Središnja medicinska knjižnica
|
|
|
- Bernard Turner
- 5 years ago
- Views:
Transcription
1 Središnja medicinska knjižnica Šmigovec I., Ðapić T., Trkulja V. (2014) Ultrasound screening for decentered hips in children with severe cerebral palsy: a preliminary evaluation. Pediatric Radiology, 44 (9). pp ISSN University of Zagreb Medical School Repository
2 Ultrasound screening for decentered hips in children with severe cerebral palsy: a preliminary evaluation Igor Šmigovec 1, Tomislav Đapić 1, Vladimir Trkulja 2 1 Department of Orthopedic Surgery, University Hospital Center Zagreb, Zagreb University School of Medicine, Zagreb, Croatia 2 Zagreb University School of Medicine, Zagreb, Croatia Corresponding author: Igor Šmigovec, MD Department of Orthopedic Surgery University Hospital Center Zagreb Zagreb University School of Medicine Šalata 6, Zagreb, Croatia ortopedija@yahoo.com phone: Authors have no conflict of interest to declare. This study received no funding/support. 1
3 Abstract Background. Ultrasound (US) is routinely used for hip screening in children with developmental hip disorder, whereas standard hip surveillance in children with cerebral palsy (CP) is based on repeated X-ray assessments. Objective. To evaluate US as a diagnostic tool in screening for decentered hips in children with CP. Patients and Methods. Prospective, diagnostic single-center assessor-blind study. Consecutive CP patients (age 2-8 years) with severe motor disability (unable to walk unaided) underwent US (lateral longitudinal scan to determine lateral head distance, LHD) and X-ray hip assessment (migration percentage, MP). Diagnostic properties of LHD in detecting hips with MP 33% (requires preventive treatment) were evaluated overall (n=100) and for hips assessed at the age (n=38) or 60< to 96 months (n=68). Fifty hips underwent US assessment by two investigators to evaluate inter-rater reliability and agreement. Results. Prevalence of MP 33% was 22.0% overall and 26.2% and 19.4% in the two age-based subsets, respectively. LHD well discriminated hips with MP 33% (areas under the ROC curves 94%, 99% and 92%, respectively). At the optimum cut-off values of LHD (5.0, 5.0 and 4.8 mm, respectively), sensitivity was 95.5%, 100% and 100% overall and in the two age-based subsets, respectively, whereas specificity was 85.9%, 96.4%, 72.0%, respectively. Consequently, positive predictive value was relatively low, but negative predictive value was 98.5% (95% CI ) overall and 100% (97.5% one-sided CI ) and 100% (97.5 one-sided CI ) in the two age-based subsets, respectively. Inter-rater reliability was high (intraclass correlation coefficient= 0.98, 95%CI ) and 95% limits of agreement were reasonably narrow ( mm to mm). Conclusion. In children with CP, US can be reliably used in screening for decentered hips and can greatly reduce the need for repeated X-ray assessments. Key words: cerebral palsy, hip migration, ultrasound, X-ray, diagnosis 2
4 Introduction At birth, children with cerebral palsy (CP) have normal hips but eccentric forces from spastic adductors and flexors tend to change the structure of the developing joint. Muscle imbalance may result in lateralization (decentered hips) and, eventually, in more advanced abnormalities hip dysplasia and hip dislocation [1]. Hip migration in CP patients is rather common, particularly among children who cannot walk unaided. The changes become noticeable around the age of two and the risk of hip dislocation is highest before seven years of age [1]. Hip migration and/or displacement can cause severe pain, loss of seating balance and comfort, progression of scoliosis (if present), whereas progressive hip contracture makes hygiene difficult [2, 3]. However, advanced hip lateralization is preventable and successful screening programs have been developed based on repeated clinical and radiological (X-ray) evaluations, typically in 6-8-month intervals and, where needed, introduction of early preventive treatments [4-6]. The classical X-ray diagnosis of decentered hips is based on determination of the migration percentage (MP) which defines the part (%) of the femoral head not covered by the acetabulum [7](Fig. 1), whereas diagnosis of acetabular dysplasia is usually based on determination of the acetabular index (AI)[8](Fig. 1). The aim is to detect hips with MP indicative of a need for preventive treatment: typically, when MP 33%, intensive conservative or preventive surgical treatment is indicated, although some authors suggest MP 25 as a threshold [9, 10]. The limitation of this screening scheme lies with the fact that infants are repeatedly exposed to X-rays. Children suffering from developmental dysplasia of the hip (DDH) also require repeated radiographic assessments in order to prevent hip dislocation. The use of ultrasound in DDH has been widely accepted during the past 20 years. Determination of the lateral head distance (LHD) which defines, in millimeters, the part of the femoral head not covered by the bony acetabulum (Fig. 1) shows good concordance with MP values (children 2 years of age) and ultrasound has replaced X-ray diagnostics in this setting to a great extent [11]. However, the experience with ultrasound in DDH cannot be simply transferred to children with CP the biomechanics of hip changes in the two conditions is considerably different. In DDH, acetabular dysplasia is a primary disorder and femoral head migration 3
5 occurs as a consequence, typically in the anterior and lateral direction [10]. In CP, muscle imbalance forces femoral head to migrate typically in the posterior and lateral direction and acetabular dysplasia is a secondary development. We therefore aimed to assess diagnostic value of the ultrasound measure LHD in screening for decentered hips in children with severe CP at the age between 2 (the earliest time to expect lateralization) and 8 years (risk of relevant lateralization disappears). Patients and methods General design and ethics This was a prospective, single-center, investigator-blind diagnostic study conducted between March 2010 and April The study was approved by the local University School of Medicine Ethics Committee. Standard hip surveillance procedure, eligibility for the present analysis and patient flow The standard hip surveillance procedure in children with CP (age 2-8 years) is based on clinical assessment (hip abduction with the hips and knees extended) and on hip X-rays [4]. Hip abduction is assessed every 6 months: if >45, regular clinical checks are continued without X-rays; if 45, a child is considered at a high risk of a relevant hip lateralization (MP 33%) and a hip X-ray is indicated (always both hips). If MP <25%, regular clinical checks are continued and X-ray is repeated annually, whereas if MP is 25% to 32%, X-ray is repeated every 6 months. In non-ambulatory children with CP, i.e., those with a severe bilateral spastic CP level IV or V according to the gross motor functions classification system (GMFCS) [12], hip abduction is most commonly 45 and X-rays are repeated in 6-8 month intervals or annually, depending on the actual MP. Monitoring is continued until a child is 8 years old. Should MP 33% be detected, monitoring after corrective interventions follows the same general scheme [4]. Eligible for the present analysis were consecutive children with CP who met the following criteria: a) informed consent (parents/guardians); b) age 24 to 96 months (inclusive); c) GMFCS level IV or V. Exclusion criteria were: a) previous surgical interventions to the hip; b) other conditions affecting the 4
6 hip, e.g., transient synovitis, Legg-Calve-Perthes disease or slipped capital femoral epiphysis. Generally, patients (hips) were assessed regardless of whether examined for the first time or at follow-up visits. In line with the indication, both hips underwent X-ray and ultrasound (US) evaluation. However, once MP 33% had been detected (unilaterally or bilaterally), further radiological assessments for this particular child were not considered for the present analysis. Hence, some patients (hips) provided X-ray/US data on more than one occasion (Fig. 2), but at each assessment the investigators were fairly unprejudiced about the local (anatomical) hip condition. Primary objective and methods to ascertain investigator blind The primary objective was to assess whether the ultrasound measure lateral head distance (LHD)[11, 13] (Fig. 1) could be meaningfully used in hip screening in children with severe CP, i.e., whether it could detect the level of hip lateralization defined as MP 33%. Clinical evaluation was performed by the same experienced investigator (IŠ, 7 years of experience as a pediatric orthopedic surgeon) and, when indicated, anteroposterior hip X-ray followed. Radiographs were evaluated by another experienced investigator (TĐ, 17 years of experience as a pediatric orthopedic surgeon, >5000 hip X- ray assessments in children) unaware of the clinical/us status. Ultrasound assessment was subsequently performed by the investigator unaware of the X-ray finding (IŠ, >3000 US hip assessments in children). Fifty hips underwent US examination by both investigators (IŠ and TĐ; TĐ with >6000 US hip assessments), independently, on the same day. No formal randomization was employed for this purpose: patients (hips) were evaluated consecutively, with no specific selection criteria or assessment order, until 50 hips were analyzed. In this case, US was performed before the X- ray evaluation. X-ray assessment (the standard of truth ) All patients (hips) underwent the same standard anterioposterior X-ray assessment (RADSpeed apparatus, Shimadzu Corp., Kyoto, Japan; tube voltage range KV; tube current range ma; entrance surface dose range mgy; dose-area product range mgy*cm 2 )[4]: children were positioned with the pelvis horizontal, flat and level and the legs were positioned almost parallel 5
7 to each other (neutral abduction/adduction) with the patellae facing upwards; in the case of a fixed flexion deformity giving a lordosis, the legs were raised until the lumbar spine flattened. Migration percentage (MP) and acetabular index (AI)(Fig. 1) were determined. In the case of the Gothic arch formation of the lateral acetabular margin, the midpoint of the arch was to be used as a reference point for calculation of MP (Fig. 1) [14]. Figure 3 shows a marked bilateral hip decentration in a 39 months old girl with MP=55%. Ultrasound assessment (the test procedure ) All patients underwent the same standardized real-time ultrasound assessment (Logiq 200 apparatus, GE Medical Systems, Milwaukee, WI, USA) being positioned in the same manner as for the X-ray, and using a method validated in DDH [11, 13]. Briefly [11, 13],scanning was performed from the lateral aspect of the hip region with a 5 MHz linear transducer. With the transducer kept parallel with the long axis of the body, a lateral longitudinal scan was employed showing the lateral anatomic landmarks of the hip joint. When depicting the central part of the femoral head, the distance from the lateral tangent of the ossification center to the lateral bony acetabular rim lateral head distance (LHD, millimeters) - was measured to represent the uncovered part of the femoral head and indicate lateralization of the femoral head relative to the acetabulum. When the entire bony femoral head was medial to the acetabular bony rim, LHD was given a negative sign.. The anatomical structures on ultrasound image are depicted 90 rotated to those on a radiograph (Fig. 1). Figure 3 shows LHD in a decentered hip (MP=55%) in a 39 months old girl. Sample size and power considerations We expected around 25% of the examined hips to have MP 33% ( event prevalence ). Considering the experience with ultrasound in DDH [11, 13], we expected LHD to have a high discriminative power defined as an area under the receiver-operating characteristic (ROC) curve of at least 90%. With the assumed event prevalence of 25% and in order to achieve 90% power to detect a difference between an area under the ROC curve of 90% (highly discriminative test) and an area under the ROC 6
