The importance of the gubernaculum in testicular migration during the human fetal period
|
|
|
- Kory Matthews
- 5 years ago
- Views:
Transcription
1 Review ARTICLE Vol. 40 (6): , November - December, 2014 doi: /S IBJU The importance of the gubernaculum in testicular migration during the human fetal period Luciano A. Favorito 1, Suelen F. Costa 1, Helce R. Julio-Junior 1, Francisco J. B. Sampaio 1 1 Urogenital Research Unit, State University of Rio de Janeiro, Brazil ABSTRACT Objectives: The objective of this review is to study the role of the gubernaculum in the testicular migration process during the human fetal period. Materials and Methods: We performed a descriptive review of the literature about the role of the gubernaculum in testicular migration during the human fetal period. Results: In the first phase of testicular migration, the gubernaculum enlarges to hold the testis near the groin and in the second phase the gubernaculum migrates across the pubic region to reach the scrotum. The proximal portion of the gubernaculum is attached to the testis and epididymis and the presence of multiple insertions in the distal gubernaculum is extremely rare. The presence of muscle and nerves in the human gubernaculum is very poor. The gubernaculum of patients with cryptorchidism has more fibrous tissue and less collagen and when the patients are submitted to hormonal treatment, the gubernaculum components alter significantly. Conclusions: The gubernaculum presents significant structural modifications during testicular migration in human fetuses. ARTICLE INFO Key words: Testicular Diseases; Cryptorchidism; Embryology; Fetus; Testis Int Braz J Urol. 2014; 40: Submitted for publication: June 20, 2014 Accepted after revision: October 31, 2014 INTRODUCTION Testicular migration is a complex process of relevant importance for the comprehension of cryptorchidism. During the human fetal period, the testes migrate from the abdomen to the scrotum, traversing the abdominal wall and the inguinal canal between the 15th and the 28th week post-conception (WPC) (1-4). Several theories have been developed to explain testicular migration. The most accepted ones are: (a) the increase in the intra-abdominal pressure (5); (b) the development of the epididymis, spermatic vessels, deferent ducts and inguinal canal (6-8); (c) the stimulus originating in the genito-femoral nerve (9); (d) the hormonal stimulus originating in the placental gonadotrophin and the testosterone produced by the fetal testes (10); and (e) the gubernaculum s development (1, 11). The gubernaculum seems to be the most important anatomical structure in the testicular migration process, by means of contraction and shortening, thus imposing traction strength on the testis (1). The objective of this review is to study the role of the gubernaculum in the process of testicular migration during the human fetal period. MATERIAL AND METHODS In this study we carried out a review of the Pubmed, Embase and Scielo databases about the role of the gubernaculum in testicular migration published in the past 40 years by using the key expressions gubernaculum testis and testicular migration. We found several papers in these databases and we included only papers 722
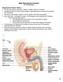
2 in English and excluded case reports, editorials and opinions of specialists. RESULTS Testicular migration happens in two distinct phases: the first phase corresponds to the testicular migration from the abdomen to the internal inguinal ring, and the second phase corresponds to the transition of the testes through the inguinal canal until their definitive arrival at the scrotum (1-3). In the first phase, the gubernaculum enlarges to hold the testes near the groin, regulated by insulin-like 3 (INLS-3) (12, 13). INSL-3 is secreted by the Leydig cells and controls gubernaculum swelling via its receptor, LGR8 (leucine-rich repeat containing G protein-coupled receptor 8, also known as GREAT or relaxin receptor 2), a process resulting in thickening of the gubernaculum because of increases in water, glycosaminoglycan and hyaluronic acid content (11-14) (Figure-1). In the second phase of testicular migration, the gubernaculum migrates across the pubic region to reach the scrotum. The androgens stimulate growth and differentiation of the muscular part of the gubernaculum bulb, which facilitates the movement of the gubernaculum through the inguinal region by the traction resulting from this growth (6, 12, 15, 16). The gubernaculum has its own nerve supply, the genito-femoral nerve (GFN), descending on the anteromedial surface of the psoas muscle from L1-L2 segments (17). The second phase of testicular descent is regulated by androgens and calcitonin gene-related peptide (CGRP), released by the sensory nucleus of the genitofemoral nerve (GFN) (10, 18). In rodents, the active proliferation of the gubernacular tip and cremaster muscle, the muscle s rhythmic contraction, and the chemotactic gradient provided by the CGRP together result in migration of the testes into the scrotum. The importance of this mechanism is corroborated by experimental models where the sectioning of the genitofemoral nerve leads to cryptorchidism (1, 15, 18). The moment when testicular migration begins is controversial. Backhouse (2) reported that Figure 1 - Image of a male fetus aged 22 weeks post-conception with both testes situated in the abdomen. The abdominal wall was dissected to show the position of the testis (T) above the internal ring (IR). The figure shows the gubernaculum (G) and the bladder (B). 723
3 this process starts at about the 24 th week post-conception, while Heyns (3) and Sampaio & Favorito (4) described cases where the migration process started as early as the 17 th week. An aspect that various authors report is that the passage of the testis through the inguinal canal occurs very quickly (2-4). Heyns (3) found only 2.6% of the testes examined in his sample located in the inguinal canal, while Sampaio & Favorito (4), in a sample of 71 human fetuses, found 20.5% of the testes located there. Furthermore, 73.3% of these testes were in fetuses with ages between 21 and 25 WPC, indicating that in this period the migration through the inguinal canal intensifies. In the same study, all the fetuses older than 30 weeks already showd the testes in the scrotum. Other authors, however, report that the testicular migration is only completed after the 32 nd week post-conception (1-3). Gubernaculum Testis The gubernaculum starts to develop in the human fetus during the sixth week of gestation, the same period when the germinative cells are arriving at the genital ridge (1, 19). In the eighth week of gestation, the testis and mesonephros are linked to the posterior abdomen wall by a peritoneal fold. As the mesonephros degenerates, the portion of this fold cranial to the testis, called the diaphragmatic ligament, also degenerates, turning into the cranial portion of the gonadal mesentery. This structure is called the caudal gonadal ligament, which gives rise to the gubernaculum testis (3, 19). Cranially, the gubernaculum approaches the mesonephric duct, while distally it approaches the inguinal region. At this moment, the future inguinal canal is still only a space in the musculature of the anterior abdominal wall, where only mesenchyme tissue exists. In this region, the genital branch of the genitofemoral nerve crosses the abdominal wall and descends to the scrotum where it will innervate the cremaster muscle, and subsequently, in the caudal to cranial direction, will provide the nerve supply to the gubernaculum (1, 2, 6, 19). Around the eight week of gestation, a portion of the epithelium starts a small invagination from the coelomic cavity, across from the gubernaculum, slowly penetrating its mesenchymal substance. This invagination occurs bilaterally and is considered as the start of the vaginal process. Some authors consider this phenomenon to be active, involving the invasion of the gubernaculum by mesothelial cells (19), while others advocate that this phenomenon is passive and secondary to the increase in intra-abdominal pressure (6, 20). The growth of the vaginal process divides the gubernaculum into three parts: (a) the main gubernaculum, which corresponds to the portion covered by the visceral layer of the peritoneum of the vaginal process; (b) the vaginal gubernaculum, which corresponds to the portion that externally surrounds the parietal portion of the vaginal process, and (c) the infra-vaginal gubernaculum, that corresponds to the caudal region of the gubernaculum, which has not been invaded by the vaginal process (19-21). Both the gubernaculum and vaginal process change in harmony during testicular migration. The maintenance of this undifferentiated mesenchyme along the inguinal canal and scrotum is essential for the downward extension of the vaginal process to occur, during which it follows the pathway created by dilation of the gubernaculum, forming the canal through which the testis will reach the scrotum (1, 2, 19, 21). The gubernaculum is a cylindrical structure, covered by a peritoneum on all sides except the posterior, where the testicular vessels and vas deferens pass. Macroscopically, it looks like the Wharton s jelly of the umbilical cord. Histologically, it is composed of undifferentiated cells with elongated shape, surrounded by a large quantity of extracellular material, where it is impossible to identify smooth or striated muscle cells except in its distal end and in the peripheral portion (22). Proximal Gubernaculum The proximal portion of the gubernaculum is adhered to the lower pole of the testis and to the epididymis. During testicular migration, these structures move through the inguinal canal as a single unit (2, 19, 23). According to Johansen & Bloom (24), in this situation the proximal gubernaculum is always adhered to the end of the vaginal 724
