Physiotherapy management
|
|
|
- Helena Boyd
- 5 years ago
- Views:
Transcription
1 Physiotherapy management
2 Pre-operative Focus is on the objective assessment looking at ROM and muscle power. Using assessment findings, knowledge of prosthetic componentry and gait patterns, provide a clinically reasoned recommended level of amputation to the consultant. Provide patient with appropriate exercises to aid post-amputation mobility.
3 Pre Surgery Teach post amputation exercises..prone lying, limb abduction, hip extension, static quads contraction Do s and Don ts contracture prevention Educate patient about phantom pain and the difference between stump and phantom pain Inform about the bandaging routine and why Fit the patient with mobility aids (axillary crutches usually the best), train him to use them, including negotiating stairs safely Be careful when talking about prosthetic options not all patients qualify, do not raise expectations But if appropriate, educate patient about their likely prosthetic option and functional capacity post amputation
4 Pre Surgery cont. Family members likely to be present and have views about amputation Try to educate them, the patient, not the family should make the decision Describe the likely functional activity level post amputation Check on home and social situation wheelchair / crutches access and former occupation If patient a smoker explain the risks and teach DB&C. (Surgeon will reinforce healing consequences of smoking.)
5 Post Surgery Day 1 Check on pain level, patient will be heavily medicated. Start static exercises, then active hip abd / add, flex / ext with PT supporting and guiding the stump. Hip extension in side lying if prone lying too painful (depends on wound location and bandaging). Position of stump in bed minimize stump / hip flexion, remove pillows if placed under stump For TT a knee extension slab may be ordered by surgeon If patient alert commence moving in the bed, S to S rolling, bridging, abduction of stump If patient alert and vital signs good you can assist patient to sit over the edge of the bed (SOOB).
6 Day 2 time to mobilise Stump exercises in bed with PT guidance. Stronger bridging exercise. SOOB. If no dizziness after 2 mins you can try a supported stand on sound limb, beside the bed in walking frame or crutches. PT must monitor patient closely and be positioned to support patient if they faint (anaesthetic and pain medications can cause nausea and hypotension, do not walk the patient if drowsy, dizzy or nauseated) Commence stump exercises in standing if patient condition allows. Gentle walking in high frame, or on crutches depending on age, strength and medical status. Important to mobilise early, if possible, to prevent muscle wasting and respiratory complications. Close monitoring by PT to prevent patient falling. Patient to mobilise generally in a wheelchair with knee extension board (or crutch) under the TT stump to prevent constant knee flexion
7 Day 3 to Discharge Patient should be mobilizing on crutches (or in wheelchair if crutches not possible due to complications, age, weight etc). If slow on crutches assist to walk daily in a walking frame Patient should lie prone 30 mins twice daily to prevent iliopsoas tightening Stump should be bandaged and positioned in the neutral position, not in flexion or abduction Patient to do stump exercises, at least twice daily Day 7 10 stitches removed and compressive stump bandaging should begin
8 Pain Differentiate between stump and phantom pain Inform Dr. if phantom pain present (different medications helpful) Stump pain will subside over first week, tenderness over the scar area will continue for some weeks Scar desensitization program may begin after suture removal (5 mins daily gentle massage with soft substance (cotton wool then gauze, then progress to rougher material), then 5 mins gentle tapping over distal end of stump with fingers, the process can take several weeks
9 Compressive Bandaging Commences post surgery, usually after suture removal. Should continue until fitting of the prosthesis. Patient should learn to do himself before discharge. Otherwise the carer should be trained. Surgeon and Nursing staff will monitor wound healing in hospital. PT to monitor any wound changes during Rehabilitation. Be aware of suture location and prevent pressure on or stretching of the suture line with the early post op exercises Stump volume can take 4 6 months to stabilize Stump socks may replace bandages in some countries
10 Why Bandage.? Helps shape the stump for prosthesis Decreases oedema (to test for oedema press your finger tip against the swelling for 1 min. Remove finger, if dimple remains = oedema). Increases distal circulation (by decreasing venous stasis) Provides skin protection In some cases a rigid bandage or POP caste may be applied post surgery for several weeks
11 Bandaging TT 11
12 Bandaging TF 12
13 Immediate post-operative prosthetic fitting It can be done especially for children The main aims are: Control of pain. Prevention of edema. Prevention of infection. Prevention of deformity/ stiffness. Prevention of DVT. Improving muscle power. Psychological confidence.
14
15 Stump Hygiene Cannot be overemphasized with patient Wash stump with soap and water daily (preferably at night) Ensure bandages are clean and dry Check skin condition daily The smallest wound / infection can be a big problem and delay wearing a prosthesis Keep stump dry, change bandages more often than daily if required
16 Psychology Patient may be depressed, think their previous life is over, tendency to hide from the world Immediately post surgery may refuse to look at or touch the stump. PT s job to address this. Then to keep them busy with exercises and focused on their training program, looking ahead Good to bring them to Rehab setting ASAP to meet and observe other amputees Use the wheelchair / crutches to re-engage with outside world. Educate carers to support the patient but also encourage independence.
17 Discharge Home Program Stump massage twice daily (5 mins per session) 2 X daily prone lying (30 mins) Stump exercises Hip / stump extension (prone), stump abduction (prone or sidelying) Knee extension (TT) in supine or sitting, 3 X 10 reps then build to a full straight leg raise Bridging on the stump (supported by firm cushion or towell) Upper limb strengthening (push up, arm or wheelchair lift, hand weights (biceps / triceps / shoulder girdle), trunk / abdominal strengthening Independent with transfers and toileting, if possible Mobilising on crutches +++, safely and on all terrain
18 Challenging Home Environment Refugees or vulnerable persons returning to refugee camp like conditions must be proficient on crutches or be given a wheelchair. Camps are placed on uneven, muddy (even flooded) ground, with few safe walking tracks, latrines located a long distance from tent, no supports in place in the latrine area Emphasize the importance of the daily stump wash with soap and water, and good drying. Stump bandages need to be cleaned regularly also. Exercises can all be done on simple mat on dry ground. Encourage patient to exercise and strengthen +++
19 POSITIONING ADVICE TO PATIENT
20 POSITIONING
21 POSITIONING To roll prone the client must turn towards the sound side, the PT ensuring that the stump is lowered gently. At first the client lies prone for 10 min only. The amputee should then build up to lying prone for 30 min 3 times a day.
