Revision Surgery for Recurrent Pain after Excision of the Accessory Navicular and Relocation of the Tibialis Posterior Tendon
|
|
|
- Sarah Price
- 5 years ago
- Views:
Transcription
1 Original Article Clinics in Orthopedic Surgery 2017;9: Revision Surgery for Recurrent Pain after Excision of the Accessory Navicular and Relocation of the Tibialis Posterior Tendon Hong Joon Choi, MD, Woo Chun Lee, MD* Department of Orthopedic Surgery, Inje University Haeundae Paik Hospital, Busan, *Department of Orthopedic Surgery, Institute for Research of Foot and Ankle Diseases, Inje University Seoul Paik Hospital, Seoul, Korea Background: The results of operative treatments for symptomatic accessory navicular are debatable. In some cases, recurrent pain may develop after the Kidner procedure. The purpose of this study is to review the reasons for recurrent pain after the Kidner procedure and to suggest possible options for revision surgery. Methods: We reviewed the clinical and radiological outcomes in 9 patients who underwent revision surgery for recurrent pain after the Kidner procedure. During the revision surgery, the tibialis posterior tendon was reattached to the navicular either by advancing the tendon in 4 patients or by lengthening the tendon in another 4 patients. In the other 1 patient, the flexor digitorum longus tendon was transferred. Surgeries for the accompanying deformities were performed simultaneously in all patients. The results were evaluated using the American Orthopaedic Foot and Ankle Society ankle-hindfoot score and a visual analog scale. The mean follow-up was 2.3 years (range, 1 to 5 years). Results: The mean American Orthopedic Foot and Ankle Society ankle-hindfoot score improved from to in the advancement group, and to in the lengthening group. The mean visual analog scale improved from 7.75 to 4.25 in the advancement group and from 7.50 to 1.75 in the lengthening group. Conclusions: Recurrent pain after the Kidner procedure was associated with pes planovalgus or hindfoot valgus deformity. In revision surgery, correction of the associated deformities and reattachment of the tibialis posterior tendon after lengthening may need to be considered. Keywords: Accessory navicular, Hindfoot valgus, Pes planovalgus, Kidner procedure The navicular bone is a common location for an accessory bone. The developmental anomaly of accessory navicular syndrome is found in approximately 10% 21% of normal feet. 1,2) The accessory navicular is classified into three types: type I is completely separated from the navicular tuberosity, type II is separated from the mother bone by a synchondrosis, and type III is united by a bony bridge to Received October 15, 2016; Accepted January 2, 2017 Correspondence to: Hong Joon Choi, MD Department of Orthopedic Surgery, Inje University Haeundae Paik Hospital, 875 Haeun-daero, Haeundae-gu, Busan 48108, Korea Tel: , Fax: cool-cool0829@hanmail.net the navicular tuberosity. 3,4) Among the different types of accessory navicular, type II is the most symptomatic. When conservative treatments for painful accessory navicular, such as shoe modification, inserts, and life style modification, fail to provide adequate pain relief, surgical treatment is recommended. The current literature supports several surgical treatment options for symptomatic accessory navicular: 3-11) simple excision; excision and relocation of the tibialis posterior (TP) tendon (the Kidner procedure); percutaneous drilling; and fusion of the accessory navicular to the body of the navicular. The results of these surgical treatments are debatable. In some cases, the Kidner procedure may hinder proper healing and cause degeneration of the relocated TP tendon. Furthermore, Copyright 2017 by The Korean Orthopaedic Association This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License ( which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. Clinics in Orthopedic Surgery pissn X eissn
2 233 if there is discontinuity at the TP tendon insertion sites, failure of the reattachment may cause severe functional deficits, including possible proximal migration of the TP tendon. 1) However, no clinical case of proximal migration of the TP tendon has been reported after surgery for symptomatic accessory navicular. We believe that the increased tension at the reattachment site is one of the reasons for recurrent pain after the Kidner procedure. Thus, we hypothesized that planovalgus or hindfoot valgus deformities are related to recurrent pain after the Kidner procedure. The purpose of this study is to review the reasons for recurrent pain after surgery for symptomatic accessory navicular and to suggest possible options for surgical revision. METHODS This is a retrospective case series. The inclusion criteria were patients who underwent revision surgery for recurrent pain after the Kidner procedure and completed at least 12-months of follow-up after the revision surgery. The exclusion criteria were patients with recurrent pain from nonunion after fusion of an accessory navicular, a history of a local steroid injection, local infection, or underlying diseases such as uncontrolled diabetic mellitus, rheumatoid arthritis, or seronegative spondyloarthropathy. Surgical treatments were performed on 10 patients from August 2004 to March Nine patients (9 feet) were included in this study because 1 patient was lost to follow-up (Table 1). Six patients underwent their initial surgery at another hospital, and the remaining 3 patients had their initial surgery performed by the author (WCL) at the study institution. The mean duration between the initial surgery and the revision surgery was 2.6 years (range, 0.5 to 5 years). The mean follow-up period was 2.3 years (range, 1 to 5 years). This study was approved by the Institutional Review Board (No. IIT ) and informed consent was obtained from all patients. In 1 patient, the TP tendon could not be reattached to the navicular due to retraction of the distal stump proximal to the tip of the medial malleolus, and so a transfer of the flexor digitorum longus (FDL) was performed instead. In 4 patients, the distal stump of the TP tendon was attached with forceful advancement alone (the advancement group). The remaining 4 patients underwent TP tendon lengthening above the ankle joint by Z-plasty, and then the distal stump was attached to the navicular with minimal force (the lengthening group). The average length of advancement or lengthening of the tendon was approximately 2 cm. Prior to the revision surgery, all patients had difficulty performing a single limb heel rise on physical examination and had hindfoot valgus deformities on radiographic evaluation. Planovalgus deformities were noted in 7 feet; the first talometatarsal angle angulated plantarward Table 1. Characteristics of the Patients Case Sex Age (yr) Follow-up (yr) MDCO LCL Length of debridement (cm) Time to revision (yr) Advancement of TP 1 Male Yes No Male Yes No Male Yes No Male No Yes Lengthening of TP 5 Female Yes Yes Male No Yes Female Yes No Male No Yes FDL transfer 9 Female Yes Yes MDCO: medial displacement calcaneal osteotomy, LCL: lateral column lengthening, TP: tibialis posterior, FDL: flexor digitorum longus.
3 234 by greater than 10 as noted on a weight-bearing foot lateral radiograph. Two patients had a hindfoot valgus deformity with normal longitudinal arches. Surgeries for the planovalgus or hindfoot valgus deformity were performed simultaneously in all patients with medial displacement calcaneal osteotomy (MDCO), lateral column lengthening (LCL), or both, to relieve the tension at the reattachment site of the TP tendon (Table 1). MDCO was performed in 6 feet, including 2 feet with hindfoot valgus with normal longitudinal arches, and LCL was performed in 5 feet. Two patients underwent both MDCO and LCL. Preoperative and postoperative clinical evaluations were performed using the American Orthopedic Foot and Ankle Society (AOFAS) ankle-hindfoot score 12,13) and a 10-point visual analog scale (VAS) for pain. Radiographic and clinical results were separately tabulated for each group (Table 2). However, the statistical power was too low to compare the groups. Therefore, only the preoperative and postoperative results of the patients were compared. The radiographic assessments were made with weight-bearing dorsoplantar (anteroposterior [AP]) and lateral radiographs of the foot and hindfoot alignment radiographs. All radiographs were digitally obtained through the Picture Archiving Communication System (Marosis Table 2. Changes in Clinical and Radiographic Parameters According to the Treatment Variable Advancement group (n = 4) Lengthening group (n = 4) FDL transfer (n = 1) AOFAS Preoperative ± ± Postoperative ± ± VAS Preoperative 7.75 ± ± Postoperative 4.25 ± ± Talonavicular coverage angle ( ) Preoperative ± ± Postoperative ± ± First talometatarsal angle (AP) ( ) Preoperative ± ± Postoperative 8.63 ± ± First talometatarsal angle (lateral) ( ) Preoperative 4.25 ± ± Postoperative 1.25 ± ± Hindfoot alignment angle ( ) Preoperative 7.38 ± ± Postoperative 1.13 ± ± Hindfoot alignment ratio Preoperative ± ± Postoperative ± ± Calcaneal pitch angle ( ) Preoperative ± ± Postoperative ± ± FDL: flexor digitorum longus, AOFAS: American Orthopedic Foot and Ankle Society ankle-hindfoot score, VAS: visual analog scale, AP: anteroposterior.
