Non-Oral Feedings. Disclosures. Feeding the Medical Complex Pediatric Patient. Pediatric Feeding Disorder. Overview.
|
|
|
- Claude Sims
- 5 years ago
- Views:
Transcription
1 Feeding the Medical Complex Pediatric Patient Brenda Sitzmann, MA, CCC-SLP (816) Disclosures Ms. Sitzmann is speech-language pathologist at Children s Mercy for which she receives a salary. Ms. Sitzmann is receiving an honorarium for presenting this workshop. Ms. Sitzmann has no non-financial relationships to disclose. 2 Pediatric Feeding Disorder Overview Goday, et al An impairment (system failure) creates a pediatric feeding disorder (PFD) that results in a dysfunction The resulting dysfunction is not considered age- appropriate Impacts at least one of these domains: medical nutrition skill and ability Non-oral feedings Eosinophilic esophagitis psychosocial Today s presentation will focus on the impact of the medical domain on skill and ability. Laryngeal cleft 3 4 Non-Oral Feedings Very useful tools Non-Oral Feedings Enables patients to receive adequate nutrition while the team addresses medical, psychosocial, and skill/ability concerns Have a plan to work towards removal before the tube is placed however this may not be the goal for all patients 5 6
2 Non-Oral Feedings Non-Oral Feedings Studies have shown that g-tubes: Improve weight gain and mid-arm circumference Reduce feeding time Improve quality of life for caregivers and patients (Gottrand et al. 2010) Today we are going to explore the following types of non-oral feedings: Nasogastric (NG) tube Nasojejunal (NJ) tube Gastrostomy (G) tube Gastro-jejunal (G/J) tube 7 8 Nasogastric (NG) Tube Nasogastric (NG) Tube A long feeding tube is inserted through the nose and passed into the stomach In GI Multidisciplinary Feeding Clinic, we often use NG tubes to trial non-oral feedings Will the patient tolerate feedings gain weight appropriately Pros: Temporary Non-surgical placement Bolus or continuous feedings into the stomach Cons: Temporary (easily pulled out, vomiting) Needs to be replaced more frequently than a g-tube Concerns that it may interfere with swallow function (unable to find research indicating that this is true) May increase oral aversion 9 10 Nasojejunal (NJ) Tube Nasojejunal (NJ) Tube Tube is inserted through the nose, passed through the stomach and placed in the jejunum (second part of the intestines) Continuous feedings (no bolus feedings) into the jejunum Limited options for formula Often used if the patient is not tolerating NG tube feedings Frequent vomiting Significant reflux concerns Pros: Temporary Non-surgical placement Can eliminate vomiting associated with NG feedings Cons: Temporary (easily pulled out; vomiting) Needs to be replaced more frequently than a g-tube Placement confirmed with x-ray Concerns that it may interfere with swallow function (unable to find research indicating that this is a valid concern) May increase oral aversion Difficult to wean to oral feedings if patient is only tolerating NJ tube feedings 11 12
3 Gastrostomy (G) Tube Gastrostomy (G) Tube Tube is inserted through the abdomen and delivers nutrition directly to the stomach Typically considered a good option if it is expected that the need for non-oral feedings will be greater than 3 months Can be used for bolus and continuous feedings gravity feedings feeding pumps Initial replacement of the tube occurs ~3 months post surgery and typically requires a visit to the surgeon Replaced every 3 months or sooner if concerns arise caregivers may be trained to replace the tube at home Gastrostomy (G) Tube Gastro-jejunal (G/J) tube Pros: Semi-permanent (can be removed) Decreased risk of oral aversion Not taped to the child s face Does not irritate the nose, pharynx, or esophagus Cons Surgical placement Complications with stoma site Granulation tissue Leaking Tube is inserted through the abdomen and delivers nutrition directly to the stomach (gtube) and also contains another tube that is passed into the jejunum (j-tube) Often start with a g-tube then progress to a g/j tube if the patient is having difficulty tolerating g-tube feedings Provide continuous feedings into the jejunum Replaced using x-ray guidance Gastro-jejunal (G/J) Tube Pros: Semi-permanent (can be removed) Decreased risk of oral aversion Not taped to the child s face Does not irritate the nose, pharynx, or esophagus J-tube is helpful when the patient is unable to tolerate g-tube feedings Cons: Surgical placement Cannot be replaced at home Continuous feedings make weaning difficult Complications with stoma site Granulation tissue Leaking Criteria typically includes: Within 90% of ideal body weight with steady weight gain Strong oral motor feeding skills Medically stable Ideally this includes being able to tolerate bolus feedings into the stomach Continuous feedings are often a sign of ongoing GI concerns and interfere with hunger signals Supportive caregivers Strong child-caregiver interactions 17 18
4 Multiple approaches STEP 1: The typical approach used by the GI Multidisciplinary Feeding Clinic at CMH is outlined in the following slides Highly individualized process Must be completed under the guidance of the patient s medical team It takes a village Feeding teams are very helpful Address medical concerns Reflux Aspiration EoE Constipation Slow gastric emptying Establish successful non-oral feedings Ensure adequate weight gain Continue oral stim program and oral feedings as tolerated expect a decrease in oral feeding initially STEP 2: Work towards bolus feedings into the stomach Pump or gravity feeds Ideally, age-appropriate volume given over 30 minutes or less Build oral motor feeding skills and normalize oral sensation if aversion is a concern STEP 3: At this point, the patient is interested in eating and taking a variety of foods orally but oral intake is limited Safe plan for liquids and intake is steadily increasing Offer oral feedings 2-3 times per day prior to non-oral feedings goal = 30 minutes or less of time in the highchair/oral feeding Provide 15 minutes to eat orally then start the non-oral feeding while the child continues to eat (if interested) work on adding variety Protein, vegetables, fruits Hydration STEP 3 (continued): Rearrange non-oral feedings to encourage hunger - Hunger provocation Work with a dietician and physician More time between feedings Provide individual feedings over a shorter period of time Decrease pump feedings from 45 minutes to 30 minutes Transition from pump feedings to a gravity feeding Condense feedings If child is receiving five 4 oz. formula boluses during the day (every three hours, example 6 am, 9 am, 12 pm, 3 pm & 6 pm), transition to four 5 oz boluses given every 4 hours (6 am, 10 am, 2 pm, 6 pm) Ideally non-oral feeding schedule will match a typical meal schedule STEP 4: As intake increases, may start counting calories and adjusting non-oral feedings based on oral intake If the child typically receives a 4 oz PediaSure bolus but drinks 2 oz orally, only 2 oz. are provided non-orally after the oral feeding More complicated when calculating intake of solids 23 24
5 STEP 4 (continued): STEP 5: Another option is to reduce all feedings by a set amount (determined by dietician based on current oral intake) then provide a catch-up feeding at the end of the day Volume of catch-up feeding depends on oral intake If the child typically receives five 6 oz. boluses, each bolus is reduced to 4 oz. If the child drinks 10 oz. of formula during that day there is no need for a supplemental feeding however if only 4 oz. are consumed orally, an additional 6 oz. feeding is provided Start eliminating non-oral bolus feedings and/or significantly reduce calories provided via non-oral feedings until the child is meeting nutritional needs via oral feedings only typically start with the meal with the best oral intake may provide a supplemental non-oral feeding at the end of the day May take a little while (few days) for the child to adjust oral intake to compensate for fewer non-oral feedings do not expect weight gain during this transition Ensure patient is drinking enough fluids (not just formula/milk) Plan for administering medication General guidelines: General guidelines (continued): Remember the big picture Weaning may not be appropriate for all patients Quality of life If the child does not seem to be recognizing hunger, medical team may consider medication Cyproheptadine/Periactin Ensure oral motor skills are appropriate before using medication Develop an appropriate long-term plan with the family ongoing discussion Typically try to avoid nighttime/overnight feedings Want to mirror an age-appropriate schedule Overnight feedings tend to interfere with oral intake in the morning Demonstrate adequate growth and weight gain for 6 months before the g-tube is removed make it through a respiratory season without using the tube Monitor weight gain closely but not too closely (no daily weight checks) Puree by g-tube/blenderized diets Intensive feeding therapy programs Eosinophilic Esophagitis (EoE) Eosinophilic Esophagitis A chronic disease of the esophagus that is often confused with gastroesophageal reflux disease but is unresponsive to treatment with proton pump inhibitors. (Chadha et al. 2014) Increasing reports of EoE most likely due to increased awareness Estimated US & European incidence = 1.3 to 12.8/100,000 children and adults (Dellon 2014) 29 30
