High tibial osteotomy (HTO), distal femoral. Rates of Deep Vein Thrombosis Occurring After Osteotomy About the Knee.
|
|
|
- Jordan Hampton
- 5 years ago
- Views:
Transcription
1 An Original Study Rates of Deep Vein Thrombosis Occurring After Osteotomy About the Knee Brandon J. Erickson, MD, Annie Tilton, MD, Rachel M. Frank, MD, William Park, BS, and Brian J. Cole, MD Abstract We conducted a study to determine the rates of symptomatic deep vein thrombosis (DVT) and pulmonary embolism (PE) after high tibial osteotomy (HTO), distal femoral osteotomy (DFO), or tibial tubercle osteotomy (TTO) in patients who did not receive postoperative chemical prophylaxis. All patients who had HTO, DFO, or TTO performed by a single surgeon between 2009 and 2014 were identified. Charts were reviewed to determine presence or absence of DVT or PE. Patient age, smoking status, oral contraceptive (OC) use, and body mass index (BMI) were recorded. Patients received no chemical or mechanical prophylaxis after surgery. We identified 141 patients (44% male, 56% female) who underwent HTO, DFO, or TTO. Mean (SD) age was (9.86) years, mean (SD) follow-up was 17.1 (4.1) months, and mean (SD) BMI was (5.11) kg/m 2. Overall, 36.7% of female patients used OCs, and 13.48% of all patients were smokers. After surgery, 2 patients (1.42%) developed below-knee DVT (unilateral in 1 case, bilateral in the other). The bilateral DVT case progressed to PE. Neither patient smoked, but the bilateral DVT/PE patient was using OCs. DVT patients mean (SD) age was (8.24) years, and their mean (SD) BMI was (0.18) kg/m 2. HTO, DFO, and TTO patients who did not receive chemical prophylaxis had low rates of DVT (1.42%) and PE (0.71%). Administration of DVT/PE prophylaxis after these osteotomies may not be warranted. High tibial osteotomy (HTO), distal femoral osteotomy (DFO), and tibial tubercle osteotomy (TTO) are viable treatment options for deformities about the knee and patella maltracking. 1-4 Although TTO can be performed in many ways (eg, anteriorization, anteromedialization, medialization), the basic idea is to move the tibial tubercle to improve patellar tracking or to offload a patellar facet that has sustained trauma or degenerated. 2 DFO is a surgical option for treating a valgus knee deformity (the lateral tibiofemoral compartment is offloaded) or for protecting a knee compartment after cartilage or meniscal restoration (medial closing wedge or lateral opening wedge). 1 Similarly, HTO is an option for treating a varus knee deformity or isolated medial compartment arthritis; the diseased compartment is offloaded, and any malalignment is corrected. Akin to DFO, HTO is often performed to protect a knee compartment, typically the medial tibiofemoral compartment, after cartilage or meniscal restoration. 2-4 Compared to most arthroscopic knee surgeries, these osteotomies are much more involved, have longer operative times, and restrict postoperative weight-bearing and range of motion. 2-4 The rates of deep vein thrombosis (DVT) and pulmonary embolism (PE) after these osteotomies are not well documented. In addition, there is no documentation of the risks in patients who smoke, are obese, or are using oral contraceptives (OCs) at time of surgery, despite the increased DVT and PE risks posed by smoking, obesity, and OC use in other surgical procedures. 5-7 Although the American Academy of Orthopaedic Surgeons (AAOS) issued clinical practice guidelines for DVT/PE prophylaxis after hip Authors Disclosure Statement: The authors report no actual or potential conflict of interest in relation to this article. January/February 2017 The American Journal of Orthopedics E23
2 Rates of DVT Occurring After Osteotomy About the Knee Take-Home Points DVT and PE are uncommon complications following osteotomies Use of oral contraceptives can increase the risk of a patient sustaining a postoperative DVT and PE following osteotomies In the absence of significant risk factors, postoperative chemical DVT prophylaxis may be unnecessary in patients undergoing osteotomies and knee arthroplasty, there is no standard prophylaxis guidelines for DVT/PE prevention after HTO, DFO, or TTO. 8,9 Last, rates of DVT after total knee arthroplasty (TKA) are well defined; they range from 2% to 12%. 10,11 These rates may be surrogates for osteotomies about the knee, but this is only conjecture. We conducted a study to determine the rates of symptomatic DVT and PE after HTO, DFO, or TTO in patients who did not receive postoperative DVT/PE prophylaxis. We also wanted to determine if age, body mass index (BMI), and smoking status have associations with the risk of developing either DVT or PE after HTO, DFO, or TTO. We hypothesized that the DVT and PE rates would both be <1%. Methods After this study was approved by our university s Institutional Review Board, we searched the surgical database of Dr. Cole, a sports medicine fellowship trained surgeon, to identify all patients who had HTO, DFO, or TTO performed between September 1, 2009 and September 30, Current Procedural Terminology (CPT) codes were used for the search. The code for HTO was 27457: osteotomy, proximal tibia, including fibular excision or osteotomy (includes correction of genu varus [bowleg] or genu valgus [knock-knee]); after epiphyseal closure). The code for DFO was 27450: osteotomy, femur, shaft or supracondylar; with fixation. Last, the code for TTO was 27418: anterior tibial tubercleplasty (eg, Maquet-type procedure). The 141 patients identified in the search were treated by Dr. Cole at a single institution and were included in the study. Study inclusion did not require a minimum follow-up. Follow-up duration was defined as the time between surgery and the final clinic note in the patient chart. No patient was excluded for lack of follow-up clinic visits, and none was lost to follow-up. Age, BMI, smoking status, and OC use were recorded for all patients. For each procedure, the surgeon s technique remained the same throughout the study period: HTO, medial opening-wedge osteotomy with plate-and-screw fixation; DFO, lateral opening-wedge osteotomy with plate-and-screw fixation; and TTO, mostly anteromedialization with screw fixation (though this was dictated by patellar contact pressures). A tourniquet was used in all cases. Each patient s hospital electronic medical record and outpatient office notes were reviewed to determine if symptomatic DVT or PE developed after surgery. The diagnosis of symptomatic DVT was based on clinical symptoms and confirmatory ultrasound, and the PE diagnosis was based on computed tomography. Doppler ultrasound was performed only in symptomatic patients (ie, it was not routinely performed). Per surgeon protocol, postoperative DVT prophylaxis was not administered. Patients were encouraged to begin dorsiflexion and plantar flexion of the ankle (ankle pumps) immediately and to mobilize as soon as comfortable. Each patient received a cold therapy machine with compression sleeve. Patients were allowed toe-touch weight-bearing for 6 weeks, and then progressed 25% per week for 4 weeks to full weight-bearing by 10 weeks. After surgery, each patient was placed in a brace, which was kept locked in extension for 10 days; when the brace was unlocked, the patient was allowed to range the knee. Continuous variable data are reported as weighted means and weighted standard deviations. Categorical variable data are reported as frequencies and percentages. Results Our database search identified 141 patients (44% male, 56% female) who underwent HTO (47 patients, 33.3%), DFO (13 patients, 9.2%), or TTO (81 patients, 57.5%). Mean (SD) age was (9.86) years, mean (SD) BMI was (5.11) kg/m 2, and mean (SD) follow-up was 17.1 (4.1) months. Of the female patients, 36.7% were using OCs at time of surgery. Of all patients, 13.48% were smokers. Two patients (1.42%) had clinical symptoms consistent with DVT. In each case, the diagnosis was confirmed with Doppler ultrasound. The below-knee DVT was unilateral in 1 case and bilateral in the other. The bilateral DVT case progressed to PE. Neither patient smoked, but the bilateral DVT/PE patient was using OCs. DVT patients mean (SD) age was (8.24) years, and their mean (SD) BMI was (0.18) kg/m 2 (Table). The unilateral DVT occurred in a patient who underwent anteromedialization of the tibial tubercle and osteochondral allograft transfer to the lateral femoral condyle for patellar maltracking and a focal trochlear defect. The DVT was diagnosed 8 days after surgery and was treated with warfarin. E24 The American Journal of Orthopedics January/February
