The Genetic Approach to Hypotonia in the Neonate Neda Zadeh and Louanne Hudgins. DOI: /neo e600
|
|
|
- Randolph Townsend
- 6 years ago
- Views:
Transcription
1 The Genetic Approach to Hypotonia in the Neonate Neda Zadeh and Louanne Hudgins NeoReviews 2009;10;e600-e607 DOI: /neo e600 The online version of this article, along with updated information and services, is located on the World Wide Web at: NeoReviews is the official journal of the American Academy of Pediatrics. A monthly publication, it has been published continuously since NeoReviews is owned, published, and trademarked by the American Academy of Pediatrics, 141 Northwest Point Boulevard, Elk Grove Village, Illinois, Copyright 2009 by the American Academy of Pediatrics. All rights reserved. Online ISSN:
2 Article genetics The Genetic Approach to Hypotonia in the Neonate Neda Zadeh, MD,* Louanne Hudgins, MD* Author Disclosure Drs Zadeh and Hudgins have disclosed no financial relationships relevant to this article. This commentary does not contain a discussion of an unapproved/ investigative use of a commercial product/ device. Objectives After completing this article, readers should be able to: 1. Describe the genetic approach to in the newborn. 2. Discuss the most common presentations of genetic disorders associated with in the newborn period. 3. Review the genetic basis of neuromuscular disorders that present with in the newborn period. 4. Understand the definition of anticipation with respect to trinucleotide repeat disorders. Abstract Numerous genetic syndromes present with during the neonatal period, including Prader-Willi syndrome, myotonic dystrophy, spinal muscular atrophy, congenital muscular dystrophies, nemaline myopathy, congenital hypomyelinating neuropathy, congenital disorders of glycosylation, and Pompe disease. This article reviews neonatal presentations and appropriate diagnostic tests and examinations for each. Awareness of possible underlying genetic causes for neonatal can aid physicians in general pediatric practice, neonatology, and other specialties in making a timely diagnosis for what may be considered rare conditions. Furthermore, early diagnosis allows for improved management of affected infants while providing invaluable information to their families with respect to potential recurrence risks in future generations. Introduction Hypotonia is defined as a subjective decrease of resistance to passive range of motion in a newborn (Fig. 1). Knowledge of genetic disorders that present most commonly with during the immediate newborn period is imperative because early diagnosis and initiation of appropriate supportive therapies allows the most beneficial outcomes for affected individuals. Molecular testing for most of these disorders is a rapid, cost-effective diagnostic approach. Most molecular tests involve acquiring a modest amount of blood, which is significantly less invasive and more cost effective than prior practices of obtaining muscle via surgical biopsy for similar diagnostic purposes. Abbreviations CDG: congenital disorder of glycosylation CHN: congenital hypomyelinating neuropathy CK: creatine kinase CMD: congenital muscular dystrophy DM1: myotonic dystrophy type 1 EMG: electromyography FCMD: Fukuyama congenital muscular dystrophy MEB: muscle-eye-brain PWS: Prader-Willi syndrome SMA: spinal muscular atrophy Prader-Willi Syndrome (PWS) Prenatal is evident with PWS, resulting in decreased fetal movement as well as abnormal positioning (ie, breech) at parturition, which causes difficulty with delivery, often necessitating cesarean section. Delivery typically is at term, with normal birth length and weight, although early failure to thrive may result in both parameters falling below the third percentile. During the immediate neonatal period, infants exhibit profound central, lethargy, decreased spontaneous movement, and weak cry. Hypogonadism is a common feature; cryptorchidism is present in 80% to 90% of affected males. Characteristic facial features of PWS in the newborn period include dolichocephaly with narrowed bifrontal diameter, almond-shaped palpebral *Department of Pediatrics, Division of Medical Genetics, Stanford University School of Medicine, Stanford, Calif. e600 NeoReviews Vol.10 No.12 December 2009
3 fissures, and a narrow nasal bridge. Infants who have PWS have poor suck and swallow, with severe cases warranting surgical insertion of a gastric tube. However, affected infants do not have respiratory insufficiency and do not require ventilatory assistance. Hypotonia improves by 2 to 3 years of age, although adolescents and adults may have evidence of mild, with subtly decreased muscle tone and bulk. Global developmental delay and excessive eating with central obesity is not seen until early childhood. PWS is caused by lack of paternal contribution of 15q11, which can be related to: Chromosome deletion of the Prader-Willi critical region (chromosome 15q11-q13) from the paternal allele Maternal uniparental disomy in which there are only two maternally derived copies of chromosome 15 Mutations of the genes responsible for imprinting control (1% of all cases) Structural chromosome abnormality (eg, translocation, duplication) involving the critical region, resulting in deletion of the paternal allele. Due to multiple causes, a number of different diagnostic tests can be undertaken to confirm the presence of PWS. Methylation study or SNRPN expression is used as first-line testing. Both forms of testing detect all four of the previously cited causes, but they cannot distinguish between the causes that have different recurrence risks. Accordingly, they often are followed by high-resolution chromosome analysis to rule out a structural chromosome abnormality involving chromosome 15, which could have implications for recurrence if one of the parents carries a balanced rearrangement. Figure 1. Hypotonia in an infant. A. Both arms fall back (instead of being held in flexion), and the baby s upper body appears to drape over the examiner s hand. B. When the infant is held in suspension, the infant appears to be slipping out of the examiner s hands. The head drops much lower than would be expected. Courtesy of Janelle L. Aby, MD. Myotonic Dystrophy (DM1) DM1 is an autosomal dominant condition that may present with and respiratory insufficiency in the neonatal period. Decreased fetal movement and polyhydramnios in utero result in breech positioning at delivery. As a result, positional malformations (clubfoot) and congenital contractures are common. At birth, infants have little-to-no spontaneous movement because of generalized muscle weakness. Bitemporal wasting, a masklike facies, and tented upper lip also may be evident. Most affected infants require respiratory assistance because of weak respiratory muscles and underdeveloped lungs. Attempts at feeding are very poor initially due to weak suck and swallow, but they improve gradually over time. Clinical diagnosis is based on facial features and the NeoReviews Vol.10 No.12 December 2009 e601
4 characteristic pattern of muscle weakness. DM1 is caused by expansion of the CTG trinucleotide repeat in the DMPK gene. Detection of trinucleotide repeat size is considered the gold standard for molecular diagnostic testing. Alleles greater than 34 repeats in length are unstable and have the ability to expand during female germline cell division (meiosis), which is also known as anticipation. Individuals who have mild DM1 possess 50 to 150 repeats; those who have the classic form have repeat sizes of 100 to 1,000. Congenital DM1 is the most severe form, with greater than 1,000 repeats. Individuals who have expansion in the premutation range frequently are asymptomatic or have very subtle clinical features. Infants who have congenital DM1 are born to affected mothers with very few exceptions. Maternal examination may reveal mild myopathic facies and sustained grip during hand shake (Fig. 2). Parents of an affected Figure 2. Myotonic dystrophy in a mother and infant. The neonate manifests signs of congenital myotonic dystrophy with tented upper lip and ; the mother has myopathic facies. infant routinely are offered testing for recurrence risk purposes and health surveillance because those who have the mild and classic forms are at risk for cataracts and arrhythmias. Spinal Muscular Atrophy (SMA) SMA is an autosomal recessive disorder characterized by symmetric and progressive muscle weakness and atrophy resulting from degeneration of anterior horn cells in the brainstem and spinal cord. There are four clinical forms of SMA; in this article, we discuss SMA type 0 and SMA I. The prenatal form of SMA (type 0) is the most severe, characterized by generalized weakness at birth as well as multiple congenital joint contractures involving at least two areas of the body (arthrogryposis multiplex congenita). Furthermore, motor milestones are not achieved and infants have a poor prognosis. Demise typically occurs at 6 months of age. SMA I also manifests early, between birth and 6 months of age. Affected infants have, muscle weakness, and mild contractures of the large joints. Deep tendon reflexes usually are absent, and on close observation, fasciculations of the tongue may be observed. This type of SMA also manifests with lack of motor development and failure to meet gross motor milestones. Intellect is usually normal. The two genes associated with SMA are known as survival motor neuron (SMN) genes. Normally, individuals have two copies of the SMN gene arranged in tandem on each chromosome, known as SMN1 (telomeric copy) and SMN2 (centromeric copy). SMA arises with the loss of function of the SMN1 gene. The remaining functional SMN2 genes cannot compensate without expression of SMN1. Molecular testing is available via blood sample for targeted mutation analysis. Congenital Muscular Dystrophy (CMD) CMD is a group of autosomal recessive disorders characterized by, joint contractures, brain malformations, eye abnormalities, generalized weakness, and elevated serum creatine kinase (CK) concentrations. We discuss merosin-deficient muscular dystrophy, Walker- Warburg syndrome, muscle-eye-brain (MEB) disease, and Fukuyama CMD (FCMD). Merosin-deficient CMD is the nonsyndromic member of this group. Affected infants have, proximal muscle weakness, and multiple large joint contractures, which worsen with age. Brain imaging results may be normal for the first 6 months after birth, followed by progressive characteristic changes of hypomyelination e602 NeoReviews Vol.10 No.12 December 2009
