Aspirin provides adequate VTE prophylaxis for patients undergoing hip preservation surgery, including periacetabular osteotomy
|
|
|
- Francine French
- 5 years ago
- Views:
Transcription
1 Journal of Hip Preservation Surgery Vol. 5, No. 2, pp doi: /jhps/hny010 Advance Access Publication 5 April 2018 Research article Aspirin provides adequate VTE prophylaxis for patients undergoing hip preservation surgery, including periacetabular osteotomy Ibrahim Azboy 1,2 *, Michael M. Kheir 1, Ronald Huang 1 and Javad Parvizi 1 1 Rothman Institute at Thomas, Jefferson University Hospital, Sheridan Building, Suite South 9th Street, Philadelphia, PA 19107, USA and 2 Department of Orthopaedics and Traumatology, Istanbul Medipol University, Kavacık Mah. Ekinciler Cad. No.19 Kavacık Kavşag - Beykoz 34810, Turkey, _Istanbul *Correspondence to: I. Azboy. ibrahimazboy@gmail.com Submitted 5 July 2017; revised version accepted 16 March 2018 ABSTRACT There are no clear guidelines regarding optimal venous thromboembolism (VTE) prophylaxis for patients undergoing hip preservation surgery (HPS), in particular pelvic osteotomy, which is considered to be a major orthopaedic procedure. The aim of this study was to determine the efficacy of aspirin for VTE prophylaxis in a large cohort of patients undergoing femoroacetabular osteoplasty (FAO) and periacetabular osteotomy (PAO). This was a retrospective study of prospectively collected data on patients undergoing HPS. A total of 603 patients (643 cases) underwent FAO and 80 patients (87 cases) underwent PAO between 2003 and The mean age of patients was 34.3 years (range years). The type of VTE prophylaxis administered changed over time with earlier patients receiving warfarin (44 cases), followed by aspirin at 325 mg twice daily (448 cases), and most recently aspirin 81 mg twice daily (238 cases). The complications of symptomatic pulmonary embolism (PE), deep venous thrombosis (DVT) and major bleeding events within 90 days of surgery were documented. There were zero patients that developed major bleeding events or required evacuation of a hematoma. One patient who underwent FAO and received aspirin 325 mg, developed post-operative symptomatic DVT. One patient who underwent PAO and received aspirin 325 mg developed DVT and PE. This study demonstrates that the incidence of VTE following joint preservation procedure is acceptably low. Administration of aspirin to patients undergoing FAO or PAO appears to be adequate in reducing the risk of VTE. Only two patients in this cohort developed VTE following HPS. INTRODUCTION Venous thromboembolism (VTE) is considered a serious complication after any surgical procedures including hip preservation surgery (HPS) [1 6]. The optimal VTE prophylaxis regimen after HPS, including femoroacetabular osteoplasty (FAO) and periacetabular osteotomy (PAO), remains unclear [2 5]. VTE prophylaxis recommendations are mainly derived from total joint arthroplasty (TJA) literature [6, 7]. These recommendations have evolved in recent years. The American College of Chest Physicians (ACCP) and the American Academy of Orthopaedic Surgeons (AAOS) accept aspirin (ASA) as an effective modality for VTE prophylaxis following TJA [1, 8]. Patients undergoing HPS surgery are relatively young, healthy and active, which places them at a lower risk for morbidity post-operatively, including VTE, compared with more elderly patients requiring joint arthroplasty [9]. In addition, recent improvements in perioperative protocols including spinal anesthesia and early mobilization may have reduced the rate of VTE regardless of prophylaxis method [10, 11]. Thus, an evidence-based recommendation for VTE prophylaxis regimen after HPS is warranted alongside these recent advances. The initial AAOS guideline in 2007 has recommended ASA 325 mg bis in die (BID) following TJA [12]. However, studies originating from both trauma and arthroplasty literature have demonstrated that lower doses of ASA areas effective for VTE prevention as higher doses VC The Author(s) Published by Oxford University Press. This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License ( which permits non-commercial re-use, distribution, and reproduction in any medium, provided the original work is properly cited. For commercial re-use, please contact journals.permissions@oup.com 125
2 126 I. Azboy et al. Table I. Demographic data of patients FAO group PAO group Number of patient (cases) 603 (643) 80 (87) Gender male/female 307/296 70/10 Age (years) 34.4 ( ) 31.3 ( ) Body mass index (kg/m 2 ) 26.9 ( ) 25.9 ( ) Charlson comorbity index (%) FAO, femoroacetabular osteoplasty; PAO: periacetabular osteotomy. of ASA [13]. As the gastrointestinal (GI) adverse effects of aspirin is dose dependent, the administration of low dose aspirin is believed to positively impact the rate of GIrelated issues [14, 15]. In the early years of our study, we utilized warfarin as the main modality for VTE prevention following joint arthroplasty and HPS. With the publication of the AAOS guidelines for prevention of VTE [8, 12] and later by the ACCP [1], endorsing aspirin as an effective chemoprophylactic drug for VTE following joint arthroplasty, we felt that aspirin could be administered to patients undergoing HPS, including those undergoing PAO. Thus, in 2005 we made a switch from the use of warfarin to aspirin. Initially higher doses of aspirin were being administered to patients undergoing HPS. The dose of aspirin was later lowered. Currently there are no VTE prophylaxis recommendations for patients undergoing HPS. In this study, we aimed to evaluate the outcomes of different VTE prophylaxis regimens in a large cohort of patients undergoing HPS, including FAO and PAO. MATERIALS AND METHODS This retrospective study consists of 645 patients (675 cases) undergoing FAO and 88 patients (96 cases) undergoing PAO between 2003 and All cases were performed by a single surgeon. Patients were followed prospectively to identify 90-day post-operative complications. The VTE prophylaxis data were available for 603 FAO patients (643 cases) and 80 PAO patients (87 cases) (Table I). The mean age of this cohort was 34.3 years (range years). The type of VTE prophylaxis administered was based on surgeon preference and mirrored VTE prophylaxis protocols in TJA at our institution (Table II). Earlier patients Table II. The distribution of venous thromboembolism prophylaxis agent in the cohort FAO group PAO group Total (n ¼ 643) (n ¼ 87) 325-mg Aspirin mg Aspirin Warfarin Total FAO, femoroacetabular osteoplasty; PAO, periacetabular osteotomy. received warfarin (44 cases), followed by aspirin at 325 mg twice daily (448 cases), and most recently aspirin 81 mg twice daily (238 cases; see Figs 1 and 2). Cases were not routinely screened for post-operative VTE. The presence of symptomatic pulmonary embolism (PE), deep venous thrombosis (DVT) and major bleeding events within 90 days of surgery were documented. The indication for FAO was the presence of a cam or pincer deformity, labral tear and the presence of persistent hip pain in the absence of advanced arthritis. The indication for PAO was hip pain in the presence of acetabular dysplasia and the absence of advanced osteoarthritis. All patients received conservative management including non-steroidal anti-inflammatory drugs and/or physical therapy or intraarticular injections prior to surgical intervention. The surgical technique for FAO consisted of a mini-open muscle-sparing anterior approach using the modified Smith Petersen approach [16].Bony impingement at thefemoral head neck junction and/or acetabular rim were addressed, and the labral and chondral lesions were treated accordingly [9]. Surgical exposure for PAO was achieved using the muscle-sparing modified Smith Petersen approach, with a 10- to 12-cm anterior incision and dissection through the plane of the tensor fascia lata and sartorius [17]. The medial aspect of the ilium was exposed, extending to the sciatic notch, and the psoas was retracted medially for exposure of the pubis. The three osteotomies, starting at the anteromedial ischium and progressing to the pubis and ilium, were performed indirectly under fluoroscopy to mobilize and reorient the acetabulum. Fully threaded 4.5 mm cortical screws were used for fixation of the osteotomy fragment. The posterior column was left intact, allowing for immediate rehabilitation without casting or a brace. As thromboprophylaxis, patients received warfarin, ASA 325 mg BID or ASA 81 mg BID for 4 weeks post-operatively, beginning on the day of surgery along with compression mechanical prophylaxis for the length of the hospital stay. The average hospital stay was 1.6 days (range
3 Aspirin provides adequate VTE prophylaxis after hip preservation surgery 127 Fig. 1. VTE: Venous thromboembolism, FAO: Femoroacetabular osteoplasty Fig. 2. VTE: Venous thromboembolism, PAO: Periacetabular osteotomy 1 5 days). The post-operative weightbearing protocol for FAO patients was 6 weeks of partial weight bearing. Postoperative partial weightbearing with crutches for 6 weeks was allowed for patients undergoing PAO. All patients were trained to start circumduction exercises at home. Patients were instructed to return for their first post-operative visit between weeks 4 and 6. Return to full activity, including high-impact sports was allowed after 3 months post-operatively. Post-operative complications occurring within 90 days after surgery were recorded, including symptomatic DVT and PE, GI complications including bleeding or ulceration, acute superficial or deep infection, and mortality. Symptomatic DVTs were detected using lower extremity ultrasound and PEs were diagnosed using chest computed tomography (CT), or ventilation perfusion (V/Q) scans. Patients were not routinely screened for VTE. Lower extremity ultrasound and chest CT/VQ scans were only performed in cases of suspected symptomatic VTE. GI complications were defined as upper GI bleeding or ulceration confirmed by endoscopy. We used only major bleeding as a clinically relevant complication related to thromboprophylaxis. Major bleeding events included fatal bleeding, bleeding into a critical organ (e.g. retroperitoneal, intracranial, intraocular, or intraspinal), clinically overt bleeding (e.g. GI) or requiring 3 units of blood transfusion after surgery, and bleeding leading to reoperation [1]. Statistical analyses were performed with SPSS 18.0 statistical software (SPSS Inc., Chicago, IL, USA). A P values less than 0.05 was considered as statistically significant. RESULTS The overall incidence of a VTE complication 90 days following FAO was one per 643 cases (0.16%). The overall
