Obsessive-compulsive disorder with comorbid major depression: What is the role of cognitive factors?
|
|
|
- Jessica Simpson
- 5 years ago
- Views:
Transcription
1 Behaviour Research and Therapy 45 (2007) Obsessive-compulsive disorder with comorbid major depression: What is the role of cognitive factors? Jonathan S. Abramowitz a,, Eric A. Storch b, Mary Keeley b, Elisabeth Cordell a a Department of Psychology, University of North Carolina at Chapel Hill, Campus Box 3270 (Davie Hall), Chapel Hill, NC , USA b University of Florida, FL, USA Received 6 January 2007; received in revised form 7 April 2007; accepted 12 April 2007 Abstract Individuals with obsessive-compulsive disorder (OCD) commonly experience comorbid mood disturbances such as major depressive disorder (MDD). Previous studies that have compared OCD patients with and without MDD have revealed differences in demographic characteristics, clinical severity, and symptom presentation between these two patient groups. Previous studies have not, however, examined whether there are differences with respect to cognitive processes. The present study therefore aimed to address this gap in the literature. Eighty patients with OCD and no unipolar mood disorders were compared with 34 OCD patients with comorbid major depression on measures of OCD symptoms, cognitions, and insight, as well as on measures of depression and functional impairment. Whereas depressed OCD patients evidenced higher scores than non-depressed OCD patients on semi-idiographic measures of OCD symptoms and cognitions, this was not the case for nomothetic measures. Functional impairment and the tendency to misinterpret innocuous intrusive thoughts as significant emerged as unique predictors of depression within the entire sample of OCD patients. Results are discussed in terms of (a) the importance of semi-idiographic assessment of OCD, (b) possible explanations for the relationship between OCD symptoms, depression, and cognitive processes, and (c) the psychological treatment of comorbid OCD and MDD. r 2007 Elsevier Ltd. All rights reserved. Keywords: Obsessive-compulsive disorder; Depression; Cognition; Insight; Semi-idiographic assessment Introduction Individuals with obsessive-compulsive disorder (OCD) commonly experience comorbid Axis I and Axis II psychopathology over the course of their illness, with mood disturbances such as major depressive disorder (MDD) among the most common additional diagnoses. Although reported comorbidity rates differ among studies due to variability in sampling and methodology, research indicates that as many as one-quarter to onehalf of OCD sufferers experience MDD (e.g., Crino & Andrews, 1996; Hong et al., 2004; Nestadt et al., 2001). Studies on the temporal nature of this comorbidity pattern indicate that in most (but not all) instances, OCD Corresponding author. Tel.: ; fax: address: jabramowitz@unc.edu (J.S. Abramowitz) /$ - see front matter r 2007 Elsevier Ltd. All rights reserved. doi: /j.brat
2 2258 J.S. Abramowitz et al. / Behaviour Research and Therapy 45 (2007) symptoms predate the depressive symptoms (Bellodi, Scioto, Diaferia, Ronchi, & Smiraldi, 1992; Demal, Lenz, Mayrhofer, Zapotoczky, & Zitterl, 1993). This suggests that the mood disturbance often occurs as a response to the distress and functional impairment associated with obsessions and compulsions. Accordingly, there is evidence that depressed OCD patients have an earlier age of OCD onset and more severe obsessions and compulsions as compared to their non-depressed counterparts (e.g., Hong et al., 2004; Tukel, Meteris, Koyuncu, Tecer, & Yazici, 2006). In addition to the aforementioned differences, depressed OCD patients show more severe general anxiety symptoms, higher rates of other comorbid conditions (e.g., anxiety disorders), higher rates of unemployment, and greater functional disability than do OCD patients without depression (Hong et al., 2004; Ricciardi & McNally, 1995; Tukel, Polat, Ozdemir, Sksut, & Turksoy, 2002; Tukel et al., 2006). Moreover, the presence of comorbid depression is associated with the occurrence of sexual and religious obsessions (Hasler, LaSalle- Ricci, & Ronquillo, 2005; Hong et al., 2004); and this is consistent with previous research indicating that these particular types of obsessions are experienced as more distressing than are other OCD symptoms (Abramowitz, Franklin, Schwartz, & Furr, 2003; McKay et al., 2004). When the prevalence and clinical severity findings reviewed above are considered in light of research demonstrating that comorbid MDD also attenuates response to the most effective treatment for OCD exposure and response prevention (e.g., Abramowitz & Foa, 2000), one recognizes the need to further study the differences between depressed and non-depressed OCD patients. The existing literature provides important information regarding differences in demographic characteristics, clinical severity, and symptom presentation between OCD patients with and without MDD; yet, there is a surprising dearth of research investigating whether these groups of patients differ with respect to relevant cognitive processes. Cognitive models of psychopathology in general (e.g., Beck, 1976) posit that emotional distress arises from dysfunctional beliefs and appraisals about external or internal stimuli. For example, Beck (1976) proposed that depression arises from specific sorts of beliefs and interpretations related to loss and selfdegradation (e.g., I am a loser who is unlovable ). As applied to obsessional problems, Rachman (1993, 1997) proposed a cognitive model in which clinical obsessions arise when normally occurring intrusive thoughts are erroneously appraised as highly significant or threatening (e.g., If I think of something terrible, I could cause it to happen ). Rachman (1993) further observed that in severe cases, such appraisals involve ideas of self-deprecation that are similar to the kinds of cognitions observed in people with MDD (e.g., The fact that I think about terrible things means I am a terrible person ). Thus, in comorbid patients, the cognitive processes involved in obsessions might also play a role in depressive symptoms. In an attempt to elucidate this role, we addressed the following two questions in the present study: (a) do depressed OCD patients evidence a greater tendency to misinterpret the significance of intrusions relative to non-depressed OCD patients? and (b) are misinterpretations of intrusions uniquely related to comorbid depressive symptoms among individuals with OCD?. A second cognitive factor that could be involved in the overlap between OCD and depression is insight the degree to which the individual recognizes the senselessness of his or her obsessions and compulsions (e.g., Kozak & Foa, 1994). Whereas most OCD patients realize to some extent that their symptoms are unrealistic and excessive, insight exists on a continuum with some individuals believing strongly that their obsessive fears are rational and their compulsive behaviors are necessary to prevent disasters (Foa & Kozak, 1995). Studies of OCD patients indicate that poor insight is associated with more severe OCD symptoms (e.g., Deacon & Abramowitz, 2005) and higher levels of self-reported symptoms of depression (Turksoy, Tukel, Ozdemir, & Karah, 2002), leading to the hypothesis that OCD patients with MDD would evidence poorer insight than non-depressed OCD patients. Although Tukel et al. (2006) reported data consistent with this prediction, poor insight was assessed as either present or absent on the basis of DSM-IV criteria, rather than as measured by a psychometrically validated continuous measure. In the present study, we therefore aimed to replicate and extend the literature on comorbid OCD and depression by examining the role of cognitive processes. Consistent with previous work, we expected to find that depressed OCD patients (i.e., with comorbid MDD) would show more severe OCD symptoms and functional disability relative to non-depressed OCD patients. We hypothesized that depressed OCD patients would also show a stronger tendency to misinterpret the significance of intrusive thoughts and evidence poorer insight into the senselessness of their OCD symptoms relative to non-depressed OCD patients. Furthermore,
3 we examined whether these cognitive factors uniquely contributed to the prediction of depressive symptoms in our OCD sample. Method Participants Participants in the present study included 114 adult (X18 years) outpatients with a primary DSM-IV-TR diagnosis of OCD seeking evaluation and treatment for this condition. Thirty-four of these patients met DSM criteria for both OCD and current MDD ( OCD-MDD group), and 80 met criteria for OCD, but for no unipolar mood disorders ( OCD-NUMD [meaning, No Unipolar Mood Disorder] group). Data were combined from consecutive referrals at two outpatient treatment facilities: 82 patients (72%) were evaluated at the Mayo Clinic in Rochester, Minnesota and 32 patients (28%) at the University of Florida in Gainesville, Florida. Procedure Diagnostic evaluations took place in OCD specialty clinics located within their respective academic medical centers. Each patient received a 1.5-h diagnostic assessment performed by a trained assessor who administered a structured diagnostic interview: the Mini International Neuropsychiatric Interview (Sheehan et al., 1998) was used at the Mayo Clinic site, and the Anxiety Disorders Interview Schedule for DSM-IV (Brown, DiNardo, & Barlow, 1994) was used at the Florida site. The interview also included the Yale Brown Obsessive Compulsive Scale (Y-BOCS; described below) and the Brown Assessment of Beliefs Scale (BABS; described below). Axis II psychopathology was assessed by means of a semi-structured interview based on DSM-IV criteria. Additional self-report measures (see below) were completed in advance of the clinic appointment. After completing the initial interview and formulating a diagnosis, the first interviewer presented the assessment data to a more expert clinician (the first or second author depending on location), who subsequently met and reviewed the assessment data with the patient. Although formal inter-rater reliability checks were not conducted, only patients for whom both interviewers agreed on diagnostic status (OCD- MDD or OCD-NUMD) were included in the study (100% inter-rater agreement). Because the design of the present study had not been conceptualized when these clinic data were collected, interviewers conducting the assessments were blind to the present study hypotheses. Individuals with additional Axis I and II disorders were included in the study as long as OCD was considered a primary (principal) diagnosis. In the OCD-MDD group, 12 patients (25.3%) evidenced additional comorbid conditions (i.e., generalized anxiety disorder, social phobia, specific phobia, eating disorders, bipolar disorder, panic disorder); in the OCD-NUMD group, 28 patients (26.2%) evidenced additional comorbid conditions (i.e., generalized anxiety disorder, panic disorder, eating disorders, phobias). w 2 -Analysis indicated that the proportion of patients with additional comorbid conditions did not differ significantly between the two groups, w 2 ¼ (N ¼ 141, df ¼ 1) ¼ 1.06, p ¼ n.s. Assessment instruments J.S. Abramowitz et al. / Behaviour Research and Therapy 45 (2007) We used a multitrait multimethod approach to assessment that included both interview and self-report measures. In addition, given the substantial heterogeneity and highly patient-specific nature of OCD symptom presentation (e.g., contamination, harm, sex, religion, washers, checkers; McKay et al., 2004), we used nomothetic as well as idiographic measures to assess obsessions, compulsions, and OCD-relevant cognitive variables. The two treatment facilities used slightly different assessment batteries. Thus, we only included data derived from measures used at both sites and with enough observations to afford adequate power for meaningful analyses. The following instruments were therefore included in the present study: Yale Brown Obsessive Compulsive Scale (Y-BOCS; Goodman, Price, Rasmussen, Mazure, Delgado et al., 1989; Goodman, Price, Rasmussen, Mazure, Fleischmann et al., 1989): Global severity of OCD was measured using the Y-BOCS, a semi-structured clinical interview that includes a symptom checklist and 10-item
