ORIGINAL ARTICLE Argininosuccinic aciduria: Clinical and biochemical phenotype findings in Malaysian children
|
|
|
- Rosaline Tyler
- 6 years ago
- Views:
Transcription
1 Malaysian J Pathol 2010; 32(2) : ORIGINAL ARTICLE Argininosuccinic aciduria: Clinical and biochemical phenotype findings in Malaysian children CHEN Bee Chin Msc, NGU Lock Hock MRCP and *ZABEDAH Md Yunus MPath Department of Genetics, Kuala Lumpur Hospital and * Biochemistry Unit, Specialized Diagnostic Centre, Institute for Medical Research, Kuala Lumpur, Malaysia. Abstract Argininosuccinic aciduria is an inborn error of the urea cycle caused by deficiency of argininosuccinate lyase (ASL). ASL-deficient patients present with progressive intoxication due to accumulation of ammonia in the body. Early diagnosis and treatment of hyperammonemia are necessary to improve survival and prevent long-term handicap. Two clinical phenotypes have been recognized neonatal acute and milder late-onset form. We investigated patients with hyperammonemia by a stepwise approach in which quantitative amino acids analysis was the core diagnostic procedure. Here, we describe the clinical phenotypes and biochemical characteristics in diagnosing this group of patients. We have identified 13 patients with argininosuccinic aciduria from 2003 till Ten patients who presented with acute neonatal hyperammonemic encephalopathy had markedly elevated blood ammonia (>430 μmol/l) within the first few days of life. Three patients with lateonset disease had more subtle clinical presentations and they developed hyperammonemia only during the acute catabolic state at two to twelve months of age. Their blood ammonia was mild to moderately elevated (> μmol/l). The diagnosis was confirmed by detection of excessive levels of argininosuccinate in the urine and/or plasma. They also have moderately increased levels of citrulline and, low levels of arginine and ornithine in their plasma. Two patients succumbed to the disease. To date, eleven patients remained well on a dietary protein restriction, oral ammonia scavenging drugs and arginine supplementation. The majority of them have a reasonable good neurological outcome. Keywords: Argininosuccinic aciduria, argininosuccinate lyase deficiency, hyperammonemia, urea cycle disorders, quantitative amino acid analysis INTRODUCTION Argininosuccinic aciduria (ASA, #MIM608310) is a rare autosomal recessive disorder caused by the deficiency of argininosuccinate lyase. It is one of the six enzymes in the urea cycle pathway that converts the toxic ammonium nitrogen into urea before being excreted in the urine (Figure 1). The gene for ASL deficiency is located on chromosome 7 and has been mapped to locus 7q ,2,3 The estimated worldwide incidence among general population is 1: 70, Two clinical phenotypes have been recognized a neonatal acute form (the classical form) and a milder late-onset form. Patients with neonatal-onset disease present with severe hyperammonemic coma within the first few days of life. They usually have an overwhelming illness that rapidly progresses from poor feeding, vomiting, lethargy or irritability and tachypnea to seizure, coma and respiratory arrest. Early clinical recognition and laboratory diagnosis, and urgent treatment to control hyperammonemia are crucial in order to prevent death and severe neurological handicap. 5 Patients with late-onset disease may present at any age outside of the newborn period. Their clinical manifestations are generally less acute and more subtle than the neonatal-onset variant, and often are precipitated by stress such as infection and anesthesia. 6,7 Their symptoms may include anorexia, recurrent vomiting, failure to thrive, epilepsy, developmental delay and behavioral problem. 1,2,3 We report here our experience in diagnosing and treating a cohort of 13 children with argininosuccinic aciduria. Address for correspondence and reprint requests: Chen Bee Chin, Biochemical Genetics Unit, Department of Genetics, Kuala Lumpur Hospital, Jalan Pahang, Kuala Lumpur, Malaysia. Tel: ext 6886, Fax: beechinmy@yahoo.com 87
2 Malaysian J Pathol December 2010 Mitochondria NAGS Ammonia CPS I N-acetylglutamate Glutamine Urea HCO 3 Ornithine Carbamyl phosphate Citrulline OTC ASS Aspartate Orotic, Orotidine & Uracil Arginase Argininosuccinate Arginine ASL Cytosol Fumarate FIG. 1: Urea cycle pathway. The Urea cycle comprises of six enzymes: N-acetyl-glutamate synthase (NAGS), Carbamyl-Phosphate-Synthetase-I (CPS I), Ornithine Transcarbamylase (OTC), Argininosuccinate Synthetase (ASS), Argininosuccinate Lyase (ASL), and Arginase. MATERIALS AND METHODS We received samples and referral from paediatricians nationwide for the diagnosis of urea cycle disorders (UCD) in children with hyperammonemia. We followed a stepwise diagnostic protocol as shown in Figure 2. Quantitative amino acid analysis in plasma and/ or urine (for patients suspected of having argininosuccinic aciduria) is the most important diagnostic tool in the evaluation for UCD. Presence of argininosuccinate in plasma or urine was mandatory in order to make a diagnosis of ASL deficiency/argininosuccinic aciduria. We reviewed retrospectively the clinical records and laboratory data of more than 360 children from 8270 samples (4.35%) received who were evaluated for hyperammonemia in our centre over a seven-year period ( ). Samples Blood and urine samples were collected from acutely ill children when the basic metabolic screen showed significant hyperammonemia. Blood (1-2 ml) was collected in a heparin tube and the plasma was separated from the blood cells immediately by centrifugation. A minimum of 2 ml urine was collected in a sterile container. Plasma and urine were frozen at -20 C if they could not be analyzed immediately. Samples were transported in an ice box and arrived frozen in the laboratory. Chemicals Argininosuccinic acid, 5-sulphosalicylic acid (SSA), and physiological standard A and B were purchased from Sigma. The ultra physiological fluid chemical kit was purchased from Biochrom Ltd., (Cambridge, UK). Instrument Amino acids were quantified by ion-exchange chromatography using a dedicated amino acids analyzer (Biochrom 30) and post column detection. In principle, the instrument system works by pumping buffers of varying ph and ionic strength through a column of cationexchange resin to separate the various amino acids. The column eluent is mixed with the ninhydrin reagent, and the mixture is then passed 88
3 ARGININOSUCCINIC ACIDURIA IN MALAYSIAN CHILDREN Hyperammonemia Plasma amino acid quantitative analysis High plasma citrulline High plasma citrulline Low plasma citrulline Arginase deficiency Argininosuccinate detection in plasma and urine urine orotic acid Detected Not detected Elevated Low/normal ASL deficiency ASS deficiency OTC deficiency CPS-I deficiency or NAGS deficiency FIG. 2: Stepwise diagnostic protocol for the investigation of hyperammonemia. ASL: Argininosuccinate Lyase; ASS: Argininosuccinate Synthetase; CPS-I: Carbamyl-Phosphate-Synthetase-I; NAGS: N-Acetyl- Glutamate Synthase; OTC: Ornithine Transcarbamylase through a high temperature reaction coil. In the reaction coil, the ninhydrin reacts with the amino acid to form a coloured compound, and the amount of coloured compound produced is directly proportional to the quantity of amino acid present. The absorbance is measured by wavelengths at 570 nm and 440 nm. The whole system is computer-controlled. Plasma amino acids analysis Plasma (100μL) was pipetted into an eppendorf tube and 100μL of 10% SSA solution was then added. The tube was capped, agitated for a few seconds, and allowed to stand for 1 hour at 4 0 C. It was then centrifuged at 10,000 rpm for 5 minutes. The supernatant was filtered through a 0.2 μm membrane to remove any remaining particulate materials prior to analysis. The filtrate was transferred into a vial and loaded into an autosampler. The filtrate (20 μl) was then injected into the amino acid analyzer. A running time of 2 hours was required for each sample. Urine amino acids analysis About 2mL of urine was required and the method for sample processing was similar to that of plasma. About 20 μl of filtrate was injected into the amino acid analyzer. The running time takes 2 hours for each sample. Creatinine concentration was determined in the urine sample by the modified Jaffe (alkalinepicrate) using Modular Biochemistry Roche Analyser and Roche reagents prior the analysis of amino acids. RESULTS We identified 13 patients (from 12 families) with argininosuccinic aciduria (four boys and nine girls). This is 0.16% of 8270 patients referred to our centre for investigation of possible inborn errors of metabolism over seven year period. Table 1 and 2 summarize the clinical presentations and laboratory data of our cohort respectively. Eleven out of thirteen patients were Malay. Parental consanguinity was noted in two families. 89
4 Malaysian J Pathol December 2010 TABLE 1: Summary of the clinical phenotypes of 13 patients with argininosuccinic aciduria Gender Ethnic Parental consanguinity Age at onset Age at diagnosis Acute treatment Current age Recurrent crises Current status Clinical symptoms 1 # B M no 3d feeding refusal, vomiting, lethargy, seizure, coma 15d a,c - no Died 2 # B M no 3d feeding refusal, vomiting, lethargy 4d a,b 3y no 1,2,3 3 G M yes 3d feeding refusal, vomiting, lethargy, coma 10d c 3.5y no 1,2,4 4 B M no 2d feeding refusal, vomiting, lethargy, coma, respiratory distress 7d a,b,c 5y yes 1,2,5 5 G C no 10d feeding refusal, vomiting, lethargy, coma 21d b,c 2y no 1,2,4 6 G M no 2d feeding refusal, vomiting, lethargy, coma 23d c 1.5y no 1,2,3 7 G M no 3d feeding refusal, vomiting, lethargy, seizure, coma 5d b,c 3m no 1,2,3 8 G I no 13d feeding refusal, vomiting, lethargy, coma 20d a,b,c 7y no 1,2,3 9 G M no 3d feeding refusal, vomiting, hyperirritability, coma 5d a,b,c 2y no 1,2,4 10 G M yes 5 d feeding refusal, vomiting, lethargy, seizure, coma 8 d a,c - no Died 11 B M no 8m feeding refusal, vomiting, lethargy, coma (following febrile illness) 14m c 4.5y no 1,2,4 12 G M no 1y developmental delay, epilepsy, brittle hair 6y - 12y no 1,2,4 13 G M yes 2m developmental delay, epilepsy, recurrent vomiting, growth failure 5y - 11y yes* 1,2,5 B: boy; G: girl; M: Malay; C: Chinese; I: Indian; d: day, m: month; y: year; acute treatment: a, acute dialysis b, intravenous ammonia scavenger drugs; c, ventilator support; current status: 1, protein restricted diet; 2, oral ammonia scavenger drugs; 3, normal development; 4, mild mental retardation; 5, moderate mental retardation. # : Patient 1 and 2 are siblings. *: until five years old. 90
