Evidence Based Care Journal
|
|
|
- Dayna Hunter
- 5 years ago
- Views:
Transcription
1 Karbandi et al 15 Evidence Based Care Journal Effects of Early Feeding Support on the Postoperative Weight Gain Status of Infants with Esophageal Atresia Marzieh Ghorbani, Akram Rezaeian, Gholamreza Khademi, Reza Shojaeian, Seyed Ali Jafari The online version of this article can be found at Evidence Based Care Journal :67 originally published online 01 July 2016 Online ISSN: X Address: Mashhad Nursing and Midwifery School, Ebn-e-Sina St., Mashhad, Iran P.O.Box: Tel.: (098 51) Fax: (098 51)
2 67 Evidence Based Care Journal, 6 (2): Original Article Effects of Early Feeding Support on the Postoperative Weight Gain Status of Infants with Esophageal Atresia Marzieh Ghorbani 1, *Akram Rezaeian 2, Gholamreza Khademi 3, Reza Shojaeian 4, Seyed Ali Jafari 5 Received: 27/05/2016 Accepted: 08/07/2016 Evidence Based Care Journal, 6 (2): Abstract Background: Infants may lose their body resources after surgery due to inadequate nutrient intake and undergoing long periods of fasting after surgery for esophageal atresia, increases risk of several complications. Aim: This study aimed to evaluate the effects of early feeding support on the postoperative weight gain status of infants with esophageal atresia. Method: This randomized, controlled clinical trial was conducted on 36 infants with esophageal atresia (type C) selected 48 hours after surgery during July 2015-March 2016 at Dr. Sheikh Hospital of Mashhad, Iran. In the intervention group, detecting no lack of leakage on chest X-ray, feeding was initiated and the control group received routine feeding. Neonatal weight changes were measured daily using a digital scale (TANITA model) since the first day after the surgery and one month after discharge from the hospital. Data was analysed using SPSS version 16 by independent T-test and Chisquare. Results: Mean neonatal weight on admission was ±337.4 grams in the intervention group and ±856 grams in the control group (P=0.47). Results of independent T-test showed that daily weight gain before and after feeding was significantly higher in the intervention group compared to the control group (P=0.01). Moreover, weight gain one month after discharge had a significant difference between infants of the intervention and control groups (P=0.03). Implications for Practice: According to the results of this study, early feeding support could improve the weight index of neonates with esophageal atresia. Considering the possible complications and long-term consequences of surgery, early initiation of feeding could be an appropriate remedial measure in infants with esophageal atresia. Keywords: Esophageal atresia, Oral feeding, Infants, Postoperative care 1. MS student in Nursing, School of Nursing and Midwifery, Mashhad University of Medical Sciences, Mashhad, Iran 2. Evidence Based Care Research Centre, Instructor of Pediatric Nursing, School of Nursing and Midwifery, Mashhad University of Medical Sciences, Mashhad, Iran 3. Associate Professor of Pediatric intensive care, School of Medicine, Mashhad University of Medical Sciences, Mashhad, Iran 4. Assistant Professor of Pediatric surgery, School of Medicine, Mashhad University of Medical Sciences, Mashhad, Iran 5. Associate Professor of Pediatric Gastroenterology, School of Medicine, Mashhad University of Medical Sciences, Mashhad, Iran Corresponding author, Rezaeiana@mums.ac.ir
3 Ghorbani et al. Effects of Early Feeding on Weight of Operated Infant 68 Introduction Esophageal atresia (EA) is a developmental defect of the upper gastrointestinal tract and a congenital anomaly, which leads to the failure of the esophagus to develop as a continuous passage, as well as the failure of the trachea and esophagus to separate into distinct structures. These abnormalities may occur separately or simultaneously (1). There are various forms of tracheoesophageal fistula and EA; in 85-90% of the cases, the most common form of these anomalies is discontinuous upper esophagus and distal esophagus connected to the trachea through the fistula (EA type C). Other forms of EA are comparatively rare. In 50% of the cases, EA is associated with other birth abnormalities, such as vertebral column, anorectal, and cardiac, spinal, renal and limbs defects. Therefore, early diagnosis of EA is essential to the effective treatment and prevention of these complications (1, 2). Global incidence of EA is approximately one case per 2,500-3,000 live births, which has been reported to be slightly higher in male neonates compared to female ones. In addition, preterm infants are at a higher risk of EA (1, 3). If EA remains undiagnosed or untreated, it poses significant risk to the health of neonates; as such, nursing interventions are required immediately after birth in order to detect this anomaly (1). Early diagnosis of EA is associated with a higher treatment success rate. According to statistics, survival rate of patients with tracheoesophageal fistula with no abnormalities or other complications is more than 90%. However, the complications and associated disorders are more common in preterm or low-birth-weight infants, with the mortality rate estimated at approximately 50% (4). According to the literature, birth weight and significant cardiac abnormalities are the main influential factors in the survival of infants with EA, so that the survival rate of infants with birth weight of less than 1500 grams is 20% lower than those with birth weight of more than 1500 grams. Furthermore, mortality rate of neonates with significant cardiac anomalies is 20% higher compared to other patients (5). Patients with EA require immediate surgical intervention, which is considered the ultimate treatment for this condition. However, surgery might be delayed in these patients due to factors such as premature birth, other birth defects or complications caused by aspiration pneumonia. Surgery could be performed on EA neonates with no cardiopulmonary disorders and other intestinal abnormalities within the first 24 hours of birth. Some EA patients have an uncomplicated postoperative period, while others are likely to present with various esophageal complications, as well as respiratory and nutritional problems. These complications could significantly affect the ability of EA infants to develop adaptive behaviors in adulthood. Among the most important complications of EA are anastomotic leakage, stenosis, gastroesophageal reflux, esophageal motility disorder, recurrent fistula, scoliosis, chest wall deformity, respiratory disorders, growth retardation, and malnutrition (6). Moreover, the most frequent, early complications associated with EA are breathing difficulty and feeding intolerance (3). In infants with EA, a hypermetabolic response occurs immediately after surgery, which leads to the emergence of potential complications, such as hypoglycemia, gluconeogenesis, protein catabolism, fat oxidation, and increased need for energy. In this regard, clinical and experimental studies have suggested that early nutritional support could diminish these complications. For instance, José Paulo et al. (1994) reported the reduced incidence of sepsis and length of hospital stay in patients receiving early enteral nutrition after gastrointestinal surgeries (6). Furthermore, it was stated that these complications were more severe in infants, followed by more adverse consequences, since the health problems of infants undergoing surgery were more complex than adults. Infants have a smaller body, higher growth rate, lack of evolved body systems and limited calorie reserves. In addition, neonates undergoing surgery have increased need for calorie intake (7). Therefore, it is anticipated that feeding support in infants undergoing surgery could remarkably affect their surgical outcomes. Researchers have suggested that adequate calorie intake could restore infant growth after response to the acute injuries caused by surgery since it drastically increases resting energy expenditure (REE), especially within 4-6 hours after surgery. On the other hand, infections and other postoperative complications increase the severity of postoperative REE despite the fact that newborns have limited energy storage. Consequently, if these infants do not receive sufficient feeding support, their physical resources deplete immediately, giving
4 69 Evidence Based Care Journal, 6 (2): rise to catabolic processes and increased need for energy, which exposes neonates to growth disorders (8). Early feeding in patients with EA has been rarely addressed in the literature. In a study, Sweed et al. (1991) carried out early feeding in EA patients via a soft silastic nasogastric tube, and the patients were orally fed one day after surgery (9). Similarly, Kevin et al. (1996) initiated early oral feeding in EA patients via transanastomotic feeding tubes one day after surgery (10). In the aforementioned studies, early feeding was not associated with the increased incidence or clinical complications of anastomotic stenosis and leakage. Furthermore, it could reduce the length of hospital stay and treatment costs (9, 10). Currently, infants with EA are unable to feed orally before surgery due to the defects in the upper digestive system; therefore, they should receive caloric requirements through parenteral nutrition only. After the surgical repair of EA, parenteral nutrition continues for 5-7 days, and oral feeding is delayed for at least 5-7 days in order to repair the surgical points. After the removal of nasogastric tube and ensuring the lack of anastomotic leakage, oral feeding is started with 5% glucose serum, followed by breastfeeding. This might challenge the initiation of oral feeding since long-term effects of fasting on infants leads to the delayed development of the digestive system, increasing the risk of cholestasis, accelerated catabolic processes, delayed wound healing, weight loss, and increased length of hospital stay (10). Although the quality nutrition in neonates after this operation is considered an indicator of acute malnutrition (7), scientific evidence is scarce on the complications associated with long-term postoperative fasting in infants (6). In nursing care, nutritional support is an inherent element of health care, especially in the case of high-risk infants. In this study, we attempted to determine whether early nutritional support in patients with EA could minimize the complications caused by long-term fasting and if concurrent parenteral nutrition could provide the necessary energy and induce weight gain in EA infants. Considering the incidence rate of EA, high costs of the surgery and treatment and the associated complications, early oral nutrition might play a key role in the prevention of these complications and improvement of the survival rate of EA infants (6, 8). It is recommended that further studies be conducted on reducing the incidence of EA complications and improving the quality of life of these patients. This study aimed to investigate the effects of early feeding support on the postoperative weight gain status of infants with EA. Methods This randomized, controlled clinical trial was conducted on infants with EA (type C), who met the inclusion criteria and underwent surgery, during July 2015-March 2016 at Dr. Sheikh Hospital of Mashhad, Iran. Since this hospital is the only center of pediatric surgery in the north-east of Iran, it was selected as the research environment. Sample size was calculated using the "comparison of means" formula at the confidence level of 95% and test power of 80%. In a pilot study, weight change rates were determined at 17.1±6.8 grams for the control group and 24.9±9.3 grams for the intervention group. In total, 36 subjects were selected via convenience sampling and randomly divided into two groups of intervention and control (18 infants in each group). To ensure reliability, at last 20 patients were allocated to each study group. Inclusion criteria were as follows: 1) gap of two bags <3 cm; 2) weight of 1800 grams; 3) physiological stability (heart rate= , respiratory rate=30-60, SPO 2=88-93%, pink colour skin and perfect tonicity) and 4) gestational age of 34 weeks (11). Exclusion criteria of the study were as follows: 1) ventilator dependence; 2) delayed removal of the patient from ventilator (>48 hours); 3) clinical signs of anastomotic leakage; 4) lack of cooperation of parents or physicians in the study; 5) twice feeding intolerance and 6) impossibility of feeding for any reason (e.g., increased bile secretion or apnea on day seven of surgery) in the control group. Based on the inclusion and exclusion criteria, demographic data of the infants were collected using data entry forms, which were developed based on previous studies and measured weight of infants using a digital scale with gram accuracy (TANITA model). During weight measurement, infants were minimally clothed, and weight of the diaper was deducted from the total baby weight. In addition, accuracy of the measurement device was controlled daily with a standard weight of 100 grams.
