Changing parenteral nutrition administration sets every 24 h versus every 48 h in newborn infants
|
|
|
- Berenice Banks
- 5 years ago
- Views:
Transcription
1 CLINICAL GASTROENTEROLOGY Changing parenteral nutrition administration sets every 24 h versus every 48 h in newborn infants Miriam Fox RN MN, Marion Molesky RN MSN, John E Van Aerde MD PhD, Sarah Muttitt MD M Fox, M Molesky, JE Van Aerde, S Muttitt. Changing parenteral nutrition administration sets every 24 h versus every 48 h in newborn infants. Can J Gastroenterol 1999;13(2): OBJECTIVE: To determine whether changing total parenteral nutrition fluid administration sets (TAS) every 48 h rather than every 24 h results in a greater infusate contamination rate. PATIENTS AND METHODS: Prospectively, 166 infants were assigned at random to have TAS changed either every 24 h or every 48 h. Samples of the infusate were cultured to determine contamination rates of the infusate in the sets and were tested from 149 of these infants. TAS was replaced every 24 h in the control group, and 445 amino acid plus dextrose solutions (AADS) and 449 lipid emulsions samples were taken for bacterial culture. Fungal cultures were also performed on 449 samples. The study group had TAS replaced every 48 h, and 454 samples of AADS were cultured for bacteria. The numbers of lipid emulsion samples sent for bacterial culture and fungal culture were 449 and 440, respectively. Information on type of intravenous access device, administration of antibiotics and blood cultures was also collected. RESULTS: There was no difference in bacterial contamination rates for AADS or lipid emulsion from TAS changed every 24 or 48 h ( 2, P>0.05). Lipid emulsion sampled from the 24 h group showed a statistically significant higher rate of fungal contamination than specimens from the 48 h group (P<0.01). CONCLUSIONS: Changing TAS every 48 h versus 24 h does not increase the contamination rate of infusate in newborns. Key Words: Infection, Neonate, Total parenteral nutrition Changer les dispositifs d administration d alimentation parentérale chez les nourrissons toutes les 24 heures ou toutes les 48 heures? OBJECTIF : Déterminer si le changement des dispositifs d administration d alimentation parentérale totale toutes les 48 heures plutôt que toutes les 24 heures peut s accompagner d un plus fort taux de contamination de la solution perfusée. PATIENTS ET MÉTHODES : De façon prospective, 166 nourrissons ont été assignés aléatoirement à l un de deux groupes selon que le dispositif de perfusion était changé toutes les 24 ou toutes les 48 heures. Des échantillons des solutions perfusées ont été mis en culture afin de vérifier les taux de contamination dans les dispositifs d administration et ils ont été vérifiés pour 149 de ces nourrissons. Le dispositif a été remplacé toutes les 24 heures dans le groupe témoin et 454 échantillons de solutions d acides aminés plus dextrose (SAAD) et 449 échantillons d émulsion de lipides ont été prélevés pour cultures. Des cultures fongiques ont en outre été effectuées sur 449 prélèvements. Pour l autre groupe, on a remplacé le dispositif toutes les 48 heures et 454 échantillons de SAAD ont été mis en culture pour y déceler la présence de bactéries. Les nombres d échantillons d émulsion de lipides testés pour culture bactérienne et culture fongique ont été 449 et 440, respectivement. Des renseignements relatifs aux différents types d accès intraveineux, à l antibiothérapie et aux hémocultures ont également été recueillis. RÉSULTATS : On n a noté aucune différence quant à la contamination bactérienne des SAAD ou des émulsions de lipides dans les dispositifs d administration changés toutes les 24 ou 48 heures ( 2, P > 0,05). Pour les échantillons d émulsion de lipides recueillis chez le groupe 24 heures, on a noté une élévation du taux de contamination fongique statistiquement significative par rapport aux spécimens prélevés dans le groupe 48 heures (P < 0,01). CONCLUSONS : Le fait de changer les dispositifs d administration de l ali- Neonatal Intensive Care Unit, Department of Pediatrics, Stollery Children s Health Centre, University of Alberta Hospitals, Edmonton, Alberta Correspondence and reprints: Ms Miriam Fox, Neonatal Intensive Care Unit, Stollery Children s Health Centre, 3A3.31 W Can J Gastroenterol Vol 13 No 2 March
2 Fox et al Sick neonates, especially those who are premature, are frequently unable to tolerate enteral feedings and have limited nutritional reserves (1). Although total parenteral nutrition (TPN) is critical to growth and recovery, complications are associated with its use, including infection due to the presence of intravenous access devices in immunocompromised patients (2). Potential sources of infection are related to intravenous access device problems such as direct invasion by microorganisms at the site of catheter insertion, hematogenous seeding of the catheter during periods of bacteremia or fungemia, and catheter hub colonization or contamination of infusate (3-6). Both the use of central venous catheters and TPN therapy have been associated with increased risk of sepsis in both adults and neonates (7,8). In adults, there has been a trend in practice to change TPN administration sets (TAS) at intervals longer than 24 h. Although cost savings without an increased incidence of contamination or patient bacteremia have been demonstrated, the data are based on adult populations, primarily with clear intravenous solutions; only two studies included amino acid plus dextrose solutions (AADS), and none reported on lipid emulsions (9-14). The current practice in the neonatal intensive care unit (NICU) at the Stollery Children s Health Centre, University of Alberta Hospitals, Edmonton, Alberta, is to change TAS every 24 h using an aseptic technique. We conducted a prospective, randomized study of contamination rates for TAS changed at 24 h versus 48 h intervals. The objective was to examine whether differences in contamination rates would occur. Figure 1) Sites for sampling fluid for analysis of parenteral nutrition administration set. X Sampling site PATIENTS AND METHODS Patient enrolment and sample collection: For 12 months, all neonates receiving TPN in the level III NICU at the Children s Health Centre were entered in the study. The study was approved by the Ethics Committee of the University of Alberta Hospitals; the Ethics Committee considered it unnecessary for informed consent to be obtained. After enrolment, a random number table was used to allocate infants in a one to two ratio to either 24 h or 48 h changes of their TAS. Group assignment remained the same for the length of each infant s hospitalization in the NICU. The bag containing AADS was prepared in the hospital pharmacy and was changed daily in both groups. Lipid emulsion bottles were changed with the line sets. For infants in the 48 h group, the AADS bag was removed, and the new one added using the same TAS for 48 h. The TAS was changed by the bedside nurse assigned to care for the patient according to NICU procedure. Samples of solutions were sent for culture at the assigned time intervals regardless of changes in intravenous access devices. The two types of TAS used during the study period were determined by the type of intravenous pump in use. One preassembled set had an in-line buretrol and a 0.22 m filter for the AADS Y-connected to an in-line buretrol line for lipid emulsion. The second TAS type required a 0.22 m filter to be added to an in-line buretrol set for the AADS, which was joined to an in-line buretrol set for lipid emulsion with a connector. This connector was not used for medication administration. After the required tubing was assembled, the connections between tubing sections and intravenous access devices were swabbed with povidone-iodine. The AADS bag and the lipid emulsion bottle were added, and the solutions were run through the tubing. When the TPN was administered by a peripheral intravenous device, the tubing was assembled using an aseptic technique over a sterile field. If the TPN was administered by a central line, the nurse wore sterile gloves while assembling the tubing over a sterile field. Line care was standardized across both groups and included administering medications through the TAS and adding electrolytes to AADS buretrols when necessary. For peripheral TAS, the injection ports were swabbed with alcohol before punctures, and central TAS injection ports were swabbed with both povidone-iodine and alcohol before punctures. If TAS were disconnected from the intravenous access device for any reason between line changes, the lines were capped with a sterile end. Immediately before a line change, the TAS lines at the sampling sites were disinfected with povidone-iodine and alcohol, and samples were drawn by the nurse caring for the patient. The sampling site in the AADS TAS was the tubing immediately past the bacterial filter, and the sample was taken from the tubing in the lipid emulsion TAS as close to the patient as possible but before the connection with the AADS (Figure 1). With the line clamped at the T- connectors distal to the intravenous access device, a 25- gauge needle attached to a sterile syringe was used to puncture the cleansed tubing at the sampling site, and 3 ml of the infusate was withdrawn to obtain an upstream sample. The fluid was sent in sterile tubes for analysis. Diagnosis, including the need for blood cultures, and treatment of suspected or proven sepsis were determined by the attending clinician. Bacteremia was diagnosed by positive blood cultures. Microbiology: According to standard laboratory practice, 148 Can J Gastroenterol Vol 13 No 2 March 1999
