Reverse Total Shoulder Arthroplasty Improves Function in Cuff Tear Arthropathy
|
|
|
- Hugo Lawson
- 5 years ago
- Views:
Transcription
1 Clin Orthop Relat Res (2011) 469: DOI /s z SYMPOSIUM: REVERSE TOTAL SHOULDER ARTHROPLASTY Reverse Total Shoulder Arthroplasty Improves Function in Cuff Tear Arthropathy Betsy M. Nolan MD, Elizabeth Ankerson BS, J. Michael Wiater MD Published online: 30 November 2010 Ó The Association of Bone and Joint Surgeons Abstract Background Early failure due to glenoid loosening with anatomic total shoulder arthroplasty in patients with severe rotator cuff deficiency led to the development of the reverse ball-and-socket shoulder prosthesis. The literature reports improved short-term pain and function scores following modern reverse total shoulder arthroplasty (RTSA) in patients with cuff tear arthropathy (CTA). Questions/purposes We therefore sought to confirm previously reported short-term improvements in pain, function scores, and range of motion, in patients treated with RTSA for CTA and to identify clinical complications and radiographic notching. Methods We retrospectively reviewed 67 patients who underwent 71 primary RTSAs for CTA. The average age was 74 years (range, years). All were preoperatively and postoperatively assessed using Constant-Murley and One or more of the authors (JMW) is a paid consultant, and he or she has or may receive payments or benefits from a commercial entity related to this work (Zimmer Inc., Warsaw, IN). This study was funded by a grant from the William Beaumont Hospital Research Institute. Each author certifies that his or her institution approved the human protocol for this investigation and that all investigations were conducted in conformity with ethical principles of research, and that informed consent for participation in the study was obtained. B. M. Nolan Indiana University School of Medicine, Indiana University, 541 Clinical Drive, Suite 600, Indianapolis, IN 46202, USA shoulderandelbowdoc@gmail.com E. Ankerson, J. M. Wiater (&) William Beaumont School of Medicine, William Beaumont Hospital, Oakland University, 3535 West Thirteen Mile Road, Suite 744, Royal Oak, MI 48073, USA jmwiater@aol.com American Shoulder and Elbow Society (ASES) scores. We identified complications and examined radiographs for notching. The minimum followup was 12 months (average, 24 months; range, months). Results Average Constant-Murley scores improved from 28 preoperatively to 62 postoperatively. Average ASES scores improved from 26 to 76. Subjective Shoulder Value (SSV) improved from 23 to 77. Active forward flexion improved from 61 preoperatively (range, ) to 121 postoperatively (range, ). Active external rotation was not affected. Thirty-five of the 71 shoulders (49%) showed radiographic notching. The overall complication rate was 23%. No patient required reoperation. One patient required closed reduction of a perioperative dislocation. Conclusions RTSA for CTA results in functional improvement, with a low complication rate. However, the longevity of the device is currently unknown. Level of Evidence Level IV, therapeutic study. See Guidelines for Authors for a complete description of levels of evidence. Introduction Rotator CTA is a difficult clinical problem, and the etiology is not completely understood. First described in 1857, it was considered a localized form of rheumatic arthritis [1]. Neer et al. [20] coined the term cuff tear arthropathy in 1983 to describe the clinical scenario of a massive rotator cuff tear associated with glenohumeral joint degeneration. It is often associated with anterosuperior subluxation of the humeral head, which allows articulation of the humeral head with the acromion. Clinically, weakness or pseudoparalysis of forward elevation and abduction are seen, and patients complain of pain with motion. Attritional rupture of the
2 Volume 469, Number 9, September 2011 RTSA for Cuff Tear Arthropathy 2477 Table 1. Hamada classification for massive rotator cuff tears Hamada grade Radiographic findings 1 Acromiohumeral interval at least 6 mm 2 Acromiohumeral interval less than 6 mm 3 Acetabularization of the acromion 4 Arthrosis of the glenohumeral joint 5 Humeral head collapse Table 2. Visotsky classifications for cuff tear arthroplasty Visotsky classification IA IB IIA IIB Position and stability of humeral head Centered and stable Centered but medialized Not centered with some limited stability Not centered and unstable long head of the biceps tendon is common. A bald humeral head can often be seen intraoperatively. In 1990, Hamada et al. [15] described the progression of glenohumeral joint degeneration associated with rotator cuff tears. In this classification, only types IV and V included CTA (Table 1). Visotsky et al. [27] further subclassified these two groups based on whether the humeral head is centered on the glenoid and its stability (Table 2). Prior to the advent of modern Grammont-type RTSA [3, 9, 10], surgical options for CTA included open or arthroscopic débridement, resection arthroplasty, arthrodesis, and humeral head arthroplasty (HHA) with or without an extended coverage head. Anatomic total shoulder arthroplasty in CTA led to eccentric loading of the glenoid component (rocking horse phenomenon) and early failure via glenoid loosening [8]; it has since been abandoned for CTA. Although HHA was once the preferred option, it has unpredictable functional outcomes and is unable to restore stability. HHA remains a treatment option, but is usually reserved for types IA and IIA, as described by Visotsky et al. [27]. HHA reportedly has 89% successful results with limited goal criteria [27]. RTSA, utilizing a deltopectoral or superolateral approach, results in substantial improvement in pain and function when used for the treatment of CTA [3, 6, 7, 9, 11 13, 21 25, 29, 30]. It has been successfully used in Europe for over 20 years. Our PubMed search found over 100 articles on RTSA, a procedure that the FDA first approved for use in the United States in late Thus, a great deal of interest has been generated for RTSA in a short time. The literature reports improved pain and function scores with RTSA for multiple indications [9, 11 13, 20, 22 25, 31]. Many of these series include revisions for failed arthroplasties. Inclusion of other diagnoses, including acute proximal humeral fracture, tuberosity malunion, and pseudo-paralysis due to rotator cuff deficiency without arthrosis, further complicates interpretation of the existing data. The results of RTSA as a salvage procedure may be less favorable than as an initial arthroplasty. Wall et al. [29] showed RTSA resulted in smaller functional gains and higher complication rates in patients with posttraumatic arthritis or prior failed shoulder arthroplasty than in patients having RTSA for other indications. Therefore, we sought to confirm previously reported improvements in pain, functional scores, and range of motion in patients treated with RTSA for CTA. We identified clinical complications and radiographic notching. Patients and Methods We enrolled all patients undergoing RTSA in a prospective database. Between December 2004 and February 2009, the senior author (JMW) performed 277 RTSAs in 265 patients. Of these, 184 shoulders in 174 patients were available for clinical and radiographic evaluation with minimum 12-month followup. We excluded 93 RTSAs in 91 patients with less than 12 months followup. Additionally, we excluded 113 shoulders in 107 patients with diagnoses other than CTA. This left 71 shoulders in 67 patients diagnosed preoperatively with CTA and with at least 12 months followup. No patient had previous ipsilateral shoulder arthroplasty. We did not offer RTSA to any patient with a nonfunctioning deltoid or known infection. Patients with rotator cuff tears without glenohumeral joint involvement (Hamada I through III) did not meet the criteria for diagnosis of CTA. We did not exclude patients with previous rotator cuff repairs and/or débridements. Of the patients in the study, 20 were men and 47 women. We performed 56 procedures on the right shoulder and 15 on the left. Four patients underwent bilateral RTSA. The average age at the time of surgery was 74.2 years (range, 54 92). The minimum followup was 12 months (average, 24 months; range, months). No patients were lost to followup. We did not recall any patients specifically for this study; all data were obtained from medical records and radiographs. We clinically evaluated all patients prior to RTSA. Patients gave informed consent to participate. The William Beaumont Hospital Human Investigations Committee approved this study, HIC # Clinical examination included range of motion and strength testing, neurovascular examination of the involved extremity, and Visual Analog Scale (VAS) pain rating on a scale of 0 (none) to 10 (maximal) [17]. We noted the presence or absence of a preoperative external rotation lag sign, but these were not recorded in six patients preoperatively. All other preoperative and postoperative data