6 Eosinophilic Esophagitis (EoE) Eosinophilic Esophagitis (EoE) Common symptoms: Long-term complications: Young children Fibrosis Vomiting Stricture formation Poor appetite Food impaction Poor growth Older children Abdominal pain (Chawla et al, 2016) Diagnosed via an EDG (esophagogastricduodenoscopy) Endoscopy that examines the esophagus, stomach, and first portion of the duodenum (small intestine) completed under anesthesia Obtain biopsies that are examined for the presence of eosinophils Must see a minimum density of a predetermined number of eosinophils per biopsy to diagnosis EoE Eosinophilic Esophagitis (EoE) Eosinophilic Esophagitis (EoE) Common course of treatment at CMH: Dietary therapy: High-dose PPI Empiric six-food elimination diet Re-scope in 8 weeks If EoE is still present, options include: Dairy, egg, wheat, soy, peanut/tree nuts, seafood Targeted elimination diet Dietary therapy foods are eliminated based on allergy testing (skin-prick) Topical steroids Elemental diet Therapy plan amino acid based with fats, sugars, vitamins and minerals Skill building EO28 Splash, Neocate, Elecare, Nutramigen AA Address oral aversion When the EoE is well managed, begin feeding therapy to add foods and increase volume of oral intake Very challenging to implement dietary changes when intake is restricted and/or variety is very limited Eosinophilic Esophagitis (EoE) Topical Steroids: Swallowed budesonide Swallowed fluticasone Stopping the topical steroid will result in elevated eosinophils because the foods that are causing the issue have not been eliminated Commonly used in our GI MDFC population As oral intake improves, may transition to an elimination diet 35 36
7 Most common reasons for tracheostomy in pediatrics: Congenital and acquired airway stenosis Neurological conditions that require long-term ventilation or pulmonary toilet Bilateral vocal insufficiency Infectious compromise of the upper airway Many studies have found that as management of airway concerns improves, tracheostomies are decreasing. Campisi et al Dysphagia in patients with trachs is often multifactoral: Trach itself can impair swallow function Open system - atypical subglottic pressures Tethers hyo-laryngeal elevation May be more pronounced with a cuffed tract Airway concerns Prematurity Atypical feeding development due to medical concerns Use of non-oral feedings Adverse oral experiences Respiratory concerns Reflux Impaired parent-child interactions Norman et al infants and toddlers Large pediatric referral hospital in South Africa Trach between 0-3 years of age 68.75% were performed on patients less than 1 year of age cannulated for more than 1 month Most common reason = upper airway obstruction (71.25%) long-term ventilation (13.75) Norman et al (continued) 64 (80%) of the patients demonstrated dysphagia Oral = 81.25% (52) oral motor concerns (94%, 48) oral sensory issues (61.5%, 32) Pharyngeal = 60.9% (39) delayed absent swallow (48%, 19) nasopharyngeal backflow (85%, 33) laryngeal penetration (56%, 22) aspiration (51%, 20) Pooling and residue (41%, 16) Norman et al (continued) Esophageal = 79.7% (51) Gastroesophageal reflux (92%, 47) Structural abnormalities (19.6%, 10) Patients with tracheostomies are at risk for dysphagia so how do we help? Passy Muir Speaking Valve Questionable impact Clinical feeding & swallowing assessment Dysmotility (22%, 11) will explore in more detail FEES excellent view of pharyngeal anatomy VFSS Able to assess oral and pharyngeal phases Feeding therapy 41 42
8 The Effect of a Speaking Valve on Laryngeal Aspiration and Penetration in Children with Tracheotomies (Ongkasuwan et al. 2013) 12 patients Median age at time of trach = 2 months Median age at time of MBS = 16 months Reasons for trach Ongkasuwan et al (continued) Administered thin liquids and purees to each patient while wearing a Passy Muir Valve (PMV) and a sham valve Assessed via MBS upper airway obstruction (7) respiratory insufficiency (4) neurological disorder (1) Feeding status primarily oral intake = 7 primarily g-tube = 3 oral feedings during the day and g-tube feedings at night = 2 Thin liquids 5 patients has penetration or aspiration with the sham valve that improved with the PMV 4 patients had a worse penetration-aspiration scale (PAS) with PMV 3 patients - no difference Ongkasuwan et al (continued) Purees Clinical Assessment of Swallow Safety Considerations: 1 patient = improved PAS with PMV 1 patient = worse PAS with PMV Conclusions laryngeal penetration and aspiration was less with purees vs. liquids for all patients, regardless of valve PMV decreased piriform sinus residue No decrease in laryngeal penetration or aspiration with a PMV Medically stable Trials approved by the medical team Have a nurse/respiratory therapist/caregiver present to suction the patient as needed I prefer to complete trials within a hospital setting (inpatient or outpatient within a hospital) Studies with adults have been mixed. Need more research Clinical assessment of swallow safety for secretions: Monitor for swallowing at rest Establish a baseline for suctioning needs Dye secretions Assess laryngeal movement Up and forward (superior-anterior) movement Monitor for clinical signs of aspiration Coughing (may see dye in secretions) before, during or after the swallow Choking wet breath or vocal sounds Suction and evaluate for signs of the dye If excessive aspiration is seen, consider an inflated cuff Clinical assessment of swallow safety for liquids: Dye the liquid Typically start with thin liquids Assess laryngeal movement Up and forward (superior-anterior) movement Monitor for clinical signs of aspiration Coughing (may see dye in the secretions that are removed) before, during or after the swallow Choking Wet breath or vocal sounds Suction and evaluate for signs of the dye If the child shows signs of aspiration with thin liquids, you can assess thickened liquids but I typically prefer an instrumental study 47 48
9 Clinical assessment of swallow safety for purees: Dye the puree Follow set-up for assessing liquids Assessing safety for soft and hard solids Proceed with caution work on non-food chewing tasks then progress to highly dissolvable solids if skills are present Dye the solid and follow protocol for liquids If there are concerns about safety with thin liquids, avoid juicy fruit (watermelon, diced fruit cups) and items that are liquid at room temperature (ex. Popsicles, ice cream) A congenital anomaly of the larynx leading to inward collapse of the supraglottic airway with inspiration. Most common congenital laryngeal anomaly Most frequent cause of stridor in infants starts in the first few weeks of life Diagnosed via flexible endoscopy Characteristics include: Inspiratory prolapse of the arytenoids Redundant arytenoid mucosa Shortened aryepiglottic folds Peaks at ~6 months of age Most symptoms resolve by months Commonly associated with: GERD Feeding difficulties Dysphagia including aspiration Omega-shaped or tubular epiglottis Obstructive sleep apnea (Bedwell et al. 2016; Simons et al. 2015) (Bedwell et al. 2016; Simons et al. 2015) Possible causes Anatomic tissue redundancy that leads to supraglottic obstruction Immature or weak laryngeal cartilage contributes to obstruction Inflammatory GERD (associated but unclear if it is a cause) Neurological Hypotonia Dysphagia & Feeding Difficulties Incidence of dysphagia and aspiration in patients with laryngomalacia is unknown (Simons et al. 2015) Impacts coordination of the suckswallow-breath pattern Impaired neuromuscular control (Bedwell et al. 2016; Simons et al. 2015) 53 54
