A Comparison of Cyclic Valgus Loading on Reconstructed Ulnar Collateral Ligament of the Elbow
|
|
|
- Conrad Jenkins
- 6 years ago
- Views:
Transcription
1 Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine 2007 A Comparison of Cyclic Valgus Loading on Reconstructed Ulnar Collateral Ligament of the Elbow Roshan Pradip Shah Follow this and additional works at: Part of the Medicine and Health Sciences Commons Recommended Citation Shah, Roshan Pradip, "A Comparison of Cyclic Valgus Loading on Reconstructed Ulnar Collateral Ligament of the Elbow" (2007). Yale Medicine Thesis Digital Library This Open Access Thesis is brought to you for free and open access by the School of Medicine at EliScholar A Digital Platform for Scholarly Publishing at Yale. It has been accepted for inclusion in Yale Medicine Thesis Digital Library by an authorized administrator of EliScholar A Digital Platform for Scholarly Publishing at Yale. For more information, please contact elischolar@yale.edu.
2 A Comparison of Cyclic Valgus Loading on Reconstructed Ulnar Collateral Ligament of the Elbow A Thesis Submitted to the Yale University School of Medicine In Partial Fulfillment of the Requirements for the Degree of Doctor of Medicine by Roshan Pradip Shah 2007
3 2 Abstract A COMPARISON OF CYCLIC VALGUS LOADING ON RECONSTRUCTED ULNAR COLLATERAL LIGAMENT OF THE ELBOW. Roshan P. Shah, Derek P. Lindsey, Gannon W. Sungar, Timothy R. McAdams. Section of Sports Medicine, Department of Orthopaedic Surgery, Stanford University, Stanford CA. (Sponsored by Michael J. Medvecky, Department of Orthopaedic Surgery, Yale University School of Medicine.) This study compares the biomechanics of early cyclic valgus loading of the ulnar collateral ligament (UCL) of the elbow repaired by either the Jobe technique or the docking technique. Better understanding of the biomechanical properties of each reconstruction may help surgeons choose the optimal surgical technique, particularly in planning earlier rehabilitation programs. Sixteen fresh frozen cadaver limbs (eight pairs) were randomized to either the Jobe cohort or the docking cohort. First intact UCLs were tested, followed by the repaired constructions. A Bionix MTS apparatus applied a constant valgus load to the elbows at 70 o flexion, and valgus displacement was measured and then used to calculate valgus angle displacement. The docking group had significantly less valgus angle displacement than the Jobe group at cycles 100 and 1,000 (p = and , respectively). Four of the eight specimens in the Jobe group failed at the tendon-suture interface before reaching 1,000 cycles, at cycles 7, 24, 250, and 362. None of the docking specimens failed before reaching 1,000 cycles. In this cadaveric study, the docking technique resulted in less angulation of the elbow in response to cyclic valgus loading as compared to the Jobe technique. The better response to valgus loading of the docking reconstruction may translate into a better response to early rehabilitation. Further study is needed to determine if this difference translates into improved clinical outcomes.
4 3 Acknowledgements Many thanks to Timothy R. McAdams, M.D. for his guidance, support, and teachings. Special thanks to Derek P. Lindsey, M.S. at the VA-Palo Alto and Michael J. Medvecky, M.D. and Jonathan N. Grauer, M.D. at the Yale School of Medicine. This work was supported through the Yale University School of Medicine Medical Student Research Fellowship.
5 4 Table of Contents I. Introduction... 5 a. Anatomy b. Injury to the Ulnar Collateral Ligament c. Therapeutic Course d. Surgical Repair Techniques e. Prior Investigations II. III. Statement of Purpose..12 Methods..13 a. Preparation of Specimens b. Biomechanical Testing of the Intact UCLs c. Surgical Reconstructions d. Calculating Valgus Angle Displacement e. Statistical Analysis f. Statement of Duties IV. Results..21 V. Discussion..25 VI. References..30
6 5 Introduction The ulnar collateral ligament (UCL) of the elbow is commonly injured in overhead throwing sports (i.e., baseball or javelin, but also racket sports and ice hockey) or post-traumatically after a fall on an outstretched arm. A combination of valgus and external rotation forces are involved in the UCL injuries caused by trauma. In throwing athletes, attenuation and laxity of the UCL is due primarily to repetitive valgus stress to the elbow. Laxity in the UCL results in instability, pain, and impaired performance. Operative repair of the UCL is generally reserved for competitive throwing athletes and for those involved in heavy manual labor. (1, 2, 3, 4, 5) Anatomy The elbow joint is stabilized by its congruous bony articulations, its lateral and medial (ulnar) collateral ligaments, its capsule, and its secondary soft tissue stabilizers. The elbow comprises articulations between the humerus, ulna, and radius. The radial head contributes to stability of the ulnohumeral joint to valgus loads. (1) The lateral collateral ligament resists varus force and stabilizes the humerus to the annular ligament and proximal ulna. (1) The flexor and pronator muscles originate at the medial epicondyle and contribute additional support, mostly notably from the flexor carpi ulnaris and the flexor digitorum superficialis. (1). The UCL resists valgus force and supports the ulnohumeral joint. (1) The UCL originates on the central 65% of the anteroinferior surface of the medial
7 6 epicondyle, just posterior to the axis of the elbow. It inserts on average 18.4 mm dorsal to the coronoid tip. (6) The UCL is comprised of three bundles: the anterior, the posterior, and the transverse bundles. The anterior bundle is the strongest and stiffest ligament of the elbow, with an average load to failure of 260 N. (1, 7) The anterior bundle consists of the anterior and posterior bands. The anterior band is taut from full extension to 60 degrees flexion; the posterior band is taut from 60 to 120 degrees flexion. (1) Based on anatomic considerations and previous observations, an elbow in 70 degrees of flexion has been chosen for evaluating the effect of valgus loading on the UCL. Sojbjerg et al. found the maximum valgus angle after transection of the UCL occurred at 60 to 70 degrees of flexion. (8) Hechtman et al. found that at 70 degrees of elbow flexion, both the anterior and posterior bands of the anterior bundle are tight in the native and reconstructed UCL. (9) Importantly, the elbow extends rapidly from approximately 125 to 25 degrees during late cocking to ball release. (10) A 70 degree angle falls in the mid-range of this phase of throwing, when angular velocities are highest. Injury to the Ulnar Collateral Ligament During the acceleration phase of overhead throwing, intense valgus forces act on the elbow. During this phase, the forearm and hand lag behind the arm, generating the valgus stress. The static torque on the UCL has been estimated at 32 N-m during late cocking and acceleration phases of baseball pitching. (10)
8 7 Significantly, the average load-to-failure of the UCL is about 33 N-m. (11) Thus, every pitch approaches the maximum torque of the UCL. When the valgus force surpasses the threshold that the UCL can withstand, injury occurs, either as chronic microscopic tears or acute gross rupture. Therapeutic Course Rehabilitation following surgical reconstruction of the UCL can take more than six months and has been described as a four phase process. (12) The first phase begins with one week of post-operative immobilization in a posterior splint of the elbow in 90 degrees flexion. This immobilization is thought to be necessary for initial would healing. A range of motion brace is used from week two to week eight and gradually allows for increased range of flexion. During this time, wrist and hand range-of-motion exercises, grasping exercises, and isometric shoulder and arm exercises are performed. Phase two generally occurs concurrently during phase one, between weeks four and eight. This phase involves elbow range-of-motion exercises and isotonic resistance strengthening of the shoulder and arm. Phase three, usually occurring between weeks nine and twelve, involves advanced strengthening through sport-specific exercises. Phase four begins around week fourteen and extends through week twenty-six or later. This phase reintroduces throwing in an interval throwing program. It is believed that earlier rehabilitation following UCL reconstruction will lead to improved clinical outcomes for the overhead throwing athlete, just as
9 8 earlier rehabilitation following anterior cruciate ligament surgery leads to better outcomes in the knee (13, 14). The first step in developing earlier rehabilitation protocols is to investigate how the various surgical reconstruction techniques perform with early cyclic valgus loading. Later clinical studies can then investigate whether better biomechanical performance of a surgical technique correlates with improved clinical outcomes. It is believed that methods using ligament fixture through bone tunnels requires longer duration of post-operative immobilization than methods utilizing interference screw fixation (13). Thus, it will be important to extend this study to include an investigation of the biomechanical performance of surgical reconstructions involving interference screws. Surgical Repair Techniques Surgical reconstruction of the UCL in high performance athletes was originally described by Jobe in (4) The procedure, popularly known as the Tommy John procedure, has evolved over the last thirty-two years. Today, thousands of ulnar collateral ligament reconstructions are performed each year. (15) Jobe s technique used a tendon graft pulled through bone tunnels in the sublime tubercle of the proximal ulna and medial epicondyle of the distal humerus. Additional techniques have modified Jobe s original technique in an effort to minimize dissection, improve tendon graft fixation, and decrease ulnar nerve complications. (9, 16, 17, 18) Efforts to minimize dissection and decrease ulnar
10 9 nerve complications motivated the use of a muscle splitting approach rather than detaching the flexor-pronator origin. (3, 12, 19) Maintaining the flexor-pronator origin intact turns out to preserve an important dynamic stabilizer of the elbow in response to valgus torque; the flexor carpi ulnaris and flexor digitorum superficialis are notable for this contribution. (20) Consequently, it can be reasonably postulated that preservation of the flexor-pronator origin will facilitate rehabilitation after elbow UCL reconstruction. Altchek et al. reported the docking procedure in 2002, a significant modification of Jobe s technique. (21) This technique used Jobe s muscle splitting approach, but with more widely spaced ulnar tunnels. Locking sutures were placed on each end of the tendon graft, and the free ends were docked into the medial epicondyle of the humerus. The sutures were tied over a proximal medial epicondyle bone bridge. This aspect allowed for easier and greater initial tensioning of the graft, and this was proffered as an operative improvement over the Jobe technique. Ahmad et al. described a significant alteration of this technique using proximal and distal interference screw fixation. (16) Interference screws for soft tissue fixation had been used with great success in fixation of anterior cruciate ligament grafts, and new instrumentation made this a reasonable alternative for elbow ligament reconstruction. (13) The method used two 5.0 x 15.0 mm cannulated metal screws that locked to a soft tissue graft with four strands of strong nonabsorbable suture. This suture reinforced fixation was thought to be essential for the strength of the reconstruction. Ahmad et al. found that the
11 10 ultimate moment of the interference screw technique compared favorably to studies of the classic Jobe technique and suture anchor fixation technique (30.5 N-m versus 15.4 N-m and 13.6 N-m, respectively). (4, 9, 16) A newer technique, the DANE procedure, is a hybrid of the docking method and the interference screw method. A medial epicondyle docking technique is combined with a distal ulna interference screw. The distal fixation of the graft into a single tunnel may more closely recreate the isometry of the native ligament. (16, 20) These recent advances in UCL reconstruction have come in a relatively short time frame. Careful analysis and comparison of each technique is necessary before settling on the preferred method of treatment. Selection of the optimal procedure will be of primary importance in returning competitive athletes to their prior level of performance. Prior Investigations Previously in this lab, McAdams et al. performed a biomechanical evaluation with cyclic loading to compare the docking technique with bioabsorbable interference screw fixation. (13) The interference screw fixation technique was found to be significantly stiffer than the docking technique in resistance to valgus torque at 10 and 100 cycles. These results suggest that, between these two techniques, the interference screw fixation technique may lead to less laxity at early phases of rehabilitation as compared to the docking technique.
