Assessment and problem solving: starting with a temporary prosthesis
|
|
|
- Barry Warren
- 5 years ago
- Views:
Transcription
1 Assessment and problem solving: starting with a temporary prosthesis Stump assessment Skin Colour, temperature, appearance sensitivity and allergies to materials Integrity eg frail, thin, dry Abrasions, skin tears and location of same ie on weight bearing surfaces or under strap. Presence of skin grafts (especially traumatic) Wound and scar Healed or open MUST allow to close before fitting the prosthesis especially with vascular insufficiency. Consider location of wound high/low risk areas. Prominent/raised. Tethered or mobile Scar massage for 1min duration at each point where skin/scar is tethered. Patient to do daily when they bathe. Increase comfort, decrease pain and risk of skin breakdown 2 to rubbing within socket. Deep circular motions or frictions perpendicular to line of scar Oedema Palpate especially distal stump. Firm, soft, pitting etc Take circumferential measures at 3, 6, 9, 12cm (+/- 14/15cm) from inf. pole of patella weekly to monitor stump volume and shape. For AKA choose relevant landmark for consistency eg scar line. Once the stump is stable (consistent measures over 2+ weeks) it is suitable for the definitive. Managed with stump bandages or shrinker socks and effleurage type massage. Bandages and socks are to be applied at all times except when washing or massaging bandaging must be reapplied frequently throughout day (at least 6 hourly). Skin must be dry before reapplying bandages or socks. Consider wound condition prior to changing to shrinker sock Sensation Simple assessment of stump sensation.
2 Considerations with prothesis fit. - Is patient able to give feedback of incorrect fit or monitor as stump shape/size changes? Eg end bearing, dropping off, rubbing, scratching - If sensation is impaired patient must be v. diligent in checking stump/skin condition regularly. Stump pain - Sensitivity to touch/pressure. Tolerate prosthesis? - Consult with medical staff re pharmacological management. - Massage at least 5mins 3-4 times a day decease swelling increase stump tolerance, helpful in reducing phantom pain. Also important for reducing/treating neuromas. - Tapping and desensitisation. Done 2-3 minutes twice daily. Cotton ball paper towel terry cloth. Boney prominences Consideration for socket relief and padding. May utilize additional padding (silicon) for very sensitive areas. ROM Assessment Amputated AND intact limb. - Intact limb especially DF, knee extension and hip extension ranges sufficient to allow balanced standing and ambulation - Amputated limb depending on level knee ranges, hip ranges Presence of contractures hamstrings, hip flexors associated with prolonged wheelchair use. - Ideally minimised through good post op management however treated with stretching program eg prone lying and long sitting with overpressure. Surgical release. - TTA 20 knee flex contracture for prosthetic use. - TFA 5 hip flexion contracture for prosthetic use. Strength Amputated AND intact limb - Compensations for missing limb segments and contribution to gait pattern. - Hip extensors++ amputated side - PF, quads, hip extensors intact side. Power AND endurance - Manual muscle testing and functional testing eg STS (height, no. in 60sec, to fatigue), mob endurance, 10MWT etc
3 - Energy (oxygen) cost of mobility progressively increases the higher the level of amputation - Consider reason for amputation (traumatic vs vascular) and age of patient decreased physical work capacity and VO2 max associated with increased age and poor cardiovascular function. - Aerobic conditioning exercises have been shown to both increase walking speed (8%) and decrease rate of oxygen consumption (6-10%) with TT and TF amputations. (Waters RL, Mulroy S) Are they suitable/ready for a prosthesis Stump condition ROM and strength considerations (intact and amputated). Ability to hop prosthetic gait training. Medical issues preventing training. Cognitive function ability to learn complicated task of gait retraining and safety in using prosthesis, medical issues affecting cognitive function eg dementia, stroke. Social situation. Attitude and motivation. Basic principles of prosthetic alignment and adjustment BKA Weight bearing surfaces Patella tendon, medial tibial flare and lateral tibial muscle bulk. Triangular shaped socket, with counterpressure in popliteal fossa. Pressure intolerant areas end stump, boney prominences eg fibula head, tibial spine, distal tib or fib, tibial tuberosity, elsewhere. Alignment patellar shelf horizontal and level with popliteal counter pressure, knee in 5 flexion (plus contracture), central brim of socket 1cm anterior to pole, mid-pole 1cm medial to mid socket. AKA Weight bearing surfaces Ischial tuberosity with anterior counterpressure on quads, medial and lateral thigh surfaces. Quadrilateral shaped socket. Pressure intolerant areas end stump and boney prominences, adductor tendons, groin.
4 Alignment posterior brim is horizontal, medial brim horizontal and in line of progression (straight ahead), ischial tuberosity sits 1/3 of the way along the brim and 1.5cm medial to centre of the knee joint. Midline of brim should sit 1cm anterior to knee joint. Prosthetic fit Patient feedback comfort (will be somewhat uncomfortable/painful especially at first) areas of pressure location, height, movement within socket. Alignment on patient in balanced upright standing with even weight distribution (compared with bench alignment) adjust prosthesis with Allen keys. Inspection of stump sock marks and red marks (consider cast is total contact). Adjustment Add layers of socks end bearing, too loose, dropping off Grind/file out relief in areas of rubbing, tenderness Change alignment to alter weight distribution Medial Lateral
5 Build up or pad sections eg patellar shelf or counter pressure. New prosthesis contracture resolved and unable to change alignment any further, change in stump shape with oedema resolution. When can they take them home? Prosthesis fits properly good alignment, pressure in pressure tolerant areas, not rubbing. They or carer knows how and what to monitor on stump ie when to add socks, pressure areas, when to stop using. The patient or carer is able to don prosthesis correctly. Patient is compliant with exercise program and will follow instructions won t do anything stupid!
