Parenteral Nutrition Policy
|
|
|
- Kory Hunter
- 5 years ago
- Views:
Transcription
1 Parenteral Nutrition Policy This is a new procedural document, please read in full Did you print this document yourself? The Trust discourages the retention of hard copies of policies and can only guarantee that the policy on the Trust website is the most up-to-date version. If, for exceptional reasons, you need to print a policy off, it is only valid for 24 hours. Author/reviewer: (this version) Date written/revised: February 2016 Approved by: Date of approval: 31/03/2016 Date issued: 12 April 2016 Next review date: February 2019 Target audience: Dr Jo Sayer - Consultant Gastroenterologist, Hannah Stirland - Nutrition Nurse Specialist, Chioma Nnamdi Specialist Pharmacist, Andrew Gregory Specialist Dietician Nutrition Steering Committee Clinical Staff, Trust wide Page 1 of 17
2 Amendment Form Please record brief details of the changes made alongside the next version number. If the procedural document has been reviewed without change, this information will still need to be recorded although the version number will remain the same. Version Date Issued Brief Summary of Changes Author Version 1 12 April 2016 This is a new procedural document, please read in full J Sayer H Stirland C Nnamdi A Gregory Page 2 of 17
3 Section Contents 1 Introduction 4 2 Purpose 4 Page No Duties and Responsibilities 3.1 Nutrition support team 3.2 Ward medical and nursing teams Procedure 4.1 Indication for parenteral nutrition (PN) 4.2 Referral process 4.3 Requirements for referral 4.4 Appropriate route 4.5 Prescribing pabrinex 4.6 Ward inpatients requiring PN 4.7 Patients on critical care requiring PN 4.8 Stopping parenteral nutrition 4.9 Patients on home PN who require hospitalisation Training/Support 5.1 Pharmaceutical stability 5.2 The prescription 5.3 Management of PN Monitoring Compliance with the Procedural Document 12 7 Definitions 12 8 Equality Impact Assessment 13 9 Associated Trust Procedural Documents References 13 Appendices Appendix 1 Parenteral nutrition pathway of care 14 Appendix 2 Specimen home PN transcription 16 Appendix 3 Equality Impact Assessment Form 17 Page 3 of 17
4 1. INTRODUCTION The aim of this policy is to ensure parenteral nutrition (PN) is delivered to appropriate inpatients safely and in line with NICE guidance (2006). PN is a specialised treatment which carries significant risks to patients, for this reason correct delivery and management of the PN is essential. This policy outlines the indications for PN, how to refer to the nutrition support team and how to manage a patient receiving parenteral nutrition. The nutrition support team is a multidisciplinary team which consists of a consultant gastroenterologist, nutrition nurse specialist, pharmacist and dietitian. The team assess and monitor all patients receiving PN and provide support to ward nursing and medical staff in the safe delivery of parenteral nutrition. 2. PURPOSE Parenteral Nutrition (PN) is a method of feeding patients intravenously when the patient is unable to absorb enough nutrients from the gut to meet their nutritional needs. It may be used as the sole form of nutrition or it may be combined with other forms of feeding (oral or enteral). It may be required to address specific nutritional deficiencies, for example patients with high output fistula or to meet all nutritional requirements. PN is an expensive option. It also carries a significant risk of adverse events or complications from the delivery of nutrients via an unnatural route, some of which may be serious or even fatal. Therefore it is important for patient safety and for effective treatment that this resource should be used only for those patients where the benefit outweighs the risk. 3. DUTIES AND RESPONSIBILITIES 3.1 Nutrition support team The nutrition support team provides support for decision-making when considering starting a patient on parenteral nutrition. While the final decision regarding starting the parenteral nutrition rests with the consultant managing that patient, the nutrition support team will make recommendations regarding the most appropriate, safest and most cost effective way to meet the patient s nutritional requirements. The nutrition support team will assess all adults on inpatient wards who have been referred for consideration of parenteral nutrition. The nutrition support team will be informed by the pharmacist covering DCC of all adult inpatients on DCC/ITU being considered for parenteral nutrition; however where the patient is under the care of an intensivist and another consultant the decision whether to start PN will be made by the intensivist and the consultant managing the patient Page 4 of 17
5 The nutrition support team will agree nutritional targets with the referring medical team and will advise how these nutritional targets can be achieved. For most referrals this will include a prescription of parenteral nutrition. The Nutrition Support team will provide an initial assessment of the patient s nutritional needs and how these can be met. They will monitor on a daily basis (Monday to Friday) the impact of the nutritional treatment and will be responsible for the prescription of parenteral nutrition on a seven day/week basis. Where it is necessary to prescribe other treatments in order to minimize harm from the parenteral nutrition (e.g. prescription of insulin for a patient with persistently raised blood glucose on parenteral nutrition), the nutrition support team will take responsibility for prescribing these medications, provided that there is no or low impact on the ongoing management of the patient s medical condition. If there is concern that the new treatment may impact on the patient s other medical problems, the nutrition support team will make a recommendation and it will be the responsibility of the medical team managing the patient to decide whether to prescribe the treatment. 3.2 Ward medical and nursing teams The ward medical team will be responsible for ensuring that all baseline and monitoring blood tests have been obtained (see section 4.3), that the patient has appropriate vascular access for delivery of parenteral nutrition and that the patient understands the proposed treatment and the risks associated with it. Please refer to central venous access device (CVAD) policy. The medical team also has a responsibility for reviewing and overseeing the fluid balance needs of the patient. If the patient just requires maintenance fluids, then the PN will often deliver an appropriate amount of fluids to meet the patient s needs. If this is the case then any additional fluid should be stopped. If the patient has a fluid deficit or on-going fluid losses, then additional fluids may be needed on top of the PN. The medical team has a responsibility for assessing the patient s fluid status and requirements on a daily basis and ensuring that these are met and not exceeded by a combination of PN and intravenous fluids as appropriate. The volume of fluid delivered in the PN needs to be factored into these calculations. The ward nursing team will be responsible for monitoring the patient and ensuring that all appropriate observations have been documented; including 4 hourly clinical observations, at least daily blood sugar, twice weekly weight, accurate fluid balance and food chart if applicable. They will also be responsible for daily monitoring of the CVC and for collecting specimens e.g. swabs from CVC entry sites. 4. PROCEDURE All patients should have a MUST score before making a referral to the nutrition support team or a dietitian. Once referred the patient must have a dietitian review as part of the nutrition support team s assessment. The only exception to this is patients in a critical care bed (DCC/ITU) where the consultant intensivist may choose to initiate parenteral nutrition over a weekend. It is not appropriate to start parenteral nutrition over a weekend unless the patient is in a critical care bed. Page 5 of 17
6 PN should never be started in the evenings or weekends unless the expertise is available to assess and monitor the patient adequately, hence the only area where this should happen is on critical care and only if the clinical condition of the patient deems this necessary prior to a full dietician assessment. 4.1 Indications for parenteral nutrition (PN) Parenteral nutrition is a treatment with a significant risk of complications. It should only be considered as a treatment for nutritional support after all oral and enteral options have been explored. The main indications for parenteral nutrition are: Intestinal perforation which is being managed conservatively (non-operatively) and where feeding the patient orally may exacerbate sepsis Intestinal obstruction which is being managed conservatively (non-operatively) Intestinal dysmotility, including prolonged post- operative ileus and intestinal pseudoobstruction leading to malabsorption Acute pancreatitis where oral, nasogastric or nasojejunal feeding is not tolerated High output stoma or high output fistula where the surgical consultant has recommended a trial period of Nil by mouth Short bowel syndrome where absorption is not sufficient to meet patient s nutritional targets There may be other cases which would benefit from parenteral nutrition. These should be discussed on an individual case basis with the nutrition support team. The decision to start parenteral nutrition needs to take account of the patient s co-morbidities, life expectancy and quality of life. For patients who are being considered for long term parenteral nutrition or home parenteral nutrition, the patient s social and psychological state should also be considered, as well as the patient s wishes. 4.2 Referral process The decision to initiate a referral for parenteral nutrition must involve the consultant managing the patient and this must be documented in the medical notes. The referral must then be completed using the online system and by bleeping the nutrition support team on bleep An to a member of the nutrition support team from the referring consultant will also be accepted. The nutrition support team can be contacted by bleep (Monday to Friday 8.00 to 16.00). Page 6 of 17
