Christina Diaz, M.D. Assistant Professor of Pediatric Anesthesiology, Children s Hospital of Wisconsin, Milwaukee, WI
|
|
|
- Cameron Peters
- 5 years ago
- Views:
Transcription
1 SPA Spring 2013 PBLD Title: Opening Pandora s Box: A 2-day-old neonate with duodenal atresia, found to have a critical airway anomaly during induction! Moderators: Christina Diaz, M.D. Assistant Professor of Pediatric Anesthesiology, Children s Hospital of Wisconsin, Milwaukee, WI Farzana Afroze, M.D. Assistant Professor of Pediatric Anesthesiology, Albany Medical Center, Albany, NY Goals: At the end of the PBLD, participants will be able to: Case: Discuss the differential diagnosis of neonatal airway abnormalities, including structural and vascular anomalies associated with airway compression/compromise. Describe the various anesthetic management styles regarding a patient with poor vascular access and requiring urgent/emergent surgery on a full stomach. Review the ASA difficult airway algorithm regarding management of a difficult airway. Discuss/debate the need for an airway evaluation and work-up on a neonate with unknown airway anomalies, prior to proceeding with a general anesthetic for an urgent procedure. Time permitting; the group will discuss the repair of complete tracheal rings. Your surgery colleagues call you; they have just posted a case of a 2-day-old neonate for a duodenal atresia repair. The baby will arrive in our NICU shortly and will be transferred back to the outside hospital POD #2 if everything goes well. The infant was born full term via C-section and per the outside hospital the prenatal ultrasound was negative for any major anomalies. The baby lost its first IV and after multiple unsuccessful attempts, the outside hospital deferred placing the IV with the expectation that anesthesia could place it intra-operatively. What is duodenal atresia? Are there any other anomalies that are associated with duodenal atresia? Can this surgery be postponed until the infant is older? What things / problems would we expect to commonly be found on the prenatal ultrasound? Do you have any concerns because the outside hospital has been unable to establish a PIV? How would you induce this baby without an IV? (Find an IV, mask induction, etc.) The baby arrives in the NICU and you send your trainee to assess the infant. He reports that the baby is slightly tachypnic and tachycardic and is on ½ L nasal cannula O2. The baby has mild retrognathia and is making some mild inspiratory
2 noises that is not relieved by repositioning. The baby s extremities are slightly cooler and with slightly decrease capillary refill. What do you attribute the baby s need for oxygen to? What is your potential differential diagnosis for the mild inspiratory noises? What do you attribute the cool extremities and decreased perfusion to? The baby arrives in the OR crying and is gagging on copious secretions. You attempt to suction the baby and are unable to pass a suction catheter down either nares. However, when you remove the nasal cannula from the nares the sats drop to the mid 80 s. You successfully suction the oral airway and set to work finding a PIV. After establishing a 24g PIV in the left foot, you take the time to give the baby a 10 ml/kg fluid bolus of LR and the baby settles under the warming lights. Does the inability to pass your suction catheter down the nares raise any concerns? What is your differential diagnosis concerning the airway? Is the infant appropriately resuscitated? Would you like any laboratory values? Do you need a T&C? The infant s extremities are now warm and with appropriate capillary refill times. The infant is now asleep on the operating table under the heat lights with only slight inspiratory noises noted and the following vital signs: HR 120, BP 69/43, RR 45, T Axillary, and SpO2 of 99 on ½ L NC., Wt. 3.3 Kg How would you induce this patient? You elect to perform a modified rapid sequence induction. After switching to oxygen via your mask, the nurse positions herself to give cricoid. You give small incremental boluses of Propofol for a total of 10 mg and instruct your trainee to adjust the airway and give small breaths to supplement the baby s breathing. Would you give a paralytic now? Would you consider a Propofol only induction? Are there any problems associated with high dose Propofol? Which drug would you choose to paralyze with? You are able to ventilate the infant well and elect to give Rocuronium 2mg. After waiting the appropriate time, your trainee intubates the infant with a 3.0 cuffed ETT but reports significant resistance and can not push the ETT past the vocal cords. You then have the trainee reintubate the patient with a 3.0 uncuffed ETT. He reports the ETT passed the vocal cords but meets some resistance past the vocal cords. You ask him to step aside and slightly withdraw the ETT and try passing it yourself. You agree that there is more resistance than expected but are able to get EtCO2 and chest rise from ventilating the endotracheal tube. The infant remains well perfused and the saturations are %.
3 What is in your differential diagnosis with regard to the airway? What would be your next anticipated move? What doses the ASA difficult airway algorithm suggests? Do you ask for any help from your colleagues? Do you request an ENT consult? What do you tell your surgeon? You proceed to personally place a 2.5 uncuffed ETT in this term infant that moves freely and has a leak noted at 22 cm of H2O pressure. You discuss with your surgeon that you have now found two airway anomalies in this infant and would like to have ENT evaluate the airway before proceeding with the laparotomy. The surgeon is worried you may cancel the case but agrees to discuss the matter after ENT comes into the room for an evaluation. The ENT surgeon had been working in the next room and arrives quickly. You discuss with him your findings and he wishes to proceed with a rigid bronchoscopy. During the rigid bronchocscopy, the neonate is noted to have complete tracheal rings along the entire trachea. The ENT surgeon also reports a tortuous airway with unusual take offs. What does this mean for the infant? Do you elect to proceed with the laparotomy? If there is a pulsatile wall/ bulge noted by the ENT, does that change your differential diagnosis? Would you proceed with the duodenal atresia repair now? The 2.5 uncuffed ETT is replaced. You continue to be able to ventilate the patient well. After discussing the risks and benefits with your surgeons, you allow the surgeon to proceed with the duodenal repair. At the end of the surgery, the patient is transferred back the NICU intubated. Considering the airway anomalies and recent surgery, would you extubate? What further evaluations do you expect this infant to undergo? How do we correct complete tracheal rings? What about vascular rings?
