A Guideline to Good Practice in Total Knee Replacement in South Africa 2016
|
|
|
- Osborne Barton
- 6 years ago
- Views:
Transcription
1 A Guideline to Good Practice in Total Knee Replacement in South Africa 2016 CONTENTS 1. Introduction. 2. Indications for operation. 3. Outpatient consultation 4. Pre-admission assessment. 5. Hospital Admission 6. Hospital facilities required for TKR 7. Required operating theatre resources. 8. The Surgeon. 9. The Anaesthetist and Anaesthetic Technique 10. Record keeping and the operation notes. 11. The choice of implant. 12. Prophylaxis against venous thrombosis and pulmonary embolus. 13. Prophylaxis against infection. 14. Surgical technique. 15. Early post-operative care. 16. The follow up of patients after total knee replacement 17. Document review date. Steering committee 1. INTRODUCTION 1.1 This document is a statement of best practice in primary Total Knee Replacement (TKR) and from available data, the document identifies current best practice in general terms. It is not a statement which claims to be applicable to all patients or in all circumstances and is not a protocol but a guideline to assist the Surgeon, aiming to improve patient outcomes. 1.2 It has been adapted for South African circumstances from the Guide to Good Practice in Knee Replacement Surgery from the British Association for Surgery of the Knee and the amendments thereof in the New Zealand Guidelines. 1.3 The Guideline has been drawn up by the SA Arthroplasty (SAAS) and SA Knee Societies(SAKS) and is endorsed by the SA Orthopaedic Association (SAOA).
2 2. THE INDICATIONS FOR THE OPERATION 2.1 Severe pain and disability arising predominantly from osteoarthritis or inflammatory arthritis with accompanying radiological changes in the knee are almost always the indications for the operation, in patients where conservative treatment has failed or is futile. 2.2 Occasionally there may be an indication to replace a knee because of progressive deformity and/or instability, and pain may not necessarily be the most significant factor. Where comorbidities exist, risk benefit considerations may rule out the operation in an individual patient. 2.3 Occasionally periarticular fractures of the distal femur in elderly patients 2.4 Tumors about the knee 3. THE OUTPATIENT CONSULTATION 3.1 Usually the patient will have consulted their General Practitioner (GP) or Health Care Professional (HCP) who will seek the opinion of an Orthopaedic Surgeon The SAAS/SAKS regards minutes as the minimum time allowed for the first consultation 3.3 A confidential environment with access for relatives, and the reliable availability of notes and radiographs are essential for the consultation. 3.4 After clinical examination and general medical assessment the surgeon should provide the patient with an explanation of the problem in understandable language and discuss the available treatment options. An individual patient may have added risk factors present (such as cardiovascular disease, obesity, predisposition to venous thromboembolism, neurological disease or diabetes) and should be made aware of the added risks when these factors are present. The surgeon should try to verify that the patient has understood the information. 3.5 The Surgeon must offer information on the risks and benefits of any suggested treatment and the outcomes of performance of any proposed knee arthroplasty where appropriate. The precise reasons for the operation should be given. 3.6 A letter to the patient s GP and/or the referring HCP should confirm that these discussions have taken place and that the patient wishes to proceed with surgery. 4. PRE-ADMISSION ASSESSMENT 4.1 A managed system of pre-admission assessment is recommended as good practice and should take place within six weeks of the operation. 4.2 Routine investigation of blood, urine, blood pressure and relevant microbiological assessment are best carried out at the pre-admission assessment which should allow enough time to optimise the patient prior to surgery.
3 4.3 There is strong evidence that obese patients have poorer outcomes after TKR and a delay of up to 8 months will not worsen outcomes, thus allowing time for weight control programmes. 4.4 Routine screening for Methicillin Resistant Staphlococcus Aureus (MRSA) should be considered in patients that have been transferred from other health care facilities, patients with a history of recent admission to a health care facility and patients with a prior history of MRSA infection. All patients with a positive test should be decolonised with Mupurocin ointment and chlorhexidine or betadine body wash. 4.5 Disease-modifying agents for Rheumatoid Arthritis should be stopped prior to elective TJA ( although this is not universally accepted, with current controversy relating mainly to biologics.) The timing of drug discontinuation should be based on the specific medication and the individual patient. The cessation of immunosuppressant medications should be performed in consultation and under the direction of the treating physician. 4.6 The knee should be assessed for previous surgical and other scars and if necessary a Plastic Surgeon should be consulted 4.7 The X-Rays must be fully evaluated for any difficulties that may be encountered and in particular any hardware that may need to be removed. 4.8 Provisional discharge planning should take place in the pre-operative assessment. The planning takes into consideration age, co-morbidities, home circumstances and the availability of carers. 4.9 Access to rehabilitation beds should be available particularly for the elderly and the more severely disabled As same-day admission and early discharge has become more frequent, all these arrangements become vital for the safe passage of the patient through the peri-operative phase 4.11 Information about the operation may be given to the patient or relatives in leaflet, pamphlet or electronic format. It should be constructed in language that is understandable to the patient 5. HOSPITAL ADMISSION 5.1 All patients should be admitted to hospital with sufficient time before their knee replacement to allow pre-operative and pre-anaesthetic procedures to be completed. 5.2 The limb for operation should be marked in an area which is still visible after draping, and an explanation of anaesthesia be given by the anaesthetist involved 5.3 The patient must give consent to the operation which may be given in the outpatients, the preadmission clinic, or in the ward. 6. HOSPITAL FACILITIES REQURIED FOR TKR 6.1 Primary knee replacement operations are best carried out in hospitals where back-up from other medical and surgical disciplines is readily available. 6.2 Access to a High Care Unit and/or Intensive Care facilities is desirable. Such units should have staff trained in the management of arthroplasty patients.
4 6.3 Adequate numbers of trained nurses and the skills of Allied Medical Professionals, especially Physiotherapists, must be available. 6.4 In order to reduce the risk of infection, knee replacement patients should be nursed in orthopaedic wards in areas separate from patients who pose a potential risk of cross infection and wards which are staffed by a team experienced in the management of arthroplasty patients. 7. REQUIRED OPERATING THEATRE RESOURCES 7.1 Infection following operation is catastrophic for the patient and surgeon as well as very expensive to the Health Care provider. 7.2 The use of ultra clean air theatres is considered to be best practice for units performing knee replacement operations. The quality of ultra-clean air should be checked regularly. 7.3 The operating theatre should be dedicated to clean elective orthopaedic surgery or joint arthroplasty. Shared facilities with other clean surgical disciplines is acceptable practice when using ultra clean air, but data supporting this practice is not available. 7.4 In ultra-clean air theatres, interposition of theatre personnel between the air source and wound can increase rates of infection so provision of efficient occlusive clothing is critical 7.5 A combination of ultra-clean air theatres, systemic antibiotics active against coagulase negative staphylococci and, where applicable antibiotic impregnated cement with occlusive theatre clothing provides the most effective prophylaxis against infection. These reduce the rate of deep infection by a factor of 18 compared to conventional theatres without additional prophylactic measures. A combination of all these prophylactic measures is recommended. 7.6 Appropriate impenetrable clothing and drapes are essential. 7.7 The surgeon should have trained assistance during the operation, and a trained scrub nurse fully familiar with the required complex instrumentation is mandatory. Sometimes more than one assistant is required. 7.8 A full range of specialised implants and instruments must be readily available to address intraoperative complications such as fracture must be readily available. Non-orthopaedic emergencies such as vascular injury may occasionally occur and specialised instrumentation should be available to manage such situations. 8. THE SURGEON 8.1 Knee Replacement surgery may only be performed by a qualified Medical Professional registered with the Health Professionals Council of SA (HPCSA) and should have had sufficient training to perform the procedure to an acceptable standard. 8.2 The theoretical and practical skills of the Surgeon performing primary arthroplasty operations must be maintained by continuous professional development. 8.3 Surgeons who perform few TKR s per year should be aware than they have a statistically significantly higher risk of complications, re-admissions and revisions. They should consider having a higher volume or experienced Surgeon assist them in their TKR s
5 8.4 The operation requires an anaesthetist with the appropriate skills and techniques for TKR. 9. THE ANAESTHETIST AND THE ANAESTHETIC TECHNIQUE 9.1 The surgeon and anaesthetic team should collaborate to define the most appropriate local hospital protocol for patients including prophylactic antibiotic policy and policies for venous thromboembolism prevention. [See Sections 12 and 13] 9.2 The SA Society of Anaesthesiology (SASA) will shortly be drawing up their guidelines for Knee Replacement Surgery which will then be incorporated into this document. 10. RECORD KEEPING AND THE OPERATION NOTES 10.1 Good clinical records are a basic tool of clinical practice, are absolutely essential and should be comprehensive and legible 10.2 Regardless of the medium in which clinical data is recorded or stored, good clinical practice necessitates communication of clinical information and immediate access for postoperative instructions. It is essential that clinical records be reproducible and transmittable without delay, information loss or inaccuracy Within the record the general medical condition of the patient as well as fitness for operation should be recorded. It should contain the clinical history, the full clinical examination findings, preexisting medical history and all current disabilities and complaints. The diagnosis of the condition and the purpose of the operation should be stated and all medication should be listed 10.4 The process of fully-informed consent should be recorded correctly and the patient s signature witnessed as appropriate. The process should ensure that the patient is aware of the risks and benefits of the procedure being offered, as well as the option of not performing any procedure The operating surgeon should ideally complete his/her own consent form with the patient. In certain circumstances (for example Unicompartmental Replacement surgery) patients must be made aware of the fact that if intra-operative findings indicate that the procedure would be inappropriate then an alternative procedure (usually TKR) may be performed. This should be recorded A second consent is signed by the patient as part of the Hospital s pre-operative process and should be checked by the Surgeon before the procedure It is best practice that operative notes be made in writing, or dictated for typing and signed by the operating surgeon. If a pre-arranged pro forma is being used the operating surgeon should personally complete the pro forma A record of the operation should be made immediately following surgery and should include: The name of the operating surgeon, anaesthetist and assistant/s The diagnosis and the procedure performed. Details of the incision and any additional procedures to achieve satisfactory exposure, Description of the findings.