7 The following: should be documented in the medical notes at the time of referral: PAT/T 66 v.1 Medical condition leading to gut failure and leading to need for parenteral nutrition Purpose of the parenteral nutrition ( to meet nutritional targets or to prevent further nutritional losses) Whether the parenteral nutrition will be sole form of feeding or combined with enteral or oral feeding Intended stopping point e.g. when patient is able to meet nutritional targets orally or enterally, or a time limited trial for example patient with high output stoma., to be nil by mouth for 2 weeks If this information is not available the nutrition support team will see and assess the patient but the PN will not be ordered from the Pharmacy until the above criteria have been agreed between the nutrition support team and the team managing the patient. 4.3 Requirements for referral The ward team should ensure that the following have been put in place: Up to date MUST score Up to date baseline bloods. As a minimum these include: o U+E, Ca, phosphate, magnesium, glucose, LFT, FBC and clottingo Further blood testing may then be requested by the nutrition support team. Central venous access (usually PICC line) requested on ICE Patient monitoring for strict fluid balance and twice weekly weight, at least BD blood glucose monitoring even if not diabetic Patients at risk of re-feeding syndrome started on Pabrinex. 4.4 Appropriate Route The most common route for PN administration is via a dedicated peripherally inserted central catheter (PICC). Other central vein catheterisation via the subclavian or jugular veins may be used for patients on DCC where appropriate. For long term PN, a tunnelled central venous catheter is most appropriate. Peripheral access may be used after due consideration by the nutrition support team if PN is considered for short term (<5 days). Only a limited number of PN bags are appropriate for peripheral administration and this would be documented on the prescription and on the product. 4.5 Prescribing Pabrinex Pabrinex is an Intravenous preparation of water soluble vitamins including high dose thiamine, to reduce risk of thiamine deficiency syndromes e.g. Wernicke s for patients at risk of re-feeding syndrome. Page 7 of 17
8 All at risk patients who are starting parenteral nutrition should be prescribed Pabrinex to reduce the risk of neurological complications of re-feeding syndrome, such as Wernicke s encephalopathy. Pabrinex should be prescribed using the TPN plus pabrinex (one pair daily for 10 days) option on JAC. If the patient has been admitted with alcohol related problems they should always be prescribed the alcohol regime on JAC. The nutrition support team will decide if pabrinex needs to be continued as part of their full assessment. 4.6 Ward inpatients requiring PN Location of adult inpatients requiring parenteral nutrition Wards managing adult patients with parenteral nutrition must be able to ensure: 1. Sufficient trained nursing staff with up to date certification for management of central venous catheters so that there will be at least 1 trained member of staff certified competent to manage the feeding line on for each shift, to set up and take down the parenteral nutrition 2. All nursing staff including healthcare assistants are familiar with the monitoring and documentation required for managing patients on parenteral nutrition. This monitoring is detailed in the Parenteral Nutrition Pathway of Care (see appendix 1). 3. Fridge with sufficient capacity to store parenteral nutrition bags 4. Means to weigh patients including access to hoist weighing scales 5. Daily medical review of patients by consultant or middle grade doctor including Saturday and Sunday. The following wards/areas have been designated for managing adult patients who require parenteral nutrition: DCC Doncaster ITU Bassetlaw Ward A5 Bassetlaw Ward 18 Doncaster Ward 20 Doncaster Ward 21 Doncaster Ward 24 Doncaster Ward S11 Doncaster If a patient who is not on one of these wards requires parenteral nutrition, the parenteral nutrition will not be ordered until the patient has been transferred to one of these wards. For patients with other complex medical needs, these will need to be discussed with either the nutrition support team or with one of the consultant intensivists (e.g. intra-dialysis parenteral nutrition). If due to complex needs it is not possible to transfer to one of these wards escalate to clinical lead /matron who will need to ensure appropriate support given to ward to allow safe administration. Page 8 of 17
9 Any adult patient who is on home parenteral nutrition who requires hospital admission must be admitted to one of the wards designated above. Please discuss with the site manager and nutrition support team to ensure the patient is admitted to the correct ward. Once the medical team managing the patient and the nutrition support team have agreed to start a patient on parenteral nutrition, the nutrition support team will be responsible for prescribing the parenteral nutrition. They will review the patient daily (Monday to Friday) and all patients receiving parenteral nutrition will be discussed at the weekly nutrition support team MDT meeting. The nutrition support team will review the patient s fluid and electrolyte balance and blood glucose control and make recommendations to the team managing the patient. Where it is deemed to be in the patient s best interests, the team may prescribe fluids or other medication relating to the nutritional care of the patient. The medical team managing the patient will be responsible for ensuring timely insertion of a central catheter for feeding, prescribing of additional intravenous fluids where appropriate and collection of bloods and other samples to monitor the patient for complications of the parenteral nutrition. The medical team will follow the guidance set out in the Parenteral Nutrition Pathway of Care (appendix 1). The ward nursing team managing the patient will be responsible for monitoring the patient s observations including blood glucose and fluid balance, as set out in the Parenteral Nutrition Pathway of Care. The ward nursing team will also be responsible for dressing the skin site of entry of the feeding line and watching for evidence of catheter related sepsis. 4.7 Patients on critical care requiring PN Adult patients on DCC will be managed by the consultant intensivists, ward pharmacist and ward dietician. Decisions to start and stop parenteral nutrition while the patient remains on DCC will not involve the nutrition support team. The nutrition nurse (or another member of the nutrition support team) will be made aware of all adult patients on the critical care unit who are requiring parenteral nutrition and will be responsible for ensuring that the nutrition support team review the patient once they are transferred to level 2 or level 1 care. Once the patient has been transferred off DCC, the nutrition support team will be responsible for prescribing and stopping parenteral nutrition. 4.8 Stopping parenteral nutrition For patients who are not in a critical care bed, the nutrition support team will make the decision when to stop the parenteral nutrition. In most instances this will follow a discussion between the medical team caring for the patient and the nutrition support team. Page 9 of 17
10 4.9 Patients on home PN who require hospitalisation Home parenteral nutrition patients must be admitted to one of the wards designated for parenteral nutrition. The designated wards are: DCC Doncaster ITU Bassetlaw A5 Bassetlaw Ward 18 Doncaster Ward 20 Doncaster Ward 21 Doncaster Ward 24 Doncaster Ward S11 Doncaster If the patient has complex medical needs that cannot be met on one of the designated wards the patient must be discussed with the nutrition support team (bleep 1812) or with a consultant intensivist. The nutrition support team MUST be informed if a home parenteral nutrition patient is admitted to Doncaster and Bassetlaw Hospitals. The team should be informed on the day of admission or on the next working day (bleep 1812). The nutrition nurse or another member of the nutrition support team will contact the Intestinal Failure centre responsible for the nutritional care of the home parenteral nutrition patient to discuss their nutritional management while the patient is in hospital. This may include transfer to the Intestinal Failure centre, where the admission is related to a complication of the parenteral nutrition. Unless advised otherwise by the Intestinal Failure centre, the patient will be managed according to the Trust Parenteral Nutrition Pathway of Care. The patient will be reviewed on a daily basis by the Nutrition support team (Monday to Friday) and will be discussed at the Nutrition team MDT meeting. The patients are required to bring their home PN bags on admission and the NST will transcribe their prescription onto the Trust PN prescription forms during working hours. If the patients are admitted out-of- hours or over the weekend, the on-call doctor covering the respective ward should complete the transcription. Transcription involves getting the home PN bag for the day and copying out the name, constituents, electrolytes and trace elements as indicated on the label and then adding the batch number and expiry dates. See specimen in appendix 1. The PN prescription forms are stocked on the appropriate wards including ward 20, 21, 24, DCC and ITU. The nutrition support team will be responsible for contacting the Intestinal Failure Unit to inform them of the patient s discharge from hospital, within 24 hours of discharge. Page 10 of 17
11 5. TRAINING/SUPPORT The members of the nutrition support team have a responsibility to provide education and training to the medical, nursing and allied health professionals caring for the patient regarding nutritional issues and in particular with reference to safe delivery and monitoring of parenteral nutrition. All nurses delivering PN via a central line must complete the central venous access device (CVAD) package and training provided by clinical skills. Revalidation of these skills will also be provided by clinical skills and nurses must be updated at least every three years. 5.1 Pharmaceutical Stability A ready to use bag of PN (with additives) has got a 7-day shelf life if stored between C. Once allowed to reach room temperature on the wards and in medicine preparation areas, the expiry is reduced to 24hours. Once PN is hung for administration any left-over product should be discarded after 24hours. If the patient has got additional IV fluids or medication, they should be given via a separate lumen or peripheral cannula as admixtures of PN and certain medication could result in instability of the formulation. 5.2 The Prescription Prescriptions will be completed by the NST after patient review on a daily basis and will be based upon a comprehensive patient assessment. The prescription will detail the type of bag, any additives, rate of infusion and the route of administration. 5.3 Management of PN All adult patients receiving parenteral nutrition within the Trust will be managed according to the guidance in the Parenteral Nutrition Pathway of Care The nutrition support team will be responsible for reviewing the pathway of care on an annual basis and ensuring that this recommends best practice and follows national and local guidance. They will consult with other interested parties such as consultant intensivists so that the guidance will be applicable for all adult patients. Page 11 of 17
