Innovating image-guided surgery: Introducing multimodal approaches for sentinel node detection Brouwer, O.R.
|
|
|
- Godwin Davidson
- 5 years ago
- Views:
Transcription
1 UvA-DARE (Digital Academic Repository) Innovating image-guided surgery: Introducing multimodal approaches for sentinel node detection Brouwer, O.R. Link to publication Citation for published version (APA): Brouwer, O. R. (2013). Innovating image-guided surgery: Introducing multimodal approaches for sentinel node detection General rights It is not permitted to download or to forward/distribute the text or part of it without the consent of the author(s) and/or copyright holder(s), other than for strictly personal, individual use, unless the work is under an open content license (like Creative Commons). Disclaimer/Complaints regulations If you believe that digital publication of certain material infringes any of your rights or (privacy) interests, please let the Library know, stating your reasons. In case of a legitimate complaint, the Library will make the material inaccessible and/or remove it from the website. Please Ask the Library: or a letter to: Library of the University of Amsterdam, Secretariat, Singel 2, 1012 WP Amsterdam, The Netherlands. You will be contacted as soon as possible. UvA-DARE is a service provided by the library of the University of Amsterdam ( Download date: 11 Dec 2018
2 1 --
3 APPENDIX Clinical application of SPECT/CT and intraoperative radioguided sentinel bode biopsy in cancers of the male reproductive system In: Atlas of Lymphoscintigraphy and Sentinel Lymph Node Mapping, Springer, Oscar R. Brouwer, Willem Meinhardt, Simon Horenblas, Renato A. Valdés Olmos
4 1 Introduction This chapter describes the principles of lymphatic mapping and sentinel node (SN) biopsy for cancers of the male reproductive system, which includes penile, prostate, and testicular cancer. Penile cancer is a relatively rare disease in the western world, with an incidence of approximately 1 per 100, Nearly all penile tumors are squamous cell carcinomas. The presence of lymph node involvement is the single most important prognostic factor for cancer-specific death. 2 Since the introduction of the concept in penile carcinoma by Cabañas et al. in 1977, the SN procedure has evolved into a reliable staging technique, with a low complication rate compared to (prophylactic) inguinal lymphadenectomy. 3 Prostate cancer In prostate cancer, lymph node staging may be important for both prognosis and therapeutic management. The presence of lymph node metastases may lead to avoidance of local therapy with curative intents, such as radiotherapy or radical (salvage) prostatectomy, and influences the duration of androgen-deprivation therapy. To date, none of the available noninvasive diagnostic imaging modalities provide a reliable assessment of lymph node (micro)metastases. Therefore, surgical staging by extended pelvic lymphadenectomy (EPL) is still the current standard of care. However, SNB is emerging as an alternative staging method, with a lower incidence of complications and with the potential to identify relevant lymph nodes outside the standard EPL field. Testicular cancer Testicular cancer is the most frequent malignancy in young men, and the incidence has risen by almost 100% in the last 20 years. At the time of diagnosis, approximately two-thirds of patients have clinical stage I disease. 6 The optimal management of regional lymph nodes in stage I testicular cancer remains controversial. A surveillance policy requires intensive, frequent follow-up visits, with costly examinations, and defers detection and treatment of lymph node metastases to a later stage. There is a need for diagnostic techniques that enable patients with lymph node metastasis to be treated at an early stage, while preventing unnecessary treatment for those patients without metastasis. In this respect, the SN procedure is potentially highly valuable. 7,8 The clinical problem Penile cancer There is no consensus on the management of patients with clinically node-negative (cn0) penile carcinoma, in whom radical inguinal lymph node dissection (ILND) is routine. 9 However, only 20 2% of these patients harbor occult nodal metastasis. This means that, although prophylactic inguinal lymphadenectomy offers the best 232 Innovating image-guided surgery: Introducing multimodal approaches for sentinel node detection
5 chance of cure, it is unnecessary in approximately 7 80% of patients. 9 In addition, this procedure is associated with substantial morbidity, such as lymphedema and infections. As currently available non-invasive staging techniques lack sufficient accuracy, mini- mally invasive staging remains necessary for the time being. However, since its clinical introduction in 199, there have been reservations about the use of SNB for penile cancer, because of the supposedly long learning curve associated with the procedure and the possibility of false-negative cases (reported in up to 21% of the procedures). 10 After analysis of false-negative cases, several modifications were made to the dynamic SN biopsy (DSNB) procedure, to increase its sensitivity Prostate cancer Although EPL is the gold standard for the identification of lymph node metastasis in patients with prostate cancer, the incidence of postoperative complications increases with the number of excised lymph nodes, ranging from 10.% for 1 lymph nodes to 2.3% when dissection includes more than 20 lymph nodes. The advantages of the SN node dissection are a lower incidence of complications and the possibility of identifying tumor-draining lymph nodes outside the field of an EPL. However, accurate laparoscopic localization of SNs in the pelvis can be challenging, especially when SNs are located near the prostatic injection site (because of the high radioactive background signal), or in the case of aberrantly located SNs (e.g. para- aortic). 12 Testicular cancer To date, large-scale randomized clinical studies to validate and assess the added benefit of SNB for testicular cancer are still lacking. This may be partially due to the fact that pa- tients are usually referred to tertiary, specialized centers only after orchidectomy has already been performed, thus after removal of the potential injection site. Furthermore, although lymphatic drainage of the testis is mainly directed towards the areas along the aorta and vena cava, aberrant drainage has also been observed. 8 The identification of these SNs in relation to the anatomical structures can be difficult using two-dimensional (2D) lymphoscintigraphy alone. Indications and contraindications for sentinel node biopy Penile cancer Patients with >T1G2 tumors and cn0 groins defined by ultrasound-guided fine needle cytology are eligible for SNB. Repeat SNB after tumor recurrence is also a validated procedure. 13 If the SN is tumor positive, completion ipsilateral lymphadenectomy is performed. Groins with tumor-free lymph nodes are managed with close surveillance, thereby avoiding the morbidity associated with lymphadenectomy. Chapter 1: Appendix 233
6 1 Prostate cancer The chances of having lymph node metastasis from prostate cancer increase with the serum level of prostate-specific antigen (PSA), the biopsy grade (Gleason score), and clinical T stage. SNB is generally reserved for patients in the intermediate-risk group (clinical stage >T2b/T3, PSA >10 ng/l, or Gleason >6). Nevertheless, SNB has been able to identify metastases in as many as 6.8% to 10.7% of patients with favorable risk factors. 1 In the intermediate-risk group, a tumor-bearing SN may influence the boundaries of the radiotherapy field and duration of hormonal (androgen-deprivation) therapy. Another possible indication is to select patients who are eligible for salvage treatment of the prostate, as the usual parameters to stratify patients in risk groups do not apply to patients with intraprostatic recurrence. Since salvage treatment of the prostate may result in serious complications, it should be considered when the prostate is actually the only tumor-bearing site. Testicular cancer SNB was introduced for patients with stage I disease. Clinical stage I seminoma and non-seminoma are defined by a negative computed tomography (CT) scan of the chest, abdomen, and pelvis, plus normal or normalized serum values of alpha-fetoprotein (AFP), human chorionic gonadotropin (HCG), and lactate dehydrogenase (LDH). In the case of mixed seminomatous/non-seminomatous tumors, treatment decisions are based on the factor with the highest malignant potential, which is the non-seminoma component. Generally, the absence of lymph nodes larger than 1 cm results in assignment of clinical stage I. Radiocolloid and modalities of injection Penile cancer The tracer (technetium-99 [ 99m Tc]-nanocolloid in most European countries) is injected intradermally. In fact, subcutaneous administration is easier to accomplish, but may not accurately identify the route of drainage from an overlying cutaneous site. Furthermore, lymphatic drainage from the dermis is much faster than drainage from subcutaneous tissue. Application of a spray containing xylocaine 10%, 30 minutes before tracer administration, is recommended. As an alternative, a lidocaine/prilocaine-based crème can be used. This local anesthesia ensures that the radiocolloid injections are well tolerated and relatively easy to perform. A volume of 0.3 ml containing 7 MBq divided into three depots (0.1 ml each) is subsequently administered intradermally around the tumor. Each depot is injected raising a bleb. The radiocolloid is injected proximally from the tumor. For large tumors not restricted to the glans, the radiocolloid can be injected in the prepuce. Injection margins within 1 cm from the primary tumor are recommended. A reproducibility rate of 100% for penile lymphoscintigraphy has been reported with an injection distance of mm. 1 In patients with a previous excision biopsy scar, injections may also be administered using similar margins. 23 Innovating image-guided surgery: Introducing multimodal approaches for sentinel node detection
7 Prostate cancer Most of the experience in the SN procedure for prostate cancer has been acquired in European countries and the most frequently used radiopharmaceutical has been 99m Tc-nanocolloid. Transrectal intraprostatic injection is guided by (transrectal) ultrasound, injecting the radiocolloid under continuous monitoring using a needle of mm (Fig. 1). Prostate cancer may be multifocal; therefore injections are performed in both lobes. An activity of about 20 MBq in 0. ml is recommended. The lymph node visualization rate tends to be less optimal when lower activities are used. The particle concentration also appears to be important, and the use of a reduced labeling dilution volume (0. ml 99mTc per 0.2 mg nanocolloid) yields more visualized SNs with higher radioactivity count rates. 16 The radiocolloid is divided into 2 injections, depending on the prostate volume. A three-way system is recommended, and after each depot saline is used for flushing the residual radioactivity in the needle. 1 Testicular cancer The route of administration of 99m Tc-nanocolloid was evaluated in a feasibility study in stage I testicular cancer. 7 While funicular administration showed only lymph node uptake in the inguinal region (which does not reflect the actual testicular tumor drainage pattern), intratesticular administration resulted in visualization of retroperitoneal SN(s), in accordance with known drainage patterns. No side effects were observed using the latter method, which proved to be easy to perform and was well tolerated under local anesthesia (funicular block using lidocaine 2%, performed by the urologist in the outpatient clinic). Generally, a single aliquot of radioactivity (approximately 100 MBq) in a volume of 0.2 ml is injected into the testicular parenchyma with a fine needle. Preoperative imaging of sentinel nodes and lymphoscintigraphy interpretation Based on lymphoscintigraphy, the main criteria to identify lymph nodes as SNs are the visualization of lymphatic ducts, the time of appearance, the lymph node basin, and the intensity of lymph node uptake. Following these criteria visualized radioactive lymph nodes may be classified as: 1) Definitely SNs: this category includes all lymph nodes draining from the site of the primary tumour through an own lymphatic vessel, or a single radioactive lymph node in a lymph node basin. 2) Highly probable SNs: this category includes lymph nodes appearing between the injection site and a first draining node, or nodes with increasing uptake appearing in other lymph node stations. 3) Less probable SNs: all higher echelon nodes (in trunk and extremities) or lower Chapter 1: Appendix 23
