LANGERHANS CELL HISTIOCYTOSIS
|
|
|
- Morgan Warren
- 5 years ago
- Views:
Transcription
1 Review article DOI /p LANGERHANS CELL HISTIOCYTOSIS Nada KRSTOVSKI Medical Faculty University of Belgrade University Childrens Hospital Belgrade, Serbia Nada Krstovski Medical faculty University of Belgrade University Children s hospital Tirsova Belgrade Serbia nada.krstovski@udk.bg.ac.rs Tel.: Fax: Langerhans cell histiocytosis is a rare disease in children, its initial presentation is variable, the clinical course, prognosis and survival are mostly unpredictable. LCH is a proliferative disorder where pathologic Langerhans cells accumulate in a variety of organs. Historically, the nomenclature regarding this entity has been confusing because the disease was subcategorized as eosinophilic granuloma, Hand-Schüller-Christian disease and Abt-Letterer- Siwe disease, simply based upon the different clinical manifestations. This nomenclature remains valuable and preserves the important historic perspective of these disorders. Currently, LCH can be divided according to disease extent and localisation of the disease at the time of evaluation. The following clinical categories have been defined: single- or multi-system disease. This article summarizes the classification, history, pathophysiology, diagnostic criteria, different clinical manifestations, treatment, prognosis and long-term sequelae of LCH in children. Key words: Histiocytosis Children Langerhans cell histiocytosis Pediatric oncology Received: May 5, 2011 Accepted: July 11, 2011 Copyright 2011 by University Clinical Center Tuzla. for permission to publish: paediatricstoday@ukctuzla.ba Introduction Histiocytic disorders are defined as disorders caused by an abnormal accumulation of cells of the mononuclear phagocytic system (MFS), consisting of dendritic cells and macrophages. They include a wide range of different conditions that affect both children and adults (1). Histiocytic disorders are classified in the group of hematological diseases since dendritic and monocyte/macrophage cells are the main pathological substrate. There is still nosological confusion regarding histiocytic disorders considering the fact that histiocytes have many different 71
2 metabolic potential and line orientations, their ubiquitous nature, their role in the regulation of hematopoiesis, the role of immune and inflammatory response as well as the uncertain ontological origin of dendritic and monocyte/ macrophage cells. The same principle was formed as in the classification of lymphoid disorders and the latest classification of histiocyte disorders is based on information about their cellular origin and biological behaviour, based on pathological and immunochemical criteria (2, 3) (Figure 1). A working group of the International Society for Histiocytosis (HS) and the Committee for Histiocytic/Reticulum Cell Proliferation of the World Health Organization (WHO) continuously monitor new laboratory and clinical findings and accordingly pronounce a classification of histiocytic disorders (1,4). Histiocytic disorders are divided into two main groups: "diseases of different biological behaviour" and "malignant disorders" which are then subclassified to dendritic (antigen presenting cells) or monocyte-macrophage (antigen processing) cells disorders (Table 1). History The history of histiocytosis dates back to 1865, when Dr Thomas Smith published the case of four year old child with impetigo and three large bone defects on the calvary. At the same time Paul Langerhans described nonpigmented dendritic cells of the epidermis, which he considered initially to be nerveous and then corrected himself later. These unique histiocytes are now called Langerhans cells. Alfred Hand in 1893, Artur Schüller in 1915 and Henry Christian in 1919 independently of each other described patients with exophthalmos, polyuria and thirst (5, 6, 7). There is also the eponym, Hand Schüller Christian disease, which is still used to describe a child over two years old with symptoms of exophthalmos, diabetes insipidus (DI) and bone lesions of the skull. Dr Erich Letterer 1924 described a six-month old infant with fulminant nonleukemic reticuloendothelial system disorder (8). Nine years later, the Swedish physician Sture Siwe described similar symptoms in a 1.5 year old child. His Legend: CFU-GEMM- Colony Forming Unit-Granulocyte, Eritocyte, Megakariocyte, Monocyte, CFU-GM -. Colony Forming Unit-Granulocyte, Monocyte, CFU-DC/M - Colony Forming Unit-Denritic cell/monocyte, CFU-M - Colony Forming Unit-/Monocyte, LC Langerhans cell, IDC - interdigitating dendritic cell Figure 1 Histiocyte development 72
3 N. Krstovski Langerhans cell histiocytosis Table 1 Classification of Histiocytic Disorders (1) Disorders of varied biologic behaviour Dendritic cell related Langerhans cell histiocytosis Secondary dendritic cell processes Juvenile xanthogranuloma and related disorders Solitary histiocytomas of various dendritic cell phenotypes Macrophage related Hemophagocytic syndromes Primary Hemophagocytic lymphohistiocytosis Secondary hemophagocytic syndromes Infection-associated Malignancy-associated Other Rosai-Dorfman disease (sinus histiocytosis with massive lymphadenopathy) Solitary histiocytoma with macrophage phenotype Malignant disorders Monocyte-related Leukemias (FAB and revised FAB classifications) Monocytic leukemia M5A and B Acute myelomonocytic leukemia M4 Chronic myelomonocytic leukemia Dendritic cell related histiocyte sarcoma (localized or disseminated) Macrophage-related histiocytic sarcoma (localized or disseminated) work provided an overview of the literature and the disease is defined pathologically as a separate entity. He described the presence of marked splenomegaly, hepatomegaly, lymphadenopathy, localized bone tumours, bleeding tendency, anaemia and secondary generalized hyperplasia of macrophages, which do not contain lipids, in various organs (9). A few years later, Arthur Abt and Denenholc Edward published a paper showing 9 patients and a disease named Letterer Siwe. In 1940 two similar works appeared which described bone lesions. The first paper was written by the doctors, Sadao Otani and Ehrlich Josef, who named the disease as solitary granuloma of the bone. The second paper was written by Louis Lichtenstein and Henry Jaffe who called the disease eosinophilic granuloma (10, 11). In 1953 Luis Liechtenstein introduced the term histiocytosis X, bringing under the same heading eosinophilic granuloma, Hand-Schüller-Christian and Letterer-Siwe disease, indicating that they are the same clinical entity with a similar pathophysiological mechanism of origin. The next significant discovery was by Birbeck (Clive Stanley Michael Birbeck) in 1961, with a description of characteristic organelles seen under an electron microscope, initially called Langerhans bodies. Today they are called Birbeck granules. Christian Nezelof, a pathologist, finally in 1973 introduced the name Langerhans Cell Histiocytosis - LCH. He also became a founding member and the first president of the International Histiocyte Society (HS) established in 1985 in Philadelphia. This society is actively working on the standardization of nomenclature, clinical 73
4 and pathological criteria and provides the basic guidelines and recommendations for the treatment of this disease (12). Etiopathogenesis The pathogenesis of LCH is unclear. Still there is debate whether LCH is a neoplasm or a reactive disorder or immune dysfunction. The often spontaneous remission of the disease argues against its malignant nature which occurs even in patients with multiple changes in multiple organs, extensive secretion of numerous cytokines, a so-called cytokine storm, and the generally high survival rates of patients (2, 10, 13, 14). Also a number of genetic studies of DNA ploidy, karyotype, single nucleotide polimorphisms - SNP, characterization of gene expression (array based comparative genomic hybridization) have not shown the existence of significant and consistent abnormalities. These observations support the theory that LCH is a reactive disorder. On the other hand, pathological tissue infiltration of cells with clonal character, the occasionally lethal outcome of the disease and cytostatic therapy, which is primarily used for the treatment of malignant disease, supports the theory that LCH is a neoplasm. Clonality was identified in localized and in the multisystemic form of the disease (15). The identification of clonality does not mean malignancy. Pathologically, Langerhans cells are characterized by functionally immature immunophenotypes that can mature in vitro after exposure to CD40 ligand (16). There are data showing that there are certain specific regions of chromosomes that exhibit microsatellite instability and loss of heterozygosity, which is characteristic of cancer cells (17). Significant matches of genetic changes are observed in twins with LCH (18). Furthermore, an aberrant expression of proteins that influence the promotion of or block the cell cycle was detected in LCH (19). However, the typical genetic disorders found in LCH cells have not been identified in other cells. All these data suggest that LCH is a clonal proliferative disorder of the immature Langerhans cells, with varying clinical behaviour. Recent studies of gene expression of CD207+ (LCH cell marker) LCH lesions and epidermal CD207+ cells have showed a difference in expression over 2000 genes. These differences were found in genes involved in cell cycle regulation, apoptosis, signalling pathways and myeloid differentiation, but not in the expression of proliferative markers, so we can assume that the LCH is a disease of abnormal cell accumulation (20). The extensive variation in gene expression between these cell populations has prompted speculation that LCH cells develop from a population of cells that are different from the LCH cells of the epidermis. The hypothesis is that dendritic cells are recruited to specific anatomical sites where they interact with T cells, and they arise as a consequence of local immune modulation responsible for the characteristic lesions of LCH. Some evidence suggests an important role of immune dysfunction in the pathogenesis of LCH. In fact, immunochemical analysis of LCH lesions indicates that immature cells stimulate the expansion of LCH polyclonal regulatory T cells. These regulatory T cells can then inhibit the immune system (the action of interleukin (IL) -10) by preventing the regeneration of LCH lesions (21). The finding of high serum levels of proinflammatory IL 17A cytokine in patients with LCH has encouraged speculation that IL-17A is also involved in the pathogenesis of the disease. Further exploration of this phenomenon has shown that IL-17A causes the fusion of dendritic cells/langerhans cells in multinuclear giant cells, which then recruit other inflammatory cells and cause local destruction of tissue, creating the characteristic lesions of LCH. However, these findin- 74
5 N. Krstovski Langerhans cell histiocytosis gs have not been confirmed and the role of IL-17A in the pathogenesis of LCH remains still controversial (21, 22). Some studies have shown that the expression of vascular endothelial growth factor - VEGF, Bcl-2 family proteins and FADD, FLICE and FLIP protein in the Fas signalling path may be involved in the pathogenesis of LCH. E-cadherin-beta-katenin-Wnt signalling pathway is also involved in the pathogenesis of LCH. Disturbance of regulation of E-cadherin is related to disease dissemination (23). Epidemiology The prevalence of LCH is approximately 1:50,000, with an incidence of about 5-10 cases per year per million children under the age of 15. Male children are affected more often, the relationship of the disease is 2:1 in favour of male children. LCH affects primarily infants and children, while in adults the disease occurs significantly less frequently (3). Clinical Manifestations Symptoms and signs of LCH vary depending on which organs are infiltrated with Langerhans and associated immunoreactive cells. Bone, skin, teeth, gums, ears, endocrine organs, lungs, liver, spleen, lymph nodes, bone marrow, CNS (pituitary/hypothalamic regions) and other organs may be affected by the pathological process and manifest dysfunction as a result of cellular infiltration. With this wide spectrum of clinical manifestations, the division is fairly traditional. Forms such as eosinophilic granuloma, Hand-Schüller- Christian disease and Abt-Letterer-Siwe disease only have historical significance but are still often used in everyday clinical practice. Multifocal or solitary eosinophilic granuloma is mainly seen in older children and young adults, usually within the first three decades of life. The incidence peaks between 5 and 10 years. This form of LCH is approximately 60% to 80% of LCH. Hand-Schüller-Christian disease is a multisystemic form of the disease, seen in all age groups, most often described in younger children, aged 2 to 5 years. This form of the disease is found in 15% to 40% of all patients with LCH. Abt-Letterer-Siwe disease is the rarest (10% of cases) and most severe form of LCH. Typically, patients are younger than 2 years with a rough seborrhoeic and ekcematoid skin rash which sometimes is purpuric, involving mostly the head, ear canal, abdominal wall, intertriginated region, face and neck. Today, patients with LCH, for decisions about treatment, are stratified into one of two groups depending on the number of affected organs: the involvement of an organ/organic system, Single System, SS-LCH or multisystem organ involvement - MS-LCH (Table 5). Bones Bone lesions are usually manifested by swelling and pain of the affected region during exercise. The most often affected are the flat bones, skull, ribs, pelvis and shoulder blade, while the hand and feet bones are rarely affected. Complications of osteolytic lesions are anatomically defined, for example, chronic middle ear inflammation is caused by mastoid and petrous infiltration of the temporal bone. Inflammation of the external ear canal are also seen (24). Exophthalmos is due to the presence of a tumour in the orbital cavity and infiltration of the roof and lateral wall orbital cavity (skeletal involvement, although not always found). Infiltration of the orbit can cause loss of vision or strabismus. Periorbital infiltration may cause proptosis. The skull can be extensively infiltrated, with many irregular fields that give the appearance of the so-called geographical fields. The long bones and lumbosacral regions of the spinal column are less commonly affected, usu- 75
