Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature reduction -Testes wall made of fibrous connective
Chapter 28: REPRODUCTIVE SYSTEM: MALE
 Chapter 28: REPRODUCTIVE SYSTEM: MALE I. FUNCTIONAL ANATOMY (Fig. 28.1) A. Testes: glands which produce male gametes, as well as glands producing testosterone 2. Seminiferous tubules (Fig.28.3; 28.5) a.
Chapter 28: REPRODUCTIVE SYSTEM: MALE I. FUNCTIONAL ANATOMY (Fig. 28.1) A. Testes: glands which produce male gametes, as well as glands producing testosterone 2. Seminiferous tubules (Fig.28.3; 28.5) a.
Reversible Conditions Organising More Information semen analysis Male Infertility at Melbourne IVF Fertility Preservation
 Male Infertility Understanding fertility in men Conceiving a baby depends on a number of factors, including healthy sperm. After a woman s age, this can be the biggest issue. Reproduction, although simple
Male Infertility Understanding fertility in men Conceiving a baby depends on a number of factors, including healthy sperm. After a woman s age, this can be the biggest issue. Reproduction, although simple
What You Need to Know
 UW MEDICINE PATIENT EDUCATION What You Need to Know Facts about male infertility This handout explains what causes male infertility, how it is diagnosed, and possible treatments. Infertility is defined
UW MEDICINE PATIENT EDUCATION What You Need to Know Facts about male infertility This handout explains what causes male infertility, how it is diagnosed, and possible treatments. Infertility is defined
Reproductive System Purpose General Structures Male Structures Functions Female Anatomy Structures Functions Clinical Applications
 The Reproductive System: Male, Ch 23 Outline of class lecture After studying the male reproductive system you should be able to: 1. Define the purpose of reproduction and identify the general organs of
The Reproductive System: Male, Ch 23 Outline of class lecture After studying the male reproductive system you should be able to: 1. Define the purpose of reproduction and identify the general organs of
**Florida licensees, please note: This exercise will appear in CE Broker under the specialty of Andrology.
 EDUCATIONAL COMMENTARY SEMEN ANALYSIS AND FERTILITY Commentary provided by: Henry C. Lee, CLS, MASCP, CPHQ Laboratory Manager Arrowhead Regional Medical Center Colton, CA Educational commentary is provided
EDUCATIONAL COMMENTARY SEMEN ANALYSIS AND FERTILITY Commentary provided by: Henry C. Lee, CLS, MASCP, CPHQ Laboratory Manager Arrowhead Regional Medical Center Colton, CA Educational commentary is provided
Male Reproductive System. Dr Maan Al-Abbasi PhD, MSc, MBChB, MD
 Male Reproductive System Dr Maan Al-Abbasi PhD, MSc, MBChB, MD Learning Objectives 1. Describe the General Anatomy of the Male Reproductive System 2. Identify the structures that are related to the prostate.
Male Reproductive System Dr Maan Al-Abbasi PhD, MSc, MBChB, MD Learning Objectives 1. Describe the General Anatomy of the Male Reproductive System 2. Identify the structures that are related to the prostate.