8 1 echelon nodes (head and neck) may be included in this category. Early planar images are essential to identify first draining lymph nodes as SNs by visualization of their lymphatic ducts. These nodes (category 1) can be distinguished from secondary lymph nodes (category 3) mostly appearing on delayed planar images. In other cases a single lymph node is seen on early and/or delayed images. This node is also considered as a definite SN (category 1). In some cases SPECT/CT can detect additional lymph nodes in other basins. This may occur for instance in the pelvis when two basins are located at the same level and there is superposition of the radioactive nodes on planar images. These nodes can be considered as definite (category 1) or highly probable SNs (category 2). Less frequently a radioactive lymph node may appear between the injection site and a first draining node; its increasing uptake can confirm this node as a highly probable SN (category 2) and it helps to differentiate this node from prolonged valve activity in a lymphatic duct, which mostly decreases in intensity on delayed images. Penile cancer As aforementioned, lymphoscintigraphy after radiocolloid injection consists of two phases: (a) dynamic scintigraphy, performed during the first 10 minutes after radiocolloid injection, preferably in both the anterior and lateral views. The dynamic study is helpful to identify lymphatic ducts and the first directly draining lymph nodes; (b) static planar imaging at minutes and at 2 hours. The early planar images visualize the first draining lymph nodes in about 8% of cases. Additional images at hours, or radiocolloid reinjection are recommended when no SNs are visualized. Generally, the lymph nodes draining directly from the injection site are classified as SNs. In the case of multiple visible nodes without visible afferent vessels, the first node appearing in a basin is considered to be the SN. Prostate cancer In the pelvis, lymphatic ducts are seldom visualized and the relatively slower deep lymphatic drainage renders dynamic lymphoscintigraphy less useful. Early planar images of lymphoscintigraphy acquired 1 minutes after radiocolloid administration can visualize the first draining lymph nodes in almost 88% of cases. 17 Delayed imaging may be performed 2 hours after injection. On delayed imaging, the lymph node visualization rate increases to more than 9%. Comparing the early and delayed images enables differentiation of second-echelon lymph nodes from the first draining nodes. This discrimination is based on the anatomical lymph node basins of the pelvis. As a rule, late-appearing lymph nodes located higher in the same basin are considered as second-echelon lymph nodes. Late-appearing lymph nodes in distal or more ventral and dorsal basins suggest direct draining from the prostate. These lymph nodes may also be considered as SNs. If no single photon emission computed tomography (SPECT)/CT is available, lateral planar images can differentiate between dorsal and more ventrally located SNs. 236 Innovating image-guided surgery: Introducing multimodal approaches for sentinel node detection
9 Testicular cancer The fast lymphatic drainage from the testicle requires dynamic gamma camera acquisition to facilitate differentiation between first- and second-echelon lymph nodes in the retroperitoneum. Immediately following radiocolloid injection, anterior and lateral dynamic images are obtained with a dual-head gamma camera over 10 minutes, and the lymphatic flow and early-draining lymph nodes are visualized in almost all cases. Static images are obtained minutes after the dynamic study. Late static images are obtained 2 hours after injection and are required to differentiate first-echelon nodes from higher-echelon nodes (if there is no visualization of SNs on the early dynamic and static images), and to identify unexpected drainage patterns. 1 Lymphatic drainage Penile cancer The most frequently visualized lymphatic drainage pattern is bilateral drainage to both groins (80%). This pattern is, however, asynchronous in two-thirds of cases, and visualization of the contralateral lymph nodes is often only possible on delayed imaging. 18 Drainage from the injection site mostly occurs through one or two visualized afferent lymphatic ducts leading to one or two SNs in each groin. In some cases, a cluster of inguinal lymph nodes is observed. Prostate cancer The main lymph node basins where the prostate drains generally follow the iliac vessels. 19 The common iliac lymph nodes are located caudally of the aortic bifurcation and are subdivided into a lateral, medial, and middle group. This latter basin is located in the lumbosacral fossa and is demarcated by the promontorium, the psoas muscle, and the common iliac vessels. The external iliac lymph nodes are located caudally to the bifurcation of the common iliac vessels and cranially to the inguinal ligament; they are also subdivided into lateral, middle, and medial groups. The lateral (lateral of the artery) and middle (between the artery and the vein) lymph nodes are located more in the proximity of the anterior abdominal wall, while the medial nodes are located along the cranial segment of the external iliac artery. Although the object of some debate, the obturator lymph nodes are generally considered to be part of the medial subgroup. The internal iliac lymph nodes are located more posteriorly in the pelvis and include the lateral sacral nodes (adjacent to the paired lateral sacral arteries), the presacral nodes (anterior to the sacrum and posterior to the mesorectal fascia), and the anterior nodes (at the origin of the proximal branches of the anterior division of the internal iliac artery; this subgroup includes the hypogastric nodes). Chapter 1: Appendix 237
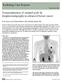
10 1 Testicular cancer Lymphatics from the right testis drain primarily to regions lateral, anterior, and medial to the vena cava and anterior to the aorta (Fig. 2). Lymphatic drainage from the left testis is primarily directed towards areas lateral, anterior, and medial to the aorta. SNs may therefore be preoperatively detected at interaortocaval, para-aortic, or pre-aortic locations. Intraoperative detection of sentinel nodes Penile cancer As is customary for SNB in melanoma and breast cancer, intraoperative SN detection is guided by a gamma-ray detection probe and blue dye. After excision of all pre-operatively defined SNs, it is important to carefully search for any residual radioactivity using the probe, to ensure that no remaining/additional SNs are left behind. Furthermore, intraoperative palpation of the wound should take place, to identify suspicious lymph nodes that failed to pick up any radiocolloid. 20 Prostate cancer Initial validation of the SNB in prostate cancer was based on open surgery and the use of a gamma-ray detection probe to guide detection of the radioactive SNs. More recently, laparoscopic SNB has been validated, and the feasibility of robot-assisted SNB has been demonstrated. In either approach, SN localization is guided by a laparoscopic gamma probe. 21 Deeply located SNs can be difficult to localize using a gamma-ray detection probe, because of tissue attenuation and because the large amount of radioactivity at the injection site may cause SNs located nearby to be missed. Testicular cancer SNB in testicular cancer was introduced in a laparoscopic setting. As such, intraoperative SN localization is also guided by the acoustic signals originated by a laparoscopic gamma-ray detection probe.8 Implementation and contribution of SPECT/CT SPECT/CT has successfully been incorporated in the SN procedure. SPECT/ CT does not replace lymphoscintigraphy. The principal aim of SPECT/CT is to anatomically localize SNs already visualized on planar images. However, SPECT/CT can also detect additional SNs. Technical aspects of SPECT/CT for SN imaging Protocols for SPECT/CT are determined by the objectives of the SN procedure. SPECT/CT is essentially oriented to the anatomical localisation of SNs. This explains why SPECT/CT is acquired using a low dose CT. Acquisition of a diagnostic high dose CT, with or without intravenous contrast, is not really necessary because 238 Innovating image-guided surgery: Introducing multimodal approaches for sentinel node detection
11 the SN procedure primarily aims to identify subclinical metastases in lymph nodes that are not enlarged. However, for SN localisation the CT component of SPECT/ CT must be of sufficient quality to provide optimal anatomical information. The second generation of SPECT/CT cameras enables the evaluation of the lymph nodes corresponding with the radioactive nodes on fused SPECT/CT images by acquiring a low dose (0 mas) CT. In superficial areas such as the groin, mm slides may provide adequate anatomical details. For more complex anatomical areas (pelvis, abdomen) 2 mm slides may be necessary. With this approach SPECT/CT can accurately localize SNs in relation to the vascular structures in deep anatomical areas. The CT component is also used to correct the SPECT signal for tissue attenuation and scattering. After these corrections SPECT can be fused with CT. A grey scale is used to display the morphology in the background image (CT) whereas a colour scale is used to display the SN in the foreground image (SPECT). To read images SPECT/CT is mostly displayed in a similar manner as that of conventional tomography. Multiplanar reconstruction (MPR) enables two-dimensional display of fused images in relation to CT and SPECT. The use of cross-reference lines allows for the navigation between axial, coronal and sagittal views. At the same time this tool leads to correlate radioactive SNs seen on fused SPECT/CT with lymph nodes seen on CT. Most frequently, a radioactive SN corresponds with a single lymph node on CT but in some cases it correlates with a cluster of lymph nodes. This information may be helpful for the intraoperative procedure and the post-excision control using portable gamma cameras or probes as more radioactive SNs may be harvested at the same location. Fused SPECT/CT images can also be three-dimensionally displayed using volume-rendering. In this modality different colours are assigned to anatomical structures such as vessels, muscle, bone and skin. This results in better anatomical reference points and incorporate an additional dimension in the recognition of SNs, for instance in relation to the vasculature or muscles. 1 Penile cancer SPECT/CT images are usually acquired after the 2-hour planar images, and contribute to better understanding of the location of the SNs in penile carcinoma (Fig. 3). SPECT/CT enables anatomical localization of the SNs that were previously identified by lymphoscintigraphy. For instance, the modality can differentiate inguinal from iliac (most frequently second-echelon) lymph nodes. Moreover, SPECT/ CT enables visualization of the SNs in the so-called Daseler s superior and central inguinal zones, which are superior and directly overlying to the saphenofemoral junction, respectively (Fig. 3). SPECT/CT has confirmed that in the majority of patients, SNs are found in the superior medial (73%), superior lateral (9%), and central quadrants (18%). Lymphatic drainage to the inferior quadrants is rare. Finally, SPECT/CT is able to identify contamination of the skin with the radiocolloid, an occurrence that can sometimes be erroneously interpreted on planar lymphoscintigrams as lymph nodes. Chapter 1: Appendix 239