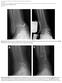
4 235 Enterprise PACS, Marosis Enterprise PACS; Infinitt, Seoul, Korea). On the weight-bearing foot AP radiographs, the talonavicular coverage angle, and the first talometatarsal angle were measured. On the weight-bearing foot lateral radiographs, the first talometatarsal angle and the calcaneal pitch angle were measured. On the hindfoot alignment view, the hindfoot alignment angle and the hindfoot alignment ratio were obtained.14) The hindfoot alignment angle, which is the angle between the tibial axis and the calcaneal axis, was measured and expressed as a positive number when it was in the valgus position. The hindfoot alignment ratio was obtained by dividing the width from the calcaneus medial to the tibial axis by the calcaneal width at its widest portion on the alignment view. If the tibial axis line passed through more medial side compared to the medial calcaneal cortex, the measurements were expressed as negative values. Statistical analysis was not performed owing to the insufficient sample size; in order to achieve sufficient power for statistical analysis (β 0.20, power 0.80), each group needed 15 patients. A C Surgical Technique The MDCO and LCL procedures were performed before the soft tissue reconstruction. LCL was performed by fusing the calcaneocuboid joint in 2 feet, and by osteotomy at the anterior calcaneus in 3 feet by using the Evans procedure. TP Advancement (4 Cases) For the TP tendon advancement, the degenerative segment of the TP tendon was excised and the distal end of the tendon was advanced to the navicular, with the foot positioned in approximately 20 of plantarflexion and inversion. The tendon was securely fixed with one or two 2.7-mm suture anchors (Arthrex, Naples, FL, USA). Additional sutures were applied between the tendon and the adjacent soft tissues. TP Lengthening (4 Cases) To lengthen the TP tendon, a 6-cm longitudinal incision was made on the posterior aspect of the medial border of the tibia, after excision of the degenerative segment of the TP tendon. After exposure of the tendon, Z-plasty lengthening was performed via a 5-cm longitudinal incision B Fig. 1. (A) The intraoperative finding revealed degeneration of the tibialis posterior tendon. (B) To lengthen the tibialis posterior tendon, a 6-cm longitudinal incision was made on the posterior aspect of the medial border of the tibia. (C) The tibialis posterior tendon was lengthened by 2 cm and repaired with interrupted 3-0 nylon sutures and the distal end of the tibialis posterior tendon was securely fixed using 2.7-mm suture anchors.
5 236 in the middle of the tendon (Fig. 1). The TP tendon was lengthened by 2 cm and repaired with interrupted 3-0 nylon sutures. The distal end of the TP tendon was securely fixed using one or two 2.7-mm suture anchors. FDL Transfer (1 Case) For the FDL transfer, the master knot of Henry was dissected and the FDL tendon was transected distal to that point. Using 2-0 Ethibond polyester suture (Ethicon, New Brunswick, NJ, USA), a single strand was placed into the distal end of the FDL tendon. The FDL tendon was then rerouted from the plantar to the dorsal direction of the navicular through a 5-mm bone tunnel. The FDL was then sutured back onto itself with two simple interrupted 2-0 Ethibond polyester sutures. Postoperative Care Postoperatively, all patients were immobilized in a short leg non-weight-bearing cast for 6 weeks. For the first 3 weeks, the ankle was placed in 10 of plantarflexion and inversion, and this was followed by 3 weeks of casting in a neutral position. Weight-bearing as tolerated was permitted once the ankle was cast in the neutral position. After 6 weeks of postoperative care, the cast was removed and a stirrup brace was applied and maintained for another 6 weeks. RESULTS The intraoperative findings of all the patients revealed different degrees of degeneration of the TP tendon. After the revision surgery, all the patients had normal muscle strength when examined by manual resistance of the TP and all the patients were able to perform a single heel rise. In all the patients, the AOFAS score, VAS, and radiographic parameters improved after surgery (Table 2). The mean AOFAS score improved from (range, 67 to 76) to (range, 67 to 100) in all patients: from (range, 67 to 76) to (range, 67 to 88) in the advancement group, and from (range, 67 to 75) to (range, 84 to 100) in the lengthening group. The mean VAS improved from 7.62 (range, 7 to 8) to 3.00 (range, 1 to 6) in all patients: from 7.75 (range, 7 to 8) to 4.25 (range, 2 to 6) in the advancement group, and from 7.50 (range, 7 to 8) to 1.75 (range, 1 to 3) in the lengthening group. Two of the 4 patients in the advancement group reported a pain VAS 4 in contrast to none in the lengthening group. The 1 patient with FDL transfer reported satisfactory results. One patient in the advancement group complained of unsatisfactory results including pain and difficulty with rehabilitation after undergoing reattachment in the extreme inversion position. This patient underwent an additional surgery (TP tendon lengthening and FDL transfer) 4 years after the revision surgery. DISCUSSION This study was conducted to investigate the characteristics of the feet and the outcomes of surgical treatment for recurrent pain after the Kidner procedure. In the total 9 patients available for this study, reattachment of the TP tendon with lengthening (the lengthening group) showed better clinical results than the forceful reattachment of the TP tendon (the advancement group). In this series, all patients were reoperated on because of severe pain at the attachment site of the TP tendon; they could not perform a single heel rise on the affected foot at the time of the revision. The decision about which procedure to perform was not made on clear-cut criteria, and the characteristics and severity of the patients symptoms varied. However, the authors noted that all the feet had pes planovalgus or hindfoot valgus deformity, and all patients showed degenerative changes of the TP tendon at its reattachment site. Although several articles have reported on patients with persistent symptoms after the Kidner procedure, no current literature reviews the possible treatment options and outcomes in these patients. 3,11,15,16) The authors believe that this is the first review of revision surgery for persistent pain after the Kidner procedure. The relationship between painful accessory navicular and flatfoot is controversial, and it is not clear whether flatfoot is the cause of painful accessory navicular or vice versa. 3,8,16,17) Vaughan and Singh 18) reported that pes planus may contribute to ongoing pain after excision of the accessory navicular. Seven of the 9 patients in the present study had planovalgus deformity; however, 2 patients had normal longitudinal arches with only hindfoot valgus deformity. We believe that both planovalgus and hindfoot valgus deformities can be associated with recurrent pain after the Kidner procedure, because both flatfoot and hindfoot valgus can increase the tension on the TP tendon and result in degeneration of the tendon, thereby causing recurrent pain. In the study patients, the TP tendon already has been advanced during the initial surgery to close the gap after excision of the accessory navicular. During revision surgery, an additional gap was created after debridement of the degenerated segment of TP tendon discovered in all the cases of this series, and additional advancement of the TP tendon was required. In this series, the mean length of
6 237 advancement or lengthening of the tendon was 2 cm, after the degenerated portion was debrided. Because the excursion of the TP tendon was only 2 cm, excessive tension was inevitable at the TP tendon reattachment site after advancing the TP tendon. 19) Although patients in the advancement group showed improvements after the revision surgery, they complained of pain after prolonged standing or walking. In contrast, all the patients in the lengthening group showed good results. After experiencing poor results from advancement of the TP tendon during the initial treatment, the tendon was lengthened to reduce the tension at the reattachment site. Corrective surgery to reduce strain on the TP tendon should be determined according to the deformity in each individual case. In the presence of hindfoot valgus deformity without forefoot abduction or low longitudinal arch, MDCO was sufficient to reduce the tension. In the cases involving planovalgus deformity, the authors independently decided to use either the MDCO or LCL method of correction, or combination of both procedures. To avoid problems associated with the Kidner procedure, the accessory navicular should be soundly fused to the mother bone. 4,11) However, secure fixation of such a small bone is difficult, and assessment of the progression of the fusion is challenging owing to the small opposing surfaces between the accessory bone and the body of the navicular. Another option for closing the gap of the TP tendon is a FDL transfer. 20) In cases with stage 2 adult acquired flatfoot, an intercalary defect is created, centered at approximately 3 5 cm proximal to the insertion after debridement of the degenerated TP tendon; an FDL transfer is a common method to reconstruct the invertor function. The TP tendon has multiple insertions besides the primary insertion at the navicular; therefore, it cannot be proximally retracted even though the TP tendon is detached from its insertion after surgery for painful accessory navicular. One patient in the present study showed proximal migration and needed FDL transfer. We believe that the major portion of the TP tendon was inserted only to the accessory navicular in this case. Kiter et al. 1) have reported that disruption at the reattachment site may cause proximal migration of the tendon when the TP tendon mainly inserts at the accessory navicular. Although the clinical result of the patient treated with FDL transfer was satisfactory, other cases were not treated with an FDL transfer for the reconstruction of the gap at the insertion of the TP tendon. We believe that reattachment of the TP tendon would be better in the long-term, rather than sacrificing the FDL. However, FDL transfer is as an alternative method of treatment when reattachment of the TP tendon is not feasible. There are several limitations in this study. The first limitation is the small number of cases, which means that statistically significant results could not be obtained. In order to achieve sufficient statistical power (β 0.20, power 0.80), 15 cases would have been needed in each group. As the symptoms of most patients are typically improved after excision of the accessory navicular, revision surgery is not common. However, we think this report on a small number of patients is meaningful because severe disability may be caused by persistent pain after the Kidner procedure. The second limitation is that the degree of associated preoperative and postoperative deformity was not significantly different between the groups. Interestingly, better clinical results were obtained in the lengthening group, which had a smaller talonavicular coverage angle, lower arch, and greater hindfoot valgus on the postoperative radiographs. These findings suggest that the lower degree of postoperative pain in the lengthening group cannot be explained by better correction of the flatfoot deformity. The third limitation is that the size of the accessory navicular was not assessed at the time of the initial surgery. As the TP tendon should be advanced a farther distance when a larger accessory navicular is excised, assessment of the size is an important factor. In this current study, 6 of the 9 patients had their initial surgery at another hospital and the size of the accessory navicular could not be determined. Therefore, we cannot assess whether a larger defect at the primary surgery was a contributing factor to the recurrent pain. The fourth limitation is that the TP tendon force was not measured with an objective method. Although all revision procedures and examinations were performed by the authors, the power of the TP tendon on manual examination, the single limb heel rise postoperatively, and subtle weakness after lengthening may not have been noticed by manual examination. In addition, further follow-up is needed to determine whether there are any long-term problems with the strength of the TP tendon. In this study, recurrent pain after the Kidner procedure was associated with pes planovalgus or hindfoot valgus deformity. Reattachment of the TP tendon after lengthening demonstrated better outcome compared to advancement of the tendon. Additional procedures to correct the planovalgus or hindfoot valgus deformity should be considered to treat recurrent pain after surgery for symptomatic accessory navicular.