6 ally the front of the vertebral body. The spread of infiltrate into the medullary canal of the long bones can cause destruction of the cortex which stimulates the formation of periosteal reaction and swelling of the soft tissue. Differential diagnoses include Ewing's sarcoma, bone lymphoma, benign bone tumour and, cysts and infections. Oral involvement is manifested with gum and palatal infiltration. Dental radiography can show characteristic floating teeth. The erosion of the gingiva causes premature eruption, decay and tooth loss. Bone involvement is seen in % of LCH patients. Radiography is the first method of choice for the detection of bone lesions. The lesions are sharply marginated, round or oval, and usually have edges that give the appearance of depth (24) (Figure 2). in about 10% of children, mainly in male infants. Spontaneous regression is common in such cases. Rarely, the disease may be manifested only by deep subcutaneous nodules, as previously described Hashimoto-Pritzker syndrome. LCH of the skin is often misdiagnosed as seborrheic dermatitis and delayed diagnosis is common. Lymph nodes The lymph nodes are affected at the presentation of the disease in less than 10% of patients and usually as part of disseminated disease or as part of the local involvement of the skin or bones. The neck lymph nodes are affected most often. Sometimes a massive increase in the lymph nodes is seen. LCH may have a strictly nodal presentation and should not be identified with sinus histiocytosis with massive lymphadenopathy, also known as Rosai-Dorfman disease. This form of LCH is characterized by a significant increase in several groups of lymph nodes, with little or no other signs of disease (24). Figure 2 Skull bone lesions Skin The skin is affected in one third of children with LCH (25). The areas most often affected are the scalp and folds (groin, perianal area, neck and axilla). The rash can be maculopapular or nodulopapular. Ulcers can occur, especially in intertriginous regions. Ulcers and other skin damage may be the entry place for the infection which can cause sepsis. Isolated cutaneous forms of LCH have been described in children and adults. They occur Bone marrow Although pancytopenia is common in patients with a disseminated form of the disease, bone marrow infiltration of Langerhans cells (not normally found in bone marrow) is rarely seen (26). Liver and spleen Although enlargement of the liver is common in patients with the disseminated form of the disease, the causes of this increase are not yet fully understood. Systemic inflammatory hyperactivation of the monocyte macrophage system can lead to Kupffer cell hyperplasia. Liver infiltration by Langerhans cells has to be histologically documented because in some cases it is the main cause of liver en- 76
7 N. Krstovski Langerhans cell histiocytosis largement. Liver enlargement can be caused by massive periportal lymphadenomegaly with cholestatic hepatomegaly. Persistent infiltration of the liver initially causes mild cholestasis, portal infiltration, and then cholangitis, which can progress to fibrosis (sclerosing cholangitis) and biliary cirrhosis. This damage can occur regardless of whether the disease is active. Liver transplantation may be indicated in patients with LCH (27). An enlarged spleen is seen in at least 5% of patients at the beginning of the disease. Lungs Pulmonary disease is diagnosed in almost half of children with MS-LCH. Isolated pulmonary LCH is usually seen in young adults in the third or fourth decade of life and occasionally in adolescents. The clinical picture varies. It can be detected on radiography during clinical assessment of patients. Coughing and dyspnea are commonly seen. The disease can have severe, chronic course and is often clinically manifested as pneumothorax. Smoking has a significant impact on the occurrence of primary pulmonary histiocytosis. The course of the disease is usually mild, although fulminant forms are described. The radiograph picture varies, from diffuse infiltration as bilateral interstitial pneumonia, to changes which are described as a "honeycomb lung" (Figure 3). Gastrointestinal system Involvement of the gastrointestinal tract is not common and ranges from 2% to 3% (28). Although some children with a systemic form of LCH lose weight, intestinal malabsorption is not always the cause. Vomiting, diarrhoea or enteropathy with protein loss are rare and gastrointestinal LCH has to be confirmed histologically, by bowel biopsy Insipid diabetes and endocrine system Diabetes insipidus (DI) occurs in 5% to 40% of patients with LCH. Most cases of DI occur in children with the systemic form of the disease and bone involvement of the skull and orbit. Polydipsia and polyuria as initial symptoms of LCH are found in less than a third of children. Most children develop DI within four years of diagnosis. DI occurs due to infiltration of the hypothalamus with or without involvement of the pituitary gland. DI can occur at any time during the LCH disease. Patients with LCH should be familiar with the symptoms of DI in order to avoid serious complications due to dehydration and electrolyte imbalance (29). Low growth is seen in up to 40% of children with the systemic form of LCH. The chronic course of the disease and steroid therapy play an important role in the development of this disorder. Short stature may also be due to damage of the anterior pituitary gland and growth hormone deficiency, which can occur in at least half of patients with early signs of pituitary dysfunction. Other endocrine manifestations may occur, such as hypogonadism and hyperprolactinemia. Infiltration of the pancreas and thyroid gland has also been described (30). Figure 3 Lung LCH Central nervous system Involvement of the central nervous system (CNS), without the hypothalamus and pituitary region is among the worst forms of LCH and is seen in less than 1% of children with LCH. Most patients with CNS involvement 77
8 also have skull, orbit or mastoid infiltration. Nuclear magnetic resonance imaging is the method of choice for identification of CNS lesions. The hypothalamus-pituitary region is the most common site of lesions in the CNS, followed by the cerebellum, pons and cerebral hemispheres. Lesions of the basal ganglia, spinal cord and optic nerve have also been described. CNS involvement is usually manifest many years after onset. Infiltrative and atrophic lesions of the cerebellum and pons often lead to severe sequelae, which are characterized primarily as neurodegenerative. The aetiology of this neurodegenerative process is unknown but is believed to be an immunemediated paraneoplastic response that occurs as a consequence of cytokines due to occult cerebellar infiltration of LCH cells (31). Prognosis Prognosis depends on the number of affected organs and the degree of dysfunction of involved organs (32). Adolescents or adults with a solitary bone lesions have the best prognosis, while infants with a large number of affected organs have the worst prognosis. Children older than 2 years have a good prognosis, whereas patients younger than two years have less favourable outcome. Age itself is not of prognostic significance but younger children usually have more affected organs, which show some degree of dysfunction. Involvement of less than four organic systems is a relatively good prognostic sign. Dysfunction of the liver, spleen and bone marrow is an extremely important predictor of unfavourable outcome (24). When LCH occurs after 65 years of age, the prognosis is poor regardless of the number and type of affected organs. In assessing the outcome of the disease it is necessary to distinguish organ dysfunction from organ involvement without functional disorder (eg, hypoproteinemia, hyperbilirubinemia vs hepatomegaly), because involvement is not itself always a negative prognostic sign as a dysfunction. Histopathology The diagnosis of LCH is based on histological and immunophenotypic examination of biopsymaterial, usually bone, affected by a pathological process. LCH is characterized by a pathological lesion of mixed cellular infiltrate. The main characteristic of the disease is the proliferation and accumulation of immature Langerhans cells, which do not show cellular atypia characteristic of most malignant diseases and variable number of macrophages, T cells, aeosinophils and multinucleate giant cells. Langerhans cells are characterized by Birbeck granules, which are seen ultrastructurally as pentalaminar tennis racquet-shaped structures (33). The classic diagnostic criteria, defined in 1987, is the presence of Birbeck granules (BG) on the electron microscope and immunochemical demonstration of CD1 +. Today it is easier to prove the presence of BG by immunochemical staining of langerin (CD207). Langerin is a relatively new monoclonal antibody directed to a type II transmembrane C-type lectin. It was shown that Langerin expression confirms the presence of BG and ultrastructural demonstration of these granules is no longer set as the gold standard for definitive diagnosis of LCH. These criteria formally verify HS (34, 35). The histopathological findings in patients with localized and systemic clinical forms of the disease are the same and attempts to define favourable and unfavourable histologic forms have failed. Lesions in patients with aeosinophilic granuloma are similar if not identical, to those in the multisystem disease (24). Differential diagnosis Differential diagnosis of LCH depends on the clinical presentation of the disease. It includes immunodeficiency syndromes with graft-versus-host disease (GVHD), viral infections, infiltrative malignancies such as leukaemia, lymphoma or metastasis of solid 78
9 N. Krstovski Langerhans cell histiocytosis tumours, storage disease, congenital infections, benign and malignant bone tumours and cysts, papular xanthoma etc. Work up After the diagnosis, along with medical history and physical examination it is necessary to perform complete, clinical, laboratory and radiological investigations in order to identify all the affected places (Table 2). The medical history must be detailed and particular attention should be paid to pain, swelling, skin changes, otorrhoea, ear, fever, loss of appetite, diarrhoea, changes in activity level, polydipsia, polyuria, fatigue, smoking, changes in behaviour and neurological changes. Physical examination must also be detailed, it is necessary in all patients to determine pubertal status, to perform dental examination, the characterization of changes to the skin, to pay attention to the presence of jaundice, oedema, lymphadenopathy, secretions from the ear, lesions in the genital area and anal mucosa, tachypnoea, intercostal feeding space, ascites, liver and spleen size. For neurological evaluation (the presence of cranial nerve abnormalities, loss of deep muscle reflexes, visual disturbances and cerebellar dysfunction) it is necessary to do a detailed neurological examination and appropriate specific tests. Laboratory tests include complete blood count, routine biochemical analysis, coagulation treatment, abdominal ultrasound and radiography of the complete skeleton. For a definitive diagnosis of DI, measurement of osmolality and electrolytes in serum and urine before and after a few hours of water deprivation should be performed. The level of vasopressin may be measured in order to document the vasopressin deficiency. Testing of infants and young children should be carefully monitored in hospital conditions to avoid severe dehydration. Finally, desmopressin acetate (DDAVP) is applied in order to achieve an increase in urine concentration. These tests are done in all children with LCH. Other tests, such as dental panoramic Table 2 Recommended baseline evaluation upon diagnosis LCH (35) Full blood count Haemoglobin, white blood cell and differential count, platelet count Blood chemistry: - Total protein, albumin, bilirubin, ALT(SGPT), AST(SGOT), alkalinephosphatase, γgt - BUN, creatinine, electrolytes - Ferritin Coagulation studies - INR/PT, APTT/PTT, fibrinogen Early morning urine sample - Specific gravity and osmolality Abdominal ultrasound - Size and structure of liver and spleen Chest radiograph - Skeletal radiograph survey* INR= International Normalized Ratio; PT= Prothrombin time; APTT= activated partial thromboplastin time; PTT= partial thromboplastin time. *Functional imaging such as bone scan is optional and can be performed in addition to skeletal survey. PET scan has proven to be the most sensitive functional test used in the identification of LCH lesions and in evaluating patient response to therapy. However, PET scan is currently expensive and not widely available (36) 79