4 process. Jackson (25), studying 60 boys submitted to orchiopexy, found the gubernaculum adhered to the lower testicular pole in all cases, but did not mention its relationship with the epididymis. Other studies have shown that changes in the proximal insertion of the gubernaculum are associated with epididymal anomalies and can contribute to the occurrence or cryptorchidism (26). Attah & Hutson (6), in a study with rats, demonstrated the importance of the integrity of the proximal portion of the gubernaculum for proper testicular migration. The proximal portion is important by uniting the scrotal region and serves as a guide for testicular migration. In this experiment, the authors performed transection of the proximal gubernaculum. After this procedure, the testicular migration was only completed in 26 of the 70 rats (37%), and of these animals 24 showed testicular torsion. The results of this study indicate that the proximal gubernaculum is important both to guide testicular migration and to limit the mobility of the testes and prevent testicular torsion. Abe (27), in a study of 44 patients with cryptorchidism, found an elongated epididymis in 42.5% of the cases. Among the patients with elongated epididymis, alterations in the proximal gubernaculum were found in 73.9% of the cases. In other study of human fetuses, the authors found a low rate of epididymal anomalies (2.75%) (28). Distal Gubernaculum The insertion site of the gubernaculum during testicular migration is variable. Studies have shown that in the period before the end of testicular migration, the distal gubernaculum is not firmly attached to the scrotum (1, 5, 18). While the testis is located inside the abdomen, the gubernaculum is firmly attached to the inguinal canal (1,18). The insertion site of the distal gubernaculum is one of the factors involved in testicular ectopia (29). Several papers have reported that the distal gubernaculum has six extensions: abdominal, pubopenile, femoral, perineal, contralateral scrotal and scrotal (1, 5, 29, 30). It is speculated that these branches of the distal gubernaculum exist during the beggining of fetal development and disappear during testicular migration (1, 3, 29, 30). If any of these extensions of the distal portion persist, the individual can develop testicular ectopia (30). Various theories have been proposed to explain testicular ectopia. The most accepted are: (a) failure of the gubernaculum to dilate the inguinal canal, enabling the testis to migrate through other pathways and not reach the scrotum (29); (b) invasion of the gubernaculum by abdominal wall fascias near the inguinal canal, blocking the passage of the testis to the scrotum and diverting it to ectopic sites (1, 30); and (c) the existence of multiple distal insertions of the gubernaculum testis, guiding the testis to the main ectopic sites (1, 2, 30). The most accepted theory to explain testicular ectopia is the existence of multiple distal insertions of the gubernaculum. According to this theory, proposed by Lockwood in nineteenth century (29), the gubernaculum presents six distal insertion sites, in decreasing order of frequency: scrotal, interstitial (abdominal), femoral, perineal, transverse (contralateral scrotal) and pubopenile. Multiple distal insertions of the gubernaculum exist at the beggining of fetal development and disappear during testicular migration (1, 29, 30). Pubopenile testicular ectopia is considered the rarest form of this anomaly, but in one study with fetuses, the only two cases of anomalous insertion of the gubernaculum were located in the pubopenile region (31). Structure of the gubernaculum during testicular migration The different parts of the gubernaculum undergo varied changes during testicular migration. The vaginal and infra-vaginal portions become proportionally longer as the testis starts to descend to the scrotum. At the same time, their diameter increases, a fact considered by Heyns (3) to be one of the most important mechanisms for dilating the inguinal canal to allow the testis to pass. The gubernaculum s growth is divided into two phases, triggered by different hormonal stimuli (12, 18). In the first, its volume increases and in the second it decreases in size, coinciding with the complete descent of the testis (32). The cremaster muscle presents structural alterations during this period as well (33). This muscle allows rhythmic contraction to guide the testis into the scro- 725
5 tum in rats and in humans, leading to eversion of the distal portion of the gubernaculum and contributing to its migration to the scrotum (33). The first phase is characterized by pronounced cell multiplication and accumulation of glycosaminoglycans, mainly hyaluronic acid. These substances act as hydrophilic agents and raise the quantity of water. There is also an increase in the amount of extracellular material, explaining the low cell density found at some points (34, 35). The presence of myoblasts intensifies and there are changes in the number and arrangement of the collagen fibers and alterations of the elastic system. In the second phase, the gubernaculum shrinks, particularly its length, normally accompanied by descent of the testis. This phenomenon appears to be androgen-dependent and brings substantial degradation of the glycosaminoglycans previously accumulated in the extracellular material, with consequent dehydration of this space and condensation of the gubernaculum (22). Although no estimates are available of the degree of shortening, some authors believe this occurs along with other factors, causing the gubernaculum to convey the testis to the scrotum (3, 18). Understanding the relationship between regression of the gubernaculum and descent of the testis is vital to comprehension of how androgens control testicular migration. Studies have demonstrated an association between androgen deficiency, on the one hand, and failed regression of the gubernaculum and cryptorchidism on the other. In this situation, the gubernaculum appears to act as an obstacle to testicular descent (36, 37). Differences between the proximal and distal portions of the gubernaculum have been reported. In one study, in fetuses aged 15 to 35 WPC the authors observed a greater number of muscle cells in the distal portion, arranged in isolated groups, while in the proximal portion the muscle tissue was present in smaller quantity and was arranged peripherally. With increasing age, the quantity of muscle tissue was found to decrease. In fetuses between 28 and 29 WPC, the authors observed a large quantity of elastic fibers and almost no muscle fibers in the entire gubernaculum (22). In the early fetal period (15 and 16 WPC), when the testes are still in the abdomen, the connective tissue is loose and poor in collagen (Figure-2A). As the gestational time increases and the testes migrate from the abdominal cavity, the connective tissue becomes progressively denser and richer in collagen (Figure-2B). In fetuses with 28 to 29 WPC, the gubernaculum presents very dense organization of the Figure 2 - A) Photomicrograph of a male fetus with 15 weeks post-conception with both testes situated in the abdomen. A low concentration of collagen and elastic fibers in the gubernaculum can be observed (HE, 400x). B) Photomicrograph of a male fetus with 35 weeks post-conception with both testes situated in the scrotum. A condensation of the gubernaculum with a large amount of collagen and elastic fibers can be observed. Masson s trichrome, 200x. A B 726
6 collagen fibers and predominance of fibroblasts, with sharp directional orientation of the fibers and cells (22). Likewise, the reticular fibers, which are arranged more loosely in the gubernaculum at the beggining of the fetal period (15 and 16 WPC) are very dense in the gubernacula of fetuses with 28 and 29 WPC (22). Changes in the tissue components of the gubernaculum during the fetal period have been reported in various experimental studies (34, 35). The relative presence of muscle tissue appears to be one of the factors that affect the traction the gubernaculum exerts on the testis during its migration (1, 3, 6). At the beggining of the fetal period, a good deal of muscle tissue is present, but it starts to diminish with time, while the elastic tissue, which is sparse at the start, is markedly higher when the fetus reaches 25 WPC. At 28 and 29 WPC, under normal circumstances the testes have already completed their migration and are located in the scrotum. At this point of gestational age, Costa (22) observed very sparse muscle fibers and a large quantity of elastic fibers in the gubernaculum, especially in the distal portion. The connective tissue of the gubernaculum undergoes remodeling, so that at the end of migration it has essentially become a fibrous structure, rich in collagen and elastic tissue (22). The tissue changes in the gubernaculum testis during the fetal period suggest that it plays an active role in testicular migration. In summary, the morphological alterations of the extracellular matrix of the gubernaculum likely lead to a reduction of its length and volume. Although there is not sufficient evidence to estimate the degree of shortening, this change probably acts synergistically with other factors, causing the gubernaculum to guide the testis to the scrotum (22). Testicular descent is therefore a complex and multifactor event, and cryptorchidism should be viewed as a disease with multiple etiologies. One of the factors involved in cryptorchidism is the failure of the gubernaculum to migrate all the way to the scrotum (38). Structural studies conducted in patients with cryptorchidism reveal significant changes in the gubernaculum s structure, with a higher quantity of fibrous tissue and lower concentration of collagen than in the fetal gubernaculum (39). The influence of fetal androgens on the fetal gubernaculum s development is very important for the alterations of this structure, and the changes in its secretions can be one of the factors involved in cryptorchidism (40). For example, in a study analyzing the structure of the gubernaculum in patients treated with hcg, the authors observed that the gubernacular components change significantly when submitted to hormonal treatment, with an increase in the concentration of elastic and striated muscle fibers and a decrease in the volumetric density of collagen (41). CONCLUSIONS In the first phase of testicular migration, the gubernaculum enlarges to hold the testis near the groin and in the second phase the gubernaculum migrates across the pubic region to reach the scrotum. The proximal portion of the gubernaculum is attached to the testis and epididymis and the presence of multiple insertions in the distal gubernaculum is extremely rare. The presence of muscles and nerves in the human gubernaculum is very poor. The gubernaculum presents significant structural modifications during testicular migration in human fetuses. The gubernaculum of patients with cryptorchidism has more fibrous tissue and less collagen, and when patients are submitted to hormonal treatment, the gubernacular components change significantly. Acknowledgments Supported by grants of CNPQ and FAPERJ. CONFLICT OF INTEREST REFERENCES None declared. 1. Heyns CF, Hutson JM. Historical review of theories on testicular descent. J Urol. 1995;153(3 Pt 1):
