Occurrence of Pituitary Dysfunction following Traumatic Brain Injury
|
|
|
- Eustace Lamb
- 6 years ago
- Views:
Transcription
1 JOURNAL OF NEUROTRAUMA Volume 21, Number 6, 2004 Mary Ann Liebert, Inc. Pp Occurrence of Pituitary Dysfunction following Traumatic Brain Injury MARTA BONDANELLI, 1 LAURA DE MARINIS, 2 MARIA ROSARIA AMBROSIO, 1 MARCELLO MONESI, 1 DOMENICO VALLE, 1 MARIA CHIARA ZATELLI, 2 ALESSANDRA FUSCO, 2 ANTONIO BIANCHI, 2 MARCO FARNETI, 4 and ETTORE C. DEGLI UBERTI 1 ABSTRACT Traumatic brain injury (TBI) may be associated with impairment of pituitary hormone secretion, which may contribute to long-term physical, cognitive, and psychological disability. We studied the occurrence and risk factors of pituitary dysfunction, including growth hormone deficiency (GHD) in 50 patients (mean age years; 40 males, age years; 10 females, age years) with TBI over 5 years. Cranial or facial fractures were documented in 12 patients, and neurosurgery was performed in 14. According to the Glasgow Coma Scale (GCS), 16 patients had suffered from mild, seven moderate, and 27 severe TBI. Glasgow Outcome Scale (GOS) indicated severe disability in five, moderate disability in 11, and good recovery in 34 cases. Basal pituitary hormone evaluation, performed once at times variable from 12 to 64 months after TBI, showed hypogonadotrophic hypogonadism in seven (14%), central hypothyroidism in five (10%), low prolactin (PRL) levels in four (8%), and high PRL levels in four (8%) cases. All subjects had normal corticotrophic and posterior pituitary function. Seven patients showed low insulin-like growth factor I (IGF-I) levels for age and sex. Results of GHRH plus arginine testing indicated partial GHD in 10 (20%) and severe GHD in four (8%) cases. Patients with GHD were older (p 0.05) than patients with normal GH secretion. Magnetic resonance imaging demonstrated pituitary abnormalities in two patients; altogether pituitary dysfunction was observed in 27 (54%) patients. Six patients (12%) showed a combination of multiple abnormalities. Occurrence of pituitary dysfunction was 37.5%, 57.1%, and 59.3% in the patients with mild, moderate, and severe TBI, respectively. GCS scores were significantly (p 0.02) lower in patients with pituitary dysfunction compared to those with normal pituitary function ( vs ). No relationship was detected between pituitary dysfunction and years since TBI, type of injury, and outcome from TBI. In conclusion, subjects with a history of TBI frequently develop pituitary dysfunction, especially GHD. Therefore, evaluation of pituitary hormone secretion, including GH, should be included in the long-term follow-up of all TBI patients so that adequate hormone replacement therapy may be administered. Key words: growth hormone deficiency; head trauma; pituitary function 1 Department of Biomedical Sciences and Advanced Therapies Section of Endocrinology, University of Ferrara, Ferrara, Italy. 2 Institute of Endocrinology and 3 Internal Medicine, Catholic University, Rome, Italy. 4 Division of Neurosurgery, St. Anna Hospital, Ferrara, Italy. 685
2 BONDANELLI ET AL. INTRODUCTION TRAUMATIC BRAIN INJURY (TBI) is one of the main causes of death and disability in young adults, with consequences ranging from physical disabilities to longterm cognitive, behavioral, psychological, and social defects (Salazar, 2000). Clinical evidence has demonstrated that TBI may cause impairment of hypothalamic-hypophyseal function, which may contribute to a delayed or hampered recovery in many of the head-injured patients (Bondanelli et al., 2002; Cernak et al., 1999; Della Corte et al., 1998; Edwards and Clark, 1986; Woolf et al., 1992). Hypopituitarism may rapidly develop after TBI, with a sudden onset of overt symptoms of cortisol, thyroid hormone, and/or gonadal steroid deficiencies (Clark et al., 1988; De Marinis et al., 1999; Edwards and Clark, 1986; Hackl et al., 1991). However, alterations in pituitary hormone secretion can develop subtly, escaping detection for months or years (Benvenga et al., 2000). Therefore, longterm follow-up is necessary to reveal the development of all pituitary hormone deficiencies. To date, few systematic studies are available in order to define the occurrence of long-term pituitary dysfunctions in head-injured patients. A recent review indicated that hypopituitarism occurs in about 60% of head-injured patients and may became clinically evident at any time after trauma with a lag time of diagnosis ranging from a few months to 40 years (Benvenga et al., 2000). In the series reported by Kelly et al. (2000), hypopituitarism occurred in 40% of 22 TBI patients studied from 3 months to 23 years after moderate or severe head trauma. Lieberman et al. (2001) reported pituitary abnormalities in 69% of 70 head-injured patients examined from 1 month to 23 years after trauma. Injury severity and secondary cerebral damage have been suggested to be risk factors for the development of hypopituitarism (Benvenga et al., 2000; Hackl et al., 1991; Kelly et al., 2000). However, currently available data are not sufficient to identify predictive and/or risk factors for hypopituitarism following head trauma. Dysfunctions of the growth hormone (GH) and gonadotrophic axes appear to be the most common deficiencies in patients with TBI. These pituitary cells are particularly vulnerable to a variety of insults, including trauma (Benvenga et al., 2000; Edwards and Clark, 1986). In the last years, the syndrome of growth hormone deficiency (GHD) in adults has been clearly defined. It is characterized by significant alterations in body composition, decreased muscular strength, exercise capacity, and bone mineral content, and impairment in the patient s sense of well-being and quality of life (Gilchrist et al., 2002; Simpson et al., 2002). Moreover, growing evidence indicates that GH plays an important role in the recovery of the central nervous system from experimental brain injury (Scheepens et al., 2000, 2001). Thus, it is possible that undiagnosed GHD may contribute to the physical, psychological, and cognitive disabilities following TBI. Therefore, the purpose of the present study was to evaluate the occurrence of long-term pituitary dysfunction, including GHD, in a cohort of adult patients admitted to the Neurosurgery Sections of the Hospital of Ferrara and of the Gemelli Hospital of Rome over 5 years ( ) after a closed or penetrating head injury. In order to assess the occurrence of specific risk factors for posttraumatic hypopituitarism, the relationships among pituitary function, the overall severity and outcome of TBI, and the time since TBI were evaluated. MATERIALS AND METHODS Subjects Eligible patients included adult patients who had been admitted to the Neurosurgery Sections of the Hospital of Ferrara or of the Gemelli Hospital of Rome over 5 years ( ) for a closed or penetrating TBI, and survived. One hundred and twenty head-injured patients (or their family representatives) were asked to participate in the study, but only 76 accepted voluntarily. Among these 76 patients, 50 (40 males, 10 females) underwent all study procedures defined in the protocol previously approved by the local Ethical Committees. Informed consent was obtained from subjects or next of kin. Criteria for patient exclusion were as follows: age of 18 years; history of preexisting metabolic, endocrine, neurological, cardiac or pulmonary diseases; liver or renal failure, or infectious diseases; alcohol and drug misuse; treatment with barbiturates, or medications that could affect GH secretion (except for the treatment administered during the acute phase after the injury). Moreover, subjects receiving parenteral nutrition and/or mechanical ventilation and/or requiring corticosteroid treatment during the previous 2 months were not included. The age of recruited patients ranged from 20 to 87 years (mean years, median 30 years), and the body mass index (BMI) ranged from 20.0 to 33.9 kg/m 2 (mean kg/m 2, median 24). Patients were studied once at variable times (12 64 months after TBI) over the 5-year period. The severity of injury was assessed by the post resuscitation Glasgow Coma Scale (GCS) score (severe head injury, GSC score of 8 or less; moderate head injury, GSC score 9 12; mild head injury, GSC score 13 15) (Teasdale and Jennett, 1974). 686
3 PITUITARY DYSFUNCTION AFTER HEAD TRAUMA The type of head injury was characterized by computerized tomography (CT) scan according to Marshall s classification (Marshall et al., 1992): diffuse injury I (no visible damage); diffuse injury II (cisterns are present with midline shift of 0 5 mm and/or no large lesion of 25 cc); diffuse injury III (diffuse brain swelling, cisterns compressed with midline shift 0 5 mm, no large lesion of 25 cc); diffuse injury IV (midline shift of 5 mm, no large lesion of 25 cc); evacuated mass lesion (EM, any lesion surgically evacuated); non-evacuated mass lesion of 25 cc. Long-term outcome was defined using the Glasgow Outcome Scale (GOS) score (1 death; 2 persistent vegetative state; 3 severe disability; 4 moderate disability; 5 good recovery) at 12 months after TBI (Jennett and Bond, 1975). Experimental Procedures In all subjects, after an overnight fast, baseline venous blood samples were drawn, at 0800 h, for determinations of insulin-like growth factor I (IGF-I), thyroid stimulating hormone (TSH), free-thyroxine (FT4), adrenocorticotrophic hormone (ACTH), cortisol, luteinizing hormone (LH), follicle-stimulating hormone (FSH), and testosterone (T) or estradiol (E 2 ) plasma levels. Three baseline blood samples were drawn at 15-min intervals for prolactin (PRL) determination. Posterior pituitary function was assessed by measurement of serum sodium, creatinine, and osmolality, as well as urine osmolality and specific gravity. GHD was assessed by GH-releasing hormone (GHRH) plus arginine (ARG) testing. On a different day, an indwelling intravenous (iv) cannula was inserted in both forearms at 0730 h after an overnight fast (10 12 h) and kept open with a slow infusion of 0.9% saline for separate blood sampling and drug administration. An equilibration period of 1 h was allowed before baseline blood samples were obtained. GHRH (Geref, Serono, Milan, Italy) was administered (1 g/kg bolus) at time 0, followed by L-arginine hydrochloride (30 g in 60 ml of saline) infused over a 30-min period, from time 0 to 30 min of the study. Blood samples were collected at 30, 0, 15, 30, 45, 60, 90, and 120 min for GH measurements. A GH response peak higher than 16.5 g/l was considered normal, less than 9.0 g/l was considered diagnostic for severe GHD, and between 16.5 and 9.0 g/l indicative of partial GHD, as previously defined by Aimaretti et al. (1998). Premenopausal (n 5) women were studied in the follicular phase of the menstrual cycle. Analytical Proce1dures Blood samples were drawn into pre-cooled glass tubes containing 1 mg/ml ethylene-diamine tetraacetic acid disodium salt (EDTA-2Na), for hormone determinations. They were promptly centrifuged at 3000 g for 15 min at 4 C, and then the plasma was frozen at 80 C until analysis. All samples for each hormone were processed in duplicate in the same assay. GH was measured by immunoradiometric assay (IRMA) with reagents supplied by Nichols Institute Diagnostics (San Juan Capistrano, CA). The limit of detection was 0.02 g/l, with intra- and interassay variation coefficients respectively of 4.2% and 7.2%, at concentration of 1.4 g/l, and of 2.8% and 4.6%, at concentration of 12.2 g/l. Plasma IGF-I was determined by radioimmunoassay (RIA) using a commercially available kit (Medgenix