5 ARGININOSUCCINIC ACIDURIA IN MALAYSIAN CHILDREN TABLE 2: Biochemical phenotypes of 13 patients with argininosuccinic aciduria Plasma Urine Urine Plasma Amino Acid ammonia orotic Arginino Arginino Citrulline Arginine Glutamine Alanine PATIENT succinate succinate 1 1,586 not done 1, ,993 3, , , ,172 not done 1, , , , not done , , , , , ,719 1, ,600* 229* , ,848 not done 2, elevated 5, , not detected , ,646 1, elevated 1, , Reference Neonate: absent absent < range <110μmol/L, older mmol/mol (μmol/mmol μmol/l μmol/l μmol/l μmol/l child 50-80μmol/L creatinine of creatinine) *Argininosuccinic acid was detected after protein challenge 91
6 Malaysian J Pathol December 2010 Ten patients (Patient 1 to 10) had the acute neonatal form of the disease, with symptoms of hyperammonemia appearing between the second and thirteenth day after birth. The blood ammonia level ranged from 430μmol/L to 1,848μmol/L. Nine of the ten patients had argininosuccinic acid detected in blood (Fig. 3a) during the acute episode. Argininosuccinate was detected in the blood of Patient 8 only after a protein challenge. Argininosuccinate found in the urine was two to ten times higher in the plasma levels. Plasma glutamine and citrulline levels were elevated in all patients, whereas arginine and ornithine levels were low. Urine orotic acid was measured in five patients and; all of them had raised orotic acids levels, three to thirty times the normal limit. Three patients presented later (between the age of two months and twelve months) with milder clinical symptoms. Late-onset patients excreted significantly less argininosuccinate compared to the neonatal-onset group. In one of the patient, argininosuccinic acid was detected only in urine. Two patients (Patient 1 and 10) with neonatal-onset disease died at the age of 12 days and 4 months when they had a recurrent hyperammonemic coma. However, nine patients survived with a reasonably good neurological outcome; four patients have normal developmental status and five have mild delayed development. Two patients (patient 4 and 13) have severe neurological disabilities as a consequence of recurrent hyperammonemic episodes. DISCUSSION Argininosuccinic aciduria is the second most common disorder of inborn errors of the urea cycle in European countries and the United States. The reported incidence is about 1 in 70,000 live births in the United States. 8 Our study shows a prevalent of 0.16% (13 positive) from 8270 patients referred to our centre for investigation of various inborn errors of metabolism disorder. It is also considered to be the most common disorder of urea cycle diagnosed in our country. The clinical presentation of argininosuccinic aciduria is rather non-specific, just like other urea cycle disorders. Neonatal disease resembles a neonatal infection whereas late-onset disease can mimic many other neurological disorders. 1,2 As such the recognition of argininosuccinic aciduria heavily relies on biochemical laboratory testing. The first clue to alert the clinician and laboratory scientist that he/she may be dealing with argininosuccinic aciduria or a urea cycle disorder in a sick child is raised blood ammonia. It is, therefore, essential to measure ammonia early in every sick child without a clear diagnosis. After excluding false hyperammonemia such as improper sample collection and transportation, struggling or a haemolysed blood sample, blood ammonia more than 200 μmol/l in a previously healthy term newborn or more than 150 μmol/l in an older child is strongly suggestive of an underlying urea cycle disorders such as argininosuccinic aciduria. 2,9 This should prompt the clinician to contact the diagnostic laboratory for urgent plasma and urine amino acids analysis. Plasma quantitative amino acid analysis is necessary to confirm a specific diagnosis of urea cycle disorder. Argininosuccinic aciduria is one of the 3 urea cycle disorders (the other two are citrullinemia and arginase deficiency) in which changes in amino acids are usually diagnostic without the need for further enzymatic or molecular testing. 2,9,10 Presence of argininosuccinate is the characteristic marker for diagnosis of argininosuccinic aciduria, which is usually not detected in a normal person. 11 Other significant amino acids are citrulline and orotic acid. In patients with argininosuccinic aciduria, the plasma citrulline is usually elevated to levels of 150 to 250 μmol/l. Hyperglutaminemia and hyperalaninemia are also often present. Elevated glutamine signifies a hyperammonemic state as glutamine is an ammonia scavenger. Raised plasma alanine is a non specific finding. Under normal circumstances, arginine is produced from argininosuccinate. Hypoargininemia will, therefore, be expected and is a common finding in argininosuccinic aciduria. 11 Although plasma amino acid quantification is diagnostic, potential pitfalls in amino acid analysis need to be recognized. Firstly, argininosuccinic acid is not one of the usual amino acids routinely detected in an amino acids analysis and can easily be misidentified, because it may co-elute with other amino acids especially leucine (Fig 3b). 12 Secondly, argininosuccinate acid is highly soluble and rapidly cleared from blood. Therefore, the amount present may be too little to be detected. As such urinary amino acid analysis is helpful in confirming argininosuccinic aciduria because of the marked excretion of argininosuccinate acid in urine. 11 In addition, urine samples treated with heat or barium precipitation prior 92
7 ARGININOSUCCINIC ACIDURIA IN MALAYSIAN CHILDREN FIG. 3a: Plasma Amino Acid Chromatogram for Patient 1 with Argininosuccinate Lyase Deficiency This chromatogram was obtained at 570nm. The amino acids can be separated because of different pka and hence eluted with different retention times. In this chromatogram, argininosiccinate was eluted immediately after leucine. 1. Aspartic acid, 2. Threonine, 3. Serine, 4. Asparagine, 5. Glutamic acid, 6. Glutamine, 7. Glycine, 8. Alanine, 9. Citrulline 10.Valine, 11. Methionine, 12. Leucine, 13. Tyrosine, 14. Phenylalanine, 15. Ammonium, 16. Ornithine, 17. Lysine, 18. Histidine, 19. Arginine. 93
8 Malaysian J Pathol December 2010 FIG. 3b: Urine Amino Acid Chromatogram for Patient 1 with Argininosuccinate Lyase Deficiency. In ASL deficiency, argininosuccinate which is the characteristic urinary marker, is excreted in large amount (1084 μmol/mmol creatinine ), and some of these are converted into anhydride forms. In this chromatogram, the two anhydrides of argininosuccinate are eluted at the retention time of homocysteine and gaba peaks, whereas argininosuccinate is eluted closely after the leucine peak. 1. Aspartic acid, 2. Threonine, 3. Serine, 4. Asparagine, 5. Glutamic acid, 6. Glutamine, 7. Glycine, 8. Alanine, 9. Citrulline 10. Valine, 11. Methionine, 12. Leucine, 13. Tyrosine, 14. Phenylalanine, 15. Ammonium, 16. Ornithine, 17. Lysine, 18. Histidine, 19. Arginine. 94
9 ARGININOSUCCINIC ACIDURIA IN MALAYSIAN CHILDREN to analysis will further improve the sensitivity of detection by converting the argininosuccinic acid into anhydrides. 12 Nevertheless, quantitative analysis of urine amino acids is generally not useful for diagnosis of most amino acid disorders and other urea cycle disorders. This is because urine amino acids concentrations do not reflect the true amino acid concentration in blood due to the effect of renal reabsorption. Urine argininosuccinate quantitative analysis is one of the few exceptions. A favourable outcome can be achieved if argininosuccinic aciduria is diagnosed early. Immediate treatment may include acute dialysis to rapidly remove ammonia which is extremely toxic to the brain. Long term treatment will normally include dietary protein restriction, arginine supplementation, use of pharmacological ammonia scavengers such as sodium benzoate and sodium phenylbutyrate. 13 In conclusion, clinicians should always consider the possibility of a child with unexplained illness, or without a clear explanation, having an inborn error of metabolism such as argininosuccinic aciduria. Close collaboration with the laboratory is potentially life saving. ACKNOWLEDGEMENT The authors like to thank all the paediatricians who have referred patients to us, all the patients and their families, and the staff of Metabolic Clinic (Ms Balktiah Mat and Ms Norzawani Che Johari) for assisting in the retrieval of medical records. The authors also wish to thank Dr Keng Wee Teik, Dr. Shanti B, Dr Ch ng Gaik Siew for their clinical support, and the staff of Biochemical Genetics Unit ( Ms Huzaimah bte Sani, Ms Tengku Rosmaliza, Mr Mohd Helmi and Miss Komalam) for their excellent technical assistance. metabolic diseases. Heidelberg, Germany: Springer; p Nagata N, Matsuda I, Oyanagi K. Estimated frequency of urea cycle enzymopathies in Japan, Am J Med Genet. 1991; 39: Berry GT, Steiner RD. Long-term management of patients with urea cycle disorders. J Pediatr 2001;138 (Suppl 1): S56 S Leonard JV. Inherited hyperammonemias. In: Blau N, Hoffmann GF, Leonard VJ, Clarke JTR. editors. Physician s guide to the treatment and follow-up of metabolic diseases. Springer-Verlag Berlin; Heidelberg, 2006.p Bourrier P, Varache N, Alquier P, Rabier D, Kamoun P, Lorre G, Alhayek G. Cerebral edema with hyperammonemia in valpromide poisoning. Manifestation in an adult, of a partial deficit in type I carbamylphosphate synthetase. Presse Med.1988; 17: Scaglia F, Brunetti-Pierr N, Kleppe S, et al. Clinical consequences of urea cycle enzyme deficiencies and potential links to arginine and nitric oxide metabolism. J Nutr. 2004; 134 (10 Suppl): 2775S- 2782S. 9. Barsotti RJ. Measurement of ammonia in blood. J Pediatr 2001; 138 (1 Suppl): S Tuchman M, Yudkoff M. Blood levels of ammonia and nitrogen scavenging amino acids in patients with inherited hyperammonemia. Mol Genet Metab. 1999; 66: Palmer T, Oberholzer VG, Levin B, Burges EA. Urinary excretion of argininosuccinic acid. Clin Chim Acta. 1973; 47: Steiner RD, Cederbaum SD. Laboratory evaluation of urea cycle disorders. J Pediatr. 2001; 138 (1 Suppl):: S Enns GM, Berry SA, Berry GT, Rhead WJ, Brusilow SW, Hamosh A. Survival after treatment with phenylacetate and benzoate for urea-cycle disorders. N Engl J Med. 2007; 356(22): REFERENCES 1. Brusilow SW, Horwich AL. Urea cycle enzymes. In: Scriver CR, Beaudet AL, Sly WS, Valle D, editors; Childs B, Kinzler KW, Vogelstein B, assoc. editors. The metabolic and molecular bases of inherited disease, 8th ed. New York: McGraw-Hill; p Leonard JV. Disorders of the Urea Cycle and Related Enzymes In: John Fernandes, Jean-Marie Saudubray, Georges van den Berghe, John H. Walter, editors. Inborn metabolic diseases. Heidelberg: Springer Medizin Verlag; p Bachmann C. Inherited hyperammonemias. In: Blau N, Hoffmann GE, Leonard J, Clarke JTR. editors. Physician s guide to the laboratory diagnosis of 95