10 Table 3 Laboratory investigations, imaging and specialized clinical assessments recommended for specific clinical scenarios Indication Assessment/Test - Bicytopenia, pancytopenia or persistent - Bone marrow aspirate or trephine biopsy single cytopenia - Liver dysfunction - Liver biopsy only recommended if there is clinically significant liver involvement and the result will alter treatment (i.e. to differentiate between active LCH and sclerosing cholangitis) - Lung involvement (abnormal CXR or symptoms/signs suggestive for lung involvement) - Abnormal lung CT and findings not characteristic for LCH - Suspected craniofacial bone lesions including maxilla and mandible - Lung high resolution computed tomography (HR-CT) Lung function test (if age appropriate) - Bronchoalveolar lavage (BAL): >5 % CD1a positive cells in BAL fluid is diagnostic in non-smokers - Lung biopsy (if BAL is not diagnostic) - MRI of head* - Suspected vertebral lesions - MRI of spine (to exclude spinal cord compression) - Suspected endocrine abnormality (i.e. short stature, growth failure, polyuria, polydipsia, hypothalamic syndromes, precocious or delayed puberty) - Aural discharge or suspected hearing impairment/mastoid involvement - Unexplained chronic diarrhoea, failure to thrive, or evidence of malabsorption - Endocrine assessment (including water deprivation test and dynamic tests of the anterior pituitary and thyroid) - Formal hearing assessment, MRI of head*, HR- CT of temporal bone - Endoscopy and biopsy *MRI of head should include the brain, hypothalamus - pituitary axis and all craniofacial bones. The use of intravenous contrast (Gadolinium DTPA) is mandatory. X radiography, pulmonary function tests, CT and NMR of the brain and middle ear, and bone marrow examination should be done if there is suspected involvement of certain organs (Table 3). The criteria for the definition risk organ involvement gave HS (Treatment guidelines 2009) (35). Therapy As our knowledge about the effectiveness of certain therapeutic modalities progressed so the therapy changed. The generally accepted standard for initial treatment of patients with LCH is to use the least toxic therapy. Patients with the diagnosis of potentially life-threate- ning signs and symptoms or development of serious pathological conditions require the application of aggressive treatment. Such an individual approach to treatment emphasizes the need for implementation of clinical protocols in which the optimal therapy is applied to patients by aligning risk groups based on carefully balanced risk assessment. HS has initiated a randomized clinical trial in which to test the effectiveness of certain drugs, vinblastine and corticosteroids first, and then to classify patients into risk groups to predict the outcome of disease. Based on the results of several clinical studies, a widely accepted system for the disease classifying has been developed and treatment guidelines were published in 2009 (35). (Table 4 and 5). 80
11 N. Krstovski Langerhans cell histiocytosis Table 4 Definition of risk organ involvement Hematopoietic involvement: (with or without bone marrow involvement*) Spleen involvement Liver involvement Lung involvement At least 2 of the following: Anaemia: haemoglobin <10 g/dl, infants <9 g/dl (not due to other causes; e.g. iron deficiency) Leukocytopenia: leukocytes <4.0 Trombocitopenija: trombociti < /l Enlargement >2 cm below costal margin in the midclavicular line Enlargement >3 cm below costal margin in the midclavicular line and/ or liver dysfunction (i.e. hypoproteinemia <55 g/l, hypoalbuminemia <25 g/l not due to other causes) and/or histopathological diagnosis Typical changes on HR-CT and/or histopathological/cytological diagnosis *Bone marrow involvement is defined as demonstration of CD1a positive cells on bone marrow smears. Table 5 Clinical classification of LCH (35) Multisystem LCH (MS-LCH) - Two or more organs/systems involved, with or without involvement of Risk Organs Single System LCH (SS-LCH) - One organ/system involved (unifocal or multifocal) - Bone: unifocal (single bone) or multifocal (>1 bone) - Skin - Lymph node (not the draining lymph node of another LCH lesion) - Lungs - Hypothalamic-pituitary/Central nervous system - Other (e.g. thyroid, thymus) Table 6 Localisations and disease extent categories are considered indications for systemic therapy SS LCH with CNS-risk lesions SS LCH with multifocal bone lesions (MFB) SS LCH with special site lesions MS-LCH - with/without involvement of risk organs Initial treatment - the involvement of one organ system (SS-LCH) There is a very high likelihood of spontaneous resolution and a favourable outcome for patients with SS-LCH disease with skin or bone involvement. Local therapy is sufficient. Further treatment may be necessary only in certain circumstances (Table 6). Bone lesions heal spontaneously, usually within a few months to years. In most cases of bone lesions, curettage and biopsy leads to diagnosis and the healing process begins. Surgical resection is usually not necessary and can lead to deformity. The criteria for further treatment are pain, risk of deformity, dysfunction due to infiltration or secondary pathological fractures, prevention of epifiseal extensions and neurological signs. In these cases local measures might be applied, such as surgical resection, intralesional corticosteroids or low doses of radiation. Intralesional infiltration of corticosteroids is effective in relieving pain and for the process of healing 81
12 (37). Today, radiation therapy is reserved for emergencies, to prevent serious damage such as optic nerve or spinal cord compression (38) Special sites - In certain situations, such as cervical vertebra and the second vertebral lesions with intraspinal propagation of soft tissue, abnormal tissue is found on functionally and anatomically critical sites. Local therapy (biopsy and curettage) of the region carries a significant risk of a life-threatening condition and permanent nerve damage. Those lesions are considered as "special places". Application of chemotherapy in isolated involvement of the special sites is indicated. Vertebral lesions, such as vertebra plana (spondylitis in which the vertebral body is reduced to a sclerotic disk) without infiltration of soft tissues do not come into this group. CNS risk lesions - Recent findings indicate that long-term involvement of the skull bones (except the calvary, such as the craniofacial bones, involvement of the eyes, ears and mouth predispose to DI appearance (39). Craniofacial bone involvement includes changes in the orbital, temporal, mastoid, sphenoidal, zygomatic or ethmoidal bones, maxilla and paranasal sinuses, or cranial fossa, with intracranial propagation of soft tissue. Eye involvement is defined if there are proptosis, exophthalmos or lesions in the orbit, zygomatic or sphenoidal bones. Ear involvement is defined if there is external otitis, otitis media, otorrhoea or changes in the temporal bone, mastoid or petrous bone. Involvement of the oral cavity is defined if there is a lesion on the oral mucosa, gums, palatal bone, maxilla and mandible. Patients with the MFB (multifocal bone involvement) form of the disease have a favourable prognosis (survival of 100%), but they also have a high propensity for reactivation of disease (30-50%) and permanent consequences. The probability that these patients will develop DI, other endocrinopathies and parenchymal diseases of the brain is 40%. The greatest risk for severe disabilities is parenchymal brain disease in the basal ganglia and cerebellum. The therapy in this group of patients is used for the prevention of reactivation of disease, disability and permanent consequences. Data from nonrandomized prospective DAL-HX 83 and DAL-HX 90 studies show the favourable effect of chemotherapy, vinblastine, prednisone and 6-mercaptopurine in reducing the incidence of reactivation of the disease and frequency of permanent consequences compared to historical controls (40). Based on these data, the HS recommended chemotherapy in these patients Disease localised in the skin, especially in infants, most often resolves spontaneously so treatment is not necessary. In severe forms, corticosteroids are applied locally. Disseminated and very severe forms of skin refractory to corticosteroids are treated with phototherapy, topical mustin application or even chemotherapy (41). Initial treatment - a multisystem disease According to preliminary data of LCH-III clinical trials, a total of 12 months treatment reduces the risk of disease reactivation compared with shorter (six months) treatment. Patients with MS-LCH have a variable disease outcome. Patients with good response to initial therapy and without involvement of risk organs have a good prognosis. A combination of prednisone and vinblastine has been proven effective and minimally toxic therapy and it is recommended as the standard for initial therapy in all patients in whom systemic therapy is necessary. Patients with RO involvement who react poorly to initial therapy, especially if there is a clinical disease progression, have a very poor prognosis (42, 43). For such patients, the use of early intensive therapy is warranted. 82
13 N. Krstovski Langerhans cell histiocytosis The initial therapy of vinblastine and prednisone for 6 weeks is recommended for all patients with MS-LCH, irrespective of whether they are affected by RO. Further therapy depends on the initial response to the applied treatment. Evaluation of the disease after 6 weeks must be performed. Patients with RO involvement who do not have a favourable therapeutic response are candidates for application of various types of intensive care. The same is recommended for patients who develop disease progression during therapy and involvement of RO. For patients without involvement of the RO without improvement on initial therapy and patients with RO involvement at diagnosis, who have a favourable therapeutic response, it is advisable to continue treatment with prednisone and vinblastine. It is also recommended that all patients who have complete resolution of disease after the initial 6 or 12 weeks therapy should continue maintenance therapy. Maintenance therapy consists of vinblastine and prednisone pulses every 3 weeks with continuous application of 6-mercaptopurine (6MP) for a total of 12 months of treatment. In patients with RO involvement where there is no improvement after 12 weeks of therapy, the recommended therapy is salvage therapy while in patients without the involvement of RO second-line therapy is advised, that is, the use of alternative medicines. Second line treatment Salvage therapy Currently, there are no recommendations for optimal treatment of severe progressive MS-LCH, which does not respond to standard therapy. Promising results with 2-chlorodeoxyadenosine (2-CDA, Cladribine, Leustatin) and cytarabine (Ara-C) combinations have been published and also of bone marrow transplantation after reduced intensity conditioning (RIC-SCT) (44, 45). These results must be confirmed by prospective clinical studies. Treatment of patients with CNS involvement depends on the type of change, the extensiveness of the changes and prior therapy, and must be conducted on a strictly individual basis. Second line therapy in patients without RO involvement The optimal treatment for this group of patients is not yet known. Intralesional use of corticosteroids, the combination of vincristine, cytarabine and prednisone and 2-CDA as monotherapy were effective. Long-term consequences of LCH, permanent sequelae Long-term sequelae of LCH and its treatment can severely impair the quality of life of survivors. Consequences according to some statistics are seen in 40-65% of survivors. They are more frequent in MS LCH and can become manifest many years after initial diagnosis with a wide spectrum of clinical presentations. DI is the most common complication seen in 35-50% of MS LCH. About 25% of patients with bone changes develop mainly orthopaedic complications. Better diagnostics, patient stratification and application of less invasive treatment techniques, without the use of radiotherapy, without the extensive surgical interventions done in the past, will contribute to a fall in the frequency of these complications. Hearing loss, various neurological problems, short stature, dental disorders, deficiency of sex and thyroid hormones are also complications that may be seen in LCH (39, 46, 47). Secondary malignancies are more common than in the general population and are most likely caused by chemotherapy. Long-term monitoring of these patients is necessary in order to prevent reactivation and late complications of the disease (48). 83