5 and hypodensity of the white matter. These specific central nervous system findings have been attributed to blood-brain barrier dysfunction causing abnormal water distribution in the cerebral white matter. Nocturnal hypopnea is a common occurrence and may require respiratory assistance via mechanical ventilation. Gross motor milestones develop poorly, with lack of ambulation during childhood. Cognitive impairment is usually mild but depends greatly on the presence and severity of brain abnormalities. The lifespan is shortened, with death occurring between the first decades of life and early adulthood. Diagnostic testing requires a muscle biopsy to evaluate histology and immunostaining for merosin and other muscle proteins. Molecular testing on a clinical basis involves sequencing of the laminin, alpha-2 chain (LAMA2) gene known to be associated with the disorder. Walker-Warburg syndrome presents with generalized neonatal and weakness as well as contractures at the elbows. Eye findings may include congenital cataracts, microphthalmia, and Peter anomaly (an anterior segment defect with corneal opacities). Severe brain malformations are common and include absence of the corpus callosum, fusion of cerebral hemispheres, and lissencephaly. Prognosis is poor, with demise occurring during early infancy. Molecular diagnostic testing for Walker- Warburg syndrome involves sequencing of protein O-mannosyl-transferase (POMT1 and POMT2) genes. MEB disease manifests with generalized neonatal, muscle weakness, eye malformations (glaucoma, progressive retinal atrophy, and juvenile cataracts), hydrocephalus, and cerebral white matter changes. There is also global developmental delay, with a very slow natural progression of milestones. Most affected individuals are nonambulatory by the third decade of life. Molecular diagnostic testing for MEB is by gene sequencing of protein O-mannoside beta-1, 2-Nacetylglucosaminyltransferase 1 (POMGNT1), which is offered clinically. FCMD is observed primarily in the Japanese population, with generalized, muscle weakness, and large joint contractures (elbows, hips, and knees) evident before 12 months of age. Neuroimaging often reveals cobblestone lissencephaly. Ophthalmologic examination is important to assess for retinal detachment and cataracts. Children fail to ambulate and exhibit severe cognitive impairment. Prognosis is poor, with a shortened lifespan due to complications from cardiomyopathy or respiratory failure. Fukutin is the only known associated gene, and clinical testing is available via gene sequencing. The evaluation strategy for this group of disorders includes neuroimaging (preferably magnetic resonance imaging), serum CK assessment, and ophthalmology and neurology evaluations. Molecular testing for Walker- Warburg syndrome, MEB disease, and FCMD are clinically available, as described previously. Nemaline Myopathy Nemaline myopathy may present early in utero with poor fetal movement and polyhydramnios. The neonatal period is notable for severe proximal muscle weakness,, dilated cardiomyopathy, arthrogryposis multiplex congenita, and absence of deep tendon reflexes. Due to generalized weakness and poor suck and swallow coordination, feeding difficulties are expected. The prognosis is poor, with demise during the first postnatal year. Screening studies reveal a normal serum CK value. If a muscle biopsy is performed, histology is abnormal on modified Gomori trichrome staining, with illustration of nemaline inclusion bodies (which appear rodlike ) scattered throughout muscle fibers. These inclusion bodies are made up of several Z-line proteins and alpha actinin and are not unique to this disorder. Five genes are known to be associated with nemaline myopathy. Unfortunately, only two tests, ACTA1 sequencing and NEB deletion/duplication analysis, are available on a clinical basis at the time of this writing. Congenital Hypomyelinating Neuropathy (CHN) CHN is an autosomal recessive disorder that presents with neonatal, generalized weakness, arthrogryposis multiplex congenita, areflexia, and respiratory insufficiency. These findings are evident during the newborn period in the neonatal form of this disorder. CHN is considered a neuromuscular disorder and usually is associated with an early demise due to the need for mechanical ventilation and subsequent complications of respiratory infections. Diagnostic evaluation should begin with molecular testing rather than more invasive methods. Molecular testing involves sequencing of MPZ, PMP22, or EGR2 genes, which are known to be associated with CHN. We do not recommend the more invasive diagnostic methods of electromyography (EMG) and nerve biopsy as first-line testing. Peripheral nerve biopsy reveals thin-toabsent myelin sheaths consistent with hypomyelination and suggestive of an intrinsic defect of myelin synthesis. Of interest, EMG often shows normal patterns when sampled at a proximal muscle site and denervation at distal muscle sites. NeoReviews Vol.10 No.12 December 2009 e603
6 Figure 3. Congenital disorders of glycosylation and unusual fat distribution. A. Inverted nipples and unusual abdominal and thigh fat distribution. B and C. Unusual suprailiac and suprapubic fat pads. Reprinted with permission from Enns GM, Steiner RD, Buist N, et al. Clinical and molecular features of congenital disorder of glycosylation in patients with type 1 sialotransferrin pattern and diverse ethnic origins. J Pediatr. 2002;141: Congenital Disorders of Glycosylation (CDGs) CDGs are a group of disorders inherited in an autosomal recessive pattern and caused by defective synthesis of N-linked oligosaccharides, which play an important role in the synthesis of glycoproteins and glycolipids throughout the body. A CDG may manifest during early infancy with and microcephaly. Examination of an affected neonate reveals an abnormal distribution of fat, most prominently notable in the suprapubic, iliac, and buttock regions, as well as the finding of inverted nipples (Fig. 3). Strabismus is very common. Other potential systemic manifestations include cardiomyopathy, protein-losing enteropathy, hypoglycemia, coagulation defects, and seizures. Neuroimaging often reveals progressive diffuse cerebellar atrophy. The variable neurologic phenotype ranges from mild impairment to severe psychomotor retardation, with motor skills more severely affected than cognition. CDG type Ib is treatable with mannose supplementation, but no curative treatment exists for the other forms. Ophthalmology, hematology, cardiology, and endocrinology evaluations are warranted. First-line diagnostic testing for CDG is carbohydrate-deficient transferrin analysis, which is detected by mass spectrometry. Mutation analysis of PMM2 is reserved for second-tier testing. The causative enzymes are known for most CDG subtypes, but enzymatic assays are not available on a clinical basis. Thus, clarification of particular CDG subtype requires molecular testing of the specific gene associated with the subtype. Pompe Disease Pompe disease is an autosomal recessive disorder manifested by profound central along with generalized weakness, respiratory insufficiency, cardiomegaly, and feeding difficulties. The condition is also known as glycogen storage disease type II and is caused by deficiency of the lysosomal enzyme acid alpha glucosidase. Dysfunction of this enzyme leads to abnormal lysosomal glycogen storage throughout the body, with skeletal, cardiac, and smooth muscle involved most prominently. Additional manifestations include macroglossia, hepatomegaly, and hearing deficits. The initial evaluation for affected infants involves echocardiography to screen for hypertrophic cardiomyopathy, assessment of pulmonary function, and measurement of serum transaminases and CK. CK concentrations may be elevated in this disorder, which is a sensitive but nonspecific marker for Pompe disease. Characteristic electrocardiographic findings include tall QRS complexes, shortened PR intervals, and arrhythmias that include Wolf-Parkinson-White syndrome. Arrhythmias are due to glycogen deposition in cardiac muscle, which acts as an electrical conductor. Untreated cardiac insufficiency may lead to heart failure and rapid demise. Molecular testing should be performed for diagnostic confirmation. The possibility of mass spectrometry newborn screening is on the horizon and may be performed on all infants to screen for this disorder in the near future. Molecular testing is GAA gene sequencing or skin fibroblast culture for enzymatic assay. Prompt diagnosis of this disorder can lead to early referral to a metabolic center for initiation of enzyme replacement therapy. Approach to the Hypotonic Infant Because neonatal has many different genetic causes, thorough physical and neurologic examinations are warranted before embarking on diagnostic testing. Careful attention should be paid to overall appearance, facial features, respiratory status, muscle bulk and tone, joint assessment for contractions, and genital development. After ruling out infection, infarction, perinatal trauma, electrolyte abnormalities, or isolated congenital e604 NeoReviews Vol.10 No.12 December 2009