3 2478 Nolan et al. Clinical Orthopaedics and Related Research 1 were recorded and available for this analysis. Patients were also evaluated both preoperatively and postoperatively using Constant-Murley scores [4], ASES scores [18], and SSV [10]. Preoperatively, we obtained radiographs that consisted of an AP Grashey view [13], scapular Y view, and axillary view of the shoulder, as well as AP and lateral full-length humerus films. All clinical measurements and radiographic assessments were performed by an independent observer. We performed the procedure in all patients using a limited 5 cm to 10 cm skin incision for the deltopectoral approach. The subscapularis was intact in 70 of 71 shoulders, and was tenotomized and repaired following placement of the prosthesis using heavy nonabsorbable sutures. In 56 patients, we released a portion of the pectoralis major insertion to aid in exposure, which we then repaired at the conclusion of the case. In cases of major soft-tissue contracture, we elevated a small portion of the anterior deltoid insertion. The long head of the biceps tendon was tenodesed in 28 of 71 patients. In the remaining 43 patients, the tendon had a pre-existing attritional rupture. The osteotomy was made in neutral version for patients with tearing of the teres minor and a preoperative external rotation lag sign [28]. We made the osteotomy in 20 of retroversion for patients with an intact teres minor and a preoperative negative external rotation lag sign. We routinely performed a 360 release of adhesions around the subscapularis. We placed the guide inferiorly on the glenoid so that the base plate was fully supported by bone and flush with the inferior glenoid margin. We placed the guide wire in approximately 10 to 15 inferior tilt, as this position minimized the risk of scapular notching [25]. Seven patients required bone graft for glenoid bony deficiency. We placed two superior and inferior locking 4.5 mm screws through the holes in the baseplate with bone purchase into the base of the coracoid and inferior scapular border. We inserted the glenosphere with its inferior border slightly overhanging the inferior glenoid margin. Polyethylene insert thickness was chosen based on soft-tissue tension during trial reduction. In judging proper soft-tissue tension, our goal was minimal shuck (1 2 mm) with tension on conjoint tendon, which was taught, but not so tight as to cause bowstringing of the tendon. Our goals for passive intraoperative range of motion included 130 forward elevation and 45 external rotations, both in neutral flexion and extension. We also attempted to manually dislocate the humerus superiorly off the glenosphere with the arm in slight abduction and neutral rotation. It required a moderate laterally directed force to do this. We routinely used two drains. In addition to RTSA, five patients underwent combined latissimus dorsi and teres major transfers, and one had transfer of the latissimus dorsi only. Table 3. Sirveaux classification of scapular notching Sirveaux notching grade Patients were placed in an abduction sling for 4 weeks. The initiation of progressive range of motion with low intensity supervised physical therapy began 2 weeks after surgery, progressive from active assist range of motion to full active range of motion. Passive external rotation was initially avoided to protect the repair of the subscapularis tendon. We instructed patients not to lift anything heavier than a gallon of milk during the recovery period. Postoperatively, we evaluated patients clinically and radiographically at 2 weeks, 3 months, 6 months, 1 year, and then yearly thereafter. Constant-Murley scores and ASES scores were recorded at yearly visits. Patients rated their shoulder using the SSV and VAS both preoperatively and postoperatively. We recorded the postoperative Constant-Murley score, ASES score, SSV, VAS pain level, and range of motion. We defined major complications as those which prolonged the hospital stay or required reoperation; we considered all other complications to be minor [26]. Postoperatively, we performed a standard three-view shoulder series at each visit. An independent observer, not involved in any of these surgical cases (BMN), evaluated all radiographs for signs of fracture or dislocation, scapular notching according to Sirveaux et al. [24] (Table 3), heterotopic ossification or spur formation, and prosthetic failure due to loosening, dissociation, wear, migration, or breakage. We measured the prosthesis-scapular border angle (PSBA) at a distance of 6 cm from the inferior margin of the baseplate (Fig. 1). There were no missing radiographs. Results Extent of involvement 1 Notch limited to scapular pillar 2 Extends to inferior screw 3 Extends beyond inferior screw 4 Notch reaches baseplate The mean ASES score, SSV, Constant-Murley score, and VAS were all substantially improved (Table 4). Range of motion improved in active forward elevation, but active external rotation was not substantially improved (Table 4). Preoperatively, 24 patients had an external rotation lag sign, while 41 had intact external rotation; we did not record the preoperative external rotation lag sign in six patients. Average postoperative active external rotation was 8 in the group with preoperative external rotation lag signs, and 17 in the group with intact preoperative external rotation (Table 5). We observed the following grades of scapular notching: 36 shoulders were Grade 0; 11 were Grade 1; 15 were
4 Volume 469, Number 9, September 2011 RTSA for Cuff Tear Arthropathy 2479 Grade 2; seven were Grade 3; one was Grade 4. Notching occurred in the early postoperative period and tended to be nonprogressive. We did not include the one shoulder with superior migration of the glenoid component in the notching analysis. The PSBA averaged 135 (range, ). Twenty-six patients had spur formation or heterotopic ossification at the inferior glenoid neck, and nine (13%) had lucency behind the baseplate. Surgery typically improved positioning (Fig. 2A D) and improved forward elevation (Fig. 2E). We identified 16 complications in 14 patients, including of 10 perioperative complications and six late complications. Perioperative complications included two patients with deep venous thrombosis that lead to pulmonary embolism, two patients with broken hardware (one broken retained drill bit and one broken anterior screw head), and one patient each with: periprosthetic humerus fracture, retinal artery thrombosis, postoperative pneumonia, and musculocutaneous mononeuropathy. An additional patient had an intraoperative anterior glenoid rim fracture beneath the baseplate, but did not prevent the placement of the glenoid implant, and healed without any alteration to the postoperative course. None of these patients required further operation. One patient sustained a perioperative dislocation, underwent closed reduction the same day of surgery, and has remained stable. Late complications included one patient with superior glenosphere migration, one with an acromial fracture at 5 weeks, one with a acute coracoid process fracture, and one who had nonunited insufficiency fractures of the scapular spine and distal clavicle at 32 months. Another patient had a self-reduced dislocation at 33 months, followed by recurrent subluxations, but was satisfied. No patient required further surgery. The patient with the coracoid fracture was treated with a sling for 6 weeks, and the shoulder remains stable Table 5. Clinical results according to preoperative external rotation lag sign Variable Preoperative external rotation lag sign* Preoperative intact active external rotation* Active forward 120 (62 to 150) (52 to 170) elevation (degrees) Active external 8.1 ( 15 to 55) 17.1 ( 44 to 60) rotation (degrees) ASES score 72.7 (40 to 98.3) 76 (21 to 100) SSV 76.5 (50 to 100) 75.2 (35 to 100) Constant-Murley score 59.4 (40 to 75) 61.1 (30 to 73) VAS pain 1.3 (0 to 6) 1.7 (0 to 8) Fig. 1 A diagram of measurement of prosthesis-scapular border angle (PSBA) is shown. * Measurements average (range); ASES - American Shoulder and Elbow Society; SSV - Subjective Shoulder Value; VAS - Visual Analog Scale. Table 4. Clinical results of RTSA for CTA Variable Preoperative average value Preoperative range Postoperative average value Postoperative range Active forward elevation (degrees) to to 170 Active external rotation to to 60 (degrees) ASES score to to 100 SSV 23 0 to to 100 Constant-Murley score to to 87 VAS pain 7 0 to to 8 RTSA - reverse total shoulder arthroplasty; CTA - cuff tear arthropathy.
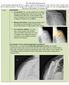
5 2480 Nolan et al. Clinical Orthopaedics and Related Research 1 Fig. 2A E Preoperative AP views of the (A) right and (B) left shoulders in a 69-year-old woman demonstrate bilateral cuff tear arthropathy with glenohumeral joint degeneration and severe narrowing of the acromiohumeral distance, allowing articulation of the humeral head with the acromion. Acetabularization of the acromion is seen. A right acromial insufficiency fracture is noted preoperatively. Postoperative AP views demonstrate reverse total shoulder prostheses in good position. Postoperative radiographs of the patient following bilateral RTSA for bilateral show improved alignment of the (C) right and (D) left shoulder. (E) After bilateral RTSA, the patient demonstrates improved forward elevation despite a right acromial fracture. at latest followup. Overall, there were four major and 12 minor complications. Discussion Relatively high rates of glenoid loosening of anatomic total shoulder arthroplasty in patients with severe CTA led to the development of the RTSA. The literature suggests pain and function is improved following modern reverse total shoulder arthroplasty in patients with CTA, although the long-term durability is unknown. Our purpose was to confirm previously reported short-term improvements in pain and function scores, as well as range of motion, in patients treated with RTSA for CTA. We also reported radiographic notching and clinical complications. We note several limitations associated with our study. First, the minimum followup of 12 months (average, 24 months) is too short to determine the longevity of the implant, or evaluate the long-term implications of radiographic findings, such as notching. The longevity of the implant remains to be determined, as it has only been FDA approved for use in the United States for 6 years. Further study with long-term followup is needed. Further, the implications of notching are not yet well understood; although concern exists regarding possible glenoid loosening in patients with scapular notching, that association is not present in the literature. Second, we did not compare results of patients treated with RTSA for CTA to those treated with RTSA for other reasons. Since CTA is the most common indication for RTSA, we believe it helpful to evaluate the outcomes of a series of patients with one diagnosis. To compare these results with the results of RTSA for other etiologies would be difficult due to the heterogeneous nature of the other diagnoses. However, this does make it difficult to compare these results to those of other authors, since those series report groups of patients with varying diagnoses. Third, we did not use fluoroscopy for postoperative radiographic analysis, thus the frequency of lucent lines may be underestimated. No symptomatic loosening has yet to occur at latest followup. Our series, limited to RTSA for CTA, experienced substantial improvements in mean Constant-Murley scores, ASES scores, SSV, VAS, and forward elevation. These findings confirm those from studies reporting RTSA for all indications (Table 6) [9, 12, 14, 19, 24, 25, 31]. The exclusion of other diagnoses, such as pseudoparalysis without glenohumeral arthrosis, acute fracture, malunion, and revision arthroplasties, may explain our outcomes. The results of RTSA depend upon indication; functional scores of RTSA in revision settings are inferior to primary RTSA with more complications [13, 25, 29, 30]. Werner et al. [30] suggested RTSA with a Grammont-type prosthesis can restore forward elevation and abduction, but not external rotation. Our patients had no change in mean external rotation after surgery. In the six patients who underwent tendon transfer in addition to RTSA, external rotation decreased from an average of 13.5 preoperatively to 9.8 postoperatively. This does not appear to support the recommendation of Gerber et al. [9] for latissimus dorsi transfer in patients with profound external rotation