10 Malaysian J Pathol December 2010 Mitochondria NAGS Ammonia CPS I N-acetylglutamate Glutamine Urea HCO 3 Ornithine Carbamyl phosphate Citrulline OTC ASS Aspartate Orotic, Orotidine & Uracil Arginase Argininosuccinate Arginine ASL Cytosol Fumarate FIG. 1: Urea cycle pathway. The Urea cycle comprises of six enzymes: N-acetyl-glutamate synthase (NAGS), Carbamyl-Phosphate-Synthetase-I (CPS I), Ornithine Transcarbamylase (OTC), Argininosuccinate Synthetase (ASS), Argininosuccinate Lyase (ASL), and Arginase. MATERIALS AND METHODS We received samples and referral from paediatricians nationwide for the diagnosis of urea cycle disorders (UCD) in children with hyperammonemia. We followed a stepwise diagnostic protocol as shown in Figure 2. Quantitative amino acid analysis in plasma and/ or urine (for patients suspected of having argininosuccinic aciduria) is the most important diagnostic tool in the evaluation for UCD. Presence of argininosuccinate in plasma or urine was mandatory in order to make a diagnosis of ASL deficiency/argininosuccinic aciduria. We reviewed retrospectively the clinical records and laboratory data of more than 360 children from 8270 samples (4.35%) received who were evaluated for hyperammonemia in our centre over a seven-year period ( ). Samples Blood and urine samples were collected from acutely ill children when the basic metabolic screen showed significant hyperammonemia. Blood (1-2 ml) was collected in a heparin tube and the plasma was separated from the blood cells immediately by centrifugation. A minimum of 2 ml urine was collected in a sterile container. Plasma and urine were frozen at -20 C if they could not be analyzed immediately. Samples were transported in an ice box and arrived frozen in the laboratory. Chemicals Argininosuccinic acid, 5-sulphosalicylic acid (SSA), and physiological standard A and B were purchased from Sigma. The ultra physiological fluid chemical kit was purchased from Biochrom Ltd., (Cambridge, UK). Instrument Amino acids were quantified by ion-exchange chromatography using a dedicated amino acids analyzer (Biochrom 30) and post column detection. In principle, the instrument system works by pumping buffers of varying ph and ionic strength through a column of cationexchange resin to separate the various amino acids. The column eluent is mixed with the ninhydrin reagent, and the mixture is then passed 88
11 ARGININOSUCCINIC ACIDURIA IN MALAYSIAN CHILDREN Hyperammonemia Plasma amino acid quantitative analysis High plasma citrulline High plasma citrulline Low plasma citrulline Arginase deficiency Argininosuccinate detection in plasma and urine urine orotic acid Detected Not detected Elevated Low/normal ASL deficiency ASS deficiency OTC deficiency CPS-I deficiency or NAGS deficiency FIG. 2: Stepwise diagnostic protocol for the investigation of hyperammonemia. ASL: Argininosuccinate Lyase; ASS: Argininosuccinate Synthetase; CPS-I: Carbamyl-Phosphate-Synthetase-I; NAGS: N-Acetyl- Glutamate Synthase; OTC: Ornithine Transcarbamylase through a high temperature reaction coil. In the reaction coil, the ninhydrin reacts with the amino acid to form a coloured compound, and the amount of coloured compound produced is directly proportional to the quantity of amino acid present. The absorbance is measured by wavelengths at 570 nm and 440 nm. The whole system is computer-controlled. Plasma amino acids analysis Plasma (100μL) was pipetted into an eppendorf tube and 100μL of 10% SSA solution was then added. The tube was capped, agitated for a few seconds, and allowed to stand for 1 hour at 4 0 C. It was then centrifuged at 10,000 rpm for 5 minutes. The supernatant was filtered through a 0.2 μm membrane to remove any remaining particulate materials prior to analysis. The filtrate was transferred into a vial and loaded into an autosampler. The filtrate (20 μl) was then injected into the amino acid analyzer. A running time of 2 hours was required for each sample. Urine amino acids analysis About 2mL of urine was required and the method for sample processing was similar to that of plasma. About 20 μl of filtrate was injected into the amino acid analyzer. The running time takes 2 hours for each sample. Creatinine concentration was determined in the urine sample by the modified Jaffe (alkalinepicrate) using Modular Biochemistry Roche Analyser and Roche reagents prior the analysis of amino acids. RESULTS We identified 13 patients (from 12 families) with argininosuccinic aciduria (four boys and nine girls). This is 0.16% of 8270 patients referred to our centre for investigation of possible inborn errors of metabolism over seven year period. Table 1 and 2 summarize the clinical presentations and laboratory data of our cohort respectively. Eleven out of thirteen patients were Malay. Parental consanguinity was noted in two families. 89
12 Malaysian J Pathol December 2010 TABLE 1: Summary of the clinical phenotypes of 13 patients with argininosuccinic aciduria Gender Ethnic Parental consanguinity Age at onset Age at diagnosis Acute treatment Current age Recurrent crises Current status Clinical symptoms 1 # B M no 3d feeding refusal, vomiting, lethargy, seizure, coma 15d a,c - no Died 2 # B M no 3d feeding refusal, vomiting, lethargy 4d a,b 3y no 1,2,3 3 G M yes 3d feeding refusal, vomiting, lethargy, coma 10d c 3.5y no 1,2,4 4 B M no 2d feeding refusal, vomiting, lethargy, coma, respiratory distress 7d a,b,c 5y yes 1,2,5 5 G C no 10d feeding refusal, vomiting, lethargy, coma 21d b,c 2y no 1,2,4 6 G M no 2d feeding refusal, vomiting, lethargy, coma 23d c 1.5y no 1,2,3 7 G M no 3d feeding refusal, vomiting, lethargy, seizure, coma 5d b,c 3m no 1,2,3 8 G I no 13d feeding refusal, vomiting, lethargy, coma 20d a,b,c 7y no 1,2,3 9 G M no 3d feeding refusal, vomiting, hyperirritability, coma 5d a,b,c 2y no 1,2,4 10 G M yes 5 d feeding refusal, vomiting, lethargy, seizure, coma 8 d a,c - no Died 11 B M no 8m feeding refusal, vomiting, lethargy, coma (following febrile illness) 14m c 4.5y no 1,2,4 12 G M no 1y developmental delay, epilepsy, brittle hair 6y - 12y no 1,2,4 13 G M yes 2m developmental delay, epilepsy, recurrent vomiting, growth failure 5y - 11y yes* 1,2,5 B: boy; G: girl; M: Malay; C: Chinese; I: Indian; d: day, m: month; y: year; acute treatment: a, acute dialysis b, intravenous ammonia scavenger drugs; c, ventilator support; current status: 1, protein restricted diet; 2, oral ammonia scavenger drugs; 3, normal development; 4, mild mental retardation; 5, moderate mental retardation. # : Patient 1 and 2 are siblings. *: until five years old. 90
13 ARGININOSUCCINIC ACIDURIA IN MALAYSIAN CHILDREN TABLE 2: Biochemical phenotypes of 13 patients with argininosuccinic aciduria Plasma Urine Urine Plasma Amino Acid ammonia orotic Arginino Arginino Citrulline Arginine Glutamine Alanine PATIENT succinate succinate 1 1,586 not done 1, ,993 3, , , ,172 not done 1, , , , not done , , , , , ,719 1, ,600* 229* , ,848 not done 2, elevated 5, , not detected , ,646 1, elevated 1, , Reference Neonate: absent absent < range <110μmol/L, older mmol/mol (μmol/mmol μmol/l μmol/l μmol/l μmol/l child 50-80μmol/L creatinine of creatinine) *Argininosuccinic acid was detected after protein challenge 91
14 Malaysian J Pathol December 2010 Ten patients (Patient 1 to 10) had the acute neonatal form of the disease, with symptoms of hyperammonemia appearing between the second and thirteenth day after birth. The blood ammonia level ranged from 430μmol/L to 1,848μmol/L. Nine of the ten patients had argininosuccinic acid detected in blood (Fig. 3a) during the acute episode. Argininosuccinate was detected in the blood of Patient 8 only after a protein challenge. Argininosuccinate found in the urine was two to ten times higher in the plasma levels. Plasma glutamine and citrulline levels were elevated in all patients, whereas arginine and ornithine levels were low. Urine orotic acid was measured in five patients and; all of them had raised orotic acids levels, three to thirty times the normal limit. Three patients presented later (between the age of two months and twelve months) with milder clinical symptoms. Late-onset patients excreted significantly less argininosuccinate compared to the neonatal-onset group. In one of the patient, argininosuccinic acid was detected only in urine. Two patients (Patient 1 and 10) with neonatal-onset disease died at the age of 12 days and 4 months when they had a recurrent hyperammonemic coma. However, nine patients survived with a reasonably good neurological outcome; four patients have normal developmental status and five have mild delayed development. Two patients (patient 4 and 13) have severe neurological disabilities as a consequence of recurrent hyperammonemic episodes. DISCUSSION Argininosuccinic aciduria is the second most common disorder of inborn errors of the urea cycle in European countries and the United States. The reported incidence is about 1 in 70,000 live births in the United States. 8 Our study shows a prevalent of 0.16% (13 positive) from 8270 patients referred to our centre for investigation of various inborn errors of metabolism disorder. It is also considered to be the most common disorder of urea cycle diagnosed in our country. The clinical presentation of argininosuccinic aciduria is rather non-specific, just like other urea cycle disorders. Neonatal disease resembles a neonatal infection whereas late-onset disease can mimic many other neurological disorders. 1,2 As such the recognition of argininosuccinic aciduria heavily relies on biochemical laboratory testing. The first clue to alert the clinician and laboratory scientist that he/she may be dealing with argininosuccinic aciduria or a urea cycle disorder in a sick child is raised blood ammonia. It is, therefore, essential to measure ammonia early in every sick child without a clear diagnosis. After excluding false hyperammonemia such as improper sample collection and transportation, struggling or a haemolysed blood sample, blood ammonia more than 200 μmol/l in a previously healthy term newborn or more than 150 μmol/l in an older child is strongly suggestive of an underlying urea cycle disorders such as argininosuccinic aciduria. 2,9 This should prompt the clinician to contact the diagnostic laboratory for urgent plasma and urine amino acids analysis. Plasma quantitative amino acid analysis is necessary to confirm a specific diagnosis of urea cycle disorder. Argininosuccinic aciduria is one of the 3 urea cycle disorders (the other two are citrullinemia and arginase deficiency) in which changes in amino acids are usually diagnostic without the need for further enzymatic or molecular testing. 2,9,10 Presence of argininosuccinate is the characteristic marker for diagnosis of argininosuccinic aciduria, which is usually not detected in a normal person. 11 Other significant amino acids are citrulline and orotic acid. In patients with argininosuccinic aciduria, the plasma citrulline is usually elevated to levels of 150 to 250 μmol/l. Hyperglutaminemia and hyperalaninemia are also often present. Elevated glutamine signifies a hyperammonemic state as glutamine is an ammonia scavenger. Raised plasma alanine is a non specific finding. Under normal circumstances, arginine is produced from argininosuccinate. Hypoargininemia will, therefore, be expected and is a common finding in argininosuccinic aciduria. 11 Although plasma amino acid quantification is diagnostic, potential pitfalls in amino acid analysis need to be recognized. Firstly, argininosuccinic acid is not one of the usual amino acids routinely detected in an amino acids analysis and can easily be misidentified, because it may co-elute with other amino acids especially leucine (Fig 3b). 12 Secondly, argininosuccinate acid is highly soluble and rapidly cleared from blood. Therefore, the amount present may be too little to be detected. As such urinary amino acid analysis is helpful in confirming argininosuccinic aciduria because of the marked excretion of argininosuccinate acid in urine. 11 In addition, urine samples treated with heat or barium precipitation prior 92