Diagnostic S.A, Fleurus, Belgium), after acid-ethanol extraction from EDTA plasma. The sensitivity of the method was 0.1 g/l. The intra- and interassay coefficients of variation were 9.6% and 6.1%, respectively, in the concentration range of g/l. ACTH was determined by IRMA (Nichols Institute Diagnostics). Cortisol, E 2 and T were determined by RIA (Diagnostic Products Corp., Los Angeles, CA). LH and FSH were measured with a two-site chemiluminometric immunoassay (ACS; Ciba Corning Diagnostic Corp., Medfield, MA). PRL, TSH, and FT4 were measured using an automated chemiluminescence system (ACS Centaur; Chiron Diagnostics Corp., East Walpole, MA). The intra- and interassay coefficients of variation for all methods were less than 5.8% and 7.8%, respectively. The age-specific normal ranges for IGF-I were g/l (20 30 years), g/l (31 40 years), g/l (41 50 years), g/l (51 60 years); and g/l (60 years). The normal ranges for the other assays were as follows: ACTH, pmol/l; cortisol, mol/l (8 10 AM); TSH, miu/l; FT4, pmol/l; PRL, 4 24 g/l in women and 2 16 g/l in men; E 2, pmol/l (follicular phase) and 180 pmol/l (menopausal women); T, nmol/l; LH, U/L (follicular phase) and U/L (menopausal women); LH, 1 10 U/L in men; FSH, U/L (follicular phase) and U/L (menopausal women); FSH, 1 7 U/L in men. Serum sodium and osmolality, urinary osmolality, and specific gravity were determined by standard methods. Normal range values were as follows: serum sodium mmol/l, serum osmolality mosm/kg, urine osmolality mosm/kg, and specific gravity greater than All patients underwent magnetic resonance imaging (MRI) of the hypothalamic-pituitary region (0.5 T and 1 T scanners, T1-weighted sequence, and 3-mm slices in sagittal and coronal sections), before and after after intravenous injection of gadolinium chelate. 687
4 BONDANELLI ET AL. Statistical Analysis All results are expressed as the mean SEM. PRL levels were obtained from the mean (SEM) of the three determinations. Baseline levels of GH were obtained from the mean (SEM) of the two values determined at times 30 and 0 min of the test. GH plasma concentrations were expressed both as absolute values (g/l) and as areas under the curves from 0 to 120 min (AUC min, g/l min) calculated by trapezoidal method, after GHRH plus ARG administration. Comparison between groups of continuous variables was assessed by using Student s t test or one-way ANOVA and the post-hoc analysis of Student-Newman-Keuls for multiple variables. Percentage comparison was made with Fisher s exact test. Correlations between hormonal values and clinical measures of trauma severity and outcome, or years from TBI or characteristics of patients were performed by linear regression analysis. Values were considered statistically significant when p was RESULTS Clinical Characteristics of Patients Sixteen patients had mild (GCS 13 15), seven moderate (GCS 9 12), and 27 severe (GCS 3 8) TBI (Fig. 1). According to Marshall s classification, nine patients had no visible damage (grade I), 20 patients had diffuse injury (grade II), and seven belonged to grade III; a mass lesion was surgically evacuated (EM) in 14 cases. Fractures of the skull and/or facial bones were observed in 12 cases. GOS indicated severe disability in five patients, moderate disability in 11 patients, and good recovery in 34 patients. When the patients were divided into five groups (Table 1), according to the time that had elapsed since trauma, the distribution of cases in each group was as follows: six patients (12%; three severe, two moderate, one mild) were evaluated 1 year but 2 years since TBI (group 1); 11 patients (22%; two severe, one moderate, eight mild) were evaluated 2 years but 3 years since TBI (group 2); four patients (8%; one severe, one moderate, two mild) were evaluated 3 years but 4 years since TBI (group 3); 18 patients (36%; 13 severe, three moderate, two mild) were evaluated 4 years but 5 years since TBI (group 4); 11 patients (22%; nine severe, one moderate, one mild) were evaluated 5 years but 6 years since TBI (group 5). The mean values of GCS and GOS as well as mean age and BMI of each group of the patients did not significantly differ among the five groups. Seven patients had suffered from temporary diabetes insipidus, which resolved spontaneously within a few days. T1 F1 GH Response to GHRH plus ARG As shown in Figure 2, GHRH plus ARG test demonstrated normal GH response in 36 (72%) patients (20 se- F2 FIG. 1. Characteristics of 50 adult patients with a history of traumatic brain injury (TBI) during the previous 5 years. GCS, Glasgow Coma Scale score: mild, 9 12 moderate, 8 severe TBI (Teasdale and Jennett, 1974); Marshall s classification of the type of head injury by initial computerized tomography scan: I, no visible pathology; II, cisterns are present with midline shift 0 5 mm and/or no large lesion of 25 cc; III, diffuse brain swelling, cisterns compressed with midline shift 0 5 mm, no large lesion of 25 cc; EM, evacuated mass lesion (Marshall et al., 1992); the presence or absence of cranial and/or facial fractures; GOS, Glasgow Outcome Scale score: 3 severe disability; 4 moderate disability; 5 good recovery (Jennett and Bond, 1975). 688
5 PITUITARY DYSFUNCTION AFTER HEAD TRAUMA TABLE 1. CLINICAL CHARACTERISTICS OF THE PATIENTS DIVIDED INTO FIVE GROUPS ACCORDING TO THE TIME ELAPSED SINCE HEAD TRAUMA Sex Marshall Years from Age BMI GCS GOS trauma (years) (kg/m 2 ) M F (mean SEM) (mean SEM) I II III EM Total Group 1, 1 year but 2 years since TBI; 2 years but 3 years since TBI; 3 years but 4 years since TBI; 4 years but 5 years since TBI; 5 years but 6 years since TBI. Age, age at time of head injury. Values are expressed as the mean SEM. vere, four moderate, and 12 mild TBI) with the mean (SEM) peak value of g/l. Ten (20%) subjects (five severe, two moderate, and three mild TBI) showed a GH response indicative of partial GHD, with a mean peak value of g/l, and four (8%) patients (two severe, one moderate, and one mild TBI) had severe GHD, with a mean peak value of g/l. No significant differences were observed in GH responses to GHRH plus ARG among patients with severe (peak g/l, AUC g/l min), moderate (peak g/l, AUC g/l min) and mild (peak g/l, AUC g/l min) TBI. No significant differences were observed among the five groups of patients divided according to the time that had elapsed since trauma, either in the GH peak values or in the AUCs after GHRH plus ARG. No differences in GH response to GHRH plus ARG were detected among patients with different GOS scores. The mean (SEM) BMI was not significantly different between patients with normal GH secretion ( kg/m 2 ) and those with GHD ( kg/m 2 ). The mean (SEM) age was significantly (p 0.05) higher in patients with partial or severe GHD ( years) as compared to the group showing normal GH secretion ( years). All subjects showed spontaneously normal levels of serum sodium and osmolality, as well as of urinary osmolality and specific gravity. As indicated in Table 2, seven (14%) of 50 patients had low blood T concentrations associated with low or normal plasma LH and FSH concentrations when compared to normal range. Five (10%) patients had low blood FT4 concentrations with low or normal TSH concentrations, indicating the presence of central hypothyroidism. Plasma PRL concentrations were slightly elevated in four patients (8%; three males) and low in four patients (8%; three males). Seven (14%) of 50 patients showed low IGF-I concentrations when compared to age- and sex-matched normal ranges. All patients had plasma ACTH and cortisol levels within the normal range. MRI revealed the presence of morphological abnormalities in two TBI patients (empty sella and slight pituitary stalk dislocation). T2 Basal Hormone Values and MRI FIG. 2. GH peak concentration after GH-releasing hormone plus arginine administration in 50 patients with a history of TBI divided according to GCS score. A GH response higher than 16.5 g/l was considered normal, 9.0 g/l was considered diagnostic for severe GH deficiency (GHD), and between 16.5 and 9.0 g/l indicative of partial GHD (Aimaretti et al., 1998). GCS score: mild; 9 12 moderate; 8 severe TBI. 689
6 BONDANELLI ET AL. Relationship between Pituitary Dysfunction and Time, Outcome, or Severity of Trauma No significant correlations were found between either IGF-I levels or GH responses to GHRH plus ARG (GH peak and AUC) and clinical scores of trauma severity (GCS). Similarly, no significant correlations were present between the indices of GH axis function and GOS scores. The number of years since TBI was significantly correlated (r 0.389, p 0.005) with serum IGF-I levels but not with either GH peak or AUC after GHRH plus ARG administration. As expected, the age of patients negatively correlated with both IGF-I levels (r 0.313, p 0.05) and GH responses to GHRH plus ARG (peak, r 0.411, p 0001; AUC, r 0.387, p 0.005). Altogether pituitary dysfunction was observed in 27 (54%) patients. Among these 27 patients, partial or severe GHD was detected in 51.8%, hypogonadism in 25.9%, hypothyroidism in 18.5%, hyperprolactinemia in 14.8%, and hypoprolactinemia in 14.8% of the patients. Six patients showed a combination of multiple hormone abnormalities. Two patients had partial GHD and low PRL. One patient had LH, FSH, and TSH deficiencies. One patient had LH, FSH, and TSH deficiencies and low PRL. One patient had low FT4 with inappropriately normal TSH and high PRL. One patient had low T with inappropriately normal LH and FSH and high PRL. Only two out of 27 (7.4%) patients with pituitary dysfunction showed anatomic pituitary abnormalities on MRI scans (Table 2). As indicated in Table 3, the mean age ( years) and BMI ( kg/m 2 ) of the patients with pituitary dysfunction did not significantly differ from that observed in patients with normal pituitary hormone se- T3 TABLE 2. SUMMARY OF THE CLINICAL, HORMONAL, AND PITUITARY IMAGING DATA FOR THE 27 PATIENTS WITH DOCUMENTED ABNORMALITIES OF PITUITARY HORMONE SECRETION Years Cranial/ Basal hormone values GH response Age, from facial to MRI sex trauma GCS Marshall fractures GOS PRL LH FSH TSH T FT4 IGF-I GHRHARG abnormalities 58, f 5 8 EM No 5 pghd 65, m 5 11 EM No 5 pghd 57, m 5 7 EM No 5 pghd 44, m No 5 Normal 31, m No 5 pghd 30, m No 4 GHD 30, m No 4 Normal 37, f Yes 5 Normal 38, f 4 9 EM No 5 pghd 64, m Yes 5 Normal 37, m 4 8 EM No 4 pghd 32, m 4 6 EM Yes 5 Normal 28, m No 3 Normal 25, m No 3 Normal 24, m No 4 pghd 23, m No 5 pghd 61, m No 5 pghd 67, f Yes 5 pghd Stalk dislocation 54, f No 5 pghd 23, f No 5 pghd 28, m Yes 5 Normal 23, m No 4 Normal 21, m No 3 Normal 44, m Yes 5 Normal Empty sella 68, m No 5 GHD 26, m No 5 Normal 24, m 1 7 EM No 5 Normal Age, age at time of head injury; GDH, severe growth hormone deficiency; pghd, partial GHD;, decreased;, increased;, normal range. For other definitions, see Fig. 1 legend. 690