3 B. J. Erickson et al Low-molecular-weight heparin (LMWH) was used as a bridge until the warfarin level was therapeutic (4 days). This male patient had no significant medical history. The bilateral DVT with PE occurred in a patient who underwent a medial opening-wedge HTO for a varus deformity with right medial compartment osteoarthritis and a meniscal tear. The DVT and PE were diagnosed 48 hours after surgery, when the patient complained of lightheadedness and lost consciousness. She had no medical problems but was using OCs at time of surgery. The patient died 3 days after surgery and subsequently was found to have a maternal-side family history of DVT (the patient and her family physician had been unaware of this history). Discussion As the rates of DVT and PE after osteotomies about the knee have not been well studied, we wanted to determine these rates after HTO, DFO, and TTO in patients who did not receive postoperative DVT prophylaxis. We hypothesized that DVT and PE rates would both be <1%, and this hypothesis was partly confirmed: The rate of PE after HTO, DFO, and TTO was <1%, and the rate of symptomatic DVT was >1%. Similarly, the patients who developed these complications were nonsmokers and had a BMI no higher than that of the patients who did not develop DVT or PE. In addition, only 1 patient developed DVT and PE, and she was using OCs and had a family history of DVT. Last, the patients who developed these complications were on average 14 years older than the patients who did not develop DVT or PE. Although there is a plethora of reports on the incidence of DVT and PE after TKA, there is little on the incidence after osteotomies 8,12 The rate of DVT after TKA varies, but many studies place it between 2% and 12%, and routinely find a PE rate of <0.5%. 10,11,13,14 Although the AAOS issued a clinical practice guideline for postoperative DVT prophylaxis after TKA, and evaluated the best available evidence, it could not reach consensus on a specific type of DVT prophylaxis, though the workgroup did recommend that patients be administered postoperative DVT prophylaxis of some kind. 8,9 Similarly, the American College of Chest Physicians (ACCP) issued clinical practice guidelines for preventing DVT and PE after elective TKA and total hip arthroplasty. 15 According to the ACCP guidelines, patients should receive prophylaxis LMWH, fondaparinux, apixaban, dabigatran, Table. Demographics of Patients Who Developed and Patients Who Did Not Develop DVT or PE Demographic Postoperative DVT/PE No rivaroxaban, low-dose unfractionated heparin, adjusted-dose vitamin K antagonist, aspirin, or an intermittent pneumatic compression device for a minimum of 14 days. Unfortunately, though there are similarities between TKAs and peri-knee osteotomies, these procedures are markedly different, and it is difficult to extrapolate and adapt recommendations and produce a consensus statement for knee arthroplasties. In addition, guidelines exist for hospitalized patients who are being treated for medical conditions or have undergone surgery, but all the patients in the present study had their osteotomies performed on an outpatient basis. Martin and colleagues 16 reviewed 323 cases of medial opening-wedge HTO and found a DVT rate of 1.4% in the absence of routine DVT prophylaxis, except in patients with a history of DVT. Their rate is almost identical to ours, but we also included other osteotomies in our study. Miller and colleagues 17 reviewed 46 cases of medial opening-wedge HTO and found a 4.3% DVT rate, despite routine prophylaxis with once-daily 325-mg aspirin and ankle pumps. This finding contrasts with our 1.42% DVT rate in the absence of postoperative chemical DVT prophylaxis. Motycka and colleagues 18 reviewed 65 HTO cases in which DVT prophylaxis (oral anticoagulant) was given for 6 weeks, and they found a DVT rate of 9.7%. Turner and colleagues 19 performed venous ultrasound on 81 consecutive patients who underwent HTO and received DVT prophylaxis (twice-daily subcutaneous heparin), and they found a DVT rate of 41% and a PE rate of 1.2%, though only 8.6% of the DVT cases were symptomatic. Of note, whereas Yes Age, y (Mean [SD]) (9.86) (8.24) BMI, kg/m (5.11) (0.18) Male 44% 50% Smoker 13.48% 0% Oral contraceptive user 20.60% 50% Abbreviations: BMI, body mass index; DVT, deep vein thrombosis; PE, pulmonary embolism. January/February 2017 The American Journal of Orthopedics E25
4 Rates of DVT Occurring After Osteotomy About the Knee the lowest postoperative DVT rate was for patients who did not receive postoperative DVT prophylaxis, the rate of symptomatic DVT after these osteotomies ranged from 1.4% to 8.6% in patients who received prophylaxis. 16,19 Given this evidence and our study results, it appears routine chemical DVT prophylaxis after osteotomies about the knee may not be necessary, though higher level evidence is needed in order to make definitive recommendations. In the present study, the 2 patients who developed symptomatic DVT (1 subsequently developed PE) were nonsmokers in good health. The female patient (DVT plus PE) was using OCs at time of surgery. Studies have shown that patients who smoke and who use OCs are at increased risk for developing DVT or PE after surgery. 5,6,12 Given that only 2 of our patients developed DVT/PE, and neither was a smoker, smoking was not associated with increased DVT or PE risk in this study population, in which 13.48% of patients were smokers at time of surgery. In addition, given that the 1 female patient who developed DVT/PE was using OCs and that 36.7% of all female patients in the study were using OCs, it is difficult to conclude whether OC use increased the female patient s risk for DVT or PE. Furthermore, neither the literature nor the AAOS consensus statement supports discontinuing OCs for this surgical procedure. Patients in this study did not receive chemical or mechanical DVT prophylaxis after surgery. Regarding various post-tka DVT prophylaxis regimens, aspirin is as effective as LMWH in preventing DVT, and the risk for postoperative blood loss and wound complications is lower with aspirin than with rivaroxaban. 20,21 Given that the present study s postoperative rates of DVT (1.42%) and PE (0.71%) are equal to or less than rates already reported in the literature, routine DVT prophylaxis after osteotomies about the knee may be unnecessary in the absence of other significant risk factors. 16,19 However, our study considered only symptomatic DVT and PE, so it is possible that the number of asymptomatic DVT cases is higher in this patient population. Definitively answering our study s clinical question will require a multicenter registry study (prospective cohort study). Study Limitations The strengths of this study include the large number of patients treated by a single surgeon using the same postoperative protocol. Limitations of this study include the lack of a control group. Although we found a DVT rate of 1.42% and a PE rate of 0.71%, the literature on the accepted risks for DVT and PE after HTO, DFO, and TTO is unclear. With our results stratified by procedure, the DVT rate was 2% in the HTO group, 0% in the DFO group, and 1% in the TTO group. However, we were unable to reliably stratify these results by each specific procedure, as the number of patients in each group would be too low. This study involved reviewing charts; as patients were not contacted, it is possible a patient developed DVT or PE, was treated at an outside facility, and then never followed up with the treating surgeon. Patients were identified by CPT codes, so, if a patient underwent HTO, DFO, or TTO that was recorded under a different CPT code, it is possible the patient was missed by our search. All patients were seen after surgery, and we reviewed the outpatient office notes that were taken, so unless the DVT or PE occurred after a patient s final postoperative visit, it would have been recorded. Similarly, the DVT and PE rates reported here cannot be extrapolated to overall risks for DVT and PE after osteotomies about the knee in all patients only in patients who did not receive DVT prophylaxis after surgery. Conclusion The rates of DVT and PE after HTO, DFO, and TTO in patients who did not receive chemical prophylaxis are low: 1.42% and 0.71%, respectively. After these osteotomies, DVT/PE prophylaxis in the absence of known risk factors may not be warranted. Dr. Erickson is an Orthopedic Surgery Resident, Rush University Medical Center, Chicago, Illinois. Dr. Tilton is an Orthopedic Surgery Resident, Northwestern University Medical Center, Chicago, Illinois. Dr. Frank is an Orthopedic Surgery Sports Medicine Fellow, Rush University Medical Center, Chicago, Illinois. Mr. Park is an Orthopedic Surgery Research Assistant, Chicago Medical School, North Chicago, Illinois. Dr. Cole is a Sports Medicine Orthopedic Surgeon and Chicago Bulls Team Physician, Midwest Orthopaedics at Rush, Rush University Medical Center, Chicago, Illinois. Address correspondence to: Brandon J. Erickson, MD, Midwest Orthopaedics at Rush, Rush University Medical Center, 1611 W Harrison St, Suite 300, Chicago, IL (tel, ; fax, ; , berickso.24@gmail.com). Am J Orthop. 2017;46(1):E23-E27. Copyright Frontline Medical Communications Inc All rights reserved. E26 The American Journal of Orthopedics January/February
