Group Meeting Clinical Director of Pharmacy
|
|
|
- Justin Benson
- 6 years ago
- Views:
Transcription
1 Title: MIU Lower leg, ankle and foot injuries- management of Ref No: 1960 Version 2 Document Author: Ratified by: Senior Manager MIU Services/Nurse Consultant Emergency Care Care and Clinical Policies Group Meeting Clinical Director of Pharmacy Date 18 October 2017 Date: 18 October December 2017 Review date: 12 January 2021 Links to policies: 1. Purpose of this document: This clinical protocol provides a clear framework for nurse/paramedic practitioners employed by Torbay & South Devon NHS Foundation Trust when providing care to patients over 2 years of age presenting at Minor injury Units with lower leg, ankle and foot injuries. 2. Scope of the Policy: This protocol is for the use by Minor Injury Unit (MIU) and Emergency Department (ED) practitioners employed by Torbay and South Devon NHS Foundation Trust who have achieved the agreed Trust clinical competencies to work under this protocol. 2.1 Exclusions All patients presented with a lower limb injury will be triaged/assessed. Those patients outside clinical protocols including x-ray protocol will be referred to the appropriated clinical setting. Red Flag: Ensure all patients on anticoagulants i.e. Warfarin, Dabigatran etexilate (Pradaxa ), Apixaban (eliquis ) and Rivaroxaban (Xarelto ) have appropriate medical follow up/review, blood tests INR review where risk of bleeding NB Be aware of limb threatening conditions such as ankle fracture dislocations and refer via 999 ambulance immediately from an MIU setting. In ED setting seek support to reduce fracture immediately with adequate pain relief. 3. Assessment 3.1. Presenting signs and symptoms; may include some of the following; Pain, swelling, bruising/redness, wounds, inflammation/heat, inability or difficulty to weight bear, reduced or loss of function, deformity/dislocation 3.2. History; refer to protocol for History taking and Clinical Documentation and the Protocol for the Management of soft tissue limb injuries; Specific: Establish when, where and how the injury occurred. Establish the exact mechanism, e.g. inversion or eversion. Was there a fall from a height? Ask whether the patient could weight bear immediately after the injury A crack felt or heard does not necessarily indicate a fracture Was there immediate swelling to the injured limb. Pain score at time of injury and on presentation First aid treatment received. Version 2 (January 2018) Page 1 of 10
2 The amount of swelling may depend on whether ice and elevation have been applied The amount of pain on examination may depend on whether analgesia has been taken Past medical history including previous injuries to effected limb Refer all patients on anticoagulation for medical urgent follow up/review. Where concerns e.g. significant swelling refer to orthopaedics or Emergency department for review. 4. Clinical Examination Observe where possible patients gait, balance, mobility, ability to weight bear Look Symmetry Deformity/dislocations Swelling, particularly below the medial and lateral malleoli Bruising/discoloration, Wounds/grazing Feel: (palpate from knee down) Note any tenderness over: Proximal fibula Tibia and fibular shaft Lateral malleolus and ligaments, including the anterior talofibular ligament Medial malleolus and deltoid ligament Calcaneum Talus, navicular, cuboid, cuneiforms Metatarsal bones including the base of 5 th metatarsal Phalanges Move Inversion/eversion Dorsi/planter flexion Internal/external rotation Flexion/extension of toes. Ability to weight bear Special tests Sensation/circulation Anterior draw test (Gently pull the foot forward on the tibia to test for Anterior/posterior laxity Of the anterior talofibular ligament) Achilles tendon: Simmons/Thomson test Talar tilt test (Gently invert the ankle, if tolerable, to test for laxity of the whole lateral ligament complex). Assess for foot drop (peroneal nerve) Interpreting Radiographs: Request ankle or foot views using the Ottawa ankle rule below Fractures are usually obvious, but may only be seen on one view If one fracture is seen, look carefully for another fracture or joint space widening Accessory ossicles adjacent to the tips of the medial and lateral malleoli are common as are fracture fragments. A larger accessory ossicle, the os trigonum, is sometimes seen at the back of the talus on Lateral view. Clinical correlation is important. In addition, and accessory ossicle has a well defined Version 2 (January 2018) Page 2 of 10
3 (I.e. sclerotic) outline; a fracture fragment is usually ill defined on one of its sides Ankle Anterior/posterior mortice view: The joint space should be uniform all the way around. Widening of the medial joint space indicates damage to the medial ligament Look for a small bone fragment within the joint or a defect in the cortex of the talus, which indicates an osteochondral fracture Inspect the lateral and medial malleoli Lateral view: Inspect the lateral and medial malleoli, and the posterior aspect of the tibia Inspect the calcaneum, as well as the navicular and base of 5 th metacarpal if shown The Ottawa Ankle Rule The rule avoids unnecessary X-rays by identifying patients likely to have significant ankle fractures It has almost 100% specificity for clinically significant fractures, and can save up to 40% of X- rays It is based on assessment of the ability to bear weight (four steps), and the areas of bony tenderness It applies to children and adults presenting with acute (within 10 days) ankle injuries The Ottawa Ankle Rule Version 2 (January 2018) Page 3 of 10
4 1. A 2-view ankle series (Anterior/posterior (AP) and lateral) is required only if there is any pain in the malleolar zone and any of the following: Bone tenderness at A, the posterior edge or tip of the lateral malleolus Bone tenderness at B, the posterior edge or tip of the medial malleolus Inability to bear weight both immediately and in the Emergency Department 2. A 3-view foot series (Anterior/posterior (AP), oblique and lateral) is required only if there is pain in the midfoot zone and any of the following: Bone tenderness at D, the navicular Inability to bear weight both immediately and in the Emergency Department 3. A 2-view foot series (Anterior/posterior (AP) and oblique) is required only if there is any pain in the midfoot zone and: Bone tenderness at C, the base of the fifth metatarsal Note: Allow a lower threshold for radiography in the very young, the elderly, those who are difficult to assess (e.g. intoxication, learning difficulties, stroke, presence of other injuries), and after injury from violent mechanism, (e.g. fall from a height, road traffic collision). The rule does not apply to heel injuries e.g. fall from a height. These must be assessed independently with calcaneal views if relevant history and local tenderness 5. Treatment: 5.1 Management of Ankle Sprains All patients who are unable to weight bear when seen must be followed up. This may be by physiotherapy, GP, Minor injury unit (MIU), Emergency department (ED)Clinic or even Fracture Clinic depending on your concerns and the patient s circumstances Most avulsion or flake fractures can be treated the same as sprains. If in doubt get senior advice The threshold for referral to physiotherapy should take into account the patient s expectations, including work, sport, hobbies etc., as well as the severity Moderate Sprain, able to weight bear Rest, elevate above hip level Apply ice for periods of 20 minutes over the first 48 hours Strapping. Stick if necessary Give analgesia as per Patient Group Direction or advice on over the counter analgesia e.g. Non-steroidal anti-inflammatory drugs (if tolerated), paracetamol Exercise sheet. Begin weight bearing as soon as symptoms allow Consider physiotherapy if recurrent Moderate to severe sprain, unable to weight bear As above, crutches Refer to physiotherapy Follow up in 5 to 7 days by GP or MIU. Exceptionally, consider a lightweight walking cast for 7 to 10 days - for very severe symptoms or difficult social circumstances, e.g. the elderly or difficulty with crutches Severe sprain, ankle unstable Give analgesia as per patient group direction. Refer to the Orthopaedic team. Version 2 (January 2018) Page 4 of 10
5 Minor avulsion or flake fracture Treat symptomatically as above 5.2 Ankle fractures Isolated lateral malleolus fracture (no deltoid ligament tenderness) Assess pain score and give analgesia as per patient group direction(pgd) or advise on over the counter analgesia e.g. Non-steroidal anti-inflammatory drugs and/or paracetamol Apply below knee Plaster of Paris backslab in neutral, using entonox if necessary as per patient group direction Take check radiographs in Plaster of Paris where manipulation required. Elevation, crutches, analgesia as per PGD or advice over the counter analgesia, Trauma Triage follow up Lateral malleolus fracture with talar shift Assess pain score and give analgesia as per patient group direction. Gentle manipulation as pain allows supported with pain relief including entonox Apply temporary below knee POP backslab and re x-ray Refer to the Orthopaedic team on call Undisplaced isolated medial or posterior malleolus fracture Assess pain score and give analgesia as per patient group direction or advise over the counter analgesia e.g. Non-steroidal anti-inflammatory drugs and/or paracetamol. Apply below knee plaster of Paris backslab in neutral, using entonox if necessary Take check radiographs in Plaster Elevation, crutches, analgesia as per PGD or advice over the counter analgesia, Trauma Triage Displaced medial or posterior malleolus fracture, bimalleolar or trimalleolar fracture Assess pain score and give analgesia as per Patient Group Direction. Apply temporary below knee Plaster of Paris backslab, Check X-ray. Refer to the Orthopaedic team. 5.3 Tibia and Fibula fractures Isolated fractures of proximal and upper midshaft of Fibula NB examine popliteal nerve (include observation for foot drop, if present refer to orthopaedics) Give analgesia as per patient group direction. Apply tubigrib. Temporary below knee POP backslab may be considered in patients with low risk of thrombosis and with a high pain score.. Provide crutches. Refer to Trauma Triage Undisplaced fractures of Tibia and Fibula Assess pain score and give analgesia as per patient group direction. Apply temporary full leg POP backslab and provide crutches. Refer to the Orthopaedic team on call for further advice and follow up.. NB Assess for Compartment syndrome and risk of thrombosis. Version 2 (January 2018) Page 5 of 10
