Early endocrine alterations reflect prolonged stress and relate to 1-year functional outcome in patients with severe brain injury
|
|
|
- Randell Rich
- 5 years ago
- Views:
Transcription
1 Clinical Study D Marina and others Endocrine alterations and 172: Early endocrine alterations reflect prolonged stress and relate to 1-year in patients with severe brain injury Djordje Marina, Marianne Klose, Annette Nordenbo 1, Annette Liebach 1 and Ulla Feldt-Rasmussen Department of Medical Endocrinology PE2131, Rigshospital, Copenhagen University Hospital, Copenhagen, Denmark and 2 Traumatic Brain Injury Unit, Department of Neurorehabilitation, Glostrup Hospital, Copenhagen University Hospital, Glostrup, Denmark Correspondence should be addressed to U Feldt-Rasmussen ufeldt@rh.dk Abstract Objective: Severe brain injury may increase the risk of developing acute and chronic hypopituitarism. Pituitary hormone alterations developed in the early recovery phase after brain injury may have implications for long-term functional recovery. The objective of the present study was to assess the pattern and prevalence of pituitary hormone alterations 3 months after a severe brain injury with relation to at a 1-year follow-up. Design: Prospective study at a tertiary university referral centre. Methods: A total of 163 patients admitted to neurorehabilitation after severe traumatic brain injury (TBI, nz111) or non-tbi (nz52) were included. The main outcome measures were endocrine alterations 3.3 months (median) after the brain injury and their relationship to the functioning and ability of the patients at a 1-year follow-up, as measured by the Functional Independence Measure and the Glasgow Outcome Scale-Extended. Results: Three months after the injury, elevated stress hormones (i.e. 30 min stimulated cortisol, prolactin and/or IGF1) and/or suppressed gonadal or thyroid hormones were recorded in 68 and 32% of the patients respectively. At 1 year after the injury, lower functioning level (Functional Independence Measure) and lower capability of performing normal life activities (Glasgow Outcome Scale-Extended) were related to both the elevated stress hormones (P%0.01) and the reduced gonadal and/or thyroid hormones (P%0.01) measured at 3 months. Conclusion: The present study suggests that brain injury-related endocrine alterations that mimic secondary hypogonadism and hypothyroidism and that occur with elevated stress hormones most probably reflect a prolonged stress response 2 5 months after severe brain injury, rather than pituitary insufficiency per se. These endocrine alterations thus seem to reflect a more severe disease state and relate to 1-year. European Journal of Endocrinology (2015) 172, Introduction Acquired traumatic brain injury (TBI) and non-tbi are recognised as major critical health problems worldwide (1), and health authorities expect TBI to become the leading cause of death and disability by the year 2020 (2). Both TBI and non-tbi may be complicated by short- and long-term pituitary dysfunction, which has possible implications for the recovery and s of patients (3). The reported prevalence of acute and chronic hypopituitarism after TBI and non-tbi has varied considerably between studies, ranging from 13 to 56% in the acute phase after TBI (4, 5, 6) and from negligible to well above 50% in the chronic phase (4, 5, 6, 7, 8, 9). Such discrepancies probably reflect differences in study populations and diagnostic set-up, as has been recently discussed (8, 10). Also, non-tbi conditions, such as aneurysmal subarachnoid haemorrhage (11), DOI: /EJE Ñ 2015 European Society of Endocrinology Printed in Great Britain Published by Bioscientifica Ltd.
2 172:6 814 chronic subdural haematoma (12) and ischaemic stroke (13), have been related to an increased prevalence of hypopituitarism in some studies but not in others (14, 15). Previous assessments of the relationship between post-traumatic hypopituitarism and outcomes have shown conflicting results. Some have suggested that hypopituitarism was related to increased disability (16) and a decreased quality of life (16, 17), whereas others have suggested that quality-of-life deficits were more closely associated with intracerebral haemorrhagic lesions than with hypopituitarism per se (18). Peak growth hormone (GH) has been shown to be an independent predictor of poorer outcomes, as measured by rehabilitation scales that evaluate cognition and disability (19), but such relations were recently questioned (20). Reduced testosterone concentrations were also recently described as being related to worse s in TBI patients (21, 22), which led the authors to suggest that secondary hypogonadism may limit the pace of recovery during neurorehabilitation. Based on early reports that suggested a high risk of post-traumatic hypopituitarism, a screening programme was introduced to assess pituitary function at the Department of Neurorehabilitation s Traumatic Brain Injury Unit at Copenhagen University Hospital, Glostrup. We hypothesised that the results from pituitary hormone assessment in the post-acute phase (i.e. w3 months postinjury) would relate to functional and cognitive outcomes at 1-year follow-up. Subjects and methods Subjects In Denmark, the post-acute rehabilitation of patients with the most severe TBI and non-tbi is centralised at two hospitals, each of which covers w50% of the Danish population of 5.5 million. Highest priority for admission is given to the most severely brain-injured patients, who are defined as having a Glasgow Coma Scale score of 3 12 in the first days after the cessation of sedation. Patients with a Glasgow Coma Scale score of in the first days after the cessation of sedation are also admitted if they have severe focal neurological deficits or are severely agitated. From 1st June 2007 until 31st May 2011, a total of 272 patients R15 years old were admitted to the Department of Neurorehabilitation s Traumatic Brain Injury Unit in Copenhagen. Patients with known pituitary disease or clinically significant renal disease or who were pregnant or breast-feeding were not considered for inclusion. Twelve patients died, and 51 were discharged to home within 2 months of their initial admission to neurorehabilitation without pituitary testing for unknown reasons. Pituitary assessment was also not performed in 46 patients who had longer stays at the Neurorehabilitation Unit (in 15 patients because of severe agitation and in 31 patients for unknown reasons). Thus, we included 163 patients who had available pituitary hormone measurements: 111 TBI and 52 non-tbi patients. The non-tbi patients included 28 with subarachnoid, intracerebral and non-traumatic haemorrhage, nine with anoxic brain injury, four with occlusion or stenosis of cerebral arteries not causing cerebral infarction, three with brain inflammation (meningitis), two with cerebral oedema, two with sepsis and one each with cerebral infarction, arteriovenous malformation, traumatic fat embolism and central pontine myelinolysis. The study was approved by the Local Ethical Committee (J.nr. H-D ) and the Danish Data Protection Agency (J.nr ). According to the Danish Act on Processing of Personal Data, a registry study without contact to the persons involved does not require verbal or written consent. Endocrine function testing and diagnostic criteria for endocrine alterations Pituitary function testing was performed at a median of 3.3 months (range ) after the brain injury and related to 1-year outcome data of functioning and ability as part of routine assessment in the department. Hormone assessment was performed between 0800 and 1300 h, and it included baseline measurements of follicle-stimulating hormone (FSH), luteinising hormone (LH), testosterone (males), oestrogen (females), thyroid-stimulating hormone (TSH), free thyroxine (FT 4 ), prolactin and insulin-like growth factor 1 (IGF1). The hypothalamic pituitary adrenal axis was assessed using an adrenocorticotrophic hormone (ACTH) stimulation test that measured cortisol concentrations at baseline and 30 min after the i.v. administration of 250 mg Synacthen (Defiante Farmacêutica S.A., Funchal, Madeira Portugal). If patients presented with thirst and/or increased urine volumes, diabetes insipidus was assumed and vasopressin therapy was initiated. Insufficiencies were defined in relation to local sex- and age-related reference ranges. Secondary hypogonadism in postmenopausal women was defined as inappropriately low gonadotrophins (FSH and LH) for age, in premenopausal women as the presence of
3 172:6 815 amenorrhoea or oligomenorrhoea associated with low oestrogen and inappropriately low gonadotrophins and in men as low testosterone associated with inappropriately low gonadotrophins. Secondary hypothyroidism was defined as subnormal FT 4 concentration associated with an inappropriately low TSH concentration. Normal reference ranges for the Immulite assay for serum cortisol was based on 100 healthy controls, with reference intervals given as the 2.5th and 97.5th percentiles (23). Thus, adrenal insufficiency was defined as!500 nmol/l 30 min cortisol in response to the Synacthen test, and elevated basal cortisol was described as concentrations of O665 nmol/l and stimulated cortisol as concentrations of O841 nmol/l. Three of the 52 female patients had been using contraceptive pills, which were discontinued at least 8 weeks prior to endocrine evaluation. At the time of endocrine evaluation, 12 patients were being treated with antipsychotics, 18 with antidepressants, 23 with antiemetics and 37 with antiepileptic drugs (the majority using Gabapentin and Fenytoin (nz19), a minority using Lamotrigin (nz2) and 16 using other antiepileptic medications). Function and ability assessments Outcome measures of functioning and ability were assessed at admission and discharge from neurorehabilitation and at a 1-year follow-up. The Functional Independence Measure is a scale consisting of 18 items describing various activities in daily living. These 18 items are further divided into physical (13 items) and cognitive domains (five items). Each item is rated on a seven-point scale from 1 (total assistance needed) to 7 (full independence). The added scores of the 18 items give a minimum total score of 18 and a maximum score of 126. For practical purposes, the overall total scores were divided into three subgroups that indicated the assistance required in order for the individual to carry out daily activities: complete dependency (18 55), moderate dependency (56 74) and low-level dependency to complete independency (75 126). Further, the Functional Independence Measure score can be divided into a motor score, with a maximum of 91, and a cognitive score, with a maximum of 35. The Functional Independence Measure was performed at admission to neurorehabilitation, at discharge and at the 1-year follow-up. The Glasgow Outcome Scale-Extended is an eightpoint scale used to describe the actual functioning of the patient in the period after the brain injury; it refers to independence at and outside the home, different social activities, work capability and return to normal life. For practical purposes, it is divided into two groups: lower scores range from 1 (coma) to 4 (upper severe disability), and higher scores range from 5 (lower moderate disability) to 8 (upper good recovery). Patients with scores from 1 to 4 are more dependent on assistance, whereas patients scoring between 5 and 8 need less assistance performing activities at and outside the home. The Glasgow Outcome Scale-Extended was performed at discharge from neurorehabilitation and at the 1-year follow-up. In addition, data on post-traumatic amnesia was assessed in the TBI patients using the Galveston Orientation and Amnesia Test. The period of post-traumatic amnesia was defined as the number of days between the date of the TBI and the date when the patient was out of the post-traumatic confused state. Post-traumatic amnesia that lasted for more than 4 weeks indicated a very severe TBI. Assays The type and performance characteristics of the assays used for the hormone measurements are shown in Supplementary Table 1, see section on supplementary data given at the end of this article. Statistical analyses Categorical data are presented as n (%), continuous as mean (GS.D.) if normally distributed and otherwise as median (range). Categorical data were compared by a c 2 test. Cramer s V coefficient was used to evaluate associations between two nominal variables. Between-group comparisons of normally distributed continuous data were analysed by Student s t-test or by Mann Whitney U test. Regression analyses were conducted to analyse the relation between outcome measures (Functional Independence Measure and Glasgow Outcome Scale-Extended) and dependent covariates (injury characteristics, medication, including analgesics, antidepressants and antiepileptic drugs, and hormonal hypo/hyper secretion). Basal and stimulated cortisol concentrations of the patients were compared to 100 healthy persons in which a Synacthen test was performed and cortisol was measured by Immulite assay (23). Associations were performed on the pooled data from the TBI and non-tbi groups, because no significant difference was observed in the prevalence of hormone alterations between the groups. A difference was