12 11 Using the same apparatus employed in this study, all intact specimens this prior study reached 1,000 cycles of loading. One interference screw treated elbow failed at cycle 873 by tendon rupture distal to the humerus interference screw site. No gross slippage at the interference screw site was evident. Two docking technique treated elbows failed prior to 100 cycles with failure at the suture-bone interface. In one, the suture pulled through the humerus bone bridge at cycle 79, and in the other, the suture failed at the knot tied over the humerus bone bridge at cycle 20. For all cycles there were no differences between the intact specimens that were randomly assigned to the docking and the interference screw groups. At cycle 1, the valgus angle was not different between the treated and intact cases. By cycle 10, the valgus angle for the docking technique was greater than both the intact (11.0 o vs. 4.4 o ; p = ) and the interference screw technique (11.0 o vs. 7.4 o ; p = ). Likewise at cycle 100, the valgus angle for the docking technique was greater than both the intact (17.5 o vs. 4.9 o ; p = ) and the interference screw technique (17.5 o vs. 9.8 o ; p = ). By the 1,000th cycle, both the docking and the interference screw techniques were larger than their respective intact specimens (19.3 o vs. 5.7 o ; p = ) and (16.8 o vs. 5.6 o ; p = ), and no difference was measured between the two techniques. Based on that study, it appeared that the bioabsorbable interference screw technique may resist slippage better than the docking technique, as evidenced by a decreased valgus angle in response to valgus torque at cycles 10 and 100. This advantage seems to equilibrate at cycle 1,000. Significant healing
13 12 occurs over the first 12 weeks after implantation of a tendon into the metaphyseal tunnel of bone, after which time the fixation sites are no longer the weakest points in the construct. (22) Further study is needed to compare these techniques with the Jobe technique and the DANE technique. This study addresses the comparison between the docking technique and the Jobe technique. Statement of Purpose This study compares the biomechanical properties of two surgical techniques to repair the ulnar collateral ligament (UCL) of the elbow: the Jobe procedure and the docking procedure. Better understanding of the biomechanical properties of each reconstruction may help the surgeon choose the optimal surgical technique in terms of early rehabilitation. This study will help us understand which reconstruction performs better (i.e., results in less valgus angle displacement) in early cyclic valgus loading of the elbow. This information is relevant to predicting the effect of earlier rehabilitation after UCL reconstruction. Our hypothesis is that the docking technique will results in less valgus displacement than the Jobe technique in elbow reconstruction. This technique has two obvious advantages: (a) the strength of the Krackow stitches and (b) it avoids a contemplated weakness in the strength of Jobe s three-ligand fixation, which results from suturing each limb together, i.e., the suture-tendon interface.
14 13 The null hypothesis for the biomechanical study is that both methods result in a statistically insignificant difference in valgus angle displacement at each cycle. Future work will include a similar evaluative technique of two additional surgical procedures: the DANE technique and the all-interference screw technique. A thorough comparison of all four techniques will allow for a full analysis of early cyclic valgus loading on UCL reconstruction surgery. With further clinical correlation, this information may lead to optimizing UCL reconstruction surgery for early rehabilitation of the elbow. Methods Preparation of Specimens Eight matched pairs of fresh-frozen cadaveric elbows were dissected to the capsule and the medial and lateral ligament complexes. Either the palmaris longus tendon (fifteen limbs) or the flexor carpi radialis tendon (one limb) was harvested from each tissue sample. The bone was sectioned 14 cm proximal and distal to the elbow joint and potted in neutral forearm rotation. The humerus and ulna/radius was potted in PMA cement inside 1.5 inch PVC piping. The elbows and grafts were kept moist throughout the preparation and testing by using sterile gauze soaked in normal saline. Biomechanical Testing of Intact UCLs The MTS apparatus is comprised of an MTS machine from Bionix and a digital video camera for motion analysis and capture of failure mechanisms. The
15 14 elbows were placed into the apparatus at 70 degrees flexion. The radius/ulna was fixed on the MTS machine and the humerus was maintained in a position parallel to the floor. (Figures 1a and 1b.) The MTS actuator applied a constant force and the displacement will be measured. A 0.5 N-m pre-load was applied, followed by a 5 N-m valgus moment (50 N force applied 10 cm from the elbow joint). This moment was applied in a cyclical fashion at a rate of 1 cycle/second for 1,000 cycles. The actuator displacement was recorded throughout the testing. An actuator limit of 70 mm was used to prevent instability of the MTS. Any specimen reaching this limit prior to 1,000 cycles was stopped automatically and the cycle was recorded. Cycles 1, 10, 100, and 1,000 were analyzed to determine the maximal actuator displacement, which was converted to the valgus angle. Specimens stopped before reaching 1,000 cycles were recorded to have a valgus angle of 35 degrees for all remaining cycles.
16 15 Figure 1a. A schematic of the MTS apparatus used for data collection. (Note that this figure shows the elbow in the opposite orientation to that used in this experiment, i.e., the medial side should face upwards such that the MTS applies a downward force to create the valgus load.) Figure 1b. The MTS apparatus used for data collection.
17 16 Surgical Reconstructions After testing the native ligament, the UCL was excised and the elbows from each matched pair were randomly divided into two groups. The first group underwent the Jobe procedure and the second underwent the docking procedure. The procedures was performed on each elbow by a single surgeon who specializes in upper extremity sports medicine (Timothy R. McAdams, M.D.). The posterior capsule and lateral ligament complex were preserved throughout the investigation. For the Jobe reconstruction, tunnels were made anterior and posterior to the sublime tubercle by using a 3 mm burr that created a 2 cm bone bridge between the tunnels. The tunnels were connected using a small, curved curette, and care was taken not to violate the bone bridge. A longitudinal humeral tunnel was created up the axis of the medial epicondyle to a depth of 15 mm using a 4 mm burr. Two adjacent tunnels were made on the upper border of the epicondyle just anterior to the remnants of the intramuscular septum. A small, curved curette was used to connect this y-shaped tunnel. A No. 2 Fiberwire was used to pass a looped suture through each tunnel in order to retrieve the graft. A palmaris longus graft was pulled through the tunnels in a figure-of-eight fashion. The elbow was reduced with maximum forearm supination and gentle varus stress while tension was held on each free limb of the graft. The two free limbs were sutured to the bridging section of graft to form a three-ligand band. (Figure 2.)
18 17 Figure 2. The Jobe technique of surgical reconstruction of the UCL. The tendon graft is pulled through bone tunnels in the ulna and the humerus. The three ligands are sutured together at the joint. The docking technique followed a previously reported technique (18) and is described here as modified by laboratory conventions. Tunnels were made anterior and posterior to the sublime tubercle by using a 3 mm burr to create a 2 cm bone bridge between the tunnels. The tunnels were connected using a small, curved curette, and care was taken not to violate the bone bridge. A No. 2 Fiberwire was used to pass a looped suture. The humeral tunnel was made in the anterior half of the medial epicondyle in the anterior position of the existing MCL. A longitudinal tunnel was created up the axis of the medial epicondyle to a depth of 15 mm by using a 4 mm burr. Exit punctures were placed on the upper border of the epicondyle just anterior to the remnants of the intramuscular septum. A small drill bit was used to make 2 small exit punctures separated by 5 mm to 1 cm. A suture passer was used from each of the two exit punctures to pass a looped suture which was then used for passage of the graft sutures.
19 18 The limb of the graft that had sutures already in place was passed into the humeral tunnel, and the sutures were pulled through one of the small superior humeral punctures. With one limb of the graft securely docked in the humerus, the elbow was reduced with maximum forearm supination and gentle varus stress. While tension was maintained on the graft, the specimen was moved so that the elbow ranged from flexion to extension to eliminate potential creep within the graft. The final length of the graft was estimated by placing the free limb of the graft adjacent to the humeral tunnel and visually estimating the length of the graft that would allow the graft to be tensioned within the humeral tunnel. The excess graft was excised immediately. A No. 1 braided nonabsorbable suture was placed in a Krackow fashion on this limb. This end of the graft was docked securely in the humeral tunnel with the sutures exiting the small puncture holes. Final graft tensioning was performed by again placing the elbow through a full range of motion with varus stress placed on the elbow. Once the surgeon was satisfied with the graft tension, the two sets of graft sutures were tied over the bone bridge on the humeral epicondyle. (Figures 3a and 3b.) Reconstructed elbow specimens were then tested in the MTS apparatus previously described. Load-displacement characteristics were measured at 1, 10, 100, and 1,000 cycles using the same protocol as for the intact elbows. In addition, India Ink markers at the aperture-tendon junction, and real-time video analysis was performed.
20 19 Figure 3a. A schematic of the docking technique of surgical reconstruction of the UCL. The tendon graft is pulled through ulnar bone tunnels and is docked in a humeral bone tunnel with small exit punctures for the graft sutures. Figure 3b. The docking technique of surgical reconstruction of the UCL. Calculating Valgus Angle Displacement The raw data collected from experiments gave the magnitude of displacement in millimeters. To find the maximal displacement per cycle of
21 20 concern, the entire data set of the cycle was examined, i.e., the ramp up and the ramp down, which gave around fifty data points. The point with maximal load was isolated, and the displacement at that point was used. The moment arm of the valgus load was constantly applied at 100 mm from the joint line. Thus, the displacement angle in radians was calculated by finding the arctangent of the ratio of the displacement over the moment arm. This value was converted from radians to degrees. Statistical Analysis For each cycle 1, 10, 100, and 1,000, the valgus angles for the intact and reconstructed specimens were compared using an analysis of variance with a significance criterion of Differences between groups were analyzed using a Fisher s Protected Least Square Difference (PLSD) test. The statistics were computed using the Statview computer software package. Statement of Duties Dissection and preparation of the tissue samples were performed by the author, Gannon W. Sungar, and Timothy R. McAdams, M.D. Surgical repair was performed by Timothy R. McAdams, M.D. Biomechanical analysis was performed by the author and Derek Lindsey, M.S. Statistical analysis was performed by the author and Derek Lindsey, M.S.
22 21 Results Eight pairs of fresh frozen cadaver arms, with an average age of 74.5 years, were tested (Table 1). Table 1. Specimen demographics. Specimen Age (y) Sex 1 57 M 2 80 M 3 88 F 4 50 F 5 81 F 6 66 M 7 93 M 8 81 M Avg. Age 74.5 Tables 2a and 2b show the valgus angle displacement data for each limb and Table 3 shows the means. Figure 4 shows the average valgus angles at cycles 1, 10, 100, and 1,000 for the intact UCLs and the reconstructed UCLs.
