Contributors T A B L E O F C O N T E N T S
|
|
|
- Phyllis Leona Johns
- 5 years ago
- Views:
Transcription
1 JOINT TRAUMA SYS TEM CLINICAL PRACTIC E GUIDELINE (JTS CPG ) Urologic Trauma Management (CPG ID: 42) Provides indications for and the procedures associated with the initial management of genitourinary (GU) trauma sustained in combat casualties. Contributors COL James Jezoir, MC, USA MAJ Steve Hudak, MC, USA LTC Jack Walters, MC, USA CAPT Zsolt Stockinger, MC, USN COL(ret) Steve Waxman, MC, USA First Publication Date: 18 Nov 2004 Publication Date: 01 Nov 2017 Supersedes CPG dated 02 Apr 2012 Opinions, interpretations, conclusions, and recommendations are those of the authors and are not necessarily endorsed by the Services or DoD. T A B L E O F C O N T E N T S Background... 2 Evaluation and Treatment... 2 Initial Evaluation... 2 Renal Trauma... 4 Bladder Trauma... 5 Urethral Trauma... 5 External Genitalia... 5 Performance Improvement (PI) Monitoring... 6 Intent (Expected Outcomes)... 6 Performance/Adherence Measures... 6 Data Source... 7 System Reporting & Frequency... 7 Responsibilities... 7 References... 7 Appendix A: Urological Diagnosis and Treatments... 9 Appendix B: Additional Information Regarding Off-Label Uses in CPGs... 12
2 BACKGROUND Genitourinary (GU) trauma accounts for 10% of all combat casualties incurred during current US conflicts. 1 Management requires a systematic approach to imaging and treatment that adheres to established surgical and trauma principals. These guidelines provide direction for the identification of life threatening GU injuries, control of hemorrhage, establishment of urinary drainage, and the preservation of function where possible. Critical to initial evaluation is the hemodynamic stability of the patient. Stable patients are afforded a rigorous radiographic evaluation that identifies genitourinary sites of hemorrhage and injury and allows for the safe establishment of urinary drainage. Unstable patients benefit from rapid surgical evaluation and hemorrhage control. Preservation of as much tissue as possible, particularly when dealing with the external genitalia, should be an additional goal for far forward surgical units. 2 Current combat care principles allow for multiple surgical evaluations along the path of evacuation to tertiary centers outside the theater of operations where tissue reevaluation, wound irrigation, and further debridement can occur. 3 EVALUATION AND TREATMENT Ten percent of all combat casualties in current U.S. conflicts have GU injuries, which may be blunt or penetrating in nature. The extensive use of improvised explosive devices (IED) has resulted in a substantial number of penetrating injuries that include GU organs as part of a complex wounding pattern with trauma to the abdomen, pelvis, perineum, and extremities. 1,4-7 A significant reduction in kidney injuries has been noted in combat casualties wearing body armor. 8 Not surprisingly, given the mechanism of injury, the most commonly injured GU structures are the external genitalia and lower urinary tract (bladder and urethra). 4,9,10 A thorough trauma evaluation is therefore mandatory in all severely injured patients and should include proper Advanced Trauma Life Support (ATLS) based initial evaluation and management. INITIAL EVALUATION Severely injured patients typically warrant immediate urethral catheter placement to facilitate urinary drainage and assist with hemodynamic monitoring via hourly assessment of urine output. Prior to catheter placement, if blood is present at the urethral meatus, urethral injury is likely and retrograde urethrography is needed (See Figure 1. Algorithm for Urologic Trauma below. 11 A urinalysis should be obtained after successful catheter placement and the presence of gross hematuria should be immediately noted. Evaluation for renal injury is necessary in hemodynamically stable blunt trauma patients with gross hematuria or microscopic hematuria and systolic BP < 90 mmhg; or in patients with mechanism of injury or physical examination findings suggestive of renal injury (i.e. rapid deceleration, rib fracture(s), flank ecchymosis, or a penetrating injury to the abdomen, flank, or lower chest). 11 The stability of the patient, operational environment and capabilities of the medical treatment facility will dictate what resources for radiographic and surgical evaluation are available at each echelon of care. The preferred imaging test to evaluate for renal and ureteral injury is an intravenous (IV) contrast enhanced computed tomography (CT) with delayed imaging. 11 If unavailable, one shot Intravenous Pyelography (IVP) can be performed. During the initial evaluation of patients with hematuria, it is important to note that the severity of hematuria (gross or microscopic) does not necessarily correlate to the severity of injury. 12 For example, it is possible to have minimal hematuria despite high grade renal injury such as disruption of the ureteropelvic junction, pedicle injuries, and segmental arterial thrombosis. 9 Conversely, low grade renal injury can result in ongoing gross hematuria. Thus, proper injury staging is critical regardless of hematuria severity. In cases of blunt renal trauma, most injuries can be managed conservatively. The grading scale is listed in Renal Injury in Appendix A: Urological Diagnosis and Treatments.) Guideline Only/Not a Substitute for Clinical Judgment 2
3 Figure 1. Algorithm for Urologic Trauma Guideline Only/Not a Substitute for Clinical Judgment 3
4 RENAL TRAUMA Patients with penetrating renal injuries often have associated injuries to other intra-abdominal organs that require laparotomy. Evidence based guidance on direct evaluation of the kidney for high velocity penetrating trauma during laparotomy is lacking. Generally, a hematoma confined to the retroperitoneum is left undisturbed; persistent bleeding and expanding or medial hematomas suggesting a hilar, aortic, or caval injury warrant direct evaluation. 11 The decision as to repair or remove the damaged kidney at that time depends on the salvage-ability of the kidney and the ability of the patient to tolerate the procedure. High velocity kidney injuries are difficult to reconstruct and often result in nephrectomy. (See Nephrectomy in Appendix A: Urological Diagnosis and Treatments.) 12 Ureteral injuries are nearly always secondary to penetrating trauma and a high index of suspicion based upon suspected bullet or fragment trajectory is necessary to avoid missing the diagnosis; IVP can be helpful if it can be performed in the operating room. 13,14 Hematuria may be absent and the only clue may be injuries to organs close to the path of the ureter or an unexplained rise in serum creatinine. (See Appendix A: Urological Diagnosis and Treatments.) 14 An algorithmic approach to renal trauma management is presented in Figure 2 below. Figure 2. Renal Trauma Algorithm Guideline Only/Not a Substitute for Clinical Judgment 4
5 BLADDER TRAUMA Bladder injuries may be secondary to blunt or penetrating trauma. Bladder rupture from blunt trauma is typically associated with pelvic fracture and results in gross hematuria. Thus, the combination of these two findings (hematuria + pelvic fracture) warrants retrograde plain film or CT cystography to evaluate for bladder injury. 11 Penetrating bladder injury must be excluded when the trajectory of the penetrating object is near the pelvis or lower abdomen. 15 Retrograde (plain film or CT) cystography should be performed prior to exploratory laparotomy if possible. However, when imaging is not possible prior to abdominal exploration, large intraperitoneal bladder injuries can be rapidly excluded by filling the bladder in a retrograde fashion with ml of sterile saline or dilute methylene blue via the Foley catheter and inspecting for leakage of the fluid into the peritoneal cavity. Extraperitoneal injuries cannot be reliably excluded using this technique. Extraperitoneal injuries may benefit from immediate repair when pelvic fractures result in exposed bone spicules in the bladder lumen, concurrent rectal or vaginal lacerations may lead to fistula formation to the ruptured bladder, for bladder neck injuries that may not heal with catheter drainage alone, or when the patient is undergoing open repair of concurrent abdominal pelvic injuries in the stable patient. 11 Bladder injury from penetrating trauma will often have an entrance and exit wound and have a high incidence of concurrent rectal injury. 15 While intraperitoneal bladder rupture must be repaired, extraperitoneal rupture can be managed non operatively with Foley catheter drainage. Bladder repair is performed using a 2 layer closure with absorbable sutures and bladder catheter drainage. (See Bladder Injuries in Appendix A: Urological Diagnosis and Treatments.) Bladder injury from penetrating trauma has a high incidence of concurrent rectal injury. 15 URETHRAL TRAUMA Urethral injuries are identified by retrograde urethrography. Blunt anterior urethral injuries should be stented with a urethral catheter when possible or diverted with a suprapubic cystostomy. 11 Posterior urethral injuries, however, can be managed with suprapubic cystostomy alone. 11 A judicious attempt to realign the urethra endoscopically can be performed at subsequent operative evaluations when the patient is clinically stable several days following injury. 11 Penetrating anterior urethral injuries can be primarily repaired with fine absorbable suture over a urethral catheter when the degree of soft tissue injury/contamination is limited. However, when complex blast injury results in anterior urethral injury associated with significant soft tissue loss of the perineum and/or genitalia, urinary diversion alone (transurethral or suprapubic) is sufficient to facilitate urinary drainage until the patient can be evaluated by a urologist who can assist with the wound care and complex urethrogenital reconstruction frequently needed in these cases. EXTERNAL GENITALIA With the rise in dismounted complex battle injuries from explosive devices in current combat operations and polytrauma involvement of the lower extremities, perineum, pelvis, and lower abdomen; greater attention has turned to the management of soft tissue injury to the external genitalia and urethra. Initial operative management involves a thorough assessment of the injury sites with removal of wound contaminants and debridement of non-viable tissue. This is done in conjunction with copious, low-pressure irrigation of the wound. 3 Testicular injuries are easily missed due to small scrotal entry wounds in some cases and require a high index of suspicion when evaluating patients with significant blast injury. (See External Genitalia Injuries in Appendix A: Urological Diagnosis and Treatments.) It is imperative to preserve all viable tissue when addressing injuries to the external genitalia to improve functional outcomes on recovery. 16 In addition to arterial bleeding, vascular structures of the penis and scrotum should be addressed on initial surgery, specifically, the corpora cavernosa, corpus spongiosum, and bilateral testes. Lacerations to the corpora Guideline Only/Not a Substitute for Clinical Judgment 5