7 2. Backhouse KM. Embryology of testicular descent and maldescent. Urol Clin North Am. 1982;9: Heyns CF. The gubernaculum during testicular descent in the human fetus. J Anat. 1987;153: Sampaio FJ, Favorito LA. Analysis of testicular migration during the fetal period in humans. J Urol. 1998;159: Attah AA, Hutson JM. The role of intra-abdominal pressure in cryptorchidism. J Urol. 1993;150: Hadziselimovi F. Mechanism of testicular descent. Urol Res. 1984;12: Hadziselimovic F, Herzog B. The development and descent of the epididymis. Eur J Pediatr. 1993;152(Suppl 2):S Hadziselimovic F, Kruslin E. The role of the epididymis in descensus testis and the topographical relationship between the testis and epididymis from the sixth month of pregnancy until immediately after birth. Anat Embryol (Berl). 1979;155: Clarnette TD, Hutson JM. The genitofemoral nerve may link testicular inguinoscrotal descent with congenital inguinal hernia. Aust N Z J Surg. 1996;66: Levard G, Laberge JM. The fate of undescended testes in patients with gastroschisis. Eur J Pediatr Surg. 1997;7: Gill B, Kogan S. Cryptorchidism. Current concepts. Pediatr Clin North Am. 1997;44: Hutson JM, Southwell BR, Li R, Lie G, Ismail K, Harisis G, Chen N. The regulation of testicular descent and the effects of cryptorchidism. Endocr Rev. 2013;34: Nation TR, Balic A, Southwell BR, Newgreen DF, Hutson JM. The hormonal control of testicular descent. Pediatr Endocrinol Rev. 2009;7: Fu P, Layfield S, Ferraro T, Tomiyama H, Hutson J, Otvos L Jr, et al. Synthesis, conformation, receptor binding and biological activities of monobiotinylated human insulin-like peptide 3. J Pept Res. 2004;63: Hutson JM, Hasthorpe S. Abnormalities of testicular descent. Cell Tissue Res. 2005;322: Allnutt B, Buraundi S, Farmer P, Southwell BR, Hutson JM, Balic A. The common fetal development of the mammary fat pad and gubernaculum. J Pediatr Surg. 2011;46: Su S, Farmer PJ, Li R, Sourial M, Buraundi S, Bodemer D, et al. Regression of the mammary branch of the genitofemoral nerve may be necessary for testicular descent in rats. J Urol. 2012;188(4 Suppl): Husmann DA, Levy JB. Current concepts in the pathophysiology of testicular undescent. Urology. 1995;46: Wensing CJ. The embryology of testicular descent. Horm Res. 1988;30: Frey HL, Rajfer J. Role of the gubernaculum and intraabdominal pressure in the process of testicular descent. J Urol. 1984;131: Ludwig KS. The development of the caudal ligaments of the mesonephros and of the gonads: a contribution to the development of the human gubernaculums (Hunteri). Anat Embryol (Berl). 1993;188: Costa WS, Sampaio FJ, Favorito LA, Cardoso LE. Testicular migration: remodeling of connective tissue and muscle cells in human gubernaculum testis. J Urol. 2002;167: Beasley SW, Hutson JM. The role of the gubernaculum in testicular descent. J Urol. 1988;140(5 Pt 2): Johansen TE, Blom GP. Histological studies of gubernaculum testis taken during orchiopexies. Scand J Urol Nephrol. 1988;22: Jackson MB, Gough MH, Dudley NE. Anatomical findings at orchiopexy. Br J Urol. 1987;59: Favorito LA, Sampaio FJ, Javaroni V, Cardoso LE, Costa WS. Proximal insertion of gubernaculum testis in normal human fetuses and in boys with cryptorchidism. J Urol. 2000;164(3 Pt 1): Abe T, Aoyama K, Gotoh T, Akiyama T, Iwamura Y, Kumori K. Cranial attachment of the gubernaculum associated with undescended testes. J Pediatr Surg. 1996;31: Favorito LA, Sampaio FJ. Anatomical relationships between testis and epididymis during the fetal period in humans (10-36 weeks postconception). Eur Urol. 1998;33: Nightingale SS, Al Shareef YR, Hutson JM. Mythical Tails of Lockwood. ANZ J Surg. 2008;78: Ramareddy RS, Alladi A, Siddappa OS. Ectopic testis in children: experience with seven cases. J Pediatr Surg. 2013;48: Favorito LA, Klodja CAB, Costa SW, Sampaio FJ. Distal insertions of gubernaculum testis and their relationships with testicular ectopia. J Urol. 2003; 170: Fentener van Vlissingen JM, Koch CA, Delpech B, Wensing CJ. Growth and differentiation of the gubernaculum testis during testicular descent in the pig: changes in the extracellular matrix, DNA content, and hyaluronidase, beta-glucuronidase, and beta- N-acetylglucosaminidase activities. J Urol. 1989;142: Lie G, Hutson JM. The role of cremaster muscle in testicular descent in humans and animal models. Pediatr Surg Int. 2011;27: Heyns CF, Human HJ, De Klerk DP. Hyperplasia and hypertrophy of the gubernaculum during testicular descent in the fetus. J Urol. 1986;135: Heyns CF, Human HJ, Werely CJ, De Klerk DP. The glycosaminoglycans of the gubernaculum during testicular descent in the fetus. J Urol. 1990;143: Elder JS, Isaacs JT, Walsh PC. Androgenic sensitivity of the gubernaculums testis: evidence for hormonal/mechanical interactions in testicular descent. J Urol. 1982;127: Barthold JS, Kumasi-Rivers K, Upadhyay J, Shekarriz B, Imperato-Mcginley J. Testicular position in the androgen insensitivity syndrome: implications for the role of androgens in testicular descent. J Urol. 2000;164:
8 38. Hutson JM, Balic A, Nation T, Southwell B. Cryptorchidism. Semin Pediatr Surg. 2010;19: Soito IC, Favorito LA, Costa WS, Sampaio FJ, Cardoso LE. Extracellular matrix remodeling in the human gubernaculum during fetal testicular descent and in cryptorchidic children. World J Urol. 2011;29: Nation T, Balic A, Buraundi S, Farmer P, Newgreen D, Southwell B, et al. The antiandrogen flutamide perturbs inguinoscrotal testicular descent in the rat and suggests a link with mammary development. J Pediatr Surg. 2009;44: El Zoghbi CS, Favorito LA, Costa WS, Sampaio FJ. Structural analysis of gubernaculum testis in cryptorchid patients submitted to treatment with human chorionic gonadotrophin. Int Braz J Urol. 2007;33:223-9; discusson 230. Correspondence address: Luciano Alves Favorito, MD, PhD Rua Professor Gabizo, 104/201 Tijuca, Rio de Janeiro, RJ, , Brazil Fax: lufavorito@yahoo.com.br 729
TESTICULAR DESCEND, HOW AND WHY: A REVIEW ARTICLE
 CASE REPORT TESTICULAR DESCEND, HOW AND WHY: A REVIEW ARTICLE SUJAN NARAYAN AGRAWAL, 1 Associate professor, Department of Surgery. Late SBRKM Government Medical College, Jagdalpur (Bastar) C.G. PIN 494001,
CASE REPORT TESTICULAR DESCEND, HOW AND WHY: A REVIEW ARTICLE SUJAN NARAYAN AGRAWAL, 1 Associate professor, Department of Surgery. Late SBRKM Government Medical College, Jagdalpur (Bastar) C.G. PIN 494001,
TESTICULAR MIGRATION: REMODELING OF CONNECTIVE TISSUE AND MUSCLE CELLS IN HUMAN GUBERNACULUM TESTIS
 0022-5347/02/1675-2171/0 THE JOURNAL OF UROLOGY Vol. 167, 2171 2176, May 2002 Copyright 2002 by AMERICAN UROLOGICAL ASSOCIATION, INC. Printed in U.S.A. TESTICULAR MIGRATION: REMODELING OF CONNECTIVE TISSUE
0022-5347/02/1675-2171/0 THE JOURNAL OF UROLOGY Vol. 167, 2171 2176, May 2002 Copyright 2002 by AMERICAN UROLOGICAL ASSOCIATION, INC. Printed in U.S.A. TESTICULAR MIGRATION: REMODELING OF CONNECTIVE TISSUE
W.S. O University of Hong Kong
 W.S. O University of Hong Kong Development of the Genital System 1. Sexual differentiation 2. Differentiation of the gonads a. Germ cells extragonadal in origin b. Genital ridge intermediate mesoderm consisting
W.S. O University of Hong Kong Development of the Genital System 1. Sexual differentiation 2. Differentiation of the gonads a. Germ cells extragonadal in origin b. Genital ridge intermediate mesoderm consisting
Surgical management of the undescended testis is performed
 Undescended Testes/Orchiopexy James C.Y. Dunn, MD, PhD, 1 Akemi L. Kawaguchi, MD, 2 and Eric W. Fonkalsrud, MD 1 Surgical management of the undescended testis is performed to prevent the potential complications
Undescended Testes/Orchiopexy James C.Y. Dunn, MD, PhD, 1 Akemi L. Kawaguchi, MD, 2 and Eric W. Fonkalsrud, MD 1 Surgical management of the undescended testis is performed to prevent the potential complications
Midgut. Over its entire length the midgut is supplied by the superior mesenteric artery
 Gi Embryology 3 Midgut the midgut is suspended from the dorsal abdominal wall by a short mesentery and communicates with the yolk sac by way of the vitelline duct or yolk stalk Over its entire length the
Gi Embryology 3 Midgut the midgut is suspended from the dorsal abdominal wall by a short mesentery and communicates with the yolk sac by way of the vitelline duct or yolk stalk Over its entire length the
under its influence, male development occurs; in its absence, female development is established.