5 Ghorbani et al. Effects of Early Feeding on Weight of Operated Infant 70 Data entry forms consisted of a table to collect daily data on weight, nutrient intake and feeding modes within the past 24 hours. Moreover, data on anastomotic leakage within the first 48 hours of surgery were recorded in this table for the intervention and control groups (on day seven of surgery in the control group). The second section of data entry forms evaluated the weight of neonates one month after discharge from the hospital. Neonatal weight was measured by the researcher at the intensive care unit (ICU) of the clinic using similar scales, the reliability and validity of which had been confirmed. Required data in this regard were collected over an interval between the surgery and discharge, as well as one month after discharge from the hospital. After the surgery, infants who met the inclusion criteria were enrolled in the study. In the intervention group, non-anastomotic leakage was confirmed via chest X-ray 48 hours after the surgery. Following that, feeding by serum glucose (5%) (Low volume: 2cc/kg) was performed via a nasogastric tube every three hours based on the surgeon s expert opinion (8). After repeating this regimen three times, breastfeeding was started with the volume of 2cc/kg every two hours. At the surgeon s discretion, the nasogastric tube was removed 72 hours after the surgery in infants with feeding tolerance and lack of anastomotic leakage signs. In the presence of feeding tolerance at the mentioned breastfeeding volume, feeding continued with the same process based on the medical supervision of ICU fellowship (Table 1) (12). Since oral intake reached up to 100 ml/kg/d, equivalent calories were obtained from milk, and 60% of the received milk volume was deducted from the serum volume of the patient. Finally, parenteral nutrition was discontinued, while oral feeding continued. Infants were controlled by the researcher and nurses in terms of feeding intolerance (abdominal distention, hemodynamic changes, nausea and vomiting) during the feeding process. If the infant showed one of the mentioned criteria of feeding intolerance, fed up with not getting medical supervision Fellowship ICU but with very low volume cc 1 every two hours continued to maintain the intestinal enzyme evolution of intestinal function (13). On the following day, if the same volume was tolerated, feeding would continue (Table 1). If these manifestations persisted (or in the presence of anastomotic leakage), the infant would be kept fasting and excluded from the study. Since the morning after surgery until discharge from the neonatal intensive care unit (NICU), weight gain status of the infants was assessed daily by nurses using a scale at the beginning of the morning shift after diaper change. In this study, infants of the control group remained on routine fasting until six days after surgery and received parenteral nutrition. On day seven of surgery, chest X-ray was carried out on the infants using contrast agents to investigate anastomotic leakage. If no finding confirmed anastomotic leakage, the nasogastric tube would be removed at the surgeon s discretion, and oral feeding would continue in the intervention group. In addition, infants of the intervention group were evaluated daily in terms of body weight changes during NICU admission. To respect the rights of the patients in this study, the researcher was fully introduced to the parents of neonates before the intervention, and an overview of the study was presented as well. Moreover, parents were assured of the safety of all the procedures. As explained to the parents and ICU authorities and personnel, participation and withdrawal from the study were optional. Informed consent was obtained from all the parents before the study, and possible risk factors were considered in the exclusion criteria. In the presence of risk factors, the infant would be excluded from the study immediately to receive care under the supervision of surgeons and ICU fellowship. At the end of the study, one infant was excluded from the intervention group due to the malfunctioning of the chest tube and episodes of apnea during transfer to the operation room. In addition, another infant was excluded due to the lack of cooperation by the parents and surgeon. Finally, 18 infants remained in the intervention group. In the control group, one patient was excluded due to increased bile secretion on day eight after surgery, and another infant was eliminated due to apnea (severe respiratory distress associated with ventilator dependence). In total, 18 neonates remained in the control group. Data analysis was performed in SPSS version 16 using Kolmogorov-Smirnov and Shapiro-Wilk tests to assess the quantitative data for normal distribution. Moreover, descriptive statistics, including distribution index, central tendency index (mean and standard deviation) and frequency distribution, were used to describe neonatal characteristics in the intervention and control groups.
6 71 Evidence Based Care Journal, 6 (2): Independent T-test was used to analyze quantitative variables with normal distribution, and Chisquare test was applied for nominal variables, which were assessed in the study groups in terms of homogeneity. In addition, To compare clinical outcomes in cases where the normal distribution was Quantitative in both groups, independent t-test was used.in all statistical analyses, confidence interval and significance level were determined at 95% and 0.05, respectively. To compare clinical outcomes in cases where the normal distribution was Quantitative in both groups, independent t-test was used. Table 1. Feeding protocol in high-risk infants (12) Total daily volume Increase Volume every two hours (per hour) (ml/kg) Stage 12 cc/kg (increase up to 24 ml/kg/d) 36 ml/kg (increase up to 24 ml/kg/d) 60 ml/kg (increase up to 24 ml/kg/d) 84 ml/kg (increase up to 24 ml/kg/d) 108 ml/kg (increase up to 24 ml/kg/d) 132 ml/kg (increase up to 24 ml/kg/d) 156 ml/kg To be continued by paediatrician 8 Results In this study, mean age of 10 infants in the intervention group (2.8±1.7 days) was higher compared to the control group (2.0±1.1 days); however, this difference was not significant according to the results of independent T-test (P=0.27). Infants of the intervention and control groups were matched in terms of the mean age on admission (Table 3). Mean weight of the subjects in the intervention group (2558.1±337.4 grams) was higher compared to the control group (2547.6±85 grams); however, results of independent T-test showed no significant difference in this regard (P=0.47). Moreover, infants of the intervention and control groups were matched in terms of mean weight on admission. Mean gestational age in the intervention group (37.2±1.2 weeks) was slightly higher compared to the control group (37±1.0 weeks); however, results of independent T-test indicated no significant difference in this regard (P=0.56). Infants of the intervention and control groups were matched in terms of mean gestational age (Table 2). Table 2. Comparison of demographic characteristics of infants in intervention and control groups Groups Mean±SD Test Control Intervention Method Results Age (day) 2.0± ±1.7 Independent T-test P=0.27 Weight (gram) ± ±337.4 Independent T-test P=0.47 Gestational age (week) 37± ±1.2 Independent T-test P=0.56 Before feeding (the first 48 hours after surgery), mean daily weight gain in the intervention group was 17.8±3.7 grams, while it was 24.3±3.5 grams after feeding (48 hours after surgery). As for the control group, mean daily weight gain before feeding (before day seven of surgery) was 13.2±3.1 grams, while it was 17.1±1.6 grams after feeding (after day seven of surgery). The difference in the daily weight gain of the neonates was considered significant in both stages (P<0.05). One month after discharge from the hospital, mean weight gain in the intervention group was 731.9±58.1 grams, while it was 578.9±48.8 grams in the control group. In comparison with the mean weight on admission, this variable had a statistically significant difference between the two groups (P=0.030).
