Patellofemoral pain syndrome
|
|
|
- Bernard Owens
- 6 years ago
- Views:
Transcription
1 CHRISTINE A. IVERSON, PT, DPT¹ PT, PhD, OCS² PT, DPT³ PT, DPT 4 PT, DPT 5 PT, DScPT, OCS, FAAOMPT 6 PT, PhD, SCS, ATC 7 PT, PhD, ECS, OCS, FAAOMPT 8 Lumbopelvic Manipulation for the Treatment of Patients With Patellofemoral Pain Syndrome: Development of a Clinical Prediction Rule Patellofemoral pain syndrome (PFPS) is a significant clinical problem and one of the most common knee disorders in young, active individuals. 13,52,63,64,80 Despite its prevalence, the etiology of PFPS is not well understood. 12,37,41,52,59,72,79 It has been proposed that abnormal neuromuscular 8,9,11,22,41,54 and biomechanical 5,23,34,40,51,62,73 factors alter patellar tracking and contribute to increased patellofemoral joint contact pressures that ultimately lead to pain and dysfunction. 16,52,72 Because the etiology is unclear, and due to variations in the clinical presentation of patients with PFPS, numerous nonoperative interventions have been proposed for the disorder. A common goal of most treatment regimens for PFPS is the restoration of quadriceps muscle strength and function. 11,12,26,52,71,72 Suter and colleagues 67,68 recently showed that sacro- knees of patients with PFPS. Similarly, Hillermann et al 28 reported that quadriceps muscle strength increased sigiliac joint (SIJ) or lumbopelvic region manipulation led to a significant decrease in quadriceps inhibition in the involved Prospective cohort/predictive validity study. To determine the predictive validity of selected clinical exam items and to develop a clinical prediction rule (CPR) to determine which patients with patellofemoral pain syndrome (PFPS) have a positive immediate response to lumbopelvic manipulation. Quadriceps muscle function in patients with PFPS was recently shown to improve following treatment with lumbopelvic manipulation. No previous study has determined if individuals with PFPS experience symptomatic relief of activity-related pain immediately following this manipulation technique. Fifty subjects (26 male, 24 female; age range, years) with PFPS underwent a standardized history and physical examination. After the evaluation, each subject performed 3 typically pain-producing functional activities (squatting, stepping up a 20-cm step, and stepping down a 20-cm step). The pain level perceived during each activity was rated on a numerical pain scale (0 representing no pain and 10 the worst possible pain). Following the assessment, all subjects were treated with a lumbopelvic manipulation, which was immediately followed by retesting the 3 functional activities to determine if there was any change in pain ratings. An immediate overall 50% or greater reduction in pain, or moderate or greater improvement on a global rating of change questionnaire, was considered a treatment success. Likelihood ratios (LRs) were calculated to determine which examination items were most predictive of treatment outcome. Data for 49 subjects were included in the data analysis, of which 22 (45%) had a successful outcome. Five predictor variables were identified. The most powerful predictor of treatment success was a side-to-side difference in hip internal rotation range of motion greater than 14 (+LR, 4.9). If this variable was present, the chance of experiencing a successful outcome with the lumbopelvic manipulation improved from 45% to 80%. A CPR was developed to predict an immediate successful response to lumbopelvic manipulation in patients with PFPS. However, in light of a limited sample size and potential omission of meaningful predictor variables, future studies are necessary to validate the CPR. Prognosis, level 2b. J Orthop Sports Phys Ther 2008;38(6): doi: /jospt anterior knee pain, physical examination, rehabilitation, spinal manipulation 1 Staff Physical Therapist, Blanchfield Army Community Hospital, Fort Campbell, KY. 2 Associate Professor, US Army-Baylor University Doctoral Program in Physical Therapy, San Antonio, TX. 3 Staff Physical Therapist, Winn Army Community Hospital, Fort Stewart, GA. 4 Staff Physical Therapist, Reynolds Army Community Hospital, Fort Sill, OK. 5 Staff Physical Therapist, Moncrief Army Community Hospital, Fort Jackson, SC. 6 Assistant Chief, Physical Therapy, Brooke Army Medical Center, San Antonio, TX. 7 Professor and Director, US Army- Baylor University Doctoral Program in Physical Therapy, Fort Sam Houston, TX. 8 Associate Professor, Physical Therapy, Texas State University, San Marcos, TX. The protocol of this study was approved by The Institutional Review Board of Brooke Army Medical Center, Fort Sam Houston, TX. Opinions or assertions herein are the private views of the authors and are not to be construed as official or as reflecting the views of the United States Army or the Department of Defense. Address correspondence to Thomas G. Sutlive, US Army-Baylor University Doctoral Program in Physical Therapy, 3150 Stanley Road, Room 1303, ATTN: MCCS-HMT, Fort Sam Houston, TX thomas.sutlive@amedd.army.mil journal of orthopaedic & sports physical therapy volume 38 number 6 june
2 Procedures Each subject made 1 visit to the clinic. Following the history (completion of questionnaire shown in and submission of general demographic data), the subject was instructed to remove his or her shoes and socks and to sit on the examining table. The examiner performed a neurological screening examination of the lower extremities that consisted of manual muscle tests, muscle stretch reflex testing, and sharp/dull sensation testing to rule out lumbosacral nerve root compression. The examiner then performed selected tests and measures of each subject s low back and lower extremities ( ). The subject was instructed to lie prone on the examining table. The symptomatic lower extremity was extended so that the ipsilateral foot hung off the end of the table and the contralateral knee was flexed to 90, with the hip externally rotated (figure-four position, as described by Donatelli 15 ). Pen marks were made on the following anatomical landmarks of each subject s lower leg and foot for measurement purposes: the calcaneus and Achilles tendon was binificantly following SIJ manipulation in patients with the disorder. However, the investigators did not measure the patients symptomatic response to the treatment in any of these previous manipulation studies. 28,67,68 While recent evidence suggests that lumbopelvic manipulation can be effective in restoring quadriceps function in patients with PFPS, there is no evidence that patients with PFPS will experience symptomatic relief following the intervention. Furthermore, no published study has identified specific clinical examination variables that are predictive of which patients with PFPS, if any, will respond successfully to lumbopelvic manipulation. Identification of these clinical examination items could lead to the development of a clinical prediction rule (CPR) to identify patients likely to respond positively to lumbopelvic manipulation. Such a CPR could potentially enhance clinical decision making, reduce treatment time, and optimize outcomes. 38,44 Therefore, the purpose of our study was to (1) determine the predictive validity of selected clinical examination items for identifying patients with PFPS who have an immediate successful response to lumbopelvic manipulation, and (2) develop a CPR derived from these same historical and physical examination findings. Subjects Fifty subjects were recruited from the active duty military population at Fort Sam Houston, San Antonio, TX. Volunteers were included in the study if they were military healthcare beneficiaries between 18 and 50 years of age and had a clinical diagnosis of PFPS. Subjects were determined to have symptomatic PFPS if they had a complaint of anterior knee pain that was provoked by 2 or more of the following: squatting, stair ascent, stair descent, prolonged sitting, kneeling, or isometric quadriceps contraction. 11,43,55,61 Exclusion criteria included pregnancy, signs of nerve root compression, palpation tenderness of the tibiofemoral joint lines or patellar tendon, or a positive finding on any special tests aimed to identify knee ligament or meniscal injuries. Volunteers were also excluded if they had a history of any of the following: prior surgery on the spine or the symptomatic knee, osteoporosis, compression fracture, or a history of systemic, connective tissue, or neurological diseases. Individuals currently receiving treatment for their knee pain were also excluded. Informed consent was obtained from each subject prior to participation, and the rights of each subject were protected. This study was approved by the Institutional Review Board of Brooke Army Medical Center, Fort Sam Houston, San Antonio, TX. Instrumentation Numeric Pain Rating Scale The numeric pain rating scale (NPRS) was used to establish the subject s pain level after each functional test. The NPRS is an 11-point scale that ranges from 0 (no pain) to 10 (worst imaginable pain). This type of scale has been shown to be a reliable, generalizable, and internally consistent measure of clinical and experimental pain sensation intensity. 57,58 After performing each of the 3 functional tests, subjects were instructed to circle the number on the NPRS that best represented their knee pain. Subjects with bilateral PFPS were instructed to complete the NPRS based on their most symptomatic knee. The most symptomatic knee was determined by the subject s self-report. 48 A composite NPRS score (total score from the 3 functional tests) was established for each subject and used for data analysis. Global Rating of Change Questionnaire The global rating of change questionnaire (GRC) is a single-item, self-report instrument used to measure the subject s impression of the change in his or her condition following an intervention ( ). A GRC measures the overall changes in the quality of life of individuals. 33 The use of a GRC is a common, feasible, and useful method for assessing outcome, 31 and has been shown to be a valid measurement of change in patient status in other populations complaining of pain. 21 Each subject was instructed to mark the statement that best represented his/her status in response to the intervention on a 15-point GRC. Examination Items Each subject completed a medical history questionnaire ( ) and received a standardized physical examination. A list of all clinical tests and measures performed on each subject, along with their operational definitions and measurement properties, is shown in. The symptomatic knee was considered the unit of analysis. All measurements were taken on the side of the symptomatic knee (or most symptomatic knee for those with bilateral PFPS), and all angular measurements were taken with a 17.8-cm plastic goniometer. 298 june 2008 volume 38 number 6 journal of orthopaedic & sports physical therapy
3 sected with a marker, and the navicular tuberosity was marked with a dot. The battery of clinical measurements then commenced as listed in on the side of the symptomatic knee only. A second examiner repeated the series of tests and measures on the first 25 subjects prior to the functional testing to assess the interrater reliability of the measurements. An assistant recorded all measurements that were taken by both the first and second examiners. To prevent order effects, as well as to expedite the examination process, the examiner order (first or second examiner) was alternated sequentially. Following completion of the examination, subjects were asked to complete 3 functional activities (stepping up a 20-cm step, stepping down a 20-cm step, and squatting). After each functional test, the subject immediately assessed his or her knee pain during the activity and circled the number that represented this pain on the NPRS. During the squat test, the angle of knee flexion at which the subject first experienced pain was measured with a plastic goniometer and recorded. By doing this, the subject was able to assess the pain experienced when he or she squatted to the same angle following the intervention. After the first set of functional tests was completed, the subject returned to the examination table and was treated with a lumbopelvic manipulation to the symptomatic side, performed as previously described 3,19 and illustrated in. A video demonstration of the manipulation technique has previously been published on-line. 7 The second examiner always performed the manipulation if the subject was part of the interrater reliability study (ie, 1 of the first 25 subjects). If the subject or examiner felt a cavitation at any point during the setup for the manipulation or during the first manipulation, the intervention was considered complete. If no cavitation was heard or felt by the subject or examiner after the first manipulation, the examiner repeated the manipulation on the same Therapist performing the lumbopelvic manipulation technique used in this study. side. If a cavitation was still not felt or heard by manipulating the symptomatic side, the examiner repeated the manipulation on the opposite side in the exact same manner. Therefore, each subject received up to a maximum of 2 manipulations on each side. Following the intervention, the subject then repeated each functional test and again rated the pain experienced during each activity on the NPRS. The subject concluded the visit by assessing the overall change in his or her condition on the GRC. All statistical analyses were performed using Microsoft Excel 2000 (Microsoft Corp, Redmond, WA) and SPSS for Windows, Version 12.0 (SPSS Inc, Chicago, IL). Interrater reliability statistics were computed using intraclass correlation coefficients (ICC 2,1 ) for continuous variables and Cohen s kappa coefficients for categorical measurements. For the predictive validity portion of the study, each subject was first classified as either a treatment success or nonsuccess. The reference criterion used to define treatment success was either a 50% or greater improvement on the composite NPRS or a score of +4 (moderately better or improved) or higher on the GRC. It has been proposed that a 30% change on a NPRS represents a clinically meaningful reduction in pain in subjects with a variety of disorders. 