salivary secretion to stimulus frequency was ml min-' g-1 Hz-l. Hong Kong
|
|
|
- Bridget Foster
- 5 years ago
- Views:
Transcription
1 Journal of Physiology (199), 431, pp With 7 figures Printed in Great Britain VARIATIONS IN BLOOD FLOW ON MANDIBULAR GLANDULAR SECRETION TO AUTONOMIC NERVOUS STIMULATIONS IN ANAESTHETIZED DOGS BY MARY A. LUNG From the Department of Physiology, Faculty of Medicine, University of Hong Kong, Hong Kong (Received 28 March 199) SUMMARY 1. Continuous stimulation of the preganglionic parasympathetic nerve (the ramus communicans of the mandibular ganglion) for 1-2 min at supramaximal voltage (5 V) and pulse duration (1 ms) increased salivary gland arterial inflow and this was accompanied by copious salivary secretion. The responses were recorded continuously during the period of stimulation. The frequency for initiating the responses was 5 Hz. Maximal responses occurred at 16 Hz. The response coefficient of arterial inflow to stimulus frequency was 417 ml min-1 g-' Hz-1 and that of secretion to stimulus frequency was -16 ml min-' g-1 Hz-'. 2. The secretory response to low and moderate levels of parasympathetic nerve stimulation (below 8 Hz) was not affected by a reduction or cessation in arterial inflow whereas the response to high level parasympathetic nerve stimulation (above 8 Hz) was significantly alleviated if blood flow to the gland was maintained (via controlled vascular perfusion) at a level less than that of the resting arterial inflow. However, when the gland was already secreting near-maximally (stimulated at 8 Hz), sudden cessation of blood flow for a short period of time (-5-2 min) had no effect on the salivary flow. 3. Continuous stimulation of the cervical sympathetic nerve for 1-2 min at supramaximal voltage (2 V) and pulse duration (1 ms) decreased arterial inflow and this was accompanied by scanty salivary secretion. The vascular response persisted during the period of stimulation. The secretory response was 15 s late in onset and might continue for 1 min after stimulation. The frequency for initiating the responses was 1-4 Hz. Maximal responses occurred at Hz. The response coefficient of arterial inflow to stimulus frequency was - -4 ml min-' g-1 Hz-' and that of salivary secretion to stimulus frequency was 1 ml min-' g-1 Hz-l. 4. The secretory response to sympathetic nerve stimulation at different frequencies in glands with blood flow maintained at resting rate (via controlled vascular perfusion) resembled that in glands with spontaneous blood flow. 5. Sympathetic nerve stimulation was found to retard salivary secretion caused by parasympathetic stimulation, irrespective of whether the gland received spontaneous arterial inflow or controlled vascular perfusion at a resting flow rate. 6. The results suggest that the salivary secretion to stimulation of para- MS 834
2 48 M. A. LUNG sympathetic nerve is independent of blood flow over a wide range of stimulus frequencies; however, the response to high frequency stimulation of the parasympathetic nerve may be affected by fluctuations in blood flow. Retardation of parasympathetic-induced salivary flow by superimposed sympathetic nerve stimulation may not be related to blood flow changes. INTRODUCTION In experimental animals, mandibular salivary secretion evoked by supramaximal parasympathetic nerve stimulation is usually diminished by concurrent sympathetic nerve stimulation. This effect has been thought to be the result of a reduced blood flow brought about by sympathetic vasoconstriction (Langley, 1878; Emmelin, 1955a). Salivary secretion induced by pilocarpine is also retarded, as in the case of parasympathetic secretion, by procedures believed to reduce blood flow, such as carotid arterial occlusion, vagal stimulation, sympathetic stimulation or injection of adrenaline (Emmelin, 1955b). In the dog, the salivary response to sympathetic nerve stimulation is usually scanty. However, in the presence of an alpha-adrenoreceptor blockade the salivary response is enhanced. The adrenoreceptor blockade agent is believed to prevent sympathetic vasoconstriction and hence leading to the loss of the indirect inhibitory action on secretion (Emmelin & Gjorstrup, 1976). These studies suggest that salivary secretion is influenced by the volume of blood supply to the gland. Nevertheless, the procedures taken to reduce blood flow to the gland may modify salivation via direct or indirect actions on the secretory apparatus. Sympathetic stimulation or application of adrenoreceptor agonists and antagonists may act directly on the secretory cells, whereas carotid arterial occlusion or vagal stimulation often causes systemic changes which may result in a secondary reflex action on the gland (Hockman, Hagstrom & Hoff, 1965). No systematic study has yet been carried out to show the relationship between fluctuations in blood supply and salivary gland secretion. We have established a method of direct measurement of spontaneous arterial inflow and saliva secretion in the mandibular gland of the dog (Lung & Wang, 199). Recently, we also described a technique for vascular perfusion of the gland (Wang & Lung, 1989). These methods have been used in the present study which examines the relationship between acute changes in arterial inflow and salivary secretion during stimulation of the autonomic nerves. Some preliminary results have already been communicated in a scientific meeting (Wang & Lung, 1989). METHODS Mongrel dogs (body weight kg; n = 24) of either sex were anaesthetized by intravenously administered sodium pentobarbitone (25 mg kg-'); supplementary doses were given when necessary. Body temperature (rectal) was maintained at 37 C by means of an electric heating pad placed beneath the animal. A femoral artery was cannulated for the measurement of systemic arterial pressure. Heparin (1 units h-') was given via a cannulated femoral vein. With the animal lying in the supine position, a longitudinal incision was made along the lingual border of the body of the mandible, extending posteriorly to the angular process. The digastricus and mylohyoideus muscles were separated to expose the facial artery (or external maxillary artery) and its glandular branch which is the major arterial supply to the mandibular gland of the dog
3 BLOOD FLOW AND SALIVARY SECRETION (Miller, Christensen & Evans, 1964). From previous dissection studies on the gland, we found that a minor arterial supply may arise from some small branches of the lingual artery. To ensure that the gland received its blood supply solely from the glandular branch, all small branches supplying the gland were ligated. Care was also taken to exclude the presence of any collateral arterial supply; this included the monitoring of the occluded glandular arterial pressure and haematocrit measurements at rest and during secreting activity (see Discussion). To monitor the occluded arterial pressure, a catheter was inserted retrogradely into the facial artery and its tip advanced to the origin of the glandular artery. When arterial inflow was stopped by a snare placed proximal to the origin of the glandular artery, the pressure monitored by the catheter reflected the occluded glandular arterial pressure. Samples of glandular arterial and venous blood were taken for haematocrit measurements. When determining the arterial inflow, an electromagnetic flow sensor (SL-7515, Statham) of appropriate size was placed around the facial artery just proximal to the origin of the glandular branch. For vascular perfusion of the mandibular gland, the facial artery proximal to the origin of the glandular branch was closed with a snare. The glandular artery was then perfused, via the facial arterial catheter, with blood from a reservoir which was continuously replenished from a cannulated femoral artery. Perfusion was carried out by means of a peristaltic pump (MHRE, MK4, Watson-Marlow). The perfusion pressure was measured from a point between the facial arterial catheter and the pump. Perfusion rate was normally adjusted to give a perfusion pressure approximating the systemic arterial pressure, although its rate could be varied according to the experimental protocol. To expose the mandibular duct, the posterior part of the mylohyoideus muscle was severed latero-medially. The duct was retrogradely cannulated and the catheter connected to a bottle in which the secreted saliva displaced a saline solution. A cannulating-type electromagnetic flow sensor (U-21, Medicon) was inserted along the outlet tube of the bottle to measure the salivary flow. Drops of saline, of -25 ml in volume, displaced from this bottle were measured by means of a drop-counter (92-1-7, E & M Instr.); salivary flow was also calculated from the time interval between falling drops. The two methods were used simultaneously to measure salivary secretion in order to evaluate if there is any discrepancy in the results obtained by electromagnetic flowmetry and drop-recording (see Discussion). All pressure and flow variables were recorded on magnetic tape (Store 14, Racal) and an oscillographic chart-recorder (28S, Gould), and mean values were calculated with the use of Universal amplifiers ( , Gould). Gould P231D transducers were used for arterial pressure measurement. All pressure transducers were zeroed to atmospheric pressure and set at the level of the mid-chest. The U-21 electromagnetic flow sensor was connected to a Statham M41 flowmeter whereas the SL-7515 Statham sensor was connected to a Statham SP-222 flowmeter. Determination of zero baseline and calibration of the sensors were carried out as previously described (Lung & Wang, 1987). In the dog, the preganglionic parasympathetic fibres to the mandibular gland follow the chorda tympani nerve and then the ramus communicans to synapse in the mandibular ganglion located in the hilus of this gland. The preganglionic sympathetic fibres pass to the cervical vagosympathetic trunk to synapse in the superior cervical ganglion (Miller et al. 1964). The ramus communicans to the mandibular ganglion, which courses alongside the mandibular duct, was exposed. The cervical sympathetic trunk just cranial to the caudal cervical ganglion was also exposed as previously described (Lung & Wang, 1986). The tied peripheral ends of both nerves were stimulated separately by bipolar platinum electrodes. Square-wave pulses were provided by a Grass S4 stimulator through an isolation unit (SI U4). Stimulation voltage ranging from 1 to 3 V, frequency from 5 to 64 Hz and pulse duration from 1 to 1-5 ms were tested as described in a previous study (Lung & Wang, 1989). Steady-state vascular and secretory responses were attained within 3 s after stimulation. Maximal vascular and salivary responses to parasympathetic nerve stimulation were obtained with an average voltage of 5 V, frequencies of 8-16 Hz and pulse durations of 8-1O ms; maximal responses to sympathetic nerve stimulation were obtained with an average voltage of 2 V, frequencies of Hz and pulse durations of 8-1 ms. Since the parasympathetic and sympathetic fibres are carried in separate nerves, the strength of stimulation could be altered by varying the frequency of stimulation. Hence, in all subsequent experiments, electrical stimulation was performed with varying frequency at fixed supramaximal voltage (5 V for parasympathetic nerve and 2 V for sympathetic nerve) and pulse duration (1 ms) for a period of 1-2 min PHY 431