14 Conclusion Nearly a century has passed since histiocytic disorders were recognized and only recently in the last few decades has seen major gains in knowledge regarding the underlying defects, clinical presentation, therapy and outcome of the histiocytic disorders. Still many quenstions remains unanswered concerning epidemiology, patophisyology and optimal treatment. Futher experimental investigations and clinical trials will ultimately lead to a better understanding and, subsequently, to a better treatment and improved outcome of patients with Langerhans cell histiocytosis. Conflict of Interest: The author declares that she has no conflict of interest. This article was not sponsored by any external organisation. References 1. Favara BE, Feller AC, Pauli M, Jaffe ES, Weiss LM, Arico M, et al, Contemporary classification of histiocytic disorders. The WHO Committee On Histiocytic/Reticulum Cell Proliferations. Reclassification Working Group of the Histiocyte Society. Med Pediatr Oncol (3): Arceci RJ. The histiocytoses: the fall of the Tower of Babel. Eur J Cancer. 1999;35(5): Aricò M, Clementi R, Caselli D, Danesino C. Histiocyte disorders. Hematol J. 2003;4: Chu T, D Angio GJ, Favara BE, Ladisch S, Nesbit M, Pritchard J. Histiocytosis syndromes in children. Lancet. 1987;2(8549): Hand AJ. Polyuria and tuberculosis. Arch Pediatrics. 1893;10: Schüller A. Über eigenartige Schädeldefekte im Jugendalter. Fortschrifte Roentgenstrahlen. 1915;23: Christian HA. Defects in membranous bones, exophthalmos and diabetes insipidus; an unusual syndrome of dyspituitarism. Med Clin North Am. 1919;3: Letterer E. Aleukämische Retikulose (Ein Beitrag zu den proliferativen Erkankungen des Retikuloendothelialapparates. Frankf Zeitschr Pathol. 1924;30: Siwe SA. Die Reticuloendotheliose-ein neues Krankheitsbild unter den Hepatosplenomegalien. Z Kinderheilk. 1933;55: Otani S, Ehrlich JC. Solitary granuloma of bone simulating primary neoplasm. Am J Pathol. 1940;16(4): Lichtenstein L, Jeffe HL. Eosinophilic granuloma of bone: With report of a case. Am J Pathol. 1940;16(5): Coppes-Zantinga A, Egeler RM. The Langerhans cell histiocytosis X files revealed. Br J Haematol. 2002;116(1): Arceci RJ, Longley BJ, Emanuel PD. Atypical cellular disorders. Hematology Am Soc Hematol Educ Program. 2002; Zelger B. Langerhans cell histiocytosis: A reactive or neoplastic disorder?. Med Pediatr Oncol. 2001;37(6): Yu RC, Chu C, Buluwela L, Chu AC. Clonal proliferation of Langerhans cells in Langerhans cell histiocytosis. Lancet. 1994;343(8900): Geissmann F, Lepelletier Y, Fraitag S, Valladeau J, Bodemer C, Debré M,Leborgne M, Saeland S, Brousse N. Differentiation of Langerhans cells in Langerhans cell histiocytosis. Blood (5): Betts DR, Leibundgut KE, Feldges A, Pluss HJ, Niggli FK. Cytogenetic abnormalities in Langerhans cell histiocytosis. Br J Cancer. 1998;77(4): Aricò M, Nichols K, Whitlock JA, Arceci R, Haupt R, Mittler U, et al. Familial clustering of Langerhans cell histiocytosis. Br J Haematol. 1999;107(4): Petersen BL, Rengtved P, Bank MI, Carstensen H. High expression of markers of apoptosis in Langerhans cell histiocytosis. Histopathology. 2003;42(2): Allen CE, Li L, Peters TL, Leung HC, Yu A, Man TK. Cell-specific gene expression in Langerhans cell histiocytosis lesions reveals a distinct profile compared with epidermal Langerhans cells. J Immunol. 2010;184(8):
15 N. Krstovski Langerhans cell histiocytosis 21. Senechal B, Elain G, Jeziorski E, Grondin V, Patey- Mariaud de Serre N, Jaubert F, et al. Expansion of regulatory T cells in patients with Langerhans cell histiocytosis. PLoS Med.2007;4(8):e Coury F, Annels N, Rivollier A, Olsson S, Santoro A, Speziani C, et al. Langerhans cell histiocytosis reveals a new IL-17A-dependent pathway of dendritic cell fusion. Nat Med. 2008;14(1): Bank MI, Gudbrand C, Rengtved P, Carstensen H, Fadeel B, Henter JI, et al. Immunohistochemical detection of the apoptosis-related proteins FADD, FLICE,and FLIP in Langerhans cell histiocytosis. J Pediatr Hematol Oncol. 2005;27(6): Lipton JM, Arceci RJ. Histiocytic disorders. In: Hoffman R. editor. Hematology: Basic Principles and Practice, 5th ed. Philadelphia (USA): Churchill Livingstone, an imprint of Elsevier Inc; Ch Munn S, Chu AC. Langerhans cell histiocytosis of the skin. Hematol Oncol Clin North Am. 1998;12: Ladisch S, Gadner H, Aricò M, Broadbent V, Grois N, Jacobson A, et al. LCH-I: a randomized trial of etoposide vs. vinblastine in disseminated Langerhans cell histiocytosis. The Histiocyte Society. Med Pediatr Oncol. 1994;23(2): Melendez HV, Dhawan A, Mieli-Vergani G, Rela M, Heaton ND, Pritchard J, et al. Liver transplantation for Langerhans cell histiocytosis--a case report and literature review. Transplantation Oct 27;62(8): Gadner H, Heitger A, Grois N, Gatterer-Menz I, Ladisch S. Treatment strategy for disseminated Langerhans cell histiocytosis. DAL HX-83 Study Group. Med Pediatr Oncol. 1994;23(2): Prosch H, Grois N, Bökkerink J, Prayer D, Leuschner I, Minkov M et al. Central diabetes insipidus: Is it Langerhans cell histiocytosis of the pituitary stalk? A diagnostic pitfall. Pediatr Blood Cancer. 2006;46(3): Braunstein GD, Kohler PO. Endocrine manifestations of histiocytosis. Am J Pediatr Hematol Oncol. 1981;3(1): Grois NG, Favara BE, Mostbeck GH, Prayer D. Central nervous system disease in Langerhans cell histiocytosis. Hematol Oncol Clin North Am. 1998;12(12): Lahey E. Histiocytosis X-An analysis of prognostic factors. J Pediatr. 1975;87(2): Wright-Browne V, McClain KL, Talpaz M, Ordonez N, Estrov Z. Physiology and pathophysiology of dendritic cells. Hum Pathol. 1997;28: Histiocytosis syndromes in children. Writing Group of the Histiocyte Society. Lancet. 1987;1(8526): Histiocyte Society.org [homepage on the Internet]. Langerans Cell Histiocytosis: Histiocyte Society Eavaluation and Treatment Guidlines [updated 2009 April 16]. Available from:htp:// 36. Phillips M, Allen C, Gerson P, McClain K. Comparison of FDG-PET scans to conventional radiography and bone scans in management of Langerhans cell histiocytosis. Pediatr Blood Cancer. 2009;52(1): Egeler RM, Thompson RC, Jr., Voute PA, Nesbit ME, Jr. Intralesional infiltration of corticosteroids in localized Langerhans cell histiocytosis. J Pediatr Orthop. 1992;12(6): Ugarriza FL, Cabezudo JM, Porras LF, Lorenzana LM. Solitary eosinophilic granuloma of the cervicothoracic junction causing neurological deficit. Br J Neurosurg. 2003;17: Grois N, Pötschger U, Prosch H, Minkov M, Arico M, Braier J, et al. Risk factors for diabetes insipidus in langerhans cell histiocytosis. Pediatr Blood Cancer. 2006;46(2): Titgemeyer C, Grois N, Minkov M, Flucher-Wolfram B, Gatterer-Menz I, Gadner H. Pattern and course of single-system disease in Langerhans cell histiocytosis data from the DAL-HX 83- and 90-study. Med Pediatr Oncol. 2001;37(2): Hoeger PH, Nanduri VR, Harper JI, Atherton DA, Pritchard J. Long term follow up of topical mustine treatment for cutaneous langerhans cell histiocytosis. Arch Dis Child. 2000;82: Minkov M, Grois N, Heitger A, Pötschger U, Westermeier T, Gadner H. Improved outcome in multisystem Langerhans cell histiocytosis is associated with therapy intensification. Blood. 2008;111(5): Minkov M, Grois N, Heitger A, Potschger U, Westermeier T, Gadner H. Response to initial treatment of multisystem Langerhans cell histiocytosis: an important prognostic indicator. Med Pediatr Oncol. 2002;39(6): Bernard F, Thomas C, Bertrand Y, Munzer M, Landman Parker J, Ouache M, et al. Multi-centre pi- 85
16 lot study of 2-chlorodeoxyadenosine and cytosine arabinoside combined chemotherapy in refractory Langerhans cell histiocytosis with haematological dysfunction. Eur J Cancer. 2005;41(17): Steiner M, Matthes-Martin S, Attarbaschi A, Minkov M, Grois N, Unger E, et al. Improved outcome of treatment-resistant high-risk Langerhans cell histiocytosis after allogeneic stem cell transplantation with reduced-intensity conditioning. Bone Marrow Transplant. 2005;36(3): Haupt R, Nanduri V, Calevo MG, Bernstrand C, Braier JL, Broadbent V, et al. Permanent consequences in Langerhans cell histiocytosis patients: a pilot study from the Histiocyte Society-Late Effects Study Group. Pediatr Blood Cancer. 2004;42: Nanduri VR, Pritchard J, Levitt G, Glaser AW. Long term morbidity and health related quality of life after multi-system Langerhans cell histiocytosis. Eur J Cancer. 2006;42: Willis B, Ablin A, Weinberg V, Zoger S, Wara WM, Matthay KK. Disease course and late sequelae of Langerhans cell histiocytosis: 25-year experience at the University of California, San Francisco. J Clin Oncol. 1996;14: Citation: Krstovski N. Langerhans cell histiocytosis. Paediatrics Today. 2011;7(2):
TREATMENT AND SURVIVAL ANALYSIS FOR PEDIATRIC PATIENTS WITH LANGERHANS CELL HISTIOCYTOSIS A SINGLE INSTITUTION REVIEW
 TREATMENT AND SURVIVAL ANALYSIS FOR PEDIATRIC PATIENTS WITH LANGERHANS CELL HISTIOCYTOSIS A SINGLE INSTITUTION REVIEW HEMANT MENGHANI, MD; CORI MORRISON, MD PEDIATRIC HEMATOLOGY ONCOLOGY, LSUHSC AND CHILDREN
TREATMENT AND SURVIVAL ANALYSIS FOR PEDIATRIC PATIENTS WITH LANGERHANS CELL HISTIOCYTOSIS A SINGLE INSTITUTION REVIEW HEMANT MENGHANI, MD; CORI MORRISON, MD PEDIATRIC HEMATOLOGY ONCOLOGY, LSUHSC AND CHILDREN
PHYSIOLOGY AND MANAGEMENT OF HISTIOCYTIC DISEASE. Brant Ward, MD, PhD Division of Rheumatology, Allergy, and Immunology
 PHYSIOLOGY AND MANAGEMENT OF HISTIOCYTIC DISEASE Brant Ward, MD, PhD Division of Rheumatology, Allergy, and Immunology What do histiocytes do? Apoptotic body removal Phagocytosis Antigen presentation Types
PHYSIOLOGY AND MANAGEMENT OF HISTIOCYTIC DISEASE Brant Ward, MD, PhD Division of Rheumatology, Allergy, and Immunology What do histiocytes do? Apoptotic body removal Phagocytosis Antigen presentation Types
Spectrum of clinical presentations
 Spectrum of clinical presentations Case History A 7-day-old male patient born full-term via uncomplicated vaginal delivery was seen for multiple erythematous red-brown purpuric lesions that were present
Spectrum of clinical presentations Case History A 7-day-old male patient born full-term via uncomplicated vaginal delivery was seen for multiple erythematous red-brown purpuric lesions that were present
PET Imaging in Langerhans Cell Histiocytosis
 PET Imaging in Langerhans Cell Histiocytosis Christiane Franzius Bremen, Germany Histiocytosis Histiocytosis Idiopathic proliferation of histiocytes Two types of histiocytes macrophages: antigen processing
PET Imaging in Langerhans Cell Histiocytosis Christiane Franzius Bremen, Germany Histiocytosis Histiocytosis Idiopathic proliferation of histiocytes Two types of histiocytes macrophages: antigen processing
Langerhans Cell Histiocytosis: An Overview
 Langerhans Cell Histiocytosis: An Overview Milen Minkov International LCH Study Reference Center Children s Cancer Research Institute St. Anna Children s Hospital Vienna, Austria Achievements Case description
Langerhans Cell Histiocytosis: An Overview Milen Minkov International LCH Study Reference Center Children s Cancer Research Institute St. Anna Children s Hospital Vienna, Austria Achievements Case description
LANGERHANS CELL HISTIOCYTOSIS LCH-CHILDREN
 LANGERHANS CELL HISTIOCYTOSIS LCH-CHILDREN Histiocytosis UK Introduction Despite the misery it causes, Histiocytosis is too rare a disease to have generated substantial research in medical circles. Unfortunately,
LANGERHANS CELL HISTIOCYTOSIS LCH-CHILDREN Histiocytosis UK Introduction Despite the misery it causes, Histiocytosis is too rare a disease to have generated substantial research in medical circles. Unfortunately,
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/20594 holds various files of this Leiden University dissertation. Author: Bechan, Indiradevi Gitanjali Title: Langerhans cell histiocytosis : clues on pathogenesis
Cover Page The handle http://hdl.handle.net/1887/20594 holds various files of this Leiden University dissertation. Author: Bechan, Indiradevi Gitanjali Title: Langerhans cell histiocytosis : clues on pathogenesis
LANGERHANS CELL HISTIOCYTOSIS LCH-CHILDREN
 LANGERHANS CELL HISTIOCYTOSIS LCH-CHILDREN Histiocytosis UK Introduction Despite the misery it causes, Histiocytosis is too rare a disease to have generated substantial research in medical circles. Unfortunately,
LANGERHANS CELL HISTIOCYTOSIS LCH-CHILDREN Histiocytosis UK Introduction Despite the misery it causes, Histiocytosis is too rare a disease to have generated substantial research in medical circles. Unfortunately,
LANGERHANS CELL HISTIOCYTOSIS LCH-ADULTS
 LANGERHANS CELL HISTIOCYTOSIS LCH-ADULTS Histiocytosis UK Introduction Despite the misery it causes, Histiocytosis is too rare a disease to have generated substantial research in medical circles. Unfortunately,
LANGERHANS CELL HISTIOCYTOSIS LCH-ADULTS Histiocytosis UK Introduction Despite the misery it causes, Histiocytosis is too rare a disease to have generated substantial research in medical circles. Unfortunately,
Pediatric Oncology. Vlad Radulescu, MD
 Pediatric Oncology Vlad Radulescu, MD Objectives Review the epidemiology of childhood cancer Discuss the presenting signs and symptoms, general treatment principles and overall prognosis of the most common
Pediatric Oncology Vlad Radulescu, MD Objectives Review the epidemiology of childhood cancer Discuss the presenting signs and symptoms, general treatment principles and overall prognosis of the most common
CASE REPORT. ACUTE DISSEMINATED LANGERHANS CELL DISEASE A RARE CASE REPORT Sunitha. M, R. Rajesh
 ACUTE DISSEMINATED LANGERHANS CELL DISEASE A RARE CASE REPORT Sunitha. M, R. Rajesh 1. Professor, Department of Oral Medicine & Radiology, Noorul Islam Dental College, Thiruvananthapuram, Kerala 2. Professor,
ACUTE DISSEMINATED LANGERHANS CELL DISEASE A RARE CASE REPORT Sunitha. M, R. Rajesh 1. Professor, Department of Oral Medicine & Radiology, Noorul Islam Dental College, Thiruvananthapuram, Kerala 2. Professor,
Canine Histiocytic Disorders DR. MEREDITH GAUTHIER, DVM DACVIM (ONCOLOGY) OCTOBER 29, 2015
 Canine Histiocytic Disorders DR. MEREDITH GAUTHIER, DVM DACVIM (ONCOLOGY) OCTOBER 29, 2015 Canine Histiocytes! Cells derived from CD34+ stem cells and blood monocytes! Macrophages! Dendritic cells (DC)!