10 and Swallowing Function in Children (Simons et al. 2015) 324 patients Mild laryngomalacia = 62.7% Moderate = 28.7% Severe = 8.6% Severity was not impacted by gender, age of onset or medical comorbidities Severe laryngomalacia tended to lead to earlier diagnosis and greater prevalence of symptoms such as apnea, cyanosis, failure to thrive and retractions Simons et al (continued) Medical comorbidities included: GERD (226, 69.8%) patients with moderate to severe laryngomalacia were more likely to have GERD compared to mild cases Down syndrome (3.1%) Neurological impairment (6.5%) Congenital heart disease (0.9%) Simons et al (continued) Results: Dysphagia or feeding difficulties =163 of 324 patients (50.3%) Severity of laryngomalacia did not have a significant effect on swallowing dysfunction Failure to thrive/poor weight gain = 31 patients (9.6%) Comorbidities were not associated with increased severity of laryngomalacia Swallow studies are frequently abnormal in laryngomalacia patients presenting both with and without subjective symptoms of dysphagia or feeding difficulty. How to help: Researchers from the Simons et al study planned to implement the following clinical care pathway in ADT Clinic: Caregiver report (guided questioning) re: swallowing symptoms Clinical swallowing evaluation with speech pathology At least one baseline instrumental swallowing assessment The sensitivity of clinical evaluation to detect laryngeal penetration and tracheal aspiration was low, as the majority of aspiration events were silent (Gasparin et al. 2017) 10 Patients with laryngomalacia and 19 with glossoptosis How to help (continued): External respiratory pacing to improve suck-swallow-breathe coordination After the baby takes 2-3 sucks, tip the bottle down to remove the milk from the nipple (do not remove the nipple from the baby s mouth). After the baby swallows and takes a breath, tip the bottle up to fill the nipple with milk. Repeat this cycle as needed throughout the feeding. If the baby swallows and takes a breathe after 2-3 sucks, you do not need to tip the bottle down. As the baby s feeding skills improve, the need for pacing should decrease Typically teach this skill with bottle feedings then improved pacing transfers to breastfeeding How to help (continued): Positioning Elevated side-lying Adjusting flow rate for bottle feedings Just right balance Thickened liquids may be helpful based on VFSS or FEES Do not recommend thickening without an instrumental swallow study 59 60
11 A rare congenital anomaly in which there is incomplete separation of the aerodigestive tract due to a midline defect in the common wall between the laryngotracheal and esophageal lumens. (Osborn et al. 2014) Grade I to IV I = gap located above the vocal folds is this a variant of normal? II = below the vocal folds III = extends below the larynx into the trachea IV = may go all the way to the bottom of the trachea Causes dysphagia because the patient may not be able to adequately close the airway and boluses enter the trachea through the cleft Commonly associated with other airway anomalies or syndromes with craniofacial, aerodigestive or neurological effects (Osborn et al. 2014) Also see the need for long-term non-oral feedings in some patients Diagnosed via microlarygoscopy and bronchoscopy Unable to identify on a VFSS or FEES May be able to see signs that would warrant a referral to ENT Where is the barium entering the sub glottal space Treatment options Small clefts (type I and II) May not cause symptoms If symptomatic, manage with medical and feeding modifications Some small clefts and all type III and IV surgical intervention goal = prevent aspiration and pulmonary compromise At Children s Mercy, typical options include Gel foam injection Supraglottoplasty (Osborn et al. 2014) Swallowing Function After Repair: More than Just Fixing the Cleft (Osborn et al. 2014) 60 patients Grade I = 21 Grade II = 21 Grade III = 17 Grade IV = 1 After repair (and possible revision) 34 children has a normal swallow 12 = some degree of penetration 14 = some degree of aspiration 65 66
12 Swallowing Function After Repair: More than Just Fixing the Cleft (Osborn et al. 2014; continued) Feeding recommendations 43 were able to take all consistencies by mouth with no-minimal modifications 11 = modified consistencies 6 = unsafe for oral intake Swallowing Function After Repair: More than Just Fixing the Cleft (Osborn et al. 2014; continued) No association between cleft type and final feeding recommendations Neurological comorbidities (CHARGE, Opitz, cerebral palsy, trisomy 21, global developmental delays) and g- tube use were associated with feeding modifications 6 times greater risk for neurological concerns 3.6 times greater need for diet modification 32 patients were cleared for oral intake of all consistencies within 1 year 11 took more than 1 year Swallowing Function After Repair: More than Just Fixing the Cleft (Osborn et al. 2014; continued) Results: 28% of children remained NPO or required the use of thickeners to achieve adequate airway protection after surgery Neurodevelopmental delay = most likely to fall in this category Recommendations: swallow evaluations at 3, 6, 12 and 24 months post repair chance of recovering normal swallow function greater than 2 years post-repair is small How to help: Clinical feeding evaluation and an instrumental swallow study prior to repair Follow-up swallow assessments following repair Revisions May still be at risk for aspiration even with a successful repair Type of instrumental assessment and timing is important Hersh et al found that each child participated in 3.24 VFSS which was the equivalent of 30.6 chest x-rays Modifications may be helpful: Thickened liquids Positioning Pacing Referral to ENT References Bedwell, J., & Zalzal, G Seminars in Pediatric Surgery. dx.doi.org/ /j.sempedsurg Chadha, S.N., Wang, L., Correa, H., Moulton, D., & Hummell, D.S Pediatric eosinophilic esophagitis: the Vanderbilt experience. Annuals of Allergy, Asthma and Immunology. 113: Chawla, N., Deshmukh, M., Sharma, A., Parole, S Strategies for Medical Management of Pediatric Eosinophilic Esophagitis. Journal of Pediatric Gastroenterology and Nutrition. 63(6): Dellon, E.S Epidemiology of eosinophilic esophagitis. Gastroenterology Clinics of North America. 43: Garuti, G., Reverberi, C., Briganti, A., Massobrio, M., Lombardi, F., & Lusuardi, M Swallowing disorders in tracheostomised patients: a multidisciplinary/multiprofessionsal approach in decannulation protocols. Multidisciplinary Respiratory Medicine Journal. 9:36. Goday, P.S., Lukens, C.T., Dodrill, P. & Feuling, M.B Pediatric Feeding Disorders: Proposed Consensus Definition and Consensus Framework. Phoenix: Feeding Matters. References 71 72
13 References Gottrand, F. & Sullivan, P.B Gastrostomy tube feeding: when to start, what to feed and how to stop. European Journal of Clinical Nutrition. 64:S17-S21. Hersh, C., Wentland, C., Sally, S., de Stadler, M., Hardy, S., Fracchia, M.S., Liu, B., & Hartnick, C Radiation exposure from videofluoroscopic swallow studies in children with a type 1 laryngeal cleft and pharyngeal dysphagia: A retrospective review. International Journal of Pediatric Otorhinolaryngology. 89: Norman, V., Louw, B., & Kritzinger, A Incidence and description of dysphagia in infants and toddlers with tracheostomies: A retrospective review. International Journal of Pediatric Otorhinolaryngology. 71: Ongkasuwan, J., Turk, C.L., Rappazzo, C.A., Lavergne, K.A., O Brian Smith, E, & Friedman, E.M The effect of a speaking valve on laryngeal aspiration and penetration in children with tracheostomies. The Laryngoscope. 124: Osborn, A.J., de Alarcon, A., Tabangin, M.E., Miller, C.K., Cotton, R.T., & Rutter, M.J Swallowing function after laryngeal cleft repair: More than just fixing the cleft. The Laryngoscope. 124: Simons, J.P., Greenberg, L.L., Deepak, K.M., Fabio, A., Maguire, R.C. & Mandell, D.L and swallowing function in children. The Laryngoscope. 126: Questions? Thank you! Brenda Sitzmann, MA, CCC-SLP bksitzmann@cmh.edu (816)
FEEDING THE MEDICAL COMPLEX PEDIATRIC PATIENT. Brenda Sitzmann, MA, CCC-SLP (816)
 FEEDING THE MEDICAL COMPLEX PEDIATRIC PATIENT Brenda Sitzmann, MA, CCC-SLP bksitzmann@cmh.edu (816) 302-8037 DISCLOSURES Ms. Sitzmann is speech-language pathologist at Children s Mercy for which she receives
FEEDING THE MEDICAL COMPLEX PEDIATRIC PATIENT Brenda Sitzmann, MA, CCC-SLP bksitzmann@cmh.edu (816) 302-8037 DISCLOSURES Ms. Sitzmann is speech-language pathologist at Children s Mercy for which she receives
Reluctance or refusal to feed or eat. Understanding Feeding Aversion in a City Full of Foodies. Presentation Outline. Learning Objectives
 Understanding Feeding Aversion in a City Full of Foodies Amy Houtrow, MD, MPH Pediatric Physical Medicine & Rehabilitation UCSF Department of Pediatrics June 2, 2007 Learning Objectives Learners will be
Understanding Feeding Aversion in a City Full of Foodies Amy Houtrow, MD, MPH Pediatric Physical Medicine & Rehabilitation UCSF Department of Pediatrics June 2, 2007 Learning Objectives Learners will be
FLOOVIDEOFLUOROSCOPIC SWALLOW STUDIES: LOOKING BEYOND ASPIRATION. Brenda Sitzmann, MA, CCC-SLP (816)
 FLOOVIDEOFLUOROSCOPIC SWALLOW STUDIES: LOOKING BEYOND ASPIRATION Brenda Sitzmann, MA, CCC-SLP bksitzmann@cmh.edu (816) 302-8037 DISCLOSURES Ms. Sitzmann is speech-language pathologist at Children s Mercy
FLOOVIDEOFLUOROSCOPIC SWALLOW STUDIES: LOOKING BEYOND ASPIRATION Brenda Sitzmann, MA, CCC-SLP bksitzmann@cmh.edu (816) 302-8037 DISCLOSURES Ms. Sitzmann is speech-language pathologist at Children s Mercy
What are the Challenges? Spreading the Word in NICU. Need for NICU Care: Impact. Baby Trachs: Use of the Passy Muir Valve in the NICU to
 What are the Challenges? Baby Trachs: Use of the Passy Muir Valve in the NICU to Optimize Swallowing and Feeding Catherine S Shaker, MS/CCC SLP, BRS S and Cari Mutnick, MS/CCC SLP Florida Hospital for
What are the Challenges? Baby Trachs: Use of the Passy Muir Valve in the NICU to Optimize Swallowing and Feeding Catherine S Shaker, MS/CCC SLP, BRS S and Cari Mutnick, MS/CCC SLP Florida Hospital for
Unilateral Supraglottoplasty for Severe Laryngomalacia in Children. Nasser A Fageeh, MD, FRCSC, FACS*
