Control and management of MRSA
|
|
|
- Abel Simmons
- 6 years ago
- Views:
Transcription
1 Control and management of MRSA Daniel Kaul M.D. Associate Professor Director, ID Fellowship Program and Transplant ID service Division of Infec?ous Diseases University of Michigan Topics MRSA an?microbial therapy? Role and limita?on of newer agents Emerging issues with vancomycin Is anything beger than vancomycin? Nosocomial pneumonia Blood stream infec?on Treatment route and dura?on for MRSA blood stream infec?ons Update on community- acquired MRSA Op?ons for refractory MRSA bacteremia Agents with reliable activity against MRSA Drug Comments Cau.ons Vancomcyin Caution with MIC > 1.0 ug/ml Much less expensive Renal failure with higher troughs and/or recent impurities Linezolid (Zyvox ) Daptomycin (Cubicin ) Superior to vancomycin for MRSA pneumonia Excellent bioavailability Not for pneumonia At least = to vancomycin for blood stream infections Resistance Serotonin syndrome, neuropathy Cytopenias (common) Poor GI tolerance (oral) Rare rhabdo (monitor CPK) Eosinphilic pneumonia
2 Agents with reliable activity against MRSA Drug Comments Cau.ons Dalfopristin/Quinopristin Very difficult to deliver at home (Synercid ) May be potent when combined with vancomycin Phlebitis requires central access Myalgias/arthralgias Tigecycline (Tygacil ) Broad spectrum activity (excludes Pseudomonas and other some other GNR) Increased mortality in clinical trials Nausea Not effective for blood stream infections Agents with reliable activity against MRSA Drug Comments Cau.ons Ceftaroline (Teflaro ) Like ceftriaxone + MRSA and MDR S. pneumonia Approved for SSTI and CAP Similar to other cephalosporins Telavancin (Vibativ ) Lipoglycopeptide (similar to vancomycin) Active against (VRSA, VRE) Approved cssti Renal toxicity Agents with variable activity against MRSA Drug Comments Cau.ons Clindamycin Bacteriostatic (not for endovascular infections) HA-MRSA often resistant Diarrhea Poor tolerance > 300 mg po qid Rifampin Never monotherapy (resistance) Potent p450 induction (multiple drug interactions) Doxycycline TMP/SMX HA-MRSA often resistant Not appropriate for invasive infections HA-MRSA often resistant GI intolerance Rash 2 nd or 3 rd line agent for invasive infections Cytopenias Renal toxicity
3 Tigecycline associated with increased mortality in pooled analysis hgp:// (March 22, 2012) Hospital- acquired pneumonia MRSA first or second most common pathogen in most centers Early, effec?ve treatment results in improved outcome Empiric treatment typically includes MRSA ac?ve agent Debate over last decade vancomycin versus linezolid Daptomycin,?gecycline not approriate Recently completed randomized trial comparing linezolid to vancomycin Linezolid verus vancomycin MRSA HA- pneumonia Hospital acquired or health care- associated pneumonia Culture posi?ve for MRSA Randomized to Linezolid or Vancomycin (15 mg/kg twice daily) for days GNR coverage un?l culture nega?ve Local adjustment of vancomycin dose Primary outcome Clinical cure Symptoms, radiology (no progression), no need for addi?onal an?bio?cs
4 Study population Pa.ent enrollment 1225 pa?ents enrolled 224 in each arm in mitt (many without MRSA on culture) 170 s in each arm in per protocol analysis Linezolid superior to vancomycin for nosocomial pneumonia No difference in 60 day mortality Subgroup analysis Outcomes not beger with higher vancomycin troughs Outcomes not worse with MIC > 1 ug/ml Clinical Response Linezolid Vancomycin
5 MRSA pneumonia treatment Linezolid likely superior No difference in mortality noted Unexpected nephrotoxicity associated with vancomycin $$$$$$ linezolid > vancomycin (drug cost) Comple?on therapy at home with oral linezolid Results likely extend to CA- MRSA pneumonia Consider linezolid for significant MRSA pneumonia (nosocomial or community- acquired) MIC drift and vancomycin efcicacy heteroresistance, VISA, VRSA hvisa (mixed popula?on, hard to iden?fy in lab, may be associated with improved outcome) VISA uncommon (MIC 4-8 ug/ml) VRSA very rare (MIC > 8ug/ml) Breakpoint for vancomycin lowered to <= 2 from <=4 in 2006 Never use vancomycin if MIC > 2 ug/ml Less than 1% of MRSA isolates in most hospitals Consider alterna?ve agent or change to another agent if MIC = 2 ug/ml Vancomycin MIC 2.0 INCREASED MORTALITY
6 Vancomycin MIC 2.0 ug/ml This will be listed as sensi?ve Further micro tes?ng (e.g., E- test) indicated but variably available If clinical failure or ongoing serious infec?on (par?cularly blood stream infec?on) change to alterna?ve agent Vancomycin dosing Typical dose mg/kg/dose (2-3 doses a day) Consider load (25-30 mg/kg) in cri?cally ill Troughs (but not peaks) should be monitored (prior to 4 th or 5 th dose) Troughs < 10 ug/ml associated with clinical failure Typical goal trough ug/ml Severe infec?ons- consider trough ug/ml Limited data to support this May be more nephrotoxic than previously thought Trough > 15 ug/ml associated with increased toxicity but not clearly with beger outcome Caution with vancomycin dosing (recommendations may be too high)
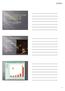
7 Renal failure more common with vancomycin Vancomycin Trough (ug/ml) Renal toxicity (%) < 15 18% % > 20 37% Case 68 year old man with a history of diabetes mellitus admit ted with 2 months of back pain significant worsened over past 72 hours Difficulty ambula?ng and unable to sleep Pain radiates down lateral aspects legs to knees No fever and no leucocytosis Blood cultures obtained Posi?ve for gram posi?ve cocci in clusters MRI Lumbar Spine Degenerative changes T2 FS T1
8 Case Slight improvement in back pain Blood cultures persistently posi?ve for 6 days on vancomycin Trans- esophageal echocardiogram without evidence of endocardi?s Discharge diagnosis (hospital day #10) Back pain secondary to degenera?ve joint disease Urinary tract infec?on S. aureus bacteremia of unknown source 2 weeks of vancomycin and PCP follow up in 2 weeks Case Re- admiged to another hospital 11 days later with increasing weakness, numbness from waist down. Barely able to liq either thigh from the bed Vancomycin had been changed to daptomycin at the subacute rehabilita?on facility T7-8 T9-10
9 MRI T- L SPINE Disci?s/osteomyeli?s at T7- T8 and T9- T10 levels with marked paravertebral phlegmon, microabscesses, and a ventral epidural phlegmon from T8 to T11 Compression of the thoracic cord with findings sugges?ve of cord edema/ischemia Moderate to severe DJD of lumbar spine Required surgery to decompress (ischemic necrosis of spinal cord) Regained only par?al neurologic func?on Case Further history obtained Undergone hip replacement 6 months earlier Staph infec?on of hip wound treated with vancomycin followed by TMP/SMX (Bactrim) Teaching points S. aureus is a high destruc?ve and s?cky organism Prolonged S. aureus bacteremia requires vigorous examina?on for metasta?c areas Bacteremia may occur without fever and leucocytosis (par?cularly in the elderly) Two week dura?on of treatment for S. aureus bacteremia can only be considered in uncomplicated cases Brief dura?on of bacteremia (< 48 hours) Must document clearance of bacteremia Rapid response to therapy (defervescence within 72 hours) No endocardi?s and no prosthesis Oqen removable focus