 Sex differentiation is a complex process that involves many genes, including some that are autosomal. The key to sexual dimorphism is the Y chromosome, which contains the testis determining gene called
Sex differentiation is a complex process that involves many genes, including some that are autosomal. The key to sexual dimorphism is the Y chromosome, which contains the testis determining gene called
M. Al-Mohtaseb. Tala Saleh. Faisal Nimri
 4 5 M. Al-Mohtaseb Tala Saleh Faisal Nimri Inguinal Hernia - An abdominal hernia is the protrusion of part of the abdominal content beyond the normal confines of the abdominal wall through weak points
4 5 M. Al-Mohtaseb Tala Saleh Faisal Nimri Inguinal Hernia - An abdominal hernia is the protrusion of part of the abdominal content beyond the normal confines of the abdominal wall through weak points
UNIVERSITY OF MEDICINE AND PHARMACY OF CRAIOVA DOCTORAL SCHOOL. PHD THESIS UNDESCENDED TESTICLE IN CHILD CLINICAL AND THERAPEUTIC ASPECTS - Abstract -
 UNIVERSITY OF MEDICINE AND PHARMACY OF CRAIOVA DOCTORAL SCHOOL PHD THESIS UNDESCENDED TESTICLE IN CHILD CLINICAL AND THERAPEUTIC ASPECTS - Abstract - SCIENTIFIC COORDINATOR: Prof. Dr. Ion GEORGESCU PHD
UNIVERSITY OF MEDICINE AND PHARMACY OF CRAIOVA DOCTORAL SCHOOL PHD THESIS UNDESCENDED TESTICLE IN CHILD CLINICAL AND THERAPEUTIC ASPECTS - Abstract - SCIENTIFIC COORDINATOR: Prof. Dr. Ion GEORGESCU PHD
ESUR SCROTAL AND PENILE IMAGING WORKING GROUP MULTIMODALITY IMAGING APPROACH TO SCROTAL AND PENILE PATHOLOGIES 2ND ESUR TEACHING COURSE
 ESUR SCROTAL AND PENILE IMAGING WORKING GROUP MULTIMODALITY IMAGING APPROACH TO SCROTAL AND PENILE PATHOLOGIES 2ND ESUR TEACHING COURSE NORMAL ANATOMY OF THE SCROTUM MICHAEL NOMIKOS M.D. F.E.B.U. UROLOGICAL
ESUR SCROTAL AND PENILE IMAGING WORKING GROUP MULTIMODALITY IMAGING APPROACH TO SCROTAL AND PENILE PATHOLOGIES 2ND ESUR TEACHING COURSE NORMAL ANATOMY OF THE SCROTUM MICHAEL NOMIKOS M.D. F.E.B.U. UROLOGICAL
حسام أبو عوض. -Dr. Mohammad Muhtasib. 1 P a g e
 5 حسام أبو عوض - -Dr. Mohammad Muhtasib 1 P a g e There are two types of inguinal hernia: direct and indirect. Hernia: protrusion of the small intestine or the greater omentum of the intra-abdominal organs
5 حسام أبو عوض - -Dr. Mohammad Muhtasib 1 P a g e There are two types of inguinal hernia: direct and indirect. Hernia: protrusion of the small intestine or the greater omentum of the intra-abdominal organs
UvA-DARE (Digital Academic Repository) Testing the undescended testis de Vries, Annebeth. Link to publication
 UvA-DARE (Digital Academic Repository) Testing the undescended testis de Vries, Annebeth Link to publication Citation for published version (APA): de Vries, A. (2014). Testing the undescended testis General
UvA-DARE (Digital Academic Repository) Testing the undescended testis de Vries, Annebeth Link to publication Citation for published version (APA): de Vries, A. (2014). Testing the undescended testis General
Development of the Genital System
 Development of the Genital System Professor Alfred Cuschieri Department of Anatomy University of Malta The mesonephros develops primitive nephrotomes draining into a mesonephric duct nephrotome mesonephric
Development of the Genital System Professor Alfred Cuschieri Department of Anatomy University of Malta The mesonephros develops primitive nephrotomes draining into a mesonephric duct nephrotome mesonephric
Maldescended testis in Adults. Dr. BG GAUDJI Urologist STEVE BIKO ACADEMIC HOSPITAL
 Maldescended testis in Adults Dr. BG GAUDJI Urologist STEVE BIKO ACADEMIC HOSPITAL Definitions Cryptorchid: testis neither resides nor can be manipulated into the scrotum Ectopic: aberrant course Retractile:
Maldescended testis in Adults Dr. BG GAUDJI Urologist STEVE BIKO ACADEMIC HOSPITAL Definitions Cryptorchid: testis neither resides nor can be manipulated into the scrotum Ectopic: aberrant course Retractile:
Inguinal Canal. It is an oblique passage through the lower part of the anterior abdominal wall. Present in both sexes
 Inguinal canal Inguinal Canal It is an oblique passage through the lower part of the anterior abdominal wall Present in both sexes It allows structures to pass to and from the testis to the abdomen in
Inguinal canal Inguinal Canal It is an oblique passage through the lower part of the anterior abdominal wall Present in both sexes It allows structures to pass to and from the testis to the abdomen in
Different surgical findings in congenital and acquired undescended testes
 BJUI BJU INTERNATIONAL Different surgical findings in congenital and acquired undescended testes Jocelyn van Brakel, Gert R. Dohle, Sabine M.P.F. de Muinck Keizer-Schrama * and Frans W. Hazebroek Urology,
BJUI BJU INTERNATIONAL Different surgical findings in congenital and acquired undescended testes Jocelyn van Brakel, Gert R. Dohle, Sabine M.P.F. de Muinck Keizer-Schrama * and Frans W. Hazebroek Urology,
10. Development of genital system. Gonads. Genital ducts. External genitalia.
 10. Development of genital system. Gonads. Genital ducts. External genitalia. Gonads, genital ducts and the external genital organs initially pass through an indifferent period of development, which is
10. Development of genital system. Gonads. Genital ducts. External genitalia. Gonads, genital ducts and the external genital organs initially pass through an indifferent period of development, which is
Persistent processus vaginalis presenting as hydrocele and hernia
 International Journal of Contemporary Pediatrics Prabakaran S et al. Int J Contemp Pediatr. 2018 Sep;5(5):1819-1823 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Original Research Article
International Journal of Contemporary Pediatrics Prabakaran S et al. Int J Contemp Pediatr. 2018 Sep;5(5):1819-1823 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Original Research Article
Human Anatomy Unit 3 REPRODUCTIVE SYSTEM
 Human Anatomy Unit 3 REPRODUCTIVE SYSTEM In Anatomy Today Male Reproductive System Gonads = testes primary organ responsible for sperm production development/maintenan ce of secondary sex characteristics
Human Anatomy Unit 3 REPRODUCTIVE SYSTEM In Anatomy Today Male Reproductive System Gonads = testes primary organ responsible for sperm production development/maintenan ce of secondary sex characteristics
Role of Human Chorionic Gonadotropin (HCG) Hormone in Undescended Testis a Prospective Study in 100 Children
 Role of Human Chorionic Gonadotropin (HCG) Hormone in Undescended Testis a Prospective Study in 100 Children BA CHEECHAK 1 MY WANI 2 A HUSSAIN 3 G HASSAN 4 This is a prospective study of 100 children (122
Role of Human Chorionic Gonadotropin (HCG) Hormone in Undescended Testis a Prospective Study in 100 Children BA CHEECHAK 1 MY WANI 2 A HUSSAIN 3 G HASSAN 4 This is a prospective study of 100 children (122
DISSECTION 8: URINARY AND REPRODUCTIVE SYSTEMS
 8546d_c01_1-42 6/25/02 4:32 PM Page 38 mac48 Mac 48: 420_kec: 38 Cat Dissection DISSECTION 8: URINARY AND REPRODUCTIVE SYSTEMS Typically, the urinary and reproductive systems are studied together, because
8546d_c01_1-42 6/25/02 4:32 PM Page 38 mac48 Mac 48: 420_kec: 38 Cat Dissection DISSECTION 8: URINARY AND REPRODUCTIVE SYSTEMS Typically, the urinary and reproductive systems are studied together, because
Male Anatomy. testes, genetically determined in mammals - testis releases hormones that then control the development of secondary sex characteristics
 Male Anatomy Male Anatomy Primary Organ testes, genetically determined in mammals - testis releases hormones that then control the development of secondary sex characteristics 1) Secondary Organs internal
Male Anatomy Male Anatomy Primary Organ testes, genetically determined in mammals - testis releases hormones that then control the development of secondary sex characteristics 1) Secondary Organs internal
Urinary system development. Male ( ) and Female ( ) Reproductive Systems Development
 Urinary system development Male ( ) and Female ( ) Reproductive Systems Development Urogenital system develops from mesodermal uro-genital ridge (intermediate mesoderm) development of male and female genital
Urinary system development Male ( ) and Female ( ) Reproductive Systems Development Urogenital system develops from mesodermal uro-genital ridge (intermediate mesoderm) development of male and female genital
Undescended testis varying presentation - Clinical research study
 Original Research Article Undescended testis varying presentation - Clinical research study S. C. Naren Kumar 1*, Bharathidasan 2, G. Ambujam 3 1 Postgraduate, 2 Associate Professor, 3 Professor and Head