4 2260 J.S. Abramowitz et al. / Behaviour Research and Therapy 45 (2007) semi-idiographic severity scale. The symptom checklist is first used to identify the patient s particular obsessions and compulsions. The severity scale then assesses the patient s main obsessions (items 1 5) and compulsions (items 6 10) on the following five parameters: (a) time, (b) interference, (c) distress, (d) resistance, and (e) degree of control. The clinician rates each item from 0 (no symptoms) to 4 (extreme) based on the past week. Two subscales (obsessions and compulsions; range 0 20) can be added to produce a total severity score that ranges from 0 to 40. The Y-BOCS interview has satisfactory psychometric properties (Goodman, Price, Rasmussen, Mazure, Delgado et al., 1989; Goodman, Price, Rasmussen, Mazure, Fleischmann et al., 1989; Storch et al., 2005) and is considered the gold standard measure of obsessivecompulsive symptoms. Brown Assessment of Beliefs Scale (BABS; Eisen et al., 1998): Insight into the senselessness of obsessions and compulsions was assessed with the BABS; a 6-item continuous measure of conviction in obsessional fears. The BABS is a semi-idiographic measure administered as a semi-structured interview. The patient and clinician first identify one or two of the patient s specific obsessional fears (e.g., I will get AIDS from flushing a public toilet, I will hit someone with my car without realizing ). Next, these beliefs are rated on the following parameters: (a) conviction in the belief, (b) perception of others views, (c) explanation of differing views, (d) fixity of the belief, (e) attempts to disprove the belief, and (f) insight (recognition of a psychiatric etiology). Item scores range from 0 (normal) to 4 (pathological) and are summed to produce a total score ranging from 0 to 24. The scale has good psychometric properties as reported by Eisen et al. (1998). Obsessive-Compulsive Inventory-Revised (OCI-R; Foa et al., 2002): Severity of OCD symptoms was assessed nomothetically using the OCI-R, an 18-item self-report questionnaire based on the earlier 84-item OCI (Foa, Kozak, Salkovskis, Coles, & Amir, 1998). Participants rate the degree to which they are bothered or distressed by OCD symptoms in the past month on a 5-point scale from 0 (not at all) to 4 (extremely). The OCI-R assesses six dimensions of OCD symptoms: (a) washing, (b) checking/doubting, (c) obsessing, (d) neutralizing, (e) ordering, and (f) hoarding. Research suggests the OCI-R possesses good internal consistency (total score alphas ¼.81 to.93 across samples) and construct validity (Abramowitz & Deacon, 2006; Foa et al., 2002). OCD is a heterogeneous condition, yet each patient presents with a specific set of obsessions and compulsions (e.g., contamination/washing, ordering/arranging). Therefore, items on the OCI-R that do not pertain to a patient s idiosyncratic presentation might be irrelevant and could suppress the representativeness of the total score. To address this issue in our analyses, we also derived scores from the OCI-R subscale that was most elevated (most severe) for each patient. Hereafter, we refer to this dependent variable as OCI-R main symptom (range ¼ 0 12). Interpretation of Intrusions Inventory (III; Obsessive Compulsive Cognitions Working Group [OCCWG], 2005): The III is a 31-item semi-idiographic questionnaire that assesses erroneous appraisals and interpretations of unwanted, distressing intrusive (obsessional) thoughts, images or impulses. After reading a definition of unwanted mental intrusions (which includes several examples), respondents were helped (by a clinician) to identify one or two obsessional thoughts they have recently experienced that are either frequent or distressing. They then rate the extent to which they believe in each of the 31 statements as related to the identified intrusive thoughts (e.g., Thinking this thought could make it happen ). Strength of belief is rated by 10 s (e.g., 0, 10, 20, etc.) from 0 ( I did not believe this idea at all ) to 100 ( I was completely convinced this idea was true ). The 31 items form three subscales: (a) importance of thoughts, (b) responsibility, and (c) control of thoughts. Thought Action Fusion Scale (TAFS; Shafran, Thordarson, & Rachman, 1996): The TAFS is a 19-item selfreport measure of the tendency to believe that thoughts are equivalent to actions. Twelve items assess moral TAF, which is the belief that thoughts are the moral equivalent of actions (e.g., Having a blasphemous thought is almost as sinful to me as a blasphemous action ). Three assess likelihood-self TAF, which is the belief that merely thinking about harm coming to oneself increases the likelihood of being harmed (e.g., If I think of myself being in a car accident this increases the risk that I will have a car accident ). The remaining four items assess likelihood-other TAF, which is the belief that thinking about harm coming to someone else increases the likelihood of that person being harmed (e.g., If I think of a relative/friend losing their job, this increases the risk that they will lose their job). Agreement with each item is rated on a scale from 0 (disagree strongly) to 4 (agree strongly). The instrument s psychometric properties are good and have been described by Shafran et al. (1996).
5 Sheehan Disability Scale (SDS; Sheehan, 1986): The SDS is a commonly used 3-item measure of the degree to which clinical symptoms interfere with work, social/leisure activities, and family/home responsibilities. It is regarded as a measure of quality of life among anxiety patients (Mendlowicz & Stein, 2000). Internal consistency of the SDS in clinical samples ranges from.56 to.86 (Mendlowicz & Stein, 2000). Beck Depression Inventory (BDI; Beck, Steer, & Brown, 1996): The BDI is a 21-item self-report scale that assesses the severity of affective, cognitive, motivational, vegetative, and psychomotor components of depression. Scores of 10 or less are considered normal; scores of 20 or greater suggest the presence of clinical depression. The BDI has excellent reliability and validity and is widely used in clinical research (Beck et al., 1996). Results Site differences In a preliminary set of analyses, we examined whether patients evaluated at the two study sites differed on demographic and psychopathology variables. These analyses indicated no such differences (p4.05) on any demographic characteristics, including group membership (OCD-MDD vs. OCD-NUMD). With two exceptions, there were also no significant site differences on the psychopathology variables. The exceptions were that participants enrolled at the University of Florida had higher scores on the Y-BOCS Total Score and on the Y-BOCS Obsessions subscale. These differences are likely due to the Florida site s specialization in the treatment of refractory patients. Because there were no site differences in the proportion of patients with comorbid MDD, we combined data from both sites in the analyses presented below. Demographic characteristics Table 1 presents demographic characteristics for the entire sample and for the OCD-MDD and OCD- NUMD groups. Between-group comparisons were made using w 2 -tests for categorical variables and t-tests for continuous variables, and these also appear in Table 1. As can be seen, no significant differences emerged on any of these variables. As expected, preliminary analyses revealed a significant between group differences on the BDI. The OCD-MDD group reported being substantially more depressed than the OCD-NUMD group. Clinical characteristics J.S. Abramowitz et al. / Behaviour Research and Therapy 45 (2007) Table 2 presents the means and standard deviations for both patient groups (and for the entire sample) on the clinical variables, as well as the results of t-tests examining differences between the OCD-MDD and OCD- NUMD groups. Between group effect sizes (Cohen s d) are also presented in Table 2. Due to the strong intercorrelations among the three SDS items (r ranged from.67 to.72) and among the three III subscales (r ranged from.72 to.82), multivariate analyses of variance were performed on these two measures. For both analyses, each dependent variable was roughly univariate normal (skewness and kurtosis estimates o1). Additionally, analysis of homogeneity of variance-covariance matrices across design cells for both analyses as indicated by the Box-M test revealed non-significant results (p4.05), suggesting that the assumption of Table 1 Demographic characteristics for the entire sample and by patient group Total sample (N ¼ 114) OCD-MDD (N ¼ 34) OCD-NUMD (N ¼ 80) Analysis (t or w 2 ) Mean (SD) age (years) (11.9) (12.2) (12.2) 0.26 Number of females (%) 50 (44.3) 16 (45.7) 34 (43.6) 0.04 Number of Caucasian (%) 82 (96.5) 24 (92.3) 58 (98.3) 2.70 Mean (SD) BDI (10.9) (10.2) (7.1) 9.23* Note: *po.01. OCD-MDD ¼ Obsessive-compulsive disorder with major depressive disorder; OCD-NUMD ¼ Obsessive-compulsive disorder with no unipolar mood disorder; BDI ¼ Beck Depression Inventory.
6 2262 J.S. Abramowitz et al. / Behaviour Research and Therapy 45 (2007) Table 2 Means (standard deviations) on clinical variables for the entire sample and each patient group Domain and variable Total sample (N ¼ 114) OCD and MDD (N ¼ 34) OCD-NUMD (N ¼ 80) F- or t-test of the difference Effect size OCD symptoms Y-BOCS (total) (5.8) (4.5) (5.9) 3.60** 0.68 Obsessions (3.0) (2.3) (3.1) 3.67** 0.69 Compulsions (3.5) (3.0) (3.6) 2.67** 0.50 OCI-R (total score) (13.2) (17.0) (11.2) Washing 4.59 (4.5) 5.39 (4.8) 4.24 (4.3) Obsessing 6.85 (3.9) 7.67 (3.7) 6.49 (3.9) Hoarding 2.93 (3.4) 3.55 (4.0) 2.66 (3.2) Ordering 4.66 (3.9) 4.78 (3.9) 4.62 (3.9) Checking 4.74 (4.0) 4.97 (4.3) 4.64 (3.8) Neutralizing 2.90 (3.6) 2.97 (4.0) 2.87 (3.5) Main symptom 9.92 (2.4) (2.4) 9.83 (2.4) Functional disability SDS work 6.26 (2.8) 7.88 (2.8) 5.57 (2.6) 14.19** 0.85 SDS social 6.35 (2.6) 7.96 (1.9) 5.68 (2.7) 15.71** 0.97 SDS family 6.75 (2.6) 8.36 (1.5) 6.00 (2.7) 17.12** 1.08 OCD-related cognition TAF Moral (12.5) (13.8) (12.0) Likelihood self 3.44 (3.3) 4.07 (3.3) 3.19 (3.3) Likelihood other 3.05 (3.8) 2.44 (3.0) 3.30 (4.1) III Importance of (251.5) (236.3) (235.5) 11.14** 0.78 thoughts Responsibility (278.7) (258.2) (271.9) 6.91* 0.62 Control of thoughts (254.6) (227.5) (248.7) 7.47** 0.65 BABS 7.37 (4.7) 8.91 (4.1) 6.73 (4.7) 1.92 a 0.36 Note: *po.05, **po.01, a p ¼.06. Degrees of freedom for t-tests ¼ 112. OCD-MDD ¼ Obsessive-compulsive disorder with major depressive disorder; OCD-NUMD ¼ Obsessive-compulsive disorder with no unipolar mood disorder; Y-BOCS ¼ Yale Brown Obsessive Compulsive Scale; OCI-R ¼ Obsessive Compulsive Inventory-Revised; BDI ¼ Beck Depression Inventory; SDS ¼ Sheehan Disability Scale; TAF ¼ Thought Action Fusion Scale; III ¼ Interpretation of Intrusions Inventory. variance-covariance was not violated. Even so, we used the relatively conservative Pillai s trace for the estimation of F-statistics in both analyses. Both groups evidenced moderate-to-severe OCD symptoms, yet whereas the OCD-MDD group demonstrated significantly more severe OCD symptoms on the Y-BOCS, no such difference was found on the OCI-R, any of its subscales, or for the OCI-R main symptom variable. The magnitudes of between group effect sizes on the Y-BOCS were moderate. Effect sizes derived from the OCI-R were small. The omnibus MANOVA for the SDS measure revealed significant between group differences in impairment ratings (F[3, 88] ¼ 7.29, po.01, Z 2 ¼.20, Pillai s trace ¼.20). Consistent with the results reported above, the OCD-MDD group indicated greater impairment in work, social, and family domains relative to the OCD-NUMD group. Effect sizes for the SDS subscales were uniformly large. Cognitive variables Our main interest in the present study was whether depressed and non-depressed OCD patients differed on cognitive variables associated with OCD. To examine our hypothesis that depressed OCD patients would
7 J.S. Abramowitz et al. / Behaviour Research and Therapy 45 (2007) Table 3 Predictors of Depression Severity (BDI) among patients with Obsessive-Compulsive Disorder in the final step of the Linear Regression Model a Variable B SE B b t Zero-order r Partial r Total Y-BOCS SDS ** III ** BABS b Note: DR 2 ¼.36, DF (3, 62) ¼ 16.90, po.001. a Model fit statistics: R 2 ¼.55, F (4, 62) ¼ 19.28, po.001. b p ¼.06, *po.05, **po.01. show a greater tendency to misinterpret the significance of intrusive thoughts, we compared the two patient groups on the TAF and III; group mean scores, F- and t-test results, and effect sizes are also presented in Table 2. As can be seen, no differences were found on any of the TAF subscales, and effect sizes were small. In contrast, the omnibus MANOVA for the III measure revealed significant between-group differences (F[3, 85] ¼ 3.71, po.05, Z 2 ¼.12, Pillai s trace ¼.12). On all three of the subscales, the OCD-MDD group evidenced significantly higher scores than did the OCD-NUMD group. The magnitudes of the between group effect sizes for the III were medium. With respect to insight into the senselessness of OCD symptoms, BABS scores indicated that both groups had reasonably good recognition that their obsessions and compulsions were excessive or unreasonable. Although the OCD-MDD group evidenced a higher mean BABS score (i.e., poorer insight) than did the OCD-NUMD group (which was in the hypothesized direction), only a non-significant trend (p ¼.06) was found. The effect size for this comparison was small to medium. Predicting MDD and depressive symptoms To further explore the relationship between cognitive factors and depressive symptomatology within OCD, we conducted hierarchical linear and logistic multiple regression analyses to examine the relative contribution of clinical and cognitive variables to the prediction of BDI scores (linear regression) and a comorbid diagnosis of MDD (logistic regression) in the entire sample (N ¼ 114). In both analyses, the Y-BOCS total score was entered in the first step to control for group differences in symptom severity. The following variables (which demonstrated significant differences between the OCD-MDD and OCD-NUMD groups) were simultaneously entered into the second step of each regression equation as predictors: SDS total score, III, and BABS. 1 Tolerance statistics for these analyses were acceptable (range.69.99) and correlations among predictor variables weak to modest (r ¼.07.37). Results of these analyses are presented in Tables 3 and 4. In the hierarchical linear multiple regression analysis, after controlling for total Y-BOCS scores, results indicated that the three predictor variables (SDS, III, and BABS) explained a significant proportion of the additional variance in BDI scores (DR 2 ¼.36, po.001), and the SDS and III contributed significant, unique variance to the model. Results from the hierarchical logistic multiple regression analysis predicting comorbid MDD also indicated that the predictors explained a significant portion of additional variance after controlling for the Y-BOCS total score (DR 2 ¼.31, po.001; see Table 4). As in the first analysis, the SDS and III again emerged as the only significant, unique predictors of MDD comorbidity. Discussion The present study examined differences between OCD patients with and without comorbid MDD with respect to clinical and cognitive variables, and to explore OCD-relevant cognitive processes as unique 1 The SDS and III total scores were used due to the strong intercorrelations between the three SDS items (r ranged from.67 to.72) and three III subscales (r ranged from.72 to.82).
