Reverse total shoulder arthroplasty in patients of varying body mass index
|
|
|
- Johnathan Barnett
- 5 years ago
- Views:
Transcription
1 J Shoulder Elbow Surg (2014) 23, Reverse total shoulder arthroplasty in patients of varying body mass index Anil K. Gupta, MD, MBA*, Peter N. Chalmers, MD, Zain Rahman, BS, Benjamin Bruce, MD, Joshua D. Harris, MD, Frank McCormick, MD, Geoffrey D. Abrams, MD, Gregory P. Nicholson, MD Section of Shoulder and Elbow Surgery, Midwest Orthopaedics at Rush, Department of Orthopedic Surgery, Rush University Medical Center, Chicago, IL, USA Background: Body mass index (BMI) is an independent predictor of complications after hip and knee arthroplasty. Whether similar trends apply to patients undergoing reverse total shoulder arthroplasty (RTSA) is unknown. Methods: A retrospective review of primary RTSAs with a minimum 90-day follow-up were included. Complications were classified as major or minor and medical or surgical. Patients were classified into 3 groups: normal BMI (BMI <25 kg/m 2 ), overweight or mildly obese (BMI kg/m 2 ), and moderately or severely obese (BMI >35 kg/m 2 ). Results: Of the 119 patients met our inclusion criteria, 30 (25%) had a BMI of less than 25 kg/m 2 ; 65 (55%) had a BMI of 25 to 35 kg/m 2, and 24 (20%) had BMI exceeding 35 kg/m 2. Complications occurred in 30 patients (25%), comprising major in 11 (9%), minor in 19 (16%), surgical in 21 (18%), and medical in 14 (12%). The most common surgical complications were acute blood loss anemia requiring transfusion (8.4%) and dislocation (4.2%). The most common medical complications were atelectasis (2.5%) and acute renal insufficiency (2.5%). Patients with a BMI exceeding 35 kg/m 2 had a significantly higher overall complication rate (P <.05) and intraoperative blood loss (P ¼.05) than the other groups. Patients with BMI of less than 25 kg/m 2 had a greater overall complication rate than those with a BMI of 25 to 35 kg/m 2 (P <.05). Multivariate regression analysis demonstrated BMI was the only significant determinant of overall complication rates and medical complication rates (P <.05). Conclusion: Patients with a BMI exceeding 35 kg/m 2 (severely obese) or a BMI of less than 25 kg/m 2 have higher rates of complication after RTSA. Level of evidence: Level III, Retrospective Cohort Study, Treatment Study. Ó 2014 Journal of Shoulder and Elbow Surgery Board of Trustees. Keywords: Complications; reverse total shoulder arthroplasty; medical; surgical; obesity The following study was Institutional Review Board Exempt. *Reprint requests: Anil K. Gupta, MD, MBA, Midwest Orthopaedics at Rush, Rush University Medical Center, 1611 W Harrison St, Chicago, IL 60612, USA. address: anilgupta07@hotmail.com (A.K. Gupta). The reverse total shoulder arthroplasty (RTSA) was first introduced in the 1980s by Grammont to treat rotator cuff tear arthropathy. Multiple series have shown significant improvement in pain and function after RTSA 4,7,13,22-24,28 Despite its success, complication rates ranging from 25% /$ - see front matter Ó 2014 Journal of Shoulder and Elbow Surgery Board of Trustees.
2 36 A.K. Gupta et al. to 50% have been reported. Intraoperative, perioperative, postoperative, surgical, and medical complications have all been reported. These include, but are not limited to, hematoma formation, instability, superficial and deep infection, periprosthetic fracture, acromial fracture, neurologic compromise, implant loosening, and medical complications. 2,6,8,11,22,26,27,30 Recent improvements in surgical techniques and implant design, however, have demonstrated lower overall complication and failure rates. 7 Body mass index (BMI) has been shown to be an independent predictor of postoperative complications in patients undergoing joint replacement. 13,14 Obesity predisposes patients to medical comorbidities such as cardiovascular disease, stroke, pulmonary embolism, and diabetes. These conditions may also serve as independent predictors of perioperative and postoperative medical and surgical complications. Preoperative medical comorbidity rates have also been shown to predict postoperative complication rates in patients undergoing orthopedic procedures. 14,17,20,25 Currently, there is a paucity of data describing the complications associated with RTSA in patients of varying BMIs. The purpose of the study was to analyze complication rates in the operative, perioperative, and early postoperative period in patients of varying BMIs undergoing RTSA. We hypothesized that BMI would serve as an independent risk factor for the development of early medical and surgical complications after RTSA. Materials and methods Patients who had undergone primary RTSA with a minimum 90- day postoperative follow-up were included. Indications for RTSA included rotator cuff tear arthropathy, massive irreparable rotator cuff tear with pseudoparalysis, end-stage glenohumeral arthritis with an irreparable rotator cuff tear, inflammatory cuff tear arthropathy, and proximal humeral malunion/nonunion with associated irreparable rotator cuff tear. Excluded were patients with previous shoulder arthroplasty, if RTSA was performed as a revision procedure for a failed prior arthroplasty (hemiarthroplasty or total shoulder arthroplasty), prior deep space infection requiring explantation, or if perioperative or operative records were incomplete. The following data were recorded in Excel X (Microsoft Corp, Redmond, WA, USA): age, sex, BMI, laterality of the dominant extremity, laterality of the RTSA, indication for operative intervention, medical comorbidities, length of procedure in minutes, estimated intraoperative blood loss in milliliters measured by anesthesia and nursing, specific implants, concomitant procedures, and the need for intraoperative or postoperative transfusion. The operative reports and the intraoperative, perioperative inpatient, and postoperative outpatient records for each patient were reviewed in detail, and all noted complications were recorded. Our institution does not have a specific transfusion threshold, and the decision to transfuse was made case-by-case according to the clinical judgement and mutual agreement of the orthopedic and internal medicine teams. The Charlson Comorbidity Index (CCI) is a validated predictive tool for complications in patients undergoing surgical procedures. 5 Specifically, it predicts the 10-year mortality of an individual based on his or her comorbid conditions, including heart disease, diabetes mellitus, and cancer. Each condition is assigned a point value of 1, 2, 3, or 6 according to the risk of death associated with the comorbidity. The higher this value, the higher the risk of death. Each patient s preoperative medical comorbidities were determined and used to calculate the CCI for planned multivariate regression analysis to determine the correlation between comorbidities and complications. Complication classification Complications were defined as any event that deviated from a normal postoperative course and were further classified as major or minor and medical or surgical. Complications were categorized according a validated classification scheme described by Dindo et al 9 : Minor complication: any deviation from the normal postoperative course requiring pharmacologic treatment. Major complication: any deviation from the normal postoperative course requiring prolonged pharmacologic treatment or surgical intervention. Medical complications: systemic events such as pulmonary emboli, cardiac events, renal failure, and atelectasis, which was a combined clinical and radiographic diagnosis. Surgical complications: local events that stemmed from the surgical site such as need for transfusion, wound complications, periprosthetic fractures, and dislocations. Statistical analysis Analyses were performed in SPSS 18 software (IBM Inc, Armonk, NY, USA), and descriptive statistics were calculated. An a priori decision was made to divide patients into 3 groups by BMI (kg/m 2 ): group 1, normal BMI (BMI <25); group 2, BMI classified as overweight or mildly obese or class I (World Health Organization Classification) obesity (BMI 25-35), and group 3, BMI classified as moderately or severely obese or class II or greater obesity (BMI >35). 29 This decision was based on our anecdotal clinical experience, the mean and standard deviation BMI of the average patient undergoing TSA and RTSA in the senior authors practice (w30.5), as well as evidence from the hip and knee arthroplasty literature suggesting complication rates may not be increased until severe obesity is reached. 17 Kolmogorov-Smirnov analysis was performed on continuous variables and all variables that significantly differed from the normal distribution (P <.05). Thus Kruskal-Wallis tests were performed to compare continuous variables among the BMI groups. Statistical comparison of categoric variables was done using c 2 tests. Given concern that multiple variables may predict complication rates, multivariable logistic regression was planned for those variables that differed between our a priori defined BMI groups to determine whether these covariates or BMI served as the primary determinant of complication rates.