7 PITUITARY DYSFUNCTION AFTER HEAD TRAUMA TABLE 3. COMPARISON BETWEEN THE PATIENTS WITH NORMAL AND ABNORMAL PITUITARY FUNCTION Normal Hypopituitarism (n 23) (n 27) Males (%) Females (%) Age, years a BMI, kg/m a Yrs from trauma a GCS score a Cranial/facial fractures (%) GOS a a p Age, age at time of head injury; BMI, body mass index; GCS, Glasgow Coma Scale score; GOS, Glasgow Outcome Scale. Unless otherwise indicated, values are expressed as the mean SEM. of 16 (37.5%) patients with mild, in four of seven (57.1%) patients with moderate, and in 16 of 27 (59.3%) patients with severe TBI (Fig. 4). Occurrence of pituitary dysfunction did not vary among patients with different types of head injury according to Marshall s classification (55.5% grade I, 50.0% grade II, 57.1% grade III, and 50.0% grade EM) (Fig. 5). Occurrence of pituitary dysfunction did not differ significantly in patients with cranial and/or facial fractures (55.3%) compared to patients without fractures (50%) (Fig. 6). Moreover, occurrence of pituitary dysfunction was similar among patients with different GOS scores (Fig. 7). DISCUSSION F4 F5 F6 F7 F3 cretion ( years and kg/m 2, respectively). Moreover, the time that had elapsed since TBI did not differ significantly between patients with ( years) or without pituitary dysfunction ( years). Considering severity of TBI, GCS scores were significantly (p 0.02) lower in patients with pituitary dysfunction ( ) compared to patients with normal pituitary function ( ). There were no significant differences in GOS values, between patients with ( ) or without ( ) pituitary dysfunction. When the patients were divided according to years since TBI, pituitary dysfunction was detected in four of six (66.7%) patients of the group 1, six of 11 (54.5%) of the group 2, two of four (50%) of the group 3, eight of 18 (44.4%) of the group 4, and seven of 11 (63.6%) of the group 5 (Fig. 3). Moreover, pituitary dysfunction was observed in six In the present study, pituitary dysfunction has been documented in a substantial proportion (54%) of the patients with a history of TBI during the last 5 years. Impaired GH secretion was the most common abnormality, being present in 28% of patients. The occurrence of pituitary dysfunction was 59% in the patients with severe TBI (according to GCS) and 37.5% in those with mild injury, suggesting that clinical severity of trauma (GCS) may be a risk factor for developing posttraumatic hypopituitarism. This is supported by the observation that GCS scores were significantly lower in patients with pituitary dysfunction compared to patients with normal pituitary function. In contrast, the type of injury (Marshall s classification and cranial fractures) and outcome from trauma did not predict of developing pituitary dysfunction. Only a minority (two out of 27, or 7.4%) of the patients with pituitary dysfunction revealed morphological alterations of the pituitary gland. FIG. 3. Occurrence of pituitary dysfunction in relationship to the time elapsed since traumatic brain injury. GHD, partial or severe GHD (for definitions, see Fig. 2 legend). patients with isolated GHD; patients with GHD associated with other pituitary dysfunction; patients with pituitary dysfunction other than GHD. 691
8 BONDANELLI ET AL. FIG. 4. Occurrence of pituitary dysfunction in relationship to severity of head trauma according to Glasgow Coma Scale (GCS) score (for definitions, see Fig. 1 legend). GHD, partial or severe GHD (for definitions, see Fig. 2 legend). patients with isolated GHD; patients with GHD associated with other pituitary dysfunction; patients with pituitary dysfunction other than GHD. The relationship between head injury and subsequent pituitary failure was first documented in 1918 (Cyran, 1918). Since 1970, several cases of pituitary dysfunction have been described in the literature, but they are mostly related to case reports and/or to data obtained from patients evaluated early after injury (Cernak et al., 1999; Della Corte et al., 1998; Clark et al., 1988; De Marinis et al., 1999; Edwards and Clark, 1986; Hackl et al., 1991; Woolf et al., 1992). However, the incidence of pituitary dysfunction following head trauma has only been reported in three previous series (Benvenga et al, 2000; Kelly et al., 2000; Lieberman et al., 2001). The present study confirms data from these three reports, indicating the presence of pituitary dysfunction in 40 69% of patients with a history of TBI (Benvenga et al., 2000; Kelly et al., 2000; Lieberman et al., 2001). The present data cannot define the precise time course of development of posttraumatic pituitary dysfunction, but they confirm the need to evaluate pituitary hormone secretion in all patients with a TBI beyond the early period after injury. In fact, although no statistically significant relationship was found between the occurrence of hypopituitarism and the time elapsed since TBI, more than 50% of the patients with a history of TBI developed pituitary dysfunction within 4 or 5 years. Accordingly, it has previously been shown that hypopituitarism may occur at any time after head trauma, even if it is more frequently (70%) diagnosed within the first year (Benvenga et al., 2000). This supports the view that signs and symptoms of hypopituitarism may frequently be unrecognized, unless careful long-term follow-up of pituitary function is performed in all patients with a history of TBI. The present data show an association between the presence of a low GCS score and endocrine abnormalities, suggesting that severity of TBI may be an important risk factor for developing posttraumatic pituitary dysfunction. Moreover, five out of six patients with multiple pituitary hormone abnormalities had severe TBI (GCS 3 8), indi- FIG. 5. Occurrence of pituitary dysfunction in relationship to the type of head injury on the initial computerized tomography (CT) scan, according to Marshall s classification (for definitions, see Fig. 1 legend; Marshall et al., 1992). GHD, partial or severe GHD (for definitions, see Fig. 2 legend). patients with isolated GHD; patients with GHD associated with other pituitary dysfunction; patients with pituitary dysfunction other than GHD. 692
9 PITUITARY DYSFUNCTION AFTER HEAD TRAUMA FIG. 6. Occurrence of pituitary dysfunction and presence of cranial and/or facial fractures. GHD, partial or severe GHD (for definitions, see Fig. 2 legend). patients with isolated GHD; patients with GHD associated with other pituitary dysfunction; patients with pituitary dysfunction other than GHD. cating a relationship between severity of injury and degree of hypopitutarism. In contrast, Marshall s classification of the type of head injury, proposed for outcome prediction (Marshall et al., 1992; Raabe et al. 1999), was not predictive of the development of pituitary dysfunction in our patients. Moreover, the outcome from head trauma, defined by the GOS, did not differ between patients with normal and impaired pituitary hormone secretion. Greater injury severity and associated cerebral insult have previously been suggested as risk factors for hypopituitarism. Kelly et al. (2000) demonstrated that diffuse swelling on initial CT scans and evidence of a hypotensive and/or hypoxic insult occurred more frequently in patients who developed hypopituitarism after TBI compared to patients who continued to have normal pituitary function. Other authors reported that occurrence of coma or unconsciousness following head trauma was followed by hypopituitarism in 93% of patients (Benvenga et al., 2000). These data suggest that the clinical severity of initial TBI may predict development of posttraumatic hypopituitarism, but further studies are necessary to clarify if the type of injury may influence longterm hypothalamic-pituitary function. In our study, the occurrence of skull and/or facial bone fractures was not predictive of subsequent post-traumatic hypopituitarism. Various reports have identified sellar fractures in association with posttraumatic hypopituitarism (Bistritzer et al., 1981; Daniel et al. 1959), but none of our patients had this type of fracture. In Crompton s study, the presence of anatomical lesions in the hypothalamus was associated with temporal-parietal blows and fractures of the skull base (Crompton, 1971). Although the majority of our patients with pituitary dysfunction had a history of severe TBI, the occurrence of anatomical lesion demonstrated by MRI was low (7.4%), as was the case in the study by Cytowic et al. (1986). These findings are in agreement with the view FIG. 7. Occurrence of pituitary dysfunction in relationship to outcome from head trauma according to the Glasgow Outcome Scale (GOS) (for definitions, see Fig. 1 legend). GHD, partial or severe GHD (for definition, see Fig. 2 legend). patients with isolated GHD; patients with GHD associated with other pituitary dysfunction; patients with pituitary dysfunction other than GHD; GOS: 3 severe disability; 4 moderate disability; 5 good recovery. 693
10 BONDANELLI ET AL. that posttraumatic hypopituitarism could be due to a hypoxic insult that leads to functional damage at the level of the hypothalamus or pituitary. Benvenga et al. (2000) reported that 93% of 89 patients with posttraumatic hypopituitarism presented with radiological abnormalities of the hypothalamus and/or pituitary region (mainly vascular insults assessed by CT or MRI). Gender or BMI of the patients did not influence development of pituitary dysfunction, however a negative correlation was present between age and GH axis function. The most frequent alteration in endocrine function detected in our study was partial or severe GHD, documented in 28% of all patients and in 52% of those affected by any pituitary abnormalities. GHD was diagnosed by combined administration of GHRH plus ARG, a potent provocative test for GH secretion (Ghigo et al., 1990; Valletto et al., 1996). This test has been shown to have a very high specificity and sensitivity for diagnosis of GHD, with less inter- and intra-individual variability than other stimulation tests. The ARG-GHRH test has been proposed to be the best diagnostic alternative to the ITT, especially for patients with contraindications for insulin-induced hypoglycemia (Aimaretti et al., 1998; Biller et al., 2002). Therefore, the ARG-GHRH test may be a useful test for evaluation of patients with TBI. However, it is possible that patients with an injury limited to the hypothalamus may have a normal response to ARG- GHRH but not to the ITT. A recent study conducted in the United States proposed lower peak GH criteria for the ARG-GHRH test, due to the higher BMI of the U.S. patients (Biller et al., 2002). However, the patients in the present study had a normal mean BMI, which supports our choice of the criteria proposed by Aimaretti et al. (1998). Eight patients with partial or complete GHD presented basal serum IGF-I concentrations within the normal range, in agreement with previous reports (Biller et al., 2002). One of the seven patients with low IGF-I had a normal GH response to GHRH plus ARG administration, indicating that low level of serum IGF-I cannot be assumed as a parameter for the definition of GHD in adult patients with a history of TBI. We found that some patients with both partial (five out of 10) and severe (two out of four) GHD were of middle or advanced age. It is well known that GH-IGF-I axis function declines with normal ageing. A 15% reduction in the 24-h GH concentrations and a 6% decrease in GH half-life for each decade have been shown after puberty (Giustina and Veldhuis, 1998; Zadik et al., 1985). Thus, the daily GH secretory rate declines from a peak of about 150 g/kg during puberty to about 25 g/kg by age 55 years. However it has been amply demonstrated that the GH response to GHRH ARG does not depend on age and that this test is able to distinguish between normal and GHD subjects with excellent reproducibility regardless of age (Ghigo et al., 1990; Valletto et al., 1996). The negative relationship between age and GH axis function suggests that aging may be a negative prognostic factor for the development of posttraumatic GHD. Perhaps the hypothalamic-pituitary region is more susceptible to injury in older individuals. Alternatively, the reduced GH secretory reserve in middle or advanced age may predispose to GHD following TBI. Although overall