12 6. MONITORING COMPLIANCE WITH THE PROCEDURAL DOCUMENT What is being Monitored Who will carry out the Monitoring How often How Reviewed/ Where Reported to The procedural document will be reviewed in the following circumstances: Audits on the usage of PN Nutrition Support Team Nutrition Support Team Every three years routinely, unless: New national or international guidance are received. Newly published evidence demonstrates need for change to current practice. Action required from Root Cause Analysis Serious Incident Investigation report Every 6 months Nutrition steering committee Clinical leads, 7. DEFINITIONS NST Nutrition Support Team MUST malnutrition universal screening tool PN parenteral nutrition DCC Department of critical care ITU - Intensive care unit CVAD- Central venous access device CVC - central venous catheter U+E Urea and electrolyte Ca Calcium LFT Liver function test FBC Full blood count Page 12 of 17
13 8. EQUALITY IMPACT ASSESSMENT An Equality Impact Assessment (EIA) has been conducted on this procedural document in line with the principles of the Equality Analysis Policy (CORP/EMP 27) and the Fair Treatment For All Policy (CORP/EMP 4). The purpose of the EIA is to minimise and if possible remove any disproportionate impact on employees on the grounds of race, sex, disability, age, sexual orientation or religious belief. No detriment was identified. (see Appendix 3). 9. ASSOCIATED TRUST PROCEDURAL DOCUMENTS Central Venous Access Device (CVADs) Care and Management Policy - PAT/T 23 Mental Capacity Act 2005 Policy and Guidance, including Deprivation of Liberty Safeguards (DoLS) - PAT/PA 19 Privacy and Dignity Policy - PAT/PA REFERENCES Nutrition support in adults: oral nutrition support, enteral tube feeding and parenteral nutrition (2006) NICE clinical guideline 32. Page 13 of 17
14 APPENDIX 1 PARENTERAL NUTRITION PATHWAY OF CARE Parenteral nutrition pathway of care Referral to NST MUST be authorised by the Consultant managing the patient 1 Is PN indicated? Y N Refer to ward Dietitian for review Contact Site manager NST on BLEEP 1812 J Sayer (Medical) T Wilson (Surgical) * Or use TPN blood profile on ICE N Refer (NST) Online referral and Bleep 1812 Is the patient on an appropriate ward? Abnormal K, Mg, PO 4? (Must be checked before PN) N Y Done Y Done 4 Order PN Bloods (FBC, U+E, LFT, Mg, bone*, Glucose, clotting) Correct abnormal K, Mg or PO 4 before PN 6 Is there a risk of refeeding? Y Prescribe Pabrinex N Done 7 Does patient have central access? N Request PICC (Complete request on ICE and liaise with DSA) PLEASE SEE EXPLANATORY NOTES OVERLEAF 8 Y Has NST reviewed patient? Done N Call NST 10 - Request further bloods* - Strict fluid balance - Regular weights Page 14 of 17 Y 9 Assess fluid and electrolyte needs
15 Indication for Parenteral Nutrition: Parenteral nutrition is a treatment with a high risk of complications. It should only be considered as a treatment for nutritional support after all oral and enteral options have been explored. The main indications for parenteral nutrition are: Intestinal perforation Intestinal obstruction Intestinal dysmotility, including prolonged post- operative ileus and intestinal pseudoobstruction leading to malabsorption Acute pancreatitis where nasojejunal feeding is not tolerated High output stoma or high output fistula where the surgical consultant has recommended a trial period of Nil by mouth Short bowel syndrome where absorption is not sufficient to meet patient s nutritional targets There may be other cases who would benefit from parenteral nutrition. These should be discussed on an individual case basis with the nutrition support team. The following wards have been designated for managing adult patients who require parenteral nutrition: DCC Doncaster Ward 18 Doncaster Ward 20 Doncaster Ward 24 Doncaster Ward 21 Doncaster Ward S11 Doncaster Ward A5 Bassetlaw ITU Bassetlaw High risk of re-feeding problems if: One or more of the following: BMI less than 16 kg/m2 Unintentional weight loss >15% within last 3-6 months Little or no nutritional intake for more than 10 days Low levels of potassium, phosphate or magnesium prior to feeding Two or more of the following: BMI less than 18.5 kg/m2 Unintentional weight loss >10% within the last 3-6 months Little or no nutritional intake for more than 5 days A history of alcohol abuse or drugs including insulin, chemotherapy, antacids or diuretics Pabrinex Information All patients who are starting parenteral nutrition should be prescribed Pabrinex to reduce the risk of neurological complications of re-feeding syndrome, such as Wernicke s encephalopathy Prescribe on JAC using the TPN plus Pabrinex option (one pair daily for ten days) Unless the patient has been admitted with alcohol related issues in which case prescribe the alcohol regimen of Pabrinex on JAC. Nursing care for all PN patients: Accurate fluid balance Blood sugar monitoring at least daily CVAD care sheet Twice weekly weight 10 Page 15 of 17
16 APPENDIX 2 SPECIMEN HOME PN TRANSCRIPTION PAT/T 66 v.1 Page 16 of 17
17 APPENDIX 3 - EQUALITY IMPACT ASSESSMENT PART 1 INITIAL SCREENING Service/Function/Policy/ Care Group/Executive Directorate and Assessor (s) New or Existing Date of Assessment Project/Strategy Department Service or Policy? Parenteral Nutrition Emergency care group Hannah Stirland New 30/03/2016 1) Who is responsible for this policy? Emergency care group 2) Describe the purpose of the service / function / policy / project/ strategy? Patients receiving parenteral nutrition (PN) and staff administering PN 3) Are there any associated objectives? NICE guidance (2006) 4) What factors contribute or detract from achieving intended outcomes? 5) Does the policy have an impact in terms of age, race, disability, gender, gender reassignment, sexual orientation, marriage/civil partnership, maternity/pregnancy and religion/belief? No If yes, please describe current or planned activities to address the impact [e.g. Monitoring, consultation] 6) Is there any scope for new measures which would promote equality? [any actions to be taken] 7) Are any of the following groups adversely affected by the policy? Affected Protected Characteristics? Impact a) Age no b) Disability no c) Gender no d) Gender Reassignment no e) Marriage/Civil Partnership no f) Maternity/Pregnancy no g) Race no h) Religion/Belief no i) Sexual Orientation no 8) Provide the Equality Rating of the service / function /policy / project / strategy tick outcome box Outcome 1 Outcome 2 Outcome 3 Outcome 4 Date for next review: February 2019 Checked by: Hannah Stirland Date: Page 17 of 17
In Hospital Management of Hypoglycaemia in Adults with Diabetes Mellitus
 In Hospital Management of Hypoglycaemia in Adults with Diabetes Mellitus This procedural document supersedes any previous guidelines in relation to this subject: PAT/T 49 v.2 In Hospital Management of
In Hospital Management of Hypoglycaemia in Adults with Diabetes Mellitus This procedural document supersedes any previous guidelines in relation to this subject: PAT/T 49 v.2 In Hospital Management of
Title The Prescription of Adult Inpatient Parenteral Nutrition (PN) Guideline. Author s job title Consultant Gastroenterologist Directorate Medicine
 Document Control Title The Prescription of Adult Inpatient Parenteral Nutrition (PN) Guideline Author Author s job title Consultant Gastroenterologist Directorate Medicine Department Medicine Version Date
Document Control Title The Prescription of Adult Inpatient Parenteral Nutrition (PN) Guideline Author Author s job title Consultant Gastroenterologist Directorate Medicine Department Medicine Version Date
Venous Thromboembolism (VTE) Prevention and Treatment of VTE in Patients Admitted to Hospital
 Please Note: This policy is currently under review and is still fit for purpose. Venous Thromboembolism (VTE) Prevention and Treatment of VTE in Patients Admitted to Hospital This procedural document supersedes
Please Note: This policy is currently under review and is still fit for purpose. Venous Thromboembolism (VTE) Prevention and Treatment of VTE in Patients Admitted to Hospital This procedural document supersedes
Parenteral Nutrition Policy
 Policy No: RM60 Version: 3.0 Name of Policy: Parenteral Nutrition Policy Effective From: 18/08/2015 Date Ratified 12/08/2015 Ratified SafeCare Council Review Date 01/08/2017 Sponsor Director of Nursing,
Policy No: RM60 Version: 3.0 Name of Policy: Parenteral Nutrition Policy Effective From: 18/08/2015 Date Ratified 12/08/2015 Ratified SafeCare Council Review Date 01/08/2017 Sponsor Director of Nursing,
Prevention of Contrast Induced Nephropathy (CIN) Guidelines
 Prevention of Contrast Induced Nephropathy (CIN) Guidelines This procedural document supersedes: PAT/T 48 v.1 - Guidelines for Prevention of Contrast Induced Nephropathy (CIN) Did you print this document
Prevention of Contrast Induced Nephropathy (CIN) Guidelines This procedural document supersedes: PAT/T 48 v.1 - Guidelines for Prevention of Contrast Induced Nephropathy (CIN) Did you print this document
Adjustable Gastric Band Management Practice Guidelines
 Adjustable Gastric Band Management Practice Guidelines This procedural document supersedes: PAT/T 47 v.2 Adjustable Gastric Band Management Practice Guidelines Did you print this document yourself? The
Adjustable Gastric Band Management Practice Guidelines This procedural document supersedes: PAT/T 47 v.2 Adjustable Gastric Band Management Practice Guidelines Did you print this document yourself? The
Intestinal Failure Referral Form
 Intestinal Failure Referral Form This form must be completed in full and emailed to UCLH.IFReferrals@nhs.net or call 07958 263178. Please complete all sections of the form. Please note that incomplete
Intestinal Failure Referral Form This form must be completed in full and emailed to UCLH.IFReferrals@nhs.net or call 07958 263178. Please complete all sections of the form. Please note that incomplete
Specialised Services Policy: CP24 Home Administered Parenteral Nutrition (HPN)
 Specialised Services Policy: CP24 Home Administered Parenteral Nutrition (HPN) Document Author: Specialist Services Planning Manager for Neurosciences and Complex Conditions Executive Lead: Director of
Specialised Services Policy: CP24 Home Administered Parenteral Nutrition (HPN) Document Author: Specialist Services Planning Manager for Neurosciences and Complex Conditions Executive Lead: Director of
Guideline scope Neonatal parenteral nutrition
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Neonatal parenteral nutrition The Department of Health in England has asked NICE to develop a new guideline on parenteral nutrition in
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Neonatal parenteral nutrition The Department of Health in England has asked NICE to develop a new guideline on parenteral nutrition in
Nutrition in Pancreatic Cancer. Edmond Sung Consultant Gastroenterologist Lead Clinician for Clinical Nutrition and Endoscopy
 Nutrition in Pancreatic Cancer Edmond Sung Consultant Gastroenterologist Lead Clinician for Clinical Nutrition and Endoscopy Overview The pancreas and nutrition Nutrition screening - can we do this well?