18 Juniper et al 33 proposed that changes of at least 4 on the GRC indicate a moderate change in the person s condition. Therefore, we felt that a 50% threshold on the NPRS or a score of +4 or greater on the GRC was sufficiently high to identify individuals who responded to the intervention. After dichotomizing the subjects into 2 outcome groups (success or nonsuccess), each element of the history and physical examination was then analyzed to determine if it was a predictor of treatment success. Sensitivity (Sn), specificity (Sp), and likelihood ratios (LR) were calculated for each variable. Sn of a test reflects the true positive rate, and Sp of a test is the true negative rate. 50 To calculate the Sn and Sp for each clinical measurement item, 2-by-2 contingency tables were used. When a zero cell value was encountered, 0.5 was added to all cell values in the table to permit calculation of LRs and their 95% confidence intervals (CI). Continuous variables were dichotomized using a receiver operator characteristic (ROC) curve. 50 We defined the cut-off of a positive test to be the point on the curve nearest the upper left-hand corner that maximized the area under the curve, representing the value with the best diagnostic accuracy. 50 Positive likelihood ratios (+LR), negative likelihood ratios ( LR), and their associated 95% CIs were also computed for all clinical measurement items. LRs were calculated as follows: +LR = Sn/(1 Sp) and LR = (1 Sn)/Sp. The LR is the statistic most often used to determine the usefulness of a CPR. 19 According to the User s Guide to Medical Literature, 25 a +LR greater than 10.0 or a LR less than 0.1 generate large and often conclusive changes from pretest to posttest probability for a given condition. LRs of 5.0 to 10.0 and 0.1 to 0.2 generate moderate shifts in pretest-to-posttest probability. LRs of 2.0 to 5.0 and 0.5 to 0.2 generate small (but sometimes important) changes in probability, and LRs of 1.0 to 2.0 and 0.5 to 1.0 alter probability to a small (and rarely important) degree. We considered a +LR greater than 1.9 and a LR less than 0.5 to be clinically meaningful. 25,31 Because several variables in our study had +LRs between 1.9 and 2.0, we included any characteristic with a +LR greater than 1.9 to avoid discarding any journal of orthopaedic & sports physical therapy volume 38 number 6 june
4 potentially useful predictors of intervention success. A binary logistic regression model was used to develop a CPR for predicting treatment success with the lumbopelvic manipulation. 29 A forward stepwise selection procedure was used to enter the variables of those who were in the treatment success group only. A liberal P value of.15 was chosen to prevent potentially useful variables from being excluded from the model. 20 Clinical measurement items selected by the regression model as predictors of treatment success were combined into a clinical cluster for the CPR and were treated as a single test item. The Sn, Sp, and LRs for the CPR were calculated as previously described for other dichotomous variables. Fifty subjects (26 male and 24 female) were enrolled in the study, and 49 were included in the data analysis. One subject was excluded from the study due to significant inconsistencies in self-reported symptoms to the 2 examiners. Subject demographics and baseline historical and physical examination items for the entire sample, as well as for the successful and nonsuccessful outcome groups, are shown in and 2. Interrater reliability data were collected on the first 25 subjects. Nine of the 26 (35%) measurements had moderate to good reliability based on a threshold greater than or equal to 0.40 for kappa values and greater than or equal to 0.50 for ICCs. 36,50 The ICCs and kappa coefficients for the clinical measurement items are listed in, along with their associated standard error of measurement (SEMs). Twenty-two (45%) of the 49 subjects were considered to be a treatment success, based on a 50% or greater improvement on the final composite NPRS or a score of at least +4 on the GRC. All 22 subjects were considered intervention successes based on just the NPRS score, and 17 of the 22 were considered successes based on the GRC score. Therefore, 17 of the subjects in the success group met the criteria for success on both the NPRS and the GRC. The composite NPRS score for each group (success, nonsuccess) at baseline and after the manipulation is depicted in. The mean SD percent NPRS improvement in the success group was 80% 17%, while in the nonsuccess group, the mean improvement was 12% 28%. The median GRC for subjects in the success group was 5 (range, 0 to 7), while the median GRC score for the nonsuccess group was 1 (range, 1 to 3). Based on the univariate analysis, 6 characteristics were identified as predictors of a successful treatment outcome based on their LRs. Of these 6 clinical predictors, 5 were identified by the logistic regression analysis to form a diagnostic test item cluster for treatment success. These 5 variables and their associated accuracy statistics are shown in. The combinations of these variables and the Demographics and Historical Characteristics of Subjects Age (y)* (18-45) (18-44) (18-45) Duration of symptoms (wk)* (1-832) (1-260) (2-832) Gender (% male) Painful side (%) Right Left Both Worst side (% right) Prior history of knee pain (%) Locking (%) Giving way (%) Clicking (%) Crepitus (%) Swelling (%) Stiffness (%) Most painful activity (%) Squatting Lifting Running Going up stairs Going down stairs * Data are mean SD (range). Percentage of subjects who demonstrated this characteristic. NPRS Success Initial Nonsuccess Final Initial and final composite numeric pain rating scale (NPRS) scores for the success and nonsuccess groups. Based on pain level with 3 activities, each rated from 0 to 10. Mean percentage change for the success group was 80% (SD, 17%). Mean percentage change for the nonsuccess group was 12% (SD, 28%) accuracy of the combinations for predicting treatment success are shown in 5. The number of subjects within each group (success, nonsuccess) that exhibited each of the predictors is shown in. 300 june 2008 volume 38 number 6 journal of orthopaedic & sports physical therapy
5 The pretest probability for the likelihood of treatment success with lumbopelvic manipulation was 45% (ie, 22 out of 49 subjects responded successfully to the intervention). The most robust predictor of treatment success was a sideto-side difference in hip internal rotation greater than 14 (+LR, 4.9; 95% CI: 1.2 to 20.8). If a subject exhibited hip internal rotation asymmetry greater than 14, the posttest probability of treatment success increased to 80%. The combination of variables that proved to be the most powerful predictor of treatment success Variables From the Baseline Clinical Examination* Quadriceps MMT (% 5/5) Hamstrings MMT (% 5/5) Gluteus medius MMT (% 5/5) Hip flexor MMT (% 5/5) Hip extensor MMT (% 5/5) Tibial torsion (deg) 20.7 (6.9) 20.5 (6.2) 20.8 (7.6) STJN-NWB (deg varus) 3.2 (1.9) 3.0 (1.8) 3.5 (1.9) Forefoot alignment (deg varus) 3.5 (1.7) 3.5 (1.9) 3.6 (1.6) Relaxed calcaneal stance (deg valgus) 6.5 (3.4) 5.4 (3.1) 7.3 (3.4) Tibial varum/valgum (deg varus) 3.8 (2.2) 4.2 (2.4) 3.4 (1.9) Navicular drop (mm) 3.5 (3.4) 4.0 (3.7) 3.0 (3.0) First MTP extension (deg) 91.3 (12.3) 91.4 (13.6) 91.3 (11.4) AROM, ankle DF (knee ext) (deg) 6.4 (3.9) 6.8 (3.3) 6.0 (4.4) AROM, ankle DF (knee flex) (deg) 16.0 (6.0) 17.1 (5.1) 15.1 (6.7) Patellar glide (% with lateral glide) Lateral pull test (% positive) Patellar tilt (% positive) McConnell test (% positive) Thomas test (% positive) Hamstring test (% positive) Ober s test (% positive) Craig s test (deg) 13.0 (5.0) 12.7 (5.2) 13.2 (5.0) Hip IR (deg) 43.0 (10.5) 41.3 (40.2) 44.4 (10.8) Side-to-side difference in hip IR (deg) 9.2 (6.5) 10.2 (7.9) 8.4 (5.2) Q-angle (deg) 11.9 (5.6) 12.4 (6.7) 11.5 (4.6) Pelvic crest asymmetry (cm) 0.1 (0.6) 0.1 (0.6) 0.01 (0.6) Standing flexion test (% positive) Sitting flexion test (% positive) Stork test (% positive) Abbreviations: AROM, active range of motion; DF, dorsiflexion; IR, internal rotation; MMT, manual muscle test; MTP, metatarsophalangeal joint; NWB, non-weight bearing; STJN, subtalar joint neutral. * Mean (SD) is shown for the continuous variables. (+LR, 18.4; 95% CI: 1.6 to 105.3) was the presence of at least 3 of the 5 predictors in, which increased the posttest probability of success to 94%. PFPS is a prevalent condition in outpatient physical therapy practice settings and management of the disorder is characterized by large variations in practice patterns. Some patients may experience significant improvement with a given intervention, while others may have symptoms and a functional status that change very little following the same treatment. The ability to predict a priori which patients will respond favorably to a specific intervention would be extremely beneficial to practicing clinicians. Therefore, the purpose of our study was to identify clinical examination items that are predictive of an immediate successful response to a specific lumbopelvic manipulation technique. To our knowledge, no previous study has shown that lumbopelvic manipulation can lead to a reduction in symptoms in patients with PFPS. Forty-five percent of the subjects in our study experienced a successful immediate response to the manipulation, as defined by the criteria for success we established in this study. Based on this pretest probability (45%) of treatment success, if a subject exhibited a side-to-side hip internal rotation asymmetry greater than 14 (+LR, 4.9), the posttest probability of success increased markedly to 80%. If a subject exhibited at least 3 of the 5 predictors, the posttest probability of success increased to 94%. The posttest probability for treatment success was 100% if a subject exhibited at least 4 of the variables constituting the CPR. However, the 3 latter combinations of predictors were associated with extremely wide CIs and in some instances crossed 1.0, creating uncertainty with the predictive accuracy and clinical application of this estimate ( 5). Based on this observation, we suggest that clinicians can have greater accuracy and confidence when determining the likelihood that a patient will exhibit a rapid response to lumbopelvic manipulation by relying on the hip internal rotation asymmetry variable alone (+LR, 4.9; 95% CI: 1.2 to 20.8). If a patient does not demonstrate hip internal rotation asymmetry greater than 14, the clinician may still opt to perform the lumbopelvic manipulation based on the presence of at least 3 of the remaining predictors. One might argue that it would be more practical for the clinician to simply try the manipulation technique to see if the patient responds to the intervention, rather journal of orthopaedic & sports physical therapy volume 38 number 6 june