5 B. J. Erickson et al References 1. Rossi R, Bonasia DE, Amendola A. The role of high tibial osteotomy in the varus knee. J Am Acad Orthop Surg. 2011;19(10): Sherman SL, Erickson BJ, Cvetanovich GL, et al. Tibial tuberosity osteotomy: indications, techniques, and outcomes. Am J Sports Med. 2014;42(8): Wright JM, Crockett HC, Slawski DP, Madsen MW, Windsor RE. High tibial osteotomy. J Am Acad Orthop Surg. 2005;13(4): Cameron JI, McCauley JC, Kermanshahi AY, Bugbee WD. Lateral opening-wedge distal femoral osteotomy: pain relief, functional improvement, and survivorship at 5 years. Clin Orthop Relat Res. 2015;473(6): Ng WM, Chan KY, Lim AB, Gan EC. The incidence of deep venous thrombosis following arthroscopic knee surgery. Med J Malaysia. 2005;60(suppl C): Platzer P, Thalhammer G, Jaindl M, et al. Thromboembolic complications after spinal surgery in trauma patients. Acta Orthop. 2006;77(5): Wallace G, Judge A, Prieto-Alhambra D, de Vries F, Arden NK, Cooper C. The effect of body mass index on the risk of post-operative complications during the 6 months following total hip replacement or total knee replacement surgery. Osteoarthritis Cartilage. 2014;22(7): Lieberman JR, Pensak MJ. Prevention of venous thromboembolic disease after total hip and knee arthroplasty. J Bone Joint Surg Am. 2013;95(19): Mont MA, Jacobs JJ. AAOS clinical practice guideline: preventing venous thromboembolic disease in patients undergoing elective hip and knee arthroplasty. J Am Acad Orthop Surg. 2011;19(12): Kim YH, Kulkarni SS, Park JW, Kim JS. Prevalence of deep vein thrombosis and pulmonary embolism treated with mechanical compression device after total knee arthroplasty in Asian patients. J Arthroplasty. 2015;30(9): Kim YH, Yoo JH, Kim JS. Factors leading to decreased rates of deep vein thrombosis and pulmonary embolism after total knee arthroplasty. J Arthroplasty. 2007;22(7): Raphael IJ, Tischler EH, Huang R, Rothman RH, Hozack WJ, Parvizi J. Aspirin: an alternative for pulmonary embolism prophylaxis after arthroplasty? Clin Orthop Relat Res. 2014;472(2): Won MH, Lee GW, Lee TJ, Moon KH. Prevalence and risk factors of thromboembolism after joint arthroplasty without chemical thromboprophylaxis in an Asian population. J Arthroplasty. 2011;26(7): Bozic KJ, Vail TP, Pekow PS, Maselli JH, Lindenauer PK, Auerbach AD. Does aspirin have a role in venous thromboembolism prophylaxis in total knee arthroplasty patients? J Arthroplasty. 2010;25(7): Falck-Ytter Y, Francis CW, Johanson NA, et al; American College of Chest Physicians. Prevention of VTE in orthopedic surgery patients: Antithrombotic Therapy and Prevention of Thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines. Chest. 2012;141(2 suppl):e278s-e325s. 16. Martin R, Birmingham TB, Willits K, Litchfield R, Lebel ME, Giffin JR. Adverse event rates and classifications in medial opening wedge high tibial osteotomy. Am J Sports Med. 2014;42(5): Miller BS, Downie B, McDonough EB, Wojtys EM. Complications after medial opening wedge high tibial osteotomy. Arthroscopy. 2009;25(6): Motycka T, Eggerth G, Landsiedl F. The incidence of thrombosis in high tibial osteotomies with and without the use of a tourniquet. Arch Orthop Trauma Surg. 2000;120(3-4): Turner RS, Griffiths H, Heatley FW. The incidence of deepvein thrombosis after upper tibial osteotomy. A venographic study. J Bone Joint Surg Br. 1993;75(6): Jiang Y, Du H, Liu J, Zhou Y. Aspirin combined with mechanical measures to prevent venous thromboembolism after total knee arthroplasty: a randomized controlled trial. Chin Med J (Engl). 2014;127(12): Zou Y, Tian S, Wang Y, Sun K. Administering aspirin, rivaroxaban and low-molecular-weight heparin to prevent deep venous thrombosis after total knee arthroplasty. Blood Coagul Fibrinolysis. 2014;25(7): This paper will be judged for the Resident Writer s Award. January/February 2017 The American Journal of Orthopedics E27
Early Ambulation Reduces the Risk of Venous Thromboembolism After Total Knee Replacement. Marilyn Szekendi, PhD, RN
 Early Ambulation Reduces the Risk of Venous Thromboembolism After Total Knee Replacement Marilyn Szekendi, PhD, RN ANA 7 th Annual Nursing Quality Conference, February 2013 Research Team Banafsheh Sadeghi,
Early Ambulation Reduces the Risk of Venous Thromboembolism After Total Knee Replacement Marilyn Szekendi, PhD, RN ANA 7 th Annual Nursing Quality Conference, February 2013 Research Team Banafsheh Sadeghi,
Japanese Deep Vein Thrombosis
 Japanese Deep Vein Thrombosis and Pulmonary Embolism after Total Knee Arthroplasty Artificial joint and cartilage implantation center, Kitasato institute hospital, Kitasato university Yasunori Tsukimura
Japanese Deep Vein Thrombosis and Pulmonary Embolism after Total Knee Arthroplasty Artificial joint and cartilage implantation center, Kitasato institute hospital, Kitasato university Yasunori Tsukimura
Aspirin or Rivaroxaban for VTE Prophylaxis after Hip or Knee Arthroplasty: The EPCAT II Trial
 Aspirin or Rivaroxaban for VTE Prophylaxis after Hip or Knee Arthroplasty: The EPCAT II Trial Wednesday, June 6, 2018, 2:00PM ET Guest Author: David R. Anderson, MD Presenter: Sara Vazquez, PharmD Moderators:
Aspirin or Rivaroxaban for VTE Prophylaxis after Hip or Knee Arthroplasty: The EPCAT II Trial Wednesday, June 6, 2018, 2:00PM ET Guest Author: David R. Anderson, MD Presenter: Sara Vazquez, PharmD Moderators:
Back out of Locking Pin with Hinge Fracture after High Tibial Osteotomy
 Case Report Knee Surg Relat Res 2018;30(2):171-175 https://doi.org/10.5792/ksrr.17.034 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Back out of Locking Pin with Hinge Fracture after
Case Report Knee Surg Relat Res 2018;30(2):171-175 https://doi.org/10.5792/ksrr.17.034 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Back out of Locking Pin with Hinge Fracture after
None. Who uses IV antibiotics before simple knee arthroscopies? 3/9/2018. Anticoagulants or Antibiotics Are they Necessary for Simple Knee Scopes?
 Anticoagulants or Antibiotics Are they Necessary for Simple Knee Scopes? Rachel M. Frank, MD Assistant Professor, Department of Orthopaedic Surgery Sports Medicine, Cartilage Restoration, and Shoulder
Anticoagulants or Antibiotics Are they Necessary for Simple Knee Scopes? Rachel M. Frank, MD Assistant Professor, Department of Orthopaedic Surgery Sports Medicine, Cartilage Restoration, and Shoulder
Periarticular knee osteotomy
 Periarticular knee osteotomy Turnberg Building Orthopaedics 0161 206 4803 All Rights Reserved 2018. Document for issue as handout. Knee joint The knee consists of two joints which allow flexion (bending)
Periarticular knee osteotomy Turnberg Building Orthopaedics 0161 206 4803 All Rights Reserved 2018. Document for issue as handout. Knee joint The knee consists of two joints which allow flexion (bending)
Incidence of Venous Thromboembolism After Arthroscopic Anterior Cruciate Ligament Reconstruction
 Incidence of Venous Thromboembolism After Arthroscopic Anterior Cruciate Ligament Reconstruction Masaki Nagashima 1,2 Toshiro Otani 3 Hiroyuki Seki 1,2 Kenichiro Takeshima 2 Nobuto Origuchi 4 Ken Ishii
Incidence of Venous Thromboembolism After Arthroscopic Anterior Cruciate Ligament Reconstruction Masaki Nagashima 1,2 Toshiro Otani 3 Hiroyuki Seki 1,2 Kenichiro Takeshima 2 Nobuto Origuchi 4 Ken Ishii
1/27/2016. Disclosure. Goals. The Risk and Prevention of Venous Thromboembolism (VTE) in Patients With Foot and Ankle Pathology
 The Risk and Prevention of Venous Thromboembolism (VTE) in Patients With Foot and Ankle Pathology STEVEN STEINLAUF, MD THE ORTHOPAEDIC FOOT AND ANKLE INSTITUTE OF SOUTH FLORIDA CLINICAL ASSISTANT PROFESSOR
The Risk and Prevention of Venous Thromboembolism (VTE) in Patients With Foot and Ankle Pathology STEVEN STEINLAUF, MD THE ORTHOPAEDIC FOOT AND ANKLE INSTITUTE OF SOUTH FLORIDA CLINICAL ASSISTANT PROFESSOR
Incidence of DVT Post- Hip or Knee Replacement. A Comparison of Incidence at Boundary Trails Health Centre to a Credible Baseline Incidence
 Incidence of DVT Post- Hip or Knee Replacement A Comparison of Incidence at Boundary Trails Health Centre to a Credible Baseline Incidence Background DVTs Pulmonary Embolisms Death Symptomatic DVTs (leg
Incidence of DVT Post- Hip or Knee Replacement A Comparison of Incidence at Boundary Trails Health Centre to a Credible Baseline Incidence Background DVTs Pulmonary Embolisms Death Symptomatic DVTs (leg
Page: 1 of 13. Post-Surgical Outpatient Use of Limb Compression Devices for Venous Thromboembolism Prophylaxis
