ARTICLE. Clinical Course and Outcomes Among Very Low-Birth-Weight Infants
|
|
|
- Laura Greene
- 6 years ago
- Views:
Transcription
1 ARTICLE Clinical Course and Outcomes Among Very Low-Birth-Weight Infants Maria Tomaszewska, MD; Eileen Stork, MD; Nori Mercuri Minich, BS; Harriet Friedman, MA; Sheila Berlin, MD; Maureen Hack, MB, ChB Objective: To describe the clinical course, neonatal morbidity, and neurodevelopmental outcomes of very lowbirth-weight ( 1500 g) children who develop pulmonary hemorrhage. Design: A retrospective case-control study in which 58 very low-birth-weight infants who developed pulmonary hemorrhage during 1990 through 1994, of whom 29 survived, were each matched to the next admitted infant who required mechanical ventilation for respiratory distress syndrome and was of the same sex, race, and birth weight (within 250 g). Setting: A regional tertiary neonatal intensive care unit and follow-up clinic for high-risk infants at University Hospitals of Cleveland, Cleveland, Ohio. Main Outcome Measures: Survival, neonatal morbidity, and neurodevelopmental outcome at 20 months corrected age. Results: hemorrhage occurred in 5.7% of the total population of very low-birth-weight infants. Despite similar severity of lung disease, significantly more infants who developed pulmonary hemorrhage received surfactant therapy compared with controls (91% vs 69%, P =.005). Infants with pulmonary hemorrhage who died had a lower birth weight and gestational age compared with those who survived (766 g vs 1023 g; 25 weeks vs 28 weeks, P.001) and more received surfactant therapy (100% vs 83%, P =.05). Survivors with pulmonary hemorrhage did not differ significantly from controls in rates of oxygen dependence at 36 weeks corrected age (52% vs 38%), grade 3 to 4 periventricular hemorrhage (28% vs 17%), or necrotizing enterocolitis (3% vs 7%), but tended to have more seizures (24% vs 3%, P =.05), periventricular leucomalacia (17% vs 0%, P =.06), and patent ductus arteriosus (79% vs 55%, P =.09). There were no significant differences in neurodevelopmental outcomes at 20 months corrected age, (cerebral palsy, 16% vs 14%; subnormal [ 70] Bayley Mental Developmental Index, 59% vs 43%; and deafness, 13% vs 10%). Conclusion: Although mortality is high, pulmonary hemorrhage does not significantly increase the risk of later pulmonary or neurodevelopmental disabilities among those who survive. Arch Pediatr Adolesc Med. 1999;153: Editor s Note: What would you suppose the long-term outcome of the surviving neonates would be? Catherine D. DeAngelis, MD From the Department of Pediatrics, Case Western Reserve University, Cleveland, Ohio. PRIOR TO 1990, neonatal pulmonary hemorrhage occurred mainly as a terminal event among infants who were small for gestational age and asphyxiated; however, after the introduction of surfactant therapy, an increased occurrence of pulmonary hemorrhage was noted among preterm infants with respiratory distress syndrome. 1-5 Depending on birth weight and the criteria used for defining pulmonary hemorrhage, reported rates of pulmonary hemorrhage among very low-birth-weight (VLBW) infants range from 0.5% to 11% Currently, approximately 50% of infants who experience pulmonary hemorrhage survive; however, there is very little information on their subsequent health and neurodevelopmental outcome We sought to describe the clinical course and associated neonatal morbidity and later neurodevelopmental outcome of VLBW ( 1500 g) children who were admitted to our neonatal intensive care unit between 1990 and 1994 and who developed pulmonary hemorrhage. We furthermore sought to identify the perinatal predictors of pulmonary hemorrhage and the correlates of death in this population. 715
2 PARTICIPANTS AND METHODS One thousand eleven VLBW infants were admitted to the Neonatal Intensive Care Unit at Rainbow Babies & Children s Hospital, University Hospitals of Cleveland, Cleveland, Ohio, between January 1, 1990, and December 31, Eight hundred fourteen infants (81%) were born at our perinatal center and the remainder were transported from community hospitals; 477 (47%) were male, 407 (40%) were white, 218 (22%) were of multiple birth, and 40 (4%) had major congenital malformations. The mean ± SD birth weight and gestational age was 1056 ± 272 g and 28.1 ± 3 weeks, respectively. Eight hundred thirty-two infants developed respiratory distress syndrome requiring assisted ventilation, of whom 474 (57%) received surfactant therapy and 662 (80%) survived to 20 months corrected age. Seventy-one VLBW infants were recorded in our neonatal database as having pulmonary hemorrhage, of whom 61 were considered to have a true pulmonary hemorrhage. This was defined as a nontraumatic gush of bloody secretion from the endotracheal tube associated with clinical deterioration requiring increased ventilatory support. 16,17 Nine children had a suspected pulmonary hemorrhage, which was defined as a persistent blood-tinged secretion suctioned from the endotracheal tube, but not associated with clinical deterioration or the need for increased ventilatory assistance. One additional infant categorized as having a pulmonary hemorrhage was excluded from the study owing to incomplete documentation of the hemorrhage. Of the 61 children with a true pulmonary hemorrhage, 1 had trisomy 18 syndrome, 1 had trisomy 21 syndrome, and 1 later developed acquired immunodeficiency syndrome. These 3 children were excluded from further analysis. The study population thus included 58 children with a true pulmonary hemorrhage. These children constituted 5.7% of the total population of VLBW infants. The rates of pulmonary hemorrhage were similar between inborn and outborn infants (5.8% vs 5.6%, P =.95). Seventeen of the infants weighed less than 750 g at birth, 23 weighed between 750 and 999 g, and 18 weighed between 1000 and 1499 g. They constituted 10%, 9%, and 3% of their respective birthweight subgroups. Twenty-nine(50%) of the 58 children with pulmonary hemorrhage survived to 20 months corrected age. A retrospective case-control method was used to select a comparison group of infants without pulmonary hemorrhage. Each infant with pulmonary hemorrhage was matched to the next admitted infant who had respiratory distress syndrome; required mechanical ventilation; and was of the same sex, race, birth weight within 250 g; and singleton or multiple birth. Because a matched comparison group of surviving children was required to examine the 20- month neurodevelopmental outcomes, survivors and nonsurvivors were matched separately. Control children with major congenital malformations and survivors who had not completed the 20 month follow-up were excluded from the matching process. Fifteen of the infants with pulmonary hemorrhage were of multiple birth (13 twins and 2 triplets), of whom 3 were matched to singletons owing to lack of a multiple-birth match. The mean birth weight and gestational age of the 58 infants with pulmonary hemorrhage and of the matched controls is presented in Table 1. In both the study and control groups, 35 (60%) of the infants were male and 24 (41%) were white. Sociodemographic characteristics of the survivors as measured by maternal age and education were similar between groups. The mean ± SD age of the mothers of children surviving pulmonary hemorrhage was 25.7 ± 5 years and of the control mothers, 27.7 ± 6 years. Seven (26%) of 27 and 2 (7%) of 28 mothers of the children with pulmonary hemorrhage and controls, respectively, had less than a high school education (difference not significant). Surfactant therapy became standard practice in our institution in December 1989 and was given as rescue therapy to infants with respiratory distress syndrome who required assisted ventilation and more than 30% inspired oxygen. Both a combination of colfosceril palmitate, cetyl RESULTS CLINICAL DESCRIPTION OF THE PULMONARY HEMORRHAGE AND THE ASSOCIATED NEONATAL COURSE Fifty-seven of the 58 infants with pulmonary hemorrhage had respiratory distress syndrome, of whom 56 required assisted ventilation and 1 oxygen via a hood. Fiftythree (91%) of the infants were treated with surfactant. They received a mean of 2 doses of surfactant (range, 1-4), with the first dose administered at a mean ±SD age of5±5 hours. The mean oxygenation index was 12 ± 7 immediately preceding the first dose of surfactant and it decreased to5±3before the pulmonary hemorrhage. For the infants who did not receive surfactant therapy, the initial oxygenation index was measured at 5 hours of life. Seventeen infants (29%) presented with prodromal episodes of a frothy reddish secretion suctioned from the endotracheal tube. These were not associated with clinical deterioration and persisted for periods of a few hours to days prior to the acute pulmonary hemorrhage. Seven infants (12%) presented with extrapulmonary bleeding prior to the pulmonary hemorrhage including severe bruising, hematuria, gastric hemorrhage, and oozing around the umbilical catheter and blood puncture sites. Eleven infants (19%) had evidence of multiorgan failure prior to the hemorrhage. Four infants (7%) had septicemia (Haemophilus influenzae, Escherichia coli, Candida albicans, Staphylococcus epidermidis) and 1 had a congenital cytomegalovirus infection. The acute episode of hemorrhage occurred at a median of 40 hours of life (range, hours). This occurred before 48 hours of life in 35 infants (60%), between 48 and 72 hours in 12 infants (21%), and beyond 72 hours of life in 11 infants (19%) (of whom 5 presented after 7 days of life). The presenting clinical signs of the pulmonary hemorrhage, in addition to the acute gush of blood, included cyanosis in all the infants and bradycardia in 35 of 58 infants. As the condition deteriorated, gasping, apnea, or an increased work of breathing with diminished breath sounds on auscultation were 716
3 alcohol, and tyloxapol (Exosurf; Burroughs Wellcome Co, Research Triangle Park, NC) and beractant (Survanta; Ross- Laboratories, Columbus, Ohio) were used during the study period. The combination of colfosceril palmitate, cetyl alcohol, and tyloxapol was administered in doses of 5 ml/kg every 12 hours and beractant at 4 ml/kg every 6 hours. A maximum of 4 doses were given. Prenatal, intrapartum, and neonatal data were examined as correlates of pulmonary hemorrhage and its outcomes. Data were extracted from the medical records at the time of the infant s discharge from the hospital. Additional details specifically pertaining to pulmonary hemorrhage were later extracted from the medical records by one of us (M.T.). These included details of surfactant administration and neonatal morbidity existing prior to the pulmonary hemorrhage, the time of occurrence and clinical presentation of the hemorrhage, vital signs, and results of arterial blood gases and ventilatory settings recorded within 6 hours prior to and 1 hour after the pulmonary hemorrhage. The oxygenation index was used as a measure of the severity of lung disease. This was calculated as the mean airway pressure times the fraction of inspired oxygen, divided by the PaO 2 times 100. Blood cell counts and results of coagulation studies and blood cultures performed within 72 hours prior to and after the hemorrhage were recorded. Septicemia was defined as a positive blood culture in the presence of clinical indices of infection. Coagulopathy included 2 or more of the following: a prothrombin time of more than 20 seconds, fibrinogen less than 1.5 g/l, D-dimer more than 0.5 mg/l, and thrombocytopenia defined as a platelet count less than /L. Multiorgan failure was defined as the presence of 3 or more of the following: respiratory insufficiency, cardiovascular instability including hypotension and poor peripheral perfusion, renal failure, intracranial hemorrhage, and metabolic abnormalities including metabolic acidosis and glucose intolerance. Intrauterine growth failure was defined as a birth weight less than 2 SDs of the mean for gestational age. 18 Chronic lung disease was defined as an oxygen dependence at 36 weeks postconceptional age. 19 Additional measures of respiratory outcome included the total number of days of oxygen and ventilator dependence and the postnatal use of steroids for chronic lung disease. Periventricular hemorrhage was defined according to Papile et al. 20 Necrotizing enterocolitis was defined according to the criteria of Bell et al. 21 The primary cause of death was respiratory distress syndrome and/or its complications, such as pulmonary hemorrhage or chronic lung disease, or infection, necrotizing enterocolitis, catastrophic cerebral hemorrhage, sudden infant death syndrome, or other causes. Follow-up information to 20 months corrected age was available from the follow-up database and included results from the Amiel-Tison neurological examination 22 and the Bayley Scales of Infant Development (BSID). 