4 482 M. A. LUNG The results are displayed as means + S.E. of the means. Student's t test was used to determine the level of significance of differences between the means. RESULTS Under resting conditions, the arterial in-flow was found to be ml min-' g-' (n = 24) and saliva secretion was absent. Table 1 shows the TABLE 1. The occluded mandibular arterial pressure and haematocrit at rest and during parasympathetic nerve stimulations OPma (mmhg) Hctv (%) At Rest Parasympathetic nerve stimulation (1 min) Atl Hz At 2Hz At 4 Hz * At 8Hz * At 16Hz * Values are given as means+ S.E. of the means. Number of animals = 6. Value of arterial haematocrit = % (n = 6). pma, occluded mandibular arterial pressure. Hctv, venous haematocrit. *P < -5, when compared to corresponding value at rest. occluded arterial pressure and venous haematocrit when the gland was at rest or in an active state (due to stimulation of the parasympathetic nerve). The occluded arterial pressure at rest was similar to that seen when the gland was stimulated. There was no difference between the resting arterial and venous haematocrit values. The venous haematocrit reading rose progressively, in parallel with the level of secreting activity induced by increasing parasympathetic nerve stimulation. Effects of parasympathetic nerve stimulation The average frequency for initiating vascular and secretory responses was -5 Hz and that for maximal responses was 16 Hz (Fig. 1). Arterial inflow increased and saliva secretion started immediately, reaching a maximum within 1 s and with a slight decline to a steady level within 3 s (Fig. 2). The magnitude of the steady responses was in direct proportion to the frequency of stimulation; the response coefficient of spontaneous arterial inflow to stimulus frequency was 17 ml min-1 g-1 Hz-' (r = 99, P < 1) and that of salivary secretion to stimulus frequency was -16 ml min-1 Hz-1 (r = -96, P < -1). Figure 3 summarizes the effects of changes in blood flow (via variations in vascular perfusion rate) on the secretory response to different levels of parasympathetic nerve stimulation in a group of six dogs. Changes in perfusion rate were effected 1-2 min prior to nerve stimulation. The duration of nerve stimulation lasted for 1-2 min. For stimulations with frequencies less than 8 Hz, the secretory response obtained under different perfusion conditions, such as normal perfusion rate, double perfusion rate, half perfusion rate or even complete cessation of perfusion, was not significantly
5 BLOOD FLOW AND SALIVARY SECRETION n= 12.3 c E E i- 2 m ?----s~~~~~~~~1. 1 -E A? 3 "I ~~~~~~~~~~~~~~~~~~.1 /~~~~~~~~~~~~~~~~~~~~~~~~~~~~~/ 4 m m a a m ma. I n VIA Stimulus frequency (Hz) Fig. 1. Actions of parasympathetic (ramus communicans to the mandibular ganglion) stimulations (5 V and 1 ms) on the mandibular arterial blood flow (@) and salivary secretion (). Values are means+s.e. of the means. n indicates number of animals. BP 15 (mmhg) 5 Qma 3 (ml min ) ol _o QSS 2[ (ml min1) Dss (4 m r') ll11! 1'---- I_i1 1 Wll1111HII _iii 1 min Stimulations Hz Fig. 2. An experimental record illustrating the effects of varying the frequency (1-8 Hz) of parasympathetic stimulation on blood flow and salivary secretion. Traces from above downwards: BP, systemic arterial pressure. Qm8, mandibular arterial inflow. QS, salivary secretion monitored by the electromagnetic flow sensor. D.., salivary drops monitored by the 'drop-recorder'. Bar, the period of stimulation. 16-2
6 484 M. A. LUNG different from that obtained with spontaneous blood flow. For stimulations with frequencies higher than 8 Hz, the secretory response under the conditions of normal perfusion rate and double perfusion rate was also not significantly different from that obtained with spontaneous blood flow; however, halving the perfusion rate or complete cessation of perfusion significantly decreased the response (P < 5). A.3 n=6 -~ I o.1 1 I I I CB...O2[ l Il l C CE.2. D.1 2IIII n=e ji i Stimulus frequency (Hz) Fig. 3. Response of salivary secretion to varying frequency (O5-32 Hz) of parasympathetic stimulation in glands with spontaneous blood flow (A ), vascular perfusion at normal resting flow rate (B), double resting flow rate (C) and half resting flow rate (D), and cessation of vascular perfusion (E). Values are given as means+ 5.E. of the means. n indicates number of animals. *P < O5, when compared to glands with spontaneous blood flow (A). Figure 4 illustrates the immediate effect of a short period of cessation of arterial inflow (O 5 min) on the secretory response to near-maximal parasympathetic nerve stimulation at 8 Hz. The glandular secretory volume was similar, either in the presence of spontaneous blood flow (A) or controlled vascular perfusion at a resting flow rate (B). Effects of sympathetic nerve stimulation The average frequency for initiating a vascular response to sympathetic nerve stimulation was 1 Hz whereas the frequency for starting the secretory response was 4 Hz. Maximal vascular and secretory responses occurred at about Hz (Fig. 5).
7 BLOOD FLOW AND SALIVARY SECRETION Arterial inflow decreased immediately and reached a steady state within 1 s, but the onset of the secretory response was usually delayed by 15-3 s with the steady state being reached within 3-6 s (Fig. 6A and B). The magnitude of the steady responses was in direct proportion to the frequency of stimulation; the response coefficient of 485 A B BP 15 M W (mmhg) 5 Qma 2 15 (mlmini) (mmhg) I t Oss 2[ 5i (ml min1).5 min - (41) mlm I Fig. 4. Experimental records illustrating the vascular and secretory responses to a short period of sudden cessation of blood flow during parasympathetic stimulation at 8 Hz in glands with spontaneous blood flow (A) and under vascular perfusion at a normal flow rate (B). Plm., mandibular vascular perfusion pressure. Other abbreviations for traces as in Fig. 2. Bar, period of stimulation. spontaneous arterial inflow to stimulus frequency was - 4 ml min-1 g-' Hz-1 (r = --91, P < -5) and that of salivary secretion to stimulus frequency was 1 ml min-' g-1 Hz-' (r = 95, P < 5). If sympathetic stimulation was performed shortly after parasympathetic stimulation, the secretory response was immediate, with the duration and volume of the initial secretion being in direct proportion to the strength of the previous parasympathetic stimulation; however, the secretory response fell gradually and reached a steady state within 3-6 s. The steady-state secretory response to sympathetic nerve stimulation was not significantly different when blood flow to the gland was maintained at resting level via controlled vascular perfusion (Figs 5B and 6B). Interaction between parasympathetic and sympathetic nerve stimulation Figure 7 illustrates the effects of interaction between parasympathetic and sympathetic nerve stimulation on arterial inflow (or perfusion pressure) and salivary secretion. In glands with spontaneous blood flow or controlled vascular perfusion at resting flow rate, steady state vascular and secretory responses were induced with a near maximal level of parasympathetic nerve stimulation (8 Hz). Concurrent maximal sympathetic nerve stimulation (16 Hz) immediately reduced the vascular response; however, the secretory response was initially enhanced before falling to a steady low level within 3-6 s. When sympathetic nerve stimulation was stopped,
8 486 M. A. LUNG both the vascular and secretory values gradually returned to the parasympatheticinduced steady-state levels. DISCUSSION For more than a century, the physiology of the salivary gland has been investigated by monitoring the venous outflow and salivary secretion with drop- ) A I E E 4-3. B CD I EE.5r.41'.31.2 j.1 j 4 r n = 6 n= O.2 E.2 X en co I... C It ) L Stimulus frequency (Hz) Fig. 5. Vascular (@) and secretory () responses to cervical sympathetic stimulations (2 V and 1 ms) in glands with spontaneous blood flow (A) and vascular perfusion at normal resting flow rate (B). Values are given as means + S.E. of the means. n indicates the number of animals. O (U U) X._ itn recorders; the venous blood or salivary secretion had to be connected to an extracorporal circuit and the rate of flow was estimated either from the time interval between falling drops or gravimetrically over a certain period of time (Langley, 1878; Emmelin, 1955a; Bloom & Edwards, 198). The present study describes the first preparation which demonstrates simultaneous measurement of arterial inflow and
9 BLOOD FLOW AND SALIVARY SECRETION secretion of the salivary gland with the use of electromagnetic flow sensors. Droprecording was also used for monitoring the salivary flow in order to evaluate the results obtained by these two methods. We found that the salivary flow rate measured by calculating the time interval between the falling drops was not significantly different from that measured by electromagnetic flowmetry (see Figs 2, 487 BP 15 (mmhg) 5 A Qma (ml min 1) 1 Dssl l l I (4 ml-') BP 15 (mmhg) 51 Ppma 25 B (mmhg) 5 Dss l_l_ l l_l (4 ml-') -5 min Fig. 6. Experimental records illustrating the vascular and secretory responses to cervical sympathetic stimulations in glands with spontaneous blood flow (A) and vascular perfusion at normal resting flow rate (B). Abbreviations for traces as in Figs 2 and 4. Bar, period of stimulation. 4 and 7). However, electromagnetic flow sensor is superior to a drop-recorder in the measurement of fluid flow because it permits instantaneous and direct recording of events. Thus, more accurate analysis of the time-related changes of the variable as well as its relation to other simultaneously measured parameters is possible. Furthermore, there is no need to divert the blood or saliva extracorporally if cufftype electromagnetic flow sensor is used; the flow rate is, therefore, measured in situ. In all previous studies on the vascular control of the salivary secretion, the measurement of vascular and secretory responses to an experimental stimulus has been performed under conditions of spontaneous arterial inflow (Emmelin 1955a,
10 488 M. A. LUNG Emmelin & Gjorstrup, 1976; Ferreira & Smaje, 1976; Andersson, Bloom, Edwards & Jarhult, 1982 a). Hence, the changes in the measured variables reflect not only the primary responses to the stimulus but also the secondary effects caused by systemic changes. This is also the first study to demonstrate vascular perfusion of the salivary BP 15[ 5 (mmnhg) A (m min ).. oss 3[ (ml min~1 l Dss (4 ml') BP 15 (mmhg) 5 Ppma 25 1 (mmhg) 5 Qss 3r (ml min-') Dss (4 ml1) B 1 min Fig. 7. Experimental records illustrating the effects of superimposed maximal cervical sympathetic stimulation (16 Hz, 2 V and 1 ms) on the vascular and secretory responses to near-maximal parasympathetic stimulation (8 Hz, 5 V, 1 ms) in glands with spontaneous blood flow (A) and vascular perfusion at normal flow rate (B). Abbreviations for traces as in Figs 2 and 4. Continuous bar, period of parasympathetic stimulation. Broken bar, period of sympathetic stimulation. gland under a controlled flow rate, enabling only the primary changes to a stimulus to be measured. Also, this vascular perfusion preparation permits actual variations in the arterial supply of the salivary gland and, thus, makes possible an accurate evaluation of the relationship between blood flow and salivary secretion. Since the aim of the study is to evaluate the effects of changes in blood flow on salivary secretion, it is essential that the mandibular gland should receive its blood supply only from the glandular artery. Hence, all small arteries to the gland were ligated. Precautions were also taken to check for the presence of any collateral arterial supply to the gland; firstly, by monitoring the occluded arterial pressure and, secondly, the haematocrit reading. When the arterial supply to a vascular bed is suddenly occluded, the arterial pressure normally falls to the level of the capillary pressure. If collateral arterial channels are present, the occluded arterial pressure will rise gradually; the magnitude of the pressure rise depends on the size of the collateral