3 Reverse shoulder arthroplasty in obesity 37 Results Demographics and intraoperative variables Of 150 possible patients assessed, 31 were revisions from a prior failed arthroplasty, leaving 119 who met the inclusion criteria. Of the total cohort, 30 patients (25%) had a normal body mass (BMI <25 kg/m 2 ; Fig 1), 24 (20%) were moderately or severely obese (BMI >35 kg/ m 2 ), and 65 (55%) were overweight or mildly obese (BMI kg/m 2 ). The mean BMI was kg/ m 2. Men and women were evenly distributed among BMI groups (P ¼.148). Rates of prior surgery were not significantly different among BMI groups (P ¼.789). Patients in group 3 (BMI >35 kg/m 2 ) tended to be significantly younger (P ¼.025), with a higher comorbidity burden (P ¼.009) than in groups 1 and 2. Indications for RTSA were similar among BMI groups (P ¼.837). Patients in group 3 had longer operative times than groups 1 and 2, but this difference did not reach statistical significance (P ¼.104; Table I). Estimated blood loss significantly differed among BMI groups, with group 3 demonstrating the greatest mean intraoperative blood loss (P ¼.050). The transfusion rate was higher in group 3 than in groups 1 and 2, but this difference did not reach statistical significance. (P ¼.174). Complication rates Among the overall patient cohort, 30 (25%) sustained 1 or more complications (Table II), including 11 (9%) with a major complication and 19 (16%) with 1 or more minor complications, mostly in the perioperative (inpatient) and postoperative period. Twenty-one patients (18%) sustained a surgical complication, 14 (12%) experienced 1 or more medical complications, and 6 (5%) sustained a medical and surgical complication. The most common surgical complications were acute blood loss anemia requiring transfusion (8.4%) and dislocation (4.2%). Infections occurred in 0.8%. The most common medical complications were atelectasis (2.5%) and acute renal insufficiency (2.5%). No deaths occurred during the study period. Complication rates differed significantly among BMI groups, with patients in groups 1 (BMI <25 kg/m 2 )and3 (BMI >35 kg/m 2 ) experiencing greater complication rates (P ¼.020). This significant difference held true when the group 1 and 2 cohorts were directly compared (P ¼.046). No significant difference was seen between groups 1 and 3 in complication rates (P ¼.529). No significant differences were seen between rates of major complications (P ¼.775), infection (P ¼.395), dislocation (P ¼.664), or death (>.99). Significantly more medical complications occurred in group 3(P ¼.006). A trend toward increased rates of surgical complications was seen in patients in groups 1 and 3 compared with group 2 (P ¼.083). The mean CCI was significantly greater for group 3 (P ¼.009). Although medical complication rates significantly correlated with CCI (P ¼.011), rates for overall complications (P ¼.115), major complications (P ¼.695), and surgical complications (P ¼.983) did not. A subgroup analysis for the patients with a BMI of less than 25 kg/m 2 showed among the patients with medical or surgical complications, or both, 6 had isolated hypertension (controlled on medication), 1 had diabetes mellitus andcoronaryarterydisease(cad),and2hadisolated CAD. The remaining patients had no comorbidities (Table III). No significant difference was found in hospital length of stay among BMI subgroups groups 1 (mean , , and days, respectively, for groups 1, 2, and 3; P ¼.15). No group 1 patients required admission to the intensive care unit (ICU). ICU admission was required immediately after surgery for 3 patients in group 2 and 2 patients in group 3. All ICU stays were for 1 night only except for 1 patient (BMI 39.6 kg/m 2 ) who required a 2-day stay in the ICU for postoperative cardiac monitoring owing to a history of paroxysmal ventricular tachycardia. Among the 5 patients admitted to the ICU, the total hospital length of stay ranged from 2 to 4 days (Table IV). Multivariate regression analysis Because age and the CCI differed significantly among the BMI groups (P ¼.009), multivariate logistic regression was performed to determine whether BMI, age, or CCI served as the primary determinant of the presence or absence of all complications, major complications, medical complications, and surgical complications. These analyses confirmed BMI was the only significant covariate with overall complication rates and medical complication rates, whereas no covariate reached significance for major complications or surgical complications (Table V). Discussion Surgical intervention on the obese population can be technically demanding. Obesity has been correlated with an increased complication rate in reports on hip and knee arthroplasty. 6,14,17,20,25 The purpose of this study was to determine if BMI correlates with complications after primary RTSA. Patients in our cohort with a BMI of less than 25 kg/m 2 or greater than 35 kg/m 2 had higher overall complication rates than those with a BMI of 25 to 35 kg/m 2. In addition, patients with a BMI greater than 35 kg/m 2 had significantly more blood loss intraoperatively and trended toward longer operations and more postoperative
4 38 A.K. Gupta et al. Figure 1 Patients were grouped according to body mass index (BMI) <25 kg/m 2 (red bars), BMI 25 to 35 kg/m 2 (green bars), and BMI >35 kg/m 2 (purple bars), with the graph showing the percentage of patients sustaining a complication, sustaining a major complication, sustaining a medical complication, sustaining a surgical complication, and the total population in that subgroup. *Indicates statistically significant differences. Table I Demographic and intraoperative characteristics segregated by body mass index (BMI) Variable BMI <25 kg/m 2 BMI kg/m 2 BMI >35 kg/m 2 Total patients P value (n ¼ 30) (n ¼ 65) (n ¼ 24) (n ¼ 119) Age, mean SD y Female, % CCI, mean SD score Patients with prior shoulder surgery, % Indications, No..837 Cuff tear arthropathy Glenohumeral osteoarthritis with irreparable cuff tear Massive/irreparable cuff tear Sequelae of a proximal humeral fracture Inflammatory arthropathy, etc Operative time, mean SD min Estimated blood loss, mean SD ml Patients requiring transfusion, % (No.) 3.3 (1) 3.1 (2) 12.5 (3) 5.0 (6).174 CCI, Charlson Comorbidity Index; SD, standard deviation. transfusions. Multivariate regression revealed BMI was the sole determinant of complications, without contributions from age or CCI. Our hypothesis that BMI would serve as an independent risk factor for the development of early medical and surgical complications after RTSA was supported. To our knowledge, this is the first series specifically evaluating varied BMI and the associated medical and surgical complications in patients undergoing RTSA. In a previous series examining outcomes of TSA in obese patients, Linberg et al 21 demonstrated improved pain and function in the morbidly obese population, although with increased intraoperative surgical time, hospital length of stay, and ICU use. Similar findings have been demonstrated in nonshoulder arthroplasty studies. Silber et al 25 demonstrated that obesity increases the intraoperative and postoperative risk and financial burden in patients undergoing
5 Reverse shoulder arthroplasty in obesity 39 Table II Complications segregated by body mass index (BMI) groups Complication BMI <25 kg/m 2 BMI kg/m 2 BMI >35 kg/m 2 Total patients P value Patients sustaining A complication, % (No.) 33 (10) 15 (10) 42 (10) 25 (30).020 A major complication, % (No.) 10 (3) 8 (5) 13 (3) 9 (11).775 A medical complication, % (No.) 13 (4) 5 (3) 29 (7) 12 (14).006 A surgical complication, % (No.) 23 (7) 11 (7) 29 (7) 18 (21).083 An infection, % (No.) 0 (0) 1.5 (1) 0 (0) 0.8 (1).664 A dislocation, % (No.) 3.3 (1) 3.1 (2) 8.3 (2) 4.2 (5).528 Mortality before final follow-up, % (No.) 0 (0) 0 (0) 0 (0) 0 (0) >.99 a variety of major operations, including hip and knee surgery, colectomy, and thoracotomy. Studies specific to hip and knee arthroplasty have shown obesity is associated with longer operative time, perioperative infection, ICU admission, and slower postoperative recovery. 1,17,18 In a level 2 prognostic study, Jain et al 16 found obesity was an independent predictor of increased postoperative complications and nonhomebound discharge in patients undergoing shoulder, hip, or knee arthroplasty. Interestingly, we did not see a significant association between hospital length of stay and BMI in this study. The mean hospital length of stay was close to 2 days for all subgroups. This difference between our findings and those in the hip and knee arthroplasty literature may be explained by the ease of mobility associated with upper extremity vs lower extremity surgery. In addition, each patient who underwent shoulder arthroplasty had a multidisciplinary approach to their care (ie, internal medicine and physical and occupational therapy consultation) to allow for expeditious management of postoperative medical or mobility issues, or both. In countries where this is not available, hospital stays for such subgroups may be prolonged, with greater expense to stakeholders. The cause for the association between an increased complication rate and a BMI of less than 25 kg/m 2 is unclear. Included among a variety of possible explanations are unmeasured or unaccounted covariates, such as malnutrition, and type I error. Our subgroup analysis did not demonstrate any patterns to suggest a correlation between a BMI of less than 25 kg/m 2 and a specific comorbidity that could have accounted for the associated complication. Only one patient had a BMI of less than 18.5 kg/m 2 (classified as underweight by the World Health Organization classification). The hip arthroplasty literature has established that malnutrition can account for failed debridement in the setting of postoperative drainage after total hip arthroplasty. 15 This subgroup did have 2 patients with deep space infection and 1 with wound dehiscence. Therefore, there is a possibility that those specific patients suffered from malnutrition. However, to accurately assess a patient for malnutrition requires a preoperative laboratory workup (ie, serum total protein, albumin, prealbumin, and transferrin level) and caloric intake counts. These data were not available for the patients in our subgroup, and therefore, a malnutrition assessment could not be performed. However, given the clinical relevance of this finding in our study, evaluation of the preoperative nutritional status of patients undergoing RSA and its association with postoperative complications including, but not limited to, infection and wound problems may be warranted in future studies. A variety of plausible causes exist to explain the complication rate in the group with a BMI exceeding 35 kg/m 2. In addition to the added technical complexity, including difficulty in gaining adequate exposure and increased intraoperative blood loss leading to increased rates of acute blood loss anemia and other surgical complications, obese patients may be less able to physiologically cope with the cardiovascular physiologic stress of surgery, leading to higher rates of postoperative medical complications such as acute renal failure. Obese patients also mobilize less readily, leading to increased rates of atelectasis. 3,12 As the United States population ages and becomes increasingly obese, the number of RTSAs performed in obese individuals will increase. 19,26 This is also true in other nations, such as Australia. 10 Surgeons need to be aware of the risks associated with RTSA in such patients in order to provide accurate, evidence-based informed consent. Individuals determining health care policy need to be aware of the increased complication rates because they may affect overall health care expenditures. In addition, because complications are costly and timeconsuming, individuals determining future public policy may want to consider altered premiums for the morbidly obese population and adjustments in surgeon compensation. Limitations of this study include short-term follow-up, varied indications for RTSA, and the possibility of missed complications due to the retrospective nature of