4 Discussion: Duodenal Atresia Congenital duodenal atresia and stenosis is a common cause of intestinal obstruction. Embryologically, it results from the failure of recanalization of the solid core of duodenum. The incidence of this congenital anomaly is about 1 per 5000 to 10,000 live births and affects boys more then girls (Holcomb &Murphy). More than 50% of those patients have associated congenital defects including pancreatic defects, intestinal malrotation with congenital bands, esophageal atresia, Tracheoesophageal fistulas, Meckel s diverticulum, imperforate anus, congenital heart disease, central nervous system defects, renal anomalies, and biliary tract anomalies. Trisomy 21 is strongly associated with duodenal atresia/stenosis/web and is present in approximately 25% to 50% of cases (5). The diagnosis of duodenal atresia is commonly made prenatally when ultrasonography demonstrates gastric and proximal duodenal dilation and polyhydramnios. The non-contrast radiographs of the infant with duodenal atresia classically demonstrate the presence of air in the stomach and in the first portion of the duodenum, the double bubble sign and absence of air beyond the second bubble. The infant with duodenal atresia is often born prematurely and clinically presents with early feeding intolerance characterized by vomiting and upper abdominal distention. Emesis is usually bilious because most lesions occur distal to the entry of the bile duct into the duodenum. Nonbilious emesis may be present in 15% to 20% of cases due to a more proximal obstruction (5). Duodenal atresia is a serious condition of neonates that has high mortality rate secondary to multiple comorbidities including prematurity, chromosomal and other associated anomalies. The pediatric anesthesiologists face a series of challenges including dehydration leading to metabolic and electrolyte disturbances and shock with end organ damage, difficult peripheral IV access and potentially challenging airway management due to airway anomalies. There is a significant risk of aspiration of gastric contents during or after induction (3). Commonly infants with duodenal atresia will arrive to operating room for surgical intervention within a few days to a few weeks of life. But prior to the OR trip these infants usually have multisystem evaluations including a genetic evaluation and a search for other associated anomalies. This evaluation is especially important in infants diagnosed postnatally. Congenital airway anomalies Congenital lesions of the airway include congenital tracheal lesions and cardiovascular causes of airway compression. Congenital tracheal lesions are rare;
5 hence experience in their management is limited and dispersed. On the other hand, vascular compression of the pediatric airway is relatively common and an often unrecognized complication of a variety of cardiovascular diseases. The intimate anatomic relationship between the cardiovascular and airway structures plays an important role in this phenomenon (1, 7). The trachea in a full-term infant is about 4 cm long, where as 11 to 13 cm long in an adult. The average diameter of the trachea in a full-term infant is 4-6 mm and 12 to 17 mm in an adult (6, 7). Because of these size differences, the pediatric airway is more susceptible to airway obstruction in the infant. The diagnosis is of a congenital tracheal anomaly or an obstructive extrinsic compression is based on a high degree of suspicion in infants and children with respiratory distress. This high index of suspicion is especially important in infants and children with recurrent respiratory difficulties, stridor, wheezing, and dysphagia or apnea unexplained by other causes. Sometimes, recurrent or persistent cough, exercise intolerance, and difficulty intubating leads to the diagnosis (1, 4, 7). If an airway anomaly is suspected, prompt diagnosis and work up is necessary to avoid further damage to the airway and possible death. There are varieties of diagnostic modalities available including plain chest radiography and echocardiogram, diagnostic investigations may include barium esophagograph, MRI, CT scans, cardiac catheterizations, and flexible and rigid bronchoscopy. The echocardiogram is essential for the evaluation of any associated congenital heart disease and is usually able to show the abnormal vascular structures. Recent advancements in CT s and MRI s can produce three-dimensional reconstructions of all anatomic elements providing more precise information about the cross-sectional area and the extent of the lesion. Despite all these noninvasive diagnostic modalities, the more invasive flexible and rigid bronchoscopy are often required for congenital acquired tracheal anomalies, e.g., tracheoesophageal fistula, traheobronchomalacia and congenital tracheal stenosis and complete tracheal stenosis (1, 4, 7). Vascular Compression of the Airway Airway compromise secondary to underlying heart/vascular pathology is mainly due to two reasons 1) the anomalous relationship between the tracheobronchial tree and vascular structures and 2) extrinsic compression by enlarged cardiac or pulmonary vascular structures (1). The term vascular ring is an aortic arch anomaly in which the trachea and esophagus are surrounded completely by vascular structures. Rings are formed by the abnormal persistence and/or regression of components of the aortic arch complex, which do not need to be patent but can cause compression of the trachea, bronchi and esophagus. A second vascular structure that can affect the airway is a vascular sling. The vascular sling
6 causes tracheal and esophageal compression without these structures being completely encircled by the vascular structures (1). Table 1: Causes of vascular compression of the airway in children (4) I. Anomalies of the aorta o Double aortic arch o Interrupted aortic arch (post- surgical repair) o Right sided aortic arch With aberrant left subclavian artery With mirror image branching and right ligamentum arteriosum o Left sided aortic arch With aberrant right subclavian artery and right ligamentum arteriosum Right sided descending aorta o Cervical aortic arch II. Absent pulmonary valve syndrome III. Aberrant left pulmonary artery (aka pulmonary artery sling) IV. Acquired cardiovascular disease o Dilated cardiomyopathy o Aneurysm Surgery is indicated in all patients with symptomatic vascular rings to prevent cartilage destruction and malacia of the infant airway, which has been observed to appear with in weeks of induced external compression. The goal of the operative repair is to divide the compressive vascular rings or slings to relieve tracheobronchial and esophageal compression and to maintain aortic perfusion (1). The most common surgical approach to vascular rings is via left thoracotomy; rarely necessitates a right thoracotomy. A sternotomy is indicated when the concomitant repair of intracardiac defects is planned or a case of pulmonary artery sling with tracheal reconstruction in which case cardiopulmonary bypass is required. Anesthesia is also complicated for these patients requiring pediatric thoracic and cardiac anesthesia skills (1). Intrinsic Tracheal Lesions Intrinsic tracheal lesions include tracheobronchomalacia (TBM), stenosis, complete tracheal rings or aberrant bronchi. In the pediatric population, primary or secondary TBM is the most common cause of significant airway collapse resulting airway obstruction. In most infants and children, TBM is self-limited and resolves within 1 to 2 years of life. Patients with dying spells, recurrent pneumonia or those who cannot be weaned from mechanical ventilation require aggressive medical and surgical intervention (7).
7 Table 2: Secondary causes of tracheobronchomalacia (7) 1. Esophageal atresia with TEF 2. Extrinsic compression a. Vascular compression b. Cardiac causes enlarged structures c. Cysts lymphatic malformations, thymic cysts, bronchogenic cysts d. Mediastinal neoplasm e. Infection 3. Prolonged intubation 4. Chondodysplasisas 5. Post traumatic result or following tracheoplasty Complete Tracheal Rings Congenial tracheal stenosis (CTS) in neonates and infants is characterized by a structural tracheal constriction, and is an often under diagnosed, life threatening respiratory anomaly, most commonly due to complete tracheal rings. The absence of the membranous portion of the trachea can create localized or generalized stenosis. More than 50% of the patients with CTS may have accompanying other malformations, including pulmonary, cardiovascular, gastrointestinal malformations or genetic anomalies. Figure 1: Normal 1-month-old infant's midtrachea with anterior cartilaginous rings and a membranous posterior (B) Three-month-old who has tracheomalacia; note the flattening of the lumen with a widened trachealis muscle. (C) Complete tracheal rings with absence of posterior membranous portion (Ho)
8 In the literature tracheal stenosis is defined as a reduction of the anatomic luminal diameter of the trachea by more than 50% compared with the remaining normal trachea (6, 7). Usually this anomaly is severe in nature and is diagnosed in the neonatal period. Sometimes diagnosis is made when patients require general anesthesia requiring an endotracheal tube or develop a respiratory tract infection resulting in further luminal narrowing. There are multiple case reports in the literature of complete tracheal rings being diagnosed months to years after birth. The condition is rare, with an incidence approximately 1 in 64,500 patients and represents 0.3 1% of all laryngotracheal stenosis. Mortality in these patients is related only to the severity of the stenosis and to the presence of other comorbid anomalies (6). The variability in the timing of diagnosis reflects the variability of stenosis. There are three types of complete tracheal rings 1) generalized hypoplasia of the trachea, 2) a funnel type stenosis, and 3) a segmental stenosis involving 2-3 rings. This anatomic description also correlates with the symptoms. Those having generalized hypoplasia, becomes symptomatic earlier in life with stridor, wheezing, and respiratory distress and where as those having segmental stenosis may be symptomatic later in life or asymptomatic altogether. Figure 2: Type I is generalized hypoplasia, Type II is funnel type stenosis with one normal end and the other one stenotic, and Type III is segmental stenosis with two or three cartilage rings involved The CTS has been managed via both conservative medical as well as surgical interventions, depending on the presentation and severity of the stenosis. Surgical techniques includes -1) enlargement, using a costal cartilage transplantation, a pericardial patch or tracheal autograft, 2) resection of the affected segment and reanastomosis of the trachea in short segment stenosis, and 3) a slide tracheoplasty in patients with long segment stenosis.
9 Figure 3: Surgicaltreatment of CTS. (I) Resection and reconstruction, suitable only for shorter stenosis. (II) Patch tracheoplasty. Incision and tracheal widening with free cartilage or pericardial grafts. Figure 4: Slide tracheoplasty. Because tracheal lesions can be due to pure congenital tracheobronchial origin or the result of cardiovascular compression and are frequently associated with other congenital anomalies, patients should have a complete cardiovascular and airway evaluation before proceeding with anesthesia for a non-emergent or urgent procedures. For any urgent/emergent procedures, the risks versus benefits of proceeding with the anesthesia and surgery should be weighted and discussed among the multidisciplinary team involved in the care of the patient. References: 1. Barry DK, Tal G, Francis XM. Cardiovascular causes of airway compression. Pediatric Anesthesia 2004; 14: Choudhary, MS, Rahman N, Boyd P, Kakhoo K. Dodenal atresia : associated anomalies, prenatal diagnosis and outcome. Pediatric Surgery Int 2009; 25:
10 3. Ciftci I, Apiliogullari S, Kara I, Gunduz E, Dumanb A. Repair of duodenal atresia under spinal anesthesia in a low-birth-weight preterm neonate: case report. Journal of Pediatric Surgery 2012; 47: E33-E35 4. Clare AM, Martin JE, Derek JR. Vascular Compression of the airway in children. Paediatric Respiratory Reviews 2008; 9: Feldman, Mark, Friedman Lawrence S, Brandt, Lawerence J. Sleisenger and Fordtran s Gastrointestinal and Liver Disease: Pathophysiology/Diagnosis/management. Piladelphia: Saunders Elsevier, th Ed 6. Ho, AS, Koltai, PJ. Pediatric tracheal stenosis. Otoraryngology clinical North Americ 2008; 41: Practice Guideline for Management of the Difficult Airway. Anesthesiology2003; 98: Sandu K, Monnier P. Congenital tracheal anomalies. Otoraryngology clinical North America 2007; 40: Trivedi P, Hardy C. A case of an unexpected airway difficulty I n the cardiac operating room.