12 1 Prostate cancer Hybrid imaging with SPECT/CT enables anatomical localization of SNs. A 98% SN visualization rate has been reported for SPECT/CT (versus 91% for planar imaging). Moreover, in 96% of cases SNs are localized inside the area of EPL; nevertheless, there is a considerable number of SNs in regions not routinely excised when performing an EPL. 22 SPECT/CT is mostly performed after the delayed planar imaging, and must be interpreted in combination with lymphoscintigraphy. Sequential planar images are able to identify the lymph nodes draining directly from the tumor site, but give only limited information about their anatomical location. With SPECT/ CT, it is possible to better localize SNs both inside and outside the pelvis. In many cases, early-appearing lymph nodes seen as a single hot spot on planar imaging are displayed as separate lymph nodes in different basins by SPECT/CT, and all of them must be considered as SNs. In other cases, intense lymph node uptake seen on fused images may correspond to a cluster of SNs as depicted on the CT component of the SPECT/ CT acquisition. As such, SPECT/CT provides valuable information for the urologist, which may lead to a significant shortening of the operation time, as less-extensive exploration might be required. Furthermore, SPECT/ CT may also provide important information for planning radiotherapy, concerning especially treatment volume and optimization of irradiation fields in the pelvis. Testicular cancer In the initial feasibility study, preoperative lymphatic mapping was performed using planar lymphoscintigraphy only. 7 However, this technique can only provide 2D information, and exact preoperative anatomical SN localization is not possible. Not only does SPECT/CT provide useful anatomic information about the location of SNs, but its improved sensitivity and the added third dimension may also lead to the detection of additional SNs (Fig. 2). Sequential planar imaging will remain important for the preoperative identification of early-appearing lymph nodes as SNs. To date, one study evaluating the use of SPECT/ CT for preoperative SN localization in testicular cancer has been published. 8 SPECT/CT enabled accurate localization of the SNs and provided anatomical reference points to plan their laparoscopic retrieval. Intraoperative imaging Penile cancer Accurate staging with SNB can only be achieved if all nodes on a direct drainage pathway from the tumor are harvested. If SNs are left behind, this constitutes one of the potential causes for false-negative results. The integration of a portable gamma camera in the intraoperative procedure may increase the detection sensitivity, as it provides an intraoperative overview image of the radioactive SNs and enables post-excision confirmation of complete removal of the SNs in the operating room. For optical visualization of the SN, vital blue dyes are traditionally used. However, SNs do not always stain blue. Recently, a hybrid tracer comprising the fluorescent 20 Innovating image-guided surgery: Introducing multimodal approaches for sentinel node detection
13 dye indocyanine green (ICG) and 99m Tc-nanocolloid has been developed. 23 Adding the fluorescent moieties does not alter the biological properties of the parental radiocolloid, and it enables near-infrared fluorescence imaging of all preoperatively identified radioactive SNs. 2 These developments may help to further refine intraoperative retrieval of SNs. Laparoscopic Surgery: Prostate cancer and testicular cancer Since the (retroperitoneal) lymphatic drainage of the prostate and testes is directed to areas deep within the abdomen that can often be complex, preoperative anatomical information about the location of the SNs is important for planning the surgical procedure. For this reason, the SPECT/CT images should be displayed in the operating room. Urological surgery has shifted from the open approach toward less- invasive laparoscopic and robot-assisted techniques. During laparoscopic surgery, the urologist localizes a SN under guidance by the sound pitch originated by the laparoscopic gamma probe. However, intraoperative spatial orientation using this device can sometimes be difficult, as a laparoscopic probe does not provide visual information. The use of a portable gamma camera helps to intraoperatively guide laparoscopic SN localization. Current portable gamma cameras are capable of detecting two different signals: the signal of 99m Tc-nanocolloid for the visualization of SNs, plus the signal of an iodine-12 ( 12 I) seed pointer placed on the tip of the laparoscopic gamma-ray detection probe. 2 The hot tip of the probe can be moved to the hot node, guided by the image of the portable camera. This approach helps navigate towards the location of the SNs. After removal of all SNs, the portable gamma camera can show whether there are any remaining SNs that have to be removed, or a second-echelon node that can confidently be left in place (Fig. ). This approach provides certainty about the completeness of the surgical procedure and complements the laparoscopic probe. Currently, intraoperative navigation approaches that are based on the preoperative (SPECT/CT) images are being developed. 26 In prostate cancer, SNs may be located in close proximity to the primary injection site (the prostate), where the high radioactive background signal may hinder radioguidance with the gamma probe. By injecting the aforementioned hybrid radioactive and fluorescent tracer ICG- 99m Tc-nanocolloid, the high resolution of near-infrared fluorescence imaging (enabled by a fluorescence endoscope) may facilitate intraoperative visualization of the SNs that were preoperatively identified by SPECT/CT (Fig. ) Chapter 1: Appendix 21
14 1 Common and rare variants Penile cancer One of the advantages of lymphatic mapping is its ability to identify SNs outside the usual nodal basins. In penile cancer, direct drainage to prepubic SNs has been described. 28 In particular, dynamic lymphoscintigraphy often shows one or two lymphatic vessels leading to the SN(s). Such vessels have also been observed to directly lead to deep inguinal and even to iliac SNs. Blockage of the lymph flow by tumor metastasis in the lymph node may cause nonvisualization and lymph rerouting, and even retrograde flow of the 99m Tc-nanocolloid containing lymphatic flow. This occurrence has been visualized by SPECT/ CT imaging. 20 Prostate cancer In prostate cancer, lymphoscintigraphy and SPECT/CT may identify SNs outside the extended dissection in 31% of cases. These aberrantly located SNs can be located proximal to the most distal part of the aorta, in the vicinity of the common iliac artery above the crossing of the ureter, around the inferior mesenteric vessels, in the perivesical area, and near the umbilical ligament. 29,30 Testicular cancer Although drainage from the testes is usually directed to paracaval, interaortocaval, and para-aortic SNs, in some patients SNs may also be seen along the testicular vessels. 8 Technical pitfalls Penile cancer The most frequent pitfall is skin contamination. The high pressure of the intradermal bleb can result in leakage during injection or after removal of the needle. The use of (surgical) lights to adequately visualize the site of injection, and of a fenestrated drape to cover the area, may help to avoid skin contamination. Furthermore, voiding of radioactive urine between the early and delayed scintigraphic imaging may also cause skin contamination. The hot spots due to contamination may be confused with SNs, thus leading to an unnecessary intraoperative pursuit. In these cases, skin decontamination is mandatory. Complementary SPECT/CT may also be helpful in detecting these artifacts. Another possible pitfall is accidental injection into the corpus cavernosum, an occurrence that will cause no visualization of lymphatic flow. Furthermore, in some cases the injection site (penis) may obscure visualization of the more inferiorly located SNs on anterior planar imaging. Prostate cancer The relatively complicated radiocolloid injection procedure for prostate cancer is probably the most frequent cause of pitfalls. Care must be taken to avoid tracer 22 Innovating image-guided surgery: Introducing multimodal approaches for sentinel node detection
15 leakage during injection, possibly resulting in subsequent contamination of the floor or of the ultrasound probe. It is therefore recommended to check for contamination of the room after injection, using a Geiger counter. During injection, incorrect needle placement may result in passage of the radiocolloid directly to the bladder or bloodstream, which in turn may cause nonvisualization during scintigraphy. By monitoring the injection procedure with a portable gamma camera, it is possible to ensure adequate radiocolloid retention in the prostate. As the injection is performed transrectally, a possible pitfall is visualization of lymphatic drainage from the rectum, leading, for example, to visualization of inguinal lymph nodes on SPECT/CT imaging. Furthermore, accidental funicular administration can also occur, possibly leading to retrograde drainage towards the scrotum. 1 Testicular cancer The route of administration of 99m Tc-nanocolloid may cause pitfalls. For instance, funicular administration may result in lymph node uptake in the inguinal region, which does not reflect testicular tumor drainage. Intratesticular administration in the parenchyma results in retroperitoneal SN visualization, in accordance with known drainage patterns. Accuracy of sentinel node biopsy Penile cancer Initially, the most significant drawback of SNB for penile cancer was found to be a relatively high false-negative rate (22%). 31 After analysis of the false-negative cases, several modifications were made to the procedure to decrease the false-negative rate and thus increase sensitivity. Histopathologic analysis was expanded with serial sectioning of the harvested SNs. Furthermore, preoperative ultrasonography of cn0 groins with fine needle aspiration cytology (FNAC) of suspicious lymph nodes was added, as well as exploration of the groin in the case of nonvisualization during scintigraphy, and intraoperative palpation of the wound to identify suspicious lymph nodes that failed to pick up any radiocolloid. Thanks to these modifications, the procedure has evolved into a reliable minimally invasive staging technique, with an associated sensitivity of 93 9% and low morbidity in experienced centers. 32 However, a recent multicenter meta-analysis reported pooled sensitivity rates of 88%. 10 One explanation for this lower sensitivity may be represented by differences in protocols (that is screening with ultrasound and FNAC to detect lymph node metastases that fail to pick up radioactivity), and/or by possibly different phases of the learning curve. Prostate cancer Original validation of SNB for prostate cancer was based on open surgery and on the use of a gamma probe to guide detection of the radioactive SNs. Out of more than 2000 evaluated patients, only 11 false-negative cases (.%) were reported. 33 Chapter 1: Appendix 23
16 More recently, SNB has been validated using a laparoscopic gamma probe during minimally invasive surgery. 17 A recent meta-analysis reported a pooled detection rate of 9% ( %) and a pooled sensitivity rate of 9% (92 97%). 3 1 Testicular cancer To date, no studies have been published other than the aforementioned feasibility studies limited by small size of the study populations (<2 patients per study), which therefore lacked the statistical power and follow-up data to assess sensitivity/false-negative rates. Although refinement of the SN procedure may enable better selection of patients who would benefit from adjuvant treatment after orchidectomy, further studies are required to substantiate the clinical value of the SN procedure in this disease. 2 Innovating image-guided surgery: Introducing multimodal approaches for sentinel node detection
17 Figures 1 Figure 1. Preoperative SN mapping in prostate cancer. A) Tracer administration with transrectal ultrasound guidance using a long needle and a three-way system. B) The radioactive dose is divided in 2 injections. The procedure is monitored using a portable gamma camera to verify adequate tracer retention within the prostate. C) Early planar lymphoscintigram showing two SNs with direct drainage from the prostate (arrows). D) The delayed lymphoscintigram enables differentiation of the SNs and a higher-echelon lymph node (arrow). E-F) Three-dimensional (3D) volume-rendered SPECT/CT image displaying the location of the SNs in more detail (arrows). g Axial fused SPECT/ CT image showing the SN on the right side along the external iliac veins, and h the SN on the left side in the obturator fossa Chapter 1: Appendix 2