6 Interrater Reliability for Continuous (ICC) and Categorical (Kappa) Variables 2,1 Quadriceps MMT* 1.00 Hamstrings MMT* 1.00 Gluteus medius MMT* 1.00 Hip flexor MMT* 1.00 Hip extensor MMT* 1.00 Tibial torsion , STJN-NWB , Forefoot alignment , Relaxed calcaneal stance , Tibial varum/valgum , Navicular drop , First MTP extension , AROM, ankle DF (ext) , AROM, ankle DF (flex) , Craig s test , Hip IR , Q-angle , Pelvic crest alignment , cm Lateral pull test 0.03 Patellar tilt 0.17 McConnell test 0.46 Thomas test 0.17 Hamstring test 0.84 Ober s test 0.17 Patellar glide Standing flexion 0.88 Sitting flexion 0.04 Stork test 1.00 Abbreviations: AROM, active range of motion; CI, confidence interval; DF, dorsiflexion; ICC, intraclass correlation coefficient; IR, internal rotation; MMT, manual muscle test; MTP, metatarsophalangeal joint; NWB, non-weight bearing; STJN, subtalar joint neutral. * All subjects had the same score, so CI and SEM could not be calculated. than taking the time to determine if the patient fits the CPR. However, given the various treatment strategies that have been proposed for the management of patients with PFPS, it seems impractical to use a trial-and-error approach for numerous possible interventions. Goniometric assessment of the most powerful predictor of treatment success, hip internal rotation, can be obtained readily in the clinic setting. Furthermore, a side-to-side difference in hip internal rotation of at least 14 is clearly evident with the patient lying in the prone position ( ). The fact that a measure related to Measurement of hip internal rotation obtained with a subject in the prone position. The side-to-side difference in hip internal rotation shown in this figure is exactly 14. hip range of motion was the most robust predictor of treatment success is consistent with recent published studies suggesting that impairment of the lumbopelvic-hip complex is associated with PFPS. 5,28,30,42,57,67,68,74 In a case report, Cibulka and Threlkeld-Watkins 5 described evaluation and intervention for a patient with a side-to-side difference in hip internal rotation of 20. The patient also exhibited weakness of the hip internal rotator and abductor muscles on the involved side, and was treated with a 2-week regimen of stretching and strengthening exercises aimed at addressing these impairments. Based on the patient s successful outcome, the authors concluded that femoral or hip joint asymmetry may be related to patellofemoral pain. Similarly, Powers 51 reported that excessive femoral rotation during weight-bearing activities may contribute to PFPS, and recommended that interventions aimed at controlling hip and pelvic motion should be considered when treating patients with PFPS. 56 Several investigators have suggested that proximal hip muscle weakness, particularly of the hip abductors and external rotators, may be associated with patellofemoral pain, 30,42,60 and Tyler and colleagues 74 showed that improvements in hip flexor strength and flexibility were associated with symptomatic improvement in patients with PFPS. The implication of the findings of these studies is that addressing proximal impairments may be an important element in the successful rehabilitation of patients with PFPS. We defined treatment success as either an at least 50% improvement on the composite NPRS or at least a 4-point change on the GRC questionnaire. By setting our reference criteria at 50%, we were confident that we identified those subjects who experienced a clinically meaningful positive immediate response to the manipulation. While results indicate an association between the manipulative intervention and outcome, our study design is not sufficient to establish a cause-and-effect relationship. In particular, the lack of a control 302 june 2008 volume 38 number 6 journal of orthopaedic & sports physical therapy
7 Sensitivity, Specificity, Likelihood Ratios (LR), and Successful Cutoff Scores for the Predictors of Intervention Success* Difference in hip IR (deg) 0.36 (0.16, 0.56) 0.93 (0.83, 1.02) 4.9 (1.2, 20.8) 0.7 (0.5, 1.0) 14 Ankle dorsiflexion with knee flexed (deg) 0.59 (0.39, 0.80) 0.70 (0.53, 0.86) 2.0 (1.0, 3.9) 0.6 (0.3, 1.0) 16 Navicular drop (mm) 0.64 (0.44, 0.84) 0.67 (0.49, 0.84) 1.91 (1.0, 3.6) 0.5 (0.3, 1.0) 3 mm No stiffness with sitting 20 min (%) 0.73 (0.54, 0.91) 0.63 (0.45, 0.81) 2.0 (1.1, 3.4) 0.4 (0.2, 0.9) NA Squatting is most painful activity 0.59 (0.39, 0.80) 0.74 (0.58, 0.91) 2.3 (1.1, 4.7) 0.6 (0.3, 1.0) NA * Success defined as an immediate 50% or greater pain reduction or moderate (+4 or greater) improvement on the Global Rating of Change scale for functional activities consisting of squatting, stepping up a 20-cm step, and stepping down a 20-cm step. 95% confidence intervals shown in parentheses. Combinations of Predictor Variables and Associated Accuracy Statistics* All 5 predictors 0.09 (0.02, 0.31) 1.00 (0.84, 1.00) Infinite (0.31, infinite) 0.91 (0.78, 1.1) 100% (20-100) At least 4 predictors 0.32 (0.15, 0.55) 1.00 (0.84, 1.00) Infinite (0.90, infinite) 0.68 (0.51, 0.92) 100% (47-100) At least 3 predictors 0.68 (0.45, 0.86) 0.96 (0.81, 1.00) 18.4 (3.6, 105.3) 0.33 (0.17, 0.55) 94% (68-99) At least 2 predictors 0.91 (0.71, 0.99) 0.56 (0.35, 0.75) 2.05 (1.3, 2.9) 0.16 (0.04, 0.69) 63% (50-70) At least 1 predictor 0.91 (0.71, 0.99) 0.15 (0.04, 0.35) 1.1 (0.87, 1.3) 0.61 (0.12, 3.0) 47% (41-52) * 95% confidence intervals in parentheses. The probability of success is calculated using the +LR and assumes a pretest probability of 45%. group or competing intervention and the fact that we measured an immediate response to the treatment leave the possibility that a placebo effect took place for those expressing a reduction of symptoms. It is important to emphasize that we developed the CPR based only on the subjects immediate response to the intervention. Although duration of symptoms did not emerge as a predictor variable in the CPR, the participants in this study generally had chronic PFPS (mean duration of symptoms, 95 weeks). Nevertheless, the development of the current CPR is a reasonable initial foray at identifying the characteristics of patients with PFPS who are most likely to experience symptomatic improvement following manipulation of the lumbopelvic region. Future validation of the proposed CPR in a randomized clinical trial is required and should include a longer follow-up period. Additionally, the CPR developed in this study was based on establishing the predictive validity of a limited number of examination variables. We recognize that the clinical examination we performed The 5 Variables Forming the Clinical Prediction Rule and the Number of Subjects in Each Group at Each Level mm 20 min was selective and may not have included some items that otherwise might have emerged as predictors of intervention success. For instance, we did not include the assessment of hip external rotator muscle strength in the physical examination. Several investigators 30,42,60 recently identified weakness of the hip external rotator muscles as a possible contributing factor in individuals with PFPS. Therefore, assessment of the strength of this muscle group should be included in future studies aimed at validation of the proposed CPR. The clinical examination items included in this study were chosen because in our opinion they (1) are routinely obtained from patients with knee pain, (2) are measures that guide clinical journal of orthopaedic & sports physical therapy volume 38 number 6 june
8 decision making for lumbopelvic manipulation, and (3) allow for comparison of the results of the present study with our previous work. 39,69 It is possible that the predictor variables that emerged in this developmental study may have occurred by chance. However, we believe that each of the physical examination variables that emerged as predictors of a successful response to lumbopelvic manipulation are biologically plausible in subjects with PFPS, and that the predictors that surfaced from the history are also relevant in this population. Nevertheless, future investigations should include all relevant clinical examination variables and larger sample sizes to minimize the possibility that predictors emerge by chance. - A reduction in distal muscle inhibition following treatment with spinal manipulation techniques is well documented. 2,27,28,66-67 In studies of patients with PFPS, Suter and colleagues 67,68 showed that SIJ manipulation led to a significant decrease in quadriceps inhibition of the involved limbs, and Hillermann et al 28 reported that quadriceps muscle strength increased significantly following SIJ manipulation in patients with the disorder. The patients symptomatic response to the treatment was not monitored in these previous studies. 28,67,68 However, improvements in quadriceps strength and a reduction in quadriceps inhibition have been associated with symptomatic relief and successful outcomes in other studies of patients with PFPS. 34,45,65 Although it was not monitored in this study, an improvement in quadriceps function immediately following the manipulation may have contributed towards the successful response observed in our subjects. An alternative explanation for the favorable response seen in our success group may be explained by the concept of regional interdependence. According to this theory, dysfunction and impairments in remote regions, both extremity and spine, may affect or contribute to a patient s primary complaint. 4,6,14,77 The biomechanical link between the lumbopelvic-hip complex and the knee region suggests that alterations in joint mobility in the lumbar spine, SIJ, or hip joint may serve as an underlying contributor to the development of patellofemoral pain. For instance, previous research has shown that femoral internal rotation during weight-bearing activities can influence patellar alignment and kinematics. 51,70 Furthermore, impairments in femoral rotation have been associated with individuals with PFPS. 53 Given that hip internal rotation asymmetry was the most powerful predictor of treatment success in the current study, it is certainly plausible that the manipulation worked by affecting lower extremity kinematics. 56 However, we did not use any imaging techniques in our study, nor did we repeat any of the clinical measurements after the manipulation and, therefore, do not know if a change in hip internal rotation asymmetry occurred following the treatment. In our subjects there was no consistent pattern with regard to hip internal rotation range of motion being greater on the side of the symptomatic versus the asymptomatic lower extremity. A current investigation in this laboratory is directed at determining whether a successful response to the manipulation is correlated with a reduction or correction of hip internal rotation asymmetry in subjects with PFPS who meet the CPR. It is interesting that the presence of a hip internal rotation measure was also a predictor of a successful response to manipulation in patients with low back pain, 3,19 suggesting that there may be a common underlying mechanism or biomechanical link for a successful response to this treatment technique. None of the subjects in the current study reported having low back pain. It is important to note that the lumbopelvic manipulation used in this study is contraindicated in individuals with serious spinal conditions, with signs of nerve root compression, who are pregnant, and who have had previous surgery to the lumbar spine, pelvis, or buttock. 3,19 In addition to developing the CPR, we examined the interrater reliability of the measurements obtained in our study. Nine of the 26 (35%) clinical measurements exhibited moderate to good reliability. 36,50 The low interrater reliability for some of the measures may pose a threat to the internal validity of our investigation and ultimately limit the interpretation and application of the CPR. Taking a mean value of multiple measurements may have provided improved reliability values, 50 but we chose to obtain each measurement just once because we believe this is most representative of what is done in clinical practice. The ICC for the measurement of hip internal rotation was 0.45, which is consistent with reliability values reported for the same measure in previous studies of healthy individuals (ICC = 0.44 to 0.51) 73 and patients with unilateral hip osteoarthritis (ICC = 0.48), 10 but much lower than the goniometric and inclinometer values reported by Ellison and colleagues 17 in their study of healthy individuals and subjects with low back pain (ICC = 0.96 to 0.99). The method error as it relates to the coefficient of variation (CV ME ) can be used when examining response stability because it reflects percentage of variation from trial to trial. 50 The CV ME for hip internal rotation was 17% (equivalent to 5-8 ), which we considered to be an acceptable level. A Cohen kappa coefficient ( ) was calculated to determine the chance-corrected agreement between raters for this predictor ( = 0.71). A more clinically meaningful way to examine the reliability data for this continuous variable is in a dichotomous fashion (greater than 14 or less than or equal to 14 ), which is how it would be used in the context of this CPR. 76 For instance, how often did the raters agree that a subject had a greater than 14 measurement of hip internal rotation asymmetry? The percent agreement between the raters using the 304 june 2008 volume 38 number 6 journal of orthopaedic & sports physical therapy