8 2264 J.S. Abramowitz et al. / Behaviour Research and Therapy 45 (2007) Table 4 Predictors of comorbidity with MDD among patients with obsessive-compulsive disorder in the final step of the Logistic Regression Model a Variable B SE Wald OR (95% CI) Total Y-BOCS ( ) SDS * 1.23 ( ) III * 1.00 ( ) BABS ( ) Note: DNagelkerke R 2 ¼.31, Dw 2 ¼ 19U46, df ¼ 3, pou001u *po.05. a Model fit statistics: Nagelkerke R 2 ¼.46, 2 log likelihood ¼ 58.01, w 2 ¼ 27U52, df ¼ 4, po.001. predictors of depressive symptoms in individuals with OCD. With regard to our between-group comparisons, and consistent with previous research (e.g., Tukel et al., 2006), depressed OCD patients experienced more severe levels of overall distress and functional impairment relative to non-depressed OCD patients. However, when all of our data are considered together, our primary hypotheses appear to receive only mixed support. Concerning OCD symptom severity, between-group differences in the predicted direction were found on the Y-BOCS, but not on the OCI-R. Similarly, with respect to the propensity toward misinterpreting the significance of intrusive thoughts, the OCD-MDD group had higher scores on the III than did the OCD-NUMD group, but no such difference was found on the TAF. Finally, only a non-significant trend in the hypothesized direction emerged regarding insight into the senselessness of OCD symptoms. Although at first glance support for our hypotheses appears mixed, a closer inspection reveals that all data from the semi-idiographic measures of OCD-related variables (i.e., the Y-BOCS, III, and BABS) are consistent (or tending to be consistent) with our predictions and with findings from earlier studies (e.g., Tukel et al., 2006); whereas this was not the case for the nomothetic OCD-relevant measures (i.e., OCI-R 2 and TAFS). Specifically, ratings based on patients specific presentation of OCD revealed that relative to nondepressed OCD patients, those with comorbid MDD had more severe obsessions and compulsions, a greater tendency to misinterpret the significance of intrusive thoughts, and poorer insight into the senselessness of their symptoms. In contrast, ratings of symptoms and cognitions assumed to be representative of people with OCD in general (i.e., on nomothetic measures) did not differ between patient groups. We believe these differential findings for semi-idiographic and nomothetic measures are consequential in light of the highly heterogeneous and idiosyncratic (patient-specific) nature of OCD (e.g., McKay et al., 2004). Because semiidiographic measures take into account the patient s specific obsessions, compulsions, and beliefs, these sorts of measures are likely to provide greater accuracy regarding the assessment of obsessive-compulsive complaints than are nomothetic measures. Our regression analyses indicated that two variables functional impairment and erroneous interpretations of intrusive thoughts evidenced unique associations with depressive symptoms and with the presence of comorbid MDD. In contrast, the severity of obsessions, compulsions, and insight into the senselessness of these symptoms, did not show such a relationship. The finding that misinterpretations of intrusive thoughts and impairment were uniquely related to depression suggests that functionality and cognitive distortions are somehow involved in depressive symptoms when they occur in the context of OCD. We cannot, however, infer the direction of this relationship since the present study was cross-sectional (correlational). Therefore, prospective and experimental studies, which are better able to resolve such causal arrow ambiguity, would be a valuable next step. 2 One might argue that the OCI-R main symptom variable represents a semi-idiosyncratic measure of OCD since it considers the patient s most severe symptom. Each OCI-R subscale, however, contains only three items. Therefore, although this variable arguably provides a measure of the severity of the patient s main or primary OCD symptom (as assessed by the OCI-R), it is still bound by the particular examples included in the three items of any particular subscale. Given the heterogeneity of obsessions and compulsions, we consider this variable a nomothetic measure of OCD.
9 J.S. Abramowitz et al. / Behaviour Research and Therapy 45 (2007) As mentioned above, the cross-sectional nature of our data precludes causal inferences regarding the nature of the relationship among cognitive processes, OCD, and depression; this relationship is likely to be complex. Our findings, however, could be considered within the context of Rachman s (1993) suggestion that in some individuals with OCD, misinterpretations of the presence and significance of intrusive obsessional thoughts become highly personalized, resulting in self-blame for having (and not being able to control) such unacceptable thoughts. Self-blame and self-deprecation lead to feelings of depression and other negative mood states (e.g., Beck, 1976). Additionally, negative mood states have been shown to increase vulnerability to intrusive obsessional thoughts (e.g., England & Dickerson, 1988; Sutherland, Newman, & Rachman, 1982). Accordingly, depression might foster obsessional thinking (Niler & Beck, 1989; Reynolds & Salkovskis, 1991), thereby completing a vicious cycle of obsessional thoughts-misinterpretations-depressed mood-more obsessional thoughts. Importantly, such a model remains speculative since we did not include measures of selfblame or self-depreciation in the present study, nor could we examine causal relationships. Although research suggests that comorbid MDD attenuates response to exposure and response prevention treatment for OCD (e.g., Abramowitz & Foa, 2000), no studies have addressed whether treatment outcome for depressed OCD patents can be improved by augmenting this therapy with additional psychological treatment techniques. One hypothesis raised by the present findings is that cognitive therapy, which is an effective treatment for uncomplicated OCD (e.g., Wilhelm & Steketee, 2006) as well as for depression (e.g., DeRubeis et al., 2005), would be a useful intervention for depressed OCD patients. Adding cognitive therapy to exposure-based therapy might help patients to explicitly identify, challenge, and modify dysfunctional beliefs and interpretations that maintain both depressive and obsessional symptoms. The use of cognitive therapy along with traditional exposure-based methods in the treatment of comorbid OCD and depression has been described elsewhere (Abramowitz, 2004). Alternatively, behavioral activation which is an effective treatment for depression that does not explicitly modify cognitions might also be considered as an augmentation strategy. Our present findings should be interpreted within the context of several limitations. As mentioned previously, our data are correlational and cross-sectional, and as such do not provide a basis for causal inferences. The relationship between depression and OCD symptoms is likely a complex one, and might differ from patient to patient. Prospective and experimental studies should be undertaken to further elucidate the nature of this relationship. Other limitations include the demographically homogeneous nature of our sample (e.g., largely Caucasian) and that we did not assess family members perceptions or experiences. Regarding the latter point, it is conceivable that family members of a patient with OCD and comorbid depression may engage in heightened levels of symptom accommodation and expressed emotion by virtue of the additional burden created by the co-occurring illnesses. Finally, the variables in our regression model accounted for only a portion of the variability in depressive symptoms. This suggests that future research is necessary to further pinpoint the processes that account for the development of clinical depression in patients with OCD. Finally, we suggest a number of avenues for future research. Firstly, additional cognitive OCD-relevant variables such as inflated responsibility, intolerance of uncertainty, perfectionism, and the need to feel that things are just right should be examined in the context of comorbid OCD and depression. Secondly, clinical observations suggest that whereas some depressed OCD patients experience separate co-principal diagnoses of these disorders, others are characterized by depression that is secondary to having OCD (e.g., I am depressed because of how my life is ruined by OCD ). Unfortunately, we did not include an assessment of this issue in the present study, yet it would be useful to examine whether these two groups of patients differ with respect to symptom severity, functional impairment, and cognitive variables. Answers to these questions might have implications for the treatment of depressed OCD patients. References Abramowitz, J. S. (2004). Treatment of obsessive-compulsive disorder in patients who have comorbid depression. Journal of Clinical Psychology, 60, (in Session). Abramowitz, J., Franklin, M., Schwartz, S., & Furr, J. (2003). Symptom presentation and outcome of cognitive-behavior therapy for obsessive-compulsive disorder. Journal of Consulting and Clinical Psychology, 71,
10 2266 J.S. Abramowitz et al. / Behaviour Research and Therapy 45 (2007) Abramowitz, J. S., & Deacon, B. J. (2006). Psychometric properties and construct validity of the obsessive-compulsive inventory-revised: Replication and extension with a clinical sample. Journal of Anxiety Disorders, 20, Abramowitz, J. S., & Foa, E. B. (2000). Does comorbid major depressive disorder influence outcome of exposure and response prevention for OCD? Behavior Therapy, 31, Beck, A. T. (1976). Cognitive therapy of the emotional disorders. New York: International Universities Press. Beck, A. T., Steer, R. A., & Brown, G. K. (1996). Manual for the Beck Depression Inventory (2nd ed). San Antonio, TX: Psychological Corporation, Harcourt Brace. Bellodi, L., Scioto, G., Diaferia, G., Ronchi, P., & Smiraldi, E. (1992). Psychiatric disorders in families of patients with obsessivecompulsive disorder. Psychiatry Research, 42, Brown, T. A., DiNardo, P., & Barlow, D. H. (1994). Anxiety disorders interview schedule for DSM-IV. San Antonio, TX, Oxford, UK: Psychological Corporation. Crino, R., & Andrews, G. (1996). Obsessive-compulsive disorder and Axis I comorbidity. Journal of Anxiety Disorders, 19, Deacon, B., & Abramowitz, J. (2005). The Yale Brown obsessive compulsive scale: Factor analysis, construct validity, and suggestions for refinement. Journal of Anxiety Disorders, 19, Demal, U., Lenz, G., Mayrhofer, A., Zapotoczky, H.