6 cavernosa can be closed with absorbable suture taking care to avoid the dorsal neurovascular structures. Aggressive over sewing of the corpus spongiosum, however, should also be avoided in favor of site specific closure to its tunical covering reducing risk of ischemic changes distal to the injury site in these complex wounds. 17 Patients with penetrating scrotal wounds or evidence of testicular rupture on exam should undergo scrotal exploration. Ruptured testes are managed with irrigation and debridement of non-viable seminiferous tubules. The tunica albuginea is then closed and returned to the scrotum. 11 A tunica vaginalis flap can be used to close the defect when there is insufficient tunica to obtain a tension free closure over the exposed tubules. 18 A delay in managing a testicular injury is acceptable when the patient is too unstable or there is insufficient expertise to manage it at initial exploration. Every attempt should be made to salvage viable testicular tissue especially when both testicles are involved or a unilateral orchiectomy is required. The injured testis should be wrapped in saline soaked gauze and protected with multiple layers of additional dressing. A vacuum assisted dressing is not appropriate if the tunica is left open. These findings should be communicated to the next echelon of care. The superficial fascia and skin layers of the penis can and should be left open following high energy trauma. Loose approximation of these layers with interrupted suture allows continued tissue evaluation and additional wound debridement. A moist gauze or negative pressure dressing is appropriate. Alternatively, Penrose drains can be placed between loosely approximated interrupted sutures. In cases where scrotal closure is impossible, the testis can be covered with a non-adherent dressing followed by a negative pressure dressing. Creation of a sub dermal thigh pouch is rarely necessary during early surgical care. With the recent introduction of female combatants to all roles in the military, we anticipate a new constellation of injuries not previously encountered. These will include labial, clitoral, and vaginal soft tissue injuries. Currently there is limited evidence-based direction in the management of these injuries. Initial care should focus on good exposure of the injured tissue with a complete examination to include the vaginal vault, urethra, and meatus with low pressure irrigation and judicious debridement of devascularized tissue. Limited debridement should be practiced around the clitoris favoring repeat examinations in the operating room with intervention as needed. This new injury pattern will need to be prospectively tracked to ensure appropriate care. PERFORMANCE IMPROVEMENT (PI) MONITORING INTENT (EXPECTED OUTCOMES) Appropriate imaging was obtained in hemodynamically stable patients. Retrograde urethrograpy is performed in patients with suspected urethral injury or blood at the meatus. Retrograde cystography is performed in patients with gross hematuria who have a mechanism of injury concerning for bladder injury, pelvic ring fracture, or findings on physical exam or imaging concerning for bladder rupture. Intravenous (IV) contrast enhanced computed tomography (CT) with delayed imaging is performed in stable blunt trauma patients with gross hematuria or microscopic hematuria and systolic blood pressure < 90mmHG, or in any stable trauma patients with mechanism of injury or physical exam findings concerning for renal injury (e.g., rapid deceleration, significant blow to flank, rib fracture, significant flank ecchymosis, penetrating injury of abdomen, flank, or lower chest). PERFORMANCE/ADHERENCE MEASURES All blunt trauma patients with gross hematuria (regardless of initial SBP) and those patients with microscopic hematuria whose initial SBP is less than 90 mmhg had contrast enhanced CT scan performed (where available) if/when they become hemodynamically stable. Guideline Only/Not a Substitute for Clinical Judgment 6
7 DATA SOURCE Patient Record Department of Defense Trauma Registry (DoDTR) SYSTEM REPORTING & FREQUENCY The above constitutes the minimum criteria for PI monitoring of this CPG. System reporting will be performed annually; additional PI monitoring and system reporting may be performed as needed. The system review and data analysis will be performed by the Joint Theater Trauma System (JTS) Director and the Performance Improvement Branch. RESPONSIBILITIES It is the trauma team leader s responsibility to ensure familiarity, appropriate compliance and PI monitoring at the local level with this CPG. REFERENCES 1. Dismounted Complex Blast Injury Task Force, Dismounted Complex Blast Injury Report of the Army, 18 Jun Accessed Mar Emergency War Surgery Handbook, 4th United States Revision Borden Institute. Walter Reed Army Medical Center, Washington, D.C. Chapter 18: Genitourinary Tract Injuries. 2013: Joint Trauma System, Management of War Wounds: Debridement and Irrigation. CPG, 25 Apr dement_irrigation_25_apr_12_id31.pdf Accessed Mar Combat Urologic Trauma in US Military Overseas Contingency Operations. F Serkin, D Soderdahl, J Hernandez, M Patterson, L Blackbourne, C Wade. J Trauma 69: S , Battlefield Urologic Injuries: The Gulf War Experience. I Thompson, S Flaherty, A Morey. J Am Coll Surg. 187: , Operative Management of Wartime Genitourinary Injuries at Balad Air Force Theater Hospital, 2005 to S Hudak, S Hakim. J Urol. 182: , Battlefield Urogenital Injuries: Changing Patterns during the Past Century. S Hudak, A Morey, T Rozanski, C Fox. Urology 65: , Genitourinary Trauma at a Combat Support Hospital during Operation Iraqi Freedom: The Impact of Body Armor, E Paquette. J Urol. 177: , Improvised explosive device-related lower genitourinary trauma in current overseas combat operations. Banti M, Walter J, Hudak S, Soderdahl D. J Trauma Acute Care Surg Jan;80(1): Penetrating trauma to the external genitalia in Operation Iraqi Freedom. Waxman S, Beekley A, Morey A, Soderdahl D. Int J Impot Res Mar-Apr;21(2): Guideline Only/Not a Substitute for Clinical Judgment 7
8 11. Urotrauma: AUA guideline. Morey AF, Brandes S, Dugi DD 3rd, Armstrong JH, Breyer BN, Broghammer JA, Erickson BA, Holzbeierlein J, Hudak SJ, Pruitt JH, Reston JT, Santucci RA, Smith TG 3rd, Wessells H; American Urological Assocation. J Urol Aug;192(2): Review of the Current Management of Upper Urinary Tract Injuries by the EAU Trauma Guidelines Panel. Serafetinides E, Kitrey ND, Djakovic N, Kuehhas FE, Lumen N, Sharma DM, Summerton DJ. Eur Urol May 67(5), Delayed Diagnoosis of Traumatic Ureteral Injuries. D Kunkle, B Kansas, A Pathak, A Goldberg, J Mydlo. J Urol. 176: , Ureteral injuries from external violence: the 25-year experience at San Francisco General Hospital. Elliott SP, McAninch JW. J Urol Oct;170(4 Pt 1): Gunshot wounds to the lower urinary tract: a single-institution experience. Cinman NM, McAninch JW, Porten SP, Myers JB, Blaschko SD, Bagga HS, Breyer BN. J Trauma Acute Care Surg Mar;74(3): Penetrating External Genital Trauma: A 30-Year Single Institution Experience. S Phonsombat, V Master, J McAninch. J Urol. 180: , Management of combat-related urological trauma in the modern era. Williams M, Jezior J. Nat Rev Urol Sep;10(9): Gunshot wound injury of the testis: the use of tunica vaginalis and polytetrafluoroethylene grafts for reconstruction. Ferguson GG, Brandes SB. J Urol Dec;178(6): Guideline Only/Not a Substitute for Clinical Judgment 8
9 APPENDIX A: UROLOGICAL DIAGNOSIS AND TREATMENTS Hematuria Diagnosis Renal Injury Renal Exploration During Abdominal Operation Nephrectomy Treatment Place Foley catheter during trauma assessment unless contra-indicated such as blood at the urethral meatus or other evidence of urethral injury (pelvic fracture). Perform a retrograde urethrogram (RUG) before attempted catheterization when there is concern for a urethral injury. RUG Obtain an oblique plain film of the pelvis with the patient s bottom leg flexed at the knee and the top leg straight. Severely injured patients or those with suspected spine fractures can be left supine. Alternately, C-arm or fluoroscopy can be used. A 12Fr Foley catheter or catheter tipped syringe is inserted into the fossa navicularis, the penis placed on traction, and 20 ml of undiluted water soluble contrast injected under gentle pressure. Images are obtained. The study is considered normal only if contrast enters the bladder without extravasation. For an anterior urethral injury, plan on repair in the operating room (OR). For a posterior urethral injury, a supra-pubic catheter can be placed in the OR, or percutaneously in the emergency department (ED) for patients who do not need surgery and an appropriate kit is available. For partial urethral disruption by RUG, a single attempt with a well-lubricated catheter may be attempted by an experienced team member in the ED. If the catheter passes, and gross hematuria is noted, proceed with GU diagnostic evaluation for bladder injury or a renal/ureteral source. CT scan with delayed images and CT cystogram are appropriate imaging studies (see technique description following). Clinicians should perform diagnostic imaging with intravenous (IV) contrast enhanced computed tomography (CT) with delayed imaging in stable blunt trauma patients with gross hematuria or microscopic hematuria and systolic blood pressure < 90mmHG or in any stable trauma patients with mechanism of injury or physical exam findings concerning for renal injury (e.g., rapid deceleration, significant blow to flank, rib fracture, significant flank ecchymosis, penetrating injury of abdomen, flank, or lower chest). Renal Injury Grading Grade 1: Sub-capsular hematoma Grade 2: Small parenchymal laceration Grade 3: Deeper parenchymal laceration without entry into collecting system Grade 4: Laceration into collecting system with extravasation; vascular injury with contained hemorrhage Grade 5: Shattered kidney or renal pedicle avulsion Hemodynamically stable patients can be managed without surgical exploration in most cases. Hemodynamically unstable patients with no or transient response to resuscitation should have immediate intervention. Vascular repair is indicated for salvageable kidneys with renal artery or vein injury. Ureteral stenting may be needed for enlarging urinoma or persistent urinary extravasation with fever, pain, ileus, fistula, or infection. Stable perirenal hematomas found at time of exploration should not be routinely opened. Renal exploration should be performed at time of laparotomy for persistent bleeding, expanding hematoma, or a central hematoma suggesting a renal hilum injury Total nephrectomy is immediately indicated in extensive renal injuries when the patient's life would be threatened by attempted renal repair. A common surgical approach is a lateral to medial mobilization of the kidney to expose the renal pedicle after incision of the peritoneal attachments of the colon to the lateral wall. While there is insufficient data to recommend initial vascular control of the renal pedicle through a mesentery window prior to exploration, this remains an acceptable principle for renal surgery. Damage control by packing the wound to control bleeding and attempting to correct metabolic and coagulation abnormalities, with a plan to return for corrective surgery within 24 hours is an option. Guideline Only/Not a Substitute for Clinical Judgment 9