 Bahrain Medical Bulletin, Vol. 37, No. 1, March 2015 Unilateral Supraglottoplasty for Severe Laryngomalacia in Children Nasser A Fageeh, MD, FRCSC, FACS* Objective: To study the efficacy of Unilateral
Bahrain Medical Bulletin, Vol. 37, No. 1, March 2015 Unilateral Supraglottoplasty for Severe Laryngomalacia in Children Nasser A Fageeh, MD, FRCSC, FACS* Objective: To study the efficacy of Unilateral
The Role of the Speech Language Pathologist & Spinal Cord Injury
 The Role of the Speech Language Pathologist & Spinal Cord Injury Facts According to the National Spinal Cord Injury Statistical Center (NSCISC) there are approxiamtely 12,000 new spinal cord injuries (SCI)
The Role of the Speech Language Pathologist & Spinal Cord Injury Facts According to the National Spinal Cord Injury Statistical Center (NSCISC) there are approxiamtely 12,000 new spinal cord injuries (SCI)
Feeding and Swallowing Problems in the Child with Special Needs
 Feeding and Swallowing Problems in the Child with Special Needs Joan Surfus, OTR/L, SWC Amy Lynch, MS, OTR/L Misericordia University This presentation is made possible, in part, by the support of the American
Feeding and Swallowing Problems in the Child with Special Needs Joan Surfus, OTR/L, SWC Amy Lynch, MS, OTR/L Misericordia University This presentation is made possible, in part, by the support of the American
VIDEOFLUOROSCOPIC SWALLOWING EXAM
 VIDEOFLUOROSCOPIC SWALLOWING EXAM INDENTIFYING INFORMATION May include the following: Name, ID/medical record number, date of birth, date of exam, referred by, reason for referral HISTORY/SUBJECTIVE INFORMATION
VIDEOFLUOROSCOPIC SWALLOWING EXAM INDENTIFYING INFORMATION May include the following: Name, ID/medical record number, date of birth, date of exam, referred by, reason for referral HISTORY/SUBJECTIVE INFORMATION
Respiratory Compromise and Swallowing
 Speech Pathology and Respiratory Care April 11, 2013 By Angela Parcaro-Tucker, MA, CCC-SLP, LSVT How can Speech Therapy help? 1 Respiratory Compromise and Swallowing Swallowing is a complex sequence of
Speech Pathology and Respiratory Care April 11, 2013 By Angela Parcaro-Tucker, MA, CCC-SLP, LSVT How can Speech Therapy help? 1 Respiratory Compromise and Swallowing Swallowing is a complex sequence of
COMMUNICATION. Communication and Swallowing post Tracheostomy. Role of SLT. Impact of Tracheostomy. Normal Speech. Facilitating Communication
 Communication and Swallowing post Tracheostomy. Role of SLT 1. 2. 3. Management of communication needs. Management of swallowing issues. Working with the multidisciplinary team to facilitate weaning. Impact
Communication and Swallowing post Tracheostomy. Role of SLT 1. 2. 3. Management of communication needs. Management of swallowing issues. Working with the multidisciplinary team to facilitate weaning. Impact
Swallow Function: Passy-Muir Valve Use for Evaluation & Rehabilitation David A. Muir Course Outline Physiology of Swallow
 Swallow Function: Passy-Muir Valve Use for Evaluation & Rehabilitation Mary Spremulli, MA, CCC-SLP Passy-Muir Clinical Consultant spre713@hotmail.com (949) 833-8255 David A. Muir 23 year-old ventilator
Swallow Function: Passy-Muir Valve Use for Evaluation & Rehabilitation Mary Spremulli, MA, CCC-SLP Passy-Muir Clinical Consultant spre713@hotmail.com (949) 833-8255 David A. Muir 23 year-old ventilator
Eosinophilic Esophagitis (EoE)
 Eosinophilic Esophagitis (EoE) 01.06.2016 EoE: immune-mediated disorder food or environmental antigens => Th2 inflammatory response. Key cytokines: IL-4, IL-5, and IL-13 stimulate the production of eotaxin-3
Eosinophilic Esophagitis (EoE) 01.06.2016 EoE: immune-mediated disorder food or environmental antigens => Th2 inflammatory response. Key cytokines: IL-4, IL-5, and IL-13 stimulate the production of eotaxin-3
Information about Feeding Tubes
 Information about Feeding Tubes By Theresa Imperato, RN and Lorraine Danowski, RD What is a feeding tube? It is a small, flexible tube, about ¼ in diameter that is an alternative route for nourishment
Information about Feeding Tubes By Theresa Imperato, RN and Lorraine Danowski, RD What is a feeding tube? It is a small, flexible tube, about ¼ in diameter that is an alternative route for nourishment
Evaluation of Failure to Thrive in a Young Child: Case Example of Jeff. Andrew Hsi, MD, MPH Family Medicine Pediatric Grand Rounds, 8 August 2012
 Evaluation of Failure to Thrive in a Young Child: Case Example of Jeff Andrew Hsi, MD, MPH Family Medicine Pediatric Grand Rounds, 8 August 2012 Objectives for Presentation At the end of this talk; the
Evaluation of Failure to Thrive in a Young Child: Case Example of Jeff Andrew Hsi, MD, MPH Family Medicine Pediatric Grand Rounds, 8 August 2012 Objectives for Presentation At the end of this talk; the
What is Eosinophilic Esophagitis (EoE)?
 EOSINOPHILIC ESOPHAGITIS What is Eosinophilic Esophagitis (EoE)? Eosinophilic esophagitis (EoE) is an illness found in the esophagus (the tube that links your mouth and stomach). EoE is the result of an
EOSINOPHILIC ESOPHAGITIS What is Eosinophilic Esophagitis (EoE)? Eosinophilic esophagitis (EoE) is an illness found in the esophagus (the tube that links your mouth and stomach). EoE is the result of an
Guideline of Videofluoroscopic Swallowing Study (VFSS) in Speech Therapy
 Page 1 of 9 Guideline of Videofluoroscopic Swallowing Study (VFSS) in Speech Therapy Version 1.0 Effective Date Document Number HKIST-C-VFG-v1 Author HKAST AR Sub-committee Custodian Chairperson of HKIST
Page 1 of 9 Guideline of Videofluoroscopic Swallowing Study (VFSS) in Speech Therapy Version 1.0 Effective Date Document Number HKIST-C-VFG-v1 Author HKAST AR Sub-committee Custodian Chairperson of HKIST
SWALLOWING DIFFICULTIES IN HD
 Nutrition, eating and swallowing needs, challenges and solutions Workshop SWALLOWING DIFFICULTIES IN HD Angela Nuzzi Speech and Language Pathologist (SLP) EHDN Language Coordinator - Italy The role of
Nutrition, eating and swallowing needs, challenges and solutions Workshop SWALLOWING DIFFICULTIES IN HD Angela Nuzzi Speech and Language Pathologist (SLP) EHDN Language Coordinator - Italy The role of
Neonatal Airway Disorders, Treatments, and Outcomes. Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center
 Neonatal Airway Disorders, Treatments, and Outcomes Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center Disclosure I have nothing to disclose Neonatal and Pediatric Tracheostomy Tracheostomy
Neonatal Airway Disorders, Treatments, and Outcomes Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center Disclosure I have nothing to disclose Neonatal and Pediatric Tracheostomy Tracheostomy
Pediatric Modified Barium Swallow Studies. Presented by Jody Bousquet, MA, CCC- SLP Susan Shonbrun, MS, CCC- SLP November 7, 2015
 Pediatric Modified Barium Swallow Studies Presented by Jody Bousquet, MA, CCC- SLP Susan Shonbrun, MS, CCC- SLP November 7, 2015 Definition * Modified Barium Swallow Study * Assesses swallow functions
Pediatric Modified Barium Swallow Studies Presented by Jody Bousquet, MA, CCC- SLP Susan Shonbrun, MS, CCC- SLP November 7, 2015 Definition * Modified Barium Swallow Study * Assesses swallow functions
Eosinophilic Esophagitis: Extraesophageal Manifestations
 Eosinophilic Esophagitis: Extraesophageal Manifestations Karen B. Zur, MD Director, Pediatric Voice Program Associate Director, Center for Pediatric Airway Disorders The Children s Hospital of Philadelphia
Eosinophilic Esophagitis: Extraesophageal Manifestations Karen B. Zur, MD Director, Pediatric Voice Program Associate Director, Center for Pediatric Airway Disorders The Children s Hospital of Philadelphia
Clinical Study Aspiration before and after Supraglottoplasty regardless of Technique
 International Otolaryngology Volume 2010, Article ID 912814, 5 pages doi:10.1155/2010/912814 Clinical Study Aspiration before and after Supraglottoplasty regardless of Technique Jeffrey C. Rastatter, 1,
International Otolaryngology Volume 2010, Article ID 912814, 5 pages doi:10.1155/2010/912814 Clinical Study Aspiration before and after Supraglottoplasty regardless of Technique Jeffrey C. Rastatter, 1,
Tracheoesophageal Fistula and Esophageal Atresia
 Patient and Family Education Tracheoesophageal Fistula and Esophageal Atresia What is tracheoesophageal fistula? The word fistula means abnormal connection. Tracheoesophageal fistula (TEF) is a condition
Patient and Family Education Tracheoesophageal Fistula and Esophageal Atresia What is tracheoesophageal fistula? The word fistula means abnormal connection. Tracheoesophageal fistula (TEF) is a condition
Complex Decision Making in Pediatric Dysphagia
 Complex Decision Making in Pediatric Dysphagia Alana Lowry, MS, CCC-SLP Fletcher Allen Health Care Kara Fletcher Larson, MS, CCC-SLP Jennifer Miller, MS, CCC-SLP Children s s Hospital Boston ASHA November
Complex Decision Making in Pediatric Dysphagia Alana Lowry, MS, CCC-SLP Fletcher Allen Health Care Kara Fletcher Larson, MS, CCC-SLP Jennifer Miller, MS, CCC-SLP Children s s Hospital Boston ASHA November
Disclosures. Repaired Esophageal Atresia and Tracheoesophageal Fistula and Chronic Dysphagia. Case Presentation. Case Presentation.