23 Twentytwo children with pulmonary hemorrhage and 28 control children had a complete developmental assessment performed at 20 months corrected age. Two of the remaining 7 children with pulmonary hemorrhage and 1 control child had been examined at 8 months corrected age. Major neurosensory abnormalities were categorized as cerebral palsy (spastic diplegia, quadriplegia, or hemiplegia), hypotonia, hypertonia, shunt-dependent hydrocephalus, unilateral or bilateral blindness, and unilateral or bilateral deafness requiring hearing aids. The children born between 1990 and 1991 (n = 19) were assessed using the original BSID, and those born between 1992 and 1994 (n = 31) were assessed using the revised BSID (BSID II). 24 Because more of the infants were tested using BSID II, which has been reported to give lower scores than the BSID, we used a correction factor for the scores of the children born prior to 1992 tested with BSID. All data were analyzed with the Statistical Program for Social Sciences (SPSS, Chicago, Ill). Children with pulmonary hemorrhage were compared with their controls in regard to perinatal and neonatal risk factors and outcomes, using 2-tailed t tests for continuous data and 2 analysis for categorical data. Continuous variables with skewed distribution were compared using nonparametric tests (eg, the Mann-Whitney test). noted in 12 infants. An acute drop in blood pressure was observed in 21 infants, extreme agitation in 3, and seizures in 3. All infants were being treated with antibiotics at the time of the hemorrhage. Management of the acute hemorrhage included an increase in ventilatory support and administration of parenteral fluids and medications. Epinephrine was administered via endotracheal tube to 32 infants and intravenously to 8 infants. Packed red blood cell transfusions were given to 41 infants, fresh-frozen plasma to 20 infants, and platelet transfusions to 10 infants. In addition, 17 infants received isotonic sodium chloride solution or a solution of 5% albumin, 12 received vasopressors, 29 received sodium bicarbonate, 37 received sedatives, and 15 received paralytic agents. The ventilatory parameters prior to and within 1 hour of the pulmonary hemorrhage are summarized in Table 2. The oxygenation index increased significantly after the hemorrhage and hypoxemia and respiratory acidosis persisted despite aggressive therapy. No additional signs of extrapulmonary hemorrhage were noted after the pulmonary hemorrhage; however, coagulopathy was documented in 10 of 24 infants tested, with thrombocytopenia in 9 of 52 infants tested. Despite blood transfusions, the mean hematocrit fell from 0.39 ± 0.7 to 0.32 ± 0.7. Among the 29 infants who survived, respiratory status gradually improved after the initial therapy and ventilatory support could be weaned to the preexisting ventilator settings within a mean of 5 days (range, 2-15 days). All surviving infants had a persistent bloody secretion suctioned from the endotracheal tube for a mean of 7 days after the acute hemorrhage (range, 2-14 days). This gradually changed from bright red to frothy pink to brown. Infants with pulmonary hemorrhage who died had a significantly lower birth weight and gestational age compared with those who survived and tended to be African American (Table 3). They had more severe respiratory disease as evidenced by a significantly higher oxygenation index. More of the infants who died received surfactant (P =.05) and their hemorrhages occurred significantly sooner after the last dose 717
4 Table 1. Birth Data and Severity of Respiratory Illness of and Their * Birth Data P Birth weight, mean ± SD, g 900 ± ± Gestational age, mean ± SD, wk 26.5 ± ± Small for gestational age 4 (14) 2 (7).67 Apgar score 6 at 1 min 43 (74) 48 (86).19 Apgar score 6 at 5 min 19 (33) 22 (39).6 Intubation in the delivery room 53 (91) 54 (93) 1.0 Oxygenation index, median (range) 10 (3-33) 12 (1-82).87 Surfactant therapy 53 (91) 40 (69).005 Indicates to 2 SDs. Oxygenation index prior to first surfactant dose or at 5 hours of life for the infants who were not treated with surfactant. Table 2. Ventilatory Parameters Prior to and Following * Prior to Within 2 Hours After Oxygenation index 5 ± 3 24 ± 20 Arterial blood gas parameters ph 7.3 ± ± 0.2 PCO 2,mmHg 42±9 63±17 PO 2,mmHg 77±28 48±33 *All values are given as mean ± SD. of surfactant than did the hemorrhages in infants who survived. There were no differences in the type of surfactant used or response to this therapy. The combination of colfosceril palmitate, cetyl alcohol, and tyloxapol was given to 18 (75%) of 24 infants who survived and to 16 (55%) of 29 infants who died (P =.23), and beractant to 7 (29%) of 24 who survived, and 13 (45%) of 29 who died (P =.38). PERINATAL RISK FACTORS AND OUTCOMES FOR INFANTS WHO DEVELOPED PULMONARY HEMORRHAGE COMPARED WITH MATCHED CONTROLS Table 3. Birth Data and the Neonatal Course of Infants With Who Survived and Those Who Died* Birth Data Survived Died P Birth weight, mean ± SD, g 1023 ± ± Gestational age, mean ± SD, wk 28 ± 2 25 ± Male 15 (52) 20 (69).28 White 16 (55) 8 (28).06 Morbidity prior to the hemorrhage Septicemia 2 (7) 2 (7) 1.0 Multiorgan failure 3 (10) 8 (28).18 Age at pulmonary hemorrhage, 50 (19-511) 35 (7-366).12 median (range), h Surfactant therapy 24 (83) 29 (100).05 Oxygenation index, mean ± SD Prior to first surfactant dose 10 ± 6 14 ± 8.03 Prior to pulmonary hemorrhage 4 ± 2 5 ± 3.07 Within 1 h after pulmonary 16 ± ± hemorrhage Hours between last surfactant dose and pulmonary hemorrhage, median (range) 27 (5-507) 14 (1-352).02 A comparison of the obstetric and delivery complications of mothers of the 58 infants who developed pulmonary hemorrhage and their matched controls revealed no significant differences between groups (Table 4). There tended, however, to be higher rates of adverse previous pregnancy outcomes and cesarean sections among the mothers of infants who developed a pulmonary hemorrhage (P =.07). The status of the infants at birth, as evidenced by low Apgar scores and the need for endotracheal intubation in the delivery room, was similar between groups (Table 1). There was no significant difference in the initial severity of lung disease, as measured by the oxygenation index; however, significantly more infants who developed pulmonary hemorrhage received surfactant therapy as compared with controls. There was no difference between groups in the type of surfactant used. The combination of colfosceril palmitate, cetyl alcohol, and tyloxapol was given to 34 (64%) of 53 infants with pulmonary hemorrhage and 30 (75%) of 40 controls (P =.37), and beractant to 20 (38%) of 53 infants with pulmonary hemorrhage and 11 (28%) of 40 controls (P =.42); these data include 1 pulmonary hemorrhage survivor and 1 control survivor who received both the combination of colfosceril palmitate, cetyl alcohol, and tyloxapol and beractant. When compared with their matched controls, significantly more infants with pulmonary hemorrhage who died did not survive beyond 28 days of life. For both groups, respiratory distress syndrome and its complications were the most common cause of death (Table 5). hemorrhage was, however, considered to be a major factor in contributing to the death of 28 of the 29 infants with pulmonary hemorrhage. The birth weight specific mortality at 20 months corrected age of the total population of VLBW infants and those with and without pulmonary hemorrhage is presented in Table 6. hemorrhage contributed to 28 (15%) of 182 of the deaths of the total VLBW population of infants admitted to the nursery. A comparison of neonatal morbidity between the infants who survived pulmonary hemorrhage and their matched controls is presented in Table 7. Although there was no significant difference between groups, the duration of ventilator dependence and rates of oxygen dependence at 28 days of life, patent ductus arteriosus, seizures, and periventricular leukomalacia tended to be higher in the pulmonary hemorrhage group. Of the 7 infants with pulmonary hemorrhage who had seizures, 1 had a seizure 2 days prior to the hemorrhage, 4 within 2 718
5 Table 4. Obstetric Data of Mothers of Infants Who Developed and * Obstetric Data P Maternal age, mean ± SD, y 24.5 ± ± 7.2 Previous adverse pregnancy 22 (38) 12 (21).07 outcome Pregnancy complications Antepartum hemorrhage 7 (12) 11 (19).44 Pregnancy-induced hypertension 8 (14) 2 (3).1 Urinary tract infection 14 (24) 16 (28).83 Chorioamnionitis 5 (9) 11 (19).18 Premature rupture of membranes 9 (16) 10 (17) 1.0 Tocolysis 19 (33) 15 (26).54 Antenatal steroids 6 (10) 6 (10) 1.0 Fetal distress 11 (19) 6 (10).29 Type of delivery Vaginal vertex 18 (31) 30 (52) Vaginal breech 7 (12) 6 (10).07 Cesarean section 33 (57) 22 (38) Included a history of previous preterm birth, stillbirth, neonatal or infant death, therapeutic and habitual abortion, or infant anomaly. Included placenta previa, abruptio placenta, or vaginal spotting defined as vaginal bleeding without a specific cause. Maternal blood pressure greater than or equal to 140/90 mm Hg during the second half of pregnancy in a previously normotensive mother. Table 5. Timing and Causes of Death of and * Timing or Cause of Death Age at death, d 7 18 (62) 16 (55) (31) 4 (14) 28 2 (7) 9 (31) Primary cause of death Respiratory distress syndrome 22 (76) 22 (76) Septicemia 3 (10) 2 (7) Intraventricular hemorrhage 2 (7) 1 (3) Necrotizing enterocolitis 1 (3) 3 (10) Sudden infant death syndrome 0 (0) 1 (3) Other 1 (3) 0 (0) *All values are given as number (percentage). P.05. Respiratory distress syndrome was considered the primary cause of death when it occurred with periventricular hemorrhage. When necrotizing enterocolitis occurred with septicemia, necrotizing enterocolitis was considered the primary cause of death. Catastrophic periventricular hemorrhage. following umbilical catheter accident. weeks after the hemorrhage, and 2 more than 4 weeks after the hemorrhage. The relative risk for oxygen dependence at 28 days among the infants with pulmonary hemorrhage was 3.39 (95% confidence interval, ); for periventricular leukomalacia, 2.2 (95% confidence interval, ), for seizures, 8.9, (95% confidence interval, ), and for patent ductus arteriosus, 3.11 (95% confidence interval, ). Table 6. Twenty-Month Birth Weight Specific Mortality of the Total Population of Very Low-Birth-Weight Infants and of Those With and Without * Birth Weight, g Total Population A comparison of the neurological and developmental outcomes at 20 months corrected age is presented in Table 8. The mean mental and psychomotor developmental indices were lower among the infants who survived pulmonary hemorrhage; however, the differences were not significant. Five of the 7 infants with pulmonary hemorrhage who had seizures also had a severe (grade 3-4) periventricular hemorrhage. All 7 children had some form of neurodevelopment impairment at 20 months corrected age (Bayley Mental Developmental Index 70, neurological abnormality, or hearing loss). COMMENT out n Deaths n Deaths n Deaths (47) (71) (44) (21) (61) (17) (8) 18 3 (17) (8) Total (18) (50) (16) *All values are given as number (percentage). Age corrected for preterm birth. Table 7. Neonatal Morbidity of the Infants Surviving and * Morbidity P Respiratory morbidity Days on ventilator, median (range) 30 (4-124) 26 (1-103).07 Days on oxygen, median (range) 56 (10-634) 31 (4-680).15 Oxygen dependence at 28 days 24 (83) 17 (59).08 Oxygen dependence at 36 weeks 15 (52) 11 (38).43 Postnatal steroid therapy 13 (45) 12 (41) 1.0 Periventricular hemorrhage Grades (35) 11 (38) 1.0 Grades (28) 5 (17).53 Periventricular leukomalacia 5 (17) 0 (0).06 Seizures 7 (24) 1 (3).05 Septicemia 9 (31) 12 (41).58 Patent ductus arteriosus 23 (79) 16 (55).09 Indomethacin therapy 14 (48) 15 (52) 1.0 Ligation 10 (35) 4 (14).12 Necrotizing enterocolitis 1 (3) 2 (7) 1.0 Maximum bilirubin level 171 µmol/l 8 (28) 5 (17).53 ( 10 mg/dl) Hospital stay, mean ± SD, d 90 ± ± Up to 20 months corrected age (680 days). hemorrhage, a rare but well-recognized complication of respiratory distress syndrome, occurred in 5.7% of the total population of VLBW infants admitted to our neonatal intensive care unit during 1990 through 1994 and 719