10 Diagnosis Renal Repair and Partial Nephrectomy Principles Ureteral Injuries Bladder Injuries Treatment Non-surgical management can result in renal preservation even with high grade injuries. Renal repair is appropriate after gaining hemorrhage control and hemodynamic stability for potentially salvageable kidneys identified during exploration. Technique: Complete renal exposure, debridement of nonviable tissue, hemostasis by individual suture ligation of bleeding vessels, watertight closure (absorbable suture), drainage of the collecting system, and coverage/approximation of the parenchymal defect. Perform partial nephrectomy if reconstruction is not possible: the collecting system must be closed and the parenchyma covered with fat or omentum. Consider the use of hemostatic agents and tissue sealants if available. Place ureteral stent for persistent urinary extravasation. Identification of ureteral injury requires a high index of suspicion. It should be evaluated with IV contrast enhanced CT with delayed imaging or direct inspection during laparotomy if preoperative imaging is not available. Ureteral contusions can be managed by stenting or judicious excision of the injured area with primary anastomosis depending on its severity. Simple ureteral lacerations should be closed primarily. Complete transections of the ureter proximal to the iliac vessels can be repaired using a tension free, end to end, spatulated anastomosis over a ureteral stent. Transections distal to the vessels should be managed with a ureteral reimplantation over a stent. A psoas hitch or Boari flap may be necessary in some cases. In cases of inadequate ureteral length to re-anastomose or hemodynamic instability of the patient intraoperatively, a pediatric feeding tube or open ended ureteral catheter may be placed in the proximal ureter and brought out through the skin and placed to closed drainage. Reconstruction of the ureter can then be performed at a future date. An ureteropelvic junction (UPJ) avulsion injury should undergo re-anastomosis of the ureter to the renal pelvis over a stent. A drain should be considered after ureteral repair. Perform retrograde cystography in patients with gross hematuria and a mechanism concerning for bladder injury, finding on exam or imaging concerning for bladder rupture, or pelvic ring fracture. Retrograde cystography can be done by CT or plain film. For CT cystogram use diluted Conray to reduce scatter artifact from the contrast. A minimum of 300 ml is needed for an adequately study. Plain film images should include a scout film and an AP image with or without oblique views both with the bladder full and again after it is drained. Extraperitoneal extravasation of contrast can be managed with Foley catheterization alone in most cases. Open repair is indicated for complicated ruptures that include pelvic fractures with exposed bone spicules in the bladder and concurrent rectal or vaginal lacerations that may lead to fistula formation. Patient s undergoing exploration for other indications that are appropriately stable and those with significant bladder neck involvement should be considered for closure. A transvesical approach can reduce disruption of the pelvic hematoma. Intraperitoneal rupture requires open repair, two-layer closure with absorbable suture, and perivesical drain placement. A large caliber urethral catheter without suprapubic catheter is usually sufficient for bladder drainage. Patients with complex lower extremity, pelvic, or perineal injuries and those requiring prolonged immobilization may benefit from suprapubic catheter drainage as well. Follow up cystography should be performed prior to catheter removal Guideline Only/Not a Substitute for Clinical Judgment 10
11 Diagnosis Urethral Injuries External Genitalia Injuries Treatment Diagnosis: A RUG should be performed in any case of suspected urethral injury. For partial urethral tears, a single attempt at urethral catheterization with a well lubricated catheter may be attempted by an experienced provider. Anterior urethral injuries: Primary repair of uncomplicated penetrating injury to the anterior urethra may be performed using fine absorbable sutures with careful mucosal to mucosal apposition over a urethral catheter. Immediate repair should not be performed in the setting of extensive tissue damage or urethral loss, patient instability, or surgeon inexperience. Bleeding from the corpus spongiosum can be controlled with site specific fine absorbable suture. Bladder drainage should be established by urethral catheterization or suprapubic drainage. Posterior urethral injuries: These injuries are typically associated with pelvic fractures or deep penetrating trauma. Suprapubic urinary drainage with delayed reconstruction is the accepted treatment for the majority of cases. Endoscopic alignment may be attempted within the first several days after injury in a hemodynamically stable patient. Aggressive attempts at realignment should be avoided. The primary goals in the management of genital injuries are hemorrhage control and tissue preservation. Hemorrhage can occur from small arteries on the dorsal penile shaft and/or the spermatic cord. These vessels can be managed with precise cautery. Large volume, low pressure, irrigation with normal saline should be performed with each surgical intervention. Delayed wound closure is appropriate for significant injuries with considerable tissue damage. Negative pressure wound dressings are well tolerated but often require creative placement techniques when applied to the genitalia. A non-adherent silicone or hydrophilic white foam dressing can be used to cover exposed testicles or freshly repaired corporal tissue when using a negative pressure dressing. Penile injury may include the corpus spongiosum or corpus cavernosa, and can result in continued hemorrhage. These can be repaired by approximation of the tunical margins with absorbable sutures in a hemostatic fashion following irrigation and debridement of necrotic or devitalized tissue. The glans is well vascularized and can generally be closed with interrupted absorbable suture. Scrotal injuries are managed in a similar fashion as other soft tissue wounds. Small penetrating injuries can result in significant testicular damage. There should be a low threshold for surgical exploration in these cases. The scrotum should undergo irrigation and debridement with primary or delayed closure. Widely spaced absorbable suture and a Penrose drain can be used in lieu of a negative pressure dressing when delayed closure is required. Testicle injuries can be diagnosed with physical exam or scrotal ultrasound. CT or sonography may also show evidence of foreign bodies or air in the scrotum or abnormality of one or both testes. Equivocal cases should be explored. Necrotic testicular tissue should be debrided and the capsule closed with absorbable suture. A tunical vaginalis flap can be used when the tunica albuginea is deficient for closure. Guideline Only/Not a Substitute for Clinical Judgment 11
12 APPENDIX B: ADDITIONAL INFORMATION REGARDING OFF-LABEL USES IN CPGS PURPOSE The purpose of this Appendix is to ensure an understanding of DoD policy and practice regarding inclusion in CPGs of off-label uses of U.S. Food and Drug Administration (FDA) approved products. This applies to off-label uses with patients who are armed forces members. BACKGROUND Unapproved (i.e., off-label ) uses of FDA-approved products are extremely common in American medicine and are usually not subject to any special regulations. However, under Federal law, in some circumstances, unapproved uses of approved drugs are subject to FDA regulations governing investigational new drugs. These circumstances include such uses as part of clinical trials, and in the military context, command required, unapproved uses. Some command requested unapproved uses may also be subject to special regulations. ADDITIONAL INFORMATION REGARDING OFF-LABEL USES IN CPGS The inclusion in CPGs of off-label uses is not a clinical trial, nor is it a command request or requirement. Further, it does not imply that the Military Health System requires that use by DoD health care practitioners or considers it to be the standard of care. Rather, the inclusion in CPGs of off-label uses is to inform the clinical judgment of the responsible health care practitioner by providing information regarding potential risks and benefits of treatment alternatives. The decision is for the clinical judgment of the responsible health care practitioner within the practitioner-patient relationship. ADDITIONAL PROCEDURES Balanced Discussion Consistent with this purpose, CPG discussions of off-label uses specifically state that they are uses not approved by the FDA. Further, such discussions are balanced in the presentation of appropriate clinical study data, including any such data that suggest caution in the use of the product and specifically including any FDA-issued warnings. Quality Assurance Monitoring With respect to such off-label uses, DoD procedure is to maintain a regular system of quality assurance monitoring of outcomes and known potential adverse events. For this reason, the importance of accurate clinical records is underscored. Information to Patients Good clinical practice includes the provision of appropriate information to patients. Each CPG discussing an unusual off-label use will address the issue of information to patients. When practicable, consideration will be given to including in an appendix an appropriate information sheet for distribution to patients, whether before or after use of the product. Information to patients should address in plain language: a) that the use is not approved by the FDA; b) the reasons why a DoD health care practitioner would decide to use the product for this purpose; and c) the potential risks associated with such use. Guideline Only/Not a Substitute for Clinical Judgment 12
Contributors. COL James Jezoir, MC, USA MAJ Steve Hudak, MC, USA LTC Jack Walters, MC, USA CAPT Zsolt Stockinger, MC, USN
 JOINT TRAUMA SYS TEM CLINICAL PRACTIC E GUIDELINE (JTS CPG ) Genitourinary (GU) Injury Trauma Management (CPG ID: 42) This CPG provides indications for and the procedures associated with the initial management
JOINT TRAUMA SYS TEM CLINICAL PRACTIC E GUIDELINE (JTS CPG ) Genitourinary (GU) Injury Trauma Management (CPG ID: 42) This CPG provides indications for and the procedures associated with the initial management
Joint Theater Trauma System Clinical Practice Guideline
 Page 1 of 10 UROLOGIC TRAUMA MANAGEMENT Original Release/Approval 18 Dec 2004 Note: This CPG requires an annual review. Reviewed: Mar 2012 Approved: 2 Apr 2012 Supersedes:, 30 June 2010 Minor Changes (or)
Page 1 of 10 UROLOGIC TRAUMA MANAGEMENT Original Release/Approval 18 Dec 2004 Note: This CPG requires an annual review. Reviewed: Mar 2012 Approved: 2 Apr 2012 Supersedes:, 30 June 2010 Minor Changes (or)
Canadian Undergraduate Urology Curriculum (CanUUC): Genitourinary Trauma. Last reviewed June 2014
 Canadian Undergraduate Urology Curriculum (CanUUC): Genitourinary Trauma Last reviewed June 2014 Session Objectives 1. Recognize hematuria as the cardinal symptom of urinary tract trauma. 1. Outline the