7 238 CONFLICT OF INTEREST No potential conflict of interest relevant to this article was reported. REFERENCES 1. Kiter E, Gunal I, Karatosun V, Korman E. The relationship between the tibialis posterior tendon and the accessory navicular. Ann Anat. 2000;182(1): Grogan DP, Gasser SI, Ogden JA. The painful accessory navicular: a clinical and histopathological study. Foot Ankle. 1989;10(3): Bennett GL, Weiner DS, Leighley B. Surgical treatment of symptomatic accessory tarsal navicular. J Pediatr Orthop. 1990;10(4): Chung JW, Chu IT. Outcome of fusion of a painful accessory navicular to the primary navicular. Foot Ankle Int. 2009;30(2): Kiter E, Gunal I, Turgut A, Kose N. Evaluation of simple excision in the treatment of symptomatic accessory navicular associated with flat feet. J Orthop Sci. 2000;5(4): Kopp FJ, Marcus RE. Clinical outcome of surgical treatment of the symptomatic accessory navicular. Foot Ankle Int. 2004;25(1): Macnicol MF, Voutsinas S. Surgical treatment of the symptomatic accessory navicular. J Bone Joint Surg Br. 1984;66(2): Sullivan JA, Miller WA. The relationship of the accessory navicular to the development of the flat foot. Clin Orthop Relat Res. 1979;(144): Nakayama S, Sugimoto K, Takakura Y, Tanaka Y, Kasanami R. Percutaneous drilling of symptomatic accessory navicular in young athletes. Am J Sports Med. 2005;33(4): Malicky ES, Levine DS, Sangeorzan BJ. Modification of the Kidner procedure with fusion of the primary and accessory navicular bones. Foot Ankle Int. 1999;20(1): Scott AT, Sabesan VJ, Saluta JR, Wilson MA, Easley ME. Fusion versus excision of the symptomatic Type II accessory navicular: a prospective study. Foot Ankle Int. 2009;30(1): Kitaoka HB, Alexander IJ, Adelaar RS, Nunley JA, Myerson MS, Sanders M. Clinical rating systems for the anklehindfoot, midfoot, hallux, and lesser toes. Foot Ankle Int. 1994;15(7): Ibrahim T, Beiri A, Azzabi M, Best AJ, Taylor GJ, Menon DK. Reliability and validity of the subjective component of the American Orthopaedic Foot and Ankle Society clinical rating scales. J Foot Ankle Surg. 2007;46(2): Lee WC, Moon JS, Lee HS, Lee K. Alignment of ankle and hindfoot in early stage ankle osteoarthritis. Foot Ankle Int. 2011;32(7): Ray S, Goldberg VM. Surgical treatment of the accessory navicular. Clin Orthop Relat Res. 1983;(177): Veitch JM. Evaluation of the Kidner procedure in treatment of symptomatic accessory tarsal scaphoid. Clin Orthop Relat Res. 1978;(131): Sella EJ, Lawson JP, Ogden JA. The accessory navicular synchondrosis. Clin Orthop Relat Res. 1986;(209): Vaughan P, Singh D. Ongoing pain and deformity after an excision of the accessory navicular. Foot Ankle Clin. 2014;19(3): Flemister AS, Neville CG, Houck J. The relationship between ankle, hindfoot, and forefoot position and posterior tibial muscle excursion. Foot Ankle Int. 2007;28(4): Myerson MS, Corrigan J. Treatment of posterior tibial tendon dysfunction with flexor digitorum longus tendon transfer and calcaneal osteotomy. Orthopedics. 1996;19(5):383-8.
Results of Calcaneal Osteotomy & Flexor Digitorum Longus transfer in Stage II Acquired Flatfoot Deformity
 Results of Calcaneal Osteotomy & Flexor Digitorum Longus transfer in Stage II Acquired Flatfoot Deformity Mr Amit Chauhan Mr Prasad Karpe Ms Maire-claire Killen Mr Rajiv Limaye University Hospital of North
Results of Calcaneal Osteotomy & Flexor Digitorum Longus transfer in Stage II Acquired Flatfoot Deformity Mr Amit Chauhan Mr Prasad Karpe Ms Maire-claire Killen Mr Rajiv Limaye University Hospital of North
The Cause of Pain in Symptomatic Accessory Navicular Syndrome : comparison between Athletes and Non-Athletes
 The Cause of Pain in Symptomatic Accessory Navicular Syndrome : comparison between Athletes and Non-Athletes Kyung Tai Lee, M.D., Young Uk Park, M.D. *, Hyuk Jegal, M.D., Young Tae Rho, M.D. KT Lee s Orthopedic
The Cause of Pain in Symptomatic Accessory Navicular Syndrome : comparison between Athletes and Non-Athletes Kyung Tai Lee, M.D., Young Uk Park, M.D. *, Hyuk Jegal, M.D., Young Tae Rho, M.D. KT Lee s Orthopedic
SUBTALAR ARTHROEREISIS IN THE OLDER PATIENT
 C H A P T E R 1 7 SUBTALAR ARTHROEREISIS IN THE OLDER PATIENT William D. Fishco, DPM, MS INTRODUCTION Arthroereisis is a surgical procedure designed to limit the motion of a joint. Subtalar joint arthroereisis
C H A P T E R 1 7 SUBTALAR ARTHROEREISIS IN THE OLDER PATIENT William D. Fishco, DPM, MS INTRODUCTION Arthroereisis is a surgical procedure designed to limit the motion of a joint. Subtalar joint arthroereisis
Modified Proximal Scarf Osteotomy for Hallux Valgus
 Original Article Clinics in Orthopedic Surgery 2018;10:479-483 https://doi.org/10.4055/cios.2018.10.4.479 Modified Proximal Scarf Osteotomy for Hallux Valgus Ki Won Young, MD, Hong Seop Lee, MD, Seong
Original Article Clinics in Orthopedic Surgery 2018;10:479-483 https://doi.org/10.4055/cios.2018.10.4.479 Modified Proximal Scarf Osteotomy for Hallux Valgus Ki Won Young, MD, Hong Seop Lee, MD, Seong
«Foot & Ankle Surgery» 04. Sept THE PAINFUL FLATFOOT. Norman Espinosa, MD
 THE PAINFUL FLATFOOT Norman Espinosa, MD Department of Orthopaedics University of Zurich Balgrist Switzerland www.balgrist.ch WHAT TO DO? INTRINSIC > EXTRINSIC ETIOLOGIES Repetitive microtrauma combined
THE PAINFUL FLATFOOT Norman Espinosa, MD Department of Orthopaedics University of Zurich Balgrist Switzerland www.balgrist.ch WHAT TO DO? INTRINSIC > EXTRINSIC ETIOLOGIES Repetitive microtrauma combined
Posterior Tibialis Tendon Dysfunction & Repair
 1 Posterior Tibialis Tendon Dysfunction & Repair Surgical Indications and Considerations Anatomical Considerations: The posterior tibialis muscle arises from the interosseous membrane and the adjacent
1 Posterior Tibialis Tendon Dysfunction & Repair Surgical Indications and Considerations Anatomical Considerations: The posterior tibialis muscle arises from the interosseous membrane and the adjacent
A Patient s Guide to Adult-Acquired Flatfoot Deformity
 A Patient s Guide to Adult-Acquired Flatfoot Deformity Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Adult-Acquired Flatfoot Deformity Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled
Changes in Dynamic Pedobarography after Extensive Plantarmedial Release for Paralytic Pes Cavovarus
 Original Article http://dx.doi.org/10.3349/ymj.2014.55.3.766 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 55(3):766-772, 2014 Changes in Dynamic Pedobarography after Extensive Plantarmedial Release
Original Article http://dx.doi.org/10.3349/ymj.2014.55.3.766 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 55(3):766-772, 2014 Changes in Dynamic Pedobarography after Extensive Plantarmedial Release
TENDON TRANSFER IN CAVUS FOOT
 TENDON TRANSFER IN CAVUS FOOT Cavovarus deformity is defined by fixed equinus of the forefoot on the hindfoot, resulting in a pathologic elevation of the longitudinal arch, with either a fixed or flexible
TENDON TRANSFER IN CAVUS FOOT Cavovarus deformity is defined by fixed equinus of the forefoot on the hindfoot, resulting in a pathologic elevation of the longitudinal arch, with either a fixed or flexible
Change of Alignment by Calcaneocuboid Distraction Arthrodesis for Acquired Flatfoot
 Change of Alignment by Calcaneocuboid Distraction Arthrodesis for Acquired Flatfoot Akira Taniguchi, Yasuhito Tanaka, Kunihiko Kadono, Kiyonori Tomiwa, So Kameda, Hiroaki Kurokawa, Takenori Matsuda, Tsukasa
Change of Alignment by Calcaneocuboid Distraction Arthrodesis for Acquired Flatfoot Akira Taniguchi, Yasuhito Tanaka, Kunihiko Kadono, Kiyonori Tomiwa, So Kameda, Hiroaki Kurokawa, Takenori Matsuda, Tsukasa
Managing Tibialis Posterior Tendon Injuries
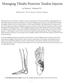 Managing Tibialis Posterior Tendon Injuries by Thomas C. Michaud, DC Published April 1, 2015 by Dynamic Chiropractic Magazine Tibialis posterior is the deepest, strongest, and most central muscle of the
Managing Tibialis Posterior Tendon Injuries by Thomas C. Michaud, DC Published April 1, 2015 by Dynamic Chiropractic Magazine Tibialis posterior is the deepest, strongest, and most central muscle of the
A Patient s Guide to Flatfoot Deformity (Pes Planus) in Children
 A Patient s Guide to Flatfoot Deformity (Pes Planus) in Children 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Flatfoot Deformity (Pes Planus) in Children 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled
Surgical correction of Hallux Valgus
 Surgical correction of Hallux Valgus complicated with adult type Pes planus Department of Orthopedic Surgery, Inje University, Ilsan Paik Hospital, Goyang-si, Korea * W Institute for Foot and Ankle Diseases
Surgical correction of Hallux Valgus complicated with adult type Pes planus Department of Orthopedic Surgery, Inje University, Ilsan Paik Hospital, Goyang-si, Korea * W Institute for Foot and Ankle Diseases
Index. Clin Podiatr Med Surg 22 (2005) Note: Page numbers of article titles are in boldface type.