10 Where does S. aureus like to go Lumbar spine > thoracic or cervical spine Oqen with extension to epidural space Psoas muscle Cardiac valves Large joints Eyes Anything possible Pericardium Thyroid Long bones brain Community- acquired MRSA Clinical syndrome CA- MRSA Fridkin et al. NEJM Volume 352:
11 A Clone of Methicillin- Resistant Staphylococcus aureus among Professional Football Players Volume 352: February 3, 2005 Number 5 MRSA St. Louis Rams NEJM 352:
12 Cultures obtained from 422 pa?ents presen?ng with skin and soq?ssue infec?ons at 11 Emergency Medicine Departments CA- MRSA (epidemiology) CA- MRSA (risk factors)
13 CA- MRSA antibiotics Fridkin et al. NEJM Volume 352: Clindamycin: inducible resistance in some CA- MRSA Inducible clindamycin resistance Lab s need to perform D- test to confirm ini?al sensi?vity to clindamycin CA- MRSA decolonization Nasal decoloniza?on mupirocin twice daily for 5 10 days AND Bleach baths (¼ cup per ¼ tub) for 15 minutes twice weekly for 2-3 months (preferred) OR Chlorhexidine (Hibclens) 3 X week for 2 weeks (drying) IF REFRACTORY Rifampin + doxy/clinda/tmp/smx for two weeks
14 CA- MRSA (teaching points) CA- MRSA typically presents as purulent soq?ssue infec?on Drainage is more important than medical treatment An?microbials indicated if significant surrounding erythema Linezolid (cost), TMP/SMX, doxycycline, clindamycin More invasive disease may occur: Necro?zing pneumonia Endovascular infec?on decoloniza?on Case 81 year old man with severe angina undergoes coronary artery bypass graqing 3 weeks post- opera?vely develops sternal wound infec?on Limited bedside debridement reveals MRSA and blood cultures are posi?ve Not a candidate for sternal debridement and flap placement Asymptoma?c but remains bacteremic for 12 weeks Evalua?on/treatment op?ons? Daptomycin non- inferior to standard therapy for Staph aureus bacteremia
15 Daptomycin may be superior to vancomycin if MIC > 1.0 ug/mi for bloodstream infection Refractory MRSA bacteremia (> 7-10 days) Evaluate for persistant source Heart valves Joints Any place that hurts Check MIC with E- test or equivalent for vancomcyin High dose daptomycin (10 mg/kg daily) Combina?on therapy Rifampin 600 mg daily Linezolid 600 mg twice daily TMP/SMX 5 mg/kg every 12 hours Aminoglycoside (probably best to avoid ) Quinopris?n/dalfopris?n + vancomycin (in vitro data) Telavancin 10 mg/kg daily Infection control basics Hand hygiene universal Contact precau?ons Most ins?tu?ons use for MRSA An?microbial stewardship Ins?tu?onal monitoring Intensified measures Cohor?ng opt out isola?on
16 Summary Vancomycin least expensive and most widely used Cau?on renal failure with higher troughs and if MIC > 1.0 ug/ml Linezolid superior for nosocomial pneumonia Daptomycin non- inferior for bacteremia MRSA is s?cky (heart valves, large joints, vertebral spine) 4-6 weeks of intravenous treatment unless brief bacteremia without deep seated focus Community- acquired MRSA most common purulent soq?ssue infec?on Invasive syndromes do occur
Session 3: New Evidence-Based Clinical Prac ce Guidelines C: Treatment of MRSA Infec ons in Adults and Children 4:15pm - 5:15pm
 January 20-22, 2012 Des Moines Marrio, 700 Grand Avenue, Des Moines, IA Session 3: New Evidence-Based Clinical Prac ce Guidelines C: Treatment of MRSA Infec ons in Adults and Children 4:15pm - 5:15pm ACPE
January 20-22, 2012 Des Moines Marrio, 700 Grand Avenue, Des Moines, IA Session 3: New Evidence-Based Clinical Prac ce Guidelines C: Treatment of MRSA Infec ons in Adults and Children 4:15pm - 5:15pm ACPE
ESCMID Online Lecture Library. by author
 Hospital Universitario Virgen Macarena, Seville New drugs against MRSA and VRE L. Eduardo López Cortés Seville, 8th July Tedizolid Oxazolidinone Ceftaroline // Ceftobiprole 5 th gen cephalosporin Overview
Hospital Universitario Virgen Macarena, Seville New drugs against MRSA and VRE L. Eduardo López Cortés Seville, 8th July Tedizolid Oxazolidinone Ceftaroline // Ceftobiprole 5 th gen cephalosporin Overview
Update in Management of Skin and So1 Tissue Infec7ons. Disclosures. None 4/23/15
 Update in Management of Skin and So1 Tissue Infec7ons Catherine Liu, MD Associate Professor UCSF, Division of Infec7ous Diseases None Disclosures 1 Overview Purulent SSTI (abscesses) Non- purulent SSTI
Update in Management of Skin and So1 Tissue Infec7ons Catherine Liu, MD Associate Professor UCSF, Division of Infec7ous Diseases None Disclosures 1 Overview Purulent SSTI (abscesses) Non- purulent SSTI
Staphylococcal Bacteremia
 Staphylococcal Bacteremia Henry F. Chambers, M.D. Professor of Medicine, UCSF Chief of Infectious Diseases San Francisco General Hospital Case 1 38 y/o man, new CHF, alcoholic cardiomyopathy, Hct = 13
Staphylococcal Bacteremia Henry F. Chambers, M.D. Professor of Medicine, UCSF Chief of Infectious Diseases San Francisco General Hospital Case 1 38 y/o man, new CHF, alcoholic cardiomyopathy, Hct = 13
The Curious Intersection of HIV and Staphylococcus aureus with a Focus on MRSA
 The Curious Intersection of HIV and Staphylococcus aureus with a Focus on MRSA Franklin D. Lowy, MD Columbia University College of Physicians & Surgeons New York, NY Topics to Be Covered Background Some
The Curious Intersection of HIV and Staphylococcus aureus with a Focus on MRSA Franklin D. Lowy, MD Columbia University College of Physicians & Surgeons New York, NY Topics to Be Covered Background Some
The Challenge of Managing Staphylococcus aureus Bacteremia
 The Challenge of Managing Staphylococcus aureus Bacteremia M A R G A R E T G R A Y B S P F C S H P C L I N I C A L P R A C T I C E M A N A G E R N O R T H / I D P H A R M A C I S T A L B E R T A H E A
The Challenge of Managing Staphylococcus aureus Bacteremia M A R G A R E T G R A Y B S P F C S H P C L I N I C A L P R A C T I C E M A N A G E R N O R T H / I D P H A R M A C I S T A L B E R T A H E A
Michael S. Niederman, M.D. Clinical Director Pulmonary and Critical Care Medicine New York Presbyterian Hospital Weill Cornell Medical Center
 CA-MRSA Pneumonia Michael S. Niederman, M.D. Clinical Director Pulmonary and Critical Care Medicine New York Presbyterian Hospital Weill Cornell Medical Center Professor of Clinical Medicine Weill Cornell
CA-MRSA Pneumonia Michael S. Niederman, M.D. Clinical Director Pulmonary and Critical Care Medicine New York Presbyterian Hospital Weill Cornell Medical Center Professor of Clinical Medicine Weill Cornell
Skin and So) Tissue Infec1ons: MRSA and Beyond
 Overview Skin and So) Tissue Infec1ons: MRSA and Beyond Catherine Liu, M.D. Assistant Clinical Professor Division of Infec1ous Diseases University of California, San Francisco 2011 IDSA MRSA Treatment
Overview Skin and So) Tissue Infec1ons: MRSA and Beyond Catherine Liu, M.D. Assistant Clinical Professor Division of Infec1ous Diseases University of California, San Francisco 2011 IDSA MRSA Treatment
Vancomycin: Class: Antibiotic.