6 Table 8. Neurodevelopmental Outcome at 20 Months Corrected Age* (n = 24) P Bayley Mental Developmental Index, 71±22 79±22.24 mean ± SD Subnormal ( 70) 13 (59) 12 (43).39 Psychomotor developmental 66±17 75±20.11 index, mean ± SD Subnormal ( 70) 14 (64) 11 (39).15 Total neurological abnormalities 9 (38) 7 (24).45 Cerebral palsy 4 (17) 4 (14).92 Hypotonia 0 (0) 1 (3).91 Hypertonia 3 (13) 3 (10).85 Shunt-dependent hydrocephalus 2 (8) 0 (0).40 Deafness 3 (13) 3 (10).85 Blindness 0 (0) 0 (0) 1.0 n = 22 for pulmonary hemorrhage survivors andn=28forcontrols. Includes 8-month neurological status of 2 children who survived pulmonary hemorrhage and 1 control child. One of the infants with cerebral palsy also had a shunt, without additional neurological impairments. Unilateral or bilateral. contributed to 15% of VLBW deaths during this time. Significantly more infants who developed pulmonary hemorrhage had received surfactant therapy compared with matched controls, despite a similar severity of lung disease. Most were showing an improvement in their respiratory status prior to the pulmonary hemorrhage. The infants who died had a significantly lower birth weight and gestational age, more severe lung disease, and more received surfactant therapy than those who survived. The survivors, after recovery from the pulmonary hemorrhage, had a neonatal course similar to their matched controls; however, they tended to require longer ventilatory support and have higher rates of patent ductus arteriosus, seizures, and periventricular leukomalacia. There were no significant differences between groups in the rates of neurodevelopmental impairment at 20 months corrected age. With the exception of an abstract by Pandit et al, 15 to our knowledge, this is the first report of the neonatal morbidity and early childhood outcomes of infants who survive pulmonary hemorrhage. Pandit et al noted an increased risk of chronic lung disease among infants with moderate to severe pulmonary hemorrhage; however, similar to our findings, the 2-year neurodevelopmental outcome of the survivors did not differ from a control population. With the exception of surfactant therapy, we could not demonstrate any perinatal or neonatal risk factors associated with the occurrence of pulmonary hemorrhage. In the presurfactant era, perinatal risk factors, which were considered to predispose to the development of pulmonary hemorrhage, included breech delivery, cesarean section for preeclampsia, multiple gestation, low birth weight, intrauterine growth failure, male sex, and birth asphyxia. 1-5 Correlates of pulmonary hemorrhage since the introduction of surfactant therapy have included the severity of respiratory distress syndrome, 7,8 the type of surfactant used, 8 the time of its administration, 7 the presence of a patent ductus arteriosus, and maternal antibiotic therapy. 14,17,25 Owing to the retrospective nature of our study and the lack of routine echocardiograms to diagnose a patent ductus arteriosus, we could not examine the association between patent ductus arteriosus and pulmonary hemorrhage in our population. A metaanalysis of the results of the randomized clinical trials of surfactant therapy indicate a 47% increased risk of pulmonary hemorrhage for infants who received surfactant therapy; however, no association with patent ductus arteriosus was demonstrated. 8 hemorrhage is considered to be a hemorrhagic edema resulting from stress failure of pulmonary capillaries associated with lung overdistension, inadequate protective surface tension, and fragility of the pulmonary capillary wall. 5,26 It is postulated that after surfactant therapy, pulmonary vascular resistance falls and that the increase in left to right shunting and lung compliance predispose to pulmonary hemorrhage. 27,28 The fact that up to 10% of infants with respiratory distress syndrome who did not receive surfactant therapy in the randomized clinical trials developed pulmonary hemorrhage and that 5 of the infants in our population developed the pulmonary hemorrhage after 7 days of life indicates that other yet-unidentified factors may also play a role in the pathogenesis of pulmonary hemorrhage. 8 The smallest and sickest infants who developed pulmonary hemorrhage died. Thus, it is not surprising that the survivors had neonatal and longer-term outcomes similar to VLBW children who did not develop pulmonary hemorrhage. We did not examine pulmonary function in our population. However, the rate of rehospitalizations was similar between groups. During the first year of life 11 (44%) of 25 of pulmonary hemorrhage survivors on whom we had information were rehospitalized at least once, compared with 10 (34%) of 29 of the controls (P =.66). In both groups, most rehospitalizations were due to pulmonary causes such as respiratory tract infection and reactive airway disease. A weakness in this study is the small population size, which might not have provided sufficient power to reveal statistically significant differences in outcome. The increased risk of neonatal seizures and periventricular leukomalacia suggested in our results may possibly be due to hypoxic ischemic encephalopathy, which could have occurred during the period of acute decompensation associated with the pulmonary hemorrhage. This might also explain the 8-point difference in the Bayley Mental Developmental Index between children surviving pulmonary hemorrhage and controls that, although not statistically significant, may be clinically meaningful. Despite this consideration, we conclude that although the mortality for infants who develop pulmonary hemorrhage is high, aggressive treatment is justified since the infants who survive do not suffer from excessive neonatal or longer-term morbidities. Accepted for publication December 16, Corresponding author: Maria Tomaszewska, MD, Division of Neonatology, Rainbow Babies & Childrens Hospital, Euclid Ave, Cleveland, OH
7 REFERENCES 1. Esterly JR, Oppenheimer EH. Massive pulmonary hemorrhage in the newborn, I: pathologic consideration. J Pediatr. 1966;69: Rowe S, Avery ME. Massive pulmonary hemorrhage in the newborn, II: clinical consideration. J Pediatr. 1966;69: Butler NR, Alberman ED, eds. Perinatal Problems. London, England: E&S Livingstone Ltd; Fedrick J, Butler NR. Certain causes of neonatal death. Biol Neonate. 1971;18: Cole VA, Normand ICS, Reynolds EOR, Rivers RPA. Pathogenesis of hemorrhagic pulmonary edema and massive pulmonary hemorrhage in the newborn. Pediatrics. 1973;51: Stevenson D, Walther F, Long W, et al. Controlled trial of a single dose of synthetic surfactant at birth in premature infants weighing 500 to 699 grams. J Pediatr. 1992;120:S3-S Zola EM, Overbach AM, Gunkel JH, et al. Treatment investigational new drug experience with Survanta (beractant). Pediatrics. 1993;91: Raju T, Langenberg P. hemorrhage and exogenous surfactant therapy: a meta-analysis. J Pediatr. 1993;123: Horbar JD, Wright LL, Soll RF, et al. A multicenter randomized trial comparing two surfactants for the treatment of neonatal respiratory distress syndrome. Pediatrics. 1993;123: Valencia G, Allen L, Claude S, Cobham A, Glass A, Anderson V. hemorrhage: a severe complication in preterm infants administered surfactant replacement therapy [abstract]. Pediatr Res. 1992;31:226A. 11. Bhandari V, Gasnon C, Hussain N, Rosenkrantz T. hemorrhage in neonates [abstract]. Pediatr Res. 1995;39:196A. 12. Geraldo V, Agrawal V, Wilks A. Does pulmonary hemorrhage contribute to excess mortality in ELBW neonates receiving surfactant therapy [abstract]? Pediatr Res. 1996;39:209A. 13. Braun K, Nielsen HC. Antecedents of neonatal pulmonary hemorrhage in the surfactant era [abstract]. Pediatr Res. 1996;39:259A. 14. Garland J, Buck R, Weinberg M. hemorrhage risk in infants with clinically diagnosed patent ductus arteriosus: a retrospective cohort study. Pediatrics. 1994;94: Pandit P, O Brien K, Dunn M, Asztalos E, Colucci E. Outcome following pulmonary hemorrhage (PH) in very low birth weight neonates treated with surfactant [abstract]. Pediatr Res. 1997;41:208A. 16. Roberton NRC. oedema/pulmonary haemorrhage. In: Greenough A, Milner AD, Roberton NRC, eds. Neonatal Respiratory Disorders. London, England: Arnold; 1996: Gonzales A, Hummler H, Sosenko IRS, Chandar J, Goldberg RN, Bancalari E. Surfactant administration, patent ductus arteriosus, and pulmonary hemorrhage in premature infants 1000 g [abstract]. Pediatr Res. 1994;35:227A. 18. Usher R, McLean F. Intrauterine growth of live-born caucasian infants at sea level: standards obtained from measurements in 7 dimensions of infants born between 25 and 44 weeks of gestation. J Pediatr. 1969;72: Shennan AT, Dunn MS, Ohlsson A, Lenox K. Abnormal pulmonary outcomes in premature infants: prediction from oxygen requirement in the neonatal period. Pediatrics. 1988;82: Papile LA, Burstein J, Burstein R, Koffler H. Incidence and evolution of subependymal and intraventricular hemorrhages: a study of infants with birthweights less than 1500 g. J Pediatr. 1978;92: Bell MJ, Ternberg JL, Feigin RD, et al. Neonatal necrotizing enterocolitis: therapeutic decisions based on clinical staging. Ann Surg. 1978;187: Amiel-Tison C, Stewart AL. Follow-up studies in the first five years of life: a pervasive assessment of neurologic function. Arch Dis Child. 1989;64: Bayley N. Bayley Scales of Infant Development. New York, NY: The Psychological Corp; Bayley N. Bayley Scales of Infant Development. 2nd ed. San Antonio, Tex: The Psychological Corp; Covert RE, Domanico RS, Barman N, et al. Prophylactic indomethacin: effect on pulmonary hemorrhage and bronchopulmonary dysplasia in surfactant-treated infants 1250 g [abstract]. Pediatr Res. 1996;39:203A. 26. West J, Mathieu-Costello O. Stress failure of pulmonary capillaries: role in lung and heart disease. Lancet. 1992;340: KääpäP, Seppänen M, Kero P, Saraste M. hemodynamics after synthetic surfactant replacement in neonatal respiratory distress syndrome. J Pediatr. 1993;123: Bhutani VK, Abbasi S, Long WA, Gerdes JS. mechanics and energetics in preterm infants who had respiratory distress syndrome treated with synthetic surfactant. J Pediatr. 1992;120:S18-S
Admission/Discharge Form for Infants Born in Please DO NOT mail or fax this form to the CPQCC Data Center. This form is for internal use ONLY.