pituitary dysfunction was more frequent in patients with severe TBI, the occurrence of partial or severe GHD was not significantly influenced by severity of trauma. This could be due to the particular vulnerability of these pituitary cells to vascular insults, which appear to be the major cause of posttraumatic hypopituitarism (Edwards and Clark, 1986; Kelly et al., 2000). Central hypogonadism was documented in 14% of all patients and in 25.9% of those affected by any pituitary abnormalities. This occurrence is lower than that observed in some previous studies, which reported the presence of hypogonadism in almost 100% of the patients with posttraumatic hypopituitarism (Edwards and Clark, 1986; Benvenga et al., 2000). In contrast, gonadotrophin deficiency was uncommon in the study of Lieberman et al. (2001). These discrepancies might be attributable to differences among the study populations, including the number of patients with hypopituitarism included in the studies. In our study, TSH deficiency was detected in 10% of all patients and in 18.5% of patients with pituitary dysfunction. Low or high PRL levels were observed in 16% of all patients and in 25.6% of patients with pituitary dysfunction even if no stalk abnormalities were demonstrated on MRI in these patients. Finally, no alteration in ACTH or cortisol levels was detected in any patient. It is possible that undiagnosed GHD and alterations in the secretion of other pituitary hormones may negatively influence the recovery and the final outcome after TBI, contributing to a diminished quality of life, or physical and/or mental impairment (Gilchrist et al., 2002; Nyberg, 2000; Simpson et al., 2002). It is well known that GHD in adult patients causes significant abnormalities in body composition, reduced bone mineral content, reduced exercise capacity, and impairment in cognitive function and sense of well being. These alterations may be improved after GH replacement therapy (Simpson et al., 2002). In this respect, growing evidence indicates that GH plays an important role in promoting recovery after experimental brain injury (Scheepens et al., 2000, 2001). However, in the present study, no significant relationship was demon- 694
11 PITUITARY DYSFUNCTION AFTER HEAD TRAUMA strated between GH axis function and outcome following TBI. Therefore, keeping in mind the beneficial neurobehavioral and physical effects of GH replacement in GHD patients, long-term evaluation of the GH axis should be performed after TBI, in order to make an early diagnosis of GHD. At present, the international consensus is that severe GHD should be treated with GH replacement therapy (Hartman, 1998). The value of GH treatment for partial GHD remains to be established. In conclusion pituitary dysfunction was identified in a substantial proportion of patients with a TBI history. Although the type and outcome of TBI, and time since TBI did not predict the occurrence of pituitary dysfunction, a greater clinical severity of TBI was associated with a higher incidence of hypopituitarism. Partial or severe GHD was the most common pituitary hormone dysfunction, especially in middle or advanced age patients. Long-term prospective studies are necessary to establish the real incidence and the time of onset of pituitary dysfunction in patients with TBI. However, the present data confirm that an accurate evaluation of pituitary hormone secretion, including the GH axis, is required for the long-term follow-up of all patients who have suffered from TBI, in order to detect the occurrence of posttraumatic hypopituitarism, independently of clinical evidence for pituitary dysfunction, and perform adequate replacement therapy. ACKNOWLEDGMENTS This work was supported by grants from the Italian Ministry of University and Scientific and Technological Research (60% 2002; MIUR ), Fondazione Cassa di Risparmio di Ferrara, and Associazione Ferrarese dell Ipertensione Arteriosa. We are deeply indebted to Dr. Mark Hartman for his critical review of the manuscript. REFERENCES AMARETTI, G., CORNELI, G., RAZZORE, P., et al. (1998). Comparison between insulin-induced hypoglycemia and growth hormone (GH) releasing hormone arginine as provocative tests for the diagnosis of GH deficiency in adults. J. Clin. Endocrinol. Metab. 83, BENVENGA, S., CAMPENNI, A., RUGGERI, R.M., et al. (2000). Hypopituitarism secondary to head trauma. J. Clin. Endocrinol. Metab. 85, BILLER, B.M., SAMUELS, M.H., ZAGAR, A., et al. (2002). Sensitivity and specificity of six tests for the diagnosis of adult GH deficiency. J. Clin. Endocrinol. Metab. 87, BISTRITZER, T., THEODOR, R., INBAR, D., et al. (1981). Anterior hypopituitarism due to fracture of the sella turcica. Am. J. Dis. Child. 135, BONDANELLI, M., AMBROSIO, M.R., MARGUTTI, A., et al. (2002). Evidence for integrity of the growth hormone/insulin-like growth factor 1 axis in patients with severe head trauma during rehabilitation. Metabolism 51, CERNAK, I., SAVIC, V.J., LAZAROV, A., et al. (1999). Neuroendocrine responses following graded traumatic brain injury in male adults. Brain Inj. 13, CLARK, J.D.A., RAGGATT, P.R., EDWARDS, O.M. (1988). Hypothalamic hypogonadism following major head injury. Clin. Endocrinol. (Oxf). 29, CROMPTON, M.R. (1971). Hypothalamic lesions following closed head injury. Brain 94, CYRAN, E. (1918). Hypophysenschadigung durch Schadelbasisfraktur. Dtsch. Med. Wschr. 44, CYTOWIC, R.E., SMITH, A., STUMP, D.A. (1986). Transient amenorrhea after closed head trauma. N. Engl. J. Med. 314, 715. DANIEL, P.M., PRICHARD, M.M.L., and TREIP, C.S. (1959). Traumatic infarction of the anterior lobe of the pituitary gland. Lancet 2, DE MARINIS, L., MANCINI, A., VALLE, D., et al. (1999). Hypothalamic derangement in traumatized patients: growth hormone (GH) and prolactin response to thyrotrophin-releasing hormone and GH-releasing hormone. Clin. Endocrinol. 50, DELLA CORTE, F., MANCINI, A., VALLE, D., et al. (1998). Provocative hypothalamo-pituitary axis tests in severe head injury: correlation with severity and prognosis. Crit. Care Med. 26, EDWARDS, O.M., and CLARK, J.D. (1986). Post-traumatic hypopituitarism. Six cases and a review of the literature. Medicine (Baltimore) 65, GHIGO, E., GOFFI, S., NICOLOSI, M., et al. (1990). Growth hormone (GH) responsiveness to combined administration of arginine and GH-releasing hormone does not vary with age in man. J. Clin. Endocrinol. Metab. 71, GILCHRIST, F.J., MURRAY, R.D., and SHALET, S.M. (2002). The effect of long-term untreated growth hormone deficiency (GHD) and 9 years of GH replacement on the quality of life (QoL) of GH-deficient adults. Clin. Endocrinol. (Oxf.) 57, GIUSTINA, A., and VELDHUIS, J.D. (1998). Pathophysiology of the neuroregulation of growth hormone secretion in experimental animals and the human. Endocrinology Rev. 19, HACKL, J.M., GOTTARDIS, M., WIESER, C., et al. (1991). Endocrine abnormalities in severe traumatic brain injury. A cue to prognosis in severe craniocerebral trauma? Intensive Care Med. 17,
12 BONDANELLI ET AL. HARTMAN, M.L. (1998). The Growth Hormone Research Society consensus guidelines for the diagnosis and treatment of adult GH deficiency. Growth. Horm. IGF Res. 8, A25 A29. JENNETT, B., and BOND, M. (1975). Assessment of come after severe brain damage: a practical scale. Lancet 1, KELLY, D.F., GONZALO, I.T., COHAN, P., et al. (2000). Hypopituitarism following traumatic brain injury and aneurysmal subarachnoid hemorrhage: a preliminary report. J. Neurosurg. 93, LIEBERMAN, S.A., OBEROI, A.L., GILKISON, C.R., et al. (2001). Prevalence of neuroendocrine dysfunction in patients recovering from traumatic brain injury. J. Clin. Endocrinol. Metab. 86, MARSHALL, L.F., MARSHALL, S.B., KLAUBER, M.R., et al. (1992). The diagnosis of head injury requires a classification based on computed axial tomography. J. Neurotrauma 9, S NYBERG, F. (2000). Growth hormone in the brain: characteristics of specific brain targets for the hormone and their functional significance. Front. Neuroendocrinol. 21, RAABE, A., GROLMS, C., SORGE, O., et al. (1999). Serum S-100B protein in severe head injury. Neurosurgery 45, SALAZAR, A.M. (2000). Rehabilitation for traumatic brain injury. J.A.M.A. 284, SCHEEPENS, A., SIRIMANNE, E.S., BREIER, B.H., et al. (2001). Growth hormone as a neuronal rescue factor during recovery from CNS injury. Neuroscience 104, SCHEEPENS, A., WILLIAMS, C.E., BREIER, B.H., et al. (2000). A role for the somatotropic axis in neural development, injury and disease. J. Pediatr. Endocrinol. Metab. 13, SIMPSON, H., SAVINE, R., SONKSEN, P., et al. (2002). Growth hormone replacement therapy for adults: into the new millennium. Growth Horm. IGF Res. 12, TEASDALE, G., and JENNETT, B. (1974). Assessment of coma and impaired consciousness: a practical scale. Lancet 2, VALETTO, M.R., BELLONE, J., BAFFONI, C., et al. (1996). Reproducibility of the growth hormone response to stimulation with growth hormone-releasing hormone plus arginine during lifespan. Eur. J. Endocrinol. 135, WOOLF, P.D. (1992). Hormonal responses to trauma. Crit. Care Med. 20, ZADIK, Z., CHALEW, S.A., MCCARTER, R.J., JR., et al. (1985). The influence of age on the 24-hour integrated concentration of growth hormone in normal individuals. J. Clin. Endocrinol. Metab. 60, Address reprint requests to: Ettore C. degli Uberti, M.D. Department of Biomedical Sciences and Advanced Therapies Section of Endocrinology University of Ferrara Via Savonarola, Ferrara, Italy ti8@unife.it 696
Medical and Rehabilitation Innovations Neuroendocrine Screening and Hormone Replacement Therapy in Trauma Related Acquired Brain Injury
 Medical and Rehabilitation Innovations Neuroendocrine Screening and Hormone Replacement Therapy in Trauma Related Acquired Brain Injury BACKGROUND Trauma related acquired brain injury (ABI) is known to
Medical and Rehabilitation Innovations Neuroendocrine Screening and Hormone Replacement Therapy in Trauma Related Acquired Brain Injury BACKGROUND Trauma related acquired brain injury (ABI) is known to
Traumatic Brain Injury and Hypopituitarism
 Mini-Review Article TheScientificWorldJOURNAL (2005) 5, 777 781 ISSN 1537-744X; DOI 10.1100/tsw.2005.100 Traumatic Brain Injury and Hypopituitarism Gianluca Aimaretti and Ezio Ghigo* Division of Endocrinology
Mini-Review Article TheScientificWorldJOURNAL (2005) 5, 777 781 ISSN 1537-744X; DOI 10.1100/tsw.2005.100 Traumatic Brain Injury and Hypopituitarism Gianluca Aimaretti and Ezio Ghigo* Division of Endocrinology
Endocrine evaluation of patients after brain injury: what else is needed to define specific clinical recommendations?
 HORMONES 2007, 6(2):132-137 Commentary Endocrine evaluation of patients after brain injury: what else is needed to define specific clinical recommendations? Gemma Sesmilo, Irene Halperin, Manuel Puig-Domingo
HORMONES 2007, 6(2):132-137 Commentary Endocrine evaluation of patients after brain injury: what else is needed to define specific clinical recommendations? Gemma Sesmilo, Irene Halperin, Manuel Puig-Domingo
Neuropsychiatric Disturbances and Hypopituitarism After Traumatic Brain Injury in an Elderly Man
 CASE REPORT Neuropsychiatric Disturbances and Hypopituitarism After Traumatic Brain Injury in an Elderly Man Yi-Cheng Chang, Jui-Chang Tsai, 1,2 Fen-Yu Tseng* Neuropsychiatric or cognitive disturbances
CASE REPORT Neuropsychiatric Disturbances and Hypopituitarism After Traumatic Brain Injury in an Elderly Man Yi-Cheng Chang, Jui-Chang Tsai, 1,2 Fen-Yu Tseng* Neuropsychiatric or cognitive disturbances
Pituitary functions in the acute phase of traumatic brain injury: Are they related to severity of the injury or mortality?