8 curve of 75% (modestly discriminative test) as significant at a two-sided alpha level 0.05, we calculated that at least 87 hips needed to be examined. Data analysis The present analysis refers to 100 X-ray/US hip images obtained from 36 children all of whom underwent bilateral radiological hip assessment at least once, whereas in 9 children the hips were assessed on repeated occasions (Fig. 2). Although the collected data were clustered by nature (two hips within a child; repeated assessments within a hip [child]) we assumed that in this specific case they could be considered numerically independent, i.e., that each pair of radiological data (Xray, US per hip) represented a different anatomical condition and corresponding (different) radiological values (MP, LHD). The assumption was based on the following reasoning: a) two hips (assessed at one time-point) in one child are not anatomically identical, i.e., each has specific key radiological measures; b) at this age and condition, anatomical hip particulars should not be expected to be identical when looked at 6-8 months apart (i.e., hip lateralization may progress or reduce between visits). To evaluate this assumption, we first determined agreement between radiological parameters (MP, LHD) established for two hips (left and right) at one visit (all included children, radiological data obtained at the first assessment point), and between radiological parameters established on two separate assessments of the same hips (children i.e., hips assessed on the first and the second assessment point, Fig. 2). As depicted in Fig. 4a, radiological measures (MP by X-ray, LHD by US) taken on two hips in the same child on one occasion showed a considerable (numerical) disagreement the 95% limits of agreement extended between -33.4% and 31.9% for MP and between -5.1 to 5.2 millimeters for LHD. Similarly, although somewhat less, the disagreement was considerable regarding repeated assessments on the same hips (Fig. 4b). In the next step, prevalence of MP 33% was analyzed by fitting several generalized linear mixed models with logit link and binomial distribution (logistic models) with LHD as a fixed effect and different modeling of random effects. The first model included patients as a G-side random effect to account for spatial clustering ( hips within patients ) and assessment point as an R-side (residual) random effect to account for 7
9 temporal clustering (repeated assessments on the same hips). However, the distribution of random effects was far from normal, residual variability was not properly modeled (Pearson Chi 2 /df= 0.07) and the amount of variability accounted for by the R-side random effect was negligible (covariance parameter estimate 0.029, standard error 0.163). The subsequent models included only G-side random effects with maximum likelihood estimation (Gauss-Hermite quadrature): a) a model with one G-side random effect to account for clustering of hips within patients (36 patients with a maximum of 8 observations per patient): b) a model with one G-side random effect that considered hips (nested in patients ) as clusters of radiological observations (1-4 per hip); c) a model with two G-side random effects (i) observations clustered in hips(patients) and (ii) patients (as a third level). The last model showed the best fit: random effects were closest to the normal distribution, - 2Log Likelihood was the lowest (51.77), residual variance was modeled better than in other models, however still poorly (Pearson Chi 2 /df= 0.21) and the test of covariance parameter estimates was not significant (df= 2; -Log Likelihood= 56.02, Chi 2 =4.26, p=0.119). The estimated effect of LHD was OR=3.44, 95% CI On the other hand, a fixed-effect model (LHD as a single independent) yielded only a slightly higher 2Log Likelihood (56.03), but with practically normal distribution of residuals and with no signs of overdispersion (Pearson Chi 2 /df= 1.02) which, generally, could indicate a need to account for correlation within data. The effect of LHD was OR=3.00, 95% CI Overall, we concluded that the most appropriate way to analyze the data is to treat them as independent observations. Discriminative properties of LHD in respect to MP 33% were evaluated by logistic regression and the receiver operating characteristics (ROC) curve analysis. Diagnostic performance of LHD was determined at a cut-off value with an optimal combination of sensitivity and specificity (sensitivity, specificity, false-positive rate, false-negative rate, proportion of correctly classified hips, positive predictive value [PPV], negative predictive value [NPV], probability of an event with a negative test, likelihood ratio for a positive test [LR+] and a negative test [LR-] and diagnostic odds ratio). Since the probability of finding incident hips with MP 33% declines with age and since children with once detected MP 33% were not further included in the present analysis, we assumed 8
10 that the event prevalence would be lower for hips assessed at older age. Since event prevalence can affect tests of diagnostic performance (i.e., PPV, NPV), the analysis was performed for the entire data set and also separately for hips assessed at the age months and hips assessed at the age 60< and 96 months. Hips that underwent ultrasound assessment by two independent investigators were used to assess inter-rater reliability (intraclass correlation coefficient, ICC) and limits of agreement for LHD. We used SAS for Windows version 9.3 (SAS Inc., Cary, NC, USA). Results The present analysis includes a total of 100 radiological (X-ray and ultrasound, US) hip assessments, 38 of which refer to hips examined at the age of months and 62 refer to hips assessed at the age of 60< and 96 months. Migration percentage (MP) 33% was detected in 22 (22%) cases overall and in 10 (26.3%) and 12 (19.4%) cases in the two age-based subsets, respectively. Other radiological particulars are summarized in Table 1. Does LHD discriminate between hips with MP 33% and MP<33%? Based on the areas under the ROC curves (all estimates >90%, all 95% CIs entirely >85%), lateral head distance (LHD) discriminated well between the hips with MP 33% and those with MP <33% - considering all hips, as well as considering hips assessed at the age months and those assessed at the later age (Fig. 5). Cut-off LHD values with optimum levels of sensitivity and specificity were 5 mm, 5 mm and 4.8 mm considering all hips and those in the two age-based subsets, respectively (Table 2). In all three (sub)sets, LHD showed very high sensitivity, i.e., 95%-100% (Table 2). Considering hips assessed at the age months, specificity was also high (96.4%), consequently false positive and false negative rates were low. In this subset, LHD showed properties of an excellent diagnostic test both considering its exclusion and confirmation properties NPV was 100% leaving no probability of MP 33% with a negative test (LHD <5 mm), and PPV exceeded 90% indicating <10% probability of no event with a positive test (LHD 5 mm) (Table 2). However, considering all hips (cut-off 5 mm) and those assessed at the older age (cut-off 4.8 mm), specificity 9
11 was relatively modest (86% and 72%, respectively) leaving a high false positive rate resulting in a poor PPV (Table 2). Still, negative predictive value in both sets was almost absolute (Table 2). In all three sets, general diagnostic test characteristics, i.e., likelihood ratios for a positive or a negative test and the overall diagnostic odds ratios were excellent (Table 2). Concordance of lateral head distance measurement by ultrasound between two raters Measurements of LHD by two raters in 50 hips were very similar regarding the means and intersubject variability (very close between-subject standard deviations) (Table 3). Intraclass correlation coefficient (0.980) indicated a high inter-rater reliability and within-subject variability (variance coefficient) was minimal (Table 2). The limits of agreement indicated that in 95% of the cases the difference between the two raters was approximately between -1.0 and 1.0 millimeter (Fig. 6). Discussion In children with cerebral palsy (CP), migration of the femoral head is rather common but severe changes of the hip joint can be precluded by timely introduction of preventive treatments. Hence, patients undergo regular clinical and X-ray assessments in order to detect whether the threshold values of migration percentage (MP) are reached [6]. In children with developmental hip dysplasia (DDH), ultrasound has greatly replaced X-ray assessments in the screening programs [11]. Considering the substantial biomechanical differences between hip lateralization in CP and DDH, we aimed to evaluate ultrasound as a diagnostic aid in screening for decentered hips specifically in children with CP. In the present preliminary analysis we embraced CP patients who are typically closely monitored for hip lateralization, i.e., those with the most severe motor disability (GMFCS levels IV and V; children with lower levels are not routinely submitted to regular X-ray assessments) at the age between 24 and 96 months since incident hip migration is rare in children above or below this age. The limitations of the study are relatively modest single-center sample and inter-rater assessment of the method based only on two assessors. However, we have ascertained a fair level of internal validity by employing an appropriate standard of truth and independence of ultrasound and 10
12 X-ray evaluations. The present results strongly suggest that using the approach implemented in hip screening in DDH (lateral longitudinal scan) [11], ultrasound measure LHD can be successfully used in screening for decentered hips in children with CP, as well. In respect to discrimination between hips with MP 33% and those with MP <33%, a commonly used threshold for introduction of preventive treatments [9], LHD shows properties of an excellent screening procedure it is quick, simple and straightforwardly excludes the need for an X-ray assessment as a definite diagnostic tool. It should be noted that NPV was consistently high at different event prevalence - 26% (age months), 19% (age 60< and 96 months) and 22% (overall). However, extension of the current study is underway that should enlarge the sample size across tighter age-based subsets possibly resulting in different prevalence of MP 33% and should allow for further evaluation of predictive values of LHD. Also, it should enable validation of LHD (and possibly other ultrasound parameters) against other diagnostic MP thresholds (e.g., 25%, 60%) and acetabular index (AI). Only four hips in the current sample had AI >30 (acetabular dysplasia), which was too few for a meaningful evaluation of discriminative properties of LHD (although all four hips had LHD well above 5 mm). Finally, inter-rater evaluation of LHD measurement indicated that it could be successfully implemented by different, comparably experienced ultrasound assessors. Conclusion The ultrasound measure lateral head distance could be used as a screening test for decentered hips in children with CP that could considerably reduce the need for repeated X-ray assessments. 11