Prosthetic Rehab Plan
 Prosthetic Rehab Plan First 4 6 weeks after surgery Until sutures are removed, follow the instructions below: Gently wash your limb daily with anti-bacterial soap and water Wear the brown stump shrinker
Prosthetic Rehab Plan First 4 6 weeks after surgery Until sutures are removed, follow the instructions below: Gently wash your limb daily with anti-bacterial soap and water Wear the brown stump shrinker
Physiotherapy management
 Physiotherapy management Pre-operative Focus is on the objective assessment looking at ROM and muscle power. Using assessment findings, knowledge of prosthetic componentry and gait patterns, provide a
Physiotherapy management Pre-operative Focus is on the objective assessment looking at ROM and muscle power. Using assessment findings, knowledge of prosthetic componentry and gait patterns, provide a
Christopher Gorrell PT, DPT May 5, 2016
 25th Annual Prosthetics Course Pre and Post-Prosthetic Rehab from a Therapist's Perspective Christopher Gorrell PT, DPT May 5, 2016 1 Objectives To review the primary goals related to treatment of a patient
25th Annual Prosthetics Course Pre and Post-Prosthetic Rehab from a Therapist's Perspective Christopher Gorrell PT, DPT May 5, 2016 1 Objectives To review the primary goals related to treatment of a patient
Application of Cast Brace for Post Acute Care of Lower Extremity Fractures
 Application of Cast Brace for Post Acute Care of Lower Extremity Fractures Roy Snelson, C.P.O.*, George Irons, C.P.O.**, and Vert Mooney, M.D.*** The fracture cast brace is designed to allow early ambulation
Application of Cast Brace for Post Acute Care of Lower Extremity Fractures Roy Snelson, C.P.O.*, George Irons, C.P.O.**, and Vert Mooney, M.D.*** The fracture cast brace is designed to allow early ambulation
Below Knee Amputation: Post-op Information
 Below Knee Amputation: Post-op Information This package contains information to help as you begin the recovery process following your amputation. The topics included are: Emotions following an amputation.
Below Knee Amputation: Post-op Information This package contains information to help as you begin the recovery process following your amputation. The topics included are: Emotions following an amputation.
Muscles of the Thigh. 6.1 Identify, describe the attachments of and deduce the actions of the muscles of the thigh: Anterior group
 Muscles of the Thigh 6.1 Identify, describe the attachments of and deduce the actions of the muscles of the thigh: Anterior group Sartorius: This is a long strap like muscle with flattened tendons at each
Muscles of the Thigh 6.1 Identify, describe the attachments of and deduce the actions of the muscles of the thigh: Anterior group Sartorius: This is a long strap like muscle with flattened tendons at each
Arthritic history is similar to that of the hip. Add history of give way and locking, swelling
 KNEE VASU PAI Arthritic history is similar to that of the hip. Add history of give way and locking, swelling INJURY MECHANISM When How Sequence Progress Disability IKDC Activity I - Strenuous activity
KNEE VASU PAI Arthritic history is similar to that of the hip. Add history of give way and locking, swelling INJURY MECHANISM When How Sequence Progress Disability IKDC Activity I - Strenuous activity
Care of the Diabetic Patient
 Care of the Diabetic Patient Aarti Deshpande, CPO Clinic Manager Zuckerberg San Francisco General Department of Orthopaedic Surgery University of California, San Francisco March 16, 2017 Diabetes Diabetes
Care of the Diabetic Patient Aarti Deshpande, CPO Clinic Manager Zuckerberg San Francisco General Department of Orthopaedic Surgery University of California, San Francisco March 16, 2017 Diabetes Diabetes
taken for a patellar-tendon-bearing socket. After these have partly dried, the balance of the shin is wrapped with a roll of plaster bandage. When the
 A PATELLAR-TENDON-BEARING ORTHOSIS Bert R. Titus, C.P.O. 1 1Associate Professor of Prosthetics and Orthotics, Director of Department of Prosthetics and Orthotics, Duke University Medical Center, P. O.
A PATELLAR-TENDON-BEARING ORTHOSIS Bert R. Titus, C.P.O. 1 1Associate Professor of Prosthetics and Orthotics, Director of Department of Prosthetics and Orthotics, Duke University Medical Center, P. O.
PCL/PLC RECONSTRUCTION REHABILITATION Revised OCTOBER 2015
 PCL/PLC RECONSTRUCTION REHABILITATION Revised OCTOBER 2015 REHABILITATION PROGRAM PHASE 1: WEEKS 0-6: PHASE I GOALS: Protect the surgical graft(s) 0-60 ROM Regain adequate quadriceps control CRUTCHES:
PCL/PLC RECONSTRUCTION REHABILITATION Revised OCTOBER 2015 REHABILITATION PROGRAM PHASE 1: WEEKS 0-6: PHASE I GOALS: Protect the surgical graft(s) 0-60 ROM Regain adequate quadriceps control CRUTCHES:
ANTERIOR CRUCTIATE LIGAMENT RECONSTRUCTION COLLATERAL LIGAMENT RECONSTRUCION/REPAIR AND MENISCUS REPAIR REHABILITATION PROTOCOL
 ANTERIOR CRUCTIATE LIGAMENT RECONSTRUCTION COLLATERAL LIGAMENT RECONSTRUCION/REPAIR AND MENISCUS REPAIR REHABILITATION PROTOCOL GENERAL GUIDELINES - The local anesthetic (similar to novacaine) in your
ANTERIOR CRUCTIATE LIGAMENT RECONSTRUCTION COLLATERAL LIGAMENT RECONSTRUCION/REPAIR AND MENISCUS REPAIR REHABILITATION PROTOCOL GENERAL GUIDELINES - The local anesthetic (similar to novacaine) in your
PRIMARY CARE EXAMINATION OF KEY JOINTS. Thomas M. Howard, MD, FACSM FFPC Sports Medicine
 PRIMARY CARE EXAMINATION OF KEY JOINTS Thomas M. Howard, MD, FACSM FFPC Sports Medicine General exam principles: Expose entire joint and opposite limb for comparison Have a Differential Diagnosis Exam
PRIMARY CARE EXAMINATION OF KEY JOINTS Thomas M. Howard, MD, FACSM FFPC Sports Medicine General exam principles: Expose entire joint and opposite limb for comparison Have a Differential Diagnosis Exam
DR. (PROF.) ANIL ARORA MS
 Hip Examination DR. (PROF.) ANIL ARORA MS (Ortho) DNB (Ortho) Dip SIROT (USA) FAPOA (Korea), FIGOF (Germany), FJOA (Japan) Commonwealth Fellow Joint Replacement (Royal National Orthopaedic Hospital, London,
Hip Examination DR. (PROF.) ANIL ARORA MS (Ortho) DNB (Ortho) Dip SIROT (USA) FAPOA (Korea), FIGOF (Germany), FJOA (Japan) Commonwealth Fellow Joint Replacement (Royal National Orthopaedic Hospital, London,
Examination of the Knee