22 POSITIONING
23 TRANSFERS / bed-chair Transfer method n 1: standing pivot transfer (patient must participate as much as possible).
24 TRANSFERS / bed-chair Transfer method n 2: backwards forwards transfer
25 TRANSFERS / bed-chair Transfer method n 3: sliding board transfer
26 Falls Prevention Transfers: Floor to Chair Good transfer technique (don t rush) Carers who are trained by the PT Sliding board helpful for TF or bilateral amputees Identify high fall risk patients and adjust their mobility program, aides and carer instructions accordingly
27 Whilst at Home Minimum 3 months required from amputation to prosthetic screening appointment, in best case scenario. Allow more time for complex cases (infections, other injuries, systemic disease) Patient should continue Home Program (2 hours work per day) in the meantime. Very important patient is mobilizing throughout day and not remaining in wheelchair or bed. Body deconditioning a major limitation for prosthetic use and outcomes
28 Preparing the stump for weight bearing After 3 months Push the end of the stump in the cushion of a chair. Push for 5 seconds and release the pressure. Repeat the procedure 20 times and several times a day.
29 Screening : Ready for a Prosthesis? No hip flexion contracture present (or at least <10 degrees) Stump volume is stable Muscle strength 4 5 (preferably 5) Balance good, able to stand on sound leg for 1 min Able to walk with mobility aid for 10 mins Energy requirements: TT - > 60 %, TF - > 120 %, Hip Disart - > 200 %
30 If not ready then more physiotherapy! Stump bandaging Intensive exercise and stretching (also passive) Intensive balance work Intensive upper limb work NB: All bilateral amputees should be issued with a wheelchair Some unilateral amputees will also need one, but guard against wheelchair dependence
31 Fitting Considerations Patient Age - the energy cost of a prosthesis may be too high for a patient over 50 in poor health Health diabetes and vascular disease may be too advanced to manage the energy and balance requirement Post op morbidity of amputation patients over 65 very high (especially with diabetes and PVD) Weight of prosthesis the lighter the prosthesis the lower the energy cost (ICRC components are light) Note: energy cost of using crutches is higher than that of a TF amputation
32 Pre-prosthetic rehabilitation???
33 Purpose of pre- prosthetic rehabilitation Physical and psychological recovery from the surgical intervention. Preparation of the body for the prosthesis. Mental preparation for a life with a prosthesis. 33
34 Aim of physiotherapy Reduce swelling. Prevent contractures. Manage pain, decreasing residual limb pain (also known as phantom pain ). Prepare people with amputations for the use of a prosthesis. 34
35 3) Pre- prosthetic training Loss of part of the body causes a change in the position of centre of gravity. Balance is disrupted and it takes time and effort to regain good control. Pre-prosthetic training influence the recovery of adequate coordination. Prepares for prosthetic rehabilitation. 35
36 3) Pre- prosthetic training Strengthening exercises ROM exercises Stretching exercises, Balance and coordination, Functional activities. 36
37 Strengthening exercises Strengthening exercises are important to enable people with amputations to get the skills needed for transfer, functional skills and ambulation. The type of strengthening exercise depend on individual muscular strength and endurance, the level of independence, access to equipment, time constraints, safety. The most usual techniques employed are: isometric strengthening; manual resistance strengthening; and concentric strengthening. The exercises should focus on the muscles of the amputated leg, the sound leg, the upper extremities and the muscles of the trunk. 37
38 Range of motion and stretching exercises Must be specific and target the adequate muscles. Movements should be slow, soft and held over time. Manual stretching passive joint mobilization passive or self-stretching contract-relax stretching 38
39 Balance Use a variety of exercises in lying, sitting and standing positions. It is important for patients to exercise in a safe environment and avoid falling (parallel bars, hand control, soft mattress). 39
40 Functional activities The greater the degree of mobility and activity gained by persons with amputations without a prosthesis, the greater the functional result with the prosthesis will likely be. Rehabilitation should also consist of a well-defined home program of exercises and exposure to activities of daily life within their usual context. 40
41
42
43
44
45
46
47
48
49
50
51 Prosthetic prescription Physiotherapist may be needed to assist in the cast appointment, to ensure a neutral alignment of the pelvis is obtained. Physiotherapy provides intervention on mobility guidance, static balance and weight bearing
52 Basically we can make 3 groups: Ready for fitting Preparation required for fitting Can not be fitted
53 Category one Yes, service user is ready for fitting: No oedema, No contracture, Free scar, No wound, No muscle weakness, General condition is good. 53
54 Category two Yes, service user is ready for fitting but pre fitting therapy is needed: Oedema, Contracture, Adherent scar, Wound, Bad hygiene, Neuroma, Bone spur, Muscle weakness. 54
55 Category three Prosthesis is technically not possible Service user is not in condition to be fitted Service user is not willing to be fitted
56 Prosthetic Training The physiotherapist takes a lead role at this stage. Beginning with educating the patient about donning and doffing the prosthesis, skin integrity and weight bearing areas on their residuum. A gait rehabilitation programme can then commence.
57 The first fitting process A continuous process of interaction between the patient, the prosthetist and the physiotherapist. Evaluations are made throughout this process to prevent, detect and correct unfavorable outcomes that might have developed (socket design/alignment). 57
58 The aim of the first fitting To reduce to a minimum the gait deviations seen as a result of the prosthetic construction (socket design/bench alignment). 58
59 The role of the physiotherapist Explain the aim and the outline of the fitting process to the person with an amputation Re-examine the person Re-examine the stump Check the prosthesis prescription Inspect the prosthesis 59
60 Fitting a prosthesis 1) Prescription and design 2) Footwear 3) Bench alignment 4) Static alignment, sitting and standing 5) Doffing- removing the prosthesis 60
61 Prosthetic training Orientation of Centre of Gravity and Weight Bearing on the Prosthesis Lateral weight shifting Forward and back weight shifting High stepping Balance board Throwing and catching Obstacle stepping Single leg standing Gait Re-Education
62 Prosthetic training Backward walking Multidirectional changes Tandem walking Stairs Slopes/hills Weight carrying Uneven surfaces Cycling Treadmill Trampoline
63 Discharge Management The physiotherapist should ensure that they include education for ongoing management, strategies for coping and training for resumption of functional activities.