6 40 A.K. Gupta et al. Table III All complications, classifications, and associated comorbidities BMI (kg/m 2 ) Complication Classification Comorbidities 18.6 Intraoperative humeral shaft fracturedcable Major surgical HTN 19.8 Blood loss anemiadtransfusion Minor surgical HTN 20.0 Blood loss anemia requiring erythropoietin, no transfusion Minor surgical CAD, DM required 22.2 Altered mental status requiring restraints Minor medical HTN 22.7 PEdanticoagulation Major medical HTN 23.6 Wound dehiscencedlocal wound care Minor surgical HTN 23.8 Hypotension, recurrent dislocationdconversion to Minor medical, major surgical CAD hemiarthroplasty 24.0 Drill bit broken in the scapula Minor Surgical None 24.9 Respiratory failure requiring supplemental oxygen Minor medical HTN 24.9 Intraoperative glenoid fracture Minor surgical HTN 25.8 Acromial stress fracture Minor surgical HTN 27.1 Acromial stress fracture Minor surgical HTN 27.9 Superficial wound infection Minor surgical HTN 28.2 Respiratory failure requiring a 2-day ICU stay Major medical HTN 28.3 PE, blood loss anemiadtransfusion Major medical, minor surgical HTN 29.7 Blood loss anemia transfusion Minor surgical HTN, CAD 30.0 Acromial stress fracture, dislocationdclosed reduction Minor surgical, major surgical Kidney cancer 31.6 CRPS in the ulnar nerve distribution Minor surgical HTN, DM 32.3 Asystole requiring pacemaker placement Major medical HTN, DM 32.4 Dislocation closed reduction Major surgical HTN 35.0 Dislocation required revision to a hemiarthroplasty Major surgical HTN 35.3 Persistent tachycardia Minor medical HTN, DM 36.0 Respiratory failure requiring supplementary oxygen Minor medical HTN, CKD 36.9 Respiratory failure, renal failure, transfusion Minor medical and surgical HTN 37.3 Renal failure resolved with medical management Minor medical HTN 37.8 Hemorrhagic traumatic hematoma Major surgical HTN 37.9 Acromial stress fracture Minor surgical HTN 40.7 Hypotension, brachial plexus palsy, dislocation Major/minor, medical/surgical HTN, PE, DM 42.4 Blood loss anemia transfusion, atelectasis Minor surgical and medical HTN, PE 43.0 Blood loss anemia transfusion, atelectasis Minor surgical and medical CAD, HTN CAD, coronary artery disease; CKD, chronic kidney disease; CRPS, complex regional pain syndrome; DM, diabetes mellitus; HTN, hypertension; IþD, irrigation and debridement; ICU, intensive care unit; PE, pulmonary embolism. Table IV Hospital length of stay (LOS) and number of intensive care unit (ICU) admissions for each body mass index (BMI) subcategory BMI, kg/m 2 LOS, d (Mean SD) ICU admission (No.) Group 1 (BMI <25) Group 2 (BMI 25-35) Group 3 (BMI >35) SD, standard deviation. Table V Significance (P values) of multivariate logistic regression analyses performed to determine whether age, body mass index (BMI) subgroup (<25, 25-35, and 35 kg/m 2 ), or Charlson Comorbidity Index (CCI) served as significant covariates with all complications, major complications, medical complications, and surgical complications after reverse total shoulder arthroplasty Variable P value Age BMI subgroup CCI All complications Major complications Medical complications Surgical complications
7 Reverse shoulder arthroplasty in obesity 41 the study. Lastly, a cost-analysis comparing RTSA in the nonobese obese populations would have strengthened the study. Conclusion Patients with a BMI exceeding 35 kg/m 2 (severe obesity) or a BMI of less than 25 kg/m 2 have higher rates of complication after RTSA. Future studies evaluating the association between causative factors, such as malnutrition in patients with a BMI of less than 25 kg/m 2, are needed. Disclaimer G.P.N. is a paid consultant for Tornier, Inc. The other authors, their immediate families, and any research foundations with which they are affiliated have not received any financial payments or other benefits from any commercial entity related to the subject of this article. References 1. AbdelSalam H, Restrepo C, Tarity TD, Sangster W, Parvizi J. Predictors of intensive care unit admission after total joint arthroplasty. J Arthroplasty 2012;27: Affonso J, Nicholson GP, Frankle MA, Walch G, Gerber C, Garzon- Muvdi J, et al. Complications of the reverse prosthesis: prevention and treatment. Instr Course Lect 2012;61: Alab HF, Zabani IA, Abdelrahman HS, Bukhari WL, Mamoun I, Ashour MA, et al. Intraoperative ventilatory strategies for prevention of pulmonary atelectasis in obese patients undergoing laparoscopic bariatric surgery. Anesth Analg 2009;109: /ANE.0b013e3181ba Boileau P, Gonzalez JF, Chuinard C, Bicknell R, Walch G. Reverse total shoulder arthroplasty after failed rotator cuff surgery. J Shoulder Elbow Surg 2009;18: jse Charlson ME, Pompei P, Ales KL, MacKenzie CR. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 1987;40: Cheung E, Willis M, Walker M, Clark R, Frankle MA. Complications in reverse total shoulder arthroplasty. J Am Acad Orthop Surg 2011; 19: Cuff D, Clark R, Pupello D, Frankle M. Reverse shoulder arthroplasty for the treatment of rotator cuff deficiency: a concise followup, at a minimum of five years, of a previous report. J Bone Joint Surg Am 2012;94: Cuff D, Pupello D, Virani N, Levy J, Frankle M. Reverse shoulder arthroplasty for the treatment of rotator cuff deficiency. J Bone Joint Surg Am 2008;90: Dindo D, Demartines N, Clavien PA. Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 2004;240: Duncan MJ, Vandelanotte C, Caperchione C, Hanley C, Mummery WK. Temporal trends in and relationships between screen time, physical activity, overweight and obesity. BMC Public Health 2012;12: Farshad M, Gerber C. Reverse total shoulder arthroplasty-from the most to the least common complication. Int Orthop 2010;34: Flier S, Knape JT. How to inform a morbidly obese patient on the specific risk to develop postoperative pulmonary complications using evidence-based methodology. Eur J Anaesthesiol 2006;23: Gallo RA, Gamradt SC, Mattern CJ, Cordasco FA, Craig EV, Dines DM. Instability after reverse total shoulder replacement. J Shoulder Elbow Surg 2011;20: Haverkamp D, Klinkenbijl MN, Somford MP, Albers GH, van der Vis HM. Obesity in total hip arthroplasty does it really matter? A meta-analysis. Acta Orthop 2011;82: / Jaberi FM, Parvizi J, Haytmanek CT, Joshi A, Purtill J. Procrastination of wound drainage and malnutrition affect the outcome of joint arthroplasty. Clin Orthop Relat Res 2008;466: org/ /s Jain NB, Guller U, Pietrobon R, Bond TK, Higgins LD. Comorbidities increase complication rates in patients having arthroplasty. Clin Orthop Relat Res 2005;435: Jamsen E, Nevalainen P, Eskelinen A, Huotari K, Kalliovalkama J, Moilanen T. Obesity, diabetes, and preoperative hyperglycemia as predictors of periprosthetic joint infection: a single-center analysis of 7181 primary hip and knee replacements for osteoarthritis. J Bone Joint Surg Am 2012;94:e J Jones CA, Cox V, Jhangri GS, Suarez-Almazor ME. Delineating the impact of obesity and its relationship on recovery after total joint arthroplasties. Osteoarthritis Cartilage 2012;20: org/ /j.joca Kaiser MJ, Bauer JM, Ramsch C, Uter W, Guigoz Y, Cederholm T, et al.., Mini Nutritional Assessment International Group. Frequency of malnutrition in older adults: a multinational perspective using the mini nutritional assessment. J Am Geriatr Soc 2010;58: doi.org/ /j x 20. Kerkhoffs GM, Servien E, Dunn W, Dahm D, Bramer JA, Haverkamp D. The influence of obesity on the complication rate and outcome of total knee arthroplasty: a meta-analysis and systematic literature review. J Bone Joint Surg Am 2012;94: doi.org/ /jbjs.k Linberg CJ, Sperling JW, Schleck CD, Cofield RH. Shoulder arthroplasty in morbidly obese patients. J Shoulder Elbow Surg 2009;18: Matsen FA 3rd, Boileau P, Walch G, Gerber C, Bicknell RT. The reverse total shoulder arthroplasty. J Bone Joint Surg Am 2007;89: Matsen FA 3rd, Boileau P, Walch G, Gerber C, Bicknell RT. The reverse total shoulder arthroplasty. Instr Course Lect 2008;57: Nolan BM, Ankerson E, Wiater JM. Reverse total shoulder arthroplasty improves function in cuff tear arthropathy. Clin Orthop Relat Res 2011;469: Silber JH, Rosenbaum PR, Kelz RR, Reinke CE, Neuman MD, Ross RN, et al. Medical and financial risks associated with surgery in the elderly obese. Ann Surg 2012;256: /SLA.0b013e ef 26. Singh JA, Sperling JW, Cofield RH. Risk factors for revision surgery after humeral head replacement: 1,431 shoulders over 3 decades. J
8 42 A.K. Gupta et al. Shoulder Elbow Surg 2012;21: jse Walch G, Bacle G, Ladermann A, Nove-Josserand L, Smithers CJ. Do the indications, results, and complications of reverse shoulder arthroplasty change with surgeon s experience? J Shoulder Elbow Surg 2012;21: jse Wall B, Nove-Josserand L, O Connor DP, Edwards TB. Walch, G. Reverse total shoulder arthroplasty: a review of results according to etiology. J Bone Joint Surg Am 2007;89: /JBJS.F World Health Organization. Classification of obesity. Available from: Accessed February 17, Zumstein MA, Pinedo M, Old J, Boileau P. Problems, complications, reoperations, and revisions in reverse total shoulder arthroplasty: a systematic review. J Shoulder Elbow Surg 2011;20:
Clinical Outcomes and Complications during the Learning Curve for Reverse Total Shoulder Arthroplasty: An Analysis of the First 40 Cases
 Original Article Clinics in Orthopedic Surgery 2017;9:213-217 https://doi.org/10.4055/cios.2017.9.2.213 Clinical Outcomes and Complications during the Learning Curve for Reverse Total Shoulder Arthroplasty:
Original Article Clinics in Orthopedic Surgery 2017;9:213-217 https://doi.org/10.4055/cios.2017.9.2.213 Clinical Outcomes and Complications during the Learning Curve for Reverse Total Shoulder Arthroplasty:
Complication rates comparing primary with revision reverse total shoulder arthroplasty
 J Shoulder Elbow Surg (2014) 23, 1647-1654 www.elsevier.com/locate/ymse Complication rates comparing primary with revision reverse total shoulder arthroplasty Bryan M. Saltzman, MD a, *, Peter N. Chalmers,
J Shoulder Elbow Surg (2014) 23, 1647-1654 www.elsevier.com/locate/ymse Complication rates comparing primary with revision reverse total shoulder arthroplasty Bryan M. Saltzman, MD a, *, Peter N. Chalmers,
Shoulder Revisions: Why Are We Here?
 Shoulder Revisions: Why Are We Here? Indications for Revision to RSA Mark A. Frankle, MD Kaitlyn N. Christmas, BS Peter Simon, PhD DJO Revision Course 2017 June 2-3 Introduction Reverse shoulder arthroplasty(rsa)
Shoulder Revisions: Why Are We Here? Indications for Revision to RSA Mark A. Frankle, MD Kaitlyn N. Christmas, BS Peter Simon, PhD DJO Revision Course 2017 June 2-3 Introduction Reverse shoulder arthroplasty(rsa)
RCR or rtsa? Massive Rotator Cuff Tears without Arthritis in Patients Older than 65 Reverse Total Shoulder Arthroplasty or Rotator Cuff Repair?
 Massive Rotator Cuff Tears without Arthritis in Patients Older than 65 Reverse Total Shoulder Arthroplasty or Rotator Cuff Repair? JESSE W. ALLERT, MD THOMAS SELLERS, MD PETER SIMON, PHD RACHEL CLARK,
Massive Rotator Cuff Tears without Arthritis in Patients Older than 65 Reverse Total Shoulder Arthroplasty or Rotator Cuff Repair? JESSE W. ALLERT, MD THOMAS SELLERS, MD PETER SIMON, PHD RACHEL CLARK,
"Stability and Instability of RTSA"
 Orthopedics Update «Reverse Total Shoulder Arthroplasty» Stability and Instability of RTSA A. LÄDERMANN Orthopaedics and Traumatology, La Tour Hospital, Meyrin, Switzerland Orthopaedics and Traumatology,
Orthopedics Update «Reverse Total Shoulder Arthroplasty» Stability and Instability of RTSA A. LÄDERMANN Orthopaedics and Traumatology, La Tour Hospital, Meyrin, Switzerland Orthopaedics and Traumatology,
Shoulder Replacement Commonly Asked Questions
 Shoulder Replacement Commonly Asked Questions Patrick J Denard, MD Shoulder Specialist 2780 E. Barnett Rd Medford, OR 97530 541-779-6250 Background Information What is the anatomy of the shoulder? The
Shoulder Replacement Commonly Asked Questions Patrick J Denard, MD Shoulder Specialist 2780 E. Barnett Rd Medford, OR 97530 541-779-6250 Background Information What is the anatomy of the shoulder? The
Why are these shoulder replacements called a reverse prosthesis?