6 Volume 469, Number 9, September 2011 RTSA for Cuff Tear Arthropathy 2481 Table 6. Current study results and published literature results Author Number of shoulders Average duration of followup (months) Active forward elevation (degrees) Active external rotation (degrees) ASES score Constant-Murley score SSV VAS pain Nolan et al. [current study] Boileau et al. [2] * * Frankle et al. [7] * * 2 Rittmeister and 8 54 * * * 63 * * Kerschbaumer [21] Sirveaux et al. [25] * 66 * * Wall et al. [29] * 60 * * Werner et al. [30] * * * Not reported. ASES - American Shoulder and Elbow Society; SSV - Subjective Shoulder Value; VAS - Visual Analog Scale. weakness, indicated by a hornblower s sign [24] or external rotation lag sign [16]. Our rate of definitive glenoid loosening was low (1.4%, 1/71). Altogether, nine patients had evidence of lucency behind the base plate, so the total percent of at-risk glenoids was 13%. This compares favorably with the 16% rate of radiographic loosening reported in the French multicenter studies [14, 25]. Our shorter followup time may account for this difference. Notching rates of 50% to 96% have been reported [21, 25, 30]. Higher grades of notching negatively correlate with Constant-Murley scores [23]. Simovitch et al. [23] calculated a notching index based on the prosthesis-scapular neck angle (PSNA) and the superior-inferior placement of the base plate on the glenoid. We have modified the PSNA to account for the anatomic variability in the scapular neck. We call this modification the prosthesis-scapular border angle (PSBA); the angle between the base plate and a line drawn from the inferior aspect of the base plate to a point 6 cm away on the lateral scapular border. We believe this is a more appropriate measurement since most notching occurs between 1 cm and 6 cm away from the base plate, rather than within 1 cm, and the scapular border is more anatomically consistent than the scapular neck. Our patients averaged 135 for the prosthesis-scapular border angle, yet our notching rate was not higher. This supports the findings of Simovitch et al. [23], which suggests inferior tilt is not the primary determinant of notching. We included all perioperative systemic complications, such as pulmonary embolism, in our analysis. However, most investigators only reported on complications directly related to the shoulder. Despite our more liberal inclusion criteria for reporting a complication, our complication rate of 23% is within the range of previous reports (Table 6). Many of ours were systemic complications and not directly implant-related. If the complications not directly related to the shoulder are removed, our complication rate is 17%. The age and medical comorbidities of CTA patients may affect the number of medical complications. No patient in this study required reoperation, and only one required formal closed reduction in the operating room for a perioperative dislocation. Two shoulders in our series suffered a dislocation, resulting in an instability rate of 2.8%, similar to those previously reported (Table 6). Instability continues to be a concern with RTSA, and is one reason that complete deltoid paralysis is considered a contraindication to RTSA. Additionally, a two-fold increased risk of instability was seen in patients with a preoperative subscapularis rupture [6]. Therefore, it is important to determine the status of the subscapularis tendon preoperatively and, if present, repair it after implantation. Authors have reported revision rates of 4.2% to 13% following RTSA [3, 5, 25]. There were no revisions in our series. It is possible that the revision rate is less due to the exclusion of patients with a previous arthroplasty and our relatively short followup. In conclusion, RTSA for CTA results in major improvements in function, and a low complication rate. Scapular notching does occur, and its relationship to pain and function scores, as well as implant longevity, requires further study. Acknowledgments We thank Mamtha Balasubramaniam, Senior Biostatistician, for help in statistical analysis. References 1. Adams R. A Treatise on Rheumatic Gout, or Chronic Rheumatic Arthritis of All the Joints. London, England: J Churchill; 1857: Boileau P, Chuinard C, Roussanne Y, Neyton L, Trojani C. Modified latissimus dorsi and teres major transfer through a single delto-pectoral approach for external rotation deficit of the
7 2482 Nolan et al. Clinical Orthopaedics and Related Research 1 shoulder: as an isolated procedure or with a reverse arthroplasty. J Shoulder Elbow Surg. 2007;16: Boileau P, Watkinson DJ, Hatzidakis AM, Balg F. Grammont reverse prosthesis: design, rationale, and biomechanics. J Shoulder Elbow Surg. 2005;14(1):147S 161S. 4. Constant CR, Murley AHG. A clinical method of functional assessment of the shoulder. Clin Orthop Relat Res. 1987;214: Ecklund KJ, Lee TQ, Tibone J, Gupta R. Rotator cuff tear arthropathy. J Am Acad Orthop Surg. 2007;15: Edwards TB, Williams MD, Labriola JE, Elkousy HA, Gartsman GM, O Connor DP. Subscapularis insufficiency and the risk of shoulder dislocation after reverse shoulder arthroplasty. J Shoulder Elbow Surg. 2009;18: Frankle M, Siegal S, Pupello D, Saleem A, Mighell M, Vasey M. The reverse shoulder prosthesis for glenohumeral arthritis associated with severe rotator cuff deficiency. A minimum 2-year follow-up study of sixty patients. J Bone Joint Surg Am. 2005; 87: Franklin JL, Barrett WP, Jackins SE, Matsen FA 3rd. Glenoid loosening in total shoulder arthroplasty. Association with rotator cuff deficiency. J Arthroplasty. 1988;3: Gerber C, Pennington SD, Lingenfelter EJ, Sukthankar A. Reverse Delta-III total shoulder replacement combined with latissimus dorsi transfer: A preliminary report. J Bone Joint Surg Am. 2007;89: Gilbart MK, Gerber C. Comparison of the subjective shoulder value and the Constant score. J Shoulder Elbow Surg. 2007;16: Grammont P, Trouillard P, Laffay JP, Deries X. Study and realization of a new shoulder prosthesis [in French]. Rhumatologie. 1987;39: Grammont PM, Baulot E. Delta shoulder prosthesis for rotator cuff rupture. Orthopedics. 1993;16: Grashey, R. Atlas of Common Radiographs [in German]. Munchen, Germany: Lehman; 1923: Guery J, Favard L, Sirveaux F, Oudet D, Mole D, Walch G. Reverse total shoulder arthroplasty. Survival analysis of eighty replacements followed for five to ten years. J Bone Joint Surg Am. 2006;88: Hamada K, Fukuda H, Mikasa M, Kobayashi Y. Roentgenographic findings in massive rotator cuff tears: A long-term observation. Clin Orthop Relat Res. 1990;254: Hertel R, Ballmer FT, Lombert SM, Gerber C. Lag signs in the diagnosis of rotator cuff rupture. J Shoulder Elbow Surg. 1996;5: Huskisson EC. Measurement of pain. Lancet. 1974; 2: Michener LA, McClure PW, Sennett BJ. American Shoulder and Elbow Surgeons Standardized Shoulder Assessment Form, patient self-report section: Reliability, validity, and responsiveness. J Shoulder Elbow Surg. 2002;11: Mole D, Favard L. Excentered scapulohumeral osteoarthritis. Rev Chir Orthop Reparatrice Appar Mot. 2007;93: Neer CS 2nd, Craig EV, Fukuda H. Cuff-tear arthropathy. J Bone Joint Surg Am. 1983;65: Rittmeister M, Kerschbaumer F. Grammont reverse total shoulder arthroplasty in patients with rheumatoid arthritis and nonreconstructible rotator cuff lesions. J Shoulder Elbow Surg. 2001;10: Simovitch RW, Helmy N, Zumstein MA, Gerber C. Impact of fatty infiltration of the teres minor muscle on the outcome of reverse total shoulder arthroplasty. J Bone Joint Surg. 2007;89: Simovitch RW, Zumstein MA, Lohri E, Helmy N, and Gerber C. Predictors of scapular notching in patients managed with the Delta III reverse total shoulder replacement. J Bone Joint Surg. 2007;89: Sirveaux F. The prosthesis of Grammant in the treatment of arthropathies of the shoulder with cuff tear: A multicenter study of 42 cases. Faculte 0 de me 0 decine de Nancy, the se del universite 0 de Nancy I 245, Sirveaux F, Favard L, Oudet D, Huquet D, Walch G, Mole D. Grammont inverted total shoulder arthroplasty in the treatment of glenohumeral osteoarthritis with massive rupture of the cuff: results of a multicentre study of 80 shoulders. J Bone Joint Surg Br. 2004;86: Swanson, KC, Valle AG, Salvati EA, Sculco TP, and Bottner, F. Perioperative morbidity after single-stage bilateral total hip arthroplasty: A matched control study. Clin Orthop Relat Res. 2006;451: Visotsky JL, Basamania C, Seebauer L, Rockwood CA, Jensen KL. Cuff tear arthropathy: Pathogenesis, classification and algorithm for treatment. J Bone Joint Surg Am. 2004;86: Walch G, Boulahia A, Calderone S, Robinson AH. The dropping and hornblower s signs in evaluation of rotator-cuff tears. J Bone Joint Surg Br. 1998;80: Wall B, Nove-Josserand L, O Connor DP, Edwards TB, Walch G. Reverse total shoulder arthroplasty: A review of results according to etiology. J Bone Joint Surg Am. 2007;89: Werner CM, Steinman PA, Gilbart M, Gerber C. Treatment of painful pseudoparesis due to irreparable rotator cuff dysfunction with the Delta III reverse-ball and-socket total shoulder prosthesis. J Bone Joint Surg Am. 2005;87: Wiater JM and Fabing MH. Shoulder arthroplasty: prosthetic options and indications. JAAOS. 2009;17:
Clinical Outcomes and Complications during the Learning Curve for Reverse Total Shoulder Arthroplasty: An Analysis of the First 40 Cases
 Original Article Clinics in Orthopedic Surgery 2017;9:213-217 https://doi.org/10.4055/cios.2017.9.2.213 Clinical Outcomes and Complications during the Learning Curve for Reverse Total Shoulder Arthroplasty:
Original Article Clinics in Orthopedic Surgery 2017;9:213-217 https://doi.org/10.4055/cios.2017.9.2.213 Clinical Outcomes and Complications during the Learning Curve for Reverse Total Shoulder Arthroplasty:
Why are these shoulder replacements called a reverse prosthesis?