Canine Histiocytic Disorders DR. MEREDITH GAUTHIER, DVM DACVIM (ONCOLOGY) OCTOBER 29, 2015 Canine Histiocytes! Cells derived from CD34+ stem cells and blood monocytes! Macrophages! Dendritic cells (DC)!
Cerebral Langerhans Cell Hystiocitosis: What the oncologist wants to know.
 Cerebral Langerhans Cell Hystiocitosis: What the oncologist wants to know. Poster No.: C-0383 Congress: ECR 2015 Type: Authors: Keywords: DOI: Educational Exhibit M. Diez Blanco, S. Sanchez Bernal, H.
Cerebral Langerhans Cell Hystiocitosis: What the oncologist wants to know. Poster No.: C-0383 Congress: ECR 2015 Type: Authors: Keywords: DOI: Educational Exhibit M. Diez Blanco, S. Sanchez Bernal, H.
Lymphoma: What You Need to Know. Richard van der Jagt MD, FRCPC
 Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
Langerhans cell histiocytosis is an intriguing
 editorial Langerhans cell histiocytosis: is there a role for genetics? haematologica 2001; 86:1009-1014 http://www.haematologica.it/2001_10/1009.htm MAURIZIO ARICÒ,* CESARE DANESINO, *Dipartimento di Pediatria,
editorial Langerhans cell histiocytosis: is there a role for genetics? haematologica 2001; 86:1009-1014 http://www.haematologica.it/2001_10/1009.htm MAURIZIO ARICÒ,* CESARE DANESINO, *Dipartimento di Pediatria,
performed to help sway the clinician in what the appropriate diagnosis is, which can substantially alter the treatment of management.
 Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
September is Histiocytosis Awareness Month
 IMMEDIATE RELEASE September is Histiocytosis Awareness Month Nationwide, September, 2011 September is Histiocytosis Awareness Month, an especially opportune time to raise visibility and funding for histiocytic
IMMEDIATE RELEASE September is Histiocytosis Awareness Month Nationwide, September, 2011 September is Histiocytosis Awareness Month, an especially opportune time to raise visibility and funding for histiocytic
Langerhans cell histiocytosis of skull: a retrospective study of 18 cases
 Original Article Langerhans cell histiocytosis of skull: a retrospective study of 18 cases Xiang-Heng Zhang, Ji Zhang, Zheng-He Chen, Ke Sai, Yin-Sheng Chen, Jian Wang, Chao Ke, Chen-Chen Guo, Zhong-Ping
Original Article Langerhans cell histiocytosis of skull: a retrospective study of 18 cases Xiang-Heng Zhang, Ji Zhang, Zheng-He Chen, Ke Sai, Yin-Sheng Chen, Jian Wang, Chao Ke, Chen-Chen Guo, Zhong-Ping
Lymphoma. Types of Lymphoma. Clinical signs
 Lymphoma Lymphoma is a tumour originating from lymphoid tissue, either nodal (lymph ) or extranodal (thymus, spleen, mucosa, conjunctiva, or skin-associated lymphoid tissue). It is one of the most common
Lymphoma Lymphoma is a tumour originating from lymphoid tissue, either nodal (lymph ) or extranodal (thymus, spleen, mucosa, conjunctiva, or skin-associated lymphoid tissue). It is one of the most common
Lymphoma (Lymphosarcoma) by Pamela A. Davol
 Lymphoma (Lymphosarcoma) by Pamela A. Davol Cells derived from the bone marrow that mature and take part in cellular immune reactions are called lymphocytes. When lymphocytes undergo transformation and
Lymphoma (Lymphosarcoma) by Pamela A. Davol Cells derived from the bone marrow that mature and take part in cellular immune reactions are called lymphocytes. When lymphocytes undergo transformation and
MULTISYSTEMIC LANGERHANS CELL HISTIOCYTOSIS IN ADULT AN UNCOMMON INCIDENCE POSING A DIAGNOSTIC CHALLENGE. Monal Trisal
 Pathology Case Report International Journal of Clinical And Diagnostic Research ISSN 2395-3403 Volume 4, Issue 4, July-Aug 2016. Glorigin Lifesciences Private Limited. MULTISYSTEMIC LANGERHANS CELL HISTIOCYTOSIS
Pathology Case Report International Journal of Clinical And Diagnostic Research ISSN 2395-3403 Volume 4, Issue 4, July-Aug 2016. Glorigin Lifesciences Private Limited. MULTISYSTEMIC LANGERHANS CELL HISTIOCYTOSIS
Histiocytic Neoplasms of the Dog and Cat
 Histiocytic Neoplasms of the Dog and Cat V.E. Valli DVM Histiocytic and Dendritic Cell Populations Both lineages are bone marrow derived. Macrophages are part of the innate immune system that are phagocytic
Histiocytic Neoplasms of the Dog and Cat V.E. Valli DVM Histiocytic and Dendritic Cell Populations Both lineages are bone marrow derived. Macrophages are part of the innate immune system that are phagocytic
Plasma cell myeloma (multiple myeloma)
 Plasma cell myeloma (multiple myeloma) Common lymphoid neoplasm, present at old age (70 years average) Remember: plasma cells are terminally differentiated B-lymphocytes that produces antibodies. B-cells
Plasma cell myeloma (multiple myeloma) Common lymphoid neoplasm, present at old age (70 years average) Remember: plasma cells are terminally differentiated B-lymphocytes that produces antibodies. B-cells
Langerhans Cell Histiocytosis in Taiwan: A Retrospective Case Series in a Medical Center
 Original Study Langerhans Cell Histiocytosis in Taiwan: A Retrospective Case Series in a Medical Center Yi-Chin Shih Wan-Lung Lin I-Hsin Shih Background: Langerhans cell histiocytosis (LCH) comprises a
Original Study Langerhans Cell Histiocytosis in Taiwan: A Retrospective Case Series in a Medical Center Yi-Chin Shih Wan-Lung Lin I-Hsin Shih Background: Langerhans cell histiocytosis (LCH) comprises a
Improved outcome in multisystem Langerhans cell histiocytosis is associated with therapy intensification
 CLINICAL TRIALS AND OBSERVATIONS Improved outcome in multisystem Langerhans cell histiocytosis is associated with therapy intensification Helmut Gadner, 1 Nicole Grois, 1 Ulrike Pötschger, 1 Milen Minkov,
CLINICAL TRIALS AND OBSERVATIONS Improved outcome in multisystem Langerhans cell histiocytosis is associated with therapy intensification Helmut Gadner, 1 Nicole Grois, 1 Ulrike Pötschger, 1 Milen Minkov,
SWISS SOCIETY OF NEONATOLOGY. A newborn with a papulonodular rash at birth
 SWISS SOCIETY OF NEONATOLOGY A newborn with a papulonodular rash at birth June 2001 2 Glanzmann R, Neonatal Intensive Care Unit, UKKB Basel, Switzerland Swiss Society of Neonatology, Thomas M Berger, Webmaster
SWISS SOCIETY OF NEONATOLOGY A newborn with a papulonodular rash at birth June 2001 2 Glanzmann R, Neonatal Intensive Care Unit, UKKB Basel, Switzerland Swiss Society of Neonatology, Thomas M Berger, Webmaster
2. Occupancy rate of beds in the hospital: Occupancy rate of at least 60%
 Appendix A Training Centre Accreditation Checklist A. Accreditation of the HOSPITAL 1. Total number of beds in the hospital : Minimum 500 beds 2. Occupancy rate of beds in the hospital: Occupancy rate
Appendix A Training Centre Accreditation Checklist A. Accreditation of the HOSPITAL 1. Total number of beds in the hospital : Minimum 500 beds 2. Occupancy rate of beds in the hospital: Occupancy rate
Langerhans cell histiocytosis (LCH), formerly
 Langerhans cell histiocytosis of bone in children: a clinicopathologic study of 108 cases Jia Wang, Xv Wu, Zheng-Jun Xi Shanghai, China Background: Langerhans cell histiocytosis (LCH) is a rare disease
Langerhans cell histiocytosis of bone in children: a clinicopathologic study of 108 cases Jia Wang, Xv Wu, Zheng-Jun Xi Shanghai, China Background: Langerhans cell histiocytosis (LCH) is a rare disease
Acute myeloid leukemia. M. Kaźmierczak 2016
 Acute myeloid leukemia M. Kaźmierczak 2016 Acute myeloid leukemia Malignant clonal disorder of immature hematopoietic cells characterized by clonal proliferation of abnormal blast cells and impaired production
Acute myeloid leukemia M. Kaźmierczak 2016 Acute myeloid leukemia Malignant clonal disorder of immature hematopoietic cells characterized by clonal proliferation of abnormal blast cells and impaired production
CHAPTER:4 LEUKEMIA. BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY 8/12/2009
 LEUKEMIA CHAPTER:4 1 BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY Leukemia A group of malignant disorders affecting the blood and blood-forming tissues of
LEUKEMIA CHAPTER:4 1 BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY Leukemia A group of malignant disorders affecting the blood and blood-forming tissues of
ISPUB.COM. Vertebra Plana. R Chahal, S Acharya INTRODUCTION CASE HISTORY
 ISPUB.COM The Internet Journal of Spine Surgery Volume 4 Number 1 R Chahal, S Acharya Citation R Chahal, S Acharya.. The Internet Journal of Spine Surgery. 2006 Volume 4 Number 1. Abstract It is not uncommon
ISPUB.COM The Internet Journal of Spine Surgery Volume 4 Number 1 R Chahal, S Acharya Citation R Chahal, S Acharya.. The Internet Journal of Spine Surgery. 2006 Volume 4 Number 1. Abstract It is not uncommon
Pathology of Hematopoietic and Lymphoid tissue
 CONTENTS Pathology of Hematopoietic and Lymphoid tissue White blood cells and lymph nodes Quantitative disorder of white blood cells Reactive lymphadenopathies Infectious lymphadenitis Tumor metastasis
CONTENTS Pathology of Hematopoietic and Lymphoid tissue White blood cells and lymph nodes Quantitative disorder of white blood cells Reactive lymphadenopathies Infectious lymphadenitis Tumor metastasis
Pathology of Hematopoietic and Lymphoid tissue