-G., & Zitterl, W. (1993). Obsessive-compulsive disorder and depression: A retrospective study on course and interaction. Psychopathology, 26, DeRubeis, R. J., Hollon, S. D., Amsterdam, J. D., Shelton, R. C., Young, P. R., Salomon, R., et al. (2005). Cognitive therapy vs. medications in the treatment of moderate to severe depression. Archives of General Psychiatry, 62, Eisen, J. L., Phillips, K. A., Baer, L., Beer, D. A., Atala, K. D., & Rasmussen, S. A. (1998). The Brown assessment of beliefs scale: Reliability and validity. American Journal of Psychiatry, 155, England, S., & Dickerson, M. (1988). Intrusive thoughts: Unpleasantness not the major cause of controllability. Behaviour Research and Therapy, 26, Foa, E. B., Huppert, J. D., Leiberg, S., Langner, R., Kichic, R., Hajcak, G., et al. (2002). The obsessive-compulsive inventory: Development and validation of a short version. Psychological Assessment, 14, Foa, E. B., & Kozak, M. J. (1995). DSM-IV field trial: Obsessive compulsive disorder. American Journal of Psychiatry, 152, Foa, E. B., Kozak, M. J., Salkovskis, P. M., Coles, M. E., & Amir, N. (1998). The validation of a new obsessive-compulsive disorder scale: The obsessive-compulsive inventory. Psychological Assessment, 10, Goodman, W. K., Price, L. H., Rasmussen, S. A., Mazure, C., Delgado, P., Heninger, G. R., et al. (1989). The Yale Brown obsessive compulsive scale: Validity. Archives of General Psychiatry, 46, Goodman, W. K., Price, L. H., Rasmussen, S. A., Mazure, C., Fleischmann, R. L., Hill, C. L., et al. (1989). The Yale Brown obsessive compulsive scale: Development, use, and reliability. Archives of General Psychiatry, 46, Hasler, G., LaSalle-Ricci, V., & Ronquillo, J. (2005). Obsessive-compulsive symptom dimensions show specific relationships to psychiatric comorbiditiy. Psychiatry Research, 135, Hong, J., Samuels, J., Bienvenu, O. J., Cannistraro, P., Grados, M., Riddle, M., et al. (2004). Clinical correlates of recurrent major depression in obsessive-compulsive disorder. Depression and Anxiety, 20, Kozak, M. J., & Foa, E. B. (1994). Obsessions, overvalued ideas, and delusions in obsessive-compulsive disorder. Behaviour Research and Therapy, 32, McKay, D., Abramowitz, J. S., Calamari, J. E., Kyrios, M., Radomsky, A. S., Sookman, D., et al. (2004). A critical evaluation of obsessive-compulsive disorder subtypes: Symptoms versus mechanisms. Clinical Psychology Review, 24, Mendlowicz, M. V., & Stein, M. B. (2000). Quality of life in individuals with anxiety disorders. American Journal of Psychiatry, 157, Nestadt, G., Samuels, J., Riddle, M., Liang, K.-Y., Bienvenu, O., Hoehn-Saric, R., et al. (2001). The relationship between obsessivecompulsive disorder and anxiety and affective disorders: Results from the Johns Hopkins OCD Family Study. Psychological Medicine, 31, Niler, E., & Beck, S. J. (1989). The relationship among guilt, dysphoria, anxiety and obsessions in a normal population. Behaviour Research and Therapy, 27, Obsessive Compulsive Cognitions Working Group. (2005). Psychometric validation of the Obsessive Beliefs questionnaire and the interpretations of intrusions inventory: Part 1. Behaviour Research and Therapy, 41, Rachman, S. (1993). Obsessions, responsibility, and guilt. Behaviour Research and Therapy, 31, Rachman, S. (1997). A cognitive theory of obsessions. Behaviour Research and Therapy, 35, Reynolds, M., & Salkovskis, P. (1991). The relationship among guilt, dysphoria, anxiety and obsessions in a normal population: an attempted replication. Behaviour Research and Therapy, 29, Ricciardi, J. N., & McNally, R. J. (1995). Depressed mood is related to obsessions but not compulsions in obsessive-compulsive disorder. Journal of Anxiety Disorders, 9, Shafran, R., Thordarson, D. S., & Rachman, S. (1996). Thought action fusion in obsessive-compulsive disorder. Journal of Anxiety Disorders, 10, Sheehan, D., Lecrubier, Y., Harnett-Sheehan, K., Amoriam, P., Janavs, J., Weiller, E., et al. (1998). The Mini International Neuropsychiatric Interview (M.I.N.I.): The development and validation of a structured diagnostic psychiatric interview. Journal of Clinical Psychiatry, 59(Suppl. 20), Sheehan, D. V. (1986). The anxiety disease. New York: Bantam Books. Storch, E. A., Shapira, N. A., Dimoulas, E., Geffken, G. R., Murphy, T. K., & Goodman, W. K. (2005). The Yale Brown obsessive compulsive scale: The dimensional structure revisited. Depression and Anxiety, 22,
11 J.S. Abramowitz et al. / Behaviour Research and Therapy 45 (2007) Sutherland, G., Newman, B., & Rachman, S. (1982). Experimental investigations of the relations between mood and intrusive unwanted cognitions. British Journal of Medical Psychology, 55, Tukel, R., Meteris, H., Koyuncu, A., Tecer, A., & Yazici, O. (2006). The clinical impact of mood disorder comorbidity on obsessivecompulsive disorder. European Archives of Psychiatry and Clinical Neuroscience, 256, Tukel, R., Polat, A., Ozdemir, O., Sksut, D., & Turksoy, N. (2002). Comorbid conditions in obsessive-compulsive disorder. Comprehensive Psychiatry, 43, Turksoy, N., Tukel, R., Ozdemir, O., & Karah, H. (2002). Comparison of clinical characteristics in good and poor insight in obsessivecompulsive disorder. Journal of Anxiety Disorders, 16, Wilhelm, S., & Steketee, G. (2006). Cognitive therapy for obsessive-compulsive disorder: A guide for professionals. Oakland: New Harbinger.
Author's personal copy
 Behaviour Research and Therapy 48 (2010) 949e954 Contents lists available at ScienceDirect Behaviour Research and Therapy journal homepage: www.elsevier.com/locate/brat The relationship between obsessive
Behaviour Research and Therapy 48 (2010) 949e954 Contents lists available at ScienceDirect Behaviour Research and Therapy journal homepage: www.elsevier.com/locate/brat The relationship between obsessive
Do Obsessive Beliefs Moderate the Relationship Between Obsessive-Compulsive and Depressive Symptoms?
 University of Richmond UR Scholarship Repository Honors Theses Student Research 2017 Do Obsessive Beliefs Moderate the Relationship Between Obsessive-Compulsive and Depressive Symptoms? Joanthan A. Teller
University of Richmond UR Scholarship Repository Honors Theses Student Research 2017 Do Obsessive Beliefs Moderate the Relationship Between Obsessive-Compulsive and Depressive Symptoms? Joanthan A. Teller
Journal of Anxiety Disorders
 Journal of Anxiety Disorders 23 (2009) 160 166 Contents lists available at ScienceDirect Journal of Anxiety Disorders Obsessive compulsive symptoms: The contribution of obsessional beliefs and experiential
Journal of Anxiety Disorders 23 (2009) 160 166 Contents lists available at ScienceDirect Journal of Anxiety Disorders Obsessive compulsive symptoms: The contribution of obsessional beliefs and experiential
Dysfunctional beliefs in the understanding & treatment of obsessive compulsive disorder Polman, Annemieke
 University of Groningen Dysfunctional beliefs in the understanding & treatment of obsessive compulsive disorder Polman, Annemieke IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's
University of Groningen Dysfunctional beliefs in the understanding & treatment of obsessive compulsive disorder Polman, Annemieke IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's
RESPONSIBILITY ATTITUDE IN A SAMPLE OF IRANIAN OBSESSIVE-COMPULSIVE PATIENTS
 RESPONSIBILITY ATTITUDE IN A SAMPLE OF IRANIAN OBSESSIVE-COMPULSIVE PATIENTS HABIBOLLAH GHASSEMZADEH, JAFAR BOLHARI, BEHROUZ BIRASHK & MOJGAN SALAVATI ABSTRACT Background: The study of distorted beliefs
RESPONSIBILITY ATTITUDE IN A SAMPLE OF IRANIAN OBSESSIVE-COMPULSIVE PATIENTS HABIBOLLAH GHASSEMZADEH, JAFAR BOLHARI, BEHROUZ BIRASHK & MOJGAN SALAVATI ABSTRACT Background: The study of distorted beliefs
treatment for contamination fear? Analyse Vazquez Thesis Director: Dr. Jesse Cougle Florida State University
 Running head: MENTAL CONTAMINATION AND ERP Does mental contamination predict treatment outcome in exposure and response prevention treatment for contamination fear? Analyse Vazquez Thesis Director: Dr.
Running head: MENTAL CONTAMINATION AND ERP Does mental contamination predict treatment outcome in exposure and response prevention treatment for contamination fear? Analyse Vazquez Thesis Director: Dr.
The Sense of Incompleteness as a Motivating Factor in Obsessive-Compulsive Symptoms: Conceptualization and Clinical Correlates
 + The Sense of Incompleteness as a Motivating Factor in Obsessive-Compulsive Symptoms: Conceptualization and Clinical Correlates Katherine Crowe & Dean McKay, Fordham University Steve Taylor, University
+ The Sense of Incompleteness as a Motivating Factor in Obsessive-Compulsive Symptoms: Conceptualization and Clinical Correlates Katherine Crowe & Dean McKay, Fordham University Steve Taylor, University
Do dysfunctional beliefs play a role in all types of obsessive compulsive disorder?
 Anxiety Disorders 20 (2006) 85 97 Do dysfunctional beliefs play a role in all types of obsessive compulsive disorder? Steven Taylor a, *, Jonathan S. Abramowitz b, Dean McKay c, John E. Calamari d, Debbie
Anxiety Disorders 20 (2006) 85 97 Do dysfunctional beliefs play a role in all types of obsessive compulsive disorder? Steven Taylor a, *, Jonathan S. Abramowitz b, Dean McKay c, John E. Calamari d, Debbie
Pathways to Inflated Responsibility Beliefs in Adolescent Obsessive-Compulsive Disorder: A Preliminary Investigation
 Behavioural and Cognitive Psychotherapy, 2011, 39, 229 234 First published online 23 November 2010 doi:10.1017/s1352465810000810 Pathways to Inflated Responsibility Beliefs in Adolescent Obsessive-Compulsive
Behavioural and Cognitive Psychotherapy, 2011, 39, 229 234 First published online 23 November 2010 doi:10.1017/s1352465810000810 Pathways to Inflated Responsibility Beliefs in Adolescent Obsessive-Compulsive
Florida Obsessive-Compulsive Inventory: Development, Reliability, and Validity
 BRIEF REPORT Florida Obsessive-Compulsive Inventory: Development, Reliability, and Validity Eric A. Storch, Daniel Bagner, Lisa J. Merlo, Nathan Andrew Shapira, Gary R. Geffken, Tanya K. Murphy, and Wayne
BRIEF REPORT Florida Obsessive-Compulsive Inventory: Development, Reliability, and Validity Eric A. Storch, Daniel Bagner, Lisa J. Merlo, Nathan Andrew Shapira, Gary R. Geffken, Tanya K. Murphy, and Wayne
Thought action fusion and its relationship to schizotypy and OCD symptoms
 Behaviour Research and Therapy 43 (2005) 29 41 www.elsevier.com/locate/brat Thought action fusion and its relationship to schizotypy and OCD symptoms Han-Joo Lee, Jesse R. Cougle, Michael J. Telch Department
Behaviour Research and Therapy 43 (2005) 29 41 www.elsevier.com/locate/brat Thought action fusion and its relationship to schizotypy and OCD symptoms Han-Joo Lee, Jesse R. Cougle, Michael J. Telch Department
Experiential Avoidance in Individuals with Hoarding Disorder
 Cogn Ther Res (2013) 37:779 785 DOI 10.1007/s10608-012-9511-2 BRIEF REPORT Experiential Avoidance in Individuals with Hoarding Disorder Michael G. Wheaton Laura E. Fabricant Noah C. Berman Jonathan S.
Cogn Ther Res (2013) 37:779 785 DOI 10.1007/s10608-012-9511-2 BRIEF REPORT Experiential Avoidance in Individuals with Hoarding Disorder Michael G. Wheaton Laura E. Fabricant Noah C. Berman Jonathan S.