 PATIENT GUIDE TO REVERSE PROSTHESIS Edward G. McFarland MD The Division of Sports Medicine and Shoulder Surgery The Department of Orthopaedic Surgery The Johns Hopkins University Baltimore MD Why are these
PATIENT GUIDE TO REVERSE PROSTHESIS Edward G. McFarland MD The Division of Sports Medicine and Shoulder Surgery The Department of Orthopaedic Surgery The Johns Hopkins University Baltimore MD Why are these
Matthew D. Saltzman, MD a, Deana M. Mercer, MD c, Winston J. Warme, MD b, Alexander L. Bertelsen, PA-C b, Frederick A. Matsen III, MD b, *
 J Shoulder Elbow Surg (2010) 19, 1028-1033 www.elsevier.com/locate/ymse A method for documenting the change in center of rotation with reverse total shoulder arthroplasty and its application to a consecutive
J Shoulder Elbow Surg (2010) 19, 1028-1033 www.elsevier.com/locate/ymse A method for documenting the change in center of rotation with reverse total shoulder arthroplasty and its application to a consecutive
Scapular notching in reverse shoulder arthroplasties: The influence of glenometaphyseal angle
 Orthopaedics & Traumatology: Surgery & Research (2011) 97S, S131 S137 ORIGINAL ARTICLE Scapular notching in reverse shoulder arthroplasties: The influence of glenometaphyseal angle V. Falaise a, C. Levigne
Orthopaedics & Traumatology: Surgery & Research (2011) 97S, S131 S137 ORIGINAL ARTICLE Scapular notching in reverse shoulder arthroplasties: The influence of glenometaphyseal angle V. Falaise a, C. Levigne
"Stability and Instability of RTSA"
 Orthopedics Update «Reverse Total Shoulder Arthroplasty» Stability and Instability of RTSA A. LÄDERMANN Orthopaedics and Traumatology, La Tour Hospital, Meyrin, Switzerland Orthopaedics and Traumatology,
Orthopedics Update «Reverse Total Shoulder Arthroplasty» Stability and Instability of RTSA A. LÄDERMANN Orthopaedics and Traumatology, La Tour Hospital, Meyrin, Switzerland Orthopaedics and Traumatology,
Biomechanical concepts of total shoulder replacement. «Shoulder Course» Day 1. Richard W. Nyffeler Orthopädie Sonnenhof Bern. 11. Sept.
 Biomechanical concepts of total shoulder replacement Richard W. Nyffeler Orthopädie Sonnenhof Bern First total shoulder prosthesis Jules Emile Péan, 1830-1898 Monobloc prostheses Charles Neer, 1917-2011
Biomechanical concepts of total shoulder replacement Richard W. Nyffeler Orthopädie Sonnenhof Bern First total shoulder prosthesis Jules Emile Péan, 1830-1898 Monobloc prostheses Charles Neer, 1917-2011
The use of the Lima reverse shoulder arthroplasty for the treatment of fracture sequelae of the proximal humerus
 J Orthop Sci (2012) 17:141 147 DOI 10.1007/s00776-011-0185-5 ORIGINAL ARTICLE The use of the Lima reverse shoulder arthroplasty for the treatment of fracture sequelae of the proximal humerus Angel Antonio
J Orthop Sci (2012) 17:141 147 DOI 10.1007/s00776-011-0185-5 ORIGINAL ARTICLE The use of the Lima reverse shoulder arthroplasty for the treatment of fracture sequelae of the proximal humerus Angel Antonio
Assessment of Scapular Morphology and Surgical Technique as Predictors of Notching in Reverse Shoulder Arthroplasty
 An Original Study Assessment of Scapular Morphology and Surgical Technique as Predictors of Notching in Reverse Shoulder Arthroplasty Vani Sabesan, MD, Mark Callanan, MD, Vinay Sharma, BA, and J. Michael
An Original Study Assessment of Scapular Morphology and Surgical Technique as Predictors of Notching in Reverse Shoulder Arthroplasty Vani Sabesan, MD, Mark Callanan, MD, Vinay Sharma, BA, and J. Michael
Scapular Notching. Recognition and Strategies to Minimize Clinical Impact. Gregory P. Nicholson MD, Eric J. Strauss MD, Seth L.
 Clin Orthop Relat Res DOI 10.1007/s11999-010-1720-y SYMPOSIUM: REVERSE TOTAL SHOULDER ARTHROPLASTY Scapular Notching Recognition and Strategies to Minimize Clinical Impact Gregory P. Nicholson MD, Eric
Clin Orthop Relat Res DOI 10.1007/s11999-010-1720-y SYMPOSIUM: REVERSE TOTAL SHOULDER ARTHROPLASTY Scapular Notching Recognition and Strategies to Minimize Clinical Impact Gregory P. Nicholson MD, Eric
SSSR. 1. Nov Shoulder Prosthesis. Postoperative Imaging. Florian M. Buck, MD
 Shoulder Prosthesis Postoperative Imaging Florian M. Buck, MD Shoulder Prosthesis Surgical Approach Findings Imaging Modalities Postoperative Problems Shoulder Prosthesis What are we talking about Anatomical
Shoulder Prosthesis Postoperative Imaging Florian M. Buck, MD Shoulder Prosthesis Surgical Approach Findings Imaging Modalities Postoperative Problems Shoulder Prosthesis What are we talking about Anatomical
Reverse Total Shoulder Arthroplasty: Early Outcome and Complication Report
 ORIGINAL ARTICLE Clinics in Shoulder and Elbow Vol. 17, No. 2, June, 2014 http://dx.doi.org/10.5397/cise.2014.17.2.68 CiSE Clinics in Shoulder and Elbow Reverse Total Shoulder Arthroplasty: Early Outcome
ORIGINAL ARTICLE Clinics in Shoulder and Elbow Vol. 17, No. 2, June, 2014 http://dx.doi.org/10.5397/cise.2014.17.2.68 CiSE Clinics in Shoulder and Elbow Reverse Total Shoulder Arthroplasty: Early Outcome
Radiology Case Reports. Scapular Spine Stress Fracture as a Complication of Reverse Shoulder Arthroplasty
 Radiology Case Reports Volume 2, Issue 2, 2007 Scapular Spine Stress Fracture as a Complication of Reverse Shoulder Arthroplasty Kimberly J. Burkholz, Catherine C. Roberts, and Steven J. Hattrup We report
Radiology Case Reports Volume 2, Issue 2, 2007 Scapular Spine Stress Fracture as a Complication of Reverse Shoulder Arthroplasty Kimberly J. Burkholz, Catherine C. Roberts, and Steven J. Hattrup We report
Reverse Total Shoulder Arthroplasty: A New Frontier (of Complications)
 Reverse Total Shoulder Arthroplasty: A New Frontier (of Complications) Emilie Cheung, MD Associate Professor Chief Shoulder Elbow Svc Stanford University Department of Orthopedic Surgery Procedure volumes
Reverse Total Shoulder Arthroplasty: A New Frontier (of Complications) Emilie Cheung, MD Associate Professor Chief Shoulder Elbow Svc Stanford University Department of Orthopedic Surgery Procedure volumes
Reverse Prostheses in Arthropathies With Cuff Tear
 Clin Orthop Relat Res (2011) 469:2469 2475 DOI 10.1007/s11999-011-1833-y SYMPOSIUM: REVERSE TOTAL SHOULDER ARTHROPLASTY Reverse Prostheses in Arthropathies With Cuff Tear Are Survivorship and Function
Clin Orthop Relat Res (2011) 469:2469 2475 DOI 10.1007/s11999-011-1833-y SYMPOSIUM: REVERSE TOTAL SHOULDER ARTHROPLASTY Reverse Prostheses in Arthropathies With Cuff Tear Are Survivorship and Function
Revision of reversed total shoulder arthroplasty. Indications and outcome
 Farshad et al. BMC Musculoskeletal Disorders 2012, 13:160 RESEARCH ARTICLE Open Access Revision of reversed total shoulder arthroplasty. Indications and outcome Mazda Farshad *, Marion Grögli, Sabrina
Farshad et al. BMC Musculoskeletal Disorders 2012, 13:160 RESEARCH ARTICLE Open Access Revision of reversed total shoulder arthroplasty. Indications and outcome Mazda Farshad *, Marion Grögli, Sabrina
Shoulder Arthroplasty. Valentin Lance 3/24/16
 Shoulder Arthroplasty Valentin Lance 3/24/16 Outline Background Pre-operative imaging assessment Total Shoulder Arthroplasty: Standard and Reverse Complications Other shoulder hardware Hemiarthroplasty
Shoulder Arthroplasty Valentin Lance 3/24/16 Outline Background Pre-operative imaging assessment Total Shoulder Arthroplasty: Standard and Reverse Complications Other shoulder hardware Hemiarthroplasty
D Degenerative joint disease, rotator cuff deficiency with, 149 Deltopectoral approach component removal with, 128
 Index A Abduction exercise, outpatient with, 193, 194 Acromioclavicular arthritis, with, 80 Acromiohumeral articulation, with, 149 Acromio-humeral interval (AHI), physical examination with, 9, 10 Active
Index A Abduction exercise, outpatient with, 193, 194 Acromioclavicular arthritis, with, 80 Acromiohumeral articulation, with, 149 Acromio-humeral interval (AHI), physical examination with, 9, 10 Active
Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty
 Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
Both anatomic (atsa) and reverse (rtsa) total
 S101 Comparison of Outcomes Using Anatomic and Reverse Total Shoulder Arthroplasty Pierre-Henri Flurin, M.D., Yann Marczuk, M.D., Martin Janout, M.D., Thomas W. Wright, M.D., Joseph Zuckerman, M.D., and
S101 Comparison of Outcomes Using Anatomic and Reverse Total Shoulder Arthroplasty Pierre-Henri Flurin, M.D., Yann Marczuk, M.D., Martin Janout, M.D., Thomas W. Wright, M.D., Joseph Zuckerman, M.D., and
Prosthetic design of reverse shoulder arthroplasty contributes to scapular notching and instability
 Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.5312/wjo.v7.i11.738 World J Orthop 2016 November 18; 7(11): 738-745 ISSN 2218-5836 (online)
Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.5312/wjo.v7.i11.738 World J Orthop 2016 November 18; 7(11): 738-745 ISSN 2218-5836 (online)
Reverse shoulder arthroplasty : Does reduced medialisation improve radiological and clinical results?