7 Ghorbani et al. Effects of Early Feeding on Weight of Operated Infant 72 Table 3. Comparison of mean weight gain of infants in intervention and control groups Groups Mean±SD Control (n=18) Intervention (n=18) Independent T-test Daily weight gain before feeding (gram) 13.2± ±3.4 P<0.001 Daily weight gain after feeding (gram) 17.1± ±3.5 P=0.010 Weight gain one month after discharge (gram) 578.9± ±58.1 P=0.030 Discussion According to the results of the present study, early feeding support could significantly increase the mean daily weight gain in neonates with EA. One month after discharge from the hospital, weight gain was observed to be higher in the intervention group compared to the control group, and this difference was statistically significant. In a study, Sashin Suri et al. (1999) evaluated the effects of early feeding after upper gastrointestinal tract surgery and concluded that weight loss was not significant in infants receiving early breastfeeding. In their study, 13 out of 14 infants weighing more than 1.5 kg were discharged from the hospital with no complications and need for readmission (14). In the mentioned study, the researchers emphasized that early feeding could prevent the metabolic complications associated with parenteral nutrition, as well as the high costs of treatment and hospitalization. Furthermore, it was stated that enteral feeding is physiologically preferred to parenteral nutrition. Findings of the study by Sashin Suri et al. are in congruence with the results of the current research. Although no advanced procedures were presented in the mentioned study to improve weight gain or weight loss, the findings indicated that early oral feeding prevents the complications caused by weight loss after upper gastrointestinal tract surgery. Moreover, in the research by Sashin Suri et al., feeding was initiated 48 hours after surgery, which is similar to the present study. In addition, selected patients in their study were infants undergoing upper gastrointestinal surgeries, which is relatively similar to our research since surgical repair of EA is part of upper gastrointestinal surgery. In the present study, a coherent program was applied for the daily measurement of body weight in the intervention and control groups. Considering that nutritional requirements and complications vary in different gastrointestinal surgeries, this study focused on the surgical repair of EA. Infants have a smaller body, higher growth rate, lack of development in several body systems, limited calorie reserves, and higher need for calorie intake after surgery (14). Postoperative fasting supplies infants with the required energy for wound healing through protein metabolism in muscles and stored body fat, which leads to the loss of weight and muscle tissues (15). According to the results of the present study, risk of oral feeding was high within 48 hours after surgery. As such, we attempted to provide the infants with the required energy for metabolism, growth and surgical repair through parenteral nutrition. During this period, the infants had daily weight gain of 17.8 grams. After applying oral feeding 48 hours after surgery, this rate reached 24.3 grams, which was significantly higher compared to the weight gain of infants before oral feeding. In the current research, daily weight gain in infants of the control group, who were kept fasting until day seven after surgery, was 13.1 grams, which was significantly lower than the intervention group. Therefore, it could be concluded that without oral feeding, the weight gain caused by parenteral nutrition would be lower than the ideal level. This could be due to the fact that weight gain declines with the age of infants because of increased caloric needs based on their weight. In another research entitled the "Long-term analysis of children with esophageal atresia and tracheoesophageal fistula", Little et al. ( ) confirmed concurrent delayed growth and weight loss in all the patients (16). Therefore, our findings regarding weight changes in the control group are consistent with the mentioned study. According to the results of the present study, weight of infants significantly increased daily in the intervention and control groups after oral feeding, which confirms the effect of nutrition on postoperative metabolic complications. However, it is noteworthy that even after daily oral feeding, weight gain in the control group was significantly lower compared to the intervention group. According to the information in Table 3, delayed weight gain was detected in infants one month after surgery, which is in line with the results of the study by Little et al. In this regard, our findings suggested that early feeding after EA surgery could affect long-term and short-term weight gain outcomes within at least one month after surgery.
8 73 Evidence Based Care Journal, 6 (2): One of the strengths of the present study was the initiation of low-volume breastfeeding in order to maintain the integrity of the small intestine, as well as the safety and nutritional needs of neonates, through the intestinal tract (7). Breast milk is the paramount nutritional option for early oral feeding in infants since it is the most wholesome, accessible and cost-efficient nutrient to meet the physiological needs of newborns. Furthermore, breast milk strengthens the emotional bond between the mother and infant since it contains multiple immunological factors, which protect the infant against various infections (17). It is predicted that early oral feeding could effectively reduce healthcare costs because with early oral feeding of the parenteral nutrition reduced and eventually stopped, which in practice it can reduce the duration of the use of parenteral nutrition., this method is cost-effective. Nevertheless, future studies are required as to compare the benefits and risks of this feeding method. Some of the limitations of our study were the long-term sampling to select the inclusion criteria and association of the disease with other disorders. Implications for Practice According to the results of this study, weight gain of infants with EA during postoperative fasting was significantly higher in the intervention group (48 hours after surgery) compared to the control group (seven days after surgery) after feeding and one month after discharge from the hospital. Therefore, it could be concluded that initiation of early feeding in the intervention group could prevent weight loss through reducing the period of fasting and increase weight gain, which positively continued up to one month after discharge in the neonates. Considering these favorable outcomes, it is recommended that future studies investigate the impact of this variable on early outcomes, such as feeding intolerance, leakage from surgical site and respiratory problems, as well as the long-term consequences, such as the narrowing of surgical site, fistula and reflux. Acknowledgments This article was extracted from an MA thesis conducted by the author at Mashhad University of Medical Sciences (No ) recorded in the Iranian Registry of Clinical Trials (code: IRCT N1). Hereby, we extend our gratitude to the Deputy of Research of Mashhad University of Medical Sciences for the financial support of this study. We would also like to thank all the nurses and physicians of the ICU of Dr. Sheikh Hospital of Mashhad for assisting us in this research project. Conflict of interest The authors declare that there is no conflict of interest. References 1. Wong D, Vilson D, Hakenbary M. esophageal atresia. Pediatric Nursing 2011;5; Hiradfar M, Bazrafshan A, Judi M, Gharavi M, Shojaeian R. An 8-year Experience of Esophageal Atresia Repair in Sarvar Children Hospital (Mashhad-IRAN).J Neonat.2011;3(1); Myrchrkhchyan M. Esophageal Atresia &Tracheo Esophageal fistula. Available from: http// Persian) 4.Chctcuti P, phelen P. Gastrointestinal Morbidity and Growth after Repair of Eesophageal Atresia and Tracheo-oesophageal Fistula. adcbmjcom. 2014;68; Pinheiro P, Simoes S,Pereira M. Current Knowledge on Esophageal Atresia. World J Gastroenterol Jul 28;18(28): pablo JV, Fernando LL, Restrepo I. Early Enteral Nutrition in Gastrointestinal Nutrition. 1996; 13(5); Wesson D. Nutrition in the Surgical Patient. Nutr Clin Pract, Apr-May;24(2): Meurling S. The Perioperative Nutritional Care of Neonates and Infants. J Nutr. 2002;44;8-11.
9 Ghorbani et al. Effects of Early Feeding on Weight of Operated Infant 74 9.Sweed J, Shoshany G. Insertion of a Soft Silastic Nasogastric Tube at Operation for Esophageal Atresia: A new technical Method. J Pediatr Surg. 1992;27(5): Kevin P, Nabil N, Burton H, Laurie A, Frank M, Timothy M. Transanastomotic Feeding Tubes in Repair of Esophageal Atresia. J Pediatr Surg. 1996;31(1): Teitelbaum D,Coran A. Perioperative Support in Pediatrics. Nutrition Support in Pediatric Surgery.1998;14(1); CormackB.NewbornServicesClinicalGuideline.Available from: May. 13.Ekingen G, Ceran C, Guvenc H, Tuzlaci A, Kahraman H. Early Enteral Feeding in Newborn Surgical Patients.2005;21(1) ; Suri S, Eradi B, Chowdhary S, Narasimhan K, Rao K. Early Postoperative Feeding and Outcome in Neonates Nutrition.2002;18; Pierro A. Metabolism and Nutritional Support in the Surgical Neonate. J Pediatr Surg Jun;37(6): Little D, Rescorla F, Scherer L. Long-Term Analysis of Children With Esophageal Atresia and Tracheoesophageal Fistula. J Pediatr Surg. 2003;38(6): Farhat A. Feeding in Premature Infants and Low Weight.Intensive Care in Newborns and Pediatrics Diseases; 2011;73-85(Persian)
An 8-year experience of esophageal atresia repair in Sarvar children hospital (Mashhad- IRAN)
 An 8-year experience of esophageal atresia repair in Sarvar children hospital (Mashhad- IRAN) Mehran Hiradfar* Ahmad Bazrafshan* Marjan Judi** Mohammad Gharavi*** - Reza Shojaeian**** * Associate professor
An 8-year experience of esophageal atresia repair in Sarvar children hospital (Mashhad- IRAN) Mehran Hiradfar* Ahmad Bazrafshan* Marjan Judi** Mohammad Gharavi*** - Reza Shojaeian**** * Associate professor
Long-gap Oesophageal Atresia
 Long-gap Atresia A guide for parents Nate (6 weeks old) Atresia Research Association Are there different types of OA? There are four main types of oesophageal atresia with or without TOF. These include
Long-gap Atresia A guide for parents Nate (6 weeks old) Atresia Research Association Are there different types of OA? There are four main types of oesophageal atresia with or without TOF. These include
Tracheoesophageal Fistula and Esophageal Atresia
 Patient and Family Education Tracheoesophageal Fistula and Esophageal Atresia What is tracheoesophageal fistula? The word fistula means abnormal connection. Tracheoesophageal fistula (TEF) is a condition
Patient and Family Education Tracheoesophageal Fistula and Esophageal Atresia What is tracheoesophageal fistula? The word fistula means abnormal connection. Tracheoesophageal fistula (TEF) is a condition
10/3/2012. Pediatric Parenteral Nutrition A Comprehensive Review
 Critical Care Nutrition Foundation for Moving Forward Justine Turner MD PhD Department of Pediatric Gastroenterology and Nutrition University of Alberta I have the following financial relationships to
Critical Care Nutrition Foundation for Moving Forward Justine Turner MD PhD Department of Pediatric Gastroenterology and Nutrition University of Alberta I have the following financial relationships to
Evaluation of Failure to Thrive in a Young Child: Case Example of Jeff. Andrew Hsi, MD, MPH Family Medicine Pediatric Grand Rounds, 8 August 2012
 Evaluation of Failure to Thrive in a Young Child: Case Example of Jeff Andrew Hsi, MD, MPH Family Medicine Pediatric Grand Rounds, 8 August 2012 Objectives for Presentation At the end of this talk; the
Evaluation of Failure to Thrive in a Young Child: Case Example of Jeff Andrew Hsi, MD, MPH Family Medicine Pediatric Grand Rounds, 8 August 2012 Objectives for Presentation At the end of this talk; the
POSTOPERATIVE CONGENITAL ESOPHAGEAL ATRESIA COMPLICATIONS: A REVIEW
 CHILDREN S HOSPITAL II POSTOPERATIVE CONGENITAL ESOPHAGEAL ATRESIA COMPLICATIONS: A REVIEW Dr. Nguyen Thuy Hanh Ngan Neonatal Department CONTENTS 1. Background 2. Classification 3. Management 4. Complications
CHILDREN S HOSPITAL II POSTOPERATIVE CONGENITAL ESOPHAGEAL ATRESIA COMPLICATIONS: A REVIEW Dr. Nguyen Thuy Hanh Ngan Neonatal Department CONTENTS 1. Background 2. Classification 3. Management 4. Complications
ENTERAL NUTRITION Identifying risk of patients for enteral feeding problems: Low risk: Moderate risk: High risk:
 ENTERAL NUTRITION Statement of best practice Feeding with mother s own breastmilk is protective against sepsis, NEC and death All mothers should be informed about this and strongly encouraged to express
ENTERAL NUTRITION Statement of best practice Feeding with mother s own breastmilk is protective against sepsis, NEC and death All mothers should be informed about this and strongly encouraged to express
An Overview of Bronchopulmonary Dysplasia and Chronic Lung Disease in Infancy
 An Overview of Bronchopulmonary Dysplasia and Chronic Lung Disease in Infancy Housekeeping: I have no financial disclosures Learning objectives: Develop an understanding of bronchopulmonary dysplasia (BPD)
An Overview of Bronchopulmonary Dysplasia and Chronic Lung Disease in Infancy Housekeeping: I have no financial disclosures Learning objectives: Develop an understanding of bronchopulmonary dysplasia (BPD)
Who Needs Parenteral Nutrition? Is Parenteral Nutrition An Appropriate Intervention?