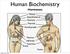
4 172:6 816 Table 1 Baseline characteristics of the included patients with traumatic brain injury (TBI) and non-tbi, with additional data on hormonal assessment. Data are given as number (%) or mean (S.D.)/median (range, 10 90%). TBI Non-TBI n Gender, men (%) 83 (75%) 28 (54%) Age at admission (years) 42.7 (18.5) 47.9 (16.0) Glasgow Coma Scale score at admission 10.2 (3.1) 11.3 (2.3) Time from trauma to neurorehabilitation (days) 20.7 (13.0) 28.6 (18.6) Length of neurorehabilitation (days) (67.2) 93.7 (40.5) CT/MR finding (TBI) Traumatic subarachnoid haemorrhage 64 (57%) / Cranial fracture 42 (38%) Shearing lesions 30 (27%) Cerebral oedema 26 (23%) Cause of injury (non-tbi) Subarachnoid haemorrhage / 16 (31%) Intracerebral haemorrhage 12 (23%) Anoxic brain injury 9 (17%) Other 15 (29%) Functional Independence Measure score at admission 18 (18 44) 18 (18 25) Post traumatic amnesia, days (%) O4 weeks 98 (88%) /!4 weeks 13 (12%) Number of patients with pituitary assessment (%) Synacthen test, including basal cortisol 102/111 (92%) 49/52 (94%) Prolactin 109/111 (98%) 50/52 (96%) Insulin-like growth factor 1 (IGF1) 109/111 (98%) 50/52 (96%) Gonadal hormones 109/111 (98%) 50/52 (96%) Free thyroxine (FT 4 ) 110/111 (99%) 50/52 (96%) Median concentration (range) of hormonal measurement Stimulated 30 min cortisol 773 nmol/l ( ) 774 nmol/l ( ) Prolactin 0.61 nmol/l ( ) 0.59 nmol/l ( ) IGF1 229 mg/l (64 486) 222 mg/l (28 461) Testosterone (males) 12 nmol/l ( ) 9.9 nmol/l ( ) FT pmol/l ( ) 14.7 pmol/l ( ) CT, computerized tomography; MR, magnetic resonance. considered significant when P!0.05. Statistical analyses were performed by SAS version 9.1 (SAS Institute, Inc., Cary, NC, USA). better Functional Independence Measure total, physical and cognitive scores one year after admission (all PZ0.02). Prevalence of endocrine alterations Results Patient characteristics The patients characteristics at admission are presented in Table 1. The Synacthen test results were missing for 12 patients (7%), whereas other hormonal measurements were missing in a minor proportion of the patients (Table 1). Patients who fulfilled the inclusion criteria but were not included (nz109) did not differ from those included (nz163) in terms of sex (PZ0.66) and age (PZ0.67), but they were less affected, as assessed by their shorter post-traumatic amnesia lengths (PZ0.001), higher Glasgow Coma Scale scores at admission (PZ0.03) and The prevalence of hormonal alterations at a median of 3.3 months after brain injury in the TBI and non-tbi patients is shown in Fig. 1. There were no significant differences in the prevalence of endocrine alterations between the TBI and non-tbi patients. The upper six panels in Fig. 1 demonstrate possible pituitary deficiencies. Hormonal alterations similar to secondary hypogonadism (24% of the TBI patients and 22% of the non-tbi patients) and hypothyroidism (9% of the TBI patients and 16% of the non-tbi patients) were the most commonly observed, whereas other deficiencies were observed in up to 5% of the TBI and non-tbi patients. The lower four panels in Fig. 1 show the prevalence of elevated stress hormones
5 172:6 817 Secondary hypogonadism Secondary hypothyroidism Secondary hypoadrenalism Diabetes insipidus Hypoprolactinaemia Reduced IGF1 Elevated prolactin Elevated IGF1 Elevated baseline cortisol Elevated stimulated cortisol TBI Non-TBI degree of dependency. Functional Independence Measures improved significantly during the rehabilitation period in both the TBI and non-tbi patients (Fig. 2). Thus, significantly fewer patients had a high degree of dependency at the 1-year follow-up as compared to baseline (i.e. at admission to neurorehabilitation) in both the TBI and non-tbi patients (P!0.01) (Table 2). In the TBI group, Functional Independence Measure scores were missing for 18 patients at the 1-year follow-up. In the non-tbi group, Functional Independence Measure scores were missing for one patient at admission, two patients at discharge and 12 patients at the 1-year follow-up visit (Table 2). Glasgow Outcome Scale-Extended (i.e. concentrations above the upper normal reference limit), including elevated prolactin (49% of the TBI patients and 50% of the non-tbi patients), IGF1 (26% of the TBI patients and 36% of the non-tbi patients), basal cortisol (5% of the TBI patients and 4% of the non-tbi patients) and 30 min cortisol (34% of the TBI patients and 29% of the non-tbi patients). The study shows that 32% of the patients had suppressed gonadal or thyroid function (1% were suppressed on both axes), whereas 68% had elevated stimulated 30 min cortisol, prolactin or IGF1 (29% had an elevated concentration of more than one hormone). Elevated stress hormones and suppressed gonadal and/or thyroid function were concomitantly registered in 40 out of 151 (26%) of the patients. Hyperprolactinaemia was related to suppressed thyroid function (PZ0.04; Cramer s VZ0.17) but not to suppressed gonadal function (PZ0.67; Cramer s VZK0.03). Elevated stimulated 30 min cortisol was related to suppressed gonadal function (PZ0.02; Cramer s VZ0.19) but not to suppressed thyroid function (PZ0.09; Cramer s VZK0.13). Functional Independence Measure Percentage of patients with hormonal alterations Figure 1 Percentage of patients with hormonal alterations presented separately in traumatic brain injury (TBI) and non-tbi groups. The shaded area represents the prevalence of elevated stress hormones. Low median Functional Independence Measure total, motor and cognitive scores at admission were in agreement with very severely injured patients that had a high At discharge, 72% of the TBI patients and 86% of the non-tbi patients had a very low Glasgow Outcome Scale-Extended score, which indicated a low degree of independent activity (Table 2). This was ameliorated at the 1-year follow-up visit in a significant number of patients in the TBI group (P!0.05). In the TBI group, Glasgow Outcome Scale-Extended scores were missing for 18 patients at the 1-year follow-up (Table 2). In the non-tbi group, Glasgow Outcome Scale-Extended scores were missing for one patient at discharge and 12 patients at the 1-year follow-up (Table 2). Relationship between early endocrine alterations and measures at the 1-year follow-up Worse Functional Independence Measure total, cognitive and physical scores at 1 year were related to lower Glasgow Coma Scale scores at referral and a need for longer rehabilitation (P!0.001; b total!k0.23; b cognitive!k0.05; b physical!k0.16) but not to shearing lesions or medical treatment with antiepileptic, antidepressant or analgesic drugs (all PO0.22). Worse Functional Independence Measure scores were also related to secondary hypogonadism (P%0.02; b total!k20; b cognitive!k4.5; b physical!k14) and increased stress hormones (P%0.02; b total!k13; b cognitive!k4; b physical!k15). Both secondary hypogonadism (PZ0.02; bz16) and increased stress hormones (PZ0.02; bz14) remained independently related to worse Functional Independence Measure scores in multivariate analyses after adjusting for the length of rehabilitation needed (P%0.01; R 2 Z0.23). A low capability for returning to normal life activities, as indicated by a low Glasgow Outcome-Extended score at 1 year, was more frequent in patients with a lower Glasgow Coma Scale score at referral and a need for longer
6 172:6 818 Functional independence measure score rehabilitation (P!0.001) but not to shearing lesions or medical treatment with antiepileptic, antidepressant or analgesic drugs (all PO0.32). A low Glasgow Outcome- Extended score was also related to reduced gonadal and/or thyroid hormones (PZ0.04; Cramer s VZK0.17) and elevated stress hormones (PZ0.006; Cramer s VZK0.23). In multivariate analyses, adjusting for the length of rehabilitation needed increased stress hormones (PZ0.01) but not secondary hypogonadism (PZ0.17), which remained independently related to a worse Glasgow Outcome-Extended score at 1 year. Discussion Total Motor Cognitive Referral One year Referral One year Traumatic brain injury Non-traumatic brain injury Figure 2 Median Functional Independence Measure scores presented with 10th and 90th percentile CIs of included patients with traumatic brain injury (TBI) and non-tbi at referral and at follow-up. Scores are divided into total, motor and cognitive scores. A Functional Independence Measure total score of 18 indicates that the patient was in need of total assistance, and a score of 126 suggests that the patient was fully independent. Maximum Functional Independence Measure scores, which are designated as optimal when the patient is completely independent, were: 126 (total), 91 (motor) and 35 (cognitive). In the present cohort of 163 patients assessed at a median of 3.3 months after a severe acquired brain injury, the most prevalent hormonal alterations were increased concentrations of stress-related hormones, followed by decreased gonadal and thyroid hormones, which concomitantly presented in 26% of the patients. Similar endocrine alterations have been reported both in patients with brain injury (4, 5, 6) and in patients with other causes of acute and severe illness (24). Although in some cases endocrine alterations may be attributed to primary or secondary injury to the hypothalamus or pituitary gland, acute severe illness involves major stress to the organism, and increased ACTH, cortisol, GH and prolactin concentrations, together with low testosterone and low triiodothyronine syndrome, have all been described as being part of important adaptive responses in the early phases following trauma, surgery and severe medical illness (24). However, distinct hormonal secretion patterns are also to be expected in the chronic phase of critical illness and in the subsequent recovery phase with the restoration of peripheral sensitivity and the loss of central drive (25). Patients included in the present study were either in the chronic phase of critical illness or in the recovery phase at the time of testing. Thus, although all of the patients still required neurorehabilitation, the cohort remained inhomogeneous, which probably explains some of the observed inter-individual differences. A Synacthen test was routinely performed in order to diagnose hypoadrenalism. At 3 months, hypoadrenalism was only registered in two non-tbi patients. Further, up to 5% of the patients in both groups had decreased basal cortisol values, which were defined as baseline total cortisol!2.5th percentile from that of healthy subjects. During critical illness, glucocorticoid secretion markedly increases and relates to stress activation of the hypothalamic pituitary adrenal axis (25) and reduced cortisol breakdown as a result of the suppressed expression and activity of cortisol-metabolising enzymes (26). The increase is, however, not necessarily discernible when only the total cortisol concentration is measured. In a study by Hamrahian et al. (27), nearly 40% of critically ill patients with hypoproteinaemia had subnormal total cortisol concentrations, even though their adrenal function was normal, as measured by free cortisol concentrations. Thus, lower cortisol binding globulin (CBG) concentrations (28) may have led to low cortisol concentrations in a subset of our patients, even though they responded appropriately to Synacthen stimulation. Furthermore, blood sampling was performed from 0800 to 1300 h, which could have influenced results because of circadian hormonal rhythms. If this was the case, we may have underestimated the prevalence of elevated basal cortisol concentrations rather than overestimating them. It is noteworthy that one-third of the patients in the present cohort had a 30 min cortisol concentration above that expected in healthy people, which suggests a