4 128 I. Azboy et al. Table III. The overall 90 day post-operative venous thromboembolism following hip preservation surgery Prophylaxis agent Number of cases VTE event (n) VTE rate (%) FAO group (n¼643) 325-mg Aspirin mg Aspirin Warfarin 21 0 PAO group (n¼87) 325-mg Aspirin mg Aspirin incidence of VTE complication after PAO was one per 87 cases (1.1%) (Table III). No major bleeding events developed in patient undergoing FAO or PAO. There was no difference between ASA 325 mg and ASA 81 mg in regards to the VTE rate after HPS (P ¼ 0.653). Also, there was no difference between ASA 325 mg and warfarin in regard to VTE rate after HPS (0.911). No difference in VTE rate was observed between ASA 325 mg and ASA 81 mg after FAO (P ¼ 0.667). Furthermore, no difference in VTE rate was observed between ASA 325 mg and ASA 81 mg after PAO (P ¼ 0.516) (Table IV). One 42-year-old female patient developed a DVT and PE after PAO. The patient was discharged on aspirin 325 mg BID. She developed episodic transient stabbing pain in the popliteal fossa and intermittent episodes of chest pain, palpitation, diaphoresis and shortness of breath 5 days post-operatively. Her symptoms progressed, and she was admitted to the emergency room on post-operative day 17. A chest X-ray was obtained which demonstrated a prominent right pulmonary trunk. A CT scan of the thorax was obtained which demonstrated a filling defect in the anterior and superior branches of the right upper lobe pulmonary artery, consistent with PE. Ultrasound of the leg Warfarin 23 0 HPS cohort (n¼730) VTE, venous thromboembolism; HPS, hip preservation surgery; FAO, femoroacetabular osteoplasty; PAO, periacetabular osteotomy. Table IV. Comparison of venous thromboembolism events between the prophylaxis agents 325-mg Aspirin 81-mg Aspirin Warfarin P value FAO group a 1 (415) 0 (207) 0 (21) b and c PAO group a 1 (33) 0 (31) 0 (23) b and c HPS cohort a 2 (448) 0 (238) 0 (44) b and c a The values are given as the number of VTE event, with the number of cases in parentheses. b A 325-mg Aspirin versus 81-mg Aspirin. c A 325-mg Aspirin versus Warfarin. VTE, venous thromboembolism; HPS, hip preservation surgery; FAO, femoroacetabular osteoplasty; PAO, periacetabular osteotomy. was positive for acute thrombus of the left posterior tibial and peroneal veins. She received intravenous heparin on admission and was transitioned to injectable low-molecular weight heparin. The patient was discharged home on enoxaparin 80 mg BID for 5 days, and warfarin 10 mg daily. The patient received warfarin for 3 months with resolution of symptoms. She was doing well at her two year follow-up with no further complications. One 44-year-old male patient had symptomatic DVT after an FAO. The patient was discharged on aspirin 325 mg BID. He developed pain and swelling in his lower extremity. The DVT was diagnosed with lower extremity ultrasound and the patient was treated with warfarin for 3 months with resolution of symptoms and no further complications. DISCUSSION HPS is a popular and effective surgical procedure for the management of young patients with minimal arthritis and symptomatic hip pathology [18]. The most effective mode of prevention of VTE following HPS remains unknown with little published on this subject matter [2 5, 9]. Recommendations for VTE prophylaxis are mainly
5 Aspirin provides adequate VTE prophylaxis after hip preservation surgery 129 based on the TJA literature [1, 6 8, 12, 13]. This is important as the demographics in the HPS population are different from that of the TJA population, with patients undergoing HPS more likely to be younger, more active, and healthier [9]. Zaltz et al. analysed the type of prophylaxis and incidence of clinically symptomatic VTE after utilizing different methods of prophylaxis for a total of 1067 periacetabular osteotomies [2]. They reported an overall incidence of VTE to be 0.94%. Polkowski et al. studied the frequency of thromboembolic disease in adult patients undergoing PAO and receiving aspirin twice daily as well as mechanical prophylaxis by assessing an ultrasound at 1 week post-operatively [3]. They found a 1.3% rate of DVT on routine screening of 136 hips, with a mean patient age of 30 years (range years). They concluded that routine post-operative screening did not detect any patients with an asymptomatic DVT. Bryan et al. reported a thromboembolic disease rate of 2 out of 75 (2.67%) patients receiving ASA 325 mg twice daily as well as mechanical prophylaxis after undergoing a Bernese PAO [11]. Another study by Thawrani et al. reported on 83 PAO cases (n ¼ 76 patients) in whom no prophylaxis was administered and found no cases of symptomatic VTE in that small cohort [4]. The symptomatic VTE rate in our study is 0.16% and 1.1% after FAO and PAO surgery, respectively, consistent with rates reported previously in the literature. Aspirin has been shown to be a safe and effective drug for VTE prophylaxis following TJA, and is supported by the most recent AAOS and ACCP guidelines [6, 19, 20]. In recent studies, aspirin, when compared with more potent anticoagulants, was found to reduce the rate of hematoma formation and subsequent wound complications, including infection, while providing similar efficacy in prevention of VTE [19 22]. Similarly, in our study, there was no significant difference in symptomatic VTE rates following HPS in patients receiving warfarin, ASA 325 mg or ASA 81 mg. This study has several limitations. First, although the number of cases are considerable for ASA 325 mg (n ¼ 448) and ASA 81 mg (n ¼ 238), the sample size is smaller for those that received warfarin (n ¼ 44). Therefore, this study was underpowered to detect a difference between VTE rates in patients receiving warfarin compared with aspirin. However, to our knowledge this is the largest cohort comparing VTE prophylaxis using different modalities in patients undergoing HPS. Second, a higher dose of ASA has been thought to increase the risk of GI complications [15]. However, in our study, no major GI bleeding or ulcer complications were recorded. Minor gastrointestinal problems were not evaluated in this study and may be better evaluated in a prospective randomized study. Lastly, a confounding variable in our study is that recent advances in perioperative protocols including the use of spinal anesthesia and early mobilization protocols may have reduced the rate of VTE events regardless of the prophylaxis regimen [10, 11]; this is difficult to account for due to the retrospective nature of the study, however we still demonstrate a very low event rate of VTE in this population (only two events in this study). In conclusion, this study suggests that aspirin is a safe and an effective modality in minimizing the risk of VTE in patients undergoing HPS including PAO. CONFLICT OF INTEREST STATEMENT None declared. REFERENCES 1. Falck-Ytter Y, Francis CW, Johanson NA et al. Prevention of VTE in orthopedic surgery patients: antithrombotic therapy and prevention of thrombosis: American College of Chest Physicians evidence-based clinical practice guidelines. CHEST 2012; 141: e278s 325S. 2. Zaltz I, Beaule P, Clohisy JC et al. Incidence of deep vein thrombosis and pulmonary embolus following periacetabular osteotomy. J Bone Joint Surg Am 2011; 93: Polkowski GG, Duncan S, Bloemke A et al. Screening for deep vein thrombosis after periacetabular osteotomy in adult patients: is it necessary? Clin Orthop Relat Res 2014; 472: Thawrani D, Sucato D, Podeszwa D, DeLaRocha A. Complications associated with the Bernese periacetabular osteotomy for hip dysplasia in adolescents. J Bone Joint Surg Am 2010; 92: Tischler EH, Ponzio DY, Diaz-Ledezma C, Parvizi J. Prevention of venous thromboembolic events following femoroacetabular osteoplasty: aspirin is enough for most. Hip Int 2014; 24: Huang RC, Parvizi J, Hozack WJ et al. Aspirin is as effective as and safer than Warfarin for patients at higher risk of venous thromboembolism undergoing total joint arthroplasty. J Arthroplasty 2016; 31: Radzak KN, Wages JJ, Hall KE, Nakasone CK. Rate of Transfusions after total knee arthroplasty in patients receiving lovenox or high-dose aspirin. J Arthroplasty 2016; 1: Mont MA, Jacobs JJ. AAOS clinical practice guideline: preventing venous thromboembolic disease in patients undergoing elective hip and knee arthroplasty. J Am Acad Orthop Surg 2011; 19: Cohen SB, Huang R, Ciccotti MG et al. Treatment of femoroacetabular impingement in athletes using a mini-direct anterior approach. Am J Sports Med 2012; 40: Atwal NS, Bedi G, Lankester BJ et al. Management of blood loss in periacetabular osteotomy. Hip Int 2008; 18:
6 130 I. Azboy et al. 11. Bryan AJ, Sanders TL, Trousdale RT, Sierra RJ. Intravenous tranexamic acid decreases allogeneic transfusion requirements in periacetabular osteotomy. Orthopedics 2016; 39: Johanson NA, Lachiewicz PF, Lieberman JR et al. Prevention of symptomatic pulmonary embolism in patients undergoing total hip or knee arthroplasty. J Am Acad Orthop Surg 2009; 17: Prevention of pulmonary embolism and deep vein thrombosis with low dose aspirin: pulmonary Embolism Prevention (PEP) trial. Lancet 2000; 355: de Abajo FJ, Garcia Rodriguez LA. Risk of upper gastrointestinal bleeding and perforation associated with low-dose aspirin as plain and enteric-coated formulations. BMC Clin Pharmacol 2001; 1: Dutch TIA, Trial Study Group. Van Gjin J, Algra A, Kapelle J et al. A comparison of two doses of aspirin (30 mg vs. 283 mg a day) in patients after a transient ischemic attack or minor ischemic stroke. N Engl J Med 1991; 325: Bender B, Nogler M, Hozack WJ. Direct anterior approach fortotal hip arthroplasty. Orthop Clin North Am 2009; 40: Troelsen A, Elmengaard B, Søballe K. A new minimally invasive transsartorial approach for periacetabular osteotomy. J Bone Joint Surg Am 2008; 90: Leunig M, Beaulé PE, Ganz R. The concept of femoroacetabular impingement: current status and future perspectives. Clin Orthop Relat Res 2009; 467: Mostafavi Tabatabaee R, Rasouli MR, Maltenfort MG et al. Costeffective prophylaxis against venous thromboembolism after total joint arthroplasty: warfarin versus aspirin. J Arthroplasty 2015; 30: Ogonda L, Hill J, Doran E et al. Aspirin for thromboprophylaxis after primary lower limb arthroplasty: early thromboembolic events and 90 day mortality in 11, 459 patients. Bone Joint J 2016; 98-B: An VV, Phan K, Levy YD, Bruce WJ. Aspirin as thromboprophylaxis in hip and knee arthroplasty: a systematic review and metaanalysis. J Arthroplasty 2016; 31: Huang R, Buckley PS, Scott B et al. Administration of aspirin as a prophylaxis agent against venous thromboembolism results in lower incidence of periprosthetic joint infection. J Arthroplasty 2015; 30:
Japanese Deep Vein Thrombosis
 Japanese Deep Vein Thrombosis and Pulmonary Embolism after Total Knee Arthroplasty Artificial joint and cartilage implantation center, Kitasato institute hospital, Kitasato university Yasunori Tsukimura
Japanese Deep Vein Thrombosis and Pulmonary Embolism after Total Knee Arthroplasty Artificial joint and cartilage implantation center, Kitasato institute hospital, Kitasato university Yasunori Tsukimura
Non-Arthroplasty Hip Surgery. Javad Parvizi MD FRCS Professor of Orthopaedic Surgery
 Non-Arthroplasty Hip Surgery Javad Parvizi MD FRCS Professor of Orthopaedic Surgery Subcapital reduction osteotomy Relative lengthening of femoral neck (Perthes) AVN surgery Femoral osteotomy Trap door
Non-Arthroplasty Hip Surgery Javad Parvizi MD FRCS Professor of Orthopaedic Surgery Subcapital reduction osteotomy Relative lengthening of femoral neck (Perthes) AVN surgery Femoral osteotomy Trap door
The Birmingham Interlocking Pelvic Osteotomy (BIPO) for Acetabular Dysplasia: 13 to 21 Year Survival Outcomes
 The Birmingham Interlocking Pelvic Osteotomy (BIPO) for Acetabular Dysplasia: 13 to 21 Year Survival Outcomes Omer Mei-Dan, MD Dylan Jewell, BSc, MSc, FRCS Tigran Garabekyan, MD Jason Brockwell, FRCSEdOrth
The Birmingham Interlocking Pelvic Osteotomy (BIPO) for Acetabular Dysplasia: 13 to 21 Year Survival Outcomes Omer Mei-Dan, MD Dylan Jewell, BSc, MSc, FRCS Tigran Garabekyan, MD Jason Brockwell, FRCSEdOrth
Aspirin or Rivaroxaban for VTE Prophylaxis after Hip or Knee Arthroplasty: The EPCAT II Trial
 Aspirin or Rivaroxaban for VTE Prophylaxis after Hip or Knee Arthroplasty: The EPCAT II Trial Wednesday, June 6, 2018, 2:00PM ET Guest Author: David R. Anderson, MD Presenter: Sara Vazquez, PharmD Moderators:
Aspirin or Rivaroxaban for VTE Prophylaxis after Hip or Knee Arthroplasty: The EPCAT II Trial Wednesday, June 6, 2018, 2:00PM ET Guest Author: David R. Anderson, MD Presenter: Sara Vazquez, PharmD Moderators:
Oral Anticoagulation Drug Class Prior Authorization Protocol
 Oral Anticoagulation Drug Class Prior Authorization Protocol Line of Business: Medicaid P & T Approval Date: February 21, 2018 Effective Date: April 1, 2018 This policy has been developed through review
Oral Anticoagulation Drug Class Prior Authorization Protocol Line of Business: Medicaid P & T Approval Date: February 21, 2018 Effective Date: April 1, 2018 This policy has been developed through review
CURRENT & FUTURE THERAPEUTIC MANAGEMENT OF VENOUS THROMBOEMBOLISM. Gordon Lowe Professor of Vascular Medicine University of Glasgow
 CURRENT & FUTURE THERAPEUTIC MANAGEMENT OF VENOUS THROMBOEMBOLISM Gordon Lowe Professor of Vascular Medicine University of Glasgow VENOUS THROMBOEMBOLISM Common cause of death and disability 50% hospital-acquired
CURRENT & FUTURE THERAPEUTIC MANAGEMENT OF VENOUS THROMBOEMBOLISM Gordon Lowe Professor of Vascular Medicine University of Glasgow VENOUS THROMBOEMBOLISM Common cause of death and disability 50% hospital-acquired
Protocol. Postsurgical Outpatient Use of Limb Compression Devices for Venous Thromboembolism Prophylaxis
 Postsurgical Outpatient Use of Limb Compression Devices for (10128) (Formerly Outpatient Use of Limb Pneumatic Compression Devices for ) Medical Benefit Effective Date: 07/01/14 Next Review Date: 03/15
Postsurgical Outpatient Use of Limb Compression Devices for (10128) (Formerly Outpatient Use of Limb Pneumatic Compression Devices for ) Medical Benefit Effective Date: 07/01/14 Next Review Date: 03/15
Slide 1. Slide 2. Slide 3. Outline of This Presentation
 Slide 1 Current Approaches to Venous Thromboembolism Prevention in Orthopedic Patients Hujefa Vora, MD Maria Fox, RN June 9, 2017 Slide 2 Slide 3 Outline of This Presentation Pathophysiology of venous
Slide 1 Current Approaches to Venous Thromboembolism Prevention in Orthopedic Patients Hujefa Vora, MD Maria Fox, RN June 9, 2017 Slide 2 Slide 3 Outline of This Presentation Pathophysiology of venous
VTE Prevention After Hip or Knee Replacement
 This Clinical Resource gives subscribers additional insight related to the Recommendations published in May 2018 ~ Resource #340506 VTE Prevention After Hip or Knee Replacement The American College of
This Clinical Resource gives subscribers additional insight related to the Recommendations published in May 2018 ~ Resource #340506 VTE Prevention After Hip or Knee Replacement The American College of
Drug Class Monograph
 Drug Class Monograph Class: Oral Anticoagulants Drug: Coumadin (warfarin), Eliquis (apixaban), Pradaxa (dabigatran), Savaysa (edoxaban), arelto (rivaroxaban) Formulary Medications: Eliquis (apixaban),
Drug Class Monograph Class: Oral Anticoagulants Drug: Coumadin (warfarin), Eliquis (apixaban), Pradaxa (dabigatran), Savaysa (edoxaban), arelto (rivaroxaban) Formulary Medications: Eliquis (apixaban),
Hip Arthroscopy in Patients with Mild to Moderate Dysplasia: When do they Fail?
 Hip Arthroscopy in Patients with Mild to Moderate Dysplasia: When do they Fail? Andrew J. Bryan 1, MD K. Poehling-Monaghan 1, MD Rohith Mohan 1, BA Nick R Johnson 1, BS Aaron J. Krych 1, MD Bruce A. Levy
Hip Arthroscopy in Patients with Mild to Moderate Dysplasia: When do they Fail? Andrew J. Bryan 1, MD K. Poehling-Monaghan 1, MD Rohith Mohan 1, BA Nick R Johnson 1, BS Aaron J. Krych 1, MD Bruce A. Levy
Incidence and Complications of Open Hip Preservation Surgery: An American Board of Orthopaedic Surgery Database Review
 Incidence and Complications of Open Hip Preservation Surgery: An American Board of Orthopaedic Surgery Database Review Jon P Hedgecock MD, 1 P Christopher Cook MD FRCS(C), 1 John Harrast PhD,2 Judith F
Incidence and Complications of Open Hip Preservation Surgery: An American Board of Orthopaedic Surgery Database Review Jon P Hedgecock MD, 1 P Christopher Cook MD FRCS(C), 1 John Harrast PhD,2 Judith F
Anticoagulation for prevention of venous thromboembolism
 Anticoagulation for prevention of venous thromboembolism Original article by: Michael Tam Note: updated in June 2009 with the eighth edition (from the seventh) evidence-based clinical practice guidelines
Anticoagulation for prevention of venous thromboembolism Original article by: Michael Tam Note: updated in June 2009 with the eighth edition (from the seventh) evidence-based clinical practice guidelines
Adam Goldfarb, M.A., D.C., D.E.S.S. Introduction
 Venous Thromboembolism Prophylaxis following Lower Extremity Orthopedic Surgery: A Review of the Biomedical Research Literature and Evidence-Based Policy in the United States. Adam Goldfarb, M.A., D.C.,
Venous Thromboembolism Prophylaxis following Lower Extremity Orthopedic Surgery: A Review of the Biomedical Research Literature and Evidence-Based Policy in the United States. Adam Goldfarb, M.A., D.C.,
Early Ambulation Reduces the Risk of Venous Thromboembolism After Total Knee Replacement. Marilyn Szekendi, PhD, RN
 Early Ambulation Reduces the Risk of Venous Thromboembolism After Total Knee Replacement Marilyn Szekendi, PhD, RN ANA 7 th Annual Nursing Quality Conference, February 2013 Research Team Banafsheh Sadeghi,
Early Ambulation Reduces the Risk of Venous Thromboembolism After Total Knee Replacement Marilyn Szekendi, PhD, RN ANA 7 th Annual Nursing Quality Conference, February 2013 Research Team Banafsheh Sadeghi,
Anesthesia for Total Hip and Knee Arthroplasty
 Anesthesia for Total Hip and Knee Arthroplasty Typical approach Describe anesthesia technique Rather Describe issues with THA and TKA How anesthesia can modify Issues Total Hip Total Knee Blood Loss ++
Anesthesia for Total Hip and Knee Arthroplasty Typical approach Describe anesthesia technique Rather Describe issues with THA and TKA How anesthesia can modify Issues Total Hip Total Knee Blood Loss ++
DVT PROPHYLAXIS IN HOSPITALIZED MEDICAL PATIENTS SAURABH MAJI SR (PULMONARY,MEDICINE)
 DVT PROPHYLAXIS IN HOSPITALIZED MEDICAL PATIENTS SAURABH MAJI SR (PULMONARY,MEDICINE) Introduction VTE (DVT/PE) is an important complication in hospitalized patients Hospitalization for acute medical illness
DVT PROPHYLAXIS IN HOSPITALIZED MEDICAL PATIENTS SAURABH MAJI SR (PULMONARY,MEDICINE) Introduction VTE (DVT/PE) is an important complication in hospitalized patients Hospitalization for acute medical illness
High tibial osteotomy (HTO), distal femoral. Rates of Deep Vein Thrombosis Occurring After Osteotomy About the Knee.