 Who Needs Parenteral Nutrition? 1 Is Parenteral Nutrition An Appropriate Intervention? Key questions to ask with initial consultation Can the gastrointestinal (GI) tract be utilized? Can the GI tract be
Who Needs Parenteral Nutrition? 1 Is Parenteral Nutrition An Appropriate Intervention? Key questions to ask with initial consultation Can the gastrointestinal (GI) tract be utilized? Can the GI tract be
4/15/2014. Nurses Take the Lead to Improve Overall Infant Growth. Improving early nutrition. Problem Identification
 Nurses Take the Lead to Improve Overall Infant Growth Cathy Lee Leon, RN, BSN, MBA, NE-BC California Pacific Medical Center-San Francisco Improving early nutrition Standardized feeding protocol Problem
Nurses Take the Lead to Improve Overall Infant Growth Cathy Lee Leon, RN, BSN, MBA, NE-BC California Pacific Medical Center-San Francisco Improving early nutrition Standardized feeding protocol Problem
SOUTHERN WEST MIDLANDS NEWBORN NETWORK
 SOUTHERN WEST MIDLANDS NEWBORN NETWORK Hereford, Worcester, Birmingham, Sandwell & Solihull Title : Person Responsible for Review : Management of Gastro-Intestinal Stomata In Neonates R. Wragg & G.Jawaheer
SOUTHERN WEST MIDLANDS NEWBORN NETWORK Hereford, Worcester, Birmingham, Sandwell & Solihull Title : Person Responsible for Review : Management of Gastro-Intestinal Stomata In Neonates R. Wragg & G.Jawaheer
Minimal Enteral Nutrition
 Abstract Minimal Enteral Nutrition Although parenteral nutrition has been used widely in the management of sick very low birth weight infants, a smooth transition to the enteral route is most desirable.
Abstract Minimal Enteral Nutrition Although parenteral nutrition has been used widely in the management of sick very low birth weight infants, a smooth transition to the enteral route is most desirable.
Total Parenteral Nutrition and Enteral Nutrition in the Home. Original Policy Date 12:2013
 MP 1.02.01 Total Parenteral Nutrition and Enteral Nutrition in the Home Medical Policy Section Durable Medical Equipment Issue Original Policy Date Last Review Status/Date Return to Medical Policy Index
MP 1.02.01 Total Parenteral Nutrition and Enteral Nutrition in the Home Medical Policy Section Durable Medical Equipment Issue Original Policy Date Last Review Status/Date Return to Medical Policy Index
Congenital Digestive Malformation and Associated Anomalies
 EUROPEAN ACADEMIC RESEARCH Vol. VI, Issue 5/ August 2018 ISSN 2286-4822 www.euacademic.org Impact Factor: 3.4546 (UIF) DRJI Value: 5.9 (B+) Congenital Digestive Malformation and Associated Anomalies AUREL
EUROPEAN ACADEMIC RESEARCH Vol. VI, Issue 5/ August 2018 ISSN 2286-4822 www.euacademic.org Impact Factor: 3.4546 (UIF) DRJI Value: 5.9 (B+) Congenital Digestive Malformation and Associated Anomalies AUREL
Nutrition. By Dr. Ali Saleh 2/27/2014 1
 Nutrition By Dr. Ali Saleh 2/27/2014 1 Nutrition Functions of nutrients: Providing energy for body processes and movement. Providing structural material for body tissues. Regulating body processes. 2/27/2014
Nutrition By Dr. Ali Saleh 2/27/2014 1 Nutrition Functions of nutrients: Providing energy for body processes and movement. Providing structural material for body tissues. Regulating body processes. 2/27/2014
Guidelines for the Provision and Assessment of Nutrition Support Therapy in the Pediatric Critically Ill Patient: ASPEN-SCCM 2017
 Number of Patients Guidelines for the Provision and Assessment of Nutrition Support Therapy in the Pediatric Critically Ill Patient: ASPEN-SCCM 2017 Jorge A. Coss-Bu, MD Associate Professor of Pediatrics
Number of Patients Guidelines for the Provision and Assessment of Nutrition Support Therapy in the Pediatric Critically Ill Patient: ASPEN-SCCM 2017 Jorge A. Coss-Bu, MD Associate Professor of Pediatrics
Guideline scope Neonatal parenteral nutrition
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Neonatal parenteral nutrition The Department of Health in England has asked NICE to develop a new guideline on parenteral nutrition in
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Neonatal parenteral nutrition The Department of Health in England has asked NICE to develop a new guideline on parenteral nutrition in
EU RISK MANAGEMENT PLAN (EU RMP) Nutriflex Omega peri emulsion for infusion , version 1.1
 EU RISK MANAGEMENT PLAN (EU RMP) Nutriflex Omega peri emulsion for infusion 13.7.2015, version 1.1 III.1. Elements for a Public Summary III.1.1. Overview of disease epidemiology Patients may need parenteral
EU RISK MANAGEMENT PLAN (EU RMP) Nutriflex Omega peri emulsion for infusion 13.7.2015, version 1.1 III.1. Elements for a Public Summary III.1.1. Overview of disease epidemiology Patients may need parenteral
PRACTICE GUIDELINES WOMEN S HEALTH PROGRAM
 C Title: NEWBORN: HYPOGLYCEMIA IN NEONATES BORN AT 35+0 WEEKS GESTATION AND GREATER: DIAGNOSIS AND MANAGEMENT IN THE FIRST 72 HOURS Authorization Section Head, Neonatology, Program Director, Women s Health
C Title: NEWBORN: HYPOGLYCEMIA IN NEONATES BORN AT 35+0 WEEKS GESTATION AND GREATER: DIAGNOSIS AND MANAGEMENT IN THE FIRST 72 HOURS Authorization Section Head, Neonatology, Program Director, Women s Health
Simulation 3: Post-term Baby in Labor and Delivery
 Simulation 3: Post-term Baby in Labor and Delivery Opening Scenario (Links to Section 1) You are an evening-shift respiratory therapist in a large hospital with a level III neonatal unit. You are paged
Simulation 3: Post-term Baby in Labor and Delivery Opening Scenario (Links to Section 1) You are an evening-shift respiratory therapist in a large hospital with a level III neonatal unit. You are paged
NUTRITIONAL REQUIREMENTS
 NUTRITION AIMS To achieve growth and nutrient accretion similar to intrauterine rates To achieve best possible neurodevelopmental outcome To prevent specific nutritional deficiencies Target population
NUTRITION AIMS To achieve growth and nutrient accretion similar to intrauterine rates To achieve best possible neurodevelopmental outcome To prevent specific nutritional deficiencies Target population
Hypoglycemia. Objectives. Glucose Metabolism
 Hypoglycemia Instructor: Janet Mendis, MSN, RNC-NIC, CNS Outline: Janet Mendis, MSN, RNC-NIC, CNS Summer Morgan, MSN, RNC-NIC, CPNP UC San Diego Health System Objectives State the blood glucose level at
Hypoglycemia Instructor: Janet Mendis, MSN, RNC-NIC, CNS Outline: Janet Mendis, MSN, RNC-NIC, CNS Summer Morgan, MSN, RNC-NIC, CPNP UC San Diego Health System Objectives State the blood glucose level at
Pediatric Learning Solutions course alignment with the Neonatal/Pediatric Specialty Examination Detailed Content Outline.
 Pediatric Learning Solutions course alignment with the Neonatal/Pediatric Specialty Examination Detailed Content Outline. The following Pediatric Learning Solutions courses align to focus areas of the
Pediatric Learning Solutions course alignment with the Neonatal/Pediatric Specialty Examination Detailed Content Outline. The following Pediatric Learning Solutions courses align to focus areas of the
Neonatal Hypoglycemia
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Neonatal Hypoglycemia. These podcasts are designed to give medical students an overview of key topics in pediatrics.
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Neonatal Hypoglycemia. These podcasts are designed to give medical students an overview of key topics in pediatrics.