3 Changing TPN lines at 24 h versus 48 h TABLE 1 Patient data (mean ± SD) for groups randomized to have parenteral nutrition administration sets changed every 24 or 48 h Randomization group 24 h (n=51) 48 h (n=97) Birth weight (g) 2004± ±1062 Gestational age (weeks) 32.7± ±5.2 Postnatal age (days) 10.9± ±20.5 Antibiotic score* 0.48± ±0.39 Line score 0.32± ±0.43 *Proportion of samples while infants on antibiotics; Proportion of samples while infants had central line. All values were not significant AADS and lipid emulsion samples were each plated on chocolate agar, and a sample of lipid emulsion was incubated on a phytone biplate. The chocolate agar plates were read, and growth identified as required after 24 and 48 h. The phytone biplates were read three times weekly for two weeks. Cultures were reported in three groups: no growth; 1 to 9 colony forming units (cfu)/ml, which was defined as questionable contamination; and 10 cfu/ml or more, which was defined as positive contamination. Blood was cultured if indicated clinically. Statistical analysis: The unit of measurement was the infusate sample not the patient. Patient data for birth weight, gestational age, postnatal age, antibiotics and type of line were expressed as mean SD and analyzed by unpaired t test. Contamination rates of the TAS sets, and the proportion of samples from infants with central lines or receiving antibiotics were analyzed by using 2 analysis, and Yates correction was applied. Previous studies in adult intensive care units have demonstrated a 4% contamination rate of AADS (5). Assuming an alpha of 0.05 and a power of 0.8, demonstration of a difference in contamination rate of 5% required a sample size of 440 cultures in each group. Infants were enrolled in the 48 h group in a two to one ratio in order to have a similar number of line changes in each arm of the study. RESULTS A total of 2686 infusate samples was taken from the lines of infants entered into the study. One hundred and sixty-six infants were randomly assigned to have TAS changed every 24 or 48 h. As per the study design, 53 infants were allocated to the 24 h group, and 113 to the 48 h group. Due to discontinuation of TPN, samples from two infants in the 24 h group and 12 in the 48 h group were not sent. Three patients in the 48 h group died before samples were taken. Samples of infusate from one infant randomly assigned to the 48 h group were incorrectly sent every 24 h. In the final analysis, TAS samples were taken from 51 infants in the 24 h group and from 97 infants in the 48 h group. TABLE 2 Contamination rates of total parenteral nutrition solutions Randomization group Parenteral solution 24 h 48 h P value AADS Bacterial 14/445 (3.1 %) 13/454 (2.9%) NS Lipid emulsion Bacterial 27/449 (6.0%) 23/449 (5.1%) NS Fungal 14/449 (3.1 %) 2/440 (0.5%) <0.01 AADS Amino acid plus dextrose solution; NS Not significant TABLE 3 Organisms in positive cultures of total parenteral nutrition solution samples Randomization group Organism 24 h (n=1343) 48 h (n=1343) Coagulase-negative staphylococci Candida species 13 0 Fungi 1 2 Enterobacter species 1 0 Enterococcus species 0 1 Streptococcus viridans 2 0 Gram-negative bacilli (glucose nonfermenting) 0 1 There was no difference between the infants in the 24 and 48 h groups for birth weight, and gestational and postnatal age (Table 1). The range of weight was 530 to 4525 g; gestational age andpostnatal age at study enrolment varied from 23 weeks to 42 weeks and one day to 64 days, respectively. About half of the cultures were taken while the patients were receiving antibiotics, a proportion similar for both groups (Table 1). For both groups, approximately one-third of the samples were taken from patients with a central line (Table 1). Bacterial contamination rates for AADS and lipid emulsion varied from 2.9% to 6.0% with an overall rate of 4.3% (Table 2). The overall bacterial contamination rate for the lipid emulsion was higher at 5.6% than that for AADS at 3.0%. Fungal contamination rates of the two interval groups were quite different at 3.1% for the 24 h group and 0.5% for the 48 h group. There was no significant difference between the 24 and 48 h groups for bacterial contamination of AADS or lipid emulsion (Table 2). Comparison of fungal contamination rates of lipid emulsion showed significantly higher contamination rates in the 24 h group than the 48 h group (P<0.01; Table 2). This difference in fungal contamination of lipid emulsion was influenced by one patient in the 24 h group; the patient had candida septicaemia and meningitis with subsequent contaminated TAS fluid cultures. When this infant was excluded from the analysis, fungal Can J Gastroenterol Vol 13 No 2 March
4 Fox et al contamination rates between the 24 and 48 h groups were similar at 0.2% and 0.5%, respectively. The organisms isolated from the TPN samples are listed in Table 3. Coagulase-negative staphylococci and candida accounted for 91% of all positive cultures. Results of blood cultures drawn for clinical indications were examined with respect to infusate cultures. Positive blood cultures were observed in 13 patients in the 24 h group, and the organism isolated was similar to that in the TPN sample in nine infants. In the 48 h group, 20 infants had positive blood cultures, and 10 infants had an organism isolated from a blood culture similar to that in the infusate samples. None of these values was statistically different between the two groups. DISCUSSION Infusate may be contaminated during attachment and/or manipulation of TAS. In adult populations, infusate contamination levels are low. Rates of 0.3% to 3.6% have been reported in studies examining infusate contamination rates for intravenous fluid administration sets replaced at 24 to 72 h (9-14). Only one of the studies showed a correlation between contaminated infusate and patient bacteremia; however, contamination of the infusate did not precede patient bacteremia (14). Two studies included AADS with other infusates, and none included lipid emulsions. Our study is the first to examine AADS and lipid emulsion exclusively, while AADS formed a small subset of the lines examined in previous adult studies. In adults, the greatest contamination rate reported of AADS infused through a central line was 3.6% (9). lnfusate contamination rates were higher in an intensive care unit setting, which was attributed to greater manipulation of the intravenous lines (9,11,12). In our study, the measured infusate contamination rate of TPN infused through peripheral and central intravenous access devices was 4.3%, which was higher than that reported for the adult population. The contamination rate measured for AADS was 3.0% in our study, which is similar to that reported in the adult literature. There are no published lipid emulsion contamination rates, so we cannot comment on the significance of the rate measured in this study. There also are no reports of infusate contamination rates for neonatal populations with which to compare rates. It is possible that TAS were manipulated to a greater extent in this population because of intravenous access problems. We did not find a higher contamination rate in neonates when TAS were changed less frequently, even when the infusate was AADS and lipid emulsion. Many of our specimens grew coagulase-negative staphylococci. This has also been reported in adult studies (9-14). These organisms may have been an outside contaminant of the TAS tubing rather than the infusate, but 10 cfu or more were required before the infusate was classified as contaminated. Because this organism is a frequent pathogen in the NICU, these results could not be ignored. Contamination of the infusate with the same organism found in a positive blood culture occurred 75% of the time, but the timing of infusate contamination varied. Infusate samples were positive before, at the same time or after positive blood cultures were obtained. Therefore, it is not possible to conclude that contaminated infusate caused blood infection in all cases. In one study, bacteremia was associated with positive infusate samples in five patients (14). Infusate contamination did not precede the onset of bacteremia. More