 Disclosures Repaired Esophageal Atresia and Tracheoesophageal Fistula and Chronic Dysphagia Dr. DeBoer is funded by Colorado Clinical and Translational Science Institute KL2 TR001080 Emily DeBoer MD Assistant
Disclosures Repaired Esophageal Atresia and Tracheoesophageal Fistula and Chronic Dysphagia Dr. DeBoer is funded by Colorado Clinical and Translational Science Institute KL2 TR001080 Emily DeBoer MD Assistant
PMV ON OR OFF WITH SWALLOWING DOES IT MAKE A DIFFERENCE?
 PMV ON OR OFF WITH SWALLOWING DOES IT MAKE A DIFFERENCE? 1 Tedd Masiongale, MA, CCC-SLP Lorry Lewis, MS, CCC-SLP REASON FOR STUDY After several years of working with trach and ventilator dependent patients,
PMV ON OR OFF WITH SWALLOWING DOES IT MAKE A DIFFERENCE? 1 Tedd Masiongale, MA, CCC-SLP Lorry Lewis, MS, CCC-SLP REASON FOR STUDY After several years of working with trach and ventilator dependent patients,
Understanding your child s videofluoroscopic swallow study report
 Understanding your child s videofluoroscopic swallow study report This leaflet is given to you during your child s appointment in order to explain some of the words used by the speech and language therapist
Understanding your child s videofluoroscopic swallow study report This leaflet is given to you during your child s appointment in order to explain some of the words used by the speech and language therapist
Oral care & swallowing
 Oral care & swallowing Oral care is important as it has a role to play in preventing healthcare associated infections. Dental plaque and the oropharynx can become colonized by bacteria and a biofilm can
Oral care & swallowing Oral care is important as it has a role to play in preventing healthcare associated infections. Dental plaque and the oropharynx can become colonized by bacteria and a biofilm can
Chapter 27 & 28. Key Terms. Digestive System. Fig. 27-1, p. 443 Also known as the Gastrointestinal System (GI system)
 Chapter 27 & 28 Nutrition & Fluids Key Terms Aspiration Dehydration Edema Dysphagia Gastrostomy tube Intravenous therapy (IV) Digestive System Fig. 27-1, p. 443 Also known as the Gastrointestinal System
Chapter 27 & 28 Nutrition & Fluids Key Terms Aspiration Dehydration Edema Dysphagia Gastrostomy tube Intravenous therapy (IV) Digestive System Fig. 27-1, p. 443 Also known as the Gastrointestinal System
Esophageal Cancer. Source: National Cancer Institute
 Esophageal Cancer Esophageal cancer forms in the tissues that line the esophagus, or the long, hollow tube that connects the mouth and stomach. Food and drink pass through the esophagus to be digested.
Esophageal Cancer Esophageal cancer forms in the tissues that line the esophagus, or the long, hollow tube that connects the mouth and stomach. Food and drink pass through the esophagus to be digested.
IAEM Clinical Guideline 9 Laryngomalacia. Version 1 September, Author: Dr Farah Mustafa
 IAEM Clinical Guideline 9 Laryngomalacia Version 1 September, 2016 Author: Dr Farah Mustafa Guideline lead: Dr Áine Mitchell, in collaboration with IAEM Clinical Guideline committee and Our Lady s Children
IAEM Clinical Guideline 9 Laryngomalacia Version 1 September, 2016 Author: Dr Farah Mustafa Guideline lead: Dr Áine Mitchell, in collaboration with IAEM Clinical Guideline committee and Our Lady s Children
Nutrition in children with special needs. Dr. Meenakshi J.
 Nutrition in children with special needs Dr. Meenakshi J. 1 Factors affecting growth and nutrition in children with special nutritional factors Inadequate intake primarily related to feeding dysfunction
Nutrition in children with special needs Dr. Meenakshi J. 1 Factors affecting growth and nutrition in children with special nutritional factors Inadequate intake primarily related to feeding dysfunction
IVOR LEWIS Esophagogastrectomy
 IVOR LEWIS Esophagogastrectomy SPEECH-LANGUAGE PATHOLOGY S ROLE MAGGIE BOYD, MS, CCC/SLP Biography Maggie Boyd, MS, CCC-SLP is a dysphagia clinical specialist at UAB hospital. She has 14 years clinical
IVOR LEWIS Esophagogastrectomy SPEECH-LANGUAGE PATHOLOGY S ROLE MAGGIE BOYD, MS, CCC/SLP Biography Maggie Boyd, MS, CCC-SLP is a dysphagia clinical specialist at UAB hospital. She has 14 years clinical
Clearing the air.. How to assist and rescue neck breathing patients. Presented by: Don Hall MCD, CCC/SLP Sarah Markel RRT, MHA
 Clearing the air.. How to assist and rescue neck breathing patients Presented by: Don Hall MCD, CCC/SLP Sarah Markel RRT, MHA Learning Objectives Define common terms identified with total (laryngectomy)
Clearing the air.. How to assist and rescue neck breathing patients Presented by: Don Hall MCD, CCC/SLP Sarah Markel RRT, MHA Learning Objectives Define common terms identified with total (laryngectomy)
Analyzing Swallow Studies in Pediatrics
 Analyzing Swallow Studies in Pediatrics About the Speaker Robert Beecher, M.S., CCC-SLP was formerly senior speech-language pahologist at the Children's Hospital of Wisconsin in Milwaukee. He is specialized
Analyzing Swallow Studies in Pediatrics About the Speaker Robert Beecher, M.S., CCC-SLP was formerly senior speech-language pahologist at the Children's Hospital of Wisconsin in Milwaukee. He is specialized
Swallowing after a Total Laryngectomy
 Swallowing after a Total Laryngectomy Diane Longnecker, M.S.,CCC-SLP, BCS-S Baylor Institute for Rehabilitation at Baylor University Medical Center Dallas, TX Disclosure Statement No relevant financial
Swallowing after a Total Laryngectomy Diane Longnecker, M.S.,CCC-SLP, BCS-S Baylor Institute for Rehabilitation at Baylor University Medical Center Dallas, TX Disclosure Statement No relevant financial
Where do we come from?
 Interdisciplinary Decision-Making with Patients Requiring Tracheostomy and Carrie Windhorst MS CCC-SLP Cheryl Wagoner MS CCC-SLP Ricque Harth MEd CCC-SLP Where do we come from? Welcome to Madonna Rehabilitation
Interdisciplinary Decision-Making with Patients Requiring Tracheostomy and Carrie Windhorst MS CCC-SLP Cheryl Wagoner MS CCC-SLP Ricque Harth MEd CCC-SLP Where do we come from? Welcome to Madonna Rehabilitation
GERD. Gastroesophageal reflux disease, or GERD, occurs when acid from the. stomach backs up into the esophagus. Normally, food travels from the
 GERD What is GERD? Gastroesophageal reflux disease, or GERD, occurs when acid from the stomach backs up into the esophagus. Normally, food travels from the mouth, down through the esophagus and into the
GERD What is GERD? Gastroesophageal reflux disease, or GERD, occurs when acid from the stomach backs up into the esophagus. Normally, food travels from the mouth, down through the esophagus and into the
Dysphagia and Swallowing. Jan Adams, DNP, MPA, RN and Karen Kern
 Dysphagia and Swallowing Jan Adams, DNP, MPA, RN and Karen Kern Scope of the Problem and Incidence 15 million people in the US have some form of Dysphagia. Every year, 1 million people are diagnosed with
Dysphagia and Swallowing Jan Adams, DNP, MPA, RN and Karen Kern Scope of the Problem and Incidence 15 million people in the US have some form of Dysphagia. Every year, 1 million people are diagnosed with
Assessing the Eating Needs of Personal Care Services (PCS) Beneficiaries Effective 12/1/2016
 Assessing the Eating Needs of Personal Care Services (PCS) Beneficiaries Effective 12/1/2016 The Freedom to Succeed November 22,2016 Content Introduction Signs and Symptoms Caring for Individuals with
Assessing the Eating Needs of Personal Care Services (PCS) Beneficiaries Effective 12/1/2016 The Freedom to Succeed November 22,2016 Content Introduction Signs and Symptoms Caring for Individuals with
Laryngomalacia and Swallowing Function in Children
 The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. TRIOLOGICAL SOCIETY CANDIDATE THESIS Laryngomalacia and Swallowing Function in Children Jeffrey P. Simons,
The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. TRIOLOGICAL SOCIETY CANDIDATE THESIS Laryngomalacia and Swallowing Function in Children Jeffrey P. Simons,
Chapter 23. Nutrition Needs. Copyright 2019 by Elsevier, Inc. All rights reserved.
 Chapter 23 Nutrition Needs Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 23.1 Define the key terms and key abbreviations in this chapter. Explain the purpose and use of the MyPlate symbol.
Chapter 23 Nutrition Needs Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 23.1 Define the key terms and key abbreviations in this chapter. Explain the purpose and use of the MyPlate symbol.
The Effect of a Speaking Valve on Laryngeal Aspiration and Penetration in Children With Tracheotomies
 The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. The Effect of a Speaking Valve on Laryngeal Aspiration and Penetration in Children With Tracheotomies Julina
The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. The Effect of a Speaking Valve on Laryngeal Aspiration and Penetration in Children With Tracheotomies Julina
Department of Pediatric Otolarygnology. ENT Specialty Programs
 Department of Pediatric Otolarygnology ENT Specialty Programs Staffed by fellowship-trained otolaryngologists, assisted by pediatric nurse practitioners, ENT (Otolaryngology) at Nationwide Children s Hospital
Department of Pediatric Otolarygnology ENT Specialty Programs Staffed by fellowship-trained otolaryngologists, assisted by pediatric nurse practitioners, ENT (Otolaryngology) at Nationwide Children s Hospital
Review of literature suggests that there are three basic theories that attempt to explain the development of laryngomalacia.