CBT Treatment. Obsessive Compulsive Disorder
 CBT Treatment Obsessive Compulsive Disorder 1 OCD DEFINITION AND DIAGNOSIS NORMAL WORRIES & COMPULSIONS DYSFUNCTIONAL/ABNORMAL OBSESSIONS DSM IV DIAGNOSIS 2 OCD DIAGNOSIS DSM IV & ICD 10 A significant
CBT Treatment Obsessive Compulsive Disorder 1 OCD DEFINITION AND DIAGNOSIS NORMAL WORRIES & COMPULSIONS DYSFUNCTIONAL/ABNORMAL OBSESSIONS DSM IV DIAGNOSIS 2 OCD DIAGNOSIS DSM IV & ICD 10 A significant
The Validation of a New Obsessive-Compulsive Disorder Scale: The Obsessive-Compulsive Inventory
 Psychological Assessment 1998. Vol. 10, No. 3. 206-214 Copyright 1998 by the American Psychological Association, Inc. 1040-3590/98/S3.00 The Validation of a New Obsessive-Compulsive Disorder Scale: The
Psychological Assessment 1998. Vol. 10, No. 3. 206-214 Copyright 1998 by the American Psychological Association, Inc. 1040-3590/98/S3.00 The Validation of a New Obsessive-Compulsive Disorder Scale: The
Dysfunctional beliefs in the understanding & treatment of obsessive compulsive disorder Polman, Annemieke
 University of Groningen Dysfunctional beliefs in the understanding & treatment of obsessive compulsive disorder Polman, Annemieke IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's
University of Groningen Dysfunctional beliefs in the understanding & treatment of obsessive compulsive disorder Polman, Annemieke IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's
Running head: SEPARATING HOARDING FROM OBSESSIVE COMPULSIVE DISORDER.
 1 Running head: SEPARATING HOARDING FROM OBSESSIVE COMPULSIVE DISORDER. Separating hoarding from OCD S. Rachman 1 *, Corinna M. Elliott 3,, Roz Shafran 2 and Adam S. Radomsky 3. 1 University of British
1 Running head: SEPARATING HOARDING FROM OBSESSIVE COMPULSIVE DISORDER. Separating hoarding from OCD S. Rachman 1 *, Corinna M. Elliott 3,, Roz Shafran 2 and Adam S. Radomsky 3. 1 University of British
A Comparative Study of Obsessive Beliefs in Obsessive-Compulsive Disorder, Anxiety Disorder Patients and a Normal Group
 ORIGINAL ARTICLE A Comparative Study of Obsessive Beliefs in Obsessive-Compulsive Disorder, Anxiety Disorder Patients and a Normal Group Giti Shams 1 and Irena Milosevic 2 1 Department of Psychiatry, Tehran
ORIGINAL ARTICLE A Comparative Study of Obsessive Beliefs in Obsessive-Compulsive Disorder, Anxiety Disorder Patients and a Normal Group Giti Shams 1 and Irena Milosevic 2 1 Department of Psychiatry, Tehran
Original Article. Predicting Obsessive Compulsive Disorder Subtypes Using Cognitive Factors
 Birth Order and Sibling Gender Ratio of a Clinical Sample Original Article Predicting Obsessive Compulsive Disorder Subtypes Using Cognitive Factors Zahra Ramezani, MA 1 Changiz Rahimi, PhD 2 Nourollah
Birth Order and Sibling Gender Ratio of a Clinical Sample Original Article Predicting Obsessive Compulsive Disorder Subtypes Using Cognitive Factors Zahra Ramezani, MA 1 Changiz Rahimi, PhD 2 Nourollah
Cognitive Behavioral Therapy Plus Motivational Interviewing Improves Outcome for Pediatric Obsessive Compulsive Disorder: A Preliminary Study
 Cognitive Behaviour Therapy Vol 39, No 1, pp. 24 27, 2010 Cognitive Behavioral Therapy Plus Motivational Interviewing Improves Outcome for Pediatric Obsessive Compulsive Disorder: A Preliminary Study Lisa
Cognitive Behaviour Therapy Vol 39, No 1, pp. 24 27, 2010 Cognitive Behavioral Therapy Plus Motivational Interviewing Improves Outcome for Pediatric Obsessive Compulsive Disorder: A Preliminary Study Lisa
Patient Adherence Predicts Outcome From Cognitive Behavioral Therapy in Obsessive-Compulsive Disorder
 Journal of Consulting and Clinical Psychology 2011 American Psychological Association 2011, Vol. 79, No. 2, 247 252 0022-006X/11/$12.00 DOI: 10.1037/a0022659 Patient Adherence Predicts Outcome From Cognitive
Journal of Consulting and Clinical Psychology 2011 American Psychological Association 2011, Vol. 79, No. 2, 247 252 0022-006X/11/$12.00 DOI: 10.1037/a0022659 Patient Adherence Predicts Outcome From Cognitive
Relationships between thought±action fusion, thought suppression and obsessive±compulsive symptoms: a structural equation modeling approach
 Behaviour Research and Therapy 38 (2000) 889±897 www.elsevier.com/locate/brat Relationships between thought±action fusion, thought suppression and obsessive±compulsive symptoms: a structural equation modeling
Behaviour Research and Therapy 38 (2000) 889±897 www.elsevier.com/locate/brat Relationships between thought±action fusion, thought suppression and obsessive±compulsive symptoms: a structural equation modeling
Event-based prospective memory and obsessive compulsive disorder intrusive obsessional thoughts
 bs_bs_banner Australian Journal of Psychology 2012; 64: 235 242 doi: 10.1111/j.1742-9536.2012.00058.x Event-based prospective memory and obsessive compulsive disorder intrusive obsessional thoughts Lynne
bs_bs_banner Australian Journal of Psychology 2012; 64: 235 242 doi: 10.1111/j.1742-9536.2012.00058.x Event-based prospective memory and obsessive compulsive disorder intrusive obsessional thoughts Lynne
Obsessive Compulsive Disorder: Advances in Psychotherapy
 Obsessive Compulsive Disorder: Advances in Psychotherapy Question from chapter 1 1) All the following are Common obsessions EXCEPT a) Fear of becoming someone else b) Unwanted violent impulses c) Fear
Obsessive Compulsive Disorder: Advances in Psychotherapy Question from chapter 1 1) All the following are Common obsessions EXCEPT a) Fear of becoming someone else b) Unwanted violent impulses c) Fear
A Programme of Research on the Role of Implicit Cognition in OCD Research. Emma Nicholson and Dermot Barnes-Holmes
 A Programme of Research on the Role of Implicit Cognition in OCD Research Emma Nicholson and Dermot Barnes-Holmes Measuring OCD Measuring OCD is difficult due to its heterogeneity and high comorbidity
A Programme of Research on the Role of Implicit Cognition in OCD Research Emma Nicholson and Dermot Barnes-Holmes Measuring OCD Measuring OCD is difficult due to its heterogeneity and high comorbidity
OBSESSIVE- COMPULSIVE DISORDER. Verena Kerschensteiner & Sonia Rogachev
 OBSESSIVE- COMPULSIVE DISORDER 05.Dez. 2013 Verena Kerschensteiner & Sonia Rogachev A Typical day of an OCD patient Chad s OCD 1. Definition OCD (Stöppler, 2012) Obsessive compulsive disorder (OCD) is
OBSESSIVE- COMPULSIVE DISORDER 05.Dez. 2013 Verena Kerschensteiner & Sonia Rogachev A Typical day of an OCD patient Chad s OCD 1. Definition OCD (Stöppler, 2012) Obsessive compulsive disorder (OCD) is
Relationship Between Religiosity and Thought Action Fusion: A Behavioral Paradigm. Noah Chase Berman
 Relationship Between Religiosity and Thought Action Fusion: A Behavioral Paradigm Noah Chase Berman A thesis submitted to the faculty of the University of North Carolina at Chapel Hill in partial fulfillment
Relationship Between Religiosity and Thought Action Fusion: A Behavioral Paradigm Noah Chase Berman A thesis submitted to the faculty of the University of North Carolina at Chapel Hill in partial fulfillment
Obsessive-Compulsive Disorder Clinical Practice Guideline Summary for Primary Care
 Obsessive-Compulsive Disorder Clinical Practice Guideline Summary for Primary Care CLINICAL ASSESSMENT AND DIAGNOSIS (ADULTS) Obsessive-Compulsive Disorder (OCD) is categorized by recurrent obsessions,
Obsessive-Compulsive Disorder Clinical Practice Guideline Summary for Primary Care CLINICAL ASSESSMENT AND DIAGNOSIS (ADULTS) Obsessive-Compulsive Disorder (OCD) is categorized by recurrent obsessions,
CHILDHOOD OCD: RESEARCH AND CLINIC
 Syllabus CHILDHOOD OCD: RESEARCH AND CLINIC - 37923 Last update 02-12-2013 HU Credits: 4 Degree/Cycle: 2nd degree (Master) Responsible Department: School of Education Academic year: 1 Semester: Yearly
Syllabus CHILDHOOD OCD: RESEARCH AND CLINIC - 37923 Last update 02-12-2013 HU Credits: 4 Degree/Cycle: 2nd degree (Master) Responsible Department: School of Education Academic year: 1 Semester: Yearly
An exploration of the relationship between mental pollution and OCD symptoms
 Journal of Behavior Therapy and Experimental Psychiatry 39 (2008) 340 353 www.elsevier.com/locate/jbtep An exploration of the relationship between mental pollution and OCD symptoms Jesse R. Cougle, Han-Joo
Journal of Behavior Therapy and Experimental Psychiatry 39 (2008) 340 353 www.elsevier.com/locate/jbtep An exploration of the relationship between mental pollution and OCD symptoms Jesse R. Cougle, Han-Joo
Journal of Psychiatric Research
 Journal of Psychiatric Research 45 (2011) 1236e1242 Contents lists available at ScienceDirect Journal of Psychiatric Research journal homepage: www.elsevier.com/locate/psychires Specificity of disgust
Journal of Psychiatric Research 45 (2011) 1236e1242 Contents lists available at ScienceDirect Journal of Psychiatric Research journal homepage: www.elsevier.com/locate/psychires Specificity of disgust
Validation of Saving Inventory-Revised (SI-R): Compulsive Hoarding Measure
 - 88 Iranian Journal of Psychiatry and Clinical Psychology, Vol. 5, No., Spring 009, - : Original Article Validation of Saving Inventory-Revised (SI-R): Compulsive Hoarding Measure Ali Mohammadzadeh* Abstract
- 88 Iranian Journal of Psychiatry and Clinical Psychology, Vol. 5, No., Spring 009, - : Original Article Validation of Saving Inventory-Revised (SI-R): Compulsive Hoarding Measure Ali Mohammadzadeh* Abstract
An adult version of the Screen for Child Anxiety Related Emotional Disorders (SCARED-A)
 Netherlands Journal of Psychology / SCARED adult version 81 An adult version of the Screen for Child Anxiety Related Emotional Disorders (SCARED-A) Many questionnaires exist for measuring anxiety; however,
Netherlands Journal of Psychology / SCARED adult version 81 An adult version of the Screen for Child Anxiety Related Emotional Disorders (SCARED-A) Many questionnaires exist for measuring anxiety; however,
Amanda N. Medley a, Daniel W. Capron a, Kristina J. Korte a & Norman B. Schmidt a a Department of Psychology, Florida State University,
 This article was downloaded by: [Florida State University] On: 15 March 2014, At: 08:05 Publisher: Routledge Informa Ltd Registered in England and Wales Registered Number: 1072954 Registered office: Mortimer
This article was downloaded by: [Florida State University] On: 15 March 2014, At: 08:05 Publisher: Routledge Informa Ltd Registered in England and Wales Registered Number: 1072954 Registered office: Mortimer
Reassuringly Calm? Self-reported patterns of responses to reassurance seeking in Obsessive. Compulsive Disorder
 Reassuringly Calm? Self-reported patterns of responses to reassurance seeking in Obsessive Compulsive Disorder Paul M. Salkovskis 1* and Osamu Kobori 2 Running head: Reassurance Seeking in OCD 1 Department
Reassuringly Calm? Self-reported patterns of responses to reassurance seeking in Obsessive Compulsive Disorder Paul M. Salkovskis 1* and Osamu Kobori 2 Running head: Reassurance Seeking in OCD 1 Department
Concurrent Validity of the Yale Brown Obsessive Compulsive Scale Symptom Checklist m
 Concurrent Validity of the Yale Brown Obsessive Compulsive Scale Symptom Checklist m Michael L. Sulkowski University of Florida m Eric A. Storch University of South Florida m Gary R. Geffken and Emily
Concurrent Validity of the Yale Brown Obsessive Compulsive Scale Symptom Checklist m Michael L. Sulkowski University of Florida m Eric A. Storch University of South Florida m Gary R. Geffken and Emily
/ *+,- )! $ %& ' # "! 9?/6=/=> 0 : 1 < :;. /! 99/8/67 0 : 1 #. /! 55/4/* 0 : /! # #! "#$ #$ % & A B ** C D B *** 3 **** F B "GH
 / // : // : // : - - * ** *** **** -.... -.. - :. - -.DSM-IV I -. - - * نويسنده مسي ول: استاديار دانشگاه پيام نور آذربايجان شرقي. ali. mohammadzadeh@gmail. com ** استاديار دانشگاه علامه طباطبايي *** دانشيار
/ // : // : // : - - * ** *** **** -.... -.. - :. - -.DSM-IV I -. - - * نويسنده مسي ول: استاديار دانشگاه پيام نور آذربايجان شرقي. ali. mohammadzadeh@gmail. com ** استاديار دانشگاه علامه طباطبايي *** دانشيار
Correspondence concerning this article should be addressed to Alishia Williams, Level 4 O Brien Building at St. Vincent s Hospital, Australia 2010