15 ARGININOSUCCINIC ACIDURIA IN MALAYSIAN CHILDREN FIG. 3a: Plasma Amino Acid Chromatogram for Patient 1 with Argininosuccinate Lyase Deficiency This chromatogram was obtained at 570nm. The amino acids can be separated because of different pka and hence eluted with different retention times. In this chromatogram, argininosiccinate was eluted immediately after leucine. 1. Aspartic acid, 2. Threonine, 3. Serine, 4. Asparagine, 5. Glutamic acid, 6. Glutamine, 7. Glycine, 8. Alanine, 9. Citrulline 10.Valine, 11. Methionine, 12. Leucine, 13. Tyrosine, 14. Phenylalanine, 15. Ammonium, 16. Ornithine, 17. Lysine, 18. Histidine, 19. Arginine. 93
16 Malaysian J Pathol December 2010 FIG. 3b: Urine Amino Acid Chromatogram for Patient 1 with Argininosuccinate Lyase Deficiency. In ASL deficiency, argininosuccinate which is the characteristic urinary marker, is excreted in large amount (1084 μmol/mmol creatinine ), and some of these are converted into anhydride forms. In this chromatogram, the two anhydrides of argininosuccinate are eluted at the retention time of homocysteine and gaba peaks, whereas argininosuccinate is eluted closely after the leucine peak. 1. Aspartic acid, 2. Threonine, 3. Serine, 4. Asparagine, 5. Glutamic acid, 6. Glutamine, 7. Glycine, 8. Alanine, 9. Citrulline 10. Valine, 11. Methionine, 12. Leucine, 13. Tyrosine, 14. Phenylalanine, 15. Ammonium, 16. Ornithine, 17. Lysine, 18. Histidine, 19. Arginine. 94
17 ARGININOSUCCINIC ACIDURIA IN MALAYSIAN CHILDREN to analysis will further improve the sensitivity of detection by converting the argininosuccinic acid into anhydrides. 12 Nevertheless, quantitative analysis of urine amino acids is generally not useful for diagnosis of most amino acid disorders and other urea cycle disorders. This is because urine amino acids concentrations do not reflect the true amino acid concentration in blood due to the effect of renal reabsorption. Urine argininosuccinate quantitative analysis is one of the few exceptions. A favourable outcome can be achieved if argininosuccinic aciduria is diagnosed early. Immediate treatment may include acute dialysis to rapidly remove ammonia which is extremely toxic to the brain. Long term treatment will normally include dietary protein restriction, arginine supplementation, use of pharmacological ammonia scavengers such as sodium benzoate and sodium phenylbutyrate. 13 In conclusion, clinicians should always consider the possibility of a child with unexplained illness, or without a clear explanation, having an inborn error of metabolism such as argininosuccinic aciduria. Close collaboration with the laboratory is potentially life saving. ACKNOWLEDGEMENT The authors like to thank all the paediatricians who have referred patients to us, all the patients and their families, and the staff of Metabolic Clinic (Ms Balktiah Mat and Ms Norzawani Che Johari) for assisting in the retrieval of medical records. The authors also wish to thank Dr Keng Wee Teik, Dr. Shanti B, Dr Ch ng Gaik Siew for their clinical support, and the staff of Biochemical Genetics Unit ( Ms Huzaimah bte Sani, Ms Tengku Rosmaliza, Mr Mohd Helmi and Miss Komalam) for their excellent technical assistance. metabolic diseases. Heidelberg, Germany: Springer; p Nagata N, Matsuda I, Oyanagi K. Estimated frequency of urea cycle enzymopathies in Japan, Am J Med Genet. 1991; 39: Berry GT, Steiner RD. Long-term management of patients with urea cycle disorders. J Pediatr 2001;138 (Suppl 1): S56 S Leonard JV. Inherited hyperammonemias. In: Blau N, Hoffmann GF, Leonard VJ, Clarke JTR. editors. Physician s guide to the treatment and follow-up of metabolic diseases. Springer-Verlag Berlin; Heidelberg, 2006.p Bourrier P, Varache N, Alquier P, Rabier D, Kamoun P, Lorre G, Alhayek G. Cerebral edema with hyperammonemia in valpromide poisoning. Manifestation in an adult, of a partial deficit in type I carbamylphosphate synthetase. Presse Med.1988; 17: Scaglia F, Brunetti-Pierr N, Kleppe S, et al. Clinical consequences of urea cycle enzyme deficiencies and potential links to arginine and nitric oxide metabolism. J Nutr. 2004; 134 (10 Suppl): 2775S- 2782S. 9. Barsotti RJ. Measurement of ammonia in blood. J Pediatr 2001; 138 (1 Suppl): S Tuchman M, Yudkoff M. Blood levels of ammonia and nitrogen scavenging amino acids in patients with inherited hyperammonemia. Mol Genet Metab. 1999; 66: Palmer T, Oberholzer VG, Levin B, Burges EA. Urinary excretion of argininosuccinic acid. Clin Chim Acta. 1973; 47: Steiner RD, Cederbaum SD. Laboratory evaluation of urea cycle disorders. J Pediatr. 2001; 138 (1 Suppl):: S Enns GM, Berry SA, Berry GT, Rhead WJ, Brusilow SW, Hamosh A. Survival after treatment with phenylacetate and benzoate for urea-cycle disorders. N Engl J Med. 2007; 356(22): REFERENCES 1. Brusilow SW, Horwich AL. Urea cycle enzymes. In: Scriver CR, Beaudet AL, Sly WS, Valle D, editors; Childs B, Kinzler KW, Vogelstein B, assoc. editors. The metabolic and molecular bases of inherited disease, 8th ed. New York: McGraw-Hill; p Leonard JV. Disorders of the Urea Cycle and Related Enzymes In: John Fernandes, Jean-Marie Saudubray, Georges van den Berghe, John H. Walter, editors. Inborn metabolic diseases. Heidelberg: Springer Medizin Verlag; p Bachmann C. Inherited hyperammonemias. In: Blau N, Hoffmann GE, Leonard J, Clarke JTR. editors. Physician s guide to the laboratory diagnosis of 95
Urea Cycle Defects. Dr Mick Henderson. Biochemical Genetics Leeds Teaching Hospitals Trust. MetBioNet IEM Introductory Training
 Urea Cycle Defects Dr Mick Henderson Biochemical Genetics Leeds Teaching Hospitals Trust The Urea Cycle The urea cycle enables toxic ammonia molecules to be converted to the readily excreted and non toxic
Urea Cycle Defects Dr Mick Henderson Biochemical Genetics Leeds Teaching Hospitals Trust The Urea Cycle The urea cycle enables toxic ammonia molecules to be converted to the readily excreted and non toxic
LOW CITRULLINE AS A MARKER FOR THE PROXIMAL UREA CYCLE DEFECTS EXPERIENCE OF THE NEW ENGLAND NEWBORN SCREENING PROGRAM
 LOW CITRULLINE AS A MARKER FOR THE PROXIMAL UREA CYCLE DEFECTS EXPERIENCE OF THE NEW ENGLAND NEWBORN SCREENING PROGRAM Inderneel Sahai, MD, FACMG Newborn Screening and Genetic Testing Symposium Oct 2014
LOW CITRULLINE AS A MARKER FOR THE PROXIMAL UREA CYCLE DEFECTS EXPERIENCE OF THE NEW ENGLAND NEWBORN SCREENING PROGRAM Inderneel Sahai, MD, FACMG Newborn Screening and Genetic Testing Symposium Oct 2014
UREA CYCLE DISORDERS - The What, Why, How and When
 UREA CYCLE DISORDERS - The What, Why, How and When George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Department of Pediatrics Icahn School of
UREA CYCLE DISORDERS - The What, Why, How and When George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Department of Pediatrics Icahn School of
Urea Cycle Disorders Prior Authorization Program Summary
 Urea Cycle Disorders Prior Authorization Program Summary FDA APPROVED INDICATIONS DOSAGE 1,2 Agent(s) Indication(s) Dosing -Adjunctive therapy in the chronic management of patients with urea cycle disorders
Urea Cycle Disorders Prior Authorization Program Summary FDA APPROVED INDICATIONS DOSAGE 1,2 Agent(s) Indication(s) Dosing -Adjunctive therapy in the chronic management of patients with urea cycle disorders
ESPEN Congress Madrid 2018
 ESPEN Congress Madrid 2018 Inborn Errors Of Metabolism Urea Cycle Disorders Diagnosis And Care F. Feillet (FR) Urea cycle disorders, diagnosis and care F Feillet National reference centre for Inborn errors
ESPEN Congress Madrid 2018 Inborn Errors Of Metabolism Urea Cycle Disorders Diagnosis And Care F. Feillet (FR) Urea cycle disorders, diagnosis and care F Feillet National reference centre for Inborn errors
Proceedings of a Consensus Conference for the
 Proceedings of a Consensus Conference for the Management of Patients with Urea Cycle Disorders Marshall Summar, MD, and Mendel Tuchman, MD In an effort to develop standards for the treatment of patients
Proceedings of a Consensus Conference for the Management of Patients with Urea Cycle Disorders Marshall Summar, MD, and Mendel Tuchman, MD In an effort to develop standards for the treatment of patients
TRANSAMINATION AND UREA CYCLE
 TRANSAMINATION AND UREA CYCLE USMAN SUMO FRIEND TAMBUNAN ARLI ADITYA PARIKESIT SEPTIANA BIOINFORMATICS GROUP DEPARTEMENT OF CHEMISTRY FACULTY OF MATHEMATIC AND SCIENCE UNIVERSITY OF INDONESIA What is transamination?
TRANSAMINATION AND UREA CYCLE USMAN SUMO FRIEND TAMBUNAN ARLI ADITYA PARIKESIT SEPTIANA BIOINFORMATICS GROUP DEPARTEMENT OF CHEMISTRY FACULTY OF MATHEMATIC AND SCIENCE UNIVERSITY OF INDONESIA What is transamination?
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Urea Cycle Disorders Page 1 of 7 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Urea Cycle Disorders Prime Therapeutics will review Prior Authorization requests
Urea Cycle Disorders Page 1 of 7 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Urea Cycle Disorders Prime Therapeutics will review Prior Authorization requests
UPDATE ON UREA CYCLE DISORDERS TREATMENT
 UPDATE ON UREA CYCLE DISORDERS TREATMENT George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Icahn School of Medicine at Mount Sinai Disclosure
UPDATE ON UREA CYCLE DISORDERS TREATMENT George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Icahn School of Medicine at Mount Sinai Disclosure
Jana Novotná, Bruno Sopko. Department of the Medical Chemistry and Clinical Biochemistry The 2nd Faculty of Medicine, Charles Univ.