64 Follow up The consultant and/or prosthetist may ask for physiotherapy input. For example if the patient is having a change of prescription, their goals have changed, their mobility has decreased/increased. The physiotherapist may be required to re-commence a gait rehabilitation programme with the patient or advice only may be required
65 Thank you
Below Knee Amputation: Positioning and Exercise Program
 Below Knee Amputation: Positioning and Exercise Program The exercises and stretches in this handout will help to prepare you to wear a prosthesis properly. The positioning instructions and exercises in
Below Knee Amputation: Positioning and Exercise Program The exercises and stretches in this handout will help to prepare you to wear a prosthesis properly. The positioning instructions and exercises in
Above Knee Amputation: Positioning and Exercise Program
 Above Knee Amputation: Positioning and Exercise Program The exercises and stretches in this handout will help to prepare you to wear a prosthesis properly. The positioning instructions and exercises in
Above Knee Amputation: Positioning and Exercise Program The exercises and stretches in this handout will help to prepare you to wear a prosthesis properly. The positioning instructions and exercises in
Overview Functional Training
 Overview Functional Training Exercises with Therapist 1. Sitting 2. Standing up vs. Sitting down 3. Standing 4. Stance phase ( Static and dynamic ) 5. Swing phase 6. Gait Evaluation 7. Walking level ground
Overview Functional Training Exercises with Therapist 1. Sitting 2. Standing up vs. Sitting down 3. Standing 4. Stance phase ( Static and dynamic ) 5. Swing phase 6. Gait Evaluation 7. Walking level ground
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
Prosthetic Rehab Plan
 Prosthetic Rehab Plan First 4 6 weeks after surgery Until sutures are removed, follow the instructions below: Gently wash your limb daily with anti-bacterial soap and water Wear the brown stump shrinker
Prosthetic Rehab Plan First 4 6 weeks after surgery Until sutures are removed, follow the instructions below: Gently wash your limb daily with anti-bacterial soap and water Wear the brown stump shrinker
Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction
 Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction Name:... Surgery Date:... Graft:... Orthopaedic Outpatient Appointment Date: Time: Location: Contact Number: Contacting
Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction Name:... Surgery Date:... Graft:... Orthopaedic Outpatient Appointment Date: Time: Location: Contact Number: Contacting
Below Knee Amputation: Post-op Information
 Below Knee Amputation: Post-op Information This package contains information to help as you begin the recovery process following your amputation. The topics included are: Emotions following an amputation.
Below Knee Amputation: Post-op Information This package contains information to help as you begin the recovery process following your amputation. The topics included are: Emotions following an amputation.
Home Exercise Program Progression and Components of the LTP Intervention. HEP Activities at Every Session Vital signs monitoring
 Home Exercise Program Progression and Components of the LTP Intervention HEP Activities at Every Session Vital signs monitoring Blood pressure, heart rate, Borg Rate of Perceived Exertion (RPE) and oxygen
Home Exercise Program Progression and Components of the LTP Intervention HEP Activities at Every Session Vital signs monitoring Blood pressure, heart rate, Borg Rate of Perceived Exertion (RPE) and oxygen
EXERCISES FOR AMPUTEES. Joanna Wojcik & Niki Marjerrison
 EXERCISES FOR AMPUTEES Joanna Wojcik & Niki Marjerrison Amputation A condition of disability resulting from the loss of one or more limbs 1.7 million people living with limb loss in the US (1 out of every
EXERCISES FOR AMPUTEES Joanna Wojcik & Niki Marjerrison Amputation A condition of disability resulting from the loss of one or more limbs 1.7 million people living with limb loss in the US (1 out of every
Assessment and problem solving: starting with a temporary prosthesis
 Assessment and problem solving: starting with a temporary prosthesis Stump assessment Skin Colour, temperature, appearance sensitivity and allergies to materials Integrity eg frail, thin, dry Abrasions,
Assessment and problem solving: starting with a temporary prosthesis Stump assessment Skin Colour, temperature, appearance sensitivity and allergies to materials Integrity eg frail, thin, dry Abrasions,
Above Knee Amputation: Post-op Information
 Above Knee Amputation: Post-op Information This package contains information to help as you begin the recovery process following your amputation. The topics included are: Emotions following an amputation.
Above Knee Amputation: Post-op Information This package contains information to help as you begin the recovery process following your amputation. The topics included are: Emotions following an amputation.
Rehabilitation programme after hemiarthroplasty surgery
 Rehabilitation programme after hemiarthroplasty surgery Information for patients at Princess Royal University Hospital This leaflet gives you advice about the things you can do after your operation both
Rehabilitation programme after hemiarthroplasty surgery Information for patients at Princess Royal University Hospital This leaflet gives you advice about the things you can do after your operation both
Total Hip Replacement Rehabilitation: Progression and Restrictions
 Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Rehabilitation. Walking after Total Knee Replacement. Continuous Passive Motion Device
 Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R
 S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H L A B R A L R E P A I R P R O T O C O L This protocol provides appropriate guidelines
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H L A B R A L R E P A I R P R O T O C O L This protocol provides appropriate guidelines
REHABILITATION FOLLOWING ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION (using Hamstring Graft)
 REHABILITATION FOLLOWING ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION (using Hamstring Graft) PHASE 1: (0-3 WEEKS) Goal: Protect graft, manage pain, decrease swelling and improve range of movement. To optimise
REHABILITATION FOLLOWING ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION (using Hamstring Graft) PHASE 1: (0-3 WEEKS) Goal: Protect graft, manage pain, decrease swelling and improve range of movement. To optimise
Therapy following a neck of femur fracture
 INFORMATION FOR PATIENTS Therapy following a neck of femur fracture Name of patient: ffffffffffffffffffffffffffffffffffffffffffff Procedure: ffffffffffffffffffffffffffffffffffffffffffffffffffff Consultant:
INFORMATION FOR PATIENTS Therapy following a neck of femur fracture Name of patient: ffffffffffffffffffffffffffffffffffffffffffff Procedure: ffffffffffffffffffffffffffffffffffffffffffffffffffff Consultant:
Heel Slides. Isometric Quad. For Appointments call:
 For Appointments call: 612-672-7100 Login ptrx.org/en/fv2d6ekjsq Exercise Prescription Date May 11, 2017 Assigning Provider Shannon Kelly PT, OCS Prescription Description - Post-op Phase 1 & 2 Heel Slides
For Appointments call: 612-672-7100 Login ptrx.org/en/fv2d6ekjsq Exercise Prescription Date May 11, 2017 Assigning Provider Shannon Kelly PT, OCS Prescription Description - Post-op Phase 1 & 2 Heel Slides
REHABILITATION AFTER ARTHROSCOPIC KNEE SURGERY
 REHABILITATION AFTER ARTHROSCOPIC KNEE SURGERY This protocol is a guideline for your rehabilitation after arthroscopic knee surgery. You may vary in your ability to do these exercises and to progress to
REHABILITATION AFTER ARTHROSCOPIC KNEE SURGERY This protocol is a guideline for your rehabilitation after arthroscopic knee surgery. You may vary in your ability to do these exercises and to progress to
Gregory H. Tchejeyan, M.D. Orthopaedic Surgery of the Hip and Knee
 TOTAL KNEE REPLACEMENT (TKR) POST-OPERATIVE REHABILITATION PROTOCOL PRE-OPERATIVE PHYSICAL THERAPY The patient is seen for a pre-operative physical therapy session which includes: o Review of the TKR protocol.