 TITLE: Current Concepts in Diagnosis and Management of Laryngomalacia SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: March 31, 2009 FACULTY PHYSICIANS: Shraddha Mukerji, MD and
TITLE: Current Concepts in Diagnosis and Management of Laryngomalacia SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: March 31, 2009 FACULTY PHYSICIANS: Shraddha Mukerji, MD and
Section 4.1 Paediatric Tracheostomy Introduction
 Bite- sized training from the GTC Section 4.1 Paediatric Tracheostomy Introduction This is one of a series of bite- sized chunks of educational material developed by the Global Tracheostomy Collaborative.
Bite- sized training from the GTC Section 4.1 Paediatric Tracheostomy Introduction This is one of a series of bite- sized chunks of educational material developed by the Global Tracheostomy Collaborative.
Multilevel airway obstruction including rare tongue base mass presenting as severe croup in an infant. Tara Brennan, MD 2,3
 Multilevel airway obstruction including rare tongue base mass presenting as severe croup in an infant Tara Brennan, MD 2,3 Jeffrey C. Rastatter, MD, FAAP 1,2 1 Department of Otolaryngology, Northwestern
Multilevel airway obstruction including rare tongue base mass presenting as severe croup in an infant Tara Brennan, MD 2,3 Jeffrey C. Rastatter, MD, FAAP 1,2 1 Department of Otolaryngology, Northwestern
An Overview of Bronchopulmonary Dysplasia and Chronic Lung Disease in Infancy
 An Overview of Bronchopulmonary Dysplasia and Chronic Lung Disease in Infancy Housekeeping: I have no financial disclosures Learning objectives: Develop an understanding of bronchopulmonary dysplasia (BPD)
An Overview of Bronchopulmonary Dysplasia and Chronic Lung Disease in Infancy Housekeeping: I have no financial disclosures Learning objectives: Develop an understanding of bronchopulmonary dysplasia (BPD)
Laryngoscopy Examinations
 Laryngoscopy Examinations Laryngoscopy is a visual examination of the back of the throat where the voice box (larynx) and vocal cords are located. The procedure is done by using hand mirrors and a light
Laryngoscopy Examinations Laryngoscopy is a visual examination of the back of the throat where the voice box (larynx) and vocal cords are located. The procedure is done by using hand mirrors and a light
Disclosure. Learning Objectives 4/25/2014. I have no disclosures
 Alka Goyal MD Division of Pediatric Gastroenterology Hepatology and Nutrition Children s Hospital of Pittsburgh of UPMC Disclosure I have no disclosures Learning Objectives Diagnosis of Eosinophilic Esophagitis
Alka Goyal MD Division of Pediatric Gastroenterology Hepatology and Nutrition Children s Hospital of Pittsburgh of UPMC Disclosure I have no disclosures Learning Objectives Diagnosis of Eosinophilic Esophagitis
Chapter 20. Assisting With Nutrition and Fluids
 Chapter 20 Assisting With Nutrition and Fluids Food and water: Are physical needs Basics of Nutrition Are necessary for life A poor diet and poor eating habits: Increase the risk for diseases and infection
Chapter 20 Assisting With Nutrition and Fluids Food and water: Are physical needs Basics of Nutrition Are necessary for life A poor diet and poor eating habits: Increase the risk for diseases and infection
Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy
 Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who are
Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who are
Enteral Nutrition. Presented by Melanie Farwell RD, LD Keene Medical Products Dietitian
 Enteral Nutrition Presented by Melanie Farwell RD, LD Keene Medical Products Dietitian What is it? Liquid feeding provided to the gastrointestinal tract via nose, stomach or small intestine -Specifically
Enteral Nutrition Presented by Melanie Farwell RD, LD Keene Medical Products Dietitian What is it? Liquid feeding provided to the gastrointestinal tract via nose, stomach or small intestine -Specifically
Swallowing Disorders and Their Management in Patients with Multiple Sclerosis
 National Multiple Sclerosis Society 733 Third Avenue New York, NY 10017-3288 Clinical Bulletin Information for Health Professionals Swallowing Disorders and Their Management in Patients with Multiple Sclerosis
National Multiple Sclerosis Society 733 Third Avenue New York, NY 10017-3288 Clinical Bulletin Information for Health Professionals Swallowing Disorders and Their Management in Patients with Multiple Sclerosis
Management of GI Issues in Duchenne. Kent Williams, MD Assistant Professor Nationwide Children s Hospital Columbus Ohio
 Management of GI Issues in Duchenne Kent Williams, MD Assistant Professor Nationwide Children s Hospital Columbus Ohio Objectives Current GI recommendations What is known and not known Case Presentation:
Management of GI Issues in Duchenne Kent Williams, MD Assistant Professor Nationwide Children s Hospital Columbus Ohio Objectives Current GI recommendations What is known and not known Case Presentation:
Barrett s Esophagus. lining of the lower esophagus that bears his name (i.e., Barrett's esophagus). We now
 Shamika Johnson Anatomy & Physiology 206 April 20, 2010 Barrett s Esophagus What is Barrett s Esophagus? Norman Barrett was a pathologist. In 1950, he described an abnormality in the lining of the lower
Shamika Johnson Anatomy & Physiology 206 April 20, 2010 Barrett s Esophagus What is Barrett s Esophagus? Norman Barrett was a pathologist. In 1950, he described an abnormality in the lining of the lower
Dysphagia Identification and Management
 Dysphagia Identification and Management Presented By Speech-Language Pathologist Developmental Disabilities Administration DC Department on Disability Services Training Objectives After this training session
Dysphagia Identification and Management Presented By Speech-Language Pathologist Developmental Disabilities Administration DC Department on Disability Services Training Objectives After this training session
Enteral Feeding Access: Your BFF or Frenemy?
 Enteral Feeding Access: Your BFF or Frenemy? Elizabeth Hood, APN/CPNP The Ann and Robert H. Lurie Children s Hospital of Chicago Chicago, IL Disclosure Information No disclosures to report Objectives The
Enteral Feeding Access: Your BFF or Frenemy? Elizabeth Hood, APN/CPNP The Ann and Robert H. Lurie Children s Hospital of Chicago Chicago, IL Disclosure Information No disclosures to report Objectives The
A Case of Severe Neonatal Dysphagia: Experience and Reason
 A Case of Severe Neonatal Dysphagia: Experience and Reason The Contemporary Management of Aerodigestive Disease in Children 2 nd Aerodigestive Meeting Vanderbilt University, Nashville, TN Friday, November
A Case of Severe Neonatal Dysphagia: Experience and Reason The Contemporary Management of Aerodigestive Disease in Children 2 nd Aerodigestive Meeting Vanderbilt University, Nashville, TN Friday, November
Feeding and Oral Hygiene: How to Address the Challenges
 Feeding and Oral Hygiene: How to Address the Challenges Paige W. Roberts, OTR/L Occupational Therapist Pediatric Feeding Disorders Program Marcus Autism Center Disclaimer: This content is for personal
Feeding and Oral Hygiene: How to Address the Challenges Paige W. Roberts, OTR/L Occupational Therapist Pediatric Feeding Disorders Program Marcus Autism Center Disclaimer: This content is for personal
Eosinophilic Esophagitis. Another Reason Not to Swallow
 Eosinophilic Esophagitis Another Reason Not to Swallow Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any form or
Eosinophilic Esophagitis Another Reason Not to Swallow Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any form or
What is Eosinophilic Esophagitis, how is it treated, and will it go away?