Nutrition in Pancreatic Cancer Edmond Sung Consultant Gastroenterologist Lead Clinician for Clinical Nutrition and Endoscopy Overview The pancreas and nutrition Nutrition screening - can we do this well?
NUTRITION. Elizabeth Viner Smith & Catherine Jones Foundations of Critical Care Nursing September 2017
 NUTRITION Elizabeth Viner Smith & Catherine Jones Foundations of Critical Care Nursing September 2017 Step One Competency 1.19 Factors contributing to nutritional impairment in critical illness. Nutritional
NUTRITION Elizabeth Viner Smith & Catherine Jones Foundations of Critical Care Nursing September 2017 Step One Competency 1.19 Factors contributing to nutritional impairment in critical illness. Nutritional
Trust Policy Adult Total Parenteral Nutrition policy
 Trust Policy Adult Total Parenteral Nutrition policy Purpose Date Version June 2017 1.0 These guidelines are aimed at adults receiving total parenteral nutrition (TPN) on general or specialist wards at
Trust Policy Adult Total Parenteral Nutrition policy Purpose Date Version June 2017 1.0 These guidelines are aimed at adults receiving total parenteral nutrition (TPN) on general or specialist wards at
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE SCOPE. Nutrition support in adults: oral supplements, enteral and parenteral feeding.
 NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE 1 Guideline title SCOPE Nutrition support in adults: oral supplements, enteral and parenteral feeding. 1.1 Short title Nutrition support 2 Background a) The National
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE 1 Guideline title SCOPE Nutrition support in adults: oral supplements, enteral and parenteral feeding. 1.1 Short title Nutrition support 2 Background a) The National
Does the patient need an enteral feed out of hours?
 Out of hours Enteral tube feeding (Nasogastric) Starter Regimen for an Adult Inpatient With Renal Failure (Including management of re-feeding syndrome) Guidance for Practice 1. Introduction 1.1 This clinical
Out of hours Enteral tube feeding (Nasogastric) Starter Regimen for an Adult Inpatient With Renal Failure (Including management of re-feeding syndrome) Guidance for Practice 1. Introduction 1.1 This clinical
Patient information leaflet. Royal Surrey County Hospital. NHS Foundation Trust. Parenteral Nutrition. Nutrition Support Team (NST)
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Parenteral Nutrition Nutrition Support Team (NST) This leaflet gives you information to help you understand what parenteral
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Parenteral Nutrition Nutrition Support Team (NST) This leaflet gives you information to help you understand what parenteral
Nutritional Protocol for Blood and Bone Marrow Transplantation (BMT)
 Nutritional Protocol for Blood and Bone Marrow Transplantation (BMT) Scope This protocol details pre, during and post BMT nutritional assessment and management for all forms of BMT undertaken by OxBMT,
Nutritional Protocol for Blood and Bone Marrow Transplantation (BMT) Scope This protocol details pre, during and post BMT nutritional assessment and management for all forms of BMT undertaken by OxBMT,
Acute management of severe malnutrition. Dr Simon Gabe St Mark s Hospital, London
 Acute management of severe malnutrition Dr Simon Gabe St Mark s Hospital, London Malnutrition definition A state resulting from lack of uptake or intake of nutrition leading to altered body composition
Acute management of severe malnutrition Dr Simon Gabe St Mark s Hospital, London Malnutrition definition A state resulting from lack of uptake or intake of nutrition leading to altered body composition
Emergency Treatment of Anaphylaxis Policy and Guidelines
 Emergency Treatment of Anaphylaxis Policy and Guidelines This procedural document supersedes: PAT/EC 3 v.6 Emergency Treatment of Anaphylaxis Policy and Guidelines This procedural document should be used
Emergency Treatment of Anaphylaxis Policy and Guidelines This procedural document supersedes: PAT/EC 3 v.6 Emergency Treatment of Anaphylaxis Policy and Guidelines This procedural document should be used
GUIDANCE NOTES. DIETETIC RISK ASSESSMENT FOR REFEEDING RECOMMENDED MEAL PLANS When commencing re-feeding: NICE (2006)
 When commencing re-feeding: NICE (2006) NICE (2006) Clinical Guideline 32 Nutrition support in adults: oral nutrition support, enteral tube feeding and parenteral nutrition (The following is based on www.nice.org.uk/cg032
When commencing re-feeding: NICE (2006) NICE (2006) Clinical Guideline 32 Nutrition support in adults: oral nutrition support, enteral tube feeding and parenteral nutrition (The following is based on www.nice.org.uk/cg032
Neonatal Parenteral Nutrition Guideline Dr M Hogan, Maire Cullen ANNP, Una Toland Ward Manager, Sandra Kilpatrick Neonatal Pharmacist
 CLINICAL GUIDELINES ID TAG Title: Author: Designation: Speciality / Division: Directorate: Neonatal Parenteral Nutrition Guideline Dr M Hogan, Maire Cullen ANNP, Una Toland Ward Manager, Sandra Kilpatrick
CLINICAL GUIDELINES ID TAG Title: Author: Designation: Speciality / Division: Directorate: Neonatal Parenteral Nutrition Guideline Dr M Hogan, Maire Cullen ANNP, Una Toland Ward Manager, Sandra Kilpatrick
Specialised Services Commissioning Policy. CP29: Bariatric Surgery
 Specialised Services Commissioning Policy CP29: Bariatric Surgery Document Author: Specialist Planner, Cardiothoracic Executive Lead: Director of Planning Approved by: Management Group Issue Date: 12 June
Specialised Services Commissioning Policy CP29: Bariatric Surgery Document Author: Specialist Planner, Cardiothoracic Executive Lead: Director of Planning Approved by: Management Group Issue Date: 12 June
September 2014 V0.17. Paediatric Daily Fluid Prescription & Balance Chart
 September 14 V0.17 Aims and outcomes of session. Aim: To provide guidance on correctly completing the paediatric daily fluid prescription & balance chart. Outcomes: Demonstrate the ability to: calculate
September 14 V0.17 Aims and outcomes of session. Aim: To provide guidance on correctly completing the paediatric daily fluid prescription & balance chart. Outcomes: Demonstrate the ability to: calculate
NON-PATIENT SLIPS, TRIPS AND FALLS GUIDANCE
 Please Note: This policy is currently under review and is still fit for purpose. NON-PATIENT SLIPS, TRIPS AND FALLS GUIDANCE This procedural document supersedes: CORP/HSFS 8 v.3 Slips, Trips and Falls
Please Note: This policy is currently under review and is still fit for purpose. NON-PATIENT SLIPS, TRIPS AND FALLS GUIDANCE This procedural document supersedes: CORP/HSFS 8 v.3 Slips, Trips and Falls
Introduction. Guidelines for patient involvement in the administration of insulin under supervision in hospital (Adult patients)
 Guidelines for patient involvement in the administration of insulin under supervision in hospital (Adult patients) Introduction This guideline is designed to provide a framework for patients to administer
Guidelines for patient involvement in the administration of insulin under supervision in hospital (Adult patients) Introduction This guideline is designed to provide a framework for patients to administer
Refeeding syndrome a practical approach
 Refeeding syndrome a practical approach PENG pre-bapen Conference Teaching Day Birmingham Monday 20 th November 2017 Rhys White Acting Clinical and Operational Lead Dietitian Guys and St Thomas NHS Foundation
Refeeding syndrome a practical approach PENG pre-bapen Conference Teaching Day Birmingham Monday 20 th November 2017 Rhys White Acting Clinical and Operational Lead Dietitian Guys and St Thomas NHS Foundation
Peripheral Venous Cannula (PVC) Management Guidelines
 Peripheral Venous Cannula (PVC) Management Guidelines This procedural document supersedes: PAT/T 45 v.2 Peripheral Venous Cannulation (PVC) Insertion and Management Guidelines Did you print this document
Peripheral Venous Cannula (PVC) Management Guidelines This procedural document supersedes: PAT/T 45 v.2 Peripheral Venous Cannulation (PVC) Insertion and Management Guidelines Did you print this document
Reducing the Door to Needle Time for Antibiotics in Suspected Neutropenic Sepsis using a Dedicated Clinical Pathway
 Reducing the Door to Needle Time for Antibiotics in Suspected Neutropenic Sepsis using a Dedicated Clinical Pathway Dr Alex Williams, Oncology Specialty Doctor. Cheltenham General Hospital Oncology Centre
Reducing the Door to Needle Time for Antibiotics in Suspected Neutropenic Sepsis using a Dedicated Clinical Pathway Dr Alex Williams, Oncology Specialty Doctor. Cheltenham General Hospital Oncology Centre
Malnutrition in Adults: Guidelines for Identification and Treatment
 Malnutrition in Adults: Guidelines for Identification and Treatment Signatures (e.g. chair of the ratifying committee and lay member) and date Signature...date Designation: Signature...date Designation
Malnutrition in Adults: Guidelines for Identification and Treatment Signatures (e.g. chair of the ratifying committee and lay member) and date Signature...date Designation: Signature...date Designation
PATIENTS PRESENTING WITH SUSPECTED OR CONFIRMED ANOREXIA NERVOSA
 Guideline for Treating Patients with Anorexia Nervosa when Admitted as a Medical Emergency Trust Reference E2/2012 PATIENTS PRESENTING WITH SUSPECTED OR CONFIRMED ANOREXIA NERVOSA AN CONFIRMED Inform Gastro
Guideline for Treating Patients with Anorexia Nervosa when Admitted as a Medical Emergency Trust Reference E2/2012 PATIENTS PRESENTING WITH SUSPECTED OR CONFIRMED ANOREXIA NERVOSA AN CONFIRMED Inform Gastro
Blood Glucose and Hyperglycaemia Management in Hospital for Adults with Diabetes Clinical Guideline V2.0. March 2018
 Blood Glucose and Hyperglycaemia Management in Hospital for Adults with Diabetes Clinical Guideline V2.0 March 2018 Page 1 of 8 Summary flow chart for monitoring of blood glucose if >11mmol/L For Adults
Blood Glucose and Hyperglycaemia Management in Hospital for Adults with Diabetes Clinical Guideline V2.0 March 2018 Page 1 of 8 Summary flow chart for monitoring of blood glucose if >11mmol/L For Adults
Contributes to CQC Outcome number: 9&12 Consulted With Post/Committee/Group Date. Pharmacist. Alison Felton Head of Pharmacy/Deputy Chief.