Canadian Undergraduate Urology Curriculum (CanUUC): Genitourinary Trauma Last reviewed June 2014 Session Objectives 1. Recognize hematuria as the cardinal symptom of urinary tract trauma. 1. Outline the
Genitourinary Tract Injuries
 Genitourinary Tract Injuries Chapter 18 Genitourinary Tract Injuries Introduction Genitourinary injuries constitute approximately 5% of the total injuries encountered in combat. Their treatment adheres
Genitourinary Tract Injuries Chapter 18 Genitourinary Tract Injuries Introduction Genitourinary injuries constitute approximately 5% of the total injuries encountered in combat. Their treatment adheres
UBC Department of Urologic Sciences Lecture Series. Urological Trauma
 UBC Department of Urologic Sciences Lecture Series Urological Trauma Disclaimer: This is a lot of information to cover and we are unlikely to cover it all today These slides are to be utilized for your
UBC Department of Urologic Sciences Lecture Series Urological Trauma Disclaimer: This is a lot of information to cover and we are unlikely to cover it all today These slides are to be utilized for your
Diagnosis & Management of Kidney Trauma. LAU - Urology Residency Program LOP Urology Residents Meeting
 Diagnosis & Management of Kidney Trauma LAU - Urology Residency Program LOP Urology Residents Meeting Outline Introduction Investigation Staging Treatment Introduction The kidneys are the most common genitourinary
Diagnosis & Management of Kidney Trauma LAU - Urology Residency Program LOP Urology Residents Meeting Outline Introduction Investigation Staging Treatment Introduction The kidneys are the most common genitourinary
Genitourinary Trauma Introduction GU Trauma overlooked
 Genitourinary Trauma Introduction GU Trauma overlooked 10-20% of all injured patients Long term morbidity Impotence Incontinence Life-threatening injuries first Urethral Injury Plan Bladder Injury Kidney
Genitourinary Trauma Introduction GU Trauma overlooked 10-20% of all injured patients Long term morbidity Impotence Incontinence Life-threatening injuries first Urethral Injury Plan Bladder Injury Kidney
West Yorkshire Major Trauma Network Clinical Guidelines 2015
 WYMTN: Pelvic fracture with urogenital trauma KEY RECOMMENDATIONS 1. During the initial exploratory survey / secondary survey, a. The external urethral meatus and the transurethral bladder catheter (if
WYMTN: Pelvic fracture with urogenital trauma KEY RECOMMENDATIONS 1. During the initial exploratory survey / secondary survey, a. The external urethral meatus and the transurethral bladder catheter (if
Urogenital Injuries The role of radiology
 Urogenital Injuries The role of radiology NORDTER 7 th Nordic Trauma Radiology Course Helsinki, Finland May 21-24, 2012 Johann Baptist Dormagen, MD, PhD Oslo University Hospital, Norway Kidney injuries
Urogenital Injuries The role of radiology NORDTER 7 th Nordic Trauma Radiology Course Helsinki, Finland May 21-24, 2012 Johann Baptist Dormagen, MD, PhD Oslo University Hospital, Norway Kidney injuries
UROLOGIC TRAUMA. Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara
 UROLOGIC TRAUMA Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara UROLOGIC TRAUMA Renal trauma Ureteral injury Bladder injury Urethral injury Injury to external genitalia
UROLOGIC TRAUMA Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara UROLOGIC TRAUMA Renal trauma Ureteral injury Bladder injury Urethral injury Injury to external genitalia
Renal Trauma: Management Options
 Renal Trauma: Management Options Immediate surgical repair Nephrectomy Conservative management Alonso RC et al. Kidney in Danger: CT Findings of Blunt and Penetrating Renal Trauma. RadioGraphics 2009;
Renal Trauma: Management Options Immediate surgical repair Nephrectomy Conservative management Alonso RC et al. Kidney in Danger: CT Findings of Blunt and Penetrating Renal Trauma. RadioGraphics 2009;
Clinical aspects in urogenital injuries
 Clinical aspects in urogenital injuries Rolf Wahlqvist Oslo Urological University Clinic Aker University Hospital Nordic Rad.2008 1 Urogenital injuries in trauma patients Renal injury Ureteral injury (infrequent/iatrogenic)
Clinical aspects in urogenital injuries Rolf Wahlqvist Oslo Urological University Clinic Aker University Hospital Nordic Rad.2008 1 Urogenital injuries in trauma patients Renal injury Ureteral injury (infrequent/iatrogenic)
Role of imaging in evaluation of genitourinary i trauma Spectrum of GU injuries Relevance of imaging findings in determining management Focus on MDCT
 Genitourinary Tract Injuries 6 th Nordic Course Scott D. Steenburg, MD Assistant Professor University of Maryland Department of Radiology Division of Trauma and Emergency Radiology R Adams Cowley Shock
Genitourinary Tract Injuries 6 th Nordic Course Scott D. Steenburg, MD Assistant Professor University of Maryland Department of Radiology Division of Trauma and Emergency Radiology R Adams Cowley Shock
Bladder Trauma Data Collection Sheet
 Bladder Trauma Data Collection Sheet If there was no traumatic injury with PENETRATION of the bladder DO NOT proceed Date of injury: / / Time of injury: Date of hospital arrival: / / Time of hospital arrival:
Bladder Trauma Data Collection Sheet If there was no traumatic injury with PENETRATION of the bladder DO NOT proceed Date of injury: / / Time of injury: Date of hospital arrival: / / Time of hospital arrival:
EAU GUIDELINES POCKET EDITION 4
 EAU GUIDELINES POCKET EDITION 4 CONTENTS: UROLOGICAL TRAUMA PAIN MANAGEMENT IN UROLOGY UROGENERIC LUTS RENAL TRANSPLANTATION 2 EAU POCKET GUIDELINES POCKET EDITION 4 Introduction 3 Introduction This is
EAU GUIDELINES POCKET EDITION 4 CONTENTS: UROLOGICAL TRAUMA PAIN MANAGEMENT IN UROLOGY UROGENERIC LUTS RENAL TRANSPLANTATION 2 EAU POCKET GUIDELINES POCKET EDITION 4 Introduction 3 Introduction This is
Question 2. What percentage of abdominal trauma involve the kidney? a) 5 % b) 10% c) 15 % d) 20 %
 Quiz Question 1 After injecting 2ml/kg of contrast for a patient needing a single-shot IVP before kidney exploration, What is the best turnaround time to take the X-ray? a) 3 minutes b) 5 minutes c) 10
Quiz Question 1 After injecting 2ml/kg of contrast for a patient needing a single-shot IVP before kidney exploration, What is the best turnaround time to take the X-ray? a) 3 minutes b) 5 minutes c) 10
GUIDELINEs ON UROLOGICAL TRAUMA
 GUIDELINEs ON UROLOGICAL TRAUMA (Text update March 2009) N. Djakovic, Th. Lynch, L. Martínez-Piñeiro, Y. Mor, E. Plas, E. Serafetinides, L. Turkeri, R.A. Santucci, M. Hohenfellner Eur Urol 2005;47(1):1-15
GUIDELINEs ON UROLOGICAL TRAUMA (Text update March 2009) N. Djakovic, Th. Lynch, L. Martínez-Piñeiro, Y. Mor, E. Plas, E. Serafetinides, L. Turkeri, R.A. Santucci, M. Hohenfellner Eur Urol 2005;47(1):1-15
GUIDELINES ON UROLOGICAL TRAUMA
 GUIDELINES ON UROLOGICAL TRAUMA (Limited text update March 2015) D.J. Summerton (Chair), N. Djakovic, N.D. Kitrey, F.E. Kuehhas, N. Lumen, E. Serafetinides, D.M. Sharma Eur Urol 2010 May;57(5):791-803
GUIDELINES ON UROLOGICAL TRAUMA (Limited text update March 2015) D.J. Summerton (Chair), N. Djakovic, N.D. Kitrey, F.E. Kuehhas, N. Lumen, E. Serafetinides, D.M. Sharma Eur Urol 2010 May;57(5):791-803
EAU GUIDELINES ON UROLOGICAL TRAUMA
 EAU GUIDELINES ON UROLOGICAL TRAUMA (Limited text update March 2016) N.D. Kitrey (Chair), N. Djakovic, M. Gonsalves, F.E. Kuehhas, N. Lumen, E. Serafetinidis, D.M. Sharma, D.J. Summerton Guidelines Associates:
EAU GUIDELINES ON UROLOGICAL TRAUMA (Limited text update March 2016) N.D. Kitrey (Chair), N. Djakovic, M. Gonsalves, F.E. Kuehhas, N. Lumen, E. Serafetinidis, D.M. Sharma, D.J. Summerton Guidelines Associates:
GUIDELINEs ON UROLOGICAL TRAUMA
 GUIDELINEs ON UROLOGICAL TRAUMA (Text update March 2009) N. Djakovic, Th. Lynch, L. Martínez-Piñeiro, Y. Mor, E. Plas, E. Serafetinides, L. Turkeri, R.A. Santucci, M. Hohenfellner Eur Urol 2005;47(1):1-15
GUIDELINEs ON UROLOGICAL TRAUMA (Text update March 2009) N. Djakovic, Th. Lynch, L. Martínez-Piñeiro, Y. Mor, E. Plas, E. Serafetinides, L. Turkeri, R.A. Santucci, M. Hohenfellner Eur Urol 2005;47(1):1-15
Surgery of urogenital trauma in condition of war or precarity
 Surgery of urogenital trauma in condition of war or precarity C. H. Rochat Multi-disciplinary Center for Robotic Surgery, Geneva (www.beaulieu.ch) Geneva Foundation for Medical Education and Research (www.gfmer.ch)
Surgery of urogenital trauma in condition of war or precarity C. H. Rochat Multi-disciplinary Center for Robotic Surgery, Geneva (www.beaulieu.ch) Geneva Foundation for Medical Education and Research (www.gfmer.ch)
Urethral Injuries: Realignment vs. Delayed Reconstruction
 Urethral Injuries: Realignment vs. Delayed Reconstruction E. Charles Osterberg, MD Assistant Professor of Surgery (Urology) Dell Medical School Chief of Urology and Genitourinary Reconstruction None Disclosures
Urethral Injuries: Realignment vs. Delayed Reconstruction E. Charles Osterberg, MD Assistant Professor of Surgery (Urology) Dell Medical School Chief of Urology and Genitourinary Reconstruction None Disclosures
Urogenital Injury. Kuncoro Adi, SpU (K) Trauma and Reconstructive Urology AMC Hasan Sadikin Hospital The 8 th Annual Acute Care Surgery Bandung
 Urogenital Injury Kuncoro Adi, SpU (K) Trauma and Reconstructive Urology AMC Hasan Sadikin Hospital The 8 th Annual Acute Care Surgery Bandung - 2018 @kuncoro202 Email: kuncoro202@gmail.com No - Disclosure
Urogenital Injury Kuncoro Adi, SpU (K) Trauma and Reconstructive Urology AMC Hasan Sadikin Hospital The 8 th Annual Acute Care Surgery Bandung - 2018 @kuncoro202 Email: kuncoro202@gmail.com No - Disclosure
Operative Management of Wartime Genitourinary Injuries at Balad Air Force Theater Hospital, 2005 to 2008
 Operative Management of Wartime Genitourinary Injuries at Balad Air Force Theater Hospital, 2005 to 2008 Steven J. Hudak and Samuel Hakim* From the Urology Service, Department of Surgery, Brooke Army Medical
Operative Management of Wartime Genitourinary Injuries at Balad Air Force Theater Hospital, 2005 to 2008 Steven J. Hudak and Samuel Hakim* From the Urology Service, Department of Surgery, Brooke Army Medical
Pelvic Injuries. Chapter 21
 Chapter 21 Introduction Injuries of the pelvis are an uncommon, but potentially lethal, battlefield injury. Blunt injuries may be associated with major hemorrhage and early mortality. Death within the
Chapter 21 Introduction Injuries of the pelvis are an uncommon, but potentially lethal, battlefield injury. Blunt injuries may be associated with major hemorrhage and early mortality. Death within the
Uroradiology For Medical Students
 Uroradiology For Medical Students Lesson 4: Cystography & Urethrography - Part 2 American Urological Association Review Cystography is useful in evaluating the bladder, the urethra and the competence of
Uroradiology For Medical Students Lesson 4: Cystography & Urethrography - Part 2 American Urological Association Review Cystography is useful in evaluating the bladder, the urethra and the competence of
Muscle spasm Diminished bowel sounds Nausea/vomiting
 3 4 5 6 7 8 9 0 Chapter 8: Abdomen and Genitalia Injuries Abdominal Injuries Abdomen is major body cavity extending from to pelvis. Contains organs that make up digestive, urinary, and genitourinary systems.