13 References 1. Rang M, Silver R, de la Garza J (1986) Cerebral palsy. In: Lovell WW, Winter RB, eds. Pediatric Orthopedics, 2 nd ed. Philadelphia, PA: JB Lippincott Co.; p Hodgkinson I, Jindrich ML, Duhaut P et al (2001) Hip pain in 234 non-ambulatory adolescents and young adults with cerebral palsy: a cross-sectional multicentre study. Dev Med Child Neurol 43: Knapp DR Jr (2002) Untreated hip dislocation in cerebral palsy. J Pediatr Orthop 22: Dobson F, Boyd RN, Parrott J et al (2002) Hip surveillance in children with cerebral palsy. J Bone Joint Surg Br 84-B: Hägglund G, Andersson S, Düppe H et al (2005) Prevention of dislocation of the hip in children with cerebral palsy. The first ten years of a population-based prevention programme. J Bone Joint Surg Br 87-B: Elkamil AI, Andersen GL, Hägglund G et al (2011) Prevalence of hip dislocation among children with cerebral palsy in regions with and without a surveillance programme: a cross sectional study in Sweden and Norway. BMC Musculoskelet Disord 12:284. doi: / Reimers J (1980) The stability of the hip in children: a radiological study of the results of muscle surgery in cerebral palsy. Acta Orthop Scand Suppl 184: Hilgenreiner H (1925) Zur frühdiagnose und frühbehandlung der angeborenen hüftgelenksverrenkung. Med Klin 21: , Hägglund G, Lauge-Pedersen H, Persson M (2007) Radiographic threshold values for hip screening in cerebral palsy. J Child Orthop 1: Miller F (2005) Cerebral palsy. New York: Springer Inc. 11. Tegnander A, Terjesen T (1999) Reliability of ultrasonography in the follow-up of hip dysplasia in children above 2 years of age. Acta Radiologica 40:
14 12. Palisano R, Rosenbaum P, Walter S et al (1997) Development and reliability of a system to classify grossmotor function in children with cerebral palsy. Dev Med Child Neurol 39: Terjesen T, Rundén TO, Johnsen HM (1991) Ultrasound in the diagnosis of congenital dysplasia and dislocation of the hip joints in children older than two years. Clin Orthop Relat Res 262: Parrott J, Boyd RN, Dobson F et al (2002) Hip displacement in spastic cerebral palsy: repeatability of radiologic measurement. J Pediatr Orthop 22:
15 Fig. 1 Schematic representation of the X-ray and ultrasound assessment of hips in children with cerebral palsy. An anteroposterior X-ray of a hip (left) is used to detectmigration percentage (MP=a/b x 100) that defines the proportion of the femoral head not covered by the acetabulum. Distance a is a distance between the acetabular rim and the lateral tangent of the femoral head, and distance b is a distance between the medial and the lateral tangent of the femoral head (both in millimeters). Acetabular index (AI) is an angle and is expressed in degrees. In the case of the Gothic arch formation of the lateral acetabular margin (middle), the midpoint of the arch is used as a reference point for calculation of MP. The diagram on the right depicts elements of the hip and surrounding structures as visualized by a longitudinal lateral ultrasound scan. Lateral head distance (LHD) is a distance (in millimeters) between the lateral tangent of the bony femoral head and iliac baseline and defines the part of the femoral head not covered by the acetabulum. LHD determined by the ultrasound corresponds to distance a determined on the anteroposterior radiograph. 14
16 Fig. 2 Patients and hips in the present analysis. All X-ray and ultrasound (US) hip assessments were always performed bilaterally. A total of 36 children were included, 27 of whom underwent only one assessment and 9 patients underwent more than one assessment (6-8-month intervals). Once migration percentage (MP) 33%had been detected (unilaterally or bilaterally), further radiological hip assessments for this particular child were not considered for the present analysis. Overall, 100 X- ray images and corresponding US hip scans were obtained. 15
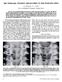
17 Fig. 3 Anteroposterior X-ray (left) of a marked bilateral hip decentration (migration percentage, MP, well above 33%) in a 39 months old girl with a severe bilateral spastic cerebral palsy (gross motor functions classification system level V) and a longitudinal lateral ultrasound scan of the right hip in the same patient (right) indicating lateral head distance (LHD) of 6.5 millimeters. In the clinical examination, passive abduction for both hips was possible to a maximum of 20 degrees. The girl underwent bilateral surgical preventive treatment. 16
18 Fig. 4 Agreement in radiological measures (migration percentage, lateral head distance) between two hips in the same child (a) and between two assessments in the same hip (b). Agreement plots with upper (UL) and lower (LL) 95% limit of agreement and mean difference ( ). 17
19 Fig. 5 Receiver-operating characteristics (ROC) curve (dashed lines) analysis for lateral head distance as a diagnostic test for migration percentage 33% regarding all assessed hips and hips assessed at different age (months). Area under the curve (AUC) is given with 95 confidence intervals. Arrows depict points with an optimum relationship between sensitivity and specificity. 18
20 Fig. 6 Agreement plot for lateral head distance (in millimeters) measurement by ultrasound based on 50 hips assessed by two investigators with upper (UL) and lower (LL) 95% limits of agreement. 19
21 Table 1 Characteristics of the analyzed hips Overall Age at assessment months Age at assessment 60< and 96 months Number of assessed hips Age at hip assessment (months) 69 (24-96) 47 (24-58) 78 (61-96) Main radiological findings Migration percentage (MP)(%)(X-ray) 25 (9-100) 25.5 ( ) 24.5 ( ) MP 33% 22 (22.0) 10 (26.3) 12 (19.4) Lateral head distance (mm)(ultrasound) 3.9 ( ) 3.1 ( ) 4.0 ( ) Other X-ray findings MP=33%-99% (subluxation) 20 (20.0) 8 (21.1) 12 (19.4) MP>60% (needs reconstruction) 3 (3.0) 3 (7.9) 0 MP=100% (luxation) 2 (2.0) 2 (5.3) 0 Acetabular index (AI)( ) 20 (10-35) 21 (10-35) 18 (12-34) AI >30 (acetabular dysplasia) 4 (3.9) 3 (7.9) 1 (1.6) Data are counts (%) or medians (range) 20
22 Table 2 Diagnostic properties of ultrasonographically measured lateral head distance (LHD) as a test for detecting hips with migration percentage 33% ( event ) considering all hips and considering hips assessed at the age months or at the age 60< and 96 months. Estimates are given with 95% confidence intervals. All assessed hips Age months Age 60< and 96 months Number of hips Event prevalence [n(%)] 22 (22.0) 10 (26.3) 12 (19.4) Optimal cut-off LHD value (mm) a Sensitivity (true positives) (%) 95.5 ( ) 100 ( ) b 100 ( ) b Specificity (true negatives) (%) 85.9 ( ) 96.4 ( ) 72.0 ( ) 1-specificity (false positives) (%) 14.1 ( ) 3.6 ( ) 28.0 ( ) 1-sensitivity (false negatives) (%) 4.5 ( ) 0 (0-30.8) b 0 (0-26.5) b Correctly classified (%) Positive predictive value (%) 65.6 ( ) 90.9 ( ) 46.2 ( ) Negative predictive value (%) 98.5 ( ) 100 ( ) b 100 ( ) b Event probability - negative test (%) 1.5 (0-7.9) 0 (0-12.8) b 0 (0-9.7) b Likelihood ratio - positive test 6.8 ( ) 28.0 ( ) 3.6 ( ) Likelihood ratio - negative test 0.05 ( ) 0 (0-0.29) 0 (0-0.34) Diagnostic odds ratio 128 ( ) a Cut-off value with an optimal level of sensitivity and specificity. LHD values cut-off are considered a positive test. Values <cut-off are considered a negative test. b One-sided 97.5 confidence interval 21
23 Table 3 Inter-rater reliability of lateral head distance (in millimeters) measurement by ultrasound based on 50 hips assessed by two investigators Rater 1 Rater 2 Mean Standard deviation Standard error % CI around mean ICC= (95% CI to 0.991) WSV coefficient = (95% CI to 0.120) ICC, intraclass correlation coefficient (coefficient of reliability); WSV, within-subject variance 22
Risk Factors for Hip Displacement in Children With Cerebral Palsy: Systematic Review
 REVIEW ARTICLE Risk Factors for Hip Displacement in Children With Cerebral Palsy: Systematic Review Blazej Pruszczynski, MD,* Julieanne Sees, DO,w and Freeman Miller, MDw Background: When hip displacement
REVIEW ARTICLE Risk Factors for Hip Displacement in Children With Cerebral Palsy: Systematic Review Blazej Pruszczynski, MD,* Julieanne Sees, DO,w and Freeman Miller, MDw Background: When hip displacement
Windswept hip deformity in children with cerebral palsy: a population-based prospective follow-up
 DOI 10.1007/s11832-016-0749-1 ORIGINAL CLINICAL ARTICLE Windswept hip deformity in children with cerebral palsy: a population-based prospective follow-up Gunnar Hägglund 1 Henrik Lauge-Pedersen 1 Måns
DOI 10.1007/s11832-016-0749-1 ORIGINAL CLINICAL ARTICLE Windswept hip deformity in children with cerebral palsy: a population-based prospective follow-up Gunnar Hägglund 1 Henrik Lauge-Pedersen 1 Måns
Hip ultrasound for developmental dysplasia: the 50% rule
 Pediatr Radiol (2017) 47:817 821 DOI 10.1007/s00247-017-3802-4 COMMENTARY Hip ultrasound for developmental dysplasia: the 50% rule H. Theodore Harcke 1 & B. Pruszczynski 2 Received: 27 October 2016 /Revised:
Pediatr Radiol (2017) 47:817 821 DOI 10.1007/s00247-017-3802-4 COMMENTARY Hip ultrasound for developmental dysplasia: the 50% rule H. Theodore Harcke 1 & B. Pruszczynski 2 Received: 27 October 2016 /Revised:
The prognostic value of the head-shaft angle on hip displacement in children with cerebral palsy
 J Child Orthop (2015) 9:129 135 DOI 10.1007/s11832-015-0654-z ORIGINAL CLINICAL ARTICLE The prognostic value of the head-shaft angle on hip displacement in children with cerebral palsy J. P. J. van der
J Child Orthop (2015) 9:129 135 DOI 10.1007/s11832-015-0654-z ORIGINAL CLINICAL ARTICLE The prognostic value of the head-shaft angle on hip displacement in children with cerebral palsy J. P. J. van der
The natural history of hip development in cerebral palsy
 DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE The natural history of hip development in cerebral palsy TERJE TERJESEN Department of Orthopaedic Surgery, Oslo University Hospital, Rikshospitalet
DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE The natural history of hip development in cerebral palsy TERJE TERJESEN Department of Orthopaedic Surgery, Oslo University Hospital, Rikshospitalet
British Columbia s Consensus on Hip Surveillance for Children with Cerebral Palsy
 British Columbia s Consensus on Hip Surveillance for Children with Cerebral Palsy Information for Health Care Professionals Caring for Children with Cerebral Palsy 2018 SUMMARY British Columbia s Consensus
British Columbia s Consensus on Hip Surveillance for Children with Cerebral Palsy Information for Health Care Professionals Caring for Children with Cerebral Palsy 2018 SUMMARY British Columbia s Consensus
A comparison of ultrasonography and radiography in the management of infants with suspected developmental dysplasia of the hip
 Acta Orthop. Belg., 2013, 79, 524-529 ORIGINAL STUDY A comparison of ultrasonography and radiography in the management of infants with suspected developmental dysplasia of the hip Hakan Atalar, Halil Dogruel,
Acta Orthop. Belg., 2013, 79, 524-529 ORIGINAL STUDY A comparison of ultrasonography and radiography in the management of infants with suspected developmental dysplasia of the hip Hakan Atalar, Halil Dogruel,
Guideline for surveillance for hip subluxation and dislocation in children and young people with cerebral palsy. Speciality: General
 Title of Guideline Contact Name and Job Title (author) Directorate & Speciality Guideline for surveillance for hip subluxation and dislocation in children and young people with cerebral palsy Janet Corderoy,
Title of Guideline Contact Name and Job Title (author) Directorate & Speciality Guideline for surveillance for hip subluxation and dislocation in children and young people with cerebral palsy Janet Corderoy,
Ultrasound and radiography findings in developmental dysplasia of the hip: a pictorial review
 Ultrasound and radiography findings in developmental dysplasia of the hip: a pictorial review Poster No.: C-2542 Congress: ECR 2012 Type: Educational Exhibit Authors: S. P. Ivanoski; Ohrid/MK Keywords:
Ultrasound and radiography findings in developmental dysplasia of the hip: a pictorial review Poster No.: C-2542 Congress: ECR 2012 Type: Educational Exhibit Authors: S. P. Ivanoski; Ohrid/MK Keywords:
Hip surveillance at your fingertips!