11 BLOOD FLOW AND SALIVARY SECRETION blood supply. Collateral arterial flow, if present, becomes very prominent during parasympathetic nerve stimulation when vasodilatation occurs, and this results in an abrupt secondary rise in the occluded arterial pressure. We found, in our preparation, that the occluded glandular arterial pressure dropped to the level of the capillary pressure without any secondary rise in pressure, irrespective of whether the gland was at rest or under the influence of parasympathetic stimulation (Table 1 and Fig. 5). This indicates that collateral blood supply, even if present, has a negligible influence. In some experiments, haematocrit readings of the glandular arterial and venous blood were taken before and immediately after parasympathetic nerve stimulation. Should the collateral arterial supply be substantial, the venous haematocrit value would remain constant despite increasing secretory activity induced by increasing levels of parasympathetic stimulation. This effect is due to dilution by blood flow via the dilated collateral channels. We found that the venous haematocrit value increased gradually with increasing level of parasympathetic stimulation, thus, confirming that the collateral blood supply to the gland was absent or insignificant. We have already shown that the total venous outflow, when monitored from the main glandular vein when all the other minor venous channels are ligated, is always lower than the arterial inflow via the glandular artery (Lung & Wang, 199). Thus, there is reasonable evidence to indicate that, in our preparations, the major or sole blood supply to the mandibular gland is from the glandular artery. Autonomic nerve fibres normally discharge their activity in bursts. Stimulation of autonomic nerves in the form of bursts has been reported to be more effective than a continuous mode of stimulation in eliciting vascular and secretory responses in the salivary gland of animals (Andersson, Bloom & Edwards, 1982b; Andersson et al. 1982a; Bloom, Edwards & Garrett, 1987). In a series of preliminary studies, we studied the effects of continuous and intermittent electrical stimulation of the autonomic nerves on the canine mandibular gland. The pattern of stimulation used by Edwards and his co-workers in cats and lambs (1 s bursts at 1 s intervals) was tested. We found that the mean vascular and secretory responses to intermittent stimulation at 2-16 Hz were even weaker than when the same total number of impulses were delivered in continuous mode (2-16 Hz). Moreover, the measured variables fluctuated greatly during the period of stimulation (Lung, unpublished observations). Hence it is questionable whether or not the tested intermittent pattern of stimulation is physiological. A species difference in the bursts pattern of autonomic nerve stimulation of a particular organ obviously cannot be excluded. Because of the uncertainty regarding the natural or physiological bursts pattern of the autonomic nerves to the canine mandibular gland, we have, therefore, used the conventional continuous mode of stimulation in this study. Effects of parasympathetic nerve stimulation We found that both the vascular and secretory responses to parasympathetic nerve stimulation were frequency dependent with maximal responses occurring at 16 Hz. The maximal secretory response was about -24 ml min-' g-1, and is within the range found by other workers (Terroux, Sekelj & Burgen, 1959; Emmelin & Holmberg, 1967). The maximal vascular response was ten-times the resting blood 489
12 49 M. A. L UNG flow rate, which is also in agreement with the findings of others (Terroux et al. 1959), although a smaller increase in blood flow has been reported (about 4-5-times the resting flow; Ferreira & Smaje, 1976). For decades, it has been believed that the rate of salivary secretion is affected greatly by blood flow (Langley, 1878; Emmelin 1955b; Emmelin & Gjorstrup, 1976). Surprisingly, we found that the secretory response to low and moderate levels of parasympathetic nerve stimulation (less than 8 Hz) was completely independent of blood flow. As long as the blood flow was maintained (via controlled vascular perfusion) at the resting level, secretory responses to maximal parasympathetic nerve stimulation (above 8 Hz) were not significantly affected. These findings suggest that, although parallel changes in blood flow and secretion occur during parasympathetic stimulation, the blood flow response is not essential for the secretory response; this could imply that the vascular and secretory changes may be separate or coincidental phenomena. Studies by Barcroft and his collaborators (Barcroft & Muller, 1912) in cats and by Terroux et al. (1959) in dogs have shown that although the rate of salivary secretion and oxygen consumption are linearly related during activity of the salivary gland, oxygen consumption and blood flow are poorly correlated. Furthermore, there is also a poor correlation between oxygen consumption and blood flow in resting conditions. Hence, it seems that metabolism is not the major controller of blood flow to the salivary gland; any increased metabolic demand caused by increased activity could be satisfied by more oxygen extraction from the blood perfusing the gland. Besides, evidence is available which suggests that the mandibular gland is able to contract an oxygen debt. The period of increased oxygen consumption accompanying secretory activity has been found to outlast the secretory response; the duration of oxygen deficit appears to be in proportion to the period of activity (Barcroft & Piper, 1912; Stromblad, 1959). Hence, when the salivary gland is active, although the blood supply is inadequate, e.g. under conditions of controlled vascular perfusion, normal secretory activity can still be maintained over a short period of time of 1-2 min through increased oxygen extraction from the blood, or by developing an oxygen debt. However, if the increased metabolic demand is in excess of the compensatory mechanisms, the secretory ability will then be impaired. This event may have caused the significant decrease in secretory response to maximal stimulation when blood flow was halved or completely stopped in our experiments. There is no doubt that salivary secretion involves an active electrolyte and water transport mechanism. However, we cannot exclude the fact that the intravascular (or capillary) hydrostatic pressure is the ultimate source of fluid supply to the secreting cells. When arterial supply is occluded (e.g. cessation of vascular perfusion in our experiments), arterial pressure drops to the level of capillary pressure (Table 1), which is sometimes even lower than the osmotic pressure of the plasma proteins. According to the Starling-Landis' concept of capillary fluid dynamics, for a normal capillary under such conditions, fluid absorption instead of filtration occurs (Landis & Pappenheimer, 1963). In this study, we found that the cessation of vascular perfusion did not affect salivary response to low and moderate stimulations. This is only possible if the secreting cells are able to incur a fluid debt, and that fluid replenishment can be made later. The ability of the secreting cells to withstand a
13 BLOOD FLOW AND SALIVARY SECRETION fluid debt of course depends on the size of the debt, which is related to the volume and duration of secretion. This could explain why there is a significant reduction of saliva secretion to maximal stimulation when the vascular perfusion is halved or stopped. Whether or not the secreting cells are indeed capable of building a fluid debt requires further investigation. Effects of sympathetic nerve stimulation Previous studies have shown that the vascular response to sympathetic stimulation is variable, being dependent on the strength and duration of stimulation. Some workers have observed an increased blood flow with brief stimulation of low intensity, and an opposite response to stimulation of high intensity; these findings suggest the presence of both vasodilating and vasoconstricting fibres (Carlson, 197). Others later found a decrease in blood flow after prolonged stimulation with low frequency and an elevated blood flow following maximal stimulation; the inhibitory response was attributed to vasoconstriction whereas the stimulatory response was thought to be due to the presence of vasodilating metabolites (Hilton & Lewis, 1956; Bhoola, Morley, Schachter & Smaje, 1965). In the present study, we found that sympathetic stimulation lowered arterial inflow and increased vascular perfusion pressure; the magnitude of the responses was greater with increasing strength of stimulation, suggesting that the primary vascular response was vasoconstriction. In glands with spontaneous blood flow, arterial inflow immediately after stimulation very often was greater than the pre-stimulation resting level (Fig. 6A). However, in glands with controlled vascular perfusion, perfusion pressure right after stimulation normally returned to pre-stimulation level (Fig. 6B). These results confirm the view that, at least in the dog, sympathetic-induced vasodilatation is probably due to the action of metabolites which accumulate because of low blood flow during stimulation. The secretory response to sympathetic stimulation is species dependent (Langley, 1878). In the dog, secretion is scanty and late in onset, and this response is confirmed by the results of the present study. Some workers believe that such a weak and delayed secretory response is due to dominant vasoconstriction since removal of vasoconstriction by adrenergic blockade results in immediate copious secretion (Emmelin & Gjorstrup, 1976). However, we found that the magnitude of the secretory response to sympathetic stimulation was the same, whether the mandibular gland was receiving spontaneous blood flow or was under controlled vascular perfusion, implying that the scanty secretion is not due to a reduced blood flow following vasoconstriction. A pharmacological antagonist, apart from its action on the blood vessels, may affect directly the secreting cells and, hence, it is difficult to predict whether the change in the secretory response after its administration is due to its effect on the secreting cells or on the blood vessels or both. If the secreting cells are capable of incurring oxygen and fluid debts (as discussed above), a short period of inadequate blood supply caused through sympathetic vasoconstriction is unlikely to have a significant effect on secretion which is so small in volume. We have confirmed the reports of others who have shown that the secretory response to sympathetic stimulation can be increased by a previous parasympathetic stimulation (Bradford, 1888; Langley, 1889). We have also found that the onset of the response is quicker and that the initial response is augmented, but the late steady 491