Neonatal Airway Disorders, Treatments, and Outcomes. Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center
 Neonatal Airway Disorders, Treatments, and Outcomes Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center Disclosure I have nothing to disclose Neonatal and Pediatric Tracheostomy Tracheostomy
Neonatal Airway Disorders, Treatments, and Outcomes Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center Disclosure I have nothing to disclose Neonatal and Pediatric Tracheostomy Tracheostomy
Tracheal stenosis in infants and children is typically characterized
 Slide Tracheoplasty for Congenital Tracheal Stenosis Peter B. Manning, MD Tracheal stenosis in infants and children is typically characterized by the presence of complete cartilaginous tracheal rings and
Slide Tracheoplasty for Congenital Tracheal Stenosis Peter B. Manning, MD Tracheal stenosis in infants and children is typically characterized by the presence of complete cartilaginous tracheal rings and
Western States Case Conference
 Western States Case Conference Annie Coates, MD Second Year Pediatric Pulmonary Fellow Lucille Packard Children s Hospital at Stanford September 21st, 2011 Outline Case Presentation Diagnosis Management
Western States Case Conference Annie Coates, MD Second Year Pediatric Pulmonary Fellow Lucille Packard Children s Hospital at Stanford September 21st, 2011 Outline Case Presentation Diagnosis Management
CONGENITAL TRACHEAL STENOSIS PRESENTING IN THE NEONATAL PERIOD
 CONGENITAL TRACHEAL STENOSIS PRESENTING IN THE NEONATAL PERIOD J Reiter, C Springer, E Erez Israel Society of Pediatric Pulmonolgy Jerusalem, September 2 nd, 2015 Topics Case Presentation Surgical Intervention
CONGENITAL TRACHEAL STENOSIS PRESENTING IN THE NEONATAL PERIOD J Reiter, C Springer, E Erez Israel Society of Pediatric Pulmonolgy Jerusalem, September 2 nd, 2015 Topics Case Presentation Surgical Intervention
Chapter 124: Congenital Disorders of the Trachea. Bruce Benjamin
 Chapter 124: Congenital Disorders of the Trachea Bruce Benjamin Investigation of the larynx and pharynx may be incomplete in infants and children with congenital abnormalities without investigation of
Chapter 124: Congenital Disorders of the Trachea Bruce Benjamin Investigation of the larynx and pharynx may be incomplete in infants and children with congenital abnormalities without investigation of
Physical Exam. Vitals stable on room air Abdomen soft, non-distented Normal external genitalia Patent anus No limb anomalies
 Case Presentation 1 day-old full-term baby girl noted to have drooling of saliva and increased secretions at birth Fetal US @32wks had shown polyhydramnios Birth weight 3515g Apgar 7@1min and 8@5min Unable
Case Presentation 1 day-old full-term baby girl noted to have drooling of saliva and increased secretions at birth Fetal US @32wks had shown polyhydramnios Birth weight 3515g Apgar 7@1min and 8@5min Unable
Wheeze. Dr Jo Harrison
 Wheeze Dr Jo Harrison 9.9.14 Wheeze - Physiology a continuous musical sound that lasts longer than 250 msec. can be high-pitched or low-pitched, consist of single or multiple notes, and occur during inspiration
Wheeze Dr Jo Harrison 9.9.14 Wheeze - Physiology a continuous musical sound that lasts longer than 250 msec. can be high-pitched or low-pitched, consist of single or multiple notes, and occur during inspiration
Tracheoesophageal Fistula and Esophageal Atresia
 Patient and Family Education Tracheoesophageal Fistula and Esophageal Atresia What is tracheoesophageal fistula? The word fistula means abnormal connection. Tracheoesophageal fistula (TEF) is a condition
Patient and Family Education Tracheoesophageal Fistula and Esophageal Atresia What is tracheoesophageal fistula? The word fistula means abnormal connection. Tracheoesophageal fistula (TEF) is a condition
Alyssa Brzenski MD May 2, 2012
 Alyssa Brzenski MD May 2, 2012 Overview Background Pre repair bronchoscopy Thorascopic repair To extubate or not? Esophageal atresia treatment of long gap esophageal atresia Complications following TEF/EA
Alyssa Brzenski MD May 2, 2012 Overview Background Pre repair bronchoscopy Thorascopic repair To extubate or not? Esophageal atresia treatment of long gap esophageal atresia Complications following TEF/EA
Subject Index. Bacterial infection, see Suppurative lung disease, Tuberculosis
 Subject Index Abscess, virtual 107 Adenoidal hypertrophy, features 123 Airway bleeding, technique 49, 50 Airway stenosis, see Stenosis, airway Anaesthesia biopsy 47 complications 27, 28 flexible 23 26
Subject Index Abscess, virtual 107 Adenoidal hypertrophy, features 123 Airway bleeding, technique 49, 50 Airway stenosis, see Stenosis, airway Anaesthesia biopsy 47 complications 27, 28 flexible 23 26
Index. Note: Page numbers of article titles are in boldface type
 Index Note: Page numbers of article titles are in boldface type A Acute coronary syndrome, perioperative oxygen in, 599 600 Acute lung injury (ALI). See Lung injury and Acute respiratory distress syndrome.
Index Note: Page numbers of article titles are in boldface type A Acute coronary syndrome, perioperative oxygen in, 599 600 Acute lung injury (ALI). See Lung injury and Acute respiratory distress syndrome.