 PATIENT GUIDE TO REVERSE PROSTHESIS Edward G. McFarland MD The Division of Sports Medicine and Shoulder Surgery The Department of Orthopaedic Surgery The Johns Hopkins University Baltimore MD Why are these
PATIENT GUIDE TO REVERSE PROSTHESIS Edward G. McFarland MD The Division of Sports Medicine and Shoulder Surgery The Department of Orthopaedic Surgery The Johns Hopkins University Baltimore MD Why are these
Instability After Reverse Total Shoulder Arthroplasty: Which Patients Dislocate?
 An Original Study Instability After Reverse Total Shoulder Arthroplasty: Which Patients Dislocate? Eric M. Padegimas, MD, Benjamin Zmistowski, MD, Camilo Restrepo, MD, Joseph A. Abboud, MD, Mark D. Lazarus,
An Original Study Instability After Reverse Total Shoulder Arthroplasty: Which Patients Dislocate? Eric M. Padegimas, MD, Benjamin Zmistowski, MD, Camilo Restrepo, MD, Joseph A. Abboud, MD, Mark D. Lazarus,
Are too many reverse TSAs being done? Problems it is causing
 Are too many reverse TSAs being done? Problems it is causing Hithem Rahmi, DO John Itamura, MD The Kerlan Jobe Orthopaedic Clinic Professor of Orthopaedic Surgery Keck School of Medicine University of
Are too many reverse TSAs being done? Problems it is causing Hithem Rahmi, DO John Itamura, MD The Kerlan Jobe Orthopaedic Clinic Professor of Orthopaedic Surgery Keck School of Medicine University of
Revision of reversed total shoulder arthroplasty. Indications and outcome
 Farshad et al. BMC Musculoskeletal Disorders 2012, 13:160 RESEARCH ARTICLE Open Access Revision of reversed total shoulder arthroplasty. Indications and outcome Mazda Farshad *, Marion Grögli, Sabrina
Farshad et al. BMC Musculoskeletal Disorders 2012, 13:160 RESEARCH ARTICLE Open Access Revision of reversed total shoulder arthroplasty. Indications and outcome Mazda Farshad *, Marion Grögli, Sabrina
Nationwide Trends in Total Shoulder Arthroplasty and Hemiarthroplasty for Osteoarthritis
 An Original Study Nationwide Trends in Total Shoulder Arthroplasty and Hemiarthroplasty for Osteoarthritis David Trofa, MD, Sean S. Rajaee, MD, and Eric L. Smith, MD Abstract Recent literature reports
An Original Study Nationwide Trends in Total Shoulder Arthroplasty and Hemiarthroplasty for Osteoarthritis David Trofa, MD, Sean S. Rajaee, MD, and Eric L. Smith, MD Abstract Recent literature reports
Gerald R. Williams, MD
 Reverse Arthroplasty: Is Overutilization a Problem? Gerald R. Williams, MD John M. Fenlin, Jr, MD Professor of Shoulder and Elbow Surgery The Rothman Institute Jefferson Medical College Royalties Conflict
Reverse Arthroplasty: Is Overutilization a Problem? Gerald R. Williams, MD John M. Fenlin, Jr, MD Professor of Shoulder and Elbow Surgery The Rothman Institute Jefferson Medical College Royalties Conflict
ORIGINAL ARTICLES SECTION II. Prevalence and Risk Factors for Symptomatic Thromboembolic Events after Shoulder Arthroplasty
 CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 448, pp. 152 156 2006 Lippincott Williams & Wilkins SECTION II ORIGINAL ARTICLES Prevalence and Risk Factors for Symptomatic Thromboembolic Events after
CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 448, pp. 152 156 2006 Lippincott Williams & Wilkins SECTION II ORIGINAL ARTICLES Prevalence and Risk Factors for Symptomatic Thromboembolic Events after
Predicting Short Term Morbidity following Revision Hip and Knee Arthroplasty
 Predicting Short Term Morbidity following Revision Hip and Knee Arthroplasty A Review of ACS-NSQIP 2006-2012 Arjun Sebastian, M.D., Stephanie Polites, M.D., Kristine Thomsen, B.S., Elizabeth Habermann,
Predicting Short Term Morbidity following Revision Hip and Knee Arthroplasty A Review of ACS-NSQIP 2006-2012 Arjun Sebastian, M.D., Stephanie Polites, M.D., Kristine Thomsen, B.S., Elizabeth Habermann,
Reverse Shoulder Arthroplasty for Management of Postinfectious Arthropathy With Rotator Cuff Deficiency
 Reverse Shoulder Arthroplasty for Management of Postinfectious Arthropathy With Rotator Cuff Deficiency Brent J. Morris, MD; Wame N. Waggenspack Jr, MD; Mitzi S. Laughlin, PhD; Hussein A. Elkousy, MD;
Reverse Shoulder Arthroplasty for Management of Postinfectious Arthropathy With Rotator Cuff Deficiency Brent J. Morris, MD; Wame N. Waggenspack Jr, MD; Mitzi S. Laughlin, PhD; Hussein A. Elkousy, MD;
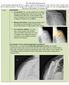
Immediate post surgical findings of soft tissue swelling, subcutaneous emphysema, and skin staples for reverse total shoulder arthroplasty.
 Immediate post surgical findings of soft tissue swelling, subcutaneous emphysema, and skin staples for reverse total shoulder arthroplasty. REVERSE TOTAL SHOULDER ARTHROPLASTY WITH FRACTURED ACROMION Above:
Immediate post surgical findings of soft tissue swelling, subcutaneous emphysema, and skin staples for reverse total shoulder arthroplasty. REVERSE TOTAL SHOULDER ARTHROPLASTY WITH FRACTURED ACROMION Above:
Assessment of Approximate Glenoid Size in Thai People
 Assessment of Approximate Glenoid Size in Thai People J Med Assoc Thai 2014; 97 (Suppl. 2): S14-S18 Full text. e-journal: http://www.jmatonline.com Pason Phonphok MD*, Nattha Kulkamthorn MD* * Division
Assessment of Approximate Glenoid Size in Thai People J Med Assoc Thai 2014; 97 (Suppl. 2): S14-S18 Full text. e-journal: http://www.jmatonline.com Pason Phonphok MD*, Nattha Kulkamthorn MD* * Division
Both anatomic (atsa) and reverse (rtsa) total
 S101 Comparison of Outcomes Using Anatomic and Reverse Total Shoulder Arthroplasty Pierre-Henri Flurin, M.D., Yann Marczuk, M.D., Martin Janout, M.D., Thomas W. Wright, M.D., Joseph Zuckerman, M.D., and
S101 Comparison of Outcomes Using Anatomic and Reverse Total Shoulder Arthroplasty Pierre-Henri Flurin, M.D., Yann Marczuk, M.D., Martin Janout, M.D., Thomas W. Wright, M.D., Joseph Zuckerman, M.D., and
MEDICAL POLICY MEDICAL POLICY DETAILS POLICY STATEMENT. Page: 1 of 6
 Page: 1 of 6 MEDICAL POLICY MEDICAL POLICY DETAILS Medical Policy Title SHOULDER ARTHROPLASTY (TOTAL, PARTIAL AND REVERSE) Policy Number 7.01.95 Category Technology Assessment Effective Date 6/21/18 Revised
Page: 1 of 6 MEDICAL POLICY MEDICAL POLICY DETAILS Medical Policy Title SHOULDER ARTHROPLASTY (TOTAL, PARTIAL AND REVERSE) Policy Number 7.01.95 Category Technology Assessment Effective Date 6/21/18 Revised
Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty
 Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
0 Introduction (20.9%) [7]
![0 Introduction (20.9%) [7] 0 Introduction (20.9%) [7]](/thumbs/92/108991709.jpg) Chinese Journal of Tissue Engineering Research www.crter.org ( 443000) DOI:10.3969/j.issn.2095-4344.0187 ORCID: 0000-0003-0005-1839() 60 120 2 60 1980 2015 443000 :R318 :A 2017-12-05 3 4 120 60 () 3 (P
Chinese Journal of Tissue Engineering Research www.crter.org ( 443000) DOI:10.3969/j.issn.2095-4344.0187 ORCID: 0000-0003-0005-1839() 60 120 2 60 1980 2015 443000 :R318 :A 2017-12-05 3 4 120 60 () 3 (P
Convertibilité. Ph. Valenti. Paris Shoulder Unit Clinique Bizet (Paris, France)
 Convertibilité Ph. Valenti Paris Shoulder Unit Clinique Bizet (Paris, France) Disclosures Arthroplasty Consultant : FH orthopaedics receive royalties Arthroscopy Consultant : Zimmer Biomet Arthrex In Last
Convertibilité Ph. Valenti Paris Shoulder Unit Clinique Bizet (Paris, France) Disclosures Arthroplasty Consultant : FH orthopaedics receive royalties Arthroscopy Consultant : Zimmer Biomet Arthrex In Last
CLINICAL GUIDELINES. CMM-318: Shoulder Arthroplasty/ Replacement/Resurfacing/ Revision/Arthrodesis. Version Effective October 22, 2018
 CLINICAL GUIDELINES CMM-318: / Replacement/Resurfacing/ Revision/Arthrodesis Version 20.0.2018 Effective October 22, 2018 Clinical guidelines for medical necessity review of speech therapy services. CMM-318:
CLINICAL GUIDELINES CMM-318: / Replacement/Resurfacing/ Revision/Arthrodesis Version 20.0.2018 Effective October 22, 2018 Clinical guidelines for medical necessity review of speech therapy services. CMM-318:
Making sense of all our measures-inclination, version, subluxation, reaming depth & implant seating
 Thursday - ANATOMIC SHOULDER ARTHROPLASTY 7:00-7:15a Welcome and Introduction of Faculty Athwal, Keener, 7:15-7:22a The ABC s of the Walch Classification Walch 7:22-7:32a How I use x-rays, CT +/- MRI for
Thursday - ANATOMIC SHOULDER ARTHROPLASTY 7:00-7:15a Welcome and Introduction of Faculty Athwal, Keener, 7:15-7:22a The ABC s of the Walch Classification Walch 7:22-7:32a How I use x-rays, CT +/- MRI for
Reverse Total Shoulder Arthroplasty: A New Frontier (of Complications)
 Reverse Total Shoulder Arthroplasty: A New Frontier (of Complications) Emilie Cheung, MD Associate Professor Chief Shoulder Elbow Svc Stanford University Department of Orthopedic Surgery Procedure volumes
Reverse Total Shoulder Arthroplasty: A New Frontier (of Complications) Emilie Cheung, MD Associate Professor Chief Shoulder Elbow Svc Stanford University Department of Orthopedic Surgery Procedure volumes
Antibiotic Spacers in Shoulder Arthroplasty: Comparison of Stemmed and Stemless Implants.