 Hip surveillance at your fingertips! HipScreen: An App for Community-Based Hip Surveillance Hip Surveillance for children with cerebral palsy can lead to early detection and treatment of hip dysplasia,
Hip surveillance at your fingertips! HipScreen: An App for Community-Based Hip Surveillance Hip Surveillance for children with cerebral palsy can lead to early detection and treatment of hip dysplasia,
Postural Therapy Update 12:45-1:30 Thursday Dec 6, Ginny Paleg, PT, DScPT Montgomery County Infants and Toddlers Program
 Postural Therapy Update 12:45-1:30 Thursday Dec 6, 2018 Ginny Paleg, PT, DScPT Montgomery County Infants and Toddlers Program ginny@paleg.com Children with contractures and deformities have pain Let s
Postural Therapy Update 12:45-1:30 Thursday Dec 6, 2018 Ginny Paleg, PT, DScPT Montgomery County Infants and Toddlers Program ginny@paleg.com Children with contractures and deformities have pain Let s
Evaluation of three ultrasound techniques used for the diagnosis of developmental dysplasia of the hip (DDH)
 Evaluation of three ultrasound techniques used for the diagnosis of developmental dysplasia of the hip (DDH) Poster No.: C-2049 Congress: ECR 2012 Type: Scientific Exhibit Authors: E. M. D. B. Pacheco,
Evaluation of three ultrasound techniques used for the diagnosis of developmental dysplasia of the hip (DDH) Poster No.: C-2049 Congress: ECR 2012 Type: Scientific Exhibit Authors: E. M. D. B. Pacheco,
Case Developmental dysplasia of hip
 Case 13303 Developmental dysplasia of hip Hidayatullah Hamidi, Sahar Maroof French medical institute for children, Kabul, Afghanistan Email: Hedayatullah.hamidi@gmail.com Maroofsahar1@gmail.com French
Case 13303 Developmental dysplasia of hip Hidayatullah Hamidi, Sahar Maroof French medical institute for children, Kabul, Afghanistan Email: Hedayatullah.hamidi@gmail.com Maroofsahar1@gmail.com French
Friday Teaching. Bones
 Friday Teaching Bones Regarding slipped femoral capital epiphysis It represents Salter Harris type V injury 20% are bilateral There is slight widening of the joint space Slip is typically posteromedial
Friday Teaching Bones Regarding slipped femoral capital epiphysis It represents Salter Harris type V injury 20% are bilateral There is slight widening of the joint space Slip is typically posteromedial
Prevalence and predictive factors of hip displacement in children with cerebral palsy at Paediatric Institute, Kuala Lumpur Hospital
 Neurology Asia 2017; 22(3) : 243 252 Prevalence and predictive factors of hip displacement in children with cerebral palsy at Paediatric Institute, Kuala Lumpur Hospital Bih-Hwa Ching MBBS MRCPCH, Teik-Beng
Neurology Asia 2017; 22(3) : 243 252 Prevalence and predictive factors of hip displacement in children with cerebral palsy at Paediatric Institute, Kuala Lumpur Hospital Bih-Hwa Ching MBBS MRCPCH, Teik-Beng
Is head shaft angle a valuable continuous risk factor for hip migration in cerebral palsy?
 DOI 10.1007/s11832-016-0774-0 ORIGINAL CLINICAL ARTICLE Is head shaft angle a valuable continuous risk factor for hip migration in cerebral palsy? Sanjay Chougule 1 John Dabis 2 Aviva Petrie 3 Karen Daly
DOI 10.1007/s11832-016-0774-0 ORIGINAL CLINICAL ARTICLE Is head shaft angle a valuable continuous risk factor for hip migration in cerebral palsy? Sanjay Chougule 1 John Dabis 2 Aviva Petrie 3 Karen Daly
Successful Pavlik treatment in late-diagnosed developmental dysplasia of the hip
 International Orthopaedics (SICOT) (2012) 36:1661 1668 DOI 10.1007/s00264-012-1587-5 ORIGINAL PAPER Successful Pavlik treatment in late-diagnosed developmental dysplasia of the hip Michiel A. J. van de
International Orthopaedics (SICOT) (2012) 36:1661 1668 DOI 10.1007/s00264-012-1587-5 ORIGINAL PAPER Successful Pavlik treatment in late-diagnosed developmental dysplasia of the hip Michiel A. J. van de
Evaluation of three ultrasound techniques used for the diagnosis of developmental dysplasia of the hip (DDH)
 Evaluation of three ultrasound techniques used for the diagnosis of developmental dysplasia of the hip (DDH) Poster No.: C-2049 Congress: ECR 2012 Type: Scientific Exhibit Authors: E. M. D. B. Pacheco,
Evaluation of three ultrasound techniques used for the diagnosis of developmental dysplasia of the hip (DDH) Poster No.: C-2049 Congress: ECR 2012 Type: Scientific Exhibit Authors: E. M. D. B. Pacheco,
Surgical release of neurological hip luxation in children H. Klima Ostschweizer Kinderspital St. Gallen Abteilung für Kinderorthopädie
 Surgical release of neurological hip luxation in children H. Klima Ostschweizer Kinderspital St. Gallen Abteilung für Kinderorthopädie Development of hip luxation At birth these hips are normal developed,
Surgical release of neurological hip luxation in children H. Klima Ostschweizer Kinderspital St. Gallen Abteilung für Kinderorthopädie Development of hip luxation At birth these hips are normal developed,
Clinical Practice & Referral Guideline - Developmental Dysplasia of the Hip
 Clinical Practice & Referral Guideline - Developmental Dysplasia of the Hip *This guideline was developed from the American Academy of Pediatrics Clinical Practice Guideline: Early Detection of Developmental
Clinical Practice & Referral Guideline - Developmental Dysplasia of the Hip *This guideline was developed from the American Academy of Pediatrics Clinical Practice Guideline: Early Detection of Developmental
Progression of Hip Displacement during Radiographic Surveillance in Patients with Cerebral Palsy
 ORIGINAL ARTICLE Musculoskeletal Disorders http://dx.doi.org/10.3346/jkms.2016.31.7.1143 J Korean Med Sci 2016; 31: 1143-1149 Progression of Hip Displacement during Radiographic Surveillance in Patients
ORIGINAL ARTICLE Musculoskeletal Disorders http://dx.doi.org/10.3346/jkms.2016.31.7.1143 J Korean Med Sci 2016; 31: 1143-1149 Progression of Hip Displacement during Radiographic Surveillance in Patients
Orthopedic Issues in Children with Special Healthcare Needs
 Orthopedic Issues in Children with Special Healthcare Needs Kathryn A Keeler, MD Assistant Professor University of Missouri-Kansas City School of Medicine, Department of Orthopaedic Surgery and Department
Orthopedic Issues in Children with Special Healthcare Needs Kathryn A Keeler, MD Assistant Professor University of Missouri-Kansas City School of Medicine, Department of Orthopaedic Surgery and Department
Ultrasound Evaluation of Pavlik Harness in Treatment of Infants with Developmental Dysplasia of the Hip: Prone Axial Approach to Harness in Situ
 Ultrasound Evaluation of Pavlik Harness in Treatment of Infants with Developmental Dysplasia of the Hip: Prone Axial Approach to Harness in Situ C Fernández, MD; M Guasp, MD; J Gómez Fernández-Montes,
Ultrasound Evaluation of Pavlik Harness in Treatment of Infants with Developmental Dysplasia of the Hip: Prone Axial Approach to Harness in Situ C Fernández, MD; M Guasp, MD; J Gómez Fernández-Montes,
A classification system for hip disease in cerebral palsy
 DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE A classification system for hip disease in cerebral palsy JONATHAN ROBIN MBBS 1 HKERRGRAHAMMD FRCS (ED) FRACS 1 RICHARD BAKER PHD CENG CSCI 2 PAULO
DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE A classification system for hip disease in cerebral palsy JONATHAN ROBIN MBBS 1 HKERRGRAHAMMD FRCS (ED) FRACS 1 RICHARD BAKER PHD CENG CSCI 2 PAULO
Treatment of congenital subluxation and dislocation of the hip by knee splint harness
 Prosthetics and Orthotics International, 1994,18, 34-39 Treatment of congenital subluxation and dislocation of the hip by knee splint harness M. FUKUSHIMA Fukushima Orthopaedic Clinic, Hiroshima City,
Prosthetics and Orthotics International, 1994,18, 34-39 Treatment of congenital subluxation and dislocation of the hip by knee splint harness M. FUKUSHIMA Fukushima Orthopaedic Clinic, Hiroshima City,
Circles are Pointless - Angles in the assessment of adult hip dysplasia are not!