 Examination of the Knee Wash your hands & Introduce the exam to the patient Positioning & Draping With the patient supine, make sure both legs are exposed in order to compare each side be sure to use draping
Examination of the Knee Wash your hands & Introduce the exam to the patient Positioning & Draping With the patient supine, make sure both legs are exposed in order to compare each side be sure to use draping
Fig. 1. Lateral view of the patient showing stockinet in place and indelible pencil marks indicating areas where modification of the positive model wi
 Femoral Immobilizer CHARLES H. PRITHAM 1 MELVIN L. STILLS 2 During the past ten years orthotics has come to play a role in the treatment of selected patients with fractures of the femur. Fundamentally,
Femoral Immobilizer CHARLES H. PRITHAM 1 MELVIN L. STILLS 2 During the past ten years orthotics has come to play a role in the treatment of selected patients with fractures of the femur. Fundamentally,
Sports Rehabilitation & Performance Center Medial Patellofemoral Ligament Reconstruction Guidelines * Follow physician s modifications as prescribed
 The following MPFL guidelines were developed by the Sports Rehabilitation and Performance Center team at Hospital for Special Surgery. Progression is based on healing constraints, functional progression
The following MPFL guidelines were developed by the Sports Rehabilitation and Performance Center team at Hospital for Special Surgery. Progression is based on healing constraints, functional progression
Training the Joint Replacement Client
 KNEE PRE-OP SAMPLE EXERCISE PLAN Quadricep: Shuttle 1 leg and 2 legs (focus on 1 leg) Leg Press 1 and 2 legs (focus on 1 leg) Sit to Stand (if no pain or compensation) Supine Circle Foam knee extension
KNEE PRE-OP SAMPLE EXERCISE PLAN Quadricep: Shuttle 1 leg and 2 legs (focus on 1 leg) Leg Press 1 and 2 legs (focus on 1 leg) Sit to Stand (if no pain or compensation) Supine Circle Foam knee extension
Muscle Testing of Knee Extensors. Yasser Moh. Aneis, PhD, MSc., PT. Lecturer of Physical Therapy Basic Sciences Department
 Muscle Testing of Knee Extensors Yasser Moh. Aneis, PhD, MSc., PT. Lecturer of Physical Therapy Basic Sciences Department Muscle Testing of Knee Extensors othe Primary muscle Quadriceps Femoris -Rectus
Muscle Testing of Knee Extensors Yasser Moh. Aneis, PhD, MSc., PT. Lecturer of Physical Therapy Basic Sciences Department Muscle Testing of Knee Extensors othe Primary muscle Quadriceps Femoris -Rectus
Bone-Patellar tendon-bone Autograft ACL Recon. Date of Surgery: Patient Name:
 Dx: o Right o Left Bone-Patellar tendon-bone Autograft ACL Recon Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: GENERAL
Dx: o Right o Left Bone-Patellar tendon-bone Autograft ACL Recon Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: GENERAL
Medial Patellofemoral Ligament Reconstruction Guidelines Brian Grawe Protocol
 Medial Patellofemoral Ligament Reconstruction Guidelines Brian Grawe Protocol Progression is based on healing constraints, functional progression specific to the patient. Phases and time frames are designed
Medial Patellofemoral Ligament Reconstruction Guidelines Brian Grawe Protocol Progression is based on healing constraints, functional progression specific to the patient. Phases and time frames are designed
Meniscal Repair Protocol-Dr. McClung
 Meniscal Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in full extension for ambulation and sleeping but drop-locked for sitting and knee ROM. Patients
Meniscal Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in full extension for ambulation and sleeping but drop-locked for sitting and knee ROM. Patients
재활의방법과시기 / 길이는얼마가적당한가?
 BK amputation 재활의방법과시기 / 길이는얼마가적당한가? Soo-Kyung, Bok. M.D., Ph.D Chungnam National University Hospital Contents Level selection of BKA Rehabilitation Preoperative management Immediate postoperative management
BK amputation 재활의방법과시기 / 길이는얼마가적당한가? Soo-Kyung, Bok. M.D., Ph.D Chungnam National University Hospital Contents Level selection of BKA Rehabilitation Preoperative management Immediate postoperative management
Home Exercise Program Progression and Components of the LTP Intervention. HEP Activities at Every Session Vital signs monitoring
 Home Exercise Program Progression and Components of the LTP Intervention HEP Activities at Every Session Vital signs monitoring Blood pressure, heart rate, Borg Rate of Perceived Exertion (RPE) and oxygen
Home Exercise Program Progression and Components of the LTP Intervention HEP Activities at Every Session Vital signs monitoring Blood pressure, heart rate, Borg Rate of Perceived Exertion (RPE) and oxygen
The causes of OA of the knee are multiple and include aging (wear and tear), obesity, and previous knee trauma or surgery. OA affects usually the
 The Arthritic Knee The causes of OA of the knee are multiple and include aging (wear and tear), obesity, and previous knee trauma or surgery. OA affects usually the medial compartment of the knee, and
The Arthritic Knee The causes of OA of the knee are multiple and include aging (wear and tear), obesity, and previous knee trauma or surgery. OA affects usually the medial compartment of the knee, and
Above Knee Amputation: Post-op Information
 Above Knee Amputation: Post-op Information This package contains information to help as you begin the recovery process following your amputation. The topics included are: Emotions following an amputation.
Above Knee Amputation: Post-op Information This package contains information to help as you begin the recovery process following your amputation. The topics included are: Emotions following an amputation.
Sheena Black, MD. Orthopaedic Surgery, Sports Medicine PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION HAMSTRING TENDON TECHNIQUE
 PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION HAMSTRING TENDON TECHNIQUE Name: Date: Post-Operative Diagnosis: Right Left ACL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures: Lateral
PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION HAMSTRING TENDON TECHNIQUE Name: Date: Post-Operative Diagnosis: Right Left ACL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures: Lateral
BELOW KNEE TEMPORARY PROSTHESIS!