 1 Thought-action fusion as a mediator of religiosity and obsessive-compulsive symptoms Alishia D. Williams a, Gloria Lau b, & Jessica R. Grisham b a The Clinical Research Unit for Anxiety and Depression,
1 Thought-action fusion as a mediator of religiosity and obsessive-compulsive symptoms Alishia D. Williams a, Gloria Lau b, & Jessica R. Grisham b a The Clinical Research Unit for Anxiety and Depression,
Pubblicato su Clinical Psychology and Psychotherapy, vol 8 (4), 2001 pag
 Pubblicato su Clinical Psychology and Psychotherapy, vol 8 (4), 2001 pag. 274-281 Articolo in press su Clinical Psychology and Psychotherapy Responsibility attitude, obsession and compulsion: a further
Pubblicato su Clinical Psychology and Psychotherapy, vol 8 (4), 2001 pag. 274-281 Articolo in press su Clinical Psychology and Psychotherapy Responsibility attitude, obsession and compulsion: a further
Psychometric Properties of Thought Fusion Instrument (TFI) in Students
 7-78 89 Iranian Journal of Psychiatry and Clinical Psychology, Vol. 6, No., Spring 00, 7-78 Short Scientific Article Psychometric Properties of Thought Fusion Instrument (TFI) in Students Kazem Khoramdel*,
7-78 89 Iranian Journal of Psychiatry and Clinical Psychology, Vol. 6, No., Spring 00, 7-78 Short Scientific Article Psychometric Properties of Thought Fusion Instrument (TFI) in Students Kazem Khoramdel*,
Jamie A. Micco, PhD APPLYING EXPOSURE AND RESPONSE PREVENTION TO YOUTH WITH PANDAS
 APPLYING EXPOSURE AND RESPONSE PREVENTION TO YOUTH WITH PANDAS Jamie A. Micco, PhD Director, Intensive Outpatient Service Child and Adolescent Cognitive Behavioral Therapy Program Massachusetts General
APPLYING EXPOSURE AND RESPONSE PREVENTION TO YOUTH WITH PANDAS Jamie A. Micco, PhD Director, Intensive Outpatient Service Child and Adolescent Cognitive Behavioral Therapy Program Massachusetts General
A Study of Depression among Individuals Suffering From Obsessive Compulsive Disorder
 The International Journal of Indian Psychology ISSN 34836 (e) ISSN: 3434 (p) Volume 6, Issue 1, DIP: 18.1.1/1861 DOI: 1.1/61.1 http://www.ijip.in January March, 18 Research Paper A Study of Depression
The International Journal of Indian Psychology ISSN 34836 (e) ISSN: 3434 (p) Volume 6, Issue 1, DIP: 18.1.1/1861 DOI: 1.1/61.1 http://www.ijip.in January March, 18 Research Paper A Study of Depression
Copyright: DOI link to article: Date deposited: Newcastle University eprints - eprint.ncl.ac.uk
 Romero-Sanchiz P, Nogueira-Arjona R, Godoy-Ávila A, Gavino-Lázaro A, Freeston MH. Narrow Specificity of Responsibility and Intolerance of Uncertainty in Obsessive-Compulsive Behavior and Generalized Anxiety
Romero-Sanchiz P, Nogueira-Arjona R, Godoy-Ávila A, Gavino-Lázaro A, Freeston MH. Narrow Specificity of Responsibility and Intolerance of Uncertainty in Obsessive-Compulsive Behavior and Generalized Anxiety
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and
 This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
Comparison of Thought-Action Fusion in Peoples with Obsessive-Compulsive Disorder and Major Depression Disorder
 International Journal of Applied Psychology 2012, 2(5): 77-82 DOI: 10.5923/j.ijap.20120205.01 Comparison of Thought-Action Fusion in Peoples with Obsessive-Compulsive Disorder and Major Depression Disorder
International Journal of Applied Psychology 2012, 2(5): 77-82 DOI: 10.5923/j.ijap.20120205.01 Comparison of Thought-Action Fusion in Peoples with Obsessive-Compulsive Disorder and Major Depression Disorder
Obsessive Compulsive Disorder. David Knight
 Obsessive Compulsive Disorder David Knight OCD is a serious anxiety-related condition a person experiences frequent intrusive and unwelcome obsessional thoughts followed by repetitive compulsions, impulses
Obsessive Compulsive Disorder David Knight OCD is a serious anxiety-related condition a person experiences frequent intrusive and unwelcome obsessional thoughts followed by repetitive compulsions, impulses
NeuRA Obsessive-compulsive disorders October 2017
 Introduction (OCDs) involve persistent and intrusive thoughts (obsessions) and repetitive actions (compulsions). The DSM-5 (Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition) defines
Introduction (OCDs) involve persistent and intrusive thoughts (obsessions) and repetitive actions (compulsions). The DSM-5 (Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition) defines
Background Paper: Obsessive Compulsive Disorder. Kristen Thomas. University of Pittsburgh
 Background Paper: Obsessive Compulsive Disorder Kristen Thomas University of Pittsburgh December 2011 2 According to the DSM-IV, obsessive compulsive disorder (OCD) will be diagnosed when the child displays
Background Paper: Obsessive Compulsive Disorder Kristen Thomas University of Pittsburgh December 2011 2 According to the DSM-IV, obsessive compulsive disorder (OCD) will be diagnosed when the child displays
Cognitive-Behavioral Assessment of Depression: Clinical Validation of the Automatic Thoughts Questionnaire
 Journal of Consulting and Clinical Psychology 1983, Vol. 51, No. 5, 721-725 Copyright 1983 by the American Psychological Association, Inc. Cognitive-Behavioral Assessment of Depression: Clinical Validation
Journal of Consulting and Clinical Psychology 1983, Vol. 51, No. 5, 721-725 Copyright 1983 by the American Psychological Association, Inc. Cognitive-Behavioral Assessment of Depression: Clinical Validation
Obsessive Compulsive Disorder. Understanding OCD & Managing Reassurance
 Obsessive Compulsive Disorder Understanding OCD & Managing Reassurance OCD What is it?? Small group brainstorm: What do you know about OCD? OCD in the Media A simplistic view How OCD are YOU? OCD obsessions
Obsessive Compulsive Disorder Understanding OCD & Managing Reassurance OCD What is it?? Small group brainstorm: What do you know about OCD? OCD in the Media A simplistic view How OCD are YOU? OCD obsessions
Michael Armey David M. Fresco. Jon Rottenberg. James J. Gross Ian H. Gotlib. Kent State University. Stanford University. University of South Florida
 Further psychometric refinement of depressive rumination: Support for the Brooding and Pondering factor solution in a diverse community sample with clinician-assessed psychopathology Michael Armey David
Further psychometric refinement of depressive rumination: Support for the Brooding and Pondering factor solution in a diverse community sample with clinician-assessed psychopathology Michael Armey David
A comparison of autogenous/reactive obsessions and worry in a nonclinical population: a test of the continuum hypothesis
 Behaviour Research and Therapy 43 (2005) 999 1010 www.elsevier.com/locate/brat A comparison of autogenous/reactive obsessions and worry in a nonclinical population: a test of the continuum hypothesis Han-Joo
Behaviour Research and Therapy 43 (2005) 999 1010 www.elsevier.com/locate/brat A comparison of autogenous/reactive obsessions and worry in a nonclinical population: a test of the continuum hypothesis Han-Joo
Journal of Behavior Therapy and Experimental Psychiatry
 J. Behav. Ther. & Exp. Psychiat. 41 (2010) 220 227 Contents lists available at ScienceDirect Journal of Behavior Therapy and Experimental Psychiatry journal homepage: www.elsevier.com/locate/jbtep The
J. Behav. Ther. & Exp. Psychiat. 41 (2010) 220 227 Contents lists available at ScienceDirect Journal of Behavior Therapy and Experimental Psychiatry journal homepage: www.elsevier.com/locate/jbtep The
Symptom Dimensions and Clinical Presentations in Obsessive Compulsive Disorder
 The International Journal of Indian Psychology ISSN 2348-5396 (e) ISSN: 2349-3429 (p) Volume 3, Issue 4, No. 59, DIP: 18.01.069/20160304 ISBN: 978-1-365-26307-1 http://www.ijip.in July-September, 2016
The International Journal of Indian Psychology ISSN 2348-5396 (e) ISSN: 2349-3429 (p) Volume 3, Issue 4, No. 59, DIP: 18.01.069/20160304 ISBN: 978-1-365-26307-1 http://www.ijip.in July-September, 2016
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and
 This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
Obsessive-Compulsive Disorder
 Get into groups of 3-4 Decide how each of you will do a low-to midlevel fear exposure over the next 3 hours Be back at 1 pm, ready to discuss what you did and the results Obsessive-Compulsive Disorder
Get into groups of 3-4 Decide how each of you will do a low-to midlevel fear exposure over the next 3 hours Be back at 1 pm, ready to discuss what you did and the results Obsessive-Compulsive Disorder
A Comparative Study of Socio Demographic and Clinical Profiles in Patient with Obsessive Compulsive Disorder and Depression
 American Journal of Psychiatry and Neuroscience 2018; 6(4): 99-103 http://www.sciencepublishinggroup.com/j/ajpn doi: 10.11648/j.ajpn.20180604.12 ISSN: 2330-4243 (Print); ISSN: 2330-426X (Online) A Comparative
American Journal of Psychiatry and Neuroscience 2018; 6(4): 99-103 http://www.sciencepublishinggroup.com/j/ajpn doi: 10.11648/j.ajpn.20180604.12 ISSN: 2330-4243 (Print); ISSN: 2330-426X (Online) A Comparative
Self-Oriented and Socially Prescribed Perfectionism in the Eating Disorder Inventory Perfectionism Subscale
 Self-Oriented and Socially Prescribed Perfectionism in the Eating Disorder Inventory Perfectionism Subscale Simon B. Sherry, 1 Paul L. Hewitt, 1 * Avi Besser, 2 Brandy J. McGee, 1 and Gordon L. Flett 3
Self-Oriented and Socially Prescribed Perfectionism in the Eating Disorder Inventory Perfectionism Subscale Simon B. Sherry, 1 Paul L. Hewitt, 1 * Avi Besser, 2 Brandy J. McGee, 1 and Gordon L. Flett 3
concerns in a non-clinical sample
 Shame, depression and eating concerns 1 Gee, A. & Troop, N.A. (2003). Shame, depressive symptoms and eating, weight and shape concerns in a non-clinical sample. Eating and Weight Disorders, 8, 72-75. Shame,
Shame, depression and eating concerns 1 Gee, A. & Troop, N.A. (2003). Shame, depressive symptoms and eating, weight and shape concerns in a non-clinical sample. Eating and Weight Disorders, 8, 72-75. Shame,
The Role of Fusion Beliefs and Metacognitions in Obsessive Compulsive Symptoms in General Population
 The Role of Fusion Beliefs and Metacognitions in Obsessive Compulsive Symptoms in General Population Shahram Mohammadkhani 1* 1. Department of Psychology, Faculty of Psycholgy & Educational Sciences, Kharazmi
The Role of Fusion Beliefs and Metacognitions in Obsessive Compulsive Symptoms in General Population Shahram Mohammadkhani 1* 1. Department of Psychology, Faculty of Psycholgy & Educational Sciences, Kharazmi
Fabrizio Didonna, Paolo Zordan, Elena Prunetti, Denise Rigoni, Marzia Zorzi, Marco Bateni Unit for Anxiety and Mood Disorders Unit for Personality
 35th International Congress of SPR 16-19 June 2004 Roma - Italy Clinical features of obsessive symptoms in Borderline Personality Disorders and Obsessive Compulsive Disorders: Differences and overlapping
35th International Congress of SPR 16-19 June 2004 Roma - Italy Clinical features of obsessive symptoms in Borderline Personality Disorders and Obsessive Compulsive Disorders: Differences and overlapping
Psychological treatment of obsessive compulsive disorder
 Psychological treatment of obsessive compulsive disorder Paul M Salkovskis Abstract NICE guidelines recommend psychological treatment (cognitive behavioural therapy, involving major elements of exposure
Psychological treatment of obsessive compulsive disorder Paul M Salkovskis Abstract NICE guidelines recommend psychological treatment (cognitive behavioural therapy, involving major elements of exposure
The Impact of Obsessive Compulsive Personality Disorder on Cognitive Behaviour Therapy for Obsessive Compulsive Disorder
 PDF For Review The Impact of Obsessive Compulsive Personality Disorder on Cognitive Behaviour Therapy for Obsessive Compulsive Disorder Journal: Behavioural and Cognitive Psychotherapy Manuscript ID BCP-0-
PDF For Review The Impact of Obsessive Compulsive Personality Disorder on Cognitive Behaviour Therapy for Obsessive Compulsive Disorder Journal: Behavioural and Cognitive Psychotherapy Manuscript ID BCP-0-
Medical utilization across the anxiety disorders
 Anxiety Disorders 22 (2008) 344 350 Medical utilization across the anxiety disorders Brett Deacon a, *, James Lickel a, Jonathan S. Abramowitz b a University of Wyoming, Department of Psychology, Dept.