 An Original Study Rates of Deep Vein Thrombosis Occurring After Osteotomy About the Knee Brandon J. Erickson, MD, Annie Tilton, MD, Rachel M. Frank, MD, William Park, BS, and Brian J. Cole, MD Abstract
An Original Study Rates of Deep Vein Thrombosis Occurring After Osteotomy About the Knee Brandon J. Erickson, MD, Annie Tilton, MD, Rachel M. Frank, MD, William Park, BS, and Brian J. Cole, MD Abstract
Reliability of Simple Radiographic Parameters for Pincer FAI
 Reliability of Simple Radiographic Parameters for Pincer FAI Sung Hoon Yang MD., Dong Hwi Kim, MD., Yong Chul Jeon, MD., Sang Hong Lee MD. PhD., Suenghwan Jo MD. PhD, Chosun University Hospital, Gwangju,
Reliability of Simple Radiographic Parameters for Pincer FAI Sung Hoon Yang MD., Dong Hwi Kim, MD., Yong Chul Jeon, MD., Sang Hong Lee MD. PhD., Suenghwan Jo MD. PhD, Chosun University Hospital, Gwangju,
1/27/2016. Disclosure. Goals. The Risk and Prevention of Venous Thromboembolism (VTE) in Patients With Foot and Ankle Pathology
 The Risk and Prevention of Venous Thromboembolism (VTE) in Patients With Foot and Ankle Pathology STEVEN STEINLAUF, MD THE ORTHOPAEDIC FOOT AND ANKLE INSTITUTE OF SOUTH FLORIDA CLINICAL ASSISTANT PROFESSOR
The Risk and Prevention of Venous Thromboembolism (VTE) in Patients With Foot and Ankle Pathology STEVEN STEINLAUF, MD THE ORTHOPAEDIC FOOT AND ANKLE INSTITUTE OF SOUTH FLORIDA CLINICAL ASSISTANT PROFESSOR
Venous Thromboembolism. Prevention
 Venous Thromboembolism Prevention August 2010 Venous Thromboembloism Prevention 1 1 Expected Practice Assess all patients upon admission to the ICU for risk factors of venous thromboembolism (VTE) and
Venous Thromboembolism Prevention August 2010 Venous Thromboembloism Prevention 1 1 Expected Practice Assess all patients upon admission to the ICU for risk factors of venous thromboembolism (VTE) and
Venous Thromboembolism Prophylaxis After Major Orthopaedic Surgery: A Pooled Analysis of Randomized Controlled Trials
 Winner of the AAHKS Award Venous Thromboembolism Prophylaxis After Major Orthopaedic Surgery: A Pooled Analysis of Randomized Controlled Trials Greg A. Brown, MD, PhD The Journal of Arthroplasty Vol. 24
Winner of the AAHKS Award Venous Thromboembolism Prophylaxis After Major Orthopaedic Surgery: A Pooled Analysis of Randomized Controlled Trials Greg A. Brown, MD, PhD The Journal of Arthroplasty Vol. 24
Society of Trauma Nurses TraumaCon 03/22/2018
 Prophylaxis Against Venous Thromboemblism (VTE) in Pediatric Trauma Society of Trauma Nurses TraumaCon 03/22/2018 Arash Mahajerin, MD, MSCr Hematology, CHOC Children s Specialists Orange, CA Disclosure
Prophylaxis Against Venous Thromboemblism (VTE) in Pediatric Trauma Society of Trauma Nurses TraumaCon 03/22/2018 Arash Mahajerin, MD, MSCr Hematology, CHOC Children s Specialists Orange, CA Disclosure
Venous thromboembolism after total knee replacement or total hip replacement: what can be learnt from root-cause analysis?
 TRAUMA AND ORTHOPAEDIC SURGERY Ann R Coll Surg Engl 2016; 98: 538 542 doi 10.1308/rcsann.2016.0202 Venous thromboembolism after total knee replacement or total hip replacement: what can be learnt from
TRAUMA AND ORTHOPAEDIC SURGERY Ann R Coll Surg Engl 2016; 98: 538 542 doi 10.1308/rcsann.2016.0202 Venous thromboembolism after total knee replacement or total hip replacement: what can be learnt from
Complications of Treatment: Nonsurgical and Surgical
 Complications of Treatment: Nonsurgical and Surgical Whenever orthopedic surgeons discuss a treatment with patients we must always consider the risks and complications of any treatment we recommend. Part
Complications of Treatment: Nonsurgical and Surgical Whenever orthopedic surgeons discuss a treatment with patients we must always consider the risks and complications of any treatment we recommend. Part
SUBJECT: LIMB PNEUMATIC COMPRESSION EFFECTIVE DATE: 06/27/13 DEVICES FOR VENOUS REVISED DATE: 06/26/14 THROMBOEMBOLISM PROPHYLAXIS
 MEDICAL POLICY SUBJECT: LIMB PNEUMATIC COMPRESSION PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical
MEDICAL POLICY SUBJECT: LIMB PNEUMATIC COMPRESSION PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical
Swiss Medical Network Musculoskeletal Conference Surgical Technique and 30-Year Results of the Periacetabular Osteotomy (PAO)
 Swiss Medical Network Musculoskeletal Conference 2017 Surgical Technique and 30-Year Results of the Periacetabular Osteotomy (PAO) Simon D. Steppacher Department of Orthopedic Surgery, Inselspital, University
Swiss Medical Network Musculoskeletal Conference 2017 Surgical Technique and 30-Year Results of the Periacetabular Osteotomy (PAO) Simon D. Steppacher Department of Orthopedic Surgery, Inselspital, University
Venous Thromboembolism Prophylaxis
 Approved by: Venous Thromboembolism Prophylaxis Vice President and Chief Medical Officer; and Vice President and Chief Operating Officer Corporate Policy & Procedures Manual Number: Date Approved January
Approved by: Venous Thromboembolism Prophylaxis Vice President and Chief Medical Officer; and Vice President and Chief Operating Officer Corporate Policy & Procedures Manual Number: Date Approved January
Management of Hip Fractures
 Management of Hip Fractures in the Elderly Patient David A. Brown MD COL U.S. Army Ret. The Center for Orthopedics and Neurosurgery Optimizing Management of Hip Fractures in the Elderly Patient Optimizing
Management of Hip Fractures in the Elderly Patient David A. Brown MD COL U.S. Army Ret. The Center for Orthopedics and Neurosurgery Optimizing Management of Hip Fractures in the Elderly Patient Optimizing
Postsurgical Home Use of Limb Compression Devices for Venous Thromboembolism Prophylaxis
 Clinical Position Statement Postsurgical Home Use of Limb Compression Devices for Venous Thromboembolism Prophylaxis Effective: October 2017 Next Review: September 2018 CLINICAL POSITION STATEMENT Postsurgical
Clinical Position Statement Postsurgical Home Use of Limb Compression Devices for Venous Thromboembolism Prophylaxis Effective: October 2017 Next Review: September 2018 CLINICAL POSITION STATEMENT Postsurgical
VTE Management in Surgical Patients: Optimizing Prophylaxis Strategies
 VTE Management in Surgical Patients: Optimizing Prophylaxis Strategies VTE in Surgical Patients: Recognizing the Patients at Risk Pathogenesis of thrombosis: Virchow s triad and VTE Risk Hypercoagulability
VTE Management in Surgical Patients: Optimizing Prophylaxis Strategies VTE in Surgical Patients: Recognizing the Patients at Risk Pathogenesis of thrombosis: Virchow s triad and VTE Risk Hypercoagulability
Objectives. Venous Thromboembolism (VTE) Prophylaxis. Case VTE WHY DO IT? Question: Who Is At Risk?