Original Research Article Undescended testis varying presentation - Clinical research study S. C. Naren Kumar 1*, Bharathidasan 2, G. Ambujam 3 1 Postgraduate, 2 Associate Professor, 3 Professor and Head
Urogenital anomalies in human male fetuses
 Early Human Development 79 (2004) 41 47 www.elsevier.com/locate/earlhumdev Urogenital anomalies in human male fetuses Luciano A. Favorito *, Themis M. Cardinot, Ana Raquel M. Morais, Francisco J.B. Sampaio
Early Human Development 79 (2004) 41 47 www.elsevier.com/locate/earlhumdev Urogenital anomalies in human male fetuses Luciano A. Favorito *, Themis M. Cardinot, Ana Raquel M. Morais, Francisco J.B. Sampaio
UCSF Pediatric Urology Child and Family Information Material
 UCSF Pediatric Urology Child and Family Information Material ------------------------------------------------------------------------ The Undescended Testicle What is an Undescended Testicle? The undescended
UCSF Pediatric Urology Child and Family Information Material ------------------------------------------------------------------------ The Undescended Testicle What is an Undescended Testicle? The undescended
PELVIS II: FUNCTION TABOOS (THE VISCERA) Defecation Urination Ejaculation Conception
 PELVIS II: FUNCTION TABOOS (THE VISCERA) Defecation Urination Ejaculation Conception REVIEW OF PELVIS I Pelvic brim, inlet Pelvic outlet True pelvis-- --viscera Tilt forward Mid-sagital views-- --how the
PELVIS II: FUNCTION TABOOS (THE VISCERA) Defecation Urination Ejaculation Conception REVIEW OF PELVIS I Pelvic brim, inlet Pelvic outlet True pelvis-- --viscera Tilt forward Mid-sagital views-- --how the
أحمد رواجبة- محمود الحربي- أحمد السالمان-
 -6 أحمد رواجبة- محمود الحربي- أحمد السالمان- 1 P a g e The Male Reproductive System The male genital system structures are divided into: Internal structures: 1- Prostate 3-Ejaculatory ducts External structures:
-6 أحمد رواجبة- محمود الحربي- أحمد السالمان- 1 P a g e The Male Reproductive System The male genital system structures are divided into: Internal structures: 1- Prostate 3-Ejaculatory ducts External structures:
The tammar wallaby (Macropus eugeni) and the Sprague-Dawley rat: comparative anatomy and physiology of inguinoscrotal testicular descent
 J. Anat. (1993) 183, pp. 441-450, with 5 figures Printed in Great Britain 441 The tammar wallaby (Macropus eugeni) and the Sprague-Dawley rat: comparative anatomy and physiology of inguinoscrotal testicular
J. Anat. (1993) 183, pp. 441-450, with 5 figures Printed in Great Britain 441 The tammar wallaby (Macropus eugeni) and the Sprague-Dawley rat: comparative anatomy and physiology of inguinoscrotal testicular
- production of two types of gametes -- fused at fertilization to form zygote
 Male reproductive system I. Sexual reproduction -- overview - production of two types of gametes -- fused at fertilization to form zygote - promotes genetic variety among members of a species -- each offspring
Male reproductive system I. Sexual reproduction -- overview - production of two types of gametes -- fused at fertilization to form zygote - promotes genetic variety among members of a species -- each offspring
GI anatomy Lecture: 2 د. عصام طارق
 GI anatomy Lecture: 2 د. عصام طارق Objectives: To define rectus sheath. To describe anatomy of inguinal canal. To relates types of inguinal hernia to the region. To explore spermatic cord. Rectus Abdominis
GI anatomy Lecture: 2 د. عصام طارق Objectives: To define rectus sheath. To describe anatomy of inguinal canal. To relates types of inguinal hernia to the region. To explore spermatic cord. Rectus Abdominis
11. SEXUAL DIFFERENTIATION. Germinal cells, gonocytes. Indifferent stage INDIFFERENT STAGE
 11. SEXUAL DIFFERENTIATION INDIFFERENT STAGE Early in pregnancy, (within 10-15 % of the pregnancy s expected length) a genital ridge is formed in the sides of the embryonic tissue, ventral to the mesonephros
11. SEXUAL DIFFERENTIATION INDIFFERENT STAGE Early in pregnancy, (within 10-15 % of the pregnancy s expected length) a genital ridge is formed in the sides of the embryonic tissue, ventral to the mesonephros
Biology 224 Human Anatomy and Physiology II Week 9; Lecture 2; Wednesday Stuart Sumida. Development and Structure, of the Reproductive System
 Biology 224 Human Anatomy and Physiology II Week 9; Lecture 2; Wednesday Stuart Sumida Development and Structure, of the Reproductive System Don t forget the relationships of the structures of the layers
Biology 224 Human Anatomy and Physiology II Week 9; Lecture 2; Wednesday Stuart Sumida Development and Structure, of the Reproductive System Don t forget the relationships of the structures of the layers
Development of the urogenital system
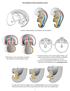 Development of the urogenital system Location of the pronephros, mesonephros and metanephros Differentiation of the intermedierm mesoderm into nephrotome and mesonephric tubules Connection between aorta
Development of the urogenital system Location of the pronephros, mesonephros and metanephros Differentiation of the intermedierm mesoderm into nephrotome and mesonephric tubules Connection between aorta
Descent of the Testis
 Descent of the Testis John M. Hutson Jørgen M. Thorup Spencer W. Beasley Descent of the Testis Second Edition John M. Hutson Royal Children s Hospital University of Melbourne Parkville, Victoria Australia
Descent of the Testis John M. Hutson Jørgen M. Thorup Spencer W. Beasley Descent of the Testis Second Edition John M. Hutson Royal Children s Hospital University of Melbourne Parkville, Victoria Australia
Laparoscopy in the Management of Impalpable Testicle
 Acta chir belg, 2005, 105, 662-666 Laparoscopy in the Management of Impalpable Testicle N. Satar, Y. Bayazıt, Ş. Doran Çukurova University, Faculty of Medicine, Department of Urology, Balcalı Hospital,
Acta chir belg, 2005, 105, 662-666 Laparoscopy in the Management of Impalpable Testicle N. Satar, Y. Bayazıt, Ş. Doran Çukurova University, Faculty of Medicine, Department of Urology, Balcalı Hospital,
The Repr duct ve System. Function: producing offspring
 The Repr duct ve System Function: producing offspring Anatomy of male reproductive system Location: The reproductive organs are classified as external and internal genitalia. The external genitalia are
The Repr duct ve System Function: producing offspring Anatomy of male reproductive system Location: The reproductive organs are classified as external and internal genitalia. The external genitalia are
Case Based Urology Learning Program
 Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 5 CBULP 2011 021 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 5 CBULP 2011 021 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature
 REPRODUCTION Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature reduction -Testes wall made of fibrous connective
REPRODUCTION Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature reduction -Testes wall made of fibrous connective
Male Reproductive System. Dr Maan Al-Abbasi PhD, MSc, MBChB, MD
 Male Reproductive System Dr Maan Al-Abbasi PhD, MSc, MBChB, MD Learning Objectives 1. Describe the General Anatomy of the Male Reproductive System 2. Identify the structures that are related to the prostate.
Male Reproductive System Dr Maan Al-Abbasi PhD, MSc, MBChB, MD Learning Objectives 1. Describe the General Anatomy of the Male Reproductive System 2. Identify the structures that are related to the prostate.
Embryology Relevant to Ultrasound Imaging of the Male Genitalia
 Embryology Relevant to Ultrasound Imaging of the Male Genitalia Gideon Richards and Bruce R. Gilbert A basic understanding of the embryologic development of the male genitalia and the male genital blood
Embryology Relevant to Ultrasound Imaging of the Male Genitalia Gideon Richards and Bruce R. Gilbert A basic understanding of the embryologic development of the male genitalia and the male genital blood
Undescended Testicle
 What is the normal descending testis? The testicle begins to form just before the second fetal month and starts to look like a testicle around the fourth fetal month. By then it has migrated down from
What is the normal descending testis? The testicle begins to form just before the second fetal month and starts to look like a testicle around the fourth fetal month. By then it has migrated down from
Embryology /organogenesis/ Week 4 Development and teratology of reproductive system.