 Clin Podiatr Med Surg 22 (2005) 309 314 Index Note: Page numbers of article titles are in boldface type. A Abductor digiti minimi muscle, myectomy of, for tailor s bunionette, 243 Achilles tendon, lengthening
Clin Podiatr Med Surg 22 (2005) 309 314 Index Note: Page numbers of article titles are in boldface type. A Abductor digiti minimi muscle, myectomy of, for tailor s bunionette, 243 Achilles tendon, lengthening
Chamnanni Rungprai, M.D.
 Comparison pre- and post-operative alignment correction in patients with stage II flatfoot deformities treated with bony realignment procedure Co-authors 1,2 Chamnanni Rungprai, M.D. 1 Tyler G. Slayman,
Comparison pre- and post-operative alignment correction in patients with stage II flatfoot deformities treated with bony realignment procedure Co-authors 1,2 Chamnanni Rungprai, M.D. 1 Tyler G. Slayman,
Outcomes after Lengthening Calcaneal Osteotomy for Flexible Flatfoot Deformity Evans- versus Hintermann-Osteotomy
 Outcomes after Lengthening Calcaneal Osteotomy for Flexible Flatfoot Deformity Evans- versus Hintermann-Osteotomy Ettinger, S. 1, Mattinger, T. 1, Yao, D. 1, Claassen, L. 1, Daniilidis, K. 2, Stukenborg-Colsman,
Outcomes after Lengthening Calcaneal Osteotomy for Flexible Flatfoot Deformity Evans- versus Hintermann-Osteotomy Ettinger, S. 1, Mattinger, T. 1, Yao, D. 1, Claassen, L. 1, Daniilidis, K. 2, Stukenborg-Colsman,
ATYPICAL MIDFOOT- DRIVEN ADULT FLATFOOT
 ATYPICAL MIDFOOT- DRIVEN ADULT FLATFOOT MICHAEL P. CLARE, MD FLORIDA ORTHOPAEDIC INSTITUTE TAMPA, FL USA DISCLOSURES 3B: BESPA, INC. (CONSULTANT) EXTREMITY MEDICAL, INC. ACKNOWLEDGMENT AK WALLING III,
ATYPICAL MIDFOOT- DRIVEN ADULT FLATFOOT MICHAEL P. CLARE, MD FLORIDA ORTHOPAEDIC INSTITUTE TAMPA, FL USA DISCLOSURES 3B: BESPA, INC. (CONSULTANT) EXTREMITY MEDICAL, INC. ACKNOWLEDGMENT AK WALLING III,
New Radiographic Parameter Assessing Hindfoot Alignment in Stage II Adult Acquired Flatfoot Deformity
 New Radiographic Parameter Assessing Hindfoot Alignment in Stage II Adult Acquired Flatfoot Deformity Emilie Williamson, BS; Jeremy Chan, MD; Jayme C Burket, PhD; Jonathan T Deland, MD; Scott Ellis, MD
New Radiographic Parameter Assessing Hindfoot Alignment in Stage II Adult Acquired Flatfoot Deformity Emilie Williamson, BS; Jeremy Chan, MD; Jayme C Burket, PhD; Jonathan T Deland, MD; Scott Ellis, MD
MIDFOOT INJURIES-ARE WE UNDERTREATING IT? Mr Rajiv Limaye Mr Prasad Karpe University Hospital of North Tees 3 rd Foot and Ankle Symposium
 MIDFOOT INJURIES-ARE WE UNDERTREATING IT? Mr Rajiv Limaye Mr Prasad Karpe University Hospital of North Tees 3 rd Foot and Ankle Symposium Introduction Increasing sports injuries RTA and traumatic injuries
MIDFOOT INJURIES-ARE WE UNDERTREATING IT? Mr Rajiv Limaye Mr Prasad Karpe University Hospital of North Tees 3 rd Foot and Ankle Symposium Introduction Increasing sports injuries RTA and traumatic injuries
Marut Arunakul, M.D. Phinit Phisitkul, M.D. Jessica Goetz, PhD. John Femino, M.D. Annunziato Amendola, M.D. University of Iowa Hospitals and Clinics
 Marut Arunakul, M.D. Phinit Phisitkul, M.D. Jessica Goetz, PhD. John Femino, M.D. Annunziato Amendola, M.D. University of Iowa Hospitals and Clinics Tripod Index Part 1: New radiographic parameter assessing
Marut Arunakul, M.D. Phinit Phisitkul, M.D. Jessica Goetz, PhD. John Femino, M.D. Annunziato Amendola, M.D. University of Iowa Hospitals and Clinics Tripod Index Part 1: New radiographic parameter assessing
Posterior Tibial Tendon Problems
 A Patient s Guide to Posterior Tibial Tendon Problems 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a
A Patient s Guide to Posterior Tibial Tendon Problems 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a
Other Congenital and Developmental Diseases of the Foot. Department of Orthopedic Surgery St. Vincent s s Hospital, The Catholic University
 Other Congenital and Developmental Diseases of the Foot Department of Orthopedic Surgery St. Vincent s s Hospital, The Catholic University Contents Metatarsus Adductus Skewfoot Hallux Valgus Hallux Valgus
Other Congenital and Developmental Diseases of the Foot Department of Orthopedic Surgery St. Vincent s s Hospital, The Catholic University Contents Metatarsus Adductus Skewfoot Hallux Valgus Hallux Valgus
A Patient s Guide to Posterior Tibial Tendon Problems
 A Patient s Guide to Posterior Tibial Tendon Problems Iain is a specialist in musculoskeletal imaging and the diagnosis of musculoskeletal pain. This information is provided with the hope that you can
A Patient s Guide to Posterior Tibial Tendon Problems Iain is a specialist in musculoskeletal imaging and the diagnosis of musculoskeletal pain. This information is provided with the hope that you can
The effect on radiographic parameters of Dwyer s osteotomy and 1 st metatarsal osteotomy for pes cavo-varus correction
 The effect on radiographic parameters of Dwyer s osteotomy and 1 st metatarsal osteotomy for pes cavo-varus correction Department of Orthopedic Surgery, Inje University, Ilsan Paik Hospital, South Korea
The effect on radiographic parameters of Dwyer s osteotomy and 1 st metatarsal osteotomy for pes cavo-varus correction Department of Orthopedic Surgery, Inje University, Ilsan Paik Hospital, South Korea
2017 AOFAS Specialty Day. Posterior Tibial Tendon Dysfunction: Stage III Getting the Most Out of Your Triple Arthrodesis
 2017 AOFAS Specialty Day Posterior Tibial Tendon Dysfunction: Stage III Getting the Most Out of Your Triple Arthrodesis Jeffrey E. Johnson, M.D. Professor, Dept. of Orthopaedic Surgery Chief, Foot and
2017 AOFAS Specialty Day Posterior Tibial Tendon Dysfunction: Stage III Getting the Most Out of Your Triple Arthrodesis Jeffrey E. Johnson, M.D. Professor, Dept. of Orthopaedic Surgery Chief, Foot and
Posterior Tibial Tendon Problems
 A Patient s Guide to Posterior Tibial Tendon Problems 2659 Professional Circle Suite 1110 Naples, FL 34119 Phone: 239-596-0100 Fax: 239-596-6737 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Posterior Tibial Tendon Problems 2659 Professional Circle Suite 1110 Naples, FL 34119 Phone: 239-596-0100 Fax: 239-596-6737 DISCLAIMER: The information in this booklet is compiled
Double calcaneal osteotomy for severe adolescent flexible flatfoot reconstruction
 Xu et al. Journal of Orthopaedic Surgery and Research (2017) 12:153 DOI 10.1186/s13018-017-0655-3 RESEARCH ARTICLE Open Access Double calcaneal osteotomy for severe adolescent flexible flatfoot reconstruction
Xu et al. Journal of Orthopaedic Surgery and Research (2017) 12:153 DOI 10.1186/s13018-017-0655-3 RESEARCH ARTICLE Open Access Double calcaneal osteotomy for severe adolescent flexible flatfoot reconstruction
.org. Posterior Tibial Tendon Dysfunction. Anatomy. Cause. Symptoms
 Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
mechanical stresses on the tendon with repetitive loading
 Tendinopathy.. How does it happen? mechanical stresses on the tendon with repetitive loading Impingement of the tendon between adjacent structures (bones, ligaments) and impaired blood supply Presentation
Tendinopathy.. How does it happen? mechanical stresses on the tendon with repetitive loading Impingement of the tendon between adjacent structures (bones, ligaments) and impaired blood supply Presentation
WHAT IS THIS CONDITION? COMMON CAUSES:
 Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT IS THIS CONDITION? The posterior tibial tendon is an important structure that is normally
Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT IS THIS CONDITION? The posterior tibial tendon is an important structure that is normally
Dorsal surface-the upper area or top of the foot. Terminology
 It is important to learn the terminology as it relates to feet to properly communicate with referring physicians when necessary and to identify the relationship between the anatomical structure of the
It is important to learn the terminology as it relates to feet to properly communicate with referring physicians when necessary and to identify the relationship between the anatomical structure of the
Copyright 2004, Yoshiyuki Shiratori. All right reserved.