 Last Review Status/Date: March 2014 Page: 1 of 13 Compression Devices for Venous Description Patients undergoing major orthopedic surgery are at increased risk for venous thromboembolism (VTE). Patients
Last Review Status/Date: March 2014 Page: 1 of 13 Compression Devices for Venous Description Patients undergoing major orthopedic surgery are at increased risk for venous thromboembolism (VTE). Patients
TITLE: Acetylsalicylic Acid for Venous Thromboembolism Prophylaxis: A Review of Clinical Evidence, Benefits and Harms
 TITLE: Acetylsalicylic Acid for Venous Thromboembolism Prophylaxis: A Review of Clinical Evidence, Benefits and Harms DATE: 23 August 2011 CONTEXT AND POLICY ISSUES: Thromboembolism occurs when a blood
TITLE: Acetylsalicylic Acid for Venous Thromboembolism Prophylaxis: A Review of Clinical Evidence, Benefits and Harms DATE: 23 August 2011 CONTEXT AND POLICY ISSUES: Thromboembolism occurs when a blood
Disclosures. Venous Thromboembolism Prophylaxis: What every orthopaedic surgeon needs to know. Published Guidelines
 Venous Thromboembolism Prophylaxis: What every orthopaedic surgeon needs to know Paul F. Lachiewicz, MD Chapel Hill Orthopedic Surgery & Sports Medicine Consulting Professor Duke Orthopaedic Surgery Disclosures
Venous Thromboembolism Prophylaxis: What every orthopaedic surgeon needs to know Paul F. Lachiewicz, MD Chapel Hill Orthopedic Surgery & Sports Medicine Consulting Professor Duke Orthopaedic Surgery Disclosures
SUBJECT: LIMB PNEUMATIC COMPRESSION EFFECTIVE DATE: 06/27/13 DEVICES FOR VENOUS REVISED DATE: 06/26/14 THROMBOEMBOLISM PROPHYLAXIS
 MEDICAL POLICY SUBJECT: LIMB PNEUMATIC COMPRESSION PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical
MEDICAL POLICY SUBJECT: LIMB PNEUMATIC COMPRESSION PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical
CPT only copyright 2014 American Medical Association. All rights reserved. 12/23/2014 Page 66 of 593
 Measure #23 (NQF 0239): Perioperative Care: Venous Thromboembolism (VTE) Prophylaxis (When Indicated in ALL Patients) National Quality Strategy Domain: Patient Safety 2015 PQRS OPTIONS FOR INDIVIDUAL MEASURES:
Measure #23 (NQF 0239): Perioperative Care: Venous Thromboembolism (VTE) Prophylaxis (When Indicated in ALL Patients) National Quality Strategy Domain: Patient Safety 2015 PQRS OPTIONS FOR INDIVIDUAL MEASURES:
Postsurgical Home Use of Limb Compression Devices for Venous Thromboembolism Prophylaxis
 Clinical Position Statement Postsurgical Home Use of Limb Compression Devices for Venous Thromboembolism Prophylaxis Effective: October 2017 Next Review: September 2018 CLINICAL POSITION STATEMENT Postsurgical
Clinical Position Statement Postsurgical Home Use of Limb Compression Devices for Venous Thromboembolism Prophylaxis Effective: October 2017 Next Review: September 2018 CLINICAL POSITION STATEMENT Postsurgical
Anticoagulation for prevention of venous thromboembolism
 Anticoagulation for prevention of venous thromboembolism Original article by: Michael Tam Note: updated in June 2009 with the eighth edition (from the seventh) evidence-based clinical practice guidelines
Anticoagulation for prevention of venous thromboembolism Original article by: Michael Tam Note: updated in June 2009 with the eighth edition (from the seventh) evidence-based clinical practice guidelines
DENOMINATOR: All surgical patients aged 18 years and older undergoing procedures for which VTE prophylaxis is indicated in all patients
 Measure #23 (NQF 0239): Perioperative Care: Venous Thromboembolism (VTE) Prophylaxis (When Indicated in ALL Patients) National Quality Strategy Domain: Patient Safety 2017 OPTIONS FOR INDIVIDUAL MEASURES:
Measure #23 (NQF 0239): Perioperative Care: Venous Thromboembolism (VTE) Prophylaxis (When Indicated in ALL Patients) National Quality Strategy Domain: Patient Safety 2017 OPTIONS FOR INDIVIDUAL MEASURES:
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Process
 Quality ID #23 (NQF 0239): Perioperative Care: Venous Thromboembolism (VTE) Prophylaxis (When Indicated in ALL Patients) National Quality Strategy Domain: Patient Safety 2018 OPTIONS FOR INDIVIDUAL MEASURES:
Quality ID #23 (NQF 0239): Perioperative Care: Venous Thromboembolism (VTE) Prophylaxis (When Indicated in ALL Patients) National Quality Strategy Domain: Patient Safety 2018 OPTIONS FOR INDIVIDUAL MEASURES:
Are There Clinical Meaning on Asymptomatic Pulmonary Embolism After Total Knee Arthroplasty?
 Are There Clinical Meaning on Asymptomatic Pulmonary Embolism After Total Knee Arthroplasty? * 1,2 ATSUSHI SATO, MD, PhD, * 1,2 Takayuki Koya, * 2,3 Hiroshi Takagi, * 2 Jun Oike,, * 2 Saki Yagura, * 2
Are There Clinical Meaning on Asymptomatic Pulmonary Embolism After Total Knee Arthroplasty? * 1,2 ATSUSHI SATO, MD, PhD, * 1,2 Takayuki Koya, * 2,3 Hiroshi Takagi, * 2 Jun Oike,, * 2 Saki Yagura, * 2
VTE Prevention After Hip or Knee Replacement
 This Clinical Resource gives subscribers additional insight related to the Recommendations published in May 2018 ~ Resource #340506 VTE Prevention After Hip or Knee Replacement The American College of
This Clinical Resource gives subscribers additional insight related to the Recommendations published in May 2018 ~ Resource #340506 VTE Prevention After Hip or Knee Replacement The American College of
Oral Anticoagulation Drug Class Prior Authorization Protocol
 Oral Anticoagulation Drug Class Prior Authorization Protocol Line of Business: Medicaid P & T Approval Date: February 21, 2018 Effective Date: April 1, 2018 This policy has been developed through review
Oral Anticoagulation Drug Class Prior Authorization Protocol Line of Business: Medicaid P & T Approval Date: February 21, 2018 Effective Date: April 1, 2018 This policy has been developed through review
Hip and Knee Replacements
 Hip and Knee Replacements What the PCP Needs to Know Derek Ward, M.D. Assistant Professor of Orthopaedic Surgery Division of Adult Reconstruction University of California, San Francisco 12/2/2017 Disclosures
Hip and Knee Replacements What the PCP Needs to Know Derek Ward, M.D. Assistant Professor of Orthopaedic Surgery Division of Adult Reconstruction University of California, San Francisco 12/2/2017 Disclosures
Page: 1 of 14. Post-Surgical Outpatient Use of Limb Compression Devices for Venous Thromboembolism Prophylaxis
 Subject: Post-Surgical Outpatient Use of Limb Page: 1 of 14 Last Review Status/Date: March 2015 Post-Surgical Outpatient Use of Limb Compression Devices for Venous Description Patients undergoing major
Subject: Post-Surgical Outpatient Use of Limb Page: 1 of 14 Last Review Status/Date: March 2015 Post-Surgical Outpatient Use of Limb Compression Devices for Venous Description Patients undergoing major
Drug Class Monograph
 Drug Class Monograph Class: Oral Anticoagulants Drug: Coumadin (warfarin), Eliquis (apixaban), Pradaxa (dabigatran), Savaysa (edoxaban), arelto (rivaroxaban) Formulary Medications: Eliquis (apixaban),
Drug Class Monograph Class: Oral Anticoagulants Drug: Coumadin (warfarin), Eliquis (apixaban), Pradaxa (dabigatran), Savaysa (edoxaban), arelto (rivaroxaban) Formulary Medications: Eliquis (apixaban),
Venous Thromboembolism. Prevention
 Venous Thromboembolism Prevention August 2010 Venous Thromboembloism Prevention 1 1 Expected Practice Assess all patients upon admission to the ICU for risk factors of venous thromboembolism (VTE) and
Venous Thromboembolism Prevention August 2010 Venous Thromboembloism Prevention 1 1 Expected Practice Assess all patients upon admission to the ICU for risk factors of venous thromboembolism (VTE) and
SUBJECT: LIMB PNEUMATIC COMPRESSION EFFECTIVE DATE: 06/27/13 DEVICES FOR VENOUS REVISED DATE: 06/26/14, 09/15/15,09/21/17. THROMBOEMBOLISM PROPHYLAXIS
 MEDICAL POLICY REVISED DATE: 06/26/14, 09/15/15,09/21/17. PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases,
MEDICAL POLICY REVISED DATE: 06/26/14, 09/15/15,09/21/17. PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases,
Misunderstandings of Venous thromboembolism prophylaxis
 Misunderstandings of Venous thromboembolism prophylaxis Veerendra Chadachan Senior Consultant Dept of General Medicine (Vascular Medicine and Hypertension) Tan Tock Seng Hospital, Singapore Case scenario
Misunderstandings of Venous thromboembolism prophylaxis Veerendra Chadachan Senior Consultant Dept of General Medicine (Vascular Medicine and Hypertension) Tan Tock Seng Hospital, Singapore Case scenario
Incidence and Complications of Open Hip Preservation Surgery: An American Board of Orthopaedic Surgery Database Review
 Incidence and Complications of Open Hip Preservation Surgery: An American Board of Orthopaedic Surgery Database Review Jon P Hedgecock MD, 1 P Christopher Cook MD FRCS(C), 1 John Harrast PhD,2 Judith F
Incidence and Complications of Open Hip Preservation Surgery: An American Board of Orthopaedic Surgery Database Review Jon P Hedgecock MD, 1 P Christopher Cook MD FRCS(C), 1 John Harrast PhD,2 Judith F