Chapter 26: Reproductive Systems. Male 11/29/2015. Male reproductive system is composed of... BIO 218 Fall Gonads (testes)
 Chapter 26: Reproductive Systems BIO 218 Fall 2015 Male Male reproductive system is composed of... Gonads (testes) Duct system (epididymis, ductus deferens, ejaculatory ducts, urethra) Accessory sex glands
Chapter 26: Reproductive Systems BIO 218 Fall 2015 Male Male reproductive system is composed of... Gonads (testes) Duct system (epididymis, ductus deferens, ejaculatory ducts, urethra) Accessory sex glands
Topic 18- Human Reproductive System. Day 2-Female (and review of) Male Reproductive Systems
 Topic 18- Human Reproductive System Day 2-Female (and review of) Male Reproductive Systems Bell Ringer (5 minutes) Bioblitz WHAT ARE WE LEARNING TODAY? Date: 12/14-12/15 Topic: Human Reproductive System
Topic 18- Human Reproductive System Day 2-Female (and review of) Male Reproductive Systems Bell Ringer (5 minutes) Bioblitz WHAT ARE WE LEARNING TODAY? Date: 12/14-12/15 Topic: Human Reproductive System
Student Academic Learning Services Page 1 of 5 Reproductive System Practice
 Student Academic Learning Services Page 1 of 5 Reproductive System Practice Fill in the blanks using the words listed: accessory glands, vas deferens, penis, scrotum, fallopian tube, testes, urethra, vagina,
Student Academic Learning Services Page 1 of 5 Reproductive System Practice Fill in the blanks using the words listed: accessory glands, vas deferens, penis, scrotum, fallopian tube, testes, urethra, vagina,
Outline. Male Reproductive System Testes and Sperm Hormonal Regulation
 Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
Physiologic Anatomy of the Male Sexual Organs
 Reproductive and Hormonal Functions of the Male The reproductive functions of the male can be divided into three major subdivisions: (1) spermatogenesis, which means simply the formation of sperm; (2)
Reproductive and Hormonal Functions of the Male The reproductive functions of the male can be divided into three major subdivisions: (1) spermatogenesis, which means simply the formation of sperm; (2)
Male Reproductive System
 Male Reproductive System organs that function in: gamete and hormone production not all in abdominal cavity paired testicles = controlled by LH & FSH duct systems accessory glands Testis: Gross Histology
Male Reproductive System organs that function in: gamete and hormone production not all in abdominal cavity paired testicles = controlled by LH & FSH duct systems accessory glands Testis: Gross Histology
SISTEMA REPRODUCTOR (LA IDEA FIJA) Copyright 2004 Pearson Education, Inc., publishing as Benjamin Cummings
 SISTEMA REPRODUCTOR (LA IDEA FIJA) How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development,
SISTEMA REPRODUCTOR (LA IDEA FIJA) How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development,
Reproductive system Presented by: Ms. Priya
 Reproductive system Presented by: Ms. Priya Reproductive system Female reproductive system has two functions: produce egg cells to protect and nourish the offspring (baby) until birth. Male reproductive
Reproductive system Presented by: Ms. Priya Reproductive system Female reproductive system has two functions: produce egg cells to protect and nourish the offspring (baby) until birth. Male reproductive
5 15/3/2012. Malik Al-Momani
 5 15/3/2012 Malik Al-Momani بسم هللا الرحمن الرحيم Spermatogenesis Note : Please refer to slides so see photos. Quick Revision : - Testis is divided by septum into testicular lobules, inside the lobules
5 15/3/2012 Malik Al-Momani بسم هللا الرحمن الرحيم Spermatogenesis Note : Please refer to slides so see photos. Quick Revision : - Testis is divided by septum into testicular lobules, inside the lobules
Male reproduction. Cross section of Human Testis ผศ.ดร.พญ.ส ว ฒณ ค ปต ว ฒ ภาคว ชาสร รว ทยา คณะแพทยศาสตร ศ ร ราชพยาบาล 1. Aims
 Aims Male reproduction Male reproductive structure Spermatogenesis ส ว ฒณ ค ปต ว ฒ ห อง 216 โทร: 7578 Hypothalamo-pituitary-testicular axis Male sex hormone action Male reproductive structure Male reproductive
Aims Male reproduction Male reproductive structure Spermatogenesis ส ว ฒณ ค ปต ว ฒ ห อง 216 โทร: 7578 Hypothalamo-pituitary-testicular axis Male sex hormone action Male reproductive structure Male reproductive
Special Parts: Gender. Why Have Sex?
