Inter-examiner reproducibility of clinical tests and criteria used to identify subacromial impingement syndrome
|
|
|
- Laureen Washington
- 5 years ago
- Views:
Transcription
1 Open Access To cite: Vind M, Bogh SB, Larsen CM, et al. Inter-examiner reproducibility of clinical tests and criteria used to identify subacromial impingement syndrome. BMJ Open 2011;1:e doi: /bmjopen < Prepublication history for this paper is available online. To view these files please visit the journal online ( bmjopen.bmj.com). Received 22 December 2010 Accepted 4 April 2011 This final article is available for use under the terms of the Creative Commons Attribution Non-Commercial 2.0 Licence; see 1 Department of Physiotherapy, University College Lillebaelt, Odense, Denmark 2 Research Unit for Musculoskeletal Function and Physiotherapy, Institute of Sports Science and Clinical Biomechanics, University of Southern Denmark, Odense, Denmark Correspondence to Mikkel Vind; vindbie@live.dk Inter-examiner reproducibility of clinical tests and criteria used to identify subacromial impingement syndrome Mikkel Vind, 1 Søren Bie Bogh, 1 Camilla Marie Larsen, 2 Hans Kromann Knudsen, 1 Karen Søgaard, 2 Birgit Juul-Kristensen 2 ABSTRACT Introduction: A specific algorithm has been proposed for classifying impingement related shoulder pain in athletes with overhead activity. Data on the interexaminer reproducibility of the suggested clinical tests and criteria and their mutual dependencies for identifying subacromial impingement symptoms (SIS) are not available. Objective: To test the inter-examiner reproducibility of selected tests and criteria suggested for classifying SIS and the mutual dependencies of each of the individual tests and SIS. Method: A standardised three-phase protocol for clinical reproducibility studies was followed, consisting of a training, an overall agreement and a study phase. To proceed to the study phase, an overall agreement of 0.80 was required. In total 10, 20 and 44 subjects were included in the three phases, respectively. The case prevalence in the study phase was 50%. The inclusion criterion for cases was $3, and for controls #1 positive test out of four. Cohen s k statistics were used for calculating agreement. Results: In the overall agreement phase, an agreement of 0.90 was obtained, while in the study phase it was 0.98 with a k of 0.95 for SIS. k Values for the individual tests varied between 0.60 and Mutual dependencies between each test and SIS showed Neer s test with anterior pain to be most often used to determine SIS. Conclusions: Inter-examiner reproducibility was moderate to almost perfect for the selected tests and criteria for SIS. The next challenge will be to establish reproducibility in clinical practice, as well as the validity of the tests and criteria for SIS. INTRODUCTION Fifty per cent of the general population experience shoulder pain every year. 1 Subacromial impingement syndrome (SIS) is the most common shoulder disorder in the population, representing 44e65% of all registered shoulder complaints in the clinical setting. 2 Its prevalence is especially high in sports with overhead activity, such as swimming, volleyball, handball and badminton. These overhead athletes have a high demand for optimal ARTICLE SUMMARY Research Article focus - This study examines the inter-tester reproducibility of Hawkins, Neer s, Jobe s and Apprehension tests, included in a recent clinical reasoning algorithm, both as individual tests and as performed as a battery of tests for screening for subacromial impingement symptoms (SIS) in overhead athletes. - Furthermore, the mutual dependency of each individual test and SIS was determined. Key messages - Overall, the reproducibility was almost perfect for tests and criteria for SIS when following a standardised test protocol for reliability and validity studies. - Mutual dependency was highest for Neer s test with anterior pain and SIS, implying that this was the test most often used to determine SIS. Strengths and limitations of this study - The strength of the study is the strict adherence to a standardised study protocol for reproducibility and validity studies, with a training and an overall agreement phase, including the requirement of a 0.50 prevalence of SIS, before performing the study phase. Since the study population consisted of overhead athletes, for whom the algorithm is intended, data can be generalised to the target population. - The limitation of the study is that the current mutual dependencies may have been deceptively high because of a possible bias due to the inclusion criteria used in this algorithm, since subjects with two out of four positive test responses are not included. However, this limitation has not biased the high reproducibility of the tests and criteria for SIS. shoulder performance and dynamic stability is required in order to prevent injury. 3e7 Until now, historical information and clinical signs have been included in the clinical examination as the most common tools for diagnosing shoulder impingement, even though radiological examinations have Vind M, Bogh SB, Larsen CM, et al. BMJ Open 2011;1:e doi: /bmjopen
2 improved the accuracy of the diagnosis. 8 MRI has recently been recommended as the best method to identify shoulder lesions, while ultrasonography is also recognised as highly accurate in detecting SIS. 910 However, neither method is able to identify subtle instability and scapula dyskinesis, while MRI findings may be unable to differentiate between symptomatic and asymptomatic shoulders or to provide a structural diagnosis. 1 Structural changes can be present without pain, thus giving a high number of false positive and negative results. 1 In the clinical setting, manual diagnostic tests are fast and easy to perform compared with imaging techniques, which are both time-consuming and expensive. A recent systematic review concluded that several clinical shoulder tests have sufficient sensitivity, but inadequate specificity. 11 Neer s and Hawkins impingement tests, in particular, have been found useful in confirming SIS, but poor at ruling out pathology. 9 12e14 Furthermore, Jobe s test and passive abduction had a relatively high sensitivity of 74% compared with MRI, and were described as good diagnostic tools. 9 A systematic review found Neer s and Hawkins tests to have a sensitivity and specificity of 79% and 53%, and 79% and 59%, respectively, and states that no shoulder test can by itself confirm impingement. 11 It is further suggested that more large, prospective, welldesigned studies should be carried out. 11 A recent prospective study of patients admitted for surgery found Neer s test, the Painful Arc test and the External Rotation Resistance test to be excellent screening tools to rule out SIS. 15 Furthermore, Painful Arc, the External Rotation Resistance test in the neutral position and Jobe s test had the highest diagnostic accuracy compared with surgical findings, and were best at confirming/ruling in SIS. Inter-examiner reliability showed k values ranging from 0.39 to 0.67, but the protocol lacked an overall agreement phase, and this may have influenced k values negatively. 15 A stronger design is therefore needed to establish more accurate k values for inter-examiner reliability. Figure 1 Algorithm for clinical reasoning in the examination of impingement related shoulder pain (from Cools et al 16 ). IR, internal rotation; GIRD, glenohumeral internal rotation deficit; ROM, range of motion; SLAP, superior labrum from anterior to posterior tear; SAT, scapular assistance test; SRT, scapular retraction test. Recently, a clinical reasoning algorithm based on clinical tests has been developed as a screening tool for the detection of different shoulder pathologies in overhead athletes (figure 1). 16 The type of impingement is decided upon, and then the underlying pathologies are examined by a battery of commonly accepted shoulder tests. For classification of SIS and internal posteriosuperior glenoid impingement, a group of four tests is performed (Jobe s test, Neer s test, Hawkins test and the Apprehension test). The use of a group of tests as a diagnostic tool is supported by the results in a recent study, where three or more positive tests out of five confirmed SIS, and less than three positive tests out of five ruled out SIS. 15 However, the algorithm has not been tested for reliability or validity, and there are no guidelines regarding how many positive test responses are required in order to differentiate between SIS and internal posteriosuperior glenoid impingement. In order to validate this algorithm, it is necessary to establish the reproducibility. Therefore, the aim of this study was to determine the inter-examiner reproducibility of selected tests and criteria for classifying SIS based on the algorithm, and second, to test the mutual dependency of the individual tests and SIS. METHODS Study design The study was carried out using the protocol for diagnostic procedures in reproducibility studies presented by the International Federation of Manual/Musculoskeletal Medicine (FIMM). 17 The protocol for a reproducibility study is a three-phase study consisting of a training phase, an overall agreement phase (>80%) and an actual study phase with a case prevalence of 50%. Two examiners (examiners A and B), with a maximum of 6 months clinical experience, blinded to their mutual test results, performed all tests. The subjects were 2 Vind M, Bogh SB, Larsen CM, et al. BMJ Open 2011;1:e doi: /bmjopen