23 22 Table 2a. Data of valgus angle displacement for each specimen in the Jobe cohort. Valgus Angle (degrees) Specimen L Intact L Jobe R Intact R Jobe R Intact R Jobe * *Failed at cycle L Intact L Jobe * *Failed at cycle R Intact R Jobe * 35* *Failed at cycle 7. 6L Intact L Jobe L Intact L Jobe L Intact L Jobe * 35* *Failed at cycle 24.
24 23 Table 2b. Data of valgus angle displacement for each specimen in the docking cohort. Valgus Angle (degrees) Specimen L Intact L Docking R Intact R Docking R Intact R Docking L Intact L Docking L Intact L Docking R Intact R Docking R Intact R Docking R Intact R Docking Table 3. Mean valgus angle displacement (degrees) by cycle. (For each cohort, n = 8.) 1 Std. Dev. 10 Std. Dev. 100 Std. Dev Std. Dev. Intact Docking Intact Jobe
25 24 Valgus Angle (degrees) Intact Docking Treated Docking Intact Jobe Treated Jobe Docking vs Jobe Cycle Figure 4. Results showing the valgus angles of intact and reconstructed elbows. All intact specimens reached 1,000 cycles of loading. All docking specimens reached 1,000 cycles of loading. Four of eight Jobe specimens failed before reaching 1,000 cycles of loading. Failures occurred at cycles 7, 24, 250, and 362. Each failure occurred by tendon rupture at the suture site. For cycles 1, 10, 100, and 1,000, there was no difference between the intact specimens that were randomly assigned to the docking group or the Jobe group. The valgus angles of the Jobe reconstructed specimens were significantly larger than the intact specimens prior to Jobe reconstruction at cycles 10 (11.89 o vs o, p = ), 100 (19.06 o vs o, p < ), and 1,000 (27.89 o vs o, p < ). The valgus angle of the Jobe reconstructed specimens was
26 25 not significantly larger than the intact specimens prior to Jobe reconstruction at cycle 1 (3.06 o vs o, p = ). The valgus angles of the docking reconstructed specimens were significantly larger than the intact specimens prior to docking reconstruction at cycles 1 (3.48 o vs o, p = ) and 1,000 (14.80 o vs o, p = ). The valgus angles of the docking reconstructed specimens were not significantly larger than the intact specimens prior to docking reconstruction at cycles 10 (7.89 o vs o, p = ) and 100 (11.10 o vs o, p = ). At cycles 1 and 10, there was no difference between the valgus angles of the reconstructed Jobe and the reconstructed docking specimens. By cycle 100, the valgus angle was significantly greater for the Jobe group as compared to the docking group (19.06 o vs o, p = ). The valgus angle remained significantly greater for the Jobe group as compared to the docking group by cycle 1,000 (27.89 o vs o, p = ). Discussion Two types of loading are commonly used to assess fixation of soft tissue to bone: cyclic loading and load-to-failure. Many studies have evaluated the failure strength of both the intact and reconstructed UCL of the elbow. (7, 9, 16, 23) Only one previous study of elbow UCL fixation using cyclic loading has been found. (24) Load-to-failure testing measures the ability of a ligament or graft to resist a sudden traumatic load. On the other hand, cyclical loading more closely resembles the clinical situation, where gradual range of motion exercise is
27 26 initiated as graft healing occurs, rather than forceful valgus loads immediately after reconstruction. Cyclic loading can assess slippage of the graft, and this is important in response to early motion therapy protocols. Clinical failures of elbow UCL reconstruction are more likely due to slippage with resultant laxity and functional impairment rather than traumatic graft rupture. (13) Armstrong et al. compared the docking technique, interference screw technique, figure-of-eight bone tunnel (Jobe technique), and an endobutton ulnar fixation technique. (24) The investigators found that the peak load-to-failure in response to valgus stress was inferior for all four reconstruction methods as compared to the native ligament. Furthermore, the docking technique was stronger than the figure-of-eight technique (peak load-to-failure of 53.0 ± 9.5 N vs ± 7.1 N, p < 0.004). The mean number of cycles sustained before failure or 5 mm of joint gapping was 701 ± 181 cycles for the docking reconstructions and 333 ± 133 cycles for the figure-of-eight reconstructions (p < 0.009). Our results found a similar relationship between the docking and the Jobe reconstructions. Four Jobe reconstructions failed before reaching 1,000 cycles in our study, while no docking reconstructions failed. Armstrong et al. used an increasing cyclic load protocol to find the peak load-to-failure for each reconstruction, beginning with 20 N applied 12 cm away (2.4 N-m valgus moment). (24) Failure occurred at a mean of 53.0 N (6.36 N-m valgus moment) for the docking reconstructions and 33.3 N (3.99 N-m valgus moment) for the Jobe procedure. We applied a constant maximal 5 N-m valgus moment throughout the cyclic testing, which is consistent with findings from Armstrong et
28 27 al. Our design illuminates more than the study from Armstrong et al. because we can judge the performance of the Jobe reconstruction in early valgus loading in a way that more closely resembles step-wise rehabilitation than peak load-tofailure tests. Paletta et al. compared the biomechanical properties of the Jobe reconstruction with those of a modified docking reconstruction (25). The modified docking reconstruction utilizes a 4-strand reconstruction by doubling the palmaris longus tendon graft. The group hypothesized that this modification would result in a reconstruction that would more closely resemble the biomechanical parameters of the native UCL. They used an MTS apparatus to test the specimens; however they applied a valgus moment at a constant rate of 1 mm/s to find the maximal moment to failure, stiffness, strain. Their study differed from ours in two other important ways: they tested the elbows in 30 degrees of flexion and used a 2-camera motion analysis system for data collection. They reported a maximal moment to failure of 18.8 ± 9.1 N-m for the native UCL, 14.3 ± 4.1 for the docking reconstruction, and 8.9 ± 3.8 for the Jobe reconstruction. The maximal moment to failure was significantly greater for intact UCLs as compared to the Jobe reconstruction (p < ). The maximal moment to failure was significantly greater for the docking reconstruction as compared to the Jobe reconstruction (p = ). The results from Paletta et al. show higher peak moments to failure than the Armstrong et al. results and as compared to our results. The difference might be attributable to the differing experimental design, the modified docking
29 28 reconstruction, and the younger elbows used in the Paletta et al. study (around 55 years as compared to 74.5 years in this study). The use of cyclic loading may weaken the reconstruction in a way that would explain why half of our Jobe reconstructions failed with a maximal moment of 5 N-m. The increased maximal moment to failure in the docking reconstructions, as compared to Armstrong et al., is likely due to the modified docking reconstruction. The 4-strand reconstruction can be reasonably expected to be stronger than the traditional 2- strand reconstruction. Despite these differences, Paletta et al. confirms the relative superiority of the docking reconstruction to the Jobe reconstruction in terms of biomechanical parameters. Our study further elucidates the improved response of the docking reconstruction to early cyclic valgus loading. Paletta et al. also reported modes of failure, which were consistent with the modes of failure seen in this study. In Paletta et al. twelve of fifteen Jobe reconstructions failed at the tendon-suture interface. Four of eight of our Jobe reconstructions failed at the tendon-suture interface. They also reported suture failure (1 of 15) and ulnar tunnel fracture (2 of 15) for the Jobe reconstructions. Paletta et al. reported suture failure in twelve of fourteen docking reconstructions, and bone tunnel fracture in two of fourteen docking reconstructions. Since we were not focused on loading our specimens to failure, we saw and expected fewer failures. Conway et al. reported Jobe s initial 13-year experience with the reconstruction. (3) This technique reported excellent outcomes in 75% of major
30 29 league players without previous surgery. An excellent outcome signifies that the patient returned to or exceeded their previous level of competition for at least 1 year. (18) Rohrbaugh et al. reported outcomes of the docking procedure on 36 patients with an average of 3.3 years of follow-up, finding that 92% (33 patients) had excellent results. (18) Similarly, Conway reported excellent outcomes in 97% of 40 throwers after undergoing the docking reconstruction. (15) Our results show less valgus angle displacement when the docking reconstruction is used as compared to the Jobe reconstruction; this finding provides biomechanical evidence to support these previously reported clinical findings. Further clinical study is required to demonstrate clinically that the docking reconstruction is more tolerant to early valgus loading than the Jobe reconstruction. Even more, additional clinical study is required to confirm that earlier rehabilitation leads to improved long-term outcomes in these patients.
31 30 References 1. Cohen, M.S. and Bruno, R.J The collateral ligaments of the elbow. Clin. Orthop. Relat. Res. 383: Andrews, J.R. and Timmerman, L.A Outcome of elbow surgery in professional baseball players. Am. J. Sports Med. 23: Conway, J.E., Jobe, F.W., Glousman, R.E., and Pink, M Medial instability of the elbow in throwing athletes. Treatment by repair or reconstruction of the ulnar collateral ligament. J. Bone Joint Surg. Am. 74: Jobe, F.W., Stark, H., and Lombardo, S.J Reconstruction of the ulnar collateral ligament in athletes. J. Bone Joint Surg. 68A: Yocum, L.A The diagnosis and nonoperative treatment of elbow problems in the athlete. Clin. Sports Med. 8: Neill Cage, D.J., Abrams, R.A., Callahan, J.J., and Botte, M.J Soft Tissue Attachments of the Ulnar Coronoid Process. Clin. Orthop. Relat. Res. 320: Regan, W.D., Korinek, S.L., Morrey, B.F., and Kai-Nan, A Biomechanical study of ligaments around the elbow joint. Clin. Orthop. Relat. Res. 271: Sojbjerg, J.O., Ovesen, J., and Nielsen, S Experimental elbow instability after transection of the medial collateral ligament. Clin. Orthop. Relat. Res. 218: Hechtman, K.S., Tjin-A-Tsoi, E.W., Zvijac, J.E., Uribe, J.W., and Latta, L.L Biomechanics of a less invasive procedure for reconstruction of the ulnar collateral ligament of the elbow. Am. J. Sports Med. 26: Fleisig, G.S., Andrews, J.R., Dillman, C.J., and Escamilla, R.F Kinetics of baseball pitching with implications about injury mechanisms. Am. J. Sports Med. 23: Langer, P., Fadale, P., and Hulstyn, M Evolution of the treatment options of ulnar collateral ligament injuries of the elbow. Br. J. Sports Med. 40: Azar, F.M., Andrews, J.R., Wilk, K.E., and Groh, D Operative treatment of ulnar collateral ligament injuries of the elbow in athletes. Am. J. Sports Med. 28:16-23.