 Why Have Sex? Lots of animals clone themselves... 100% of their genes are passed on! Sex requires sharing, it s expensive (time, mate selection, special parts, prenuptial gifts...) So why do it? Special
Why Have Sex? Lots of animals clone themselves... 100% of their genes are passed on! Sex requires sharing, it s expensive (time, mate selection, special parts, prenuptial gifts...) So why do it? Special
Chapter 14 The Reproductive System
 Biology 12 Name: Reproductive System Per: Date: Chapter 14 The Reproductive System Complete using BC Biology 12, page 436-467 14. 1 Male Reproductive System pages 440-443 1. Distinguish between gametes
Biology 12 Name: Reproductive System Per: Date: Chapter 14 The Reproductive System Complete using BC Biology 12, page 436-467 14. 1 Male Reproductive System pages 440-443 1. Distinguish between gametes
Chapter 16 Endocrine and Reproductive Health
 Note Taking Lesson 2 The Male Reproductive System Directions: Use the following outline to help organize your notes as you read through the lesson. Key Concept Consider and Reconsider Before reading the
Note Taking Lesson 2 The Male Reproductive System Directions: Use the following outline to help organize your notes as you read through the lesson. Key Concept Consider and Reconsider Before reading the
Primary sex organs (gonads): testes and ovaries. Accessory reproductive organs: ducts, glands, and external genitalia
 Male Reproductive System Primary sex organs (gonads): testes and ovaries Produce sex cells (gametes) Secrete steroid sex hormones Androgens (males) Estrogens and progesterone (females) Accessory reproductive
Male Reproductive System Primary sex organs (gonads): testes and ovaries Produce sex cells (gametes) Secrete steroid sex hormones Androgens (males) Estrogens and progesterone (females) Accessory reproductive
Reproductive Endocrinology. Isabel Hwang Department of Physiology Faculty of Medicine University of Hong Kong Hong Kong May2007
 Reproductive Endocrinology Isabel Hwang Department of Physiology Faculty of Medicine University of Hong Kong Hong Kong May2007 isabelss@hkucc.hku.hk A 3-hormone chain of command controls reproduction with
Reproductive Endocrinology Isabel Hwang Department of Physiology Faculty of Medicine University of Hong Kong Hong Kong May2007 isabelss@hkucc.hku.hk A 3-hormone chain of command controls reproduction with
Functions of male Reproductive System: produce gametes deliver gametes protect and support gametes
 Functions of male Reproductive System: produce gametes deliver gametes protect and support gametes Spermatogenesis occurs in the testes after puberty. From the testes they are deposited into the epididymas
Functions of male Reproductive System: produce gametes deliver gametes protect and support gametes Spermatogenesis occurs in the testes after puberty. From the testes they are deposited into the epididymas
Unit 15 ~ Learning Guide
 Unit 15 ~ Learning Guide Name: INSTRUCTIONS Complete the following notes and questions as you work through the related lessons. You are required to have this package completed BEFORE you write your unit
Unit 15 ~ Learning Guide Name: INSTRUCTIONS Complete the following notes and questions as you work through the related lessons. You are required to have this package completed BEFORE you write your unit
Getting Help for Obstructive Azoospermia A BASIC GUIDE TO MALE. A doctor s guide for patients developed by the American Urological Association, Inc.
 A BASIC GUIDE TO MALE Getting Help for Obstructive Azoospermia A doctor s guide for patients developed by the American Urological Association, Inc. Based on the AUA Best Practice Policy and ASRM Practice
A BASIC GUIDE TO MALE Getting Help for Obstructive Azoospermia A doctor s guide for patients developed by the American Urological Association, Inc. Based on the AUA Best Practice Policy and ASRM Practice
Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems
 CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems 3. Male Reproductive anatomy and physiology. Testes = paired
CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems 3. Male Reproductive anatomy and physiology. Testes = paired
Animal Reproduc5on. Chapter 46. Asexual and Sexual Reproduc5on. Asexual and Sexual Reproduc5on. Sexual reproduc-on
 Chapter 46 Animal Reproduc5on BIOL 223 Sexual reproduc-on Asexual and Sexual Reproduc5on crea5on of an offspring by fusion of a male gamete (sperm) and female gamete (egg) to form a zygote Asexual reproduc-on
Chapter 46 Animal Reproduc5on BIOL 223 Sexual reproduc-on Asexual and Sexual Reproduc5on crea5on of an offspring by fusion of a male gamete (sperm) and female gamete (egg) to form a zygote Asexual reproduc-on
Human Growth and Development
 Human Growth and Development 6th Grade Male Click here for teacher notes Ground Rules Use proper terminology. (Do not use slang.) Participate seriously. Share today s information with your parents. (Do
Human Growth and Development 6th Grade Male Click here for teacher notes Ground Rules Use proper terminology. (Do not use slang.) Participate seriously. Share today s information with your parents. (Do
Imaging Ejaculatory Disorders and Hematospermia
 ATHENS 4-6 October 2018 European Society of Urogenital Radiology Imaging Ejaculatory Disorders and Hematospermia Parvati Ramchandani, MD Professor, Radiology and Surgery University of Pennsylvania Medical
ATHENS 4-6 October 2018 European Society of Urogenital Radiology Imaging Ejaculatory Disorders and Hematospermia Parvati Ramchandani, MD Professor, Radiology and Surgery University of Pennsylvania Medical
Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor)
 Indifferent ducts of embryo Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Y chromosome present Y chromosome absent Phenotypic sex is depends on development of external
Indifferent ducts of embryo Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Y chromosome present Y chromosome absent Phenotypic sex is depends on development of external
Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor)
 Indifferent ducts of embryo Y chromosome present Y chromosome absent Male Female penis ovary uterus vagina testis Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Phenotypic
Indifferent ducts of embryo Y chromosome present Y chromosome absent Male Female penis ovary uterus vagina testis Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Phenotypic
Outline OVERVIEW PUBERTY PRE-TESTS PUBERTY WITH SAM AND SALLY MENSTRUATION: HOW DOES IT WORK? SPERMATOGENESIS: HOW DOES IT WORK?