 Brain Injury, April 27; 21(4): 433 439 Pituitary functions in the acute phase of traumatic brain injury: Are they related to severity of the injury or mortality? FATIH TANRIVERDI 1, HALIL ULUTABANCA 2,
Brain Injury, April 27; 21(4): 433 439 Pituitary functions in the acute phase of traumatic brain injury: Are they related to severity of the injury or mortality? FATIH TANRIVERDI 1, HALIL ULUTABANCA 2,
Hypothalamus & Pituitary Gland
 Hypothalamus & Pituitary Gland Hypothalamus and Pituitary Gland The hypothalamus and pituitary gland form a unit that exerts control over the function of several endocrine glands (thyroid, adrenals, and
Hypothalamus & Pituitary Gland Hypothalamus and Pituitary Gland The hypothalamus and pituitary gland form a unit that exerts control over the function of several endocrine glands (thyroid, adrenals, and
Causes of TBI vary with age
 Endocrinopathies after Traumatic Brain Injury Susan R. Rose, MD Professor Cincinnati Children s Hospital Medical Center University of Cincinnati Supported by Pfizer, Inc Investigator-Initiated Research
Endocrinopathies after Traumatic Brain Injury Susan R. Rose, MD Professor Cincinnati Children s Hospital Medical Center University of Cincinnati Supported by Pfizer, Inc Investigator-Initiated Research
PITUITARY: JUST THE BASICS PART 2 THE PATIENT
 PITUITARY: JUST THE BASICS PART 2 THE PATIENT DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none Steps taken to review and
PITUITARY: JUST THE BASICS PART 2 THE PATIENT DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none Steps taken to review and
Pituitary Complications in Traumatic Brain Injury
 Pituitary Complications in Traumatic Brain Injury François Lauzier, MD, MSc, FRCPC Assistant Professor Division of Critical Care Medicine Department of Anesthesiology and Critical Care Medicine Department
Pituitary Complications in Traumatic Brain Injury François Lauzier, MD, MSc, FRCPC Assistant Professor Division of Critical Care Medicine Department of Anesthesiology and Critical Care Medicine Department
9. Neuroendocrine Disorders Post ABI
 9. Neuroendocrine Disorders Post ABI 9.1 History and Epidemiology On behalf of the ERABI Research Group Neuroendocrine disorders, primarily hypopituitarism, were first diagnosed by the German researcher
9. Neuroendocrine Disorders Post ABI 9.1 History and Epidemiology On behalf of the ERABI Research Group Neuroendocrine disorders, primarily hypopituitarism, were first diagnosed by the German researcher
Evaluation and Management of Pituitary Failure. Dr S. Ali Imran MBBS, FRCP (Edin), FRCPC Professor of Medicine Dalhousie University, Halifax, NS
 Evaluation and Management of Pituitary Failure Dr S. Ali Imran MBBS, FRCP (Edin), FRCPC Professor of Medicine Dalhousie University, Halifax, NS Conflict of Interest None Objectives Diagnostic approach
Evaluation and Management of Pituitary Failure Dr S. Ali Imran MBBS, FRCP (Edin), FRCPC Professor of Medicine Dalhousie University, Halifax, NS Conflict of Interest None Objectives Diagnostic approach
The subjects were participants in a Dutch national prospective study, running from April
 Supplemental Data Subjects The subjects were participants in a Dutch national prospective study, running from April 1, 1994 to April 1, 1996. Infants with neonatal screening results indicative of CH-C
Supplemental Data Subjects The subjects were participants in a Dutch national prospective study, running from April 1, 1994 to April 1, 1996. Infants with neonatal screening results indicative of CH-C
9 - Neuroendocrine Disorders Following Acquired Brain Injury
 9 - Neuroendocrine Disorders Following Acquired Brain Injury Genevieve Sirois MD, Jo-Anne Aubut BA, Lilia Golverk MD, Robert Teasell MD FRCPC, T. Arnold Bayley, MD, FRCPC, Mark Bayley MD, FRCPC ERABI Parkwood
9 - Neuroendocrine Disorders Following Acquired Brain Injury Genevieve Sirois MD, Jo-Anne Aubut BA, Lilia Golverk MD, Robert Teasell MD FRCPC, T. Arnold Bayley, MD, FRCPC, Mark Bayley MD, FRCPC ERABI Parkwood
Endocrine part one. Presented by Dr. Mohammad Saadeh The requirements for the Clinical Chemistry Philadelphia University Faculty of pharmacy
 Endocrine part one Presented by Dr. Mohammad Saadeh The requirements for the Clinical Chemistry Philadelphia University Faculty of pharmacy HORMONES Hormones are chemicals released by a cell or a gland
Endocrine part one Presented by Dr. Mohammad Saadeh The requirements for the Clinical Chemistry Philadelphia University Faculty of pharmacy HORMONES Hormones are chemicals released by a cell or a gland
Endocrinological Outcome Among Treated Craniopharyngioma Patients
 Endocrinological Outcome Among Treated Craniopharyngioma Patients Afaf Al Sagheir, MD Head & Consultant, Section of Endocrinology/Diabetes Department of Pediatrics KFSH&RC Introduction Craniopharyngiomas
Endocrinological Outcome Among Treated Craniopharyngioma Patients Afaf Al Sagheir, MD Head & Consultant, Section of Endocrinology/Diabetes Department of Pediatrics KFSH&RC Introduction Craniopharyngiomas
Hypopituitarism following traumatic brain injury: prevalence is affected by the use of different dynamic tests and different normal values
 European Journal of Endocrinology (2010) 162 11 18 ISSN 0804-4643 REVIEW Hypopituitarism following traumatic brain injury: prevalence is affected by the use of different dynamic tests and different normal
European Journal of Endocrinology (2010) 162 11 18 ISSN 0804-4643 REVIEW Hypopituitarism following traumatic brain injury: prevalence is affected by the use of different dynamic tests and different normal
European Journal of Endocrinology (2006) ISSN
 European Journal of Endocrinology (2006) 155 553 557 ISSN 0804-4643 CLINICAL STUDY Discrepant results in the diagnosis of GH deficiency with the insulin-tolerance test and the GHRH plus arginine test in
European Journal of Endocrinology (2006) 155 553 557 ISSN 0804-4643 CLINICAL STUDY Discrepant results in the diagnosis of GH deficiency with the insulin-tolerance test and the GHRH plus arginine test in
JACK L. SNITZER, DO INTERNAL MEDICINE BOARD REVIEW COURSE 2018 PITUITARY
 JACK L. SNITZER, DO INTERNAL MEDICINE BOARD REVIEW COURSE 2018 PITUITARY JACK L. SNITZER, D.O. Peninsula Regional Endocrinology 1415 S. Division Street Salisbury, MD 21804 Phone:410-572-8848 Fax:410-572-6890
JACK L. SNITZER, DO INTERNAL MEDICINE BOARD REVIEW COURSE 2018 PITUITARY JACK L. SNITZER, D.O. Peninsula Regional Endocrinology 1415 S. Division Street Salisbury, MD 21804 Phone:410-572-8848 Fax:410-572-6890
Hypopituitarism After Traumatic Brain Injury
 Hypopituitarism After Traumatic Brain Injury Eva Fernandez-Rodriguez, MD a, Ignacio Bernabeu, MD a, Ana I. Castro a,b, Felipe F. Casanueva, MD, PhD a,b, * KEYWORDS Traumatic brain injury Hypopituitarism
Hypopituitarism After Traumatic Brain Injury Eva Fernandez-Rodriguez, MD a, Ignacio Bernabeu, MD a, Ana I. Castro a,b, Felipe F. Casanueva, MD, PhD a,b, * KEYWORDS Traumatic brain injury Hypopituitarism
Diagnosing Growth Disorders. PE Clayton School of Medical Sciences, Faculty of Biology, Medicine & Health
 Diagnosing Growth Disorders PE Clayton School of Medical Sciences, Faculty of Biology, Medicine & Health Content Normal pattern of growth and its variation Using growth charts Interpreting auxological
Diagnosing Growth Disorders PE Clayton School of Medical Sciences, Faculty of Biology, Medicine & Health Content Normal pattern of growth and its variation Using growth charts Interpreting auxological
Prolactin-Secreting Pituitary Adenomas (Prolactinomas) The Diagnostic Pathway (11-2K-234)
 Prolactin-Secreting Pituitary Adenomas (Prolactinomas) The Diagnostic Pathway (11-2K-234) Common presenting symptoms/clinical assessment: Pituitary adenomas are benign neoplasms of the pituitary gland.
Prolactin-Secreting Pituitary Adenomas (Prolactinomas) The Diagnostic Pathway (11-2K-234) Common presenting symptoms/clinical assessment: Pituitary adenomas are benign neoplasms of the pituitary gland.
/02/$15.00/0 The Journal of Clinical Endocrinology & Metabolism 87(5): Copyright 2002 by The Endocrine Society
 0013-7227/02/$15.00/0 The Journal of Clinical Endocrinology & Metabolism 87(5):2067 2079 Printed in U.S.A. Copyright 2002 by The Endocrine Society Sensitivity and Specificity of Six Tests for the Diagnosis
0013-7227/02/$15.00/0 The Journal of Clinical Endocrinology & Metabolism 87(5):2067 2079 Printed in U.S.A. Copyright 2002 by The Endocrine Society Sensitivity and Specificity of Six Tests for the Diagnosis
Melatonin and Growth Hormone Deficiency: A Contribution to the Evaluation of Neuroendocrine Disorders
 Melatonin and Growth Hormone Deficiency: A Contribution to the Evaluation of Neuroendocrine Disorders Fideleff G., Suárez M., Boquete HR, Azaretzky M., Sobrado P., Brunetto O*, Fideleff HL Endocrinology
Melatonin and Growth Hormone Deficiency: A Contribution to the Evaluation of Neuroendocrine Disorders Fideleff G., Suárez M., Boquete HR, Azaretzky M., Sobrado P., Brunetto O*, Fideleff HL Endocrinology
2. Has this plan authorized this medication in the past for this member (i.e., previous authorization is on file under this plan)?
 Pharmacy Prior Authorization AETA BETTER HEALTH KETUCK Growth Hormone (Medicaid) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information, sign and
Pharmacy Prior Authorization AETA BETTER HEALTH KETUCK Growth Hormone (Medicaid) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information, sign and
Pituitary Apoplexy. Updated: April 22, 2018 CLINICAL RECOGNITION
 Pituitary Apoplexy Zeina C Hannoush, MD. Assistant Professor of Clinical Medicine. Division of Endocrinology, Diabetes and Metabolism. University of Miami, Miller School of Medicine. Roy E Weiss, MD, PhD,
Pituitary Apoplexy Zeina C Hannoush, MD. Assistant Professor of Clinical Medicine. Division of Endocrinology, Diabetes and Metabolism. University of Miami, Miller School of Medicine. Roy E Weiss, MD, PhD,
Autoimmune hypophysitis may eventually become empty sella
 Neuroendocrinology Letters Volume 34 No. 2 2013 Autoimmune hypophysitis may eventually become empty sella Hua Gao*, You-you Gu*, Ming-cai Qiu Department of Endocrinology, Tianjin Medical University General
Neuroendocrinology Letters Volume 34 No. 2 2013 Autoimmune hypophysitis may eventually become empty sella Hua Gao*, You-you Gu*, Ming-cai Qiu Department of Endocrinology, Tianjin Medical University General
9. Neuroendocrine Function and Disorders Following Acquired Brain Injury
 9. Neuroendocrine Function and Disorders Following Acquired Brain Injury Genevieve Sirois MD, Robert Teasell MD FRCPC, Pavlina Faltynek MSc, Joshua Wiener BSc, Mark Bayley MD FRCPC ERABI Parkwood Institute
9. Neuroendocrine Function and Disorders Following Acquired Brain Injury Genevieve Sirois MD, Robert Teasell MD FRCPC, Pavlina Faltynek MSc, Joshua Wiener BSc, Mark Bayley MD FRCPC ERABI Parkwood Institute
Endocrine part two. Presented by Dr. Mohammad Saadeh The requirements for the Clinical Chemistry Philadelphia University Faculty of pharmacy
 Endocrine part two Presented by Dr. Mohammad Saadeh The requirements for the Clinical Chemistry Philadelphia University Faculty of pharmacy Cushing's disease: increased secretion of adrenocorticotropic
Endocrine part two Presented by Dr. Mohammad Saadeh The requirements for the Clinical Chemistry Philadelphia University Faculty of pharmacy Cushing's disease: increased secretion of adrenocorticotropic
ENDOCRINOLOGY COORDINATION OF PHYSIOLOGICAL PROCESSES:
 ENDOCRINOLOGY COORDINATION OF PHYSIOLOGICAL PROCESSES: -In a living organism there must be coordination of number of physiological activities taking place simultaneously such as: movement, respiration,
ENDOCRINOLOGY COORDINATION OF PHYSIOLOGICAL PROCESSES: -In a living organism there must be coordination of number of physiological activities taking place simultaneously such as: movement, respiration,
Pituitary gland diseases
 Pituitary gland diseases Pituitary Gland Weight 600 mg Is located within the sella turcica Anatomically and functionally distinct anterior and posterior lobes Pituitary Development The pituitary originate
Pituitary gland diseases Pituitary Gland Weight 600 mg Is located within the sella turcica Anatomically and functionally distinct anterior and posterior lobes Pituitary Development The pituitary originate
Pituitary Tumors and Incidentalomas. Bijan Ahrari, MD, FACE, ECNU Palm Medical Group
 Pituitary Tumors and Incidentalomas Bijan Ahrari, MD, FACE, ECNU Palm Medical Group Background Pituitary incidentaloma: a previously unsuspected pituitary lesion that is discovered on an imaging study
Pituitary Tumors and Incidentalomas Bijan Ahrari, MD, FACE, ECNU Palm Medical Group Background Pituitary incidentaloma: a previously unsuspected pituitary lesion that is discovered on an imaging study
UW MEDICINE PATIENT EDUCATION. Acromegaly Symptoms and treatments. What is acromegaly? DRAFT. What are the symptoms? How is it diagnosed?