information regarding infusate contamination compared with blood contamination would have been possible if more frequent blood culture samples had been obtained. This was not done because it would have been unethical to draw blood culture samples from stable babies. Therefore, the physician caring for the infant determined whether the clinical status of the patient warranted blood cultures. It has been speculated that a significant factor in the contamination of infusates is the number of times that intravenous administration lines are manipulated. There was no control exercised or information collected about the number of TAS manipulations (disconnection of TAS from the intravenous device or injection into the TAS). This information may have been helpful in determining why the infusate contamination rate was elevated compared with published results of other infusates, but the number of TAS manipulations proved too difficult to determine accurately. However, the current practice of multiple entries extended an additional 24 h does not lead to a significant increase in TAS infusate contamination. There are significant cost savings to the NICU if TAS are changed every 48 h rather than every 24 h. The cost of administration sets for TPN varies with the type of TAS and the type of intravenous pump used within an NICU. Currently, a complete administration set for TPN costs $8.57, and a bottle of lipid emulsion is $7.08. Therefore, a total of $15.65 can be saved for every line change eliminated. Total savings would vary with the number of patient days of TPN. During the past year, changing TAS every 48 h would have realized a savings of $15, (1982 patient days of TPN divided by two and multiplied by $15.65). These findings indicated that changing TAS every 48 h rather than every 24 h seems safe and does not increase bacterial or fungal contamination rates of AADS or lipid emulsion infusates. In addition, change to this practice would result in cost savings. ACKNOWLEDGEMENTS: This research was supported by a research grant from the Special Services and Research Committee of the University of Alberta Hospitals, Edmonton, Alberta. REFERENCES 1. Pereira GR, Balmer D. Feeding the critically ill neonate. In: Spitzer AR, ed. Intensive Care of the Fetus and Neonate. St Louis: Mosby, 1996: Spear ML. Intravenous alimentation. In: Spitzer AR, ed. Intensive Care of the Fetus and Neonate. St Louis: Mosby, 1996: Can J Gastroenterol Vol 13 No 2 March 1999
5 Changing TPN lines at 24 h versus 48 h 3. Linares J, Sitges-Serra A, Garau J, Perez JL, Martin R. Pathogenesis of catheter sepsis: a prospective study with quantitative and semiquantitative cultures of catheter hub and segments. J Clin Microbiol 1985;21: Maki DG. Infections associated with intravascular lines. In: Remington JS, Swartz MN, eds. Current Clinical Topics in Infectious Diseases, vol 3. New York: McGraw-Hill, 1982: Norwood S, Ruby A, Civetta J, Cortes V. Catheter-related infections and associated septicemia. Chest 1991;99: Sitges-Serra A, Puig P, Linares J, et al. Hub colonization as the initial step in an outbreak of catheter-related sepsis due to coagulase negative staphylococci during parenteral nutrition. J Parenter Entera Nutr 1984;8: Moro ML, Vigano EF, Cozzi Lepri A. Risk factors for central venous catheter-related infections in surgical and intensive care units. The Central Venous Catheter-Related Infections Study Group. Infect Control Hosp Epidemiol 1994;15: Wolfson P. General surgical considerations. In: Spitzer AR, ed. Intensive Care of the Fetus and Neonate. St Louis: Mosby, 1996: Maki DG, Botticelli JT, LeRoy ML, Thieike TS. Prospective study of replacing administration sets for intravenous therapy at 48- vs 72-hour intervals. 72 hours is safe and cost-effective. JAMA 1987;258: Buxton AE, Highsmith AK, Garner JS, et al. Contamination of intravenous infusion fluid: effects of changing administration sets. Ann Intern Med 1979;90: Band JD, Maki DG. Safety of changing intravenous delivery systems at longer than 24-hour intervals. Ann Intern Med 1979;91: Gorbea HF, Snydman DR, Delaney A, Stockman J, Martin WJ. Intravenous tubing with burettes can be safely changed at 48-hour intervals. JAMA 1984;251: Josephson A, Gombert ME, Sietta MF, Karanfil LV, Tansino GF. The relationship between intravenous fluid contamination and the frequency of tubing replacement. Infect Control 1985;6: Snydman DR, Donnelly-Reidy M, Perry LK, Martin WJ. Intravenous tubing containing burettes can be safely changed at 72 hour intervals. Infect Control 1987;8: Can J Gastroenterol Vol 13 No 2 March
6 MEDIATORS of INFLAMMATION The Scientific World Journal Gastroenterology Research and Practice Diabetes Research International Endocrinology Immunology Research Disease Markers Submit your manuscripts at BioMed Research International PPAR Research Obesity Ophthalmology Evidence-Based Complementary and Alternative Medicine Stem Cells International Oncology Parkinson s Disease Computational and Mathematical Methods in Medicine AIDS Behavioural Neurology Research and Treatment Oxidative Medicine and Cellular Longevity
Lab 4. Blood Culture (Media) MIC AMAL-NORA-ALJAWHARA 1
 Lab 4. Blood Culture (Media) 2018 320 MIC AMAL-NORA-ALJAWHARA 1 Blood Culture 2018 320 MIC AMAL-NORA-ALJAWHARA 2 What is a blood culture? A blood culture is a laboratory test in which blood is injected
Lab 4. Blood Culture (Media) 2018 320 MIC AMAL-NORA-ALJAWHARA 1 Blood Culture 2018 320 MIC AMAL-NORA-ALJAWHARA 2 What is a blood culture? A blood culture is a laboratory test in which blood is injected
320 MBIO Microbial Diagnosis. Aljawharah F. Alabbad Noorah A. Alkubaisi 2017
 320 MBIO Microbial Diagnosis Aljawharah F. Alabbad Noorah A. Alkubaisi 2017 Blood Culture What is a blood culture? A blood culture is a laboratory test in which blood is injected into bottles with culture
320 MBIO Microbial Diagnosis Aljawharah F. Alabbad Noorah A. Alkubaisi 2017 Blood Culture What is a blood culture? A blood culture is a laboratory test in which blood is injected into bottles with culture
SARASOTA MEMORIAL HOSPITAL
 SARASOTA MEMORIAL HOSPITAL TITLE: NURSING PROCEDURE BLOOD CULTURE COLLECTION PROCEDURE (spe20) DATE: REVIEWED: PAGES: 6/10 2/19 1 of 6 PS1094 ISSUED FOR: Nursing/Lab RESPONSIBILITY: RN, LPN II, select
SARASOTA MEMORIAL HOSPITAL TITLE: NURSING PROCEDURE BLOOD CULTURE COLLECTION PROCEDURE (spe20) DATE: REVIEWED: PAGES: 6/10 2/19 1 of 6 PS1094 ISSUED FOR: Nursing/Lab RESPONSIBILITY: RN, LPN II, select
BLOOD CULTURE POLICY FOR PAEDIATRICS
 BLOOD CULTURE POLICY FOR PAEDIATRICS 1. INTRODUCTION Blood culture to detect bacteraemia is an important investigation with major implications for the diagnosis of patients with infection and the selection
BLOOD CULTURE POLICY FOR PAEDIATRICS 1. INTRODUCTION Blood culture to detect bacteraemia is an important investigation with major implications for the diagnosis of patients with infection and the selection
The Clinical Significance of Blood Cultures. Presented BY; Cindy Winfrey, MSN, RN, CIC, DON- LTC TM, VA- BC TM
 The Clinical Significance of Blood Cultures Presented BY; Cindy Winfrey, MSN, RN, CIC, DON- LTC TM, VA- BC TM OVERVIEW Blood cultures are considered an important laboratory tool used to diagnose serious
The Clinical Significance of Blood Cultures Presented BY; Cindy Winfrey, MSN, RN, CIC, DON- LTC TM, VA- BC TM OVERVIEW Blood cultures are considered an important laboratory tool used to diagnose serious
Blood Culture Collection and Interpretation
 Blood Culture Collection and Interpretation Catherine Ernst, RN,PBT(ASCP) Blood Cultures Indications for blood culture collection Proper method for blood culture collection Interpreting a blood culture
Blood Culture Collection and Interpretation Catherine Ernst, RN,PBT(ASCP) Blood Cultures Indications for blood culture collection Proper method for blood culture collection Interpreting a blood culture
Blood culture 壢新醫院 病理檢驗科 陳啟清技術主任
 Blood culture 壢新醫院 病理檢驗科 陳啟清技術主任 A Positive Blood Culture Clinically Important Organism Failure of host defenses to contain an infection at its primary focus Failure of the physician to effectively eradicate,
Blood culture 壢新醫院 病理檢驗科 陳啟清技術主任 A Positive Blood Culture Clinically Important Organism Failure of host defenses to contain an infection at its primary focus Failure of the physician to effectively eradicate,
LABORATORY SERVICES TECHNICAL PROCEDURE
 LABORATORY SERVICES TECHNICAL PROCEDURE TITLE: BLOOD CULTURE COLLECTION PROCEDURE NUMBER: SC050.4 PERFORMING SITE(s): University Hospital, Drake Center SITE EFFECTIVE DATE 8/8/13 SUPERSEDES: 1/5/2012 RETIRED
LABORATORY SERVICES TECHNICAL PROCEDURE TITLE: BLOOD CULTURE COLLECTION PROCEDURE NUMBER: SC050.4 PERFORMING SITE(s): University Hospital, Drake Center SITE EFFECTIVE DATE 8/8/13 SUPERSEDES: 1/5/2012 RETIRED
NOTE: The first appearance of terms in bold in the body of this document (except titles) are defined terms please refer to the Definitions section.