6 5.3.3 Displaced fracture of tibia and Fibula Assess pain score and give analgesia as per patient group direction. Consider entonox as per PGD. Gentle manipulation as pain allows supported with pain relief including entonox apply temporary full leg POP backslab or await ambulance support with relevant splintage if based in MIU. Refer to the Orthopaedic team on call for further treatment. Transfer by ambulance to local Emergency Department for Ortho review id based in MIU. NB Assess for Compartment syndrome and risk of thrombosis. 5.4 Lower leg injuries Significant Lower leg swelling with no Fracture seen on X-ray: Assess pain score and give analgesia as per patient group directions. Elevate limb and provide ice treatment. Refer to Emergency department for further assessment where there is a risk of compartment syndrome or suspicion of thrombosis. (Discuss with Emergency Department Consultant or senior Doctor) Calf Strain (gastrocnemius strain) Acute gastrocnemius tears usually occur during sport, (running, twisting etc.) There is pain on weight bearing (may only be partially weight bearing on tiptoe) and tenderness and/ or swelling, usually over the medial belly. Patients may describe a feeling of been hit in the back of the leg/calf muscle. Carefully check the Achilles tendon for signs of rupture Differential diagnosis includes Deep Vein Thrombosis and ruptured Baker s cyst Treatment Minor strain Analgesia, ice application, elastic support and progressive weight bearing Treatment Severe sprain As above with crutches if necessary, physiotherapy referral and GP or minor injury unit follow up Achilles Tendon Rupture Specific history May follow sudden muscle activity, especially in sports The patient feels a sudden sharp pain or blow behind the ankle, followed by difficulty walking and standing on the toes Examine the patient prone or kneeling on a chair with the feet hanging free over the edge There may be swelling, pain or bruising and even a palpable gap in the tendon Always perform and record the result of the calf-squeeze/simmons/thomson test: Gently squeeze the calf. If the foot moves as the ankle plantar flexes, the Achilles tendon is intact. If it fails to move, the Achilles tendon is ruptured. Compare both sides. Record the test as normal or abnormal, rather than positive or negative to avoid confusion Treatment of ruptured Achilles tendon Refer all cases to the Orthopaedic team Place in equinus POP back slab and provide crutches Treatment may be conservative or surgical but requires orthopaedic review Achilles Tendonitis Symptoms may include a history of gradual onset of pain and stiffness over the tendon. Tenderness over the tendon on palpation. Crepitus and swelling. Pain on active movement. Version 2 (January 2018) Page 6 of 10
7 Treatment: Advise non -steroidal anti- inflammatory medication as per patient group directions, ice and rest. May require physiotherapy if recurrent problem or not resolving following rest. 5.5 Growth plate (epiphyseal plate); Salter Harris Type 2 fractures are common Minimally or not displaced Assess pain score and give analgesia as per patient group direction, Apply below knee POP backslab and provide crutches, Advise elevation and arrange Trauma Triage Displaced: Refer to orthopaedics Analgesia (as per patient group direction), backslab, elevate, Refer to the Orthopaedic team for manipulation Growth plate injury without fracture If no fracture is seen on radiographs but there is a lot of tenderness of the distal tibial or fibular epiphysis, treat as a growth plate injury, Analgesia as per patient group direction, below knee Plaster of Paris backslab, crutches, elevation and await x-ray report. If x-ray confirms growth plate injury refer to trauma Triage If x-ray report is normal review in 3 5 days, remove POP treat as sprain where clear improvement found. If child remains in pain or has reduced ROM of ability to weight bear re-plaster and refer to Trauma Triage. 5.6 Tarsal Bone fractures Calcaneal Fractures Specific history; Usually follows a fall from a height but may be caused by a twisting injury. Examine the calcaneum in all ankle injuries Signs and symptoms include swelling, bruising and tenderness over the heel and sides of the calcaneum. In major fractures the heel appears flattened and tilted laterally Investigations to include specific calcaneal x-rays views. Check Bohler s angle for flattening (less than 30 degrees) indicating a crush fracture Treatment. Simple Undisplaced fracture. POP back slab below knee or wool and crepe depending on patient s pain score. Advise analgesia as per patient group direction. Provide patient with crutches. Arrange Trauma Triage follow up. Treatment of all other calcaneal fractures, refer to Orthopaedics for further advice/review. NB Patients with calcaneum fractures may have further significant injury including spinal injuries. Consider referral for further assessment Minor avulsion fractures of Talus or Navicular. Assess pain score and give analgesia as per patient group direction. Apply below knee POP backslab and provide crutches. Trauma Triage follow up All other Talus or navicular fractures Assess pain score and give analgesia as per patient group direction. Refer to Orthopaedics for further management Simple Cuboid fractures with no Tarsometarsal joint involvement Assess pain score and give analgesia as per patient group direction. Apply below knee POP backslab and provide crutches. Trauma Triage follow up Version 2 (January 2018) Page 7 of 10
8 5.6.4 Tarsometatarsal (lisfrancs) injuries/dislocations There is disruption of one or more of the joints, usually with associated fracture of the metatarsal, cuboid or cuneiform bones Prompt reduction is necessary because of the risks of swelling, circulatory impairment (especially dorsalis pedis) and compartment syndrome Assess pain score and give analgesia as per patient group direction. Refer to Orthopaedics for further management. 5.7 Metatarsal Fractures Avulsion fractures of the base of 5 th Metatarsal. Usually associated with an inversion injury of the foot or ankle. Treatment: Assess pain score and give analgesia as per patient group direction Treat with tubigrib/support bandage or podlux shoe/boot if available depending on severity of pain. Weight bearing as pain allows (Provide crutches to support partial weight bearing or nonweight bearing as patient tolerates) Discharge with isolated 5 th metatarsal base fracture leaflet as per orthopaedic ED/MIU fracture and trauma triage guidelines th Metatarsal Jones fracture Tends to occur in athletes during training, it has some of the features of stress fracture Non-union is common and is often associated with early weight bearing This may happen if mistaken for a base of fifth metatarsal fracture Treatment: Assess pain score and give analgesia as per patient group direction Treat with Boot or POP backslab below knee. Non weight bearing with crutches. Trauma Triage follow up Other Metatarsal fractures Can be caused from crush injuries or sporting injuries Treatment: Undisplaced Fractures. Assess pain score and give analgesia as per patient group direction Treat with POP backslab below knee or support bandage depending on pain score Non weight bearing with crutches. Trauma Triage follow up. Treatment for multiple or displaced fractures refer to orthopaedics for further management. 5.8 Phalangeal Fractures Radiography Toe injuries Apart from the hallux, most isolated toe injuries do not require radiography X-ray only if there is obvious deformity, gross swelling, suspected dislocation, compound injury, or MTPJ tenderness Treatment Un-displaced Toe fractures: Advise simple analgesia as per Patient Group direction. Neighbour strap and advise elevation. Advise discomfort may last as bone heals over 4 6 weeks. GP follow up if pain persists. Version 2 (January 2018) Page 8 of 10
9 Treatment displaced fractures and dislocations: Following x-ray, where competent manipulate under local anaesthetic digital block, neighbour strap, check x-ray and treat as above. Refer to ED if unable to relocate displacement or dislocation. Trauma Triage Hallux fractures (Big Toe Fractures) Usually from a heavy weight falling on an unprotected foot May involve the IP joint and may be open Treatment; Trephine nail as necessary if subungal haematoma present, or remove if virtually separated Irrigate well with Normal saline. Treat open fracture with Co- Amoxiclav as per Patient Group direction. Consider need for Tetanus prophylaxis as per patient Group direction and risk of tetanus prone wound. Proximal phalanx fractures may require a walking plaster with toe platform for pain relief. Seek advice from Orthopaedics on call. Simple Undisplaced closed fractures may be treated with Toe Spica and arrange Trauma Triage. 6. Documentation 6.1. Clinical records must be written in accordance with Torbay and South Devon NHS Foundation Trust History Taking and Clinical Documentation protocol, Nursing & Midwifery Council standards including record keeping or relevant registering body e.g. Health & care professional Council (HCPC) standards including record keeping guidance A summary letter of the MIU/ED attendance and the care delivered must also be sent to the General practitioner and also the health visitor if less than 5yrs or school nurse if aged between 5yrs and 16yrs to ensure the central medical record of the patient is accurate For patients being transferred to the Emergency department, ensure clinical records are completed in a timely manner on the shared symphony IT system. A summary letter will be sent to the General practitioner in the normal manner For patients seeing the General practitioner or specialist within the next 24 hours ensure the patient has a copy of the attendance record to take with them. A summary record will be sent to the General practitioner in the normal manner. 7. Discharge information 7.1 Ensure those patients who have been referred for further acute intervention have appropriate transport to meet their needs, all relevant treatment has been prescribed and/or administered and correct information & documentation is given to the patient. 7.2 The patient /carer understand that if the condition deteriorates or they have any further concerns to seek medical advice The patient and /or carer demonstrate understanding of advice given during The patient/carer has been provided with written advice leaflet to reinforce advice given during consultation 7.4 The patient/carer demonstrates and understanding of how to manage subsequent problems 8. Training and implementation: MIU Network meeting Cascade. All staff adhering to protocols must have agreed training and proven competence to work within protocol. Each protocol must be agreed and signed by line manager. Version 2 (January 2018) Page 9 of 10
10 9. Monitoring tool Regular review of clinical practice to ensure individuals are adhering to clinical protocol. 10. References Accident & Emergency, theory into practice. Dolan B, Holt L Acute Medical Emergencies, a nursing guide. Harrison R, Daly L British National Formulary March 2017 Clinical orthopaedic Examination. McRae R. 5 th edition 2004 Differential Diagnosis. Rafley, A. Lim, E. 2 nd edition 2005 Guide to physical examination and History Taking. Bickley 2003 Nurse Practitioners, clinical skills & professional issues. Walsh M, Crumbie A, Reveley S Minor Emergencies Splinters to fractures. Butteovolli P, Stair T 2000 Minor Injuries, A Clinical guide. Purcell D. 2 nd edition 2010 South& west Devon Formulary 2 Amendment History Issue Status Date Reason for Change Authorised 1 Created February 2013 Merger of Torbay Care Trust and NHS Devon Protocols for lower leg, ankle & foot injuries 1.1 Reviewed August 2015 Reviewed no clinical changes required Documentation amendments to reflect new symphony IT system 2 Revised 12 January 2018 Trust name Emergency Department practitioner inclusion. New Orthopaedic ED/MIU fracture and Trauma triage guidelines 2 12 February 2018 Review date extended from 2 years to 3 years Senior Manager MIU Services/Nurse Consultant Emergency Care Senior Manager MIU Services/Nurse Consultant Emergency Care Care and Clinical Policies Group Clinical Director of Pharmacy Version 2 (January 2018) Page 10 of 10