 Selection Criteria Admission/Discharge Form for Infants Born in 2016 To be eligible, you MUST answer YES to at least one of the possible criteria (A-C) A. 401 1500 grams o Yes B. GA range 22 0/7 31 6/7
Selection Criteria Admission/Discharge Form for Infants Born in 2016 To be eligible, you MUST answer YES to at least one of the possible criteria (A-C) A. 401 1500 grams o Yes B. GA range 22 0/7 31 6/7
The high risk neonate
 The high risk neonate Infant classification by gestational (postmenstrual) age Preterm. Less than 37 completed weeks (259 days). Term. Thirty-seven to 416/7 weeks (260-294 days). Post-term. Forty-two weeks
The high risk neonate Infant classification by gestational (postmenstrual) age Preterm. Less than 37 completed weeks (259 days). Term. Thirty-seven to 416/7 weeks (260-294 days). Post-term. Forty-two weeks
ROLE OF EARLY POSTNATAL DEXAMETHASONE IN RESPIRATORY DISTRESS SYNDROME
 INDIAN PEDIATRICS VOLUME 35-FEBRUAKY 1998 ROLE OF EARLY POSTNATAL DEXAMETHASONE IN RESPIRATORY DISTRESS SYNDROME Kanya Mukhopadhyay, Praveen Kumar and Anil Narang From the Division of Neonatology, Department
INDIAN PEDIATRICS VOLUME 35-FEBRUAKY 1998 ROLE OF EARLY POSTNATAL DEXAMETHASONE IN RESPIRATORY DISTRESS SYNDROME Kanya Mukhopadhyay, Praveen Kumar and Anil Narang From the Division of Neonatology, Department
Hyaline membrane disease. By : Dr. Ch Sarishma Peadiatric Pg
 Hyaline membrane disease By : Dr. Ch Sarishma Peadiatric Pg Also called Respiratory distress syndrome. It occurs primarily in premature infants; its incidence is inversely related to gestational age and
Hyaline membrane disease By : Dr. Ch Sarishma Peadiatric Pg Also called Respiratory distress syndrome. It occurs primarily in premature infants; its incidence is inversely related to gestational age and
ADMISSION/DISCHARGE FORM FOR INFANTS BORN IN 2019 DO NOT mail or fax this form to the CPQCC Data Center. This form is for internal use ONLY.
 1 Any eligible inborn infant who dies in the delivery room or at any other location in your hospital within 12 hours after birth and prior to admission to the NICU is defined as a "Delivery Room Death."
1 Any eligible inborn infant who dies in the delivery room or at any other location in your hospital within 12 hours after birth and prior to admission to the NICU is defined as a "Delivery Room Death."
Uses 1,2,3 : Labeled: Prevention of respiratory distress syndrome in premature infants
 Brand Name: Surfaxin Generic Name: lucinactant Manufacturer 1 : Discovery Laboratories, Inc. Drug Class 2,3 : Synthetic lung surfactant Uses 1,2,3 : Labeled: Prevention of respiratory distress syndrome
Brand Name: Surfaxin Generic Name: lucinactant Manufacturer 1 : Discovery Laboratories, Inc. Drug Class 2,3 : Synthetic lung surfactant Uses 1,2,3 : Labeled: Prevention of respiratory distress syndrome
Noah Hillman M.D. IPOKRaTES Conference Guadalajaira, Mexico August 23, 2018
 Postnatal Steroids Use for Bronchopulmonary Dysplasia in 2018 + = Noah Hillman M.D. IPOKRaTES Conference Guadalajaira, Mexico August 23, 2018 AAP Policy Statement - 2002 This statement is intended for
Postnatal Steroids Use for Bronchopulmonary Dysplasia in 2018 + = Noah Hillman M.D. IPOKRaTES Conference Guadalajaira, Mexico August 23, 2018 AAP Policy Statement - 2002 This statement is intended for
Patent Ductus Arteriosus: Philosophy or Pathology?
 Patent Ductus Arteriosus: Philosophy or Pathology? Disclosure Ray Sato, MD is a speaker for Prolacta Biosciences, Inc. This presentation will discuss off-label uses of acetaminophen and ibuprofen. RAY
Patent Ductus Arteriosus: Philosophy or Pathology? Disclosure Ray Sato, MD is a speaker for Prolacta Biosciences, Inc. This presentation will discuss off-label uses of acetaminophen and ibuprofen. RAY
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara
 Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
Objectives. Birth Depression Management. Birth Depression Terms
 Objectives Birth Depression Management Regional Perinatal Outreach Program 2016 Understand the terms and the clinical characteristics of birth depression. Be familiar with the evidence behind therapeutic
Objectives Birth Depression Management Regional Perinatal Outreach Program 2016 Understand the terms and the clinical characteristics of birth depression. Be familiar with the evidence behind therapeutic
Massive pulmonary haemorrhage in the newborn infant
 Archives of Disease in Childhood, 1975, 50, 123. Massive pulmonary haemorrhage in the newborn infant R. TROMPETER, V. Y. H. YU, A. AYNSLEY-GREEN, and N. R. C. ROBERTON From the Department of Paediatrics,
Archives of Disease in Childhood, 1975, 50, 123. Massive pulmonary haemorrhage in the newborn infant R. TROMPETER, V. Y. H. YU, A. AYNSLEY-GREEN, and N. R. C. ROBERTON From the Department of Paediatrics,
Neurodevelopmental and Behavioral Outcome of Very Low Birth Weight Babies at Corrected Age of 2 Years
 Indian J Pediatr (2010) 77:963 967 DOI 10.1007/s12098-010-0149-3 ORIGINAL ARTICLE Neurodevelopmental and Behavioral Outcome of Very Low Birth Weight Babies at Corrected Age of 2 Years Kanya Mukhopadhyay
Indian J Pediatr (2010) 77:963 967 DOI 10.1007/s12098-010-0149-3 ORIGINAL ARTICLE Neurodevelopmental and Behavioral Outcome of Very Low Birth Weight Babies at Corrected Age of 2 Years Kanya Mukhopadhyay
SWISS SOCIETY OF NEONATOLOGY. Spontaneous intestinal perforation or necrotizing enterocolitis?