 TITLE PARENTERAL NUTRITION ADMINISTRATION AND MONITORING SCOPE Provincial: Acute Care APPROVAL AUTHORITY Clinical Operations Executive Committee SPONSOR Pharmacy Services, Nutrition Services, and Health
TITLE PARENTERAL NUTRITION ADMINISTRATION AND MONITORING SCOPE Provincial: Acute Care APPROVAL AUTHORITY Clinical Operations Executive Committee SPONSOR Pharmacy Services, Nutrition Services, and Health
Successful IV Starts Revised February 2014
 Successful IV Starts Revised February 2014 Why Intravenous Therapy? Used for access to the body s circulation Indications: Administer fluids, blood, medications, and nutrition Obtain laboratory specimens
Successful IV Starts Revised February 2014 Why Intravenous Therapy? Used for access to the body s circulation Indications: Administer fluids, blood, medications, and nutrition Obtain laboratory specimens
Bionector Ready-Sets Protected IV Management Systems For Neonates. Filter Feed Infuse Protect
 Bionector Ready-Sets Protected IV Management Systems For Neonates Filter Feed Infuse Protect vygon@vygon.co.uk www.vygon.co.uk Bionector Ready-Sets Bionector Ready-Sets can be used to meet all your infusion
Bionector Ready-Sets Protected IV Management Systems For Neonates Filter Feed Infuse Protect vygon@vygon.co.uk www.vygon.co.uk Bionector Ready-Sets Bionector Ready-Sets can be used to meet all your infusion
MICROBIOLOGICAL TESTING IN PICU
 MICROBIOLOGICAL TESTING IN PICU This is a guideline for the taking of microbiological samples in PICU to diagnose or exclude infection. The diagnosis of infection requires: Ruling out non-infectious causes
MICROBIOLOGICAL TESTING IN PICU This is a guideline for the taking of microbiological samples in PICU to diagnose or exclude infection. The diagnosis of infection requires: Ruling out non-infectious causes
Jo Kuehn, RN, MSN, CPHQ Jenell Westhoven, RN, BSN
 Jo Kuehn, RN, MSN, CPHQ Jenell Westhoven, RN, BSN Disclosure Information Intravenous Therapy and Parenteral Nutrition Administration: Nursing In- Focus Jo Kuehn, RN, MSN, CPHQ and Jenell Westhoven, RN,
Jo Kuehn, RN, MSN, CPHQ Jenell Westhoven, RN, BSN Disclosure Information Intravenous Therapy and Parenteral Nutrition Administration: Nursing In- Focus Jo Kuehn, RN, MSN, CPHQ and Jenell Westhoven, RN,
Prevention of Central Line-associated Bloodstream Infections (CLA-BSIs) associated with Arterial Catheters
 Prevention of Central Line-associated Bloodstream Infections (CLA-BSIs) associated with Arterial Catheters William R. Jarvis, M.D. President, Jason and Jarvis Associates, LLC Saxe Communications 2012 Sponsored
Prevention of Central Line-associated Bloodstream Infections (CLA-BSIs) associated with Arterial Catheters William R. Jarvis, M.D. President, Jason and Jarvis Associates, LLC Saxe Communications 2012 Sponsored
IV Fluids. Nursing B23. Objectives. Serum Osmolality
 IV Fluids Nursing B23 Objectives Discuss the purpose of IV Discuss nursing interventions in IV therapy Identify complications of IV therapy Differentiate between peripheral line, central line, and PICC
IV Fluids Nursing B23 Objectives Discuss the purpose of IV Discuss nursing interventions in IV therapy Identify complications of IV therapy Differentiate between peripheral line, central line, and PICC
IV Fluids Nursing B23 Objectives Serum Osmolality 275 to 295 Isotonic
 1 IV Fluids Nursing B23 2 Objectives 3 Serum Osmolality Serum osmolality solute concentration of a solution Higher osmolality means greater pulling power for water Normal serum osmolality is 275 to 295
1 IV Fluids Nursing B23 2 Objectives 3 Serum Osmolality Serum osmolality solute concentration of a solution Higher osmolality means greater pulling power for water Normal serum osmolality is 275 to 295
Congenital Chylothorax
 Case Study TheScientificWorldJOURNAL (2009) 9, 431 434 ISSN 1537-744X; DOI 10.1100/tsw.2009.62 Congenital Chylothorax Saad Lahmiti*, Jamila Elhoudzi, Salwa Baki, and Abdelmounaim Aboussad Neonatal Intensive
Case Study TheScientificWorldJOURNAL (2009) 9, 431 434 ISSN 1537-744X; DOI 10.1100/tsw.2009.62 Congenital Chylothorax Saad Lahmiti*, Jamila Elhoudzi, Salwa Baki, and Abdelmounaim Aboussad Neonatal Intensive
Recommendations for Hospital Quality Measures in 2011:
 Pediatric Measures: Recommendations for Hospital Quality Measures in 2011: Based on the input of a group of healthcare stakeholders, the following new hospital measures are recommended: 1) Home Management
Pediatric Measures: Recommendations for Hospital Quality Measures in 2011: Based on the input of a group of healthcare stakeholders, the following new hospital measures are recommended: 1) Home Management
If viewing a printed copy of this policy, please note it could be expired. Got to to view current policies.
 If viewing a printed copy of this policy, please note it could be expired. Got to www.fairview.org/fhipolicies to view current policies. Department Policy Code: D: PC-5555 Entity: Fairview Pharmacy Services
If viewing a printed copy of this policy, please note it could be expired. Got to www.fairview.org/fhipolicies to view current policies. Department Policy Code: D: PC-5555 Entity: Fairview Pharmacy Services
Central Venous Catheter Insertion: Assisting
 Approved by: Central Venous Catheter Insertion: Assisting Gail Cameron Senior Director, Operations, Maternal, Neonatal & Child Health Programs Dr. Santiago Ensenat Medical Director, Neonatology Neonatal
Approved by: Central Venous Catheter Insertion: Assisting Gail Cameron Senior Director, Operations, Maternal, Neonatal & Child Health Programs Dr. Santiago Ensenat Medical Director, Neonatology Neonatal
Routine endotracheal cultures for the prediction of sepsis in ventilated babies
 Archives of Disease in Childhood, 1989, 64, 34-38 Routine endotracheal cultures for the prediction of sepsis in ventilated babies T A SLAGLE, E M BIFANO, J W WOLF, AND S J GROSS Department of Pediatrics,
Archives of Disease in Childhood, 1989, 64, 34-38 Routine endotracheal cultures for the prediction of sepsis in ventilated babies T A SLAGLE, E M BIFANO, J W WOLF, AND S J GROSS Department of Pediatrics,
SARASOTA MEMORIAL HOSPITAL
 SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: PARENTERAL NUTRITION AND INTRAVENOUS FAT EMULSION (ADULT AND PEDIATRICS) Nursing DATE: REVIEWED: PAGES: RESPONSIBILITY: RN, LPN II 12/80
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: PARENTERAL NUTRITION AND INTRAVENOUS FAT EMULSION (ADULT AND PEDIATRICS) Nursing DATE: REVIEWED: PAGES: RESPONSIBILITY: RN, LPN II 12/80
Access Site and Hub Disinfection: In Vitro Testing of a Novel Device
 Access Site and Hub Disinfection: In Vitro Testing of a Novel Device Marcia A. Ryder, PhD MS RN, George Szorenyi, BS, Martin A. Hamilton, PhD, Gordon C. Hamilton, BS, Paul D. Holtom, MD University of Southern
Access Site and Hub Disinfection: In Vitro Testing of a Novel Device Marcia A. Ryder, PhD MS RN, George Szorenyi, BS, Martin A. Hamilton, PhD, Gordon C. Hamilton, BS, Paul D. Holtom, MD University of Southern
E.N : Tubal Feeding Systems ; Closed vs. Open
 E.N : Tubal Feeding Systems ; Closed vs. Open Dr:Enas Mogawer, MD Head Of Clinical Nutrition Department,AFSH Professor Of Internal Medicine Kasr El Aini Medical Consultant Of Clinical Nutrition And Obesity
E.N : Tubal Feeding Systems ; Closed vs. Open Dr:Enas Mogawer, MD Head Of Clinical Nutrition Department,AFSH Professor Of Internal Medicine Kasr El Aini Medical Consultant Of Clinical Nutrition And Obesity
IV Link Staff. Infection Prevention & Control A Learning Package for IV Link Staff
 IV Link Staff Infection Prevention & Control A Learning Package for IV Link Staff Purpose This learning package provides key infection prevention messages and direction for knowledge that you require as
IV Link Staff Infection Prevention & Control A Learning Package for IV Link Staff Purpose This learning package provides key infection prevention messages and direction for knowledge that you require as
Getting the Point of Injection Safety
 Getting the Point of Injection Safety Barbara Montana, MD, MPH, FACP Medical Director Communicable Disease Service Outbreak of Enterococcus faecalis endocarditis associated with an oral surgery practice
Getting the Point of Injection Safety Barbara Montana, MD, MPH, FACP Medical Director Communicable Disease Service Outbreak of Enterococcus faecalis endocarditis associated with an oral surgery practice
Management of Catheter Related Bloodstream Infection (CRBSI), including Antibiotic Lock Therapy.
 Management of Catheter Related Bloodstream Infection (CRBSI), including Antibiotic Lock Therapy. Written by: Dr K Gajee, Consultant Microbiologist Date: June 2017 Approved by: Drugs & Therapeutics Committee
Management of Catheter Related Bloodstream Infection (CRBSI), including Antibiotic Lock Therapy. Written by: Dr K Gajee, Consultant Microbiologist Date: June 2017 Approved by: Drugs & Therapeutics Committee
BLOOD CULTURE SPECIMEN COLLECTION. Skills: 40 points. Objectives:
 EXERCISE 7: BLOOD CULTURE SPECIMEN COLLECTION Skills: 40 points Objectives: 1. Differentiate between sterile and antiseptic techniques. 2. Define the following terms: FUO, septicemia, bacteremia, aerobic
EXERCISE 7: BLOOD CULTURE SPECIMEN COLLECTION Skills: 40 points Objectives: 1. Differentiate between sterile and antiseptic techniques. 2. Define the following terms: FUO, septicemia, bacteremia, aerobic
Central Venous Access Devices and Infection
 Central Venous Access Devices and Infection Dr Andrew Daley Microbiology & Infectious Diseases Women s & Children s Health Melbourne Background Types of infection! Local site infection! Blood stream infection!
Central Venous Access Devices and Infection Dr Andrew Daley Microbiology & Infectious Diseases Women s & Children s Health Melbourne Background Types of infection! Local site infection! Blood stream infection!