32 McAdams, T.R., Lee, A.T., Centeno, J., Giori, N.J., and Lindsey, D.P Two ulnar collateral ligament reconstruction methods: the docking technique versus bioabsorbable interference screw fixation: a biomechanical evaluation with cyclic loading. J. Shoulder Elbow Surg. In Press. 14. Frank, C.B. and Jackson, D.W Current Concepts Review The Science of Reconstruction of the Anterior Cruciate Ligament. J. Bone Joint Surg. 79: Conway, J.E The DANE TJ Procedure for Elbow Medial Ulnar Collateral Ligament Insufficiency. Techniques in Shoulder and Elbow Surgery. 7: Ahmad, C.S., Lee, T.Q., and ElAttrache, N.S Biomechanical evaluation of a new ulnar collateral ligament reconstruction technique with interference screw fixation. Am. J. Sports Med. 31: Hyman, J., Breazeale, N.M., and Altchek, D.W Valgus instability of the elbow in athletes. Clin. Sports Med. 20: Rohrbough, J.T., Altchek, D.W., Hyman, J., Williams, R.J., and Botts, J.D Medial collateral ligament reconstruction of the elbow using the docking technique. Am. J. Sports Med. 30: Thompson, W.H., Jobe, F.W., Yocum, L.A., and Pink, M.M Ulnar Collateral ligament reconstruction in athletes: Muscle-splitting approach without transposition of the ulnar nerve. J. Shoulder Elbow Surg. 10: Ochi, N., Ogura, T., Hashizuma, H., Shigeyama, Y., Senda, M., and Inoue, H Anatomic relation between the medial collateral ligament of the elbow and the humero-ulnar joint axis. J. Shoulder Elbow Surg. 8: Altchek, D., Hyman, J., Williams, R., et al Management of medial collateral ligament injuries of the elbow in throwers. Techniques in Shoulder and Elbow Surg. 1: Rodeo, S.A., Arnoczky, S.P., Torzilli, P.A., Hidaka, C., and Warren, R.F Tendon-healing in a bone tunnel: A biomechanical and histological study in the dog. J. Bone Joint Surg. Am. 75: Mullen, D.J., Goradia, V.K., Parks, B.G., and Matthews, L.S A biomechanical study of stability of the elbow to valgus stress before and
33 32 after reconstruction of the medial collateral ligament. J. Shoulder Elbow Surg. 11: Armstrong, A.D., Dunning, C.E., Ferreira, L.M., Faber, K.J., Johnson, J.A., et al A biomechanical comparison of four reconstruction techniques for the medial collateral ligament-deficient elbow. J. Shoulder Elbow Surg. 14: Paletta, G.A., Klepps, S.J., Difelice, G.S., Allen, T., Brodt, M.D., et al Biomechanical Evaluation of 2 Techniques for Ulnar Collateral Ligament Reconstruction of the Elbow. Am. J. Sports Med. 34: Callaway, G.H., Field, L.D., Deng, X.H., Torzilli, P.A., O Brien, S.J., et al Biomechanical Evaluation of the Medial Collateral Ligament of the Elbow. J. Bone Joint Surg. Am. 79:
Biomechanics of Two Reconstruction Techniques for Elbow Ulnar Collateral Ligament Insufficiency
 Biomechanics of Two Reconstruction Techniques for Elbow Ulnar Collateral Ligament Insufficiency Justin E. Chronister, MD 1, Randal P. Morris, BS 2, Clark R. Andersen, MS 2, J. Michael Bennett, MD 3, Thomas
Biomechanics of Two Reconstruction Techniques for Elbow Ulnar Collateral Ligament Insufficiency Justin E. Chronister, MD 1, Randal P. Morris, BS 2, Clark R. Andersen, MS 2, J. Michael Bennett, MD 3, Thomas
1. Scope vs No Scope. UCL Reconstruction Variations 11/19/2018. Evolutionary Pressure. Complexity of the Surgery Extensive Dissection
 UCL Reconstruction Variations Christopher S. Ahmad, MD Professor Orthopedic Surgery Chief Sports Medicine Head Team Physician New York Yankees New York City Football Club Evolutionary Pressure Complexity
UCL Reconstruction Variations Christopher S. Ahmad, MD Professor Orthopedic Surgery Chief Sports Medicine Head Team Physician New York Yankees New York City Football Club Evolutionary Pressure Complexity
Medial Collateral Instability of the Elbow. CSES Residents Course Calgary AB February 1-3, 2017 WD Regan MD
 Medial Collateral Instability of the Elbow CSES Residents Course Calgary AB February 1-3, 2017 WD Regan MD Disclosures I have no disclosures to report Anatomy Medial Collateral Ligament Anterior Oblique
Medial Collateral Instability of the Elbow CSES Residents Course Calgary AB February 1-3, 2017 WD Regan MD Disclosures I have no disclosures to report Anatomy Medial Collateral Ligament Anterior Oblique
I (and/or my co-authors) have something to disclose.
 Elbow Anatomy And Biomechanics Nikhil N Verma, MD Director, Division of Sports Medicine Professor, Department of Orthopedics Rush University Medical Center Team Physician, Chicago White Sox and Bulls I
Elbow Anatomy And Biomechanics Nikhil N Verma, MD Director, Division of Sports Medicine Professor, Department of Orthopedics Rush University Medical Center Team Physician, Chicago White Sox and Bulls I
Disclosures. Throwing is NOT Normal MCL RECONSTRUCTION: INDICATIONS, TECHNIQUE, RESULTS. Joshua S. Dines, MD. Sports Medicine and Shoulder Service
 MCL RECONSTRUCTION: INDICATIONS, TECHNIQUE, RESULTS Joshua S. Dines, MD Sports Medicine and Shoulder Service Disclosures Consultant: Arthrex, Conmed Linvatec, Ossur IP/Royalties: Conmed Linvatec Editorial
MCL RECONSTRUCTION: INDICATIONS, TECHNIQUE, RESULTS Joshua S. Dines, MD Sports Medicine and Shoulder Service Disclosures Consultant: Arthrex, Conmed Linvatec, Ossur IP/Royalties: Conmed Linvatec Editorial
Rehabilitation Guidelines for UCL Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for UCL Repair The elbow is a complex system of three joints formed from three bones; the humerus (the upper arm bone), the ulna (the larger bone
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for UCL Repair The elbow is a complex system of three joints formed from three bones; the humerus (the upper arm bone), the ulna (the larger bone
Biomechanical Comparison of Ulnar Collateral Ligament Reconstruction With the Docking Technique Versus Repair With Internal Bracing
 Biomechanical Comparison of Ulnar Collateral Ligament Reconstruction With the Docking Technique Versus Repair With Internal Bracing 5-in-5 Blake M. Bodendorfer,* MD, Austin M. Looney,* MD, Sloane L. Lipkin,
Biomechanical Comparison of Ulnar Collateral Ligament Reconstruction With the Docking Technique Versus Repair With Internal Bracing 5-in-5 Blake M. Bodendorfer,* MD, Austin M. Looney,* MD, Sloane L. Lipkin,
Throwing is NOT Normal TREATMENT OF ELBOW INJURIES. Joshua S. Dines, MD IN OVERHEAD ATHLETES: HOW HAS IT EVOLVED?
 TREATMENT OF ELBOW INJURIES IN OVERHEAD ATHLETES: HOW HAS IT EVOLVED? Joshua S. Dines, MD Sports Medicine and Shoulder Service Hospital for Special Surgery Throwing is NOT Normal Excessive Joint Forces
TREATMENT OF ELBOW INJURIES IN OVERHEAD ATHLETES: HOW HAS IT EVOLVED? Joshua S. Dines, MD Sports Medicine and Shoulder Service Hospital for Special Surgery Throwing is NOT Normal Excessive Joint Forces
ADVENTURES AND LESSONS LEARNED ON THE UCL
 ADVENTURES AND LESSONS LEARNED ON THE UCL Michael G. Ciccotti, M.D. Department of Orthopaedics The Rothman Institute Thomas Jefferson University Philadelphia, PA Eastern Athletic Trainers Association Philadelphia,
ADVENTURES AND LESSONS LEARNED ON THE UCL Michael G. Ciccotti, M.D. Department of Orthopaedics The Rothman Institute Thomas Jefferson University Philadelphia, PA Eastern Athletic Trainers Association Philadelphia,
A biomechanical evaluation of a novel surgical reconstruction technique of the ulnar collateral ligament of the elbow joint
 University of South Florida Scholar Commons Graduate Theses and Dissertations Graduate School 2008 A biomechanical evaluation of a novel surgical reconstruction technique of the ulnar collateral ligament
University of South Florida Scholar Commons Graduate Theses and Dissertations Graduate School 2008 A biomechanical evaluation of a novel surgical reconstruction technique of the ulnar collateral ligament
First awareness of problems with the ulnar collateral ligament. Ulnar Collateral Ligament Reconstruction
 Ulnar Collateral Ligament Reconstruction Richard Lehman, md Ulnar collateral ligament reconstruction, which is commonly known as Tommy John surgery, was first performed on Tommy John who was a pitcher
Ulnar Collateral Ligament Reconstruction Richard Lehman, md Ulnar collateral ligament reconstruction, which is commonly known as Tommy John surgery, was first performed on Tommy John who was a pitcher
on the elbow. Individuals, but most typically overhead athletes may injure this ligament,
 Ulnar Collateral Ligament Repair Niomi Eipp Robert Osborne Brittany Young Abstract The ulnar collateral ligament, specifically the anterior bundle, resists valgus force on the elbow. Individuals, but most
Ulnar Collateral Ligament Repair Niomi Eipp Robert Osborne Brittany Young Abstract The ulnar collateral ligament, specifically the anterior bundle, resists valgus force on the elbow. Individuals, but most
Introduction. Anatomy
 Introduction The doctors call it a UCLR ulnar collateral ligament reconstruction. Baseball players and fans call it Tommy John surgery -- named after the pitcher (Los Angeles Dodgers) who was the first
Introduction The doctors call it a UCLR ulnar collateral ligament reconstruction. Baseball players and fans call it Tommy John surgery -- named after the pitcher (Los Angeles Dodgers) who was the first
Jin-Young Park, MD, Kyung-Soo Oh, MD, Seung-Chul Bahng, MD, Seok-Won Chung, MD, Jin-Ho Choi, MD
 Original Article Clinics in Orthopedic Surgery 2014;6:190-195 http://dx.doi.org/10.4055/cios.2014.6.2.190 Does Well Maintained Graft Provide Consistent Return to Play after Medial Ulnar Collateral Ligament
Original Article Clinics in Orthopedic Surgery 2014;6:190-195 http://dx.doi.org/10.4055/cios.2014.6.2.190 Does Well Maintained Graft Provide Consistent Return to Play after Medial Ulnar Collateral Ligament
MEDIAL ELBOW INSTABILITY
 MEDIAL ELBOW INSTABILITY Felix H. Savoie III, MD Ray J. Haddad Professor & Chairman Department of Orthopaedic Surgery Tulane University New Orleans, LA Royalties: none Stock: none Stock option: Cayenne
MEDIAL ELBOW INSTABILITY Felix H. Savoie III, MD Ray J. Haddad Professor & Chairman Department of Orthopaedic Surgery Tulane University New Orleans, LA Royalties: none Stock: none Stock option: Cayenne
Minimally Invasive ACL Surgery
 Minimally Invasive ACL Surgery KOCO EATON, M.D. T A M P A B A Y R A Y S ( 1 9 9 5 P R E S E N T ) T A M P A B A Y B U C C A N E E R S ( 2 0 1 5 2 0 1 6 ) T A M P A B A Y R O W D I E S ( 2 0 1 4 2 0 1 7
Minimally Invasive ACL Surgery KOCO EATON, M.D. T A M P A B A Y R A Y S ( 1 9 9 5 P R E S E N T ) T A M P A B A Y B U C C A N E E R S ( 2 0 1 5 2 0 1 6 ) T A M P A B A Y R O W D I E S ( 2 0 1 4 2 0 1 7
Slide 1. Slide 2. Slide 3. The Thrower s Elbow: When to Operate. Medial Elbow Pain in the Athlete. Goal of This Talk
 Slide 1 The Thrower s Elbow: When to Operate Luke S. Oh, MD Massachusetts General Hospital Team Physician, Boston Red Sox Team Physician, New England Revolution Consultant, Harvard University Athletics
Slide 1 The Thrower s Elbow: When to Operate Luke S. Oh, MD Massachusetts General Hospital Team Physician, Boston Red Sox Team Physician, New England Revolution Consultant, Harvard University Athletics
Patient Education Ulnar Collateral Ligament Reconstruction
 Explanation of Procedure and/or Diagnosis Overview is commonly referred to as Tommy John Surgery. Tommy John was a baseball pitcher who played for the Los Angeles Dodgers. He was the first person to have
Explanation of Procedure and/or Diagnosis Overview is commonly referred to as Tommy John Surgery. Tommy John was a baseball pitcher who played for the Los Angeles Dodgers. He was the first person to have
Medial Elbow Instability & Ulnar Collateral Ligament Reconstruction in a Collegiate Baseball Player.