3 4 5 6 7 8 9 0 Chapter 8: Abdomen and Genitalia Injuries Abdominal Injuries Abdomen is major body cavity extending from to pelvis. Contains organs that make up digestive, urinary, and genitourinary systems.
2. Blunt abdominal Trauma
 Abdominal Trauma 1. Evaluation and management depends on: a. Mechanism (Blunt versus Penetrating) b. Injury complex in addition to abdomen c. Haemodynamic stability assessment: i. Classically patient s
Abdominal Trauma 1. Evaluation and management depends on: a. Mechanism (Blunt versus Penetrating) b. Injury complex in addition to abdomen c. Haemodynamic stability assessment: i. Classically patient s
Center for Reconstructive Urethral Surgery Guido Barbagli Center for Reconstructive Urethral Surgery Arezzo - Italy
 Guido Barbagli Arezzo - Italy E-mail: guido@rdn.it Website: www.urethralcenter.it 23 rd ANNUAL EAU CONGRESS Sub-plenary Session on Male urinary incontinence 26 29 March 2008 Milan Italy Incontinence following
Guido Barbagli Arezzo - Italy E-mail: guido@rdn.it Website: www.urethralcenter.it 23 rd ANNUAL EAU CONGRESS Sub-plenary Session on Male urinary incontinence 26 29 March 2008 Milan Italy Incontinence following
Abdomen and Genitalia Injuries. Chapter 28
 Abdomen and Genitalia Injuries Chapter 28 Hollow Organs in the Abdominal Cavity Signs of Peritonitis Abdominal pain Tenderness Muscle spasm Diminished bowel sounds Nausea/vomiting Distention Solid Organs
Abdomen and Genitalia Injuries Chapter 28 Hollow Organs in the Abdominal Cavity Signs of Peritonitis Abdominal pain Tenderness Muscle spasm Diminished bowel sounds Nausea/vomiting Distention Solid Organs
Sara Schaenzer Grand Rounds January 24 th, 2018
 Sara Schaenzer Grand Rounds January 24 th, 2018 Bladder Anatomy Ureter Anatomy Areas of Injury Bladder: Posterior bladder wall above trigone Ureter Crosses beneath uterine vessels At pelvic brim when ligating
Sara Schaenzer Grand Rounds January 24 th, 2018 Bladder Anatomy Ureter Anatomy Areas of Injury Bladder: Posterior bladder wall above trigone Ureter Crosses beneath uterine vessels At pelvic brim when ligating
Contributors. LtCol Wade Gordon, MC, USAF CDR Luke Balsamo, MC, USN LtCol Max Talbot, RCMS, CF LCDR Charles Osier, MC, USN
 JOINT TRAUMA SYSTEM CLINICAL PRACTIC E GUIDELINE (JTS CPG ) Amputation: Evaluation and Treatment (CPG 07) To provide standardization of optimal care for the performance of wound management and life-saving
JOINT TRAUMA SYSTEM CLINICAL PRACTIC E GUIDELINE (JTS CPG ) Amputation: Evaluation and Treatment (CPG 07) To provide standardization of optimal care for the performance of wound management and life-saving
Guido Barbagli. Center for Reconstructive ti Urethral lsurgery
 Guido Barbagli Center for Reconstructive ti Urethral lsurgery Arezzo - Italy E-mail: guido@rdn.it Website: www.urethralcenter.it Dedicated to Ruggero Lenzi, teacher and friend. His passing was a great
Guido Barbagli Center for Reconstructive ti Urethral lsurgery Arezzo - Italy E-mail: guido@rdn.it Website: www.urethralcenter.it Dedicated to Ruggero Lenzi, teacher and friend. His passing was a great
Guidelines on Urological Trauma
 Guidelines on Urological Trauma D. Lynch, L. Martinez-Piñeiro, E. Plas, E. Serafetinidis, L. Turkeri, R. Santucci, M. Hohenfellner European Association of Urology 2006 TABLE OF CONTENTS PAGE 1. RENAL TRAUMA
Guidelines on Urological Trauma D. Lynch, L. Martinez-Piñeiro, E. Plas, E. Serafetinidis, L. Turkeri, R. Santucci, M. Hohenfellner European Association of Urology 2006 TABLE OF CONTENTS PAGE 1. RENAL TRAUMA
Repair of Bulbar Urethra Using the Barbagli Technique
 22 Repair of Bulbar Urethra Using the Barbagli Technique G. Barbagli, M. Lazzeri 22.1 Introduction and Historical Background 182 22.2 Anatomical Remarks 182 22.3 Step-by-Step Surgical Details 183 22.3.1
22 Repair of Bulbar Urethra Using the Barbagli Technique G. Barbagli, M. Lazzeri 22.1 Introduction and Historical Background 182 22.2 Anatomical Remarks 182 22.3 Step-by-Step Surgical Details 183 22.3.1
Pelvic Fracture Care (CPG ID: 34) Provides a brief review for the stabilization and treatment of pelvic fractures sustained in combat casualties.
 JOINT TRAUMA SYS TEM CLINICAL PRACTIC E GUIDELINE (JTS CPG ) Pelvic Fracture Care (CPG ID: 34) Provides a brief review for the stabilization and treatment of pelvic fractures sustained in combat casualties.
JOINT TRAUMA SYS TEM CLINICAL PRACTIC E GUIDELINE (JTS CPG ) Pelvic Fracture Care (CPG ID: 34) Provides a brief review for the stabilization and treatment of pelvic fractures sustained in combat casualties.