Optimal timing for intravascular administration set replacement
 Optimal timing for intravascular administration set replacement Author Ullman, Amanda, Cooke, Marie, Gillies, Donna, Marsh, Nicole, Daud, Azlina, McGrail, Matthew, O#Riordan, Elizabeth, Rickard, Claire
Optimal timing for intravascular administration set replacement Author Ullman, Amanda, Cooke, Marie, Gillies, Donna, Marsh, Nicole, Daud, Azlina, McGrail, Matthew, O#Riordan, Elizabeth, Rickard, Claire
Neonatal Parenteral Nutrition Guideline Dr M Hogan, Maire Cullen ANNP, Una Toland Ward Manager, Sandra Kilpatrick Neonatal Pharmacist
 CLINICAL GUIDELINES ID TAG Title: Author: Designation: Speciality / Division: Directorate: Neonatal Parenteral Nutrition Guideline Dr M Hogan, Maire Cullen ANNP, Una Toland Ward Manager, Sandra Kilpatrick
CLINICAL GUIDELINES ID TAG Title: Author: Designation: Speciality / Division: Directorate: Neonatal Parenteral Nutrition Guideline Dr M Hogan, Maire Cullen ANNP, Una Toland Ward Manager, Sandra Kilpatrick
MANAGEMENT OF INTRAVASCULAR (IV) LINES AND THERAPY. All GCC Countries
 TITLE/DESCRIPTION: MANAGEMENT OF INTRAVASCULAR (IV) LINES AND THERAPY INDEX NUMBER: EFFECTIVE DATE: APPLIES TO: ISSUING AUTHORITY: 01/01/2009 01/01/2013 All GCC Countries GULF COOPERATION COUNCIL CENTRE
TITLE/DESCRIPTION: MANAGEMENT OF INTRAVASCULAR (IV) LINES AND THERAPY INDEX NUMBER: EFFECTIVE DATE: APPLIES TO: ISSUING AUTHORITY: 01/01/2009 01/01/2013 All GCC Countries GULF COOPERATION COUNCIL CENTRE
Chapter 64 Administration of Injectable Medications
 Chapter 64 Administration of Injectable Medications Injectable Medications Injection or intravenous (IV) infusion More invasive than administration by mouth, rectum, or through the skin Common methods
Chapter 64 Administration of Injectable Medications Injectable Medications Injection or intravenous (IV) infusion More invasive than administration by mouth, rectum, or through the skin Common methods
Enrichment culture of CSF is of limited value in the diagnosis of neonatal meningitis
 Enrichment culture of CSF is of limited value in the diagnosis of neonatal S. H. Chaudhry, D. Wagstaff, Anupam Gupta, I. C. Bowler, D. P. Webster To cite this version: S. H. Chaudhry, D. Wagstaff, Anupam
Enrichment culture of CSF is of limited value in the diagnosis of neonatal S. H. Chaudhry, D. Wagstaff, Anupam Gupta, I. C. Bowler, D. P. Webster To cite this version: S. H. Chaudhry, D. Wagstaff, Anupam
Key words: Bacteremia, Catheter
 Key words: Bacteremia, Catheter 1. ID No.: 2. Name: 3. Date of Birth: 4. Ward: Table 1 Recordings Inspection Card on Central Venous Catheter [To be filled out by physicians] 5. Type of catheter A: central
Key words: Bacteremia, Catheter 1. ID No.: 2. Name: 3. Date of Birth: 4. Ward: Table 1 Recordings Inspection Card on Central Venous Catheter [To be filled out by physicians] 5. Type of catheter A: central
ATI Skills Modules Checklist for Central Venous Access Devices
 For faculty use only Educator s name Score Date ATI Skills Modules Checklist for Central Venous Access Devices Student s name Date Verify order Patient record Assess for procedure need Identify, gather,
For faculty use only Educator s name Score Date ATI Skills Modules Checklist for Central Venous Access Devices Student s name Date Verify order Patient record Assess for procedure need Identify, gather,
Alberta Health Services Infection Prevention and Control - Initiatives and Services. Surveillance Protocol January 12, 2010 Rev.
 Alberta Health Services Infection Prevention and Control - Initiatives and Services Hospital Acquired Bloodstream Infections (HABSI) Hospital Wide- in Acute Care and Acute Rehabilitation Facilities Surveillance
Alberta Health Services Infection Prevention and Control - Initiatives and Services Hospital Acquired Bloodstream Infections (HABSI) Hospital Wide- in Acute Care and Acute Rehabilitation Facilities Surveillance
Department Policy. Code: D:PC Entity: Fairview Pharmacy Services. Department: Fairview Home Infusion. Manual: Policy and Procedure Manual
 Entity: Fairview Pharmacy Services Department: Fairview Home Infusion Manual: Policy and Procedure Manual Category: Home Infusion Subject: Midline (Extended Dwell Peripheral) Catheter Care and Management
Entity: Fairview Pharmacy Services Department: Fairview Home Infusion Manual: Policy and Procedure Manual Category: Home Infusion Subject: Midline (Extended Dwell Peripheral) Catheter Care and Management
Education for self administration of intravenous therapy HOME IV THERAPY. 30 minute - Baxter Pump Tobramycin
 HOME IV THERAPY Tobramycin Tobramycin Check the order on the drug chart This can change when the results from your blood test come through. Your doctor will change the order, if required. A copy of the
HOME IV THERAPY Tobramycin Tobramycin Check the order on the drug chart This can change when the results from your blood test come through. Your doctor will change the order, if required. A copy of the
142 BJID 2003; 7 (April)
 142 BJID 2003; 7 (April) Comparison Between the Jugular and Subclavian Vein as Insertion Site for Central Venous Catheters: Microbiological Aspects and Risk Factors for Colonization and Infection Geraldo
142 BJID 2003; 7 (April) Comparison Between the Jugular and Subclavian Vein as Insertion Site for Central Venous Catheters: Microbiological Aspects and Risk Factors for Colonization and Infection Geraldo
Central Line Care and Management
 Central Line Care and Management What is a Central Line/ CVAD? (central venous access device) A vascular infusion device that terminates at or close to the heart or in one of the great vessels (aorta,
Central Line Care and Management What is a Central Line/ CVAD? (central venous access device) A vascular infusion device that terminates at or close to the heart or in one of the great vessels (aorta,
A15b. Prevention of Hospital Acquired Infections. Session Summary. Session Objectives. References
 A15b Prevention of Hospital Acquired Infections Eric C. Eichenwald, MD Professor of Pediatrics, Assistant Dean for Children s Health Care Quality Chief, Division of Neonatal/Perinatal Medicine University
A15b Prevention of Hospital Acquired Infections Eric C. Eichenwald, MD Professor of Pediatrics, Assistant Dean for Children s Health Care Quality Chief, Division of Neonatal/Perinatal Medicine University
Blood & Blood Product Administration
 Approved by: Blood & Blood Product Administration Addendum to: Corporate Policy VII-B-397 Transfusion of Blood Components and Products- Pediatric/Neonate Gail Cameron Senior Director Operations, Maternal,
Approved by: Blood & Blood Product Administration Addendum to: Corporate Policy VII-B-397 Transfusion of Blood Components and Products- Pediatric/Neonate Gail Cameron Senior Director Operations, Maternal,
3M Tegaderm CHG Chlorhexidine Gluconate I.V. Securement Dressing Description 3M Tegaderm CHG Chlorhexidine Gluconate I.V. Securement Dressing is used
 3M Tegaderm CHG Chlorhexidine Gluconate I.V. Securement Dressing Description 3M Tegaderm CHG Chlorhexidine Gluconate I.V. Securement Dressing is used to cover and protect catheter sites and to secure devices
3M Tegaderm CHG Chlorhexidine Gluconate I.V. Securement Dressing Description 3M Tegaderm CHG Chlorhexidine Gluconate I.V. Securement Dressing is used to cover and protect catheter sites and to secure devices
Blood Sampling: Venipuncture
 Approved by: Blood Sampling: Venipuncture Gail Cameron Senor Director, Operations, Maternal, Neonatal & Child Health Programs Dr. Paul Byrne Medical Director, Neonatology Neonatal Nursery Policy & Procedures
Approved by: Blood Sampling: Venipuncture Gail Cameron Senor Director, Operations, Maternal, Neonatal & Child Health Programs Dr. Paul Byrne Medical Director, Neonatology Neonatal Nursery Policy & Procedures
Prevention of Intravascular Device-Associated Infections Peter Heeg
 Chapter 17 Prevention of Intravascular Device-Associated Infections Peter Heeg Key points Thorough hand disinfection by operator before insertion of catheter and during maintenance procedures. Thorough
Chapter 17 Prevention of Intravascular Device-Associated Infections Peter Heeg Key points Thorough hand disinfection by operator before insertion of catheter and during maintenance procedures. Thorough
MANITOBA RENAL PROGRAM
 MANITOBA RENAL PROGRAM SUBJECT Use of Closed Needleless Access Device with Hemodialysis Central Venous Catheters (CVC) SECTION CODE 30.20.04 30.20 Vascular Access AUTHORIZATION Professional Advisory Committee,
MANITOBA RENAL PROGRAM SUBJECT Use of Closed Needleless Access Device with Hemodialysis Central Venous Catheters (CVC) SECTION CODE 30.20.04 30.20 Vascular Access AUTHORIZATION Professional Advisory Committee,
Media Fill Test Kits. Manufactured by. Making USP <797> compliance easy!