9 cutoff score of greater than 14 was 76%, while the kappa coefficient ( ) was 0.32, which is considered poor to fair. 36 A possible limitation of our study was the fact that the majority of our data were taken from individuals with bilateral knee pain. Thirty-two of the 49 subjects who completed the study presented with bilateral PFPS. Therefore, one might argue that our results were potentially biased due to a lack of independence of data. To examine this issue, we compared the NPRS scores between subjects with unilateral PFPS and those with bilateral pain. Descriptive statistics were calculated for the mean percent NPRS change scores of the 17 subjects with unilateral knee pain and compared with the mean percent NPRS change scores of 17 randomly selected subjects with bilateral pain. The mean NPRS change score in the subjects with unilateral pain was 38.8% (SD, 39.2%), and the mean NPRS change score in subjects with bilateral pain was 39.1% (SD, 46.1%). These results suggested that the subjects with bilateral PFPS responded similarly to those with unilateral knee pain. While the internal validity of data from future studies of PFPS may be strengthened by including only subjects with unilateral knee pain, we believe that the inclusion of subjects with bilateral symptoms 30,46,48,49,69 is more reflective of clinical practice and will ultimately increase the generalizability of future investigations. e developed a CPR that identified the characteristics of patients with PFPS who would experience an immediate, positive response to treatment with lumbopelvic manipulation, as based on a 50% or greater reduction in the composite NPRS or a score of +4 or higher on the GRC for 3 functional tests (squatting, stepping up a 20-cm step, and stepping down a 20-cm step). Based on the results of this preliminary study, patients with PFPS who demonstrate a side-to-side difference in hip internal rotation range of motion greater than 14 and are treated with a lumbopelvic manipulation have an 80% posttest probability of experiencing a positive outcome. However, future studies are necessary in light of a limited sample size, the marginal reliability of some predictors, and the potential omission of possibly useful clinical examination variables in this study. The predictors identified in this study may help investigators assemble a more homogenous subgroup of patients with PFPS for a future validation study in the form of a randomized clinical trial, which is necessary before the CPR can be used confidently in the clinic. A preliminary CPR was developed to predict an immediate successful response to lumbopelvic manipulation in patients with patellofemoral pain syndrome (PFPS). The most robust predictor of a successful response to the manipulation was a side-to-side difference in hip internal rotation range of motion of greater than 14. The clinical prediction rule developed in this study may help clinicians identify patients with PFPS who will respond successfully to lumbopelvic manipulation. Limitations of this study included a small sample size (n = 49), marginal reliability of some predictors, and the omission of some potentially useful clinical examination variables. Future randomized clinical trials are needed to validate the findings of this study. REFERENCES 1. Joint Motion Measurement. Vol TC Washington, DC: Headquarters, Department of the Army; Bulbulian R, Burke J, Dishman JD. Spinal reflex excitability changes after lumbar spine passive flexion mobilization. J Manipulative Physiol Ther. 2002;25: Childs JD, Fritz JM, Flynn TW, et al. A clinical prediction rule to identify patients with low back pain most likely to benefit from spinal manipulation: a validation study. Ann Intern Med. 2004;141: Cibulka MT. Low back pain and its relation to the hip and foot. J Orthop Sports Phys Ther. 1999;29: Cibulka MT, Threlkeld-Watkins J. Patellofemoral pain and asymmetrical hip rotation. Phys Ther. 2005;85: Cleland JA, Childs JD, Fritz JM, Whitman JM, Eberhart SL. Development of a clinical prediction rule for guiding treatment of a subgroup of patients with neck pain: use of thoracic spine manipulation, exercise, and patient education. Phys Ther. 2007;87: org/ /ptj Cleland JA, Fritz JM, Whitman JM, Childs JD, Palmer JA. The use of a lumbar spine manipulation technique by physical therapists in patients who satisfy a clinical prediction rule: a case series. J Orthop Sports Phys Ther. 2006;36: Cowan SM, Bennell KL, Crossley KM, Hodges PW, McConnell J. Physical therapy alters recruitment of the vasti in patellofemoral pain syndrome. Med Sci Sports Exerc. 2002;34: org/ /01.mss ce Cowan SM, Bennell KL, Hodges PW, Crossley KM, McConnell J. Delayed onset of electromyographic activity of vastus medialis obliquus relative to vastus lateralis in subjects with patellofemoral pain syndrome. Arch Phys Med Rehabil. 2001;82: apmr Croft PR, Nahit ES, Macfarlane GJ, Silman AJ. Interobserver reliability in measuring flexion, internal rotation, and external rotation of the hip using a plurimeter. Ann Rheum Dis. 1996;55: Crossley K, Bennell K, Green S, Cowan S, McConnell J. Physical therapy for patellofemoral pain: a randomized, double-blinded, placebo-controlled trial. Am J Sports Med. 2002;30: Crossley K, Bennell K, Green S, McConnell J. A systematic review of physical interventions for patellofemoral pain syndrome. Clin J Sport Med. 2001;11: Devereaux MD, Lachmann SM. Patello-femoral arthralgia in athletes attending a Sports Injury Clinic. Br J Sports Med. 1984;18: Deyle GD, Henderson NE, Matekel RL, Ryder MG, Garber MB, Allison SC. Effectiveness of manual physical therapy and exercise in osteoarthritis of the knee. A randomized, controlled trial. Ann Intern Med. 2000;132: Donatelli R. The Biomechanics of the Foot and Ankle. 2nd ed. Philadelphia, PA: FA Davis Company; Dye S, Vaupel G, Dye C. Conscious neurosensory mapping of the internal structures of the human knee without intraarticular anesthesia. Am J Sports Med. 1998;26: Ellison JB, Rose SJ, Sahrmann SA. Patterns journal of orthopaedic & sports physical therapy volume 38 number 6 june
10 of hip rotation range of motion: a comparison between healthy subjects and patients with low back pain. Phys Ther. 1990;70: Farrar JT, Young JP, Jr., LaMoreaux L, Werth JL, Poole RM. Clinical importance of changes in chronic pain intensity measured on an 11-point numerical pain rating scale. Pain. 2001;94: Flynn T, Fritz J, Whitman J, et al. A clinical prediction rule for classifying patients with low back pain who demonstrate short-term improvement with spinal manipulation. Spine. 2002;27: org/ /01.brs d 20. Freedman D. A note on screening regression equations. Am Statistician. 1983;37: Fritz JM, Irrgang JJ. A comparison of a modified Oswestry Low Back Pain Disability Questionnaire and the Quebec Back Pain Disability Scale. Phys Ther. 2001;81: Gilleard W, McConnell J, Parsons D. The effect of patellar taping on the onset of vastus medialis obliquus and vastus lateralis muscle activity in persons with patellofemoral pain. Phys Ther. 1998;78: Grelsamer RP, Klein JR. The biomechanics of the patellofemoral joint. J Orthop Sports Phys Ther. 1998;28: Gross MT. Lower quarter screening for skeletal malalignment--suggestions for orthotics and shoewear. J Orthop Sports Phys Ther. 1995;21: Guyatt G, Rennie D. User s Guide to the Medical Literature: Essentials of Evidence-Based Clinical Practice. Chicago, IL: American Medical Association; Herrington L, Al-Sherhi A. A controlled trial of weight-bearing versus nonweight-bearing exercises for patellofemoral pain. J Orthop Sports Phys Ther. 2007;37: org/ /jospt Herzog W, Scheele D, Conway PJ. Electromyographic responses of back and limb muscles associated with spinal manipulative therapy. Spine. 1999;24: ; discussion Hillermann B, Gomes AN, Korporaal C, Jackson D. A pilot study comparing the effects of spinal manipulative therapy with those of extraspinal manipulative therapy on quadriceps muscle strength. J Manipulative Physiol Ther. 2006;29: jmpt Holleman DR, Jr., Simel DL. Quantitative assessments from the clinical examination. How should clinicians integrate the numerous results? J Gen Intern Med. 1997;12: Ireland ML, Willson JD, Ballantyne BT, Davis IM. Hip strength in females with and without patellofemoral pain. J Orthop Sports Phys Ther. 2003;33: Jaeschke R, Guyatt GH, Sackett DL. Users guides to the medical literature. III. How to use an article about a diagnostic test. B. What are the results and will they help me in caring for my patients? The Evidence-Based Medicine Working Group. JAMA. 1994;271: Jonson SR, Gross MT. Intraexaminer reliability, interexaminer reliability, and mean values for nine lower extremity skeletal measures in healthy naval midshipmen. J Orthop Sports Phys Ther. 1997;25: Juniper EF, Guyatt GH, Willan A, Griffith LE. Determining a minimal important change in a disease-specific Quality of Life Questionnaire. J Clin Epidemiol. 1994;47: Kannus P, Niittymaki S. Which factors predict outcome in the nonoperative treatment of patellofemoral pain syndrome? A prospective follow-up study. Med Sci Sports Exerc. 1994;26: Kendall F. Muscles Testing and Function. Philadelphia, PA: Lippincott, Williams, & Wilkins; Landis JR, Koch GG. The measurement of observer agreement for categorical data. Biometrics. 1977;33: Laprade J, Culham E. Radiographic measures in subjects who are asymptomatic and subjects with patellofemoral pain syndrome. Clin Orthop Relat Res. 2003; org/ /01.blo f5 38. Laupacis A, Sekar N, Stiell IG. Clinical prediction rules. A review and suggested modifications of methodological standards. JAMA. 1997;277: Lesher JD, Sutlive TG, Miller GA, Chine NJ, Garber MB, Wainner RS. Development of a clinical prediction rule for classifying patients with patellofemoral pain syndrome who respond to patellar taping. J Orthop Sports Phys Ther. 2006;36: jospt Magee D. Orthopedic Physical Assessment. 3rd ed. Philadelphia, PA: W.B. Saunders; Mariani PP, Caruso I. An electromyographic investigation of subluxation of the patella. J Bone Joint Surg Br. 1979;61-B: Mascal CL, Landel R, Powers C. Management of patellofemoral pain targeting hip, pelvis, and trunk muscle function: 2 case reports. J Orthop Sports Phys Ther. 2003;33: McConnell J. The management of chondromalacia patellae: a long-term solution. Aust J Physiother. 1986;32: McGinn TG, Guyatt GH, Wyer PC, Naylor CD, Stiell IG, Richardson WS. Users guides to the medical literature: XXII: how to use articles about clinical decision rules. Evidence- Based Medicine Working Group. JAMA. 2000;284: Natri A, Kannus P, Jarvinen M. Which factors predict the long-term outcome in chronic patellofemoral pain syndrome? A 7-yr prospective follow-up study. Med Sci Sports Exerc. 1998;30: Nijs J, Van Geel C, Van der auwera C, Van de Velde B. Diagnostic value of five clinical tests in patellofemoral pain syndrome. Man Ther. 2006;11: math Petrone MR, Guinn J, Reddin A, Sutlive TG, Flynn TW, Garber MP. The accuracy of the Palpation Meter (PALM) for measuring pelvic crest height difference and leg length discrepancy. J Orthop Sports Phys Ther. 2003;33: Piva SR, Fitzgerald K, Irrgang JJ, et al. Reliability of measures of impairments associated with patellofemoral pain syndrome. BMC Musculoskelet Disord. 2006;7:33. org/ / Piva SR, Goodnite EA, Childs JD. Strength around the hip and flexibility of soft tissues in individuals with and without patellofemoral pain syndrome. J Orthop Sports Phys Ther. 2005;35: Portney L, Watkins M. Foundations of Clinical Research: Applications to Practice. 2nd ed. Upper Saddle River, NJ: Prentice Hall Health; Powers CM. The influence of altered lowerextremity kinematics on patellofemoral joint dysfunction: a theoretical perspective. J Orthop Sports Phys Ther. 2003;33: Powers CM. Rehabilitation of patellofemoral joint disorders: a critical review. J Orthop Sports Phys Ther. 1998;28: Powers CM, Chen PY, Reischl SF, Perry J. Comparison of foot pronation and lower extremity rotation in persons with and without patellofemoral pain. Foot Ankle Int. 2002;23: Powers CM, Landel R, Perry J. Timing and intensity of vastus muscle activity during functional activities in subjects with and without patellofemoral pain. Phys Ther. 1996;76: ; discussion Powers CM, Perry J, Hsu A, Hislop HJ. Are patellofemoral pain and quadriceps femoris muscle torque associated with locomotor function? Phys Ther. 1997;77: ; discussion Powers CM, Ward SR, Fredericson M, Guillet M, Shellock FG. Patellofemoral kinematics during weight-bearing and nonweight-bearing knee extension in persons with lateral subluxation of the patella: a preliminary study. J Orthop Sports Phys Ther. 2003;33: Price DD, Bush FM, Long S, Harkins SW. A comparison of pain measurement characteristics of mechanical visual analogue and simple numerical rating scales. Pain. 1994;56: Price DD, McGrath PA, Rafii A, Buckingham B. The validation of visual analogue scales as ratio scale measures for chronic and experimental pain. Pain. 1983;17: Reid DC. The myth, mystic and frustration of anterior knee pain [editorial]. Clin J Sport Med. 1993;3: Robinson RL, Nee RJ. Analysis of hip strength in females seeking physical therapy treatment for unilateral patellofemoral pain syndrome. J Orthop Sports Phys Ther. 2007;37: dx.doi.org/doi: /jospt Salsich GB, Brechter JH, Farwell D, Powers CM. The effects of patellar taping on knee kinetics, kinematics, and vastus lateralis muscle activity during stair ambulation in individuals with 306 june 2008 volume 38 number 6 journal of orthopaedic & sports physical therapy