 Amino acid metabolism II. Urea cycle Jana Novotná, Bruno Sopko Department of the Medical Chemistry and Clinical Biochemistry The 2nd Faculty of Medicine, Charles Univ. Nitrogen balance Tissue proteins
Amino acid metabolism II. Urea cycle Jana Novotná, Bruno Sopko Department of the Medical Chemistry and Clinical Biochemistry The 2nd Faculty of Medicine, Charles Univ. Nitrogen balance Tissue proteins
Hyperammonemia: Diagnostic Experience At The Metabolism Laboratory
 ISPUB.COM The Internet Journal of Laboratory Medicine Volume 1 Number 2 Hyperammonemia: Diagnostic Experience At The Metabolism Laboratory A Rao, P Varma, Sumitra, S Dhanya Citation A Rao, P Varma, Sumitra,
ISPUB.COM The Internet Journal of Laboratory Medicine Volume 1 Number 2 Hyperammonemia: Diagnostic Experience At The Metabolism Laboratory A Rao, P Varma, Sumitra, S Dhanya Citation A Rao, P Varma, Sumitra,
First report of carglumic acid in a patient with citrullinemia type 1 (argininosuccinate synthetase deficiency)
 Received: 14 June 2017 Accepted: 20 June 2017 DOI: 10.1111/jcpt.12593 CASE REPORT First report of carglumic acid in a patient with citrullinemia type 1 (argininosuccinate synthetase deficiency) E. Kose
Received: 14 June 2017 Accepted: 20 June 2017 DOI: 10.1111/jcpt.12593 CASE REPORT First report of carglumic acid in a patient with citrullinemia type 1 (argininosuccinate synthetase deficiency) E. Kose
METABOLISMO DE AMINOÁCIDOS
 DEZ 2015 METABOLISMO DE AMINOÁCIDOS Licenciatura em Ciências da Saúde (Ano 2015-2016) Isabel Tavares de Almeida Faculdade de Farmácia da ULisboa PROTEIN DEGRADATION - DIGESTION AMINO ACID STRUCTURE 2-,
DEZ 2015 METABOLISMO DE AMINOÁCIDOS Licenciatura em Ciências da Saúde (Ano 2015-2016) Isabel Tavares de Almeida Faculdade de Farmácia da ULisboa PROTEIN DEGRADATION - DIGESTION AMINO ACID STRUCTURE 2-,
Carbamoyl Phosphate Synthetase (code 50470) Notice of Assessment
 Carbamoyl Phosphate Synthetase (code 50470) Notice of Assessment June 2013 DISCLAIMER: This document was originally drafted in French by the Institut national d'excellence en santé et en services sociaux
Carbamoyl Phosphate Synthetase (code 50470) Notice of Assessment June 2013 DISCLAIMER: This document was originally drafted in French by the Institut national d'excellence en santé et en services sociaux
Carbamoyl phosphate synthetase 1 deficiency: First report of this rare metabolic disorder in Kingdom of Bahrain with novel mutation
 Alsahlawi et al. 1 CASE REPORT PEER REVIEWED OPEN ACCESS Carbamoyl phosphate synthetase 1 deficiency: First report of this rare metabolic disorder in Kingdom of Bahrain with novel mutation Z. Alsahlawi,
Alsahlawi et al. 1 CASE REPORT PEER REVIEWED OPEN ACCESS Carbamoyl phosphate synthetase 1 deficiency: First report of this rare metabolic disorder in Kingdom of Bahrain with novel mutation Z. Alsahlawi,
Urea Cycle Disorders and Hyperammonemia: Diagnosable Treatable Screenable
 Urea Cycle Disorders and Hyperammonemia: Diagnosable Treatable Screenable Marshall L. Summar, M.D. Chief, Division of Genetics and Metabolism Children s National Medical Center Washington, DC, USA Disclosure
Urea Cycle Disorders and Hyperammonemia: Diagnosable Treatable Screenable Marshall L. Summar, M.D. Chief, Division of Genetics and Metabolism Children s National Medical Center Washington, DC, USA Disclosure
UNDERSTANDING UREA CYCLE DISORDERS
 UNDERSTANDING UREA CYCLE DISORDERS What is a urea cycle disorder? A urea cycle disorder is a genetic disease that affects how protein is broken down in the body. It is therefore classified as a metabolic
UNDERSTANDING UREA CYCLE DISORDERS What is a urea cycle disorder? A urea cycle disorder is a genetic disease that affects how protein is broken down in the body. It is therefore classified as a metabolic
Urea is the major end product of nitrogen catabolism in humans One nitrogen free NH3 other nitrogen aspartate. carbon oxygen CO2 liver,
 Urea is the major end product of nitrogen catabolism in humans Urea is the major disposal form of amino groups derived from amino acids, and accounts about 90% percent of the nitrogencontaining components
Urea is the major end product of nitrogen catabolism in humans Urea is the major disposal form of amino groups derived from amino acids, and accounts about 90% percent of the nitrogencontaining components
ERNDIM QC Schemes. Diagnostic Proficiency Scheme. Practice at Reporting and Interpretation
 ERNDIM QC Schemes Diagnostic Proficiency Scheme Practice at Reporting and Interpretation ERNDIM Proficiency Scheme: Design Clinical picture Lab results and interpretation Pre-investigations Amino acid
ERNDIM QC Schemes Diagnostic Proficiency Scheme Practice at Reporting and Interpretation ERNDIM Proficiency Scheme: Design Clinical picture Lab results and interpretation Pre-investigations Amino acid
Amino Acid Oxidation and the Urea Cycle
 Amino Acid Oxidation and the Urea Cycle Amino Acids: Final class of biomolecules whose oxidation contributes significantly to the generation of energy Undergo oxidation in three metabolic circumstances
Amino Acid Oxidation and the Urea Cycle Amino Acids: Final class of biomolecules whose oxidation contributes significantly to the generation of energy Undergo oxidation in three metabolic circumstances
Lab Guide 2019 Metabolic Section Lab Guide
 Lab Guide 2019 Metabolic Section Lab Guide Quantitative Amino acids Plasma Plasma. Container/Tube: Preferred EDTA, Place immediately in ice. Acceptable: lithium heparin, sodium heparin. Patient preparation:
Lab Guide 2019 Metabolic Section Lab Guide Quantitative Amino acids Plasma Plasma. Container/Tube: Preferred EDTA, Place immediately in ice. Acceptable: lithium heparin, sodium heparin. Patient preparation:
Fate of Dietary Protein
 Fate of Dietary Protein Dietary protein Stomach: l, pepsin Denatured and partially hydrolyzed protein (large polypeptides) small intestine: proteases Amino acids and dipeptides intestinal lining: proteases
Fate of Dietary Protein Dietary protein Stomach: l, pepsin Denatured and partially hydrolyzed protein (large polypeptides) small intestine: proteases Amino acids and dipeptides intestinal lining: proteases
Amino Acid Metabolism
 Amino Acid Metabolism Fate of Dietary Protein Dietary protein Stomach: l, pepsin Denatured and partially hydrolyzed protein (large polypeptides) small intestine: proteases Amino acids and dipeptides intestinal
Amino Acid Metabolism Fate of Dietary Protein Dietary protein Stomach: l, pepsin Denatured and partially hydrolyzed protein (large polypeptides) small intestine: proteases Amino acids and dipeptides intestinal
THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE
 THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE Dr. Nadeem Qureshi M.D, FAAP, FCCM Associate Professor Pediatrics School of Medicine. St Louis University Attending Physician Pediatric Emergency
THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE Dr. Nadeem Qureshi M.D, FAAP, FCCM Associate Professor Pediatrics School of Medicine. St Louis University Attending Physician Pediatric Emergency
AMINO ACID METABOLISM
 AMINO ACID METABOLISM Synthesis of Urea in Liver The series of reactions that form urea is known as the Urea Cycle or the Krebs-Henseleit Cycle. The urea cycle operates only to eliminate excess nitrogen.
AMINO ACID METABOLISM Synthesis of Urea in Liver The series of reactions that form urea is known as the Urea Cycle or the Krebs-Henseleit Cycle. The urea cycle operates only to eliminate excess nitrogen.
UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA
 UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA Hyperammonaemia results from defective catabolism of amino acids to urea. Recognition and treatment of hyperammonaemia,
UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA Hyperammonaemia results from defective catabolism of amino acids to urea. Recognition and treatment of hyperammonaemia,
AMINOACID METABOLISM FATE OF AMINOACIDS & UREA CYCLE
 AMINOACID METABOLISM FATE OF AMINOACIDS & UREA CYCLE SOURCE & FATE OF AA The aminoacids obtained from DIETARY SOURCE or BODY PROTEIN TURNOVER are utilized for protein biosynthesis and the production of
AMINOACID METABOLISM FATE OF AMINOACIDS & UREA CYCLE SOURCE & FATE OF AA The aminoacids obtained from DIETARY SOURCE or BODY PROTEIN TURNOVER are utilized for protein biosynthesis and the production of
Lecture 10 - Protein Turnover and Amino Acid Catabolism
 Lecture 10 - Protein Turnover and Amino Acid Catabolism Chem 454: Regulatory Mechanisms in Biochemistry University of Wisconsin-Eau Claire 1 Introduction 2 Proteins are degraded into amino acids. Protein
Lecture 10 - Protein Turnover and Amino Acid Catabolism Chem 454: Regulatory Mechanisms in Biochemistry University of Wisconsin-Eau Claire 1 Introduction 2 Proteins are degraded into amino acids. Protein
CASE SERIES Biochemical and molecular characteristics of Malaysian patients with lysinuric protein intolerance
 Malaysian J Pathol 2016; 38(3) : 305 310 CASE SERIES Biochemical and molecular characteristics of Malaysian patients with lysinuric protein intolerance Anasufiza HABIB MBChB, MPath, Nor Azimah AZIZE* BSc,
Malaysian J Pathol 2016; 38(3) : 305 310 CASE SERIES Biochemical and molecular characteristics of Malaysian patients with lysinuric protein intolerance Anasufiza HABIB MBChB, MPath, Nor Azimah AZIZE* BSc,
TITLE: NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH UREA CYCLE DEFECTS. Eilish O Connell, Clinical Education Facilitator, NCIMD
 NO. OF PAGES: Page 1 of 16 SUPERCEDES: N/A NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH UREA CYCLE DEFECTS NAME/ Eilish O Connell, Clinical Education Facilitator, NCIMD SIGNATURE: DATE: NAME/
NO. OF PAGES: Page 1 of 16 SUPERCEDES: N/A NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH UREA CYCLE DEFECTS NAME/ Eilish O Connell, Clinical Education Facilitator, NCIMD SIGNATURE: DATE: NAME/
Ornithine Transcarbamylase Deficiency (OTCD) Recommendations on Emergency Management of Metabolic Disease
 Ornithine Transcarbamylase Deficiency (OTCD) Recommendations on Emergency Management of Metabolic Disease Patient s Name: Date of Birth: MRN in KFSH&RC: Please read carefully. Meticulous and prompt treatment
Ornithine Transcarbamylase Deficiency (OTCD) Recommendations on Emergency Management of Metabolic Disease Patient s Name: Date of Birth: MRN in KFSH&RC: Please read carefully. Meticulous and prompt treatment
Amino Acid Metabolism
 Amino Acid Metabolism The continuous degradation and synthesis of cellular proteins occur in all forms of life. Each day humans turn over 1 2% of their total body protein, principally muscle protein. Approximately