 Acta Orthop. Belg., 2009, 75, 158-166 ORIGINAL STUDY Reverse shoulder arthroplasty : Does reduced medialisation improve radiological and clinical results? Ibrahim KALOUCHE, Nuno SEVIVAS, Abhijeet WAHEGAONKER,
Acta Orthop. Belg., 2009, 75, 158-166 ORIGINAL STUDY Reverse shoulder arthroplasty : Does reduced medialisation improve radiological and clinical results? Ibrahim KALOUCHE, Nuno SEVIVAS, Abhijeet WAHEGAONKER,
)532( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY
 )532( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE The Midterm Results of the Delta Xtend Reverse Shoulder System: A Five-Year Outcome Study John G. Horneff, MD; Thema A. Nicholson,
)532( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE The Midterm Results of the Delta Xtend Reverse Shoulder System: A Five-Year Outcome Study John G. Horneff, MD; Thema A. Nicholson,
Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis
 CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 366, pp. 39-45 0 1999 Lippincott Williams & Wilkins, Inc. Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis Jens 0. S@jbjerg,
CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 366, pp. 39-45 0 1999 Lippincott Williams & Wilkins, Inc. Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis Jens 0. S@jbjerg,
Bilateral Anatomic Total Shoulder Arthroplasty Versus Reverse Shoulder Arthroplasty
 Bilateral Anatomic Total Shoulder Arthroplasty Versus Reverse Shoulder Arthroplasty Vaqar Latif, MD; Patrick J. Denard, MD; Allan A. Young, MD; Jean-Pierre Liotard, MD; Gilles Walch, MD abstract Full article
Bilateral Anatomic Total Shoulder Arthroplasty Versus Reverse Shoulder Arthroplasty Vaqar Latif, MD; Patrick J. Denard, MD; Allan A. Young, MD; Jean-Pierre Liotard, MD; Gilles Walch, MD abstract Full article
Optimal Baseplate Rotational Alignment in Reverse Total Shoulder Arthroplasty: A Three-Dimensional Computer-Aided Design Study.
 Optimal Baseplate Rotational Alignment in Reverse Total Shoulder Arthroplasty: A Three-Dimensional Computer-Aided Design Study. Byron F. Stephens, MD 1, Casey T. Hebert 2, Thomas W. Throckmorton, MD 1,
Optimal Baseplate Rotational Alignment in Reverse Total Shoulder Arthroplasty: A Three-Dimensional Computer-Aided Design Study. Byron F. Stephens, MD 1, Casey T. Hebert 2, Thomas W. Throckmorton, MD 1,
Immediate post surgical findings of soft tissue swelling, subcutaneous emphysema, and skin staples for reverse total shoulder arthroplasty.
 Immediate post surgical findings of soft tissue swelling, subcutaneous emphysema, and skin staples for reverse total shoulder arthroplasty. REVERSE TOTAL SHOULDER ARTHROPLASTY WITH FRACTURED ACROMION Above:
Immediate post surgical findings of soft tissue swelling, subcutaneous emphysema, and skin staples for reverse total shoulder arthroplasty. REVERSE TOTAL SHOULDER ARTHROPLASTY WITH FRACTURED ACROMION Above:
Reverse Total Shoulder Arthroplasty: A Review of Results According to Etiology
 1476 COPYRIGHT 2007 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Reverse Total Shoulder Arthroplasty: A Review of Results According to Etiology By Bryan Wall, MD, Laurent Nové-Josserand, MD,
1476 COPYRIGHT 2007 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Reverse Total Shoulder Arthroplasty: A Review of Results According to Etiology By Bryan Wall, MD, Laurent Nové-Josserand, MD,
AJO DO NOT COPY. The low grade of the intrinsic stability of the shoulder. Total Reverse Shoulder Arthroplasty: European Lessons and Future Trends
 A Review Paper Total Reverse Shoulder Arthroplasty: European Lessons and Future Trends Ludwig Seebauer, MD Abstract In the late 1980s, Grammont introduced a new reverse total shoulder arthroplasty (TSA),
A Review Paper Total Reverse Shoulder Arthroplasty: European Lessons and Future Trends Ludwig Seebauer, MD Abstract In the late 1980s, Grammont introduced a new reverse total shoulder arthroplasty (TSA),
Influence of Glenosphere Design on Outcomes and Complications of Reverse Arthroplasty: A Systematic Review
 Original Article Clinics in Orthopedic Surgery 2016;8:288-297 http://dx.doi.org/10.4055/cios.2016.8.3.288 Influence of Glenosphere Design on Outcomes and Complications of Reverse Arthroplasty: A Systematic
Original Article Clinics in Orthopedic Surgery 2016;8:288-297 http://dx.doi.org/10.4055/cios.2016.8.3.288 Influence of Glenosphere Design on Outcomes and Complications of Reverse Arthroplasty: A Systematic
Massive Rotator Cuff Tears. Rafael M. Williams, MD
 Massive Rotator Cuff Tears Rafael M. Williams, MD Rotator Cuff MRI MRI Small / Partial Thickness Medium Tear Arthroscopic View Massive Tear Fatty Atrophy Arthroscopic View MassiveTears Tear is > 5cm
Massive Rotator Cuff Tears Rafael M. Williams, MD Rotator Cuff MRI MRI Small / Partial Thickness Medium Tear Arthroscopic View Massive Tear Fatty Atrophy Arthroscopic View MassiveTears Tear is > 5cm
The Deltopectoral Approach for Reverse Shoulder Arthroplasty
 The Deltopectoral Approach for Reverse Shoulder Arthroplasty George M. McCluskey III, MD, and Howard D. Routman, DO Director, St. Francis Shoulder Center, St. Francis Orthopaedic Institute, Columbus, Georgia
The Deltopectoral Approach for Reverse Shoulder Arthroplasty George M. McCluskey III, MD, and Howard D. Routman, DO Director, St. Francis Shoulder Center, St. Francis Orthopaedic Institute, Columbus, Georgia
Reverse Total Shoulder. Dr. Minoo Patel
 Reverse Total Shoulder Dr. Minoo Patel AOA VIC, Lorne, 2011 The role of the rotator cuff Depress and humeral head (against the force of the deltoid) Keep the humeral head co-apted in the glenoid Initiate
Reverse Total Shoulder Dr. Minoo Patel AOA VIC, Lorne, 2011 The role of the rotator cuff Depress and humeral head (against the force of the deltoid) Keep the humeral head co-apted in the glenoid Initiate
An evaluation of the radiological changes around the Grammont reverse geometry shoulder arthroplasty after eight to 12 years
 UPPER LIMB An evaluation of the radiological changes around the Grammont reverse geometry shoulder arthroplasty after eight to 12 years B. Melis, M. DeFranco, A. Lädermann, D. Molé, L. Favard, C. Nérot,
UPPER LIMB An evaluation of the radiological changes around the Grammont reverse geometry shoulder arthroplasty after eight to 12 years B. Melis, M. DeFranco, A. Lädermann, D. Molé, L. Favard, C. Nérot,
Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD
 General Information: Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH)
General Information: Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH)
Reverse shoulder arthroplasty for the treatment of three and four part fractures of the proximal humerus in patients older than 75 years old
 Acta Orthop. Belg., 2014, 80, 99-105 ORIGINAL STUDY Reverse shoulder arthroplasty for the treatment of three and four part fractures of the proximal humerus in patients older than 75 years old Aristotelis
Acta Orthop. Belg., 2014, 80, 99-105 ORIGINAL STUDY Reverse shoulder arthroplasty for the treatment of three and four part fractures of the proximal humerus in patients older than 75 years old Aristotelis
Reverse Total Shoulder Arthroplasty Protocol
 General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
Instability After Reverse Total Shoulder Arthroplasty: Which Patients Dislocate?
 An Original Study Instability After Reverse Total Shoulder Arthroplasty: Which Patients Dislocate? Eric M. Padegimas, MD, Benjamin Zmistowski, MD, Camilo Restrepo, MD, Joseph A. Abboud, MD, Mark D. Lazarus,
An Original Study Instability After Reverse Total Shoulder Arthroplasty: Which Patients Dislocate? Eric M. Padegimas, MD, Benjamin Zmistowski, MD, Camilo Restrepo, MD, Joseph A. Abboud, MD, Mark D. Lazarus,
The Irreparable Rotator Cuff Tear:
 The Irreparable Rotator Cuff Tear: Trauma 101: Shoulder Session #2 Brian Grawe, MD Assistant Professor Orthopaedics & Sports Medicine 5/10/2018 Brian Grawe, MD Assistant Professor Phone Number: 513-558-4516
The Irreparable Rotator Cuff Tear: Trauma 101: Shoulder Session #2 Brian Grawe, MD Assistant Professor Orthopaedics & Sports Medicine 5/10/2018 Brian Grawe, MD Assistant Professor Phone Number: 513-558-4516
Disclosures A prospective comparison between reverse and anatomic total shoulder arthroplasty
 Disclosures A prospective comparison between reverse and anatomic total shoulder arthroplasty Tuyen Kiet Micah Naimark, MD Brian T. Feeley, MD Teddy T. Chung Tatiana Gajiu Sarah L. Hall, MA C. Benjamin
Disclosures A prospective comparison between reverse and anatomic total shoulder arthroplasty Tuyen Kiet Micah Naimark, MD Brian T. Feeley, MD Teddy T. Chung Tatiana Gajiu Sarah L. Hall, MA C. Benjamin
11/13/2017. Disclosures: The Irreparable Rotator Cuff. I am a consultant for Arhtrex, Inc and Endo Pharmaceuticals.
 Massive Rotator Cuff Tears without Arthritis THE CASE FOR SUPERIOR CAPSULAR RECONSTRUCTION MICHAEL GARCIA, MD NOVEMBER 4, 2017 FLORIDA ORTHOPAEDIC INSTITUTE Disclosures: I am a consultant for Arhtrex,
Massive Rotator Cuff Tears without Arthritis THE CASE FOR SUPERIOR CAPSULAR RECONSTRUCTION MICHAEL GARCIA, MD NOVEMBER 4, 2017 FLORIDA ORTHOPAEDIC INSTITUTE Disclosures: I am a consultant for Arhtrex,
What Factors are Associated With Clinically Important Improvement After Shoulder Hemiarthroplasty for Cuff Tear Arthropathy?