7 Table. Genetic Conditions and Appropriate Diagnostic Testing Genetic Disorder Prader-Willi syndrome Myotonic Dystrophy Spinal Muscular Atrophy Congenital Muscular Dystrophies Merosin-deficient CMD Walker-Warburg syndrome Muscle-eye-brain Fukuyama CMD Nemaline myopathy Congenital hypomyelinating neuropathy Congenital disorders of glycosylation Pompe disease Diagnostic Tests First tier: Methylation studies or SNRPN expression Second tier: High-resolution chromosome analysis Detection of trinucleotide CTG repeat expansion in DMPK Targeted mutation analysis for SMN1 and SMN2 LAMA2 gene sequencing POMT1 and POMT2 gene sequencing POMGNT1 gene sequencing Fukutin gene sequencing ACTA1 sequencing and NEB deletion/duplication analysis; consider muscle histology MPZ, PMP22, or EGR2 gene sequencing First tier: Carbohydrate-deficient transferrin analysis, which is detected by mass spectrometry Second tier: Mutation analysis of PMM2 GAA gene sequencing or skin fibroblast culture for enzymatic assay brain malformations as the cause for, the neonatologist should consider a number of genetic disorders. For infants who have normal respiratory function and evidence of hypogonadism, PWS should be considered. Neonates who have large joint contractures should be evaluated for possible SMA and syndromic forms of CMDs. Neonates who have respiratory deficiency should be evaluated further for any underlying abnormality affecting muscle, including DM1, CHN, SMA, and nemaline myopathy. Laboratory evaluations should include serum CK. CK is present in cardiac and skeletal muscle and is a nonspecific marker of muscle breakdown. Mild-to-moderate elevations should raise the suspicion for CMD such as MEB disease and Walker-Warburg syndrome. Of note, the expected CK concentrations in these disorders are not as severely elevated as would be expected in males who have Duchenne muscular dystrophy, which usually is greater than 10 times the normal value. Thus, laboratory findings of elevated CK should prompt neuroimaging and formal ophthalmologic evaluation. Other laboratory evaluation should include chromosome analysis and possible comparative genomic hybridization if dysmorphic features are present. If a particular disorder is being considered, specific single gene testing is more appropriate. Congenital hypothyroidism also should be considered in the diagnostic evaluation of an infant exhibiting. Serum thyroid-stimulating hormone and free thyroxine are measured easily. Hypothyroidism is important to consider because this condition has a much better prognosis when detected early. Conclusion Many genetic and metabolic conditions may present with signs of and generalized muscle weakness. The cause and mechanism of muscle weakness depends on the disorder and underlying associated genetics. Furthermore, lack of cellular energy, abnormally functioning proteins, or accumulation of toxic metabolites may result in a similar clinical picture. The genetic approach to includes knowledge of presenting signs/symptoms of some of the most common inheritable disorders and the appropriate diagnostic tools that are available (molecular and biochemical testing) (Table). Awareness of these possible underlying causes may prove very beneficial to physicians in general pediatric practice, neonatology, and other specialties in making a timely diagnosis for conditions that may be seen more rarely and often not considered. Such early consideration allows further management and provides invaluable information to American Board of Pediatrics Neonatal-Perinatal Medicine Content Specifications Know the etiology, molecular phenotype, and clinical manifestations of disorders associated with uniparental disomy. Recognize the DNA findings, clinical manifestations, and inheritance of expanding genes, such as myotonic dystrophy. Know the basis for (including genetic), clinical and laboratory features (including associated abnormalities), differential diagnosis, management, and outcomes of neonatal /neuromuscular weakness. NeoReviews Vol.10 No.12 December 2009 e605
8 families regarding genetic counseling with respect to recurrence risk in future pregnancies. Suggested Reading Bios I, Forrest S. Spinal muscular atrophy: untangling the knot? J Med Genet. 1999;36:1 8 Cassidy SB, McCandless SE. Prader-Willi syndrome. In: Cassidy SB, Allanson JE, eds. Management of Genetic Syndromes. 2nd ed. New York, NY: Wiley-Liss; 2005: Congenital disorders of glycosylation overview, Fukuyama congenital muscular dystrophy, congenital muscular dystrophy overview, nemaline myopathy, spinal muscular atrophy, Prader-Willi syndrome, and myotonic dystrophy type 1. Gene Reviews. Clinical Genetic Information Resource. Available at: genetests.org. Accessed September 2009 Cormand B, Pinhko H, Bayes M, et al. Clinical and genetic distinction between Walker-Warburg syndrome and muscle-eye-brain disease. Neurology. 2001;56: Die-Smulders CEM. Myotonic dystrophy type 1. In: Cassidy SB, Allanson JE, eds. Management of Genetic Syndromes. 2nd ed. New York, NY: Wiley-Liss; 2005: Dobyns WB, Pagon RA, Armstrong D, et al. Diagnostic criteria for Walker-Warburg syndrome. Am J Med Genet. 1989;32: Enns G, Steiner RD, Buist N, et al. Clinical and molecular features of congenital disorder of glycosylation in patients with type 1 sialotransferrin pattern and diverse ethnic origins. J Pediatr. 2002;141: Gould SJ, Raymond GV, Valle D. The peroxisome biogenesis disorders. In: Scriver CR, Beaudet AL, Sly WS, Valle D, eds. The Metabolic and Molecular Bases of Inherited Disease. 8th ed. New York, NY: McGraw-Hill Companies, Inc; 2001: Hahn JS, Henry M, Hudgins L, Madan A. Congenital hypomyelination neuropathy in a newborn infant: unusual cause of diaphragmatic and vocal cord paralyzes. Pediatrics. 2001;108:e95 Kishnani PS, Steiner RD, Bali D, et al. Pompe disease diagnosis and management guideline. Genet Med. 2006;8: Liquori CL, Ricker K, Moseley ML, et al. Myotonic dystrophy type 2 caused by CCTG expansion in intron 1 of ZNF9. Science. 2001;293: Paro-Panjan D, Neubauer D. Congenital : is there an algorithm? J Child Neurol. 2004;19: Prasad AN, Prasad C. The floppy infant: contribution of genetic and metabolic disorders. Brain Dev. 2003;27: Stiefel L. Hypotonia in infants. Pediatr Rev. 1996;17: Thomas NH, Dubowitz V. The natural history of type I (severe) spinal muscular atrophy. Neuromuscul Disord. 1994;4: van der Ploeg A, Reuser AJ. Lysosomal storage disease 2. Pompe s disease. Lancet. 2008;372: e606 NeoReviews Vol.10 No.12 December 2009
9 NeoReviews Quiz 4. While discussing the causes of neonatal with medical students, you raise the possibility of Prader-Willi syndrome in a patient. Of the following, the most accurate statement regarding Prader-Willi syndrome is that: A. A characteristic cranial feature is brachycephaly. B. Deletion of the maternal allele from chromosome 15 is the genetic cause. C. Cryptorchidism is present in nearly all affected males. D. Hypotonia worsens with age. E. Prolonged ventilatory assistance is often necessary. 5. Molecular genetic testing is a rapid and cost-effective means of making a diagnosis in cases of neonatal. Of the following, an expansion of the CTG trinucleotide repeat in the DMPK gene is most consistent with the diagnosis of: A. Congenital hypomyelinating neuropathy. B. Merosin-deficient congenital muscular dystrophy. C. Myotonic dystrophy. D. Nemaline myopathy. E. Spinal muscular atrophy. 6. A term newborn presents with severe proximal muscle weakness, arthrogryposis multiplex congenita, and dilated cardiomyopathy. Maternal history is significant for poor fetal movement and polyhydramnios from fetal dysphagia, suggestive of prenatal onset of the neuromuscular disease. A muscle biopsy using Gomori trichrome staining reveals rodlike bodies scattered throughout the muscle fibers. Of the following, the most likely diagnosis in this infant is: A. Fukuyama congenital muscular dystrophy. B. Merosin-deficient congenital muscular dystrophy. C. Muscle-eye-brain disease. D. Nemaline myopathy. E. Walker-Warburg syndrome. 7. A 3-month-old male infant is being evaluated for severe. Physical examination reveals an abnormal distribution of fat, especially in the suprapubic, iliac, and gluteal regions. The infant has inverted nipples, strabismus, and microcephaly. Cranial magnetic resonance imaging shows diffuse cerebellar atrophy. Of the following, the most likely diagnosis for this infant is: A. Congenital disorder of glycosylation. B. Congenital hypomyelinating neuropathy. C. Congenital hypothyroidism. D. Pompe glycogen storage disease. E. Prader-Willi syndrome. NeoReviews Vol.10 No.12 December 2009 e607
10 The Genetic Approach to Hypotonia in the Neonate Neda Zadeh and Louanne Hudgins NeoReviews 2009;10;e600-e607 DOI: /neo e600 Updated Information & Services Permissions & Licensing Reprints including high-resolution figures, can be found at: s;10/12/e600 Information about reproducing this article in parts (figures, tables) or in its entirety can be found online at: Information about ordering reprints can be found online:
Neonatal Hypotonia Guideline Prepared by Dan Birnbaum MD August 27, 2012
 Neonatal Hypotonia Guideline Prepared by Dan Birnbaum MD August 27, 2012 Hypotonia: reduced tension or resistance to range of motion Localization can be central (brain), peripheral (spinal cord, nerve,
Neonatal Hypotonia Guideline Prepared by Dan Birnbaum MD August 27, 2012 Hypotonia: reduced tension or resistance to range of motion Localization can be central (brain), peripheral (spinal cord, nerve,
Neonatal Hypotonia. Encephalopathy acute No encephalopathy. Neurology Chapter of IAP
 The floppy infant assumes a frog legged position. On ventral suspension, the baby can not maintain limb posture against gravity and assumes the position of a rag doll. Encephalopathy acute No encephalopathy
The floppy infant assumes a frog legged position. On ventral suspension, the baby can not maintain limb posture against gravity and assumes the position of a rag doll. Encephalopathy acute No encephalopathy
The Floppy Baby. Clare Betteridge
 The Floppy Baby Clare Betteridge The floppy baby Identification Evaluation Investigation Diagnosis Examples What is a floppy baby? Elbows and knees loosely extended. Head control is usually poor or absent.
The Floppy Baby Clare Betteridge The floppy baby Identification Evaluation Investigation Diagnosis Examples What is a floppy baby? Elbows and knees loosely extended. Head control is usually poor or absent.
Evaluation of the Hypotonic Infant and Child
 Evaluation of the Hypotonic Infant and Child Basil T. Darras, M.D. Neuromuscular Program Boston Children s Hospital Harvard Medical School Boston, MA, USA Classification and General Clinical Evaluation
Evaluation of the Hypotonic Infant and Child Basil T. Darras, M.D. Neuromuscular Program Boston Children s Hospital Harvard Medical School Boston, MA, USA Classification and General Clinical Evaluation
NEONATAL MUSCULAR HYPOTONIA
 NEONATAL MUSCULAR HYPOTONIA Differential Diagnosis Systemic causes of neonatal hypotonia should be identified rapidly as they are usually transient if treated appropriately. Major differential diagnoses
NEONATAL MUSCULAR HYPOTONIA Differential Diagnosis Systemic causes of neonatal hypotonia should be identified rapidly as they are usually transient if treated appropriately. Major differential diagnoses
A Lawyer s Perspective on Genetic Screening Performed by Cryobanks
 A Lawyer s Perspective on Genetic Screening Performed by Cryobanks As a lawyer practicing in the area of sperm bank litigation, I have, unfortunately, represented too many couples that conceived a child
A Lawyer s Perspective on Genetic Screening Performed by Cryobanks As a lawyer practicing in the area of sperm bank litigation, I have, unfortunately, represented too many couples that conceived a child
Hypotonia Care Pathway Update: Diagnosis Garey Noritz, MD...