Anxiety Disorders 22 (2008) 344 350 Medical utilization across the anxiety disorders Brett Deacon a, *, James Lickel a, Jonathan S. Abramowitz b a University of Wyoming, Department of Psychology, Dept.
SUMMARY AND DISCUSSION
 Risk factors for the development and outcome of childhood psychopathology SUMMARY AND DISCUSSION Chapter 147 In this chapter I present a summary of the results of the studies described in this thesis followed
Risk factors for the development and outcome of childhood psychopathology SUMMARY AND DISCUSSION Chapter 147 In this chapter I present a summary of the results of the studies described in this thesis followed
Five Changes in DSM 5 Principles for Primary Care. Tom Janzen, M.D. STEGH Mental Health May 14, 2014
 Five Changes in DSM 5 Principles for Primary Care Tom Janzen, M.D. STEGH Mental Health May 14, 2014 Overall Learning Objectives Review 5 changes to DSM 5 which have significance for Family Physicians Examine
Five Changes in DSM 5 Principles for Primary Care Tom Janzen, M.D. STEGH Mental Health May 14, 2014 Overall Learning Objectives Review 5 changes to DSM 5 which have significance for Family Physicians Examine
Y-BOCS Symptom Checklist
 Y-BOCS Symptom Checklist (Yale-Brown Obsessive Compulsive Scale) Administering the Y-BOCS Symptom Checklist and Severity Ratings. 1. Establish the diagnosis of obsessive compulsive disorder. 2. Using the
Y-BOCS Symptom Checklist (Yale-Brown Obsessive Compulsive Scale) Administering the Y-BOCS Symptom Checklist and Severity Ratings. 1. Establish the diagnosis of obsessive compulsive disorder. 2. Using the
Quality of Life and Stress among Obsessive Compulsive Disorder. Caregivers and General Population
 The International Journal of Indian Psychology ISSN 2348-5396 (e) ISSN: 2349-3429 (p) Volume 3, Issue 2, No.4, DIP: 18.01.069/20160302 ISBN: 978-1-329-85570-0 http://www.ijip.in January - March, 2016 Quality
The International Journal of Indian Psychology ISSN 2348-5396 (e) ISSN: 2349-3429 (p) Volume 3, Issue 2, No.4, DIP: 18.01.069/20160302 ISBN: 978-1-329-85570-0 http://www.ijip.in January - March, 2016 Quality
ORIGINAL RESEARCH Key Words: psychometric evaluation, obsessive-compulsive disorder, co-morbidity, assessment
 025-030_PB_V39N1_de_Haan.qxd 9/21/06 5:35 PM Page 25 ORIGINAL RESEARCH Key Words: psychometric evaluation, obsessive-compulsive disorder, co-morbidity, assessment Reliability and Validity of the Yale-Brown
025-030_PB_V39N1_de_Haan.qxd 9/21/06 5:35 PM Page 25 ORIGINAL RESEARCH Key Words: psychometric evaluation, obsessive-compulsive disorder, co-morbidity, assessment Reliability and Validity of the Yale-Brown
Background. Interoceptive Exposure: An Underused Weapon in the Arsenal against OCD. Outline. Exposure Therapy for OCD
 Outline Interoceptive Exposure: An Underused Weapon in the Arsenal against OCD Shannon Blakey, MS & Jonathan Abramowitz, PhD University of North Carolina at Chapel Hill 30 July 2016 Background Anxiety
Outline Interoceptive Exposure: An Underused Weapon in the Arsenal against OCD Shannon Blakey, MS & Jonathan Abramowitz, PhD University of North Carolina at Chapel Hill 30 July 2016 Background Anxiety
Perhaps you only imagined doing it : Reality-Monitoring in Obsessive-Compulsive Checkers. Using Semi-Idiographic Stimuli
 Reality-monitoring 1 Running head: REALITY-MONITORING Perhaps you only imagined doing it : Reality-Monitoring in Obsessive-Compulsive Checkers Using Semi-Idiographic Stimuli Jesse R. Cougle 1, Paul M.
Reality-monitoring 1 Running head: REALITY-MONITORING Perhaps you only imagined doing it : Reality-Monitoring in Obsessive-Compulsive Checkers Using Semi-Idiographic Stimuli Jesse R. Cougle 1, Paul M.
Memory bias, confidence and responsibility in compulsive checking
 Behaviour Research and Therapy 39 (2001) 813 822 www.elsevier.com/locate/brat Memory bias, confidence and responsibility in compulsive checking Adam S. Radomsky *, S. Rachman, David Hammond University
Behaviour Research and Therapy 39 (2001) 813 822 www.elsevier.com/locate/brat Memory bias, confidence and responsibility in compulsive checking Adam S. Radomsky *, S. Rachman, David Hammond University
Looming Maladaptive Style as a Specific Moderator of Risk Factors for Anxiety
 Looming Maladaptive Style as a Specific Moderator of Risk Factors for Anxiety Abby D. Adler Introduction Anxiety disorders are the most common mental illness in the United States with a lifetime prevalence
Looming Maladaptive Style as a Specific Moderator of Risk Factors for Anxiety Abby D. Adler Introduction Anxiety disorders are the most common mental illness in the United States with a lifetime prevalence
The Relationship between Scrupulosity, Obsessive-Compulsive Disorder and Its Related Cognitive Styles
 The Relationship between Scrupulosity, Obsessive-Compulsive Disorder and Its Related Cognitive Styles Sara Kaviani 1*, Hossein Eskandari 1, Soghra Ebrahimi Ghavam 2 1. Department of Psychology and Educational
The Relationship between Scrupulosity, Obsessive-Compulsive Disorder and Its Related Cognitive Styles Sara Kaviani 1*, Hossein Eskandari 1, Soghra Ebrahimi Ghavam 2 1. Department of Psychology and Educational
BECOMING A DISCRIMINATING CONSUMER OF TREATMENT OUTCOMES
 BECOMING A DISCRIMINATING CONSUMER OF TREATMENT OUTCOMES BECOMING A DISCRIMINATING CONSUMER OF TREATMENT OUTCOMES Craig Johnson, PhD, FAED, CEDS, Chief Science Officer Emmett R. Bishop Jr., MD, FAED,
BECOMING A DISCRIMINATING CONSUMER OF TREATMENT OUTCOMES BECOMING A DISCRIMINATING CONSUMER OF TREATMENT OUTCOMES Craig Johnson, PhD, FAED, CEDS, Chief Science Officer Emmett R. Bishop Jr., MD, FAED,
Symmetry, Ordering and Arranging Compulsive Behaviour
 1 Symmetry, Ordering and Arranging Compulsive Behaviour Adam S. Radomsky* Concordia University and S. Rachman University of British Columbia University of British Columbia Keywords: Ordering, Arranging,
1 Symmetry, Ordering and Arranging Compulsive Behaviour Adam S. Radomsky* Concordia University and S. Rachman University of British Columbia University of British Columbia Keywords: Ordering, Arranging,
Teacher stress: A comparison between casual and permanent primary school teachers with a special focus on coping
 Teacher stress: A comparison between casual and permanent primary school teachers with a special focus on coping Amanda Palmer, Ken Sinclair and Michael Bailey University of Sydney Paper prepared for presentation
Teacher stress: A comparison between casual and permanent primary school teachers with a special focus on coping Amanda Palmer, Ken Sinclair and Michael Bailey University of Sydney Paper prepared for presentation
Obsessive Compulsive Disorder: Cognitive Behavioral Therapy via Exposure and Response Prevention
 Mako: NSU Undergraduate Student Journal Volume 4 Article 2 Winter 2-1-2012 Obsessive Compulsive Disorder: Cognitive Behavioral Therapy via Exposure and Response Prevention Dyona Augustin Nova Southeastern
Mako: NSU Undergraduate Student Journal Volume 4 Article 2 Winter 2-1-2012 Obsessive Compulsive Disorder: Cognitive Behavioral Therapy via Exposure and Response Prevention Dyona Augustin Nova Southeastern
Psychometric Properties of the French and English versions of the Vancouver Obsessional-
 1 Psychometric Properties of the French and English versions of the Vancouver Obsessional- Compulsive Inventory and the Symmetry, Ordering and Arranging Questionnaire Adam S. Radomsky 1,2, Allison J. Ouimet
1 Psychometric Properties of the French and English versions of the Vancouver Obsessional- Compulsive Inventory and the Symmetry, Ordering and Arranging Questionnaire Adam S. Radomsky 1,2, Allison J. Ouimet
DIMENSIONAL AND SUBTYPE MODELS OF OCD
 Chapter 2 DIMENSIONAL AND SUBTYPE MODELS OF OCD Steven Taylor Although obsessive-compulsive disorder (OCD) is recognized in DSM-IV as a unitary syndrome (American Psychiatric Association [APA], 2000),
Chapter 2 DIMENSIONAL AND SUBTYPE MODELS OF OCD Steven Taylor Although obsessive-compulsive disorder (OCD) is recognized in DSM-IV as a unitary syndrome (American Psychiatric Association [APA], 2000),
King s Research Portal
 King s Research Portal DOI: 10.1016/j.jocrd.2016.02.001 Document Version Peer reviewed version Link to publication record in King's Research Portal Citation for published version (APA): Veale, D., Lim,
King s Research Portal DOI: 10.1016/j.jocrd.2016.02.001 Document Version Peer reviewed version Link to publication record in King's Research Portal Citation for published version (APA): Veale, D., Lim,
Obsessive compulsive disorder
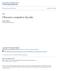 University of Northern Iowa UNI ScholarWorks Graduate Research Papers Graduate College 2010 Obsessive compulsive disorder Angela Bigelow University of Northern Iowa Copyright 2010 Angela Bigelow Follow
University of Northern Iowa UNI ScholarWorks Graduate Research Papers Graduate College 2010 Obsessive compulsive disorder Angela Bigelow University of Northern Iowa Copyright 2010 Angela Bigelow Follow
Acute Stabilization In A Trauma Program: A Pilot Study. Colin A. Ross, MD. Sean Burns, MA, LLP
 In Press, Psychological Trauma Acute Stabilization In A Trauma Program: A Pilot Study Colin A. Ross, MD Sean Burns, MA, LLP Address correspondence to: Colin A. Ross, MD, 1701 Gateway, Suite 349, Richardson,
In Press, Psychological Trauma Acute Stabilization In A Trauma Program: A Pilot Study Colin A. Ross, MD Sean Burns, MA, LLP Address correspondence to: Colin A. Ross, MD, 1701 Gateway, Suite 349, Richardson,