 Circles are Pointless - Angles in the assessment of adult hip dysplasia are not! Poster No.: C-1964 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit S. E. West, S. G. Cross, J. Adu,
Circles are Pointless - Angles in the assessment of adult hip dysplasia are not! Poster No.: C-1964 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit S. E. West, S. G. Cross, J. Adu,
Childhood hip conditions. Belen Carsi Paediatric Orthopaedic Consultant
 Childhood hip conditions Belen Carsi Paediatric Orthopaedic Consultant Developmental Dysplasia of the Hip Legg-Calve-Perthes disease Slipped Capital femoral epiphysis Limp Arthritis Developmental Dysplasia
Childhood hip conditions Belen Carsi Paediatric Orthopaedic Consultant Developmental Dysplasia of the Hip Legg-Calve-Perthes disease Slipped Capital femoral epiphysis Limp Arthritis Developmental Dysplasia
Management of knee flexion contractures in patients with Cerebral Palsy
 Management of knee flexion contractures in patients with Cerebral Palsy Emmanouil Morakis Orthopaedic Consultant Royal Manchester Children s Hospital 1. Introduction 2. Natural history 3. Pathophysiology
Management of knee flexion contractures in patients with Cerebral Palsy Emmanouil Morakis Orthopaedic Consultant Royal Manchester Children s Hospital 1. Introduction 2. Natural history 3. Pathophysiology
Ultrasound Scanning of Neonatal Hips
 Ultrasound Scanning of Neonatal Hips Dr. Dickson S F Tsang Associate Consultant Queen Mary Hospital Why? How? What? Outline IAAHS 2nd April, 2011 Outline Why? Why performing hip ultrasound (USG)? Why USG?
Ultrasound Scanning of Neonatal Hips Dr. Dickson S F Tsang Associate Consultant Queen Mary Hospital Why? How? What? Outline IAAHS 2nd April, 2011 Outline Why? Why performing hip ultrasound (USG)? Why USG?
What is Hip Surveillance and Why is It Important for My Child? Information for Parents and Caregivers of Children with Cerebral Palsy
 What is Hip Surveillance and Why is It Important for My Child? Information for Parents and Caregivers of Children with Cerebral Palsy 2018 BC s Consensus on Hip Surveillance for Children with Cerebral
What is Hip Surveillance and Why is It Important for My Child? Information for Parents and Caregivers of Children with Cerebral Palsy 2018 BC s Consensus on Hip Surveillance for Children with Cerebral
HIP SURVEILLANCE. Bottom Line Evidence-Informed Recommendations for the Hip Surveillance in Individuals with Cerebral Palsy
 Bottom Line EvidenceInformed Recommendations for the Hip Surveillance T Mayson (project manager and clinical examination subgroup leader), S Miller (radiology subgroup leader), R Cairns, K Graham, S Love,
Bottom Line EvidenceInformed Recommendations for the Hip Surveillance T Mayson (project manager and clinical examination subgroup leader), S Miller (radiology subgroup leader), R Cairns, K Graham, S Love,
HIP DYSPLASIA WITHOUT DISLOCATION IN ONE-YEAR-OLD BOYS
 HIP DYSPLASIA WITHOUT DISLOCATION IN ONE-YEAR-OLD BOYS A. B. NEVELOS, p. R. J. BURCH From Leeds/Bradford Orthopaedic Training Schetne Six boys were examined during the second year of life, each with symptoms
HIP DYSPLASIA WITHOUT DISLOCATION IN ONE-YEAR-OLD BOYS A. B. NEVELOS, p. R. J. BURCH From Leeds/Bradford Orthopaedic Training Schetne Six boys were examined during the second year of life, each with symptoms
Developmental dysplasia of the hip (DDH) is a common
 ORIGINAL ARTICLE Reliability of a New Radiographic Classification for Developmental Dysplasia of the Hip Unni Narayanan, MBBS, MSc, FRCS(S),* Kishore Mulpuri, MBBS, MS (Ortho), MHSc(Epi),w Wudbhav N. Sankar,
ORIGINAL ARTICLE Reliability of a New Radiographic Classification for Developmental Dysplasia of the Hip Unni Narayanan, MBBS, MSc, FRCS(S),* Kishore Mulpuri, MBBS, MS (Ortho), MHSc(Epi),w Wudbhav N. Sankar,
The Factor Causing Poor Results in Late Developmental Dysplasia of the Hip (DDH)
 The Factor Causing Poor Results in Late Developmental Dysplasia of the Hip (DDH) Perajit Eamsobhana MD*, Kamwong Saisamorn MD*, Tanatip Sisuchinthara MS* Thunchanok Jittivilai PN*, Kamolporn Keawpornsawan
The Factor Causing Poor Results in Late Developmental Dysplasia of the Hip (DDH) Perajit Eamsobhana MD*, Kamwong Saisamorn MD*, Tanatip Sisuchinthara MS* Thunchanok Jittivilai PN*, Kamolporn Keawpornsawan
Comparison of Botulinum Toxin Type A Injection and Soft- Tissue Surgery to Treat Hip Subluxation in Children With Cerebral Palsy
 2108 ORIGINAL ARTICLE Comparison of Botulinum Toxin Type A Injection and Soft- Tissue Surgery to Treat Hip Subluxation in Children With Cerebral Palsy Eun Joo Yang, MD, Dong-wook Rha, MD, Hyun Woo Kim,
2108 ORIGINAL ARTICLE Comparison of Botulinum Toxin Type A Injection and Soft- Tissue Surgery to Treat Hip Subluxation in Children With Cerebral Palsy Eun Joo Yang, MD, Dong-wook Rha, MD, Hyun Woo Kim,
PROGRESSSIVE HIP SUBLUXATION leading to hip dislocation
 431 Hip Migration Percentage in Children With Cerebral Palsy Treated With Botulinum Toxin Type A Frank S. Pidcock, MD, David E. Fish, MD, MPH, Doug Johnson-Greene, PhD, ABPP, Isabel Borras, MD, John McGready,
431 Hip Migration Percentage in Children With Cerebral Palsy Treated With Botulinum Toxin Type A Frank S. Pidcock, MD, David E. Fish, MD, MPH, Doug Johnson-Greene, PhD, ABPP, Isabel Borras, MD, John McGready,
The Leg Length Discrepancy in The Entire Lower Limbs after Total Hip Arthroplasty Influences The Coronal Alignment of Pelvis and Spine.
 The Leg Length Discrepancy in The Entire Lower Limbs after Total Hip Arthroplasty Influences The Coronal Alignment of Pelvis and Spine. Hiroshi Fujimaki, MD 1, Yutaka Inaba, MD, PhD 2, Naomi Kobayashi,
The Leg Length Discrepancy in The Entire Lower Limbs after Total Hip Arthroplasty Influences The Coronal Alignment of Pelvis and Spine. Hiroshi Fujimaki, MD 1, Yutaka Inaba, MD, PhD 2, Naomi Kobayashi,
Hip Dysplasia David S. Feldman, MD
 Hip Dysplasia David S. Feldman, MD Chief of Pediatric Orthopedic Surgery Professor of Orthopedic Surgery & Pediatrics NYU Langone Medical Center & NYU Hospital for Joint Diseases Overview Hip dysplasia
Hip Dysplasia David S. Feldman, MD Chief of Pediatric Orthopedic Surgery Professor of Orthopedic Surgery & Pediatrics NYU Langone Medical Center & NYU Hospital for Joint Diseases Overview Hip dysplasia
Combined Pelvic Osteotomy in the Treatment of Both Deformed and Dysplastic Acetabulum Three Years Prospective Study
 Prague Medical Report / Vol. 106 (2005) No. 2, p. 159 166 159) Combined Pelvic Osteotomy in the Treatment of Both Deformed and Dysplastic Acetabulum Three Years Prospective Study Al Razi Orthopedic Hospital,
Prague Medical Report / Vol. 106 (2005) No. 2, p. 159 166 159) Combined Pelvic Osteotomy in the Treatment of Both Deformed and Dysplastic Acetabulum Three Years Prospective Study Al Razi Orthopedic Hospital,
A novel method for assessing postoperative femoral head reduction in developmental dysplasia of the hip
 J Child Orthop (2014) 8:319 324 DOI 10.1007/s11832-014-0600-5 ORIGINAL CLINICAL ARTICLE A novel method for assessing postoperative femoral head reduction in developmental dysplasia of the hip Anthony Cooper
J Child Orthop (2014) 8:319 324 DOI 10.1007/s11832-014-0600-5 ORIGINAL CLINICAL ARTICLE A novel method for assessing postoperative femoral head reduction in developmental dysplasia of the hip Anthony Cooper
SWASH CERTIFICATION EXAM
 SWASH CERTIFICATION EXAM Sitting Walking And Standing Hip Orthosis Today s Date: Location: Name: License #: Employer: Address: Ste/Apt #: City: State: Zip: Email Address: 1) Which of the following are
SWASH CERTIFICATION EXAM Sitting Walking And Standing Hip Orthosis Today s Date: Location: Name: License #: Employer: Address: Ste/Apt #: City: State: Zip: Email Address: 1) Which of the following are
Hip joint subluxation after selective dorsal rhizotomy for spastic cerebral palsy
 J Neurosurg (Pediatrics 1) 103:10 16, 2005 Hip joint subluxation after selective dorsal rhizotomy for spastic cerebral palsy TUFAN HICDONMEZ, M.D., PAUL STEINBOK, M.B.B.S., F.R.C.S.(C), RICHARD BEAUCHAMP,
J Neurosurg (Pediatrics 1) 103:10 16, 2005 Hip joint subluxation after selective dorsal rhizotomy for spastic cerebral palsy TUFAN HICDONMEZ, M.D., PAUL STEINBOK, M.B.B.S., F.R.C.S.(C), RICHARD BEAUCHAMP,
The Pavlik harness is a positioning device commonly
 RESEARCH PAPERS Ultrasound Evaluation of Hip Position in the Pavlik Harness Leslie E. Grissom, MD*, H. Theodore Harcke, MD*, S. Jay Kumar, MOt, George S. Bassett, MOt, G. Dean MacEwen, MOt Fifty infants
RESEARCH PAPERS Ultrasound Evaluation of Hip Position in the Pavlik Harness Leslie E. Grissom, MD*, H. Theodore Harcke, MD*, S. Jay Kumar, MOt, George S. Bassett, MOt, G. Dean MacEwen, MOt Fifty infants
What is a Hip Dysplasia?