 Medial Elbow Instability & Ulnar Collateral Ligament Reconstruction in a Collegiate Baseball Player www.fisiokinesiterapia.biz PLAN for the day: Brief introduction Review of elbow anatomy Ulnar Collateral
Medial Elbow Instability & Ulnar Collateral Ligament Reconstruction in a Collegiate Baseball Player www.fisiokinesiterapia.biz PLAN for the day: Brief introduction Review of elbow anatomy Ulnar Collateral
Four-Bundle Cortical-Button Ulnar Collateral Ligament Reconstruction
 Four-Bundle Cortical-Button Ulnar Collateral Ligament Reconstruction Matthew H. Blake, MD 1 G. Russell Huffman, MD, MPH 1 1 Department of Orthopaedic Surgery University of Pennsylvania Ulnar collateral
Four-Bundle Cortical-Button Ulnar Collateral Ligament Reconstruction Matthew H. Blake, MD 1 G. Russell Huffman, MD, MPH 1 1 Department of Orthopaedic Surgery University of Pennsylvania Ulnar collateral
A Patient s Guide to. Ulnar Collateral Ligament Reconstruction (Tommy John Surgery)
 A Patient s Guide to Ulnar Collateral Ligament Reconstruction (Tommy John Surgery) 228 West Main St., Suite D Missoula, MT 59802-4345 Phone: 406-721-3072 Fax: 406-721-2619 info@eorthopod.com DISCLAIMER:
A Patient s Guide to Ulnar Collateral Ligament Reconstruction (Tommy John Surgery) 228 West Main St., Suite D Missoula, MT 59802-4345 Phone: 406-721-3072 Fax: 406-721-2619 info@eorthopod.com DISCLAIMER:
Recurrent and Chronic Elbow Instability
 Recurrent and Chronic Elbow Instability Elbow instability is a looseness in the elbow joint that may cause the joint to catch, pop, or slide out of place during certain arm movements. It most often occurs
Recurrent and Chronic Elbow Instability Elbow instability is a looseness in the elbow joint that may cause the joint to catch, pop, or slide out of place during certain arm movements. It most often occurs
Ulnar Collateral Ligament Reconstruction
 Ulnar Collateral Ligament Reconstruction 1. Defined a. The ulnar collateral ligament is critical for valgus stability of the elbow. It serves as the primary elbow stabilizer and as such, serves a very
Ulnar Collateral Ligament Reconstruction 1. Defined a. The ulnar collateral ligament is critical for valgus stability of the elbow. It serves as the primary elbow stabilizer and as such, serves a very
Adam J. Seidl, MD Assistant Professor University of Colorado School of Medicine Shoulder & Elbow Surgery Division of Sports Medicine and Shoulder
 Adam J. Seidl, MD Assistant Professor University of Colorado School of Medicine Shoulder & Elbow Surgery Division of Sports Medicine and Shoulder Surgery Division of Hand, Wrist, and Elbow Surgery Anatomy
Adam J. Seidl, MD Assistant Professor University of Colorado School of Medicine Shoulder & Elbow Surgery Division of Sports Medicine and Shoulder Surgery Division of Hand, Wrist, and Elbow Surgery Anatomy
Functional Anatomy of the Elbow
 Functional Anatomy of the Elbow Orthopedic Institute Daryl C. Osbahr, M.D. Chief of Sports Medicine, Orlando Health Chief Medical Officer, Orlando City Soccer Club Orthopedic Consultant, Washington Nationals
Functional Anatomy of the Elbow Orthopedic Institute Daryl C. Osbahr, M.D. Chief of Sports Medicine, Orlando Health Chief Medical Officer, Orlando City Soccer Club Orthopedic Consultant, Washington Nationals
Sports Medicine Unit 16 Elbow
 Sports Medicine Unit 16 Elbow I. Bones a. b. c. II. What movements does the elbow perform? a. Flexion b. c. Pronation d. III. Muscles in motion a. FLEXION (supinated) i Brachialis (pronated) ii (neutral)
Sports Medicine Unit 16 Elbow I. Bones a. b. c. II. What movements does the elbow perform? a. Flexion b. c. Pronation d. III. Muscles in motion a. FLEXION (supinated) i Brachialis (pronated) ii (neutral)
Terrible Triad: Tricks for Dealing with the Unstable Elbow
 Terrible Triad: Tricks for Dealing with the Unstable Elbow Mark A. Mighell, MD Kaitlyn N. Christmas, BS Disclosure Paid Consultation Research Support Speakers Bureau Paid Consultation Speakers Bureau The
Terrible Triad: Tricks for Dealing with the Unstable Elbow Mark A. Mighell, MD Kaitlyn N. Christmas, BS Disclosure Paid Consultation Research Support Speakers Bureau Paid Consultation Speakers Bureau The
UvA-DARE (Digital Academic Repository) Radial head fracture: a potentially complex injury Kaas, L. Link to publication
 UvA-DARE (Digital Academic Repository) Radial head fracture: a potentially complex injury Kaas, L. Link to publication Citation for published version (APA): Kaas, L. (2012). Radial head fracture: a potentially
UvA-DARE (Digital Academic Repository) Radial head fracture: a potentially complex injury Kaas, L. Link to publication Citation for published version (APA): Kaas, L. (2012). Radial head fracture: a potentially
MEDIAL EPICONDYLE FRACTURES
 MEDIAL EPICONDYLE FRACTURES Demographic 20% of elbow fractures 60% of which are associated with elbow dislocation. 75% in boys between 6-12 years 20% of elbow dislocation with ME fracture, the ME is incarcerated
MEDIAL EPICONDYLE FRACTURES Demographic 20% of elbow fractures 60% of which are associated with elbow dislocation. 75% in boys between 6-12 years 20% of elbow dislocation with ME fracture, the ME is incarcerated
Elbow Elbow Anatomy. Flexion extension. Pronation Supination. Anatomy. Anatomy. Romina Astifidis, MS., PT., CHT
 Elbow Elbow Anatomy Romina Astifidis, MS., PT., CHT Curtis National Hand Center Baltimore, MD October 6-8, 2017 Link between the arm and forearm to position the hand in space Not just a hinge Elbow = 70%
Elbow Elbow Anatomy Romina Astifidis, MS., PT., CHT Curtis National Hand Center Baltimore, MD October 6-8, 2017 Link between the arm and forearm to position the hand in space Not just a hinge Elbow = 70%
A Patient s Guide to Ulnar Collateral Ligament Injuries
 A Patient s Guide to Ulnar Collateral Ligament Injuries 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information
A Patient s Guide to Ulnar Collateral Ligament Injuries 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information
The Biomechanics of the Human Upper Extremity-The Elbow Joint C. Mirzanli Istanbul Gelisim University
 The Biomechanics of the Human Upper Extremity-The Elbow Joint C. Mirzanli Istanbul Gelisim University Structure of The Elbow Joint A simple hinge joint, actually categorized as a trochoginglymus joint
The Biomechanics of the Human Upper Extremity-The Elbow Joint C. Mirzanli Istanbul Gelisim University Structure of The Elbow Joint A simple hinge joint, actually categorized as a trochoginglymus joint
Anterior Elbow Capsulodesis
 7(1):72 76, 2006 m R E V I E W m Anterior Elbow Capsulodesis Donald H. Lee, MD, Douglas R. Weikert, and Jeffry T. Watson Department of Orthopaedic Surgery Vanderbilt Orthopaedic Institute Nashville, TN
7(1):72 76, 2006 m R E V I E W m Anterior Elbow Capsulodesis Donald H. Lee, MD, Douglas R. Weikert, and Jeffry T. Watson Department of Orthopaedic Surgery Vanderbilt Orthopaedic Institute Nashville, TN
No financial disclosures
 Thomas J. Noonan, MD Steadman Hawkins Clinic Denver University of Colorado No financial disclosures Thomas Noonan, Gregory Ford, James Genuario, Jason Kinkartz, Thomas Githens, Scott Murayama Steadman
Thomas J. Noonan, MD Steadman Hawkins Clinic Denver University of Colorado No financial disclosures Thomas Noonan, Gregory Ford, James Genuario, Jason Kinkartz, Thomas Githens, Scott Murayama Steadman
The Elbow and the cubital fossa. Prof Oluwadiya Kehinde
 The Elbow and the cubital fossa Prof Oluwadiya Kehinde www.oluwadiya.com Elbow and Forearm Anatomy The elbow joint is formed by the humerus, radius, and the ulna Bony anatomy of the elbow Distal Humerus
The Elbow and the cubital fossa Prof Oluwadiya Kehinde www.oluwadiya.com Elbow and Forearm Anatomy The elbow joint is formed by the humerus, radius, and the ulna Bony anatomy of the elbow Distal Humerus
Revision Tommy John. Disclosure. Revision UCL Recon 11/11/2016. Christopher S. Ahmad, MD
 Revision Tommy John Christopher S. Ahmad, MD Professor of Orthopaedic Surgery Chief of Sports Medicine Head Team Physician New York Yankees Disclosure 1. Basic Science Support a. Arthrex b. Smith-Nephew
Revision Tommy John Christopher S. Ahmad, MD Professor of Orthopaedic Surgery Chief of Sports Medicine Head Team Physician New York Yankees Disclosure 1. Basic Science Support a. Arthrex b. Smith-Nephew
Elbow Injuries in the Throwing Athlete
 Elbow Injuries in the Throwing Athlete Overhand throwing places extremely high stresses on the elbow. In baseball pitchers and other throwing athletes, these high stresses are repeated many times and can