7 172:6 819 Table 2 Distribution of scores in traumatic brain injury (TBI) and non-tbi patients. The table presents the number of patients with baseline and/or discharge, as well as follow-up Functional Independence Measure total scores and Glasgow Outcome Scale-Extended scores. Both scores were further divided in scoring subgroups depending on the actual level of the patients functioning. TBI Non-TBI Time of measurement Admission Discharge One-year One-year follow-up a Admission b Discharge b follow-up b Functional Independence Measure Complete dependency c (score: 18 55) Moderate dependency c (score: 56 74) Low dependency to complete independency c (score: ) Glasgow Outcome Scale-Extended Coma to upper severe disability (score: 1 4) Lower moderate disability to upper good recovery (score: 5 8) 104/111 (94%) 45/111 (41%) 23/93 (25%) d 48/51 (94%) 24/50 (48%) 10/40 (25%) d 3/111 (3%) 8/111 (7%) 5/93 (5%) 0/51 (0%) 2/50 (4%) 2/40 (5%) 4/111 (3%) 58/111 (52%) 65/93 (70%) d 3/51 (6%) 24/50 (48%) 28/40 (70%) d Not done 80/111 (72%) 47/93 (51%) Not done 44/51 (86%) 25/40 (62.5%) Not done 31/111 (28%) 46/93 (49%) e Not done 7/51 (14%) 15/40 (37.5%) a In the TBI group, Functional Independence Measure and Glasgow Outcome Scale-Extended scores were missing for 18 patients at the 1-year follow-up (two patients died before attending the follow-up visit, one patient attended the visit but that patient s score was not recorded, and 15 patients did not attend the follow-up visit for unknown reasons). b In the non-tbi group, Functional Independence Measure scores were missing for one patient at admission, two patients at discharge, and 12 patients at the 1-year follow-up visit (three patients died before attending the follow-up visit, one patient attended the follow-up visit but that patient s score was not recorded, and eight patients did not attend the follow-up visit for unknown reasons), whereas Glasgow Outcome Scale-Extended scores were missing for one patient at discharge and for the same number of patients at the 1-year follow-up as described for the Functional Independence Measure scores. c Three scoring groups (scores in parentheses) represent the actual need for help in performing basic daily activities. Patients in the lowest scoring group were completely dependent on assistance during the day. On the contrary, patients in the highest scoring group needed less assistance. d A significant number of patients switched from the complete dependency group (at admission) to the low dependency/complete independency group (at the 1-year follow-up) (P!0.01). e A significant number of patients switched from the lower-scoring group (at discharge) to the higher-scoring group (at the 1-year follow-up) (P!0.05). prolonged stress response with glucocorticoid hyperactivation. Unfortunately, neither ACTH nor CBG were measured, and thus no correlations between total and free cortisol concentrations could be made. Finally, the documented use of the Synacthen test is apt for the assessment of hypo- and not hyperactivation of the adrenal gland. The original purpose of the study was to assess hypofunction; thus, measurements of such factors as 24-h urine cortisol, which would have been preferable for assessing hyperactivation (29), were not included. Increased prolactin was the most commonly observed endocrine alteration. Hyperprolactinaemia is a wellknown phenomenon in the acute phase of a brain injury that may persist in 31% of patients during rehabilitation (30), and it was reported in up to 47% of the TBI patients who had other endocrine failures during long-term follow-up (31). Although hyperprolactinaemia may indicate pituitary stalk and/or hypothalamic injury, prolactin is one of the first hormones to increase in acute phases of severe illness, whereas prolactin is no longer as high in chronic phases (24). In acute and chronic phases of critical illness, IGF1 concentrations tended to be low (32). However,Kopczak et al. (33) showed that 14% of their patients had elevated IGF1, whereas 6% had reduced IGF1 concentrations, as measured at a median of 7 weeks after the TBI or subarachnoid haemorrhage. This was in keeping with our data of commonly registered elevated IGF1. However, it is not clear whether increased IGF1 should be considered part of neuroprotection (34) or as a result of the insulin resistance and hyperglycaemia that are commonly observed during prolonged critical illness (35). A concomitant assessment of GH concentrations might have clarified this further. Endocrine alterations similar to secondary hypogonadism and hypothyroidism were observed in 23 and 11% of the patients respectively. Similar findings have previously been observed in patients with brain injury (4, 5, 11) but also in patients with critical illness resulting from other causes and without a history of acquired brain injury (24). It is well established that prolonged critical illness alters the physiology of the reproductive axis with decreased testosterone concentrations and reduced or low to normal gonadotrophins (36); these patterns have also been observed for the thyroid axis (24). The most likely explanation for these endocrine alterations in severe prolonged illness was suggested to be impairment of the pulsatile component of pituitary hormones, such as the gonadal axis (24), but it may also involve reduced
8 172:6 820 hypothalamic stimulation of trophic hormones, which in turn leads to reduced stimulation of the target organ (25). Because secondary hypogonadism and hypothyroidism were present concomitant with elevated stress hormones in 26% of the patients, we suggest that these endocrine alterations were a result of the prolonged stress response in the period after the severe brain injury and not a result of hypothalamo-pituitary injury. Some recent outcome studies have indicated that posttraumatic hypopituitarism has clinical significance because it impacts both health-related quality of life and lipid status (17), but the findings have been inconsistent (20, 37). Ulfarsson et al. (37) tested 51 patients with severe TBI for 2 10 years after the initial trauma, which is longer than the present study, but they showed no relationship between hypopituitarism and worse psychological, cognitive or motor functioning in the longer term. In the present study, both secondary hypogonadism and increased stress hormones were related to worse 1-year follow-up scores on the Functional Independence Measure, which is well known and widely used in rehabilitation settings. A recent non-randomised retrospective study in TBI patients suggested that reduced testosterone levels at admission were related to lower admission scores, less change in scores on the Functional Independence Measure and longer hospitalisation (21). Other authors have suggested that hypogonadism may limit the pace of recovery during rehabilitation (22) because of the well-known effects of testosterone on muscle mass and strength, cognition and perception of the quality of life. Whether the same pattern of action can be applied to people with acquired severe brain injuries remains to be investigated. Kopczak et al. (33) went a step further and treated 13 male patients after TBI or subarachnoid haemorrhage with testosterone replacement. The Barthel index (a measurement of independence and recovery) and haemoglobin concentrations before and after treatment were measured, and haemoglobin had increased in four patients in 4 weeks O2 g/dl (1.24 mmol/l), which was a surrogate sign of testosterone replacement benefit (33). However, the distinction between primary and secondary hypogonadism was unclear, because gonadotrophins were not measured. Further studies are needed to predict if male patients diagnosed with hypogonadism after an acquired brain injury, irrespective of its cause, would achieve a better neurorehabilitation outcome with testosterone treatment. Low Glasgow Outcome Scale-Extended scores were significantly improved from discharge to the 1-year follow-up, which implies that more patients became capable of returning to normal activities both inside and outside of their homes. However, low Glasgow Outcome Scale-Extended scores were more frequent in patients with reduced gonadal and/or thyroid hormones and increased stress hormones, whereas only increased stress hormones remained independently related to a worse Glasgow Outcome Scale-Extended score at the 1-year follow-up. Santarsieri et al. (38) recently measured cortisol in the cerebrospinal fluid of the TBI patients and showed persistently elevated cortisol during the first 6 days after trauma, which was associated with poorer outcomes, as measured by Glasgow Outcome Scale scores and Functional Independence Measure cognitive scores 6 months after the injury. Recently, pituitary abnormalities in 27% of patients 3 6 months after a subarachnoid haemorrhage were significantly related to lower median Glasgow Outcome Scale scores at follow-up, with more prevalent endocrine abnormalities occurring when bleeding sites were closer to the hypothalamus (39). In contrast to the present and previously mentioned studies, other authors did not find an association between endocrine alterations and Glasgow Outcome Scale-Extended score measures (37, 40) or other quality-of-life questionnaires (18, 20). Some limitations of the present study should be addressed. GH stimulation tests were not part of the routine screening programme at the neurorehabilitation centre, and GH measurements are thus not available, although they could have potentially clarified the significance of the observed changes in IGF1 values. BMI has been shown to influence both GH and IGF1, the latter being decreased with BMI exceeding 32.5 kg/m 2 as well as with low BMI (41). Unfortunately, at the time of testing, BMI was not available for our patients, and we could thus not correct for it. Another limitation is the aetiologic difference with variable prognoses and influence on the Functional Independence Measure score. However, the number of patients within each aetiologic subgroup was too small for subgroup analyses. Although the patients in the present study represented a heterogeneous group, especially among the non-tbi patients, the vast majority had very severe trauma, which was indicated by very low physical and cognitive scores at the time of admission to neurorehabilitation, w3 weeks after the initial trauma. Finally, the influence of medications such as antidepressants, antipsychotics and antiemetics could be additional factors for the observed frequency of such conditions as hyperprolactinaemia. In the present study, hormonal assessment was performed w3 months after injury. The development of post-traumatic hypopituitarism later than 3 months after injury has been suggested (6). It remains speculative, however, if such new deficiencies would have affected
9 172:6 821 our data. The insufficiencies reported in the present study were retested by repeat measurement w12 months after the injury (D Marina, M Klose and U Feldt-Rasmussen, unpublished data). Most had resolved, and none of the patients had any replacements initiated after the 3-month testing. In conclusion, the present study suggested that endocrine alterations similar to secondary hypogonadism and hypothyroidism at a median of 3.3 months after an acquired severe brain injury most probably reflected a prolonged stress response rather than brain damage per se. Accordingly, not only secondary hypogonadism and hypothyroidism but also elevated stress hormones were related to worse 1-year s. Thus, we suggest that post-brain injury endocrine alterations are not necessarily a consequence of hypothalamic or pituitary damage; rather, they may represent physiological stress adaptations to acute critical illness, with a subsequent prolonged stress response at least 3 months post-injury. Therefore, routine pituitary assessment in the early phases (e.g. within a year) after acquired brain injury should be limited to patients that present with typical clinical features suggestive of hypopituitarism (4, 7). Supplementary data This is linked to the online version of the paper at EJE Declaration of interest U Feldt-Rasmussen received unrestricted research and travel grants and speaker s fees from Novartis and Ipsen, research grants, speaker s fees and advisory board honoraria from Pfizer and a research grant from Arvid Nilsson s Fund. M Klose received an unrestricted research grant from Novo Nordic and speaker fees from Pfizer and Novartis. D Marina, A Nordenbo and A Liebach have nothing to disclose. Funding This research did not receive any specific grant from any funding agency in the public, commercial or not-for-profit sector. Author contribution statement D Marina wrote the paper; A Nordenbo and A Liebach were supervisors during the whole period of the study and collected the data; M Klose and U Feldt-Rasmussen initiated the study and supervised all aspects of the process; all authors contributed to the writing of the paper. Acknowledgements U Feldt-Rasmussen s research salary was supported by a grant from Arvid Nilsson s fund. We thank Lars Westergaard for his assistance in collecting data and constructing the patient database used in the present study. References 1 Greenwald BD, Burnett DM & Miller MA. Congenital and acquired brain injury. 