Dethroning the Clinical Prediction Rule WPTA Fall Conference 2017
 Course objectives 1. Understand the methodology for developing clinical prediction rules. 2. Assess clinical prediction rule methodology in prescriptive rules used in rehabilitation. 3. Discuss methods
Course objectives 1. Understand the methodology for developing clinical prediction rules. 2. Assess clinical prediction rule methodology in prescriptive rules used in rehabilitation. 3. Discuss methods
Knee Capsular Disorder. ICD-9-CM: Stiffness in joint of lower leg, not elsewhere classified
 1 Knee Capsular Disorder "Knee Capsulitis" ICD-9-CM: 719.56 Stiffness in joint of lower leg, not elsewhere classified Diagnostic Criteria History: Physical Exam: Stiffness Aching with prolonged weight
1 Knee Capsular Disorder "Knee Capsulitis" ICD-9-CM: 719.56 Stiffness in joint of lower leg, not elsewhere classified Diagnostic Criteria History: Physical Exam: Stiffness Aching with prolonged weight
Research Theme. Cal PT Fund Research Symposium 2015 Christopher Powers. Patellofemoral Pain to Pathology Continuum. Applied Movement System Research
 Evaluation and Treatment of Movement Dysfunction: A Biomechanical Approach Research Theme Christopher M. Powers, PhD, PT, FAPTA Understanding injury mechanisms will lead to the development of more effective
Evaluation and Treatment of Movement Dysfunction: A Biomechanical Approach Research Theme Christopher M. Powers, PhD, PT, FAPTA Understanding injury mechanisms will lead to the development of more effective
APTA Intro to Identity. The Movement System The Kinesiopathologic Model Movement System Impairment Syndromes of the Knee THE HUMAN MOVEMENT SYSTEM
 The Movement System The Kinesiopathologic Model Movement System Impairment Syndromes of the Knee Shirley Sahrmann, PT, PhD, FAPTA Professor Emerita Statement of Privacy To protect the privacy of the subjects
The Movement System The Kinesiopathologic Model Movement System Impairment Syndromes of the Knee Shirley Sahrmann, PT, PhD, FAPTA Professor Emerita Statement of Privacy To protect the privacy of the subjects
Do Persons with PFP. PFJ Loading? Biomechanical Factors Contributing to Patellomoral Pain: The Dynamic Q Angle. Patellofemoral Pain: A Critical Review
 Biomechanical Factors Contributing to Patellomoral Pain: The Dynamic Q Angle Division Biokinesiology & Physical Therapy Co Director, oratory University of Southern California Movement Performance Institute
Biomechanical Factors Contributing to Patellomoral Pain: The Dynamic Q Angle Division Biokinesiology & Physical Therapy Co Director, oratory University of Southern California Movement Performance Institute
Dynamic Stabilization of the Patellofemoral Joint: Stabilization from above & below
 Dynamic Stabilization of the Patellofemoral Joint: Stabilization from above & below Division Biokinesiology & Physical Therapy Co Director, oratory University of Southern California Movement Performance
Dynamic Stabilization of the Patellofemoral Joint: Stabilization from above & below Division Biokinesiology & Physical Therapy Co Director, oratory University of Southern California Movement Performance
Disclosures. Objectives. Overview. Patellofemoral Syndrome. Etiology. Management of Patellofemoral Pain
 Management of Patellofemoral Pain Implications of Top Down Mechanics Disclosures I have no actual or potential conflict of interest in relation to this presentation David Nolan, PT, DPT, MS, OCS, SCS,
Management of Patellofemoral Pain Implications of Top Down Mechanics Disclosures I have no actual or potential conflict of interest in relation to this presentation David Nolan, PT, DPT, MS, OCS, SCS,
World Medical & Health Games
 Management of Patellofemoral Pain Syndrome João Barroso Orthopaedic department ULS Matosinhos Portugal Introduction Anterior Knee Pain affects 1 in 4 athletes very common! (Knowles et al) Patellofemoral
Management of Patellofemoral Pain Syndrome João Barroso Orthopaedic department ULS Matosinhos Portugal Introduction Anterior Knee Pain affects 1 in 4 athletes very common! (Knowles et al) Patellofemoral
Paradigm Shift. Biomedical Model. Regional Interdependence Model. Evidence to Support R-I Exam
 A Clinical Approach to Assessing and Addressing Movement Pattern Dysfunction Models of Adverse Health Regional Interdependence Evidence to Support R-I Systematic Assessment Case Studies using System Implementation
A Clinical Approach to Assessing and Addressing Movement Pattern Dysfunction Models of Adverse Health Regional Interdependence Evidence to Support R-I Systematic Assessment Case Studies using System Implementation
Total Hip Replacement Rehabilitation: Progression and Restrictions
 Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Prevalence of Patellofemoral Pain (PFP)
 10/11/2017 Evaluation of a Sequential Cognitive and Physical Treatment Approach for Patients with Patellofemoral Pain: A Randomized Controlled Trial Mitchell Selhorst, Todd Degenhart, Michael Jackowski,
10/11/2017 Evaluation of a Sequential Cognitive and Physical Treatment Approach for Patients with Patellofemoral Pain: A Randomized Controlled Trial Mitchell Selhorst, Todd Degenhart, Michael Jackowski,
Patellofemoral pain syndrome (PFPS) is a common orthopedic
 Ryan L. Robinson, MPT, DPT 1 Robert J. Nee, PT, MAppSc, ATC 2 Analysis of Hip Strength in Females Seeking Physical Therapy Treatment for Unilateral Patellofemoral Pain Syndrome Patellofemoral pain syndrome
Ryan L. Robinson, MPT, DPT 1 Robert J. Nee, PT, MAppSc, ATC 2 Analysis of Hip Strength in Females Seeking Physical Therapy Treatment for Unilateral Patellofemoral Pain Syndrome Patellofemoral pain syndrome
Standard of Care: Patellofemoral Pain Syndrome (PFS)
 Department of Rehabilitation Services Physical Therapy Case Type / Diagnosis: Patellofemoral Pain Syndrome (719.46) Patellofemoral Pain syndrome A general category of anterior knee pain from patella malalignment.
Department of Rehabilitation Services Physical Therapy Case Type / Diagnosis: Patellofemoral Pain Syndrome (719.46) Patellofemoral Pain syndrome A general category of anterior knee pain from patella malalignment.
Muscle Testing of Knee Extensors. Yasser Moh. Aneis, PhD, MSc., PT. Lecturer of Physical Therapy Basic Sciences Department
 Muscle Testing of Knee Extensors Yasser Moh. Aneis, PhD, MSc., PT. Lecturer of Physical Therapy Basic Sciences Department Muscle Testing of Knee Extensors othe Primary muscle Quadriceps Femoris -Rectus
Muscle Testing of Knee Extensors Yasser Moh. Aneis, PhD, MSc., PT. Lecturer of Physical Therapy Basic Sciences Department Muscle Testing of Knee Extensors othe Primary muscle Quadriceps Femoris -Rectus
Balanced Body Movement Principles
 Balanced Body Movement Principles How the Body Works and How to Train it. Module 3: Lower Body Strength and Power Developing Strength, Endurance and Power The lower body is our primary source of strength,
Balanced Body Movement Principles How the Body Works and How to Train it. Module 3: Lower Body Strength and Power Developing Strength, Endurance and Power The lower body is our primary source of strength,
A Comparison of the Immediate Effects of Eccentric Training vs Static Stretch on Hamstring Flexibility in Basketball Players Dr.
 A Comparison of the Immediate Effects of Eccentric Training vs Static Stretch on Hamstring Flexibility in Basketball Players Dr. Mandeep Thour* *Assistant Professor, Department of Physical Education SGGS
A Comparison of the Immediate Effects of Eccentric Training vs Static Stretch on Hamstring Flexibility in Basketball Players Dr. Mandeep Thour* *Assistant Professor, Department of Physical Education SGGS
Does the Manual Therapy Technique Matter?
 Does the Manual Therapy Technique Matter? Joshua A. Cleland, DPT, OCS Assistant Professor, Physical Therapy Program, Franklin Pierce College, Concord, NH and Physical Therapist, Rehabilitation Services
Does the Manual Therapy Technique Matter? Joshua A. Cleland, DPT, OCS Assistant Professor, Physical Therapy Program, Franklin Pierce College, Concord, NH and Physical Therapist, Rehabilitation Services
ORIGINAL CONTRIBUTION
 Interexaminer Reliability of Three Methods of Combining Test Results to Determine Side of Sacral Restriction, Sacral Base Position, and Innominate Bone Position Henry C. Tong, MD; Oscar G. Heyman, DO;
Interexaminer Reliability of Three Methods of Combining Test Results to Determine Side of Sacral Restriction, Sacral Base Position, and Innominate Bone Position Henry C. Tong, MD; Oscar G. Heyman, DO;
Kavitha Shetty, Lawrence Mathias, Mahesh V. Hegde & Sukumar Shanmugam 1,3. Assistant Professors, Nitte Institute of Physiotherapy, Nitte University 2
 Original Article NUJHS Vol. 6, No.1, March 216, ISSN 2249-711 Short - Term Effects of Eccentric Hip Abductors and Lateral Rotators Strengthening In Sedentary People with Patellofemoral Pain Syndrome on
Original Article NUJHS Vol. 6, No.1, March 216, ISSN 2249-711 Short - Term Effects of Eccentric Hip Abductors and Lateral Rotators Strengthening In Sedentary People with Patellofemoral Pain Syndrome on
Hyperpronation of the foot causes many different
 IMMEDIATE CHANGES IN THE QUADRICEPS FEMORIS ANGLE AFTER INSERTION OF AN ORTHOTIC DEVICE D. Robert Kuhn, DC, a Terry R. Yochum, DC, b Anton R. Cherry, c and Sean S. Rodgers c ABSTRACT Objective: To measure
IMMEDIATE CHANGES IN THE QUADRICEPS FEMORIS ANGLE AFTER INSERTION OF AN ORTHOTIC DEVICE D. Robert Kuhn, DC, a Terry R. Yochum, DC, b Anton R. Cherry, c and Sean S. Rodgers c ABSTRACT Objective: To measure
BIOMECHANICAL EXAMINATION OF THE PEDIATRIC LOWER EXTREMITY
 BIOMECHANICAL EXAMINATION OF THE PEDIATRIC LOWER EXTREMITY B.Resseque, D.P.M. ARCH HEIGHT OFF WEIGHTBEARING Evaluate arch height by placing a ruler from the heel to the first metatarsal head Compare arch
BIOMECHANICAL EXAMINATION OF THE PEDIATRIC LOWER EXTREMITY B.Resseque, D.P.M. ARCH HEIGHT OFF WEIGHTBEARING Evaluate arch height by placing a ruler from the heel to the first metatarsal head Compare arch
Effect of VMO strengthening with and without hip strengthening on pain and function in patients with Patellofemoral Pain Syndrome
 2017; 4(4): 408-412 P-ISSN: 2394-1685 E-ISSN: 2394-1693 Impact Factor (ISRA): 5.38 IJPESH 2017; 4(4): 408-412 2017 IJPESH www.kheljournal.com Received: 18-05-2017 Accepted: 20-06-2017 Anusha. M RV College
2017; 4(4): 408-412 P-ISSN: 2394-1685 E-ISSN: 2394-1693 Impact Factor (ISRA): 5.38 IJPESH 2017; 4(4): 408-412 2017 IJPESH www.kheljournal.com Received: 18-05-2017 Accepted: 20-06-2017 Anusha. M RV College
7/20/14. Patella Instability. Alignment. PF contact areas. Tissue Restraints. Pain. Acute Blunt force trauma Disorders of the Patellafemoral Joint
 Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Supplemental Video Available at
 The Use of a Lumbar Spine Manipulation Technique by Physical Therapists in Patients Who Satisfy a Clinical Prediction Rule: A Case Series Joshua A. Cleland, DPT, PhD, OCS 1 Julie M. Fritz, PT, PhD, ATC
The Use of a Lumbar Spine Manipulation Technique by Physical Therapists in Patients Who Satisfy a Clinical Prediction Rule: A Case Series Joshua A. Cleland, DPT, PhD, OCS 1 Julie M. Fritz, PT, PhD, ATC
CLINICAL REASONING TOOLS
 CLINICAL REASONING TOOLS FRANK TUDINI PT, DSC,OCS,FAAOMPT MATT WALK PT, DPT,OCS, FAAOMPT Rothstein, Echternach and Riddle 2003 Hypothesis-Oriented Algorithm for Clinicians Patient-centered conceptual framework
CLINICAL REASONING TOOLS FRANK TUDINI PT, DSC,OCS,FAAOMPT MATT WALK PT, DPT,OCS, FAAOMPT Rothstein, Echternach and Riddle 2003 Hypothesis-Oriented Algorithm for Clinicians Patient-centered conceptual framework
APPLICATION OF THE MOVEMENT SYSTEMS MODEL TO THE MANAGEMENT COMMON HIP PATHOLOGIES
 APPLICATION OF THE MOVEMENT SYSTEMS MODEL TO THE MANAGEMENT COMMON HIP PATHOLOGIES Tracy Porter, PT, DPT Des Moines University Department of Physical Therapy Objectives Review current literature related
APPLICATION OF THE MOVEMENT SYSTEMS MODEL TO THE MANAGEMENT COMMON HIP PATHOLOGIES Tracy Porter, PT, DPT Des Moines University Department of Physical Therapy Objectives Review current literature related
Patellofemoral Joint. Question? ANATOMY
 Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
Checklist for Physical Examination of the Knee Muscuoskeletal Block -- Chris McGrew MD, Andrew Ashbaugh DO
 Checklist for Physical Examination of the Knee Muscuoskeletal Block -- Chris McGrew MD, Andrew Ashbaugh DO This handout is for use as a rough guide and study aid. Your instructor may perform certain maneuvers
Checklist for Physical Examination of the Knee Muscuoskeletal Block -- Chris McGrew MD, Andrew Ashbaugh DO This handout is for use as a rough guide and study aid. Your instructor may perform certain maneuvers
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes
 Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Obesity is associated with reduced joint range of motion (Park, 2010), which has been partially
 INTRODUCTION Obesity is associated with reduced joint range of motion (Park, 2010), which has been partially attributed to adipose tissues around joints limiting inter-segmental rotations (Gilleard, 2007).