3 instructed not to give information about results from previous tests. In the training phase, the test manual was refined on the basis of feedback, and the performance and interpretation of the tests were evaluated in order to remove potential errors. The four tests (Jobe, Neer, Hawkins and Apprehension) were used as a battery of tests to detect SIS. In the overall agreement phase, examiner A tested one sample first (11 players) and examiner B tested another sample first (nine players), and then the examiners switched samples and agreements were calculated. In the study phase, the 0.50 prevalence method was applied in order to obtain an accurate k coefficient. In this phase, one examiner selected and tested a minimum of 20 subjects (10 cases and 10 controls) and sent them to the other examiner, and vice versa. The criterion for inclusion of subjects in the study phase was therefore either SIS ($3 positive tests) for cases or no-sis (#1 positive tests out of four) for controls. A prevalence of 50% was obtained through this method (figure 2). This method is recommended when one diagnostic test is performed, and therefore all four tests were reduced to one diagnostic criterion classification, either SIS or no-sis. Figure 2 Flow diagram of the 0.50 prevalence method (study phase). Examiners A and B perform the battery of tests on their own groups of subjects. Both examiners sent the same number of positive and negative tests to each other (minimum of 10 positive and 10 negative). Materials According to the study protocol, the training phase was carried out on 10 subjects (three male and seven female physiotherapy students with a mean6sd age of years), and the overall agreement phase was carried out on 20 subjects (active male handball players with a mean6sd age of years) with the dominant shoulder being tested, comprising 15 right and five left shoulders. In total, 30 males and 14 females with a mean6sd age of years, comprising 35 right and nine left shoulders, respectively (n¼44), met the criteria for inclusion in the study phase. To include these 44 subjects, 134 shoulders of active overhead athletes were tested (figure 3). The study was approved by the Ethics Committee in Science of the Region of Southern Denmark. Clinical tests The tests were performed according to the recommendations of Cools et al 16 (table 1). Jobe s test/empty can test Jobe s test/empty can test was performed with the subject standing, and the arm to be examined in 908 elevation in the scapular plane in maximal internal rotation. The angle of the scapular plane was set to 408 as mentioned elsewhere in the literature This angle was marked on the floor to guide subject movement. Manual resistance prevented further elevation of the arm. The test was positive if the subject experienced pain. 16 Jobe s test, as a single test for impingement, has been found to have almost perfect levels of agreement. 12 Neer s test Neer s test was performed with the subject sitting on a chair. The examiner performed a maximal forward flexion of the subject s arm, while elevation of the scapula was prevented. The test was positive when pain was located in the anterior aspect of the shoulder (Neer ant ). Pain to the posterior aspect was also recorded. Combined with reports of anterior pain, these reports were called Neer general (Neer gen ). Hawkins test Hawkins test was performed with the subject sitting on the examination table with feet on the ground. The arm was held in 908 forward flexion, elbow flexed to 908. Passive internal rotation of the shoulder was performed. The test was positive if pain was reported. Hawkins test Figure 3 phase. Flow diagram of the subjects included in the study Vind M, Bogh SB, Larsen CM, et al. BMJ Open 2011;1:e doi: /bmjopen
4 Table 1 Introduction Preparation Jobe s Neer s Hawkins Performance of the clinical tests for SIS (from Cools et al 16 ), described as if performed on the right shoulder 1. I am going to perform four shoulder tests on you. 2. For each different test I will ask if you experience any pain, and you must answer either yes or no. 3. Sometimes I will ask if the pain is in the front or the back of your shoulder, and you use your judgement. Pain down to the insertion of the deltoid muscle is accepted as a positive response (show!). For Jobe s test a line is marked on the floor, on which the subject is asked to stand. On this line an angle of 408 is marked, which is used to point out the plane of the scapula. Description Placing of hands, etc Evaluation Subject is standing. The right shoulder is elevated 908 in the plane of the scapula and maximally internally rotated (empty can position). The examiner resists further elevation of the arm (isometric hold). Subject is sitting. The scapula is fixated/stabilised in a depressed position, while the shoulder is maximally forwardly flexed. Subject is sitting on the examination table. The shoulder is placed in 908 of forward flexion and passively internally rotated as far as possible (elbow flexed 908). The left hand of the examiner is placed on the arm of the subject proximally to the wrist and downward pressure is applied. The left hand of the examiner is placed over the scapula. The right hand grasps distally to the elbow, and subsequently passively flexes the right shoulder of the subject. The examiner stands in front of the subject. The right arm of the subject is placed in 908 of flexion. The left hand of the examiner is placed on the left shoulder of the subject, and serves to support the right arm of the subject. The examiner grasps the right arm of the subject proximally to the wrist and performs internal rotation of the right shoulder of the subject as far as possible. Does this hurt your shoulder? Yes/no Does this hurt your shoulder? Yes/no Does it hurt in the front of the shoulder or in the back? Does this hurt your shoulder? Yes/no Continued 4 Vind M, Bogh SB, Larsen CM, et al. BMJ Open 2011;1:e doi: /bmjopen
5 Table 1 Continued Apprehension Results are noted on the score sheet by the examiner. SIS, subacromial impingement syndrome. was found to have almost perfect levels of agreement, 12 and the test has been recommended for use in screening for impingement. 11 The Apprehension test The Apprehension test was carried out with the subject lying supine on the examination table. The shoulder (908 abduction, the elbow in 908 flexion) was passively placed in maximal external rotation. The test was considered positive if the subject reported pain from the anterior aspect of the shoulder. 16 Statistics For the dichotomous data, Cohen s k statistics were used to calculate levels of agreement between the two examiners (inter-examiner reproducibility) with 95% CIs, and the relationship between the individual tests and the classification of SIS (mutual dependency). Furthermore, values for observed agreement, prevalence and expected agreement were calculated. Data were analysed in Microsoft Office Excel 2007, using 232 contingency tables. The k values were interpreted at five levels according to Landis and Koch. 20 RESULTS The groups of cases and controls were comparable on age with mean (6SD) ages of years and Description Placing of hands, etc Evaluation Subject is supine on the examination table. The subject is asked to move to the edge of the table. The shoulder is placed in 908 of horizontal abduction and is externally rotated to the end of range. The examiner grasps the lower arm and performs a passive external rotation. The right hand of the examiner grasps the humerus for support. Does this hurt your shoulder? Yes/no Does it hurt in the front of the shoulder or in the back? years, respectively. The overall agreement phase was completed with an observed agreement of 90% (table 2), meaning that the criterion of a minimum of agreement of 80% was met. In the study phase, an almost perfect k value of 0.95 was calculated for SIS (table 3), while k values for the specific tests varied between 0.60 and k for Neer s test was calculated as 0.86 for anterior pain (Neer ant ) and as 0.95 for pain in general (Neer gen ). The k values for mutual dependency indicate that Neer s test with anterior pain (Neer ant ) was the most frequently used test for classifying SIS, with Jobe s test being the least frequently used (table 4). The highest k values were obtained on the Neer ant with k values for examiner A and B of 0.82 and 0.91, respectively, followed by Apprehension ant with k¼0.77 and k¼0.73, Hawkins with k¼0.73 and k¼0.68 and Jobe s with k¼0.64 and k¼0.60. DISCUSSION The results from this study showed an almost perfect k value for SIS (k¼0.95) and for the individual tests (k values between 0.60 and 0.90). Calculations of mutual dependencies found the highest k values for the Neer ant test followed by the Apprehension ant test, Hawkins test and Jobe s test. Our study included an overall agreement phase and a 50% case prevalence, which may explain the Table 2 Agreement regarding number (%) of positive and negative tests in the overall agreement and study phases for SIS, with calculations of observed agreement and k values SIS Total agreement in positive tests (n, %) Total agreement in negative tests (n, %) Total agreement (n, %) Overall agreement phase (n¼20) 6 (30%) 12 (60%) 18/20 (90%) e Study phase (n¼44) 22 (50%) 21 (48%) 43/44 (98%) 0.95 SIS, subacromial impingement syndrome. k Value Vind M, Bogh SB, Larsen CM, et al. BMJ Open 2011;1:e doi: /bmjopen