Bladder & Urethral Trauma. Bohyun Kim Professor of Radiology Mayo Clinic College of Medicine
 Bladder & Urethral Trauma Bohyun Kim Professor of Radiology Mayo Clinic College of Medicine Disclosure None Acknowledgement Akira Kawashima, Mayo Clinic Scottsdale, AZ Eric Lantz, Mayo Clinic Rochester,
Bladder & Urethral Trauma Bohyun Kim Professor of Radiology Mayo Clinic College of Medicine Disclosure None Acknowledgement Akira Kawashima, Mayo Clinic Scottsdale, AZ Eric Lantz, Mayo Clinic Rochester,
Injuries to the Hands and Feet
 Injuries to the Hands and Feet Chapter 26 Injuries to the Hands and Feet Introduction Combat injuries to the hands and feet differ from those of the arms and legs in terms of mortality and morbidity. Death
Injuries to the Hands and Feet Chapter 26 Injuries to the Hands and Feet Introduction Combat injuries to the hands and feet differ from those of the arms and legs in terms of mortality and morbidity. Death
Genitourinary Tract Trauma. Wen-xuan Chen Department of urology Tianjin medical university General hospital
 Genitourinary Tract Trauma Wen-xuan Chen Department of urology Tianjin medical university General hospital Introduction About 10% of all injuries in the emergency room are genitourinary injuries. The most
Genitourinary Tract Trauma Wen-xuan Chen Department of urology Tianjin medical university General hospital Introduction About 10% of all injuries in the emergency room are genitourinary injuries. The most
FIG The inferior and posterior peritoneal reflection is easily
 PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
THE USE OF DEEPITHELIALIZATION
 THE USE OF DEEPITHELIALIZATION IN URETHROPLASTY - Deepithelialization Stratum corneum - Epidermis Papillary dermis Reticular dermis Skin Healing in any reconstructive surgery depends on not only the intact
THE USE OF DEEPITHELIALIZATION IN URETHROPLASTY - Deepithelialization Stratum corneum - Epidermis Papillary dermis Reticular dermis Skin Healing in any reconstructive surgery depends on not only the intact
Guidelines and Protocols
 TITLE: PELVIC TRAUMA PURPOSE: Develop a protocol of care that will insure rapid identification and treatment of these patients PROCESS: I. CARE OF PATIENTS WITH PELVIC TRAUMA A. Patients in hemorrhagic
TITLE: PELVIC TRAUMA PURPOSE: Develop a protocol of care that will insure rapid identification and treatment of these patients PROCESS: I. CARE OF PATIENTS WITH PELVIC TRAUMA A. Patients in hemorrhagic
11 Genitourinary Trauma and Emergencies
 Página 1 de 26 11 Genitourinary Trauma and Emergencies Meir Daller Gennaro Carpinito A urologic emergency arises when a condition requires rapid diagnosis and immediate treatment. This chapter focuses
Página 1 de 26 11 Genitourinary Trauma and Emergencies Meir Daller Gennaro Carpinito A urologic emergency arises when a condition requires rapid diagnosis and immediate treatment. This chapter focuses
ISPUB.COM. Traumatic Uretero-Pelvic Junction Disruption. G Kraushaar, S Harder, K Visvanathan INTRODUCTION CASE REPORT
 ISPUB.COM The Internet Journal of Radiology Volume 4 Number 1 Traumatic Uretero-Pelvic Junction Disruption G Kraushaar, S Harder, K Visvanathan Citation G Kraushaar, S Harder, K Visvanathan. Traumatic
ISPUB.COM The Internet Journal of Radiology Volume 4 Number 1 Traumatic Uretero-Pelvic Junction Disruption G Kraushaar, S Harder, K Visvanathan Citation G Kraushaar, S Harder, K Visvanathan. Traumatic
Amputations. Chapter 23
 Amputations Chapter 23 Amputations Introduction Battle casualties who sustain amputations have the most severe extremity injuries. Historically, 1 in 3 patients with a major amputation (proximal to the
Amputations Chapter 23 Amputations Introduction Battle casualties who sustain amputations have the most severe extremity injuries. Historically, 1 in 3 patients with a major amputation (proximal to the
Contributors. LCDR Charles Osier, MC, USN LCDR Chris Smith, MC, USN MAJ Daniel Stinner, MC, USA MAJ Jessica Rivera, MC, USA
 JOINT TRAUMA SYSTEM CLINICAL PRACTIC E GUIDELINE (JTS CPG ) Orthopaedic Trauma: Extremity Fractures (CPG ID: 56) To describe the initial non-surgical and surgical management of extremity fractures and
JOINT TRAUMA SYSTEM CLINICAL PRACTIC E GUIDELINE (JTS CPG ) Orthopaedic Trauma: Extremity Fractures (CPG ID: 56) To describe the initial non-surgical and surgical management of extremity fractures and
Joint Theater Trauma System Clinical Practice Guideline
 Page 1 of 7 Joint Theater Trauma System Clinical Practice Guideline TRAUMA AIRWAY MANAGEMENT Original Release/Approval 18 Dec 2004 Note: This CPG requires an annual review. Reviewed: May 2012 Approved:
Page 1 of 7 Joint Theater Trauma System Clinical Practice Guideline TRAUMA AIRWAY MANAGEMENT Original Release/Approval 18 Dec 2004 Note: This CPG requires an annual review. Reviewed: May 2012 Approved:
Role of Imaging in the evaluation of Renal Trauma
 Role of Imaging in the evaluation of Renal Trauma M. H. Ather,M.A. Noor ( Department of Surgery, The Aga Khan University, Karachi. ) Trauma is the leading cause of morbidity and mortality among young adults
Role of Imaging in the evaluation of Renal Trauma M. H. Ather,M.A. Noor ( Department of Surgery, The Aga Khan University, Karachi. ) Trauma is the leading cause of morbidity and mortality among young adults
Contributors T A B L E O F C O N T E N T S
 JOINT TRAUMA SYS TEM CLINICAL PRACTIC E GUIDELINE (JTS CPG ) High Bilateral Amputations and Dismounted Complex Blast Injury (CPG ID: 22) To review indications for and the procedures associated with the
JOINT TRAUMA SYS TEM CLINICAL PRACTIC E GUIDELINE (JTS CPG ) High Bilateral Amputations and Dismounted Complex Blast Injury (CPG ID: 22) To review indications for and the procedures associated with the
ORIGINAL ARTICLE. Complications Following Renal Trauma
 ORIGINAL ARTICLE Complications Following Renal Trauma Margaret Starnes, MD; Demetrios Demetriades, MD, PhD; Pantelis Hadjizacharia, MD; Kenji Inaba, MD; Charles Best, MD; Linda Chan, PhD Objectives: To
ORIGINAL ARTICLE Complications Following Renal Trauma Margaret Starnes, MD; Demetrios Demetriades, MD, PhD; Pantelis Hadjizacharia, MD; Kenji Inaba, MD; Charles Best, MD; Linda Chan, PhD Objectives: To
Conservative Management of Renal Trauma: Ten Years Experience Reem Al-Bareeq MRCSI, CABU* Kadem Zabar CABS** Mohammed Al-Tantawi CABS***
 Bahrain Medical Bulletin, Vol. 28, No. 3, September 2006 Conservative Management of Renal Trauma: Ten Years Experience Reem Al-Bareeq MRCSI, CABU* Kadem Zabar CABS** Mohammed Al-Tantawi CABS*** Objective:
Bahrain Medical Bulletin, Vol. 28, No. 3, September 2006 Conservative Management of Renal Trauma: Ten Years Experience Reem Al-Bareeq MRCSI, CABU* Kadem Zabar CABS** Mohammed Al-Tantawi CABS*** Objective:
3. Urinary Catheters. Indications. Methods of Bladder Catheterization. Hashim Hashim
 3. Urinary Catheters Hashim Hashim Indications Urinary catheters are used to drain urine from the bladder. The main indications are: A. Diagnostic Measure post-void residual in the absence of ultrasound
3. Urinary Catheters Hashim Hashim Indications Urinary catheters are used to drain urine from the bladder. The main indications are: A. Diagnostic Measure post-void residual in the absence of ultrasound
Guidelines on Urological Trauma
 Guidelines on Urological Trauma N. Djakovic, E. Plas, L. Martínez-Piñeiro, Th. Lynch, Y. Mor, R.A. Santucci, E. Serafetinidis, L.N. Turkeri, M. Hohenfellner European Association of Urology 2012 TABLE OF
Guidelines on Urological Trauma N. Djakovic, E. Plas, L. Martínez-Piñeiro, Th. Lynch, Y. Mor, R.A. Santucci, E. Serafetinidis, L.N. Turkeri, M. Hohenfellner European Association of Urology 2012 TABLE OF
CHAPTER 10 PENILE INJURIES
 PENILE INJURIES 175 CHAPTER 10 PENILE INJURIES GU Tract Ch 2 Ch 3 Ch 4,5 Ch 6,7,8,11 Ch 8,9 Ch 8,9 Ch 8,10 Structure Kidney Ureter Bladder Urethra Scrotum Spermatic Penis Testis Cord No. Patients 132 36
PENILE INJURIES 175 CHAPTER 10 PENILE INJURIES GU Tract Ch 2 Ch 3 Ch 4,5 Ch 6,7,8,11 Ch 8,9 Ch 8,9 Ch 8,10 Structure Kidney Ureter Bladder Urethra Scrotum Spermatic Penis Testis Cord No. Patients 132 36
Procedure related complications and how to prevent them
 Procedure related complications and how to prevent them Rama Jayanthi, M.D. Section of Urology Nationwide Children s Hospital The Ohio State University Retroperitoneoscopic surgery Inadvertent peritoneal
Procedure related complications and how to prevent them Rama Jayanthi, M.D. Section of Urology Nationwide Children s Hospital The Ohio State University Retroperitoneoscopic surgery Inadvertent peritoneal
Urethral Stricture Management. AUA Guidelines. Michael Coburn, MD Scott Department of Urology Baylor College of Medicine Houston, Texas
 Urethral Stricture Management AUA Guidelines Michael Coburn, MD Scott Department of Urology Baylor College of Medicine Houston, Texas Urethral Stricture Guidelines Systematic peer-reviewed literature review
Urethral Stricture Management AUA Guidelines Michael Coburn, MD Scott Department of Urology Baylor College of Medicine Houston, Texas Urethral Stricture Guidelines Systematic peer-reviewed literature review
Guido Barbagli. Center for Reconstructive ti Urethral lsurgery
 Guido Barbagli Center for Reconstructive ti Urethral lsurgery Arezzo - Italy E-mail: guido@rdn.it Website: www.urethralcenter.it Portuguese Andrological Association National Meeting June 21-23, 2008 Oporto
Guido Barbagli Center for Reconstructive ti Urethral lsurgery Arezzo - Italy E-mail: guido@rdn.it Website: www.urethralcenter.it Portuguese Andrological Association National Meeting June 21-23, 2008 Oporto
Hemorrhage Control. Chapter 6
 Chapter 6 The hemorrhage that take[s] place when a main artery is divided is usually so rapid and so copious that the wounded man dies before help can reach him. Colonel H. M. Gray, 1919 Stop the Bleeding!
Chapter 6 The hemorrhage that take[s] place when a main artery is divided is usually so rapid and so copious that the wounded man dies before help can reach him. Colonel H. M. Gray, 1919 Stop the Bleeding!