INTRODUCTION Obesity is associated with reduced joint range of motion (Park, 2010), which has been partially attributed to adipose tissues around joints limiting inter-segmental rotations (Gilleard, 2007).
The effect of patellofemoral pain syndrome on the hip and knee neuromuscular control on dynamic postural control task
 The University of Toledo The University of Toledo Digital Repository Theses and Dissertations 2009 The effect of patellofemoral pain syndrome on the hip and knee neuromuscular control on dynamic postural
The University of Toledo The University of Toledo Digital Repository Theses and Dissertations 2009 The effect of patellofemoral pain syndrome on the hip and knee neuromuscular control on dynamic postural
RN(EC) ENC(C) GNC(C) MN ACNP *** MECHANISM OF INJURY.. MOST IMPORTANT *** - Useful in determining mechanism of injury / overuse
 HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient Sport / Occupation - Certain conditions are more prevalent in particular age groups (Osgood Schlaters in youth / Degenerative Joint Disease
HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient Sport / Occupation - Certain conditions are more prevalent in particular age groups (Osgood Schlaters in youth / Degenerative Joint Disease
Female Athlete Injury Prevention
 Female Athlete Injury Prevention Startling Facts Huge rise in knee ligament injuries among young females engaging in sport and exercise Females athletes participating in jumping and pivoting sports are
Female Athlete Injury Prevention Startling Facts Huge rise in knee ligament injuries among young females engaging in sport and exercise Females athletes participating in jumping and pivoting sports are
LUMBAR SPINE CASE 3. Property of VOMPTI, LLC. For Use of Participants Only. No Use or Reproduction Without Consent 1. L4-5, 5-S1 disc, facet (somatic)
 LUMBAR SPINE CASE 3 A.J. Lievre, PT, DPT, OCS, CMPT Aaron Hartstein, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Richmond 2018-2019 L4-5, 5-S1 disc, facet (somatic) L5/S1 Radiculopathy
LUMBAR SPINE CASE 3 A.J. Lievre, PT, DPT, OCS, CMPT Aaron Hartstein, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Richmond 2018-2019 L4-5, 5-S1 disc, facet (somatic) L5/S1 Radiculopathy
Relative Isometric Force of the Hip Abductor and Adductor Muscles
 Relative Isometric Force of the Hip Abductor and Adductor Muscles WARREN W. MAY, Captain, AMSC A-LTHOUGH THE CONCEPT of the muscular force curve is not new, its clinical application has been generally
Relative Isometric Force of the Hip Abductor and Adductor Muscles WARREN W. MAY, Captain, AMSC A-LTHOUGH THE CONCEPT of the muscular force curve is not new, its clinical application has been generally
Patellofemoral Pain and Asymmetrical Hip Rotation. Hip rotation, Patellofemoral pain, Physical therapy.
 Case Report Key Words: Patellofemoral Pain and Asymmetrical Hip Rotation Background and Purpose. Patellofemoral joint problems are the most common overuse injury of the lower extremity, and altered femoral
Case Report Key Words: Patellofemoral Pain and Asymmetrical Hip Rotation Background and Purpose. Patellofemoral joint problems are the most common overuse injury of the lower extremity, and altered femoral
A.J. Lievre, PT, DPT, OCS, CMPT Aaron Hartstein, PT, DPT, OCS, FAAOMPT
 LUMBAR SPINE CASE #3 A.J. Lievre, PT, DPT, OCS, CMPT Aaron Hartstein, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 L4-5, 5-S1 disc, facet (somatic) L5/S1 Radiculopathy
LUMBAR SPINE CASE #3 A.J. Lievre, PT, DPT, OCS, CMPT Aaron Hartstein, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 L4-5, 5-S1 disc, facet (somatic) L5/S1 Radiculopathy
The Truth on Fitness: LEG EXTENSIONS
 The Truth on Fitness: LEG EXTENSIONS Paul M. Juris, Ed.D. Executive Director, CYBEX Institute The Truth on Fitness: LEG EXTENSIONS Of the many highly scrutinized exercises used in fitness and rehabilitation
The Truth on Fitness: LEG EXTENSIONS Paul M. Juris, Ed.D. Executive Director, CYBEX Institute The Truth on Fitness: LEG EXTENSIONS Of the many highly scrutinized exercises used in fitness and rehabilitation
Patellofemoral syndrome (PFS) is one of the most common
 Patellofemoral Rehabilitation Vincent E. Perez, PT Patellofemoral syndrome is one of the most common conditions encountered by orthopedic surgeons and physical therapists. These patients present with a
Patellofemoral Rehabilitation Vincent E. Perez, PT Patellofemoral syndrome is one of the most common conditions encountered by orthopedic surgeons and physical therapists. These patients present with a
The iliotibial (IT) tract,
 Use of an Inclinometer to Measure Flexibility of the Iliotibial Band Using the Ober Test and the Modified Ober Test: Differences in Magnitude and Reliability of Measurements Nancy B. Reese, PT, PhD 1 William
Use of an Inclinometer to Measure Flexibility of the Iliotibial Band Using the Ober Test and the Modified Ober Test: Differences in Magnitude and Reliability of Measurements Nancy B. Reese, PT, PhD 1 William
BIOMECHANICAL EXAMINATION OF THE PEDIATRIC LOWER EXTREMITY 2017
 BIOMECHANICAL EXAMINATION OF THE PEDIATRIC LOWER EXTREMITY 2017 B. RESSEQUE, D.P.M., D.A.B.P.O. Professor, N.Y. College of Podiatric Medicine ARCH HEIGHT OFF WEIGHTBEARING Evaluate arch height by placing
BIOMECHANICAL EXAMINATION OF THE PEDIATRIC LOWER EXTREMITY 2017 B. RESSEQUE, D.P.M., D.A.B.P.O. Professor, N.Y. College of Podiatric Medicine ARCH HEIGHT OFF WEIGHTBEARING Evaluate arch height by placing
Diagnostic and Treatment Approach to the Active Patient with Complex Spine Pathology
 Physical Therapy Diagnostic and Treatment Approach to the Active Patient with Complex Spine Pathology Scott Behjani, DPT, OCS Introduction Prevalence 1-year incidence of first-episode LBP ranges from
Physical Therapy Diagnostic and Treatment Approach to the Active Patient with Complex Spine Pathology Scott Behjani, DPT, OCS Introduction Prevalence 1-year incidence of first-episode LBP ranges from
A Regional Interdependent Approach For The Treatment Of Symptoms For An. Adult Female Long Distance Runner With Patellar-Femoral Pain Syndrome
 A Regional Interdependent Approach For The Treatment Of Symptoms For An Adult Female Long Distance Runner With Patellar-Femoral Pain Syndrome Justin Lin, DPT, CSCS Marymount University 0 ABSTRACT In recent
A Regional Interdependent Approach For The Treatment Of Symptoms For An Adult Female Long Distance Runner With Patellar-Femoral Pain Syndrome Justin Lin, DPT, CSCS Marymount University 0 ABSTRACT In recent
CHAPTER 8: THE BIOMECHANICS OF THE HUMAN LOWER EXTREMITY
 CHAPTER 8: THE BIOMECHANICS OF THE HUMAN LOWER EXTREMITY _ 1. The hip joint is the articulation between the and the. A. femur, acetabulum B. femur, spine C. femur, tibia _ 2. Which of the following is
CHAPTER 8: THE BIOMECHANICS OF THE HUMAN LOWER EXTREMITY _ 1. The hip joint is the articulation between the and the. A. femur, acetabulum B. femur, spine C. femur, tibia _ 2. Which of the following is
Evaluation of Gait Mechanics Using Computerized Plantar Surface Pressure Analysis and it s Relation to Common Musculoskeletal Problems
 Evaluation of Gait Mechanics Using Computerized Plantar Surface Pressure Analysis and it s Relation to Common Musculoskeletal Problems Laws of Physics effecting gait Ground Reaction Forces Friction Stored
Evaluation of Gait Mechanics Using Computerized Plantar Surface Pressure Analysis and it s Relation to Common Musculoskeletal Problems Laws of Physics effecting gait Ground Reaction Forces Friction Stored
Application of Motor Learning Principles in the Intervention of Patellofemoral Pain
 Application of Motor Learning Principles in the Intervention of Patellofemoral Pain Dorothy Beatty, SPT Virginia Commonwealth University September 29, 2016 Patient Introduction 22 y/o white female presenting
Application of Motor Learning Principles in the Intervention of Patellofemoral Pain Dorothy Beatty, SPT Virginia Commonwealth University September 29, 2016 Patient Introduction 22 y/o white female presenting
EFFECIVENESS OF THE WILLIAMS EXCERCISE IN MECHANICAL LOW BACK PAIN
 EFFECIVENESS OF THE WILLIAMS EXCERCISE IN MECHANICAL LOW BACK PAIN Dr.U.Ganapathy Sankar, Ph.D Dean I/C, SRM College of Occupational Therapy, SRMUniversity, Kattankulathur, KancheepuramDistrict, Tamil
EFFECIVENESS OF THE WILLIAMS EXCERCISE IN MECHANICAL LOW BACK PAIN Dr.U.Ganapathy Sankar, Ph.D Dean I/C, SRM College of Occupational Therapy, SRMUniversity, Kattankulathur, KancheepuramDistrict, Tamil
Functional Movement Screen (Cook, 2001)
 Functional Movement Screen (Cook, 2001) TEST 1 DEEP SQUAT Purpose - The Deep Squat is used to assess bilateral, symmetrical, mobility of the hips, knees, and ankles. The dowel held overhead assesses bilateral,
Functional Movement Screen (Cook, 2001) TEST 1 DEEP SQUAT Purpose - The Deep Squat is used to assess bilateral, symmetrical, mobility of the hips, knees, and ankles. The dowel held overhead assesses bilateral,
A Syndrome (Pattern) Approach to Low Back Pain. History
 A Syndrome (Pattern) Approach to Low Back Pain Hamilton Hall MD FRCSC Professor, Department of Surgery, University of Toronto Medical Director, CBI Health Group Executive Director, Canadian Spine Society
A Syndrome (Pattern) Approach to Low Back Pain Hamilton Hall MD FRCSC Professor, Department of Surgery, University of Toronto Medical Director, CBI Health Group Executive Director, Canadian Spine Society
Assessment of Lower Extremity Posture: Qualitative and Quantitative Clinical Skills
 CLINICAL EVALUATION & TESTING Darin A. Padua. PhD, ATC, Column Editor Assessment of Lower Extremity Posture: Qualitative and Quantitative Clinical Skills Marjorie A. King, PhD. ATC, PT Plymouth State University
CLINICAL EVALUATION & TESTING Darin A. Padua. PhD, ATC, Column Editor Assessment of Lower Extremity Posture: Qualitative and Quantitative Clinical Skills Marjorie A. King, PhD. ATC, PT Plymouth State University
Int J Physiother. Vol 1(3), , August (2014) ISSN:
 Int J Physiother. Vol 1(3), 120-126, August (2014) ISSN: 2348-8336 ABSTRACT Sreekar Kumar Reddy.R 1 B. Siva kumar 2 N. Vamsidhar 2 G. Haribabu 3 Background: Patellofemoral pain syndrome is a very common
Int J Physiother. Vol 1(3), 120-126, August (2014) ISSN: 2348-8336 ABSTRACT Sreekar Kumar Reddy.R 1 B. Siva kumar 2 N. Vamsidhar 2 G. Haribabu 3 Background: Patellofemoral pain syndrome is a very common
Reliability of Measuring Trunk Motions in Centimeters
 Reliability of Measuring Trunk Motions in Centimeters MARGARET ROST, SANDRA STUCKEY, LEE ANNE SMALLEY, and GLENDA DORMAN A method of measuring trunk motion and two related motions using a tape measure
Reliability of Measuring Trunk Motions in Centimeters MARGARET ROST, SANDRA STUCKEY, LEE ANNE SMALLEY, and GLENDA DORMAN A method of measuring trunk motion and two related motions using a tape measure
HIP CASESTUDY 3. Body Chart-Initial Hypothesis: Property of VOMPTI, LLC. For Use of Participants Only. No Use or Reproduction Without Consent 1
 Body Chart-Initial Hypothesis: HIP CASESTUDY 3 Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 Eric Magrum DPT OCS FAAOMPT Hamstring Strain HS Tendinopathy Lumbar Radiculopathy Lumbar
Body Chart-Initial Hypothesis: HIP CASESTUDY 3 Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 Eric Magrum DPT OCS FAAOMPT Hamstring Strain HS Tendinopathy Lumbar Radiculopathy Lumbar
IFAST Assessment. Name: Date: Sport: Review Health Risk Assessment on initial consult form. List Client Goals (what brings you here?