TOTAL KNEE REPLACEMENT (TKR) POST-OPERATIVE REHABILITATION PROTOCOL PRE-OPERATIVE PHYSICAL THERAPY The patient is seen for a pre-operative physical therapy session which includes: o Review of the TKR protocol.
Advice: After the Removal of a Lower Leg Cast
 Advice: After the Removal of a Lower Leg Cast The aim of this leaflet is to give you some understanding of the problems you have with your condition and to provide some advice on how to manage this. It
Advice: After the Removal of a Lower Leg Cast The aim of this leaflet is to give you some understanding of the problems you have with your condition and to provide some advice on how to manage this. It
Rehabilitation. Walkers, Crutches, Canes
 Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Exercise Therapy for Patients with Knee OA Knee Exercise Protocol Knee Home Exercise Programme
 Chapter FOUR Exercise Therapy for Patients with Knee OA Knee Exercise Protocol Knee Home Exercise Programme Chris Higgs Cathy Chapple Daniel Pinto J. Haxby Abbott 99 n n 100 General Guidelines Knee Exercise
Chapter FOUR Exercise Therapy for Patients with Knee OA Knee Exercise Protocol Knee Home Exercise Programme Chris Higgs Cathy Chapple Daniel Pinto J. Haxby Abbott 99 n n 100 General Guidelines Knee Exercise
POSTNATAL EXERCISES. (Early In Patient Postnatal Days Until Six Weeks Post Delivery)
 POSTNATAL EXERCISES (Early In Patient Postnatal Days Until Six Weeks Post Delivery) Exercise Regularly This brochure is intended to educate women about mobility and exercises while as an In Patient and
POSTNATAL EXERCISES (Early In Patient Postnatal Days Until Six Weeks Post Delivery) Exercise Regularly This brochure is intended to educate women about mobility and exercises while as an In Patient and
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R
 S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H This protocol provides appropriate guidelines for the rehabilitation of patients following
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H This protocol provides appropriate guidelines for the rehabilitation of patients following
Exercises and advice following your breast reconstruction surgery
 Exercises and advice following your breast reconstruction surgery This leaflet gives information to people who have had breast reconstructive surgery. It contains exercises that your physiotherapist would
Exercises and advice following your breast reconstruction surgery This leaflet gives information to people who have had breast reconstructive surgery. It contains exercises that your physiotherapist would
GETTING READY FOR TOTAL HIP REPLACEMENT
 GETTING READY FOR TOTAL HIP REPLACEMENT Pre-Op Exercises for a Better Recovery Your Recovery Begins Now Even if your hip replacement surgery is weeks or months away, start getting ready now. People who
GETTING READY FOR TOTAL HIP REPLACEMENT Pre-Op Exercises for a Better Recovery Your Recovery Begins Now Even if your hip replacement surgery is weeks or months away, start getting ready now. People who
Mosaicplasty and OATS Rehabilitation Protocol
 Mosaicplasty and OATS Rehabilitation Protocol PHASE 1: 0 2 weeks after surgery You will go home with crutches, cryocuff cold therapy unit and a CPM machine. GOALS: 1. Protect the cartilage transfer avoid
Mosaicplasty and OATS Rehabilitation Protocol PHASE 1: 0 2 weeks after surgery You will go home with crutches, cryocuff cold therapy unit and a CPM machine. GOALS: 1. Protect the cartilage transfer avoid
Posterior/Direct Total Hip Arthroplasty Rehabilitation Guideline
 Posterior/Direct Total Hip Arthroplasty Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for
Posterior/Direct Total Hip Arthroplasty Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for
Internal Rotation (turning toes/knee toward other leg) 30 degree limit. limit
 Hip Arthroscopy Patient Education Use of Brace and Crutches: - Wear the brace all times of weight bearing for the first 3 weeks after surgery. This is done to protect your hip and motion into hip extension
Hip Arthroscopy Patient Education Use of Brace and Crutches: - Wear the brace all times of weight bearing for the first 3 weeks after surgery. This is done to protect your hip and motion into hip extension
Mr Paul Y F Lee All in side - ACL Reconstruction Version 2.2. Sports Knee Surgery. Rehabilitation protocol. ACL Reconstruction.