18 1 Figure 2. Intratesticular injection of hybrid ICG 99mTc-nanocolloid in a 2-year-old male patient with a seminoma in his left testicle, followed by lymphoscintigraphy and SPECT/ CT. A) Early planar anterior image showing drainage from the left testicle towards an abdominal SN (arrow). B) The delayed lymphoscintigram reveals an additional sentinel node just below the SN that was visualized on the early image (upper arrows), a second- echelon node to the right, and an additional hotspot located more caudally (lower arrow), which was therefore also defined as a SN. C) Fused SPECT/CT image displayed with 3D volume rendering, showing the cranial two SNs alongside the aorta, the interaortocaval second- echelon node, and the more caudal SN (arrow) next to the funiculus. D) Axial fused SPECT/CT image depicting the caudal SN along the external iliac vessels next to the funiculus. All SNs were excised during laparoscopy guided by a laparoscopic gamma probe and fluorescence endoscope. E) Ex-vivo fluorescence image of a para-aortic SN, revealing the location of the node within the excised tissue specimen 26 Innovating image-guided surgery: Introducing multimodal approaches for sentinel node detection
19 1 Figure 3. Lymphatic drainage in penile cancer and the five inguinal zones of Daseler: in the majority of patients, SNs are seen in the superior medial quadrant (73%), superior lateral (9%), and central (18%). Drainage to the inferior quadrants is rare (A). B) Lymphoscintigraphy shows drainage to a SN in both groins (arrows) and bilateral higher-echelon drainage. C) 3D volume-rendered image revealing that both SNs are located in the central zone of Daseler. D-E) Axial fused SPECT/CT images depicting both radioactive SNs, with the corresponding lymph nodes on CT (arrows) Chapter 1: Appendix 27
20 1 Figure. A) Early lymphoscintigraphy after transrectal intraprostatic visualization of bilateral lymphatic drainage with an early-appearing SN along the great abdominal vessels (arrow). B) Axial SPECT/CT image showing the exact location of this SN next to the common iliac artery (arrow). C) 3D volume- rendered SPECT/CT image providing an overview of all SNs: the upper SN next to the common ilac artery (upper arrow), two along the external iliac vessels on the left side, one along the external iliac artery on the right side, but also an additional SN located more mediocaudally (lower arrow). D) The axial image shows that this SN is located paravesically. E) All SNs were harvested laparoscopically, aided by a portable gamma camera (arrow) and a laparoscopic gamma probe. F) Intraoperative visualization of a SN(s) (arrow) using a portable gamma camera, allowing post-excision confirmation that the SN has been removed completely. After excision (right screen), no significant remaining activity is seen Figure. Aberrant drainage afterr transrectal intraprostatic injection of hybrid radioactive and fluorescent ICG 99mTc-nanocolloid in a 9-year-old male patient with intermediate-risk prostate cancer. A) Delayed planar lymphoscintigram showing retrograde drainage towards the scrotum on the right side, due to partial funicular tracer administration as well as drainage to sentinel nodes on both sides (obturator fossa); and a sentinel node located more caudally on the left side (arrow). B-C) The 3D volume-rendered and axial SPECT/ CT images reveal that the most caudal sentinel node on the left side reflects aberrant drainage ventrally against the abdominal wall (arrow). The sentinel nodes were harvested during robot-assisted laparoscopy guided by a laparoscopic gamma probe and fluorescence endoscope. D) Fluorescence endoscope image showing the sentinel node against the abdominal wall along the umbilical ligament (green). This sentinel node (and an iliac sentinel node on the right side) contained metastases at histopathology 28 Innovating image-guided surgery: Introducing multimodal approaches for sentinel node detection
21 References 1. Hernandez BY, Barnholtz-Sloan J, German RR et al (2008) Bur- den of invasive squamous cell carcinoma of the penis in the United States, Cancer 113: Horenblas S, van Tinteren H. Squamous cell carcinoma of the penis. IV. Prognostic factors of survival: analysis of tumor, nodes and metastasis classification system. J Urol 199;11: Leijte JAP, Hughes B, Graafland NM et al. Two-center evaluation of dynamic sentinel node biopsy for squamous cell car- cinoma of the penis. J Clin Oncol 2009;27: Meinhardt W. Sentinel node evaluation in prostate cancer. EAU-EBU Update Series 2007;: Meinhardt W, van der Poel H, Bex A et al. Laparoscopic sentinel lymph node biopsy for prostate cancer: the relevance of locations outside the extended dissection area. Prostate Cancer. 2012;(7173):1. 6. Bray F, Richiardi L, Ekbom A et al.trends in testicular cancer incidence and mortality in 22 European countries: continu- ing increases in incidence and declines in mortality. Int J Cancer. 2006;118: Tanis PJ, Horenblas S, Valdés-Olmos RA et al. Feasibility of sentinel node lymphoscintigraphy in stage I testicular cancer. Eur J Nucl Med Mol Imaging 2002;29: Brouwer OR, Valdés-Olmos RA, Vermeeren L et al.spect/ CT and a portable gamma-camera for image-guided laparoscopic sentinel node biopsy in testicular cancer. J Nucl Med. 2011;2:1. 9. Wespes E. The management of regional lymph nodes in pa- tients with penile carcinoma and reliability of sentinel node biopsy. Eur Urol. 2007;2: Sadeghi R, Gholami H, Zakavi SR et al. Accuracy of sentinel lymph node biopsy for inguinal lymph node staging of penile squamous cell carcinoma: systematic review and meta-analysis of the literature. J Urol. 2012;187: Kroon BK, Horenblas S, Estourgie SH et al. How to avoid false-negative dynamic sentinel node procedures in penile carci- noma. J Urol. 200;171: Vermeeren L, Valdés-Olmos RA, Meinhardt W et al. Intraoperative imaging for sentinel node identification in prostate carcinoma: its use in combination with other techniques. J Nucl Med. 2011;2: Graafland NM, Leijte JAP, Valdés-Olmos RA et al. Repeat dynamic sentinel node biopsy in locally recurrent penile carcinoma. BJU Int. 2009;10: Chapter 1: Appendix 29
22 1 1. Weckermann D, Wawroschek F, Harzmann R. Is there a need for pelvic lymph node dissection in low risk prostate cancer patients prior to definitive local therapy? Eur Urol. 200;7: Kroon BK, Valdés-Olmos RA, van Tinteren H et al. Reproducibility of lymphoscintigraphy for lymphatic mapping in patients with penile carcinoma. J Urol. 200;17: Vermeeren L, Muller SH, Meinhardt W et al. Optimizing the colloid particle concentration for improved preoperative and intraoperative image-guided detection of sentinel nodes in prostate cancer. Eur J Nucl Med Mol Imaging 2010;37: Meinhardt W, Valdés-Olmos RA, van der Poel HG et al. Laparoscopic sentinel node dissection for prostate carcinoma: tech- nical and anatomical observations. BJU Int. 2008;102: Valdés Olmos RA, Tanis PJ, Hoefnagel CA et al. Penile lymphoscintigraphy for sentinel node identification. Eur J Nucl Med. 2001;28: McMahon CJ, Rofsky NM, Pedrosa I. Lymphatic metastases from pelvic tumors: anatomic classification, characterization, and staging. Radiology 2010;2: Leijte JAP, van der Ploeg IMC, Valdés-Olmos RA et al. Visualization of tumor blockage and rerouting of lymphatic drainage in penile cancer patients by use of SPECT/ CT. J Nucl Med. 2009;0: Jeschke S, Nambirajan T, Leeb K et al. Detection of early lymph node metastases in prostate cancer by laparoscopic radioisotope guided sentinel lymph node dissection. J Urol. 200;173: Vermeeren L, Valdés-Olmos RA, Meinhardt W et al. Value of SPECT/CT for detection and anatomic localization of sentinel lymph nodes before laparoscopic sentinel node lymphadenectomy in prostate carcinoma. J Nucl Med. 2009;0: van Leeuwen AC, Buckle T, Bendle G et al. Tracer-cocktail injections for combined pre- and intraoperative multimodal imaging of lymph nodes in a spontaneous mouse prostate tumor model. J Biomed Opt. 2011;16: Brouwer OR, Buckle T, Vermeeren L et al. Comparing the novel hybrid radioactive/ fluorescent tracer ICG-99mTc-nanocolloid with 99mTc-nanocolloid for sentinel node identification: a validation study using lymphoscintigraphy and SPECT/CT. J Nucl Med. 2012;3: Vermeeren L, Valdés Olmos RA, Meinhardt W et al. Intraoperative radioguidance with a portable gamma camera: a novel technique for laparoscopic sentinel node localisation in urological malignancies. Eur J Nucl Med Mol Imaging 2009;36: Innovating image-guided surgery: Introducing multimodal approaches for sentinel node detection
23 26. Brouwer OR, Buckle T, Bunschoten A et al. Image navigation as a means to expand the boundaries of fluorescence guided surgery. Phys Med Biol. 2012;7: van der Poel HG, Buckle T, Brouwer OR et al. Intraoperative laparoscopic fluorescence guidance to the sentinel lymph node in prostate cancer patients: clinical proof of concept of an integrated functional imaging approach using a multimodal tracer. Eur Urol. 2011;60: Kroon BK, Vald s Olmos RA, van der Poel HG et al. Prepubic sentinel node location in penile carcinoma. Clin Nucl Med. 200;30: Vermeeren L, Meinhardt W, Valdés-Olmos RA. Prostatic lymphatic drainage with sentinel nodes at the ventral abdominal wall visualized with SPECT/CT: a case series. Clin Nucl Med. 2010;3: Vermeeren L, Meinhardt W, Bex A et al. Paraaortic sentinel lymph nodes: toward optimal detection and intraoperative localization using SPECT/CT and intraoperative real-time imaging. J Nucl Med. 2010;1: Tanis PJ, Lont AP, Meinhardt W et al. Dynamic sentinel node biopsy for penile cancer: reliability of a staging technique. J Urol. 2002;168: Leijte JAP, Kroon BK, Valdés-Olmos RA et al. Reliability and safety of current dynamic sentinel node biopsy for penile carcinoma. Eur Urol. 2007;2: Holl G, Dorn R, Wengenmair H, Weckermann D et al. Validation of sentinel lymph node dissection in prostate cancer: experience in more than 2000 patients. Eur J Nucl Med Mol Imaging 2009;36: Sadeghi R, Tabasi KT, Bazaz SMM et al. Sentinel node mapping in the prostate cancer. Nuklearmedizin 2011;0: Chapter 1: Appendix 21
The GOSTT concept. (radio)guided intraoperative Scintigraphic Tumor Targeting. Emmanuel Deshayes. GOSTT = Radioguided Surgery
 IAEA WorkShop, November 2017 Emmanuel Deshayes With the kind help of Pr Francesco Giammarile The GOSTT concept GOSTT = Radioguided Surgery (radio)guided intraoperative Scintigraphic Tumor Targeting 1 Radioguided
IAEA WorkShop, November 2017 Emmanuel Deshayes With the kind help of Pr Francesco Giammarile The GOSTT concept GOSTT = Radioguided Surgery (radio)guided intraoperative Scintigraphic Tumor Targeting 1 Radioguided
Radionuclide detection of sentinel lymph node
 Radionuclide detection of sentinel lymph node Sophia I. Koukouraki Assoc. Professor Department of Nuclear Medicine Medicine School, University of Crete 1 BACKGROUND The prognosis of malignant disease is
Radionuclide detection of sentinel lymph node Sophia I. Koukouraki Assoc. Professor Department of Nuclear Medicine Medicine School, University of Crete 1 BACKGROUND The prognosis of malignant disease is
Innovating image-guided surgery: Introducing multimodal approaches for sentinel node detection Brouwer, O.R.
 UvA-DARE (Digital Academic Repository) Innovating image-guided surgery: Introducing multimodal approaches for sentinel node detection Brouwer, O.R. Link to publication Citation for published version (APA):
UvA-DARE (Digital Academic Repository) Innovating image-guided surgery: Introducing multimodal approaches for sentinel node detection Brouwer, O.R. Link to publication Citation for published version (APA):
A specific mapping study using fluorescence sentinel lymph node detection in patients with
 1 2 3 A specific mapping study using fluorescence sentinel lymph node detection in patients with intermediate- and high-risk prostate cancer undergoing extended pelvic lymph node dissection 4 5 6 Daniel
1 2 3 A specific mapping study using fluorescence sentinel lymph node detection in patients with intermediate- and high-risk prostate cancer undergoing extended pelvic lymph node dissection 4 5 6 Daniel
Innovating image-guided surgery: Introducing multimodal approaches for sentinel node detection Brouwer, O.R.
 UvA-DARE (Digital Academic Repository) Innovating image-guided surgery: Introducing multimodal approaches for sentinel node detection Brouwer, O.R. Link to publication Citation for published version (APA):
UvA-DARE (Digital Academic Repository) Innovating image-guided surgery: Introducing multimodal approaches for sentinel node detection Brouwer, O.R. Link to publication Citation for published version (APA):
The Concept of GOSTT
 IAEA Regional Training Course on Sentinel Lymph Node Mapping and Radioguided Surgery The Concept of GOSTT Giuliano Mariani Regional Center of Nuclear Medicine, University of Pisa Medical School, Pisa,
IAEA Regional Training Course on Sentinel Lymph Node Mapping and Radioguided Surgery The Concept of GOSTT Giuliano Mariani Regional Center of Nuclear Medicine, University of Pisa Medical School, Pisa,
Innovating image-guided surgery: Introducing multimodal approaches for sentinel node detection Brouwer, O.R.