Medical - Clinical Research & Reviews
 Research Article Research Article Medical - Clinical Research & Reviews ISSN 2575-6087 Management of Kidney in Saiful Anwar General Hospital Malang Indonesia Besut Daryanto, I Made Udiyana Indradiputra,
Research Article Research Article Medical - Clinical Research & Reviews ISSN 2575-6087 Management of Kidney in Saiful Anwar General Hospital Malang Indonesia Besut Daryanto, I Made Udiyana Indradiputra,
Algorithms for managing the common trauma patient
 ALGORITHMS Algorithms for managing the common trauma patient J John, MB ChB Department of Urology, Frere Hospital, East London Hospital Complex, East London, South Africa Corresponding author: J John (jeffveenajohn@gmail.com)
ALGORITHMS Algorithms for managing the common trauma patient J John, MB ChB Department of Urology, Frere Hospital, East London Hospital Complex, East London, South Africa Corresponding author: J John (jeffveenajohn@gmail.com)
Management of Blunt Renal Trauma in Srinagarind Hospital: 10-Year Experience
 Management of Blunt Renal Trauma in Srinagarind Hospital: 10-Year Experience Chaiyut Thanapaisal MD*, Wichien Sirithanaphol MD* * Department of Surgery, Faculty of Medicine, Khon Kaen University, Khon
Management of Blunt Renal Trauma in Srinagarind Hospital: 10-Year Experience Chaiyut Thanapaisal MD*, Wichien Sirithanaphol MD* * Department of Surgery, Faculty of Medicine, Khon Kaen University, Khon
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 9 Urinary Tract and Perineum Key Points 2 9.1 Urinary Bladder & Urinary Retention Acute retention of urine is an indication for emergency drainage of the bladder
Surgical Care at the District Hospital 1 9 Urinary Tract and Perineum Key Points 2 9.1 Urinary Bladder & Urinary Retention Acute retention of urine is an indication for emergency drainage of the bladder
Dr. Syah Mirsya Warli, SpU Dr. Bungaran Sihombing,SpU Div. of Urology, Surgery Dept. Medical Faculty, University of Sumatera Utara
 Emergency Room Urology Dr. Syah Mirsya Warli, SpU Dr. Bungaran Sihombing,SpU Div. of Urology, Surgery Dept. Medical Faculty, University of Sumatera Utara Ref : Clinical Manual of Urology, (Philip M. Hanno
Emergency Room Urology Dr. Syah Mirsya Warli, SpU Dr. Bungaran Sihombing,SpU Div. of Urology, Surgery Dept. Medical Faculty, University of Sumatera Utara Ref : Clinical Manual of Urology, (Philip M. Hanno
Management of High-grade Blunt Renal Trauma
 ORIGINAL ARTICLE J Trauma Inj 2017;30(4):192-196 http://doi.org/10.20408/jti.2017.30.4.192 JOURNAL OF TRAUMA AND INJURY Management of High-grade Blunt Renal Trauma Min A Lee, M.D., Myung Jin Jang, M.S.,
ORIGINAL ARTICLE J Trauma Inj 2017;30(4):192-196 http://doi.org/10.20408/jti.2017.30.4.192 JOURNAL OF TRAUMA AND INJURY Management of High-grade Blunt Renal Trauma Min A Lee, M.D., Myung Jin Jang, M.S.,
PENETRATING COLON TRAUMA: THE CURRENT EVIDENCE
 PENETRATING COLON TRAUMA: THE CURRENT EVIDENCE Samuel Hawkins MD CASE PRESENTATION 22M BIBEMS s/p multiple GSW ABCs intact Normotensive, non-tachycardic Secondary Survey: 4 truncal bullet holes L superior
PENETRATING COLON TRAUMA: THE CURRENT EVIDENCE Samuel Hawkins MD CASE PRESENTATION 22M BIBEMS s/p multiple GSW ABCs intact Normotensive, non-tachycardic Secondary Survey: 4 truncal bullet holes L superior
LIVER INJURIES PROFF. S.FLORET
 LIVER INJURIES PROFF. S.FLORET Abdominal injuries For anatomical consideration: Abdomen can be divided in four areas Intra thoracic abdomen True abdomen Pelvic abdomen Retroperitoneal abdomen ETIOLOGY
LIVER INJURIES PROFF. S.FLORET Abdominal injuries For anatomical consideration: Abdomen can be divided in four areas Intra thoracic abdomen True abdomen Pelvic abdomen Retroperitoneal abdomen ETIOLOGY
Delayed Presentation of Traumatic Bladder Injury: A case report and review of current treatment trends
 ISPUB.COM The Internet Journal of Urology Volume 5 Number 1 Delayed Presentation of Traumatic Bladder Injury: A case report and review of current treatment trends S Deem, C Lavender, S Agarwal Citation
ISPUB.COM The Internet Journal of Urology Volume 5 Number 1 Delayed Presentation of Traumatic Bladder Injury: A case report and review of current treatment trends S Deem, C Lavender, S Agarwal Citation
Decision-Making in the Acute Management of Blunt and Penetrating Wounds Mary Somerville, DVM, DACVS
 Decision-Making in the Acute Management of Blunt and Penetrating Wounds Mary Somerville, DVM, DACVS Providing the best quality care and service for the patient, the client, and the referring veterinarian.
Decision-Making in the Acute Management of Blunt and Penetrating Wounds Mary Somerville, DVM, DACVS Providing the best quality care and service for the patient, the client, and the referring veterinarian.
RECTAL INJURY IN UROLOGIC SURGERY. Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences.
 RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
Joint Theater Trauma System Clinical Practice Guideline
 CERVICAL SPINE EVALUATION & N-SURGICAL MANAGEMENT Original Release/Approval: 1 March 2010 Note: This CPG requires an annual review Reviewed: Feb 2012 Approved: 19 Mar 2012 Supersedes: Cervical Spine Evaluation,
CERVICAL SPINE EVALUATION & N-SURGICAL MANAGEMENT Original Release/Approval: 1 March 2010 Note: This CPG requires an annual review Reviewed: Feb 2012 Approved: 19 Mar 2012 Supersedes: Cervical Spine Evaluation,
Damage Control in Abdominal and Pelvic Injuries
 Damage Control in Abdominal and Pelvic Injuries Raul Coimbra, MD, PhD, FACS The Monroe E. Trout Professor of Surgery Surgeon-in Chief UCSD Medical Center Hillcrest Campus Executive Vice-Chairman Department
Damage Control in Abdominal and Pelvic Injuries Raul Coimbra, MD, PhD, FACS The Monroe E. Trout Professor of Surgery Surgeon-in Chief UCSD Medical Center Hillcrest Campus Executive Vice-Chairman Department
Pediatric Abdomen Trauma
 Pediatric Abdomen Trauma Susan D. John, MD, FACR Pediatric Trauma Trauma is leading cause of death and disability in children and adolescents Causes and effects vary between age groups Blunt trauma predominates
Pediatric Abdomen Trauma Susan D. John, MD, FACR Pediatric Trauma Trauma is leading cause of death and disability in children and adolescents Causes and effects vary between age groups Blunt trauma predominates
SURGERY FOR PEYRONIE S DISEASE. PEYRONIE S DISEASE WITHOUT IMPOTENCE Exposure and Mobilization of Dorsal Nerves and Vessels
 SURGERY FOR 25 PEYRONIE S DISEASE PEYRONIE S DISEASE WITHOUT Exposure and Mobilization of Dorsal Nerves and Vessels FIG. 25-1. Most surgeons use a degloving procedure via a circumferential skin incision
SURGERY FOR 25 PEYRONIE S DISEASE PEYRONIE S DISEASE WITHOUT Exposure and Mobilization of Dorsal Nerves and Vessels FIG. 25-1. Most surgeons use a degloving procedure via a circumferential skin incision
We have reviewed this material in accordance with U.S. Copyright Law and have tried to maximize your ability to
 Author(s): Patrick Carter, Daniel Wachter, Rockefeller Oteng, Carl Seger, 2009-2010. License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution
Author(s): Patrick Carter, Daniel Wachter, Rockefeller Oteng, Carl Seger, 2009-2010. License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution
Coding Companion for Urology/Nephrology. A comprehensive illustrated guide to coding and reimbursement
 Coding Companion for Urology/Nephrology A comprehensive illustrated guide to coding and reimbursement 2014 Contents Getting Started with Coding Companion...i Integumentary...1 Arteries and Veins...15 Lymph
Coding Companion for Urology/Nephrology A comprehensive illustrated guide to coding and reimbursement 2014 Contents Getting Started with Coding Companion...i Integumentary...1 Arteries and Veins...15 Lymph
Guideline of guidelines: a review of urological trauma guidelines
 Guideline of guidelines: a review of urological trauma guidelines Darren J. Bryk and Lee C. Zhao Department of Urology, NYU School of Medicine, New York, NY, USA [Corrections added after initial acceptance
Guideline of guidelines: a review of urological trauma guidelines Darren J. Bryk and Lee C. Zhao Department of Urology, NYU School of Medicine, New York, NY, USA [Corrections added after initial acceptance
Traumatic Renocaval Fistula With Pseudoaneurysm Leading To Renal Atrophy
 ISPUB.COM The Internet Journal of Radiology Volume 6 Number 2 Traumatic Renocaval Fistula With Pseudoaneurysm Leading To Renal Atrophy M Kukkady, A Deena, S Raj, Ramachandra Citation M Kukkady, A Deena,
ISPUB.COM The Internet Journal of Radiology Volume 6 Number 2 Traumatic Renocaval Fistula With Pseudoaneurysm Leading To Renal Atrophy M Kukkady, A Deena, S Raj, Ramachandra Citation M Kukkady, A Deena,
Combat Extremity Vascular Trauma
 Combat Extremity Vascular Trauma Training teams to be a TEAM Chatt A. Johnson LTC, MC, USA 08 March 2010 US Army Trauma Training Center Core Discussion Series Outline: Combat Vascular Injury Physiologic
Combat Extremity Vascular Trauma Training teams to be a TEAM Chatt A. Johnson LTC, MC, USA 08 March 2010 US Army Trauma Training Center Core Discussion Series Outline: Combat Vascular Injury Physiologic
Case Report Delayed Presentation of Traumatic Intraperitoneal Rupture of Urinary Bladder
 Case Reports in Urology Volume 2012, Article ID 430746, 4 pages doi:10.1155/2012/430746 Case Report Delayed Presentation of Traumatic Intraperitoneal Rupture of Urinary Bladder Hazim H. Alhamzawi, 1 Husham