11 The Mental Capacity Act 2005 The Mental Capacity Act provides a statutory framework for people who lack capacity to make decisions for themselves, or who have capacity and want to make preparations for a time when they lack capacity in the future. It sets out who can take decisions, in which situations, and how they should go about this. It covers a wide range of decision making from health and welfare decisions to finance and property decisions Enshrined in the Mental Capacity Act is the principle that people must be assumed to have capacity unless it is established that they do not. This is an important aspect of law that all health and social care practitioners must implement when proposing to undertake any act in connection with care and treatment that requires consent. In circumstances where there is an element of doubt about a person s ability to make a decision due to an impairment of or disturbance in the functioning of the mind or brain the practitioner must implement the Mental Capacity Act. The legal framework provided by the Mental Capacity Act 2005 is supported by a Code of Practice, which provides guidance and information about how the Act works in practice. The Code of Practice has statutory force which means that health and social care practitioners have a legal duty to have regard to it when working with or caring for adults who may lack capacity to make decisions for themselves. The Act is intended to assist and support people who may lack capacity and to discourage anyone who is involved in caring for someone who lacks capacity from being overly restrictive or controlling. It aims to balance an individual s right to make decisions for themselves with their right to be protected from harm if they lack the capacity to make decisions to protect themselves. (3) All Trust workers can access the Code of Practice, Mental Capacity Act 2005 Policy, Mental Capacity Act 2005 Practice Guidance, information booklets and all assessment, checklists and Independent Mental Capacity Advocate referral forms on icare Infection Control All staff will have access to Infection Control Policies and comply with the standards within them in the work place. All staff will attend Infection Control Training annually as part of their mandatory training programme. Version 2 (January 2018) The Mental Capacity Act Page 1 of 1
12 Rapid (E)quality Impact Assessment (EqIA) (for use when writing policies) Policy Title (and number) Version and Date Policy Author An (e)quality impact assessment is a process designed to ensure that policies do not discriminate or disadvantage people whilst advancing equality. Consider the nature and extent of the impact, not the number of people affected. Who may be affected by this document? Patients/ Service Users Staff Other, please state Could the policy treat people from protected groups less favorably than the general population? PLEASE NOTE: Any Yes answers may trigger a full EIA and must be referred to the equality leads below Age Yes No Gender Reassignment Yes No Sexual Orientation Yes No Race Yes No Disability Yes No Religion/Belief (non) Yes No Gender Yes No Pregnancy/Maternity Yes No Marriage/ Civil Partnership Yes No Is it likely that the policy could affect particular Inclusion Health groups less favourably than Yes No the general population? (substance misuse; teenage mums; carers 1 ; travellers 2 ; homeless 3 ; convictions; social isolation 4 ; refugees) Please provide details for each protected group where you have indicated Yes. VISION AND VALUES: Policies must aim to remove unintentional barriers and promote inclusion Is inclusive language 5 used throughout? Yes No NA Are the services outlined in the policy fully accessible 6? Yes No NA Does the policy encourage individualised and person-centred care? Yes No NA Could there be an adverse impact on an individual s independence or autonomy 7? Yes No NA EXTERNAL FACTORS Is the policy a result of national legislation which cannot be modified in any way? Yes No What is the reason for writing this policy? (Is it a result in a change of legislation/ national research?) Who was consulted when drafting this policy? Patients/ Service Users Trade Unions Protected Groups (including Trust Equality Groups) Staff General Public Other, please state What were the recommendations/suggestions? Does this document require a service redesign or substantial amendments to an existing Yes No process? PLEASE NOTE: Yes may trigger a full EIA, please refer to the equality leads below ACTION PLAN: Please list all actions identified to address any impacts Action Person responsible Completion date AUTHORISATION: By signing below, I confirm that the named person responsible above is aware of the actions assigned to them Name of person completing the form Signature Validated by (line manager) Signature Please contact the Equalities team for guidance: For South Devon & Torbay CCG, please call or marisa.cockfield@nhs.net Version 2 (January 2018) Rapid (E)quality Impact Assessment Page 1 of 2
13 For Torbay and South Devon NHS Trusts, please call or This form should be published with the policy and a signed copy sent to your relevant organisation. 1 Consider any additional needs of carers/ parents/ advocates etc, in addition to the service user 2 Travelers may not be registered with a GP - consider how they may access/ be aware of services available to them 3 Consider any provisions for those with no fixed abode, particularly relating to impact on discharge 4 Consider how someone will be aware of (or access) a service if socially or geographically isolated 5 Language must be relevant and appropriate, for example referring to partners, not husbands or wives 6 Consider both physical access to services and how information/ communication in available in an accessible format 7 Example: a telephone-based service may discriminate against people who are d/deaf. Whilst someone may be able to act on their behalf, this does not promote independence or autonomy Version 2 (January 2018) Rapid (E)quality Impact Assessment Page 2 of 2
14 Clinical and Non-Clinical Policies New Data Protection Regulation (NDPR) Torbay and South Devon NHS Foundation Trust (TSDFT) has a commitment to ensure that all policies and procedures developed act in accordance with all relevant data protection regulations and guidance. This policy has been designed with the EU New Data Protection Regulation (NDPR) in mind and therefore provides the reader with assurance of effective information governance practice. NDPR intends to strengthen and unify data protection for all persons; consequently, the rights of individuals have changed. It is assured that these rights have been considered throughout the development of this policy. Furthermore, NDPR requires that the Trust is open and transparent with its personal identifiable processing activities and this has a considerable effect on the way TSDFT holds, uses, and shares personal identifiable data. The most effective way of being open is through data mapping. Data mapping for NDPR was initially undertaken in November 2017 and must be completed on a triannual (every 3 years) basis to maintain compliance. This policy supports the data mapping requirement of the NDPR. For more information: Contact the Data Access and Disclosure Office on dataprotection.tsdft@nhs.net, See TSDFT s Data Protection & Access Policy, Visit our GDPR page on ICON. Version 2 (January 2018) New Data Protection Regulation Page 1 of 1
Last Review Date August 2015 Version 1.1 Page 1 of 11
 1960 Title: Protocol for the Management of Lower Leg, Ankle and Foot Injuries Document Owner: Deirdre Molloy Document Author: Deirdre Molloy Presented to: Care & Clinical Policies Date: August 2015 Ratified
1960 Title: Protocol for the Management of Lower Leg, Ankle and Foot Injuries Document Owner: Deirdre Molloy Document Author: Deirdre Molloy Presented to: Care & Clinical Policies Date: August 2015 Ratified
3.2. History; refer to protocol for History taking and Clinical Documentation and the Protocol for the Management of soft tissue limb injuries;
 Title: MIU Elbow injuries- management of Ref No: 1953 Version 2 Document Author: Ratified by: Senior Manager MIU Services Nurse Consultant Emergency care Care & Clinical Policies Group Meeting Clinical
Title: MIU Elbow injuries- management of Ref No: 1953 Version 2 Document Author: Ratified by: Senior Manager MIU Services Nurse Consultant Emergency care Care & Clinical Policies Group Meeting Clinical
Title Management of Ankle and Lower Limb Injuries Protocol in MIUs and WICs
 Document Control Title Management of Ankle and Lower Limb Injuries Protocol in MIUs and WICs Author Author s job title Professional Lead, Minor Injuries Unit Directorate Emergency Services, Logistics and
Document Control Title Management of Ankle and Lower Limb Injuries Protocol in MIUs and WICs Author Author s job title Professional Lead, Minor Injuries Unit Directorate Emergency Services, Logistics and
Title: MIU Upper leg and knee injuries- management of. Ref No: 1971 Version 3
 Title: MIU Upper leg and knee injuries- management of Ref No: 1971 Version 3 Document Author: Ratified by: Senior Manager MIU Services Nurse Consultant Emergency Care Care & Clinical Policies Group Meeting
Title: MIU Upper leg and knee injuries- management of Ref No: 1971 Version 3 Document Author: Ratified by: Senior Manager MIU Services Nurse Consultant Emergency Care Care & Clinical Policies Group Meeting
1. Purpose of this document
 Guideline Ref No: 0900 Version 4 Title: Document Author: Ratified by: Specialist Orthopaedic Physiotherapist Care and Clinical Policies Group Date: 13 February 2017 Date: 19 April 2017 Review date: 5 May
Guideline Ref No: 0900 Version 4 Title: Document Author: Ratified by: Specialist Orthopaedic Physiotherapist Care and Clinical Policies Group Date: 13 February 2017 Date: 19 April 2017 Review date: 5 May
Senior Manager MIU Services/Nurse Consultant Emergency care
 Title: MIU Forearm and wrist injuries - management of Ref No: 1955 Version 2 Document Author: Ratified by: Senior Manager MIU Services/Nurse Consultant Emergency care Care & Clinical Polices Group Meeting
Title: MIU Forearm and wrist injuries - management of Ref No: 1955 Version 2 Document Author: Ratified by: Senior Manager MIU Services/Nurse Consultant Emergency care Care & Clinical Polices Group Meeting
BCCH Emergency Department LOWER LIMB INJURIES Resource pack
 1 BCCH Emergency Department LOWER LIMB INJURIES Resource pack Developed by: Rena Heathcote RN. 2 Knee Injuries The knee joint consists of a variety of structures including: 3 bones (excluding the patella)
1 BCCH Emergency Department LOWER LIMB INJURIES Resource pack Developed by: Rena Heathcote RN. 2 Knee Injuries The knee joint consists of a variety of structures including: 3 bones (excluding the patella)
Prevention and Treatment of Injuries. Anatomy. Anatomy. Tibia: the second longest bone in the body
 Prevention and Treatment of Injuries The Ankle and Lower Leg Westfield High School Houston, Texas Anatomy Tibia: the second longest bone in the body Serves as the principle weight-bearing bone of the leg.