 Prescribing paracetamol in adult inpatients at MEHT Type: Clinical Guideline Register No: 18005 Status: Public on ratification Developed in response to: In line with Basildon Contributes to CQC Outcome
Prescribing paracetamol in adult inpatients at MEHT Type: Clinical Guideline Register No: 18005 Status: Public on ratification Developed in response to: In line with Basildon Contributes to CQC Outcome
POLICY DOCUMENT. Pharmacy MMG/MPG. Approved By and Date Medicines Management roup March March 2016
 POLICY DOCUMENT Document Title High dose and combination antipsychotic guidance Reference Number n/a Policy Type Prescribing and Treatment Guideline Electronic File/Location Clinical Resources/Pharmacy/Prescribing
POLICY DOCUMENT Document Title High dose and combination antipsychotic guidance Reference Number n/a Policy Type Prescribing and Treatment Guideline Electronic File/Location Clinical Resources/Pharmacy/Prescribing
Methods of Nutrition Support KNH 406
 Methods of Nutrition Support KNH 406 Malnutrition 30 50% of hospitalized patients 95% of nursing home patients Resulting in reduced quality of life & increased health care costs May be remedied by providing
Methods of Nutrition Support KNH 406 Malnutrition 30 50% of hospitalized patients 95% of nursing home patients Resulting in reduced quality of life & increased health care costs May be remedied by providing
The Newcastle upon Tyne Hospitals NHS Foundation Trust. Pre-filled Patient Controlled Analgesia (PCA) syringes
 The Newcastle upon Tyne Hospitals NHS Foundation Trust Pre-filled Patient Controlled Analgesia (PCA) syringes Version.: 2.2 Effective From: 1 June 2016 Expiry Date: 1 June 2019 Date Ratified: 20 April
The Newcastle upon Tyne Hospitals NHS Foundation Trust Pre-filled Patient Controlled Analgesia (PCA) syringes Version.: 2.2 Effective From: 1 June 2016 Expiry Date: 1 June 2019 Date Ratified: 20 April
CHEMOTHERAPY NETWORK GROUP POLICY FOR ADMINISTRATION OF CYTOTOXIC CHEMOTHERAPY
 CHEMOTHERAPY NETWORK GROUP POLICY FOR ADMINISTRATION OF CYTOTOXIC CHEMOTHERAPY Version 4.0 March 2016 Review date March 2018 Introduction It is the purpose of this policy to provide clear guidelines that
CHEMOTHERAPY NETWORK GROUP POLICY FOR ADMINISTRATION OF CYTOTOXIC CHEMOTHERAPY Version 4.0 March 2016 Review date March 2018 Introduction It is the purpose of this policy to provide clear guidelines that
Parenteral Nutrition Policy for Adults
 Parenteral Nutrition Policy for Adults East Cheshire NHS Trust: CNSG002 Parenteral Nutrition Policy for Adults Page 1 of 24 Policy Title: Parenteral Nutrition Policy for Adults Executive Summary: To optimise
Parenteral Nutrition Policy for Adults East Cheshire NHS Trust: CNSG002 Parenteral Nutrition Policy for Adults Page 1 of 24 Policy Title: Parenteral Nutrition Policy for Adults Executive Summary: To optimise
Appropriate Use of Prescribed Oral Nutritional Supplement (ONS) in the Community
 Appropriate Use of Prescribed Oral Nutritional Supplement (ONS) in the Community Aim This guideline sets out a recommended procedure for the identification and treatment of malnutrition to ensure Oral
Appropriate Use of Prescribed Oral Nutritional Supplement (ONS) in the Community Aim This guideline sets out a recommended procedure for the identification and treatment of malnutrition to ensure Oral
Index No: MMG11/1. Version: 1. Date ratified: 12 th November 2013
 Index No: Intravenous fluid prescription in children For previously well children aged one month to 16 years (excluding renal, cardiac, diabetic ketoacidosis and acute burns patients) Version: 1 Date ratified:
Index No: Intravenous fluid prescription in children For previously well children aged one month to 16 years (excluding renal, cardiac, diabetic ketoacidosis and acute burns patients) Version: 1 Date ratified:
28 th September Author Jeremy Gilbert Bariatric Nurse Specialist
 POLICY FOR SELF ADMINISTRATION OF CONTINUOUS POSITIVE AIRWAY PRESSURE BY COMPETENT PATIENTS COMING IN FOR METABOLIC AND OBESITY SURGERY (BARIATRIC SURGERY) TO PENDENNIS WARD 28 th September 2014 Author
POLICY FOR SELF ADMINISTRATION OF CONTINUOUS POSITIVE AIRWAY PRESSURE BY COMPETENT PATIENTS COMING IN FOR METABOLIC AND OBESITY SURGERY (BARIATRIC SURGERY) TO PENDENNIS WARD 28 th September 2014 Author
Managing Hyperglycaemia in Acute (Adult) Inpatients Requiring Enteral Feeding Guidelines
 Document Control Title Managing Hyperglycaemia in Acute (Adult) Inpatients Requiring Author Author s job title Specialist Nurse Consultant Physician Department Directorate Unscheduled Care Version Date
Document Control Title Managing Hyperglycaemia in Acute (Adult) Inpatients Requiring Author Author s job title Specialist Nurse Consultant Physician Department Directorate Unscheduled Care Version Date
UK Inflammatory Bowel Disease Audit. A summary report on the quality of healthcare provided to people with inflammatory bowel disease
 UK Inflammatory Bowel Disease Audit A summary report on the quality of healthcare provided to people with inflammatory bowel disease Section heading UK IBD Audit summary report 2014 This summary report
UK Inflammatory Bowel Disease Audit A summary report on the quality of healthcare provided to people with inflammatory bowel disease Section heading UK IBD Audit summary report 2014 This summary report
Care Homes - Homely Remedies Protocol
 Care Homes - Homely Remedies Protocol A homely remedy is a medicine for the short-term treatment of a minor ailment, such as indigestion, a cough, mild to moderate pain or constipation, and can be obtained
Care Homes - Homely Remedies Protocol A homely remedy is a medicine for the short-term treatment of a minor ailment, such as indigestion, a cough, mild to moderate pain or constipation, and can be obtained
Use of Oral Nutritional Supplements in Primary Care Version 1 September 2017
 Use of Oral Nutritional Supplements in Primary Care Version 1 September 2017 VERSION CONTROL Version Date Amendments made Version 1 Sept 2017 New document. AG. Contents Page 2. Introduction 2. Malnutrition
Use of Oral Nutritional Supplements in Primary Care Version 1 September 2017 VERSION CONTROL Version Date Amendments made Version 1 Sept 2017 New document. AG. Contents Page 2. Introduction 2. Malnutrition
Nutrition care plan for surgical patients. Objectives
 Slide 1 Nutrition care plan for surgical patients Surgical Nutrition Training Module Level 1 Philippine Society of General Surgeons Committee on Surgical Training In this session we will discuss the most
Slide 1 Nutrition care plan for surgical patients Surgical Nutrition Training Module Level 1 Philippine Society of General Surgeons Committee on Surgical Training In this session we will discuss the most
A Guide to Prescribing Adult Oral Nutritional Supplements in West Kent CCG
 A Guide to Prescribing Adult Oral Nutritional Supplements in West Kent CCG Aim This guideline has been designed to support primary care prescribers initiating nutrition support for adults in West Kent.