 Pathology of Hematopoietic and Lymphoid tissue Peerayut Sitthichaiyakul, M.D. Department of Pathology and Forensic Medicine Faculty of Medicine, Naresuan University CONTENTS White blood cells and lymph
Pathology of Hematopoietic and Lymphoid tissue Peerayut Sitthichaiyakul, M.D. Department of Pathology and Forensic Medicine Faculty of Medicine, Naresuan University CONTENTS White blood cells and lymph
الفتوي الاصفر الحبيبوم = Xanthogranuloma_Juvenile JUVENILE XANTHOGRANULOMA 1 / 9
 JUVENILE XANTHOGRANULOMA 1 / 9 Clinical Findings CUTANEOUS LESIONS JXG is a benign, self-healing disorder that is characterized by asymptomatic yellowish papulonodular lesions of the skin and other organs
JUVENILE XANTHOGRANULOMA 1 / 9 Clinical Findings CUTANEOUS LESIONS JXG is a benign, self-healing disorder that is characterized by asymptomatic yellowish papulonodular lesions of the skin and other organs
Mast Cell Tumors in Dogs
 Mast Cell Tumors in Dogs 803-808-7387 www.gracepets.com These notes are provided to help you understand the diagnosis or possible diagnosis of cancer in your pet. For general information on cancer in pets
Mast Cell Tumors in Dogs 803-808-7387 www.gracepets.com These notes are provided to help you understand the diagnosis or possible diagnosis of cancer in your pet. For general information on cancer in pets
Tumors of the Spleen
 Tumors of the Spleen 803-808-7387 www.gracepets.com These notes are provided to help you understand the diagnosis or possible diagnosis of cancer in your pet. For general information on cancer in pets
Tumors of the Spleen 803-808-7387 www.gracepets.com These notes are provided to help you understand the diagnosis or possible diagnosis of cancer in your pet. For general information on cancer in pets
WHAT ARE PAEDIATRIC CANCERS
 WHAT ARE PAEDIATRIC CANCERS INTRODUCTION Childhood cancers are RARE 0.5% of all cancers in the West Overall risk that a child will develop cancer during first 15 years of life is 1 in 450 and 1 in 600
WHAT ARE PAEDIATRIC CANCERS INTRODUCTION Childhood cancers are RARE 0.5% of all cancers in the West Overall risk that a child will develop cancer during first 15 years of life is 1 in 450 and 1 in 600
Primary Cutaneous CD30-Positive T-cell Lymphoproliferative Disorders
 Primary Cutaneous CD30-Positive T-cell Lymphoproliferative Disorders Definition A spectrum of related conditions originating from transformed or activated CD30-positive T-lymphocytes May coexist in individual
Primary Cutaneous CD30-Positive T-cell Lymphoproliferative Disorders Definition A spectrum of related conditions originating from transformed or activated CD30-positive T-lymphocytes May coexist in individual
Case Report Langerhans cell histiocytosis (LCH) occurring in the skull: report of 3 cases and review of the literature
 Int J Clin Exp Pathol 2017;10(1):695-701 www.ijcep.com /ISSN:1936-2625/IJCEP0041815 Case Report Langerhans cell histiocytosis (LCH) occurring in the skull: report of 3 cases and review of the literature
Int J Clin Exp Pathol 2017;10(1):695-701 www.ijcep.com /ISSN:1936-2625/IJCEP0041815 Case Report Langerhans cell histiocytosis (LCH) occurring in the skull: report of 3 cases and review of the literature
City Pediatric Meet-Dec 2011 SPECTRUM OF HLH. Spectrum of HLH. Dr.Revathi Raj s unit, Apollo Children s Hospital.
 City Pediatric Meet-Dec 2011 SPECTRUM OF HLH Spectrum of HLH Dr.Revathi Raj s unit, Apollo Children s Hospital. Case 1 4 month male child /thriving well Fever - 5 days with cough O/E hepatospenomegaly
City Pediatric Meet-Dec 2011 SPECTRUM OF HLH Spectrum of HLH Dr.Revathi Raj s unit, Apollo Children s Hospital. Case 1 4 month male child /thriving well Fever - 5 days with cough O/E hepatospenomegaly
Group of malignant disorders of the hematopoietic tissues characteristically associated with increased numbers of white cells in the bone marrow and
 Group of malignant disorders of the hematopoietic tissues characteristically associated with increased numbers of white cells in the bone marrow and / or peripheral blood Classified based on cell type
Group of malignant disorders of the hematopoietic tissues characteristically associated with increased numbers of white cells in the bone marrow and / or peripheral blood Classified based on cell type
Haemophagocytic Lymphohistiocytosis Complicating Myelodysplasia
 Haemophagocytic Lymphohistiocytosis Complicating Myelodysplasia Geraldine Quintero- Platt a, Carima Belleyo- Belkasem a, Taida Martín- Santos b, Onán Pérez- Hernández a, Emilio González- Reimers a a Internal
Haemophagocytic Lymphohistiocytosis Complicating Myelodysplasia Geraldine Quintero- Platt a, Carima Belleyo- Belkasem a, Taida Martín- Santos b, Onán Pérez- Hernández a, Emilio González- Reimers a a Internal
Done By : WESSEN ADNAN BUTHAINAH AL-MASAEED
 Done By : WESSEN ADNAN BUTHAINAH AL-MASAEED Acute Myeloid Leukemia Firstly we ll start with this introduction then enter the title of the lecture, so be ready and let s begin by the name of Allah : We
Done By : WESSEN ADNAN BUTHAINAH AL-MASAEED Acute Myeloid Leukemia Firstly we ll start with this introduction then enter the title of the lecture, so be ready and let s begin by the name of Allah : We
Adstock Science Club. Parvathy Elacode Harikumar. PhD student/research Assistant Clore Laboratory University of Buckingham
 Adstock Science Club Parvathy Elacode Harikumar PhD student/research Assistant Clore Laboratory University of Buckingham My Background Finished school education in India Completed A-Levels in London BSc
Adstock Science Club Parvathy Elacode Harikumar PhD student/research Assistant Clore Laboratory University of Buckingham My Background Finished school education in India Completed A-Levels in London BSc
Melanoma Case Scenario 1
 Melanoma Case Scenario 1 History and physical 11/5/16 Patient is a single, 48-year-old male in good health who presented to his primary physician for a yearly physical exam during which a 3.4 x 2.8 x 1.5
Melanoma Case Scenario 1 History and physical 11/5/16 Patient is a single, 48-year-old male in good health who presented to his primary physician for a yearly physical exam during which a 3.4 x 2.8 x 1.5
Hemophagocytic Lymphohistiocytosis Secondary to T cell/histiocyte-rich Large B-cell Lymphoma
 Hemophagocytic Lymphohistiocytosis Secondary to T cell/histiocyte-rich Large B-cell Lymphoma Katherine Devitt, M.D., Benjamin Chen, M.D., Ph.D., Hongbo Yu, M.D., Ph.D., Bruce Woda, M.D. 1 1 Department
Hemophagocytic Lymphohistiocytosis Secondary to T cell/histiocyte-rich Large B-cell Lymphoma Katherine Devitt, M.D., Benjamin Chen, M.D., Ph.D., Hongbo Yu, M.D., Ph.D., Bruce Woda, M.D. 1 1 Department
Melanoma Case Scenario 1
 Melanoma Case Scenario 1 History and physical 11/5/16 Patient is a single, 48-year-old male in good health who presented to his primary physician for a yearly physical exam during which a 3.4 x 2.8 x 1.5
Melanoma Case Scenario 1 History and physical 11/5/16 Patient is a single, 48-year-old male in good health who presented to his primary physician for a yearly physical exam during which a 3.4 x 2.8 x 1.5
Central Nervous System Disease in Langerhans Cell Histiocytosis
 Br. J. Cancer (1994), 70, (Suppl. XXIII) S24-S28 Br. J. Cancer (1994),70,(Suppl. XXIII) S24-S28 (~~~~~) Macmillan Press Ltd., 1994- Central Nervous System Disease in Langerhans Cell Histiocytosis Nicole
Br. J. Cancer (1994), 70, (Suppl. XXIII) S24-S28 Br. J. Cancer (1994),70,(Suppl. XXIII) S24-S28 (~~~~~) Macmillan Press Ltd., 1994- Central Nervous System Disease in Langerhans Cell Histiocytosis Nicole
LYMPHOMA Joginder Singh, MD Medical Oncologist, Mercy Cancer Center
 LYMPHOMA Joginder Singh, MD Medical Oncologist, Mercy Cancer Center Lymphoma is cancer of the lymphatic system. The lymphatic system is made up of organs all over the body that make up and store cells
LYMPHOMA Joginder Singh, MD Medical Oncologist, Mercy Cancer Center Lymphoma is cancer of the lymphatic system. The lymphatic system is made up of organs all over the body that make up and store cells
What is head and neck cancer? How is head and neck cancer diagnosed and evaluated? How is head and neck cancer treated?
 Scan for mobile link. Head and Neck Cancer Head and neck cancer is a group of cancers that start in the oral cavity, larynx, pharynx, salivary glands, nasal cavity or paranasal sinuses. They usually begin
Scan for mobile link. Head and Neck Cancer Head and neck cancer is a group of cancers that start in the oral cavity, larynx, pharynx, salivary glands, nasal cavity or paranasal sinuses. They usually begin
Contents. vii. Preface... Acknowledgments... v xiii
 Contents Preface... Acknowledgments... v xiii SECTION I 1. Introduction... 3 Knowledge-Based Diagnosis... 4 Systematic Examination of the Lymph Node... 7 Cell Type Identification... 9 Cell Size and Cellularity...
Contents Preface... Acknowledgments... v xiii SECTION I 1. Introduction... 3 Knowledge-Based Diagnosis... 4 Systematic Examination of the Lymph Node... 7 Cell Type Identification... 9 Cell Size and Cellularity...