 Panelists What is Eosinophilic Esophagitis, how is it treated, and will it go away? Bradley A. Becker, M.D. Professor of Pediatrics and Internal Medicine Division of Allergy and Immunology Saint Louis
Panelists What is Eosinophilic Esophagitis, how is it treated, and will it go away? Bradley A. Becker, M.D. Professor of Pediatrics and Internal Medicine Division of Allergy and Immunology Saint Louis
SWALLOW PHYSIOLOGY IN PATIENTS WITH TRACH CUFF INFLATED OR DEFLATED: A RETROSPECTIVE STUDY
 SWALLOW PHYSIOLOGY IN PATIENTS WITH TRACH CUFF INFLATED OR DEFLATED: A RETROSPECTIVE STUDY Ruiying Ding, PhD, 1 Jeri A. Logemann, PhD 2 1 University of Wisconsin-Whitewater, Department of Communicative
SWALLOW PHYSIOLOGY IN PATIENTS WITH TRACH CUFF INFLATED OR DEFLATED: A RETROSPECTIVE STUDY Ruiying Ding, PhD, 1 Jeri A. Logemann, PhD 2 1 University of Wisconsin-Whitewater, Department of Communicative
Objectives. Disclosures. Eosinophilic Esophagitis and Nutritional Consequences. Food Allergy In Schools
 Eosinophilic Esophagitis and Nutritional Consequences Douglas T. Johnston, DO, FACAAI, FAAAAI Assistant Professor of Internal Medicine / Allergy & Immunology Edward Via College of Osteopathic Medicine
Eosinophilic Esophagitis and Nutritional Consequences Douglas T. Johnston, DO, FACAAI, FAAAAI Assistant Professor of Internal Medicine / Allergy & Immunology Edward Via College of Osteopathic Medicine
POSTOPERATIVE CONGENITAL ESOPHAGEAL ATRESIA COMPLICATIONS: A REVIEW
 CHILDREN S HOSPITAL II POSTOPERATIVE CONGENITAL ESOPHAGEAL ATRESIA COMPLICATIONS: A REVIEW Dr. Nguyen Thuy Hanh Ngan Neonatal Department CONTENTS 1. Background 2. Classification 3. Management 4. Complications
CHILDREN S HOSPITAL II POSTOPERATIVE CONGENITAL ESOPHAGEAL ATRESIA COMPLICATIONS: A REVIEW Dr. Nguyen Thuy Hanh Ngan Neonatal Department CONTENTS 1. Background 2. Classification 3. Management 4. Complications
Video Fluoroscopic Swallowing Exam (VFSE)
 Scan for mobile link. Video Fluoroscopic Swallowing Exam (VFSE) A video fluoroscopic swallowing exam (VFSE) uses a form of real-time x-ray called fluoroscopy to evaluate a patient s ability to swallow
Scan for mobile link. Video Fluoroscopic Swallowing Exam (VFSE) A video fluoroscopic swallowing exam (VFSE) uses a form of real-time x-ray called fluoroscopy to evaluate a patient s ability to swallow
Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing
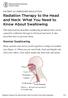 PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
Learning Objectives. Disclaimer 9/8/2015. Jean Marie Osborne MS, RN, ANP-C
 Jean Marie Osborne MS, RN, ANP-C Learning Objectives 1. Understand the pathophysiologic process of EoE. 2. Dietary indiscretions 3. Management None to report Disclaimer 1 History EoE as an allergic disease
Jean Marie Osborne MS, RN, ANP-C Learning Objectives 1. Understand the pathophysiologic process of EoE. 2. Dietary indiscretions 3. Management None to report Disclaimer 1 History EoE as an allergic disease
GASTROINTESTINAL TRACT IN EBS generalized severe
 GASTROINTESTINAL TRACT IN EBS generalized severe 1. Introduction In some forms of EB formation of blisters on the mucous membranes of the mouth and esophagus can occur. This causes various problems; the
GASTROINTESTINAL TRACT IN EBS generalized severe 1. Introduction In some forms of EB formation of blisters on the mucous membranes of the mouth and esophagus can occur. This causes various problems; the
Eosinophilic esophagitis. Kathleen Boynton MD University of Utah Gastroenterology Division
 Eosinophilic esophagitis Kathleen Boynton MD University of Utah Gastroenterology Division Financial disclosures: Janssen Genetech UCB All for research support Learning Objectives To identify the clinical
Eosinophilic esophagitis Kathleen Boynton MD University of Utah Gastroenterology Division Financial disclosures: Janssen Genetech UCB All for research support Learning Objectives To identify the clinical
OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices OPTICS
 OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices Educational Booklet for Families Version April 26 th 2016 Page 1 of 12 This information booklet was originally
OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices Educational Booklet for Families Version April 26 th 2016 Page 1 of 12 This information booklet was originally
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY LARYNGOMALACIA Laryngomalacia is characterised by collapse of the supraglottic tissues on inspiration, and is the most common cause of
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY LARYNGOMALACIA Laryngomalacia is characterised by collapse of the supraglottic tissues on inspiration, and is the most common cause of
Diarrhea may be: Acute (short-term, usually lasting several days), which is usually related to bacterial or viral infections.
 Pediatric Gastroenterology Conditions Evaluated and Treated Having a child suffer with abdominal pain, chronic eating problems, or other gastrointestinal disorders can be a very trying time for a parent.
Pediatric Gastroenterology Conditions Evaluated and Treated Having a child suffer with abdominal pain, chronic eating problems, or other gastrointestinal disorders can be a very trying time for a parent.
Dysphagia. A Problem Swallowing Foods or Liquids
 Dysphagia A Problem Swallowing Foods or Liquids What Is Dysphagia? If you have a problem swallowing foods or liquids, you may have dysphagia. It has a number of causes. Your doctor can find out what is
Dysphagia A Problem Swallowing Foods or Liquids What Is Dysphagia? If you have a problem swallowing foods or liquids, you may have dysphagia. It has a number of causes. Your doctor can find out what is
TREATMENT OF DYSPHAGIA IN PATIENTS AFTER STROKE IN ESTONIA
 TREATMENT OF DYSPHAGIA IN PATIENTS AFTER STROKE IN ESTONIA ANNE URIKO SPORTS MEDICINE AND REHABILITATION CLINIG OF TARTU UNIVERSITY HOSPITAL 17.09.2010 DYSPHAGIA DIFFICULTY MOVING FOOD FROM MOUTH TO STOMACH
TREATMENT OF DYSPHAGIA IN PATIENTS AFTER STROKE IN ESTONIA ANNE URIKO SPORTS MEDICINE AND REHABILITATION CLINIG OF TARTU UNIVERSITY HOSPITAL 17.09.2010 DYSPHAGIA DIFFICULTY MOVING FOOD FROM MOUTH TO STOMACH
Having a PEG tube inserted
 Having a PEG tube inserted This information leaflet is for patients who are having a PEG (Percutaneous Endoscopic Gastrostomy) tube inserted. It explains what is involved, what to expect and what significant
Having a PEG tube inserted This information leaflet is for patients who are having a PEG (Percutaneous Endoscopic Gastrostomy) tube inserted. It explains what is involved, what to expect and what significant
OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices OPTICS
 OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices Educational Booklet for Families Version June 16 2014 Page 1 of 11 This information booklet was originally
OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices Educational Booklet for Families Version June 16 2014 Page 1 of 11 This information booklet was originally
Evidence-Based Swallowing Related Issues in Patients with Tracheotomy Tubes
 Evidence-Based Swallowing Related Issues in Patients with Tracheotomy Tubes Steven B. Leder, Ph.D. Yale University School of Medicine Debra M. Suiter,, Ph.D. University of Memphis Impetus Swallowing Rx
Evidence-Based Swallowing Related Issues in Patients with Tracheotomy Tubes Steven B. Leder, Ph.D. Yale University School of Medicine Debra M. Suiter,, Ph.D. University of Memphis Impetus Swallowing Rx
Back to Basics: What Imaging Test should I order? Jeanne G. Hill, M.D. Pediatric Radiology Medical University of South Carolina
 Back to Basics: What Imaging Test should I order? Jeanne G. Hill, M.D. Pediatric Radiology Medical University of South Carolina Disclosure Neither I nor any member of my immediate family has a relevant
Back to Basics: What Imaging Test should I order? Jeanne G. Hill, M.D. Pediatric Radiology Medical University of South Carolina Disclosure Neither I nor any member of my immediate family has a relevant
Speech and Language Therapy. Kerrie McCarthy Senior Speech and Language Therapist
 Speech and Language Therapy Kerrie McCarthy Senior Speech and Language Therapist Contents 1. Voice disorders 2. Swallow disorders 3. Videofluroscopy 4. Adult Acquired Communication Disorders 5. How to
Speech and Language Therapy Kerrie McCarthy Senior Speech and Language Therapist Contents 1. Voice disorders 2. Swallow disorders 3. Videofluroscopy 4. Adult Acquired Communication Disorders 5. How to
Gastroesophageal Reflux in Infants. Kathleen Borowitz, MS, CCC-SLP Speech-Language Pathologist University of Virginia Children s Hospital
 Gastroesophageal Reflux in Infants Kathleen Borowitz, MS, CCC-SLP Speech-Language Pathologist University of Virginia Children s Hospital Disclaimers Speech-language pathologist, not a pediatrician Married
Gastroesophageal Reflux in Infants Kathleen Borowitz, MS, CCC-SLP Speech-Language Pathologist University of Virginia Children s Hospital Disclaimers Speech-language pathologist, not a pediatrician Married
Tracheostomy and Ventilator Education Program Module 10: Communication Supplies
 Tracheostomy and Ventilator Education Program Module 10: Communication Supplies Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who
Tracheostomy and Ventilator Education Program Module 10: Communication Supplies Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who
WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)?
 WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)? The term gastroesophageal reflux describes the movement (or reflux) of stomach contents back up into the esophagus, the muscular tube that extends from the
WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)? The term gastroesophageal reflux describes the movement (or reflux) of stomach contents back up into the esophagus, the muscular tube that extends from the
Management of Pediatric Tracheostomy
 Management of Pediatric Tracheostomy Deepak Mehta Associate Professor Of Otolaryngology Director Pediatric Aerodigestive Center Definitions Tracheotomy: The making of an incision in the trachea The name
Management of Pediatric Tracheostomy Deepak Mehta Associate Professor Of Otolaryngology Director Pediatric Aerodigestive Center Definitions Tracheotomy: The making of an incision in the trachea The name
Here are some types of gastric bypass surgery:
 Gastric Bypass- Definition By Mayo Clinic staff Weight-loss (bariatric) surgeries change your digestive system, often limiting the amount of food you can eat. These surgeries help you lose weight and can
Gastric Bypass- Definition By Mayo Clinic staff Weight-loss (bariatric) surgeries change your digestive system, often limiting the amount of food you can eat. These surgeries help you lose weight and can
GASTROINTESTINAL TRACT IN EBS generalized intermediate
 GASTROINTESTINAL TRACT IN EBS generalized intermediate 1. Introduction In some forms of EB formation of blisters on the mucous membranes of the mouth and esophagus can occur. This causes various problems;
GASTROINTESTINAL TRACT IN EBS generalized intermediate 1. Introduction In some forms of EB formation of blisters on the mucous membranes of the mouth and esophagus can occur. This causes various problems;
DYSPHAGIA MANAGEMENT IN ACUTE CARE AMANDA HEREFORD, MA, CCC- SLP
 DYSPHAGIA MANAGEMENT IN ACUTE CARE AMANDA HEREFORD, MA, CCC- SLP OVERVIEW Decision making re: swallowing in the medically compromised patient Swallow evaluation vs. Nursing Swallow Screening Instrumental
DYSPHAGIA MANAGEMENT IN ACUTE CARE AMANDA HEREFORD, MA, CCC- SLP OVERVIEW Decision making re: swallowing in the medically compromised patient Swallow evaluation vs. Nursing Swallow Screening Instrumental
Colonic (Large Intestine) Manometry
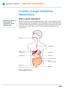 Patient and Family Education Colonic (Large Intestine) Manometry Manometry measures the pressure of contractions of the digestive tract. What is colonic manometry? The colon (also known as the large intestine)
Patient and Family Education Colonic (Large Intestine) Manometry Manometry measures the pressure of contractions of the digestive tract. What is colonic manometry? The colon (also known as the large intestine)
ORIGINAL ARTICLE. Synchronous Airway Lesions and Outcomes in Infants With Severe Laryngomalacia Requiring Supraglottoplasty
 ORIGINAL ARTICLE Synchronous Airway Lesions and Outcomes in Infants With Severe Laryngomalacia Requiring Supraglottoplasty James W. Schroeder Jr, MD; Naveen D. Bhandarkar, MD; Lauren D. Holinger, MD Objective:
ORIGINAL ARTICLE Synchronous Airway Lesions and Outcomes in Infants With Severe Laryngomalacia Requiring Supraglottoplasty James W. Schroeder Jr, MD; Naveen D. Bhandarkar, MD; Lauren D. Holinger, MD Objective:
Day 2 Pulmonary Breakout Interventional Pulmonology
 Day 2 Pulmonary Breakout Interventional Pulmonology R. Paul Boesch, DO, MS Assistant Professor, Pulmonary Medicine Mayo Clinic Children s Center Interventional Pediatric Pulmonology or Pulm/ENT airway
Day 2 Pulmonary Breakout Interventional Pulmonology R. Paul Boesch, DO, MS Assistant Professor, Pulmonary Medicine Mayo Clinic Children s Center Interventional Pediatric Pulmonology or Pulm/ENT airway
Inflammation of the Esophagus (Esophagitis) Basics
 Inflammation of the Esophagus (Esophagitis) Basics OVERVIEW Inflammation of the esophagus typically involves the tubular area of the esophagus itself (known as the esophageal body ) and the muscular area
Inflammation of the Esophagus (Esophagitis) Basics OVERVIEW Inflammation of the esophagus typically involves the tubular area of the esophagus itself (known as the esophageal body ) and the muscular area
Definition. Failure to Thrive. No clear consensus Growth below the 3 rd or 5 th percentile Decreased growth crossing 2 major growth percentiles
 Failure to Thrive Karen Swarts, MD 6/4/2004 Definition No clear consensus Growth below the 3 rd or 5 th percentile Decreased growth crossing 2 major growth percentiles 1 Nelson Textbook of Pediatrics,
Failure to Thrive Karen Swarts, MD 6/4/2004 Definition No clear consensus Growth below the 3 rd or 5 th percentile Decreased growth crossing 2 major growth percentiles 1 Nelson Textbook of Pediatrics,
Pediatric Gastroenterology Referral Guidelines
 Suggested Pre-Referral Workup This is a general suggestion of possible testing to confirm a suspected diagnosis. Although referrals will be accepted without the suggested work up being complete, to ensure
Suggested Pre-Referral Workup This is a general suggestion of possible testing to confirm a suspected diagnosis. Although referrals will be accepted without the suggested work up being complete, to ensure
4/11/2013. & approaches to management. Disclosure. No financial support
 Laryngomalacia: ay aaca pese presentations tato s & approaches to management Hamdy El-Hakim FRCS(Ed) FRCS(ORL) Associate Professor Pediatric Otolaryngology Division of Otolaryngology Head & Neck Surgery
Laryngomalacia: ay aaca pese presentations tato s & approaches to management Hamdy El-Hakim FRCS(Ed) FRCS(ORL) Associate Professor Pediatric Otolaryngology Division of Otolaryngology Head & Neck Surgery
When Eating Becomes A Challenge Dysphagia
 When Eating Becomes A Challenge Dysphagia 1. DYSPHAGIA, WHAT IS IT? 2. IMPLICATIONS 3. ASSESSMENT 4. COMPENSATORY SWALLOWING AND EXERCISES 5. DIET TEXTURE ADJUSTMENTS Swallowing Dysfunction = Dysphagia
When Eating Becomes A Challenge Dysphagia 1. DYSPHAGIA, WHAT IS IT? 2. IMPLICATIONS 3. ASSESSMENT 4. COMPENSATORY SWALLOWING AND EXERCISES 5. DIET TEXTURE ADJUSTMENTS Swallowing Dysfunction = Dysphagia
SWALLOWING: HOW CAN WE HELP
 SWALLOWING: HOW CAN WE HELP Carol Romero-Clark, M.S., CCC-SLP University of New Mexico Hospital Speech Pathology Department November 10, 2017 What happens when you swallow? Mouth (Oral Phase) Your tongue
SWALLOWING: HOW CAN WE HELP Carol Romero-Clark, M.S., CCC-SLP University of New Mexico Hospital Speech Pathology Department November 10, 2017 What happens when you swallow? Mouth (Oral Phase) Your tongue
Swallowing Screen Why? How? and So What? พญ.พวงแก ว ธ ต สก ลช ย ภาคว ชาเวชศาสตร ฟ นฟ คณะแพทยศาสตร ศ ร ราชพยาบาล
 Swallowing Screen Why? How? and So What? พญ.พวงแก ว ธ ต สก ลช ย ภาคว ชาเวชศาสตร ฟ นฟ คณะแพทยศาสตร ศ ร ราชพยาบาล Dysphagia in Stroke The incidence of dysphagia after stroke ranging from 23-50% 1 Location
Swallowing Screen Why? How? and So What? พญ.พวงแก ว ธ ต สก ลช ย ภาคว ชาเวชศาสตร ฟ นฟ คณะแพทยศาสตร ศ ร ราชพยาบาล Dysphagia in Stroke The incidence of dysphagia after stroke ranging from 23-50% 1 Location
Gastroesophageal Reflux Disease in Infants and Children
 Gastroesophageal Reflux Disease in Infants and Children 4 Marzo 2017 Drssa Chiara Leoni Drssa Valentina Giorgio pediatriagastro@gmail.com valentinagiorgio1@gmail.com Definitions: GER GER is the passage
Gastroesophageal Reflux Disease in Infants and Children 4 Marzo 2017 Drssa Chiara Leoni Drssa Valentina Giorgio pediatriagastro@gmail.com valentinagiorgio1@gmail.com Definitions: GER GER is the passage
15/11/2011. Swallowing
 Swallowing Swallowing starts from placement of the food in the mouth and continues until food enters the stomach. Dysphagia: any difficulty in moving food from mouth to stomach. Pharynx is shared for both
Swallowing Swallowing starts from placement of the food in the mouth and continues until food enters the stomach. Dysphagia: any difficulty in moving food from mouth to stomach. Pharynx is shared for both
CHILDREN: NUTRITIONALS Prescription Required Provided by the Wisconsin WIC Program to Children (1 through 4 Years of Age)
 P-40077C (03/2016) CHILDREN: NUTRITIONALS Prescription Required Provided by the Wisconsin WIC Program to Children (1 through 4 Years of Age) A Prescription, for treatment of a diagnosed medical condition,
P-40077C (03/2016) CHILDREN: NUTRITIONALS Prescription Required Provided by the Wisconsin WIC Program to Children (1 through 4 Years of Age) A Prescription, for treatment of a diagnosed medical condition,
Upper Gastrointestinal (GI) Tract X-ray (Radiography)
 Upper Gastrointestinal (GI) Tract X-ray (Radiography) What is Upper Gastrointestinal (GI) Tract Radiography? What are some common uses of the procedure? How should I prepare? What does the equipment look
Upper Gastrointestinal (GI) Tract X-ray (Radiography) What is Upper Gastrointestinal (GI) Tract Radiography? What are some common uses of the procedure? How should I prepare? What does the equipment look