 Sports Knee Surgery Rehabilitation protocol ACL Reconstruction ACL Repair Meniscus Repair Surgeon: Paul Y F Lee MBBch, MFSEM, MSc, PhD, FRCS (T&O) Why ACL Reconstruction? The ACL helps to stabilize the
Sports Knee Surgery Rehabilitation protocol ACL Reconstruction ACL Repair Meniscus Repair Surgeon: Paul Y F Lee MBBch, MFSEM, MSc, PhD, FRCS (T&O) Why ACL Reconstruction? The ACL helps to stabilize the
KNEE AND LEG EXERCISE PROGRAM
 KNEE AND LEG EXERCISE PROGRAM These exercises are specifically designed to rehabilitate the muscles of the hip and knee by increasing the strength and flexibility of the involved leg. This exercise program
KNEE AND LEG EXERCISE PROGRAM These exercises are specifically designed to rehabilitate the muscles of the hip and knee by increasing the strength and flexibility of the involved leg. This exercise program
Information and exercises following a proximal femoral replacement
 Physiotherapy Department Information and exercises following a proximal femoral replacement Introduction The hip joint is a type known as a ball and socket joint. The cup side of the joint is known as
Physiotherapy Department Information and exercises following a proximal femoral replacement Introduction The hip joint is a type known as a ball and socket joint. The cup side of the joint is known as
PCL/PLC RECONSTRUCTION REHABILITATION Revised OCTOBER 2015
 PCL/PLC RECONSTRUCTION REHABILITATION Revised OCTOBER 2015 REHABILITATION PROGRAM PHASE 1: WEEKS 0-6: PHASE I GOALS: Protect the surgical graft(s) 0-60 ROM Regain adequate quadriceps control CRUTCHES:
PCL/PLC RECONSTRUCTION REHABILITATION Revised OCTOBER 2015 REHABILITATION PROGRAM PHASE 1: WEEKS 0-6: PHASE I GOALS: Protect the surgical graft(s) 0-60 ROM Regain adequate quadriceps control CRUTCHES:
Exercises following Copeland Surface Replacement Arthroplasty (CSRA)
 Physiotherapy patient information Copeland Surface Replacement Arthroplasty Exercises following Copeland Surface Replacement Arthroplasty (CSRA) Introduction The Copeland Surface Replacement as it s name
Physiotherapy patient information Copeland Surface Replacement Arthroplasty Exercises following Copeland Surface Replacement Arthroplasty (CSRA) Introduction The Copeland Surface Replacement as it s name
Anterior Cruciate Ligament Hamstring Rehabilitation Protocol
 Anterior Cruciate Ligament Hamstring Rehabilitation Protocol Focus on exercise quality avoid overstressing the donor area while it heals. Typically, isolated hamstring strengthening begins after the 6
Anterior Cruciate Ligament Hamstring Rehabilitation Protocol Focus on exercise quality avoid overstressing the donor area while it heals. Typically, isolated hamstring strengthening begins after the 6
Handling Skills Used in the Management of Adult Hemiplegia: A Lab Manual
 Handling Skills Used in the Management of Adult Hemiplegia: A Lab Manual 2nd Edition Isabelle M. Bohman, M.S., P.T., NDT Coordinator Instructor TM Published by Clinician s View Albuquerque, NM 505-880-0058
Handling Skills Used in the Management of Adult Hemiplegia: A Lab Manual 2nd Edition Isabelle M. Bohman, M.S., P.T., NDT Coordinator Instructor TM Published by Clinician s View Albuquerque, NM 505-880-0058
For more information on arthritis and knee replacements please see:
 Chester Knee Clinic at Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Consultant Orthopaedic Surgeon: Vladimir Bobic, MD, FRCSEd www.kneeclinic.info office@kneeclinic.info
Chester Knee Clinic at Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Consultant Orthopaedic Surgeon: Vladimir Bobic, MD, FRCSEd www.kneeclinic.info office@kneeclinic.info
Rehabilitation programme after cannulated hip screw surgery
 Rehabilitation programme after cannulated hip screw surgery Information for patients at Princess Royal University Hospital This leaflet gives you advice about the things you can do after your operation
Rehabilitation programme after cannulated hip screw surgery Information for patients at Princess Royal University Hospital This leaflet gives you advice about the things you can do after your operation
Physiotherapy Services. Physiotherapy Guide. Hip Replacement
 Physiotherapy Services Physiotherapy Guide to Hip Replacement AGH 01535 293656 Bingley Hospital 01274 563438 Ilkley Coronation Hospital 01943 609666 ext 241 Skipton General Hospital 01756 701726 Settle
Physiotherapy Services Physiotherapy Guide to Hip Replacement AGH 01535 293656 Bingley Hospital 01274 563438 Ilkley Coronation Hospital 01943 609666 ext 241 Skipton General Hospital 01756 701726 Settle
GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction
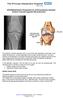 GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction Femur ACL Graft Fibula Tibia The Anterior Cruciate Ligament (ACL) is one of the main ligaments in the
GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction Femur ACL Graft Fibula Tibia The Anterior Cruciate Ligament (ACL) is one of the main ligaments in the
Lumbar decompression or discectomy
 Information and exercises Lumbar decompression or discectomy Introduction A lumbar decompression or discectomy is done to relieve pressure on the nerves in order to relieve pain and altered sensation.
Information and exercises Lumbar decompression or discectomy Introduction A lumbar decompression or discectomy is done to relieve pressure on the nerves in order to relieve pain and altered sensation.
P.I.R.P.A.G Gym Ball Exercises for Amputee Rehabilitation
 P.I.R.P.A.G Gym Ball Exercises for Amputee Rehabilitation Set Up Gym Ball always to be placed on a non-slip mat Choose correct size of Gym Ball - ensure hips and knees at 90 º angles Consider where to
P.I.R.P.A.G Gym Ball Exercises for Amputee Rehabilitation Set Up Gym Ball always to be placed on a non-slip mat Choose correct size of Gym Ball - ensure hips and knees at 90 º angles Consider where to
Protocol for the Management of Hip Arthroscopy Surgery
 Overall Aims of Surgery To decrease pain To increase range of motion (ROM) To increase hip/pelvis and lumbar stability To enable return to activities of daily living and sport Initial Post-operative Objectives
Overall Aims of Surgery To decrease pain To increase range of motion (ROM) To increase hip/pelvis and lumbar stability To enable return to activities of daily living and sport Initial Post-operative Objectives
Physiotherapy following peri acetabular osteotomy (PAO) surgery
 Physiotherapy following peri acetabular osteotomy (PAO) surgery This leaflet explains more about returning to your everyday activities after your peri acetabular osteotomy (PAO). It explains the exercises
Physiotherapy following peri acetabular osteotomy (PAO) surgery This leaflet explains more about returning to your everyday activities after your peri acetabular osteotomy (PAO). It explains the exercises
Information and exercises following dynamic hip screw
 Physiotherapy Department Information and exercises following dynamic hip screw Introduction A dynamic hip screw is performed where the neck of femur has been fractured and where there is a good chance
Physiotherapy Department Information and exercises following dynamic hip screw Introduction A dynamic hip screw is performed where the neck of femur has been fractured and where there is a good chance
Training the Joint Replacement Client
 KNEE PRE-OP SAMPLE EXERCISE PLAN Quadricep: Shuttle 1 leg and 2 legs (focus on 1 leg) Leg Press 1 and 2 legs (focus on 1 leg) Sit to Stand (if no pain or compensation) Supine Circle Foam knee extension