CASE PRIMERS. Pediatric Anesthesia Fellowship Program. Laryngotracheal Reconstruction (LTR) Tufts Medical Center
 CASE PRIMERS Pediatric Anesthesia Fellowship Program Tufts Medical Center Department of Anesthesiology and Perioperative Medicine Division of Pediatric Anesthesia 800 Washington Street, Box 298 Boston,
CASE PRIMERS Pediatric Anesthesia Fellowship Program Tufts Medical Center Department of Anesthesiology and Perioperative Medicine Division of Pediatric Anesthesia 800 Washington Street, Box 298 Boston,
AORTIC COARCTATION. Synonyms: - Coarctation of the aorta
 AORTIC COARCTATION Synonyms: - Coarctation of the aorta Definition: Aortic coarctation is a congenital narrowing of the aorta, usually located after the left subclavian artery, near the ductus or the ligamentum
AORTIC COARCTATION Synonyms: - Coarctation of the aorta Definition: Aortic coarctation is a congenital narrowing of the aorta, usually located after the left subclavian artery, near the ductus or the ligamentum
Unusual presentation of complete tracheal rings in a 15 year old trauma patient
 Unusual presentation of complete tracheal rings in a 15 year old trauma patient B. S. Schmidt 1, E. J. Herschmiller 2, R. J. Jarrah 1, T. A. Nakagawa 1 1 Department of Anesthesiology (Section on Pediatric
Unusual presentation of complete tracheal rings in a 15 year old trauma patient B. S. Schmidt 1, E. J. Herschmiller 2, R. J. Jarrah 1, T. A. Nakagawa 1 1 Department of Anesthesiology (Section on Pediatric
All bedside percutaneously placed tracheostomies
 Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
90 th Annual Meeting The American Association for Thoracic Surgery May 1, 2010 Toronto, Ontario, Canada. Slide Tracheoplasty
 90 th Annual Meeting The American Association for Thoracic Surgery May 1, 2010 Toronto, Ontario, Canada Congenital Skills Course Slide Tracheoplasty Carl Lewis Backer, MD A.C. Buehler Professor of Surgery
90 th Annual Meeting The American Association for Thoracic Surgery May 1, 2010 Toronto, Ontario, Canada Congenital Skills Course Slide Tracheoplasty Carl Lewis Backer, MD A.C. Buehler Professor of Surgery
Society of Rural Physicians of Canada 26TH ANNUAL RURAL AND REMOTE MEDICINE COURSE ST. JOHN'S NEWFOUNDLAND AND LABRADOR APRIL 12-14, 2018
 Society of Rural Physicians of Canada 26TH ANNUAL RURAL AND REMOTE MEDICINE COURSE ST. JOHN'S NEWFOUNDLAND AND LABRADOR APRIL 12-14, 2018 Dr. Andrea Losier OTTAWA ON 332 PEDS ER CASES Pediatric ED Cases
Society of Rural Physicians of Canada 26TH ANNUAL RURAL AND REMOTE MEDICINE COURSE ST. JOHN'S NEWFOUNDLAND AND LABRADOR APRIL 12-14, 2018 Dr. Andrea Losier OTTAWA ON 332 PEDS ER CASES Pediatric ED Cases
MRSA pneumonia mucus plug burden and the difficult airway
 Case report Crit Care Shock (2016) 19:54-58 MRSA pneumonia mucus plug burden and the difficult airway Ann Tsung, Brian T. Wessman An 80-year-old female with a past medical history of chronic obstructive
Case report Crit Care Shock (2016) 19:54-58 MRSA pneumonia mucus plug burden and the difficult airway Ann Tsung, Brian T. Wessman An 80-year-old female with a past medical history of chronic obstructive
Large veins of the thorax Brachiocephalic veins
 Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Aberrant Right Subclavian Artery
 A Doubtful Cause of Symptoms Thomas P. Comer, M.D., Malvin Weinberger, M.D., and Howard D. Sirak, M.D. ABSTRACT Ten patients with surgically treated aberrant right subclavian artery are reviewed. In half,
A Doubtful Cause of Symptoms Thomas P. Comer, M.D., Malvin Weinberger, M.D., and Howard D. Sirak, M.D. ABSTRACT Ten patients with surgically treated aberrant right subclavian artery are reviewed. In half,
IAEM Clinical Guideline 9 Laryngomalacia. Version 1 September, Author: Dr Farah Mustafa
 IAEM Clinical Guideline 9 Laryngomalacia Version 1 September, 2016 Author: Dr Farah Mustafa Guideline lead: Dr Áine Mitchell, in collaboration with IAEM Clinical Guideline committee and Our Lady s Children
IAEM Clinical Guideline 9 Laryngomalacia Version 1 September, 2016 Author: Dr Farah Mustafa Guideline lead: Dr Áine Mitchell, in collaboration with IAEM Clinical Guideline committee and Our Lady s Children
Home FAQ Archives ABP Topics NeoReviews.org My Bookmarks CME Information Help. Print this Page Add to my Bookmarks Page 3 of 10
 Welcome Kristin Ingstrup [ Logout ] SEARCH Home FAQ Archives ABP Topics NeoReviews.org My Bookmarks CME Information Help Overview Editorial Board My Learning Plan January February March May June July August
Welcome Kristin Ingstrup [ Logout ] SEARCH Home FAQ Archives ABP Topics NeoReviews.org My Bookmarks CME Information Help Overview Editorial Board My Learning Plan January February March May June July August
Simulation 3: Post-term Baby in Labor and Delivery
 Simulation 3: Post-term Baby in Labor and Delivery Opening Scenario (Links to Section 1) You are an evening-shift respiratory therapist in a large hospital with a level III neonatal unit. You are paged
Simulation 3: Post-term Baby in Labor and Delivery Opening Scenario (Links to Section 1) You are an evening-shift respiratory therapist in a large hospital with a level III neonatal unit. You are paged
Airway Management in a Patient with Klippel-Feil Syndrome Using Extracorporeal Membrane Oxygenator
 Airway Management in a Patient with Klippel-Feil Syndrome Using Extracorporeal Membrane Oxygenator Beckerman Z*, Cohen O, Adler Z, Segal D, Mishali D and Bolotin G Department of Cardiac Surgery, Rambam
Airway Management in a Patient with Klippel-Feil Syndrome Using Extracorporeal Membrane Oxygenator Beckerman Z*, Cohen O, Adler Z, Segal D, Mishali D and Bolotin G Department of Cardiac Surgery, Rambam
VASCULAR RINGS A CASE - BASED REVIEW
 VASCULAR RINGS A CASE - BASED REVIEW Beverley Newman, BSc. MB.Bch. FACR Professor of Radiology Stanford University and Lucile Packard Children s Hospital Q1,2,3 Frontal chest radiographs on three different
VASCULAR RINGS A CASE - BASED REVIEW Beverley Newman, BSc. MB.Bch. FACR Professor of Radiology Stanford University and Lucile Packard Children s Hospital Q1,2,3 Frontal chest radiographs on three different
24. An infant with recurrent pneumonia underwent a frontal chest radiograph (Fig 24-A) followed by
 24. An infant with recurrent pneumonia underwent a frontal chest radiograph (Fig 24-A) followed by diagnosis? ndings, what is the most likely A. Pulmonary sequestration B. Congenital pulmonary airway malformation
24. An infant with recurrent pneumonia underwent a frontal chest radiograph (Fig 24-A) followed by diagnosis? ndings, what is the most likely A. Pulmonary sequestration B. Congenital pulmonary airway malformation
Screening for Critical Congenital Heart Disease
 Screening for Critical Congenital Heart Disease Caroline K. Lee, MD Pediatric Cardiology Disclosures I have no relevant financial relationships or conflicts of interest 1 Most Common Birth Defect Most
Screening for Critical Congenital Heart Disease Caroline K. Lee, MD Pediatric Cardiology Disclosures I have no relevant financial relationships or conflicts of interest 1 Most Common Birth Defect Most
Section 4.1 Paediatric Tracheostomy Introduction
 Bite- sized training from the GTC Section 4.1 Paediatric Tracheostomy Introduction This is one of a series of bite- sized chunks of educational material developed by the Global Tracheostomy Collaborative.
Bite- sized training from the GTC Section 4.1 Paediatric Tracheostomy Introduction This is one of a series of bite- sized chunks of educational material developed by the Global Tracheostomy Collaborative.
Options for Airway Management During Complex Resection and Reconstruction
 Options for Airway Management During Complex Resection and Reconstruction Brian E. Louie MD, FACS, FRCSC, MHA, MPH Director, Thoracic Research and Education Co-Director, Minimally Invasive Thoracic Surgery
Options for Airway Management During Complex Resection and Reconstruction Brian E. Louie MD, FACS, FRCSC, MHA, MPH Director, Thoracic Research and Education Co-Director, Minimally Invasive Thoracic Surgery
Review of Neonatal Respiratory Problems
 Review of Neonatal Respiratory Problems Respiratory Distress Occurs in about 7% of infants Clinical presentation includes: Apnea Cyanosis Grunting Inspiratory stridor Nasal flaring Poor feeding Tachypnea
Review of Neonatal Respiratory Problems Respiratory Distress Occurs in about 7% of infants Clinical presentation includes: Apnea Cyanosis Grunting Inspiratory stridor Nasal flaring Poor feeding Tachypnea
Lung sequestration and Scimitar syndrome
 Lung sequestration and Scimitar syndrome Imaging approaches M. Mearadji International Foundation for Pediatric Imaging Aid Rotterdam, The Netherlands Pulmonary sequestration Pulmonary sequestration (PS)
Lung sequestration and Scimitar syndrome Imaging approaches M. Mearadji International Foundation for Pediatric Imaging Aid Rotterdam, The Netherlands Pulmonary sequestration Pulmonary sequestration (PS)
There are four general types of congenital lung disorders:
 Pediatric Pulmonology Conditions Evaluated and Treated As a parent, watching a child suffer from a respiratory disorder can be frightening and worrisome. Our respiratory specialists provide compassionate
Pediatric Pulmonology Conditions Evaluated and Treated As a parent, watching a child suffer from a respiratory disorder can be frightening and worrisome. Our respiratory specialists provide compassionate
Disclosures. Learning Objectives. Coeditor/author. Associate Science Editor, American Heart Association
 Tracheotomy Challenges for airway specialists Elizabeth H. Sinz, MD Professor of Anesthesiology & Neurosurgery Associate Dean for Clinical Simulation Disclosures Coeditor/author Associate Science Editor,
Tracheotomy Challenges for airway specialists Elizabeth H. Sinz, MD Professor of Anesthesiology & Neurosurgery Associate Dean for Clinical Simulation Disclosures Coeditor/author Associate Science Editor,
Topics for discussion. Pediatric General Surgery. Physiology. Surgical Newborns. Neonatal Intestinal Obstruction
 Topics for discussion Pediatric General Surgery Professor General & Thoracic Surgery What makes Pediatric Surgery unique? Neonatal intestinal obstruction Abdominal wall defects Inguinal hernias Appendicitis
Topics for discussion Pediatric General Surgery Professor General & Thoracic Surgery What makes Pediatric Surgery unique? Neonatal intestinal obstruction Abdominal wall defects Inguinal hernias Appendicitis
TRACHEOSTOMY. Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion
 TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
Cricoid pressure: useful or dangerous?