 UNIT FIVE: PUBERTY HiTOPS, Inc./Princeton Center for Leadership Training OVERVIEW PUBERTY PRE-TESTS Outline PUBERTY WITH SAM AND SALLY MENSTRUATION: HOW DOES IT WORK? SPERMATOGENESIS: HOW DOES IT WORK?
UNIT FIVE: PUBERTY HiTOPS, Inc./Princeton Center for Leadership Training OVERVIEW PUBERTY PRE-TESTS Outline PUBERTY WITH SAM AND SALLY MENSTRUATION: HOW DOES IT WORK? SPERMATOGENESIS: HOW DOES IT WORK?
Testosterone Therapy-Male Infertility
 Testosterone Therapy-Male Infertility Testosterone Therapy-Male Infertility Many men are prescribed testosterone for a variety of reasons. Low testosterone levels (Low T) with no symptoms, general symptoms
Testosterone Therapy-Male Infertility Testosterone Therapy-Male Infertility Many men are prescribed testosterone for a variety of reasons. Low testosterone levels (Low T) with no symptoms, general symptoms
The Male Reproductive System
 The Male Reproductive System YONG-MEI CHEN ( 陈咏梅 ) Dept. of Anatomy, Histology & Embryology Peking Union Medical College Tel:69156461 E-mail address: pumc_he@126.com Content Spermatogenesis Spermiogenesis
The Male Reproductive System YONG-MEI CHEN ( 陈咏梅 ) Dept. of Anatomy, Histology & Embryology Peking Union Medical College Tel:69156461 E-mail address: pumc_he@126.com Content Spermatogenesis Spermiogenesis
Importance of Papanicolaou Staining for Sperm Morphologic Analysis Comparison With an Automated Sperm Quality Analyzer
 Anatomic Pathology / Pap Staining for Sperm Morphologic Analysis Importance of Papanicolaou Staining for Sperm Morphologic Analysis Comparison With an Automated Sperm Quality Analyzer Smita Singh, MD,
Anatomic Pathology / Pap Staining for Sperm Morphologic Analysis Importance of Papanicolaou Staining for Sperm Morphologic Analysis Comparison With an Automated Sperm Quality Analyzer Smita Singh, MD,
MALE REPRODUCTIVE SYSTEM
 MALE REPRODUCTIVE SYSTEM The male reproductive system consists of primary sex organs (testes) and secondary or accessory sex organs. The secondary organs consist of a series of genital ducts (ductules
MALE REPRODUCTIVE SYSTEM The male reproductive system consists of primary sex organs (testes) and secondary or accessory sex organs. The secondary organs consist of a series of genital ducts (ductules
Chapter 36 Active Reading Guide Reproduction and Development
 Name: AP Biology Mr. Croft Chapter 36 Active Reading Guide Reproduction and Development Section 1 1. Distinguish between sexual reproduction and asexual reproduction. 2. Which form of reproduction: a.
Name: AP Biology Mr. Croft Chapter 36 Active Reading Guide Reproduction and Development Section 1 1. Distinguish between sexual reproduction and asexual reproduction. 2. Which form of reproduction: a.