 Clin Orthop Relat Res (2016) 474:2682 2688 DOI 10.1007/s11999-016-5037-3 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons CLINICAL RESEARCH What Factors
Clin Orthop Relat Res (2016) 474:2682 2688 DOI 10.1007/s11999-016-5037-3 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons CLINICAL RESEARCH What Factors
Evaluating Scapular Notching after Reverse Total Shoulder Arthroplasty
 ORIGINAL ARTICLE Clinics in Shoulder and Elbow Vol. 18, No. 4, December, 2015 http://dx.doi.org/10.5397/cise.2015.18.4.248 CiSE Clinics in Shoulder and Elbow Evaluating Scapular Notching after Reverse
ORIGINAL ARTICLE Clinics in Shoulder and Elbow Vol. 18, No. 4, December, 2015 http://dx.doi.org/10.5397/cise.2015.18.4.248 CiSE Clinics in Shoulder and Elbow Evaluating Scapular Notching after Reverse
Reverse arthroplasty of the shoulder for treating rotator cuff arthropathy,
 rev bras ortop. 2014;49(3):279 285 www.rbo.org.br Original Article Reverse arthroplasty of the shoulder for treating rotator cuff arthropathy, Marcus Vinicius Galvão Amaral, José Leonardo Rocha de Faria,
rev bras ortop. 2014;49(3):279 285 www.rbo.org.br Original Article Reverse arthroplasty of the shoulder for treating rotator cuff arthropathy, Marcus Vinicius Galvão Amaral, José Leonardo Rocha de Faria,
3/9/2018. Algorithm for Massive RCT s. Massive Rotator Cuff Tears: When is Reverse TSA the only option?
 Massive Rotator Cuff Tears: When is Reverse TSA the only option? Anthony A. Romeo, MD Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Team Physician, Chicago White Sox
Massive Rotator Cuff Tears: When is Reverse TSA the only option? Anthony A. Romeo, MD Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Team Physician, Chicago White Sox
Index. B Backslap technique depth assessment, 82, 83 diaphysis distal trocar, 82 83
 Index A Acromial impingement, 75, 76 Aequalis intramedullary locking avascular necrosis, 95 central humeral head, 78, 80 clinical and functional outcomes, 95, 96 design, 77, 79 perioperative complications,
Index A Acromial impingement, 75, 76 Aequalis intramedullary locking avascular necrosis, 95 central humeral head, 78, 80 clinical and functional outcomes, 95, 96 design, 77, 79 perioperative complications,
Reverse Total Shoulder Protocol
 Marion Herring, M.D. OrthoVirginia PH: (804) 270-1305 FX: (804) 273-9294 www.orthovirginia.com Reverse Total Shoulder Protocol General Information: Reverse Total Shoulder Arthroplasty (rtsa) is designed
Marion Herring, M.D. OrthoVirginia PH: (804) 270-1305 FX: (804) 273-9294 www.orthovirginia.com Reverse Total Shoulder Protocol General Information: Reverse Total Shoulder Arthroplasty (rtsa) is designed
Proximal Humeral Fractures RSA v HHR. Proximal Humeral Fractures RSA v HHR. Introduction
 Proximal Humeral Fractures RSA v HHR Xavier A. Duralde, MD Peachtree Orthopaedic Clinic Atlanta, GA Proximal Humeral Fractures RSA v HHR Consultant: Smith+Nephew Board of Directors: CORR Introduction Incidence
Proximal Humeral Fractures RSA v HHR Xavier A. Duralde, MD Peachtree Orthopaedic Clinic Atlanta, GA Proximal Humeral Fractures RSA v HHR Consultant: Smith+Nephew Board of Directors: CORR Introduction Incidence
RCR or rtsa? Massive Rotator Cuff Tears without Arthritis in Patients Older than 65 Reverse Total Shoulder Arthroplasty or Rotator Cuff Repair?
 Massive Rotator Cuff Tears without Arthritis in Patients Older than 65 Reverse Total Shoulder Arthroplasty or Rotator Cuff Repair? JESSE W. ALLERT, MD THOMAS SELLERS, MD PETER SIMON, PHD RACHEL CLARK,
Massive Rotator Cuff Tears without Arthritis in Patients Older than 65 Reverse Total Shoulder Arthroplasty or Rotator Cuff Repair? JESSE W. ALLERT, MD THOMAS SELLERS, MD PETER SIMON, PHD RACHEL CLARK,
ANATOMIC TOTAL SHOULDER REPLACEMENT:
 The Shoulder Replacement A total shoulder arthroplasty (TSA) is a surgery to replace the damaged parts of the ball and socket shoulder joint with an artificial prosthesis. The damage to the shoulder can
The Shoulder Replacement A total shoulder arthroplasty (TSA) is a surgery to replace the damaged parts of the ball and socket shoulder joint with an artificial prosthesis. The damage to the shoulder can
Total Shoulder Arthroplasty
 1 Total Shoulder Arthroplasty Surgical indications and contraindications Anatomical Considerations: Total shoulder arthroplasty surgery involves the replacement of the humeral head and the glenoid articulating
1 Total Shoulder Arthroplasty Surgical indications and contraindications Anatomical Considerations: Total shoulder arthroplasty surgery involves the replacement of the humeral head and the glenoid articulating
Results of a stemless reverse shoulder prosthesis at more than 58 months mean without loosening
 J Shoulder Elbow Surg (2013) 22, e1-e6 www.elsevier.com/locate/ymse Results of a stemless reverse shoulder prosthesis at more than 58 months mean without loosening Richard Ballas, MD a, *, Laurent Beguin,
J Shoulder Elbow Surg (2013) 22, e1-e6 www.elsevier.com/locate/ymse Results of a stemless reverse shoulder prosthesis at more than 58 months mean without loosening Richard Ballas, MD a, *, Laurent Beguin,
Post-Operative Physical Therapy Management of a Reverse Total Shoulder Arthroplasty (rtsa)
 Post-Operative Physical Therapy Management of a Reverse Total Shoulder Arthroplasty (rtsa) Steve Volpe PT, MBA, OCS, CHT, CSCS Regional Director of Rehabilitation Services, ProMedica Health System South
Post-Operative Physical Therapy Management of a Reverse Total Shoulder Arthroplasty (rtsa) Steve Volpe PT, MBA, OCS, CHT, CSCS Regional Director of Rehabilitation Services, ProMedica Health System South
Effect of Prosthesis Design on Muscle Length and Moment Arms in Reverse Total Shoulder Arthroplasty
 S31 Effect of Prosthesis Design on Muscle Length and Moment Arms in Reverse Total Shoulder Arthroplasty Matthew A. Hamilton, Ph.D., Christopher P. Roche, M.S., M.B.A., Phong Diep, B.S., Pierre- Henri Flurin,
S31 Effect of Prosthesis Design on Muscle Length and Moment Arms in Reverse Total Shoulder Arthroplasty Matthew A. Hamilton, Ph.D., Christopher P. Roche, M.S., M.B.A., Phong Diep, B.S., Pierre- Henri Flurin,
Nationwide Trends in Total Shoulder Arthroplasty and Hemiarthroplasty for Osteoarthritis
 An Original Study Nationwide Trends in Total Shoulder Arthroplasty and Hemiarthroplasty for Osteoarthritis David Trofa, MD, Sean S. Rajaee, MD, and Eric L. Smith, MD Abstract Recent literature reports
An Original Study Nationwide Trends in Total Shoulder Arthroplasty and Hemiarthroplasty for Osteoarthritis David Trofa, MD, Sean S. Rajaee, MD, and Eric L. Smith, MD Abstract Recent literature reports
WHAT YOU IS BACK WITHIN ARM S REACH
 YOUR TOTAL SHOULDER REPLACEMENT SURGERY STEPS TO RETURNING TO A LIFESTYLE YOU DESERVE WHAT YOU IS BACK WITHIN ARM S REACH Nathan Richardson, MD Orthopedics, Shoulder & Elbow Surgeon Board Certified in
YOUR TOTAL SHOULDER REPLACEMENT SURGERY STEPS TO RETURNING TO A LIFESTYLE YOU DESERVE WHAT YOU IS BACK WITHIN ARM S REACH Nathan Richardson, MD Orthopedics, Shoulder & Elbow Surgeon Board Certified in
Shoulder Joint Examination. Shoulder Joint Examination. Inspection. Inspection Palpation Movement. Look Feel Move
 Shoulder Joint Examination History Cuff Examination Instability Examination AC Joint Examination Biceps Tendon Examination Superior Labrum Examination Shoulder Joint Examination Inspection Palpation Movement
Shoulder Joint Examination History Cuff Examination Instability Examination AC Joint Examination Biceps Tendon Examination Superior Labrum Examination Shoulder Joint Examination Inspection Palpation Movement
Reverse Shoulder Arthroplasty A Literature Review
 Send Orders for Reprints to reprints@benthamscience.net 366 The Open Orthopaedics Journal, 2013, 7, (Suppl 3: M13) 366-372 Reverse Shoulder Arthroplasty A Literature Review Open Access Aatif Mahmood, Joby
Send Orders for Reprints to reprints@benthamscience.net 366 The Open Orthopaedics Journal, 2013, 7, (Suppl 3: M13) 366-372 Reverse Shoulder Arthroplasty A Literature Review Open Access Aatif Mahmood, Joby
What are the options for shoulder replacement today?