 Objectives Venous Thromboembolism (VTE) Prophylaxis Rishi Garg, MD Department of Medicine Identify patients at risk for VTE Options for VTE prophylaxis Current Recommendations (based on The Seventh ACCP
Objectives Venous Thromboembolism (VTE) Prophylaxis Rishi Garg, MD Department of Medicine Identify patients at risk for VTE Options for VTE prophylaxis Current Recommendations (based on The Seventh ACCP
Aspirin as Venous Thromboprophylaxis
 Canadian Society of Internal Medicine Nov 2, 2017 Aspirin as Venous Thromboprophylaxis Bill Geerts, MD, FRCPC Thromboembolism Consultant, Sunnybrook HSC Professor of Medicine, University of Toronto Disclosures
Canadian Society of Internal Medicine Nov 2, 2017 Aspirin as Venous Thromboprophylaxis Bill Geerts, MD, FRCPC Thromboembolism Consultant, Sunnybrook HSC Professor of Medicine, University of Toronto Disclosures
Clinical Practice Guideline for Patients Requiring Total Hip Replacement
 Clinical Practice Guideline for Patients Requiring Total Hip Replacement Inclusions Patients undergoing elective total hip replacement Exclusions Patients with active local or systemic infection or medical
Clinical Practice Guideline for Patients Requiring Total Hip Replacement Inclusions Patients undergoing elective total hip replacement Exclusions Patients with active local or systemic infection or medical
Does Surgeon Experience Impact the Risk of Complications After Bernese Periacetabular Osteotomy?
 Clin Orthop Relat Res (2017) 475:1110 1117 DOI 10.1007/s11999-016-5010-1 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons SYMPOSIUM: 2016 BERNESE HIP
Clin Orthop Relat Res (2017) 475:1110 1117 DOI 10.1007/s11999-016-5010-1 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons SYMPOSIUM: 2016 BERNESE HIP
Connecticut Joint Replacement Institute (CJRI) Outcomes Report
 Connecticut Joint Replacement Institute () Outcomes Report Our Highlights: Nationally recognized Over 27,000 surgeries performed Devoted to excellence in patient care Proven superior outcomes that matter.
Connecticut Joint Replacement Institute () Outcomes Report Our Highlights: Nationally recognized Over 27,000 surgeries performed Devoted to excellence in patient care Proven superior outcomes that matter.
Research Article. Abstract
 Research Article Trends in Deep Vein Thrombosis Prophylaxis and Deep Vein Thrombosis Rates After Total Hip and Knee Arthroplasty Harpreet Bawa, MD Jack W. Weick, MD Douglas R. Dirschl, MD Hue H. Luu, MD
Research Article Trends in Deep Vein Thrombosis Prophylaxis and Deep Vein Thrombosis Rates After Total Hip and Knee Arthroplasty Harpreet Bawa, MD Jack W. Weick, MD Douglas R. Dirschl, MD Hue H. Luu, MD
Incidence of DVT Post- Hip or Knee Replacement. A Comparison of Incidence at Boundary Trails Health Centre to a Credible Baseline Incidence
 Incidence of DVT Post- Hip or Knee Replacement A Comparison of Incidence at Boundary Trails Health Centre to a Credible Baseline Incidence Background DVTs Pulmonary Embolisms Death Symptomatic DVTs (leg
Incidence of DVT Post- Hip or Knee Replacement A Comparison of Incidence at Boundary Trails Health Centre to a Credible Baseline Incidence Background DVTs Pulmonary Embolisms Death Symptomatic DVTs (leg
EAST MULTICENTER STUDY DATA DICTIONARY
 EAST MULTICENTER STUDY DATA DICTIONARY Does the Addition of Daily Aspirin to Standard Deep Venous Thrombosis Prophylaxis Reduce the Rate of Venous Thromboembolic Events? Data Entry Points and appropriate
EAST MULTICENTER STUDY DATA DICTIONARY Does the Addition of Daily Aspirin to Standard Deep Venous Thrombosis Prophylaxis Reduce the Rate of Venous Thromboembolic Events? Data Entry Points and appropriate
Periacetabular Osteotomy (PAO)
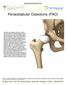 Periacetabular Osteotomy (PAO) At the top of your thigh bone, the femur, is a ball shaped structure called the femoral head, which fits in a socket in the pelvis, called the acetabulum. Both of these structures
Periacetabular Osteotomy (PAO) At the top of your thigh bone, the femur, is a ball shaped structure called the femoral head, which fits in a socket in the pelvis, called the acetabulum. Both of these structures
SUBJECT: LIMB PNEUMATIC COMPRESSION EFFECTIVE DATE: 06/27/13 DEVICES FOR VENOUS REVISED DATE: 06/26/14, 09/15/15,09/21/17. THROMBOEMBOLISM PROPHYLAXIS
 MEDICAL POLICY REVISED DATE: 06/26/14, 09/15/15,09/21/17. PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases,
MEDICAL POLICY REVISED DATE: 06/26/14, 09/15/15,09/21/17. PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases,
NOTE: The first appearance of terms in bold in the body of this document (except titles) are defined terms please refer to the Definitions section.
 TITLE VENOUS THROMBOEMBOLISM PROPHYLAXIS SCOPE Provincial Acute and Sub-Acute Care Facilities APPROVAL AUTHORITY Alberta Health Services Executive Committee SPONSOR Vice President, Quality and Chief Medical
TITLE VENOUS THROMBOEMBOLISM PROPHYLAXIS SCOPE Provincial Acute and Sub-Acute Care Facilities APPROVAL AUTHORITY Alberta Health Services Executive Committee SPONSOR Vice President, Quality and Chief Medical
1. SCOPE of GUIDELINE:
 Page 1 of 35 CLINICAL PRACTICE GUIDELINE: Venous Thromboembolism (VTE) Prevention Guideline: Thromboprophylaxis AUTHORIZATION: VP, Medicine Date Approved: May 17, 2012 Date Revised: Vancouver Coastal Health
Page 1 of 35 CLINICAL PRACTICE GUIDELINE: Venous Thromboembolism (VTE) Prevention Guideline: Thromboprophylaxis AUTHORIZATION: VP, Medicine Date Approved: May 17, 2012 Date Revised: Vancouver Coastal Health
Orthopedic Surgery for Adults with Cerebral Palsy- Medical Considerations. Disclosures. Objectives. Adults with Cerebral Palsy
 Orthopedic Surgery for Adults with Cerebral Palsy- Medical Considerations American Academy for Cerebral Palsy and Developmental Medicine, 2013, IC 6 Garey Noritz, MD, FAAP, FACP Nationwide Children s Hospital
Orthopedic Surgery for Adults with Cerebral Palsy- Medical Considerations American Academy for Cerebral Palsy and Developmental Medicine, 2013, IC 6 Garey Noritz, MD, FAAP, FACP Nationwide Children s Hospital
CADTH Rapid Response Report: ASA for Venous Thromboembolism Prophylaxis: Evidence for Clinical Benefit and Harm
 CADTH Rapid Response Report: ASA for Venous Thromboembolism Prophylaxis: Evidence for Clinical Benefit and Harm P. Timothy Pollak, MD, PhD University of Calgary Rocky Mountain/ACP Internal Medicine Meeting,
CADTH Rapid Response Report: ASA for Venous Thromboembolism Prophylaxis: Evidence for Clinical Benefit and Harm P. Timothy Pollak, MD, PhD University of Calgary Rocky Mountain/ACP Internal Medicine Meeting,
Challenges in Anticoagulation and Thromboembolism
 Challenges in Anticoagulation and Thromboembolism Ethan Cumbler M.D. Assistant Professor of Medicine Hospitalist Medicine Section University of Colorado Denver May 2010 No Conflicts of Interest Objectives
Challenges in Anticoagulation and Thromboembolism Ethan Cumbler M.D. Assistant Professor of Medicine Hospitalist Medicine Section University of Colorado Denver May 2010 No Conflicts of Interest Objectives
Primary VTE Prophylaxis. Ponlapat Rojnuckarin, MD PhD Chulalongkorn University Bangkok, Thailand
 Primary VTE Prophylaxis Ponlapat Rojnuckarin, MD PhD Chulalongkorn University Bangkok, Thailand A 70-yr-old female before THA BMI 31 kg/m 2 with varicose vein What do you recommend for VTE prevention?
Primary VTE Prophylaxis Ponlapat Rojnuckarin, MD PhD Chulalongkorn University Bangkok, Thailand A 70-yr-old female before THA BMI 31 kg/m 2 with varicose vein What do you recommend for VTE prevention?