6 Details of all soft tissue release procedures. Details of significant tissue excision, transposition or augmentation. Details of serial numbers of prostheses and other implanted materials. Details of bone grafting. Details of component alignment Post implantation stability. Details of method of closure and sutures used. An accurate description of any difficulties or complications encountered and how these were overcome. Immediate post-operative instructions Progress after operations, including early complications, should be listed. The date of discharge and arrangements for continuity of care should be recorded All notes should be contemporaneous and should not be altered; errors should be identified. Orthopaedic records within general hospital records should be easily identified within the case notes Follow-up notes should allow another doctor to assume the care of the patient at any time. Details of written and verbal information given to general practitioners, patients, relatives and carers, whether at admission or later, must be recorded. Details of all investigations considered and whether the investigation has actually been requested should be noted. Ideally, at least one entry each day recording the patient s progress, but it is recognised that with pressures of work this is not always achievable particularly at weekends. An entry when the management of the patient is changed or when there is an additional procedure. An entry should be made whenever a doctor is called to see a patient. Deletions should be made with a single line and signed and dated All patients should have good quality antero-posterior and lateral (and if applicable a skyline Merchant view) radiographs of the operated knee before discharge from hospital, or at the first post-operative outpatient visit
7 10.13 Records and images should be retained to permit long-term follow-up and facilitate revision should it be required although this is not legally required according to HPCSA rules Patient, operative and prosthesis details should be entered into the South African Joint Registry 11. THE CHOICE OF IMPLANT 11.1 Orthopaedic Surgeons have large numbers of knee devices from which to choose. Many of these devices have not been subject to studies of outcome for as long as 10 years and should be used with caution and the patient must be made aware of this Care should be taken when using the term "total knee replacement" as this implies that all articular surfaces in the knee have been replaced including resurfacing of the patella. The issue of patellar resurfacing remains controversial as there is no strong data to support resurfacing or non resurfacing. Surgeons practising knee replacement therefore fall into three groups, those who always resurface, those who never resurface and those who selectively resurface. In primary knee arthroplasty implants may be unconstrained i.e., there is no direct mechanical linkage between the tibial and femoral components. Most prostheses have varying degrees of constraint and at present there is no compelling evidence to support the use of any particular design. Degenerative joint disease may be confined to one of the three compartments and in these circumstances implants are currently available which replace both sides of the single diseased compartment Concerns about the long term effect of polyethylene wear debris have resulted in the development of implants which involve the use of mobile polythene bearings in both total knee replacement and uni-compartmental tibio-femoral knee replacement. Both fixed and mobile bearing devices have good long term records but can be device dependant Many factors determine surgeon preference for an individual implant. Influences include their trainers, consultant colleagues, a desire to improve their own results or the perceived outcomes of existing devices. The manufacturers of knee devices can also have a significant effect on choice through the service they provide The choice of prosthesis should be governed by evidence of the effective performance of that implant 11.6 The choice of implant may be influenced by cost. Surgeons and their teams should ensure that the cost of the implant does not result in the use of an unproven or sub-standard implant 11.7 A Surgeon should not gain financially from the choice of a particular implant. The HPCSA Ethical rules state: 7. Fees and commission (1) A practitioner shall not accept commission or any material consideration, (monetary or otherwise) from a person or from another practitioner or institution in return for the purchase,
8 sale or supply of any goods, substances or materials used by him or her in the conduct of his or her professional practice Published results of many knee implants offer little help to the surgeon wishing to make an informed choice. Most outcome research is short term, non-comparative and does not take into account case-mix and variations in the operative technique of the operating surgeon. Importantly, there is no agreed standardisation of outcome measures for knee replacement A further confounding factor for the surgeon is that knee devices with apparently good published results have in the meantime been modified by the manufacturers and the clinically tested design is no longer available. There has been a failure to realise that even minor modifications to design, material, surface finish, or fixation techniques can dramatically alter the performance of a knee replacement The selection of knee prostheses for general use should normally be based on evidence published in peer reviewed journals. These include national arthroplasty registers such as the NJR in England and Wales, the Scandinavian, Australian and New Zealand registries. A clinical follow-up of at least 10 years with a published life table and survivorship curve calculated according to best statistical practice are recommended criteria in support of the use of a particular knee prosthesis. There should be at least a 90% ten year survival for knee prostheses In the absence of peer reviewed evidence of outcome at ten years, a device must be subject to ongoing surveillance and be part of a properly conducted controlled prospective trial. The use of such devices should have ethical approval. 12. PROPHYLAXIS AGAINST VENOUS THROMBOSIS AND PULMONARY EMBOLISM It is well recognised that venous thromboembolism does occur after primary knee replacement but there is debate regarding the precise incidence of this complication. Recent evidence suggests that the prevalence of fatal pulmonary embolism, even in the absence of chemical prophylaxis, is very low following both knee and hip replacement, and much lower than quoted in historical papers There is no doubt that deep venous thrombosis occurs fairly commonly after primary knee replacement and can be demonstrated, by venography, in between 30 and 60% of cases at any level and 10 to 20% of cases proximally. Only a very few of these develop a clinical event causing death or morbidity There is no good evidence to suggest that the use of chemical prophylaxis reduces either overall mortality or fatal pulmonary embolism, and there is a known morbidity from the use of chemical prophylaxis. In contemporary practice TKR should be regarded as moderate risk for death from pulmonary embolism. Chemical prophylaxis may reduce the risk of non-fatal pulmonary embolism (PE), but rigorous scientific evidence is not available. There are usually no long term sequelae from a non-fatal PE There is strong evidence for the effectiveness of low dose heparin, low molecular weight heparin and Warfarin in reducing radiological DVT by 40 to 60% but death from other causes may be
9 increased. There is also significant concern regarding possible bleeding complications which may put the knee replacement at considerable risk There should be a combination of mechanical and pharmacological prophylaxis. Mechanical prophylaxis encompasses either well-fitting stockings, foot or calf pumps and walking as soon as feasible. Pharmacological prophylaxis includes any of LMWH, Fondaparinux, Dabigatran, Rivaroxaban or aspirin started after 12 hours and continued for 4 to 6 weeks 12.6 Under normal circumstances, early mobilisation (6 to24 hours) after surgery should always be considered as should the use of mechanical methods of reducing deep venous thrombosis although rigorous scientific evidence that these are effective is also lacking. These measures are free of significant side effects In patients with proven thrombophilia, or a history of proximal DVT or PE full prolonged anticoagulation with oral agents is recommended. If the risk assessment indicates that the consequences of bleeding outweigh the benefits of pharmacological prophylaxis, surgeons may choose not to prescribe them but the reasons should be documented fully. Wound haematoma, significant haemarthrosis and failure of primary healing are strongly associated with an increased rate of deep infection 13. PROPHYLAXIS AGAINST INFECTION 13.1 Patients, prior to knee replacement, should be clinically screened for active infection Although there is no specific data relating to TKR, we believe that all patients should receive an intravenous broad spectrum antibiotic within an hour of induction of anaesthesia and with a further 24 hours of post-operative antibiotic administration The TKR should be performed in ultra clean air theatres with minimisation of personnel and foot traffic through theatre 13.4 A combination of systemic antibiotics active against coagulase negative staphylococci, ultraclean air theatres and either body exhaust suits or occlusive theatre clothing provides the most effective prophylaxis against infection Surgery should not be unduly prolonged and soft tissues should be handled gently. Haemostasis should be meticulously obtained pre closure, especially if no drain is to be used There does not appear to be an increased risk of urinary tract infection if an indwelling urinary catheter is used for only a short time in the immediate post-operative period There is strong evidence to support the use of Tranexamic Acid as it decreases postoperative blood loss, reduces haematomas and the necessity of postoperative transfusions and has no known contraindications. 14 SURGICAL TECHNIQUE 14.1 There is strong evidence that the use of a tourniquet in TKR increases short-term postoperative pain and, if used, should be for as short a period as possible and at the lowest effective pressure Any anterior incision which allows adequate exposure of the distal end of the femur, proximal end of the tibia and the posterior articular surface of the patella is acceptable.