 SWISS SOCIETY OF NEONATOLOGY Spontaneous intestinal perforation or necrotizing enterocolitis? June 2004 2 Stocker M, Berger TM, Neonatal and Pediatric Intensive Care Unit, Children s Hospital of Lucerne,
SWISS SOCIETY OF NEONATOLOGY Spontaneous intestinal perforation or necrotizing enterocolitis? June 2004 2 Stocker M, Berger TM, Neonatal and Pediatric Intensive Care Unit, Children s Hospital of Lucerne,
COMPARISON OF THE EFFICIENCY OF CAFFEINE VERSUS AMINOPHYLLINE FOR THE TREATMENT OF APNOEA OF PREMATURITY
 CASE STUDIES COMPARISON OF THE EFFICIENCY OF CAFFEINE VERSUS AMINOPHYLLINE FOR THE TREATMENT OF APNOEA OF PREMATURITY Gabriela Ildiko Zonda 1, Andreea Avasiloaiei 1, Mihaela Moscalu 2, Maria Stamatin 1
CASE STUDIES COMPARISON OF THE EFFICIENCY OF CAFFEINE VERSUS AMINOPHYLLINE FOR THE TREATMENT OF APNOEA OF PREMATURITY Gabriela Ildiko Zonda 1, Andreea Avasiloaiei 1, Mihaela Moscalu 2, Maria Stamatin 1
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC
 Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
1
 1 2 3 RIFAI 5 6 Dublin cohort, retrospective review. Milrinone was commenced at an initial dose of 0.50 μg/kg/minute up to 0.75 μg/kg/minute and was continued depending on clinical response. No loading
1 2 3 RIFAI 5 6 Dublin cohort, retrospective review. Milrinone was commenced at an initial dose of 0.50 μg/kg/minute up to 0.75 μg/kg/minute and was continued depending on clinical response. No loading
Update on mangement of patent ductus arteriosus in preterm infants. Dr. Trinh Thi Thu Ha
 Update on mangement of patent ductus arteriosus in preterm infants Dr. Trinh Thi Thu Ha Outline 1. Overview of PDA 2. Timing of screening PDA? 3. When to treat PDA? Timing of ductal closure Prenatal
Update on mangement of patent ductus arteriosus in preterm infants Dr. Trinh Thi Thu Ha Outline 1. Overview of PDA 2. Timing of screening PDA? 3. When to treat PDA? Timing of ductal closure Prenatal
Birth Asphyxia - Summary of the previous meeting and protocol overview
 Birth Asphyxia - Summary of the previous meeting and protocol overview Dr Ornella Lincetto, WHO Geneve Milano, 11June 2007 Vilka är Personality egenskaper med den astrologiska Tvillingarna? Objective of
Birth Asphyxia - Summary of the previous meeting and protocol overview Dr Ornella Lincetto, WHO Geneve Milano, 11June 2007 Vilka är Personality egenskaper med den astrologiska Tvillingarna? Objective of
SAMPLE. V.12.1 Special Report: Very Low Birthweight Neonates. I. Introduction
 I. Introduction V.12.1 Special Report: Very Low Birthweight Neonates The delivery of a very low birth weight infant continues to present many challenges to families and health care providers in spite of
I. Introduction V.12.1 Special Report: Very Low Birthweight Neonates The delivery of a very low birth weight infant continues to present many challenges to families and health care providers in spite of
Neonatal Resuscitation. Dustin Coyle, M.D. Anesthesiology
 Neonatal Resuscitation Dustin Coyle, M.D. Anesthesiology Recognize complications Maternal-fetal factors Maternal DM PIH Chronic HTN Previous stillbirth Rh sensitization Infection Substance abuse/certain
Neonatal Resuscitation Dustin Coyle, M.D. Anesthesiology Recognize complications Maternal-fetal factors Maternal DM PIH Chronic HTN Previous stillbirth Rh sensitization Infection Substance abuse/certain
Benefits of Caffeine Citrate: Neurodevelopmental Outcomes of ELBW Infants
 St. Catherine University SOPHIA Master of Arts in Nursing Theses Nursing 12-2011 Benefits of Caffeine Citrate: Neurodevelopmental Outcomes of ELBW Infants Teri Johnson St. Catherine University Follow this
St. Catherine University SOPHIA Master of Arts in Nursing Theses Nursing 12-2011 Benefits of Caffeine Citrate: Neurodevelopmental Outcomes of ELBW Infants Teri Johnson St. Catherine University Follow this
Research Article Timing of Caffeine Therapy and Neonatal Outcomes in Preterm Infants: A Retrospective Study
 International Pediatrics Volume 2016, Article ID 9478204, 6 pages http://dx.doi.org/10.1155/2016/9478204 Research Article Timing of Caffeine Therapy and Neonatal Outcomes in Preterm Infants: A Retrospective
International Pediatrics Volume 2016, Article ID 9478204, 6 pages http://dx.doi.org/10.1155/2016/9478204 Research Article Timing of Caffeine Therapy and Neonatal Outcomes in Preterm Infants: A Retrospective
Bubble CPAP for Respiratory Distress Syndrome in Preterm Infants
 R E S E A R C H P A P E R Bubble CPAP for Respiratory Distress Syndrome in Preterm Infants JAGDISH KOTI*, SRINIVAS MURKI, PRAMOD GADDAM, ANUPAMA REDDY AND M DASARADHA RAMI REDDY From Fernandez Hospital
R E S E A R C H P A P E R Bubble CPAP for Respiratory Distress Syndrome in Preterm Infants JAGDISH KOTI*, SRINIVAS MURKI, PRAMOD GADDAM, ANUPAMA REDDY AND M DASARADHA RAMI REDDY From Fernandez Hospital
Difficulties at Birth: Long Term Developmental Outcomes
 Difficulties at Birth: Long Term Developmental Outcomes Alan D. Bedrick MD Division of Neonatology and Developmental Biology Department of Pediatrics University of Arizona Tucson, Arizona DISCLOSURE I
Difficulties at Birth: Long Term Developmental Outcomes Alan D. Bedrick MD Division of Neonatology and Developmental Biology Department of Pediatrics University of Arizona Tucson, Arizona DISCLOSURE I
An Overview of Bronchopulmonary Dysplasia and Chronic Lung Disease in Infancy
 An Overview of Bronchopulmonary Dysplasia and Chronic Lung Disease in Infancy Housekeeping: I have no financial disclosures Learning objectives: Develop an understanding of bronchopulmonary dysplasia (BPD)
An Overview of Bronchopulmonary Dysplasia and Chronic Lung Disease in Infancy Housekeeping: I have no financial disclosures Learning objectives: Develop an understanding of bronchopulmonary dysplasia (BPD)
Extensive cystic periventricular leukomalacia following early-onset group B streptococcal sepsis in a very low birth weight infant
 SWISS SOCIETY OF NEONATOLOGY Extensive cystic periventricular leukomalacia following early-onset group B streptococcal sepsis in a very low birth weight infant July 2012 2 Berger TM, Caduff JC, Neonatal
SWISS SOCIETY OF NEONATOLOGY Extensive cystic periventricular leukomalacia following early-onset group B streptococcal sepsis in a very low birth weight infant July 2012 2 Berger TM, Caduff JC, Neonatal
5 Million neonatal deaths each year worldwide. 20% caused by neonatal asphyxia. Improvement of the outcome of 1 million newborns every year
 1 5 Million neonatal deaths each year worldwide 20% caused by neonatal asphyxia Improvement of the outcome of 1 million newborns every year International Liaison Committee on Resuscitation (ILCOR) American
1 5 Million neonatal deaths each year worldwide 20% caused by neonatal asphyxia Improvement of the outcome of 1 million newborns every year International Liaison Committee on Resuscitation (ILCOR) American
Cover Page. The handle holds various files of this Leiden University dissertation
 Cover Page The handle http://hdl.handle.net/1887/22368 holds various files of this Leiden University dissertation Author: Lugt, Neeltje Margaretha van der Title: Neonatal pearls : safety and efficacy of
Cover Page The handle http://hdl.handle.net/1887/22368 holds various files of this Leiden University dissertation Author: Lugt, Neeltje Margaretha van der Title: Neonatal pearls : safety and efficacy of
Planning Committee: Jeffery D. Horbar, MD, Madge E. Buus-Frank, RN, MS, APRN-BC, FAAN, Roger F. Soll, MD
 Title of Program: What has Cochrane Neonatal Done For Babies? Speakers/Moderators: Roger F. Soll, MD Planning Committee: Jeffery D. Horbar, MD, Madge E. Buus-Frank, RN, MS, APRN-BC, FAAN, Roger F. Soll,
Title of Program: What has Cochrane Neonatal Done For Babies? Speakers/Moderators: Roger F. Soll, MD Planning Committee: Jeffery D. Horbar, MD, Madge E. Buus-Frank, RN, MS, APRN-BC, FAAN, Roger F. Soll,
Permissive Hypotension in Extremely Low Birth Weight Infants ( 1000 gm)
 Original Article http://dx.doi.org/./ymj.2.3.4.7 pissn: 3-79, eissn: 97-2437 Yonsei Med J 3(4):7-77, 2 Permissive Hypotension in Extremely Low Birth Weight Infants ( gm) So Yoon Ahn, Eun Sun Kim, Jin Kyu
Original Article http://dx.doi.org/./ymj.2.3.4.7 pissn: 3-79, eissn: 97-2437 Yonsei Med J 3(4):7-77, 2 Permissive Hypotension in Extremely Low Birth Weight Infants ( gm) So Yoon Ahn, Eun Sun Kim, Jin Kyu
Early seizures indicate quality of perinatal care
 Archives of Disease in Childhood, 1985, 6, 89-813 Early seizures indicate quality of perinatal care R J DERHAM, T G MATTHEWS, AND T A CLARKE Rotunda Hospital, Dublin, Ireland SUMMARY An analysis of antepartum,
Archives of Disease in Childhood, 1985, 6, 89-813 Early seizures indicate quality of perinatal care R J DERHAM, T G MATTHEWS, AND T A CLARKE Rotunda Hospital, Dublin, Ireland SUMMARY An analysis of antepartum,
** SURFACTANT THERAPY**
 ** SURFACTANT THERAPY** Full Title of Guideline: Surfactant Therapy Author (include email and role): Stephen Wardle (V4) Reviewed by Dushyant Batra Consultant Neonatologist Division & Speciality: Division:
** SURFACTANT THERAPY** Full Title of Guideline: Surfactant Therapy Author (include email and role): Stephen Wardle (V4) Reviewed by Dushyant Batra Consultant Neonatologist Division & Speciality: Division:
SWISS SOCIETY OF NEONATOLOGY. Severe apnea and bradycardia in a term infant
 SWISS SOCIETY OF NEONATOLOGY Severe apnea and bradycardia in a term infant October 2014 2 Walker JH, Arlettaz Mieth R, Däster C, Division of Neonatology, University Hospital Zurich, Switzerland Swiss Society
SWISS SOCIETY OF NEONATOLOGY Severe apnea and bradycardia in a term infant October 2014 2 Walker JH, Arlettaz Mieth R, Däster C, Division of Neonatology, University Hospital Zurich, Switzerland Swiss Society
SWISS SOCIETY OF NEONATOLOGY. Neonatal gastric perforation
 SWISS SOCIETY OF NEONATOLOGY Neonatal gastric perforation September 2002 2 Zankl A, Stähelin J, Roth K, Boudny P and Zeilinger G, Children s Hospital of Aarau (ZA, SJ, RK, ZG) and Institute of Pathology
SWISS SOCIETY OF NEONATOLOGY Neonatal gastric perforation September 2002 2 Zankl A, Stähelin J, Roth K, Boudny P and Zeilinger G, Children s Hospital of Aarau (ZA, SJ, RK, ZG) and Institute of Pathology
Original Policy Date
 MP 8.01.17 Inhaled Nitric Oxide Medical Policy Section Therapy Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return to Medical Policy Index
MP 8.01.17 Inhaled Nitric Oxide Medical Policy Section Therapy Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return to Medical Policy Index
The Case Begins. The case continued. Necrotizing Enterocolitis
 Bugs, Drugs and Things that go Bump in the Night From ghoulies to ghosties and long leggety beasties & things that go bump in the night, good lord deliver us Old Cornish Prayer Caring for premature infant
Bugs, Drugs and Things that go Bump in the Night From ghoulies to ghosties and long leggety beasties & things that go bump in the night, good lord deliver us Old Cornish Prayer Caring for premature infant
The Basics. Editorial Team. Editorial Team 9/28/2017
 Title of Program: What has Cochrane Neonatal Done For Babies? Speakers/Moderators: Roger F. Soll, MD Planning Committee: Jeffery D. Horbar, MD, Madge E. Buus-Frank, RN, MS, APRN-BC, FAAN, Roger F. Soll,
Title of Program: What has Cochrane Neonatal Done For Babies? Speakers/Moderators: Roger F. Soll, MD Planning Committee: Jeffery D. Horbar, MD, Madge E. Buus-Frank, RN, MS, APRN-BC, FAAN, Roger F. Soll,
Short-Term Outcome Of Different Treatment Modalities Of Patent Ductus Arteriosus In Preterm Infants. Five Years Experiences In Qatar
 ISPUB.COM The Internet Journal of Cardiovascular Research Volume 7 Number 2 Short-Term Outcome Of Different Treatment Modalities Of Patent Ductus Arteriosus In Preterm Infants. Five Years Experiences In
ISPUB.COM The Internet Journal of Cardiovascular Research Volume 7 Number 2 Short-Term Outcome Of Different Treatment Modalities Of Patent Ductus Arteriosus In Preterm Infants. Five Years Experiences In
Premature: is live born infants delivered before 37 wk from the 1 st day of the last menstrual period.