1. Brain injury: epidemiology and pathophysiology. Archives of Physical Medicine and Rehabilitation S3 S7. (doi: /apmr ) 2 Hyder AA, Wunderlich CA, Puvanachandra P, Gururaj G & Kobusingye OC. The impact of traumatic brain injuries: a global perspective. NeuroRehabilitation Schneider HJ, Kreitschmann-Andermahr I, Ghigo E, Stalla GK & Agha A. Hypothalamopituitary dysfunction following traumatic brain injury and aneurysmal subarachnoid hemorrhage: a systematic review. Journal of the American Medical Association (doi: /jama ) 4 Klose M, Juul A, Struck J, Morgenthaler NG, Kosteljanetz M & Feldt- Rasmussen U. Acute and long-term pituitary insufficiency in traumatic brain injury: a prospective single-centre study. Clinical Endocrinology (doi: /j x) 5 Schneider HJ, Schneider M, Saller B, Petersenn S, Uhr M, Husemann B, von Rosen F & Stalla GK. Prevalence of anterior pituitary insufficiency 3 and 12 months after traumatic brain injury. European Journal of Endocrinology (doi: /eje ) 6 Tanriverdi F, Senyurek H, Unluhizarci K, Selcuklu A, Casanueva FF & Kelestimur F. High risk of hypopituitarism after traumatic brain injury: a prospective investigation of anterior pituitary function in the acute phase and 12 months after trauma. Journal of Clinical Endocrinology and Metabolism (doi: /jc ) 7 Klose M, Juul A, Poulsgaard L, Kosteljanetz M, Brennum J & Feldt- Rasmussen U. Prevalence and predictive factors of post-traumatic hypopituitarism. Clinical Endocrinology (doi: / j x) 8 Klose M, Stochholm K, Janukonyte J, Lehman CL, Frystyk J, Andersen M, Laurberg P, Christiansen JS & Feldt-Rasmussen U. Prevalence of posttraumatic growth hormone deficiency is highly dependent on the diagnostic set-up: results from The Danish National Study on Posttraumatic Hypopituitarism. Journal of Clinical Endocrinology and Metabolism (doi: /jc ) 9 van der Eerden AW, Twickler MT, Sweep FC, Beems T, Hendricks HT, Hermus AR & Vos PE. Should anterior pituitary function be tested during follow-up of all patients presenting at the emergency department because of traumatic brain injury? European Journal of Endocrinology (doi: /eje ) 10 Kokshoorn NE, Wassenaar MJ, Biermasz NR, Roelfsema F, Smit JW, Romijn JA & Pereira AM. Hypopituitarism following traumatic brain injury: prevalence is affected by the use of different dynamic tests and different normal values (doi: /eje ) 11 Aimaretti G, Ambrosio MR, Di Somma C, Fusco A, Cannavo S, Gasperi M, Scaroni C, De Marinis L, Benvenga S, degli Uberti EC et al. Traumatic brain injury and subarachnoid haemorrhage are conditions at high risk for hypopituitarism: screening study at 3 months after the brain injury. Clinical Endocrinology (doi: / j x) 12 Hana V, Kosak M, Masopust V, Netuka D, Lacinova Z, Krsek M, Marek J & Pecen L. Hypothalamo-pituitary dysfunction in patients with chronic subdural hematoma. Physiological Research Bondanelli M, Ambrosio MR, Carli A, Bergonzoni A, Bertocchi A, Zatelli MC, Ceruti S, Valle D, Basaglia N & degli Uberti EC. Predictors of pituitary dysfunction in patients surviving ischemic stroke. Journal of Clinical Endocrinology and Metabolism (doi: / jc ) 14 Klose M, Brennum J, Poulsgaard L, Kosteljanetz M, Wagner A & Feldt- Rasmussen U. Hypopituitarism is uncommon after aneurysmal subarachnoid haemorrhage. Clinical Endocrinology (doi: /j x)
10 172: Gardner CJ, Javadpour M, Stoneley C, Purthuran M, Biswas S, Daousi C, Macfarlane IA & Cuthbertson DJ. Low prevalence of hypopituitarism after subarachnoid haemorrhage using confirmatory testing and with BMI-specific growth hormone cut-off levels. European Journal of Endocrinology (doi: /eje ) 16 Bavisetty S, Bavisetty S, McArthur DL, Dusick JR, Wang C, Cohan P, Boscardin WJ, Swerdloff R, Levin H, Chang DJ et al. Chronic hypopituitarism after traumatic brain injury: risk assessment and relationship to outcome. Neurosurgery (doi: /01.neu a) 17 Klose M, Watt T, Brennum J & Feldt-Rasmussen U. Posttraumatic hypopituitarism is associated with an unfavorable body composition and lipid profile, and decreased quality of life 12 months after injury. Journal of Clinical Endocrinology and Metabolism (doi: /jc ) 18 Wachter D, Gundling K, Oertel MF, Stracke H & Boker DK. Pituitary insufficiency after traumatic brain injury. Journal of Clinical Neuroscience (doi: /j.jocn ) 19 Bondanelli M, Ambrosio MR, Cavazzini L, Bertocchi A, Zatelli MC, Carli A, Valle D, Basaglia N & Uberti EC. Anterior pituitary function may predict functional and cognitive outcome in patients with traumatic brain injury undergoing rehabilitation. Journal of Neurotrauma (doi: /neu ) 20 Pavlovic D, Pekic S, Stojanovic M, Zivkovic V, Djurovic B, Jovanovic V, Miljic N, Medic-Stojanoska M, Doknic M, Miljic D et al. Chronic cognitive sequelae after traumatic brain injury are not related to growth hormone deficiency in adults. European Journal of Neurology (doi: /j x) 21 Young TP, Hoaglin HM & Burke DT. The role of serum testosterone and TBI in the in-patient rehabilitation setting. Brain Injury (doi: / ) 22 Carlson NE, Brenner LA, Wierman ME, Harrison-Felix C, Morey C, Gallagher S & Ripley D. Hypogonadism on admission to acute rehabilitation is correlated with lower functional status at admission and discharge. Brain Injury (doi: / ) 23 Klose M, Lange M, Rasmussen AK, Skakkebaek NE, Hilsted L, Haug E, Andersen M & Feldt-Rasmussen U. Factors influencing the adrenocorticotropin test: role of contemporary cortisol assays, body composition, and oral contraceptive agents. Journal of Clinical Endocrinology and Metabolism (doi: /jc ) 24 Van Den Berghe G. Endocrine evaluation of patients with critical illness. Endocrinology and Metabolism Clinics of North America (doi: /s (03) ) 25 Boonen E & Van Den Berghe G. Endocrine responses to critical illness: novel insights and therapeutic implications. Journal of Clinical Endocrinology and Metabolism (doi: / jc ) 26 Boonen E, Vervenne H, Meersseman P, Andrew R, Mortier L, Declercq PE, Vanwijngaerden YM, Spriet I, Wouters PJ, Vander PS et al. Reduced cortisol metabolism during critical illness. New England Journal of Medicine (doi: / NEJMoa ) 27 Hamrahian AH, Oseni TS & Arafah BM. Measurements of serum free cortisol in critically ill patients. New England Journal of Medicine (doi: /nejmoa020266) 28 Beishuizen A, Thijs LG & Vermes I. Patterns of corticosteroid-binding globulin and the free cortisol index during septic shock and multitrauma. Intensive Care Medicine (doi: / s ) 29 Carroll TB & Findling JW. The diagnosis of Cushing s syndrome. Reviews in Endocrine & Metabolic Disorders (doi: /s ) 30 Agha A, Rogers B, Mylotte D, Taleb F, Tormey W, Phillips J & Thompson CJ. Neuroendocrine dysfunction in the acute phase of traumatic brain injury. Clinical Endocrinology (doi: /j x) 31 Benvenga S, Campenni A, Ruggeri RM & Trimarchi F. Clinical review 113: Hypopituitarism secondary to head trauma. Journal of Clinical Endocrinology and Metabolism (doi: / jcem ) 32 Mesotten D & Van Den Berghe G. Changes within the growth hormone/insulin-like growth factor I/IGF binding protein axis during critical illness. Endocrinology and Metabolism Clinics of North America , ix x. (doi: /j.ecl ) 33 Kopczak A, Kilimann I, von Rosen F, Krewer C, Schneider HJ, Stalla GK & Schneider M. Screening for hypopituitarism in 509 patients with traumatic brain injury or subarachnoid hemorrhage. Journal of Neurotrauma (doi: /neu ) 34 Rubovitch V, Edut S, Sarfstein R, Werner H & Pick CG. The intricate involvement of the insulin-like growth factor receptor signaling in mild traumatic brain injury in mice. Neurobiological Disorders Van den Berghe G. How does blood glucose control with insulin save lives in intensive care? Journal of Clinical Investigation (doi: /jci23506) 36 Spratt DI. Altered gonadal steroidogenesis in critical illness: is treatment with anabolic steroids indicated? Best Practice & Research. Clinical Endocrinology & Metabolism (doi: / beem ) 37 Ulfarsson T, Gudnason GA, Rosen T, Blomstrand C, Stibrant SK, Lundgren-Nilsson A & Nilsson M. Pituitary function and functional outcome in adults after severe traumatic brain injury: the long-term perspective. Journal of Neurotrauma (doi: /neu ) 38 Santarsieri M, Niyonkuru C, McCullough E, Dobos J, Dixon CE, Berga S & Wagner AK. CSF cortisol and progesterone profiles and outcomes prognostication after severe TBI. Journal of Neurotrauma (doi: /neu ) 39 Kronvall E, Valdemarsson S, Saveland H & Nilsson OG. Pituitary dysfunction after aneurysmal subarachnoid hemorrhage is associated with impaired early outcome. World Neurosurgery (doi: /j.wneu ) 40 Wagner J, Dusick JR, McArthur DL, Cohan P, Wang C, Swerdloff R, Boscardin WJ & Kelly DF. Acute gonadotroph and somatotroph hormonal suppression after traumatic brain injury. Journal of Neurotrauma (doi: /neu ) 41 Schneider HJ, Saller B, Klotsche J, Marz W, Erwa W, Wittchen HU & Stalla GK. Opposite associations of age-dependent insulin-like growth factor-i standard deviation scores with nutritional state in normal weight and obese subjects (doi: /eje ) Received 28 December 2014 Revised version received 10 March 2015 Accepted 30 March 2015
Hypopituitarism following traumatic brain injury: prevalence is affected by the use of different dynamic tests and different normal values
 European Journal of Endocrinology (2010) 162 11 18 ISSN 0804-4643 REVIEW Hypopituitarism following traumatic brain injury: prevalence is affected by the use of different dynamic tests and different normal
European Journal of Endocrinology (2010) 162 11 18 ISSN 0804-4643 REVIEW Hypopituitarism following traumatic brain injury: prevalence is affected by the use of different dynamic tests and different normal
Endocrine evaluation of patients after brain injury: what else is needed to define specific clinical recommendations?
 HORMONES 2007, 6(2):132-137 Commentary Endocrine evaluation of patients after brain injury: what else is needed to define specific clinical recommendations? Gemma Sesmilo, Irene Halperin, Manuel Puig-Domingo
HORMONES 2007, 6(2):132-137 Commentary Endocrine evaluation of patients after brain injury: what else is needed to define specific clinical recommendations? Gemma Sesmilo, Irene Halperin, Manuel Puig-Domingo
Hypopituitarism After Traumatic Brain Injury
 Hypopituitarism After Traumatic Brain Injury Eva Fernandez-Rodriguez, MD a, Ignacio Bernabeu, MD a, Ana I. Castro a,b, Felipe F. Casanueva, MD, PhD a,b, * KEYWORDS Traumatic brain injury Hypopituitarism
Hypopituitarism After Traumatic Brain Injury Eva Fernandez-Rodriguez, MD a, Ignacio Bernabeu, MD a, Ana I. Castro a,b, Felipe F. Casanueva, MD, PhD a,b, * KEYWORDS Traumatic brain injury Hypopituitarism
Hypothalamo pituitary dysfunction in patients with chronic subdural hematoma
 Hypothalamo pituitary dysfunction in patients with chronic subdural hematoma Václav Hána 1, Mikuláš Kosák 1, Václav Masopust 2, David Netuka 2, Zdena Lacinová 1, Michal Kršek 1, Josef Marek 1, Ladislav
Hypothalamo pituitary dysfunction in patients with chronic subdural hematoma Václav Hána 1, Mikuláš Kosák 1, Václav Masopust 2, David Netuka 2, Zdena Lacinová 1, Michal Kršek 1, Josef Marek 1, Ladislav
Medical and Rehabilitation Innovations Neuroendocrine Screening and Hormone Replacement Therapy in Trauma Related Acquired Brain Injury
 Medical and Rehabilitation Innovations Neuroendocrine Screening and Hormone Replacement Therapy in Trauma Related Acquired Brain Injury BACKGROUND Trauma related acquired brain injury (ABI) is known to
Medical and Rehabilitation Innovations Neuroendocrine Screening and Hormone Replacement Therapy in Trauma Related Acquired Brain Injury BACKGROUND Trauma related acquired brain injury (ABI) is known to
Pituitary functions in the acute phase of traumatic brain injury: Are they related to severity of the injury or mortality?
 Brain Injury, April 27; 21(4): 433 439 Pituitary functions in the acute phase of traumatic brain injury: Are they related to severity of the injury or mortality? FATIH TANRIVERDI 1, HALIL ULUTABANCA 2,
Brain Injury, April 27; 21(4): 433 439 Pituitary functions in the acute phase of traumatic brain injury: Are they related to severity of the injury or mortality? FATIH TANRIVERDI 1, HALIL ULUTABANCA 2,
Previously, loss of pituitary function caused by traumatic
 ORIGINAL ARTICLE Endocrine Care Prevalence of Posttraumatic Growth Hormone Deficiency Is Highly Dependent on the Diagnostic Set-up: Results From The Danish National Study on Posttraumatic Hypopituitarism
ORIGINAL ARTICLE Endocrine Care Prevalence of Posttraumatic Growth Hormone Deficiency Is Highly Dependent on the Diagnostic Set-up: Results From The Danish National Study on Posttraumatic Hypopituitarism
Traumatic Brain Injury and Hypopituitarism
 Mini-Review Article TheScientificWorldJOURNAL (2005) 5, 777 781 ISSN 1537-744X; DOI 10.1100/tsw.2005.100 Traumatic Brain Injury and Hypopituitarism Gianluca Aimaretti and Ezio Ghigo* Division of Endocrinology
Mini-Review Article TheScientificWorldJOURNAL (2005) 5, 777 781 ISSN 1537-744X; DOI 10.1100/tsw.2005.100 Traumatic Brain Injury and Hypopituitarism Gianluca Aimaretti and Ezio Ghigo* Division of Endocrinology
Traumatic Brain Injury-Related Hypopituitarism: A Review and Recommendations for Screening Combat Veterans
 MILITARY MEDICINE, 175, 8:574, 2010 Traumatic Brain Injury-Related Hypopituitarism: A Review and Recommendations for Screening Combat Veterans CPT(P) Arthur F. Guerrero, MC USA ; MAJ Abel Alfonso, MC USA
MILITARY MEDICINE, 175, 8:574, 2010 Traumatic Brain Injury-Related Hypopituitarism: A Review and Recommendations for Screening Combat Veterans CPT(P) Arthur F. Guerrero, MC USA ; MAJ Abel Alfonso, MC USA
Endocrine part one. Presented by Dr. Mohammad Saadeh The requirements for the Clinical Chemistry Philadelphia University Faculty of pharmacy
 Endocrine part one Presented by Dr. Mohammad Saadeh The requirements for the Clinical Chemistry Philadelphia University Faculty of pharmacy HORMONES Hormones are chemicals released by a cell or a gland
Endocrine part one Presented by Dr. Mohammad Saadeh The requirements for the Clinical Chemistry Philadelphia University Faculty of pharmacy HORMONES Hormones are chemicals released by a cell or a gland
Antipituitary antibodies after traumatic brain injury: is head trauma-induced pituitary dysfunction associated with autoimmunity?