Protocol. Postsurgical Outpatient Use of Limb Compression Devices for Venous Thromboembolism Prophylaxis
 Postsurgical Outpatient Use of Limb Compression Devices for (10128) (Formerly Outpatient Use of Limb Pneumatic Compression Devices for ) Medical Benefit Effective Date: 07/01/14 Next Review Date: 03/15
Postsurgical Outpatient Use of Limb Compression Devices for (10128) (Formerly Outpatient Use of Limb Pneumatic Compression Devices for ) Medical Benefit Effective Date: 07/01/14 Next Review Date: 03/15
Adam Goldfarb, M.A., D.C., D.E.S.S. Introduction
 Venous Thromboembolism Prophylaxis following Lower Extremity Orthopedic Surgery: A Review of the Biomedical Research Literature and Evidence-Based Policy in the United States. Adam Goldfarb, M.A., D.C.,
Venous Thromboembolism Prophylaxis following Lower Extremity Orthopedic Surgery: A Review of the Biomedical Research Literature and Evidence-Based Policy in the United States. Adam Goldfarb, M.A., D.C.,
Slide 1. Slide 2. Slide 3. Outline of This Presentation
 Slide 1 Current Approaches to Venous Thromboembolism Prevention in Orthopedic Patients Hujefa Vora, MD Maria Fox, RN June 9, 2017 Slide 2 Slide 3 Outline of This Presentation Pathophysiology of venous
Slide 1 Current Approaches to Venous Thromboembolism Prevention in Orthopedic Patients Hujefa Vora, MD Maria Fox, RN June 9, 2017 Slide 2 Slide 3 Outline of This Presentation Pathophysiology of venous
10/8/2012. Disclosures. Making Sense of AT9: Review of the 2012 ACCP Antithrombotic Guidelines. Goals and Objectives. Outline
 Disclosures Making Sense of AT9: Review of the 2012 ACCP Antithrombotic Guidelines No relevant conflicts of interest related to the topic presented. Cyndy Brocklebank, PharmD, CDE Chronic Disease Management
Disclosures Making Sense of AT9: Review of the 2012 ACCP Antithrombotic Guidelines No relevant conflicts of interest related to the topic presented. Cyndy Brocklebank, PharmD, CDE Chronic Disease Management
PRIMARY TOTAL KNEE & HIP
 Clinical Guideline Version 2.0 Title: PRIMARY TOTAL KNEE & HIP Venous ThromboEmbolic (VTE) Guideline Target Audience: thopedic Surgeons and their Advanced Practice Practitioner partners; Hospitalists,
Clinical Guideline Version 2.0 Title: PRIMARY TOTAL KNEE & HIP Venous ThromboEmbolic (VTE) Guideline Target Audience: thopedic Surgeons and their Advanced Practice Practitioner partners; Hospitalists,
Getting Started Kit VENOUS THROMBOEMBOLISM PREVENTION. Section 2: Evidence-Based Appropriate VTE Prophylaxis
 Reducing Harm Improving Healthcare Protecting Canadians VENOUS THROMBOEMBOLISM PREVENTION Getting Started Kit Section 2: Evidence-Based Appropriate VTE Prophylaxis January 2017 www.patientsafetyinstitute.ca
Reducing Harm Improving Healthcare Protecting Canadians VENOUS THROMBOEMBOLISM PREVENTION Getting Started Kit Section 2: Evidence-Based Appropriate VTE Prophylaxis January 2017 www.patientsafetyinstitute.ca
Disclosures. DVT: Diagnosis and Treatment. Questions To Ask. Dr. Susanna Shin - DVT: Diagnosis and Treatment. Acute Venous Thromboembolism (VTE) None
 Disclosures DVT: Diagnosis and Treatment None Susanna Shin, MD, FACS Assistant Professor University of Washington Acute Venous Thromboembolism (VTE) Deep Venous Thrombosis (DVT) Pulmonary Embolism (PE)
Disclosures DVT: Diagnosis and Treatment None Susanna Shin, MD, FACS Assistant Professor University of Washington Acute Venous Thromboembolism (VTE) Deep Venous Thrombosis (DVT) Pulmonary Embolism (PE)
Comparison of high-flex and conventional implants for bilateral total knee arthroplasty
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 14 Number 1 Comparison of high-flex and conventional implants for bilateral total knee arthroplasty C Martin-Hernandez, M Guillen-Soriano, A
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 14 Number 1 Comparison of high-flex and conventional implants for bilateral total knee arthroplasty C Martin-Hernandez, M Guillen-Soriano, A
Objectives. Venous Thromboembolism (VTE) Prophylaxis. Case VTE WHY DO IT? Question: Who Is At Risk?
 Objectives Venous Thromboembolism (VTE) Prophylaxis Rishi Garg, MD Department of Medicine Identify patients at risk for VTE Options for VTE prophylaxis Current Recommendations (based on The Seventh ACCP
Objectives Venous Thromboembolism (VTE) Prophylaxis Rishi Garg, MD Department of Medicine Identify patients at risk for VTE Options for VTE prophylaxis Current Recommendations (based on The Seventh ACCP
2/22/2018. Goals. What are We Concerned About?
 DVT Prophylaxis - Concerns in Foot and Ankle Pathology CSFA Tampa, Feb. 2018 STEVEN STEINLAUF, MD THE ORTHOPAEDIC FOOT AND ANKLE INSTITUTE OF SOUTH FLORIDA CLINICAL ASSISTANT PROFESSOR THE UNIVERSITY OF
DVT Prophylaxis - Concerns in Foot and Ankle Pathology CSFA Tampa, Feb. 2018 STEVEN STEINLAUF, MD THE ORTHOPAEDIC FOOT AND ANKLE INSTITUTE OF SOUTH FLORIDA CLINICAL ASSISTANT PROFESSOR THE UNIVERSITY OF
MEDICAL POLICY SUBJECT: LIMB PNEUMATIC COMPRESSION DEVICES FOR VENOUS THROMBOEMBOLISM PROPHYLAXIS
 MEDICAL POLICY SUBJECT: LIMB PNEUMATIC COMPRESSION REVISED DATE: 06/26/14, 10/15/15, 06/16/16, PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria
MEDICAL POLICY SUBJECT: LIMB PNEUMATIC COMPRESSION REVISED DATE: 06/26/14, 10/15/15, 06/16/16, PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria
VTE Management in Surgical Patients: Optimizing Prophylaxis Strategies
 VTE Management in Surgical Patients: Optimizing Prophylaxis Strategies VTE in Surgical Patients: Recognizing the Patients at Risk Pathogenesis of thrombosis: Virchow s triad and VTE Risk Hypercoagulability
VTE Management in Surgical Patients: Optimizing Prophylaxis Strategies VTE in Surgical Patients: Recognizing the Patients at Risk Pathogenesis of thrombosis: Virchow s triad and VTE Risk Hypercoagulability
Fatal P.E. Historic 1-2% Current %
 Dr. (Prof.) Anil Arora MS (Ortho) DNB (Ortho) Dip SIROT (USA) FAPOA (Korea), FIGOF (Germany), FJOA (Japan) Commonwealth Fellow Joint Replacement (Royal National Orthopaedic Hospital, London, UK) Senior
Dr. (Prof.) Anil Arora MS (Ortho) DNB (Ortho) Dip SIROT (USA) FAPOA (Korea), FIGOF (Germany), FJOA (Japan) Commonwealth Fellow Joint Replacement (Royal National Orthopaedic Hospital, London, UK) Senior
Primary VTE Prophylaxis. Ponlapat Rojnuckarin, MD PhD Chulalongkorn University Bangkok, Thailand
 Primary VTE Prophylaxis Ponlapat Rojnuckarin, MD PhD Chulalongkorn University Bangkok, Thailand A 70-yr-old female before THA BMI 31 kg/m 2 with varicose vein What do you recommend for VTE prevention?
Primary VTE Prophylaxis Ponlapat Rojnuckarin, MD PhD Chulalongkorn University Bangkok, Thailand A 70-yr-old female before THA BMI 31 kg/m 2 with varicose vein What do you recommend for VTE prevention?
Deep Vein Thrombosis Prevention in Total Knee Arthroplasty. A Review -
 International Journal of Orthopedics: Research & Therapy Review Article Deep Vein Thrombosis Prevention in Total Knee Arthroplasty. A Review - Julio Cesar Gali* Faculty of Medical Science and Health Catholic
International Journal of Orthopedics: Research & Therapy Review Article Deep Vein Thrombosis Prevention in Total Knee Arthroplasty. A Review - Julio Cesar Gali* Faculty of Medical Science and Health Catholic
Prophylaxis for Venous Thromboembolism Following Total Knee Arthroplasty: A Survey of Korean Knee Surgeons
 Original Article Knee Surg Relat Res 2016;28(3):207-212 http://dx.doi.org/10.5792/ksrr.2016.28.3.207 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Prophylaxis for Venous Thromboembolism
Original Article Knee Surg Relat Res 2016;28(3):207-212 http://dx.doi.org/10.5792/ksrr.2016.28.3.207 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Prophylaxis for Venous Thromboembolism
AN AUDIT: THROMBOPROPHYLAXIS FOR TOTAL HIP REPLACEMENT PATIENTS AT NORTHWICK PARK AND CENTRAL MIDDLESEX HOSPITALS
 The West London Medical Journal 2010 Vol 2 No 4 pp 19-24 AN AUDIT: THROMBOPROPHYLAXIS FOR TOTAL HIP REPLACEMENT PATIENTS AT NORTHWICK PARK AND CENTRAL MIDDLESEX HOSPITALS Soneji ND Agni NR Acharya MN Anjari
The West London Medical Journal 2010 Vol 2 No 4 pp 19-24 AN AUDIT: THROMBOPROPHYLAXIS FOR TOTAL HIP REPLACEMENT PATIENTS AT NORTHWICK PARK AND CENTRAL MIDDLESEX HOSPITALS Soneji ND Agni NR Acharya MN Anjari
Primary VTE Thromboprophylaxis
 Primary VTE Thromboprophylaxis Controversies in Hematology 53 rd Annual Meeting of Thai Society of Hematology Bundarika Suwanawiboon, MD Division of Hematology Department of Medicine Faculty of Medicine
Primary VTE Thromboprophylaxis Controversies in Hematology 53 rd Annual Meeting of Thai Society of Hematology Bundarika Suwanawiboon, MD Division of Hematology Department of Medicine Faculty of Medicine
Venous thromboembolism after total knee replacement or total hip replacement: what can be learnt from root-cause analysis?