 UvA-DARE (Digital Academic Repository) Innovating image-guided surgery: Introducing multimodal approaches for sentinel node detection Brouwer, O.R. Link to publication Citation for published version (APA):
UvA-DARE (Digital Academic Repository) Innovating image-guided surgery: Introducing multimodal approaches for sentinel node detection Brouwer, O.R. Link to publication Citation for published version (APA):
UvA-DARE (Digital Academic Repository)
 UvA-DARE (Digital Academic Repository) In search of the sentinel node : validation and sophistication of lymphatic mapping and sentinel node biopsy in breast cancer and melanoma van der Ploeg, I.M.C. Link
UvA-DARE (Digital Academic Repository) In search of the sentinel node : validation and sophistication of lymphatic mapping and sentinel node biopsy in breast cancer and melanoma van der Ploeg, I.M.C. Link
SPECT/CT Imaging of the Sentinel Lymph Node
 IAEA Regional Training Course on Hybrid Imaging SPECT/CT Imaging of the Sentinel Lymph Node Giuliano Mariani Regional Center of Nuclear Medicine, University of Pisa Medical School, Pisa, Italy Vilnius,
IAEA Regional Training Course on Hybrid Imaging SPECT/CT Imaging of the Sentinel Lymph Node Giuliano Mariani Regional Center of Nuclear Medicine, University of Pisa Medical School, Pisa, Italy Vilnius,
GOSTT General concept
 GOSTT General concept Francesco GIAMMARILE «Aut tace aut loquere meliora silentio» Presentation Outline Introduction: GOSTT and radioguided surgery The Sentinel Node Concept Latest technological knowledge
GOSTT General concept Francesco GIAMMARILE «Aut tace aut loquere meliora silentio» Presentation Outline Introduction: GOSTT and radioguided surgery The Sentinel Node Concept Latest technological knowledge
UvA-DARE (Digital Academic Repository)
 UvA-DARE (Digital Academic Repository) In search of the sentinel node : validation and sophistication of lymphatic mapping and sentinel node biopsy in breast cancer and melanoma van der Ploeg, I.M.C. Link
UvA-DARE (Digital Academic Repository) In search of the sentinel node : validation and sophistication of lymphatic mapping and sentinel node biopsy in breast cancer and melanoma van der Ploeg, I.M.C. Link
STAGING AND FOLLOW-UP STRATEGIES
 ATHENS 4-6 October 2018 European Society of Urogenital Radiology STAGING AND FOLLOW-UP STRATEGIES Ahmet Tuncay Turgut, MD Professor of Radiology Hacettepe University, Faculty of Medicine Ankara 2nd ESUR
ATHENS 4-6 October 2018 European Society of Urogenital Radiology STAGING AND FOLLOW-UP STRATEGIES Ahmet Tuncay Turgut, MD Professor of Radiology Hacettepe University, Faculty of Medicine Ankara 2nd ESUR
«Aut tace aut loquere meliora silentio» Francesco GIAMMARILE
 «Aut tace aut loquere meliora silentio» Francesco GIAMMARILE Presentation Outline Introduction: the GOSTT Concept The EANM Guideline in Melanoma Future trends and concluding remarks I sort of thought your
«Aut tace aut loquere meliora silentio» Francesco GIAMMARILE Presentation Outline Introduction: the GOSTT Concept The EANM Guideline in Melanoma Future trends and concluding remarks I sort of thought your
Austin Radiological Association Nuclear Medicine Procedure LYMPHOSCINTIGRAPHY (Tc-99m-Sulfur Colloid [Filtered])
![Austin Radiological Association Nuclear Medicine Procedure LYMPHOSCINTIGRAPHY (Tc-99m-Sulfur Colloid [Filtered]) Austin Radiological Association Nuclear Medicine Procedure LYMPHOSCINTIGRAPHY (Tc-99m-Sulfur Colloid [Filtered])](/thumbs/87/95258373.jpg) Austin Radiological Association Nuclear Medicine Procedure LYMPHOSCINTIGRAPHY (Tc-99m-Sulfur Colloid [Filtered]) Overview Indications The Lymphoscintigraphy Study demonstrates the flow of lymph from the
Austin Radiological Association Nuclear Medicine Procedure LYMPHOSCINTIGRAPHY (Tc-99m-Sulfur Colloid [Filtered]) Overview Indications The Lymphoscintigraphy Study demonstrates the flow of lymph from the
GUIDELINES ON PENILE CANCER
 GUIDELINES ON PENILE CANCER (Text updated March 2005) G. Pizzocaro (chairman), F. Algaba, S. Horenblas, H. van der Poel, E. Solsona, S. Tana, N. Watkin 58 Penile Cancer Eur Urol 2004;46(1);1-8 Introduction
GUIDELINES ON PENILE CANCER (Text updated March 2005) G. Pizzocaro (chairman), F. Algaba, S. Horenblas, H. van der Poel, E. Solsona, S. Tana, N. Watkin 58 Penile Cancer Eur Urol 2004;46(1);1-8 Introduction
Sentinel Node Localisation of Melanoma
 Sentinel Node Localisation of Melanoma V Bongers, Diakonessenhuis, Utrecht 1. Introduction A melanoma is mostly a malignancy of the skin. The sentinel lymph node (SLN) concept of sequential progression
Sentinel Node Localisation of Melanoma V Bongers, Diakonessenhuis, Utrecht 1. Introduction A melanoma is mostly a malignancy of the skin. The sentinel lymph node (SLN) concept of sequential progression
AMORE (Ablative surgery, MOulage technique brachytherapy and REconstruction) for childhood head and neck rhabdomyosarcoma Buwalda, J.
 UvA-DARE (Digital Academic Repository) AMORE (Ablative surgery, MOulage technique brachytherapy and REconstruction) for childhood head and neck rhabdomyosarcoma Buwalda, J. Link to publication Citation
UvA-DARE (Digital Academic Repository) AMORE (Ablative surgery, MOulage technique brachytherapy and REconstruction) for childhood head and neck rhabdomyosarcoma Buwalda, J. Link to publication Citation
EUROPEAN UROLOGY 63 (2013)
 EUROPEAN UROLOGY 63 (2013) 657 663 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Penile Cancer Editorial by Nicola Nicolai on pp. 664 666 of this issue
EUROPEAN UROLOGY 63 (2013) 657 663 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Penile Cancer Editorial by Nicola Nicolai on pp. 664 666 of this issue
Citation for published version (APA): Bartels, S. A. L. (2013). Laparoscopic colorectal surgery: beyond the short-term effects
 UvA-DARE (Digital Academic Repository) Laparoscopic colorectal surgery: beyond the short-term effects Bartels, S.A.L. Link to publication Citation for published version (APA): Bartels, S. A. L. (2013).
UvA-DARE (Digital Academic Repository) Laparoscopic colorectal surgery: beyond the short-term effects Bartels, S.A.L. Link to publication Citation for published version (APA): Bartels, S. A. L. (2013).
Comparison of intra-operative gamma probe detection with postoperative SPECT/CT of sentinel nodes related to the ovary.
 Journal of Nuclear Medicine, published on October 13, 2016 as doi:10.2967/jnumed.116.183426 Comparison of intra-operative gamma probe detection with postoperative SPECT/CT of sentinel nodes related to
Journal of Nuclear Medicine, published on October 13, 2016 as doi:10.2967/jnumed.116.183426 Comparison of intra-operative gamma probe detection with postoperative SPECT/CT of sentinel nodes related to
MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER
 10 MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER Recommendations from the EAU Working Party on Muscle Invasive and Metastatic Bladder Cancer G. Jakse (chairman), F. Algaba, S. Fossa, A. Stenzl, C. Sternberg
10 MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER Recommendations from the EAU Working Party on Muscle Invasive and Metastatic Bladder Cancer G. Jakse (chairman), F. Algaba, S. Fossa, A. Stenzl, C. Sternberg
by Gamma and Fluorescence
 Double Detection of Sentinel Lymph Nodes by Gamma and Fluorescence Sarl au capital de 15 000 RCS PARIS 432 607 562 Siret 432 607 562 00027 APE4646Z 13 rue Raymond Losserand 75014 Paris- France Tél : 33(0)
Double Detection of Sentinel Lymph Nodes by Gamma and Fluorescence Sarl au capital de 15 000 RCS PARIS 432 607 562 Siret 432 607 562 00027 APE4646Z 13 rue Raymond Losserand 75014 Paris- France Tél : 33(0)
Citation for published version (APA): Veenstra, H. J. (2013). Melanoma surgery and the impact of sentinel node biopsy.
 UvA-DARE (Digital Academic Repository) Melanoma surgery and the impact of sentinel node biopsy Veenstra, H.J. Link to publication Citation for published version (APA): Veenstra, H. J. (2013). Melanoma
UvA-DARE (Digital Academic Repository) Melanoma surgery and the impact of sentinel node biopsy Veenstra, H.J. Link to publication Citation for published version (APA): Veenstra, H. J. (2013). Melanoma
GUIDELINES ON PENILE CANCER
 46 E. Solsona (chairman), F. Algaba, S. Horenblas, G. Pizzocaro, T. Windahl Eur Urol 2002;42(3):199-203 Introduction Penile carcinoma is an uncommon malignant disease with an incidence ranging from 0.1
46 E. Solsona (chairman), F. Algaba, S. Horenblas, G. Pizzocaro, T. Windahl Eur Urol 2002;42(3):199-203 Introduction Penile carcinoma is an uncommon malignant disease with an incidence ranging from 0.1
Sentinel lymph node imaging in urologic oncology
 Review Article Sentinel lymph node imaging in urologic oncology Sherif Mehralivand 1,2,3, Henk van der Poel 4, Alexander Winter 5, Peter L. Choyke 3, Peter A. Pinto 2, Baris Turkbey 3 1 Department of Urology
Review Article Sentinel lymph node imaging in urologic oncology Sherif Mehralivand 1,2,3, Henk van der Poel 4, Alexander Winter 5, Peter L. Choyke 3, Peter A. Pinto 2, Baris Turkbey 3 1 Department of Urology
Integrating new imaging modalities in breast cancer management Pouw, Bas
 UvA-DARE (Digital Academic Repository) Integrating new imaging modalities in breast cancer management Pouw, Bas Link to publication Citation for published version (APA): Pouw, B. (2016). Integrating new
UvA-DARE (Digital Academic Repository) Integrating new imaging modalities in breast cancer management Pouw, Bas Link to publication Citation for published version (APA): Pouw, B. (2016). Integrating new
Technical Considerations. Imaging Considerations
 354 CUTANEOUS MALIGNANCY OF THE HEAD AND NECK desmoplastic melanomas are characterized by a uniform desmoplasia that is prominent throughout the entire tumor (termed pure desmoplastic melanoma), whereas
354 CUTANEOUS MALIGNANCY OF THE HEAD AND NECK desmoplastic melanomas are characterized by a uniform desmoplasia that is prominent throughout the entire tumor (termed pure desmoplastic melanoma), whereas
Citation for published version (APA): Vermeeren, L. (2011). Sentinel nodes in complex areas: innovating radioguided surgery
 UvA-DARE (Digital Academic Repository) Sentinel nodes in complex areas: innovating radioguided surgery Vermeeren, L. Link to publication Citation for published version (APA): Vermeeren, L. (2011). Sentinel
UvA-DARE (Digital Academic Repository) Sentinel nodes in complex areas: innovating radioguided surgery Vermeeren, L. Link to publication Citation for published version (APA): Vermeeren, L. (2011). Sentinel
Role and extension of lymph node dissection in kidney, bladder and prostate cancer. Omar Ghanem (PGY3 ) Moderator: Dr A. Noujem 30 th March 2017
 Role and extension of lymph node dissection in kidney, bladder and prostate cancer Omar Ghanem (PGY3 ) Moderator: Dr A. Noujem 30 th March 2017 Bladder Cancer LN dissection in Bladder cancer 25% of patients
Role and extension of lymph node dissection in kidney, bladder and prostate cancer Omar Ghanem (PGY3 ) Moderator: Dr A. Noujem 30 th March 2017 Bladder Cancer LN dissection in Bladder cancer 25% of patients
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman
 Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Case 1: 79 yr-old woman with a lump in upper outer quadrant of left breast.