 Ankle and Leg Evaluation 1. History Chief Complaint: A. What happened? B. Is it a sharp or dull pain? C. How long have you had the pain? D. Can you pinpoint the pain? E. Do you have any numbness or tingling?
Ankle and Leg Evaluation 1. History Chief Complaint: A. What happened? B. Is it a sharp or dull pain? C. How long have you had the pain? D. Can you pinpoint the pain? E. Do you have any numbness or tingling?
5 COMMON CONDITIONS IN THE FOOT & ANKLE
 5 COMMON CONDITIONS IN THE FOOT & ANKLE MICHAEL P. CLARE, MD FLORIDA ORTHOPAEDIC INSTITUTE TAMPA, FL USA IN A NUTSHELL ~ ALL ANATOMY & BIOMECHANICS >90% OF CONDITIONS IN FOOT & ANKLE DIAGNISED FROM GOOD
5 COMMON CONDITIONS IN THE FOOT & ANKLE MICHAEL P. CLARE, MD FLORIDA ORTHOPAEDIC INSTITUTE TAMPA, FL USA IN A NUTSHELL ~ ALL ANATOMY & BIOMECHANICS >90% OF CONDITIONS IN FOOT & ANKLE DIAGNISED FROM GOOD
Correction of Traumatic Ankle Valgus and Procurvatum using the Taylor Spatial Frame: A Case Report
 The Foot and Ankle Online Journal Official publication of the International Foot & Ankle Foundation Correction of Traumatic Ankle Valgus and Procurvatum using the Taylor Spatial Frame: A Case Report by
The Foot and Ankle Online Journal Official publication of the International Foot & Ankle Foundation Correction of Traumatic Ankle Valgus and Procurvatum using the Taylor Spatial Frame: A Case Report by
SURGICAL TECHNIQUE THE TENDON ANCHOR SYSTEM
 SURGICAL TECHNIQUE THE TENDON ANCHOR SYSTEM TABLE OF CONTENTS Introduction PAGE 1 Features and Benefits PAGE 1-2 Applications PAGE 3 Ordering Information PAGE 4 Indications & Contra-indications PAGE 5
SURGICAL TECHNIQUE THE TENDON ANCHOR SYSTEM TABLE OF CONTENTS Introduction PAGE 1 Features and Benefits PAGE 1-2 Applications PAGE 3 Ordering Information PAGE 4 Indications & Contra-indications PAGE 5
Physical Examination of the Foot & Ankle
 Inspection Standing, feet straight forward facing toward examiner Swelling Deformity Flatfoot (pes planus and hindfoot valgus) High arch (pes cavus and hindfoot varus) Peek-a-boo heel Varus Too many toes
Inspection Standing, feet straight forward facing toward examiner Swelling Deformity Flatfoot (pes planus and hindfoot valgus) High arch (pes cavus and hindfoot varus) Peek-a-boo heel Varus Too many toes
Subtalar joint kinematics and arthroscopy: insight in the subtalar joint range of motion and aspects of subtalar joint arthroscopy Beimers, L.
 UvA-DARE (Digital Academic Repository) Subtalar joint kinematics and arthroscopy: insight in the subtalar joint range of motion and aspects of subtalar joint arthroscopy Beimers, L. Link to publication
UvA-DARE (Digital Academic Repository) Subtalar joint kinematics and arthroscopy: insight in the subtalar joint range of motion and aspects of subtalar joint arthroscopy Beimers, L. Link to publication
Extraarticular Lateral Ankle Impingement
 Extraarticular Lateral Ankle Impingement Poster No.: C-1282 Congress: ECR 2016 Type: Educational Exhibit Authors: C. Cevikol; Keywords: Trauma, Diagnostic procedure, MR, CT, Musculoskeletal system, Musculoskeletal
Extraarticular Lateral Ankle Impingement Poster No.: C-1282 Congress: ECR 2016 Type: Educational Exhibit Authors: C. Cevikol; Keywords: Trauma, Diagnostic procedure, MR, CT, Musculoskeletal system, Musculoskeletal
Claw toes after tibial fracture in children
 J Child Orthop (2009) 3:339 343 DOI 10.1007/s11832-009-0200-y ORIGINAL CLINICAL ARTICLE Claw toes after tibial fracture in children Frank Fitoussi Æ Brice Ilharreborde Æ Florent Guerin Æ Philippe Souchet
J Child Orthop (2009) 3:339 343 DOI 10.1007/s11832-009-0200-y ORIGINAL CLINICAL ARTICLE Claw toes after tibial fracture in children Frank Fitoussi Æ Brice Ilharreborde Æ Florent Guerin Æ Philippe Souchet
Assessment of percutaneous V osteotomy of the calcaneus with Ilizarov application for correction of complex foot deformities
 Acta Orthop. Belg., 2004, 70, 586-590 ORIGINAL STUDY Assessment of percutaneous V osteotomy of the calcaneus with Ilizarov application for correction of complex foot deformities Hani EL-MOWAFI From Mansoura
Acta Orthop. Belg., 2004, 70, 586-590 ORIGINAL STUDY Assessment of percutaneous V osteotomy of the calcaneus with Ilizarov application for correction of complex foot deformities Hani EL-MOWAFI From Mansoura
Complications associated with Mitchell s Osteotomy for Hallux Valgus Correction: A retrospective hospital review
 The Foot and Ankle Online Journal Official publication of the International Foot & Ankle Foundation Complications associated with Mitchell s Osteotomy for Hallux Valgus Correction: A retrospective hospital
The Foot and Ankle Online Journal Official publication of the International Foot & Ankle Foundation Complications associated with Mitchell s Osteotomy for Hallux Valgus Correction: A retrospective hospital
Rippstein, Trnka, Saragas, Narramore
 THURS 25th MAY 07:45 07:55 Welcome and Introductions Paulo Ferrao Lecture 1: 08:00 10:20 Forefoot I: Hallux Valgus and Lesser Toes Mark Easley 30 mins 08:00 08:30 Surgical Management of Hallux Valgus Saragas,
THURS 25th MAY 07:45 07:55 Welcome and Introductions Paulo Ferrao Lecture 1: 08:00 10:20 Forefoot I: Hallux Valgus and Lesser Toes Mark Easley 30 mins 08:00 08:30 Surgical Management of Hallux Valgus Saragas,
How to avoid complications of distraction osteogenesis for first brachymetatarsia
 220 Acta Orthopaedica 2009; 80 (2): 220 225 How to avoid complications of distraction osteogenesis for first brachymetatarsia Keun-Bae Lee, Hyun-Kee Yang, Jae-Yoon Chung, Eun-Sun Moon, and Sung-Taek Jung
220 Acta Orthopaedica 2009; 80 (2): 220 225 How to avoid complications of distraction osteogenesis for first brachymetatarsia Keun-Bae Lee, Hyun-Kee Yang, Jae-Yoon Chung, Eun-Sun Moon, and Sung-Taek Jung
2017 SAFSA CONGRESS PROGRAMME
 2017 SAFSA CONGRESS PROGRAMME THURSDAY, MAY 25 07h45 07h55: WELCOME & INTRODUCTIONS Forefoot I: Hallux Valgus and Lesser Toes (08h00-10h00 Lectures) 08h00 08h30: Surgical Management of Hallux Valgus Rippstein,
2017 SAFSA CONGRESS PROGRAMME THURSDAY, MAY 25 07h45 07h55: WELCOME & INTRODUCTIONS Forefoot I: Hallux Valgus and Lesser Toes (08h00-10h00 Lectures) 08h00 08h30: Surgical Management of Hallux Valgus Rippstein,
Foot and ankle update
 Foot and ankle update Mr Ian Garnham Consultant Foot and Ankle Surgeon Whipps Cross University Hospital Hallux Rigidus Symptoms first ray and 1st MTP pain and swelling worse with push off or forced dorsiflexion
Foot and ankle update Mr Ian Garnham Consultant Foot and Ankle Surgeon Whipps Cross University Hospital Hallux Rigidus Symptoms first ray and 1st MTP pain and swelling worse with push off or forced dorsiflexion
Tendon split lengthening technique for flexor hallucis longus tendon rupture
 Park et al. Journal of Orthopaedic Surgery and Research (2017) 12:165 DOI 10.1186/s13018-017-0668-y RESEARCH ARTICLE Open Access Tendon split lengthening technique for flexor hallucis longus tendon rupture
Park et al. Journal of Orthopaedic Surgery and Research (2017) 12:165 DOI 10.1186/s13018-017-0668-y RESEARCH ARTICLE Open Access Tendon split lengthening technique for flexor hallucis longus tendon rupture
Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus
 Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus Yui Akiyama, Takaaki Hirano, Hiroyuki Mitsui Shingo Maeda, Hisateru Niki Department
Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus Yui Akiyama, Takaaki Hirano, Hiroyuki Mitsui Shingo Maeda, Hisateru Niki Department
Dr Nabil khouri MD. MSc. Ph.D
 Dr Nabil khouri MD. MSc. Ph.D Foot Anatomy The foot consists of 26 bones: 14 phalangeal, 5 metatarsal, and 7 tarsal. Toes are used to balance the body. Metatarsal Bones gives elasticity to the foot in
Dr Nabil khouri MD. MSc. Ph.D Foot Anatomy The foot consists of 26 bones: 14 phalangeal, 5 metatarsal, and 7 tarsal. Toes are used to balance the body. Metatarsal Bones gives elasticity to the foot in
There are few conditions in foot and ankle surgery that elicit
 SPECIAL FOCUS The Adult Acquired Flatfoot Deformity: A Treatment Algorithm Troy Watson, MD Abstract: The presentation of an adult with acquired flatfoot deformity is highly variable with a wide range of
SPECIAL FOCUS The Adult Acquired Flatfoot Deformity: A Treatment Algorithm Troy Watson, MD Abstract: The presentation of an adult with acquired flatfoot deformity is highly variable with a wide range of
The Flower Medial Column Fusion Plate
 The Flower Medial Column Fusion Plate PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION
The Flower Medial Column Fusion Plate PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION
How to approach the pediatric flatfoot
 Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.5312/wjo.v7.i1.1 World J Orthop 2016 January 18; 7(1): 1-7 ISSN 2218-5836 (online) 2016 Baishideng
Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.5312/wjo.v7.i1.1 World J Orthop 2016 January 18; 7(1): 1-7 ISSN 2218-5836 (online) 2016 Baishideng
*Rippstein, Trnka, Saragas, Hoffman
 THURS 25th MAY 07:00 07:10 Welcome and Introductions Paulo Ferrao Lecture 1: 07:10 09:45 Forefoot I: Hallux Valgus and Lesser Toes Mark Easley 40 mins 07:10 07:50 Surgical Management of Hallux Valgus 30
THURS 25th MAY 07:00 07:10 Welcome and Introductions Paulo Ferrao Lecture 1: 07:10 09:45 Forefoot I: Hallux Valgus and Lesser Toes Mark Easley 40 mins 07:10 07:50 Surgical Management of Hallux Valgus 30
Cavus Foot: Subtle and Not-So-Subtle AOFAS Resident Review Course September 28, 2013
 Cavus Foot: Subtle and Not-So-Subtle Course September 28, 2013 Matthew M. Roberts, MD Associate Professor of Clinical Orthopaedic Surgery Co-Chief, Foot and Ankle Service Hospital for Special Surgery Disclosure
Cavus Foot: Subtle and Not-So-Subtle Course September 28, 2013 Matthew M. Roberts, MD Associate Professor of Clinical Orthopaedic Surgery Co-Chief, Foot and Ankle Service Hospital for Special Surgery Disclosure
ANKLE PLANTAR FLEXION
 ANKLE PLANTAR FLEXION Evaluation and Measurements By Isabelle Devreux 1 Ankle Plantar Flexion: Gastrocnemius and Soleus ROM: 0 to 40-45 A. Soleus: Origin: Posterior of head of fibula and proximal1/3 of
ANKLE PLANTAR FLEXION Evaluation and Measurements By Isabelle Devreux 1 Ankle Plantar Flexion: Gastrocnemius and Soleus ROM: 0 to 40-45 A. Soleus: Origin: Posterior of head of fibula and proximal1/3 of
Technique Guide. VersiTomic. ReelX STT Double-Row Achilles G-Lok. J. Martin Leland III, M.D. J. Martin Leland III, M.D. Proximal Biceps Tenodesis
 Technique Guide VersiTomic ReelX STT Double-Row Achilles G-Lok Tendon Sub-Pectoral Repair Proximal Biceps Tenodesis J. Martin Leland III, M.D. J. Martin Leland III, M.D. The opinions expressed are those
Technique Guide VersiTomic ReelX STT Double-Row Achilles G-Lok Tendon Sub-Pectoral Repair Proximal Biceps Tenodesis J. Martin Leland III, M.D. J. Martin Leland III, M.D. The opinions expressed are those
POSTOP FOLLOW-UP & REHABILITATION FOLLOWING FOOT & ANKLE SURGERY
 1 POSTOP FOLLOW-UP & REHABILITATION FOLLOWING FOOT & ANKLE SURGERY The following instructions are general guidelines, but surgeon post-op instructions will dictate the individual patient's post-op management
1 POSTOP FOLLOW-UP & REHABILITATION FOLLOWING FOOT & ANKLE SURGERY The following instructions are general guidelines, but surgeon post-op instructions will dictate the individual patient's post-op management
Case. 15 Y old boy presented with pain in the foot. No history of injury or any constitutional symptoms. Your diagnosis?
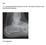 Case 15 Y old boy presented with pain in the foot. No history of injury or any constitutional symptoms Your diagnosis? Diagnosis: Calcaneo-navicular tarsal coalition. C sign Talar beaking Ant eaters nose
Case 15 Y old boy presented with pain in the foot. No history of injury or any constitutional symptoms Your diagnosis? Diagnosis: Calcaneo-navicular tarsal coalition. C sign Talar beaking Ant eaters nose
Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow.
 Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow. Berezhnoy Sergey. Percutaneous First Metatarsocuneiform Joint Arthrodesis in a Treatment of Metatarsus Primus Varus: a Prospective
Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow. Berezhnoy Sergey. Percutaneous First Metatarsocuneiform Joint Arthrodesis in a Treatment of Metatarsus Primus Varus: a Prospective
Chronic insertional achilles tendon ruptures treated by suture anchor repair and augmentation with flexor hallucis longus tendon transfer
 International Journal of Research in Orthopaedics Athar AMA et al. Int J Res Orthop. 2018 Mar;4(2):227-231 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20180442
International Journal of Research in Orthopaedics Athar AMA et al. Int J Res Orthop. 2018 Mar;4(2):227-231 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20180442
Evaluating midcalcaneal length after Evans calcaneal osteotomy: a comparison of the locking plate and tricortical allograft wedge
 IFFAS AOFAS Chicago, 2014 Evaluating midcalcaneal length after Evans calcaneal osteotomy: a comparison of the locking plate and tricortical allograft wedge Garrett M. Wobst, DPM, AACFAS, Nicole M. Protzman,
IFFAS AOFAS Chicago, 2014 Evaluating midcalcaneal length after Evans calcaneal osteotomy: a comparison of the locking plate and tricortical allograft wedge Garrett M. Wobst, DPM, AACFAS, Nicole M. Protzman,
Scar Engorged veins. Size of the foot [In clubfoot, small foot]
![Scar Engorged veins. Size of the foot [In clubfoot, small foot] Scar Engorged veins. Size of the foot [In clubfoot, small foot]](/thumbs/78/77722241.jpg) 6. FOOT HISTORY Pain: Walking, Running Foot wear problem Swelling; tingly feeling Deformity Stiffness Disability: At work; recreation; night; walk; ADL, Sports Previous Rx Comorbidities Smoke, Sugar, Steroid
6. FOOT HISTORY Pain: Walking, Running Foot wear problem Swelling; tingly feeling Deformity Stiffness Disability: At work; recreation; night; walk; ADL, Sports Previous Rx Comorbidities Smoke, Sugar, Steroid
The Valgus Foot in Cerebral Palsy Equinovalgus not Plano-Valgus. Alfred D. Grant, M.D. David Feldman, M.D.
 The Valgus Foot in Cerebral Palsy Equinovalgus not Plano-Valgus Alfred D. Grant, M.D. David Feldman, M.D. Norman Otsuka, MD M.D. THE PURPOSE OF THIS PRESENTATION IS TO STATE CLEARLY THAT THE VALGUS FOOT
The Valgus Foot in Cerebral Palsy Equinovalgus not Plano-Valgus Alfred D. Grant, M.D. David Feldman, M.D. Norman Otsuka, MD M.D. THE PURPOSE OF THIS PRESENTATION IS TO STATE CLEARLY THAT THE VALGUS FOOT
Financial Disclosure. The authors have not received any financial support for the preparation of this work.