Recommendations for Hospital Quality Measures in 2011:
 Pediatric Measures: Recommendations for Hospital Quality Measures in 2011: Based on the input of a group of healthcare stakeholders, the following new hospital measures are recommended: 1) Home Management
Pediatric Measures: Recommendations for Hospital Quality Measures in 2011: Based on the input of a group of healthcare stakeholders, the following new hospital measures are recommended: 1) Home Management
Infection. Risk factor for infection ACoRN alerting sign with * Clinical deterioration. Problem List. Respiratory. Cardiovascular
 The ACoRN Process Baby at risk Unwell Risk factors Post-resuscitation requiring stabilization Resuscitation Ineffective breathing Heart rate < 100 bpm Central cyanosis Support Infection Risk factor for
The ACoRN Process Baby at risk Unwell Risk factors Post-resuscitation requiring stabilization Resuscitation Ineffective breathing Heart rate < 100 bpm Central cyanosis Support Infection Risk factor for
SWISS SOCIETY OF NEONATOLOGY. Unusual cause of pneumoperitoneum in a spontaneously breathing 1-day-old term infant
 SWISS SOCIETY OF NEONATOLOGY Unusual cause of pneumoperitoneum in a spontaneously breathing 1-day-old term infant March 2012 2 Berger TM, Winiker H, Neonatal and Pediatric Intensive Care Unit (BTM), Pediatric
SWISS SOCIETY OF NEONATOLOGY Unusual cause of pneumoperitoneum in a spontaneously breathing 1-day-old term infant March 2012 2 Berger TM, Winiker H, Neonatal and Pediatric Intensive Care Unit (BTM), Pediatric
Case Study. Synopsis. Introduction/overview. Hannah Roberts Specialist Paediatric Dietitian County Durham and Darlington Foundation Trust
 Case Study The use of a 1.5 kcal/ml whey peptide based feed to help promote gastric emptying and feed tolerance in a paediatric patient with neurodisability age y im ar Libr Hannah Roberts Specialist Paediatric
Case Study The use of a 1.5 kcal/ml whey peptide based feed to help promote gastric emptying and feed tolerance in a paediatric patient with neurodisability age y im ar Libr Hannah Roberts Specialist Paediatric
Gastroschisis Sequelae and Management
 Gastroschisis Sequelae and Management Mary Finn Gillian Lieberman, MD Primary Care Radiology Beth Israel Deaconess Medical Center Harvard Medical School April 2014 Outline I. Definition and Epidemiology
Gastroschisis Sequelae and Management Mary Finn Gillian Lieberman, MD Primary Care Radiology Beth Israel Deaconess Medical Center Harvard Medical School April 2014 Outline I. Definition and Epidemiology
CONTINUING EDUCATION COURSES
 CONTINUING EDUCATION COURSES FOR HEALTHCARE PROFESSIONALS Visit ANHI MISSION To connect and empower people through science-based nutrition resources to optimize health worldwide ANHI VISION To improve
CONTINUING EDUCATION COURSES FOR HEALTHCARE PROFESSIONALS Visit ANHI MISSION To connect and empower people through science-based nutrition resources to optimize health worldwide ANHI VISION To improve
The jury is still out: changes in gastroschisis management over the last decade are associated with both benefits and shortcomings
 Journal of Pediatric Surgery (2012) 47, 119 124 www.elsevier.com/locate/jpedsurg The jury is still out: changes in gastroschisis management over the last decade are associated with both benefits and shortcomings
Journal of Pediatric Surgery (2012) 47, 119 124 www.elsevier.com/locate/jpedsurg The jury is still out: changes in gastroschisis management over the last decade are associated with both benefits and shortcomings
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE SCOPE. Nutrition support in adults: oral supplements, enteral and parenteral feeding.
 NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE 1 Guideline title SCOPE Nutrition support in adults: oral supplements, enteral and parenteral feeding. 1.1 Short title Nutrition support 2 Background a) The National
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE 1 Guideline title SCOPE Nutrition support in adults: oral supplements, enteral and parenteral feeding. 1.1 Short title Nutrition support 2 Background a) The National
Mehmet Melek 1 and Ufuk Cobanoglu Introduction. 2. Material and Method
 Gastroenterology Research and Practice Volume 2011, Article ID 527323, 4 pages doi:10.1155/2011/527323 Methodology Report A New Technique in Primary Repair of Congenital Esophageal Atresia Preventing Anastomotic
Gastroenterology Research and Practice Volume 2011, Article ID 527323, 4 pages doi:10.1155/2011/527323 Methodology Report A New Technique in Primary Repair of Congenital Esophageal Atresia Preventing Anastomotic
Neonatal Intensive Care Unit Skills Checklist
 _ XXX-XX- Print Name Last 4 of SS # Date Completed Directions Please circle a value for each question to provide us and the interested facilities with an assessment of your clinical experience. These values
_ XXX-XX- Print Name Last 4 of SS # Date Completed Directions Please circle a value for each question to provide us and the interested facilities with an assessment of your clinical experience. These values
Gastrointestinal Feedings Post Op: What s the deal on beginning oral feedings?
 Gastrointestinal Feedings Post Op: What s the deal on beginning oral feedings? Kate Willcutts, DCN, RD, CNSC University of Virginia Health System Charlottesville, VA kfw3w@virginia.edu Objectives 1. Discuss
Gastrointestinal Feedings Post Op: What s the deal on beginning oral feedings? Kate Willcutts, DCN, RD, CNSC University of Virginia Health System Charlottesville, VA kfw3w@virginia.edu Objectives 1. Discuss
Provide guidelines for the management of mechanical ventilation in infants <34 weeks gestation.
 Page 1 of 5 PURPOSE: Provide guidelines for the management of mechanical ventilation in infants
Page 1 of 5 PURPOSE: Provide guidelines for the management of mechanical ventilation in infants
[No conflicts of interest]
![[No conflicts of interest] [No conflicts of interest]](/thumbs/86/94144068.jpg) [No conflicts of interest] Patients and staff at: Available evidence pre-calories Three meta-analyses: Gramlich L et al. Does enteral nutrition compared to parenteral nutrition result in better outcomes
[No conflicts of interest] Patients and staff at: Available evidence pre-calories Three meta-analyses: Gramlich L et al. Does enteral nutrition compared to parenteral nutrition result in better outcomes
Neonatal Airway Disorders, Treatments, and Outcomes. Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center
 Neonatal Airway Disorders, Treatments, and Outcomes Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center Disclosure I have nothing to disclose Neonatal and Pediatric Tracheostomy Tracheostomy
Neonatal Airway Disorders, Treatments, and Outcomes Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center Disclosure I have nothing to disclose Neonatal and Pediatric Tracheostomy Tracheostomy
Slow versus Fast Enteral Feed Advancements in Very Low Birth Weight Infants: A Randomized Controlled Trial. A. Salhotra and S.
 Original Article Slow versus Fast Enteral Feed Advancements in Very Low Birth Weight Infants: A Randomized Controlled Trial A. Salhotra and S. Ramji From the Neonatal Division, Department of Pediatrics,
Original Article Slow versus Fast Enteral Feed Advancements in Very Low Birth Weight Infants: A Randomized Controlled Trial A. Salhotra and S. Ramji From the Neonatal Division, Department of Pediatrics,
Wali R Johnson et. al. / International Journal of New Technologies in Science and Engineering Vol. 2, Issue 4, October 2015, ISSN
 Enteral Feeding via Percutaneous Endoscopic Gastrojejunostomy(PEGJ) Tubes Decreases Risk of Aspiration and Tube Dislodgement Related Complications Compared to PEGs. Wali R Johnson, MSIV, L Ray Matthews,
Enteral Feeding via Percutaneous Endoscopic Gastrojejunostomy(PEGJ) Tubes Decreases Risk of Aspiration and Tube Dislodgement Related Complications Compared to PEGs. Wali R Johnson, MSIV, L Ray Matthews,
Nutritional Support in the Perioperative Period
 Nutritional Support in the Perioperative Period Topic 17 Module 17.3 Nutritional Support in the Perioperative Period Ken Fearon Learning Objectives Understand the principles behind nutritional care for
Nutritional Support in the Perioperative Period Topic 17 Module 17.3 Nutritional Support in the Perioperative Period Ken Fearon Learning Objectives Understand the principles behind nutritional care for
Gastric Residuals in Preterm Infants
 Neonatal Nursing Education Brief: Gastric Residuals in the Preterm Infant https://www.seattlechildrens.org/healthcareprofessionals/education/continuing-medical-nursing-education/neonatalnursing-education-briefs/
Neonatal Nursing Education Brief: Gastric Residuals in the Preterm Infant https://www.seattlechildrens.org/healthcareprofessionals/education/continuing-medical-nursing-education/neonatalnursing-education-briefs/
Pediatric Surgery MUHC MCH Siste. Objectives of Training
 Preamble A rotation in Pediatric Surgery must give residents the opportunity to become familiar with the unique needs of infants and children as surgical patients. Some of the surgical diseases encountered
Preamble A rotation in Pediatric Surgery must give residents the opportunity to become familiar with the unique needs of infants and children as surgical patients. Some of the surgical diseases encountered
Nutrition in the preterm - current menu Dr Heena Hooker Consulting Neonatal Paediatrician Aga Khan University Hospital, Nairobi
 Nutrition in the preterm - current menu Dr Heena Hooker Consulting Neonatal Paediatrician Aga Khan University Hospital, Nairobi Outline O Background O Challenges in preterm nutrition O Parenteral Nutrition
Nutrition in the preterm - current menu Dr Heena Hooker Consulting Neonatal Paediatrician Aga Khan University Hospital, Nairobi Outline O Background O Challenges in preterm nutrition O Parenteral Nutrition
Efficacy of Breast Milk Gastric Lavage in Preterm Neonates. Archana B. Patel and Samiuddin Shaikh
 Research Papers Efficacy of Breast Milk Gastric Lavage in Preterm Neonates Archana B. Patel and Samiuddin Shaikh From the Department of Pediatrics and Clinical Epidemiology Unit, Indira Gandhi Medical
Research Papers Efficacy of Breast Milk Gastric Lavage in Preterm Neonates Archana B. Patel and Samiuddin Shaikh From the Department of Pediatrics and Clinical Epidemiology Unit, Indira Gandhi Medical
Neurodevelopmental Risk?