 TRAUMA AND ORTHOPAEDIC SURGERY Ann R Coll Surg Engl 2016; 98: 538 542 doi 10.1308/rcsann.2016.0202 Venous thromboembolism after total knee replacement or total hip replacement: what can be learnt from
TRAUMA AND ORTHOPAEDIC SURGERY Ann R Coll Surg Engl 2016; 98: 538 542 doi 10.1308/rcsann.2016.0202 Venous thromboembolism after total knee replacement or total hip replacement: what can be learnt from
DVT PROPHYLAXIS IN HOSPITALIZED MEDICAL PATIENTS SAURABH MAJI SR (PULMONARY,MEDICINE)
 DVT PROPHYLAXIS IN HOSPITALIZED MEDICAL PATIENTS SAURABH MAJI SR (PULMONARY,MEDICINE) Introduction VTE (DVT/PE) is an important complication in hospitalized patients Hospitalization for acute medical illness
DVT PROPHYLAXIS IN HOSPITALIZED MEDICAL PATIENTS SAURABH MAJI SR (PULMONARY,MEDICINE) Introduction VTE (DVT/PE) is an important complication in hospitalized patients Hospitalization for acute medical illness
Post-Surgical Outpatient Use of Limb Compression Devices for Venous Thromboembolism Prophylaxis
 Post-Surgical Outpatient Use of Limb Compression Devices for Venous Thromboembolism Prophylaxis Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary,
Post-Surgical Outpatient Use of Limb Compression Devices for Venous Thromboembolism Prophylaxis Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary,
THROMBOPROPHYLAXIS: NON-ORTHOPEDIC SURGERY
 THROMBOPROPHYLAXIS: NON-ORTHOPEDIC SURGERY OBJECTIVE: To outline a practical approach for the prevention of venous thromboembolism (VTE) in patients undergoing non-orthopedic surgery. BACKGROUND: VTE is
THROMBOPROPHYLAXIS: NON-ORTHOPEDIC SURGERY OBJECTIVE: To outline a practical approach for the prevention of venous thromboembolism (VTE) in patients undergoing non-orthopedic surgery. BACKGROUND: VTE is
Distal Femoral Osteotomy to Treat Patellar Instability with Valgus Lower Extremity Alignment in Adolescents
 Distal Femoral Osteotomy to Treat Patellar Instability with Valgus Lower Extremity Alignment in Adolescents Sheena R. Black, MD, Henry B. Ellis, MD, Philip L. Wilson, MD, David A. Podeszwa, MD LLRS Annual
Distal Femoral Osteotomy to Treat Patellar Instability with Valgus Lower Extremity Alignment in Adolescents Sheena R. Black, MD, Henry B. Ellis, MD, Philip L. Wilson, MD, David A. Podeszwa, MD LLRS Annual
Venous Thromboembolism Prophylaxis - Why Should We Care? Harry Gibbs FRACP FCSANZ Vascular Physician The Alfred Hospital
 Venous Thromboembolism Prophylaxis - Why Should We Care? Harry Gibbs FRACP FCSANZ Vascular Physician The Alfred Hospital VTE is common and dangerous 5 VTE is Common VTE Incidence: 1.5 / 1000 per year
Venous Thromboembolism Prophylaxis - Why Should We Care? Harry Gibbs FRACP FCSANZ Vascular Physician The Alfred Hospital VTE is common and dangerous 5 VTE is Common VTE Incidence: 1.5 / 1000 per year
ACL Athletic Career. ACL Rupture - Warning Features Intensive pain Immediate swelling Locking Feel a Pop Dead leg Cannot continue to play
 FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
These are guidelines only and can be deviated from if it is thought to be in the patient s best interest.
 Clinical Guideline Venothromboembolism prophylaxis: Trauma and Orthopaedics Venous thromboembolism (VTE) is a recognised complication associated with inactivity and surgical procedures. Therefore, all
Clinical Guideline Venothromboembolism prophylaxis: Trauma and Orthopaedics Venous thromboembolism (VTE) is a recognised complication associated with inactivity and surgical procedures. Therefore, all
Venous Thromboembolism Prophylaxis After Major Orthopaedic Surgery: A Pooled Analysis of Randomized Controlled Trials
 Winner of the AAHKS Award Venous Thromboembolism Prophylaxis After Major Orthopaedic Surgery: A Pooled Analysis of Randomized Controlled Trials Greg A. Brown, MD, PhD The Journal of Arthroplasty Vol. 24
Winner of the AAHKS Award Venous Thromboembolism Prophylaxis After Major Orthopaedic Surgery: A Pooled Analysis of Randomized Controlled Trials Greg A. Brown, MD, PhD The Journal of Arthroplasty Vol. 24
Prevalence of Symptomatic Venous Thrombo-Embolism in Patients with Total Contact Cast for Diabetic foot Complications A Retrospective Case Series.
 Prevalence of Symptomatic Venous Thrombo-Embolism in Patients with Total Contact Cast for Diabetic foot Complications A Retrospective Case Series. Dr R King, Miss GE Jackson, Mr SR Platt Wirral University
Prevalence of Symptomatic Venous Thrombo-Embolism in Patients with Total Contact Cast for Diabetic foot Complications A Retrospective Case Series. Dr R King, Miss GE Jackson, Mr SR Platt Wirral University
Index. orthopedic.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acetabular fractures thromboembolic disease after, 341 Achilles tendon rupture ACL. See Anterior cruciate ligament (ACL) Adolescent idiopathic
Index Note: Page numbers of article titles are in boldface type. A Acetabular fractures thromboembolic disease after, 341 Achilles tendon rupture ACL. See Anterior cruciate ligament (ACL) Adolescent idiopathic
Venous Thromboembolism Prophylaxis: Checked!
 Venous Thromboembolism Prophylaxis: Checked! William Geerts, MD, FRCPC Director, Thromboembolism Program, Sunnybrook HSC Professor of Medicine, University of Toronto National Lead, VTE Prevention, Safer
Venous Thromboembolism Prophylaxis: Checked! William Geerts, MD, FRCPC Director, Thromboembolism Program, Sunnybrook HSC Professor of Medicine, University of Toronto National Lead, VTE Prevention, Safer
What evidence exists that describes the efficacy of mechanical prophylaxis for venous thromboembolism (VTE) in adult surgical patients?
 July 2015 Rapid Review Evidence Summary McGill University Health Centre: Division of Nursing Research and MUHC Libraries What evidence exists that describes the efficacy of mechanical prophylaxis for venous
July 2015 Rapid Review Evidence Summary McGill University Health Centre: Division of Nursing Research and MUHC Libraries What evidence exists that describes the efficacy of mechanical prophylaxis for venous
Functional Outcome of Uni-Knee Arthroplasty in Asians with six-year Follow-up
 Functional Outcome of Uni-Knee Arthroplasty in Asians with six-year Follow-up Ching-Jen Wang, M.D. Department of Orthopedic Surgery Kaohsiung Chang Gung Memorial Hospital Chang Gung University College
Functional Outcome of Uni-Knee Arthroplasty in Asians with six-year Follow-up Ching-Jen Wang, M.D. Department of Orthopedic Surgery Kaohsiung Chang Gung Memorial Hospital Chang Gung University College
DEEP VEIN THROMBOSIS (DVT): TREATMENT
 DEEP VEIN THROMBOSIS (DVT): TREATMENT OBJECTIVE: To provide an evidence-based approach to treatment of patients presenting with deep vein thrombosis (DVT). BACKGROUND: An estimated 45,000 patients in Canada
DEEP VEIN THROMBOSIS (DVT): TREATMENT OBJECTIVE: To provide an evidence-based approach to treatment of patients presenting with deep vein thrombosis (DVT). BACKGROUND: An estimated 45,000 patients in Canada
Life. Uncompromised. The KineSpring Knee Implant System Surgeon Handout
 Life Uncompromised The KineSpring Knee Implant System Surgeon Handout 2 Patient Selection Criteria Patient Selection Criteria Medial compartment degeneration must be confirmed radiographically or arthroscopically
Life Uncompromised The KineSpring Knee Implant System Surgeon Handout 2 Patient Selection Criteria Patient Selection Criteria Medial compartment degeneration must be confirmed radiographically or arthroscopically
Results from RE-COVER RE-COVER II RE-MEDY RE-SONATE EXECUTIVE SUMMARY
 Assessment of the safety and efficacy of dabigatran etexilate (Pradaxa ) in the treatment of deep vein thrombosis (DVT) and pulmonary embolism (PE) and the prevention of recurrent DVT and PE Results from
Assessment of the safety and efficacy of dabigatran etexilate (Pradaxa ) in the treatment of deep vein thrombosis (DVT) and pulmonary embolism (PE) and the prevention of recurrent DVT and PE Results from
Venothromboembolism prophylaxis: Trauma and Orthopaedics Clinical guideline, V2
 Clinical Guideline Venothromboembolism prophylaxis: Trauma and Orthopaedics 11/11/11 TEMPORARY GUIDANCE There is no prophylactic tinzaparin available in the Trust currently. Please substitute enoxaparin
Clinical Guideline Venothromboembolism prophylaxis: Trauma and Orthopaedics 11/11/11 TEMPORARY GUIDANCE There is no prophylactic tinzaparin available in the Trust currently. Please substitute enoxaparin
Osteoarthrosis, unspecified whether generalized or localized, lower leg. Osteoarthrosis, localized, not specified whether primary or secondary, pelvic
 Page 1 Appendix TABLE E-1 Codes (and Definitions) in Humana Database Used for Study Inclusion and Exclusion of Patients Who Underwent,, or 1 to 2-Level Inclusion ICD-9-P-8154 Total knee replacement ICD-9-D-71596