 Embryology /organogenesis/ Week 4 Development and teratology of reproductive system. Male or female sex is determined by spermatozoon Y in the moment of fertilization SRY gene, on the short arm of the
Embryology /organogenesis/ Week 4 Development and teratology of reproductive system. Male or female sex is determined by spermatozoon Y in the moment of fertilization SRY gene, on the short arm of the
Clinical Study Laparoscopic Management of Intra-Abdominal Testis: 5-Year Single-Centre Experience A Retrospective Descriptive Study
 Minimally Invasive Surgery Volume 2012, Article ID 878509, 4 pages doi:10.1155/2012/878509 Clinical Study Laparoscopic Management of Intra-Abdominal Testis: 5-Year Single-Centre Experience A Retrospective
Minimally Invasive Surgery Volume 2012, Article ID 878509, 4 pages doi:10.1155/2012/878509 Clinical Study Laparoscopic Management of Intra-Abdominal Testis: 5-Year Single-Centre Experience A Retrospective
Outline. Male Reproductive System Testes and Sperm Hormonal Regulation
 Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
Reproductive System Purpose General Structures Male Structures Functions Female Anatomy Structures Functions Clinical Applications
 The Reproductive System: Male, Ch 23 Outline of class lecture After studying the male reproductive system you should be able to: 1. Define the purpose of reproduction and identify the general organs of
The Reproductive System: Male, Ch 23 Outline of class lecture After studying the male reproductive system you should be able to: 1. Define the purpose of reproduction and identify the general organs of
Proceedings of the 12th International Congress of the World Equine Veterinary Association WEVA
 www.ivis.org Proceedings of the 12th International Congress of the World Equine Veterinary Association WEVA November 2-5, 2011 Hyderabad, India Reprinted in IVIS with the Permission of WEVA Organizers
www.ivis.org Proceedings of the 12th International Congress of the World Equine Veterinary Association WEVA November 2-5, 2011 Hyderabad, India Reprinted in IVIS with the Permission of WEVA Organizers
Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization
 Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization may occur! A. Scrotum 1. Muscular pouch that holds the
Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization may occur! A. Scrotum 1. Muscular pouch that holds the
PERSISTANT MULLERIAN DUCT SYNDROME ASSOCIATED WITH TRANSVERSE TESTICULAR ECTOPIA
 PERSISTANT MULLERIAN DUCT SYNDROME ASSOCIATED WITH TRANSVERSE TESTICULAR ECTOPIA Dr. Abdulrahman A. Al-Bassam, FRCS(Ed) Assistant Professor & Consultant Paediatric Surgeon King Khalid University Hospital
PERSISTANT MULLERIAN DUCT SYNDROME ASSOCIATED WITH TRANSVERSE TESTICULAR ECTOPIA Dr. Abdulrahman A. Al-Bassam, FRCS(Ed) Assistant Professor & Consultant Paediatric Surgeon King Khalid University Hospital
The Scrotum & Testes Prof. Dr. Imran Qureshi
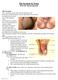 The Scrotum & Testes Prof. Dr. Imran Qureshi The Scrotum It is a cutaneous pouch of the anterior abdominal wall. Most layers of the abdominal wall are represented in its structure. It contains the testes
The Scrotum & Testes Prof. Dr. Imran Qureshi The Scrotum It is a cutaneous pouch of the anterior abdominal wall. Most layers of the abdominal wall are represented in its structure. It contains the testes
Reproductive System. Where it all begins
 Reproductive System Where it all begins When it comes the reproductive anatomy of my gender, I would rate my knowledge (1 very poor, 10 excellent) When it comes the reproductive anatomy of the opposite
Reproductive System Where it all begins When it comes the reproductive anatomy of my gender, I would rate my knowledge (1 very poor, 10 excellent) When it comes the reproductive anatomy of the opposite
MALE REPRODUCTIVE SYSTEM
 MALE REPRODUCTIVE SYSTEM 1. The male reproductive system is made up of the following structures, EXCEPT: a. prostate; b. testicle; c. spermatic ducts; d. vestibular bulbs; e. seminal vesicles. 2.The testicle:
MALE REPRODUCTIVE SYSTEM 1. The male reproductive system is made up of the following structures, EXCEPT: a. prostate; b. testicle; c. spermatic ducts; d. vestibular bulbs; e. seminal vesicles. 2.The testicle:
Urogenital System. PUMC Dept. of Anat. Hist. & Embry. 钱晓菁 XIAO-JING QIAN Dept. of Anatomy, Histology & Embryology Peking Union Medical College
 Urogenital System 钱晓菁 XIAO-JING QIAN Dept. of Anatomy, Histology & Embryology Peking Union Medical College intermediate mesoderm urogenital ridge mesonephric ridge genital ridge I. Urinary System 1. kidney
Urogenital System 钱晓菁 XIAO-JING QIAN Dept. of Anatomy, Histology & Embryology Peking Union Medical College intermediate mesoderm urogenital ridge mesonephric ridge genital ridge I. Urinary System 1. kidney
Connective Tissue. Consists of two basic elements: Cells and Extra-cellular matrix
 Connective Tissue Consists of two basic elements: Cells and Extra-cellular matrix True Connective Tissue Cells Fibroblasts: Secrete both fibers and ground substance of the matrix (wandering) Macrophages:
Connective Tissue Consists of two basic elements: Cells and Extra-cellular matrix True Connective Tissue Cells Fibroblasts: Secrete both fibers and ground substance of the matrix (wandering) Macrophages:
Bronchioles. Alveoli. Type I alveolar cells are very thin simple squamous epithelial cells and form most of the lining of an alveolus.
 276 Bronchioles Bronchioles continue on to form bronchi. The primary identifying feature is the loss of hyaline cartilage. The epithelium has become simple ciliated columnar, and there is a complete ring
276 Bronchioles Bronchioles continue on to form bronchi. The primary identifying feature is the loss of hyaline cartilage. The epithelium has become simple ciliated columnar, and there is a complete ring
Scrotal pain and Swelling
 Scrotal pain and Swelling Color index : Important Further explanation Done By: Nada Alamri Editing link Acute Scrotal Pain DDx: 1) Testicular torsion : Twisting and strangulation of the testicle on the
Scrotal pain and Swelling Color index : Important Further explanation Done By: Nada Alamri Editing link Acute Scrotal Pain DDx: 1) Testicular torsion : Twisting and strangulation of the testicle on the
ABDOMINAL WALL & RECTUS SHEATH
 ABDOMINAL WALL & RECTUS SHEATH Learning Objectives Describe the anatomy, innervation and functions of the muscles of the anterior, lateral and posterior abdominal walls. Discuss their functional relations
ABDOMINAL WALL & RECTUS SHEATH Learning Objectives Describe the anatomy, innervation and functions of the muscles of the anterior, lateral and posterior abdominal walls. Discuss their functional relations
Bio& 241 Unit 1 / Lecture 4
 Bio& 241 Unit 1 / Lecture 4 Connective Tissue Consists of two basic elements: Cells and Extra-cellular matrix 1 True Connective Tissue Cells Fibroblasts: Secrete both fibers and ground substance of the
Bio& 241 Unit 1 / Lecture 4 Connective Tissue Consists of two basic elements: Cells and Extra-cellular matrix 1 True Connective Tissue Cells Fibroblasts: Secrete both fibers and ground substance of the
Male Reproductive System
 Male Reproductive System organs that function in: gamete and hormone production not all in abdominal cavity paired testicles = controlled by LH & FSH duct systems accessory glands Testis: Gross Histology
Male Reproductive System organs that function in: gamete and hormone production not all in abdominal cavity paired testicles = controlled by LH & FSH duct systems accessory glands Testis: Gross Histology
Primary sex organs (gonads): testes and ovaries. Accessory reproductive organs: ducts, glands, and external genitalia
 Male Reproductive System Primary sex organs (gonads): testes and ovaries Produce sex cells (gametes) Secrete steroid sex hormones Androgens (males) Estrogens and progesterone (females) Accessory reproductive
Male Reproductive System Primary sex organs (gonads): testes and ovaries Produce sex cells (gametes) Secrete steroid sex hormones Androgens (males) Estrogens and progesterone (females) Accessory reproductive
MANAGEMENT OF UNDESCENDED TESTES IN A TERTIARY CARE HOSPITAL: A STUDY FROM CENTRAL INDIA M. Maheshwari 1, Roshan Chanchlani 2
 MANAGEMENT OF UNDESCENDED TESTES IN A TERTIARY CARE HOSPITAL: A STUDY FROM CENTRAL INDIA M. Maheshwari 1, Roshan Chanchlani 2 HOW TO CITE THIS ARTICLE: M. Maheshwari, Roshan Chanchlani. Management of Undescended
MANAGEMENT OF UNDESCENDED TESTES IN A TERTIARY CARE HOSPITAL: A STUDY FROM CENTRAL INDIA M. Maheshwari 1, Roshan Chanchlani 2 HOW TO CITE THIS ARTICLE: M. Maheshwari, Roshan Chanchlani. Management of Undescended
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,350 108,000 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,350 108,000 1.7 M Open access books available International authors and editors Downloads Our
Development of the Urinary System. 3 Distinct Embryonic Kidney Structures
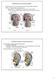 Development of the Urinary System Excretory portion of urinary system derived from intermediate mesoderm Week 4: 1 st nephrons/renal corpuscles form Nephrotomes form and develop hollow lumens to form nephric
Development of the Urinary System Excretory portion of urinary system derived from intermediate mesoderm Week 4: 1 st nephrons/renal corpuscles form Nephrotomes form and develop hollow lumens to form nephric
Male Reproductive System Dr. Gary Mumaugh
 Male Reproductive System Dr. Gary Mumaugh Reproductive System Basics Primary sex organs (gonads) testes in males, ovaries in females Gonads produce sex cells called gametes (gametes means spouses) and
Male Reproductive System Dr. Gary Mumaugh Reproductive System Basics Primary sex organs (gonads) testes in males, ovaries in females Gonads produce sex cells called gametes (gametes means spouses) and