6 Table 3 k Statistics and 95% CIs for SIS and each of the specific tests in the study phase k Value (95% CI) higher strength/validity of the present k values compared to those found in earlier studies examining the reproducibility of clinical shoulder tests. Without including an overall agreement phase, the risk of a systematic bias cannot be excluded. Only one study has examined the reproducibility of several tests as a group. Michener et al found that three positive tests out of five were most likely to confirm SIS. 15 The conflicting results in the three studies mentioned above, however, together with the almost perfect levels of agreement in the current study, indicate a need for methodologically stronger study designs in order to minimise errors due to systematic bias. Implementation of a training phase, an overall agreement phase ($80%) and a study phase including the 0.50 prevalence method in future studies is therefore recommended. In the current study, Jobe s test produced the highest k value (k¼0.90) of all the individual tests (table 3), even though the prevalence of 0.34 weakens the credibility of the k value compared to a prevalence of For Neer s test for anterior pain (Neer ant ) and Neer s test for pain in general (Neer gen ), where pain is located either anteriorly and/or posteriorly in the shoulder, the k values were 0.86 and 0.95, respectively, with a prevalence close to 0.50 (table 3). These results show that a high level of agreement was still obtained even when differentiating between anterior and posterior pain. Prevalence of the index condition Observed agreement SIS 0.95 (0.87 to 1.00) Test Jobe s 0.90 (0.76 to 1.00) Neer s (ant pain) 0.86 (0.71 to 1.00) Neer s (general pain) 0.95 (0.86 to 1.00) Hawkins 0.60 (0.34 to 0.85) Apprehension (ant pain) 0.71 (0.59 to 0.98) ant, anterior; SIS, subacromial impingement syndrome. Table 4 Test k Statistics for mutual dependency of the individual tests and the diagnosis of SIS k Value Prevalence of the index condition Expected agreement by chance Dromerick et al examined Neer s test and presented a substantial k value of Johansson et al 12 examined, among others, Jobe s test, Neer s test and Hawkins test. High k values were obtained for all three tests (Jobe s k¼0.94, Neer s test k¼1.0, Hawkins test k¼0.91), but only Jobe s test was performed with a prevalence close to Michener et al also examined Jobe s, Neer s and Hawkins tests for reproducibility and found k values ranging from 0.39 to 0.47, with a prevalence of SIS of 0.29, 15 which may explain the relatively low k. The Apprehension test obtained a k value of 0.71, with a prevalence of 0.39 making the result slightly weaker compared with a prevalence of The Apprehension test was carried out in accordance with the classical protocol described by Cools et al (908 abduction and maximal external rotation). 16 However, disagreement was found, since Cools et al 16 refer to Meister et al 22 where the test is described and performed differently (with the shoulder abducted 90e1108 and in slight extension). Meister et al conclude that posterior pain is a sign of posterio-superior glenoid impingement. 22 However, there are no references in the literature suggesting that the Apprehension test with anterior pain can be used for the detection of SIS. The validity of this modified test, therefore, needs to be verified, that is, the use of a modification of this test, originally designed for internal posterio-superior glenoid impingement, for the Observed agreement Jobe s Examiner A Examiner B Neer s (anterior pain) Examiner A Examiner B Hawkins Examiner A Examiner B Apprehension (anterior pain) Examiner A Examiner B SIS, subacromial impingement syndrome. Expected agreement by chance 6 Vind M, Bogh SB, Larsen CM, et al. BMJ Open 2011;1:e doi: /bmjopen
7 detection of SIS, which is regarded as an external anterio-superior glenoid impingement syndrome. According to our results, there is clear coherence between a positive Apprehension ant test and SIS, shown by the substantial k values for mutual dependency (k¼0.77 for examiner A, k¼0.73 for examiner B). The high k values could be attributed to an actual relationship between anterior pain/instability and impingement symptoms, as argued by Meister et al. 22 This k value should therefore be considered with some caution, since this was not a study on the validity of the tests. Whether there is a clear relationship between pain from the anterior aspect of the shoulder in the Apprehension test and SIS, can only be verified by imaging techniques. Also Neer ant and Hawkins tests had a relatively high mutual dependency, showing these tests to be closely related to SIS, in contrast to Jobe s test. However, we have no further explanation for this difference in mutual dependency between tests. The current mutual dependencies could have been influenced by our inclusion criteria, since subjects with two out of four positive test responses were excluded, meaning that our results for mutual dependency are deceptively high. However, the Neer ant and the Apprehension tests have the highest values of mutual dependency, which indicates that these two tests should carry more weight than Jobe s test and Hawkins s test. No prior studies were found that addressed the mutual dependencies of these tests. The limitation of the study is that the current mutual dependencies may have been deceptively high because of a possible bias due to the inclusion criteria used in this algorithm, since subjects with two out of four positive test responses are not included. However, this limitation has not biased the high reproducibility of the tests and criteria for SIS. Another limitation is the unknown reproducibility of the current tests carried out by untrained clinicians, which of course might be different from the reproducibility of trained examiners. This means that reproducibility also needs to be tested in a normal clinical environment. In case inexperienced examiners have a low inter-examiner test reproducibility, our study has shown that it should be possible through education and training to obtain high enough skills to perform the tests in a reproducible way. Reproducibility is only the first step on the path to establishing the diagnostic value of these tests. Therefore, the validity (ie, concurrent, discriminative, predictive, prescriptive) and the diagnostic accuracy (ie, sensitivity and specificity) of this clinical reasoning algorithm must be determined. With respect to internal impingement, exactly the same procedures (tests for reliability and validity) need to be performed. The strength of the study lies in its design, which followed a standardised protocol, originally presented by FIMM. 17 The two examiners undertook a training phase in order to minimise the risk of bias in the performance of the tests, and an overall agreement of 90% was achieved before carrying out the study phase. The study phase was performed using the 0.50 prevalence method, which strengthens the k values. Finally, the study was carried out in overhead athletes, for whom the algorithm is intended, making the results relevant for screening purposes within this group. CONCLUSIONS The current study on overhead athletes showed almost perfect inter-examiner reproducibility of the tests and criteria for SIS, based on a clinical reasoning algorithm. Also each of the selected tests (Jobe s, Neer s, Hawkins and Apprehension) presented high levels of agreement and reproducibility. Based on the mutual dependency of each of the individual tests and SIS, Neer s test with anterior pain (Neer ant ) had the highest level of agreement, and is therefore important in the classification of SIS. Although showing excellent levels of agreement, it is recommended that further research be carried out in order to establish reproducibility in clinical practice, and also the validity of this clinical algorithm. Acknowledgements The authors wish to thank the National Research Fund for Health and Disease, the Research Fund for the Region of Southern Denmark, the Arthritis Research Association, and the Danish Physiotherapy Research Foundation for supporting this project. Category: Clinical study. Funding The National Research Fund for Health and Disease, the Research Fund for the Region of Southern Denmark, the Arthritis Research Association, and the Danish Physiotherapy Research Foundation. Competing interests None. Patient consent Obtained. Ethics approval The study was approved by the Ethics Committee in Science of the Region of Southern Denmark. Contributors MV contributed to the conception, design of the study and writing of the article, the description of the tests and practical performance of the study, conducted the statistical analysis, and drafted and approved the final manuscript. SBB contributed to the conception, design of the study and writing of the article, the description of the test manual and practical performance of the study, conducted the statistical analysis, and drafted and approved the final manuscript. CML contributed to the description of the test manual and revised and approved the final manuscript. HKK contributed to the conception and design of the study, contributed to the description of the test manual, and revised and approved the final manuscript. KS contributed to the conception and design of the study, and revised and approved the final manuscript. BJK contributed to the conception, design of the study and writing of the article, and the description of the test manual, and revised and approved the final manuscript. All the authors will act as guarantors for the paper. Provenance and peer review Not commissioned; externally peer reviewed. Data sharing statement Data in 232 contingency tables, and the dataset are available from the corresponding author at vindbie@live.dk. Participants gave informed consent for data sharing. REFERENCES 1. Lewis JS. Rotator cuff tendinopathy/subacromial impingement syndrome: is it time for a new method of assessment? Br J Sports Med 2009;43:259e Michener LA, McClure PW, Karduna AR. Anatomical and biomechanical mechanisms of subacromial impingement syndrome. Clin Biomech (Bristol, Avon) 2003;18:369e Belling Sorensen AK, Jorgensen U. Secondary impingement in the shoulder. An improved terminology in impingement. Scand J Med Sci Sports 2000;10:266e78. Vind M, Bogh SB, Larsen CM, et al. BMJ Open 2011;1:e doi: /bmjopen