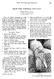 BELOW KNEl!: TEMPORARY PROSTHESIS 195 BELOW KNEE TEMPORARY PROSTHESIS! PATRICIA BAKER, 1\1.A.P.A. Caulfield Hospital, Vi'ctoria There are definite advantages in using temporary prostheses. Their use reduces
BELOW KNEl!: TEMPORARY PROSTHESIS 195 BELOW KNEE TEMPORARY PROSTHESIS! PATRICIA BAKER, 1\1.A.P.A. Caulfield Hospital, Vi'ctoria There are definite advantages in using temporary prostheses. Their use reduces
Balanced Body Movement Principles
 Balanced Body Movement Principles How the Body Works and How to Train it. Module 3: Lower Body Strength and Power Developing Strength, Endurance and Power The lower body is our primary source of strength,
Balanced Body Movement Principles How the Body Works and How to Train it. Module 3: Lower Body Strength and Power Developing Strength, Endurance and Power The lower body is our primary source of strength,
A Single-Bar Above-Knee Orthosis
 A Single-Bar Above-Knee Orthosis Robert O. Nitschke,* C.P.O. I would like to present a different approach to the design of aboveknee, or "long leg", orthoses. When weight-bearing is not necessary, I have
A Single-Bar Above-Knee Orthosis Robert O. Nitschke,* C.P.O. I would like to present a different approach to the design of aboveknee, or "long leg", orthoses. When weight-bearing is not necessary, I have
ARTHROSCOPIC KNEE SURGERY REHABILITATION PROTOCOL MENISCUS REPAIR
 GENERAL GUIDELINES ARTHROSCOPIC KNEE SURGERY REHABILITATION PROTOCOL MENISCUS REPAIR - The local anesthetic (similar to novacaine) in your knee lasts 6-12 hours - Start taking the pain medication as soon
GENERAL GUIDELINES ARTHROSCOPIC KNEE SURGERY REHABILITATION PROTOCOL MENISCUS REPAIR - The local anesthetic (similar to novacaine) in your knee lasts 6-12 hours - Start taking the pain medication as soon
Musculoskeletal Examination Benchmarks
 Musculoskeletal Examination Benchmarks _ The approach to examining the musculoskeletal system is the same no matter what joint or limb is being examined. The affected and contralateral region should both
Musculoskeletal Examination Benchmarks _ The approach to examining the musculoskeletal system is the same no matter what joint or limb is being examined. The affected and contralateral region should both
Sheena Black, MD. Orthopaedic Surgery, Sports Medicine PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION PATELLAR TENDON/ BTB TECHNIQUE
 PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION PATELLAR TENDON/ BTB TECHNIQUE Name: Date: Post-Operative Diagnosis: Right Left ACL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures:
PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION PATELLAR TENDON/ BTB TECHNIQUE Name: Date: Post-Operative Diagnosis: Right Left ACL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures:
MEDIAL PATELLOFEMORAL LIGAMENT REPAIR & TIBIAL TUBERCLE OSTEOTOMY
 MEDIAL PATELLOFEMORAL LIGAMENT REPAIR & TIBIAL TUBERCLE OSTEOTOMY Revised SEP 2013 SPECIAL PRECAUTIONS/ LIMITATIONS: 1) CRUTCHES/ WEIGHT BEARING: Partial weight bearing at day 1 in brace locked at 0 extension
MEDIAL PATELLOFEMORAL LIGAMENT REPAIR & TIBIAL TUBERCLE OSTEOTOMY Revised SEP 2013 SPECIAL PRECAUTIONS/ LIMITATIONS: 1) CRUTCHES/ WEIGHT BEARING: Partial weight bearing at day 1 in brace locked at 0 extension
Technical Manual. Transtibial Hand Casting & Modification Version no. 2
 Transtibial Hand Casting & Modification Version no. 2 Introduction The successful fitting of Transtibial prosthesis is dependent on the fit of the hard socket. Appropriate socket design is fundamental
Transtibial Hand Casting & Modification Version no. 2 Introduction The successful fitting of Transtibial prosthesis is dependent on the fit of the hard socket. Appropriate socket design is fundamental
Protocol G Arthroscopic Surgery: Therapist Information
 Protocol G Arthroscopic Surgery: Therapist Information Please read entire protocol prior to initiating therapy Please do not hesitate to contact Dr. Wolff with questions or concerns. Rest is a vital component
Protocol G Arthroscopic Surgery: Therapist Information Please read entire protocol prior to initiating therapy Please do not hesitate to contact Dr. Wolff with questions or concerns. Rest is a vital component
Management of knee flexion contractures in patients with Cerebral Palsy
 Management of knee flexion contractures in patients with Cerebral Palsy Emmanouil Morakis Orthopaedic Consultant Royal Manchester Children s Hospital 1. Introduction 2. Natural history 3. Pathophysiology
Management of knee flexion contractures in patients with Cerebral Palsy Emmanouil Morakis Orthopaedic Consultant Royal Manchester Children s Hospital 1. Introduction 2. Natural history 3. Pathophysiology
Post-Operative Physical Therapy Protocol for Autograft ACL Reconstruction
 Adam J. Farber, MD Sports Medicine and Orthopaedic Surgery Board Certified; Fellowship-trained in Sports Medicine & Arthroscopic Surgery P: 480-219-3342; F: 480-219-3271 Post-Operative Physical Therapy
Adam J. Farber, MD Sports Medicine and Orthopaedic Surgery Board Certified; Fellowship-trained in Sports Medicine & Arthroscopic Surgery P: 480-219-3342; F: 480-219-3271 Post-Operative Physical Therapy
Overview Functional Training
 Overview Functional Training Exercises with Therapist 1. Sitting 2. Standing up vs. Sitting down 3. Standing 4. Stance phase ( Static and dynamic ) 5. Swing phase 6. Gait Evaluation 7. Walking level ground
Overview Functional Training Exercises with Therapist 1. Sitting 2. Standing up vs. Sitting down 3. Standing 4. Stance phase ( Static and dynamic ) 5. Swing phase 6. Gait Evaluation 7. Walking level ground
Total Hip Replacement Rehabilitation: Progression and Restrictions
 Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Fig. 1. Antero-medial view of the knee cylinder. Fig. 2. Lateral view of the knee cylinder. thought of as for asuprapatellar/supracondylar PTB prosthe
 Knee Cylinder CHARLES H. PRITHAM 1 MELVIN STILLS2 For a variety of reasons it is not uncommon to wish to hold the knee it difficult to lock the joints of the orthosis about all edges of the orthosis, but
Knee Cylinder CHARLES H. PRITHAM 1 MELVIN STILLS2 For a variety of reasons it is not uncommon to wish to hold the knee it difficult to lock the joints of the orthosis about all edges of the orthosis, but
Hip Arthroscopy with Labral Repair and Osteoplasties PT Rehab Protocol