Elbow Injuries in the Throwing Athlete Overhand throwing places extremely high stresses on the elbow. In baseball pitchers and other throwing athletes, these high stresses are repeated many times and can
Risk Factors Leading to UCL Reconstruction and Revision Surgery: A Case Report of a Division I Collegiate Pitcher
 Skyline - The Big Sky Undergraduate Journal Volume 2 Issue 1 Article 2 2014 Risk Factors Leading to UCL Reconstruction and Revision Surgery: A Case Report of a Division I Collegiate Pitcher Taylor M. Bennett
Skyline - The Big Sky Undergraduate Journal Volume 2 Issue 1 Article 2 2014 Risk Factors Leading to UCL Reconstruction and Revision Surgery: A Case Report of a Division I Collegiate Pitcher Taylor M. Bennett
Double Bundle PCL Reconstruction. Surgical Technique
 Double Bundle PCL Reconstruction Surgical Technique Double Bundle PCL Reconstruction With recent interest in double tunnel endoscopic PCL reconstruction, Arthrex has created a series of Femoral PCL Drill
Double Bundle PCL Reconstruction Surgical Technique Double Bundle PCL Reconstruction With recent interest in double tunnel endoscopic PCL reconstruction, Arthrex has created a series of Femoral PCL Drill
MUCL REPAIR. Felix H. Savoie III, MD Ray J. Haddad Professor & Chairman Department of Orthopaedic Surgery Tulane University New Orleans, LA
 MUCL REPAIR Felix H. Savoie III, MD Ray J. Haddad Professor & Chairman Department of Orthopaedic Surgery Tulane University New Orleans, LA MUCL INJURY EPIDEMIC Frequency increasing despite major efforts
MUCL REPAIR Felix H. Savoie III, MD Ray J. Haddad Professor & Chairman Department of Orthopaedic Surgery Tulane University New Orleans, LA MUCL INJURY EPIDEMIC Frequency increasing despite major efforts
Bipolar Radial Head System
 Bipolar Radial Head System Katalyst Surgical Technique DESCRIPTION The Katalyst Telescoping Bipolar Radial Head implant restores the support and bearing surface of the radial head in the face of fracture,
Bipolar Radial Head System Katalyst Surgical Technique DESCRIPTION The Katalyst Telescoping Bipolar Radial Head implant restores the support and bearing surface of the radial head in the face of fracture,
Elbow Anatomy, Growth and Physical Exam. Donna M. Pacicca, MD Section of Sports Medicine Division of Orthopaedic Surgery Children s Mercy Hospital
 Elbow Anatomy, Growth and Physical Exam Donna M. Pacicca, MD Section of Sports Medicine Division of Orthopaedic Surgery Children s Mercy Hospital Contributing Factors to Elbow Injury The elbow is affected
Elbow Anatomy, Growth and Physical Exam Donna M. Pacicca, MD Section of Sports Medicine Division of Orthopaedic Surgery Children s Mercy Hospital Contributing Factors to Elbow Injury The elbow is affected
The Upper Limb. Elbow Rotation 4/25/18. Dr Peter Friis
 The Upper Limb Dr Peter Friis Elbow Rotation Depending upon the sport, the elbow moves through an arc of approximately 75⁰ to 100⁰ in about 20 to 35 msec. The resultant angular velocity is between 1185
The Upper Limb Dr Peter Friis Elbow Rotation Depending upon the sport, the elbow moves through an arc of approximately 75⁰ to 100⁰ in about 20 to 35 msec. The resultant angular velocity is between 1185
Other Elbow Concerns in Overhead Athletes
 Other Elbow Concerns in Overhead Athletes John A. Steubs, M.D. Team Physician, Minnesota Twins TRIA Orthopaedic Center Disclosures None relevant to this presentation. Other Elbow Problems Valgus extension
Other Elbow Concerns in Overhead Athletes John A. Steubs, M.D. Team Physician, Minnesota Twins TRIA Orthopaedic Center Disclosures None relevant to this presentation. Other Elbow Problems Valgus extension
Upper Limb Biomechanics SCHOOL OF HUMAN MOVEMENT STUDIES
 Upper Limb Biomechanics Phases of throwing motion 1. Wind up Starts: initiate first movement Ends: lead leg is lifted & throwing hand removed from glove COG raised 2. Early Cocking Start: lead leg is lifted
Upper Limb Biomechanics Phases of throwing motion 1. Wind up Starts: initiate first movement Ends: lead leg is lifted & throwing hand removed from glove COG raised 2. Early Cocking Start: lead leg is lifted
Rehabilitation after Total Elbow Arthroplasty
 Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
Disclosures. UCL Reconstruction: Technical Variations 11/18/2016. UCLR: Technical Variations
 UCL Reconstruction: Technical Variations Anthony A. Romeo, MD Professor, Department of Orthopedics Rush University Medical Center Section Head, Shoulder and Elbow Chicago, Illinois Disclosures 1. Royalties:
UCL Reconstruction: Technical Variations Anthony A. Romeo, MD Professor, Department of Orthopedics Rush University Medical Center Section Head, Shoulder and Elbow Chicago, Illinois Disclosures 1. Royalties:
Key Factors: Rehabilitation After Elbow Dislocation
 VOLUME 21 ISSUE 2 SUMMER 2014 TIMES THE NEWSLETTER OF THE AMERICAN SOCIETY OF HAND THERAPISTS CONTENTS 1 Key Factors: Rehabilitation After Elbow Dislocation 3 President s Message 4 Editor s Letter 5 Meet
VOLUME 21 ISSUE 2 SUMMER 2014 TIMES THE NEWSLETTER OF THE AMERICAN SOCIETY OF HAND THERAPISTS CONTENTS 1 Key Factors: Rehabilitation After Elbow Dislocation 3 President s Message 4 Editor s Letter 5 Meet
Elbow Injuries in the Adult Athlete. Tamara A. Scerpella, MD Professor, Orthopedic Surgery University of Wisconsin
 Elbow Injuries in the Adult Athlete Tamara A. Scerpella, MD Professor, Orthopedic Surgery University of Wisconsin Acute Elbow Dislocation Fracture Distal humerus Olecranon Radial head Distal Biceps Rupture
Elbow Injuries in the Adult Athlete Tamara A. Scerpella, MD Professor, Orthopedic Surgery University of Wisconsin Acute Elbow Dislocation Fracture Distal humerus Olecranon Radial head Distal Biceps Rupture
Extensor Mechanism Rupture
 Extensor Mechanism Rupture Repair or Augmentation Michael J. Stuart MD Mayo Clinic Rochester, MN Michael J. Stuart MD February 25, 2018 Financial Relationships Consultant & Royalties- Arthrex Research
Extensor Mechanism Rupture Repair or Augmentation Michael J. Stuart MD Mayo Clinic Rochester, MN Michael J. Stuart MD February 25, 2018 Financial Relationships Consultant & Royalties- Arthrex Research
Throwing Injuries and Prevention: The Physical Therapy Perspective
 Throwing Injuries and Prevention: The Physical Therapy Perspective Andrew M Jordan, PT, DPT, OCS Staff Physical Therapist, Cayuga Medical Center Physical Therapy and Sports Medicine ajordan@cayugamed.org
Throwing Injuries and Prevention: The Physical Therapy Perspective Andrew M Jordan, PT, DPT, OCS Staff Physical Therapist, Cayuga Medical Center Physical Therapy and Sports Medicine ajordan@cayugamed.org
Elbow & Forearm H O W V I T A L I S T H E E L B O W T O O U R D A I L Y L I V E S?
 Elbow & Forearm H O W V I T A L I S T H E E L B O W T O O U R D A I L Y L I V E S? Clarification of Terms The elbow includes: 3 bones (humerus, radius, and ulna) 2 joints (humeroulnar and humeroradial)
Elbow & Forearm H O W V I T A L I S T H E E L B O W T O O U R D A I L Y L I V E S? Clarification of Terms The elbow includes: 3 bones (humerus, radius, and ulna) 2 joints (humeroulnar and humeroradial)
Upper Extremity Injuries in Youth Baseball: Causes and Prevention
 Upper Extremity Injuries in Youth Baseball: Causes and Prevention Biomechanics Throwing a baseball is an unnatural movement Excessively high forces are generated at the elbow and shoulder Throwing requires
Upper Extremity Injuries in Youth Baseball: Causes and Prevention Biomechanics Throwing a baseball is an unnatural movement Excessively high forces are generated at the elbow and shoulder Throwing requires
Elbow Joint Anatomy ELBOW ANATOMY, BIOMECHANICS. Bone Anatomy. Bone Anatomy. Property of VOMPTI, LLC
 ELBOW ANATOMY, BIOMECHANICS AND PATHOLOGY Kristin Kelley, DPT, OCS, FAAOMPT Elbow Joint Anatomy Joint articulations Humeroulnar Radiohumeral Radioulnar (proximal and distal) Orthopaedic Manual Physical
ELBOW ANATOMY, BIOMECHANICS AND PATHOLOGY Kristin Kelley, DPT, OCS, FAAOMPT Elbow Joint Anatomy Joint articulations Humeroulnar Radiohumeral Radioulnar (proximal and distal) Orthopaedic Manual Physical
ACL Primary Repair Surgical Technique
 ACL Primary Repair Surgical Technique ACL Primary Repair ACL Primary Repair BioComposite SwiveLock and Labral Scorpion Suture Passing Technology There has been a recent resurgence of interest in the possibility
ACL Primary Repair Surgical Technique ACL Primary Repair ACL Primary Repair BioComposite SwiveLock and Labral Scorpion Suture Passing Technology There has been a recent resurgence of interest in the possibility
Osteology of the Elbow and Forearm Complex. The ability to perform many activities of daily living (ADL) depends upon the elbow.