 Case 1: 79 yr-old woman with a lump in upper outer quadrant of left breast. Giuliano Mariani Regional Center of Nuclear Medicine, University of Pisa Medical School, Pisa (Italy) Relevant history 79-yr
Case 1: 79 yr-old woman with a lump in upper outer quadrant of left breast. Giuliano Mariani Regional Center of Nuclear Medicine, University of Pisa Medical School, Pisa (Italy) Relevant history 79-yr
performed to help sway the clinician in what the appropriate diagnosis is, which can substantially alter the treatment of management.
 Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Investigating the role of SPECT/CT in dynamic sentinel lymph node biopsy for penile cancers
 Eur J Nucl Med Mol Imaging (2017) 44:1176 1184 DOI 10.1007/s00259-017-3636-1 ORIGINAL ARTICLE Investigating the role of SPECT/CT in dynamic sentinel lymph node biopsy for penile cancers Ziauddin Zia Saad
Eur J Nucl Med Mol Imaging (2017) 44:1176 1184 DOI 10.1007/s00259-017-3636-1 ORIGINAL ARTICLE Investigating the role of SPECT/CT in dynamic sentinel lymph node biopsy for penile cancers Ziauddin Zia Saad
Cover Page. The handle holds various files of this Leiden University dissertation
 Cover Page The handle http://hdl.handle.net/1887/44147 holds various files of this Leiden University dissertation Author: Berg, Nynke van den Title: Advancing surgical guidance : from (hybrid) molecule
Cover Page The handle http://hdl.handle.net/1887/44147 holds various files of this Leiden University dissertation Author: Berg, Nynke van den Title: Advancing surgical guidance : from (hybrid) molecule
The Template of the Primary Lymphatic Landing Sites of the Prostate Should Be Revisited: Results of a Multimodality Mapping Study
 european urology 53 (2008) 118 125 available at www.sciencedirect.com journal homepage: www.europeanurology.com Prostate Cancer The Template of the Primary Lymphatic Landing Sites of the Prostate Should
european urology 53 (2008) 118 125 available at www.sciencedirect.com journal homepage: www.europeanurology.com Prostate Cancer The Template of the Primary Lymphatic Landing Sites of the Prostate Should
UvA-DARE (Digital Academic Repository) Vascular factors in dementia and apathy Eurelings, Lisa. Link to publication
 UvA-DARE (Digital Academic Repository) Vascular factors in dementia and apathy Eurelings, Lisa Link to publication Citation for published version (APA): Eurelings, L. S. M. (2016). Vascular factors in
UvA-DARE (Digital Academic Repository) Vascular factors in dementia and apathy Eurelings, Lisa Link to publication Citation for published version (APA): Eurelings, L. S. M. (2016). Vascular factors in
UvA-DARE (Digital Academic Repository)
 UvA-DARE (Digital Academic Repository) In search of the sentinel node : validation and sophistication of lymphatic mapping and sentinel node biopsy in breast cancer and melanoma van der Ploeg, I.M.C. Link
UvA-DARE (Digital Academic Repository) In search of the sentinel node : validation and sophistication of lymphatic mapping and sentinel node biopsy in breast cancer and melanoma van der Ploeg, I.M.C. Link
Regional metastatic melanoma. Aspects of treatment and prognostic factors Strobbe, L.J.A.
 UvA-DARE (Digital Academic Repository) Regional metastatic melanoma. Aspects of treatment and prognostic factors Strobbe, L.J.A. Link to publication Citation for published version (APA): Strobbe, L. J.
UvA-DARE (Digital Academic Repository) Regional metastatic melanoma. Aspects of treatment and prognostic factors Strobbe, L.J.A. Link to publication Citation for published version (APA): Strobbe, L. J.
UvA-DARE (Digital Academic Repository) An electronic nose in respiratory disease Dragonieri, S. Link to publication
 UvA-DARE (Digital Academic Repository) An electronic nose in respiratory disease Dragonieri, S. Link to publication Citation for published version (APA): Dragonieri, S. (2012). An electronic nose in respiratory
UvA-DARE (Digital Academic Repository) An electronic nose in respiratory disease Dragonieri, S. Link to publication Citation for published version (APA): Dragonieri, S. (2012). An electronic nose in respiratory
Nonvisualization of sentinel node by lymphoscintigraphy in advanced breast cancer
 Radiology Case Reports Nonvisualization of sentinel node by lymphoscintigraphy in advanced breast cancer Volume 5, Issue 3, 2010 Brian Wosnitzer, MD; Rosna Mirtcheva, MD; and Munir Ghesani, MD Previous
Radiology Case Reports Nonvisualization of sentinel node by lymphoscintigraphy in advanced breast cancer Volume 5, Issue 3, 2010 Brian Wosnitzer, MD; Rosna Mirtcheva, MD; and Munir Ghesani, MD Previous
Practice of Axilla Surgery
 Summer School of Breast Disease 2016 Practice of Axilla Surgery Axillary Lymph Node Dissection & Sentinel Lymph Node Biopsy 연세의대외과 박세호 Contents Anatomy of the axilla Axillary lymph node dissection (ALND)
Summer School of Breast Disease 2016 Practice of Axilla Surgery Axillary Lymph Node Dissection & Sentinel Lymph Node Biopsy 연세의대외과 박세호 Contents Anatomy of the axilla Axillary lymph node dissection (ALND)
GUIDELINES ON PROSTATE CANCER
 10 G. Aus (chairman), C. Abbou, M. Bolla, A. Heidenreich, H-P. Schmid, H. van Poppel, J. Wolff, F. Zattoni Eur Urol 2001;40:97-101 Introduction Cancer of the prostate is now recognized as one of the principal
10 G. Aus (chairman), C. Abbou, M. Bolla, A. Heidenreich, H-P. Schmid, H. van Poppel, J. Wolff, F. Zattoni Eur Urol 2001;40:97-101 Introduction Cancer of the prostate is now recognized as one of the principal
Characterizing scaphoid nonunion deformity using 2-D and 3-D imaging techniques ten Berg, P.W.L.
 UvA-DARE (Digital Academic Repository) Characterizing scaphoid nonunion deformity using 2-D and 3-D imaging techniques ten Berg, P.W.L. Link to publication Citation for published version (APA): ten Berg,
UvA-DARE (Digital Academic Repository) Characterizing scaphoid nonunion deformity using 2-D and 3-D imaging techniques ten Berg, P.W.L. Link to publication Citation for published version (APA): ten Berg,
Surgeons Perspective: LN as a Draining Pattern. Jose A. Karam, MD, FACS Associate Professor Department of Urology
 Surgeons Perspective: LN as a Draining Pattern Jose A. Karam, MD, FACS Associate Professor Department of Urology Disclosures EMD Serono, Pfizer, Novartis: Advisory board/consultant Disclosures I perform
Surgeons Perspective: LN as a Draining Pattern Jose A. Karam, MD, FACS Associate Professor Department of Urology Disclosures EMD Serono, Pfizer, Novartis: Advisory board/consultant Disclosures I perform
BREAST CANCER SURGERY. Dr. John H. Donohue
 Dr. John H. Donohue HISTORY References to breast surgery in ancient Egypt (ca 3000 BCE) Mastectomy described in numerous medieval texts Petit formulated organized approach in 18 th Century Improvements
Dr. John H. Donohue HISTORY References to breast surgery in ancient Egypt (ca 3000 BCE) Mastectomy described in numerous medieval texts Petit formulated organized approach in 18 th Century Improvements
Citation for published version (APA): Wijkerslooth de Weerdesteyn, T. R. (2013). Population screening for colorectal cancer by colonoscopy
 UvA-DARE (Digital Academic Repository) Population screening for colorectal cancer by colonoscopy de Wijkerslooth, T.R. Link to publication Citation for published version (APA): Wijkerslooth de Weerdesteyn,
UvA-DARE (Digital Academic Repository) Population screening for colorectal cancer by colonoscopy de Wijkerslooth, T.R. Link to publication Citation for published version (APA): Wijkerslooth de Weerdesteyn,
Cardiff MRCS OSCE Courses Testicular Cancer
 Testicular Cancer Scenario: A 40-year-old male presents to the surgical out-patient clinic with a 6-8 week history of a painless lump in his left scrotum. He however complains of a dull ache in the scrotum
Testicular Cancer Scenario: A 40-year-old male presents to the surgical out-patient clinic with a 6-8 week history of a painless lump in his left scrotum. He however complains of a dull ache in the scrotum
Clinical Study Sentinel Lymph Node Detection Using Laser-Assisted Indocyanine Green Dye Lymphangiography in Patients with Melanoma
 International Surgical Oncology Volume 2013, Article ID 904214, 4 pages http://dx.doi.org/10.1155/2013/904214 Clinical Study Sentinel Lymph Node Detection Using Laser-Assisted Indocyanine Green Dye Lymphangiography
International Surgical Oncology Volume 2013, Article ID 904214, 4 pages http://dx.doi.org/10.1155/2013/904214 Clinical Study Sentinel Lymph Node Detection Using Laser-Assisted Indocyanine Green Dye Lymphangiography
Prostate cancer presents in various ways, including
 Case Report 840 Presentation of Prostate Carcinoma with Cervical Lymphadenopathy: Report of Three Cases Hung-Jen Wang, MD; Po-Hui Chiang, PhD; Jyh-Ping Peng 1, MD; Tsan-Jeng Yu, MD The most common method
Case Report 840 Presentation of Prostate Carcinoma with Cervical Lymphadenopathy: Report of Three Cases Hung-Jen Wang, MD; Po-Hui Chiang, PhD; Jyh-Ping Peng 1, MD; Tsan-Jeng Yu, MD The most common method
Canadian Scientific Journal. Intraoperative color detection of lymph nodes metastases in thyroid cancer
 Canadian Scientific Journal 2 (2014) Contents lists available at Canadian Scientific Journal Canadian Scientific Journal journal homepage: Intraoperative color detection of lymph nodes metastases in thyroid
Canadian Scientific Journal 2 (2014) Contents lists available at Canadian Scientific Journal Canadian Scientific Journal journal homepage: Intraoperative color detection of lymph nodes metastases in thyroid
Sentinel Lymph Node Biopsy in Other Tumours: Sentinel Lymph Node Biopsy in Other Tumours. Methodology. Results. Key Questions to Consider
 Sentinel Lymph Node Biopsy in Other Tumours Dr. Rona Cheifetz Surgical Oncology Update November 24, 2006 Sentinel Lymph Node Biopsy in Other Tumours: An Operation Looking for an Application Dr. Rona Cheifetz
Sentinel Lymph Node Biopsy in Other Tumours Dr. Rona Cheifetz Surgical Oncology Update November 24, 2006 Sentinel Lymph Node Biopsy in Other Tumours: An Operation Looking for an Application Dr. Rona Cheifetz
Molecular Imaging and Breast Cancer
 Molecular Imaging and Breast Cancer Breast cancer forms in tissues of the breast usually in the ducts, tubes that carry milk to the nipple, and lobules, the glands that make milk. It occurs in both men
Molecular Imaging and Breast Cancer Breast cancer forms in tissues of the breast usually in the ducts, tubes that carry milk to the nipple, and lobules, the glands that make milk. It occurs in both men
Whole Body MRI. Dr. Nina Tunariu. Prostate Cancer recurrence, progression and restaging
 Whole Body MRI Prostate Cancer recurrence, progression and restaging Dr. Nina Tunariu Consultant Radiology Drug Development Unit and Prostate Targeted Therapies Group 12-13 Janeiro 2018 Evolving Treatment
Whole Body MRI Prostate Cancer recurrence, progression and restaging Dr. Nina Tunariu Consultant Radiology Drug Development Unit and Prostate Targeted Therapies Group 12-13 Janeiro 2018 Evolving Treatment
Renal vascular evaluation with 64 Multislice Computerized Tomography Daniela Stoisa, Fabrizzio E. Galiano, Andrés Quaranta, Roberto L.