 Cricoid pressure: useful or dangerous? Francis VEYCKEMANS Cliniques Universitaires Saint Luc Bruxelles (2009) Controversial issue - Can J Anaesth 1997 JR Brimacombe - Pediatr Anesth 2002 JG Brock-Utne
Cricoid pressure: useful or dangerous? Francis VEYCKEMANS Cliniques Universitaires Saint Luc Bruxelles (2009) Controversial issue - Can J Anaesth 1997 JR Brimacombe - Pediatr Anesth 2002 JG Brock-Utne
Infection. Risk factor for infection ACoRN alerting sign with * Clinical deterioration. Problem List. Respiratory. Cardiovascular
 The ACoRN Process Baby at risk Unwell Risk factors Post-resuscitation requiring stabilization Resuscitation Ineffective breathing Heart rate < 100 bpm Central cyanosis Support Infection Risk factor for
The ACoRN Process Baby at risk Unwell Risk factors Post-resuscitation requiring stabilization Resuscitation Ineffective breathing Heart rate < 100 bpm Central cyanosis Support Infection Risk factor for
HOW TO IMAGE AND DESCRIBE CONGENITAL LUNG MALFORMATIONS
 HOW TO IMAGE AND DESCRIBE CONGENITAL LUNG MALFORMATIONS Paul Thacker, MD Assistant Professor Departments of Radiology and Pediatrics Medical University of South Carolina DISCLOSURES I have no relevant
HOW TO IMAGE AND DESCRIBE CONGENITAL LUNG MALFORMATIONS Paul Thacker, MD Assistant Professor Departments of Radiology and Pediatrics Medical University of South Carolina DISCLOSURES I have no relevant
Intravascular Ultrasound (IVUS) and Optical Coherence Tomography (OCT)
 Intravascular Ultrasound (IVUS) and Optical Coherence Tomography (OCT) Clare McLaren Great Ormond Street Hospital London Introduction IVUS and OCT supplementary techniques to angiography provide information
Intravascular Ultrasound (IVUS) and Optical Coherence Tomography (OCT) Clare McLaren Great Ormond Street Hospital London Introduction IVUS and OCT supplementary techniques to angiography provide information
POSTOPERATIVE CONGENITAL ESOPHAGEAL ATRESIA COMPLICATIONS: A REVIEW
 CHILDREN S HOSPITAL II POSTOPERATIVE CONGENITAL ESOPHAGEAL ATRESIA COMPLICATIONS: A REVIEW Dr. Nguyen Thuy Hanh Ngan Neonatal Department CONTENTS 1. Background 2. Classification 3. Management 4. Complications
CHILDREN S HOSPITAL II POSTOPERATIVE CONGENITAL ESOPHAGEAL ATRESIA COMPLICATIONS: A REVIEW Dr. Nguyen Thuy Hanh Ngan Neonatal Department CONTENTS 1. Background 2. Classification 3. Management 4. Complications
Audra Fuller MD, Mark Sigler MD, Shrinivas Kambali MD, Raed Alalawi MD
 Clinical Series Successful treatment of post-intubation tracheal stenosis with balloon dilation, argon plasma coagulation, electrocautery and application of mitomycin C Audra Fuller MD, Mark Sigler MD,
Clinical Series Successful treatment of post-intubation tracheal stenosis with balloon dilation, argon plasma coagulation, electrocautery and application of mitomycin C Audra Fuller MD, Mark Sigler MD,
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Varied Presentation and Management of Tracheal Polyps in Children Vinod M Raj 1, Varun Hathiramani 2, Swathi
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Varied Presentation and Management of Tracheal Polyps in Children Vinod M Raj 1, Varun Hathiramani 2, Swathi
Cuffed or uncuffed ETT in pediatric anesthesia? Dr. Renata Haghedooren Dr. Sophie Chullikal Dr. Julie Lauweryns
 Cuffed or uncuffed ETT in pediatric anesthesia? Dr. Renata Haghedooren Dr. Sophie Chullikal Dr. Julie Lauweryns Overview History Survey Tradition Pro-Con Debate Conclusions History of intubation 1878:
Cuffed or uncuffed ETT in pediatric anesthesia? Dr. Renata Haghedooren Dr. Sophie Chullikal Dr. Julie Lauweryns Overview History Survey Tradition Pro-Con Debate Conclusions History of intubation 1878:
An 8-year experience of esophageal atresia repair in Sarvar children hospital (Mashhad- IRAN)
 An 8-year experience of esophageal atresia repair in Sarvar children hospital (Mashhad- IRAN) Mehran Hiradfar* Ahmad Bazrafshan* Marjan Judi** Mohammad Gharavi*** - Reza Shojaeian**** * Associate professor
An 8-year experience of esophageal atresia repair in Sarvar children hospital (Mashhad- IRAN) Mehran Hiradfar* Ahmad Bazrafshan* Marjan Judi** Mohammad Gharavi*** - Reza Shojaeian**** * Associate professor
Suspected Foreign Body Ingestion
 Teresa Liang Suspected Foreign Body Ingestion 1. General Presentation Background: Of more than 100,000 cases of foreign body ingestion reported each year in the United States, 80% occur in children, with
Teresa Liang Suspected Foreign Body Ingestion 1. General Presentation Background: Of more than 100,000 cases of foreign body ingestion reported each year in the United States, 80% occur in children, with
A novel plain abdominal radiograph sign to diagnose malrotation with volvulus
 A novel plain abdominal radiograph sign to diagnose malrotation with volvulus Nataraja RM 1, Mahomed AA 1* 1. Department of Paediatric Surgery, Royal Alexandra Hospital for Sick Children, Brighton,UK *
A novel plain abdominal radiograph sign to diagnose malrotation with volvulus Nataraja RM 1, Mahomed AA 1* 1. Department of Paediatric Surgery, Royal Alexandra Hospital for Sick Children, Brighton,UK *
PEPP Course: PEPP BLS Pretest
 PEPP Course: PEPP BLS Pretest 1. What is the best way to administer oxygen to a child in moderate respiratory distress? Nasal cannula Simple mask Nonrebreathing mask Bag-valve-mask device 2. A 2-year-old
PEPP Course: PEPP BLS Pretest 1. What is the best way to administer oxygen to a child in moderate respiratory distress? Nasal cannula Simple mask Nonrebreathing mask Bag-valve-mask device 2. A 2-year-old
Aortic arch pathology. Cerebral ischemia following carotid artery stenosis.