 European Journal of Endocrinology (2008) 159 7 13 ISSN 0804-4643 CLINICAL STUDY Antipituitary antibodies after traumatic brain injury: is head trauma-induced pituitary dysfunction associated with autoimmunity?
European Journal of Endocrinology (2008) 159 7 13 ISSN 0804-4643 CLINICAL STUDY Antipituitary antibodies after traumatic brain injury: is head trauma-induced pituitary dysfunction associated with autoimmunity?
European Journal of Endocrinology (2006) ISSN
 European Journal of Endocrinology (2006) 155 553 557 ISSN 0804-4643 CLINICAL STUDY Discrepant results in the diagnosis of GH deficiency with the insulin-tolerance test and the GHRH plus arginine test in
European Journal of Endocrinology (2006) 155 553 557 ISSN 0804-4643 CLINICAL STUDY Discrepant results in the diagnosis of GH deficiency with the insulin-tolerance test and the GHRH plus arginine test in
Causes of TBI vary with age
 Endocrinopathies after Traumatic Brain Injury Susan R. Rose, MD Professor Cincinnati Children s Hospital Medical Center University of Cincinnati Supported by Pfizer, Inc Investigator-Initiated Research
Endocrinopathies after Traumatic Brain Injury Susan R. Rose, MD Professor Cincinnati Children s Hospital Medical Center University of Cincinnati Supported by Pfizer, Inc Investigator-Initiated Research
PITUITARY: JUST THE BASICS PART 2 THE PATIENT
 PITUITARY: JUST THE BASICS PART 2 THE PATIENT DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none Steps taken to review and
PITUITARY: JUST THE BASICS PART 2 THE PATIENT DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none Steps taken to review and
Endocrine part two. Presented by Dr. Mohammad Saadeh The requirements for the Clinical Chemistry Philadelphia University Faculty of pharmacy
 Endocrine part two Presented by Dr. Mohammad Saadeh The requirements for the Clinical Chemistry Philadelphia University Faculty of pharmacy Cushing's disease: increased secretion of adrenocorticotropic
Endocrine part two Presented by Dr. Mohammad Saadeh The requirements for the Clinical Chemistry Philadelphia University Faculty of pharmacy Cushing's disease: increased secretion of adrenocorticotropic
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Traumatic brain injury: endocrine consequences in children and adults
 DOI 10.1007/s12020-013-0049-1 REVIEW Traumatic brain injury: endocrine consequences in children and adults Erick Richmond Alan D. Rogol Received: 25 June 2013 / Accepted: 27 August 2013 Ó Springer Science+Business
DOI 10.1007/s12020-013-0049-1 REVIEW Traumatic brain injury: endocrine consequences in children and adults Erick Richmond Alan D. Rogol Received: 25 June 2013 / Accepted: 27 August 2013 Ó Springer Science+Business
Acromegaly resolution after traumatic brain injury: a case report
 Cob Journal of Medical Case Reports 2014, 8:290 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Acromegaly resolution after traumatic brain injury: a case report Alejandro Cob Abstract Introduction:
Cob Journal of Medical Case Reports 2014, 8:290 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Acromegaly resolution after traumatic brain injury: a case report Alejandro Cob Abstract Introduction:
Critical illness and endocrinology. ICU Fellowship Training Radboudumc
 Critical illness and endocrinology ICU Fellowship Training Radboudumc Critical illness Ultimate form of severe physical stress Generates an orchestrated endocrine response to provide the energy for fight
Critical illness and endocrinology ICU Fellowship Training Radboudumc Critical illness Ultimate form of severe physical stress Generates an orchestrated endocrine response to provide the energy for fight
Antipituitary antibodies after traumatic brain injury: Is head trauma induced pituitary dysfunction associated with autoimmunity?
 Page 1 of 24 Accepted Preprint first posted on 7 May 2008 as Manuscript EJE-08-0050 Antipituitary antibodies after traumatic brain injury: Is head trauma induced pituitary dysfunction associated with autoimmunity?
Page 1 of 24 Accepted Preprint first posted on 7 May 2008 as Manuscript EJE-08-0050 Antipituitary antibodies after traumatic brain injury: Is head trauma induced pituitary dysfunction associated with autoimmunity?
Prediction of Adrenocortical Insufficiency After Pituitary Adenoma Surgery Using Postoperative Basal Cortisol Levels
 Physiol. Res. 64: 531-536, 2015 Prediction of Adrenocortical Insufficiency After Pituitary Adenoma Surgery Using Postoperative Basal Cortisol Levels V. HÁNA Jr. 1, J. JEŽKOVÁ 1, M. KOSÁK 1, M. KRŠEK 1,
Physiol. Res. 64: 531-536, 2015 Prediction of Adrenocortical Insufficiency After Pituitary Adenoma Surgery Using Postoperative Basal Cortisol Levels V. HÁNA Jr. 1, J. JEŽKOVÁ 1, M. KOSÁK 1, M. KRŠEK 1,
Anterior Pituitary Hormones Changes After Spontaneous Subarachnoid Hemorrhage
 ISPUB.COM The Internet Journal of Neurosurgery Volume 13 Number 1 Anterior Pituitary Hormones Changes After Spontaneous Subarachnoid Hemorrhage H Eldawoody, A Elawadly, A Shaker, A Mesbah, M Hegazy Citation
ISPUB.COM The Internet Journal of Neurosurgery Volume 13 Number 1 Anterior Pituitary Hormones Changes After Spontaneous Subarachnoid Hemorrhage H Eldawoody, A Elawadly, A Shaker, A Mesbah, M Hegazy Citation
It has been suggested that aneurysmal subarachnoid hemorrhage
 High Incidence of Neuroendocrine Dysfunction in Long-Term Survivors of Aneurysmal Subarachnoid Hemorrhage Ioanna Dimopoulou, MD; Andreas T. Kouyialis, MD; Marinella Tzanella, MD; Apostolos Armaganidis,
High Incidence of Neuroendocrine Dysfunction in Long-Term Survivors of Aneurysmal Subarachnoid Hemorrhage Ioanna Dimopoulou, MD; Andreas T. Kouyialis, MD; Marinella Tzanella, MD; Apostolos Armaganidis,
Hypothalamus & Pituitary Gland
 Hypothalamus & Pituitary Gland Hypothalamus and Pituitary Gland The hypothalamus and pituitary gland form a unit that exerts control over the function of several endocrine glands (thyroid, adrenals, and
Hypothalamus & Pituitary Gland Hypothalamus and Pituitary Gland The hypothalamus and pituitary gland form a unit that exerts control over the function of several endocrine glands (thyroid, adrenals, and
Evaluation and Management of Pituitary Failure. Dr S. Ali Imran MBBS, FRCP (Edin), FRCPC Professor of Medicine Dalhousie University, Halifax, NS
 Evaluation and Management of Pituitary Failure Dr S. Ali Imran MBBS, FRCP (Edin), FRCPC Professor of Medicine Dalhousie University, Halifax, NS Conflict of Interest None Objectives Diagnostic approach
Evaluation and Management of Pituitary Failure Dr S. Ali Imran MBBS, FRCP (Edin), FRCPC Professor of Medicine Dalhousie University, Halifax, NS Conflict of Interest None Objectives Diagnostic approach
9. Neuroendocrine Disorders Post ABI
 9. Neuroendocrine Disorders Post ABI 9.1 History and Epidemiology On behalf of the ERABI Research Group Neuroendocrine disorders, primarily hypopituitarism, were first diagnosed by the German researcher
9. Neuroendocrine Disorders Post ABI 9.1 History and Epidemiology On behalf of the ERABI Research Group Neuroendocrine disorders, primarily hypopituitarism, were first diagnosed by the German researcher
Endocrine system overview
 Endocrine system overview Nature of the hormonal system -Major integrator of body function Classification of hormones Endocrine vs paracrine Nature of hormone-receptor systems Role of the hypothalamuspituitary
Endocrine system overview Nature of the hormonal system -Major integrator of body function Classification of hormones Endocrine vs paracrine Nature of hormone-receptor systems Role of the hypothalamuspituitary
Traumatic brain injury induced hypothalamic-pituitary dysfunction: a paediatric perspective
 Pituitary (2007) 10:373 380 DOI 10.1007/s11102-007-0052-8 Traumatic brain injury induced hypothalamic-pituitary dysfunction: a paediatric perspective Carlo L. Acerini Æ Robert C. Tasker Published online:
Pituitary (2007) 10:373 380 DOI 10.1007/s11102-007-0052-8 Traumatic brain injury induced hypothalamic-pituitary dysfunction: a paediatric perspective Carlo L. Acerini Æ Robert C. Tasker Published online:
9. Neuroendocrine Function and Disorders Following Acquired Brain Injury
 9. Neuroendocrine Function and Disorders Following Acquired Brain Injury Genevieve Sirois MD, Robert Teasell MD FRCPC, Pavlina Faltynek MSc, Joshua Wiener BSc, Mark Bayley MD FRCPC ERABI Parkwood Institute
9. Neuroendocrine Function and Disorders Following Acquired Brain Injury Genevieve Sirois MD, Robert Teasell MD FRCPC, Pavlina Faltynek MSc, Joshua Wiener BSc, Mark Bayley MD FRCPC ERABI Parkwood Institute
ENDOCRINOLOGY COORDINATION OF PHYSIOLOGICAL PROCESSES:
 ENDOCRINOLOGY COORDINATION OF PHYSIOLOGICAL PROCESSES: -In a living organism there must be coordination of number of physiological activities taking place simultaneously such as: movement, respiration,
ENDOCRINOLOGY COORDINATION OF PHYSIOLOGICAL PROCESSES: -In a living organism there must be coordination of number of physiological activities taking place simultaneously such as: movement, respiration,
Growth Hormone Deficiency after Traumatic Brain Injury: improvement in quality of. life with GH therapy - analysis of the KIMS database
 Page 1 of 27 Accepted Preprint first posted on 12 January 2015 as Manuscript EJE-14-0654 Growth Hormone Deficiency after Traumatic Brain Injury: improvement in quality of life with GH therapy - analysis
Page 1 of 27 Accepted Preprint first posted on 12 January 2015 as Manuscript EJE-14-0654 Growth Hormone Deficiency after Traumatic Brain Injury: improvement in quality of life with GH therapy - analysis
The prevalence of growth hormone deficiency in survivors of subarachnoid haemorrhage: results from a large single centre study
 DOI 10.1007/s11102-017-0825-7 The prevalence of growth hormone deficiency in survivors of subarachnoid haemorrhage: results from a large single centre study Sumithra Giritharan 1,7 Joanna Cox 2 Calvin
DOI 10.1007/s11102-017-0825-7 The prevalence of growth hormone deficiency in survivors of subarachnoid haemorrhage: results from a large single centre study Sumithra Giritharan 1,7 Joanna Cox 2 Calvin
Received: 24 Jun 2008 Revisions requested: 14 Jul 2008 Revisions received: 30 Aug 2008 Accepted: 13 Oct 2008 Published: 13 Oct 2008
 Available online http://ccforum.com/content/12/5/r126 Vol 12 No 5 Research Open Access Pituitary-adrenal function in patients with acute subarachnoid haemorrhage: a prospective cohort study Stepani Bendel
Available online http://ccforum.com/content/12/5/r126 Vol 12 No 5 Research Open Access Pituitary-adrenal function in patients with acute subarachnoid haemorrhage: a prospective cohort study Stepani Bendel
Human Biochemistry. Hormones
 Human Biochemistry Hormones THE ENDOCRINE SYSTEM THE ENDOCRINE SYSTEM THE ENDOCRINE SYSTEM The ENDOCRINE SYSTEM = the organ system that regulates internal environment conditions by secreting hormones into
Human Biochemistry Hormones THE ENDOCRINE SYSTEM THE ENDOCRINE SYSTEM THE ENDOCRINE SYSTEM The ENDOCRINE SYSTEM = the organ system that regulates internal environment conditions by secreting hormones into
Neuropsychiatric Disturbances and Hypopituitarism After Traumatic Brain Injury in an Elderly Man
 CASE REPORT Neuropsychiatric Disturbances and Hypopituitarism After Traumatic Brain Injury in an Elderly Man Yi-Cheng Chang, Jui-Chang Tsai, 1,2 Fen-Yu Tseng* Neuropsychiatric or cognitive disturbances
CASE REPORT Neuropsychiatric Disturbances and Hypopituitarism After Traumatic Brain Injury in an Elderly Man Yi-Cheng Chang, Jui-Chang Tsai, 1,2 Fen-Yu Tseng* Neuropsychiatric or cognitive disturbances
PROOF ONLY. Neuroendocrine surveillance and management of neurosurgical patients MANAGEMENT OF ENDOCRINE DISEASE. Review. Abstract.