 Normal Newborn During transitional hypoglycemia normal newborns have an enhanced ketogenic response to fasting. Newborn brains have enhanced capability to use ketone bodies for fuel Allows newborns to
Normal Newborn During transitional hypoglycemia normal newborns have an enhanced ketogenic response to fasting. Newborn brains have enhanced capability to use ketone bodies for fuel Allows newborns to
Evidence-Based Update: Using Glucose Gel to Treat Neonatal Hypoglycemia
 Neonatal Nursing Education Brief: Evidence-Based Update: Using Glucose Gel to Treat Neonatal Hypoglycemia http://www.seattlechildrens.org/healthcare-professionals/education/continuing-medicalnursing-education/neonatal-nursing-education-briefs/
Neonatal Nursing Education Brief: Evidence-Based Update: Using Glucose Gel to Treat Neonatal Hypoglycemia http://www.seattlechildrens.org/healthcare-professionals/education/continuing-medicalnursing-education/neonatal-nursing-education-briefs/
Optimal Distribution and Utilization of Donated Human Breast Milk: A Novel Approach
 653738JHLXXX10.1177/0890334416653738Journal of Human LactationSimpson et al research-article2016 Original Research: Brief Report Optimal Distribution and Utilization of Donated Human Breast Milk: A Novel
653738JHLXXX10.1177/0890334416653738Journal of Human LactationSimpson et al research-article2016 Original Research: Brief Report Optimal Distribution and Utilization of Donated Human Breast Milk: A Novel
Oklahoma Dietetic Association. Ainsley Malone, MS, RD, LD, CNSD April, 16, 2008 Permissive Underfeeding: What, Where and Why? Mt.
 The What, Why and When of Permissive Ainsley Malone, MS, RD, CNSD Nutrition Support Team Mt. Carmel West Hospital Mt. Carmel West 500 bed academic center Non-physician based NST Dietitian, pharmacist and
The What, Why and When of Permissive Ainsley Malone, MS, RD, CNSD Nutrition Support Team Mt. Carmel West Hospital Mt. Carmel West 500 bed academic center Non-physician based NST Dietitian, pharmacist and
Original Effective Date: 9/10/09
 Subject: Oral and Tube Fed Enteral Nutrition Policy Number: MCR-070 *(This MCR replaces and combines MCG-070 & 071) Original Effective Date: 9/10/09 Revision Date(s): 6/29/12, 8/7/14 This MCR is no longer
Subject: Oral and Tube Fed Enteral Nutrition Policy Number: MCR-070 *(This MCR replaces and combines MCG-070 & 071) Original Effective Date: 9/10/09 Revision Date(s): 6/29/12, 8/7/14 This MCR is no longer
A Randomized Controlled Clinical Trial of Olive Oil Added to Human Breast Milk for Weight Gaining in Very Low Birth Weight Infants
 A Randomized Controlled Clinical Trial of Olive Oil Added to Human Breast Milk for Weight Gaining in Very Low Birth Weight Infants Elaheh Amini; M.D.,2, Mamak Shariat; M.D.,2, Fatemeh Nayeri; M.D.,2, Firuzeh
A Randomized Controlled Clinical Trial of Olive Oil Added to Human Breast Milk for Weight Gaining in Very Low Birth Weight Infants Elaheh Amini; M.D.,2, Mamak Shariat; M.D.,2, Fatemeh Nayeri; M.D.,2, Firuzeh
Acquired pediatric esophageal diseases Imaging approaches and findings. M. Mearadji International Foundation for Pediatric Imaging Aid
 Acquired pediatric esophageal diseases Imaging approaches and findings M. Mearadji International Foundation for Pediatric Imaging Aid Acquired pediatric esophageal diseases The clinical signs of acquired
Acquired pediatric esophageal diseases Imaging approaches and findings M. Mearadji International Foundation for Pediatric Imaging Aid Acquired pediatric esophageal diseases The clinical signs of acquired
Learning Objectives. At the conclusion of this module, participants should be better able to:
 Learning Objectives At the conclusion of this module, participants should be better able to: Treat asymptomatic neonatal hypoglycemia with buccal dextrose gel Develop patient-specific approaches to intravenous
Learning Objectives At the conclusion of this module, participants should be better able to: Treat asymptomatic neonatal hypoglycemia with buccal dextrose gel Develop patient-specific approaches to intravenous
WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)?
 WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)? The term gastroesophageal reflux describes the movement (or reflux) of stomach contents back up into the esophagus, the muscular tube that extends from the
WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)? The term gastroesophageal reflux describes the movement (or reflux) of stomach contents back up into the esophagus, the muscular tube that extends from the
NEONATAL INTENSIVE CARE SKILLS CHECKLIST
 NEONATAL INTENSIVE CARE SKILLS CHECKLIST NAME: DATE: Please check the appropriate letter of proficiency for the following types of clinical situations and equipment. GENERAL Gestational assessment Physical
NEONATAL INTENSIVE CARE SKILLS CHECKLIST NAME: DATE: Please check the appropriate letter of proficiency for the following types of clinical situations and equipment. GENERAL Gestational assessment Physical
Topics for discussion. Pediatric General Surgery. Physiology. Surgical Newborns. Neonatal Intestinal Obstruction
 Topics for discussion Pediatric General Surgery Professor General & Thoracic Surgery What makes Pediatric Surgery unique? Neonatal intestinal obstruction Abdominal wall defects Inguinal hernias Appendicitis
Topics for discussion Pediatric General Surgery Professor General & Thoracic Surgery What makes Pediatric Surgery unique? Neonatal intestinal obstruction Abdominal wall defects Inguinal hernias Appendicitis
Thoracoscopic repair of esophageal atresia with a distal fistula lessons from the first 10 operations
 Original paper Thoracoscopic repair of esophageal atresia with a distal fistula lessons from the first 10 operations Paweł Nachulewicz 1, Kamila Zaborowska 1, Błażej Rogowski 1, Anita Kalińska 1, Marzena
Original paper Thoracoscopic repair of esophageal atresia with a distal fistula lessons from the first 10 operations Paweł Nachulewicz 1, Kamila Zaborowska 1, Błażej Rogowski 1, Anita Kalińska 1, Marzena
Scott A. Lynch, MD, MPH,FAAFP Assistant Professor
 Scott A. Lynch, MD, MPH,FAAFP Assistant Professor Lynch.Scott@mayo.edu 2015 MFMER 3543652-1 Nutrition in the Hospital Mayo School of Continuous Professional Development 2nd Annual Inpatient Medicine for
Scott A. Lynch, MD, MPH,FAAFP Assistant Professor Lynch.Scott@mayo.edu 2015 MFMER 3543652-1 Nutrition in the Hospital Mayo School of Continuous Professional Development 2nd Annual Inpatient Medicine for
Small bowel atresia. Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families
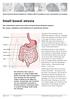 Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Small bowel atresia This information sheet from Great Ormond Street Hospital explains the causes, symptoms and treatment
Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Small bowel atresia This information sheet from Great Ormond Street Hospital explains the causes, symptoms and treatment
Introduction to Clinical Nutrition
 M-III Introduction to Clinical Nutrition Donald F. Kirby, MD Chief, Section of Nutrition Division of Gastroenterology 1 Things We Take for Granted Air to Breathe Death Taxes Another Admission Our Next
M-III Introduction to Clinical Nutrition Donald F. Kirby, MD Chief, Section of Nutrition Division of Gastroenterology 1 Things We Take for Granted Air to Breathe Death Taxes Another Admission Our Next
Int. Med J Vol. 6 No 1 June 2007 Enteral Nutrition In Intensive Care: Tiger Tube For Small Bowel Feeding In Acute Pancreatitis.