 Vancomycin: Class: Antibiotic. Indications: Treatment of patients with infections caused by staphylococcal species and streptococcal Species. Available dosage form in the hospital: 1G VIAL, 500MG VIAL.
Vancomycin: Class: Antibiotic. Indications: Treatment of patients with infections caused by staphylococcal species and streptococcal Species. Available dosage form in the hospital: 1G VIAL, 500MG VIAL.
Bone and Joint Infections in Diabetics: Diagnosis and Management of Diabetic Foot and Other Common Lower Extremity Infections
 Bone and Joint Infections in Diabetics: Diagnosis and Management of Diabetic Foot and Other Common Lower Extremity Infections Objectives How do you to diagnose, classify and manage DFI? How do you diagnose
Bone and Joint Infections in Diabetics: Diagnosis and Management of Diabetic Foot and Other Common Lower Extremity Infections Objectives How do you to diagnose, classify and manage DFI? How do you diagnose
Skin and soft tissue (SSTI) sepsis (surgery, antimicrobial therapy and more)
 Skin and soft tissue (SSTI) sepsis (surgery, antimicrobial therapy and more) Christian Eckmann Antibiotic Stewardship Expert ECDC Chief of Staff Department of General, Visceral and Thoracic Surgery Klinikum
Skin and soft tissue (SSTI) sepsis (surgery, antimicrobial therapy and more) Christian Eckmann Antibiotic Stewardship Expert ECDC Chief of Staff Department of General, Visceral and Thoracic Surgery Klinikum
Vancomycin powder to reduce surgical site infection in spine surgery
 Vancomycin powder to reduce surgical site infection in spine surgery 2014/03/25 EBM Spine Fellow 林東儀 Post-Op infection in spine surgery Wound infection: 0.7% to 11.9% Infection rates of 2.8% to 6.0% for
Vancomycin powder to reduce surgical site infection in spine surgery 2014/03/25 EBM Spine Fellow 林東儀 Post-Op infection in spine surgery Wound infection: 0.7% to 11.9% Infection rates of 2.8% to 6.0% for
Consideration of some other specific indications: Bacteremia
 European Medicines Agency Workshop on Antibacterials, London 7-8 February 2011 Consideration of some other specific indications: Bacteremia Harald Seifert Institut für Medizinische Mikrobiologie, Immunologie
European Medicines Agency Workshop on Antibacterials, London 7-8 February 2011 Consideration of some other specific indications: Bacteremia Harald Seifert Institut für Medizinische Mikrobiologie, Immunologie
Rochester Patient Safety C. difficile Prevention Collaborative: Long Term Care Antimicrobial Stewardship (funded by NYSDOH)
 Rochester Patient Safety C. difficile Prevention Collaborative: Long Term Care Antimicrobial Stewardship (funded by NYSDOH) Clinical Practice Guideline* for the Diagnosis and Management of Acute Bacterial
Rochester Patient Safety C. difficile Prevention Collaborative: Long Term Care Antimicrobial Stewardship (funded by NYSDOH) Clinical Practice Guideline* for the Diagnosis and Management of Acute Bacterial
Options for Complicated Skin and Skin Structure Infections. Andrew F. Shorr, MD, MPH Washington Hospital Center Georgetown Univ.
 Options for Complicated Skin and Skin Structure Infections Andrew F. Shorr, MD, MPH Washington Hospital Center Georgetown Univ. Disclosures I have served as a consultant to, researcher/investigator for,
Options for Complicated Skin and Skin Structure Infections Andrew F. Shorr, MD, MPH Washington Hospital Center Georgetown Univ. Disclosures I have served as a consultant to, researcher/investigator for,
Invasive Staphylococcal Infections
 Invasive Staphylococcal Infections Henry F. Chambers, M.D. Professor of Medicine, UCSF San Francisco General Hospital Disclosures AstraZeneca advisory board Cubist research grant, advisory panel Genentech
Invasive Staphylococcal Infections Henry F. Chambers, M.D. Professor of Medicine, UCSF San Francisco General Hospital Disclosures AstraZeneca advisory board Cubist research grant, advisory panel Genentech
Objectives. Define classes of uncomplicated skin and soft tissue infection (SSTI) that drive empiric antimicrobial selection
 Objectives Define classes of uncomplicated skin and soft tissue infection (SSTI) that drive empiric antimicrobial selection Purulent SSTI Non-purulent SSTI Recognize conditions that suggest complications
Objectives Define classes of uncomplicated skin and soft tissue infection (SSTI) that drive empiric antimicrobial selection Purulent SSTI Non-purulent SSTI Recognize conditions that suggest complications
arguably the greatest risk to human health comes in the form of antibiotic-resistant bacteria. We live in a bacterial world where we will never be
 arguably the greatest risk to human health comes in the form of antibiotic-resistant bacteria. We live in a bacterial world where we will never be able to stay ahead of the mutation curve. A test of our
arguably the greatest risk to human health comes in the form of antibiotic-resistant bacteria. We live in a bacterial world where we will never be able to stay ahead of the mutation curve. A test of our
Infections Amenable to OPAT. (Nabin Shrestha + Ajay Mathur)
 3 Infections Amenable to OPAT (Nabin Shrestha + Ajay Mathur) Decisions regarding outpatient treatment of infections vary with the institution, the prescribing physician, the individual patient s condition
3 Infections Amenable to OPAT (Nabin Shrestha + Ajay Mathur) Decisions regarding outpatient treatment of infections vary with the institution, the prescribing physician, the individual patient s condition
Responders as percent of overall members in each category: Region: New England 50 (58% of 86 members) 19 (51% of 37 members) 3 (33% of 9 members)
 Infectious Diseases Society of America Emerging Infections Network Report for Query: Prosthetic Joint Infections (PJI) in Adults Overall response rate: 556/118 (4.2%) physicians responded from 5/16/12
Infectious Diseases Society of America Emerging Infections Network Report for Query: Prosthetic Joint Infections (PJI) in Adults Overall response rate: 556/118 (4.2%) physicians responded from 5/16/12
Development of Drugs for Bacteremia
 Development of Drugs for Bacteremia Mark Kunkel MD EFPIA - Bacteremia comments 1 Bacteremia Guidance Issues EMA guidance suggests that bacteremia is not a primary diagnosis but represents isolation from
Development of Drugs for Bacteremia Mark Kunkel MD EFPIA - Bacteremia comments 1 Bacteremia Guidance Issues EMA guidance suggests that bacteremia is not a primary diagnosis but represents isolation from
Angel 12 year old F Airedale Terrier
 December 2014 Dr. Norman Ackerman served the University of Florida, College of Veterinary Medicine with distinction as Professor of Radiology from 1979 to 1994. A concerned teacher of veterinary students
December 2014 Dr. Norman Ackerman served the University of Florida, College of Veterinary Medicine with distinction as Professor of Radiology from 1979 to 1994. A concerned teacher of veterinary students
Osteomyelitis Samir S. Shah, MD, MSCE
 Osteomyelitis Samir S. Shah, MD, MSCE Professor, Department of Pediatrics University of Cincinnati College of Medicine Director, Division of Hospital Medicine Attending Physician in Infectious Diseases
Osteomyelitis Samir S. Shah, MD, MSCE Professor, Department of Pediatrics University of Cincinnati College of Medicine Director, Division of Hospital Medicine Attending Physician in Infectious Diseases
CLINICAL USE OF GLYCOPEPTIDES. Herbert Spapen Intensive Care Department University Hospital Vrije Universiteit Brussel
 CLINICAL USE OF GLYCOPEPTIDES Herbert Spapen Intensive Care Department University Hospital Vrije Universiteit Brussel Glycopeptides Natural Vancomycin introduced in 1958 Teicoplanin introduced in Europe
CLINICAL USE OF GLYCOPEPTIDES Herbert Spapen Intensive Care Department University Hospital Vrije Universiteit Brussel Glycopeptides Natural Vancomycin introduced in 1958 Teicoplanin introduced in Europe
MRSA: Implications in Sports Medicine
 MRSA: Implications in Sports Medicine Staphylococcus aureus, often referred to as staph, are bacteria commonly carried on the skin or in the nose of healthy people Staphylococcus Aureus Occasionally, staph
MRSA: Implications in Sports Medicine Staphylococcus aureus, often referred to as staph, are bacteria commonly carried on the skin or in the nose of healthy people Staphylococcus Aureus Occasionally, staph
Osteomyelitis and Septic Joints; Practical Considerations. Coleen K. Cunningham
 Osteomyelitis and Septic Joints; Practical Considerations Coleen K. Cunningham Goals/objectives To improve understanding of the diagnosis, treatment, and follow-up of pediatric bone and joint infections
Osteomyelitis and Septic Joints; Practical Considerations Coleen K. Cunningham Goals/objectives To improve understanding of the diagnosis, treatment, and follow-up of pediatric bone and joint infections
WHO posi)on paper on pneumococcal vaccines. Geneva, Switzerland Published in the Weekly Epidemiological Record on 6 Apr 2012
 WHO posi)on paper on pneumococcal vaccines Geneva, Switzerland Published in the Weekly Epidemiological Record on 6 Apr 2012 WHO posi)on paper on pneumococcal vaccines, April 2012 The current posi)on paper
WHO posi)on paper on pneumococcal vaccines Geneva, Switzerland Published in the Weekly Epidemiological Record on 6 Apr 2012 WHO posi)on paper on pneumococcal vaccines, April 2012 The current posi)on paper
Hospital-acquired Pneumonia
 Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
Vertebral and Paravertebral Diseases
 Department of Radiology University of California San Diego Vertebral and Paravertebral Diseases John R. Hesselink, M.D. Vertebral / Paravertebral Disease (Extradural) Metastatic disease Primary bone tumors
Department of Radiology University of California San Diego Vertebral and Paravertebral Diseases John R. Hesselink, M.D. Vertebral / Paravertebral Disease (Extradural) Metastatic disease Primary bone tumors
Skin and so* +ssue infec+on. N.Nuntachit MD.