 Important: -Subclavian Steal Syndrome -Cerebral ischemia Aortic arch pathology. Cerebral ischemia following carotid artery stenosis. Mina Aubeed & Alba Hernández Pinilla Aortic arch pathology Common arch
Important: -Subclavian Steal Syndrome -Cerebral ischemia Aortic arch pathology. Cerebral ischemia following carotid artery stenosis. Mina Aubeed & Alba Hernández Pinilla Aortic arch pathology Common arch
Complex Airway problems - Paediatric Perspective
 Complex Airway problems - Paediatric Perspective Dave Albert BACO Liverpool 2009 www.albert.uk.com Complex Ξ not simple, multiple parts Multiple problems with airway Combined Web/stenosis/multiple levels
Complex Airway problems - Paediatric Perspective Dave Albert BACO Liverpool 2009 www.albert.uk.com Complex Ξ not simple, multiple parts Multiple problems with airway Combined Web/stenosis/multiple levels
Therapeutic Bronchoscopy Etiology - Benign Stenosis Post - intubation Trauma Post - operative Inflammatory Idiopathic
 Endobronchial Palliation of Airway Disease Douglas E. Wood, MD Professor and Chief Division of Cardiothoracic Surgery Vice-Chair, Department of Surgery Endowed Chair in Lung Cancer Research University
Endobronchial Palliation of Airway Disease Douglas E. Wood, MD Professor and Chief Division of Cardiothoracic Surgery Vice-Chair, Department of Surgery Endowed Chair in Lung Cancer Research University
A case of a neonate with a congenital laryngeal web: management of a difficult airway and intra-operative complications
 A case of a neonate with a congenital laryngeal web: management of a difficult airway and intra-operative complications Moderators: Marcellene Franzen, MD Fellow in Pediatric Anesthesiology Medical College
A case of a neonate with a congenital laryngeal web: management of a difficult airway and intra-operative complications Moderators: Marcellene Franzen, MD Fellow in Pediatric Anesthesiology Medical College
Anatomy and Physiology. The airways can be divided in to parts namely: The upper airway. The lower airway.
 Airway management Anatomy and Physiology The airways can be divided in to parts namely: The upper airway. The lower airway. Non-instrumental airway management Head Tilt and Chin Lift Jaw Thrust Advanced
Airway management Anatomy and Physiology The airways can be divided in to parts namely: The upper airway. The lower airway. Non-instrumental airway management Head Tilt and Chin Lift Jaw Thrust Advanced
Development of Respiratory System. Dr. Sanaa Alshaarawy& Dr. Saeed Vohra
 Development of Respiratory System Dr. Sanaa Alshaarawy& Dr. Saeed Vohra OBJECTIVES At the end of the lecture the students should be able to: Identify the development of the laryngeotracheal (respiratory)
Development of Respiratory System Dr. Sanaa Alshaarawy& Dr. Saeed Vohra OBJECTIVES At the end of the lecture the students should be able to: Identify the development of the laryngeotracheal (respiratory)
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 14 Practical Anesthesia Key Points 2 14.1 General Anesthesia Have a clear plan before starting anesthesia Never use an unfamiliar anesthetic technique in an emergency
Surgical Care at the District Hospital 1 14 Practical Anesthesia Key Points 2 14.1 General Anesthesia Have a clear plan before starting anesthesia Never use an unfamiliar anesthetic technique in an emergency
The Role of ECMO in Thoracic Surgery. Matthew Hartwig, MD
 The Role of ECMO in Thoracic Surgery Matthew Hartwig, MD Disclosure Slide Consultant for Mallincrodkt and Quark Pharmaceuticals Case #1 28 y.o. female with tracheal mass No previous medical or surgical
The Role of ECMO in Thoracic Surgery Matthew Hartwig, MD Disclosure Slide Consultant for Mallincrodkt and Quark Pharmaceuticals Case #1 28 y.o. female with tracheal mass No previous medical or surgical
Objectives. Objectives 10/12/2011. Case Study: Initial Assessment of the Critically Ill Child. By Rebecca Saul, MSN, CRNP
 Case Study: Initial Assessment of the Critically Ill Child By Rebecca Saul, MSN, CRNP Objectives Define the anatomic variations between children and adults Recognize and implement exam techniques useful
Case Study: Initial Assessment of the Critically Ill Child By Rebecca Saul, MSN, CRNP Objectives Define the anatomic variations between children and adults Recognize and implement exam techniques useful
Original Article. Double Aortic Arch in Infants and Children CH XIE, FQ GONG, GP JIANG, SL FU. Key words. Background
 HK J Paediatr (new series) 2018;23:233-238 Original Article Double Aortic Arch in Infants and Children CH XIE, FQ GONG, GP JIANG, SL FU Abstract Key words Background: This study aimed to report the diagnosis,
HK J Paediatr (new series) 2018;23:233-238 Original Article Double Aortic Arch in Infants and Children CH XIE, FQ GONG, GP JIANG, SL FU Abstract Key words Background: This study aimed to report the diagnosis,
Original Report. Imaging Findings in Pediatric Patients with Persistent Airway Symptoms After Surgery for Double Aortic Arch
 Robert J. Fleck 1,2 Preeyacha Pacharn 1,3 Bradley L. Fricke 1 Matthew A. Ziegler 1 Robin T. Cotton 4 Lane F. Donnelly 1 Received August 30, 2001; accepted after revision October 22, 2001. 1 Department
Robert J. Fleck 1,2 Preeyacha Pacharn 1,3 Bradley L. Fricke 1 Matthew A. Ziegler 1 Robin T. Cotton 4 Lane F. Donnelly 1 Received August 30, 2001; accepted after revision October 22, 2001. 1 Department
Paediatric Resuscitation. EMS Rounds Gurinder Sangha MD Paediatric Emergency Fellow June 18, 2009
 Paediatric Resuscitation EMS Rounds Gurinder Sangha MD Paediatric Emergency Fellow June 18, 2009 Essentials of Resuscitation Airway Breathing Circulation AIRWAY Differences in Paediatric Airway Shorter
Paediatric Resuscitation EMS Rounds Gurinder Sangha MD Paediatric Emergency Fellow June 18, 2009 Essentials of Resuscitation Airway Breathing Circulation AIRWAY Differences in Paediatric Airway Shorter
Thoracoscopic division of vascular rings in infants and children
 Journal of Pediatric Surgery (2007) 42, 1357 1361 www.elsevier.com/locate/jpedsurg Thoracoscopic division of vascular rings in infants and children Abdulrahman Al-Bassam a, *, Mohammad Saquib Mallick a,
Journal of Pediatric Surgery (2007) 42, 1357 1361 www.elsevier.com/locate/jpedsurg Thoracoscopic division of vascular rings in infants and children Abdulrahman Al-Bassam a, *, Mohammad Saquib Mallick a,
Final FRCA Written PAEDIATRICS Past Paper Questions November March 2014
 Final FRCA Written PAEDIATRICS Past Paper Questions November 1996- March 2014 March 2014 A 5-year-old patient presents for a myringotomy and grommet insertion as a day case. During your pre-operative assessment
Final FRCA Written PAEDIATRICS Past Paper Questions November 1996- March 2014 March 2014 A 5-year-old patient presents for a myringotomy and grommet insertion as a day case. During your pre-operative assessment
Duct Dependant Congenital Heart Disease
 Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease This guideline has been agreed by both NTS & CATS Document Control Information Author CATS/NTS Author Position
Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease This guideline has been agreed by both NTS & CATS Document Control Information Author CATS/NTS Author Position
Respiratory distress in patients with central airway obstruction
 Indian J Thorac Cardiovasc Surg (2010) 26:151 156 DOI 10.1007/s12055-010-0021-0 ORIGINAL ARTICLE Respiratory distress in patients with central airway obstruction Mohamed Abdel Hamied Regal & Yasser Ahmed
Indian J Thorac Cardiovasc Surg (2010) 26:151 156 DOI 10.1007/s12055-010-0021-0 ORIGINAL ARTICLE Respiratory distress in patients with central airway obstruction Mohamed Abdel Hamied Regal & Yasser Ahmed
Trauma. Neck trauma zones. Neck Injuries 1/3/2018. Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure
 Trauma 45 minutes highest points Ahmed Mahmoud, MD Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure Neck trauma zones Airway ;Rapid sequence intubation Breathing ;Needle
Trauma 45 minutes highest points Ahmed Mahmoud, MD Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure Neck trauma zones Airway ;Rapid sequence intubation Breathing ;Needle
CONGENITAL HEART DISEASE (CHD)
 CONGENITAL HEART DISEASE (CHD) DEFINITION It is the result of a structural or functional abnormality of the cardiovascular system at birth GENERAL FEATURES OF CHD Structural defects due to specific disturbance
CONGENITAL HEART DISEASE (CHD) DEFINITION It is the result of a structural or functional abnormality of the cardiovascular system at birth GENERAL FEATURES OF CHD Structural defects due to specific disturbance
9/8/2009 < 1 1,2 3,4 5,6 7,8 9,10 11,12 13,14 15,16 17,18 > 18. Tetralogy of Fallot. Complex Congenital Heart Disease.