8 4. Cools AM, Witvrouw EE, Declercq GA, et al. Scapular muscle recruitment patterns: trapezius muscle latency with and without impingement symptoms. Am J Sports Med 2003;31:542e9. 5. Bak K, Fauno P. Clinical findings in competitive swimmers with shoulder pain. Am J Sports Med 1997;25:254e Pink MM, Tibone JE. The painful shoulder in the swimming athlete. Orthop Clin North Am 2000;31:247e Fu FH, Harner CD, Klein AH. Shoulder impingement syndrome. A critical review. Clin Orthop Relat Res 1991;269:162e Ardic F, Kahraman Y, Kacar M, et al. Shoulder impingement syndrome: relationships between clinical, functional, and radiologic findings. Am J Phys Med Rehabil 2006;85:53e Silva L, Andreu JL, Munoz P, et al. Accuracy of physical examination in subacromial impingement syndrome. Rheumatology (Oxford) 2008;47:679e Fodor D, Poanta L, Felea I, et al. Shoulder impingement syndrome: correlations between clinical tests and ultrasonographic findings. Ortop Traumatol Rehabil 2009;11:120e Hegedus EJ, Goode A, Campbell S, et al. Physical examination tests of the shoulder: a systematic review with meta-analysis of individual tests. Br J Sports Med 2008;42:80e92. discussion Johansson K, Ivarson S. Intra- and interexaminer reliability of four manual shoulder maneuvers used to identify subacromial pain. Man Ther 2009;14:231e Calis M, Akgun K, Birtane M, et al. Diagnostic values of clinical diagnostic tests in subacromial impingement syndrome. Ann Rheum Dis 2000;59:44e Tennent TD, Beach WR, Meyers JF. A review of the special tests associated with shoulder examination. Part I: the rotator cuff tests. Am J Sports Med 2003;31:154e Michener LA, Walsworth MK, Doukas WC, et al. Reliability and diagnostic accuracy of 5 physical examination tests and combination of tests for subacromial impingement. Arch Phys Med Rehabil 2009;90:1898e Cools AM, Cambier D, Witvrouw EE. Screening the athlete s shoulder for impingement symptoms: a clinical reasoning algorithm for early detection of shoulder pathology. Br J Sports Med 2008;42:628e Patijn J, Remvig L. Reproducibility And Validity 2007-Protocol Formats For Diagnostics Procedures In Manual/Musculoskeletal Medicine Dayanidhi S, Orlin M, Kozin S, et al. Scapular kinematics during humeral elevation in adults and children. Clin Biomech (Bristol, Avon) 2005;20:600e McFarland EG, Kim TK. Examination Of The Shoulder: The Complete Edition. United States of America, New York: Thieme Medical Publishers, Landis JR, Koch GG. The measurement of observer agreement for categorical data. Biom 1977;33:159e Dromerick AW, Kumar A, Volshteyn O, et al. Hemiplegic shoulder pain syndrome: interrater reliability of physical diagnosis signs. Arch Phys Med Rehabil 2006;87:294e Meister K, Buckley B, Batts J. The posterior impingement sign: diagnosis of rotator cuff and posterior labral tears secondary to internal impingement in overhand athletes. Am J Orthop 2004;33:412e15. PAGE fraction trail=7.5 BMJ Open: first published as /bmjopen on 18 May Downloaded from on 17 February 2019 by guest. Protected by copyright. 8 Vind M, Bogh SB, Larsen CM, et al. BMJ Open 2011;1:e doi: /bmjopen
BMJ Open INTER-EXAMINER REPRODUCIBILITY OF CLINICAL TESTS AND CRITERIA TO IDENTIFY SUBACROMIAL IMPINGEMENT SYNDROME
 INTER-EXAMINER REPRODUCIBILITY OF CLINICAL TESTS AND CRITERIA TO IDENTIFY SUBACROMIAL IMPINGEMENT SYNDROME Journal: BMJ Open Manuscript ID: BMJ Open-0-0000 Article Type: Research Date Submitted by the
INTER-EXAMINER REPRODUCIBILITY OF CLINICAL TESTS AND CRITERIA TO IDENTIFY SUBACROMIAL IMPINGEMENT SYNDROME Journal: BMJ Open Manuscript ID: BMJ Open-0-0000 Article Type: Research Date Submitted by the
DIFFERENTIAL DIAGNOSIS: Looking for the causes of impingement
 DIFFERENTIAL DIAGNOSIS: Looking for the causes of Ann Cools, PT, PhD Ghent University - Belgium Dept of Rehabilitation Sciences & Physiotherapy Ann.Cools@UGent.be «thinking about.» Which special tests
DIFFERENTIAL DIAGNOSIS: Looking for the causes of Ann Cools, PT, PhD Ghent University - Belgium Dept of Rehabilitation Sciences & Physiotherapy Ann.Cools@UGent.be «thinking about.» Which special tests
IMPINGEMENT-TESTSTESTS
 «thinking about.» DIFFERENTIAL DIAGNOSIS: Looking for the causes of Which special tests do you use in your shoulder examination? Ann Cools, PT, PhD Ghent University - Belgium Dept of Rehabilitation Sciences
«thinking about.» DIFFERENTIAL DIAGNOSIS: Looking for the causes of Which special tests do you use in your shoulder examination? Ann Cools, PT, PhD Ghent University - Belgium Dept of Rehabilitation Sciences
The Effectiveness of Shoulder Stretching and Joint Mobilizations on Posterior Shoulder Tightness
 Journal of Sport Rehabilitation, 2013, 22, 313-319 2013 Human Kinetics, Inc. www.jsr-journal.com CRITICALLY APPRAISED TOPIC The Effectiveness of Shoulder Stretching and Joint Mobilizations on Posterior
Journal of Sport Rehabilitation, 2013, 22, 313-319 2013 Human Kinetics, Inc. www.jsr-journal.com CRITICALLY APPRAISED TOPIC The Effectiveness of Shoulder Stretching and Joint Mobilizations on Posterior
Physical Examination of the Shoulder
 General setup Patient will be examined in both the seated and supine position so exam table needed 360 degree access to patient Expose neck and both shoulders (for comparison); female in gown or sports
General setup Patient will be examined in both the seated and supine position so exam table needed 360 degree access to patient Expose neck and both shoulders (for comparison); female in gown or sports
Shoulder Joint Examination. Shoulder Joint Examination. Inspection. Inspection Palpation Movement. Look Feel Move
 Shoulder Joint Examination History Cuff Examination Instability Examination AC Joint Examination Biceps Tendon Examination Superior Labrum Examination Shoulder Joint Examination Inspection Palpation Movement
Shoulder Joint Examination History Cuff Examination Instability Examination AC Joint Examination Biceps Tendon Examination Superior Labrum Examination Shoulder Joint Examination Inspection Palpation Movement
Evidence- Based Examination of the Shoulder Presented by Eric Hegedus, PT, DPT, MHSC, OCS, CSCS Practice Sessions/Skill Check- offs
 Evidence- Based Examination of the Shoulder Practice Session & Skills Check- offs Evidence- Based Examination of the Shoulder Presented by Eric Hegedus, PT, DPT, MHSC, OCS, CSCS Practice Sessions/Skill
Evidence- Based Examination of the Shoulder Practice Session & Skills Check- offs Evidence- Based Examination of the Shoulder Presented by Eric Hegedus, PT, DPT, MHSC, OCS, CSCS Practice Sessions/Skill
Labral Tears. Fig 1: Intact labrum and biceps tendon
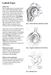 Labral Tears What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone that is
Labral Tears What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone that is
Review shoulder anatomy Review the physical exam of the shoulder Discuss some common causes of acute shoulder pain Discuss some common causes of
 Review shoulder anatomy Review the physical exam of the shoulder Discuss some common causes of acute shoulder pain Discuss some common causes of chronic shoulder pain Review with some case questions Bones:
Review shoulder anatomy Review the physical exam of the shoulder Discuss some common causes of acute shoulder pain Discuss some common causes of chronic shoulder pain Review with some case questions Bones:
Breakout Session #7: Manual therapy for shoulder pain and limited mobility
 Northwestern University Feinberg School of Medicine Breakout Session #7: Manual therapy for shoulder pain and limited mobility @Amee_S Objectives 1. Demonstrate the examination procedures and describe
Northwestern University Feinberg School of Medicine Breakout Session #7: Manual therapy for shoulder pain and limited mobility @Amee_S Objectives 1. Demonstrate the examination procedures and describe
TIPS FOR SUCCESSFUL SHOULDER TREATMENT. In Service Training 16 th May 2014
 TIPS FOR SUCCESSFUL SHOULDER TREATMENT In Service Training 16 th May 2014 Training day aims to address: Controversies of impingement syndrome diagnosis Controversies of MRI/USS imaging Clinical diagnosis
TIPS FOR SUCCESSFUL SHOULDER TREATMENT In Service Training 16 th May 2014 Training day aims to address: Controversies of impingement syndrome diagnosis Controversies of MRI/USS imaging Clinical diagnosis
Describe methods to evaluate for scapular. Perform a scapular dyskinesis examination. With humeral elevation, the scapula:
 Describe methods to evaluate for scapular dyskinesis Perform a scapular dyskinesis examination Lori Michener, PhD, PT, ATC Virginia Commonwealth University Richmond, VA Ant / Post Tilting Internal / External
Describe methods to evaluate for scapular dyskinesis Perform a scapular dyskinesis examination Lori Michener, PhD, PT, ATC Virginia Commonwealth University Richmond, VA Ant / Post Tilting Internal / External
Musculoskeletal dysfunctions associated with swimmer s shoulder
 Musculoskeletal dysfunctions associated with swimmer s shoulder SURPRISING? Control Strength Endurance Mobility Elite swimmers: 14km/day 2500 shoulder revolution/day 16 000 shoulder revolutions/week Shoulder
Musculoskeletal dysfunctions associated with swimmer s shoulder SURPRISING? Control Strength Endurance Mobility Elite swimmers: 14km/day 2500 shoulder revolution/day 16 000 shoulder revolutions/week Shoulder
Journal of Sport Rehabilitation. The reliability of strength tests performed in elevated shoulder positions using a hand-held dynamometer
 The reliability of strength tests performed in elevated shoulder positions using a hand-held dynamometer Journal: Manuscript ID: JSR.2015-0034.R2 Manuscript Type: Technical Report Keywords: dynamometry,
The reliability of strength tests performed in elevated shoulder positions using a hand-held dynamometer Journal: Manuscript ID: JSR.2015-0034.R2 Manuscript Type: Technical Report Keywords: dynamometry,
Subacromial Impingement (diagnostic methods )
 Subacromial Impingement (diagnostic methods ) M.N. Naderi Fellowship in shoulder and arthroscopic surgery Neer : Definition Impingement on the tendinous portion of the rotator cuff by the coracoacromial
Subacromial Impingement (diagnostic methods ) M.N. Naderi Fellowship in shoulder and arthroscopic surgery Neer : Definition Impingement on the tendinous portion of the rotator cuff by the coracoacromial
RN(EC) ENC(C) GNC(C) MN ACNP *** MECHANISM OF INJURY.. MOST IMPORTANT ***
 HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age - Certain conditions are more prevalent in particular age groups (i.e. Full rotator cuff tears are more common over the age of 45, traumatic injuries
HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age - Certain conditions are more prevalent in particular age groups (i.e. Full rotator cuff tears are more common over the age of 45, traumatic injuries
Nonoperative Treatment For Rotator Cuff Tendinitis/ Partial Thickness Tear Dr. Trueblood
 Nonoperative Treatment For Rotator Cuff Tendinitis/ Partial Thickness Tear Dr. Trueblood Relieving Pain Patients who present with SIS will have shoulder pain that is exacerbated with overhead activities.