Reproductive Systems. BIOLOGY OF HUMANS Concepts, Applications, and Issues. Judith Goodenough Betty McGuire
 BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 17 Reproductive Systems Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 17 Reproductive Systems Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems
 CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems Review of Male Reproductive Anatomy Fig 15.9 Vas deferens
CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems Review of Male Reproductive Anatomy Fig 15.9 Vas deferens
Web Activity: Simulation Structures of the Female Reproductive System
 differentiate. The epididymis is a coiled tube found along the outer edge of the testis where the sperm mature. 3. Testosterone is a male sex hormone produced in the interstitial cells of the testes. It
differentiate. The epididymis is a coiled tube found along the outer edge of the testis where the sperm mature. 3. Testosterone is a male sex hormone produced in the interstitial cells of the testes. It
Information Sheet. Male Infertility
 Infertility National Public Awareness Campaign Information Sheet Male Infertility In approximately half of couples complaining of infertility part of the problem lies with the male. Male infertility has
Infertility National Public Awareness Campaign Information Sheet Male Infertility In approximately half of couples complaining of infertility part of the problem lies with the male. Male infertility has
HEALTHY GROWTH & SEXUALITY
 HEALTHY GROWTH & SEXUALITY Y T LI X E S A U SEX GEND ER https://youtu.be/df2yow4xad4 First, egg cells are produced in two almond shaped organs known as the ovaries. During the process of ovulation,
HEALTHY GROWTH & SEXUALITY Y T LI X E S A U SEX GEND ER https://youtu.be/df2yow4xad4 First, egg cells are produced in two almond shaped organs known as the ovaries. During the process of ovulation,
Sperm production. Sperm production. Meiosis. Mitosis. The cells of Leydig in testes secrete
 Sperm production Ductus deferens Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Sperm production Ductus deferens Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Sperm production. Sperm production. Controlling sperm production. Meiosis. Mitosis. The cells of Leydig in testes secrete
 Ductus deferens Sperm production Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Ductus deferens Sperm production Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Male and Female Reproduction
 Male and Female Reproduction Similarities / Differences Develop very similar structures of sex glands Two genital tubes Manufacture the hormones of the other sex. Hormones of one sex are often used to
Male and Female Reproduction Similarities / Differences Develop very similar structures of sex glands Two genital tubes Manufacture the hormones of the other sex. Hormones of one sex are often used to
Histology of Male Reproductive system (1)
 Histology of Male Reproductive system (1) Prof. Dr. Malak A. Al-yawer Learning Objectives At the end of this lecture, the medical student will be able to: State the organization of the testis Define seminiferous
Histology of Male Reproductive system (1) Prof. Dr. Malak A. Al-yawer Learning Objectives At the end of this lecture, the medical student will be able to: State the organization of the testis Define seminiferous
The Male Reproductive System
 The Male Reproductive System The male reproductive system Testes Genital ducts Accessory sex glands: seminal vesicles prostate bulbourethral glands External genitalia: penis Structure of the Testis Tunica
The Male Reproductive System The male reproductive system Testes Genital ducts Accessory sex glands: seminal vesicles prostate bulbourethral glands External genitalia: penis Structure of the Testis Tunica
Grade 9 Science - Human Reproduction
 Grade 9 Science - Human Reproduction The human reproductive system is a series of organs that work together for one purpose: reproduction (creating new humans). Each part has a specific role in the reproductive
Grade 9 Science - Human Reproduction The human reproductive system is a series of organs that work together for one purpose: reproduction (creating new humans). Each part has a specific role in the reproductive
Chapter 7. Male Reproductive System
 Chapter 7 Male Reproductive System 1 Sexual Reproduction Sexual reproduction two individuals produce offspring that have genetic characteristics from both parents Sexual reproduction introduces new gene
Chapter 7 Male Reproductive System 1 Sexual Reproduction Sexual reproduction two individuals produce offspring that have genetic characteristics from both parents Sexual reproduction introduces new gene
Ch 20: Reproduction. Keypoints: Human Chromosomes Gametogenesis Fertilization Early development Parturition
 Ch 20: Reproduction Keypoints: Human Chromosomes Gametogenesis Fertilization Early development Parturition SLOs Contrast mitosis/meiosis, haploid/diploid, autosomes/sex chromosomes. Outline the hormonal
Ch 20: Reproduction Keypoints: Human Chromosomes Gametogenesis Fertilization Early development Parturition SLOs Contrast mitosis/meiosis, haploid/diploid, autosomes/sex chromosomes. Outline the hormonal
VideoTesT-Sperm 2.1 VideoTesT-Sperm 2.1 Motility Morphology Motility Standard Method Morphology Standard Method Database
 VideoTesT-Sperm 2.1 CASA is designed to equip the workplace of specialists dealing with sperm analysis. The analyzer enables experts to count the amount of spermatozoa and to estimate their motility parameters
VideoTesT-Sperm 2.1 CASA is designed to equip the workplace of specialists dealing with sperm analysis. The analyzer enables experts to count the amount of spermatozoa and to estimate their motility parameters
a. the tail disappears b. they become spermatids c. they undergo capacitation d. they have been stored in the uterus for several days
 (2 points each) Multiple Choice. Read each question thoroughly before answering. From the choices available, choose the answer that is the most correct. Place all answers on the accompanying answer sheet.