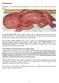 Prematurity Premature: is live born infants delivered before 37 wk from the 1 st day of the last menstrual period. Low birth weight (LBW): (birth weight
Prematurity Premature: is live born infants delivered before 37 wk from the 1 st day of the last menstrual period. Low birth weight (LBW): (birth weight
Hazards and Benefits of Postnatal Steroids. David J. Burchfield, MD Professor and Chief, Neonatology University of Florida
 Hazards and Benefits of Postnatal Steroids David J. Burchfield, MD Professor and Chief, Neonatology University of Florida Disclosures I have no financial affiliations or relationships to disclose. I will
Hazards and Benefits of Postnatal Steroids David J. Burchfield, MD Professor and Chief, Neonatology University of Florida Disclosures I have no financial affiliations or relationships to disclose. I will
Neonatal Therapeutic Hypothermia. A Wasunna Professor of Neonatal Medicine and Pediatrics School of Medicine, University of Nairobi
 Neonatal Therapeutic Hypothermia A Wasunna Professor of Neonatal Medicine and Pediatrics School of Medicine, University of Nairobi Definition of Perinatal Asphyxia *No agreed universal definition ACOG/AAP
Neonatal Therapeutic Hypothermia A Wasunna Professor of Neonatal Medicine and Pediatrics School of Medicine, University of Nairobi Definition of Perinatal Asphyxia *No agreed universal definition ACOG/AAP
Received: Jun 15, 2013; Accepted: Nov 08, 2013; First Online Available: Jan 24, 2014
 Original Article Iran J Pediatr Feb 2014; Vol 24 (No 1), Pp: 57-63 Management of Neonatal Respiratory Distress Syndrome Employing ACoRN Respiratory Sequence Protocol versus Early Nasal Continuous Positive
Original Article Iran J Pediatr Feb 2014; Vol 24 (No 1), Pp: 57-63 Management of Neonatal Respiratory Distress Syndrome Employing ACoRN Respiratory Sequence Protocol versus Early Nasal Continuous Positive
Research Roundtable Summary
 Research Roundtable Summary 10 TENTH in a Series of Seminars on MCHB-funded Research Projects Early Cortisol Deficiency and Bronchopulmonary Dysplasia October 18, 1995 Parklawn Building Potomac Conference
Research Roundtable Summary 10 TENTH in a Series of Seminars on MCHB-funded Research Projects Early Cortisol Deficiency and Bronchopulmonary Dysplasia October 18, 1995 Parklawn Building Potomac Conference
Minimal Enteral Nutrition
 Abstract Minimal Enteral Nutrition Although parenteral nutrition has been used widely in the management of sick very low birth weight infants, a smooth transition to the enteral route is most desirable.
Abstract Minimal Enteral Nutrition Although parenteral nutrition has been used widely in the management of sick very low birth weight infants, a smooth transition to the enteral route is most desirable.
ETIOLOGY AND PATHOGENESIS OF HYPOXIC-ISCHEMIC ENCEPHALOPATHY
 ETIOLOGY AND PATHOGENESIS OF HYPOXIC-ISCHEMIC ENCEPHALOPATHY HYPOXIC-ISCHEMIC ENCEPHALOPATHY Hypoxic-İschemic Encephalopathy Encephalopathy due to hypoxic-ischemic injury [Hypoxic-ischemic encephalopathy
ETIOLOGY AND PATHOGENESIS OF HYPOXIC-ISCHEMIC ENCEPHALOPATHY HYPOXIC-ISCHEMIC ENCEPHALOPATHY Hypoxic-İschemic Encephalopathy Encephalopathy due to hypoxic-ischemic injury [Hypoxic-ischemic encephalopathy
TRAINING NEONATOLOGY SILVANA PARIS
 TRAINING ON NEONATOLOGY SILVANA PARIS RESUSCITATION IN DELIVERY ROOM INTRODUCTION THE GLOBAL RESUSCITATION BURDEN IN NEWBORN 136 MILL NEWBORN BABIES EACH YEAR (WHO WORLD REPORT) 5-8 MILL NEWBORN INFANTS
TRAINING ON NEONATOLOGY SILVANA PARIS RESUSCITATION IN DELIVERY ROOM INTRODUCTION THE GLOBAL RESUSCITATION BURDEN IN NEWBORN 136 MILL NEWBORN BABIES EACH YEAR (WHO WORLD REPORT) 5-8 MILL NEWBORN INFANTS
Lectures 4 Early fetal assessment, screening, ultrasound and treatment modalities during pregnancy. II. Asphyxia and Resuscitation (3 lectures)...
 Outline of a 2 year Neonatology educational course (80 lectures) PLUS 2 graduate level courses (GENETICS and BIOSTATISTICS & EPIDEMIOLOGY Approximate Percent in Examination I. Maternal-Fetal Medicine (6
Outline of a 2 year Neonatology educational course (80 lectures) PLUS 2 graduate level courses (GENETICS and BIOSTATISTICS & EPIDEMIOLOGY Approximate Percent in Examination I. Maternal-Fetal Medicine (6
Hypernatraemia as a cause of intracranial haemorrhage
 Archives of Disease in Childhood, 1975, 50, 938. Hypernatraemia as a cause of intracranial haemorrhage N. R. C. ROBERTON and P. HOWAT From the Department of Paediatrics, University of Oxford, John Radcliffe
Archives of Disease in Childhood, 1975, 50, 938. Hypernatraemia as a cause of intracranial haemorrhage N. R. C. ROBERTON and P. HOWAT From the Department of Paediatrics, University of Oxford, John Radcliffe
INTRODUCTION The effect of CPAP works on lung mechanics to improve oxygenation (PaO 2
 2 Effects of CPAP INTRODUCTION The effect of CPAP works on lung mechanics to improve oxygenation (PaO 2 ). The effect on CO 2 is only secondary to the primary process of improvement in lung volume and
2 Effects of CPAP INTRODUCTION The effect of CPAP works on lung mechanics to improve oxygenation (PaO 2 ). The effect on CO 2 is only secondary to the primary process of improvement in lung volume and
Correlation of Neurodevelopmental Outcome and brain MRI/EEG findings in term HIE infants
 Correlation of Neurodevelopmental Outcome and brain MRI/EEG findings in term HIE infants Ajou University School of Medicine Department of Pediatrics Moon Sung Park M.D. Hee Cheol Jo, M.D., Jang Hoon Lee,
Correlation of Neurodevelopmental Outcome and brain MRI/EEG findings in term HIE infants Ajou University School of Medicine Department of Pediatrics Moon Sung Park M.D. Hee Cheol Jo, M.D., Jang Hoon Lee,
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials
 Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
Name and title of the investigators responsible for conducting the research: Dr Anna Lavizzari, Dr Mariarosa Colnaghi
 Protocol title: Heated, Humidified High-Flow Nasal Cannula vs Nasal CPAP for Respiratory Distress Syndrome of Prematurity. Protocol identifying number: Clinical Trials.gov NCT02570217 Name and title of
Protocol title: Heated, Humidified High-Flow Nasal Cannula vs Nasal CPAP for Respiratory Distress Syndrome of Prematurity. Protocol identifying number: Clinical Trials.gov NCT02570217 Name and title of
Effects of Indomethacin Prophylaxis Timing on IVH and PDA in Extremely Low Birth Weight (ELBW) Infants
 Effects of Indomethacin Prophylaxis Timing on IVH and PDA in Extremely Low Birth Weight (ELBW) Infants Hussnain Mirza, University of Central Florida Abbot R. Laptook, Brown University William Oh, Brown
Effects of Indomethacin Prophylaxis Timing on IVH and PDA in Extremely Low Birth Weight (ELBW) Infants Hussnain Mirza, University of Central Florida Abbot R. Laptook, Brown University William Oh, Brown
TRANSIENT NEUROLOGICAL ABNORMALITIES: EARLY SCHOOL OUTCOMES IN EXTREMELY PREMATURE INFANTS HEIDI HARMON, M.D. Master of Science
 TRANSIENT NEUROLOGICAL ABNORMALITIES: EARLY SCHOOL OUTCOMES IN EXTREMELY PREMATURE INFANTS by HEIDI HARMON, M.D. Submitted in partial fulfillment of the requirements for the degree of Master of Science
TRANSIENT NEUROLOGICAL ABNORMALITIES: EARLY SCHOOL OUTCOMES IN EXTREMELY PREMATURE INFANTS by HEIDI HARMON, M.D. Submitted in partial fulfillment of the requirements for the degree of Master of Science
Recommendations for Hospital Quality Measures in 2011:
 Pediatric Measures: Recommendations for Hospital Quality Measures in 2011: Based on the input of a group of healthcare stakeholders, the following new hospital measures are recommended: 1) Home Management
Pediatric Measures: Recommendations for Hospital Quality Measures in 2011: Based on the input of a group of healthcare stakeholders, the following new hospital measures are recommended: 1) Home Management
Avoiding hyperoxia in infants p1250 g is associated with improved short- and long-term outcomes
 (2006) 26, 700 705 r 2006 Nature Publishing Group All rights reserved. 0743-8346/06 $30 www.nature.com/jp ORIGINAL ARTICLE Avoiding hyperoxia in infants p1250 g is associated with improved short- and long-term
(2006) 26, 700 705 r 2006 Nature Publishing Group All rights reserved. 0743-8346/06 $30 www.nature.com/jp ORIGINAL ARTICLE Avoiding hyperoxia in infants p1250 g is associated with improved short- and long-term
AEROSURF Phase 2 Program Update Investor Conference Call
 AEROSURF Phase 2 Program Update Investor Conference Call November 12, 2015 Forward Looking Statement To the extent that statements in this presentation are not strictly historical, including statements
AEROSURF Phase 2 Program Update Investor Conference Call November 12, 2015 Forward Looking Statement To the extent that statements in this presentation are not strictly historical, including statements
Neonatal Seizure. Dr.Nawar Yahya. Presented by: Sarah Khalil Zeina Shamil Zainab Waleed Zainab Qahtan. Supervised by:
 Neonatal Seizure Supervised by: Dr.Nawar Yahya Presented by: Sarah Khalil Zeina Shamil Zainab Waleed Zainab Qahtan Objectives: What is neonatal seizure Etiology Clinical presentation Differential diagnosis
Neonatal Seizure Supervised by: Dr.Nawar Yahya Presented by: Sarah Khalil Zeina Shamil Zainab Waleed Zainab Qahtan Objectives: What is neonatal seizure Etiology Clinical presentation Differential diagnosis
Insults to the Developing Brain & Effect on Neurodevelopmental Outcomes
 Insults to the Developing Brain & Effect on Neurodevelopmental Outcomes Ira Adams-Chapman, MD Assistant Professor of Pediatrics Director, Developmental Progress Clinic Emory University School of Medicine
Insults to the Developing Brain & Effect on Neurodevelopmental Outcomes Ira Adams-Chapman, MD Assistant Professor of Pediatrics Director, Developmental Progress Clinic Emory University School of Medicine
Infection. Risk factor for infection ACoRN alerting sign with * Clinical deterioration. Problem List. Respiratory. Cardiovascular
 The ACoRN Process Baby at risk Unwell Risk factors Post-resuscitation requiring stabilization Resuscitation Ineffective breathing Heart rate < 100 bpm Central cyanosis Support Infection Risk factor for
The ACoRN Process Baby at risk Unwell Risk factors Post-resuscitation requiring stabilization Resuscitation Ineffective breathing Heart rate < 100 bpm Central cyanosis Support Infection Risk factor for
Historical Perspectives on the Etiology of Cerebral Palsy 233 Tonse N.K. Raju
 PERINATAL CAUSES OF CEREBRAL PALSY Preface Marcus C. Hermansen xv Historical Perspectives on the Etiology of Cerebral Palsy 233 Tonse N.K. Raju This essay presents the early history on the evolution of
PERINATAL CAUSES OF CEREBRAL PALSY Preface Marcus C. Hermansen xv Historical Perspectives on the Etiology of Cerebral Palsy 233 Tonse N.K. Raju This essay presents the early history on the evolution of
New Zealand Data Sheet. Poractant alfa (Phospholipid fraction of porcine lung) 80 mg/ml
 CUROSURF New Zealand Data Sheet Poractant alfa (Phospholipid fraction of porcine lung) 80 mg/ml Presentation Sterile suspension in single-dose vials for intratracheal or intrabronchial administration.