 Persistent Clubfoot Deformity Following Treatment by the Ponseti Method W.B. Lehman, M.D. Alice Chu, M.D. New York Ponseti Clubfoot Center Department of Pediatric Orthopaedic Surgery Financial Disclosure
Persistent Clubfoot Deformity Following Treatment by the Ponseti Method W.B. Lehman, M.D. Alice Chu, M.D. New York Ponseti Clubfoot Center Department of Pediatric Orthopaedic Surgery Financial Disclosure
An Anatomical Cadaveric Study Comparing Medial vs. Plantar Approach for FDL or FHL Tendon Harvest for PTTD Reconstruction
 An Anatomical Cadaveric Study Comparing Medial vs. Plantar Approach for FDL or FHL Tendon Harvest for PTTD Reconstruction Mena Abdelmalak, BS, MBF Umur Aydogan, MD Penn State Hershey Medical Center Penn
An Anatomical Cadaveric Study Comparing Medial vs. Plantar Approach for FDL or FHL Tendon Harvest for PTTD Reconstruction Mena Abdelmalak, BS, MBF Umur Aydogan, MD Penn State Hershey Medical Center Penn
Surgical Correction of Lower Extremity Deformities by Triple Arthrodesis
 Surgical Correction of Lower Extremity Deformities by Triple Arthrodesis 足踝畸形矯治 振興醫療財團法人振興醫院 骨科部 熊永萬醫師 Introduction: The primary goals of a triple arthrodesis are to relieve pain from arthritic, deformed,
Surgical Correction of Lower Extremity Deformities by Triple Arthrodesis 足踝畸形矯治 振興醫療財團法人振興醫院 骨科部 熊永萬醫師 Introduction: The primary goals of a triple arthrodesis are to relieve pain from arthritic, deformed,
FACTS 1. Most need only Gastro aponeurotic release [in positive Silverskiold test]
![FACTS 1. Most need only Gastro aponeurotic release [in positive Silverskiold test] FACTS 1. Most need only Gastro aponeurotic release [in positive Silverskiold test]](/thumbs/83/88335212.jpg) FOOT IN CEREBRAL PALSY GAIT IN CEREBRAL PALSY I True Equinus II Jump gait III Apparent Equinus IV Crouch gait Group I True Equinus Extended hip and knee Equinus at ankle II Jump Gait [commonest] Equinus
FOOT IN CEREBRAL PALSY GAIT IN CEREBRAL PALSY I True Equinus II Jump gait III Apparent Equinus IV Crouch gait Group I True Equinus Extended hip and knee Equinus at ankle II Jump Gait [commonest] Equinus
Financial Disclosure. Turf Toe
 Seth O Brien, CP, LP Financial Disclosure Mr. Seth O'Brien has no relevant financial relationships with commercial interests to disclose. Turf Toe Common in athletes playing on firm, artificial turf Forceful
Seth O Brien, CP, LP Financial Disclosure Mr. Seth O'Brien has no relevant financial relationships with commercial interests to disclose. Turf Toe Common in athletes playing on firm, artificial turf Forceful
Hallux Valgus Deformity: Preoperative Radiologic Assessment
 119 Pictorial Essay H............ - Hallux Valgus Deformity: Preoperative Radiologic Assessment David Karasick1 and Keith L. Wapner An estimated 40% of the American adult population experiences foot problems,
119 Pictorial Essay H............ - Hallux Valgus Deformity: Preoperative Radiologic Assessment David Karasick1 and Keith L. Wapner An estimated 40% of the American adult population experiences foot problems,
Case Report A Case Report of Isolated Cuboid Nutcracker Fracture
 Case Reports in Orthopedics Volume 2016, Article ID 3264172, 5 pages http://dx.doi.org/10.1155/2016/3264172 Case Report A Case Report of Isolated Cuboid Nutcracker Fracture Takaaki Ohmori, 1,2 Shinichi
Case Reports in Orthopedics Volume 2016, Article ID 3264172, 5 pages http://dx.doi.org/10.1155/2016/3264172 Case Report A Case Report of Isolated Cuboid Nutcracker Fracture Takaaki Ohmori, 1,2 Shinichi
Classifications in Brief: Johnson and Strom Classification of Adult-acquired Flatfoot Deformity
 Clin Orthop Relat Res DOI 10.1007/s11999-015-4581-6 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons IN BRIEF Classifications in Brief: Johnson and
Clin Orthop Relat Res DOI 10.1007/s11999-015-4581-6 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons IN BRIEF Classifications in Brief: Johnson and
The Lower Limb VII: The Ankle & Foot. Anatomy RHS 241 Lecture 7 Dr. Einas Al-Eisa
 The Lower Limb VII: The Ankle & Foot Anatomy RHS 241 Lecture 7 Dr. Einas Al-Eisa Ankle joint Synovial, hinge joint Allow movement of the foot in the sagittal plane only (1 degree of freedom): dorsiflexion:
The Lower Limb VII: The Ankle & Foot Anatomy RHS 241 Lecture 7 Dr. Einas Al-Eisa Ankle joint Synovial, hinge joint Allow movement of the foot in the sagittal plane only (1 degree of freedom): dorsiflexion:
بسم هللا الرحمن الرحيم
 بسم هللا الرحمن الرحيم Laboratory RHS 221 Manual Muscle Testing Theory 1 hour practical 2 hours Dr. Ali Aldali, MS, PT Department of Physical Therapy King Saud University Talocrural and Subtalar Joint
بسم هللا الرحمن الرحيم Laboratory RHS 221 Manual Muscle Testing Theory 1 hour practical 2 hours Dr. Ali Aldali, MS, PT Department of Physical Therapy King Saud University Talocrural and Subtalar Joint
MR Imaging Findings of Painful Type II Accessory Navicular Bone: Correlation with Surgical and Pathologic Studies
 MR Imaging Findings of Painful Type II Accessory Navicular Bone: Correlation with Surgical and Pathologic Studies Yun Sun Choi, MD 1 Kyung Tai Lee, MD 2 Heung Sik Kang, MD 3 Eun Kyung Kim, MD 4 Index terms:
MR Imaging Findings of Painful Type II Accessory Navicular Bone: Correlation with Surgical and Pathologic Studies Yun Sun Choi, MD 1 Kyung Tai Lee, MD 2 Heung Sik Kang, MD 3 Eun Kyung Kim, MD 4 Index terms:
Therapeutic Foot Care Certificate Program Part I: Online Home Study Program
 Therapeutic Foot Care Certificate Program Part I: Online Home Study Program 1 Anatomy And Terminology Of The Lower Extremity Joan E. Edelstein, MA, PT, FISPO Associate Professor of Clinical Physical Therapy
Therapeutic Foot Care Certificate Program Part I: Online Home Study Program 1 Anatomy And Terminology Of The Lower Extremity Joan E. Edelstein, MA, PT, FISPO Associate Professor of Clinical Physical Therapy
Forefoot Procedures to Heal and Prevent Recurrence. Watermark. Diabetic Foot Update 2015 San Antonio, Texas
 Forefoot Procedures to Heal and Prevent Recurrence Diabetic Foot Update 2015 San Antonio, Texas J. Randolph Clements, DPM Assistant Professor of Orthopaedics Virginia Tech- Carilion School of Medicine
Forefoot Procedures to Heal and Prevent Recurrence Diabetic Foot Update 2015 San Antonio, Texas J. Randolph Clements, DPM Assistant Professor of Orthopaedics Virginia Tech- Carilion School of Medicine
Satisfaction analysis of Figure 8 (open heel) short leg cast
 Chan Kang, MD, PhD Dong-Hun Kang, MD Jae-Hwang Song, MD Min-Gu Jang, MD Ki-Jun Ahn, MD Ki-Soo, Lee, MD Department of Orthopedic Surgery, Chungnam National University School of Medicine. Daejeon, Republic
Chan Kang, MD, PhD Dong-Hun Kang, MD Jae-Hwang Song, MD Min-Gu Jang, MD Ki-Jun Ahn, MD Ki-Soo, Lee, MD Department of Orthopedic Surgery, Chungnam National University School of Medicine. Daejeon, Republic
Anterior Transfer of Tibialis Posterior through the Interosseous Membranes in Post Injection Drop Foot: The Expirence at CORU.