 Skin and so* +ssue infec+on N.Nuntachit MD. Non purulent SSTI Impe+go, ecthyma Celluli+s, Erysipelas Erysipeloid Necro+zing infec+on Etc eg Glanders, bubonic plaque Purulent SSTI Furuncle Carbuncle Abscess
Skin and so* +ssue infec+on N.Nuntachit MD. Non purulent SSTI Impe+go, ecthyma Celluli+s, Erysipelas Erysipeloid Necro+zing infec+on Etc eg Glanders, bubonic plaque Purulent SSTI Furuncle Carbuncle Abscess
Methicillin-Resistant Staphylococcus aureus (MRSA) S urveillance Report 2008 Background Methods
 Methicillin-Resistant Staphylococcus aureus (MRSA) Surveillance Report 2008 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Department of Human Services
Methicillin-Resistant Staphylococcus aureus (MRSA) Surveillance Report 2008 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Department of Human Services
Pneumonia Community-Acquired Healthcare-Associated
 Pneumonia Community-Acquired Healthcare-Associated Edwin Yu Clin Infect Dis 2007;44(S2):27-72 Am J Respir Crit Care Med 2005; 171:388-416 IDSA / ATS Guidelines Microbiology Principles and Practice of Infectious
Pneumonia Community-Acquired Healthcare-Associated Edwin Yu Clin Infect Dis 2007;44(S2):27-72 Am J Respir Crit Care Med 2005; 171:388-416 IDSA / ATS Guidelines Microbiology Principles and Practice of Infectious
Aciphin Ceftriaxone Sodium
 Aciphin Ceftriaxone Sodium Only for the use of Medical Professionals Description Aciphin is a bactericidal, long-acting, broad spectrum, parenteral cephalosporin preparation, active against a wide range
Aciphin Ceftriaxone Sodium Only for the use of Medical Professionals Description Aciphin is a bactericidal, long-acting, broad spectrum, parenteral cephalosporin preparation, active against a wide range
Division of Vascular and Endovascular Surgery University of South Florida School of Medicine Tampa, Florida
 Division of Vascular and Endovascular Surgery University of South Florida School of Medicine Tampa, Florida Appearance: oearly < 3 mo. olate > 3 mo.. Extent: Szilagyi Classification: Grade I: infection
Division of Vascular and Endovascular Surgery University of South Florida School of Medicine Tampa, Florida Appearance: oearly < 3 mo. olate > 3 mo.. Extent: Szilagyi Classification: Grade I: infection
Severe β-lactam allergy. Alternative (use for mild-moderate β-lactam allergy) therapy
 Recommended Empirical Antibiotic Regimens for MICU Patients Notes: The antibiotic regimens shown are general guidelines and should not replace clinical judgment. Always assess for antibiotic allergies.
Recommended Empirical Antibiotic Regimens for MICU Patients Notes: The antibiotic regimens shown are general guidelines and should not replace clinical judgment. Always assess for antibiotic allergies.
PATIENT DEMOGRAPHICS. Surname. Given name. Pacific Islander (non-maori) ADMISSION DETAILS
 Reviewer / hospital Date review started PATIENT DEMOGRAPHICS MRN DOB Sex Patient sticky label if available, else enter details here Surname Post-code Given name Australian Aborigine / TSI Middle Eastern
Reviewer / hospital Date review started PATIENT DEMOGRAPHICS MRN DOB Sex Patient sticky label if available, else enter details here Surname Post-code Given name Australian Aborigine / TSI Middle Eastern
Clostridium difficile coli%s. John K. Midturi January 2013
 Clostridium difficile coli%s John K. Midturi January 2013 Objec%ves Describe pathogenesis of C. Diff coli%s Review methods of diagnosis of C. Diff coli%s Discuss treatment op%ons first episode refractory
Clostridium difficile coli%s John K. Midturi January 2013 Objec%ves Describe pathogenesis of C. Diff coli%s Review methods of diagnosis of C. Diff coli%s Discuss treatment op%ons first episode refractory
Community-acquired pneumonia (CAP)
 Community-acquired pneumonia (CAP) Keith F Barker, MD GlaxoSmithKline 1 CAP: Key issues Definitions and patient population Use of prior antibiotics Microbiologically Evaluable population Efficacy endpoints
Community-acquired pneumonia (CAP) Keith F Barker, MD GlaxoSmithKline 1 CAP: Key issues Definitions and patient population Use of prior antibiotics Microbiologically Evaluable population Efficacy endpoints
Superhero or Superzero? Vancomycin vs. Linezolid for MRSA Pneumonia
 Superhero or Superzero? Vancomycin vs. Linezolid for MRSA Pneumonia Brandon Dionne, PharmD, BCPS, AAHIVP Assistant Clinical Professor Northeastern University Seth Housman, PharmD, MPA Clinical Assistant
Superhero or Superzero? Vancomycin vs. Linezolid for MRSA Pneumonia Brandon Dionne, PharmD, BCPS, AAHIVP Assistant Clinical Professor Northeastern University Seth Housman, PharmD, MPA Clinical Assistant
Cubicin (Daptomycin) Priv.Doz. Dr. med. Markus Rothenburger
 Cubicin (Daptomycin) Priv.Doz. Dr. med. Markus Rothenburger Cubicin (Daptomycin): A new generation of antibiotics First-in-class cyclic natural lipopeptide Activity against major gram positive pathogens
Cubicin (Daptomycin) Priv.Doz. Dr. med. Markus Rothenburger Cubicin (Daptomycin): A new generation of antibiotics First-in-class cyclic natural lipopeptide Activity against major gram positive pathogens
Pediatric Infections: Treatment of Resistant Pathogens. Focus : MRSA and DRSP Infections, Including Pneumonia. Blaise L. Congeni M.D.