 IFAST Assessment Name: Date: Sport: Review Health Risk Assessment on initial consult form List Client Goals (what brings you here?) Cardiovascular Measurements Blood Pressure Resting Heart Rate Body Composition
IFAST Assessment Name: Date: Sport: Review Health Risk Assessment on initial consult form List Client Goals (what brings you here?) Cardiovascular Measurements Blood Pressure Resting Heart Rate Body Composition
The Role of Hip Muscle Function in the Treatment of Patellofemoral Pain Syndrome
 The Role of Hip Muscle Function in the Treatment of Patellofemoral Pain Syndrome Timothy F. Tyler,* MS, PT, ATC, Stephen J. Nicholas, MD, Michael J. Mullaney, MPT, and Malachy P. McHugh, PhD From the Nicholas
The Role of Hip Muscle Function in the Treatment of Patellofemoral Pain Syndrome Timothy F. Tyler,* MS, PT, ATC, Stephen J. Nicholas, MD, Michael J. Mullaney, MPT, and Malachy P. McHugh, PhD From the Nicholas
The Effect of Patellar Taping on Knee Kinematics during Stair Ambulation in Individuals with Patellofemoral Pain. Abdelhamid Akram F
 The Effect of Patellar Taping on Knee Kinematics during Stair Ambulation in Individuals with Patellofemoral Pain Abdelhamid Akram F Department of Orthopedic Physical Therapy, Faculty of Physical Therapy,
The Effect of Patellar Taping on Knee Kinematics during Stair Ambulation in Individuals with Patellofemoral Pain Abdelhamid Akram F Department of Orthopedic Physical Therapy, Faculty of Physical Therapy,
Keys to the Office Based Evaluation of the Youth Runner
 Keys to the Office Based Evaluation of the Youth Runner Michelle Cappello, PT, SCS Clinical Director of Physical Therapy and Athletic Training Sports Medicine Center for Young Athletes UCSF Benioff Children
Keys to the Office Based Evaluation of the Youth Runner Michelle Cappello, PT, SCS Clinical Director of Physical Therapy and Athletic Training Sports Medicine Center for Young Athletes UCSF Benioff Children
INITIAL REHABILITATION PHASE 0-4 weeks. Posterolateral Corner Injury
 Posterolateral Corner Injury Indications for Surgery The main indication of PLC reconstruction surgery is symptomatic instability following PLC injury. The aim of PLC reconstruction surgery is to restore
Posterolateral Corner Injury Indications for Surgery The main indication of PLC reconstruction surgery is symptomatic instability following PLC injury. The aim of PLC reconstruction surgery is to restore
Exercise Therapy for Patients with Knee OA Knee Exercise Protocol Knee Home Exercise Programme
 Chapter FOUR Exercise Therapy for Patients with Knee OA Knee Exercise Protocol Knee Home Exercise Programme Chris Higgs Cathy Chapple Daniel Pinto J. Haxby Abbott 99 n n 100 General Guidelines Knee Exercise
Chapter FOUR Exercise Therapy for Patients with Knee OA Knee Exercise Protocol Knee Home Exercise Programme Chris Higgs Cathy Chapple Daniel Pinto J. Haxby Abbott 99 n n 100 General Guidelines Knee Exercise
Evaluating the Athlete Questionnaire
 Evaluating the Athlete Questionnaire Prior to developing the strength and conditioning training plan the coach should first evaluate factors from the athlete s questionnaire that may impact the strength
Evaluating the Athlete Questionnaire Prior to developing the strength and conditioning training plan the coach should first evaluate factors from the athlete s questionnaire that may impact the strength
Comparison of Range of Motion of Knee and Hip in Athletes With and Without Patellofemoral Pain Syndrome
 Journal of Research in Applied sciences. Vol., 1(3): 70-77, 2014 Available online at http://www.jrasjournal.com ISSN 2148-6662 Copyright 2014 ORIGINAL ARTICLE Comparison of Range of Motion of Knee and
Journal of Research in Applied sciences. Vol., 1(3): 70-77, 2014 Available online at http://www.jrasjournal.com ISSN 2148-6662 Copyright 2014 ORIGINAL ARTICLE Comparison of Range of Motion of Knee and
When Clinical Reasoning Overrules the Evidence
 When Clinical Reasoning Overrules the Evidence Breakout session Paul Mintken PT, DPT, OCS, FAAOMPT Kristin Carpenter PT, DPT, OCS, FAAOMPT Amy McDevitt PT, DPT, OCS, FAAOMPT Objectives Break Out Session
When Clinical Reasoning Overrules the Evidence Breakout session Paul Mintken PT, DPT, OCS, FAAOMPT Kristin Carpenter PT, DPT, OCS, FAAOMPT Amy McDevitt PT, DPT, OCS, FAAOMPT Objectives Break Out Session
Improving Decision-Making in Low Back Pain: How to Target the Right Treatment at the Right Patient
 Evidence Based Examination Stats No not stats Patient Values & Expectations SNNOUT Sensitivity a highly 'SeNsitive' test, when Negative rules OUT disease (SN-N-OUT). Individual Clinical Expertise EBM Best
Evidence Based Examination Stats No not stats Patient Values & Expectations SNNOUT Sensitivity a highly 'SeNsitive' test, when Negative rules OUT disease (SN-N-OUT). Individual Clinical Expertise EBM Best
Musculoskeletal Examination Benchmarks
 Musculoskeletal Examination Benchmarks _ The approach to examining the musculoskeletal system is the same no matter what joint or limb is being examined. The affected and contralateral region should both
Musculoskeletal Examination Benchmarks _ The approach to examining the musculoskeletal system is the same no matter what joint or limb is being examined. The affected and contralateral region should both
CORE STABILIZATION EXERCISE. Vincent J. Hudson, PhD, DPT, MBA, ATC Chief Operating Officer OAA Orthopaedic Specialists Allentown, PA
 CORE STABILIZATION EXERCISE Vincent J. Hudson, PhD, DPT, MBA, ATC Chief Operating Officer OAA Orthopaedic Specialists Allentown, PA Stepping Back What are the goals? What is the value? Is it Sport Specific
CORE STABILIZATION EXERCISE Vincent J. Hudson, PhD, DPT, MBA, ATC Chief Operating Officer OAA Orthopaedic Specialists Allentown, PA Stepping Back What are the goals? What is the value? Is it Sport Specific
Anterior Knee Pain in Children. Joseph Chorley, MD Associate Professor, Pediatrics Baylor College of Medicine
 Anterior Knee Pain in Children Joseph Chorley, MD Associate Professor, Pediatrics Baylor College of Medicine Goals and Objectives To learn how to care for patients with chronic knee pain To be able to
Anterior Knee Pain in Children Joseph Chorley, MD Associate Professor, Pediatrics Baylor College of Medicine Goals and Objectives To learn how to care for patients with chronic knee pain To be able to
A Comparison of Two Stretching Protocols on Hip Range of Motion: Implications for Total Daily Stretch Duration
 Journal of Strength and Conditioning Research, 2003, 17(2), 274 278 2003 National Strength & Conditioning Association A Comparison of Two Stretching Protocols on Hip Range of Motion: Implications for Total
Journal of Strength and Conditioning Research, 2003, 17(2), 274 278 2003 National Strength & Conditioning Association A Comparison of Two Stretching Protocols on Hip Range of Motion: Implications for Total
What is Medial Plica Syndrome?
 What is Medial Plica Syndrome? It is a congenital disorder in which the thin wall of fibrous tissue extends from the synovial capsule of the knee. Pain usually occurs when the synovial capsule becomes
What is Medial Plica Syndrome? It is a congenital disorder in which the thin wall of fibrous tissue extends from the synovial capsule of the knee. Pain usually occurs when the synovial capsule becomes
Mechanisms Underlying Patellofemoral Pain: Lessons Learned over the Past 20 Years. Christopher M. Powers, PT, PhD, FASCM, FAPTA
 Mechanisms Underlying Patellofemoral Pain: Lessons Learned over the Past 20 Years Christopher M. Powers, PT, PhD, FASCM, FAPTA Although recognized as one of the most common lower extremity disorders encountered
Mechanisms Underlying Patellofemoral Pain: Lessons Learned over the Past 20 Years Christopher M. Powers, PT, PhD, FASCM, FAPTA Although recognized as one of the most common lower extremity disorders encountered
Evidence- Based Examination of the Lumbar Spine Presented by Chad Cook, PT, PhD, MBA, FAAOMPT Practice Sessions/Skill Check- offs
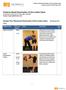 Evidence- Based Examination of the Lumbar Spine Presented by Chad Cook, PT, PhD, MBA, FAAOMPT Practice Sessions/Skill Check- offs Chapter Five: Movement Examination of the Lumbar Spine Time) (45 minutes
Evidence- Based Examination of the Lumbar Spine Presented by Chad Cook, PT, PhD, MBA, FAAOMPT Practice Sessions/Skill Check- offs Chapter Five: Movement Examination of the Lumbar Spine Time) (45 minutes
Internal Rotation (turning toes/knee toward other leg) 30 degree limit. limit
 Hip Arthroscopy Patient Education Use of Brace and Crutches: - Wear the brace all times of weight bearing for the first 3 weeks after surgery. This is done to protect your hip and motion into hip extension
Hip Arthroscopy Patient Education Use of Brace and Crutches: - Wear the brace all times of weight bearing for the first 3 weeks after surgery. This is done to protect your hip and motion into hip extension
Comparison Of Bilateral Quadriceps Angle In Asymptomatic And Symptomatic Males With Unilateral Anterior Knee Pain
 ISPUB.COM The Internet Journal of Pain, Symptom Control and Palliative Care Volume 6 Number 1 Comparison Of Bilateral Quadriceps Angle In Asymptomatic And Symptomatic Males With Unilateral A Sra, T Ba,
ISPUB.COM The Internet Journal of Pain, Symptom Control and Palliative Care Volume 6 Number 1 Comparison Of Bilateral Quadriceps Angle In Asymptomatic And Symptomatic Males With Unilateral A Sra, T Ba,
ACE s Essentials of Exercise Science for Fitness Professionals TRUNK
 ACE s Essentials of Exercise Science for Fitness Professionals TRUNK Posture and Balance Posture refers to the biomechanical alignment of the individual body parts and the orientation of the body to the
ACE s Essentials of Exercise Science for Fitness Professionals TRUNK Posture and Balance Posture refers to the biomechanical alignment of the individual body parts and the orientation of the body to the
Scapulothoracic muscle strength in individuals with neck pain
 Journal of Back and Musculoskeletal Rehabilitation 29 (2016) 549 555 549 DOI 10.3233/BMR-160656 IOS Press Scapulothoracic muscle strength in individuals with neck pain Shannon M. Petersen a,,nathana.domino
Journal of Back and Musculoskeletal Rehabilitation 29 (2016) 549 555 549 DOI 10.3233/BMR-160656 IOS Press Scapulothoracic muscle strength in individuals with neck pain Shannon M. Petersen a,,nathana.domino
Lumbar Spine Applied Anatomy. Jason Zafereo, PT, OCS, FAAOMPT Clinical Orthopedic Rehabilitation Education
 Lumbar Spine Applied Anatomy Jason Zafereo, PT, OCS, FAAOMPT Clinical Orthopedic Rehabilitation Education Objectives Discuss concepts relevant to pathophysiology and differential diagnosis for lumbar radiculopathy
Lumbar Spine Applied Anatomy Jason Zafereo, PT, OCS, FAAOMPT Clinical Orthopedic Rehabilitation Education Objectives Discuss concepts relevant to pathophysiology and differential diagnosis for lumbar radiculopathy
Gluteal Strengthening Exercises: A Review of the Literature
 Common Imbalances Female Athlete Hip Injuries: Exploring the CORE of Patterns and Prevention Kelly McInnis, DO Irene Davis, PhD, PT, FAPTA, FACSM, FASB David Nolan, PT, DPT, MS, OCS, SCS, CSCS Gluteal
Common Imbalances Female Athlete Hip Injuries: Exploring the CORE of Patterns and Prevention Kelly McInnis, DO Irene Davis, PhD, PT, FAPTA, FACSM, FASB David Nolan, PT, DPT, MS, OCS, SCS, CSCS Gluteal