 Thomas Jefferson University Jefferson Digital Commons Department of Orthopaedic Surgery Faculty Papers Department of Orthopaedic Surgery 12-1-2017 Antibiotic Spacers in Shoulder Arthroplasty: Comparison
Thomas Jefferson University Jefferson Digital Commons Department of Orthopaedic Surgery Faculty Papers Department of Orthopaedic Surgery 12-1-2017 Antibiotic Spacers in Shoulder Arthroplasty: Comparison
Balgrist Shoulder Course 2017
 Diagnosis and Management of Infection in Revision Shoulder Arthroplasty Joseph P. Iannotti MD, PhD Maynard Madden Professor and Chairman Orthopaedic and Rheumatologic Institute Cleveland Clinic Conflict
Diagnosis and Management of Infection in Revision Shoulder Arthroplasty Joseph P. Iannotti MD, PhD Maynard Madden Professor and Chairman Orthopaedic and Rheumatologic Institute Cleveland Clinic Conflict
Management of arthritis of the shoulder. Omar Haddo Consultant Orthopaedic Surgeon
 Management of arthritis of the shoulder Omar Haddo Consultant Orthopaedic Surgeon Diagnosis Pain - with activity initially. As disease progresses night pain is common and sleep difficult Stiffness trouble
Management of arthritis of the shoulder Omar Haddo Consultant Orthopaedic Surgeon Diagnosis Pain - with activity initially. As disease progresses night pain is common and sleep difficult Stiffness trouble
Matthew D. Saltzman, MD a, Deana M. Mercer, MD c, Winston J. Warme, MD b, Alexander L. Bertelsen, PA-C b, Frederick A. Matsen III, MD b, *
 J Shoulder Elbow Surg (2010) 19, 1028-1033 www.elsevier.com/locate/ymse A method for documenting the change in center of rotation with reverse total shoulder arthroplasty and its application to a consecutive
J Shoulder Elbow Surg (2010) 19, 1028-1033 www.elsevier.com/locate/ymse A method for documenting the change in center of rotation with reverse total shoulder arthroplasty and its application to a consecutive
Shoulder Arthroplasty. Valentin Lance 3/24/16
 Shoulder Arthroplasty Valentin Lance 3/24/16 Outline Background Pre-operative imaging assessment Total Shoulder Arthroplasty: Standard and Reverse Complications Other shoulder hardware Hemiarthroplasty
Shoulder Arthroplasty Valentin Lance 3/24/16 Outline Background Pre-operative imaging assessment Total Shoulder Arthroplasty: Standard and Reverse Complications Other shoulder hardware Hemiarthroplasty
The use of the Lima reverse shoulder arthroplasty for the treatment of fracture sequelae of the proximal humerus
 J Orthop Sci (2012) 17:141 147 DOI 10.1007/s00776-011-0185-5 ORIGINAL ARTICLE The use of the Lima reverse shoulder arthroplasty for the treatment of fracture sequelae of the proximal humerus Angel Antonio
J Orthop Sci (2012) 17:141 147 DOI 10.1007/s00776-011-0185-5 ORIGINAL ARTICLE The use of the Lima reverse shoulder arthroplasty for the treatment of fracture sequelae of the proximal humerus Angel Antonio
SHOULDER ARTHROPLASTY (TOTAL, HEMI, REVERSE)/ARTHRODESIS
 evicore healthcare. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Imaging requests for patients with atypical symptoms or clinical presentations
evicore healthcare. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Imaging requests for patients with atypical symptoms or clinical presentations
Disclosures A prospective comparison between reverse and anatomic total shoulder arthroplasty
 Disclosures A prospective comparison between reverse and anatomic total shoulder arthroplasty Tuyen Kiet Micah Naimark, MD Brian T. Feeley, MD Teddy T. Chung Tatiana Gajiu Sarah L. Hall, MA C. Benjamin
Disclosures A prospective comparison between reverse and anatomic total shoulder arthroplasty Tuyen Kiet Micah Naimark, MD Brian T. Feeley, MD Teddy T. Chung Tatiana Gajiu Sarah L. Hall, MA C. Benjamin
3/9/2018. Algorithm for Massive RCT s. Massive Rotator Cuff Tears: When is Reverse TSA the only option?
 Massive Rotator Cuff Tears: When is Reverse TSA the only option? Anthony A. Romeo, MD Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Team Physician, Chicago White Sox
Massive Rotator Cuff Tears: When is Reverse TSA the only option? Anthony A. Romeo, MD Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Team Physician, Chicago White Sox
Not relevant to this presentation.
 Nolan R. May, MD Kearney, NE Heartland Surgery Center, Kearney NE Not relevant to this presentation. 1 What are the indications for total shoulder arthroplasty? What are the differences between total shoulder
Nolan R. May, MD Kearney, NE Heartland Surgery Center, Kearney NE Not relevant to this presentation. 1 What are the indications for total shoulder arthroplasty? What are the differences between total shoulder
Retrospective Analysis of Arthroscopic Management of Glenohumeral Degenerative Disease
 Retrospective Analysis of Arthroscopic Management of Glenohumeral Degenerative Disease Geoffrey S. Van Thiel, M.D., M.B.A., Steven Sheehan, B.S., Rachel M. Frank, B.S., Mark Slabaugh, M.D., Brian J. Cole,
Retrospective Analysis of Arthroscopic Management of Glenohumeral Degenerative Disease Geoffrey S. Van Thiel, M.D., M.B.A., Steven Sheehan, B.S., Rachel M. Frank, B.S., Mark Slabaugh, M.D., Brian J. Cole,
Degenerative joint disease of the shoulder, while
 Arthroscopic Debridement of the Shoulder for Osteoarthritis David M. Weinstein, M.D., John S. Bucchieri, M.D., Roger G. Pollock, M.D., Evan L. Flatow, M.D., and Louis U. Bigliani, M.D. Summary: Twenty-five
Arthroscopic Debridement of the Shoulder for Osteoarthritis David M. Weinstein, M.D., John S. Bucchieri, M.D., Roger G. Pollock, M.D., Evan L. Flatow, M.D., and Louis U. Bigliani, M.D. Summary: Twenty-five
Prosthetic design of reverse shoulder arthroplasty contributes to scapular notching and instability
 Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.5312/wjo.v7.i11.738 World J Orthop 2016 November 18; 7(11): 738-745 ISSN 2218-5836 (online)
Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.5312/wjo.v7.i11.738 World J Orthop 2016 November 18; 7(11): 738-745 ISSN 2218-5836 (online)
Cigna Medical Coverage Policies Musculoskeletal Shoulder Arthroplasty (Total, Hemi, Reverse)/Arthrodesis
 Cigna Medical Coverage Policies Musculoskeletal Shoulder Arthroplasty (Total, Hemi, Reverse)/Arthrodesis Effective January 1, 2016 Instructions for use The following coverage policy applies to health benefit
Cigna Medical Coverage Policies Musculoskeletal Shoulder Arthroplasty (Total, Hemi, Reverse)/Arthrodesis Effective January 1, 2016 Instructions for use The following coverage policy applies to health benefit
Influence of Glenosphere Design on Outcomes and Complications of Reverse Arthroplasty: A Systematic Review
 Original Article Clinics in Orthopedic Surgery 2016;8:288-297 http://dx.doi.org/10.4055/cios.2016.8.3.288 Influence of Glenosphere Design on Outcomes and Complications of Reverse Arthroplasty: A Systematic
Original Article Clinics in Orthopedic Surgery 2016;8:288-297 http://dx.doi.org/10.4055/cios.2016.8.3.288 Influence of Glenosphere Design on Outcomes and Complications of Reverse Arthroplasty: A Systematic
)19( COPYRIGHT 2019 BY THE ARCHIVES OF BONE AND JOINT SURGERY
 )19( COPYRIGHT 2019 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE Failure of Anatomic Total Shoulder Arthroplasty with Revision to Another Anatomic Total Shoulder Arthroplasty Mihir Sheth,
)19( COPYRIGHT 2019 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE Failure of Anatomic Total Shoulder Arthroplasty with Revision to Another Anatomic Total Shoulder Arthroplasty Mihir Sheth,
Scapular Notching. Recognition and Strategies to Minimize Clinical Impact. Gregory P. Nicholson MD, Eric J. Strauss MD, Seth L.