KNEE PRE-OP SAMPLE EXERCISE PLAN Quadricep: Shuttle 1 leg and 2 legs (focus on 1 leg) Leg Press 1 and 2 legs (focus on 1 leg) Sit to Stand (if no pain or compensation) Supine Circle Foam knee extension
High Tibial Osteotomy (HTO) Rehabilitation Protocols
 High Tibial Osteotomy (HTO) Rehabilitation Protocols Targets Upon Discharge from Hospital Protected weight-bearing (feather-weight -bearing) Ambulating with crutches Rehab brace without range of motion
High Tibial Osteotomy (HTO) Rehabilitation Protocols Targets Upon Discharge from Hospital Protected weight-bearing (feather-weight -bearing) Ambulating with crutches Rehab brace without range of motion
Ex Fix Rehab Phase II Strengthening
 Perform repetitions of each exercise, twice daily. Increase to repetitions. Ankle Pumps: With leg resting on bed and knee straight, slowly pump ankle up and down as far as possible. Quad sets: Tighten
Perform repetitions of each exercise, twice daily. Increase to repetitions. Ankle Pumps: With leg resting on bed and knee straight, slowly pump ankle up and down as far as possible. Quad sets: Tighten
Essential intervention No.1 Health education and self-care KEY OBJECTIVES
 Essential intervention No.1 Health education and self-care Health education bridges the gap between health information and behaviour. The person affected by BU must have the knowledge, skills, resources,
Essential intervention No.1 Health education and self-care Health education bridges the gap between health information and behaviour. The person affected by BU must have the knowledge, skills, resources,
ACL RECONSTRUCTION PROTOCOL
 ACL RECONSTRUCTION PROTOCOL Name of Protocol/Regime ACL Reconstruction Consultant Updated On Updated By Review Date Mr Dawson 5/5/16 Barbara Pinguey/ Rachael Edgar 6/18 Please note that surgeons may have
ACL RECONSTRUCTION PROTOCOL Name of Protocol/Regime ACL Reconstruction Consultant Updated On Updated By Review Date Mr Dawson 5/5/16 Barbara Pinguey/ Rachael Edgar 6/18 Please note that surgeons may have
Dr Schock High Tibial Osteotomy
 Dr Schock High Tibial Osteotomy Goals for phase 1 Control pain Control edema Initiate ROM and quad strengthening Maintain WB restrictions Appropriate brace wear Criteria for progression to Phase 2 Edema
Dr Schock High Tibial Osteotomy Goals for phase 1 Control pain Control edema Initiate ROM and quad strengthening Maintain WB restrictions Appropriate brace wear Criteria for progression to Phase 2 Edema
Ellipse Rehab Phase 2 Strengthening
 Strengthening Perform reps of each exercise, twice daily. Increase to reps Ankle Pumps: With leg resting on bed and knee straight, slowly pump ankle up and down as far as possible. Quad sets: Tighten thigh
Strengthening Perform reps of each exercise, twice daily. Increase to reps Ankle Pumps: With leg resting on bed and knee straight, slowly pump ankle up and down as far as possible. Quad sets: Tighten thigh
While it s unlikely you ll meet all of us you can expect to see more than one physio during your stay in hospital.
 Introduction: This information is provided to give you and your family a basic knowledge of the total hip replacement operation, outlining the things you should know, both before and after surgery. The
Introduction: This information is provided to give you and your family a basic knowledge of the total hip replacement operation, outlining the things you should know, both before and after surgery. The
REHABILITATION PROTOCOL FOR ROTATOR CUFF SURGERY SMALL TO MEDIUM TEARS PHYSIOTHERAPY GUIDELINES
 MATTHEW EVANS MBBS, FRACS (Orth), FAOrthA ORTHOPAEDIC SURGEON Knee and Shoulder Surgery Provider No 202767JX Phone: 9529 3820 Fax: 9573 9693 Email:mevans@mog.com.au www.matthewevans.com.au REHABILITATION
MATTHEW EVANS MBBS, FRACS (Orth), FAOrthA ORTHOPAEDIC SURGEON Knee and Shoulder Surgery Provider No 202767JX Phone: 9529 3820 Fax: 9573 9693 Email:mevans@mog.com.au www.matthewevans.com.au REHABILITATION
Above Knee Amputation Exercises with Prosthesis
 Above Knee Amputation Exercises with Prosthesis These exercises help you improve your balance and strengthen the muscles to best use your prosthetic leg. Do these exercises as directed by your therapist
Above Knee Amputation Exercises with Prosthesis These exercises help you improve your balance and strengthen the muscles to best use your prosthetic leg. Do these exercises as directed by your therapist
The SUPPORT Trial: SUbacromial impingement syndrome and Pain: a randomised controlled trial Of exercise and injection
 The SUPPORT Trial: SUbacromial impingement syndrome and Pain: a randomised controlled trial Of exercise and injection SUPPORT Physiotherapy Intervention Training Manual Authors: Sue Jackson (SJ) Julie
The SUPPORT Trial: SUbacromial impingement syndrome and Pain: a randomised controlled trial Of exercise and injection SUPPORT Physiotherapy Intervention Training Manual Authors: Sue Jackson (SJ) Julie
A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY
 A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY Georgia Bouffard Student Physiotherapist Colin Walker Orthopaedic Knee Specialist Frank Gilroy BSc MSCP 1 CONTENTS Anatomy of the knee
A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY Georgia Bouffard Student Physiotherapist Colin Walker Orthopaedic Knee Specialist Frank Gilroy BSc MSCP 1 CONTENTS Anatomy of the knee
Knee Replacement PROGRAM. Nightingale. Home Healthcare
 Knee Replacement PROGRAM TM Nightingale Home Healthcare With the help of Nightingale s experienced and professional rehabilitation team, you will be guided through a more complete and successful recovery
Knee Replacement PROGRAM TM Nightingale Home Healthcare With the help of Nightingale s experienced and professional rehabilitation team, you will be guided through a more complete and successful recovery
Below Knee Amputee Home Exercise Program
 Below Knee Amputee Home Exercise Program It is important that you take an active role in your rehabilitation. The following exercises must be done every day to prevent complications. After below the knee
Below Knee Amputee Home Exercise Program It is important that you take an active role in your rehabilitation. The following exercises must be done every day to prevent complications. After below the knee
GALLAND/KIRBY ISOLATED MENISCAL REPAIR POST- SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY ISOLATED MENISCAL REPAIR POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered, continue
GALLAND/KIRBY ISOLATED MENISCAL REPAIR POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered, continue
Medial Collateral Ligament Repair Protocol-Dr. McClung
 Medial Collateral Ligament Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in 30 degrees for ambulation and sleeping but drop-locked for sitting and knee
Medial Collateral Ligament Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in 30 degrees for ambulation and sleeping but drop-locked for sitting and knee
GALLAND/KIRBY ACL RECONSTRUCTION: BONE-TENDON- BONE AUTO / ALLOGRAFT POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY ACL RECONSTRUCTION: BONE-TENDON- BONE AUTO / ALLOGRAFT POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing,
GALLAND/KIRBY ACL RECONSTRUCTION: BONE-TENDON- BONE AUTO / ALLOGRAFT POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing,
Hip Arthroscopy Protocol
 The intent of this protocol is to provide guidelines for progression of rehabilitation, it is not intended to serve as a substitute for clinical decision making. Progression through each phase of rehabilitation