10 14.3 The surgical approach selected should achieve these aims without the need to apply excessive forces to skin, soft tissue or bone The recognised complications of particular approaches should be explained to the patient Implants may be inserted with or without cement. In cemented knee replacement the bone surfaces should be cleaned, irrigated and dried before application of bone cement and cement should be compressed where possible. Current evidence does not support the use of antibiotic loaded cement For cementless knee replacement, adequate preparation of the bone and stable fixation of the implants must be achieved at operation Where possible, tension in the medial and lateral soft tissue structures should be balanced in both flexion and extension whilst excessive tension or laxity on one side in either flexion or extension should be avoided Rotation of the femoral and tibial components must be thoroughly checked and internal rotation of either should be avoided unless in exceptional circumstances After implantation the patellar tracking should be checked and appropriate adjustment made if not satisfactory. It is essential to check the integrity of the extensor mechanism before closure Leg length equality cannot be achieved in every case and is dictated by ligament tension which is more important, except in fully constrained prostheses Pre-operative flexion deformity should always be corrected at the time of surgery to gain full extension, but may still be noted at follow-up despite appropriate post-operative rehabilitation. Patients with marked limitation of flexion pre-operatively should be informed that they may not achieve full range of movement post-operatively In appropriate cases, bilateral simultaneous or sequential knee replacement may be performed under the same anaesthetic. There is evidence to suggest that rehabilitation is more rapid than after staged procedures, but there are some concerns about the morbidity of such major surgery. Patients undergoing bilateral surgery should ideally have no co-morbidities and be managed post-operatively in a high care unit Patient Specific Instrumentation, intra-operative navigation using imageless and CT guided techniques have been developed with the intention of improving the accuracy with which components are positioned. No differences in outcomes or complications have been shown compared with conventional instrumentation The use of minimally invasive (minimal incision) techniques have been described for TKA. The claimed benefits of minimally invasive TKR have not been reproduced in randomized clinical trials and concerns have been raised about increased complication rates using these techniques Surgeons should ensure that, when using new techniques or techniques new to them, they are capable and competent to perform these. Any specific risk associated with these new techniques, together with the surgeon s own experience in them, should be shared with the patient as part of the informed consent process There is variation in the use of wound drains and suture materials. Current evidence does not support the use of drains
11 15. EARLY POST-OPERATIVE CARE 15.1 It is important to confirm neurovascular integrity in the operated limb at an early stage Drains, catheters and other indwelling access should be removed as soon as clinically indicated Strong evidence supports that rehabilitation started on the day of TKR reduces the length of stay in the hospital Mobilisation, the achievement of full extension and an increasing flexion range should be supervised by a physiotherapist experienced in the management of patients following knee replacement. Patients undergoing knee replacement at the end of the working week should have access to physiotherapy at the weekend. Adequate provision for outpatient physiotherapy is also required There is no evidence to support the use of continuous passive motion (CPM) machines. 16. THE FOLLOW-UP OF PATIENTS AFTER TOTAL KNEE REPLACEMENT 16.1 Patients should be followed up by the Surgeon or by an HCP experienced in TKR follow up at days post operatively in uncomplicated cases and as clinically indicated where there have been concerns. An assessment should be made at 6 weeks to ensure rehabilitation is progressing adequately 16.2 Primary TKR may fail between five and ten years but the majority fail after ten years. For best practice, patients should be followed up clinically and radiologically in the long term We believe that ideally a minimum requirement is an AP and Lateral X-ray at five years, and each five years thereafter Failure from aseptic loosening of a TKR is often silent the patient does not complain. Regular follow-up identifies the patient at risk of progressive failure. Exchange or revision operations should be planned and performed before massive bone destruction occurs, as delay may result in the need for much more extensive surgery which is more demanding of resources and has a greater risk of failure. Revision procedures are less successful than primary operations Follow-up by using questionnaires with X-ray checks by non-medically qualified practitioners is used in some centres, but there is no audit evidence of the efficacy of such arrangements The establishment of a national knee arthroplasty register must be seen as a priority and must be adequately funded. Every Surgeon should make it his responsibility to ensure that his TKR s are captured on the South African Joint registry. 17. DOCUMENT REVIEW DATE 17.1 This document should be reviewed five years from the date of publication or more frequently should the situation arise.
12 STEERING COMMITTEE 20 th August 2016 SA Arthroplasty Society Dr Rob McLennan-Smith (President) Dr Jan de Vos ( Incoming President) Dr Lipalo Mokete (Secretary) Dr Allan van Zyl ( Past President) SA Knee Society Dr Brad Gelbart (President) Dr Ponky Firer ( Past President) SA Orthopaedic Association Dr Robert Fraser (President)
CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR
 CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR Evolution of TKR In 1860, Verneuil proposed interposition arthroplasty, involving the insertion of soft tissue
CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR Evolution of TKR In 1860, Verneuil proposed interposition arthroplasty, involving the insertion of soft tissue
FOOT AND ANKLE ARTHROSCOPY
 FOOT AND ANKLE ARTHROSCOPY Information for Patients WHAT IS FOOT AND ANKLE ARTHROSCOPY? The foot and the ankle are crucial for human movement. The balanced action of many bones, joints, muscles and tendons
FOOT AND ANKLE ARTHROSCOPY Information for Patients WHAT IS FOOT AND ANKLE ARTHROSCOPY? The foot and the ankle are crucial for human movement. The balanced action of many bones, joints, muscles and tendons
Bilateral total knee arthroplasty: One mobile-bearing and one fixed-bearing
 Journal of Orthopaedic Surgery 2001, 9(1): 45 50 Bilateral total knee arthroplasty: One mobile-bearing and one fixed-bearing KY Chiu, TP Ng, WM Tang and P Lam Department of Orthopaedic Surgery, The University
Journal of Orthopaedic Surgery 2001, 9(1): 45 50 Bilateral total knee arthroplasty: One mobile-bearing and one fixed-bearing KY Chiu, TP Ng, WM Tang and P Lam Department of Orthopaedic Surgery, The University
British Orthopaedic Association PATRON: H.R.H. THE PRINCE OF WALES
 British Orthopaedic Association PATRON: H.R.H. THE PRINCE OF WALES PRIMARY TOTAL HIP REPLACEMENT: A GUIDE TO GOOD PRACTICE First published by the British Orthopaedic Association, 1999; Revised Aug 2006,
British Orthopaedic Association PATRON: H.R.H. THE PRINCE OF WALES PRIMARY TOTAL HIP REPLACEMENT: A GUIDE TO GOOD PRACTICE First published by the British Orthopaedic Association, 1999; Revised Aug 2006,
RISKS AND COMPLICATIONS
 PATIENT INFORMATION SHEET RISKS AND COMPLICATIONS TOTAL HIP REPLACEMENT Page 1 of 12 RISKS AND COMPLICATIONS - TOTAL HIP REPLACEMENT Index Pages INTRODUCTION 3 (1) ANAESTHETIC AND MEDICAL: 4 (2) BLOOD
PATIENT INFORMATION SHEET RISKS AND COMPLICATIONS TOTAL HIP REPLACEMENT Page 1 of 12 RISKS AND COMPLICATIONS - TOTAL HIP REPLACEMENT Index Pages INTRODUCTION 3 (1) ANAESTHETIC AND MEDICAL: 4 (2) BLOOD
PARTIAL KNEE REPLACEMENT
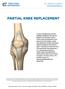 PARTIAL KNEE REPLACEMENT A partial knee replacement removes damaged cartilage from the knee and replaces it with prosthetic implants. Unlike a total knee replacement, which removes all of the cartilage,
PARTIAL KNEE REPLACEMENT A partial knee replacement removes damaged cartilage from the knee and replaces it with prosthetic implants. Unlike a total knee replacement, which removes all of the cartilage,
Total Hip Replacement
 AFFIX PATIENT DETAIL STICKER HERE and on each subsequent page Forename.. Male Female Surname Hospital Number... Consultant D.O.B.././ OPERATION: Total Hip Replacement PROCEDURE: The hip joint is a ball
AFFIX PATIENT DETAIL STICKER HERE and on each subsequent page Forename.. Male Female Surname Hospital Number... Consultant D.O.B.././ OPERATION: Total Hip Replacement PROCEDURE: The hip joint is a ball
RISKS AND COMPLICATIONS
 PATIENT INFORMATION SHEET RISKS AND COMPLICATIONS TOTAL HIP REPLACEMENT Page 1 of 8 INTRODUCTION A hip replacement is an extremely successful operation. At least 95% of patients are satisfied with their
PATIENT INFORMATION SHEET RISKS AND COMPLICATIONS TOTAL HIP REPLACEMENT Page 1 of 8 INTRODUCTION A hip replacement is an extremely successful operation. At least 95% of patients are satisfied with their
WHAT IS HIP ARTHROSCOPY?