 Clin Orthop Relat Res DOI 10.1007/s11999-010-1720-y SYMPOSIUM: REVERSE TOTAL SHOULDER ARTHROPLASTY Scapular Notching Recognition and Strategies to Minimize Clinical Impact Gregory P. Nicholson MD, Eric
Clin Orthop Relat Res DOI 10.1007/s11999-010-1720-y SYMPOSIUM: REVERSE TOTAL SHOULDER ARTHROPLASTY Scapular Notching Recognition and Strategies to Minimize Clinical Impact Gregory P. Nicholson MD, Eric
ANATOMIC TOTAL SHOULDER REPLACEMENT:
 The Shoulder Replacement A total shoulder arthroplasty (TSA) is a surgery to replace the damaged parts of the ball and socket shoulder joint with an artificial prosthesis. The damage to the shoulder can
The Shoulder Replacement A total shoulder arthroplasty (TSA) is a surgery to replace the damaged parts of the ball and socket shoulder joint with an artificial prosthesis. The damage to the shoulder can
continued TABLE E-1 Potential Predictors of Short-Term Complications and Reoperations* Comparison Group OR 95% CI P Value
 Page 1 of 7 TABLE E-1 Potential Predictors of Short-Term Complications and Reoperations* Pulmonary embolism Charlson comorbidity index 1.2 1.0 to 1.4 0.06 Hospital volume percentile, 40-79 80-100 0.8 0.4
Page 1 of 7 TABLE E-1 Potential Predictors of Short-Term Complications and Reoperations* Pulmonary embolism Charlson comorbidity index 1.2 1.0 to 1.4 0.06 Hospital volume percentile, 40-79 80-100 0.8 0.4
Management of Hip Fractures
 Management of Hip Fractures in the Elderly Patient David A. Brown MD COL U.S. Army Ret. The Center for Orthopedics and Neurosurgery Optimizing Management of Hip Fractures in the Elderly Patient Optimizing
Management of Hip Fractures in the Elderly Patient David A. Brown MD COL U.S. Army Ret. The Center for Orthopedics and Neurosurgery Optimizing Management of Hip Fractures in the Elderly Patient Optimizing
Good functional outcomes expected after shoulder arthroplasty irrespective of body mass index
 J Shoulder Elbow Surg (2018) 27, S43 S49 www.elsevier.com/locate/ymse Good functional outcomes expected after shoulder arthroplasty irrespective of body mass index David D. Savin, MD a, *, Rachel M. Frank,MD
J Shoulder Elbow Surg (2018) 27, S43 S49 www.elsevier.com/locate/ymse Good functional outcomes expected after shoulder arthroplasty irrespective of body mass index David D. Savin, MD a, *, Rachel M. Frank,MD
SSSR. 1. Nov Shoulder Prosthesis. Postoperative Imaging. Florian M. Buck, MD
 Shoulder Prosthesis Postoperative Imaging Florian M. Buck, MD Shoulder Prosthesis Surgical Approach Findings Imaging Modalities Postoperative Problems Shoulder Prosthesis What are we talking about Anatomical
Shoulder Prosthesis Postoperative Imaging Florian M. Buck, MD Shoulder Prosthesis Surgical Approach Findings Imaging Modalities Postoperative Problems Shoulder Prosthesis What are we talking about Anatomical
Periprosthetic joint infection: are patients with multiple prosthetic joints at risk?
 Thomas Jefferson University Jefferson Digital Commons Rothman Institute Rothman Institute 6-1-2012 Periprosthetic joint infection: are patients with multiple prosthetic joints at risk? S Mehdi Jafari The
Thomas Jefferson University Jefferson Digital Commons Rothman Institute Rothman Institute 6-1-2012 Periprosthetic joint infection: are patients with multiple prosthetic joints at risk? S Mehdi Jafari The
The Irreparable Rotator Cuff Tear:
 The Irreparable Rotator Cuff Tear: Trauma 101: Shoulder Session #2 Brian Grawe, MD Assistant Professor Orthopaedics & Sports Medicine 5/10/2018 Brian Grawe, MD Assistant Professor Phone Number: 513-558-4516
The Irreparable Rotator Cuff Tear: Trauma 101: Shoulder Session #2 Brian Grawe, MD Assistant Professor Orthopaedics & Sports Medicine 5/10/2018 Brian Grawe, MD Assistant Professor Phone Number: 513-558-4516
The Role of Concomitant Biceps Tenodesis in Shoulder Arthroplasty for Primary Osteoarthritis: Results of a Multicentric Study
 4edwards.qxd 4/6/04 3:53 PM Page 401 The Role of Concomitant Biceps Tenodesis in Shoulder Arthroplasty for Primary Osteoarthritis: Results of a Multicentric Study GIUSEPPE FAMA, MD*; T. BRADLEY EDWARDS,
4edwards.qxd 4/6/04 3:53 PM Page 401 The Role of Concomitant Biceps Tenodesis in Shoulder Arthroplasty for Primary Osteoarthritis: Results of a Multicentric Study GIUSEPPE FAMA, MD*; T. BRADLEY EDWARDS,
EPO-144 Patients with Morbid Obesity and Congestive Heart Failure Have Longer Operative Time and Room Time in Total Hip Arthroplasty
 SESUG 2016 EPO-144 Patients with Morbid Obesity and Congestive Heart Failure Have Longer Operative Time and Room Time in Total Hip Arthroplasty ABSTRACT Yubo Gao, University of Iowa Hospitals and Clinics,
SESUG 2016 EPO-144 Patients with Morbid Obesity and Congestive Heart Failure Have Longer Operative Time and Room Time in Total Hip Arthroplasty ABSTRACT Yubo Gao, University of Iowa Hospitals and Clinics,
Managing acromial fractures: prevention and treatment, both nonoperative and operative
 Review Article Page 1 of 8 Managing acromial fractures: prevention and treatment, both nonoperative and operative Christopher D. Joyce, Adam J. Seidl Department of Orthopaedics, University of Colorado,
Review Article Page 1 of 8 Managing acromial fractures: prevention and treatment, both nonoperative and operative Christopher D. Joyce, Adam J. Seidl Department of Orthopaedics, University of Colorado,
Insulin Dependence Heralds Adverse Events After Hip And Knee Arthroplasty
 Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine 1-1-2016 Insulin Dependence Heralds Adverse Events After Hip And Knee
Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine 1-1-2016 Insulin Dependence Heralds Adverse Events After Hip And Knee
Percutaneous Fluoroscopic Synovial Biopsy as a New Diagnostic Test for Periprosthetic Infection after Shoulder Arthroplasty: A Feasibility Study
 Percutaneous Fluoroscopic Synovial Biopsy as a New Diagnostic Test for Periprosthetic Infection after Shoulder Arthroplasty: A Feasibility Study J Quon, K Hynes, P Lapner, A Sheikh The Ottawa Hospital
Percutaneous Fluoroscopic Synovial Biopsy as a New Diagnostic Test for Periprosthetic Infection after Shoulder Arthroplasty: A Feasibility Study J Quon, K Hynes, P Lapner, A Sheikh The Ottawa Hospital
)532( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY
 )532( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE The Midterm Results of the Delta Xtend Reverse Shoulder System: A Five-Year Outcome Study John G. Horneff, MD; Thema A. Nicholson,
)532( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE The Midterm Results of the Delta Xtend Reverse Shoulder System: A Five-Year Outcome Study John G. Horneff, MD; Thema A. Nicholson,
Reverse Shoulder System. Abstracts
 TM Reverse Shoulder System s 2 Contents Introduction 2 Reverse shoulder arthroplasty components and surgical techniques that restore glenohumeralmotion 3 Isometric strength, range of motion, and impairment
TM Reverse Shoulder System s 2 Contents Introduction 2 Reverse shoulder arthroplasty components and surgical techniques that restore glenohumeralmotion 3 Isometric strength, range of motion, and impairment
L. Favard a,, D. Katz b, M. Colmar c, T. Benkalfate d, H. Thomazeau e, S. Emily c WORKSHOPS OF THE SOO (2011, LA BAULE).
 Orthopaedics & Traumatology: Surgery & Research (2012) 98, S41 S47 Available online at www.sciencedirect.com WORKSHOPS OF THE SOO (2011, LA BAULE). ORIGINAL ARTICLE Total shoulder arthroplasty Arthroplasty
Orthopaedics & Traumatology: Surgery & Research (2012) 98, S41 S47 Available online at www.sciencedirect.com WORKSHOPS OF THE SOO (2011, LA BAULE). ORIGINAL ARTICLE Total shoulder arthroplasty Arthroplasty
Hip and Knee Replacements
 Hip and Knee Replacements What the PCP Needs to Know Derek Ward, M.D. Assistant Professor of Orthopaedic Surgery Division of Adult Reconstruction University of California, San Francisco 12/2/2017 Disclosures
Hip and Knee Replacements What the PCP Needs to Know Derek Ward, M.D. Assistant Professor of Orthopaedic Surgery Division of Adult Reconstruction University of California, San Francisco 12/2/2017 Disclosures
Biomechanical concepts of total shoulder replacement. «Shoulder Course» Day 1. Richard W. Nyffeler Orthopädie Sonnenhof Bern. 11. Sept.
 Biomechanical concepts of total shoulder replacement Richard W. Nyffeler Orthopädie Sonnenhof Bern First total shoulder prosthesis Jules Emile Péan, 1830-1898 Monobloc prostheses Charles Neer, 1917-2011
Biomechanical concepts of total shoulder replacement Richard W. Nyffeler Orthopädie Sonnenhof Bern First total shoulder prosthesis Jules Emile Péan, 1830-1898 Monobloc prostheses Charles Neer, 1917-2011
Comparison of Pegged and Keeled Glenoid Components for Total Shoulder Arthroplasty: A Systematic Review
 Review Article Comparison of Pegged and Keeled Glenoid Components for Total Shoulder Arthroplasty: A Systematic Review Journal of Shoulder and Elbow Arthroplasty Volume 1: 1 7! The Author(s) 2017 Reprints
Review Article Comparison of Pegged and Keeled Glenoid Components for Total Shoulder Arthroplasty: A Systematic Review Journal of Shoulder and Elbow Arthroplasty Volume 1: 1 7! The Author(s) 2017 Reprints
Malnutrition: An independent Risk Factor for Postoperative Complications
 Malnutrition: An independent Risk Factor for Postoperative Complications Bryan P. Hooks, D.O. University of Pittsburgh-Horizon June 24, 2017 Orthopedic Surgeon-Adult Reconstruction Disclosures: None Objectives:
Malnutrition: An independent Risk Factor for Postoperative Complications Bryan P. Hooks, D.O. University of Pittsburgh-Horizon June 24, 2017 Orthopedic Surgeon-Adult Reconstruction Disclosures: None Objectives:
ABSTRACT TITLE: Near-OR Perioperative Interventions to Decrease Hospital Length
 ABSTRACT NUMBER: 020-0094 ABSTRACT TITLE: Near-OR Perioperative Interventions to Decrease Hospital Length of Stay AUTHORS: Mark J. Lenart, MD Vanderbilt University 1301 Medical Center Drive Nashville,
ABSTRACT NUMBER: 020-0094 ABSTRACT TITLE: Near-OR Perioperative Interventions to Decrease Hospital Length of Stay AUTHORS: Mark J. Lenart, MD Vanderbilt University 1301 Medical Center Drive Nashville,
Perioperative Optimization
 Perioperative Optimization AAHKS 2017 Peter Caccavallo, MD, MS Internal Medicine Perioperative Orthopedic Hospitalist Director of Indianapolis Perioperative Medicine 2003-Present ppcaccav@yahoo.com Disclosures
Perioperative Optimization AAHKS 2017 Peter Caccavallo, MD, MS Internal Medicine Perioperative Orthopedic Hospitalist Director of Indianapolis Perioperative Medicine 2003-Present ppcaccav@yahoo.com Disclosures
TORNIER AEQUALIS FX. Shoulder System SYSTEM OVERVIEW
 TORNIER AEQUALIS FX Shoulder System SYSTEM OVERVIEW Simple in design, but used for the most complex fractures Each year, approximately 4 million people in the United States seek medical care for shoulder
TORNIER AEQUALIS FX Shoulder System SYSTEM OVERVIEW Simple in design, but used for the most complex fractures Each year, approximately 4 million people in the United States seek medical care for shoulder
Functional outcomes of reverse shoulder arthroplasty compared with hemiarthroplasty for acute proximal humeral fractures
 J Shoulder Elbow Surg (2013) 22, 32-37 www.elsevier.com/locate/ymse Functional outcomes of reverse shoulder arthroplasty compared with hemiarthroplasty for acute proximal humeral fractures Matthew J. Boyle,
J Shoulder Elbow Surg (2013) 22, 32-37 www.elsevier.com/locate/ymse Functional outcomes of reverse shoulder arthroplasty compared with hemiarthroplasty for acute proximal humeral fractures Matthew J. Boyle,
Ankle fractures are one of
 Elevated Risks of Ankle Fracture Surgery in Patients With Diabetes Nelson F. SooHoo, MD, Lucie Krenek, MD, Michael Eagan, MD, and David S. Zingmond, MD, PhD Ankle fractures are one of the most common types
Elevated Risks of Ankle Fracture Surgery in Patients With Diabetes Nelson F. SooHoo, MD, Lucie Krenek, MD, Michael Eagan, MD, and David S. Zingmond, MD, PhD Ankle fractures are one of the most common types
Arthroplasty Of The Shoulder
 Arthroplasty Of The Shoulder 1 / 7 2 / 7 3 / 7 Arthroplasty Of The Shoulder About Your Shoulder. Ligaments and tendons hold it together. Ligaments connect the bones, while tendons connect muscles to the
Arthroplasty Of The Shoulder 1 / 7 2 / 7 3 / 7 Arthroplasty Of The Shoulder About Your Shoulder. Ligaments and tendons hold it together. Ligaments connect the bones, while tendons connect muscles to the
YEAR EXPERIENCE WITH STEMLESS ARTHROPLASTY. Disclosures INDICATIONS FOR STEMMLES TSA
 5-10 YEAR EXPERIENCE WITH STEMLESS ARTHROPLASTY PETER HABERMEYER DEUTSCHES SCHULTERZENTRUM MUNICH Germany Disclosures Consultant for Arthrex Inc. Royalties Arthrex Inc. INDICATIONS FOR STEMMLES TSA 1.