 Renal vascular evaluation with 64 Multislice Computerized Tomography Daniela Stoisa, Fabrizzio E. Galiano, Andrés Quaranta, Roberto L. Villavicencio Footnote Diagnóstico Médico Oroño. Bv. Oroño 1515. 2000.
Renal vascular evaluation with 64 Multislice Computerized Tomography Daniela Stoisa, Fabrizzio E. Galiano, Andrés Quaranta, Roberto L. Villavicencio Footnote Diagnóstico Médico Oroño. Bv. Oroño 1515. 2000.
Melanoma Surgery Update James R. Ouellette, DO FACS Premier Health Cancer Institute Wright State University Chief, Surgical Oncology Division
 Melanoma Surgery Update 2018 James R. Ouellette, DO FACS Premier Health Cancer Institute Wright State University Chief, Surgical Oncology Division Surgery for Melanoma Mainstay of treatment for potentially
Melanoma Surgery Update 2018 James R. Ouellette, DO FACS Premier Health Cancer Institute Wright State University Chief, Surgical Oncology Division Surgery for Melanoma Mainstay of treatment for potentially
Citation for published version (APA): Donker, M. (2014). Improvements in locoregional treatment of breast cancer
 UvA-DARE (Digital Academic Repository) Improvements in locoregional treatment of breast cancer Donker, Mila Link to publication Citation for published version (APA): Donker, M. (2014). Improvements in
UvA-DARE (Digital Academic Repository) Improvements in locoregional treatment of breast cancer Donker, Mila Link to publication Citation for published version (APA): Donker, M. (2014). Improvements in
THE ROLE OF CONTEMPORARY IMAGING AND HYBRID METHODS IN THE DIAGNOSIS OF CUTANEOUS MALIGNANT MELANOMA(CMM) AND MERKEL CELL CARCINOMA (MCC)
 THE ROLE OF CONTEMPORARY IMAGING AND HYBRID METHODS IN THE DIAGNOSIS OF CUTANEOUS MALIGNANT MELANOMA(CMM) AND MERKEL CELL CARCINOMA (MCC) I.Kostadinova, Sofia, Bulgaria CMM some clinical facts The incidence
THE ROLE OF CONTEMPORARY IMAGING AND HYBRID METHODS IN THE DIAGNOSIS OF CUTANEOUS MALIGNANT MELANOMA(CMM) AND MERKEL CELL CARCINOMA (MCC) I.Kostadinova, Sofia, Bulgaria CMM some clinical facts The incidence
Imaging in gastric cancer
 Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
EAU GUIDELINES ON PENILE CANCER
 EAU GUIDELINES ON PENILE CANCER (Text update April 2014) O.W. Hakenberg (Chair), N. Watkin, E. Compérat, S. Minhas, A. Necchi, C. Protzel Introduction and epidemiology The incidence of penile cancer increases
EAU GUIDELINES ON PENILE CANCER (Text update April 2014) O.W. Hakenberg (Chair), N. Watkin, E. Compérat, S. Minhas, A. Necchi, C. Protzel Introduction and epidemiology The incidence of penile cancer increases
Is Sentinel Node Biopsy Practical?
 Breast Cancer Is Sentinel Node Biopsy Practical? Benefits and Limitations JMAJ 45(10): 444 448, 2002 Shigeru IMOTO *1, Satoshi EBIHARA *2 and Noriyuki MORIYAMA *3 *1 Breast Surgery Division, National Cancer
Breast Cancer Is Sentinel Node Biopsy Practical? Benefits and Limitations JMAJ 45(10): 444 448, 2002 Shigeru IMOTO *1, Satoshi EBIHARA *2 and Noriyuki MORIYAMA *3 *1 Breast Surgery Division, National Cancer
UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication
 UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication Citation for published version (APA): van Bergen, C. J. A. (2014). Treatment
UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication Citation for published version (APA): van Bergen, C. J. A. (2014). Treatment
is time consuming and expensive. An intra-operative assessment is not going to be helpful if there is no more tissue that can be taken to improve the
 My name is Barry Feig. I am a Professor of Surgical Oncology at The University of Texas MD Anderson Cancer Center in Houston, Texas. I am going to talk to you today about the role for surgery in the treatment
My name is Barry Feig. I am a Professor of Surgical Oncology at The University of Texas MD Anderson Cancer Center in Houston, Texas. I am going to talk to you today about the role for surgery in the treatment
Scanning with 18F-FDG-PET/CT for Detection of Pelvic Nodal Involvement in Inguinal Node-Positive Penile Carcinoma
 EUROPEAN UROLOGY 56 (2009) 339 345 available at www.sciencedirect.com journal homepage: www.europeanurology.com Penile Cancer Scanning with 18F-FDG-PET/CT for Detection of Pelvic Nodal Involvement in Inguinal
EUROPEAN UROLOGY 56 (2009) 339 345 available at www.sciencedirect.com journal homepage: www.europeanurology.com Penile Cancer Scanning with 18F-FDG-PET/CT for Detection of Pelvic Nodal Involvement in Inguinal
Doppler ultrasound of the abdomen and pelvis, and color Doppler
 - - - - - - - - - - - - - Testicular tumors are rare in children. They account for only 1% of all pediatric solid tumors and 3% of all testicular tumors [1,2]. The annual incidence of testicular tumors
- - - - - - - - - - - - - Testicular tumors are rare in children. They account for only 1% of all pediatric solid tumors and 3% of all testicular tumors [1,2]. The annual incidence of testicular tumors
Minimally invasive function-preserving surgery based on sentinel node concept in early gastric cancer
 Review Article Minimally invasive function-preserving surgery based on sentinel node concept in early gastric cancer Hiroya Takeuchi, Yuko Kitagawa Department of Surgery, Keio University School of Medicine,
Review Article Minimally invasive function-preserving surgery based on sentinel node concept in early gastric cancer Hiroya Takeuchi, Yuko Kitagawa Department of Surgery, Keio University School of Medicine,
Testicular Malignancies /8/15
 Collecting Cancer Data: Testis 2014-2015 NAACCR Webinar Series January 8, 2015 Q&A Please submit all questions concerning webinar content through the Q&A panel. Reminder: If you have participants watching
Collecting Cancer Data: Testis 2014-2015 NAACCR Webinar Series January 8, 2015 Q&A Please submit all questions concerning webinar content through the Q&A panel. Reminder: If you have participants watching
IMAGING GUIDELINES - COLORECTAL CANCER
 IMAGING GUIDELINES - COLORECTAL CANCER DIAGNOSIS The majority of colorectal cancers are diagnosed on colonoscopy, with some being diagnosed on Ba enema, ultrasound or CT. STAGING CT chest, abdomen and
IMAGING GUIDELINES - COLORECTAL CANCER DIAGNOSIS The majority of colorectal cancers are diagnosed on colonoscopy, with some being diagnosed on Ba enema, ultrasound or CT. STAGING CT chest, abdomen and
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER
 MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
Citation Acta medica Nagasakiensia. 1963, 8(
 NAOSITE: Nagasaki University's Ac Title Radical Operation For Prostatic Car Author(s) Kondoh, Atushi Citation Acta medica Nagasakiensia. 1963, 8( Issue Date 1963-12-25 URL http://hdl.handle.net/10069/15473
NAOSITE: Nagasaki University's Ac Title Radical Operation For Prostatic Car Author(s) Kondoh, Atushi Citation Acta medica Nagasakiensia. 1963, 8( Issue Date 1963-12-25 URL http://hdl.handle.net/10069/15473
Glossary of Terms Primary Urethral Cancer
 Patient Information English Glossary of Terms Primary Urethral Cancer Advanced cancer A tumour that grows into deeper layers of tissue, adjacent organs, or surrounding muscles. Anaesthesia (general, spinal,
Patient Information English Glossary of Terms Primary Urethral Cancer Advanced cancer A tumour that grows into deeper layers of tissue, adjacent organs, or surrounding muscles. Anaesthesia (general, spinal,
GUIDELINES ON RENAL CELL CANCER
 20 G. Mickisch (chairman), J. Carballido, S. Hellsten, H. Schulze, H. Mensink Eur Urol 2001;40(3):252-255 Introduction is characterised by a constant rise in incidence over the last 50 years, with a predominance
20 G. Mickisch (chairman), J. Carballido, S. Hellsten, H. Schulze, H. Mensink Eur Urol 2001;40(3):252-255 Introduction is characterised by a constant rise in incidence over the last 50 years, with a predominance
UvA-DARE (Digital Academic Repository)
 UvA-DARE (Digital Academic Repository) Clinical studies and tissue analyses in the earliest phases of rheumatoid arthritis: In search of the transition from being at risk to having clinically apparent
UvA-DARE (Digital Academic Repository) Clinical studies and tissue analyses in the earliest phases of rheumatoid arthritis: In search of the transition from being at risk to having clinically apparent
EAU GUIDELINES ON PENILE CANCER
 EAU GUIDELINES ON PENILE CANCER (Text update April 2014) O.W. Hakenberg (Chair), E. Compérat, S. Minhas, A. Necchi, C. Protzel, N. Watkin Guidelines Associate: R. Robinson Introduction and epidemiology
EAU GUIDELINES ON PENILE CANCER (Text update April 2014) O.W. Hakenberg (Chair), E. Compérat, S. Minhas, A. Necchi, C. Protzel, N. Watkin Guidelines Associate: R. Robinson Introduction and epidemiology
UvA-DARE (Digital Academic Repository)
 UvADARE (Digital Academic Repository) In search of the sentinel node : validation and sophistication of lymphatic mapping and sentinel node biopsy in breast cancer and melanoma van der Ploeg, I.M.C. Link
UvADARE (Digital Academic Repository) In search of the sentinel node : validation and sophistication of lymphatic mapping and sentinel node biopsy in breast cancer and melanoma van der Ploeg, I.M.C. Link
Alexander Winter, MD 1, Joachim Woenkhaus, MD 2, and Friedhelm Wawroschek, MD 1
 Ann Surg Oncol (2014) 21:4390 4396 DOI 10.1245/s10434-014-4024-8 ORIGINAL ARTICLE UROLOGIC ONCOLOGY A Novel Method for Intraoperative Sentinel Lymph Node Detection in Prostate Cancer Patients Using Superparamagnetic
Ann Surg Oncol (2014) 21:4390 4396 DOI 10.1245/s10434-014-4024-8 ORIGINAL ARTICLE UROLOGIC ONCOLOGY A Novel Method for Intraoperative Sentinel Lymph Node Detection in Prostate Cancer Patients Using Superparamagnetic
Eight false negative sentinel node procedures in breast cancer: what went wrong?