 What is a Hip Dysplasia? Hip dysplasia, developmental dysplasia of the hip (DDH)[1] or congenital dysplasia of the hip (CDH)[2] is a congenital or acquired deformation or misalignment of the hip joint.
What is a Hip Dysplasia? Hip dysplasia, developmental dysplasia of the hip (DDH)[1] or congenital dysplasia of the hip (CDH)[2] is a congenital or acquired deformation or misalignment of the hip joint.
Effect of Superior Placement of the Hip Center on Abductor Muscle Strength in Total Hip Arthroplasty
 The Journal of Arthroplasty Vol. 24 No. 2 2009 Effect of Superior Placement of the Hip Center on Abductor Muscle Strength in Total Hip Arthroplasty Takahiko Kiyama, MD, Masatoshi Naito, MD, PhD, Hiroshi
The Journal of Arthroplasty Vol. 24 No. 2 2009 Effect of Superior Placement of the Hip Center on Abductor Muscle Strength in Total Hip Arthroplasty Takahiko Kiyama, MD, Masatoshi Naito, MD, PhD, Hiroshi
Radiographic Evaluation Of Dynamic Hip Instability In Lequesne s False Profile View
 Radiographic Evaluation Of Dynamic Hip Instability In Lequesne s False Profile View Ryo Mori 1, Yuji Yasunaga 2, Takuma Yamasaki 1, Michio Hamanishi 1, Takeshi Shoji 1, Sotaro Izumi 1, Susumu Hachisuka
Radiographic Evaluation Of Dynamic Hip Instability In Lequesne s False Profile View Ryo Mori 1, Yuji Yasunaga 2, Takuma Yamasaki 1, Michio Hamanishi 1, Takeshi Shoji 1, Sotaro Izumi 1, Susumu Hachisuka
Introduction To The New AACPDM Hip Surveillance Care Pathway For Children With Cerebral Palsy: What's the Consensus? How Can It Be Implemented?
 Introduction To The New AACPDM Hip Surveillance Care Pathway For Children With Cerebral Palsy: What's the Consensus? How Can It Be Implemented? September 15, 2017 Montreal Quebec Canada 1 CARE PATHWAYS
Introduction To The New AACPDM Hip Surveillance Care Pathway For Children With Cerebral Palsy: What's the Consensus? How Can It Be Implemented? September 15, 2017 Montreal Quebec Canada 1 CARE PATHWAYS
Developmental Dysplasia of the Hip
 Developmental Dysplasia of the Hip Abnormal relationship of femoral head to the acetabulum Formerly known as congenital hip dislocation Believed to be developmental Most dislocations are evident at births
Developmental Dysplasia of the Hip Abnormal relationship of femoral head to the acetabulum Formerly known as congenital hip dislocation Believed to be developmental Most dislocations are evident at births
Hip Joint DX 612 Orthopedics and Neurology
 Hip Joint DX 612 Orthopedics and Neurology James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Hip Anatomy Palpation Point tenderness Edema Symmetry Hip ROM Hip Contracture
Hip Joint DX 612 Orthopedics and Neurology James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Hip Anatomy Palpation Point tenderness Edema Symmetry Hip ROM Hip Contracture
Hip Anatomy. Hip Joint DX 612 Orthopedics and Neurology. Hip ROM. Palpation
 Hip Joint DX 612 Orthopedics and Neurology Hip Anatomy James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Palpation Hip ROM Point tenderness Edema Symmetry Hip Contracture
Hip Joint DX 612 Orthopedics and Neurology Hip Anatomy James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Palpation Hip ROM Point tenderness Edema Symmetry Hip Contracture
Case Report Ipsilateral Hip Dysplasia in Patients with Sacral Hemiagenesis: A Report of Two Cases
 Case Reports in Orthopedics Volume 2015, Article ID 854151, 4 pages http://dx.doi.org/10.1155/2015/854151 Case Report Ipsilateral Hip Dysplasia in Patients with Sacral Hemiagenesis: A Report of Two Cases
Case Reports in Orthopedics Volume 2015, Article ID 854151, 4 pages http://dx.doi.org/10.1155/2015/854151 Case Report Ipsilateral Hip Dysplasia in Patients with Sacral Hemiagenesis: A Report of Two Cases
Guidelines, Policies and Statements. Statement on the Use of Ultrasound in the Diagnosis of Developmental Hip Dysplasia and Dislocation
 Guidelines, Policies and Statements Statement on the Use of Ultrasound in the Diagnosis of Developmental Hip Dysplasia and Dislocation Approved by Council June 2018 Disclaimer and Copyright The ASUM Standards
Guidelines, Policies and Statements Statement on the Use of Ultrasound in the Diagnosis of Developmental Hip Dysplasia and Dislocation Approved by Council June 2018 Disclaimer and Copyright The ASUM Standards
Anterior Knee Pain in Patients with Cerebral Palsy
 Original Article Clinics in Orthopedic Surgery 2014;6:426-431 http://dx.doi.org/10.4055/cios.2014.6.4.426 Anterior Knee Pain in Patients with Cerebral Palsy Young Choi, MD a, Sang Hyeong Lee, MD* a, Chin
Original Article Clinics in Orthopedic Surgery 2014;6:426-431 http://dx.doi.org/10.4055/cios.2014.6.4.426 Anterior Knee Pain in Patients with Cerebral Palsy Young Choi, MD a, Sang Hyeong Lee, MD* a, Chin
HIP DYSPLASIA AND HYPOTONIA CAN STANDING IN ABDUCTION HELP?
 HIP DYSPLASIA AND HYPOTONIA CAN STANDING IN ABDUCTION HELP? Written by: MARY MILES, PT, DPT, ATP THIS CASE STUDY IS SPONSORED BY ALTIMATE MEDICAL Standing with hips in abduction has evolved as the new
HIP DYSPLASIA AND HYPOTONIA CAN STANDING IN ABDUCTION HELP? Written by: MARY MILES, PT, DPT, ATP THIS CASE STUDY IS SPONSORED BY ALTIMATE MEDICAL Standing with hips in abduction has evolved as the new
ASJ. Magnification Error in Digital Radiographs of the Cervical Spine Against Magnetic Resonance Imaging Measurements. Asian Spine Journal
 Asian Spine Journal Asian Spine Clinical Journal Study Asian Spine J 2013;7(4):267-272 Magnification http://dx.doi.org/10.4184/asj.2013.7.4.267 error in cervical spine 267 Magnification Error in Digital
Asian Spine Journal Asian Spine Clinical Journal Study Asian Spine J 2013;7(4):267-272 Magnification http://dx.doi.org/10.4184/asj.2013.7.4.267 error in cervical spine 267 Magnification Error in Digital
The Limping Child: Differential Diagnosis
 The Limping Child: Differential Diagnosis Kathryn A Keeler, MD Assistant Professor University of Missouri-Kansas City School of Medicine, Department of Orthopaedic Surgery and Department of Pediatrics
The Limping Child: Differential Diagnosis Kathryn A Keeler, MD Assistant Professor University of Missouri-Kansas City School of Medicine, Department of Orthopaedic Surgery and Department of Pediatrics
BIOMECHANICAL EXAMINATION OF THE PEDIATRIC LOWER EXTREMITY
 BIOMECHANICAL EXAMINATION OF THE PEDIATRIC LOWER EXTREMITY B.Resseque, D.P.M. ARCH HEIGHT OFF WEIGHTBEARING Evaluate arch height by placing a ruler from the heel to the first metatarsal head Compare arch
BIOMECHANICAL EXAMINATION OF THE PEDIATRIC LOWER EXTREMITY B.Resseque, D.P.M. ARCH HEIGHT OFF WEIGHTBEARING Evaluate arch height by placing a ruler from the heel to the first metatarsal head Compare arch
Hip subluxation and dislocation in cerebral palsy : Outcome of bone surgery in 21 hips
 Acta Orthop. Belg., 2008, 74, 609-614 ORIGINAL STUDY Hip subluxation and dislocation in cerebral palsy : Outcome of bone surgery in 21 hips Pietro PERSIANI, Iakov MOLAYEM, Alessandro CALISTRI, Stefano
Acta Orthop. Belg., 2008, 74, 609-614 ORIGINAL STUDY Hip subluxation and dislocation in cerebral palsy : Outcome of bone surgery in 21 hips Pietro PERSIANI, Iakov MOLAYEM, Alessandro CALISTRI, Stefano
Society for Pediatric Radiology 2015 Hands on Session. DDH: Pitfalls and Practical Tips
 Society for Pediatric Radiology 2015 Hands on Session DDH: Pitfalls and Practical Tips Michael A. DiPietro, M.D. John F. Holt Collegiate Professor of Radiology Professor of Pediatrics and Communicable
Society for Pediatric Radiology 2015 Hands on Session DDH: Pitfalls and Practical Tips Michael A. DiPietro, M.D. John F. Holt Collegiate Professor of Radiology Professor of Pediatrics and Communicable
Stephanie W. Mayer, MD. Director of Child and Young Adult Hip Preservation Sports Medicine Center Children s Hospital Colorado
 Stephanie W. Mayer, MD Director of Child and Young Adult Hip Preservation Sports Medicine Center Children s Hospital Colorado University of Colorado Sports Medicine Assistant Team Physician, Colorado Avalanche
Stephanie W. Mayer, MD Director of Child and Young Adult Hip Preservation Sports Medicine Center Children s Hospital Colorado University of Colorado Sports Medicine Assistant Team Physician, Colorado Avalanche
Radiological Sequelae of developmental dysplasia of the hip: a Review