Incidence of Venous Thromboembolism After Arthroscopic Anterior Cruciate Ligament Reconstruction
 Incidence of Venous Thromboembolism After Arthroscopic Anterior Cruciate Ligament Reconstruction Masaki Nagashima 1,2 Toshiro Otani 3 Hiroyuki Seki 1,2 Kenichiro Takeshima 2 Nobuto Origuchi 4 Ken Ishii
Incidence of Venous Thromboembolism After Arthroscopic Anterior Cruciate Ligament Reconstruction Masaki Nagashima 1,2 Toshiro Otani 3 Hiroyuki Seki 1,2 Kenichiro Takeshima 2 Nobuto Origuchi 4 Ken Ishii
Deep Vein Thrombosis and Pulmonary Embolism: Patient Information
 Deep Vein Thrombosis and Pulmonary Embolism: Patient Information A Deep Vein Thrombosis (DVT) and a Pulmonary Embolism (PE) are both disorders of unwanted blood clotting. Unwanted blood clots can occur
Deep Vein Thrombosis and Pulmonary Embolism: Patient Information A Deep Vein Thrombosis (DVT) and a Pulmonary Embolism (PE) are both disorders of unwanted blood clotting. Unwanted blood clots can occur
Proper Diagnosis of Venous Thromboembolism (VTE)
 Proper Diagnosis of Venous Thromboembolism (VTE) Whal Lee, M.D. Seoul National University Hospital Department of Radiology 2 nd EFORT Asia Symposium, 3 rd November 2010, Taipei DVT - Risk Factors Previous
Proper Diagnosis of Venous Thromboembolism (VTE) Whal Lee, M.D. Seoul National University Hospital Department of Radiology 2 nd EFORT Asia Symposium, 3 rd November 2010, Taipei DVT - Risk Factors Previous
Drug Class Review Newer Oral Anticoagulant Drugs
 Drug Class Review Newer Oral Anticoagulant Drugs Final Original Report May 2016 The purpose of reports is to make available information regarding the comparative clinical effectiveness and harms of different
Drug Class Review Newer Oral Anticoagulant Drugs Final Original Report May 2016 The purpose of reports is to make available information regarding the comparative clinical effectiveness and harms of different
CPT only copyright 2014 American Medical Association. All rights reserved. 12/23/2014 Page 66 of 593
 Measure #23 (NQF 0239): Perioperative Care: Venous Thromboembolism (VTE) Prophylaxis (When Indicated in ALL Patients) National Quality Strategy Domain: Patient Safety 2015 PQRS OPTIONS FOR INDIVIDUAL MEASURES:
Measure #23 (NQF 0239): Perioperative Care: Venous Thromboembolism (VTE) Prophylaxis (When Indicated in ALL Patients) National Quality Strategy Domain: Patient Safety 2015 PQRS OPTIONS FOR INDIVIDUAL MEASURES:
AN AUDIT: THROMBOPROPHYLAXIS FOR TOTAL HIP REPLACEMENT PATIENTS AT NORTHWICK PARK AND CENTRAL MIDDLESEX HOSPITALS
 The West London Medical Journal 2010 Vol 2 No 4 pp 19-24 AN AUDIT: THROMBOPROPHYLAXIS FOR TOTAL HIP REPLACEMENT PATIENTS AT NORTHWICK PARK AND CENTRAL MIDDLESEX HOSPITALS Soneji ND Agni NR Acharya MN Anjari
The West London Medical Journal 2010 Vol 2 No 4 pp 19-24 AN AUDIT: THROMBOPROPHYLAXIS FOR TOTAL HIP REPLACEMENT PATIENTS AT NORTHWICK PARK AND CENTRAL MIDDLESEX HOSPITALS Soneji ND Agni NR Acharya MN Anjari
Page: 1 of 13. Post-Surgical Outpatient Use of Limb Compression Devices for Venous Thromboembolism Prophylaxis
 Last Review Status/Date: March 2014 Page: 1 of 13 Compression Devices for Venous Description Patients undergoing major orthopedic surgery are at increased risk for venous thromboembolism (VTE). Patients
Last Review Status/Date: March 2014 Page: 1 of 13 Compression Devices for Venous Description Patients undergoing major orthopedic surgery are at increased risk for venous thromboembolism (VTE). Patients
Venous Thromboembolism Prophylaxis: Checked!
 Venous Thromboembolism Prophylaxis: Checked! William Geerts, MD, FRCPC Director, Thromboembolism Program, Sunnybrook HSC Professor of Medicine, University of Toronto National Lead, VTE Prevention, Safer
Venous Thromboembolism Prophylaxis: Checked! William Geerts, MD, FRCPC Director, Thromboembolism Program, Sunnybrook HSC Professor of Medicine, University of Toronto National Lead, VTE Prevention, Safer
Mitchell McDowell, DO**, Daljeet Sagoo, DO*, Michael P. Muldoon, MD*, Richard Santore, MD*
 Mitchell McDowell, DO**, Daljeet Sagoo, DO*, Michael P. Muldoon, MD*, Richard Santore, MD* *Orthopedic Medical Group,7910 Frost St. #200 San Diego, California 92123, USA **Riverside County Regional Medical
Mitchell McDowell, DO**, Daljeet Sagoo, DO*, Michael P. Muldoon, MD*, Richard Santore, MD* *Orthopedic Medical Group,7910 Frost St. #200 San Diego, California 92123, USA **Riverside County Regional Medical
EBM. Comparative Systematic Review of the Open Dislocation, Mini-Open, and Arthroscopic Surgeries for Femoroacetabular Impingement
 EBM Comparative Systematic Review of the Open Dislocation, Mini-Open, and Arthroscopic Surgeries for Femoroacetabular Impingement ~ Arthroscopy: The Journal of Arthroscopic and Related Surgery, Vol 27,
EBM Comparative Systematic Review of the Open Dislocation, Mini-Open, and Arthroscopic Surgeries for Femoroacetabular Impingement ~ Arthroscopy: The Journal of Arthroscopic and Related Surgery, Vol 27,
DENOMINATOR: All surgical patients aged 18 years and older undergoing procedures for which VTE prophylaxis is indicated in all patients
 Measure #23 (NQF 0239): Perioperative Care: Venous Thromboembolism (VTE) Prophylaxis (When Indicated in ALL Patients) National Quality Strategy Domain: Patient Safety 2017 OPTIONS FOR INDIVIDUAL MEASURES:
Measure #23 (NQF 0239): Perioperative Care: Venous Thromboembolism (VTE) Prophylaxis (When Indicated in ALL Patients) National Quality Strategy Domain: Patient Safety 2017 OPTIONS FOR INDIVIDUAL MEASURES:
PRIMARY TOTAL KNEE & HIP
 Clinical Guideline Version 2.0 Title: PRIMARY TOTAL KNEE & HIP Venous ThromboEmbolic (VTE) Guideline Target Audience: thopedic Surgeons and their Advanced Practice Practitioner partners; Hospitalists,
Clinical Guideline Version 2.0 Title: PRIMARY TOTAL KNEE & HIP Venous ThromboEmbolic (VTE) Guideline Target Audience: thopedic Surgeons and their Advanced Practice Practitioner partners; Hospitalists,
Measure #23 (NQF 0239): Perioperative Care: Venous Thromboembolism (VTE) Prophylaxis (When Indicated in ALL Patients)
 Measure #23 (NQF 0239): Perioperative Care: Venous Thromboembolism (VTE) Prophylaxis (When Indicated in ALL Patients) 2013 PQRS OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS, REGISTRY DESCRIPTION: Percentage
Measure #23 (NQF 0239): Perioperative Care: Venous Thromboembolism (VTE) Prophylaxis (When Indicated in ALL Patients) 2013 PQRS OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS, REGISTRY DESCRIPTION: Percentage
What You Should Know
 1 New 2018 ASH Clinical Practice Guidelines on Venous Thromboembolism: What You Should Know New 2018 ASH Clinical Practice Guidelines on Venous Thromboembolism: What You Should Know The American Society
1 New 2018 ASH Clinical Practice Guidelines on Venous Thromboembolism: What You Should Know New 2018 ASH Clinical Practice Guidelines on Venous Thromboembolism: What You Should Know The American Society
TITLE: Acetylsalicylic Acid for Venous Thromboembolism Prophylaxis: A Review of Clinical Evidence, Benefits and Harms
 TITLE: Acetylsalicylic Acid for Venous Thromboembolism Prophylaxis: A Review of Clinical Evidence, Benefits and Harms DATE: 23 August 2011 CONTEXT AND POLICY ISSUES: Thromboembolism occurs when a blood
TITLE: Acetylsalicylic Acid for Venous Thromboembolism Prophylaxis: A Review of Clinical Evidence, Benefits and Harms DATE: 23 August 2011 CONTEXT AND POLICY ISSUES: Thromboembolism occurs when a blood
Σάββας Σουρμελής Διευθυντής Β Ορθοπαιδικής Κλινικής ΔΘΚΑ «Υγεία» Αναγνώριση παραγόντων κινδύνου της φλεβικής θρόμβωσης.
 Σάββας Σουρμελής Διευθυντής Β Ορθοπαιδικής Κλινικής ΔΘΚΑ «Υγεία» Αναγνώριση παραγόντων κινδύνου της φλεβικής θρόμβωσης. VTE: deep vein thrombosis (DVT) and pulmonary embolism (PE) PE Migration Embolus
Σάββας Σουρμελής Διευθυντής Β Ορθοπαιδικής Κλινικής ΔΘΚΑ «Υγεία» Αναγνώριση παραγόντων κινδύνου της φλεβικής θρόμβωσης. VTE: deep vein thrombosis (DVT) and pulmonary embolism (PE) PE Migration Embolus
MEDICAL POLICY SUBJECT: LIMB PNEUMATIC COMPRESSION DEVICES FOR VENOUS THROMBOEMBOLISM PROPHYLAXIS
 MEDICAL POLICY SUBJECT: LIMB PNEUMATIC COMPRESSION REVISED DATE: 06/26/14, 10/15/15, 06/16/16, PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria
MEDICAL POLICY SUBJECT: LIMB PNEUMATIC COMPRESSION REVISED DATE: 06/26/14, 10/15/15, 06/16/16, PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria
PREVENTION AND TREATMENT OF VENOUS THROMBOEMBOLISM
 PREVENTION AND TREATMENT OF VENOUS THROMBOEMBOLISM International Consensus Statement 2013 Guidelines According to Scientific Evidence Developed under the auspices of the: Cardiovascular Disease Educational
PREVENTION AND TREATMENT OF VENOUS THROMBOEMBOLISM International Consensus Statement 2013 Guidelines According to Scientific Evidence Developed under the auspices of the: Cardiovascular Disease Educational
VTE in the Trauma Population
 VTE in the Trauma Population Erik Peltz, D.O. February 11 th, 2015 * contributions from Eduardo Gonzalez, M.D. University of Colorado T-32 Research Fellow The problem. VTE - Scope of the Problem One of
VTE in the Trauma Population Erik Peltz, D.O. February 11 th, 2015 * contributions from Eduardo Gonzalez, M.D. University of Colorado T-32 Research Fellow The problem. VTE - Scope of the Problem One of
Comparison of Venothromboembolism Prophylaxis Practices in a Winnipeg Tertiary Care Hospital to Chest Guidelines: A Quality Improvement Project
 Comparison of Venothromboembolism Prophylaxis Practices in a Winnipeg Tertiary Care Hospital to Chest Guidelines: A Quality Improvement Project Dr. Jonathan Laxton, FRCPC, R5 GIM University of Manitoba
Comparison of Venothromboembolism Prophylaxis Practices in a Winnipeg Tertiary Care Hospital to Chest Guidelines: A Quality Improvement Project Dr. Jonathan Laxton, FRCPC, R5 GIM University of Manitoba
Results from RE-COVER RE-COVER II RE-MEDY RE-SONATE EXECUTIVE SUMMARY
 Assessment of the safety and efficacy of dabigatran etexilate (Pradaxa ) in the treatment of deep vein thrombosis (DVT) and pulmonary embolism (PE) and the prevention of recurrent DVT and PE Results from
Assessment of the safety and efficacy of dabigatran etexilate (Pradaxa ) in the treatment of deep vein thrombosis (DVT) and pulmonary embolism (PE) and the prevention of recurrent DVT and PE Results from
Are There Clinical Meaning on Asymptomatic Pulmonary Embolism After Total Knee Arthroplasty?