 Current Indications for Pediatric CTA S Bruce Greenberg Professor of Radiology Arkansas Children s Hospital University of Arkansas for Medical Sciences greenbergsbruce@uams.edu 45 40 35 30 25 20 15 10
Current Indications for Pediatric CTA S Bruce Greenberg Professor of Radiology Arkansas Children s Hospital University of Arkansas for Medical Sciences greenbergsbruce@uams.edu 45 40 35 30 25 20 15 10
Pediatric Surgery MUHC MCH Siste. Objectives of Training
 Preamble A rotation in Pediatric Surgery must give residents the opportunity to become familiar with the unique needs of infants and children as surgical patients. Some of the surgical diseases encountered
Preamble A rotation in Pediatric Surgery must give residents the opportunity to become familiar with the unique needs of infants and children as surgical patients. Some of the surgical diseases encountered
Pediatric Shock. Hypovolemia. Sepsis. Most common cause of pediatric shock Small blood volumes (80cc/kg)
 Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Tracheal Trauma: Management and Treatment. Kosmas Iliadis, MD, PhD, FECTS
 Tracheal Trauma: Management and Treatment Kosmas Iliadis, MD, PhD, FECTS Thoracic Surgeon Director of Thoracic Surgery Department Hygeia Hospital, Athens INTRODUCTION Heterogeneous group of injuries mechanism
Tracheal Trauma: Management and Treatment Kosmas Iliadis, MD, PhD, FECTS Thoracic Surgeon Director of Thoracic Surgery Department Hygeia Hospital, Athens INTRODUCTION Heterogeneous group of injuries mechanism
Congenital Lung Malformations: Radiologic-Pathologic Correlation
 Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 51-60, Abr.-Jun., 2006 Congenital Lung Malformations: Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 51-60, Abr.-Jun., 2006 Congenital Lung Malformations: Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
Pediatric Ingestion Injuries: Assessment & Treatment
 Pediatric Ingestion Injuries: Assessment & Treatment Benjamin L. Eithun, MSN, CRNP, RN, CPNP-AC, CCRN, TCRN Andrea L. Williams, PhD, RN UW Health & AFCH Case #1 Presentation Dispatched to Sandstone Ridge
Pediatric Ingestion Injuries: Assessment & Treatment Benjamin L. Eithun, MSN, CRNP, RN, CPNP-AC, CCRN, TCRN Andrea L. Williams, PhD, RN UW Health & AFCH Case #1 Presentation Dispatched to Sandstone Ridge
Congenital tracheal stenosis (CTS) in neonates and infants is an underdiagnosed,
 Simultaneous management of congenital tracheal stenosis and cardiac anomalies in infants Tsvetomir Loukanov, MD, a Christian Sebening, MD, a Wolfgang Springer, MD, b Herbert Ulmer, MD, PhD, b and Siegfried
Simultaneous management of congenital tracheal stenosis and cardiac anomalies in infants Tsvetomir Loukanov, MD, a Christian Sebening, MD, a Wolfgang Springer, MD, b Herbert Ulmer, MD, PhD, b and Siegfried
NON INVASIVE LIFE SAVERS. Non Invasive Ventilation (NIV)
 Table 1. NIV: Mechanisms Of Action Decreases work of breathing Increases functional residual capacity Recruits collapsed alveoli Improves respiratory gas exchange Reverses hypoventilation Maintains upper
Table 1. NIV: Mechanisms Of Action Decreases work of breathing Increases functional residual capacity Recruits collapsed alveoli Improves respiratory gas exchange Reverses hypoventilation Maintains upper
PULMONARY VENOLOBAR SYNDROME. Dr.C.Anandhi DNB Resident, Southern Railway Headquarters Hospital.
 PULMONARY VENOLOBAR SYNDROME Dr.C.Anandhi DNB Resident, Southern Railway Headquarters Hospital. Presenting complaint: 10 yrs old girl with recurrent episodes of lower respiratory tract infection from infancy.
PULMONARY VENOLOBAR SYNDROME Dr.C.Anandhi DNB Resident, Southern Railway Headquarters Hospital. Presenting complaint: 10 yrs old girl with recurrent episodes of lower respiratory tract infection from infancy.
Evaluation & Management of Penetrating Wounds to the NECK
 Evaluation & Management of Penetrating Wounds to the NECK Goal Effectively identify patients with a high probability of injury requiring surgical intervention Define the role of diagnostic tests in assessing
Evaluation & Management of Penetrating Wounds to the NECK Goal Effectively identify patients with a high probability of injury requiring surgical intervention Define the role of diagnostic tests in assessing
Course n : (ex: Course 6) Sub-category: (ex: 6.4.) Date: ( ) Language:English/Romanian City:Bucharest Country:Romania Speaker: (Radu T.
 Course n : (ex: Course 6) Sub-category: (ex: 6.4.) Date: (9-12-2015) Language:English/Romanian City:Bucharest Country:Romania Speaker: (Radu T. Stoica) Dificulties in Pediatric Thoracic Anesthesia Dr.
Course n : (ex: Course 6) Sub-category: (ex: 6.4.) Date: (9-12-2015) Language:English/Romanian City:Bucharest Country:Romania Speaker: (Radu T. Stoica) Dificulties in Pediatric Thoracic Anesthesia Dr.