Non-Hodgkin lymphoma
 Non-Hodgkin lymphoma Non-Hodgkin s lymphoma Definition: - clonal tumours of mature and immature B cells, T cells or NK cells - highly heterogeneous, both histologically and clinically Non-Hodgkin lymphoma
Non-Hodgkin lymphoma Non-Hodgkin s lymphoma Definition: - clonal tumours of mature and immature B cells, T cells or NK cells - highly heterogeneous, both histologically and clinically Non-Hodgkin lymphoma
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL)
 Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
Primary bone tumors > metastases from other sites Primary bone tumors widely range -from benign to malignant. Classified according to the normal cell
 Primary bone tumors > metastases from other sites Primary bone tumors widely range -from benign to malignant. Classified according to the normal cell counterpart and line of differentiation. Among the
Primary bone tumors > metastases from other sites Primary bone tumors widely range -from benign to malignant. Classified according to the normal cell counterpart and line of differentiation. Among the
( Rosai Dorfman disease)
 Sinus histiocytosis with massive lymphadenopathy ( Rosai Dorfman disease) BIBI SHAIN SHAMSIAN Rosai Dorfman disease Rosai-Dorfman Disease (RDD) or Sinus Histiocytosis with massive lymhadenopathy (SHML):
Sinus histiocytosis with massive lymphadenopathy ( Rosai Dorfman disease) BIBI SHAIN SHAMSIAN Rosai Dorfman disease Rosai-Dorfman Disease (RDD) or Sinus Histiocytosis with massive lymhadenopathy (SHML):
CNS TUMORS. D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria)
 CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
Overview of Cutaneous Lymphomas: Diagnosis and Staging. Lauren C. Pinter-Brown MD, FACP Health Sciences Professor of Medicine and Dermatology
 Overview of Cutaneous Lymphomas: Diagnosis and Staging Lauren C. Pinter-Brown MD, FACP Health Sciences Professor of Medicine and Dermatology Definition of Lymphoma A cancer or malignancy that comes from
Overview of Cutaneous Lymphomas: Diagnosis and Staging Lauren C. Pinter-Brown MD, FACP Health Sciences Professor of Medicine and Dermatology Definition of Lymphoma A cancer or malignancy that comes from
Hematology 101. Rachid Baz, M.D. 5/16/2014
 Hematology 101 Rachid Baz, M.D. 5/16/2014 Florida 101 Epidemiology Estimated prevalence 8,000 individuals in U.S (compare with 80,000 MM patients) Annual age adjusted incidence 3-8/million-year 1 More
Hematology 101 Rachid Baz, M.D. 5/16/2014 Florida 101 Epidemiology Estimated prevalence 8,000 individuals in U.S (compare with 80,000 MM patients) Annual age adjusted incidence 3-8/million-year 1 More
MALIGNANT TUMOURS OF THE JAWS
 MALIGNANT TUMOURS OF THE JAWS MALIGNANT TUMOURS OF THE JAWS Squamous cell carcinoma Osteogenic sarcoma Chondrosarcoma Fibrosarcoma Malignant lymphomas (incl. Burkitt s) Multiple myeloma Ameloblastoma Secondary
MALIGNANT TUMOURS OF THE JAWS MALIGNANT TUMOURS OF THE JAWS Squamous cell carcinoma Osteogenic sarcoma Chondrosarcoma Fibrosarcoma Malignant lymphomas (incl. Burkitt s) Multiple myeloma Ameloblastoma Secondary
ISPUB.COM. Spectrum Of MRI Findings In Musculoskeletal Tuberculosis: Pictoral Essay. P Chudgar INTRODUCTION SPINE
 ISPUB.COM The Internet Journal of Radiology Volume 8 Number 2 Spectrum Of MRI Findings In Musculoskeletal Tuberculosis: Pictoral Essay P Chudgar Citation P Chudgar.. The Internet Journal of Radiology.
ISPUB.COM The Internet Journal of Radiology Volume 8 Number 2 Spectrum Of MRI Findings In Musculoskeletal Tuberculosis: Pictoral Essay P Chudgar Citation P Chudgar.. The Internet Journal of Radiology.
Case Presentation. Maha Akkawi, MD, Fatima Obeidat, MD, Tariq Aladily, MD. Department of Pathology Jordan University Hospital Amman, Jordan
 Case Presentation Maha Akkawi, MD, Fatima Obeidat, MD, Tariq Aladily, MD Department of Pathology Jordan University Hospital Amman, Jordan The 25th Annual Congress of the ADIAP The 8/11/2013 1 5th International
Case Presentation Maha Akkawi, MD, Fatima Obeidat, MD, Tariq Aladily, MD Department of Pathology Jordan University Hospital Amman, Jordan The 25th Annual Congress of the ADIAP The 8/11/2013 1 5th International
New lung lesion in a 55 year-old male treated with chemoradiation for non-small cell lung carcinoma
 July 2016 New lung lesion in a 55 year-old male treated with chemoradiation for non-small cell lung carcinoma Contributed by: Laurel Rose, MD, Resident Physician, Indiana University School of Medicine,
July 2016 New lung lesion in a 55 year-old male treated with chemoradiation for non-small cell lung carcinoma Contributed by: Laurel Rose, MD, Resident Physician, Indiana University School of Medicine,
Langerhans Cell Histiocytosis
 Kansas Journal of Medicine 2012 Langerhans Cell Histiocytosis Introduction Langerhans Cell Histiocytosis (LCH) is a rare disease characterized by aberrant proliferation of a specific dendritic (Langerhans)
Kansas Journal of Medicine 2012 Langerhans Cell Histiocytosis Introduction Langerhans Cell Histiocytosis (LCH) is a rare disease characterized by aberrant proliferation of a specific dendritic (Langerhans)
An overlooked case of mandibular histiocytosis: Case report and review of the literature
 Int J Case Rep Images 2018;9:100993Z01KI2019. CASE REPORT Imrani et al. 1 PEER REVIEWED OPEN ACCESS An overlooked case of mandibular histiocytosis: Case report and review of the literature Kaoutar Imrani,
Int J Case Rep Images 2018;9:100993Z01KI2019. CASE REPORT Imrani et al. 1 PEER REVIEWED OPEN ACCESS An overlooked case of mandibular histiocytosis: Case report and review of the literature Kaoutar Imrani,
Neoplasia part I. Dr. Mohsen Dashti. Clinical Medicine & Pathology nd Lecture
 Neoplasia part I By Dr. Mohsen Dashti Clinical Medicine & Pathology 316 2 nd Lecture Lecture outline Review of structure & function. Basic definitions. Classification of neoplasms. Morphologic features.
Neoplasia part I By Dr. Mohsen Dashti Clinical Medicine & Pathology 316 2 nd Lecture Lecture outline Review of structure & function. Basic definitions. Classification of neoplasms. Morphologic features.
Leukemia. There are different types of leukemia and several treatment options for each type.
 Leukemia Introduction Leukemia is the name of a group of cancers of the blood cells. Hundreds of thousands of people worldwide are diagnosed with leukemia each year. There are different types of leukemia
Leukemia Introduction Leukemia is the name of a group of cancers of the blood cells. Hundreds of thousands of people worldwide are diagnosed with leukemia each year. There are different types of leukemia
The Lymphomas. An overview..
 The Lymphomas An overview.. Peter Anglin MD, FRCPC, MBA Stronach Regional Cancer Centre Newmarket, ON The lymphomas are an important part of the history of medicine 1666 Magpighi publishes first recorded
The Lymphomas An overview.. Peter Anglin MD, FRCPC, MBA Stronach Regional Cancer Centre Newmarket, ON The lymphomas are an important part of the history of medicine 1666 Magpighi publishes first recorded
Burkitt lymphoma. Sporadic Endemic in Africa associated with EBV Translocations involving MYC gene on chromosome 8
 Heme 8 Burkitt lymphoma Sporadic Endemic in Africa associated with EBV Translocations involving MYC gene on chromosome 8 Most common is t(8;14) Believed to be the fastest growing tumor in humans!!!! Morphology
Heme 8 Burkitt lymphoma Sporadic Endemic in Africa associated with EBV Translocations involving MYC gene on chromosome 8 Most common is t(8;14) Believed to be the fastest growing tumor in humans!!!! Morphology
Cancers of unknown primary : Knowing the unknown. Prof. Ahmed Hossain Professor of Medicine SSMC
 Cancers of unknown primary : Knowing the unknown Prof. Ahmed Hossain Professor of Medicine SSMC Definition Cancers of unknown primary site (CUPs) Represent a heterogeneous group of metastatic tumours,
Cancers of unknown primary : Knowing the unknown Prof. Ahmed Hossain Professor of Medicine SSMC Definition Cancers of unknown primary site (CUPs) Represent a heterogeneous group of metastatic tumours,
Wilms Tumor and Neuroblastoma
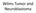 Wilms Tumor and Neuroblastoma Wilm s Tumor AKA: Nephroblastoma the most common intra-abdominal cancer in children. peak incidence is 2 to 3 years of age Biology somatic mutations restricted to tumor tissue
Wilms Tumor and Neuroblastoma Wilm s Tumor AKA: Nephroblastoma the most common intra-abdominal cancer in children. peak incidence is 2 to 3 years of age Biology somatic mutations restricted to tumor tissue
Clinical & Laboratory Assessment
 Clinical & Laboratory Assessment Dr Roger Pool NHLS & University of Pretoria Clinical Assessment (History) Anaemia ( haemoglobin) Dyspnoea (shortness of breath) Tiredness Angina Headache Clinical Assessment
Clinical & Laboratory Assessment Dr Roger Pool NHLS & University of Pretoria Clinical Assessment (History) Anaemia ( haemoglobin) Dyspnoea (shortness of breath) Tiredness Angina Headache Clinical Assessment
Acute Lymphoblastic Leukaemia
 Acute Lymphoblastic Leukaemia Terri Boyer 17 th October 2006 Overview Disease information: Aetiology of ALL proposed theory, contributing factors Symptoms Complications Diagnostic approaches - morphology
Acute Lymphoblastic Leukaemia Terri Boyer 17 th October 2006 Overview Disease information: Aetiology of ALL proposed theory, contributing factors Symptoms Complications Diagnostic approaches - morphology
Langerhans cell histiocytosis: update for the pediatrician Sheila Weitzman a and R. Maarten Egeler b
 Langerhans cell histiocytosis: update for the pediatrician Sheila Weitzman a and R. Maarten Egeler b a Division of Pediatric Hematology/Oncology, The Hospital for Sick Children, Toronto and University
Langerhans cell histiocytosis: update for the pediatrician Sheila Weitzman a and R. Maarten Egeler b a Division of Pediatric Hematology/Oncology, The Hospital for Sick Children, Toronto and University
Head and Neck Cancer. What is head and neck cancer?