 Are There Clinical Meaning on Asymptomatic Pulmonary Embolism After Total Knee Arthroplasty? * 1,2 ATSUSHI SATO, MD, PhD, * 1,2 Takayuki Koya, * 2,3 Hiroshi Takagi, * 2 Jun Oike,, * 2 Saki Yagura, * 2
Are There Clinical Meaning on Asymptomatic Pulmonary Embolism After Total Knee Arthroplasty? * 1,2 ATSUSHI SATO, MD, PhD, * 1,2 Takayuki Koya, * 2,3 Hiroshi Takagi, * 2 Jun Oike,, * 2 Saki Yagura, * 2
Slide 1: Perioperative Management of Anticoagulation
 Perioperative Management of Anticoagulation by Steven L. Cohn, MD, FACP Director, Medical Consultation Service, Kings County Hospital Center, Clinical Professor of Medicine, SUNY Downstate, Brooklyn, NY
Perioperative Management of Anticoagulation by Steven L. Cohn, MD, FACP Director, Medical Consultation Service, Kings County Hospital Center, Clinical Professor of Medicine, SUNY Downstate, Brooklyn, NY
Corporate Medical Policy
 Corporate Medical Policy Postsurgical Home Use of Limb Compression Devices for Venous File Name: Origination: Last CAP Review: Next CAP Review: Last Review: postsurgical_home_use_of_limb_ compression_devices_for_vte_prophylaxis
Corporate Medical Policy Postsurgical Home Use of Limb Compression Devices for Venous File Name: Origination: Last CAP Review: Next CAP Review: Last Review: postsurgical_home_use_of_limb_ compression_devices_for_vte_prophylaxis
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Process
 Quality ID #23 (NQF 0239): Perioperative Care: Venous Thromboembolism (VTE) Prophylaxis (When Indicated in ALL Patients) National Quality Strategy Domain: Patient Safety 2018 OPTIONS FOR INDIVIDUAL MEASURES:
Quality ID #23 (NQF 0239): Perioperative Care: Venous Thromboembolism (VTE) Prophylaxis (When Indicated in ALL Patients) National Quality Strategy Domain: Patient Safety 2018 OPTIONS FOR INDIVIDUAL MEASURES:
SCORES FOR 4 TH QUARTER, RD QUARTER, 2014
 SCORES FOR 4 TH QUARTER, 2013 3 RD QUARTER, 2014 PATIENT SATISFACTION SCORES (HCAHPS): 4 STARS OUT OF 5 (ONLY 4 AREA ACUTE CARE HOSPITALS RECEIVED A 4-STAR RATING. NONE ACHIEVED 5-STARS). STRUCTURAL MEASURES:
SCORES FOR 4 TH QUARTER, 2013 3 RD QUARTER, 2014 PATIENT SATISFACTION SCORES (HCAHPS): 4 STARS OUT OF 5 (ONLY 4 AREA ACUTE CARE HOSPITALS RECEIVED A 4-STAR RATING. NONE ACHIEVED 5-STARS). STRUCTURAL MEASURES:
Rapidly Progressive Osteoarthritis after Arthroscopic Labral Repair for Dysplasia. Dean K. Matsuda, MD Monti Khatod, MD Los Angeles, California, USA
 Rapidly Progressive Osteoarthritis after Arthroscopic Labral Repair for Dysplasia Dean K. Matsuda, MD Monti Khatod, MD Los Angeles, California, USA Recent reports of poor clinical outcomes after arthroscopic
Rapidly Progressive Osteoarthritis after Arthroscopic Labral Repair for Dysplasia Dean K. Matsuda, MD Monti Khatod, MD Los Angeles, California, USA Recent reports of poor clinical outcomes after arthroscopic
Hip and Knee Replacements
 Hip and Knee Replacements What the PCP Needs to Know Derek Ward, M.D. Assistant Professor of Orthopaedic Surgery Division of Adult Reconstruction University of California, San Francisco 12/2/2017 Disclosures
Hip and Knee Replacements What the PCP Needs to Know Derek Ward, M.D. Assistant Professor of Orthopaedic Surgery Division of Adult Reconstruction University of California, San Francisco 12/2/2017 Disclosures
What evidence exists that describes the efficacy of mechanical prophylaxis for venous thromboembolism (VTE) in adult surgical patients?
 July 2015 Rapid Review Evidence Summary McGill University Health Centre: Division of Nursing Research and MUHC Libraries What evidence exists that describes the efficacy of mechanical prophylaxis for venous
July 2015 Rapid Review Evidence Summary McGill University Health Centre: Division of Nursing Research and MUHC Libraries What evidence exists that describes the efficacy of mechanical prophylaxis for venous
Deep vein thrombosis and its prevention in critically ill adults Attia J, Ray J G, Cook D J, Douketis J, Ginsberg J S, Geerts W H
 Deep vein thrombosis and its prevention in critically ill adults Attia J, Ray J G, Cook D J, Douketis J, Ginsberg J S, Geerts W H Authors' objectives To systematically review the incidence of deep vein
Deep vein thrombosis and its prevention in critically ill adults Attia J, Ray J G, Cook D J, Douketis J, Ginsberg J S, Geerts W H Authors' objectives To systematically review the incidence of deep vein
Triple Pelvic Osteotomy
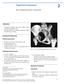 Triple Pelvic Osteotomy Peter Templeton and Peter V. Giannoudis 2 Indications Acetabular dysplasia with point loading, lateral migration, and painful limp. Hip joint should be reasonably congruent in abduction
Triple Pelvic Osteotomy Peter Templeton and Peter V. Giannoudis 2 Indications Acetabular dysplasia with point loading, lateral migration, and painful limp. Hip joint should be reasonably congruent in abduction
Management of Post-Thrombotic Syndrome
 Management of Post-Thrombotic Syndrome Thanainit Chotanaphuti Phramongkutklao College of Medicine Bangkok, Thailand President of CAOS Asia President of Thai Hip & Knee Society President of ASEAN Arthroplasty
Management of Post-Thrombotic Syndrome Thanainit Chotanaphuti Phramongkutklao College of Medicine Bangkok, Thailand President of CAOS Asia President of Thai Hip & Knee Society President of ASEAN Arthroplasty
INDICATIONS FOR THROMBO-PROPHYLAXIS AND WHEN TO STOP ANTICOAGULATION BEFORE ELECTIVE SURGERY
 INDICATIONS FOR THROMBO-PROPHYLAXIS AND WHEN TO STOP ANTICOAGULATION BEFORE ELECTIVE SURGERY N.E. Pearce INTRODUCTION Preventable death Cause of morbidity and mortality Risk factors Pulmonary embolism
INDICATIONS FOR THROMBO-PROPHYLAXIS AND WHEN TO STOP ANTICOAGULATION BEFORE ELECTIVE SURGERY N.E. Pearce INTRODUCTION Preventable death Cause of morbidity and mortality Risk factors Pulmonary embolism
Combined Hip Arthroscopy and Periacetabular Osteotomy: Intra-Articular Pathology
 Combined Hip Arthroscopy and Periacetabular Osteotomy: Intra-Articular Pathology URMC Sports Medicine and Hip Preservation Raymond J. Kenney, MD Kelly L. Adler, MEd, ATC P. Christopher Cook, MD Brian D.
Combined Hip Arthroscopy and Periacetabular Osteotomy: Intra-Articular Pathology URMC Sports Medicine and Hip Preservation Raymond J. Kenney, MD Kelly L. Adler, MEd, ATC P. Christopher Cook, MD Brian D.
COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP)
 The European Agency for the Evaluation of Medicinal Products Evaluation of Medicines for Human Use London, 16 December 1999 COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP) NOTE FOR GUIDANCE ON CLINICAL
The European Agency for the Evaluation of Medicinal Products Evaluation of Medicines for Human Use London, 16 December 1999 COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP) NOTE FOR GUIDANCE ON CLINICAL
Updates in Medical Management of Pulmonary Embolism and Deep Vein Thrombosis. By: Justin Youtsey, Elliott Reiff, William Montgomery, Grant Finlan
 Updates in Medical Management of Pulmonary Embolism and Deep Vein Thrombosis By: Justin Youtsey, Elliott Reiff, William Montgomery, Grant Finlan Objectives Describe the prevalence of PE and DVT as it relates
Updates in Medical Management of Pulmonary Embolism and Deep Vein Thrombosis By: Justin Youtsey, Elliott Reiff, William Montgomery, Grant Finlan Objectives Describe the prevalence of PE and DVT as it relates
Prevention and management of deep venous thrombosis (DVT) John Fletcher Wound Care Association of New South Wales
 Prevention and management of deep venous thrombosis (DVT) John Fletcher Wound Care Association of New South Wales Merimbula, 6 th November 2010 University of Sydney Department of Surgery Westmead Hospital
Prevention and management of deep venous thrombosis (DVT) John Fletcher Wound Care Association of New South Wales Merimbula, 6 th November 2010 University of Sydney Department of Surgery Westmead Hospital
Prevention of Venous Thromboembolism
 Prevention of Venous Thromboembolism Surgical Care Improvement Project Dale W. Bratzler, DO, MPH President and CEO Dale W. Bratzler, DO, MPH Oklahoma Foundation for Medical Quality QIOSC Medical Director
Prevention of Venous Thromboembolism Surgical Care Improvement Project Dale W. Bratzler, DO, MPH President and CEO Dale W. Bratzler, DO, MPH Oklahoma Foundation for Medical Quality QIOSC Medical Director
Hip arthroscopy. Anatomy The hip is functionally a ball and socket joint.
 Hip arthroscopy The term arthroscopy (or keyhole surgery) refers to the viewing of the inside of a joint through a small operating telescope. First described in the 1970s, arthroscopic techniques have
Hip arthroscopy The term arthroscopy (or keyhole surgery) refers to the viewing of the inside of a joint through a small operating telescope. First described in the 1970s, arthroscopic techniques have
Radiographic and Clinical Risk Factors for the Extent of Labral Injury at the Time of Hip Arthroscopy
 Radiographic and Clinical Risk Factors for the Extent of Labral Injury at the Time of Hip Arthroscopy John M. Redmond, MD Jon E. Hammarstedt, BS Asheesh Gupta, MD MPH Christine E. Stake, DHA Kevin F. Dunne,
Radiographic and Clinical Risk Factors for the Extent of Labral Injury at the Time of Hip Arthroscopy John M. Redmond, MD Jon E. Hammarstedt, BS Asheesh Gupta, MD MPH Christine E. Stake, DHA Kevin F. Dunne,
AJO. An Original Study. Ashley Levack, MAS, Atul F. Kamath, MD, and Jess H. Lonner, MD
 An Original Study Ashley Levack, MAS, Atul F. Kamath, MD, and Jess H. Lonner, MD dvances in surgical technique, patient selection, and prosthetic design for patellofemoral arthroplasty (PFA) have generated
An Original Study Ashley Levack, MAS, Atul F. Kamath, MD, and Jess H. Lonner, MD dvances in surgical technique, patient selection, and prosthetic design for patellofemoral arthroplasty (PFA) have generated
Perioperative VTE Prophylaxis
 Perioperative VTE Prophylaxis Gregory J. Misky, M.D. Assistant Professor of Medicine University Of Colorado Denver You recommend the following 72 y.o. man admitted for an elective R hip repair. Patient
Perioperative VTE Prophylaxis Gregory J. Misky, M.D. Assistant Professor of Medicine University Of Colorado Denver You recommend the following 72 y.o. man admitted for an elective R hip repair. Patient
Outcome LMWH ASA LMWH ASA
 Page 1 of 15 TABLE E-1 Incidence of Postoperative VTE Events and Major Bleeding* Total Hip Arthroplasty Total Knee Arthroplasty Outcome LMWH ASA LMWH ASA Symptomatic DVT 0.011 0.017 0.024 0.038 Symptomatic
Page 1 of 15 TABLE E-1 Incidence of Postoperative VTE Events and Major Bleeding* Total Hip Arthroplasty Total Knee Arthroplasty Outcome LMWH ASA LMWH ASA Symptomatic DVT 0.011 0.017 0.024 0.038 Symptomatic
Bone Bangalore
 Dr Suresh Annamalai MBBS, MRCS(Edn), FRCS( Tr & Orth)(Edn), FEBOT(European Board), Young Hip and Knee Fellowship(Harrogate, UK) HOD & Consultant Arthroplasty and Arthroscopic Surgeon Manipal Hospital,
Dr Suresh Annamalai MBBS, MRCS(Edn), FRCS( Tr & Orth)(Edn), FEBOT(European Board), Young Hip and Knee Fellowship(Harrogate, UK) HOD & Consultant Arthroplasty and Arthroscopic Surgeon Manipal Hospital,
Indications of Anticoagulants; Which Agent to Use for Your Patient? Marc Carrier MD MSc FRCPC Thrombosis Program Ottawa Hospital Research Institute
 Indications of Anticoagulants; Which Agent to Use for Your Patient? Marc Carrier MD MSc FRCPC Thrombosis Program Ottawa Hospital Research Institute Disclosures Research Support/P.I. Employee Leo Pharma
Indications of Anticoagulants; Which Agent to Use for Your Patient? Marc Carrier MD MSc FRCPC Thrombosis Program Ottawa Hospital Research Institute Disclosures Research Support/P.I. Employee Leo Pharma
Case Study: Nadine. Conditions Treated Hip Dysplasia. Age Range During Treatment 39 years
 Case Study: Nadine Conditions Treated Hip Dysplasia Age Range During Treatment 39 years David S. Feldman, MD Chief of Pediatric Orthopedic Surgery Professor of Orthopedic Surgery & Pediatrics NYU Langone
Case Study: Nadine Conditions Treated Hip Dysplasia Age Range During Treatment 39 years David S. Feldman, MD Chief of Pediatric Orthopedic Surgery Professor of Orthopedic Surgery & Pediatrics NYU Langone
10/8/2012. Disclosures. Making Sense of AT9: Review of the 2012 ACCP Antithrombotic Guidelines. Goals and Objectives. Outline
 Disclosures Making Sense of AT9: Review of the 2012 ACCP Antithrombotic Guidelines No relevant conflicts of interest related to the topic presented. Cyndy Brocklebank, PharmD, CDE Chronic Disease Management
Disclosures Making Sense of AT9: Review of the 2012 ACCP Antithrombotic Guidelines No relevant conflicts of interest related to the topic presented. Cyndy Brocklebank, PharmD, CDE Chronic Disease Management
VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS
 VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS KANSAS ASSOCIATION OF OSTEOPATHIC MEDICINE ANNUAL CME CONVENTION APRIL 13, 2018 THREE
VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS KANSAS ASSOCIATION OF OSTEOPATHIC MEDICINE ANNUAL CME CONVENTION APRIL 13, 2018 THREE
Treatment Of Heterotopic Ossification After Hip Arthroscopy
 Treatment Of Heterotopic Ossification After Hip Arthroscopy ISHA Annual Scientific Meeting 2012 Boston, MA Crispin Ong MD, Michael Hall MD, Thomas Youm MD Disclosures Consultancy: Arthrex, Depuy Lectures/speakers
Treatment Of Heterotopic Ossification After Hip Arthroscopy ISHA Annual Scientific Meeting 2012 Boston, MA Crispin Ong MD, Michael Hall MD, Thomas Youm MD Disclosures Consultancy: Arthrex, Depuy Lectures/speakers
CLINICS IN SPORTS MEDICINE
 Clin Sports Med 25 (2006) 365 369 CLINICS IN SPORTS MEDICINE A Acetabular labrum, tears of, hip arthroscopy in, 264 Acetabular rim, trimming of, and labral repair, new method for, 293 297 Acetabulum, femoral
Clin Sports Med 25 (2006) 365 369 CLINICS IN SPORTS MEDICINE A Acetabular labrum, tears of, hip arthroscopy in, 264 Acetabular rim, trimming of, and labral repair, new method for, 293 297 Acetabulum, femoral
New Antithrombotic and Antiplatelet Drugs in CAD : (Factor Xa inhibitors, Direct Thrombin inhibitors and Prasugrel)
 New Antithrombotic and Antiplatelet Drugs in CAD : (Factor Xa inhibitors, Direct Thrombin inhibitors and Prasugrel) Limitations and Advantages of UFH and LMWH Biological limitations of UFH : 1. immune-mediated
New Antithrombotic and Antiplatelet Drugs in CAD : (Factor Xa inhibitors, Direct Thrombin inhibitors and Prasugrel) Limitations and Advantages of UFH and LMWH Biological limitations of UFH : 1. immune-mediated
Abstract Introduction Currently there are no consensuses in the national guidance on
 THIEME Review Article e191 A Systematic Review on the Use of Aspirin in the Prevention of Deep Vein Thrombosis in Major Elective Lower Limb Orthopedic Surgery: An Update from the Past 3 Years Dylan A.
THIEME Review Article e191 A Systematic Review on the Use of Aspirin in the Prevention of Deep Vein Thrombosis in Major Elective Lower Limb Orthopedic Surgery: An Update from the Past 3 Years Dylan A.
*Corresponding Author:
 Audit of venous thromboembolism prophylaxis administered to general surgical patients undergoing elective and emergency operations at National Hospital, Sri Lanka *Migara Seneviratne 1, Asanka Hemachandra
Audit of venous thromboembolism prophylaxis administered to general surgical patients undergoing elective and emergency operations at National Hospital, Sri Lanka *Migara Seneviratne 1, Asanka Hemachandra