 UW MEDICINE PATIENT EDUCATION Acromegaly Symptoms and treatments This handout explains a health condition called acromegaly. It describes tests that are used to diagnose the condition and gives basic instructions
UW MEDICINE PATIENT EDUCATION Acromegaly Symptoms and treatments This handout explains a health condition called acromegaly. It describes tests that are used to diagnose the condition and gives basic instructions
Traumatic brain injury: endocrine consequences in children and adults
 DOI 10.1007/s12020-013-0049-1 REVIEW Traumatic brain injury: endocrine consequences in children and adults Erick Richmond Alan D. Rogol Received: 25 June 2013 / Accepted: 27 August 2013 Ó Springer Science+Business
DOI 10.1007/s12020-013-0049-1 REVIEW Traumatic brain injury: endocrine consequences in children and adults Erick Richmond Alan D. Rogol Received: 25 June 2013 / Accepted: 27 August 2013 Ó Springer Science+Business
Imaging pituitary gland tumors
 November 2005 Imaging pituitary gland tumors Neel Varshney,, Harvard Medical School Year IV Two categories of presenting signs of a pituitary mass Functional tumors present with symptoms due to excess
November 2005 Imaging pituitary gland tumors Neel Varshney,, Harvard Medical School Year IV Two categories of presenting signs of a pituitary mass Functional tumors present with symptoms due to excess
PROOF ONLY. Neuroendocrine surveillance and management of neurosurgical patients MANAGEMENT OF ENDOCRINE DISEASE. Review. Abstract.
 Review A Garrahy and others Hypopituitarism in 176:5 R217 R233 MANAGEMENT OF ENDOCRINE DISEASE Neuroendocrine surveillance and management of Aoife Garrahy 1, Mark Sherlock 2 and Christopher J Thompson
Review A Garrahy and others Hypopituitarism in 176:5 R217 R233 MANAGEMENT OF ENDOCRINE DISEASE Neuroendocrine surveillance and management of Aoife Garrahy 1, Mark Sherlock 2 and Christopher J Thompson
Prospective study of hypothalamo-hypophyseal dysfunction in children and adolescents following traumatic brain injury
 Prospective study of hypothalamo-hypophyseal dysfunction in children and adolescents following traumatic brain injury David Krahulik a, Darina Aleksijevic b, Vratislav Smolka b, Eva Klaskova b, Petra Venhacova
Prospective study of hypothalamo-hypophyseal dysfunction in children and adolescents following traumatic brain injury David Krahulik a, Darina Aleksijevic b, Vratislav Smolka b, Eva Klaskova b, Petra Venhacova
panhypopituitarism Pattawan Wongwijitsook Maharat Nakhon Ratchasima hospital 17 Nov 2013
 panhypopituitarism Pattawan Wongwijitsook Maharat Nakhon Ratchasima hospital 17 Nov 2013 PITUITARY GLAND (HYPOPHYSIS CEREBRI) The master of endocrine glands master of endocrine glands It is a small oval
panhypopituitarism Pattawan Wongwijitsook Maharat Nakhon Ratchasima hospital 17 Nov 2013 PITUITARY GLAND (HYPOPHYSIS CEREBRI) The master of endocrine glands master of endocrine glands It is a small oval
X/00/$03.00/0 Vol. 85, No. 5 The Journal of Clinical Endocrinology & Metabolism Copyright 2000 by The Endocrine Society
 0021-972X/00/$03.00/0 Vol. 85, No. 5 The Journal of Clinical Endocrinology & Metabolism Printed in U.S.A. Copyright 2000 by The Endocrine Society The Dominant Role of Increased Intrasellar Pressure in
0021-972X/00/$03.00/0 Vol. 85, No. 5 The Journal of Clinical Endocrinology & Metabolism Printed in U.S.A. Copyright 2000 by The Endocrine Society The Dominant Role of Increased Intrasellar Pressure in
Pituitary Adenomas: Evaluation and Management. Fawn M. Wolf, MD 10/27/17
 Pituitary Adenomas: Evaluation and Management Fawn M. Wolf, MD 10/27/17 Over 18,000 pituitaries examined at autopsy: -10.6% contained adenomas (1.5-27%) -Frequency similar for men and women and across
Pituitary Adenomas: Evaluation and Management Fawn M. Wolf, MD 10/27/17 Over 18,000 pituitaries examined at autopsy: -10.6% contained adenomas (1.5-27%) -Frequency similar for men and women and across
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/33195 holds various files of this Leiden University dissertation. Author: Appelman-Dijkstra, Natasha Mireille Title: Long-term consequences of growth hormone
Cover Page The handle http://hdl.handle.net/1887/33195 holds various files of this Leiden University dissertation. Author: Appelman-Dijkstra, Natasha Mireille Title: Long-term consequences of growth hormone
Acromegaly resolution after traumatic brain injury: a case report
 Cob Journal of Medical Case Reports 2014, 8:290 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Acromegaly resolution after traumatic brain injury: a case report Alejandro Cob Abstract Introduction:
Cob Journal of Medical Case Reports 2014, 8:290 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Acromegaly resolution after traumatic brain injury: a case report Alejandro Cob Abstract Introduction:
Traumatic Brain Injury-Related Hypopituitarism: A Review and Recommendations for Screening Combat Veterans
 MILITARY MEDICINE, 175, 8:574, 2010 Traumatic Brain Injury-Related Hypopituitarism: A Review and Recommendations for Screening Combat Veterans CPT(P) Arthur F. Guerrero, MC USA ; MAJ Abel Alfonso, MC USA
MILITARY MEDICINE, 175, 8:574, 2010 Traumatic Brain Injury-Related Hypopituitarism: A Review and Recommendations for Screening Combat Veterans CPT(P) Arthur F. Guerrero, MC USA ; MAJ Abel Alfonso, MC USA
Aetna Better Health of Virginia
 Genotropin Nutropin Serostim Zomacton Humatrope Omnitrope Zorbtive somatropin Norditropin Saizen General Criteria for Approval: Omnitrope vial formulation is the preferred Growth Hormone product; consideration
Genotropin Nutropin Serostim Zomacton Humatrope Omnitrope Zorbtive somatropin Norditropin Saizen General Criteria for Approval: Omnitrope vial formulation is the preferred Growth Hormone product; consideration
ABNORMAL PITUITARY FUNCTION
 Overview ABNORMAL PITUITARY FUNCTION Specialist Portfolio Seminar Katie Jones Sandwell and West Birmingham Hospitals NHS Trust Anterior pituitary overview Posterior pituitary overview Pituitary dysfunction
Overview ABNORMAL PITUITARY FUNCTION Specialist Portfolio Seminar Katie Jones Sandwell and West Birmingham Hospitals NHS Trust Anterior pituitary overview Posterior pituitary overview Pituitary dysfunction
Many patients with head injuries show severely impaired
 J Neurosurg 113:532 538, 2010 Negative effect of hypopituitarism following brain trauma in patients with diffuse axonal injury Clinical article Ja e Hy u n Je o n g, M.D., Yo u n g Zo o n Kim, M.D., Yo
J Neurosurg 113:532 538, 2010 Negative effect of hypopituitarism following brain trauma in patients with diffuse axonal injury Clinical article Ja e Hy u n Je o n g, M.D., Yo u n g Zo o n Kim, M.D., Yo
Functional disorders of the hypothalamic-pituitaryadrenal axis in patients with severe brain injury
 GMJ, ASM 212;1(S1):S31-S37 Functional disorders of the hypothalamic-pituitaryadrenal axis in patients with severe brain injury Munzir J M Al-Zabin 1 *, Thomas Kemmer 2 1 Department of Neurosurgery, Gulf
GMJ, ASM 212;1(S1):S31-S37 Functional disorders of the hypothalamic-pituitaryadrenal axis in patients with severe brain injury Munzir J M Al-Zabin 1 *, Thomas Kemmer 2 1 Department of Neurosurgery, Gulf
Hypothalamo pituitary dysfunction in patients with chronic subdural hematoma
 Hypothalamo pituitary dysfunction in patients with chronic subdural hematoma Václav Hána 1, Mikuláš Kosák 1, Václav Masopust 2, David Netuka 2, Zdena Lacinová 1, Michal Kršek 1, Josef Marek 1, Ladislav
Hypothalamo pituitary dysfunction in patients with chronic subdural hematoma Václav Hána 1, Mikuláš Kosák 1, Václav Masopust 2, David Netuka 2, Zdena Lacinová 1, Michal Kršek 1, Josef Marek 1, Ladislav
Marshall Scale for Head Trauma Mark C. Oswood, MD PhD Department of Radiology Hennepin County Medical Center, Minneapolis, MN
 Marshall Scale for Head Trauma Mark C. Oswood, MD PhD Department of Radiology Hennepin County Medical Center, Minneapolis, MN History of Marshall scale Proposed by Marshall, et al in 1991 to classify head
Marshall Scale for Head Trauma Mark C. Oswood, MD PhD Department of Radiology Hennepin County Medical Center, Minneapolis, MN History of Marshall scale Proposed by Marshall, et al in 1991 to classify head
Traumatic brain injury induced hypothalamic-pituitary dysfunction: a paediatric perspective
 Pituitary (2007) 10:373 380 DOI 10.1007/s11102-007-0052-8 Traumatic brain injury induced hypothalamic-pituitary dysfunction: a paediatric perspective Carlo L. Acerini Æ Robert C. Tasker Published online:
Pituitary (2007) 10:373 380 DOI 10.1007/s11102-007-0052-8 Traumatic brain injury induced hypothalamic-pituitary dysfunction: a paediatric perspective Carlo L. Acerini Æ Robert C. Tasker Published online:
Humatrope*, Norditropin*, Genotropin, Nutropin, Nutropin AQ, Omnitrope, Saizen
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.08.11 Subject: Growth Hormone Adult Page: 1 of 6 Last Review Date: December 5, 2014 Growth Hormone Adult
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.08.11 Subject: Growth Hormone Adult Page: 1 of 6 Last Review Date: December 5, 2014 Growth Hormone Adult
HYPOTHALAMO PITUITARY GONADAL AXIS
 HYPOTHALAMO PITUITARY GONADAL AXIS Physiology of the HPG axis Endogenous opioids and the HPG axis (exerciseinduced menstrual disturbances) Effects of the immune system on the HPG axis (cytokines: interleukins
HYPOTHALAMO PITUITARY GONADAL AXIS Physiology of the HPG axis Endogenous opioids and the HPG axis (exerciseinduced menstrual disturbances) Effects of the immune system on the HPG axis (cytokines: interleukins
The reproductive system
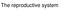 The reproductive system THE OVARIAN CYCLE HORMONAL REGULATION OF OOGENSIS AND OVULATION hypothalamic-pituitary-ovary axis Overview of the structures of the endocrine system Principal functions of the
The reproductive system THE OVARIAN CYCLE HORMONAL REGULATION OF OOGENSIS AND OVULATION hypothalamic-pituitary-ovary axis Overview of the structures of the endocrine system Principal functions of the
Peri-op Pituitary / Diabetes Insipidus/ Apoplexy Dr. Stan Van Uum, MD, PhD, FRCPC
 10 th Annual Canadian Endocrine Update 3 rd Canadian Endocrine Review Course Peri-op Pituitary / Diabetes Insipidus/ Apoplexy Dr. Stan Van Uum, MD, PhD, FRCPC 10 th Annual Canadian Endocrine Update Dr.