 Review A Garrahy and others Hypopituitarism in 176:5 R217 R233 MANAGEMENT OF ENDOCRINE DISEASE Neuroendocrine surveillance and management of Aoife Garrahy 1, Mark Sherlock 2 and Christopher J Thompson
Review A Garrahy and others Hypopituitarism in 176:5 R217 R233 MANAGEMENT OF ENDOCRINE DISEASE Neuroendocrine surveillance and management of Aoife Garrahy 1, Mark Sherlock 2 and Christopher J Thompson
The Endocrine System/Hormones
 The Endocrine System/Hormones Controls many body functions exerts control by releasing special chemical substances into the blood called hormones Hormones affect other endocrine glands or body systems
The Endocrine System/Hormones Controls many body functions exerts control by releasing special chemical substances into the blood called hormones Hormones affect other endocrine glands or body systems
Living Control Mechanisms
 Living Control Mechanisms Dr Kate Earp MBChB MRCP Specialty Registrar Chemical Pathology & Metabolic Medicine kate.earp@sth.nhs.uk 15/10/2015 Contents Aims & objectives Homeostasis Cell communication Introduction
Living Control Mechanisms Dr Kate Earp MBChB MRCP Specialty Registrar Chemical Pathology & Metabolic Medicine kate.earp@sth.nhs.uk 15/10/2015 Contents Aims & objectives Homeostasis Cell communication Introduction
ABNORMAL PITUITARY FUNCTION
 Overview ABNORMAL PITUITARY FUNCTION Specialist Portfolio Seminar Katie Jones Sandwell and West Birmingham Hospitals NHS Trust Anterior pituitary overview Posterior pituitary overview Pituitary dysfunction
Overview ABNORMAL PITUITARY FUNCTION Specialist Portfolio Seminar Katie Jones Sandwell and West Birmingham Hospitals NHS Trust Anterior pituitary overview Posterior pituitary overview Pituitary dysfunction
Pituitary Complications in Traumatic Brain Injury
 Pituitary Complications in Traumatic Brain Injury François Lauzier, MD, MSc, FRCPC Assistant Professor Division of Critical Care Medicine Department of Anesthesiology and Critical Care Medicine Department
Pituitary Complications in Traumatic Brain Injury François Lauzier, MD, MSc, FRCPC Assistant Professor Division of Critical Care Medicine Department of Anesthesiology and Critical Care Medicine Department
Endocrinological Outcome Among Treated Craniopharyngioma Patients
 Endocrinological Outcome Among Treated Craniopharyngioma Patients Afaf Al Sagheir, MD Head & Consultant, Section of Endocrinology/Diabetes Department of Pediatrics KFSH&RC Introduction Craniopharyngiomas
Endocrinological Outcome Among Treated Craniopharyngioma Patients Afaf Al Sagheir, MD Head & Consultant, Section of Endocrinology/Diabetes Department of Pediatrics KFSH&RC Introduction Craniopharyngiomas
Neuroendocrine Disturbances after Brain Damage: An Important and Often Undiagnosed Disorder
 J. Clin. Med. 2015, 4, 847-857; doi:10.3390/jcm4050847 Review OPEN ACCESS Journal of Clinical Medicine ISSN 2077-0383 www.mdpi.com/journal/jcm Neuroendocrine Disturbances after Brain Damage: An Important
J. Clin. Med. 2015, 4, 847-857; doi:10.3390/jcm4050847 Review OPEN ACCESS Journal of Clinical Medicine ISSN 2077-0383 www.mdpi.com/journal/jcm Neuroendocrine Disturbances after Brain Damage: An Important
Adrenal Glands. Adrenal Glands. Adrenal Glands. Adrenal Glands. Adrenal Glands 4/12/2016. Controlled by both nerves and hormones.
 Glands http://www.hawaiilife.com/articles/2012/03/good-news-vacation-rental-owners/ 70 Figure 10.14a gland Glands cortex Mineralocorticoids Gonadocorticoids Glucocorticoids medulla Epinephrine Norepinephrine
Glands http://www.hawaiilife.com/articles/2012/03/good-news-vacation-rental-owners/ 70 Figure 10.14a gland Glands cortex Mineralocorticoids Gonadocorticoids Glucocorticoids medulla Epinephrine Norepinephrine
Endocrine System. Chemical Control
 Endocrine System Chemical Control Endocrine System - the system that secretes hormones in the body - hormones can last for minutes or for hours - a major gland, once called the master gland, is the pituitary
Endocrine System Chemical Control Endocrine System - the system that secretes hormones in the body - hormones can last for minutes or for hours - a major gland, once called the master gland, is the pituitary
Checking the Right Box at the Right Age: the Art of Pediatric Endocrine Testing
 Checking the Right Box at the Right Age: the Art of Pediatric Endocrine Testing Jean-Pierre Chanoine, MD Endocrinology and Diabetes Unit British Columbia s Children s Hospital Objectives 1. Interpret the
Checking the Right Box at the Right Age: the Art of Pediatric Endocrine Testing Jean-Pierre Chanoine, MD Endocrinology and Diabetes Unit British Columbia s Children s Hospital Objectives 1. Interpret the
Endocrine System. Modified by M. Myers
 Endocrine System Modified by M. Myers 1 The Endocrine System 2 Endocrine Glands The endocrine system is made of glands & tissues that secrete hormones. Hormones are chemicals messengers influencing a.
Endocrine System Modified by M. Myers 1 The Endocrine System 2 Endocrine Glands The endocrine system is made of glands & tissues that secrete hormones. Hormones are chemicals messengers influencing a.
62-year-old woman with severe headache. Celeste Thomas November 1, 2012
 62-year-old woman with severe headache Celeste Thomas November 1, 2012 History of Present Illness History of hypertension and hyperlipidemia Presented to outside hospital after awakening from sleep with
62-year-old woman with severe headache Celeste Thomas November 1, 2012 History of Present Illness History of hypertension and hyperlipidemia Presented to outside hospital after awakening from sleep with
David Henley. Sir Charles Gairdner Hospital, Nedlands WA University of Western Australia. ESA Seminar Weekend, Melbourne Vic 27 th May 2017
 David Henley Sir Charles Gairdner Hospital, Nedlands WA University of Western Australia ESA Seminar Weekend, Melbourne Vic 27 th May 2017 Disclosures Received honoraria from Ipsen, Novartis, Servier, Bristol-Myers
David Henley Sir Charles Gairdner Hospital, Nedlands WA University of Western Australia ESA Seminar Weekend, Melbourne Vic 27 th May 2017 Disclosures Received honoraria from Ipsen, Novartis, Servier, Bristol-Myers
Introduction to Endocrinology. Hypothalamic and Pituitary diseases Prolactinoma + Acromegaly
 Introduction to Endocrinology. Hypothalamic and Pituitary diseases Prolactinoma + Acromegaly Dr. Peter Igaz MD PhD DSc 2nd Department of Medicine Semmelweis University Fields of Endocrinology Diseases
Introduction to Endocrinology. Hypothalamic and Pituitary diseases Prolactinoma + Acromegaly Dr. Peter Igaz MD PhD DSc 2nd Department of Medicine Semmelweis University Fields of Endocrinology Diseases
Prediction of adrenocortical insufficiency after pituitary adenoma surgery using postoperative basal cortisol levels
 Prediction of adrenocortical insufficiency after pituitary adenoma surgery using postoperative basal cortisol levels Václav Hána jr. 1, Jana Ježková 1, Mikuláš Kosák 1, Michal Kršek 1, Josef Marek 1, David
Prediction of adrenocortical insufficiency after pituitary adenoma surgery using postoperative basal cortisol levels Václav Hána jr. 1, Jana Ježková 1, Mikuláš Kosák 1, Michal Kršek 1, Josef Marek 1, David
Unit Eleven - The Endocrine System
 Unit Eleven - The Endocrine System I. Introduction A. Overview: the endocrine system and nervous system work to control homeostasis within the body. The endocrine system operates at a much pace but the
Unit Eleven - The Endocrine System I. Introduction A. Overview: the endocrine system and nervous system work to control homeostasis within the body. The endocrine system operates at a much pace but the
Chapter 8.2 The Endocrine System
 Major Endocrine Organs Hypothalamus Pineal Gland Pituitary Gland Thyroid Gland Thymus Gland Adrenal Glands Pancreas Ovaries (Female) Testis (Male) Chapter 8.2 The Endocrine System The endocrine system
Major Endocrine Organs Hypothalamus Pineal Gland Pituitary Gland Thyroid Gland Thymus Gland Adrenal Glands Pancreas Ovaries (Female) Testis (Male) Chapter 8.2 The Endocrine System The endocrine system
Prolactin-Secreting Pituitary Adenomas (Prolactinomas) The Diagnostic Pathway (11-2K-234)
 Prolactin-Secreting Pituitary Adenomas (Prolactinomas) The Diagnostic Pathway (11-2K-234) Common presenting symptoms/clinical assessment: Pituitary adenomas are benign neoplasms of the pituitary gland.
Prolactin-Secreting Pituitary Adenomas (Prolactinomas) The Diagnostic Pathway (11-2K-234) Common presenting symptoms/clinical assessment: Pituitary adenomas are benign neoplasms of the pituitary gland.