 Derek Plausinis, MASC, MD, FRCSC What are the options for shoulder replacement today? Anatomic total shoulder replacement continues to provide excellent outcomes in cases of advanced osteoarthritis, while
Derek Plausinis, MASC, MD, FRCSC What are the options for shoulder replacement today? Anatomic total shoulder replacement continues to provide excellent outcomes in cases of advanced osteoarthritis, while
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD
 Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
Management of arthritis of the shoulder. Omar Haddo Consultant Orthopaedic Surgeon
 Management of arthritis of the shoulder Omar Haddo Consultant Orthopaedic Surgeon Diagnosis Pain - with activity initially. As disease progresses night pain is common and sleep difficult Stiffness trouble
Management of arthritis of the shoulder Omar Haddo Consultant Orthopaedic Surgeon Diagnosis Pain - with activity initially. As disease progresses night pain is common and sleep difficult Stiffness trouble
The Reverse Total Shoulder Arthroplasty
 This is an enhanced PDF from The Journal of Bone and Joint Surgery The PDF of the article you requested follows this cover page. The Reverse Total Shoulder Arthroplasty Frederick A. Matsen, III, Pascal
This is an enhanced PDF from The Journal of Bone and Joint Surgery The PDF of the article you requested follows this cover page. The Reverse Total Shoulder Arthroplasty Frederick A. Matsen, III, Pascal
Or thopaedic Surger y
 Article Improved external rotation with concomitant reverse total shoulder arthroplasty and latissimus dorsi tendon transfer: A systematic review Journal of Or thopaedic Surger y Journal of Orthopaedic
Article Improved external rotation with concomitant reverse total shoulder arthroplasty and latissimus dorsi tendon transfer: A systematic review Journal of Or thopaedic Surger y Journal of Orthopaedic
Reverse Total Shoulder Arthroplasty with Latissimus dorsi tendon transfer Protocol:
 Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Reverse Total Shoulder Arthroplasty with Latissimus dorsi tendon transfer Protocol: General Information:
Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Reverse Total Shoulder Arthroplasty with Latissimus dorsi tendon transfer Protocol: General Information:
Making sense of all our measures-inclination, version, subluxation, reaming depth & implant seating
 Thursday - ANATOMIC SHOULDER ARTHROPLASTY 7:00-7:15a Welcome and Introduction of Faculty Athwal, Keener, 7:15-7:22a The ABC s of the Walch Classification Walch 7:22-7:32a How I use x-rays, CT +/- MRI for
Thursday - ANATOMIC SHOULDER ARTHROPLASTY 7:00-7:15a Welcome and Introduction of Faculty Athwal, Keener, 7:15-7:22a The ABC s of the Walch Classification Walch 7:22-7:32a How I use x-rays, CT +/- MRI for
Managing acromial fractures: prevention and treatment, both nonoperative and operative
 Review Article Page 1 of 8 Managing acromial fractures: prevention and treatment, both nonoperative and operative Christopher D. Joyce, Adam J. Seidl Department of Orthopaedics, University of Colorado,
Review Article Page 1 of 8 Managing acromial fractures: prevention and treatment, both nonoperative and operative Christopher D. Joyce, Adam J. Seidl Department of Orthopaedics, University of Colorado,
P. Trouilloud M. Gonzalvez P. Martz H. Charles F. Handelberg R. W. Nyffeler E. Baulot DuocentricÒ Group
 DOI 10.1007/s00590-013-1213-2 ORIGINAL ARTICLE Duocentric Ò reversed shoulder prosthesis and Personal Fit Ò templates: innovative strategies to optimize prosthesis positioning and prevent scapular notching
DOI 10.1007/s00590-013-1213-2 ORIGINAL ARTICLE Duocentric Ò reversed shoulder prosthesis and Personal Fit Ò templates: innovative strategies to optimize prosthesis positioning and prevent scapular notching
Options for the Irreparable RCT 3/9/2018. Your Patient has an Irreparable RC Tear: What Now? Asheesh Bedi, MD
 Your Patient has an Irreparable RC Tear: What Now? Asheesh Bedi, MD Harold and Helen W. Gehring Professor Chief, Sports Medicine & Shoulder Surgery MedSport, Department of Orthopedic Surgery Head Team
Your Patient has an Irreparable RC Tear: What Now? Asheesh Bedi, MD Harold and Helen W. Gehring Professor Chief, Sports Medicine & Shoulder Surgery MedSport, Department of Orthopedic Surgery Head Team
MEDICAL POLICY MEDICAL POLICY DETAILS POLICY STATEMENT. Page: 1 of 6
 Page: 1 of 6 MEDICAL POLICY MEDICAL POLICY DETAILS Medical Policy Title SHOULDER ARTHROPLASTY (TOTAL, PARTIAL AND REVERSE) Policy Number 7.01.95 Category Technology Assessment Effective Date 6/21/18 Revised
Page: 1 of 6 MEDICAL POLICY MEDICAL POLICY DETAILS Medical Policy Title SHOULDER ARTHROPLASTY (TOTAL, PARTIAL AND REVERSE) Policy Number 7.01.95 Category Technology Assessment Effective Date 6/21/18 Revised
Name of Policy: Shoulder Resurfacing
 Name of Policy: Shoulder Resurfacing Policy #: 366 Latest Review Date: November 2010 Category: Surgery Policy Grade: Active policy but no longer scheduled for regular literature reviews and update. Background/Definitions:
Name of Policy: Shoulder Resurfacing Policy #: 366 Latest Review Date: November 2010 Category: Surgery Policy Grade: Active policy but no longer scheduled for regular literature reviews and update. Background/Definitions:
Uncommon Indications for Reverse Total Shoulder Arthroplasty
 Review Article Clinics in Orthopedic Surgery 2013;5:243-255 http://dx.doi.org/10.4055/cios.2013.5.4.243 Uncommon Indications for Reverse Total Shoulder Arthroplasty Yoon Suk Hyun, MD, Gazi Huri, MD, Nickolas
Review Article Clinics in Orthopedic Surgery 2013;5:243-255 http://dx.doi.org/10.4055/cios.2013.5.4.243 Uncommon Indications for Reverse Total Shoulder Arthroplasty Yoon Suk Hyun, MD, Gazi Huri, MD, Nickolas
Index. ESSKA 2018 G. Milano et al. (eds.), Management of Failed Shoulder Surgery,
 A Acromial fractures, 186 Acromioclavicular joint (ACJ) instability, 55, 97 case study, 98 100 classification, 85 clinical relevant situations, 86 dislocation, 97 98 insufficient fixation, 87 88 operative
A Acromial fractures, 186 Acromioclavicular joint (ACJ) instability, 55, 97 case study, 98 100 classification, 85 clinical relevant situations, 86 dislocation, 97 98 insufficient fixation, 87 88 operative
Indications for reverse shoulder replacement
 INSTRUCTIONAL REVIEW: UPPER LIMB Indications for reverse shoulder replacement A SYSTEMATIC REVIEW C. D. Smith, P. Guyver, T. D. Bunker From Princess Elizabeth Orthopaedic Centre, Exeter, United Kingdom
INSTRUCTIONAL REVIEW: UPPER LIMB Indications for reverse shoulder replacement A SYSTEMATIC REVIEW C. D. Smith, P. Guyver, T. D. Bunker From Princess Elizabeth Orthopaedic Centre, Exeter, United Kingdom
Bulletin of the Hospital for Joint Diseases 2013;71(4):284-93
 284 Impact of Inferior Glenoid Tilt, Humeral Retroversion, Bone Grafting, and Design Parameters on Muscle Length and Wrapping in Reverse Shoulder Arthroplasty Christopher P. Roche, M.S., M.B.A., Phong
284 Impact of Inferior Glenoid Tilt, Humeral Retroversion, Bone Grafting, and Design Parameters on Muscle Length and Wrapping in Reverse Shoulder Arthroplasty Christopher P. Roche, M.S., M.B.A., Phong
Shoulder hemiarthroplasty in the management of humeral head fractures
 Acta Orthop. Belg., 2004, 70, 214-218 ORIGINAL STUDY Shoulder hemiarthroplasty in the management of humeral head fractures Joseph J. CHRISTOFORAKIS, George M. KONTAKIS, Pavlos G. KATONIS, Konstantinos
Acta Orthop. Belg., 2004, 70, 214-218 ORIGINAL STUDY Shoulder hemiarthroplasty in the management of humeral head fractures Joseph J. CHRISTOFORAKIS, George M. KONTAKIS, Pavlos G. KATONIS, Konstantinos
Chapter 7. Arthroplasty and Rotator Cuff Deficiency. Gregory P. Nicholson
 Chapter 7 Arthroplasty and Rotator Cuff Deficiency Gregory P. Nicholson Rotator cuff deficient shoulders with degenerative joint disease are a treatment challenge. Most patients present primarily due to
Chapter 7 Arthroplasty and Rotator Cuff Deficiency Gregory P. Nicholson Rotator cuff deficient shoulders with degenerative joint disease are a treatment challenge. Most patients present primarily due to
Les séquelles traumatiques. Ph. Valenti, J. Kany, D. Katz
 Indications et Techniques Les séquelles traumatiques Ph. Valenti, J. Kany, D. Katz Paris Shoulder Unit Clinique Bizet (Paris, France) Disclosures Arthroplasty Consultant : FH orthopaedics receive royalties
Indications et Techniques Les séquelles traumatiques Ph. Valenti, J. Kany, D. Katz Paris Shoulder Unit Clinique Bizet (Paris, France) Disclosures Arthroplasty Consultant : FH orthopaedics receive royalties
Advantages to medialize less
 Advantages to medialize less less RSP? Clinical and radiological results Ph Valenti, D Katz, Ph Sauzieres J Kany, K Elkolti, P Gleyze Paris, Lorient, Toulouse, Lyon, Colmar Delta RSP CTA pseudoparalytic
Advantages to medialize less less RSP? Clinical and radiological results Ph Valenti, D Katz, Ph Sauzieres J Kany, K Elkolti, P Gleyze Paris, Lorient, Toulouse, Lyon, Colmar Delta RSP CTA pseudoparalytic
 Use of a partial humeral head resurfacing system for management of an osseous mechanic... Page 1 of 12 Int J Shoulder Surg. 2011 Jan-Mar; 5(1): 17 20. doi: 10.4103/0973-6042.80465. PMCID: PMC3109768 Copyright
Use of a partial humeral head resurfacing system for management of an osseous mechanic... Page 1 of 12 Int J Shoulder Surg. 2011 Jan-Mar; 5(1): 17 20. doi: 10.4103/0973-6042.80465. PMCID: PMC3109768 Copyright
FUNCTIONAL ANATOMY OF SHOULDER JOINT