 Page 1 of 6 Int. Med J Vol. 6 No 1 June 2007 Enteral Nutrition In Intensive Care: Tiger Tube For Small Bowel Feeding In Acute Pancreatitis. Case Report Mohd Basri bin Mat Nor. Department of Anaesthesiology
Page 1 of 6 Int. Med J Vol. 6 No 1 June 2007 Enteral Nutrition In Intensive Care: Tiger Tube For Small Bowel Feeding In Acute Pancreatitis. Case Report Mohd Basri bin Mat Nor. Department of Anaesthesiology
Management of pharynx fistula after upper digestive tract instrumentation
 RESEARCH ROJSP 2017, Vol. 2 (issue 1): E 35-40. Management of pharynx fistula after upper digestive tract instrumentation Popescu Bogdan 1,2, Voiculescu Ștefan 1, Scăunașu Răzvan 1, Alexandra Oana Păun
RESEARCH ROJSP 2017, Vol. 2 (issue 1): E 35-40. Management of pharynx fistula after upper digestive tract instrumentation Popescu Bogdan 1,2, Voiculescu Ștefan 1, Scăunașu Răzvan 1, Alexandra Oana Păun
4/7/2015. Conflicts of Interest. None Heather Rush
 Heather Rush, APRN, CDE Wendy L Novak Diabetes Care Center Louisville, KY Conflicts of Interest None Heather Rush A conflict of interest exists when an individual is in a position to profit directly or
Heather Rush, APRN, CDE Wendy L Novak Diabetes Care Center Louisville, KY Conflicts of Interest None Heather Rush A conflict of interest exists when an individual is in a position to profit directly or
ETHICAL CHALLENGES IN PEDIATRIC PALLIATIVE CARE
 ETHICAL CHALLENGES IN PEDIATRIC PALLIATIVE CARE Disclosure I have no financial relationships to disclose. Glen Medellin, MD, FAAP, FAAHPM Learning Objectives Define the basic principles of ethical analysis
ETHICAL CHALLENGES IN PEDIATRIC PALLIATIVE CARE Disclosure I have no financial relationships to disclose. Glen Medellin, MD, FAAP, FAAHPM Learning Objectives Define the basic principles of ethical analysis
MORTALITY RISK FACTORS FOR NEONATAL INTESTINAL OBSTRUCTION
 Basrah Journal Of Surgery MORTALITY RISK FACTORS FOR NEONATAL INTESTINAL OBSTRUCTION Haithem Hussein Ali Almoamin MB, ChB, FIBMS Pediatric Surgery, Lecturer, Department of Surgery, College of Medicine,
Basrah Journal Of Surgery MORTALITY RISK FACTORS FOR NEONATAL INTESTINAL OBSTRUCTION Haithem Hussein Ali Almoamin MB, ChB, FIBMS Pediatric Surgery, Lecturer, Department of Surgery, College of Medicine,
Nutritional intervention in hospitalised paediatric patients. Dr Y.K.Amdekar
 Nutritional intervention in hospitalised paediatric patients Dr Y.K.Amdekar Back to basics Suboptimal nutrient intake is always dangerous in health and more so in disease to feed or not to feed is it a
Nutritional intervention in hospitalised paediatric patients Dr Y.K.Amdekar Back to basics Suboptimal nutrient intake is always dangerous in health and more so in disease to feed or not to feed is it a
Indian Pediatrics - Editorial
 Page 1 of 7 Home Past Issue About IP About IAP Feedback Links Author Info. Subscription Original Articles Indian Pediatrics 2004; 41:435-441 Slow versus Fast Enteral Feed Advancements in Very Low Birth
Page 1 of 7 Home Past Issue About IP About IAP Feedback Links Author Info. Subscription Original Articles Indian Pediatrics 2004; 41:435-441 Slow versus Fast Enteral Feed Advancements in Very Low Birth
Principles of nutrition in the preterm infant. Importance of nutrition: Undernutrition is very common in VLBW infants
 Principles of nutrition in the preterm infant Dr. S. Navarro-Psihas Pädiatrie IV, Klinik für Neonatologie Medizinische Universität Innsbruck Importance of nutrition: Undernutrition is very common in VLBW
Principles of nutrition in the preterm infant Dr. S. Navarro-Psihas Pädiatrie IV, Klinik für Neonatologie Medizinische Universität Innsbruck Importance of nutrition: Undernutrition is very common in VLBW
Wessex Care Pathway for Term Infants Referred with Bilious Vomiting for Exclusion of Malrotation
 Wessex Care Pathway for Term Infants Referred with Bilious Vomiting for Exclusion of Malrotation Version: 1.3 Issued: Review date: Author: Melanie Drewett The procedural aspects of this guideline can be
Wessex Care Pathway for Term Infants Referred with Bilious Vomiting for Exclusion of Malrotation Version: 1.3 Issued: Review date: Author: Melanie Drewett The procedural aspects of this guideline can be
Research Roundtable Summary
 Research Roundtable Summary 10 TENTH in a Series of Seminars on MCHB-funded Research Projects Early Cortisol Deficiency and Bronchopulmonary Dysplasia October 18, 1995 Parklawn Building Potomac Conference
Research Roundtable Summary 10 TENTH in a Series of Seminars on MCHB-funded Research Projects Early Cortisol Deficiency and Bronchopulmonary Dysplasia October 18, 1995 Parklawn Building Potomac Conference
The Case Begins. The case continued. Necrotizing Enterocolitis
 Bugs, Drugs and Things that go Bump in the Night From ghoulies to ghosties and long leggety beasties & things that go bump in the night, good lord deliver us Old Cornish Prayer Caring for premature infant
Bugs, Drugs and Things that go Bump in the Night From ghoulies to ghosties and long leggety beasties & things that go bump in the night, good lord deliver us Old Cornish Prayer Caring for premature infant
8/20/12. Discuss the importance of thermoregulation in the neonate.
 Sharon Rush MSN NNP-BC Discuss the importance of thermoregulation in the neonate. To maintain correct body temperature range in order to: Reduce oxygen consumption Reduce calorie expenditure Maximize metabolic
Sharon Rush MSN NNP-BC Discuss the importance of thermoregulation in the neonate. To maintain correct body temperature range in order to: Reduce oxygen consumption Reduce calorie expenditure Maximize metabolic
Neonatal Hypoglycemia. Presented By : Kamlah Olaimat 25\7\2010
 Neonatal Hypoglycemia Presented By : Kamlah Olaimat 25\7\2010 Definition The S.T.A.B.L.E. Program defines hypoglycemia as: Glucose delivery or availability is inadequate to meet glucose demand (Karlsen,
Neonatal Hypoglycemia Presented By : Kamlah Olaimat 25\7\2010 Definition The S.T.A.B.L.E. Program defines hypoglycemia as: Glucose delivery or availability is inadequate to meet glucose demand (Karlsen,
Post Discharge Nutrition. Jatinder Bhatia, MD, FAAP
 Post Discharge Nutrition Jatinder Bhatia, MD, FAAP Declaration of potential conflicts of interest Regarding this presentation the following relationships could be perceived as potential conflicts of interest:
Post Discharge Nutrition Jatinder Bhatia, MD, FAAP Declaration of potential conflicts of interest Regarding this presentation the following relationships could be perceived as potential conflicts of interest:
Amanda Hernandez FND October 17, 2011 Enteral Feeding Case Study
 Amanda Hernandez FND 430-001 October 17, 2011 Enteral Feeding Case Study 1. Nutritional Assessment to determine energy and protein needs Percent Usual Body Weight [(current body weight/usual body weight)
Amanda Hernandez FND 430-001 October 17, 2011 Enteral Feeding Case Study 1. Nutritional Assessment to determine energy and protein needs Percent Usual Body Weight [(current body weight/usual body weight)
Nutrition in the NICU ANDI MARKELL RD, LD
 Nutrition in the NICU ANDI MARKELL RD, LD PORTLAND, OREGON ANDI MARKELL NUTRITION CONSULTANT Conflict of Interest I had no conflict of interest until 2015 when I was asked to join the Nutrition Advisory
Nutrition in the NICU ANDI MARKELL RD, LD PORTLAND, OREGON ANDI MARKELL NUTRITION CONSULTANT Conflict of Interest I had no conflict of interest until 2015 when I was asked to join the Nutrition Advisory
Long Term Follow-up. 6 Month 1 Year Annual enter year #: What is the assessment date: / / Unknown. Is the patient alive? Yes No
 Long Term Follow-up 6 Month 1 Year Annual enter year #: What is the assessment date: / / Unknown Is the patient alive? Yes No Was an exam performed by a bariatric physician or PA/NP? Yes No Was the patient
Long Term Follow-up 6 Month 1 Year Annual enter year #: What is the assessment date: / / Unknown Is the patient alive? Yes No Was an exam performed by a bariatric physician or PA/NP? Yes No Was the patient
Division of Acute Care Surgery Clinical Practice Policies, Guidelines, and Algorithms: Enteral Nutrition Algorithm Clinical Practice Guideline
 Division of Acute Care Surgery Clinical Practice Policies, Guidelines, and Algorithms: Enteral Nutrition Algorithm Clinical Practice Guideline Original Date: 08/2011 Purpose: To promote the early use of
Division of Acute Care Surgery Clinical Practice Policies, Guidelines, and Algorithms: Enteral Nutrition Algorithm Clinical Practice Guideline Original Date: 08/2011 Purpose: To promote the early use of
Feeding the critically ill child
 Feeding the critically ill child Khaw Sia (1913 1984) Lee Jan Hau, MBBS, MRCPCH, MCI Children s Intensive Care Unit September 2018 1 2 3 No disclosures Outline Is there a need to optimize enteral nutrition?
Feeding the critically ill child Khaw Sia (1913 1984) Lee Jan Hau, MBBS, MRCPCH, MCI Children s Intensive Care Unit September 2018 1 2 3 No disclosures Outline Is there a need to optimize enteral nutrition?
Nutrition in the premie World
 SURVIVAL AND GROWTH NUTRITION ESSENTIALS Nutrition in the premie World DR VISH SUBRAMANIAN MD MRCP (UK) FAAP NEONATAL CRITICAL CARE MERCY CHILDRENS HOSPITAL., SPRINGFIELD MO Prematurity Nutritional Requirements
SURVIVAL AND GROWTH NUTRITION ESSENTIALS Nutrition in the premie World DR VISH SUBRAMANIAN MD MRCP (UK) FAAP NEONATAL CRITICAL CARE MERCY CHILDRENS HOSPITAL., SPRINGFIELD MO Prematurity Nutritional Requirements
Prediction Of Feeding Difficulties In Post- Operative Neonates
 Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine January 2014 Prediction Of Feeding Difficulties In Post- Operative
Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine January 2014 Prediction Of Feeding Difficulties In Post- Operative
An Overview on Pediatric Esophageal Disorders. Annamaria Staiano Department of Translational Medical Sciences University of Naples Federico II
 An Overview on Pediatric Esophageal Disorders Annamaria Staiano Department of Translational Medical Sciences University of Naples Federico II Case report F.C. 3 year old boy Preterm born from emergency
An Overview on Pediatric Esophageal Disorders Annamaria Staiano Department of Translational Medical Sciences University of Naples Federico II Case report F.C. 3 year old boy Preterm born from emergency
Fast Track Surgery and Surgical Carepath in Optimising Colorectal Surgery. R Sim Centre for Advanced Laparoscopic Surgery, TTSH
 Fast Track Surgery and Surgical Carepath in Optimising Colorectal Surgery R Sim Centre for Advanced Laparoscopic Surgery, TTSH Conventional Surgery Postop care Nasogastric tube Enteral feeds when ileus
Fast Track Surgery and Surgical Carepath in Optimising Colorectal Surgery R Sim Centre for Advanced Laparoscopic Surgery, TTSH Conventional Surgery Postop care Nasogastric tube Enteral feeds when ileus
By; Ashraf El Houfi MD MS (pulmonology) MRCP (UK) FRCP (London) EDIC Consultant ICU Dubai Hospital
 By; Ashraf El Houfi MD MS (pulmonology) MRCP (UK) FRCP (London) EDIC Consultant ICU Dubai Hospital Introduction The significance of nutrition in hospital setting (especially the ICU) cannot be overstated.