Assessing Adrenal Function in Ill, Hospitalized Patients. Bruce Redmon, MD Division of Endocrinology, Diabetes and Metabolism
 Assessing Adrenal Function in Ill, Hospitalized Patients Bruce Redmon, MD Division of Endocrinology, Diabetes and Metabolism Disclosures Very surprised when I received an email two weeks ago disclosing
Assessing Adrenal Function in Ill, Hospitalized Patients Bruce Redmon, MD Division of Endocrinology, Diabetes and Metabolism Disclosures Very surprised when I received an email two weeks ago disclosing
JACK L. SNITZER, DO INTERNAL MEDICINE BOARD REVIEW COURSE 2018 PITUITARY
 JACK L. SNITZER, DO INTERNAL MEDICINE BOARD REVIEW COURSE 2018 PITUITARY JACK L. SNITZER, D.O. Peninsula Regional Endocrinology 1415 S. Division Street Salisbury, MD 21804 Phone:410-572-8848 Fax:410-572-6890
JACK L. SNITZER, DO INTERNAL MEDICINE BOARD REVIEW COURSE 2018 PITUITARY JACK L. SNITZER, D.O. Peninsula Regional Endocrinology 1415 S. Division Street Salisbury, MD 21804 Phone:410-572-8848 Fax:410-572-6890
MANAGEMENT OF PATIENTS WITH PITUITARY DISORDERS ON THE NEUROSUGERY WARDS RESPONSIBILITIES OF THE METABOLIC REGISTRAR
 MANAGEMENT OF PATIENTS WITH PITUITARY DISORDERS ON THE NEUROSUGERY WARDS RESPONSIBILITIES OF THE METABOLIC REGISTRAR We have clear links with DCN and a responsibility for the management of patients with
MANAGEMENT OF PATIENTS WITH PITUITARY DISORDERS ON THE NEUROSUGERY WARDS RESPONSIBILITIES OF THE METABOLIC REGISTRAR We have clear links with DCN and a responsibility for the management of patients with
9 - Neuroendocrine Disorders Following Acquired Brain Injury
 9 - Neuroendocrine Disorders Following Acquired Brain Injury Genevieve Sirois MD, Jo-Anne Aubut BA, Lilia Golverk MD, Robert Teasell MD FRCPC, T. Arnold Bayley, MD, FRCPC, Mark Bayley MD, FRCPC ERABI Parkwood
9 - Neuroendocrine Disorders Following Acquired Brain Injury Genevieve Sirois MD, Jo-Anne Aubut BA, Lilia Golverk MD, Robert Teasell MD FRCPC, T. Arnold Bayley, MD, FRCPC, Mark Bayley MD, FRCPC ERABI Parkwood
Diagnosing Growth Disorders. PE Clayton School of Medical Sciences, Faculty of Biology, Medicine & Health
 Diagnosing Growth Disorders PE Clayton School of Medical Sciences, Faculty of Biology, Medicine & Health Content Normal pattern of growth and its variation Using growth charts Interpreting auxological
Diagnosing Growth Disorders PE Clayton School of Medical Sciences, Faculty of Biology, Medicine & Health Content Normal pattern of growth and its variation Using growth charts Interpreting auxological
Pituitary Tumors and Incidentalomas. Bijan Ahrari, MD, FACE, ECNU Palm Medical Group
 Pituitary Tumors and Incidentalomas Bijan Ahrari, MD, FACE, ECNU Palm Medical Group Background Pituitary incidentaloma: a previously unsuspected pituitary lesion that is discovered on an imaging study
Pituitary Tumors and Incidentalomas Bijan Ahrari, MD, FACE, ECNU Palm Medical Group Background Pituitary incidentaloma: a previously unsuspected pituitary lesion that is discovered on an imaging study
Pituitary Adenomas: Evaluation and Management. Fawn M. Wolf, MD 10/27/17
 Pituitary Adenomas: Evaluation and Management Fawn M. Wolf, MD 10/27/17 Over 18,000 pituitaries examined at autopsy: -10.6% contained adenomas (1.5-27%) -Frequency similar for men and women and across
Pituitary Adenomas: Evaluation and Management Fawn M. Wolf, MD 10/27/17 Over 18,000 pituitaries examined at autopsy: -10.6% contained adenomas (1.5-27%) -Frequency similar for men and women and across
Endocrine Glands: Hormone-secreting organs are called endocrine glands
 University of Jordan Department of Physiology and Biochemistry Nursing students, Academic year 2017/2018. ******************************************************************* Ref: Principles of Anatomy
University of Jordan Department of Physiology and Biochemistry Nursing students, Academic year 2017/2018. ******************************************************************* Ref: Principles of Anatomy
Peri-op Pituitary / Diabetes Insipidus/ Apoplexy Dr. Stan Van Uum, MD, PhD, FRCPC
 10 th Annual Canadian Endocrine Update 3 rd Canadian Endocrine Review Course Peri-op Pituitary / Diabetes Insipidus/ Apoplexy Dr. Stan Van Uum, MD, PhD, FRCPC 10 th Annual Canadian Endocrine Update Dr.
10 th Annual Canadian Endocrine Update 3 rd Canadian Endocrine Review Course Peri-op Pituitary / Diabetes Insipidus/ Apoplexy Dr. Stan Van Uum, MD, PhD, FRCPC 10 th Annual Canadian Endocrine Update Dr.
Occurrence of Pituitary Dysfunction following Traumatic Brain Injury
 JOURNAL OF NEUROTRAUMA Volume 21, Number 6, 2004 Mary Ann Liebert, Inc. Pp. 000 000 Occurrence of Pituitary Dysfunction following Traumatic Brain Injury MARTA BONDANELLI, 1 LAURA DE MARINIS, 2 MARIA ROSARIA
JOURNAL OF NEUROTRAUMA Volume 21, Number 6, 2004 Mary Ann Liebert, Inc. Pp. 000 000 Occurrence of Pituitary Dysfunction following Traumatic Brain Injury MARTA BONDANELLI, 1 LAURA DE MARINIS, 2 MARIA ROSARIA
Robert Wadlow and his father
 Robert Wadlow and his father 1 Robert Wadlow Wadlow reached 8 ft 11.1 in (2.72 m) in height and weighed 485 lb (220 kg) at his death at age 22. Born in Illinois. His great size and his continued growth
Robert Wadlow and his father 1 Robert Wadlow Wadlow reached 8 ft 11.1 in (2.72 m) in height and weighed 485 lb (220 kg) at his death at age 22. Born in Illinois. His great size and his continued growth
HYPOTHALAMO PITUITARY GONADAL AXIS
 HYPOTHALAMO PITUITARY GONADAL AXIS Physiology of the HPG axis Endogenous opioids and the HPG axis (exerciseinduced menstrual disturbances) Effects of the immune system on the HPG axis (cytokines: interleukins
HYPOTHALAMO PITUITARY GONADAL AXIS Physiology of the HPG axis Endogenous opioids and the HPG axis (exerciseinduced menstrual disturbances) Effects of the immune system on the HPG axis (cytokines: interleukins
Functional disorders of the hypothalamic-pituitaryadrenal axis in patients with severe brain injury
 GMJ, ASM 212;1(S1):S31-S37 Functional disorders of the hypothalamic-pituitaryadrenal axis in patients with severe brain injury Munzir J M Al-Zabin 1 *, Thomas Kemmer 2 1 Department of Neurosurgery, Gulf
GMJ, ASM 212;1(S1):S31-S37 Functional disorders of the hypothalamic-pituitaryadrenal axis in patients with severe brain injury Munzir J M Al-Zabin 1 *, Thomas Kemmer 2 1 Department of Neurosurgery, Gulf
Pituitary Apoplexy. Updated: April 22, 2018 CLINICAL RECOGNITION
 Pituitary Apoplexy Zeina C Hannoush, MD. Assistant Professor of Clinical Medicine. Division of Endocrinology, Diabetes and Metabolism. University of Miami, Miller School of Medicine. Roy E Weiss, MD, PhD,
Pituitary Apoplexy Zeina C Hannoush, MD. Assistant Professor of Clinical Medicine. Division of Endocrinology, Diabetes and Metabolism. University of Miami, Miller School of Medicine. Roy E Weiss, MD, PhD,
Pituitary for the General Practitioner. Marilyn Lee Consultant physician and endocrinologist
 Pituitary for the General Practitioner Marilyn Lee Consultant physician and endocrinologist Pituitary tumours Anterior/posterior pituitary Extension of adenoma upwards/downwards/sideways Producing too
Pituitary for the General Practitioner Marilyn Lee Consultant physician and endocrinologist Pituitary tumours Anterior/posterior pituitary Extension of adenoma upwards/downwards/sideways Producing too
panhypopituitarism Pattawan Wongwijitsook Maharat Nakhon Ratchasima hospital 17 Nov 2013
 panhypopituitarism Pattawan Wongwijitsook Maharat Nakhon Ratchasima hospital 17 Nov 2013 PITUITARY GLAND (HYPOPHYSIS CEREBRI) The master of endocrine glands master of endocrine glands It is a small oval
panhypopituitarism Pattawan Wongwijitsook Maharat Nakhon Ratchasima hospital 17 Nov 2013 PITUITARY GLAND (HYPOPHYSIS CEREBRI) The master of endocrine glands master of endocrine glands It is a small oval
BACKGROUND AND KEY TERMS RELATED TO THIS EXERCISE
 Downloaded from advan.physiology.org on April 15, 2012 LABORATORY EXERCISE BACKGROUND AND KEY TERMS RELATED TO THIS EXERCISE Questions are integrated throughout the text to serve as a source of discussion
Downloaded from advan.physiology.org on April 15, 2012 LABORATORY EXERCISE BACKGROUND AND KEY TERMS RELATED TO THIS EXERCISE Questions are integrated throughout the text to serve as a source of discussion
Female Reproductive Endocrinology
 Female Reproductive Endocrinology Dr. Channa Jayasena PhD MRCP FRCPath Clinical Senior Lecturer & Consultant Endocrinologist Department of Gynaecology, Hammersmith Hospital Anovulation is a common cause
Female Reproductive Endocrinology Dr. Channa Jayasena PhD MRCP FRCPath Clinical Senior Lecturer & Consultant Endocrinologist Department of Gynaecology, Hammersmith Hospital Anovulation is a common cause
WARD INSTRUCTIONS WEBSITE
 DEPARTMENT OF CLINICAL CHEMISTRY NEW CROSS HOSPITAL WOLVERHAMPTON WARD INSTRUCTIONS WEBSITE Edition 1.1 SOP E1.120P.CHE Date issued: June 2016 Review interval: Authorised copy: Printed copies Author Location
DEPARTMENT OF CLINICAL CHEMISTRY NEW CROSS HOSPITAL WOLVERHAMPTON WARD INSTRUCTIONS WEBSITE Edition 1.1 SOP E1.120P.CHE Date issued: June 2016 Review interval: Authorised copy: Printed copies Author Location
I. Provide patient care that is compassionate, appropriate and effective for the prevention and treatment of endocrinologic disorders.
 Endocrinology Curriculum Goal Endocrinology is the diagnosis and care of disorders of the endocrine system. The principal endocrine problems handled by the general internist include goiter, thyroid nodules,
Endocrinology Curriculum Goal Endocrinology is the diagnosis and care of disorders of the endocrine system. The principal endocrine problems handled by the general internist include goiter, thyroid nodules,
PATIENT INFORMATION HYPOPITUITARISM YOUR QUESTIONS ANSWERED
 PATIENT INFORMATION HYPOPITUITARISM YOUR QUESTIONS ANSWERED Contents What is hypopituitarism? 1 What causes hypopituitarism? 2 What are the symptoms and signs of hypopituitarism? 4 How is hypopituitarism
PATIENT INFORMATION HYPOPITUITARISM YOUR QUESTIONS ANSWERED Contents What is hypopituitarism? 1 What causes hypopituitarism? 2 What are the symptoms and signs of hypopituitarism? 4 How is hypopituitarism
Process / Evidence Class. Clinical Assessment / III
 Table 2: Endocrine Author Cozzi et al (2009) 1 Study Design: Prospectively followed case series. Fourteen patients had pre-op hypocortisolism. Patient Population: Seventy-two adult patients who underwent
Table 2: Endocrine Author Cozzi et al (2009) 1 Study Design: Prospectively followed case series. Fourteen patients had pre-op hypocortisolism. Patient Population: Seventy-two adult patients who underwent
This is a published version of a paper published in Scandinavian Journal of Trauma, Resuscitation and Emergency Medicine.