Prevention and Treatment of Injuries The Ankle and Lower Leg Westfield High School Houston, Texas Anatomy Tibia: the second longest bone in the body Serves as the principle weight-bearing bone of the leg.
Surgery-Ortho. Fractures of the tibia and fibula. Management. Treatment of low energy fractures. Fifth stage. Lec-6 د.
 Fifth stage Lec-6 د. مثنى Surgery-Ortho 28/4/2016 Indirect force: (low energy) Fractures of the tibia and fibula Twisting: spiral fractures of both bones Angulatory: oblique fractures with butterfly segment.
Fifth stage Lec-6 د. مثنى Surgery-Ortho 28/4/2016 Indirect force: (low energy) Fractures of the tibia and fibula Twisting: spiral fractures of both bones Angulatory: oblique fractures with butterfly segment.
Ankle Sprains and Their Imitators
 Ankle Sprains and Their Imitators Mark Halstead, MD Dr. Mark Halstead is the Associate Professor of the Departments of Orthopedics and Pediatrics at Washington University School of Medicine; Director of
Ankle Sprains and Their Imitators Mark Halstead, MD Dr. Mark Halstead is the Associate Professor of the Departments of Orthopedics and Pediatrics at Washington University School of Medicine; Director of
Ankle Fracture Orthopaedic Department Patient Information Leaflet. Under review. Page 1
 Ankle Fracture Orthopaedic Department Patient Information Leaflet Page 1 Ankle Fracture Welcome to the Dudley Group NHS Foundation Trust. This leaflet will provide you with information regarding the diagnosis
Ankle Fracture Orthopaedic Department Patient Information Leaflet Page 1 Ankle Fracture Welcome to the Dudley Group NHS Foundation Trust. This leaflet will provide you with information regarding the diagnosis
Outline. Ankle/Foot Anatomy Ankle Sprains Ottawa Ankle Rules DDx: The Sprain That Wasn t
 Ankle Injuries Outline Ankle/Foot Anatomy Ankle Sprains Ottawa Ankle Rules DDx: The Sprain That Wasn t Anatomy: Ankle Mortise Bony Anatomy Lateral Ligament Complex Medial Ligament Complex Ankle Sprains
Ankle Injuries Outline Ankle/Foot Anatomy Ankle Sprains Ottawa Ankle Rules DDx: The Sprain That Wasn t Anatomy: Ankle Mortise Bony Anatomy Lateral Ligament Complex Medial Ligament Complex Ankle Sprains
Title Protocol for the Management of Shoulder Injuries in MIUs and WICs
 Document Control Title in MIUs and WICs Author Author s job title Professional Lead, Minor Injuries Unit Directorate, Logistics and Resilience Department Emergency Department Version Date Issued Status
Document Control Title in MIUs and WICs Author Author s job title Professional Lead, Minor Injuries Unit Directorate, Logistics and Resilience Department Emergency Department Version Date Issued Status
Acute Ankle Injuries, Part 1: Office Evaluation and Management
 t June 08, 2009 Obesity [1] Each acute ankle injury commonly seen in the office has associated with it a mechanism by which it can be injured, trademark symptoms that the patient experiences during the
t June 08, 2009 Obesity [1] Each acute ankle injury commonly seen in the office has associated with it a mechanism by which it can be injured, trademark symptoms that the patient experiences during the
Title Management of Knee Injuries Protocol in MIUs and WICs
 Document Control Title Management of Knee Injuries Protocol in MIUs and WICs Author Author s job title Professional Lead, Minor Injuries Unit Directorate Emergency Services, Logistics and Resilience Department
Document Control Title Management of Knee Injuries Protocol in MIUs and WICs Author Author s job title Professional Lead, Minor Injuries Unit Directorate Emergency Services, Logistics and Resilience Department
Leg and Ankle Problems in Primary Care.
 Leg and Ankle Problems in Primary Care www.fisiokinesiterapia.biz Leg and Ankle Presentations 4Trauma 4Pain Ankle Trauma 41. Twist and Fall--Fracture or Sprain 42. Patient hears/feels a pop--tendon or
Leg and Ankle Problems in Primary Care www.fisiokinesiterapia.biz Leg and Ankle Presentations 4Trauma 4Pain Ankle Trauma 41. Twist and Fall--Fracture or Sprain 42. Patient hears/feels a pop--tendon or
Physical Examination of the Foot & Ankle
 Inspection Standing, feet straight forward facing toward examiner Swelling Deformity Flatfoot (pes planus and hindfoot valgus) High arch (pes cavus and hindfoot varus) Peek-a-boo heel Varus Too many toes
Inspection Standing, feet straight forward facing toward examiner Swelling Deformity Flatfoot (pes planus and hindfoot valgus) High arch (pes cavus and hindfoot varus) Peek-a-boo heel Varus Too many toes
Copyright 2004, Yoshiyuki Shiratori. All right reserved.
 Ankle and Leg Evaluation 1. History Chief Complaint: A. What happened? B. Is it a sharp or dull pain? C. How long have you had the pain? D. Can you pinpoint the pain? E. Do you have any numbness or tingling?
Ankle and Leg Evaluation 1. History Chief Complaint: A. What happened? B. Is it a sharp or dull pain? C. How long have you had the pain? D. Can you pinpoint the pain? E. Do you have any numbness or tingling?
Foot Injuries. Dr R B Kalia
 Foot Injuries Dr R B Kalia Overview Dramatic impact on the overall health, activity, and emotional status More attention and aggressive management Difficult appendage to study and diagnose. Aim- a stable
Foot Injuries Dr R B Kalia Overview Dramatic impact on the overall health, activity, and emotional status More attention and aggressive management Difficult appendage to study and diagnose. Aim- a stable
Journal reading. Introduction. Introduction. Ottawa Ankle Rules. Method
 Journal reading Presenter: PGY 林聖傑 Supervisor: Dr. 林俊龍 102.12.23 The accuracy of ultrasound evaluation in foot and ankle trauma Salih Ekinci, MD American Journal of Emergency Medicine 31 (2013) 1551 1555
Journal reading Presenter: PGY 林聖傑 Supervisor: Dr. 林俊龍 102.12.23 The accuracy of ultrasound evaluation in foot and ankle trauma Salih Ekinci, MD American Journal of Emergency Medicine 31 (2013) 1551 1555
Scar Engorged veins. Size of the foot [In clubfoot, small foot]
![Scar Engorged veins. Size of the foot [In clubfoot, small foot] Scar Engorged veins. Size of the foot [In clubfoot, small foot]](/thumbs/78/77722241.jpg) 6. FOOT HISTORY Pain: Walking, Running Foot wear problem Swelling; tingly feeling Deformity Stiffness Disability: At work; recreation; night; walk; ADL, Sports Previous Rx Comorbidities Smoke, Sugar, Steroid
6. FOOT HISTORY Pain: Walking, Running Foot wear problem Swelling; tingly feeling Deformity Stiffness Disability: At work; recreation; night; walk; ADL, Sports Previous Rx Comorbidities Smoke, Sugar, Steroid
SOFT TISSUE KNEE INJURIES
 SOFT TISSUE KNEE INJURIES Soft tissue injuries of the knee commonly occur in all sports or in any activity that requires sudden changes in activity or movement. The knee is a complex joint and any injury
SOFT TISSUE KNEE INJURIES Soft tissue injuries of the knee commonly occur in all sports or in any activity that requires sudden changes in activity or movement. The knee is a complex joint and any injury
AAP Boot Camp KNEE AND ANKLE EXAM
 AAP Boot Camp KNEE AND ANKLE EXAM Disclosures I have no relevant financial relationships with the manufacturers of any commercial products and or providers of commercial services discussed in this CME
AAP Boot Camp KNEE AND ANKLE EXAM Disclosures I have no relevant financial relationships with the manufacturers of any commercial products and or providers of commercial services discussed in this CME
This guideline was adapted in collaboration with Dr Georgina Walker and the Palliative Care Team at Rowcroft Hospice. With thanks.