 Hypotonia Care Pathway Update: Diagnosis Garey Noritz, MD Disclosure Information- AACPDM 72 nd Annual Meeting October 9-13, 2018 Speaker Name: Garey Noritz, MD Disclosure of Relevant Financial Relationships
Hypotonia Care Pathway Update: Diagnosis Garey Noritz, MD Disclosure Information- AACPDM 72 nd Annual Meeting October 9-13, 2018 Speaker Name: Garey Noritz, MD Disclosure of Relevant Financial Relationships
DEVELOPING A FOLLOW-UP FRAMEWORK FOR POMPE DISEASE
 DEVELOPING A FOLLOW-UP FRAMEWORK FOR POMPE DISEASE Presenter: Sarah Bradley, MS, CGC Genetic Counselor, NYS Newborn Screening Program Authors: S. Bradley, D. Kronn, B. Vogel, M. Caggana, J. Orsini, K.
DEVELOPING A FOLLOW-UP FRAMEWORK FOR POMPE DISEASE Presenter: Sarah Bradley, MS, CGC Genetic Counselor, NYS Newborn Screening Program Authors: S. Bradley, D. Kronn, B. Vogel, M. Caggana, J. Orsini, K.
Learn the steps to identify pediatric muscle weakness and signs of neuromuscular disease.
 Learn the steps to identify pediatric muscle weakness and signs of neuromuscular disease. Listen Observe Evaluate Test Refer Guide for primary care providers includes: Surveillance Aid: Assessing Weakness
Learn the steps to identify pediatric muscle weakness and signs of neuromuscular disease. Listen Observe Evaluate Test Refer Guide for primary care providers includes: Surveillance Aid: Assessing Weakness
Prader-Willi Syndrome: an underrecognized
 www.jpnim.com Open Access eissn: 2281-0692 Journal of Pediatric and Neonatal Individualized Medicine 2018;7(1):e070107 doi: 10.7363/070107 Received: 2017 Aug 06; revised: 2017 Aug 24; accepted: 2017 Aug
www.jpnim.com Open Access eissn: 2281-0692 Journal of Pediatric and Neonatal Individualized Medicine 2018;7(1):e070107 doi: 10.7363/070107 Received: 2017 Aug 06; revised: 2017 Aug 24; accepted: 2017 Aug
Disorders of Muscle. Disorders of Muscle. Muscle Groups Involved in Myopathy. Needle Examination of EMG. History. Muscle Biopsy
 Disorders of Muscle Disorders of Muscle Zakia Bell, M.D. Associate Professor of Neurology and Physical Medicine & Rehabilitation Virginia Commonwealth University Cardinal symptom of diseases of the muscle
Disorders of Muscle Disorders of Muscle Zakia Bell, M.D. Associate Professor of Neurology and Physical Medicine & Rehabilitation Virginia Commonwealth University Cardinal symptom of diseases of the muscle
Neuromuscular in the Pediatric Clinic: Recognition and Referral
 Neuromuscular in the Pediatric Clinic: Recognition and Referral Matthew Harmelink, MD Assistant Professor, Pediatric Neurology Medical College of Wisconsin Objectives: 1. Understand common presentations
Neuromuscular in the Pediatric Clinic: Recognition and Referral Matthew Harmelink, MD Assistant Professor, Pediatric Neurology Medical College of Wisconsin Objectives: 1. Understand common presentations
Spinal Muscular Atrophy: Case Study. Spinal muscular atrophy (SMA) is a fairly common genetic disorder, affecting
 Spinal Muscular Atrophy: Case Study Spinal muscular atrophy (SMA) is a fairly common genetic disorder, affecting approximately one in 6,000 babies. It is estimated that one in every 40 Americans carries
Spinal Muscular Atrophy: Case Study Spinal muscular atrophy (SMA) is a fairly common genetic disorder, affecting approximately one in 6,000 babies. It is estimated that one in every 40 Americans carries
Muscular Dystrophies. Pinki Munot Consultant Paediatric Neurologist Great Ormond Street Hospital Practical Neurology Study days April 2018
 Muscular Dystrophies Pinki Munot Consultant Paediatric Neurologist Great Ormond Street Hospital Practical Neurology Study days April 2018 Definition and classification Clinical guide to recognize muscular
Muscular Dystrophies Pinki Munot Consultant Paediatric Neurologist Great Ormond Street Hospital Practical Neurology Study days April 2018 Definition and classification Clinical guide to recognize muscular
Genetic diagnosis of limb girdle muscular dystrophy type 2A, A Case Report
 Genetic diagnosis of limb girdle muscular dystrophy type 2A, A Case Report Roshanak Jazayeri, MD, PhD Assistant Professor of Medical Genetics Faculty of Medicine, Alborz University of Medical Sciences
Genetic diagnosis of limb girdle muscular dystrophy type 2A, A Case Report Roshanak Jazayeri, MD, PhD Assistant Professor of Medical Genetics Faculty of Medicine, Alborz University of Medical Sciences
Recognizing Genetic Red Flags in Clinical Evaluations
 Recognizing Genetic Red Flags in Clinical Evaluations ACGME Sub-competencies / Developmental Milestones Addressed Patient Care: Gather essential and accurate information about the patient; Make informed
Recognizing Genetic Red Flags in Clinical Evaluations ACGME Sub-competencies / Developmental Milestones Addressed Patient Care: Gather essential and accurate information about the patient; Make informed
1/28/2019. OSF HealthCare INI Care Center Team. Neuromuscular Disease: Muscular Dystrophy. OSF HealthCare INI Care Center Team: Who are we?
 Neuromuscular Disease: Muscular Dystrophy Muscular Dystrophy Association (MDA) and OSF HealthCare Illinois Neurological Institute (INI) Care Center Team The Neuromuscular clinic is a designated MDA Care
Neuromuscular Disease: Muscular Dystrophy Muscular Dystrophy Association (MDA) and OSF HealthCare Illinois Neurological Institute (INI) Care Center Team The Neuromuscular clinic is a designated MDA Care
CURRENT GENETIC TESTING TOOLS IN NEONATAL MEDICINE. Dr. Bahar Naghavi
 2 CURRENT GENETIC TESTING TOOLS IN NEONATAL MEDICINE Dr. Bahar Naghavi Assistant professor of Basic Science Department, Shahid Beheshti University of Medical Sciences, Tehran,Iran 3 Introduction Over 4000
2 CURRENT GENETIC TESTING TOOLS IN NEONATAL MEDICINE Dr. Bahar Naghavi Assistant professor of Basic Science Department, Shahid Beheshti University of Medical Sciences, Tehran,Iran 3 Introduction Over 4000
When to suspect Prader Willi Syndrome and how to diagnose it?
 When to suspect Prader Willi Syndrome and how to diagnose it? Dr Chirita-Emandi Adela Dr Dobrescu Andreea Victor Babes University of Medicine and Pahrmacy Timisoara Emergency Hospital for Children Louis
When to suspect Prader Willi Syndrome and how to diagnose it? Dr Chirita-Emandi Adela Dr Dobrescu Andreea Victor Babes University of Medicine and Pahrmacy Timisoara Emergency Hospital for Children Louis
Next-generation sequencing-based molecular diagnosis of neonatal hypotonia in Chinese
 Title page Next-generation sequencing-based molecular diagnosis of neonatal hypotonia in Chinese Population Yan Wang 1, #,Wei peng 1,#, Hong-Yan Guo 3,4, Hui Li 3,4, Jie Tian 3,4, Yu-Jing Shi 3,4, Xiao
Title page Next-generation sequencing-based molecular diagnosis of neonatal hypotonia in Chinese Population Yan Wang 1, #,Wei peng 1,#, Hong-Yan Guo 3,4, Hui Li 3,4, Jie Tian 3,4, Yu-Jing Shi 3,4, Xiao
Diagnosis, management and new treatments for Spinal Muscular Atrophy Special Focus: SMA Type 1
 Diagnosis, management and new treatments for Spinal Muscular Atrophy Special Focus: SMA Type 1 17 th April 2018 Adnan Manzur Consultant Paediatric Neurologist Dubowitz Neuromuscular Centre, GOSH & ICH,
Diagnosis, management and new treatments for Spinal Muscular Atrophy Special Focus: SMA Type 1 17 th April 2018 Adnan Manzur Consultant Paediatric Neurologist Dubowitz Neuromuscular Centre, GOSH & ICH,
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: nusinersen_spinraza 03/2017 10/2017 10/2018 10/2017 Description of Procedure or Service Spinal muscular atrophy
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: nusinersen_spinraza 03/2017 10/2017 10/2018 10/2017 Description of Procedure or Service Spinal muscular atrophy
What s New in Newborn Screening?
 What s New in Newborn Screening? Funded by: Illinois Department of Public Health Information on Newborn Screening Newborn screening in Illinois is administered by the Illinois Department of Public Health.
What s New in Newborn Screening? Funded by: Illinois Department of Public Health Information on Newborn Screening Newborn screening in Illinois is administered by the Illinois Department of Public Health.