 Matthew T. Mantell, MD 128 Medical Circle Winchester, VA 22601 Phone: 540-667-8975 Email: mattmantellmd@gmail.com Web: www.mattmantellmd.com Hip Arthroscopy with Labral Repair and Osteoplasties PT Rehab
Matthew T. Mantell, MD 128 Medical Circle Winchester, VA 22601 Phone: 540-667-8975 Email: mattmantellmd@gmail.com Web: www.mattmantellmd.com Hip Arthroscopy with Labral Repair and Osteoplasties PT Rehab
GALLAND/KIRBY ACL RECONSTRUCTION: BONE-TENDON- BONE AUTO / ALLOGRAFT POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY ACL RECONSTRUCTION: BONE-TENDON- BONE AUTO / ALLOGRAFT POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing,
GALLAND/KIRBY ACL RECONSTRUCTION: BONE-TENDON- BONE AUTO / ALLOGRAFT POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing,
Medial Collateral Ligament Repair Protocol-Dr. McClung
 Medial Collateral Ligament Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in 30 degrees for ambulation and sleeping but drop-locked for sitting and knee
Medial Collateral Ligament Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in 30 degrees for ambulation and sleeping but drop-locked for sitting and knee
RN(EC) ENC(C) GNC(C) MN ACNP *** MECHANISM OF INJURY.. MOST IMPORTANT *** - Useful in determining mechanism of injury / overuse
 HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient Sport / Occupation - Certain conditions are more prevalent in particular age groups (Osgood Schlaters in youth / Degenerative Joint Disease
HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient Sport / Occupation - Certain conditions are more prevalent in particular age groups (Osgood Schlaters in youth / Degenerative Joint Disease
GALLAND/KIRBY ACL RECONSTRUCTION REVISION POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY ACL RECONSTRUCTION REVISION POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered, continue
GALLAND/KIRBY ACL RECONSTRUCTION REVISION POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered, continue
Jennifer L. Cook, MD
 Jennifer L. Cook, MD Florida Joint Replacement and Sports Medicine Center 5243 Hanff Lane New Port Richey, FL 34652 Phone: (727)848-4249 Fax: (727) 841-8934 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE
Jennifer L. Cook, MD Florida Joint Replacement and Sports Medicine Center 5243 Hanff Lane New Port Richey, FL 34652 Phone: (727)848-4249 Fax: (727) 841-8934 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE
Meniscus Repair Rehabilitation Protocol
 Meniscus Repair Rehabilitation Protocol GENERAL GUIDELINES - Use the cryotherapy cuff continuously for the first 72 hours, then as needed thereafter - Ensure that the cuff never contacts the skin directly
Meniscus Repair Rehabilitation Protocol GENERAL GUIDELINES - Use the cryotherapy cuff continuously for the first 72 hours, then as needed thereafter - Ensure that the cuff never contacts the skin directly
Stump Bandaging of the Lower-Extremity Amputee*
 Stump Bandaging of the Lower-Extremity Amputee* By BELLA J. MAY, B.A. In many rehabilitation centers and hospitals throughout the country, the physical therapist must wait for the amputee to be referred
Stump Bandaging of the Lower-Extremity Amputee* By BELLA J. MAY, B.A. In many rehabilitation centers and hospitals throughout the country, the physical therapist must wait for the amputee to be referred
Post-Op Physical Therapy Protocol for ACL-MCL Reconstruction. Post-Operative Weeks 0-2: Weight-bearing: 1. Non-weightbearing x 4 weeks.
 Adam J. Farber, MD Sports Medicine and Orthopaedic Surgery Board Certified; Fellowship-trained in Sports Medicine & Arthroscopic Surgery P: 480-219-3342; F: 480-219-3271 Post-Op Physical Therapy Protocol
Adam J. Farber, MD Sports Medicine and Orthopaedic Surgery Board Certified; Fellowship-trained in Sports Medicine & Arthroscopic Surgery P: 480-219-3342; F: 480-219-3271 Post-Op Physical Therapy Protocol
Personalized Blood Flow Restriction Rehabilitation. Anterior Cruciate Reconstruction with Meniscal Repair
 Personalized Blood Flow Restriction Rehabilitation Anterior Cruciate Reconstruction with Meniscal Repair ACL with Meniscus Repair 2 PHASE 1 (PROTECTED PHASE) Typically, after an anterior cruciate reconstruction
Personalized Blood Flow Restriction Rehabilitation Anterior Cruciate Reconstruction with Meniscal Repair ACL with Meniscus Repair 2 PHASE 1 (PROTECTED PHASE) Typically, after an anterior cruciate reconstruction
A NEW CONCEPT IN FUNCTIONAL ORTHOSES
 A NEW CONCEPT IN FUNCTIONAL ORTHOSES THE KNEE in movement! Climbing stairs, walking and running are everyday actions that we can perform thanks to our knees. The knee joint is one of the most exposed and
A NEW CONCEPT IN FUNCTIONAL ORTHOSES THE KNEE in movement! Climbing stairs, walking and running are everyday actions that we can perform thanks to our knees. The knee joint is one of the most exposed and
What is arthroscopy? Normal knee anatomy
 What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction
 Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction Name:... Surgery Date:... Graft:... Orthopaedic Outpatient Appointment Date: Time: Location: Contact Number: Contacting
Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction Name:... Surgery Date:... Graft:... Orthopaedic Outpatient Appointment Date: Time: Location: Contact Number: Contacting
Patella Tendon Repair
 Alta View Sports Medicine Dr. James R. Meadows, MD Orthopedic Surgery & Sports Medicine 74 Kimballs Ln Ste 230, Draper, UT 84020 9844 S. 1300 E. Ste 100, Sandy, UT 84094 (801) 571-9433 www.meadowsmd.com
Alta View Sports Medicine Dr. James R. Meadows, MD Orthopedic Surgery & Sports Medicine 74 Kimballs Ln Ste 230, Draper, UT 84020 9844 S. 1300 E. Ste 100, Sandy, UT 84094 (801) 571-9433 www.meadowsmd.com
Overview Ligament Injuries. Anatomy. Epidemiology Very commonly injured joint. ACL Injury 20/06/2016. Meniscus Tears. Patellofemoral Problems
 Overview Ligament Injuries Meniscus Tears Pankaj Sharma MBBS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon Manchester Royal Infirmary Patellofemoral Problems Knee Examination Anatomy Epidemiology Very
Overview Ligament Injuries Meniscus Tears Pankaj Sharma MBBS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon Manchester Royal Infirmary Patellofemoral Problems Knee Examination Anatomy Epidemiology Very
Case Study: Christopher