The intent of this protocol is to provide guidelines for progression of rehabilitation, it is not intended to serve as a substitute for clinical decision making. Progression through each phase of rehabilitation
Meniscal Repair Protocol-Dr. McClung
 Meniscal Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in full extension for ambulation and sleeping but drop-locked for sitting and knee ROM. Patients
Meniscal Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in full extension for ambulation and sleeping but drop-locked for sitting and knee ROM. Patients
Reversed geometry shoulder replacement
 Information and exercises Reversed geometry shoulder replacement Introduction The reversed geometry total shoulder replacement is designed for use in shoulders that have a deficient rotator cuff, arthritis
Information and exercises Reversed geometry shoulder replacement Introduction The reversed geometry total shoulder replacement is designed for use in shoulders that have a deficient rotator cuff, arthritis
Knee Arthroscopy Exercise Programme
 Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: office@kneeclinic.info
Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: office@kneeclinic.info
Lumbar Decompression GUIDELINES FOR PATIENTS HAVING A. Lumbar Decompression
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING A Lumbar Decompression Please stick addresograph
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING A Lumbar Decompression Please stick addresograph
Recovery after a Breastbone Repair
 Page 1 of 8 Recovery after a Breastbone Repair with Nuss Surgery For 6 to 12 weeks: Do not lie on your side. Do not log roll to your side. Do not twist your upper trunk to the right or left. You should
Page 1 of 8 Recovery after a Breastbone Repair with Nuss Surgery For 6 to 12 weeks: Do not lie on your side. Do not log roll to your side. Do not twist your upper trunk to the right or left. You should
Physiotherapy following cardiac surgery. Information for patients Cardiac Surgery
 Physiotherapy following cardiac surgery Information for patients Cardiac Surgery Physiotherapy is an essential part of your recovery from your operation. The physiotherapist will see you before you have
Physiotherapy following cardiac surgery Information for patients Cardiac Surgery Physiotherapy is an essential part of your recovery from your operation. The physiotherapist will see you before you have
Cervical Surgeries. DO NOT twist or bend your neck, or lift with your arms, without getting clearance from your doctor.
 Precautions: Cervical Surgeries DO NOT twist or bend your neck, or lift with your arms, without getting clearance from your doctor. If you must bend down to pick up an object, use a grabber instead. Tighten
Precautions: Cervical Surgeries DO NOT twist or bend your neck, or lift with your arms, without getting clearance from your doctor. If you must bend down to pick up an object, use a grabber instead. Tighten
Protocol G Arthroscopic Surgery: Therapist Information
 Protocol G Arthroscopic Surgery: Therapist Information Please read entire protocol prior to initiating therapy Please do not hesitate to contact Dr. Wolff with questions or concerns. Rest is a vital component
Protocol G Arthroscopic Surgery: Therapist Information Please read entire protocol prior to initiating therapy Please do not hesitate to contact Dr. Wolff with questions or concerns. Rest is a vital component
Single leg bridging with prosthesis. Hip extension side-lying against wall with prosthesis. Side plank with prosthesis
 Single leg bridging with prosthesis Hold your sound limb in air, with your prosthetic foot on the bed with your knee bent. Squeeze your buttocks and lift your hips as high as you can toward the ceiling.
Single leg bridging with prosthesis Hold your sound limb in air, with your prosthetic foot on the bed with your knee bent. Squeeze your buttocks and lift your hips as high as you can toward the ceiling.
Guide To ACL Reconstruction Rehabilitation
 Guide To ACL Reconstruction Rehabilitation Welcome to our ACL Reconstruction Rehabilitation video series. The goal of these videos is to help maximize your recovery following ACL reconstruction surgery.
Guide To ACL Reconstruction Rehabilitation Welcome to our ACL Reconstruction Rehabilitation video series. The goal of these videos is to help maximize your recovery following ACL reconstruction surgery.
Benefits of Weight bearing increased awareness of the involved side decreased fear improved symmetry regulation of muscle tone
 From the information we have gathered during our Evaluation, the Clinical Reasoning we used to identify key problem areas and the Goals Established with functional outcomes we now have enough information
From the information we have gathered during our Evaluation, the Clinical Reasoning we used to identify key problem areas and the Goals Established with functional outcomes we now have enough information
Tibia intramedullary nail operation physiotherapy advice
 Tibia intramedullary nail operation physiotherapy advice This leaflet gives you advice about recovering after your operation. It also explains exercises you should do each day, things to look out for and
Tibia intramedullary nail operation physiotherapy advice This leaflet gives you advice about recovering after your operation. It also explains exercises you should do each day, things to look out for and
Anterior Cruciate Ligament Reconstruction
 Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
Posture. In this article
 Posture Posture is the way we hold our bodies against gravity and maintaining a good posture involves training yourself to become aware of how you hold yourself in all activities as your posture is constantly
Posture Posture is the way we hold our bodies against gravity and maintaining a good posture involves training yourself to become aware of how you hold yourself in all activities as your posture is constantly
Move your ankle inward toward your other foot and then outward away from your other foot.
 TOTAL HIP REPLACEMENT POST OPERATIVE EXERCISES Regular exercises to restore your normal hip motion and strength and a gradual return to everyday activities are important for your full recovery. Dr. Robertson
TOTAL HIP REPLACEMENT POST OPERATIVE EXERCISES Regular exercises to restore your normal hip motion and strength and a gradual return to everyday activities are important for your full recovery. Dr. Robertson
MATTHEW EVANS MBBS, FRACS (Orth), FAOrthA ORTHOPAEDIC SURGEON Knee and Shoulder Surgery Provider No JX
 MATTHEW EVANS MBBS, FRACS (Orth), FAOrthA ORTHOPAEDIC SURGEON Knee and Shoulder Surgery Provider No 202767JX Phone: 9529 3820 Fax: 9573 9693 Email:mevans@mog.com.au www.matthewevans.com.au REHABILITATION
MATTHEW EVANS MBBS, FRACS (Orth), FAOrthA ORTHOPAEDIC SURGEON Knee and Shoulder Surgery Provider No 202767JX Phone: 9529 3820 Fax: 9573 9693 Email:mevans@mog.com.au www.matthewevans.com.au REHABILITATION
Post-operative information Total knee replacement
 Post-operative information Total knee replacement Day of operation You will arrive on the ward following your surgery. You may have had a spinal anaesthetic which will wear off after a couple of hours.
Post-operative information Total knee replacement Day of operation You will arrive on the ward following your surgery. You may have had a spinal anaesthetic which will wear off after a couple of hours.