5-10 YEAR EXPERIENCE WITH STEMLESS ARTHROPLASTY PETER HABERMEYER DEUTSCHES SCHULTERZENTRUM MUNICH Germany Disclosures Consultant for Arthrex Inc. Royalties Arthrex Inc. INDICATIONS FOR STEMMLES TSA 1.
Optimal Baseplate Rotational Alignment in Reverse Total Shoulder Arthroplasty: A Three-Dimensional Computer-Aided Design Study.
 Optimal Baseplate Rotational Alignment in Reverse Total Shoulder Arthroplasty: A Three-Dimensional Computer-Aided Design Study. Byron F. Stephens, MD 1, Casey T. Hebert 2, Thomas W. Throckmorton, MD 1,
Optimal Baseplate Rotational Alignment in Reverse Total Shoulder Arthroplasty: A Three-Dimensional Computer-Aided Design Study. Byron F. Stephens, MD 1, Casey T. Hebert 2, Thomas W. Throckmorton, MD 1,
Vitamin D deficiency is associated with longer hospital stay and lower functional outcome after total knee arthroplasty.
 Reference number to be mentioned by correspondence : ORTHO/- Acta Orthop. Belg., 2015, 83, 00-00 ORIGINAL STUDY Vitamin D deficiency is associated with longer hospital stay and lower functional outcome
Reference number to be mentioned by correspondence : ORTHO/- Acta Orthop. Belg., 2015, 83, 00-00 ORIGINAL STUDY Vitamin D deficiency is associated with longer hospital stay and lower functional outcome
Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis
 CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 366, pp. 39-45 0 1999 Lippincott Williams & Wilkins, Inc. Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis Jens 0. S@jbjerg,
CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 366, pp. 39-45 0 1999 Lippincott Williams & Wilkins, Inc. Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis Jens 0. S@jbjerg,
Reverse Total Shoulder Arthroplasty: Early Outcome and Complication Report
 ORIGINAL ARTICLE Clinics in Shoulder and Elbow Vol. 17, No. 2, June, 2014 http://dx.doi.org/10.5397/cise.2014.17.2.68 CiSE Clinics in Shoulder and Elbow Reverse Total Shoulder Arthroplasty: Early Outcome
ORIGINAL ARTICLE Clinics in Shoulder and Elbow Vol. 17, No. 2, June, 2014 http://dx.doi.org/10.5397/cise.2014.17.2.68 CiSE Clinics in Shoulder and Elbow Reverse Total Shoulder Arthroplasty: Early Outcome
ISSUES FROM AN ORTHOPEDIC PERSPECTIVE
 ISSUES FROM AN ORTHOPEDIC PERSPECTIVE John Brown, MD The Core Institute Objectives: Understand the common orthopedic problems of the geriatric population. Describe the standard treatment algorithms for
ISSUES FROM AN ORTHOPEDIC PERSPECTIVE John Brown, MD The Core Institute Objectives: Understand the common orthopedic problems of the geriatric population. Describe the standard treatment algorithms for
Bilateral Anatomic Total Shoulder Arthroplasty Versus Reverse Shoulder Arthroplasty
 Bilateral Anatomic Total Shoulder Arthroplasty Versus Reverse Shoulder Arthroplasty Vaqar Latif, MD; Patrick J. Denard, MD; Allan A. Young, MD; Jean-Pierre Liotard, MD; Gilles Walch, MD abstract Full article
Bilateral Anatomic Total Shoulder Arthroplasty Versus Reverse Shoulder Arthroplasty Vaqar Latif, MD; Patrick J. Denard, MD; Allan A. Young, MD; Jean-Pierre Liotard, MD; Gilles Walch, MD abstract Full article
Zimmer Patient Specific Instruments (PSI) for Reverse Shoulder Arthroplasty
 Zimmer Patient Specific Instruments (PSI) for Reverse Shoulder Arthroplasty Ryan Krupp, M.D. Norton Orthopaedic Specialists Louisville, KY Anand Murthi, M.D. MedStar Union Memorial Hospital Baltimore,
Zimmer Patient Specific Instruments (PSI) for Reverse Shoulder Arthroplasty Ryan Krupp, M.D. Norton Orthopaedic Specialists Louisville, KY Anand Murthi, M.D. MedStar Union Memorial Hospital Baltimore,
WHAT YOU IS BACK WITHIN ARM S REACH
 YOUR TOTAL SHOULDER REPLACEMENT SURGERY STEPS TO RETURNING TO A LIFESTYLE YOU DESERVE WHAT YOU IS BACK WITHIN ARM S REACH Nathan Richardson, MD Orthopedics, Shoulder & Elbow Surgeon Board Certified in
YOUR TOTAL SHOULDER REPLACEMENT SURGERY STEPS TO RETURNING TO A LIFESTYLE YOU DESERVE WHAT YOU IS BACK WITHIN ARM S REACH Nathan Richardson, MD Orthopedics, Shoulder & Elbow Surgeon Board Certified in
Risk Factors for Readmission and Revision Surgery Following Rotator Cuff Repair
 Clin Orthop Relat Res (2008) 466:608 613 DOI 10.1007/s11999-008-0116-8 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Risk Factors for Readmission and Revision Surgery Following Rotator Cuff Repair Seth
Clin Orthop Relat Res (2008) 466:608 613 DOI 10.1007/s11999-008-0116-8 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Risk Factors for Readmission and Revision Surgery Following Rotator Cuff Repair Seth
Shoulder Arthroplasty
 Shoulder Arthroplasty Nathan G. Everding, MD Specializing in Hand, Wrist, Elbow & Shoulder Surgery Syracuse Orthopedic Specialists SJH Family Practice Refresher course 3/8/19 Shoulder Arthroplasty Rate
Shoulder Arthroplasty Nathan G. Everding, MD Specializing in Hand, Wrist, Elbow & Shoulder Surgery Syracuse Orthopedic Specialists SJH Family Practice Refresher course 3/8/19 Shoulder Arthroplasty Rate
Shoulder Joint Replacement
 Shoulder Joint Replacement Although shoulder joint replacement is less common than knee or hip replacement, it is just as successful in relieving joint pain. Shoulder replacement surgery was first performed
Shoulder Joint Replacement Although shoulder joint replacement is less common than knee or hip replacement, it is just as successful in relieving joint pain. Shoulder replacement surgery was first performed
Considerations 3/9/2018. Asheesh Bedi, MD. I have no disclosures or conflicts of interest related to the content of this presentation.