Amino Acid Metabolism The continuous degradation and synthesis of cellular proteins occur in all forms of life. Each day humans turn over 1 2% of their total body protein, principally muscle protein. Approximately
Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis)
 Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis) 1) Argininosuccinic acidemia (ASA) a) Incidence: ~1 in 70,000 b) Deficiency in an enzyme of
Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis) 1) Argininosuccinic acidemia (ASA) a) Incidence: ~1 in 70,000 b) Deficiency in an enzyme of
Senior Vice President, Medical Affairs and Health Outcomes, 150 South Saunders Road, Lake Forest, IL 60045, Horizon Pharma USA, Inc, USA
 Research Hyperammonemic crises in patients with urea cycle disorders on chronic nitrogen scavenger therapy with either sodium phenylbutyrate or glycerol phenylbutyrate Jeffrey D Kent 1, Robert J Holt,2
Research Hyperammonemic crises in patients with urea cycle disorders on chronic nitrogen scavenger therapy with either sodium phenylbutyrate or glycerol phenylbutyrate Jeffrey D Kent 1, Robert J Holt,2
ARGININOSUCCINIC ACIDEMIA (or ARGININOSUCCINATE LYASE DEFICIENCY) RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES
 ARGININOSUCCINIC ACIDEMIA (or ARGININOSUCCINATE LYASE DEFICIENCY) RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt
ARGININOSUCCINIC ACIDEMIA (or ARGININOSUCCINATE LYASE DEFICIENCY) RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt
Biochemistry: A Short Course
 Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 30 Amino Acid Degradation and the Urea Cycle 2013 W. H. Freeman and Company In the cytosol of a cell amino groups from amino acids
Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 30 Amino Acid Degradation and the Urea Cycle 2013 W. H. Freeman and Company In the cytosol of a cell amino groups from amino acids
Urea cycle disorders (UCD) compromise a group of inherited metabolic disorders with an estimated overall prevalence
 Early Clinical Manifestations and Eating Patterns in Patients with Urea Cycle Disorders Thatjana Gardeitchik, MD 1,2, Maureen Humphrey, APD 1,3, Judy Nation, APD 1,3, and Avihu Boneh, MD, PhD 1,4 Objectives
Early Clinical Manifestations and Eating Patterns in Patients with Urea Cycle Disorders Thatjana Gardeitchik, MD 1,2, Maureen Humphrey, APD 1,3, Judy Nation, APD 1,3, and Avihu Boneh, MD, PhD 1,4 Objectives
Survival after Treatment with Phenylacetate and Benzoate for Urea-Cycle Disorders
 T h e n e w e ng l a nd j o u r na l o f m e dic i n e original article Survival after Treatment with Phenylacetate and Benzoate for Urea-Cycle Disorders Gregory M. Enns, M.B., Ch.B., Susan A. Berry, M.D.,
T h e n e w e ng l a nd j o u r na l o f m e dic i n e original article Survival after Treatment with Phenylacetate and Benzoate for Urea-Cycle Disorders Gregory M. Enns, M.B., Ch.B., Susan A. Berry, M.D.,
Amino Acid Analyzer AAA400
 Amino Acid Analyzer AAA400 Determination of amino acid of hydrolyzates (food and feed) Column: LG ANB OSTION 3.6x340 12μm Eluents: sodium-citrate buffers, 0.2 M NaOH Aspartic Acid, Threonine, Serine, Glutamic
Amino Acid Analyzer AAA400 Determination of amino acid of hydrolyzates (food and feed) Column: LG ANB OSTION 3.6x340 12μm Eluents: sodium-citrate buffers, 0.2 M NaOH Aspartic Acid, Threonine, Serine, Glutamic
NITROGEN METABOLISM An Overview
 1 University of Papua New Guinea School of Medicine and Health Sciences Division of Basic Medical Sciences Discipline of Biochemistry and Molecular Biology PBL Seminar & Health Sciences NITROGEN METABOLISM
1 University of Papua New Guinea School of Medicine and Health Sciences Division of Basic Medical Sciences Discipline of Biochemistry and Molecular Biology PBL Seminar & Health Sciences NITROGEN METABOLISM
Quantitative Analysis of Underivatized Amino Acids in Plant Matrix by Hydrophilic Interaction Chromatography (HILIC) with LC/MS Detection
 Application Note Food Testing, Metabolomics, Agricultural Chemistry, Environmental Quantitative Analysis of Underivatized Amino Acids in Plant Matrix by Hydrophilic Interaction Chromatography (HILIC) with
Application Note Food Testing, Metabolomics, Agricultural Chemistry, Environmental Quantitative Analysis of Underivatized Amino Acids in Plant Matrix by Hydrophilic Interaction Chromatography (HILIC) with
NITROGEN METABOLISM: An Overview
 NITROGEN METABOLISM: An Overview University of PNG School of Medicine and Health Sciences Division of Basic Medical Sciences Discipline of Biochemistry & Molecular Biology VJ Temple 1 How are nitrogen-containing
NITROGEN METABOLISM: An Overview University of PNG School of Medicine and Health Sciences Division of Basic Medical Sciences Discipline of Biochemistry & Molecular Biology VJ Temple 1 How are nitrogen-containing
M1 - Renal, Fall 2007
 University of Michigan Deep Blue deepblue.lib.umich.edu 2007-09 M1 - Renal, Fall 2007 Lyons, R.; Burney, R. Lyons, R., Burney, R. (2008, August 07). Renal. Retrieved from Open.Michigan - Educational Resources
University of Michigan Deep Blue deepblue.lib.umich.edu 2007-09 M1 - Renal, Fall 2007 Lyons, R.; Burney, R. Lyons, R., Burney, R. (2008, August 07). Renal. Retrieved from Open.Michigan - Educational Resources
Biochemistry: A Short Course
 Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 30 Amino Acid Degradation and the Urea Cycle 2013 W. H. Freeman and Company Chapter 30 Outline Amino acids are obtained from the
Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 30 Amino Acid Degradation and the Urea Cycle 2013 W. H. Freeman and Company Chapter 30 Outline Amino acids are obtained from the
New developments in Urea Cycle Disorders and its impact on patients
 New developments in Urea Cycle Disorders and its impact on patients Johannes Häberle University Children s Hospital Zurich, Division of Metabolism 16 June 2015 SFEIM 2015, Lille, France The urea cycle
New developments in Urea Cycle Disorders and its impact on patients Johannes Häberle University Children s Hospital Zurich, Division of Metabolism 16 June 2015 SFEIM 2015, Lille, France The urea cycle
Age-related reference ranges
 Authoriser: Peter Beresford Page 1 of 6 Age-related reference ranges Alkaline Phosphatase (ALP) IU/L Both less than 14 days 90 273 Both 14 days
Authoriser: Peter Beresford Page 1 of 6 Age-related reference ranges Alkaline Phosphatase (ALP) IU/L Both less than 14 days 90 273 Both 14 days
Advances in UCD treatment and management of UCDs
 Advances in UCD treatment and management of UCDs Brendan Lee M.D.,Ph.D. Howard Hughes Medical Institute Department of Molecular and Human Genetics Baylor College of Medicine Nitrogen and the urea cycle
Advances in UCD treatment and management of UCDs Brendan Lee M.D.,Ph.D. Howard Hughes Medical Institute Department of Molecular and Human Genetics Baylor College of Medicine Nitrogen and the urea cycle
Amino acid metabolism
 Amino acid metabolism The important reaction commonly employed in the breakdown of an amino acid is always the removal of its -amino group. The product ammonia is excreted after conversion to urea or other
Amino acid metabolism The important reaction commonly employed in the breakdown of an amino acid is always the removal of its -amino group. The product ammonia is excreted after conversion to urea or other
Effect of Excess of Individual Essential Amino Acids in Diets on Chicks
 135 Effect of Excess of Individual Essential Amino Acids in Diets on Chicks Jun-ichi OKUMURA and Kiyoto YAMAGUCHI Laboratory of Animal Nutrition, Faculty of Agriculture, Nagoya University, Nagoya-shi 464
135 Effect of Excess of Individual Essential Amino Acids in Diets on Chicks Jun-ichi OKUMURA and Kiyoto YAMAGUCHI Laboratory of Animal Nutrition, Faculty of Agriculture, Nagoya University, Nagoya-shi 464
Analysis of Amino Acids Derived Online Using an Agilent AdvanceBio AAA Column
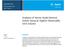 Application Note Pharmaceutical and Food Testing Analysis of Amino Acids Derived Online Using an Agilent AdvanceBio AAA Column Author Lu Yufei Agilent Technologies, Inc. Abstract A liquid chromatographic
Application Note Pharmaceutical and Food Testing Analysis of Amino Acids Derived Online Using an Agilent AdvanceBio AAA Column Author Lu Yufei Agilent Technologies, Inc. Abstract A liquid chromatographic
Amino acid Catabolism
 Enzymatic digestion of dietary proteins in gastrointestinal-tract. Amino acid Catabolism Amino acids: 1. There are 20 different amino acid, they are monomeric constituents of proteins 2. They act as precursors
Enzymatic digestion of dietary proteins in gastrointestinal-tract. Amino acid Catabolism Amino acids: 1. There are 20 different amino acid, they are monomeric constituents of proteins 2. They act as precursors
Volume 3 (2017) Issue 10 ISSN Keywords. Introduction. Case Report. Open Journal of Clinical & Medical Case Reports
 Open Journal of Clinical & Medical Case Reports Volume 3 (2017) Issue 10 ISSN 2379-1039 Recurrent hyperammonemia in an 80-year-old woman with congenital urea cycle abnormality Junji Yamaguchi, MD*; Koichi
Open Journal of Clinical & Medical Case Reports Volume 3 (2017) Issue 10 ISSN 2379-1039 Recurrent hyperammonemia in an 80-year-old woman with congenital urea cycle abnormality Junji Yamaguchi, MD*; Koichi
Nitrogen Metabolism. Overview
 Nitrogen Metabolism Pratt and Cornely Chapter 18 Overview Nitrogen assimilation Amino acid biosynthesis Nonessential aa Essential aa Nucleotide biosynthesis Amino Acid Catabolism Urea Cycle Juicy Steak
Nitrogen Metabolism Pratt and Cornely Chapter 18 Overview Nitrogen assimilation Amino acid biosynthesis Nonessential aa Essential aa Nucleotide biosynthesis Amino Acid Catabolism Urea Cycle Juicy Steak
Module : Clinical correlates of disorders of metabolism Block 3, Week 2
 Module : Clinical correlates of disorders of metabolism Block 3, Week 2 Department of Paediatrics and Child Health University of Pretoria Tutor : Prof DF Wittenberg : dwittenb@medic.up.ac.za Aim of this
Module : Clinical correlates of disorders of metabolism Block 3, Week 2 Department of Paediatrics and Child Health University of Pretoria Tutor : Prof DF Wittenberg : dwittenb@medic.up.ac.za Aim of this
BCH 447. Estimation of Serum Urea
 BCH 447 Estimation of Serum Urea 1 Objective: Estimation of Blood urea nitrogen (BUN) in serum sample. 2 -Urea: Urea is the highest non-protein nitrogen compound in the blood. Urea is the major excretory