 Pediatric Infections: Treatment of Resistant Pathogens Focus : MRSA and DRSP Infections, Including Pneumonia Blaise L. Congeni M.D. Patient 1-LP 8 yo with 8 days of fever and 6 days of cough. She had consistently
Pediatric Infections: Treatment of Resistant Pathogens Focus : MRSA and DRSP Infections, Including Pneumonia Blaise L. Congeni M.D. Patient 1-LP 8 yo with 8 days of fever and 6 days of cough. She had consistently
Management of severe staphylococcal infections
 Management of severe staphylococcal infections Dilip Nathwani BSAC April 7 th 2009 Ninewells Hospital & Medical School Dundee DD1 9SY Objectives Mortality related to MSSA and MRSA infections Glycopeptides
Management of severe staphylococcal infections Dilip Nathwani BSAC April 7 th 2009 Ninewells Hospital & Medical School Dundee DD1 9SY Objectives Mortality related to MSSA and MRSA infections Glycopeptides
2018 CNISP HAI Surveillance Case definitions
 2018 CNISP HAI Surveillance Case definitions The following case definitions for the surveillance of healthcare-associated infections (HAIs) are used by all acute-care hospitals that participate in the
2018 CNISP HAI Surveillance Case definitions The following case definitions for the surveillance of healthcare-associated infections (HAIs) are used by all acute-care hospitals that participate in the
Cellulitis and Soft Tissue Infections. Sally Williams MD
 Cellulitis and Soft Tissue Infections Sally Williams MD Cellulitis: A very common infection 25 cases per 1000 patient years More common in men, obese patients 60% occurs in the lower extremities 74% handled
Cellulitis and Soft Tissue Infections Sally Williams MD Cellulitis: A very common infection 25 cases per 1000 patient years More common in men, obese patients 60% occurs in the lower extremities 74% handled
Medical/Surgical Asepsis. Presented by: Cynthia Bartlau, RN, PHN, MSN
 Medical/Surgical Asepsis Presented by: Cynthia Bartlau, RN, PHN, MSN Objectives At the completion of this lesson the student will be able to Discuss concepts related to the chain of infection Differentiate
Medical/Surgical Asepsis Presented by: Cynthia Bartlau, RN, PHN, MSN Objectives At the completion of this lesson the student will be able to Discuss concepts related to the chain of infection Differentiate
Cubicin A Guide to Dosing
 Cubicin A Guide to Dosing Cubicin (Daptomycin) powder for solution for injection or infusion Indications (see SmPC) 1 : Cubicin is indicated for the treatment of the following infections (see sections
Cubicin A Guide to Dosing Cubicin (Daptomycin) powder for solution for injection or infusion Indications (see SmPC) 1 : Cubicin is indicated for the treatment of the following infections (see sections
Vancomycin: A 50-something-yearold antibiotic we still don t understand
 Current Drug Therapy CME CREDIT EDUCATIONAL OBJECTIVES: Readers will use vancomycin appropriately Amy Schilling, PharmD Department of Pharmacy, The University of Texas Medical Branch, Galveston Elizabeth
Current Drug Therapy CME CREDIT EDUCATIONAL OBJECTIVES: Readers will use vancomycin appropriately Amy Schilling, PharmD Department of Pharmacy, The University of Texas Medical Branch, Galveston Elizabeth
Management of Gram-Positive Coccal Bacteremia and Hemodialysis
 In Practice Management of Gram-Positive Coccal Bacteremia and Hemodialysis Lynn N. Fitzgibbons, MD, 1 Darcy L. Puls, MD, 1 Kimberly Mackay, PharmD, 2 and Graeme N. Forrest, MBBS 3 Gram-positive cocci are
In Practice Management of Gram-Positive Coccal Bacteremia and Hemodialysis Lynn N. Fitzgibbons, MD, 1 Darcy L. Puls, MD, 1 Kimberly Mackay, PharmD, 2 and Graeme N. Forrest, MBBS 3 Gram-positive cocci are
6/18/2014. John K. Midturi, DO, MPH June 5 th, 2014
 John K. Midturi, DO, MPH June 5 th, 2014 Heterogeneous disease Disease of antiquity Evolved from disease of high mortality disease with high morbidity One of the most difficult infections to treat Thomas
John K. Midturi, DO, MPH June 5 th, 2014 Heterogeneous disease Disease of antiquity Evolved from disease of high mortality disease with high morbidity One of the most difficult infections to treat Thomas
Community Acquired & Nosocomial Pneumonias
 Community Acquired & Nosocomial Pneumonias IDSA/ATS 2007 & 2016 Guidelines José Luis González, MD Clinical Assistant Professor of Medicine Outline Intro - Definitions & Diagnosing CAP treatment VAP & HAP
Community Acquired & Nosocomial Pneumonias IDSA/ATS 2007 & 2016 Guidelines José Luis González, MD Clinical Assistant Professor of Medicine Outline Intro - Definitions & Diagnosing CAP treatment VAP & HAP
OSTEOMYELITIS. If it occurs in adults, then the axial skeleton is the usual site.
 OSTEOMYELITIS Introduction Osteomyelitis is an acute or chronic inflammatory process of the bone and its structures secondary to infection with pyogenic organisms. Pathophysiology Osteomyelitis may be
OSTEOMYELITIS Introduction Osteomyelitis is an acute or chronic inflammatory process of the bone and its structures secondary to infection with pyogenic organisms. Pathophysiology Osteomyelitis may be
Treatment of febrile neutropenia in patients with neoplasia
 Treatment of febrile neutropenia in patients with neoplasia George Samonis MD, PhD Medical Oncologist Infectious Diseases Specialist Professor of Medicine The University of Crete, Heraklion,, Crete, Greece
Treatment of febrile neutropenia in patients with neoplasia George Samonis MD, PhD Medical Oncologist Infectious Diseases Specialist Professor of Medicine The University of Crete, Heraklion,, Crete, Greece
Osteomyelitis Revisited
 Osteomyelitis Revisited Alan Jay Block, DPM, MS, FASPS, FACFAS Co-Chairman My Leg My Choice Assistant Professor Dept Of Orthopeadics The Ohio State University Medical Board Kent State University Editor-in
Osteomyelitis Revisited Alan Jay Block, DPM, MS, FASPS, FACFAS Co-Chairman My Leg My Choice Assistant Professor Dept Of Orthopeadics The Ohio State University Medical Board Kent State University Editor-in
December 3, 2015 Severe Sepsis and Septic Shock Antibiotic Guide
 Severe Sepsis and Septic Shock Antibiotic Guide Surviving Sepsis: The choice of empirical antimicrobial therapy depends on complex issues related to the patient s history, including drug intolerances,
Severe Sepsis and Septic Shock Antibiotic Guide Surviving Sepsis: The choice of empirical antimicrobial therapy depends on complex issues related to the patient s history, including drug intolerances,
Development of Drugs for Bacteremia
 Development of Drugs for Bacteremia Charles Knirsch, MD, MPH VP, Clinical Research Pfizer Inc 1 Bacteremia Guidance Issues EMA guidance suggests that bacteremia is not a primary diagnosis but represents
Development of Drugs for Bacteremia Charles Knirsch, MD, MPH VP, Clinical Research Pfizer Inc 1 Bacteremia Guidance Issues EMA guidance suggests that bacteremia is not a primary diagnosis but represents
Sponsored by Virox Technologies Inc. C. difficile 101 A brief review of guidelines and controversies
 Controlling Clostridium difficile Outbreaks: Going Beyond the Guidelines Michael Gardam Infec
Controlling Clostridium difficile Outbreaks: Going Beyond the Guidelines Michael Gardam Infec
Brice Taylor Assistant Professor Division of Pulmonary and Critical Care Medicine
 Brice Taylor Assistant Professor Division of Pulmonary and Critical Care Medicine Discuss advances in predicting prognosis Understand dwhat we know (and don t know) about the Microbiology Recognize important
Brice Taylor Assistant Professor Division of Pulmonary and Critical Care Medicine Discuss advances in predicting prognosis Understand dwhat we know (and don t know) about the Microbiology Recognize important
Clinical management of Staphylococcus aureus bacteremia an updated proposal of protocol