By; Ashraf El Houfi MD MS (pulmonology) MRCP (UK) FRCP (London) EDIC Consultant ICU Dubai Hospital Introduction The significance of nutrition in hospital setting (especially the ICU) cannot be overstated.
Experience. Initials Medical Staffing Network Rev. 06/15 F01201 NNICU 2 of 5
 Neonatal Intensive Care Unit Self Assessment Directions Please circle a value for each question to provide us and the interested facilities with an assessment of your clinical experience. These values
Neonatal Intensive Care Unit Self Assessment Directions Please circle a value for each question to provide us and the interested facilities with an assessment of your clinical experience. These values
PARENTERAL NUTRITION
 PARENTERAL NUTRITION DEFINITION Parenteral nutrition [(PN) or total parenteral nutrition (TPN)] is the intravenous infusion of some or all nutrients for tissue maintenance, metabolic requirements and growth
PARENTERAL NUTRITION DEFINITION Parenteral nutrition [(PN) or total parenteral nutrition (TPN)] is the intravenous infusion of some or all nutrients for tissue maintenance, metabolic requirements and growth
Melinda Elliott, MD Senior Director, Clinical Education and Professional Development, Prolacta Bioscience Neonatologist, Pediatrix Medical Group of
 Melinda Elliott, MD Senior Director, Clinical Education and Professional Development, Prolacta Bioscience Neonatologist, Pediatrix Medical Group of Maryland Breast Milk is for Babies, Cows Milk is for
Melinda Elliott, MD Senior Director, Clinical Education and Professional Development, Prolacta Bioscience Neonatologist, Pediatrix Medical Group of Maryland Breast Milk is for Babies, Cows Milk is for
ENTERAL NUTRITION IN THE CRITICALLY ILL
 ENTERAL NUTRITION IN THE CRITICALLY ILL 1 Ebb phase Flow phase acute response (catabolic) adoptive response (anabolic) 2 3 Metabolic Response to Stress (catabolic phase) Glucose and Protein Metabolism
ENTERAL NUTRITION IN THE CRITICALLY ILL 1 Ebb phase Flow phase acute response (catabolic) adoptive response (anabolic) 2 3 Metabolic Response to Stress (catabolic phase) Glucose and Protein Metabolism
Nutrition and Medicine, 2006 Tufts University School of Medicine Nutrition and Acute Illness: Learning Objectives
 Nutrition and Medicine, 2006 Tufts University School of Medicine Nutrition and Acute Illness: Learning Objectives Margo N. Woods, D.Sc. 1. Define protein-calorie, or protein-energy malnutrition (PEM) and
Nutrition and Medicine, 2006 Tufts University School of Medicine Nutrition and Acute Illness: Learning Objectives Margo N. Woods, D.Sc. 1. Define protein-calorie, or protein-energy malnutrition (PEM) and
Nutritional Issues in Cholestatic Disease
 THE HOSPITAL FOR SICK CHILDREN Nutritional Issues in Cholestatic Disease NASPGHAN-CPNP Joint Session Binita M. Kamath, MBBChir MRCP MTR Associate Professor Division of Gastroenterology, Hepatology and
THE HOSPITAL FOR SICK CHILDREN Nutritional Issues in Cholestatic Disease NASPGHAN-CPNP Joint Session Binita M. Kamath, MBBChir MRCP MTR Associate Professor Division of Gastroenterology, Hepatology and
The use of a 1.5kcal/ml whey peptide based feed to help promote gastric emptying and feed tolerance in a paediatric patient with neurodisability.
 The use of a 1.5kcal/ml whey peptide based feed to help promote gastric emptying and feed tolerance in a paediatric patient with neurodisability. Hannah Roberts Specialist Paediatric Dietitian County Durham
The use of a 1.5kcal/ml whey peptide based feed to help promote gastric emptying and feed tolerance in a paediatric patient with neurodisability. Hannah Roberts Specialist Paediatric Dietitian County Durham
PROTOCOL FOR PARENTERAL NUTRITION
 PROTOCOL FOR PARENTERAL NUTRITION Based on; Roberton s textbook of neonatology. 4 th edition. 2005. Sudha Chaudari and Sandeep Kumar.TPN in neonates. Indian Paediatrics. November 2006 Deepak Chawla, Anu
PROTOCOL FOR PARENTERAL NUTRITION Based on; Roberton s textbook of neonatology. 4 th edition. 2005. Sudha Chaudari and Sandeep Kumar.TPN in neonates. Indian Paediatrics. November 2006 Deepak Chawla, Anu
Professor Joseph HADDAD Pediatric Department Saint George Univ Hosp Balamand Univ Beirut Lebanon
 Nutrition & Growth in Premature Infant Professor Joseph HADDAD Pediatric Department Saint George Univ Hosp Balamand Univ Beirut Lebanon PART ONE : THE GROWTH OF THE PREMATURE INFANT ARE WE ON THE RIGHT
Nutrition & Growth in Premature Infant Professor Joseph HADDAD Pediatric Department Saint George Univ Hosp Balamand Univ Beirut Lebanon PART ONE : THE GROWTH OF THE PREMATURE INFANT ARE WE ON THE RIGHT
Product Catalog. Pediatric Learning Solutions. Listing of all current products (as of May, 2013) offered by Children's Hospital Association.
 Product Catalog Pediatric Learning Solutions Listing of all current products (as of May, 2013) offered by Children's Hospital Association. Acquired Heart Disease in Children WBT Acute Respiratory Distress
Product Catalog Pediatric Learning Solutions Listing of all current products (as of May, 2013) offered by Children's Hospital Association. Acquired Heart Disease in Children WBT Acute Respiratory Distress
A Crash Course in Failure to Thrive April 5, Kelly E. Wood, MD Clinical Assistant Professor Stead Family Department of Pediatrics
 A Crash Course in Failure to Thrive April 5, 2016 Kelly E. Wood, MD Clinical Assistant Professor Stead Family Department of Pediatrics Disclosures I have nothing to disclose Educational Objectives Define
A Crash Course in Failure to Thrive April 5, 2016 Kelly E. Wood, MD Clinical Assistant Professor Stead Family Department of Pediatrics Disclosures I have nothing to disclose Educational Objectives Define
NUTRITIONAL OPTIMIZATION IN PRE LIVER TRANSPLANT PATIENTS
 NUTRITIONAL OPTIMIZATION IN PRE LIVER TRANSPLANT PATIENTS ACHIEVING NUTRITIONAL ADEQUACY Dr N MURUGAN Consultant Hepatologist Apollo Hospitals Chennai NUTRITION IN LIVER FAILURE extent of problem and consequences
NUTRITIONAL OPTIMIZATION IN PRE LIVER TRANSPLANT PATIENTS ACHIEVING NUTRITIONAL ADEQUACY Dr N MURUGAN Consultant Hepatologist Apollo Hospitals Chennai NUTRITION IN LIVER FAILURE extent of problem and consequences
ESPEN Congress Florence 2008
 ESPEN Congress Florence 2008 PN Guidelines presentation PN Guidelines in pancreas diseases L. Gianotti (Italy) ESPEN Guidelines on Parenteral Nutrition: Pancreas L.Gianotti, R.Meier, D.N.Lobo, C.Bassi,
ESPEN Congress Florence 2008 PN Guidelines presentation PN Guidelines in pancreas diseases L. Gianotti (Italy) ESPEN Guidelines on Parenteral Nutrition: Pancreas L.Gianotti, R.Meier, D.N.Lobo, C.Bassi,
Lung Function Abnormalities Following Repaired Esophageal Atresia and Tracheoesophageal Fistula
 Bahrain Medical Bulletin, Vol. 27, No.4, December 2005 Lung Function Abnormalities Following Repaired Esophageal Atresia and Tracheoesophageal Fistula Hanaa Banjar, MD, FRCPC* Introduction: Esophageal
Bahrain Medical Bulletin, Vol. 27, No.4, December 2005 Lung Function Abnormalities Following Repaired Esophageal Atresia and Tracheoesophageal Fistula Hanaa Banjar, MD, FRCPC* Introduction: Esophageal
Apneas in Infants with Postconceptional Age bellow 60 Weeks Undergoing Herniorrhaphy
 Original Article Iran J Pediatr Apr 2014; Vol 24 (No 2), Pp: 179-183 Apneas in Infants with Postconceptional Age bellow 60 Weeks Undergoing Herniorrhaphy Mohamad Gharavi-Fard, MD; Mehryar Taghavi-Gilani,
Original Article Iran J Pediatr Apr 2014; Vol 24 (No 2), Pp: 179-183 Apneas in Infants with Postconceptional Age bellow 60 Weeks Undergoing Herniorrhaphy Mohamad Gharavi-Fard, MD; Mehryar Taghavi-Gilani,
NEC. cathy e. shin childrens hospital los angeles department of surgery university of southern california keck school of medicine
 NEC cathy e. shin childrens hospital los angeles department of surgery university of southern california keck school of medicine Necrotizing enterocolitis (NEC) the most common and most lethal disease
NEC cathy e. shin childrens hospital los angeles department of surgery university of southern california keck school of medicine Necrotizing enterocolitis (NEC) the most common and most lethal disease