Approach to the Child with Developmental Delay
 Approach to the Child with Developmental Delay Arwa Nasir Department of Pediatrics University of Nebraska Medical Center DISCLOSURE DECLARATION Approach to the Child with Developmental Delay Arwa Nasir
Approach to the Child with Developmental Delay Arwa Nasir Department of Pediatrics University of Nebraska Medical Center DISCLOSURE DECLARATION Approach to the Child with Developmental Delay Arwa Nasir
AMERICAN BOARD OF MEDICAL GENETICS AND GENOMICS
 AMERICAN BOARD OF MEDICAL GENETICS AND GENOMICS Logbook Guidelines for Certification in Clinical Genetics and Genomics for the 2017 Examination as of 10/5/2015 Purpose: The purpose of the logbook is to
AMERICAN BOARD OF MEDICAL GENETICS AND GENOMICS Logbook Guidelines for Certification in Clinical Genetics and Genomics for the 2017 Examination as of 10/5/2015 Purpose: The purpose of the logbook is to
LSD WORKSHOP WHAT EVERY PEDIATRICIAN SHOULD KNOW. Amal Al Tenaiji Pediatric Metabolic Genetics SKMC Abu Dhabi
 LSD WORKSHOP WHAT EVERY PEDIATRICIAN SHOULD KNOW Amal Al Tenaiji Pediatric Metabolic Genetics SKMC Abu Dhabi CASE A 1 month old infant presents with difficulty feeding and respiratory distress. Mom and
LSD WORKSHOP WHAT EVERY PEDIATRICIAN SHOULD KNOW Amal Al Tenaiji Pediatric Metabolic Genetics SKMC Abu Dhabi CASE A 1 month old infant presents with difficulty feeding and respiratory distress. Mom and
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Genetics
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Genetics 1. GOAL: Understand the role of the pediatrician in preventing genetic disease, and in counseling and screening
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Genetics 1. GOAL: Understand the role of the pediatrician in preventing genetic disease, and in counseling and screening
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: nusinersen_spinraza 03/2017 10/2018 10/2019 10/2018 Description of Procedure or Service Spinal muscular atrophy
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: nusinersen_spinraza 03/2017 10/2018 10/2019 10/2018 Description of Procedure or Service Spinal muscular atrophy
What s New in Newborn Screening?
 What s New in Newborn Screening? Funded by: Illinois Department of Public Health Information on Newborn Screening Newborn screening in Illinois is mandated and administered by the Illinois Department of
What s New in Newborn Screening? Funded by: Illinois Department of Public Health Information on Newborn Screening Newborn screening in Illinois is mandated and administered by the Illinois Department of
Case 1 A 65 year old college professor came to the neurology clinic referred by her family physician because of frequent falling. She had a history of
 Peripheral Nervous System Case 1 A 65 year old college professor came to the neurology clinic referred by her family physician because of frequent falling. She had a history of non-insulin dependent diabetes
Peripheral Nervous System Case 1 A 65 year old college professor came to the neurology clinic referred by her family physician because of frequent falling. She had a history of non-insulin dependent diabetes
A rare case of muscular dystrophy with POMT2 and FKRP gene mutation. Present by : Ghasem Khazaei Supervisor :Dr Mina Mohammadi Sarband
 A rare case of muscular dystrophy with POMT2 and FKRP gene mutation Present by : Ghasem Khazaei Supervisor :Dr Mina Mohammadi Sarband Index : Congenital muscular dystrophy (CMD) Dystroglycanopathies Walker-Warburg
A rare case of muscular dystrophy with POMT2 and FKRP gene mutation Present by : Ghasem Khazaei Supervisor :Dr Mina Mohammadi Sarband Index : Congenital muscular dystrophy (CMD) Dystroglycanopathies Walker-Warburg
Patient L.L. KRISTEN ARREDONDO, MD CHILD NEUROLOGY PGY5, UT SOUTHWESTERN
 Patient L.L. KRISTEN ARREDONDO, MD CHILD NEUROLOGY PGY5, UT SOUTHWESTERN Birth History LL was born to a healthy first time mother with an uncomplicated pregnancy Delivered at 38 weeks via C-section due
Patient L.L. KRISTEN ARREDONDO, MD CHILD NEUROLOGY PGY5, UT SOUTHWESTERN Birth History LL was born to a healthy first time mother with an uncomplicated pregnancy Delivered at 38 weeks via C-section due
Corporate Medical Policy
 Corporate Medical Policy Genetic Testing for Duchenne and Becker Muscular Dystrophy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_duchenne_and_becker_muscular_dystrophy
Corporate Medical Policy Genetic Testing for Duchenne and Becker Muscular Dystrophy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_duchenne_and_becker_muscular_dystrophy
Unusual Modes of Inheritance. Wayne Lam
 Unusual Modes of Inheritance Wayne Lam wayne.lam@ed.ac.uk New Genetics Non-Mendelian Genomic Imprinting Digenic Inheritance Triallelic inheritance Mitochondrial Inheritance Chromosomal Telomeric deletions
Unusual Modes of Inheritance Wayne Lam wayne.lam@ed.ac.uk New Genetics Non-Mendelian Genomic Imprinting Digenic Inheritance Triallelic inheritance Mitochondrial Inheritance Chromosomal Telomeric deletions
Nemaline (rod) myopathies
 Nemaline (rod) myopathies Nemaline, or rod, myopathies are a group of conditions which fall under the umbrella of congenital myopathies. They are characterised by rod-like structures in the muscle cells,
Nemaline (rod) myopathies Nemaline, or rod, myopathies are a group of conditions which fall under the umbrella of congenital myopathies. They are characterised by rod-like structures in the muscle cells,
Pompe. Lysosomal Disorders. Introduction
 Introduction disease is an inherited, genetic disorder which results in the lack of an enzyme 'acid alpha-glucosidase. disease is also known as acid maltase deficiency or glycogen storage disease type
Introduction disease is an inherited, genetic disorder which results in the lack of an enzyme 'acid alpha-glucosidase. disease is also known as acid maltase deficiency or glycogen storage disease type
Spinal Muscular Atrophy Newborn Screening
 10.2018 Spinal Muscular Atrophy Newborn Screening Melissa Gibbons, MS, CGC Erica Wright, MS, CGC Clinical Genetics and Metabolism Department of Pediatrics Children s Hospital Colorado/ University of Colorado
10.2018 Spinal Muscular Atrophy Newborn Screening Melissa Gibbons, MS, CGC Erica Wright, MS, CGC Clinical Genetics and Metabolism Department of Pediatrics Children s Hospital Colorado/ University of Colorado
PRADER-WILLI SYNDROME HOWARD WONG 3UU PER. 6 GENETICS SBS11QHG2 #24
 PRADER-WILLI SYNDROME HOWARD WONG 3UU PER. 6 GENETICS SBS11QHG2 #24 PHYSIOLOGY Fig. 1 Fig. 2 Prader-Willi Syndrome affects both the physical and mental state of a person, starting from birth until the
PRADER-WILLI SYNDROME HOWARD WONG 3UU PER. 6 GENETICS SBS11QHG2 #24 PHYSIOLOGY Fig. 1 Fig. 2 Prader-Willi Syndrome affects both the physical and mental state of a person, starting from birth until the
Approach to the Genetic Diagnosis of Neurological Disorders
 Approach to the Genetic Diagnosis of Neurological Disorders Dr Wendy Jones MBBS MRCP Great Ormond Street Hospital for Children National Hospital for Neurology and Neurosurgery What is a genetic diagnosis?
Approach to the Genetic Diagnosis of Neurological Disorders Dr Wendy Jones MBBS MRCP Great Ormond Street Hospital for Children National Hospital for Neurology and Neurosurgery What is a genetic diagnosis?
MEDICAL GENETICS CLINICAL CARE ROTATION
 Medical Genetics Clinical Care Rotation 1 MEDICAL GENETICS CLINICAL CARE ROTATION Overview: The Medical Genetics Clinical Care Rotation (MGC) is the backbone of the clinical genetics experience for the
Medical Genetics Clinical Care Rotation 1 MEDICAL GENETICS CLINICAL CARE ROTATION Overview: The Medical Genetics Clinical Care Rotation (MGC) is the backbone of the clinical genetics experience for the
Systematizing in vivo modeling of pediatric disorders
 Systematizing in vivo modeling of pediatric disorders Nicholas Katsanis, Ph.D. Duke University Medical Center Center for Human Disease Modeling Rescindo Therapeutics www.dukegenes.org Task Force for
Systematizing in vivo modeling of pediatric disorders Nicholas Katsanis, Ph.D. Duke University Medical Center Center for Human Disease Modeling Rescindo Therapeutics www.dukegenes.org Task Force for
III./10.4. Diagnosis. Introduction. A.) Laboratory tests. Laboratory tests, electrophysiology, muscle biopsy, genetic testing, imaging techniques
 III./10.4. Diagnosis Laboratory tests, electrophysiology, muscle biopsy, genetic testing, imaging techniques After studying this chapter, you will become familiar with the most commonly used diagnostic
III./10.4. Diagnosis Laboratory tests, electrophysiology, muscle biopsy, genetic testing, imaging techniques After studying this chapter, you will become familiar with the most commonly used diagnostic
AMERICAN ACADEMY OF PEDIATRICS
 AMERICAN ACADEMY OF PEDIATRICS The Role of the Primary Care Pediatrician in the Management of High-risk Newborn Infants ABSTRACT. Quality care for high-risk newborns can best be provided by coordinating
AMERICAN ACADEMY OF PEDIATRICS The Role of the Primary Care Pediatrician in the Management of High-risk Newborn Infants ABSTRACT. Quality care for high-risk newborns can best be provided by coordinating
Pompe Disease. Family Education Booklet. Division of Pediatric Genetics Metabolism and Genomic Medicine
 Pompe Disease Family Education Booklet Division of Pediatric Genetics Metabolism and Genomic Medicine Table of Contents What is Pompe disease?... 1 How common is Pompe disease?... 1 Basic genetic concepts...
Pompe Disease Family Education Booklet Division of Pediatric Genetics Metabolism and Genomic Medicine Table of Contents What is Pompe disease?... 1 How common is Pompe disease?... 1 Basic genetic concepts...