 Case Study: Christopher Conditions Treated Anterior Knee Pain, Severe Crouch Gait, & Hip Flexion Contracture Age Range During Treatment 23 Years to 24 Years David S. Feldman, MD Chief of Pediatric Orthopedic
Case Study: Christopher Conditions Treated Anterior Knee Pain, Severe Crouch Gait, & Hip Flexion Contracture Age Range During Treatment 23 Years to 24 Years David S. Feldman, MD Chief of Pediatric Orthopedic
Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS)
 Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650
Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650
RN(EC) ENC(C) GNC(C) MN ACNP *** MECHANISM OF INJURY.. MOST IMPORTANT ***
 HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient - Certain conditions are more prevalent in particular age groups (Hip pain in children may refer to the knee from Legg-Calve-Perthes
HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient - Certain conditions are more prevalent in particular age groups (Hip pain in children may refer to the knee from Legg-Calve-Perthes
GO Competency Lab Manual Therapy: Soft Tissue Mobilization (STM) 1. Basic Considerations of Manual Therapy
 Manual Therapy: Soft Tissue Mobilization (STM) 1 Upon completion of this lab, clinicians will be able to: 1. Demonstrate the ability to assess soft tissue relative to an orthopedic patient 2. Understand
Manual Therapy: Soft Tissue Mobilization (STM) 1 Upon completion of this lab, clinicians will be able to: 1. Demonstrate the ability to assess soft tissue relative to an orthopedic patient 2. Understand
ACL Reconstruction Rehabilitation Bone Patellar Tendon Bone Graft Kyle F. Chun, MD
 ACL Reconstruction Rehabilitation Bone Patellar Tendon Bone Graft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT
ACL Reconstruction Rehabilitation Bone Patellar Tendon Bone Graft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT
Checklist for Physical Examination of the Knee Muscuoskeletal Block -- Chris McGrew MD, Andrew Ashbaugh DO
 Checklist for Physical Examination of the Knee Muscuoskeletal Block -- Chris McGrew MD, Andrew Ashbaugh DO This handout is for use as a rough guide and study aid. Your instructor may perform certain maneuvers
Checklist for Physical Examination of the Knee Muscuoskeletal Block -- Chris McGrew MD, Andrew Ashbaugh DO This handout is for use as a rough guide and study aid. Your instructor may perform certain maneuvers
AAP Boot Camp KNEE AND ANKLE EXAM
 AAP Boot Camp KNEE AND ANKLE EXAM Disclosures I have no relevant financial relationships with the manufacturers of any commercial products and or providers of commercial services discussed in this CME
AAP Boot Camp KNEE AND ANKLE EXAM Disclosures I have no relevant financial relationships with the manufacturers of any commercial products and or providers of commercial services discussed in this CME
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas Phone: Fax:
 Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 MENISCAL REPAIR PROTOCOL Longitudinal Meniscal Repair This rehabilitation
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 MENISCAL REPAIR PROTOCOL Longitudinal Meniscal Repair This rehabilitation
Below Knee Amputation: Positioning and Exercise Program
 Below Knee Amputation: Positioning and Exercise Program The exercises and stretches in this handout will help to prepare you to wear a prosthesis properly. The positioning instructions and exercises in
Below Knee Amputation: Positioning and Exercise Program The exercises and stretches in this handout will help to prepare you to wear a prosthesis properly. The positioning instructions and exercises in
5 minutes: Attendance and Breath of Arrival. 50 minutes: Problem Solving Ankles and Feet
 5 minutes: Attendance and Breath of Arrival 50 minutes: Problem Solving Ankles and Feet Punctuality- everybody's time is precious: o o Be ready to learn by the start of class, we'll have you out of here
5 minutes: Attendance and Breath of Arrival 50 minutes: Problem Solving Ankles and Feet Punctuality- everybody's time is precious: o o Be ready to learn by the start of class, we'll have you out of here
Patient Information & Exercise Folder
 MEDIAL PATELLO-FEMORAL LIGAMENT RECONSTRUCTION Patient Information & Exercise Folder Mr D Raj FRCS (Tr & Orth) Consultant Lower Limb Orthopaedic Surgeon Pilgrim Hospital, Sibsey Road, Boston Lincolnshire
MEDIAL PATELLO-FEMORAL LIGAMENT RECONSTRUCTION Patient Information & Exercise Folder Mr D Raj FRCS (Tr & Orth) Consultant Lower Limb Orthopaedic Surgeon Pilgrim Hospital, Sibsey Road, Boston Lincolnshire
From Childhood to Adulthood OMT for LOWER EXTREMITY Hip, Knee, Ankle, Foot. Objectives
 From Childhood to Adulthood OMT for LOWER EXTREMITY Hip, Knee, Ankle, Foot Jan Hendryx, DO, FAAO Peek n Peak CME March 1, 2019 Objectives 1. Demonstrate knowledge of the anatomy of the lower extremity-
From Childhood to Adulthood OMT for LOWER EXTREMITY Hip, Knee, Ankle, Foot Jan Hendryx, DO, FAAO Peek n Peak CME March 1, 2019 Objectives 1. Demonstrate knowledge of the anatomy of the lower extremity-
Exercise Therapy for Patients with Knee OA Knee Exercise Protocol Knee Home Exercise Programme
 Chapter FOUR Exercise Therapy for Patients with Knee OA Knee Exercise Protocol Knee Home Exercise Programme Chris Higgs Cathy Chapple Daniel Pinto J. Haxby Abbott 99 n n 100 General Guidelines Knee Exercise
Chapter FOUR Exercise Therapy for Patients with Knee OA Knee Exercise Protocol Knee Home Exercise Programme Chris Higgs Cathy Chapple Daniel Pinto J. Haxby Abbott 99 n n 100 General Guidelines Knee Exercise
GALLAND/KIRBY ISOLATED MENISCAL REPAIR POST- SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY ISOLATED MENISCAL REPAIR POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered, continue
GALLAND/KIRBY ISOLATED MENISCAL REPAIR POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered, continue
GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: - POD 1: Debulk dressing, TED Hose in place - POD 2: Change
GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: - POD 1: Debulk dressing, TED Hose in place - POD 2: Change
A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY
 A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY Georgia Bouffard Student Physiotherapist Colin Walker Orthopaedic Knee Specialist Frank Gilroy BSc MSCP 1 CONTENTS Anatomy of the knee