(2 points each) Multiple Choice. Read each question thoroughly before answering. From the choices available, choose the answer that is the most correct. Place all answers on the accompanying answer sheet.
AP Biology Ch ANIMAL REPRODUCTION. Using only what you already know (you cannot look up anything) complete the chart below.
 AP Biology Ch. 46 - ANIMAL REPRODUCTION Using only what you already know (you cannot look up anything) complete the chart below. I. Overview of Animal Reproduction A. Both asexual and sexual reproduction
AP Biology Ch. 46 - ANIMAL REPRODUCTION Using only what you already know (you cannot look up anything) complete the chart below. I. Overview of Animal Reproduction A. Both asexual and sexual reproduction
Animal Reproductive Systems. Chapter 42
 Animal Reproductive Systems Chapter 42 Impacts, Issues Male or Female? Body or Genes? Body and genes don t always match male or female characteristics also depend on hormones mutations can result in intersex
Animal Reproductive Systems Chapter 42 Impacts, Issues Male or Female? Body or Genes? Body and genes don t always match male or female characteristics also depend on hormones mutations can result in intersex
Chapter 14 Reproduction Review Assignment
 Date: Mark: _/45 Chapter 14 Reproduction Review Assignment Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Use the diagram above to answer the next question.
Date: Mark: _/45 Chapter 14 Reproduction Review Assignment Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Use the diagram above to answer the next question.
Adapted from Preg. & Part., Senger
 MALE ENDOCRINOLOGY AND SPERMATOGENESIS (Chapter 10) AVS 222 (Instructor: Dr. Amin Ahmadzadeh) I. MALE ENDOCRINOLOGY (Figure10-1 to 10-3) A. Glands and their respective hormones 1) Hypothalamic hormone:
MALE ENDOCRINOLOGY AND SPERMATOGENESIS (Chapter 10) AVS 222 (Instructor: Dr. Amin Ahmadzadeh) I. MALE ENDOCRINOLOGY (Figure10-1 to 10-3) A. Glands and their respective hormones 1) Hypothalamic hormone:
REPRODUCCIÓN. La idea fija. Copyright 2004 Pearson Education, Inc., publishing as Benjamin Cummings
 REPRODUCCIÓN La idea fija How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development, birth
REPRODUCCIÓN La idea fija How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development, birth
Testicular Biopsy and Sperm Extraction for Fertility Preservation
 Testicular Biopsy and Sperm Extraction for Fertility Preservation This fact sheet aims to provide information about why and when a testicular biopsy or aspiration might be offered, what it involves and
Testicular Biopsy and Sperm Extraction for Fertility Preservation This fact sheet aims to provide information about why and when a testicular biopsy or aspiration might be offered, what it involves and
Efferent Ducts and Epididymis
 increase) the secretion of each of the androgen regulated proteins. Regulation of spermatogenesis is therefore an extremely complex cascade of cell-cell interactions with the Leydig cells supporting germ
increase) the secretion of each of the androgen regulated proteins. Regulation of spermatogenesis is therefore an extremely complex cascade of cell-cell interactions with the Leydig cells supporting germ
Sample Provincial exam Q s: Reproduction
 Sample Provincial exam Q s: Reproduction 11. Functions Testosterone Makes the male sex organs function normally, and also inhibits hypothalamus s release of GnRH and thus LH & FSH and thus testosterone
Sample Provincial exam Q s: Reproduction 11. Functions Testosterone Makes the male sex organs function normally, and also inhibits hypothalamus s release of GnRH and thus LH & FSH and thus testosterone
The Male Reproductive System
 The Male Reproductive System Male Reproductive System The male sex cell is a sperm cell The whole purpose is to produce and deliver sperm to the egg Structure of a Human Sperm Cell Streamlined, built to
The Male Reproductive System Male Reproductive System The male sex cell is a sperm cell The whole purpose is to produce and deliver sperm to the egg Structure of a Human Sperm Cell Streamlined, built to