BCH 447 Estimation of Serum Urea 1 Objective: Estimation of Blood urea nitrogen (BUN) in serum sample. 2 -Urea: Urea is the highest non-protein nitrogen compound in the blood. Urea is the major excretory
Metabolic Disorders. Chapter Thomson - Wadsworth
 Metabolic Disorders Chapter 28 1 Metabolic Disorders Inborn errors of metabolism group of diseases that affect a wide variety of metabolic processes; defective processing or transport of amino acids, fatty
Metabolic Disorders Chapter 28 1 Metabolic Disorders Inborn errors of metabolism group of diseases that affect a wide variety of metabolic processes; defective processing or transport of amino acids, fatty
Hyperammonemia due to urea cycle disorders: a potentially fatal condition in the intensive care setting
 Machado and Pinheiro da Silva Journal of Intensive Care 2014, 2:22 REVIEW Open Access Hyperammonemia due to urea cycle disorders: a potentially fatal condition in the intensive care setting Marcel Cerqueira
Machado and Pinheiro da Silva Journal of Intensive Care 2014, 2:22 REVIEW Open Access Hyperammonemia due to urea cycle disorders: a potentially fatal condition in the intensive care setting Marcel Cerqueira
Scottish Medicines Consortium
 Scottish Medicines Consortium carglumic acid 200mg dispersible tablets (Carbaglu ) No. 299/06 Orphan Europe 8 September 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the
Scottish Medicines Consortium carglumic acid 200mg dispersible tablets (Carbaglu ) No. 299/06 Orphan Europe 8 September 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the
Newborn Screening & Methods for Diagnosing Inborn Errors of Metabolism
 Newborn Screening & Methods for Diagnosing Inborn Errors of Metabolism Patricia Jones, PhD DABCC FACB UT Southwestern Medical Center Children s Medical Center Dallas, Texas Learning Objectives Justify
Newborn Screening & Methods for Diagnosing Inborn Errors of Metabolism Patricia Jones, PhD DABCC FACB UT Southwestern Medical Center Children s Medical Center Dallas, Texas Learning Objectives Justify
Urea cycle disorder presenting as bilateral mesial temporal sclerosis an unusual cause of seizures: a case report and review of the literature
 Wang et al. Journal of Medical Case Reports (2018) 12:208 https://doi.org/10.1186/s13256-018-1750-8 CASE REPORT Open Access Urea cycle disorder presenting as bilateral mesial temporal sclerosis an unusual
Wang et al. Journal of Medical Case Reports (2018) 12:208 https://doi.org/10.1186/s13256-018-1750-8 CASE REPORT Open Access Urea cycle disorder presenting as bilateral mesial temporal sclerosis an unusual
Annual Report ERNDIM-EQAS Quantitative Amino Acids 2002
 Annual Report ERNDIM-EQAS Quantitative Amino Acids 2002 1. Purpose The purpose of the ERNDIM External Quality Assurance Scheme for Quantitative Organic Acids is the monitoring of the analytical quality
Annual Report ERNDIM-EQAS Quantitative Amino Acids 2002 1. Purpose The purpose of the ERNDIM External Quality Assurance Scheme for Quantitative Organic Acids is the monitoring of the analytical quality
Amino acids. Ing. Petrová Jaroslava. Workshop on Official Controls of Feed AGR 46230, , Ankara. Turkey ÚKZÚZ - NRL RO Praha 1
 Amino acids Ing. Petrová Jaroslava Workshop on Official Controls of Feed AGR 46230, 6. 7. 12. 2011, Ankara. Turkey 6.12.2011 ÚKZÚZ - NRL RO Praha 1 Content of this presentation 1. Function of amino acids
Amino acids Ing. Petrová Jaroslava Workshop on Official Controls of Feed AGR 46230, 6. 7. 12. 2011, Ankara. Turkey 6.12.2011 ÚKZÚZ - NRL RO Praha 1 Content of this presentation 1. Function of amino acids
Amino Acid Disorders. What is ASAL deficiency? Genetic Fact Sheets for Parents
 Genetic Fact Sheets for Parents Amino Acid Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social issues
Genetic Fact Sheets for Parents Amino Acid Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social issues
0010 Amino Acids 40 Profile - Plasma
 Accession #: Order #: G1234567 Date Collected: Date Received: 01/22/2013 Reference #: Patient: Date of Birth: 02/05/1962 Date of Report: Telephone: 7704464583 Ordering Physician: 1234 Main St. Anywhere,
Accession #: Order #: G1234567 Date Collected: Date Received: 01/22/2013 Reference #: Patient: Date of Birth: 02/05/1962 Date of Report: Telephone: 7704464583 Ordering Physician: 1234 Main St. Anywhere,
[ APPLICATION NOTE ] UPLC-MS/MS Analysis of 45 Amino Acids Using the Kairos Amino Acid Kit for Biomedical Research INTRODUCTION APPLICATION BENEFITS
![[ APPLICATION NOTE ] UPLC-MS/MS Analysis of 45 Amino Acids Using the Kairos Amino Acid Kit for Biomedical Research INTRODUCTION APPLICATION BENEFITS [ APPLICATION NOTE ] UPLC-MS/MS Analysis of 45 Amino Acids Using the Kairos Amino Acid Kit for Biomedical Research INTRODUCTION APPLICATION BENEFITS](/thumbs/88/117895443.jpg) UPLC-MS/MS Analysis of 45 Amino Acids Using the Kairos Amino Acid Kit for Biomedical Research Padhraic Rossiter, 1 Jaime Salcedo Dominguez, 1 Jennifer Warren, 1 Norma Breen, 1 Lisa Calton 2 1 Waters Corporation,
UPLC-MS/MS Analysis of 45 Amino Acids Using the Kairos Amino Acid Kit for Biomedical Research Padhraic Rossiter, 1 Jaime Salcedo Dominguez, 1 Jennifer Warren, 1 Norma Breen, 1 Lisa Calton 2 1 Waters Corporation,
Diagnostic Proficiency Testing Survey Annual Report
 ERNDIM DPT Centre Basel University Children s Hospital Metabolic Unit Postfach, CH-4005 Basel, Switzerland phone: ++41 61 704 2826 Diagnostic Proficiency Testing Survey 2010 Annual Report prepared by Brian
ERNDIM DPT Centre Basel University Children s Hospital Metabolic Unit Postfach, CH-4005 Basel, Switzerland phone: ++41 61 704 2826 Diagnostic Proficiency Testing Survey 2010 Annual Report prepared by Brian
Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT
 Great Ormond Street Hospital London 20/04/2018 Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT Spyros P. Batzios, MD, MSc, PhD OAs & UCDs How do they present? neonatal
Great Ormond Street Hospital London 20/04/2018 Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT Spyros P. Batzios, MD, MSc, PhD OAs & UCDs How do they present? neonatal
Estimation of Serum Urea
 Estimation of Serum Urea 1 -Urea: Urea is the highest non-protein nitrogen compound in the blood. Urea is the major excretory product of protein metabolism. It is formed by urea cycle in the liver from
Estimation of Serum Urea 1 -Urea: Urea is the highest non-protein nitrogen compound in the blood. Urea is the major excretory product of protein metabolism. It is formed by urea cycle in the liver from
Medical Foods for Inborn Errors of Metabolism
 Medical Foods for Inborn Errors of Metabolism Policy Number: Original Effective Date: MM.02.014 02/18/2000 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 08/23/2013 Section: Medicine Place(s)
Medical Foods for Inborn Errors of Metabolism Policy Number: Original Effective Date: MM.02.014 02/18/2000 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 08/23/2013 Section: Medicine Place(s)
SYNTHESIS OF NON-ESSENTIAL AMINO ACIDS [LIPPINCOTT S ] Deeba S. Jairajpuri
![SYNTHESIS OF NON-ESSENTIAL AMINO ACIDS [LIPPINCOTT S ] Deeba S. Jairajpuri SYNTHESIS OF NON-ESSENTIAL AMINO ACIDS [LIPPINCOTT S ] Deeba S. Jairajpuri](/thumbs/80/80689583.jpg) SYNTHESIS OF NON-ESSENTIAL AMINO ACIDS [LIPPINCOTT S 267-274] Deeba S. Jairajpuri TYPES OF AMINO ACIDS Amino acids that cannot be synthesized by the human body and are required to be taken in the diet
SYNTHESIS OF NON-ESSENTIAL AMINO ACIDS [LIPPINCOTT S 267-274] Deeba S. Jairajpuri TYPES OF AMINO ACIDS Amino acids that cannot be synthesized by the human body and are required to be taken in the diet
Lynne A. Wolfe, MS, ACNP, PNP, BC Department of Genetics Yale School of Medicine
 Lynne A. Wolfe, MS, ACNP, PNP, BC Department of Genetics Yale School of Medicine Harvey Levy, MD Mark Korson, MD Piero Rinaldo, MD, PhD Larry Sweetman, PhD K. Michael Gibson, PhD Charlie Roe, MD Jerry
Lynne A. Wolfe, MS, ACNP, PNP, BC Department of Genetics Yale School of Medicine Harvey Levy, MD Mark Korson, MD Piero Rinaldo, MD, PhD Larry Sweetman, PhD K. Michael Gibson, PhD Charlie Roe, MD Jerry
The spectrum and outcome of the. neonates with inborn errors of. metabolism at a tertiary care hospital
 The spectrum and outcome of the neonates with inborn errors of metabolism at a tertiary care hospital Dr. Sevim Ünal Neonatology Division, Ankara Children s Hematology Oncology Research Hospital, Ankara,
The spectrum and outcome of the neonates with inborn errors of metabolism at a tertiary care hospital Dr. Sevim Ünal Neonatology Division, Ankara Children s Hematology Oncology Research Hospital, Ankara,
Amino Acid Metabolism (Nitrogen Metabolism) Dec Dr. Robert Lyons
 1 Amino Acid Metabolism (itrogen Metabolism) Dec 9-11 008 Dr. Robert Lyons See: http://seqcore.brcf.med.umich.edu/mcb500 for supplementary (non-required) course materials. Medical relevance of amino acid
1 Amino Acid Metabolism (itrogen Metabolism) Dec 9-11 008 Dr. Robert Lyons See: http://seqcore.brcf.med.umich.edu/mcb500 for supplementary (non-required) course materials. Medical relevance of amino acid
Inborn errors of metabolism
 ESPEN Congress Nice 2010 From child to adult nutrition Inborn errors of metabolism Pascal Crenn Inborn errors of metabolism: from child to adult Pascal Crenn Hôpital Raymond Poincaré 92380 Garches. France
ESPEN Congress Nice 2010 From child to adult nutrition Inborn errors of metabolism Pascal Crenn Inborn errors of metabolism: from child to adult Pascal Crenn Hôpital Raymond Poincaré 92380 Garches. France
PROTEIN METABOLISM: SPECIFIC WAYS OF AMINO ACIDS CATABOLISM AND SYNTHESIS
 PROTEIN METABOLISM: SPECIFIC WAYS OF AMINO ACIDS CATABOLISM AND SYNTHESIS SPECIFIC WAYS OF AMINO ACID CATABOLISM After removing of amino group the carbon skeletons of amino acids are transformed into metabolic
PROTEIN METABOLISM: SPECIFIC WAYS OF AMINO ACIDS CATABOLISM AND SYNTHESIS SPECIFIC WAYS OF AMINO ACID CATABOLISM After removing of amino group the carbon skeletons of amino acids are transformed into metabolic
Chapter 26. Outline. Nitrogen. Nitrogen and Amino Acid Metabolism. BCH 4054 Spring 2001 Chapter 26 Lecture Notes. Slide 1. Slide 2
 BCH 4054 Spring 2001 Chapter 26 Lecture Notes 1 Chapter 26 Nitrogen and Amino Acid Metabolism 2 utline No time to cover entire chapter, therefore concentrate on a few focal points Assimilation of inorganic
BCH 4054 Spring 2001 Chapter 26 Lecture Notes 1 Chapter 26 Nitrogen and Amino Acid Metabolism 2 utline No time to cover entire chapter, therefore concentrate on a few focal points Assimilation of inorganic
Test de aminoácidos. Orina.