 EJSO 2003; 29: 336±340 doi:10.1053/ejso.2002.1379 Eight false negative sentinel node procedures in breast cancer: what went wrong? S. H. Estourgie*, O. E. Nieweg*, R. A. ValdeÂs Olmos², E. J. Th. Rutgers*,
EJSO 2003; 29: 336±340 doi:10.1053/ejso.2002.1379 Eight false negative sentinel node procedures in breast cancer: what went wrong? S. H. Estourgie*, O. E. Nieweg*, R. A. ValdeÂs Olmos², E. J. Th. Rutgers*,
SENTINEL LYMPH NODE CONCEPT IN OESOPHAGEAL CANCER
 SENTINEL LYMPH NODE CONCEPT IN OESOPHAGEAL CANCER Sarah K Thompson, M.D. Queenstown ANZGOSA Mtg, 2010 Sentinel Lymph Node (SLN) Sentinel Lymph Node (SLN) Not always on a direct drainage pathway Not always
SENTINEL LYMPH NODE CONCEPT IN OESOPHAGEAL CANCER Sarah K Thompson, M.D. Queenstown ANZGOSA Mtg, 2010 Sentinel Lymph Node (SLN) Sentinel Lymph Node (SLN) Not always on a direct drainage pathway Not always
GUIDELINES ON PENILE CANCER
 GUIDELINES ON PENILE CANCER (Text update April 2010) G. Pizzocaro, F. Algaba, S. Horenblas, E. Solsona, S. Tana, H. Van Der Poel, N. Watkin 78 Penile Cancer Eur Urol 2010 Jun;57(6):1002-12 Introduction
GUIDELINES ON PENILE CANCER (Text update April 2010) G. Pizzocaro, F. Algaba, S. Horenblas, E. Solsona, S. Tana, H. Van Der Poel, N. Watkin 78 Penile Cancer Eur Urol 2010 Jun;57(6):1002-12 Introduction
MRI and metastases of PCa
 MRI and metastases of PCa François CORNUD Céline COUVIDAT David EISS Arnaud LEFEVRE IRM Paris 16, France, Paris, France Université Paris Descartes, Paris, France When imaging should be considered for detection
MRI and metastases of PCa François CORNUD Céline COUVIDAT David EISS Arnaud LEFEVRE IRM Paris 16, France, Paris, France Université Paris Descartes, Paris, France When imaging should be considered for detection
General information about prostate cancer
 Prostate Cancer General information about prostate cancer Key points Prostate cancer is a disease in which malignant (cancer) cells form in the tissues of the prostate. Signs of prostate cancer include
Prostate Cancer General information about prostate cancer Key points Prostate cancer is a disease in which malignant (cancer) cells form in the tissues of the prostate. Signs of prostate cancer include
EUROPEAN UROLOGY 58 (2010)
 EUROPEAN UROLOGY 58 (2010) 742 747 available at www.sciencedirect.com journal homepage: www.europeanurology.com Penile Cancer Prognostic Factors for Occult Inguinal Lymph Node Involvement in Penile Carcinoma
EUROPEAN UROLOGY 58 (2010) 742 747 available at www.sciencedirect.com journal homepage: www.europeanurology.com Penile Cancer Prognostic Factors for Occult Inguinal Lymph Node Involvement in Penile Carcinoma
ANNEX 1 OBJECTIVES. At the completion of the training period, the fellow should be able to:
 1 ANNEX 1 OBJECTIVES At the completion of the training period, the fellow should be able to: 1. Breast Surgery Evaluate and manage common benign and malignant breast conditions. Assess the indications
1 ANNEX 1 OBJECTIVES At the completion of the training period, the fellow should be able to: 1. Breast Surgery Evaluate and manage common benign and malignant breast conditions. Assess the indications
COMPARATIVE ANALYSIS OF COLON AND RECTAL CANCERS IN SENTINEL LYMPH NODE MAPPING
 Trakia Journal of Sciences, Vol. 5, No. 1, pp 10-14, 2007 Copyright 2007 Trakia University Available online at: http://www.uni-sz.bg ISSN 1312-1723 Original Contribution COMPARATIVE ANALYSIS OF COLON AND
Trakia Journal of Sciences, Vol. 5, No. 1, pp 10-14, 2007 Copyright 2007 Trakia University Available online at: http://www.uni-sz.bg ISSN 1312-1723 Original Contribution COMPARATIVE ANALYSIS OF COLON AND
Index. Surg Oncol Clin N Am 16 (2007) Note: Page numbers of article titles are in boldface type.
 Surg Oncol Clin N Am 16 (2007) 465 469 Index Note: Page numbers of article titles are in boldface type. A Adjuvant therapy, preoperative for gastric cancer, staging and, 339 B Breast cancer, metabolic
Surg Oncol Clin N Am 16 (2007) 465 469 Index Note: Page numbers of article titles are in boldface type. A Adjuvant therapy, preoperative for gastric cancer, staging and, 339 B Breast cancer, metabolic
Perineum. done by : zaid al-ghnaneem
 Perineum done by : zaid al-ghnaneem Hello everyone, this sheet will talk about 2 nd Lecture which is Perineum but there are some slides and info from 1 st Lecture. Everything included Slides + Pics Let
Perineum done by : zaid al-ghnaneem Hello everyone, this sheet will talk about 2 nd Lecture which is Perineum but there are some slides and info from 1 st Lecture. Everything included Slides + Pics Let
UvA-DARE (Digital Academic Repository) Improving aspects of palliative care for children Jagt, C.T. Link to publication
 UvA-DARE (Digital Academic Repository) Improving aspects of palliative care for children Jagt, C.T. Link to publication Citation for published version (APA): Jagt, C. T. (2017). Improving aspects of palliative
UvA-DARE (Digital Academic Repository) Improving aspects of palliative care for children Jagt, C.T. Link to publication Citation for published version (APA): Jagt, C. T. (2017). Improving aspects of palliative
Prostate Cancer Local or distant recurrence?
 Prostate Cancer Local or distant recurrence? Diagnostic flowchart Vanessa Vilas Boas Urologist VFX Hospital FEBU PSA - only recurrence PSA recurrence: 27-53% of all patients undergoing treatment with curative
Prostate Cancer Local or distant recurrence? Diagnostic flowchart Vanessa Vilas Boas Urologist VFX Hospital FEBU PSA - only recurrence PSA recurrence: 27-53% of all patients undergoing treatment with curative
The Use of PET Scanning in Urologic Oncology
 The Use of PET Scanning in Urologic Oncology Dr Nicholas C. Buchan Uro-oncology Fellow 1 2 Aims To understand the basic concepts underlying PET scanning. Understand the emerging role of PET Scanning for
The Use of PET Scanning in Urologic Oncology Dr Nicholas C. Buchan Uro-oncology Fellow 1 2 Aims To understand the basic concepts underlying PET scanning. Understand the emerging role of PET Scanning for
Introduction. Mitsuru Koizumi 1 Masamichi Koyama 1
 https://doi.org/10.1007/s12149-018-1319-z ORIGINAL ARTICLE Comparison between single photon emission computed tomography with computed tomography and planar scintigraphy in sentinel node biopsy in breast
https://doi.org/10.1007/s12149-018-1319-z ORIGINAL ARTICLE Comparison between single photon emission computed tomography with computed tomography and planar scintigraphy in sentinel node biopsy in breast
Q&A. Overview. Collecting Cancer Data: Prostate. Collecting Cancer Data: Prostate 5/5/2011. NAACCR Webinar Series 1
 Collecting Cancer Data: Prostate NAACCR 2010-2011 Webinar Series May 5, 2011 Q&A Please submit all questions concerning webinar content through the Q&A panel Overview NAACCR 2010-2011 Webinar Series 1
Collecting Cancer Data: Prostate NAACCR 2010-2011 Webinar Series May 5, 2011 Q&A Please submit all questions concerning webinar content through the Q&A panel Overview NAACCR 2010-2011 Webinar Series 1
NCDB Special Study: Post-Active Treatment Surveillance in Prostate Cancer Webinar #5: NCRA /9/17 Eileen Tonner, MS
 NCDB Special Study: Post-Active Treatment Surveillance in Prostate Cancer Webinar #5: NCRA 2017-044 5/9/17 Eileen Tonner, MS Purpose of the Study For patients who have received curative-intent prostate
NCDB Special Study: Post-Active Treatment Surveillance in Prostate Cancer Webinar #5: NCRA 2017-044 5/9/17 Eileen Tonner, MS Purpose of the Study For patients who have received curative-intent prostate
Chapter 2: Initial treatment for endometrial cancer (including histologic variant type)
 Chapter 2: Initial treatment for endometrial cancer (including histologic variant type) CQ01 Which surgical techniques for hysterectomy are recommended for patients considered to be stage I preoperatively?
Chapter 2: Initial treatment for endometrial cancer (including histologic variant type) CQ01 Which surgical techniques for hysterectomy are recommended for patients considered to be stage I preoperatively?
Cervical Cancer 3/25/2019. Abnormal vaginal bleeding
 Cervical Cancer Abnormal vaginal bleeding Postcoital, intermenstrual or postmenopausal Vaginal discharge Pelvic pain or pressure Asymptomatic In most patients who are not sexually active due to symptoms
Cervical Cancer Abnormal vaginal bleeding Postcoital, intermenstrual or postmenopausal Vaginal discharge Pelvic pain or pressure Asymptomatic In most patients who are not sexually active due to symptoms
UvA-DARE (Digital Academic Repository) The artificial pancreas Kropff, J. Link to publication
 UvA-DARE (Digital Academic Repository) The artificial pancreas Kropff, J. Link to publication Citation for published version (APA): Kropff, J. (2017). The artificial pancreas: From logic to life General
UvA-DARE (Digital Academic Repository) The artificial pancreas Kropff, J. Link to publication Citation for published version (APA): Kropff, J. (2017). The artificial pancreas: From logic to life General
GUIDELINES ON TESTICULAR CANCER
 38 (Text updated March 2005) P. Albers (chairman), W. Albrecht, F. Algaba, C. Bokemeyer, G. Cohn-Cedermark, A. Horwich, O. Klepp, M.P. Laguna, G. Pizzocaro Introduction Compared with other types of cancer
38 (Text updated March 2005) P. Albers (chairman), W. Albrecht, F. Algaba, C. Bokemeyer, G. Cohn-Cedermark, A. Horwich, O. Klepp, M.P. Laguna, G. Pizzocaro Introduction Compared with other types of cancer
16/09/2015. ACOSOG Z011 changing practice. Presentation outline. Nodal mets #1 prognostic tool. Less surgery no change in oncologic outcomes
 ACOSOG Z011 changing practice The end of axillary US/FNA? Preoperative staging of the axilla in the era of Z011 Adena S Scheer MD MSc FRCSC Surgical Oncologist, St. Michael s Hospital Assistant Professor,
ACOSOG Z011 changing practice The end of axillary US/FNA? Preoperative staging of the axilla in the era of Z011 Adena S Scheer MD MSc FRCSC Surgical Oncologist, St. Michael s Hospital Assistant Professor,
Appendix 1: Regional Lymph Node Stations for Staging Esophageal Cancer
 Appendix 1: Regional Lymph Node Stations for Staging Esophageal Cancer Locoregional (N stage) disease was redefined in the seventh edition of the AJCC Cancer Staging Manual as any periesophageal lymph
Appendix 1: Regional Lymph Node Stations for Staging Esophageal Cancer Locoregional (N stage) disease was redefined in the seventh edition of the AJCC Cancer Staging Manual as any periesophageal lymph
Citation for published version (APA): Luijendijk, P. (2014). Aortic coarctation: late complications and treatment strategies.
 UvA-DARE (Digital Academic Repository) Aortic coarctation: late complications and treatment strategies Luijendijk, P. Link to publication Citation for published version (APA): Luijendijk, P. (2014). Aortic
UvA-DARE (Digital Academic Repository) Aortic coarctation: late complications and treatment strategies Luijendijk, P. Link to publication Citation for published version (APA): Luijendijk, P. (2014). Aortic