A Guide to Prescribing Adult Oral Nutritional Supplements in West Kent CCG Aim This guideline has been designed to support primary care prescribers initiating nutrition support for adults in West Kent.
PARENTERAL NUTRITION
 PARENTERAL NUTRITION DEFINITION Parenteral nutrition [(PN) or total parenteral nutrition (TPN)] is the intravenous infusion of some or all nutrients for tissue maintenance, metabolic requirements and growth
PARENTERAL NUTRITION DEFINITION Parenteral nutrition [(PN) or total parenteral nutrition (TPN)] is the intravenous infusion of some or all nutrients for tissue maintenance, metabolic requirements and growth
High Intensity Chemotherapy Guidelines for Haematology Patients at ASPH
 High Intensity Chemotherapy Guidelines for Haematology Patients at ASPH Contents: Page No. 1. Overview 2 2. Admission 3 3. Admission Checklist 5 4. Inpatient management during chemotherapy 6 5. Inpatient
High Intensity Chemotherapy Guidelines for Haematology Patients at ASPH Contents: Page No. 1. Overview 2 2. Admission 3 3. Admission Checklist 5 4. Inpatient management during chemotherapy 6 5. Inpatient
Suboptimal hydration harms patients.
 Suboptimal hydration harms patients. NHS Fife is committed to improving hydration management. To achieve this we need your help! In 2014 new fluid balance charts were implemented in the Victoria Hospital,
Suboptimal hydration harms patients. NHS Fife is committed to improving hydration management. To achieve this we need your help! In 2014 new fluid balance charts were implemented in the Victoria Hospital,
HOMES AND SENIORS SERVICES. APPROVAL DATE: February 2011 REVISION DATE: January 2015; July 2018
 POLICY: Page 1 of 6 A resident requiring enteral (tube) feeding as a sole source or adjunctive nutrition support have access to a comprehensive enteral feeding program and receive appropriate support from
POLICY: Page 1 of 6 A resident requiring enteral (tube) feeding as a sole source or adjunctive nutrition support have access to a comprehensive enteral feeding program and receive appropriate support from
Initiation of Clozapine Treatment Community Patients
 Initiation of Clozapine Treatment Community Patients Who Should Read This Policy Target Audience All clinical staff working in the community N/A N/A Initiation of Clozapine Treatment for Patients in the
Initiation of Clozapine Treatment Community Patients Who Should Read This Policy Target Audience All clinical staff working in the community N/A N/A Initiation of Clozapine Treatment for Patients in the
Please inform the Diabetes Nurse Specialist that this patient has been admitted within 24hrs of admission.
 Adult Diabetic Ketoacidosis Care Bundle (V1. Issued October 2014 Review October 2015) Improving patient care This pack includes: DKA Management Guideline Name: (Patient Addressograph) DOB: Hospital No:
Adult Diabetic Ketoacidosis Care Bundle (V1. Issued October 2014 Review October 2015) Improving patient care This pack includes: DKA Management Guideline Name: (Patient Addressograph) DOB: Hospital No:
Consultation Group: Dr Amalia Mayo, Paediatric Consultant. Review Date: March Uncontrolled when printed. Version 2. Executive Sign-Off
 Policy For The Adjustment Of Insulin Injections By Paediatric Diabetes Specialist Nurses/Community Paediatric Nurses Diabetes Working With Children Within NHS Grampian Co-ordinators: Lead Paediatric Diabetes
Policy For The Adjustment Of Insulin Injections By Paediatric Diabetes Specialist Nurses/Community Paediatric Nurses Diabetes Working With Children Within NHS Grampian Co-ordinators: Lead Paediatric Diabetes
- Arterial line safety Learning from a serious untoward incident on the Intensive Care Unit.
 - Arterial line safety Learning from a serious untoward incident on the Intensive Care Unit. Margi Jenkins Ex-Senior Sister Intensive care unit Royal United Hospital Bath Specialist Nurse Organ Donation
- Arterial line safety Learning from a serious untoward incident on the Intensive Care Unit. Margi Jenkins Ex-Senior Sister Intensive care unit Royal United Hospital Bath Specialist Nurse Organ Donation
Integrated Care Pathway (ICP) for the. Management of clozapine COMMUNITY INITIATION
 Document Reference MM 049 Integrated Care Pathway (ICP) for the Management of clozapine COMMUNITY INITIATION Surname Title Address Forenames Date of Birth RT/NHS number Care Co-ordinator GP CS number Consultant
Document Reference MM 049 Integrated Care Pathway (ICP) for the Management of clozapine COMMUNITY INITIATION Surname Title Address Forenames Date of Birth RT/NHS number Care Co-ordinator GP CS number Consultant
Policy Compliance Procedure
 Policy Compliance Procedure Safe Handling of Adult Intravenous Potassium Chloride Preparations This PCP relates to NSW Health PD NSW Health Policy Directive PD2005_342 Safe Handling of Intravenous Potassium
Policy Compliance Procedure Safe Handling of Adult Intravenous Potassium Chloride Preparations This PCP relates to NSW Health PD NSW Health Policy Directive PD2005_342 Safe Handling of Intravenous Potassium
Start. What is the serum phosphate concentration? Moderate Hypophosphataemia mmol/l. Replace using oral. phosphate. (See section 3.
 CLINICAL GUIDELINE FOR THE MANAGEMENT OF HYPOPHOSPHATAEMIA IN ADULTS Summary. Key: General Notes GP/SWASFT ED/MAU/SRU/Acute GP/Amb-Care In-patient wards Start What is the serum concentration? Mild Hypophosphataemia
CLINICAL GUIDELINE FOR THE MANAGEMENT OF HYPOPHOSPHATAEMIA IN ADULTS Summary. Key: General Notes GP/SWASFT ED/MAU/SRU/Acute GP/Amb-Care In-patient wards Start What is the serum concentration? Mild Hypophosphataemia
NUTRITION SUPPORT TEAM. Consensus guideline for best practice in intestinal failure in paediatrics. John Puntis
 NUTRITION SUPPORT TEAM Consensus guideline for best practice in intestinal failure in paediatrics. John Puntis Nutritional Support Team What is a Nutritional Support Team? nutrition is a multidisciplinary
NUTRITION SUPPORT TEAM Consensus guideline for best practice in intestinal failure in paediatrics. John Puntis Nutritional Support Team What is a Nutritional Support Team? nutrition is a multidisciplinary
DIAGNOSIS AND MANAGEMENT OF PYLORIC STENOSIS IN CHILDREN CLINICAL GUIDELINE V3.0
 DIAGNOSIS AND MANAGEMENT OF PYLORIC STENOSIS IN CHILDREN CLINICAL GUIDELINE V3.0 1. Aim/Purpose of this Guideline This guideline is relevant to all medical and nursing staff caring for children with Pyloric
DIAGNOSIS AND MANAGEMENT OF PYLORIC STENOSIS IN CHILDREN CLINICAL GUIDELINE V3.0 1. Aim/Purpose of this Guideline This guideline is relevant to all medical and nursing staff caring for children with Pyloric
Falls The Assessment, Prevention and Management of Patient Falls (Adult Services) 1.34
 SECTION: 1 PATIENT CARE Including Physical Healthcare POLICY /PROCEDURE: 1.34 NATURE AND SCOPE: SUBJECT (Title): POLICY AND PROCEDURE - TRUST WIDE FALLS: THE ASSESSMENT, PREVENTION AND MANAGEMENT OF PATIENT
SECTION: 1 PATIENT CARE Including Physical Healthcare POLICY /PROCEDURE: 1.34 NATURE AND SCOPE: SUBJECT (Title): POLICY AND PROCEDURE - TRUST WIDE FALLS: THE ASSESSMENT, PREVENTION AND MANAGEMENT OF PATIENT
Parenteral nutrition (PN) therapy
 Parenteral nutrition (PN) therapy Nutrition Nurse Specialists Information for Patients i University Hospitals of Leicester NHS Trust Introduction This leaflet aims to tell you about your intravenous feed
Parenteral nutrition (PN) therapy Nutrition Nurse Specialists Information for Patients i University Hospitals of Leicester NHS Trust Introduction This leaflet aims to tell you about your intravenous feed
Patient Group Directions Policy
 Patient Group Directions Policy Category: Summary: Equality Analysis undertaken: Valid From: Date of Next Review: Approval Date/ Via: Distribution: Related Documents: Author(s): Further Information: This
Patient Group Directions Policy Category: Summary: Equality Analysis undertaken: Valid From: Date of Next Review: Approval Date/ Via: Distribution: Related Documents: Author(s): Further Information: This
A three month project September December 2016
 Improving Insulin Safety in the Clinical Decision Unit A three month project September December 2016 Sarah Gregory - In-Patient DSN, QEQM Hospital Julie Gammon - Ward Manager, CDU, QEQM Hospital 1 The
Improving Insulin Safety in the Clinical Decision Unit A three month project September December 2016 Sarah Gregory - In-Patient DSN, QEQM Hospital Julie Gammon - Ward Manager, CDU, QEQM Hospital 1 The
PPP 1. Continuation, modification, and discontinuation of a medication
 PRESCRIBING POLICIES: 4.7 PHARMACIST AUTHORITY The College of Pharmacists of BC Professional Practice Policy (PPP) 58 Medication Management (Adapting a Prescription) became effective April 1, 2009. The
PRESCRIBING POLICIES: 4.7 PHARMACIST AUTHORITY The College of Pharmacists of BC Professional Practice Policy (PPP) 58 Medication Management (Adapting a Prescription) became effective April 1, 2009. The
concentrate intravenous solution and other strong potassium solutions
 Policy for the use of potassium chloride concentrate intravenous solution and other strong potassium solutions CLINICAL GUIDELINES ID TAG Policy for the use of potassium chloride Title: concentrate intravenous
Policy for the use of potassium chloride concentrate intravenous solution and other strong potassium solutions CLINICAL GUIDELINES ID TAG Policy for the use of potassium chloride Title: concentrate intravenous
Alcohol Issues in the Acute General Hospital Setting
 Alcohol Issues in the Acute General Hospital Setting (Guidelines and Management) This procedural document supersedes: PAT/T 25 version 3 - Guidelines for the Management of Alcohol Issues in the Acute General
Alcohol Issues in the Acute General Hospital Setting (Guidelines and Management) This procedural document supersedes: PAT/T 25 version 3 - Guidelines for the Management of Alcohol Issues in the Acute General
NCEPOD - Measuring the Units; A review of patients who died with alcohol-related liver disease
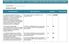 NCEPOD - Measuring the Units; A review of patients who died with alcohol-related liver disease Hospital Number Admission to hospital 5. Trusts should ensure that medical patients are reviewed by a consultant
NCEPOD - Measuring the Units; A review of patients who died with alcohol-related liver disease Hospital Number Admission to hospital 5. Trusts should ensure that medical patients are reviewed by a consultant
Alcohol Detoxification (Inpatient) Prescribing Guidelines
 Alcohol Detoxification (Inpatient) Prescribing Guidelines Author: Sponsor/Executive: Responsible committee: Consultation & Approval: (Committee/Groups which signed off the procedure, including date) This
Alcohol Detoxification (Inpatient) Prescribing Guidelines Author: Sponsor/Executive: Responsible committee: Consultation & Approval: (Committee/Groups which signed off the procedure, including date) This
Clinical guideline Published: 22 February 2006 nice.org.uk/guidance/cg32
 Nutrition support for adults: oral nutrition support, enteral tube feeding and parenteral al nutrition Clinical guideline Published: 22 February 2006 nice.org.uk/guidance/cg32 NICE 2018. All rights reserved.