 FUNCTIONAL ANATOMY OF SHOULDER JOINT ARTICULATION Articulation is between: The rounded head of the Glenoid cavity humerus and The shallow, pear-shaped glenoid cavity of the scapula. 2 The articular surfaces
FUNCTIONAL ANATOMY OF SHOULDER JOINT ARTICULATION Articulation is between: The rounded head of the Glenoid cavity humerus and The shallow, pear-shaped glenoid cavity of the scapula. 2 The articular surfaces
SHOULDER ARTHROPLASTY (TOTAL, HEMI, REVERSE)/ARTHRODESIS
 evicore healthcare. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Imaging requests for patients with atypical symptoms or clinical presentations
evicore healthcare. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Imaging requests for patients with atypical symptoms or clinical presentations
CLINICAL GUIDELINES. CMM-318: Shoulder Arthroplasty/ Replacement/Resurfacing/ Revision/Arthrodesis. Version Effective October 22, 2018
 CLINICAL GUIDELINES CMM-318: / Replacement/Resurfacing/ Revision/Arthrodesis Version 20.0.2018 Effective October 22, 2018 Clinical guidelines for medical necessity review of speech therapy services. CMM-318:
CLINICAL GUIDELINES CMM-318: / Replacement/Resurfacing/ Revision/Arthrodesis Version 20.0.2018 Effective October 22, 2018 Clinical guidelines for medical necessity review of speech therapy services. CMM-318:
TORNIER AEQUALIS FX. Shoulder System SYSTEM OVERVIEW
 TORNIER AEQUALIS FX Shoulder System SYSTEM OVERVIEW Simple in design, but used for the most complex fractures Each year, approximately 4 million people in the United States seek medical care for shoulder
TORNIER AEQUALIS FX Shoulder System SYSTEM OVERVIEW Simple in design, but used for the most complex fractures Each year, approximately 4 million people in the United States seek medical care for shoulder
Fixed and Variable Geometry Total Shoulder Arthroplasty
 Fixed and Variable Geometry Total Shoulder Arthroplasty RECOVERY FUNCTION SURVIVORSHIP DePuy believes in an approach to total shoulder replacement that places equal importance on recovery, function and
Fixed and Variable Geometry Total Shoulder Arthroplasty RECOVERY FUNCTION SURVIVORSHIP DePuy believes in an approach to total shoulder replacement that places equal importance on recovery, function and
The reverse shoulder prosthesis in the treatment of fractures of the proximal humerus in the elderly
 The reverse shoulder prosthesis in the treatment of fractures of the proximal humerus in the elderly J.-F. Cazeneuve, D.-J. Cristofari From Orthopaedic Centre, Centre Hospitalier, Laon, France We have
The reverse shoulder prosthesis in the treatment of fractures of the proximal humerus in the elderly J.-F. Cazeneuve, D.-J. Cristofari From Orthopaedic Centre, Centre Hospitalier, Laon, France We have
Investigation performed at the Mayo Clinic and Mayo Foundation, Rochester, Minnesota
 1814 COPYRIGHT 2001 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Shoulder Hemiarthroplasty for Glenohumeral Arthritis Associated with Severe Rotator Cuff Deficiency BY JOAQUIN SANCHEZ-SOTELO,
1814 COPYRIGHT 2001 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Shoulder Hemiarthroplasty for Glenohumeral Arthritis Associated with Severe Rotator Cuff Deficiency BY JOAQUIN SANCHEZ-SOTELO,
P V S MEMORIAL HOSPITAL LTD.
 SHOULDER XRAYS Instability Series o True AP (Grashey s) o Axillary o Stryker Notch view o True AP in Internal rotation o Scapular Y view o West Point view for Bony Bankart ( looks like modif axillary view)
SHOULDER XRAYS Instability Series o True AP (Grashey s) o Axillary o Stryker Notch view o True AP in Internal rotation o Scapular Y view o West Point view for Bony Bankart ( looks like modif axillary view)
STATE OF CONNECTICUT ETHICS BOARD NONE ARTHREX INC ARTHREX INC
 Rationale, Biomechanics,Early Results after Superior Capsular Reconstruction Augustus D Mazzocca MS, MD Director of the New England Musculoskeletal Institute Chairman Department of Orthopaedic Surgery
Rationale, Biomechanics,Early Results after Superior Capsular Reconstruction Augustus D Mazzocca MS, MD Director of the New England Musculoskeletal Institute Chairman Department of Orthopaedic Surgery
How does scapula motion change after reverse total shoulder arthroplasty? - a preliminary report
 Kim et al. BMC Musculoskeletal Disorders 2012, 13:210 RESEARCH ARTICLE Open Access How does scapula motion change after reverse total shoulder arthroplasty? - a preliminary report Myung-Sun Kim 1, Keun-Young
Kim et al. BMC Musculoskeletal Disorders 2012, 13:210 RESEARCH ARTICLE Open Access How does scapula motion change after reverse total shoulder arthroplasty? - a preliminary report Myung-Sun Kim 1, Keun-Young
Rotator Cuff Tear Arthropathy
 Rotator Cuff Tear Arthropathy Kier J. Ecklund, MD Thay Q. Lee, PhD James Tibone, MD Ranjan Gupta, MD Dr. Ecklund is Chief Resident, Department of Orthopaedic Surgery, University of California, Irvine,
Rotator Cuff Tear Arthropathy Kier J. Ecklund, MD Thay Q. Lee, PhD James Tibone, MD Ranjan Gupta, MD Dr. Ecklund is Chief Resident, Department of Orthopaedic Surgery, University of California, Irvine,
Shoulder joint Assessment and General View
 Shoulder joint Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The shoulder contains
Shoulder joint Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The shoulder contains
Comparison of Pegged and Keeled Glenoid Components for Total Shoulder Arthroplasty: A Systematic Review
 Review Article Comparison of Pegged and Keeled Glenoid Components for Total Shoulder Arthroplasty: A Systematic Review Journal of Shoulder and Elbow Arthroplasty Volume 1: 1 7! The Author(s) 2017 Reprints
Review Article Comparison of Pegged and Keeled Glenoid Components for Total Shoulder Arthroplasty: A Systematic Review Journal of Shoulder and Elbow Arthroplasty Volume 1: 1 7! The Author(s) 2017 Reprints
THE REVERSE SHOULDER REPLACEMENT
 THE REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is a newly approved implant that has been used successfully for over ten years in Europe. It was approved by the FDA for use in the U.S.A.
THE REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is a newly approved implant that has been used successfully for over ten years in Europe. It was approved by the FDA for use in the U.S.A.
Surgical. Technique. AEQUALIS Spherical Base Glenoid. Shoulder Prosthesis.
 Surgical Technique Shoulder Prosthesis AEQUALIS Spherical Base Glenoid www.tornier.com CONTENTS CONTENTS 1. Subscapularis 2. Anterior capsule 3. Humeral protector 4. Inserting retractors 1. DESIGN FEATURES
Surgical Technique Shoulder Prosthesis AEQUALIS Spherical Base Glenoid www.tornier.com CONTENTS CONTENTS 1. Subscapularis 2. Anterior capsule 3. Humeral protector 4. Inserting retractors 1. DESIGN FEATURES
Cigna Medical Coverage Policies Musculoskeletal Shoulder Arthroplasty (Total, Hemi, Reverse)/Arthrodesis
 Cigna Medical Coverage Policies Musculoskeletal Shoulder Arthroplasty (Total, Hemi, Reverse)/Arthrodesis Effective January 1, 2016 Instructions for use The following coverage policy applies to health benefit
Cigna Medical Coverage Policies Musculoskeletal Shoulder Arthroplasty (Total, Hemi, Reverse)/Arthrodesis Effective January 1, 2016 Instructions for use The following coverage policy applies to health benefit
ROTATOR CUFF DISORDERS/IMPINGEMENT
 ROTATOR CUFF DISORDERS/IMPINGEMENT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH
ROTATOR CUFF DISORDERS/IMPINGEMENT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH
Reversed Revised : What to do when it goes wrong?
 Acta Orthop. Belg., 2014, 80, 314-321 ORIGINAL STUDY Reversed Revised : What to do when it goes wrong? Bart Middernacht, Alexander Van Tongel, Lieven De Wilde From Department of Orthopaedics, University
Acta Orthop. Belg., 2014, 80, 314-321 ORIGINAL STUDY Reversed Revised : What to do when it goes wrong? Bart Middernacht, Alexander Van Tongel, Lieven De Wilde From Department of Orthopaedics, University
REVERSE SHOULDER REPLACEMENT
 REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is designed specifically for the use in shoulders with a deficient rotator cuff and arthritis, as well as other difficult shoulder reconstructive
REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is designed specifically for the use in shoulders with a deficient rotator cuff and arthritis, as well as other difficult shoulder reconstructive
A symptom-based classification for shoulders with massive rotator cuff defects
 International Orthopaedics (SICOT) (2010) 34:63 69 DOI 10.1007/s00264-009-0725-1 ORIGINAL PAPER A symptom-based classification for shoulders with massive rotator cuff defects Markus Loew & Patric Raiss
International Orthopaedics (SICOT) (2010) 34:63 69 DOI 10.1007/s00264-009-0725-1 ORIGINAL PAPER A symptom-based classification for shoulders with massive rotator cuff defects Markus Loew & Patric Raiss
Reverse Total Shoulder
 Rehabilitation Protocol: Reverse Total Shoulder Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Rehabilitation Protocol: Reverse Total Shoulder Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Keywords Arthroplasty; Replacement; Joint Diseases; Rotator Cuff
 ORIGINAL article Results of Surgical Treatment of Denerative Arthropathy of the Rotator Cuff using Hemiarthroplasty- CTA Rômulo Brasil Filho 1, Fabiano Rebouças Ribeiro 1, Antonio Carlos Tenor Junior 1,
ORIGINAL article Results of Surgical Treatment of Denerative Arthropathy of the Rotator Cuff using Hemiarthroplasty- CTA Rômulo Brasil Filho 1, Fabiano Rebouças Ribeiro 1, Antonio Carlos Tenor Junior 1,