 SPECIMEN VALIDITY per creatinine INTERVAL 2.5 th 16 th 50 th 84 th 97.5 th Creatinine 57 mg/dl 15-120 Glutamine/Glutamate 4.3 5-160 Ammonia Level (NH 4 ) 42800 μm/g 18000-100000 Specimen Validity Index
SPECIMEN VALIDITY per creatinine INTERVAL 2.5 th 16 th 50 th 84 th 97.5 th Creatinine 57 mg/dl 15-120 Glutamine/Glutamate 4.3 5-160 Ammonia Level (NH 4 ) 42800 μm/g 18000-100000 Specimen Validity Index
So Much More Than The PKU Test
 Newborn Metabolic Screening So Much More Than The PKU Test Sarah Viall, MSN, PPCNP BC Newborn Screening Program Coordinator Division of Genetics & Metabolism Conflicts of Interest I have no conflicts of
Newborn Metabolic Screening So Much More Than The PKU Test Sarah Viall, MSN, PPCNP BC Newborn Screening Program Coordinator Division of Genetics & Metabolism Conflicts of Interest I have no conflicts of
Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review -
 Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review - Guideline development group International interdisciplinary guideline
Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review - Guideline development group International interdisciplinary guideline
Take a closer look at UCD management
 Take a closer look at UCD management An evaluation tool to help determine whether patients with urea cycle disorders (UCDs) may be experiencing treatment failure What is treatment failure and how do you
Take a closer look at UCD management An evaluation tool to help determine whether patients with urea cycle disorders (UCDs) may be experiencing treatment failure What is treatment failure and how do you
retardation in infants. A wide variety of analytical methods for the analysis of
 IN THE NAME OF GOD Diagnosis and measurment of Phenylalanine in plasma and dried bilood spot (DBS) by a simple and sensitive HPLC method and compaire with Recipe Reference Health Laboratory Research Center,
IN THE NAME OF GOD Diagnosis and measurment of Phenylalanine in plasma and dried bilood spot (DBS) by a simple and sensitive HPLC method and compaire with Recipe Reference Health Laboratory Research Center,
Col Rama Krishna Sanjeev Military Hospital Chennai Prof Shanmughasundaram Mehta Hospital, Chennai
 Col Rama Krishna Sanjeev Military Hospital Chennai Prof Shanmughasundaram Mehta Hospital, Chennai 11 day old male neonate admitted on 26/6 to our Hospital with c/olethargy -since day1 abnormal movements
Col Rama Krishna Sanjeev Military Hospital Chennai Prof Shanmughasundaram Mehta Hospital, Chennai 11 day old male neonate admitted on 26/6 to our Hospital with c/olethargy -since day1 abnormal movements
Subject: Ravicti (glycerol phenylbutyrate) Original Effective Date: 03/16/15. Policy Number: MCP-242. Revision Date(s):
 Subject: Ravicti (glycerol phenylbutyrate) Original Effective Date: 03/16/15 Policy Number: MCP-242 Revision Date(s): Review Date(s): 12/15/2016; 6/22/2017 DISCLAIMER This Medical Policy is intended to
Subject: Ravicti (glycerol phenylbutyrate) Original Effective Date: 03/16/15 Policy Number: MCP-242 Revision Date(s): Review Date(s): 12/15/2016; 6/22/2017 DISCLAIMER This Medical Policy is intended to
CLINICAL PHARMACOLOGY
 BUPHENYL (sodium phenylbutyrate) Tablets BUPHENYL (sodium phenylbutyrate) Powder [bu fen-ǝl] (sodium phenylbutyrate) Rx Only DESCRIPTION BUPHENYL (sodium phenylbutyrate) Tablets for oral administration
BUPHENYL (sodium phenylbutyrate) Tablets BUPHENYL (sodium phenylbutyrate) Powder [bu fen-ǝl] (sodium phenylbutyrate) Rx Only DESCRIPTION BUPHENYL (sodium phenylbutyrate) Tablets for oral administration
AMINO ACID METABOLISM. Sri Widia A Jusman Dept. of Biochemistry & Molecular Biology FMUI
 AMINO ACID METABOLISM Sri Widia A Jusman Dept. of Biochemistry & Molecular Biology FMUI Amino acids derived from dietary protein absorbed from intestine through blood taken up by tissues used for biosynthesis
AMINO ACID METABOLISM Sri Widia A Jusman Dept. of Biochemistry & Molecular Biology FMUI Amino acids derived from dietary protein absorbed from intestine through blood taken up by tissues used for biosynthesis
Nitrogen Metabolism. Pratt and Cornely Chapter 18
 Nitrogen Metabolism Pratt and Cornely Chapter 18 Overview Nitrogen assimilation Amino acid biosynthesis Nonessential aa Essential aa Nucleotide biosynthesis Amino Acid Catabolism Urea Cycle Juicy Steak
Nitrogen Metabolism Pratt and Cornely Chapter 18 Overview Nitrogen assimilation Amino acid biosynthesis Nonessential aa Essential aa Nucleotide biosynthesis Amino Acid Catabolism Urea Cycle Juicy Steak
How to dose RAVICTI (glycerol phenylbutyrate) Oral Liquid
 How to dose RAVICTI (glycerol phenylbutyrate) Oral Liquid A REFERENCE GUIDE FOR DOSING, ADMINISTRATION, AND SUPPORT RAVICTI is so easy to take... It s just one little moment. Isaac, Age 20 Actual RAVICTI
How to dose RAVICTI (glycerol phenylbutyrate) Oral Liquid A REFERENCE GUIDE FOR DOSING, ADMINISTRATION, AND SUPPORT RAVICTI is so easy to take... It s just one little moment. Isaac, Age 20 Actual RAVICTI
Analysis of L- and D-Amino Acids Using UPLC Yuta Mutaguchi 1 and Toshihisa Ohshima 2*
 Analysis of L- and D-Amino Acids Using UPLC Yuta Mutaguchi 1 and Toshihisa Ohshima 2* 1 Department of Biotechnology, Akita Prefectural University, Akita City, Japan; 2 Department of Biomedical Engineering,
Analysis of L- and D-Amino Acids Using UPLC Yuta Mutaguchi 1 and Toshihisa Ohshima 2* 1 Department of Biotechnology, Akita Prefectural University, Akita City, Japan; 2 Department of Biomedical Engineering,
Diagnostic Proficiency Testing Survey Annual Report
 ERNDIM DPT Centre Basel University Children s Hospital Metabolic Unit Postfach, CH-4005 Basel, Switzerland phone: ++41 61 685 62 75 or ++41 61 685 63 23 Diagnostic Proficiency Testing Survey 2009 Annual
ERNDIM DPT Centre Basel University Children s Hospital Metabolic Unit Postfach, CH-4005 Basel, Switzerland phone: ++41 61 685 62 75 or ++41 61 685 63 23 Diagnostic Proficiency Testing Survey 2009 Annual
Fundamentals of Organic Chemistry CHEM 109 For Students of Health Colleges
 Fundamentals of Organic Chemistry CHEM 109 For Students of Health Colleges Credit hrs.: (2+1) King Saud University College of Science, Chemistry Department CHEM 109 CHAPTER 9. AMINO ACIDS, PEPTIDES AND
Fundamentals of Organic Chemistry CHEM 109 For Students of Health Colleges Credit hrs.: (2+1) King Saud University College of Science, Chemistry Department CHEM 109 CHAPTER 9. AMINO ACIDS, PEPTIDES AND
Part III => METABOLISM and ENERGY. 3.5 Protein Catabolism 3.5a Protein Degradation 3.5b Amino Acid Breakdown 3.5c Urea Cycle
 Part III => METABOLISM and ENERGY 3.5 Protein Catabolism 3.5a Protein Degradation 3.5b Amino Acid Breakdown 3.5c Urea Cycle Section 3.5a: Protein Degradation Synopsis 3.5a - Dietary proteins are degraded
Part III => METABOLISM and ENERGY 3.5 Protein Catabolism 3.5a Protein Degradation 3.5b Amino Acid Breakdown 3.5c Urea Cycle Section 3.5a: Protein Degradation Synopsis 3.5a - Dietary proteins are degraded
AMINO ACID METABOLISM
 AMINO ACID METABOLISM PHL-285 Biochemistry-2 Mahmoud N. Nagi, Ph.D. Professor of Biochemistry Overview of amino acid metabolism. Classification of amino acids. Biosynthesis of nonessential amino acids.
AMINO ACID METABOLISM PHL-285 Biochemistry-2 Mahmoud N. Nagi, Ph.D. Professor of Biochemistry Overview of amino acid metabolism. Classification of amino acids. Biosynthesis of nonessential amino acids.
3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES
 3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt treatment
3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt treatment
Lecture: Amino Acid catabolism: Nitrogen-The Urea cycle
 BIOC 423: Introductory Biochemistry Biochemistry Education Department of Biochemistry & Molecular Biology University of New Mexico Lecture: Amino Acid catabolism: Nitrogen-The Urea cycle OBJECTIVES Describe
BIOC 423: Introductory Biochemistry Biochemistry Education Department of Biochemistry & Molecular Biology University of New Mexico Lecture: Amino Acid catabolism: Nitrogen-The Urea cycle OBJECTIVES Describe
ISOVALERIC ACIDAEMIA -ACUTE DECOMPENSATION (standard version)
 Contact Details Name: Hospital Telephone: This protocol has 5 pages ISOVALERIC ACIDAEMIA -ACUTE DECOMPENSATION (standard version) Please read carefully. Meticulous treatment is very important as there
Contact Details Name: Hospital Telephone: This protocol has 5 pages ISOVALERIC ACIDAEMIA -ACUTE DECOMPENSATION (standard version) Please read carefully. Meticulous treatment is very important as there
Nitrogen Metabolism. Overview
 Nitrogen Metabolism Pratt and Cornely Chapter 18 Overview Nitrogen assimilation Amino acid biosynthesis Nonessential aa Essential aa Nucleotide biosynthesis Amino Acid Catabolism Urea Cycle Juicy Steak
Nitrogen Metabolism Pratt and Cornely Chapter 18 Overview Nitrogen assimilation Amino acid biosynthesis Nonessential aa Essential aa Nucleotide biosynthesis Amino Acid Catabolism Urea Cycle Juicy Steak
XURIDEN (uridine triacetate) oral granules
 XURIDEN (uridine triacetate) oral granules Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy
XURIDEN (uridine triacetate) oral granules Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy
Diagnostic Proficiency Testing Survey Annual Report
 ERNDIM DPT Centre Basel University Children s Hospital Metabolic Unit Postfach, CH-4005 Basel, Switzerland phone: ++41 61 685 62 75 or ++41 61 685 63 23 Diagnostic Proficiency Testing Survey 2008 Annual
ERNDIM DPT Centre Basel University Children s Hospital Metabolic Unit Postfach, CH-4005 Basel, Switzerland phone: ++41 61 685 62 75 or ++41 61 685 63 23 Diagnostic Proficiency Testing Survey 2008 Annual
SUMMARY OF PRODUCT CHARACTERISTICS
 SUMMARY OF PRODUCT CHARACTERISTICS 1. NAME OF THE MEDICINAL PRODUCT PRIMENE 10% 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Each litre of the infusion solution contains: L-Isoleucine L-Leucine L-Valine
SUMMARY OF PRODUCT CHARACTERISTICS 1. NAME OF THE MEDICINAL PRODUCT PRIMENE 10% 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Each litre of the infusion solution contains: L-Isoleucine L-Leucine L-Valine
NIH Public Access Author Manuscript Pediatr Res. Author manuscript; available in PMC 2010 July 1.
 NIH Public Access Author Manuscript Published in final edited form as: Pediatr Res. 2009 July ; 66(1): 96 101. doi:10.1203/pdr.0b013e3181a27a16. Intellectual, Adaptive, and Behavioral Functioning in Children
NIH Public Access Author Manuscript Published in final edited form as: Pediatr Res. 2009 July ; 66(1): 96 101. doi:10.1203/pdr.0b013e3181a27a16. Intellectual, Adaptive, and Behavioral Functioning in Children