A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY Georgia Bouffard Student Physiotherapist Colin Walker Orthopaedic Knee Specialist Frank Gilroy BSc MSCP 1 CONTENTS Anatomy of the knee
GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing,
GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing,
Hip Pain. Anatomy of the hip
 Hip Pain Anatomy of the hip The hip is a ball and socket joint, the ball is on the head of femur (the top of the thigh bone) and the socket (acetabulum) is a part of the pelvis. It s surrounded by tendons
Hip Pain Anatomy of the hip The hip is a ball and socket joint, the ball is on the head of femur (the top of the thigh bone) and the socket (acetabulum) is a part of the pelvis. It s surrounded by tendons
Noyes Knee Institute Rehabilitation Protocol: Posterolateral Knee Reconstruction
 Noyes Knee Institute Rehabilitation Protocol: Posterolateral Knee Reconstruction Brace: Bivalved cylinder cast Custom medial unloader or hinged soft tissue brace minimum goals: 0-90 0-110 0-120 0-130 Weight
Noyes Knee Institute Rehabilitation Protocol: Posterolateral Knee Reconstruction Brace: Bivalved cylinder cast Custom medial unloader or hinged soft tissue brace minimum goals: 0-90 0-110 0-120 0-130 Weight
Practical 1 Worksheet
 Practical 1 Worksheet ANATOMICAL TERMS 1. Use the word bank to fill in the missing words. reference side stand body arms palms anatomical forward All anatomical terms have a(n) point which is called the
Practical 1 Worksheet ANATOMICAL TERMS 1. Use the word bank to fill in the missing words. reference side stand body arms palms anatomical forward All anatomical terms have a(n) point which is called the
th Maccabiah Games Handbook Australian Swim Team Information Pack
 SELF CARE/RECOVERY STRETCHING: Stretching is a vitally important part of the conditioning aspect of your training. Stretching helps in the recovery of muscles. It lengthens and realigns shortened muscle
SELF CARE/RECOVERY STRETCHING: Stretching is a vitally important part of the conditioning aspect of your training. Stretching helps in the recovery of muscles. It lengthens and realigns shortened muscle
DON T JUST PROVIDE A BAND-AID ELIZABETH COLE, MSPT, ATP U.S. Rehab / VGM
 DON T JUST PROVIDE A BAND-AID ELIZABETH COLE, MSPT, ATP U.S. Rehab / VGM Selecting the most appropriate product solutions for specific postural problems should be a thoughtful exercise in analyzing the
DON T JUST PROVIDE A BAND-AID ELIZABETH COLE, MSPT, ATP U.S. Rehab / VGM Selecting the most appropriate product solutions for specific postural problems should be a thoughtful exercise in analyzing the
Knee disarticulation versus above-knee amputation*
 Prosthetics and Orthotics International, 1979, 3, 15-19 Knee disarticulation versus above-knee amputation* R. F. BAUMGARTNER Balgrist Orthopaedic Hospital, University of Zurich. Abstract If below-knee
Prosthetics and Orthotics International, 1979, 3, 15-19 Knee disarticulation versus above-knee amputation* R. F. BAUMGARTNER Balgrist Orthopaedic Hospital, University of Zurich. Abstract If below-knee
Mr Paul Y F Lee All in side - ACL Reconstruction Version 2.2. Sports Knee Surgery. Rehabilitation protocol. ACL Reconstruction.
 Sports Knee Surgery Rehabilitation protocol ACL Reconstruction ACL Repair Meniscus Repair Surgeon: Paul Y F Lee MBBch, MFSEM, MSc, PhD, FRCS (T&O) Why ACL Reconstruction? The ACL helps to stabilize the
Sports Knee Surgery Rehabilitation protocol ACL Reconstruction ACL Repair Meniscus Repair Surgeon: Paul Y F Lee MBBch, MFSEM, MSc, PhD, FRCS (T&O) Why ACL Reconstruction? The ACL helps to stabilize the
Bunion (hallux valgus deformity) surgery
 Bunion (hallux valgus deformity) surgery Bunion surgery is generally reserved for bunions that are severe and impacting on function. There most frequent surgical procedure used involves a medial incision
Bunion (hallux valgus deformity) surgery Bunion surgery is generally reserved for bunions that are severe and impacting on function. There most frequent surgical procedure used involves a medial incision
North of England Bone and Soft Tissue Tumour Service
 North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after proximal tibial replacement Proximal tibial replacement surgery is usually carried out as part of treatment for
North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after proximal tibial replacement Proximal tibial replacement surgery is usually carried out as part of treatment for
Hip Arthroscopy Rehabilitation Protocol
 Hip Arthroscopy Rehabilitation Protocol 1. Concepts: a. Range of motion and weight bearing restrictions must be adhered to during the initial rehab process (4 total weeks of ROM and weight bearing restrictions)
Hip Arthroscopy Rehabilitation Protocol 1. Concepts: a. Range of motion and weight bearing restrictions must be adhered to during the initial rehab process (4 total weeks of ROM and weight bearing restrictions)
Anterior Cruciate Ligament (ACL) Rehabilitation
 Thomas D. Rosenberg, M.D. Vernon J. Cooley, M.D. Anterior Cruciate Ligament (ACL) Rehabilitation Dear Enclosed you will find a copy of our Anterior Cruciate Ligament (ACL) Rehabilitation program and the
Thomas D. Rosenberg, M.D. Vernon J. Cooley, M.D. Anterior Cruciate Ligament (ACL) Rehabilitation Dear Enclosed you will find a copy of our Anterior Cruciate Ligament (ACL) Rehabilitation program and the
Knee Capsular Disorder. ICD-9-CM: Stiffness in joint of lower leg, not elsewhere classified
 1 Knee Capsular Disorder "Knee Capsulitis" ICD-9-CM: 719.56 Stiffness in joint of lower leg, not elsewhere classified Diagnostic Criteria History: Physical Exam: Stiffness Aching with prolonged weight
1 Knee Capsular Disorder "Knee Capsulitis" ICD-9-CM: 719.56 Stiffness in joint of lower leg, not elsewhere classified Diagnostic Criteria History: Physical Exam: Stiffness Aching with prolonged weight
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
7/20/14. Patella Instability. Alignment. PF contact areas. Tissue Restraints. Pain. Acute Blunt force trauma Disorders of the Patellafemoral Joint
 Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Foot and ankle. Achilles tendon rupture repair. After surgery
 Foot and ankle Achilles tendon rupture repair There is no agreed single best treatment for Achilles tendon ruptures. Similar results can be achieved with non-surgical and surgical treatments. There is