 Osteology of the Elbow and Forearm Complex The ability to perform many activities of daily living (ADL) depends upon the elbow. Activities of Daily Living (ADL) Can you think of anything that you do to
Osteology of the Elbow and Forearm Complex The ability to perform many activities of daily living (ADL) depends upon the elbow. Activities of Daily Living (ADL) Can you think of anything that you do to
Lateral Ulnar Collateral Ligament Reconstruction: An Analysis of Ulnar Tunnel Locations
 An Original Study Lateral Ulnar Collateral Ligament Reconstruction: An Analysis of Ulnar Tunnel Locations Oke A. Anakwenze, MD, Krishn Khanna, MD, William N. Levine, MD, and Christopher S. Ahmad, MD Abstract
An Original Study Lateral Ulnar Collateral Ligament Reconstruction: An Analysis of Ulnar Tunnel Locations Oke A. Anakwenze, MD, Krishn Khanna, MD, William N. Levine, MD, and Christopher S. Ahmad, MD Abstract
Grundkurs SGSM-SSMS Sion Sports Elbow. Dr Stéphane Kämpfen
 Grundkurs SGSM-SSMS Sion 2015 Sports Elbow Dr Stéphane Kämpfen Type of pathologies! Acute:! Fractures - dislocation! Sprain! Chronic:! Overload syndrome Fractures - Radial head: Mason classification Mason
Grundkurs SGSM-SSMS Sion 2015 Sports Elbow Dr Stéphane Kämpfen Type of pathologies! Acute:! Fractures - dislocation! Sprain! Chronic:! Overload syndrome Fractures - Radial head: Mason classification Mason
The American Journal of Sports Medicine
 The American Journal of Sports Medicine http://ajs.sagepub.com/ Outcome of Ulnar Collateral Ligament Reconstruction of the Elbow in 1281 Athletes : Results in 743 Athletes With Minimum 2-Year Follow-up
The American Journal of Sports Medicine http://ajs.sagepub.com/ Outcome of Ulnar Collateral Ligament Reconstruction of the Elbow in 1281 Athletes : Results in 743 Athletes With Minimum 2-Year Follow-up
Main Menu. Wrist and Hand Joints click here. The Power is in Your Hands
 1 The Wrist and Hand Joints click here Main Menu K.5 http://www.handsonlineeducation.com/classes/k5/k5entry.htm[3/23/18, 1:40:40 PM] Bones 29 bones, including radius and ulna 8 carpal bones in 2 rows of
1 The Wrist and Hand Joints click here Main Menu K.5 http://www.handsonlineeducation.com/classes/k5/k5entry.htm[3/23/18, 1:40:40 PM] Bones 29 bones, including radius and ulna 8 carpal bones in 2 rows of
Triceps Tendon Fascia for Collateral Ligament Reconstruction About the Elbow: A Clinical and Biomechanical Evaluation
 An Original Study Triceps Tendon Fascia for Collateral Ligament Reconstruction About the Elbow: A Clinical and Biomechanical Evaluation C. Ryan Martin, MD, Kevin A. Hildebrand, MD, FRCSC James Baergen,
An Original Study Triceps Tendon Fascia for Collateral Ligament Reconstruction About the Elbow: A Clinical and Biomechanical Evaluation C. Ryan Martin, MD, Kevin A. Hildebrand, MD, FRCSC James Baergen,
Inspection. Physical Examination of the Elbow. Anterior Elbow 2/14/2017. Inspection. Carrying angle. Lateral dimple. Physical Exam of the Elbow
 of the Elbow Anthony A. Romeo, MD Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Rush University President-Elect, American Shoulder Elbow Surgeons Team Physician, Chicago
of the Elbow Anthony A. Romeo, MD Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Rush University President-Elect, American Shoulder Elbow Surgeons Team Physician, Chicago
AFX. Femoral Implant. System. The AperFix. AM Portal Surgical Technique Guide. with the. The AperFix System with the AFX Femoral Implant
 The AperFix System AFX with the Femoral Implant AM Portal Surgical Technique Guide The Cayenne Medical AperFix system with the AFX Femoral Implant is the only anatomic system for soft tissue ACL reconstruction
The AperFix System AFX with the Femoral Implant AM Portal Surgical Technique Guide The Cayenne Medical AperFix system with the AFX Femoral Implant is the only anatomic system for soft tissue ACL reconstruction
Early Elbow Motion Protocol Ligament Repair of the elbow
 499 Blossom Hill Rd, San Jose, Ca 95123 Tel: 408-268-8536 Fax: 408-268-8727 www.handsoncaretherapy.com Early Elbow Motion Protocol Ligament Repair of the elbow EARLY MOTION PROTOCOL 1-3 DAYS POST OP LIGAMENT
499 Blossom Hill Rd, San Jose, Ca 95123 Tel: 408-268-8536 Fax: 408-268-8727 www.handsoncaretherapy.com Early Elbow Motion Protocol Ligament Repair of the elbow EARLY MOTION PROTOCOL 1-3 DAYS POST OP LIGAMENT
AJSM PreView, published on March 29, 2010 as doi: /
 AJSM PreView, published on March 29, 2010 as doi:10.1177/0363546509359060 Clinical Follow-up of Professional Baseball Players Undergoing Ulnar Collateral Ligament Reconstruction Using the New Kerlan-Jobe
AJSM PreView, published on March 29, 2010 as doi:10.1177/0363546509359060 Clinical Follow-up of Professional Baseball Players Undergoing Ulnar Collateral Ligament Reconstruction Using the New Kerlan-Jobe
2.7 mm/3.5 mm Variable Angle LCP Elbow System DJ9257-B 1
 2.7 mm/3.5 mm Variable Angle LCP Elbow System DJ9257-B 1 System overview Simply complete: A comprehensive system, consisting of five (5) distal humerus plates and three (3) types of olecranon plates Implant
2.7 mm/3.5 mm Variable Angle LCP Elbow System DJ9257-B 1 System overview Simply complete: A comprehensive system, consisting of five (5) distal humerus plates and three (3) types of olecranon plates Implant
Clinical Orthopaedic Rehabilitation Volume 1 and 2
 Clinical Orthopaedic Rehabilitation Volume 1 and 2 COURSE DESCRIPTION This program is a practical, clinical guide that provides guidance on the evaluation, differential diagnosis, treatment, and rehabilitation
Clinical Orthopaedic Rehabilitation Volume 1 and 2 COURSE DESCRIPTION This program is a practical, clinical guide that provides guidance on the evaluation, differential diagnosis, treatment, and rehabilitation
Evaluation of Elbow and Shoulder Problems in Professional Baseball Pitchers
 An Original Sudy Evaluation of Elbow and Shoulder Problems in Professional Baseball Pitchers William A. Grana, MD, MPH, James B. Boscardin, MD, Herman J. Schneider, ATC/L, Scott H. Takao, MEd, ATC/L, Tomas
An Original Sudy Evaluation of Elbow and Shoulder Problems in Professional Baseball Pitchers William A. Grana, MD, MPH, James B. Boscardin, MD, Herman J. Schneider, ATC/L, Scott H. Takao, MEd, ATC/L, Tomas
Platelet-Rich Plasma Can Be Used to Successfully Treat Elbow Ulnar Collateral Ligament Insufficiency in High- Level Throwers
 Platelet-Rich Plasma Can Be Used to Successfully Treat Elbow Ulnar Collateral Ligament Insufficiency in High- Level Throwers Am J Orthop. 2016 May;45(4):296-300 Authors: Dines JS Williams PN Elattrache
Platelet-Rich Plasma Can Be Used to Successfully Treat Elbow Ulnar Collateral Ligament Insufficiency in High- Level Throwers Am J Orthop. 2016 May;45(4):296-300 Authors: Dines JS Williams PN Elattrache
Terrible triad of the elbow
 Terrible triad of the elbow Vasu Pai ? Terrible triad of the elbow" Posterior dislocation of the elbow + Fractures of the radial head + Fracture of coronoid process Uncommon injury 5% of dislocation Problems
Terrible triad of the elbow Vasu Pai ? Terrible triad of the elbow" Posterior dislocation of the elbow + Fractures of the radial head + Fracture of coronoid process Uncommon injury 5% of dislocation Problems
Meniscus cartilage replacement with cadaveric
 Technical Note Meniscal Allografting: The Three-Tunnel Technique Kevin R. Stone, M.D., and Ann W. Walgenbach, R.N.N.P., M.S.N. Abstract: This technical note describes an improved arthroscopic technique
Technical Note Meniscal Allografting: The Three-Tunnel Technique Kevin R. Stone, M.D., and Ann W. Walgenbach, R.N.N.P., M.S.N. Abstract: This technical note describes an improved arthroscopic technique
ARM Brachium Musculature
 ARM Brachium Musculature Coracobrachialis coracoid process of the scapula medial shaft of the humerus at about its middle 1. flexes the humerus 2. assists to adduct the humerus Blood: muscular branches
ARM Brachium Musculature Coracobrachialis coracoid process of the scapula medial shaft of the humerus at about its middle 1. flexes the humerus 2. assists to adduct the humerus Blood: muscular branches
A Patient s Guide to Biceps Rupture. William T. Grant, MD
 A Patient s Guide to Biceps Rupture Dr. Grant is a talented orthopedic surgeon with more than 30 years of experience helping people return to their quality of life. He and GM Pugh, PA-C pride themselves
A Patient s Guide to Biceps Rupture Dr. Grant is a talented orthopedic surgeon with more than 30 years of experience helping people return to their quality of life. He and GM Pugh, PA-C pride themselves
1 Humeral fractures 1.13 l Distal humeral fractures Treatment with a splint
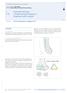 1 Executive Editor: Chris Colton Authors: Mariusz Bonczar, Daniel Rikli, David Ring 1 Humeral fractures 1.13 l Distal humeral fractures Treatment with a splint Indication All 13-A type fractures, excluding
1 Executive Editor: Chris Colton Authors: Mariusz Bonczar, Daniel Rikli, David Ring 1 Humeral fractures 1.13 l Distal humeral fractures Treatment with a splint Indication All 13-A type fractures, excluding
Ligaments of Elbow hinge: sagittal plane so need lateral and medial ligaments
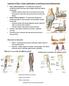 Ligaments of Elbow hinge: sagittal plane so need lateral and medial ligaments Ulnar Collateral ligament on medial side; arising from medial epicondyle and stops excess valgus movement (lateral movement)
Ligaments of Elbow hinge: sagittal plane so need lateral and medial ligaments Ulnar Collateral ligament on medial side; arising from medial epicondyle and stops excess valgus movement (lateral movement)
Non-operative Management of UCL Injuries
 Non-operative Management of UCL Injuries Mark S. Schickendantz, MD Professor of Surgery Director of Sports Medicine Cleveland Clinic Head Team Physician Cleveland Indians Disclosures Arthrex DJO Smith
Non-operative Management of UCL Injuries Mark S. Schickendantz, MD Professor of Surgery Director of Sports Medicine Cleveland Clinic Head Team Physician Cleveland Indians Disclosures Arthrex DJO Smith
Technique Guide. 2.4 mm Variable Angle LCP Distal Radius System. For fragment-specific fracture fixation with variable angle locking technology.