14 492 M. A. LUNG response is not much different from the one without previous parasympathetic stimulation. The initial augmentation in secretion may be due to contraction of the myoepithelial cells (Emmelin, Garrett & Ohlin, 1969) or heightened excitability of the secretory cells caused by a previous parasympathetic stimulation (Langley, 1889; Babkin, 195). Interaction between sympathetic and parasympathetic nerve stimulation We found that superimposition of strong electrical stimulation of the sympathetic nerve (at 16 Hz) during the course of near-maximal stimulation by the parasympathetic nerve caused the previously good flow of secretion to increase further initially but to decrease significantly later (Fig. 7A). The initial short augmentation in secretion may be related to stimulation of myoepithelial cells or heightened excitability of the secreting cells caused by parasympathetic stimulation (as discussed above). The late decrease in secretion is believed to be due to vasoconstriction which leads to reduced blood flow and diminished secretion (Emmelin, 1955a, b). However, the late retardation in secretion also occurs in the gland with controlled vascular perfusion, suggesting that the cause is not related to a change in blood flow (Fig. 7B). We have already demonstrated that vascular perfusion at normal resting rate is adequate for supporting maximal secretory activity (Fig. 3). Besides, we have shown in Fig. 4 that when a gland is secreting at near-maximal level (with parasympathetic nerve stimulation at 8 Hz), sudden complete cessation of blood flow for a very short period of time does not lead to a significant impairment in secretion; this impairment in secretion is very much smaller than that which is evoked by superimposed sympathetic stimulation of similar duration. Hence, our findings strongly suggest that inhibition of parasympathetic-induced salivary secretion by sympathetic nerve activation is not due to vasoconstriction but to some presently unknown mechanism(s). Further studies are needed. This work has been supported by the University of Hong Kong Research Fund (337/34/11) and Lee Wing Tat Medical Research Fund (377/3/784). The author is grateful to Professor C. W. Ogle and Dr J. C. C. Wang for helpful advice, and to Mr K. K. Tsang and Mr Y. M. Lo for technical assistance. REFERENCES ANDERSSON, P. O., BLOOM, S. R. & EDWARDS, A. V. (1982b). Parotid responses to stimulation of the parasympathetic innervation in weaned lambs. Journal of Physiology 33, ANDERSSON, P. O., BLOOM, S. R., EDWARDS, A. V. & JARHULT, J. (1982a). Effects of stimulation of the chorda tympani in bursts on submaxillary responses in the cat. Journal of Physiology 322, BABKIN, B. P. (195). Secretory Mechanism of the Digestive Glands, 2nd edn. Hoeber, New York. BARCROFT, J. & MULLER, F. (1912). The relation of blood flow to metabolism of salivary gland. Journal of Physiology 44, BARCROFT, J. & PIPER, H. (1912). The gaseous metabolism of the submaxillary gland with reference especially to the effect of adrenaline and the time relation of the stimulus to the oxidation. Journal of Physiology 44, BHOOLA, K. D., MORLEY, J., SCHACHTER, M. & SMAJE, L. H. (1965). Vasodilatation in the submaxillary gland of the cat. Journal of Physiology 179,
15 BLOOD FLOW AND SALIVARY SECRETION BLOOM, S. R. & EDWARDS, A. V. (198). Vasoactive intestinal peptide in relation to atropine resistant vasodilatation in the submaxillary gland of the cat. Journal of Physiology 3, BLOOM, S. R., EDWARDS, A. V. & GARRETT, J. R. (1987). Effects of stimulating the sympathetic innervation in bursts on submandibular vascular and secretory function in cats. Journal of Physiology 393, BRADFORD, J. R. (1888). Some points in the physiology of gland nerves. Journal of Physiology 9, CARLSON, A. J. (197). Vasodilator fibers to the submaxillary gland in the cervical sympathetic of the cat. American Journal of Physiology 19, EMMELIN, N. (1955 a). On the innervation of the submaxillary gland cells in cats. Acta physiologica scandinavica 34, EMMELIN, N. (1955 b). Blood flow and rate of secretion in the submaxillary gland. Acta physiologica scandinavica 34, EMMELIN, N., GARRETT, J. R. & OHLIN, P. (1969). Motor nerves of salivary myoepithelial cells in dogs. Journal of Physiology 2, EMMELIN, N. & GJORSTRUP, P. (1976). Interactions between sympathetic and parasympathetic salivary nerves in dogs. Archives of Oral Biology 21, EMMELIN, N. & HOLMBERG, J. (1967). Impulse frequency in secretory nerves of salivary glands. Journal of Physiology 191, FERREIRA, S. H. & SMAJE, L. H. (1976). Bradykinin and functional vasodilatation in the salivary gland. British Journal of Pharmacology 58, HILTON, S. M. & LEWIS, G. P. (1956). The relationship between glandular activity, bradykinin formation and functional vasodilatation in the submandibular salivary gland. Journal of Physiology 134, HOCKMAN, C. H., HAGSTROM, E. C. & HOFF, F. C. (1965). Salivary response to stimulation of gastric branches of vagus nerve. American Journal of Physiology 29, LANGLEY, J. N. (1878). On the physiology of the salivary secretion. I. The influence of the chorda tympani and sympathetic nerves upon the secretion of the submaxillary gland of the cat. Journal of Physiology 1, LANGLEY, J. N. (1889). On the physiology of the salivary secretion. V. The effects of stimulating the cerebral secretory nerves upon the amount of saliva obtained by stimulating the sympathetic nerve. Journal of Physiology 1, LANDIS, E. M. & PAPPENHEIMER, J. R. (1963). Exchange of substances through the capillary walls. In Handbook of Physiology, section 2, vol. II, ed. HAMILTON, W. F. & Dow, P., pp American Physiological Society, Washington DC. LUNG, M. A. & WANG, J. C. C. (1986). Effects of hypercapnia and hypoxia on nasal vasculature and airflow resistance in the dog. Journal of Physiology 373, LUNG, M. A. & WANG, J. C. C. (1987). Arterial supply, venous drainage and collateral circulation in the nose of the anaesthetized dog. Journal of Physiology 391, LUNG, M. A. & WANG, J. C. C. (1989). Autonomic nervous control of nasal vasculature and airflow resistance in the anaesthetized dog. Journal of Physiology 419, LUNG, M. A. & WANG, J. C. C. (199). Direct measurement of arterial inflow, venous outflow and saliva secretion of mandibular gland in anaesthetized dogs: effects of parasympathetic stimulation. Journal of Physiology 422, 8P. MILLER, M. E., CHRISTENSEN, J. C. & EVANS, H. E. (1964). Anatomy of the Dog. W. B. Saunders Company, Philadelphia, London. STROMBLAD, B. C. R. (1959). Gaseous metabolism of the normal and denervated submaxillary gland of the cat. Journal of Physioloy 145, TERROUX, K. G., SEKELJ, P. & BURGEN, A. S. V. (1959). Oxygen consumption and blood flow in the submaxillary gland of the dog. Canadian Journal of Biochemistry and Physiology 37, WANG, J. C. C. & LUNG, M. A. (1989). Blood flow and saliva secretion of canine mandibular gland. Abstracts of University of Hong Kong Dental Faculty Annual Scientific Meeting 1989,
Action of drugs on denervated myoepithelial cells of salivary glands
 Br. J. Pharmac. (1973), 48, 73-79. Action of drugs on denervated myoepithelial cells of salivary glands N. EMMELIN AND A. THULIN Institute of Physiology, University of Lund, Sweden Summary 1. The pressure
Br. J. Pharmac. (1973), 48, 73-79. Action of drugs on denervated myoepithelial cells of salivary glands N. EMMELIN AND A. THULIN Institute of Physiology, University of Lund, Sweden Summary 1. The pressure
auriculo-temporal nerve. The secretory response to various cholinesterase
 Quarterly Journal of Experimental Phy8iology (1974) 59, 11-17 THE SECRETORY INNERVATION OF THE PAROTID GLAND OF THE CAT: AN UNEXPECTED COMPONENT. By J. EKSTROM and N. EMMELIN. From the Institute of Physiology,
Quarterly Journal of Experimental Phy8iology (1974) 59, 11-17 THE SECRETORY INNERVATION OF THE PAROTID GLAND OF THE CAT: AN UNEXPECTED COMPONENT. By J. EKSTROM and N. EMMELIN. From the Institute of Physiology,
LEAKAGE OF TRANSMITTERS IN SALIVARY GLANDS
 Brit. J. Pharmacol. (1964), 22, 119-125. LEAKAGE OF TRANSMITTERS IN SALIVARY GLANDS BY N. ASSARSON AND N. EMMELIN From the Institute of Physiology, University of Lund, Sweden (Received October 8, 1963)
Brit. J. Pharmacol. (1964), 22, 119-125. LEAKAGE OF TRANSMITTERS IN SALIVARY GLANDS BY N. ASSARSON AND N. EMMELIN From the Institute of Physiology, University of Lund, Sweden (Received October 8, 1963)
gland, the tongue and the sweat glands of the cat. The submaxillary
 306 547.435-292:6I2.8I7 THE LIBERATION OF ACETYLCHOLINE BY POTASSIUM. BY W. FELDBERG1 AND J. A. GUIMARAIS1,2. (From the National Institute for Medical Research, London, N.W. 3.) (Received November 22,
306 547.435-292:6I2.8I7 THE LIBERATION OF ACETYLCHOLINE BY POTASSIUM. BY W. FELDBERG1 AND J. A. GUIMARAIS1,2. (From the National Institute for Medical Research, London, N.W. 3.) (Received November 22,
REINNERVATION OF SUBMAXILLARY GLANDS AFTER PARTIAL. mainly in sympathetic ganglia, in which marked sprouting has been shown
 Q. Jl exp. Phy8iol. (1968) 53, 1-18 REINNERVATION OF SUBMAXILLARY GLANDS AFTER PARTIAL POSTGANGLIONIC DENERVATION. By N. EMMELIN and C. PEREC*. From the Institute of Physiology, University of Lund, Sweden.
Q. Jl exp. Phy8iol. (1968) 53, 1-18 REINNERVATION OF SUBMAXILLARY GLANDS AFTER PARTIAL POSTGANGLIONIC DENERVATION. By N. EMMELIN and C. PEREC*. From the Institute of Physiology, University of Lund, Sweden.
it by the sympathetic nerve.
 OBSERVATIONS ON AUGMENTED SALIVARY SECRETION. BY G. V. ANREP. * (From the Institute of Physiology, University College, London.) IN 1889 Langley described a peculiar effect of stimulation of the cerebral
OBSERVATIONS ON AUGMENTED SALIVARY SECRETION. BY G. V. ANREP. * (From the Institute of Physiology, University College, London.) IN 1889 Langley described a peculiar effect of stimulation of the cerebral
however, reduced after parasympathetic denervation [Nordenfelt et al., 1960]. opposite to those caused by parasympathetic denervation.
![however, reduced after parasympathetic denervation [Nordenfelt et al., 1960]. opposite to those caused by parasympathetic denervation. however, reduced after parasympathetic denervation [Nordenfelt et al., 1960]. opposite to those caused by parasympathetic denervation.](/thumbs/90/101412039.jpg) CHOLINE ACETYLASE IN SALIVARY GLANDS OF THE CAT AFTER SYMPATHETIC DENERVATION. By IVAR NORDENFELT. From the Institute of Physiology, University of Lund, Sweden. (Received for publication 20th April 1964)
CHOLINE ACETYLASE IN SALIVARY GLANDS OF THE CAT AFTER SYMPATHETIC DENERVATION. By IVAR NORDENFELT. From the Institute of Physiology, University of Lund, Sweden. (Received for publication 20th April 1964)
SUPERSENSITIVITY OF THE SUBMAXILLARY GLAND FOLLOWING EXCLUSION OF THE POSTGANGLIONIC PARASYMPATHETIC NEURONE
 Brit. J. Pharmacol. (1960), 15, 356. SUPERSENSITIVITY OF THE SUBMAXILLARY GLAND FOLLOWING EXCLUSION OF THE POSTGANGLIONIC PARASYMPATHETIC NEURONE BY N. EMMELIN From the Institute of Physiology, University
Brit. J. Pharmacol. (1960), 15, 356. SUPERSENSITIVITY OF THE SUBMAXILLARY GLAND FOLLOWING EXCLUSION OF THE POSTGANGLIONIC PARASYMPATHETIC NEURONE BY N. EMMELIN From the Institute of Physiology, University
6I :6I2.I83 BY ALISON S. DALE. concluded that the apparent vaso-constriction obtained by F r6 hli c h and
 6I2.313.87:6I2.I83 A REVERSED ACTION OF THE CHORDA TYMPANI ON THE VENOUS OUTFLOW FROM THE SUBMAXILLARY GLAND. BY ALISON S. DALE. (From the Physiological Laboratory, Cambridcgel.) INTRODUCTORY. FROiHLICH
6I2.313.87:6I2.I83 A REVERSED ACTION OF THE CHORDA TYMPANI ON THE VENOUS OUTFLOW FROM THE SUBMAXILLARY GLAND. BY ALISON S. DALE. (From the Physiological Laboratory, Cambridcgel.) INTRODUCTORY. FROiHLICH
Autonomic nervous control of myoepithelial cells and secretion in submandibular gland of anaesthetized dogs
 J Physiol (2003), 546.3, pp. 837 850 DOI: 10.1113/jphysiol.2002.029686 The Physiological Society 2002 www.jphysiol.org Autonomic nervous control of myoepithelial cells and secretion in submandibular gland
J Physiol (2003), 546.3, pp. 837 850 DOI: 10.1113/jphysiol.2002.029686 The Physiological Society 2002 www.jphysiol.org Autonomic nervous control of myoepithelial cells and secretion in submandibular gland
Observations on the function of the gland after denervation have usually
 Quarterly Journal of Experimental Phy8iology (1974) 59,1-9 REINNERVATION OF THE DENERVATED PAROTID GLAND OF THE CAT. By J. EKSTROM and N. EMMELIN. From the Institute of Physiology, University of Lund,
Quarterly Journal of Experimental Phy8iology (1974) 59,1-9 REINNERVATION OF THE DENERVATED PAROTID GLAND OF THE CAT. By J. EKSTROM and N. EMMELIN. From the Institute of Physiology, University of Lund,
THE ACTION OF NICOTINE ON THE CILIARY GANGLION
 Brit. J. Pharmnacol. (1952), 7, 665. THE ACTION OF NICOTINE ON THE CILIARY GANGLION BY BRENDA M. SCHOFIELD From the Department of Pharmacology, University of Oxford (Received June 7, 1952) The existing
Brit. J. Pharmnacol. (1952), 7, 665. THE ACTION OF NICOTINE ON THE CILIARY GANGLION BY BRENDA M. SCHOFIELD From the Department of Pharmacology, University of Oxford (Received June 7, 1952) The existing
(From the Physiological Laboratory, Cambridge.)