CUROSURF New Zealand Data Sheet Poractant alfa (Phospholipid fraction of porcine lung) 80 mg/ml Presentation Sterile suspension in single-dose vials for intratracheal or intrabronchial administration.
Kimberly M. Thornton, 1,2 Hongying Dai, 3 Seth Septer, 2,4 and Joshua E. Petrikin 1,2. 1. Introduction
 International Pediatrics, Article ID 643689, 7 pages http://dx.doi.org/10.1155/2014/643689 Research Article Effects of Whole Body Therapeutic Hypothermia on Gastrointestinal Morbidity and Feeding Tolerance
International Pediatrics, Article ID 643689, 7 pages http://dx.doi.org/10.1155/2014/643689 Research Article Effects of Whole Body Therapeutic Hypothermia on Gastrointestinal Morbidity and Feeding Tolerance
The Turkish Journal of Pediatrics 2014; 56:
 The Turkish Journal of Pediatrics 2014; 56: 232-237 Original INSURE method (INtubation-SURfactant-Extubation) in early and late premature neonates with respiratory distress: factors affecting the outcome
The Turkish Journal of Pediatrics 2014; 56: 232-237 Original INSURE method (INtubation-SURfactant-Extubation) in early and late premature neonates with respiratory distress: factors affecting the outcome
Visual defects in children of low birthweight
 Archives of Disease in Childhood, 1982, 57, 818-822 Visual defects in children of low birthweight EVA ALBERMAN, JULIA BENSON, AND STEPHEN EVANS Department of Clinical Epidemiology, London Hospital Medical
Archives of Disease in Childhood, 1982, 57, 818-822 Visual defects in children of low birthweight EVA ALBERMAN, JULIA BENSON, AND STEPHEN EVANS Department of Clinical Epidemiology, London Hospital Medical
Premature Infants with Patent Ductus Arteriosus and Res iratory Distress: Selection for mdap Ligation
 Premature Infants with Patent Ductus Arteriosus and Res iratory Distress: Selection for mdap Ligation George S. Hall, M.D., James A. Helmsworth, M.D., J. Tracy Schreiber, M.D., Jens G. Rosenkrantz, M.D.,
Premature Infants with Patent Ductus Arteriosus and Res iratory Distress: Selection for mdap Ligation George S. Hall, M.D., James A. Helmsworth, M.D., J. Tracy Schreiber, M.D., Jens G. Rosenkrantz, M.D.,
Original Article. Associated Anomalies and Clinical Outcomes in Infants with Omphalocele: A Single-centre 10-year Review
 HK J Paediatr (new series) 2018;23:220-224 Original Article Associated Anomalies and Clinical Outcomes in Infants with Omphalocele: A Single-centre 10-year Review YY CHEE, MSC WONG, RMS WONG, KY WONG,
HK J Paediatr (new series) 2018;23:220-224 Original Article Associated Anomalies and Clinical Outcomes in Infants with Omphalocele: A Single-centre 10-year Review YY CHEE, MSC WONG, RMS WONG, KY WONG,
The Effectiveness of Surfactant Replacement Therapy for Preterm Infants with Respiratory Dis~ress Syndrome
 The Effectiveness of Surfactant Replacement Therapy for Preterm Infants with Respiratory Dis~ress Syndrome W L Lim, MRCP, C T Lim, FRCP, J K Chye, FRACP, Department of Paediatrics, U nive.rsity of Malaya,
The Effectiveness of Surfactant Replacement Therapy for Preterm Infants with Respiratory Dis~ress Syndrome W L Lim, MRCP, C T Lim, FRCP, J K Chye, FRACP, Department of Paediatrics, U nive.rsity of Malaya,
Paediatrica Indonesiana. Echocardiographic patterns in asphyxiated neonates. Maswin Masyhur, Idham Amir, Sukman Tulus Putra, Alan Roland Tumbelaka
 Paediatrica Indonesiana VOLUME 49 July NUMBER 4 Original Article Echocardiographic patterns in asphyxiated neonates Maswin Masyhur, Idham Amir, Sukman Tulus Putra, Alan Roland Tumbelaka Abstract Background
Paediatrica Indonesiana VOLUME 49 July NUMBER 4 Original Article Echocardiographic patterns in asphyxiated neonates Maswin Masyhur, Idham Amir, Sukman Tulus Putra, Alan Roland Tumbelaka Abstract Background
The Premature Infant CHAPTER DEFINITIONS RESPIRATORY DISTRESS SYNDROME
 4206 Litman-10.qxd 1/19/04 2:33 PM Page 68 CHAPTER 10 The Premature Infant RONALD S. LITMAN, D.O. Definitions Respiratory Distress Syndrome Intraoperative Ventilator Management Outcome of RDS Apnea of
4206 Litman-10.qxd 1/19/04 2:33 PM Page 68 CHAPTER 10 The Premature Infant RONALD S. LITMAN, D.O. Definitions Respiratory Distress Syndrome Intraoperative Ventilator Management Outcome of RDS Apnea of
PROFESSOR DR. NUMAN NAFIE HAMEED الاستاذ الدكتور نعمان نافع الحمداني
 Lecture 6 PROFESSOR DR. NUMAN NAFIE HAMEED الاستاذ الدكتور نعمان نافع الحمداني Neonatal Resuscitation Program (NRP) 2010 MCQ? In neonatal resuscitation program, the preterm neonates need special preparations
Lecture 6 PROFESSOR DR. NUMAN NAFIE HAMEED الاستاذ الدكتور نعمان نافع الحمداني Neonatal Resuscitation Program (NRP) 2010 MCQ? In neonatal resuscitation program, the preterm neonates need special preparations
NEONATAL-PERINATAL MEDICINE ROTATION Competency Based Goals and Objectives
 NEONATAL-PERINATAL MEDICINE ROTATION Competency Based Goals and Objectives Competency 1. Patient Care: Provide family centered patient care that is developmentally and age appropriate, compassionate, and
NEONATAL-PERINATAL MEDICINE ROTATION Competency Based Goals and Objectives Competency 1. Patient Care: Provide family centered patient care that is developmentally and age appropriate, compassionate, and
Diuretics: Increased risk of renal dysfunction. (7) See 17 for PATIENT COUNSELING INFORMATION. Revised: 10/2017 FULL PRESCRIBING INFORMATION: CONTENTS
 HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use NEOPROFEN safely and effectively. See full prescribing information for NEOPROFEN. NEOPROFEN (ibuprofen
HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use NEOPROFEN safely and effectively. See full prescribing information for NEOPROFEN. NEOPROFEN (ibuprofen
T he main purpose of neonatal intensive care is to promote
 15 ORIGINAL ARTICLE The Questionnaire: achieving concordance with published criteria H P Jones, Z E S Guildea, J H Stewart, P H T Cartlidge... See end of article for authors affiliations... Correspondence
15 ORIGINAL ARTICLE The Questionnaire: achieving concordance with published criteria H P Jones, Z E S Guildea, J H Stewart, P H T Cartlidge... See end of article for authors affiliations... Correspondence
Kugelman A, Riskin A, Said W, Shoris I, Mor F, Bader D.