 Technique Guide 2.4 mm Variable Angle LCP Distal Radius System. For fragment-specific fracture fixation with variable angle locking technology. Table of Contents Introduction 2.4 mm Variable Angle LCP
Technique Guide 2.4 mm Variable Angle LCP Distal Radius System. For fragment-specific fracture fixation with variable angle locking technology. Table of Contents Introduction 2.4 mm Variable Angle LCP
ARTICLE IN PRESS. Technical Note
 Technical Note Hybrid Anterior Cruciate Ligament Reconstruction: Introduction of a New Technique for Anatomic Anterior Cruciate Ligament Reconstruction Darren A. Frank, M.D., Gregory T. Altman, M.D., and
Technical Note Hybrid Anterior Cruciate Ligament Reconstruction: Introduction of a New Technique for Anatomic Anterior Cruciate Ligament Reconstruction Darren A. Frank, M.D., Gregory T. Altman, M.D., and
Rehabilitation Guidelines for Labral/Bankert Repair
 Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Chapter 6 The Elbow and Radioulnar Joints
 The Elbow & Radioulnar Chapter 6 The Elbow and Radioulnar Manual of Structural Kinesiology R.T. Floyd, EdD, ATC, CSCS Most upper extremity movements involve the elbow & radioulnar joints Usually grouped
The Elbow & Radioulnar Chapter 6 The Elbow and Radioulnar Manual of Structural Kinesiology R.T. Floyd, EdD, ATC, CSCS Most upper extremity movements involve the elbow & radioulnar joints Usually grouped
Elbow Instability. Derrick G. Hickey, M.D., and Mark I. Loebenberg, M.D. Anatomy. Biomechanics of Elbow Instability
 166 Bulletin of the NYU Hospital for Joint Diseases Volume 64, Numbers 3 & 4, 2006 Elbow Instability Derrick G. Hickey, M.D., and Mark I. Loebenberg, M.D. A variety of conditions can manifest as elbow
166 Bulletin of the NYU Hospital for Joint Diseases Volume 64, Numbers 3 & 4, 2006 Elbow Instability Derrick G. Hickey, M.D., and Mark I. Loebenberg, M.D. A variety of conditions can manifest as elbow
the radial collateral ligament, the lateral ulnar collateral ligament, and the annular ligament 13
 1823 COPYRIGHT 2001 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Ligamentous Stabilizers Against Posterolateral Rotatory Instability of the Elbow BY CYNTHIA E. DUNNING, PHD, ZANE D.S. ZARZOUR,
1823 COPYRIGHT 2001 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Ligamentous Stabilizers Against Posterolateral Rotatory Instability of the Elbow BY CYNTHIA E. DUNNING, PHD, ZANE D.S. ZARZOUR,
Unstable elbow dislocations: a case report of a new surgical technique
 SICOT J 2016, 2, 15 Ó The Authors, published by EDP Sciences, 2016 DOI: 10.1051/sicotj/2016010 Available online at: www.sicot-j.org CASE REPORT OPEN ACCESS Unstable elbow dislocations: a case report of
SICOT J 2016, 2, 15 Ó The Authors, published by EDP Sciences, 2016 DOI: 10.1051/sicotj/2016010 Available online at: www.sicot-j.org CASE REPORT OPEN ACCESS Unstable elbow dislocations: a case report of
The Elbow 3/5/2015. The Elbow Scanning Sequence. * Anterior Joint (The anterior Pyramid ) * Lateral Epicondyle * Medial Epicondyle * Posterior Joint
 Scanning Sequence * Anterior Joint (The anterior Pyramid ) * Lateral Epicondyle * Medial Epicondyle * Posterior Joint Anterior Elbow Pyramid Courtesy of Jay Smith, MD. Vice chair PMR Mayo Clinic Rochester,
Scanning Sequence * Anterior Joint (The anterior Pyramid ) * Lateral Epicondyle * Medial Epicondyle * Posterior Joint Anterior Elbow Pyramid Courtesy of Jay Smith, MD. Vice chair PMR Mayo Clinic Rochester,
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD
 Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
Forearm and Wrist Regions Neumann Chapter 7
 Forearm and Wrist Regions Neumann Chapter 7 REVIEW AND HIGHLIGHTS OF OSTEOLOGY & ARTHROLOGY Radius dorsal radial tubercle radial styloid process Ulna ulnar styloid process ulnar head Carpals Proximal Row
Forearm and Wrist Regions Neumann Chapter 7 REVIEW AND HIGHLIGHTS OF OSTEOLOGY & ARTHROLOGY Radius dorsal radial tubercle radial styloid process Ulna ulnar styloid process ulnar head Carpals Proximal Row
Introduction & Question 1
 Page 1 of 7 www.medscape.com To Print: Click your browser's PRINT button. NOTE: To view the article with Web enhancements, go to: http://www.medscape.com/viewarticle/424981 Case Q & A Shoulder Pain, Part
Page 1 of 7 www.medscape.com To Print: Click your browser's PRINT button. NOTE: To view the article with Web enhancements, go to: http://www.medscape.com/viewarticle/424981 Case Q & A Shoulder Pain, Part
Biceps Tendon Tear at the Elbow
 DISEASES & CONDITIONS Biceps Tendon Tear at the Elbow The biceps muscle is located in the front of your upper arm. It is attached to the bones of the shoulder and elbow by tendons strong cords of fibrous
DISEASES & CONDITIONS Biceps Tendon Tear at the Elbow The biceps muscle is located in the front of your upper arm. It is attached to the bones of the shoulder and elbow by tendons strong cords of fibrous
Bio-Tenodesis Screw Fixation
 Bio-Tenodesis Screw Fixation in Tendon Enhanced Ankle Ligament Reconstruction Surgical Technique Kevin O'Shea, M.D. with contributions from Thomas Clanton, M.D., and William McGarvey, M.D. Bio-Tenodesis
Bio-Tenodesis Screw Fixation in Tendon Enhanced Ankle Ligament Reconstruction Surgical Technique Kevin O'Shea, M.D. with contributions from Thomas Clanton, M.D., and William McGarvey, M.D. Bio-Tenodesis
SHOULDER INSTABILITY
 SHOULDER INSTABILITY Your shoulder is the most flexible joint in your body, allowing you to throw fastballs, lift a heavy suitcase, scratch your back, and reach in almost any direction. Your shoulder joint
SHOULDER INSTABILITY Your shoulder is the most flexible joint in your body, allowing you to throw fastballs, lift a heavy suitcase, scratch your back, and reach in almost any direction. Your shoulder joint
Integra. Katalyst Bipolar Radial Head System SURGICAL TECHNIQUE
 Integra Katalyst Bipolar Radial Head System SURGICAL TECHNIQUE Surgical Technique As the manufacturer of this device, Integra does not practice medicine and does not recommend this or any other surgical
Integra Katalyst Bipolar Radial Head System SURGICAL TECHNIQUE Surgical Technique As the manufacturer of this device, Integra does not practice medicine and does not recommend this or any other surgical
WEEKEND 2 Elbow. Elbow Range of Motion Assessment
 Virginia Orthopedic Manual Physical Therapy Institute - 2016 Technique Manual WEEKEND 2 Elbow Elbow Range of Motion Assessment - Patient Positioning: Sitting or supine towards the edge of the bed - Indications:
Virginia Orthopedic Manual Physical Therapy Institute - 2016 Technique Manual WEEKEND 2 Elbow Elbow Range of Motion Assessment - Patient Positioning: Sitting or supine towards the edge of the bed - Indications:
The Elbow and Radioulnar Joints Kinesiology. Dr Cüneyt Mirzanli Istanbul Gelisim University
 The Elbow and Radioulnar Joints Kinesiology Dr Cüneyt Mirzanli Istanbul Gelisim University 1 The Elbow & Radioulnar Joints Most upper extremity movements involve the elbow & radioulnar joints. Usually
The Elbow and Radioulnar Joints Kinesiology Dr Cüneyt Mirzanli Istanbul Gelisim University 1 The Elbow & Radioulnar Joints Most upper extremity movements involve the elbow & radioulnar joints. Usually
BTB ACL Reconstruction with the ToggleLoc Fixation Device with ZipLoop Technology. Surgical Technique by James R. Andrews, M.D.
 BTB ACL Reconstruction with the ToggleLoc Fixation Device with ZipLoop Technology Surgical Technique by James R. Andrews, M.D. Table of Contents Femoral Tunnel Preparation... 4 Prepare ToggleLoc Device...
BTB ACL Reconstruction with the ToggleLoc Fixation Device with ZipLoop Technology Surgical Technique by James R. Andrews, M.D. Table of Contents Femoral Tunnel Preparation... 4 Prepare ToggleLoc Device...
LCP Proximal Radius Plates 2.4. Plates for radial head rim and for radial head neck address individual fracture patterns of the proximal radius.
 Technique Guide LCP Proximal Radius Plates 2.4. Plates for radial head rim and for radial head neck address individual fracture patterns of the proximal radius. Table of Contents Introduction LCP Proximal
Technique Guide LCP Proximal Radius Plates 2.4. Plates for radial head rim and for radial head neck address individual fracture patterns of the proximal radius. Table of Contents Introduction LCP Proximal
Locking Radial Head Plates
 Locking Radial Head Plates Locking Radial Head Plates Since 1988, Acumed has been designing solutions to the demanding situations facing orthopaedic surgeons, hospitals and their patients. Our strategy
Locking Radial Head Plates Locking Radial Head Plates Since 1988, Acumed has been designing solutions to the demanding situations facing orthopaedic surgeons, hospitals and their patients. Our strategy
The Cryo/Cuff provides two functions: 1. Compression - to keep swelling down. 2. Ice Therapy - to keep swelling down and to help minimize pain. Patien
 The Cryo/Cuff provides two functions: 1. Compression - to keep swelling down. 2. Ice Therapy - to keep swelling down and to help minimize pain. Patients, for the most part, experience less pain and/or
The Cryo/Cuff provides two functions: 1. Compression - to keep swelling down. 2. Ice Therapy - to keep swelling down and to help minimize pain. Patients, for the most part, experience less pain and/or
REHABILITATION FOR SHOULDER FRACTURES & SURGERIES. Clavicle fractures Proximal head of humerus fractures
 REHABILITATION FOR SHOULDER FRACTURES & SURGERIES Clavicle fractures Proximal head of humerus fractures By Dr. Mohamed Behiry Lecturer Department of physical therapy for Orthopaedic and its surgery. Delta
REHABILITATION FOR SHOULDER FRACTURES & SURGERIES Clavicle fractures Proximal head of humerus fractures By Dr. Mohamed Behiry Lecturer Department of physical therapy for Orthopaedic and its surgery. Delta
Top Elbow Problems: Tennis Elbow, Anyone?
 Disclosure Top Elbow Problems: Tennis Elbow, Anyone? Founder, RunSafe, RaceSafe Founder, SportZPeak Inc. Sanofi, Investigator initiated grant Anthony Luke MD, MPH, CAQ (Sport Med) UCSF Sports Medicine
Disclosure Top Elbow Problems: Tennis Elbow, Anyone? Founder, RunSafe, RaceSafe Founder, SportZPeak Inc. Sanofi, Investigator initiated grant Anthony Luke MD, MPH, CAQ (Sport Med) UCSF Sports Medicine