 HIP ARTHROSCOPY Information for patients WHAT IS HIP ARTHROSCOPY? Hip arthroscopy is a minimally invasive procedure. An arthroscopic camera provides a magnified image of all parts of the joint. With the
HIP ARTHROSCOPY Information for patients WHAT IS HIP ARTHROSCOPY? Hip arthroscopy is a minimally invasive procedure. An arthroscopic camera provides a magnified image of all parts of the joint. With the
Introduction. Peripheral arterial disease. Hospital inpatient data - 5,498 FCE (2009/10), & 530 deaths in England alone
 1 Introduction 2 Introduction Peripheral arterial disease Affects 20% adults in Europe and North America In the UK 500-1000/million PAD, 1-2% require amputation LLA 8-15% in people with diabetes with up
1 Introduction 2 Introduction Peripheral arterial disease Affects 20% adults in Europe and North America In the UK 500-1000/million PAD, 1-2% require amputation LLA 8-15% in people with diabetes with up
North of England Bone and Soft Tissue Tumour Service
 North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after proximal tibial replacement Proximal tibial replacement surgery is usually carried out as part of treatment for
North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after proximal tibial replacement Proximal tibial replacement surgery is usually carried out as part of treatment for
About Knee Replacements
 Why have I received this leaflet? About Knee Replacements You have decided or are considering undergoing total knee replacement surgery. I will have discussed with you in clinic that knee replacements
Why have I received this leaflet? About Knee Replacements You have decided or are considering undergoing total knee replacement surgery. I will have discussed with you in clinic that knee replacements
Partial Knee Replacement
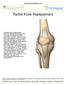 Partial Knee Replacement A partial knee replacement removes damaged cartilage from the knee and replaces it with prosthetic implants. Unlike a total knee replacement, which removes all of the cartilage,
Partial Knee Replacement A partial knee replacement removes damaged cartilage from the knee and replaces it with prosthetic implants. Unlike a total knee replacement, which removes all of the cartilage,
Venous Thromboembolism (VTE) Prevention and Treatment of VTE in Patients Admitted to Hospital
 Please Note: This policy is currently under review and is still fit for purpose. Venous Thromboembolism (VTE) Prevention and Treatment of VTE in Patients Admitted to Hospital This procedural document supersedes
Please Note: This policy is currently under review and is still fit for purpose. Venous Thromboembolism (VTE) Prevention and Treatment of VTE in Patients Admitted to Hospital This procedural document supersedes
Periarticular knee osteotomy
 Periarticular knee osteotomy Turnberg Building Orthopaedics 0161 206 4803 All Rights Reserved 2018. Document for issue as handout. Knee joint The knee consists of two joints which allow flexion (bending)
Periarticular knee osteotomy Turnberg Building Orthopaedics 0161 206 4803 All Rights Reserved 2018. Document for issue as handout. Knee joint The knee consists of two joints which allow flexion (bending)
Original Date: December 2015 Page 1 of 8 FOR CMS (MEDICARE) MEMBERS ONLY
 National Imaging Associates, Inc. Clinical guidelines TOTAL JOINT ARTHROPLASTY -Total Hip Arthroplasty -Total Knee Arthroplasty -Replacement/Revision Hip or Knee Arthroplasty CPT4 Codes: Please refer to
National Imaging Associates, Inc. Clinical guidelines TOTAL JOINT ARTHROPLASTY -Total Hip Arthroplasty -Total Knee Arthroplasty -Replacement/Revision Hip or Knee Arthroplasty CPT4 Codes: Please refer to
Dynamic Hip Screw - DHS
 Dynamic Hip Screw - DHS Turnberg Building Orthopaedics 0161 206 4898 All Rights Reserved 2017. Document for issue as handout. Procedure Alternative procedure The hip is an important ball and socket joint.
Dynamic Hip Screw - DHS Turnberg Building Orthopaedics 0161 206 4898 All Rights Reserved 2017. Document for issue as handout. Procedure Alternative procedure The hip is an important ball and socket joint.
YOUR TOTAL KNEE REPLACEMENT
 YOUR TOTAL KNEE REPLACEMENT Dr. M.S. Barrow Barrow Physiotherapy MBBch (Wits), FCS (SA) Orth. Waterfall City Hospital Orthopaedic Surgeon Tel: 011 304 7829 Suite 5, East Wing, Sunninghill Hospital www.barrowphysiotherapy.co.za
YOUR TOTAL KNEE REPLACEMENT Dr. M.S. Barrow Barrow Physiotherapy MBBch (Wits), FCS (SA) Orth. Waterfall City Hospital Orthopaedic Surgeon Tel: 011 304 7829 Suite 5, East Wing, Sunninghill Hospital www.barrowphysiotherapy.co.za
Fractured neck of femur
 PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label What is a fractured neck of femur? A healthy hip joint is vital to normal walking
PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label What is a fractured neck of femur? A healthy hip joint is vital to normal walking
UNICOMPARTMENTAL KNEE REPLACEMENT (UKR) PATIENT INFORMATION
 UNICOMPARTMENTAL KNEE REPLACEMENT (UKR) PATIENT INFORMATION The following information is to help you understand what is going to happen when you have a UKR. It is only a guide and some aspects will vary
UNICOMPARTMENTAL KNEE REPLACEMENT (UKR) PATIENT INFORMATION The following information is to help you understand what is going to happen when you have a UKR. It is only a guide and some aspects will vary
Simple removal of the kidney (simple nephrectomy): procedure-specific information
 PATIENT INFORMATION Simple removal of the kidney (simple nephrectomy): procedure-specific information What is the evidence base for this information? This leaflet includes advice from consensus panels,
PATIENT INFORMATION Simple removal of the kidney (simple nephrectomy): procedure-specific information What is the evidence base for this information? This leaflet includes advice from consensus panels,
Venous thromboembolism - reducing the risk
 Venous thromboembolism - reducing the risk Reducing the risk of venous thromboembolism (deep vein thrombosis and pulmonary embolism) in patients admitted to hospital NICE guideline Draft for consultation,
Venous thromboembolism - reducing the risk Reducing the risk of venous thromboembolism (deep vein thrombosis and pulmonary embolism) in patients admitted to hospital NICE guideline Draft for consultation,
TOTAL KNEE ARTHROPLASTY (Total Knee Replacement) The Knee Joint
 (Total Knee Replacement) The Knee Joint The knee is a hinge joint, formed by the end of the femur (thighbone) and the end of the tibia (shinbone). The bones are coated in cartilage, which acts as a cushion
(Total Knee Replacement) The Knee Joint The knee is a hinge joint, formed by the end of the femur (thighbone) and the end of the tibia (shinbone). The bones are coated in cartilage, which acts as a cushion
Venous thromboembolism: reducing the risk
 Issue date: January 2010 Venous thromboembolism: reducing the risk Reducing the risk of venous thromboembolism (deep vein thrombosis and pulmonary embolism) in patients admitted to hospital This guideline
Issue date: January 2010 Venous thromboembolism: reducing the risk Reducing the risk of venous thromboembolism (deep vein thrombosis and pulmonary embolism) in patients admitted to hospital This guideline
Venothromboembolism prophylaxis: Trauma and Orthopaedics Clinical guideline, V2
 Clinical Guideline Venothromboembolism prophylaxis: Trauma and Orthopaedics 11/11/11 TEMPORARY GUIDANCE There is no prophylactic tinzaparin available in the Trust currently. Please substitute enoxaparin
Clinical Guideline Venothromboembolism prophylaxis: Trauma and Orthopaedics 11/11/11 TEMPORARY GUIDANCE There is no prophylactic tinzaparin available in the Trust currently. Please substitute enoxaparin
Hip hemi-arthroplasty
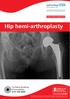 Hip hemi-arthroplasty Turnberg Building Orthopaedics 0161 206 4898 All Rights Reserved 2017. Document for issue as handout. Procedure The hip joint is a ball and socket joint. It is a very important joint