 Clinical management of Staphylococcus aureus bacteremia an updated proposal of protocol Promotor : Prof. dr. W. Peetermans Second reader : Prof. dr. E. Van Wijngaerden Master s Thesis Internal Medicine
Clinical management of Staphylococcus aureus bacteremia an updated proposal of protocol Promotor : Prof. dr. W. Peetermans Second reader : Prof. dr. E. Van Wijngaerden Master s Thesis Internal Medicine
Antibiotics to treat multi-drug-resistant bacterial infections
 Antibiotics to treat multi-drug-resistant bacterial infections July 2013 JUNE 2013 Copyright 2013 Tetraphase Pharmaceuticals, Inc. 1 Forward Looking Statements and Other Important Cautions Any statements
Antibiotics to treat multi-drug-resistant bacterial infections July 2013 JUNE 2013 Copyright 2013 Tetraphase Pharmaceuticals, Inc. 1 Forward Looking Statements and Other Important Cautions Any statements
An Update in the Management of Candidiasis
 An Update in the Management of Candidiasis Daniel B. Chastain, Pharm.D., AAHIVP Infectious Diseases Pharmacy Specialist Phoebe Putney Memorial Hospital Adjunct Clinical Assistant Professor UGA College
An Update in the Management of Candidiasis Daniel B. Chastain, Pharm.D., AAHIVP Infectious Diseases Pharmacy Specialist Phoebe Putney Memorial Hospital Adjunct Clinical Assistant Professor UGA College
Cystic Fibrosis: Pulmonary Exacerbations Management Guidelines
 Cystic Fibrosis: Pulmonary Exacerbations Management Guidelines Inclusion Criteria: Age 1 year with cystic fibrosis admitted for a pulmonary exacerbation. Exclusion Criteria: ICU Admission Newborn with
Cystic Fibrosis: Pulmonary Exacerbations Management Guidelines Inclusion Criteria: Age 1 year with cystic fibrosis admitted for a pulmonary exacerbation. Exclusion Criteria: ICU Admission Newborn with
(telavancin) Healthcare Professional s Guide. Version 2, 4 November 2014
 VIBATIV (telavancin) Healthcare Professional s Guide Version 2, 4 November 2014 1 Table of Contents Introduction... 3 About Vibativ / Therapeutic indications... 3 Antimicrobial spectrum of activity for
VIBATIV (telavancin) Healthcare Professional s Guide Version 2, 4 November 2014 1 Table of Contents Introduction... 3 About Vibativ / Therapeutic indications... 3 Antimicrobial spectrum of activity for
Infectious Disease Hot Topics: 2008
 Infectious Disease Hot Topics: 2008 Joseph Domachowske MD Professor of Pediatrics, Microbiology and Immunology Golisano Children s Hospital at SUNY Upstate Medical University Topic 1: COMMUNITY-ASSOCIATED
Infectious Disease Hot Topics: 2008 Joseph Domachowske MD Professor of Pediatrics, Microbiology and Immunology Golisano Children s Hospital at SUNY Upstate Medical University Topic 1: COMMUNITY-ASSOCIATED
Upper...and Lower Respiratory Tract Infections
 Upper...and Lower Respiratory Tract Infections Robin Jump, MD, PhD Cleveland Geriatric Research Education and Clinical Center (GRECC) Louis Stokes Cleveland VA Medical Center Case Western Reserve University
Upper...and Lower Respiratory Tract Infections Robin Jump, MD, PhD Cleveland Geriatric Research Education and Clinical Center (GRECC) Louis Stokes Cleveland VA Medical Center Case Western Reserve University
HEALTHCARE-ASSOCIATED PNEUMONIA: EPIDEMIOLOGY, MICROBIOLOGY & PATHOPHYSIOLOGY
 HEALTHCARE-ASSOCIATED PNEUMONIA: EPIDEMIOLOGY, MICROBIOLOGY & PATHOPHYSIOLOGY David Jay Weber, M.D., M.P.H. Professor of Medicine, Pediatrics, & Epidemiology Associate Chief Medical Officer, UNC Health
HEALTHCARE-ASSOCIATED PNEUMONIA: EPIDEMIOLOGY, MICROBIOLOGY & PATHOPHYSIOLOGY David Jay Weber, M.D., M.P.H. Professor of Medicine, Pediatrics, & Epidemiology Associate Chief Medical Officer, UNC Health
Continuous Infusion of Antibiotics In The ICU: What Is Proven? Professor of Medicine Vice-Chairman, Department of Medicine SUNY at Stony Brook
 Continuous Infusion of Antibiotics In The ICU: What Is Proven? Michael S. Niederman, M.D. Chairman, Department of Medicine Winthrop-University Hospital Mineola, NY Professor of Medicine Vice-Chairman,
Continuous Infusion of Antibiotics In The ICU: What Is Proven? Michael S. Niederman, M.D. Chairman, Department of Medicine Winthrop-University Hospital Mineola, NY Professor of Medicine Vice-Chairman,
GROUP A STREPTOCOCCUS (GAS) INVASIVE
 GROUP A STREPTOCOCCUS (GAS) INVASIVE Case definition CONFIRMED CASE Laboratory confirmation of infection with or without clinical evidence of invasive disease: isolation of group A streptococcus (Streptococcus
GROUP A STREPTOCOCCUS (GAS) INVASIVE Case definition CONFIRMED CASE Laboratory confirmation of infection with or without clinical evidence of invasive disease: isolation of group A streptococcus (Streptococcus
EDUCATIONAL COMMENTARY VANCOMYCIN MONITORING
 EDUCATIONAL COMMENTARY VANCOMYCIN MONITORING Commentary provided by: Julie Hall, MHS, MT (ASCP) Assistant Dean, College of Health Professions Assistant Professor, Medical Laboratory Science Grand Valley
EDUCATIONAL COMMENTARY VANCOMYCIN MONITORING Commentary provided by: Julie Hall, MHS, MT (ASCP) Assistant Dean, College of Health Professions Assistant Professor, Medical Laboratory Science Grand Valley
Infectious Disease in the Critically Ill Patient
 Infectious Disease in the Critically Ill Patient Heather L. Evans, MD MS FACS Director of Surgical Infectious Disease Harborview Medical Center Asst. Professor UW Department of Surgery New Antibiotics:
Infectious Disease in the Critically Ill Patient Heather L. Evans, MD MS FACS Director of Surgical Infectious Disease Harborview Medical Center Asst. Professor UW Department of Surgery New Antibiotics:
The EM Educator Series
 The EM Educator Series The EM Educator Series: Why is my patient with gallbladder pathology so sick? Author: Alex Koyfman, MD (@EMHighAK) // Edited by: Brit Long, MD (@long_brit) and Manpreet Singh, MD
The EM Educator Series The EM Educator Series: Why is my patient with gallbladder pathology so sick? Author: Alex Koyfman, MD (@EMHighAK) // Edited by: Brit Long, MD (@long_brit) and Manpreet Singh, MD
Staphylococci. What s to be Covered. Clinical Scenario #1
 Staphylococci Micrococcus, which, when limited in its extent and activity, causes acute suppurative inflammation (phlegmon), produces, when more extensive and intense in its action on the human system,
Staphylococci Micrococcus, which, when limited in its extent and activity, causes acute suppurative inflammation (phlegmon), produces, when more extensive and intense in its action on the human system,
Updated Clostridium difficile Treatment Guidelines
 Updated Clostridium difficile Treatment Guidelines Arielle Arnold, PharmD, BCPS Clinical Pharmacist Saint Alphonsus Regional Medical Center September 29 th, 2018 Disclosures Nothing to disclose Learning
Updated Clostridium difficile Treatment Guidelines Arielle Arnold, PharmD, BCPS Clinical Pharmacist Saint Alphonsus Regional Medical Center September 29 th, 2018 Disclosures Nothing to disclose Learning
Osteomieliti STEOMIE
 OsteomielitiSTEOMIE Osteomyelitis is the inflammation of bone caused by pyogenic organisms. Major sources of infection: - haematogenous spread - tracking from adjacent foci of infection - direct inoculation
OsteomielitiSTEOMIE Osteomyelitis is the inflammation of bone caused by pyogenic organisms. Major sources of infection: - haematogenous spread - tracking from adjacent foci of infection - direct inoculation
Evidence for the use of new and old agents for MRSA infection. Dr Charis Marwick Ninewells Hospital & Medical School Dundee
 Evidence for the use of new and old agents for MRSA infection Dr Charis Marwick Ninewells Hospital & Medical School Dundee 32 year old man Admitted unwell for few days Cough, fever, short of breath, pleuritic
Evidence for the use of new and old agents for MRSA infection Dr Charis Marwick Ninewells Hospital & Medical School Dundee 32 year old man Admitted unwell for few days Cough, fever, short of breath, pleuritic
What's New in Infectious Diseases Pharmacotherapy?