Foot and ankle Achilles tendon rupture repair There is no agreed single best treatment for Achilles tendon ruptures. Similar results can be achieved with non-surgical and surgical treatments. There is
Protocol for the Management of Hip Arthroscopy Surgery
 Overall Aims of Surgery To decrease pain To increase range of motion (ROM) To increase hip/pelvis and lumbar stability To enable return to activities of daily living and sport Initial Post-operative Objectives
Overall Aims of Surgery To decrease pain To increase range of motion (ROM) To increase hip/pelvis and lumbar stability To enable return to activities of daily living and sport Initial Post-operative Objectives
Physical Examination of the Knee
 History: Pain Traumatic vs. atraumatic Acute vs Chronic Mechanism of injury Swelling, catching, instability Previous evaluation and treatment General Setup Examine standing, sitting and supine Evaluate
History: Pain Traumatic vs. atraumatic Acute vs Chronic Mechanism of injury Swelling, catching, instability Previous evaluation and treatment General Setup Examine standing, sitting and supine Evaluate
Goals &Objectives. 1. Review the anatomy of the knee 2. Practice your hands-on skills 3. By the end of the workshop:
 Clinical Knee Exam Goals &Objectives 1. Review the anatomy of the knee 2. Practice your hands-on skills 3. By the end of the workshop: Be able to categorize knee injuries Understand the significance of
Clinical Knee Exam Goals &Objectives 1. Review the anatomy of the knee 2. Practice your hands-on skills 3. By the end of the workshop: Be able to categorize knee injuries Understand the significance of
Section Three: The Leg, Ankle, and Foot Lecture: Review of Clinical Anatomy, Patterns of Dysfunction and Injury, and
 Section Three: The Leg, Ankle, and Foot Lecture: Review of Clinical Anatomy, Patterns of Dysfunction and Injury, and Treatment Implications for the Leg, Ankle, and Foot Levels I and II Demonstration and
Section Three: The Leg, Ankle, and Foot Lecture: Review of Clinical Anatomy, Patterns of Dysfunction and Injury, and Treatment Implications for the Leg, Ankle, and Foot Levels I and II Demonstration and
Heidi Sanders, OTR/L. Amy Shuckra, MPT
 Adaptive Equipment Heidi Sanders, OTR/L University of New Mexico Health Sciences Center, Los Pasos Program Amy Shuckra, MPT Shriners Hospitals for Children Salt Lake City, Utah What is Adaptive Equipment?
Adaptive Equipment Heidi Sanders, OTR/L University of New Mexico Health Sciences Center, Los Pasos Program Amy Shuckra, MPT Shriners Hospitals for Children Salt Lake City, Utah What is Adaptive Equipment?
GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction
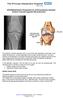 GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction Femur ACL Graft Fibula Tibia The Anterior Cruciate Ligament (ACL) is one of the main ligaments in the
GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction Femur ACL Graft Fibula Tibia The Anterior Cruciate Ligament (ACL) is one of the main ligaments in the
Non Surgical Hip Therapy Athletic Hip Injury: Therapist Information
 Non Surgical Hip Therapy Athletic Hip Injury: Therapist Information Please read entire protocol prior to initiating therapy Please note: Individual hip injuries vary widely. This therapy protocol should
Non Surgical Hip Therapy Athletic Hip Injury: Therapist Information Please read entire protocol prior to initiating therapy Please note: Individual hip injuries vary widely. This therapy protocol should
GENERAL EXERCISES KNEE BMW MANUFACTURING CO. PZ-AM-G-US I July 2017
 GENERAL EXERCISES KNEE BMW MANUFACTURING CO. PZ-AM-G-US I July 2017 Disclosure: The exercises, stretches, and mobilizations provided in this presentation are for educational purposes only are not to be
GENERAL EXERCISES KNEE BMW MANUFACTURING CO. PZ-AM-G-US I July 2017 Disclosure: The exercises, stretches, and mobilizations provided in this presentation are for educational purposes only are not to be
Non Surgical Management Of Hip And Knee Osteoarthritis Toolkit. Evaluation and Diagnosis of Osteoarthritis in Primary Care
 Non Surgical Management Of Hip And Knee Osteoarthritis Toolkit Evaluation and Diagnosis of Osteoarthritis in Primary Care OA-HxPE-716.indd 1 TABLE OF CONTENTS HISTORY TAKING... 3 EVALUATION OF SUSPECTED
Non Surgical Management Of Hip And Knee Osteoarthritis Toolkit Evaluation and Diagnosis of Osteoarthritis in Primary Care OA-HxPE-716.indd 1 TABLE OF CONTENTS HISTORY TAKING... 3 EVALUATION OF SUSPECTED
Above Knee Amputation: Positioning and Exercise Program
 Above Knee Amputation: Positioning and Exercise Program The exercises and stretches in this handout will help to prepare you to wear a prosthesis properly. The positioning instructions and exercises in
Above Knee Amputation: Positioning and Exercise Program The exercises and stretches in this handout will help to prepare you to wear a prosthesis properly. The positioning instructions and exercises in
Physical Examination of the Knee
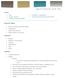 History: Pain Traumatic vs. atraumatic? Acute vs Chronic Previous procedures done on the knee? Swelling, catching, instability General Setup Examine standing, sitting and supine Evaluate gait Examine hip
History: Pain Traumatic vs. atraumatic? Acute vs Chronic Previous procedures done on the knee? Swelling, catching, instability General Setup Examine standing, sitting and supine Evaluate gait Examine hip
Chapter 29 Orthopaedic Injuries Principles of Splinting Types of Muscles
 1 2 3 4 5 6 7 Chapter 29 Orthopaedic Injuries Principles of Splinting Types of Muscles Striated Skeletal Smooth Anatomy and Physiology of the Musculoskeletal System Skeletal System Skeletal System Functions
1 2 3 4 5 6 7 Chapter 29 Orthopaedic Injuries Principles of Splinting Types of Muscles Striated Skeletal Smooth Anatomy and Physiology of the Musculoskeletal System Skeletal System Skeletal System Functions
ARTHROSCOPIC LABRAL REPAIR WITH CAPSULAR PLICATION PHYSICAL THERAPY PROTOCOL
 ARTHROSCOPIC LABRAL REPAIR WITH CAPSULAR PLICATION PHYSICAL THERAPY PROTOCOL Jovan R. Laskovski, M.D. Hip Arthroscopy Sports Medicine & Orthopaedic Surgery Crystal Clinic Orthopaedic Center Please use
ARTHROSCOPIC LABRAL REPAIR WITH CAPSULAR PLICATION PHYSICAL THERAPY PROTOCOL Jovan R. Laskovski, M.D. Hip Arthroscopy Sports Medicine & Orthopaedic Surgery Crystal Clinic Orthopaedic Center Please use