 Radiological Assessment of the Rotator Cuff What predicts outcomes? Asheesh Bedi, MD Harold and Helen W. Gehring Professor Chief, Sports Medicine & Shoulder Surgery MedSport, Department of Orthopedic Surgery
Radiological Assessment of the Rotator Cuff What predicts outcomes? Asheesh Bedi, MD Harold and Helen W. Gehring Professor Chief, Sports Medicine & Shoulder Surgery MedSport, Department of Orthopedic Surgery
Anaesthesia for the Over 75s. Chris Edge
 Anaesthesia for the Over 75s Chris Edge Topics to be Covered Post-operative cognitive management Morbidity and mortality General anaesthesia a good idea or not? Multiple comorbidities and assessment of
Anaesthesia for the Over 75s Chris Edge Topics to be Covered Post-operative cognitive management Morbidity and mortality General anaesthesia a good idea or not? Multiple comorbidities and assessment of
Surface Replacement for the Active Patient with GH DJD. Disclosures. Popularized by Copeland 3/1/2018
 Surface Replacement for the Active Patient with GH DJD E. Rhett Hobgood, M.D. MS Sports Medicine Jackson, MS Disclosures Consultant for Exactech No royalties from any company Fellowship support from Mitek,
Surface Replacement for the Active Patient with GH DJD E. Rhett Hobgood, M.D. MS Sports Medicine Jackson, MS Disclosures Consultant for Exactech No royalties from any company Fellowship support from Mitek,
Conversion of Anatomic TSA to RSA
 Conversion of Anatomic TSA to RSA Joseph A. Abboud, M.D. Professor of Shoulder and Elbow Surgery Senior Vice-President at the Rothman Institute Philadelphia, PA Disclosures Joseph A. Abboud, MD Depuy Synthes
Conversion of Anatomic TSA to RSA Joseph A. Abboud, M.D. Professor of Shoulder and Elbow Surgery Senior Vice-President at the Rothman Institute Philadelphia, PA Disclosures Joseph A. Abboud, MD Depuy Synthes
Revision of the humeral component for aseptic loosening in arthroplasty of the shoulder
 Revision of the humeral component for aseptic loosening in arthroplasty of the shoulder A. Cil, C. J. H. Veillette, J. Sanchez-Sotelo, J. W. Sperling, C. Schleck, R. H. Cofield From the Mayo Clinic, Rochester,
Revision of the humeral component for aseptic loosening in arthroplasty of the shoulder A. Cil, C. J. H. Veillette, J. Sanchez-Sotelo, J. W. Sperling, C. Schleck, R. H. Cofield From the Mayo Clinic, Rochester,
A Patient s Guide to Anatomic Total Shoulder Replacement (Standard Shoulder Shoulder)
 A Patient s Guide to Anatomic Total Shoulder Replacement (Standard Shoulder Shoulder) Introduction Yearly, there are approximately 50,000 shoulder replacements performed annually in the USA. Anatomic shoulder
A Patient s Guide to Anatomic Total Shoulder Replacement (Standard Shoulder Shoulder) Introduction Yearly, there are approximately 50,000 shoulder replacements performed annually in the USA. Anatomic shoulder
Common Shoulder Problems and Treatment Options. Benjamin W. Szerlip D.O. Austin Shoulder Institute
 Common Shoulder Problems and Treatment Options Benjamin W. Szerlip D.O. Austin Shoulder Institute Speaker Disclosure Dr. Szerlip has disclosed that he has no actual or potential conflict of interest in
Common Shoulder Problems and Treatment Options Benjamin W. Szerlip D.O. Austin Shoulder Institute Speaker Disclosure Dr. Szerlip has disclosed that he has no actual or potential conflict of interest in
Assessment of Scapular Morphology and Surgical Technique as Predictors of Notching in Reverse Shoulder Arthroplasty
 An Original Study Assessment of Scapular Morphology and Surgical Technique as Predictors of Notching in Reverse Shoulder Arthroplasty Vani Sabesan, MD, Mark Callanan, MD, Vinay Sharma, BA, and J. Michael
An Original Study Assessment of Scapular Morphology and Surgical Technique as Predictors of Notching in Reverse Shoulder Arthroplasty Vani Sabesan, MD, Mark Callanan, MD, Vinay Sharma, BA, and J. Michael
Reverse total shoulder arthroplasty for acute proximal humeral fracture: comparison to open reduction internal fixation and hemiarthroplasty
 J Shoulder Elbow Surg (2014) 23, 197-204 www.elsevier.com/locate/ymse Reverse total shoulder arthroplasty for acute proximal humeral fracture: comparison to open reduction internal fixation and hemiarthroplasty
J Shoulder Elbow Surg (2014) 23, 197-204 www.elsevier.com/locate/ymse Reverse total shoulder arthroplasty for acute proximal humeral fracture: comparison to open reduction internal fixation and hemiarthroplasty
Optimizing Patient Outcomes Following Orthopedic Surgery: The Role of Albumin and the Case For Fast- Track
 Optimizing Patient Outcomes Following Orthopedic Surgery: The Role of Albumin and the Case For Fast- Track Andrew Ng Robin Wang Mentor: Atul Kamath, MD Outline - The Role of Albumin as a Risk Factor for
Optimizing Patient Outcomes Following Orthopedic Surgery: The Role of Albumin and the Case For Fast- Track Andrew Ng Robin Wang Mentor: Atul Kamath, MD Outline - The Role of Albumin as a Risk Factor for
Outcomes of Shoulder Arthroplasty Performed for Postinfectious Arthritis
 Original Article Clinics in Orthopedic Surgery 2018;10:344-351 https://doi.org/10.4055/cios.2018.10.3.344 Outcomes of Shoulder Arthroplasty Performed for Postinfectious Arthritis Eric Michael Padegimas,
Original Article Clinics in Orthopedic Surgery 2018;10:344-351 https://doi.org/10.4055/cios.2018.10.3.344 Outcomes of Shoulder Arthroplasty Performed for Postinfectious Arthritis Eric Michael Padegimas,
Scapular notching in reverse shoulder arthroplasties: The influence of glenometaphyseal angle
 Orthopaedics & Traumatology: Surgery & Research (2011) 97S, S131 S137 ORIGINAL ARTICLE Scapular notching in reverse shoulder arthroplasties: The influence of glenometaphyseal angle V. Falaise a, C. Levigne
Orthopaedics & Traumatology: Surgery & Research (2011) 97S, S131 S137 ORIGINAL ARTICLE Scapular notching in reverse shoulder arthroplasties: The influence of glenometaphyseal angle V. Falaise a, C. Levigne
Effect of age, sex, co morbidities, delay in surgery and complications on outcome in elderly with proximal femur fractures
 2018; 4(3): 498-506 ISSN: 2395-1958 IJOS 2018; 4(3): 498-506 2018 IJOS www.orthopaper.com Received: 27-05-2018 Accepted: 28-06-2018 P Venu Gopala Reddy Assistant Professor, Department of Orthopaedic Surgery,
2018; 4(3): 498-506 ISSN: 2395-1958 IJOS 2018; 4(3): 498-506 2018 IJOS www.orthopaper.com Received: 27-05-2018 Accepted: 28-06-2018 P Venu Gopala Reddy Assistant Professor, Department of Orthopaedic Surgery,
ARTICLE IN PRESS. All-Patient Refined Diagnosis- Related Groups in Primary Arthroplasty
 The Journal of Arthroplasty Vol. 00 No. 0 2009 All-Patient Refined Diagnosis- Related Groups in Primary Arthroplasty Carlos J. Lavernia, MD,*y Artit Laoruengthana, MD,y Juan S. Contreras, MD,y and Mark
The Journal of Arthroplasty Vol. 00 No. 0 2009 All-Patient Refined Diagnosis- Related Groups in Primary Arthroplasty Carlos J. Lavernia, MD,*y Artit Laoruengthana, MD,y Juan S. Contreras, MD,y and Mark
Curriculum Vitae. Derek J. Cuff
 Curriculum Vitae Derek J. Cuff Suncoast Orthopaedic Surgery and Sports Medicine 836 Sunset Lake Blvd, Building A Suite 205 Venice, FL 34292 Office:941-485-1505, Email: dcuff001@hotmail.com, web:www.suncoastshoulder-elbow.com
Curriculum Vitae Derek J. Cuff Suncoast Orthopaedic Surgery and Sports Medicine 836 Sunset Lake Blvd, Building A Suite 205 Venice, FL 34292 Office:941-485-1505, Email: dcuff001@hotmail.com, web:www.suncoastshoulder-elbow.com
Clinical Practice Guideline for Patients Requiring Total Hip Replacement
 Clinical Practice Guideline for Patients Requiring Total Hip Replacement Inclusions Patients undergoing elective total hip replacement Exclusions Patients with active local or systemic infection or medical
Clinical Practice Guideline for Patients Requiring Total Hip Replacement Inclusions Patients undergoing elective total hip replacement Exclusions Patients with active local or systemic infection or medical
The complex characteristics of 282 unsatisfactory shoulder arthroplasties
 The complex characteristics of 282 unsatisfactory shoulder arthroplasties Amy K. Franta, MD, a Tim R. Lenters, MD, a Doug Mounce, MSc, a Blazej Neradilek, MSc, b and Frederick A. Matsen, III, MD, a Seattle,
The complex characteristics of 282 unsatisfactory shoulder arthroplasties Amy K. Franta, MD, a Tim R. Lenters, MD, a Doug Mounce, MSc, a Blazej Neradilek, MSc, b and Frederick A. Matsen, III, MD, a Seattle,
Reverse Total Shoulder Arthroplasty Improves Function in Cuff Tear Arthropathy
 Clin Orthop Relat Res (2011) 469:2476 2482 DOI 10.1007/s11999-010-1683-z SYMPOSIUM: REVERSE TOTAL SHOULDER ARTHROPLASTY Reverse Total Shoulder Arthroplasty Improves Function in Cuff Tear Arthropathy Betsy
Clin Orthop Relat Res (2011) 469:2476 2482 DOI 10.1007/s11999-010-1683-z SYMPOSIUM: REVERSE TOTAL SHOULDER ARTHROPLASTY Reverse Total Shoulder Arthroplasty Improves Function in Cuff Tear Arthropathy Betsy
Reverse Prostheses in Arthropathies With Cuff Tear
 Clin Orthop Relat Res (2011) 469:2469 2475 DOI 10.1007/s11999-011-1833-y SYMPOSIUM: REVERSE TOTAL SHOULDER ARTHROPLASTY Reverse Prostheses in Arthropathies With Cuff Tear Are Survivorship and Function
Clin Orthop Relat Res (2011) 469:2469 2475 DOI 10.1007/s11999-011-1833-y SYMPOSIUM: REVERSE TOTAL SHOULDER ARTHROPLASTY Reverse Prostheses in Arthropathies With Cuff Tear Are Survivorship and Function
Hip Arthroscopy in Patients with Mild to Moderate Dysplasia: When do they Fail?
 Hip Arthroscopy in Patients with Mild to Moderate Dysplasia: When do they Fail? Andrew J. Bryan 1, MD K. Poehling-Monaghan 1, MD Rohith Mohan 1, BA Nick R Johnson 1, BS Aaron J. Krych 1, MD Bruce A. Levy
Hip Arthroscopy in Patients with Mild to Moderate Dysplasia: When do they Fail? Andrew J. Bryan 1, MD K. Poehling-Monaghan 1, MD Rohith Mohan 1, BA Nick R Johnson 1, BS Aaron J. Krych 1, MD Bruce A. Levy
A comparison of peri-operative outcomes between elective and non-elective total hip arthroplasties
 Original Article Page 1 of 8 A comparison of peri-operative outcomes between elective and non-elective total hip arthroplasties Hiba K. Anis 1, Nipun Sodhi 2, Marine Coste 2, Joseph O. Ehiorobo 2, Jared
Original Article Page 1 of 8 A comparison of peri-operative outcomes between elective and non-elective total hip arthroplasties Hiba K. Anis 1, Nipun Sodhi 2, Marine Coste 2, Joseph O. Ehiorobo 2, Jared