 Radiological Sequelae of developmental dysplasia of the hip: a Review Poster No.: P-0037 Congress: ESSR 2012 Type: Scientific Exhibit Authors: S. G. Flanagan, J. Sarkodieh, K. Mcdonald, M. Ramachandran,
Radiological Sequelae of developmental dysplasia of the hip: a Review Poster No.: P-0037 Congress: ESSR 2012 Type: Scientific Exhibit Authors: S. G. Flanagan, J. Sarkodieh, K. Mcdonald, M. Ramachandran,
The Effects of Botulinum Toxin Type-A on Spasticity and Motor Function in Children with Cerebral Palsy
 Pacific University CommonKnowledge PT Critically Appraised Topics School of Physical Therapy 2014 The Effects of Botulinum Toxin Type-A on Spasticity and Motor Function in Children with Cerebral Palsy
Pacific University CommonKnowledge PT Critically Appraised Topics School of Physical Therapy 2014 The Effects of Botulinum Toxin Type-A on Spasticity and Motor Function in Children with Cerebral Palsy
Hip Biomechanics and Osteotomies
 Hip Biomechanics and Osteotomies Organization Introduction Hip Biomechanics Principles of Osteotomy Femoral Osteotomies Pelvic Osteotomies Summary Inroduction Osteoarthritis is very prevalent Primary OA
Hip Biomechanics and Osteotomies Organization Introduction Hip Biomechanics Principles of Osteotomy Femoral Osteotomies Pelvic Osteotomies Summary Inroduction Osteoarthritis is very prevalent Primary OA
Bioscience Research Print ISSN: Online ISSN:
 Available online freely at www.isisn.org Bioscience Research Print ISSN: 1811-9506 Online ISSN: 2218-3973 Journal by Innovative Scientific Information & Services Network RESEARCH ARTICLE BIOSCIENCE RESEARCH,
Available online freely at www.isisn.org Bioscience Research Print ISSN: 1811-9506 Online ISSN: 2218-3973 Journal by Innovative Scientific Information & Services Network RESEARCH ARTICLE BIOSCIENCE RESEARCH,
L ecografia cerebrale: accuratezza diagnostica Dr Patrizio Prati Neurologia CIDIMU Torino
 L ecografia cerebrale: accuratezza diagnostica Dr Patrizio Prati Neurologia CIDIMU Torino Ecografia cerebrale: l accuratezza diagnostica. Lo studio NOBIS Dr Patrizio Prati Neurologia CIDIMU Torinorin Normal
L ecografia cerebrale: accuratezza diagnostica Dr Patrizio Prati Neurologia CIDIMU Torino Ecografia cerebrale: l accuratezza diagnostica. Lo studio NOBIS Dr Patrizio Prati Neurologia CIDIMU Torinorin Normal
Developmental Dysplasia of the Hip
 1 Developmental Dysplasia of the Hip Developmental dysplasia of the hip (DDH) or otherwise known as congenital dislocation of the hip (CDH) is a developmental (ongoing) process, which can often go undetected
1 Developmental Dysplasia of the Hip Developmental dysplasia of the hip (DDH) or otherwise known as congenital dislocation of the hip (CDH) is a developmental (ongoing) process, which can often go undetected
A Useful Reference Guide for the Stem Anteversion During Total Hip Arthroplasty in the Dysplastic Femur
 A Useful Reference Guide for the Stem Anteversion During Total Hip Arthroplasty in the Dysplastic Femur Tadashi Tsukeoka, Yoshikazu Tsuneizumi, TaeHyun Lee. Chiba Rehabilitation Center, Chiba, Japan. Disclosures:
A Useful Reference Guide for the Stem Anteversion During Total Hip Arthroplasty in the Dysplastic Femur Tadashi Tsukeoka, Yoshikazu Tsuneizumi, TaeHyun Lee. Chiba Rehabilitation Center, Chiba, Japan. Disclosures:
Developmental Dysplasia of the Hip, (DDH) including Femoral and Pelvic Osteotomy
 Developmental Dysplasia of the Hip, (DDH) including Femoral and Pelvic Osteotomy Leicester Children s Hospital Information for Patients, Parents and Carers DRAFT What is developmental dysplasia of the
Developmental Dysplasia of the Hip, (DDH) including Femoral and Pelvic Osteotomy Leicester Children s Hospital Information for Patients, Parents and Carers DRAFT What is developmental dysplasia of the
Case Presentations The Child with a Limp
 Case Presentations The Child with a Limp Douglas G. Armstrong, M.D. Professor, PennState Hershey College of Medicine Division Head, Pediatric Orthopaedics Dept. of Orthopaedics and Rehabilitation PennState
Case Presentations The Child with a Limp Douglas G. Armstrong, M.D. Professor, PennState Hershey College of Medicine Division Head, Pediatric Orthopaedics Dept. of Orthopaedics and Rehabilitation PennState
Changes in lower limb rotation after soft tissue surgery in spastic diplegia
 Acta Orthopaedica 2010; 81 (2): 245 249 245 Changes in lower limb rotation after soft tissue surgery in spastic diplegia 3-dimensional gait analysis in 28 children Bjørn Lofterød 1 and Terje Terjesen 2
Acta Orthopaedica 2010; 81 (2): 245 249 245 Changes in lower limb rotation after soft tissue surgery in spastic diplegia 3-dimensional gait analysis in 28 children Bjørn Lofterød 1 and Terje Terjesen 2
SUMMARY. Applied exercise physiology in rehabilitation of children with cerebral palsy
 S SUMMARY Applied exercise physiology in rehabilitation of children with cerebral palsy Summary Cerebral palsy (CP) is the most common cause of physical disability in childhood. CP is defined as a group
S SUMMARY Applied exercise physiology in rehabilitation of children with cerebral palsy Summary Cerebral palsy (CP) is the most common cause of physical disability in childhood. CP is defined as a group
DDH. Abnormal hip development Traditionally CDH (congenital dysplasia of the hip) Today DDH(developmental dysplasia of the hip)
 DDH Update on Screening Kathryn A Keeler, MD Assistant Professor University of Missouri-Kansas City School of Medicine, Department of Orthopaedic Surgery and Department of Pediatrics Children s Mercy Kansas
DDH Update on Screening Kathryn A Keeler, MD Assistant Professor University of Missouri-Kansas City School of Medicine, Department of Orthopaedic Surgery and Department of Pediatrics Children s Mercy Kansas
Adult Hip Dysplasia David S. Feldman, MD
 Adult Hip Dysplasia David S. Feldman, MD Chief of Pediatric Orthopedic Surgery Professor of Orthopedic Surgery & Pediatrics NYU Langone Medical Center & NYU Hospital for Joint Diseases Overview Adult hip
Adult Hip Dysplasia David S. Feldman, MD Chief of Pediatric Orthopedic Surgery Professor of Orthopedic Surgery & Pediatrics NYU Langone Medical Center & NYU Hospital for Joint Diseases Overview Adult hip
)371( COPYRIGHT 2016 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE. Research performed at Dr. Sheikh Children Hospital, Mashhad, Iran
 )371( COPYRIGHT 2016 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE Assessment of Diagnostic Value of Single View Static & Dynamic Technique in Diagnosis of Developmental Dysplasia of Hip:
)371( COPYRIGHT 2016 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE Assessment of Diagnostic Value of Single View Static & Dynamic Technique in Diagnosis of Developmental Dysplasia of Hip:
Primary osteoathrosis of the hip and Heberden's nodes
 Annals of the Rheumatic Diseases, 1979, 38, 107-111 Primary osteoathrosis of the hip and Heberden's nodes J. S. MARKS, I. M. STEWART, AND K. HARDINGE From the Wrightington Hospital, Wigan, Lancs SUMMARY
Annals of the Rheumatic Diseases, 1979, 38, 107-111 Primary osteoathrosis of the hip and Heberden's nodes J. S. MARKS, I. M. STEWART, AND K. HARDINGE From the Wrightington Hospital, Wigan, Lancs SUMMARY
Orthopedics. 1. GOAL: Understand the pediatrician's role in preventing and screening for
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Orthopedics 1. GOAL: Understand the pediatrician's role in preventing and screening for orthopedic injury, disease and dysfunction.
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Orthopedics 1. GOAL: Understand the pediatrician's role in preventing and screening for orthopedic injury, disease and dysfunction.
A 4 year old with hip pain: Legg-Calvé-Perthes Disease
 A 4 year old with hip pain: Legg-Calvé-Perthes Disease Cyndie Seraphin Harvard Medical School Year III Our Patient A 4 year-old boy is complaining of severe L hip pain. The differential diagnosis of acute
A 4 year old with hip pain: Legg-Calvé-Perthes Disease Cyndie Seraphin Harvard Medical School Year III Our Patient A 4 year-old boy is complaining of severe L hip pain. The differential diagnosis of acute
THE HIP. Cooler than cool, the pinnacle of what is "it". Beyond all trends and conventional coolness.