Nonoperative Treatment For Rotator Cuff Tendinitis/ Partial Thickness Tear Dr. Trueblood Relieving Pain Patients who present with SIS will have shoulder pain that is exacerbated with overhead activities.
SHOULDER PAIN. A Real Pain in the Neck. Michael Wolk, MD Northeastern Rehabilitation Associates October 31, 2017
 SHOULDER PAIN A Real Pain in the Neck Michael Wolk, MD Northeastern Rehabilitation Associates October 31, 2017 THE SHOULDER JOINT (S) 1. glenohumeral 2. suprahumeral 3. acromioclavicular 4. scapulocostal
SHOULDER PAIN A Real Pain in the Neck Michael Wolk, MD Northeastern Rehabilitation Associates October 31, 2017 THE SHOULDER JOINT (S) 1. glenohumeral 2. suprahumeral 3. acromioclavicular 4. scapulocostal
MOON SHOULDER GROUP NONOPERATIVE TREATMENT OF ROTATOR CUFF TENDONOPATHY PHYSICAL THERAPY GUIDELINES
 MOON SHOULDER GROUP NONOPERATIVE TREATMENT OF ROTATOR CUFF TENDONOPATHY PHYSICAL THERAPY GUIDELINES From: Kuhn JE. Exercise in the treatment of rotator cuff impingement. A systematic review and synthesized
MOON SHOULDER GROUP NONOPERATIVE TREATMENT OF ROTATOR CUFF TENDONOPATHY PHYSICAL THERAPY GUIDELINES From: Kuhn JE. Exercise in the treatment of rotator cuff impingement. A systematic review and synthesized
REMINDER. Obtain medical clearance and physician s release prior to beginning an exercise program for clients with medical or orthopedic concerns
 Understanding Shoulder Dysfunction REMINDER Obtain medical clearance and physician s release prior to beginning an exercise program for clients with medical or orthopedic concerns What is a healthy shoulder?
Understanding Shoulder Dysfunction REMINDER Obtain medical clearance and physician s release prior to beginning an exercise program for clients with medical or orthopedic concerns What is a healthy shoulder?
Table 17: Provocative tests performed in a neutral shoulder position, i.e. the arm is at the patient s side.
 Page 1 of 1 Table 17: Provocative tests performed in a neutral shoulder position, i.e. the arm is at the patient s side. Description Click Image Positive Indicator Study Painful Arc of Abduction Also reported
Page 1 of 1 Table 17: Provocative tests performed in a neutral shoulder position, i.e. the arm is at the patient s side. Description Click Image Positive Indicator Study Painful Arc of Abduction Also reported
Rehabilitation of Overhead Shoulder Injuries
 Rehabilitation of Overhead Shoulder Injuries 16 th Annual Primary Care Orthopaedic & Sports Medicine Symposium January 29, 2016 Jeremy Sherman, PT, MPT Disclosures No financial disclosures to note. Jeremy
Rehabilitation of Overhead Shoulder Injuries 16 th Annual Primary Care Orthopaedic & Sports Medicine Symposium January 29, 2016 Jeremy Sherman, PT, MPT Disclosures No financial disclosures to note. Jeremy
C. Christopher Smith, M.D. Associate Professor of Medicine Harvard Medical School Beth Israel Deaconess Medical Center
 Evaluation and Treatment of the Painful Shoulder in the Primary Care Setting C. Christopher Smith, M.D. Associate Professor of Medicine Harvard Medical School Beth Israel Deaconess Medical Center A 65-year-old
Evaluation and Treatment of the Painful Shoulder in the Primary Care Setting C. Christopher Smith, M.D. Associate Professor of Medicine Harvard Medical School Beth Israel Deaconess Medical Center A 65-year-old
WEEKEND 2 Shoulder. Shoulder Active Range of Motion Assessment
 Virginia Orthopedic Manual Physical Therapy Institute - 2016 Technique Manual WEEKEND 2 Shoulder Shoulder Active Range of Motion Assessment - Patient Positioning: Standing, appropriately undressed so that
Virginia Orthopedic Manual Physical Therapy Institute - 2016 Technique Manual WEEKEND 2 Shoulder Shoulder Active Range of Motion Assessment - Patient Positioning: Standing, appropriately undressed so that
Biceps Tenodesis Protocol
 Biceps Tenodesis Protocol A biceps tenodesis procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum and then anchoring the tendon along its anatomical
Biceps Tenodesis Protocol A biceps tenodesis procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum and then anchoring the tendon along its anatomical
Lab Workbook. ANATOMY Manual Muscle Testing Lower Trapezius Patient: prone
 ANATOMY Manual Muscle Testing Lower Trapezius Patient: prone Lab Workbook Fixation: place on hand below the scapula on the opposite side Test: adduction and depression of the scapula with lateral rotation
ANATOMY Manual Muscle Testing Lower Trapezius Patient: prone Lab Workbook Fixation: place on hand below the scapula on the opposite side Test: adduction and depression of the scapula with lateral rotation
EBP - An Examination of Special Tests for the Shoulder- Module 8 Exam
 We recommend that you download and print this exam to use as a worksheet. As you study the course material, add your answers to the worksheet. After studying, you will submit the answers. After you submit
We recommend that you download and print this exam to use as a worksheet. As you study the course material, add your answers to the worksheet. After studying, you will submit the answers. After you submit
EBP- An Examination of Special Tests for the Shoulder Module 4 Questions
 EBP- An Examination of Special Tests for the Shoulder Module 4 Questions 51-100 Question 51 The Active Compression test using pain or a click as a positive test indicator provides a more accurate diagnosis
EBP- An Examination of Special Tests for the Shoulder Module 4 Questions 51-100 Question 51 The Active Compression test using pain or a click as a positive test indicator provides a more accurate diagnosis
Biceps Tenodesis Protocol
 Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Biceps Tenodesis Protocol The intent of this protocol is to provide the clinician with a
Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Biceps Tenodesis Protocol The intent of this protocol is to provide the clinician with a
Acromioplasty. Surgical Indications and Considerations
 1 Acromioplasty Surgical Indications and Considerations Anatomical Considerations: Any abnormality that disrupts the intricate relationship within the subacromial space may lead to impingement. Both intrinsic
1 Acromioplasty Surgical Indications and Considerations Anatomical Considerations: Any abnormality that disrupts the intricate relationship within the subacromial space may lead to impingement. Both intrinsic
Type II SLAP lesions are created when the biceps anchor has pulled away from the glenoid attachment.
 Arthroscopic Superior Labral (SLAP) Repair Protocol-Type II, IV, and Complex Tears The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of
Arthroscopic Superior Labral (SLAP) Repair Protocol-Type II, IV, and Complex Tears The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of
Anterior Labrum Repair Protocol
 Anterior Labrum Repair Protocol Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain scapular
Anterior Labrum Repair Protocol Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain scapular
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is
Structure and Function of the Bones and Joints of the Shoulder Girdle
 Structure and Function of the Bones and Joints of the Shoulder Girdle LEARNING OBJECTIVES: At the end of this laboratory exercise the student will be able to: Palpate the important skeletal landmarks of
Structure and Function of the Bones and Joints of the Shoulder Girdle LEARNING OBJECTIVES: At the end of this laboratory exercise the student will be able to: Palpate the important skeletal landmarks of
Rehabilitation Guidelines for Labral/Bankert Repair
 Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Superior Labrum Repair Protocol - SLAP
 Superior Labrum Repair Protocol - SLAP Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain
Superior Labrum Repair Protocol - SLAP Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain
APPENDIX: The Houston Astros Stretching Program
 Vol. 35, No. 4, 2007 Glenohumeral Internal Rotation Deficits 1 APPENDIX: The Houston Astros Stretching Program Our Flexibility program consists of 5 positions. Four of the 5 have 2 variations of each position.
Vol. 35, No. 4, 2007 Glenohumeral Internal Rotation Deficits 1 APPENDIX: The Houston Astros Stretching Program Our Flexibility program consists of 5 positions. Four of the 5 have 2 variations of each position.