 Title: Directorate: Responsible for review: Ratified by: DIABETES, MANAGEMENT OF IN PALLIATIVE CARE PATIENTS General Medicine Diabetes Specialist Nurse Service Delivery Unit Clinical Director of Pharmacy
Title: Directorate: Responsible for review: Ratified by: DIABETES, MANAGEMENT OF IN PALLIATIVE CARE PATIENTS General Medicine Diabetes Specialist Nurse Service Delivery Unit Clinical Director of Pharmacy
Ankle Arthroscopy.
 Ankle Arthroscopy Key words: Ankle pain, ankle arthroscopy, ankle sprain, ankle stiffness, day case surgery, articular cartilage, chondral injury, chondral defect, anti-inflammatory medication Our understanding
Ankle Arthroscopy Key words: Ankle pain, ankle arthroscopy, ankle sprain, ankle stiffness, day case surgery, articular cartilage, chondral injury, chondral defect, anti-inflammatory medication Our understanding
Tendo Achilles rupture
 Tendo Achilles rupture Conservative and surgical management Therapy Department 01935 475 122 yeovilhospital.nhs.uk What is the Achilles tendon? The Achilles tendon is a large tendon at the back of the
Tendo Achilles rupture Conservative and surgical management Therapy Department 01935 475 122 yeovilhospital.nhs.uk What is the Achilles tendon? The Achilles tendon is a large tendon at the back of the
Review relevant anatomy of the foot and ankle. Learn the approach to examining the foot and ankle
 Objectives Review relevant anatomy of the foot and ankle Learn the approach to examining the foot and ankle Learn the basics of diagnosis and treatment of ankle sprains Overview of other common causes
Objectives Review relevant anatomy of the foot and ankle Learn the approach to examining the foot and ankle Learn the basics of diagnosis and treatment of ankle sprains Overview of other common causes
KNEE EXAMINATION. Tips & Tricks from an Emergency Physician Perspective. EM Physicians Less Exposed to MSK Medicine
 KNEE EXAMINATION Tips & Tricks from an Emergency Physician Perspective Dr P O CONNOR Emergency Medicine Physician EUSEM 10/09/2018 EM Physicians Less Exposed to MSK Medicine Musculoskeletal Medicine becoming
KNEE EXAMINATION Tips & Tricks from an Emergency Physician Perspective Dr P O CONNOR Emergency Medicine Physician EUSEM 10/09/2018 EM Physicians Less Exposed to MSK Medicine Musculoskeletal Medicine becoming
Anatomy and evaluation of the ankle.
 Anatomy and evaluation of the ankle www.fisiokinesiterapia.biz Ankle Anatomical Structures Tibia Fibular Talus Tibia This is the strongest largest bone of the lower leg. It bears weight and the bone creates
Anatomy and evaluation of the ankle www.fisiokinesiterapia.biz Ankle Anatomical Structures Tibia Fibular Talus Tibia This is the strongest largest bone of the lower leg. It bears weight and the bone creates
Orthopaedics. Assessment and management of foot and ankle fractures TIME OUT 1
 By reading this article and writing a practice profile, you can gain ten continuing education points (CEPs). You have up to a year to send in your practice profile. Guidelines on how to write and submit
By reading this article and writing a practice profile, you can gain ten continuing education points (CEPs). You have up to a year to send in your practice profile. Guidelines on how to write and submit
radiologymasterclass.co.uk
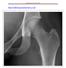 http://radiologymasterclass.co.uk Hip X-ray anatomy - Normal AP (anterior-posterior) Shenton's line is formed by the medial edge of the femoral neck and the inferior edge of the superior pubic ramus Loss
http://radiologymasterclass.co.uk Hip X-ray anatomy - Normal AP (anterior-posterior) Shenton's line is formed by the medial edge of the femoral neck and the inferior edge of the superior pubic ramus Loss
X-Ray Rounds: (Plain) Radiographic Evaluation of the Ankle.
 X-Ray Rounds: (Plain) Radiographic Evaluation of the Ankle www.fisiokinesiterapia.biz Anatomy Complex hinge joint Articulations among: Fibula Tibia Talus Tibial plafond Distal tibial articular surface
X-Ray Rounds: (Plain) Radiographic Evaluation of the Ankle www.fisiokinesiterapia.biz Anatomy Complex hinge joint Articulations among: Fibula Tibia Talus Tibial plafond Distal tibial articular surface
Dr Nabil khouri MD. MSc. Ph.D
 Dr Nabil khouri MD. MSc. Ph.D Foot Anatomy The foot consists of 26 bones: 14 phalangeal, 5 metatarsal, and 7 tarsal. Toes are used to balance the body. Metatarsal Bones gives elasticity to the foot in
Dr Nabil khouri MD. MSc. Ph.D Foot Anatomy The foot consists of 26 bones: 14 phalangeal, 5 metatarsal, and 7 tarsal. Toes are used to balance the body. Metatarsal Bones gives elasticity to the foot in
Bones = phalanges 5 metatarsals 7 tarsals
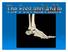 The Foot (Bones) Bones = 26 14 phalanges 5 metatarsals 7 tarsals Toes (Phalanges) Designed to give wider base for balance and propelling the body forward. 1st toe (Hallux) Two sesamoid bones located under
The Foot (Bones) Bones = 26 14 phalanges 5 metatarsals 7 tarsals Toes (Phalanges) Designed to give wider base for balance and propelling the body forward. 1st toe (Hallux) Two sesamoid bones located under
MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg)
 MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg) Description Expected Outcome Medial head gastrocnemius tear is a strain of the inner part (medial head) of the major calf muscle (gastrocnemius muscle). Muscle
MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg) Description Expected Outcome Medial head gastrocnemius tear is a strain of the inner part (medial head) of the major calf muscle (gastrocnemius muscle). Muscle
LRI Emergency Department
 LRI Emergency Department Guideline for the management of: Finger Tip Injuries in Children In the Paediatric Emergency Department (UHL Category C Guidance) Staff relevant to: ED Medical and Nursing staff
LRI Emergency Department Guideline for the management of: Finger Tip Injuries in Children In the Paediatric Emergency Department (UHL Category C Guidance) Staff relevant to: ED Medical and Nursing staff
Peggers Super Summaries: Foot Injuries
 Lisfranc Injury ANATOMY Roman arch with recessed 2 nd MT base AP medial side of intermediate cuneiform to 2 nd MT base Oblique medial side of lateral cuneiform with 3 rd MT base and 4 th with medial boarder
Lisfranc Injury ANATOMY Roman arch with recessed 2 nd MT base AP medial side of intermediate cuneiform to 2 nd MT base Oblique medial side of lateral cuneiform with 3 rd MT base and 4 th with medial boarder
Surgical repair of achilles tendon
 Surgical repair of achilles tendon Turnberg Building Orthopaedics 0161 206 4898 All Rights Reserved 2017. Document for issue as handout. Procedure Alternative procedure A tendon is a band of tissue that
Surgical repair of achilles tendon Turnberg Building Orthopaedics 0161 206 4898 All Rights Reserved 2017. Document for issue as handout. Procedure Alternative procedure A tendon is a band of tissue that
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
Ankle and Foot Orthopaedic Tests Orthopedics and Neurology DX 612
 Ankle and Foot Orthopaedic Tests Orthopedics and Neurology DX 612 James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Ankle & Foot Anatomy Stability of the ankle is dependent
Ankle and Foot Orthopaedic Tests Orthopedics and Neurology DX 612 James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Ankle & Foot Anatomy Stability of the ankle is dependent
ASSESSMENT AND MANAGEMENT OF THE KNEE AND LOWER LIMB.