Hip hemi-arthroplasty Turnberg Building Orthopaedics 0161 206 4898 All Rights Reserved 2017. Document for issue as handout. Procedure The hip joint is a ball and socket joint. It is a very important joint
Venous Thromboembolism Prophylaxis
 Approved by: Venous Thromboembolism Prophylaxis Vice President and Chief Medical Officer; and Vice President and Chief Operating Officer Corporate Policy & Procedures Manual Number: Date Approved January
Approved by: Venous Thromboembolism Prophylaxis Vice President and Chief Medical Officer; and Vice President and Chief Operating Officer Corporate Policy & Procedures Manual Number: Date Approved January
*Corresponding Author:
 Audit of venous thromboembolism prophylaxis administered to general surgical patients undergoing elective and emergency operations at National Hospital, Sri Lanka *Migara Seneviratne 1, Asanka Hemachandra
Audit of venous thromboembolism prophylaxis administered to general surgical patients undergoing elective and emergency operations at National Hospital, Sri Lanka *Migara Seneviratne 1, Asanka Hemachandra
Clinical Practice Guideline for Patients Requiring Total Hip Replacement
 Clinical Practice Guideline for Patients Requiring Total Hip Replacement Inclusions Patients undergoing elective total hip replacement Exclusions Patients with active local or systemic infection or medical
Clinical Practice Guideline for Patients Requiring Total Hip Replacement Inclusions Patients undergoing elective total hip replacement Exclusions Patients with active local or systemic infection or medical
A study of functional outcome after Primary Total Knee Arthroplasty in elderly patients
 Original Research Article A study of functional outcome after Primary Total Knee Arthroplasty in elderly patients Ragesh Chandran 1*, Sanath K Shetty 2, Ashwin Shetty 3, Bijith Balan 1, Lawrence J Mathias
Original Research Article A study of functional outcome after Primary Total Knee Arthroplasty in elderly patients Ragesh Chandran 1*, Sanath K Shetty 2, Ashwin Shetty 3, Bijith Balan 1, Lawrence J Mathias
PATIENT INFORMATION Cartiva implant surgery
 PATIENT INFORMATION Cartiva implant surgery Introduction This leaflet will explain what will happen when you come to the hospital for an operation to have a Cartiva implant inserted into your toe joint.
PATIENT INFORMATION Cartiva implant surgery Introduction This leaflet will explain what will happen when you come to the hospital for an operation to have a Cartiva implant inserted into your toe joint.
Unicondylar Knee Vs Total Knee Replacement: Is Less Better In the Middle Aged Athlete
 Unicondylar Knee Vs Total Knee Replacement: Is Less Better In the Middle Aged Athlete Chair: Maurilio Marcacci, MD Alois Franz "Basic principles and considerations of the Unis" Joao M. Barretto "Sport
Unicondylar Knee Vs Total Knee Replacement: Is Less Better In the Middle Aged Athlete Chair: Maurilio Marcacci, MD Alois Franz "Basic principles and considerations of the Unis" Joao M. Barretto "Sport
Reducing the risk of venous thrombo-embolism (VTE) in hospital and after discharge
 Reducing the risk of venous thrombo-embolism (VTE) in hospital and after discharge What is a venous thromboembolism (VTE)? This is a medical term that describes a blood clot that develops in a deep vein
Reducing the risk of venous thrombo-embolism (VTE) in hospital and after discharge What is a venous thromboembolism (VTE)? This is a medical term that describes a blood clot that develops in a deep vein
Stefan Rahm MD University Hospital Balgrist
 Knee Prosthesis Models & Materials, Surgical Techniques and Approaches Stefan Rahm MD University Hospital Balgrist INTRODUCTION VARUS VALGUS 46 Y OLD MALE Pain in the medial compartment left more than
Knee Prosthesis Models & Materials, Surgical Techniques and Approaches Stefan Rahm MD University Hospital Balgrist INTRODUCTION VARUS VALGUS 46 Y OLD MALE Pain in the medial compartment left more than
Laparoscopic partial removal of the kidney
 Laparoscopic partial removal of the kidney Department of Urology 2 Patient Information What evidence is this information based on? This booklet includes advice from consensus panels, the British Association
Laparoscopic partial removal of the kidney Department of Urology 2 Patient Information What evidence is this information based on? This booklet includes advice from consensus panels, the British Association
Unicompartmental Knee Resurfacing
 Disclaimer This movie is an educational resource only and should not be used to manage knee pain. All decisions about the management of knee pain must be made in conjunction with your Physician or a licensed
Disclaimer This movie is an educational resource only and should not be used to manage knee pain. All decisions about the management of knee pain must be made in conjunction with your Physician or a licensed
Audit of perioperative management of patients with fracture neck of femur
 Audit of perioperative management of patients with fracture neck of femur *M Dissanayake 1, N Wijesuriya 2 Registrar in Anaesthesia 1, Consultant Anaesthetist 2, North Colombo Teaching Hospital, Ragama,
Audit of perioperative management of patients with fracture neck of femur *M Dissanayake 1, N Wijesuriya 2 Registrar in Anaesthesia 1, Consultant Anaesthetist 2, North Colombo Teaching Hospital, Ragama,
TOTAL HIP ARTHROPLASTY (Total Hip Replacement)
 (Total Hip Replacement) The Hip Joint The hip is a ball and socket joint. The joint is formed by the head of the femur (thighbone) and the acetabulum (pelvis). The bones are coated in cartilage, which
(Total Hip Replacement) The Hip Joint The hip is a ball and socket joint. The joint is formed by the head of the femur (thighbone) and the acetabulum (pelvis). The bones are coated in cartilage, which
EARLY CLINICAL RESULTS OF PRIMARY CEMENTLESS TOTAL KNEE ARTHROPLASTY
 EARLY CLINICAL RESULTS OF PRIMARY CEMENTLESS TOTAL KNEE ARTHROPLASTY Benkovich V. Perry T., Bunin A., Bilenko V., Unit for Joint Arthroplasty, Soroka Medical Center Ben Gurion University of Negev Beer
EARLY CLINICAL RESULTS OF PRIMARY CEMENTLESS TOTAL KNEE ARTHROPLASTY Benkovich V. Perry T., Bunin A., Bilenko V., Unit for Joint Arthroplasty, Soroka Medical Center Ben Gurion University of Negev Beer
Prevention and Management of Hip Fracture in Older People
 Scottish Intercollegiate Guidelines Network 56 Prevention and Management of Hip Fracture in Older People A national clinical guideline 1 Introduction 1 2 Prevention of hip fracture 4 3 Pre-hospital management
Scottish Intercollegiate Guidelines Network 56 Prevention and Management of Hip Fracture in Older People A national clinical guideline 1 Introduction 1 2 Prevention of hip fracture 4 3 Pre-hospital management
Hemiarthroplasty (half hip replacement)
 Hemiarthroplasty (half hip replacement) Trauma and Orthopaedics Patient Information Leaflet Introduction This leaflet is about an operation called a half hip replacement. It gives information about the
Hemiarthroplasty (half hip replacement) Trauma and Orthopaedics Patient Information Leaflet Introduction This leaflet is about an operation called a half hip replacement. It gives information about the
Misunderstandings of Venous thromboembolism prophylaxis
 Misunderstandings of Venous thromboembolism prophylaxis Veerendra Chadachan Senior Consultant Dept of General Medicine (Vascular Medicine and Hypertension) Tan Tock Seng Hospital, Singapore Case scenario
Misunderstandings of Venous thromboembolism prophylaxis Veerendra Chadachan Senior Consultant Dept of General Medicine (Vascular Medicine and Hypertension) Tan Tock Seng Hospital, Singapore Case scenario
Subcapital hip fracture surgery. Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Subcapital hip fracture surgery Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the
Subcapital hip fracture surgery Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the
Ankle Arthroscopy.