Pearson Education Limited Edinburgh Gate Harlow Essex CM20 2JE England and Associated Companies throughout the world
 Pearson Education Limited Edinburgh Gate Harlow Essex CM20 2JE England and Associated Companies throughout the world Visit us on the World Wide Web at: www.pearsoned.co.uk Pearson Education Limited 2014
Pearson Education Limited Edinburgh Gate Harlow Essex CM20 2JE England and Associated Companies throughout the world Visit us on the World Wide Web at: www.pearsoned.co.uk Pearson Education Limited 2014
Throwing Athlete Rehabilitation. Brett Schulz LAT/CMSS Sport and Spine Physical Therapy
 Throwing Athlete Rehabilitation Brett Schulz LAT/CMSS Sport and Spine Physical Therapy Disclosure No conflicts to disclose Throwing Athlete Dilemma The shoulder must have enough range of motion to allow
Throwing Athlete Rehabilitation Brett Schulz LAT/CMSS Sport and Spine Physical Therapy Disclosure No conflicts to disclose Throwing Athlete Dilemma The shoulder must have enough range of motion to allow
Unit 8 SPECIFIC SPORTS INJURIES Upper Extremity Case Study
 Unit 8 SPECIFIC SPORTS INJURIES Upper Extremity Case Study Swimming Shoulder Pain Identifying the Source By Tamara Stelting, ATC As swimming season kicks into gear, many shoulders will start feeling fatigued
Unit 8 SPECIFIC SPORTS INJURIES Upper Extremity Case Study Swimming Shoulder Pain Identifying the Source By Tamara Stelting, ATC As swimming season kicks into gear, many shoulders will start feeling fatigued
The Shoulder. Anatomy and Injuries PSK 4U Unit 3, Day 4
 The Shoulder Anatomy and Injuries PSK 4U Unit 3, Day 4 Shoulder Girdle Shoulder Complex is the most mobile joint in the body. Scapula Clavicle Sternum Humerus Rib cage/thorax Shoulder Girdle It also includes
The Shoulder Anatomy and Injuries PSK 4U Unit 3, Day 4 Shoulder Girdle Shoulder Complex is the most mobile joint in the body. Scapula Clavicle Sternum Humerus Rib cage/thorax Shoulder Girdle It also includes
Clinical pearls for the shoulder/arm exam and the treatment. What is seeing youare you seeing it
 Clinical pearls for the shoulder/arm exam and the treatment What is seeing youare you seeing it W. Ben Kibler, MD Medical director Case 1 18 y/o R hand dominant high school pitcher, with 6 week hx gradual
Clinical pearls for the shoulder/arm exam and the treatment What is seeing youare you seeing it W. Ben Kibler, MD Medical director Case 1 18 y/o R hand dominant high school pitcher, with 6 week hx gradual
IJSPT ORIGINAL RESEARCH ABSTRACT
 IJSPT ORIGINAL RESEARCH THE EFFECTS OF A DAILY STRETCHING PROTOCOL ON PASSIVE GLENOHUMERAL INTERNAL ROTATION IN OVERHEAD THROWING COLLEGIATE ATHLETES Roy Aldridge, PT, EdD 1 J. Stephen Guffey, PT, EdD
IJSPT ORIGINAL RESEARCH THE EFFECTS OF A DAILY STRETCHING PROTOCOL ON PASSIVE GLENOHUMERAL INTERNAL ROTATION IN OVERHEAD THROWING COLLEGIATE ATHLETES Roy Aldridge, PT, EdD 1 J. Stephen Guffey, PT, EdD
Biceps Tenotomy Protocol
 Biceps Tenotomy Protocol A biceps tenotomy procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum. A biceps tenotomy is typically done when there is
Biceps Tenotomy Protocol A biceps tenotomy procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum. A biceps tenotomy is typically done when there is
Total Shoulder Rehab Protocol Dr. Payne
 Total Shoulder Rehab Protocol Dr. Payne Phase I Immediate Post Surgical Phase (0-4 weeks): Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase passive range of motion (PROM)
Total Shoulder Rehab Protocol Dr. Payne Phase I Immediate Post Surgical Phase (0-4 weeks): Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase passive range of motion (PROM)
Rotator Cuff Repair +/- Acromioplasty/Mumford. Phase I: 0 to 2 weeks after surgery
 Rotator Cuff Repair +/- Acromioplasty/Mumford 2. Ensure wound healing Phase I: 0 to 2 weeks after surgery 1. Sling: Use your sling all of the time. 2. Use of the affected arm: You may use your hand on
Rotator Cuff Repair +/- Acromioplasty/Mumford 2. Ensure wound healing Phase I: 0 to 2 weeks after surgery 1. Sling: Use your sling all of the time. 2. Use of the affected arm: You may use your hand on
Anterior Stabilization of the Shoulder: Distal Tibial Allograft
 Anterior Stabilization of the Shoulder: Distal Tibial Allograft Name: Diagnosis: Date: Date of Surgery: Phase I Immediate Post Surgical Phase (approximately Weeks 1-3) Minimize shoulder pain and inflammatory
Anterior Stabilization of the Shoulder: Distal Tibial Allograft Name: Diagnosis: Date: Date of Surgery: Phase I Immediate Post Surgical Phase (approximately Weeks 1-3) Minimize shoulder pain and inflammatory
Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines
 Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington
Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington
11/6/2013. Keely Behning, PT, SCS, ATC MNPTA Fall Conference November 16, 2013
 Keely Behning, PT, SCS, ATC MNPTA Fall Conference November 16, 2013 Upon completion of this course, attendees should be able to: Understand pertinent anatomy and biomechanics as they relate to specific
Keely Behning, PT, SCS, ATC MNPTA Fall Conference November 16, 2013 Upon completion of this course, attendees should be able to: Understand pertinent anatomy and biomechanics as they relate to specific
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS
 Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
PROM is not stretching!
 Dx: o Right o Left Shoulder Replacement/Hemiarthroplasty Rehab Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: The intent
Dx: o Right o Left Shoulder Replacement/Hemiarthroplasty Rehab Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: The intent
Biceps Tenotomy Protocol
 Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that has undergone
Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that has undergone
SHOULDER REHABILITATION PART II
 SHOULDER REHABILITATION PART II Ann Cools, PT, PhD Ghent University - Belgium Dept of Rehabilitation Sciences & Physiotherapy Ann.Cools@UGent.be Shoulder rehab course level I Shoulder pathology and clinical
SHOULDER REHABILITATION PART II Ann Cools, PT, PhD Ghent University - Belgium Dept of Rehabilitation Sciences & Physiotherapy Ann.Cools@UGent.be Shoulder rehab course level I Shoulder pathology and clinical
D: Doorway Stretch E: Towel Stretch for Pectoralis Minor Blackburn Exercises: 6 Positions A: Prone Horizontal Abduction (Neutral)
 D: Doorway Stretch Bring your shoulder into a horizontal position out to your side (abduction) and flex your elbow 90û Place your elbow against the edge of a doorway Lead forward and downwards with your
D: Doorway Stretch Bring your shoulder into a horizontal position out to your side (abduction) and flex your elbow 90û Place your elbow against the edge of a doorway Lead forward and downwards with your
Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol
 Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol The intent of this protocol is to provide the therapist with a guideline of the postoperative rehabilitation course of a patient that has
Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol The intent of this protocol is to provide the therapist with a guideline of the postoperative rehabilitation course of a patient that has
Since the description of the superior labral lesions. Biceps Load Test II: A Clinical Test for SLAP Lesions of the Shoulder
 Biceps Load Test II: A Clinical Test for SLAP Lesions of the Shoulder Seung-Ho Kim, M.D., Ph.D., Kwon-Ick Ha, M.D., Ph.D., Jin-Hwan Ahn, M.D., Ph.D., Sang-Hyun Kim, M.D., and Hee-Joon Choi, M.D. Purpose:
Biceps Load Test II: A Clinical Test for SLAP Lesions of the Shoulder Seung-Ho Kim, M.D., Ph.D., Kwon-Ick Ha, M.D., Ph.D., Jin-Hwan Ahn, M.D., Ph.D., Sang-Hyun Kim, M.D., and Hee-Joon Choi, M.D. Purpose:
REMINDER. an exercise program. Senior Fitness Obtain medical clearance and physician s release prior to beginning
 Functional Forever: Exercise for Independent Living REMINDER Obtain medical clearance and physician s release prior to beginning an exercise program for clients with medical or orthopedic concerns. What
Functional Forever: Exercise for Independent Living REMINDER Obtain medical clearance and physician s release prior to beginning an exercise program for clients with medical or orthopedic concerns. What
BMJ Open is committed to open peer review. As part of this commitment we make the peer review history of every article we publish publicly available.