Development of pancreas and Small Intestine. ANATOMY DEPARTMENT DR.SANAA AL-AlSHAARAWY DR.ESSAM Eldin Salama
 Development of pancreas and Small Intestine ANATOMY DEPARTMENT DR.SANAA AL-AlSHAARAWY DR.ESSAM Eldin Salama OBJECTIVES At the end of the lecture, the students should be able to : Describe the development
Development of pancreas and Small Intestine ANATOMY DEPARTMENT DR.SANAA AL-AlSHAARAWY DR.ESSAM Eldin Salama OBJECTIVES At the end of the lecture, the students should be able to : Describe the development
Penetrating Neck Injuries. Jason Levine MD Lutheran Medical Center July 22, 2010
 Penetrating Neck Injuries Jason Levine MD Lutheran Medical Center July 22, 2010 CASE PRESENTATION 19 YO M 3 Stab Wounds Right zone I neck SW 2 SW anterior abdomen Left epigastrium anterior axillary line
Penetrating Neck Injuries Jason Levine MD Lutheran Medical Center July 22, 2010 CASE PRESENTATION 19 YO M 3 Stab Wounds Right zone I neck SW 2 SW anterior abdomen Left epigastrium anterior axillary line
DOUBLE AORTIC ARCH SURGERY
 DOUBLE AORTIC ARCH SURGERY *Suraj Wasudeo Nagre 1 and Dwarkanath V. Kulkarni 2 1 Department of C.V.T.S., Grant Medical College, Mumbai 2 Department of C.V.T.S., G.S. Medical College, Mumbai *Author for
DOUBLE AORTIC ARCH SURGERY *Suraj Wasudeo Nagre 1 and Dwarkanath V. Kulkarni 2 1 Department of C.V.T.S., Grant Medical College, Mumbai 2 Department of C.V.T.S., G.S. Medical College, Mumbai *Author for
MODULE VII. Delivery and Immediate Neonatal Care
 MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia Main cause of perinatal and neonatal
MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia Main cause of perinatal and neonatal
Ventilating the paediatric patient. Lizzie Barrett Nurse Educator November 2016
 Ventilating the paediatric patient Lizzie Barrett Nurse Educator November 2016 Acknowledgements Kate Leutert NE PICU Children's Hospital Westmead Dr. Chloe Tetlow VMO Anaesthetist and Careflight Overview
Ventilating the paediatric patient Lizzie Barrett Nurse Educator November 2016 Acknowledgements Kate Leutert NE PICU Children's Hospital Westmead Dr. Chloe Tetlow VMO Anaesthetist and Careflight Overview
Table 1: The major changes in AHA / AAP neonatal resuscitation guidelines2010 compared to previous recommendations in 2005
 Table 1: The major changes in AHA / AAP neonatal guidelines2010 compared to previous recommendations in 2005 Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE 1) Assessment
Table 1: The major changes in AHA / AAP neonatal guidelines2010 compared to previous recommendations in 2005 Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE 1) Assessment
Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of
 Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of Washington Seattle Children s Hospital Objectives Define
Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of Washington Seattle Children s Hospital Objectives Define
TRAINING NEONATOLOGY SILVANA PARIS
 TRAINING ON NEONATOLOGY SILVANA PARIS RESUSCITATION IN DELIVERY ROOM INTRODUCTION THE GLOBAL RESUSCITATION BURDEN IN NEWBORN 136 MILL NEWBORN BABIES EACH YEAR (WHO WORLD REPORT) 5-8 MILL NEWBORN INFANTS
TRAINING ON NEONATOLOGY SILVANA PARIS RESUSCITATION IN DELIVERY ROOM INTRODUCTION THE GLOBAL RESUSCITATION BURDEN IN NEWBORN 136 MILL NEWBORN BABIES EACH YEAR (WHO WORLD REPORT) 5-8 MILL NEWBORN INFANTS
Pitfalls of the Pediatric Chest and Abdomen SPR 2017
 Pitfalls of the Pediatric Chest and Abdomen SPR 2017 Richard I. Markowitz, MD, FACR Children s Hospital of Philadelphia Perelman School of Medicine University of Pennsylvania No Disclosures Cognitive Perceptual
Pitfalls of the Pediatric Chest and Abdomen SPR 2017 Richard I. Markowitz, MD, FACR Children s Hospital of Philadelphia Perelman School of Medicine University of Pennsylvania No Disclosures Cognitive Perceptual
Small bowel atresia. Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families
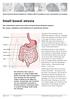 Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Small bowel atresia This information sheet from Great Ormond Street Hospital explains the causes, symptoms and treatment
Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Small bowel atresia This information sheet from Great Ormond Street Hospital explains the causes, symptoms and treatment
Capnography: The Most Vital Sign
 Capnography: The Most Vital Sign Mike McEvoy, PhD, NRP, RN, CCRN Cardiac Surgical ICU RN & Chair Resuscitation Committee Albany Medical Center EMS Coordinator Saratoga County, NY www.mikemcevoy.com CO
Capnography: The Most Vital Sign Mike McEvoy, PhD, NRP, RN, CCRN Cardiac Surgical ICU RN & Chair Resuscitation Committee Albany Medical Center EMS Coordinator Saratoga County, NY www.mikemcevoy.com CO
5 Million neonatal deaths each year worldwide. 20% caused by neonatal asphyxia. Improvement of the outcome of 1 million newborns every year
 1 5 Million neonatal deaths each year worldwide 20% caused by neonatal asphyxia Improvement of the outcome of 1 million newborns every year International Liaison Committee on Resuscitation (ILCOR) American
1 5 Million neonatal deaths each year worldwide 20% caused by neonatal asphyxia Improvement of the outcome of 1 million newborns every year International Liaison Committee on Resuscitation (ILCOR) American
Duct Dependant Congenital Heart Disease
 Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease Document Control Information Author CATS/NTS Author Position CC Transport Services Document Owner E. Polke
Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease Document Control Information Author CATS/NTS Author Position CC Transport Services Document Owner E. Polke
Extracorporeal Life Support Organization (ELSO) Guidelines for Pediatric Respiratory Failure
 Extracorporeal Life Support Organization (ELSO) Guidelines for Pediatric Respiratory Failure Introduction This pediatric respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Extracorporeal Life Support Organization (ELSO) Guidelines for Pediatric Respiratory Failure Introduction This pediatric respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Long-gap Oesophageal Atresia
 Long-gap Atresia A guide for parents Nate (6 weeks old) Atresia Research Association Are there different types of OA? There are four main types of oesophageal atresia with or without TOF. These include
Long-gap Atresia A guide for parents Nate (6 weeks old) Atresia Research Association Are there different types of OA? There are four main types of oesophageal atresia with or without TOF. These include
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials
 Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
Respiratory Anesthetic Emergencies in Oral and Maxillofacial Surgery. By: Lillian Han
 Respiratory Anesthetic Emergencies in Oral and Maxillofacial Surgery By: Lillian Han Background: Respiratory anesthetic emergencies are the most common complications during the administration of anesthesia
Respiratory Anesthetic Emergencies in Oral and Maxillofacial Surgery By: Lillian Han Background: Respiratory anesthetic emergencies are the most common complications during the administration of anesthesia
The RESPIRATORY System. Unit 3 Transportation Systems
 The RESPIRATORY System Unit 3 Transportation Systems Functions of the Respiratory System Warm, moisten, and filter incoming air Resonating chambers for speech and sound production Oxygen and Carbon Dioxide
The RESPIRATORY System Unit 3 Transportation Systems Functions of the Respiratory System Warm, moisten, and filter incoming air Resonating chambers for speech and sound production Oxygen and Carbon Dioxide
The blue baby. Case 4
 Case 4 The blue baby Mrs Smith has brought her baby to A&E because she says he has started turning blue. What are your immediate differential diagnoses? 1 Respiratory causes: Congenital respiratory disorder.
Case 4 The blue baby Mrs Smith has brought her baby to A&E because she says he has started turning blue. What are your immediate differential diagnoses? 1 Respiratory causes: Congenital respiratory disorder.
AORTIC DISSECTIONS Current Management. TOMAS D. MARTIN, MD, LAT Professor, TCV Surgery Director UF Health Aortic Disease Center University of Florida
 AORTIC DISSECTIONS Current Management TOMAS D. MARTIN, MD, LAT Professor, TCV Surgery Director UF Health Aortic Disease Center University of Florida DISCLOSURES Terumo Medtronic Cook Edwards Cryolife AORTIC
AORTIC DISSECTIONS Current Management TOMAS D. MARTIN, MD, LAT Professor, TCV Surgery Director UF Health Aortic Disease Center University of Florida DISCLOSURES Terumo Medtronic Cook Edwards Cryolife AORTIC
Surgical indications: Non-malignant pulmonary diseases. Punnarerk Thongcharoen
 Surgical indications: Non-malignant pulmonary diseases Punnarerk Thongcharoen Non-malignant Malignant as a pathological term: Cancer Non-malignant = not cancer Malignant as an adjective: Disposed to cause
Surgical indications: Non-malignant pulmonary diseases Punnarerk Thongcharoen Non-malignant Malignant as a pathological term: Cancer Non-malignant = not cancer Malignant as an adjective: Disposed to cause
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
I enjoy open airway surgery In 2010: LTRs 28 CTRs 6 Clefts 4 Slides 20
 Michael J. Rutter, FRACS Department of Pediatric Otolaryngology- Head & Neck Surgery Aerodigestive and Esophageal Center Cincinnati Children s Hospital Medical Center Cincinnati, Ohio IPSA Denver, CO June
Michael J. Rutter, FRACS Department of Pediatric Otolaryngology- Head & Neck Surgery Aerodigestive and Esophageal Center Cincinnati Children s Hospital Medical Center Cincinnati, Ohio IPSA Denver, CO June
The Fetal Care Center at NewYork-Presbyterian/ Weill Cornell Medicine
 The Fetal Care Center at NewYork-Presbyterian/ Weill Cornell Medicine Prompt and Personalized Care for Women with Complex Pregnancies A Team of Experts additional training in maternal and fetal complications
The Fetal Care Center at NewYork-Presbyterian/ Weill Cornell Medicine Prompt and Personalized Care for Women with Complex Pregnancies A Team of Experts additional training in maternal and fetal complications