 Media Fill Test Kits Manufactured by Making USP compliance easy! Compliance was never so easy! Microbial Contamination Testing for CSPs Hardy Diagnostics offers all the products you need to easily
Media Fill Test Kits Manufactured by Making USP compliance easy! Compliance was never so easy! Microbial Contamination Testing for CSPs Hardy Diagnostics offers all the products you need to easily
CATHETER-ASSOCIATED URINARY TRACT INFECTIONS
 CATHETER-ASSOCIATED URINARY TRACT INFECTIONS Hamid Emadi M.D Associate professor of Infectious diseases Department Tehran university of medical science The most common nosocomial infection The urinary
CATHETER-ASSOCIATED URINARY TRACT INFECTIONS Hamid Emadi M.D Associate professor of Infectious diseases Department Tehran university of medical science The most common nosocomial infection The urinary
Reducing Blood Culture Contamination in Hospitalized Pediatric Patients
 ISSN: 2319-7706 Volume 4 Number 12 (2015) pp. 200-208 http://www.ijcmas.com Original Research Article Reducing Blood Culture Contamination in Hospitalized Pediatric Patients S. H. Khater Enas 1 * and Taha
ISSN: 2319-7706 Volume 4 Number 12 (2015) pp. 200-208 http://www.ijcmas.com Original Research Article Reducing Blood Culture Contamination in Hospitalized Pediatric Patients S. H. Khater Enas 1 * and Taha
ESPEN Congress Brussels How to take care of central venous access devices (CVAD)? Eva Johansson
 ESPEN Congress Brussels 2005 How to take care of central venous access devices (CVAD)? Eva Johansson How to take care of central venous access devices (CVAD)? Eva Johansson, RN, PhD Division of Hematology
ESPEN Congress Brussels 2005 How to take care of central venous access devices (CVAD)? Eva Johansson How to take care of central venous access devices (CVAD)? Eva Johansson, RN, PhD Division of Hematology
The Impact of Healthcare Associated Infection (HCAI)
 Instructions for use Save this presentation Feel free to add or delete slides as necessary, change information to suit local needs and as new guidance or evidence is published Disclaimer: Whilst the working
Instructions for use Save this presentation Feel free to add or delete slides as necessary, change information to suit local needs and as new guidance or evidence is published Disclaimer: Whilst the working
A Multicentre Study about Pattern and Organisms Isolated in Follow-up Blood Cultures
 Ann Clin Microbiol Vol., No., March, 0 http://dx.doi.org/0./acm.0... ISSN -0 A Multicentre Study about Pattern and Organisms Isolated in Follow-up Blood Cultures Jeong Hwan Shin, Eui Chong Kim, Sunjoo
Ann Clin Microbiol Vol., No., March, 0 http://dx.doi.org/0./acm.0... ISSN -0 A Multicentre Study about Pattern and Organisms Isolated in Follow-up Blood Cultures Jeong Hwan Shin, Eui Chong Kim, Sunjoo
Emergency clamp should always be readily available in case of accidental catheter fracture
 Note: Please see individual policies for further information. Flushing best practice: Always use a 10 diameter syringe or larger when first accessing and when flushing vascular access device (VAD) Use
Note: Please see individual policies for further information. Flushing best practice: Always use a 10 diameter syringe or larger when first accessing and when flushing vascular access device (VAD) Use
Parenteral Nutrition
 Approved by: Parenteral Nutrition Gail Cameron Senior Director Operations, Maternal, Neonatal & Child Health Programs Dr. Paul Byrne Medical Director, Neonatology Neonatal Policy & Procedures Manual :
Approved by: Parenteral Nutrition Gail Cameron Senior Director Operations, Maternal, Neonatal & Child Health Programs Dr. Paul Byrne Medical Director, Neonatology Neonatal Policy & Procedures Manual :
Microbiological diagnosis of infective endocarditis; what is new?
 Microbiological diagnosis of infective endocarditis; what is new? Dr Amani El Kholy, MD Professor of Clinical Pathology (Microbiology), Faculty of Medicine, Cairo University ESC 2017 1 Objectives Lab Diagnostic
Microbiological diagnosis of infective endocarditis; what is new? Dr Amani El Kholy, MD Professor of Clinical Pathology (Microbiology), Faculty of Medicine, Cairo University ESC 2017 1 Objectives Lab Diagnostic
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A AAP. See American Academy of Pediatrics (AAP) Acyclovir dosing in infants, 185 187 American Academy of Pediatrics (AAP) COFN of, 199 204 Amphotericin
Note: Page numbers of article titles are in boldface type. A AAP. See American Academy of Pediatrics (AAP) Acyclovir dosing in infants, 185 187 American Academy of Pediatrics (AAP) COFN of, 199 204 Amphotericin
4 PARENTERAL THERAPY
 WOMEN AND NEWBORN HEALTH SERVICE CLINICAL GUIDELINES SECTION A: GUIDELINES RELEVANT TO OBSTETRICS AND GYNAECOLOGY 4 PARENTERAL THERAPY 4.11 TOTAL PARENTERAL NUTRITION Authorised by: OGCCU Review Team:
WOMEN AND NEWBORN HEALTH SERVICE CLINICAL GUIDELINES SECTION A: GUIDELINES RELEVANT TO OBSTETRICS AND GYNAECOLOGY 4 PARENTERAL THERAPY 4.11 TOTAL PARENTERAL NUTRITION Authorised by: OGCCU Review Team:
Vascular access device selection & placement. Alisa Seangleulur, MD Anesthesiology Department, Faculty of Medicine, Thammasat University
 Vascular access device selection & placement Alisa Seangleulur, MD Anesthesiology Department, Faculty of Medicine, Thammasat University How to make the right choice of vascular access device.. Peripheral
Vascular access device selection & placement Alisa Seangleulur, MD Anesthesiology Department, Faculty of Medicine, Thammasat University How to make the right choice of vascular access device.. Peripheral
NOTTINGHAM CHILDREN S HOSPITAL Nursing Guideline. P07 Care and Management of Children with a Totally Implantable Venous Access Device (Portacath).
 NOTTINGHAM CHILDREN S HOSPITAL Nursing Guideline P07 Care and Management of Children with a Totally Implantable Venous Access Device (Portacath). Introduction A Portacath is a central venous access device
NOTTINGHAM CHILDREN S HOSPITAL Nursing Guideline P07 Care and Management of Children with a Totally Implantable Venous Access Device (Portacath). Introduction A Portacath is a central venous access device
The relationship between intravenous infusate colonisation and fluid container hang time
 The relationship between intravenous infusate colonisation and fluid container hang time Author Rickard, Claire, Vannapraseuth, Boun, McGrail, Matthew, Keene, Lorraine, Rambaldo, Sam, Smith, Chloe, Ray-Barruel,
The relationship between intravenous infusate colonisation and fluid container hang time Author Rickard, Claire, Vannapraseuth, Boun, McGrail, Matthew, Keene, Lorraine, Rambaldo, Sam, Smith, Chloe, Ray-Barruel,
Catheter-Associated Urinary Tract Infection (CAUTI) Event
 Catheter-Associated Urinary Tract Infection () Event Introduction: The urinary tract is the most common site of healthcare-associated infection, accounting for more than 30% of infections reported by acute
Catheter-Associated Urinary Tract Infection () Event Introduction: The urinary tract is the most common site of healthcare-associated infection, accounting for more than 30% of infections reported by acute
Infection Screening for Newborn Babies
 Infection Screening for Newborn Babies Patient Information Leaflet If you require a translation or an alternative format of this leaflet please speak to the nurse in charge or call the Patient Advice Liaison
Infection Screening for Newborn Babies Patient Information Leaflet If you require a translation or an alternative format of this leaflet please speak to the nurse in charge or call the Patient Advice Liaison
Stability and Compatibility of Granisetron Alone and in Combination with Dexamethasone in 0.9% Sodium Chloride and 5% Dextrose in Water Solutions
 ARTICLE Stability and Compatibility of Granisetron Alone and in Combination with Dexamethasone in 0.9% Sodium Chloride and 5% Dextrose in Water Solutions Scott E. Walker and Shirley Law ABSTRACT Background:
ARTICLE Stability and Compatibility of Granisetron Alone and in Combination with Dexamethasone in 0.9% Sodium Chloride and 5% Dextrose in Water Solutions Scott E. Walker and Shirley Law ABSTRACT Background:
PARENTERAL NUTRITION- ASSOCIATED LIVER DISEASE IN CHILDREN
 PARENTERAL NUTRITION- ASSOCIATED LIVER DISEASE IN CHILDREN Praveen Goday MBBS CNSC Associate Professor Pediatric Gastroenterology Medical College of Wisconsin Milwaukee, WI Parenteral Nutrition-Associated
PARENTERAL NUTRITION- ASSOCIATED LIVER DISEASE IN CHILDREN Praveen Goday MBBS CNSC Associate Professor Pediatric Gastroenterology Medical College of Wisconsin Milwaukee, WI Parenteral Nutrition-Associated
Y s A P. n n. C o. e c. t o r s E R. e s. e l. e e d l I V. e d o s C l. vadsite The Transparent, Split Septum, Needleless Connector
 I V T H N E R e e d l A P e l e s Y s C o n n e c t o r s e d o s C l vadsite The Transparent, Split Septum, Needleless Connector What is vadsite? vadsite is a Neutral Displacement Needleless Connector
I V T H N E R e e d l A P e l e s Y s C o n n e c t o r s e d o s C l vadsite The Transparent, Split Septum, Needleless Connector What is vadsite? vadsite is a Neutral Displacement Needleless Connector
Bloodstream Infections
 GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER NUMBER 30: Bloodstream Infections Authors Larry Lutwick MD Gonzalo Bearman MD, MPH Chapter Editor Ziad A. Memish, MD, FRCPC, FACP Topic Outline Definition
GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER NUMBER 30: Bloodstream Infections Authors Larry Lutwick MD Gonzalo Bearman MD, MPH Chapter Editor Ziad A. Memish, MD, FRCPC, FACP Topic Outline Definition
SAFE INJECTION PRACTICES. Barbara J Connell MS,MT(ASCP)SH VP Clinical Services Medline Industries, Inc.