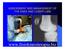 ASSESSMENT AND MANAGEMENT OF THE KNEE AND LOWER LIMB www.fisiokinesiterapia.biz Overview History Examination X-rays Fractures and Dislocations. Soft Tissue Injuries Other Knee/Lower limb Problems Anatomy
ASSESSMENT AND MANAGEMENT OF THE KNEE AND LOWER LIMB www.fisiokinesiterapia.biz Overview History Examination X-rays Fractures and Dislocations. Soft Tissue Injuries Other Knee/Lower limb Problems Anatomy
WHAT IS THIS CONDITION? COMMON CAUSES:
 Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT IS THIS CONDITION? The posterior tibial tendon is an important structure that is normally
Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT IS THIS CONDITION? The posterior tibial tendon is an important structure that is normally
Achilles Tendonitis and Tears
 Achilles Tendonitis and Tears The Achilles tendon is an important structure for normal ankle motion and normal function, even for daily activities such as walking. Achilles tendonitis can occur in patients
Achilles Tendonitis and Tears The Achilles tendon is an important structure for normal ankle motion and normal function, even for daily activities such as walking. Achilles tendonitis can occur in patients
ANKLE PLANTAR FLEXION
 ANKLE PLANTAR FLEXION Evaluation and Measurements By Isabelle Devreux 1 Ankle Plantar Flexion: Gastrocnemius and Soleus ROM: 0 to 40-45 A. Soleus: Origin: Posterior of head of fibula and proximal1/3 of
ANKLE PLANTAR FLEXION Evaluation and Measurements By Isabelle Devreux 1 Ankle Plantar Flexion: Gastrocnemius and Soleus ROM: 0 to 40-45 A. Soleus: Origin: Posterior of head of fibula and proximal1/3 of
An older systematic review looked at the evidence behind the best approach to evaluate acute knee pain in primary care (Ann Int Med.2003;139:575).
 There is so much we don't know in medicine that could make a difference, and often we focus on the big things, and the little things get forgotten. To highlight some smaller but important issues, we've
There is so much we don't know in medicine that could make a difference, and often we focus on the big things, and the little things get forgotten. To highlight some smaller but important issues, we've
Ankle Arthritis PATIENT INFORMATION. The ankle joint. What is ankle arthritis?
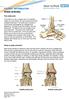 PATIENT INFORMATION Ankle Arthritis The ankle joint The ankle is a very complex joint. It is actually made up of two joints: the true ankle joint and the subtalar ankle joint. The ankle joint consists
PATIENT INFORMATION Ankle Arthritis The ankle joint The ankle is a very complex joint. It is actually made up of two joints: the true ankle joint and the subtalar ankle joint. The ankle joint consists
Anterior Cruciate Ligament Reconstruction
 Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
Anterior Cruciate Ligament (ACL) Reconstruction
 Further information Information on who to contact, i.e. web sites / telephone numbers of other departments / organisations which may be of help. How to contact us Watford General Hospital West Hertfordshire
Further information Information on who to contact, i.e. web sites / telephone numbers of other departments / organisations which may be of help. How to contact us Watford General Hospital West Hertfordshire
ANKLE JOINT ANATOMY 3. TALRSALS = (FOOT BONES) Fibula. Frances Daly MSc 1 CALCANEUS 2. TALUS 3. NAVICULAR 4. CUBOID 5.
 ANKLE JOINT ANATOMY The ankle joint is a synovial joint of the hinge type. The joint is formed by the distal end of the tibia and medial malleolus, the fibula and lateral malleolus and talus bone. It is
ANKLE JOINT ANATOMY The ankle joint is a synovial joint of the hinge type. The joint is formed by the distal end of the tibia and medial malleolus, the fibula and lateral malleolus and talus bone. It is
Everything. You Should Know. About Your Ankles
 Everything You Should Know About Your Ankles How Your Ankle Works The ankle joint is a hinge type joint that participates in movement and is involved in lower limb stability. There are 2 types of motions
Everything You Should Know About Your Ankles How Your Ankle Works The ankle joint is a hinge type joint that participates in movement and is involved in lower limb stability. There are 2 types of motions
Tibialis Posterior Tendon Dysfunction. Orthopaedic Department Patient Information Leaflet
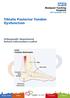 Tibialis Posterior Tendon Dysfunction Orthopaedic Department Patient Information Leaflet What is Tibialis Posterior Tendon Dysfunction? The Tibialis Posterior Tendon (see diagram) is an important structure
Tibialis Posterior Tendon Dysfunction Orthopaedic Department Patient Information Leaflet What is Tibialis Posterior Tendon Dysfunction? The Tibialis Posterior Tendon (see diagram) is an important structure
CHRONIC FOOT PROBLEMS FOOT and ANKLE BASICS
 CHRONIC FOOT PROBLEMS FOOT and ANKLE BASICS ABC s of Comprehensive Musculoskeletal Care December 1 st, 2007 Stephen Pinney MD Chief, UCSF Foot and Ankle Service Chronic problems typically occur gradually
CHRONIC FOOT PROBLEMS FOOT and ANKLE BASICS ABC s of Comprehensive Musculoskeletal Care December 1 st, 2007 Stephen Pinney MD Chief, UCSF Foot and Ankle Service Chronic problems typically occur gradually
Calcaneus (Heel Bone) Fractures
 Page 1 of 8 Calcaneus (Heel Bone) Fractures A fracture of the calcaneus, or heel bone, can be a painful and disabling injury. This type of fracture commonly occurs during a high-energy event such as a
Page 1 of 8 Calcaneus (Heel Bone) Fractures A fracture of the calcaneus, or heel bone, can be a painful and disabling injury. This type of fracture commonly occurs during a high-energy event such as a
Plantar Fasciitis and Heel Pain
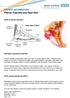 PATIENT INFORMATION Plantar Fasciitis and Heel Pain What is plantar fasciitis? Heel pain and plantar fasciitis Plantar fasciitis causes pain under your heel. It usually goes in time. Treatment may speed
PATIENT INFORMATION Plantar Fasciitis and Heel Pain What is plantar fasciitis? Heel pain and plantar fasciitis Plantar fasciitis causes pain under your heel. It usually goes in time. Treatment may speed
ANKLE SPRAINS. Explanation. Causes. Symptoms
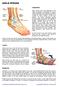 ANKLE SPRAINS Explanation Ankle sprains occur when ligaments in the ankle are partially or completely torn due to sudden stretching, either laterally or medially, or when the ankle is suddenly twisted
ANKLE SPRAINS Explanation Ankle sprains occur when ligaments in the ankle are partially or completely torn due to sudden stretching, either laterally or medially, or when the ankle is suddenly twisted
Ankle instability surgery
 Ankle instability surgery Ankle instability surgery is generally reserved for people with chronic ankle instability who have failed to respond to conservative treatment. The surgical technique used will
Ankle instability surgery Ankle instability surgery is generally reserved for people with chronic ankle instability who have failed to respond to conservative treatment. The surgical technique used will
Paul Alley MD,DPM,MS,FACS,FAAOS,BFD Eby Orthopaedics,Jasper,Indiana
 Paul Alley MD,DPM,MS,FACS,FAAOS,BFD Eby Orthopaedics,Jasper,Indiana Very common Bone=fractures Description (cracked,broke,busted,or smashed) A=anatomic area of bone eg: head,neck,shaft B=bone involved
Paul Alley MD,DPM,MS,FACS,FAAOS,BFD Eby Orthopaedics,Jasper,Indiana Very common Bone=fractures Description (cracked,broke,busted,or smashed) A=anatomic area of bone eg: head,neck,shaft B=bone involved
Main Menu. Ankle and Foot Joints click here. The Power is in Your Hands
 1 The Ankle and Foot Joints click here Main Menu Copyright HandsOn Therapy Schools 2009 K.8 http://www.handsonlineeducation.com/classes/k8/k8entry.htm[3/27/18, 1:40:03 PM] Ankle and Foot Joint 26 bones
1 The Ankle and Foot Joints click here Main Menu Copyright HandsOn Therapy Schools 2009 K.8 http://www.handsonlineeducation.com/classes/k8/k8entry.htm[3/27/18, 1:40:03 PM] Ankle and Foot Joint 26 bones
Recognizing common injuries to the lower extremity
 Recognizing common injuries to the lower extremity Bones Femur Patella Tibia Tibial Tuberosity Medial Malleolus Fibula Lateral Malleolus Bones Tarsals Talus Calcaneus Metatarsals Phalanges Joints - Knee
Recognizing common injuries to the lower extremity Bones Femur Patella Tibia Tibial Tuberosity Medial Malleolus Fibula Lateral Malleolus Bones Tarsals Talus Calcaneus Metatarsals Phalanges Joints - Knee
Columbia/NYOH FOOT and ANKLE ROTATION-SPECIFIC OBJECTIVES
 Updated 2/8/10 Columbia/NYOH FOOT and ANKLE ROTATION-SPECIFIC OBJECTIVES INTERPERSONAL AND COMMUNICATION SKILLS Resident will at all times demonstrate behavior that is beyond reproach. Residents must be
Updated 2/8/10 Columbia/NYOH FOOT and ANKLE ROTATION-SPECIFIC OBJECTIVES INTERPERSONAL AND COMMUNICATION SKILLS Resident will at all times demonstrate behavior that is beyond reproach. Residents must be
ANKLE FRACTURES. Contents The Ankle Joint... 3
 Contents The Ankle Joint................................................. 3 What is a fractured ankle?........................................ 4 YOUR GUIDE TO ANKLE FRACTURES What treatment can I receive?.....................................