Recognizing common injuries to the lower extremity
 Recognizing common injuries to the lower extremity Bones Femur Patella Tibia Tibial Tuberosity Medial Malleolus Fibula Lateral Malleolus Bones Tarsals Talus Calcaneus Metatarsals Phalanges Joints - Knee
Recognizing common injuries to the lower extremity Bones Femur Patella Tibia Tibial Tuberosity Medial Malleolus Fibula Lateral Malleolus Bones Tarsals Talus Calcaneus Metatarsals Phalanges Joints - Knee
Functional Movement Test. Deep Squat
 Functional Movement Test Put simply, the FMS is a ranking and grading system that documents movement patterns that are key to normal function. By screening these patterns, the FMS readily identifies functional
Functional Movement Test Put simply, the FMS is a ranking and grading system that documents movement patterns that are key to normal function. By screening these patterns, the FMS readily identifies functional
Common Lower Limb Pathology Related to Running. Catherine Irwin, PT, OCS January 10, 2012
 Common Lower Limb Pathology Related to Running Catherine Irwin, PT, OCS January 10, 2012 Objectives Pathology Treatment Shoe guidelines Pathology Shin Splints Posterior Tibialis Tendonitis Achilles Tendonopathy/Sever
Common Lower Limb Pathology Related to Running Catherine Irwin, PT, OCS January 10, 2012 Objectives Pathology Treatment Shoe guidelines Pathology Shin Splints Posterior Tibialis Tendonitis Achilles Tendonopathy/Sever
Stress Fracture Rehabilitation Guideline
 Stress Fracture Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation following
Stress Fracture Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation following
Runner with Recurrent Achilles Tendon Pain 4/21/2017
 Young Runner with Recurrent Achilles Pain In alphabetical order: Kornelia Kulig PT, PhD, FAPTA Los Angeles, CA Lisa Meyer PT, DPT, OCS isports Physical Therapy Los Angeles, CA Liz Poppert MS, DPT, OCS
Young Runner with Recurrent Achilles Pain In alphabetical order: Kornelia Kulig PT, PhD, FAPTA Los Angeles, CA Lisa Meyer PT, DPT, OCS isports Physical Therapy Los Angeles, CA Liz Poppert MS, DPT, OCS
Patellofemoral pain syndrome (PFPS) is one of the most
 LAURA KOOIKER, PT, MSc 1 INGRID G.L. VAN DE PORT, PhD 1,2 ADAM WEIR, MBBS, PhD 3 MAARTEN H. MOEN, MD, PhD 2,4 Effects of Physical Therapist Guided Quadriceps-Strengthening Exercises for the Treatment of
LAURA KOOIKER, PT, MSc 1 INGRID G.L. VAN DE PORT, PhD 1,2 ADAM WEIR, MBBS, PhD 3 MAARTEN H. MOEN, MD, PhD 2,4 Effects of Physical Therapist Guided Quadriceps-Strengthening Exercises for the Treatment of
Physical Therapy for the Lower Extremity: What You and Your Patient Should Expect from Rehab
 1 Physical Therapy for the Lower Extremity: What You and Your Patient Should Expect from Rehab Thomas Clennell, PT, DPT, SCS Physical Therapist UCSF Benioff Children s Hospital Oakland Sports Medicine
1 Physical Therapy for the Lower Extremity: What You and Your Patient Should Expect from Rehab Thomas Clennell, PT, DPT, SCS Physical Therapist UCSF Benioff Children s Hospital Oakland Sports Medicine
Relationship between Body Core Stabilization and Athletic Function in. Football, Basketball and Swimming Athletes
 Relationship between Body Core Stabilization and Athletic Function in Football, Basketball and Swimming Athletes Fatemeh Pouya (Msc) 1, Farahnaz Ghaffarinejad (Msc) 2 1. Department of Anatomy, Kerman University
Relationship between Body Core Stabilization and Athletic Function in Football, Basketball and Swimming Athletes Fatemeh Pouya (Msc) 1, Farahnaz Ghaffarinejad (Msc) 2 1. Department of Anatomy, Kerman University
5/14/2013. Acute vs Chronic Mechanism of Injury:
 Third Annual Young Athlete Conference: The Lower Extremity February 22, 2013 Audrey Lewis, DPT Acute vs Chronic Mechanism of Injury: I. Direct: blow to the patella II. Indirect: planted foot with a valgus
Third Annual Young Athlete Conference: The Lower Extremity February 22, 2013 Audrey Lewis, DPT Acute vs Chronic Mechanism of Injury: I. Direct: blow to the patella II. Indirect: planted foot with a valgus
Active-Assisted Stretches
 1 Active-Assisted Stretches Adequate flexibility is fundamental to a functional musculoskeletal system which represents the foundation of movement efficiency. Therefore a commitment toward appropriate
1 Active-Assisted Stretches Adequate flexibility is fundamental to a functional musculoskeletal system which represents the foundation of movement efficiency. Therefore a commitment toward appropriate
Lumbar Spine Applied Anatomy. Jason Zafereo, PT, OCS, FAAOMPT
 Lumbar Spine Applied Anatomy Jason Zafereo, PT, OCS, FAAOMPT Clinical i l Orthopedic Rehabilitation ti Education 1 Objectives Apply key concepts from the cervical anatomy/kinesiology self-study to aid
Lumbar Spine Applied Anatomy Jason Zafereo, PT, OCS, FAAOMPT Clinical i l Orthopedic Rehabilitation ti Education 1 Objectives Apply key concepts from the cervical anatomy/kinesiology self-study to aid
Conservative Correction of Leg-Length Discrepancies of 10 mm or Less for the Relief of Chronic Low Back Pain
 Conservative Correction of Leg-Length Discrepancies of 10 mm or Less for the Relief of Chronic Low Back Pain Archives of Physical Medicine and Rehabilitation November 2005, Volume 86, Issue 11, pp 2075-2080
Conservative Correction of Leg-Length Discrepancies of 10 mm or Less for the Relief of Chronic Low Back Pain Archives of Physical Medicine and Rehabilitation November 2005, Volume 86, Issue 11, pp 2075-2080
Factors Related to Extension Lag at the Knee Joint
 01 96-6011 /82/0304-Ol78$02.00/0 THE JOURNAL OF ORTHOPAEDIC AND SPORTS PHYSICAL THERAPY Copyright 0 1982 by The Orthopaedic and Sports Physical Therapy Sections of the American Physical Therapy Association
01 96-6011 /82/0304-Ol78$02.00/0 THE JOURNAL OF ORTHOPAEDIC AND SPORTS PHYSICAL THERAPY Copyright 0 1982 by The Orthopaedic and Sports Physical Therapy Sections of the American Physical Therapy Association
Correlations Between Hip Strength and Static Foot and Knee Posture
 J Sport Rehabil. 2006, 15, 12-23 2006 Human Kinetics, Inc. Correlations Between Hip Strength and Static Foot and Knee Posture John H. Hollman, Kimberly E. Kolbeck, Jamie L. Hitchcock, Jonathan W. Koverman,
J Sport Rehabil. 2006, 15, 12-23 2006 Human Kinetics, Inc. Correlations Between Hip Strength and Static Foot and Knee Posture John H. Hollman, Kimberly E. Kolbeck, Jamie L. Hitchcock, Jonathan W. Koverman,
Myology of the Knee. PTA 105 Kinesiology
 Myology of the Knee PTA 105 Kinesiology Objectives Describe the planes of motion and axes of rotation of the knee joint Visualize the origins and insertions of the muscles about the knee List the innervations
Myology of the Knee PTA 105 Kinesiology Objectives Describe the planes of motion and axes of rotation of the knee joint Visualize the origins and insertions of the muscles about the knee List the innervations
Improving Thoracic Mobility
 Improving Thoracic Mobility By William J. Hanney DPT, PhD, ATC, CSCS Course Description A lack of thoracic mobility can have broad clinical implications and evidence suggests addressing mobility in this
Improving Thoracic Mobility By William J. Hanney DPT, PhD, ATC, CSCS Course Description A lack of thoracic mobility can have broad clinical implications and evidence suggests addressing mobility in this
What do we want? Cervicothoracic Workgroup. ICF Scheme. start with end in mind. What do consumers want?
 Cervicothoracic Workgroup Use of the International Classification of Functioning to Develop Evidence-Based Treatment Guidelines for the Management of Cervicothoracic Conditions John D. Childs, PT, PhD,
Cervicothoracic Workgroup Use of the International Classification of Functioning to Develop Evidence-Based Treatment Guidelines for the Management of Cervicothoracic Conditions John D. Childs, PT, PhD,
Running Injuries. Rebecca Christenson
 Running Injuries Rebecca Christenson Improve your time? Don t get injured! Think about your training graph Recovery Causes of Overuse Injuries Biomechanics Sudden increase in training Poor recovery strategies
Running Injuries Rebecca Christenson Improve your time? Don t get injured! Think about your training graph Recovery Causes of Overuse Injuries Biomechanics Sudden increase in training Poor recovery strategies
Validity of Data Extraction Techniques on the Kinetic Communicator (KinCom) Isokinetic Device
 Validity of Data Extraction Techniques on the Kinetic Communicator (KinCom) Isokinetic Device By: Laurie L. Tis, PhD, AT,C * and David H. Perrin, PhD, AT,C Tis, L.L., & Perrin, D.H. (1993). Validity of
Validity of Data Extraction Techniques on the Kinetic Communicator (KinCom) Isokinetic Device By: Laurie L. Tis, PhD, AT,C * and David H. Perrin, PhD, AT,C Tis, L.L., & Perrin, D.H. (1993). Validity of
EVect of stretching duration on active and passive range of motion in the lower extremity
 Br J Sports Med 1999;33:259 263 259 School of Health Sciences, University of Sunderland J M Roberts K Wilson Correspondence to: J M Roberts, School of Health Sciences, University of Sunderland, Chester
Br J Sports Med 1999;33:259 263 259 School of Health Sciences, University of Sunderland J M Roberts K Wilson Correspondence to: J M Roberts, School of Health Sciences, University of Sunderland, Chester
Movement System Diagnoses. Movement System Impairment Syndromes of the Lumbar Spine. MSI Syndrome - Assumptions. Return From Forward Bending
 Movement System Diagnoses Kinesiopathologic Pathokinesiologic Movement System Impairment Syndromes of the Lumbar Spine Shirley Sahrmann, PT, PhD, FAPTA Washington University St. Louis School of Medicine
Movement System Diagnoses Kinesiopathologic Pathokinesiologic Movement System Impairment Syndromes of the Lumbar Spine Shirley Sahrmann, PT, PhD, FAPTA Washington University St. Louis School of Medicine
FIT IN LINE EXAMPLE REPORT (15/03/11) THE WHITE HOUSE PHYSIOTHERAPY CLINIC PRESENT
 THE WHITE HOUSE PHYSIOTHERAPY CLINIC PRESENT FIT IN LINE EXAMPLE REPORT (15/03/11) A 12 part assessment tool to screen your athletic performance in 4 key components: Flexibility, Balance, Strength & Core
THE WHITE HOUSE PHYSIOTHERAPY CLINIC PRESENT FIT IN LINE EXAMPLE REPORT (15/03/11) A 12 part assessment tool to screen your athletic performance in 4 key components: Flexibility, Balance, Strength & Core
PTA 210 PTA Techniques
 PTA 210 PTA Techniques Patient Positioning and Draping INTRO Patient Positioning Must be considered before, during and after treatment AND when the patient is to be at rest for a prolonged period of time
PTA 210 PTA Techniques Patient Positioning and Draping INTRO Patient Positioning Must be considered before, during and after treatment AND when the patient is to be at rest for a prolonged period of time
Solving Today s Pain and Injury Puzzle with Erik Dalton An Online Workshop for ABMP Members Session 4 Handout
 Solving Today s Pain and Injury Puzzle with Erik Dalton An Online Workshop for ABMP Members Session 4 Handout Please Note: Erik Dalton teaches his Myoskeletal Alignment Techniques with the expectation
Solving Today s Pain and Injury Puzzle with Erik Dalton An Online Workshop for ABMP Members Session 4 Handout Please Note: Erik Dalton teaches his Myoskeletal Alignment Techniques with the expectation