10 th Annual Canadian Endocrine Update 3 rd Canadian Endocrine Review Course Peri-op Pituitary / Diabetes Insipidus/ Apoplexy Dr. Stan Van Uum, MD, PhD, FRCPC 10 th Annual Canadian Endocrine Update Dr.
A Combined Case of Macroprolactinoma, Growth Hormone Excess and Graves' Disease
 A Combined Case of Macroprolactinoma, Growth Hormone Excess and Graves' Disease Z Hussein, MRCP*, B Tress**, P G Cohnan, FRACP***... 'Department of Medicine, Hospital Putrajaya, Putrajaya, Presint 7, 62250
A Combined Case of Macroprolactinoma, Growth Hormone Excess and Graves' Disease Z Hussein, MRCP*, B Tress**, P G Cohnan, FRACP***... 'Department of Medicine, Hospital Putrajaya, Putrajaya, Presint 7, 62250
High and Low GH: an update of diagnosis and management of GH disorders
 High and Low GH: an update of diagnosis and management of GH disorders Georgia Chapter-AACE 2017 Laurence Katznelson, MD Professor of Medicine and Neurosurgery Associate Dean of Graduate Medical Education
High and Low GH: an update of diagnosis and management of GH disorders Georgia Chapter-AACE 2017 Laurence Katznelson, MD Professor of Medicine and Neurosurgery Associate Dean of Graduate Medical Education
Pituitary for the General Practitioner. Marilyn Lee Consultant physician and endocrinologist
 Pituitary for the General Practitioner Marilyn Lee Consultant physician and endocrinologist Pituitary tumours Anterior/posterior pituitary Extension of adenoma upwards/downwards/sideways Producing too
Pituitary for the General Practitioner Marilyn Lee Consultant physician and endocrinologist Pituitary tumours Anterior/posterior pituitary Extension of adenoma upwards/downwards/sideways Producing too
Diseases of pituitary gland
 Diseases of pituitary gland A brief introduction Anterior lobe = adenohypophysis Posterior lobe = neurohypophysis The production of most pituitary hormones is controlled in large part by positively and
Diseases of pituitary gland A brief introduction Anterior lobe = adenohypophysis Posterior lobe = neurohypophysis The production of most pituitary hormones is controlled in large part by positively and
What we will cover. Evaluation of the Child with Suspected Pituitary Disease. ituitary
 Evaluation of the Child with Suspected Pituitary Disease Craig Alter, MD University of Pennsylvania Children s Hospital of Philadelphia What we will cover * What laboratory tests to order * MRI: common
Evaluation of the Child with Suspected Pituitary Disease Craig Alter, MD University of Pennsylvania Children s Hospital of Philadelphia What we will cover * What laboratory tests to order * MRI: common
Case Report Rapid Pituitary Apoplexy Regression: What Is the Time Course of Clot Resolution?
 Case Reports in Radiology Volume 2015, Article ID 268974, 5 pages http://dx.doi.org/10.1155/2015/268974 Case Report Rapid Pituitary Apoplexy Regression: What Is the Time Course of Clot Resolution? Devon
Case Reports in Radiology Volume 2015, Article ID 268974, 5 pages http://dx.doi.org/10.1155/2015/268974 Case Report Rapid Pituitary Apoplexy Regression: What Is the Time Course of Clot Resolution? Devon
62-year-old woman with severe headache. Celeste Thomas November 1, 2012
 62-year-old woman with severe headache Celeste Thomas November 1, 2012 History of Present Illness History of hypertension and hyperlipidemia Presented to outside hospital after awakening from sleep with
62-year-old woman with severe headache Celeste Thomas November 1, 2012 History of Present Illness History of hypertension and hyperlipidemia Presented to outside hospital after awakening from sleep with
ENDOCRINE SYSTEM. Endocrine
 ENDOCRINE SYSTEM Endocrine Function Help regulate internal functions Use chemical messengers Recall: Endocrine vs. Exocrine glands Nervous System vs Endocrine System Target Specificity Lock n Key action
ENDOCRINE SYSTEM Endocrine Function Help regulate internal functions Use chemical messengers Recall: Endocrine vs. Exocrine glands Nervous System vs Endocrine System Target Specificity Lock n Key action
BIOM2010 (till mid sem) Endocrinology. e.g. anterior pituitary gland, thyroid, adrenal. Pineal Heart GI Female
 BIOM2010 (till mid sem) Endocrinology Endocrine system Endocrine gland : a that acts by directly into the which then to other parts of the body to act on (cells, tissues, organs) : found at e.g. anterior
BIOM2010 (till mid sem) Endocrinology Endocrine system Endocrine gland : a that acts by directly into the which then to other parts of the body to act on (cells, tissues, organs) : found at e.g. anterior
Pathology of pituitary gland. By: Shifaa Qa qa
 Pathology of pituitary gland By: Shifaa Qa qa Sella turcica Adenohypophysis (80%): - epithelial cells - acidophil, basophil, chromophobe - Somatotrophs, Mammosomatotrophs, Corticotrophs, Thyrotrophs, Gonadotrophs
Pathology of pituitary gland By: Shifaa Qa qa Sella turcica Adenohypophysis (80%): - epithelial cells - acidophil, basophil, chromophobe - Somatotrophs, Mammosomatotrophs, Corticotrophs, Thyrotrophs, Gonadotrophs
THE ANTERIOR PITUITARY. Embryology cont. Embryology of the pituitary BY MISPA ZUH HS09A179. Embryology cont. THE PITUIYARY GLAND Anatomy:
 THE ANTERIOR PITUITARY BY MISPA ZUH HS09A179 Embryology of the pituitary The pituitary is formed early in embryonic life from the fusion of the Rathke s pouch (anterior) and the diencephalon ( posterior)
THE ANTERIOR PITUITARY BY MISPA ZUH HS09A179 Embryology of the pituitary The pituitary is formed early in embryonic life from the fusion of the Rathke s pouch (anterior) and the diencephalon ( posterior)
Endocrine system overview
 Endocrine system overview Nature of the hormonal system -Major integrator of body function Classification of hormones Endocrine vs paracrine Nature of hormone-receptor systems Role of the hypothalamuspituitary
Endocrine system overview Nature of the hormonal system -Major integrator of body function Classification of hormones Endocrine vs paracrine Nature of hormone-receptor systems Role of the hypothalamuspituitary
Anterior pituitary dysfunction following traumatic brain injury (TBI)
 Clinical Endocrinology (2006) 64, 481 488 doi: 10.1111/j.1365-2265.2006.02517.x CLINICAL PRACTICE UPDATE Blackwell Publishing Ltd Anterior pituitary dysfunction following traumatic brain injury (TBI) Amar
Clinical Endocrinology (2006) 64, 481 488 doi: 10.1111/j.1365-2265.2006.02517.x CLINICAL PRACTICE UPDATE Blackwell Publishing Ltd Anterior pituitary dysfunction following traumatic brain injury (TBI) Amar
Pituitary apoplexy 台北榮總內分泌新陳代謝科主治醫師林怡君
 Pituitary apoplexy 台北榮總內分泌新陳代謝科主治醫師林怡君 Williams text book of endocrinology 11 th e Anterior pituitary hormone 10-20% of pituitary cells, increase to 40% during AP PRL releasing factors: TRH, oxytocin,
Pituitary apoplexy 台北榮總內分泌新陳代謝科主治醫師林怡君 Williams text book of endocrinology 11 th e Anterior pituitary hormone 10-20% of pituitary cells, increase to 40% during AP PRL releasing factors: TRH, oxytocin,
CIGNA HealthCare Prior Authorization Form - Growth Hormone Medications -
 Pharmacy Services Phone: (800)244-6224 Fax: (800)390-9745 CIGNA HealthCare Prior Authorization Form - Growth Hormone Medications - Notice: Failure to complete this form in its entirety may result in delayed
Pharmacy Services Phone: (800)244-6224 Fax: (800)390-9745 CIGNA HealthCare Prior Authorization Form - Growth Hormone Medications - Notice: Failure to complete this form in its entirety may result in delayed
A Boy with Optic Glioma
 Clin Pediatr Endocrinol 1994;3(Suppl 4): 169-173 Copyright(C)1994 by The Japanese Society for Pediatric Endocrinology Taisuke Okada, Sumitaka Dohno, Yousei Shimasaki, Takashi Tomoda, Makiko Koga, Kumiko
Clin Pediatr Endocrinol 1994;3(Suppl 4): 169-173 Copyright(C)1994 by The Japanese Society for Pediatric Endocrinology Taisuke Okada, Sumitaka Dohno, Yousei Shimasaki, Takashi Tomoda, Makiko Koga, Kumiko
PRACTICE GUIDELINE. DEFINITIONS: Mild head injury: Glasgow Coma Scale* (GCS) score Moderate head injury: GCS 9-12 Severe head injury: GCS 3-8
 PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Pituitary Stalk Interruption Syndrome. Leena Shahla, MD, PGY5 Endocrinology, Diabetes and Metabolism Fellowship University of Massachusetts
 Pituitary Stalk Interruption Syndrome Leena Shahla, MD, PGY5 Endocrinology, Diabetes and Metabolism Fellowship University of Massachusetts 11/12/2016 Case: NP, 42 year old female, from Dominican Republic.
Pituitary Stalk Interruption Syndrome Leena Shahla, MD, PGY5 Endocrinology, Diabetes and Metabolism Fellowship University of Massachusetts 11/12/2016 Case: NP, 42 year old female, from Dominican Republic.
Art labeling Activity: Figure 16.1
 ANP 1105D Winter 2013 Assignment 6 part I: The Endocrine Sy... Assignment 6 part I: The Endocrine System, Chapter 16 Due: 11:59pm on Monday, March 4, 2013 Note: To understand how points are awarded, read
ANP 1105D Winter 2013 Assignment 6 part I: The Endocrine Sy... Assignment 6 part I: The Endocrine System, Chapter 16 Due: 11:59pm on Monday, March 4, 2013 Note: To understand how points are awarded, read
Hormonal Replacement in Hypopituitarism in Adults: An Endocrine Society Clinical Practice Guideline
 Hormonal Replacement in Hypopituitarism in Adults: An Endocrine Society Clinical Practice Guideline Task Force Members Maria Fleseriu, MD Ibrahim A. Hashim, PhD Niki Karavitaki, PhD Shlomo Melmed, MD M.
Hormonal Replacement in Hypopituitarism in Adults: An Endocrine Society Clinical Practice Guideline Task Force Members Maria Fleseriu, MD Ibrahim A. Hashim, PhD Niki Karavitaki, PhD Shlomo Melmed, MD M.