Nutrition support for adults: oral nutrition support, enteral tube feeding and parenteral al nutrition Clinical guideline Published: 22 February 2006 nice.org.uk/guidance/cg32 NICE 2018. All rights reserved.
GUIDELINE FOR ENTERAL TUBE FEEDING (NASOGASTRIC OR PEG) IN PATIENTS WITH DIABETES MELLITUS TREATED WITH INSULIN
 GUIDELINE FOR ENTERAL TUBE FEEDING (NASOGASTRIC OR PEG) IN PATIENTS WITH DIABETES MELLITUS TREATED WITH INSULIN This guidance does not override the individual responsibility of health professionals to
GUIDELINE FOR ENTERAL TUBE FEEDING (NASOGASTRIC OR PEG) IN PATIENTS WITH DIABETES MELLITUS TREATED WITH INSULIN This guidance does not override the individual responsibility of health professionals to
TOTAL PARENTERAL NUTRITION
 TOTAL PARENTERAL NUTRITION Indication See algorithm. Timing Start TPN as indicated on algorithm 1. There is no need to build up TPN volume. The volume of TPN (including lipids) should equate to the total
TOTAL PARENTERAL NUTRITION Indication See algorithm. Timing Start TPN as indicated on algorithm 1. There is no need to build up TPN volume. The volume of TPN (including lipids) should equate to the total
Percutaneous removal of kidney stone(s): procedurespecific information
 PATIENT INFORMATION Percutaneous removal of kidney stone(s): procedurespecific information What is the evidence base for this information? This leaflet includes advice from consensus panels, the British
PATIENT INFORMATION Percutaneous removal of kidney stone(s): procedurespecific information What is the evidence base for this information? This leaflet includes advice from consensus panels, the British
Out of Hours Emergency Enteral Feeding Regimen (Including Risk Reduction for Re-feeding Syndrome)
 Out of Hours Emergency Enteral Feeding Regimen (Including Risk Reduction for Re-feeding Syndrome) This guidance does not override the individual responsibility of health professionals to make appropriate
Out of Hours Emergency Enteral Feeding Regimen (Including Risk Reduction for Re-feeding Syndrome) This guidance does not override the individual responsibility of health professionals to make appropriate
Southern Trust Home IV Service. Guidelines for the administration of IV antibiotics
 Southern Trust Home IV Service Guidelines for the administration of IV antibiotics Title: Author: CLINICAL GUIDELINES ID TAG Antibiotic guidelines - Southern Trust Home IV service guidelines for the administration
Southern Trust Home IV Service Guidelines for the administration of IV antibiotics Title: Author: CLINICAL GUIDELINES ID TAG Antibiotic guidelines - Southern Trust Home IV service guidelines for the administration
DOCUMENT CONTROL PAGE
 DOCUMENT CONTROL PAGE Title Title: UNDERGOING SPINAL DEFORMITY SURGERY Version: 2 Reference Number: Supersedes Supersedes: all other versions Description of Amendment(s): Revision of analgesia requirements
DOCUMENT CONTROL PAGE Title Title: UNDERGOING SPINAL DEFORMITY SURGERY Version: 2 Reference Number: Supersedes Supersedes: all other versions Description of Amendment(s): Revision of analgesia requirements
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Centre for Clinical Practice SCOPE Clinical guideline title: Intravenous fluid therapy in adults in hospital Quality standard title: Intravenous fluid
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Centre for Clinical Practice SCOPE Clinical guideline title: Intravenous fluid therapy in adults in hospital Quality standard title: Intravenous fluid
Acute Alcohol Withdrawal Protocol
 Acute Alcohol Withdrawal Protocol Controlled document This document is uncontrolled when downloaded or printed Reference number Version 1 Author WHHT: C268 Dr Mohamed Shariff Date ratified August 2014
Acute Alcohol Withdrawal Protocol Controlled document This document is uncontrolled when downloaded or printed Reference number Version 1 Author WHHT: C268 Dr Mohamed Shariff Date ratified August 2014
Haemodialysis central venous catheter-related sepsis management guideline Version 3. NAME M. Letheren Chair Clinical Effectiveness Advisory Group
 Lancashire Teaching Hospitals NHS Foundation Trust Haemodialysis central venous catheter-related sepsis management guideline Version 3 AUTHOR APPROVED BY DATE AUTH REF. NO NAME REBG/00018/July12 Michael
Lancashire Teaching Hospitals NHS Foundation Trust Haemodialysis central venous catheter-related sepsis management guideline Version 3 AUTHOR APPROVED BY DATE AUTH REF. NO NAME REBG/00018/July12 Michael
Pharmaceutical risk management strategies for parenteral nutrition. J. Eastwood (UK)
 ESPEN Congress Leipzig 2013 Pharmaceutical Session Pharmaceutical risk management strategies for parenteral nutrition J. Eastwood (UK) Pharmaceutical risk management strategies for parenteral nutrition
ESPEN Congress Leipzig 2013 Pharmaceutical Session Pharmaceutical risk management strategies for parenteral nutrition J. Eastwood (UK) Pharmaceutical risk management strategies for parenteral nutrition
CLINICAL GUIDELINE FOR THE ADMINISTRATION OF MESNA WITH IFOSFAMIDE AND CYCLOPHOSPHAMIDE Summary.