Page 1 Appendix TABLE E-1 Codes (and Definitions) in Humana Database Used for Study Inclusion and Exclusion of Patients Who Underwent,, or 1 to 2-Level Inclusion ICD-9-P-8154 Total knee replacement ICD-9-D-71596
Research Article. Abstract
 Research Article Trends in Deep Vein Thrombosis Prophylaxis and Deep Vein Thrombosis Rates After Total Hip and Knee Arthroplasty Harpreet Bawa, MD Jack W. Weick, MD Douglas R. Dirschl, MD Hue H. Luu, MD
Research Article Trends in Deep Vein Thrombosis Prophylaxis and Deep Vein Thrombosis Rates After Total Hip and Knee Arthroplasty Harpreet Bawa, MD Jack W. Weick, MD Douglas R. Dirschl, MD Hue H. Luu, MD
Epidemiology of Venous Thromboembolism in the East. Heng Joo NG Department of Haematology Singapore General Hospital Singapore
 Epidemiology of Venous Thromboembolism in the East Heng Joo NG Department of Haematology Singapore General Hospital Singapore Early Literature Tinckler LF Br Med J 1964;1:502 Propagating a notion.. Hwang
Epidemiology of Venous Thromboembolism in the East Heng Joo NG Department of Haematology Singapore General Hospital Singapore Early Literature Tinckler LF Br Med J 1964;1:502 Propagating a notion.. Hwang
Results of arthroscopic surgery, with or without high Tibial osteotomy, in osteoarthritis of knee
 2018; 2(3): 100-105 ISSN (P): 2521-3466 ISSN (E): 2521-3474 Clinical Orthopaedics www.orthoresearchjournal.com 2018; 2(3): 100-105 Received: 17-05-2018 Accepted: 18-06-2018 Dr. Tarkik Amin Assistant Professor,
2018; 2(3): 100-105 ISSN (P): 2521-3466 ISSN (E): 2521-3474 Clinical Orthopaedics www.orthoresearchjournal.com 2018; 2(3): 100-105 Received: 17-05-2018 Accepted: 18-06-2018 Dr. Tarkik Amin Assistant Professor,
27/01/12. Revising the stiff TKA. Warm up: Case NV. Literature. Definition. Definition. Flexion requirements for ADL
 Revising the stiff TKA Warm up: Case NV Literature Definition o Bong MR, Di Cesare PE: Stiffness after total knee arthroplasty. J Am Acad Orthop Surg 2004;12:164-171 o Scranton PE: Management of knee pain
Revising the stiff TKA Warm up: Case NV Literature Definition o Bong MR, Di Cesare PE: Stiffness after total knee arthroplasty. J Am Acad Orthop Surg 2004;12:164-171 o Scranton PE: Management of knee pain
National Quality Improvement Project 2018/2019 VTE Risk in Lower Limb Immobilisation Information Pack
 National Quality Improvement Project 2018/2019 VTE Risk in Lower Limb Immobilisation Information Pack Introduction... 2 Methodology... 3 Flow of data searches to identify audit cases... 3 Data entry information...
National Quality Improvement Project 2018/2019 VTE Risk in Lower Limb Immobilisation Information Pack Introduction... 2 Methodology... 3 Flow of data searches to identify audit cases... 3 Data entry information...
Clinical Practice Guideline for Patients Requiring Total Hip Replacement
 Clinical Practice Guideline for Patients Requiring Total Hip Replacement Inclusions Patients undergoing elective total hip replacement Exclusions Patients with active local or systemic infection or medical
Clinical Practice Guideline for Patients Requiring Total Hip Replacement Inclusions Patients undergoing elective total hip replacement Exclusions Patients with active local or systemic infection or medical
Ideal Candidate for Cartilage Restoration. Large or Complex Lesions
 Complex Biological Knee Reconstruction: Bipolar, Multifocal Lesions and Osteoarthritis William Bugbee, MD Attending Physician, Scripps Clinic 18 th International Sports Medicine Fellow s Conference Ideal
Complex Biological Knee Reconstruction: Bipolar, Multifocal Lesions and Osteoarthritis William Bugbee, MD Attending Physician, Scripps Clinic 18 th International Sports Medicine Fellow s Conference Ideal
Disclosures. Why Osteotomy? Osteotomies of the Knee Indications, Techniques and Outcomes
 Osteotomies of the Knee Indications, Techniques and Outcomes Tom Minas MD MS Director, Cartilage Repair Center BWH Associate Professor HMS, Boston Ma www.cartilagerepaircenter.org Disclosures Vericel (
Osteotomies of the Knee Indications, Techniques and Outcomes Tom Minas MD MS Director, Cartilage Repair Center BWH Associate Professor HMS, Boston Ma www.cartilagerepaircenter.org Disclosures Vericel (
21/01/10. Disclosures. Results of High Tibial Osteotomy Osteotomy: Review of the Literature. Introduction. OW osteotomy and bone graft
 3rd Annual Advanced Course on Knee Surgery January 17-22, 2010, Val D Isere, Results of High Tibial Osteotomy Osteotomy: Review of the Literature Disclosures Conflict of interest related to this presentation:
3rd Annual Advanced Course on Knee Surgery January 17-22, 2010, Val D Isere, Results of High Tibial Osteotomy Osteotomy: Review of the Literature Disclosures Conflict of interest related to this presentation:
High Tibial Osteotomy
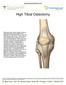 High Tibial Osteotomy With each step, forces equal to three to eight times your body weight travel between the thigh bone (femur) and shin bone (tibia) in your knee. These forces are dampened by a meniscus
High Tibial Osteotomy With each step, forces equal to three to eight times your body weight travel between the thigh bone (femur) and shin bone (tibia) in your knee. These forces are dampened by a meniscus
Survivorship After Meniscal Allograft Transplantation According To Articular Cartilage Status
 # 154134 Survivorship After Meniscal Allograft Transplantation According To Articular Cartilage Status Jun-Gu Park, Seong-Il Bin, Jong-Min Kim, Bum Sik Lee Department of Orthopaedic Surgery, Asan Medical
# 154134 Survivorship After Meniscal Allograft Transplantation According To Articular Cartilage Status Jun-Gu Park, Seong-Il Bin, Jong-Min Kim, Bum Sik Lee Department of Orthopaedic Surgery, Asan Medical
Prevention and management of deep venous thrombosis (DVT) John Fletcher Wound Care Association of New South Wales
 Prevention and management of deep venous thrombosis (DVT) John Fletcher Wound Care Association of New South Wales Merimbula, 6 th November 2010 University of Sydney Department of Surgery Westmead Hospital
Prevention and management of deep venous thrombosis (DVT) John Fletcher Wound Care Association of New South Wales Merimbula, 6 th November 2010 University of Sydney Department of Surgery Westmead Hospital
PREVENTION AND TREATMENT OF VENOUS THROMBOEMBOLISM
 PREVENTION AND TREATMENT OF VENOUS THROMBOEMBOLISM International Consensus Statement 2013 Guidelines According to Scientific Evidence Developed under the auspices of the: Cardiovascular Disease Educational
PREVENTION AND TREATMENT OF VENOUS THROMBOEMBOLISM International Consensus Statement 2013 Guidelines According to Scientific Evidence Developed under the auspices of the: Cardiovascular Disease Educational
General. Recommendations. Guideline Title. Bibliographic Source(s) Guideline Status. Major Recommendations
 General Guideline Title Prevention of deep vein thrombosis and pulmonary embolism. Bibliographic Source(s) American College of Obstetricians and Gynecologists (ACOG). Prevention of deep vein thrombosis
General Guideline Title Prevention of deep vein thrombosis and pulmonary embolism. Bibliographic Source(s) American College of Obstetricians and Gynecologists (ACOG). Prevention of deep vein thrombosis
Proximal fibular osteotomy: a new surgery for pain relief and improvement of joint function in patients with knee osteoarthritis
 Clinical Report Proximal fibular osteotomy: a new surgery for pain relief and improvement of joint function in patients with knee osteoarthritis Journal of International Medical Research 2017, Vol. 45(1)
Clinical Report Proximal fibular osteotomy: a new surgery for pain relief and improvement of joint function in patients with knee osteoarthritis Journal of International Medical Research 2017, Vol. 45(1)
Measure #23 (NQF 0239): Perioperative Care: Venous Thromboembolism (VTE) Prophylaxis (When Indicated in ALL Patients)
 Measure #23 (NQF 0239): Perioperative Care: Venous Thromboembolism (VTE) Prophylaxis (When Indicated in ALL Patients) 2013 PQRS OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS, REGISTRY DESCRIPTION: Percentage
Measure #23 (NQF 0239): Perioperative Care: Venous Thromboembolism (VTE) Prophylaxis (When Indicated in ALL Patients) 2013 PQRS OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS, REGISTRY DESCRIPTION: Percentage
Abstract Introduction Currently there are no consensuses in the national guidance on
 THIEME Review Article e191 A Systematic Review on the Use of Aspirin in the Prevention of Deep Vein Thrombosis in Major Elective Lower Limb Orthopedic Surgery: An Update from the Past 3 Years Dylan A.