 is committed to open peer review. As part of this commitment we make the peer review history of every article we publish publicly available. When an article is published we post the peer reviewers comments
is committed to open peer review. As part of this commitment we make the peer review history of every article we publish publicly available. When an article is published we post the peer reviewers comments
Total Shoulder Arthroplasty / Hemiarthroplasty Protocol
 Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Shoulder Arthroplasty / Hemiarthroplasty Protocol The intent of this protocol is to provide the
Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Shoulder Arthroplasty / Hemiarthroplasty Protocol The intent of this protocol is to provide the
Anterior Stabilization of the Shoulder: Latarjet Protocol
 Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Stabilization of the Shoulder: Latarjet Protocol The intent of this protocol is
Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Stabilization of the Shoulder: Latarjet Protocol The intent of this protocol is
Shoulder Instability. Fig 1: Intact labrum and biceps tendon
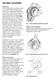 Shoulder Instability What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone
Shoulder Instability What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone
Throwing Injuries and Prevention: The Physical Therapy Perspective
 Throwing Injuries and Prevention: The Physical Therapy Perspective Andrew M Jordan, PT, DPT, OCS Staff Physical Therapist, Cayuga Medical Center Physical Therapy and Sports Medicine ajordan@cayugamed.org
Throwing Injuries and Prevention: The Physical Therapy Perspective Andrew M Jordan, PT, DPT, OCS Staff Physical Therapist, Cayuga Medical Center Physical Therapy and Sports Medicine ajordan@cayugamed.org
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
2015 OPSC Annual Convention. syllabus. February 4-8, 2015 Hyatt Regency Mission Bay San Diego, California
 2015 OPSC Annual Convention syllabus February 4-8, 2015 Hyatt Regency Mission Bay San Diego, California THURSDAY, FEBRUARY 5, 2015: 3:30pm - 4:30pm The Shoulder: 2 View or Not 2 View * Presented by Alexandra
2015 OPSC Annual Convention syllabus February 4-8, 2015 Hyatt Regency Mission Bay San Diego, California THURSDAY, FEBRUARY 5, 2015: 3:30pm - 4:30pm The Shoulder: 2 View or Not 2 View * Presented by Alexandra
Rehabilitation for MDI in the Female Athlete. John Dale PT, DPT, SCS, ATC, CSCS Andrew Naylor PT, DPT, SCS
 Rehabilitation for MDI in the Female Athlete John Dale PT, DPT, SCS, ATC, CSCS Andrew Naylor PT, DPT, SCS Disclosure No relevant financial relationship exists Session Learning Objectives Discuss etiology
Rehabilitation for MDI in the Female Athlete John Dale PT, DPT, SCS, ATC, CSCS Andrew Naylor PT, DPT, SCS Disclosure No relevant financial relationship exists Session Learning Objectives Discuss etiology
Burwood Road, Concord 160 Belmore Road, Randwick
 www.orthosports.com.au 47 49 Burwood Road, Concord 160 Belmore Road, Randwick Conservative management of subacromial pathology Mel Cusi MBBS, Cert Sp Med, FACSP, FFSEM (UK) Presenting symptoms Shoulder
www.orthosports.com.au 47 49 Burwood Road, Concord 160 Belmore Road, Randwick Conservative management of subacromial pathology Mel Cusi MBBS, Cert Sp Med, FACSP, FFSEM (UK) Presenting symptoms Shoulder
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Open Bankart Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Open Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Open Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared
After Arthroscopic Subacromial Decompression Intact Rotator Cuff (Distal Clavicle Resection)
 After Arthroscopic Subacromial Decompression Intact Rotator Cuff (Distal Clavicle Resection) Rehabilitation Protocol Phase 1: Weeks 0-4 Restrictions ROM 140 degrees of forward flexion 40 degrees of external
After Arthroscopic Subacromial Decompression Intact Rotator Cuff (Distal Clavicle Resection) Rehabilitation Protocol Phase 1: Weeks 0-4 Restrictions ROM 140 degrees of forward flexion 40 degrees of external
The Relationship of Periscapular Strength on Scapular Upward Rotation in Professional Baseball Pitchers
 Journal of Sport Rehabilitation, 2008, 17, 95-105 2008 Human Kinetics, Inc. Original Research Reports The Relationship of Periscapular Strength on Scapular Upward Rotation in Professional Baseball Pitchers
Journal of Sport Rehabilitation, 2008, 17, 95-105 2008 Human Kinetics, Inc. Original Research Reports The Relationship of Periscapular Strength on Scapular Upward Rotation in Professional Baseball Pitchers
Reverse Total Shoulder Arthroplasty Protocol
 General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
Mastering the Musculoskeletal Exam UCSF Essentials of Women s Health July 7, 2016 Carlin Senter, M.D. Henry Crevensten, M.D.
 Mastering the Musculoskeletal Exam UCSF Essentials of Women s Health July 7, 2016 Carlin Senter, M.D. Henry Crevensten, M.D. I have nothing to disclose Outline Knee exam Shoulder exam Knee Anatomy The
Mastering the Musculoskeletal Exam UCSF Essentials of Women s Health July 7, 2016 Carlin Senter, M.D. Henry Crevensten, M.D. I have nothing to disclose Outline Knee exam Shoulder exam Knee Anatomy The
Secrets and Staples of Training the Athletic Shoulder
 Secrets and Staples of Training the Athletic Shoulder Eric Beard Corrective Exercise Specialist Athletic Performance Enhancement Specialist EricBeard.com AthleticShoulder.com Presentation Overview Rationale
Secrets and Staples of Training the Athletic Shoulder Eric Beard Corrective Exercise Specialist Athletic Performance Enhancement Specialist EricBeard.com AthleticShoulder.com Presentation Overview Rationale
Conservative Posterior Capsular Instability Protocol
 SPORTS & ORTHOPAEDIC SPECIALISTS Conservative Posterior Capsular Instability Protocol 4-6 visits over 6 weeks Primary instability often experiences secondary impingement. Therefore, to treat posterior
SPORTS & ORTHOPAEDIC SPECIALISTS Conservative Posterior Capsular Instability Protocol 4-6 visits over 6 weeks Primary instability often experiences secondary impingement. Therefore, to treat posterior
SHOULDER PAIN LESSONS FROM THE SPORTS FIELD MOVEMENT RESTRICTIONS. Steve McCaig
 SHOULDER PAIN LESSONS FROM THE SPORTS FIELD MOVEMENT RESTRICTIONS 1 Steve McCaig Senior Physiotherapist England Development Programme, ECB, Loughborough, United Kingdom Throwing High forces upper limb
SHOULDER PAIN LESSONS FROM THE SPORTS FIELD MOVEMENT RESTRICTIONS 1 Steve McCaig Senior Physiotherapist England Development Programme, ECB, Loughborough, United Kingdom Throwing High forces upper limb
Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears:
 Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears: The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that
Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears: The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that
Anatomical Considerations/ Pathophysiology The shoulder is the most mobile joint in the body. : Three bones:
 Introduction Musculoskeletal training is generally underrepresented in medical training and residency curriculums. There is a general deficit in musculoskeletal knowledge amongst current medical students,
Introduction Musculoskeletal training is generally underrepresented in medical training and residency curriculums. There is a general deficit in musculoskeletal knowledge amongst current medical students,
SHOULDER DISLOCATION & INSTABILITY Rehabilitation Considerations
 SHOULDER DISLOCATION & INSTABILITY Rehabilitation Considerations Meagan Pehnke, MS, OTR/L, CHT, CLT March 1 st, 2019 Philadelphia Surgery & Rehabilitation of the Hand: Pediatric Pre-course OUTLINE Discuss
SHOULDER DISLOCATION & INSTABILITY Rehabilitation Considerations Meagan Pehnke, MS, OTR/L, CHT, CLT March 1 st, 2019 Philadelphia Surgery & Rehabilitation of the Hand: Pediatric Pre-course OUTLINE Discuss
Reverse Total Shoulder Protocol
 Marion Herring, M.D. OrthoVirginia PH: (804) 270-1305 FX: (804) 273-9294 www.orthovirginia.com Reverse Total Shoulder Protocol General Information: Reverse Total Shoulder Arthroplasty (rtsa) is designed
Marion Herring, M.D. OrthoVirginia PH: (804) 270-1305 FX: (804) 273-9294 www.orthovirginia.com Reverse Total Shoulder Protocol General Information: Reverse Total Shoulder Arthroplasty (rtsa) is designed
Get Rhythm or what s the link between scapular dyskinesis and Algorithm?
 Get Rhythm or what s the link between scapular dyskinesis and Algorithm? Rehabilitation of scapular dyskinesis: from the office worker to the elite overhead athlete Adapted Critical appraised Paper and
Get Rhythm or what s the link between scapular dyskinesis and Algorithm? Rehabilitation of scapular dyskinesis: from the office worker to the elite overhead athlete Adapted Critical appraised Paper and
Clinical Assessment of Scapular Motion
 Clinical Assessment of Scapular Motion BRADY L. TRIPP, MEd, ATC, and TIM L. UHL, PhD, ATC, PT University of Kentucky Key Points Many athletic therapists appreciate the role that scapular function plays
Clinical Assessment of Scapular Motion BRADY L. TRIPP, MEd, ATC, and TIM L. UHL, PhD, ATC, PT University of Kentucky Key Points Many athletic therapists appreciate the role that scapular function plays
Rehab protocol. Phase I: Immediate Post-Surgical Phase: Typically 0-4 weeks; 2 PT visits. Goals:
 Reverse Total shoulder arthroplasty Rehab protocol Phase I: Immediate Post-Surgical Phase: Typically 0-4 weeks; 2 PT visits Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase
Reverse Total shoulder arthroplasty Rehab protocol Phase I: Immediate Post-Surgical Phase: Typically 0-4 weeks; 2 PT visits Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase
OrthoCarolina. Arthroscopic SLAP Lesion (Type II) Repair Protocol
 OrthoCarolina Arthroscopic SLAP Lesion (Type II) Repair Protocol Surgical Overview: SLAP, which stands for superior labrum anterior to posterior, lesions are labral detachments that originate posterior
OrthoCarolina Arthroscopic SLAP Lesion (Type II) Repair Protocol Surgical Overview: SLAP, which stands for superior labrum anterior to posterior, lesions are labral detachments that originate posterior
Continuing Education: Shoulder Stability
 Continuing Education: Shoulder Stability Anatomy & Kinesiology: The GHJ consists of the articulation of three bones: the scapula, clavicle and humerus. The scapula has three protrusions: the coracoid,
Continuing Education: Shoulder Stability Anatomy & Kinesiology: The GHJ consists of the articulation of three bones: the scapula, clavicle and humerus. The scapula has three protrusions: the coracoid,
Rehabilitation Guidelines for Arthroscopic Capsular Shift
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Arthroscopic Capsular Shift The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee.