 Scan for mobile link. Head and Neck Cancer Head and neck cancer is a group of cancers that usually originate in the squamous cells that line the mouth, nose and throat. Typical symptoms include a persistent
Scan for mobile link. Head and Neck Cancer Head and neck cancer is a group of cancers that usually originate in the squamous cells that line the mouth, nose and throat. Typical symptoms include a persistent
Hematologic Malignancies of the Liver : Spectrum of Disease. Zhou Jian
 Hematologic Malignancies of the Liver : Spectrum of Disease Zhou Jian 2015-7-8 Hematologic malignancies include a wide spectrum of lymphoproliferative and myeloproliferative disorders with nodal and extranodal
Hematologic Malignancies of the Liver : Spectrum of Disease Zhou Jian 2015-7-8 Hematologic malignancies include a wide spectrum of lymphoproliferative and myeloproliferative disorders with nodal and extranodal
Indolent Lymphomas. Dr. Melissa Toupin The Ottawa Hospital
 Indolent Lymphomas Dr. Melissa Toupin The Ottawa Hospital What does indolent mean? Slow growth Often asymptomatic Chronic disease with periods of relapse (long natural history possible) Incurable with
Indolent Lymphomas Dr. Melissa Toupin The Ottawa Hospital What does indolent mean? Slow growth Often asymptomatic Chronic disease with periods of relapse (long natural history possible) Incurable with
Evaluation of Neck Mass. Disclosure. Learning Objectives 3/24/2014. Karen T. Pitman MD, FACS Banner MDACC, Gilbert AZ. Nothing to disclose
 Evaluation of Neck Mass Karen T. Pitman MD, FACS Banner MDACC, Gilbert AZ Nothing to disclose Disclosure Learning Objectives 1. Describe a systematic method to evaluate a patient with a neck mass 2. Select
Evaluation of Neck Mass Karen T. Pitman MD, FACS Banner MDACC, Gilbert AZ Nothing to disclose Disclosure Learning Objectives 1. Describe a systematic method to evaluate a patient with a neck mass 2. Select
9/25/2017. Disclosure. I have nothing to disclose. Young S. Kim MD Dept. of Pathology
 Disclosure MAST CELLNEOPLASM I have nothing to disclose. Young S. Kim MD Dept. of Pathology 1 Objectives What is mast cell lineage? Changes in updated WHO 2016 mastocytosis Issues of Mastocytosis CD30
Disclosure MAST CELLNEOPLASM I have nothing to disclose. Young S. Kim MD Dept. of Pathology 1 Objectives What is mast cell lineage? Changes in updated WHO 2016 mastocytosis Issues of Mastocytosis CD30
Erdheim Chester Disease Mark Heaney MD PhD
 Erdheim Chester Disease 2017 Mark Heaney MD PhD Erdheim-Chester Disease Described as Lipid Granulomatosis by Jakob Erdheim and William Chester in 1930 Lipid-laden macrophages and Touton giant cells CD
Erdheim Chester Disease 2017 Mark Heaney MD PhD Erdheim-Chester Disease Described as Lipid Granulomatosis by Jakob Erdheim and William Chester in 1930 Lipid-laden macrophages and Touton giant cells CD
LEUKAEMIA and LYMPHOMA. Dr Mubarak Abdelrahman Assistant Professor Jazan University
 LEUKAEMIA and LYMPHOMA Dr Mubarak Abdelrahman Assistant Professor Jazan University OBJECTIVES Identify etiology and epidemiology for leukemia and lymphoma. Discuss common types of leukemia. Distinguish
LEUKAEMIA and LYMPHOMA Dr Mubarak Abdelrahman Assistant Professor Jazan University OBJECTIVES Identify etiology and epidemiology for leukemia and lymphoma. Discuss common types of leukemia. Distinguish
Principles of Surgical Oncology. Winnie Achilles Tierklinik Hollabrunn Lastenstrasse Hollabrunn
 Principles of Surgical Oncology Winnie Achilles Tierklinik Hollabrunn Lastenstrasse 2 2020 Hollabrunn boexi@gmx.de The first surgery provides the best chance for a cure in an animal with a tumor Clinical
Principles of Surgical Oncology Winnie Achilles Tierklinik Hollabrunn Lastenstrasse 2 2020 Hollabrunn boexi@gmx.de The first surgery provides the best chance for a cure in an animal with a tumor Clinical
Optic Pathway Gliomas, Germinomas, Spinal Cord Tumours. Colin Kennedy March 2015
 Optic Pathway Gliomas, Germinomas, Spinal Cord Tumours Colin Kennedy March 2015 Glioma of the optic chiasm. T1-weighted MRI with gadolinium enhancement, showing intense irregular uptake of contrast. The
Optic Pathway Gliomas, Germinomas, Spinal Cord Tumours Colin Kennedy March 2015 Glioma of the optic chiasm. T1-weighted MRI with gadolinium enhancement, showing intense irregular uptake of contrast. The
Case 2. Dr. Sathima Natarajan M.D. Kaiser Permanente Medical Center Sunset
 Case 2 Dr. Sathima Natarajan M.D. Kaiser Permanente Medical Center Sunset History 24 year old male presented with a 3 day history of right flank pain, sharp in nature Denies fever, chills, hematuria or
Case 2 Dr. Sathima Natarajan M.D. Kaiser Permanente Medical Center Sunset History 24 year old male presented with a 3 day history of right flank pain, sharp in nature Denies fever, chills, hematuria or
Pediatric TB Intensive Houston, Texas
 Pediatric TB Intensive Houston, Texas November 13, 2009 Radiographic Manifestations of Pediatric TB Susan D. John, MD, FACR November 13, 2009 Radiologic Presentation of Childhood TB Susan D. John, MD,
Pediatric TB Intensive Houston, Texas November 13, 2009 Radiographic Manifestations of Pediatric TB Susan D. John, MD, FACR November 13, 2009 Radiologic Presentation of Childhood TB Susan D. John, MD,
The AML subtypes are based on how mature (developed) the cancer cells are at the time of diagnosis and how different they are from normal cells.
 What is Acute Myeloid Leukemia (AML)? Acute myeloid leukemia (AML) is a cancer of cells in the blood, bone marrow and lymph nodes. AML is also called acute nonlymphocytic leukemia, acute myeloblastic leukemia,
What is Acute Myeloid Leukemia (AML)? Acute myeloid leukemia (AML) is a cancer of cells in the blood, bone marrow and lymph nodes. AML is also called acute nonlymphocytic leukemia, acute myeloblastic leukemia,
1 Introduction. 1.1 Cancer. Introduction
 Introduction 1 1.1 Cancer 1 Introduction Cancer is the most precarious disease characterized by uncontrolled proliferation of cells without any physiological demands of the organism. Cancer may be defined
Introduction 1 1.1 Cancer 1 Introduction Cancer is the most precarious disease characterized by uncontrolled proliferation of cells without any physiological demands of the organism. Cancer may be defined
7 Omar Abu Reesh. Dr. Ahmad Mansour Dr. Ahmad Mansour
 7 Omar Abu Reesh Dr. Ahmad Mansour Dr. Ahmad Mansour -Leukemia: neoplastic leukocytes circulating in the peripheral bloodstream. -Lymphoma: a neoplastic process in the lymph nodes, spleen or other lymphatic
7 Omar Abu Reesh Dr. Ahmad Mansour Dr. Ahmad Mansour -Leukemia: neoplastic leukocytes circulating in the peripheral bloodstream. -Lymphoma: a neoplastic process in the lymph nodes, spleen or other lymphatic
Cover Page. Author: Quispel, W.T. Title: Langerhans cell histiocytosis : genetic and immunologic fingerprinting Issue Date:
 Cover Page The handle http://hdl.handle.net/887/4387 holds various files of this Leiden University dissertation Author: Quispel, W.T. Title: Langerhans cell histiocytosis : genetic and immunologic fingerprinting
Cover Page The handle http://hdl.handle.net/887/4387 holds various files of this Leiden University dissertation Author: Quispel, W.T. Title: Langerhans cell histiocytosis : genetic and immunologic fingerprinting
Case Workshop of Society for Hematopathology and European Association for Haematopathology
 Case 148 2007 Workshop of Society for Hematopathology and European Association for Haematopathology Robert P Hasserjian Department of Pathology Massachusetts General Hospital Boston, MA Clinical history
Case 148 2007 Workshop of Society for Hematopathology and European Association for Haematopathology Robert P Hasserjian Department of Pathology Massachusetts General Hospital Boston, MA Clinical history
MS.4/ Acute Leukemia: AML. Abdallah Al Abbadi.MD.FRCP.FRCPath Feras Fararjeh MD
 MS.4/ 27.02.2019 Acute Leukemia: AML Abdallah Al Abbadi.MD.FRCP.FRCPath Feras Fararjeh MD Case 9: Acute Leukemia 29 yr old lady complains of fever and painful gums for 1 week. She developed easy bruising
MS.4/ 27.02.2019 Acute Leukemia: AML Abdallah Al Abbadi.MD.FRCP.FRCPath Feras Fararjeh MD Case 9: Acute Leukemia 29 yr old lady complains of fever and painful gums for 1 week. She developed easy bruising
Pediatric TB Intensive Houston, Texas October 14, 2013
 Pediatric TB Intensive Houston, Texas October 14, 2013 Radiologic Presentation of Childhood TB Susan D. John, MD, FACR October 14, 2013 Disclosures I have no disclosures or conflicts of interest to report
Pediatric TB Intensive Houston, Texas October 14, 2013 Radiologic Presentation of Childhood TB Susan D. John, MD, FACR October 14, 2013 Disclosures I have no disclosures or conflicts of interest to report
Pediatric Retroperitoneal Masses Radiologic-Pathologic Correlation
 Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 61-70, Abr.-Jun., 2006 Pediatric Retroperitoneal Masses Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 61-70, Abr.-Jun., 2006 Pediatric Retroperitoneal Masses Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
Endocrinological Outcome Among Treated Craniopharyngioma Patients
 Endocrinological Outcome Among Treated Craniopharyngioma Patients Afaf Al Sagheir, MD Head & Consultant, Section of Endocrinology/Diabetes Department of Pediatrics KFSH&RC Introduction Craniopharyngiomas
Endocrinological Outcome Among Treated Craniopharyngioma Patients Afaf Al Sagheir, MD Head & Consultant, Section of Endocrinology/Diabetes Department of Pediatrics KFSH&RC Introduction Craniopharyngiomas
155.2 Malignant neoplasm of liver not specified as primary or secondary. C22.9 Malignant neoplasm of liver, not specified as primary or secondary
 ICD-9 TO ICD-10 Reference ICD-9 150.9 Malignant neoplasm of esophagus unspecified site C15.9 Malignant neoplasm of esophagus, unspecified 151.9 Malignant neoplasm of stomach unspecified site C16.9 Malignant
ICD-9 TO ICD-10 Reference ICD-9 150.9 Malignant neoplasm of esophagus unspecified site C15.9 Malignant neoplasm of esophagus, unspecified 151.9 Malignant neoplasm of stomach unspecified site C16.9 Malignant
Information. about cancer
 1 Information about cancer This chapter may help you answer simple questions about what cancer is and how it is treated. There are more than 200 different types of cancer and a range of treatments. Being
1 Information about cancer This chapter may help you answer simple questions about what cancer is and how it is treated. There are more than 200 different types of cancer and a range of treatments. Being
Paediatric Manifestations of Langerhans Cell Histiocytosis: a Review of the Clinical and Radiological Findings
 Clinical Radiology (2003) 58: 269 278 doi:10.1016/s0009-9260(02)00537-8, available online at www.sciencedirect.com Review Paediatric Manifestations of Langerhans Cell Histiocytosis: a Review of the Clinical
Clinical Radiology (2003) 58: 269 278 doi:10.1016/s0009-9260(02)00537-8, available online at www.sciencedirect.com Review Paediatric Manifestations of Langerhans Cell Histiocytosis: a Review of the Clinical
Therapy prolongation improves outcome in multisystem Langerhans cell histiocytosis
 Regular Article CLINICAL TRIALS AND OBSERVATIONS Therapy prolongation improves outcome in multisystem Langerhans cell histiocytosis Helmut Gadner, 1 Milen Minkov, 1 Nicole Grois, 1 Ulrike Pötschger, 1
Regular Article CLINICAL TRIALS AND OBSERVATIONS Therapy prolongation improves outcome in multisystem Langerhans cell histiocytosis Helmut Gadner, 1 Milen Minkov, 1 Nicole Grois, 1 Ulrike Pötschger, 1
Hodgkin's Lymphoma. Symptoms. Types
 Hodgkin's lymphoma (Hodgkin's disease) usually develops in the lymphatic system, a part of the body's immune system. This system carries disease-fighting white blood cells throughout the body. Lymph tissue
Hodgkin's lymphoma (Hodgkin's disease) usually develops in the lymphatic system, a part of the body's immune system. This system carries disease-fighting white blood cells throughout the body. Lymph tissue
What is a hematological malignancy? Hematology and Hematologic Malignancies. Etiology of hematological malignancies. Leukemias
 Hematology and Hematologic Malignancies Cancer of the formed elements of the blood What is a hematological malignancy? A hematologic malignancy is a malignancy (or cancer) of any of the formed elements
Hematology and Hematologic Malignancies Cancer of the formed elements of the blood What is a hematological malignancy? A hematologic malignancy is a malignancy (or cancer) of any of the formed elements
Recurrent torticollis secondary to Langerhans Cell Histiocytosis : A case report
 Acta Orthop. Belg., 2005, 71, 102-106 CASE REPORT Recurrent torticollis secondary to Langerhans Cell Histiocytosis : A case report Stavroula KOSTARIDOU, John ANASTASOPOULOS, Charalambos VELIOTIS, John
Acta Orthop. Belg., 2005, 71, 102-106 CASE REPORT Recurrent torticollis secondary to Langerhans Cell Histiocytosis : A case report Stavroula KOSTARIDOU, John ANASTASOPOULOS, Charalambos VELIOTIS, John