THIEME Review Article e191 A Systematic Review on the Use of Aspirin in the Prevention of Deep Vein Thrombosis in Major Elective Lower Limb Orthopedic Surgery: An Update from the Past 3 Years Dylan A.
Symptomatic Venous Thromboembolism after Shoulder Arthroscopy
 Symptomatic Venous Thromboembolism after Shoulder Arthroscopy Diane Thi Tran, MD Sports Medicine Fellow, TRIA Orthopaedic Center Jonathan P. Braman, MD Associate Professor, Department of Orthopaedic Surgery,
Symptomatic Venous Thromboembolism after Shoulder Arthroscopy Diane Thi Tran, MD Sports Medicine Fellow, TRIA Orthopaedic Center Jonathan P. Braman, MD Associate Professor, Department of Orthopaedic Surgery,
Incidence of Symptomatic Pulmonary Embolism in Spinal Surgery
 Incidence of Symptomatic Pulmonary Embolism in Spinal Surgery Chatupon Chotigavanichaya MD*, Monchai Ruangchainikom MD*, Choompon Piyavanno MD*, Ekkapoj Korwutthikulrangsri MD*, Sirichai Wilartratsami
Incidence of Symptomatic Pulmonary Embolism in Spinal Surgery Chatupon Chotigavanichaya MD*, Monchai Ruangchainikom MD*, Choompon Piyavanno MD*, Ekkapoj Korwutthikulrangsri MD*, Sirichai Wilartratsami
Medical Patients: A Population at Risk
 Case Vignette A 68-year-old woman with obesity was admitted to the Medical Service with COPD and pneumonia and was treated with oral corticosteroids, bronchodilators, and antibiotics. She responded well
Case Vignette A 68-year-old woman with obesity was admitted to the Medical Service with COPD and pneumonia and was treated with oral corticosteroids, bronchodilators, and antibiotics. She responded well
Deep venous thrombosis (DVT) occurs frequently
 Ann Vasc Dis Vol.5, No.3; 2012; pp 328 333 2012 Annals of Vascular Diseases doi: 10.3400/avd.oa.12.00049 Original Article Deep Vein Thrombosis in Orthopedic Surgery of the Lower Extremities Masatoshi Motohashi,
Ann Vasc Dis Vol.5, No.3; 2012; pp 328 333 2012 Annals of Vascular Diseases doi: 10.3400/avd.oa.12.00049 Original Article Deep Vein Thrombosis in Orthopedic Surgery of the Lower Extremities Masatoshi Motohashi,
Venous Thromboembolism Prophylaxis
 Approved by: Venous Thromboembolism Prophylaxis Vice President and Chief Medical Officer; and Vice President and Chief Operating Officer Corporate Policy & Procedures Manual Number: Date Approved January
Approved by: Venous Thromboembolism Prophylaxis Vice President and Chief Medical Officer; and Vice President and Chief Operating Officer Corporate Policy & Procedures Manual Number: Date Approved January
Anesthesia for Total Hip and Knee Arthroplasty
 Anesthesia for Total Hip and Knee Arthroplasty Typical approach Describe anesthesia technique Rather Describe issues with THA and TKA How anesthesia can modify Issues Total Hip Total Knee Blood Loss ++
Anesthesia for Total Hip and Knee Arthroplasty Typical approach Describe anesthesia technique Rather Describe issues with THA and TKA How anesthesia can modify Issues Total Hip Total Knee Blood Loss ++
AJO. An Original Study. Ashley Levack, MAS, Atul F. Kamath, MD, and Jess H. Lonner, MD
 An Original Study Ashley Levack, MAS, Atul F. Kamath, MD, and Jess H. Lonner, MD dvances in surgical technique, patient selection, and prosthetic design for patellofemoral arthroplasty (PFA) have generated
An Original Study Ashley Levack, MAS, Atul F. Kamath, MD, and Jess H. Lonner, MD dvances in surgical technique, patient selection, and prosthetic design for patellofemoral arthroplasty (PFA) have generated
Clinical Policy: Dalteparin (Fragmin) Reference Number: ERX.SPA.207 Effective Date:
 Clinical Policy: (Fragmin) Reference Number: ERX.SPA.207 Effective Date: 01.11.17 Last Review Date: 02.18 Revision Log See Important Reminder at the end of this policy for important regulatory and legal
Clinical Policy: (Fragmin) Reference Number: ERX.SPA.207 Effective Date: 01.11.17 Last Review Date: 02.18 Revision Log See Important Reminder at the end of this policy for important regulatory and legal
PRELIMINARY PROGRAM. AOSSM & ISAKOS Surgical Skills Course
 SURGICAL SKILLS AOSSM & ISAKOS Surgical Skills Course Osteotomies Around the Knee: From Ligament Insufficiency to Cartilage/Meniscus Pathologies and Arthritis April 12 13, 2019 OLC Education and Conference
SURGICAL SKILLS AOSSM & ISAKOS Surgical Skills Course Osteotomies Around the Knee: From Ligament Insufficiency to Cartilage/Meniscus Pathologies and Arthritis April 12 13, 2019 OLC Education and Conference
Nurse Initiated Sequential Compression Device Application Program for Total Knee Replacement Patient
 Nurse Initiated Sequential Compression Device Application Program for Total Knee Replacement Patient Cheung Shuk Shan, Susana (APN,O&T, PYNEH) 15 May, 2013 Total Knee Replacement (TKR) TKR is a common
Nurse Initiated Sequential Compression Device Application Program for Total Knee Replacement Patient Cheung Shuk Shan, Susana (APN,O&T, PYNEH) 15 May, 2013 Total Knee Replacement (TKR) TKR is a common
Prevention of VTE in Orthopedic Surgery Patients
 CHEST Supplement ANTITHROMBOTIC THERAPY AND PREVENTION OF THROMBOSIS, 9TH ED: ACCP GUIDELINES Prevention of VTE in Orthopedic Surgery Patients Antithrombotic Therapy and Prevention of Thrombosis, 9th ed:
CHEST Supplement ANTITHROMBOTIC THERAPY AND PREVENTION OF THROMBOSIS, 9TH ED: ACCP GUIDELINES Prevention of VTE in Orthopedic Surgery Patients Antithrombotic Therapy and Prevention of Thrombosis, 9th ed:
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/01/2012 Radiology Quiz of the Week # 101 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/01/2012 Radiology Quiz of the Week # 101 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Aspirin provides adequate VTE prophylaxis for patients undergoing hip preservation surgery, including periacetabular osteotomy
 Journal of Hip Preservation Surgery Vol. 5, No. 2, pp. 125 130 doi: 10.1093/jhps/hny010 Advance Access Publication 5 April 2018 Research article Aspirin provides adequate VTE prophylaxis for patients undergoing
Journal of Hip Preservation Surgery Vol. 5, No. 2, pp. 125 130 doi: 10.1093/jhps/hny010 Advance Access Publication 5 April 2018 Research article Aspirin provides adequate VTE prophylaxis for patients undergoing
Perioperative VTE Prophylaxis
 Perioperative VTE Prophylaxis Gregory J. Misky, M.D. Assistant Professor of Medicine University Of Colorado Denver You recommend the following 72 y.o. man admitted for an elective R hip repair. Patient
Perioperative VTE Prophylaxis Gregory J. Misky, M.D. Assistant Professor of Medicine University Of Colorado Denver You recommend the following 72 y.o. man admitted for an elective R hip repair. Patient
NOTE: The first appearance of terms in bold in the body of this document (except titles) are defined terms please refer to the Definitions section.
 TITLE VENOUS THROMBOEMBOLISM PROPHYLAXIS SCOPE Provincial Acute and Sub-Acute Care Facilities APPROVAL AUTHORITY Alberta Health Services Executive Committee SPONSOR Vice President, Quality and Chief Medical
TITLE VENOUS THROMBOEMBOLISM PROPHYLAXIS SCOPE Provincial Acute and Sub-Acute Care Facilities APPROVAL AUTHORITY Alberta Health Services Executive Committee SPONSOR Vice President, Quality and Chief Medical
Osteotomy of the Knee
 Osteotomy of the Knee Osteotomy literally means "cutting of the bone." In a knee osteotomy, either the tibia (shinbone) or femur (thighbone) is cut and then reshaped to relieve pressure on the knee joint.
Osteotomy of the Knee Osteotomy literally means "cutting of the bone." In a knee osteotomy, either the tibia (shinbone) or femur (thighbone) is cut and then reshaped to relieve pressure on the knee joint.
Knee Surg Relat Res 2016;28(3): pissn eissn Knee Surgery & Related Research
 Original Article Knee Surg Relat Res 2016;28(3):213-218 http://dx.doi.org/10.5792/ksrr.2016.28.3.213 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Incidences of Deep Vein Thrombosis and
Original Article Knee Surg Relat Res 2016;28(3):213-218 http://dx.doi.org/10.5792/ksrr.2016.28.3.213 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Incidences of Deep Vein Thrombosis and
Case Study: Christopher
 Case Study: Christopher Conditions Treated Anterior Knee Pain, Severe Crouch Gait, & Hip Flexion Contracture Age Range During Treatment 23 Years to 24 Years David S. Feldman, MD Chief of Pediatric Orthopedic
Case Study: Christopher Conditions Treated Anterior Knee Pain, Severe Crouch Gait, & Hip Flexion Contracture Age Range During Treatment 23 Years to 24 Years David S. Feldman, MD Chief of Pediatric Orthopedic