 CLINICAL GUIDELINE FOR THE ADMINISTRATION OF MESNA WITH IFOSFAMIDE AND CYCLOPHOSPHAMIDE Summary. Yes Is patient prescribed ifosfamide or cyclophosphamide >1g/m 2? Chemotherapy prescription on Aria should
CLINICAL GUIDELINE FOR THE ADMINISTRATION OF MESNA WITH IFOSFAMIDE AND CYCLOPHOSPHAMIDE Summary. Yes Is patient prescribed ifosfamide or cyclophosphamide >1g/m 2? Chemotherapy prescription on Aria should
Paediatric Prescribing Pocket Guide September 2014 (Version 1)
 PAGE 1 Paediatric Prescribing Pocket Guide September 2014 (Version 1) In children, the risk of medication errors is often exacerbated by the need for calculations to determine the dose. Prescribing errors
PAGE 1 Paediatric Prescribing Pocket Guide September 2014 (Version 1) In children, the risk of medication errors is often exacerbated by the need for calculations to determine the dose. Prescribing errors
Guidelines for the Management of Dyspepsia and GORD. Gastroenterology/ Acute Adult Governance. Drugs and Therapeutics Committee
 Guidelines for the Management of Dyspepsia and GORD Document type: Version: 3.0 Author (name): Author (designation): Validated by Prescribing Dr. G. Lipscomb Date validated October 2015 Ratified by: Date
Guidelines for the Management of Dyspepsia and GORD Document type: Version: 3.0 Author (name): Author (designation): Validated by Prescribing Dr. G. Lipscomb Date validated October 2015 Ratified by: Date
National Diabetes Inpatient Audit (NaDIA) 2016
 National Diabetes Inpatient Audit (NaDIA) 2016 DIABETES A summary report for people with diabetes and anyone interested in the quality of care for people with diabetes when they stay in hospital. Based
National Diabetes Inpatient Audit (NaDIA) 2016 DIABETES A summary report for people with diabetes and anyone interested in the quality of care for people with diabetes when they stay in hospital. Based
02/GMS/0030 ADULT EPILEPSY SERVICE CCP for General Medical and Surgical POOLE HOSPITAL NHS FOUNDATION TRUST
 Service Specification No. Service Commissioner Leads 02/GMS/0030 ADULT EPILEPSY SERVICE CCP for General Medical and Surgical Provider Lead POOLE HOSPITAL NHS FOUNDATION TRUST Period 1 April 2013 to 31
Service Specification No. Service Commissioner Leads 02/GMS/0030 ADULT EPILEPSY SERVICE CCP for General Medical and Surgical Provider Lead POOLE HOSPITAL NHS FOUNDATION TRUST Period 1 April 2013 to 31
Dietetic Outcomes in Home Parenteral Nutrition
 Dietetic Outcomes in Home Parenteral Nutrition Dr Alison Culkin Research Dietitian Intestinal Failure & Home Parenteral Nutrition St Mark s Hospital PENG Meeting November 2011 The Dietetic Outcomes Model
Dietetic Outcomes in Home Parenteral Nutrition Dr Alison Culkin Research Dietitian Intestinal Failure & Home Parenteral Nutrition St Mark s Hospital PENG Meeting November 2011 The Dietetic Outcomes Model
Nutrition support in adults: oral supplements, enteral and parenteral feeding
 Nutrition support in adults: oral supplements, enteral and parenteral feeding NICE guideline First draft for consultation, May 2005 If you wish to comment on this version of the guideline, please be aware
Nutrition support in adults: oral supplements, enteral and parenteral feeding NICE guideline First draft for consultation, May 2005 If you wish to comment on this version of the guideline, please be aware
Laser vaporisation of prostate (Green light laser prostate surgery): procedure-specific information
 PATIENT INFORMATION Laser vaporisation of prostate (Green light laser prostate surgery): procedure-specific information What is the evidence base for this information? This leaflet includes advice from
PATIENT INFORMATION Laser vaporisation of prostate (Green light laser prostate surgery): procedure-specific information What is the evidence base for this information? This leaflet includes advice from
Developed By Name Signature Date
 Patient Group Direction 2155 version 2.0 Administration / Supply of Inhaled Salbutamol in Asthma by Registered Practitioners employed by Torbay and South Devon NHS Foundation Trust Date of Introduction:
Patient Group Direction 2155 version 2.0 Administration / Supply of Inhaled Salbutamol in Asthma by Registered Practitioners employed by Torbay and South Devon NHS Foundation Trust Date of Introduction:
Care homes - Homely remedies
 Bulletin 72 August 2014 Care homes - Homely remedies Care home staff have a recognised duty of care to be able to respond to minor symptoms experienced by residents. A homely remedy is a medicinal product
Bulletin 72 August 2014 Care homes - Homely remedies Care home staff have a recognised duty of care to be able to respond to minor symptoms experienced by residents. A homely remedy is a medicinal product
Specialised Services Policy:
 Specialised Services Policy: CP35 Cochlear Implants Document Author: Specialised Planner for Women & Children s Services Executive Lead: Director of Planning Approved by: Executive Board Issue Date: 05
Specialised Services Policy: CP35 Cochlear Implants Document Author: Specialised Planner for Women & Children s Services Executive Lead: Director of Planning Approved by: Executive Board Issue Date: 05
NHS Grampian Staff Guideline For The Management Of Acute Hypophosphataemia In Adults
 NHS Grampian Staff Guideline For The Management Of Acute Hypophosphataemia In Adults Co-ordinators: Medicine Information Pharmacist Consultation Group: See Page 5 Approver: Medicine Guidelines and Policies
NHS Grampian Staff Guideline For The Management Of Acute Hypophosphataemia In Adults Co-ordinators: Medicine Information Pharmacist Consultation Group: See Page 5 Approver: Medicine Guidelines and Policies
Unit 11. Objectives. Indications for IV Therapy. Intravenous Access Devices & Common IV Fluids. 3 categories. Maintenance Replacement Restoration
 Unit 11 Fluids, Electrolytes and Acid Base Imbalances Intravenous Access Devices & Common IV Fluids Objectives Review the purpose and types of intravenous (IV) therapy. Recall the nursing care related
Unit 11 Fluids, Electrolytes and Acid Base Imbalances Intravenous Access Devices & Common IV Fluids Objectives Review the purpose and types of intravenous (IV) therapy. Recall the nursing care related
IDPN. A Piece of the Puzzle for Dialysis Patients Nutrition. Toll Free: Toll Free:
 IDPN A Piece of the Puzzle for Dialysis Patients Nutrition Toll Free: 844-633-3448 Toll Free: 844-633-3448 Executive Infusion is pleased to announce our nutritional services which include Intradialytic
IDPN A Piece of the Puzzle for Dialysis Patients Nutrition Toll Free: 844-633-3448 Toll Free: 844-633-3448 Executive Infusion is pleased to announce our nutritional services which include Intradialytic
Penile Straightening Nesbit tuck, Lue vein patch or synthetic graft operation): procedure-specific information
 PATIENT INFORMATION Penile Straightening Nesbit tuck, Lue vein patch or synthetic graft operation): procedure-specific information This information is intended to supplement any advice you may already
PATIENT INFORMATION Penile Straightening Nesbit tuck, Lue vein patch or synthetic graft operation): procedure-specific information This information is intended to supplement any advice you may already
Prescribing Guidelines for Oral Nutritional Supplements (ONS) for adults
 Worcestershire Area Prescribing Committee Prescribing Guidelines for Oral Nutritional Supplements (ONS) for adults September 2017 Review Date September 2020 Version 3.0 1 Version Control: Version Type
Worcestershire Area Prescribing Committee Prescribing Guidelines for Oral Nutritional Supplements (ONS) for adults September 2017 Review Date September 2020 Version 3.0 1 Version Control: Version Type
North Derbyshire OPAT (Outpatient Parenteral Antimicrobial Therapy) Pathway for Primary Care (Step-Up Pathway/Admission Avoidance)
 North Derbyshire OPAT (Outpatient Parenteral Antimicrobial Therapy) Pathway for Primary Care (Step-Up Pathway/Admission Avoidance) Introduction OPAT services provide intravenous (IV) antibiotics to patients
North Derbyshire OPAT (Outpatient Parenteral Antimicrobial Therapy) Pathway for Primary Care (Step-Up Pathway/Admission Avoidance) Introduction OPAT services provide intravenous (IV) antibiotics to patients
Formulary and Prescribing Guidelines
 Formulary and Prescribing Guidelines SECTION 15: TREATMENT OF EATING DISORDERS 15.1 Introduction Please review the Trust document Guidelines for the assessment and treatment of eating disorders in the
Formulary and Prescribing Guidelines SECTION 15: TREATMENT OF EATING DISORDERS 15.1 Introduction Please review the Trust document Guidelines for the assessment and treatment of eating disorders in the
Integrated Care Pathway (ICP) for the. Management of clozapine INPATIENT INITIATION
 Document Reference MM 048 Integrated Care Pathway (ICP) for the Management of clozapine INPATIENT INITIATION Surname Title Address Forenames Date of Birth RT/NHS number Care Co-ordinator GP CS number Consultant
Document Reference MM 048 Integrated Care Pathway (ICP) for the Management of clozapine INPATIENT INITIATION Surname Title Address Forenames Date of Birth RT/NHS number Care Co-ordinator GP CS number Consultant
The Newcastle upon Tyne Hospitals NHS Foundation Trust. Essential Out-of Hours Cancer Chemotherapy
 The Newcastle upon Tyne Hospitals NHS Foundation Trust Essential Out-of Hours Cancer Chemotherapy Version No.: 4.0 Effective From: 27 December 2017 Expiry Date: 27 December 2020 Date Ratified: 19 July
The Newcastle upon Tyne Hospitals NHS Foundation Trust Essential Out-of Hours Cancer Chemotherapy Version No.: 4.0 Effective From: 27 December 2017 Expiry Date: 27 December 2020 Date Ratified: 19 July
Trust Policy 218 Ionising Radiation Safety Policy
 Trust Policy 218 Ionising Radiation Safety Policy Purpose Date Version August 2016 7 To ensure that Plymouth Hospitals NHS Trust complies with all relevant legislation with regard to the use of ionising
Trust Policy 218 Ionising Radiation Safety Policy Purpose Date Version August 2016 7 To ensure that Plymouth Hospitals NHS Trust complies with all relevant legislation with regard to the use of ionising