 Disclosure What's New in Infectious Diseases Pharmacotherapy? Nothing to Disclose Douglas Slain, Pharm.D., BCPS, FCCP, FASHP Associate Professor Infectious Diseases Clinical Specialist West Virginia University
Disclosure What's New in Infectious Diseases Pharmacotherapy? Nothing to Disclose Douglas Slain, Pharm.D., BCPS, FCCP, FASHP Associate Professor Infectious Diseases Clinical Specialist West Virginia University
Morbid Obesity: Multi system Considerations for Acute Care
 Morbid Obesity: Multi system Considerations for Acute Care BRENDA ENGLER, MSN, ACNP BC, CCRN GEISINGER MEDICAL CENTER Disclosures None 1 Obesity Statistics 30 % of the adult population of Pennsylvania
Morbid Obesity: Multi system Considerations for Acute Care BRENDA ENGLER, MSN, ACNP BC, CCRN GEISINGER MEDICAL CENTER Disclosures None 1 Obesity Statistics 30 % of the adult population of Pennsylvania
Division of Vascular and Endovascular Surgery University of South Florida School of Medicine Tampa, Florida
 Division of Vascular and Endovascular Surgery University of South Florida School of Medicine Tampa, Florida Appearance: oearly < 3 mo. olate > 3 mo.. Extent: Szilagyi Classification: Grade I: infection
Division of Vascular and Endovascular Surgery University of South Florida School of Medicine Tampa, Florida Appearance: oearly < 3 mo. olate > 3 mo.. Extent: Szilagyi Classification: Grade I: infection
Infected cardiac-implantable electronic devices: diagnosis, and treatment
 Infected cardiac-implantable electronic devices: diagnosis, and treatment The incidence of infection following implantation of cardiac implantable electronic devices (CIEDs) is increasing at a faster rate
Infected cardiac-implantable electronic devices: diagnosis, and treatment The incidence of infection following implantation of cardiac implantable electronic devices (CIEDs) is increasing at a faster rate
Mortality Rate was unsightly!!! 4/24/2013. Sepsis Quality Improvement Project
 Libby, MT Sepsis Quality Improvement Project Barb Dumont RN, Director of Quality and Risk Management Mike Julius RN, ED Manager Cathy Wolfe RN, Chief Nursing Officer. Mortality Rate was unsightly!!! percent
Libby, MT Sepsis Quality Improvement Project Barb Dumont RN, Director of Quality and Risk Management Mike Julius RN, ED Manager Cathy Wolfe RN, Chief Nursing Officer. Mortality Rate was unsightly!!! percent
Enhancement of Infection Control for MRSA in Renal Unit
 Enhancement of Infection Control for MRSA in Renal Unit Ms Ida Yip SNO (Infection Control) Hong Kong East Cluster Hospital 19 August 2011 IC Forum (19-8-2011) 1 MRSA Common Multi Drug Resistant Organisms
Enhancement of Infection Control for MRSA in Renal Unit Ms Ida Yip SNO (Infection Control) Hong Kong East Cluster Hospital 19 August 2011 IC Forum (19-8-2011) 1 MRSA Common Multi Drug Resistant Organisms
Development of C sporins. Beta-lactam antibiotics - Cephalosporins. Second generation C sporins. Targets - PBP s
 Beta-lactam antibiotics - Cephalosporins Development of C sporins Targets - PBP s Activity - Cidal - growing organisms (like the penicillins) Principles of action - Affinity for PBP s Permeability properties
Beta-lactam antibiotics - Cephalosporins Development of C sporins Targets - PBP s Activity - Cidal - growing organisms (like the penicillins) Principles of action - Affinity for PBP s Permeability properties
ESPID New Bone and Joint Infection Guidelines
 ESPID New Bone and Joint Infection Guidelines Theoklis Zaoutis, MD, MSCE Professor of Pediatrics and Epidemiology Perelman School of Medicine at the University of Pennsylvania Chief, Division of Infectious
ESPID New Bone and Joint Infection Guidelines Theoklis Zaoutis, MD, MSCE Professor of Pediatrics and Epidemiology Perelman School of Medicine at the University of Pennsylvania Chief, Division of Infectious
Neutropenic Fever. CID 2011; 52 (4):e56-e93
 Neutropenic Fever www.idsociety.org CID 2011; 52 (4):e56-e93 Definitions Fever: Single oral temperature of 101 F (38.3 C) Temperature 100.4 F (38.0 C) over 1 hour Neutropenia: ANC < 500 cells/mm 3 Expected
Neutropenic Fever www.idsociety.org CID 2011; 52 (4):e56-e93 Definitions Fever: Single oral temperature of 101 F (38.3 C) Temperature 100.4 F (38.0 C) over 1 hour Neutropenia: ANC < 500 cells/mm 3 Expected
ORIGINAL ARTICLE DOI: (e) ISSN Online: (p) ISSN Print: Anand Kumar Singh 1, Poonam Verma 2. Sciences, Dehradun
 ORIGINAL ARTICLE CLINICAL ASSESSMENT OF NEPHROTOXICITY ASSOCIATED WITH VANCOMYCIN TROUGH CONCENTRATIONS DURING TREATMENT OF DEEP-SEATED INFECTIONS: A RETROSPECTIVE ANALYSIS Anand Kumar Singh 1, Poonam
ORIGINAL ARTICLE CLINICAL ASSESSMENT OF NEPHROTOXICITY ASSOCIATED WITH VANCOMYCIN TROUGH CONCENTRATIONS DURING TREATMENT OF DEEP-SEATED INFECTIONS: A RETROSPECTIVE ANALYSIS Anand Kumar Singh 1, Poonam
Curbside Consultation: Answering the Most Common Infection Prevention and Control Questions. Disclosures. Learning Objectives
 Curbside Consultation: Answering the Most Common Infection Prevention and Control Questions Michelle A. Barron, MD Medical Director, University of Colorado Hospital, Infection Prevention and Control Professor
Curbside Consultation: Answering the Most Common Infection Prevention and Control Questions Michelle A. Barron, MD Medical Director, University of Colorado Hospital, Infection Prevention and Control Professor
declara&ons Clostridium difficile infec&on. Time to wake up and smell the..., um, nevermind. OK, next slide please. Bruce Dalton, BScPhm. PharmD.