 Anterior Transfer of Tibialis Posterior through the Interosseous Membranes in Post Injection Drop Foot: The Expirence at CORU. J Okello,F Franceschi, A Loro, D Kintu, I Otim. CORU Mengo Hospital, Kampala,
Anterior Transfer of Tibialis Posterior through the Interosseous Membranes in Post Injection Drop Foot: The Expirence at CORU. J Okello,F Franceschi, A Loro, D Kintu, I Otim. CORU Mengo Hospital, Kampala,
BLUE SKY SCHOOL OF PROFESSIONAL MASSAGE AND THERAPEUTIC BODYWORK Musculoskeletal Anatomy & Kinesiology KNEE & ANKLE MUSCLES
 BLUE SKY SCHOOL OF PROFESSIONAL MASSAGE AND THERAPEUTIC BODYWORK Musculoskeletal Anatomy & Kinesiology KNEE & ANKLE MUSCLES MSAK201-I Session 3 1) REVIEW a) THIGH, LEG, ANKLE & FOOT i) Tibia Medial Malleolus
BLUE SKY SCHOOL OF PROFESSIONAL MASSAGE AND THERAPEUTIC BODYWORK Musculoskeletal Anatomy & Kinesiology KNEE & ANKLE MUSCLES MSAK201-I Session 3 1) REVIEW a) THIGH, LEG, ANKLE & FOOT i) Tibia Medial Malleolus
Duration of Follow-up (mo)
 Page 1 of 7 Fig. E-1 Fig. E-2 Fig. E-1 Medial ankle arthritis with medial translation of the talus and mortise widening. Note the shape of the medial malleolus (white arrow). Fig. E-2 Measurement of mortise
Page 1 of 7 Fig. E-1 Fig. E-2 Fig. E-1 Medial ankle arthritis with medial translation of the talus and mortise widening. Note the shape of the medial malleolus (white arrow). Fig. E-2 Measurement of mortise
Triple Arthrodesis of Foot for Correction of Lower Extremity Deformities
 Triple Arthrodesis of Foot for Correction of Lower Extremity Deformities 振興醫療財團法人振興醫院骨科部 * 熊永萬 A triple arthrodesis consists of surgical fusion of the talocalcaneal (TC), talonavicular (TN), and calcaneocuboid
Triple Arthrodesis of Foot for Correction of Lower Extremity Deformities 振興醫療財團法人振興醫院骨科部 * 熊永萬 A triple arthrodesis consists of surgical fusion of the talocalcaneal (TC), talonavicular (TN), and calcaneocuboid
Foot. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Foot Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Dorsum of the Foot Sole of the Foot Plantar aponeurosis It is a triangular thickening of deep fascia in the sole of the foot Attachments:
Foot Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Dorsum of the Foot Sole of the Foot Plantar aponeurosis It is a triangular thickening of deep fascia in the sole of the foot Attachments:
Proper Logging of Surgical Procedures (Effective July 1, 2018)
 Proper Logging of Surgical Procedures (Effective July 1, 2018) GENERAL GUIDELINES: 1) For the procedure codes listed below, the program director must review each entry to determine proper usage. The following
Proper Logging of Surgical Procedures (Effective July 1, 2018) GENERAL GUIDELINES: 1) For the procedure codes listed below, the program director must review each entry to determine proper usage. The following
Aetiology: Pressure of Distal intermetatarsal ligament against common digital nerve. Lumbar radiculopathy Instability MTPJ joint or inflammatory MPJ
 MORTON S NEUROMA 80% III web space (next common is II). Never occurs in III or IV Common in females in fifties Aetiology: Pressure of Distal intermetatarsal ligament against common digital nerve Rule out
MORTON S NEUROMA 80% III web space (next common is II). Never occurs in III or IV Common in females in fifties Aetiology: Pressure of Distal intermetatarsal ligament against common digital nerve Rule out
The Leg. Prof. Oluwadiya KS
 The Leg Prof. Oluwadiya KS www.oluwadiya.sitesled.com Compartments of the leg 4 Four Compartments: 1. Anterior compartment Deep fibular nerve Dorsiflexes the foot and toes 2. Lateral Compartment Superficial
The Leg Prof. Oluwadiya KS www.oluwadiya.sitesled.com Compartments of the leg 4 Four Compartments: 1. Anterior compartment Deep fibular nerve Dorsiflexes the foot and toes 2. Lateral Compartment Superficial
Split tendon transfers for the correction of spastic varus foot deformity: a case series study
 JOURNAL OF FOOT AND ANKLE RESEARCH RESEARCH Open Access Split tendon transfers for the correction of spastic varus foot deformity: a case series study Maria Vlachou 1*, Dimitris Dimitriadis 1,2 Abstract
JOURNAL OF FOOT AND ANKLE RESEARCH RESEARCH Open Access Split tendon transfers for the correction of spastic varus foot deformity: a case series study Maria Vlachou 1*, Dimitris Dimitriadis 1,2 Abstract
PTTD Reconstruction-Turning Failure into Your Guide to Success Michael D. Dujela DPM, FACFAS
 PTTD Reconstruction-Turning Failure into Your Guide to Success Michael D. Dujela DPM, FACFAS Visiting Fellowship Alumnus, Orthopedic Foot and Ankle Center A.O. Fellowship Orthopaedic Foot and Ankle Alumnus
PTTD Reconstruction-Turning Failure into Your Guide to Success Michael D. Dujela DPM, FACFAS Visiting Fellowship Alumnus, Orthopedic Foot and Ankle Center A.O. Fellowship Orthopaedic Foot and Ankle Alumnus
Investigation performed at the Department of Orthopaedic and Trauma Surgery, Glasgow Royal Infirmary, Glasgow, United Kingdom
 748 COPYRIGHT 2005 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Long-Term Results of the Modified Hoffman Procedure in the Rheumatoid Forefoot BY S. THOMAS, MBCHB, BSC, MRCS, A.W.G. KINNINMONTH,
748 COPYRIGHT 2005 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Long-Term Results of the Modified Hoffman Procedure in the Rheumatoid Forefoot BY S. THOMAS, MBCHB, BSC, MRCS, A.W.G. KINNINMONTH,
Evaluation of hindfoot alignment change before and after total knee arthroplasty
 Evaluation of hindfoot alignment change before and after total knee arthroplasty Ohashi S, Ikoma K, Hara Y, Arai Y Nagasawa K, Maki M, Kubo T Department of Orthopaedics, Graduate School of Medical Science,
Evaluation of hindfoot alignment change before and after total knee arthroplasty Ohashi S, Ikoma K, Hara Y, Arai Y Nagasawa K, Maki M, Kubo T Department of Orthopaedics, Graduate School of Medical Science,
Calcaneal lengthening osteotomy for treatment of idiopathic flexible flat foot in children
 International Journal of Research in Orthopaedics Soudy SE-E. Int J Res Orthop. 2016 Dec;2(4):340-345 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20164165
International Journal of Research in Orthopaedics Soudy SE-E. Int J Res Orthop. 2016 Dec;2(4):340-345 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20164165
Anatomy of Foot and Ankle
 Anatomy of Foot and Ankle Surface anatomy of the ankle & foot Surface anatomy of the ankle & foot Medial orientation point medial malleous sustentaculum tali tuberosity of navicular TA muscle TP muscle
Anatomy of Foot and Ankle Surface anatomy of the ankle & foot Surface anatomy of the ankle & foot Medial orientation point medial malleous sustentaculum tali tuberosity of navicular TA muscle TP muscle
Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity
 Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity Amber M. Shane, DPM, FACFAS 1, Christopher L. Reeves, DPM, FACFAS 1 1. Orlando Foot & Ankle Clinic, Orlando, FL Abstract
Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity Amber M. Shane, DPM, FACFAS 1, Christopher L. Reeves, DPM, FACFAS 1 1. Orlando Foot & Ankle Clinic, Orlando, FL Abstract
CHRONIC FOOT PROBLEMS FOOT and ANKLE BASICS
 CHRONIC FOOT PROBLEMS FOOT and ANKLE BASICS ABC s of Comprehensive Musculoskeletal Care December 1 st, 2007 Stephen Pinney MD Chief, UCSF Foot and Ankle Service Chronic problems typically occur gradually
CHRONIC FOOT PROBLEMS FOOT and ANKLE BASICS ABC s of Comprehensive Musculoskeletal Care December 1 st, 2007 Stephen Pinney MD Chief, UCSF Foot and Ankle Service Chronic problems typically occur gradually
Biokinesiology of the Ankle Complex
 Rehabilitation Considerations Following Ankle Fracture: Impact on Gait & Closed Kinetic Chain Function Disclosures David Nolan, PT, DPT, MS, OCS, SCS, CSCS I have no actual or potential conflict of interest
Rehabilitation Considerations Following Ankle Fracture: Impact on Gait & Closed Kinetic Chain Function Disclosures David Nolan, PT, DPT, MS, OCS, SCS, CSCS I have no actual or potential conflict of interest
PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION. At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral)
 PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral) They are contained within the tendons of Flexor Hallucis Brevis
PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral) They are contained within the tendons of Flexor Hallucis Brevis
Plantar fasciopathy (PFs)
 Plantar fasciopathy (PFs) 2016. 04. 30. Jung-Soo Lee, M.D., Ph.D. Department of Rehabilitation Medicine, Uijeongbu St. Mary's Hospital, College of Medicine, The Catholic University of Korea Anatomy of
Plantar fasciopathy (PFs) 2016. 04. 30. Jung-Soo Lee, M.D., Ph.D. Department of Rehabilitation Medicine, Uijeongbu St. Mary's Hospital, College of Medicine, The Catholic University of Korea Anatomy of
Achilles Tendon Anatomy. Achilles Tendon Anatomy. Acute Achilles Rupture. Acute Achilles Rupture 8/19/14. Primary plantarflexor
 Disclosure Conditions of the Achilles Tendon Brian Clowers, M.D. I have no financial relationships that would influence the content of this presentation Oklahoma Sports and Orthopedic Institute September
Disclosure Conditions of the Achilles Tendon Brian Clowers, M.D. I have no financial relationships that would influence the content of this presentation Oklahoma Sports and Orthopedic Institute September
No disclosures relevant to this topic Acknowledgement: some clinical pictures were obtained from the OTA fracture lecture series and AO fracture
 CALCANEUS FRACTURES No disclosures relevant to this topic Acknowledgement: some clinical pictures were obtained from the OTA fracture lecture series and AO fracture lecture series INCIDENCE 2% of all fractures
CALCANEUS FRACTURES No disclosures relevant to this topic Acknowledgement: some clinical pictures were obtained from the OTA fracture lecture series and AO fracture lecture series INCIDENCE 2% of all fractures
HOW TO CITE THIS ARTICLE:
 MANAGEMENT OF CHRONIC ACHILLES TENDON RUPTURES BY RECONSTRUCTING WITH FLEXOR HALLUCIS LONGUS AND PERONEUS BREVIS TENDONS: A COMPARATIVE STUDY Ananthula Krishna Reddy 1, Bachu Srinivas 2, V. Prashanth 3,
MANAGEMENT OF CHRONIC ACHILLES TENDON RUPTURES BY RECONSTRUCTING WITH FLEXOR HALLUCIS LONGUS AND PERONEUS BREVIS TENDONS: A COMPARATIVE STUDY Ananthula Krishna Reddy 1, Bachu Srinivas 2, V. Prashanth 3,
A new radiographic view of the hindfoot
 Ikoma et al. Journal of Foot and Ankle Research 2013, 6:48 JOURNAL OF FOOT AND ANKLE RESEARCH RESEARCH Open Access A new radiographic view of the hindfoot Kazuya Ikoma 1*, Masahiko Noguchi 2, Koji Nagasawa
Ikoma et al. Journal of Foot and Ankle Research 2013, 6:48 JOURNAL OF FOOT AND ANKLE RESEARCH RESEARCH Open Access A new radiographic view of the hindfoot Kazuya Ikoma 1*, Masahiko Noguchi 2, Koji Nagasawa