 THE HIP Cooler than cool, the pinnacle of what is "it". Beyond all trends and conventional coolness. Objectives Hip anatomy Causes of hip pain Hip exam Anatomy Bones Ilium Anterior Superior Iliac Spine
THE HIP Cooler than cool, the pinnacle of what is "it". Beyond all trends and conventional coolness. Objectives Hip anatomy Causes of hip pain Hip exam Anatomy Bones Ilium Anterior Superior Iliac Spine
Non-inflammatory joint pain
 Non-inflammatory joint pain Lawrence Owino Okong o, Mmed (UoN); Mphil. (UCT). Lecturer, Department of Paediatrics and Child Health, University of Nairobi. Paediatrician/ Rheumatologist. INTRODUCTION Musculoskeletal
Non-inflammatory joint pain Lawrence Owino Okong o, Mmed (UoN); Mphil. (UCT). Lecturer, Department of Paediatrics and Child Health, University of Nairobi. Paediatrician/ Rheumatologist. INTRODUCTION Musculoskeletal
Association between Sacral Slanting and Adjacent Structures in Patients with Adolescent Idiopathic Scoliosis
 Original Article Clinics in Orthopedic Surgery 17;9:57-62 https://doi.org/10.4055/cios.17.9.1.57 Association between Sacral Slanting and Adjacent Structures in Patients with Adolescent Idiopathic Scoliosis
Original Article Clinics in Orthopedic Surgery 17;9:57-62 https://doi.org/10.4055/cios.17.9.1.57 Association between Sacral Slanting and Adjacent Structures in Patients with Adolescent Idiopathic Scoliosis
Clinical Application of Computed Radiography in Orthopedic Surgery
 Clinical Application of Computed Radiography in Orthopedic Surgery Satoru Fujita, Masamichi Tanaka, Sigeaki Hirota, and Takeshi Fuji Since 1988, Fuji Computed Radiography (FCR) system (Fuji Medical Systems,
Clinical Application of Computed Radiography in Orthopedic Surgery Satoru Fujita, Masamichi Tanaka, Sigeaki Hirota, and Takeshi Fuji Since 1988, Fuji Computed Radiography (FCR) system (Fuji Medical Systems,
Avascular necrosis as a complication of the treatment of dislocation of the hip in children with cerebral palsy
 CHILDREN S ORTHOPAEDICS Avascular necrosis as a complication of the treatment of dislocation of the hip in children with cerebral palsy A. Koch, M. Jozwiak, M. Idzior, M. Molinska-Glura, A. Szulc From
CHILDREN S ORTHOPAEDICS Avascular necrosis as a complication of the treatment of dislocation of the hip in children with cerebral palsy A. Koch, M. Jozwiak, M. Idzior, M. Molinska-Glura, A. Szulc From
Bilateral hip pain with right proximal femoral lesion
 Bilateral hip pain with right proximal femoral lesion Legg-Calve-Perthes Idiopathic osteonecrosis of the femoral head epiphysis during childhood First described by Arthur Thorton Legg in 1909 and published
Bilateral hip pain with right proximal femoral lesion Legg-Calve-Perthes Idiopathic osteonecrosis of the femoral head epiphysis during childhood First described by Arthur Thorton Legg in 1909 and published
Effects of Immobilization. N24 Pedi Musculoskeletal Spring 2012, Week 14. Cabrillo ADN/C. Madsen RN, MSN 1. Physical effects on other systems
 Common Orthopedic Problems of Children Congenital Acquired Bones Neuromuscular Physical effects on other systems Pulmonary Cardiac Skin integrity Elimination GI GU 1 4 General Nursing Considerations any
Common Orthopedic Problems of Children Congenital Acquired Bones Neuromuscular Physical effects on other systems Pulmonary Cardiac Skin integrity Elimination GI GU 1 4 General Nursing Considerations any
Elisabet Rodby-Bousquet 1,2, Atli Ágústsson 3, Guðný Jónsdóttir 3, Tomasz Czuba 4, Ann-Christin Johansson 2 and Gunnar Hägglund 1
 465423CRE28110.1177/0269215512465423Clinical RehabilitationRodby-Bousquet et al. 2012 Article CLINICAL REHABILITATION Interrater reliability and construct validity of the Posture and Postural Ability Scale
465423CRE28110.1177/0269215512465423Clinical RehabilitationRodby-Bousquet et al. 2012 Article CLINICAL REHABILITATION Interrater reliability and construct validity of the Posture and Postural Ability Scale
The Efficacy of Pavlik Harness as a Treatment of Developmental Dislocation of the Hip
 The Efficacy of Pavlik Harness as a Treatment of Developmental Dislocation of the Hip Firas A. Suleiman, MD*, Fadi Al Rousan, MD*, Ahmad Almarzoq, MD *, Razi Altarawneh, MD*, Hidar Soudi, MD* ABSTRACT
The Efficacy of Pavlik Harness as a Treatment of Developmental Dislocation of the Hip Firas A. Suleiman, MD*, Fadi Al Rousan, MD*, Ahmad Almarzoq, MD *, Razi Altarawneh, MD*, Hidar Soudi, MD* ABSTRACT
Orthopaedics Springer-Verlag 1987
 International Orthopaedics (SICOT) (1987) 11:83-87 International Orthopaedics Springer-Verlag 1987 The correlation of arthrography with the results of treatment in late diagnosed congenital dislocation
International Orthopaedics (SICOT) (1987) 11:83-87 International Orthopaedics Springer-Verlag 1987 The correlation of arthrography with the results of treatment in late diagnosed congenital dislocation
Joints of the lower limb
 Joints of the lower limb 1-Type: Hip joint Synovial ball-and-socket joint 2-Articular surfaces: a- head of femur b- lunate surface of acetabulum Which is deepened by the fibrocartilaginous labrum acetabulare
Joints of the lower limb 1-Type: Hip joint Synovial ball-and-socket joint 2-Articular surfaces: a- head of femur b- lunate surface of acetabulum Which is deepened by the fibrocartilaginous labrum acetabulare
Main Menu. Joint and Pelvic Girdle click here. The Power is in Your Hands
 1 Hip Joint and Pelvic Girdle click here Main Menu K.6 http://www.handsonlineeducation.com/classes//k6entry.htm[3/23/18, 2:01:12 PM] Hip Joint (acetabular femoral) Relatively stable due to : Bony architecture
1 Hip Joint and Pelvic Girdle click here Main Menu K.6 http://www.handsonlineeducation.com/classes//k6entry.htm[3/23/18, 2:01:12 PM] Hip Joint (acetabular femoral) Relatively stable due to : Bony architecture
New, specific ultrasonographic findings for the diagnosis of pulled elbow
 Clin Exp Emerg Med 2014;1(2):109-113 http://dx.doi.org/10.15441/ceem.14.009 New, specific ultrasonographic findings for the diagnosis of pulled elbow Yu Sung Lee, You Dong Sohn, Young Teak Oh Department
Clin Exp Emerg Med 2014;1(2):109-113 http://dx.doi.org/10.15441/ceem.14.009 New, specific ultrasonographic findings for the diagnosis of pulled elbow Yu Sung Lee, You Dong Sohn, Young Teak Oh Department
Anterior Displacement of Ulnar Nerve at the Elbow in Children Based on Ultrasonography
 108472 NV-OA8 pg29-33.qxd 11/05/2007 05:05 PM Page 29 (Black plate) Anterior Displacement of Ulnar Nerve at the Elbow in Children Based on Ultrasonography H Shamsul, MS (Ortho)*, A Saw, FRCS*, G John,
108472 NV-OA8 pg29-33.qxd 11/05/2007 05:05 PM Page 29 (Black plate) Anterior Displacement of Ulnar Nerve at the Elbow in Children Based on Ultrasonography H Shamsul, MS (Ortho)*, A Saw, FRCS*, G John,
Case Report Anterior Hip Subluxation due to Lumbar Degenerative Kyphosis and Posterior Pelvic Tilt
 Case Reports in Orthopedics, Article ID 806157, 4 pages http://dx.doi.org/10.1155/2014/806157 Case Report Anterior Hip Subluxation due to Lumbar Degenerative Kyphosis and Posterior Pelvic Tilt Hiroyuki
Case Reports in Orthopedics, Article ID 806157, 4 pages http://dx.doi.org/10.1155/2014/806157 Case Report Anterior Hip Subluxation due to Lumbar Degenerative Kyphosis and Posterior Pelvic Tilt Hiroyuki
ORIGINAL PAPER. Department of Orthopedic Surgery, Hamamatsu Medical Center ABSTRACT
 Nagoya J. Med. Sci. 71. 145 ~ 150, 2009 ORIGINAL PAPER AUTOGENOUS BULK STRUCTURAL BONE GRAFTING FOR RECONSTRUCTION OF THE ACETABLUM IN PRIMARY TOTAL HIP ARTHROPLASTY: AVERAGE 12-YEAR FOLLOW-UP TETSUO MASUI,
Nagoya J. Med. Sci. 71. 145 ~ 150, 2009 ORIGINAL PAPER AUTOGENOUS BULK STRUCTURAL BONE GRAFTING FOR RECONSTRUCTION OF THE ACETABLUM IN PRIMARY TOTAL HIP ARTHROPLASTY: AVERAGE 12-YEAR FOLLOW-UP TETSUO MASUI,
Where to Draw the Line:
 Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
EXAMINATION OF HIP. A. Inspection Examination
 EXAMINATION OF HIP History: What is your trouble? Pain, stiffness, limp Please tell me more about your problem?.listen Listen for at least one minute: Let patient do the talking Do not ask leading question
EXAMINATION OF HIP History: What is your trouble? Pain, stiffness, limp Please tell me more about your problem?.listen Listen for at least one minute: Let patient do the talking Do not ask leading question
Femoral Acetabular Impingement 10/22/2016
 Femoral Acetabular Impingement 10/22/2016 Disclosures No Disclosures to report Questions Does FAI lead to early development of osteoarthritis? Is surgical correction an effective treatment for FAI? Who
Femoral Acetabular Impingement 10/22/2016 Disclosures No Disclosures to report Questions Does FAI lead to early development of osteoarthritis? Is surgical correction an effective treatment for FAI? Who
Conservative Correction of Leg-Length Discrepancies of 10 mm or Less for the Relief of Chronic Low Back Pain
 Conservative Correction of Leg-Length Discrepancies of 10 mm or Less for the Relief of Chronic Low Back Pain Archives of Physical Medicine and Rehabilitation November 2005, Volume 86, Issue 11, pp 2075-2080
Conservative Correction of Leg-Length Discrepancies of 10 mm or Less for the Relief of Chronic Low Back Pain Archives of Physical Medicine and Rehabilitation November 2005, Volume 86, Issue 11, pp 2075-2080
Scoliosis in Patients with Severe Cerebral Palsy: Three Different Courses in Adolescents
 Original Article http ://escholarship.lib.okayama-u.ac.jp/amo/ Scoliosis in Patients with Severe Cerebral Palsy: Three Different Courses in Adolescents Yoshiaki Oda a*, Tomoyuki Takigawa a, Yoshihisa Sugimoto
Original Article http ://escholarship.lib.okayama-u.ac.jp/amo/ Scoliosis in Patients with Severe Cerebral Palsy: Three Different Courses in Adolescents Yoshiaki Oda a*, Tomoyuki Takigawa a, Yoshihisa Sugimoto
Significance of radiological appearance of ossific femoral nucleus in diagnosis of developmental hip dysplasia
 Significance of radiological appearance of ossific femoral nucleus in diagnosis of developmental hip dysplasia, MBChB, D Orth, MSc. Abstract: The aim of the study to determine the benefit of delaying appearance
Significance of radiological appearance of ossific femoral nucleus in diagnosis of developmental hip dysplasia, MBChB, D Orth, MSc. Abstract: The aim of the study to determine the benefit of delaying appearance
CLINICAL GUIDELINES ID TAG Developmental Dysplasia of hips Regional Guideline Mr Aidan Cosgrove. Title:
 Title: Author: Designation: Speciality / Division: Directorate: CLINICAL GUIDELINES ID TAG Developmental Dysplasia of hips Regional Guideline Mr Aidan Cosgrove Paediatric Orthopaedics Orthopaedic Orthopaedics
Title: Author: Designation: Speciality / Division: Directorate: CLINICAL GUIDELINES ID TAG Developmental Dysplasia of hips Regional Guideline Mr Aidan Cosgrove Paediatric Orthopaedics Orthopaedic Orthopaedics