Post Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction
 Post Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction
Post Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction
Jennifer L. Cook, MD
 Jennifer L. Cook, MD Florida Joint Replacement and Sports Medicine Center 5243 Hanff Lane New Port Richey, FL 34652 Phone: (727)848-4249 Fax: (727) 841-8934 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE
Jennifer L. Cook, MD Florida Joint Replacement and Sports Medicine Center 5243 Hanff Lane New Port Richey, FL 34652 Phone: (727)848-4249 Fax: (727) 841-8934 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE
POST OP CLOSED BANKART PROCEDURE
 POST OP CLOSED BANKART PROCEDURE WEEKS 1-6 Do 1. Wear sling until advised otherwise 2. Keep dressing clean and dry 3. Do passive pendulum exercises to 90 degrees 4. Ice for 15 minutes after exercising
POST OP CLOSED BANKART PROCEDURE WEEKS 1-6 Do 1. Wear sling until advised otherwise 2. Keep dressing clean and dry 3. Do passive pendulum exercises to 90 degrees 4. Ice for 15 minutes after exercising
KNEE REHABILITATION PROGRAMME
 Jessica Barrow BSc Physiotherapy, SPT1 www.barrowphysiotherapy.co.za Cell: 083 256 0434 Room GF03 Waterfall Hospital Cnr. Magwa Crescent and Mac Mac Avenue Tel: 011 304-7829 Fax: 011 304-7941 KNEE REHABILITATION
Jessica Barrow BSc Physiotherapy, SPT1 www.barrowphysiotherapy.co.za Cell: 083 256 0434 Room GF03 Waterfall Hospital Cnr. Magwa Crescent and Mac Mac Avenue Tel: 011 304-7829 Fax: 011 304-7941 KNEE REHABILITATION
Total knee replacement
 Total knee replacement Inpatient and home exercises Information for patients MSK Orthopaedic Inpatients (Therapy) When you go home from hospital following your knee replacement, a referral will be made
Total knee replacement Inpatient and home exercises Information for patients MSK Orthopaedic Inpatients (Therapy) When you go home from hospital following your knee replacement, a referral will be made
Jennifer L. Cook, MD. Total Hip Arthroplasty /Hemi Arthroplasty Protocol
 Jennifer L. Cook, MD Florida Joint Replacement and Sports Medicine Center 5243 Hanff Lane New Port Richey, FL 34652 Phone: (727)848-4249 Fax: (727) 841-8934 Total Hip Arthroplasty /Hemi Arthroplasty Protocol
Jennifer L. Cook, MD Florida Joint Replacement and Sports Medicine Center 5243 Hanff Lane New Port Richey, FL 34652 Phone: (727)848-4249 Fax: (727) 841-8934 Total Hip Arthroplasty /Hemi Arthroplasty Protocol
ACHILLES TENDON REPAIR REHAB GUIDELINES
 ACHILLES TENDON REPAIR REHAB GUIDELINES Typically patients are discharged on the day of the operation or the next day. The leg is usually immobilized in a cast or hinged brace, ranging from 4-8 weeks.
ACHILLES TENDON REPAIR REHAB GUIDELINES Typically patients are discharged on the day of the operation or the next day. The leg is usually immobilized in a cast or hinged brace, ranging from 4-8 weeks.
GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: - POD 1: Debulk dressing, TED Hose in place - POD 2: Change
GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: - POD 1: Debulk dressing, TED Hose in place - POD 2: Change
What is arthroscopy? Normal knee anatomy
 What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
GALLAND/KIRBY ACL RECONSTRUCTION REVISION POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY ACL RECONSTRUCTION REVISION POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered, continue
GALLAND/KIRBY ACL RECONSTRUCTION REVISION POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered, continue
Postoperative Days 1-7
 ACL RECONSTRUCTION REHABILITATION PROTOCOL Postoperative Days 1-7 *IT IS EXTREMELY IMPORTANT THAT YOU WORK ON EXTENSION IMMEDIATELY Goals: * Control pain and swelling * Care for the knee and dressing *
ACL RECONSTRUCTION REHABILITATION PROTOCOL Postoperative Days 1-7 *IT IS EXTREMELY IMPORTANT THAT YOU WORK ON EXTENSION IMMEDIATELY Goals: * Control pain and swelling * Care for the knee and dressing *
Speed Your Recovery. After your knee surgery, you will need to perform exercises to strengthen the muscles that affect the replacement joint.
 FO R THE TO TAL KNEE REPLACEMENT PATIENT Speed Your Recovery After your knee surgery, you will need to perform exercises to strengthen the muscles that affect the replacement joint. The exercises may
FO R THE TO TAL KNEE REPLACEMENT PATIENT Speed Your Recovery After your knee surgery, you will need to perform exercises to strengthen the muscles that affect the replacement joint. The exercises may
Exercises following arthroscopic subacromial decompression and/or acromioclavicular joint excision and/or excision of calcific deposits
 Physiotherapy patient information Exercises following arthroscopic subacromial decompression and/or acromioclavicular joint excision and/or excision of calcific deposits Introduction The subacromial area
Physiotherapy patient information Exercises following arthroscopic subacromial decompression and/or acromioclavicular joint excision and/or excision of calcific deposits Introduction The subacromial area
TOTAL HIP REPLACEMENT GUIDE
 TOTAL HIP REPLACEMENT GUIDE This manual was made by physical therapists and Patient, Family and Community Education at City of Hope. Your physical therapist is: who can be reached at 626-256-HOPE (4673),
TOTAL HIP REPLACEMENT GUIDE This manual was made by physical therapists and Patient, Family and Community Education at City of Hope. Your physical therapist is: who can be reached at 626-256-HOPE (4673),
GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing,
GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing,
Range of motion and positioning
 Range of motion and positioning Learning guide Why is motion important? Most people take free, comfortable movement for granted. Motion is meant to be smooth and painless. The ligaments, tendons, muscles,
Range of motion and positioning Learning guide Why is motion important? Most people take free, comfortable movement for granted. Motion is meant to be smooth and painless. The ligaments, tendons, muscles,
Advice and exercises for managing knee and hip osteoarthritis October 2018 V1.2 April 2018 April 2021
 Advice and exercises for managing knee and hip osteoarthritis 0496 October 2018 V1.2 April 2018 April 2021 This advice and exercise booklet has been produced by senior physiotherapists working for DynamicHealth.
Advice and exercises for managing knee and hip osteoarthritis 0496 October 2018 V1.2 April 2018 April 2021 This advice and exercise booklet has been produced by senior physiotherapists working for DynamicHealth.