 SAFE INJECTION PRACTICES Barbara J Connell MS,MT(ASCP)SH VP Clinical Services Medline Industries, Inc. DISCLOSURES»Employee of Medline Industries, Inc.»Opinions expressed are my own and not necessarily
SAFE INJECTION PRACTICES Barbara J Connell MS,MT(ASCP)SH VP Clinical Services Medline Industries, Inc. DISCLOSURES»Employee of Medline Industries, Inc.»Opinions expressed are my own and not necessarily
Optimal nutrition in critically ill children
 Optimal nutrition in critically ill children MODULE 4 Good safety practices required for nutritional therapy Developed by The Asia Pacific Middle East Consensus Working Group on Nutrition Therapy in the
Optimal nutrition in critically ill children MODULE 4 Good safety practices required for nutritional therapy Developed by The Asia Pacific Middle East Consensus Working Group on Nutrition Therapy in the
Infusion Skills Competency Checklist To be used at annual skills fair or at any other time for IV Competency
 Employee Profile Infusion Skills Checklist Last Name First Name Middle Initial Employee Number Employee Discipline Check one: RN LPN Per state specific LPN Practice Acts Direct Supervisor s Name: Date
Employee Profile Infusion Skills Checklist Last Name First Name Middle Initial Employee Number Employee Discipline Check one: RN LPN Per state specific LPN Practice Acts Direct Supervisor s Name: Date
Introduction to IV Therapy. BY Terry White, MBA, BSN
 Introduction to IV Therapy BY Terry White, MBA, BSN Important It is West Virginia State Law that nursing students (LPN and RN) are forbidden to start IVs or draw blood samples on patients Taking this class
Introduction to IV Therapy BY Terry White, MBA, BSN Important It is West Virginia State Law that nursing students (LPN and RN) are forbidden to start IVs or draw blood samples on patients Taking this class
URINARY TRACT INFECTIONS 3 rd Y Med Students. Prof. Dr. Asem Shehabi Faculty of Medicine, University of Jordan
 URINARY TRACT INFECTIONS 3 rd Y Med Students Prof. Dr. Asem Shehabi Faculty of Medicine, University of Jordan Urinary Tract Infections-1 Normal urine is sterile.. It contains fluids, salts, and waste products,
URINARY TRACT INFECTIONS 3 rd Y Med Students Prof. Dr. Asem Shehabi Faculty of Medicine, University of Jordan Urinary Tract Infections-1 Normal urine is sterile.. It contains fluids, salts, and waste products,
Exchange Transfusion
 Approved by: Exchange Transfusion Gail Cameron Director, Maternal, Neonatal & Child Health Programs Neonatal Nursery Policy & Procedures Manual : Next Review March 2016 Dr. Ensenat Medical Director, Neonatology
Approved by: Exchange Transfusion Gail Cameron Director, Maternal, Neonatal & Child Health Programs Neonatal Nursery Policy & Procedures Manual : Next Review March 2016 Dr. Ensenat Medical Director, Neonatology
Dialysis Event Protocol
 Dialysis Event Protocol Introduction In 2009, more than 370,000 patients were treated with maintenance hemodialysis in the United States. 1 Hemodialysis patients require a vascular access, which can be
Dialysis Event Protocol Introduction In 2009, more than 370,000 patients were treated with maintenance hemodialysis in the United States. 1 Hemodialysis patients require a vascular access, which can be
Neonatal Meningitis: Risk Factors, Causes, and Neurologic Complications
 original ARTICLE Neonatal Meningitis: Risk Factors, Causes, and Neurologic Complications How to Cite This Article: Khalessi N, Afsharkhas L. Neonatal Meningitis: Risk Factors, Causes and Neurologic Complications.
original ARTICLE Neonatal Meningitis: Risk Factors, Causes, and Neurologic Complications How to Cite This Article: Khalessi N, Afsharkhas L. Neonatal Meningitis: Risk Factors, Causes and Neurologic Complications.
590 La Revue de Santé de la Méditerranée orientale, Vol. 14, N o 3, 2008
 590 La Revue de Santé de la Méditerranée orientale, Vol. 4, N o 3, 2008 Rubella serology in pregnant women attending health centres of Tehran University of Medical Sciences F. Majlessi, A. Batebi, M. Shariat,
590 La Revue de Santé de la Méditerranée orientale, Vol. 4, N o 3, 2008 Rubella serology in pregnant women attending health centres of Tehran University of Medical Sciences F. Majlessi, A. Batebi, M. Shariat,
Guideline scope Neonatal parenteral nutrition
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Neonatal parenteral nutrition The Department of Health in England has asked NICE to develop a new guideline on parenteral nutrition in
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Neonatal parenteral nutrition The Department of Health in England has asked NICE to develop a new guideline on parenteral nutrition in
5. Use of antibiotics, which disturbs balance of normal flora. 6. Poor nutritional status.
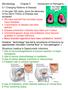 Microbiology Chapter 5 Introduction to Pathogens 5:1 Changing Patterns of Disease In the past 100 years, since the discovery of the Germ Theory of Disease was accepted: We have learned that microbes cause
Microbiology Chapter 5 Introduction to Pathogens 5:1 Changing Patterns of Disease In the past 100 years, since the discovery of the Germ Theory of Disease was accepted: We have learned that microbes cause
Bacterial colony counts during vaginal surgery
 Infect Dis Obstet Gynecol 2003;11:161 165 Patrick Culligan 1, Michael Heit 1, Linda Blackwell 1, Miles Murphy 1, Carol A. Graham 1 and James Snyder 2 1 Division of Urogynecology and Reconstructive Pelvic
Infect Dis Obstet Gynecol 2003;11:161 165 Patrick Culligan 1, Michael Heit 1, Linda Blackwell 1, Miles Murphy 1, Carol A. Graham 1 and James Snyder 2 1 Division of Urogynecology and Reconstructive Pelvic
Blood cultures in ED. Dr Sebastian Chang MBBS FACEM
 Blood cultures in ED Dr Sebastian Chang MBBS FACEM Why do we care about blood cultures? blood cultures are the most direct method for detecting bacteraemia in patients a positive blood culture: 1. can
Blood cultures in ED Dr Sebastian Chang MBBS FACEM Why do we care about blood cultures? blood cultures are the most direct method for detecting bacteraemia in patients a positive blood culture: 1. can
original article Improving access to care by allowing self-referral to a hepatitis C clinic
 original article Improving access to care by allowing self-referral to a hepatitis C clinic Karen Doucette MD MSc FRCPC 1, Vicki Robson RN 2, Stephen Shafran MD 1, Dennis Kunimoto MD 1 K Doucette, V Robson,
original article Improving access to care by allowing self-referral to a hepatitis C clinic Karen Doucette MD MSc FRCPC 1, Vicki Robson RN 2, Stephen Shafran MD 1, Dennis Kunimoto MD 1 K Doucette, V Robson,
Parkland Health & Hospital System Women & Infant Specialty Health
 Parkland Health & Hospital System Women & Infant Specialty Health NS 1700.04 Nursery Services Procedure Manual Arterial Puncture Practice Statement Upon the written order of the provider, the credentialled
Parkland Health & Hospital System Women & Infant Specialty Health NS 1700.04 Nursery Services Procedure Manual Arterial Puncture Practice Statement Upon the written order of the provider, the credentialled
Work up of Respiratory & Wound Cultures:
 Work up of Respiratory & Wound Cultures: Culture work up 2 Systematic approaches 1 Work up of Respiratory & Wound Cultures Resident flora Colonizing organisms Pathogens 2 Work up of Respiratory & Wound
Work up of Respiratory & Wound Cultures: Culture work up 2 Systematic approaches 1 Work up of Respiratory & Wound Cultures Resident flora Colonizing organisms Pathogens 2 Work up of Respiratory & Wound
If viewing a printed copy of this policy, please note it could be expired. Got to to view current policies.