Contents The Ankle Joint................................................. 3 What is a fractured ankle?........................................ 4 YOUR GUIDE TO ANKLE FRACTURES What treatment can I receive?.....................................
AMERICAN RED CROSS FIRST AID RESPONDING TO EMERGENCIES FOURTH EDITION Copyright 2006 by The American National Red Cross All rights reserved.
 Musculoskeletal injuries are most commonly caused by Mechanical forms of energy. Chemicals. Electrical energy. Heat Mechanical energy produces direct, indirect, twisting and contracting forces. Can be
Musculoskeletal injuries are most commonly caused by Mechanical forms of energy. Chemicals. Electrical energy. Heat Mechanical energy produces direct, indirect, twisting and contracting forces. Can be
METATARSAL FRACTURE (Including Jones and Dancer s Fractures)
 METATARSAL FRACTURE (Including Jones and Dancer s Fractures) Description Possible Complications Metatarsal fracture is a broken bone (fracture) in the middle Nonunion (fracture does not heal, particularly
METATARSAL FRACTURE (Including Jones and Dancer s Fractures) Description Possible Complications Metatarsal fracture is a broken bone (fracture) in the middle Nonunion (fracture does not heal, particularly
BUCKS MSK: FOOT AND ANKLE PATHWAY GP MANAGEMENT. Hallux Valgus. Assessment: Early Management. (must be attempted prior to any referral to imsk):
 Hallux Valgus Common condition: affecting around 28% of the adult population. Prevalence increases with age and in females. Observation: Lateral deviation of the great toe. May cause secondary irritation
Hallux Valgus Common condition: affecting around 28% of the adult population. Prevalence increases with age and in females. Observation: Lateral deviation of the great toe. May cause secondary irritation
Bunion (hallux valgus deformity) surgery
 Bunion (hallux valgus deformity) surgery Bunion surgery is generally reserved for bunions that are severe and impacting on function. There most frequent surgical procedure used involves a medial incision
Bunion (hallux valgus deformity) surgery Bunion surgery is generally reserved for bunions that are severe and impacting on function. There most frequent surgical procedure used involves a medial incision
Sports Injuries of the Foot and Ankle. Mark McEleney, MD University of Iowa College of Medicine Refresher Course for the Family Physician 4/4/2018
 Sports Injuries of the Foot and Ankle Mark McEleney, MD University of Iowa College of Medicine Refresher Course for the Family Physician 4/4/2018 I. Objectives A. By the end of the lecture attendees will
Sports Injuries of the Foot and Ankle Mark McEleney, MD University of Iowa College of Medicine Refresher Course for the Family Physician 4/4/2018 I. Objectives A. By the end of the lecture attendees will
June 2013 Case Study. Author: T. Walker Robinson, MD, MPH, Nationwide Children s Hospital
 June 2013 Case Study Author: T. Walker Robinson, MD, MPH, Nationwide Children s Hospital Chief Complaint: Right ankle pain HPI: A 10 year old female dancer presents to the clinic with a five day history
June 2013 Case Study Author: T. Walker Robinson, MD, MPH, Nationwide Children s Hospital Chief Complaint: Right ankle pain HPI: A 10 year old female dancer presents to the clinic with a five day history
Therapy following a neck of femur fracture
 INFORMATION FOR PATIENTS Therapy following a neck of femur fracture Name of patient: ffffffffffffffffffffffffffffffffffffffffffff Procedure: ffffffffffffffffffffffffffffffffffffffffffffffffffff Consultant:
INFORMATION FOR PATIENTS Therapy following a neck of femur fracture Name of patient: ffffffffffffffffffffffffffffffffffffffffffff Procedure: ffffffffffffffffffffffffffffffffffffffffffffffffffff Consultant:
ACHILLES TENDON RUPTURE
 ACHILLES TENDON RUPTURE Description Expected Outcome Achilles tendon rupture is a complete tear of the Achilles tendon. This tendon, sometimes called the heel cord, is the tendon attachment of the calf
ACHILLES TENDON RUPTURE Description Expected Outcome Achilles tendon rupture is a complete tear of the Achilles tendon. This tendon, sometimes called the heel cord, is the tendon attachment of the calf
Developed By Name Signature Date
 Patient Group Direction 2155 version 2.0 Administration / Supply of Inhaled Salbutamol in Asthma by Registered Practitioners employed by Torbay and South Devon NHS Foundation Trust Date of Introduction:
Patient Group Direction 2155 version 2.0 Administration / Supply of Inhaled Salbutamol in Asthma by Registered Practitioners employed by Torbay and South Devon NHS Foundation Trust Date of Introduction:
THE LOWER EXTREMITY EXAM FOR THE FAMILY PRACTITIONER
 THE LOWER EXTREMITY EXAM FOR THE FAMILY PRACTITIONER Melinda A. Scott, D.O. Orthopedic Associates of Dayton Board Certified in Primary Care Sports Medicine GOALS Identify landmarks necessary for exam of
THE LOWER EXTREMITY EXAM FOR THE FAMILY PRACTITIONER Melinda A. Scott, D.O. Orthopedic Associates of Dayton Board Certified in Primary Care Sports Medicine GOALS Identify landmarks necessary for exam of
NICE guideline Published: 17 February 2016 nice.org.uk/guidance/ng38
 Fractures (non-complex): assessment and management NICE guideline Published: 17 February 2016 nice.org.uk/guidance/ng38 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Fractures (non-complex): assessment and management NICE guideline Published: 17 February 2016 nice.org.uk/guidance/ng38 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Ankle Arthroscopy PATIENT INFORMATION. What is an ankle arthroscopy? Common disorders in which ankle arthroscopy is useful.
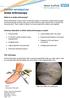 PATIENT INFORMATION Ankle Arthroscopy What is an ankle arthroscopy? Ankle arthroscopy is also known as keyhole surgery or minimally invasive ankle surgery. Ankle arthroscopy involves using very small incisions
PATIENT INFORMATION Ankle Arthroscopy What is an ankle arthroscopy? Ankle arthroscopy is also known as keyhole surgery or minimally invasive ankle surgery. Ankle arthroscopy involves using very small incisions
ANKLE SPRAIN, ACUTE. Description
 Description ANKLE SPRAIN, ACUTE An acute ankle sprain involves the stretching and tearing of one or more ligaments in the ankle. A two-ligament sprain causes more disability than a single-ligament sprain.
Description ANKLE SPRAIN, ACUTE An acute ankle sprain involves the stretching and tearing of one or more ligaments in the ankle. A two-ligament sprain causes more disability than a single-ligament sprain.
A Patient s Guide to Adult-Acquired Flatfoot Deformity
 A Patient s Guide to Adult-Acquired Flatfoot Deformity Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Adult-Acquired Flatfoot Deformity Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled
Foot and ankle. Achilles tendon rupture repair. After surgery
 Foot and ankle Achilles tendon rupture repair There is no agreed single best treatment for Achilles tendon ruptures. Similar results can be achieved with non-surgical and surgical treatments. There is
Foot and ankle Achilles tendon rupture repair There is no agreed single best treatment for Achilles tendon ruptures. Similar results can be achieved with non-surgical and surgical treatments. There is
PRIMARY CARE EXAMINATION OF KEY JOINTS. Thomas M. Howard, MD, FACSM FFPC Sports Medicine
 PRIMARY CARE EXAMINATION OF KEY JOINTS Thomas M. Howard, MD, FACSM FFPC Sports Medicine General exam principles: Expose entire joint and opposite limb for comparison Have a Differential Diagnosis Exam
PRIMARY CARE EXAMINATION OF KEY JOINTS Thomas M. Howard, MD, FACSM FFPC Sports Medicine General exam principles: Expose entire joint and opposite limb for comparison Have a Differential Diagnosis Exam
Lapidus procedure and Akin osteotomy
 Lapidus procedure and Akin osteotomy Bunion surgery Information for patients Department of Podiatric Surgery What is a bunion? A bunion is a bony deformity of the joint at the base of the big toe (hallux).
Lapidus procedure and Akin osteotomy Bunion surgery Information for patients Department of Podiatric Surgery What is a bunion? A bunion is a bony deformity of the joint at the base of the big toe (hallux).
Managing Tibialis Posterior Tendon Injuries
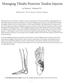 Managing Tibialis Posterior Tendon Injuries by Thomas C. Michaud, DC Published April 1, 2015 by Dynamic Chiropractic Magazine Tibialis posterior is the deepest, strongest, and most central muscle of the
Managing Tibialis Posterior Tendon Injuries by Thomas C. Michaud, DC Published April 1, 2015 by Dynamic Chiropractic Magazine Tibialis posterior is the deepest, strongest, and most central muscle of the
But it s only an ankle sprain. Ankle injuries are the most common injury to the lower limb as a result of sports.