ORIGINAL ARTICLE. CLINICAL STUDY AND MANAGEMENT OF CHILDREN WITH IMPERFECT DESCENT OF TESTIS Sathyanarayana B.A 1, Ramachandra J 2
 CLINICAL STUDY AND MANAGEMENT OF CHILDREN WITH IMPERFECT DESCENT OF TESTIS Sathyanarayana B.A 1, Ramachandra J 2 HOW TO CITE THIS ARTICLE: Sathyanarayana B.A, Ramachandra J. Clinical Study And Management
CLINICAL STUDY AND MANAGEMENT OF CHILDREN WITH IMPERFECT DESCENT OF TESTIS Sathyanarayana B.A 1, Ramachandra J 2 HOW TO CITE THIS ARTICLE: Sathyanarayana B.A, Ramachandra J. Clinical Study And Management
Human Reproductive System
 Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
Systematic Anatomy. Shanghai Medical College,Fudan University. Dr.Hongqi Zhang ( 张红旗 )
 Systematic Anatomy Department of Anatomy,Histology & Embryology Shanghai Medical College,Fudan University Dr.Hongqi Zhang ( 张红旗 ) Email: zhanghq58@yahoo.com.cn Office: Building 9,Room308, 54237151-9308
Systematic Anatomy Department of Anatomy,Histology & Embryology Shanghai Medical College,Fudan University Dr.Hongqi Zhang ( 张红旗 ) Email: zhanghq58@yahoo.com.cn Office: Building 9,Room308, 54237151-9308
Urinary Bladder. Prof. Imran Qureshi
 Urinary Bladder Prof. Imran Qureshi Urinary Bladder It develops from the upper end of the urogenital sinus, which is continuous with the allantois. The allantois degenerates and forms a fibrous cord in
Urinary Bladder Prof. Imran Qureshi Urinary Bladder It develops from the upper end of the urogenital sinus, which is continuous with the allantois. The allantois degenerates and forms a fibrous cord in
Femoral Triangle and Adductor Canal. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Femoral Triangle and Adductor Canal Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Femoral Triangle and Adductor Canal Femoral triangle Is a triangular depressed area located in the upper
Femoral Triangle and Adductor Canal Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Femoral Triangle and Adductor Canal Femoral triangle Is a triangular depressed area located in the upper
Rama Nada. - Ensherah Mokheemer. - Ahmed salman. 1 P a g e
 - 5 - Rama Nada - Ensherah Mokheemer - Ahmed salman 1 P a g e We will continue talking about the urinary bladder The ligaments of the bladder: 1-Median umbilical ligament: Continuous with apex of the bladder
- 5 - Rama Nada - Ensherah Mokheemer - Ahmed salman 1 P a g e We will continue talking about the urinary bladder The ligaments of the bladder: 1-Median umbilical ligament: Continuous with apex of the bladder
Chapter 14 The Reproductive System
 Biology 12 Name: Reproductive System Per: Date: Chapter 14 The Reproductive System Complete using BC Biology 12, page 436-467 14. 1 Male Reproductive System pages 440-443 1. Distinguish between gametes
Biology 12 Name: Reproductive System Per: Date: Chapter 14 The Reproductive System Complete using BC Biology 12, page 436-467 14. 1 Male Reproductive System pages 440-443 1. Distinguish between gametes
Structural analysis of testicular appendices in patients with cryptorchidism
 ORIGINL rticle Vol. 39 (2): 240-247, March - pril, 2013 doi: 10.1590/S1677-5538.IJU.2013.02.13 Structural analysis of testicular appendices in patients with cryptorchidism Guilherme D. Tostes, Suelen F.
ORIGINL rticle Vol. 39 (2): 240-247, March - pril, 2013 doi: 10.1590/S1677-5538.IJU.2013.02.13 Structural analysis of testicular appendices in patients with cryptorchidism Guilherme D. Tostes, Suelen F.
Epithelial Tissues. Types of Epithelial Tissues: Lining of Kidney
 Epithelial Tissues Covers the entire body surface and most of the body s inner cavities Outer epidermis (skin) protects from injury and drying out Inner epidermal tissue (on internal surfaces) often serves
Epithelial Tissues Covers the entire body surface and most of the body s inner cavities Outer epidermis (skin) protects from injury and drying out Inner epidermal tissue (on internal surfaces) often serves
Chapter 22 Reproductive Systems. Male Reproductive Organs. Male Reproductive Organs. Specialized to produce, maintain the male sex cells (sperm)
 Chapter 22 Reproductive Systems Male reproductive organs 1 Male Reproductive Organs posterior view 2 Male Reproductive Organs Specialized to produce, maintain the male sex cells (sperm) Transport these
Chapter 22 Reproductive Systems Male reproductive organs 1 Male Reproductive Organs posterior view 2 Male Reproductive Organs Specialized to produce, maintain the male sex cells (sperm) Transport these
The Male and Female Internal Genitalia. Dr Oluwadiya Kehinde
 The Male and Female Internal Genitalia Dr Oluwadiya Kehinde www.oluwadiya.com Overview The reproductive role of the male is to produce sperm, deliver them to the female Primary sex organs are the gonads
The Male and Female Internal Genitalia Dr Oluwadiya Kehinde www.oluwadiya.com Overview The reproductive role of the male is to produce sperm, deliver them to the female Primary sex organs are the gonads
HOLE S ANATOMY CHAPTER 5, PART II Lecture notes
 HOLE S ANATOMY CHAPTER 5, PART II Lecture notes I. Connective Tissue A. Structure 1. have few cells that are spaced apart and can divide; two categories: a. fixed cells cells that are present in tissue
HOLE S ANATOMY CHAPTER 5, PART II Lecture notes I. Connective Tissue A. Structure 1. have few cells that are spaced apart and can divide; two categories: a. fixed cells cells that are present in tissue
Development of the Digestive System. W.S. O The University of Hong Kong
 Development of the Digestive System W.S. O The University of Hong Kong Plan for the GI system Then GI system in the abdomen first develops as a tube suspended by dorsal and ventral mesenteries. Blood
Development of the Digestive System W.S. O The University of Hong Kong Plan for the GI system Then GI system in the abdomen first develops as a tube suspended by dorsal and ventral mesenteries. Blood
THE INS AND OUTS OF HERNIAS WHERE TO START? WHAT IS A HERNIA? CLINICAL INDICATIONS THE INGUINAL CANAL THE CLINICAL QUESTION 18/09/2018
 THE INS AND OUTS OF HERNIAS Cassandra Harrison BA/BSc, MMRU, AMS WHERE TO START? The Clinical Question Essential anatomy Inguinal hernia Scanning technique Variations WHAT IS A HERNIA? CLINICAL INDICATIONS
THE INS AND OUTS OF HERNIAS Cassandra Harrison BA/BSc, MMRU, AMS WHERE TO START? The Clinical Question Essential anatomy Inguinal hernia Scanning technique Variations WHAT IS A HERNIA? CLINICAL INDICATIONS
Study of different tissues Abnormal cells and tissues can be compared to normal tissues to identify disease, such as cancer Being able to know and
 CHAPTER 4 Study of different tissues Abnormal cells and tissues can be compared to normal tissues to identify disease, such as cancer Being able to know and recognize normal tissues under the microscope
CHAPTER 4 Study of different tissues Abnormal cells and tissues can be compared to normal tissues to identify disease, such as cancer Being able to know and recognize normal tissues under the microscope
Physiologic Anatomy of the Male Sexual Organs
 Reproductive and Hormonal Functions of the Male The reproductive functions of the male can be divided into three major subdivisions: (1) spermatogenesis, which means simply the formation of sperm; (2)
Reproductive and Hormonal Functions of the Male The reproductive functions of the male can be divided into three major subdivisions: (1) spermatogenesis, which means simply the formation of sperm; (2)
Unit 15 ~ Learning Guide
 Unit 15 ~ Learning Guide Name: INSTRUCTIONS Complete the following notes and questions as you work through the related lessons. You are required to have this package completed BEFORE you write your unit
Unit 15 ~ Learning Guide Name: INSTRUCTIONS Complete the following notes and questions as you work through the related lessons. You are required to have this package completed BEFORE you write your unit
THE DESCENT OF THE TESTIS
 Arch. Dis. Childh., 1964, 39, 605. THE DESCENT OF THE TESTIS BY C. G. SCORER From Hillingdon Hospital, Uxbridge This study is based on observations made on boys at birth, during infancy, and throughout
Arch. Dis. Childh., 1964, 39, 605. THE DESCENT OF THE TESTIS BY C. G. SCORER From Hillingdon Hospital, Uxbridge This study is based on observations made on boys at birth, during infancy, and throughout
Human Reproductive System
 Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male=s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male=s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
Developmental Changes of Müllerian and Wolffian Ducts in Domestic Cat Fetuses
 Exp. Anim. 58(1), 41 45, 2009 Note Developmental Changes of Müllerian and Wolffian Ducts in Domestic Cat Fetuses Tomo INOMATA 1), Hiroyoshi NINOMIYA 1), Katsuyasu SAKITA 1), Naomi KASHIWAZAKI 2), Junya
Exp. Anim. 58(1), 41 45, 2009 Note Developmental Changes of Müllerian and Wolffian Ducts in Domestic Cat Fetuses Tomo INOMATA 1), Hiroyoshi NINOMIYA 1), Katsuyasu SAKITA 1), Naomi KASHIWAZAKI 2), Junya
Yes, cranially with ovarian, caudally with vaginal. Yes, with uterine artery (collateral circulation between abdominal +pelvic source)
 Blood supply to internal female genitalia: uterine Internal iliac Sup. large branch: uterus, inf. Small branch: cervix+ sup. Vagina Yes, cranially with ovarian, caudally with vaginal Medially in base of
Blood supply to internal female genitalia: uterine Internal iliac Sup. large branch: uterus, inf. Small branch: cervix+ sup. Vagina Yes, cranially with ovarian, caudally with vaginal Medially in base of
Science and Health THE HUMAN REPRODUCTIVE SYSTEM
 5 Module 1 Science and Health THE HUMAN REPRODUCTIVE SYSTEM Male Female A DepEd-BEAM Distance Learning Program supported by the Australian Agency for International Development NOTICE Section 9 of the Presidential
5 Module 1 Science and Health THE HUMAN REPRODUCTIVE SYSTEM Male Female A DepEd-BEAM Distance Learning Program supported by the Australian Agency for International Development NOTICE Section 9 of the Presidential
What do we mean by male infertility?