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Arthroscopic Capsular Shift The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee.
Strength and muscle activity of shoulder external rotation of subjects with and
 Strength and muscle activity of shoulder external rotation of subjects with and without scapular dyskinesis DAISUKE UGA, RPT, MS 1,2), RIE NAKAZAWA, RPT, PhD 2), MASAAKI SAKAMOTO, RPT, PhD 2) 1) Jobu Hospital
Strength and muscle activity of shoulder external rotation of subjects with and without scapular dyskinesis DAISUKE UGA, RPT, MS 1,2), RIE NAKAZAWA, RPT, PhD 2), MASAAKI SAKAMOTO, RPT, PhD 2) 1) Jobu Hospital
Shoulder Instability and Tendon Injuries
 Shoulder Instability and Tendon Injuries Shoulder Update Spire Hospital Leeds November 2017 Simon Boyle Consultant Shoulder and Elbow Surgeon Simon Boyle York and Leeds Nuffield Trained in Yorkshire, Annecy,
Shoulder Instability and Tendon Injuries Shoulder Update Spire Hospital Leeds November 2017 Simon Boyle Consultant Shoulder and Elbow Surgeon Simon Boyle York and Leeds Nuffield Trained in Yorkshire, Annecy,
Returning the Shoulder Back to Optimal Function. Scapula. Clavicle. Humerus. Bones of the Shoulder (Osteology) Joints of the Shoulder (Arthrology)
 Returning the Shoulder Back to Optimal Function Sternum Clavicle Ribs Scapula Humerus Bones of the Shoulder (Osteology) By Rick Kaselj Clavicle Scapula Medial Left Anterior Clavicle Inferior View 20 degree
Returning the Shoulder Back to Optimal Function Sternum Clavicle Ribs Scapula Humerus Bones of the Shoulder (Osteology) By Rick Kaselj Clavicle Scapula Medial Left Anterior Clavicle Inferior View 20 degree
Shoulder Impingement Rehabilitation Recommendations
 Shoulder Impingement Rehabilitation Recommendations The following protocol can be utilized for conservative care of shoulder impingement as well as post- operative subacromial decompression (SAD) surgery.
Shoulder Impingement Rehabilitation Recommendations The following protocol can be utilized for conservative care of shoulder impingement as well as post- operative subacromial decompression (SAD) surgery.
S3 EFFECTIVE FOR SHOULDER PATHOLOGIES -Dr. Steven Smith
 S3 EFFECTIVE FOR SHOULDER PATHOLOGIES -Dr. Steven Smith Introduction: Scapular function and its role in shoulder biomechanics has gained increased notoriety in the pathogenesis of shoulder dysfunction
S3 EFFECTIVE FOR SHOULDER PATHOLOGIES -Dr. Steven Smith Introduction: Scapular function and its role in shoulder biomechanics has gained increased notoriety in the pathogenesis of shoulder dysfunction
Advanced Treatment of VEO in the Thrower
 Advanced Treatment of VEO in the Thrower by Toko Nguyen PT, DPT, OCS, SCS, FAAOMPT, CSCS Ben Renfrow PT, DPT, OCS, SCS, FAAOMPT AAOMPT Annual Conference 2015 Lexington, KY Define VEO IAR OBJECTIVES Discuss
Advanced Treatment of VEO in the Thrower by Toko Nguyen PT, DPT, OCS, SCS, FAAOMPT, CSCS Ben Renfrow PT, DPT, OCS, SCS, FAAOMPT AAOMPT Annual Conference 2015 Lexington, KY Define VEO IAR OBJECTIVES Discuss
Addressing Core and Balance Deficits to Maximize Return to Sport in Overhead Athletes
 Addressing Core and Balance Deficits to Maximize Return to Sport in Overhead Athletes Meg Jacobs P.T. Momentum Physical Therapy and Sports Rehab Hands on care for faster results www.wegetyouhealthy.com
Addressing Core and Balance Deficits to Maximize Return to Sport in Overhead Athletes Meg Jacobs P.T. Momentum Physical Therapy and Sports Rehab Hands on care for faster results www.wegetyouhealthy.com
POST-SURGICAL POSTERIOR GLENOHUMERAL STABILIZATION REHABILITATION PROTOCOL (Capsulolabral Repair)
 Gregory N. Lervick, MD Andrew Anderson, PA-C 952-456-7111 POST-SURGICAL POSTERIOR GLENOHUMERAL STABILIZATION REHABILITATION PROTOCOL (Capsulolabral Repair) Open Arthroscopic Phase 1: Weeks 0-4 No shoulder
Gregory N. Lervick, MD Andrew Anderson, PA-C 952-456-7111 POST-SURGICAL POSTERIOR GLENOHUMERAL STABILIZATION REHABILITATION PROTOCOL (Capsulolabral Repair) Open Arthroscopic Phase 1: Weeks 0-4 No shoulder
Rehabilitation Guidelines for Total Shoulder Arthroplasty and Hemi-arthroplasty
 Rehabilitation Guidelines for Total Shoulder Arthroplasty and Hemi-arthroplasty Josef K. Eichinger, MD General Information Total Recovery time is between 4-6 months depending on factors such as injury
Rehabilitation Guidelines for Total Shoulder Arthroplasty and Hemi-arthroplasty Josef K. Eichinger, MD General Information Total Recovery time is between 4-6 months depending on factors such as injury
Exploring the Rotator Cuff
 Exploring the Rotator Cuff Improving one s performance in sports and daily activity is a factor of neuromuscular efficiency and metabolic enhancements. To attain proficiency, reaction force must be effectively
Exploring the Rotator Cuff Improving one s performance in sports and daily activity is a factor of neuromuscular efficiency and metabolic enhancements. To attain proficiency, reaction force must be effectively
Page 2 of 13 Fig. E-2A Fig. E-2B Fig. E-2C Fig. E-2D Figs. E-2A through E-2D Treatment to relax the upper part of the trapezius muscle. Fig. E-2A Pati
 Page 1 of 13 Fig. E-1A Fig. E-1B Figs. E-1A through E-1C Correction of the sitting position to increase the patient s awareness for the correct sitting position and the interscapular muscles. Fig. E-1A
Page 1 of 13 Fig. E-1A Fig. E-1B Figs. E-1A through E-1C Correction of the sitting position to increase the patient s awareness for the correct sitting position and the interscapular muscles. Fig. E-1A
SHOULDERS MADE DR DR CHRIS MILNE SPORTS PHYSICIAN
 SHOULDERS MADE SHOULDERS MADE SIMPLE SIMPLE Yeah Right DR DR CHRIS MILNE MILNE SPORTS PHYSICIAN SPORTS PHYSICIAN Yeah Right SHOULDER ANATOMY OUTLINE History Examination Investigations MY SHOULDER HURTS!
SHOULDERS MADE SHOULDERS MADE SIMPLE SIMPLE Yeah Right DR DR CHRIS MILNE MILNE SPORTS PHYSICIAN SPORTS PHYSICIAN Yeah Right SHOULDER ANATOMY OUTLINE History Examination Investigations MY SHOULDER HURTS!
G roin pain is associated with many sports and
 446 ORIGINAL ARTICLE Clinical examination of athletes with groin pain: an intraobserver and interobserver reliability study PHölmich, L R Hölmich, A M Bjerg... See end of article for authors affiliations...
446 ORIGINAL ARTICLE Clinical examination of athletes with groin pain: an intraobserver and interobserver reliability study PHölmich, L R Hölmich, A M Bjerg... See end of article for authors affiliations...
Phase I : Immediate Postoperative Phase- Protected Motion. (0-2 Weeks)
 Phase I : Immediate Postoperative Phase- Protected Motion (0-2 Weeks) Appointments Progression Criteria 2 weeks after surgery Rehabilitation appointments begin within 7-10 days of surgery, continue 1-2
Phase I : Immediate Postoperative Phase- Protected Motion (0-2 Weeks) Appointments Progression Criteria 2 weeks after surgery Rehabilitation appointments begin within 7-10 days of surgery, continue 1-2