Study of the correlation between growth hormone deficiency and serum leptin, adiponectin, and visfatin levels in adults
 Study of the correlation between growth hormone deficiency and serum leptin, adiponectin, and visfatin levels in adults Z.-P. Li 1, M. Zhang 2, J. Gao 3, G.-Y. Zhou 3, S.-Q. Li 1 and Z.-M. An 3 1 Golden
Study of the correlation between growth hormone deficiency and serum leptin, adiponectin, and visfatin levels in adults Z.-P. Li 1, M. Zhang 2, J. Gao 3, G.-Y. Zhou 3, S.-Q. Li 1 and Z.-M. An 3 1 Golden
Endocrine Glands: Hormone-secreting organs are called endocrine glands
 University of Jordan Department of Physiology and Biochemistry Nursing students, Academic year 2017/2018. ******************************************************************* Ref: Principles of Anatomy
University of Jordan Department of Physiology and Biochemistry Nursing students, Academic year 2017/2018. ******************************************************************* Ref: Principles of Anatomy
Growth hormone therapy for short stature in adolescents the experience in the University Medical Unit, National Hospital of Sri Lanka
 Growth hormone therapy for short stature in adolescents Growth hormone therapy for short stature in adolescents the experience in the University Medical Unit, National Hospital of Sri Lanka K K K Gamage,
Growth hormone therapy for short stature in adolescents Growth hormone therapy for short stature in adolescents the experience in the University Medical Unit, National Hospital of Sri Lanka K K K Gamage,
MANAGEMENT OF PATIENTS WITH PITUITARY DISORDERS ON THE NEUROSUGERY WARDS RESPONSIBILITIES OF THE METABOLIC REGISTRAR
 MANAGEMENT OF PATIENTS WITH PITUITARY DISORDERS ON THE NEUROSUGERY WARDS RESPONSIBILITIES OF THE METABOLIC REGISTRAR We have clear links with DCN and a responsibility for the management of patients with
MANAGEMENT OF PATIENTS WITH PITUITARY DISORDERS ON THE NEUROSUGERY WARDS RESPONSIBILITIES OF THE METABOLIC REGISTRAR We have clear links with DCN and a responsibility for the management of patients with
Lab Exercise Endocrine System
 Lab Exercise Endocrine System Name Date Materials: Human torso model Compound light microscope Prepared slides of the pituitary gland, pineal gland, thyroid gland, parathyroid glands, thymus gland, adrenal
Lab Exercise Endocrine System Name Date Materials: Human torso model Compound light microscope Prepared slides of the pituitary gland, pineal gland, thyroid gland, parathyroid glands, thymus gland, adrenal
Chapter 13 worksheet
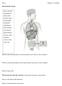 Name: Chapter 13 worksheet The Endocrine System Please label the: hypothalamus pineal gland pituitary gland thyroid gland parathyroid gland thymus heart stomach liver adrenal glands kidneys pancreas small
Name: Chapter 13 worksheet The Endocrine System Please label the: hypothalamus pineal gland pituitary gland thyroid gland parathyroid gland thymus heart stomach liver adrenal glands kidneys pancreas small
The Neuroendocrine Effects of Traumatic Brain Injury
 SPECIAL ARTICLES The Neuroendocrine Effects of Traumatic Brain Injury Micol S. Rothman, M.D. David B. Arciniegas, M.D. Christopher M. Filley, M.D. Margaret E. Wierman, M.D. Neuroendocrine dysfunction after
SPECIAL ARTICLES The Neuroendocrine Effects of Traumatic Brain Injury Micol S. Rothman, M.D. David B. Arciniegas, M.D. Christopher M. Filley, M.D. Margaret E. Wierman, M.D. Neuroendocrine dysfunction after
Initials:.. Number of patient in the registry:... Date of visit:.. Gender (genetic): female / male
 1. Patient personal details Institute code: Physician code: Initials:.. Number of patient in the registry:... Date of visit:.. Gender (genetic): female / male 2. Changes in acromegaly-specific medical
1. Patient personal details Institute code: Physician code: Initials:.. Number of patient in the registry:... Date of visit:.. Gender (genetic): female / male 2. Changes in acromegaly-specific medical
Pituitary Disorders. Eiman Ali Basheir Mob: /1/2019
 Pituitary Disorders Eiman Ali Basheir Mob: 0915020385 31/1/2019 Objectives By the end of this lecture the students will be able to: Understand basic Pituitary axis physiology State the common causes of
Pituitary Disorders Eiman Ali Basheir Mob: 0915020385 31/1/2019 Objectives By the end of this lecture the students will be able to: Understand basic Pituitary axis physiology State the common causes of
Original Article Pituitary imaging in 129 children with growth hormone deficiency: A spectrum of findings
 Original Article Pituitary imaging in 129 children with growth hormone deficiency: A spectrum of findings Rushaid N A AlJurayyan (1), Nasir A M AlJurayyan (2), Hala G Omer (2), Sharifah D A Alissa (2),
Original Article Pituitary imaging in 129 children with growth hormone deficiency: A spectrum of findings Rushaid N A AlJurayyan (1), Nasir A M AlJurayyan (2), Hala G Omer (2), Sharifah D A Alissa (2),
CEREBROVASCULAR DISEASE has a high prevalence
 0021-972X/06/$15.00/0 The Journal of Clinical Endocrinology & Metabolism 91(10):3928 3934 Printed in U.S.A. Copyright 2006 by The Endocrine Society doi: 10.1210/jc.2006-1040 Predictive Value of Circulating
0021-972X/06/$15.00/0 The Journal of Clinical Endocrinology & Metabolism 91(10):3928 3934 Printed in U.S.A. Copyright 2006 by The Endocrine Society doi: 10.1210/jc.2006-1040 Predictive Value of Circulating
General Approval Criteria for ALL Growth Hormone agents: (ALL criteria must be met)
 Growth Hormone Agents Prior Authorization Criteria for Louisiana Fee for Service and MCO Medicaid Recipients Page 1 of 7 Preferred Agents Somatropin Pen (Norditropin ) Somatropin Pen (Nutropin AQ ) Non-Preferred
Growth Hormone Agents Prior Authorization Criteria for Louisiana Fee for Service and MCO Medicaid Recipients Page 1 of 7 Preferred Agents Somatropin Pen (Norditropin ) Somatropin Pen (Nutropin AQ ) Non-Preferred
Endocrine System Notes
 Endocrine System Notes is the tendency to maintain a stable internal environment. - parts of the body that secrete hormones directly into the body. - parts of the body that make secretions which travel
Endocrine System Notes is the tendency to maintain a stable internal environment. - parts of the body that secrete hormones directly into the body. - parts of the body that make secretions which travel
Process / Evidence Class. Clinical Assessment / III
 Table 2: Endocrine Author Cozzi et al (2009) 1 Study Design: Prospectively followed case series. Fourteen patients had pre-op hypocortisolism. Patient Population: Seventy-two adult patients who underwent
Table 2: Endocrine Author Cozzi et al (2009) 1 Study Design: Prospectively followed case series. Fourteen patients had pre-op hypocortisolism. Patient Population: Seventy-two adult patients who underwent
CLINICAL REVIEW 113 Hypopituitarism Secondary to Head Trauma
 0021-972X/00/$03.00/0 Vol. 85, No. 4 The Journal of Clinical Endocrinology & Metabolism Printed in U.S.A. Copyright 2000 by The Endocrine Society CLINICAL REVIEW 113 Hypopituitarism Secondary to Head Trauma
0021-972X/00/$03.00/0 Vol. 85, No. 4 The Journal of Clinical Endocrinology & Metabolism Printed in U.S.A. Copyright 2000 by The Endocrine Society CLINICAL REVIEW 113 Hypopituitarism Secondary to Head Trauma
Moron General Hospital Ciego de Avila Cuba. Department of Neurological Surgery
 Moron General Hospital Ciego de Avila Cuba Department of Neurological Surgery Early decompressive craniectomy in severe head injury with intracranial hypertension Angel J. Lacerda MD PhD, Daisy Abreu MD,
Moron General Hospital Ciego de Avila Cuba Department of Neurological Surgery Early decompressive craniectomy in severe head injury with intracranial hypertension Angel J. Lacerda MD PhD, Daisy Abreu MD,
Assessment of pituitary function in patients with nasopharyngeal carcinoma: The effect of radiotherapy
 Available online at www.medicinescience.org ORIGINAL RESEARCH Medicine Science International Medical Journal Medicine Science 2019; ( ): Assessment of pituitary function in patients with nasopharyngeal
Available online at www.medicinescience.org ORIGINAL RESEARCH Medicine Science International Medical Journal Medicine Science 2019; ( ): Assessment of pituitary function in patients with nasopharyngeal
4/23/2018. Endocrine System: Overview. Endocrine System: Overview
 Endocrine System: Overview With nervous system, coordinates and integrates activity of body cells Influences metabolic activities via hormones transported in blood Response slower but longer lasting than
Endocrine System: Overview With nervous system, coordinates and integrates activity of body cells Influences metabolic activities via hormones transported in blood Response slower but longer lasting than
Endocrine Glands. Endocrine glands
 ENDOCRINOLOGY Endocrine Glands Endocrine glands Produce substances called hormones. Ductless glands, i.e., they release hormones directly into the bloodstream Hormones only act at their target tissue where
ENDOCRINOLOGY Endocrine Glands Endocrine glands Produce substances called hormones. Ductless glands, i.e., they release hormones directly into the bloodstream Hormones only act at their target tissue where
Checking the Right Box at the Right Age: the Art of Pediatric Endocrine Testing
 Checking the Right Box at the Right Age: the Art of Pediatric Endocrine Testing Jean-Pierre Chanoine, MD Endocrinology and Diabetes Unit British Columbia s Children s Hospital Objectives 1. Interpret the
Checking the Right Box at the Right Age: the Art of Pediatric Endocrine Testing Jean-Pierre Chanoine, MD Endocrinology and Diabetes Unit British Columbia s Children s Hospital Objectives 1. Interpret the
Human Biochemistry. Hormones
 Human Biochemistry Hormones THE ENDOCRINE SYSTEM THE ENDOCRINE SYSTEM THE ENDOCRINE SYSTEM The ENDOCRINE SYSTEM = the organ system that regulates internal environment conditions by secreting hormones into
Human Biochemistry Hormones THE ENDOCRINE SYSTEM THE ENDOCRINE SYSTEM THE ENDOCRINE SYSTEM The ENDOCRINE SYSTEM = the organ system that regulates internal environment conditions by secreting hormones into
Clinical Guideline POSITION STATEMENT ON THE INVESTIGATION AND TREATMENT OF GROWTH HORMONE DEFICIENCY IN TRANSITION
 Clinical Guideline POSITION STATEMENT ON THE INVESTIGATION AND TREATMENT OF GROWTH HORMONE DEFICIENCY IN TRANSITION Date of First Issue 01/04/2015 Approved 28/01/2016 Current Issue Date 28/01/2016 Review
Clinical Guideline POSITION STATEMENT ON THE INVESTIGATION AND TREATMENT OF GROWTH HORMONE DEFICIENCY IN TRANSITION Date of First Issue 01/04/2015 Approved 28/01/2016 Current Issue Date 28/01/2016 Review
Imaging The Turkish Saddle. Russell Goodman, HMS III Dr. Gillian Lieberman
 Imaging The Turkish Saddle Russell Goodman, HMS III Dr. Gillian Lieberman Learning Objectives Review the anatomy of the sellar region Discuss the differential diagnosis of sellar masses Discuss typical
Imaging The Turkish Saddle Russell Goodman, HMS III Dr. Gillian Lieberman Learning Objectives Review the anatomy of the sellar region Discuss the differential diagnosis of sellar masses Discuss typical
Reproductive FSH. Analyte Information
 Reproductive FSH Analyte Information 1 Follicle-stimulating hormone Introduction Follicle-stimulating hormone (FSH, also known as follitropin) is a glycoprotein hormone secreted by the anterior pituitary
Reproductive FSH Analyte Information 1 Follicle-stimulating hormone Introduction Follicle-stimulating hormone (FSH, also known as follitropin) is a glycoprotein hormone secreted by the anterior pituitary