 Ankle Arthroscopy Key words: Ankle pain, ankle arthroscopy, ankle sprain, ankle stiffness, day case surgery, articular cartilage, chondral injury, chondral defect, anti-inflammatory medication Our understanding
Ankle Arthroscopy Key words: Ankle pain, ankle arthroscopy, ankle sprain, ankle stiffness, day case surgery, articular cartilage, chondral injury, chondral defect, anti-inflammatory medication Our understanding
Important notice: the device(s) can be prescribed and implanted only by a doctor legally authorized to perform this type of surgery.
 rev.10 CAUTION Federal law (USA) restricts this device to sale, by or on the order of a physician. ENGLISH - EVOLIS/GMK KNEE PROSTHESIS - INSTRUCTIONS FOR USE Important notice: the device(s) can be prescribed
rev.10 CAUTION Federal law (USA) restricts this device to sale, by or on the order of a physician. ENGLISH - EVOLIS/GMK KNEE PROSTHESIS - INSTRUCTIONS FOR USE Important notice: the device(s) can be prescribed
Radical removal of the kidney (radical nephrectomy): procedure-specific information
 PATIENT INFORMATION Radical removal of the kidney (radical nephrectomy): procedure-specific information What is the evidence base for this information? This leaflet includes advice from consensus panels,
PATIENT INFORMATION Radical removal of the kidney (radical nephrectomy): procedure-specific information What is the evidence base for this information? This leaflet includes advice from consensus panels,
JRI Thompson Hemiarthroplasty
 JRI ORTHOPAEDICS LTD 18 Churchill Way, 35A Business Park, Chapeltown, Sheffield, S35 2PY, UK Instructions for Use JRI Thompson Hemiarthroplasty Page 1 of 6 English 3 Page 2 of 6 Important Information Please
JRI ORTHOPAEDICS LTD 18 Churchill Way, 35A Business Park, Chapeltown, Sheffield, S35 2PY, UK Instructions for Use JRI Thompson Hemiarthroplasty Page 1 of 6 English 3 Page 2 of 6 Important Information Please
... Anterior Cruciate Ligament (ACL) Reconstruction (arthroscopic) using autograft
 AFFIX PATIENT DETAIL STICKER HERE and on each subsequent page Forename.. Male Female Surname Hospital Number... Consultant.. D.O.B.././ OPERATION:..... Anterior Cruciate Ligament (ACL) Reconstruction (arthroscopic)
AFFIX PATIENT DETAIL STICKER HERE and on each subsequent page Forename.. Male Female Surname Hospital Number... Consultant.. D.O.B.././ OPERATION:..... Anterior Cruciate Ligament (ACL) Reconstruction (arthroscopic)
Arthroscopy. This booklet can also be provided in large print on request. Please call Delivering Excellence. Nuffield Orthopaedic Centre
 This booklet can also be provided in large print on request. Please call 01865 738126 Nuffield Orthopaedic Centre NHS Trust www.noc.nhs.uk NHS Arthroscopy Marketing & Communications Nuffield Orthopaedic
This booklet can also be provided in large print on request. Please call 01865 738126 Nuffield Orthopaedic Centre NHS Trust www.noc.nhs.uk NHS Arthroscopy Marketing & Communications Nuffield Orthopaedic
TOTAL KNEE ARTHROPLASTY (TKA)
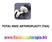 TOTAL KNEE ARTHROPLASTY (TKA) 1 Anatomy, Biomechanics, and Design 2 Femur Medial and lateral condyles Convex, asymmetric Medial larger than lateral 3 Tibia Tibial plateau Medial tibial condyle: concave
TOTAL KNEE ARTHROPLASTY (TKA) 1 Anatomy, Biomechanics, and Design 2 Femur Medial and lateral condyles Convex, asymmetric Medial larger than lateral 3 Tibia Tibial plateau Medial tibial condyle: concave
Total Knee Original System Primary Surgical Technique
 Surgical Procedure Total Knee Original System Primary Surgical Technique Where as a total hip replacement is primarily a bony operation, a total knee replacement is primarily a soft tissue operation. Excellent
Surgical Procedure Total Knee Original System Primary Surgical Technique Where as a total hip replacement is primarily a bony operation, a total knee replacement is primarily a soft tissue operation. Excellent
You and Your Knee Joint Replacement. Joint School Surgical Rehabilitation Team
 You and Your Knee Joint Replacement Joint School Surgical Rehabilitation Team Housekeeping Length of Session Questions during the session Fire Toilet Facilities Moving around to relieve discomfort Enhanced
You and Your Knee Joint Replacement Joint School Surgical Rehabilitation Team Housekeeping Length of Session Questions during the session Fire Toilet Facilities Moving around to relieve discomfort Enhanced
Total knee replacement: The enhanced recovery programme
 INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, to outline certain common
INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, to outline certain common
Surgical Technique Final Trial Reduction and Component Implantation of
 Surgical Technique Final Trial Reduction and Component Implantation of TC *smith&nephew TC-PLUS PRIMARY Mobile Bearing TC-PLUS PRIMARY Mobile Bearing Final Trial Reduction and Component Implantation of
Surgical Technique Final Trial Reduction and Component Implantation of TC *smith&nephew TC-PLUS PRIMARY Mobile Bearing TC-PLUS PRIMARY Mobile Bearing Final Trial Reduction and Component Implantation of
Total knee replacement
 PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label What is a total knee replacement? In a total knee replacement the cartilage surfaces
PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label What is a total knee replacement? In a total knee replacement the cartilage surfaces
Hospital Acquired VTE: update on national guidance
 Hospital Acquired VTE: update on national guidance Rebecca Chanda Consultant Pharmacist - Thrombosis and Haemostasis Guy s and St Thomas Hospitals NHS Foundation Trust Chair of the UK Clinical Pharmacy
Hospital Acquired VTE: update on national guidance Rebecca Chanda Consultant Pharmacist - Thrombosis and Haemostasis Guy s and St Thomas Hospitals NHS Foundation Trust Chair of the UK Clinical Pharmacy
Ankle Fracture Orthopaedic Department Patient Information Leaflet. Under review. Page 1
 Ankle Fracture Orthopaedic Department Patient Information Leaflet Page 1 Ankle Fracture Welcome to the Dudley Group NHS Foundation Trust. This leaflet will provide you with information regarding the diagnosis
Ankle Fracture Orthopaedic Department Patient Information Leaflet Page 1 Ankle Fracture Welcome to the Dudley Group NHS Foundation Trust. This leaflet will provide you with information regarding the diagnosis
How to prevent blood clots whilst in hospital and after your return home
 How to prevent blood clots whilst in hospital and after your return home Patient information WHAT What IS is DEEP deep VEIN vein THROMBOSIS? thrombosis? Deep Vein Thrombosis DVT is a blood clot within
How to prevent blood clots whilst in hospital and after your return home Patient information WHAT What IS is DEEP deep VEIN vein THROMBOSIS? thrombosis? Deep Vein Thrombosis DVT is a blood clot within
Mr Aslam Mohammed FRCS, FRCS (Orth) Consultant Orthopaedic Surgeon Specialising in Lower Limb Arthroplasty and Sports Injury
 Mr Aslam Mohammed FRCS, FRCS (Orth) Consultant Orthopaedic Surgeon Specialising in Lower Limb Arthroplasty and Sports Injury I qualified from the Welsh National School of Medicine in Cardiff in 1984. I
Mr Aslam Mohammed FRCS, FRCS (Orth) Consultant Orthopaedic Surgeon Specialising in Lower Limb Arthroplasty and Sports Injury I qualified from the Welsh National School of Medicine in Cardiff in 1984. I
These are guidelines only and can be deviated from if it is thought to be in the patient s best interest.