ASSESSMENT OF NEONATAL HYPOTONIA CLINICAL GUIDELINE 1. Aim/Purpose of this Guideline
 ASSESSMENT OF NEONATAL HYPOTONIA CLINICAL GUIDELINE 1. Aim/Purpose of this Guideline 1.1. To provide guidance on the management of hypotonic infants. All involved will benefit from the improvement in service
ASSESSMENT OF NEONATAL HYPOTONIA CLINICAL GUIDELINE 1. Aim/Purpose of this Guideline 1.1. To provide guidance on the management of hypotonic infants. All involved will benefit from the improvement in service
SMA IS A SEVERE NEUROLOGICAL DISORDER [1]
![SMA IS A SEVERE NEUROLOGICAL DISORDER [1] SMA IS A SEVERE NEUROLOGICAL DISORDER [1]](/thumbs/72/67086153.jpg) SMA OVERVIEW SMA IS A SEVERE NEUROLOGICAL DISORDER [1] Autosomal recessive genetic inheritance 1 in 50 people (approximately 6 million Americans) are carriers [2] 1 in 6,000 to 1 in 10,000 children born
SMA OVERVIEW SMA IS A SEVERE NEUROLOGICAL DISORDER [1] Autosomal recessive genetic inheritance 1 in 50 people (approximately 6 million Americans) are carriers [2] 1 in 6,000 to 1 in 10,000 children born
What is myotonic dystrophy?
 What is myotonic dystrophy? Myotonic dystrophy is a muscle condition that falls under the umbrella term muscular dystrophy. The muscular dystrophies all have three features in common; they are hereditary,
What is myotonic dystrophy? Myotonic dystrophy is a muscle condition that falls under the umbrella term muscular dystrophy. The muscular dystrophies all have three features in common; they are hereditary,
Medical Conditions Resulting in High Probability of Developmental Delay and DSCC Screening Information
 Jame5. L.Jma5, ~reuiry Medical Conditions Medical Conditions Resulting in High Probability of Developmental Delay and DSCC Screening Information I Not Listed later Children with medical conditions which
Jame5. L.Jma5, ~reuiry Medical Conditions Medical Conditions Resulting in High Probability of Developmental Delay and DSCC Screening Information I Not Listed later Children with medical conditions which
Orthopedic and Surgical Features in Patients with Prader Willi Syndrome
 Orthopedic and Surgical Features in Patients with Prader Willi Syndrome Vlad David, Alexandra Pal Victor Babes University of Medicine and Pharmacy Timisoara Louis Turcanu Emergency Children s Hospital
Orthopedic and Surgical Features in Patients with Prader Willi Syndrome Vlad David, Alexandra Pal Victor Babes University of Medicine and Pharmacy Timisoara Louis Turcanu Emergency Children s Hospital
Keith Bachmann, MD UVA Department of Orthopaedic Surgery
 Keith Bachmann, MD UVA Department of Orthopaedic Surgery Definition Spinal deformity secondary to either neurologic or muscle pathology. Etiology Imbalance of muscle forces Lack of truncal support Similar
Keith Bachmann, MD UVA Department of Orthopaedic Surgery Definition Spinal deformity secondary to either neurologic or muscle pathology. Etiology Imbalance of muscle forces Lack of truncal support Similar
Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists
 Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists What is NCS/EMG? NCS examines the conduction properties of sensory and motor peripheral nerves. For both
Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists What is NCS/EMG? NCS examines the conduction properties of sensory and motor peripheral nerves. For both
Infantile-onset glycogen storage disease type II
 Case Report 379 Infantile-Onset Glycogen Storage Disease Type II (Pompe Disease): Report of a Case with Genetic Diagnosis and Pathological Findings Yao-Tun Teng, MD; Wen-Jen Su, MD; Jia-Wei Hou 1, MD,
Case Report 379 Infantile-Onset Glycogen Storage Disease Type II (Pompe Disease): Report of a Case with Genetic Diagnosis and Pathological Findings Yao-Tun Teng, MD; Wen-Jen Su, MD; Jia-Wei Hou 1, MD,
Presentation and investigation of mitochondrial disease in children
 Presentation and investigation of mitochondrial disease in children Andrew Morris Willink Unit, Manchester Mitochondrial function Carbohydrate Fat Respiratory chain Energy Mitochondria are the product
Presentation and investigation of mitochondrial disease in children Andrew Morris Willink Unit, Manchester Mitochondrial function Carbohydrate Fat Respiratory chain Energy Mitochondria are the product
DSS-1. No financial disclosures
 DSS-1 No financial disclosures Clinical History 9 year old boy with past medical history significant for cerebral palsy, in-turning right foot, left clubfoot that was surgically corrected at 3 years of
DSS-1 No financial disclosures Clinical History 9 year old boy with past medical history significant for cerebral palsy, in-turning right foot, left clubfoot that was surgically corrected at 3 years of
Cardiac Considerations and Care in Children with Neuromuscular Disorders
 Cardiac Considerations and Care in Children with Neuromuscular Disorders - importance of early and ongoing treatment, management and available able medications. Dr Bo Remenyi Department of Cardiology The
Cardiac Considerations and Care in Children with Neuromuscular Disorders - importance of early and ongoing treatment, management and available able medications. Dr Bo Remenyi Department of Cardiology The
A novel POMT2 mutation causes mild congenital muscular dystrophy with normal brain MRI
 Brain & Development 31 (2009) 465 468 Case report A novel POMT2 mutation causes mild congenital muscular dystrophy with normal brain MRI Terumi Murakami a,b, Yukiko K. Hayashi a, *, Megumu Ogawa a, Satoru
Brain & Development 31 (2009) 465 468 Case report A novel POMT2 mutation causes mild congenital muscular dystrophy with normal brain MRI Terumi Murakami a,b, Yukiko K. Hayashi a, *, Megumu Ogawa a, Satoru
Muscular Dystrophy. Biol 405 Molecular Medicine
 Muscular Dystrophy Biol 405 Molecular Medicine Duchenne muscular dystrophy Duchenne muscular dystrophy is a neuromuscular disease that occurs in ~ 1/3,500 male births. The disease causes developmental
Muscular Dystrophy Biol 405 Molecular Medicine Duchenne muscular dystrophy Duchenne muscular dystrophy is a neuromuscular disease that occurs in ~ 1/3,500 male births. The disease causes developmental
Hypoglycemia. Objectives. Glucose Metabolism
 Hypoglycemia Instructor: Janet Mendis, MSN, RNC-NIC, CNS Outline: Janet Mendis, MSN, RNC-NIC, CNS Summer Morgan, MSN, RNC-NIC, CPNP UC San Diego Health System Objectives State the blood glucose level at
Hypoglycemia Instructor: Janet Mendis, MSN, RNC-NIC, CNS Outline: Janet Mendis, MSN, RNC-NIC, CNS Summer Morgan, MSN, RNC-NIC, CPNP UC San Diego Health System Objectives State the blood glucose level at
SALSA MLPA KIT P060-B2 SMA
 SALSA MLPA KIT P6-B2 SMA Lot 111, 511: As compared to the previous version B1 (lot 11), the 88 and 96 nt DNA Denaturation control fragments have been replaced (QDX2). Please note that, in contrast to the
SALSA MLPA KIT P6-B2 SMA Lot 111, 511: As compared to the previous version B1 (lot 11), the 88 and 96 nt DNA Denaturation control fragments have been replaced (QDX2). Please note that, in contrast to the
Gaucher disease 3/22/2009. Mendelian pedigree patterns. Autosomal-dominant inheritance
 Mendelian pedigree patterns Autosomal-dominant inheritance Autosomal dominant Autosomal recessive X-linked dominant X-linked recessive Y-linked Examples of AD inheritance Autosomal-recessive inheritance
Mendelian pedigree patterns Autosomal-dominant inheritance Autosomal dominant Autosomal recessive X-linked dominant X-linked recessive Y-linked Examples of AD inheritance Autosomal-recessive inheritance
LIST OF ABBREVIATIONS
 PAPER 2006 Royal College of Physicians of Edinburgh Myotonic dystrophy C Longman Department of Clinical Genetics, Guy s Hospital, London, England ABSTRACT Myotonic dystrophy is the most common form of
PAPER 2006 Royal College of Physicians of Edinburgh Myotonic dystrophy C Longman Department of Clinical Genetics, Guy s Hospital, London, England ABSTRACT Myotonic dystrophy is the most common form of
Introduction and aims of the study
 Introduction and aims of the study 1 Chapter 1 Motor neuron diseases include the most incapacitating and life-threatening illnesses but also rather benign disorders with only mild symptoms and slow progression.
Introduction and aims of the study 1 Chapter 1 Motor neuron diseases include the most incapacitating and life-threatening illnesses but also rather benign disorders with only mild symptoms and slow progression.
Basic Facts About PWS:
 Phone: 800-926-4797 or 941-312-0400 Your membership provides this website - Join Today! Basic Facts About PWS: A Diagnosis and Reference Guide for Physicians and Other Health Professionals What is Prader-Willi
Phone: 800-926-4797 or 941-312-0400 Your membership provides this website - Join Today! Basic Facts About PWS: A Diagnosis and Reference Guide for Physicians and Other Health Professionals What is Prader-Willi
The 2017 Update of the Standard of Care Recommendations for Spinal Muscular Atrophy
 Richard Finkel, MD Nemours Children s Hospital Orlando, FL, USA Thomas Crawford, MD Johns Hopkins Hospital Baltimore, MD, USA The 2017 Update of the Standard of Care Recommendations for Spinal Muscular
Richard Finkel, MD Nemours Children s Hospital Orlando, FL, USA Thomas Crawford, MD Johns Hopkins Hospital Baltimore, MD, USA The 2017 Update of the Standard of Care Recommendations for Spinal Muscular
Red flags for clinical practice - guidance on indicators that your patient may have a genetic condition
 Red flags for clinical practice - guidance on indicators that your patient may have a genetic condition General red flags for clinical practice One or more of these red flags that may indicate a high genetic
Red flags for clinical practice - guidance on indicators that your patient may have a genetic condition General red flags for clinical practice One or more of these red flags that may indicate a high genetic
Myotonic Dystrophy OUTLINE
 OUTLINE Myotonic Dystrophy INTRODUCTION: 1). GENERAL OVERVIEW 2). SYMPTOMS 3). DIAGNOSIS 4). CAUSES and PATHOLOGY 5). GENETICS 6). TREATMENT and MEDICAL MANAGEMENT 7). LIFESTYLE IMPACTS 8). RESEARCH 9).