TESTING THE AUTOGENOUS REACTIVE MODEL OF OBSESSIONS
 DEPRESSION AND ANXIETY 21:118 129 (2005) Research Article TESTING THE AUTOGENOUS REACTIVE MODEL OF OBSESSIONS Han-Joo Lee, 1 Seok-Man Kwon, 2 Jun Soo Kwon, 3 and Michael J. Telch 1n Two independent studies
DEPRESSION AND ANXIETY 21:118 129 (2005) Research Article TESTING THE AUTOGENOUS REACTIVE MODEL OF OBSESSIONS Han-Joo Lee, 1 Seok-Man Kwon, 2 Jun Soo Kwon, 3 and Michael J. Telch 1n Two independent studies
Exploring the relationship between fear of positive evaluation and social anxiety
 Journal of Anxiety Disorders 22 (2008) 386 400 Exploring the relationship between fear of positive evaluation and social anxiety Justin W. Weeks a, Richard G. Heimberg a, *, Thomas L. Rodebaugh b, Peter
Journal of Anxiety Disorders 22 (2008) 386 400 Exploring the relationship between fear of positive evaluation and social anxiety Justin W. Weeks a, Richard G. Heimberg a, *, Thomas L. Rodebaugh b, Peter
BRIEF REPORT. Gerald J. Haeffel. Zachary R. Voelz and Thomas E. Joiner, Jr. University of Wisconsin Madison, Madison, WI, USA
 COGNITION AND EMOTION 2007, 21 (3), 681688 BRIEF REPORT Vulnerability to depressive symptoms: Clarifying the role of excessive reassurance seeking and perceived social support in an interpersonal model
COGNITION AND EMOTION 2007, 21 (3), 681688 BRIEF REPORT Vulnerability to depressive symptoms: Clarifying the role of excessive reassurance seeking and perceived social support in an interpersonal model
Metacognitive therapy for generalized anxiety disorder: An open trial
 Journal of Behavior Therapy and Experimental Psychiatry 37 (2006) 206 212 www.elsevier.com/locate/jbtep Metacognitive therapy for generalized anxiety disorder: An open trial Adrian Wells a,, Paul King
Journal of Behavior Therapy and Experimental Psychiatry 37 (2006) 206 212 www.elsevier.com/locate/jbtep Metacognitive therapy for generalized anxiety disorder: An open trial Adrian Wells a,, Paul King
I can t stop thinking about my child s flaws : An investigation of parental preoccupation with. their children s perceived flaws
 I can t stop thinking about my child s flaws : An investigation of parental preoccupation with their children s perceived flaws 1 Guy Doron 2 Danny Derby 3 Ohad Szepsenwol 1 School of Psychology, Interdisciplinary
I can t stop thinking about my child s flaws : An investigation of parental preoccupation with their children s perceived flaws 1 Guy Doron 2 Danny Derby 3 Ohad Szepsenwol 1 School of Psychology, Interdisciplinary
The relationship between obsessive compulsive and posttraumatic stress symptoms in clinical and non-clinical samples
 Anxiety Disorders 19 (2005) 127 136 The relationship between obsessive compulsive and posttraumatic stress symptoms in clinical and non-clinical samples Jonathan D. Huppert a,*, Jason S. Moser a, Beth
Anxiety Disorders 19 (2005) 127 136 The relationship between obsessive compulsive and posttraumatic stress symptoms in clinical and non-clinical samples Jonathan D. Huppert a,*, Jason S. Moser a, Beth
Treatment of Anxiety as a Cooccurring Disorder
 Treatment of Anxiety as a Cooccurring Disorder John J. Arnold, Ph.D., Sanctuary at Lake Chelan Community Hospital Presented at the 2016 Washington Behavioral Healthcare Conference Learning Objectives Learn
Treatment of Anxiety as a Cooccurring Disorder John J. Arnold, Ph.D., Sanctuary at Lake Chelan Community Hospital Presented at the 2016 Washington Behavioral Healthcare Conference Learning Objectives Learn
Anxiety Disorders. Fear & Anxiety. Anxiety Disorder? 26/5/2014. J. H. Atkinson, M.D. Fear. Anxiety. An anxiety disorder is present when
 Anxiety s J. H. Atkinson, M.D. HIV Neurobehavioral Research Center University of California, San Diego Department of Psychiatry & Veterans Affairs Healthcare System, San Diego Materials courtesy of Dr.
Anxiety s J. H. Atkinson, M.D. HIV Neurobehavioral Research Center University of California, San Diego Department of Psychiatry & Veterans Affairs Healthcare System, San Diego Materials courtesy of Dr.
Running head: NEGATIVE PROBLEM ORIENTATION 1. Fergus, T. A., Valentiner, D. P., Wu, K. D., & McGrath, P. B. (2015). Examining the symptomlevel
 Running head: NEGATIVE PROBLEM ORIENTATION 1 Fergus, T. A., Valentiner, D. P., Wu, K. D., & McGrath, P. B. (2015). Examining the symptomlevel specificity of negative problem orientation in a clinical sample.
Running head: NEGATIVE PROBLEM ORIENTATION 1 Fergus, T. A., Valentiner, D. P., Wu, K. D., & McGrath, P. B. (2015). Examining the symptomlevel specificity of negative problem orientation in a clinical sample.
Not just right experiences : perfectionism, obsessive compulsive features and general psychopathology
 Behaviour Research and Therapy 41 (2003) 681 700 www.elsevier.com/locate/brat Not just right experiences : perfectionism, obsessive compulsive features and general psychopathology Meredith E. Coles a,,
Behaviour Research and Therapy 41 (2003) 681 700 www.elsevier.com/locate/brat Not just right experiences : perfectionism, obsessive compulsive features and general psychopathology Meredith E. Coles a,,
Psychiatry Research 225 (2015) Contents lists available at ScienceDirect. Psychiatry Research
 Psychiatry Research 225 (2015) 236 246 Contents lists available at ScienceDirect Psychiatry Research journal homepage: www.elsevier.com/locate/psychres Review article Efficacy of cognitive-behavioral therapy
Psychiatry Research 225 (2015) 236 246 Contents lists available at ScienceDirect Psychiatry Research journal homepage: www.elsevier.com/locate/psychres Review article Efficacy of cognitive-behavioral therapy
P1: OTA/XYZ P2: ABC JWST176-c01 JWST176-Zohar March 23, :25 Printer Name: Yet to Come SECTION 1. Assessment and Treatment COPYRIGHTED MATERIAL
 SECTION 1 Assessment and Treatment COPYRIGHTED MATERIAL CHAPTER 1 Assessment Jose M. Menchon Department of Psychiatry, Hospital Universitari de Bellvitge-IDIBELL, Hospitalet de Llobregat (Barcelona),
SECTION 1 Assessment and Treatment COPYRIGHTED MATERIAL CHAPTER 1 Assessment Jose M. Menchon Department of Psychiatry, Hospital Universitari de Bellvitge-IDIBELL, Hospitalet de Llobregat (Barcelona),
Randomised controlled trial of parent-enhanced CBT compared with individual CBT for. Obsessive Compulsive Disorder in young people. Shirley A Reynolds
 Randomised controlled trial of parent-enhanced CBT compared with individual CBT for Obsessive Compulsive Disorder in young people Shirley A Reynolds Charlie Waller Institute, University of Reading Sarah
Randomised controlled trial of parent-enhanced CBT compared with individual CBT for Obsessive Compulsive Disorder in young people Shirley A Reynolds Charlie Waller Institute, University of Reading Sarah
CHILDREN S YALE-BROWN OBSESSIVE COMPULSIVE SCALE (CY-BOCS) DEVELOPED BY:
 First Edition 10/1/86 (Revised 2/9/11) CHILDREN S YALE-BROWN OBSESSIVE COMPULSIVE SCALE (CY-BOCS) DEVELOPED BY: WAYNE K. GOODMAN, M.D. 1 STEVEN A. RASMUSSEN, M.D. 2 LAWRENCE H. PRICE, M.D. 2 ERIC STORCH,
First Edition 10/1/86 (Revised 2/9/11) CHILDREN S YALE-BROWN OBSESSIVE COMPULSIVE SCALE (CY-BOCS) DEVELOPED BY: WAYNE K. GOODMAN, M.D. 1 STEVEN A. RASMUSSEN, M.D. 2 LAWRENCE H. PRICE, M.D. 2 ERIC STORCH,
Study of Meditational Role of Self-Esteem in the Relationship Between Perfectionism and Competitive Anxiety Elite Athletes
 American Journal of Psychology and Cognitive Science Vol. 4, No. 3, 2018, pp. 26-30 http://www.aiscience.org/journal/ajpcs ISSN: 2381-7453 (Print); ISSN: 2381-747X (Online) Study of Meditational Role of
American Journal of Psychology and Cognitive Science Vol. 4, No. 3, 2018, pp. 26-30 http://www.aiscience.org/journal/ajpcs ISSN: 2381-7453 (Print); ISSN: 2381-747X (Online) Study of Meditational Role of
Specificity of disgust sensitivity in the prediction of behavioral avoidance in contamination fear
 Behaviour Research and Therapy 45 (2007) 2110 2120 www.elsevier.com/locate/brat Specificity of disgust sensitivity in the prediction of behavioral avoidance in contamination fear Brett Deacon a,, Bunmi
Behaviour Research and Therapy 45 (2007) 2110 2120 www.elsevier.com/locate/brat Specificity of disgust sensitivity in the prediction of behavioral avoidance in contamination fear Brett Deacon a,, Bunmi
Adam S. Radomsky 1,2, Allison J. Ouimet 1, Andrea R. Ashbaugh 1, Stefanie L. Lavoie 1, Chris L. Parrish 1 and Kieron P. O Connor 2
 Cognitive Behaviour Therapy Vol 35, No 3, pp. 164 173, 2006 Psychometric Properties of the French and English Versions of the Vancouver Obsessional-Compulsive Inventory and the Symmetry Ordering and Arranging
Cognitive Behaviour Therapy Vol 35, No 3, pp. 164 173, 2006 Psychometric Properties of the French and English Versions of the Vancouver Obsessional-Compulsive Inventory and the Symmetry Ordering and Arranging
BroadcastMed Bipolar, Borderline, Both? Diagnostic/Formulation Issues in Mood and Personality Disorders
 BroadcastMed Bipolar, Borderline, Both? Diagnostic/Formulation Issues in Mood and Personality Disorders BRIAN PALMER: Hi. My name is Brian Palmer. I'm a psychiatrist here at Mayo Clinic. Today, we'd like
BroadcastMed Bipolar, Borderline, Both? Diagnostic/Formulation Issues in Mood and Personality Disorders BRIAN PALMER: Hi. My name is Brian Palmer. I'm a psychiatrist here at Mayo Clinic. Today, we'd like