 Clinical Guideline Venothromboembolism prophylaxis: Trauma and Orthopaedics Venous thromboembolism (VTE) is a recognised complication associated with inactivity and surgical procedures. Therefore, all
Clinical Guideline Venothromboembolism prophylaxis: Trauma and Orthopaedics Venous thromboembolism (VTE) is a recognised complication associated with inactivity and surgical procedures. Therefore, all
AN AUDIT: THROMBOPROPHYLAXIS FOR TOTAL HIP REPLACEMENT PATIENTS AT NORTHWICK PARK AND CENTRAL MIDDLESEX HOSPITALS
 The West London Medical Journal 2010 Vol 2 No 4 pp 19-24 AN AUDIT: THROMBOPROPHYLAXIS FOR TOTAL HIP REPLACEMENT PATIENTS AT NORTHWICK PARK AND CENTRAL MIDDLESEX HOSPITALS Soneji ND Agni NR Acharya MN Anjari
The West London Medical Journal 2010 Vol 2 No 4 pp 19-24 AN AUDIT: THROMBOPROPHYLAXIS FOR TOTAL HIP REPLACEMENT PATIENTS AT NORTHWICK PARK AND CENTRAL MIDDLESEX HOSPITALS Soneji ND Agni NR Acharya MN Anjari
Radial head fractures; ORIF radial head; radial head arthroplasty; coronoid process fracture; ligament repair Elbow Anatomy Spectrum of injuries
 Radial head fractures; ORIF radial head; radial head arthroplasty; coronoid process fracture; ligament repair This information aims to help you understand your condition and gain maximum benefit from your
Radial head fractures; ORIF radial head; radial head arthroplasty; coronoid process fracture; ligament repair This information aims to help you understand your condition and gain maximum benefit from your
For more information on arthritis and knee replacements please see:
 Chester Knee Clinic at Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Consultant Orthopaedic Surgeon: Vladimir Bobic, MD, FRCSEd www.kneeclinic.info office@kneeclinic.info
Chester Knee Clinic at Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Consultant Orthopaedic Surgeon: Vladimir Bobic, MD, FRCSEd www.kneeclinic.info office@kneeclinic.info
Patient information. Total Ankle Replacement Trauma and Orthopaedic Directorate PIF 1335 V2
 Patient information Total Ankle Replacement Trauma and Orthopaedic Directorate PIF 1335 V2 Your Consultant has advised you that you are suitable to have a total ankle replacement. The aim of surgery is
Patient information Total Ankle Replacement Trauma and Orthopaedic Directorate PIF 1335 V2 Your Consultant has advised you that you are suitable to have a total ankle replacement. The aim of surgery is
KNEE ARTHROSCOPY PATIENT INFORMATION SHEET
 KNEE ARTHROSCOPY PATIENT INFORMATION SHEET Introduction It has been recommended that you undergo an arthroscopy of your knee. This information sheet is designed to explain what is involved in an arthroscopy,
KNEE ARTHROSCOPY PATIENT INFORMATION SHEET Introduction It has been recommended that you undergo an arthroscopy of your knee. This information sheet is designed to explain what is involved in an arthroscopy,
A Patient s Guide to Partial Knee Resurfacing
 A Patient s Guide to Partial Knee Resurfacing Surgical Outcomes System (SOS ) www.orthoillustrated.com OrthoIllustrated is a leading Internet-based resource for patient education. Please visit this website
A Patient s Guide to Partial Knee Resurfacing Surgical Outcomes System (SOS ) www.orthoillustrated.com OrthoIllustrated is a leading Internet-based resource for patient education. Please visit this website
CEC ARTICLE: Special Medical Conditions Part 3: Hip and Knee Replacement C. Eggers
 CEC ARTICLE: Special Medical Conditions Part 3: Hip and Knee Replacement C. Eggers Joint replacement surgery removes a damaged joint and replaces it with a prosthesis or artificial joint. The purpose of
CEC ARTICLE: Special Medical Conditions Part 3: Hip and Knee Replacement C. Eggers Joint replacement surgery removes a damaged joint and replaces it with a prosthesis or artificial joint. The purpose of
Appendix E : Evidence table 9 Rehabilitation: Other Key Documents
 Appendix E : Evidence table 9 Rehabilitation: Other Key Documents 1. Cameron et al. Geriatric rehabilitation following following fractures in older people: a systematic review. Health Technology Assessment
Appendix E : Evidence table 9 Rehabilitation: Other Key Documents 1. Cameron et al. Geriatric rehabilitation following following fractures in older people: a systematic review. Health Technology Assessment
Venous thromboembolism after total knee replacement or total hip replacement: what can be learnt from root-cause analysis?
 TRAUMA AND ORTHOPAEDIC SURGERY Ann R Coll Surg Engl 2016; 98: 538 542 doi 10.1308/rcsann.2016.0202 Venous thromboembolism after total knee replacement or total hip replacement: what can be learnt from
TRAUMA AND ORTHOPAEDIC SURGERY Ann R Coll Surg Engl 2016; 98: 538 542 doi 10.1308/rcsann.2016.0202 Venous thromboembolism after total knee replacement or total hip replacement: what can be learnt from
THE RECOVERY PROCESS
 THE RECOVERY PROCESS PART II If you're considering a major Orthopaedic surgical procedure to relieve pain in your back, knee, or hip, there's a lot to consider. These procedures, while common, do come
THE RECOVERY PROCESS PART II If you're considering a major Orthopaedic surgical procedure to relieve pain in your back, knee, or hip, there's a lot to consider. These procedures, while common, do come
Massive Varus- Overview. Massive Varus- Classification. Massive Varus- Definition 07/02/14. Correction of Massive Varus Deformity in TKR
 07/02/14 Massive Varus- Overview Correction of Massive Varus Deformity in TKR Myles Coolican Val d Isere 2014 Massive Varus- Classification Classification Intra articular Massive Varus- Classification Classification
07/02/14 Massive Varus- Overview Correction of Massive Varus Deformity in TKR Myles Coolican Val d Isere 2014 Massive Varus- Classification Classification Intra articular Massive Varus- Classification Classification
Internal fixation of a hip fracture. Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Internal fixation of a hip fracture Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained
Internal fixation of a hip fracture Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained
The in-hospital management of COPD-exacerbation includes three core processes:
 Appendix 1A. Process flow for in-hospital management of COPDexacerbation The in-hospital management of COPD-exacerbation includes three core processes: 1. Diagnostic assessment 2. Pharmacological management
Appendix 1A. Process flow for in-hospital management of COPDexacerbation The in-hospital management of COPD-exacerbation includes three core processes: 1. Diagnostic assessment 2. Pharmacological management
CAUTION Federal law (USA) restricts this device to sale, by or on the order of a physician.
 CAUTION Federal law (USA) restricts this device to sale, by or on the order of a physician. ENGLISH Mpact 3D Metal Implants and Augments 3D Metal INSTRUCTION FOR USE Important notice: the device(s) can
CAUTION Federal law (USA) restricts this device to sale, by or on the order of a physician. ENGLISH Mpact 3D Metal Implants and Augments 3D Metal INSTRUCTION FOR USE Important notice: the device(s) can
Deep Vein Thrombosis and Pulmonary Embolism: Risks, Prevention & Treatment
 Deep Vein Thrombosis and Pulmonary Embolism: Risks, Prevention & Treatment Other formats If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast,
Deep Vein Thrombosis and Pulmonary Embolism: Risks, Prevention & Treatment Other formats If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast,
A Best Practice Clinical Care Pathway for Major Amputation Surgery
 A Best Practice Clinical Care Pathway for Major Amputation Surgery April 2016 Introduction The perioperative mortality rate after major lower limb amputation in the UK is unacceptably high in modern medical
A Best Practice Clinical Care Pathway for Major Amputation Surgery April 2016 Introduction The perioperative mortality rate after major lower limb amputation in the UK is unacceptably high in modern medical
Orthopaedic Mortality
 Orthopaedic Mortality Lessons from VASM Nigel Broughton Orthopaedic Surgeon, Peninsula Health AOA Rep on VASM Colin Russell Founder of VASM Director of Surgery, Peninsula Health 1993-2007 First Clinical
Orthopaedic Mortality Lessons from VASM Nigel Broughton Orthopaedic Surgeon, Peninsula Health AOA Rep on VASM Colin Russell Founder of VASM Director of Surgery, Peninsula Health 1993-2007 First Clinical
Knee Replacement Complications
 Knee Replacement Complications Knee replacements have become a routine surgery in the United States. Nearly 700,000 people each year receive this life-improving surgery and are able to enjoy richer, more
Knee Replacement Complications Knee replacements have become a routine surgery in the United States. Nearly 700,000 people each year receive this life-improving surgery and are able to enjoy richer, more
Lancashire Teaching Hospitals NHS Foundation Trust Information for Patients having a Breast Reduction Operation
 Lancashire Teaching Hospitals NHS Foundation Trust Information for Patients having a Breast Reduction Operation Plastic Surgery Department Leaflet Number 2 Produced: October 2007 Review date: October 2010
Lancashire Teaching Hospitals NHS Foundation Trust Information for Patients having a Breast Reduction Operation Plastic Surgery Department Leaflet Number 2 Produced: October 2007 Review date: October 2010
Total Knee Replacement
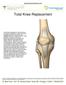 Total Knee Replacement A total knee replacement, also known as total knee arthroplasty, involves removing damaged portions of the knee, and capping the bony surfaces with man-made prosthetic implants.