OUTLINE Myotonic Dystrophy INTRODUCTION: 1). GENERAL OVERVIEW 2). SYMPTOMS 3). DIAGNOSIS 4). CAUSES and PATHOLOGY 5). GENETICS 6). TREATMENT and MEDICAL MANAGEMENT 7). LIFESTYLE IMPACTS 8). RESEARCH 9).
Statutory Approvals Committee minutes
 Statutory Approvals Committee minutes Centre 0102 (Guys Hospital) Pre-implantation Genetic Diagnosis (PGD) application for Muscular Dystrophy, Congenital, LMNA-related, (MDCL) OMIM #613205 Thursday, 25
Statutory Approvals Committee minutes Centre 0102 (Guys Hospital) Pre-implantation Genetic Diagnosis (PGD) application for Muscular Dystrophy, Congenital, LMNA-related, (MDCL) OMIM #613205 Thursday, 25
Miller-Dieker syndrome. William B Dobyns, MD
 Miller-Dieker syndrome William B Dobyns, MD MDS phenotype Early clinical course Prenatal Prenatal growth DEF 11/26 Polyhydramnios 13/24 Neonatal Neonatal resuscitation 06/20 Neonatal jaundice 08/21 Growth
Miller-Dieker syndrome William B Dobyns, MD MDS phenotype Early clinical course Prenatal Prenatal growth DEF 11/26 Polyhydramnios 13/24 Neonatal Neonatal resuscitation 06/20 Neonatal jaundice 08/21 Growth
Muscle Pathology Surgical Pathology Unknown Conference. November, 2008 Philip Boyer, M.D., Ph.D.
 Muscle Pathology Surgical Pathology Unknown Conference November, 2008 Philip Boyer, M.D., Ph.D. Etiologic Approach to Differential Diagnosis Symptoms / Signs / Imaging / Biopsy / CSF Analysis Normal Abnormal
Muscle Pathology Surgical Pathology Unknown Conference November, 2008 Philip Boyer, M.D., Ph.D. Etiologic Approach to Differential Diagnosis Symptoms / Signs / Imaging / Biopsy / CSF Analysis Normal Abnormal
Klinefelter syndrome ( 47, XXY )
 Sex Chromosome Abnormalities, Sex Chromosome Aneuploidy It has been estimated that, overall, approximately one in 400 infants have some form of sex chromosome aneuploidy. A thorough discussion of sex chromosomes
Sex Chromosome Abnormalities, Sex Chromosome Aneuploidy It has been estimated that, overall, approximately one in 400 infants have some form of sex chromosome aneuploidy. A thorough discussion of sex chromosomes
Diseases of Muscle and Neuromuscular Junction
 Diseases of Muscle and Neuromuscular Junction Diseases of Muscle and Neuromuscular Junction Neuromuscular Junction Muscle Myastenia Gravis Eaton-Lambert Syndrome Toxic Infllammatory Denervation Atrophy
Diseases of Muscle and Neuromuscular Junction Diseases of Muscle and Neuromuscular Junction Neuromuscular Junction Muscle Myastenia Gravis Eaton-Lambert Syndrome Toxic Infllammatory Denervation Atrophy
A CASE OF GIANT AXONAL NEUROPATHY HEMANANTH T SECOND YEAR POST GRADUATE IN PAEDIATRICS INSTITUTE OF SOCIAL PAEDIATRICS GOVERNMENT STANLEY HOSPITAL
 A CASE OF GIANT AXONAL NEUROPATHY HEMANANTH T SECOND YEAR POST GRADUATE IN PAEDIATRICS INSTITUTE OF SOCIAL PAEDIATRICS GOVERNMENT STANLEY HOSPITAL CASE HISTORY Nine year old male child Second born Born
A CASE OF GIANT AXONAL NEUROPATHY HEMANANTH T SECOND YEAR POST GRADUATE IN PAEDIATRICS INSTITUTE OF SOCIAL PAEDIATRICS GOVERNMENT STANLEY HOSPITAL CASE HISTORY Nine year old male child Second born Born
Tel: , Fax: ,
 1 Nemaline Myopathy Type 2 (NEM2): Two Novel Mutations in the Nebulin (NEB) Gene Anna Gajda MD 1*, Emese Horváth MD 2*, Tibor Hortobágyi MD, PhD 3, Gyurgyinka Gergev MA 1,4, Hajnalka Szabó MD, PhD 1, Katalin
1 Nemaline Myopathy Type 2 (NEM2): Two Novel Mutations in the Nebulin (NEB) Gene Anna Gajda MD 1*, Emese Horváth MD 2*, Tibor Hortobágyi MD, PhD 3, Gyurgyinka Gergev MA 1,4, Hajnalka Szabó MD, PhD 1, Katalin
LIMP BABIES - WHAT MAY THAT MEAN?
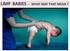 LIMP BABIES - WHAT MAY THAT MEAN? ARE WE LOOKING WHERE WE SHOULD? FLOPPY = LIMP = FLACCID = WEAK Poor head control when pulled C-posture sitting, or in ventral susp. Frog-leg lying Dropping arms Casey
LIMP BABIES - WHAT MAY THAT MEAN? ARE WE LOOKING WHERE WE SHOULD? FLOPPY = LIMP = FLACCID = WEAK Poor head control when pulled C-posture sitting, or in ventral susp. Frog-leg lying Dropping arms Casey
Should Universal Carrier Screening be Universal?
 Should Universal Carrier Screening be Universal? Disclosures Research funding from Natera Mary E Norton MD University of California, San Francisco Antepartum and Intrapartum Management June 15, 2017 Burden
Should Universal Carrier Screening be Universal? Disclosures Research funding from Natera Mary E Norton MD University of California, San Francisco Antepartum and Intrapartum Management June 15, 2017 Burden
SEX-LINKED INHERITANCE. Dr Rasime Kalkan
 SEX-LINKED INHERITANCE Dr Rasime Kalkan Human Karyotype Picture of Human Chromosomes 22 Autosomes and 2 Sex Chromosomes Autosomal vs. Sex-Linked Traits can be either: Autosomal: traits (genes) are located
SEX-LINKED INHERITANCE Dr Rasime Kalkan Human Karyotype Picture of Human Chromosomes 22 Autosomes and 2 Sex Chromosomes Autosomal vs. Sex-Linked Traits can be either: Autosomal: traits (genes) are located
THIAMINE TRANSPORTER TYPE 2 DEFICIENCY
 THIAMINE TRANSPORTER TYPE 2 DEFICIENCY WHAT IS THE THIAMINE TRANSPORTER TYPE 2 DEFICIENCY (hthtr2)? The thiamine transporter type 2 deficiency (hthtr2) is a inborn error of thiamine metabolism caused by
THIAMINE TRANSPORTER TYPE 2 DEFICIENCY WHAT IS THE THIAMINE TRANSPORTER TYPE 2 DEFICIENCY (hthtr2)? The thiamine transporter type 2 deficiency (hthtr2) is a inborn error of thiamine metabolism caused by
Putting Neuromotor Screening Into Practice: Webinar 3. June 27, :00 am Central
 Putting Neuromotor Screening Into Practice: Webinar 3 June 27, 2013 11:00 am Central 1 AGENDA Agenda Item Speaker Time Welcome and Project Introduction Pat Heinrich, RN, MSN, QI Advisor 5 min Discuss Action
Putting Neuromotor Screening Into Practice: Webinar 3 June 27, 2013 11:00 am Central 1 AGENDA Agenda Item Speaker Time Welcome and Project Introduction Pat Heinrich, RN, MSN, QI Advisor 5 min Discuss Action
Clinical Summaries. CLN1 Disease, infantile onset and others
 Clinical Summaries CLN1 Disease, infantile onset and others The gene called CLN1 lies on chromosome 1. CLN1 disease is inherited as an autosomal recessive disorder, which means that both chromosomes carry
Clinical Summaries CLN1 Disease, infantile onset and others The gene called CLN1 lies on chromosome 1. CLN1 disease is inherited as an autosomal recessive disorder, which means that both chromosomes carry
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier/Additional Provider
 Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier/Additional Provider TEST DISEASE/CONDITION POPULATION TRIAD Submitting laboratory: Manchester RGC Approved: September 2013
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier/Additional Provider TEST DISEASE/CONDITION POPULATION TRIAD Submitting laboratory: Manchester RGC Approved: September 2013
Unifactorial or Single Gene Disorders. Hanan Hamamy Department of Genetic Medicine and Development Geneva University Hospital
 Unifactorial or Single Gene Disorders Hanan Hamamy Department of Genetic Medicine and Development Geneva University Hospital Training Course in Sexual and Reproductive Health Research Geneva 2011 Single
Unifactorial or Single Gene Disorders Hanan Hamamy Department of Genetic Medicine and Development Geneva University Hospital Training Course in Sexual and Reproductive Health Research Geneva 2011 Single
To Be Your Local Expert A General Pediatrician s Story
 To Be Your Local Expert A General Pediatrician s Story DDC Clinic mission: To enhance the quality of life for people with special needs caused by rare genetic disorders What Does It Take to Be Your Local
To Be Your Local Expert A General Pediatrician s Story DDC Clinic mission: To enhance the quality of life for people with special needs caused by rare genetic disorders What Does It Take to Be Your Local
Supplementary Online Content
 Supplementary Online Content Honein MA, Dawson AL, Petersen E, et al; US Zika Pregnancy Registry Collaboration. Birth Defects Among Fetuses and Infants of US Women With Laboratory Evidence of Possible
Supplementary Online Content Honein MA, Dawson AL, Petersen E, et al; US Zika Pregnancy Registry Collaboration. Birth Defects Among Fetuses and Infants of US Women With Laboratory Evidence of Possible
Genetic evaluation of the pediatric patient with hypotonia: perspective from a hypotonia specialty clinic and review of the literature
 DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY REVIEW Genetic evaluation of the pediatric patient with hypotonia: perspective from a hypotonia specialty clinic and review of the literature EMILY C LISI RONALDDCOHN
DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY REVIEW Genetic evaluation of the pediatric patient with hypotonia: perspective from a hypotonia specialty clinic and review of the literature EMILY C LISI RONALDDCOHN
Neonatal manifestations of lysosomal storage diseases
 Neonatal manifestations of lysosomal storage diseases Nadia ALhashmi MD Metabolic &genetic disorder Royal hospital 2 nd Oman international pediatric and neonatal conference 13 th -15 th April 2017 Muscat
Neonatal manifestations of lysosomal storage diseases Nadia ALhashmi MD Metabolic &genetic disorder Royal hospital 2 nd Oman international pediatric and neonatal conference 13 th -15 th April 2017 Muscat
MRC-Holland MLPA. Description version 19;
 SALSA MLPA probemix P6-B2 SMA Lot B2-712, B2-312, B2-111, B2-511: As compared to the previous version B1 (lot B1-11), the 88 and 96 nt DNA Denaturation control fragments have been replaced (QDX2). SPINAL
SALSA MLPA probemix P6-B2 SMA Lot B2-712, B2-312, B2-111, B2-511: As compared to the previous version B1 (lot B1-11), the 88 and 96 nt DNA Denaturation control fragments have been replaced (QDX2). SPINAL
Below are photos from a 6 month old child with Werdnig-Hoffman s disease.