 Umeå University This is a published version of a paper published in Scandinavian Journal of Trauma, Resuscitation and Emergency Medicine. Citation for the published paper: Olivecrona, Z., Dahlqvist, P.,
Umeå University This is a published version of a paper published in Scandinavian Journal of Trauma, Resuscitation and Emergency Medicine. Citation for the published paper: Olivecrona, Z., Dahlqvist, P.,
Hormones. Introduction to Endocrine Disorders. Hormone actions. Modulation of hormone levels. Modulation of hormone levels
 Introduction to Endocrine Disorders Hormones Self-regulating system (homeostasis) Affect: Growth Metabolism Reproduction Fluid and electrolyte balance Hormone actions Endocrine gland Hormone synthesis
Introduction to Endocrine Disorders Hormones Self-regulating system (homeostasis) Affect: Growth Metabolism Reproduction Fluid and electrolyte balance Hormone actions Endocrine gland Hormone synthesis
Anterior pituitary dysfunction following traumatic brain injury (TBI)
 Clinical Endocrinology (2006) 64, 481 488 doi: 10.1111/j.1365-2265.2006.02517.x CLINICAL PRACTICE UPDATE Blackwell Publishing Ltd Anterior pituitary dysfunction following traumatic brain injury (TBI) Amar
Clinical Endocrinology (2006) 64, 481 488 doi: 10.1111/j.1365-2265.2006.02517.x CLINICAL PRACTICE UPDATE Blackwell Publishing Ltd Anterior pituitary dysfunction following traumatic brain injury (TBI) Amar
Endocrine System. Chapter 9
 Endocrine System Chapter 9 Endocrine Organs Hormones Chemical messengers that are released from one tissue and transported through blood to a target tissue. Chemical classification: amino acids, steroids,
Endocrine System Chapter 9 Endocrine Organs Hormones Chemical messengers that are released from one tissue and transported through blood to a target tissue. Chemical classification: amino acids, steroids,
Polycystic Ovary Syndrome
 Polycystic Ovary Syndrome Definition: the diagnostic criteria Evidence of hyperandrogenism, biochemical &/or clinical (hirsutism, acne & male pattern baldness). Ovulatory dysfunction; amenorrhoea; oligomenorrhoea
Polycystic Ovary Syndrome Definition: the diagnostic criteria Evidence of hyperandrogenism, biochemical &/or clinical (hirsutism, acne & male pattern baldness). Ovulatory dysfunction; amenorrhoea; oligomenorrhoea
ENDOCRINOLOGY. Dr.AZZA SAJID ALKINANY 2 nd STAGE
 ENDOCRINOLOGY Dr.AZZA SAJID ALKINANY 2 nd STAGE THE RELATIONSHIP AMONG THE HYPOTHALMUS,POSTERIOR PITUITARY AND TARGET TISSUES. The posterior pituitary does not produce its own hormones, but stores and
ENDOCRINOLOGY Dr.AZZA SAJID ALKINANY 2 nd STAGE THE RELATIONSHIP AMONG THE HYPOTHALMUS,POSTERIOR PITUITARY AND TARGET TISSUES. The posterior pituitary does not produce its own hormones, but stores and
CATEGORY Endocrine System Review. Provide labels for the following diagram CHAPTER 13 BLM
 CHAPTER 13 BLM 13.1.1 CATEGORY Endocrine System Review Provide labels for the following diagram. 1. 6. 2. 7. 3. 8. 4. 9. 5. 10. CHAPTER 13 BLM 13.1.2 OVERHEAD Glands and Their Secretions Endocrine gland
CHAPTER 13 BLM 13.1.1 CATEGORY Endocrine System Review Provide labels for the following diagram. 1. 6. 2. 7. 3. 8. 4. 9. 5. 10. CHAPTER 13 BLM 13.1.2 OVERHEAD Glands and Their Secretions Endocrine gland
BACKGROUND AND SCIENTIFIC RATIONALE. Protocol Code: ISRCTN V 1.0 date 30 Jan 2012
 BACKGROUND AND SCIENTIFIC RATIONALE Protocol Code: ISRCTN15088122 V 1.0 date 30 Jan 2012 Traumatic Brain Injury 10 million killed or hospitalised every year 90% in low and middle income countries Mostly
BACKGROUND AND SCIENTIFIC RATIONALE Protocol Code: ISRCTN15088122 V 1.0 date 30 Jan 2012 Traumatic Brain Injury 10 million killed or hospitalised every year 90% in low and middle income countries Mostly
Endocrine secretion cells secrete substances into the extracellular fluid
 Animal Hormones Concept 30.1 Hormones Are Chemical Messengers Endocrine secretion cells secrete substances into the extracellular fluid Exocrine secretion cells secrete substances into a duct or a body
Animal Hormones Concept 30.1 Hormones Are Chemical Messengers Endocrine secretion cells secrete substances into the extracellular fluid Exocrine secretion cells secrete substances into a duct or a body
Hypothalamic pituitary insufficiency following infectious diseases of the central nervous system
 European Journal of Endocrinology (2008) 158 3 9 ISSN 0804-4643 CLINICAL STUDY Hypothalamic pituitary insufficiency following infectious diseases of the central nervous system S Schaefer, N Boegershausen,
European Journal of Endocrinology (2008) 158 3 9 ISSN 0804-4643 CLINICAL STUDY Hypothalamic pituitary insufficiency following infectious diseases of the central nervous system S Schaefer, N Boegershausen,
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/33195 holds various files of this Leiden University dissertation. Author: Appelman-Dijkstra, Natasha Mireille Title: Long-term consequences of growth hormone
Cover Page The handle http://hdl.handle.net/1887/33195 holds various files of this Leiden University dissertation. Author: Appelman-Dijkstra, Natasha Mireille Title: Long-term consequences of growth hormone
Interrelation between Neuroendocrine Disturbances and Medical Complications Encountered during Rehabilitation after TBI
 J. Clin. Med. 2015, 4, 1815-1840; doi:10.3390/jcm4091815 Review OPEN ACCESS Journal of Clinical Medicine ISSN 2077-0383 www.mdpi.com/journal/jcm Interrelation between Neuroendocrine Disturbances and Medical
J. Clin. Med. 2015, 4, 1815-1840; doi:10.3390/jcm4091815 Review OPEN ACCESS Journal of Clinical Medicine ISSN 2077-0383 www.mdpi.com/journal/jcm Interrelation between Neuroendocrine Disturbances and Medical
BIOLOGY - CLUTCH CH.45 - ENDOCRINE SYSTEM.
 !! www.clutchprep.com Chemical signals allow cells to communicate with each other Pheromones chemical signals released to the environment to communicate with other organisms Autocrine signaling self-signaling,
!! www.clutchprep.com Chemical signals allow cells to communicate with each other Pheromones chemical signals released to the environment to communicate with other organisms Autocrine signaling self-signaling,
Pathology of pituitary gland. By: Shifaa Qa qa
 Pathology of pituitary gland By: Shifaa Qa qa Sella turcica Adenohypophysis (80%): - epithelial cells - acidophil, basophil, chromophobe - Somatotrophs, Mammosomatotrophs, Corticotrophs, Thyrotrophs, Gonadotrophs
Pathology of pituitary gland By: Shifaa Qa qa Sella turcica Adenohypophysis (80%): - epithelial cells - acidophil, basophil, chromophobe - Somatotrophs, Mammosomatotrophs, Corticotrophs, Thyrotrophs, Gonadotrophs
ROLE OF HORMONAL ASSAY IN DIAGNOSING PCOD DR GAANA SREENIVAS (JSS,MYSURU)
 ROLE OF HORMONAL ASSAY IN DIAGNOSING PCOD DR GAANA SREENIVAS (JSS,MYSURU) In 1935, Stein and Leventhal described 7 women with bilateral enlarged PCO, amenorrhea or irregular menses, infertility and masculinizing
ROLE OF HORMONAL ASSAY IN DIAGNOSING PCOD DR GAANA SREENIVAS (JSS,MYSURU) In 1935, Stein and Leventhal described 7 women with bilateral enlarged PCO, amenorrhea or irregular menses, infertility and masculinizing
Impaired Pituitary Axes Following Traumatic Brain Injury
 J. Clin. Med. 2015, 4, 1463-1479; doi:10.3390/jcm4071463 Review OPEN ACCESS Journal of Clinical Medicine ISSN 2077-0383 www.mdpi.com/journal/jcm Impaired Pituitary Axes Following Traumatic Brain Injury
J. Clin. Med. 2015, 4, 1463-1479; doi:10.3390/jcm4071463 Review OPEN ACCESS Journal of Clinical Medicine ISSN 2077-0383 www.mdpi.com/journal/jcm Impaired Pituitary Axes Following Traumatic Brain Injury
The Endocrine System
 The Endocrine System What is the system? 1. Made up of glands that produce and secrete hormones (chemical messengers) 2. Regulation of growth, metabolism, sexual development 3. Responses to stress and
The Endocrine System What is the system? 1. Made up of glands that produce and secrete hormones (chemical messengers) 2. Regulation of growth, metabolism, sexual development 3. Responses to stress and
I. Endocrine System & Hormones Figure 1: Human Endocrine System
 I. Endocrine System & Hormones Figure 1: Human Endocrine System Endocrine System: a) Endocrine glands are ductless since they lack specific vessels for the transport of hormones throughout the body. Instead,
I. Endocrine System & Hormones Figure 1: Human Endocrine System Endocrine System: a) Endocrine glands are ductless since they lack specific vessels for the transport of hormones throughout the body. Instead,
Additional Case Study: Glands and Hormones
 Student Worksheet Additional Case Study: Glands and Hormones LSM 8.5-2 This activity can be done individually or in pairs. Prepare the pieces ahead of time. Materials For each student (or pair): one copy
Student Worksheet Additional Case Study: Glands and Hormones LSM 8.5-2 This activity can be done individually or in pairs. Prepare the pieces ahead of time. Materials For each student (or pair): one copy
BIOM2010 (till mid sem) Endocrinology. e.g. anterior pituitary gland, thyroid, adrenal. Pineal Heart GI Female
 BIOM2010 (till mid sem) Endocrinology Endocrine system Endocrine gland : a that acts by directly into the which then to other parts of the body to act on (cells, tissues, organs) : found at e.g. anterior
BIOM2010 (till mid sem) Endocrinology Endocrine system Endocrine gland : a that acts by directly into the which then to other parts of the body to act on (cells, tissues, organs) : found at e.g. anterior
Non-Functioning Tumours and Pituitary Hormone Testing. Miguel Debono Consultant in Endocrinology
 Non-Functioning Tumours and Pituitary Hormone Testing Miguel Debono Consultant in Endocrinology Agenda Pituitary masses Non functioning pituitary adenomas Testing pituitary function Pituitary Hormone Replacement
Non-Functioning Tumours and Pituitary Hormone Testing Miguel Debono Consultant in Endocrinology Agenda Pituitary masses Non functioning pituitary adenomas Testing pituitary function Pituitary Hormone Replacement
BIOCHEMICAL TESTS FOR THE INVESTIGATION OF COMMON ENDOCRINE PROBLEMS IN THE MALE
 Authoriser: Moya O Doherty Page 1 of 7 BIOCHEMICAL TESTS FOR THE INVESTIGATION OF COMMON ENDOCRINE PROBLEMS IN THE MALE The purpose of this protocol is to describe common tests used for the investigation
Authoriser: Moya O Doherty Page 1 of 7 BIOCHEMICAL TESTS FOR THE INVESTIGATION OF COMMON ENDOCRINE PROBLEMS IN THE MALE The purpose of this protocol is to describe common tests used for the investigation
Autoimmune hypophysitis may eventually become empty sella
 Neuroendocrinology Letters Volume 34 No. 2 2013 Autoimmune hypophysitis may eventually become empty sella Hua Gao*, You-you Gu*, Ming-cai Qiu Department of Endocrinology, Tianjin Medical University General
Neuroendocrinology Letters Volume 34 No. 2 2013 Autoimmune hypophysitis may eventually become empty sella Hua Gao*, You-you Gu*, Ming-cai Qiu Department of Endocrinology, Tianjin Medical University General
What we will cover. Evaluation of the Child with Suspected Pituitary Disease. ituitary
 Evaluation of the Child with Suspected Pituitary Disease Craig Alter, MD University of Pennsylvania Children s Hospital of Philadelphia What we will cover * What laboratory tests to order * MRI: common
Evaluation of the Child with Suspected Pituitary Disease Craig Alter, MD University of Pennsylvania Children s Hospital of Philadelphia What we will cover * What laboratory tests to order * MRI: common
THE ANTERIOR PITUITARY. Embryology cont. Embryology of the pituitary BY MISPA ZUH HS09A179. Embryology cont. THE PITUIYARY GLAND Anatomy:
 THE ANTERIOR PITUITARY BY MISPA ZUH HS09A179 Embryology of the pituitary The pituitary is formed early in embryonic life from the fusion of the Rathke s pouch (anterior) and the diencephalon ( posterior)
THE ANTERIOR PITUITARY BY MISPA ZUH HS09A179 Embryology of the pituitary The pituitary is formed early in embryonic life from the fusion of the Rathke s pouch (anterior) and the diencephalon ( posterior)