 THE INNERVATION OF THE PYLORIC SPHINCTER OF THE RAT. BY M. NAKANISHI. (From the Physiological Laboratory, Cambridge.) WHILST numerous observations have been made on the behaviour of the pyloric region
THE INNERVATION OF THE PYLORIC SPHINCTER OF THE RAT. BY M. NAKANISHI. (From the Physiological Laboratory, Cambridge.) WHILST numerous observations have been made on the behaviour of the pyloric region
EFFECT OF DENERVATION AND OF COCAINE ON THE ACTION OF SYMPATHOMIMETIC AMINES
 Brit. J. Pharmacol. (1960), 15, 328. EFFECT OF DENERVATION AND OF COCAINE ON THE ACTION OF SYMPATHOMIMETIC AMINES BY B. C. R. STROMBLAD From the Institute of Physiology, Lund, Sweden (RECEIVED FEBRUARY
Brit. J. Pharmacol. (1960), 15, 328. EFFECT OF DENERVATION AND OF COCAINE ON THE ACTION OF SYMPATHOMIMETIC AMINES BY B. C. R. STROMBLAD From the Institute of Physiology, Lund, Sweden (RECEIVED FEBRUARY
KALLIKREIN AND VASODILATION IN THE SUBMAXILLARY GLAND
 GASTROENTEROLOGY Copyright 1967 by The Williams & Wilk' ns Co. Vol. 52, No.2, Part 2 Printed in U.S.A. KALLIKREIN AND VASODILATION IN THE SUBMAXILLARY GLAND MELVILLE SCHACHTER, M.D., AND SUSANNE BEILENSON,
GASTROENTEROLOGY Copyright 1967 by The Williams & Wilk' ns Co. Vol. 52, No.2, Part 2 Printed in U.S.A. KALLIKREIN AND VASODILATION IN THE SUBMAXILLARY GLAND MELVILLE SCHACHTER, M.D., AND SUSANNE BEILENSON,
Autonomic Nervous System Dr. Ali Ebneshahidi
 Autonomic Nervous System Dr. Ali Ebneshahidi Nervous System Divisions of the nervous system The human nervous system consists of the central nervous System (CNS) and the Peripheral Nervous System (PNS).
Autonomic Nervous System Dr. Ali Ebneshahidi Nervous System Divisions of the nervous system The human nervous system consists of the central nervous System (CNS) and the Peripheral Nervous System (PNS).
Franklin, 1933; Waterman, 1933]; indeed, the only negative findings, [Waterman, 1933]. Inasmuch, then, as Donegan was misled with
![Franklin, 1933; Waterman, 1933]; indeed, the only negative findings, [Waterman, 1933]. Inasmuch, then, as Donegan was misled with Franklin, 1933; Waterman, 1933]; indeed, the only negative findings, [Waterman, 1933]. Inasmuch, then, as Donegan was misled with](/thumbs/91/106294335.jpg) 381 6I2.I34:6I2.893 THE CONSTRICTOR RESPONSE OF THE INFERIOR VENA CAVA TO STIMULATION OF THE SPLANCHNIC NERVE BY K. J. FRANKLIN AND A. D. McLACHLIN (From the University Department of Pharmacology, Oxford)
381 6I2.I34:6I2.893 THE CONSTRICTOR RESPONSE OF THE INFERIOR VENA CAVA TO STIMULATION OF THE SPLANCHNIC NERVE BY K. J. FRANKLIN AND A. D. McLACHLIN (From the University Department of Pharmacology, Oxford)
SCHOOL OF ANATOMICAL SCIENCES Mock Run Questions. 4 May 2012
 SCHOOL OF ANATOMICAL SCIENCES Mock Run Questions 4 May 2012 1. With regard to the muscles of the neck: a. the platysma muscle is supplied by the accessory nerve. b. the stylohyoid muscle is supplied by
SCHOOL OF ANATOMICAL SCIENCES Mock Run Questions 4 May 2012 1. With regard to the muscles of the neck: a. the platysma muscle is supplied by the accessory nerve. b. the stylohyoid muscle is supplied by
The Autonomic Nervous System Outline of class lecture for Physiology
 The Autonomic Nervous System Outline of class lecture for Physiology 1 After studying the endocrine system you should be able to: 1. Describe the organization of the nervous system. 2. Compare and contrast
The Autonomic Nervous System Outline of class lecture for Physiology 1 After studying the endocrine system you should be able to: 1. Describe the organization of the nervous system. 2. Compare and contrast
following its stimulation. joined each superior thyroid artery and was found just cephalad to
 612.44: 612.817 THE THYROID NERVE IN THE DOG AND ITS FUNCTION. By W. DONALD Ross 1 and V. H. K. MOORHOUSE. From the Department of Physiology, Faculty of Medicine, University of Manitoba. (Received for
612.44: 612.817 THE THYROID NERVE IN THE DOG AND ITS FUNCTION. By W. DONALD Ross 1 and V. H. K. MOORHOUSE. From the Department of Physiology, Faculty of Medicine, University of Manitoba. (Received for
possibility of a secretion of adrenaline from the suprarenal glands resulting
 355 J Physiol. (I942) IOI, 355-36I 6i2.014.465:577 I74.5 THE EFFECT OF ANAESTHESIA ON THE ADRENALINE CONTENT OF THE SUPRARENAL GLANDS BY P. C. ELMES AND A. A. JEFFERSON From the Department of Pharmacology,
355 J Physiol. (I942) IOI, 355-36I 6i2.014.465:577 I74.5 THE EFFECT OF ANAESTHESIA ON THE ADRENALINE CONTENT OF THE SUPRARENAL GLANDS BY P. C. ELMES AND A. A. JEFFERSON From the Department of Pharmacology,
increasing the pressure within the vessels of the human forearm, and if so, Bayliss in 1902 and Folkow in 1949 found that increasing or decreasing the
 501 J. Physiol. (I954) I25, 50I-507 THE BLOOD FLOW IN THE HUMAN FOREARM FOLLOWING VENOUS CONGESTION By G. C. PATTERSON AND J. T. SHEPHERD From the Department of Physiology, The Queen's University of Belfast
501 J. Physiol. (I954) I25, 50I-507 THE BLOOD FLOW IN THE HUMAN FOREARM FOLLOWING VENOUS CONGESTION By G. C. PATTERSON AND J. T. SHEPHERD From the Department of Physiology, The Queen's University of Belfast
Cardiovascular Physiology. Heart Physiology. Introduction. The heart. Electrophysiology of the heart
 Cardiovascular Physiology Heart Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through
Cardiovascular Physiology Heart Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through
Properties of Pressure
 OBJECTIVES Overview Relationship between pressure and flow Understand the differences between series and parallel circuits Cardiac output and its distribution Cardiac function Control of blood pressure
OBJECTIVES Overview Relationship between pressure and flow Understand the differences between series and parallel circuits Cardiac output and its distribution Cardiac function Control of blood pressure
(From the Physiological Laboratories of University College, London and Cambridge University.) extracts2, etc.). dilation of the vessels.
 THE OXYGEN EXCHANGE OF THE PANCREAS. BY J. BARCROFT AND E. H. STARLING. (From the Physiological Laboratories of University College, London and Cambridge University.) THE interest of the investigations,
THE OXYGEN EXCHANGE OF THE PANCREAS. BY J. BARCROFT AND E. H. STARLING. (From the Physiological Laboratories of University College, London and Cambridge University.) THE interest of the investigations,
Chapter 16. APR Enhanced Lecture Slides
 Chapter 16 APR Enhanced Lecture Slides See separate PowerPoint slides for all figures and tables pre-inserted into PowerPoint without notes and animations. Copyright The McGraw-Hill Companies, Inc. Permission
Chapter 16 APR Enhanced Lecture Slides See separate PowerPoint slides for all figures and tables pre-inserted into PowerPoint without notes and animations. Copyright The McGraw-Hill Companies, Inc. Permission
I. Neural Control of Involuntary Effectors. Chapter 9. Autonomic Motor Nerves. Autonomic Neurons. Autonomic Ganglia. Autonomic Neurons 9/19/11
 Chapter 9 I. Neural Control of Involuntary Effectors The Autonomic Nervous System Lecture PowerPoint Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Autonomic
Chapter 9 I. Neural Control of Involuntary Effectors The Autonomic Nervous System Lecture PowerPoint Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Autonomic
WHILE it is generally agreed that elevation
 The Derivation of Coronary Sinus Flow During Elevation of Right Ventricular Pressure By HERMAN M. GELLER, B.S., M.D., MARTIN BRANDFONBRENEU, M.D., AND CARL J. WIGGERS, M.D., The derivation of coronary
The Derivation of Coronary Sinus Flow During Elevation of Right Ventricular Pressure By HERMAN M. GELLER, B.S., M.D., MARTIN BRANDFONBRENEU, M.D., AND CARL J. WIGGERS, M.D., The derivation of coronary
INTRODUCTION. IN a previous paper(l) we have been able to show that adrenaline may
 REVERSAL OF THE ACTION OF ADRENALINE. BY B. A. McSWINEY AND G. L. BROWN. (From the Department of Physiology, University of Manchester.) INTRODUCTION. IN a previous paper(l) we have been able to show that
REVERSAL OF THE ACTION OF ADRENALINE. BY B. A. McSWINEY AND G. L. BROWN. (From the Department of Physiology, University of Manchester.) INTRODUCTION. IN a previous paper(l) we have been able to show that
Dr.Ban I.S. head & neck anatomy 2 nd y. جامعة تكريت كلية طب االسنان املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102
 جامعة تكريت كلية طب االسنان التشريح مادة املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102 Parotid region The part of the face in front of the ear and below the zygomatic arch is the parotid region. The
جامعة تكريت كلية طب االسنان التشريح مادة املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102 Parotid region The part of the face in front of the ear and below the zygomatic arch is the parotid region. The
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1
 BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
Separation of Responses of Arteries and Veins to Sympathetic Stimulation
 Separation of Responses of Arteries and Veins to Sympathetic Stimulation By Ben G. Zimmerman, Ph.D. The sympathetic innervation of the vascular tree consists of postganglionic fibers derived from the sympathetic
Separation of Responses of Arteries and Veins to Sympathetic Stimulation By Ben G. Zimmerman, Ph.D. The sympathetic innervation of the vascular tree consists of postganglionic fibers derived from the sympathetic
Cardiac Output 1 Fox Chapter 14 part 1
 Vert Phys PCB3743 Cardiac Output 1 Fox Chapter 14 part 1 T. Houpt, Ph.D. Regulation of Heart & Blood Pressure Keep Blood Pressure constant if too low, not enough blood (oxygen, glucose) reaches tissues
Vert Phys PCB3743 Cardiac Output 1 Fox Chapter 14 part 1 T. Houpt, Ph.D. Regulation of Heart & Blood Pressure Keep Blood Pressure constant if too low, not enough blood (oxygen, glucose) reaches tissues
Chapter 14 The Autonomic Nervous System Chapter Outline
 Chapter 14 The Autonomic Nervous System Chapter Outline Module 14.1 Overview of the Autonomic Nervous System (Figures 14.1 14.3) A. The autonomic nervous system (ANS) is the involuntary arm of the peripheral
Chapter 14 The Autonomic Nervous System Chapter Outline Module 14.1 Overview of the Autonomic Nervous System (Figures 14.1 14.3) A. The autonomic nervous system (ANS) is the involuntary arm of the peripheral
Cardiovascular Physiology
 Cardiovascular Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through two vascular systems
Cardiovascular Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through two vascular systems
Contents. Page 1. Homework 11 Chapter Blood Vessels Due: Week 6 Lec 11
 Page 1 Homework 11 Chapter 18-19 Blood Vessels Due: Week 6 Lec 11 Contents When printing, make sure that you specify the page range that you want to print out! Learning objectives for Lecture 11:...pg
Page 1 Homework 11 Chapter 18-19 Blood Vessels Due: Week 6 Lec 11 Contents When printing, make sure that you specify the page range that you want to print out! Learning objectives for Lecture 11:...pg
Human Anatomy and Physiology - Problem Drill 15: The Autonomic Nervous System
 Human Anatomy and Physiology - Problem Drill 15: The Autonomic Nervous System Question No. 1 of 10 Which of the following statements is correct about the component of the autonomic nervous system identified
Human Anatomy and Physiology - Problem Drill 15: The Autonomic Nervous System Question No. 1 of 10 Which of the following statements is correct about the component of the autonomic nervous system identified
Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus
 Outline of content Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus Boundary Content Communication Mandibular division of trigeminal
Outline of content Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus Boundary Content Communication Mandibular division of trigeminal
ANTERIOR CERVICAL TRIANGLE (Fig. 2.1 )
 2 Neck Anatomy ANTERIOR CERVICAL TRIANGLE (Fig. 2.1 ) The boundaries are: Lateral: sternocleidomastoid muscle Superior: inferior border of the mandible Medial: anterior midline of the neck This large triangle
2 Neck Anatomy ANTERIOR CERVICAL TRIANGLE (Fig. 2.1 ) The boundaries are: Lateral: sternocleidomastoid muscle Superior: inferior border of the mandible Medial: anterior midline of the neck This large triangle
Lec [8]: Mandibular nerve:
![Lec [8]: Mandibular nerve: Lec [8]: Mandibular nerve:](/thumbs/94/121295776.jpg) Lec [8]: Mandibular nerve: The mandibular branch from the trigeminal ganglion lies in the middle cranial fossa lateral to the cavernous sinus. With the motor root of the trigeminal nerve [motor roots lies
Lec [8]: Mandibular nerve: The mandibular branch from the trigeminal ganglion lies in the middle cranial fossa lateral to the cavernous sinus. With the motor root of the trigeminal nerve [motor roots lies
THE NATURE OF THE ATRIAL RECEPTORS RESPONSIBLE FOR A REFLEX INCREASE IN ACTIVITY IN EFFERENT CARDIAC SYMPATHETIC NERVES
 Quaterly Journal of Experimental Physiology (1982), 67, 143-149 Printed in Great Britain THE NATURE OF THE ATRIAL RECEPTORS RESPONSIBLE FOR A REFLEX INCREASE IN ACTIVITY IN EFFERENT CARDIAC SYMPATHETIC
Quaterly Journal of Experimental Physiology (1982), 67, 143-149 Printed in Great Britain THE NATURE OF THE ATRIAL RECEPTORS RESPONSIBLE FOR A REFLEX INCREASE IN ACTIVITY IN EFFERENT CARDIAC SYMPATHETIC
Fig Glossopharyngeal nerve transmits signals to medulla oblongata. Integrating center. Receptor. Baroreceptors sense increased blood pressure
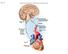 Fig. 5. Integrating center Glossopharyngeal nerve transmits signals to medulla oblongata Receptor 3 Vagus nerve transmits inhibitory signals to cardiac pacemaker Baroreceptors sense increased blood pressure
Fig. 5. Integrating center Glossopharyngeal nerve transmits signals to medulla oblongata Receptor 3 Vagus nerve transmits inhibitory signals to cardiac pacemaker Baroreceptors sense increased blood pressure
Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa :
![Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa : Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa :](/thumbs/88/115294566.jpg) Lec [5] / Temporal fossa : Borders of the Temporal Fossa: Superior: Superior temporal line. Inferior: gap between zygomatic arch and infratemporal crest of sphenoid bone. Anterior: Frontal process of the
Lec [5] / Temporal fossa : Borders of the Temporal Fossa: Superior: Superior temporal line. Inferior: gap between zygomatic arch and infratemporal crest of sphenoid bone. Anterior: Frontal process of the
Cardiovascular Physiology
 Cardiovascular Physiology Lecture 1 objectives Explain the basic anatomy of the heart and its arrangement into 4 chambers. Appreciate that blood flows in series through the systemic and pulmonary circulations.
Cardiovascular Physiology Lecture 1 objectives Explain the basic anatomy of the heart and its arrangement into 4 chambers. Appreciate that blood flows in series through the systemic and pulmonary circulations.
AUTONOMIC NERVOUS SYSTEM PART I: SPINAL CORD
 AUTONOMIC NERVOUS SYSTEM PART I: SPINAL CORD How is the organization of the autonomic nervous system different from that of the somatic nervous system? Peripheral Nervous System Divisions Somatic Nervous
AUTONOMIC NERVOUS SYSTEM PART I: SPINAL CORD How is the organization of the autonomic nervous system different from that of the somatic nervous system? Peripheral Nervous System Divisions Somatic Nervous
Peripheral Collateral Blood Flow and Vascular Reactivity
 tournal of Clinical Investigation Vol. 45, No. 6, 1966 Peripheral Collateral Blood Flow and Vascular Reactivity in the Dog * JAY D. COFFMAN t (From the Department of Medicine, University Hospital, Boston
tournal of Clinical Investigation Vol. 45, No. 6, 1966 Peripheral Collateral Blood Flow and Vascular Reactivity in the Dog * JAY D. COFFMAN t (From the Department of Medicine, University Hospital, Boston
PTERYGOPALATINE FOSSA
 PTERYGOPALATINE FOSSA Outline Anatomical Structure and Boundaries Foramina and Communications with other spaces and cavities Contents Pterygopalatine Ganglion Especial emphasis on certain arteries and
PTERYGOPALATINE FOSSA Outline Anatomical Structure and Boundaries Foramina and Communications with other spaces and cavities Contents Pterygopalatine Ganglion Especial emphasis on certain arteries and
Temporal region. temporal & infratemporal fossae. Zhou Hong Ying Dept. of Anatomy
 Temporal region temporal & infratemporal fossae Zhou Hong Ying Dept. of Anatomy Temporal region is divided by zygomatic arch into temporal & infratemporal fossae. Temporal Fossa Infratemporal fossa Temporal
Temporal region temporal & infratemporal fossae Zhou Hong Ying Dept. of Anatomy Temporal region is divided by zygomatic arch into temporal & infratemporal fossae. Temporal Fossa Infratemporal fossa Temporal
J. Physiol. (I956) I33,
 232 J. Physiol. (I956) I33, 232-242 A STUDY OF THE EFFECT OF THE PATTERN OF ELECTRICAL STIMULATION OF THE AORTIC NERVE ON THE REFLEX DEPRESSOR RESPONSES By W. W. DOUGLAS, J. M. RITCHIE AND W. SCHAUMANN*
232 J. Physiol. (I956) I33, 232-242 A STUDY OF THE EFFECT OF THE PATTERN OF ELECTRICAL STIMULATION OF THE AORTIC NERVE ON THE REFLEX DEPRESSOR RESPONSES By W. W. DOUGLAS, J. M. RITCHIE AND W. SCHAUMANN*
Autonomic Nervous System
 Autonomic Nervous System Keri Muma Bio 6 Organization of the Nervous System Efferent Division Somatic Nervous System Voluntary control Effector = skeletal muscles Muscles must be excited by a motor neuron
Autonomic Nervous System Keri Muma Bio 6 Organization of the Nervous System Efferent Division Somatic Nervous System Voluntary control Effector = skeletal muscles Muscles must be excited by a motor neuron
Composed by Natalia Leonidovna Svintsitskaya, Associate professor of the Chair of Human Anatomy, Candidate of Medicine
 Theoretical background to the study of the autonomic nervous system. Sympathetic and parasympathetic divisions of the autonomic nervous system. Features of the structure, function Composed by Natalia Leonidovna
Theoretical background to the study of the autonomic nervous system. Sympathetic and parasympathetic divisions of the autonomic nervous system. Features of the structure, function Composed by Natalia Leonidovna
The Autonomic Nervous System
 The Autonomic Nervous System Responsible for control of visceral effectors and visceral reflexes: smooth muscle, glands, the heart. e.g. blood pressure, cardiac output, plasma glucose The autonomic system
The Autonomic Nervous System Responsible for control of visceral effectors and visceral reflexes: smooth muscle, glands, the heart. e.g. blood pressure, cardiac output, plasma glucose The autonomic system
(Received 13 March 1981)
 J. Physiol. (1982), 322, pp. 469-483 469 With 12 text-ftgure8 Printed in Great Britain EFFETS OF STIMULATION OF THE HORDA TYMPANI IN BURSTS ON SUBMAXILLARY RESPONSES IN THE AT BY P-O. ANDERSSON*, S. R.
J. Physiol. (1982), 322, pp. 469-483 469 With 12 text-ftgure8 Printed in Great Britain EFFETS OF STIMULATION OF THE HORDA TYMPANI IN BURSTS ON SUBMAXILLARY RESPONSES IN THE AT BY P-O. ANDERSSON*, S. R.
Veins of the Face and the Neck
 Veins of the Face and the Neck Facial Vein The facial vein is formed at the medial angle of the eye by the union of the supraorbital and supratrochlear veins. connected through the ophthalmic veins with
Veins of the Face and the Neck Facial Vein The facial vein is formed at the medial angle of the eye by the union of the supraorbital and supratrochlear veins. connected through the ophthalmic veins with
CAROTID SINUS REFLEX AND CONTRACTION
 Brit. J. Pharmacol. (1950), 5, 505. CAROTID SINUS REFLEX AND CONTRACTION OF THE SPLEEN BY ROBERT L. DRIVER AND MARTHE VOGT From the Department of Pharmacology, University of Edinburgh (Received July 12,
Brit. J. Pharmacol. (1950), 5, 505. CAROTID SINUS REFLEX AND CONTRACTION OF THE SPLEEN BY ROBERT L. DRIVER AND MARTHE VOGT From the Department of Pharmacology, University of Edinburgh (Received July 12,
Cardiovascular System B L O O D V E S S E L S 2
 Cardiovascular System B L O O D V E S S E L S 2 Blood Pressure Main factors influencing blood pressure: Cardiac output (CO) Peripheral resistance (PR) Blood volume Peripheral resistance is a major factor
Cardiovascular System B L O O D V E S S E L S 2 Blood Pressure Main factors influencing blood pressure: Cardiac output (CO) Peripheral resistance (PR) Blood volume Peripheral resistance is a major factor
Ch 9. The Autonomic Nervous System
 Ch 9 The Autonomic Nervous System SLOs Review the organization of the ANS Describe how neural regulation of smooth and cardiac muscles differs from that of skeletal muscles Describe the structure and innervation
Ch 9 The Autonomic Nervous System SLOs Review the organization of the ANS Describe how neural regulation of smooth and cardiac muscles differs from that of skeletal muscles Describe the structure and innervation
Chapter 14 Blood Vessels, Blood Flow and Pressure Exam Study Questions
 Chapter 14 Blood Vessels, Blood Flow and Pressure Exam Study Questions 14.1 Physical Law Governing Blood Flow and Blood Pressure 1. How do you calculate flow rate? 2. What is the driving force of blood
Chapter 14 Blood Vessels, Blood Flow and Pressure Exam Study Questions 14.1 Physical Law Governing Blood Flow and Blood Pressure 1. How do you calculate flow rate? 2. What is the driving force of blood
REGULATION OF CARDIOVASCULAR SYSTEM
 REGULATION OF CARDIOVASCULAR SYSTEM Jonas Addae Medical Sciences, UWI REGULATION OF CARDIOVASCULAR SYSTEM Intrinsic Coupling of cardiac and vascular functions - Autoregulation of vessel diameter Extrinsic
REGULATION OF CARDIOVASCULAR SYSTEM Jonas Addae Medical Sciences, UWI REGULATION OF CARDIOVASCULAR SYSTEM Intrinsic Coupling of cardiac and vascular functions - Autoregulation of vessel diameter Extrinsic
612.I73:6I2.I3. mammary and mediastinal vessels tied off. The thoracic wall on the left
 612.I73:6I2.I3 CARDIAC OUTPUT AND BLOOD DISTRIBUTION. By H. BAR CROFT (Harmsworth Scholar, St Mary's Hospital, London). (From the Physiological Laboratory, Cambridge.) THE methods for the measurement of
612.I73:6I2.I3 CARDIAC OUTPUT AND BLOOD DISTRIBUTION. By H. BAR CROFT (Harmsworth Scholar, St Mary's Hospital, London). (From the Physiological Laboratory, Cambridge.) THE methods for the measurement of
Grossman, 1953), and there is little information so far concerning its function
 52 J. Physiol. (I957) I35, 52-57 A SURGICAL APPROACH TO THE SUPERIOR CERVICAL GANGLION AND RELATED STRIJCTURES IN THE SHEEP BY THE LATE A. B. APPLETON* AND G. M. H. WAITES From the Zoological Society of
52 J. Physiol. (I957) I35, 52-57 A SURGICAL APPROACH TO THE SUPERIOR CERVICAL GANGLION AND RELATED STRIJCTURES IN THE SHEEP BY THE LATE A. B. APPLETON* AND G. M. H. WAITES From the Zoological Society of
(Received February 6, 1934.)