 PBL 4 Sadie s story Sadie s Story Objectives of PBL: 1) Review and be able to answer questions about normal skeletal muscle organization and structure. 2) Review and be able to answer questions about spinal
PBL 4 Sadie s story Sadie s Story Objectives of PBL: 1) Review and be able to answer questions about normal skeletal muscle organization and structure. 2) Review and be able to answer questions about spinal
A. Definitions... CD-157. B. General Information... CD-158
 CD Part 10 Multiple Body System Disorders A. Definitions... CD-157 B. General Information... CD-158 C. Specific Listings and Residual Functional Capacity... CD-158 1. Listing 10.06: Non-Mosaic Down Syndrome
CD Part 10 Multiple Body System Disorders A. Definitions... CD-157 B. General Information... CD-158 C. Specific Listings and Residual Functional Capacity... CD-158 1. Listing 10.06: Non-Mosaic Down Syndrome
Myotubular (centronuclear) myopathy
 Myotubular (centronuclear) myopathy Myotubular, or centronuclear, myopathy falls under the umbrella of congenital myopathies. It is characterised by a specific pattern in the muscle tissue when viewed
Myotubular (centronuclear) myopathy Myotubular, or centronuclear, myopathy falls under the umbrella of congenital myopathies. It is characterised by a specific pattern in the muscle tissue when viewed
Lab #10: Karyotyping Lab
 Lab #10: Karyotyping Lab INTRODUCTION A karyotype is a visual display of the number and appearance of all chromosomes from a single somatic cell. A normal human karyotype would reveal 46 chromosomes (22
Lab #10: Karyotyping Lab INTRODUCTION A karyotype is a visual display of the number and appearance of all chromosomes from a single somatic cell. A normal human karyotype would reveal 46 chromosomes (22
Sialic Acid Storage Diseases
 Sialic Acid Storage Diseases Class: BIOL 10001 Instructor: Dr. Vivegananthan Submitted by: Lyndsay Grover Date Submitted: Thursday March 24 th, 2011 Introduction to Sialic Acid Storage Diseases Sialic
Sialic Acid Storage Diseases Class: BIOL 10001 Instructor: Dr. Vivegananthan Submitted by: Lyndsay Grover Date Submitted: Thursday March 24 th, 2011 Introduction to Sialic Acid Storage Diseases Sialic
Association of motor milestones and SMN2 copy and outcome in spinal muscular. atrophy types 0 4
 jnnp-2016-314292 1 - SUPPLEMENTARY FILE - Methods and additional data on clinical characteristics and motor development Association of motor milestones and SMN2 copy and outcome in spinal muscular atrophy
jnnp-2016-314292 1 - SUPPLEMENTARY FILE - Methods and additional data on clinical characteristics and motor development Association of motor milestones and SMN2 copy and outcome in spinal muscular atrophy
Prenatal Prediction of The Neurologically Impaired Neonate By Ultrasound
 Prenatal Prediction of The Neurologically Impaired Neonate By Ultrasound Robert H. Debbs, D.O.,F.A.C.O.O.G. Professor of OB-GYN Perelman School of Medicine, University of Pennsylvania Director, Pennsylvania
Prenatal Prediction of The Neurologically Impaired Neonate By Ultrasound Robert H. Debbs, D.O.,F.A.C.O.O.G. Professor of OB-GYN Perelman School of Medicine, University of Pennsylvania Director, Pennsylvania
Nusinersen Use in Spinal Muscular Atrophy
 Nusinersen Use in Spinal Muscular Atrophy Report by: Guideline Development, Dissemination, and Implementation Subcommittee of the American Academy of Neurology Slide 1 Evidence in Focus Endorsement and
Nusinersen Use in Spinal Muscular Atrophy Report by: Guideline Development, Dissemination, and Implementation Subcommittee of the American Academy of Neurology Slide 1 Evidence in Focus Endorsement and
GENETICS: A BASIC HUMAN GENETICS PRIMER: PART II ORIGIN OF GENETIC DISEASE
 GENETICS: A BASIC HUMAN GENETICS PRIMER: PART II Goal: Understand the basic principles of medical genetics. After completing this activity participants will be able to: Explain aneuploidy and common structural
GENETICS: A BASIC HUMAN GENETICS PRIMER: PART II Goal: Understand the basic principles of medical genetics. After completing this activity participants will be able to: Explain aneuploidy and common structural
Warm Up! Test review (already! ;))
 Warm Up! Test review (already! ;)) Write a question you might find on the Unit 5 test next week! (Multiple choice, matching, fill in, or short answer!) - challenge yourself and be ready to share!!! PowerPoint
Warm Up! Test review (already! ;)) Write a question you might find on the Unit 5 test next week! (Multiple choice, matching, fill in, or short answer!) - challenge yourself and be ready to share!!! PowerPoint
Feeding Disorders and Growth in Williams Syndrome
 Feeding Disorders and Growth in Williams Syndrome Sharon M. Greis M.A., CCC/SLP BRS-S and Paige Kaplan M.B.B.Ch. Williams Syndrome Clinic The Children s Hospital of Philadelphia Pediatric Feeding & Swallowing
Feeding Disorders and Growth in Williams Syndrome Sharon M. Greis M.A., CCC/SLP BRS-S and Paige Kaplan M.B.B.Ch. Williams Syndrome Clinic The Children s Hospital of Philadelphia Pediatric Feeding & Swallowing
Critical Illness Polyneuropathy CIP and Critical Illness Myopathy CIM. Andrzej Sladkowski
 Critical Illness Polyneuropathy CIP and Critical Illness Myopathy CIM Andrzej Sladkowski Potential causes of weakness in the ICU-1 Muscle disease Critical illness myopathy Inflammatory myopathy Hypokalemic
Critical Illness Polyneuropathy CIP and Critical Illness Myopathy CIM Andrzej Sladkowski Potential causes of weakness in the ICU-1 Muscle disease Critical illness myopathy Inflammatory myopathy Hypokalemic
Congenital Muscular Dystrophy: Hospital Based Study in Egyptian Pediatric Patients
 World Journal of Medical Sciences 10 (4): 503-507, 2014 ISSN 1817-3055 IDOSI Publications, 2014 DOI: 10.5829/idosi.wjms.2014.10.4.953 Congenital Muscular Dystrophy: Hospital Based Study in Egyptian Pediatric
World Journal of Medical Sciences 10 (4): 503-507, 2014 ISSN 1817-3055 IDOSI Publications, 2014 DOI: 10.5829/idosi.wjms.2014.10.4.953 Congenital Muscular Dystrophy: Hospital Based Study in Egyptian Pediatric
W E HAVE recently seen two youngsters whose pnesenting complaints were highly suggestive of spinal cord disease but
 AMERICAN ACADEMY OF PEDIATRICS CLINICAL CONFERENCE BONY LESIONS OF THE LOWER EXTREMITIES SIMULATING CENTRAL NERVOUS SYSTEM DISEASE Irving H. Rozenfeld, M.D. W E HAVE recently seen two youngsters whose
AMERICAN ACADEMY OF PEDIATRICS CLINICAL CONFERENCE BONY LESIONS OF THE LOWER EXTREMITIES SIMULATING CENTRAL NERVOUS SYSTEM DISEASE Irving H. Rozenfeld, M.D. W E HAVE recently seen two youngsters whose