Total Knee Replacement A total knee replacement, also known as total knee arthroplasty, involves removing damaged portions of the knee, and capping the bony surfaces with man-made prosthetic implants.
JOINT RULER. Surgical Technique For Knee Joint JRReplacement
 JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
National Joint Replacement Registry. Lay Summary 2015 Annual Report Hip and Knee Replacement
 National Joint Replacement Registry Lay Summary 2015 Annual Report Hip and Knee Replacement SUPPLEMENTARY REPORT 2015 TABLE OF CONTENTS Introduction... 1 A brief history of the Registry origins... 1 The
National Joint Replacement Registry Lay Summary 2015 Annual Report Hip and Knee Replacement SUPPLEMENTARY REPORT 2015 TABLE OF CONTENTS Introduction... 1 A brief history of the Registry origins... 1 The
Totally Hip Preservation to Revision. Gothenburg, Sweden 29 March - 1 April 2017 WEDNESDAY 29 MARCH. Arrivals THURSDAY 30 MARCH
 Totally Hip 2017 Preservation to Revision Gothenburg, Sweden 29 March - 1 April 2017 WEDNESDAY 29 MARCH Arrivals THURSDAY 30 MARCH 08:00 08:30 Welcome from the Chairmen, Co Chairmen and technical intro
Totally Hip 2017 Preservation to Revision Gothenburg, Sweden 29 March - 1 April 2017 WEDNESDAY 29 MARCH Arrivals THURSDAY 30 MARCH 08:00 08:30 Welcome from the Chairmen, Co Chairmen and technical intro
Dynamic hip screw (sliding hip screw)
 Dynamic hip screw (sliding hip screw) Trauma and Orthopaedics Patient Information Leaflet Introduction This leaflet is about an operation called a dynamic hip screw, sometimes also known as a sliding hip
Dynamic hip screw (sliding hip screw) Trauma and Orthopaedics Patient Information Leaflet Introduction This leaflet is about an operation called a dynamic hip screw, sometimes also known as a sliding hip
Tibial shaft fracture surgery (tibial nailing)
 Tibial shaft fracture surgery (tibial nailing) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we
Tibial shaft fracture surgery (tibial nailing) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION
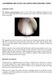 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION INTRODUCTION The anterior cruciate ligament (ACL) is one of the major stabilising ligaments in the knee. It is a strong rope like structure located in the centre
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION INTRODUCTION The anterior cruciate ligament (ACL) is one of the major stabilising ligaments in the knee. It is a strong rope like structure located in the centre
Page 1 of 6. Appendix 1
 Page 1 Appendix 1 Rotation Objectives and Schedule 1. Introductory Month 4 weeks 2. Total Joints 4 weeks a. Diagnosis and management of hip and knee arthritis b. Indications for surgery c. Implant selection;
Page 1 Appendix 1 Rotation Objectives and Schedule 1. Introductory Month 4 weeks 2. Total Joints 4 weeks a. Diagnosis and management of hip and knee arthritis b. Indications for surgery c. Implant selection;
Osteoarthritis (OA) of the Knee. Patient Information Leaflet
 Osteoarthritis (OA) of the Knee Patient Information Leaflet What is osteoarthritis (OA)? Osteoarthritis is a condition that affects the joints causing pain and stiffness. The knee is one of the more commonly
Osteoarthritis (OA) of the Knee Patient Information Leaflet What is osteoarthritis (OA)? Osteoarthritis is a condition that affects the joints causing pain and stiffness. The knee is one of the more commonly
Total elbow replacement. Information for patients Orthopaedics - Upper Limb
 Total elbow replacement Information for patients Orthopaedics - Upper Limb Introduction The Upper Limb Unit team would like you and your family to understand as much as possible about the operation you
Total elbow replacement Information for patients Orthopaedics - Upper Limb Introduction The Upper Limb Unit team would like you and your family to understand as much as possible about the operation you
NOTE: The first appearance of terms in bold in the body of this document (except titles) are defined terms please refer to the Definitions section.
 TITLE VENOUS THROMBOEMBOLISM PROPHYLAXIS SCOPE Provincial Acute and Sub-Acute Care Facilities APPROVAL AUTHORITY Alberta Health Services Executive Committee SPONSOR Vice President, Quality and Chief Medical
TITLE VENOUS THROMBOEMBOLISM PROPHYLAXIS SCOPE Provincial Acute and Sub-Acute Care Facilities APPROVAL AUTHORITY Alberta Health Services Executive Committee SPONSOR Vice President, Quality and Chief Medical
DOCUMENT CONTROL PAGE
 DOCUMENT CONTROL PAGE Title Title: UNDERGOING SPINAL DEFORMITY SURGERY Version: 2 Reference Number: Supersedes Supersedes: all other versions Description of Amendment(s): Revision of analgesia requirements
DOCUMENT CONTROL PAGE Title Title: UNDERGOING SPINAL DEFORMITY SURGERY Version: 2 Reference Number: Supersedes Supersedes: all other versions Description of Amendment(s): Revision of analgesia requirements
REVISION TOTAL KNEE REPLACEMENT
 PATIENT INFORMATION SHEET YOU ARE GOING TO UNDERGO REVISION TOTAL KNEE REPLACEMENT and sports traumatology ORTHOPAEDIC SURGERY Doctor Philippe Paillard Office YOU HAVE A LOOSENING OF THE KNEE PROSTHESIS
PATIENT INFORMATION SHEET YOU ARE GOING TO UNDERGO REVISION TOTAL KNEE REPLACEMENT and sports traumatology ORTHOPAEDIC SURGERY Doctor Philippe Paillard Office YOU HAVE A LOOSENING OF THE KNEE PROSTHESIS
Section of total knee replacement. Total Knee Replacement System. Knieendoprothesen System. Système de prothèse totale de genou
 Section of total knee replacement Total Knee Replacement System Knieendoprothesen System Système de prothèse totale de genou Introduction: This knee system features great versality with its modular component
Section of total knee replacement Total Knee Replacement System Knieendoprothesen System Système de prothèse totale de genou Introduction: This knee system features great versality with its modular component
DENOMINATOR: All surgical patients aged 18 years and older undergoing procedures for which VTE prophylaxis is indicated in all patients
 Measure #23 (NQF 0239): Perioperative Care: Venous Thromboembolism (VTE) Prophylaxis (When Indicated in ALL Patients) National Quality Strategy Domain: Patient Safety 2017 OPTIONS FOR INDIVIDUAL MEASURES:
Measure #23 (NQF 0239): Perioperative Care: Venous Thromboembolism (VTE) Prophylaxis (When Indicated in ALL Patients) National Quality Strategy Domain: Patient Safety 2017 OPTIONS FOR INDIVIDUAL MEASURES:
Optimum implant geometry
 Surgical Technique Optimum implant geometry Extending proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
Surgical Technique Optimum implant geometry Extending proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
5A* ODEP. Conserving bone. Preserving soft tissue. Restoring biomechanics. rating
 MiniHip is designed to give patients the advantages of a traditional hip replacement whilst also preserving the natural anatomy. MiniHip potentially allows for future revisions and so provides a pre-primary
MiniHip is designed to give patients the advantages of a traditional hip replacement whilst also preserving the natural anatomy. MiniHip potentially allows for future revisions and so provides a pre-primary
Sign up to receive ATOTW weekly -
 ANAESTHESIA FOR TOTAL KNEE REPLACEMENT ANAESTHESIA TUTORIAL OF THE WEEK 76 3RD DECEMBER 2007 Dr Helen Bromhead, Locum Consultant Anaesthetist Royal Hampshire County Hospital UK e mail: hjbromhead@hotmail.com
ANAESTHESIA FOR TOTAL KNEE REPLACEMENT ANAESTHESIA TUTORIAL OF THE WEEK 76 3RD DECEMBER 2007 Dr Helen Bromhead, Locum Consultant Anaesthetist Royal Hampshire County Hospital UK e mail: hjbromhead@hotmail.com