 Heated, Humidified High-Flow Nasal Cannula (HHHFNC) vs. Nasal Intermittent Positive Pressure Ventilation (NIPPV) for the Primary Treatment of RDS, A Randomized, Controlled, Prospective, Pilot Study Kugelman
Heated, Humidified High-Flow Nasal Cannula (HHHFNC) vs. Nasal Intermittent Positive Pressure Ventilation (NIPPV) for the Primary Treatment of RDS, A Randomized, Controlled, Prospective, Pilot Study Kugelman
Study of renal functions in neonatal asphyxia
 Original article: Study of renal functions in neonatal asphyxia *Dr. D.Y.Shrikhande, **Dr. Vivek Singh, **Dr. Amit Garg *Professor and Head, **Senior Resident Department of Pediatrics, Pravara Institute
Original article: Study of renal functions in neonatal asphyxia *Dr. D.Y.Shrikhande, **Dr. Vivek Singh, **Dr. Amit Garg *Professor and Head, **Senior Resident Department of Pediatrics, Pravara Institute
CLINICAL AUDIT SUMMARY CLINICAL AUDIT SUMMARY. Diagnosis and Recognition of Congenital Cytomegalovirus in Northern Ireland
 Regional Virology Issue Date: 08/09/14 Page(s): Page 1 of 6 1.0 Name of audit Diagnosis and Recognition of Congenital Cytomegalovirus in Northern Ireland 2.0 Personnel involved Peter Coyle, Han Lu, Daryl
Regional Virology Issue Date: 08/09/14 Page(s): Page 1 of 6 1.0 Name of audit Diagnosis and Recognition of Congenital Cytomegalovirus in Northern Ireland 2.0 Personnel involved Peter Coyle, Han Lu, Daryl
State of Florida Systemic Supportive Care Guidelines. Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology
 State of Florida Systemic Supportive Care Guidelines Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology I. FEN 1. What intravenous fluids should be initiated upon admission
State of Florida Systemic Supportive Care Guidelines Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology I. FEN 1. What intravenous fluids should be initiated upon admission
Advanced Necrotizing Enterocolitis Part 1: Mortality
 8 Original Article Advanced Necrotizing Enterocolitis Part 1: Mortality M. Thyoka 1 P. de Coppi 1 S. Eaton 1 K. Khoo 1 N.J. Hall 1 J. Curry 1 E. Kiely 1 D. Drake 1 K. Cross 1 A. Pierro 1 1 Department of
8 Original Article Advanced Necrotizing Enterocolitis Part 1: Mortality M. Thyoka 1 P. de Coppi 1 S. Eaton 1 K. Khoo 1 N.J. Hall 1 J. Curry 1 E. Kiely 1 D. Drake 1 K. Cross 1 A. Pierro 1 1 Department of
Extracorporeal Membrane Oxygenation (ECMO)
 Extracorporeal Membrane Oxygenation (ECMO) Policy Number: Original Effective Date: MM.12.006 05/16/2006 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 11/01/2014 Section: Other/Miscellaneous
Extracorporeal Membrane Oxygenation (ECMO) Policy Number: Original Effective Date: MM.12.006 05/16/2006 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 11/01/2014 Section: Other/Miscellaneous
Neurodevelopmental Outcomes of Premature Infants Treated with Inhaled Nitric Oxide
 The new england journal of medicine original article Neurodevelopmental Outcomes of Premature Infants Treated with Inhaled Nitric Oxide Karen K.L. Mestan, M.D., Jeremy D. Marks, Ph.D., M.D., Kurt Hecox,
The new england journal of medicine original article Neurodevelopmental Outcomes of Premature Infants Treated with Inhaled Nitric Oxide Karen K.L. Mestan, M.D., Jeremy D. Marks, Ph.D., M.D., Kurt Hecox,
You admitted a previously healthy nullipara at 36 weeks gestation who presented with new-onset periorbital edema and is found to have blood pressure
 Preeclampsia Case report You admitted a previously healthy nullipara at 36 weeks gestation who presented with new-onset periorbital edema and is found to have blood pressure readings of 150/100 to 155/105
Preeclampsia Case report You admitted a previously healthy nullipara at 36 weeks gestation who presented with new-onset periorbital edema and is found to have blood pressure readings of 150/100 to 155/105
ARTIFICIAL INTELLIGENCE FOR PREDICTION OF SEPSIS IN VERY LOW BIRTH WEIGHT INFANTS
 ARTIFICIAL INTELLIGENCE FOR PREDICTION OF SEPSIS IN VERY LOW BIRTH WEIGHT INFANTS Markus Leskinen MD PhD, Neonatologist Children s Hospital, University of Helsinki and Helsinki University Hospital The
ARTIFICIAL INTELLIGENCE FOR PREDICTION OF SEPSIS IN VERY LOW BIRTH WEIGHT INFANTS Markus Leskinen MD PhD, Neonatologist Children s Hospital, University of Helsinki and Helsinki University Hospital The
Hummi Micro Draw Blood Transfer Device. An Important Addition to Your IVH Bundle
 Hummi Micro Draw Blood Transfer Device An Important Addition to Your IVH Bundle Hummi Micro Draw & Micro T Connector For Infec6on Control and IVH Risk Reduc6on The Next Genera6on System for Closed Micro
Hummi Micro Draw Blood Transfer Device An Important Addition to Your IVH Bundle Hummi Micro Draw & Micro T Connector For Infec6on Control and IVH Risk Reduc6on The Next Genera6on System for Closed Micro
Study of role of MRI brain in evaluation of hypoxic ischemic encephalopathy
 Original article: Study of role of MRI brain in evaluation of hypoxic ischemic encephalopathy *Dr Harshad Bhagat, ** Dr Ravindra Kawade, ***Dr Y.P.Sachdev *Junior Resident, Department Of Radiodiagnosis,
Original article: Study of role of MRI brain in evaluation of hypoxic ischemic encephalopathy *Dr Harshad Bhagat, ** Dr Ravindra Kawade, ***Dr Y.P.Sachdev *Junior Resident, Department Of Radiodiagnosis,
Comparison of Two Phototherapy Methods (Prophylactic vs Therapeutic) for Management of Hyperbilirubinemia in Very Low Birth Weight Newborns
 Original Article Iran J Pediatr Dec 2011; Vol 21 (No 4), Pp: 425-430 Comparison of Two Phototherapy Methods (Prophylactic vs Therapeutic) for Management of Hyperbilirubinemia in Very Low Birth Weight Newborns
Original Article Iran J Pediatr Dec 2011; Vol 21 (No 4), Pp: 425-430 Comparison of Two Phototherapy Methods (Prophylactic vs Therapeutic) for Management of Hyperbilirubinemia in Very Low Birth Weight Newborns
abstract n engl j med 376;7 nejm.org February 16,
 The new england journal of medicine established in 1812 February 16, 2017 vol. 376 no. 7 Survival and Neurodevelopmental Outcomes among Periviable Infants Noelle Younge, M.D., M.H.S., Ricki F. Goldstein,
The new england journal of medicine established in 1812 February 16, 2017 vol. 376 no. 7 Survival and Neurodevelopmental Outcomes among Periviable Infants Noelle Younge, M.D., M.H.S., Ricki F. Goldstein,
INTRAVENOUS FLUID THERAPY
 INTRAVENOUS FLUID THERAPY PRINCIPLES Postnatal physiological weight loss is approximately 5 10% in first week of life Preterm neonates have more total body water and may lose 10 15% of their weight in
INTRAVENOUS FLUID THERAPY PRINCIPLES Postnatal physiological weight loss is approximately 5 10% in first week of life Preterm neonates have more total body water and may lose 10 15% of their weight in
Clinical Study Pulmonary Effects of Neonatal Hydrocortisone Treatment in Ventilator-Dependent Preterm Infants
 International Pediatrics Volume 2011, Article ID 783893, 7 pages doi:10.1155/2011/783893 Clinical Study Pulmonary Effects of Neonatal Hydrocortisone Treatment in Ventilator-Dependent Preterm Infants Sandra
International Pediatrics Volume 2011, Article ID 783893, 7 pages doi:10.1155/2011/783893 Clinical Study Pulmonary Effects of Neonatal Hydrocortisone Treatment in Ventilator-Dependent Preterm Infants Sandra
Ashley Robson Canyon Creek Dr. Mckinney, TX 75070
 1 Ashley Robson 2212 Canyon Creek Dr. Mckinney, TX 75070 September 2 nd 2014 Debra Brandon PhD, RN, CCNS, FAAN Duke University School of Nursing Durham, NC Dear Mrs. Brandon- I would like the opportunity
1 Ashley Robson 2212 Canyon Creek Dr. Mckinney, TX 75070 September 2 nd 2014 Debra Brandon PhD, RN, CCNS, FAAN Duke University School of Nursing Durham, NC Dear Mrs. Brandon- I would like the opportunity
National follow-up program CPUP Pediatric Neurology paper form
 National follow-up program CPUP Pediatric Neurology paper form 110206 1 National Follow-Up program- CPUP Pediatric Neurology Personal nr (unique identifier): Last name: First name: Region child belongs
National follow-up program CPUP Pediatric Neurology paper form 110206 1 National Follow-Up program- CPUP Pediatric Neurology Personal nr (unique identifier): Last name: First name: Region child belongs
INTRAVENOUS FLUIDS PRINCIPLES
 INTRAVENOUS FLUIDS PRINCIPLES Postnatal physiological weight loss is approximately 5-10% Postnatal diuresis is delayed in Respiratory Distress Syndrome (RDS) Preterm babies have limited capacity to excrete
INTRAVENOUS FLUIDS PRINCIPLES Postnatal physiological weight loss is approximately 5-10% Postnatal diuresis is delayed in Respiratory Distress Syndrome (RDS) Preterm babies have limited capacity to excrete
Quality Improvement Approaches to BPD. Jay P. Goldsmith, M.D. Tulane University New Orleans, Louisiana
 Quality Improvement Approaches to BPD Jay P. Goldsmith, M.D. Tulane University New Orleans, Louisiana goldsmith.jay@gmail.com No conflicts of interest to declare There is nothing more dangerous to the
Quality Improvement Approaches to BPD Jay P. Goldsmith, M.D. Tulane University New Orleans, Louisiana goldsmith.jay@gmail.com No conflicts of interest to declare There is nothing more dangerous to the
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Actinobacteria, 413 Active treatment, survival rate and, 294 296 Air displacement plethysmography, 397 Airway obstruction, 309 310 Aluminum
Note: Page numbers of article titles are in boldface type. A Actinobacteria, 413 Active treatment, survival rate and, 294 296 Air displacement plethysmography, 397 Airway obstruction, 309 310 Aluminum
DOWNLOAD OR READ : PERINATAL EVENTS AND BRAIN DAMAGE IN SURVIVING CHILDREN BASED ON PAPERS PRESENTED AT AN INTERNATIONA PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : PERINATAL EVENTS AND BRAIN DAMAGE IN SURVIVING CHILDREN BASED ON PAPERS PRESENTED AT AN INTERNATIONA PDF EBOOK EPUB MOBI Page 1 Page 2 perinatal events and brain damage in surviving
DOWNLOAD OR READ : PERINATAL EVENTS AND BRAIN DAMAGE IN SURVIVING CHILDREN BASED ON PAPERS PRESENTED AT AN INTERNATIONA PDF EBOOK EPUB MOBI Page 1 Page 2 perinatal events and brain damage in surviving
Review of Neonatal Respiratory Problems
 Review of Neonatal Respiratory Problems Respiratory Distress Occurs in about 7% of infants Clinical presentation includes: Apnea Cyanosis Grunting Inspiratory stridor Nasal flaring Poor feeding Tachypnea
Review of Neonatal Respiratory Problems Respiratory Distress Occurs in about 7% of infants Clinical presentation includes: Apnea Cyanosis Grunting Inspiratory stridor Nasal flaring Poor feeding Tachypnea
Medical Follow-up of the High-Risk NICU Graduate
 Medical Follow-up of the High-Risk NICU Graduate Silvia Fajardo-Hiriart, M.D. Medical Director High-Risk Infant Follow-Up/Early Intervention Program University of Miami Miller School of Medicine Department
Medical Follow-up of the High-Risk NICU Graduate Silvia Fajardo-Hiriart, M.D. Medical Director High-Risk Infant Follow-Up/Early Intervention Program University of Miami Miller School of Medicine Department
Prophylactic Aminophylline for Prevention of Apnea at Higher-Risk Preterm Neonates
 Iran Red Crescent Med J. 2014 August; 16(8): e12559. Published online 2014 August 5. DOI: 10.5812/ircmj.12559 Research Article Prophylactic Aminophylline for Prevention of Apnea at Higher-Risk Preterm
Iran Red Crescent Med J. 2014 August; 16(8): e12559. Published online 2014 August 5. DOI: 10.5812/ircmj.12559 Research Article Prophylactic Aminophylline for Prevention of Apnea at Higher-Risk Preterm