Case Reports in Urology Volume 2012, Article ID 430746, 4 pages doi:10.1155/2012/430746 Case Report Delayed Presentation of Traumatic Intraperitoneal Rupture of Urinary Bladder Hazim H. Alhamzawi, 1 Husham
Uroradiology Tutorial For Medical Students
 Uroradiology Tutorial For Medical Students Lesson 3: Cystography & Urethrography Part 1 American Urological Association Introduction Conventional radiography of the urinary tract includes several diagnostic
Uroradiology Tutorial For Medical Students Lesson 3: Cystography & Urethrography Part 1 American Urological Association Introduction Conventional radiography of the urinary tract includes several diagnostic
COMPLEX RECONSTRUCTIONS IN HYPOSPADIAS: - - P
 COMPLEX RECONSTRUCTIONS IN HYPOSPADIAS: - Penile straightening - Penile lengthening - Glans and penile skin resurfacing Rados P. Djinovic, Belgrade Growing number of adult patients Majority had multiple
COMPLEX RECONSTRUCTIONS IN HYPOSPADIAS: - Penile straightening - Penile lengthening - Glans and penile skin resurfacing Rados P. Djinovic, Belgrade Growing number of adult patients Majority had multiple
THE operation of reimplantation of the ureter into the bladder has undergone
 REIMPLANTATION OF THE URETER INTO THE BLADDER J. G. WARDEN, M.D., and C. C. HIGGINS, M.D. Department of Urology THE operation of reimplantation of the ureter into the bladder has undergone a stormy course
REIMPLANTATION OF THE URETER INTO THE BLADDER J. G. WARDEN, M.D., and C. C. HIGGINS, M.D. Department of Urology THE operation of reimplantation of the ureter into the bladder has undergone a stormy course
Acute Groin Pain Following Trauma
 Lehigh Valley Health Network LVHN Scholarly Works Department of Family Medicine Acute Groin Pain Following Trauma Victoria Chen MD Lehigh Valley Health Network, victoria.chen@lvhn.org Follow this and additional
Lehigh Valley Health Network LVHN Scholarly Works Department of Family Medicine Acute Groin Pain Following Trauma Victoria Chen MD Lehigh Valley Health Network, victoria.chen@lvhn.org Follow this and additional
Surgical management of the undescended testis is performed
 Undescended Testes/Orchiopexy James C.Y. Dunn, MD, PhD, 1 Akemi L. Kawaguchi, MD, 2 and Eric W. Fonkalsrud, MD 1 Surgical management of the undescended testis is performed to prevent the potential complications
Undescended Testes/Orchiopexy James C.Y. Dunn, MD, PhD, 1 Akemi L. Kawaguchi, MD, 2 and Eric W. Fonkalsrud, MD 1 Surgical management of the undescended testis is performed to prevent the potential complications
Genitourinary. Common Clinical Scenarios Protocoling Module. Patty Ojeda & Mariam Shehata
 The following training module was developed as a quality improvement project to serve as an educational tool for junior radiology residents. The following diagnostic radiology protocoling modules were
The following training module was developed as a quality improvement project to serve as an educational tool for junior radiology residents. The following diagnostic radiology protocoling modules were
Male External Genital Injuries; Pattern of Presentation and Management at the Jos University Teaching Hospital
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 10 Ver. IV (Oct. 2014), PP 67-72 Male External Genital Injuries; Pattern of Presentation and
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 10 Ver. IV (Oct. 2014), PP 67-72 Male External Genital Injuries; Pattern of Presentation and
Morbidity Audit and Logbook Tool SNOMED Board Reporting Terms for SET and IMG Urology ENDOSCOPIC LOWER URINARY TRACT
 ENDOSCOPIC LOWER URINARY TRACT Cystolitholapaxy Cystoscopic removal of foreign body from bladder Cystoscopic removal of ureteric stent Cystoscopy and cystodiathermy Cystoscopy and transurethral biopsy
ENDOSCOPIC LOWER URINARY TRACT Cystolitholapaxy Cystoscopic removal of foreign body from bladder Cystoscopic removal of ureteric stent Cystoscopy and cystodiathermy Cystoscopy and transurethral biopsy
DISSECTION 8: URINARY AND REPRODUCTIVE SYSTEMS
 8546d_c01_1-42 6/25/02 4:32 PM Page 38 mac48 Mac 48: 420_kec: 38 Cat Dissection DISSECTION 8: URINARY AND REPRODUCTIVE SYSTEMS Typically, the urinary and reproductive systems are studied together, because
8546d_c01_1-42 6/25/02 4:32 PM Page 38 mac48 Mac 48: 420_kec: 38 Cat Dissection DISSECTION 8: URINARY AND REPRODUCTIVE SYSTEMS Typically, the urinary and reproductive systems are studied together, because
PROTOCOLS. Lap-belt syndrome. Principal investigator. Background
 Lap-belt syndrome Principal investigator Claude Cyr, MD, Centre hospitalier universitaire de Sherbrooke, 3001 12 e Avenue Nord, Sherbrooke QC J1H 5N4; tel.: (819) 346-1110, ext. 14634; fax: (819) 564-5398;
Lap-belt syndrome Principal investigator Claude Cyr, MD, Centre hospitalier universitaire de Sherbrooke, 3001 12 e Avenue Nord, Sherbrooke QC J1H 5N4; tel.: (819) 346-1110, ext. 14634; fax: (819) 564-5398;
SciFed Journal of Public Health. Endoscopic Management of Obstetrical Uretero-Uterine Fistula. Case Report and Review of Literature
 SciFed Journal of Public Health Case Report Open Access Endoscopic Management of Obstetrical Uretero-Uterine Fistula. Case Report and Review of Literature * Yasin Idweini * Chairperson of Urology Department
SciFed Journal of Public Health Case Report Open Access Endoscopic Management of Obstetrical Uretero-Uterine Fistula. Case Report and Review of Literature * Yasin Idweini * Chairperson of Urology Department
Japanese Neurogenic Bladder Society Meeting. Kofu - Japan. September 29th - October 1st, 2010
 Japanese Neurogenic Bladder Society Meeting Kofu - Japan September 29th - October 1st, 2010 Reconstruction of penile and bulbar urethra Evaluation of anterior urethral stricture Urethrography Retrograde
Japanese Neurogenic Bladder Society Meeting Kofu - Japan September 29th - October 1st, 2010 Reconstruction of penile and bulbar urethra Evaluation of anterior urethral stricture Urethrography Retrograde
DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis.
 DISCHARGE SUMMARY DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis. OPERATIONS/PROCEDURES: Living related renal transplantation. HISTORY: For full details
DISCHARGE SUMMARY DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis. OPERATIONS/PROCEDURES: Living related renal transplantation. HISTORY: For full details
ANATOMY OF PELVICAYCEAL SYSTEM -DR. RAHUL BEVARA
 1 ANATOMY OF PELVICAYCEAL SYSTEM -DR. RAHUL BEVARA 2 KIDNEY:ANATOMY OVERVIEW Kidneys are retroperitoneal, in posterior abdominal region, extending from T12 L3 Bean-shaped Right kidney is lower than left
1 ANATOMY OF PELVICAYCEAL SYSTEM -DR. RAHUL BEVARA 2 KIDNEY:ANATOMY OVERVIEW Kidneys are retroperitoneal, in posterior abdominal region, extending from T12 L3 Bean-shaped Right kidney is lower than left
MALE GENITAL SURGICAL PROCEDURES
 Male Genital Surgical ProceduresDecember 22, 2015 (effective March 1, 201) PENIS Slit of prepuce (complete care) S5 - newborn... 14.35 S58 - infant... 21.50 S59 - adult or child... 30.25 EXCISION Circumcision
Male Genital Surgical ProceduresDecember 22, 2015 (effective March 1, 201) PENIS Slit of prepuce (complete care) S5 - newborn... 14.35 S58 - infant... 21.50 S59 - adult or child... 30.25 EXCISION Circumcision
Lecture 56 Kidney and Urinary System
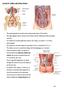 Lecture 56 Kidney and Urinary System The adrenal glands are located on the superomedial aspect of the kidney The right diagram shows a picture of the kidney with the abdominal walls and organs removed
Lecture 56 Kidney and Urinary System The adrenal glands are located on the superomedial aspect of the kidney The right diagram shows a picture of the kidney with the abdominal walls and organs removed
Staged urethroplasty in the management of complex anterior urethral stricture disease
 Review Article Staged urethroplasty in the management of complex anterior urethral stricture disease Ryan L. Mori 1, Kenneth W. Angermeier 2 1 Geisinger Medical Center, Danville, PA 17822, USA; 2 Center
Review Article Staged urethroplasty in the management of complex anterior urethral stricture disease Ryan L. Mori 1, Kenneth W. Angermeier 2 1 Geisinger Medical Center, Danville, PA 17822, USA; 2 Center
Management of Bleeding Pelvic Fractures
 Management of Bleeding Pelvic Fractures Clay Cothren Burlew, MD FACS Professor of Surgery Program Director, SCC and TACS Fellowships Director, Surgical Intensive Care Unit Denver Health Medical Center/University
Management of Bleeding Pelvic Fractures Clay Cothren Burlew, MD FACS Professor of Surgery Program Director, SCC and TACS Fellowships Director, Surgical Intensive Care Unit Denver Health Medical Center/University
The number following the procedure code is the TRICARE payment group. KIDNEY
 TRICARE/CHAMPUS POLICY MANUAL 6010.47-M JUNE 25, 1999 S POLICY CHAPTER 13 SECTION 9.1 ADDENDUM 1, SECTION 8 TRICARE-APPROVED AMBULATORY SURGERY S - URINARY SYSTEM The number following the procedure code
TRICARE/CHAMPUS POLICY MANUAL 6010.47-M JUNE 25, 1999 S POLICY CHAPTER 13 SECTION 9.1 ADDENDUM 1, SECTION 8 TRICARE-APPROVED AMBULATORY SURGERY S - URINARY SYSTEM The number following the procedure code
Primary Realignment of Posterior Urethral Rupture
 Urology Journal UNRC/IUA Vol. 2, No. 4, 211-215 Autumn 2005 Printed in IRAN Mehdi Salehipour, Abdolaziz Khezri, Rashid Askari,* Parham Masoudi Department of Surgery, Division of Urology, Faghihi Hospital,
Urology Journal UNRC/IUA Vol. 2, No. 4, 211-215 Autumn 2005 Printed in IRAN Mehdi Salehipour, Abdolaziz Khezri, Rashid Askari,* Parham Masoudi Department of Surgery, Division of Urology, Faghihi Hospital,