 Chapter1 What do we mean by male infertility? What do we mean by male infertility? This may be a strange question to ask at the beginning of a book on male infertility but it is an important one and, as
Chapter1 What do we mean by male infertility? What do we mean by male infertility? This may be a strange question to ask at the beginning of a book on male infertility but it is an important one and, as
The posterior abdominal wall. Prof. Oluwadiya KS
 The posterior abdominal wall Prof. Oluwadiya KS www.oluwadiya.sitesled.com Posterior Abdominal Wall Lumbar vertebrae and discs. Muscles opsoas, quadratus lumborum, iliacus, transverse, abdominal wall
The posterior abdominal wall Prof. Oluwadiya KS www.oluwadiya.sitesled.com Posterior Abdominal Wall Lumbar vertebrae and discs. Muscles opsoas, quadratus lumborum, iliacus, transverse, abdominal wall
SURGICAL PROCEDURE DESCRIPTIONS
 SURGICAL PROCEDURE DESCRIPTIONS GONADECTOMY: CASTRATION USING SCROTAL METHOD 1. The animal is anesthetized and placed in dorsal recumbency with the tail toward the surgeon. 2. The abdominal and scrotal
SURGICAL PROCEDURE DESCRIPTIONS GONADECTOMY: CASTRATION USING SCROTAL METHOD 1. The animal is anesthetized and placed in dorsal recumbency with the tail toward the surgeon. 2. The abdominal and scrotal
The Reproductive System
 16 PART A The Reproductive System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Reproductive
16 PART A The Reproductive System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Reproductive
Sexual differentiation:
 Abnormal Development of Female Genitalia Dr. Maryam Fetal development of gonads, external genitalia, Mullerian ducts and Wolffian ducts can be disrupted at a variety of points, leading to a wide range
Abnormal Development of Female Genitalia Dr. Maryam Fetal development of gonads, external genitalia, Mullerian ducts and Wolffian ducts can be disrupted at a variety of points, leading to a wide range
Different aspects of congenital undescended testis
 Different aspects of congenital undescended testis chapter : DIFFERENT ASPECTS OF CONGENITAL UNDESCENDED TESTIS Synopsis: In this chapter the surgical aspects of congenital undescended testis, as found
Different aspects of congenital undescended testis chapter : DIFFERENT ASPECTS OF CONGENITAL UNDESCENDED TESTIS Synopsis: In this chapter the surgical aspects of congenital undescended testis, as found
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 3. October 17, 2014
 STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 3 October 17, 2014 PART l. Answer in the space provided. (12 pts) 1. Identify the structures. (2 pts) A. B. A B C. D. C D 2. Identify the structures. (2
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 3 October 17, 2014 PART l. Answer in the space provided. (12 pts) 1. Identify the structures. (2 pts) A. B. A B C. D. C D 2. Identify the structures. (2
Histology of Male Reproductive system (1)
 Histology of Male Reproductive system (1) Prof. Dr. Malak A. Al-yawer Learning Objectives At the end of this lecture, the medical student will be able to: State the organization of the testis Define seminiferous
Histology of Male Reproductive system (1) Prof. Dr. Malak A. Al-yawer Learning Objectives At the end of this lecture, the medical student will be able to: State the organization of the testis Define seminiferous
Abdominal Hernia Omar alnoubani MD,MRCS
 Abdominal Hernia Omar alnoubani MD,MRCS Definition of hernia Anatomical landmarks Overview of types of hernia Presentation and Management of common types of hernia What is the definition of a hernia? An
Abdominal Hernia Omar alnoubani MD,MRCS Definition of hernia Anatomical landmarks Overview of types of hernia Presentation and Management of common types of hernia What is the definition of a hernia? An
Muscle Tissue. General concepts. Classification of muscle. I. Functional classification is based on the type of neural control.
 Muscle Tissue LEARNING OBJECTIVES 1. Identify the three types of muscle tissue at the light microscopic level. 2. List and compare the structural and functional features of each of the three muscle fiber
Muscle Tissue LEARNING OBJECTIVES 1. Identify the three types of muscle tissue at the light microscopic level. 2. List and compare the structural and functional features of each of the three muscle fiber
STRUCTURE AND FUNCTION OF THE MALE REPRODUCTIVE SYSTEM
 Unit 7A STRUCTURE AND FUNCTION OF THE MALE REPRODUCTIVE SYSTEM LEARNING OBJECTIVES 1. Learn the structures of the male reproductive system. 2. Learn the functions of the male reproductive system. 3. Learn
Unit 7A STRUCTURE AND FUNCTION OF THE MALE REPRODUCTIVE SYSTEM LEARNING OBJECTIVES 1. Learn the structures of the male reproductive system. 2. Learn the functions of the male reproductive system. 3. Learn
Fareed Khdair, MD Assistant Professor Chief, Section of Pediatric Gastroenterology, Hepatology, and Nutrition University of Jordan School of Medicine
 Fareed Khdair, MD Assistant Professor Chief, Section of Pediatric Gastroenterology, Hepatology, and Nutrition University of Jordan School of Medicine Outline Lecture one : Gut formation Foregut: esophagus,
Fareed Khdair, MD Assistant Professor Chief, Section of Pediatric Gastroenterology, Hepatology, and Nutrition University of Jordan School of Medicine Outline Lecture one : Gut formation Foregut: esophagus,
Histology. Study of body tissues
 Histology Study of body tissues 2 Introduction to Body Tissues 1. Composed of specialized cells of similar structure and perform a common function 2. Four major types (4 Cs) a. Epithelial - Cover b. Connective
Histology Study of body tissues 2 Introduction to Body Tissues 1. Composed of specialized cells of similar structure and perform a common function 2. Four major types (4 Cs) a. Epithelial - Cover b. Connective
Chapter 6: Skeletal System: Bones and Bone Tissue
 Chapter 6: Skeletal System: Bones and Bone Tissue I. Functions A. List and describe the five major functions of the skeletal system: 1. 2. 3.. 4. 5.. II. Cartilage A. What do chondroblasts do? B. When
Chapter 6: Skeletal System: Bones and Bone Tissue I. Functions A. List and describe the five major functions of the skeletal system: 1. 2. 3.. 4. 5.. II. Cartilage A. What do chondroblasts do? B. When
Human Sexuality - Ch. 2 Sexual Anatomy (Hock)
 Human Sexuality - Ch. 2 Sexual Anatomy (Hock) penis penile glans corona frenulum penile shaft erection foreskin circumcision corpora cavernosa corpus spongiosum urethra scrotum spermatic cords testicles
Human Sexuality - Ch. 2 Sexual Anatomy (Hock) penis penile glans corona frenulum penile shaft erection foreskin circumcision corpora cavernosa corpus spongiosum urethra scrotum spermatic cords testicles