 218 6I2.327:6I2.826 THE EFFECTS OF HYPOTHALAMIC STIMULATION ON GASTRIC MOTILITY. BY J. BEATTIE AND D. SHE E HAN (Rockefeller Research Fellow). (From the Department of Anatomy, McGill University, Montreal.)
218 6I2.327:6I2.826 THE EFFECTS OF HYPOTHALAMIC STIMULATION ON GASTRIC MOTILITY. BY J. BEATTIE AND D. SHE E HAN (Rockefeller Research Fellow). (From the Department of Anatomy, McGill University, Montreal.)
Posted: 11/27/2011 on Medscape; Published Br J Anaesth. 2011;107(2): Oxford University Press
 Posted: 11/27/2011 on Medscape; Published Br J Anaesth. 2011;107(2):209-217. 2011 Oxford University Press Effect of Phenylephrine and Ephedrine Bolus Treatment on Cerebral Oxygenation in Anaesthetized
Posted: 11/27/2011 on Medscape; Published Br J Anaesth. 2011;107(2):209-217. 2011 Oxford University Press Effect of Phenylephrine and Ephedrine Bolus Treatment on Cerebral Oxygenation in Anaesthetized
Asmusssen, Hald & Larsen (1948) observed that the infusion of acetaldehyde
 234 J. Physiol. (1963), 168, pp. 234-237 With 2 plates and 1 text-figure Printed in Great Britain THE ACTION OF ACETALDEHYDE ON THE CHEMO- RECEPTORS OF THE CAROTID GLOMUS BY N. JOELS AND E. NEIL From the
234 J. Physiol. (1963), 168, pp. 234-237 With 2 plates and 1 text-figure Printed in Great Britain THE ACTION OF ACETALDEHYDE ON THE CHEMO- RECEPTORS OF THE CAROTID GLOMUS BY N. JOELS AND E. NEIL From the
Cardiac Output (C.O.) Regulation of Cardiac Output
 Cardiac Output (C.O.) Is the volume of the blood pumped by each ventricle per minute (5 Litre) Stroke volume: Is the volume of the blood pumped by each ventricle per beat. Stroke volume = End diastolic
Cardiac Output (C.O.) Is the volume of the blood pumped by each ventricle per minute (5 Litre) Stroke volume: Is the volume of the blood pumped by each ventricle per beat. Stroke volume = End diastolic
Autonomic Nervous System. Ms. DS Pillay Room 2P24
 Autonomic Nervous System Ms. DS Pillay Room 2P24 OVERVIEW OF THE NERVOUS SYSTEM NERVOUS SYSTEM CNS PNS BRAIN SPINAL CORD SOMATIC ANS SYMPATHEIC PARASYMPATHEIC LOCATION OF GANGLIA IN THE ANS Short post-ganglionic
Autonomic Nervous System Ms. DS Pillay Room 2P24 OVERVIEW OF THE NERVOUS SYSTEM NERVOUS SYSTEM CNS PNS BRAIN SPINAL CORD SOMATIC ANS SYMPATHEIC PARASYMPATHEIC LOCATION OF GANGLIA IN THE ANS Short post-ganglionic
CHAPTER 15 LECTURE OUTLINE
 CHAPTER 15 LECTURE OUTLINE I. INTRODUCTION A. The autonomic nervous system (ANS) regulates the activity of smooth muscle, cardiac muscle, and certain glands. B. Operation of the ANS to maintain homeostasis,
CHAPTER 15 LECTURE OUTLINE I. INTRODUCTION A. The autonomic nervous system (ANS) regulates the activity of smooth muscle, cardiac muscle, and certain glands. B. Operation of the ANS to maintain homeostasis,
Structure and organization of blood vessels
 The cardiovascular system Structure of the heart The cardiac cycle Structure and organization of blood vessels What is the cardiovascular system? The heart is a double pump heart arteries arterioles veins
The cardiovascular system Structure of the heart The cardiac cycle Structure and organization of blood vessels What is the cardiovascular system? The heart is a double pump heart arteries arterioles veins
Central and peripheral fatigue in sustained maximum voluntary contractions of human quadriceps muscle
 Clinical Science and Molecular Medicine (1978) 54,609-614 Central and peripheral fatigue in sustained maximum voluntary contractions of human quadriceps muscle B. BIGLAND-RITCHIE*, D. A. JONES, G. P. HOSKING
Clinical Science and Molecular Medicine (1978) 54,609-614 Central and peripheral fatigue in sustained maximum voluntary contractions of human quadriceps muscle B. BIGLAND-RITCHIE*, D. A. JONES, G. P. HOSKING
Human Anatomy. Autonomic Nervous System
 Human Anatomy Autonomic Nervous System 1 Autonomic Nervous System ANS complex system of nerves controls involuntary actions. Works with the somatic nervous system (SNS) regulates body organs maintains
Human Anatomy Autonomic Nervous System 1 Autonomic Nervous System ANS complex system of nerves controls involuntary actions. Works with the somatic nervous system (SNS) regulates body organs maintains
Razi Kittaneh & Leen Osama. Marah Bitar. Mohammad Khatatbeh
 11 Razi Kittaneh & Leen Osama Marah Bitar Mohammad Khatatbeh Notes on the previous lecture o Spatial summation: input (postsynaptic potentials) from multiple presynaptic neurons. These postsynaptic potentials
11 Razi Kittaneh & Leen Osama Marah Bitar Mohammad Khatatbeh Notes on the previous lecture o Spatial summation: input (postsynaptic potentials) from multiple presynaptic neurons. These postsynaptic potentials
The Nervous System: Autonomic Nervous System Pearson Education, Inc.
 17 The Nervous System: Autonomic Nervous System Introduction The autonomic nervous system: Functions outside of our conscious awareness Makes routine adjustments in our body s systems The autonomic nervous
17 The Nervous System: Autonomic Nervous System Introduction The autonomic nervous system: Functions outside of our conscious awareness Makes routine adjustments in our body s systems The autonomic nervous
PHYSIOLOGY MeQ'S (Morgan) All the following statements related to blood volume are correct except for: 5 A. Blood volume is about 5 litres. B.
 PHYSIOLOGY MeQ'S (Morgan) Chapter 5 All the following statements related to capillary Starling's forces are correct except for: 1 A. Hydrostatic pressure at arterial end is greater than at venous end.
PHYSIOLOGY MeQ'S (Morgan) Chapter 5 All the following statements related to capillary Starling's forces are correct except for: 1 A. Hydrostatic pressure at arterial end is greater than at venous end.
Role of the Autonomic Nervous System in the Release of Rat Submandibular Gland Kallikrein into the Circulation
 635 Role of the Autonomic Nervous System in the Release of Rat Kallikrein into the Circulation S.F. Rabito, T.B. 0rstavik, A.G. Scicli, A. Schork, and O.A. Carretero From the Hypertension Research Laboratory,
635 Role of the Autonomic Nervous System in the Release of Rat Kallikrein into the Circulation S.F. Rabito, T.B. 0rstavik, A.G. Scicli, A. Schork, and O.A. Carretero From the Hypertension Research Laboratory,
Skeletal muscle. Flow increases and decreases with each muscular contraction - as a result of compression of the blood vessels by contracted muscle
 Regional blood flow Skeletal muscle Extreme increases during exercises Flow increases and decreases with each muscular contraction - as a result of compression of the blood vessels by contracted muscle
Regional blood flow Skeletal muscle Extreme increases during exercises Flow increases and decreases with each muscular contraction - as a result of compression of the blood vessels by contracted muscle
ansesthesia; an oncometer was used for measurement of the splenic Laboratory, Cambridge.)