 If viewing a printed copy of this policy, please note it could be expired. Got to www.fairview.org/fhipolicies to view current policies. Department Policy Code: D: PC-5575 Entity: Fairview Pharmacy Services
If viewing a printed copy of this policy, please note it could be expired. Got to www.fairview.org/fhipolicies to view current policies. Department Policy Code: D: PC-5575 Entity: Fairview Pharmacy Services
International Journal of Medical Science and Education pissn eissn
 CATHETER ASSOCIATED URINARY TRACT INFECTION (CAUTI) INDUCED NOSOCOMIAL INFECTION WITH REFERENCE TO INCIDENCE, DURATION AND ORGANISM IN A TERTIARY CARE TEACHING HOSPITAL Dr.Trilok Patil* Associate Professor,
CATHETER ASSOCIATED URINARY TRACT INFECTION (CAUTI) INDUCED NOSOCOMIAL INFECTION WITH REFERENCE TO INCIDENCE, DURATION AND ORGANISM IN A TERTIARY CARE TEACHING HOSPITAL Dr.Trilok Patil* Associate Professor,
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE
 SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: Nursing DATE: REVIEWED: PAGES: 11/78 4/18 1 of 10 RESPONSIBILITY: RN (for chemo), LPN (nonchemo) PURPOSE: OBJECTIVE: To introduce medication
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: Nursing DATE: REVIEWED: PAGES: 11/78 4/18 1 of 10 RESPONSIBILITY: RN (for chemo), LPN (nonchemo) PURPOSE: OBJECTIVE: To introduce medication
Effect of changing lipid formulation in Parenteral Nutrition in the Newborn Experimental Pathology BSc
 Effect of changing lipid formulation in Parenteral Nutrition in the Newborn Experimental Pathology BSc Word count: 6939 0 CONTENTS Abstract...2 Acknowledgements...3 Introduction...4 Materials and Methods...11
Effect of changing lipid formulation in Parenteral Nutrition in the Newborn Experimental Pathology BSc Word count: 6939 0 CONTENTS Abstract...2 Acknowledgements...3 Introduction...4 Materials and Methods...11
IV Therapy January, 08 Tip of the Month
 Every Hub Every Time IV Therapy January, 08 Tip of the Month Every Hub Every Time No matter what the occasion, SCRUB the catheter ports every single time before access. Evidence Supports SCRUBBING using
Every Hub Every Time IV Therapy January, 08 Tip of the Month Every Hub Every Time No matter what the occasion, SCRUB the catheter ports every single time before access. Evidence Supports SCRUBBING using
Duygu Perçin 1, Gülin Güler 2
 Duygu Perçin 1, Gülin Güler 2 1 Department of Clinical Microbiology and 2 Department of Anesthesiology and Reanimation, Erciyes University Faculty of Medicine, Kayseri, TURKEY They are used to fill vaporizers
Duygu Perçin 1, Gülin Güler 2 1 Department of Clinical Microbiology and 2 Department of Anesthesiology and Reanimation, Erciyes University Faculty of Medicine, Kayseri, TURKEY They are used to fill vaporizers
Direct Intravenous (IV) Medication Administration Procedure
 Approved by: Chief Medical Officer; and Chief Operating Officer Direct Intravenous (IV) Medication Administration Procedure Corporate Policy & Procedures Manual Number: VII-B-310 Date Approved January
Approved by: Chief Medical Officer; and Chief Operating Officer Direct Intravenous (IV) Medication Administration Procedure Corporate Policy & Procedures Manual Number: VII-B-310 Date Approved January
Staphylococci. Gram stain: gram positive cocci arranged in clusters.
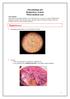 Microbiology lab Respiratory system Third medical year Lab contents: Gram positive bacteria (Staphylococcus and Streptococcus spp), two types of filamentous fungi (Aspergillus and Penicillium spp), and
Microbiology lab Respiratory system Third medical year Lab contents: Gram positive bacteria (Staphylococcus and Streptococcus spp), two types of filamentous fungi (Aspergillus and Penicillium spp), and
High Impact Intervention Peripheral intravenous cannula care bundle
 High Impact Intervention Peripheral intravenous cannula care bundle Aim To reduce the incidence of peripheral intravenous cannula infections. Introduction The aim of the care bundle, as set out in this
High Impact Intervention Peripheral intravenous cannula care bundle Aim To reduce the incidence of peripheral intravenous cannula infections. Introduction The aim of the care bundle, as set out in this
Venenkatheter-assoziierte Infektionen
 Update Infektionen in der Hämatologie und Onkologie Venenkatheter-assoziierte Infektionen Georg Maschmeyer Potsdam www.dghoinfektionen.de Aktuelle Leitlinie der AGIHO...unter Berücksichtigung von: Ann
Update Infektionen in der Hämatologie und Onkologie Venenkatheter-assoziierte Infektionen Georg Maschmeyer Potsdam www.dghoinfektionen.de Aktuelle Leitlinie der AGIHO...unter Berücksichtigung von: Ann
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE
 SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: INTERMITTENT FLUID AND MEDICATION THERAPY Nursing DATE: REVIEWED: PAGES: RESPONSIBILITY: RN, LPN I, LPN II Per Job Description 03/81 8/09
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: INTERMITTENT FLUID AND MEDICATION THERAPY Nursing DATE: REVIEWED: PAGES: RESPONSIBILITY: RN, LPN I, LPN II Per Job Description 03/81 8/09
BLOOD CULTURE GUIDELINE FOR RED CROSS WAR MEMORIAL CHILDREN S HOSPITAL
 BLOOD CULTURE GUIDELINE FOR RED CROSS WAR MEMORIAL CHILDREN S HOSPITAL Lead author: Harsha Lochan Contributing authors: Brian Eley, Colleen Bamford, James Nuttall, Andrew Argent Posted: 7 August 2014 Comments:
BLOOD CULTURE GUIDELINE FOR RED CROSS WAR MEMORIAL CHILDREN S HOSPITAL Lead author: Harsha Lochan Contributing authors: Brian Eley, Colleen Bamford, James Nuttall, Andrew Argent Posted: 7 August 2014 Comments:
Peripherally Inserted Central Catheter (PICC) Booklet
 Aintree University Hospital FT PICC Booklet: a real world example This local booklet is an example used in the NICE medical technology guidance adoption support resource for SecurAcath for securing percutaneous
Aintree University Hospital FT PICC Booklet: a real world example This local booklet is an example used in the NICE medical technology guidance adoption support resource for SecurAcath for securing percutaneous
Blood Cultures at Central Line Insertion in the Intensive Care Unit: Comparison with Peripheral Venipuncture
 JOURNAL OF CLINICAL MICROBIOLOGY, July 2011, p. 2398 2403 Vol. 49, No. 7 0095-1137/11/$12.00 doi:10.1128/jcm.02546-10 Copyright 2011, American Society for Microbiology. All Rights Reserved. Blood Cultures
JOURNAL OF CLINICAL MICROBIOLOGY, July 2011, p. 2398 2403 Vol. 49, No. 7 0095-1137/11/$12.00 doi:10.1128/jcm.02546-10 Copyright 2011, American Society for Microbiology. All Rights Reserved. Blood Cultures
Yield of Suprapubic Aspirate versus Bag Collection in Diagnosis of UTI in Children 0 to 6 Months of Age
 Proceeding S.Z.P.G.M.I. Vol: 25(2): pp. 61-65, 2011. Yield of Suprapubic Aspirate versus Bag Collection in Diagnosis of UTI in Children 0 to 6 Months of Age Lubna Riaz, Muhammad Aslam, Waqar Hussain, Anita
Proceeding S.Z.P.G.M.I. Vol: 25(2): pp. 61-65, 2011. Yield of Suprapubic Aspirate versus Bag Collection in Diagnosis of UTI in Children 0 to 6 Months of Age Lubna Riaz, Muhammad Aslam, Waqar Hussain, Anita
Rapid publication. Evaluation of a novel endoluminal brush method. for in situ diagnosis of catheter related sepsis
 278 2J Clin Pathol 1997;50:278-282 Rapid publication Department of Microbiology, University of Leeds, The General Infirmary, Leeds, United Kingdom P Kite M H Wilcox W N Fawley A J L Kindon D Thomas Department
278 2J Clin Pathol 1997;50:278-282 Rapid publication Department of Microbiology, University of Leeds, The General Infirmary, Leeds, United Kingdom P Kite M H Wilcox W N Fawley A J L Kindon D Thomas Department
Cover Page. The handle holds various files of this Leiden University dissertation
 Cover Page The handle http://hdl.handle.net/1887/22368 holds various files of this Leiden University dissertation Author: Lugt, Neeltje Margaretha van der Title: Neonatal pearls : safety and efficacy of
Cover Page The handle http://hdl.handle.net/1887/22368 holds various files of this Leiden University dissertation Author: Lugt, Neeltje Margaretha van der Title: Neonatal pearls : safety and efficacy of