 But it s only an ankle sprain Ankle injuries are the most common injury to the lower limb as a result of sports. Fortunately, most of them are minor and require little specific treatment, however, some
But it s only an ankle sprain Ankle injuries are the most common injury to the lower limb as a result of sports. Fortunately, most of them are minor and require little specific treatment, however, some
How is 1st MTP joint fusion carried out? Patient Information: Big Toe Fusion Metatarsophalangeal (MTP)
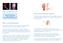 Patient Information: Big Toe Fusion Metatarsophalangeal (MTP) How is 1st MTP joint fusion carried out? You will be asked to wash your feet thoroughly on the day of operation and keep them clean, as this
Patient Information: Big Toe Fusion Metatarsophalangeal (MTP) How is 1st MTP joint fusion carried out? You will be asked to wash your feet thoroughly on the day of operation and keep them clean, as this
Lesser toe sequential repair
 Lesser toe sequential repair For the correction of lesser toe deformity Information for patients Department of Podiatric Surgery What is lesser toe deformity? The lesser toes are those other than your
Lesser toe sequential repair For the correction of lesser toe deformity Information for patients Department of Podiatric Surgery What is lesser toe deformity? The lesser toes are those other than your
BLUE SKY SCHOOL OF PROFESSIONAL MASSAGE AND THERAPEUTIC BODYWORK Musculoskeletal Anatomy & Kinesiology KNEE & ANKLE MUSCLES
 BLUE SKY SCHOOL OF PROFESSIONAL MASSAGE AND THERAPEUTIC BODYWORK Musculoskeletal Anatomy & Kinesiology KNEE & ANKLE MUSCLES MSAK201-I Session 3 1) REVIEW a) THIGH, LEG, ANKLE & FOOT i) Tibia Medial Malleolus
BLUE SKY SCHOOL OF PROFESSIONAL MASSAGE AND THERAPEUTIC BODYWORK Musculoskeletal Anatomy & Kinesiology KNEE & ANKLE MUSCLES MSAK201-I Session 3 1) REVIEW a) THIGH, LEG, ANKLE & FOOT i) Tibia Medial Malleolus
.org. Ankle Fractures (Broken Ankle) Anatomy
 Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
What Happens to the Paediatric Flat Foot? Peter J Briggs Freeman Hospital Newcastle upon Tyne
 What Happens to the Paediatric Flat Foot? Peter J Briggs Freeman Hospital Newcastle upon Tyne We don t know!! Population Studies 2300 children aged 4-13 years Shoe wearers Flat foot 8.6% Non-shoe wearers
What Happens to the Paediatric Flat Foot? Peter J Briggs Freeman Hospital Newcastle upon Tyne We don t know!! Population Studies 2300 children aged 4-13 years Shoe wearers Flat foot 8.6% Non-shoe wearers
MIDFOOT INJURIES-ARE WE UNDERTREATING IT? Mr Rajiv Limaye Mr Prasad Karpe University Hospital of North Tees 3 rd Foot and Ankle Symposium
 MIDFOOT INJURIES-ARE WE UNDERTREATING IT? Mr Rajiv Limaye Mr Prasad Karpe University Hospital of North Tees 3 rd Foot and Ankle Symposium Introduction Increasing sports injuries RTA and traumatic injuries
MIDFOOT INJURIES-ARE WE UNDERTREATING IT? Mr Rajiv Limaye Mr Prasad Karpe University Hospital of North Tees 3 rd Foot and Ankle Symposium Introduction Increasing sports injuries RTA and traumatic injuries
Medical Practice for Sports Injuries and Disorders of the Lower Limb
 Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Lower Limb JMAJ 48(1): 25 29, 2005 Motonobu NATSUYAMA Chief Surgeon, Department of Orthopedic Surgery, Kantoh
Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Lower Limb JMAJ 48(1): 25 29, 2005 Motonobu NATSUYAMA Chief Surgeon, Department of Orthopedic Surgery, Kantoh
Physiotherapy information for Achilles Tendinopathy
 Physiotherapy information for Achilles Tendinopathy What is Achilles Tendinopathy? Achilles Tendinopathy is a condition that can cause pain, swelling and weakness of the Achilles Tendon. This joins your
Physiotherapy information for Achilles Tendinopathy What is Achilles Tendinopathy? Achilles Tendinopathy is a condition that can cause pain, swelling and weakness of the Achilles Tendon. This joins your
Hany El-Rashidy and Anand Vora
 Chapter 194 Lisfranc Injuries Chapter 194 Lisfranc Injuries Hany El-Rashidy and Anand Vora 8 ICD-9 CODE 838.03 Lisfranc (Tarsometatarsal) Fracture-Dislocation Key Concepts The Lisfranc joint represents
Chapter 194 Lisfranc Injuries Chapter 194 Lisfranc Injuries Hany El-Rashidy and Anand Vora 8 ICD-9 CODE 838.03 Lisfranc (Tarsometatarsal) Fracture-Dislocation Key Concepts The Lisfranc joint represents
Results of Calcaneal Osteotomy & Flexor Digitorum Longus transfer in Stage II Acquired Flatfoot Deformity
 Results of Calcaneal Osteotomy & Flexor Digitorum Longus transfer in Stage II Acquired Flatfoot Deformity Mr Amit Chauhan Mr Prasad Karpe Ms Maire-claire Killen Mr Rajiv Limaye University Hospital of North
Results of Calcaneal Osteotomy & Flexor Digitorum Longus transfer in Stage II Acquired Flatfoot Deformity Mr Amit Chauhan Mr Prasad Karpe Ms Maire-claire Killen Mr Rajiv Limaye University Hospital of North
Weber B ankle fracture Information for patients Outpatient Fracture Care Team: Shared care plan
 Weber B ankle fracture Information for patients Outpatient Fracture Care Team: Shared care plan Orthopaedic Department Tunbridge Wells Hospital Tonbridge Road Pembury TN2 4QJ Telephone: 07734370108 Email:
Weber B ankle fracture Information for patients Outpatient Fracture Care Team: Shared care plan Orthopaedic Department Tunbridge Wells Hospital Tonbridge Road Pembury TN2 4QJ Telephone: 07734370108 Email:
A Patient s Guide to Post-Operative Advice Following Pes Cavus
 A Patient s Guide to Post-Operative Advice Following Pes Cavus The Foot and Ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of three specialist
A Patient s Guide to Post-Operative Advice Following Pes Cavus The Foot and Ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of three specialist
Achilles Tendon Rupture
 43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353 Website: philip-bayliss.com Achilles Tendon Rupture Summary Achilles tendon ruptures commonly occur in athletic individuals in their
43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353 Website: philip-bayliss.com Achilles Tendon Rupture Summary Achilles tendon ruptures commonly occur in athletic individuals in their
.org. Tibia (Shinbone) Shaft Fractures. Anatomy. Types of Tibial Shaft Fractures
 Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
OBJECTIVES: Define basic assessments skills needed to identify orthopedic injuries. Differentiate when an orthopedic injury is a medical emergency
 1 2 How to Triage Orthopaedic Care David W. Gray, M.D. OBJECTIVES: Define basic assessments skills needed to identify orthopedic injuries Differentiate when an orthopedic injury is a medical emergency
1 2 How to Triage Orthopaedic Care David W. Gray, M.D. OBJECTIVES: Define basic assessments skills needed to identify orthopedic injuries Differentiate when an orthopedic injury is a medical emergency
Foot and ankle fractures
 Foot and ankle fractures Some fractures can be managed without surgery, but others require surgery to achieve the best possible outcome. Fractures and injuries to joints have a high risk of developing
Foot and ankle fractures Some fractures can be managed without surgery, but others require surgery to achieve the best possible outcome. Fractures and injuries to joints have a high risk of developing
Orthopaedic (Ankles & Feet) Referral Guidelines
 Orthopaedic (Ankles & Feet) Referral Guidelines Austin Health Orthopaedic Clinic holds weekly multidisciplinary meetings to discuss and plan the treatment of patients with Orthopaedic and Fracture conditions.
Orthopaedic (Ankles & Feet) Referral Guidelines Austin Health Orthopaedic Clinic holds weekly multidisciplinary meetings to discuss and plan the treatment of patients with Orthopaedic and Fracture conditions.
Goals. Initial management skeletal trauma. Physical Exam ABC OF PRIMARY CARE MEDICINE FRACTURE MANAGEMENT 12/4/2010
 ABC OF PRIMARY CARE MEDICINE FRACTURE MANAGEMENT Brian Feeley, MD UCSF Sports Medicine and Shoulder Surgery Goals Discuss common fractures and initial management, treatment guidelines Let your patients
ABC OF PRIMARY CARE MEDICINE FRACTURE MANAGEMENT Brian Feeley, MD UCSF Sports Medicine and Shoulder Surgery Goals Discuss common fractures and initial management, treatment guidelines Let your patients
Non weight bearing advice (post operative)
 Non weight bearing advice (post operative) Physiotherapy Department Patient information leaflet Who is this booklet for? This booklet is for post-operative patients who have been told that they will have
Non weight bearing advice (post operative) Physiotherapy Department Patient information leaflet Who is this booklet for? This booklet is for post-operative patients who have been told that they will have
LISFRANC FRACTURE-DISLOCATION
 LISFRANC FRACTURE-DISLOCATION Napoleon at Mont St. Bernard, Jacques-Louis David, 1800, Oil on Canvas, Musee du Louvre, Paris. This is Jacques-Louis David s immortal depiction of a young Napoleon Bonaparte,
LISFRANC FRACTURE-DISLOCATION Napoleon at Mont St. Bernard, Jacques-Louis David, 1800, Oil on Canvas, Musee du Louvre, Paris. This is Jacques-Louis David s immortal depiction of a young Napoleon Bonaparte,