 Clostridium difficile infec&on. Time to wake up and smell the..., um, nevermind. OK, next slide please. Bruce Dalton, BScPhm. PharmD. declara&ons No financial disclosures Personal acquaintance, co- worker,
Clostridium difficile infec&on. Time to wake up and smell the..., um, nevermind. OK, next slide please. Bruce Dalton, BScPhm. PharmD. declara&ons No financial disclosures Personal acquaintance, co- worker,
Bad Bugs in the Blood!
 Bad Bugs in the Blood! How to Work Up and Treat Bloodstream Infections Sharanjeet Thind M.D. Director of Inpatient Infectious Diseases, VA Medical Center Assistant Professor of Medicine, OUHSC, College
Bad Bugs in the Blood! How to Work Up and Treat Bloodstream Infections Sharanjeet Thind M.D. Director of Inpatient Infectious Diseases, VA Medical Center Assistant Professor of Medicine, OUHSC, College
Serum C-reactive protein levels correlate with clinical response in patients treated with antibiotics for wound infections after spinal surgery
 The Spine Journal 6 (2006) 311 315 Serum C-reactive protein levels correlate with clinical response in patients treated with antibiotics for wound infections after spinal surgery Mustafa H. Khan, MD a,
The Spine Journal 6 (2006) 311 315 Serum C-reactive protein levels correlate with clinical response in patients treated with antibiotics for wound infections after spinal surgery Mustafa H. Khan, MD a,
Optimizing Antibiotic Therapy in the ICU For Pneumonia Current and Future Approaches
 Optimizing Antibiotic Therapy in the ICU For Pneumonia Current and Future Approaches Andrew F. Shorr, MD, MPH Washington Hospital Center Georgetown Univ. Disclosures I have served as a consultant to, researcher/investigator
Optimizing Antibiotic Therapy in the ICU For Pneumonia Current and Future Approaches Andrew F. Shorr, MD, MPH Washington Hospital Center Georgetown Univ. Disclosures I have served as a consultant to, researcher/investigator
What s to be Covered. Microbiology of staphylococci Epidemiology of S. aureus infections Pathogenesis of S. aureus infections
 Staphylococci Micrococcus, which, when limited in its extent and activity, causes acute suppurative inflammation (phlegmon), produces, when more extensive and intense in its action on the human system,
Staphylococci Micrococcus, which, when limited in its extent and activity, causes acute suppurative inflammation (phlegmon), produces, when more extensive and intense in its action on the human system,
Respiratory Tract Infec1ons Long Term Care. Dr Karsten Hammond Infec1ous Diseases 28 March 2015
 Respiratory Tract Infec1ons Long Term Care Dr Karsten Hammond Infec1ous Diseases 28 March 2015 Disclosures I have no financial rela1onships to disclose 82 yo Female In LTC for two years, total care from
Respiratory Tract Infec1ons Long Term Care Dr Karsten Hammond Infec1ous Diseases 28 March 2015 Disclosures I have no financial rela1onships to disclose 82 yo Female In LTC for two years, total care from
Hospital Communicable Diseases Surveillance Protocols Primer. Key Infec:on Preven:on and Control Lapses in the Clinical Office
 OEMAC 33 rd Scien/fic Conference September 29, 2015; 2:50-3:15 Hospital Communicable Diseases Surveillance Protocols Primer Key Infec:on Preven:on and Control Lapses in the Clinical Office Se@ng Dr. Maureen
OEMAC 33 rd Scien/fic Conference September 29, 2015; 2:50-3:15 Hospital Communicable Diseases Surveillance Protocols Primer Key Infec:on Preven:on and Control Lapses in the Clinical Office Se@ng Dr. Maureen
Modifiable Risk Factors in Orthopaedic Infections
 Modifiable Risk Factors in Orthopaedic Infections AAOS Patient Safety Committee Burden US Surgical Site Infections (SSI) by the Numbers ~300,000 SSIs/yr (17% of all HAI; second to UTI) 2%-5% of patients
Modifiable Risk Factors in Orthopaedic Infections AAOS Patient Safety Committee Burden US Surgical Site Infections (SSI) by the Numbers ~300,000 SSIs/yr (17% of all HAI; second to UTI) 2%-5% of patients
Osteomyelitis Revisited
 Osteomyelitis Revisited Alan Jay Block, DPM, MS, FASPS, FACFAS Assistant Professor Dept Of Orthopeadics The Ohio State University Medical Board Kent State University Editor-in -Chief The Journal of the
Osteomyelitis Revisited Alan Jay Block, DPM, MS, FASPS, FACFAS Assistant Professor Dept Of Orthopeadics The Ohio State University Medical Board Kent State University Editor-in -Chief The Journal of the
New Strategies to Reduce MRSA in ICUs
 New Strategies to Reduce MRSA in ICUs Susan Huang, MD MPH Associate Professor, UC Irvine Health Medical Director, Epidemiology & Infection Prevention Division of Infectious Diseases & Health Policy Research
New Strategies to Reduce MRSA in ICUs Susan Huang, MD MPH Associate Professor, UC Irvine Health Medical Director, Epidemiology & Infection Prevention Division of Infectious Diseases & Health Policy Research
Decolonization to Reduce MDROs in Healthcare: Who, What, Where, When, and Why?
 Live broadcast from Decolonization to Reduce MDROs in Healthcare: Who, What, Where, When, and Why? Susan Huang, MD MPH Professor of Medicine Medical Director, Epidemiology & Infection Prevention Division
Live broadcast from Decolonization to Reduce MDROs in Healthcare: Who, What, Where, When, and Why? Susan Huang, MD MPH Professor of Medicine Medical Director, Epidemiology & Infection Prevention Division
Antibiotic Management of Pediatric Osteomyelitis
 Reprinted from www.antimicrobe.org Sandra Arnold, M.D. Antibiotic Management of Pediatric Osteomyelitis Several points uncertainty exist regarding the antimicrobial management of acute hematogenous osteomyelitis,
Reprinted from www.antimicrobe.org Sandra Arnold, M.D. Antibiotic Management of Pediatric Osteomyelitis Several points uncertainty exist regarding the antimicrobial management of acute hematogenous osteomyelitis,
Open Forum Infectious Diseases MAJOR ARTICLE
 Open Forum Infectious Diseases MAJOR ARTICLE Efficacy and Safety of Oritavancin Relative to Vancomycin for Patients with Acute Bacterial Skin and Skin Structure Infections (ABSSSI) in the Outpatient Setting:
Open Forum Infectious Diseases MAJOR ARTICLE Efficacy and Safety of Oritavancin Relative to Vancomycin for Patients with Acute Bacterial Skin and Skin Structure Infections (ABSSSI) in the Outpatient Setting:
New Medicines Committee Briefing. July Fosfomycin trometamol for the treatment of multidrug resistant urinary tract infection
 New Medicines Committee Briefing July 2014 Fosfomycin trometamol for the treatment of multidrug resistant urinary tract infection (unlicensed indication) Fosfomycin trometamol to be reviewed for use within:
New Medicines Committee Briefing July 2014 Fosfomycin trometamol for the treatment of multidrug resistant urinary tract infection (unlicensed indication) Fosfomycin trometamol to be reviewed for use within:
Appendix A: Summary of evidence from surveillance
 Appendix A: Summary of evidence from surveillance 8-year surveillance (2017) Surgical site infections: prevention and treatment (2008) NICE guideline CG74 Summary of evidence from surveillance... 1 Research
Appendix A: Summary of evidence from surveillance 8-year surveillance (2017) Surgical site infections: prevention and treatment (2008) NICE guideline CG74 Summary of evidence from surveillance... 1 Research