 6I2.4I3:6I2.I43 CAUSE OF RHYTHMICAL. CONTRACTION OF THE SPLEEN. BY J. BARCROFT AN Y. NISIMARU' (Okayama). (From the Physiological Laboratory, Cambridge.) Roy [1881] was the first to discover the rhythmical
6I2.4I3:6I2.I43 CAUSE OF RHYTHMICAL. CONTRACTION OF THE SPLEEN. BY J. BARCROFT AN Y. NISIMARU' (Okayama). (From the Physiological Laboratory, Cambridge.) Roy [1881] was the first to discover the rhythmical
blood-vessels of the isolated perfused lungs of the rat. Both Hirakawa
 547.435-292: 547.781.5: 577.174.5: 612.215 THE ACTION OF ADRENALINE, ACETYLCHOLINE, AND HIS- TAMINE ON THE LUNGS OF THE RAT. By P. FoGGIE. From the Physiology Department, University of Edinburgh. (Received
547.435-292: 547.781.5: 577.174.5: 612.215 THE ACTION OF ADRENALINE, ACETYLCHOLINE, AND HIS- TAMINE ON THE LUNGS OF THE RAT. By P. FoGGIE. From the Physiology Department, University of Edinburgh. (Received
... Glandular Mechanisms of Salivary Secretion
 Glandular Mechanisms of Salivary Secretion.. Frontiers of Oral Biology Vol. 10 Series Editor R.W.A. Linden, London Glandular Mechanisms of Salivary Secretion Volume Editors J.R. Garrett, London J. Ekström,
Glandular Mechanisms of Salivary Secretion.. Frontiers of Oral Biology Vol. 10 Series Editor R.W.A. Linden, London Glandular Mechanisms of Salivary Secretion Volume Editors J.R. Garrett, London J. Ekström,
Physiological processes in the GI tract:
 Gastrointestinal physiology for medical students General principal of gastrointestinal function Motility, nervous control and blood circulation Physiological processes in the GI tract: Motility Secretion
Gastrointestinal physiology for medical students General principal of gastrointestinal function Motility, nervous control and blood circulation Physiological processes in the GI tract: Motility Secretion
Divisions of ANS. Divisions of ANS 2 Divisions dualing innervate most organs. Autonomic Nervous System (Chapter 9)
 Autonomic Nervous System (Chapter 9) Autonomic Nervous System (ANS) general properties anatomy Autonomic Effects on Target Organs Subs of Nervous System Central nervous system Brain Spinal cord Peripheral
Autonomic Nervous System (Chapter 9) Autonomic Nervous System (ANS) general properties anatomy Autonomic Effects on Target Organs Subs of Nervous System Central nervous system Brain Spinal cord Peripheral
The Autonomic Nervous
 Autonomic Nervous System The Autonomic Nervous Assess Prof. Fawzia Al-Rouq System Department of Physiology College of Medicine King Saud University LECTUR (1) Functional Anatomy & Physiology of Autonomic
Autonomic Nervous System The Autonomic Nervous Assess Prof. Fawzia Al-Rouq System Department of Physiology College of Medicine King Saud University LECTUR (1) Functional Anatomy & Physiology of Autonomic
Neuropsychiatry Block
 Neuropsychiatry Block Physiology of the Autonomic Nervous System By Laiche Djouhri, PhD Dept. of Physiology Email: ldjouhri@ksu.edu.sa Ext:71044 References The Autonomic Nervous System and the Adrenal
Neuropsychiatry Block Physiology of the Autonomic Nervous System By Laiche Djouhri, PhD Dept. of Physiology Email: ldjouhri@ksu.edu.sa Ext:71044 References The Autonomic Nervous System and the Adrenal
PHYSIOLOGY WEEK 9. vascular physiology - ED Primary Exam Teaching
 PHYSIOLOGY WEEK 9 vascular physiology - ED Primary Exam Teaching CONCEPTS OF BLOOD FLOW Vascular distensibility - when pressure in the arterioles is increased, this dilates the arterioles and therefore
PHYSIOLOGY WEEK 9 vascular physiology - ED Primary Exam Teaching CONCEPTS OF BLOOD FLOW Vascular distensibility - when pressure in the arterioles is increased, this dilates the arterioles and therefore
QUIZ 2. Tuesday, April 6, 2004
 Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
by Starling [1914] and Daly [1925].
![by Starling [1914] and Daly [1925]. by Starling [1914] and Daly [1925].](/thumbs/83/88889966.jpg) 612.13 PROPERTIES OF THE PERIPHERAL VASCULAR SYSTEM AND THEIR RELATION TO THE SYSTEMIC OUTPUT. BY HENRY BARCROFT. Harmsworth Scholar, St Mary's Hospital, London. (Experiments performed in the Physiological
612.13 PROPERTIES OF THE PERIPHERAL VASCULAR SYSTEM AND THEIR RELATION TO THE SYSTEMIC OUTPUT. BY HENRY BARCROFT. Harmsworth Scholar, St Mary's Hospital, London. (Experiments performed in the Physiological
AUTONOMIC NERVOUS SYSTEM (ANS):
 University of Jordan Faculty of Medicine Department of Physiology & Biochemistry Medical 1 st year students, 2017/2018. ++++++++++++++++++++++++++++++++++++++++++++++++++ Textbook of Medical Physiology,
University of Jordan Faculty of Medicine Department of Physiology & Biochemistry Medical 1 st year students, 2017/2018. ++++++++++++++++++++++++++++++++++++++++++++++++++ Textbook of Medical Physiology,
skeletal muscle, it was concluded that the vasodilatation is brought about by
 289 J. Physiol. (I954) I23, 289-3 THE EFFECTS OF NICOTINE ON THE BLOOD VESSELS OF SKELETAL MUSCLE IN THE CAT. AN INVESTIGATION OF VASOMOTOR AXON REFLEXES BY S. M. HILTON From the Physiological Laboratory,
289 J. Physiol. (I954) I23, 289-3 THE EFFECTS OF NICOTINE ON THE BLOOD VESSELS OF SKELETAL MUSCLE IN THE CAT. AN INVESTIGATION OF VASOMOTOR AXON REFLEXES BY S. M. HILTON From the Physiological Laboratory,
Functional components
 Facial Nerve VII cranial nerve Emerges from Pons Two roots Functional components: 1. GSA (general somatic afferent) 2. SA (Somatic afferent) 3. GVE (general visceral efferent) 4. BE (Special visceral/branchial
Facial Nerve VII cranial nerve Emerges from Pons Two roots Functional components: 1. GSA (general somatic afferent) 2. SA (Somatic afferent) 3. GVE (general visceral efferent) 4. BE (Special visceral/branchial
Chp. 16: AUTONOMIC N.S. (In Review: Peripheral N. S.)
 Chp. 16: AUTONOMIC N.S. (In Review: Peripheral N. S.) Peripheral nerves contain both motor and sensory neurons Among the motor neurons, some of these are somatic and innervate skeletal muscles while some
Chp. 16: AUTONOMIC N.S. (In Review: Peripheral N. S.) Peripheral nerves contain both motor and sensory neurons Among the motor neurons, some of these are somatic and innervate skeletal muscles while some
Circulatory System Review
 Circulatory System Review 1. Know the diagrams of the heart, internal and external. a) What is the pericardium? What is myocardium? What is the septum? b) Explain the 4 valves of the heart. What is their
Circulatory System Review 1. Know the diagrams of the heart, internal and external. a) What is the pericardium? What is myocardium? What is the septum? b) Explain the 4 valves of the heart. What is their
Departments of Physiology and Anaestliesiology, K. G's Medical College, Luck now,
 VAGAL r HIBITKO OF HEART :n.n HYPOXi:C DOGS. S. KUMAR, P. D. JAIN AND R. P. BADOLA Departments of Physiology and Anaestliesiology, K. G's Medical College, Luck now, Slowing of heart can be brought about
VAGAL r HIBITKO OF HEART :n.n HYPOXi:C DOGS. S. KUMAR, P. D. JAIN AND R. P. BADOLA Departments of Physiology and Anaestliesiology, K. G's Medical College, Luck now, Slowing of heart can be brought about
[ANATOMY #12] April 28, 2013
![[ANATOMY #12] April 28, 2013 [ANATOMY #12] April 28, 2013](/thumbs/86/93473883.jpg) Sympathetic chain : Sympathetic chain is each of the pair of ganglionated longitudinal cords of the sympathetic nervous system; extend from level of atlas (base of skull) till coccyx. It is paravertebral
Sympathetic chain : Sympathetic chain is each of the pair of ganglionated longitudinal cords of the sympathetic nervous system; extend from level of atlas (base of skull) till coccyx. It is paravertebral
(Received April 6, 1936)
 275 6I2.26 RESPIRATION AND FUNCTIONAL ACTIVITY BY W. DEUTSCH AND H. S. RAPER (From the Department of Physiology, University of Manchester) (Received April 6, 1936) IT has long been established that in
275 6I2.26 RESPIRATION AND FUNCTIONAL ACTIVITY BY W. DEUTSCH AND H. S. RAPER (From the Department of Physiology, University of Manchester) (Received April 6, 1936) IT has long been established that in
Lujain Hamdan. Ayman Musleh & Yahya Salem. Mohammed khatatbeh
 12 Lujain Hamdan Ayman Musleh & Yahya Salem Mohammed khatatbeh the last lecture, we have studied the differences between the two divisions of the ANS: sympathetic and parasympathetic pathways which work
12 Lujain Hamdan Ayman Musleh & Yahya Salem Mohammed khatatbeh the last lecture, we have studied the differences between the two divisions of the ANS: sympathetic and parasympathetic pathways which work
Chronotropic and Inotropic Effects of 3 Kinds of Alpha-Adrenergic Blockers on the Isolated Dog Atria
 Chronotropic and Inotropic Effects of 3 Kinds of Alpha-Adrenergic Blockers on the Isolated Dog Atria Shigetoshi CHIBA, M.D., Yasuyuki FURUKAWA, M.D., and Hidehiko WATANABE, M.D. SUMMARY Using the isolated
Chronotropic and Inotropic Effects of 3 Kinds of Alpha-Adrenergic Blockers on the Isolated Dog Atria Shigetoshi CHIBA, M.D., Yasuyuki FURUKAWA, M.D., and Hidehiko WATANABE, M.D. SUMMARY Using the isolated
Integrated Cardiopulmonary Pharmacology Third Edition
 Integrated Cardiopulmonary Pharmacology Third Edition Chapter 3 Pharmacology of the Autonomic Nervous System Multimedia Directory Slide 19 Slide 37 Slide 38 Slide 39 Slide 40 Slide 41 Slide 42 Slide 43
Integrated Cardiopulmonary Pharmacology Third Edition Chapter 3 Pharmacology of the Autonomic Nervous System Multimedia Directory Slide 19 Slide 37 Slide 38 Slide 39 Slide 40 Slide 41 Slide 42 Slide 43
Biology 218 Human Anatomy
 Chapter 20 Adapted form Tortora 10 th ed. LECTURE OUTLINE A. Introduction (p. 632) 1. The autonomic nervous system (ANS) regulates the activity of smooth muscle, cardiac muscle, and certain glands. 2.
Chapter 20 Adapted form Tortora 10 th ed. LECTURE OUTLINE A. Introduction (p. 632) 1. The autonomic nervous system (ANS) regulates the activity of smooth muscle, cardiac muscle, and certain glands. 2.
London, N.W. 7. Tubocurarine perfused through the cerebral ventricles of cats produces
 J. Physiol. (1962), 164, pp. 301-317 301 With 7 text-figures Printed in Great Britain THE RELATION BETWEEN SEIZURE DISCHARGE AND MYOCLONUS DURING PERFUSION OF THE CEREBRAL VENTRICLES WITH TUBOCURARINE
J. Physiol. (1962), 164, pp. 301-317 301 With 7 text-figures Printed in Great Britain THE RELATION BETWEEN SEIZURE DISCHARGE AND MYOCLONUS DURING PERFUSION OF THE CEREBRAL VENTRICLES WITH TUBOCURARINE
Investigation of human cardiovascular physiology is very interesting, but many
 6 E X E R C I S E Frog Cardiovascular Physiology O B J E C T I V E S 1. To list the properties of cardiac muscle as automaticity and rhythmicity, and to define each. 2. To explain the statement, Cardiac
6 E X E R C I S E Frog Cardiovascular Physiology O B J E C T I V E S 1. To list the properties of cardiac muscle as automaticity and rhythmicity, and to define each. 2. To explain the statement, Cardiac
Autonomic Nervous System. Autonomic (Visceral) Nervous System. Visual Anatomy & Physiology First Edition. Martini & Ober
 Visual Anatomy & Physiology First Edition Martini & Ober Chapter 14 Autonomic Nervous System Lecture 21 1 Autonomic (Visceral) Nervous System CNS PNS 2 Autonomic Nervous System functions without conscious
Visual Anatomy & Physiology First Edition Martini & Ober Chapter 14 Autonomic Nervous System Lecture 21 1 Autonomic (Visceral) Nervous System CNS PNS 2 Autonomic Nervous System functions without conscious