Clinical evaluation of infertility
 Clinical evaluation of infertility DR. FARIBA KHANIPOUYANI OBSTETRICIAN & GYNECOLOGIST PRENATOLOGIST Definition: inability to achieve conception despite one year of frequent unprotected intercourse. Male
Clinical evaluation of infertility DR. FARIBA KHANIPOUYANI OBSTETRICIAN & GYNECOLOGIST PRENATOLOGIST Definition: inability to achieve conception despite one year of frequent unprotected intercourse. Male
Health Science: the structures & functions of the reproductive system
 Health Science: the structures & functions of the reproductive BELLWORK 1. List (4) careers that are r/t the Reproductive, Urinary, and Endocrine Systems 2. Copy down the following terms: -ologist = one
Health Science: the structures & functions of the reproductive BELLWORK 1. List (4) careers that are r/t the Reproductive, Urinary, and Endocrine Systems 2. Copy down the following terms: -ologist = one
Male fertility disorders
 Male fertility disorders Etiology diagnosis therapeutic approaches Dr. Cornelia Roggenbuck September 29, 2009 Orthomol pharmazeutische Vertriebs GmbH Content Fertility Facts and figures Factors of influence
Male fertility disorders Etiology diagnosis therapeutic approaches Dr. Cornelia Roggenbuck September 29, 2009 Orthomol pharmazeutische Vertriebs GmbH Content Fertility Facts and figures Factors of influence
Animal Reproduction Chapter 46. Fission. Budding. Parthenogenesis. Fragmentation 11/27/2017
 Animal Reproduction Chapter 46 Both asexual and sexual reproduction occur in the animal kingdom Sexual reproduction is the creation of an offspring by fusion of a male gamete (sperm) and female gamete
Animal Reproduction Chapter 46 Both asexual and sexual reproduction occur in the animal kingdom Sexual reproduction is the creation of an offspring by fusion of a male gamete (sperm) and female gamete
What to do about infertility?
 What to do about infertility? Dr. M.A. Fischer Section Head, Division of Urology, Department of Surgery Assistant Clinical Professor, Department of Obstetrics and Gynecology Hamilton Health Sciences, Hamilton,
What to do about infertility? Dr. M.A. Fischer Section Head, Division of Urology, Department of Surgery Assistant Clinical Professor, Department of Obstetrics and Gynecology Hamilton Health Sciences, Hamilton,
Human Sexuality - Ch. 2 Sexual Anatomy (Hock)
 Human Sexuality - Ch. 2 Sexual Anatomy (Hock) penis penile glans corona frenulum penile shaft erection foreskin circumcision corpora cavernosa corpus spongiosum urethra scrotum spermatic cords testicles
Human Sexuality - Ch. 2 Sexual Anatomy (Hock) penis penile glans corona frenulum penile shaft erection foreskin circumcision corpora cavernosa corpus spongiosum urethra scrotum spermatic cords testicles
Lecture 28, The Reproductive System
 Fundamentals of Anatomy & Physiology Lecture 28, The Reproductive System SIXTH EDITION Frederic H. Martini Lecturer: Dr. Barjis Room: P313 Phone: (718) 260-5285 E-Mail: ibarjis@citytech.cuny.edu Copyright
Fundamentals of Anatomy & Physiology Lecture 28, The Reproductive System SIXTH EDITION Frederic H. Martini Lecturer: Dr. Barjis Room: P313 Phone: (718) 260-5285 E-Mail: ibarjis@citytech.cuny.edu Copyright
REPRODUCTIVE SYSTEM OBJECTIVES
 REPRODUCTIVE SYSTEM OBJECTIVES OBJECTIVES: 1. List the organs and functions of the reproductive system. Female Organs Male Organs Functions 1 OVARIES 1 TESTES 1 Produce gametes 2 fallopian tubes 2 scrotum
REPRODUCTIVE SYSTEM OBJECTIVES OBJECTIVES: 1. List the organs and functions of the reproductive system. Female Organs Male Organs Functions 1 OVARIES 1 TESTES 1 Produce gametes 2 fallopian tubes 2 scrotum
Urinary System Chapter 16
 Urinary System Chapter 16 1 Urology- the branch of medicine that treats male and female urinary systems as well as the male reproductive system. Nephrology- the scientific study of the anatomy, physiology,
Urinary System Chapter 16 1 Urology- the branch of medicine that treats male and female urinary systems as well as the male reproductive system. Nephrology- the scientific study of the anatomy, physiology,
